Guidelines for the Laboratory Investigation of Heritable Disorders of Platelet Function
|
|
|
- Barry Owen
- 10 years ago
- Views:
Transcription
1 Guidelines for the Laboratory Investigation of Heritable Disorders of Platelet Function British Committee for Standards in Haematology Writing group: Paul Harrison 1, Ian Mackie 2, Andrew Mumford 3, Carol Briggs 4, Ri Liesner 5, Mark Winter 6, Sam Machin 2 Address for correspondence: BCSH Secretary British Society for Haematology 100 White Lion Street London N1 9PF [email protected] Published in August 2011 The guideline will be reviewed in August 2013 unless BCSH considers that new evidence or information necessitates an earlier review. Any amendments to the guideline and the date when the guideline was last reviewed will be published on the BCSH website. Disclaimer While the advice and information in these guidelines is believed to be true and accurate at the time of going to press, neither the authors, the British Society for Haematology nor the publishers accept any legal responsibility for the content of these guidelines. 1 Oxford Haemophilia & Thrombosis Centre, Churchill Hospital, Oxford 2 Haemostasis Research Unit, Department of Haematology, University College London 3 Bristol Haemophilia Centre, Bristol Haematology and Oncology Centre, Bristol 4 Department of Haematology, University College London Hospitals NHS Trust, London, W1T 4EU. 5 Haemophilia Comprehensive Care Centre, Great Ormond Street Hospital for Children NHS Trust, London 6 Kent Haemophilia Centre, Kent and Canterbury Hospital 1
2 Table of contents: Methodology Introduction Pre-analytical variables Tests and assays Specific assays of platelet function... 1Error! Bookmark not defined. 5 Other tests Diagnostic features Diagnosis in infants and small children Table 1: drugs, compounds, foods that affect platelet function Table 2: agonists used for LTA and receptor targets Table 3: minimun diagnostic criteria for platelet defects Figure 1: LTA patterns and diagnosis Appendix 1: Grading of evidence and recommendations Acknowledgements and declarations of interests References
3 METHODOLOGY The guideline writing group was selected to be representative of UK-based medical experts. MEDLINE was systematically searched for publications in English up to the Summer of 2009 using key words platelet, platelet function testing and platelet aggregometry. Relevant references generated from initial papers and published guidelines/reviews were also examined. Meeting abstracts were not included. The writing group produced the draft guideline which was subsequently revised and agreed by consensus. Further comment was made by members of the Haemostasis and Thrombosis Task Force of the British Committee for Standards in Haematology. The guideline was then reviewed by a sounding board of approximately 40 UK haematologists, the BCSH (British Committee for Standards in Haematology) and the British Society for Haematology Committee and comments incorporated where appropriate. Criteria used to quote levels and grades of evidence are as outlined in appendix 1 of this guideline. The objective of this guideline is to provide healthcare professionals with clear guidance on platelet function testing in patients with suspected bleeding disorders. The guidance may not be appropriate to patients receiving antiplatelet therapy and in all cases individual patient circumstances may dictate an alternative approach. Guideline update A previous BCSH guideline was published in 1988 (The British Society for Haematology BCSH Haemostasis and Thrombosis Task Force, 1988) and the new guideline is designed to completely replace this. 3
4 1 INTRODUCTION The diagnostic evaluation of platelet disorders is complex, poorly standardised and time consuming. This coupled with the wide spectrum of a known range of disorders some of which are very rare, presents a significant challenge to even the best diagnostic laboratory. (Bolton-Maggs et al, 2006; Hayward & Favaloro, 2009; Pai & Hayward, 2009; Watson et al, 2010). Many new tests (e.g. use of the PFA-100 and flow cytometry) have become available since the last BCSH guideline (The British Society for Haematology BCSH Haemostasis and Thrombosis Task Force, 1988) and the bleeding time (BT) is now used less frequently. A number of recent surveys have shown large variations between laboratories in platelet function testing practice and clearly demonstrate that new guidelines are urgently required (Jennings et al, 2008;Moffat et al, 2005;Cattaneo et al, 2009). These surveys have revealed why many types of mild platelet defects, (e.g. primary secretion defects) may be missed. This is not only because of the heterogeneity and rarity of some defects, but is also probably related to the failure to apply certain key platelet tests. This document outlines a new standardised approach which could be adopted by most clinical laboratories for the investigation of heritable platelet bleeding disorders. When the clinical picture and/or laboratory results suggest an inherited platelet disorder, referral to an expert reference centre should also be considered. Platelet function tests used specifically for monitoring antiplatelet drugs and/or detecting platelet hyperfunction will not be discussed in these guidelines. An evaluation of patients with abnormal bleeding requires objective clinical assessment of bleeding history, any family history and physical examination followed, when appropriate, by laboratory investigations. During this process it is essential to recognise that numerical and/or functional platelet disorders are prevalent amongst patients with abnormal bleeding and may be clinically indistinguishable from other haemostatic disorders, particularly von Willebrand disease (VWD).(Hayward, 2008;Cattaneo, 2003) Platelet disorders can also sometimes co-exist with other coagulation factor defects or VWD. (Daly et al, 2009;Quiroga et al, 2007) Laboratory investigations of platelet number and function are therefore recommended in any patient where bleeding symptoms are not fully explained by standard clinical laboratory investigations. Further information on the clinical presentation of patients with platelet disorders and the differential diagnosis 4
5 is available in detail elsewhere.(bolton-maggs et al, 2006) The current guideline focuses on the laboratory investigation of suspected platelet function disorders that should be performed in UK haematology laboratories. However, laboratory tests should ultimately be interpreted in terms of the clinical information. 2 PRE-ANALYTICAL VARIABLES 2.1 Specimen collection Venipuncture Ideally, samples for platelet function studies should only be collected from fasting and resting subjects who have refrained from smoking and caffeine ingestion on the day of testing. If the patient is taking medication known to affect platelet function, e.g. non-steroidal anti-inflammatory drugs (George & Shattil, 1991), testing should, if possible, be deferred for days after the last dose. Herbal remedies, garlic, alcohol and certain foods may also cause acquired platelet dysfunction. (George & Shattil, 1991) See table 1 for a list of drugs and other agents that are known to affect platelet function. In normal clinical practice it is difficult to avoid some of these patient related variables and so a pragmatic approach is to consider proceeding with platelet function tests, but if they are abnormal, collecting a fresh sample under more suitable conditions and repeating the tests. Blood should be collected by experienced phlebotomists using a standardised, atraumatic protocol, from the antecubital fossa, by clean venipuncture using minimum tourniquet pressure. Needles should be gauge (butterfly cannulae are suitable, providing blood flow is not restricted) and either evacuated tube systems or plastic syringes may be used. A discard tube should be used before collecting successive citrate tubes. Where tubes with a variety of anticoagulant types are required, the citrate tubes should be collected before EDTA- or heparincontaining tubes wherever possible to avoid the potential for carryover.(favaloro et al, 2008) 5
6 2.1.2 Anticoagulants Blood should be collected into a 1/10 volume of trisodium citrate ( mmol/l final concentration) for clinical platelet function testing. Buffered citrate solutions that maintain the sample ph are preferred. Care must be taken to ensure that tubes are correctly filled Specimen processing All specimens must be maintained at room temperature (20-25 C) and should not be placed on ice, in a refrigerator or a water bath. Immediately after blood collection, all tubes should be mixed by gentle inversion at least 6 times (and discarded if there is any evidence of clotting). Tubes should be kept capped at room temperature and not subjected to any vibration, shaking, vortexing, continuous mixing or agitation; they should not be transported via pneumatic tube systems. The time delay between collection, transport and analysis should ideally be preferably between 30 minutes and 2 hours but not more than 4 hours. Recommendations A complete record of current medication taken by patients or controls should be taken prior to blood collection to either prevent unwanted drug interference or help interpretation of test results (1A) Collect blood using a standardised, atraumatic protocol, with minimal stasis (2C) Use needles between 19 and 21 gauge; evacuated tube systems or syringes are acceptable (2C) The first 3-5ml of blood should not be used for platelet function tests (2C) Use mmol/l buffered trisodium citrate tubes (2C) Maintain specimens at room temperature (1B) Keep tubes upright and capped; do not subject to excessive mixing or agitation; do not use pneumatic transport systems (2C) 6
7 Samples should be tested between 30 minutes and no more than 4 hours from blood collection (2C) 3 TESTS AND ASSAYS Laboratory tests for platelet disorders comprise: i. Measurement of platelet number and size ii. iii. Global screening tests of platelet haemostatic function Specific assays of platelet haemostatic function 3.1 Platelet number, size and morphology Performance of the modern Full Blood Count investigation on whole blood is an essential investigation in patients with abnormal bleeding. The measurement of platelet number and size using automated cell counters and blood film analysis is highly sensitive and specific for numerical platelet disorders and is therefore valuable early in the investigation. Normal results will eliminate thrombocytopenia and anaemia as potential causes of bleeding and ensure that subsequent platelet function tests are not going to be affected by low platelet counts. Low platelet counts indeed affect most platelet function tests discussed below except flow cytometry Thrombocytosis, which may underlie abnormal bleeding, will also be revealed. If abnormalities in either platelet count, size (mean platelet volume, MPV) or distribution are flagged by the instrument then it is recommended that a blood film be examined to look for abnormalities in platelet number, size and/or granule content.(briggs et al, 2007)(Althaus & Greinacher, 2009) More recently, multiple light scatter parameters and/or fluorescence, rather than impedance sizing alone have been introduced into commercial analysers. This has improved their ability to distinguish large platelets from red cells and can sometimes provide more accurate counts (e.g. in samples from patients with macrothrombocytopenia where counts are usually underestimated).(harrison et al, 2000) Immunocounting by flow cytometry should also be considered when accurate counts are required in mactothrombocytopenia. (Harrison et al, 2000) 7
8 3.2 Global tests of platelet haemostatic function Global tests of platelet function are often used during the investigation of individuals with pathological bleeding. Since global tests do not enable a diagnosis of a specific platelet disorder, they are normally performed as the first part of a strategy which requires further testing with more specialised assays of platelet function. (Zeidan et al, 2007)(Harrison & Mumford, 2009) Normal test results may therefore theoretically be used to exclude the diagnosis of platelet function disorder so that further specialised testing can be avoided. For this reason, global platelet function tests are usually performed at the same time as global assays of coagulation pathway function (prothrombin time (PT) and activated partial thromboplastin time (aptt), von Willebrand Factor (VWF) screening tests (VWF:Ag, VWF:RCo and F:VIII:C) and measurement of platelet number). Guidelines for the systematic investigation of patients with suspected VWD and other coagulation factor deficiencies have recently been published elsewhere and are not discussed further in this review.(laffan et al, 2004;Bolton-Maggs et al, 2004) The most widely performed tests for screening platelet function disorders are currently the template BT and the Platelet Function Analyser (PFA-100 ; Siemens Diagnostics) closure time. Other commercial platelet function assay systems are also available, including those designed to measure the effect of antiplatelet drugs. (Harrison et al, 2007) Thromboelastography (TEG) and Rotational Thromboelastometry (ROTEM) ROTEM and TEG provide global tests of haemostasis and platelet function and are mainly used withinthe surgical setting.(perry, 2010) The utility of most of these assay systems including TEG/ROTEM for the screening and diagnosis of platelet function defects has not yet been examined systematically and their use for this application is therefore not currently recommended Template bleeding time The bleeding time described by Duke in 1910 is the oldest test of platelet function.(duke, 1910) Although the BT was previously recommended as a clinically useful test of platelet function,(the British Society for Haematology BCSH Haemostasis and Thrombosis Task Force, 1988) and surprisingly it remains in wide 8
9 use in the UK (Jennings et al, 2008), there is considerable variation in methodology between laboratories. The BT is highly dependent on operator technique, is subjective and is influenced by patient variables unrelated to haemostasis, such as age, gender, haematocrit, vascular pattern, skin thickness and skin temperature.(rodgers & Levin, 1990;Peterson et al, 1998) The BT therefore has poor reproducibility, sensitivity and specificity, as well as being invasive; for these reasons it is not recommended Closure time by the Platelet Function Analyser Assay principle The PFA-100 device is a test system in which citrated whole blood is aspirated at high shear rates ( s -1 ) through disposable cartridges containing an aperture coated with either collagen and epinephrine (CEPI) or collagen and ADP (CADP).(Kundu et al, 1995;Jilma, 2001;Kratzer & Born, 1985) These agonists trigger platelet adhesion, activation and aggregation leading to rapid occlusion of the aperture and cessation of blood flow.(kundu et al, 1995) The end-points for each test are time to occlusion of blood flow (closure time [CT]) or non-closure if the CT exceeds 300 seconds. The PFA-100 assay system requires small quantities of citrated venous blood (0.8 ml per cartridge) and is therefore useful for studying paediatric samples. Accordingly, the PFA-100 device is widely used as a screening tool to measure global platelet haemostatic function.(jennings et al, 2008;Moffat et al, 2005) Factors that influence PFA-100 closure time The choice of anticoagulant, specimen collection and transportation techniques and time between sampling and analysis (see Specimen Collection section above for guidance) all have critical effects on CT results.(jilma, 2001) (Harrison et al, 1999;Heilmann et al, 1997). Recent evidence reinforces the need for a discard tube during blood collection for PFA-100 testing (Kunicki et al, 2009). It is important that each laboratory establishes a reference range preferably within mmol/l buffered trisodium citrate tubes. Further guidance for the quality control of the PFA- 9
10 100 is published elsewhere. (Christie et al, 2008;Harrison, 2004;Hayward & Eikelboom, 2007)(Favaloro, 2009) There are extensive general reviews of the clinical utility of the PFA-100. (Favaloro, 2008)(Hayward et al, 2006) Knowledge of the full blood count is critical for interpreting CT results from the PFA Thrombocytopenia (< 100 x 10 9 /l) and anaemia (< 20% haematocrit) often results in prolongation of the CT. (Kundu et al, 1995;Harrison et al, 1999) CT also correlates inversely with plasma VWF activity in normal subjects and may therefore be longer in patients with blood group O.(Lippi et al, 2001) The Collagen/Epinephrine (CEPI) CT, but not the Collagen/ADP (CADP) CT, is usually prolonged by COX-1 inhibitors such as aspirin.(jilma, 2001) PFA-100 CT and VWD Abnormal CT on both cartridges are typical for types 2A, 2B, 2M and 3 VWD with a sensitivity of > 98%.(Franchini, 2005) When type 1 VWD is included, the overall sensitivity of CT to VWD is reported to be lower (85-90%),(Favaloro, 2006) but there is a clear relationship between VWF level and CT,(Moeller et al, 2001). Type 2N gives normal results. The PFA-100 may also be useful for monitoring desmopressin therapy in VWD patients.(cattaneo et al, 1999;Favaloro et al, 2001;Franchini et al, 2002;Hayward et al, 2006;van Vliet et al, 2008) PFA-100 CT and diagnosis of heritable platelet function disorders Greater abnormalities in CT in both cartridges occur with the severe platelet function defects, such as Glanzmann thrombasthenia (GT), Bernard Soulier syndrome (BSS) and platelet type or pseudo-vwd in which non-closure is typical.(harrison et al, 1999;Harrison, 2005;Hayward et al, 2006; Mammen et al, 1998) In many less severe platelet function defects, the CT may be either normal or prolonged; abnormal results are more frequently reported with the CEPI than the CADP cartridge.(hayward et al, 2006;Harrison et al, 2002) There are rare reports of abnormal CADP but with normal CEPI CTs suggesting that the CEPI cartridge cannot be used exclusively as a screening test. It is not currently possible to accurately determine the sensitivity of 10
11 the PFA-100 for most mild, heritable platelet function defects since most reported studies comprise small patient numbers, with varying mixtures of these defects.(hayward et al, 2006;Harrison, 2005) The PFA-100 CT exhibits poor sensitivity for mild platelet defects in a small number of prospective studies in patients with an unequivocal personal and family history of mucocutaneous bleeding.(quiroga et al, 2004;Cattaneo, 2004;Podda et al, 2007) Other retrospective cohort studies of patients with previously diagnosed platelet function defects indicate sensitivities up to >80% for prolonged CT, although many of these studies included subjects with severe phenotypes (e.g. GT, BSS) and VWD. (Harrison et al, 1999;Harrison et al, 2004;Kerenyi et al, 1999;Posan et al, 2003) A recent metaanalysis concluded that the overall sensitivity and specificity of the CEPI cartridge for disorders in primary haemostasis was 83% and 89% respectively. CADP sensitivity was lower at 67% with an equivalent specificity of 86%. (Karger et al, 2007). The PFA-100 has shown good sensitivity (> 90%) in screening patients with menorrhagia for VWD and platelet function defects.(james et al, 2004;Philipp et al, 2005;Acharya et al, 2008) Guidelines on the utility and practice of using the PFA-100 for clinical assessment of platelet disorders are provided by various international and national organisations. (Hayward et al, 2006;Bolton-Maggs et al, 2006; Christie et al, 2008). It is reasonable to use normal PFA closure times to rule out a significant platelet defect in patients who have a low clinical suspicion of such a defect, however if the clinical suspicion of a platelet defect is high, then a normal PFA result should not be used to rule out this possibility and specific assays of platelet function are indicated. Recommendations Perform a full blood count on all patients (1A) In samples with abnormalities in platelet count or size distribution (as indicated by an automated analyser), a blood film should be examined (1B) The bleeding time is not recommended (1B) 11
12 The PFA-100 provides an optional screening test, but this must be interpreted with caution and in the context of the clinical background, as the test is not diagnostic or sensitive for mild platelet disorders (1B) Both PFA-100 CADP and CEPI cartridges should be used for screening (1B) 4 SPECIFIC ASSAYS OF PLATELET FUNCTION 4.1 Light transmission aggregometry Light transmission aggregometry (LTA) was invented in the early 1960s and is still regarded as the gold standard for platelet function testing. Despite its widespread use, the test is poorly standardised and there are wide variations in laboratory practice(jennings et al, 2008;Moffat et al, 2005;Cattaneo et al, 2009). Guidelines specific for LTA have also recently been published (Christie et al, 2008; Cattaneo et al, 2011; Hayward et al, 2010) Sample preparation for LTA Citrated blood samples obtained as described above are centrifuged to prepare platelet rich plasma (PRP) and platelet poor plasma (PPP). To prepare PRP, whole blood tubes should be centrifuged at g for 10 minutes in a swing-out rotor at room temperature (RT) without application of the brake. Autologous PPP is prepared by centrifugation (after removal of PRP or using whole samples) at least 1500 g for at least 15 minutes at RT (Christie et al, 2008). At the end of the centrifugation steps a plastic pipette should be used to separate the top 2/3rds of PRP or PPP should be carefully removed without disturbing the buffy coat layer and red cells. PRP or PPP should then be transferred into separate polypropylene tubes capped and stored upright at RT. The PRP should then be left for at least 30 minutes prior to testing. Visual inspection of the samples is important as icteric, lipaemic, red cell contaminated and haemolysed samples should not be tested. A platelet count should be performed on the PRP and unless it is greater than 600 x 10 9 /L, the platelet count should not be adjusted using PPP, as this may cause artefactual inhibition of platelet aggregation (Linnemann et al, 2008;Cattaneo et al, 2007). Analysis of PRP with a 12
13 platelet count <150 x 10 9 /L is possible, but the results should be treated with caution (ideally a normal control should be analysed, where the PRP count is adjusted to equal that of the test, by dilution with buffer instead of PPP) (to prevent artefacts). PRP with low counts can still be tested to exclude severe platelet disorders such as BSS and type 2B and platelet type VWD. Agonists for LTA ADP, epinephrine, collagen (type I, tendon), arachidonic acid and ristocetin are the traditional baseline panel of agonists for LTA. (see Table 2) (The British Society for Haematology BCSH Haemostasis and Thrombosis Task Force, 1988) An extended panel of agonists can include gamma Thrombin, Thrombin Receptor Activating Peptides (TRAP), Collagen-Related Peptide, endoperoxide analogue U46619 and calcium ionophore A23187, which may all be useful when a more detailed investigation of the exact nature of the defect is required (see Table 2). Most laboratories perform dose response curves for ADP ( M), collagen ( g/ml) and epinephrine ( M). Although this provides a detailed pharmacological approach, more recent evidence supports the use of single doses of a panel of agonists, which significantly increases the likelihood of detecting a platelet defect (odds ratio 32).(Hayward et al, 2009b) (Dawood et al, 2007) A recommended baseline example panel therefore comprises: 2.5 M ADP, 1.25 g/ml collagen, 5 M epinephrine, 1.2 mg/ml ristocetin, and 1.0 mm arachidonic acid (all final concentrations in PRP). If the initial aggregation results with ADP, collagen or epinephrine are abnormal then retesting should be performed at higher concentrations of the agonist(s) and even to supranormal concentrations to confirm a specific defect. It should be noted that a significant proportion of normal samples may not always give a full aggregation response to epinephrine (due to natural variations in adrenoreceptor numbers) and have no related platelet defect. If the aggregation to ristocetin is normal then retesting should additionally be performed with low dose ( mg/ml) ristocetin to check for hyperfunction or gain of function (associated with Type 2B and platelet type VWD). If results with 1.2 mg/ml ristocetin are absent then retesting can be performed with addition of an external source of VWF (e.g. cryoprecipitate or a VWF concentrate) to confirm either a VWF or GpIb 13
14 defect. If arachidonic acid aggregation is abnormal then further testing should be performed with 1.0 M U46619 to test for any thromboxane receptor abnormalities. An extended panel of tests (usually only available within more specialised centres) could also be considered including gamma thrombin (which does not cause clotting), PAR-1 (SFLLRN) and PAR-4 (AYPGKF) TRAP peptides (if gamma thrombin is abnormal) Collagen-Related Peptide (CRP), calcium ionophore and PMA (Phorbol 12-myristate 13 acetate) if abnormalities in the thrombin receptors, GpVI, calcium mobilisation and protein kinase C respectively, are suspected. Performing aggregometry A maximum of 1/10 volume of agonist is added to PRP to initiate aggregation and the final concentration of agonist within PRP is recorded (taking into account the 10 fold dilution factor). It is imperative that new batches of agonist are checked against the previous batch for performance, using normal control samples. Platelet aggregometers measure the change in optical density (or light transmittance) over time of stirred PRP in cuvettes at 37 C after addition of the agonists. They are calibrated for transmission using autologous PPP (100%) and PRP (0%). A stir speed of rpm is normally recommended. It is important that samples are pre-incubated for at least 5 minutes at 37 C prior to assay to obtain stable baseline traces. The appropriate agonists must then be added directly to the PRP and not pipetted onto the side of the tube. It is important that no air bubbles are introduced at any stage of the procedure as these can interfere with transmission measurement. The aggregation tracing should be observed for at least 5 minutes, but preferably 10 minutes to monitor the lag phase, shape change (negative deflection), primary and secondary aggregation and any delayed platelet responses e.g. reversible or spontaneous aggregation. The assay is then terminated and results printed and stored for visual inspection. It is recommended that local, normal cut-off values are established, using nonparametric statistics. However, it is recognised that this is not possible for most clinical laboratories due to the inherent variability of the test and the large number of subjects that would be required (i.e. >40). For this reason, most clinical laboratory staff subjectively evaluate the shape of the aggregation curves. The following 14
15 parameters should always be considered: lag phase, maximal amplitude, primary aggregation slope, and disaggregation, for each commonly used agonist concentration.(hayward et al, 2009b;Hayward et al, 2008). It is important that the overall shape of the aggregation responses obtained with each agonist are fully described and interpreted by experienced staff (e.g. is the response fully reversible and is there a significant lag phase; what is the maximal amplitude of the response). See Figure 1 for typical examples of normal and abnormal aggregometry curves in various classical defects. Recommendations Platelet counts >600x10 9 /L (1B) in platelet rich plasma should be diluted. Repeat all unexpected, abnormal light transmission aggregometry tests with a fresh sample, in parallel with a normal control sample (2C) Only experienced individuals should interpret tracings and results (1C) Assess performance of new batches of agonists by comparison with a previous batch (1A) 4.2 Flow cytometry The most commonly used flow cytometry tests relevant to platelet function are the quantification of glycoprotein receptor density in the diagnosis of defects such as GT and BSS, and detecting their heterozygous states. Flow cytometry can also be used to measure the collagen (GpIa/IIa and GpVI) and PAR-1 receptor densities if LTA testing suggests any abnormalities in these receptors. There are also tests available to measure: platelet activation in response to classical agonists, dense granule content, and exposure of anionic phospholipids As flow cytometry is expensive, time consuming and requires specialised training, only those patients with an appropriate clinical history and/or abnormalities of other platelet function tests should be assessed for receptor defects. Guidelines and protocols on flow cytometry of 15
16 platelets have been published elsewhere.(schmitz et al, 1998;Goodall & Appleby, 2004;Michelson et al, 2007) It is recommended that analysis should be performed using fresh, citrated whole blood, to avoid platelet activation and loss of platelet subpopulations during centrifugation. If measuring platelet activation and function it is important to control for ex-vivo activation caused by delays in analysis from blood sampling for example. Fluorescently labelled antibodies are added to the blood samples and after incubation at room temperature, in the dark, the samples are diluted to a final volume of between 1-2 ml with buffer (e.g. Hepes buffered saline, ph 7.4), or a mild fixative before analysis. All buffers must be filtered (e.g. using a 0.2 µm filter) and tubes should not be vortexed, but mixed gently by tapping, otherwise platelet aggregation will occur. Matched isotype control fluorescent antibodies should be tested at the same time in control tubes. It is recommended that normal positive control samples are analysed in parallel to verify assay performance and that the antibodies are efficiently binding to their respective receptors particularly if a receptor is completely absent in GT or BS for example. Some commercial assays are now available that can give absolute quantification of the copy number of individual receptors of interest. Normal ranges can be established for either fluorescence or copy number of individual glycoproteins Neonates may also have significantly lower receptor densities than adults. The lower limit of detection if ~500 receptors/platelet so the test cannot always be used reliably to detect low copy number receptors. It is possible to measure platelet procoagulant activity, apoptosis (and microparticles) by incubating samples with high affinity probes against phosphatidyl serine (e.g. Annexin-V) and activating the cells with calcium ionophore, collagen-related peptide or combinations of thrombin and collagen. This enables the diagnosis of Scott syndrome and related disorders although these defects are indeed very rare. Recommendations Flow cytometry should be used in the investigation or confirmation of Glanzmann thrombasthenia, Bernard Soulier Syndrome (1B) and Scott syndrome (1C); and may also be used to investigate abnormalities in the collagen (GpVI and GpIa/IIa) and thrombin receptors (PAR-1) (1B) 16
17 Whole blood platelet assays are preferable although PRP can be used for BSS diagnosis (1B) Analyse normal controls in parallel with test samples (1A) 4.3 Measurement of total and released nucleotides The measurement of total and/or released adenine nucleotides provides an important additional diagnostic tool usually in conjunction with aggregometry for determining whether there is any specific deficiency in dense granule numbers or their content (e.g. storage pool disease), or specific defect(s) in degranulation (e.g. release defects). There is evidence to suggest that these defects can be misdiagnosed if relying on platelet aggregometry alone.(nieuwenhuis et al, 1987;Israels et al, 1990)(Hayward et al, 2009b)(Cattaneo, 2009) It is therefore recommended that laboratories perform an independent measurement of the release reaction. However, although nucleotide measurement is very straightforward and normally involves measuring ATP by simple bioluminescent assays (using firefly luciferin/luciferase assays), recent surveys indicate that many laboratories do not measure platelet nucleotides.(jennings et al, 2008;Moffat et al, 2005) This suggests that many platelet storage and secretion defects are potentially being underdiagnosed with current practice. The simplest assay of released platelet nucleotides can be performed in real time with a Lumi-Aggregometer (either LTA or whole blood aggregometry, WBA). (Dawood et al, 2007; Christie et al, 2008; Watson et al, 2010)These instruments provide a rapid assessment of ATP levels during platelet aggregation and normally demonstrate release of ATP during the secondary aggregation phase in LTA. The amount of ATP released is easily calibrated using commercially available ATP standards analysed in the same channels of the aggregometer. However, it is impossible to distinguish between storage and release defects using this approach. Many laboratories therefore determine the total platelet content of both ADP and ATP with lysed platelet preparations (at standardised platelet counts) and sometimes after a degranulation step to induce release. Adenine nucleotides are measured in platelet lysates using either luminometers (Summerfield et al, 1981 or by HPLC (Greaves & Preston, 1985), with conversion of ADP to ATP (using pyruvate kinase). 17
18 Calibration is performed using an ATP standard. These assays have the advantage that samples can be frozen and shipped to more specialised laboratories that regularly perform nucleotide measurements. There are two nucleotide pools within the platelet:- the metabolic pool and the dense granular/storage pool, the latter comprising about 60% of the total content. The ratio of ATP:ADP is therefore of fundamental diagnostic importance as there are pronounced differences between the relative concentrations in the two pools. Any storage defects are associated with a decrease in the amount of stored and released ADP with an increased ratio of ATP:ADP. Normal ADP levels and ATP:ADP ratios but decreased ADP release are indicative of a release-defect. Normal ranges should be established locally, but typical values are and nmol/10 9 platelets for total ADP and ATP respectively (ATP:ADP ratio ). Typical normal ranges for released nucleotides are: and 8-20 nmol/10 9 platelets for ADP and ATP respectively (ATP:ADP ratio ) (Chanarin, 1989). Serotonin (5-HT) is actively taken up and stored within the platelet dense granules and it is possible to measure the uptake and release of radiolabelled serotonin into and from the platelets with standardised assays.(the British Society for Haematology BCSH Haemostasis and Thrombosis Task Force, 1988;Zhou & Schmaier, 2005) ELISA assays for platelet serotonin content are also available. Mepacrine uptake and release by the dense granules can be measured by flow cytometry(wall et al, 1995;Gordon et al, 1995). Recommendations When there is a high clinical suspicion of a platelet function defect, adenine nucleotides should be measured even if the aggregation is normal (1B) If aggregation results suggest storage pool disease or a release defect, measure stored and released nucleotides (1B) 18
19 4.4 Whole blood aggregometry In impedance aggregometry, whole blood is stirred at 37 C and aggregation is detected by the accretion of platelets to the surface of two fine, precious metal, wire electrodes.(fritsma, 2007) Adherent platelets increase the electrical impedance between the electrodes, which can be displayed as a wave of aggregation.(cardinal & Flower, 1980) Impedance aggregation measurements in whole blood may be influenced by: haematocrit (>0.35 L/L), platelet count, and elevated white cell count, while the agonist responsiveness differs from LTA. (Mackie et al, 1984;Ingerman- Wojenski et al, 1983;Sweeney et al, 1989) Impedance and LTA methods show similar dose responsiveness to equine tendon collagen, but higher ADP concentrations are required to induce aggregation by the impedance technique and low doses (e.g. 1 M) give no impedance response. Reversible aggregation and biphasic responses to ADP cannot be demonstrated by whole blood impedance,(mackie et al, 1984;Ingerman- Wojenski et al, 1983) while epinephrine responses tend to be absent or very weak,(mackie et al, 1984;Swart et al, 1984). A study by UK NEQAS surveyed 169 haemostasis centres, (119 UK and 50 non-uk) and found that only 4/88 performed whole blood platelet aggregation studies.(jennings et al, 2008) Some of the technical problems of whole blood impedance aggregation have been overcome by the development of disposable electrodes, standardised reagents and the availability of a 5 channel multiple electrode platelet aggregometer (Dynabyte, Munich, Germany)). (Toth et al, 2006) There is very sparse peer review literature comparing impedance and LTA methods and a lack of clinical validation in the diagnosis of heritable platelet function defects. 5 OTHER TESTS Platelet alpha granule proteins (e.g. Platelet Factor 4 (PF4) and Beta- Thromboglobulin ( TG)) can be measured by ELISA, RIA or western blotting and may be helpful for the diagnosis of Quebec platelet disorder (Kahr et al, 2001). Electron microscopy has also proven very useful for defining ultrastructural abnormalities associated with a variety of platelet defects.(clauser & Cramer-Borde, 2009). The simpler whole mount electron microscopy technique has proven useful for confirming dense granule defects(hayward et al, 2009a). 19
20 Molecular genetic diagnosis of heritable platelet disorders may offer valuable confirmation of diagnosis in affected individuals, in family members where phenotypic testing of platelets is impractical and for ante-natal diagnosis. Molecular diagnosis is most feasible in GT and BSS where the number of candidate genes is small and there are already accessible databases containing large patient groups to help confirm that observed nucleotide variations are pathogenic ( and sinaicentral.mssm.edu). Clinical diagnostic services for GT and BSS by direct sequencing of PCR-amplified genomic DNA are now offered in a small number of clinical genetic laboratories in the UK. For mild platelet function or platelet number disorders individual candidate genes can occasionally be identified using clinical and laboratory phenotypic features (e.g. MYH9 related disorder, CAMT, TAR, WAS) or by laboratory phenotype alone (e.g. thromboxane and P2Y 12 ADP receptor defects, GPVI defects). (Nurden et al, 2009 ; Watson et al, 2010). However, molecular genetic analysis of these disorders is currently available only in research laboratories. Since there is limited repertoire of reported mutations, it is usually difficult to assign pathogenicity to observed nucleotide variations without expression studies. In some patient populations where a specific pathogenic mutation is prevalent (e.g. 16bp deletion in HPS1 in Peurto Rican descent patients with Hermansky-Pudlak syndrome), allele specific mutation detection strategies may enable rapid molecular diagnosis of selected disorders. In all cases when molecular genetic diagnosis is considered, families should undergo careful genetic counselling and provide written consent in accordance with current best practice guidelines. (Ludlam et al, 2005). 6 DIAGNOSTIC FEATURES Typical clinical and laboratory findings of platelet function tests in many different platelet defects are detailed in Table 3. For more diagnosis and treatment of all platelet disorders including the inherited thrombocytopenias see Bolton-Maggs et al, 2006(Bolton-Maggs et al, 2006). 20
21 7 DIAGNOSING PLATELET FUNCTION DISORDERS IN INFANTS AND SMALL CHILDREN Severe platelet disorders such as GT and BSS usually present in infancy or early childhood but the diagnosis of these disorders in the very young is more challenging than in older children or adults for a number of reasons, mainly pre-analytical. Junior paediatricians commonly take blood using heelpricks, fingerpricks or a standard venipuncture needle inserted into a vein, collecting the drops from the end of the needle. None of these methods is appropriate for assessment of platelet function which should be done on a free-flowing venepuncture sample though in practice indwelling arterial and central venous catheters have also been used to facilitate getting the necessary volumes from small children. The minimum volume of blood required for full platelet LTA and nucleotide testing is usually 20 ml; this may be 8-10% of the blood volume in neonates and could cause hypovolaemic symptoms. The usual needle gauge for blood sampling in infants and smaller children is 23G as the recommended size of 19-21G can be too big for small peripheral veins and is also more likely to cause trauma to subcutaneous tissues which may be significant if a severe platelet disorder is present. It is therefore recommended that the control sample is also taken with a 23G needle to ensure that the patient sample is processed along with a similarly taken sample. Validation of platelet function tests in age-matched normal control populations of infants and children is rarely possible due to ethical issues of taking large volumes of blood from healthy normals. Although there are scanty data on LTA in normal neonates and infants, there are no known comprehensive studies looking at nucleotide values at different ages through the 1 st year of life. The available literature suggests that in infancy the platelets are generally hyporeactive (except to ristocetin and variably collagen) but beyond infancy reactiveness of platelets, both aggregation and nucleotide release reactions, is very similar to that in adults (Knofler et al, 1998 ; Bonduel et al, 2007). Therefore the usual and pragmatic approach is to assess platelet function in children > 1 year of age using adult controls and normal ranges (Hayward et al, 2010). Family testing may also be useful not only to confirm a given defect but to discern the potential inheritance pattern. As there is few data, results of investigations taken in the first year should be viewed with more caution and should always be repeated, particularly if the apparent abnormalities are 21
22 relatively subtle and if the putative diagnosis is one of the usually milder disorders such as a granule or secretion defect. Results of investigations in infants with the severe function defects GT or BSS are usually very clear-cut at all ages and it could be argued that the safest way to diagnose these disorders in an infant is to limit the investigations to those that can be performed on relatively small volumes of blood; with a full blood count, PFA-100 (which will reliably show non-closure with both cartridges in both GT and BSS), and flow cytometry. Flow cytometry if performed carefully (see above section) can also be utilised to study platelet function/activation in small volumes of blood by determining responsiveness to various agonists at differing concentrations. Confirmatory LTA can then be done when possible but demonstration of a severe defect of primary haemostasis using the PFA-100 in combination with absent or very low levels of the affected receptor, and macro-thrombocytopenia in BSS, is highly suggestive and enough to guide appropriate treatment for bleeding. Conversely, both GT and BSS can effectively be excluded in infants if the PFA-100 shows normal closure times this can be of crucial clinical use in unexplained severe bleeding such as intracranial haemorrhage when there is a query as to whether this is an inflicted injury or it is due to spontaneous bleeding in association with a severe bleeding diathesis. A detailed diagnostic approach to platelet disorders in children has recently been published (Israels et al, 2011) 22
23 TABLE 1 A list of drugs, compounds and dietary components/herbs that can affect platelet function (Reprinted and modified with permission from Kottke-Marchant and Corcoran G. The laboratory diagnosis of platelet disorders. Arch Pathol Lab Med 2002:126: with permission from Archives of Pathology & Laboratory Medicine. Copyright College of American Pathologists. Cyclo-oxygenase (COX)-1 inhibitors (irreversible) Aspirin and all proprietary or over-the-counter preparations containing acetylsalicylic acid. COX-1 and COX-2 inhibitors (reversible) (Nonsteroidal anti-inflammatory drugs (NSAIDs) Ibuprofen Indomethacin, naproxen Mefenamic acid Inhibitors of Platelet Receptors Abciximab, tirofiban, eptifibatide ( IIb 3) Ticlopidine, clopidogrel, prasugrel (irreversible), cangrelor (reversible), ticagrelor (reversible) (P2Y 12 ) Phosphodiesterase Inhibitors Dipyridamole Cilostazole Anticoagulants Heparinoids, vitamin K antagonists and direct thrombin inhibitors may indirectly influence platelet function due to inhibition of thrombin. Cardiovascular Agents -adrenergic blockers (propranolol) Vasodilators (nitroprusside, nitroglycerin) Diuretics (furosemide) Calcium channel blockers Antimicrobials lactams (penicillins, cephalosporins) Amphotericin (antifungal) Hydroxychloroquine (antimalarial) Nitrofurantoin Chemotherapeutic agents Asparaginase Plicamycin Vincristine Psychotropics and Anaesthetics 23
24 Tricyclic antidepressants (imipramine) Phenothiazines (chloropromazine) Local and general anaesthesia (halothane) Thrombolytic Agents Streptokinase Urokinase Tissue Plasminogen Activator (TPA) Miscellaneous Clofibrate Dextrans Guaifenesin (expectorant) Radiographic contrast media Food/Herbs (at high concentrations) Alcohol Caffeine (methylxanthine) Cumin Dong quai Fenugreek Garlic, onion, ginger Ginseng Fish Oil Tamarind Turmeric Willow Vitamins C and E Black Tree Fungus ( Chinese mushroom ). N.B.: This is only a partial list and many other agents are also known to affect platelet function. A full drug and relevant dietary history should always be taken for each subject tested for platelet function. If abnormal results are obtained then retesting can confirm if any defect is transiently acquired or not. 24
25 TABLE 2 A list of the basic and extended panels of platelet agonists used for LTA recommended starting concentrations and the range of final concentrations (after dilution into the PRP) normally used, the receptor target and effect of defects on the aggregation response Agonist Recommend Starting concentration s In PRP Baseline Panel Range of Final concentration s in PRP Receptor Targets ADP 0.5 P2Y 1 and P2Y 12 Epinephrin e Arachidonic acid Collagen (type I tendon) 1 mm mm (single dose) Ristocetin mg/ml and mg/ml (single doses) Extended Panel Gammathrombin U Collagenrelated peptide Adrenoreceptors Testing Thromboxane generation and TX receptor 1.0 GpVI and GpIa/IIa receptors GpIb/VWF axis ng/ml Thrombin receptors but without clotting Thromboxane receptor dose ng/ml GpVI stimulation Convulxin TRAP peptides ng/ml SFLLRN (PAR-1) PAR-1 and PAR-4 Calcium ionophore A23187 PMA (Phorbol 12- myristate 13 acetate AYPGKF (PAR- 4) Calcium mobilisation and procoagulant function 30 nm Protein kinase C 25
26 TABLE 3 Minimal Diagnostic Criteria for various platelet defects. The pattern of expected platelet function test results are listed for the most common platelet disorders. GT Glanzmann Thrombasthenia, BSS - Bernard Soulier Syndrome. PCI Prothrombin Consumption Index. ETP Endogenous Thrombin Potential. The result for a potential P2Y 1 defect are hypothetical as none described yet. Disorder Type 1, 2A and 3 VWD Platelet type or type 2B VWD Platelet Count/Morphology Normal PFA CADP/CEPI both equally prolonged. Very prolonged in 2A and 3. LTA Pattern Defective response to high dose ristocetin (correctable by VWF source). Normal Both abnormal Platelets aggregate on addition of plasma or cryoprecipitate Gain of function with low dose ristocetin GT Normal CADP/CEPI both very prolonged BSS Dense Granule Defects Mild to moderate macrothrombocytopenia Low to normal count Reduced electron dense granules by whole mount EM CADP/CEPI both very prolonged CADP normal CEPI sometimes prolonged Profound impairment to all agonists except high dose ristocetin Defective aggregation to high dose ristocetin (not correctable by addition of VWF source) Decreased secondary aggregation to ADP and epinephrine Nucleotid es Flow Cytometry Other Normal Normal VWF panel will confirm subtype Normal Increased VWF binding to platelets Abnormal VWF panel in Type 2B VWD/ Loss of high MW VWF in platelet type VWD Normal Significantly reduced copy number of Normal to high levels Increased ATP:ADP ratio with reduced ADP level. Reduced ATP release defective functioning can be investigated) Significantly reduced copy number of GpIb (heterozygotes can also be measured) Reduced Mepacrine uptake and release Reduced Serotonin Release Hermansky Pudlak and Chediak- 26
27 Secretion defect Aspirin-like defect Thromboxane receptor defect Giant platelet syndrome Collagen receptor defects Normal Normal Normal Macrothrombocytopenia Normal CADP normal CEPI sometimes prolonged CADP normal CEPI normally prolonged (NB can by bypassed by high VWF levels) CADP normal CEPI sometimes prolonged Sometimes normal Both abnormal Decreased secondary aggregation to ADP and epinephrine Absent arachidonic acid response but normal to U Decreased secondary aggregation to ADP and epinephrine Absent Arachidonic Acid and U46619 response Normal response to ristocetin Decreased Collagen aggregation. Decreased CRP response if GpVI defect P2Y 12 defect Normal Normal Decreased ADP aggregation. Reversible response at high doses. by luminoaggreg ometry Normal but with defective release. reduced ATP release by luminoaggreg ometry Normal Normal Normal to high Normal Normal Normal mepacrine uptake but defective release Normal-High receptor copy numbers per platelet Low GpIa/IIa or GpVI levels by flow cytometry Low P2Y 12 copy number using radioligand binding assay Higashi syndromes are autosomal recessive and associated with oculocutaneou s albinism Retest or defer for 10 days if patient taking aspirin or NSAIDs Retest or defer if patient taking clopidogrel or 27
28 Reduced secondary responses P2Y 1 defect Unknown Unknown Decreased response Normal to ADP no shape change and curves not reversible Scott Normal Normal Normal Normal Reduced expression of phosphatidyl syndrome serine on activated platelets by flow cytometry using Annexin-V other anti- P2Y12 drugs Reduced PCI And ETP 28
29 FIGURE 1: Illustration of how LTA patterns can be used to diagnose a range of rare platelet defects. Note that these are generalised illustrations and actual patterns may differ slightly between patients with similar defects. The 0% baseline (bottom of y axes) has been set with undiluted PRP and the 100% aggregation (top of y axes) limit set with autologous PPP. After establishment of a stable baseline for a few minutes the following agonists were added to these final concentrations, 10 M ADP, 2 g./ml collagen, 5 M epinephrine, 1.0 mm arachidonic acid and low ( mg/ml) and high dose ( mg/ml) ristocetin. Aggregation was then monitored for up to 10 minutes (x axes from left to right) Example tracings are shown for a normal subject, a patient with Glanzmann thrombasthenia (GT), patients with VWD or Bernard Soulier Syndrome (BSS), Type 2B VWD/pseudo-VWD, GpVI deficiency, P2Y 12 deficiency, an aspirin-like defect, storage pool and release defects and a P2Y 1 defect. Normals will give an initial shape change (slight negative deflection) followed by a rapid and irreversible aggregation response to high concentrations of ADP. Lower doses can be used to determine the threshold for secondary aggregation. High dose collagen will give a characteristic lag phase followed by a shape change (slight negative deflection) followed by a rapid and irreversible aggregation. Epinephrine will give the classical biphasic response (primary and secondary aggregation) with no shape change. Arachidonic acid will give a shape change followed by full aggregation. Only high dose ristocetin will give a normal agglutination response in normals. The GT patient shows no aggregation to any agonist except high dose ristocetin (which is reversible). Flow cytometry and molecular biology can then be used to confirm the defect in IIb 3. Patients with BSS and VWD do not respond to ristocetin but VWD samples (but not BSS) will be correctable after addition of a source VWF to the plasma. VWD should be confirmed with a VWF panel of tests/molecular biology and BSS confirmed by flow cytometry and molecular biology. Type 2B and pseudo-vwd show the gain of function with a response to low dose ristocetin. A VWF panel/molecular biology will confirm type 2B VWD and molecular biology will confirm the diagnosis of pseudo-vwd in the GpIb gene. Gp VI deficiency gives no response to collagen which can be confirmed using CRP, by flow cytometry (see extended panel of agonists) or molecular biology. A P2Y 12 defect shows a reduced and 29
30 reversible response to ADP. In a homozygous P2Y 12 defect, only minimal primary aggregation to all concentrations of ADP will be present. In a heterozygous P2Y 12 defect there will be absence of secondary aggregation but disaggregation tends to begin < 10 M ADP with a biphasic response to epinephrine. An aspirin-like defect will show reduced secondary aggregation responses to ADP and epinephrine and absent arachidonic acid aggregation. A defect in the thromboxane receptor can then be checked for using U46619 (see extended panel of agonists). Patients with storage pool disease or release defects will give an identical pattern as the aspirinlike defect except giving a good primary aggregation response to arachidonic acid. The P2Y defect pattern is based upon in vitro response to anti-p2y 1 antagonists as no patients with a P2Y 1 defect have ever been described. This figure was significantly modified with permission from Figure 12.3, page 115 in Chapter 12 Diagnostic Assessment of platelet function by P.Nurden and A. Nurden in Quality in Laboratory Hemostasis and Thrombosis edited by Kitchen S, Olson JD & Preston FE and published by Wiley-Blackwell in
31 (Figure 1) 31
32 (Figure 1cont...) 32
33 Appendix 1: Grading of recommendations and levels of evidence: The GRADE Nomenclature: STRENGTH OF RECOMMENDATIONS: Strong (grade 1): Strong recommendations (grade 1) are made when there is confidence that the benefits do or do not outweigh harm and burden. Grade 1 recommendations can be applied uniformly to most patients. Regard as 'recommend'. Weak (grade 2): Where the magnitude of benefit or not is less certain a weaker grade 2 recommendation is made. Grade 2 recommendations require judicious application to individual patients. Regard as suggest. QUALITY OF EVIDENCE The quality of evidence is graded as high (A), moderate (B) or low (C). To put this in context it is useful to consider the uncertainty of knowledge and whether further research could change what we know or our certainty. (A) High Further research is very unlikely to change confidence in the estimate of effect. Current evidence derived from randomised clinical trials without important limitations. (B) Moderate Further research may well have an important impact on confidence in the estimate of effect and may change the estimate. Current evidence derived from randomised clinical trials with important limitations (e.g. inconsistent results, imprecision - wide confidence intervals or methodological flaws - e.g. lack of blinding, large losses to follow up, failure to adhere to intention to treat analysis),or very strong evidence from observational studies or case series (e.g. large or very large and consistent estimates of the magnitude of a treatment effect or demonstration of a dose-response gradient). (C) Low Further research is likely to have an important impact on confidence in the estimate of effect and is likely to change the estimate. Current evidence from observational studies, case series or just opinion. More information on the GRADE nomenclature can be found at 33
34 ACKNOWLEDGEMENTS AND DECLARATIONS OF CONFLICTS OF INTEREST Paul Harrison is a consultant for Sysmex UK and has received a research grant from Siemens Diagnostics and Eli Lilly. Carol Briggs has received an unrestricted educational grant from Sysmex Europe and is a consultant to Beckman Coulter. The authors would also like to thank Dr. Elizabeth Chalmers, Professor Steve Watson, Dr. Ban Dawood, the ISTH platelet physiology SSC and the CLSI subcommittee on platelet function testing for helpful discussions and suggestions. Paul Harrison, Ian Mackie, Andrew Mumford, Carol Briggs, Ri Liesner, Mark Winter & Sam Machin all contributed to the design, writing and editing of this guideline. The BCSH Haemostasis and Thrombosis Task Force at the time of publication of this guideline consists of: David Keeling (Chair), Henry Watson (Secretary), Mike Laffan, Andrew Mumford, Ian Jennings, Isobel Walker, Elaine Gray, Campbell Tait, Mike Makris 34
35 REFERENCES Acharya,S., Barraclough,J., Ibrahim,M.S., Oxby,C., Jones,S.E., Parapia,L., & O'donovan,P. (2008) The usefulness of the platelet function analyser (PFA-100) in screening for underlying bleeding disorders in women with menorrhagia. J Obstet.Gynaecol., 28, Althaus,K. & Greinacher,A. (2009) MYH9-related platelet disorders. Semin.Thromb.Hemost., 35, Bolton-Maggs,P.H., Chalmers,E.A., Collins,P.W., Harrison,P., Kitchen,S., Liesner,R.J., Minford,A., Mumford,A.D., Parapia,L.A., Perry,D.J., Watson,S.P., Wilde,J.T., & Williams,M.D. (2006) A review of inherited platelet disorders with guidelines for their management on behalf of the UKHCDO. Br.J Haematol., 135, Bolton-Maggs,P.H., Perry,D.J., Chalmers,E.A., Parapia,L.A., Wilde,J.T., Williams,M.D., Collins,P.W., Kitchen,S., Dolan,G., & Mumford,A.D. (2004) The rare coagulation disorders-- review with guidelines for management from the United Kingdom Haemophilia Centre Doctors' Organisation. Haemophilia., 10, Bonduel, M., Frontroth, J.P., Hepner, M., Sciuccati, G., Feliu-Torres, A. (2007) Platelet aggregation and adenosine triphosphate release values in children and adults. J.Thromb.Haemost Briggs,C., Harrison,P., & Machin,S.J. (2007) Platelet Counting. Platelets (ed. by A. D. Michelson), pp Academic Press, San Diego. Cardinal,D.C. & Flower,R.J. (1980) The electronic aggregometer: a novel device for assessing platelet behavior in blood. J.Pharmacol.Methods, 3, Cattaneo, M et al (2011) ISTH platelet physiology SSC guidelines on LTA. Manuscript in Preparation Cattaneo,M. (2009) Light transmission aggregometry and ATP release for the diagnostic assessment of platelet function. Semin.Thromb.Hemost., 35, Cattaneo,M. (2003) Inherited platelet-based bleeding disorders. J.Thromb.Haemost., 1, Cattaneo,M. (2004) Are the bleeding time and PFA-100 useful in the initial screening of patients with mucocutaneous bleedings of hereditary nature? J.Thromb.Haemost., 2, Cattaneo,M., Federici,A.B., Lecchi,A., Agati,B., Lombardi,R., Stabile,F., & Bucciarelli,P. (1999) Evaluation of the PFA-100 system in the diagnosis and therapeutic monitoring of patients with von Willebrand disease. Thromb.Haemost., 82, Cattaneo,M., Hayward,C.P., Moffat,K.A., Pugliano,M.T., Liu,Y., & Michelson,A.D. (2009) Results of a worldwide survey on the assessment of platelet function by light transmission aggregometry: a report from the platelet physiology subcommittee of the SSC of the ISTH. J Thromb.Haemost., 7,
36 Cattaneo,M., Lecchi,A., Zighetti,M.L., & Lussana,F. (2007) Platelet aggregation studies: autologous platelet-poor plasma inhibits platelet aggregation when added to platelet-rich plasma to normalize platelet count. Haematologica, 92, Chanarin, I. (1989) Platelet Function Tests. In : Laboratory Haematology. Churchill Livingstone, Edinburgh, Christie,D.J., Avari,T., Carrington,LR., Cohen,E., DeBiase,B., Harrison,P., Kickler,T., Kottke-Marchant,K., Ledford-Kraemer,M.R., Rand,M.L., Schmaier,A.H., & McCabe White,M. (2008) Platelet Function Testing by Aggregometry: Approved Guideline. Wayne PA: Clinical and Laboratory Standards Institute, 28, Clauser,S. & Cramer-Borde,E. (2009) Role of platelet electron microscopy in the diagnosis of platelet disorders. Semin.Thromb.Hemost., 35, Daly,M.E., Dawood,B.B., Lester,W.A., Peake,I.R., Rodeghiero,F., Goodeve,A.C., Makris,M., Wilde,J.T., Mumford,A.D., Watson,S.P., & Mundell,S.J. (2009) Identification and characterization of a novel P2Y 12 variant in a patient diagnosed with type 1 von Willebrand disease in the European MCMDM-1VWD study. Blood, 113, Dawood,B.B., Wilde,J., & Watson,S.P. (2007) Reference curves for aggregation and ATP secretion to aid diagnose of platelet-based bleeding disorders: effect of inhibition of ADP and thromboxane A(2) pathways. Platelets., 18, Duke,W.W. The relation of blood platelets to hemorrhagic disease. Description of a method for determining the bleeding time and the coagulation time and report of three cases of hemorrahagic disease relieved by blood transfusion. JAMA 55, Favaloro,E.J. (2006) The utility of the PFA-100 in the identification of von Willebrand disease: a concise review. Semin.Thromb.Hemost., 32, Favaloro,E.J. (2008) Clinical utility of the PFA-100. Semin.Thromb.Hemost., 34, Favaloro,E.J. (2009) Internal quality control and external quality assurance of platelet function tests. Semin.Thromb.Hemost., 35, Favaloro,E.J., Kershaw,G., Bukuya,M., Hertzberg,M., & Koutts,J. (2001) Laboratory diagnosis of von Willebrand disorder (vwd) and monitoring of DDAVP therapy: efficacy of the PFA-100 and vwf:cba as combined diagnostic strategies. Haemophilia., 7, Favaloro,E.J., Lippi,G., & Adcock,D.M. (2008) Preanalytical and postanalytical variables: the leading causes of diagnostic error in hemostasis? Semin.Thromb.Hemost., 34, Franchini,M. (2005) The platelet function analyzer (PFA-100): an update on its clinical use. Clin.Lab, 51, Franchini,M., Gandini,G., Manzato,F., & Lippi,G. (2002) Evaluation of the PFA-100 system for monitoring desmopressin therapy in patients with type 1 von Willebrand's disease. Haematologica, 87, 670. Fritsma,G.A. (2007) Platelet function testing: aggregometry and lumiaggregometry. Clin.Lab Sci., 20,
37 George,J.N. & Shattil,S.J. (1991) The clinical importance of acquired abnormalities of platelet function. N.Engl.J Med, 324, Goodall,A.H. & Appleby,J. (2004) Flow-cytometric analysis of platelet-membrane glycoprotein expression and platelet activation. Methods Mol.Biol., 272, Gordon,N., Thom,J., Cole,C., & Baker,R. (1995) Rapid detection of hereditary and acquired platelet storage pool deficiency by flow cytometry. Br.J.Haematol., 89, Greaves, M., & Preston, F.E. (1985) The laboratory investigation of acquired and platelet disorders. In Thomson J.M. (ed) Blood Coagulation and Haemostasis: A Practical Guide. Churchill Livingstone, Edinburgh, Harrison,P. (2005) The role of PFA-100 testing in the investigation and management of haemostatic defects in children and adults. Br.J.Haematol., 130, Harrison,P. (2004) In vitro measurement of high-shear platelet adhesion and aggregation by the PFA-100. Methods Mol.Biol., 272, Harrison,P., Frelinger,A.L., III, Furman,M.I., & Michelson,A.D. (2007) Measuring antiplatelet drug effects in the laboratory. Thromb.Res., 120, Harrison,P., Horton,A., Grant,D., Briggs,C., & Machin,S. (2000) Immunoplatelet counting: a proposed new reference procedure. Br.J Haematol., 108, Harrison,P. & Mumford,A. (2009) Screening tests of platelet function: update on their appropriate uses for diagnostic testing. Semin.Thromb.Hemost., 35, Harrison,P., Robinson,M., Liesner,R., Khair,K., Cohen,H., Mackie,I., & Machin,S. (2002) The PFA-100: a potential rapid screening tool for the assessment of platelet dysfunction. Clin.Lab Haematol., 24, Harrison,P., Robinson,M.S., Mackie,I.J., Joseph,J., McDonald,S.J., Liesner,R., Savidge,G.F., Pasi,J., & Machin,S.J. (1999) Performance of the platelet function analyser PFA-100 in testing abnormalities of primary haemostasis. Blood Coagul.Fibrinolysis, 10, Harrison,P., Segal,H., Furtado,C., Verjee,S., Sukhu,K., & Murphy,M.F. (2004) High incidence of defective high-shear platelet function among platelet donors. Transfusion, 44, Hayward,C.P. (2008) Diagnostic approach to platelet function disorders. Transfus.Apher.Sci., 38, Hayward,C.P. & Eikelboom,J. (2007) Platelet function testing: quality assurance. Semin.Thromb.Hemost., 33, Hayward,C.P. & Favaloro,E.J. (2009) Diagnostic evaluation of platelet disorders: the past, the present, and the future. Semin.Thromb.Hemost., 35,
38 Hayward,C.P., Harrison,P., Cattaneo,M., Ortel,T.L., & Rao,A.K. Platelet function analyser (PFA-100) closure time in the evaluation of platelet disorders and platelet function. Journal of Thrombosis and Haemostasis 4, Hayward,C.P., Moffat,K.A., Pai,M., Liu,Y., Seecharan,J., McKay,H., Webert,K.E., Cook,R.J., & Heddle,N.M. (2008) An evaluation of methods for determining reference intervals for light transmission platelet aggregation tests on samples with normal or reduced platelet counts. Thromb.Haemost., 100, Hayward,C.P., Moffat,K.A., Spitzer,E., Timleck,M., Plumhoff,E., Israels,S.J., & White,J. (2009a) Results of an external proficiency testing exercise on platelet dense-granule deficiency testing by whole mount electron microscopy. Am.J Clin.Pathol., 131, Hayward,C.P., Pai,M., Liu,Y., Moffat,K.A., Seecharan,J., Webert,K.E., Cook,R.J., & Heddle,N.M. (2009b) Diagnostic utility of light transmission platelet aggregometry: results from a prospective study of individuals referred for bleeding disorder assessments. J Thromb.Haemost. 7, Hayward CP, Moffat KA, Raby A, Israels S, Plumhoff E, Flynn G & Zehnder (2010) Development of North American Consensus Guidelines for Medical Laboratories that Perform and Interpret Platelet Function Testing Using Light Transmission Aggregometry. Am J Clin Path, 134, Heilmann,E.J., Kundu,S.K., Sio,R., Garcia,C., Gomez,R., & Christie,D.J. (1997) Comparison of four commercial citrate blood collection systems for platelet function analysis by the PFA- 100 system. Thromb.Res., 87, Ingerman-Wojenski,C., Smith,J.B., & Silver,M.J. (1983) Evaluation of electrical aggregometry: comparison with optical aggregometry, secretion of ATP, and accumulation of radiolabeled platelets. J Lab Clin.Med, 101, Israels,S.J., McNicol,A., Robertson,C., & Gerrard,J.M. (1990) Platelet storage pool deficiency: diagnosis in patients with prolonged bleeding times and normal platelet aggregation. Br.J.Haematol., 75, Israels, S.J., Kahr, W.H.A, Blanchette, V.S., Luban, N.L.C., Rivard, G.E., & Rand, M.L. (2011) Platelet disorders in children : A diagnostic approach. Pediatr. Blood Cancer, 56, James,A.H., Lukes,A.S., Brancazio,L.R., Thames,E., & Ortel,T.L. (2004) Use of a new platelet function analyzer to detect von Willebrand disease in women with menorrhagia. Am.J.Obstet.Gynecol., 191, Jennings,I., Woods,T.A., Kitchen,S., & Walker,I.D. (2008) Platelet function testing: practice among UK National External Quality Assessment Scheme for Blood Coagulation participants, J Clin.Pathol., 61, Jilma,B. (2001) Platelet function analyzer (PFA-100): a tool to quantify congenital or acquired platelet dysfunction. J.Lab Clin.Med., 138, Kahr,W.H., Zheng,S., Sheth,P.M., Pai,M., Cowie,A., Bouchard,M., Podor,T.J., Rivard,G.E., & Hayward,C.P. (2001) Platelets from patients with the Quebec platelet disorder contain 38
39 and secrete abnormal amounts of urokinase-type plasminogen activator. Blood, 98, Karger,R., Donner-Banzhoff,N., Muller,H.H., Kretschmer,V., & Hunink,M. (2007) Diagnostic performance of the platelet function analyzer (PFA-100) for the detection of disorders of primary haemostasis in patients with a bleeding history-a systematic review and metaanalysis. Platelets., 18, Kerenyi,A., Schlammadinger,A., Ajzner,E., Szegedi,I., Kiss,C., Pap,Z., Boda,Z., & Muszbek,L. (1999) Comparison of PFA-100 closure time and template bleeding time of patients with inherited disorders causing defective platelet function. Thromb.Res., 96, Knofler, R., Weissbach, G., Kuhlisch, E. (1998) Platelet function tests in childhood. Measuring aggregation and release reaction in whole blood. Semin Thromb Hemost Kratzer,M.A. & Born,G.V. (1985) Simulation of primary haemostasis in vitro. Haemostasis, 15, Kundu,S.K., Heilmann,E.J., Sio,R., Garcia,C., Davidson,R.M., & Ostgaard,R.A. (1995) Description of an in vitro platelet function analyzer--pfa-100. Semin.Thromb.Hemost., 21 Suppl 2, Laffan,M., Brown,S.A., Collins,P.W., Cumming,A.M., Hill,F.G., Keeling,D., Peake,I.R., & Pasi,K.J. (2004) The diagnosis of von Willebrand disease: a guideline from the UK Haemophilia Centre Doctors' Organization. Haemophilia., 10, Linnemann,B., Schwonberg,J., Mani,H., Prochnow,S., & Lindhoff-Last,E. (2008) Standardization of light transmittance aggregometry for monitoring antiplatelet therapy: an adjustment for platelet count is not necessary. J Thromb.Haemost. Lippi,G., Franchini,M., Brocco,G., & Manzato,F. (2001) Influence of the ABO blood type on the platelet function analyzer PFA-100. Thromb.Haemost., 85, Ludlam, C.A., Pasi, K.J., Bolton-Maggs, P., Collins, P.W., Cumming, A.M., Dolan, G., Fryer, A., Harrington, C., Hill, F.G., Peake, I.R., Perry, D.J., Skirton, H., & Smith, M. (2005) UK Haemophilia Centre Doctors' Organisation. A framework for genetic service provision for haemophilia and other inherited bleeding disorders. Haemophilia. 2, Mackie,I.J., Jones,R., & Machin,S.J. (1984) Platelet impedance aggregation in whole blood and its inhibition by antiplatelet drugs. J Clin.Pathol., 37, Mammen,E.F., Comp,P.C., Gosselin,R., Greenberg,C., Hoots,W.K., Kessler,C.M., Larkin,E.C., Liles,D., & Nugent,D.J. (1998) PFA-100 system: a new method for assessment of platelet dysfunction. Semin.Thromb.Hemost., 24, Michelson,A.D., Linden,M., Barnard,M.R., Furman,M.I., & Frelinger,A.L. (2007) Flow Cytometry. Platelets (ed. by A. D. Michelson), pp Academic Press. Moeller,A., Weippert-Kretschmer,M., Prinz,H., & Kretschmer,V. (2001) Influence of ABO blood groups on primary hemostasis. Transfusion, 41,
40 Moffat,K.A., Ledford-Kraemer,M.R., Nichols,W.L., & Hayward,C.P. (2005) Variability in clinical laboratory practice in testing for disorders of platelet function: results of two surveys of the North American Specialized Coagulation Laboratory Association. Thromb.Haemost., 93, Nieuwenhuis,H.K., Akkerman,J.W., & Sixma,J.J. (1987) Patients with a prolonged bleeding time and normal aggregation tests may have storage pool deficiency: studies on one hundred six patients. Blood, 70, Nurden,A.T., Fiore,M., Pillois,X., & Nurden,P. (2009) Genetic testing in the diagnostic evaluation of inherited platelet disorders. Semin.Thromb.Hemost., 35, Pai,M. & Hayward,C.P. (2009) Diagnostic assessment of platelet disorders: what are the challenges to standardization? Semin.Thromb.Hemost., 35, Perry,D.J., Fitzmaurice, D.A., Kitchen, S., Mackie, I.J., & Mallet, S. (2010) Point of care testing in Haemostasis. Br.J.Haematol, 150 (5) Peterson,P., Hayes,T.E., Arkin,C.F., Bovill,E.G., Fairweather,R.B., Rock,W.A., Jr., Triplett,D.A., & Brandt,J.T. (1998) The preoperative bleeding time test lacks clinical benefit: College of American Pathologists' and American Society of Clinical Pathologists' position article. Arch.Surg., 133, Philipp,C.S., Miller,C.H., Faiz,A., Dilley,A., Michaels,L.A., Ayers,C., Bachmann,G., Dowling,N., & Saidi,P. (2005) Screening women with menorrhagia for underlying bleeding disorders: the utility of the platelet function analyser and bleeding time. Haemophilia., 11, Podda,G.M., Bucciarelli,P., Lussana,F., Lecchi,A., & Cattaneo,M. (2007) Usefulness of PFA-100 testing in the diagnostic screening of patients with suspected abnormalities of hemostasis: comparison with the bleeding time. J Thromb.Haemost., 5, Posan,E., McBane,R.D., Grill,D.E., Motsko,C.L., & Nichols,W.L. (2003) Comparison of PFA- 100 testing and bleeding time for detecting platelet hypofunction and von Willebrand disease in clinical practice. Thromb.Haemost., 90, Quiroga,T., Goycoolea,M., Munoz,B., Morales,M., Aranda,E., Panes,O., Pereira,J., & Mezzano,D. (2004) Template bleeding time and PFA-100 have low sensitivity to screen patients with hereditary mucocutaneous hemorrhages: comparative study in 148 patients. J.Thromb.Haemost., 2, Quiroga,T., Goycoolea,M., Panes,O., Aranda,E., Martinez,C., Belmont,S., Munoz,B., Zuniga,P., Pereira,J., & Mezzano,D. (2007) High prevalence of bleeders of unknown cause among patients with inherited mucocutaneous bleeding. A prospective study of 280 patients and 299 controls. Haematologica, 92, Rodgers,R.P. & Levin,J. (1990) A critical reappraisal of the bleeding time. Semin.Thromb.Hemost., 16, Schmitz,G., Rothe,G., Ruf,A., Barlage,S., Tschope,D., Clemetson,K.J., Goodall,A.H., Michelson,A.D., Nurden,A.T., & Shankey,T.V. (1998) European Working Group on Clinical 40
41 Cell Analysis: Consensus protocol for the flow cytometric characterisation of platelet function. Thromb.Haemost., 79, Summerfield, G.P., Keenan, J.P., Brodie, N.J., & Bellingham, A.J. (1981) Bioluminescent assay of adenine nucleotides: rapid analysis of ATP and ADP in red cells and platelets using the LKB luminometer. Clin Lab Haem., 3, Swart,S.S., Pearson,D., Wood,J.K., & Barnett,D.B. (1984) Effects of adrenaline and alpha adrenergic antagonists on platelet aggregation in whole blood: evaluation of electrical impedance aggregometry. Thromb.Res., 36, Sweeney,J.D., Hoernig,L.A., Michnik,A., & Fitzpatrick,J.E. (1989) Whole blood aggregometry. Influence of sample collection and delay in study performance on test results. Am.J Clin.Pathol., 92, The British Society for Haematology BCSH Haemostasis and Thrombosis Task Force (1988) Guidelines on platelet function testing. J.Clin.Pathol., 41, Toth, O., Calatzis, A., Losonczy, H., Siess, W. (2006) Multiple electrode aggregometry: a new device to measure platelet aggregation in whole blood. Thromb. Haemost., 96, van Vliet,H.H., Kappers-Klunne,M.C., Leebeek,F.W., & Michiels,J.J. (2008) PFA-100 monitoring of von Willebrand factor (VWF) responses to desmopressin (DDAVP) and factor VIII/VWF concentrate substitution in von Willebrand disease type 1 and 2. Thromb.Haemost., 100, Wall,J.E., Buijs-Wilts,M., Arnold,J.T., Wang,W., White,M.M., Jennings,L.K., & Jackson,C.W. (1995) A flow cytometric assay using mepacrine for study of uptake and release of platelet dense granule contents. Br.J.Haematol., 89, Watson S., Daly M., Dawood B., Gissen P., Makris M., Mundell S., Wilde J., & Mumford A. (2010) Phenotypic approaches to gene mapping in platelet function disorrders. Hamostaseologie., 30, Zeidan,A.M., Kouides,P.A., Tara,M.A., & Fricke,W.A. (2007) Platelet function testing: state of the art. Expert.Rev.Cardiovasc.Ther., 5, Zhou,L. & Schmaier,A.H. (2005) Platelet aggregation testing in platelet-rich plasma: description of procedures with the aim to develop standards in the field. Am.J.Clin.Pathol., 123,
Screening Tests of Platelet Function: Update on their appropriate uses for diagnostic testing
 Screening Tests of Platelet Function: Update on their appropriate uses for diagnostic testing Paul Harrison Oxford Haemophilia & Thrombosis Centre Churchill Hospital Oxford, UK 10 th February 2011 Namur
Screening Tests of Platelet Function: Update on their appropriate uses for diagnostic testing Paul Harrison Oxford Haemophilia & Thrombosis Centre Churchill Hospital Oxford, UK 10 th February 2011 Namur
Bleeding disorders or haemorrhagic diatheses are a group of disorders characterised by defective haemostasis with abnormal bleeding.
 Bleeding disorders or haemorrhagic diatheses are a group of disorders characterised by defective haemostasis with abnormal bleeding. Bleeding may be spontaneous in the form of small haemorrhages into the
Bleeding disorders or haemorrhagic diatheses are a group of disorders characterised by defective haemostasis with abnormal bleeding. Bleeding may be spontaneous in the form of small haemorrhages into the
Platelet Transmission Electron Microscopy and Flow Cytometry 11/15/2015
 Welcome to Mayo Medical Laboratories Hot Topics. These presentations provide short discussion of current topics and may be helpful to you in your practice. Today our topic looks at hereditary platelet
Welcome to Mayo Medical Laboratories Hot Topics. These presentations provide short discussion of current topics and may be helpful to you in your practice. Today our topic looks at hereditary platelet
Platelet Function analysis using Multiple Electrode Aggregometry (Multiplate )
 Platelet Function analysis using Multiple Electrode Aggregometry (Multiplate ) Multiplate platelet function analysis in whole blood based on impedance aggregometry Multiplate instrument 5 channels for
Platelet Function analysis using Multiple Electrode Aggregometry (Multiplate ) Multiplate platelet function analysis in whole blood based on impedance aggregometry Multiplate instrument 5 channels for
510(k) SUBSTANTIAL EQUIVALENCE DETERMINATION DECISION SUMMARY
 510(k) SUBSTANTIAL EQUIVALENCE DETERMINATION DECISION SUMMARY A. 510(k) Number: k103555 B. Purpose for Submission: New submission C. Measurand: Platelet aggregation D. Type of Test: Platelet aggregometer
510(k) SUBSTANTIAL EQUIVALENCE DETERMINATION DECISION SUMMARY A. 510(k) Number: k103555 B. Purpose for Submission: New submission C. Measurand: Platelet aggregation D. Type of Test: Platelet aggregometer
Multiplate platelet function analysis - application and interpretation
 Dr. Andreas Calatzis PD Dr. Michael Spannagl Department for Haemostasis and Transfusion Medicine Munich University Clinic Ludwig-Maximilians University Ziemssen Str. 1 80336 Munich, Germany [email protected]
Dr. Andreas Calatzis PD Dr. Michael Spannagl Department for Haemostasis and Transfusion Medicine Munich University Clinic Ludwig-Maximilians University Ziemssen Str. 1 80336 Munich, Germany [email protected]
Platelet Aggregation Testing in Platelet-Rich Plasma Description of Procedures With the Aim to Develop Standards in the Field
 Coagulation and Transfusion Medicine / PLATELET FUNCTION TESTING Platelet Aggregation Testing in Platelet-Rich Plasma Description of Procedures With the Aim to Develop Standards in the Field Lan Zhou,
Coagulation and Transfusion Medicine / PLATELET FUNCTION TESTING Platelet Aggregation Testing in Platelet-Rich Plasma Description of Procedures With the Aim to Develop Standards in the Field Lan Zhou,
510(k) SUBSTANTIAL EQUIVALENCE DETERMINATION DECISION SUMMARY DEVICE AND INSTRUMENT TEMPLATE
 510(k) SUBSTANTIAL EQUIVALENCE DETERMINATION DECISION SUMMARY DEVICE AND INSTRUMENT TEMPLATE A. 510(k) Number: K041502 B. Purpose for Submission: To change the name of a previously cleared analyzer, and
510(k) SUBSTANTIAL EQUIVALENCE DETERMINATION DECISION SUMMARY DEVICE AND INSTRUMENT TEMPLATE A. 510(k) Number: K041502 B. Purpose for Submission: To change the name of a previously cleared analyzer, and
Note: Page numbers in italics indicate figures. Page numbers followed by a t indicate tables.
 INDEX Note: Page numbers in italics indicate figures. Page numbers followed by a t indicate tables. Acquired bleeding disorders, 37-57 acquired combined inhibitor to factor V and thrombin, 55 acquired
INDEX Note: Page numbers in italics indicate figures. Page numbers followed by a t indicate tables. Acquired bleeding disorders, 37-57 acquired combined inhibitor to factor V and thrombin, 55 acquired
University of Utah CME Statement
 University of Utah CME Statement The University of Utah School of Medicine adheres to ACCME Standards regarding industry support of continuing medical education. Speakers are also expected to openly disclose
University of Utah CME Statement The University of Utah School of Medicine adheres to ACCME Standards regarding industry support of continuing medical education. Speakers are also expected to openly disclose
Platelet storage pool disease case discussions. Tzu-Fei Wang The Hemostasis and Thrombosis Center The Ohio State University
 Platelet storage pool disease case discussions Tzu-Fei Wang The Hemostasis and Thrombosis Center The Ohio State University Case I 29 yo WF presented for evaluation of possible platelet storage pool disease,
Platelet storage pool disease case discussions Tzu-Fei Wang The Hemostasis and Thrombosis Center The Ohio State University Case I 29 yo WF presented for evaluation of possible platelet storage pool disease,
INR = (patient PT/mean normal PT) ISI.
 The Relationship of the International Normalized Ratio () to the Prothrombin Time (PT) By: William DePond MD, President and Chief Medical Officer MEDLAB In 1983, it was determined that patients receiving
The Relationship of the International Normalized Ratio () to the Prothrombin Time (PT) By: William DePond MD, President and Chief Medical Officer MEDLAB In 1983, it was determined that patients receiving
Contents. Abstract... i. Committee Membership... iii. Foreword... vii. 1 Scope... 1. 2 Introduction... 1. 3 Standard Precautions...
 Vol. 28 No. 20 Replaces H47-A Vol. 16 No. 3 One-Stage Prothrombin Time (PT) Test and Activated Partial Thromboplastin Time (APTT) Test; Approved Guideline Second Edition This document provides guidelines
Vol. 28 No. 20 Replaces H47-A Vol. 16 No. 3 One-Stage Prothrombin Time (PT) Test and Activated Partial Thromboplastin Time (APTT) Test; Approved Guideline Second Edition This document provides guidelines
Clinical Guideline N/A. November 2013
 State if the document is a Trust Policy/Procedure or a Clinical Guideline Clinical Guideline Document Title: Document Number 352 Version Number 1 Name and date and version number of previous document (if
State if the document is a Trust Policy/Procedure or a Clinical Guideline Clinical Guideline Document Title: Document Number 352 Version Number 1 Name and date and version number of previous document (if
Collection Guidelines for Routine & Special Coagulation Testing
 Revised May 2010 Collection Guidelines for Routine & Special Coagulation Testing Best samples come from peripheral stick with evacuated tube system 19 to 22 gauge needle (smaller or bigger could cause
Revised May 2010 Collection Guidelines for Routine & Special Coagulation Testing Best samples come from peripheral stick with evacuated tube system 19 to 22 gauge needle (smaller or bigger could cause
Abnormal Basic Coagulation Testing Laboratory Testing Algorithms
 Global Coagulation Testing Abnormal Basic Coagulation Testing Laboratory Testing Algorithms Jeffrey S. Jhang, M.D. No single global laboratory test Bleeding history is the strongest predictor of bleeding
Global Coagulation Testing Abnormal Basic Coagulation Testing Laboratory Testing Algorithms Jeffrey S. Jhang, M.D. No single global laboratory test Bleeding history is the strongest predictor of bleeding
Platelet Review July 2012. Thomas S. Kickler M.D. Johns Hopkins University School of Medicine
 Platelet Review July 2012 Thomas S. Kickler M.D. Johns Hopkins University School of Medicine Hemostasis Hemostasis is the process that leads to the stopping of bleeding Hemostasis involves blood vessels,
Platelet Review July 2012 Thomas S. Kickler M.D. Johns Hopkins University School of Medicine Hemostasis Hemostasis is the process that leads to the stopping of bleeding Hemostasis involves blood vessels,
Use of Antithrombotic Agents In The Presence Of Neuraxial Anesthesia
 Use of Antithrombotic Agents In The Presence Of Neuraxial Anesthesia Insertion, removal or presence of a catheter in selected sites can place a patient who is antithrombotic agent at risk for a local bleeding
Use of Antithrombotic Agents In The Presence Of Neuraxial Anesthesia Insertion, removal or presence of a catheter in selected sites can place a patient who is antithrombotic agent at risk for a local bleeding
ADP/ATP Ratio Assay Kit (Bioluminescent)
 ab65313 ADP/ATP Ratio Assay Kit (Bioluminescent) Instructions for Use For the rapid, sensitive and accurate measurement of the ratio of ADP/ATP in various samples. This product is for research use only
ab65313 ADP/ATP Ratio Assay Kit (Bioluminescent) Instructions for Use For the rapid, sensitive and accurate measurement of the ratio of ADP/ATP in various samples. This product is for research use only
Mouse Creatine Kinase MB isoenzyme (CKMB) ELISA
 KAMIYA BIOMEDICAL COMPANY Mouse Creatine Kinase MB isoenzyme (CKMB) ELISA For the quantitative determination of mouse CKMB in serum, plasma, cell culture fluid and other biological fluids Cat. No. KT-57681
KAMIYA BIOMEDICAL COMPANY Mouse Creatine Kinase MB isoenzyme (CKMB) ELISA For the quantitative determination of mouse CKMB in serum, plasma, cell culture fluid and other biological fluids Cat. No. KT-57681
INTRODUCTION Thrombophilia deep vein thrombosis DVT pulmonary embolism PE inherited thrombophilia
 INTRODUCTION Thrombophilia (Hypercoagulability) is a condition in which a person forms blood clots more than normal. Blood clots may occur in the arms or legs (e.g., deep vein thrombosis DVT), the lungs
INTRODUCTION Thrombophilia (Hypercoagulability) is a condition in which a person forms blood clots more than normal. Blood clots may occur in the arms or legs (e.g., deep vein thrombosis DVT), the lungs
Blood Plasma Sample Collection and Handling for Proteomics Analysis - A guide to obtain optimal plasma samples -
 Blood Plasma Sample Collection and Handling for Proteomics Analysis - A guide to obtain optimal plasma samples - 1 Introduction Blood can be regarded as a complex liquid tissue that comprises cells and
Blood Plasma Sample Collection and Handling for Proteomics Analysis - A guide to obtain optimal plasma samples - 1 Introduction Blood can be regarded as a complex liquid tissue that comprises cells and
Thrombophilia. Steven R. Lentz, M.D. Ph.D. Carver College of Medicine The University of Iowa May 2003
 Thrombophilia Steven R. Lentz, M.D. Ph.D. Carver College of Medicine The University of Iowa May 2003 Thrombophilia Hereditary and acquired risk factors for thrombosis Venous thromboembolism Arterial thromboembolism
Thrombophilia Steven R. Lentz, M.D. Ph.D. Carver College of Medicine The University of Iowa May 2003 Thrombophilia Hereditary and acquired risk factors for thrombosis Venous thromboembolism Arterial thromboembolism
Analytical Specifications RIVAROXABAN
 Page 1 of 9 ANALYTE NAME AND STRUCTURE - RIVAROXABAN SYNONYMS Xarelto CATEGORY Anticoagulant TEST CODE PURPOSE Therapeutic Drug Monitoring GENERAL RELEVANCY BACKGROUND Xarelto (rivaroxaban) is an orally
Page 1 of 9 ANALYTE NAME AND STRUCTURE - RIVAROXABAN SYNONYMS Xarelto CATEGORY Anticoagulant TEST CODE PURPOSE Therapeutic Drug Monitoring GENERAL RELEVANCY BACKGROUND Xarelto (rivaroxaban) is an orally
Learning Objectives. Qualitative and Quantitative Platelet Disorders. Platelet Signaling. Platelet vs. Coagulation Bleeding.
 Learning Objectives Qualitative and Quantitative Platelet isorders Jeffrey S. Jhang, M.. Assistant Professor of Clinical Pathology College of Physicians and Surgeons New York, New York Understand the evaluation
Learning Objectives Qualitative and Quantitative Platelet isorders Jeffrey S. Jhang, M.. Assistant Professor of Clinical Pathology College of Physicians and Surgeons New York, New York Understand the evaluation
Application Guide... 2
 Protocol for GenomePlex Whole Genome Amplification from Formalin-Fixed Parrafin-Embedded (FFPE) tissue Application Guide... 2 I. Description... 2 II. Product Components... 2 III. Materials to be Supplied
Protocol for GenomePlex Whole Genome Amplification from Formalin-Fixed Parrafin-Embedded (FFPE) tissue Application Guide... 2 I. Description... 2 II. Product Components... 2 III. Materials to be Supplied
INTRODUCTION Thrombophilia deep vein thrombosis DVT pulmonary embolism PE inherited thrombophilia
 INTRODUCTION Thrombophilia (Hypercoagulability) is a condition in which a person forms blood clots more than normal. Blood clots may occur in the arms or legs (e.g., deep vein thrombosis DVT), the lungs
INTRODUCTION Thrombophilia (Hypercoagulability) is a condition in which a person forms blood clots more than normal. Blood clots may occur in the arms or legs (e.g., deep vein thrombosis DVT), the lungs
Canine creatine kinase MB isoenzyme (CK-MB)ELISA Kit
 Canine creatine kinase MB isoenzyme (CK-MB)ELISA Kit Catalog No. CSB-E15852c (96T) This immunoassay kit allows for the in vitro quantitative determination of canine CK-MB concentrations in serum and plasma.
Canine creatine kinase MB isoenzyme (CK-MB)ELISA Kit Catalog No. CSB-E15852c (96T) This immunoassay kit allows for the in vitro quantitative determination of canine CK-MB concentrations in serum and plasma.
Creatine Kinase (CK) Enzymatic Assay Kit Manual Catalog #: 3460-07
 Creatine Kinase (CK) Enzymatic Assay Kit Manual Catalog #: 3460-07 TABLE OF CONTENTS GENERAL INFORMATION... 2 Product Description... 2 Procedure Overview... 2 Kit Contents, Storage and Shelf Life... 3
Creatine Kinase (CK) Enzymatic Assay Kit Manual Catalog #: 3460-07 TABLE OF CONTENTS GENERAL INFORMATION... 2 Product Description... 2 Procedure Overview... 2 Kit Contents, Storage and Shelf Life... 3
QuantiFERON TB Gold In Tube Method (QGIT Test) Manufacturer: Cellestis Inc. (USA) a QIAGEN Company
 QuantiFERON TB Gold In Tube Method (QGIT Test) Manufacturer: Cellestis Inc. (USA) a QIAGEN Company P1078 TB APPRISE TB Ante vs. Postpartum Prevention with INH in HIV Seropositive mothers and their Exposed
QuantiFERON TB Gold In Tube Method (QGIT Test) Manufacturer: Cellestis Inc. (USA) a QIAGEN Company P1078 TB APPRISE TB Ante vs. Postpartum Prevention with INH in HIV Seropositive mothers and their Exposed
RealStar HBV PCR Kit 1.0 11/2012
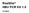 RealStar HBV PCR Kit 1.0 11/2012 RealStar HBV PCR Kit 1.0 For research use only! (RUO) Product No.: 201003 96 rxns INS-201000-GB-02 Store at -25 C... -15 C November 2012 altona Diagnostics GmbH Mörkenstraße
RealStar HBV PCR Kit 1.0 11/2012 RealStar HBV PCR Kit 1.0 For research use only! (RUO) Product No.: 201003 96 rxns INS-201000-GB-02 Store at -25 C... -15 C November 2012 altona Diagnostics GmbH Mörkenstraße
Instructions. Torpedo sirna. Material. Important Guidelines. Specifications. Quality Control
 is a is a state of the art transfection reagent, specifically designed for the transfer of sirna and mirna into a variety of eukaryotic cell types. is a state of the art transfection reagent, specifically
is a is a state of the art transfection reagent, specifically designed for the transfer of sirna and mirna into a variety of eukaryotic cell types. is a state of the art transfection reagent, specifically
HANDBOOK OF DIAGNOSTIC HEMOSTASIS AND THROMBOSIS TESTS
 HANDBOOK OF DIAGNOSTIC HEMOSTASIS AND THROMBOSIS TESTS Offered by University of Washington Department of Laboratory Medicine Reference Laboratory Services Third Edition 2005 UNIVERSITY OF WASHINGTON DEPARTMENT
HANDBOOK OF DIAGNOSTIC HEMOSTASIS AND THROMBOSIS TESTS Offered by University of Washington Department of Laboratory Medicine Reference Laboratory Services Third Edition 2005 UNIVERSITY OF WASHINGTON DEPARTMENT
75515-7 Lupus anticoagulant aptt & drvvt screening panel W Reflex
 75515-7 file:///c:/users/cholck/appdata/local/temp/relma_2_49_user_75515-... Page 1 of 1 75515-7 Lupus anticoagulant aptt & drvvt screening panel W Reflex PANEL HIERARCHY LOINC# LOINC Name R/O/C CardinalityEx.
75515-7 file:///c:/users/cholck/appdata/local/temp/relma_2_49_user_75515-... Page 1 of 1 75515-7 Lupus anticoagulant aptt & drvvt screening panel W Reflex PANEL HIERARCHY LOINC# LOINC Name R/O/C CardinalityEx.
Standard Operating Procedure (SOP) Work Package 8. Sample Collection and Storage
 Standard Operating Procedure (SOP) Work Package 8 Sample Collection and Storage May 2008 SOP WP 8 - Sample collection Table of Contents 1 SAMPLE COLLECTION... 3 1.1 Sample collection -summary... 3 1.2
Standard Operating Procedure (SOP) Work Package 8 Sample Collection and Storage May 2008 SOP WP 8 - Sample collection Table of Contents 1 SAMPLE COLLECTION... 3 1.1 Sample collection -summary... 3 1.2
Human Free Testosterone(F-TESTO) ELISA Kit
 Human Free Testosterone(F-TESTO) ELISA Kit Catalog Number. MBS700040 For the quantitative determination of human free testosterone(f-testo) concentrations in serum, plasma. This package insert must be
Human Free Testosterone(F-TESTO) ELISA Kit Catalog Number. MBS700040 For the quantitative determination of human free testosterone(f-testo) concentrations in serum, plasma. This package insert must be
A Patient s Guide to Primary and Secondary Prevention of Cardiovascular Disease Using Blood-Thinning (Anticoagulant) Drugs
 A Patient s Guide to Primary and Secondary Prevention of PATIENT EDUCATION GUIDE What Is Cardiovascular Disease? Cardiovascular disease (CVD) is a broad term that covers any disease of the heart and circulatory
A Patient s Guide to Primary and Secondary Prevention of PATIENT EDUCATION GUIDE What Is Cardiovascular Disease? Cardiovascular disease (CVD) is a broad term that covers any disease of the heart and circulatory
Rat Creatine Kinase MB isoenzyme,ck-mb ELISA Kit
 Rat Creatine Kinase MB isoenzyme,ck-mb ELISA Kit Catalog No: E0479r 96 Tests Operating instructions www.eiaab.com FOR RESEARCH USE ONLY; NOT FOR THERAPEUTIC OR DIAGNOSTIC APPLICATIONS! PLEASE READ THROUGH
Rat Creatine Kinase MB isoenzyme,ck-mb ELISA Kit Catalog No: E0479r 96 Tests Operating instructions www.eiaab.com FOR RESEARCH USE ONLY; NOT FOR THERAPEUTIC OR DIAGNOSTIC APPLICATIONS! PLEASE READ THROUGH
Creatine Kinase Activity Assay Kit (Colorimetric)
 ab155901 Creatine Kinase Activity Assay Kit (Colorimetric) Instructions for Use For the sensitive and accurate measurement of Creatine Kinase activity in various samples. This product is for research use
ab155901 Creatine Kinase Activity Assay Kit (Colorimetric) Instructions for Use For the sensitive and accurate measurement of Creatine Kinase activity in various samples. This product is for research use
Lupus anticoagulant Pocket card
 Lupus anticoagulant Pocket card Issue number 5 2012 Antiphospholipid Syndrome 1 The antiphospholipid syndrome (APS) is diagnosed in patients with recurrent thromboembolic events and /or pregnancy loss
Lupus anticoagulant Pocket card Issue number 5 2012 Antiphospholipid Syndrome 1 The antiphospholipid syndrome (APS) is diagnosed in patients with recurrent thromboembolic events and /or pregnancy loss
Mouse Insulin ELISA. For the quantitative determination of insulin in mouse serum and plasma
 Mouse Insulin ELISA For the quantitative determination of insulin in mouse serum and plasma Please read carefully due to Critical Changes, e.g., Calculation of Results. For Research Use Only. Not For Use
Mouse Insulin ELISA For the quantitative determination of insulin in mouse serum and plasma Please read carefully due to Critical Changes, e.g., Calculation of Results. For Research Use Only. Not For Use
Instructions for Use
 PN 14438.A.1 2012 09 14 Instructions for Use Technical Support: (US) 1 800 643 1640 (Outside US) +1 858 643 1600 MDSS: +1 858 643 1600 1 INTENDED USE The VerifyNow PRUTest is a whole blood test used in
PN 14438.A.1 2012 09 14 Instructions for Use Technical Support: (US) 1 800 643 1640 (Outside US) +1 858 643 1600 MDSS: +1 858 643 1600 1 INTENDED USE The VerifyNow PRUTest is a whole blood test used in
Hemostasis analyzer system
 Hemostasis analyzer system Providing fast, actionable results to help you reduce risks, complications and costs Get the whole picture with TEG Hemostasis analyzer system For more than forty years, hospitals
Hemostasis analyzer system Providing fast, actionable results to help you reduce risks, complications and costs Get the whole picture with TEG Hemostasis analyzer system For more than forty years, hospitals
Perioperative management of Dual Antiplatelet therapy post drug eluting stent-changing time
 Perioperative management of Dual Antiplatelet therapy post drug eluting stent-changing time Robert Chilton DO, FACOI, FACC, FAHA Professor of Medicine University of Texas Health Science Center Director
Perioperative management of Dual Antiplatelet therapy post drug eluting stent-changing time Robert Chilton DO, FACOI, FACC, FAHA Professor of Medicine University of Texas Health Science Center Director
LABORATORY DIAGNOSIS OF BLEEDING DISORDERS
 LABORATORY DIAGNOSIS OF BLEEDING DISORDERS Secondary Hemostasis CIRCULATORY SYSTEM Low volume, high pressure system Efficient for nutrient delivery to tissues Prone to leakage 2º 2 to endothelial surface
LABORATORY DIAGNOSIS OF BLEEDING DISORDERS Secondary Hemostasis CIRCULATORY SYSTEM Low volume, high pressure system Efficient for nutrient delivery to tissues Prone to leakage 2º 2 to endothelial surface
JOINT COMMISSION INTERNATIONAL ACCREDITATION STANDARDS FOR. 2nd Edition
 JOINT COMMISSION INTERNATIONAL ACCREDITATION STANDARDS FOR CliniCAl laboratories 2nd Edition Effective 1 April 2010 International Patient Safety Goals (IPSG) Goals The following is a list of all goals.
JOINT COMMISSION INTERNATIONAL ACCREDITATION STANDARDS FOR CliniCAl laboratories 2nd Edition Effective 1 April 2010 International Patient Safety Goals (IPSG) Goals The following is a list of all goals.
Point-of-care testing Thrombelastography and platelet transfusion
 Point-of-care testing Thrombelastography and platelet transfusion Gisela Scharbert Department of Anesthesiology, Intensive Care and Pain Management Vienna Medical University, Austria Trauma-induced coagulopathy
Point-of-care testing Thrombelastography and platelet transfusion Gisela Scharbert Department of Anesthesiology, Intensive Care and Pain Management Vienna Medical University, Austria Trauma-induced coagulopathy
The Golden Rule of Specimen Collection: The Patient Test Result is Only as Good as the Sample We Get
 The Golden Rule of Specimen Collection: The Patient Test Result is Only as Good as the Sample We Get Jan Frerichs, MLS (ASCP) The University of Iowa [email protected] Importance of Phlebotomist
The Golden Rule of Specimen Collection: The Patient Test Result is Only as Good as the Sample We Get Jan Frerichs, MLS (ASCP) The University of Iowa [email protected] Importance of Phlebotomist
Evaluation of a Platelet Function Analyser (PFA-100 ) in patients with a bleeding tendency
 Original article Peer reviewed article SWISS MED WKLY 2002;132:443 448 www.smw.ch 443 Evaluation of a Platelet Function Analyser (PFA-100 ) in patients with a bleeding tendency Walter A. Wuillemin a, Katharina
Original article Peer reviewed article SWISS MED WKLY 2002;132:443 448 www.smw.ch 443 Evaluation of a Platelet Function Analyser (PFA-100 ) in patients with a bleeding tendency Walter A. Wuillemin a, Katharina
Whole Blood Flow Cytometry
 Whole Blood Flow Cytometry y Nailin Li Department t of Medicine, i Clinical i l Pharmacology Unit Karolinska Institute/University Hospital, 171 76 Stockholm Department of Pathology & Pathophysiology Zhejiang
Whole Blood Flow Cytometry y Nailin Li Department t of Medicine, i Clinical i l Pharmacology Unit Karolinska Institute/University Hospital, 171 76 Stockholm Department of Pathology & Pathophysiology Zhejiang
ab185915 Protein Sumoylation Assay Ultra Kit
 ab185915 Protein Sumoylation Assay Ultra Kit Instructions for Use For the measuring in vivo protein sumoylation in various samples This product is for research use only and is not intended for diagnostic
ab185915 Protein Sumoylation Assay Ultra Kit Instructions for Use For the measuring in vivo protein sumoylation in various samples This product is for research use only and is not intended for diagnostic
STAINING OF PBF AND INTERPRETATION OF NORMAL AND ABNORMAL RED CELL MORPHOLOGY
 9 STAINING OF PBF AND INTERPRETATION OF NORMAL AND ABNORMAL RED CELL MORPHOLOGY 9.1 INTRODUCTION A peripheral blood smear (peripheral blood film) is a glass microscope slide coated on one side with a thin
9 STAINING OF PBF AND INTERPRETATION OF NORMAL AND ABNORMAL RED CELL MORPHOLOGY 9.1 INTRODUCTION A peripheral blood smear (peripheral blood film) is a glass microscope slide coated on one side with a thin
4/24/2015. Urgent, STAT, Super STAT, ASAP! Achieving timely lab testing for the Emergency Department. Learning Objectives.
 Urgent, STAT, Super STAT, ASAP! Achieving timely lab testing for the Emergency Department Nichole Korpi-Steiner, PhD, DABCC, FACB University of North Carolina Chapel Hill, NC Learning Objectives Describe
Urgent, STAT, Super STAT, ASAP! Achieving timely lab testing for the Emergency Department Nichole Korpi-Steiner, PhD, DABCC, FACB University of North Carolina Chapel Hill, NC Learning Objectives Describe
THE INTERNET STROKE CENTER PRESENTATIONS AND DISCUSSIONS ON STROKE MANAGEMENT
 THE INTERNET STROKE CENTER PRESENTATIONS AND DISCUSSIONS ON STROKE MANAGEMENT Stroke Prevention in Atrial Fibrillation Gregory Albers, M.D. Director Stanford Stroke Center Professor of Neurology and Neurological
THE INTERNET STROKE CENTER PRESENTATIONS AND DISCUSSIONS ON STROKE MANAGEMENT Stroke Prevention in Atrial Fibrillation Gregory Albers, M.D. Director Stanford Stroke Center Professor of Neurology and Neurological
IgM ELISA. For the quantitative determination of IgM in human serum and plasma. For Research Use Only. Not For Use In Diagnostic Procedures.
 IgM ELISA For the quantitative determination of IgM in human serum and plasma For Research Use Only. Not For Use In Diagnostic Procedures. Please read carefully due to Critical Changes, e.g., Calibrator
IgM ELISA For the quantitative determination of IgM in human serum and plasma For Research Use Only. Not For Use In Diagnostic Procedures. Please read carefully due to Critical Changes, e.g., Calibrator
Standardization, Calibration and Quality Control
 Standardization, Calibration and Quality Control Ian Storie Flow cytometry has become an essential tool in the research and clinical diagnostic laboratory. The range of available flow-based diagnostic
Standardization, Calibration and Quality Control Ian Storie Flow cytometry has become an essential tool in the research and clinical diagnostic laboratory. The range of available flow-based diagnostic
Transfection reagent for visualizing lipofection with DNA. For ordering information, MSDS, publications and application notes see www.biontex.
 METAFECTENE FluoR Transfection reagent for visualizing lipofection with DNA For ordering information, MSDS, publications and application notes see www.biontex.com Description Cat. No. Size METAFECTENE
METAFECTENE FluoR Transfection reagent for visualizing lipofection with DNA For ordering information, MSDS, publications and application notes see www.biontex.com Description Cat. No. Size METAFECTENE
Diabetes mellitus. Lecture Outline
 Diabetes mellitus Lecture Outline I. Diagnosis II. Epidemiology III. Causes of diabetes IV. Health Problems and Diabetes V. Treating Diabetes VI. Physical activity and diabetes 1 Diabetes Disorder characterized
Diabetes mellitus Lecture Outline I. Diagnosis II. Epidemiology III. Causes of diabetes IV. Health Problems and Diabetes V. Treating Diabetes VI. Physical activity and diabetes 1 Diabetes Disorder characterized
Mouse Keyhole Limpet Hemocyanin antibody(igm) ELISA Kit
 Mouse Keyhole Limpet Hemocyanin antibody(igm) ELISA Kit Catalog No. MBS702810 (96 tests) This immunoassay kit allows for the in vitro semi-quantitative determination of mouse KLH(IgM)antibody concentrations
Mouse Keyhole Limpet Hemocyanin antibody(igm) ELISA Kit Catalog No. MBS702810 (96 tests) This immunoassay kit allows for the in vitro semi-quantitative determination of mouse KLH(IgM)antibody concentrations
Planning: Patient Goals and Expected Outcomes The patient will: Remain free of unusual bleeding Maintain effective tissue perfusion Implementation
 Obtain complete heath history including allergies, drug history and possible drug Assess baseline coagulation studies and CBC Assess for history of bleeding disorders, GI bleeding, cerebral bleed, recent
Obtain complete heath history including allergies, drug history and possible drug Assess baseline coagulation studies and CBC Assess for history of bleeding disorders, GI bleeding, cerebral bleed, recent
Inc. Wuhan. Quantity Pre-coated, ready to use 96-well strip plate 1 Plate sealer for 96 wells 4 Standard (liquid) 2
 Uscn Life Science Inc. Wuhan Website: www.uscnk.com Phone: +86 27 84259552 Fax: +86 27 84259551 E-mail: [email protected] ELISA Kit for Human Prostaglandin E1(PG-E1) Instruction manual Cat. No.: E0904Hu
Uscn Life Science Inc. Wuhan Website: www.uscnk.com Phone: +86 27 84259552 Fax: +86 27 84259551 E-mail: [email protected] ELISA Kit for Human Prostaglandin E1(PG-E1) Instruction manual Cat. No.: E0904Hu
NHS FIFE WIDE POLICY - HAEMATOLOGY MANAGEMENT OF ANTICOAGULATION THERAPY DURING MAJOR AND MINOR ELECTIVE SURGERY
 MANAGEMENT OF ANTICOAGULATION THERAPY DURING MAJOR AND MINOR ELECTIVE SURGERY The scope of this guideline is to simplify the management of patients on oral anticoagulation undergoing major and minor surgery.
MANAGEMENT OF ANTICOAGULATION THERAPY DURING MAJOR AND MINOR ELECTIVE SURGERY The scope of this guideline is to simplify the management of patients on oral anticoagulation undergoing major and minor surgery.
Cold Agglutination Titer detecting Cold Reacting Antibodies
 Objectives: Cold Agglutination Titer detecting Cold Reacting Antibodies 1. Perform a serial dilution to determine the amount of cold reacting antibody present in a patient specimen with the results obtained
Objectives: Cold Agglutination Titer detecting Cold Reacting Antibodies 1. Perform a serial dilution to determine the amount of cold reacting antibody present in a patient specimen with the results obtained
INMA LABORATORY MANUAL
 INMA LABORATORY MANUAL NUTRITION BIOMARKERS Cohorte-VALENCIA This manual describes the collection, separation, storage and transport of blood samples for the INMA study. Careful collection of samples is
INMA LABORATORY MANUAL NUTRITION BIOMARKERS Cohorte-VALENCIA This manual describes the collection, separation, storage and transport of blood samples for the INMA study. Careful collection of samples is
Genomic DNA Extraction Kit INSTRUCTION MANUAL
 Genomic DNA Extraction Kit INSTRUCTION MANUAL Table of Contents Introduction 3 Kit Components 3 Storage Conditions 4 Recommended Equipment and Reagents 4 Introduction to the Protocol 4 General Overview
Genomic DNA Extraction Kit INSTRUCTION MANUAL Table of Contents Introduction 3 Kit Components 3 Storage Conditions 4 Recommended Equipment and Reagents 4 Introduction to the Protocol 4 General Overview
Diagnosis of HIV-1 Infection. Estelle Piwowar-Manning HPTN Central Laboratory The Johns Hopkins University
 Diagnosis of HIV-1 Infection Estelle Piwowar-Manning HPTN Central Laboratory The Johns Hopkins University Tests Used to Diagnose HIV-1 Infection HIV antibody (today s topic) HIV p24 antigen HIV DNA HIV
Diagnosis of HIV-1 Infection Estelle Piwowar-Manning HPTN Central Laboratory The Johns Hopkins University Tests Used to Diagnose HIV-1 Infection HIV antibody (today s topic) HIV p24 antigen HIV DNA HIV
Coagulation Disorders In Pregnancy
 Coagulation Disorders In Pregnancy Dr Rashmi Sharma, M.D, FRCA SpR Anaesthetics Blackburn Royal Infirmary Dr Anna Bewlay FRCA Consultant Anaesthetist Royal Preston Hospital Physiological changes in pregnancy
Coagulation Disorders In Pregnancy Dr Rashmi Sharma, M.D, FRCA SpR Anaesthetics Blackburn Royal Infirmary Dr Anna Bewlay FRCA Consultant Anaesthetist Royal Preston Hospital Physiological changes in pregnancy
Seahorse XF Cell Mito Stress Test Kit
 Seahorse XF Cell Mito Stress Test Kit Part # 103015-100 User Guide For use with Seahorse XF e and XF Extracellular Flux Analyzers For Research Use Only 1 Table of Contents Product Description... 2 Introduction...
Seahorse XF Cell Mito Stress Test Kit Part # 103015-100 User Guide For use with Seahorse XF e and XF Extracellular Flux Analyzers For Research Use Only 1 Table of Contents Product Description... 2 Introduction...
INTRODUCTION. Viral shedding is crucial for Gene Therapy Products Safety linked with shedding data
 INTRODUCTION Viral shedding is crucial for Gene Therapy Products Safety linked with shedding data For the patient For families and friends For the environment No treatment possible without good safety
INTRODUCTION Viral shedding is crucial for Gene Therapy Products Safety linked with shedding data For the patient For families and friends For the environment No treatment possible without good safety
Duration of Dual Antiplatelet Therapy After Coronary Stenting
 Duration of Dual Antiplatelet Therapy After Coronary Stenting C. DEAN KATSAMAKIS, DO, FACC, FSCAI INTERVENTIONAL CARDIOLOGIST ADVOCATE LUTHERAN GENERAL HOSPITAL INTRODUCTION Coronary artery stents are
Duration of Dual Antiplatelet Therapy After Coronary Stenting C. DEAN KATSAMAKIS, DO, FACC, FSCAI INTERVENTIONAL CARDIOLOGIST ADVOCATE LUTHERAN GENERAL HOSPITAL INTRODUCTION Coronary artery stents are
Dr Gordon Royle Haematologist, Middlemore Hospital
 The New Oral Anticoagulants (NOACs) Dr Gordon Royle Haematologist, Middlemore Hospital Disclaimers Boehringer-Ingelheim Bayer Sanofi Douglas Pharmaceuticals Preventing disasters: lessons learned A cautionary
The New Oral Anticoagulants (NOACs) Dr Gordon Royle Haematologist, Middlemore Hospital Disclaimers Boehringer-Ingelheim Bayer Sanofi Douglas Pharmaceuticals Preventing disasters: lessons learned A cautionary
Application Sheet for Rivaroxaban (Xarelto ) Standard Range with. BIOPHEN Heparin LRT (#221011/221013) RUO
 Instrument Adaptation The attached instrument adaptation has been prepared and validated by the reagent manufacturer, Hyphen-Biomed. Instrument Siemens BCS-XP Product BIOPHEN Heparin LRT Analyte Rivaroxaban
Instrument Adaptation The attached instrument adaptation has been prepared and validated by the reagent manufacturer, Hyphen-Biomed. Instrument Siemens BCS-XP Product BIOPHEN Heparin LRT Analyte Rivaroxaban
Dr Gordon Royle Haematologist, Middlemore Hospital
 The New Oral Anticoagulants (NOACs) Dr Gordon Royle Haematologist, Middlemore Hospital Disclaimers Boehringer-Ingelheim Bayer Sanofi Douglas Pharmaceuticals Preventing disasters: lessons learned A cautionary
The New Oral Anticoagulants (NOACs) Dr Gordon Royle Haematologist, Middlemore Hospital Disclaimers Boehringer-Ingelheim Bayer Sanofi Douglas Pharmaceuticals Preventing disasters: lessons learned A cautionary
Session 3 Topics. Argatroban. Argatroban. Drug Use and Adverse Effects. Laboratory Monitoring of Anticoagulant Therapy
 ~~Marshfield Labs Presents~~ Laboratory Monitoring of Anticoagulant Therapy Session 3 of 4 Michael J. Sanfelippo, M.S. Technical Director, Coagulation Services Session 3 Topics Direct Thrombin Inhibitors:
~~Marshfield Labs Presents~~ Laboratory Monitoring of Anticoagulant Therapy Session 3 of 4 Michael J. Sanfelippo, M.S. Technical Director, Coagulation Services Session 3 Topics Direct Thrombin Inhibitors:
Genetic testing. The difference diagnostics can make. The British In Vitro Diagnostics Association
 6 Genetic testing The difference diagnostics can make The British In Vitro Diagnostics Association Genetic INTRODUCTION testing The Department of Health published Our Inheritance, Our Future - Realising
6 Genetic testing The difference diagnostics can make The British In Vitro Diagnostics Association Genetic INTRODUCTION testing The Department of Health published Our Inheritance, Our Future - Realising
Mouse krebs von den lungen 6 (KL-6) ELISA
 KAMIYA BIOMEDICAL COMPANY Mouse krebs von den lungen 6 (KL-6) ELISA For the quantitative determination of mouse KL-6 in serum, plasma, cell culture supernatants, body fluid and tissue homogenate Cat. No.
KAMIYA BIOMEDICAL COMPANY Mouse krebs von den lungen 6 (KL-6) ELISA For the quantitative determination of mouse KL-6 in serum, plasma, cell culture supernatants, body fluid and tissue homogenate Cat. No.
Direct Antiglobulin Test (DAT)
 Exercise 8 Exercise 9 Direct Antiglobulin Test (DAT) Elution Study Task Aim Introduction To perform the DAT and elution procedure with correct interpretation of results. To perform with 100% accuracy the
Exercise 8 Exercise 9 Direct Antiglobulin Test (DAT) Elution Study Task Aim Introduction To perform the DAT and elution procedure with correct interpretation of results. To perform with 100% accuracy the
Rat creatine kinase MM isoenzyme (CK-MM) ELISA Kit
 Rat creatine kinase MM isoenzyme (CK-MM) ELISA Kit Catalog Number. CSB-E14405r For the quantitative determination of rat creatine kinase MM isoenzyme (CK-MM) concentrations in serum, plasma and tissue
Rat creatine kinase MM isoenzyme (CK-MM) ELISA Kit Catalog Number. CSB-E14405r For the quantitative determination of rat creatine kinase MM isoenzyme (CK-MM) concentrations in serum, plasma and tissue
PFA-100 Platelet Function Analyzer In vitro method for platelet function testing
 PFA-100 Platelet Function Analyzer In vitro method for platelet function testing Clinical issue Insufficient bleeding tendency assessment before operation------- history taking, CBC,aPTT, PT, BT (Koscient
PFA-100 Platelet Function Analyzer In vitro method for platelet function testing Clinical issue Insufficient bleeding tendency assessment before operation------- history taking, CBC,aPTT, PT, BT (Koscient
Safety indicators for inpatient and outpatient oral anticoagulant care
 Safety indicators for inpatient and outpatient oral anticoagulant care 1 Recommendations from the British Committee for Standards in Haematology (BCSH) & National Patient Safety Agency (NPSA) Address for
Safety indicators for inpatient and outpatient oral anticoagulant care 1 Recommendations from the British Committee for Standards in Haematology (BCSH) & National Patient Safety Agency (NPSA) Address for
123count ebeads Catalog Number: 01-1234 Also known as: Absolute cell count beads GPR: General Purpose Reagents. For Laboratory Use.
 Page 1 of 1 Catalog Number: 01-1234 Also known as: Absolute cell count beads GPR: General Purpose Reagents. For Laboratory Use. Normal human peripheral blood was stained with Anti- Human CD45 PE (cat.
Page 1 of 1 Catalog Number: 01-1234 Also known as: Absolute cell count beads GPR: General Purpose Reagents. For Laboratory Use. Normal human peripheral blood was stained with Anti- Human CD45 PE (cat.
Rational for secondary prophylaxis in VWD
 Rational for secondary prophylaxis in VWD Susan Halimeh Medical Thrombosis and Haemophilia treatment Center, Duisburg, Germany Dr. med. Susan Halimeh When is prophylaxis in patients with VWD recommended?
Rational for secondary prophylaxis in VWD Susan Halimeh Medical Thrombosis and Haemophilia treatment Center, Duisburg, Germany Dr. med. Susan Halimeh When is prophylaxis in patients with VWD recommended?
NHS FORTH VALLEY RIVAROXABAN AS TREATMENT FOR DEEP VEIN THROMBOSIS AND PULMONARY EMBOLISM IN ADULTS
 NHS FORTH VALLEY RIVAROXABAN AS TREATMENT FOR DEEP VEIN THROMBOSIS AND PULMONARY EMBOLISM IN ADULTS Date of First Issue 01/12/ 2012 Approved 15/11/2012 Current Issue Date 29/10/2014 Review Date 29/10/2016
NHS FORTH VALLEY RIVAROXABAN AS TREATMENT FOR DEEP VEIN THROMBOSIS AND PULMONARY EMBOLISM IN ADULTS Date of First Issue 01/12/ 2012 Approved 15/11/2012 Current Issue Date 29/10/2014 Review Date 29/10/2016
STEP-BY-STEP INSTRUCTIONS FOR INVESTIGATIONAL USE. Rapid HCV Antibody Test FOR ORAQUICK RAPID HCV ANTIBODY TEST
 Before performing testing, all operators MUST read and become familiar with Universal Precautions for Prevention of Transmission of Human Immunodeficiency Virus, Hepatitis B Virus, and other Blood-borne
Before performing testing, all operators MUST read and become familiar with Universal Precautions for Prevention of Transmission of Human Immunodeficiency Virus, Hepatitis B Virus, and other Blood-borne
Title of Guideline. Thrombosis Pharmacist)
 Title of Guideline Contact Name and Job Title (author) Guideline for patients receiving Rivaroxaban (Xarelto ) requiring Emergency Surgery or treatment for Haemorrhage Julian Holmes (Haemostasis and Thrombosis
Title of Guideline Contact Name and Job Title (author) Guideline for patients receiving Rivaroxaban (Xarelto ) requiring Emergency Surgery or treatment for Haemorrhage Julian Holmes (Haemostasis and Thrombosis
Acute Myocardial Infarction (the formulary thrombolytic for AMI at AAMC is TNK, please see the TNK monograph in this manual for information)
 ANNE ARUNDEL MEDICAL CENTER CRITICAL CARE MEDICATION MANUAL DEPARTMENT OF NURSING AND PHARMACY Guidelines for Use of Intravenous Alteplase (Tissue Plasminogen Activator (t-pa)), Activase in the Treatment
ANNE ARUNDEL MEDICAL CENTER CRITICAL CARE MEDICATION MANUAL DEPARTMENT OF NURSING AND PHARMACY Guidelines for Use of Intravenous Alteplase (Tissue Plasminogen Activator (t-pa)), Activase in the Treatment
User Manual. CelluLyser Lysis and cdna Synthesis Kit. Version 1.4 Oct 2012 From cells to cdna in one tube
 User Manual CelluLyser Lysis and cdna Synthesis Kit Version 1.4 Oct 2012 From cells to cdna in one tube CelluLyser Lysis and cdna Synthesis Kit Table of contents Introduction 4 Contents 5 Storage 5 Additionally
User Manual CelluLyser Lysis and cdna Synthesis Kit Version 1.4 Oct 2012 From cells to cdna in one tube CelluLyser Lysis and cdna Synthesis Kit Table of contents Introduction 4 Contents 5 Storage 5 Additionally
East Kent Prescribing Group
 East Kent Prescribing Group Rivaroxaban (Xarelto ) Safety Information Approved by the East Kent Prescribing Group. Approved by: East Kent Prescribing Group (Representing Ashford CCG, Canterbury and Coastal
East Kent Prescribing Group Rivaroxaban (Xarelto ) Safety Information Approved by the East Kent Prescribing Group. Approved by: East Kent Prescribing Group (Representing Ashford CCG, Canterbury and Coastal
The new oral anticoagulants & the future of haemostasis laboratory testing. Alcohol: the good, the bad and the ugly
 The new oral anticoagulants & the future of haemostasis laboratory testing Emmanuel J Favaloro Diagnostic Haemostasis Laboratory, Institute of Clinical Pathology & Medical Research, ICPMR, Pathology West,
The new oral anticoagulants & the future of haemostasis laboratory testing Emmanuel J Favaloro Diagnostic Haemostasis Laboratory, Institute of Clinical Pathology & Medical Research, ICPMR, Pathology West,
BLOOD BANK SPECIMEN COLLECTION PROCEDURE
 BLOOD BANK SPECIMEN COLLECTION PROCEDURE INTRODUCTION Scientific and technical advances in blood group serology have made the transfusion of blood a relatively safe procedure, but serious adverse effects
BLOOD BANK SPECIMEN COLLECTION PROCEDURE INTRODUCTION Scientific and technical advances in blood group serology have made the transfusion of blood a relatively safe procedure, but serious adverse effects
Dual Antiplatelet Therapy. Stephen Monroe, MD FACC Chattanooga Heart Institute
 Dual Antiplatelet Therapy Stephen Monroe, MD FACC Chattanooga Heart Institute Scope of Talk Identify the antiplatelet drugs and their mechanisms of action Review dual antiplatelet therapy in: The medical
Dual Antiplatelet Therapy Stephen Monroe, MD FACC Chattanooga Heart Institute Scope of Talk Identify the antiplatelet drugs and their mechanisms of action Review dual antiplatelet therapy in: The medical
Minimal residual disease detection in Acute Myeloid Leukaemia on a Becton Dickinson flow cytometer
 Minimal residual disease detection in Acute Myeloid Leukaemia on a Becton Dickinson flow cytometer Purpose This procedure gives instruction on minimal residual disease (MRD) detection in patients with
Minimal residual disease detection in Acute Myeloid Leukaemia on a Becton Dickinson flow cytometer Purpose This procedure gives instruction on minimal residual disease (MRD) detection in patients with
Thrombin Generation Assay
 Thrombin Generation Assay Kit insert Version: February 2013 Summary Thrombin is a key enzyme of the coagulation cascade. Its measurement gives direct information about the thrombogenicity of a biomaterial
Thrombin Generation Assay Kit insert Version: February 2013 Summary Thrombin is a key enzyme of the coagulation cascade. Its measurement gives direct information about the thrombogenicity of a biomaterial
CORD BLOOD COLLECTION / ANALYSIS- AT BIRTH
 WOMEN AND NEWBORN HEALTH SERVICE King Edward Memorial Hospital CLINICAL GUIDELINES OBSTETRICS AND MIDWIFERY King Edward Memorial Hospital WOMEN AND NEWBORN HEALTH SERVICE INTRAPARTUM CARE SPECIMEN COLLECTION
WOMEN AND NEWBORN HEALTH SERVICE King Edward Memorial Hospital CLINICAL GUIDELINES OBSTETRICS AND MIDWIFERY King Edward Memorial Hospital WOMEN AND NEWBORN HEALTH SERVICE INTRAPARTUM CARE SPECIMEN COLLECTION
MCHENRY WESTERN LAKE COUNTY EMS SYSTEM OPTIONAL CE ADVANCED LEVEL (EMTP, PHRN, ECRN) August 2013. Anticoagulants
 MCHENRY WESTERN LAKE COUNTY EMS SYSTEM OPTIONAL CE ADVANCED LEVEL (EMTP, PHRN, ECRN) August 2013 Anticoagulants Anticoagulants are agents that prevent the formation of blood clots. Before we can talk about
MCHENRY WESTERN LAKE COUNTY EMS SYSTEM OPTIONAL CE ADVANCED LEVEL (EMTP, PHRN, ECRN) August 2013 Anticoagulants Anticoagulants are agents that prevent the formation of blood clots. Before we can talk about
Low Molecular Weight Heparin. All Wales Medicines Strategy Group (AWMSG) Recommendations and advice
 Low Molecular Weight Heparin All Wales Medicines Strategy Group (AWMSG) Recommendations and advice Starting Point Low Molecular Weight Heparin (LMWH): Inhibits factor Xa and factor IIa (thrombin) Small
Low Molecular Weight Heparin All Wales Medicines Strategy Group (AWMSG) Recommendations and advice Starting Point Low Molecular Weight Heparin (LMWH): Inhibits factor Xa and factor IIa (thrombin) Small
Collect and label sample according to standard protocols. Gently invert tube 8-10 times immediately after draw. DO NOT SHAKE. Do not centrifuge.
 Complete Blood Count CPT Code: CBC with Differential: 85025 CBC without Differential: 85027 Order Code: CBC with Differential: C915 Includes: White blood cell, Red blood cell, Hematocrit, Hemoglobin, MCV,
Complete Blood Count CPT Code: CBC with Differential: 85025 CBC without Differential: 85027 Order Code: CBC with Differential: C915 Includes: White blood cell, Red blood cell, Hematocrit, Hemoglobin, MCV,
