Self-injectable, infused and oral specialty drugs 2014 Aetna Specialty CareRx SM Benefits Plan Drug List
|
|
|
- Antonia Parrish
- 8 years ago
- Views:
Transcription
1 Quality health plans & benefits Healthier living Financial well-being Intelligent solutions Self-injectable, infused and oral specialty drugs 2014 Aetna Specialty CareRx SM Benefits Plan Drug List F (1/14)
2 What you should know to get started What is Aetna Specialty CareRx? Aetna Specialty CareRx is a pharmacy benefits/insurance plan that covers certain specialty drugs. You may get your first fill of these drugs at a retail pharmacy. To achieve best coverage, all refills must come from an in-network specialty pharmacy, like Aetna Specialty Pharmacy medicine and support services. Please review your plan documents for more about the requirements and limitations of your pharmacy benefits and insurance plan. What is a specialty drug? Specialty drugs treat complex, chronic diseases. Because of the complex therapy needed, a pharmacist or nurse should check in with you often during your treatment. These drugs may be injected, infused or taken by mouth. They may need to be refrigerated. They are often expensive and may not be available at retail pharmacies. Specialty medicine through Aetna Specialty Pharmacy and the Specialty Pharmacy Network may not be available to California HMO members. Talk to your doctor about the appropriate way to get the specialty medicines you need. Doctors may have agreed to dispense and administer these drugs to you themselves. Or they may write a prescription so you can fill them at any participating retail or mail-order pharmacy you choose. Key PR Precertification required under most plans * Drug may not be available through Aetna Specialty Pharmacy. QL Quantity limit applies under most plans ** Specialty tier drugs that are also available through a retail pharmacy or through Aetna Specialty Pharmacy. ST Step therapy applies under most plans + If your doctor supplies and administers these drugs, he or she may continue to do so. Your drug may continue to be covered by your medical plan. Category Generic medicine Brand-name medicine Antineoplastic Agents Antineoplastics (oral) tretinoin QL capecitabine temozolomide ST AFINITOR AFINITOR DIS BOSULIF CAPRELSA * COMETRIQ ERIVEDGE GILOTRIF * GLEEVEC HYCAMTIN ST ICLUSIG ST INLYTA IRESSA * QL JAKAFI * MEKINIST ST NEXAVAR OFORTA * POMALYST REVLIMID PR ST SPRYCEL STIVARGA SUTENT TAFINLAR TARCEVA TASIGNA TEMODAR THALOMID TYKERB VOTRIENT XELODA XALKORI * ZELBORAF ZOLINZA 2 Health benefits and health insurance plans are offered, administered and/or underwritten by Aetna Health Inc., Aetna Health of California Inc., Aetna Health Insurance Company of New York, Aetna Health Insurance Company and/or Aetna Life Insurance Company (Aetna). In Florida, by Aetna Health Inc. and/or Aetna Life Insurance Company. In Maryland, by Aetna Health Inc., 151 Farmington Avenue, Hartford, CT Each insurer has sole financial responsibility for its own products. Aetna Pharmacy Management refers to an internal business unit of Aetna Health Management, LLC.
3 Antineoplastics Hormonal agents leuprolide ELIGARD FASLODEX + FIRMAGON PR + LUPRON LUPRON DEPOT + TRELSTAR MIX + TRELSTAR DEPOT + TRELSTAR LA + VANTAS + ST XTANDI * ZOLADEX + + ZYTIGA Antineoplastics Miscellaneous ACTIMMUNE PR ALFERON N PR + INTRON-A PR SYLATRON Blood Products Modifiers Volume Expanders Anticoagulants Heparins fondaparinux ** FRAGMIN ** INNOHEP ** IPRIVASK ** Anti-inhibitor Coagulant Complex FEIBA NF PR FEIBA VH PR Blood Clotting Factor VIIa (recombinant) NOVOSEVEN PR NOVOSEVEN RT PR Blood Clotting Factor VIII (human) ALPHANATE PR CORIFACT PR HEMOFIL M PR HUMATE-P PR KOATE-DVI PR MONOCLATE-P PR WILATE PR Blood Clotting Factor VIII (recombinant) ADVATE PR HELIXATE FS PR KOGENATE FS PR RECOMBINATE PR REFACTO PR XYNTHA PR Blood Clotting Factor IX (non-recombinant) ALPHANINE SD PR MONONINE PR PROFILNINE PR Blood Clotting Factor IX (recombinant) BEBULIN VH PR BENEFIX PR PROPLEX T PR Fibrinogen Concentrate (Human) RIASTAP + RIXUBIS PR Hematopoietic Growth Factors ARANESP PR + EPOGEN PR + LEUKINE + NEULASTA + NEUMEGA + NEUPOGEN + NPLATE + PROCRIT PR + PROMACTA PR + Hereditary Angioedema BERINERT PR + CINRYZE * PR + FIRAZYR PR + KALBITOR * PR + Paroxysmal Nocturnal Hemoglobinuria (PNH) SOLIRIS PR + Cardiovascular System ST Hypertension VECAMYL Inherited homozygous familial hypercholesterolemia JUXTAPID * ST ST KYNAMRO 3
4 Pulmonary Hypertension Agents epoprostenol * PR + ADCIRCA sildenafil ADEMPAS * FLOLAN * PR + LETAIRIS PR + REMODULIN * REVATIO TRACLEER PR TYVASO * PR VELETRI * PR + VENTAVIS * PR Central Nervous System Analgesics Non-Narcotic PRIALT + Anticonvulsants GABA Modulators SABRIL * PR tablets only Huntington s Disease Chorea XENAZINE * Multiple Sclerosis Agents AMPYRA AVONEX ST AUBAGIO BETASERON COPAXONE PR EXTAVIA ST GILENYA REBIF PR ST TECFIDERA + TYSABRI Dermatological Agents ST Antineoplastic-Alkylating Agents VALCHLOR Gel * Antipsoriatics AMEVIVE PR + ENBREL PR HUMIRA PR KINERET PR REMICADE PR + SIMPONI PR + STELARA PR + Endocrine System Acromegaly octreotide + SANDOSTATIN + SOMATULINE + SANDOSTATIN LAR + SOMAVERT Corticotropin ACTHAR HP PR + Cushing s Disease SIGNIFOR Diagnostic Drugs THYROGEN + Fabry Disease FABRAZYME PR + Fertility Agents chorionic gonadotropin PR leuprolide novarel PR pregnyl PR BRAVELLE PR CETROTIDE PR FOLLISTIM AQ PR GANIRELIX PR GONAL-F PR GONAL-F RFF PR LUPRON LUVERIS PR MENOPUR PR OVIDREL PR REPRONEX PR Gaucher Disease CEREDASE PR + CEREZYME PR + ELELYSO * PR + VPRIV PR + ZAVESCA * PR + 4
5 Growth Factors, Insulin-like INCRELEX PR Growth Hormone Agents GENOTROPIN HUMATROPE NORDITROPIN NUTROPIN NUTROPIN AQ NUTROPIN AQ NUSPIN OMNITROPE PR SAIZEN SEROSTIM TEV-TROPIN ZORBTIVE PR Hereditary Tyrosinemia ORFADIN * Homocystinuria CYSTADANE Hormone Replacement Progestins MAKENA Hunter Syndrome ELAPRASE * PR + Hyperammonemia AMMONUL + BUPHENYL Hyperparathyroidism HECTOROL SENSIPAR ZEMPLAR LHRH/GnRH Agonist Analog Pituitary Suppressants SUPPRELIN LA + SYNAREL Mucopolysaccharidosis I ALDURAZYME PR + Mucopolysaccharidosis VI NAGLAZYME PR + Phenylketonuria KUVAN * Pompe Disease LUMIZYME PR + MYOZYME PR + Vasopressin Receptor Antagonists SAMSCA * PR Gastrointestinal System + Crohn s Disease CIMZIA REMICADE PR + HUMIRA PR Short bowel syndrome GATTEX * Infections and Infestations Antiretrovirals Fusion Inhibitors FUZEON Antivirals CMV Agents foscarnet + ganciclovir CYTOGAM + CYTOVENE + VALCYTE VALCYTE SOL VISTIDE 5
6 Antivirals Hepatitis Agents ribapak ribasphere ribavirin BARACLUDE COPEGUS EPIVIR HBV HEPSERA INCIVEK PR INFERGEN PR + PEGASYS PR PEG-INTRON PR REBETOL TYZEKA VICTRELIS PR Musculoskeletal System Bone Modifying Agents pamidronate PR + AREDIA PR + zoledronic acid PR + BONIVA (inj only) FORTEO PR + GANITE + + PROLIA PR + RECLAST PR + XGEVA PR + ZOMETA PR + Enzymes XIAFLEX + Gout KRYSTEXXA PR + Interleukin-1beta Blockers ILARIS * PR + Interleukin-1 Blockers ARCALYST * PR + Neuromuscular Blocking Agent Neurotoxins BOTOX PR + MYOBLOC PR + DYSPORT PR + XEOMIN PR + Osteoarthritis EUFLEXXA PR + + GEL-ONE INJ + HYALGAN ORTHOVISC PR + Rheumatoid Arthritis + ACTEMRA + CIMZIA ENBREL PR HUMIRA PR KINERET + ORENCIA + SUPARTZ + SYNVISC + SYNVISC ONE REMICADE PR + RITUXAN PR SIMPONI PR SIMPONI ARIA PR ST XELJANZ Ophthalmic Agents Macular Degeneration EYLEA + Macular Edema OZURDEX + LUCENTIS + MACUGEN + VISUDYNE + Vitreomacular adhesion JETREA + Respiratory Tract Agents Alpha-Proteinase Inhibitors ARALAST PR + ARALAST NP PR + GLASSIA * PR + PROLASTIN * PR + PROLASTIN-C * PR + ZEMAIRA * PR + Antiasthmatic Monoclonal Antibodies XOLAIR PR + 6
7 Cystic Fibrosis colistimethate sodium + BETHKIS NEB CAYSTON * COLY-MYCIN-M + KALYDECO PULMOZYME PR TOBI TOBI podhaler Respiratory Syncytial Virus Monoclonal Antibodies SYNAGIS PR + ST Tuberculosis SIRTURO Therapeutic Nutrients Vitamins Minerals Electrolytes Mineral Supplements nulecit + FERRLECIT + VENOFER + Toxicologic Agents Alcohol Dependence VIVITROL + Antidotes deferoxamine mesylate + DESFERAL + EXJADE Vaccines, Toxoids and Biologics Immune Globulin Cytomegalovirus (CMV) CYTOGAM + HYZENTRA PR + Immune Globulin Immune Disorders ADAGEN PR + BIVIGAM PR + CARIMUNE NANOFILTERED PR + FLEBOGAMMA PR + GAMASTAN S/D PR + GAMMAGARD PR + GAMMAGARD S/D PR + GAMMAKED PR GAMMAPLEX PR + GAMUNEX PR + GAMUNEX-C PR + HIZENTRA PR + OCTAGAM PR + PRIVIGEN PR + VIVAGLOBIN PR + Immune Globulin Hepatitis B HEPAGAM B + HYPERHEP B + NABI-HB + Immune Globulin Rabies HYPERRAB S/D + IMOGAM RABIES + Immune Globulin Rh Isoimmunization HYPERRHO S/D + MICRHOGAM ULTRA-FILTERED + RHOGAM ULTRA-FILTERED PLUS + RHOPHYLAC + WINRHO SDF + Immune Globulin Tetanus HYPERTET S/D + Miscellaneous Cystinosis CYSTARAN * ST PROCYSBI 7
8 Immunosuppressive Agents azathioprine (inj only) + cyclosporine (inj only) + tacrolimus ASTAGRAF ATGAM + MYFORTIC NEORAL NULOJIX + ORTHOCLONE OKT3 + PROGRAF RAPAMUNE SANDIMMUNE SIMULECT + THYMOGLOBULIN + ZORTRESS + Systemic Lupus Erythematosus Agents BENLYSTA PR + Urea Cycle Disorder RAVICTI * PR For more information on Aetna Specialty Pharmacy, call ASRX ( ) or TDD: ASRX ( ). Or visit Commercial fully insured members in Louisiana and Texas (except Federal Employee Health Benefit Plan members) who have coverage for medications that are added to or removed from the Aetna Specialty CareRx List, National Precertification List, Precertification Safety Edit List, Precertification List, Step-therapy List or Quantity Limit List, or have Quantity Limits modified, during the plan year will continue to have those medications covered at the same benefit level under their plan prior to the addition, removal or change, until their plan s renewal date. The term precertification means the utilization review process to determine whether the requested service, procedure, prescription drug or medical device meets the company s clinical criteria for coverage. It does not mean precertification as defined by Texas law, as a reliable representation of payment of care or services to fully insured HMO and PPO members. In accordance with state law, fully insured Commercial California HMO members (except Federal Employee Health Benefit Plan members) who are receiving coverage for medications that are added to the Precertification or Step-therapy Lists will continue to have those medications covered, for as long as the treating physician continues prescribing them, provided that the drug is appropriately prescribed and is considered safe and effective for treating the enrollee s medical condition. In accordance with state law, fully insured Commercial Connecticut PPO members (except Federal Employee Health Benefit Plan members) who are receiving coverage for medications that are added to the Precertification or Step-therapy Lists will continue to have those medications covered for as long as the treating physician prescribes them, provided the drug is medically necessary and more medically beneficial than other covered drugs. Nothing in this section shall preclude the prescribing provider from prescribing another drug covered by the plan that is medically appropriate for the enrollee, nor shall anything in this section be construed to prohibit generic drug substitutions. This material is for information only. Health benefits and health insurance plans contain exclusions and limitations. Not all health services are covered. See plan documents for a complete description of benefits, exclusions, limitations and conditions of coverage. Providers are independent contractors and are not agents of Aetna. Provider participation may change without notice. Aetna does not provide care or guarantee access to health services. Aetna Specialty Pharmacy refers to Aetna Specialty Pharmacy, LLC, a licensed pharmacy subsidiary of Aetna Inc. that operates through specialty pharmacy prescription fulfillment. Information is believed to be accurate as of the production date; however, it is subject to change. For more information about Aetna plans, refer to Policy forms issued in OK include: HMO OK COC-5 09/07, HMO/OK GA-3 11/01, HMO OK POS RIDER 08/07, GR-23 and/or GR-29/GR-29N Aetna Inc F (1/14)
Specialty Drug Program RX Benefit Member Guide
 Specialty Drug Program RX Benefit Member Guide bcbsm.com Enrollment Form for Walgreens Specialty Pharmacy, LLC. How to place your initial order with Walgreens Specialty Pharmacy: 1) Print and complete
Specialty Drug Program RX Benefit Member Guide bcbsm.com Enrollment Form for Walgreens Specialty Pharmacy, LLC. How to place your initial order with Walgreens Specialty Pharmacy: 1) Print and complete
MEDICAL ASSISTANCE BULLETIN
 ISSUE DATE August 20, 2015 SUBJECT EFFECTIVE DATE September 28, 2015 MEDICAL ASSISTANCE BULLETIN NUMBER 99-15-08 BY Specialty Pharmacy Drug Program Pharmacy Services Leesa M. Allen, Deputy Secretary Office
ISSUE DATE August 20, 2015 SUBJECT EFFECTIVE DATE September 28, 2015 MEDICAL ASSISTANCE BULLETIN NUMBER 99-15-08 BY Specialty Pharmacy Drug Program Pharmacy Services Leesa M. Allen, Deputy Secretary Office
Alameda Alliance for Health SPECIALTY PHARMACY PROGRAM FOR ALLIANCE MEDI-CAL AND GROUP CARE MEMBERS PROGRAM DESCRIPTION
 Alameda Alliance for Health SPECIALTY PHARMACY PROGRAM FOR ALLIANCE MEDI-CAL AND GROUP CARE MEMBERS PROGRAM DESCRIPTION Contents Page Program Overview 1 Process for Obtaining Authorization 2 Contacts 2
Alameda Alliance for Health SPECIALTY PHARMACY PROGRAM FOR ALLIANCE MEDI-CAL AND GROUP CARE MEMBERS PROGRAM DESCRIPTION Contents Page Program Overview 1 Process for Obtaining Authorization 2 Contacts 2
Pain management for cancer patients Acute Ischemic Stroke. Hemophilia, Von willebrand disease & Bleeding disorders. Infectious Disease
 Cigna Specialty Pharmacy Services Limited Distribution and Risk Evaluation Mitigation (RE) Drug List Last updated on 04/06/2015 Medication Brand Name Condition Actemra Rheumatroid Arthritis Acthar Seizure
Cigna Specialty Pharmacy Services Limited Distribution and Risk Evaluation Mitigation (RE) Drug List Last updated on 04/06/2015 Medication Brand Name Condition Actemra Rheumatroid Arthritis Acthar Seizure
STAT Bulletin. Drug Therapy Guideline Updates. May 11, 2012 Volume: 18 Issue: 12
 STAT Bulletin May 11, 2012 Volume: 18 Issue: 12 To: All primary care physicians and specialists Contracts Affected: All Lines of Business Drug Therapy Guideline Updates Why you re receiving this Stat What
STAT Bulletin May 11, 2012 Volume: 18 Issue: 12 To: All primary care physicians and specialists Contracts Affected: All Lines of Business Drug Therapy Guideline Updates Why you re receiving this Stat What
encourages correct prescription drug use for a particular diagnosis, promotes the safe use of prescription drugs, and helps reduce drug costs.
 Prior Authorization Your health plan participates in a Prior Authorization (PA) program for specific prescription drugs. This means that Caremark must review certain information provided by your doctor
Prior Authorization Your health plan participates in a Prior Authorization (PA) program for specific prescription drugs. This means that Caremark must review certain information provided by your doctor
Great-West s Drug Prior Authorization
 Great-West s Drug Prior Authorization Great-West Life s prior authorization process is designed to provide an effective approach to managing claims for specific prescription drugs. Approval for coverage
Great-West s Drug Prior Authorization Great-West Life s prior authorization process is designed to provide an effective approach to managing claims for specific prescription drugs. Approval for coverage
CONNECTICARE, INC. & AFFILIATES
 CONNECTICARE, INC. & AFFILIATES INSERT PAGE FOR PRE-CERTIFICATION AND PRE- AUTHORIZATION LISTS UPDATE Applies to all ConnectiCare health plans, except the ConnectiCare Network USA-PPO Plan and as otherwise
CONNECTICARE, INC. & AFFILIATES INSERT PAGE FOR PRE-CERTIFICATION AND PRE- AUTHORIZATION LISTS UPDATE Applies to all ConnectiCare health plans, except the ConnectiCare Network USA-PPO Plan and as otherwise
Prescription Drug Benefit Description
 Prescription Drug Benefit Description Herein called Description Prescription Drug Program For State of Kansas Employees Health Plan This booklet describes the Prescription Drug benefits available through
Prescription Drug Benefit Description Herein called Description Prescription Drug Program For State of Kansas Employees Health Plan This booklet describes the Prescription Drug benefits available through
N/A N/A N/A. Supporting statement of diagnosis from the N/A. physician and documented trial of 1 generic. formulary alternative
 Actimmune Amlodipine Androderm Anticonvulsant Antidepressants Antineoplastics Antipsychotics Arcalyst Butalbital Colony Stimulating Factors ESRD Therapy Actimmune Norvasc Androderm Banzel Keppra Mysoline
Actimmune Amlodipine Androderm Anticonvulsant Antidepressants Antineoplastics Antipsychotics Arcalyst Butalbital Colony Stimulating Factors ESRD Therapy Actimmune Norvasc Androderm Banzel Keppra Mysoline
Provider Manual. This manual is to help you learn more about The Ohio State University s medical plans, administered by OSU Health Plan Inc.
 2014 Provider Manual This manual is to help you learn more about The Ohio State University s medical plans, administered by OSU Health Plan Inc. We hope you find this information and the enclosed documents
2014 Provider Manual This manual is to help you learn more about The Ohio State University s medical plans, administered by OSU Health Plan Inc. We hope you find this information and the enclosed documents
REVISING SPECIALTY TIERS
 WHITE PAPER REVISING SPECIALTY TIERS PROTECTING MEDICARE PART D BENEFICIARIES FROM BURDENSOME COST SHIFTING Gary G., Michigan Gary thought he had his financial assistance grant set up to cover his out-of-pocket
WHITE PAPER REVISING SPECIALTY TIERS PROTECTING MEDICARE PART D BENEFICIARIES FROM BURDENSOME COST SHIFTING Gary G., Michigan Gary thought he had his financial assistance grant set up to cover his out-of-pocket
COVERAGE MANAGEMENT PROGRAMS
 COVERAGE MANAGEMENT PROGRAMS The purpose of coverage management programs is to help improve the quality of care by encouraging the right patient and provider behaviors to avoid compromised care and unnecessary
COVERAGE MANAGEMENT PROGRAMS The purpose of coverage management programs is to help improve the quality of care by encouraging the right patient and provider behaviors to avoid compromised care and unnecessary
Drugs Requiring Prior Authorization. Olysio. Subsys. Prolia. Tecfidera
 Abstral Acthar Hp Adcirca Adempas Affinitor Amitiza Amitriptyline Ampyra Androgel Androderm Androxy Aranesp Arcalyst Aubagio Avonex Bosulif Bydureon Byetta Cimzia Cinryze Clomipramine Cometriq Copaxone
Abstral Acthar Hp Adcirca Adempas Affinitor Amitiza Amitriptyline Ampyra Androgel Androderm Androxy Aranesp Arcalyst Aubagio Avonex Bosulif Bydureon Byetta Cimzia Cinryze Clomipramine Cometriq Copaxone
Humana 2015 Autorización previa
 Humana 2015 Autorización previa Los medicamentos a continuación requerirán autorización previa en 2015. Para información sobre el nivel de copago, visite Humana.com. Abstral 100 mcg sublingual tablet Abstral
Humana 2015 Autorización previa Los medicamentos a continuación requerirán autorización previa en 2015. Para información sobre el nivel de copago, visite Humana.com. Abstral 100 mcg sublingual tablet Abstral
January 1, 2016 At A Glance. CSEA Civil Service Employees Association
 January 1, 2016 At A Glance CSEA Civil Service Employees Association For Employees of the State of New York represented by Civil Service Employees Association (CSEA) and for their enrolled Dependents;
January 1, 2016 At A Glance CSEA Civil Service Employees Association For Employees of the State of New York represented by Civil Service Employees Association (CSEA) and for their enrolled Dependents;
Specialty Pharmacy: Understanding the Market and Solution. Your Goals. Presented by Chris Brown November 2009
 Specialty Pharmacy: Understanding the Market and Solution Presented by Chris Brown November 2009 Your Goals What What is a Specialty is a specialty Medication? medication? Specialty drugs are injectable,
Specialty Pharmacy: Understanding the Market and Solution Presented by Chris Brown November 2009 Your Goals What What is a Specialty is a specialty Medication? medication? Specialty drugs are injectable,
UMASTER PREFERRED DRUG LIST (DRUG FORMULARY) Effective July 1, 2015 RA05/15.654
 UMASTER PREFERRED DRUG LIST (DRUG FORMULARY) Effective July 1, 2015 1PU 2PU 3PU 4PU UPU UPU UPU UPU P P P P P Tier Master List (PDL) (Drug Formulary) Effective July 1, 2015 THE BLUEGRASS FAMILY HEALTH
UMASTER PREFERRED DRUG LIST (DRUG FORMULARY) Effective July 1, 2015 1PU 2PU 3PU 4PU UPU UPU UPU UPU P P P P P Tier Master List (PDL) (Drug Formulary) Effective July 1, 2015 THE BLUEGRASS FAMILY HEALTH
2016 MDwise HIP Medical Services that Require Prior Authorization
 2016 MDwise HIP Medical Services that Require Prior Authorization Medical services that require Prior Authorization Type of Service Coding All Out of Network services Facility to facility ambulance transport
2016 MDwise HIP Medical Services that Require Prior Authorization Medical services that require Prior Authorization Type of Service Coding All Out of Network services Facility to facility ambulance transport
ICORE Healthcare: Injectable Drug Utilization Management Program Overview for EmblemHealth Providers. May 1, 2012
 ICORE Healthcare: Injectable Drug Utilization Management Program Overview for EmblemHealth Providers May 1, 2012 Agenda Topics for Today 1. Program Summary Specialty Injectable Drugs in scope EmblemHealth
ICORE Healthcare: Injectable Drug Utilization Management Program Overview for EmblemHealth Providers May 1, 2012 Agenda Topics for Today 1. Program Summary Specialty Injectable Drugs in scope EmblemHealth
Medi-Cal Expansion, Mental Health Services and Changes to Medi-Cal Prior Authorization Requirements
 REGULATORY DECEMBER 19, 2013 UPDATE 13-545 12 PAGES Medi-Cal Expansion, Mental Health Services and Changes to Medi-Cal Beginning January 1, 2014, Medi-Cal coverage is expanding under the Affordable Care
REGULATORY DECEMBER 19, 2013 UPDATE 13-545 12 PAGES Medi-Cal Expansion, Mental Health Services and Changes to Medi-Cal Beginning January 1, 2014, Medi-Cal coverage is expanding under the Affordable Care
Effective: July 28, 2015. Arizona Prior Authorization Requirements Health Net Access, Inc.
 Effective: July 28, 2015 Arizona Prior Authorization Requirements Health Net Access, Inc. The following services, procedures and equipment are subject to prior authorization requirements (unless noted
Effective: July 28, 2015 Arizona Prior Authorization Requirements Health Net Access, Inc. The following services, procedures and equipment are subject to prior authorization requirements (unless noted
Your pharmacy, as near as your mailbox Aetna Rx Home Delivery
 Quality health plans & benefits Healthier living Financial well-being Intelligent solutions Your pharmacy, as near as your mailbox Aetna Rx Home Delivery www.aetna.com 05.02.308.1-KC B (12/13) Start saving
Quality health plans & benefits Healthier living Financial well-being Intelligent solutions Your pharmacy, as near as your mailbox Aetna Rx Home Delivery www.aetna.com 05.02.308.1-KC B (12/13) Start saving
Specialty Pharmacy. Business Plan. July 8, 2013. 2013 RUSH University Medical Center
 Specialty Pharmacy Business Plan July 8, 2013 Specialty Pharmaceuticals What are they? Biotech/gene-based therapy Require special handling Newer products oral or self- administered One third have REMS
Specialty Pharmacy Business Plan July 8, 2013 Specialty Pharmaceuticals What are they? Biotech/gene-based therapy Require special handling Newer products oral or self- administered One third have REMS
2016 MDwise HIP Medical Services that Require Prior Authorization
 2016 MDwise HIP Medical Services that Require Prior Authorization Medical services that require Prior Authorization Type of Service Coding All Out of Network services Facility to facility ambulance transport
2016 MDwise HIP Medical Services that Require Prior Authorization Medical services that require Prior Authorization Type of Service Coding All Out of Network services Facility to facility ambulance transport
INPATIENT SERVICES Commercial Medicare. Notification required only, as soon as possible, but no later than 24 hours
 Effective: January 1, 2016 Arizona Prior Authorization Requirements HMO (including CommunityCare HMO) Point-of-Service (POS) PPO Advantage (MA) HMO The following services, procedures or equipment are subject
Effective: January 1, 2016 Arizona Prior Authorization Requirements HMO (including CommunityCare HMO) Point-of-Service (POS) PPO Advantage (MA) HMO The following services, procedures or equipment are subject
This information is also available in large print. Call 1-800-286-4242. TTY users should call toll-free 1-800-361-2629.
 Your prescription drug program 2015 This information is also available in large print. Call 1-800-286-4242. TTY users should call toll-free 1-800-361-2629. Table of Contents Your Prescription Drug Program...
Your prescription drug program 2015 This information is also available in large print. Call 1-800-286-4242. TTY users should call toll-free 1-800-361-2629. Table of Contents Your Prescription Drug Program...
April 30, 2009. The Honorable Edward M. Kennedy Chairman Committee on Health, Education, Labor, and Pensions United States Senate
 United States Government Accountability Office Washington, DC 20548 April 30, 2009 The Honorable Edward M. Kennedy Chairman Committee on Health, Education, Labor, and Pensions United States Senate Subject:
United States Government Accountability Office Washington, DC 20548 April 30, 2009 The Honorable Edward M. Kennedy Chairman Committee on Health, Education, Labor, and Pensions United States Senate Subject:
Medical Prior Authorization List For prescription drug requirements, see plan formularies.
 For prescription drug requirements, see plan formularies. General Information These requirements are administered by Health First Health Plans ( Health Plans ). Benefits are determined by the plan. Items
For prescription drug requirements, see plan formularies. General Information These requirements are administered by Health First Health Plans ( Health Plans ). Benefits are determined by the plan. Items
Specialty drug trend
 2 0 0 8 Specialty drug trend r e p o r t Specialty Pharmacy A n E x p r e s s S c r i p t s C o m p a n y Lead Authors Emily Cox, PhD, RPh Yakov Svirnovskiy, MA Chris Peterson, PharmD Aimee Tharaldson,
2 0 0 8 Specialty drug trend r e p o r t Specialty Pharmacy A n E x p r e s s S c r i p t s C o m p a n y Lead Authors Emily Cox, PhD, RPh Yakov Svirnovskiy, MA Chris Peterson, PharmD Aimee Tharaldson,
Prescription Drug Benefit
 Prescription Drug Benefit The Cleveland Clinic Employee Health Plan (EHP) Total Care Prescription Drug Benefit is administered through CVS Caremark. CVS Caremark has a dedicated, toll-free Customer Service
Prescription Drug Benefit The Cleveland Clinic Employee Health Plan (EHP) Total Care Prescription Drug Benefit is administered through CVS Caremark. CVS Caremark has a dedicated, toll-free Customer Service
Brand Generic J-Code Covered Uses Required Medical Information and Criteria
 FIDELIS CARE NEW YORK DEPARTMENT OF PHARMACY SERVICES J-Code Prior Authorizations & Required Clinical Information Medicaid, Family Health Plus, Child Health Plus, NY State of Health Brand Generic J-Code
FIDELIS CARE NEW YORK DEPARTMENT OF PHARMACY SERVICES J-Code Prior Authorizations & Required Clinical Information Medicaid, Family Health Plus, Child Health Plus, NY State of Health Brand Generic J-Code
ACTEMRA. Cigna Medicare Rx (PDP) 2014 Cigna Medicare Rx Secure Plan (PDP) Formulary. Products Affected Actemra. Prior Authorization Criteria
 Cigna Medicare Rx (PDP) Medicare Part D Prescription Drug Plans 2014 Cigna Medicare Rx Secure Plan (PDP) Formulary Prior Authorization ACTEMRA Products Affected Actemra PA Details Age Other Authorization
Cigna Medicare Rx (PDP) Medicare Part D Prescription Drug Plans 2014 Cigna Medicare Rx Secure Plan (PDP) Formulary Prior Authorization ACTEMRA Products Affected Actemra PA Details Age Other Authorization
Prescription Drug Summary Plan Description
 Prescription Drug Summary Plan Description About This Summary Plan Description (SPD) The Prescription Drug Program is a component program in the Tenet Employee Benefit Plan (TEBP). The TEBP is a comprehensive
Prescription Drug Summary Plan Description About This Summary Plan Description (SPD) The Prescription Drug Program is a component program in the Tenet Employee Benefit Plan (TEBP). The TEBP is a comprehensive
Prior Authorization FID 16157 VER.7 UPDATED 8/2015
 Prior Authorization FID 16157 VER.7 UPDATED 8/2015 Prior Authorization 2016 MAPD Leon 3 Tier Last Updated: 10/22/2015 ACTEMRA Products Affected Actemra INJ 162MG/0.9ML PA Details Other 1 ACTIMMUNE Products
Prior Authorization FID 16157 VER.7 UPDATED 8/2015 Prior Authorization 2016 MAPD Leon 3 Tier Last Updated: 10/22/2015 ACTEMRA Products Affected Actemra INJ 162MG/0.9ML PA Details Other 1 ACTIMMUNE Products
2013 Prior Authorization (PA) Criteria
 2013 Prior Authorization (PA) Criteria Certain drugs require prior authorization from EmblemHealth Medicare PDP Medicare Plans. This means that your doctor must contact us to get approval before prescribing
2013 Prior Authorization (PA) Criteria Certain drugs require prior authorization from EmblemHealth Medicare PDP Medicare Plans. This means that your doctor must contact us to get approval before prescribing
January 1, 2014. Participating Agencies
 January 1, 2014 PA Participating Agencies For Active Employees, Retirees, Vestees and Dependent Survivors, Enrollees covered under Preferred List Provisions, their Dependents, COBRA enrollees and Young
January 1, 2014 PA Participating Agencies For Active Employees, Retirees, Vestees and Dependent Survivors, Enrollees covered under Preferred List Provisions, their Dependents, COBRA enrollees and Young
HealthPartners, Inc. 2013 Medicare Part D Formulary ID 13142, Version 22 Prior Authorization Criteria. Last Updated: 11/01/2013
 ACTEMRA Actemra (1) DIAGNOSIS OF MODERATELY TO SEVERELY ACTIVE RHEUMATOID ARTHRITIS, OR (2) JUVENILE IDIOPATHIC ARTHRITIS, AND (3) DOCUMENTATION OF MEDICAL CONTRAINDICATIONS OR FAILURE WITH ENBREL OR HUMIRA.
ACTEMRA Actemra (1) DIAGNOSIS OF MODERATELY TO SEVERELY ACTIVE RHEUMATOID ARTHRITIS, OR (2) JUVENILE IDIOPATHIC ARTHRITIS, AND (3) DOCUMENTATION OF MEDICAL CONTRAINDICATIONS OR FAILURE WITH ENBREL OR HUMIRA.
Items Covered Benefit for Preferred Vendor Contact Information. Medicaid ONLY Integra Phone 718-369-0012
 Department Of Pharmacy (Medicaid, Child Health Plus, Medicare Part B, Qualified Health Plan) Medications Requiring Authorization under Medical Benefit - Fax request to (718) 536-3383 (Last Revised 8/4/15)
Department Of Pharmacy (Medicaid, Child Health Plus, Medicare Part B, Qualified Health Plan) Medications Requiring Authorization under Medical Benefit - Fax request to (718) 536-3383 (Last Revised 8/4/15)
Medicare Part D Drugs that Require Prior-Authorization Effective 12/01/2015
 Medicare Drugs that Require Prior- Effective 12/01/2015 Prior Actemra IV Actemra All FDAapproved Required Medical Information Age Prescriber 2. For Rheumatoid Arthritis: Patient must have tried and failed
Medicare Drugs that Require Prior- Effective 12/01/2015 Prior Actemra IV Actemra All FDAapproved Required Medical Information Age Prescriber 2. For Rheumatoid Arthritis: Patient must have tried and failed
Prescription Drug Utilization and Cost Trends, 2009-2013
 Agenda Item 7 Attachment 1 Prescription Drug Utilization and Cost Trends, 2009-2013 Pension and Health Benefits Committee October 14, 2014 Melissa Mantong, PharmD CalPERS Pharmacist Overview Trends in
Agenda Item 7 Attachment 1 Prescription Drug Utilization and Cost Trends, 2009-2013 Pension and Health Benefits Committee October 14, 2014 Melissa Mantong, PharmD CalPERS Pharmacist Overview Trends in
22 Medicare Provider Manual
 22 Medicare Provider Manual Table of Contents Title Page Introduction 2 Important Contact Information 4 Member Eligibility & Plan Design 5 ID card sample 8 Provider Reconsideration Process 9 Member Grievance
22 Medicare Provider Manual Table of Contents Title Page Introduction 2 Important Contact Information 4 Member Eligibility & Plan Design 5 ID card sample 8 Provider Reconsideration Process 9 Member Grievance
Prescription Access resources. NeedyMeds. RxAssist.org. Together RX Access 800-444-4106. TogetherRxAccess.com
 Prescription Access resources NeedyMeds RxAssist.org Together RX Access 800-444-4106 TogetherRxAccess.com The Partnership for Prescription Access 888-4PPA-NOW (888-477-2669) www.pparx.org By Company: ABBOTT
Prescription Access resources NeedyMeds RxAssist.org Together RX Access 800-444-4106 TogetherRxAccess.com The Partnership for Prescription Access 888-4PPA-NOW (888-477-2669) www.pparx.org By Company: ABBOTT
Prior Authorization Criteria 2014
 Prior Authorization Criteria 2014 For information on obtaining an updated coverage determination or an exception to a coverage determination please contact Easy Choice Health Plan of New York s Member
Prior Authorization Criteria 2014 For information on obtaining an updated coverage determination or an exception to a coverage determination please contact Easy Choice Health Plan of New York s Member
Medical School for Actuaries. June 12, 2013. Baltimore, Maryland
 Medical School for Actuaries June 12, 2013 Baltimore, Maryland Developments in the Treatment of Conditions Treated with Specialty Mediations (Cancer, MS, RA, Hemophilia) Mark S. Matusik, PharmD Developments
Medical School for Actuaries June 12, 2013 Baltimore, Maryland Developments in the Treatment of Conditions Treated with Specialty Mediations (Cancer, MS, RA, Hemophilia) Mark S. Matusik, PharmD Developments
NDC HCPCS HCPCS Description NDC Description Effective Date End Date X-Over Only
 Updated 5.5.14 NDC HCPCS HCPCS Description NDC Description Effective Date End Date X-Over Only 68152-0103-03 A9543 YTTRIUM Y-90 IBRITUMOMAB TIUXETAN ZEVALIN Y-90 VIAL 9/1/2013 12/31/2013 50419-0320-05
Updated 5.5.14 NDC HCPCS HCPCS Description NDC Description Effective Date End Date X-Over Only 68152-0103-03 A9543 YTTRIUM Y-90 IBRITUMOMAB TIUXETAN ZEVALIN Y-90 VIAL 9/1/2013 12/31/2013 50419-0320-05
Immune Modulating Drugs Prior Authorization Request Form
 Patient: HPHC member ID #: Requesting provider: Phone: Servicing provider: Diagnosis: Contact for questions (name and phone #): Projected start and end date for requested Requesting provider NPI: Fax:
Patient: HPHC member ID #: Requesting provider: Phone: Servicing provider: Diagnosis: Contact for questions (name and phone #): Projected start and end date for requested Requesting provider NPI: Fax:
PATIENT ASSISTANCE PROGRAMS
 PATIENT ASSISTANCE PROGRAMS Definitions SAP Class I Class II BC Cancer Agency Health Canada Special Access Program Reimbursed for active cancer or approved treatment or approved indication only Reimbursed
PATIENT ASSISTANCE PROGRAMS Definitions SAP Class I Class II BC Cancer Agency Health Canada Special Access Program Reimbursed for active cancer or approved treatment or approved indication only Reimbursed
Rheumatic Diseases, Psoriasis, and Crohn s Disease
 Rheumatic Diseases, Psoriasis, and Crohn s Disease What does this handout cover? This handout has information about rheumatic disease, psoriasis, and Crohn s disease. It also has information on how these
Rheumatic Diseases, Psoriasis, and Crohn s Disease What does this handout cover? This handout has information about rheumatic disease, psoriasis, and Crohn s disease. It also has information on how these
Express Scripts/Medco Prescription Plan Information For Drug Coverage Review, Prior Authorization Process and Personalized Medicine Information
 Express Scripts/Medco Prescription Plan Information For Drug Coverage Review, Prior Authorization Process and Personalized Medicine Information The endowed health plan offers faculty and staff members
Express Scripts/Medco Prescription Plan Information For Drug Coverage Review, Prior Authorization Process and Personalized Medicine Information The endowed health plan offers faculty and staff members
Wendy Clary Nash, PharmD BCPS CPG FASCP. Neil Medical Group Sept 30, 2014
 Wendy Clary Nash, PharmD BCPS CPG FASCP Neil Medical Group Sept 30, 2014 Do you feel like You re in a daze? A healthcare craze? A medication maze? Quack, Quack If it walks like a duck, talks like a duck
Wendy Clary Nash, PharmD BCPS CPG FASCP Neil Medical Group Sept 30, 2014 Do you feel like You re in a daze? A healthcare craze? A medication maze? Quack, Quack If it walks like a duck, talks like a duck
To start using DocFind today, go to www.aetna.com/docfind/custom/uva. Registration is not required.
 Dear University of Virginia Faculty and Staff: Welcome to Aetna! One of the nation's leading health benefits companies, Aetna provides members with information and resources to help you make smart decisions
Dear University of Virginia Faculty and Staff: Welcome to Aetna! One of the nation's leading health benefits companies, Aetna provides members with information and resources to help you make smart decisions
SUMMARY PLAN DESCRIPTION 2014-2015 STUDENT HEALTH PLAN Designed Especially for Students of
 SUMMARY PLAN DESCRIPTION 2014-2015 STUDENT HEALTH PLAN Designed Especially for Students of Table of Contents Privacy Policy 3 Eligibility 3 Qualifying Event 3 Effective and Termination Dates 3 General
SUMMARY PLAN DESCRIPTION 2014-2015 STUDENT HEALTH PLAN Designed Especially for Students of Table of Contents Privacy Policy 3 Eligibility 3 Qualifying Event 3 Effective and Termination Dates 3 General
4Precertification. and Referrals. Precertification...59 Referrals (Gated Plans Only)...73
 4Precertification and Referrals Precertification.....................59 Referrals (Gated Plans Only)............73 Section 4 Precertification and Referrals 58 www.oxfordhealth.com Precertification and
4Precertification and Referrals Precertification.....................59 Referrals (Gated Plans Only)............73 Section 4 Precertification and Referrals 58 www.oxfordhealth.com Precertification and
Winter 2013. Changing landscapes, pipeline products and plan sponsor impact
 Winter 2013 Changing landscapes, pipeline products and plan sponsor impact Changing landscapes, pipeline products and plan sponsor impact The pharmaceutical landscape is changing as is the profile of blockbuster
Winter 2013 Changing landscapes, pipeline products and plan sponsor impact Changing landscapes, pipeline products and plan sponsor impact The pharmaceutical landscape is changing as is the profile of blockbuster
Drugs That Require Prior Authorization (PA) Before Being Approved for Coverage PRIOR AUTHORIZATION MEDICATIONS
 That Require Prior Authorization (PA) Before Being Approved for Coverage PRIOR AUTHORIZATION MEDICATIONS ACNE Approve for those 12 years of age and older AVITA, RETIN-A MICRO, TRETINOIN ACTHAR HP All FDA-approved
That Require Prior Authorization (PA) Before Being Approved for Coverage PRIOR AUTHORIZATION MEDICATIONS ACNE Approve for those 12 years of age and older AVITA, RETIN-A MICRO, TRETINOIN ACTHAR HP All FDA-approved
ACNE PRODUCTS. Affected Drugs: Epiduo Retin-A Tretinoin. Covered Uses: All FDA-approved indications not otherwise excluded from Part D
 ACNE PRODUCTS Epiduo Retin-A Tretinoin Exclusion Criteria: Esthetic purposes N/A N/A TSA 2015 Royal, Classic, Vital and Vital Plus Formulary Page 1 of 148 ACTEMRA Actemra Exclusion Criteria: 1) Active
ACNE PRODUCTS Epiduo Retin-A Tretinoin Exclusion Criteria: Esthetic purposes N/A N/A TSA 2015 Royal, Classic, Vital and Vital Plus Formulary Page 1 of 148 ACTEMRA Actemra Exclusion Criteria: 1) Active
FREE PRESCRIPTION DISCOUNT CARD AVAILABLE TO WELD COUNTY RESIDENTS
 FREE PRESCRIPTION DISCOUNT CARD AVAILABLE TO WELD COUNTY RESIDENTS Money is tight for everyone these days. Many families work hard to stay within a budget, and, if they are lucky, they are also able to
FREE PRESCRIPTION DISCOUNT CARD AVAILABLE TO WELD COUNTY RESIDENTS Money is tight for everyone these days. Many families work hard to stay within a budget, and, if they are lucky, they are also able to
Prescription Plan FAQ s
 Prescription Plan FAQ s What is a specialty medication? Specialty medication is the term used to describe certain medications and a set of services designed to meet the particular needs of people who take
Prescription Plan FAQ s What is a specialty medication? Specialty medication is the term used to describe certain medications and a set of services designed to meet the particular needs of people who take
www.oxfordhealth.com
 www.oxfordhealth.com Oxford s HMO products are underwritten by Oxford Health Plans (NY), Inc., Oxford Health Plans (NJ), Inc., and Oxford Health Plans (CT), Inc., and insurance products are underwritten
www.oxfordhealth.com Oxford s HMO products are underwritten by Oxford Health Plans (NY), Inc., Oxford Health Plans (NJ), Inc., and Oxford Health Plans (CT), Inc., and insurance products are underwritten
Coverage and Pricing. of Drugs That Can Be Covered Under. Part B and Part D
 Coverage and Pricing Elizabeth Hargrave NORC at the University of Chicago Jack Hoadley of Drugs That Can Be Covered Under Part B and Part D Jennifer Thompson Georgetown University MedPAC A study conducted
Coverage and Pricing Elizabeth Hargrave NORC at the University of Chicago Jack Hoadley of Drugs That Can Be Covered Under Part B and Part D Jennifer Thompson Georgetown University MedPAC A study conducted
The Basics of Pharmacy Benefits Management (PBM) 2009
 The Basics of Pharmacy Benefits Management (PBM) 2009 Andrew Kingery Pharmacy Account Management Virginia CE Forum 2009 Course# 201719 Objectives & Introduction Provide basic components of a PBM Define
The Basics of Pharmacy Benefits Management (PBM) 2009 Andrew Kingery Pharmacy Account Management Virginia CE Forum 2009 Course# 201719 Objectives & Introduction Provide basic components of a PBM Define
drug trend and therapy class review CuraScript Specialty Pharmacy Management Guide & Trend Report
 drug trend and therapy class review CuraScript Specialty Pharmacy Management Guide & Trend Report Drug Trend and Therapy Class Review The growth of specialty drugs continues to outpace the traditional
drug trend and therapy class review CuraScript Specialty Pharmacy Management Guide & Trend Report Drug Trend and Therapy Class Review The growth of specialty drugs continues to outpace the traditional
Coverage and a smart way to help pay for it Aetna HealthFund Health Savings Account (HSA) Plan
 Quality health plans & benefits Healthier living Financial well-being Intelligent solutions Coverage and a smart way to help pay for it Aetna HealthFund Health Savings Account (HSA) Plan www.aetna.com
Quality health plans & benefits Healthier living Financial well-being Intelligent solutions Coverage and a smart way to help pay for it Aetna HealthFund Health Savings Account (HSA) Plan www.aetna.com
Monoclonal antibody (mab) products are currently a fast
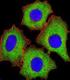 Antibody Monoclonal Therapeutics Janice M. Reichert, Ph.D. Monoclonal antibody (mab) products are currently a fast growing category of drugs. Like antibodies produced naturally by the human immune system,
Antibody Monoclonal Therapeutics Janice M. Reichert, Ph.D. Monoclonal antibody (mab) products are currently a fast growing category of drugs. Like antibodies produced naturally by the human immune system,
Understanding specialty drugs
 Group Benefits Understanding specialty drugs What your pharmaceutical benefits plan may look like over the next decade Between 2011 and 2014, the percentage of total drug spend represented by specialty
Group Benefits Understanding specialty drugs What your pharmaceutical benefits plan may look like over the next decade Between 2011 and 2014, the percentage of total drug spend represented by specialty
Stretching your health care dollars Aetna HealthFund Health Reimbursement Arrangement (HRA) Plan
 Quality health plans & benefits Healthier living Financial well-being Intelligent solutions Stretching your health care dollars Aetna HealthFund Health Reimbursement Arrangement (HRA) Plan www.aetna.com
Quality health plans & benefits Healthier living Financial well-being Intelligent solutions Stretching your health care dollars Aetna HealthFund Health Reimbursement Arrangement (HRA) Plan www.aetna.com
PULMONARY ARTERIAL HYPERTENSION AGENTS
 Approvable Criteria: PULMONARY ARTERIAL HYPERTENSION AGENTS Brand Name Generic Name Length of Authorization Revatio Sildenafil citrate Calendar Year Adcirca Tadalafil Calendar Year Letairis Ambrisentan
Approvable Criteria: PULMONARY ARTERIAL HYPERTENSION AGENTS Brand Name Generic Name Length of Authorization Revatio Sildenafil citrate Calendar Year Adcirca Tadalafil Calendar Year Letairis Ambrisentan
Princeton University Prescription Drug Plan Summary Plan Description
 Princeton University Prescription Drug Plan Summary Plan Description Princeton University Prescription Drug Plan Summary Plan Description January 2015 Contents Introduction... 1 How the Plan Works... 2
Princeton University Prescription Drug Plan Summary Plan Description Princeton University Prescription Drug Plan Summary Plan Description January 2015 Contents Introduction... 1 How the Plan Works... 2
Your pharmacy, as near as your mailbox Aetna Rx Home Delivery
 Quality health plans & benefits Healthier living Financial well-being Intelligent solutions Your pharmacy, as near as your mailbox Aetna Rx Home Delivery www.aetna.com 05.02.308.1-KC B WEB (6/13) Our mail-order
Quality health plans & benefits Healthier living Financial well-being Intelligent solutions Your pharmacy, as near as your mailbox Aetna Rx Home Delivery www.aetna.com 05.02.308.1-KC B WEB (6/13) Our mail-order
REFERRAL/AUTHORIZATION GUIDELINES Commercial Plans
 Moda Health Referral/Authorization Guidelines Oregon updated September 2014 Page 1 of 7 REFERRAL/AUTHORIZATION GUIDELINES Commercial Plans Referral & Authorization Information Referral and authorization
Moda Health Referral/Authorization Guidelines Oregon updated September 2014 Page 1 of 7 REFERRAL/AUTHORIZATION GUIDELINES Commercial Plans Referral & Authorization Information Referral and authorization
Drug Formulary Update, July 2013
 Drug Formulary Update, July 2013 Updates to the HealthPartners Drug Formularies are listed below. Updates for the Commercial Drug Formularies and the Minnesota Health Care Programs (Medicaid and Minnesota
Drug Formulary Update, July 2013 Updates to the HealthPartners Drug Formularies are listed below. Updates for the Commercial Drug Formularies and the Minnesota Health Care Programs (Medicaid and Minnesota
Medicare Part D Plans Deliver Significant Savings on Innovative, Breakthrough Medicines
 Medicare Part D Plans Deliver Significant Savings on Innovative, Breakthrough Medicines Survey Finds Private Sector Negotiations Provide Both Savings and Choice, Making Government Interference Unnecessary
Medicare Part D Plans Deliver Significant Savings on Innovative, Breakthrough Medicines Survey Finds Private Sector Negotiations Provide Both Savings and Choice, Making Government Interference Unnecessary
Commercial Medicines Unit
 Commercial Medicines Unit Procurement guidance For The provision of homecare delivery service of medicines to patients at home Issue date: May 2011 Review date: Sep 2012 1 September 2012 Crown Copyright
Commercial Medicines Unit Procurement guidance For The provision of homecare delivery service of medicines to patients at home Issue date: May 2011 Review date: Sep 2012 1 September 2012 Crown Copyright
How To Use Aetna Health Fund Health Savings Account (Hsa) Plan
 Quality health plans & benefits Healthier living Financial well-being Intelligent solutions Coverage and a smart way to help pay for it Aetna HealthFund Health Savings Account (HSA) Plan www.aetna.com
Quality health plans & benefits Healthier living Financial well-being Intelligent solutions Coverage and a smart way to help pay for it Aetna HealthFund Health Savings Account (HSA) Plan www.aetna.com
MEDICATION GUIDE. ACTEMRA (AC-TEM-RA) (tocilizumab) Solution for Intravenous Infusion
 MEDICATION GUIDE ACTEMRA (AC-TEM-RA) (tocilizumab) Solution for Intravenous Infusion ACTEMRA (AC-TEM-RA) (tocilizumab) Injection, Solution for Subcutaneous Administration Read this Medication Guide before
MEDICATION GUIDE ACTEMRA (AC-TEM-RA) (tocilizumab) Solution for Intravenous Infusion ACTEMRA (AC-TEM-RA) (tocilizumab) Injection, Solution for Subcutaneous Administration Read this Medication Guide before
Student Employee Health Plan (SEHP) for Graduate Student Employees
 New York State Health Insurance Program Student Employee Health Plan (SEHP) for Graduate Student Employees January 1, 2009 For Graduate Student Employees and for their enrolled Dependents and for COBRA
New York State Health Insurance Program Student Employee Health Plan (SEHP) for Graduate Student Employees January 1, 2009 For Graduate Student Employees and for their enrolled Dependents and for COBRA
Coverage and a smart way to help pay for it Aetna HealthFund Health Savings Account (HSA) Plan
 Quality health plans & benefits Healthier living Financial well-being Intelligent solutions Coverage and a smart way to help pay for it Aetna HealthFund Health Savings Account (HSA) Plan www.aetna.com
Quality health plans & benefits Healthier living Financial well-being Intelligent solutions Coverage and a smart way to help pay for it Aetna HealthFund Health Savings Account (HSA) Plan www.aetna.com
Local Coverage Article: Self-Administered Drug Exclusion List (A51866)
 Local Coverage Article: Self-Administered Drug Exclusion List (A51866) Contractor Information Contractor Name Novitas Solutions, Inc. Article Information General Information Article ID A51866 General Article
Local Coverage Article: Self-Administered Drug Exclusion List (A51866) Contractor Information Contractor Name Novitas Solutions, Inc. Article Information General Information Article ID A51866 General Article
Coverage and a smart way to help pay for it Aetna HealthFund Health Savings Account (HSA) Plan
 Quality health plans & benefits Healthier living Financial well-being Intelligent solutions Coverage and a smart way to help pay for it Aetna HealthFund Health Savings Account (HSA) Plan www.aetna.com
Quality health plans & benefits Healthier living Financial well-being Intelligent solutions Coverage and a smart way to help pay for it Aetna HealthFund Health Savings Account (HSA) Plan www.aetna.com
University of Nebraska Prescription Drug Program 2014
 University of Nebraska Prescription Drug Program 2014 The University of Nebraska s prescription benefit program is administered by CVS Caremark, a leading national provider of prescription drug benefit
University of Nebraska Prescription Drug Program 2014 The University of Nebraska s prescription benefit program is administered by CVS Caremark, a leading national provider of prescription drug benefit
scriptsourcing THE NEXT 5 YEARS OF RX COSTS AND HOW THEY WILL IMPACT YOUR BOTTOM LINE ScriptSourcing Prescription Advocacy Services
 scriptsourcing THE NEXT 5 YEARS OF RX COSTS AND HOW THEY WILL IMPACT YOUR BOTTOM LINE ScriptSourcing Prescription Advocacy Services Gary Becker, CEO Benefit Consultant, Risk Mitigation Expert, and Author
scriptsourcing THE NEXT 5 YEARS OF RX COSTS AND HOW THEY WILL IMPACT YOUR BOTTOM LINE ScriptSourcing Prescription Advocacy Services Gary Becker, CEO Benefit Consultant, Risk Mitigation Expert, and Author
Illinois Department of Revenue Regulations TITLE 86: REVENUE CHAPTER I: DEPARTMENT OF REVENUE
 Illinois Department of Revenue Regulations Title 86 Part 530 Section 530.110 Covered Prescription Drugs TITLE 86: REVENUE CHAPTER I: DEPARTMENT OF REVENUE PART 530 SENIOR CITIZENS AND DISABLED PERSONS
Illinois Department of Revenue Regulations Title 86 Part 530 Section 530.110 Covered Prescription Drugs TITLE 86: REVENUE CHAPTER I: DEPARTMENT OF REVENUE PART 530 SENIOR CITIZENS AND DISABLED PERSONS
Important health care reform notice Women s preventive services covered with no member cost share
 Quality health plans & benefits Healthier living Financial well-being Intelligent solutions Important health care reform notice Women s preventive services covered with no member cost share www.aetna.com
Quality health plans & benefits Healthier living Financial well-being Intelligent solutions Important health care reform notice Women s preventive services covered with no member cost share www.aetna.com
Special Authorization
 Special Authorization Certain medications in the Reformulary require Special Authorization from your insurance company before your prescription is eligible for coverage. What is Special Authorization?
Special Authorization Certain medications in the Reformulary require Special Authorization from your insurance company before your prescription is eligible for coverage. What is Special Authorization?
Contents General Information... 1. General Information
 Contents General Information... 1 Preferred Drug List... 2 Pharmacies... 3 Prescriptions... 4 Generic and Preferred Drugs... 5 Express Scripts Website and Mobile App... 5 Specialty Medicines... 5 Prior
Contents General Information... 1 Preferred Drug List... 2 Pharmacies... 3 Prescriptions... 4 Generic and Preferred Drugs... 5 Express Scripts Website and Mobile App... 5 Specialty Medicines... 5 Prior
Stretching your health care dollars Aetna HealthFund Health Reimbursement Arrangement (HRA) Plan
 Quality health plans & benefits Healthier living Financial well-being Intelligent solutions Stretching your health care dollars Aetna HealthFund Health Reimbursement Arrangement (HRA) Plan 32.02.301.1
Quality health plans & benefits Healthier living Financial well-being Intelligent solutions Stretching your health care dollars Aetna HealthFund Health Reimbursement Arrangement (HRA) Plan 32.02.301.1
Outpatient Prescription Drug Benefit
 Outpatient Prescription Drug Benefit GENERAL INFORMATION This supplemental Evidence of Coverage and Disclosure Form is provided in addition to your Member Handbook and Health Plan Benefits and Coverage
Outpatient Prescription Drug Benefit GENERAL INFORMATION This supplemental Evidence of Coverage and Disclosure Form is provided in addition to your Member Handbook and Health Plan Benefits and Coverage
MEDICAL ASSISTANCE HANDBOOK PRIOR AUTHORIZATION OF PHARMACEUTICAL SERVICES `I. Requirements for Prior Authorization of Cytokine and CAM Antagonists
 MEDICAL ASSISTANCE HBOOK `I. Requirements for Prior Authorization of Cytokine and CAM Antagonists A. Prescriptions That Require Prior Authorization All prescriptions for Cytokine and CAM Antagonists must
MEDICAL ASSISTANCE HBOOK `I. Requirements for Prior Authorization of Cytokine and CAM Antagonists A. Prescriptions That Require Prior Authorization All prescriptions for Cytokine and CAM Antagonists must
MEDICAL ASSISTANCE BULLETIN
 ISSUE DATE May 11, 2015 SUBJECT EFFECTIVE DATE May 18, 2015 MEDICAL ASSISTANCE BULLETIN NUMBER *See below BY Prior Authorization of Multiple Sclerosis Agents Pharmacy Service Leesa M. Allen, Deputy Secretary
ISSUE DATE May 11, 2015 SUBJECT EFFECTIVE DATE May 18, 2015 MEDICAL ASSISTANCE BULLETIN NUMBER *See below BY Prior Authorization of Multiple Sclerosis Agents Pharmacy Service Leesa M. Allen, Deputy Secretary
GENERAL INFORMATION. With Express Scripts, you have access to:
 CONTENTS GENERAL INFORMATION... 1 PREFERRED DRUG LIST....2 PHARMACIES... 3 PRESCRIPTIONS... 4 GENERIC AND PREFERRED DRUGS... 5 EXPRESS SCRIPTS WEBSITE AND MOBILE APP... 5 SPECIALTY MEDICATIONS... 6 PRIOR
CONTENTS GENERAL INFORMATION... 1 PREFERRED DRUG LIST....2 PHARMACIES... 3 PRESCRIPTIONS... 4 GENERIC AND PREFERRED DRUGS... 5 EXPRESS SCRIPTS WEBSITE AND MOBILE APP... 5 SPECIALTY MEDICATIONS... 6 PRIOR
Prescription Drug Plan
 Prescription Drug Plan The prescription drug plan helps you pay for prescribed medications using either a retail pharmacy or the mail order program. For More Information Administrative details and procedures
Prescription Drug Plan The prescription drug plan helps you pay for prescribed medications using either a retail pharmacy or the mail order program. For More Information Administrative details and procedures
WESTCHESTER COMMUNITY COLLEGE Valhalla, NY 10595. COURSE TITLE: Pharmacology (for Nursing and Health Fields) COURSE NUMBER: Biology 202
 WESTCHESTER COMMUNITY COLLEGE Valhalla, NY 10595 SYLLABUS FORM COURSE TITLE: Pharmacology (for Nursing and Health Fields) COURSE NUMBER: Biology 202 1. NAME OF COURSE: Pharmacology (for Nursing and Health
WESTCHESTER COMMUNITY COLLEGE Valhalla, NY 10595 SYLLABUS FORM COURSE TITLE: Pharmacology (for Nursing and Health Fields) COURSE NUMBER: Biology 202 1. NAME OF COURSE: Pharmacology (for Nursing and Health
SPECIALTY TREND MANAGEMENT
 SPECIALTY TREND MANAGEMENT Table of Contents Specialty drives pharmacy trend... Chapter 1 Managing price, mix and utilization... Chapter 2 Expand preferred drug strategies... Chapter 3 Cost-effective site
SPECIALTY TREND MANAGEMENT Table of Contents Specialty drives pharmacy trend... Chapter 1 Managing price, mix and utilization... Chapter 2 Expand preferred drug strategies... Chapter 3 Cost-effective site
MEDICAL BENEFIT BOOKLET
 MEDICAL BENEFIT BOOKLET For Administered By Si usted necesita ayuda en español para entender este documento, puede solicitarla gratuitamente llamando a Servicios al Cliente al número que se encuentra en
MEDICAL BENEFIT BOOKLET For Administered By Si usted necesita ayuda en español para entender este documento, puede solicitarla gratuitamente llamando a Servicios al Cliente al número que se encuentra en
Kaiser Permanente s Evaluation And Management Of Biotech Drugs: Assessing, Measuring, And Affecting Use
 Perspective Kaiser Permanente s Evaluation And Management Of Biotech Drugs: Assessing, Measuring, And Affecting Use A large integrated delivery system reports on its management of specialty pharmaceuticals.
Perspective Kaiser Permanente s Evaluation And Management Of Biotech Drugs: Assessing, Measuring, And Affecting Use A large integrated delivery system reports on its management of specialty pharmaceuticals.
Control costs while helping employees manage health expenses Aetna HealthFund One-to-One for small businesses. www.aetna.com
 Quality health plans & benefits Healthier living Financial well-being Intelligent solutions Control costs while helping employees manage health expenses Aetna HealthFund One-to-One for small businesses
Quality health plans & benefits Healthier living Financial well-being Intelligent solutions Control costs while helping employees manage health expenses Aetna HealthFund One-to-One for small businesses
Summary of Drug Coverage Location - Georgia SHBP
 Summary of Drug Coverage Location - Georgia SHBP Last Update: 12/07/2015 Therapeutic Category Description Trade Name Description SHBP Coverage Location Route Description Date of Revision to Document ADJUNCTIVE
Summary of Drug Coverage Location - Georgia SHBP Last Update: 12/07/2015 Therapeutic Category Description Trade Name Description SHBP Coverage Location Route Description Date of Revision to Document ADJUNCTIVE
Cytokine and CAM Antagonists
 Texas Prior Authorization Program Clinical Edit Criteria Drug/Drug Class Clinical Edit Information Included in this Document Actemra (Tocilizumab) Drugs requiring prior authorization: the list of drugs
Texas Prior Authorization Program Clinical Edit Criteria Drug/Drug Class Clinical Edit Information Included in this Document Actemra (Tocilizumab) Drugs requiring prior authorization: the list of drugs
How To Treat Rheumatoid Arthritis
 Pharmacy Prior Authorization Non-Formulary, Prior Authorization and Step-Therapy Guidelines Scroll down to see PA Criteria by drug class, or Ctrl+F to search document by drug name Non-Formulary Medication
Pharmacy Prior Authorization Non-Formulary, Prior Authorization and Step-Therapy Guidelines Scroll down to see PA Criteria by drug class, or Ctrl+F to search document by drug name Non-Formulary Medication
