2014 Quality Improvement and Utilization Management Evaluation Summary
|
|
|
- Cory Cooper
- 10 years ago
- Views:
Transcription
1 2014 Quality Improvement and Utilization Management Evaluation Summary INTRODUCTION The Quality Improvement (QI) and Utilization Management (UM) Program Evaluation summarizes the completed and ongoing quality improvement and utilization management activities and evaluates the overall effectiveness of Kentucky Health Cooperative (KYHC) Quality Improvement Program (QIP). The Clinical Care Integration Department has established annual reporting of QI/UM initiatives, activities, results and analysis by completing the QI/UM Program Evaluation for this first reporting period, plan year At this time, it does not allow for timely reporting of Healthcare Effectiveness Data and Information Set (HEDIS ) results and other annual measurements since this is the first year baseline evaluation. Therefore, this evaluation is focused on activities completed between January 1, 2014 and December 31, It addresses the Quality Improvement (QI) Program Description, the Utilzation Management (UM) Program Description, the QI/UM Work Plan and related QI/UM projects, studies and initiatives during this defined time frame. The 2014 QI/UM Evaluation also provides an overview and summary of the results of KYHC s clinical and service initiatives which affect its membership. The 2014 program results are evaluated, tracked and trended herein for the purpose of overall program evaluation and planning for the year The 2014 QI/UM Work Plan was developed to meet the obligations outlined in the QI/UM Program Descriptions, NCQA accreditation standards and both state and federal contractual requirements; it includes quality improvement goals and objectives for the year. The KYHC Board of Directors approves the QI/UM Program Evaluation in order to fulfill its responsibility to managed care members, the community, regulatory agencies and accreditation bodies. The QI Program Description, the UM Program Description, the QI/UM Work Plan and QI/UM Program Evaluation are reviewed and approved at least annually by the Quality Improvement Committee (QIC) and the KYHC Board of Directors (BOD). MISSION STATEMENT Kentucky Health Cooperative exists to promote community health and well-being by engaging the members and practitioners it serves in the valued delivery of quality coverage of integarated health care services. The organization s mission encompasses outreach to all eligible individuals with a particular focus on population segments previously ignored by other health insurers. Commonly known as the working uninsured, Kentucky Health Cooperative will seek to help those individuals who need health insurance coverage, but are not eligible for public assistance in other forms. As Kentucky Health Cooperative will operate as a statewide organization, it will devote equal effort to promote coverage of individuals and small groups in rural as well as urban settings.
2 PURPOSE The purpose of the QI/UM Program Evaluation is to plan, implement and monitor ongoing efforts that demonstrate improvements in member safety, health status, outcomes, and satisfaction. The quality improvement program is evaluated to determine its effectiveness and how the program has improved care and service to members. PROGRAM OVERVIEW Clinical Care Integration (CCI) Department Structure and Resources The CCI Department resources did not always meet the needs of the QI/UM Program during 2014, resulting in the need to hire, train and maintain both UM Nurse Managers and Intake Coordinators. The following positions and staff were involved in various QI/UM Program activities: Vice President for Clinical Care Integration (VPCCI) serves as the Senior Executive for Quality Initiatives Director, Quality Improvement (RN) Director, Utilization and Case Management (RN) Appeals Coordinators (1) Case Management Coordinators (2) Disease Management Coordinators (2) Intake Coordinators (4) Pharmacy Coordinator (2) Program Coordinator (1) QI Coordinators (1) QI Project Manager (1) Utilization Management Nurses (6) Chief Medical Officer (1) (part-time) Committee Structure During 2014, the following Committees supported the QI/UM Program: Board of Directors KYHC s Board of Directors (BOD) has the ultimate authority and accountability for the QI/UM Program. The Board of Directors delegates the authority of the QI/UM Program to KYHC s CEO who delegates the daily operations of the QI/UM Program to the Vice President of Clinical Care Integration (VPCCI). The BOD met eleven times during At each meeting, QI/UM activities were reviewed, evaluated, and approved and/or recommendations were made related to the activities.
3 Quality Improvement Committee (QIC) The Quality Improvement Committee (QIC) is a key committee at KYHC and provides delegated oversight of the QI/UM Program on behalf of the BOD and is charged with developing and implementing the QI/UM Program. The QIC reports directly to the BOD. The QIC provided direction to, and oversight of, those management and subcommittee functions responsible for the provision of clinical care and services. The QIC is responsible for approval of the annual QI and UM Program Descriptions, review of the QI/UM Work Plan and Annual QI/UM Evaluations. The QIC is also responsible for the review and approval of clinical and preventive health guidelines, UM criteria, under- and over-utilization findings, clinical and service audit findings, and administrative policies that have an impact on the member s health care. The QIC provided recommendations regarding practitioner education and interventions, health education programs, and other Plan initiatives. It is charged with accountability for the review of member complaints for quality of care and sentinel events having the potential for an adverse effect on members. The QIC reviewed the aggregate data of member complaints and surveys, as well as the results of practitioner audits. The QIC met seven times during Credentialing Committee (CC) The CC is responsible for managing the Credentialing Program to credential and re-credential providers, practitioners, facilities, and ancillary providers. The CC is a statewide committee that incorporates data identified through QI and UM process as indicated in its ongoing monitoring and re-credentialing process. The CC reports directly to the QIC; it met eight times during Utilization Management Committee (UMC) The UMC is responsible for the review and appropriate approval of medical necessity criteria, protocols, policies and procedures. The UMC monitors and analyzes relevant data to detect and correct patterns of potential or actual inappropriate under- or over-utilization, which may affect health care services, as well as the coordination of care, appropriate use of services, resources and member and practitioner satisfaction with the UM process. Annually, the UMC reviews and approves the Utilization Management Program Description, Work Plan and Program Evaluation. The UMC reports directly to the QIC; it met five times during Complaint and Appeals Committee (CAC) The CAC oversees all member complaints and appeals activities to maintain compliance with the contractual regulatory and accreditation requirements and reviews. The CAC also oversees delegated entity complaints for KYHC members. The CAC monitors all follow-up review resolutions related to member complaints and appeals and they review member complaints and appeals for trends and/or patterns and categorizes accordingly. The CAC reports directly to the QIC and meets quarterly. The CAC met once during 4 th quarter and reviewed 1 st, 2 nd and 3 rd quarter complaints and appeals.
4 QI/UM PROGRAM EFFECTIVENESS During 2014 the QI/UM Program continued its collaboration with all organizational departments to facilitate continuous improvement in performance by empowering all stakeholders through education, communication, and evaluation. KYHC has continued to improve the quality of care and services provided to the membership through continuous assessment of patterns and trends and identification of barriers to quality outcomes. Strengths and Accomplishments 1. All Plan Policies and Procedures were reviewed and updated as needed 2. Developed multiple QI/UM initiatives 3. Maintained ongoing audits of Denial and Appeal Files 4. Access goals for Primary Care and High Volume Specialist were exceeded 5. HIPAA Audits were conducted by Compilance on all KYHC employees 6. Completed verification of licensure on 100% of licensed employees 7. All UM Medical Necessity Appeals met Turn Around Time (TAT) less than or equal to 30 days 8. All DOI complaints resolutions were completed in a timely manner 9. KYHC Provider Manual was made available to practitioners on the provider tab of the KYHC public website 10. Placed links on the Clinical Care web page for Clinical Practice Guidelines and Preventive Care Guidelines adopted by KYHC 11. New direct contract practitioner orientation program is conducted monthly 12. Annual Compliance Training completed for all KYHC employees in Identified various process flows for managing prior authorizations and educated the practitioner network of the various UM requirements 14. Maintained consistency in utilization care manager application of InterQual medical necessity criteria. 15. Established ongoing delegated oversight with Behavioral Health, Pharmacy, Vision Services and Helpline Opportunities for Improvement 1. Maintain regularly scheduled committee meetings 2. Increase the number of participating practitioners in the following committees a. Quality Improvement Committee b. Credentialing Committee 3. Educate participating practitioners on KYHC appointment and after hours standards 4. Initiate the Complex Case Management Program 5. Increase resources in the CCI department 6. Obtain Baseline HEDIS Data 7. Obtain Baseline CAHPS Qualified Health Plan Member Experience Data 8. Increase the Complaints and Appeals Workgroup Meetings to four times a year 9. Meet TAT for UM Medical Necessity initial determinations
5 10. Initiate Perinatal Depression Screening Awareness Program 11. Initiate Medical and Behavioral Health Continuity and Coordination Meetings between KYHC and MHNet 12. Develop health and wellness programs utilizing self-management tools 13. Develop tools to assist members in obtaining information regarding claims processing, ordering an ID card and managing pharmacy benefits online Conclusion The above evaluation focuses not only on KYHC strengths and accomplishments, but identifies several opportunities for improvements in our processes, our training methods, and ways in which KYHC procures and shares information. The evaluation highlights the need for continuous quality improvement with regard to stabilize KYHCs operational components affecting responsiveness to members, with regard to member services call center operations, UM staffing and administrative processes. Attracting almost double the anticipated enrollment into the KYHC plan offerings significantly challenged the ability of the plan to have administrative processes and procedures in place to meet the needs of members, particularly given the unusual mix of consumers without previous health plan experience and the adverse selection that occurred with the enrolled patient mix. According to the Exchange, KYHC received approximately 90% of the State s High Risk Pool population that enrolled with a Qualified Health Plan in Based upon the existing patient demographics and utilization patterns, KYHCs patient mix maintains a higher level of acuity than most traditional commercial populations. KYHC has taken actions to avoid significant net new enrollments, and has adjusted staffing, or engaged external resources to better meet the needs of its members going forward. Conversely, KYHC was able to offer health benefit plans that appealed to more consumers than it had anticipated. This allowed the plan to enroll a sufficient membership base to begin baseline assessments of population-based underlying health status, evaluation of chronic health care needs, and identification of disease specific conditions, as well as early identification of opportunities for improvement. These opportunities align closely with the KYHCs mission of providing quality health insurance benefits access to consumers in both urban and rural areas of the state. The first year of operations resulted in providing an exciting new choice in Kentucky for consumers. KYHC is committed to continuous quality improvement in its operational functions to better focus on its mission: identifying member needs, designing programs/interventions that lower costs while continuing to maintain quality, and helping improve health outcomes for KYHC members. KYHC has the ability, with its relatively small size, to be nimble and responsive to marketplace demands, to engage with members and practitioners in communities, and to be
6 innovative with regard to utilization strategies that lead to health outcomes improvement. Being one of only two statewide issuers on the Kentucky Exchange provides KYHC with the unique opportunity to work in small rural communities, considering the social determinants such as lack of education, transportation, income, cultural, or other common social barriers which may negatively affect patient compliance, use of preventive measures, and achievement of personal health outcomes. The opportunity to positively affect change in these areas is further strengthened by KYHC s proximity to its membership. In addition, the baseline data gathered reflects opportunities for KYHC to provide focused education to its members, practitioners, and others in regard to the benefits of maintaining health insurance, the importance of health improvement and health maintenance, and the prevention of health complications. This not only impacts the members themselves, but extends to other stakeholders, such as their families, their communities, and employers. Many of our members report anecdotally that they have never had consistent insurance coverage prior to enrolling this year. This may explain the unique profile that is the average KYHC member. Our members are still learning how to appropriately access and engage the healthcare system. Many are for the first time in a long-time establishing care with a provider. Even more are just beginning to learn how to be their own healthcare advocates. They are learning how their health insurance works and how to receive benefits. There is a learning curve to this process which may explain the utilization rates we are experiencing. While the goals described are ambitious, given the strides made this past year as a brand new start-up insurer, KYHC is confident we will continue to develop multiple strategies for improving our product, our member s access to health care and the quality of care provided to our members. The CO-OP concept, (i.e. nonprofit, member-governed health plans), has proven a very attractive option to both rural and urban constituents. Cooperatives engender a greater level of trust from members and practitioners than typical commercial insurers tend to experience. Member trust in a health plan is a foundational building block for a positive working relationship. Offering a reliable benefits plan, with quality coverage, at a fair price, with a broad network of providers, affords us the trust of our members to educate them, advocate for them and expand their options for care, and in the process, positively change members lives. It also provides a platform which extends beyond the Member, and integrates working with their practitioners s and healthcare facilities, to achieve improved overall health outcomes for the Member, their families, their employers and the greater community, and ultimately, for a healthier Kentucky
Making the Grade! A Closer Look at Health Plan Performance
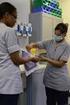
 Primary Care Update August 2011 Making the Grade! A Closer Look at Health Plan Performance HEDIS (Healthcare Effectiveness Data and Information Set) is a set of standardized measures designed to track
Primary Care Update August 2011 Making the Grade! A Closer Look at Health Plan Performance HEDIS (Healthcare Effectiveness Data and Information Set) is a set of standardized measures designed to track
Clinical Affairs. Quality Management and Improvement and Utilization Management Program Evaluation July 1 December 31 Calendar Year 2011
 Clinical Affairs July 1, 2011 December 31, 2011 Annual Evaluation of the Quality Management and Improvement Program. This evaluation is organized into sections which include Clinical Practice Guidelines,
Clinical Affairs July 1, 2011 December 31, 2011 Annual Evaluation of the Quality Management and Improvement Program. This evaluation is organized into sections which include Clinical Practice Guidelines,
Coventry Health Care of Florida, Inc. Coventry Health Plan of Florida, Inc. Summit Health Plan of Florida
 Coventry Health Care of Florida, Inc. Coventry Health Plan of Florida, Inc. Summit Health Plan of Florida Medicare Quality Management Program Overview Quality Improvement (QI) Overview At Coventry, we
Coventry Health Care of Florida, Inc. Coventry Health Plan of Florida, Inc. Summit Health Plan of Florida Medicare Quality Management Program Overview Quality Improvement (QI) Overview At Coventry, we
2014 Quality Improvement Program Description
 2014 Quality Improvement Program Description Table of Contents BACKGROUND AND HISTORY 2 MISSION STATEMENT 3 AUTHORITY 3 SCOPE 3 QI ACTIVITES TO FULFILL THE SCOPE 4 PURPOSE 6 GOALS 7 OBJECTIVES 7 DELEGATION
2014 Quality Improvement Program Description Table of Contents BACKGROUND AND HISTORY 2 MISSION STATEMENT 3 AUTHORITY 3 SCOPE 3 QI ACTIVITES TO FULFILL THE SCOPE 4 PURPOSE 6 GOALS 7 OBJECTIVES 7 DELEGATION
Coventry Health Care of Florida, Inc. Coventry Health Plan of Florida, Inc. Coventry Health and Life Insurance Company Commercial Lines of Business
 Coventry Health Care of Florida, Inc. Coventry Health Plan of Florida, Inc. Coventry Health and Life Insurance Company Commercial Lines of Business Quality Management Program 2012 Overview Quality Improvement
Coventry Health Care of Florida, Inc. Coventry Health Plan of Florida, Inc. Coventry Health and Life Insurance Company Commercial Lines of Business Quality Management Program 2012 Overview Quality Improvement
A. IEHP Quality Management Program Description
 A. IEHP Quality Management Program Description A. Purpose: The purpose of the QM Program is to provide operational direction necessary to monitor and evaluate the quality and appropriateness of care, identify
A. IEHP Quality Management Program Description A. Purpose: The purpose of the QM Program is to provide operational direction necessary to monitor and evaluate the quality and appropriateness of care, identify
Riverside Physician Network Utilization Management
 Subject: Program Riverside Physician Network Author: Candis Kliewer, RN Department: Product: Commercial, Senior Revised by: Linda McKevitt, RN Approved by: Effective Date January 1997 Revision Date 1/21/15
Subject: Program Riverside Physician Network Author: Candis Kliewer, RN Department: Product: Commercial, Senior Revised by: Linda McKevitt, RN Approved by: Effective Date January 1997 Revision Date 1/21/15
Quality and Performance Improvement Program Description 2016
 Quality and Performance Improvement Program Description 2016 Introduction and Purpose Contra Costa Health Plan (CCHP) is a federally qualified, state licensed, county sponsored Health Maintenance Organization
Quality and Performance Improvement Program Description 2016 Introduction and Purpose Contra Costa Health Plan (CCHP) is a federally qualified, state licensed, county sponsored Health Maintenance Organization
Quality Improvement Program Description
 2015 Quality Improvement Program Description Approved by the Board of Directors: March 19, 2002; April 22, 2003; April 20, 2004; April 26, 2005, April 25, 2006, February 27, 2007, March 25, 2008, March
2015 Quality Improvement Program Description Approved by the Board of Directors: March 19, 2002; April 22, 2003; April 20, 2004; April 26, 2005, April 25, 2006, February 27, 2007, March 25, 2008, March
Quality Improvement Program
 Quality Improvement Program Section M-1 Additional information on the Quality Improvement Program (QIP) and activities is available on our website at www.molinahealthcare.com Upon request in writing, Molina
Quality Improvement Program Section M-1 Additional information on the Quality Improvement Program (QIP) and activities is available on our website at www.molinahealthcare.com Upon request in writing, Molina
How To Manage Health Care Needs
 HEALTH MANAGEMENT CUP recognizes the importance of promoting effective health management and preventive care for conditions that are relevant to our populations, thereby improving health care outcomes.
HEALTH MANAGEMENT CUP recognizes the importance of promoting effective health management and preventive care for conditions that are relevant to our populations, thereby improving health care outcomes.
Aetna Better Health Aetna Better Health Kids. Quality Management Utilization Management. 2013 Program Evaluation
 Aetna Better Health Aetna Better Health Kids Quality Management Utilization Management 2013 Program Evaluation EXECUTIVE SUMMARY Introduction Aetna Better Health implemented its Medicaid Physical Health-Managed
Aetna Better Health Aetna Better Health Kids Quality Management Utilization Management 2013 Program Evaluation EXECUTIVE SUMMARY Introduction Aetna Better Health implemented its Medicaid Physical Health-Managed
HEALTH ALLIANCE MEDICAL PLANS 2015 QUALITY and MEDICAL MANAGEMENT PROGRAM STRUCTURE
 HEALTH ALLIANCE MEDICAL PLANS 2015 QUALITY and MEDICAL MANAGEMENT PROGRAM STRUCTURE The Quality and Medical Management (QMM) Program integrates the primary functions of Quality, Medical Management and
HEALTH ALLIANCE MEDICAL PLANS 2015 QUALITY and MEDICAL MANAGEMENT PROGRAM STRUCTURE The Quality and Medical Management (QMM) Program integrates the primary functions of Quality, Medical Management and
URAC Issue Brief: Best Practices in Network Management
 1220 L Street, NW, Suite 400 Washington, DC 20005 202.216.9010 Best Practices in Network Management Introduction As consumers enroll in health plans through newly formed Health Insurance Marketplaces,
1220 L Street, NW, Suite 400 Washington, DC 20005 202.216.9010 Best Practices in Network Management Introduction As consumers enroll in health plans through newly formed Health Insurance Marketplaces,
Utilization Management Program. [January 2016-January 2017]
![Utilization Management Program. [January 2016-January 2017] Utilization Management Program. [January 2016-January 2017]](/thumbs/39/18083548.jpg) Utilization Management Program [January 2016-January 2017] Table of Contents Program Overview... 5 Program Goals... 6 Scope... 6 UM Committee Structure [UM1A:1 & 3; UM2A:4-5; UM1B; UM1C; UM1D]... 7 Use
Utilization Management Program [January 2016-January 2017] Table of Contents Program Overview... 5 Program Goals... 6 Scope... 6 UM Committee Structure [UM1A:1 & 3; UM2A:4-5; UM1B; UM1C; UM1D]... 7 Use
504 Lavaca Street Suite 850 Austin, Texas 78701 PROVIDER NEWSLETTER
 504 Lavaca Street Suite 850 Austin, Texas 78701 PROVIDER NEWSLETTER PROVIDER REPORT www.cenpatico.com Welcome to the first Cenpatico provider report for 2013. We re excited to share with you details on
504 Lavaca Street Suite 850 Austin, Texas 78701 PROVIDER NEWSLETTER PROVIDER REPORT www.cenpatico.com Welcome to the first Cenpatico provider report for 2013. We re excited to share with you details on
Regal Medical Group & QUALITY IMPROVEMENT (QI) PROGRAM 2015
 Regal Medical Group & QUALITY IMPROVEMENT (QI) PROGRAM 2015 Approval Signatures: Kenneth Epstein, MD, Committee Chair 1/23/2015 Date: QUALITY IMPROVEMENT (QI) PROGRAM Contents REGAL MEDICAL GROUP & LAKESIDE
Regal Medical Group & QUALITY IMPROVEMENT (QI) PROGRAM 2015 Approval Signatures: Kenneth Epstein, MD, Committee Chair 1/23/2015 Date: QUALITY IMPROVEMENT (QI) PROGRAM Contents REGAL MEDICAL GROUP & LAKESIDE
Louisiana CMC MAGELLAN HEALTH SERVICES MAGELLAN HEALTH UTILIZATION MANAGEMENT PROGRAM DESCRIPTION FOR MEDICAID MANAGED CARE
 Louisiana CMC MAGELLAN HEALTH SERVICES MAGELLAN HEALTH UTILIZATION MANAGEMENT PROGRAM DESCRIPTION FOR MEDICAID MANAGED CARE MARCH 1, 2014 FEBRUARY 28, 2015 Table of Contents Section I: Overview of Program
Louisiana CMC MAGELLAN HEALTH SERVICES MAGELLAN HEALTH UTILIZATION MANAGEMENT PROGRAM DESCRIPTION FOR MEDICAID MANAGED CARE MARCH 1, 2014 FEBRUARY 28, 2015 Table of Contents Section I: Overview of Program
OROVILLE HOSPITAL JOB DESCRIPTION. Department: Dept.#: Last Updated:
 OROVILLE HOSPITAL JOB DESCRIPTION Job Description for VICE PRESIDENT OF NURSING Department: Dept.#: Last Updated: Nursing Administration 8720 TITLE: REPORTS TO: VICE PRESIDENT OF NURSING CHIEF EXECUTIVE
OROVILLE HOSPITAL JOB DESCRIPTION Job Description for VICE PRESIDENT OF NURSING Department: Dept.#: Last Updated: Nursing Administration 8720 TITLE: REPORTS TO: VICE PRESIDENT OF NURSING CHIEF EXECUTIVE
Functions: The UM Program consists of the following components:
 1.0 Introduction Alameda County Behavioral Health Care Services (ACBHCS) includes a Utilization Management (UM) Program and Behavioral Health Managed Care Plan (MCP). They are dedicated to delivering cost
1.0 Introduction Alameda County Behavioral Health Care Services (ACBHCS) includes a Utilization Management (UM) Program and Behavioral Health Managed Care Plan (MCP). They are dedicated to delivering cost
California Networks for EHR Adoption
 California Networks for EHR Adoption Request for Proposals: Phase I - Planning A program jointly sponsored by: Community Clinics Initiative A joint program of Tides and The California Endowment California
California Networks for EHR Adoption Request for Proposals: Phase I - Planning A program jointly sponsored by: Community Clinics Initiative A joint program of Tides and The California Endowment California
HealthCare Partners of Nevada. Heart Failure
 HealthCare Partners of Nevada Heart Failure Disease Management Program 2010 HF DISEASE MANAGEMENT PROGRAM The HealthCare Partners of Nevada (HCPNV) offers a Disease Management program for members with
HealthCare Partners of Nevada Heart Failure Disease Management Program 2010 HF DISEASE MANAGEMENT PROGRAM The HealthCare Partners of Nevada (HCPNV) offers a Disease Management program for members with
In Quality Management/Risk Management (QM/RM), PHQCI is responsible for overseeing the
 Title: Population Health and Quality of Care Improvement Director (PHQCI) Job Summary: Reporting directly to the COO the PHQCI is responsible for the day to day activities of National Health Services (NHS)
Title: Population Health and Quality of Care Improvement Director (PHQCI) Job Summary: Reporting directly to the COO the PHQCI is responsible for the day to day activities of National Health Services (NHS)
Standards of Practice & Scope of Services. for Health Care Delivery System Case Management and Transitions of Care (TOC) Professionals
 A M E R I C A N C A S E M A N A G E M E N T A S S O C I A T I O N Standards of Practice & Scope of Services for Health Care Delivery System Case Management and Transitions of Care (TOC) Professionals O
A M E R I C A N C A S E M A N A G E M E N T A S S O C I A T I O N Standards of Practice & Scope of Services for Health Care Delivery System Case Management and Transitions of Care (TOC) Professionals O
Guidelines for a Successful OC Survey
 Guidelines for a Successful OC Survey 2007 Standards Welcome to the NCQA Organization Certification (OC) survey process. The guidelines and resources contained in this appendix will help you prepare for
Guidelines for a Successful OC Survey 2007 Standards Welcome to the NCQA Organization Certification (OC) survey process. The guidelines and resources contained in this appendix will help you prepare for
Quality Improvement Program Description
 ABH 2013 Quality Improvement Program Description, Work Plan, and Evaluation 1 Appendix A Quality Improvement Program Description ABH 2013 Quality Improvement Program Description, Work Plan, and Evaluation
ABH 2013 Quality Improvement Program Description, Work Plan, and Evaluation 1 Appendix A Quality Improvement Program Description ABH 2013 Quality Improvement Program Description, Work Plan, and Evaluation
EQR PROTOCOL 1 ASSESSING MCO COMPLIANCE WITH MEDICAID AND CHIP MANAGED CARE REGULATIONS
 EQR PROTOCOL 1 ASSESSING MCO COMPLIANCE WITH MEDICAID AND CHIP MANAGED CARE REGULATIONS Attachment D: The purpose of this Attachment to Protocol 1 is to provide the reviewer(s) with sample review questions
EQR PROTOCOL 1 ASSESSING MCO COMPLIANCE WITH MEDICAID AND CHIP MANAGED CARE REGULATIONS Attachment D: The purpose of this Attachment to Protocol 1 is to provide the reviewer(s) with sample review questions
2015 Quality Improvement Program Description
 Horizon Blue Cross Blue Shield of New Jersey Horizon Healthcare of New Jersey, Inc. Horizon Insurance Company 2015 Quality Improvement Program Description QIC approval 1/26/2015 Table of Contents I. INTRODUCTION
Horizon Blue Cross Blue Shield of New Jersey Horizon Healthcare of New Jersey, Inc. Horizon Insurance Company 2015 Quality Improvement Program Description QIC approval 1/26/2015 Table of Contents I. INTRODUCTION
HEALTH ALLIANCE MEDICAL PLANS 2013 QUALITY and MEDICAL MANAGEMENT PROGRAM STRUCTURE
 HEALTH ALLIANCE MEDICAL PLANS 2013 QUALITY and MEDICAL MANAGEMENT PROGRAM STRUCTURE The Quality and Medical Management (QMM) Program integrates the primary functions of Quality, Medical Management and
HEALTH ALLIANCE MEDICAL PLANS 2013 QUALITY and MEDICAL MANAGEMENT PROGRAM STRUCTURE The Quality and Medical Management (QMM) Program integrates the primary functions of Quality, Medical Management and
Regulatory and Legislative Action Since the September 2010 Membership Meeting:
 MEMBERSHIP MEETING January 19, 2011 Delivery System Reform: Healthcare Workforce Issue: The passage of health reform will bring millions of newly insured individuals into the system and drive patients
MEMBERSHIP MEETING January 19, 2011 Delivery System Reform: Healthcare Workforce Issue: The passage of health reform will bring millions of newly insured individuals into the system and drive patients
FIRST COAST HEALTH ALLIANCE, LLC CHARTER AUDIT, FINANCE, AND NETWORK CONTRACTS COMMITTEE
 AUDIT, FINANCE, AND NETWORK CONTRACTS COMMITTEE 1. Establishment and Purpose. The Audit, Finance, and Networks Contracts Committee is established by the Board for the purpose of overseeing the integrity
AUDIT, FINANCE, AND NETWORK CONTRACTS COMMITTEE 1. Establishment and Purpose. The Audit, Finance, and Networks Contracts Committee is established by the Board for the purpose of overseeing the integrity
Crosswalk: CMS Shared Savings Rules & NCQA ACO Accreditation Standards 12/1/2011
 Crosswalk: CMS Shared Savings Rules & NCQA ACO Accreditation Standards 12/1/2011 The table below details areas where NCQA s ACO Accreditation standards overlap with the CMS Final Rule CMS Pioneer ACO CMS
Crosswalk: CMS Shared Savings Rules & NCQA ACO Accreditation Standards 12/1/2011 The table below details areas where NCQA s ACO Accreditation standards overlap with the CMS Final Rule CMS Pioneer ACO CMS
Blue Shield Mental Health Service Administrator (MHSA) Quality Improvement Program
 Blue Shield Mental Health Service Administrator (MHSA) Quality Improvement Program Blue Shield of California s mental health service administrator (MHSA) administers behavioral health and substance use
Blue Shield Mental Health Service Administrator (MHSA) Quality Improvement Program Blue Shield of California s mental health service administrator (MHSA) administers behavioral health and substance use
PROVIDER MANUAL. HPN Clinical Services Department
 2015 PROVIDER MANUAL HPN Clinical Services Department 1 TABLE OF CONTENTS Page # GENERAL INFORMATION... 3 HERITAGE PROVIDER NETWORK, INC. STRUCTURE... 4 HPN, INC. MISSION, VISION AND VALUES... 5 CULTURAL
2015 PROVIDER MANUAL HPN Clinical Services Department 1 TABLE OF CONTENTS Page # GENERAL INFORMATION... 3 HERITAGE PROVIDER NETWORK, INC. STRUCTURE... 4 HPN, INC. MISSION, VISION AND VALUES... 5 CULTURAL
Colorado Choice Health Plans
 Quality Overview Colorado Choice Health Plans Accreditation Exchange Product Accrediting Organization: Accreditation Status: URAC Health Plan Accreditation (Marketplace HMO) Provisional Accreditation Commercial
Quality Overview Colorado Choice Health Plans Accreditation Exchange Product Accrediting Organization: Accreditation Status: URAC Health Plan Accreditation (Marketplace HMO) Provisional Accreditation Commercial
Response to Serving the Medi Cal SPD Population in Alameda County
 Expanding Health Coverage and Increasing Access to High Quality Care Response to Serving the Medi Cal SPD Population in Alameda County As the State has acknowledged in the 1115 waiver concept paper, the
Expanding Health Coverage and Increasing Access to High Quality Care Response to Serving the Medi Cal SPD Population in Alameda County As the State has acknowledged in the 1115 waiver concept paper, the
RFP HTH 460-12-02. Attachment I. CAMHD Quality Assurance and Improvement Program
 Attachment I CAMHD Table of Contents 1. Purpose of the................... 3 2. Goals and Objectives of the QAIP......................................... 4 3. Methods Used to Systematically Monitor Care
Attachment I CAMHD Table of Contents 1. Purpose of the................... 3 2. Goals and Objectives of the QAIP......................................... 4 3. Methods Used to Systematically Monitor Care
Compliance Department No. COMP.1000.18 Title: EFFECTIVE SYSTEM FOR ROUTINE MONITORING, AUDITING, AND IDENTIFICATION OF COMPLIANCE RISKS (ELEMENT 6)
 Page: 1 of 9 I. SCOPE: This policy applies to (1) Tenet Healthcare Corporation and its wholly-owned subsidiaries and affiliates (each, an Affiliate ); and (2) any other entity or organization in which
Page: 1 of 9 I. SCOPE: This policy applies to (1) Tenet Healthcare Corporation and its wholly-owned subsidiaries and affiliates (each, an Affiliate ); and (2) any other entity or organization in which
More than a score: working together to achieve better health outcomes while meeting HEDIS measures
 NEVADA ProviderNews Vol. 3 2014 More than a score: working together to achieve better health outcomes while meeting HEDIS measures We know you ve heard of Healthcare Effectiveness Data and Information
NEVADA ProviderNews Vol. 3 2014 More than a score: working together to achieve better health outcomes while meeting HEDIS measures We know you ve heard of Healthcare Effectiveness Data and Information
Quality Management Plan 1
 BIGHORN VALLEY HEALTH CENTER PRINCIPLES OF PRACTICE Category: Quality Title: C3 Quality Management Plan Quality Management Plan 1 I. STRUCTURE OF THE QUALITY MANAGEMENT PROGRAM A. Definition of Quality
BIGHORN VALLEY HEALTH CENTER PRINCIPLES OF PRACTICE Category: Quality Title: C3 Quality Management Plan Quality Management Plan 1 I. STRUCTURE OF THE QUALITY MANAGEMENT PROGRAM A. Definition of Quality
Medicare Managed Care Manual Chapter 5 - Quality Assessment
 Medicare Managed Care Manual Chapter 5 - Quality Assessment Transmittals Issued for this Chapter Table of Contents (Rev. 117, 08-08-14) 10 Introduction 20 Medicare Quality Improvement Program 20.1 Chronic
Medicare Managed Care Manual Chapter 5 - Quality Assessment Transmittals Issued for this Chapter Table of Contents (Rev. 117, 08-08-14) 10 Introduction 20 Medicare Quality Improvement Program 20.1 Chronic
For any questions not answered by materials provided within this profile, please contact Wayne Pendleton, CEO of LIFE, at [email protected].
 For More Information For any questions not answered by materials provided within this profile, please contact Wayne Pendleton, CEO of LIFE, at [email protected]. Or contact Shawn Bloom, President
For More Information For any questions not answered by materials provided within this profile, please contact Wayne Pendleton, CEO of LIFE, at [email protected]. Or contact Shawn Bloom, President
NORTH COUNTRY COMMUNITY MENTAL HEALTH NORTHERN AFFILIATION UTILIZATION MANAGEMENT PLAN November 1, 2001. Revised January 2013
 NORTH COUNTRY COMMUNITY MENTAL HEALTH NORTHERN AFFILIATION UTILIZATION MANAGEMENT PLAN November 1, 2001 Revised January 2013 I. Mission II. III. IV. Scope Philosophy Authority V. Utilization Management
NORTH COUNTRY COMMUNITY MENTAL HEALTH NORTHERN AFFILIATION UTILIZATION MANAGEMENT PLAN November 1, 2001 Revised January 2013 I. Mission II. III. IV. Scope Philosophy Authority V. Utilization Management
2015 ASHP STRATEGIC PLAN
 2015 ASHP STRATEGIC PLAN ASHP Vision ASHP s vision is that medication use will be optimal, safe, and effective for all people all of the time. ASHP Mission The mission of pharmacists is to help people
2015 ASHP STRATEGIC PLAN ASHP Vision ASHP s vision is that medication use will be optimal, safe, and effective for all people all of the time. ASHP Mission The mission of pharmacists is to help people
Introduction to Medication Management Systems, Inc. Comprehensive Medication Therapy Management Solutions
 Introduction to Medication Management Systems, Inc. Comprehensive Medication Therapy Management Solutions Vision Medication Management Systems, Inc. (MMS) envisions a health care system in which all patients
Introduction to Medication Management Systems, Inc. Comprehensive Medication Therapy Management Solutions Vision Medication Management Systems, Inc. (MMS) envisions a health care system in which all patients
VENDOR AUDIT LETTER TEMPLATE
 VENDOR AUDIT LETTER TEMPLATE Date Mr/Ms. Vendor Contact Name Title Company Name Company Address City, State Zip Dear Mr/Ms.: As part of our Vendor Management Program, (Name) Health Plan performs oversight
VENDOR AUDIT LETTER TEMPLATE Date Mr/Ms. Vendor Contact Name Title Company Name Company Address City, State Zip Dear Mr/Ms.: As part of our Vendor Management Program, (Name) Health Plan performs oversight
Indiana Coalition for Human Services ICHS) Comments on the Healthy Indiana Plan (HIP) 2.0 Waiver Application (submitted 9/20/14)
 Indiana Coalition for Human Services ICHS) Comments on the Healthy Indiana Plan (HIP) 2.0 Waiver Application (submitted 9/20/14) Indiana Coalition for Human Services (ICHS) appreciates the opportunity
Indiana Coalition for Human Services ICHS) Comments on the Healthy Indiana Plan (HIP) 2.0 Waiver Application (submitted 9/20/14) Indiana Coalition for Human Services (ICHS) appreciates the opportunity
Linking the Parish Mobile Clinic - Strategic Plan
 19 Linking the Parish Mobile Clinic - Strategic Plan Introduction Strategic planning for this project focuses on assessing needs and resources, defining a target patient base, and establishing a set of
19 Linking the Parish Mobile Clinic - Strategic Plan Introduction Strategic planning for this project focuses on assessing needs and resources, defining a target patient base, and establishing a set of
OPTUM PIERCE BEHAVIORAL HEALTH ORGANIZATION
 OPTUM PIERCE BEHAVIORAL HEALTH ORGANIZATION QUALITY ASSURANCE/PERFORMANCE IMPROVEMENT POLICIES AND PROCEDURES Quality Assurance/Performance Improvement (QA/PI) Committee Structure Policy: QA-06 Section:
OPTUM PIERCE BEHAVIORAL HEALTH ORGANIZATION QUALITY ASSURANCE/PERFORMANCE IMPROVEMENT POLICIES AND PROCEDURES Quality Assurance/Performance Improvement (QA/PI) Committee Structure Policy: QA-06 Section:
Pamela Tropiano, RN, CCM, BSN, MPA. CareSource
 Annual Education Conference September 30 October 3, 2012 Orlando, FL 1.7 Creative Case Management Pamela Tropiano, RN, CCM, BSN, MPA Senior Vice President, Health hservices CareSource Mission: The CareSource
Annual Education Conference September 30 October 3, 2012 Orlando, FL 1.7 Creative Case Management Pamela Tropiano, RN, CCM, BSN, MPA Senior Vice President, Health hservices CareSource Mission: The CareSource
CLASS FAMILY: Business Operations and Administrative Management
 OCCUPATIONAL GROUP: Business Administration CLASS FAMILY: Business Operations and Administrative Management CLASS FAMILY DESCRIPTION: This family of positions includes those which perform administrative
OCCUPATIONAL GROUP: Business Administration CLASS FAMILY: Business Operations and Administrative Management CLASS FAMILY DESCRIPTION: This family of positions includes those which perform administrative
Special Needs Plans Structure & Process Measures. Policy Clarifications and Frequently Asked Questions (FAQs)
 Effective June 4, 2010 Special Needs Plans Structure & Process Measures Policy Clarifications and Frequently Asked Questions (FAQs) CMS Contract No. HHSM-500-2006-00060C Contents General Questions Q1:
Effective June 4, 2010 Special Needs Plans Structure & Process Measures Policy Clarifications and Frequently Asked Questions (FAQs) CMS Contract No. HHSM-500-2006-00060C Contents General Questions Q1:
NCQA Health Plan Accreditation. Creating Value by Improving Health Care Quality
 NCQA Health Plan Accreditation Creating Value by Improving Health Care Quality NCQA Health Plan Accreditation Creating Value by Improving Health Care Quality Purchasers, consumers and health plans pay
NCQA Health Plan Accreditation Creating Value by Improving Health Care Quality NCQA Health Plan Accreditation Creating Value by Improving Health Care Quality Purchasers, consumers and health plans pay
UNIVERSITY OF MISSISSIPPI MEDICAL CENTER RISK MANAGEMENT PLAN
 UNIVERSITY OF MISSISSIPPI MEDICAL CENTER RISK MANAGEMENT PLAN 2013 1 RISK MANAGEMENT PLAN 2013 PROGRAM GOALS The University of Mississippi Medical Center is committed to providing the highest level of
UNIVERSITY OF MISSISSIPPI MEDICAL CENTER RISK MANAGEMENT PLAN 2013 1 RISK MANAGEMENT PLAN 2013 PROGRAM GOALS The University of Mississippi Medical Center is committed to providing the highest level of
Performance Appraisal Process for the CEO 1
 www.simonejoyaux.com Simone P. Joyaux, ACFRE Performance Appraisal Process for the CEO 1 Note: This process and appraisal tool along with Joyaux CEO job description applies, in general to any organization.
www.simonejoyaux.com Simone P. Joyaux, ACFRE Performance Appraisal Process for the CEO 1 Note: This process and appraisal tool along with Joyaux CEO job description applies, in general to any organization.
IX. Network Management
 A. ValueOptions' Network Department As part of the efforts to develop a state-of-the-art behavioral health system in Texas, ValueOptions recognizes and acknowledges the provider network is not only crucial
A. ValueOptions' Network Department As part of the efforts to develop a state-of-the-art behavioral health system in Texas, ValueOptions recognizes and acknowledges the provider network is not only crucial
MNsure Compliance Program Strategic Plan. December 17, 2014
 MNsure Compliance Program Strategic Plan December 17, 2014 Page 2 of 12 TABLE OF CONTENTS Introduction... 3 Compliance Program Mission... 3 Compliance Department Mission... 3 Regulatory Profile... 4 Key
MNsure Compliance Program Strategic Plan December 17, 2014 Page 2 of 12 TABLE OF CONTENTS Introduction... 3 Compliance Program Mission... 3 Compliance Department Mission... 3 Regulatory Profile... 4 Key
Brazos Valley Community Action Agency, Inc Community Health Centers (HealthPoint) Quality Management (QM) Plan
 Brazos Valley Community Action Agency, Inc Community Health Centers (HealthPoint) Quality Management (QM) Plan TABLE OF CONTENTS PURPOSE OBJECTIVES STRUCTURE AND ROLES OF QUALITY MANAGEMENT PROGRAM I.
Brazos Valley Community Action Agency, Inc Community Health Centers (HealthPoint) Quality Management (QM) Plan TABLE OF CONTENTS PURPOSE OBJECTIVES STRUCTURE AND ROLES OF QUALITY MANAGEMENT PROGRAM I.
MERCY MARICOPA INTEGRATED CARE Job list*
 MERCY MARICOPA INTEGRATED CARE Job list* Position Integrated Health Care Development Officer Chief Clinical Officer Arizona-licensed clinical practitioner Children's Medical Arizona-licensed physician,
MERCY MARICOPA INTEGRATED CARE Job list* Position Integrated Health Care Development Officer Chief Clinical Officer Arizona-licensed clinical practitioner Children's Medical Arizona-licensed physician,
Conifer Health Solutions Tenet Investor Webinar
 Conifer Health Solutions Tenet Investor Webinar May 16, 2012 Stephen Mooney President, Conifer Health Solutions 1 2012 Conifer Health Solutions, LLC. All Rights Reserved. Forward Looking Statements Certain
Conifer Health Solutions Tenet Investor Webinar May 16, 2012 Stephen Mooney President, Conifer Health Solutions 1 2012 Conifer Health Solutions, LLC. All Rights Reserved. Forward Looking Statements Certain
CHAPTER 535 HEALTH HOMES. Background... 2. Policy... 2. 535.1 Member Eligibility and Enrollment... 2. 535.2 Health Home Required Functions...
 TABLE OF CONTENTS SECTION PAGE NUMBER Background... 2 Policy... 2 535.1 Member Eligibility and Enrollment... 2 535.2 Health Home Required Functions... 3 535.3 Health Home Coordination Role... 4 535.4 Health
TABLE OF CONTENTS SECTION PAGE NUMBER Background... 2 Policy... 2 535.1 Member Eligibility and Enrollment... 2 535.2 Health Home Required Functions... 3 535.3 Health Home Coordination Role... 4 535.4 Health
The City of Calgary, 2009 PSC Operational Review Final Report
 1. The City of Calgary, 2009 PSC Operational Review Final Report Prepared by Framework Partners Inc. & Emergency Services Consulting International April 20, 2010 Table of Contents Executive Summary...
1. The City of Calgary, 2009 PSC Operational Review Final Report Prepared by Framework Partners Inc. & Emergency Services Consulting International April 20, 2010 Table of Contents Executive Summary...
5. Case Studies: Implementation of Performance Improvement Strategies
 5. Case Studies: Implementation of Performance Improvement Strategies Case Study #1: Best Practices for Call Center Operations, Consumer- Focused Staff, and Sharing Effective Solutions The Case of Blue
5. Case Studies: Implementation of Performance Improvement Strategies Case Study #1: Best Practices for Call Center Operations, Consumer- Focused Staff, and Sharing Effective Solutions The Case of Blue
Exhibit 2.9 Utilization Management Program
 Exhibit 2.9 Utilization Management Program Access HealthSource, Inc. Utilization Management Company is licensed as a Utilization Review Agent with the Texas Department of Insurance. The Access HealthSource,
Exhibit 2.9 Utilization Management Program Access HealthSource, Inc. Utilization Management Company is licensed as a Utilization Review Agent with the Texas Department of Insurance. The Access HealthSource,
Quality Improvement Project (QIP) Reporting Tool
 Quality Improvement Project (QIP) Reporting Tool A. Medicare Advantage Organization (MAO) Information MAO Name Contract # Identification # MAO Location Contact Person Name Title Telephone Email MAO Plan
Quality Improvement Project (QIP) Reporting Tool A. Medicare Advantage Organization (MAO) Information MAO Name Contract # Identification # MAO Location Contact Person Name Title Telephone Email MAO Plan
GENESEE COUNTY Date Issued: 01-1999 COMMUNITY MENTAL HEALTH Date Revised: 08-2011 PIHP POLICY MANUAL SUBJECT:
 GENESEE COUNTY Date Issued: 01-1999 COMMUNITY MENTAL HEALTH Date Revised: 08-2011 PIHP POLICY MANUAL SUBJECT: Page 1 of 7 WRITTEN BY: T. Deeghan, COO TECHNICAL REVIEW BY: T. Deeghan, S. Mason AUTHORIZED
GENESEE COUNTY Date Issued: 01-1999 COMMUNITY MENTAL HEALTH Date Revised: 08-2011 PIHP POLICY MANUAL SUBJECT: Page 1 of 7 WRITTEN BY: T. Deeghan, COO TECHNICAL REVIEW BY: T. Deeghan, S. Mason AUTHORIZED
DTCC RISK COMMITTEE CHARTER
 DTCC RISK COMMITTEE CHARTER Purpose The ability to identify, manage and mitigate risk is fundamental to the services that The Depository Trust & Clearing Corporation ( DTCC ) provides to its members and
DTCC RISK COMMITTEE CHARTER Purpose The ability to identify, manage and mitigate risk is fundamental to the services that The Depository Trust & Clearing Corporation ( DTCC ) provides to its members and
High Desert Medical Group Connections for Life Program Description
 High Desert Medical Group Connections for Life Program Description POLICY: High Desert Medical Group ("HDMG") promotes patient health and wellbeing by actively coordinating services for members with multiple
High Desert Medical Group Connections for Life Program Description POLICY: High Desert Medical Group ("HDMG") promotes patient health and wellbeing by actively coordinating services for members with multiple
ACCREDITATION STANDARDS AND CRITERIA FOR ACADEMIC QUALITY OF POST-SECONDARY AND HIGHER DEGREE PROGRAMS IN NURSING
 III. ACCREDITATION STANDARDS AND CRITERIA FOR ACADEMIC QUALITY OF POST-SECONDARY AND HIGHER DEGREE PROGRAMS IN NURSING A. NLNAC Definition of Quality The core values of accreditation emphasize learning,
III. ACCREDITATION STANDARDS AND CRITERIA FOR ACADEMIC QUALITY OF POST-SECONDARY AND HIGHER DEGREE PROGRAMS IN NURSING A. NLNAC Definition of Quality The core values of accreditation emphasize learning,
BOARD AND CEO ROLES DIFFERENT JOBS DIFFERENT TASKS
 BOARD AND CEO ROLES DIFFERENT JOBS DIFFERENT TASKS Introduction Local boards of trustees and chief executive officers play different roles and have different responsibilities in leading their districts.
BOARD AND CEO ROLES DIFFERENT JOBS DIFFERENT TASKS Introduction Local boards of trustees and chief executive officers play different roles and have different responsibilities in leading their districts.
Section 10. Compliance
 Section 10. Compliance Fraud, Waste, and Abuse Introduction Molina Healthcare of [state] maintains a comprehensive Fraud, Waste, and Abuse program. The program is held accountable for the special investigative
Section 10. Compliance Fraud, Waste, and Abuse Introduction Molina Healthcare of [state] maintains a comprehensive Fraud, Waste, and Abuse program. The program is held accountable for the special investigative
DEFINITIONS: The following definitions will apply to this Policy:
 CLASSIFICATION: MEDICAL STAFF POLICY NUMBER: MS004 EFFECTIVE DATE: 08/91 SUBJECT: Allied Health Professionals DATE REVIEWED/ REVISED: 03/97, 09/01, 06/03, 12/03, 09/04, 11/08, 2/09, 2/10, 3/12, 2/13, 3/13,
CLASSIFICATION: MEDICAL STAFF POLICY NUMBER: MS004 EFFECTIVE DATE: 08/91 SUBJECT: Allied Health Professionals DATE REVIEWED/ REVISED: 03/97, 09/01, 06/03, 12/03, 09/04, 11/08, 2/09, 2/10, 3/12, 2/13, 3/13,
Quality Management Program I. PURPOSE...2 II. SCOPE...2 MTM S MISSION AND VISION...3 IV. RESOURCES...3 V. OBJECTIVES...3
 Table of Contents I. PURPOSE...2 II. SCOPE...2 III. MTM S MISSION AND VISION...3 IV. RESOURCES...3 V. OBJECTIVES...3 VI. STRATEGIES...4 A. OVERSIGHT OF CUSTOMER SERVICE CENTERS...4 B. TRANSPORTATION PROVIDER
Table of Contents I. PURPOSE...2 II. SCOPE...2 III. MTM S MISSION AND VISION...3 IV. RESOURCES...3 V. OBJECTIVES...3 VI. STRATEGIES...4 A. OVERSIGHT OF CUSTOMER SERVICE CENTERS...4 B. TRANSPORTATION PROVIDER
CORPORATE GOVERNANCE GUIDELINES. (Adopted as of June 2, 2014)
 CORPORATE GOVERNANCE GUIDELINES (Adopted as of June 2, 2014) The following corporate governance guidelines have been approved and adopted by the Board of Directors (the Board ) of Arista Networks, Inc.
CORPORATE GOVERNANCE GUIDELINES (Adopted as of June 2, 2014) The following corporate governance guidelines have been approved and adopted by the Board of Directors (the Board ) of Arista Networks, Inc.
MODULE 11: Developing Care Management Support
 MODULE 11: Developing Care Management Support In this module, we will describe the essential role local care managers play in health care delivery improvement programs and review some of the tools and
MODULE 11: Developing Care Management Support In this module, we will describe the essential role local care managers play in health care delivery improvement programs and review some of the tools and
MUTUAL HOUSING MANAGEMENT
 J O B D E S C R I P T I O N Job Title: Location: Department: Reports To: FSLA Status: Director of Property Management Sacramento Property Management Chief Executive Officer Exempt (professional) Updated:
J O B D E S C R I P T I O N Job Title: Location: Department: Reports To: FSLA Status: Director of Property Management Sacramento Property Management Chief Executive Officer Exempt (professional) Updated:
Kaiser Permanente Southern California Depression Care Program
 Kaiser Permanente Southern California Depression Care Program Abstract In 2001, Kaiser Permanente of Southern California (KPSC) adopted the IMPACT model of collaborative care for depression, developed
Kaiser Permanente Southern California Depression Care Program Abstract In 2001, Kaiser Permanente of Southern California (KPSC) adopted the IMPACT model of collaborative care for depression, developed
LogistiCare Solutions, LLC
 June 16, 2014 LogistiCare Solutions, LLC Non Emergency Medical Transportation Program June 11, 2014 LogistiCare empowers passionate people to provide quality access to human and healthcare services through
June 16, 2014 LogistiCare Solutions, LLC Non Emergency Medical Transportation Program June 11, 2014 LogistiCare empowers passionate people to provide quality access to human and healthcare services through
[SAMPLE RISK MANAGEMENT PLAN] [ORGANIZATION NAME BUSINESS ADDRESS CITY, ST, ZIP TELEPHONE NUMBER FACSIMILE NUMBER WEBSITE ADDRESS EMAIL ADDRESS]
![[SAMPLE RISK MANAGEMENT PLAN] [ORGANIZATION NAME BUSINESS ADDRESS CITY, ST, ZIP TELEPHONE NUMBER FACSIMILE NUMBER WEBSITE ADDRESS EMAIL ADDRESS] [SAMPLE RISK MANAGEMENT PLAN] [ORGANIZATION NAME BUSINESS ADDRESS CITY, ST, ZIP TELEPHONE NUMBER FACSIMILE NUMBER WEBSITE ADDRESS EMAIL ADDRESS]](/thumbs/38/17924683.jpg) Risk management is an integral component of a healthcare firm's standard business practice. Healthcare Providers Service Organization (HPSO) and Nurses Service Organization (NSO), the administrators of
Risk management is an integral component of a healthcare firm's standard business practice. Healthcare Providers Service Organization (HPSO) and Nurses Service Organization (NSO), the administrators of
CHAPTER 59A-23 WORKERS COMPENSATION MANAGED CARE ARRANGEMENTS 59A-23.001 Scope. 59A-23.002 Definitions. 59A-23.003 Authorization Procedures.
 CHAPTER 59A-23 WORKERS COMPENSATION MANAGED CARE ARRANGEMENTS 59A-23.001 Scope. 59A-23.002 Definitions. 59A-23.003 Authorization Procedures. 59A-23.004 Quality Assurance. 59A-23.005 Medical Records and
CHAPTER 59A-23 WORKERS COMPENSATION MANAGED CARE ARRANGEMENTS 59A-23.001 Scope. 59A-23.002 Definitions. 59A-23.003 Authorization Procedures. 59A-23.004 Quality Assurance. 59A-23.005 Medical Records and
