Call us Managing the side effects of treatment for head and neck cancers
|
|
|
- Benedict Lindsey
- 8 years ago
- Views:
Transcription
1 Call us Managing the side effects of treatment for head and neck cancers Last reviewed June 2012 Contents Dry mouth Mouth sores and ulcers Changes in taste, smell and appetite Nausea and vomiting Difficulty swallowing Weight loss Tube feeding Changes to speech Loss of speech Having speech therapy Tracheostomy Tracheostomy tube Stoma Information reviewed by Head and neck cancer, and its treatment, can cause many side effects that may be temporary or permanent. This section lists some possible side effects and ways to manage them. Dry mouth A dry mouth can make chewing difficult and increases your risk of developing cavities in your teeth, so it Is important to maintaingood oral hygiene. Speak to your dentist about an oral care plan. Regular dentist visits and frequent, correct oral care at home can reduce dental complications. Ask your medical team, dentist or pharmacist about using mouth lubricants and mouthwashes Cut food into small pieces. Have frequent sips of fluid with your meals. Avoid dry, hard lollies, crisps and biscuits if your mouth is sore as well as dry. Avoid fluids that are dehydrating e.g. alcohol or highly caffeinated drinks. Try sugar-free pastilles, mints or jubes to increase saliva. If your mouth is not sore, try tangy foods such as lemons or fruit, to stimulate saliva. Make soft, moist meals e.g. add gravies or sauces, use minced meat, have soups and casseroles and add custard or cream to desserts. Sip water frequently; carry a water bottle with you. Mouth sores and ulcers Mouth sores are common during chemotherapy and radiotherapy treatment. The sores, which can form on any soft tissue in your mouth, make it difficult to eat, talk and swallow. If you have mouth sores your doctor can treat them by giving you medicines that reduce the pain when you eat, drink or speak. You may also use painkillers that can be applied directly to the mouth sores to numb them. Avoid foods that sting your mouth such as vinegar, spices, salty foods, alcohol, very hot or very cold foods and drinks, and citrus or tomato-based food or juice. Drink diluted non-citrus fruit juices such as pear or mango. Avoid dry, rough or crunchy foods such as chips, nuts, crackers or toast.
2 Chop or blend food, or add stock, milk, sauce or gravy so it s easier to swallow. Rinse your mouth and throat with warm saltwater or a mix of one teaspoon salt, one teaspoon baking soda and four cups of water. Use a straw for drinking if you have mouth ulcers. Talk to your doctor about mouthwashes or medication to relieve ulcers or thrush (a white coating in the mouth) and to keep your mouth fresh. Don t use mouthwashes with alcohol as they may irritate ulcers. Use a soft-bristled toothbrush and gently brush your teeth after meals and before bed. Replace your toothbrush regularly to reduce infections. Tell your doctor or dietitian if you have ongoing or severe difficulty swallowing. Changes in taste, smell and appetite Treatment can affect your sense of taste and smell. It can take several months for your sense of taste to return to normal. You may never regain your full sense of smell. Taste changes may make you lose your appetite or this can happen as a result of stress. Try to find ways to make mealtimes more appealing. Marinate meat, fish, poultry or tofu to add extra flavour. Freshen your mouth with sugar-free mints or chewing gum and brush your teeth after meals. If you smoke, try to quit. As well as damaging your health, smoking reduces appetite and changes the taste of food. Add lemon, ginger and vinegar to your cooking to stimulate your digestive juices and appetite. These ingredients also help to add flavour to your food. Use salt, lemon juice or coffee powder if food is too sweet; try sugar or honey if food tastes metallic or salty. You can add flavour to food with spices, garlic, herbs, cheese or bacon. Use a drinking straw to bypass your tastebuds. Ask your family or friends to prepare meals for you or try pre-cooked frozen meals if you don t feel like cooking or eating. Eat small meals and snacks throughout the day. If you lose your sense of smell take precautions such as installing smoke detectors in your home and checking the use-by dates of foods because you may not be able to smell smoke or foods that are off. Nausea and vomiting Feeling sick (nausea) and vomiting are common side effects of chemotherapy. Some people feel nauseous before, during or after treatment. Eat small meals often not eating can make nausea worse. Try sour or salty foods such as dry savoury biscuits and potato crisps. Sugar-free fizzy drinks are also good. Try a small snack such as dry toast if you wake up nauseous. Eat cold foods which may be easier to manage than hot, fried, greasy or spicy foods e.g. sandwiches, cold meats, salads and cold milk puddings. Eat or drink ginger-based foods such as candied ginger, lemon and ginger tea, dry ginger ale or ginger beer. Talk to your doctor about medication to ease ongoing nausea. If the medication is not helpful ask your doctor about trying a new type. Difficulty swallowing Many people with head and neck cancer have trouble swallowing (dysphagia) before or after treatment. Radiotherapy can cause dryness, pain and changes to the strength of the muscles used in swallowing. Surgery may also reduce your ability to swallow. If swallowing is painful ask your doctor about taking painkillers. You may also be able to use other types of soothing agents to prevent your mouth and throat from becoming too irritated. A speech pathologist can assess how you swallow and suggest changes to your diet and swallowing action to help reduce any discomfort or concerns of food going down the wrong way (aspiration). If these problems persist you may need tube feeding. Weight loss
3 You may lose weight because you may find it difficult to eat. It is important to keep your body as well nourished as possible. This is because significant weight loss can lead to reduced energy and strength, and reduced quality of life. It is also important to maintain a good weight during treatment because a change in weight can influence the accuracy of radiotherapy or the dose of chemotherapy. Eat small meals frequently. Try to eat and drink nourishing meals or snacks e.g. drink milk rather than cordial; eat biscuits rather than lollies. To gain weight add extra ingredients to recipes such as whey powder to full-cream milk, other dairy products (sour cream, butter, mayonnaise or cheese), oil, eggs, honey, sugar or golden syrup. Ask your dietitian about nutritional supplement drinks which may help you gain weight. Tube feeding After treatment many people need a temporary feeding tube. In some cases people experience long-term eating difficulties. For example, they may be at risk of aspirating food or drink into their lungs and need a different way of getting nutrition. Tube feeding (also called enteral feeding) can help you stay well-nourished if you are having difficulties eating. If the treatment team thinks you will need assistance with your nutrition during treatment they will recommend a feeding tube be placed before treatment. This will be discussed with you. A temporary feeding tube is a tube inserted through your nasal passageway (nasogastric or NG tube). It will usually be used for a few days or weeks. A long-term or permanent feeding tube is a tube inserted into your stomach while you are anaesthetised (gastrostomy). This may be referred to as a PEG (percutaneous endoscopic gastrostomy) or a RIG (radiologically inserted gastrostomy) depending on how it is inserted. If you have a long-term feeding tube THE flexible tubing may protrude eight to ten centimetres from your abdomen. Your health care team will advise you on how to keep the tube clean to prevent wear and leakage, ways to prevent blockages, and when the tubing needs to be replaced. A dietitian will tell you what kind of feeding formula and the amount you need to use. Tube feeding helps control your food intake (nutrition), fluid intake (hydration) and your overall well-being. Many people find that having a feeding tube eases the discomfort of eating and the pressure of having to
4 eat meals. If medications can t be swallowed these can also be given through the feeding tube. Having a feeding tube inserted is a significant change and it is common to feel upset about it. Talking to your family, a counsellor, dietitian or nurse may help you adjust to the change. Changes to speech Communication is one of the most important parts of life. Most people take their ability to communicate for granted. If you lose your voice or your ability to speak clearly it is natural to feel distressed, frustrated and angry at times. People around you may need to learn new ways to communicate with you. It will probably help them to take more time to listen carefully. If your voice or speech has changed some people might pretend to understand what you re saying so they don t upset you or because they re embarrassed to say they don t understand. It can be frustrating when people aren t prepared to take extra time to communicate and you may feel uncomfortable or alienated. It is important for your family and friends to provide you with understanding, sympathy and support. Loss of speech Some people lose the ability to speak clearly or produce voice due to surgery to their mouth or the removal of their voice box. Immediately after surgery you can communicate in other ways. You may find it helpful to: gesture, point, nod, smile or mouth words ring a bell to call people keep pads of paper and pens handy write on a whiteboard or point to a board with pictures or words use a computer, mobile phone or other device to type messages use the National Relay Service join an online support group such as Cancer Council s You will work with a speech pathologist to improve your speech and teach you strategies for communicating with your family and friends. Although this can be challenging sometimes most people who have had surgery are able to learn techniques to talk again. A counsellor or social worker can help you address any problems or frustrations. Having speech therapy If you are learning to talk after a total laryngectomy there are three main methods your speech pathologist may try with you: Oesophageal speech. You swallow air and force it up through your oesophagus to produce a voice like a low-pitched burp. Most people find this technique difficult to learn. Tracheoesophageal speech. Your surgeon may create a puncture between your trachea and oesophagus during the laryngectomy or later on. Your speech pathologist can then fit you with a voice prosthesis (or valve) to direct air from your trachea into the oesophagus. This creates a low-pitch, throaty voice. Mechanical speech. A battery-powered device (such as an electrolarynx) creates an external vibrating sound when it is held against the neck or cheek or placed inside the mouth. You press a button attached to the device when you want to speak. Whichever method you choose talking will take time and practice. You will also have to get used to the way your new voice sounds. If you are feeling self-conscious about the change counselling may help. Tracheostomy A tracheostomy is an operation to create an artificial opening (stoma) through the neck into the windpipe (trachea). This opening, which looks like a small hole, allows you to breathe. If you are having another surgical procedure the tracheostomy is usually done at the same time under general anaesthetic. The stoma may be temporary or permanent, and it may have tubes inserted in it. When laryngeal or pharyngeal cancer becomes advanced it can block your airways. You may have a tracheostomy before treatment. If you are recovering from surgery that has caused a swollen mouth or has interfered with breathing through the upper airways you will probably have a temporary stoma for a few weeks.
5 If you have had a total laryngectomy you will learn how to breathe through a permanent stoma. Tracheostomy tube If you have a tracheostomy tube your trachea is still connected with your upper airway. A plastic outer tube is inserted in the hole to keep it from closing. An inner tube can be removed for cleaning. It is unlikely that you will be able to speak at first because for most patients, air will not pass up through the tube into the voice box and mouth. However some patients who have a small tube or a tube with a hole (fenestrated tracheostomy tube) will be able to speak. Your nursing staff or speech pathologist will teach you how to achieve voice with these tubes. After a recovery period the tracheostomy tube will probably be removed and the stoma will close up. At first your voice may be weak and breathy but it should return to normal once the stoma has healed. Occasionally people need a tracheostomy tube for several weeks during radiotherapy or on a permanent basis. Your health care team will discuss this with you if needed. Stoma People who have a total laryngectomy breathe through a permanent stoma. During the laryngectomy the trachea is stitched permanently to an opening at the front of the neck and is no longer connected to the mouth and nose in the upper airway. You may have a tube inserted into the stoma immediately after the surgery. This makes sure the stoma stays the same size and keeps your airway open for breathing while you are healing. Your nurses will teach you and your carers how to clean the tube. You will probably be able to remove the tube during the day and eventually you probably won t need it at all. Your speech pathologist or nurse will show you products to cover the stoma and provide heat and moisture for the trachea. Feeling embarrassed or self-conscious about the way the stoma makes you look and speak is not unusual. Addressing concerns may help you come to terms with the change. Call Cancer Council with any questions. Information reviewed by: Dr Tim Iseli, ENT Surgeon, Royal Melbourne Hospital; Katrina Blyth, Senior Speech Pathologist, Royal Prince Alfred Hospital, NSW; Dr David Boadle, Staff Specialist, Medical Oncology, Royal Hobart Hospital; Geoffrey Booth, Consumer; Teresa Brown, Team Leader, Royal Brisbane and Women s Hospital; Marty Doyle, Co-founder and Facilitator, Head and Neck Cancer Support Group, Brisbane; Dr Peter Foltyn, Dental Department, St Vincent s Hospital, NSW; Noelene Hunt, Consumer; Dr Michael Jackson, Director, Radiation Oncology Department, Prince of Wales Hospital, NSW; Len McDowall, Consumer; and Cancer Council SA Helpline Consultant. Content printed from This website is made possible by the generous support of South Australians.
6 Copyright Cancer Council SA
Common nutritional problems and cancer
 Information Prescriptions Information Prescriptions are a quick and easy way to provide information about your condition and local services. www.nhs.uk/ips Acknowledgement With many thanks to the Queensland
Information Prescriptions Information Prescriptions are a quick and easy way to provide information about your condition and local services. www.nhs.uk/ips Acknowledgement With many thanks to the Queensland
Managing Eating Problems In Cancer Patients
 Managing Eating Problems In Cancer Patients Patient Information Nutrition and Dietetic Department Author ID: LB Leaflet Number: Diet 004 Version: 2 Name of Leaflet: Managing Eating Problems in Cancer Patients
Managing Eating Problems In Cancer Patients Patient Information Nutrition and Dietetic Department Author ID: LB Leaflet Number: Diet 004 Version: 2 Name of Leaflet: Managing Eating Problems in Cancer Patients
Dental care for patients with head and neck cancer
 Dental care for patients with head and neck cancer This leaflet explains why it is important to see a dentist before and after your treatment for head and neck cancer. It also explains what you can expect
Dental care for patients with head and neck cancer This leaflet explains why it is important to see a dentist before and after your treatment for head and neck cancer. It also explains what you can expect
Nutrition after chemotherapy and radiation for head and neck cancer
 Nutrition after chemotherapy and radiation for head and neck cancer Good nutrition is important while you are recovering from the side effects of your treatment for head and neck cancer. You may have:
Nutrition after chemotherapy and radiation for head and neck cancer Good nutrition is important while you are recovering from the side effects of your treatment for head and neck cancer. You may have:
Living With Congestive Heart Failure
 Living With Congestive Heart Failure Information for patients and their families Patient information developed by EPICORE Centre, Division of Cardiology, University of Alberta The REACT study: supported
Living With Congestive Heart Failure Information for patients and their families Patient information developed by EPICORE Centre, Division of Cardiology, University of Alberta The REACT study: supported
Mouth care during chemotherapy
 Some people having chemotherapy treatment find that their mouth gets sore. This information gives some tips about how you can look after your mouth before and during your chemotherapy treatment. In this
Some people having chemotherapy treatment find that their mouth gets sore. This information gives some tips about how you can look after your mouth before and during your chemotherapy treatment. In this
Managing Side Effects of Palliative Radiation Therapy
 RADIATION THERAPY SYMPTOM MANAGEMENT Managing Side Effects of Palliative Radiation Therapy In this booklet you will learn about: Common side effects when you receive palliative radiation therapy Tips on
RADIATION THERAPY SYMPTOM MANAGEMENT Managing Side Effects of Palliative Radiation Therapy In this booklet you will learn about: Common side effects when you receive palliative radiation therapy Tips on
Managing Mouth Sores
 Managing Mouth Sores The following information is based on the general experiences of many prostate cancer patients. Your experience may be different. If you have any questions about what prostate cancer
Managing Mouth Sores The following information is based on the general experiences of many prostate cancer patients. Your experience may be different. If you have any questions about what prostate cancer
Mouth Problems. How to Manage Your. This patient guide will help you understand:
 How to Manage Your Mouth Problems This patient guide will help you understand: What are cancer-related mouth problems? pg 2 What causes cancer-related mouth problems? pg 3 What can I do to help my mouth
How to Manage Your Mouth Problems This patient guide will help you understand: What are cancer-related mouth problems? pg 2 What causes cancer-related mouth problems? pg 3 What can I do to help my mouth
Dietary advice for people starting treatment for Hepatitis C. Information for patients Sheffield Dietetics
 Dietary advice for people starting treatment for Hepatitis C Information for patients Sheffield Dietetics Do I need to follow a special diet? You don t need to have a special diet but you should try and
Dietary advice for people starting treatment for Hepatitis C Information for patients Sheffield Dietetics Do I need to follow a special diet? You don t need to have a special diet but you should try and
FOLFOX Chemotherapy. This handout provides information about FOLFOX chemotherapy. It is sometimes called as FLOX chemotherapy.
 FOLFOX Chemotherapy This handout provides information about FOLFOX chemotherapy. It is sometimes called as FLOX chemotherapy. What is chemotherapy? Chemotherapy is a method of treating cancer by using
FOLFOX Chemotherapy This handout provides information about FOLFOX chemotherapy. It is sometimes called as FLOX chemotherapy. What is chemotherapy? Chemotherapy is a method of treating cancer by using
Side Effects of Chemotherapy Treatment
 Side Effects of Chemotherapy Treatment Chemotherapy drugs affect all body cells. They affect cancer cells and also normal cells. That's the reason for some of the side effects. Chemotherapy drugs especially
Side Effects of Chemotherapy Treatment Chemotherapy drugs affect all body cells. They affect cancer cells and also normal cells. That's the reason for some of the side effects. Chemotherapy drugs especially
Oxford Centre for Head and Neck Oncology. Sore Mouth or Throat (Mucositis) Dry Mouth (Xerostomia) Oral Thrush (Candida) Information for patients
 Oxford Centre for Head and Neck Oncology Sore Mouth or Throat (Mucositis) Dry Mouth (Xerostomia) Oral Thrush (Candida) Information for patients This leaflet gives you some suggested remedies which previous
Oxford Centre for Head and Neck Oncology Sore Mouth or Throat (Mucositis) Dry Mouth (Xerostomia) Oral Thrush (Candida) Information for patients This leaflet gives you some suggested remedies which previous
Managing Bowel Problems after Cancer Treatment
 Managing Bowel Problems after Cancer Treatment UHN Information for cancer survivors Read this pamphlet to learn: What bowel problems are What causes bowel problems What you can do to manage your bowel
Managing Bowel Problems after Cancer Treatment UHN Information for cancer survivors Read this pamphlet to learn: What bowel problems are What causes bowel problems What you can do to manage your bowel
Important Information for Patients Who Receive Radiation Therapy to the Head & Neck Region. Therapeutic Radiation & Oral Heath
 Important Information for Patients Who Receive Radiation Therapy to the Head & Neck Region Therapeutic Radiation & Oral Heath This leaflet should be given to patients attending the Head and Neck Cancer
Important Information for Patients Who Receive Radiation Therapy to the Head & Neck Region Therapeutic Radiation & Oral Heath This leaflet should be given to patients attending the Head and Neck Cancer
Eating problems and cancer
 This information is an extract from the booklet Eating problems and cancer. You may find the full booklet helpful. We can send you a copy free see page 13. Contents Eating problems Specialist diets Dietitians
This information is an extract from the booklet Eating problems and cancer. You may find the full booklet helpful. We can send you a copy free see page 13. Contents Eating problems Specialist diets Dietitians
Healthy Eating For Your Kidneys
 Winter 14 Healthy Eating For Your Kidneys (For People Not on Dialysis) BC Provincial Renal Agency If you have kidney disease, you may need to change the food you eat. Changes will depend on your appetite,
Winter 14 Healthy Eating For Your Kidneys (For People Not on Dialysis) BC Provincial Renal Agency If you have kidney disease, you may need to change the food you eat. Changes will depend on your appetite,
Meal Planning for a Mushy Soft Diet After Laparoscopic Myotomy
 Meal Planning for a Mushy Soft Diet After Laparoscopic Myotomy Name: Date: Dietitian: Telephone: Why is it necessary to follow this diet? This diet is necessary for individuals who have had some types
Meal Planning for a Mushy Soft Diet After Laparoscopic Myotomy Name: Date: Dietitian: Telephone: Why is it necessary to follow this diet? This diet is necessary for individuals who have had some types
MEAL PLANNING FOR MECHANICAL SOFT DIET
 MEAL PLANNING FOR MECHANICAL SOFT DIET Definition of Terms Calories Protein Blenderized Pureed Units of energy. A nutrient used by your body for growth and repair. The best sources are milk, meats, fish,
MEAL PLANNING FOR MECHANICAL SOFT DIET Definition of Terms Calories Protein Blenderized Pureed Units of energy. A nutrient used by your body for growth and repair. The best sources are milk, meats, fish,
Meal Planning for a Mushy Soft Diet After Nissen Fundoplication
 Meal Planning for a Mushy Soft Diet After Nissen Fundoplication Name: Date: Dietitian: Telephone: Questions? CALL YOUR DIETITIAN! Patient Food and Nutrition Services University of Michigan Hospital 1500
Meal Planning for a Mushy Soft Diet After Nissen Fundoplication Name: Date: Dietitian: Telephone: Questions? CALL YOUR DIETITIAN! Patient Food and Nutrition Services University of Michigan Hospital 1500
Information for people being discharged with a naso-gastric (NG) feeding tube
 Information for people being discharged with a naso-gastric (NG) feeding tube The aim of this leaflet is to provide patients with the relevant information for the use of a nasogastric tube. It will include:
Information for people being discharged with a naso-gastric (NG) feeding tube The aim of this leaflet is to provide patients with the relevant information for the use of a nasogastric tube. It will include:
Head and Neck Cancer
 Head and Neck Cancer Radiation Treatment Information for patients receiving radiation therapy for cancers of the head and neck Reading this booklet can help answer some questions you may have about your
Head and Neck Cancer Radiation Treatment Information for patients receiving radiation therapy for cancers of the head and neck Reading this booklet can help answer some questions you may have about your
Instructions Following Dental Implant Surgery
 Instructions Following Dental Implant Surgery Swelling is to be expected and usually reaches its maximum in 2-3 days. To minimize swelling, cold packs or ice bag wrapped in a towel should be applied to
Instructions Following Dental Implant Surgery Swelling is to be expected and usually reaches its maximum in 2-3 days. To minimize swelling, cold packs or ice bag wrapped in a towel should be applied to
Bariatric Surgery: Step III Diet
 Bariatric Surgery: Step III Diet This diet is blended foods with one new solid food added daily. The portions are very small to help prevent vomiting. Warning: This diet does not have enough calories,
Bariatric Surgery: Step III Diet This diet is blended foods with one new solid food added daily. The portions are very small to help prevent vomiting. Warning: This diet does not have enough calories,
Michael Abufaris, DDS, PA 201 N Lakemont Ave, Suite 600 Winter Park, FL 32792 407.629.6400
 Michael Abufaris, DDS, PA 201 N Lakemont Ave, Suite 600 Winter Park, FL 32792 407.629.6400 Oral lichen Oral lichen planus is an inflammatory condition of the mucus membranes (mucosa) and/or skin. The cause
Michael Abufaris, DDS, PA 201 N Lakemont Ave, Suite 600 Winter Park, FL 32792 407.629.6400 Oral lichen Oral lichen planus is an inflammatory condition of the mucus membranes (mucosa) and/or skin. The cause
Nutrition and Chronic Kidney Disease
 Nutrition and Chronic Kidney Disease I have been told I have early kidney failure. What does this mean? What can I expect? This means that your kidneys are not doing as good a job as they should to help
Nutrition and Chronic Kidney Disease I have been told I have early kidney failure. What does this mean? What can I expect? This means that your kidneys are not doing as good a job as they should to help
Duke Center for Metabolic and Weight Loss Surgery Pre-op Nutrition Questionnaire
 Duke Center for Metabolic and Weight Loss Surgery Pre-op Nutrition Questionnaire Name Date How long have you been considering weight loss surgery? Which procedure are you interested in having? Gastric
Duke Center for Metabolic and Weight Loss Surgery Pre-op Nutrition Questionnaire Name Date How long have you been considering weight loss surgery? Which procedure are you interested in having? Gastric
Tooth Decay. What Is Tooth Decay? Tooth decay happens when you have an infection of your teeth.
 Tooth Decay What Is Tooth Decay? Tooth decay happens when you have an infection of your teeth. When you eat food and drink, it is broken down into acid. This acid helps to make plaque (a sticky substance).
Tooth Decay What Is Tooth Decay? Tooth decay happens when you have an infection of your teeth. When you eat food and drink, it is broken down into acid. This acid helps to make plaque (a sticky substance).
Eating Hints. National Cancer Institute. Before, During, and After Cancer Treatment. Support for People With Cancer. National Institutes of Health
 National Cancer Institute Support for People With Cancer Eating Hints Before, During, and After Cancer Treatment U.S. Department of Health and Human Services National Institutes of Health About this Book
National Cancer Institute Support for People With Cancer Eating Hints Before, During, and After Cancer Treatment U.S. Department of Health and Human Services National Institutes of Health About this Book
Healthy Eating During Pregnancy
 Healthy Eating During Pregnancy Pregnancy is a time of great change. Your body is changing to allow your baby to grow and develop. Good nutrition will help you meet the extra demands of pregnancy while
Healthy Eating During Pregnancy Pregnancy is a time of great change. Your body is changing to allow your baby to grow and develop. Good nutrition will help you meet the extra demands of pregnancy while
Dental Care and Chronic Conditions. Respiratory Disease Cardiovascular Disease Diabetes
 Dental Care and Chronic Conditions Respiratory Disease Cardiovascular Disease Diabetes Shape Up Your Smile and Avoid Some Complications of Chronic Diseases When you take good care of your oral health,
Dental Care and Chronic Conditions Respiratory Disease Cardiovascular Disease Diabetes Shape Up Your Smile and Avoid Some Complications of Chronic Diseases When you take good care of your oral health,
Laryngeal Cancer. Understanding your diagnosis
 Laryngeal Cancer Understanding your diagnosis Laryngeal Cancer Understanding your diagnosis When you first hear that you have cancer, you may feel alone and afraid. You may be overwhelmed by the large
Laryngeal Cancer Understanding your diagnosis Laryngeal Cancer Understanding your diagnosis When you first hear that you have cancer, you may feel alone and afraid. You may be overwhelmed by the large
How To Eat Without Getting Sick
 Level 2 Dysphagia Mechanically Altered* This diet consists of foods that are moist, soft-textured and easily formed into a bolus. All foods on Level 1 are. Meats and other select foods may be ground or
Level 2 Dysphagia Mechanically Altered* This diet consists of foods that are moist, soft-textured and easily formed into a bolus. All foods on Level 1 are. Meats and other select foods may be ground or
First line nutrition support dietary advice
 First line nutrition support dietary advice For patients referred to the Dietetic Telephone Clinic 1 You have been given this leaflet because it was highlighted during your outpatient attendance that
First line nutrition support dietary advice For patients referred to the Dietetic Telephone Clinic 1 You have been given this leaflet because it was highlighted during your outpatient attendance that
U.S. Department of Health and Human Services National Institutes of Health National Institute of Dental and Craniofacial Research
 U.S. Department of Health and Human Services National Institutes of Health National Institute of Dental and Craniofacial Research What do I need to know about dry mouth? Dry mouth is the feeling that
U.S. Department of Health and Human Services National Institutes of Health National Institute of Dental and Craniofacial Research What do I need to know about dry mouth? Dry mouth is the feeling that
Having a PEG tube inserted?
 Having a PEG tube inserted? Information for Patients and Carers Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Having a PEG tube inserted? Information for Patients and Carers Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
For the Patient: GDP Other names: LYGDP
 1 For the Patient: GDP Other names: LYGDP G D P Gemcitabine Dexamethasone (taken by mouth) CISPlatin Uses: GDP is a drug treatment given for Non-Hodgkins and Hodgkin Lymphoma with the expectation of destroying
1 For the Patient: GDP Other names: LYGDP G D P Gemcitabine Dexamethasone (taken by mouth) CISPlatin Uses: GDP is a drug treatment given for Non-Hodgkins and Hodgkin Lymphoma with the expectation of destroying
Sick Day Management for People with Type 2 Diabetes Using Insulin
 Sick Day Management for People with Type 2 Diabetes Using Insulin When you are sick, controlling your blood sugar (glucose) can be a challenge. Nausea, vomiting, illness and changes in eating will affect
Sick Day Management for People with Type 2 Diabetes Using Insulin When you are sick, controlling your blood sugar (glucose) can be a challenge. Nausea, vomiting, illness and changes in eating will affect
Registered Trade Mark
 2008 High Energy, High Protein, Low Fiber Guidelines Registered Trade Mark High Energy, High Protein, Low Fibre Guidelines Eating well, even though you may not feel hungry, is an important part of taking
2008 High Energy, High Protein, Low Fiber Guidelines Registered Trade Mark High Energy, High Protein, Low Fibre Guidelines Eating well, even though you may not feel hungry, is an important part of taking
Low Fat Diet after Cardiac Surgery With or Without Chyle Leak
 Low Fat Diet after Cardiac Surgery With or Without Chyle Leak What is chyle? Chyle (sounds like kyle) is a milky white fluid that contains protein, fat, cholesterol, lymphocytes, and electrolytes. It is
Low Fat Diet after Cardiac Surgery With or Without Chyle Leak What is chyle? Chyle (sounds like kyle) is a milky white fluid that contains protein, fat, cholesterol, lymphocytes, and electrolytes. It is
Learning about Mouth Cancer
 Learning about Mouth Cancer Creation of this material was made possible in part by a pioneering grant from CBCC-USA. Distributed by India Cancer Initiative What is mouth cancer? Our bodies are made up
Learning about Mouth Cancer Creation of this material was made possible in part by a pioneering grant from CBCC-USA. Distributed by India Cancer Initiative What is mouth cancer? Our bodies are made up
Dental health following cancer treatment
 Dental health following cancer treatment Treatment for cancer often increases the risk for dental problems. As a cancer survivor, it is important for you to understand the reasons why dental care is especially
Dental health following cancer treatment Treatment for cancer often increases the risk for dental problems. As a cancer survivor, it is important for you to understand the reasons why dental care is especially
Understanding Dental Implants
 Understanding Dental Implants Comfort and Confidence Again A new smile It s no fun when you re missing teeth. You may not feel comfortable eating or speaking. You might even avoid smiling in public. Fortunately,
Understanding Dental Implants Comfort and Confidence Again A new smile It s no fun when you re missing teeth. You may not feel comfortable eating or speaking. You might even avoid smiling in public. Fortunately,
Dental care and treatment for patients with head and neck cancer. Department of Restorative Dentistry Information for patients
 Dental care and treatment for patients with head and neck cancer Department of Restorative Dentistry Information for patients i Why have I been referred to the Restorative Dentistry Team? Treatment of
Dental care and treatment for patients with head and neck cancer Department of Restorative Dentistry Information for patients i Why have I been referred to the Restorative Dentistry Team? Treatment of
EMBRACE Your Journey Nutrition During Treatment
 Nutrition is an important part of your cancer treatment. As you prepare for treatment, it is important to focus on eating a well-balanced diet so that your body is as healthy as it can be. When your body
Nutrition is an important part of your cancer treatment. As you prepare for treatment, it is important to focus on eating a well-balanced diet so that your body is as healthy as it can be. When your body
simple steps give you for good bowel health
 simple steps give you for good bowel health This booklet contains simple steps you can take to help achieve good bowel health. This is important to everyone, as these small changes will help your digestive
simple steps give you for good bowel health This booklet contains simple steps you can take to help achieve good bowel health. This is important to everyone, as these small changes will help your digestive
Diet for Oral Surgery/Wired Jaw
 Diet for Oral Surgery/Wired Jaw After oral surgery no chewing is allowed for a period of 4-8 weeks. During this time you will need a blenderized or liquid diet. This pamphlet will help you to get adequate
Diet for Oral Surgery/Wired Jaw After oral surgery no chewing is allowed for a period of 4-8 weeks. During this time you will need a blenderized or liquid diet. This pamphlet will help you to get adequate
Nutrition and Chronic Kidney Disease
 Nutrition and Chronic Kidney Disease National Kidney Foundation s Kidney Disease Outcomes Quality Initiative (NKF-K/DOQI TM ) The National Kidney Foundation is developing guidelines for clinical care to
Nutrition and Chronic Kidney Disease National Kidney Foundation s Kidney Disease Outcomes Quality Initiative (NKF-K/DOQI TM ) The National Kidney Foundation is developing guidelines for clinical care to
Undergoing an Oesophageal Endoscopic Resection (ER)
 Contact Information If you have an enquiry about your appointment time/date please contact the Booking Office on 0300 422 6350. For medication enquiries please call 0300 422 8232, this is an answer machine
Contact Information If you have an enquiry about your appointment time/date please contact the Booking Office on 0300 422 6350. For medication enquiries please call 0300 422 8232, this is an answer machine
NUTRITION AND HEMODIALYSIS
 NUTRITION AND HEMODIALYSIS www.kidney.org National Kidney Foundation's Kidney Disease Outcomes Quality Initiative Did you know that the National Kidney Foundation's Kidney Disease Outcomes Quality Initiative
NUTRITION AND HEMODIALYSIS www.kidney.org National Kidney Foundation's Kidney Disease Outcomes Quality Initiative Did you know that the National Kidney Foundation's Kidney Disease Outcomes Quality Initiative
Enhanced recovery after laparoscopic surgery (ERALS) programme: patient information and advice 2
 This booklet is funded by, and developed in collaboration between University Hospital Southampton NHS Foundation Trust and Pfizer Limited. NPKAM0198 March 2014 Enhanced recovery after laparoscopic surgery
This booklet is funded by, and developed in collaboration between University Hospital Southampton NHS Foundation Trust and Pfizer Limited. NPKAM0198 March 2014 Enhanced recovery after laparoscopic surgery
Radiation Treatment and Your Mouth
 Radiation Treatment and Your Mouth Oral Health, Cancer Care, and You Fitting the Pieces Together Oral Health, Cancer Care, and You Fitting the Pieces Together Oral Health, Cancer Care, and You is an awareness
Radiation Treatment and Your Mouth Oral Health, Cancer Care, and You Fitting the Pieces Together Oral Health, Cancer Care, and You Fitting the Pieces Together Oral Health, Cancer Care, and You is an awareness
Lesson 2: Save your Smile from Tooth Decay
 Lesson 2: Save your Smile from Tooth Decay OVERVIEW Objectives: By the end of the lesson, the Lay Health Worker will be able to: 1. Describe what tooth decay is and how it happens. 2. State the causes
Lesson 2: Save your Smile from Tooth Decay OVERVIEW Objectives: By the end of the lesson, the Lay Health Worker will be able to: 1. Describe what tooth decay is and how it happens. 2. State the causes
Gastric Banding. Liquid Diet - Two weeks post-operatively. Fawkner Park Nutrition Services. The Avenue Clinic, 42 The Avenue, Windsor.
 LAP BANDING - INITIAL 2 WEEKS POST GP Gastric Banding Liquid Diet - Two weeks post-operatively Fawkner Park Nutrition Services The Avenue Clinic, 42 The Avenue, Windsor Phone 9076 3063 FAWKNER' PARK NUTRITION
LAP BANDING - INITIAL 2 WEEKS POST GP Gastric Banding Liquid Diet - Two weeks post-operatively Fawkner Park Nutrition Services The Avenue Clinic, 42 The Avenue, Windsor Phone 9076 3063 FAWKNER' PARK NUTRITION
Day Case Unit, Horton General Hospital Advice after dental extractions Information for patients
 Day Case Unit, Horton General Hospital Advice after dental extractions Information for patients page 2 For the first 24 hours after your dental surgery you should avoid: any food or drinks that are very
Day Case Unit, Horton General Hospital Advice after dental extractions Information for patients page 2 For the first 24 hours after your dental surgery you should avoid: any food or drinks that are very
ENDOSCOPY UNIT. Duodenum Stomach. Having an oesophageal stent. Patient information leaflet
 Trafford Hospitals ENDOSCOPY UNIT Gastroscope Oesophagus Lungs Duodenum Stomach Having an oesophageal stent Patient information leaflet If you are unable to keep your appointment, please telephone the
Trafford Hospitals ENDOSCOPY UNIT Gastroscope Oesophagus Lungs Duodenum Stomach Having an oesophageal stent Patient information leaflet If you are unable to keep your appointment, please telephone the
UNDERGOING OESOPHAGEAL STENT INSERTION
 UNDERGOING OESOPHAGEAL STENT INSERTION Information Leaflet Your Health. Our Priority. Page 2 of 5 Introduction This leaflet tells you about the procedure known as oesophageal stent insertion, explains
UNDERGOING OESOPHAGEAL STENT INSERTION Information Leaflet Your Health. Our Priority. Page 2 of 5 Introduction This leaflet tells you about the procedure known as oesophageal stent insertion, explains
Pancreatoduodenectomy (Whipple s Procedure)
 Pancreatoduodenectomy (Whipple s Procedure) Your doctor has arranged to surgically remove part of your pancreas or Whipple s procedure. We have written this pamphlet to help you learn about your surgery
Pancreatoduodenectomy (Whipple s Procedure) Your doctor has arranged to surgically remove part of your pancreas or Whipple s procedure. We have written this pamphlet to help you learn about your surgery
For the Patient: Paclitaxel injection Other names: TAXOL
 For the Patient: Paclitaxel injection Other names: TAXOL Paclitaxel (pak'' li tax' el) is a drug that is used to treat many types of cancer. It is a clear liquid that is injected into a vein. Tell your
For the Patient: Paclitaxel injection Other names: TAXOL Paclitaxel (pak'' li tax' el) is a drug that is used to treat many types of cancer. It is a clear liquid that is injected into a vein. Tell your
My Spinal Surgery: Going Home
 My Spinal Surgery: Going Home The Spinal Surgery Team has prepared this insert containing information to help prepare you and your family for going home after your spinal surgery. Please visit the UHN
My Spinal Surgery: Going Home The Spinal Surgery Team has prepared this insert containing information to help prepare you and your family for going home after your spinal surgery. Please visit the UHN
LAPAROSCOPIC ADJUSTABLE GASTRIC BANDING (LAP-BAND TM or Realize TM Band)
 1 LAPAROSCOPIC ADJUSTABLE GASTRIC BANDING (LAP-BAND TM or Realize TM Band) DIET INSTRUCTIONS Name: Date: Dietitian: Phone: Revision 06/16/2013 2 PRESURGICAL DIET Your diet is important in the months and
1 LAPAROSCOPIC ADJUSTABLE GASTRIC BANDING (LAP-BAND TM or Realize TM Band) DIET INSTRUCTIONS Name: Date: Dietitian: Phone: Revision 06/16/2013 2 PRESURGICAL DIET Your diet is important in the months and
Bariatric Care Center Adjustable Gastric Band Post-Op Diet
 Bariatric Care Center Adjustable Gastric Band Post-Op Diet Nothing by Mouth (Night of Surgery) Clear Liquids (DAYS 1-3) Starts the day after surgery Clear liquids must be plain or sugar-free. In general,
Bariatric Care Center Adjustable Gastric Band Post-Op Diet Nothing by Mouth (Night of Surgery) Clear Liquids (DAYS 1-3) Starts the day after surgery Clear liquids must be plain or sugar-free. In general,
BREAKFAST. 2 poached eggs 1 envelope Instant Breakfast 1 cup warm milk 8 oz milk
 WHAT CAN I EAT NOW? While you are recovering from your surgery, good nutrition will be vitally important. Even though all food will need to be in liquid form, you can still enjoy mealtimes and promote
WHAT CAN I EAT NOW? While you are recovering from your surgery, good nutrition will be vitally important. Even though all food will need to be in liquid form, you can still enjoy mealtimes and promote
Oesophageal Stent. Patient Information
 Oesophageal Stent Patient Information Introduction You have been advised to have a flexible metal tube inserted into your oesophagus (gullet). This is called an oesophageal stent. The stent will hopefully
Oesophageal Stent Patient Information Introduction You have been advised to have a flexible metal tube inserted into your oesophagus (gullet). This is called an oesophageal stent. The stent will hopefully
Having a RIG tube inserted
 Having a RIG tube inserted Information for patients and carers Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Having a RIG tube inserted Information for patients and carers Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Laparoscopic Antireflux Surgery Information Sheet
 Laparoscopic Antireflux Surgery Information Sheet What is Laparoscopic Antireflux Surgery? Antireflux surgery (also known as fundoplication) is the standard surgical method of treating gastro-oesophageal
Laparoscopic Antireflux Surgery Information Sheet What is Laparoscopic Antireflux Surgery? Antireflux surgery (also known as fundoplication) is the standard surgical method of treating gastro-oesophageal
Days 1 and 2: Bariatric Clear Liquids
 Gastric Bypass Diet Days 1 and 2: Bariatric Clear Liquids Duration: 2 days Food consistency: Bariatric clear liquids, which includes clear, non-carbonated, noncalorie, caffeine-free liquids such as: o
Gastric Bypass Diet Days 1 and 2: Bariatric Clear Liquids Duration: 2 days Food consistency: Bariatric clear liquids, which includes clear, non-carbonated, noncalorie, caffeine-free liquids such as: o
Radiotherapy for a mesothelioma
 Oxford University Hospitals NHS Trust The Radiotherapy Department Radiotherapy for a mesothelioma Information for patients Introduction This leaflet is for people who have been recommended treatment with
Oxford University Hospitals NHS Trust The Radiotherapy Department Radiotherapy for a mesothelioma Information for patients Introduction This leaflet is for people who have been recommended treatment with
Chemotherapy. What is chemotherapy? How does it work? What is cancer? How will I be given chemotherapy? Cannula
 INFORMATION SHEET This information sheet has been written to help you understand more about chemotherapy. The sheet discusses the support and information your doctors, nurses and the Cancer Society can
INFORMATION SHEET This information sheet has been written to help you understand more about chemotherapy. The sheet discusses the support and information your doctors, nurses and the Cancer Society can
Understanding Cytotoxic Chemotherapy
 Understanding Cytotoxic Chemotherapy Introduction Chemotherapy is part of your continuing treatment. This booklet has been compiled in an effort to help you understand cytotoxic chemotherapy. It is your
Understanding Cytotoxic Chemotherapy Introduction Chemotherapy is part of your continuing treatment. This booklet has been compiled in an effort to help you understand cytotoxic chemotherapy. It is your
Cancer Care Oral Mucositis Managing Oral Care After Radiation or Chemotherapy. May 08
 Cancer Care Oral Mucositis Managing Oral Care After Radiation or Chemotherapy May 08 Halton Region Health Department Mission Statement Together with the Halton community, the Health Department works to
Cancer Care Oral Mucositis Managing Oral Care After Radiation or Chemotherapy May 08 Halton Region Health Department Mission Statement Together with the Halton community, the Health Department works to
Colon Cancer Surgery and Recovery. A Guide for Patients and Families
 Colon Cancer Surgery and Recovery A Guide for Patients and Families This Booklet You are receiving this booklet because you will be having surgery shortly. This booklet tells you what to do before, during,
Colon Cancer Surgery and Recovery A Guide for Patients and Families This Booklet You are receiving this booklet because you will be having surgery shortly. This booklet tells you what to do before, during,
Diet and haemodialysis
 Diet and haemodialysis This leaflet is for patients with kidney disease who are receiving haemodialysis treatment. If you have any further questions, please contact us using the details below and on the
Diet and haemodialysis This leaflet is for patients with kidney disease who are receiving haemodialysis treatment. If you have any further questions, please contact us using the details below and on the
Table 1. How Cancer Treatments Can Affect Eating
 Table 1. How Cancer Treatments Can Affect Eating Cancer Treatment How it Can Affect Eating Surgery Increases the need for good nutrition. May slow digestion. May lessen the ability of the mouth, throat,
Table 1. How Cancer Treatments Can Affect Eating Cancer Treatment How it Can Affect Eating Surgery Increases the need for good nutrition. May slow digestion. May lessen the ability of the mouth, throat,
Ear Infections Gastroenteritis gastroenteritis
 Ear Gastroenteritis Infections gastroenteritis Gastroenteritis can be caused by many different germs, and the effects of gastro on babies and children depend on several things including: the age of the
Ear Gastroenteritis Infections gastroenteritis Gastroenteritis can be caused by many different germs, and the effects of gastro on babies and children depend on several things including: the age of the
Eating for life with a gastric band
 Eating for life with a gastric band This information leaflet should only be used from at least 6 weeks after your band placement and when you are tolerating normal textured food. A reminder on how the
Eating for life with a gastric band This information leaflet should only be used from at least 6 weeks after your band placement and when you are tolerating normal textured food. A reminder on how the
A breastfed baby s bowel motions are soft, a bright yellow colour and often very frequent, but each baby is different. Breastfed babies don t usually
 2 A breastfed baby s bowel motions are soft, a bright yellow colour and often very frequent, but each baby is different. Breastfed babies don t usually get constipated, even though some babies only have
2 A breastfed baby s bowel motions are soft, a bright yellow colour and often very frequent, but each baby is different. Breastfed babies don t usually get constipated, even though some babies only have
DIABETES & HEALTHY EATING
 DIABETES & HEALTHY EATING Food gives you the energy you need for healthy living. Your body changes most of the food you eat into a sugar called glucose. (glucose) Insulin helps your cells get the sugar
DIABETES & HEALTHY EATING Food gives you the energy you need for healthy living. Your body changes most of the food you eat into a sugar called glucose. (glucose) Insulin helps your cells get the sugar
SICK DAY PLANS FOR ALL CHILDREN WITH DIABETES
 SICK DAY PLANS FOR ALL CHILDREN WITH DIABETES High blood sugar Any child with diabetes may at times have high blood sugars; it may be for a single blood test or for several tests. High blood sugar can
SICK DAY PLANS FOR ALL CHILDREN WITH DIABETES High blood sugar Any child with diabetes may at times have high blood sugars; it may be for a single blood test or for several tests. High blood sugar can
Oesophageal Stent Insertion
 Oesophageal Stent Insertion What is a Stent? A stent is a tube made of a flexible metal mesh. It is passed by mouth into the oesophagus (gullet) and positioned across the area that has narrowed. This is
Oesophageal Stent Insertion What is a Stent? A stent is a tube made of a flexible metal mesh. It is passed by mouth into the oesophagus (gullet) and positioned across the area that has narrowed. This is
Oral health care is vital for seniors
 Oral health care is vital for seniors (NC) Statistics Canada estimates seniors represent the fastest growing segment of the Canadian population, a segment expected to reach 9.2 million by 2041. As more
Oral health care is vital for seniors (NC) Statistics Canada estimates seniors represent the fastest growing segment of the Canadian population, a segment expected to reach 9.2 million by 2041. As more
Chemotherapy Side Effects Worksheet
 Page 1 of 6 Chemotherapy Side Effects Worksheet Medicines or drugs that destroy cancer cells are called cancer chemotherapy. It is sometimes the first choice for treating many cancers. Chemotherapy differs
Page 1 of 6 Chemotherapy Side Effects Worksheet Medicines or drugs that destroy cancer cells are called cancer chemotherapy. It is sometimes the first choice for treating many cancers. Chemotherapy differs
Blenderized & Pureed Recipes
 Blenderized & Pureed Recipes While you are having difficulty chewing or swallowing, use these recipes for preparing pureed meals. Use the recipes as a base for developing your own recipes. Be creative!
Blenderized & Pureed Recipes While you are having difficulty chewing or swallowing, use these recipes for preparing pureed meals. Use the recipes as a base for developing your own recipes. Be creative!
Why does my child need to follow a milk and dairy free diet?
 Milk and dairy free diet Why does my child need to follow a milk and dairy free diet? Your child has an allergy to milk and dairy products, and their ingredients. An allergic reaction to milk and dairy
Milk and dairy free diet Why does my child need to follow a milk and dairy free diet? Your child has an allergy to milk and dairy products, and their ingredients. An allergic reaction to milk and dairy
Virtual or CT Colonography
 Virtual or CT Colonography CT Department Ground Floor, Lanesborough Wing Please contact the CT department on 020 8725 1730 to confirm your appointment. This information leaflet is for patients who are
Virtual or CT Colonography CT Department Ground Floor, Lanesborough Wing Please contact the CT department on 020 8725 1730 to confirm your appointment. This information leaflet is for patients who are
Information for adult patients. Common questions about tonsil surgery. Why do we have tonsils? How is the operation performed? What happens now?
 Information for adult patients The purpose of this information is to help everyone who undergoes tonsil surgery to feel as good as possible after the operation and to return to normal food and normal activities
Information for adult patients The purpose of this information is to help everyone who undergoes tonsil surgery to feel as good as possible after the operation and to return to normal food and normal activities
Radiation Therapy for Breast Cancer
 Radiation Therapy for Breast Cancer www.cpmc.org/learning i learning about your health What Is? Radiation therapy is a treatment for cancer that uses high-energy x-rays to destroy cancer cells. (Radiation
Radiation Therapy for Breast Cancer www.cpmc.org/learning i learning about your health What Is? Radiation therapy is a treatment for cancer that uses high-energy x-rays to destroy cancer cells. (Radiation
Oesophageal stent insertion
 Oesophageal stent insertion Exceptional healthcare, personally delivered Oesophageal Stent Insertion Introduction This leaflet tells you about the procedure known as oesophageal stent insertion, explains
Oesophageal stent insertion Exceptional healthcare, personally delivered Oesophageal Stent Insertion Introduction This leaflet tells you about the procedure known as oesophageal stent insertion, explains
Sick Day Management of Adults with Type 2 Diabetes. CONSUMER RESOURCE December 2014
 Sick Day Management of Adults with Type 2 Diabetes CONSUMER RESOURCE December 2014 Acknowledgement The 2014 Sick Day Management of Adults with Type 2 Diabetes Consumer resource is develop based on the
Sick Day Management of Adults with Type 2 Diabetes CONSUMER RESOURCE December 2014 Acknowledgement The 2014 Sick Day Management of Adults with Type 2 Diabetes Consumer resource is develop based on the
A guide to eating and drinking with a Gastric Band
 The London Bariatric Group A guide to eating and drinking with a Gastric Band Information for patients and carers A practical guide to changes in eating and drinking after adjustable gastric band surgery
The London Bariatric Group A guide to eating and drinking with a Gastric Band Information for patients and carers A practical guide to changes in eating and drinking after adjustable gastric band surgery
GUIDELINES FOR CONSISTENCY MODIFICATIONS OF FOODS AND LIQUIDS
 GUIDELINES FOR CONSISTENCY MODIFICATIONS OF FOODS AND LIQUIDS 1. Alterations to the consistency of foods and/ or liquids presented to the individual are made in accordance with the recommendation of an
GUIDELINES FOR CONSISTENCY MODIFICATIONS OF FOODS AND LIQUIDS 1. Alterations to the consistency of foods and/ or liquids presented to the individual are made in accordance with the recommendation of an
How to prepare for your colonoscopy using bowel preparation Type 1 and type 2 diabetes - insulin treated diabetes management (Evening appointment)
 South of Tyne Bowel Cancer Screening Programme How to prepare for your colonoscopy using bowel preparation Type 1 and type 2 diabetes - insulin treated diabetes management (Evening appointment) December
South of Tyne Bowel Cancer Screening Programme How to prepare for your colonoscopy using bowel preparation Type 1 and type 2 diabetes - insulin treated diabetes management (Evening appointment) December
Managing mouth problems after head and neck cancer treatment
 Managing mouth problems after head and neck cancer treatment This information is an extract from the booklet Managing the late effects of head and neck cancer treatment. You may find the full booklet helpful.
Managing mouth problems after head and neck cancer treatment This information is an extract from the booklet Managing the late effects of head and neck cancer treatment. You may find the full booklet helpful.
Recovery plan: radical cystectomy Information for patients
 Recovery plan: radical cystectomy Information for patients Help for you following a bereavement 5 This leaflet will help you know what to expect during your time with us. Please take some time to read
Recovery plan: radical cystectomy Information for patients Help for you following a bereavement 5 This leaflet will help you know what to expect during your time with us. Please take some time to read
How to prepare for your colonoscopy using bowel preparation Type 1 and type 2 diabetes / insulin treated diabetes management. (Morning appointment)
 South of Tyne Bowel Cancer Screening Programme How to prepare for your colonoscopy using bowel preparation Type 1 and type 2 diabetes / insulin treated diabetes management. (Morning appointment) June 2012
South of Tyne Bowel Cancer Screening Programme How to prepare for your colonoscopy using bowel preparation Type 1 and type 2 diabetes / insulin treated diabetes management. (Morning appointment) June 2012
Oesophageal Stent Insertion
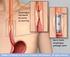 Oesophageal Stent Insertion Endoscopy Department Central Operations Group This leaflet has been designed to give you important information about your condition / procedure, and to answer some common queries
Oesophageal Stent Insertion Endoscopy Department Central Operations Group This leaflet has been designed to give you important information about your condition / procedure, and to answer some common queries
Laparoscopic Fundoplication for Reflux
 Laparoscopic Fundoplication for Reflux Exceptional healthcare, personally delivered Understanding Reflux General Reflux happens when acid from the stomach washes up into the gullet (oesophagus) from the
Laparoscopic Fundoplication for Reflux Exceptional healthcare, personally delivered Understanding Reflux General Reflux happens when acid from the stomach washes up into the gullet (oesophagus) from the
A guide to eating and drinking with a Gastric Band
 A guide to eating and drinking with a Gastric Band Information for patients and carers A practical guide to changes in eating and drinking after adjustable gastric band surgery Contents Introduction 3
A guide to eating and drinking with a Gastric Band Information for patients and carers A practical guide to changes in eating and drinking after adjustable gastric band surgery Contents Introduction 3
Useful Websites for more information. www.eatwell.gov.uk. www.lovefoodhatewaste.com. www.nutrition.org.uk. www.bda.uk.com
 Useful Websites for more information www.eatwell.gov.uk www.lovefoodhatewaste.com www.nutrition.org.uk www.bda.uk.com Community Development Dietitians 2010 This Leaflet has been awarded: Commendation from
Useful Websites for more information www.eatwell.gov.uk www.lovefoodhatewaste.com www.nutrition.org.uk www.bda.uk.com Community Development Dietitians 2010 This Leaflet has been awarded: Commendation from
Managing Acute Side Effects of Pelvic Radiation for Gynaecological Cancers
 RADIATION THERAPY SYMPTOM MANAGEMENT Managing Acute Side Effects of Pelvic Radiation for Gynaecological Cancers In this booklet you will learn about: Common side effects when you receive radiation therapy
RADIATION THERAPY SYMPTOM MANAGEMENT Managing Acute Side Effects of Pelvic Radiation for Gynaecological Cancers In this booklet you will learn about: Common side effects when you receive radiation therapy
