HIP ARTHROSCOPY : PATIENT INFORMATION
|
|
|
- Gladys Carr
- 10 years ago
- Views:
Transcription
1 !!
2
3 HIP ARTHROSCOPY : PATIENT INFORMATION Contents Diagram of a labral tear 2 Operative technique 4 Operating time 6 Complications 6 After hip arthroscopy 7 Further reading : Femoro-Acetabular Impingement What is femoro-acetabular impingement? 9 Dealing with the acetabular cartilage and labrum 12 Addressing the underlying bony deformity 13 What is the post-operative rehabilitation? 14 Contact us
4 In the past, patients suffering from hip problems had limited options. In most cases, they were forced to live with the pain until a total hip replacement was required. With the advent of arthroscopic hip surgery, however, there are now less invasive treatment options available that can provide relief or significant improvement for a number of conditions. Most people who suffer pain or experience decreased mobility due to hip impingement, labral tears, cartilage injuries, loose bodies in the joint, or other conditions may benefit from a minimally invasive surgical procedure. Hip arthroscopy (key hole surgery of the hip) is used to assist the diagnosis and treatment of a variety of disorders of the adult hip: Labral tears Removal of lose bodies Osteochondral injuries Synovial disease Ligamentum teres tears Treatment of septic arthritis Surgery for femoro-acetabular impingement Evaluation of undiagnosed hip pain Diagram of a labral tear Hip arthroscopy also has diagnostic and therapeutic applications for hip disorders in children and adolescents. Like arthroscopy of other joints, hip arthroscopy benefits from minimal invasiveness and shorter recovery periods than with open procedures. Hip arthroscopy, however, is not widely available as it requires specialist equipment and takes a long time to learn. 2
5 Hip arthroscopy is carried out under a general anaesthetic and usually involves an overnight stay in hospital Perhaps the two most common current indications for hip arthroscopy include the presence of symptomatic FAI or an acetabular labral tear, or both. These will be considered in more detail here: 1) Femoroacetabular Impingement (FAI) FAI is a condition affecting the hip joint (Figure 1) and is characterised by abnormal contact between the femoral head (hip ball ) and the rim of the acetabulum (hip socket) leading to damage to the articular cartilage (lining or gristle) in the acetabulum, or to the labrum of the hip, or both. The labrum is a ring of cartilage that surrounds the acetabulum and looks very like the meniscus of a knee joint, although its function is different. Damage to the labrum and/or articular cartilage will likely cause pain. An abnormality in the shape of the femoral head or acetabulum, or both, may cause FAI. Activities that involve recurrent hip motion can increase the frequency of this abnormal contact, e.g. kicking sports. FAI generally presents in three forms: cam impingement, pincer impingement and mixed impingement (involving both cam and pincer type). FAI can affect all age groups from the early teens to throughout adult life and is being increasingly recognised as one of the predisposing factors for osteoarthritis of the hip. Although scientific evidence is still slightly sketchy, it is felt by many that without early intervention surgery, there is a high likelihood of developing osteoarthritis ( wear and tear ), with the subsequent requirement for either a hip replacement or other major hip operations. Hip arthroscopy can be used to reshape the femoral head and socket to prevent impingement, and aims to protect the hip from developing osteoarthritis, as well relieving current symptoms. There is a more comprehensive explanation of FAI later in the booklet. 2) Acetabular labral tears The labrum, which surrounds the acetabulum, can be partially damaged or torn. This is usually associated with FAI, but not always so. With hip arthroscopy, the labrum can be either debrided (remove the damaged tissue only) or repaired. Occasionally a labrum can also be grafted. MRI and/or CT scans, although often performed before hip arthroscopic surgery is undertaken, do not always reveal every labral tear. 3
6 & ' & ' Operative technique The patient is positioned on a fracture table (special traction table) with a well padded perineal post pressing against the inner aspect of the proximal thigh (very close to the groin). The legs are held apart as shown on the diagram and traction is applied to each leg via the foot plates. The image intensifier (special X-ray) is used to confirm adequate distraction (to allow the telescope to pass into the joint) before starting the procedure. 4
7 The leg is then prepared and draped using waterproof drapes. The image intensifier is also draped and positioned from the opposite side and the distraction is reapplied and verified to allow the procedure to begin. The bones of the hip joint (the ball and socket) are separated by approximately 1cm by applying traction to the foot while wearing a special boot. By distracting the hip, this provides enough room for a small telescope ( arthroscope ) to be introduced into the joint. Initially, air and/or fluid are injected into the hip, under x-ray guidance. Once correct placement of the instrument has been confirmed, two, three, or sometimes four small incisions are made on the side of the hip. Each of these incisions generally measures approximately 5-10 mm in length. Through these small holes, the telescope and instruments are passed into the joint. The surgeon will then be able to visualise the hip joint, identify the problem(s), and proceed appropriately. Very occasionally it is not possible to insert an arthroscope into the hip joint. Typically three or four such portals are created during hip arthroscopy to allow the visualisation and treatment of the hip abnormalities or injuries. The additional portals allow the passage of specialist instruments into the hip joint to carry out the required procedures. Fluid is passed through the joint under high pressure to clear any debris. Hip arthroscopy involves the assessment of both the central compartment (ball and socket joint) and the peripheral compartment (head-neck junction and soft tissues just outside the ball and socket joint). The traction is released (and the traction post sometimes removed) and the hip and knee are flexed to allow access to the peripheral compartment. At the end of the procedure medications may be injected into the hip to minimise pain after the surgery. The small holes are often closed with one to two stitches each or tapes. Finally, a further dressing is placed over the holes. 5
8 Operating time Operating time varies from patient to patient and is dependant on what needs to be done in each individual case. Typically it can take at least minutes to carry out the required procedures in the central compartment and then a further hour to change the position of the leg, gain access to the peripheral compartment and then carry out the procedure in this compartment ( e.g. reshape the femoral head-neck junction). Complications Any surgical procedure carries a risk of potential complications, regardless of how competent the surgeon is. The surgeon and patient need to work together to minimise the risk of complications. Complications can be described as being related to surgery generally (general complications) or related to hip arthroscopy specifically (specific complications). General Complications (common to most lower limb operations): postoperative chest infection inability to pass urine after surgery inability to open bowels blood clots in leg veins, or bleeding into leg heart attack Specific Complications (specifically related to hip arthroscopy): There is a less than 5% chance that the hip arthroscopy may make symptoms worse (particularly in the arthritic hip). Typically can expect discomfort for two weeks and may have intermittent symptoms for up to three months. Associated with traction post (pressure effects): Skin perineal splitting (in females) or pressure sores Nerve damage Pudendal neuropraxia (numbness between the legs) Damage to other nerves can also rarely happen Nerve damage is usually temporary, but rarely can be permanent Bleeding very rarely Infection very rarely 6
9 After hip arthroscopy: Usually, you will feel some discomfort in your hip. In addition, the discomfort can be experienced in the lower back, buttock, knee and ankle. The discomfort can normally be reduced with the appropriate pain relief. In the majority, there will be some swelling in the groin, buttock and thigh. This is caused by the fluid used during the surgery. The swelling reduces over the following few days. You are likely to be seen by a physiotherapist following your surgery. They will make sure you are safe to mobilise with or without the aid of crutches. This will depend on the instructions received from your surgeon. In some circumstances you may be asked to limit the amount of weight you put through your operated leg, while in others you may be allowed to fully weight-bear immediately after surgery.. Consequently, you may require crutches for a few days, or weeks depending on what specific surgery has been undertaken. Your surgeon and physiotherapist will decide when it is appropriate for you to stop using the crutches. Observe the wound for any signs of infection (increasing pain, redness or swelling). The skin incisions can sometimes leak fluid or blood slightly for a few days; this is normal At a variable point after surgery you will be reviewed by your surgical team. At this appointment, your wound may be inspected and, in some cases, the sutures removed if that has not already been performed. A further explanation of the surgery undertaken can then be provided and there will also be an opportunity for specific queries to be answered. Any subsequent appointments will be arranged and will be guided by the surgery performed. Your surgeon and physiotherapist will develop an appropriate rehabilitation programme for you following the surgery. Your physiotherapist will guide your return to sporting activities (running etc.) depending on your progress. This is extremely variable between individuals, depending on the surgical findings and the length of symptoms prior to surgery. In the majority, by 8 weeks after surgery you should be walking relatively pain-free. By this 8 week point, running can be commenced if that is your wish. Remember, however, that it may take 3 to 6 months (or more) to return to an elite level of competition/fitness. Any unexpected increase in pain can be treated with ice packs and anti-inflammatory medication. The broad strategy for rehabilitation is to regain early range of movement and stability, followed by strength and endurance. Return to work will depend on pain levels and the nature of your job. 7
10 There are some activities to avoid or take care with up to 8 weeks following surgery. These include the following : - Prolonged standing, especially on hard surfaces. Prolonged walking i.e.; around shopping centres. Heavy lifting Squatting / crouching Sleeping on your side. Try to sleep on your back. If you must sleep on your side, sleep on the unoperated side, with a pillow under your operated leg to hold that leg level with the body. Clutch use in manual cars (for left hips) may flare up symptoms in the first couple of weeks and is best avoided. Exchange cars if possible. Sitting with the hips at 90 degrees a more open seat angle is recommended i.e.; 120 degrees. Car seats should be tilted backwards slightly in order to open the hips out. 8
11 FURTHER READING : FEMORO-ACETABULAR IMPINGEMENT What is femoroacetabular impingement? Femoroacetabular Impingement (FAI) is a condition in which there is abnormal contact (impingement) between the rim of the acetabulum (hip joint socket) and femoral head-neck junction (the bone just below the ball part of the thigh bone), on movement of the hip. The most common movement that brings on pain is hip flexion (knee towards chest). Patients will experience pain, usually in the groin, but sometimes further down the front of the thigh, side or back of the hip. There may be episodes of clicking in the hip, or the sensation that it is coming out of joint. Certain activities, particularly those which involve hip flexion (e.g football, dancing, ballet, aerobics) will make the pain worse. Patients often find that sitting for a prolonged period of time e.g long car journey, will bring on groin pain, and they often struggle to move into a more comfortable position. Diagram of hip joint How does FAI occur? The mechanism of FAI was only described as recently as It is important to understand that all hips will impinge in asymptomatic people, but only at the extremes of movement. The difference between a normal hip and one with FAI is that the hip impinges much earlier in a patient with FAI. This occurs because of subtle differences in the anatomy of the hip joint. 9
12 Essentially this difference is an excess of bone, either on the edge of the acetabulum, or on the femoral head-neck junction, or both. If the acetabulum is tilted backwards (retroverted), the same effect occurs. The diagrams below illustrate this mechanism. Normal hip joint, viewed from the side no impingement at 90 degrees of hip flexion Hip joint with impingement at 90 degrees of hip flexion, because of excess bone at the head-neck junction. This type of impingement is termed Cam impingement. The red arrows indicate the shear force applied to the acetabular cartilage (right arrow) and the displacing force applied to the acetabular labrum (left arrow) Hip joint with impingement at 90 degrees of hip flexion, because of excess bone in the anterior rim of the acetabulum. This type of impingement is termed Pincer impingement. This results in direct damage to the labrum (left arrow) and the femoral head is levered posteriorly, damaging the cartilage at the back of the joint (right arrow) 10
13 Why does FAI cause hip pain? As can be seen from the diagrams above, FAI results in damage to the cartilage (shiny shock absorbing layer) of the hip joint, and to the acetabular labrum (gristly bumper around the edge of the socket that helps to seal the joint). The labrum has lots of nerve endings so damage to it is painful. Cartilage does not contain nerves, but it is likely that the increased force applied to the bone beneath the cartilage, which does contain nerves, causes the pain. Why is FAI important? FAI is important for two reasons. First, it is a common cause of groin pain in young adults. Because FAI has only recently been understood, in the past such patients may have been misdiagnosed as having other conditions such as a muscle strain (groin strain), hernia, or inflammatory joint disease. The second reason is that many surgeons believe that if untreated, FAI may result in hip arthritis, which may ultimately require a hip replacement. It is important to understand however, that there are not currently any studies that show that this is definitely the case, and that there are no studies yet that show that treatment of FAI prevents progressive wearing out of the joint and arthritis. What causes FAI? Some patients have a previous history of hip problems (such as injury, childhood hip conditions) and develop FAI as a secondary consequence. For the vast majority of patients however, there is no obvious reason why FAI occurs. The primary problem is the subtle deformity in the joint shape, but this may or may not cause problems depending on the activity level of the patient and how easily their cartilage and labrum are damaged. Recent research from Oxford has shown a strong genetic predisposition to the condition. How is FAI investigated? Initial consultation with your surgeon will focus on establishing if the pain is likely to be coming from the hip joint, and to exclude other sources and identify any predisposing factors. You will then be examined and a number of provocative manoeuvres will be performed (such as the impingement test shown below), to demonstrate the impingement. 11
14 Impingement test Following the clinical assessment, xrays of the hip will be taken to look for signs of arthritis, any other cause of hip pain, and the subtle bony deformities that are associated with FAI. It is likely that an MRI scan of your hip will also be done, usually with dye injected into the joint (MR Arthrogram), to look in detail to see if the labrum is torn or if there is any sign of damage to the cartilage. It may be that the radiologist also injects local anaesthetic into the hip with the dye, to help determine if your pain is coming from within the joint. How is FAI treated? Some patients may find that modification of activity, with or without simple analgesics, is adequate to limit their symptoms to a satisfactory degree. Patients who wish to continue their activities may be advised to consider surgery. There are two main principles in the surgical management of FAI: 1) Deal with the damage caused to the acetabular cartilage and labrum 2) Address the underlying bony deformity that caused the impingement in the first place Surgery may be performed via an open procedure, or via a keyhole (arthroscopic) technique. FAI is now the most common indication for a hip arthroscopy. There isn t any evidence as yet as to whether open or arthroscopic surgery is best. Our preferred approach is arthroscopic, because we believe that the rehabilitation is quicker and there is less scarring that may compromise further procedures in the future. Dealing with the damaged acetabular cartilage and labrum Usually, simple debridement (removal) of the damaged tissue is all that is necessary to improve mechanical symptoms. Unfortunately this tissue is not capable of healing itself. It is important to ensure that all unstable areas of cartilage are removed to 12
15 prevent further damage. Occasionally, it is necessary to repair the labrum if it is detached. This is done using suture anchors into the bone of the acetabulum. If the cartilage has been worn away by the impingement, microfracture of the exposed bone (whereby the surface is scratched using a small pick) may encourage new cartilage to form, but the long-term results of this procedure are not known. Probe showing an unstable flap of acetabular cartilage, before (left) and after (right) debridement Degenerate labrum, before (left) and after (right) debridement Addressing the underlying bony deformity Excess bone on the rim of the acetabulum and femoral head may be removed using a burr, visualising the resection directly using the camera. The aim is to remove enough bone so that there is no longer any impingement within a normal range of movement. Adequate bony resection is confirmed with the camera and xray equipment, and a dynamic impingement test performed (see below). 13
16 Schematic diagrams to illustrate the removal of bone from the femoral headneck junction (left), and acetabular rim (right). Arthroscopic view of excess bone at femoral head-neck junction, before and after removal with a burr. The xrays below show the resection of bone, termed a femoral osteochondroplasty Dynamic impingement test. This can be performed at the end of the arthroscopic procedure to ensure that an adequate bony resection has been performed. This test reproduces the impingement position (as described above) and thereby confirms that there is no residual impingement. What is the post-operative rehabilitation? This will depend according to the surgical procedure performed. Some patients are able to go home the same day or day after surgery. Patients who have a femoral osteochondroplasty will usually be asked to touch-weightbear for one to two weeks after surgery, and for up to 6 weeks if acetabular microfracture is performed. If a labral repair, or extensive debridement is performed, then flexion will be limited for up 14
17 to six weeks. Your rehabilitation will be carefully supervised by your physiotherapist. It is important to keep the joint mobile to prevent post-operative scar formation. Hydrotherapy is commonly employed from the third post-operative week. Does treatment of FAI improve symptoms? The published evidence indicates that surgical treatment of FAI improves symptoms in the short term. There is no evidence to indicate the best methods of treatment as yet. The success of surgery will largely be determined by the degree of pre-existing damage to the cartilage and labrum. Patients with focal areas of full-thickness cartilage loss will likely develop progressive arthritis in spite of surgery, although may gain improvement in their range of motion in the short-term. There is no evidence as to whether treatment of FAI slows or prevents the progression of arthritis currently. What are the complications of arthroscopic surgery for FAI? The complications are the same as for a normal hip arthroscopy. In addition, femoral osteochondroplasty may theoretically weaken the bone leading to a risk of fracture, however in practice this is extremely rare. The main risk is that the procedure does not improve the patient s symptoms significantly, or that they deteriorate after initial benefit. 15
18 CONTACT US!"#$%&'()$*(&+,"( 789:!;7957-8'&++<1:!4<9<8<-8$1-=3'51!"#$%&$'()*+(,-./-0,!!!!!!!! F&+I!"JK!?#L!?"LH!4(MI!"JK!?#L!??LL!"#$%&'$()*+,-.-$/#(01( *(267*68# $ $!"#$-%'.&$+)'(&$ ;7957-N=481:!;>98-2/@6/@1:!49-=3'518$:!;;&6-=3'51-N9F1!"#$%&$'()*+(.1230,4!!!!!!!! >//,!#"?:!9+(3&,/@'!A/.BC'(+:!;(C@!>/(6!-/DD!EC+6&3@&..!>61: 9+(3&,/@':!9(B&!F/G@:!HH"#! F&+I!"JK!?#L!?"LH!4(MI!"JK!?#L!??LL!"#$%&'049-$,.+,-.-$/#(01( *(267*68# $ 16
19
20 $!!!
This is my information booklet: Introduction
 Hip arthroscopy is a relatively new procedure which allows the surgeon to diagnose and treat hip disorders by providing a clear view of the inside of the hip with very small incisions. This is a more complicated
Hip arthroscopy is a relatively new procedure which allows the surgeon to diagnose and treat hip disorders by providing a clear view of the inside of the hip with very small incisions. This is a more complicated
Hip arthroscopy Frequently Asked Questions
 Hip arthroscopy Frequently Asked Questions What is a hip arthroscopy? Hip arthroscopy is key hole surgery. Usually 2-3 small incisions (about 1 cm long) are made on the side of your hip. Through these
Hip arthroscopy Frequently Asked Questions What is a hip arthroscopy? Hip arthroscopy is key hole surgery. Usually 2-3 small incisions (about 1 cm long) are made on the side of your hip. Through these
ARTHROSCOPIC HIP SURGERY
 ARTHROSCOPIC HIP SURGERY Hip Arthroscopy is a relatively simple procedure whereby common disorders of the hip can be diagnosed and treated using keyhole surgery. Some conditions, which previously were
ARTHROSCOPIC HIP SURGERY Hip Arthroscopy is a relatively simple procedure whereby common disorders of the hip can be diagnosed and treated using keyhole surgery. Some conditions, which previously were
Arthroscopy of the Hip
 Arthroscopy of the Hip Professor Ernest Schilders FRCS, FFSEM Consultant Orthopaedic Surgeon Specialist in Shoulder and Hip Arthroscopy, Groin and Sports Injuries Private consulting rooms The London Hip
Arthroscopy of the Hip Professor Ernest Schilders FRCS, FFSEM Consultant Orthopaedic Surgeon Specialist in Shoulder and Hip Arthroscopy, Groin and Sports Injuries Private consulting rooms The London Hip
What to Expect from your Hip Arthroscopy Surgery A Guide for Patients
 What to Expect from your Hip Arthroscopy Surgery A Guide for Patients Sources of Information: http://orthoinfo.aaos.org http://dev.aana.org/portals/0/popups/animatedsurgery.htm http://www.isha.net/ http://
What to Expect from your Hip Arthroscopy Surgery A Guide for Patients Sources of Information: http://orthoinfo.aaos.org http://dev.aana.org/portals/0/popups/animatedsurgery.htm http://www.isha.net/ http://
When is Hip Arthroscopy recommended?
 HIP ARTHROSCOPY Hip arthroscopy is a minimally invasive surgical procedure that uses a camera inserted through very small incisions to examine and treat problems in the hip joint. The camera displays pictures
HIP ARTHROSCOPY Hip arthroscopy is a minimally invasive surgical procedure that uses a camera inserted through very small incisions to examine and treat problems in the hip joint. The camera displays pictures
Femoral Acetabular Impingement And Labral Tears of the Hip James Genuario, MD MS
 Femoral Acetabular Impingement And Labral Tears of the Hip James Genuario, MD MS Steadman Hawkins Clinic Denver at Lone Tree 10103 RidgeGate Pkwy, Aspen Bldg#110 Lone Tree, CO 80124 Phone: 303-586-9500
Femoral Acetabular Impingement And Labral Tears of the Hip James Genuario, MD MS Steadman Hawkins Clinic Denver at Lone Tree 10103 RidgeGate Pkwy, Aspen Bldg#110 Lone Tree, CO 80124 Phone: 303-586-9500
A patient s s guide to: Arthroscopy of the Hip
 A patient s s guide to: Arthroscopy of the Hip Brian J. White MD Assistant Team Physician Denver Nuggets Western Orthopaedics - Denver, Colorado Introduction This is designed to provide you with a better
A patient s s guide to: Arthroscopy of the Hip Brian J. White MD Assistant Team Physician Denver Nuggets Western Orthopaedics - Denver, Colorado Introduction This is designed to provide you with a better
PHYSIOTHERAPY REHAB AFTER HIP ARTHROSCOPY
 PHYSIOTHERAPY REHAB AFTER HIP ARTHROSCOPY Information Leaflet Your Health. Our Priority. Page 2 of 6 Introduction This leaflet has been compiled by the Physiotherapy Team to help you understand the hip
PHYSIOTHERAPY REHAB AFTER HIP ARTHROSCOPY Information Leaflet Your Health. Our Priority. Page 2 of 6 Introduction This leaflet has been compiled by the Physiotherapy Team to help you understand the hip
Hip Replacement. Department of Orthopaedic Surgery Tel: 01473 702107
 Information for Patients Hip Replacement Department of Orthopaedic Surgery Tel: 01473 702107 DMI ref: 0134-08.indd(RP) Issue 3: February 2008 The Ipswich Hospital NHS Trust, 2005-2008. All rights reserved.
Information for Patients Hip Replacement Department of Orthopaedic Surgery Tel: 01473 702107 DMI ref: 0134-08.indd(RP) Issue 3: February 2008 The Ipswich Hospital NHS Trust, 2005-2008. All rights reserved.
YOUR GUIDE TO TOTAL HIP REPLACEMENT
 A Partnership for Better Healthcare A Partnership for Better Healthcare YOUR GUIDE TO TOTAL HIP REPLACEMENT PEI Limited M50 Business Park Ballymount Road Upper Ballymount Dublin 12 Tel: 01-419 6900 Fax:
A Partnership for Better Healthcare A Partnership for Better Healthcare YOUR GUIDE TO TOTAL HIP REPLACEMENT PEI Limited M50 Business Park Ballymount Road Upper Ballymount Dublin 12 Tel: 01-419 6900 Fax:
Y O U R S U R G E O N S. choice of. implants F O R Y O U R S U R G E R Y
 Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Your Surgeon Has Chosen the C 2 a-taper Acetabular System The
Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Your Surgeon Has Chosen the C 2 a-taper Acetabular System The
OPERATION:... Proximal tibial osteotomy Distal femoral osteotomy
 AFFIX PATIENT DETAIL STICKER HERE Forename.. Surname NHS Organisation. Responsible surgeon. Job Title Hospital Number... D.O.B.././ No special requirements OPERATION:..... Proximal tibial osteotomy Distal
AFFIX PATIENT DETAIL STICKER HERE Forename.. Surname NHS Organisation. Responsible surgeon. Job Title Hospital Number... D.O.B.././ No special requirements OPERATION:..... Proximal tibial osteotomy Distal
SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS?
 SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS? The spinal canal is best imagined as a bony tube through which nerve fibres pass. The tube is interrupted between each pair of adjacent
SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS? The spinal canal is best imagined as a bony tube through which nerve fibres pass. The tube is interrupted between each pair of adjacent
Rehabilitation Programme following Hip Arthroscopy
 Rehabilitation Programme following Hip Arthroscopy Updated May 2010 Hip Arthroscopy Patient information and rehabilitation programme: The Hip Joint The hip is a ball-and-socket joint and is the largest
Rehabilitation Programme following Hip Arthroscopy Updated May 2010 Hip Arthroscopy Patient information and rehabilitation programme: The Hip Joint The hip is a ball-and-socket joint and is the largest
Shoulder Arthroscopy
 Copyright 2011 American Academy of Orthopaedic Surgeons Shoulder Arthroscopy Arthroscopy is a procedure that orthopaedic surgeons use to inspect, diagnose, and repair problems inside a joint. The word
Copyright 2011 American Academy of Orthopaedic Surgeons Shoulder Arthroscopy Arthroscopy is a procedure that orthopaedic surgeons use to inspect, diagnose, and repair problems inside a joint. The word
Anterior Hip Replacement
 Disclaimer This movie is an educational resource only and should not be used to manage Orthopaedic health. All decisions about the management of hip replacement and arthritis management must be made in
Disclaimer This movie is an educational resource only and should not be used to manage Orthopaedic health. All decisions about the management of hip replacement and arthritis management must be made in
A Patient s Guide to Post-Operative Physiotherapy. Following Anterior Cruciate Ligament Reconstruction of the Knee
 A Patient s Guide to Post-Operative Physiotherapy Following Anterior Cruciate Ligament Reconstruction of the Knee Introduction The anterior cruciate ligament (ACL) is one of the main supporting ligaments
A Patient s Guide to Post-Operative Physiotherapy Following Anterior Cruciate Ligament Reconstruction of the Knee Introduction The anterior cruciate ligament (ACL) is one of the main supporting ligaments
Orthopaedic Spine Center. Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs
 Orthopaedic Spine Center Graham Calvert MD James Woodall MD PhD Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs The cervical spine consists of the bony vertebrae, discs, nerves and other structures.
Orthopaedic Spine Center Graham Calvert MD James Woodall MD PhD Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs The cervical spine consists of the bony vertebrae, discs, nerves and other structures.
KNEE ARTHROSCOPY. Dr C.S. Waller. Orthopaedic Surgeon
 KNEE ARTHROSCOPY Dr C.S. Waller Orthopaedic Surgeon Specializing in surgery of the hip and knee 83826199 What is Arthroscopy? Arthroscopy involves the inspection of the inside of the knee joint with a
KNEE ARTHROSCOPY Dr C.S. Waller Orthopaedic Surgeon Specializing in surgery of the hip and knee 83826199 What is Arthroscopy? Arthroscopy involves the inspection of the inside of the knee joint with a
Frequently Asked Questions following Anterior Cruciate Ligament Reconstruction Surgery 1
 Frequently Asked Questions following Anterior Cruciate Ligament Reconstruction Surgery 1 Will my knee be normal after surgery and recovery? Unfortunately, even with an ACL reconstructive procedure, it
Frequently Asked Questions following Anterior Cruciate Ligament Reconstruction Surgery 1 Will my knee be normal after surgery and recovery? Unfortunately, even with an ACL reconstructive procedure, it
Arthritis of the hip. Normal hip In an x-ray of a normal hip, the articular cartilage (the area labeled normal joint space ) is clearly visible.
 Arthritis of the hip Arthritis of the hip is a condition in which the smooth gliding surfaces of your hip joint (articular cartilage) have become damaged. This usually results in pain, stiffness, and reduced
Arthritis of the hip Arthritis of the hip is a condition in which the smooth gliding surfaces of your hip joint (articular cartilage) have become damaged. This usually results in pain, stiffness, and reduced
HEADER TOTAL HIP REPLACEMENT SURGERY FROM PREPARATION TO RECOVERY
 HEADER TOTAL HIP REPLACEMENT SURGERY FROM PREPARATION TO RECOVERY ABOUT THE HIP JOINT The hip joint is a ball and socket joint that connects the body to the legs. The leg bone is called the femur. The
HEADER TOTAL HIP REPLACEMENT SURGERY FROM PREPARATION TO RECOVERY ABOUT THE HIP JOINT The hip joint is a ball and socket joint that connects the body to the legs. The leg bone is called the femur. The
A Patient s Guide to Arthritis of the Big Toe (Hallux Rigidus) With Discussion on Cheilectomy and Fusion
 A Patient s Guide to Arthritis of the Big Toe (Hallux Rigidus) With Discussion on Cheilectomy and Fusion The foot and ankle unit at the Royal National Orthopaedic Hospital (RNOH) is a multi-disciplinary
A Patient s Guide to Arthritis of the Big Toe (Hallux Rigidus) With Discussion on Cheilectomy and Fusion The foot and ankle unit at the Royal National Orthopaedic Hospital (RNOH) is a multi-disciplinary
Dr. Benjamin Hewitt. Subacramial Decompression & Rotator Cuff Repair
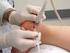 Please contactmethroughthegoldcoasthospitaswityouhaveanyproblemsafteryoursurgery. Dr. Benjamin Hewitt Orthopaedic Surgeon Subacramial Decompression & Rotator Cuff Repair The Rotator Cuff consists of four
Please contactmethroughthegoldcoasthospitaswityouhaveanyproblemsafteryoursurgery. Dr. Benjamin Hewitt Orthopaedic Surgeon Subacramial Decompression & Rotator Cuff Repair The Rotator Cuff consists of four
KNEE ARTHROSCOPY POST-OPERATIVE REHABILITATION PROGRAMME
 KNEE ARTHROSCOPY POST-OPERATIVE REHABILITATION PROGRAMME ABOUT THE OPERATION The arthroscope is a fibre-optic telescope that can be inserted into a joint. A camera is attached to the arthroscope and the
KNEE ARTHROSCOPY POST-OPERATIVE REHABILITATION PROGRAMME ABOUT THE OPERATION The arthroscope is a fibre-optic telescope that can be inserted into a joint. A camera is attached to the arthroscope and the
Hip Replacement Surgery Understanding the Risks
 Hip Replacement Surgery Understanding the Risks Understanding the Risks of Hip Replacement Surgery Introduction This booklet is designed to help your doctor talk to you about the most common risks you
Hip Replacement Surgery Understanding the Risks Understanding the Risks of Hip Replacement Surgery Introduction This booklet is designed to help your doctor talk to you about the most common risks you
Arthroscopic shoulder stabilisation. Patient Information to be retained by patient
 PLEASE PRINT WHOLE FORM DOUBLE SIDED ON YELLOW PAPER Patient Information to be retained by patient affix patient label Shoulder instability The shoulder is the most common joint in the body to dislocate.
PLEASE PRINT WHOLE FORM DOUBLE SIDED ON YELLOW PAPER Patient Information to be retained by patient affix patient label Shoulder instability The shoulder is the most common joint in the body to dislocate.
Total Hip Replacement
 Please contactmethroughthegoldcoasthospitaswityouhaveanyproblemsafteryoursurgery. Dr. Benjamin Hewitt Orthopaedic Surgeon Total Hip Replacement The hip joint is a ball and socket joint that connects the
Please contactmethroughthegoldcoasthospitaswityouhaveanyproblemsafteryoursurgery. Dr. Benjamin Hewitt Orthopaedic Surgeon Total Hip Replacement The hip joint is a ball and socket joint that connects the
Knee arthroscopy advice sheet
 Knee arthroscopy advice sheet During an arthroscopy, a camera is inserted into the knee through two or three small puncture wounds. It allows the surgeon to look at the joint surfaces, cartilage and the
Knee arthroscopy advice sheet During an arthroscopy, a camera is inserted into the knee through two or three small puncture wounds. It allows the surgeon to look at the joint surfaces, cartilage and the
Patient Information. Posterior Cervical Surgery. Here to help. Respond Deliver & Enable
 Here to help Our Health Information Centre (HIC) provides advice and information on a wide range of health-related topics. We also offer: Services for people with disabilities. Information in large print,
Here to help Our Health Information Centre (HIC) provides advice and information on a wide range of health-related topics. We also offer: Services for people with disabilities. Information in large print,
Posterior Cervical Decompression
 Posterior Cervical Decompression Spinal Unit Tel: 01473 702032 or 702097 Issue 2: January 2009 Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed with a
Posterior Cervical Decompression Spinal Unit Tel: 01473 702032 or 702097 Issue 2: January 2009 Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed with a
After Hip Arthroscopy
 After Hip Arthroscopy On your road to recovery... Rehabilitation is essential to help you return to an active life and reach your personal goals. This booklet provides goals, activities and milestones
After Hip Arthroscopy On your road to recovery... Rehabilitation is essential to help you return to an active life and reach your personal goals. This booklet provides goals, activities and milestones
1 of 6 1/22/2015 10:06 AM
 1 of 6 1/22/2015 10:06 AM 2 of 6 1/22/2015 10:06 AM This cross-section view of the shoulder socket shows a typical SLAP tear. Injuries to the superior labrum can be caused by acute trauma or by repetitive
1 of 6 1/22/2015 10:06 AM 2 of 6 1/22/2015 10:06 AM This cross-section view of the shoulder socket shows a typical SLAP tear. Injuries to the superior labrum can be caused by acute trauma or by repetitive
Medial patellofemoral ligament (MPFL) reconstruction
 Medial patellofemoral ligament (MPFL) reconstruction Introduction Mal-tracking (when the knee cap doesn t move smoothly in the grove below) and instability of the patella (knee Normal patella (above) on
Medial patellofemoral ligament (MPFL) reconstruction Introduction Mal-tracking (when the knee cap doesn t move smoothly in the grove below) and instability of the patella (knee Normal patella (above) on
Knee Microfracture Surgery Patient Information Leaflet
 ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 Knee Microfracture Surgery Patient Information Leaflet Table of Contents 1. Introduction
ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 Knee Microfracture Surgery Patient Information Leaflet Table of Contents 1. Introduction
Arthroscopy of the Hand and Wrist
 Arthroscopy of the Hand and Wrist Arthroscopy is a minimally invasive procedure whereby a small camera is inserted through small incisions of a few millimeters each around a joint to view the joint directly.
Arthroscopy of the Hand and Wrist Arthroscopy is a minimally invasive procedure whereby a small camera is inserted through small incisions of a few millimeters each around a joint to view the joint directly.
KNEE ARTHROSCOPIC SURGERY IN INJURY AND DISEASE
 KNEE ARTHROSCOPIC SURGERY IN INJURY AND DISEASE INFORMATION FOR PATIENTS and peri-oerative health WORKERS IN GHANA AND SUB-SAHARAN AFRICA RACHEL GEVEL (chartered physiotherapist) & P OFORI-ATTA (orthopaedic
KNEE ARTHROSCOPIC SURGERY IN INJURY AND DISEASE INFORMATION FOR PATIENTS and peri-oerative health WORKERS IN GHANA AND SUB-SAHARAN AFRICA RACHEL GEVEL (chartered physiotherapist) & P OFORI-ATTA (orthopaedic
.org. Herniated Disk in the Lower Back. Anatomy. Description
 Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
.org. Rotator Cuff Tears: Surgical Treatment Options. When Rotator Cuff Surgery is Recommended. Surgical Repair Options
 Rotator Cuff Tears: Surgical Treatment Options Page ( 1 ) The following article provides in-depth information about surgical treatment for rotator cuff injuries, and is a continuation of the article Rotator
Rotator Cuff Tears: Surgical Treatment Options Page ( 1 ) The following article provides in-depth information about surgical treatment for rotator cuff injuries, and is a continuation of the article Rotator
.org. Arthritis of the Hand. Description
 Arthritis of the Hand Page ( 1 ) The hand and wrist have multiple small joints that work together to produce motion, including the fine motion needed to thread a needle or tie a shoelace. When the joints
Arthritis of the Hand Page ( 1 ) The hand and wrist have multiple small joints that work together to produce motion, including the fine motion needed to thread a needle or tie a shoelace. When the joints
TOWN CENTER ORTHOPAEDIC ASSOCIATES P.C. Labral Tears
 Labral Tears The shoulder is your body s most flexible joint. It is designed to let the arm move in almost any direction. But this flexibility has a price, making the joint prone to injury. The shoulder
Labral Tears The shoulder is your body s most flexible joint. It is designed to let the arm move in almost any direction. But this flexibility has a price, making the joint prone to injury. The shoulder
Total hip replacement
 Patient Information to be retained by patient What is a total hip replacement? In a total hip replacement both the ball (femoral or thigh bone) side of the hip joint and the socket (acetabular or pelvic
Patient Information to be retained by patient What is a total hip replacement? In a total hip replacement both the ball (femoral or thigh bone) side of the hip joint and the socket (acetabular or pelvic
SHOULDER ACROMIOPLASTY/ SHOULDER DECOMPRESSION
 ORTHOPAEDIC WARD: 01-293 8687 /01-293 6602 BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 GUIDELINES FOR PATIENTS HAVING A SHOULDER ACROMIOPLASTY/ SHOULDER DECOMPRESSION
ORTHOPAEDIC WARD: 01-293 8687 /01-293 6602 BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 GUIDELINES FOR PATIENTS HAVING A SHOULDER ACROMIOPLASTY/ SHOULDER DECOMPRESSION
Knee Arthroscopy Exercise Programme
 Chester Knee Clinic & Cartilage Repair Centre Nuffield Health, The Grosvenor Hospital Chester Wrexham Road Chester CH4 7QP Hospital Telephone: 01244 680 444 CKC Website: www.kneeclinic.info Email: [email protected]
Chester Knee Clinic & Cartilage Repair Centre Nuffield Health, The Grosvenor Hospital Chester Wrexham Road Chester CH4 7QP Hospital Telephone: 01244 680 444 CKC Website: www.kneeclinic.info Email: [email protected]
What Is Femoral Acetabular Impingement? Patient Guide into Joint Preservation
 What Is Femoral Acetabular Impingement? Patient Guide into Joint Preservation Normal Hip Joint The hip joint, also known as a ball and socket joint is located where the femur (the thigh bone) meets the
What Is Femoral Acetabular Impingement? Patient Guide into Joint Preservation Normal Hip Joint The hip joint, also known as a ball and socket joint is located where the femur (the thigh bone) meets the
Procedure Information Guide
 Procedure Information Guide Total hip replacement Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made every effort to ensure that the
Procedure Information Guide Total hip replacement Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made every effort to ensure that the
.org. Achilles Tendinitis. Description. Cause. Achilles tendinitis is a common condition that causes pain along the back of the leg near the heel.
 Achilles Tendinitis Page ( 1 ) Achilles tendinitis is a common condition that causes pain along the back of the leg near the heel. The Achilles tendon is the largest tendon in the body. It connects your
Achilles Tendinitis Page ( 1 ) Achilles tendinitis is a common condition that causes pain along the back of the leg near the heel. The Achilles tendon is the largest tendon in the body. It connects your
Dr. Benjamin Hewitt. Shoulder Stabilisation
 Please contactmethroughthegoldcoasthospitaswityouhaveanyproblemsafteryoursurgery. Dr. Benjamin Hewitt Orthopaedic Surgeon Shoulder Stabilisation The shoulder is the most flexible joint in the body, allowing
Please contactmethroughthegoldcoasthospitaswityouhaveanyproblemsafteryoursurgery. Dr. Benjamin Hewitt Orthopaedic Surgeon Shoulder Stabilisation The shoulder is the most flexible joint in the body, allowing
.org. Fractures of the Thoracic and Lumbar Spine. Cause. Description
 Fractures of the Thoracic and Lumbar Spine Page ( 1 ) Spinal fractures can vary widely in severity. While some fractures are very serious injuries that require emergency treatment, other fractures can
Fractures of the Thoracic and Lumbar Spine Page ( 1 ) Spinal fractures can vary widely in severity. While some fractures are very serious injuries that require emergency treatment, other fractures can
Patient Information. Anterior Cervical Surgery. Here to help. Respond Deliver & Enable
 Here to help Our Health Information Centre (HIC) provides advice and information on a wide range of health-related topics. We also offer: Services for people with disabilities. Information in large print,
Here to help Our Health Information Centre (HIC) provides advice and information on a wide range of health-related topics. We also offer: Services for people with disabilities. Information in large print,
Surgery for cervical disc prolapse or cervical osteophyte
 Mr Paul S. D Urso MBBS(Hons), PhD, FRACS Neurosurgeon Provider Nº: 081161DY Epworth Centre Suite 6.1 32 Erin Street Richmond 3121 Tel: 03 9421 5844 Fax: 03 9421 4186 AH: 03 9483 4040 email: [email protected]
Mr Paul S. D Urso MBBS(Hons), PhD, FRACS Neurosurgeon Provider Nº: 081161DY Epworth Centre Suite 6.1 32 Erin Street Richmond 3121 Tel: 03 9421 5844 Fax: 03 9421 4186 AH: 03 9483 4040 email: [email protected]
Shoulder stabilisation surgery. Information for patients Orthopaedics
 Shoulder stabilisation surgery Information for patients Orthopaedics page 2 of 20 Introduction The upper limb unit team wants you and your family to understand as much as possible about the operation you
Shoulder stabilisation surgery Information for patients Orthopaedics page 2 of 20 Introduction The upper limb unit team wants you and your family to understand as much as possible about the operation you
ARTHROSCOPIC (KEY-HOLE) SHOULDER SURGERY
 ARTHROSCOPIC (KEY-HOLE) SHOULDER SURGERY Information Leaflet Your Health. Our Priority. Page 2 of 8 What is arthroscopic ( key-hole ) surgery? Key-hole surgery is the technique of performing surgery though
ARTHROSCOPIC (KEY-HOLE) SHOULDER SURGERY Information Leaflet Your Health. Our Priority. Page 2 of 8 What is arthroscopic ( key-hole ) surgery? Key-hole surgery is the technique of performing surgery though
Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865
 Write questions or notes here: Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865 Document Title: Total Knee Replacement Further Information and Feedback: Tell us how useful
Write questions or notes here: Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865 Document Title: Total Knee Replacement Further Information and Feedback: Tell us how useful
SHOULDER INSTABILITY. E. Edward Khalfayan, MD
 SHOULDER INSTABILITY E. Edward Khalfayan, MD Instability of the shoulder can occur from a single injury or as the result of repetitive activity such as overhead sports. Dislocations of the shoulder are
SHOULDER INSTABILITY E. Edward Khalfayan, MD Instability of the shoulder can occur from a single injury or as the result of repetitive activity such as overhead sports. Dislocations of the shoulder are
X-Plain Hip Replacement Surgery - Preventing Post Op Complications Reference Summary
 X-Plain Hip Replacement Surgery - Preventing Post Op Complications Reference Summary Introduction Severe arthritis in the hip can lead to severe pain and inability to walk. To relieve the pain and improve
X-Plain Hip Replacement Surgery - Preventing Post Op Complications Reference Summary Introduction Severe arthritis in the hip can lead to severe pain and inability to walk. To relieve the pain and improve
Posterior Lumbar Decompression for Spinal Stenosis
 Posterior Lumbar Decompression for Spinal Stenosis Spinal Unit Tel: 01473 702032 or 702097 Issue 5: August 2014 Review date: July 2017 Following your recent MRI scan and consultation with your spinal surgeon
Posterior Lumbar Decompression for Spinal Stenosis Spinal Unit Tel: 01473 702032 or 702097 Issue 5: August 2014 Review date: July 2017 Following your recent MRI scan and consultation with your spinal surgeon
HIP JOINT REPLACEMENT
 HIP JOINT REPLACEMENT Information for Patients WHAT IS HIP JOINT REPLACEMENT? The hip joint is a ball-and-socket joint formed by the upper part of the thigh bone (femoral head) and a part of the pelvis
HIP JOINT REPLACEMENT Information for Patients WHAT IS HIP JOINT REPLACEMENT? The hip joint is a ball-and-socket joint formed by the upper part of the thigh bone (femoral head) and a part of the pelvis
Further information You can get more information and share your experience at www.aboutmyhealth.org
 OS01 Total Hip Replacement Further information You can get more information and share your experience at www.aboutmyhealth.org Local information You can get information locally from: Taunton and Somerset
OS01 Total Hip Replacement Further information You can get more information and share your experience at www.aboutmyhealth.org Local information You can get information locally from: Taunton and Somerset
J F de Beer, K van Rooyen, D Bhatia. Rotator Cuff Tears
 1 J F de Beer, K van Rooyen, D Bhatia Rotator Cuff Tears Anatomy The shoulder consists of a ball (humeral head) and a socket (glenoid). The muscles around the shoulder act to elevate the arm. The large
1 J F de Beer, K van Rooyen, D Bhatia Rotator Cuff Tears Anatomy The shoulder consists of a ball (humeral head) and a socket (glenoid). The muscles around the shoulder act to elevate the arm. The large
Ankle Stabilisation Procedure
 Ankle Stabilisation Procedure Exceptional healthcare, personally delivered Following your consultation with a member of the Foot and Ankle team you have been diagnosed with an unstable ankle. This leaflet
Ankle Stabilisation Procedure Exceptional healthcare, personally delivered Following your consultation with a member of the Foot and Ankle team you have been diagnosed with an unstable ankle. This leaflet
Rehabilitation guidelines for patients undergoing knee arthroscopy
 Rehabilitation guidelines for patients undergoing knee arthroscopy At the RNOH, our emphasis is patient specific, which encourages recognition of those who may progress slower then others. We also want
Rehabilitation guidelines for patients undergoing knee arthroscopy At the RNOH, our emphasis is patient specific, which encourages recognition of those who may progress slower then others. We also want
Inguinal Hernia (Female)
 Inguinal Hernia (Female) WHAT IS AN INGUINAL HERNIA? 2 WHAT CAUSES AN INGUINAL HERNIA? 2 WHAT DOES TREATMENT / MANAGEMENT INVOLVE? 3 DAY SURGERY MANAGEMENT 3 SURGICAL REPAIR 4 WHAT ARE THE RISKS/COMPLICATIONS
Inguinal Hernia (Female) WHAT IS AN INGUINAL HERNIA? 2 WHAT CAUSES AN INGUINAL HERNIA? 2 WHAT DOES TREATMENT / MANAGEMENT INVOLVE? 3 DAY SURGERY MANAGEMENT 3 SURGICAL REPAIR 4 WHAT ARE THE RISKS/COMPLICATIONS
Rehabilitation Guidelines for Knee Arthroscopy
 Rehabilitation Guidelines for Knee Arthroscopy Arthroscopy is a common surgical procedure in which a joint is viewed using a small camera. This technique allows the surgeon to have a clear view of the
Rehabilitation Guidelines for Knee Arthroscopy Arthroscopy is a common surgical procedure in which a joint is viewed using a small camera. This technique allows the surgeon to have a clear view of the
Arthritis of the Shoulder
 Arthritis of the Shoulder In 2011, more than 50 million people in the United States reported that they had been diagnosed with some form of arthritis, according to the National Health Interview Survey.
Arthritis of the Shoulder In 2011, more than 50 million people in the United States reported that they had been diagnosed with some form of arthritis, according to the National Health Interview Survey.
.org. Shoulder Pain and Common Shoulder Problems. Anatomy. Cause
 Shoulder Pain and Common Shoulder Problems Page ( 1 ) What most people call the shoulder is really several joints that combine with tendons and muscles to allow a wide range of motion in the arm from scratching
Shoulder Pain and Common Shoulder Problems Page ( 1 ) What most people call the shoulder is really several joints that combine with tendons and muscles to allow a wide range of motion in the arm from scratching
Total knee replacement
 Patient Information to be retained by patient What is a total knee replacement? In a total knee replacement the cartilage surfaces of the thigh bone (femur) and leg bone (tibia) are replaced. The cartilage
Patient Information to be retained by patient What is a total knee replacement? In a total knee replacement the cartilage surfaces of the thigh bone (femur) and leg bone (tibia) are replaced. The cartilage
Varicose Veins Operation. Patient information Leaflet
 Varicose Veins Operation Patient information Leaflet 22 nd August 2014 WHAT IS VARICOSE VEIN SURGERY (HIGH LIGATION AND MULTIPLE AVULSIONS) The operation varies from case to case, depending on where the
Varicose Veins Operation Patient information Leaflet 22 nd August 2014 WHAT IS VARICOSE VEIN SURGERY (HIGH LIGATION AND MULTIPLE AVULSIONS) The operation varies from case to case, depending on where the
Total Shoulder Arthroplasty
 Specialists in Joint Replacement, Spinal Surgery, Orthopaedics and Sport Injuries Total Shoulder Arthroplasty Ms. Ruth Delaney Consultant Orthopaedic Surgeon www.sportssurgeryclinic.com Introduction Arthritis
Specialists in Joint Replacement, Spinal Surgery, Orthopaedics and Sport Injuries Total Shoulder Arthroplasty Ms. Ruth Delaney Consultant Orthopaedic Surgeon www.sportssurgeryclinic.com Introduction Arthritis
Open Discectomy. North American Spine Society Public Education Series
 Open Discectomy North American Spine Society Public Education Series What Is Open Discectomy? Open discectomy is the most common surgical treatment for ruptured or herniated discs of the lumbar spine.
Open Discectomy North American Spine Society Public Education Series What Is Open Discectomy? Open discectomy is the most common surgical treatment for ruptured or herniated discs of the lumbar spine.
Posterior Lumbar Decompression for Spinal Stenosis
 Posterior Lumbar Decompression for Spinal Stenosis Issue 6: March 2016 Review date: February 2019 Following your recent MRI scan and consultation with your spinal surgeon you have been diagnosed with
Posterior Lumbar Decompression for Spinal Stenosis Issue 6: March 2016 Review date: February 2019 Following your recent MRI scan and consultation with your spinal surgeon you have been diagnosed with
Your Practice Online
 P R E S E N T S Your Practice Online Disclaimer This information is an educational resource only and should not be used to make a decision on Revision Hip Replacement or arthritis management. All decisions
P R E S E N T S Your Practice Online Disclaimer This information is an educational resource only and should not be used to make a decision on Revision Hip Replacement or arthritis management. All decisions
Recurrent Varicose Veins
 Information for patients Recurrent Varicose Veins Sheffield Vascular Institute Northern General Hospital You have been diagnosed as having Varicose Veins that have recurred (come back). This leaflet explains
Information for patients Recurrent Varicose Veins Sheffield Vascular Institute Northern General Hospital You have been diagnosed as having Varicose Veins that have recurred (come back). This leaflet explains
ACL RECONSTRUCTION POST-OPERATIVE REHABILITATION PROGRAMME
 ACL RECONSTRUCTION POST-OPERATIVE REHABILITATION PROGRAMME ABOUT THE OPERATION The aim of your operation is to reconstruct the Anterior Cruciate Ligament (ACL) to restore knee joint stability. A graft,
ACL RECONSTRUCTION POST-OPERATIVE REHABILITATION PROGRAMME ABOUT THE OPERATION The aim of your operation is to reconstruct the Anterior Cruciate Ligament (ACL) to restore knee joint stability. A graft,
Lumbar Laminectomy and Interspinous Process Fusion
 Lumbar Laminectomy and Interspinous Process Fusion Introduction Low back and leg pain caused by pinched nerves in the back is a common condition that limits your ability to move, walk, and work. This condition
Lumbar Laminectomy and Interspinous Process Fusion Introduction Low back and leg pain caused by pinched nerves in the back is a common condition that limits your ability to move, walk, and work. This condition
Calcaneus (Heel Bone) Fractures
 Copyright 2010 American Academy of Orthopaedic Surgeons Calcaneus (Heel Bone) Fractures Fractures of the heel bone, or calcaneus, can be disabling injuries. They most often occur during high-energy collisions
Copyright 2010 American Academy of Orthopaedic Surgeons Calcaneus (Heel Bone) Fractures Fractures of the heel bone, or calcaneus, can be disabling injuries. They most often occur during high-energy collisions
KNEE LIGAMENT REPAIR AND RECONSTRUCTION INFORMED CONSENT INFORMATION
 KNEE LIGAMENT REPAIR AND RECONSTRUCTION INFORMED CONSENT INFORMATION The purpose of this document is to provide written information regarding the risks, benefits and alternatives of the procedure named
KNEE LIGAMENT REPAIR AND RECONSTRUCTION INFORMED CONSENT INFORMATION The purpose of this document is to provide written information regarding the risks, benefits and alternatives of the procedure named
The Knee: Problems and Solutions
 The Knee: Problems and Solutions Animals, like people, may suffer a variety of disorders of the knee that weaken the joint and cause significant pain if left untreated. Two common knee problems in companion
The Knee: Problems and Solutions Animals, like people, may suffer a variety of disorders of the knee that weaken the joint and cause significant pain if left untreated. Two common knee problems in companion
world-class orthopedic care right in your own backyard.
 world-class orthopedic care right in your own backyard. Patient Promise: At Adventist Hinsdale Hospital, our Patient Promise means we strive for continued excellence in everything we do. This means you
world-class orthopedic care right in your own backyard. Patient Promise: At Adventist Hinsdale Hospital, our Patient Promise means we strive for continued excellence in everything we do. This means you
Arthroscopic Ankle Fusion (Arthrodesis)
 Arthroscopic Ankle Fusion (Arthrodesis) Exceptional healthcare, personally delivered Following your consultation with a member of the Foot and Ankle team you have been diagnosed with ankle arthritis and
Arthroscopic Ankle Fusion (Arthrodesis) Exceptional healthcare, personally delivered Following your consultation with a member of the Foot and Ankle team you have been diagnosed with ankle arthritis and
Patient Information. Lumbar Spine Segmental Decompression. Royal Devon and Exeter NHS Foundation Trust
 Lumbar Spine Segmental Decompression Royal Devon and Exeter NHS Foundation Trust Patient Information Lumbar Spine Segmental Decompression Reference Number: TO 05 004 004 (version date: June 2015) Introduction
Lumbar Spine Segmental Decompression Royal Devon and Exeter NHS Foundation Trust Patient Information Lumbar Spine Segmental Decompression Reference Number: TO 05 004 004 (version date: June 2015) Introduction
.org. Knee Arthroscopy. Description. Preparing for Surgery. Surgery
 Knee Arthroscopy Page ( 1 ) Arthroscopy is a common surgical procedure in which a joint (arthro-) is viewed (-scopy) using a small camera. Arthroscopy gives doctors a clear view of the inside of the knee.
Knee Arthroscopy Page ( 1 ) Arthroscopy is a common surgical procedure in which a joint (arthro-) is viewed (-scopy) using a small camera. Arthroscopy gives doctors a clear view of the inside of the knee.
.org. Distal Radius Fracture (Broken Wrist) Description. Cause
 Distal Radius Fracture (Broken Wrist) Page ( 1 ) The radius is the larger of the two bones of the forearm. The end toward the wrist is called the distal end. A fracture of the distal radius occurs when
Distal Radius Fracture (Broken Wrist) Page ( 1 ) The radius is the larger of the two bones of the forearm. The end toward the wrist is called the distal end. A fracture of the distal radius occurs when
Rehabilitation Guidelines for Meniscal Repair
 UW Health Sports Rehabilitation Rehabilitation Guidelines for Meniscal Repair There are two types of cartilage in the knee, articular cartilage and cartilage. Articular cartilage is made up of collagen,
UW Health Sports Rehabilitation Rehabilitation Guidelines for Meniscal Repair There are two types of cartilage in the knee, articular cartilage and cartilage. Articular cartilage is made up of collagen,
Knee Arthroscopy Post-operative Instructions
 Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Knee Arthroscopy Post-operative Instructions PLEASE READ ALL OF THESE INSTRUCTIONS CAREFULLY. THEY WILL ANSWER MOST OF YOUR QUESTIONS. 1. You may walk
Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Knee Arthroscopy Post-operative Instructions PLEASE READ ALL OF THESE INSTRUCTIONS CAREFULLY. THEY WILL ANSWER MOST OF YOUR QUESTIONS. 1. You may walk
Shoulder Dislocation or Instability Surgery: A Guide to Recovery After Surgery
 What is Shoulder Instability? What is a Shoulder Dislocation? The shoulder joint is a ball in socket joint and is the most mobile joint in the human body. The socket, however, is quite shallow which means
What is Shoulder Instability? What is a Shoulder Dislocation? The shoulder joint is a ball in socket joint and is the most mobile joint in the human body. The socket, however, is quite shallow which means
The main surgical options for treating early stage cervical cancer are:
 INFORMATION LEAFLET ON TOTAL LAPAROSCOPIC RADICAL HYSTERECTOMY (TLRH) FOR EARLY STAGE CERVICAL CANCER (TREATING EARLY STAGE CERVICAL CANCER BY RADICAL HYSTERECTOMY THROUGH KEYHOLE SURGERY) Aim of the leaflet
INFORMATION LEAFLET ON TOTAL LAPAROSCOPIC RADICAL HYSTERECTOMY (TLRH) FOR EARLY STAGE CERVICAL CANCER (TREATING EARLY STAGE CERVICAL CANCER BY RADICAL HYSTERECTOMY THROUGH KEYHOLE SURGERY) Aim of the leaflet
Femoral Hernia Repair
 Femoral Hernia Repair WHAT IS A FEMORAL HERNIA REPAIR? 2 WHAT CAUSES A FEMORAL HERNIA? 2 WHAT DOES TREATMENT/ MANAGEMENT INVOLVE? 3 DAY SURGERY MANAGEMENT 3 SURGICAL REPAIR 4 WHAT ARE THE RISKS/COMPLICATIONS
Femoral Hernia Repair WHAT IS A FEMORAL HERNIA REPAIR? 2 WHAT CAUSES A FEMORAL HERNIA? 2 WHAT DOES TREATMENT/ MANAGEMENT INVOLVE? 3 DAY SURGERY MANAGEMENT 3 SURGICAL REPAIR 4 WHAT ARE THE RISKS/COMPLICATIONS
Trochanteric Bursitis Self Management for Patients
 Trochanteric Bursitis Self Management for Patients Updated May 2010 What is the Trochanteric Bursa? The trochanteric bursa is a fluid-filled sac that functions as a gliding surface to reduce friction between
Trochanteric Bursitis Self Management for Patients Updated May 2010 What is the Trochanteric Bursa? The trochanteric bursa is a fluid-filled sac that functions as a gliding surface to reduce friction between
A compressive dressing that you apply around your ankle, and
 Ankle Injuries & Treatment The easiest way to remember this is: R.I.C.E. Each of these letters stands for: Rest. Rest your ankle. Do not place weight on it if it is very tender. Avoid walking long distances.
Ankle Injuries & Treatment The easiest way to remember this is: R.I.C.E. Each of these letters stands for: Rest. Rest your ankle. Do not place weight on it if it is very tender. Avoid walking long distances.
Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865
 Write questions or notes here: Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865 Document Title: Revision Total Hip Replacement Further Information and Feedback: Tell us how
Write questions or notes here: Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865 Document Title: Revision Total Hip Replacement Further Information and Feedback: Tell us how
.org. Ankle Fractures (Broken Ankle) Anatomy
 Ankle Fractures (Broken Ankle) Page ( 1 ) A broken ankle is also known as an ankle fracture. This means that one or more of the bones that make up the ankle joint are broken. A fractured ankle can range
Ankle Fractures (Broken Ankle) Page ( 1 ) A broken ankle is also known as an ankle fracture. This means that one or more of the bones that make up the ankle joint are broken. A fractured ankle can range
Pre - Operative Rehabilitation Program for Anterior Cruciate Ligament Reconstruction
 Pre - Operative Rehabilitation Program for Anterior Cruciate Ligament Reconstruction This protocol is designed to assist you with your preparation for surgery and should be followed under the direction
Pre - Operative Rehabilitation Program for Anterior Cruciate Ligament Reconstruction This protocol is designed to assist you with your preparation for surgery and should be followed under the direction
Total Knee Replacement
 Dr C.S. Waller MB BS FRCS(Ed) FRACS FA(Orth)A Specialist Hip and Knee Surgeon Total Knee Replacement If your knee is severely damaged by arthritis or injury, it may be hard for you to perform simple activities
Dr C.S. Waller MB BS FRCS(Ed) FRACS FA(Orth)A Specialist Hip and Knee Surgeon Total Knee Replacement If your knee is severely damaged by arthritis or injury, it may be hard for you to perform simple activities
Adult Forearm Fractures
 Adult Forearm Fractures Your forearm is made up of two bones, the radius and ulna. In most cases of adult forearm fractures, both bones are broken. Fractures of the forearm can occur near the wrist at
Adult Forearm Fractures Your forearm is made up of two bones, the radius and ulna. In most cases of adult forearm fractures, both bones are broken. Fractures of the forearm can occur near the wrist at
