brief report: A Comparison of Clients With a Dual Diagnosis Referred to Specialized Clinical and Crisis-Support Programs Abstract
|
|
|
- Alicia Hutchinson
- 8 years ago
- Views:
Transcription
1 brief report: A Comparison of Clients With a Dual Diagnosis Referred to Specialized Clinical and Crisis-Support Programs Abstract Authors Stacy E. White, 1 Yona Lunsky, 1,2 Clara Ko, 1,2 Jillian Carlyle, 1 Trevor Lumb 3 1 Dual Diagnosis Program, Centre for Addiction and Mental Health 2 University of Toronto 3 Griffin Community Support Network Correspondence stacyewhite@yahoo.ca Keywords dual diagnosis, crisis, specialized clinical services The Dual Diagnosis Program (DDP) at the Centre for Addiction and Mental Health and the Griffin Community Support Network (GCSN) work in partnership to serve individuals with a dual diagnosis in Toronto. The present study compared clients referred to the DDP, a specialized clinical service (n = 51), to those referred to the GCSN, a crisis-support program (n = 51). Client groups differed with respect to service needs, referral sources, place of residence and legal involvement. Similarities included demographics, psychiatric profile, and history of mental health hospitalization. Implications for dual diagnosis service provision and directions for future research are discussed. The term dual diagnosis is used to describe individuals with an intellectual or developmental disability and mental health needs (Ministry of Health and Long-Term Care & Ministry of Community and Social Services, 2008). It is estimated that in Ontario, there are over 125,000 individuals with intellectual disabilities (ID), at least 30% of whom have a dual diagnosis (MOHLTC & MCSS, 2008; Yu & Atkinson, 1993). In Ontario, services for this population are provided by two separate sectors (Ministry of Health and Ministry of Community and Social Services), and have been criticized as fragmented, in that clients and caregivers have trouble seeking services from both sectors at the same time (Lunsky & Puddicombe, 2005; MOHLTC & MCCS, 2008). Even within each sector, the system is difficult to navigate, particularly for service users. The recent Joint Policy Guideline (MOHLTC & MCSS, 2008) stipulates that services for this population should be integrated, coordinated and operate responsively and proactively both within and across sectors (p.1). To help create a continuum of dual diagnosis services in Toronto, a partnership was developed in the late 1990s between the Dual Diagnosis Program at the Centre for Addiction and Mental Health and the Griffin Community Support Network. Description of Programs Through direct services and referrals to respite, residential safebeds, short-term case management, clinical services and day programming, the Griffin Community Support Network (GCSN) provides time limited crisis and transitional support to adults 16 years and over with a developmental dis ability or a dual diagnosis. The Dual Diagnosis Program (DDP) provides assessment, diagnosis, consultation,
2 90 Wh i t e et a l. education, and training to indi viduals with a dual diagnosis and their care givers, through interdisciplinary teams including behaviour therapy, occupational therapy, psychology, psychiatry, nursing and social work. Description of Clients A review of studies on individuals with ID accessing crisis-intervention or emergency services for psychiatric or behavioural crises highlights several key characteristics of this group. These clients are often younger adults with milder disabilities (Cowley et al., 2005; Davidson et al., 1999; Gustaffson, 1997). Environmental triggers include the absence of appropriate residential supports (Lunsky, Gracey, & Gelfand, 2008), and some crises may occur because of activities or behaviour requiring legal involvement. Clients utilizing specialized dual diagnosis services are more likely to be young adult males with levels of ID ranging from mild to profound. Research also shows that they are more likely than clients with psychiatric diagnoses without ID to present with externalizing behaviour difficulties as opposed to internalizing problems (Lunsky et al., 2006), and rates of serious mental illness, such as psychotic disorder, tend to be high (Bouras et al., 2003). Although previous studies have examined the profile of these two related client groups, no studies have yet compared them. Such compari sons are important, if clinical and crisis services are to be linked as part of a continuum of supports for this complex population. In the present study, we aimed to delineate the differences in clients referred to the DDP and GCSN, and to better understand the factors that lead clients to use one service rather than the other. Participants Method The sample comprised 51 clients referred to the DDP and 51 referred to the GCSN, between April and November Excluded from analyses were clients using both programs simultaneously. Measures All client data were collected using the Referral and Intake Form (RIF), a structured interview jointly developed by both organizations (for more information or to obtain the form, contact the authors).. This tool captures current and historical data on clients regarding presenting problems, linkages to other service providers, behavioural risks, diagnoses, medical problems, and other areas. Data in this tool are entered into an Internet-based database shared by the DDP and GCSN. Procedure Through a retrospective review of electronic charts, data gathered for each client at the time of referral were analyzed. For this study, data on the following variables were examined: demographics; primary psychiatric diagnosis; level of ID; medication use; place of residence; referral source sector; history of challenging behaviour, forensic involvement, and mental health hospitalization; and primary reasons for referral. This study was approved by the Research Ethics Board at the Centre for Addiction and Mental Health. Results Detailed results for chi-square analyses are presented in Table 1. No statistically significant differences were found between client groups in gender distribution, age and marital status; overall, clients in both groups were predominantly male and unmarried, with mean ages of 33.9 (DDP) and 30.4 (GCSN) (t(100)=1.48, p=0.14). The diagnostic profiles of each client group did not differ significantly. The majority of individuals referred to both services did not have an Axis I disorder recorded at intake. The least common disorders in both groups were anxiety disorders (3.9% DDP, 2.0% GCSN) and autism (3.9% DDP, 5.9 % GCSN), with psychotic disorders as the most common diagnoses (13.7% DDP and GCSN). There was a trend for clients referred to the GCSN to be diagnosed more frequently with Borderline/Mild ID than were those referred to the specialized program. The percentage of clients in each group using at least one psychotropic medication, as well as JoDD
3 Comparison of Clinical and Crisis Service Clients 91 Table 1. Chi square comparisons of client characteristics DDP % (n) GCSN % (n) χ 2 Gender (% male) 52.9 (27) 62.7 (32) Marital Status (% single) 82.4 (42) 84.3 (43) Primary Psychiatric Diagnoses Psychotic Disorder 13.7 (7) 13.7 (7) Mood Disorder 9.8 (5) 13.7 (7) Anxiety Disorder 5.9 (3) Substance-related Disorder Autism Spectrum Disorder No Axis I Diagnosis 54.9 (28) 49.0 (25) Other/unknown 7.8 (4) Level of Intellectual Disability Borderline/Mild ID Moderate/Severe ID ID Unknown/Unspecified 35.6 (16) 31.1 (14) 33.3 (15) 58.0 (29) 26.0 (13) 16.0 (8) 5.676*** % using psychotropic medications 51.0 (26) 54.9 (28) Referral Source Sectors Community Health 15.7 (8) * Correctional Developmental 49.0 (25) 39.2 (20) Family/Self 17.6 (9) 17.6 (9) Housing Mental Health 11.8 (6) 11.8 (6) Specialized Dual Diagnosis 15.7 (8) Place of Residence Group home/sil Boarding/nursing home Family/foster home Other temporary housing Independent Unknown 33.3 (17) 5.9 (3) 39.2 (20) 17.6 (9) 14.0 (7) 6.0 (3) 50.0 (25) 24.0 (12) 4.0 (2) ** History of challenging behaviour 47.1 (24) 60.8 (31) Previous legal involvement 11.8 (6) 27.5 (14) 3.980* Previous psychiatric hospitalization 29.4 (15) 45.1 (23) Primary Reasons for Referral Diagnostic clarification Assess challenging/aggressive behaviour Involvement with legal system Extra staffing needed Housing support inadequate Client unattached to service systems Case management required * p < 0.05; **p < 0.01; *** non-significant trend Only items for which a significant difference was found are listed 23.5 (12) 41.2 (21) 9.8 (5) 5.9 (3) 15.7 (8) 33.3 (17) 15.7 (8) 17.6 (9) 29.4 (15) ** ** 8.681** ** 5.971* 4.993* 6.220* v.15 n.2
4 92 Wh i t e et a l. the mean number of medications, did not differ significantly. Just over half of the clients using each service took psychotropic medications (DDP: 51.0%, GCSN: 54.9%), and used more than 2 medications each (DDP: mean=2.50; GCSN: mean=2.29; t(52) = 0.66, p=0.51). A significantly higher proportion of DDP clients lived in supported housing arrangements, such as group homes and Supported Independent Living. GCSN clients were more likely to reside in temporary or more unstable housing, including homeless shelters, transitional homes, safebeds, and correctional facilities. Service sectors from which clients were referred differed somewhat between programs, in that clients referred to the GCSN were significantly more likely to have been referred by other specialized dual diagnosis programs, whereas DDP clients were more frequently referred by community health care providers (including hospitals, general practitioners, and community-based psychiatrists). Although a higher proportion of GCSN clients had previously been involved with the legal system, no significant differences were found with regard to history of challenging behaviour or psychiatric hospitalization. Finally, clients accessing the DDP were significantly more likely to be referred for clinical services, such as diagnostic clarification and behavioural assessment, whereas clients using the GCSN were more often referred for reasons reflecting a need for increased supports, or services to intervene in an environmentally-based problem, including inadequate housing support, involvement with the legal system, and a need for case management. Discussion Clients using the specialized clinical and crisissupport programs differed in many respects, such as service needs, referral sources, place of residence, history of forensic involvement, and perhaps level of ID. Individuals using the GCSN were more likely to be referred by other specialized dual diagnosis program. Our expectation that referral reasons for GCSN clients would be more crisis based and that the residential settings of these clients would be more likely to be unstable or at risk was confirmed. One explanation for differences in referral sources is that health care providers may be more comfortable and familiar with referring clients to other hospital-based services (such as the DDP), but less familiar with community-based resources (such as the GCSN). If this is the case, further education of health professionals on crisis services may be warranted. It is interesting to note that GCSN clients were more likely to have both unstable housing and previous forensic involvement, as these experiences may be causally linked. Individuals needing housing and social support may more often engage in activity leading to legal involvement, perhaps out of perceived necessity, which may, in turn, lead to a crisis situation. Alternatively, users and non-users of crisis-support programs may be equally likely to be involved in potentially illegal activity; however, supported individuals may be deemed less risky by law enforcement officials and/or be less likely to be charged with an offence. As suggested by Holland, Clare, & Mukhopadhyay (2002), appropriate social support for individuals with ID, along with clinical intervention, may lower the risk for offending behaviour. In general, the profile of clients using the crisis service is consistent with the literature describing individuals with ID who experience crises. The profile of clients referred to dual diagnosis services also matches what has been reported in the literature. It is interesting, however, that the two groups are quite simi lar with regard to gender distribution, age, psychotropic medication use, presence of psychiatric disorders, and history of challeng ing behaviour and mental health hospitalization. This leads us to ask why these two comparable groups do not access more similar services. It appears that individuals who are better supported and in more stable situations are those who are directed towards dual diagnosis clinical services. In contrast, less supported individuals may not access clinical services, even though they would likely also benefit from them. These findings further highlight the need for a collaborative approach to service provision for this population. We are concerned that clients and caregivers in crisis may not seek clinical services once their immediate needs are met JoDD
5 Comparison of Clinical and Crisis Service Clients 93 and they are no longer in an acute crisis situation. If this occurs and underlying mental health issues go unaddressed, one might argue that this can contribute to future episodes of crisis. More research on clients pathway to crisis and to service is needed. This is a preliminary study based on informa tion collected over only a six-month period. Future research comparing client characteristics should include a larger sample referred over a longer time frame. It would also be beneficial to examine the profile of clients accessing both services simultaneously, and to study whether crisis clients do ultimately access clinic al services when their crisis resolves. It is important for crisis and clinical service agencies to know that despite different approaches, the two types of programs serve similar clients; this knowledge may help to strengthen and better integrate the services they each provide. References Bouras, N., Cowley, A., Holt, G., Newton, J.T., & Sturmey, P. (2003). Referral trends of people with intellectual disabilities and psychiatric disorders. Journal of Intellectual Disability Research, 47(6), Cowley, A., Newton, J., Sturmey, P, Bouras, N., & Holt, G. (2005). Psychiatric inpatient admissions of adults with intellectual disabilities: Predictive factors. American Journal on Mental Retardation, 110, Davidson, P.W., Houser, K.D., Cain, N.N., Sloane-Reeves, J., Quijano, L., Matons, L., Giesow, V., & Ladrigan, P.M. (1999). Characteristics of older adults with intellectual disabilities referred for crisis intervention. Journal of Intellectual Disability Research, 43(1), Griffin Community Support Network (GCSN) tss.asp Gustaffson, C. (1997). The prevalence of people with intellectual disability admitted to general hospital psychiatric units: Level of handicap, psychiatric diagnoses and care utilization. Journal of Intellectual Disability Research, 41(6), Holland, T., Clare, I.C.H., & Mukhopadhyay, T. (2002). Prevalence of criminal offending by men and women with intellectual disability and the characteristics of offenders : Implications for research and service development. Journal of Intellectual Disability Research, 46(1), 620. Lunsky, Y., Bradley, E., Durbin, J., Koegl, C., Canrinus, M., & Goering, P., (2006). The clinical profile and service needs of hospitalized adults with mental retardation and a psychiatric diagnosis. Psychiatric Services, 57(1), Lunsky, Y., Gracey, C., & Gelfand, S. (2008). Emergency psychiatric services for individuals with intellectual disabilities: Perspectives of hospital staff. Intellectual and Developmental Disabilities, 46(6) Lunsky, Y., & Puddicombe, J. (2005). Dual diagnosis in Ontario s speciality (psychiatric) hospitals: Qualitative findings and recommendations (Phase II Summary report). : Centre for Addiction and Mental Health. Ministry of Health and Long-Term Care & Ministry of Community and Social Services. (2008). Joint policy guideline for the provision of community mental health and developmental services for adults with a dual diagnosis. Queen s Printer for Ontario. Yu, D., & Atkinson, L. (1993). Developmental disability with and without psychiatric involvement: Prevalence estimates for Ontario. Journal on Developmental Disabilities, 2(1), 16. v.15 n.2
Aggression and Dual Diagnosis: Implications for Ontario's Developmental Services. Abstract
 JOURNAL ON DEVELOPMENTAL DISABILITIES, VOLUME 13 NUMBER 1, 2007 Aggression and Dual Diagnosis: Implications for Ontario's Developmental Services Jennifer Puddicombe and Yona Lunsky Abstract Aggression
JOURNAL ON DEVELOPMENTAL DISABILITIES, VOLUME 13 NUMBER 1, 2007 Aggression and Dual Diagnosis: Implications for Ontario's Developmental Services Jennifer Puddicombe and Yona Lunsky Abstract Aggression
Dual Diagnosis or Dual Confusion: Limitations When Utilizing Non-specialist Clinical Data. Abstract
 JOURNAL ON DEVELOPMENTAL DISABILITIES, VOLUME 13 NUMBER 1, 2007 Dual Diagnosis or Dual Confusion: Limitations When Utilizing Non-specialist Clinical Data Yona Lunsky and Elspeth Bradley Abstract In this
JOURNAL ON DEVELOPMENTAL DISABILITIES, VOLUME 13 NUMBER 1, 2007 Dual Diagnosis or Dual Confusion: Limitations When Utilizing Non-specialist Clinical Data Yona Lunsky and Elspeth Bradley Abstract In this
Crisis prevention and management tool
 Crisis prevention and management tool INTRODUCTION In September 2005, the Dual Diagnosis Resource Service (DDRS) at the Centre for Addiction and Mental Health (CAMH), the Griffin Community Support Network
Crisis prevention and management tool INTRODUCTION In September 2005, the Dual Diagnosis Resource Service (DDRS) at the Centre for Addiction and Mental Health (CAMH), the Griffin Community Support Network
Joint Policy Guideline for the Provision of Community Mental Health and Developmental Services for Adults with a Dual Diagnosis
 Ministry of Health and Long-Term Care and Ministry of Community and Social Services Joint Policy Guideline for the Provision of Community Mental Health and Developmental Services for Adults with a Dual
Ministry of Health and Long-Term Care and Ministry of Community and Social Services Joint Policy Guideline for the Provision of Community Mental Health and Developmental Services for Adults with a Dual
GREY BRUCE DUAL DIAGNOSIS PROGRAM. A Successful Community Collaboration Model
 GREY BRUCE DUAL DIAGNOSIS PROGRAM A Successful Community Collaboration Model DEFINITION OF DUAL DIAGNOSIS People with a dual diagnosis have 2 specific diagnoses: 1) a developmental disability and 2) mental
GREY BRUCE DUAL DIAGNOSIS PROGRAM A Successful Community Collaboration Model DEFINITION OF DUAL DIAGNOSIS People with a dual diagnosis have 2 specific diagnoses: 1) a developmental disability and 2) mental
DUAL DIAGNOSIS IN ONTARIO S SPECIALTY (PSYCHIATRIC) HOSPITALS: QUALITATIVE FINDINGS AND RECOMMENDATIONS
 DUAL DIAGNOSIS IN ONTARIO S SPECIALTY (PSYCHIATRIC) HOSPITALS: QUALITATIVE FINDINGS AND RECOMMENDATIONS PHASE II SUMMARY REPORT Dr. Yona Lunsky 1,2,3 and Jennifer Puddicombe 1 DECEMBER 2005 This study
DUAL DIAGNOSIS IN ONTARIO S SPECIALTY (PSYCHIATRIC) HOSPITALS: QUALITATIVE FINDINGS AND RECOMMENDATIONS PHASE II SUMMARY REPORT Dr. Yona Lunsky 1,2,3 and Jennifer Puddicombe 1 DECEMBER 2005 This study
How To Treat A Mental Illness At Riveredge Hospital
 ABOUT US n Riveredge Hospital maintains the treatment philosophy of Trauma Informed Care. n Our commitment to providing the highest quality of care includes offering Animal Assisted Therapy, and Expressive
ABOUT US n Riveredge Hospital maintains the treatment philosophy of Trauma Informed Care. n Our commitment to providing the highest quality of care includes offering Animal Assisted Therapy, and Expressive
Mental Health Needs Assessment Personality Disorder Prevalence and models of care
 Mental Health Needs Assessment Personality Disorder Prevalence and models of care Introduction and definitions Personality disorders are a complex group of conditions identified through how an individual
Mental Health Needs Assessment Personality Disorder Prevalence and models of care Introduction and definitions Personality disorders are a complex group of conditions identified through how an individual
West Virginia Bureau for Behavioral Health and Health Facilities Covered Services 2012
 Assessment/Diagnostic & Treatment Services CATEGORY A & CATEGORY B Assessment/Diagnostic & Treatment Services are covered by Medicaid/Other third party payor or Charity Care - Medicaid Covered Services:
Assessment/Diagnostic & Treatment Services CATEGORY A & CATEGORY B Assessment/Diagnostic & Treatment Services are covered by Medicaid/Other third party payor or Charity Care - Medicaid Covered Services:
2C: Community Rehabilitation and Treatment Programs
 2C: Community Rehabilitation and Treatment Programs 100% SERVICES PROVIDED 75% 50% 25% 0% Clinical Planning Community Supports Crisis Outpatient Day Services Employment - 63 - TABLE 2C-1 AGE AND GENDER
2C: Community Rehabilitation and Treatment Programs 100% SERVICES PROVIDED 75% 50% 25% 0% Clinical Planning Community Supports Crisis Outpatient Day Services Employment - 63 - TABLE 2C-1 AGE AND GENDER
COMMUNITY SERVICES 238 HUMAN SERVICES. Mission Statement. Mandates. Expenditure Budget: $37,580,036 30.7% of Human Services
 Mission Statement We are committed to improving the quality of life for people with or at risk of developing mental disabilities and substance abuse problems and to preventing the occurrences of these
Mission Statement We are committed to improving the quality of life for people with or at risk of developing mental disabilities and substance abuse problems and to preventing the occurrences of these
Behavioral Health Rehabilitation Services: Brief Treatment Model
 Behavioral Health Rehabilitation Services: Brief Treatment Model Presented by Allegheny HealthChoices, Inc. 444 Liberty Avenue, Pittsburgh, PA 15222 Phone: 412/325-1100 Fax 412/325-1111 April 2006 AHCI
Behavioral Health Rehabilitation Services: Brief Treatment Model Presented by Allegheny HealthChoices, Inc. 444 Liberty Avenue, Pittsburgh, PA 15222 Phone: 412/325-1100 Fax 412/325-1111 April 2006 AHCI
Complete Program Listing
 Complete Program Listing Mental Health (MH) Services Division Adult Mental Health Outpatient Clinics - Provide outpatient mental health services to individuals 18 years and older who live with severe and
Complete Program Listing Mental Health (MH) Services Division Adult Mental Health Outpatient Clinics - Provide outpatient mental health services to individuals 18 years and older who live with severe and
length of stay in hospital, sex, marital status, discharge status and diagnostic categories. Mean age and mean length of stay were compared for the
 Clinical and Demographic Characteristics of Psychiatric Inpatients admitted via Emergency and Non-Emergency routes at a University Hospital in Pakistan E.U. Syed,R. Atiq ( Departments of Psychiatry, Aga
Clinical and Demographic Characteristics of Psychiatric Inpatients admitted via Emergency and Non-Emergency routes at a University Hospital in Pakistan E.U. Syed,R. Atiq ( Departments of Psychiatry, Aga
CLINICAL PRACTICE GUIDELINES Treatment of Schizophrenia
 CLINICAL PRACTICE GUIDELINES Treatment of Schizophrenia V. Service Delivery Service Delivery and the Treatment System General Principles 1. All patients should have access to a comprehensive continuum
CLINICAL PRACTICE GUIDELINES Treatment of Schizophrenia V. Service Delivery Service Delivery and the Treatment System General Principles 1. All patients should have access to a comprehensive continuum
Needs Identification and Development of Specialized Services for Persons with a Dual Diagnosis within the Province of Ontario
 Needs Identification and Development of Specialized Services for Persons with a Dual Diagnosis within the Province of Ontario Tony Vipond Marnie McDermott Canadian Statistics There are more than 300,000
Needs Identification and Development of Specialized Services for Persons with a Dual Diagnosis within the Province of Ontario Tony Vipond Marnie McDermott Canadian Statistics There are more than 300,000
Fax # s for CAMH programs and services
 INFORMATION AND INSTRUCTIONS STEP 1 BEFORE COMPLETING THE REFERRAL FORM CATS Program / General Psychiatry Memory Clinic, Geriatric Mental Health Program Go to www.camh.net for detailed information on each
INFORMATION AND INSTRUCTIONS STEP 1 BEFORE COMPLETING THE REFERRAL FORM CATS Program / General Psychiatry Memory Clinic, Geriatric Mental Health Program Go to www.camh.net for detailed information on each
Systems Analysis of Health and Community Services for Acquired Brain Injury in Ontario
 Systems Analysis of Health and Community Services for Acquired Brain Injury in Ontario July 2010 Report provided to the Ontario Neurotrauma Foundation by the Research Team: Dr. Susan Jaglal Principal Investigator
Systems Analysis of Health and Community Services for Acquired Brain Injury in Ontario July 2010 Report provided to the Ontario Neurotrauma Foundation by the Research Team: Dr. Susan Jaglal Principal Investigator
Who We Serve Adults with severe and persistent mental illnesses such as schizophrenia, bipolar disorder and major depression.
 We Serve Adults with severe and persistent mental illnesses such as schizophrenia, bipolar disorder and major depression. We Do Provide a comprehensive individually tailored group treatment program in
We Serve Adults with severe and persistent mental illnesses such as schizophrenia, bipolar disorder and major depression. We Do Provide a comprehensive individually tailored group treatment program in
Schizophrenia N= 16. Male N= 14 Female N= 2 Other psychotic disorders N=0. Substance-related and addictive
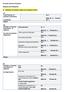 Forensic Service Provision Request and Response A. Forensic Cases as in-patient in 2013 A1. in-patients: A2. by main diagnosis: Schizophrenia 16 37 Male 26 11 Male 14 2 Other psychotic disorders 0 Personality
Forensic Service Provision Request and Response A. Forensic Cases as in-patient in 2013 A1. in-patients: A2. by main diagnosis: Schizophrenia 16 37 Male 26 11 Male 14 2 Other psychotic disorders 0 Personality
Specialist mental health service components
 Specialist mental health service components The specialist public mental health system consists of clinical services and psychiatric disability rehabilitation and support services (PDRSS). Clinical mental
Specialist mental health service components The specialist public mental health system consists of clinical services and psychiatric disability rehabilitation and support services (PDRSS). Clinical mental
LEVEL I SA: OUTPATIENT INDIVIDUAL THERAPY - Adult
 LEVEL I SA: OUTPATIENT INDIVIDUAL THERAPY - Adult Definition The following is based on the Adult Criteria of the Patient Placement Criteria for the Treatment of Substance-Related Disorders of the American
LEVEL I SA: OUTPATIENT INDIVIDUAL THERAPY - Adult Definition The following is based on the Adult Criteria of the Patient Placement Criteria for the Treatment of Substance-Related Disorders of the American
Medical Necessity Criteria
 Medical Necessity Criteria 2015 Updated 03/04/2015 Appendix B Medical Necessity Criteria Purpose: In order to promote consistent utilization management decisions, all utilization and care management staff
Medical Necessity Criteria 2015 Updated 03/04/2015 Appendix B Medical Necessity Criteria Purpose: In order to promote consistent utilization management decisions, all utilization and care management staff
Integrated Delivery of Rehabilitation Services:
 Integrated Delivery of Rehabilitation Services: Guidelines SPECIAL for NEEDS Children s STRATEGY Community Agencies, Health Guidelines Service for Providers Local Implementation and District School of
Integrated Delivery of Rehabilitation Services: Guidelines SPECIAL for NEEDS Children s STRATEGY Community Agencies, Health Guidelines Service for Providers Local Implementation and District School of
COMMUNITY CRISIS STABILIZATION (CCS)
 COMMUNITY CRISIS STABILIZATION (CCS) Providers contracted for this level of care or service are expected to comply with all requirements of these service-specific performance specifications. Additionally,
COMMUNITY CRISIS STABILIZATION (CCS) Providers contracted for this level of care or service are expected to comply with all requirements of these service-specific performance specifications. Additionally,
STRUCTURED OUTPATIENT ADDICTION PROGRAM (SOAP)
 STRUCTURED OUTPATIENT ADDICTION PROGRAM (SOAP) Providers contracted for this level of care or service are expected to comply with all requirements of these service-specific performance specifications.
STRUCTURED OUTPATIENT ADDICTION PROGRAM (SOAP) Providers contracted for this level of care or service are expected to comply with all requirements of these service-specific performance specifications.
treatment effectiveness and, in most instances, to result in successful treatment outcomes.
 Key Elements of Treatment Planning for Clients with Co Occurring Substance Abuse and Mental Health Disorders (COD) [Treatment Improvement Protocol, TIP 42: SAMHSA/CSAT] For purposes of this TIP, co occurring
Key Elements of Treatment Planning for Clients with Co Occurring Substance Abuse and Mental Health Disorders (COD) [Treatment Improvement Protocol, TIP 42: SAMHSA/CSAT] For purposes of this TIP, co occurring
Mental Health and Addiction Services Overview
 Mental Health and Addiction Services Overview CEAC 0216 January 2015 Mental Health and Addiction Services Management Team Executive Director (306) 766-7930 Manager, Rural Mental Health & Addictions (306)
Mental Health and Addiction Services Overview CEAC 0216 January 2015 Mental Health and Addiction Services Management Team Executive Director (306) 766-7930 Manager, Rural Mental Health & Addictions (306)
Collaborative and Individualized Resource (CAIR): PILOT FINDINGS 2011-2013
 Collaborative and Individualized Resource (CAIR): PILOT FINDINGS 2011-2013 Report For: Report By: Barbara Macdonald, Griffin Centre on behalf of CAIR Service Team, TNSC and MCSS Service Provider Committee
Collaborative and Individualized Resource (CAIR): PILOT FINDINGS 2011-2013 Report For: Report By: Barbara Macdonald, Griffin Centre on behalf of CAIR Service Team, TNSC and MCSS Service Provider Committee
Professional Treatment Services in Facility-Based Crisis Program Children and Adolescents
 Professional Treatment Services in Facility-Based Crisis Program Children and Adolescents Medicaid and North Carolina Health Choice (NCHC) Billable Service WORKING DRAFT Revision Date: September 11, 2014
Professional Treatment Services in Facility-Based Crisis Program Children and Adolescents Medicaid and North Carolina Health Choice (NCHC) Billable Service WORKING DRAFT Revision Date: September 11, 2014
Guidelines for Managing the Client with Intellectual Disability in the Emergency Room
 Guidelines for Managing the Client with Intellectual Disability in the Emergency Room Guidelines for Managing the Client with Intellectual Disability in the Emergency Room Prepared by Elspeth Bradley and
Guidelines for Managing the Client with Intellectual Disability in the Emergency Room Guidelines for Managing the Client with Intellectual Disability in the Emergency Room Prepared by Elspeth Bradley and
Community Center Readiness Guide Additional Resource #17 Protocol for Physician Assistants and Advanced Practice Nurses
 Community Center Readiness Guide Additional Resource #17 Protocol for Physician Assistants and Advanced Practice Nurses PROTOCOL FOR PHYSICIAN ASSISTANTS AND ADVANCED PRACTICE NURSES 1. POLICY Advanced
Community Center Readiness Guide Additional Resource #17 Protocol for Physician Assistants and Advanced Practice Nurses PROTOCOL FOR PHYSICIAN ASSISTANTS AND ADVANCED PRACTICE NURSES 1. POLICY Advanced
How To Run An Acquired Brain Injury Program
 ` Acquired Brain Injury Program Regional Rehabilitation Centre at the Hamilton General Hospital Table of Contents Page Introduction... 3-4 Acquired Brain Injury Program Philosophy... 3 Vision... 3 Service
` Acquired Brain Injury Program Regional Rehabilitation Centre at the Hamilton General Hospital Table of Contents Page Introduction... 3-4 Acquired Brain Injury Program Philosophy... 3 Vision... 3 Service
Mental Health Fact Sheet
 Mental Health Fact Sheet Substance Abuse and Treatment Branch (SATB), Community Supervision Services Re-Entry and Sanctions Center (RSC), Office of Community Justice Programs Adult Probationers / Parolees
Mental Health Fact Sheet Substance Abuse and Treatment Branch (SATB), Community Supervision Services Re-Entry and Sanctions Center (RSC), Office of Community Justice Programs Adult Probationers / Parolees
Position Statement #37 POLICY ON MENTAL HEALTH SERVICES
 THE ROYAL AUSTRALIAN AND NEW ZEALAND COLLEGE OF PSYCHIATRISTS Position Statement #37 POLICY ON MENTAL HEALTH SERVICES Mental disorder is a major cause of distress in the community. It is one of the remaining
THE ROYAL AUSTRALIAN AND NEW ZEALAND COLLEGE OF PSYCHIATRISTS Position Statement #37 POLICY ON MENTAL HEALTH SERVICES Mental disorder is a major cause of distress in the community. It is one of the remaining
Assertive Community Treatment (ACT)
 Assertive Community Treatment (ACT) Definition The Assertive Community Treatment (ACT) Team provides high intensity services, and is available to provide treatment, rehabilitation, and support activities
Assertive Community Treatment (ACT) Definition The Assertive Community Treatment (ACT) Team provides high intensity services, and is available to provide treatment, rehabilitation, and support activities
A Program Framework for: Mental Health Diversion/ Court Support Services
 A Program Framework for: Mental Health Diversion/ Court Support Services February 2006 Table of Contents 2 Preface 3 Chapter 1: Introduction to Mental Health Diversion/Court Support Services 3 1.1 Introduction
A Program Framework for: Mental Health Diversion/ Court Support Services February 2006 Table of Contents 2 Preface 3 Chapter 1: Introduction to Mental Health Diversion/Court Support Services 3 1.1 Introduction
Program of Assertive Community Services (PACT)
 Program of Assertive Community Services (PACT) Service/Program Definition Program of Assertive Community Services (PACT) entails the provision of an array of services delivered by a community-based, mobile,
Program of Assertive Community Services (PACT) Service/Program Definition Program of Assertive Community Services (PACT) entails the provision of an array of services delivered by a community-based, mobile,
IAC 9/30/15 Human Services[441] Ch 24, p.1
![IAC 9/30/15 Human Services[441] Ch 24, p.1 IAC 9/30/15 Human Services[441] Ch 24, p.1](/thumbs/27/9939915.jpg) IAC 9/30/15 Human Services[441] Ch 24, p.1 CHAPTER 24 ACCREDITATION OF PROVIDERS OF SERVICES TO PERSONS WITH MENTAL ILLNESS, INTELLECTUAL DISABILITIES, OR DEVELOPMENTAL DISABILITIES PREAMBLE The mental
IAC 9/30/15 Human Services[441] Ch 24, p.1 CHAPTER 24 ACCREDITATION OF PROVIDERS OF SERVICES TO PERSONS WITH MENTAL ILLNESS, INTELLECTUAL DISABILITIES, OR DEVELOPMENTAL DISABILITIES PREAMBLE The mental
Mental Health Emergency Service Interventions for Children, Youth and Families
 State of Rhode Island Department of Children, Youth and Families Mental Health Emergency Service Interventions for Children, Youth and Families Regulations for Certification May 16, 2012 I. GENERAL PROVISIONS
State of Rhode Island Department of Children, Youth and Families Mental Health Emergency Service Interventions for Children, Youth and Families Regulations for Certification May 16, 2012 I. GENERAL PROVISIONS
IAC 10/15/14 Human Services[441] Ch 24, p.1
![IAC 10/15/14 Human Services[441] Ch 24, p.1 IAC 10/15/14 Human Services[441] Ch 24, p.1](/thumbs/24/2340167.jpg) IAC 10/15/14 Human Services[441] Ch 24, p.1 CHAPTER 24 ACCREDITATION OF PROVIDERS OF SERVICES TO PERSONS WITH MENTAL ILLNESS, INTELLECTUAL DISABILITIES, OR DEVELOPMENTAL DISABILITIES PREAMBLE The mental
IAC 10/15/14 Human Services[441] Ch 24, p.1 CHAPTER 24 ACCREDITATION OF PROVIDERS OF SERVICES TO PERSONS WITH MENTAL ILLNESS, INTELLECTUAL DISABILITIES, OR DEVELOPMENTAL DISABILITIES PREAMBLE The mental
Subacute Inpatient MH - Adult
 Subacute Inpatient MH - Adult Definition Subacute Inpatient hospital psychiatric services are medically necessary short-term psychiatric services provided to a client with a primary psychiatric diagnosis
Subacute Inpatient MH - Adult Definition Subacute Inpatient hospital psychiatric services are medically necessary short-term psychiatric services provided to a client with a primary psychiatric diagnosis
STRUCTURED OUTPATIENT ADDICTION PROGRAM (SOAP)
 STRUCTURED OUTPATIENT ADDICTION PROGRAM (SOAP) Providers contracted for this level of care or service will be expected to comply with all requirements of these service-specific performance specifications.
STRUCTURED OUTPATIENT ADDICTION PROGRAM (SOAP) Providers contracted for this level of care or service will be expected to comply with all requirements of these service-specific performance specifications.
Billing Frequently Asked Questions
 Billing Frequently Asked Questions What are the general conditions which must be met in order to bill for a service? All billed services except assessment must be medically necessary for the treatment
Billing Frequently Asked Questions What are the general conditions which must be met in order to bill for a service? All billed services except assessment must be medically necessary for the treatment
North Bay Regional Health Centre
 Addictions and Mental Health Division Programs Central Intake Referral Form The Central Intake Referral Form is used in the District of Nipissing by the North Bay Regional Health Centre s Addictions and
Addictions and Mental Health Division Programs Central Intake Referral Form The Central Intake Referral Form is used in the District of Nipissing by the North Bay Regional Health Centre s Addictions and
Beth Merriam, M.A., OATR, ATR-BC, CCC Email: bmerriam@rogers.com
 Beth Merriam, M.A., OATR, ATR-BC, CCC Email: bmerriam@rogers.com EDUCATION 1992: M.A in, Art Therapy, Norwich University, Vermont, U.S.A, 1990: B.F.A., with major in art education, Concordia University,
Beth Merriam, M.A., OATR, ATR-BC, CCC Email: bmerriam@rogers.com EDUCATION 1992: M.A in, Art Therapy, Norwich University, Vermont, U.S.A, 1990: B.F.A., with major in art education, Concordia University,
THE OFFICE OF SUBSTANCE ABUSE SERVICES REQUIREMENTS FOR THE PROVISION OF RESIDENTIAL DETOXIFICATION SERVICES BY PROVIDERS FUNDED WITH DBHDS RESOURCES
 THE OFFICE OF SUBSTANCE ABUSE SERVICES REQUIREMENTS FOR THE PROVISION OF RESIDENTIAL DETOXIFICATION SERVICES BY PROVIDERS FUNDED WITH DBHDS RESOURCES PURPOSE: The goal of this document is to describe the
THE OFFICE OF SUBSTANCE ABUSE SERVICES REQUIREMENTS FOR THE PROVISION OF RESIDENTIAL DETOXIFICATION SERVICES BY PROVIDERS FUNDED WITH DBHDS RESOURCES PURPOSE: The goal of this document is to describe the
LEVEL III.5 SA: SHORT TERM RESIDENTIAL - Adult (DUAL DIAGNOSIS CAPABLE)
 LEVEL III.5 SA: SHT TERM RESIDENTIAL - Adult (DUAL DIAGNOSIS CAPABLE) Definition The following is based on the Adult Criteria of the Patient Placement Criteria for the Treatment of Substance-Related Disorders
LEVEL III.5 SA: SHT TERM RESIDENTIAL - Adult (DUAL DIAGNOSIS CAPABLE) Definition The following is based on the Adult Criteria of the Patient Placement Criteria for the Treatment of Substance-Related Disorders
Continuum of Community Mental Health and Addictions Services. Page 1 of 18
 Continuum of Community Mental Health and Addictions Services Page 1 of 18 List of Services for People with Severe Addictions and Mental Illness (SAMI) General Health System Primary care Assessment, treatment
Continuum of Community Mental Health and Addictions Services Page 1 of 18 List of Services for People with Severe Addictions and Mental Illness (SAMI) General Health System Primary care Assessment, treatment
DRAFT. Child and Youth Mental Health Service Framework
 DRAFT Child and Youth Mental Health Service Framework September, 2013 DRAFT CHILD AND YOUTH MENTAL HEALTH SERVICE FRAMEWORK Table of Contents SECTION 1: CONTEXT... 4 CHILD AND YOUTH MENTAL HEALTH SERVICES...
DRAFT Child and Youth Mental Health Service Framework September, 2013 DRAFT CHILD AND YOUTH MENTAL HEALTH SERVICE FRAMEWORK Table of Contents SECTION 1: CONTEXT... 4 CHILD AND YOUTH MENTAL HEALTH SERVICES...
EMERGENCY DEPARTMENT DIVERSION (EDD) PROJECT
 EMERGENCY DEPARTMENT DIVERSION (EDD) PROJECT AN INTEGRATED RESPONSE TO MENTAL HEALTH PATIENTS PRESENTING IN HOSPITAL EMERGENCY DEPARTMENT NORTH YORK GENERAL HOSPITAL * SAINT ELIZABETH HEALTH CARE * ACCESS
EMERGENCY DEPARTMENT DIVERSION (EDD) PROJECT AN INTEGRATED RESPONSE TO MENTAL HEALTH PATIENTS PRESENTING IN HOSPITAL EMERGENCY DEPARTMENT NORTH YORK GENERAL HOSPITAL * SAINT ELIZABETH HEALTH CARE * ACCESS
Psychiatric Rehabilitation Services
 DEFINITION Psychiatric or Psychosocial Rehabilitation Services provide skill building, peer support, and other supports and services to help adults with serious and persistent mental illness reduce symptoms,
DEFINITION Psychiatric or Psychosocial Rehabilitation Services provide skill building, peer support, and other supports and services to help adults with serious and persistent mental illness reduce symptoms,
ACUTE TREATMENT SERVICES (ATS) FOR SUBSTANCE USE DISORDERS LEVEL III.7
 ACUTE TREATMENT SERVICES (ATS) FOR SUBSTANCE USE DISORDERS LEVEL III.7 Providers contracted for this level of care or service are expected to comply with all requirements of these service-specific performance
ACUTE TREATMENT SERVICES (ATS) FOR SUBSTANCE USE DISORDERS LEVEL III.7 Providers contracted for this level of care or service are expected to comply with all requirements of these service-specific performance
Collaborative Care: Aging & Dual Diagnosis (CCADD) Presented by: Annalee King, RN, GNC(C) Marc Simpson, RSW
 1 Collaborative Care: Aging & Dual Diagnosis (CCADD) Presented by: Annalee King, RN, GNC(C) Marc Simpson, RSW Today s Objectives 2 Background information Subspecialty populations Development of work group
1 Collaborative Care: Aging & Dual Diagnosis (CCADD) Presented by: Annalee King, RN, GNC(C) Marc Simpson, RSW Today s Objectives 2 Background information Subspecialty populations Development of work group
Public Consultation 2009 Submission to the Second Independent Monitoring Group for A Vision for Change
 Public Consultation 2009 Submission to the Second Independent Monitoring Group for A Vision for Change Response of the National Council for the Professional Development of Nursing and Midwifery The National
Public Consultation 2009 Submission to the Second Independent Monitoring Group for A Vision for Change Response of the National Council for the Professional Development of Nursing and Midwifery The National
Charting the System for Persons with Autism Spectrum Disorder. Page 1
 EI Early Intervention Families with eligible children receive an Individualized Family Service Plan (IFSP), which lists the s and supports that are needed for the child to achieve his/her outcomes. Services
EI Early Intervention Families with eligible children receive an Individualized Family Service Plan (IFSP), which lists the s and supports that are needed for the child to achieve his/her outcomes. Services
Mental Health Services for Children and Youth in Nova Scotia
 Mental Health Services for Children and Youth in Nova Scotia Presentation to the Standing Committee on Community Services - June 1, 2010 Patricia Murray, Director of Children s Services Mental Health,
Mental Health Services for Children and Youth in Nova Scotia Presentation to the Standing Committee on Community Services - June 1, 2010 Patricia Murray, Director of Children s Services Mental Health,
3.1 TWELVE CORE FUNCTIONS OF THE CERTIFIED COUNSELLOR
 3.1 TWELVE CORE FUNCTIONS OF THE CERTIFIED COUNSELLOR The Case Presentation Method is based on the Twelve Core Functions. Scores on the CPM are based on the for each core function. The counsellor must
3.1 TWELVE CORE FUNCTIONS OF THE CERTIFIED COUNSELLOR The Case Presentation Method is based on the Twelve Core Functions. Scores on the CPM are based on the for each core function. The counsellor must
Planning Services for Persons with Developmental Disabilities and Mental Health Diagnoses
 Planning Services for Persons with Developmental Disabilities and Mental Health Diagnoses Persons with Intellectual Disabilities (ID) have mental disorders three to four times more frequently than do persons
Planning Services for Persons with Developmental Disabilities and Mental Health Diagnoses Persons with Intellectual Disabilities (ID) have mental disorders three to four times more frequently than do persons
Rehabilitation and high support services
 Rehabilitation and high support services REHABILITATION AND RECOVERY UNIT Introduction Pennine Care NHS Foundation Trust is a leading provider of mental health and community services predominantly for
Rehabilitation and high support services REHABILITATION AND RECOVERY UNIT Introduction Pennine Care NHS Foundation Trust is a leading provider of mental health and community services predominantly for
COMMUNITY MENTAL HEALTH RESOURCES
 COMMUNITY MENTAL HEALTH RESOURCES (Adult Mental Health Initiative) Ramsey & Washington Information gathered by: MN. State Advisory Council on Mental Health 17-25 Year Old Committee Mental Health Services
COMMUNITY MENTAL HEALTH RESOURCES (Adult Mental Health Initiative) Ramsey & Washington Information gathered by: MN. State Advisory Council on Mental Health 17-25 Year Old Committee Mental Health Services
Dual Diagnosis Treatment Team (DDT T)
 Dual Diagnosis Treatment Team (DDT T) Objectives To gain an overall understanding of the structure of the DDTT To understand the dynamics of this team s approach To understand the effectiveness of this
Dual Diagnosis Treatment Team (DDT T) Objectives To gain an overall understanding of the structure of the DDTT To understand the dynamics of this team s approach To understand the effectiveness of this
Mental Health Services Follow-up
 Mental Health Services Follow-up REGIONAL SUMMARY Performance Review Unit Department of Health, Social Services and Public Safety CONTENTS page BACKGROUND... 3 STRATEGIC DIRECTION... 6 PROVISION OF SERVICES...
Mental Health Services Follow-up REGIONAL SUMMARY Performance Review Unit Department of Health, Social Services and Public Safety CONTENTS page BACKGROUND... 3 STRATEGIC DIRECTION... 6 PROVISION OF SERVICES...
OUTPATIENT SERVICES. Components of Service
 OUTPATIENT SERVICES Providers contracted for this level of care or service are expected to comply with all requirements of these service-specific performance specifications. Additionally, providers contracted
OUTPATIENT SERVICES Providers contracted for this level of care or service are expected to comply with all requirements of these service-specific performance specifications. Additionally, providers contracted
ARKANSAS DEPARTMENT OF EDUCATION SCHOOL - BASED DAY TREATMENT PROGRAMS GUIDELINES
 ARKANSAS DEPARTMENT OF EDUCATION SCHOOL - BASED DAY TREATMENT PROGRAMS GUIDELINES I. DESCRIPTION A. Day Treatment is the most intensive non-residential program that can be provided over an extended period
ARKANSAS DEPARTMENT OF EDUCATION SCHOOL - BASED DAY TREATMENT PROGRAMS GUIDELINES I. DESCRIPTION A. Day Treatment is the most intensive non-residential program that can be provided over an extended period
Outcomes for People on Allegheny County Community Treatment Teams
 Allegheny HealthChoices, Inc. Winter 2010 Outcomes for People on Allegheny County Community Treatment Teams Community Treatment Teams (CTTs) in Allegheny County work with people who have some of the most
Allegheny HealthChoices, Inc. Winter 2010 Outcomes for People on Allegheny County Community Treatment Teams Community Treatment Teams (CTTs) in Allegheny County work with people who have some of the most
907 KAR 9:005. Level I and II psychiatric residential treatment facility service and coverage policies.
 907 KAR 9:005. Level I and II psychiatric residential treatment facility service and coverage policies. RELATES TO: KRS 205.520, 216B.450, 216B.455, 216B.459 STATUTORY AUTHORITY: KRS 194A.030(2), 194A.050(1),
907 KAR 9:005. Level I and II psychiatric residential treatment facility service and coverage policies. RELATES TO: KRS 205.520, 216B.450, 216B.455, 216B.459 STATUTORY AUTHORITY: KRS 194A.030(2), 194A.050(1),
Med-QUEST Division Behavioral Health Protocol
 Attachment F Med-QUEST Division Behavioral Health Protocol I. OVERVIEW The Med-QUEST Division (MQD) is responsible for providing behavioral health to all its beneficiaries. MQD provides standard behavioral
Attachment F Med-QUEST Division Behavioral Health Protocol I. OVERVIEW The Med-QUEST Division (MQD) is responsible for providing behavioral health to all its beneficiaries. MQD provides standard behavioral
Pennsylvania Dual Diagnosis Direct Support Curriculum Training Summaries
 Pennsylvania Dual Diagnosis Direct Support Curriculum Training Summaries The PA Dual Diagnosis Direct Support Curriculum Initiative The commonwealth of Pennsylvania, Office of Mental Health and Substance
Pennsylvania Dual Diagnosis Direct Support Curriculum Training Summaries The PA Dual Diagnosis Direct Support Curriculum Initiative The commonwealth of Pennsylvania, Office of Mental Health and Substance
Public Act No. 15-226
 Public Act No. 15-226 AN ACT CONCERNING HEALTH INSURANCE COVERAGE FOR MENTAL OR NERVOUS CONDITIONS. Be it enacted by the Senate and House of Representatives in General Assembly convened: Section 1. Section
Public Act No. 15-226 AN ACT CONCERNING HEALTH INSURANCE COVERAGE FOR MENTAL OR NERVOUS CONDITIONS. Be it enacted by the Senate and House of Representatives in General Assembly convened: Section 1. Section
To precertify inpatient admissions or transitional care services, call 1-866-688-3400 and select option #1.
 Security Health Plan provides coverage of various mental health/aoda (alcohol and other drug abuse) benefits to individual and employer group members. These benefits are managed by Security Health Plan.
Security Health Plan provides coverage of various mental health/aoda (alcohol and other drug abuse) benefits to individual and employer group members. These benefits are managed by Security Health Plan.
WORKERS COMPENSATION PROTOCOLS WHEN PRIMARY INJURY IS PSYCHIATRIC/PSYCHOLOGICAL
 WORKERS COMPENSATION PROTOCOLS WHEN PRIMARY INJURY IS PSYCHIATRIC/PSYCHOLOGICAL General Guidelines for Treatment of Compensable Injuries Patient must have a diagnosed mental illness as defined by DSM-5
WORKERS COMPENSATION PROTOCOLS WHEN PRIMARY INJURY IS PSYCHIATRIC/PSYCHOLOGICAL General Guidelines for Treatment of Compensable Injuries Patient must have a diagnosed mental illness as defined by DSM-5
Documentation Guidelines for ADD/ADHD
 Documentation Guidelines for ADD/ADHD Hope College Academic Success Center This document was developed following the best practice recommendations for disability documentation as outlined by the Association
Documentation Guidelines for ADD/ADHD Hope College Academic Success Center This document was developed following the best practice recommendations for disability documentation as outlined by the Association
October 28, 2014. Dear Ms. Albanese,
 Ministry of Community and Social Services Minister s Office Hepburn Block Queen s Park Toronto ON M7A 1E9 Tel.: (416) 325-5225 Fax: (416) 325-3347 Ministère des Services sociaux et communautaires Bureau
Ministry of Community and Social Services Minister s Office Hepburn Block Queen s Park Toronto ON M7A 1E9 Tel.: (416) 325-5225 Fax: (416) 325-3347 Ministère des Services sociaux et communautaires Bureau
Concurrent Disorder Comprehensive Assessment: Every Interaction is an Intervention
 Concurrent Disorder Comprehensive Assessment: Every Interaction is an Intervention Presented by: Kristin Falconer, Gillian Hutton & Stacey Whitman November 12, 2015 Disclosure Statement We have not received
Concurrent Disorder Comprehensive Assessment: Every Interaction is an Intervention Presented by: Kristin Falconer, Gillian Hutton & Stacey Whitman November 12, 2015 Disclosure Statement We have not received
MEDICAL ASSOCIATES HEALTH PLANS HEALTH CARE SERVICES POLICY AND PROCEDURE MANUAL POLICY NUMBER: PP 27
 POLICY TITLE: RESIDENTIAL TREATMENT CRITERIA POLICY STATEMENT: Provide consistent criteria when determining coverage for Residential Mental Health and Substance Abuse Treatment. NOTE: This policy applies
POLICY TITLE: RESIDENTIAL TREATMENT CRITERIA POLICY STATEMENT: Provide consistent criteria when determining coverage for Residential Mental Health and Substance Abuse Treatment. NOTE: This policy applies
INTRODUCTION...2 GUIDING PRINCIPLES...3 PURPOSE...3 FRAMEWORK FOR THE DELIVERY OF MENTAL HEALTH AND DISABILITY SERVICES IN QUEENSLAND...
 TABLE OF CONTENTS INTRODUCTION...2 GUIDING PRINCIPLES...3 PURPOSE...3 FRAMEWORK FOR THE DELIVERY OF MENTAL HEALTH AND DISABILITY SERVICES IN QUEENSLAND...4 WHO SHOULD USE THE GUIDELINES...6 COMMUNICATION
TABLE OF CONTENTS INTRODUCTION...2 GUIDING PRINCIPLES...3 PURPOSE...3 FRAMEWORK FOR THE DELIVERY OF MENTAL HEALTH AND DISABILITY SERVICES IN QUEENSLAND...4 WHO SHOULD USE THE GUIDELINES...6 COMMUNICATION
CLINIC, REHABILITATION, TARGETED CASE MANAGEMENT OPTIONS AND BHHF CONTRACT PROVIDERS
 APS UTILIZATION MANAGEMENT GUIDELINES West Virginia MEDICAID, CLINIC, REHABILITATION, TARGETED CASE MANAGEMENT OPTIONS AND BHHF CONTRACT PROVIDERS APS Healthcare, Inc.- West Virginia West Virginia Clinic,
APS UTILIZATION MANAGEMENT GUIDELINES West Virginia MEDICAID, CLINIC, REHABILITATION, TARGETED CASE MANAGEMENT OPTIONS AND BHHF CONTRACT PROVIDERS APS Healthcare, Inc.- West Virginia West Virginia Clinic,
CLINICAL REHABILITATION COUNSELING
 CLINICAL REHABILITATION COUNSELING Students who are preparing to work as rehabilitation counselors will demonstrate the professional knowledge, skills, and practices necessary to address a wide variety
CLINICAL REHABILITATION COUNSELING Students who are preparing to work as rehabilitation counselors will demonstrate the professional knowledge, skills, and practices necessary to address a wide variety
12 Core Functions. Contact: IBADCC PO Box 1548 Meridian, ID 83680 Ph: 208.468.8802 Fax: 208.466.7693 e-mail: ibadcc@ibadcc.org www.ibadcc.
 Contact: IBADCC PO Box 1548 Meridian, ID 83680 Ph: 208.468.8802 Fax: 208.466.7693 e-mail: ibadcc@ibadcc.org www.ibadcc.org Page 1 of 9 Twelve Core Functions The Twelve Core Functions of an alcohol/drug
Contact: IBADCC PO Box 1548 Meridian, ID 83680 Ph: 208.468.8802 Fax: 208.466.7693 e-mail: ibadcc@ibadcc.org www.ibadcc.org Page 1 of 9 Twelve Core Functions The Twelve Core Functions of an alcohol/drug
Behavioral Health Forum 2014 Description of 4 Mental Health Service areas
 Behavioral Health Forum 2014 Description of 4 Mental Health Service areas Terri Timberlake, Ph.D. Director, Adult Mental Health Department of Behavioral Health and Developmental Disabilities Core Eligibility
Behavioral Health Forum 2014 Description of 4 Mental Health Service areas Terri Timberlake, Ph.D. Director, Adult Mental Health Department of Behavioral Health and Developmental Disabilities Core Eligibility
How To Know If You Can Get Help For An Addiction
 2014 FLORIDA SUBSTANCE ABUSE LEVEL OF CARE CLINICAL CRITERIA SUBSTANCE ABUSE LEVEL OF CARE CLINICAL CRITERIA Overview Psychcare strives to provide quality care in the least restrictive environment. An
2014 FLORIDA SUBSTANCE ABUSE LEVEL OF CARE CLINICAL CRITERIA SUBSTANCE ABUSE LEVEL OF CARE CLINICAL CRITERIA Overview Psychcare strives to provide quality care in the least restrictive environment. An
DEVELOPMENTAL DISABILITIES ADMINISTRATION Olympia, Washington TITLE: CROSS SYSTEM CRISIS PLANS POLICY 5.18
 DEVELOPMENTAL DISABILITIES ADMINISTRATION Olympia, Washington TITLE: CROSS SYSTEM CRISIS PLANS POLICY 5.18 Authority: Chapter 71A RCW Developmental Disabilities Reference: DDA Policy 5.14 Positive Behavior
DEVELOPMENTAL DISABILITIES ADMINISTRATION Olympia, Washington TITLE: CROSS SYSTEM CRISIS PLANS POLICY 5.18 Authority: Chapter 71A RCW Developmental Disabilities Reference: DDA Policy 5.14 Positive Behavior
Financial Tips for Parents of Children with Special Needs
 Financial Tips for Parents of Children with Special Needs Children and youth with special needs have medical, emotional, developmental, mental or behavioural problems that require ongoing help and support.
Financial Tips for Parents of Children with Special Needs Children and youth with special needs have medical, emotional, developmental, mental or behavioural problems that require ongoing help and support.
SOMERSET DUAL DIAGNOSIS PROTOCOL OCTOBER 2011
 SOMERSET DUAL DIAGNOSIS PROTOCOL OCTOBER 2011 This document is intended to be used with the Somerset Dual Diagnosis Operational Working guide. This document provides principles governing joint working
SOMERSET DUAL DIAGNOSIS PROTOCOL OCTOBER 2011 This document is intended to be used with the Somerset Dual Diagnosis Operational Working guide. This document provides principles governing joint working
Protocol to Support Individuals with a Dual Diagnosis in Central Alberta
 Protocol to Support Individuals with a Dual Diagnosis in Central Alberta Partners David Thompson Health Region Canadian Mental Health Association, Central Alberta Region Persons with Developmental Disabilities
Protocol to Support Individuals with a Dual Diagnosis in Central Alberta Partners David Thompson Health Region Canadian Mental Health Association, Central Alberta Region Persons with Developmental Disabilities
DEPARTMENT OF PSYCHIATRY. 1153 Centre Street Boston, MA 02130
 DEPARTMENT OF PSYCHIATRY 1153 Centre Street Boston, MA 02130 Who We Are Brigham and Women s Faulkner Hospital (BWFH) Department of Psychiatry is the largest clinical psychiatry site in the Brigham / Faulkner
DEPARTMENT OF PSYCHIATRY 1153 Centre Street Boston, MA 02130 Who We Are Brigham and Women s Faulkner Hospital (BWFH) Department of Psychiatry is the largest clinical psychiatry site in the Brigham / Faulkner
Training Needs of Psychiatric Nursing Staff in Acute Wards. An Empirical Study in the Psychiatric Hospital of Thessaloniki, Greece.
 Training Needs of Psychiatric Nursing Staff in Acute Wards. An Empirical Study in the Psychiatric Hospital of Thessaloniki, Greece. Anatoli Moschovopoulou Qualified Mental Health Nurse, 3 rd Acute ward
Training Needs of Psychiatric Nursing Staff in Acute Wards. An Empirical Study in the Psychiatric Hospital of Thessaloniki, Greece. Anatoli Moschovopoulou Qualified Mental Health Nurse, 3 rd Acute ward
Accomplishments of the Emergency Department Mental Health & Addiction Review
 October 2014 Accomplishments of the Emergency Department Mental Health & Addiction Review Caring for people with mental health and addiction needs, while ensuring public safety What was the review about?
October 2014 Accomplishments of the Emergency Department Mental Health & Addiction Review Caring for people with mental health and addiction needs, while ensuring public safety What was the review about?
Telecare Corporation A GUIDE TO OUR SERVICES. Our Background. Our Clients
 Our Background is one of the nation s largest providers of services and supports to individuals with serious mental illness (SMI). Our Clients Telecare s clients are typically adults (18-55), older adults
Our Background is one of the nation s largest providers of services and supports to individuals with serious mental illness (SMI). Our Clients Telecare s clients are typically adults (18-55), older adults
Partial Hospitalization - MH - Adult (Managed Medicaid only Service)
 Partial Hospitalization - MH - Adult (Managed Medicaid only Service) Definition Partial hospitalization is a nonresidential treatment program that is hospital-based. The program provides diagnostic and
Partial Hospitalization - MH - Adult (Managed Medicaid only Service) Definition Partial hospitalization is a nonresidential treatment program that is hospital-based. The program provides diagnostic and
DUAL DIAGNOSIS CAPABILITY IN ADDICTION TREATMENT (DDCAT) VERSION 3.2 RATING SCALE COVER SHEET
 DUAL DIAGNOSIS CAPABILITY IN ADDICTION TREATMENT (DDCAT) VERSION 3.2 Program Identification RATING SCALE COVER SHEET Date: Rater(s): Time Spent (Hours): Agency Name: Program Name: Address: Zip Code: Contact
DUAL DIAGNOSIS CAPABILITY IN ADDICTION TREATMENT (DDCAT) VERSION 3.2 Program Identification RATING SCALE COVER SHEET Date: Rater(s): Time Spent (Hours): Agency Name: Program Name: Address: Zip Code: Contact
Treatment Services for Individuals with Co-Occurring Mental Health and Intellectual Disability/Developmental Disabilities
 Two types of individuals 1. People with primary diagnosis of intellectual disability/developmental disability Mental health diagnosis is secondary Primary services through ID/DD system Residential/Housing
Two types of individuals 1. People with primary diagnosis of intellectual disability/developmental disability Mental health diagnosis is secondary Primary services through ID/DD system Residential/Housing
LEVEL II.1 SA: INTENSIVE OUTPATIENT - Adult
 LEVEL II.1 SA: INTENSIVE OUTPATIENT - Adult Definition The following is based on the Adult Criteria of the Patient Placement Criteria for the Treatment of Substance- Related Disorders of the American Society
LEVEL II.1 SA: INTENSIVE OUTPATIENT - Adult Definition The following is based on the Adult Criteria of the Patient Placement Criteria for the Treatment of Substance- Related Disorders of the American Society
Service Coordination Core Training Module Component 1
 Service Coordination Core Training Module Component 1 It is important to remember that the purpose of this training program is to provide general information about case management services for eligible
Service Coordination Core Training Module Component 1 It is important to remember that the purpose of this training program is to provide general information about case management services for eligible
Published Date: January 1, 2016 Table of Contents
 NC Division of Mental Health, Facility-Based Developmental Disabilities & Crisis Service for Children Substance Abuse Services and Adolescents Published Date: January 1, 2016 Table of Contents Description
NC Division of Mental Health, Facility-Based Developmental Disabilities & Crisis Service for Children Substance Abuse Services and Adolescents Published Date: January 1, 2016 Table of Contents Description
TEFRA Care Coordinator Manual. Issued by: Terry Hamm DPA Long Term Care Coordinator/TEFRA Oversight
 Issued by: Terry Hamm DPA Long Term Care Coordinator/TEFRA Oversight Table of Contents Table of Contents... 2 What is TEFRA Medicaid?... 4 Eligibility Requirements... 4 Overview... 4 Age Requirements...
Issued by: Terry Hamm DPA Long Term Care Coordinator/TEFRA Oversight Table of Contents Table of Contents... 2 What is TEFRA Medicaid?... 4 Eligibility Requirements... 4 Overview... 4 Age Requirements...
Department of Psychiatry, St Joseph's Health Centre offers training in the following areas:
 ST. JOSEPH S HEALTH CENTRE 30 The Queensway Toronto, ON M6R 1B5 TEL 416-530-6000 FAX 416-530-6393 Dr. Nagi Ghabbour, Site Coordinator E-mail: ghabbn@stjoe.on.ca Ext: 4061 n/a, Education Assistant E-mail:
ST. JOSEPH S HEALTH CENTRE 30 The Queensway Toronto, ON M6R 1B5 TEL 416-530-6000 FAX 416-530-6393 Dr. Nagi Ghabbour, Site Coordinator E-mail: ghabbn@stjoe.on.ca Ext: 4061 n/a, Education Assistant E-mail:
PSYCHIATRY PROFILE. GENERAL INFORMATION (Sources: Pathway Evaluation Program, the Canadian Medical Residency Guide, and the Royal College)
 PSYCHIATRY PROFILE GENERAL INFORMATION (Sources: Pathway Evaluation Program, the Canadian Medical Residency Guide, and the Royal College) Psychiatry is the medical specialty that deals with the diseases
PSYCHIATRY PROFILE GENERAL INFORMATION (Sources: Pathway Evaluation Program, the Canadian Medical Residency Guide, and the Royal College) Psychiatry is the medical specialty that deals with the diseases
TRANSITIONAL RESIDENTIAL TREATMENT PROGRAM Session Law 2007-323 House Bill 1473, Section 10.49(i)
 REPORT TO THE THE JOINT LEGISLATIVE OVERSIGHT COMMITTEE ON MENTAL HEALTH, DEVELOPMENTAL DISABILITIES AND SUBSTANCE ABUSE SERVICES TRANSITIONAL RESIDENTIAL TREATMENT PROGRAM Session Law 2007-323 House Bill
REPORT TO THE THE JOINT LEGISLATIVE OVERSIGHT COMMITTEE ON MENTAL HEALTH, DEVELOPMENTAL DISABILITIES AND SUBSTANCE ABUSE SERVICES TRANSITIONAL RESIDENTIAL TREATMENT PROGRAM Session Law 2007-323 House Bill
