ANNUAL REPORT. (See Appendix A for the evaluation of the BSRT program goals for the academic goals.)
|
|
|
- Elvin Warner
- 10 years ago
- Views:
Transcription
1 ANNUAL REPORT I. ASSESSMENT ACTIVITIES: A. Program Goals The goals of the St. Mary s/marshall University Cooperative Bachelor of Science in Respiratory Care are congruent with the mission of Marshall University. Our goals must also be congruent with St. Mary's Medical Center. Our goals were therefore revised and approved by the Faculty Organization in its May 2006 meeting. The revised goals also included objectives which are sealed in measurable terms. (See Appendix A for the evaluation of the BSRT program goals for the academic goals.) A formal Systematic Evaluation Plan is in place for the St. Mary's/ Marshall University Cooperative BSRT Program. The components being evaluated include: Mission and Governance Faculty Student Curriculum and Instruction Resources Integrity Educational Effectiveness The assessment plan is implemented by ad hoc committees out of the St. Mary's Center for Education Faculty Organization. The program is scheduled to be evaluated by site visitors from the Committee on Accreditation for Respiratory Care (CoARC) during the fall of A letter of intent to start a BSRT program was submitted to CoARC and approved in September of A thorough self-study was submitted to CoARC in May of CoARC reviewed the self study issued and approved the program to begin following a few revisions. The school will have an on site visit by CoARC within six months following the graduation of the first class. There were three standards that CoARC sought revision of and those have been addressed. (See Appendix B for letter from CoARC) The faculty reviews the evaluation data to be used for program development, maintenance and revision. Therefore, the faculty members of St. Mary's/Marshall University Cooperative BSRT Program have reviewed the revision of the standards and criteria and are in the process of updating the program's systematic plan. The faculty approved a calendar for reviewing each component at the May 2006 meeting of the Faculty Organization. A revised template was also approved at this same meeting. (A copy of the schedule and the Systematic Evaluation Plan is included in Appendix C.)
2 B./C. LEARNING OUTCOMES/DATA COLLECTION/RESULTS The Committee for Accreditation for Respiratory Care (CoARC) is the recognized accrediting body for Respiratory Care and has specific guidelines in the standards that a Respiratory Care program must demonstrate to be in compliance with the program outcome criteria. These specific standards and goals of the Bachelor of Science Degree in Respiratory Care are incorporated into the courses. The course and clinical objectives reflect these competencies. See Appendix D for course and clinical syllabi. The program outcomes used to evaluate the Cooperative BSRT Program are performance on licensure examination, job placement rates, program satisfaction, and graduation rates. Our outcomes and definitions were changed to reflect the CoARC outcomes. Criteria for each of the required and selected outcomes are measured at the end of the program during the students' final semester. In addition course evaluations are administered at the end of each semester. The results of these course evaluations are reviewed by the faculty and any deficiencies are corrected and implemented into the appropriate course instruction. Definition of Outcomes: 1. Clinical Assessment: Assessment is evaluated each semester for application of procedures that have or are presently being instructed. If a negative review has been noted by a faculty member then the student is re-instructed in the procedure and reevaluated by another faculty member. If the student is again found to be deficient the student is re-instructed by the faculty member. A final review is done with the student by the director of the respiratory care program. If it is determined the student is in fact deficient in the competency a failing grade will be recorded. 2. Licensure Pass Rate: Performance on licensing examination (NBRC) is the percentage of graduates passing the NBRC entry level examination on the first attempt. Defined Level of Achievement: The BSRT program has not graduated any students at this point. At this time there is no information to submit. The currently enrolled class will not be eligible to sit for their examination until January Our goal is for each class that sits for the NBRC entry level licensure examination that we will meet or exceed the national pass rate on their first attempt.
3 This data is collected from reports submitted to each school by the Committee on Accreditation for Respiratory Care. Table 1: Licensure Pass Rate CLASS # OF GRADS % PASSING NBRC PASS RATE NBRC NATIONAL 2009 N/A N/A N/A RATE N/A 2010 N/A N/A N/A N/A Job Placement Rates: The first class will not graduate until December of There is no information to report at this time. Defined Level of Achievement: 90% or greater of graduates seeking employment as a CRT or RRT will be employed within 6 months of graduation. This data is collected by the faculty. The employment data does indicate that the graduates who are seeking employment do work as graduate CRT or RRT s. Table 2, Job Placement Rates reflects this data. Table 2: Job Placement Rates CLASS # GRADUATES # EMPLOYED & % NO INFORMATION # NOT SEEKING AVAILABLE EMPLOYMENT 2009 N/A N/A N/A N/A 2010 N/A N/A N/A N/A Program Satisfaction: Program satisfaction is the degree to which the current students rate the effectiveness and quality of the Respiratory Care program. The students evaluate each course of instruction at the completion of the
4 semester and assigned a rating of 1-5 on a Likert scale. Program satisfaction is the degree to which the graduates rate the effectiveness and quality of The Respiratory Care program. Defined Level of Achievement: Current students enrolled in the program evaluate each course of instruction at the completion of the semester and assigned a rating of 1-5 on a Likert scale. Current students will indicate satisfaction with the program with 2.5 or higher on a Likert scale of 1-5. To assess satisfaction with the class progression and the program, the St. Mary's School of Respiratory Care course evaluations is considered one of the primary sources of data. Graduates will indicate satisfaction with the program with 2.5 or higher on a Likert scale of 1-5. To assess graduate satisfaction with the program, the St. Mary's School of Respiratory Care Graduate Survey Questionnaire is one of the primary sources of data. At this time there are no graduates from the school of respiratory care. The first survey is to be conducted in the summer of The data collected will be trended and will indicate overall graduate satisfaction. Table 3, Program Satisfaction illustrates the data. Table 3: Program Satisfaction CLASS STUDENT ALUMNI MU GRADUATING SURVEY QUESTIONNAIRE SENIOR 2009 N/A N/A QUESTIONNAIRE N/A 2010 N/A N/A N/A Likert Scale: 1 = Highest; 5 = Lowest *Likert Scale: 5 = Highest; 1 = Lowest **Percent of those responding to agree/valuable or higher ***Alumni Questionnaire results compiled for Classes of (N/A) 1. Graduation Rates: Graduation rates are defined as the percentage of students successfully completing the program within four years. Defined Level of Achievement:
5 75% or greater of students who enter the program will graduate within four years of the start of the program. No graduation rates have been calculated since the first graduating class will not be complete all course requirements until December 2008 but will be based on criteria that the students must graduate in the specified time of four years. Table 4 demonstrates the admission/retention/graduation rates. This data is collected on a continual basis by the Director. This attrition report is filed annually with CoARC. See Appendix E for annual report filed with CoARC. The faculty of St. Mary s School of Respiratory Care is committed to be available to all students. Each student is assigned an advisor at the beginning of each year of the program. The faculty member meets during the year with each advisee. The faculty also makes every effort to contact their respective advisees who are experiencing difficulty in the program to assess the problems and problem solve for solutions. It is a requirement that any student scoring below a 75% on any unit exam meet with the assigned advisor to review the exam. Table 4: Admission/Retention/Graduation Rates CLASS ADMISSI Admitted ONS - 2 Withdrawals 12 currently enrolled Admitted - 5 Failure to Maintain C Average 8 currently enrolled 2011 GRADUATED RETENTION RATE N/A 86% N/A 61%
6 2014 Academic difficulty is not the only reason a student may withdraw from the program. It is important to look at the number of students who withdraw for other reasons. Table 5 demonstrates reasons for withdrawal over the past 3 years. Table 5: Reason for Withdrawal CLASS ACADEMIC HEALTH PERSONAL OTHER N/A 1 N/A 2011 N/A N/A N/A N/A 2012 N/A N/A N/A N/A 2013 N/A N/A N/A N/A 2014 N/A N/A N/A N/A 2015 N/A N/A N/A N/A 2016 N/A N/A N/A N/A 2017 N/A N/A N/A N/A St. Mary s/marshall University will make graduation comparison rates with the ACT news release ( once the first class has graduated Class Public Institutions Private Institutions All Institutions 2012 N/A N/A N/A 2011 N/A N/A N/A 2010 N/A N/A N/A 2009 N/A N/A N/A Table 6 Retention Rates for NCAA At the end of each semester, the St. Mary's Bachelor of Science Academic Planning and Standards Committee reviews course and clinical syllabi for activities and evaluation criteria related to the learning outcomes. Copies of course syllabi are submitted with this report. See Appendix F In order to successfully complete the required courses, students must demonstrate the satisfactory achievement of the following learning outcomes from the RRT NBRC Job Matrix:
7 See Appendix G Table 7 illustrates the data that will be obtained from St. Mary's/Marshall University Graduate Questionnaire. Table 7: Learning Outcomes Class of 2014 Class of 2013 Class of 2012 Class of 2011 Class of 2010 Class of 2009 Respiratory N/A N/A N/A N/A N/A N/A Process Therapeutic N/A N/A N/A N/A N/A N/A Respiratory Interventions Managing Care N/A N/A N/A N/A N/A N/A Teaching/ Learning N/A N/A N/A N/A N/A N/A Critical Thinking N/A N/A N/A N/A N/A N/A Likert Scale: 1 = Excellent; 5 = Poor At the end of each course, students complete evaluations of the course. The required learning outcomes are a part of these evaluations. See Appendix - Course Evaluations Prior to graduation, students complete a written evaluation of the BSRT program. This evaluation also includes the learning outcomes. Graduating students also complete the Marshall University Graduating Student Outcomes Questionnaire. This survey was not available at the time this report was completed. Performance on NBRC Entry Level Examination is described in Section II, Senate Bill 653 Compliance, and also in Table 1 in Section I. II. SENATE BILL 653 COMPLIANCE: St. Mary's/Marshall University Cooperative BSRT Program meets the requirements of Senate Bill 653. The program implements a Systematic Evaluation and evaluates achievement of goals annually. Both the Systematic evaluation and the goals are attached to this report in the appendices. The national standard for assessing the knowledge and skills of graduates of respiratory care programs in the
8 licensing examination (NBRC Entry Level). The benchmark established by the faculty of the St. Mary's/Marshall University Cooperative BSRT Program is: To meet or exceed the cut score established by the NBRC on their first attempt. This cut score changes from examination to examination based on national pass rates for all candidates. See Table 1 in Section I. III. PLANS FOR THE CURRENT YEAR: The plans for the academic year include the implementation of the Systematic Program Evaluation Plan in the areas of Mission and Governance, Curriculum, and Evaluation. This will be done during the Fall of 2008 semester. A comprehensive standardized testing package will begin with the Class of The tests are produced by the National Board for Respiratory Care (NBRC). Beginning in the Fall of 2008, prior to the first day of class, every respiratory student will be required to take three tests: 1. Test of Essential Academic Skills (TEAS) 2. Critical thinking 3. Self Assessment Inventory. Students who do not achieve pre-determined scores on these tests will be required to attend Strive for Success classes weekly for 10 weeks. Strive for Success classes were developed by two nursing faculty members from the St. Mary s Center for Education. The classes will focus on study skills, learning styles, etc. Also, each student who does not pass a unit exam with a 76% or above will be required to meet with the instructors who developed the test and complete a remediation assignment. The Goals for academic years are included in Appendix F. IV. ASSISTANCE NEEDED: The continued timely return of course and graduate evaluation data is greatly appreciated. V. IMPORTANT THING LEARNED: As with any assessment, the faculty members always find that program strengths and weaknesses are identified. Therefore, the faculty can try to correct weaknesses and continue to build upon strengths. The faculty members continue to work diligently to assist students who are having academic difficulty. We did revise our criteria for admission to the school for the next pool of applicants. It will be interesting to see if that assists in increasing our retention rate. The chart titled "Assessment of Student Outcomes: Component/Course/Program Level" is completed and may be reviewed below.
9 Marshall University Assessment of Student Outcomes: Component/Course/Program Level Component Area/Program/Discipline: St Mary's/Marshall University School of Respiratory Care Student Outcomes as Required by CoARC Person or Office Responsible Assessment Tool or Approach Standards/ Benchmark Results Analysis Action Taken Job Placement Rates Chuck Zuhars, Director, And Brent Blevins, Clinical Director Graduate/Employer Survey Roster with names and places of employment 80% or greater of respiratory graduates seeking employment as a CRT or RRT will be employed within 6 months of graduation N/A N/A & Faculty Performance on Licensure Examinations Chuck Zuhars, Director, And Brent Blevins, Clinical Director & Data from National ent. Board of Respiratory Care (NBRC) St. Mary s/marshall University School of Respiratory graduates will meet or exceed the cut score as set by the NBRC student pass the on the first attempt. N/A N/A Faculty
10 Graduation Rates Chuck Zuhars, Director, And Brent Blevins, Clinical Director Roster of names with data. 75% or greater of students who enter the program will graduate within four years. N/A N/A Program Satisfaction Chuck Zuhars, Director And Brent Blevins, Clinical Director St Mary's Graduate Questionnaire. Graduates will indicate satisfaction with the program with an average of 2.5 or greater on scale of 1-5. (Liked Scale: 1 = highest;5 = lowest) N/A N/A
11 Appendix A
12 St. Mary's/Marshall University Cooperative School of Respiratory BSRT Program Goals and Objectives: Service 1. Maintain a satisfactory graduation rate. a. Achieve a graduation rate of 80% or greater. The first class does not graduate until December There are no statistics to report. 2. Provide academic support to students at risk of academic failure. a. Continue enhancing the existing services and resources for the students. Goal Met: Various computer instructed cd roms are provided to the student to
13 enhance their learning experience. The Center for Education has purchased various manikins to enhance the students experience and training level prior to practice in the clinical area. The Center for Education has purchased periodicals to enhance and support their learning experience. This information is located in the student library. b. Identify at risk students and assist them with a remediation plan that will assist them in achieving success in the respiratory program. Goal Met: The faculty of the School of Respiratory Care has a mandatory conference with the students at mid term. Quality Weaknesses are identified at this point and discussed with the student. A remediation plan is designed and available for the student and assistance is rendered by the faculty to enhance the students learning experience. 1. Faculty will maintain membership in professional organizations. a. All faculty will be a member of a professional organization. Goal Met: All faculty members are members of the American Association of Respiratory Care and the National Board for Respiratory Care. b. Fifty percent (50%) of faculty will serve in a leadership role (officer, board member, committee member) in a professional organization. Goal Not Met: 2 faculty members have had the opportunity to be nominated for a leadership role in the West Virginia Society for Respiratory Care. The formal election has not been held as of this report. 2. Prepare graduates for entry level CRT/RRT positions as indicated on
14 standardized tests. a. Meet or exceed the national mean on standardized tests. There has not been a graduating class from the School of Respiratory Care. The first class will graduate in December Graduates will be prepared for entry level CRT/RRT positions as indicated by the National Board of Respiratory Care (NBRC). a. The graduates will meet or exceed the national pass rate as determined by the National Board of Respiratory Care (NBRC). There has not been a graduating class from the School of Respiratory Care. The first class will graduate in December Maintain graduate satisfaction with the program. a. The graduates will rate "program satisfaction" as a 2 or below on the St. Mary's Graduate Questionnaire. There has not been a graduating class from the School of Respiratory Care. The first class will graduate in December Enhance critical thinking skills. a. The graduates will have a group mean score on the ATI Critical Thinking EXIT EXAM that meets or exceeds the ATI Critical Thinking ENTRANCE EXAM group mean. This testing phase will begin with the class that enters in the Fall of Implement the PDA bulk-buying program for all incoming Year I students. Goal Met: PDA s were purchased and given to the students
15 Financial People 1. Enhance financial resources. a. In collaboration with the SMMC Foundation, submit a grant through the Center for Education Grant Committee for student or faculty use. Goal Met: The faculty members of the School of Respiratory Care have participated in several grant applications to benefit the Center for Education. 2. Faculty will support the capital campaign for the Center for Education. Goal Met: The faculty members have participated in activities that directly support the capital campaign. 3. Faculty will seek support of area clinical affiliates to secure donations of supplies and equipment. Goal Met: The faculty and staff have solicited and obtained donations to assist the School of Respiratory Care. 1. Caring will be a concept of the curriculum. a. Students will rate the courses as enhancing the "ability to be a caring professional" as evidenced by a mean of 2.5 or less on the St. Mary's Course Evaluation. Goal Met: The students complete course evaluations at the completion of each semester. The course evaluations have a rating for understanding of students needs. The faculty rating in this area is continues to rate above the cut score.
16 Growth 2. Student communication skills will be developed. a. Students will rate the courses as facilitating "the development of my communication skills" as evidenced by a mean score of 2.5 or less on the St. Mary's Course Evaluation. Goal Met: The students complete course evaluations at the completion of each semester. The course evaluations have a rating for understanding of students needs. The faculty rating in this area is continues to rate above the cut score. 1. Demonstrate a continued need for the BSRT Program. a. Recruit a pool of qualified applicants for each space in the program. Total space allocation for the program is 15 students. Goal Met: The School of Respiratory Care has met the number of qualified applicant for the currently enrolled class and for the class beginning in January The sophomore class had 14 students enrolled. The current enrollment is student dropped because she married and moved out of the state. 1 student dropped and changed her major to elementary education. The freshman class had a total enrollment of 13 students 1 student dropped due to personal reasons 4 were dropped due to failure to maintain a C average b. Ninety percent (90%) of the graduates seeking a position in respiratory care will have a job offer within 6 months of graduation. There has not been a graduating class from the School of Respiratory
17 Care. The first class will graduate in December 2008 Community 2. Demonstrate a plan to enhance the physical facilities of the School of Respiratory Care. a. Faculty will continue to participate in the planning for the Center for Education. Goal Met: The Respiratory Care program has been moved to another section of the school and has doubled the space previously held. There is ample space provided for the classes and labs to be conducted. The faculty of the School of Respiratory Care has been actively involved with the planning committee for the new Center for Education. The faculty have provided input and assisted with the allocated space for classroom and labs for their program. 3. Implement a plan to address the respiratory shortage. a. Achieve and implement a plan to attract the CRT s employed within a 50 mile radius of the school and recruit them for enrollment into the RRT program. Goal Met: Dr. Shelia Kyle, Vice President, School of Nursing and Health Professions, and St. Mary s Center for Education and the faculty of the School of Respiratory Care have worked diligently this academic year and have seen qualified applicants for admission increase. Encourage faculty involvement in community health related activities.
18 a. All faculty will participate in a community health related activities. Goal Met: The faculty members have participated in health fairs throughout the tri-state area to promote health and wellness for the population of our service area. 2. Enhance the students' ability to provide service to the community. a. All students will participate in a community health project. Goal Met: Students will be assisting with the community health fair conducted in December of The respiratory care students will be working in unison with the nursing and radiology students. b. Students will rate the courses as enhancing the "ability to provide service to the community" as evidenced by an average score of 2.5 or greater on a Likert scale of 1-5 on the St. Mary's Course Evaluation. Goal Not Met: This will be conducted in the December of 2007
19 Appendix
20 B Executive Office Sponsored By: The American Association of Respiratory Care The American College of Chest Physicians The American Society of Anesthesiologists The American Thoracic Society MEMORANDUM TO: FROM: SUBJECT: St. Mary's Medical Center Richard T. Walker, MBA, RRT CoARC, Executive Director "APPROVAL OF INTENT" TO ESTABLISH A RESPIRATORY CARE PROGRAM
21 Date: September 16, 2004 This "Memorandum" serves as formal approval to begin the process of establishing an educational program in Respiratory Care. Please be advised that a qualified Program Director should be appointed and will be responsible for of the initial review process. The initial review process will consist of the following: 1. Self-Study #1 For Programs seeking a "Letter of Review" 2. Self-Study #2 For programs seeking "Initial Accreditation" 3. The On-Site Visit, to occur after the program's first class graduates 4. Response to the Site Visit Report following the On-Site Visit The following items can be found on the CoARC Web Site: 1. The CoARC Standards and Guidelines for the Profession of Respiratory Care 2. CoARC Accreditation Handbook see "New or Re-Accreditation" section NOTE: The Program Director should feel free to call me for any assistance needed during the remainder of the accreditation process ( , Ext. 101) Harwood Road Bedford, Texas (817) Fax (817) (800) June 9, 2005 Chuck Zuhars, RRT, MS Program Director Respiratory Care Program St. Mary's School of Respiratory Care/ Marshall University 2900 is! Avenue Huntington, West Virginia Dear Mr. Zuhars: RE: I have completed my review of your self study and will be contacting you by telephone to discuss my findings. In
22 preparation for your next self study and your annual program evaluation, please re-address the following Standards. Standard V. A. 2. Fair Practices Program accreditation status must be stated in the college catalog. Note the following statement which should be in the college catalog. Any information that you send prospective students must also include program accreditation status. Program Statement: The Respiratory Care program is accredited by the Commission on Accreditation of the Allied Health Education Programs (CAAHEP), in collaboration with the Committee on Accreditation for Respiratory Care (CoARC), 1248 Harwood Road Bedford, TX 76021, , Standard III. A. Resources, Type & Amount and B. 1Key Administrative Personnel I am concerned with the limited administrative hours for the program director and director of clinical education as well as the very high (10:1) lab and clinical teaching ratios. Please consult with your administrative officers regarding adjustments in both these areas. Standard III, D Resource Assessment I wish to advise you to include the advisory committee members in your surveying. Please refer to the CoARC evaluation instruments Web page which states that the Personnel-Program Resource Survey, edition , is to be administered annually at the program advisory Board meeting. This survey instrument is to be completed by program faculty, the Medical Director, and advisory board members. I also recommend revising your purposes statements for the library to include computer resources and electronic reference materials and financial resources to include fiscal support for the retention of personnel and the acquisition and maintenance of equipment and supplies. Please call me at (727) or reply via should you require further assistance. Send your documents electronically or in hard copy form to the CoARC Executive Office and to me. Sincerely, Stephen Mikles, EdS, RRT Referee
23 Appendix C Standardized Progress Report Questions - Program Attrition % Success Directions to the Program: The following questions have been developed by CoARC to guide your analysis and action plan, directed toward improving your outcomes on Program Attrition. Your Threshold Level of Success results on this outcome have triggered an accreditation dialogue consisting of assigning a referee and requiring this progress report. The referee is available to assist
24 you with your preparation of this report and the identification of possible changes to improve your attrition results. REMINDER: Upon completion of these questions, please forward a copy electronically to the Executive Office and Referee. Each program is encouraged to utilize the NBRC electronic filing system. Program Name: St. Mary's/Marshall University School of Respiratory Care CoARC Program Number: Your referee is: Stephen Mikles The progress report is due by: September 2009 For those Students leaving for non-academic reasons: 1. Could the attrition have been predicted at the time of the student's admission? For example, did the student expect to work part-time or full time during the program? Did the student have inadequate language skills to complete the program? If the answer is yes to any of the above, was the student adequately counseled about the rigors and time requirements of the program? The attrition of students could not be predicted at the time of admission. 1 student in the class of 2008 entered the program with aspirations of being in respiratory therapy. After attending the introductory classes she made the decision that respiratory care was not what she wanted to do as a career. The student in the class of 2009 dropped because of personal reasons that she stated was not due to anything or anyone in the program. She stated it was purely for personal reasons she did not feel free to discuss. The 2nd student was engaged to be married when accepted in the respiratory class. During the summer 2006 session her fiancé accepted employment in another state and she withdrew to move out of state with him. The other 4 students in the class of 2009 were forced to leave the program for academic reasons. All 4 students stated they did not realize the complexity of the program and due to other commitments this greatly decreased their performance. All the students had the appropriate language skills to be successful in this program. All the students were counseled prior to admission to the respiratory care program as to the time commitment required to be successful in this program. Revised November, 2002
25 2. Did the student know what he/she was getting into? For example, does the program require prospective students to `shadow' a Respiratory Therapist at one of its clinical sites before acceptance into program? Were potential or alleged health hazards explained to the student prior to acceptance? Does the program require a prospective student to speak with current students to get a feel for the physical and academic rigors of the program and profession? If some of the mandatory clinical sites are extremely distant, was this made clear to the student prior to admission? It is the opinion of both the Program Director and the Director of Clinical Education that all the students were explained the processes and commitment required to be successful in the respiratory program. It is a requirement of our program that prior to entry they must attend a shadowing experience at a local hospital. The potential hazards of the respiratory care field were explained in depth prior to acceptance into the program as well as information presented in the class room. At this time it is not required for the prospective student to speak with previous classes. We did strongly recommend that they contact respiratory therapists at local hospitals to further explore the field. Due to our program being located in rural Appalachia, we did address the issue of travel distance required to attend some of our distant clinical sites. 3. Was adequate and timely financial aid and personal counseling available to students? Did students have a clear understanding of all financial requirements of the Program prior to admission? Do students in the program have access to all services available to students in other programs? The students did have available to them a financial aid counselor. Our financial aid counselor does assist the students through the whole process to insure their process is done correctly and is not an unpleasant experience The financial requirements are explained in depth by our financial aid counselor prior to admission to the program. This process is a very important commitment for our students and is necessary for the student to understand. The students in the respiratory program have the same privileges and availability of services as any other student in any of our other allied health programs. 4. Were students apprised of professional behavioral expectations prior to admission? Were students adequately counseled as to the significance and importance of these behaviors as problems occurred? The professional behaviors expectations were explained to each student prior to entry tom the
26 program. This was reinforced in the introductory academic classes as well. The students did not exhibit any behavioral problems For students who leave for Academic reasons: 1. Could this have been predicted prior to admission based upon the student's prior academic performance? If so, was the student counseled that such an outcome was likely? The admissions director does a very thorough job screening applicants that may have difficulty in progressing in this program. Once the admissions director screens the applicants for all admissions criteria, the Vice President for the Center for Education, the Program Director and the Director of Clinical Education also review the applicants for admission. 2. If the program has data demonstrating that a certain level of academic competence (e.g., GPA, aptitude tests) is required to succeed in the program, is this information used to set entrance requirements? In institutions with an "open admissions" policy, do all programs have the same academic entrance requirements? The Nursing program and the Respiratory Program do have the same admissions requirements. 3. Does the program use non-respiratory prerequisite courses as a predictor of success? Yes 4. Are students regularly informed and counseled about their academic progress? Is academic counseling and systematic remediation (e.g., tutoring) available for students who are having difficulties? Yes, all students not successfully passing an examination are remediated and retested to ensure academic success. 5. Can academic difficulties be traced to a particular instructor (didactic, laboratory, or clinical rotations)? Does the program regularly evaluate all of its instructors (e.g., Resource Assessment, course evaluations) and address any problems identified?
27 No. All students are given a course evaluation to complete at the end of the semester. The instructors are rated on a Likert scale of 1-5. No deficiencies have been noted as of this date. 6. Can the students' academic difficulties be traced to a particular instructor or course (regardless of instructor)? No S T A N D A R D P R O G R E S S R E P O R T F O R M A T T R I T I O N Program Name: Marshall University/St. Mary's Medical Center - School of Respiratory Care CoARC Program # Was attrition due to: x General Education Courses x RT Core Courses X Non-Academic Analysis: The Program Director and the Director of Clinical Education feel that adequate pre admission qualifications are in place. There is no way to predict family situations (marriage)that occur in an individuals life and the subsequent timing of this. The student that left for a change of major, we did see some indicators after class began that maybe this was not the appropriate career for this student. The student who left for personal reasons would not reveal the circumstances that forced her to leave. The students that were unable to advance for academic reasons did not realize the time commitment required for this course of study. Action Plan: The faculty are going to reevaluate the form used for shadowing and see if it adequately covers what is required for a therapist to perform their functions. This will be reviewed by the advisory committee for their input as well.
28 Date Expected to Re-evaluate: Fall 2008 Revised November, PROGRAM RESOURCE ASSESSMENT RESOURCE: ADVISORY COMMITTEE PURPOSE(S): To actively develop, promote, support and evaluate the goals of the respiratory therapy program. MEASUREMENT SYSTEM(S): 1. Program Personnel Program Resource Survey 2. Advisory Committee Minutes and Actions. DATE(S) OF MEASUREMENT:
29 1. May of each year. 2. May of each year. RESULTS: 2007 The advisory Committee felt like the goals and objectives were met for the academic school year. ACTION PLAN(S): No actions were noted to be taken 2007 PROGRAM RESOURCE ASSESSMENT RESOURCE: MEDICAL DIRECTOR PURPOSE(S): 1. To provide input into curriculum including review of appropriateness of medical content. 2. To provide review of selected respiratory care topics in a format that encourages student interaction with a physician. 3. To assist in the development of physician "communication skills and to assist in
30 the evaluation of student attainment of these skills. MEASUREMENT SYSTEM(s): Program Course and Resource Survey(s) completed by the students. Program Resource Survey completed by the faculty and advisory committee. Medical Director written evaluation(s) of student communication skills. DATE(S) OF MEASUREMENT: Program Resource Surveys are completed annually at the end of the spring semester. Course Surveys are completed at the end of each semester. Medical Director evaluation of student "communication skills"-minimum of once per semester. RESULTS: No deficiencies were noted in the medical direction of the program. ACTION PLAN(S): It was the consensus of the Program full-time personnel that no specific changes in medical director activities were indicated based on the 2007 assessments PROGRAM RESOURCE ASSESSMENT RESOURCE: FACULTY PURPOSE(S):
31 Program Director: To provide classroom, lab, and clinical instruction and to coordinate the overall program activities. Director of Clinical Education: To provide classroom, lab, and clinical instruction and to coordinate the clinical education of the students. Additional Full-time Faculty: To teach selected classroom and labs and to supervise the clinical rotation at various clinical sites. Adjunct Clinical Faculty: to provide focused review on specific procedures and provide "formative evaluations" in the clinical setting. Medical Director: See Medical Director Resource Assessment. MEASUREMENT SYSTEM(S): Program Resource Survey(s) completed by the students. Program Personnel Resource Surveys completed by the faculty, Note: Starting in 2006, also by: advisory committee, and Medical Director. DATE(S) OF MEASUREMENT: Student Exit/Resource Survey: End of each academic year (May) Advisory Committee and Medical Director Survey: Spring Advisory meeting. RESULTS: 2007 No deficiencies were noted. ACTION PLAN(S): 1. Will monitor feedback on faculty performance by students. 2. Implement newest CoARC Program resource surveys this academic year, that include feedback from advisory committee and Medical director PROGRAM RESOURCE ASSESSMENT
32 RESOURCE: Support Personnel PURPOSE(S): To provide adequate secretarial support for primary program faculty. MEASUREMENT SYSTEM: Faculty Resource survey DATE(S) OF MEASUREMENT: Program Resource Surveys are completed annually at the end of the spring semester. RESULTS: 2007 Faculty felt there was not enough secretarial support for the program. ACTION PLAN(S): Next years budget will ask for a secretary for the respiratory care division.
33 2007 PROGRAM RESOURCE ASSESSMENT RESOURCE: PHYSICAL RESOURCES / LABORATORY PURPOSE(S): 1. To provide adequate physical resources (classroom and lab) for effective delivery of the program curriculum. 2. To provide each student an opportunity to practice with equipment and procedures prior to being responsible for the equipment or skill in the clinical environment. MEASUREMENT SYSTEM(s): Program Resource Survey(s) completed by the students. Program Resource Survey completed by the faculty. DATE(S) OF MEASUREMENT: Program Resource Surveys are completed annually at the end of the spring semester. RESULTS: 2007 The students there was not adequate space for classrooms and lab. ACTION PLAN(S): The respiratory care department was moved to a larger area on the 3 rd floor of the center for education.
34 2007 PROGRAM RESOURCE ASSESSMENT RESOURCE: LABORATORY EQUIPMENT & SUPPLIES PURPOSE(S): 1. To provide adequate laboratory resources (equipment and supplies) for effective delivery of laboratory exercises. 2. To provide each student an opportunity to practice with equipment and procedures prior to being responsible for the equipment or skill in the clinical environment. MEASUREMENT SYSTEM(s): Program Resource Survey(s) completed by the students. Program Resource Survey completed by the faculty. DATE(S) OF MEASUREMENT: Program Resource Surveys are completed annually at the end of the spring semester. RESULTS: 2007 The respiratory students felt there was not adequate space allocated for the laboratory exercises.
35 ACTION PLAN(S): The respiratory class room and lab was moved to a larger area on the 3 rd floor for the center of education PROGRAM RESOURCE ASSESSMENT RESOURCE: LEARNING RESOURCES PURPOSE(S): 1. To provide a quiet place to study (Library). 2. To provide reference material when required to complete class assignments. 3. To provide sufficient computer support for students to complete assignments (computer lab). MEASUREMENT SYSTEM(S): Program Resource Survey(s) completed by the students. Program Resource Survey completed by the faculty. DATE(S) OF MEASUREMENT: Program Resource Surveys are completed annually at the end of the spring semester. RESULTS: 2005 The students felt the library area was adequate for their learning experience.
36 ACTION PLAN(S): No action necessary 2007 PROGRAM RESOURCE ASSESSMENT RESOURCE: FINANCIAL RESOURCES PURPOSE(S): To provide adequate financial support to support program needs as identified during the various outcome (product) assessments. MEASUREMENT SYSTEM: Faculty Resource survey DATE(S) OF MEASUREMENT:
37 Program Resource Surveys are completed annually at the end of the spring semester. RESULTS: 2005 The faculty felt more money should be allocated to capital purchases for the laboratory. ACTION PLAN(S): A proposed increase in the budget for fiscal year 2009 will be submitted PROGRAM RESOURCE ASSESSMENT RESOURCE: CLINICAL RESOURCES PURPOSE(S): St. Mary s Medical Center: To provide sufficient clinical experience at a large teaching medical university in order to: (1) develop the student's ability to perform respiratory critical care procedures as identified in the program's clinical activities summary log. (2) facilitate the student's development of patient assessment skills. (3) develop students "physician interaction" skills (4) provide clinical instruction with periodic "formative evaluations" to assist the student and the program in identifying progress in clinical skills development.
38 All other clinical affiliates (except Neonatal Intensive Care Units): To provide sufficient clinical experience at teaching and community hospitals in order to: (1) develop the student's ability to perform respiratory care procedures as identified in the program's clinical activities summary log. (2) facilitate the student's development of patient assessment skills. (3) develop students "physician interaction" skills Neonatal Intensive Care Units: To provide sufficient clinical experience in Neonatal Intensive Care in order to: (1) familarize the student with neonatal respiratory care. (2) develop students "physician interaction" skills MEASUREMENT SYSTEM(s): Program Resource Survey(s) completed by the students. Program Resource Survey completed by the faculty. Faculty Review of student Clinical Summary Logs. DATE(S) OF MEASUREMENT: Program Resource Surveys are completed annually at the end of the spring semester. Clinical Summary logs are reviewed on an on-going basis as well as being formally reviewed twice each semester RESULTS: The students did not feel their pediatric/neonatal rotation was adequate for their educational goals ACTION PLAN: CAMC has been added for the pediatric/neonatal rotation PROGRAM RESOURCE ASSESSMENT RESOURCE: PHYSICAIN INPUT - INSTRUCTIONAL PURPOSE(S): 1. The primary purpose of physician interaction in the clinical setting is to assist the students in developing their "professional communication" skills to facilitate their
39 effective interaction in the clinical setting. 2. Physician input by the Medical Director is to assist in the development and evaluation of practitioner/physician "communication skills". MEASUREMENT SYSTEM(s): 1. Program Resource Survey(s) completed by the students. 2. Program Resource Survey completed by the faculty. 3. Physician Interaction documentation forms. 4. Daily clinical log documentation of physician interaction. 5. Medical Director written evaluation(s) of student communication skills. 6. Pulmonologist written assessment of student assessment and communication skills. DATE(S) OF MEASUREMENT: 1. Exit survey conducted at end of academic year (May). 2. May each year per semester required / reviewed and approved by program faculty. 4. Clinical Activity logs are reviewed weekly by program faculty. 5. Medical Director evaluation of student "communication skills" performed a minimum of once each semester based on bedside clinical rounds. 6. Written evaluations are performed by Dr. Pete Ottavanio twice during Fall and Spring semesters based on clinical interaction during "patient assessment" and "Ventilator rounds" activities at St. Mary s Medical Center. RESULTS: 2007 The students felt physician interaction was good and beneficial in both their classroom and clinical experience. ACTION PLAN(S): No action necessary
40 Appendix D
41 The Respiratory Care faculty believe: that all people have dignity and worth. RESPIRATORY CARE PROGRAM Statement of Philosophy that these programs should serve people regardless of race, creed, sex, disadvantage, or handicap. in the of within that the cognitive base, psychomotor skills, and effective domain are of equal importance training of respiratory care practitioners. that the graduates of these programs should possess competence in the technical phases respiratory care and a sound understanding of the scientific principles of respiratory care. that graduates should have developed the ability to make independent clinical judgments the limits of the respiratory therapy technician s responsibilities. that graduates should exhibit strong ethical behavior and attitudes. team. that competent respiratory care technicians are significant participants on the health care
42 RESPIRATORY CARE PROGRAM Goals: 1. Provide instruction necessary to enable individuals to function as competent entry level respiratory care practitioners. 2. To help satisfy the need in local and regional communities for competent respiratory care practitioners. The Respiratory Care Program prepare graduates to: 1. Recognize the role of the respiratory care practitioner as a member of the health care team. 2. Develop a caring ethical behavior. 3. Develop a respect for the dignity and worth of the patient. 4. Develop effective communication skills. 5. Utilize a knowledge base in the sciences and technologies for the practice of respiratory care at the technician level. 6. Demonstrate an ability to practice independent clinical judgment under the direction of a physician. 7. Assume responsibility for continued learning following graduation.
43 RESPIRATORY CARE PROGRAM TASK LIST A. Administering Medical Gas Therapy 1. Identify, transport, and store medical gas cylinders 2. Select, attach, and use regulating devices 3. Operate, and perform general maintenance of air compressors and oxygen concentrators 4. Select, obtain, and assemble oxygen delivery devices appropriate to the respiratory care plan 5. Administer oxygen via low flow systems 6. Administer oxygen via high flow systems 7. Administer oxygen utilizing precision metering devices] 8. Perform oxygen analysis 9. Evaluate patient response to oxygen therapy, and recommend modification as indicated B. Administering Humidity and Aerosol Therapy 1. Select, obtain, and assemble humidifying devices appropriate to the respiratory care plan 2. Administer humidity therapy
44 3. Select, obtain, and assemble nebulizing devices appropriate to the respiratory care plan 4. Administer aerosol therapy via pneumatic nebulizers 5. Administer aerosol therapy via ultrasonic nebulizers 6. Administer aerosol therapy via tents 7. Evaluate patient response to humidity or aerosol therapy and recommend modifications as indicated C. Administering Therapeutic Procedures 1. Select, obtain, and assemble therapeutic equipment appropriate to the respiratory care plan 2. Administer incentive spirometry 3. Administer intermittent positive pressure breathing (IPPB) therapy 4. Administer mask CPAP (continuous positive airway pressure) therapy 5. Administer chest physiotherapy 6. Evaluate patient response to therapeutic procedures and recommend modification as indicated D. Administering Pulmonary Medications 1. Obtain and prepare prescribed dosage of medication 2. Administer prescribed agents via aerosol, inhalation, or metered dose inhaler 3. Monitor and evaluate patient response to the medications administered, and recommend modification as indicated E. Providing Airway Management 1. Select, obtain, and assemble airway management equipment 2. Position the patient to assure a patent airway 3. Insert appropriate oral and nasal pharyngeal airways 4. Perform oral endotracheal intubation 5. Change tracheostomy tubes 6. Maintain proper cuff inflation and position of endotracheal and tracheostomy tubes 7. Extubate patients 8. Remove esophageal obturator airways 9. Suction artificial airways 10. Perform naso-tracheal suctioning 11. Perform tracheal suctioning for specimen collection 12. Monitor and evaluate patient response to airway management procedures
45 and recommend modification as indicated F. Select, Reviewing, Obtaining, and Interpreting Patient Data 1. Review existing data in the patient record, and recommend diagnostic procedures 2. Assess patient s respiratory status by inspection 3. Assess patient s respiratory status by palpation 4. Assess patient s respiratory status by auscultation 5. Inspect the chest x-ray for gross abnormalities 6. Interview the patient 7. Measure and assess the patient s vital signs 8. Recommend procedures for obtaining additional data G. Cardiopulmonary Testing and Evaluation 1. Measure and interpret tidal volume, respiratory rate, and minute volume 2. Calculate I:E (inspiratory to expiratory) ratio 3. Measure and evaluate the negative inspiratory force 4. Measure and evaluate peak flow I. Providing Respiratory Care in Special Settings 1. Provides respiratory care to pediatric and neonatal patients 2. Provide respiratory care in the home environment 3. Provide respiratory care in emergency situations 4. Provide respiratory care to pulmonary rehabilitation patients J. Maintaining Infection Control 1. Utilize aseptic techniques while providing respiratory care 2. Practice isolation techniques 3. Disinfect respiratory care equipment 4. Sterilize respiratory care equipment 5. Measure and evaluate the vital capacity 6. Measure and evaluate timed forced expiratory volumes 7. Perform and evaluate spirometry pre- and post- bronchodilator 8. Measure and evaluate lung volumes 9. Evaluate the results of closing volume determination 10. Evaluate the results of diffusion studies 11. Evaluate the results of volume of isoflow measurement 12. Evaluate flow volume curves 13. Obtain samples for arterial blood gas measurement 14. Measure arterial blood gases 15. Interpret arterial blood gases 16. Perform and interpret oximetry
46 17. Perform and interpret capnography 18. Calculate and evaluate A-aDO2 19. Calculate and evaluate shunt 20. Calculate and evaluate VD/VT 21. Perform electrocardiography 22. Recognize basic cardiac arrhythmias 23. Measure and evaluate blood pressure 24. Interpret arterial pressure tracings 25. Interpret central venous pressure measurements 26. Evaluate (basic) hemodynamic patterns from pulmonary artery catheters 27. Inspect the chest x-ray to find gross abnormalities H. Providing ventilatory Support 1. Assess the patient s need for ventilatory support 2. Select, assemble and prepare appropriate ventilators 3. Select appropriate ventilatory parameters 4. Adjust the mechanical ventilator to comply with physician orders or established protocol 5. Recommend modification of ventilatory parameters based on patient data 6. Initiate, adjust, and monitor effects of CPAP and PEEP 7. Replace ventilator circuits as needed 8. Institutes modifications of ventilator circuitry following established protocol 9. Institute and modify weaning procedures 10. Monitor, record, and react to changing conditions related to mechanical ventilation RSP 100 Respiratory Pharmacology
47 This 3 credit hour will introduce the student to the basic principles of pharmacology. This will include regulatory agencies, dosage calculations, and the physiology of the autonomic nervous system as it is related to respiratory care pharmacology. Major topics of discussion include; sympathomimetics, parasympolytics, xanthines, prostaglandins, Mucokinetics, cortiocosteriods, cromlyn sodium, other broncho-active agents, and neuromuscular blockers. Additionally, central nervous system agents, cardiovascular and diuretic agents, and antimicrobials are included. RSP 101 Introduction to Respiratory Care This 2 credit hour course will introduce the student to the History of Respiratory Care and Professional Organization. Emphasis is on exploring the role of the respiratory therapist or technician as a member of the health care team. Ethical and medicolegal dimensions of health care are presented. Basic techniques of patient evaluation are covered. Included are: Chest physical examination, measurement of the vital signs, patient interview and history, evaluation of the chest x-ray, and spirometry. Pre- requisites Admission into the Respiratory Care Program RSP 102 Introduction to Respiratory Care Procedures This introduction course is 3 credit hours in length. The administration of medical gases, humidity and aerosol therapy is covered. Emphasis is placed on the safe handling of medical gases and safety in administration. Principles and techniques of therapeutic procedures used in basic respiratory care are covered. Also included are: Techniques of chest inflation therapy, chest physical therapy, breathing exercises, bronchial hygiene. The physiologic effects, indications, and contraindications of each therapy are stressed. Detailed study of isolation, equipment and supplies used in these therapies is included. Pre-requisites Admission into the Respiratory Care Program. RSP 102L - Respiratory Care Procedures Lab This 1 hour laboratory class will give the student the opportunity to practice techniques and use of technology covered in Respiratory Care Procedures and Introduction to Respiratory Care. Lab exercises will be given for the student to complete. Pre-requisites Successful completion of program sequence. RSP 201 Pulmonary Pathophysiology This 3 credit hour course is designed to supplement the information presented in Introduction to Respiratory Care. The most frequently encountered diseases and syndromes are presented in detail. Emphasis is placed on the etiology, signs and symptoms, pathology, clinical manifestations, sequellae, and treatment. The respiratory therapists role in the recognition and treatment of pulmonary diseases is given special emphasis. The student completing the course is expected to have a firm understanding of the diseases covered. Pre-requisites Successful completion of program sequence
48 RSP 202 Mechanical Ventilation Technology & Management This 3 credit hour course provides an introduction to the fundamentals of mechanical ventilation techniques and terminology is presented. Various classes of mechanical ventilators are discussed and compared, emphasizing the differences required in their uses. The technology of adult continuous mechanical ventilation is covered. The design, function, and operation of representative mechanical ventilators of the various classifications are examined in detail. Management of continuous adult mechanical ventilation is covered with emphasis on the physiologic effects of various techniques and selection of optimal methods. Monitoring, quality control, and the ability to solve clinical problems relating to mechanical ventilation are emphasized. Pre-requisites Successful completion of program sequence RSP 202L - Mechanical Ventilation Technology & Management Lab This 1 hour laboratory class will give the student the opportunity to practice techniques and use of technology covered in Mechanical Ventilation & Management. Lab exercises will be given for the student to complete. Pre-requisites Successful completion of program sequence RSP 203 Respiratory Internship 1 This 4 credit hour course is designed to introduce the student to the clinical facility and to clinical education. Opportunity is given for observation of the various aspects of respiratory care. Practice in gathering information from the patient record, patient evaluation, oxygen administration, and record keeping is provided. Techniques of cardiopulmonary resuscitation are covered with laboratory practice and evaluation. Pre-requisites Successful completion of program sequence. RSP 204 Cardiopulmonary Diagnostics This 3 credit hour course will cover advanced techniques of pulmonary function testing. Topics include lung volume determination, tests of small airways, diffusion, and distribution of ventilation. Invasive and non-invasive methods of arterial blood gas sampling, analysis, and interpretation are also covered. The technology and methodology of invasive and non-invasive cardiovascular testing including electrocardiography and hemodynamic monitoring are presented. Fundamental interpretation of these tests is covered. Pre-requisites Successful completion of program sequence. RSP 205 Neonatal/Pediatric Respiratory Care This introductory course is 3 credit hours. It is designed to provide the student with detailed knowledge to the needs of neonatal and pediatric patients. Fetal cardiopulmonary development and changes at birth are covered. Equipment, procedures and methods used in the care and evaluation of neonatal and pediatric patients are also covered (Neonatal Vents). Also included are cardiopulmonary conditions and diseases particular to neonate and pediatric patients.
49 Pre-requisites Successful completion of program sequence. RSP 206 Introduction to Critical Care Management This introductory course is 3 credit hours and is designed to provide the student with detailed knowledge to the principles and techniques of therapeutic procedures used in Respiratory Care as covered: Airway management, transtracheal oxygen therapy and aspiration, bronchoscopy, thoracentisis and pleural chest tubes, arterial lines, ABG interpretation and analysis, transports, and electrocardiogram interpretation. Pre-requisites Successful completion of program sequence. RSP 207 Pulmonary Rehabilitation/Home Care This 1 credit hour course will cover care of the patient with long term pulmonary disability. Psychosocial and physical needs of the patient are addressed with emphasis on motivating and conditioning the patient with the goal of improving both quality of life and cardiopulmonary reserve. Special requirements for the patient in the home who requires respiratory care are covered. Pre-requisites Successful completion of program sequence. RSP 208 Seminar in Respiratory Care This 1 credit hour course introduces the student to NBRC exam taking skills, mock examinations of the NBRC matrix, and self-evaluation studies. Study methods and application are also covered. A study of realistic clinical problems and situations, with emphasis on analyzing and evaluating these problems to formulate acceptable respiratory care modalities. Practice will be provided in the necessary techniques to take the NBRC clinical simulation examination. Computer simulations are an integral part of this course. Pre-requisites Successful completion of program sequence. RSP 209 Respiratory Internship 2 This course is 4 credit hour course is designed to introduce the student to aspects of Respiratory Care learned in RSP 102 and RSP 101. Emphasis is on the supervised practice of basic respiratory care techniques covered in Introduction to Respiratory Care Procedures and in Introduction to Respiratory Care. Opportunity for respiratory care techniques such as oxygen therapy, humidity and aerosol therapy, aerosol drug therapy, lung inflation therapy is provided. Also, observation and supervised practice in the techniques used in electrocardiography. Pre-requisites Successful completion of program sequence. RSP 210 Respiratory Internship 3 This course is 4 credit hour course is designed to provide the student with additional experience in the practice of fundamental respiratory care techniques. Emphasis is given to the development of efficiency in the practice of these techniques. Opportunities for observation and strictly supervised practice in the techniques of arterial blood gas sampling and analysis, arterial line management and chest tube management. are also provided. Also, included is critical care observation, supervised practice of techniques used in electrocardiography and observation of hemodynamic measurement and monitoring. Additional experiences in the application of all previously covered respiratory care techniques are also provided.
50 Neonatal/Pediatric assessment and care will be provided in addition to mechanical ventilation, airway management, critical care respiratory therapy, pulmonary function testing and sleep studies. Emphasis will be placed in pulmonary rehab/home care and neonatal/pediatric respiratory care. The student of this course will maintain daily records of all activities. The student will submit and present a detailed case study. Pre-requisites Successful completion of program sequence. RSP 211 ACLS/PALS This 1 credit hour course is designed to provide the student, upon successful completion, the Advanced Cardiac Life Support and Pediatric Advanced Life Support certification. This course will cover topics required by the American Heart Association for certification. Pre-requisites Successful completion of program sequence. RSP 212 Cardiopulmonary/Renal Anatomy & Physiology This 3 credit hour course will cover the anatomy and physiology of the respiratory systems in detail. Emphasis is placed on the interaction of systems in gas exchange renal and acid base balance. The structure and function of the chest cage, mechanics of breathing, and control of respiration are also included. Pre-requisites Successful completion of program sequence. RSP 301 Introduction to Management Introduction to basic principles of management and their application in the current healthcare environment. Course content includes: management theory, scope of management, quality issues, budgeting, personnel issues, and evaluation and application of management concepts. RSP 302 Directed Reading/Seminar Critical Care This course affords the senior respiratory care student with the opportunity to practice advanced evaluative and procedural skills in the intensive care setting. Emphasis is placed on cardiopulmonary assessment and treatment of trauma, post-surgical, cardiac and renal patients, quantitative assessment techniques, refinement of monitoring procedures, and interpretation of data. RSP Respiratory Education This 3 credit hour course is designed as an introduction to clinical teaching in a respiratory care program. The course includes self-directed study in instructional and evaluation strategies and development of performance objectives. The student performs functions required of a clinical instructor in a respiratory care program. The student will be required to set up Prerequisite: RSP Respiratory Cost Management & Solutions This 3 credit hour course introduces the student to management decision making and providing costs solutions for a respiratory department. Topics covered will be annual budgets, purchasing decisions, effective staffing, inventory and supply controls as well as searching for other methods to contain costs in the healthcare environment. Prerequisite: RSP 305 Respiratory Care Performance Improvement
51 Provides basic principles associated with Total Quality Management (TQM) and Continuous Quality Improvement (CQI). Aids identification and quality problem-solving found in all healthcare organizations utilizing continuous quality improvement (CQI) tools and techniques. Through the use of case studies, current events, and textbook materials, students will learn how to identify problems, recommend improvements, and collect data to demonstrate process improvement. RSP 306 Advanced Neonatal & Pediatrics This 3 credit hour course provides an in-depth study of neonatal/pediatric anatomy, physiology, growth and development; physical, radiological, laboratory, and risk assessment; general principles of management of the sick neonate and child; and special considerations in neonatal/pediatric pharmacology as each applies to respiratory care of the neonatal/pediatric patient. An in-depth study of neonatal/pediatric pathophysiology including parenchymal disease, obstructive airway disease, lesions of the lungs and airways, congenital abnormalities, respiratory distress syndrome, apnea disorders, neurological disorders, and trauma as each applies to respiratory care of the neonatal/pediatric patient will also be covered in detail. RSP 307 Advanced Techniques in Adult Critical Care This 3 hour credit course introduces the student to current respiratory care procedures for the critically ill adult patient along with an exploration into newer and experimental techniques. Topics include independent lung ventilation, ECMO, high frequency ventilation, inverse ratio, and disease specific ventilatory support. Attendance at clinical sites is required. Prerequisite: RSP 402 Introduction to Sleep Disorders Course Description: This 3 credit hour course is designed to teach the student the process of procuring an effective sleep history and physical examination relevant to a sleep disorders patient, identify the more common relevant sleep disorders, have a general understanding of how a polysomnogram is performed, know the major categories of sleep disorders, and have a good sense of the presenting symptoms of sleep apnea, narcolepsy, psychophysiological insomnia, and sleep disturbance due to depression. The student will also be able to recognize a typical example of obstructive sleep apnea on a polysomnogram upon successful completion of this course. Prerequisites: RSP Respiratory Management Course Description: This 3 credit hour course is designed to examine the healthcare delivery system in the Appalachian region. The course examines the entire health care delivery system in general. This course will assist in the development of recommendations for future developments. This course will address the key issues confronting healthcare today, examine the causes, and develop reasonable solutions to the current set of problems.
52 Prerequisites: RSP 404 Respiratory Care Research This course is 3 semester credit hours and is designed to provide the student knowledge about survey of research problems, methods, and designs utilized in respiratory care, with emphasis on data presentation and analysis. RSP 405 Advanced Respiratory Care Diagnosis A method of instruction providing detailed education, training and work- based experience and direct patient/client care, generally at a clinical site. Specific detailed learning objectives are developed for each course by the faculty. On-site clinical instruction, supervision, evaluation and placement is the responsibility of the College faculty. Clinical experiences are unpaid external learning experiences. RSP 420 Capstone in Respiratory Care Course Goals: Introduction to Respiratory Care A. To identify appropriate behavior in promoting and practicing effective human relationships in health care settings and recognize patient well-being as the ultimate concern of the respiratory technician. B. To make necessary communication with patients and health team members, using appropriate methods and terminology and practice ethical behavior in health care situations. C. Recognize the significance of respiratory therapy education its evolution, growth and contributions in providing manpower in the health care system.
53 D. Identify the legal factors that affect his/her functions as a student and practitioner in respiratory therapy and as a member of the health care team. E. Develop a concept of future opportunities in the health field and his/her responsibility for self improvement through continuing education programs. F. To develop and practice good study habits. I. Study Skills TOPICAL OUTLINE: RSP 101 INTRODUCTION TO RESPIRATORY CARE II. Respiratory Care Profession A. Roles and Responsibilities
54 B. Professional and Credentialing Organizations C. Code of Ethics III. Team Medicine A. Benefits of Patient B. Benefits to Health Care Professionals IV. Grief Responses and Resolutions A. Patient B. Practitioner V. Medicolegal Aspects A. Negligence B. Malpractice C. Patient Rights VI. Record Keeping and Hospital Communication A. Medical Terminology B. Charting C. Incident Reports D. Verbal Reporting E. Communication with Physicians VII. Continuing Education A. Need B. Benefits INSTRUCTIONAL OBJECTIVES RSP 101 INTRODUCTION TO RESPIRATORY CARE
55 Upon completion of appropriate units of instruction, the student will demonstrate on examination the ability to: 1. Describe the role of the respiratory therapy technician in providing health care. 2. Relate the role of the technician to that of the therapist, physician, patient, nurse, and the remainder of the health care team. 3. Explain the concept and advantages of team medicine. 4. Describe the history of respiratory care. 5. Explain the role of the American Association for Respiratory Care and the National Board for Respiratory Care. 6. Describe the levels of employment in respiratory care and the necessary examination procedures for the various credentials. 7. Explain the effect of licensure. 8. Describe the mechanisms of grief resolution. 9. Identify the stages of grief resolution. 10. Outline methods of avoiding and relieving stress. 11. Recognize and apply current standards of ethical practice of respiratory care. 12. Given common respiratory care situations, identify those meeting current standards of ethical practice. 13. Recognize and avoid common causes of negligence and malpractice in the practice of respiratory care. 14. Given common respiratory care situations, identify those which illustrate negligence and malpractice. 15. Identify the criteria of proper charting and discuss their importance. 16. Given examples of charting, identify incorrect records and explain why there are incorrect. 17. Explain the use and results of the incident report.
56 18. Identify situations requiring an incident report. 19. Correctly use and define standard medical terms and abbreviations. 20. Explain why respiratory care practitioners must continue their education beyond credentialing. 21. Discuss the need for continuing education of all allied health practitioners.
57 RSP 101 INTRODUCTION TO RESPIRATORY CARE ORIENTATION TO HEALTH CARE TOPICS ASSIGNMENTS Introduction Respiratory Care Profession Burton, pp Handouts Team Medicine Burton, pp Burton, pp Ross, pp Examination #1 Grief Responses and Resolution Ross, pp Medicolegal Aspects Burton, pp Record Keeping and Hospital Communication Handout Burton, pp Examination #2 Continuing Education Burton, pp Comprehensive Final
58 TOPICAL OUTLINE: RSP INTRODUCTION TO RESPIRATORY CARE PROCEDURES I. Chest Physical Examination A. Reference Landmarks B. Observation/Inspection C. Palpation D. Percussion E. Auscultation F. Causes of Abnormal Findings II. Vital Signs A. Pulse Assessment B. Respiration Assessment C. Blood Pressure Assessment III. Patient Interview A. History B. Present Illness C. Activities and Exercise Tolerance IV. Chest Radiograph A. Normal Findings B. Placement of Tubes C. Gross Abnormalities V. Pulmonary Measuring and Monitoring Devices A. Respirometers B. Spirometers C. Peak Flow Meters D. Body Plethysmograph VI. Basic Pulmonary Measurements
59 A. Minute Ventilation B. Tidal Volume C. Vital Capacity D. Peak Flow E. Inspiratory Force VII. Routine Pulmonary Function A. Lung Volumes Definition B. Spirometry C. MVV D. Pre-/Post- Bronchodilator Studies INSTRUCTIONAL OBJECTIVES RSP INTRODUCTION TO RESPIRATORY CARE PROCEDURES Upon completion of appropriate units of instruction, the student will demonstrate on examination the ability to: 1. Describe the anatomic landmarks which will be used to localize findings of chest physical examination. 2. Summarize the process of inspecting the patient to determine: respiratory rate, use of accessory muscles, symmetry of chest expansion, presence of retractions, rhythmicity of breathing, general appearance, peripheral edema, diaphoresis, digital clubbing, cyanosis, chest configuration, nasal flaring, character of cough, amount and character of sputum. 3. List the findings expected when palpating the thorax to determine: symmetry of chest expansion, presence of fremitus, pulse (rate, rhythm, force), tracheal deviation. 4. Explain the process of auscultation. 5. Describe the character of normal and abnormal breath sounds and adventitious sounds.
60 6. List the physical findings expected with common pathologic conditions including: atelectasis, hyperinflation, pneumothorax, pleural effusion, subcutaneous emphysema, and consolidation. 7. List the steps of measuring the blood pressure using the sphygmomanometer. 8. Recognize normal range for the vital signs. 9. Outline the process of interviewing the patient to determine: level of consciousness, orientation, emotional state, ability to cooperate, presence of dyspnea and orthopnea, sputum production, exercise tolerance, and activities of daily living. 10. Describe the process used in making chest x-ray. 11. Describe normal anatomic structures in a chest x-ray. 12. Explain the process of evaluating the chest x-ray to determine: position of endotracheal or tracheostomy tubes, presence of pneumothorax, segmental or lobar atelectasis or consolidation, hyperinflation, pulmonary edema, large pleural effusions. 13. Calculate the patient s minute volume using the tidal volume and respiratory rate. 14. Explain the mechanism of common volumetric devices. 15. Describe the process of measuring the negative inspiratory force. 16. List factors which influence the maximum inspiratory and expiratory pressures. 17. Describe the significance of peak flow measurements. 18. Describe the mechanisms of common devices used in pulmonary function testing. 19. List, define, and give normal values for the various lung volumes and capacities. 20. List factors which influence the successful measurement of pulmonary function. 21. Provide a rationale for performing pulmonary function tests. 22. Summarize the process of administering a spirometry test. 23. Use a spirometry tracing to measure and calculate Vt, IRV, ERV, IV, FVC, FEV1, FEV2, FEV3, FEVT%s, FEF , FEF 25-75%. 24. Describe the maximum voluntary ventilation test.
61 25. Describe the equipment used for flow volume testing. 26. Given a flow volume curve, identify: inspiratory and expiratory flow, vital capacity, peak flow, FEF %. 27. Determine whether a flow volume curve represents fixed or variable large or small airway obstruction. 28. Evaluate pre/post bronchodilator spirometry results. TOPICAL OUTLINE: RSP INTRODUCTION TO RESPIRATORY CARE PROCEDURES I. Gas Storage A. Atmospheric and Medical Gases B. Cylinders C. Bulk Systems D. Liquid Systems
62 II. Gas Delivery A. Hospital Piping Systems B. Medical Gas Piping Systems C. Compressors D. Oxygen Concentrators III. Medical Gas Administration A. Regulators B. Flow Meters C. Blenders D. Low Flow Administration Devices E. High Flow Administration Devices F. Treatment of Hypoxia G. Carbogen Therapy H. Helium Therapy IV. Oxygen Analyzers A. Electrical B. Physical C. Electrochemical V. Humidity Therapy A. Basic Concepts B. Humidifier Mechanisms C. Methods of Administration VI. Aerosol Therapy A. Penetration and Deposition B. Pneumatic Nebulizers C. Ultrasonic Nebulizers D. Hydronamic nebulizers E. Administration Devices F. Methods of Administration VII. Chest Physical Therapy (Indications, Goals, Methods, Hazards) A. Postural Drainage B. Percussion
63 C. Vibration D. Cough Assistance E. Breathing Exercises VIII. Lung Inflation Therapies (Indications, Goals, Methods, Hazards) A. Intermittent Positive Pressure Breathing B. Incentive Spirometry C. Mask CPAP
64 INSTRUCTIONAL OBJECTIVES RSP INTRODUCTION TO RESPIRATORY CARE PROCEDURES MEDICAL GAS THERAPY Upon completion of appropriate units of instruction, the student will demonstrate on examination the ability to: 1. List the gases composing the atmosphere and relate these to Dalton s Law. 2. Describe the methods of manufacturing oxygen. 3. Identify the color code, size, capacity, and construction of various medical gas cylinders. 4. Categorize various medical gases as to use and flammability. 5. List the steps in gas cylinder testing. 6. Identify and explain gas cylinder markings. 7. Calculate the duration of flow for a gas cylinder. 8. Describe the requirements of a hospital bulb oxygen storage and delivery system. 9. Compare the use of liquid and gaseous bulk oxygen. 10. Define the roles of the various regulatory agencies in manufacture, transport, and storage of medical gases. 11. List safety standards for handling compressed gases. 12. Define, compare, and contrast the compressed gas connector safety systems. 13. Explain the basic design and function of the various types of gas pressure regulators to include: preset, adjustable, single, and multistage. 14. Given a diagram of a regulator, identify its components.
65 INSTRUCTIONAL OBJECTIVES RSP INTRODUCTION TO RESPIRATORY CARE PROCEDURES HUMIDITY AND AEROSOL THERAPY Upon completion of appropriate units of instruction, the student will demonstrate on examination the ability to: 1. Describe the pathophysiology of retained secretions. 2. List and explain the etiologies of retained secretions. 3. Describe how to prevent or correct retained secretions. 4. Describe the concept of humidity and its thermodynamics. 5. Calculate relative humidity or absolute humidity. 6. Calculate the humidity deficit. 7. Describe the design and function of Passover, bubble diffusion, cascade, hygroscopic, and room humidifiers. 8. List the factors which influence the effectiveness of humidifiers. 9. Given an illustration, identify the components of a humidifier. 10. Describe the clinical uses and appropriate applications of the various humidifiers. 11. Explain the safety factors involved in the use of heaters used for humidity and aerosol therapy. 12. Define aerosol and describe the uses of aerosol in medicine. 13. Describe the factors which influence the penetration, deposition, and stability of aerosols. 14. List methods for optimizing deposition of therapeutic aerosols. 15. List and recognize the hazards of aerosol therapy.
66 16. Describe the mechanisms of aerosol clearance from the pulmonary system. 17. Describe the design and function of jet, hydronamic, and ultrasonic nebulizers. 18. Given illustrations, identify the type of a nebulizer and its components. 19. List the goals of aerosol therapy and methods of achieving these goals. 20. Describe the use of aerosol masks, face tents, t-pieces, tracheotomy masks, and patient enclosures. 21. List the advantages and disadvantages of the various devices used to administer aerosol therapy. 22. Given illustrations or described situations, identify correct and incorrect methods of administration of aerosol therapy and give reasons for your selection.
67 INSTRUCTIONAL OBJECTIVES: RSP INTRODUCTION TO RESPIRATORY CARE PROCEDURES BRONCHIAL HYGIENE & LUNG INFLATION THERAPIES Upon completion of appropriate units of instruction, the student will demonstrate on examination the ability to: 1. List the indications, contraindications, hazards, the therapeutic goals of the various techniques of chest physical therapy. 2. List the postural drainage position and the anatomical landmarks for each lung segment. 3. Describe the proper techniques of therapeutic percussion, vibration, and postural drainage. 4. Explain the rationale for diaphragmatic and pursed lip breathing. 5. Describe the techniques of diaphragmatic and pursed lip breathing. 6. Describe the techniques for localized expansion exercises. 7. List the factors to be monitored during chest physiotherapy. 8. List the indications, contraindications, hazards, physiologic effects, and clinical goals of intermittent positive pressure breathing therapy. 9. Describe the adjustment of the equipment used for IPPB therapy to achieve the goals of the therapy.
68 10. List and explain the instructions given to a patient during IPPB to achieve maximal lung volume. 11. List the patient parameters to be monitored during IPPB therapy for safety and effectiveness. 12. Summarize the rational for the use of incentive breathing devices. 13. Describe the technique for incentive spirometry. 14. Explain the methods of coaching the patient during incentive spirometry (sustained maximal inspiration). 15. List parameters to be monitored with the patient during incentive spirometry therapy for safety and effectiveness. 16. Describe the cough mechanism. 17. Outline the methods for instructing and assisting the patient in effective coughing. 18. List the indications, contraindications, physiologic effects, hazards, and clinical goals of mask CPAP therapy. 19. Describe the method of administering mask CPAP for lung inflation therapy. 20. Explain the function of a mask CPAP system. 21. List the parameters to be monitored in a patient receiving mask CPAP for safety and effectiveness.
69 TOPICAL OUTLINE: CARDIOPULMONARY ANATOMY AND PHYSIOLOGY I. Respiratory System A. General Structure and Function B. Upper Airways C. Lower Airways D. Defense Mechanisms E. Acinus F. Histology G. Thoracic Cage H. Mechanics of Breathing I. Ventilation Perfusion Matching & Mismatch
70 II. Cardiovascular System A. Organization B. Electrophysiology C. Mechanics III. Blood Gas Transport A. Oxygen Transport B. CO 2 Transport C. Acid Base Regulation D. Evaluation IV. Control of Respiration A. Central B. Peripheral C. Reflexes D. Breathing Patterns INSTRUCTIONAL OBJECTIVES CARDIOPULMONARY ANATOMY AND PHYSIOLOGY Upon completion of appropriate units of instruction, the student will on examination demonstrate the ability to: 1. List the functions of the respiratory system. 2. Differentiate between breathing, ventilation, internal, and external respiration.
71 3. On a illustration, identify the structures of the upper airway and describe their function in detail. 4. List the cartilages of the larynx and describe its structure and function. 5. On an illustration, identify the structures of the tracheobronchial tree and describe their functions. 6. Describe the histology of the airways and changes found in the various airway generations. 7. Identify the various defense mechanisms of the pulmonary system and explain their importance. 8. Describe the structure and function of the acinus. 9. State the cell types of the alveolar epithelium and describe their functions. 10. List the origin, composition, function and explain the significance of the surfactant. 11. On an illustration, identify the various lung lobes and segments. 12. Describe the structure and function of the components of the thoracic cavity. 13. List the major and minor muscles of respiration and describe their role in breathing. 14. Explain the physiology of ventilation and state the effects of compliance, resistance, and pressure gradients. 15. Describe the elastic forces of the lung and chest wall and explain their effect on lung volume. 16. Summarize the effects of resistance on breathing. 17. Define work of breathing and delineate factors which change it. 18. Describe the normal breathing cycle and calculate the I;E ratio. 19. Relate ventilation perfusion matching and the effects of shunt and dead space. 20. Describe regional differences in ventilation, perfusion, and ventilation perfusion matching.
72 21. Explain the process of diffusion relating factors which influence the efficiency of diffusion. 22. On an illustration, identify the structures of the heart and describe their function. 23. On an illustration, trace the flow of blood through the pulmonary and systemic circulatory systems. 24. Describe the electrophysiology of the heart and relate the events of cardiac conduction to the electrocardiogram. 25. Relate the events of myocardial contraction to Starling s Law. 26. Draw, label, and define the components of the normal electrocardiogram. 27. Explain, compare, and contrast the mechanisms of oxygen transport in the erythrocyte and in plasma. 28. Describe the structure and function of hemoglobin and relate the differences in major abnormal forms. 29. Draw the oxyhemoglobin dissociation curve. 30. Describe the effects of temperature, ph, PCO 2, and 2,3-DPG on the binding of oxyhemoglobin. 31. Describe the Bohr effect. 32. List the normal values of arterial and venous oxygen tensions and saturations. 33. Give PaO 2 calculate the oxygen content when the hemoglobin concentration is known. 34. Define hypoxia and hypoxemia, list common causes, and determine the severity when given PaO 2 values. 35. Describe the various mechanisms of carbon dioxide transport. 36. Summarize the Haldane effect. 37. Describe the effect of carbon dioxide on the acid base status of the patient. 38. Classify the acid base status of blood when given ph and PaCO 2 values. 39. Describe the identify the mechanism of compensation for acid base derangements.
73 40. Given levels of VO 2 and VCO 2 calculate the respiratory quotient. 41. Explain how the respiratory quotient affects the need for ventilation. 42. Calculate the A-aDO 2 and relate its value to impairment of the cardiopulmonary systems. 43. Compare the use of A-aDO 2 to the FiO 2 / PaO 2 ratio and Pa/aO 2 ratios. 44. List the components of the medullary and pontine respiratory centers and describe their interaction in controlling ventilatory drive. 45. Describe the mechanism of the central chemoreceptors and relate their function in normal and abnormal breathing patterns. 46. Describe the influence of the cerebrum over ventilation. 47. Locate and describe the function of the peripheral chemoreceptors. 48. Describe the effects of the various reflexes on breathing. 49. Recognize common abnormal breathing patterns.
74 TOPICAL OUTLINE: Pulmonary Pathophysiology I. Infectious Pneumonias A. Etiologies B. Susceptibilities C. Diagnostic techniques D. Clinical manifestations E. Pathology F. Treatment II. Asthma A. Etiology B. Pathology C. Biochemical reactions D. Clinical manifestations E. Prognosis F. Treatments III. Chronic Obstructive Pulmonary Diseases A. Definitions B. Etiologies C. Pathology D. Clinical manifestations E. Prognosis F. Treatment G. Rehabilitation IV. Adult Respiratory Distress Syndrome
75 A. Definition B. Etiologies C. Pathogenesis D. Clinical manifestations E. Diagnostic techniques F. Treatment G. Sequellae H. Prognosis V. Pulmonary Embolism A. Etiologies B. Clinical manifestations C. Diagnostic techniques D. Treatment E. Prognosis VI. Pulmonary Hypertension A. Definition B. Etiologies C. Clinical manifestations D. Treatment E. Prognosis VII. Hypersensitivity Pneumonitis A. Hypersensitivity reaction types B. Etiologies C. Clinical manifestations D. Treatment E. Pathology F. Prognosis VIII. Pulmonary Tuberculosis A. Etiology B. Pathology C. Clinical manifestations D. Diagnostic techniques E. Chemotherapy F. Control G. Complications H. Prognosis
76 IX. Pulmonary Fungus Diseases A. Etiologies B. Pathology C. Clinical manifestations D. Treatments X. Bronchiectasis A. Etiology B. Diagnostic techniques C. Pathology D. Clinical manifestations E. Treatment XI. Lung Abscess A. Etiologies B. Pathology C. Clinical manifestations D. Treatment XII. Pleural Effusions A. Etiologies B. Treatment C. Clinical manifestations XIII. Pneumothorax and Pneumomediastinum A. Pathogenesis B. Clinical manifestations C. Treatment D. Precautions XIV. Pulmonary Neoplasms A. Types B. Incidence C. Clinical manifestations D. Treatments E. Prognosis F. Post-operative care
77 XV. Interstitial Pneumonias A. Types B. Etiologies C. Pathology D. Treatment E. Clinical manifestations XVI. Pneumoconioses A. Types B. Etiologies C. Diagnostic techniques D. Treatment E. Rehabilitation XVII. Connective Tissue Diseases A. Types B. Etiologies C. Treatment D. Clinical manifestations XVIII. Myasthenia Gravis A. Etiology B. Clinical manifestations C. Monitoring D. Treatment XIX. Diseases Affecting Control of Ventilation A. Etiologies B. Clinical manifestations C. Treatments XX. Myocardial Infarction and Congestive Heart Failure A. Etiologies B. Clinical manifestations C. Treatments D. Prognosis
78 TOPICAL OUTLINE: CARDIOPULMONARY PATHOPHYSIOLOGY I. Cardiovascular Pathology A. Myocardial Infarction B. Congestive Heart Failure II. Obstructive Pulmonary Disease A. Bronchitis B. Emphysema C. Asthma D. Cystic Fibrosis E. Bronchiectasis
79 III. Infectious Diseases A. Pneumonia B. Pulmonary Fungus Disease C. Tuberculosis D. Lung Abcess IV. Restrictive Lung Diseases A. Sarcoidosis B. Pneumonitis C. Rheumatoid Lung Diseases D. Lung Abcess V. Pulmonary Vascular Diseases A. Pulmonary Emboli B. Pulmonary Hypertension C. Cor Pulmonale VI. Conditions of Thoracic Cage and Pleura A. Pneumothorax B. Pleural Effusion C. Kyphoscoliosis VII. Lung cancer A. Primary B. Metastatic VIII. Environmental Lung Diseases A. Pneumoconiosis B. Noxious Gas Inhalation IX. Neuromuscular Diseases and Disorders of Respiratory Control A. Guillian Barre' B. Myasthenia Gravis C. Polio D. Sleep Apnea and Hypoventilation E. Paralysis
80 F. Intracranial Pressure X. Trauma and Surgery of the Chest A. Thoracic Surgery B. Abdominal Surgery C. Atelectasis D. Flair chest E. Lung contusion INSTRUCTIONAL OBJECTIVES CARDIOPULMONARY PATHOPHYSIOLOGY Upon completion of appropriate units of instruction, the student will demonstrate on examination the ability to:
81 1. Outline the factors which pre-dispose a patient to the development of myocardial infarction. 2. List the etiologies of myocardial infarction. 3. Describe the clinical manifestations of myocardial infarction. 4. Describe the pathogenesis and manifestations of congestive heart failure. 5. List the common treatments of MI and CHF. 6. Recognize the signs and symptoms of cardiopulmonary arrest. 7. recognize the signs and symptoms of cardiovascular decompensation. 8. List the diseases commonly associated with COPD. 9. List the pre-disposing factors for COPD. 10. Differentiate the pathology and clinical symptomatology of patients with predominately chronic bronchitis versus emphysema. 11. Compare and contrast centrilobular versus panlobular emphysema. 12. Outline and justify the treatments of COPD. 13. Describe the impact of COPD on the patient, family and society. 14. Describe the pathogenesis and prognosis of COPD. 15. Describe the etiology and pathophysiology of bronchiectasis. 16. Describe the treatment and prognosis of bronchiectasis. 17. Describe the pathogenesis of cystic fibrosis and differentiate its treatment compared to other chronic obstructive diseases. 18. Recognize and delineate the special needs of the patient with cystic fibrosis. 19. Explain the role of pulmonary rehabilitation in chronic obstructive pulmonary diseases. 20. Outline the etiology and pathophysiology of asthma.
82 21. Describe the cellular events that take place during an asthma attack and list the chemical mediators of bronchospasm. 22. Justify the treatments of asthma. 23. Differentiate between the various common infectious pneumonias with regard to: causative organism, clinical manifestations, pathogenesis, and prognosis. 24. Outline the various treatments for pneumonia. 25. List the most common pulmonary fungus diseases and their causative organism, differentiating their likely sources to include: histoplasmosis, coccidioidomycosis, blastomycosis, and candidiasis. 26. Describe the pathophysiology of pulmonary fungus diseases. 27. List the treatments of pulmonary fungus diseases. 28. Outline the pathogenesis and manifestations of tuberculosis. 29. List the treatments of tuberculosis. 30. Describe the special requirements of infection control with tuberculosis patients in the hospital or in the community. 31. Describe the special requirements for treatment of lung abscess. 32. List factors pre-disposing to lung abscess formation and its prognosis. 33. Summarize the pathophysiology of sarcoidosis. 34. Describe the clinical manifestations of sarcoidosis and its management. 35. List the causes of hypersensitivity pneumonitis. 36. Describe the pathology and clinical manifestations of hypersensitivity pneumonitis. 37. List the treatments of hypersensitivity pneumonitis. 38. Describe the pathophysiology and clinical manifestations of common rheumatoid lung diseases. 39. List major etiologies of the Adult Respiratory Distress Syndrome.
83 40. Describe the clinical manifestations of ARDS. 41. Outline the treatment of ARDS and its prognosis. 42. List factors which pre-dispose a patient to pulmonary embolic disease. 43. Describe the clinical manifestations of pulmonary emboli. 44. Outline the treatment of pulmonary emboli. 45. Describe the etiologies, manifestations, and treatment of pleural effusions. 46. List common etiologies of pleural effusions. 47. List the clinical manifestations and treatment of pleural effusions. 48. List the common causes of pneumothorax and describe its treatment. 49. Describe the components and function of common chest drainage systems. 50. Recognize the signs and symptoms and special treatment considerations of a patient with pneumothorax. 51. Outline the occurrence etiology, treatment, and prognosis of common pulmonary neoplasms. 52. Describe the techniques used in the treatment and diagnosis of pulmonary neoplasms. 53. Describe the etiologies, clinical manifestations, and treatment of interstitial pneumonitis. 54. Explain the etiologies and pathogenesis of the more common pneumoconiosis. 55. Define black lung and coal workers pneumoconiosis. 56. Describe the methods of decreasing the incidence of pneumoconiosis. 57. Outline the treatment of pneumoconiosis. 58. Describe the etiology and clinical manifestations of Myasthenia Gravis. 59. Summarize the special requirements of respiratory monitoring for the patient with Myasthenia Gravis.
84 60. Outline the pharmacologic and respiratory treatment of Myasthenia Gravis. 61. Explain the pharmacologic treatment of muscarinic crisis. 62. Describe the monitoring and necessary support for patients with Guillain Barre' Syndrome. 63. Describe the pathophysiology of Guillain Barre' Syndrome. 64. List the pre-disposing and complicating factors associated with the various forms of sleep apnea and hypoventilation. 65. Summarize the methods of diagnosis and treatment for the sleep apnea syndromes. 66. Describe the pathophysiology and treatment of polio. 67. Explain the special complications and needs of patients with respiratory muscle paralysis. 68. Relate the role of ventilation in control of intracranial pressure. 69. Describe the special considerations of providing respiratory care to neurosurgical patients. 70. Summarize the effects of thoracic and abdominal surgery on the patient s pulmonary status. 71. Outline the effects of the various modes of respiratory care in preventing and treating postoperative pulmonary complications. 72. List the clinical signs and symptoms of atelectasis. 73. Describe the pathophysiology, clinical manifestations, and treatment of pulmonary aspiration, including foreign body, gastric contents, and hydrocarbons. 74. Define the terms: flail chest and lung contusion. Outline the pathophysiology and treatment of these conditions.
85 TOPICAL OUTLINE RSP MECHANICAL VENTILATION TECHNOLOGY & MANAGEMENT I. TERMINOLOGY A. Modes B. Cycling Mechanisms C. Drive Mechanisms II. VENTILATOR CLASSIFICATION SYSTEM A. Bennett B. Bird IV. TIME CYCLED VENTILATORS A. Rotary Drive B. Pneumatically Powdered Electrically Controlled V. VOLUME CYCLED VENTILATORS
86 A. Bellows Type B. Fluidic C. Microprocessor Controlled D. Portable Home Care Type VI. MANUAL RESUSCITATORS A. Types B. Use TOPICAL OUTLINE: RSP MECHANICAL VENTILATION TECHNOLOGY & MANAGEMENT I. Terminology A. Modes B. Cycling Mechanisms C. Drive Mechanisms II. Ventilator Classification System A. Bennett B. Bird III. Time Cycles Ventilators A. Rotary Drive B. Pneumatically Powered Electrically Controlled
87 IV. Volume Cycled Ventilators A. Bellows Type B. Fluidic C. Microprocessor Controlled D. Portable Home Care Type V. Manual Resuscitators A. Types B. Uses INSTRUCTIONAL OBJECTIVES RSP MECHANICAL VENTILATION TECHNOLOGY & MANAGEMENT Upon completion of appropriate units of instruction, the student will demonstrate on examination the ability to: 1. Describe the characteristics of the various modes of mechanical ventilation and recognize their pressure curves. 2. Explain the different cycling mechanisms (pressure, volume, time, flow) and describe the variability of their effects in ventilating patients. 3. Explain the classification system used to describe mechanical ventilators.
88 4. Classify the Bird MK VII ventilator. 5. Explain, in detail, the function of the Bird MK VII and its component parts. 6. Describe the effects of each of the controls of the Bird ventilator with respect to ventilation, oxygenation, and interrelationship with other controls. 7. Classify the Bennett PR 2 ventilator. 8. Describe the function of the component parts of the Bennett PR 2 and the interrelationship of its controls. 9. Classify and explain the mechanism of a representative electrically powered, time cycled, rotary drive, piston type ventilator, specified by the program (example: Emerson 3PV, IMV). 10. Classify and explain the mechanism of at least one electrically powered, compressor driven, bellows type, double circuit ventilator, specified by the program (example: Ma-1, MA-2, Ohio CCV2). 11. Define fluidics and describe its use in mechanical ventilators. 12. Describe the coanda effect. 13. Explain the function of common fluidic devices. 14. Classify and explain the mechanism of a representative, fluidically controlled mechanical ventilator, specified by the program (example: Monaghan). 15. Classify and explain the mechanism of at least tow pneumatically powered, electrically controlled, adult mechanical ventilators, specified by the program (example: Bear 1 & 2, Servo 900C). 16. Classify and explain the mechanism of at least one microprocessor controlled, adult mechanical ventilator, specified by the program (example: Bear V, Bennett 7200, Hamilton, Engstrom Erica). 17. Describe the mechanism and explain the use of a representative, electrically powered portable ventilator commonly used by home bound patients. 18. List performance characteristics of commonly used manual resuscitators. 19. Illustrate and explain the function of representative manual resuscitators.
89 20. List criteria for verifying adequate function of manual resuscitators. 21. Describe the proper use of manual resuscitators. 22. Explain the importance of periodic monitoring of technical performance of mechanical ventilators. 23. Outline a procedure for verifying function of mechanical ventilators. 24. Given a description of a malfunctioning mechanical ventilator, recognize likely causes of the malfunction and describe the role of the technician in correcting it. RSP MECHANICAL VENTILATION TECHNOLOGY & MANAGEMENT Ventilator Maintenance REFERENCE: Clinical Application of Respiratory Care, Shapiro, Chapter 20
90 PERFORMANCE OBJECTIVES: 1. Define the terminology used in ventilator care. 2. Recognize the ventilator used by reading pressure curves. 3. Discuss the different cycling mechanisms of mechanical ventilators and the variability of ventilator parameters while using these. 4. List the ventilator parameters which are used and monitored in ventilator care. 5. When given blood gas parameters for a patient, discuss changes which should be made in the ventilator parameters. Course Competencies: 1. List the indications for mechanical ventilation. 2. List and explain the causes and effects of respiratory failure. 3. Define the terminology of mechanical ventilation. 4. Provide a rationale for ventilator commitment. 5. Describe the hemodynamic effects of mechanical ventilation. 6. List the factors which must be optimized prior to weaning. 7. Discuss the psychological impact of mechanical ventilator on the patient and the family. 8. Knows various techniques, indications, contraindications of weaning. 9. List the parameters which must be monitored in mechanical ventilation. 10. Describe the various methods of mechanical ventilation, and give criteria. 11. Recognize the ventilator mode by reading pressure and flow patterns. 12. Discuss the different cycling mechanisms of mechanical ventilators, and the variability of ventilator parameters while using these.
91 TOPICAL OUTLINE: RSP MECHANICAL VENTILATION TECHNOLOGY & MANAGEMENT I. Indications A. Respiratory Failure B. Ventilatory Failure C. Cardiopulmonary Reserve D. Parameters/Measurements II. Goals of Mechanical Ventilation A. Desired Parameters B. Effects IV. IV. Complications Methods A. Modes B. Parameters 1. Volume 2. Flow 3. Rate 4. Pressures C. Special Methods 1. PEEP 2. CPAP D. Modification V. Monitoring A. Volume B. Pressures C. Compliance D. Resistance E. FiO 2 F. Alarm Systems G. Recording and Reporting VI. Weaning
92 A. Methods B. Monitoring C. Special Considerations INSTRUCTIONAL OBJECTIVES RSP MECHANICAL VENTILATION TECHNOLOGY & MANAGEMENT Upon completion of appropriate units of instruction, the student will demonstrate on examination the ability to: 1. Define critically ill. 2. Differentiate between respiratory and ventilatory failure. 3. List common causes of respiratory and ventilatory failure. 4. Recognize the signs and symptoms and respiratory and ventilatory failure. 5. Outline methods of assessing cardiopulmonary reserve. 6. List the indications for mechanical ventilation. 7. List the goals of mechanical ventilation. 8. Explain the importance of early ventilator commitment. 9. Identify the moral and ethical problems associated with life support systems. 10. Delineate the sequence of steps in ventilator commitment. 11. Outline the use of and special considerations of the various modes of mechanical ventilation including: control, assist, assist-control, IMV, SIMV, IDV, EMMV, pressure support. 12. Describe the physiologic effects and hazards of mechanical ventilation. 13. Describe the psychological impact of mechanical ventilation. 14. Summarize the use of PEEP including indications, contraindications, effects, and hazards. 15. Select the optimal PEEP level for a patient based on physiologic response. 16. List the indications, contraindications, and hazards of CPAP.
93 17. Describe the application of CPAP and its monitoring. 18. Given simulated or common clinical situations, determine changes to be made in mechanical ventilation modes or parameters to restore blood gas values or other physiologic responses to appropriate levels. 19. List parameters that should be monitored during the course of mechanical ventilation and describe the significance of those measurements. 20. Calculate static compliance and dynamic characteristics of a mechanical ventilation patient. 21. Calculate and correct for lost volume due to compression in the ventilator circuitry. 22. Determine safe limits for alarms used during mechanical ventilation. 23. Identify the parameters to be measured in monitoring the patient s physiologic response to mechanical ventilation. 24. List the indications for weaning from mechanical ventilation. 25. List the physiologic factors which must be optimized prior to successful weaning from mechanical ventilation. 26. Describe the procedure and special considerations for conventional weaning techniques. 27. Summarize the use of IMV and associated techniques for weaning and describe the procedures used. 28. Explain special considerations for weaning from PEEP and high oxygen concentrations. 29. List the steps to be accomplished in weaning.
94 TOPICAL OUTLINE: RSP MECHANICAL VENTILATION TECHNOLOGY & MANAGEMENT I. Assessment of Cardiopulmonary Reserve II. Respiratory Failure A. Causes B. Effects III. IV. Mechanical Ventilation Terminology Pressure Patterns V. Flow Patterns VI. VII. VIII. Ventilation Commitment Effects of Mechanical Ventilation Weaning from the Mechanical Ventilator PERFORMANCE OBJECTIVES: Upon completion of this unit, the student will demonstrate on examination, the ability to:
95 1. Define critically ill. 2. Describe how and why to assess mechanical pulmonary reserve. 3. List normal and abnormal levels of: a. tidal volume b. respiratory rate c. I:E ratio d. Vital capacity e. Negative inspiratory force f. Dead space and V D /V T 4. Describe the methods of assessing the cardiovascular reserve. 5. List and describe normal and abnormal limits of: a. EKG b. blood pressure c. pre-load and after-load d. central venous pressure e. pulmonary artery pressure f. pulmonary capillary wedge pressure g. 6. Differentiate between primary and secondary (relative) hypovolemia. 7. List the clinical signs used to assess perfusion. 8. Discuss the importance of blood constituents, and micro-circulation in relation to perfusion. 9. Assess the levels of gas exchange and reserve when given blood gas parameters. 10. List the normal and critical levels of blood gas parameters. 11. When given a clinical description of a patient s status in relation to parameters of cardiopulmonary reserve, make a decision as to need for cardiovascular or mechanical pulmonary support.
96 RSP MECHANICAL VENTILATION TECHNOLOGY & MANAGEMENT Ventilator Commitment PERFORMANCE OBJECTIVES: Upon completion of this unit, the student will demonstrate on examination, the ability to: 1. Discuss the importance of early ventilator commitment. 2. List the goals of mechanical ventilation. 3. List the indications for mechanical ventilation. 4. Describe moral and ethical problems associated with mechanical ventilators and life-support systems. 5. Discuss the five steps of ventilator commitment as listed by Shapiro.
97 INSTRUCTIONAL OBJECTIVES RSP 204 CARDIOPULMONARY DIAGNOSTICS TRANSTRACHEAL ASPIRATION AND OXYGEN THERAPY Upon completion of appropriate units of instruction, the student will demonstrate on examination the ability to: 1. List and explain the indications for transtracheal aspiration. 2. List the equipment needed to perform transtracheal aspiration and oxygen therapy.
98 3. Explain the procedure for insertion of a transtracheal catheter. 4. Describe the uses of a transtracheal catheter. 5. List the hazards and complications of transtracheal catheter insertion. INSTRUCTIONAL OBJECTIVES RSP 204 CARDIOPULMONARY DIAGNOSTICS BRONCHOSCOPY
99 Upon completion of appropriate units of instruction, the student will demonstrate on examination the ability to: 1. Explain the diagnostic and therapeutic uses of rigid and fiberoptic bronchoscopy. 2. Describe the advantages and disadvantages of rigid and fiberoptic bronchoscopy. 3. Explain the procedure of rigid and fiberoptic bronchoscopy. 4. On an illustration, identify and label the parts of a fiberoptic bronchoscope. 5. Identify the hazards and complications of bronchoscopy. 6. Explain the therapeutic treatment for each of the hazards and complications of bronchoscopy. INSTRUCTIONAL OBJECTIVES
100 RSP 204 CARDIOPULMONARY DIAGNOSTICS THORACENTESIS AND PLEURAL CHEST TUBES Upon completion of appropriate units of instruction, the student will demonstrate on examination the ability to: 1. Anatomy and physiology review of the pleural space. 2. Describe the optimal positioning of a client for a thoracentesis. 3. Explain the procedure of a thoracentesis. 4. List the signs and symptoms that would indicate the need for a thoracentesis. 5. Define the following terms; empyema, chyle, loculated, purulent, mucopurulent, serosanguinous. 6. Differentiate characteristics of transudative and exudative effusions. 7. List the disease processes that cause transudative and exudative effusions. 8. List abnormal conditions requiring chest tube placement. 9. Describe the anatomical location of chest tube insertion. 10. Describe the use of chest tube drainage systems. 11. Describe the function of a one bottle/chamber drainage system. 12. Identify the bottles used in a two bottle/chamber drainage system. 13. Explain when it is recommended to use a two bottle/chamber system over a one bottle system. 14. Identify the bottles used in a three bottle/chamber suction drainage system and describe their function. 15. Identify and correct various problems that occur when using a one, two, and three bottle/chamber drainage system.
101 INSTRUCTIONAL OBJECTIVES RSP 204 CARDIOPULMONARY DIAGNOSTICS ARTERIAL LINE MANAGEMENT Upon completion of appropriate units of instruction, the student will demonstrate on examination the ability to: 1. Explain the procedure of performing an Allen test. 2. Explain other procedures that provide accurate assessment of ulnar collateral blood flow to the hand. 3. Identify advantages and disadvantages associated with percutaneous cannulation of the following arterial sites; radial artery, brachial artery, axillary artery, and the femoral artery. 4. Identify and name the anatomic locations of the arteries of the arm. 5. Explain the procedure for percutaneous cannulation of the radial artery. 6. Explain specific complications associated with percutaneous cannulation of arterial insertion sites. 7. Explain what physiologic events occur and their relationship with arterial systole and arterial diastole pressures. 8. Define and calculate stroke volume. 9. Calculate Mean Arterial Pressure (MAP) when given cardiac output (CO) and systemic vascular resistance (SVR). 10. Differentiate between arterial pressures being measured via a transducer vs an anaeroid manometer. 11. Explain the procedure of setting up an arterial pressure system using a transducer and pressure IV bag. 12. Identify and label a normal arterial pressure waveform.
102 13. Identify and label an abnormal arterial pressure waveform demonstrating marked reduction in stroke volume and pulse pressure associated with a run of PVC s aortic stenosis, hypertrophic cardiomyopathy, aortic insufficiency. 14. Identify problems and causes, and give prevention techniques and treatment of problems encountered with arterial catheters. 15. Identify signs and symptoms of infection of arterial sites and list preventive techniques and treatment. 16. Explain the steps for obtaining arterial blood from an arterial catheter. INSTRUCTIONAL OBJECTIVES RSP 207 PULMONARY REHAB/HOME CARE SLEEP APNEA Upon completion of appropriate units of instruction, the student will demonstrate on examination the ability to: 1. Explain the physiologic effects of rapid eye movement (REM) and non-rem (NREM) sleep. 2. Explain the physiologic changes in respiration during sleep. 3. Explain the influence of chemical stimuli during wakefulness and sleep. 4. Define the three classifications of sleep apnea. 1. central sleep apnea 2. obstructive sleep apnea 3. mixed disorder sleep apnea 5. Explain the clinical features, diagnosis, and treatment of central, obstructive, and mixed disorder sleep apnea.
103 INSTRUCTIONAL OBJECTIVES RSP 204 CARDIOPULMONARY DIAGNOSTICS TRANSPORTS Upon completion of appropriate units of instruction, the student will demonstrate on examination the ability to: 1. Outline field triage criteria for trauma patients. 2. Describe the criteria used in patient assessment using the Glascow Coma Scale. 3. Describe the physiologic effects of altitude during aviation transport. 4. Predict in-flight arterial oxygen tension from cabin altitude and preflight arterial oxygen tension using a nomogram. 5. Explain the operational characteristics and features of the following transports ventilators: 1. Impact Uni-vent 2. Hamilton MAX 3. Pneu-Pac 2-R or HARV 4. Auto Vent 2000 and Stein Gates Omni Vent 6. Define the terms capnometry, capnogram and capnography. List clinical situations in which they are useful.
104 7. Describe the basic components of a nondispersive double-beam, positive-filter infrared CO2 detector. 8. Describe the basic components of a single-beam, negative-filter infrared CO2 detector. 9. Identify and label, on an illustration, a normal capnogram waveform. 10. List advantages and disadvantages of capnometry. INSTRUCTIONAL OBJECTIVES RSP 204 CARDIOPULMONARY DIAGNOSTICS ELECTROCARDIOGRAM INTERPRETATION Upon completion of appropriate units of instruction, the student will demonstrate on examination the ability to: 1. Identify and label, on an illustration, the electro conduction system of the heart. 2. Describe and label the electrophysiological events represented by the normal sinus electrocardiogram. 3. Explain the ten features that should be examined in the interpretation of an electrocardiogram. 4. Identify and label, on an illustration, the following ECG tracings: 1. normal sinus rhythm 2. sinus arrhythmia 3. sinus tachycardia 4. sinus bradycardia
105 5. paroxysmal atrial tachycardia 6. atrial flutter 7. atrial fibrillation 8. first degree atrioventricular (AV) block 9. second degree AV block Mobitz type I (wenckebach) 10. second degree AV block Mobitz type II 11. third degree (complete) AV block 12. premature ventricular contraction (PVC) 13. ventricular tachycardia 14. ventricular fibrillation 5. Explain the procedure and indications for cardiovension. 6. Explain the procedure and indications for defibrillation. 7. Explain the hazards and complications of cardioversion and defibrillation. TOPICAL OUTLINE RSP 206 INTRODUCTION TO CRITICAL CARE MANAGEMENT I. Airway Management A. Upper airway anatomy. B. Airway obstruction. C. Artificial airways. D. Endotracheal intubation/extubation E. Cuff management. F. Tracheostomy tubes and care. G. Suctioning. H. Manual resuscitators II. Transtracheal Aspiration and Oxygen Therapy A. Indications. B. Equipment needed. C. Transtracheal oxygen catheter placement.
106 D. Procedure for transtracheal aspiration. III. Bronchoscopy A. Indications. B. Rigid vs Fiberoptic 1. advantages 2. disadvantages C. Bronchoscopy procedure D. Risks IV. Thoracentesis and Pleural Chest Tubes A. Indications. B. Procedures. 1. thoracentesis 2. pleural chest tube C. Pleural drainage systems. D. Three chamber vs four chamber. E. Troubleshooting complications. V. Arterial Lines VI. VII. A. Arterial access. B. Physiologic review. C. Clinical applications. D. Intra-arterial pressure measurement. E. Waveforms. F. Complications and troubleshooting. G. Prevention of infection. H. Arterial blood sampling. Sleep Apnea A. Physiology of sleep. B. Respiratory physiologic process during sleep. C. Obstructive sleep apnea. D. Central sleep apnea. Transports A. Prehospital Respiratory Care. B. Transport ventilation. C. Capnography VIII. Electrocardiogram interpretation A. Electroconduction system of the heart. B. EKG interpretation
107 C. Cardioversion D. Defibrillation INSTRUCTIONAL OBJECTIVES RSP 204 CARDIOPULMONARY DIAGNOSTICS AIRWAY MANAGEMENT
108 Upon completion of appropriate units of instruction, the student will demonstrate on examination the ability to: 1. Define the role of the Respiratory Therapist in airway management. 2. Locate and identify the anatomical structures of the upper airway. 3. Explain the anatomical structures and their effects on airway maintenance. 4. List the causes of airway obstruction. 5. List the signs and circumstantial signs of airway obstruction. 6. Discuss the development and use of the Heimlich maneuver. 7. List the specific steps in performing the Heimlich maneuver with the victim standing, sitting and lying. 8. Discuss the use of artificial airways in the prevention of airway obstruction. 9. List the general indications for artificial airways. 10. Name the general classifications or artificial airways. 11. Identify the advantages and problems associated with artificial airways. 12. Explain the proper insertion techniques of the oropharyngeal and nasopharyngeal airway. 13. Explain the procedure in the selection of an artificial airway. 14. Identify parts of an endotracheal tube. 15. Identify the parts and list the indications for the double-channeled endotracheal tube. 16. Identify the different types of endotracheal tube cuffs and explain how they are classified according to volume and pressure. 17. Discuss and explain the techniques for performing the minimal occlusive volume (MOV), minimal leak volume (MLV) and actual measurement using a pressure manometer. 18. List the hazards of tracheal tubes and cuffs.
109 19. Discuss what measures can be done to prevent tracheal damage. 20. Discuss the composition of tracheal tubes. 21. Explain the steps involved in determining the correct size tracheal tube. 22. Identify and list the equipment needed for tracheal intubation. 23. Differentiate between the use of various laryngoscope blades. 24. On an illustration, identify anatomical landmarks used in endotracheal intubation. 25. Discuss the process of endotracheal intubation. 26. List the hazards of oral and nasal intubation. 27. List the potential results of improper airway insertion techniques during endotracheal intubation. 28. List the methods and criteria of monitoring, securing and verifying the position of oral and nasal endotracheal tubes. 29. Identify the hazards of excessive cuff pressure. 30. List the rationales and hazards of a tracheotomy. 31. Identify the parts of a tracheostomy tube. 32. List and identify the various styles of tracheostomy tubes. 33. Describe the techniques of tracheostomy tube care. 34. List the indications, contraindications, and hazards of endotracheal suctioning. 35. List and explain the different types of endotracheal suctioning techniques. 36. List the signs and symptoms expected as a result of complications during airway suctioning. 37. Describe the method of monitoring the patient being suctioned for safety and effectiveness. 38. List criteria indicating that suctioning is effective. 39. Describe the use of a sterile trap for sputum collection during airway suctioning.
110 40. List the pressures and time used when suctioning adults, infants, and children. 41. Identify appropriately sized suction catheters. 42. List the standards for the design and construction of manual resuscitators set by the American Society for Testing and Materials (ASTM). 43. Identify the various brands of manual resuscitators and the type of patient valve and pressure relief valve that each incorporate into their system. 44. List the indications for the use of manual resuscitators. 45. Identify and correct a malfunction of a manual resuscitator when given a clinical situation.
111 Appendix E
112 ST. MARY ' S/MARSHALL UNIVERSITY COOPERATIVE B.S. RESPIRATORY CARE PROGRAM DATE: COURSE EVALUATION COURSE: This evaluation is designed for the student to evaluate the course and the instructors. Use a number 2 pencil for marking the appropriate circle on the computer answer sheet. If an item does not apply, leave the answer sheet blank for that item. You are also asked to provide comments for each section. Please explain your reasons for rating an item (instructor, unit, etc.), especially if you had a problem or concern. Use the space provided on this evaluation sheet for your comments. Use the following rating scale (A-E) to rate each item. A Strongly Agree B Agree C Neutral D Disagree E Strongly Disagree EVALUATE THE FOLLOWING COURSE RELATED ITEMS, USING TIM ABOVE SCALE. PUT YOUR COMMENTS IN THE DESIGNATED AREA OF THE SCORING SHEET. 1. This course had clearly stated course objectives. 2. This course had achievable course objectives. 3. Course assignments are relevant to course objectives. 4. The grading method is appropriate for course content. 5. There is sufficient time in class for questions and discussions. 6. Exams accurately assess what I have learned in this course. 7. The course content built on my previous knowledge. 8. Lecture information is adequately supplemented by other work. 9. The course content facilitated the development of critical thinking (questioning, reasoning, analyzing, etc.) 10. The course facilitated the development of my communication skills (verbal, non-verbal). 11. The course content enhanced my knowledge and skills necessary to provide patient care. 12. The course content will assist me in providing service to the community and the profession. 13. The syllabus provided guidance for my learning. 14. The syllabus identified objectives, course content and teaching methods. 15. The syllabus described evaluation methods. 16. The course content enhanced my ability to be a caring professional.
113 ST. MARY ' S/MARSHALL UNIVERSITY COOPERATIVE B.S. RESPIRATORY CARE PROGRAM COURSE EVALUATION DATE: COURSE: This evaluation is designed for the student to evaluate the course and the instructors. Use a number 2 pencil for marking the appropriate circle on the computer answer sheet. If an item does not apply, leave the answer sheet blank for that item. You are also asked to provide comments for each section. Please explain your reasons for rating an item (instructor, unit, etc.), especially if you had a problem or concern. Use the space provided on this evaluation sheet for your comments. Use the following rating scale (A-E) to rate each item. A Strongly Agree B Agree C Neutral D Disagree E Strongly Disagree INSTRUCTOR PERFORMANCE: Evaluate only those classroom or clinical instructors to which you were assigned. Instructor presented content in a knowledgeable manner. 17. Brent Blevins 18. Chuck Zuhars Instructor presented content in an organized manner. 19. Brent Blevins 20. Chuck Zuhars Instructor demonstrated knowledge in assigned clinical area. 21. Brent Blevins 22. Chuck Zuhars The instructor provided additional explanation or resource material when requested Brent Blevins 24. Chuck Zuhars The instructor provided additional assistance with clinical aspects of the course as needed. 25. Brent Blevins 26. Chuck Zuhars Written/verbal feedback in the classroom/clinical from instructor was beneficial. 27. Brent Blevins 28. Chuck Zuhars Instructor promoted an environment of learning. 29. Brent Blevins 30. Chuck Zuhars Comment: Identify the instructor (by name) and provide any pertinent comments regarding any of the above topics.
114 DATE: ST. MARY ' S/MARSHALL UNIVERSITY COOPERATIVE B.S. RESPIRATORY CARE PROGRAM COURSE EVALUATION COURSE: This evaluation is designed for the student to evaluate the course and the instructors. Use a number 2 pencil for marking the appropriate circle on the computer answer sheet. If an item does not apply, leave the answer sheet blank for that item. You are also asked to provide comments for each section. Please explain your reasons for rating an item (instructor, unit, etc.), especially if you had a problem or concern. Use the space provided on this evaluation sheet for your comments. Use the following rating scale (A-E) to rate each item. A Strongly Agree B Agree C Neutral D Disagree E Strongly Disagree CLINICAL ROTATIONS/AGENCY: Evaluate only those units to which you actually were assigned. Clinical rotations were appropriate for application of course content. 45. St. Mary s Medical Center 46. Holzer Medical Center Comment: Identify the clinical experience by number above and provide pertinent comments: 47. Student was able to collaborate with staff on assigned unit in an effective manner. 48. Staff modeled the professional respiratory therapists role. 49. Staff members on assigned units were helpful. Comment: Please make comments regarding staff on units by first identifying the unit or agency and then provide any pertinent comments: TEXTBOOKS: 50. The textbook was useful in understanding classroom presentation and clinical situations Comment: Identify the text by number above and then provide any pertinent comments: LEARNING RESOURCES 51. When I needed additional learning resources for this course, the library, Academic Support Center, and/or the computer lab had what I needed. Comment: 52. Instructional aids, such as Power Point presentations, videos, and handouts given by the instructors were beneficial. Comment:
115 DATE: ST. MARY ' S/MARSHALL UNIVERSITY COOPERATIVE BSRT PROGRAM COURSE EVALUATION COURSE: This evaluation is designed for the student to evaluate the course and the instructors. Use a number 2 pencil for marking the appropriate circle on the computer answer sheet. If an item does not apply, leave the answer sheet blank for that item. You are also asked to provide comments for each section. Please explain your reasons for rating an item (instructor, unit, etc.), especially if you had a problem or concern. Use the space provided on this evaluation sheet for your comments. Use the following rating scale (A-E) to rate each item A Strongly Agree B Agree C Neutral D Disagree E Strongly Disagree 53. Classroom, library and laboratory facilities were adequate to meet my learning needs. Comment: 54. What was your advisor's name? Did you find him/her helpful? Yes No If not, explain: 55. Identify the grade that you expected to receive in this course. 10/95 10/99 06/00 03/04 11/05 9/06
116 Appendix F
117 COURSE SYLLABI
118 COURSE NAME: RSP Pharmacology SCHOOL OF RESPIRATORY THERAPY ST. MARY S/MARSHALL UNIVERSITY COURSE CURRICULUM CLASS HOURS: 45 LAB HOURS: 0 PREREQUISITES: Successful completion of program sequence. COURSE DESCRIPTION: This two credit hour course consists of two hours of lecture each week. This course is a presentation of topics related to drug groups commonly used in respiratory therapy; their physiologic mechanisms; pharmacological mode of action; drug doses; pharmacy calculations; and related drug product review. COURSE OBJECTIVES: 1. Gain a thorough understanding of the drug groups used in respiratory therapy practice. 2. Gain a thorough understanding of the mechanism of action of various classes of drugs. 3. Become familiar with various generic and brand names of medications commonly used in respiratory therapy. 4. Become familiar with appropriate adult and pediatric respiratory medication dosages. 5. Gain a thorough understanding of the rational for drug administration. 6. Become familiar with and be able to recognize complications associated with use of various respiratory medications. 7. List contraindications of various classes of respiratory medications. METHODS OF TEACHING: Lecture/Discussion Through the Teaching/Learning Process Exercises to Assist with Problem Solving In-Class Activities Handouts Reference Readings Paper/Pen Examinations
119 COURSE MATERIAL: Required Textbooks: Rau: Respiratory Care Pharmacology, 6 th Ed., Elsevier 2002 Reference and Resource Material: Hill, F.: Respiratory Care Drug Reference, Delmar, Kacmarek, Mack, Dimas: The Essentials of Respiratory Therapy, 4 th Ed., Elsevier 2005 Physicians Desk Reference Wilkins, Stoller, Scanlan: Egan s Fundamentals of Respiratory Care, 8 th Ed., Elsevier 2003 SAFETY PRACTICES: Safety is an important component of respiratory care and technical skills taught throughout the semester. Features of each unit are given below: Unit 1: General Principles of Pharmacology- A general overview of pharmacology is given. Unit 2: Calculating Drug Dosages- The students are instructed how to calculate and administer appropriate dosages for respiratory medication for the adult and pediatric patient. Unit 3: The Central and Peripheral Nervous Systems- The effects of various pharmacological agents on the central and peripheral nervous system is presented. Unit 4: Sympathomimetic Bronchodilators- The generic and trade names, indications, appropriate dosages, contraindications, proper administration, and side effects of sympathomimetic bronchodilators is presented. Unit 5: Parasympatholytic Bronchodilators- The generic and trade names, indications, appropriate dosages, contraindications, proper administration, and side effects of parasympatholytic bronchodilators is presented. Unit 6: Xanthines- The generic and trade names, indications, appropriate dosages, contraindications, proper administration, and side effects of xanthines is presented.
120 Unit 7: Mucus Controlling Agents- The generic and trade names, indications, appropriate dosages, contraindications, proper administration, and side effects of mucus controlling agents is presented. Unit 8: Surfactant Agents- The generic and trade names, indications, appropriate dosages, contraindications, proper administration, and side effects of surfactant agents is presented. Unit 9: Corticosteroids in Respiratory Care- The generic and trade names, indications, appropriate dosages, contraindications, proper administration, and side effects of corticosteriods is presented. Unit 10: Antiasthmatic Aerosol Agents- The generic and trade names, indications, appropriate dosages, contraindications, proper administration, and side effects of antiasthmatic agents is presented. Unit 11: Aerosolized Anti-Infective Agents- The generic and trade names, indications, appropriate dosages, contraindications, proper administration, and side effects of aerosolized anti-infective agents is presented. Unit 12: Anti-Microbial Agents- The generic and trade names, indications, appropriate dosages, contraindications, proper administration, and side effects of anti-microbial agents is presented. Unit 13: Neuromuscular Agents- The generic and trade names, indications, appropriate dosages, contraindications, proper administration, and side effects of neuromuscular agents is presented. Unit 14: Cardiovascular Agents- The generic and trade names, indications, appropriate dosages, contraindications, proper administration, and side effects of various cardiovascular agents is presented. Unit 15: Diuretic Agents- The generic and trade names, indications, appropriate dosages, contraindications, proper administration, and side effects of diuretics is presented..
121 SCHOOL OF RESPIRATORY THERAPY ST. MARY S/MARSHALL UNIVERSITY 12 EVALUATION OF THE STUDENT EVALUATION The purpose of evaluation is to indicate, to some degree, the extent to which the student has learned the concepts presented. Frequent testing will encourage the student to study and learn at a regular and constant pace throughout the course. The teaching-learning process meets the expected outcome goal. Evaluation is also utilized as a learning tool. Questions are designed to stimulate problem solving. The examinations are reviewed to provide feedback and promote discussion. Students who require additional support outside of that given during class hours may set-up personal meetings with the instructor during office hours. Students with math difficulties will be referred to ABE or URG Learning Center for tutoring. 1. Examinations/Quizzes A. Unit Exams B. Quizzes SPECIFIC FACTORS 4 Exams: Each exam is worth 15% of the final grade for a total of 60%. Exams will be approximately 30 questions in length and may include multiple choice, matching, listing, labeling, short answer, and essay style questions. An hour will be given for each unit exam. Quizzes: There will be a total of 15 quizzes administered after the completion of each unit. All quizzes will be averaged to consist of 10% of the final grade Quizzes will be approximately 10 questions in length and questions may include multiple choice, short answer, listing, and labeling. C. Final Examination Final Exam: The Final exam will be comprehensive and may include multiple choice, matching, listing, labeling, short answer, and essay style questions. The final exam will be worth 30% of the final grade. The final exam will be administered during Finals Week. 2. Homework/Classwork
122 It will be the student s responsibility to complete homework/classwork assignments. There are no scheduled homework assignments in this course. However, additional assignments may be given at the instructor s discretion Class Participation: Class participation will include discussions and workgroups. 4. Grading Scale: Theory: Laboratory Skills 93%-100%: A Excellent No lab scheduled for this course. 85%-92%: B Good 76%-84%: C Satisfactory 0%-75%: Failing 5. Final Grade Calculation The factors below will be used to determine the final grade for the course: A. The unit exams are worth 60% of the final grade. The unit quizzes are worth 10% of the final grade. The final exam is worth 30% of the final grade.
123 12 RESPIRATORY THERAPY St. Mary s/marshall University COURSE CURRICULUM COURSE NAME: RSP Introduction to Respiratory Care Instructors: Contact Information: Chuck Zuhars, RRT, M.S. Chris Trotter, RRT, B.A. Chuck Zuhars Chris Trotter Phone: (304) (304) [email protected] [email protected] Office hours : by appointment PREREQUISITES: Successful completion of program sequence COURSE DESCRIPTION: This 2 credit hour course will cover the history of Respiratory Care and our Professional Organization. Emphasis is on exploring the role of the respiratory therapist or technician as a member of the health care team. Ethical and medico-legal dimensions of health care are presented. Basic techniques of patient evaluation are covered. Included are: Chest physical examination, measurement of the vital signs, patient interview and history, evaluation of the chest x-ray, and electrocardiography. COURSE OBJECTIVES: Upon successful completion of this course, the student will: 1. The student will gain a basic understanding of the Respiratory Care Profession including its evolution, medical and professional ethics, and required professional interaction skills. 2. The student will demonstrate comprehension of patient assessment skills to include inspection, percussion, palpation, auscultation, chest radiology, and electrocardiogram procedure and basic interpretation. 3. The student will gain knowledge of infection control procedure, universal precautions, and proper equipment processing.
124 12 Methods of Evaluation: Assignments/course book - 10% Quizzes -10% Exams (2) - 20% Final Exam 20% Lab 20% Attendance 20% Grade Scale points A points B points C points D <60 points F Methods of Teaching: Academic Progress: University Statement on Equality, Tolerance and Affirmative Action: This course consists of weekly lectures and includes a variety other teaching methods (i.e., discussion, simulation, audiovisuals etc.) Information regarding the Student's academic progress in this course will be shared with their Academic Advisor and/or Department Chair. Please indicate by the end of the 2 nd week of the course if you will need accommodations under the Americans with Disabilities Act. Academic Integrity: Course Evaluations: Academic dishonesty includes, but is not limited to, cheating, plagiarism, collusion, the submission for credit of any work or materials that are attributable in whole or in part to another person, taking an examination for another person, and any act designed to give unfair advantage to a student or the attempt to commit such an act. Students will be given the opportunity to evaluate the performance of the instructor and course near the end of the course/semester. When submitting course evaluations students must follow the guidelines provided by the course instructor or department. MEHODS OF TEACHING: Lecture/Discussion through the Teaching/Learning Process Exercises to Assist with Problem Solving In-Class Activities Handouts Reference Readings Paper/Pen Examinations Laboratory Simulations and Exercises
125 12 COURSE MATERIAL: Required Textbooks: Wilkins, Stoller, Scanlan: Egan s Fundamentals of Respiratory Care, 8 th Ed., Elsevier 2003 White, G.C.: Basic Lab Competencies for Respiratory Care, 4 th Ed., Delmar, Reference and Resource Material: Kacmarek, Mack, Dimas: The Essentials of Respiratory Therapy, 4 th Ed., Elsevier 2005 SAFETY PRACTICES: Safety is an important component of respiratory care and technical skills taught throughout the semester.
126 Features of each unit are given below: 12 Unit #1: The Respiratory Care Professional - An overview of the evolution of respiratory therapy is provided. The roles and responsibilities of the respiratory therapist are introduced. The professional and credentialing agencies of respiratory therapy and their functions are defined. An overview of the continuing education requirements and the justification of those requirements are defined. Unit #2: Medical, Legal, and Ethical Issues of Respiratory Care- Various medico-legal aspects of respiratory care are introduced. Included are negligence, malpractice and patient rights. The AARC Code of Ethics is provided as a guideline for therapist behavior. Unit #3: Hospital Procedures- The fundamental operating procedures of a hospital are introduced. This includes: team medicine, record keeping, communication between therapists and other healthcare professionals, communication between therapist and physician, charting procedures, incident reports, and verbal reports. Finally, an overview of appropriate grief responses are provided. Unit #4: Introduction to Patient Assessment The technique of physical assessment is introduced. The patient interview process is detailed. The components of physical assessment are defined. The rationale for palpation, percussion, and auscultation is introduced. The procedure for observation and detailed inspection is given. Normal and abnormal chest physical examination findings are discussed. Unit #5: Patient Assessment, Part 2 The four vital signs are described and normal values given. Basic bedside evaluation of work of breathing and ventilatory reserve is described. The chest radiograph is introduced. Anatomical landmarks are described. Normal and abnormal findings are discussed. Unit #6: Introduction to Medical Laboratory Procedures Basic laboratory values that are significant to the respiratory therapist are discussed. Normal values are provided. A basic overview of infection control techniques is discussed. The respiratory therapist s role in infection control is described.
127 12 Features of each laboratory session is given below: Lab 1: Appropriate professional interaction is demonstrated. Examples of appropriate and inappropriate behavior in the clinical setting will be given. Hospital safety procedure are introduced. The following safety topics are covered: proper body mechanics, responding to hospital emergency codes, and electrical safety. The student will be given time to practice techniques presented in Units 1, 2, and 3. Lab 2: The correct procedure for inspection, palpation, percussion, and auscultation will be demonstrated. Students will be given time to practice techniques presented in Unit 4. Lab 3: Proper procedure for obtaining vital signs will be demonstrated. The correct method for obtaining bedside respiratory parameters will be demonstrated as well. Sample chest radiographs will be presented. The student will be given time to practice techniques presented in 5. Lab 4: Proper infection control techniques will be demonstrated. These include: hand washing, use of personal protective equipment, and proper handling of needles and other sharp instruments. The student will be given time to practice techniques presented in Unit 6.
128 RSP-102 Introduction to Respiratory Care Procedures RESPIRATORY THERAPY ST.MARY S/MARSHALL UNIVERSITY EVALUATION OF THE STUDENT EVALUATION The purpose of evaluation is to indicate, to some degree, the extent to which the student has learned the concepts presented. Frequent testing will encourage the student to study and learn at a regular and constant pace throughout the course. The teaching-learning process meets the expected outcome goal. Evaluation is also utilized as a learning tool. Questions are designed to stimulate problem solving. The examinations are reviewed to provide feedback and promote discussion. Laboratory simulations and exercises will further enhance the learning process through a supervised hands-on approach. Students who require additional support outside of that given during class hours may set-up personal meetings with the instructor during office hours. 1. Examinations/Quizzes SPECIFIC FACTORS A. Unit Examinations: 2 Exams: Each exam is worth 20% of the final grade for a total of 40%. Exams will be approximately 50 questions in length and may include multiple choice, matching, listing, labeling, short answer, and essay style questions. An hour will be given for each unit exam. B. Quizzes Quizzes: There will be a total of 2 quizzes administered. All quizzes will be averaged to consist of 10% of the final grade Quizzes will be approximately 10 questions in length and questions may include multiple choice, short answer, listing, and labeling. C. Final Examination: The Final exam will be comprehensive and may include multiple choice, matching, listing, labeling, short answer, and essay style questions. The final exam will be worth 20% of the final grade. The final exam will be administered during Finals Week. 128
129 RSP-102 Introduction to Respiratory Care Procedures D. Course Notebook: The course book will be turned in at the completion of this class. Your notes will be reviewed for content & correctness. This will equal 10% of your grade. 2. Laboratory Exercise Check-Offs Students will complete 2 laboratory check-offs with the instructor on techniques learned in the course. Each laboratory check-off will be worth 5%, for a total of 10% of the final grade. 3. Homework/Classwork 4. Class Participation: 5. Grading Scale: It will be the student s responsibility to complete homework/classwork assignments. There are no scheduled homework assignments in this course. However, additional assignments may be given at the instructor s discretion. Class participation will include discussions, workgroups, and laboratory exercises. Theory: Laboratory Skills 90%-100%: A Excellent 2: Excellent 80%-89%: B Good 1: Needs Improvement 70%-79%: C Satisfactory 0: Failed to meet the basic 0%-69%: Failing objectives of exercise 129
130 RSP-102 Introduction to Respiratory Care Procedures COURSE OUTLINE Time: TBA Room: hr = 45 hrs/semester WEEK DATE DAY TIME CONTENT INSTRUCTOR 1 5/14/07 Mon 30 MIN Syllabus and questions CZ 45 MIN Unit 1 CZ 5/15/07 Tue 40 Unit 1 CZ 35 Unit 2 CZ 5/16/07 Wed 35 MIN Unit 2 CZ 40 MIN Unit 3 CZ 2 5/22/07 Tue 30 MIN Unit 3 CT 45 MIN Unit 4 CT 5/23/07 Wed 30 MIN QUIZ 1 CT 45 MIN Unit 4 CT 3 5/29/07 Tue 75 MIN Unit 4 CZ CZ/BB 5/30/07 Wed 75 MIN Unit 4 CZ 4 6/04/07 Mon 30 MIN QUIZ 2 CT 45 MIN Unit 4 CT 6/05/07 Tue 75 MIN Unit 4 CT 6/06/07 Wed 75 MIN TEST 1 UNITS 1-4 CT 5 6/11/07 Mon 75 MIN Unit 5 CT 6/12/07 Tue 75 MIN Unit5 CT 130
131 RSP-102 Introduction to Respiratory Care Procedures 6/13/07 Wed 30 MIN QUIZ 3 CZ 45 MIN Unit 6 CZ 6 6/18/07 Mon 75 MIN Unit 6 CZ 6/19/07 Tue 75 MIN Unit 6 CZ 6/20/07 Wed 75 MIN Unit 6 CZ 7 6/25/07 Mon 30 MIN QUIZ 4 CZ 45 MIN Review 6/26/07 Tue 75 MIN TEST 2 Units 5-6 CZ 6/27/07 Wed 75 MIN Review CZ/CT 8 7/02/07 Mon 75 MIN FINAL EXAM UNITS 1 6 CZ/CT 7/03/07 Tue TBA Neo/Peds presentations attendance is extra credit Class of
132 RSP-102 Introduction to Respiratory Care Procedures Student Outcome Goals Essential Content Student References 132
133 RSP-102 Introduction to Respiratory Care Procedures Identify significant developments in the field of respiratory therapy. Describe the role of the respiratory therapist in providing health care. Explain the role of the AARC and NBRC to the respiratory therapist. Explain the effect of licensure. Describe the various levels of employment in respiratory therapy and the necessary examination procedures for the various credentials. Discuss the need for continuing education. Unit 1: The Respiratory Care Professional Lesson 1: Lecture 7 hours (Includes Lab) 1. Evolution of Respiratory Therapy a. Historical developments relating to respiratory therapy b. Developments in the profession of respiratory therapy 2. Roles and responsibilities of the Respiratory Therapist 3. Credentialing and Licensing Process a. The NBRC b. CRT c. RRT d. Ohio License 4. Continuing Education a. Required amount 5. Professional Agencies a. AARC 6. Respiratory Therapy Department Functions a. Chain of Command 7. Respiratory Care Protocols a. Definition Egan s Chapter 1, pp Handout 1-a Prominent Figures in Respiratory Therapy Handout 1-b Historical Developments Respiratory Therapy Unit 2: Medical, Legal, and Ethical Issues in Respiratory Care Recognize and apply current standards of ethical practice for Lecture 6.5 hours (Includes Lab) 1. Ethical Dilemmas of Practice and Code of Ethics a. AARC Code of Ethics 2. Guiding principles of Ethical Decision Making a. Autonomy b. Veracity c. Nonmaleficence d. Beneficence e. Confidentiality f. Justice Egan s Chapter 4, pp Handout 2-a Patient Right Statement
134 RSP-102 Introduction to Respiratory Care Procedures Instructors: Contact Information: Jim Montgomery Jim Montgomery Brent Blevins (304) (304) Chris Trotter Chuck Zuhars (304) (304) Office hours : by appointment COURSE DESCRIPTION: This 3 credit hour course includes three credit hours for lecture. This course will cover the administration of medical gases, humidity and aerosol therapy. Emphasis is placed on the safe handling of medical gases safety in the administration of medical gases. Principles and techniques of therapeutic procedures used in basic respiratory care are covered. Focus will be placed on techniques of chest inflation therapy, chest physical therapy, breathing exercises, and bronchial hygiene. The physiologic effects, indications, and contraindications of each therapy are stressed. Detailed study of the equipment and supplies used in these therapies in included. COURSE OBJECTIVES: Upon successful completion of this course, the student will have demonstrated: 1. A thorough understanding of the physical principles of gases, gas flow and the gas laws. 2. A thorough understanding of the mechanisms for the production, storage, and distribution of medical gases. 3. A thorough understanding of the indications for administration, complications, and contraindications for the administration of medical gases. 4. Knowledge of and basic skills with the following equipment and therapies: a. Intermittent Positive Pressure Ventilation b. Incentive Spirometry c. Aerosol therapy d. Chest Physical Therapy and Postural Drainage 134
135 RSP-102 Introduction to Respiratory Care Procedures e. Bronchial Hygiene Exercises Methods of Evaluation: Assignments/course book 10% Quizzes 15% Exams (3) 45% Final Exam 30% Grade Scale points A points B points C points D <60 points F Methods of Teaching: Academic Progress: University Statement on Equality, Tolerance and Affirmative Action: This course consists of weekly lectures and includes a variety other teaching methods (i.e., discussion, simulation, audiovisuals etc.) Information regarding the Student's academic progress in this course will be shared with their Academic Advisor and/or Department Chair. Please indicate by the end of the 2 nd week of the course if you will need accommodations under the Americans with Disabilities Act. Academic Integrity: Course Evaluations: Academic dishonesty includes, but is not limited to, cheating, plagiarism, collusion, the submission for credit of any work or materials that are attributable in whole or in part to another person, taking an examination for another person, and any act designed to give unfair advantage to a student or the attempt to commit such an act. Students will be given the opportunity to evaluate the performance of the instructor and course near the end of the course/semester. When submitting course evaluations students must follow the guidelines provided by the course instructor or department. 135
136 RSP-102 Introduction to Respiratory Care Procedures COURSE MATERIAL: Required Textbooks: Wilkins, Stoller, Scanlan: Egan s Fundamentals of Respiratory Care, 8 th Ed., Elsevier White, G.C.: Basic Lab Competencies for Respiratory Care, 4 th Ed., Delmar, Cairo & Pilbeam: Mosby s Respiratory Care Equipment, 7 th Ed., Elsevier, Reference and Resource Material: Kacmarek, Mack, Dimas: The Essentials of Respiratory Therapy, 4 th Ed., Elsevier 2005 SAFETY PRACTICES: Safety is an important component of respiratory care and technical skills taught throughout the semester. Features of each unit are given below: Unit #1:The Physical Property of Gases An overview of the physical property of gases is provided. Topics for discussion include: the pressure, temperature, volume, and density variables of gas. Unit #2: The Dynamics of Air Pressure 136
137 RSP-102 Introduction to Respiratory Care Procedures Elements of air pressure and their significance to the respiratory care practitioner will be introduced. The concept of barometric pressure is introduced. Specific variables of barometric pressure such as absolute humidity, relative humidity, and water vapor pressure are discussed. The gaseous composition of the atmosphere is covered as well. Unit #3: Application of Gas Laws Various gas laws and their application to respiratory therapy will be discussed. The rationale and method for correction of gases when exposed to specific conditions will be presented. Unit #4: Properties of Gases under Extreme Conditions The effect of extreme conditions on the state of gases will be presented. The various states of gas will be discussed. Unit #5: Oxygen Therapy The clinical indications of oxygen therapy are introduced. Emphasis will be placed on appropriate treatment of hypoxia and hypoxemia with oxygen. The physiological effects and hazards of oxygen therapy will be discussed. Unit #6: Medical Gases other than Oxygen The physical principles and clinical uses of medical gases other than oxygen will be presented. Gases to be discussed include: helium, carbon dioxide, nitrous oxide, and nitric oxide. Unit #7: Regulation and Supply of Medical Gases An overview of the regulation and supply systems for medical gases used in respiratory therapy is presented. The regulations regarding medical gas production, transport, and storage is discussed. Systems of medical gas supply in the healthcare facilities will be covered as well. Unit #8: Humidity Therapy The general concept of humidity is presented. The clinical indications and physiologic effects of humidity therapy are discussed. Unit #9: Aerosol Therapy An overview of the physical principles of aerosol therapy is presented. The clinical indications, physiologic effects, and hazards of aerosol therapy are discussed. Unit #10: Aerosolized Administration of Medications An overview of the use of aerosolized medications will be presented. The clinical indications, physiologic effects, and hazards of aerosolized medications will be discussed. Factors influencing the pulmonary distribution of aerosolized medications will be discussed. 137
138 RSP-102 Introduction to Respiratory Care Procedures Unit #11: Hyperbaric Oxygen Therapy An overview of hyperbaric oxygen therapy will be introduced. The goals, indications, potential hazards and methods for administering hyperbaric oxygen will be discussed. Unit #12: Introduction to Bronchopulmonary Hygiene and Lung Expansion Therapies An overview of perioperative complications will be presented. The pathologic changes of the lungs when alveolar consolidation occurs will be discussed. Prevention and treatment of pulmonary consolidation processes will be introduced. The rationale and importance of bronchopulmonary hygiene and lung expansion therapies will be discussed. Unit #13: Bronchopulmonary Drainage and Chest Physical Therapy The concept of bronchopulmonary drainage will be introduced. Clinical indications, technique, hazards, and assessment of therapy effectiveness will be discussed. Unit #14:Deep Breathing and Coughing Techniques An overview of deep breathing and coughing techniques will be discussed. The rationale, technique, clinical indications, physiologic effects, and hazards of deep breathing and cough therapies will be presented. Unit #15: Adjuncts to Bronchopulmonary Hygiene A brief overview of high frequency oscillation therapy will be presented. Specific highfrequency oscillation therapies such as intrapulmonary percussive ventilation, flutter valves, and high-frequency chest wall oscillation will be discussed. The rationale, technique, clinical indications, physiologic effects, and hazards of high frequency oscillation therapies will be presented. Unit #16: Incentive Spirometry An overview of incentive spirometry is presented. The rationale, technique, clinical indications, physiologic effects, and hazards of incentive spirometry therapies will be presented. Unit #17: Function of Positive Pressure Devices A brief overview of positive pressure ventilation will be presented. The classification of ventilators will be discussed. Topics will include: types of ventilators, powering mechanisms, driving mechanisms, cycling mechanisms, modes of ventilation, flow curves, pressure curves, and pressure versus flow generation. Unit #18: Intermittent Positive Pressure Breathing 138
139 RSP-102 Introduction to Respiratory Care Procedures The physiologic principles and therapeutic rationale for IPPB will be introduced. The clinical indications, contraindications, and hazards for IPPB therapy will be discussed. Unit #19 IPPB Equipment An overview of specific IPPB units will be presented. Emphasis will be placed on the Bennett PR 2, the Bennett AP series, and the Bird Mark series. Unit #20: Positive Airway Pressure and Bronchopulmonary Hygiene An overview of positive airway pressure therapy is presented. Specific PAP devices such as continuous positive airway pressure and positive expiratory pressure will be discussed. The rationale, technique, clinical indications, physiologic effects, and hazards of positive airway pressure therapies will be presented. 139
140 RSP-102L Respiratory Care Procedures Lab EVALUATION OF THE STUDENT EVALUATION The purpose of evaluation is to indicate, to some degree, the extent to which the student has learned the concepts presented. Frequent testing will encourage the student to study and learn at a regular and constant pace throughout the course. The teaching-learning process meets the expected outcome goal. Evaluation is also utilized as a learning tool. Questions are designed to stimulate problem solving. The examinations are reviewed to provide feedback and promote discussion. Laboratory simulations and exercises will further enhance the learning process through a supervised hands-on approach. The labs in the school of Respiratory Care will be open for your use to practice procedures or equipment from 8am to 4pm daily, Monday thru Thursday, and 8am to 12pm on Friday. There will be a white binder, designated laboratory sign in, placed on the counter outside of Brent and Jims offices each morning. Please note all extra time spent in the school labs in this book. The time and extra effort spent in the labs will be taken into consideration when the final course grades are calculated at the end of the semester. You may schedule additional time in the lab with an instructor on Fridays by ing and requesting an appointment. Please state the date and time that you want to schedule, also the topic or piece of equipment which you would like to cover. You will receive a return to confirm your appointment, or if the time requested is unavailable, an offer of alternate appointment time. The request must be received no later than 12pm, the Wednesday before the Friday that is being scheduled. Please send your requests to: [email protected] or [email protected] or [email protected] We encourage each of you to optimize your clinical experiences by practicing your skills and increasing your knowledge of the equipment that will be utilized. 140
141 RSP-102L Respiratory Care Procedures Lab SPECIFIC FACTORS 1. Examinations/Quizzes A. Unit Exams 3 Exams: Each exam is worth 15% of the final grade for a total of 45%. Exams will be approximately questions in length and may include multiple choice, matching, listing, labeling, short answer, and essay style questions. B. Quizzes Quizzes: There will be quizzes administered approximately each week. All quizzes will be averaged to consist of 10% of the final grade Quizzes will be approximately questions in length and questions may include multiple choice, short answer, listing, and labeling. C. Course Book The class course book will contain class notes on all units covered. The course syllabus will be in the front followed by notes identified/tabbed for each unit. Homework assigned and attendance will be considered into this grade. The class course book is due at the time of the final test. It is worth 10% of the final grade. D. Final Examination Final Exam: The Final exam will be comprehensive and may include multiple choice, matching, listing, labeling, short answer, and essay style questions. The final exam will be worth 30% of the final grade. The final exam will be administered during Finals Week. 2. Homework/Class work It will be the student s responsibility to complete homework and class work assignments. There are no scheduled homework assignments in this course. However, Additional assignments may be given at the instructor s discretion and will be considered with the course book. 3. Class Participation 141
142 RSP-102L Respiratory Care Procedures Lab Class participation will include discussion, workgroups, and laboratory exercises. Attendance will be monitored and influence course book grade. 3 hr = 45 hrs/semester Time: TBA Room: 300A Course Outline WEEK DATE DAY TIME CONTENT INSTRUCTOR 1 05/14/07 Mon 15 min Syllabus and questions JM 60 min Unit 1 JM 30 min Unit 2 JM 05/15/07 Tue 30 min Unit 2 JM 60 min Unit 3 JM 15 min Review and questions JM 05/16/07 Wed 60 min Unit 4 JM 30 min Unit 5 JM 15 min Review and questions JM 2 05/21/07 Mon 15 min Quiz 1 JM 30 min Unit 5 JM 45 min Unit 6 JM 15 min Review and questions JM 05/22/07 Tue 15 min Unit 6 JM 60 min Unit 7 JM 30 min Review and questions JM 05/23/07 Wed 60 min Exam 1 JM 30 min Unit 8 JM 15 min Review and questions JM 3 05/28/07 Mon Memorial Day Holiday JM 05/29/07 Tue 15 min Quiz 2 JM 30 min Unit 8 JM 45 min Unit 9 JM 142
143 RSP-102L Respiratory Care Procedures Lab 15 min Review and questions JM 05/30/07 Wed 15 min Unit 9 JM 60 min Unit 10 JM 15 min Unit 11 JM 15 Min Review and questions JM 4 06/04/07 Mon 15 min Quiz 3 JM 45 min Unit 11 JM 45 min Unit 12 JM 15 Min Review and questions JM 06/05/07 Tue 15 min Unit 12 JM 60 min Unit 13 JM 30 Min Review and questions JM 06/06/07 Wed 60 min Exam 2 JM 30 min Unit 14 JM 15 Min Review and questions JM 5 06/11/07 Mon 15 min Quiz 4 JM 30 min Unit 14 JM 45 min Unit 15 JM 15 Min Review and questions JM 06/12/07 Tue 15 min Unit 15 JM 60 min Unit 16 JM 15 min Unit 17 JM 15 Min Review and questions JM 06/13/07 Wed 45 min Unit 17 JM 45 min Unit 18 JM 15 Min Review and questions JM 6 06/18/07 Mon 15 min Quiz 5 JM 15 min Unit 18 JM 60 min Unit 19 JM 15 Min Review and questions JM 143
144 RSP-102L Respiratory Care Procedures Lab 06/19/07 Tue 60 min Unit 20 JM 45 min Review and questions JM 06/20/07 Wed 60 min Exam 3 JM 45 min Review and questions JM 7 06/25/07 Mon 1hr 45min Review and skills JM 06/26/07 Tue 1hr 45min Review and skills JM 06/27/07 Wed 1hr 45min Review and skills JM 8 07/02/07 Mon 1hr 45min FINAL EXAM/COURSE BOOK DUE JM 07/03/07 Tue 8 am 5 pm Neo/Peds Presentation Extra Credit for Attendance JM All classes are subject to change due to weather, guest speakers and out of class activities. Marshall University Registration/Schedule - Summer 2007 SPRING Session A: May 4, Friday, 8 a.m. 5 p.m. Session A Regular Registration May 7, Monday Session A First Day of Classes May 7, Monday, 8 a.m. 5 p.m. Late Registration/Schedule Adjustment Closes for Session A May 25, Friday Last Day to Drop an Individual Course May 26 May 27 University Computer Services Unavailable May 28, Monday Memorial Day Holiday University Closed 144
145 RSP-102L Respiratory Care Procedures Lab May 30 June 1 Complete Withdrawals Only June 1, Friday Last Class Day Last Day to Withdraw for Session A June 1, Friday Final Examination Day Session A Ends June 4, Monday Deadline for Submitting Final Grades for Session A Session B: Term 1 (12 Weeks) May 14 August 6 Term 2 (6 Weeks) May 14 June 25 Term 3 (6 Weeks) June 26 August 6 Term 1 May 11, Friday, 8 a.m. 5 p.m. Regular Registration Session B May 14, Monday First Class Day May 14, Monday Late Registration/Schedule Adjustment Closes for Session B May 26 May 28 University Computer Services Unavailable May 28, Monday Memorial Day Holiday University Closed July 4, Wednesday Independence Day Holiday Observed University Closed July 13, Friday Final Draft of Thesis/Dissertation Due in Advisor s Office July 20, Friday Last Day to Drop an Individual Course July 30, Monday Last Possible Date for Thesis/Dissertation Defense 145
146 RSP-102L Respiratory Care Procedures Lab August 3, Friday Last Class Day August 6, Monday Final Examination Day August 8, Wednesday Deadline for Submitting Grades August 9, Thursday Approved Thesis/Dissertation Must Be Submitted Electronically and all Paperwork/Checks Must Be in Graduate College Office Term 2 May 11, Friday, 8 a.m. 5p.m. Regular Registration Session B May 14, Monday First Class Day May 14, Monday Late Registration/Schedule Adjustment Closes for Session B May 26 May 28 University Computer Services Unavailable May 28, Monday Memorial Day Holiday University Closed June 8, Friday Final Draft of Thesis/Dissertation Due in Advisor s Office June 15, Friday Last Day to Drop an Individual Course June 22, Friday Last Class Day June 25, Monday Final Examination Day June 27, Wednesday Deadline for Submitting Grades July 5, Thursday Approved Thesis/Dissertation Due in Graduate College Office 146
147 RSP-102L Respiratory Care Procedures Lab Term 3 June 26, Tuesday First Class Day July 4, Wednesday Independence Day Holiday Observed University Closed July 13, Friday Final Draft of Thesis/Dissertation Due in Advisor s Office July 27, Friday Last Day to Drop an Individual Course July 30, Monday Last Possible Date for Thesis/Dissertation Defense August 3, Friday Last Class Day August 6, Monday Final Examination Day August 8, Wednesday Deadline for Submitting Grades August 9, Thursday Approved Thesis/Dissertation Must Be Submitted Electronically and all Paperwork/Checks Must Be in Graduate College Office Session C: June 1, Friday, 8 a.m. 5 p.m. Regular Registration Session C June 3, Sunday, 9 a.m. Residence Halls Open June 4, Monday Session C First Day of Classes June 4, Monday Late Registration/Schedule Adjustment Closes for Session C June 8, Friday Application for July Graduation Due in Academic Dean s -- Final Draft of Thesis/Dissertation Due in Advisor s Office 147
148 RSP-102L Respiratory Care Procedures Lab June 22, Friday Last Day to Drop an Individual Course June 26 July 5 Complete Withdrawals Only July 4, Wednesday Independence Day Holiday University Closed July 5, Thursday Approved Thesis/Dissertation Due in Graduate College Office July 5, Thursday Last Class Day Last Day to Withdraw from Session C July 6, Friday Final Examination Day Session C Ends Official July Graduation Date July 9, Monday Deadline for Submitting Final Grades for Session C Session D: July 9, Monday, 8 a.m. 5 p.m. Session D Regular Registration July 10, Tuesday Session D First Day of Classes July 10, Tuesday Late Registration/Schedule Adjustment Closes for Session D July 13, Friday Application for August Graduation Due in Academic Dean s Office. Final Draft of Thesis or Dissertation Due in Advisor s Office August 3, Friday Last Day to Drop an Individual Course August 6 August 10 Complete Withdrawals Only August 10, Friday Last Class Day Last Day to Withdraw from Session D Approved Thesis or Dissertation Due in Graduate College Office 148
149 RSP-102L Respiratory Care Procedures Lab August 10, Friday Final Examination Day Session D Ends Official Graduation Date for Session D August 10, Friday, 6 p.m. Residence Halls Close August 13, Monday Deadline for Submitting Final Grades for Session D Student Outcome Goals Essential Content Student References 149
150 RSP-102L Respiratory Care Procedures Lab Unit 1: The Physical Properties of Gases Describe the three states of matter. Explain how the pressure of gases is produced. Describe selected temperature scales. Convert temperatures between temperature scales. State Avogadro s Law. Describe Avogadro s number. Define density. Calculate the density of a given gas. Lesson 1: Lecture 1 hour 1. Basic Units and Relationships a. Mass b. Weight c. Velocity d. Work e. Potential and Kinetic Energy f. Pressure 2. States of Matter a. Solid b. Liquid c. Gas 3. Properties of Gases a. Kinetic Theory of Gases b. Temperature c. Pressure d. Avogadro s Law e. Molar Volume f. Density g. Specific gravity Egan s Chapter 5, pp Mosby s Chapter 1, pp. 3-4,
151 RSP-102L Respiratory Care Procedures Lab Discuss the various gases found in the atmosphere and their relative abundance. Describe the instruments used to measure atmospheric pressure. Explain Dalton s Law of Partial Pressures. Explain selected concepts of humidity. Calculate relative humidity and water vapor pressure. List the four variable affecting gas properties. Describe changes in gases as represented by the gas laws. Write the combined gas law. Rearrange the combined gas law to calculate selected variables. Calculate changes in gas conditions for dry and humidified gases. Calculate changes in gas conditions for changing pressure, Unit 2: The Dynamics of Air Pressure Lesson 2: Lecture 1 hour 1. Atmospheric Pressure 2. Composition of the atmosphere 3. Partial Pressures and Dalton s Law 4. Barometers a. Mechanism of action b. Types of barometers 5. Humidity a. Water vapor content b. Absolute humidity c. Relative humidity d. Clinical humidity terms i. Humidity deficit Unit 3: Application of Gas Laws Lesson 3: Lecture 1 hour 1. Ideal Gas Laws 2. Boyle s Law 3. Charles Law 4. Gay-Lussac s Law 5. Combined Gas Law 6. Correcting for water vapor pressure 7. Correcting for barometric pressure and temperature 8. Correcting for mass and density Unit 4: Properties of Gases Egan s Chapter 5, pp , Egan s Chapter 5, pp Mosby s Chapter 1, pp
152 RSP-102L Respiratory Care Procedures Lab Instructors: Contact Information: Jim Montgomery Jim Montgomery Brent Blevins (304) (304) Chris Trotter Chuck Zuhars (304) (304) Office hours : by appointment COURSE DESCRIPTION: This 1 hour laboratory class will give the student the opportunity to practice techniques and use of technology covered in Respiratory Care Procedures and Introduction to Respiratory Care. Lab exercises will be given for the student to complete. Pre-requisites Successful completion of program sequence. COURSE OBJECTIVES: Upon successful completion of this course, the student will have demonstrated: 5. A thorough understanding of the physical principles, mechanisms for the production, storage, and equipment used in delivery of medical gases. 6. A thorough understanding of the indications for administration, complications, and contraindications for the administration of aerosols and humidity. 7. A thorough understanding of the indications for administration, complications, and contraindications for the administration of hyperinflation therapy. 8. A thorough understanding of the physical principles, indications for administration, complications and contraindications of the administration of bronchpulmonary drainage and chest physical therapy. 9. Knowledge of and basic skills with the following equipment and therapies: a. Intermittent Positive Pressure Ventilation b. Incentive Spirometry c. Aerosol therapy d. Chest Physical Therapy and Postural Drainage e. Bronchial Hygiene Exercises f. O2 delivery 152
153 RSP-102L Respiratory Care Procedures Lab Methods of Evaluation: Course book 10% Competencies 60% Final Exam 30% Grade Scale points A points B points C points D <60 points F Methods of Teaching: Academic Progress: University Statement on Equality, Tolerance and Affirmative Action: This course consists of weekly demonstrations, hands on practice, lectures and includes a variety other teaching methods (i.e., discussion, simulation, audiovisuals etc.) Information regarding the Student's academic progress in this course will be shared with their Academic Advisor and/or Department Chair. Please indicate by the end of the 2 nd week of the course if you will need accommodations under the Americans with Disabilities Act. Academic Integrity: Course Evaluations: Academic dishonesty includes, but is not limited to, cheating, plagiarism, collusion, the submission for credit of any work or materials that are attributable in whole or in part to another person, taking an examination for another person, and any act designed to give unfair advantage to a student or the attempt to commit such an act. Students will be given the opportunity to evaluate the performance of the instructor and course near the end of the course/semester. When submitting course evaluations students must follow the guidelines provided by the course instructor or department. 153
154 RSP-102L Respiratory Care Procedures Lab COURSE MATERIAL: Required Textbooks: Wilkins, Stoller, Scanlan: Egan s Fundamentals of Respiratory Care, 8 th Ed., Elsevier White, G.C.: Basic Lab Competencies for Respiratory Care, 4 th Ed., Delmar, Cairo & Pilbeam: Mosby s Respiratory Care Equipment, 7 th Ed., Elsevier, Reference and Resource Material: Kacmarek, Mack, Dimas: The Essentials of Respiratory Therapy, 4 th Ed., Elsevier 2005 SAFETY PRACTICES: Safety is an important component of respiratory care and technical skills taught throughout the semester. Features of each lab are given below: Lab #1:Cylanders, gas pressure, and flow regulation An overview and practice with cylinders, reducing valves, regulators, and flowmeters. Lab #2 : O2 therapy delivery devices and O2 analyzers An overview and practice with low flow O2 devices, high flow O2 delivery devices, determining FIO2, total system flow, selection of O2 systems, troubleshooting O2 systems, O2 analyzers. Lab #3 : Humidity and areosal devices An overview and practice with types of humidifiers, aerosol generators, aerosol generators for medications and proper technique for delivery of medications to patients. Lab #4 : Compressors, concentrators, and gas mixing devices An overview and practice with compressors, concentrators, and gas mixing systems. Lab #5 : Bronchopulmonary drainage and chest physical therapy An overview and practice with CPT, postural drainage positions, percussion, vibration, and mechanical percussors. 154
155 RSP-102L Respiratory Care Procedures Lab Lab #6 : Incentive spirometry, deep breathing, and cough techniques An overview and practice with incentive spirometry, directed cough procedure, forced expiratory technique, active cycle of breathing, autogenic drainage, cough assistance, and breathing instruction for COPD patients. Lab #7 : Administering IPPB treatment An overview and practice with IPPB machines and technique for delivery of treatments. 155
156 EVALUATION OF THE STUDENT EVALUATION The purpose of evaluation is to indicate, to some degree, the extent to which the student has learned the concepts presented. Frequent testing will encourage the student to study and learn at a regular and constant pace throughout the course. The teaching-learning process meets the expected outcome goal. Evaluation is also utilized as a learning tool. Questions are designed to stimulate problem solving. The examinations are reviewed to provide feedback and promote discussion. Laboratory simulations and exercises will further enhance the learning process through a supervised hands-on approach. The labs in the School of Respiratory Care will be open for your use to practice procedures or equipment from 8am to 4pm daily, Monday thru Thursday, and 8am to 12pm on Friday. There will be a white binder, designated laboratory sign in, placed on the counter outside of Brent and Jims offices each morning. Please note all extra time spent in the school labs in this book. The time and extra effort spent in the labs will be taken into consideration when the final course grades are calculated at the end of the semester. You may schedule additional time in the lab with an instructor on Fridays by ing and requesting an appointment. Please state the date and time that you want to schedule, also the topic or piece of equipment which you would like to cover. You will receive a return to confirm your appointment, or if the time requested is unavailable, an offer of alternate appointment time. The request must be received no later than 12pm, the Wednesday before the Friday that is being scheduled. Please send your requests to: [email protected] Or [email protected] Or [email protected] We encourage each of you to optimize your clinical experiences by practicing your skills and increasing your knowledge of the equipment that will be utilized. 156
157 SPECIFIC FACTORS 1. Examinations/Competencies/Course book A. Competencies 14 competencies : these competencies are worth 60% of the final grade. The competencies will include cylinder safety, nasal cannula, simple O2 and partial rebreather masks, venture and non-rebreather masks, measurement of O2 concentration, aerosol and humidity therapy, heated aerosol and humidity therapy with varied FIO2, aerosol drug administration via HHN, incentive spirometry, IPPB, breathing exercises, assist with cough maneuvers, positive expiratory pressure mask therapy, Postural drainage and percussion. B. Final Exam The Laboratory Final Exam is worth 30% of the final grade. It will consist of hands on activities with equipment combined with matching, listing, and labeling problems. D. Course Book The class course book will contain class notes on all units covered and completed competencies. The course syllabus will be in the front followed by notes identified/tabbed for each unit. Homework assigned and attendance will be considered into this grade. The class course book is due at the time of the final test. It is worth 10% of the final grade. 2. Homework/Class work It will be the student s responsibility to complete homework and class work assignments. There are no scheduled homework assignments in this course. However, Additional assignments may be given at the instructor s discretion and will be considered with the course book. 3. Class Participation Class participation will include discussion, workgroups, and laboratory exercises. Attendance will be monitored and influence course book grade. 157
158 1 hr = 15 hrs/semester Time: TBA Room: 300A Course Outline WEEK DATE DAY TIME CONTENT INSTRUCTOR 1 05/17/07 Thu 2hr 45min Syllabus and Lab 1 JM 2 05/24/07 Thu 2hr 45min Lab 2 JM 3 05/31/07 Thu 2hr 45min Lab 3 JM 4 06/07/07 Thu 2hr 45min Lab 4 JM 5 06/14/07 Thu 2hr 45min Lab 5 JM 6 06/21/07 Thu 2hr 45min Lab 6 JM 7 06/28/07 Thu 2hr 45min Lab 7 and review JM 8 06/29/07 Thu 2hr 45min Final exam, course books due JM All classes are subject to change due to weather, guest speakers and out of class activities. Marshall University Registration/Schedule - Summer 2007 SPRING Session A: May 4, Friday, 8 a.m. 5 p.m. Session A Regular Registration May 7, Monday Session A First Day of Classes May 7, Monday, 8 a.m. 5 p.m. Late Registration/Schedule Adjustment Closes for Session A May 25, Friday Last Day to Drop an Individual Course 158
159 May 26 May 27 University Computer Services Unavailable May 28, Monday Memorial Day Holiday University Closed May 30 June 1 Complete Withdrawals Only June 1, Friday Last Class Day Last Day to Withdraw for Session A June 1, Friday Final Examination Day Session A Ends June 4, Monday Deadline for Submitting Final Grades for Session A Session B: Term 1 (12 Weeks) May 14 August 6 Term 2 (6 Weeks) May 14 June 25 Term 3 (6 Weeks) June 26 August 6 Term 1 May 11, Friday, 8 a.m. 5 p.m. Regular Registration Session B May 14, Monday First Class Day May 14, Monday Late Registration/Schedule Adjustment Closes for Session B May 26 May 28 University Computer Services Unavailable May 28, Monday Memorial Day Holiday University Closed July 4, Wednesday Independence Day Holiday Observed University Closed July 13, Friday Final Draft of Thesis/Dissertation Due in Advisor s Office July 20, Friday Last Day to Drop an Individual Course 159
160 July 30, Monday Last Possible Date for Thesis/Dissertation Defense August 3, Friday Last Class Day August 6, Monday Final Examination Day August 8, Wednesday Deadline for Submitting Grades August 9, Thursday Approved Thesis/Dissertation Must Be Submitted Electronically and all Paperwork/Checks Must Be in Graduate College Office Term 2 May 11, Friday, 8 a.m. 5p.m. Regular Registration Session B May 14, Monday First Class Day May 14, Monday Late Registration/Schedule Adjustment Closes for Session B May 26 May 28 University Computer Services Unavailable May 28, Monday Memorial Day Holiday University Closed June 8, Friday Final Draft of Thesis/Dissertation Due in Advisor s Office June 15, Friday Last Day to Drop an Individual Course June 22, Friday Last Class Day June 25, Monday Final Examination Day June 27, Wednesday Deadline for Submitting Grades 160
161 July 5, Thursday Approved Thesis/Dissertation Due in Graduate College Office Term 3 June 26, Tuesday First Class Day July 4, Wednesday Independence Day Holiday Observed University Closed July 13, Friday Final Draft of Thesis/Dissertation Due in Advisor s Office July 27, Friday Last Day to Drop an Individual Course July 30, Monday Last Possible Date for Thesis/Dissertation Defense August 3, Friday Last Class Day August 6, Monday Final Examination Day August 8, Wednesday Deadline for Submitting Grades August 9, Thursday Approved Thesis/Dissertation Must Be Submitted Electronically and all Paperwork/Checks Must Be in Graduate College Office Session C: June 1, Friday, 8 a.m. 5 p.m. Regular Registration Session C June 3, Sunday, 9 a.m. Residence Halls Open June 4, Monday Session C First Day of Classes June 4, Monday Late Registration/Schedule Adjustment Closes for Session C 161
162 June 8, Friday Application for July Graduation Due in Academic Dean s -- Final Draft of Thesis/Dissertation Due in Advisor s Office June 22, Friday Last Day to Drop an Individual Course June 26 July 5 Complete Withdrawals Only July 4, Wednesday Independence Day Holiday University Closed July 5, Thursday Approved Thesis/Dissertation Due in Graduate College Office July 5, Thursday Last Class Day Last Day to Withdraw from Session C July 6, Friday Final Examination Day Session C Ends Official July Graduation Date July 9, Monday Deadline for Submitting Final Grades for Session C Session D: July 9, Monday, 8 a.m. 5 p.m. Session D Regular Registration July 10, Tuesday Session D First Day of Classes July 10, Tuesday Late Registration/Schedule Adjustment Closes for Session D July 13, Friday Application for August Graduation Due in Academic Dean s Office. Final Draft of Thesis or Dissertation Due in Advisor s Office August 3, Friday Last Day to Drop an Individual Course August 6 August 10 Complete Withdrawals Only 162
163 August 10, Friday Last Class Day Last Day to Withdraw from Session D Approved Thesis or Dissertation Due in Graduate College Office August 10, Friday Final Examination Day Session D Ends Official Graduation Date for Session D August 10, Friday, 6 p.m. Residence Halls Close August 13, Monday Deadline for Submitting Final Grades for Session D Student Outcome Goals Essential Content Student References 163
164 Lab 1 : Cylinders, gas pressure, and flow regulation 5. Differentiate between medical gas supply systems 6. Describe their construction and principles of operation 7. Identify the contents of a medical gas cylinder using the U.S. and international color code system 8. Identify the markings stamped on cylinders 9. List 13 rules est. by the compressed gas Assoc. and Fire Protection Assoc. for the safe handling and storage of cylinders 10. Describe construction and principles of operation of the different O2 regulators and flowmeters Lab 1 : 2 hour 45 min 6. Cylinders a. types h. markings i. sizes j. capacities k. storage l. troubleshooting 4. Reducing valves and regulators a. types b. troubleshooting 5. Flowmeters a. types b. troubleshooting White-chapter 12 pp Mosby-chapter 2 pp Mosby-chapter 3 pp
165 Lab 2 : O2 therapy devices and O2 analyzers List indications for O2 therapy Differentiate between O2 delivery devices Classify devices as high or low flow Describe the operation of an O2 entrainment device Explain the principles of hyperbaric O2 therapy Differentiate between equip. used for mixed gas therapy and that used for O2 Lab 2 : 2 hour 45 min 7. O2 delivery devices 8. Determining FIO2 and total flow 9. Criteria for use of high and low flow O2 devices 10. Troubleshooting O2 delivery devices 11. O2 analyzers White-chapter 13 pp Mosby-chapter 3 pp Lab 3 : Humidity and aerosol devices Describe the physics of humidity and aerosol therapy Explain the principles of operation of the different types of humidifiers Explain the principles of operation of the different types of aerosol devices Explain the operation and application single dose nebs and MDIs Lab 3 : 2 hour 45 min 9. Humidifier overveiw 10. Types of humidifiers 11. Aerosol overveiw 12. Types of aerosol generators 13. Aerosol generators for medications 14. Proper technique for administration of SVN, MDI, DPI therapies White-chapter 15 pp Identify types of medical air compressors and Lab 4 : Compressors, concentrators, and gas mixing devices Lab 4 : 2 hour 45 min White-chapter
166 Marshall University College of Health Professions St. Mary s Medical Center School of Respiratory Care COURSE NAME: RSP PULMONARY PATHOPHYSIOLOGY INSTRUCTOR: James Montgomery (304) [email protected] CREDIT HOURS: 3 PREREQUISITES: RSP 102 COREQUISITES : BSC 250 COURSE DESCRIPTION: This is a 3 credit hour course designed to supplement the information presented introduction to respiratory care. The most frequently encountered diseases and syndromes are presented in detail. Emphasis is placed on the etiology, signs and symptoms, pathology, clinical manifestations, sequellae, and treatment. The respiratory therapist s role in the recognition and treatment of pulmonary diseases is highlighted. COURSE OBJECTIVES: At the end of the course the student will be able to: 1. Describe the clinical manifestations and interactions of common cardiac and pulmonary diseases. 2. Discuss pathophysiology of common chronic pulmonary diseases, clinical manifestations and commonly accepted treatment for each type of disease. 3. Identify acute manifestations of chronic cardiopulmonary conditions and appropriate treatment. 4. Predict common cardiopulmonary complications of other disease states. 5. Describe acute cardiopulmonary disease processes and emergencies and appropriate treatment. 6. Recognize the signs and symptoms of cardiopulmonary decompensation and arrest. 7. Discuss appropriate respiratory care intervention in a cardiopulmonary arrest. 166
167 METHODS OF TEACHING - LEARNING: Lecture Class participation Video Presentations Readings as assigned Exams Required Textbooks: Des Jardins: Clinical Manifestations and Assessment of Respiratory Disease, 5 th Ed., Reference and Resource Material: Kacmarek, Mack, Dimas: The Essentials of Respiratory Therapy, 4 th Ed., Elsevier 2005 Merck Manual of Medical Information, Merck, Oakes, D.: Clinical Practitioner s Pocket Guide to Respiratory Care, 6 th Ed., Health Care Educator Publishers, Pagana & Pagana: Mosby s Diagnostic and Laboratory Test Reference, 7 th Ed., Elsevier, Wilkins, Stoller, Scanlan: Egan s Fundamentals of Respiratory Care, 8 th Ed., Elsevier 2003 Wojciechowski, W.V.: Respiratory Care Sciences An Integrated Approach, 4 th Ed., Delmar, Wojciechowski, B.: Carbon monoxide poisoning. Focus Journal for Respiratory Care, Fall Wheeler, D. Bronchiectasis: A brief review. Focus Journal for Respiratory Care, 2003 Wojciechowski, B.: Pulmonary edema A Brief Review and Update. Focus Journal for Respiratory Care, 2003 Wojciechowski, B.: Cor Pulmonale Heart failure due to lung disease. Focus Journal for Respiratory Care, Winter Wojciechowski, B.: Pleural Effusion. Focus Journal for Respiratory Care, Summer,
168 Wojciechowski, B.: Asbestosis A Primer and an Update. Focus Journal for Respiratory Care, Wojciechowski, B.: Acute Respiratory Distress Syndrome. Focus Journal for Respiratory Care, Wojciechowski, B.: Guillain-Barre Syndrome. Focus Journal for Respiratory Care, Fall Wojciechowski, B.: Myasthenia Gravis. Focus Journal for Respiratory Care, Spring, Wojciechowski, B.: Congestive Heart Failure. Focus Journal for Respiratory Care, Wyka, Mathews, & Clark: Foundations of Respiratory Care, Delmar, 2002 ADA Statement: If a student wishes to be identified as having a physical, mental, or learning disability that may require accommodation, he/she must register with the Office of Accessibility, located in the Department of Health Services, prior to the end of the first week of classes for each semester. These registered students must identify themselves to their instructors and provide them with a copy of a letter from the Accessibility Office that identifies appropriate accommodations at the first class meeting and no later than the end of the first week of class for each semester. FACULTY: Brent Blevins RRT Chris Trotter RRT Chuck Zuhars RRT Dr. Pete Ottaviano GRADING SCALE: A B C D below 60 F 168
169 Features of each unit: Unit 2:Obstructive Airway Diseases The etiologies, clinical manifestations, diagnostic process, treatment, and prognosis of obstructive airway diseases will be discussed in detail. Specific pathologies to be covered include: chronic bronchitis, emphysema, bronchiectasis, asthma, and cystic fibrosis. Unit 3: Infectious Pulmonary Diseases- The etiologies, clinical manifestations, diagnostic process, treatment, and prognosis of infectious airway disease will be discussed in detail. Specific pathologies to be covered include: pneumonia, human immunodeficiency virus, lung abscess, tuberculosis, and fungal diseases of the lungs. Unit 4: Pulmonary Vascular Diseases- The etiologies, clinical manifestations, diagnostic process, treatment, and prognosis of pulmonary vascular diseases will be discussed in detail. Specific pathologies to be covered include: pulmonary edema, pulmonary embolism, pulmonary hypertension, and cor pulmonale Unit 5: Chest and Pleural Trauma- The etiologies, clinical manifestations, diagnostic process, treatment, and prognosis of chest and pleural traumas will be discussed in detail. Specific pathologies to be covered include: flail chest, pneumothorax, and lung contusions. Unit 6: Disorders of the Pleura and of the Chest Wall- The etiologies, clinical manifestations, diagnostic process, treatment, and prognosis of pleural and chest wall disorders will be discussed in detail. Specific pathologies to be covered include: pleural effusions and kyphoscoliosis. Unit 7: Environmental Lung Diseases- The etiologies, clinical manifestations, diagnostic process, treatment, and prognosis of environmental lung diseases will be discussed in detail. Specific pathologies to be covered include: pneumoconiosis and hypersensitivity pneumonitis. Unit 8: Neoplastic Disease- The etiologies, clinical manifestations, diagnostic process, treatment, and prognosis of neoplastic disease of the lungs will be discussed in detail. Specific pathologies to be covered include: primary and metastatic neoplasm of the lungs. Unit 9: Diffuse Alveolar Disease- The etiologies, clinical manifestations, diagnostic process, treatment, and prognosis of diffuse alveolar disease will be discussed in detail. Specific pathologies to be covered include: acute respiratory distress syndrome and sepsis. 169
170 Unit 10: Chronic Noninfectious Parenchymal Disease - The etiologies, clinical manifestations, diagnostic process, treatment, and prognosis of chronic noninfectious parenchymal disease will be discussed in detail. Specific pathologies to be covered include: sarcoidosis, connective tissue diseases, and pulmonary fibrosis. Unit 11: Neuromuscular Disorders and Sleep Apnea- The etiologies, clinical manifestations, diagnostic process, treatment, and prognosis of neuromuscular disorders and sleep apnea will be discussed in detail. Specific pathologies to be covered include: Guillain-Barre Syndrome, Myasthenia Gravis, and sleep apnea. Unit 13: Other Important Topics - The etiologies, clinical manifestations, diagnostic process, treatment, and prognosis of several selected pulmonary pathologies will be discussed in detail. Specific pathologies to be covered include: near drowning, smoke inhalation, and respiratory failure. 170
171 EVALUATION OF THE STUDENT The purpose of evaluation is to indicate, to some degree, the extent to which the student has learned the concepts presented. Frequent testing will encourage the student to study and learn at a regular and constant pace throughout the course. The teaching-learning process meets the expected outcome goal. Evaluation is also utilized as a learning tool. Questions are designed to stimulate problem solving. The examinations are reviewed to provide feedback and promote discussion. Laboratory simulations and exercises will further enhance the learning process through a supervised hands-on approach. The labs in the school of Respiratory Care will be open for your use to practice procedures or equipment from 8am to 4pm daily, Monday thru Thursday, and 8am to 12pm on Friday. There will be a white binder, designated laboratory sign in, placed on the counter outside of Brent and Jims offices each morning. Please note all extra time spent in the school labs in this book. The time and extra effort spent in the labs will be taken into consideration when the final course grades are calculated at the end of the semester. You may schedule additional time in the lab with an instructor on Fridays by ing and requesting an appointment. Please state the date and time that you want to schedule, also the topic or piece of equipment which you would like to cover. You will receive a return to confirm your appointment, or if the time requested is unavailable, an offer of alternate appointment time. The request must be received no later than 12pm, the Wednesday before the Friday that is being scheduled. Please send your requests to: [email protected] or [email protected] or [email protected] We encourage each of you to optimize your clinical experiences by practicing your skills and increasing your knowledge of the equipment that will be utilized. 171
172 SPECIFIC FACTORS 1. Examinations D. Unit Exams 4 Exams: Each exam is worth 15% of the final grade for a total of 60%. Exams may include multiple choices, matching, listing, labeling, short answer, and essay style questions. An hour will be given for each unit exam. E. Final Examination Final Exam: The Final exam will be comprehensive and may include multiple choice, matching, listing, labeling, short answer, and essay style questions. The final exam will be worth 25% of the final grade. The final exam will be administered during Finals Week. 2. Homework/Class work It will be the student s responsibility to complete homework/classwork assignments. There are no scheduled homework assignments in this course. However, additional assignments may be given at the instructor s discretion. 3. Class Participation: 4. Course Book Class participation will include discussions and workgroups. The class course book will contain class notes on all units covered. The course syllabus will be in the front followed by notes identified/tabbed for each unit. Homework assigned and class participation will be considered into this grade. The class course book is due at the time of the final test. It is worth 15% of the final grade. 5. Final Grade Calculation The factors below will be used to determine the final grade for the course: The unit exams are worth 60% of the final grade. The final exam is worth 25% of the final grade. The course book is worth 15% of the final grade. 172
173 ATTENDANCE/ABSENCE POLICY ATTENDANCE IS THE RESPONSIBILITY OF EACH STUDENT 1. Punctual attendance in all classes and clinical experiences is important if the student is to meet all course objectives. 2. Notify the School of Respiratory Care by contacting the course instructor as soon as possible regarding the absence. 3. The course grade will be lowered one letter grade if theory absences exceed 20% of the theory contact hours. 4. Class notes and other course material missed is the responsibility of the student, not the instructor. 5. References provided to potential employers by the faculty and/or Director will include information on attendance while the student was enrolled in the program. 6. Absences/tardiness on the Day of an Exam/Quiz a. Students who miss an exam/quiz must contact the instructor before the exam/quiz, or as soon as possible after the exam/quiz is missed. b. Documentation of the reason for the exam/quiz absence or tardiness (i.e., health care provider statement, receipt to substantiate car trouble, etc.) must be provided in order to determine eligibility for a makeup exam c. Permission for makeup will be at the discretion of the course instructor(s). d. Makeup exams/quizzes may be different than the original exams/quizzes. e. Any make-ups will be scheduled at a time convenient for the instructor. f. Student should be ready to take the make-up exam/quiz upon the first day of return, unless other plans have been arranged. g. If tardy for an exam/quiz the student must decide if it can be completed within the remaining administration time. The exam/quiz will be turned in at the same time as all other students taking it. If the student does not believe the exam/quiz can be completed within the planned administration time, a request for make-up may be submitted for consideration. h. Students may not take more than two (2) make-up exams per course. Each subsequent test missed will be scored as zero (0). 7. The faculty for each course has the option of establishing rules and consequences for tardiness and attendance. Special seating may be assigned for late-comers. NOTE: This attendance policy also applies lab/clinical check-offs. : 173
174 Test Remediation Policy Anyone who earns a grade less than 70% on an exam must remediate the test during the semester. The last test of the semester is not to be remediated. All questions missed on that failed examination must be remediated Remediation will consist of an explanation of the correct answer and why the students answer was incorrect. For Unit Exams, remediations are to be turned in to the remediation coordinator, Brent, seven days after the test is reviewed in class with the students. Remediations are to be turned in or ed to Brent ([email protected]). Each question remediated must include a reference from an assigned reading. If the answer cannot be found in an assigned reading, you may reference an instructor s or guest lecturer s presentation. Remediations will be graded S or U by the remediation coordinator. A student earning U should meet with Brent to discuss the question and remediation to ensure that the student understands the concepts being tested and the correct way to perform remediation. Student remediation will be done at the respiratory care school. Test keys will be provided at that time. Tests are not to be removed from the school. If this remediation is not completed in the permitted time, documentation will be placed in the students permanent file and consider at the end of the semester. Academic Calendar August 13, Monday August 17, Friday Registration/Schedule Adjustment August 17, Friday, 9 a.m. Residence Halls Open for Freshmen August 20, Monday, 8 a.m. First Day of Classes August 20, Monday August 24, Friday Late Registration and Add/Drop (Schedule Adjustment) August 24, Friday Last Day to Add Classes (Withdrawals Only After This Date) 174
175 August 27, Monday W Withdrawal Period Begins September 1, Saturday September 3, Monday University Computer Services Unavailable September 3, Monday Labor Day Holiday University Closed September 14, Friday Application for December Graduation Due in Academic Dean s Office September 21, Friday Last Day to Drop 1st 8 Weeks Courses October 8, Monday Final Draft of Thesis Due in Advisor s Office October 9, Tuesday Mid-Semester, 1st 8 Weeks Courses End October 10, Wednesday 2nd 8 Weeks Courses Begin October 15, Monday Deadline for Submitting Freshmen Mid Term Grades October 22, Monday Students should schedule appointments with advisors to prepare for advance registration (Required for students who have mandatory advising holds) October 26, Friday Last Day to Drop a Full Semester Individual Course October 29, Monday Recommended Date to Apply for May 2008 Graduation October 29, Monday December 4, Tuesday Complete Withdrawals Only November 5, Monday November 16, Friday Advance Registration for Spring Semester for Currently Enrolled Students 175
176 November 9, Friday Last Day to Drop 2nd 8 Weeks Courses November 17, Saturday, Noon Residence Halls Close November 19, Monday Last day for Defense of Dissertation November 19, Mon December 11, Tuesday Advance Registration for Spring Semester Open to All Admitted/Re-Admitted Students November 19, Monday November 24, Saturday Thanksgiving/Fall Break - Classes Dismissed November 22, Thursday November 25, Sunday University Computer Services Unavailable November 22, Thursday Thanksgiving Holiday University Closed November 23, Friday University Holiday University Closed November 25, Sunday, Noon Residence Halls Open November 26, Monday Classes Resume November 28, Wednesday December 4, Tuesday Dead Week December 4, Tuesday Last Class Day and Last Day to Completely Withdraw for Fall Semester December 5, Wednesday Study Day - Exams for Wednesday Classes 3 p.m. and After Will Be Held December 6, Thursday Exam Day 176
177 December 6, Thursday Approved Thesis/Dissertation Must Be Submitted Electronically and all Paperwork/Checks Must Be In Graduate College Office December 7, Friday Exam Day December 8, Saturday Exam Day for Saturday Classes (and some common finals) December 10, Monday Exam Day December 11, Tuesday Exam Day Fall Semester Closes Official Graduation Date For Fall Semester December 12, Wednesday 12 p.m.. Residence Halls Close December 12, Wednesday December 26, Wednesday Advance Registration/Schedule Adjustment for Spring Semester is Suspended December 13, Thursday, Noon Deadline for Submitting Final Set of Grades December 21, Friday January 1, 2008, Tuesday University Closed December 27, Thursday December 28, Friday On-Line Registration Resumes 177
178 Class Schedule Week Date Day Content Instructor 1 08/20 MON Syllabus - COPD overview JM 08/22 WED No class due to SMMC field trip JM 2 08/27 MON Bronchitis JM 08/29 WED Emphysema JM 3 09/03 MON No class - LDH JM 09/05 WED Bronchiectasis JM 4 09/10 MON Asthma JM 09/12 WED Cystic fibrosis/copd management JM 5 09/17 MON TEST 1 JM 09/19 WED Pneumonia JM 6 09/24 MON Hive, AIDS/Lung abscess JM / presentation 09/26 WED TB/Fungal diseases JM / presentation 7 10/01 MON Pulmonary edema JM 10/03 WED Pulmonary embolism JM / presentation 8 10/08 MON TEST 2 10/10 WED Pulmonary hypertension/cor pulmonale JM / presentation 9 10/15 MON Flail chest/pneumothorax JM / presentation 10/17 WED Pleural diseases/kyphoscoliosis JM 10 10/22 MON Pneumoconiosis/Hypersensitivity peumonitis JM / presentation 10/24 WED Lung cancer JM 11 10/29 MON TEST 3 JM 10/31 WED ARDS JM 12 11/05 MON Chronic interstitial lung disease JM 178
179 11/07 WED Guillain-Barre syndrome JM 13 11/12 MON Myasthenia gravis JM / presentation 11/14 WED TEST 4-Sleep apnea/neuromuscular JM 14 11/19 MON No class - TGH JM 11/21 WED No class - TGH JM 15 11/26 MON Near drowning/smoke inhalation/co JM poisoning 11/28 WED Respiratory Failure JM 16 12/03 MON MI JM / presentation 12/05 WED CHF JM / presentation 17 12/10 MON Final exam Course book is due JM 179
180 List the diseases commonly associated with COPD. List the predisposing factors for COPD. Differentiate the pathology and clinical symptomatology of patient with predominately chronic bronchitis versus emphysema. Compare and contrast centrilobular versus panlobular emphysema. Outline and justify the treatments of COPD. Describe the impact of COPD on the patient, family and society. Describe the pathogenesis and prognosis of COPD. Explain the role of pulmonary rehabilitation in chronic obstructive pulmonary diseases. Describe the etiology and pathophysiology of bronchiectasis. Describe the treatment and prognosis of bronchiectasis. Lesson 1 1. COPD Overview a. Prevalence b. General causes of COPD c. Physical appearance of the COPD patient d. General Pulmonary Function changes e. General radiographic findings f. Dyspnea g. Ventilatory drive and COPD h. General pattern of ABG s Lesson 2 1. Bronchitis a. Acute bronchitis i. Clinical manifestations ii. Etiology iii. Treatment b. Chronic Bronchitis i. Diagnosis ii. Etiology iii. Clinical manifestations iv. Pathophysiology v. Chest film findings vi. PFT s vii. ABG s viii. Oxygen and hemodynamic indices ix. Treatment Lesson 3 1. Emphysema a. Definition b. Etiology c. Types i. Centrilobular ii. Panlobular iii. Bullous d. Clinical manifestations e. Chest film findings f. PFT s g. ABG s h. Oxygen and hemodynamic indices Lesson 4 1. Bronchiectasis a. Definition Presentation/Handou ts Des Jardins Ch. 11, pp Des Jardins - Ch. 12 pp Des Jardins - Ch. 13, pp
181 Marshall University College of Health Professions St. Mary s Medical Center School of Respiratory Care COURSE NAME: RSP Mechanical Ventilation Technology and Management INSTRUCTOR: James Montgomery (304) [email protected] CREDIT HOURS: 3 PREREQUISITES: RSP 102 COREQUISITES : BSC 250, RSP201, RSP 203 COURSE DESCRIPTION: An introduction to the fundamentals of mechanical ventilation techniques and terminology. Monitoring and the ability to solve clinical problems relating to mechanical ventilation are emphasized. COURSE OBJECTIVES: At the end of the course the student will be able to: 8. Describe the characteristics of the various modes of mechanical ventilation and recognize their pressure curves. 9. Explain the different cycling mechanisms (pressure, volume, time, flow) and describe the variability of their efforts in ventilating patients. 10. Explain the classification system used to describe mechanical ventilators. 11. Describe the mechanism of different types of ventilators. 12. Describe the mechanism and explain the use of a representative, electrically powered portable ventilator commonly used by home bound patients. 13. List performance characteristic functions and criteria for verifying adequate functioning of commonly used manual resuscitators. 14. Demonstrate proper application of mechanical ventilators. METHODS OF TEACHING - LEARNING: Lecture Class participation Readings as assigned 181
182 Laboratory Simulations and Exercises Exams Required Textbooks: Wilkins, Stoller, Scanlan: Egan s Fundamentals of Respiratory Care, 8 th Ed., Elsevier 2003 White, G.C.: Basic Lab Competencies for Respiratory Care, 4 th Ed., Delmar, Reference and Resource Material: Kacmarek, Mack, Dimas: The Essentials of Respiratory Therapy, 4 th Ed., Elsevier 2005 Merck Manual of Medical Information, Merck, Oakes, D.: Clinical Practitioner s Pocket Guide to Respiratory Care, 6 th Ed., Health Care Educator Publishers, Pagana & Pagana: Mosby s Diagnostic and Laboratory Test Reference, 7 th Ed., Elsevier, Wojciechowski, W.V.: Respiratory Care Sciences An Integrated Approach, 4 th Ed., Delmar, Wojciechowski, B.: Carbon monoxide poisoning. Focus Journal for Respiratory Care, Fall Wheeler, D. Bronchiectasis: A brief review. Focus Journal for Respiratory Care, 2003 Wojciechowski, B.: Pulmonary edema A Brief Review and Update. Focus Journal for Respiratory Care, 2003 Wojciechowski, B.: Cor Pulmonale Heart failure due to lung disease. Focus Journal for Respiratory Care, Winter Wojciechowski, B.: Pleural Effusion. Focus Journal for Respiratory Care, Summer, Wojciechowski, B.: Asbestosis A Primer and an Update. Focus Journal for Respiratory Care, Wojciechowski, B.: Acute Respiratory Distress Syndrome. Focus Journal for Respiratory Care, Wojciechowski, B.: Guillain-Barre Syndrome. Focus Journal for Respiratory Care, Fall Wojciechowski, B.: Myasthenia Gravis. Focus Journal for Respiratory Care, Spring,
183 Wojciechowski, B.: Congestive Heart Failure. Focus Journal for Respiratory Care, Wyka, Mathews, & Clark: Foundations of Respiratory Care, Delmar, 2002 ADA Statement: If a student wishes to be identified as having a physical, mental, or learning disability that may require accommodation, he/she must register with the Office of Accessibility, located in the Department of Health Services, prior to the end of the first week of classes for each semester. These registered students must identify themselves to their instructors and provide them with a copy of a letter from the Accessibility Office that identifies appropriate accommodations at the first class meeting and no later than the end of the first week of class for each semester. FACULTY: Brent Blevins RRT Chris Ttrotter RRT Chuck Zuhars RRT GRADING SCALE: A B C D below 60 F 183
184 Features of each unit: Unit 1 Continuous Mechanical Ventilation Indications: The indications for continuous mechanical ventilation will be presented. The pathophysiology of common disease processes that often require mechanical ventilation will be discussed. Emphasis will be placed on recognizing clinical situations that require mechanical ventilation. Unit 2 Physiological Effects and Hazards of Mechanical Ventilation: The physiological effects of positive pressure ventilation will be reviewed. Hazards and possible complications of mechanical ventilation will be presented. Unit 3 Operational Overview of Patient-Ventilator Systems: A detailed discussion of the mechanical principles of ventilators will be presented. A review of classification of ventilators will be discussed. Emphasis will be placed on applying mechanical principles of ventilators to the patient-ventilator system. Unit 4 Modes of Mechanical Ventilation: The modes of mechanical ventilation will be presented. The characteristics, clinical indications, and complications of the various modes of mechanical ventilation will be discussed in detail. Unit 5 Mechanical Ventilation Parameter Relationships: The mathematical relationship of mechanical ventilation parameters will be discussed. Emphasis will be placed on the interaction of these parameters and the outcome of patient-ventilator management. Unit 6 Initiation of Mechanical Ventilation: The process for initiating mechanical ventilation in the clinical setting will be presented. Emphasis will be placed on recognizing the signs of ventilatory and respiratory failure and selecting appropriate initial settings for the ventilator. Unit 7 Ventilator Management: The principles of managing the patient-ventilator system will be presented. The various parameters that are monitored while a patient is receiving mechanical ventilation will be discussed. Emphasis will be placed on recognizing changes in the patient s cardiopulmonary status and adjusting the ventilator settings accordingly. Unit 8 Airway Graphics: The principles of airway graphics will be introduced to the student. The relationship between airway graphics and ventilator settings will be discussed. Emphasis will be placed on recognizing patient-ventilator system interactions by patterns in airway graphics. Unit 9 Troubleshooting the Patient-Ventilator System: The principles of recognizing and correcting problems in the patient-ventilator system will be presented. 184
185 Unit 10 Special Ventilatory Procedures: Special ventilatory procedures used in the intensive care units for the respiratory management of critical care cases will be presented. Emphasis will be placed on the clinical indications and uses of the procedures. Topics to be discussed will include: high frequency ventilation in the adult, tracheal gas insufflation, independent lung ventilation, and prone positioning. Unit 11 Noninvasive Ventilation: The principles of non-invasive ventilation in the critical care setting will be presented. Emphasis will be placed on the clinical indications, hazards, and uses of non-invasive ventilation in critical care. Unit 12 Continuous Mechanical Ventilation Pharmacology: Common medications used in the management of mechanically ventilated patients will be presented. The indications, side effects, and clinical uses of various pharmacological agents used in the intensive care units will be discussed. Unit 13 Weaning: The rationale and procedure for removing a patient from mechanical ventilation support will be presented. The indications and hazards of weaning ventilatory support will be discussed in detail. Emphasis will be placed on recognizing clinical situations that indicate a patient s readiness to be removed from ventilatory support. 185
186 186 EVALUATION OF THE STUDENT The purpose of evaluation is to indicate, to some degree, the extent to which the student has learned the concepts presented. Frequent testing will encourage the student to study and learn at a regular and constant pace throughout the course. The teaching-learning process meets the expected outcome goal. Evaluation is also utilized as a learning tool. Questions are designed to stimulate problem solving. The examinations are reviewed to provide feedback and promote discussion. Laboratory simulations and exercises will further enhance the learning process through a supervised hands-on approach. The labs in the school of Respiratory Care will be open for your use to practice procedures or equipment from 8am to 4pm daily, Monday thru Thursday, and 8am to 12pm on Friday. There will be a white binder, designated laboratory sign in, placed on the counter outside of Brent and Jims offices each morning. Please note all extra time spent in the school labs in this book. The time and extra effort spent in the labs will be taken into consideration when the final course grades are calculated at the end of the semester. You may schedule additional time in the lab with an instructor on Fridays by ing and requesting an appointment. Please state the date and time that you want to schedule, also the topic or piece of equipment which you would like to cover. You will receive a return to confirm your appointment, or if the time requested is unavailable, an offer of alternate appointment time. The request must be received no later than 12pm, the Wednesday before the Friday that is being scheduled. Please send your requests to: [email protected] or [email protected] or [email protected] We encourage each of you to optimize your clinical experiences by practicing your skills and increasing your knowledge of the equipment that will be utilized. 186
187 187 SPECIFIC FACTORS 2. Examinations F. Unit Exams 4 Exams: Each exam is worth 15% of the final grade for a total of 60%. Exams may include multiple choices, matching, listing, labeling, short answer, and essay style questions. An hour will be given for each unit exam. G. Final Examination Final Exam: The Final exam will be comprehensive and may include multiple choice, matching, listing, labeling, short answer, and essay style questions. The final exam will be worth 25% of the final grade. The final exam will be administered during Finals Week. 2. Homework/Class work It will be the student s responsibility to complete homework/classwork assignments. There are no scheduled homework assignments in this course. However, additional assignments may be given at the instructor s discretion. 4. Class Participation: 4. Course Book Class participation will include discussions and workgroups. The class course book will contain class notes on all units covered. The course syllabus will be in the front followed by notes identified/tabbed for each unit. Homework assigned and class participation will be considered into this grade. The class course book is due at the time of the final test. It is worth 10% of the final grade. 5. Clinical skills check-offs There will be clinical skills assessment check-offs that can be completed either in the school skills lab or at the clinical site. The time and place of each check-off will be at the discretion of the course instructor. These check-offs will be worth 5% of the final grade. 6. Final Grade Calculation The factors below will be used to determine the final grade for the course: The unit exams are worth 60% of the final grade. The final exam is worth 25% of the final grade. 187
188 The course book is worth 10% of the final grade. The clinical skills check-offs are worth 5% of the final grade. 188 ATTENDANCE/ABSENCE POLICY ATTENDANCE IS THE RESPONSIBILITY OF EACH STUDENT 1. Punctual attendance in all classes and clinical experiences is important if the student is to meet all course objectives. 2. Notify the School of Respiratory Care by contacting the course instructor as soon as possible regarding the absence. 3. The course grade will be lowered one letter grade if theory absences exceed 20% of the theory contact hours. 4. Class notes and other course material missed is the responsibility of the student, not the instructor. 5. References provided to potential employers by the faculty and/or Director will include information on attendance while the student was enrolled in the program. 6. Absences/tardiness on the Day of an Exam/Quiz i. Students who miss an exam/quiz must contact the instructor before the exam/quiz, or as soon as possible after the exam/quiz is missed. j. Documentation of the reason for the exam/quiz absence or tardiness (i.e., health care provider statement, receipt to substantiate car trouble, etc.) must be provided in order to determine eligibility for a makeup exam k. Permission for makeup will be at the discretion of the course instructor(s). l. Makeup exams/quizzes may be different than the original exams/quizzes. m. Any make-ups will be scheduled at a time convenient for the instructor. n. Student should be ready to take the make-up exam/quiz upon the first day of return, unless other plans have been arranged. o. If tardy for an exam/quiz the student must decide if it can be completed within the remaining administration time. The exam/quiz will be turned in at the same time as all other students taking it. If the student does not believe the exam/quiz can be completed within the planned administration time, a request for make-up may be submitted for consideration. p. Students may not take more than two (2) make-up exams per course. Each subsequent test missed will be scored as zero (0). 7. The faculty for each course has the option of establishing rules and consequences for tardiness and attendance. Special seating may be assigned for late-comers. 188
189 NOTE: This attendance policy also applies lab/clinical check-offs. 189 : Test Remeadiation Policy Anyone who earns a grade less than 70% on an exam must remediate the test during the semester. The last test of the semester is not to be remediated. All questions missed on that failed examination must be remediated Remediation will consist of an explanation of the correct answer and why the students answer was incorrect. For Unit Exams, remediations are to be turned in to the remediation coordinator, Brent, seven days after the test is reviewed in class with the students. Remediations are to be turned in or ed to Brent ([email protected]). Each question remediated must include a reference from an assigned reading. If the answer cannot be found in an assigned reading, you may reference an instructor s or guest lecturer s presentation. Remediations will be graded S or U by the remediation coordinator. A student earning U should meet with Brent to discuss the question and remediation to ensure that the student understands the concepts being tested and the correct way to perform remediation. Student remediation will be done at the respiratory care school. Test keys will be provided at that time. Tests are not to be removed from the school. If this remediation is not completed in the permitted time, documentation will be placed in the students permanent file and consider at the end of the semester. Class Schedule Week Date Day Content Instructor 1 08/20 MON Syllabus/Principles of Mech. Ventilation JM 08/22 WED No class due to SMMC field trip JM 2 08/27 MON Effects of PPV/Hazards of PPV JM 08/29 WED Classification of Ventilators JM 3 09/03 MON No Class - LDH JM 09/05 WED Types of Ventilators JM 189
190 /10 MON TEST 1 JM 09/12 WED Ventilator Mode Classification JM 5 09/17 MON Main Modes of Ventilation JM 09/19 WED Other Types of Vent Modes JM 6 09/24 MON Mech. Vent. Parameter Relationships JM 09/26 WED Ventilator Manipulation JM 7 10/01 MON TEST 2 JM 10/03 WED Indications for Vent Support JM 8 10/08 MON Disease Consideration in Vent. Support JM 10/10 WED Techniques for Improving Ventilation JM 9 10/15 MON Techniques for Improving Oxygenation JM 10/17 WED Improving Pt. /Vent. Interaction JM 10 10/22 MON TEST 3 JM 10/24 WED Specific Disease Management JM 11 10/29 MON Airway Graphics JM 10/31 WED Airway Graphics/Abnormal Waveforms JM 12 11/05 MON Signs of Pt. Distress JM 11/07 WED Troubleshooting the Ventilator JM 13 11/12 MON TEST 4 JM 11/14 WED Unusual Types of Ventilation JM 14 11/19 MON No class - TGH JM 11/21 WED No class - TGH JM 15 11/26 MON Non-invasive Positive Press. Ventilation JM 11/28 WED Types of NIPPV JM 16 12/03 MON Mech. Ventilation Pharmacology JM 12/05 WED Weaning and DC from Mechanical JM Ventilation 17 12/10 MON Reveiw JM 12/12 WED Final Exam - Course Book Due JM 190
191 Academic Calendar 191 August 13, Monday August 17, Friday Registration/Schedule Adjustment August 17, Friday, 9 a.m. Residence Halls Open for Freshmen August 20, Monday, 8 a.m. First Day of Classes August 20, Monday August 24, Friday Late Registration and Add/Drop (Schedule Adjustment) August 24, Friday Last Day to Add Classes (Withdrawals Only After This Date) August 27, Monday W Withdrawal Period Begins September 1, Saturday September 3, Monday University Computer Services Unavailable September 3, Monday Labor Day Holiday University Closed September 14, Friday Application for December Graduation Due in Academic Dean s Office September 21, Friday Last Day to Drop 1st 8 Weeks Courses October 8, Monday Final Draft of Thesis Due in Advisor s Office October 9, Tuesday Mid-Semester, 1st 8 Weeks Courses End October 10, Wednesday 2nd 8 Weeks Courses Begin October 15, Monday Deadline for Submitting Freshmen Mid Term Grades 191
192 192 October 22, Monday Students should schedule appointments with advisors to prepare for advance registration (Required for students who have mandatory advising holds) October 26, Friday Last Day to Drop a Full Semester Individual Course October 29, Monday Recommended Date to Apply for May 2008 Graduation October 29, Monday December 4, Tuesday Complete Withdrawals Only November 5, Monday November 16, Friday Advance Registration for Spring Semester for Currently Enrolled Students November 9, Friday Last Day to Drop 2nd 8 Weeks Courses November 17, Saturday, Noon Residence Halls Close November 19, Monday Last day for Defense of Dissertation November 19, Mon December 11, Tuesday Advance Registration for Spring Semester Open to All Admitted/Re-Admitted Students November 19, Monday November 24, Saturday Thanksgiving/Fall Break - Classes Dismissed November 22, Thursday November 25, Sunday University Computer Services Unavailable November 22, Thursday Thanksgiving Holiday University Closed November 23, Friday University Holiday University Closed November 25, Sunday, Noon Residence Halls Open 192
193 November 26, Monday Classes Resume 193 November 28, Wednesday December 4, Tuesday Dead Week December 4, Tuesday Last Class Day and Last Day to Completely Withdraw for Fall Semester December 5, Wednesday Study Day - Exams for Wednesday Classes 3 p.m. and After Will Be Held December 6, Thursday Exam Day December 6, Thursday Approved Thesis/Dissertation Must Be Submitted Electronically and all Paperwork/Checks Must Be In Graduate College Office December 7, Friday Exam Day December 8, Saturday Exam Day for Saturday Classes (and some common finals) December 10, Monday Exam Day December 11, Tuesday Exam Day Fall Semester Closes Official Graduation Date For Fall Semester December 12, Wednesday 12 p.m.. Residence Halls Close 193
194 Student Outcome Goals Essential Content Student Referenc es
195 Demonstrate proficiency in assessing the need for mechanical ventilation. Justify the conclusion from assessment. List the indications for mechanical ventilation. Discuss the appropriate methods of assessment for given pathologic processes. Explain the pathophysiologic process that necessitates mechanical ventilation. Discuss the clinical parameters that are monitored in the assessment for the need of mechanical ventilation. When presented with clinical situations, determine if mechanical ventilation is indicated. Define the objectives of mechanical ventilation. 195 Unit 1: Continuous Mechanical Ventilation Technology Lesson 1: Lecture 90 minutes 1. Principles of mechanical ventilation a. Airway resistance b. Lung compliance c. Time constants d. Deadspace 2. Pathophysiological indications for CMV a. Acute respiratory failure i. Hypoxemic respiratory failure ii. Hypercapnic respiratory failure b. Differential diagnosis of ARF c. Impending respiratory failure d. Prophylactic ventilatory support e. Hyperventilation therapy 3. Clinical parameters for CMV need a. Ventilation b. Oxygenation c. Mechanical capabilities d. Intracranial pressure 4. Physiologic objectives of mechanical ventilation a. Support of pulmonary gas exchange b. Increase lung volume c. Manipulate WOB 5. Clinical objectives of mechanical ventilation Egan s Chapter 41, pp White Chapter 26, pp Describe the action to be taken in the event of mechanical failures. Describe common hazards Unit 2: Physiologic Effects and Hazards of Mechanical Ventilation Lesson 2: Lecture 90 minutes 1. Physiologic effects of PPV a. Increased mean airway pressure b. Increased mean intrathoracic pressure c. Decreased venous return d. Decreased cardiac output e. Increased ICP f. Decreased urinary output g. Mechanical bronchodilation h. Increased deadspace ventilation i. Increased intrapulmonary shunt j. Effects on GI tract k. Effects on hepatic function l. Nutritional effects of MV m. Psychological effects of MV 195
196 196 ST. MARY S/MARSHALL UNIVERSITY SCHOOL OF RESPIRATORY THERAPY COURSE SYLLABUS COURSE NAME: RSP 203-Respiratory Internship I CREDIT HOURS: 4 PREREQUISITES: Successful completion of program sequence. Sophomore level. COREQUUISITE: RSP-201, RSP-202 INSTRUCTOR: Chuck Zuhars, RRT, M.S. Office Phone: Brent Blevins, RN, RRT Office Phone: Jim Montgomery, RRT Office Phone: Chris Trotter, RRT, B.A. Office Phone: COURSE DESCRIPTION: This is a four hour course where the emphasis is placed on information gathering from the patient record, physical evaluation of the patient and basic respiratory interventions. COURSE OBJECTIVES: At the end of this course the student will be able to: 8. Report pertinent patient data within the medical record while maintaining HIPAA standards. 9. Demonstrate correct charting methods with supervision 10. Use oxygen therapy with supervision. 11. Perform cardiopulmonary resuscitation with supervision. 12. Performs basic respiratory interventions with supervision. 13. Uses physical assessments skills to evaluate cardiopulmonary status with supervision. 196
197 METHODS OF TEACHING: 197 Lecture/Discussion through the Teaching/Learning Process Exercises to Assist with Problem Solving In-Class/clinical Activities Handouts Reference Readings Evaluation Process Clinical Attendance 35% Clinical Evaluations 15% Presentation/Assignments 15% Therapy evaluations, chart reviews, etc. Clinical notebook 15% Cognitive objectives Check offs lab and clinical Completion/organization of clinical book Exam 20% Directed readings, Charting, O2 therapy, Cardio-pulmonary resuscitation SPECIFIC FACTORS 1. Attendance and completion of required paperwork. Attendance is mandatory for all clinical rotations. All missed clinical time will be made up. 2. Cognitive objectives. The student is required to complete the provided list of cognitive objectives for the clinical instructor. It is at the instructor s discretion as to how these objectives will be assessed. 3. Completion of clinical competencies. The following clinical competencies are to be completed by the student and checked off by the instructor/preceptor. o Hand washing o Isolation techniques o Medical records o Vital signs o Arterial blood pressure o Patient positioning o Pulmonary auscultation o Bedside ventilatory assessment o Patient assessment o Cylinder Safety and Transport o Nasal Cannula o Simple O2 and Partial Rebreather Mask 197
198 o Venturi and non-rebreather Mask o Measurement of O2 concentration o Aerosol and Humidity Therapy o Heated Aerosol and Humidity Therapy with Varied FiO2 o Aerosol Drug Administration via HHN o Incentive Spirometry o Breathing Exercises Completion of minimum required procedures. The student is required to complete a minimum number of required procedures per clinical practicum. Any procedures not completed will carry over to the following clinical practicum until the required number of procedures is completed. Required procedures: a. Patient assessments 5 b. Nasal Cannula set-up 5 c. Simple O2/partial rebreather mask set-up 2 d. Venturi and non-rebreather mask set-up 2 e. Measurement of O2 concentration 2 f. Aerosol set-up 2 g. Aerosol drug administration via HHN 10 h. Incentive spirometry 2 i. Physician contact 1 hour 5. Patient assessment forms. The student will complete at least 5 therapy evaluation forms. Completed forms are to be submitted to the clinical instructor or placed in the clinical book. CLASS ATTENDANCE AND DISCIPLINE Any student who is unable to attend class must call the school stating the reason for absence. In the event a student must be absent and a call is made to the school this is not necessarily an excused absence. If a student is unable to be present for a Clinical experience, the student must notify the Clinical site and the Director of Clinical Education two hours prior to the scheduled time on duty, stating the reason for absence. Students are responsible for making up any curriculum missed when absent from class or Clinical. In the event the instructor determines a student has become disruptive in class or Clinical, the student will receive counseling from the instructor of that class or Clinical site and the Program Director 198
199 199 CLINICAL ABSENCE After two days absence from Clinical per quarter, consecutive or intermittent, the student will receive a written notice from the Director of Clinical Education notifying the student of their current attendance status. At the time of the notification the two Clinical days missed will be scheduled for make-up by the Director of Clinical Education, at the convenience of the school and the Clinical affiliate. The missed Clinical days must be completed by the last day of the current semester in which the absences occurred. The third day of absence, consecutive or intermittent, the student will be terminated from the program, unless a leave of absence has been approved prior to the absences. In the event that the absence is not made up, by the last day of the semester that the absence occurred, it will result in the immediate termination of the student from the program. Eight hours completes a Clinical day, exceptions can be made due to facility requirements. Eight hours, consecutive or intermittent, missed will be considered an absence, regardless of the number of days involved either in arriving tardy or leaving early. All hours regardless will be made up. Transportation problems are considered an unexcused absence! EXCUSED ABSENCE Excused absences will be recognized for the following reasons: -Personal illness verified by a doctor s slip. -Death in immediate family. -Required court appearance. TARDINESS Tardiness is inexcusable. However, if for some reason you will be late to class or Clinical practice. The Clinical site, school, and Director of Clinical Education, is to be notified before the scheduled time for class or Clinical duty. The student is responsible for material missed due to tardiness. It is not the responsibility of the instructor to recover the material that is missed due to tardiness. If a student has three tardy occurrences during clinicals. The student will be sent home with an unexcused absence. If the student then continues to have tardiness occurrences he/she will have a conference with Program Director for possible dismissal. 199
200 DRESS CODE 200 The student will be required to wear the regulation uniform selected for the Respiratory Therapy Program. The uniform will be worn when attending Clinical rotations and/or Clinical related activities. Forest green scrubs and white lab coat. SMRC patch on left arm. All students are required to attend all scheduled Clinical duty with the following items: -Watch with a second hand -Stethoscope -Clinical Education Module Book -St. Mary s Respiratory Therapy Program Name Badge The Clinical instructor may dismiss any student from Clinical duty for NOT ATTENDING WITH THE REQUIRED ITEMS or not arriving at the required time(instructors discretion). Any student dismissed from Clinical duty due to insubordination will be assigned an unexcused absence and be required to make-up the Clinical hours missed. Miscellaneous: Clinical schedules will be handed out the second week of class. Directed reading assignments Clinical site this semester: St. Mary s Medical Center o Emergency room o Pulmonary rehabilitation o Pulmonary Floor o Cardiac step down o 4S, 5S, 6S, SNU Floor therapy 200
201 Laboratory 201 Laboratory simulations and exercises will further enhance the learning process through a supervised hands-on approach. The labs in the school of Respiratory Care will be open for your use to practice procedures or equipment from 8am to 4pm daily(except for scheduled class labs), Monday thru Thursday, and 8am to 12pm on Friday. There is a white binder, designated laboratory sign in, placed on the counter outside of Brent and Jims offices each morning. Please note all extra time spent in the school labs in this book. The time and extra effort spent in the labs will be taken into consideration when the final course grades are calculated at the end of the semester. You may schedule additional time in the lab with an instructor on Fridays by ing and requesting an appointment. Please state the date and time that you want to schedule, also the topic or piece of equipment which you would like to cover. You will receive a return to confirm your appointment, or if the time requested is unavailable, an offer of alternate appointment time. The request must be received no later than 12pm, the Wednesday before the Friday that is being scheduled. Please send your requests to: [email protected] or [email protected] or [email protected] 201
202 CONTENT OUTLINE: I. Medical Records A. Finding information B. HIPPA Standards 202 Egan s Respiratory 8 th edition Chapter 2 pg II. Charting Skills A. SOAP Notes III. Physical Examination of the Patient A. Overview of the Patient B. Heart Sounds C. Breath Sounds D. Percussion of the chest III. Oxygen Therapy A. Types of Therapy B. Physician Orders C. Nasal Cannula D. Face Mask E. Non-rebreather mask F. Venti-mask G. Bag-valve mask Chapter 14 pg Chapter 35 pg V. Cardiopulmonary Resuscitation A. Techniques B. Standards C. Adult Chapter 31 pg **Each chapter use the chapter outline, In this chapter you will learn, key terms and key points to study for test. ** GRADING SCALE: A B C D 202
203 Below 60- F 203 Required Textbooks: Wilkins, Stoller, Scanlan: Egan s Fundamentals of Respiratory Care, 8 th Ed., Elsevier Dates to remember August 13, Monday August 17, Friday Registration/Schedule Adjustment August 17, Friday, 9 a.m. Residence Halls Open for Freshmen August 20, Monday, 8 a.m. First Day of Classes August 20, Monday August 24, Friday Late Registration and Add/Drop (Schedule Adjustment) August 24, Friday Last Day to Add Classes (Withdrawals Only After This Date) August 27, Monday W Withdrawal Period Begins September 1, Saturday September 3, Monday University Computer Services Unavailable September 3, Monday Labor Day Holiday University Closed September 14, Friday Application for December Graduation Due in Academic Dean s Office September 21, Friday Last Day to Drop 1st 8 Weeks Courses October 8, Monday Final Draft of Thesis Due in Advisor s Office October 9, Tuesday Mid-Semester, 1st 8 Weeks Courses End October 10, Wednesday 2nd 8 Weeks Courses Begin October 15, Monday Deadline for Submitting Freshmen Mid Term Grades 203
204 October 22, Monday Students should schedule appointments with advisors to prepare for advance registration (Required for students who have mandatory advising holds) 204 October 26, Friday Last Day to Drop a Full Semester Individual Course October 29, Monday Recommended Date to Apply for May 2008 Graduation October 29, Monday December 4, Tuesday Complete Withdrawals Only November 5, Monday November 16, Friday Advance Registration for Spring Semester for Currently Enrolled Students November 9, Friday Last Day to Drop 2nd 8 Weeks Courses November 17, Saturday, Noon Residence Halls Close November 19, Monday Last day for Defense of Dissertation November 19, Mon December 11, Tuesday Advance Registration for Spring Semester Open to All Admitted/Re-Admitted Students November 19, Monday November 24, Saturday Thanksgiving/Fall Break - Classes Dismissed November 22, Thursday November 25, Sunday University Computer Services Unavailable November 22, Thursday Thanksgiving Holiday University Closed November 23, Friday University Holiday University Closed November 25, Sunday, Noon Residence Halls Open November 26, Monday Classes Resume November 28, Wednesday December 4, Tuesday Dead Week December 4, Tuesday Last Class Day and Last Day to Completely Withdraw for Fall Semester December 5, Wednesday Study Day - Exams for Wednesday Classes 3 p.m. and After Will Be Held 204
205 December 6, Thursday Exam Day 205 December 6, Thursday Approved Thesis/Dissertation Must Be Submitted Electronically and all Paperwork/Checks Must Be In Graduate College Office December 7, Friday Exam Day December 8, Saturday Exam Day for Saturday Classes (and some common finals) December 10, Monday Exam Day December 11, Tuesday Exam Day Fall Semester Closes Official Graduation Date For Fall Semester December 12, Wednesday 12 p.m.. Residence Halls Close December 12, Wednesday December 26, Wednesday Advance Registration/Schedule Adjustment for Spring Semester is Suspended December 13, Thursday, Noon Deadline for Submitting Final Set of Grades December 21, Friday January 1, 2008, Tuesday University Closed December 27, Thursday December 28, Friday On-Line Registration Resumes SAFETY PRACTICES: Safety is an important component of respiratory care and technical skills taught throughout the semester. Test Remediation 1. Anyone who earns a grade less than 70% on an exam must remediate the test during the semester. 2. The last test of the semester is not to be remediated. 3. All questions missed on that failed examination must be remediated 4. Remediation will consist of an explanation of the correct answer and why the students answer was incorrect. 5. For Unit Exams, remediations are to be turned in to the remediation coordinator, Brent, seven days after the test is reviewed in class with the students. 6. Remediations are to be turned in or ed to Brent ([email protected]). 205
206 Each question remediated must include a reference from an assigned reading. If the answer cannot be found in an assigned reading, you may reference an instructor s or guest lecturer s presentation. 8. Remediations will be graded S or U by the remediation coordinator. A student earning U should meet with Brent to discuss the question and remediation to ensure that the student understands the concepts being tested and the correct way to perform remediation. 9. Student remediation will be done at the respiratory care school. Test keys will be provided at that time. Tests are not to be removed from the school. 10. If this remediation is not completed in the permitted time, documentation will be placed in the students permanent file and consider at the end of the semester. POLICY STATEMENTS ACADEMIC INTEGRITY Academic dishonesty of any kind will not be tolerated. Academic dishonesty includes cheating on exams, fabrication/falsification, plagiarism, bribes/favors/threats, and complicity. The student will be subject to penalties which may include a lower or failing grade on a project/paper/or exam, or a lower or failing course grade, or expulsion. The full policy is described in the St. Mary's Student Handbook. INCLEMENT WEATHER: As an off campus site, decisions regarding inclement weather are independent of Marshall University, St. Mary's School of Nursing does not cancel classes (theory/clinicals/labs) unless weather conditions are severe. If the decision is made to close the school, the VP of Schools of Nursing and Health Professions will leave a message on this number: 304/ Students may call this number after 6:15 a.m. for a recorded message. Television and radio announcements will be made. The full policy is in the St. Mary's Student Handbook. DISABILITY STATEMENT: St. Mary's/Marshall University Cooperative Degree Program will make accommodations for those students with recognized (medically certified) mental, physical, emotional, and/or learning disabilities provided the accommodations(s) requested do not place undo financial or physical demands on the institution. Written documentation is required from a health care provider who is qualified to diagnose learning disability disorders. This must be provided to the VP of Schools of Nursing and Health Professions. The written documentation must include the need for special accommodations related to the learning disability. In addition, the student must be able to demonstrate ability to meet the objectives of the course(s). See Student Handbook and/or school catalog for specific policy and procedure. **Refer to the Clinical Manual or Instructor for further information 206
207 207 SCHOOL OF RESPIRATORY THERAPY ST. MARY S/ MARSHALL UNIVERSITY COURSE CURRICULUM COURSE NAME: RSP 205 Cardiopulmonary Diagnostics CLASS HOURS: 30 LAB HOURS: 45 PREREQUISITES: Successful completion of program sequence COURSE DESCRIPTION: This advanced course is 3 credit hours in length. It is intended to provide the student with detailed knowledge in the rationale, methodology, and evaluation of pulmonary function testing, including lung volume determination, tests of pulmonary mechanics, diffusion ventilation, and blood flow. Arterial blood gas sampling and analysis is also studied with special attention given to the design and function of blood gas analyzers and interpretation of arterial blood gases. The student is introduced to the principles and practice of stress testing, bronchoscopy, hemodynamic monitoring, pulmonary function testing, and airway management. Throughout the course, emphasis is placed on the relationship of the test results to various cardiopulmonary disease states. COURSE OBJECTIVES: Upon completion of this course, the student will have demonstrated: 1. A thorough understanding of the techniques used for obtaining arterial blood gas samples. 2. An understanding of the equipment and techniques used to analyze arterial blood samples. 3. A thorough understanding of the body s acid-base balance. 4. An understanding of equipment used to measure lung volumes and pulmonary mechanics. 5. A thorough understanding of the techniques used for measuring lung volumes and pulmonary mechanics. 6. An ability to perform and calculate results for lung volumes and pulmonary mechanics. 207
208 An ability to interpret pulmonary function data as to normal or obstructive and restrictive disorders. 8. Demonstrate comprehension of pulmonary stress testing to include theory and techniques used in performing the test. 9. Demonstrate a general knowledge of polysomnography testing. 10. An understanding of the principles of pulmonary rehabilitation and home care procedures. MEHODS OF TEACHING: Lecture/Discussion through the Teaching/Learning Process Exercises to Assist with Problem Solving In-Class Activities Handouts Reference Readings Paper/Pen Examinations Laboratory Simulations and Exercises COURSE MATERIAL: Required Textbooks: Madama, V.C.: Pulmonary Function Testing and Cardiopulmonary Stress Testing, 2 nd Ed., Delmar, Malley, W.M.: Clinical Blood Gases, 2 nd Ed., Elsevier, Wilkins, Stoller, Scanlan: Egan s Fundamentals of Respiratory Care, 8 th Ed., Elsevier 2003 White, G.C.: Basic Lab Competencies for Respiratory Care, 4 th Ed., Delmar, Reference and Resource Material: AARC Clinical Practice Guidelines: Blood Gas Analysis and Hemoximetry Body Plethysmography Capnography/Capnometry during Mechanical Ventilation Discharge Planning for the Respiratory Care Patient Exercise Testing for Evaluation of Hypoxemia and/or Desaturation Long-Term Invasive of Mechanical Ventilation in the Home Metabolic Measurement using Indirect Calorimetry during Mechanical Ventilation Methacholine Challenge Testing Single Breath Carbon Monoxide Diffusing Capacity Polysomnography 208
209 209 Providing Patient and Caregiver Training Pulmonary Rehabilitation Pulse Oximetry Sampling for Arterial Blood Gas Analysis Spirometry Static Lung Volumes Transcutaneous Blood Gas Monitoring for Neonatal and Pediatric Patients Demint, W.C., et al.: A Manual of Standardized Terminology Techniques and Scoring System for Sleep Stages in Human Subjects. Public Health Service, Kacmarek, Mack, Dimas: The Essentials of Respiratory Therapy, 4 th Ed., Elsevier 2005 Merck Manual of Medical Information, Merck, Pagana & Pagana: Mosby s Diagnostic and Laboratory Test Reference, 7 th Ed., Elsevier, Persing, G. Respiratory Care Exam Review. 2 nd Ed., Elsevier, Oakes, D.: Clinical Practitioner s Pocket Guide to Respiratory Care, 6 th Ed., Health Care Educator Publishers, Schmidt, H.: Sleep Disorder Patient Education. Ohio Sleep Medicine Institute. Shapiro, Peruzzi, & Templin: Clinical Application of Blood Gases, 5 th Ed., Mosby, Sills, J.R.: Advanced Respiratory Therapist Exam Guide. 2 nd Ed. Mosby, White, G.C.: Equipment Theory for Respiratory Therapists, 4 th Ed., Delmar, Wilkins, Krider, & Sheldon: Clinical Assessment in Respiratory Care, 3 rd Ed., Mosby, Wojciechowski, W.V.: Respiratory Care Sciences An Integrated Approach, 4 th Ed., Delmar, Wojciechowski, B.: Evaluation of blood oxygenation. Focus Journal for Respiratory Care, Spring, Wyka, Mathews, & Clark: Foundations of Respiratory Care, Delmar, 2002 SAFETY PRACTICES: Safety is an important component of respiratory care and technical skills taught throughout the semester. 209
210 Features of each unit are given below: 210 Unit 1- Arterial Blood Gas Physiology: A review of external and internal respiration, oxygen transport, acid-base balance, and shunt-deadspace relationships is provided. The relationship of these principles to arterial blood gas sampling is discussed. Unit 2- Arterial Blood Gas Technical Issues: Possible arterial blood gas sampling errors are defined and discussed in detail. An overview of quality assurance and control measure in arterial blood gas sampling is provided. The concept of point of care testing is introduced. Unit 3-Arterial Blood Gas Calculations: The clinical equations for assessing various components contributing to the patient s overall respiratory status are presented. The clinical applications of these equations will be discussed. Unit 4- Introduction to Pulmonary Function Testing: A general introduction to the theory, rationale, and technique of pulmonary function testing is provided. Unit 5- Pulmonary Mechanics: The various pulmonary function tests for pulmonary mechanics are introduced. The discussion will include: test descriptions, test rationales, and normal values. Unit 6- Volumes and Capacities: The various pulmonary function tests for lung volumes and capacities are introduced. Specific tests discussed include: Nitrogen washout and helium dilution tests. The discussion will include: test descriptions, test rationales, and normal values. Unit 7- Gas Distribution: The various pulmonary function tests for assessment of gas distribution are introduced. Emphasis will be placed on the Single-Breath Nitrogen Washout test. The discussion will include: test descriptions, test rationales, and normal values. Unit 8- Gas Diffusion: The various pulmonary function tests for assessment of gas diffusion are introduced. Emphasis will be placed in the diffusing capacity of carbon monoxide in relation to gas diffusion assessment. The discussion will include: test descriptions, test rationales, and normal values. Unit 9- Body Plethysmography: The operating principles of body plethysmography are discussed. The use of body plethysmography in the assessment of airway resistance, lung compliance, and thoracic gas volumes is presented. Unit 10- Pulmonary Function Quality Programs: An overview of quality assurance and control programs in the pulmonary function laboratories is discussed. Unit 11- Cardiopulmonary Stress Testing: The various aspects of cardiopulmonary stress testing are introduced. Discussion will include: testing rationale, parameters evaluated during testing, contraindications, equipment, and basic interpretation. 210
211 211 Unit 12- Nutrition Overview: A brief overview of the nutritional needs and metabolic and respiratory consequences of diet will be presented. Emphasis will be placed on the nutritional management of patients with chronic pulmonary disease. Unit 13- Miscellaneous Cardiopulmonary Testing: Various cardiopulmonary tests that have not been previously covered will be discussed. Emphasis will be placed on metabolic studies. The rationale and procedure for various cardiopulmonary testing will be presented. Unit 14- Cardiac Monitors: The various aspects of specific cardiac monitors are introduced. Monitors to be discussed include: Holter, Event, and Telemetry monitors. Discussion will include: testing rationale, contraindications, and equipment. 211
212 212 Features of each lab are given below: Lab 1- Arterial Blood Gas Technique: The indications, contraindications, correct technique, and sample processing procedure for arterial blood gas sampling is discussed. The student will be given time to practice topics presented in lab and corresponding unit lectures. Lab 2- Arterial Blood Gas Interpretation: A review of arterial blood gas interpretation is presented. An in-depth discussion will be provided on arterial blood gas classification and the clinical implications of abnormal results. The student will be given time to practice topics presented in lab and corresponding unit lectures. Lab 3- Alternative Measurements: An overview of various alternative assessment techniques for the evaluation of arterial blood gases and acid-base status will be presented. Topics of discussion will include: pulse oximetry, transcutaneous oxygen/carbon dioxide monitoring, and capnography. The student will be given time to practice topics presented in lab and corresponding unit lectures. Lab 4- Pulmonary Function Equipment and Testing Regimens : A general overview of pulmonary function testing regimens and required equipment will be presented. Topics of discussion will include: test descriptions, testing rationale, testing procedure, equipment used in pulmonary function testing, and significance of findings. The student will be given time to practice topics presented in lab and corresponding unit lectures. Lab5-Performing a Complete Pulmonary Function Test: The procedure and rationale for performing a complete pulmonary function test will be presented. The student will be given time to practice topics presented in lab and corresponding unit lectures. Lab 6-Bedside Parameters: An overview of various spontaneous pulmonary parameters will be presented. Topics of discussion will include: test descriptions, testing rationale, testing procedure, equipment used in obtaining spontaneous parameters, and significance of findings. The student will be given time to practice topics presented in lab and corresponding unit lectures. Lab 7- Pulmonary Function Test Interpretation: An overview of the calculation of normal values on pulmonary function tests and interpretation of the pulmonary function test will be presented. An in-depth discussion will be provided on pulmonary function test classification and the clinical implications of abnormal results. The student will be given time to practice topics presented in lab and corresponding unit lectures. Lab 8- Performing Cardiopulmonary Testing: The process of obtaining various cardiopulmonary stress tests will be presented. The correct procedure for patient selection, exam preparation, and instruction will be emphasized. The student will be given time to practice topics presented in lab and corresponding unit lectures. Lab 9- Cardioversion: The process for assisting in the controlled cardioversion will be presented. The correct procedure for patient selection, preparation, and instruction will be 212
213 213 emphasized. The student will be given time to practice topics presented in lab and corresponding unit lectures. 213
214 214 SCHOOL OF RESPIRATORY THERAPY ST. MARY S/MARSHALL UNIVERSITY EVALUATION OF THE STUDENT EVALUATION The purpose of evaluation is to indicate, to some degree, the extent to which the student has learned the concepts presented. Frequent testing will encourage the student to study and learn at a regular and constant pace throughout the course. The teaching-learning process meets the expected outcome goal. Evaluation is also utilized as a learning tool. Questions are designed to stimulate problem solving. The examinations are reviewed to provide feedback and promote discussion. Laboratory simulations and exercises will further enhance the learning process through a supervised hands-on approach. Students who require additional support outside of that given during class hours may set-up personal meetings with the instructor during office hours. 1. Examinations/Quizzes SPECIFIC FACTORS A. Unit Examinations: 4 Exams: Each exam is worth 10% of the final grade for a total of 40%. Exams will be approximately 30 questions in length and may include multiple choice, matching, listing, labeling, short answer, and essay style questions. An hour will be given for each unit exam. B. Quizzes Quizzes: There will be quizzes administered after the completion of each unit. All quizzes will be averaged to consist of 10% of the final grade Quizzes will be approximately 10 questions in length and questions may include multiple choice, short, answer, listing, and labeling. E. Final Examination Final Exam: The Final exam will be comprehensive and may include multiple choice, matching, listing, labeling, short answer, and essay style questions. The final exam will be worth 30% of the final grade. The final exam will be administered during Finals Week. 2. Laboratory Exercise Check-Offs 214
215 215 Students will complete 2 laboratory check-offs with the instructor on techniques learned in the course. Each laboratory check-off will be worth 10%, for a total of 20% of the final grade. Additional laboratory check-offs will be administered on a pass/fail basis as deemed necessary by the instructor. 3. Homework/Classwork 4. Class Participation: 5. Grading Scale: It will be the student s responsibility to complete homework/classwork assignments. There are no scheduled homework assignments in this course. However, additional assignments may be given at the instructor s discretion. Class participation will include discussions, workgroups, and laboratory exercises. Theory: Laboratory Skills 90%-100%: A Excellent 2: Excellent 80%-89%: B Good 1: Needs Improvement 70%-79%: C Satisfactory 0: Failed to meet the basic 0%-69%: Failing objectives of exercise 6. Final Grade Calculation: The factors listed below will be used to determine the final grade for the course: A. The Unit Exams are worth 40% of the final grade. B. The Unit Quizzes are worth 10% of the final grade. C. The Final Exam is worth 30 % of the final grade. D. Laboratory Check-Offs are worth 20% of the final grade. 215
216 216 Student Outcome Goals Essential Content Student References Discuss how oxygen and carbon dioxide are transported in the body. Differentiate between total CO2 and PCO2. Explain the physiologic effect of shunting and deadspace. Differentiate between shunt and deadspace disorders. Describe the composition of the intra-alveolar spaces. Explain how electrolytes are balanced in the body. Define the components of the anion gap. Discuss the significance of base excess. Identify the various buffer systems of the body. Explain how bicarbonate is controlled by the body. Unit 1: Arterial Blood Gas Physiology Lesson 1: Lecture 60 minutes 1. Oxygen and carbon dioxide transport a. O2 cascade b. Role of O2 in the cell c. Carriage of O2 in the blood d. O2 content e. Oxyhemoglobin dissociation curve f. Bohr effect g. Carriage of CO2 in blood h. Total CO2 2. Shunting and deadspace a. Overview i. Ideal alveolarcapillary unit ii. Deadspace unit iii. Shunt unit iv. Silent unit b. Intrapulmonary shunting i. Anatomic shunt ii. Capillary shunt iii. Shunt effect c. Pulmonary deadspace i. Anatomic deadspace ii. Alveolar deadspace iii. Deadspace effect Lesson 2: Lecture 60 minutes 1. Fluid and electrolyte balance a. Introduction b. Distribution of body fluids c. Normal intake and output of fluids d. Composition of intravascular space e. Anion gap f. Strong anion difference 2. Acid-base balance a. Electrolytes b. Law of mass action c. Buffers Malley Chapters 6, 7, 8 Handout 1-a: O2-Hb Dissociation Curve Review Handout 1-b: Shunt versus Deadspace units Handout 1-c: Distribution of Body Fluids 216
217 217 d. Bicarbonate control e. Base excess/base deficit Describe the design of each of the three electrodes found on a blood gas analyzer. Describe the process for calibration of each of the three types of electrodes found in blood gas analyzers. Explain the function of a cooximeter. Explain the need for cooximeters. Describe the components of a quality assurance program for arterial blood gas analyzers. Identify acceptable and unacceptable values in the calibration process of arterial blood gas analyzers. Describe how various factors like temperature and air bubbles affect the arterial blood gas sample. Unit 2: Arterial Blood Gas Technical Issues Lesson 3: Lecture 60 minutes 1. Blood gas analyzers a. Overview b. PO2 c. ph d. PCO2 e. Co-oximeters f. Point of care testing 2. Quality control and assurance measures for ABG analyzers a. Definitions b. Calibration i. Controls ii. Levels of calibration c. Levey-Jennings charts d. Troubleshooting 3. Quality control measures while obtaining an ABG a. Syringe set up b. Icing sample 4. Typical blood gas contaminants a. Anti-coagulants b. Air bubbles 5. Temperature correction 6. Venous samples Malley Chapters 3 and 4 Handout 2-a: Levey- Jennings Charts 217
218 218 Perform the various calculations presented. Relate equations to clinical findings. Differentiate between shunt and deadspace diseases. Explain the effect of minute ventilation of PCO2. Unit 3: Arterial Blood Gas Calculations Lesson 4: Lecture 60 minutes 1. Introduction 2. Acid-base calculations a. Anion gap b. Bicarbonate correction of ph c. Rule of 8 s d. Predicted PaCO2 e. Estimation of ph changes based on PCO2 3. Oxygenation a. Alveolar air equation b. A-a gradient c. A/A ratio d. O2 content e. Arterial to mixed venous O2 content difference f. Arterial to mixed venous O2 tension difference g. O2 consumption h. O2 delivery i. O2 extraction ratio j. PaO2/FIO2 ratio k. Predicted PaO2 l. Respiratory index m. Respiratory quotient n. Respiratory exchange ratio o. V/Q ratio 4. Shunt Equation a. Classical shunt equation 5. Clinical uses of the shunt equation 6. Clinical uses of the VD/VT ratio 7. Minute volume to PaCo2 relationship 8. Guidelines for differentiating shunt from deadspace producing disease Malley Chapters 9, 11, 13 Handout 3-a: Equation Reference 218
219 219 Define the purpose of the PFT. List the indications of the PFT. Explain the contraindications for the PFT. Calculate the ideal body weight for various testing subjects. Discuss the therapist s role in performing a PFT. Unit 4: Introduction to Pulmonary Function Testing Lesson 5: Lecture 60 minutes 1. Definition of pulmonary function tests 2. Indications for the PFT 3. Contraindications for the PFT 4. Hazards and complications of the PFT 5. Limitations of the PFT 6. Ideal body weight 7. Therapist role in PFT testing Madama Text Introduction White Chapter 5, pp
220 220 Define the individual tests included in pulmonary mechanic testing. Explain the patient maneuver for obtaining pulmonary mechanic tests. Explain how the various pulmonary mechanic tests relate to anatomical regions of the lungs. Discuss the clinical significance of each pulmonary mechanic test. Unit 5: Pulmonary Mechanics Lesson 6: Lecture 60 minutes 1. Introduction 2. Forced Vital Capacity maneuvers 3. Forced Vital Capacity the measurement a. Prediction equations 4. Volume/Time Curve and Measurements a. Timed forced expiratory volumes b. Forced expiratory volume percents c. Forced expiratory flows 5. Flow/Volume Loops a. Timed forced expiratory volumes b. Forced expiratory volume percents c. Forced expiratory flows d. Forced inspiratory volumes e. Forced inspiratory flow rates 6. Peak expiratory flow 7. FVC with Heliox 8. Maximum voluntary ventilation 9. Significance of pulmonary mechanic measurements a. FVC b. FEV 0.5 c. FEV 1 d. FEV 2 e. FEV 3 f. FEV/FVC ratio g. FEF h. FEF 25-75% i. FEF 75-85% j. PEFR k. FIF 25-75% l. MVV Madama Chapter 2 Handout 5-a: FVC Overview Handout 5-b: Pulmonary Mechanics Summary 220
221 221 Define the four lung volumes and capacities. State the lung volumes and capacities that are not measurable with direct spirometry and why. Identify 3 methods for measuring the FVC. Unit 6: Volumes and Capacities Lesson 7: Lecture 60 minutes 1. Introduction 2. Lung volumes a. Inspiratory reserve volume b. Tidal volume c. Expiratory reserve volume d. Residual volume 3. Lung capacities a. Inspiratory capacity b. Functional residual capacity c. Vital capacity d. Total lung capacity 4. Slow vital capacity 5. Direct techniques for measuring lung volumes and capacities a. Direct spirometry i. Volumes measured ii. Procedure 6. Indirect techniques for measuring lung volumes and capacities a. Overview b. Nitrogen washout c. Helium dilution 7. Comparison of gas dilution techniques 8. Normal range for FVC Madama Chapter 4 Handout 6-a: Lung Volumes and Capacities Handout 6-b: Open and Closed Circuit FVC Systems Handout 6-c: Helium Dilution Circuit Handout 6-d: Open Circuit Nitrogen Washout Tracings 221
222 222 Describe the rationale for gas distribution tests. Describe the technique used for the single breath nitrogen elimination test. Define closing volume and closing capacity. Unit 7: Gas Distribution Lesson 8: Lecture 60 minutes 1. Deadspace ventilation 2. Overview of distribution of ventilation 3. Assessing distribution of ventilation with He dilution and N2 washout. 4. Single Breath Nitrogen Elimination Test a. Description b. Phases c. Closing volume d. Closing capacity e. Clinical applications of SBN2 Madama Chapter 5 Explain the rationale for diffusion studies. Explain why CO is used in diffusion studies. Differentiate between DLCOSB and DLCOSS techniques. Unit 8: Gas Diffusion Lesson 9: Lecture 60 minutes 1. Diffusion studies overview a. Significance of CO 2. Single breath method 3. Steady state method 4. Fractional CO uptake method 5. Rebreathing method 6. Test preparation 7. DLCO interpretation Madama Chapter 6 222
223 223 State the law that governs the operation of the body plethysmograph. Explain how body plethysmography measures thoracic gas volume. Define airway resistance and lung compliance. Explain the technique used for obtaining measurements for airway resistance and lung compliance. Unit 9: Body Plethysmography Lesson 10: Lecture 60 minutes 1. Thoracic gas volume 2. Boyles Law 3. Lung compliance a. Procedure for measuring b. Interpretation 4. Airway resistance a. Procedure for measuring b. Interpretation 5. Advantages and disadvantages of body plethysmography Madama Chapter 2, pp and Chapter 4, pp Handout 9-a: Schematic Overview of Body Plethysmography Handout 9-b: Operation of Body Plethysmograph 223
224 224 Discuss the purpose of quality assurance programs in the PFT lab. Explain the procedure and rationale for quality control in the following PFT equipment: o Spirometers o N2 washout equipment o He dilution equipment o Body plethysmograph o Gas analyzers Unit 10: Pulmonary Function Quality Programs Lesson 11: Lecture 60 minutes 1. Introduction 2. Maintenance of PFT equipment 3. Quality control overview 4. Quality control of spirometers 5. Quality control of N2 washout equipment 6. Quality control of He dilution equipment 7. Quality control of body plethysmograph 8. Quality control of gas analyzers Madama Chapter 16 List the types of stress tests and the purpose of each test. List the indications and contraindications for stress testing. Define the parameters that are monitored during a stress test. Unit 11: Cardiopulmonary Stress Testing Lesson 12: Lecture 60 minutes 1. Introduction 2. Types of cardiopulmonary stress tests a. Tests for evaluating general fitness b. Tests to evaluate O2 desaturation during exercise c. Tests to evaluate exercise tolerance Madama Chapters 13 and
225 225 Explain the limitations of stress testing. 3. Indications for stress testing 4. Patient evaluation prior to stress testing 5. Contraindications to stress testing 6. Parameters analyzed during stress tests a. Metabolic equivalents b. Respiratory exchange ratio c. Max O2 consumption d. Max CO2 production e. O2 pulse f. Anaerobic threshold g. Max hear rate 7. Limitations of stress testing a. Deconditioned muscles b. Pulmonary limitations c. Cardiovascular limitations Explain how carbohydrates, lipids, and protein are metabolized by the body. Give a brief explanation of how energy is derived in the body. List the essential vitamins. Explain how nutritional status can affect respiratory function. Discuss the effects of weigh loss and muscle strength loss in pulmonary patients. List several nutritional interventions that may improve patient s pulmonary status. Unit 12: Nutritional Status of the Pulmonary Patient Lesson 13: Lecture 60 minutes 1. Overview of metabolism a. Carbohydrate metabolism b. Lipid metabolism c. Protein metabolism 2. Summary of energy metabolism 3. Vitamin requirements 4. Relationship between pulmonary disease and nutritional status 5. Weight loss and pulmonary disease 6. Muscle mass and strength 7. Dietary intervention Egan s Chapter
226 226 Explain the rationale for Calorimetry. Explain the importance of Calorimetry in the overall management of the pulmonary patient. Define the occlusion pressure. Explain the ventilatory response to O2 and CO2. Discuss testing methods for assessing the ventilatory response to O2 and CO2 Unit 13: Miscellaneous Cardiopulmonary Testing Lesson 14: Lecture 60 minutes 1. Calorimetry a. Direct Calorimetry b. Indirect Calorimetry c. Significance of Calorimetry 2. Ventilatory response tests a. Occlusion pressure b. Ventilatory response to O2 c. Ventilatory response to CO2 Unit 14: Cardiac Monitors Lesson 15: Lecture 60 minutes 1. Continuous ECG monitoring 2. Holter monitors 3. Event monitors 4. Procedure for cardiac monitor setup Madama Chapter 15 List the rationale and set-up procedure for the following cardiac monitors: o Continuous ECG o Holter monitor o Event monitor Lecture Handout 14-a: Holter Monitor Set-up 226
227
228 228 RESPIRATORY THERAPY ST. MARY S/MARSHALL UNIVERSITY SCHOOL OF RESPIRATORY CARE COURSE CURRICULUM COURSE NAME: RSP 206 Neonatal and Pediatric Respiratory Care CLASS HOURS: 30 LAB HOURS: 45 PREREQUISITES: Successful completion of program sequence COURSE DESCRIPTION: This 3 credit hour course introduces the student to the special needs of the neonatal and pediatric patient. Fetal cardiopulmonary development and changes at birth are covered. Equipment, procedures, and methods used in the care and evaluation of neonatal and pediatric patients are also covered. Cardiopulmonary conditions and diseases specific to neonates and pediatrics are discussed. COURSE OBJECTIVES: Upon completion of this course, the student will have demonstrated: 1. A thorough understanding of the physiologic and anatomic differenced between the cardiopulmonary systems of the newborn, child, and adult. 2. A thorough understanding of the indications for, function of, and maintenance of the respiratory therapy equipment used in pediatric and neonatal respiratory care. 3. A proficiency in initiating, maintaining, and discontinuing mechanical ventilation of the neonate and pediatric patient. 4. An awareness of common cardiopulmonary disorders, to include their pathophysiology and treatment, in the infant and pediatric patient. 5. A thorough understanding of the techniques and uses of cardiopulmonary resuscitation in newborns and children. 6. A thorough understanding of the rationale and techniques of respiratory therapy modalities pertinent to the neonatal and pediatric respiratory patient. 228
229 229 MEHODS OF TEACHING: Lecture/Discussion through the Teaching/Learning Process Exercises to Assist with Problem Solving In-Class Activities Handouts Reference Readings Paper/Pen Examinations Laboratory Simulations and Exercises Required Textbooks: Whitaker, K.: Comprehensive Perinatal and Pediatric Respiratory Care, 3 rd Ed., Delmar, White, G.C.: Basic Lab Competencies for Respiratory Care, 4 th Ed., Delmar, Reference and Resource Material: AARC Clinical Practice Guidelines: Application of Continuous Positive Airway Pressure to Neonates via Nasal Prongs, or Nasopharyngeal Tube, or Nasal Mask Capillary Blood Gas Sampling for Neonatal and Pediatric Patients Neonatal Time-Triggered, Pressure Limited, Timed-Cycle Mechanical Ventilation Selection of an Aerosol Delivery Device for Neonatal and Pediatric Patients Selection of an Oxygen Delivery Device for Neonatal and Pediatric Patients Surfactant Replacement Therapy American Heart Association Pediatric Advanced Life Support Guidelines, Cairo, Pilbeam: Mosby s Respiratory Care Equipment, 7 th Ed., Elsevier Kacmarek, Mack, Dimas: The Essentials of Respiratory Therapy, 4 th Ed., Elsevier 2005 Merck Manual of Medical Information, Merck, Pagana & Pagana: Mosby s Diagnostic and Laboratory Test Reference, 7 th Ed., Elsevier, Persing, G. Respiratory Care Exam Review. 2 nd Ed., Elsevier,
230 230 Oakes, D.: Neonatal / Pediatric Respiratory Care A Critical Care Pocket Guide, 5 th Ed., Health Care Educator Publishers, Oakes, D.: Clinical Practitioner s Pocket Guide to Respiratory Care, 6 th Ed., Health Care Educator Publishers, Sills, J.R.: Advanced Respiratory Therapist Exam Guide. 2 nd Ed. Mosby, White, G.C.: Equipment Theory for Respiratory Therapists, 4 th Ed., Delmar, Wilkins, Stoller, and Scanlon: Egan s Fundamentals of Respiratory Care, 8 th Ed., Levier 2003 Wilkins, Krider, & Sheldon: Clinical Assessment in Respiratory Care, 3 rd Ed., Mosby, Wojciechowski, W.V.: Respiratory Care Sciences An Integrated Approach, 4 th Ed., Delmar, Wyka, Mathews, & Clark: Foundations of Respiratory Care, Delmar, 2002 SAFETY PRACTICES: Safety is an important component of respiratory care and technical skills taught throughout the semester. 230
231 231 Features of each unit are given below: Unit 1 Fetal Development: The stages of fetal development will be discussed. Emphasis will be placed on fetal pulmonary and circulation development. Anatomical changes from the fetal stage to the newborn will be presented. Possible complications of the labor and delivery process will be presented as well. Unit 2 Continuing Care of the Neonate: The principles of caring for the neonate after the birthing process will be discussed. Emphasis will be placed on thermoregulation, skin care, fluid and electrolyte balance, and developmental needs of the neonate. Unit 3 Respiratory Disorders of the Newborn: Common respiratory disorders of the newborn will be discussed. Emphasis will be placed on disease pathology and the respiratory management of the disorder. Disorders to be discussed will include: persistent pulmonary hypertension, respiratory distress syndrome, meconium aspiration, pneumothorax, pneumonia, apnea, congenital heart disease, and bronchopulmonary dysplasia. Unit 4 Mechanical Ventilation of the Neonate: The general principles of mechanically ventilating the neonate will be presented. Special considerations applicable to mechanical ventilation of the neonate will be emphasized. Unit 5 Special Procedures: Special procedures for the treatment of premature neonates with respiratory disorders will be presented. Topics to be discussed will include: nitrous oxide ventilation, high frequency oscillation, and extracorporeal life support. Unit 6 Pediatric Respiratory Disorders: Common respiratory disorders of the pediatric patient will be discussed. Emphasis will be placed on disease pathology and the respiratory management of the disorder. Disorders to be discussed include: croup, epiglottis, bronchiolitis, cystic fibrosis, foreign body aspiration, and asthma. Unit 7 Pediatric Ventilation: The general principles of mechanically ventilating the pediatric patient will be presented. Special considerations applicable to mechanical ventilation of the pediatric patient will be emphasized. Unit 8 Pharmacology: Common respiratory medications used in the treatment and management of respiratory disorders in the neonatal and pediatric patient will be discussed. Emphasis will be placed on the indications, adverse reactions, and clinical uses of applicable medications. Unit 9 Neonatal Transport: The respiratory management of the neonate during inter-hospital transport will be presented. The respiratory therapist s role in transporting the neonatal patient will be emphasized. Features of each laboratory session are given below: Lab 1 Assessment and Management of the Newborn: The principles of clinical assessment of the neonate will be presented. Emphasis will be placed on recognizing the signs of respiratory distress, the Apgar score, arterial blood gas sampling, pulse oximetry, transcutaneous monitoring, suctioning, and 231
232 232 bag and mask resuscitation. Management of the neonate in respiratory distress will be discussed as well. The student will be given time to practice topics presented in the lab session and corresponding unit lectures. Lab 2 Basic Respiratory Care: The basic modalities of respiratory care as they are applied to the neonatal and pediatric patients will be presented. Specific topics to be discussed will include: oxygen administration, aerosolized medication delivery, and bronchopulmonary hygiene techniques. The student will be given time to practice topics presented in the lab session and corresponding unit lectures. Lab 3 Continuous Positive Airway Pressure: The rationale, procedure and equipment for applying continuous positive airway pressure to the neonatal and pediatric patient will be presented. The student will be given time to practice topics presented in the lab session and corresponding unit lectures. Lab 4 Mechanical Ventilation of the Neonatal and Pediatric Patient: The rationale, procedure, and equipment for mechanically ventilating the neonatal patient will be presented. The student will be given time to practice topics presented in the lab session and corresponding unit lectures. Lab 5 Pediatric Advanced Life Support: The general principles of pediatric advanced life support will be presented. The student will be given time to practice topics presented in the lab session and corresponding unit lectures. 232
233 233 RESPIRATORY THERAPY ST. MARY S/MARSHALL UNIVERSITY SCHOOL OF RESPIRATORY CARE EVALUATION OF THE STUDENT EVALUATION The purpose of evaluation is to indicate, to some degree, the extent to which the student has learned the concepts presented. Frequent testing will encourage the student to study and learn at a regular and constant pace throughout the course. The teaching-learning process meets the expected outcome goal. Evaluation is also utilized as a learning tool. Questions are designed to stimulate problem solving. The examinations are reviewed to provide feedback and promote discussion. Laboratory simulations and exercises will further enhance the learning process through a supervised hands-on approach. Students who require additional support outside of that given during class hours may set-up personal meetings with the instructor during office hours. 1. Examinations/Quizzes SPECIFIC FACTORS A. Unit Examinations: 4 Exams: Each exam is worth 10% of the final grade for a total of 40%. Exams will be approximately 30 questions in length and may include multiple choice, matching, listing, labeling, short answer, and essay style questions. An hour will be given for each unit exam. B. Quizzes Quizzes: There will be a total of 9 quizzes administered after the completion of each unit. All quizzes will be averaged to consist of 10% of the final grade Quizzes will be approximately 10 questions in length and questions may include multiple choice, short answer, listing, and labeling. F. Final Examination Final Exam: The Final exam will be comprehensive and may include multiple choice, matching, listing, labeling, short answer, and essay style questions. The final exam will be worth 30% of the final grade. The final exam will be administered during Finals Week. 233
234 Laboratory Exercise Check-Offs 3. Clinical Simulations Students will complete 1 laboratory check-off with the instructor on initiation of mechanical ventilation on the neonate. The laboratory check-off will be worth 10% of the final grade. Additional laboratory check-offs will be administered on a pass/fail basis as deemed necessary by the instructor. Students will be given two neonatal and pediatric clinical simulation case studies to complete. The clinical simulations will be worth 5% each, for a total of 10% of the final grade. 4. Homework/Classwork 5. Class Participation: 6. Grading Scale: It will be the student s responsibility to complete homework/classwork assignments. There are no scheduled homework assignments in this course. However, additional assignments may be given at the instructor s discretion. Class participation will include discussions, workgroups, and laboratory exercises. Theory: Laboratory Skills 90%-100%: A Excellent 2: Excellent 80%-89%: B Good 1: Needs Improvement 70%-79%: C Satisfactory 0: Failed to meet the basic 0%-69%: Failing objectives of exercise 7. Final Grade Calculation: The factors listed below will be used to determine the final grade for the course: A. The Unit Exams are worth 40% of the final grade. E. The Unit Quizzes are worth 10% of the final grade. F. The Final Exam is worth 25 % of the final grade. G. Laboratory Check-Offs is worth 10% of the final grade. H. Clinical simulations are worth 15% of the final grade. 234
235 235 Student Outcome Goals Essential Content Student References Unit 1: Fetal Development List the major events of fetal lung development. Describe fetal circulation. Describe pulmonary and circulatory changes at birth. Describe post-natal lung development. Provide an overview of the changes that the cardiopulmonary system undergoes at birth. Compare neonatal respiratory anatomy that of an adult. Lesson 1: Lecture 1 hour 1. General development periods a. Fertilization period b. Embryonic period c. Fetal period 2. Perinatal and pediatric classification 3. Respiratory system development a. Upper airway b. Lower airway c. Period of lung maturation i. Embryonic period ii. Pseudoglandular period iii. Canalicular period iv. Terminal sac period 4. Fetal lung period Lesson 2: Lecture 1 hour 1. Surfactant a. Function b. Administration 2. Amniotic fluid a. Overview 3. Maternal factors a. Gravida and para b. High risk pregnancy factors c. Maternal conditions 4. The Placenta a. Function 5. Fetal circulation a. Anatomy and physiology 6. Transfer of oxygen from maternal to fetal blood a. Process overview Lesson 3: Lecture 1 hour 1. Transition from fetal circulation to newborn circulation a. Process overview b. Stage of development correlation 2. Cardiopulmonary changes at birth a. Ductus arteriosus b. Ductus venosus c. Foramen ovale d. Umbilical arteries Whitaker Chapters 1, 2, 3 Handout 1-a Fetal Development Handout 1-bMajor Divisions of Fetal Development Handout 1-c Respiratory Physiology Handout 1- dcategories of Presentation Handout 1-e Comparison of neonatal and adult respiratory anatomy 235
236 236 e. Umbilical veins f. Pulmonary arteries g. Systemic circulation 3. Comparative neonatal respiratory anatomy a. Head b. Tongue c. Neck d. Larynx e. Epiglottis f. Trachea g. Bronchi h. Thoracic cage Lesson 4: Lecture 1 hour 1. Labor and delivery a. Labor stages b. Premature labor c. Dystocia d. Placental abnormalities e. Problems associated with the umbilical cord 236
237 237 List and describe special environmental considerations in the care of he neonate including: Temperature, light, humidity, noise, FiO 2 and handling. Describe the principles of fluid management in the neonate. Unit 2: Continuing Care of the Neonate Lesson 5: Lecture 1 hour 1. Thermoregulation a. Neutral zone b. Physiology of heat loss c. Thermoregulation in the delivery room d. Equipment for thermal control 2. Controlling the NICU environment a. Effects of stress on the neonate b. Stimulation 3. Skin care of the neonate a. Physiology of neonatal skin b. Skin care recommendations Lesson 6: Lecture 1 hour 1. Fluid and electrolyte balance a. Distribution of water b. Distribution of solutes c. Electrolyte disorders d. Intake and output e. Assessing dehydration 2. Jaundice a. Overview b. Causes c. Treatment Whitaker Chapter 7 Summarize the cause and pathology of common congenital anomalies of the respiratory system including: Tracheoesophageal fistula, diaphragmatic hernia, and choanal atresia. List and explain factors which indicate high risk for neonatal distress Describe the pathophysiology of asphyxia in the newborn. List and recognize the signs and symptoms of respiratory distress in the newborn. List the factors that predispose to Unit 3: Respiratory Disorders of the Newborn Lesson 7: Lecture 1 hour 1. Persistent pulmonary hypertension in the newborn a. Etiology b. Pathophysiology c. Clinical presentation d. Diagnostic tests e. Management of PPHN Lesson 8: Lecture 1 hour 1. Respiratory distress syndrome a. Definition b. Etiology c. Risk factors for RDS Whitaker Chapters 10 and 11 Handout 3a: Surfactant Replacement Therapy 237
238 238 respiratory distress syndrome (RDS). Describe the pathophysiology of RDS. Outline the pulmonary treatment of RDS. Summarize the causes, signs and symptoms, pathophysiology, and treatment of bronchopulmonary dysplasia. Describe the pathophysiology of meconium aspiration. State the problems associated with periodic apnea and transient tachypnea of the newborn. Describe the pathology, effects, and treatment of common congenital anomalies of the circulatory system including: Persistent fetal circulation, patent ductus arteriosus, vascular stenosis, and Tetraology of Fallot. d. Pathophysiology e. Clinical presentation f. X-ray findings g. Clinical RDS scoring system h. Management of RDS Lesson 9: Lecture 1 hour 1. Meconium aspiration syndrome a. Description b. Etiology c. Predisposing factors d. Pathophysiology e. X-ray findings f. Clinical presentation g. Management of MAS 2. Air Leak syndrome a. Overview b. Description c. Etiology d. Clinical manifestations e. Treatment 3. Pneumothorax a. Etiology b. Pathophysiology c. Clinical presentation d. Diagnosis e. Management Lesson 10: Lecture 1 hour 1. Pneumonia a. Incidence in neonates b. Etiology c. Predisposing factors d. Pathophysiology e. Clinical presentation f. Management 2. Transient Tachypnea in the newborn a. Description b. Etiology c. Pathophysiology d. Clinical presentation e. Management of TTN 3. Apnea in the neonate a. Description b. Primary apnea c. Secondary apnea d. Iatrogenic causes of apnea e. Management Handout 3b: Congenital Heart Disease Overview 238
239 239 Lesson 11: Lecture 1 hour 1. Bronchopulmonary dysplasia a. Overview b. Etiology c. Predisposing factors d. Pathophysiology e. Stages of BPD f. Clinical presentation g. Management h. Complications of BPD 2. Retinopathy of prematurity a. Overview b. Etiology c. Pathophysiology d. Classification of severity e. Management and prevention of ROP Lesson 12: Lecture 1 hour 1. Congenital heart disease a. Etiology b. Signs and symptoms c. Patent ductus arteriosus d. Atrial septal defect e. Ventricular septal defect f. Aortic stenosis g. Pulmonary stenosis h. Coarctation of the aorta i. Tetraology of Fallot j. Truncus arteriosus k. Complete transposition of the great vessels l. Tricuspid atresia m. Pulmonary atresia Lesson 13: Lecture 1 hour 1. Choanal atresia a. Overview b. Clinical presentation c. Management 2. Esophageal atresia a. Overview b. Clinical presentation c. Management 3. Congenital diaphragmatic hernia a. Characteristics b. Management 4. Intraventricular hemorrhage a. Incidence 239
240 240 b. Etiology c. Pathophysiology d. Factors affecting cerebral blood flow e. Clinical presentation of intracranial hypertension f. Clinical presentation of IVH g. Management 5. Necrotizing enterocolitis a. Etiology b. Pathophysiology c. Clinical presentation of NEC d. Management List the indications for mechanical ventilation of the infant newborn. Define differences in the parameters of ventilation for neonates compared to adults. Provide typical initial settings for neonatal mechanical ventilation. Given arterial blood gases for a neonatal patient, describe mechanical ventilation changes necessary to restore those values to an acceptable range. List clinical indications for weaning the neonatal mechanical ventilation patient and recommend methods for weaning from mechanical ventilation. List the indications, contraindications, and hazards of PEEP and CPAP for neonatal patients. Unit 4: Mechanical Ventilation of the Neonate Lesson 14: Lecture 1 hour 1. Neonatal physiology affecting ventilation 2. Indications for mechanical ventilation 3. General classifications of neonatal pulmonary disorders a. Atelectatic b. Obstructive 4. Goals of mechanical ventilation 5. Hazards and complications of mechanical ventilation Lesson 15: Lecture 1 hour 6. Time constant review a. Compliance and resistance 7. Types of ventilation a. Neonatal conventional ventilation 1. Pressure control 2. Volume control 3. CPAP b. Variables affecting neonatal conventional ventilation 8. Ventilator parameters a. Tidal volume b. Peak inspiratory pressure c. Mean airway pressure d. PEEP e. Rate f. Inspiratory time g. Inspiratory flow Whitaker Chapters 14 and
241 241 h. Waveforms i. Expiratory time j. I:E ratio k. FiO2 9. Effect of ventilator parameters on blood gas values a. FiO2 b. PIP c. TV d. Rate e. PEEP f. I Time g. I flow h. MAP Lesson 16: lecture 1 hour 10. Initiating ventilatory support a. Items to consider b. Typical ABG goals c. Assessing humidification 11. Initial ventilator setting guidelines 12. Ventilator management strategies a. Oxygenation b. Ventilation 13. Suggested ventilatory strategies for common neonatal respiratory disorders a. Apnea of prematurity b. BPD c. CDH d. MAS e. PPHN f. RDS 14. Weaning from mechanical support a. SIMV b. PS 15. Extubation a. Items to consider b. Extubation readiness criteria c. Procedure overview d. Post extubation care 241
242 242 Summarize the mechanism of action, indications, benefits, and hazards of the four types of high frequency ventilation. Describe the clinical uses of inhaled nitric oxide. Describe the principle of operation for extra corporeal life support. Summarize the indications and contraindications of ECLS. Describe the principle of partial liquid ventilation. Unit 5: Special Procedures Lesson 17: Lecture 1 hour 1. High frequency ventilation a. High frequency positive pressure ventilation b. High frequency jet ventilation c. High frequency oscillation d. High frequency percussive ventilation e. Indications for HFV f. Mechanisms of gas exchange in HFV g. Ventilation and oxygenation with HFV h. Respiratory and cardiovascular effects of HFV i. Hazards of HFV j. Safety issues k. Humidification with HFV l. Initial setting on HFV 2. Inhaled nitric oxide a. Overview of NO b. Indications for ino c. Delivery d. Hazards and complications Lesson 18: Lecture - hour 3. Extracorporeal life support a. Goals of ECMO b. Indications c. Contraindications d. Method for ECLS support e. Ventilator management during ECLS f. ECLS course of care Whitaker Chapters 17 Handout 5a: High Frequency Ventilation Settings 242
243 243 g. Risks of ECLS 4. Liquid ventilation a. History b. Definitions and descriptions c. Uses d. Mechanisms or action e. Conventional ventilation during partial liquid ventilation f. Monitoring g. Outcome assessment Differentiate between the pathophysiology and treatment of bronchiolitis, croup, and epiglottitis Outline the pathophysiology and treatment of bronchiolitis, croup, epiglottitis, cystic fibrosis, and asthma Summarize the respiratory management of the patient suffering pulmonary burns or near drowning. Unit 6: Pediatric Respiratory Disorders Lesson 19: Lecture 1 hour 1. Pediatric age classification 2. Laryngotracheobronchitis a. Description b. Pathophysiology c. Clinical presentation d. CXR presentation e. Management 3. Epiglotitis a. Description b. Causes c. Pathophysiology d. Clinical presentation e. X-ray findings f. Management 4. Bronchiolitis a. Description Whitaker Chapter 243
244 244 b. Pathophysiology c. Clinical findings d. X-ray findings e. Diagnosis f. Management of mild symptoms g. Management of severe symptoms Lesson 20: Lecture 1 hour 1. Cystic Fibrosis a. Description b. Causes c. Pathophysiology d. Clinical presentation e. X-ray findings f. Management 2. Asthma a. Definition b. Etiology c. Clinical manifestations d. Classifying severity of attacks e. Classification of asthma severity in steps f. Differential diagnostic possibilities for asthma in infants and children g. Hospital based management of asthma exacerbation h. Daily management of asthma 12 Handout 6a: Presentation of Bronchiolitis Handout 6b: Pediatric Asthma Medications Lesson 21: Lecture 1 hour 1. Pulmonary burns / smoke inhalation a. Description b. Etiology c. Signs and symptoms d. Stages of pulmonary burns e. Treatment of pulmonary burns f. Indications for airway support 2. Near drowning a. Clinical presentation b. Treatment 3. Reye s syndrome a. Overview b. Clinical presentation c. Treatment Unit 7: Pediatric Ventilation List the indications for mechanical Lesson 22: Lecture 1 hour 1. Overview 244
245 245 ventilation of the pediatric patient Provide typical initial settings for pediatric mechanical ventilation. Given arterial blood gases for a pediatric patient, describe mechanical ventilation changes necessary to restore those values to an acceptable range. List clinical indications for weaning the pediatric mechanical ventilation patient and recommend methods for weaning from mechanical ventilation. List the indications, contraindications, and hazards of PEEP and CPAP for pediatric patients. 2. Indications for mechanical ventilation 3. Pediatric ventilator settings a. Initial assessment b. Mode c. Tidal volume d. Rate e. Inspiratory time f. Inspiratory flow rate g. PEEP h. FiO2 i. Lung protective ventilation Lesson 23: Lecture 1 hour 1. Monitoring during mechanical ventilation of the pediatric patient a. Arterial blood gases b. Noninvasive measures c. Physical examination d. Patient ventilator interaction 2. Weaning the pediatric patient from mechanical ventilation a. Extubation readiness test b. Weaning process 3. High frequency ventilation in the pediatric patient a. Goals b. Indications c. Guidelines d. Clinical management 4. Complications of mechanical ventilation Whitaker Chapters 14 and
246 246 List the indications, uses, and pediatric dosages for the following classes of medications: Mast cell stabilizers Anti-leukotrienes Anti-infective agents Sympathomimetic bronchodilators Parasympatholytic bronchodilators Methylxanthines Detergents Expectorants Mucolytics Respiratory enzymes Steroids Cardiovascular medications Diuretics Anti-convulsants Sedatives Calculate pediatric dosages when given patient age and weight of the drugs listed above. Unit 8: Neonatal and Pediatric Pharmacology Lesson 24: Lecture 1 hour 1. General points about neonatal drug administration 2. Calculating pediatric drug dosages a. BSA rules b. Age rules 3. Mast cell stabilizers 4. Anti-leukotrienes 5. Anti-infective agents 6. Sympathomimetic bronchodilators 7. Parasympatholytic bronchodilators 8. Methylxanthines Lesson 25: Lecture 1 hour 1. Detergents 2. Expectorants 3. Mucolytics 4. Respiratory enzymes 5. Steroids 6. Cardiovascular medications 7. Diuretics 8. Anti-convulsants 9. Sedation and control of ventilation Whitaker Chapter 8 Outline the special considerations Unit 9: Neonatal Transport Lesson 26: Lecture 1 hour 1. NICU classifications 2. Indications for transport 246
247 247 of preparing and transporting high-risk newborn. Summarize the procedure for stabilizing the newborn for transport. Describe the effect of altitude on the partial pressure of arterial oxygen. a. Neonate conditions b. Maternal conditions 3. Communications between referring and receiving hospitals a. Neonatal information b. Maternal information 4. Stabilization of the mother and newborn prior to transport a. Maternal stabilization b. Newborn stabilization 5. Preparation for transport a. Parameters to monitor 6. Procedure for transport team a. Preparation b. Delegated team c. Arranging for transport mode d. Equipment check 7. Evaluation and stabilization of the newborn by the transport team a. Items to evaluate b. Apply appropriate monitors c. Stabilize patient further 8. Special needs during transport a. RDS b. Diaphragmatic hernia c. Cyanotic congenital heart disease d. Air leaks e. T-E fistula f. Heart failure g. Seizures h. Intestinal obstruction 9. Managing enroute a. Continuous monitoring parameters 10. Review of effects of altitude on PaO2 Whitaker Chapter 18 Handout 9a: Altitude Chart 247
248 248 SCHOOL OF RESPIRATORY THERAPY ST. MARY S/MARSHALL UNIVERSITY COURSE SYLLABUS COURSE NAME: RSP 301 Introduction to Management CLASS HOURS: 3 LAB HOURS: 0 PREREQUISITES: Successful completion of program sequence. INSTRUCTOR: Chuck Zuhars, RRT, M.S. Office Phone: Brent Blevins, RN, RRT Office Phone: Chris Trotter, RRT, B.A. Office Phone: COURSE DESCRIPTION: This three credit hour course consists of three hours of lecture each week. This course is an introduction to basic principles of management and their application in the current healthcare environment. Course content includes: management theory, scope of management, quality issues, budgeting, personnel issues, and evaluation and application of management concepts. COURSE OBJECTIVES: 14. Gain a thorough understanding of the philosophy of effective team management. 15. Gain a thorough understanding of how the manager handles conflict within the organization. 16. Become familiar with various accountability basics. 17. Become familiar with appropriate leadership management styles. 248
249 Gain a thorough understanding of performance accountability and the ownership of work. 19. Become familiar with and be able to recognize complications associated with structuring and how to be effective in your support for structure 20. Understanding the process of employee recruitment. 21. Understanding the role synthesis in providing expert decision making. METHODS OF TEACHING: Lecture/Discussion Through the Teaching/Learning Process Exercises to Assist with Problem Solving In-Class Activities Handouts Reference Readings Paper/Pen Examinations COURSE MATERIAL: Required Textbooks: Porter-O Grady & Malloch: Managing for Success in Health Care, 1 st Edition Reference and Resource Material: Finkler, Kovner, & Jones: Financial Management for Nurse Managers and Executives, Third Edition. SAFETY PRACTICES: Safety is an important component of respiratory care and technical skills taught throughout the semester. Features of each unit are given below: Unit 1: Team Development and Leadership - A general overview of how to build effective teams, How to handle and resolve conflict, conducting employee evaluations, how to manage through transformation and transitions. Unit 2: Building Decision-Making Skills- How to use all resources and make effective decisions, How to lead adults in today s workforce, Creating a context for empowerment, structuring for shared decision making, engaging decision makers and leading others to lead. Unit 3: Performance Accountability- How to evaluate an employees competence for their job classification, How to hold each position accountable for their job classification, How to tie accountability and job excellence and raise the standards for all employees. 249
250 250 Unit 4: Structuring for Excellence- Building a context for employee retention, How to develop structure and define what structure is, Getting all employees support for structure, developing staff leadership, advancing the practice of respiratory care, how to maintain and sustain employee and departmental excellence. Unit 5: Searching for Excellence When Recruiting Assessing your environment and the workplace, assessing the market realities of recruiting, selling your company or organization, How to conduct an interview and select the best candidate, Socializing and orientating your new employee. Unit 6: Building the Future of Excellence - Synthesis the new roles of the department leader, How to model mentor in the leadership role, Managing your risks and vulnerability, Developing patience in a world of uncertain expectations, Building relationships in the new age of a changing workforce. SCHOOL OF RESPIRATORY THERAPY ST. MARY S/MARSHALL UNIVERSITY EVALUATION OF THE STUDENT EVALUATION The purpose of evaluation is to indicate, to some degree, the extent to which the student has learned the concepts presented. Frequent testing will encourage the student to study and learn at a regular and constant pace throughout the course. The teaching-learning process meets the expected outcome goal. Evaluation is also utilized as a learning tool. Questions are designed to stimulate problem solving. The examinations are reviewed to provide feedback and promote discussion. Students who require additional support outside of that given during class hours may set-up personal meetings with the instructor during office hours. Students with math difficulties will be referred to the Learning Center for tutoring. 1. Examinations/Quizzes H. Unit Exams SPECIFIC FACTORS 6 Exams: The total of the exams is worth 50% of the final grade. Exams will be approximately 30 questions or greater in length and may include multiple choice, matching, listing, labeling, short answer, and essay style questions. An hour will be given for each unit exam. 250
251 251 I. Quizzes Quizzes: There will be administered during the discussion of each unit. All quizzes will be averaged to consist of 10% of the final grade Quizzes will be approximately 10 questions in length and questions may include multiple choice, short answer, listing, and labeling. J. Final Examination Final Exam: The Final exam will be comprehensive and may include multiple choice, matching, listing, labeling, short answer, and essay style questions. The final exam will be worth 20% of the final grade. The final exam will be administered during Finals Week. K. Course Paper A research paper will be assigned the 2 nd week of class. The topic assigned will be given to the student by the instructor. The outline will follow AMA guidelines. 2. Homework/Classwork It will be the student s responsibility to complete homework/classwork assignments. There are scheduled homework assignments in this course. Additional assignments may be given at the instructor s discretion. 3. Class Participation: 4. Grading Scale: Class participation will include discussions and workgroups. Theory: Laboratory Skills be 90%-100%: A Excellent No lab is scheduled for this course, but may 80%- 89%: B Good conducted at the discretion of the instructor. 70%- 79%: C Satisfactory 60%- 69% D - Unsatisfactory 0%- 59%: Failing 5. Final Grade Calculation The factors below will be used to determine the final grade for the course: 251
252 252 B. The unit exams are worth 50% of the final grade. The unit quizzes are worth 10% of the final grade. The final exam is worth 20% of the final grade. The assigned paper is worth 20% of the final grade 252
253 253 ATTENDANCE/ABSENCE POLICY ATTENDANCE IS THE RESPONSIBILITY OF EACH STUDENT 1. Punctual attendance in all classes and clinical experiences is important if the student is to meet all course objectives. 2. Notify the School of Respiratory Care by contacting the course instructor as soon as possible regarding the absence. 3. The course grade will be lowered one letter grade if theory absences exceed 20% of the theory contact hours. 4. Class notes and other course material missed is the responsibility of the student, not the instructor. 5. References provided to potential employers by the faculty and/or Director will include information on attendance while the student was enrolled in the program. 6. Absences/tardiness on the Day of an Exam/Quiz q. Students who miss an exam/quiz must contact the instructor before the exam/quiz, or as soon as possible after the exam/quiz is missed. r. Documentation of the reason for the exam/quiz absence or tardiness (i.e., health care provider statement, receipt to substantiate car trouble, etc.) must be provided in order to determine eligibility for a makeup exam s. Permission for makeup will be at the discretion of the course instructor(s). t. Makeup exams/quizzes may be different than the original exams/quizzes. u. Any make-ups will be scheduled at a time convenient for the instructor. v. Student should be ready to take the make-up exam/quiz upon the first day of return, unless other plans have been arranged. w. If tardy for an exam/quiz the student must decide if it can be completed within the remaining administration time. The exam/quiz will be turned in at the same time as all other students taking it. If the student does not believe the exam/quiz can be completed within the planned administration time, a request for make-up may be submitted for consideration. x. Students may not take more than two (2) make-up exams per course. Each subsequent test missed will be scored as zero (0). 7. The faculty for each course has the option of establishing rules and consequences for tardiness and attendance. Special seating may be assigned for late-comers. NOTE: This attendance policy also applies lab/clinical check-offs. 253
254 254 POLICY STATEMENTS ACADEMIC INTEGRITY Academic dishonesty of any kind will not be tolerated. Academic dishonesty includes cheating on exams, fabrication/falsification, plagiarism, bribes/favors/threats, and complicity. The student will be subject to penalties which may include a lower or failing grade on a project/paper/or exam, or a lower or failing course grade, or expulsion. The full policy is described in the St. Mary's Student Handbook. INCLEMENT WEATHER: As an off campus site, decisions regarding inclement weather are independent of Marshall University, St. Mary's School of Nursing does not cancel classes (theory/clinicals/labs) unless weather conditions are severe. If the decision is made to close the school, the VP of Schools of Nursing and Health Professions will leave a message on this number: 304/ Students may call this number after 6:15 a.m. for a recorded message. Television and radio announcements will be made. The full policy is in the St. Mary's Student Handbook. DISABILITY STATEMENT: St. Mary's/Marshall University Cooperative Degree Program will make accommodations for those students with recognized (medically certified) mental, physical, emotional, and/or learning disabilities provided the accommodations(s) requested do not place undo financial or physical demands on the institution. Written documentation is required from a health care provider who is qualified to diagnose learning disability disorders. This must be provided to the VP of Schools of Nursing and Health Professions. The written documentation must include the need for special accommodations related to the learning disability. In addition, the student must be able to demonstrate ability to meet the objectives of the course(s). See Student Handbook and/or school catalog for specific policy and procedure. 254
255 255 Test Remediation Policy St. Mary s School of Respiratory Care Anyone who earns a grade less than 70% on an exam must remediate the test during the semester. The last test of the semester is not to be remediated. All questions missed on that failed examination must be remediated Remediation will consist of an explanation of the correct answer and why the students answer was incorrect. For Unit Exams, remediations are to be turned in to the remediation coordinator, Mr. Brent Blevins, seven days after the test is reviewed in class with the students. Remediations are to be turned in or ed to Mr. Blevins ([email protected]). Each question remediated must include a reference from an assigned reading. If the answer cannot be found in an assigned reading, you may reference an instructor s or guest lecturer s presentation. Remediations will be graded S or U by the remediation coordinator. A student earning U should meet with Mr. Blevins to discuss the question and remediation to ensure that the student understands the concepts being tested and the correct way to perform remediation. Student remediation will be done at the respiratory care school. Test keys will be provided at that time. Tests are not to be removed from the school. If this remediation is not completed in the permitted time, documentation will be placed in the students permanent file and consider at the end of the semester. 255
256 256 COURSE OUTLINE Time: TBA Room: hr = 45 hrs/semester WEEK DATE DAY TIME CONTENT INSTRUCTOR 1 8/20/07 Mon 30 MIN Syllabus and questions CZ/BB/CT 45 MIN Unit 1 CZ/BB/CT 1 8/22/07 Wed 1.5 hours Unit 1 CZ/BB/CT 2 8/27/07 Mon 1.5 hours Group Project CZ/BB/CT 2 8/29/07 Wed 1.5 hours Test 1 CZ/BB/CT 3 9/03/07 Mon No School Labor Day!!!!!! 3 9/05/07 Wed 1.5 hours Unit 2 CZ/BB/CT 4 9/10/07 Mon 1.5 hours Unit 2 CZ/BB/CT 4 9/12/07 Wed 1.5 hours Group Project CZ/BB/CT 5 9/17/07 Mon 1.5 hours Test 2 CZ/BB/CT 5 9/219/07 Wed 1.5 hours Unit 3 CZ/BB/CT 6 9/24/07 Mon 1.5 hours Unit 3 CZ/BB/CT 6 9/26/07 Wed 1.5 hours Group Project CZ/BB/CT 7 10/01/07 Mon 1.5 hours Test 3 CZ/BB/CT 7 10/03/07 Wed 1.5 hours Unit 4 CZ/BB/CT 8 10/08/07 Mon 1.5 hours Unit 4 CZ/BB/CT 8 10/10/07 Wed 1.5 hours Group Project CZ/BB/CT 9 10/15/07 Mon 1.5 hours Test 4 CZ/BB/CT 9 10/17/07 Wed 1.5 hours Unit 5 CZ/BB/CT 10 10/22/07 Mon 1.5 hours Unit 5 CZ/BB/CT 10 10/24/07 Wed 1.5 hours Group Project CZ/BB/CT 256
257 /29/07 Mon 1.5 hours Group Project CZ/BB/CT 11 10/31/07 Wed 1.5 hours Test 5 CZ/BB/CT 12 11/05/07 Mon 1.5 hours Unit 6 CZ/BB/CT 12 11/07/07 Wed 1.5 hours Unit 6 CZ/BB/CT 13 11/12/07 Mon 1.5 hours Test 6 CZ/BB/CT 13 11/14/07 Wed 1.5 hours Presentation of Papers CZ/BB/CT 14 11/19/07 Mon Thanksgiving Break CZ/BB/CT 14 11/21/07 Wed Thanksgiving Break CZ/BB/CT 15 11/26/07 Mon 1.5 hours Presentation of Papers CZ/BB/CT 15 11/28/07 Wed 1.5 hours Presentation of Papers CZ/BB/CT 12/05/07 Wed Final Exam CZ/BB/CT 257
258 258 Outline of Unit Reading Unit 1: Team Development and Leadership (Pages 1-108) A. Effective Teams Read Chapter 1 - all B. Conflict Management Read Chapter 2 - all C. Team Performance Read Chapter 3 - all D. Transformation and Transition Read Chapter 4 - all E. Transforming Teams for Decisions Read Chapter 5 - all Unit 2: Building Decision-Making Skills (Pages ) A. Making Effective Decisions Read Chapter 1 - all B. Leading the Adult- to -Adult Work Place; Who Am I Leading C. Creating a Context for Empowerment; Structuring for Shared Decision Making D. Engaging Decision Makers; Empowering Others to Lead E. The Person of the Leader; How Do I Lead Read Chapter 2 - all Read Chapter 3 - all Read Chapter 4 - all Read Chapter 5 - all Unit 3: Accountability (Pages ) A. Performance Accountability; Competence for the Work B. Role Accountability; The Ownership of Work Read Chapter 1 - all Read Chapter 2 - all C. Accountability of Excellence Read Chapter 3 - all D. Accountability and Evidence Read Chapter 4 - all 258
259 259 Unit 4: Structuring Excellence: Building a Context for Retention (Pages ) A. Structure for Excellence; What is Structure? Read Chapter 1 - all B. Supporting the Structure Read Chapter 2 - all C. Staff Leadership Read Chapter 3 - all D. Sustaining Excellence Read Chapter 5 - all Unit 5: Search for Excellence: Recruiting the Best (Pages ) A. Assessing the Work Place Read Chapter 1 - all B. Market Realities of Recruiting Read Chapter 2 - all C. Sell Your Organization Read Chapter 3 - all D. Interviewing for Excellence Read Chapter 4 - all E. Socializing New Employees Read Chapter 5 - all Unit 6: Building the Future of excellence: Mentoring, Learning, and Living Leadership (Pages ) A. Synthesis; The New Role of the Leader Read Chapter 1 - all B. Modeling and Mentoring Leadership Read Chapter 2 - all C. Managing Risk and Vulnerability Read Chapter 3 - all D. Practice in a World of Uncertain Expectations Read Chapter 4 - all E. Building Relationships in the New Age of Work Read Chapter 5 - all 259
260 260 SCHOOL OF RESPIRATORY THERAPY ST. MARY S/MARSHALL UNIVERSITY COURSE SYLLABUS COURSE NAME: RSP 302-Respiratory Internship IV/Directed Reading CREDIT HOURS: 2 PREREQUISITES: Successful completion of program sequence. Junior level INSTRUCTOR: Chuck Zuhars, RRT, M.S. Office Phone: Brent Blevins, RN, RRT Office Phone: Chris Trotter, RRT, B.A. Office Phone: COURSE DESCRIPTION: This two credit hour course will place emphasis on cardiopulmonary assessment and treatment of trauma, post-surgical, cardiac, renal, neonatal and pediatric patients with refinement of monitoring procedures and interpretation of data. COURSE OBJECTIVES: 22. Build up previous skills. 23. Apply laboratory values to clinical practice or determine clinical correlations between lab values and patient condition/care. 24. Perform clinical assessments on critically ill patients with moderate supervision. 25. Provide appropriate respiratory therapy interventions with moderate supervision for critically ill patients. 26. Prioritize care for critically ill patients with moderate supervision. 27. Select mechanical ventilators appropriate to patient needs with moderate supervision. METHODS OF TEACHING: Lecture/Discussion Through the Teaching/Learning Process Exercises to Assist with Problem Solving In-Class Activities Handouts Reference Readings Evaluation Process Clinical Attendance 30% Presentation/Assignments 20% CAMC, case studies, ventilators, etc. Clinical notebook completion 10% Cognitive objectives Check offs lab and clinical 260
261 261 Evaluations 10% Student Exam 1 15% Medical terminology Exam 2 15% Directed reading CLASS ATTENDANCE AND DISCIPLINE Any student who is unable to attend class must call the school stating the reason for absence. In the event a student must be absent and a call is made to the school this is not necessarily an excused absence. If a student is unable to be present for a Clinical experience, the student must notify the Clinical site and the Director of Clinical Education two hours prior to the scheduled time on duty, stating the reason for absence. Students are responsible for making up any curriculum missed when absent from class or Clinical. In the event the instructor determines a student has become disruptive in class or Clinical, the student will receive counseling from the instructor of that class or Clinical site and the Program Director CLINICAL ABSENCE After two days absence from Clinical per quarter, consecutive or intermittent, the student will receive a written notice from the Director of Clinical Education notifying the student of their current attendance status. At the time of the notification the two Clinical days missed will be scheduled for make-up by the Director of Clinical Education, at the convenience of the school and the Clinical affiliate. The missed Clinical days must be completed by the last day of the current semester in which the absences occurred. The third day of absence, consecutive or intermittent, the student will be terminated from the program, unless a leave of absence has been approved prior to the absences. In the event that the absence is not made up, by the last day of the semester that the absence occurred, it will result in the immediate termination of the student from the program. Eight hours completes a Clinical day, exceptions can be made due to facility requirements. Eight hours, consecutive or intermittent, missed will be considered an absence, regardless of the number of days involved either in arriving tardy or leaving early. All hours regardless will be made up. Transportation problems are considered an unexcused absence! EXCUSED ABSENCE Excused absences will be recognized for the following reasons: -Personal illness verified by a doctor s slip. -Death in immediate family. -Required court appearance. 261
262 262 TARDINESS Tardiness is inexcusable. However, if for some reason you will be late to class or Clinical practice, the Clinical site, school, and Director of Clinical Education, is to be notified before the scheduled time for class or Clinical duty. Students are expected to report to the classroom promptly. Fifteen minutes after the beginning of class the door will be locked, students arriving after the door is locked will not be admitted until the beginning or the next schedule class/schedule break. The student is responsible for material missed due to tardiness. It is not the responsibility of the instructor to recover the material that is missed due to tardiness. If a student has three tardy occurrences during clinicals. The student will be sent home with an unexcused absence. If the student then continues to have tardiness occurrences he/she will have a conference with Program Director for possible dismissal. DRESS CODE The student will be required to wear the regulation uniform selected for the Respiratory Therapy Program. The uniform will be worn when attending Clinical rotations and/or Clinical related activities. Forest green scrubs and white lab coat. SMRC patch on left arm. All students are required to attend all scheduled Clinical duty with the following items: -Watch with a second hand -Stethoscope -Clinical Education Module Book -St. Mary s Respiratory Therapy Program Name Badge The Clinical instructor may dismiss any student from Clinical duty for NOT ATTENDING WITH THE REQUIRED ITEMS or not arriving at the required time(instructors discretion). Any student dismissed from Clinical duty due to insubordination will be assigned an unexcused absence and be required to make-up the Clinical hours missed. Miscellaneous: Clinical schedules will be handed out the first week of class. Presentation assignments will also be given. Directed reading assignments Clinical sites this semester: St. Mary s Medical Center Charleston Area Medical Center 262
263 263 Laboratory Laboratory simulations and exercises will further enhance the learning process through a supervised hands-on approach. The labs in the school of Respiratory Care will be open for your use to practice procedures or equipment from 8am to 4pm daily(except for scheduled class labs), Monday thru Thursday, and 8am to 12pm on Friday. There is a white binder, designated laboratory sign in, placed on the counter outside of Brent and Jims offices each morning. Please note all extra time spent in the school labs in this book. The time and extra effort spent in the labs will be taken into consideration when the final course grades are calculated at the end of the semester. You may schedule additional time in the lab with an instructor on Fridays by ing and requesting an appointment. Please state the date and time that you want to schedule, also the topic or piece of equipment which you would like to cover. You will receive a return to confirm your appointment, or if the time requested is unavailable, an offer of alternate appointment time. The request must be received no later than 12pm, the Wednesday before the Friday that is being scheduled. Please send your requests to: [email protected] or [email protected] or [email protected] CONTENT OUTLINE: I. Laboratory Values C. ABGs D. Carboxyhemoglobin E. PT, PTT F. Hemoglobin E. Hematocrit F. Electrolytes Egan s Respiratory 8 th edition Chapter 15 pg Chapter 16 all II. Clinical Assessment A. History B. Physical Examination C. 12 Lead ECG interpretation D. Arrhythmia Recognition E. Hemodynamic Monitoring i. CVP Catheters ii. Swan-Ganz Catheters Chapter 14 all Chapter 15 pg III. Respiratory Interventions E. Oxygen Therapy F. Aerosol Therapy G. Intubation H. Mechanical Ventilation I. IABP Chapter 35 pg Chapter 32 pg
264 264 IV. J. Chest Tubes K. Arterial line placement L. ABGs M. Others Prioritizing Care D. Airway E. Breathing F. Circulation Chapter Chapter 39 all Chapter V. Mechanical Ventilation Selection D. Neonatal E. Pediatric F. Adult Chapter 39 all VI. Special Populations A. Trauma B. Emergency C. Surgical ICU D. Pediatric E. Neonatal F. Post surgical cardiac G. Post surgical renal Chapter 45 pg **Each chapter use the chapter outline, In this chapter you will learn, Key terms and Key points to study for test. ** GRADING SCALE: A B C D Below 60- F Required Textbooks: Wilkins, Stoller, Scanlan: Egan s Fundamentals of Respiratory Care, 8 th Ed., Elsevier White, G.C.: Basic Lab Competencies for Respiratory Care, 4 th Ed., Delmar, Cairo & Pilbeam: Mosby s Respiratory Care Equipment, 7 th Ed., Elsevier,
265 265 Dates to remember August 13, Monday August 17, Friday Registration/Schedule Adjustment August 17, Friday, 9 a.m. Residence Halls Open for Freshmen August 20, Monday, 8 a.m. First Day of Classes August 20, Monday August 24, Friday Late Registration and Add/Drop (Schedule Adjustment) August 24, Friday Last Day to Add Classes (Withdrawals Only After This Date) August 27, Monday W Withdrawal Period Begins September 1, Saturday September 3, Monday University Computer Services Unavailable September 3, Monday Labor Day Holiday University Closed September 14, Friday Application for December Graduation Due in Academic Dean s Office September 21, Friday Last Day to Drop 1st 8 Weeks Courses October 8, Monday Final Draft of Thesis Due in Advisor s Office October 9, Tuesday Mid-Semester, 1st 8 Weeks Courses End October 10, Wednesday 2nd 8 Weeks Courses Begin October 15, Monday Deadline for Submitting Freshmen Mid Term Grades October 22, Monday Students should schedule appointments with advisors to prepare for advance registration (Required for students who have mandatory advising holds) October 26, Friday Last Day to Drop a Full Semester Individual Course October 29, Monday Recommended Date to Apply for May 2008 Graduation October 29, Monday December 4, Tuesday Complete Withdrawals Only November 5, Monday November 16, Friday Advance Registration for Spring Semester for Currently Enrolled Students November 9, Friday Last Day to Drop 2nd 8 Weeks Courses 265
266 266 November 17, Saturday, Noon Residence Halls Close November 19, Monday Last day for Defense of Dissertation November 19, Mon December 11, Tuesday Advance Registration for Spring Semester Open to All Admitted/Re-Admitted Students November 19, Monday November 24, Saturday Thanksgiving/Fall Break - Classes Dismissed November 22, Thursday November 25, Sunday University Computer Services Unavailable November 22, Thursday Thanksgiving Holiday University Closed November 23, Friday University Holiday University Closed November 25, Sunday, Noon Residence Halls Open November 26, Monday Classes Resume November 28, Wednesday December 4, Tuesday Dead Week December 4, Tuesday Last Class Day and Last Day to Completely Withdraw for Fall Semester December 5, Wednesday Study Day - Exams for Wednesday Classes 3 p.m. and After Will Be Held December 6, Thursday Exam Day December 6, Thursday Approved Thesis/Dissertation Must Be Submitted Electronically and all Paperwork/Checks Must Be In Graduate College Office December 7, Friday Exam Day December 8, Saturday Exam Day for Saturday Classes (and some common finals) December 10, Monday Exam Day December 11, Tuesday Exam Day Fall Semester Closes Official Graduation Date For Fall Semester December 12, Wednesday 12 p.m.. Residence Halls Close December 12, Wednesday December 26, Wednesday Advance Registration/Schedule Adjustment for Spring Semester is Suspended December 13, Thursday, Noon Deadline for Submitting Final Set of Grades 266
267 267 December 21, Friday January 1, 2008, Tuesday University Closed December 27, Thursday December 28, Friday On-Line Registration Resumes SAFETY PRACTICES: Safety is an important component of respiratory care and technical skills taught throughout the semester. Test Remediation 11. Anyone who earns a grade less than 70% on an exam must remediate the test during the semester. 12. The last test of the semester is not to be remediated. 13. All questions missed on that failed examination must be remediated 14. Remediation will consist of an explanation of the correct answer and why the students answer was incorrect. 15. For Unit Exams, remediations are to be turned in to the remediation coordinator, Brent, seven days after the test is reviewed in class with the students. 16. Remediations are to be turned in or ed to Brent ([email protected]). 17. Each question remediated must include a reference from an assigned reading. If the answer cannot be found in an assigned reading, you may reference an instructor s or guest lecturer s presentation. 18. Remediations will be graded S or U by the remediation coordinator. A student earning U should meet with Brent to discuss the question and remediation to ensure that the student understands the concepts being tested and the correct way to perform remediation. 19. Student remediation will be done at the respiratory care school. Test keys will be provided at that time. Tests are not to be removed from the school. 20. If this remediation is not completed in the permitted time, documentation will be placed in the students permanent file and consider at the end of the semester. POLICY STATEMENTS ACADEMIC INTEGRITY Academic dishonesty of any kind will not be tolerated. Academic dishonesty includes cheating on exams, fabrication/falsification, plagiarism, bribes/favors/threats, and complicity. The student will be subject to penalties which may include a lower or failing grade on a project/paper/or exam, or a lower or failing course grade, or expulsion. The full policy is described in the St. Mary's Student Handbook. INCLEMENT WEATHER: As an off campus site, decisions regarding inclement weather are independent of Marshall University, St. Mary's School of Nursing does not cancel classes (theory/clinicals/labs) unless weather conditions are severe. If the decision is made to close the school, the VP of Schools of Nursing and Health Professions will leave a message on this number: 304/ Students may call this number after 6:15 a.m. for a recorded message. Television and radio announcements will be made. The full policy is in the St. Mary's Student Handbook. 267
268 268 DISABILITY STATEMENT: St. Mary's/Marshall University Cooperative Degree Program will make accommodations for those students with recognized (medically certified) mental, physical, emotional, and/or learning disabilities provided the accommodations(s) requested do not place undo financial or physical demands on the institution. Written documentation is required from a health care provider who is qualified to diagnose learning disability disorders. This must be provided to the VP of Schools of Nursing and Health Professions. The written documentation must include the need for special accommodations related to the learning disability. In addition, the student must be able to demonstrate ability to meet the objectives of the course(s). See Student Handbook and/or school catalog for specific policy and procedure. **Refer to the Clinical Manual or Instructor for further information 268
269 269 SCHOOL OF RESPIRATORY THERAPY ST. MARY S/MARSHALL UNIVERSITY COURSE SYLLABUS COURSE NAME: RSP 303 Respiratory Education CREDIT HOURS: 3 LAB HOURS: 0 PREREQUISITES: Successful completion of program sequence. INSTRUCTORS: Chuck Zuhars, RRT, M.S. Office Phone: (304) Brent Blevins, RN, RRT Office Phone: (304) Chris Trotter, RRT, BA Office Phone: (304) COURSE DESCRIPTION: This 3 credit hour course is designed as an introduction to clinical teaching in a respiratory care program. The course includes self-directed study in instructional and evaluation strategies as well as development of performance objectives. The student performs functions required of a clinical instructor in a respiratory care program. The student will become the educator and discover that knowing a topic well and being able to teach a topic well are two different things. Both of these activities require different talents and skills that must be learned and improved upon. COURSE OBJECTIVES: Upon successful completion of this course, the student will: 1. Have a better understanding of the clinical instruction as related to the amount of time required in preparation of taking new students into the clinical setting. 2. Have a greater knowledge of the different challenges that develop in educating people to be a healthcare professional. 3. Understand some of the different types of students and ways to reach each of them to better meet their needs in the education process. 4. Design and develop a lesson plan that includes learning objectives. 5. Formulate a course syllabus that includes learning objectives. 6. Prepare one course-specific teaching module. 7. Compose a set of course specific evaluation questions to be completed by students at the end of the course. 269
270 270 METHODS OF TEACHING: Lecture/Discussion through the Teaching/Learning Process Exercises to Assist with Problem Solving In-Class Activities Handouts Reference Readings Paper/Pen Examinations Simulations and Exercises COURSE MATERIAL: Required Textbooks: Davis, Barbra Gross: Tools for Teaching, Jossey-Bass 1993 Reference and Resource Material: Deck, Michele L.: Instant Teaching Tools for the New Millennium, Elsevier 2004 SAFETY PRACTICES: Safety is an important component of respiratory care and technical skills taught throughout the semester. Features of each unit are given below: Unit #1: Getting Under Way- This unit will help the student understand where and how to get started when preparing to teach a class. This section covers topics that include: preparing or revising a course, creating a course syllabus, and the first day of class. Unit #2: Responding to a Diverse Student Body- This unit will give the students a little insight into the challenges of teaching many different types of students. Some of the topics in this section include: academic accommodations for students with disabilities, diversity and complexity in the classroom, reentry students, and teaching academically diverse students. Unit #3: Discussion Strategies This unit covers way for an instructor to lead class room instruction that promotes interaction with the students and learning the material. Some of the methods taught include: Leading a discussion, encouraging student participation in discussion, asking questions, and fielding student questions. Unit #4: Lecture Strategies This unit will address what it takes to prepare a lecture that gets the information to students. The strategies discussed include: preparing to teach the lecture course, delivering a lecture, explaining clearly, personalizing the large lecture class, supplements and alternatives to lecturing, and maintaining structural quality. 270
271 271 Unit #5: Collaborative and Experiential Strategies- This unit will go over some concepts of group learning. The topics covered here will include: collaborative learning, role playing and case studies, and field work. Unit #6: Enhancing Students Learning and Motivation This unit will help the student understand what is like trying to deliver information and how hard it can be to keep students motivated. Some of the topic covered include: helping students learn, learning styles and preference, and motivating students. Unit #7: Writing Skills and Homework Assignments This unit is designed to help the student have a better idea of what instructors must focus in when creating and reviewing assignments. The topics covered include: helping students write better in class, designing effective writing assignments, evaluating students written work, and homework. Unit #8: Testing and Grading- This unit covers strategies of making and developing good tests. Some of the topics include: spending adequate amounts of time developing tests, matching test to content, making test valid, a variety of testing methods, and writing test questions that test skill and not recall. Unit #9: Instructional Media and Technology This unit covers different types of ways to present material. Some of the methods discussed include: chalkboards, flipcharts, transparencies and overhead projectors, slides, films and videotapes, and computers and multimedia. Unit #10: Evaluation to Improve Teaching This unit discusses way that educators can be evaluated to improve their teaching techniques. The methods that will be covered include: watching yourself on videotape, self-evaluation and student feedback. Unit #11: Teaching Outside the classroom This unit will cover the role the teacher has outside of the classroom. It will cover topics including: holding office hours, academic advising and mentoring, and guiding, training, and supervising graduate students. Unit #12: Finishing Up: The final unit will pull every thing together that would need to be discussed at the end of a semester. The topics will include: the last day of class, student rating forms, and writing letters of recommendation. 271
272 272 SCHOOL OF RESPIRATORY THERAPY ST. MARY S/MARSHALL UNIVERSITY EVALUATION OF THE STUDENT EVALUATION The purpose of evaluation is to indicate, to some degree, the extent to which the student has learned the concepts presented. Frequent testing will encourage the student to study and learn at a regular and constant pace throughout the course. The teaching-learning process meets the expected outcome goal. Evaluation is also utilized as a learning tool. Questions are designed to stimulate problem solving. The examinations are reviewed to provide feedback and promote discussion. Laboratory simulations and exercises will further enhance the learning process through a supervised hands-on approach. Students who require additional support outside of that given during class hours may set-up personal meetings with the instructor during office hours. Students with math difficulties will be referred to the Learning Center for tutoring. SPECIFIC FACTORS 1. Examinations A. Unit Examinations: Exams are worth a total of 20% of the final grade. Exams will be approximately 30 questions in length and may include multiple choice, matching, listing, labeling, short answer, and essay style questions. An hour will be given for each unit exam. B. Final Examination: The Final exam will be comprehensive and may include multiple choice, matching, listing, labeling, short answer, and essay style questions. The final exam will be worth 20% of the final grade. The final exam will be administered during Finals Week. 2. Classroom Exercise Students will participate in the classroom exercises that focus on techniques learned in the course. The participation in these exercises is worth a total of 15% of the final grade. 272
273 Homework/Class work 4. Evaluations: 5. Presentations: 7. Grading Scale: It will be the student s responsibility to complete homework/class work assignments. There are no scheduled homework assignments in this course. However, additional assignments may be given at the instructor s discretion. The students will be evaluated frequently by the underclassmen who they instruct. These evaluations will be worth 25% of the final grade. Each Student will prepare a lesson and present it to the class. The lesson may cover any health care topic of the students choice with the instructor s approval. The lesson will contain a tool created by the student. The tool should be similar to the ones we use in the class. The tool is to reinforce the lessons subject. The class will fill out an evaluation on each presentation and will discuss the effectiveness of the presentation. These evaluations will be completed by the class, and will determine the grade for the presentation. This presentation is worth 20% of the final course grade. 90%-100%: A Excellent 88%- 89%: B Good 70%-79%: C Satisfactory 60%- 69% D- Unsatisfactory 0%- 59%: Failing 8. Final Grade Calculation The factors below will be used to determine the final grade for the course: Exams - 20% Final Exam - 20% Participation 15% Evaluations - 25% Presentation 20% 273
274 274 ATTENDANCE/ABSENCE POLICY ATTENDANCE IS THE RESPONSIBILITY OF EACH STUDENT 1. Punctual attendance in all classes and clinical experiences is important if the student is to meet all course objectives. 2. Notify the School of Respiratory Care by contacting the course instructor as soon as possible regarding the absence. 3. The course grade will be lowered one letter grade if theory absences exceed 20% of the theory contact hours. 4. Class notes and other course material missed is the responsibility of the student, not the instructor. 5. References provided to potential employers by the faculty and/or Director will include information on attendance while the student was enrolled in the program. 6. Absences/tardiness on the Day of an Exam/Quiz y. Students who miss an exam/quiz must contact the instructor before the exam/quiz, or as soon as possible after the exam/quiz is missed. z. Documentation of the reason for the exam/quiz absence or tardiness (i.e., health care provider statement, receipt to substantiate car trouble, etc.) must be provided in order to determine eligibility for a makeup exam aa. Permission for makeup will be at the discretion of the course instructor(s). bb. Makeup exams/quizzes may be different than the original exams/quizzes. cc. Any make-ups will be scheduled at a time convenient for the instructor. dd. Student should be ready to take the make-up exam/quiz upon the first day of return, unless other plans have been arranged. ee. If tardy for an exam/quiz the student must decide if it can be completed within the remaining administration time. The exam/quiz will be turned in at the same time as all other students taking it. If the student does not believe the exam/quiz can be completed within the planned administration time, a request for make-up may be submitted for consideration. ff. Students may not take more than two (2) make-up exams per course. Each subsequent test missed will be scored as zero (0). 7. The faculty for each course has the option of establishing rules and consequences for tardiness and attendance. Special seating may be assigned for late-comers. NOTE: This attendance policy also applies lab/clinical check-offs. 274
275 275 POLICY STATEMENTS ACADEMIC INTEGRITY Academic dishonesty of any kind will not be tolerated. Academic dishonesty includes cheating on exams, fabrication/falsification, plagiarism, bribes/favors/threats, and complicity. The student will be subject to penalties which may include a lower or failing grade on a project/paper/or exam, or a lower or failing course grade, or expulsion. The full policy is described in the St. Mary's Student Handbook. INCLEMENT WEATHER: As an off campus site, decisions regarding inclement weather are independent of Marshall University, St. Mary's School of Nursing does not cancel classes (theory/clinicals/labs) unless weather conditions are severe. If the decision is made to close the school, the VP of Schools of Nursing and Health Professions will leave a message on this number: 304/ Students may call this number after 6:15 a.m. for a recorded message. Television and radio announcements will be made. The full policy is in the St. Mary's Student Handbook. DISABILITY STATEMENT: St. Mary's/Marshall University Cooperative Degree Program will make accommodations for those students with recognized (medically certified) mental, physical, emotional, and/or learning disabilities provided the accommodations(s) requested do not place undo financial or physical demands on the institution. Written documentation is required from a health care provider who is qualified to diagnose learning disability disorders. This must be provided to the VP of Schools of Nursing and Health Professions. The written documentation must include the need for special accommodations related to the learning disability. In addition, the student must be able to demonstrate ability to meet the objectives of the course(s). See Student Handbook and/or school catalog for specific policy and procedure. 275
276 276 Test Remediation Policy St. Mary s School of Respiratory Care Anyone who earns a grade less than 70% on an exam must remediate the test during the semester. The last test of the semester is not to be remediated. All questions missed on that failed examination must be remediated Remediation will consist of an explanation of the correct answer and why the students answer was incorrect. For Unit Exams, remediations are to be turned in to the remediation coordinator, Mr. Brent Blevins, seven days after the test is reviewed in class with the students. Remediations are to be turned in or ed to Mr. Blevins ([email protected]). Each question remediated must include a reference from an assigned reading. If the answer cannot be found in an assigned reading, you may reference an instructor s or guest lecturer s presentation. Remediations will be graded S or U by the remediation coordinator. A student earning U should meet with Mr. Blevins to discuss the question and remediation to ensure that the student understands the concepts being tested and the correct way to perform remediation. Student remediation will be done at the respiratory care school. Test keys will be provided at that time. Tests are not to be removed from the school. If this remediation is not completed in the permitted time, documentation will be placed in the students permanent file and consider at the end of the semester. 276
277 277 COURSE OUTLINE Time: TBA Room: hr = 45 hrs/semester WEEK DATE DAY TIME CONTENT INSTRUCTOR 1 8/20/07 Mon 30 MIN Syllabus and questions CZ/BB/CT 45 MIN Unit 1 CZ/BB/CT 1 8/22/07 Wed 1.5 hours Unit 1 CZ/BB/CT 2 8/27/07 Mon 1.5 hours Units 2 CZ/BB/CT 2 8/29/07 Wed 1.5 hours Units 2 CZ/BB/CT 3 9/03/07 Mon NO SCHOOL LABOR DAY!! 3 9/05/07 Wed 1.5 hours Unit 3 CZ/BB/CT 4 9/10/07 Mon 1.5 hours Unit 3 CZ/BB/CT 4 9/12/07 Wed 1.5 hours Test 1 CZ/BB/CT 5 9/17/07 Mon 1.5 hours Unit 4 CZ/BB/CT 5 9/19/07 Wed 1.5 hours Unit 4 CZ/BB/CT 6 9/24/07 Mon 1.5 hours Unit 5 CZ/BB/CT 6 9/26/07 Wed 1.5 hours Unit 5 CZ/BB/CT 7 10/01/07 Mon 1.5 hours Unit 6 CZ/BB/CT 7 10/03/07 Wed 1.5 hours Unit 6 CZ/BB/CT 8 10/08/07 Mon 1.5 hours Unit 7 CZ/BB/CT 8 10/10/07 Wed 1.5 hours Unit 7 CZ/BB/CT 9 10/15/07 Mon 1.5 hours Test 2 CZ/BB/CT 9 10/17/07 Wed 1.5 hours Unit 8 CZ/BB/CT 277
278 278 CZ/BB/CT 10 10/22/07 Mon 1.5 hours Unit /24/07 Wed 1.5 hours Unit 9 CZ/BB/CT 11 10/29/07 Mon 1.5 hours Unit 9 CZ/BB/CT 11 10/31/07 Wed 1.5 hours Unit 10 CZ/BB/CT 12 11/05/07 Mon 1.5 hours Test 3 CZ/BB/CT 12 11/07/07 Wed 1.5 hours Unit 10 CZ/BB/CT 13 11/12/07 Mon 1.5 hours Unit 11 CZ/BB/CT 13 11/14/07 Wed 1.5 hours Unit 11 CZ/BB/CT 14 11/19/07 Mon Thanksgiving Break 14 11/21/07 Wed Thanksgiving Break 15 11/26/07 Mon 1.5 hours Unit 12 CZ/BB/CT 15 11/28/07 Wed 1.5 hours Unit 12 CZ/BB/CT 12/06/07 Wed Final Exam CZ/BB/CT 278
279 279 Outline of Unit Reading Unit 1: Getting Under Way Chapter 1- Preparing or Revising a Course Chapter 2- The course Syllabus Chapter 3- The First Day of Class Unit 2: Responding to a Diverse Student Body Chapter 4- Academic Accommodations for the Students with Disabilities Chapter 5- Diversity and Complexity in the Classroom Chapter 6- Reentry Students Chapter 7- Teaching Academically Diverse Students Unit 3: Discussion Strategies Chapter 8- Leading a Discussion Chapter 9- Encouraging Student Participation in Discussion Chapter 10- Asking Questions Chapter 11- Fielding Students Questions Unit 4: Lecture Strategies Chapter 12- Preparing to Teach the Large Lecture Course Chapter 13- Delivering a lecture Chapter 14- Explaining Clearly Chapter 15- Personalizing the Large Lecture Class Chapter 16- Supplements and Alternatives to Lecturing Chapter 17- Maintaining Instructional Quality with Limited Resources 279
280 280 Unit 5: Collaborative and Experiential Strategies Chapter 18- Collaborative Learning Chapter 19- Role Playing and Case Studies Chapter 20- Fieldwork Unit 6: Enhancing Students Learning and Motivation Chapter 21- Helping Students Learn Chapter 22- Learning Styles and Preferences Chapter 23- Motivating Students Unit 7: Writing Skills and Homework Assignments Chapter 24- Helping Students Write Better in All Courses Chapter 25- Designing Effective Writing Assignments Chapter 26- Evaluating Students Written Work Chapter 27- Homework Unit 8: Testing and Grading Chapter 28- Quizzes, Tests, and Exams Chapter 29- Allaying Students Anxieties About Tests Chapter 30- Multiple-Choice and Matching Tests Chapter 31- Short-Answer and Essay Test Chapter 32- Grading Practices Chapter 33- Calculating and Assigning Grades Chapter 34- Preventing Academic Dishonesty 280
281 281 Unit 9: Instructional Media and Technology Chapter 35- Chalkboards Chapter 36- Flipcharts Chapter 37- Transparencies and Overhead Projectors Chapter 38- Slides Chapter 39- Films and Videotapes Chapter 40- Computers and Multimedia Unit 10: Evaluation to Improve Teaching Chapter 41- Fast Feedback Chapter 42- Watching Yourself on Videotape Chapter 43- Self-Evaluation and Teaching Dossier Unit 11: Teaching Outside the Classroom Chapter 44 Holding Office Hours Chapter 45- Academic Advising and Mentoring Undergraduates Chapter 46- Guiding, Training, and Supervising Graduate Student Instructors Unit 12: Finishing Up Chapter 47- The Last Day Chapter 48- Student Rating Forms Chapter 49- Writing Letters of Recommendation 281
282 282 Presentation Evaluations Each class member will fill out a critique of each class presentation given by a student. This feedback helps the student that gave the presentation by allowing them to learn from their peers how to give better presentations in the future. The critique will have the evaluator's name removed before it is distributed to the members of the presenting team. This evaluation task should receive a great deal of professional attention by the evaluator; the critique should be given in as constructive a manner as possible. The presentation will be evaluated for style and content on a numeric scale from 1 (worst possible) to 10 (best possible). Outstanding individual contributions to the presentation should be noted. The evaluator will also note major strengths and weaknesses of the presentation and the delivery methods used. Each student will be evaluated, and then an average rating from all evaluators will be computed. These are the ten areas being evaluated: organization of the material knowledge of the material ability to convey information ability to answer questions use of supporting materials clarity of speech eye contact appearance professionalism of presentation Approximately ten minutes will be provided following the presentation for you to complete your evaluation. Notice that this is not THREE minutes, but TEN minutes. This is given so that your evaluation can be complete, with well-reasoned comments in each section. Your signature is required, though it will be removed before your comments are given to the presenting student. 282
283 283 PRESENTATION EVALUATION Name of presenter: Organization of the material Knowledge of the material Ability to convey information Ability to answer questions Use of supporting materials (Tool) Clarity of speech Eye contact
284 284 Appearance Professionalism of presentation COMMENTS: Evaluators Name: Date: 284
285 285 SCHOOL OF RESPIRATORY THERAPY ST. MARY S/MARSHALL UNIVERSITY COURSE SYLLABUS COURSE NAME: RSP 304 Respiratory Cost Management and Solutions CLASS HOURS: 3 LAB HOURS: 0 PREREQUISITES: Successful completion of program sequence. INSTRUCTOR: Chuck Zuhars, RRT, M.S. Office Phone: Brent Blevins, RN, RRT Office Phone: Chris Trotter, RRT, B.A. Office Phone: COURSE DESCRIPTION: This three credit hour course consists of three hours of lecture each week. This course introduces the students to cost solutions for respiratory departments. Topics include annual budgets, purchasing decisions, effective staffing, inventory and supply controls, and cost-containment methods. COURSE OBJECTIVES: 28. Formulate par levels and measure service levels for a respiratory department. 29. Determine 10 ways that profits can be improved by reducing inventories while simultaneously improving service. 30. Assemble a purchasing manual. 31. Design a staffing matrix. 32. Discuss problems encountered in designing levels for fluctuating acuity levels. 33. Describe factors involved in developing an annual budget for a respiratory department. 34. Prepare a mock annual budget for a respiratory care department. METHODS OF TEACHING: Lecture/Discussion Through the Teaching/Learning Process Exercises to Assist with Problem Solving In-Class Activities Handouts Reference Readings Paper/Pen Examinations COURSE MATERIAL: Required Textbooks: Berger, Steven: Fundamentals of Health Care Financial Management, Second Edition. Jossey-Bass
286 286 Reference and Resource Material: Finkler, Kovner, & Jones: Financial Management for Nurse Managers and Executives, Third Edition. SAFETY PRACTICES: Safety is an important component of respiratory care and technical skills taught throughout the semester. 286
287 287 Features of each unit are given below: The units are the names of the months. The reason for this is to cover the aspects as they occur throughout the year. The topics will be covered in the month in which they occur. Unit #1: January - In this unit the class will learn about principles and theories of financial management, the importance of financial management, living with the financial committee and board of directors, and year-end closing. Unit #2: February - This unit of the course will deal with topics including: accounting principles, objectives of financial reporting, basic accounting concepts, uses of financial information and preparing for auditors. Unit #3: March - In this unit the topics will include: strategic financial planning, ratio analysis, capitol affordability, and the capital plan and its relationship to the strategic plan. Unit #4: April - This unit discusses such topics as: Medicare and Medicaid net revenue concepts, calculating Medicare and Medicaid contractual adjustments, managing care net revenue concepts, and implications of management letter comments proposed by auditors. Unit #5: May - This unit will cover topics including: fundamentals of accounts receivable management, patient registration, calculation of allowance for doubtful accounts and bad-debt expense, and calculation of allowance for contractual adjustments. Unit #6: June - In this unit the topics that will be discussed will include: budget preparation (beginning), budget calendar, volume issues, capital budgeting, and accounting and finance department responsibilities. Unit #7: July - The focus of this unit will be on items such as: budget preparation (middle), capital budgeting (July), regulatory and legal environment, corporate compliance, and accreditation issues. Unit #8: August - This unit will discuss topics that include: capital budget (August), operating budget, budget variance analysis, cost accounting and analysis, and August finance committee special agenda items. Unit #9: September - In this unit of the class the topics will include: operating budget, capital budget (September), cash budget, and physical practice management issues. Unit #10: October - This section will cover topics that include: information systems implications for health care financial management, information technology strategic plan initiatives, HIPPA implementation, and the impact of the internet. 287
288 288 Unit #11: November - This unit will connect previous units just a s this month would tie together past months. Some topics discussed include: preparation of the budget results and delivery to the department managers, budgeting and spreading contractual adjustments by department, how to improve the organization s cost structure, and benefits of tax status to the health care organization. Unit #12: December - This final unit of the class will pull the past units together. The topics that will be discussed will include: getting ready for year end reporting and looking to the future of health care finance. 288
289 289 SCHOOL OF RESPIRATORY THERAPY ST. MARY S/MARSHALL UNIVERSITY EVALUATION OF THE STUDENT EVALUATION The purpose of evaluation is to indicate, to some degree, the extent to which the student has learned the concepts presented. Frequent testing will encourage the student to study and learn at a regular and constant pace throughout the course. The teaching-learning process meets the expected outcome goal. Evaluation is also utilized as a learning tool. Questions are designed to stimulate problem solving. The examinations are reviewed to provide feedback and promote discussion. Students who require additional support outside of that given during class hours may set-up personal meetings with the instructor during office hours. Students with math difficulties will be referred to the Learning Center for tutoring. 1. Examinations/Quizzes L. Unit Exams M. Quizzes SPECIFIC FACTORS Exams: The total of all exams is worth 50% the final grade. Exams will be approximately 30 questions or greater in length and may include multiple choice, matching, listing, labeling, short answer, and essay style questions. An hour will be given for each unit exam. Quizzes: There will be administered during the discussion of each unit. All quizzes will be averaged to consist of 10% of the final grade. Quizzes will be approximately 10 questions in length and questions may include multiple choice, short answer, listing, and labeling. N. Final Examination Final Exam: The Final exam will be comprehensive and may include multiple choice, matching, listing, labeling, short answer, and essay style questions. The final exam will be worth 20% of the final grade. The final exam will be administered during Finals Week. O. Course Paper A research paper will be assigned the 2 nd week of class. The topic assigned will be given to the student by the instructor. The outline will follow AMA guidelines. 289
290 Homework/Classwork It will be the student s responsibility to complete homework/classwork assignments. There are scheduled homework assignments in this course. Additional assignments may be given at the instructor s discretion. 3. Class Participation: 4. Grading Scale: Class participation will include discussions and workgroups. Theory: Laboratory Skills 90%-100%: A Excellent No lab is scheduled for 80%- 89%: B Good this course, but may be 70%- 79%: C Satisfactory conducted at the discretion 60%- 69%: D Unsatisfactory of the instructor. 0%- 59%: E -Failing. 5. Final Grade Calculation The factors below will be used to determine the final grade for the course: C. The unit exams are worth 50% of the final grade. The unit quizzes are worth 10% of the final grade. The final exam is worth 20% of the final grade. The assigned paper is worth 20% of the final grade 290
291 291 ATTENDANCE/ABSENCE POLICY ATTENDANCE IS THE RESPONSIBILITY OF EACH STUDENT 1. Punctual attendance in all classes and clinical experiences is important if the student is to meet all course objectives. 2. Notify the School of Respiratory Care by contacting the course instructor as soon as possible regarding the absence. 3. The course grade will be lowered one letter grade if theory absences exceed 20% of the theory contact hours. 4. Class notes and other course material missed is the responsibility of the student, not the instructor. 5. References provided to potential employers by the faculty and/or Director will include information on attendance while the student was enrolled in the program. 6. Absences/tardiness on the Day of an Exam/Quiz gg. Students who miss an exam/quiz must contact the instructor before the exam/quiz, or as soon as possible after the exam/quiz is missed. hh. Documentation of the reason for the exam/quiz absence or tardiness (i.e., health care provider statement, receipt to substantiate car trouble, etc.) must be provided in order to determine eligibility for a makeup exam ii. Permission for makeup will be at the discretion of the course instructor(s). jj. Makeup exams/quizzes may be different than the original exams/quizzes. kk. Any make-ups will be scheduled at a time convenient for the instructor. ll. Student should be ready to take the make-up exam/quiz upon the first day of return, unless other plans have been arranged. mm. If tardy for an exam/quiz the student must decide if it can be completed within the remaining administration time. The exam/quiz will be turned in at the same time as all other students taking it. If the student does not believe the exam/quiz can be completed within the planned administration time, a request for make-up may be submitted for consideration. nn. Students may not take more than two (2) make-up exams per course. Each subsequent test missed will be scored as zero (0). 7. The faculty for each course has the option of establishing rules and consequences for tardiness and attendance. Special seating may be assigned for late-comers. NOTE: This attendance policy also applies lab/clinical check-offs. 291
292 292 POLICY STATEMENTS ACADEMIC INTEGRITY Academic dishonesty of any kind will not be tolerated. Academic dishonesty includes cheating on exams, fabrication/falsification, plagiarism, bribes/favors/threats, and complicity. The student will be subject to penalties which may include a lower or failing grade on a project/paper/or exam, or a lower or failing course grade, or expulsion. The full policy is described in the St. Mary's Student Handbook. INCLEMENT WEATHER: As an off campus site, decisions regarding inclement weather are independent of Marshall University, St. Mary's School of Nursing does not cancel classes (theory/clinicals/labs) unless weather conditions are severe. If the decision is made to close the school, the VP of Schools of Nursing and Health Professions will leave a message on this number: 304/ Students may call this number after 6:15 a.m. for a recorded message. Television and radio announcements will be made. The full policy is in the St. Mary's Student Handbook. DISABILITY STATEMENT: St. Mary's/Marshall University Cooperative Degree Program will make accommodations for those students with recognized (medically certified) mental, physical, emotional, and/or learning disabilities provided the accommodations(s) requested do not place undo financial or physical demands on the institution. Written documentation is required from a health care provider who is qualified to diagnose learning disability disorders. This must be provided to the VP of Schools of Nursing and Health Professions. The written documentation must include the need for special accommodations related to the learning disability. In addition, the student must be able to demonstrate ability to meet the objectives of the course(s). See Student Handbook and/or school catalog for specific policy and procedure. 292
293 293 Test Remediation Policy St. Mary s School of Respiratory Care Anyone who earns a grade less than 70% on an exam must remediate the test during the semester. The last test of the semester is not to be remediated. All questions missed on that failed examination must be remediated Remediation will consist of an explanation of the correct answer and why the students answer was incorrect. For Unit Exams, remediations are to be turned in to the remediation coordinator, Mr. Brent Blevins, seven days after the test is reviewed in class with the students. Remediations are to be turned in or ed to Mr. Blevins ([email protected]). Each question remediated must include a reference from an assigned reading. If the answer cannot be found in an assigned reading, you may reference an instructor s or guest lecturer s presentation. Remediations will be graded S or U by the remediation coordinator. A student earning U should meet with Mr. Blevins to discuss the question and remediation to ensure that the student understands the concepts being tested and the correct way to perform remediation. Student remediation will be done at the respiratory care school. Test keys will be provided at that time. Tests are not to be removed from the school. If this remediation is not completed in the permitted time, documentation will be placed in the students permanent file and consider at the end of the semester. 293
294 294 COURSE OUTLINE Time: TBA Room: hr = 45 hrs/semester WEEK DATE DAY TIME CONTENT INSTRUCTOR 1 8/20/07 Mon 30 MIN Syllabus and questions CZ/BB/CT 45 MIN Unit 1 & 2 CZ/BB/CT 1 8/22/07 Wed 1.5 hours Unit 1 & 2 CZ/BB/CT 2 8/27/07 Mon 1.5 hours Units 3 & 4 CZ/BB/CT 2 8/29/07 Wed 1.5 hours Units 3 & 4 CZ/BB/CT 3 9/03/07 Mon NO SCHOOL LABOR DAY!! 3 9/05/07 Wed 1.5 hours Unit 5 CZ/BB/CT 4 9/10/07 Mon 1.5 hours Test 1 CZ/BB/CT 4 9/12/07 Wed 1.5 hours Unit 6 CZ/BB/CT 5 9/17/07 Mon 1.5 hours Unit 6 CZ/BB/CT 5 9/19/07 Wed 1.5 hours Unit 7 CZ/BB/CT 6 9/24/07 Mon 1.5 hours Unit 7 CZ/BB/CT 6 9/26/07 Wed 1.5 hours Unit 8 CZ/BB/CT 7 10/01/07 Mon 1.5 hours Unit 8 CZ/BB/CT 7 10/03/07 Wed 1.5 hours Unit 9 CZ/BB/CT 8 10/08/07 Mon 1.5 hours Unit 9 & 10 CZ/BB/CT 8 10/10/07 Wed 1.5 hours Test 2 CZ/BB/CT 9 10/15/07 Mon 1.5 hours Unit 10 CZ/BB/CT 9 10/17/07 Wed 1.5 hours Unit 11 CZ/BB/CT CZ/BB/CT 10 10/22/07 Mon 1.5 hours Unit /24/07 Wed 1.5 hours Unit 12 CZ/BB/CT 294
295 /29/07 Mon 1.5 hours Unit 12 CZ/BB/CT 11 10/31/07 Wed 1.5 hours Test 3 CZ/BB/CT 12 11/05/07 Mon 1.5 hours Group Project 1 Paper Due CZ/BB/CT 12 11/07/07 Wed 1.5 hours Group Project 2 CZ/BB/CT 13 11/12/07 Mon 1.5 hours Group Project 3 CZ/BB/CT 13 11/14/07 Wed 1.5 hours Group Project 4 CZ/BB/CT 14 11/19/07 Mon Thanksgiving Break 14 11/21/07 Wed Thanksgiving Break 15 11/26/07 Mon 1.5 hours Group Project 5 CZ/BB/CT 15 11/28/07 Wed 1.5 hours Group Project 6 CZ/BB/CT 12/06/07 Wed Final Exam CZ/BB/CT 295
296 296 Outline of Unit Reading Unit 1: January (pg 1-27) What is Health Care? What is Management? What is Financial Management? Why is Financial Management Important? Ridgeland Heights Medical Center: The Primary Statistics Pro Forma Development Living with the Financial Committee and Board of Directors Calendar Year-End Closing Unit 2: February (pg 28-54) Accounting Principles and Practices Objectives of Financial Reporting Basic Accounting Concepts Basic Financial Statements of a Health Care Organization Uses of Financial Information The financial Statement Preparing for the Auditors February Finance Committee Special Reports Unit 3: March (pg 55-83) Strategic Financial Planning: Five-Year Projections RHMC Strategic Financial Planning Ratio Analysis The Capital Plan and its Relationship to the Strategic Plan Capital Affordability Unit 4: April (pg ) Medicare and Medicaid Net Revenue Concepts Calculation of Medicare and Medicaid Contractual Adjustments Implications of the Balanced Budget Act of 1997 Managed Care Net Revenue Concepts Preparation of the Medicare and Medicaid Cost Report Presentation of Audited Financial Statements to the Finance Committee Implications of Management Letter Comments Proposed by Auditors 296
297 297 Unit 5: May (pg ) Fundamentals of Accounts Receivable Management Patient Registration: Which Division should it Report To? Calculation of Allowance for Doubtful Accounts and Bad-Debt Expense Calculation of Allowance for Contractual Adjustments Unit 6: June (pg ) Budget Preparation: The Beginning Budget Calendar Volume Issues Capital Budgeting (June) Accounting and Finance Department Responsibilities June Finance Committee Special Agenda Items Unit 7: July (pg ) Budget Preparation: The Middle Months Capital Budgeting (July) Regulatory and Legal Environment Other Regulatory and Business Compliance Issues Corporate Compliance Accreditation Issues Patient Satisfaction Issues Unit 8: August (pg ) Capital Budgeting (August) Operating Budget Budget Variance Analysis Cost Accounting and Analysis August Financial Committee Special Agenda Items Unit 9: September (pg ) Operating Budget Capital Budget (September) Cash Budget Physician Practice Management Issues 297
298 298 Unit 10: October (pg ) Information System Implications for Health Care Financial Management Information Technology Strategic Plan Initiatives HIPPA Implementation Issues Impact of the Internet Budget Presentation to the Board Finance Committee October Finance Committee Special Agenda Items Unit 11: November (pg ) Preparation of the Budget Results and Delivery to the Department Managers Budgeting and Spreading Contractual Adjustments by Department Issues Involving RHMC s Cost Structure How to Improve the Organization s Cost Structure Materials Management in Health Care Benefits of Tax Status to the Health Care Organization Preparation and Implications of the Annual IRS 990 Report Unit 12: December (pg ) Getting Ready for Year-End Reporting..Again Open Heart Surgery Pro Forma December Finance Committee Special Agenda Items Looking into the Future of Health Care Finance 298
299 299 APPENDIX G 299
300 300 Word 97 for Windows NBRC Detailed Content Outline for RRT Written Examination Task Recall Application I. Select, Review, Obtain and Interpret Data SETTING: In any patient care setting, the advanced respiratory therapist reviews existing clinical data and collects or recommends obtaining additional pertinent clinical data. The therapist evaluates all data to determine the appropriateness of the prescribed respiratory care plan, and participates in the development of the respiratory care plan. 3 3 A. Review patient record and recommend diagnostic procedures. 1* 1 1. Review existing data in the patient record: a. patient history [e.g., present illness, admission notes, respiratory care orders, progress notes] X** b. physical examination [e.g., vital signs, physical findings] X c. lab data [e.g., CBC, chemistries/electrolytes, coagulation studies, Gram stain, culture and sensitivities, urinalysis] X X d. pulmonary function and blood gas results X X e. radiologic studies [e.g., radiographs of chest/upper airway, CT, MRI] X X f. monitoring data (1) fluid balance (intake and output) (2) pulmonary mechanics [e.g., maximum inspiratory pressure (MIP), vital capacity] (3) respiratory monitoring [e.g., rate, tidal volume, minute volume, I:E, inspiratory and expiratory pressures; flow, volume and pressure waveforms] X X X X (4) lung compliance, airway resistance, work of breathing X X (5) noninvasive monitoring [e.g., capnography, pulse oximetry, transcutaneous O 2/CO 2] X X 300
301 301 g. results of cardiovascular monitoring Task Recall Application (1) ECG, blood pressure, heart rate X X (2) hemodynamic monitoring [e.g., central venous pressure, cardiac output, pulmonary capillary wedge pressure, pulmonary artery pressures, mixed venous O 2,, shunt studies ( )] h. maternal and perinatal/neonatal history and data [e.g., Apgar scores, gestational age, L/S ratio, pre/post-ductal oxygenation studies] i. other diagnostic studies [e.g., EEG, intracranial pressure monitoring, metabolic studies (, nutritional assessment), ventilation/perfusion scan, pulmonary angiography, sleep studies, other ultrasonography] 2. Recommend the following procedures to obtain additional data: X X X a. CBC, electrolytes, other blood chemistries b. radiograph of chest and upper airway, CT scan, bronchoscopy, ventilation/perfusion lung scan, barium swallow X X c. Gram stain, culture and sensitivities X X d. spirometry before and/or after bronchodilator, maximum voluntary ventilation, diffusing capacity, functional residual capacity, flow-volume loops, body plethysmography, nitrogen washout distribution test, total lung capacity, CO 2 response curve, closing volume, airway resistance, bronchoprovocation, maximum inspiratory pressure (MIP), maximum expiratory pressure (MEP) e. blood gas analysis, insertion of arterial, umbilical and/or central venous, pulmonary artery monitoring lines X X X X f. lung compliance, airway resistance, lung mechanics, work of breathing X X g. ECG, echocardiography, pulse oximetry, transcutaneous O 2/CO 2 monitoring X X h. V D/V T,, cardiac output, cardiopulmonary stress testing B. Collect and evaluate clinical information Assess patient s overall cardiopulmonary status by inspection to determine: a. general appearance, muscle wasting, venous distention, peripheral edema, diaphoresis, digital clubbing, cyanosis, capillary refill X X Task Recall Application b. chest configuration, evidence of diaphragmatic movement, breathing pattern, accessory muscle activity, asymmetrical chest movement, intercostal and/or sternal retractions, nasal flaring, character of cough, amount and character of sputum X X c. transillumination of chest, Apgar score, gestational age X X 2. Assess p at ient s o verall card iop ulm o nar y st at us b y p alp at io n t o d et er m ine: a. h eart r at e, r h yt hm, f or ce X X b. asym m et r ical ch est m o vem en t s, t act ile f r em it us, crep it us, t end ern ess, secret io ns in t he air w ay, t r acheal d eviat ion, en d o t rach eal t ub e p lacem ent 3. Assess p at ient s o verall card iop ulm o nar y st at us b y p er cussion t o d et er m ine d iap hragm at ic excursion an d ar eas o f alt ered reso nan ce X X X X 301
302 Assess patient s overall cardiopulmonary status by auscultation to determine presence of: a. breath sounds [e.g., normal, bilateral, increased, decreased, absent, unequal, rhonchi or crackles (râles), wheezing, stridor, friction rub] X X b. heart sounds, dysrhythmias, murmurs, bruits X X c. blood pressure X X 5. Assess patient s learning needs [e.g., age and language appropriateness, education level, prior disease and medication knowledge] 6. Interview patient to determine: a. level of consciousness, orientation to time, place and person, emotional state, ability to cooperate b. presence of dyspnea and/or orthopnea, work of breathing, sputum production, exercise tolerance and activities of daily living X X X X X X c. physical environment, social support systems, nutritional status X X 7. Review chest radiograph to determine: a. presence of, or changes in, pneumothorax or subcutaneous emphysema, other extra-pulmonary air, consolidation and/or atelectasis, pulmonary infiltrates X X b. presence and position of foreign bodies X X c. position of endotracheal or tracheostomy tube, evidence of endotracheal or tracheostomy tube cuff hyperinflation X X Task Recall Application d. position of chest tube(s), nasogastric and/or feeding tube, pulmonary artery catheter, pacemaker, CVP, and other catheters e. position of, or changes in, hemidiaphragms, hyperinflation, pleural fluid, pulmonary edema, mediastinal shift, patency and size of major airways 8. Review lateral neck radiograph to determine: X X X a. presence of epiglottitis and subglottic edema X X b. presence or position of foreign bodies X X c. airway narrowing X X 9. Per f o rm b ed sid e p r o ced ures t o d et er m ine: a. ECG, pulse oximetry, transcutaneous O 2/CO 2 monitoring, capnography, mass spectrometry X X b. tidal volume, minute volume, I:E X X c. blood gas analysis, P(A-a)O 2, alveolar ventilation, V D/V T,, mixed venous sampling X X d. peak flow, maximum inspiratory pressure, maximum expiratory pressure, forced vital capacity, timed forced expiratory volumes [e.g., FEV 1], lung compliance, lung mechanics e. cardiac output, pulmonary capillary wedge pressure, central venous pressure, pulmonary artery pressures, fluid balance (intake and output) f. pulmonary vascular resistance and systemic vascular resistance X X g. apnea monitoring, sleep studies, respiratory impedance plethysmography X X 302
303 303 h. t rach eal t ub e cuf f p r essur e, vo lum e 10. In t erp ret result s o f b ed sid e p r o ced ures t o d et er m ine: a. ECG, pulse oximetry, transcutaneous O 2/CO 2 monitoring, capnography, mass spectrometry X X X X b. tidal volume, minute volume, I:E X X c. blood gas analysis, P(A-a)O 2, alveolar ventilation, V D/V T,,mixed venous sampling X X d. peak flow, maximum inspiratory pressure, maximum expiratory pressure, forced vital capacity, timed forced expiratory volumes [e.g., FEV 1], lung compliance, lung mechanics X X Task Recall Application e. cardiac output, pulmonary capillary wedge pressure, central venous pressure, pulmonary artery pressures, fluid balance (intake and output) f. pulmonary vascular resistance and systemic vascular resistance g. apnea monitoring, sleep studies, respiratory impedance plethysmography X X h. t rach eal t ub e cuf f p r essur e, vo lum e X X C. Perform procedures and interpret results, determine appropriateness of and participate in developing and recommending modifications to respiratory care plan Perform and/or measure the following: a. spirometry before and/or after bronchodilator, maximum voluntary ventilation, diffusing capacity, functional residual capacity, flow-volume loops, body plethysmography, nitrogen washout distribution test, total lung capacity, CO 2 response curve, closing volume, airway resistance X X b. ECG, pulse oximetry, transcutaneous O 2/CO 2 monitoring X X c. V D/V T,,mixed venous sampling, cardiac output, pulmonary capillary wedge pressure, central venous pressure, pulmonary artery pressures, cardiopulmonary stress testing d. fluid balance (intake and output) e. arterial sampling and blood gas analysis, co-oximetry, P(A-a)O 2 X X f. sleep studies, metabolic studies [e.g., indirect calorimetry] g. ventilator flow, volume and pressure waveforms, lung compliance X X 2. In t erp ret result s o f t h e f o llo w in g: a. spirometry before and/or after bronchodilator, maximum voluntary ventilation, diffusing capacity, functional residual capacity, flow-volume loops, body plethysmography, nitrogen washout distribution test, total lung capacity, CO 2 response curve, closing volume, airway resistance, bronchoprovocation X X b. ECG, pulse oximetry, transcutaneous O 2/CO 2 monitoring X X 303
304 304 Task Recall Application c. V D/V T,, mixed venous sampling,, cardiac output, pulmonary capillary wedge pressure, central venous pressure, pulmonary artery pressures, cardiopulmonary stress testing d. fluid balance (intake and output) e. arterial sampling and blood gas analysis, co-oximetry, P(A-a)O 2 X X f. peripheral venipuncture or insertion of intravenous line g. sleep studies, metabolic studies [e.g., indirect calorimetry] h. insertion of arterial and umbilical monitoring lines i. ventilator flow, volume, and pressure waveforms, lung compliance X X 3. Det er m in e t he ap p rop r iat eness o f t he p rescr ib ed r esp irat or y car e p lan an d r eco m m end m o d if icat io ns w her e ind icat ed : a. perform respiratory care quality assurance X X b. develop quality improvement program X X c. review interdisciplinary patient and family care plan X X 4. Par t icip at e in d evelop m ent o f resp ir at or y care p lan [e.g., case managem en t, d evelop and ap p ly p r ot o co ls, d isease m anagem en t ed ucat ion ] II. Select, Assemble and Check Equipment for Proper Function, Operation and Cleanliness SETTING: In an y p at ien t car e set t in g, t h e ad van ced resp ir at or y t h erap ist select s, assem b les, an d assures clean liness o f all eq uip m en t used in p ro vid in g resp ir at or y car e. Th e t h erap ist ch ecks all eq uip m ent and corr ect s m alf unct io ns. A. Select and obtain equipment, and assure equipment cleanliness. X X Select and o b t ain eq uip m ent ap p rop r iat e t o t he resp irat or y care p lan : a. oxygen administration devices (1) n asal cann ula, m ask, reser vo ir m ask (p ar t ial reb reat hin g, n o nr eb r eat h ing), f ace t en t s, t ranst r ach eal o xygen cat het er, o xygen con ser vin g cann ulas X X Task Recall Application (2) air -ent r ainm en t d evices, t racheost o m y co llar and T-p iece, o xygen h o od s an d t ent s X X (3) CPAP d evices X X b. humidifiers [e.g., bubble, passover, cascade, wick, heat moisture exchanger] X X c. aerosol generators [e.g., pneumatic nebulizer, ultrasonic nebulizer] X X d. resuscitation devices [e.g., manual resuscitator (bag-valve), pneumatic (demandvalve), mouth-to-valve mask resuscitator] X X 304
305 305 e. ventilators (1) pneumatic, electric, microprocessor, fluidic X X (2) high frequency (3) noninvasive positive pressure X X f. artificial airways (1) oro- and nasopharyngeal airways X X (2) oral, nasal and double-lumen endotracheal tubes X X (3) tracheostomy tubes and buttons X X (4) intubation equipment [e.g., laryngoscope and blades, exhaled CO 2 detection devices] (5) o t h er air w ays [e.g., lar yn geal m ask air w ay (LMA), Esop hageal Trach eal Co m b it ub e (ETC)] g. suctioning devices [e.g., suction catheters, specimen collectors, oropharyngeal suction devices] h. gas delivery, metering and clinical analyzing devices (1) regulators, reducing valves, connectors and flowmeters, air/oxygen blenders, pulse-dose systems X X X X X X (2) oxygen concentrators, air compressors, liquid oxygen systems X X (3) gas cylinders, bulk systems and manifolds X X Task Recall Application (4) capnograph, blood gas analyzer and sampling devices, co-oximeter, transcutaneous O 2/CO 2 monitor, pulse oximeter X X (5) CO, He, O 2 and specialty gas analyzers X X i. patient breathing circuits (1) IPPB, continuous mechanical ventilation X X (2) CPAP, PEEP valve assembly X X (3) H-valve assembly j. environmental devices (1) in cub at ors, rad iant w arm ers (2) aerosol (mist) tents X X (3) scavenging systems X k. positive expiratory pressure device (PEP) l. Flutter mucous clearance device 305
306 306 m. other therapeutic gases [e.g., O 2/CO 2, He/O 2] n. manometers and gauges (1) manometers water, mercury and aneroid, inspiratory/expiratory pressure meters, cuff pressure manometers X X (2) p ressure t ransd ucers X X o. respirometers [e.g., flow-sensing devices (pneumotachometer), volume displacement] p. electrocardiography devices [e.g., ECG oscilloscope monitors, ECG machines (12-lead), Holter monitors] q. hemodynamic monitoring devices (1) central venous catheters, pulmonary artery catheters, cardiac output, continuous monitors X X X X Task Recall Application (2) arterial catheters r. vacuum systems [e.g., pumps, regulators, collection bottles, pleural drainage devices] X X s. metered dose inhalers (MDI), MDI spacers X X t. Small Particle Aerosol Generators (SPAG) X X u. bronchoscopes X X 2. Assur e select ed eq uip m ent clean liness [e.g., select or d et er m ine ap p r op r iat e agent and t ech n iq ue f or d isin f ect ion and /or st er ilizat io n, p er f o rm p ro ced ur es f or d isinf ect io n and /or st er ilizat ion, m on it o r ef f ect iven ess o f st er ilizat io n p ro ced ures] X X B. Assemble and check equipment function, identify and correct equipment malfunctions, and perform quality control Assemble, check for proper function, and identify malfunctions of equipment: a. oxygen administration devices (1) nasal cannula, mask, reservoir mask (partial rebreathing, nonrebreathing), face tents, transtracheal oxygen catheter, oxygen conserving cannulas (2) air-entrainment devices, tracheostomy collar and T-piece, oxygen hoods and tents X X X X (3) CPAP devices X X b. humidifiers [e.g., bubble, passover, cascade, wick, heat moisture exchanger] X X c. aerosol generators [e.g., pneumatic nebulizer, ultrasonic nebulizer] X X d. resuscitation devices [e.g., manual resuscitator (bag-valve), pneumatic (demand-valve), mouth-to-valve mask resuscitator] e. ventilators X X (1) p neum at ic, elect r ic, m icr op r ocessor, f luid ic X X (2) h igh f r eq uen cy 306
307 307 (3) n o n in vasive p osit ive p ressur e X X f. artificial airways Task Recall Application (1) oro- and nasopharyngeal airways X X (2) oral, nasal and double-lumen endotracheal tubes X X (3) tracheostomy tubes and buttons X X (4) intubation equipment [e.g., laryngoscope and blades, exhaled CO 2 detection devices] g. suctioning devices [e.g., suction catheters, specimen collectors, oropharyngeal suction devices] h. gas delivery, metering and clinical analyzing devices (1) r egulat o rs, r ed ucin g valves, co n nect ors an d f lo w m et ers, air /o xygen b lend ers, p u lse-d o se syst em s X X X X X X (2) o xygen con cent rat or s, air co m p r essors, liq uid o xygen syst em s X X (3) gas cylin d ers, b ulk syst em s and m an if o ld s X X (4) capnograph, blood gas analyzer and sampling devices, co-oximeter, transcutaneous O 2/CO 2 monitor, pulse oximeter X X (5) CO, He, O 2 an d sp ecialt y gas an alyzers X X i. p at ient b r eat h ing circuit s (1) IPPB, continuous mechanical ventilation X X (2) CPAP, PEEP valve assem b ly X X (3) H-valve assem b ly X j. environmental devices (1) incubators, radiant warmers (2) aerosol (mist) tents X X Task Recall Application k. positive expiratory pressure devices (PEP) l. Flutter mucous clearance device m. other therapeutic gases [e.g., O 2/CO 2, He/O 2] n. m ano m et ers and gauges (1) m ano m et ers w at er, m ercur y and an er o id, in sp irat or y/exp irat or y p r essur e m et er s, cuf f p r essure m ano m et ers X X 307
308 308 (2) p ressure t ransd ucers o. respirometers [e.g., flow-sensing devices (pneumotachometer), volume displacement] p. electrocardiography devices [e.g., ECG oscilloscope monitors, ECG machines (12-lead), Holter monitors] q. hemodynamic monitoring devices (1) cent r al ven o us cat h et ers, p ulm o nar y ar t er y cat het ers, card iac o ut p ut, cont in uous m o n it ors (2) arterial catheters r. vacuum systems [e.g., pumps, regulators, collection bottles, pleural drainage devices] s. bronchoscopes X X X X X X 2. Take act io n t o corr ect m alf unct io ns of eq uip m ent : a. oxygen administration devices (1) nasal cannula, mask, reservoir mask (partial rebreathing, nonrebreathing), face tents, transtracheal oxygen catheter, oxygen conserving cannulas (2) air-entrainment devices, tracheostomy collar and T-piece, oxygen hoods and tents X X X X (3) CPAP devices X X b. humidifiers [e.g., bubble, passover, cascade, wick, heat moisture exchanger] X X Task Recall Application c. aerosol generators [e.g., pneumatic nebulizer, ultrasonic nebulizer] X X d. resuscitation devices [e.g., manual resuscitator (bag-valve), pneumatic (demandvalve), mouth-to-valve mask resuscitator] e. ventilators X X (1) p neum at ic, elect r ic, m icr op r ocessor, f luid ic X X (2) h igh f r eq uen cy (3) n o n in vasive p osit ive p ressur e X X f. artificial airways (1) oro- and nasopharyngeal airways X X (2) oral, nasal and double lumen endotracheal tubes X X (3) tracheostomy tubes and buttons X X (4) intubation equipment [e.g., laryngoscope and blades, exhaled CO 2 detection devices g. suctioning devices [e.g., suction catheters, specimen collectors, oropharyngeal suction devices h. gas delivery, metering and clinical analyzing devices X X X X 308
309 309 (1) r egulat o rs, r ed ucin g valves, co n nect ors an d f lo w m et ers, air /o xygen b lend ers, p ulse-d o se syst em s X X (2) o xygen con cent rat or s, air co m p r essors, liq uid o xygen syst em s X X (3) gas cylin d ers, b ulk syst em s and m an if o ld s X X (4) capnograph, blood gas analyzer and sampling devices, co-oximeter, transcutaneous O 2/CO 2 monitor, pulse oximeter (5) CO, He, O 2 an d sp ecialt y gas an alyzers X X i. p at ient b r eat h ing circuit s (1) IPPB, continuous mechanical ventilation X X Task Recall Application (2) CPAP, PEEP valve assem b ly X X (3) H-valve assem b ly j. environmental devices (1) incubators, radiant warmers (2) aerosol (mist) tents X X k. positive expiratory pressure devices (PEP) l. Flutter mucous clearance device m. other therapeutic gases [e.g., O 2/CO 2, He/O 2] n. m ano m et ers and gauges (1) m ano m et ers w at er, m ercur y and an er o id, in sp irat or y/exp irat or y p r essur e m et er s, cuf f p r essure m ano m et ers (2) p ressure t ransd ucers X X o. respirometers [e.g., flow-sensing devices (pneumotachometer), volume displacement] p. electrocardiography devices [e.g., ECG oscilloscope monitors, ECG machines (12-lead), Holter monitors] q. hemodynamic monitoring devices (1) cent r al ven o us cat h et ers, p ulm o nar y ar t er y cat het ers, card iac o ut p ut, cont in uous m o n it ors (2) arterial catheters r. vacuum systems [e.g., pumps, regulators, collection bottles, pleural drainage devices] s. Small Particle Aerosol Generators (SPAG) X X X X t. bronchoscopes 309
310 310 Task Recall Application 3. Per f o rm q ualit y co nt r o l p r oced ur es f o r : a. blood gas analyzers and sampling devices, co-oximeters X X b. pulmonary function equipment, ventilator volume/flow/pressure calibration X X c. gas metering devices X X d. noninvasive monitors [e.g., transcutaneous] III. Initiate, Conduct, and Modify Prescribed Therapeutic Procedures SETTING: In an y p at ien t car e set t in g, t h e ad van ced resp ir at or y t h erap ist evaluat es, m o n it o rs and r ecor d s p at ient s r esp on se t o care. Th e t h er ap ist m aint ains p at ient record s and com m un icat es w it h o t her h ealt h care t eam m em b ers. The t herap ist in it iat es, co nd uct s, and m od if ies p rescr ib ed t herap eut ic p ro ced ur es t o ach ieve t h e d esired ob ject ives. Th e t herap ist p ro vid es car e in em er gen cy set t in gs, assist s t he p h ysician an d co nd uct s p ulm on ar y rehab ilit at ion and h om e car e. A. Evaluate, monitor, and record patient's response to respiratory care Evaluate and monitor patient s response to respiratory care: a. recommend and review chest radiograph X X b. perform arterial puncture, capillary blood gas sampling, and venipuncture; obtain blood from arterial or pulmonary artery lines; perform transcutaneous O 2/CO 2, pulse oximetry, co-oximetry, and capnography monitoring c. observe changes in sputum production and consistency, note patient s subjective response to therapy and mechanical ventilation d. measure and record vital signs, monitor cardiac rhythm, evaluate fluid balance (intake and output) e. perform spirometry/determine vital capacity, measure lung compliance and airway resistance, interpret ventilator flow, volume, and pressure waveforms, measure peak flow f. determine and record central venous pressure, pulmonary artery pressures, pulmonary capillary wedge pressure and/or cardiac output g. recommend measurement of electrolytes, hemoglobin, CBC and/or chemistries h. monitor mean airway pressure, adjust and check alarm systems, measure tidal volume, respiratory rate, airway pressures, I:E, and maximum inspiratory pressure (MIP) X X X X X X X X X X Task Recall Application i. measure F IO 2 and/or liter flow X X J. monitor endotracheal or tracheostomy tube cuff pressure X X k. auscultate chest and interpret changes in breath sounds X X l. perform hemodynamic calculations [e.g., shunt studies ( ), cardiac output, cardiac index, pulmonary vascular resistance and systemic vascular resistance, stroke volume] m. in t erp r et hem od yn am ic calculat io ns: (1) calculate and interpret P(A-a)O 2,, 310
311 311 (2) interpret exhaled CO 2 monitoring, V D/V T (3) cardiac output, cardiac index, pulmonary vascular resistance and systemic vascular resistance, stroke volume 2. Maintain records and communication: a. record therapy and results using conventional terminology as required in the healthcare setting and/or by regulatory agencies by noting and interpreting: (1) patient's response to therapy including the ef f ect s of t h erap y, ad verse r eact ion s, p at ient s sub ject ive and at t it ud inal resp on se t o t herap y (2) auscult at or y f ind in gs, co ugh and sp ut um p r od uct ion and ch aract er ist ics (3) vit al signs [e.g., heart rat e, r esp irat or y rat e, b lo od p ressur e, b od y t em p erat ure] X X X X X X (4) pulse oximetry, heart rhythm, capnography X X b. ver if y co m p ut at ions and n ot e err on eo us d at a X X c. apply computer technology to patient management [e.g., ventilator waveform analysis, electronic charting, patient care algorithms] X X d. co m m un icat e result s of t h er ap y and alt er t h erap y p er p r ot o co l(s) X X 311
312 312 Task Recall Application B. Conduct therapeutic procedures to maintain a patent airway, achieve adequate ventilation and oxygenation, and remove bronchopulmonary secretions Main t ain a p at en t air w ay includ in g t h e car e o f art if icial air w ays: a. insert oro- and nasopharyngeal airway, select endotracheal or tracheostomy tube, perform endotracheal intubation, change tracheostomy tube, maintain proper cuff inflation, position of endotracheal or tracheostomy tube X X b. maintain adequate humidification X X c. extubate the patient X X d. properly position patient X X e. identify endotracheal tube placement by available means X X 2. Achieve adequate spontaneous and artificial ventilation: a. initiate and adjust IPPB therapy X X b. initiate and select appropriate settings for high frequency ventilation c. initiate and adjust ventilator modes [e.g., A/C, SIMV, pressure support ventilation (PSV), pressure control ventilation (PCV)] d. initiate and adjust independent (differential) lung ventilation 3. Rem o ve b ro nch op ulm o nar y secret io ns b y inst r uct ing and encouraging bronchopulmonary hygiene techniques [e.g., coughing techniques, autogenic drainage, positive expiratory pressure device (PEP), intrapulmonary percussive ventilation (IPV), Flutter, High Frequency Chest Wall Oscillation (HFCWO)] 4. Achieve adequate arterial and tissue oxygenation: X X X X a. initiate and adjust CPAP, PEEP, and noninvasive positive pressure X X b. initiate and adjust combinations of ventilatory techniques [e.g., SIMV, PEEP, PS, PCV] X X 312
313 313 Task Recall Application c. position patient to minimize hypoxemia, administer oxygen (on or off ventilator), prevent procedure-associated hypoxemia [e.g., oxygenate before and after suctioning and equipment changes] X X C. Make necessary modifications in therapeutic procedures based on patient response Mod if y IPPB: a. adjust sensitivity, flow, volume, pressure, F IO 2 X X b. adjust expiratory retard X X c. change patient machine interface [e.g., mouthpiece, mask] X X 2. Mod if y p at ient b reat h in g p at t er n d ur in g aer oso l t h er ap y X X 3. Mod if y o xygen t h erap y: a. change mode of administration, adjust flow, and F IO 2 X X b. set up an O 2 concentrator or liquid O 2 system X X 4. Modify specialty gas [e.g., He/O 2, O 2 /CO 2] therapy [e.g., change mode of administration, adjust flow, adjust gas concentration] 5. Modify bronchial hygiene therapy [e.g., alter position of patient, alter duration of treatment and techniques, coordinate sequence of therapies, alter equipment used and PEP therapy] 6. Modify artificial airway management: a. alter endotracheal or tracheostomy tube position, change endotracheal or tracheostomy tube X X X X X b. in it iat e suct io n in g X X c. in f lat e and d ef lat e t h e cuf f X X 7. Modify suctioning: a. alter frequency and duration of suctioning X X Task Recall Application b. change size and type of catheter X X c. alter negative pressure X X d. instill irrigating solutions X X 8. Modify mechanical ventilation: a. change patient breathing circuitry, change type of ventilator X X b. measure volume loss through chest tube(s) X 313
314 314 c. change mechanical dead space X X D. Initiate, conduct, or modify respiratory care techniques in an emergency setting Treat cardiopulmonary collapse according to: a. BCLS X X b. ACLS X X c. PALS X X d. NRP X X 2. Treat tension pneumothorax 3. Participate in land/air patient transport E. Assist physician, initiate and conduct pulmonary rehabilitation Act as an assistant to the physician performing special procedures including: a. bronchoscopy X X b. thoracentesis X X c. transtracheal aspiration Task Recall Application d. tracheostomy X X e. cardiopulmonary stress testing f. percutaneous needle biopsies of the lung g. sleep studies h. cardioversion X X i. intubation X X j. insertion of chest tubes k. insertion of lines for invasive monitoring [e.g., central venous pressure, pulmonary artery catheters, arterial lines] l. conscious sedation 2. Initiate and conduct pulmonary rehabilitation and home care within the prescription: a. monitor and maintain home respiratory care equipment, maintain apnea monitors b. explain planned therapy and goals to patient in understandable terms to achieve optimal therapeutic outcome, counsel patient and family concerning smoking cessation, disease management X X 314
315 315 c. assure safety and infection control X X d. modify respiratory care procedures for use in the home X X e. implement and monitor graded exercise program f. conduct patient education and disease management programs X X TOTALS * The number in each column is the number of items in that content area and cognitive level contained in each examination. For example, in category I.A., one item will be asked at the recall level, one item at the application level and three items at the analysis level. The items could be asked relative to any tasks listed (1-2) under category I.A. ** Note: An x denotes the examination does NOT contain items for the given task at the cognitive level indicated in the respective column (Recall, Application, Analysis). 315
316 316 COURSE EVALUATIONS 316
317 317 ST. MARY ' S/MARSHALL UNIVERSITY COOPERATIVE B.S. RESPIRATORY CARE PROGRAM COURSE EVALUATION DATE: Spring 2006 COURSE: RSP 100 This evaluation is designed for the student to evaluate the course and the instructors. Use a number 2 pencil for marking the appropriate circle on the computer answer sheet. If an item does not apply, leave the answer sheet blank for that item. You are also asked to provide comments for each section. Please explain your reasons for rating an item (instructor, unit, etc.), especially if you had a problem or concern. Use the space provided on this evaluation sheet for your comments. Use the following rating scale (A-E) to rate each item. A Strongly Agree B Agree C Neutral D Disagree E Strongly Disagree EVALUATE THE FOLLOWING COURSE RELATED ITEMS, USING TIM ABOVE SCALE. PUT YOUR COMMENTS IN THE DESIGNATED AREA OF THE SCORING SHEET. 9. This course had clearly stated course objectives. Strongly Agree Agree Neutral Disagree Strongly Disagree This course had achievable course objectives. Strongly Agree Agree Neutral Disagree Strongly Disagree Course assignments are relevant to course objectives. Strongly Agree Agree Neutral Disagree Strongly Disagree The grading method is appropriate for course content. Strongly Agree Agree Neutral Disagree Strongly Disagree There is sufficient time in class for questions and discussions. Strongly Agree Agree Neutral Disagree Strongly Disagree Exams accurately assess what I have learned in this course. Strongly Agree Agree Neutral Disagree Strongly Disagree
318 The course content built on my previous knowledge. Strongly Agree Agree Neutral Disagree Strongly Disagree Lecture information is adequately supplemented by other work. Strongly Agree Agree Neutral Disagree Strongly Disagree The course content facilitated the development of critical thinking (questioning, reasoning, analyzing, etc.) Strongly Agree Agree Neutral Disagree Strongly Disagree The course facilitated the development of my communication skills (verbal, non-verbal). Strongly Agree Agree Neutral Disagree Strongly Disagree The course content enhanced my knowledge and skills necessary to provide patient care. Strongly Agree Agree Neutral Disagree Strongly Disagree The course content will assist me in providing service to the community and the profession. Strongly Agree Agree Neutral Disagree Strongly Disagree The syllabus provided guidance for my learning. Strongly Agree Agree Neutral Disagree Strongly Disagree The syllabus identified objectives, course content and teaching methods. Strongly Agree Agree Neutral Disagree Strongly Disagree The syllabus described evaluation methods. Strongly Agree Agree Neutral Disagree Strongly Disagree
319 The course content enhanced my ability to be a caring professional. Strongly Agree Agree Neutral Disagree Strongly Disagree COMMENTS: 319
320 320 ST. MARY ' S/MARSHALL UNIVERSITY COOPERATIVE B.S. RESPIRATORY CARE PROGRAM COURSE EVALUATION DATE: COURSE: RSP 101 This evaluation is designed for the student to evaluate the course and the instructors. Use a number 2 pencil for marking the appropriate circle on the computer answer sheet. If an item does not apply, leave the answer sheet blank for that item. You are also asked to provide comments for each section. Please explain your reasons for rating an item (instructor, unit, etc.), especially if you had a problem or concern. Use the space provided on this evaluation sheet for your comments. Use the following rating scale (A-E) to rate each item. A Strongly Agree B Agree C Neutral D Disagree E Strongly Disagree INSTRUCTOR PERFORMANCE: Evaluate only those classroom or clinical instructors to which you were assigned. Instructor presented content in a knowledgeable manner. 31. Brent Blevins Strongly Agree Agree Neutral Disagree Strongly Disagree Chuck Zuhars Strongly Agree Agree Neutral Disagree Strongly Disagree Instructor presented content in an organized manner. 33. Brent Blevins Strongly Agree Agree Neutral Disagree Strongly Disagree Chuck Zuhars Strongly Agree Agree Neutral Disagree Strongly Disagree Instructor demonstrated knowledge in assigned clinical area. 35. Brent Blevins Strongly Agree Agree Neutral Disagree Strongly Disagree
321 Chuck Zuhars Strongly Agree Agree Neutral Disagree Strongly Disagree The instructor provided additional explanation or resource material when requested Brent Blevins Strongly Agree Agree Neutral Disagree Strongly Disagree Chuck Zuhars Strongly Agree Agree Neutral Disagree Strongly Disagree The instructor provided additional assistance with clinical aspects of the course as needed. 39. Brent Blevins Strongly Agree Agree Neutral Disagree Strongly Disagree Chuck Zuhars Strongly Agree Agree Neutral Disagree Strongly Disagree Written/verbal feedback in the classroom/clinical from instructor was beneficial. 41. Brent Blevins Strongly Agree Agree Neutral Disagree Strongly Disagree Chuck Zuhars Strongly Agree Agree Neutral Disagree Strongly Disagree Instructor promoted an environment of learning. 43. Brent Blevins Strongly Agree Agree Neutral Disagree Strongly Disagree
322 Chuck Zuhars Strongly Agree Agree Neutral Disagree Strongly Disagree Comment: Identify the instructor (by name) and provide any pertinent comments regarding any of the above topics. 322
323 323 ST. MARY ' S/MARSHALL UNIVERSITY COOPERATIVE B.S. RESPIRATORY CARE PROGRAM COURSE EVALUATION DATE: COURSE: RSP 101 This evaluation is designed for the student to evaluate the course and the instructors. Use a number 2 pencil for marking the appropriate circle on the computer answer sheet. If an item does not apply, leave the answer sheet blank for that item. You are also asked to provide comments for each section. Please explain your reasons for rating an item (instructor, unit, etc.), especially if you had a problem or concern. Use the space provided on this evaluation sheet for your comments. Use the following rating scale (A-E) to rate each item. A Strongly Agree B Agree C Neutral D Disagree E Strongly Disagree CLINICAL ROTATIONS/AGENCY: Evaluate only those units to which you actually were assigned. Clinical rotations were appropriate for application of course content. 31. St. Mary s Medical Center Strongly Agree Agree Neutral Disagree Strongly Disagree Holzer Medical Center Strongly Agree Agree Neutral Disagree Strongly Disagree Comment: Identify the clinical experience by number above and provide pertinent comments: 33. Student was able to collaborate with staff on assigned unit in an effective manner. Strongly Agree Agree Neutral Disagree Strongly Disagree Staff modeled the professional respiratory therapists role. Strongly Agree Agree Neutral Disagree Strongly Disagree Staff members on assigned units were helpful. Strongly Agree Agree Neutral Disagree Strongly Disagree
324 324 Comment: Please make comments regarding staff on units by first identifying the unit or agency and then provide any pertinent comments: TEXTBOOKS: 36. The textbook was useful in understanding classroom presentation and clinical situations Strongly Agree Agree Neutral Disagree Strongly Disagree Comment: Identify the text by number above and then provide any pertinent comments: LEARNING RESOURCES 37. When I needed additional learning resources for this course, the library, Academic Support Center, and/or the computer lab had what I needed. Strongly Agree Agree Neutral Disagree Strongly Disagree Comment: 38. Instructional aids, such as Power Point presentations, videos, and handouts given by the instructors were beneficial. Strongly Agree Agree Neutral Disagree Strongly Disagree Comment: 324
325 325 ST. MARY ' S/MARSHALL UNIVERSITY COOPERATIVE BSRT PROGRAM COURSE EVALUATION DATE: COURSE: RSP 101 This evaluation is designed for the student to evaluate the course and the instructors. Use a number 2 pencil for marking the appropriate circle on the computer answer sheet. If an item does not apply, leave the answer sheet blank for that item. You are also asked to provide comments for each section. Please explain your reasons for rating an item (instructor, unit, etc.), especially if you had a problem or concern. Use the space provided on this evaluation sheet for your comments. Use the following rating scale (A-E) to rate each item A Strongly Agree B Agree C Neutral D Disagree E Strongly Disagree 39.. Classroom, library and laboratory facilities were adequate to meet my learning needs. Strongly Agree Agree Neutral Disagree Strongly Disagree Comment: 40. What was your advisor's name? Did you find him/her helpful? Yes No If not, explain: 41. Identify the grade that you expected to receive in this course. 10/95 10/99 06/00 03/04 11/05 9/06 325
326 326 ST. MARY ' S/MARSHALL UNIVERSITY COOPERATIVE B.S. RESPIRATORY CARE PROGRAM COURSE EVALUATION DATE: Summer 2006 COURSE: RSP 102 This evaluation is designed for the student to evaluate the course and the instructors. Use a number 2 pencil for marking the appropriate circle on the computer answer sheet. If an item does not apply, leave the answer sheet blank for that item. You are also asked to provide comments for each section. Please explain your reasons for rating an item (instructor, unit, etc.), especially if you had a problem or concern. Use the space provided on this evaluation sheet for your comments. Use the following rating scale (A-E) to rate each item. A Strongly Agree B Agree C Neutral D Disagree E Strongly Disagree EVALUATE THE FOLLOWING COURSE RELATED ITEMS, USING TIM ABOVE SCALE. PUT YOUR COMMENTS IN THE DESIGNATED AREA OF THE SCORING SHEET. 17. This course had clearly stated course objectives. Strongly Agree Agree Neutral Disagree Strongly Disagree This course had achievable course objectives. Strongly Agree Agree Neutral Disagree Strongly Disagree Course assignments are relevant to course objectives. Strongly Agree Agree Neutral Disagree Strongly Disagree The grading method is appropriate for course content. Strongly Agree Agree Neutral Disagree Strongly Disagree There is sufficient time in class for questions and discussions. Strongly Agree Agree Neutral Disagree Strongly Disagree Exams accurately assess what I have learned in this course. Strongly Agree Agree Neutral Disagree Strongly Disagree
327 The course content built on my previous knowledge. Strongly Agree Agree Neutral Disagree Strongly Disagree Lecture information is adequately supplemented by other work. Strongly Agree Agree Neutral Disagree Strongly Disagree The course content facilitated the development of critical thinking (questioning, reasoning, analyzing, etc.) Strongly Agree Agree Neutral Disagree Strongly Disagree The course facilitated the development of my communication skills (verbal, non-verbal). Strongly Agree Agree Neutral Disagree Strongly Disagree The course content enhanced my knowledge and skills necessary to provide patient care. Strongly Agree Agree Neutral Disagree Strongly Disagree The course content will assist me in providing service to the community and the profession. Strongly Agree Agree Neutral Disagree Strongly Disagree The syllabus provided guidance for my learning. Strongly Agree Agree Neutral Disagree Strongly Disagree The syllabus identified objectives, course content and teaching methods. Strongly Agree Agree Neutral Disagree Strongly Disagree The syllabus described evaluation methods. Strongly Agree Agree Neutral Disagree Strongly Disagree
328 The course content enhanced my ability to be a caring professional. Strongly Agree Agree Neutral Disagree Strongly Disagree COMMENTS: 328
329 329 ST. MARY ' S/MARSHALL UNIVERSITY COOPERATIVE B.S. RESPIRATORY CARE PROGRAM COURSE EVALUATION DATE: COURSE: RSP 101 This evaluation is designed for the student to evaluate the course and the instructors. Use a number 2 pencil for marking the appropriate circle on the computer answer sheet. If an item does not apply, leave the answer sheet blank for that item. You are also asked to provide comments for each section. Please explain your reasons for rating an item (instructor, unit, etc.), especially if you had a problem or concern. Use the space provided on this evaluation sheet for your comments. Use the following rating scale (A-E) to rate each item. A Strongly Agree B Agree C Neutral D Disagree E Strongly Disagree INSTRUCTOR PERFORMANCE: Evaluate only those classroom or clinical instructors to which you were assigned. Instructor presented content in a knowledgeable manner. 45. Brent Blevins Strongly Agree Agree Neutral Disagree Strongly Disagree Chuck Zuhars Strongly Agree Agree Neutral Disagree Strongly Disagree Instructor presented content in an organized manner. 47. Brent Blevins Strongly Agree Agree Neutral Disagree Strongly Disagree Chuck Zuhars Strongly Agree Agree Neutral Disagree Strongly Disagree Instructor demonstrated knowledge in assigned clinical area. 49. Brent Blevins Strongly Agree Agree Neutral Disagree Strongly Disagree
330 Chuck Zuhars Strongly Agree Agree Neutral Disagree Strongly Disagree The instructor provided additional explanation or resource material when requested Brent Blevins Strongly Agree Agree Neutral Disagree Strongly Disagree Chuck Zuhars Strongly Agree Agree Neutral Disagree Strongly Disagree The instructor provided additional assistance with clinical aspects of the course as needed. 53. Brent Blevins Strongly Agree Agree Neutral Disagree Strongly Disagree Chuck Zuhars Strongly Agree Agree Neutral Disagree Strongly Disagree Written/verbal feedback in the classroom/clinical from instructor was beneficial. 55. Brent Blevins Strongly Agree Agree Neutral Disagree Strongly Disagree Chuck Zuhars Strongly Agree Agree Neutral Disagree Strongly Disagree Instructor promoted an environment of learning. 57. Brent Blevins Strongly Agree Agree Neutral Disagree Strongly Disagree
331 Chuck Zuhars Strongly Agree Agree Neutral Disagree Strongly Disagree Comment: Identify the instructor (by name) and provide any pertinent comments regarding any of the above topics. 331
332 332 ST. MARY ' S/MARSHALL UNIVERSITY COOPERATIVE B.S. RESPIRATORY CARE PROGRAM COURSE EVALUATION DATE: COURSE: RSP 102 This evaluation is designed for the student to evaluate the course and the instructors. Use a number 2 pencil for marking the appropriate circle on the computer answer sheet. If an item does not apply, leave the answer sheet blank for that item. You are also asked to provide comments for each section. Please explain your reasons for rating an item (instructor, unit, etc.), especially if you had a problem or concern. Use the space provided on this evaluation sheet for your comments. Use the following rating scale (A-E) to rate each item. A Strongly Agree B Agree C Neutral D Disagree E Strongly Disagree CLINICAL ROTATIONS/AGENCY: Evaluate only those units to which you actually were assigned. Clinical rotations were appropriate for application of course content. 31. St. Mary s Medical Center Strongly Agree Agree Neutral Disagree Strongly Disagree Holzer Medical Center Strongly Agree Agree Neutral Disagree Strongly Disagree Comment: Identify the clinical experience by number above and provide pertinent comments: 37. Student was able to collaborate with staff on assigned unit in an effective manner. Strongly Agree Agree Neutral Disagree Strongly Disagree Staff modeled the professional respiratory therapists role. Strongly Agree Agree Neutral Disagree Strongly Disagree Staff members on assigned units were helpful. Strongly Agree Agree Neutral Disagree Strongly Disagree Comment: Please make comments regarding staff on units by first identifying the unit or agency and then provide any pertinent comments: 332
333 333 TEXTBOOKS: 40. The textbook was useful in understanding classroom presentation and clinical situations Strongly Agree Agree Neutral Disagree Strongly Disagree Comment: Identify the text by number above and then provide any pertinent comments: LEARNING RESOURCES 37. When I needed additional learning resources for this course, the library, Academic Support Center, and/or the computer lab had what I needed. Strongly Agree Agree Neutral Disagree Strongly Disagree Comment: 38. Instructional aids, such as Power Point presentations, videos, and handouts given by the instructors were beneficial. Strongly Agree Agree Neutral Disagree Strongly Disagree Comment: 333
334 334 ST. MARY ' S/MARSHALL UNIVERSITY COOPERATIVE BSRT PROGRAM COURSE EVALUATION DATE: COURSE: RSP 102 This evaluation is designed for the student to evaluate the course and the instructors. Use a number 2 pencil for marking the appropriate circle on the computer answer sheet. If an item does not apply, leave the answer sheet blank for that item. You are also asked to provide comments for each section. Please explain your reasons for rating an item (instructor, unit, etc.), especially if you had a problem or concern. Use the space provided on this evaluation sheet for your comments. Use the following rating scale (A-E) to rate each item A Strongly Agree B Agree C Neutral D Disagree E Strongly Disagree 39.. Classroom, library and laboratory facilities were adequate to meet my learning needs. Strongly Agree Agree Neutral Disagree Strongly Disagree Comment: 40. What was your advisor's name? Did you find him/her helpful? Yes No If not, explain: 41. Identify the grade that you expected to receive in this course. 10/95 10/99 06/00 03/04 11/05 9/06 334
335 335 ST. MARY ' S/MARSHALL UNIVERSITY COOPERATIVE B.S. RESPIRATORY CARE PROGRAM DATE: Summer 2006 COURSE EVALUATION COURSE: RSP 102L This evaluation is designed for the student to evaluate the course and the instructors. Use a number 2 pencil for marking the appropriate circle on the computer answer sheet. If an item does not apply, leave the answer sheet blank for that item. You are also asked to provide comments for each section. Please explain your reasons for rating an item (instructor, unit, etc.), especially if you had a problem or concern. Use the space provided on this evaluation sheet for your comments. Use the following rating scale (A-E) to rate each item. A Strongly Agree B Agree C Neutral D Disagree E Strongly Disagree EVALUATE THE FOLLOWING COURSE RELATED ITEMS, USING TIM ABOVE SCALE. PUT YOUR COMMENTS IN THE DESIGNATED AREA OF THE SCORING SHEET. 25. This course had clearly stated course objectives. Strongly Agree Agree Neutral Disagree Strongly Disagree This course had achievable course objectives. Strongly Agree Agree Neutral Disagree Strongly Disagree Course assignments are relevant to course objectives. Strongly Agree Agree Neutral Disagree Strongly Disagree The grading method is appropriate for course content. Strongly Agree Agree Neutral Disagree Strongly Disagree There is sufficient time in class for questions and discussions. Strongly Agree Agree Neutral Disagree Strongly Disagree Exams accurately assess what I have learned in this course. Strongly Agree Agree Neutral Disagree Strongly Disagree
336 The course content built on my previous knowledge. Strongly Agree Agree Neutral Disagree Strongly Disagree Lecture information is adequately supplemented by other work. Strongly Agree Agree Neutral Disagree Strongly Disagree The course content facilitated the development of critical thinking (questioning, reasoning, analyzing, etc.) Strongly Agree Agree Neutral Disagree Strongly Disagree The course facilitated the development of my communication skills (verbal, non-verbal). Strongly Agree Agree Neutral Disagree Strongly Disagree The course content enhanced my knowledge and skills necessary to provide patient care. Strongly Agree Agree Neutral Disagree Strongly Disagree The course content will assist me in providing service to the community and the profession. Strongly Agree Agree Neutral Disagree Strongly Disagree The syllabus provided guidance for my learning. Strongly Agree Agree Neutral Disagree Strongly Disagree The syllabus identified objectives, course content and teaching methods. Strongly Agree Agree Neutral Disagree Strongly Disagree The syllabus described evaluation methods. Strongly Agree Agree Neutral Disagree Strongly Disagree
337 The course content enhanced my ability to be a caring professional. Strongly Agree Agree Neutral Disagree Strongly Disagree COMMENTS: 337
338 338 ST. MARY ' S/MARSHALL UNIVERSITY COOPERATIVE B.S. RESPIRATORY CARE PROGRAM DATE: COURSE EVALUATION COURSE: RSP 102L This evaluation is designed for the student to evaluate the course and the instructors. Use a number 2 pencil for marking the appropriate circle on the computer answer sheet. If an item does not apply, leave the answer sheet blank for that item. You are also asked to provide comments for each section. Please explain your reasons for rating an item (instructor, unit, etc.), especially if you had a problem or concern. Use the space provided on this evaluation sheet for your comments. Use the following rating scale (A-E) to rate each item. A Strongly Agree B Agree C Neutral D Disagree E Strongly Disagree INSTRUCTOR PERFORMANCE: Evaluate only those classroom or clinical instructors to which you were assigned. Instructor presented content in a knowledgeable manner. 59. Brent Blevins Strongly Agree Agree Neutral Disagree Strongly Disagree Chuck Zuhars Strongly Agree Agree Neutral Disagree Strongly Disagree Instructor presented content in an organized manner. 61. Brent Blevins Strongly Agree Agree Neutral Disagree Strongly Disagree Chuck Zuhars Strongly Agree Agree Neutral Disagree Strongly Disagree Instructor demonstrated knowledge in assigned clinical area. 63. Brent Blevins Strongly Agree Agree Neutral Disagree Strongly Disagree
339 Chuck Zuhars Strongly Agree Agree Neutral Disagree Strongly Disagree The instructor provided additional explanation or resource material when requested Brent Blevins Strongly Agree Agree Neutral Disagree Strongly Disagree Chuck Zuhars Strongly Agree Agree Neutral Disagree Strongly Disagree The instructor provided additional assistance with clinical aspects of the course as needed. 67. Brent Blevins Strongly Agree Agree Neutral Disagree Strongly Disagree Chuck Zuhars Strongly Agree Agree Neutral Disagree Strongly Disagree Written/verbal feedback in the classroom/clinical from instructor was beneficial. 69. Brent Blevins Strongly Agree Agree Neutral Disagree Strongly Disagree Chuck Zuhars Strongly Agree Agree Neutral Disagree Strongly Disagree Instructor promoted an environment of learning. 71. Brent Blevins Strongly Agree Agree Neutral Disagree Strongly Disagree
340 Chuck Zuhars Strongly Agree Agree Neutral Disagree Strongly Disagree Comment: Identify the instructor (by name) and provide any pertinent comments regarding any of the above topics. 340
341 341 ST. MARY ' S/MARSHALL UNIVERSITY COOPERATIVE B.S. RESPIRATORY CARE PROGRAM DATE: COURSE EVALUATION COURSE: RSP 102L This evaluation is designed for the student to evaluate the course and the instructors. Use a number 2 pencil for marking the appropriate circle on the computer answer sheet. If an item does not apply, leave the answer sheet blank for that item. You are also asked to provide comments for each section. Please explain your reasons for rating an item (instructor, unit, etc.), especially if you had a problem or concern. Use the space provided on this evaluation sheet for your comments. Use the following rating scale (A-E) to rate each item. A Strongly Agree B Agree C Neutral D Disagree E Strongly Disagree CLINICAL ROTATIONS/AGENCY: Evaluate only those units to which you actually were assigned. Clinical rotations were appropriate for application of course content. 31. St. Mary s Medical Center Strongly Agree Agree Neutral Disagree Strongly Disagree Holzer Medical Center Strongly Agree Agree Neutral Disagree Strongly Disagree Comment: Identify the clinical experience by number above and provide pertinent comments: 41. Student was able to collaborate with staff on assigned unit in an effective manner. Strongly Agree Agree Neutral Disagree Strongly Disagree Staff modeled the professional respiratory therapists role. Strongly Agree Agree Neutral Disagree Strongly Disagree Staff members on assigned units were helpful. Strongly Agree Agree Neutral Disagree Strongly Disagree Comment: Please make comments regarding staff on units by first identifying the unit or agency and then provide any pertinent comments: 341
342 342 TEXTBOOKS: 44. The textbook was useful in understanding classroom presentation and clinical situations Strongly Agree Agree Neutral Disagree Strongly Disagree Comment: Identify the text by number above and then provide any pertinent comments: LEARNING RESOURCES 37. When I needed additional learning resources for this course, the library, Academic Support Center, and/or the computer lab had what I needed. Strongly Agree Agree Neutral Disagree Strongly Disagree Comment: 38. Instructional aids, such as Power Point presentations, videos, and handouts given by the instructors were beneficial. Strongly Agree Agree Neutral Disagree Strongly Disagree Comment: 342
343 343 DATE: ST. MARY ' S/MARSHALL UNIVERSITY COOPERATIVE BSRT PROGRAM COURSE EVALUATION COURSE: RSP 102L This evaluation is designed for the student to evaluate the course and the instructors. Use a number 2 pencil for marking the appropriate circle on the computer answer sheet. If an item does not apply, leave the answer sheet blank for that item. You are also asked to provide comments for each section. Please explain your reasons for rating an item (instructor, unit, etc.), especially if you had a problem or concern. Use the space provided on this evaluation sheet for your comments. Use the following rating scale (A-E) to rate each item A Strongly Agree B Agree C Neutral D Disagree E Strongly Disagree 39.. Classroom, library and laboratory facilities were adequate to meet my learning needs. Strongly Agree Agree Neutral Disagree Strongly Disagree Comment: 40. What was your advisor's name? Did you find him/her helpful? Yes No If not, explain: 41. Identify the grade that you expected to receive in this course. 10/95 10/99 06/00 03/04 11/05 9/06 343
CENTRAL NEW MEXICO COMMUNITY COLLEGE Respiratory Therapy Program STUDENT HANDBOOK
 CENTRAL NEW MEXICO COMMUNITY COLLEGE Respiratory Therapy Program STUDENT HANDBOOK In the event of a conflict between information contained in the student handbook and the CNM catalog, the catalog takes
CENTRAL NEW MEXICO COMMUNITY COLLEGE Respiratory Therapy Program STUDENT HANDBOOK In the event of a conflict between information contained in the student handbook and the CNM catalog, the catalog takes
Respiratory Care Technology (RC)
 Cincinnati State 1 Cincinnati State offers a comprehensive program in Respiratory Technology. Students develop a wide range of clinical skills in traditional and nontraditional roles and gain proficiency
Cincinnati State 1 Cincinnati State offers a comprehensive program in Respiratory Technology. Students develop a wide range of clinical skills in traditional and nontraditional roles and gain proficiency
Respiratory Therapist Program Description
 Program Description Respiratory Therapy is a health profession that specializes in the evaluation, treatment, education and rehabilitation of patients with lung and heart disease, under the direction of
Program Description Respiratory Therapy is a health profession that specializes in the evaluation, treatment, education and rehabilitation of patients with lung and heart disease, under the direction of
Accreditation Standards. for the. Profession of Respiratory Care
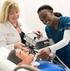 Accreditation Standards for the Profession of Respiratory Care Essentials/Standards initially adopted in 1962; revised in 1972, 1977, 1986, 2000, 2003, and 2010 Adopted by the AMERICAN ASSOCIATION FOR
Accreditation Standards for the Profession of Respiratory Care Essentials/Standards initially adopted in 1962; revised in 1972, 1977, 1986, 2000, 2003, and 2010 Adopted by the AMERICAN ASSOCIATION FOR
SELF-STUDY REPORT DIVIDERS
 SELF-STUDY REPORT DIVIDERS Outlined below are the supporting documents that are required to be submitted with the Self- Study Report. These additional details are designed to provide the Program Director
SELF-STUDY REPORT DIVIDERS Outlined below are the supporting documents that are required to be submitted with the Self- Study Report. These additional details are designed to provide the Program Director
ST. ROSE HOSPITAL Job Description
 ST. ROSE HOSPITAL Job Description JOB TITLE/CLASSIFICATION... REGISTERED RESPIRATORY THERAPIST (RRT) (163) DEPARTMENT... PULMONARY SERVICES STATUS... NON-EXEMPT RELATIONSHIPS Reports to... PULMONARY SUPERVISOR
ST. ROSE HOSPITAL Job Description JOB TITLE/CLASSIFICATION... REGISTERED RESPIRATORY THERAPIST (RRT) (163) DEPARTMENT... PULMONARY SERVICES STATUS... NON-EXEMPT RELATIONSHIPS Reports to... PULMONARY SUPERVISOR
Respiratory Therapy. Associate in Science Degree. GENERAL EDUCATION ACADEMIC ADVISEMENT: Students must meet with a regular ELAC academic
 Respiratory Therapy Associate in Science Degree This program provides students with a strong academic foundation and the clinical proficiency to utilize modern respiratory devices (under the direction
Respiratory Therapy Associate in Science Degree This program provides students with a strong academic foundation and the clinical proficiency to utilize modern respiratory devices (under the direction
Part III. Self-Study Report Template
 Part 3 Ministry Of Education And Higher Education Directorate General of Higher Education Part III Self-Study Report Template LABE SELF-STUDY QUESTIONNAIRE http://www.labe.org.lb General Instructions Introduction
Part 3 Ministry Of Education And Higher Education Directorate General of Higher Education Part III Self-Study Report Template LABE SELF-STUDY QUESTIONNAIRE http://www.labe.org.lb General Instructions Introduction
02 DEPARTMENT OF PROFESSIONAL AND FINANCIAL REGULATION. Summary: This chapter defines certain professional terms used throughout the board s rules.
 02 DEPARTMENT OF PROFESSIONAL AND FINANCIAL REGULATION 343 BOARD OF RESPIRATORY CARE PRACTITIONERS Chapter 1: DEFINITIONS Summary: This chapter defines certain professional terms used throughout the board
02 DEPARTMENT OF PROFESSIONAL AND FINANCIAL REGULATION 343 BOARD OF RESPIRATORY CARE PRACTITIONERS Chapter 1: DEFINITIONS Summary: This chapter defines certain professional terms used throughout the board
Letter of Intent. Respiratory Therapist Program. AAS Degree in Respiratory Therapy
 Letter of Intent Respiratory Therapist Program AAS Degree in Respiratory Therapy Office of the Provost and Department of Nursing Table of Contents 1. Purposes and goals 2. Need for the Curriculum 3. Students
Letter of Intent Respiratory Therapist Program AAS Degree in Respiratory Therapy Office of the Provost and Department of Nursing Table of Contents 1. Purposes and goals 2. Need for the Curriculum 3. Students
Respiratory Therapy Program Technical Standards
 Respiratory Therapy Program Technical Standards Technical Standards define the observational, communication, cognitive, affective, and physical capabilities deemed essential to complete this program and
Respiratory Therapy Program Technical Standards Technical Standards define the observational, communication, cognitive, affective, and physical capabilities deemed essential to complete this program and
Commission on Accreditation of Allied Health Education Programs
 Standards and Guidelines for the Accreditation of Educational Programs in Surgical Technology Essentials/Standards initially adopted in l972; revised in 1991, 2000, 2002, and 2004 by the: American College
Standards and Guidelines for the Accreditation of Educational Programs in Surgical Technology Essentials/Standards initially adopted in l972; revised in 1991, 2000, 2002, and 2004 by the: American College
Program Effectiveness Plan (PEP) Training Manual
 Program Effectiveness Plan (PEP) Training Manual ABHES 7777 Leesburg Pike, Suite 314N Falls Church, Virginia 22043 703.917.9503 / www.abhes.org January 2010 1 TABLE OF CONTENTS The Purpose of the PEP...
Program Effectiveness Plan (PEP) Training Manual ABHES 7777 Leesburg Pike, Suite 314N Falls Church, Virginia 22043 703.917.9503 / www.abhes.org January 2010 1 TABLE OF CONTENTS The Purpose of the PEP...
RESPIRATORY THERAPY AAS DEGREE School of Nursing and Allied Health. Information Package. Distance Education. Revised 25-Jun-13
 RESPIRATORY THERAPY AAS DEGREE School of Nursing and Allied Health Information Package Distance Education Revised 25-Jun-13 Dear Prospective Respiratory Therapy Student, Thank you for expressing an interest
RESPIRATORY THERAPY AAS DEGREE School of Nursing and Allied Health Information Package Distance Education Revised 25-Jun-13 Dear Prospective Respiratory Therapy Student, Thank you for expressing an interest
RESPIRATORY THERAPY PROGRAM
 TEXAS SOUTHERN UNIVERSITY COLLEGE OF PHARMACY & HEALTH SCIENCES DEPARTMENT OF HEALTH SCIENCES RESPIRATORY THERAPY PROGRAM Application for Spring 2016 Admission - Deadline NOVEMBER 30, 2015 (Applications
TEXAS SOUTHERN UNIVERSITY COLLEGE OF PHARMACY & HEALTH SCIENCES DEPARTMENT OF HEALTH SCIENCES RESPIRATORY THERAPY PROGRAM Application for Spring 2016 Admission - Deadline NOVEMBER 30, 2015 (Applications
Respiratory Therapists
 SOC 29-1126: Assess, treat, and care for patients with breathing disorders. Assume primary responsibility for all respiratory care modalities, including the supervision of respiratory therapy technicians.
SOC 29-1126: Assess, treat, and care for patients with breathing disorders. Assume primary responsibility for all respiratory care modalities, including the supervision of respiratory therapy technicians.
High School GPA: 3.0 on a 4.0 scale SAT: 1000 or Above ACT: 21 or Above
 APPLICATION PROCEDURES The Occupational Therapy Admissions Committee selects students for admission after they have met the general Tuskegee University requirements for admission to the Graduate Program.
APPLICATION PROCEDURES The Occupational Therapy Admissions Committee selects students for admission after they have met the general Tuskegee University requirements for admission to the Graduate Program.
Respiratory Care Associate in Science Degree
 2011-12 See your Career Program Advisor to help you get in the right classes. Respiratory Care Associate in Science Degree Set Yourself Up for a Great Career Respiratory therapists are an integral member
2011-12 See your Career Program Advisor to help you get in the right classes. Respiratory Care Associate in Science Degree Set Yourself Up for a Great Career Respiratory therapists are an integral member
RESPIRATORY THERAPY AAS DEGREE School of Nursing and Allied Health. Information Package. Revised 25-Jun-13
 RESPIRATORY THERAPY AAS DEGREE School of Nursing and Allied Health Information Package Revised 25-Jun-13 Dear Prospective Respiratory Therapy Student, Thank you for expressing an interest in the Respiratory
RESPIRATORY THERAPY AAS DEGREE School of Nursing and Allied Health Information Package Revised 25-Jun-13 Dear Prospective Respiratory Therapy Student, Thank you for expressing an interest in the Respiratory
How To Manage Nursing Education
 NLNAC STANDARDS AND CRITERIA ASSOCIATE DEGREE PROGRAMS I. Mission and Governance There are clear and publicly stated mission and/or philosophy and purposes appropriate to postsecondary or higher education
NLNAC STANDARDS AND CRITERIA ASSOCIATE DEGREE PROGRAMS I. Mission and Governance There are clear and publicly stated mission and/or philosophy and purposes appropriate to postsecondary or higher education
National Standards. Council for Standards in Human Service Education. http://www.cshse.org 2013 (2010, 1980, 2005, 2009)
 Council for Standards in Human Service Education National Standards ASSOCIATE DEGREE IN HUMAN SERVICES http://www.cshse.org 2013 (2010, 1980, 2005, 2009) I. GENERAL PROGRAM CHARACTERISTICS A. Institutional
Council for Standards in Human Service Education National Standards ASSOCIATE DEGREE IN HUMAN SERVICES http://www.cshse.org 2013 (2010, 1980, 2005, 2009) I. GENERAL PROGRAM CHARACTERISTICS A. Institutional
Respiratory Care. A Life and Breath Career for You!
 Respiratory Care A Life and Breath Career for You! Respiratory Care Makes a Difference At 9:32 am, Lori Moreno brought a newborn baby struggling to breathe back to life What have you accomplished today?
Respiratory Care A Life and Breath Career for You! Respiratory Care Makes a Difference At 9:32 am, Lori Moreno brought a newborn baby struggling to breathe back to life What have you accomplished today?
Appendix K. Nutrition and Dietetics Department Dietetics Student Handbook. Bluffton University Bluffton, Ohio
 Appendix K Nutrition and Dietetics Department Dietetics Student Handbook Bluffton University Bluffton, Ohio Revised June, 2014 Table of Contents Page Welcome... 3 Program Information Mission Statement...
Appendix K Nutrition and Dietetics Department Dietetics Student Handbook Bluffton University Bluffton, Ohio Revised June, 2014 Table of Contents Page Welcome... 3 Program Information Mission Statement...
4. Appendices - supplemental information that supports the documentation related to the standards provided in the report.
 Oklahoma Board of Nursing 2915 North Classen Boulevard, Suite 524 Oklahoma City, OK 73106 (405) 962-1800 GUIDELINES FOR SURVEY VISITS OF NURSING EDUCATION PROGRAMS Preparing for the Survey Visit Each nursing
Oklahoma Board of Nursing 2915 North Classen Boulevard, Suite 524 Oklahoma City, OK 73106 (405) 962-1800 GUIDELINES FOR SURVEY VISITS OF NURSING EDUCATION PROGRAMS Preparing for the Survey Visit Each nursing
Program in Rehabilitation Counseling
 Program in Rehabilitation Counseling The RC Profession Work and working are highly valued in our society. Rehabilitation Counselors provide and coordinate services for individuals with a range of physical,
Program in Rehabilitation Counseling The RC Profession Work and working are highly valued in our society. Rehabilitation Counselors provide and coordinate services for individuals with a range of physical,
HOUSE OF REPRESENTATIVES - FLOOR VERSION
 HOUSE OF REPRESENTATIVES - FLOOR VERSION STATE OF OKLAHOMA nd Session of the rd Legislature () HOUSE BILL By: Mulready of the House and Brinkley of the Senate AS INTRODUCED An Act relating to professions
HOUSE OF REPRESENTATIVES - FLOOR VERSION STATE OF OKLAHOMA nd Session of the rd Legislature () HOUSE BILL By: Mulready of the House and Brinkley of the Senate AS INTRODUCED An Act relating to professions
2015-2016. University of Houston Victoria. Counseling Psychology Graduate Student Handbook D E P A R T M E N T O F A R T S & S C I E N C E S
 2015-2016 University of Houston Victoria Counseling Psychology Graduate Student Handbook D E P A R T M E N T O F A R T S & S C I E N C E S Welcome and Overview Welcome to the UHV Masters Program in Counseling
2015-2016 University of Houston Victoria Counseling Psychology Graduate Student Handbook D E P A R T M E N T O F A R T S & S C I E N C E S Welcome and Overview Welcome to the UHV Masters Program in Counseling
RESPIRATORY THERAPY PROGRAM INFORMATION
 RESPIRATORY THERAPY PROGRAM INFORMATION Respiratory therapists work with physicians and other allied health professionals to diagnose and treat patients with disorders associated with the respiratory and
RESPIRATORY THERAPY PROGRAM INFORMATION Respiratory therapists work with physicians and other allied health professionals to diagnose and treat patients with disorders associated with the respiratory and
National Standards. Council for Standards in Human Service Education. http://www.cshse.org 2013 (2010, 1980, 2005, 2009)
 Council for Standards in Human Service Education National Standards BACCALAUREATE DEGREE IN HUMAN SERVICES http://www.cshse.org 2013 (2010, 1980, 2005, 2009) I. GENERAL PROGRAM CHARACTERISTICS A. Institutional
Council for Standards in Human Service Education National Standards BACCALAUREATE DEGREE IN HUMAN SERVICES http://www.cshse.org 2013 (2010, 1980, 2005, 2009) I. GENERAL PROGRAM CHARACTERISTICS A. Institutional
C. Responsibilities of Sponsor The Sponsor must ensure that the provisions of these Standards and Guidelines are met.
 NOTE: This document contains the changes that the 2015 Standards includes. There are some minor wording changes that have not been included, but the focus is on the change in requirements. Please see the
NOTE: This document contains the changes that the 2015 Standards includes. There are some minor wording changes that have not been included, but the focus is on the change in requirements. Please see the
This policy and procedure describes the requirements, selection process, and admission status types for the respiratory therapy program at NPCC.
 This policy and procedure describes the requirements, selection process, and admission status types for the respiratory therapy program at NPCC. 1. General Statements a. Curriculum is offered on a full-time
This policy and procedure describes the requirements, selection process, and admission status types for the respiratory therapy program at NPCC. 1. General Statements a. Curriculum is offered on a full-time
Clinical Preceptor Handbook Respiratory Care Practitioner Program Wheeling Jesuit University
 Clinical Preceptor Handbook Respiratory Care Practitioner Program Wheeling Jesuit University 2 Contents I. Objective 3 II. The role of the clinical preceptor (CP) 3 III. Criteria for selection of clinical
Clinical Preceptor Handbook Respiratory Care Practitioner Program Wheeling Jesuit University 2 Contents I. Objective 3 II. The role of the clinical preceptor (CP) 3 III. Criteria for selection of clinical
STATE OF NEBRASKA STATUTES RELATING TO RESPIRATORY CARE PRACTICE ACT
 2012 STATE OF NEBRASKA STATUTES RELATING TO RESPIRATORY CARE PRACTICE ACT Department of Health and Human Services Division of Public Health Licensure Unit 301 Centennial Mall South, Third Floor PO Box
2012 STATE OF NEBRASKA STATUTES RELATING TO RESPIRATORY CARE PRACTICE ACT Department of Health and Human Services Division of Public Health Licensure Unit 301 Centennial Mall South, Third Floor PO Box
Office of the President
 Office of the President Dr. Belle Wheelan, President, Commission on Colleges Southern Association of Colleges and Schools 1866 Southern Lane, Decatur, GA 30033 December 13, 2010 In keeping with the Southern
Office of the President Dr. Belle Wheelan, President, Commission on Colleges Southern Association of Colleges and Schools 1866 Southern Lane, Decatur, GA 30033 December 13, 2010 In keeping with the Southern
NLNAC STANDARDS AND CRITERIA BACCALAUREATE DEGREE PROGRAMS
 NLNAC STANDARDS AND CRITERIA BACCALAUREATE DEGREE PROGRAMS I. Mission and Governance There are clear and publicly stated mission and/or philosophy and purposes appropriate to postsecondary or higher education
NLNAC STANDARDS AND CRITERIA BACCALAUREATE DEGREE PROGRAMS I. Mission and Governance There are clear and publicly stated mission and/or philosophy and purposes appropriate to postsecondary or higher education
15. Policy on Institutions Participating in Title IV Programs
 15. Policy on Institutions Participating in Title IV Programs This policy sets forth the Accrediting Commission s procedures for the institutions to seek to establish eligibility to participate in, Federal
15. Policy on Institutions Participating in Title IV Programs This policy sets forth the Accrediting Commission s procedures for the institutions to seek to establish eligibility to participate in, Federal
SENATE STAFF ANALYSIS AND ECONOMIC IMPACT STATEMENT
 SENATE STAFF ANALYSIS AND ECONOMIC IMPACT STATEMENT (This document is based on the provisions contained in the legislation as of the latest date listed below.) BILL: CS/SB 476 SPONSOR: SUBJECT: Health,
SENATE STAFF ANALYSIS AND ECONOMIC IMPACT STATEMENT (This document is based on the provisions contained in the legislation as of the latest date listed below.) BILL: CS/SB 476 SPONSOR: SUBJECT: Health,
Respiratory Care Program Information Packet
 Respiratory Care Program Information Packet www.collin.edu/rcp Table of Contents Page Number Page Number Minimum Prerequisites 2 Class Times and Costs 9 Admissions Requirements 2-3 PSB Information 10 Selective
Respiratory Care Program Information Packet www.collin.edu/rcp Table of Contents Page Number Page Number Minimum Prerequisites 2 Class Times and Costs 9 Admissions Requirements 2-3 PSB Information 10 Selective
This standard is 100% met for the baccalaureate program. This standard is 100% met for the master s program.
 STANDARD 6 - Outcomes Evaluation of student learning demonstrates that graduates have achieved identified competencies consistent with the institutional mission and professional standards and that the
STANDARD 6 - Outcomes Evaluation of student learning demonstrates that graduates have achieved identified competencies consistent with the institutional mission and professional standards and that the
it s all about Choices School of Health Related Professions Diagnostic Imaging Technologies
 D E P A R T M E N T O F D I A G N O S T I C I M A G I N G T E C H N O L O G Y it s all Choices about S H R P School of Health Related Professions Diagnostic Imaging Technologies D I A G N O S T I C M E
D E P A R T M E N T O F D I A G N O S T I C I M A G I N G T E C H N O L O G Y it s all Choices about S H R P School of Health Related Professions Diagnostic Imaging Technologies D I A G N O S T I C M E
El Camino College ADN Nursing Program
 El Camino College ADN Nursing Program Upward Mobility Program (LVN-RN and Transfer Applicants) FILING PERIOD: The El Camino College Nursing Program accepts applications twice a year beginning the third
El Camino College ADN Nursing Program Upward Mobility Program (LVN-RN and Transfer Applicants) FILING PERIOD: The El Camino College Nursing Program accepts applications twice a year beginning the third
Illinois Institute of Technology M.S. in Rehabilitation Counseling Program Annual Program Assessment Report (Covers from 8/1/2011 7/31/2012)
 Illinois Institute of Technology M.S. in Rehabilitation Counseling Program Annual Program Assessment Report (Covers from 8/1/2011 7/31/2012) The goal of the rehabilitation counseling master s program at
Illinois Institute of Technology M.S. in Rehabilitation Counseling Program Annual Program Assessment Report (Covers from 8/1/2011 7/31/2012) The goal of the rehabilitation counseling master s program at
Physician Assistant Studies
 Physician Assistant Studies Physician Assistant Phone: (540) 568-8171 Website: http://www.jmu.edu/heathsci/paweb Interim Academic Unit Head Dr. Paula Maxwell Graduate Program Director Mr. James Hammond,
Physician Assistant Studies Physician Assistant Phone: (540) 568-8171 Website: http://www.jmu.edu/heathsci/paweb Interim Academic Unit Head Dr. Paula Maxwell Graduate Program Director Mr. James Hammond,
RESPIRATORY THERAPIST CLASSIFICATION SERIES
 STATE OF WISCONSIN CLASSIFICATION SPECIFICATION RESPIRATORY THERAPIST CLASSIFICATION SERIES Effective Date: June 16, 1985 Modified Effective: November 5, 2000 Modified Effective: May 6, 2001 Modified Effective:
STATE OF WISCONSIN CLASSIFICATION SPECIFICATION RESPIRATORY THERAPIST CLASSIFICATION SERIES Effective Date: June 16, 1985 Modified Effective: November 5, 2000 Modified Effective: May 6, 2001 Modified Effective:
RESPIRATORY THERAPY PROGRAM ASSOCIATE in SCIENCE DEGREE
 Mt. San Antonio College Technology and Health Division RESPIRATORY THERAPY PROGRAM ASSOCIATE in SCIENCE DEGREE This Respiratory Therapy Program, which is accredited by the Committee on Accreditation for
Mt. San Antonio College Technology and Health Division RESPIRATORY THERAPY PROGRAM ASSOCIATE in SCIENCE DEGREE This Respiratory Therapy Program, which is accredited by the Committee on Accreditation for
SCHOOL OF NURSING Baccalaureate Study in Nursing Goals and Assessment of Student Learning Outcomes
 SCHOOL OF NURSING Baccalaureate Study in Nursing Goals and Assessment of Student Learning Outcomes The baccalaureate program prepares students for beginning professional nursing practice. The School of
SCHOOL OF NURSING Baccalaureate Study in Nursing Goals and Assessment of Student Learning Outcomes The baccalaureate program prepares students for beginning professional nursing practice. The School of
OCCUPATIONAL GROUP: Health Services. CLASS FAMILY: Allied Health CLASS FAMILY DESCRIPTION:
 OCCUPATIONAL GROUP: Health Services CLASS FAMILY: Allied Health CLASS FAMILY DESCRIPTION: This family of positions is comprised of health care practitioners with formal education and clinical training
OCCUPATIONAL GROUP: Health Services CLASS FAMILY: Allied Health CLASS FAMILY DESCRIPTION: This family of positions is comprised of health care practitioners with formal education and clinical training
Georgia Regents University M.Ed. Counselor Education Program
 Georgia Regents University M.Ed. Counselor Education Program Information for Prospective Students The Counselor Education Master of Education (M.Ed.) degree graduate program at Georgia Regents University
Georgia Regents University M.Ed. Counselor Education Program Information for Prospective Students The Counselor Education Master of Education (M.Ed.) degree graduate program at Georgia Regents University
Fulton County Medical Center Job Description
 Fulton County Medical Center Job Description POSITION TITLE: Staff Respiratory Therapy Technician REPORTS TO: Director of Cardiopulmonary Services REVISION DATE: July 28, 2010 I. POSITION SUMMARY: To provide
Fulton County Medical Center Job Description POSITION TITLE: Staff Respiratory Therapy Technician REPORTS TO: Director of Cardiopulmonary Services REVISION DATE: July 28, 2010 I. POSITION SUMMARY: To provide
Respiratory Therapy (A45720)
 Respiratory Therapy (A45720) Associate in Applied Science The Respiratory Therapy curriculum prepares individuals to function as respiratory therapists. In these roles, individuals perform diagnostic testing,
Respiratory Therapy (A45720) Associate in Applied Science The Respiratory Therapy curriculum prepares individuals to function as respiratory therapists. In these roles, individuals perform diagnostic testing,
Master of Science in Counseling Psychology
 Certificates Addictions Counseling Psychology Child and Family Counseling Psychology Providing training in professional psychology at the graduate level, the program is designed for those pursuing further
Certificates Addictions Counseling Psychology Child and Family Counseling Psychology Providing training in professional psychology at the graduate level, the program is designed for those pursuing further
SHAWNEE STATE UNIVERSITY RESPIRATORY THERAPY PROGRAM Application for Admission and Autobiography Form
 SHAWNEE STATE UNIVERSITY RESPIRATORY THERAPY PROGRAM Application for Admission and Autobiography Form Name Student ID Street City State Zip Phone: Day ( ) Evening ( ) Cell ( ) Email Address Applying to
SHAWNEE STATE UNIVERSITY RESPIRATORY THERAPY PROGRAM Application for Admission and Autobiography Form Name Student ID Street City State Zip Phone: Day ( ) Evening ( ) Cell ( ) Email Address Applying to
Accreditation Standards and Rules and Regulations for Mississippi Nursing Degree Programs
 Accreditation Standards and Rules and Regulations for Mississippi Nursing Degree Programs Revised July 1, 1992 Revised July 1, 1993 Amended April 1995 Amended June 1998 Amended July 1999 Revised November
Accreditation Standards and Rules and Regulations for Mississippi Nursing Degree Programs Revised July 1, 1992 Revised July 1, 1993 Amended April 1995 Amended June 1998 Amended July 1999 Revised November
Accreditation Council for Occupational Therapy Education (ACOTE ) Guide to Compliance with the 2006 Master s-level OT Standards
 Accreditation Council for Occupational Therapy Education (ACOTE ) Guide to Compliance with the 2006 Master s-level OT Standards PREAMBLE: The rapidly changing and dynamic nature of contemporary health
Accreditation Council for Occupational Therapy Education (ACOTE ) Guide to Compliance with the 2006 Master s-level OT Standards PREAMBLE: The rapidly changing and dynamic nature of contemporary health
American Academy of Forensic Sciences
 American Academy of Forensic Sciences Forensic Science Education Programs Accreditation Commission (FEPAC) ACCREDITATION STANDARDS Adopted by FEPAC May 16, 2003 Approved by the AAFS Board of Directors
American Academy of Forensic Sciences Forensic Science Education Programs Accreditation Commission (FEPAC) ACCREDITATION STANDARDS Adopted by FEPAC May 16, 2003 Approved by the AAFS Board of Directors
9. ACADEMIC QUALITY PLANNING PROCESS AND OUTCOME ASSESSMENT
 Page 1 of 32 STANDARDS AND CRITERIA FOR ACCREDITATION OF POSTSECONDARY CONSTRUCTION EDUCATION DEGREE PROGRAMS TABLE OF CONTENTS 1. INTRODUCTION 2. GOVERNANCE AND ADMINISTRATION 3. CURRICULUM 4. FACULTY
Page 1 of 32 STANDARDS AND CRITERIA FOR ACCREDITATION OF POSTSECONDARY CONSTRUCTION EDUCATION DEGREE PROGRAMS TABLE OF CONTENTS 1. INTRODUCTION 2. GOVERNANCE AND ADMINISTRATION 3. CURRICULUM 4. FACULTY
CHAPTER SIX STANDARDS FOR NURSING EDUCATION PROGRAMS
 Agency #067.00 CHAPTER SIX STANDARDS FOR NURSING EDUCATION PROGRAMS SECTION I APPROVAL OF PROGRAMS This chapter presents the Standards established by the Arkansas State Board of Nursing for nursing education
Agency #067.00 CHAPTER SIX STANDARDS FOR NURSING EDUCATION PROGRAMS SECTION I APPROVAL OF PROGRAMS This chapter presents the Standards established by the Arkansas State Board of Nursing for nursing education
Guidelines For Graduate Studies In Biology The Master of Science in Biology
 Guidelines For Graduate Studies In Biology The Master of Science in Biology Department of Biology Virginia Commonwealth University 1000 W. Cary St. Richmond, VA 23284-2012 Telephone: (804) 828-1562 Fax:
Guidelines For Graduate Studies In Biology The Master of Science in Biology Department of Biology Virginia Commonwealth University 1000 W. Cary St. Richmond, VA 23284-2012 Telephone: (804) 828-1562 Fax:
Application Dates: February 15 th to March 30 th
 Effective 3/12 to 3/13 Application Dates: February 15 th to March 30 th OHLONE COLLEGE (IN COOPERATION WITH DIABLO VALLEY COLLEGE, PLEASANT HILL) APPLICATION F ADMISSION TO THE RESPIRATY THERAPIST PROGRAM
Effective 3/12 to 3/13 Application Dates: February 15 th to March 30 th OHLONE COLLEGE (IN COOPERATION WITH DIABLO VALLEY COLLEGE, PLEASANT HILL) APPLICATION F ADMISSION TO THE RESPIRATY THERAPIST PROGRAM
September 7, 2006. Dr. Bettie Rose Horne, Chair, and Members, Committee on Academic Affairs and Licensing
 CAAL 9/7/06 Agenda Item 4b September 7, 2006 MEMORANDUM To: From: Dr. Bettie Rose Horne, Chair, and Members, Committee on Academic Affairs and Licensing Dr. R. Lynn Kelley, Acting Director of Academic
CAAL 9/7/06 Agenda Item 4b September 7, 2006 MEMORANDUM To: From: Dr. Bettie Rose Horne, Chair, and Members, Committee on Academic Affairs and Licensing Dr. R. Lynn Kelley, Acting Director of Academic
College of Health Sciences Department of Health Master of Public Health Program ***************** Council on Education for Public Health
 College of Health Sciences Department of Health Master of Public Health Program ***************** Council on Education for Public Health Accreditation Self-Study Report September, 2013 1 WEST CHESTER UNIVERSITY
College of Health Sciences Department of Health Master of Public Health Program ***************** Council on Education for Public Health Accreditation Self-Study Report September, 2013 1 WEST CHESTER UNIVERSITY
Augusta University Counselor Education Program. Information for Prospective Student (M.Ed.)
 Augusta University Counselor Education Program Information for Prospective Student (M.Ed.) The Counselor Education Master of Education (M.Ed.) degree graduate program at Augusta University prepares students
Augusta University Counselor Education Program Information for Prospective Student (M.Ed.) The Counselor Education Master of Education (M.Ed.) degree graduate program at Augusta University prepares students
2015 2016 Forensic Psychology Handbook
 University of Houston Victoria College of Arts & Sciences Competence Theory Justice 2015 2016 Forensic Psychology Handbook Knowledge Skill Welcome and Overview Welcome to the UHV Masters Program in Forensic
University of Houston Victoria College of Arts & Sciences Competence Theory Justice 2015 2016 Forensic Psychology Handbook Knowledge Skill Welcome and Overview Welcome to the UHV Masters Program in Forensic
Title 32: PROFESSIONS AND OCCUPATIONS
 Title 32: PROFESSIONS AND OCCUPATIONS Chapter 97: RESPIRATORY CARE PRACTITIONERS Table of Contents Section 9701. DECLARATION OF PURPOSE... 3 Section 9702. DEFINITIONS... 3 Section 9703. BOARD OF RESPIRATORY
Title 32: PROFESSIONS AND OCCUPATIONS Chapter 97: RESPIRATORY CARE PRACTITIONERS Table of Contents Section 9701. DECLARATION OF PURPOSE... 3 Section 9702. DEFINITIONS... 3 Section 9703. BOARD OF RESPIRATORY
Cerritos College Associate Degree Nursing Program
 Cerritos College Associate Degree Nursing Program The California Board of Registered Nursing 2010-2011 Annual School Report reflected that 61% of nursing programs in California are Associate Degree programs.
Cerritos College Associate Degree Nursing Program The California Board of Registered Nursing 2010-2011 Annual School Report reflected that 61% of nursing programs in California are Associate Degree programs.
Accreditation Standards for Nuclear Medicine Technologist Education
 Accreditation Standards for Nuclear Medicine Technologist Education DRAFT 2 FOR PUBLIC COMMENT Joint Review Committee on Educational Programs In Nuclear Medicine Technology??? A table of contents and introduction
Accreditation Standards for Nuclear Medicine Technologist Education DRAFT 2 FOR PUBLIC COMMENT Joint Review Committee on Educational Programs In Nuclear Medicine Technology??? A table of contents and introduction
it s all about Choices S H R P School of Health Related Professions Physician Assistant Program
 D E P A R T M E N T O F P R I M A R Y C A R E it s all Choices about S H R P School of Health Related Professions Physician Assistant Program P H Y S I C I A N A S S I S T A N T Choices Students who choose
D E P A R T M E N T O F P R I M A R Y C A R E it s all Choices about S H R P School of Health Related Professions Physician Assistant Program P H Y S I C I A N A S S I S T A N T Choices Students who choose
Master of Science in Counseling Psychology
 Emphasis Options Addictions Counseling Psychology Child and Family Counseling Psychology Providing training in professional psychology at the graduate level, the program is designed for those pursuing
Emphasis Options Addictions Counseling Psychology Child and Family Counseling Psychology Providing training in professional psychology at the graduate level, the program is designed for those pursuing
Appendix A Components for the Review of Institutions of Higher Education
 Appendix A Components for the Review of Institutions of Higher Education Appendix A: Components for the Review of Institutions of Higher Education The PI 34 requirements for program approval are organized
Appendix A Components for the Review of Institutions of Higher Education Appendix A: Components for the Review of Institutions of Higher Education The PI 34 requirements for program approval are organized
2014-15 Spring 2015. Master of Arts in counseling degree programs Handbook. And Certificates of Graduate Study
 2014-15 Spring 2015 Master of Arts in counseling degree programs Handbook And Certificates of Graduate Study School of Psychology & Counseling 1000 Regent University Drive Virginia Beach, VA 23464 regent.edu/acad/schcou
2014-15 Spring 2015 Master of Arts in counseling degree programs Handbook And Certificates of Graduate Study School of Psychology & Counseling 1000 Regent University Drive Virginia Beach, VA 23464 regent.edu/acad/schcou
2014-15 Revised September 2014
 2014-15 Revised September 2014 Master of Arts in Counseling Degree Program Handbook And Certificates of Graduate Study School of Psychology & Counseling 1000 Regent University Drive Virginia Beach, VA
2014-15 Revised September 2014 Master of Arts in Counseling Degree Program Handbook And Certificates of Graduate Study School of Psychology & Counseling 1000 Regent University Drive Virginia Beach, VA
Standards and Guidelines for the Accreditation of Educational Programs for the Medical Scribe Specialist
 Standards and Guidelines for the Accreditation of Educational Programs for the Medical Scribe Specialist Standards initially adopted in 201x Adopted by the The American College of Medical Scribe Specialists
Standards and Guidelines for the Accreditation of Educational Programs for the Medical Scribe Specialist Standards initially adopted in 201x Adopted by the The American College of Medical Scribe Specialists
Graduate Student HANDBOOK. Rehabilitation Counseling Program
 Graduate Student HANDBOOK Rehabilitation Counseling Program 2014-2015 Dear Rehabilitation Counseling Students, On behalf of the Rehabilitation Counseling faculty, staff, and second year students, I would
Graduate Student HANDBOOK Rehabilitation Counseling Program 2014-2015 Dear Rehabilitation Counseling Students, On behalf of the Rehabilitation Counseling faculty, staff, and second year students, I would
Itawamba Community College Program Review Career-Technical and Health Science Programs
 Itawamba Community College Program Review Career-Technical and Health Science Programs I. Program Information 1. Name of Program: Physical Therapist Assistant Program 2. Submission Date of Program Review:
Itawamba Community College Program Review Career-Technical and Health Science Programs I. Program Information 1. Name of Program: Physical Therapist Assistant Program 2. Submission Date of Program Review:
Coding Guidelines for Certain Respiratory Care Services July 2014
 Coding Guidelines for Certain Respiratory Care Services Overview From time to time the AARC receives inquiries about respiratory-related coding and coverage issues through its Help Line or Coding Listserv.
Coding Guidelines for Certain Respiratory Care Services Overview From time to time the AARC receives inquiries about respiratory-related coding and coverage issues through its Help Line or Coding Listserv.
Frequency of Assessment. Every three years and at any time of change of mission/philo sophy of the parent institution or the program.
 BSN PROGRAM CCNE Standard I: The mission, philosophy, and expected outcomes of the program are congruent with those of the parent institution, reflect professional nursing standards and guidelines, and
BSN PROGRAM CCNE Standard I: The mission, philosophy, and expected outcomes of the program are congruent with those of the parent institution, reflect professional nursing standards and guidelines, and
Policy and Procedure Manual 2015-2016
 2015-2016 The provisions in this manual are based on Hartnell College policies and services and are subject to change. Material cited does not constitute an irrevocable contract between any applicant or
2015-2016 The provisions in this manual are based on Hartnell College policies and services and are subject to change. Material cited does not constitute an irrevocable contract between any applicant or
