Short Communications. Isolated or Predominant Ocular Motor Nerve Palsy As a Manifestation of Brain Stem Stroke
|
|
|
- Winifred Evans
- 8 years ago
- Views:
Transcription
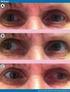
1 Short Communications 581 Isolated or Predominant Ocular Motor Nerve Palsy As a Manifestation of Brain Stem Stroke Jong S. Kim, MD; Joong K. Kang, MD; Sang A. Lee, MD; and Myoung C. Lee, MD Background and Purpose: There have been few reports of strokes producing isolated or predominant ocular motor nerve palsies as a clinical manifestation. Methods: We studied seven patients with brain stem stroke who had ocular motor palsies as the only or the predominant neurological manifestation, and we correlated their clinical features with radiological findings. Results: Five patients had small strokes in the area of oculomotor nuclei or fascicles and showed various combinations of oculomotor disturbances. Three of these patients showed vertical gaze paresis of the opposite eye. One patient with a small hemorrhage near the aqueduct of Sylvius showed fourth nerve palsy on the contralateral side, and a patient with a small infarct in the pontine tegmentum showed isolated sixth nerve palsy. Nonocular minor neurological signs included trigeminal sensory changes in four patients and clumsy arm in two. Ocular and nonocular dysfunctions generally improved within several months. Radiologicalfindingsof the brain stem correlated well with the ocular signs. Conclusions: We conclude that acute brain stem stroke should be included in the differential diagnosis of isolated ocular motor nerve palsies and that appropriate diagnostic investigations should be performed in these cases. (Stroke 1993;24: ) KEY WORDS brain stem cerebrovascular disorders oculomotor nerve A lthough stroke has not been recognized as an / \ important cause of isolated ocular motor nerve *- A. palsy in the previous review articles, 1 " 8 recent reports 910 suggest that intrinsic brain stem lesions including strokes may be an important cause of isolated ocular nerve palsy. Reports of strokes that produce isolated oculomotor palsy without significant nonocular signs have been rare. Biller et al 11 described a patient with brain stem infarction identified by computed tomographic (CT) scan who showed bilateral oculomotor paresis and transient Babinski signs. More recently, a series of reports described patients with midbrain hemorrhage 1213 or infarction who exhibited oculomotor palsy as a predominant neurological manifestation. Reports of isolated fourth or sixth nerve palsy secondary to stroke are also rare. A few patients were described in whom midbrain infarct 18 or hemorrhage 19 " 21 caused fourth nerve palsy, and three recent reports 22 " 24 described pontine lacunes that produced isolated sixth nerve palsy. However, aside from these sporadic case reports there have been no studies in which a sufficient number of cases were described with detailed clinicalradiological correlation. From the Department of Neurology, University of Ulsan, Asan Medical Center, Seoul, Korea. Presented in part at the 44th Annual Meeting of the American Academy of Neurology, San Diego, Calif., May Address for correspondence: Jong S. Kim, MD, Department of Neurology, Henry Ford Hospital, 2799 West Grand Boulevard, Detroit, MI Received September 8, 1992;finalrevision received December 24, 1992; accepted January 11, Subjects and Methods We studied seven patients with acute brain stem stroke with ocular motor nerve palsy as the sole or a predominant neurological sign and correlated their clinical features with radiological findings. One patient was evaluated by CT (GE/9800) scan and six by magnetic resonance imaging (MRI) with a 1.5-T superconducting unit (GE). Axial T2- (repetition time [TR], 2,500 msec; echo time [TE], 80 msec) and Tl- (TR, 600 msec; TE, 20 msec) weighted and sagittal Tl-weighted scans were generated with a slice thickness of 5 mm. Angiography was performed in two patients. Case Reports Third nerve palsy. Patient 1, a 60-year-old hypertensive male smoker, developed sudden dizziness and diplopia. Examination showed right oculomotor nerve palsy without definite ptosis or pupillary changes. In primary position, his right eye deviated outward and downward; in the opposite eye, upward and downward gaze pareses were noted. In addition, he exhibited a clumsy left hand and dysesthesia on pinprick and touch on the left side of his face and left hand. Results of routine laboratory tests were normal. Brain MRI showed a small infarct in the right midbrain (Figure 1). The patient's oculomotor function normalized 6 months after onset. Patient 2, a 58-year-old hypertensive woman, became drowsy and complained of diplopia and numbness in the right upper peribuccal area. Examination showed left oculomotor nerve palsy, with bilateral ptosis worse in her left eye. Attempted adduction of the left eye was accompanied by transient abducting nystagmus of the
2 582 Stroke Vol 24, No 4 April 1993 FIGURE 1. Patient 1. T2-weighted magnetic resonance image shows an infarct (arrows) in the right midbrain probably involving the oculomotor fascicles, rostral interstitial nucleus of the medial longitudinal fasciculus, trigeminal lemniscus, and a portion of the medial lemniscus. right eye. The pupil size was bigger in the left eye (6 mm) than the right (3 mm), and the light reflex was sluggish in the left. There was upward gaze limitation of the right eye, although it was in the neutral position on straight gaze. Neurological examination showed dysesthesia in the right upper peribuccal area and a mildly weak and ataxic right arm. On gait, she tended to veer to the right. Brain MRI showed a small infarct in the left midbrain (Figure 2). Her right-arm weakness resolved within 2 days, and oculomotor abnormalities were normalized 5 months after onset. Patient 3, a 53-year-old man with a history of angina and hyperlipidemia, had sudden diplopia and painful left facial numbness. Examination showed right-sided oculomotor nerve palsy with ptosis. His right eye was mildly deviated downward and outward on primary gaze. Pupils were equal and reactive on both sides. Ocular movements of his left eye were normal. Sensory examination revealed facial hyperalgia in the left VI and V2 areas. Brain MRI showed ischemic changes in the right midbrain (Figure 3). Three months later, the patient's ocular motor function was fully recovered. Patient 4, a hypertensive 38-year-old man with a history of congestive heart failure, developed sudden headache and diplopia. Examination showed left-sided complete oculomotor nerve palsy, including ptosis, and dilated, fixed pupil. On primary gaze, his left eye deviated outward and downward; in addition, upward gaze limitation was noted in his right eye. Brain CT scan showed a small hemorrhage in the left midbrain (Figure 4). An angiogram showed normal findings. During 7 FIGURE 2. Patient 2. T2-weighted magnetic resonance image shows an infarct (arrows) in the left paramedian midbrain probably involving the oculomotor nucleus, rostral interstitial nucleus of the medial longitudinal fasciculus, and trigeminal lemniscus. days of admission, there was a slight improvement in his oculomotor function. After discharge, however, he was lost to follow-up. FIGURE 3. Patient 3. T2-weighted magnetic resonance image shows scattered infarcts (arrows) in the right midbrain probably involving the oculomotor fascicles and trigeminal lemniscus.
3 Kim et al Ocular Nerve Palsy and Brain Stem Stroke 583 FIGURE 4. Patient 4. Computed tomographic scan shows a hemorrhage in the left paramedian midbrain probably involving the oculomotor fascicles (arrows, left panel). Note the extension of the hemorrhage in the most rostral midbrain that may involve the pupillary fibers (arrows, right panel). Patient 5, a previously healthy 42-year-old woman, developed sudden dizziness and diplopia on downward gaze. Examination showed isolated inferior rectus paresis of her right eye, with a mild hypertropia of the right eye in primary gaze. Pupils were equal, and ptosis was absent in both eyes. Results of laboratory tests were normal except for positive lupus anticoagulant. Brain MRI showed a small infarct in the right midbrain (Figure 5). Two months later her ocular motor function had improved, but she still had diplopia on looking downward. Fourth nerve palsy. Patient 6 (previously described 25 ), a 38-year-old man, developed a dull headache and dizziness associated with diplopia on looking downward. He also experienced a tingling sensation in his right cheek. Three weeks later, when he came to Asan Medical Center, examination showed isolated right superior oblique palsy: limitation of his right eye in the left downward direction and 10 prism diopters of right hypertropia with his head tilted to the right. Pupil sizes and light reflexes were normal in both eyes. In addition there was decreased facial sensation over the right V2 and V3 areas. Tl- and T2-weighted MRI showed a linear low-intensity signal in the left midbrain (Figure 6). An angiogram showed normal findings. One month later his facial paresthesia improved, and ocular movements were completely recovered 4 months later. Sixth nerve palsy. Patient 7, a hypertensive 76-year-old man, developed dizziness and diplopia. He exhibited a right lateral rectus paresis with a slight esotropia of the right eye on straight gaze. Otherwise, his neurological examination was normal. Brain MRI revealed a small infarct in the right pontine tegmentum (Figure 7). His oculomotor dysfunction fully improved 3 months later. Results In this series, we studied seven patients (five men and two women, [mean, 52] years of age). Five had small infarcts, and two had hemorrhages. The risk FIGURE 5. Patient 5. Magnetic resonance image shows a small infarct (arrows) in the left paramedian rostral midbrain that may selectively involve the subnucleus of the inferior rectus.
4 584 Stroke Vol 24, No 4 April 1993 Pupillary changes were observed in two patients. Four patients had weakness of all muscles innervated by the oculomotor nerve, whereas one showed a selective paresis of the inferior rectus. Three patients showed vertical gaze palsy on the opposite eye (upward gaze palsy in two and upward and downward gaze palsy in one). One patient had trochlear nerve palsy, and one showed isolated lateral rectus palsy. In all patients, diplopia secondary to ocular paresis was the only symptom or the major symptom. Minor nonocular neurological manifestations included facial numbness in four (with additional sensory change in the hand of one patient) and ataxic and clumsy arm in two. One patient was drowsy initially. In all, ocular motor dysfunctions improved within 6 months, although one patient was not adequately followed up. Radiological evaluation showed lesions in the brain stem (midbrain in six and pontine tegmentum in one) that correlated well with clinical manifestations (see "Discussion"). FIGURE 6. Patient 6. Tl-weighted magnetic resonance image shows an area of low signal intensity near the aqueduct (arrow) probably involving the trochlear nerve fascicles and trigeminal lemniscus. factors for stroke included hypertension in four, smoking in one, hyperlipidemia in one, and coronary heart disease in one. One patient showed a positive result for lupus anticoagulant. One young man (patient 6) suffered small hemorrhage probably due to vascular malformation. Five patients showed third nerve palsies; ptosis was noted in three, one of them bilaterally. FIGURE 7. Patient 7. T2-weighted magnetic resonance image shows a small infarct (arrow) in the right pontine tegmentum probably involving the abducens nerve fascicles. Discussion MRI findings in our patients suggest that patients 2 and 5 had lesions in the third nerve nucleus complex; therefore, the bilateral ptosis of patient 2 was probably due to the involvement of the central caudal nucleus, which is known to bilaterally innervate the levator palpebrae. There have been occasional reports of a single nuclear lesion causing bilateral ptosis, 16 ' 2627 and Conway et al 28 reported an unusual patient with isolated bilateral complete ptosis secondary to lesions confined to the central caudal nuclear complex. It is of interest that patient 5 had isolated inferior rectus paresis. Although rare, there have been reports of isolated inferior rectus paresis due to intra-axial brain stem lesions It is not clear whether the responsible lesion in these cases is in the fascicles or nucleus. Recently, Pusateri et al 32 described a patient with isolated inferior rectus paresis in whom MRI findings correlated with the autopsy findings of metastasis on the third nerve nucleus. According to Warwick's scheme, 33 the inferior rectus subnucleus is isolated from other subnuclei at the most rostral part of the oculomotor complex. Therefore, selective involvement of this area may cause the isolated inferior rectus paresis. 30 ' 32 Clinical and MRI findings of patients 1, 3, and 4 suggest lesions are in the oculomotor nerve fascicles. Fascicular lesions were reported to cause various combinations of signs such as isolated inferior oblique paresis, 34 isolated pupillary changes, 35 or divisional nerve paresis that suggests intra-axial divisional differentiation. 36 ' 37 However, Castro et al 34 suggested topographical arrangement of the fibers from lateral to medial as follows: inferior oblique, superior rectus, medial rectus, levator palpebrae, inferior rectus, and pupillary fibers. Our patients with fascicular lesion showed diffuse involvement of the fibers, which did not support any particular topographical arrrangement. However, the spared pupillary dysfunction in two cases (patients 1 and 3) deserves mention. Fascicular lesions sparing the pupil have been described by a number of authors, ' whereas patients described by othersi3,i4,i7,35 showed pupillary involvement; the patients described by Keane 1 3 and one (case 2) reported by Shuaib and Murphy 12 had paramedian midbrain hem-
5 Kim et al Ocular Nerve Palsy and Brain Stem Stroke 585 orrhage extending rostrally to the hypothalamus. Shuaib et al 35 described an unusual patient with isolated pupillary deficit who had a small hemorrhage in the paramedian, rostral midbrain. In our series, patient 4 (the only one with a fascicular lesion who showed pupillary involvement) had a hemorrhage extending into the most central-rostral portion of the midbrain (Figure 4, right panel), whereas patients 1 and 3 showed lesions situated more caudally. Therefore, within widespread fascicles, the pupillary fibers seem to run in the most rostral and central portion. It is noteworthy that three patients with third nerve palsy showed vertical gaze palsy in the opposite eye. Vertical saccade for both upward and downward gaze has been known to be related to the cell groups of the rostral interstitial nucleus of medial longitudinal fasciculus (RiMLF), 41 which is located in the anterosuperior portion of the oculomotor complex. It has recently been documented that a unilateral lesion of RiMLF can result in bilateral vertical gaze paresis Our patients 1,2, and 4 probably had lesions involving the RiMLF. In patient 2, the possibility of contralateral superior rectus paresis secondary to nuclear involvement cannot be ruled out. However, the patient's contralateral eye was not hypotropic on straight gaze, and there was a limitation of the eye movements in the inferior oblique direction, both of which support a diagnosis of supranuclear upward gaze defect. Patients with nuclear lesions with 17 or without 16 involvement of the contralateral superior rectus have been reported, and Bogousslavsky et al 27 described a patient with midbrain infarction that caused contralateral superior rectus paresis, probably due to the involvement of the prenuclear fibers. There have been only a few reports in which fourth nerve palsy was an isolated or predominant manifestation of stroke Patient 6 showed isolated trochlear nerve palsy and trigeminal sensory change in the contralateral side of the lesion, probably due to involvement of the trochlear fascicles and ascending trigeminothalamic fibers. Including patient 6, four of our patients showed trigeminal sensory changes, sometimes in the restricted area of the face. This can be explained by the close association of the trigeminothalamic second-order neurons with the oculomotor or trochlear nucleus in the human brain stem The patients described by Growdon et al 26 and Breen et al 15 also showed facial sensory changes on the side contralateral to the lesion. Therefore, careful examination of facial sensation may help localize the lesion in patients with ocular motor nerve palsy. Patient 1 had additional numbness in the hand, thus demonstrating a cheiro-oral sensory syndrome. Midbrain lesion as a cause of cheirooral syndrome has been previously described. 48 To our knowledge, there have been three reports that described small pontine infarcts as a cause of isolated sixth nerve palsy MRI of our patient 7 revealed a tiny pontine infarct impinging on the abducens fascicles but probably sparing the corticospinal tracts and the medial lemniscus. Our patient and previously reported cases did not show any signs or symptoms of brain stem dysfunction, and their sixth nerve palsies improved completely within several months. Therefore, it seems impossible to distinguish a central from a peripheral cause of sixth nerve palsy in these cases. It is suggested that pontine infarcts be considered as a possible cause of isolated sixth nerve palsy in elderly patients with hypertension or diabetes mellitus. However, it remains to be determined whether every patient should be evaluated by MRI. In conclusion, clinical findings in our patients suggest that brain stem stroke can manifest itself with isolated or predominant ocular motor nerve palsy, which is sometimes indistinguishable from peripheral nerve lesions (patients 3, 4, and 7). As with peripheral lesions, the prognosis for these patients is generally good, and ocular motor dysfunction tends to improve or resolve within several months. Subtle signs and symptoms such as trigeminal sensory change, vertical paresis of the contralateral eye, clumsy hands, or transient drowsiness may help localize the brain stem lesion and warrant MRI evaluation, which usually correlates well with ocular and nonocular signs in these patients. References 1. Rucker CW: Paralysis of third, fourth and sixth cranial nerves. Am J Ophthalmol 1958;46: Green WR, Hackett ER, Schlezinger NS: Neuro-ophthalmologic evaluation of oculomotor nerve paralysis. Arch Ophthalmol 1964; 72: Rucker CW: The causes of paralysis of the third, fourth and sixth cranial nerves. Am J Ophthalmol 1966;61: Keane JR: Bilateral sixth nerve palsy: Analysis of 125 cases. Arch Neurol 1976;33: Younge BR, Sutula F: Analysis of trochlear nerve palsies: Diagnosis, etiology, and treatment. Mayo Clin Proc 1977;52: Rush JA, Younge BR: Paralysis of cranial nerves III, IV, and VI: Cause and prognosis in 1000 cases,. Arch Ophthalmol 1981;99: Mansour AM, Reinecke RD: Central trochlear palsy. Surv Ophthalmol 1986;30: Ksiazek S, Behar R, Sasvino P, Sergott R, Bosley TM: Isolated acquired fourth nerve palsies, (abstract) Neurology 1988;38 (suppl 1): Hopf HC, Gutmann L: Diabetic 3rd nerve palsy: Evidence for a mesencephalic lesion. Neurology 1990;40: Brazis PW: Localization of lesions of the oculomotor nerve: Recent concepts. Mayo Clin Proc 1991;66: Biller J, Shapiro R, Evans LS, Haag JR, Fine M: Oculomotor nuclear complex infarction: Clinical and radiological correlation. Arch Neurol 1984;41: Shuaib A, Murphy W: Mesencephalic hemorrhage and third nerve palsy. / Comput Tomogr 1987;11: Keane JR: Isolated brain-stem third nerve palsy. Arch Neurol 1988; 45: Ferbert A, Mullges W, Biniek R: Fascicular third nerve palsy with decreased vertical saccade velocity of the contralateral eye. Neuro- Ophthalmology 1990;10: Breen LA, Hopf HC, Farris BK, Gutmann L: Pupil-sparing oculomotor nerve palsy due to midbrain infarction. Arch Neurol 1991; 48: Liu GT, Carrazana EJ, Charness ME: Unilateral oculomotor palsy and bilateral ptosis from paramedian midbrain infarction. Arch Neurol 1991;48: Yasuda Y, Akiguchi I, Kameyama M: Crossed innervation of the superior rectus. Clin Neurol Neurosurg 1991;93: Cobbs WH, Schatz NJ, Savino PJ: Nontraumatic bilateral fourth nerve palsies: A dorsal midbrain sign, (abstract) Ann Neurol 1980; 8: Sand JJ, Biller J, Corbett JJ, Adams HP Jr, Dunn V: Partial dorsal mesencephalic hemorrhages: Report of three cases. Neurology 1986;36: Kamei T, Uchiyama F, Hukuyama J: Primary tectal mesencephalic hemorrhage with isolated trochlear nerve palsy: A case report. Clin Neurol 1987;27: Tachibana H, Mimura O, Shioma M, Oono T: Bilateral trochlear nerve palsies from a brainstem hematoma. J Clin Neuro Ophthalmol 1990;10: Donaldson D, Rosenberg N: Infarction of abducens nerve fascicle as cause of isolated sixth nerve palsy related to hypertension. Neurology 1988;38:1654
6 586 Stroke Vol 24, No 4 April Johnson LN, Hepler RS: Isolated abducens nerve paresis from intrapontine fascicular abducens nerve injury. Am J Ophthalmol 1989;108: Fukutake T, Hirayama K: Isolated abducens nerve palsy from pontine infarction in a diabetic patient. Neurology 1992;42: Kim JS, Kang JK: Contralateral trochlear palsy and facial sensory change due to a probable brain stem vascular malformation. Neuro- Ophthalmology 1992;12: Growdon JH, Winkler GF, Wray SH: Midbrain ptosis: A case with clinicopathologic correlation. Arch Neurol 1974;30: Bogousslavsky J, Regli F, Ghika J, Hungerbuhler JP: Internuclear ophthalmoplegia, prenuclear paresis of contralateral superior rectus, and bilateral ptosis. / Neurol 1983;230: Conway VH, Rozdilsky B, Schneider RJ, Sundaram M: Isolated bilateral complete ptosis. Can J Ophthalmol 1983;18: Roper-Hall G, Burde RM: Inferior rectus palsies as a manifestation of atypical IHrd cranial nerve disease. Am OrthoptJ 1975;25: Warren W, Burde RM, Klingele TG, Roper-Hall G: Atypical oculomotor paresis. / Clin Neuro Ophthalmol 1982;2: Eustace P: Partial nuclear third nerve palsies. Neuro-Ophthalmology 1985;5: Pusateri TJ, Sedwick LA, Margo CE: Isolated inferior rectus muscle palsy from a solitary metastasis to the oculomotor nucleus. Arch Ophthalmol 1987;105: Warwick R: Representation of the extra-ocular muscles in the oculomotor nuclei of the monkey. / Comp Neurol 1953;98: Castro O, Johnson LN, Mamourian AC: Isolated inferior oblique paresis from brain-stem infarction: Perspective on oculomotor fascicular organization in the ventral midbrain tegmentum. Arch Neurol 1990;47: Shuaib A, Israelian G, Lee MA: Mesencephalic hemorrhage and unilateral pupillary deficit. / Clin Neuro Ophthalmol 1989;9: Ksiazek SM, Repka MX, Maguire A, Harbour RC, Savino PJ, Miller NR, Sergott RC, Bosley TM: Divisional oculomotor nerve paresis caused by intrinsic brainstem disease. Ann Neurol 1989;26: Abdollah A, Francis GS: Demyelinating disease presenting as a partial oculomotor nerve paresis. Can J Neurol Sci 1989;16: Wilkins DE, Samhouri AM: Isolated bilateral oculomotor paresis due to lymphoma. Neurology 1979;29: Nadeau SE, Trobe JD: Pupil sparing in oculomotor palsy: A brief review. Ann Neurol 1983;13: Newman N, Lessell S: Isolated pupil-sparing third nerve palsy as the presenting sign of multiple sclerosis. Arch Neurol 1990;47: Buttner-Ennever JA, Buttner U, Cohen B, Baumgartner G: Vertical gaze paralysis and the rostral interstitial nucleus of the medial longitudinal fasciculus. Brain 1982;105: Ranalli PJ, Sharpe JA, Fletcher WA: Palsy of upward and downward saccadic, pursuit, and vestibular movements with a unilateral midbrain lesion: Pathophysiologic correlations. Neurology 1988;38: Bogousslavsky J, Miklosssy, Regli F, Janzer R: Vertical gaze palsy and selective unilateral infarction of the rostral interstitial nucleus of the medial longitudinal fasciculus (rimlf). / Neurol Neurosurg Psychiatry 1990;53: Hommel M, Bogousslavsky J: The spectrum of vertical gaze palsy following unilateral brainstem stroke. Neurology 1991;41: Leigh RJ, Zee DS: The Neurology of Eye Movements, ed 2. Philadelphia, Pa, FA Davis Co, 1991, pp Carpenter MB, Sutin J: Human Neuroanatomy, ed 8. Baltimore, Md, Williams & Wilkins, 1983, pp Bradley WG Jr: MR of the brain stem: A practical approach. Radiology 1991;179: Ono S, Inoue K: Cheiro-oral syndrome following midbrain hemorrhage. / Neurol 1985;232:
Pseudoabducens palsy: When a VI nerve palsy is not a VI nerve palsy
 Pseudoabducens palsy: When a VI nerve palsy is not a VI nerve palsy Emily S. Birkholz, MD, and Michael Wall, MD December 30, 2009 CC: 44 year old male with diplopia HPI: This 44 year old man with a history
Pseudoabducens palsy: When a VI nerve palsy is not a VI nerve palsy Emily S. Birkholz, MD, and Michael Wall, MD December 30, 2009 CC: 44 year old male with diplopia HPI: This 44 year old man with a history
Primary Motor Pathway
 Understanding Eye Movements Abdullah Moh. El-Menaisy, MD, FRCS Chief, Neuro-ophthalmology ophthalmology & Investigation Units, Dhahran Eye Specialist Hospital, Dhahran, Saudi Arabia Primary Motor Pathway
Understanding Eye Movements Abdullah Moh. El-Menaisy, MD, FRCS Chief, Neuro-ophthalmology ophthalmology & Investigation Units, Dhahran Eye Specialist Hospital, Dhahran, Saudi Arabia Primary Motor Pathway
Original Article. A 3 Year Review of Cranial Nerve Palsies from the University of Port Harcourt Teaching Hospital Eye Clinic, Nigeria
 Original Article A 3 Year Review of Cranial Nerve Palsies from the University of Port Harcourt Teaching Hospital Eye Clinic, Nigeria Chinyere Nnenne Pedro Egbe, Bassey Fiebai, Elizabeth Akon Awoyesuku
Original Article A 3 Year Review of Cranial Nerve Palsies from the University of Port Harcourt Teaching Hospital Eye Clinic, Nigeria Chinyere Nnenne Pedro Egbe, Bassey Fiebai, Elizabeth Akon Awoyesuku
Management Approach to Isolated Ocular Motor Nerve Palsies
 Management Approach to Isolated Ocular Motor Nerve Palsies Alfredo A. Sadun, MD, PhD Thornton Professor of Vision Doheny Eye Institute Departments of Ophthalmology and Neurosurgery Keck/USC School of Medicine
Management Approach to Isolated Ocular Motor Nerve Palsies Alfredo A. Sadun, MD, PhD Thornton Professor of Vision Doheny Eye Institute Departments of Ophthalmology and Neurosurgery Keck/USC School of Medicine
Common visual symptoms and findings in MS: Clues and Identification
 Common visual symptoms and findings in MS: Clues and Identification Teresa C Frohman, PA-C, MSCS Neuro-ophthalmology Research Manager, UT Southwestern Medical Center at Dallas Professor Biomedical Engineering,
Common visual symptoms and findings in MS: Clues and Identification Teresa C Frohman, PA-C, MSCS Neuro-ophthalmology Research Manager, UT Southwestern Medical Center at Dallas Professor Biomedical Engineering,
Fourth Nerve Palsy (a.k.a. Superior Oblique Palsy)
 Hypertropia Hypertropia is a type of strabismus characterized by vertical misalignment of the eyes. Among the many causes of vertical strabismus, one of the most common is a fourth nerve palsy (also known
Hypertropia Hypertropia is a type of strabismus characterized by vertical misalignment of the eyes. Among the many causes of vertical strabismus, one of the most common is a fourth nerve palsy (also known
Eye movement problems in adults
 Eye movement problems in adults 07/12/2015 A. Dahlmann-Noor Dr med PhD FRCOphth FRCS(Ed) DipMedEd Consultant Ophthalmologist Clinical Trials Lead Paediatric Ophthalmology Horizontal misalignment (Cyclo)vertical
Eye movement problems in adults 07/12/2015 A. Dahlmann-Noor Dr med PhD FRCOphth FRCS(Ed) DipMedEd Consultant Ophthalmologist Clinical Trials Lead Paediatric Ophthalmology Horizontal misalignment (Cyclo)vertical
207-2. Selective Saccadic Palsy
 207-2 Selective Saccadic Palsy Selective Saccadic Palsy after Cardiac Surgery Selective loss of all forms of saccades (voluntary and reflexive quick phases of nystagmus) with sparing of other eye movements.
207-2 Selective Saccadic Palsy Selective Saccadic Palsy after Cardiac Surgery Selective loss of all forms of saccades (voluntary and reflexive quick phases of nystagmus) with sparing of other eye movements.
Internuclear ophthalmoplegia: recovery and plasticity
 Internuclear ophthalmoplegia: recovery and plasticity M. J. Doslak, L. B. Kline, L. F. Dell'Osso, and R. B. Daroff We studied refixational eye movements of a patient during the gradual resolution of an
Internuclear ophthalmoplegia: recovery and plasticity M. J. Doslak, L. B. Kline, L. F. Dell'Osso, and R. B. Daroff We studied refixational eye movements of a patient during the gradual resolution of an
Cranial Nerves. Cranial Nerve 1: Olfactory Nerve. Cranial Nerve 1: Olfactory Nerve. Cranial Nerve 2: Optic Nerve. Cranial Nerve 2: Optic Nerve
 Cranial Nerves Examination of Cranial Nerves and Palsies Drs Nathan Kerr and Shenton Chew 1 Olfactory On 2 Optic Old 3 Oculomotor Olympus 4 Trochlear Towering 5 Trigeminal Top 6 Abducens A 7 Facial Finn
Cranial Nerves Examination of Cranial Nerves and Palsies Drs Nathan Kerr and Shenton Chew 1 Olfactory On 2 Optic Old 3 Oculomotor Olympus 4 Trochlear Towering 5 Trigeminal Top 6 Abducens A 7 Facial Finn
How to test ocular movements in PSP Jan Kassubek
 How to test ocular movements in PSP Jan Kassubek Universitätsklinik für Neurologie, Ulm Bedside Screening: PSP initially slowing of vertical saccades slowing of downward saccades is considered the hallmark
How to test ocular movements in PSP Jan Kassubek Universitätsklinik für Neurologie, Ulm Bedside Screening: PSP initially slowing of vertical saccades slowing of downward saccades is considered the hallmark
Doctor, I See Double : Managing Cranial Nerve Palsies
 1 Doctor, I See Double : Managing Cranial Nerve Palsies Joseph W. Sowka, OD, FAAO, Diplomate Professor of Optometry Nova Southeastern University, College of Optometry 3200 South University Drive Fort Lauderdale,
1 Doctor, I See Double : Managing Cranial Nerve Palsies Joseph W. Sowka, OD, FAAO, Diplomate Professor of Optometry Nova Southeastern University, College of Optometry 3200 South University Drive Fort Lauderdale,
Outcome of Surgery for Bilateral Third Nerve Palsy
 CLINICAL INVESTIGATIONS Outcome of Surgery for Bilateral Third Nerve Palsy Kazuhiro Aoki, Tatsushi Sakaue, Nobue Kubota and Toshio Maruo Department of Ophthalmology, Teikyo University School of Medicine,
CLINICAL INVESTIGATIONS Outcome of Surgery for Bilateral Third Nerve Palsy Kazuhiro Aoki, Tatsushi Sakaue, Nobue Kubota and Toshio Maruo Department of Ophthalmology, Teikyo University School of Medicine,
STROKE PREVENTION AND TREATMENT MARK FISHER, MD PROFESSOR OF NEUROLOGY UC IRVINE
 STROKE PREVENTION AND TREATMENT MARK FISHER, MD PROFESSOR OF NEUROLOGY UC IRVINE CASE REPORT: ACUTE STROKE MANAGEMENT 90 YEAR OLD WOMAN, PREVIOUSLY ACTIVE AND INDEPENDENT, CHRONIC ATRIAL FIBRILLATION,
STROKE PREVENTION AND TREATMENT MARK FISHER, MD PROFESSOR OF NEUROLOGY UC IRVINE CASE REPORT: ACUTE STROKE MANAGEMENT 90 YEAR OLD WOMAN, PREVIOUSLY ACTIVE AND INDEPENDENT, CHRONIC ATRIAL FIBRILLATION,
How To Diagnose Stroke In Acute Vestibular Syndrome
 Danica Dummer, PT, DPT, University of Utah Abigail Reid, PT, DPT, Kessler Institute for Rehabilitation Online Journal Club-Article Review Article Citation Study Objective/Purpose (hypothesis) Study Design
Danica Dummer, PT, DPT, University of Utah Abigail Reid, PT, DPT, Kessler Institute for Rehabilitation Online Journal Club-Article Review Article Citation Study Objective/Purpose (hypothesis) Study Design
Ocular motor nerve palsies: implications for diagnosis and mechanisms of repair
 C. Kennard & R.J. Leigh (Eds.) Progress in Brain Research, Vol. 171 ISSN 0079-6123 Copyright r 2008 Elsevier B.V. All rights reserved CHAPTER 1.9 Ocular motor nerve palsies: implications for diagnosis
C. Kennard & R.J. Leigh (Eds.) Progress in Brain Research, Vol. 171 ISSN 0079-6123 Copyright r 2008 Elsevier B.V. All rights reserved CHAPTER 1.9 Ocular motor nerve palsies: implications for diagnosis
DIAGNOSTIC CRITERIA OF STROKE
 DIAGNOSTIC CRITERIA OF STROKE Diagnostic criteria are used to validate clinical diagnoses. Here below MONICA diagnostic criteria are reported. MONICA - MONItoring trends and determinants of CArdiovascular
DIAGNOSTIC CRITERIA OF STROKE Diagnostic criteria are used to validate clinical diagnoses. Here below MONICA diagnostic criteria are reported. MONICA - MONItoring trends and determinants of CArdiovascular
The Many Faces of MS
 The Many Faces of MS Patricia A. Modica, OD, FAAO SUNY College of Optometry Kelly Malloy, OD, FAAO Pennsylvania College of Optometry at Salus University Multiple Sclerosis (MS) Most common acquired disease
The Many Faces of MS Patricia A. Modica, OD, FAAO SUNY College of Optometry Kelly Malloy, OD, FAAO Pennsylvania College of Optometry at Salus University Multiple Sclerosis (MS) Most common acquired disease
Management of sixth nerve palsy different approaches
 100 Prună et al Management of sixth nerve palsy Management of sixth nerve palsy different approaches Violeta-Ioana Prună 1,4, Ligia Gabriela Tătăranu 3, V.M. Prună 2, Daniela Cioplean 4, R.M. Gorgan 3
100 Prună et al Management of sixth nerve palsy Management of sixth nerve palsy different approaches Violeta-Ioana Prună 1,4, Ligia Gabriela Tătăranu 3, V.M. Prună 2, Daniela Cioplean 4, R.M. Gorgan 3
Basic Cranial Nerve Examination
 Basic Cranial Nerve Examination WIPE Wash hands Introduce yourself Permission Position (Patient sitting facing you, maintain comparable eye level) Exposure (Face exposed only, i.e. remove hats etc) Identify
Basic Cranial Nerve Examination WIPE Wash hands Introduce yourself Permission Position (Patient sitting facing you, maintain comparable eye level) Exposure (Face exposed only, i.e. remove hats etc) Identify
NEUROLOCALIZATION MADE EASY
 NEUROLOCALIZATION MADE EASY Jared B. Galle, DVM, Diplomate ACVIM (Neurology) Dogwood Veterinary Referral Center 4920 Ann Arbor-Saline Road Ann Arbor, MI 48103 Localizing a neurologic problem to an anatomical
NEUROLOCALIZATION MADE EASY Jared B. Galle, DVM, Diplomate ACVIM (Neurology) Dogwood Veterinary Referral Center 4920 Ann Arbor-Saline Road Ann Arbor, MI 48103 Localizing a neurologic problem to an anatomical
Paralytic Strabismus: Third, Fourth, and Sixth Nerve Palsy
 Paralytic Strabismus: Third, Fourth, and Sixth Nerve Palsy Sashank Prasad, MD a, *, Nicholas J. Volpe, MD b KEYWORDS Paralytic strabismus Nerve palsy Ocular motor nerves Eye movement abnormalities ANATOMY
Paralytic Strabismus: Third, Fourth, and Sixth Nerve Palsy Sashank Prasad, MD a, *, Nicholas J. Volpe, MD b KEYWORDS Paralytic strabismus Nerve palsy Ocular motor nerves Eye movement abnormalities ANATOMY
Paediatric Bell s Palsy Paediatric Update November 2014
 Paediatric Bell s Palsy Paediatric Update November 2014 Richard Webster, Paediatric Neurologist Children s Hospital at Westmead Typical history Unilateral LMN facial weakness Acute onset over a day or
Paediatric Bell s Palsy Paediatric Update November 2014 Richard Webster, Paediatric Neurologist Children s Hospital at Westmead Typical history Unilateral LMN facial weakness Acute onset over a day or
Surgical Outcome Of Incomitant Exotropia In Patients With Partial Third Nerve Palsy
 Surgical Outcome Of Incomitant Exotropia In Patients With Partial Third Nerve Palsy Amit Mohan, MS ; Sudhir Singh, MS ; Dr V.C. Bhatnagar, MS, DNB Dr Amit Mohan, MS Jr.Consultant Global Hospital Institute
Surgical Outcome Of Incomitant Exotropia In Patients With Partial Third Nerve Palsy Amit Mohan, MS ; Sudhir Singh, MS ; Dr V.C. Bhatnagar, MS, DNB Dr Amit Mohan, MS Jr.Consultant Global Hospital Institute
ICTUS CEREBELOSOS. Carlos S. Kase, M.D. Department of Neurology Boston University Boston, MA
 ICTUS CEREBELOSOS Carlos S. Kase, M.D. Department of Neurology Boston University Boston, MA CEREBELLAR STROKES CEREBELLAR INFARCTION CEREBELLAR HEMORRHAGE Distribution of Pathologically Confirmed Cerebellar
ICTUS CEREBELOSOS Carlos S. Kase, M.D. Department of Neurology Boston University Boston, MA CEREBELLAR STROKES CEREBELLAR INFARCTION CEREBELLAR HEMORRHAGE Distribution of Pathologically Confirmed Cerebellar
Ptosis. Ptosis and Pupils. Ptosis. Palpebral fissure. Blepharospasm. Blepharospasm or ptosis? Bilateral, longstanding, familial: Palpebral fissure
 Ptosis and Pupils Ptosis Jack CF Chong, MS, MD 99/03/06 Ptosis Bilateral, longstanding, familial: CPEO (chronic progressive external ophthalmoplegia) D/D: Acute, recent, unilateral Palpebral fissure Palpebral
Ptosis and Pupils Ptosis Jack CF Chong, MS, MD 99/03/06 Ptosis Bilateral, longstanding, familial: CPEO (chronic progressive external ophthalmoplegia) D/D: Acute, recent, unilateral Palpebral fissure Palpebral
Evaluation of Diplopia: An Anatomic and Systematic Approach
 Clinical Review Article Evaluation of Diplopia: An Anatomic and Systematic Approach Victoria S. Pelak, MD Double vision, or diplopia, is a symptom with many potential causes that can involve many different
Clinical Review Article Evaluation of Diplopia: An Anatomic and Systematic Approach Victoria S. Pelak, MD Double vision, or diplopia, is a symptom with many potential causes that can involve many different
The Work Up of Isolated Ocular Motor Palsy: Who to Scan and Why
 The Work Up of Isolated Ocular Motor Palsy: Who to Scan and Why Nicholas Volpe, MD Scheie Eye Institute, University of Pennsylvania Philadelphia, Pennsylvania LEARNING OBJECTIVES 1. To identify common
The Work Up of Isolated Ocular Motor Palsy: Who to Scan and Why Nicholas Volpe, MD Scheie Eye Institute, University of Pennsylvania Philadelphia, Pennsylvania LEARNING OBJECTIVES 1. To identify common
Esotropia (Crossed Eye(s))
 Esotropia (Crossed Eye(s)) Esotropia is a type of strabismus or eye misalignment in which the eyes are "crossed," that is, while one eye looks straight ahead, the other eye is turned in toward the nose.
Esotropia (Crossed Eye(s)) Esotropia is a type of strabismus or eye misalignment in which the eyes are "crossed," that is, while one eye looks straight ahead, the other eye is turned in toward the nose.
Return to same game if sx s resolve within 15 minutes. Return to next game if sx s resolve within one week Return to Competition
 Assessment Skills of the Spine on the Field and in the Clinic Ron Burke, MD Cervical Spine Injuries Sprains and strains Stingers Transient quadriparesis Cervical Spine Injuries Result in critical loss
Assessment Skills of the Spine on the Field and in the Clinic Ron Burke, MD Cervical Spine Injuries Sprains and strains Stingers Transient quadriparesis Cervical Spine Injuries Result in critical loss
Pathoanatomical Changes of the Brachial Plexus and of C5-C6 Following Whiplash-Type Injury: A Case Report
 Pathoanatomical Changes of the Brachial Plexus and of C5-C6 Following Whiplash-Type Injury: A Case Report 1 Journal Of Whiplash & Related Disorders Vol. 1, No, 1, 2002 Gunilla Bring, Halldor Jonsson Jr.,
Pathoanatomical Changes of the Brachial Plexus and of C5-C6 Following Whiplash-Type Injury: A Case Report 1 Journal Of Whiplash & Related Disorders Vol. 1, No, 1, 2002 Gunilla Bring, Halldor Jonsson Jr.,
Differentiating Cervical Radiculopathy and Peripheral Neuropathy. Adam P. Smith, MD
 Differentiating Cervical Radiculopathy and Peripheral Neuropathy Adam P. Smith, MD I have no financial, personal, or professional conflicts of interest to report Radiculopathy versus Neuropathy Radiculopathy
Differentiating Cervical Radiculopathy and Peripheral Neuropathy Adam P. Smith, MD I have no financial, personal, or professional conflicts of interest to report Radiculopathy versus Neuropathy Radiculopathy
Acute diplopia associated with systemic hypertension - A case Report
 Standard Research Journal of Medicine and Medical Sciences Vol 3(2): 042-046, February 2015 (ISSN: 2409-0638) http://www.standresjournals.org/journals/srjmms Case Report Acute diplopia associated with
Standard Research Journal of Medicine and Medical Sciences Vol 3(2): 042-046, February 2015 (ISSN: 2409-0638) http://www.standresjournals.org/journals/srjmms Case Report Acute diplopia associated with
CERVICAL DISC HERNIATION
 CERVICAL DISC HERNIATION Most frequent at C 5/6 level but also occur at C 6 7 & to a lesser extent at C4 5 & other levels In relatively younger persons soft disk protrusion is more common than hard disk
CERVICAL DISC HERNIATION Most frequent at C 5/6 level but also occur at C 6 7 & to a lesser extent at C4 5 & other levels In relatively younger persons soft disk protrusion is more common than hard disk
Isolated Ocular Motor Nerve Palsies
 539 Nathan H. Kung, MD 1 Gregory P. Van Stavern, MD 2 1 Department of Neurology, Washington University in St. Louis, St. Louis, Missouri 2 Department of Ophthalmology, Washington University in St. Louis,
539 Nathan H. Kung, MD 1 Gregory P. Van Stavern, MD 2 1 Department of Neurology, Washington University in St. Louis, St. Louis, Missouri 2 Department of Ophthalmology, Washington University in St. Louis,
Stuart B Black MD, FAAN Chief of Neurology Co-Medical Director: Neuroscience Center Baylor University Medical Center at Dallas
 Billing and Coding in Neurology and Headache Stuart B Black MD, FAAN Chief of Neurology Co-Medical Director: Neuroscience Center Baylor University Medical Center at Dallas CPT Codes vs. ICD Codes Category
Billing and Coding in Neurology and Headache Stuart B Black MD, FAAN Chief of Neurology Co-Medical Director: Neuroscience Center Baylor University Medical Center at Dallas CPT Codes vs. ICD Codes Category
PUPILS AND NEAR VISION. Akilesh Gokul PhD Research Fellow Department of Ophthalmology
 PUPILS AND NEAR VISION Akilesh Gokul PhD Research Fellow Department of Ophthalmology Iris Anatomy Two muscles: Radially oriented dilator (actually a myo-epithelium) - like the spokes of a wagon wheel Sphincter/constrictor
PUPILS AND NEAR VISION Akilesh Gokul PhD Research Fellow Department of Ophthalmology Iris Anatomy Two muscles: Radially oriented dilator (actually a myo-epithelium) - like the spokes of a wagon wheel Sphincter/constrictor
Diplopia, or double vision, is a frequently encountered. Binocular Diplopia. A Practical Approach ORIGINAL ARTICLE
 ORIGINAL ARTICLE A Practical Approach Janet C. Rucker, MD, and Robert L. Tomsak, MD, PhD Background: Diplopia is a common complaint in both inpatient and outpatient neurologic practice. Its causes are
ORIGINAL ARTICLE A Practical Approach Janet C. Rucker, MD, and Robert L. Tomsak, MD, PhD Background: Diplopia is a common complaint in both inpatient and outpatient neurologic practice. Its causes are
Acute demyelinating optic neuritis Rod Foroozan, MD, Lawrence M. Buono, MD, Peter J. Savino, MD, and Robert C. Sergott, MD
 Acute demyelinating optic neuritis Rod Foroozan, MD, Lawrence M. Buono, MD, Peter J. Savino, MD, and Robert C. Sergott, MD Acute demyelinating optic neuritis associated with multiple sclerosis (MS) is
Acute demyelinating optic neuritis Rod Foroozan, MD, Lawrence M. Buono, MD, Peter J. Savino, MD, and Robert C. Sergott, MD Acute demyelinating optic neuritis associated with multiple sclerosis (MS) is
Examination Approach. Case 1: Mental Status. Examination Approach. The Neurological Exam In the ICU: High Yield Techniques 5/30/2013
 The Neurological Exam In the ICU: High Yield Techniques S. Andrew Josephson MD Carmen Castro-Franceschi and Gladyne K. Mitchell Neurohospitalist Distinguished Professor Vice Chairman, Parnassus Programs
The Neurological Exam In the ICU: High Yield Techniques S. Andrew Josephson MD Carmen Castro-Franceschi and Gladyne K. Mitchell Neurohospitalist Distinguished Professor Vice Chairman, Parnassus Programs
Aetna Nerve Conduction Study Policy
 Aetna Nerve Conduction Study Policy Policy Aetna considers nerve conduction velocity (NCV) studies medically necessary when both of the following criteria are met: 1. Member has any of the following indications:
Aetna Nerve Conduction Study Policy Policy Aetna considers nerve conduction velocity (NCV) studies medically necessary when both of the following criteria are met: 1. Member has any of the following indications:
Mini-atlas of the Marmoset Brain
 Mini-atlas of the Marmoset Brain http://marmoset-brain.org Aya Senoo Tokyo University of Agriculture and Technology Hironobu Tokuno Tokyo Metropolitan Institute of Medical Science Charles Watson Curtin
Mini-atlas of the Marmoset Brain http://marmoset-brain.org Aya Senoo Tokyo University of Agriculture and Technology Hironobu Tokuno Tokyo Metropolitan Institute of Medical Science Charles Watson Curtin
Original Contributions
 doi:10.1016/j.jemermed.2007.04.020 The Journal of Emergency Medicine, Vol. 35, No. 3, pp. 239 246, 2008 Copyright 2008 Elsevier Inc. Printed in the USA. All rights reserved 0736-4679/08 $ see front matter
doi:10.1016/j.jemermed.2007.04.020 The Journal of Emergency Medicine, Vol. 35, No. 3, pp. 239 246, 2008 Copyright 2008 Elsevier Inc. Printed in the USA. All rights reserved 0736-4679/08 $ see front matter
Whiplash injuries can be visible by functional magnetic resonance imaging. Pain Research and Management Autumn 2006; Vol. 11, No. 3, pp.
 Whiplash injuries can be visible by functional magnetic resonance imaging 1 Bengt H Johansson, MD FROM ABSTRACT: Pain Research and Management Autumn 2006; Vol. 11, No. 3, pp. 197-199 Whiplash trauma can
Whiplash injuries can be visible by functional magnetic resonance imaging 1 Bengt H Johansson, MD FROM ABSTRACT: Pain Research and Management Autumn 2006; Vol. 11, No. 3, pp. 197-199 Whiplash trauma can
Guideline for the Management of Acute Peripheral Facial nerve palsy. Bells Palsy in Children
 Guideline for the Management of Acute Peripheral Facial nerve palsy Definition Bells Palsy in Children Bell palsy is an acute, idiopathic unilateral lower motor neurone facial nerve palsy that is not associated
Guideline for the Management of Acute Peripheral Facial nerve palsy Definition Bells Palsy in Children Bell palsy is an acute, idiopathic unilateral lower motor neurone facial nerve palsy that is not associated
Multifocal Motor Neuropathy. Jonathan Katz, MD Richard Lewis, MD
 Multifocal Motor Neuropathy Jonathan Katz, MD Richard Lewis, MD What is Multifocal Motor Neuropathy? Multifocal Motor Neuropathy (MMN) is a rare condition in which multiple motor nerves are attacked by
Multifocal Motor Neuropathy Jonathan Katz, MD Richard Lewis, MD What is Multifocal Motor Neuropathy? Multifocal Motor Neuropathy (MMN) is a rare condition in which multiple motor nerves are attacked by
ß-interferon and. ABN Guidelines for 2007 Treatment of Multiple Sclerosis with. Glatiramer Acetate
 ABN Guidelines for 2007 Treatment of Multiple Sclerosis with ß-interferon and Glatiramer Acetate Published by the Association of British Neurologists Ormond House, 27 Boswell Street, London WC1N 3JZ Contents
ABN Guidelines for 2007 Treatment of Multiple Sclerosis with ß-interferon and Glatiramer Acetate Published by the Association of British Neurologists Ormond House, 27 Boswell Street, London WC1N 3JZ Contents
The Physiology of the Senses Lecture 11 - Eye Movements www.tutis.ca/senses/
 The Physiology of the Senses Lecture 11 - Eye Movements www.tutis.ca/senses/ Contents Objectives... 2 Introduction... 2 The 5 Types of Eye Movements... 2 The eyes are rotated by 6 extraocular muscles....
The Physiology of the Senses Lecture 11 - Eye Movements www.tutis.ca/senses/ Contents Objectives... 2 Introduction... 2 The 5 Types of Eye Movements... 2 The eyes are rotated by 6 extraocular muscles....
Reversibility of Acute Demyelinating Lesions in relapsingremitting
 Reversibility of Acute Demyelinating Lesions in relapsingremitting Multiple Sclerosis Omar A. Khan ( Division of Neuroimmunology, Department of Neurology, Neurology and Research Services. Veterans Affairs
Reversibility of Acute Demyelinating Lesions in relapsingremitting Multiple Sclerosis Omar A. Khan ( Division of Neuroimmunology, Department of Neurology, Neurology and Research Services. Veterans Affairs
1 PYRAMIDS - CORTICOSPINAL FIBERS
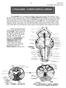 151 Brain stem Pyramids/Corticospinal Tract 1 PYRAMIDS - CORTICOSPINAL FIBERS The pyramids are two elongated swellings on the ventral aspect of the medulla. Each pyramid contains approximately 1,000,000
151 Brain stem Pyramids/Corticospinal Tract 1 PYRAMIDS - CORTICOSPINAL FIBERS The pyramids are two elongated swellings on the ventral aspect of the medulla. Each pyramid contains approximately 1,000,000
Paraneoplastic Antibodies in Clinical Practice. Mohammed El lahawi New Cross Hospital Wolverhampton
 Paraneoplastic Antibodies in Clinical Practice Mohammed El lahawi New Cross Hospital Wolverhampton 1 Effects of Neoplasm Direct mass ( pressure ) effect Metastasis effect Remote effect 2 The Nervous System
Paraneoplastic Antibodies in Clinical Practice Mohammed El lahawi New Cross Hospital Wolverhampton 1 Effects of Neoplasm Direct mass ( pressure ) effect Metastasis effect Remote effect 2 The Nervous System
*A discrete, hypersensitive nodule within tight band of muscle or fascia that present with classic pattern of pain referral that does not follow
 A patient presents with c/o cervical spine pain and chronic headaches that radiates across the top of his head. He also experiences frequent bouts of nausea, dizziness and indigestion. The patient also
A patient presents with c/o cervical spine pain and chronic headaches that radiates across the top of his head. He also experiences frequent bouts of nausea, dizziness and indigestion. The patient also
Optic Neuritis. The optic nerve fibers are coated with myelin to help them conduct the electrical signals back to your brain.
 Optic Neuritis Your doctor thinks that you have had an episode of optic neuritis. This is the most common cause of sudden visual loss in a young patient. It is often associated with discomfort in or around
Optic Neuritis Your doctor thinks that you have had an episode of optic neuritis. This is the most common cause of sudden visual loss in a young patient. It is often associated with discomfort in or around
Neurology Clerkship Learning Objectives
 Neurology Clerkship Learning Objectives Clinical skills Perform a neurological screening examination of the cranial nerves, motor system, reflexes, and sensory system under the observation and guidance
Neurology Clerkship Learning Objectives Clinical skills Perform a neurological screening examination of the cranial nerves, motor system, reflexes, and sensory system under the observation and guidance
CLINICAL NEUROPHYSIOLOGY
 CLINICAL NEUROPHYSIOLOGY Barry S. Oken, MD, Carter D. Wray MD Objectives: 1. Know the role of EMG/NCS in evaluating nerve and muscle function 2. Recognize common EEG findings and their significance 3.
CLINICAL NEUROPHYSIOLOGY Barry S. Oken, MD, Carter D. Wray MD Objectives: 1. Know the role of EMG/NCS in evaluating nerve and muscle function 2. Recognize common EEG findings and their significance 3.
ALS and Lyme Disease Questions from Patient and Families Responses from Medical Experts
 ALS and Lyme Disease Questions from Patient and Families Responses from Medical Experts Introduction: When anyone receives a diagnosis of ALS, it is normal and understandable to ask why you ve developed
ALS and Lyme Disease Questions from Patient and Families Responses from Medical Experts Introduction: When anyone receives a diagnosis of ALS, it is normal and understandable to ask why you ve developed
Ocular torsion and perceived vertical in oculomotor, trochlear and abducens nerve palsies
 Brain (1993), 116, 1095-1104 Ocular torsion and perceived vertical in oculomotor, trochlear and abducens nerve palsies Marianne Dieterich and Thomas Brandt Department of Neurology, Klinikum Grosshadern,
Brain (1993), 116, 1095-1104 Ocular torsion and perceived vertical in oculomotor, trochlear and abducens nerve palsies Marianne Dieterich and Thomas Brandt Department of Neurology, Klinikum Grosshadern,
List of diagnostic flowcharts
 List of diagnostic flowcharts Chapter 3 Visual loss Transient visual loss 43 Sudden or rapidly progressive visual loss 46 Gradual visual loss 61 Chapter 4 The red eye One red eye, decreased vision 83 One
List of diagnostic flowcharts Chapter 3 Visual loss Transient visual loss 43 Sudden or rapidly progressive visual loss 46 Gradual visual loss 61 Chapter 4 The red eye One red eye, decreased vision 83 One
Peripheral nervous system (PNS) Consists of: 12 pairs of cranial nerves 31 pairs of spinal nerves The autonomic nervous system
 Peripheral nervous system (PNS) Consists of: 12 pairs of cranial nerves 31 pairs of spinal nerves The autonomic nervous system Nerves and neurons Cranial nerves There are 12 pairs They are numbered according
Peripheral nervous system (PNS) Consists of: 12 pairs of cranial nerves 31 pairs of spinal nerves The autonomic nervous system Nerves and neurons Cranial nerves There are 12 pairs They are numbered according
Vision Health: Conditions, Disorders & Treatments NEUROOPTHALMOLOGY
 Vision Health: Conditions, Disorders & Treatments NEUROOPTHALMOLOGY Neuroophthalmology focuses on conditions caused by brain or systemic abnormalities that result in visual disturbances, among other symptoms.
Vision Health: Conditions, Disorders & Treatments NEUROOPTHALMOLOGY Neuroophthalmology focuses on conditions caused by brain or systemic abnormalities that result in visual disturbances, among other symptoms.
Neuro-ophthalmology: Disorders of the Efferent Visual Pathway
 neurology Board Review Manual Statement of Editorial Purpose The Hospital Physician Neurology Board Review Manual is a peer-reviewed study guide for residents and practicing physicians preparing for board
neurology Board Review Manual Statement of Editorial Purpose The Hospital Physician Neurology Board Review Manual is a peer-reviewed study guide for residents and practicing physicians preparing for board
.org. Herniated Disk in the Lower Back. Anatomy. Description
 Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
EMG and the Electrodiagnostic Consultation for the Family Physician
 EMG and the Electrodiagnostic Consultation for the Family Physician Stephanie Kopey, D.O., P.T. 9/27/15 The American Association of Neuromuscular & Electrodiagnostic Medicine (AANEM) Marketing Committee
EMG and the Electrodiagnostic Consultation for the Family Physician Stephanie Kopey, D.O., P.T. 9/27/15 The American Association of Neuromuscular & Electrodiagnostic Medicine (AANEM) Marketing Committee
Chapter 7 Complex Ocular Motor Disorders in Children
 Chapter 7 Complex Ocular Motor Disorders in Children Introduction A number of complex ocular motility disorders are discussed in this chapter. The diversity of these conditions reflects the need for the
Chapter 7 Complex Ocular Motor Disorders in Children Introduction A number of complex ocular motility disorders are discussed in this chapter. The diversity of these conditions reflects the need for the
MANAGEMENT OF VITH NERVE PALSY-AVOIDING UNNECESSARY SURGERY
 MANAGEMENT OF VITH NERVE PALSY-AVOIDING UNNECESSARY SURGERY P. RIORDAN-E VA and J. P. LEE London SUMMARY Unresolved Vlth nerve palsy that is not adequately controlled by an abnormal head posture or prisms
MANAGEMENT OF VITH NERVE PALSY-AVOIDING UNNECESSARY SURGERY P. RIORDAN-E VA and J. P. LEE London SUMMARY Unresolved Vlth nerve palsy that is not adequately controlled by an abnormal head posture or prisms
Brown-Sequard Syndrome Caused by Cervical Disc Herniation
 62 CASE REPORT Brown-Sequard Syndrome Caused by Cervical Disc Herniation Chih-Hsiu Wang, Chun-Chung Chen, Der-Yang Cho Department of Neurosurgery, China Medical University Hospital, Taichung, Taiwan, R.O.C.
62 CASE REPORT Brown-Sequard Syndrome Caused by Cervical Disc Herniation Chih-Hsiu Wang, Chun-Chung Chen, Der-Yang Cho Department of Neurosurgery, China Medical University Hospital, Taichung, Taiwan, R.O.C.
2014 Fall CE@SCO. COURSE 3 Doc, I m Seeing Double. COPE Course 40262-NO
 2014 Fall CE@SCO COURSE 3 Doc, I m Seeing Double COPE Course 40262-NO SCO HOMECOMING / FALL CE WEEKEND OCTOBER 9-12, 2014 Levels of disease Dennis Mathews, O.D. Partner, Eye Specialty Group Associate
2014 Fall CE@SCO COURSE 3 Doc, I m Seeing Double COPE Course 40262-NO SCO HOMECOMING / FALL CE WEEKEND OCTOBER 9-12, 2014 Levels of disease Dennis Mathews, O.D. Partner, Eye Specialty Group Associate
UAMS / CAVHS Adult Neurology Neuro-Ophthalmology Curriculum 6/13/08
 UAMS / CAVHS Adult Neurology Neuro-Ophthalmology Curriculum 6/13/08 Summary Description of Rotation The adult neurology neuro-ophthalmology rotation is an extremely important rotation for 1 month during
UAMS / CAVHS Adult Neurology Neuro-Ophthalmology Curriculum 6/13/08 Summary Description of Rotation The adult neurology neuro-ophthalmology rotation is an extremely important rotation for 1 month during
Concussion/MTBI Certification Series. Featuring: Frederick R Carrick, DC, PhD Distinguished Professor of Neurology, Life University
 Concussion/MTBI Certification Series Featuring: Frederick R Carrick, DC, PhD Distinguished Professor of Neurology, Life University Please note that spaces are limited for this specialty certification program.
Concussion/MTBI Certification Series Featuring: Frederick R Carrick, DC, PhD Distinguished Professor of Neurology, Life University Please note that spaces are limited for this specialty certification program.
NEUROIMAGING in Parkinsonian Syndromes
 NEUROIMAGING in Parkinsonian Syndromes (Focus on Structural Techniques: CT and MRI) Dr. Roberto Cilia Parkinson Institute, ICP, Milan, Italy OUTLINE Primary Parkinsonism Idiopathic Parkinson s Disease
NEUROIMAGING in Parkinsonian Syndromes (Focus on Structural Techniques: CT and MRI) Dr. Roberto Cilia Parkinson Institute, ICP, Milan, Italy OUTLINE Primary Parkinsonism Idiopathic Parkinson s Disease
Skew deviation is a vertical strabismus caused by
 AAPOS Workshops Understanding skew deviation and a new clinical test to differentiate it from trochlear nerve palsy Agnes M. F. Wong, MD, PhD SUMMARY Skew deviation is a vertical strabismus caused by a
AAPOS Workshops Understanding skew deviation and a new clinical test to differentiate it from trochlear nerve palsy Agnes M. F. Wong, MD, PhD SUMMARY Skew deviation is a vertical strabismus caused by a
Angela Wilkin May 2013
 Angela Wilkin May 2013 Upper Motor Neuron v Lower Motor Neuron Lesions UMN Lesion LMN Lesion Forehead usually unaffected (bilateral innervation) Forehead affected Contralateral side Ipsilateral side Often
Angela Wilkin May 2013 Upper Motor Neuron v Lower Motor Neuron Lesions UMN Lesion LMN Lesion Forehead usually unaffected (bilateral innervation) Forehead affected Contralateral side Ipsilateral side Often
Eye Movement Abnormalities in Multiple Sclerosis
 Eye Movement Abnormalities in Multiple Sclerosis Sashank Prasad, MD a, *, Steven L. Galetta, MD b KEYWORDS Multiple sclerosis Eye movement abnormalities Neuroanatomy Neuroimaging Multiple sclerosis (MS)
Eye Movement Abnormalities in Multiple Sclerosis Sashank Prasad, MD a, *, Steven L. Galetta, MD b KEYWORDS Multiple sclerosis Eye movement abnormalities Neuroanatomy Neuroimaging Multiple sclerosis (MS)
Vocabulary & General Concepts of Brain Organization
 Vocabulary & General Concepts of Brain Organization Jeanette J. Norden, Ph.D. Professor Emerita Vanderbilt University School of Medicine Course Outline Lecture 1: Vocabulary & General Concepts of Brain
Vocabulary & General Concepts of Brain Organization Jeanette J. Norden, Ph.D. Professor Emerita Vanderbilt University School of Medicine Course Outline Lecture 1: Vocabulary & General Concepts of Brain
6.0 Management of Head Injuries for Maxillofacial SHOs
 6.0 Management of Head Injuries for Maxillofacial SHOs As a Maxillofacial SHO you are not required to manage established head injury, however an awareness of the process is essential when dealing with
6.0 Management of Head Injuries for Maxillofacial SHOs As a Maxillofacial SHO you are not required to manage established head injury, however an awareness of the process is essential when dealing with
FastTest. You ve read the book... ... now test yourself
 FastTest You ve read the book...... now test yourself To ensure you have learned the key points that will improve your patient care, read the authors questions below. The answers will refer you back to
FastTest You ve read the book...... now test yourself To ensure you have learned the key points that will improve your patient care, read the authors questions below. The answers will refer you back to
AMERICAN ACADEMY OF NEUROLOGY NEURO-OPHTHALMOLOGY/NEURO-OTOLOGY FELLOWSHIP CORE CURRICULUM
 AMERICAN ACADEMY OF NEUROLOGY NEURO-OPHTHALMOLOGY/NEURO-OTOLOGY FELLOWSHIP CORE CURRICULUM A CURRICULUM FOR NEURO-OPHTHALMOLOGY Definition and Scope Neuro-ophthalmology focuses on brain and systemic abnormalities
AMERICAN ACADEMY OF NEUROLOGY NEURO-OPHTHALMOLOGY/NEURO-OTOLOGY FELLOWSHIP CORE CURRICULUM A CURRICULUM FOR NEURO-OPHTHALMOLOGY Definition and Scope Neuro-ophthalmology focuses on brain and systemic abnormalities
Nonoperative Management of Herniated Cervical Intervertebral Disc With Radiculopathy. Spine Volume 21(16) August 15, 1996, pp 1877-1883
 Nonoperative Management of Herniated Cervical Intervertebral Disc With Radiculopathy 1 Spine Volume 21(16) August 15, 1996, pp 1877-1883 Saal, Joel S. MD; Saal, Jeffrey A. MD; Yurth, Elizabeth F. MD FROM
Nonoperative Management of Herniated Cervical Intervertebral Disc With Radiculopathy 1 Spine Volume 21(16) August 15, 1996, pp 1877-1883 Saal, Joel S. MD; Saal, Jeffrey A. MD; Yurth, Elizabeth F. MD FROM
Thyroid Eye Disease. Anatomy: There are 6 muscles that move your eye.
 Thyroid Eye Disease Your doctor thinks you have thyroid orbitopathy. This is an autoimmune condition where your body's immune system is producing factors that stimulate enlargement of the muscles that
Thyroid Eye Disease Your doctor thinks you have thyroid orbitopathy. This is an autoimmune condition where your body's immune system is producing factors that stimulate enlargement of the muscles that
Anatomy: The sella is a depression in the sphenoid bone that makes up part of the skull base located behind the eye sockets.
 Pituitary Tumor Your doctor thinks you may have a pituitary tumor. Pituitary tumors are benign (non-cancerous) overgrowth of cells that make up the pituitary gland (the master gland that regulates other
Pituitary Tumor Your doctor thinks you may have a pituitary tumor. Pituitary tumors are benign (non-cancerous) overgrowth of cells that make up the pituitary gland (the master gland that regulates other
UBC Pain Medicine Residency Program: CanMEDS Goals and Objectives of the Neurology Rotation
 UBC Pain Medicine Residency Program: CanMEDS Goals and Objectives of the Neurology Rotation Goals of the Program To acquire the knowledge and skills necessary to assess and provide a management plan for
UBC Pain Medicine Residency Program: CanMEDS Goals and Objectives of the Neurology Rotation Goals of the Program To acquire the knowledge and skills necessary to assess and provide a management plan for
Symptoms and Signs of Irritation of the Brachial Plexus in Whiplash Injuries
 1 Symptoms and Signs of Irritation of the Brachial Plexus in Whiplash Injuries J Bone Joint Surg (Br) 2001 Mar;83(2):226-9 Ide M, Ide J, Yamaga M, Takagi K Department of Orthopaedic Surgery, Kumamoto University
1 Symptoms and Signs of Irritation of the Brachial Plexus in Whiplash Injuries J Bone Joint Surg (Br) 2001 Mar;83(2):226-9 Ide M, Ide J, Yamaga M, Takagi K Department of Orthopaedic Surgery, Kumamoto University
Natural Modality in the Treatment of Primary Headaches. William S. Mihin, D.C. Catharine Helms, M.S. Michelle M. Anderson, M.S.N., F.N.P.
 Natural Modality in the Treatment of Primary Headaches William S. Mihin, D.C. Catharine Helms, M.S. Michelle M. Anderson, M.S.N., F.N.P. Abstract Headaches are both a prevalent and disabling condition.
Natural Modality in the Treatment of Primary Headaches William S. Mihin, D.C. Catharine Helms, M.S. Michelle M. Anderson, M.S.N., F.N.P. Abstract Headaches are both a prevalent and disabling condition.
NEURO MRI PROTOCOLS TABLE OF CONTENTS
 TABLE OF CONTENTS NEURO MRI PROTOCOLS BRAIN...2 Brain 1 Screen... 2 Brain 2 Brain Tumor... 2 Brain 3 Brain Infection / Meningitis... 2 Brain 4 Trauma... 3 Brain 5 Hemorrhage... 3 Brain 6 Demyelinating
TABLE OF CONTENTS NEURO MRI PROTOCOLS BRAIN...2 Brain 1 Screen... 2 Brain 2 Brain Tumor... 2 Brain 3 Brain Infection / Meningitis... 2 Brain 4 Trauma... 3 Brain 5 Hemorrhage... 3 Brain 6 Demyelinating
Sheep Brain Dissection
 Sheep Brain Dissection http://www.carolina.com/product/preserved+organisms/preserved+animals+%28mammal s%29/sheep+organs/preserved+sheep+dissection.do Michigan State University Neuroscience Program Brain
Sheep Brain Dissection http://www.carolina.com/product/preserved+organisms/preserved+animals+%28mammal s%29/sheep+organs/preserved+sheep+dissection.do Michigan State University Neuroscience Program Brain
Exotropias: A Brief Review. Leila M. Khazaeni, MD November 2, 2008
 Exotropias: A Brief Review Leila M. Khazaeni, MD November 2, 2008 Exotropia Myths Myth #1 He/she will grow out of it FALSE 75% of XTs show progression over a 3 year period Myth #2 The only treatment choice
Exotropias: A Brief Review Leila M. Khazaeni, MD November 2, 2008 Exotropia Myths Myth #1 He/she will grow out of it FALSE 75% of XTs show progression over a 3 year period Myth #2 The only treatment choice
The Nuts and Bolts of Multiple Sclerosis. Rebecca Milholland, M.D., Ph.D. Center for Neurosciences
 The Nuts and Bolts of Multiple Sclerosis Rebecca Milholland, M.D., Ph.D. Center for Neurosciences Objectives Discuss which patients are at risk for Multiple Sclerosis Discuss the diagnostic criteria for
The Nuts and Bolts of Multiple Sclerosis Rebecca Milholland, M.D., Ph.D. Center for Neurosciences Objectives Discuss which patients are at risk for Multiple Sclerosis Discuss the diagnostic criteria for
doi: 10.1016/j.jocn.2010.10.005
 doi: 10.1016/j.jocn.2010.10.005 A remote desktop-based telemedicine system Yasushi Shibata, MD, PhD Department of Neurosurgery, Mito Medical Center, University of Tsukuba Mito, Ibaraki, 310-0015, Japan
doi: 10.1016/j.jocn.2010.10.005 A remote desktop-based telemedicine system Yasushi Shibata, MD, PhD Department of Neurosurgery, Mito Medical Center, University of Tsukuba Mito, Ibaraki, 310-0015, Japan
06/06/2012. The Impact of Multiple Sclerosis in the Pacific Northwest. James Bowen, MD. Swedish Neuroscience Institute
 The Impact of Multiple Sclerosis in the Pacific Northwest James Bowen, MD Multiple Sclerosis Center Multiple Sclerosis Center Swedish Neuroscience Institute 1 2 Motor Symptoms of MS Weakness Spasticity
The Impact of Multiple Sclerosis in the Pacific Northwest James Bowen, MD Multiple Sclerosis Center Multiple Sclerosis Center Swedish Neuroscience Institute 1 2 Motor Symptoms of MS Weakness Spasticity
What You Should Know About Cerebral Aneurysms
 What You Should Know About Cerebral Aneurysms From the Cerebrovascular Imaging and Interventions Committee of the American Heart Association Cardiovascular Radiology Council Randall T. Higashida, M.D.,
What You Should Know About Cerebral Aneurysms From the Cerebrovascular Imaging and Interventions Committee of the American Heart Association Cardiovascular Radiology Council Randall T. Higashida, M.D.,
Neurological Assessment of the School Age Child
 O U T R E A C H E D U C A T I O N Neurological Assessment of the School Age Child April 3, 2008 Program Handouts This information is provided as a courtesy by Children's Health Care System and its related
O U T R E A C H E D U C A T I O N Neurological Assessment of the School Age Child April 3, 2008 Program Handouts This information is provided as a courtesy by Children's Health Care System and its related
 THE EYES IN CHARGE: FOR THE OPHTHALMOLOGIST Roberta A. Pagon, M.D. Division of Medical Genetics, CH-25, Children's Hospital /Medical Center, Box C5371, Seattle, WA 98105-0371 bpagon@u.washington.edu (206)
THE EYES IN CHARGE: FOR THE OPHTHALMOLOGIST Roberta A. Pagon, M.D. Division of Medical Genetics, CH-25, Children's Hospital /Medical Center, Box C5371, Seattle, WA 98105-0371 bpagon@u.washington.edu (206)
A 34-year-old female with a history of multiple sclerosis (MS) returns to the neurology clinic for follow-up.
 Complementary and Alternative Medicine in Multiple Sclerosis Case Presentation: A 34-year-old female with a history of multiple sclerosis (MS) returns to the neurology clinic for follow-up. The patient
Complementary and Alternative Medicine in Multiple Sclerosis Case Presentation: A 34-year-old female with a history of multiple sclerosis (MS) returns to the neurology clinic for follow-up. The patient
Khaled s Radiology report
 Khaled s Radiology report Patient Name: Khaled Adli Moustafa Date 06/15/2014 The patient is not present. And the following report is based upon what was in the MRI of the cervical and lumbar spine report
Khaled s Radiology report Patient Name: Khaled Adli Moustafa Date 06/15/2014 The patient is not present. And the following report is based upon what was in the MRI of the cervical and lumbar spine report
Vertebrobasilar Disease
 The Vascular Surgery team at the University of Michigan is dedicated to providing exceptional treatments for in the U-M Cardiovascular Center (CVC), our new state-of-the-art clinical facility. Treatment
The Vascular Surgery team at the University of Michigan is dedicated to providing exceptional treatments for in the U-M Cardiovascular Center (CVC), our new state-of-the-art clinical facility. Treatment
A Flow Chart For Classification Of Nystagmus
 A Flow Chart For Classification Of Nystagmus Is fixation impaired because of a slow drift, or an intrusive saccade, away from the target? If a slow drift is culprit Jerk Pendular Unidrectional (constant
A Flow Chart For Classification Of Nystagmus Is fixation impaired because of a slow drift, or an intrusive saccade, away from the target? If a slow drift is culprit Jerk Pendular Unidrectional (constant
Cervicogenic Headache: A Review of Diagnostic and Treatment Strategies
 Cervicogenic Headache: A Review of Diagnostic and Treatment Strategies 1 Journal of the American Osteopathic Association April 2005, Vol. 105, No. 4 supplement, pp. 16-22 David M. Biondi, DO FROM ABSTRACT:
Cervicogenic Headache: A Review of Diagnostic and Treatment Strategies 1 Journal of the American Osteopathic Association April 2005, Vol. 105, No. 4 supplement, pp. 16-22 David M. Biondi, DO FROM ABSTRACT:
Characterization of small renal lesions: Problem solving with MRI Gary Israel, MD
 Characterization of small renal lesions: Problem solving with MRI Gary Israel, MD With the widespread use of cross-sectional imaging, many renal masses are incidentally found. These need to be accurately
Characterization of small renal lesions: Problem solving with MRI Gary Israel, MD With the widespread use of cross-sectional imaging, many renal masses are incidentally found. These need to be accurately
Substandard Underwriting Structured Settlements
 Substandard Underwriting Structured Settlements Structures 101-Back to Basics February 20-22, 2013 Las Vegas, Nevada Rosemary Brindamour BSN CSSC Chief Medical Underwriter Structured Settlement Underwriting
Substandard Underwriting Structured Settlements Structures 101-Back to Basics February 20-22, 2013 Las Vegas, Nevada Rosemary Brindamour BSN CSSC Chief Medical Underwriter Structured Settlement Underwriting

![Bell s Palsy ]]> <![CDATA[Bell's Palsy]]> Bell s Palsy ]]> <![CDATA[Bell's Palsy]]>](/thumbs/27/10105461.jpg)