Differentiation of bone marrow stem cells into functional pancreatic insulin-producing cells
|
|
|
- Augustus Farmer
- 8 years ago
- Views:
Transcription
1 Differentiation of bone marrow stem cells into functional pancreatic insulin-producing cells Von der Fakultät für Lebenswissenschaften der Technischen Universität Carolo-Wilhelmina zu Braunschweig zur Erlangung des Grades einer Doktorin der Naturwissenschaften (Dr. rer. nat.) genehmigte D i s s e r t a t i o n von Tayaramma Thatava aus Vijayawada / Indien
2 1. Referent: Professor Dr. Martin Korte 2. Referent: Privatdozent Dr. Peter Paul Müller Eingereicht am: Mündliche Prüfung (Disputation) am: Druckjahr 2007
3 Vorveröffentlichungen der Dissertation Teilergebnisse aus dieser Arbeit wurden mit Genehmigung der Fakultät für Lebenswissenschaften, vertreten durch die Mentorin/den Mentor* der Arbeit, in folgenden Beiträgen vorab veröffentlicht: Publikationen Chromatin-remodeling factors allow differentiation of bone marrow cells into insulinproducing cells. Tayaramma Thatava, Bin Ma, Manfred Rhode, Hubert Mayer 1* Stem Cells, Vol.24, No.12; December 2006, Page No Tagungsbeiträge Efficient differentiation of adult stem cells into glucose regulated insulin producing cells using histone deacetylating agents Tayaramma Thatava, Hubert Mayer, 3rd International Stem Cell Meeting, Münster, Germany, May 15 16, 2006 (poster presentation). Glucose regulated release of insulin from intracellular vesicles in differentiated bone marrow cells Thatava Tayaramma, Hubert Mayer. German Society for Cell Biology Annual Meeting, Braunschweig, Germany, March 29-April 1, 2006 (Poster presentation) Human MSC differentiation into endodermal lineages Thatava Tayaramma, Hubert Mayer. 2nd International Meeting of the Stem Cell Network: New Horizons in Cell Differentiation, Bonn, Germany, April 1-2, 2004 (Poster presentation)
4 Contents 1 Contents Abbreviations 5 Summary 7 1 Introduction Regulation of blood glucose Role of Glucagon Anatomy and functions of pancreas Anatomy General functions Functions of pancreatic β-cells Insulin secretion Pancreas organogenesis Genes and transcription factors involved in the development of pancreas Pancreatic diseases Diabetes mellitus Type 1 diabetes Type 2 diabetes Pathology of diabetes Short-term acute complications Long-term chronic complications 28
5 Contents Microvascular disease Macrovascular disease Treatment of diabetes mellitus Treatment of type 1 diabetes Treatment of type 2 diabetes Side effects Strategies to cure diabetes Transplantation of islets and whole pancreas Transplantation of insulin-secreting cell lines Pancreatic progenitors as a source of islet cells Embryonic stem (ES) cells as a source for islet cells Generation of islet-like cells from adult stem and progenitor cells Adult stem cells Transdifferentiation Chromatin remodeling of stem cells Aim of the study Material and Methods Chromatin remodeling factors Trichostatin A Dimethyl sulfoxide (DMSO) Sodium butyrate Azacytidine Mice 43
6 Contents Isolation of mouse bone marrow cells Culturing and differentiation of BM stem cells Isolation of pancreatic islets Dithizone staining Newport Green DCF labeling Immunocytochemistry Confocal microscopy Three-dimensional (3D) reconstruction of differentiated cluster ELISA Quantification of secreted insulin Intracellular insulin detection Co-immunoprecipitation Western blot RNA extraction Reverse Transcription/polymerase chain reaction (RT PCR) Electron microscopy Nuclear imaging Microarray analysis RNA isolation DNA microarray hybridization Data analysis Sources of chemicals Statistical analysis 65
7 Contents 4 4. Results 4.1 Chromatin remodeling factors induce differentiation of bone marrow cells Detection of insulin containing cells in islet-like clusters Detection of pancreas-specific hormones Three-dimensional (3D) reconstruction image of islet like cell cluster Glucose regulated insulin secretion from differentiated BMSC Endocrine-specific gene expression in differentiated islet-like clusters Ultrastructural analysis of insulin-producing cell clusters Chromatin morphology after treatment with TSA Genes expressed at different time points of differentiation Discussion Chromatin remodeling factors induce differentiation of BMSC Detection of insulin-producing cells in the culture Presence of transcription factors and genes specific for pancreas Expression of pancreas-specific hormones in differentiated cells Regulation of insulin secretion in differentiated islet-like cells Presence of insulin in secretory vesicles of differentiated BMSC Effect of TSA treatment on cells Outlook 102 Literature 104 Acknowledgements 122 Curriculum Vitae
8 Abbreviations 5 Abbreviations β -cells Beta cells BM Bone marrow BMSC Bone marrow stem cells BSA Bovine serum albumin bp Base pair bhlh basic helix-loop-helix cdna Complementary Deoxyribonucleic Acid Cy3 Cyanine-3-Tyramide DAPI 4', 6-Diamidino-2-phenylindole DMSO Dimethyl sulfoxide DNA Deoxyribonucleic acid dl deciliter ECM extracellular matrix ELISA Enzyme-Linked Immunosorbent Assay EDTA Ethylenediaminetetraacetic acid EGF epidermal growth factor ESC Embryonic stem cells FBS Fetal Bovine Serum FITC Fluorescein isothiocyanate g Gram GLP 1 glucagon-like peptide 1 GLUT 2 glucose transporter 2 HBSS Hank`s balanced salt solution hr Hour HEPES 4-(2-hydroxyethyl)-1-piperazineethanesulfonic acid HGF hepatocyte growth factor HNF hepatocytes nuclear factor
9 Abbreviations 6 HSC Hematopoietic stem cells IAPP Islet amyloid polypeptide IGF insulin-like growth factor Isl-1 Islet-1 kda Kilo Dalton l liter M Molar MODY maturity-onset diabetes of young mrna messenger Ribonucleic Acid Min Minute MSC Mesenchymal stem cells µ Micron N Normal NGF nerve growth factor NGN neurogenin PBS Phosphate buffered saline PCR Polymerase chain reaction PDX1/IPF1 pancreatic duodenal homeobox 1/insulin promoter factor 1 PFA Paraformaldehyde PP pancreatic polypeptide RNA Ribonucleic Acid RNase Ribonuclease rpm rounds per minute RT Room temperature/reverse transcriptase s Seconds SD Standard deviation SDS-PAGE Sodium dodecyl sulfate polyacrylamide gel electrophoresis TEM Transmission electron microscopy TF Transcription factor TSA Trichostatin A
10 Summary 7 Summary Diabetes mellitus (DM) is a common metabolic disorder affecting millions of people worldwide and is characterized by abnormally high levels of glucose in blood. Type 1 diabetes is caused by the destruction of pancreatic β-cells by T cells of the immune system. The common therapy of diabetes is daily injections of insulin. However, this therapy does not overcome the serious long-term complications that, result in overall shortened life expectancy of diabetic patients. Therefore, great efforts have been undertaken to develop novel strategies. A promising alternative to present treatments would be the generation and implantation of pancreatic islets from adult stem cells. Conditions were investigated that allow BM stem cells (BMSC) to differentiate into insulin-producing cells. A novel in vitro differentiation method was developed by using the histone deacetylase inhibitor (HDACi), Trichostatin A (TSA). BMSC, cultured in the presence of TSA. BMSCs differentiated into islet-like clusters under these culture conditions. These clusters were similar to the cells of the islets of the pancreas. The cells in the clusters showed endoderm specific gene expression typical for pancreatic β-cell development and function, such as insulin (I and II), glucagon, somatostatin, GLUT-2, pancreatic duodenal homeobox-1 (PDX-1), and Pax 4. To show that cells of the islet-like clusters synthesized pancreatic hormones, the co-localization of insulin and C-Peptide
11 Summary 8 was analyzed by immunocytochemistry. Enzyme-linked immunosorbent assay (ELISA) analysis demonstrated that insulin secretion was regulated by glucose concentration. Western blot analysis showed the presence of intracellular stored insulin. Electron microscopy of the islet-like cells revealed that they possessed an ultrastructure similar to that of pancreatic β-cells, which contain insulin granules within secretory vesicles. These findings suggest that histone-deacetylating agents help to promote differentiation of BMSC into functional insulin-producing β-cells. In addition, gene expression analysis confirmed the presence of new signaling pathways that are important in endocrine pancreas development. A subset of known and novel genes was temporally regulated, including genes that spatially define developing endocrine cells from BMSC. The development of new protocols to stimulate the differentiation of BMSC into pancreatic β- like cells may contribute to future cell therapeutic treatments of type 1 diabetes.
12 Introduction 9 1. Introduction A major source of energy for all cells is glucose, and all major food types are first broken-down to glucose prior to being used. Glucose is released from the gut into the blood stream, is taken up by cells in all tissues of the body, and is used as a fuel to generate energy that allows us to undertake all our major activities such as walking, running, and reading. Any excess sugar that is not used up immediately is stored in the cells as a backup source of energy. In healthy individuals, the level of circulating blood sugar is strictly regulated. This state of equilibrium, normoglycemia (normal glucose level), is tightly controlled by the hormone insulin, which is secreted in specific cells in the pancreas, the β-cells. This balance in glucose level is achieved through the regulation of the amount of insulin that is secreted to down-regulate increased blood sugar levels after consumption of sugar containing nutrients. 1.1 Regulation of blood glucose Blood glucose levels are not always constant; they rise and fall depending upon the body s needs and are regulated by hormones. This results in glucose levels normally ranging from 70 to 110 mg/dl. The blood glucose level can rise for three reasons: diet, breakdown of glycogen, or hepatic synthesis of glucose. Eating produces a rise in blood glucose, the extent of which depends on a number of factors such as the amount and the type of carbohydrate eaten (i.e., the glycemic index), the rate of digestion, and the rate of
13 Introduction 10 absorption. Because glucose is a polar molecule, its absorption across the hydrophobic gut wall requires specialized glucose transporters (GLUTS). The liver releases glucose from the breakdown of glycogen and also synthesizes glucose from intermediates of carbohydrate, protein, and fat metabolism. The liver is a major regulator of glucose and can buffer blood glucose levels. It receives glucose-rich blood directly from the digestive tract via the portal vein. The portal vein drains almost all of the blood coming from the digestive tract and empties directly into the liver. The liver can quickly remove large amounts of glucose from the circulation so that even after a meal, blood glucose levels rarely rise above 110 mg/dl. The rise in blood glucose following a meal is detected by the pancreatic beta (β) cells, which respond by releasing insulin. Insulin increases the uptake and use of glucose by tissues such as skeletal muscle and fat cells. This rise in glucose also inhibits the release of glucagon, inhibiting the production of glucose from other sources, e.g., by glycogen breakdown. Once inside the cell, some of the glucose is used immediately via glycolysis. During the well-fed state, the high levels of insulin and low levels of glucagon stimulate glycolysis, which releases energy and produces carbohydrate intermediates that can be used in other metabolic pathways. Brain consumes more than 80% glucose. The liver and muscle take up any glucose that is not used immediately, where it can be converted into glycogen. Insulin stimulates glycogenesis in the liver by inducing hepatic glycogen synthetase (the enzyme that catalyzes glycogen synthesis in the liver). Insulin prevents the breakdown of stored glycogen (glycogenolysis) and the synthesis of new glucose (gluconeogenesis). Insulin also encourages glycogen formation in muscle, but by a different method. Here, it
14 Introduction 11 increases the number of glucose transporters (GLUT4) on the cell surface. This leads to a rapid uptake of glucose that is converted into muscle glycogen. When glycogen stores are fully replenished, excess glucose is converted into fat in a process called lipogenesis. Glucose is converted into fatty acids that are further processed to triglycerides for storage. Insulin promotes lipogenesis by increasing the number of glucose transporters (GLUT4) expressed on the surface of the fat cell, causing a rapid uptake of glucose. In addition to promoting fat synthesis, insulin also inhibits fat breakdown by inhibiting hormone-sensitive lipase. As a result, levels of fatty acids in the blood stream decrease. Insulin also has an anabolic effect on protein metabolism. It stimulates both the entry of amino acids into cells and protein production from amino acids.
15 Introduction 12 Figure 1.1 Mechanisms of glucose balance Under basal conditions, 80% of circulating glucose is taken up by the brain. When food is ingested, there is a parallel rise in blood glucose level (yellow arrow). This increase in blood glucose is sensed by the β-cells in the pancreas, and as a result, insulin is secreted (pale blue arrows). Insulin circulates through the body and signals to the major insulin sensitive organs (muscle, liver, and fat) to increase their glucose intake (red arrows). Insulin simultaneously leads to a reduction of glucose production from the liver and other organs (blue arrows). In this way, the hormone insulin counteracts the rise of glucose in the blood, thereby returning the system to its equilibrium. (This figure is adopted from Sanger Institute).
16 Introduction Role of Glucagon A drop in blood sugar levels inhibits insulin secretion and stimulates glucagon release. Glucagon opposes many actions of insulin. Most importantly, glucagon raises blood sugar levels by stimulating the mobilization of glycogen stores in the liver, providing a rapid burst of glucose. During continued fasting, glycogen stores are depleted under such conditions; glucagon stimulates glucose production by stimulating the hepatic uptake of amino acids, the carbon skeletons of which are used to synthesize glucose. 1.2 Anatomy and functions of pancreas Anatomy The human pancreas is an elongated tapered organ lying behind the stomach and across the back of the abdomen. The pancreas is made up of two types of tissues: exocrine and endocrine tissue. The cells of the exocrine tissue secrete digestive enzymes into the digestive tract. These enzymes break down all categories of digestible foods. The endocrine pancreas produces hormones that affect carbohydrate metabolism. The endocrine tissue, which consists of the islets of Langerhans, secretes these hormones into the bloodstream. The islets of Langerhans contain insulin-producing β-cells (60 80% of the islet cells), glucagon-releasing alpha-cells (10-20%), somatostatin-secreting deltacells (3-10%), and a few pancreatic polypeptide-containing (PP) cells. Most of the insulin-containing cells occur in cell groups in the islets of Langerhans. The number and size of the pancreatic islets vary among species and seem to be regulated by developmental, nutrient, and hormonal factors. Pancreatic β-cells compose more than 60% of the adult islet volume. Single islet β-cells rapidly and spontaneously reaggregate into spherical particles that can establish a mantle by associating with other islet
17 Introduction 14 endocrine cells. This reaggregation of islet β-cells is thought to be calcium-dependent and stimulated by glucose and cyclic AMP. Figure.1.2 Schematic diagram of the anatomy of the pancreas The pancreas is located in the curve of duodenum. The exocrine pancreas contains acinar cells, whereas the endocrine pancreas contains four different populations of cells: alpha-cells, β-cells, delta-cells, and PP cells. (This figure is adopted from the website General functions The pancreas has digestive and hormonal functions. The enzymes secreted by the exocrine tissue in the pancreas help to break down carbohydrates, fats, proteins, and acids in the duodenum. These enzymes travel down the pancreatic duct into the bile duct in an
18 Introduction 15 inactive form. When they enter the duodenum, they are activated. The exocrine tissue also secretes bicarbonate to neutralize stomach acid in the duodenum. The hormones secreted by the endocrine tissue in the pancreas are insulin and glucagon (which regulate the level of glucose in the blood), and somatostatin (which prevents the release of the other two hormones) Functions of pancreatic β-cells The main function of pancreatic β-cells is the production and controlled release of insulin. The insulin gene is present as a single copy in all species, with the exception of rat and mouse, where there are two non-allelic insulin genes. The human insulin gene is located near the end of the short arm of chromosome 11 and is flanked on the 5 -side with the gene for tyrosine hydroxylase and on the 3 -side with the gene for IGF-II. The structure of the gene is highly conserved. Insulin is a small hormone composed of two polypeptide chains (A and B) linked by two disulfide bonds and has a molecular weight of about 6000 daltons. The A chain consists of 21 amino acids and the B chain of 30 amino acids. Insulin is a small protein and is produced as part of a larger protein to ensure it folds properly. In the protein assembly of insulin, the messenger RNA transcript is translated into an inactive protein called preproinsulin (Figure 1.3). Preproinsulin contains an amino terminal signal sequence that is required in order for the precursor hormone to pass through the membrane of the endoplasmic reticulum(er) for post-translational processing. The post-translational processing clips away those portions not needed for the bioactive hormone. Upon entering the ER, the preproinsulin signal sequence, now useless, is proteolytically removed from proinsulin. Once the post-translational formation of three vital disulfide
19 Introduction 16 bonds occurs, specific peptidases cleave proinsulin. The final product of the biosyntheis is mature and active insulin. Finally, insulin is packaged and stored in secretory granules, which accumulate in the cytoplasm, until release is triggered. The secretory vesicles contain up to 80% of insulin related proteins. These are principally insulin and C-Peptide, both being present in equimolar amounts, and a much smaller amount of proinsulin and its intermediate conversion products. Insulin molecules are stored in crystalline form, occupying the electron-dense portion of the secretory granules. An adult pancreatic β-cell has a store of approximately 50 pg insulin per cell. Insulin molecules in storage granules are secreted by granule membrane fusion with the plasma membrane of the cell. Insulin molecules have a tendency to form dimers in solution because of hydrogen-bonding between the C-termini of the B chains. Additionally, in the presence of zinc ions, insulin dimers associate into hexamers.
20 Introduction 17 Figure 1.3 Schematic representation of insulin synthesis Insulin production involved intermediate steps. Initially, preproinsulin is the inactive form that is secreted into the endoplasmic reticulum. Post-translational processing clips the N-terminal signal sequence and forms the disulfide bridges. Lastly, the polypeptide is clipped at two positions to release the intervening chain C. This and active insulin are finally packaged into secretory granules for storage. (This picture is adopted from Beta cell biology consortium)
21 Introduction Insulin secretion Increasing levels of glucose (above 10 mm) inside the pancreatic β-cells trigger the release of insulin. However, insulin release is also induced by other factors, such as high amino acid and fatty acid levels in the blood, hormones released from the stomach and intestine, and neurotransmitters (Lang, 1999). Glucose is transported into the β-cell by type 2 glucose transporters (GLUT2). Once inside, the first step in glucose metabolism is the phosphorylation of glucose to produce glucose-6-phosphate. This step is catalyzed by glucokinase; this is the rate-limiting step in glycolysis, and it effectively traps glucose inside the cell. As glucose metabolism proceeds, ATP is produced in the mitochondria. The increase in the ATP:ADP ratio closes ATP-gated potassium channels in the β-cell membrane. Positively charged potassium ions (K + ) are now prevented from leaving the β-cell. The rise in the positive charge inside the β-cell causes depolarization. Voltage-gated calcium channels open, allowing calcium ions (Ca 2+ ) to flood into the cell. The increase in the intracellular calcium concentration triggers the secretion of insulin via exocytosis (Figure 1.4).
22 Introduction 19 Figure 1.4 Schematic presentation of mechanism of insulin secretion Insulin secretion in beta cells is triggered by rising blood glucose levels. Starting with the uptake of glucose by the GLUT2 transporter, the glycolytic phosphorylation of glucose causes a rise in the ATP:ADP ratio. The rise inactivates the potassium channel that depolarizes the membrane, causing the calcium channel to open up allowing calcium ions to flow inward. The ensuing rise in levels of calcium leads to the exocytotic release of insulin from their storage granule. (This picture is adopted from Beta cell biology consortium.)
23 Introduction 20 There are two phases of insulin release in response to a rise in glucose. The first is an immediate release of insulin. This is attributable to the release of preformed insulin, which is stored in secretory granules. Once depleted, a second phase of insulin release is initiated. This latter release is prolonged since insulin has to be synthesized, processed, and secreted for the duration of the increase of blood glucose. Furthermore, beta cells also have to regenerate the stores of insulin initially depleted in the fast response phase. As important as insulin is to preventing too high of a blood glucose level, it is just as important that there not be too much insulin and hypoglycemia. As one step in monitoring insulin levels, the enzyme insulinase (found in the liver and kidneys) breaks down blood-circulating insulin resulting in a half-life of about six minutes for the hormone. This degradative process ensures that levels of circulating insulin are modulated and that blood glucose levels do not get dangerously low. 1.3 Pancreas organogenesis After gastrulation, mammalian endoderm, which is a sheet of undifferentiated cells, eventually forms the epithelial components of the gastrointestinal tract (esophagus, stomach, and intestine) and the glands derived from it (thyroid, thymus, pancreas, and liver) (Well et al., 1999). Pancreas arises from the endoderm as a dorsal and a ventral bud that fuse together to form a single organ (Slack, 1995). In mice, the pancreas begins to develop at embryonic day E9.5 from evaginations of the foregut endoderm at the level of the anterior intestinal portal (AIP), forming two primordia (dorsal and ventral) capped by mesenchymal cells (Pictet et al., 1972, Wells and Melton, 1999, Wessels and Cohen, 1967), which subsequently form a single gland at
24 Introduction 21 around E13.5. This period of pancreatic organogenesis is called primary transition, referring to the changing of the pre-pancreatic endoderm (Edlund, 1999, 2000). Proliferation of the pancreatic epithelium results in the formation of branching cords from which clusters of endocrine and exocrine cells progressively differentiate (Herrera et al., 1991, Slack, 1995). This differentiation wave occurs during the secondary transition, between E13.5 and E15.5 (Pictet and Rutter et al., 1972).
25 Introduction Genes and transcription factors involved in the development of pancreas The genes and transcription factors involved in the pancreas development were listed in Table 1. Table 1. Major pancreatic transcription factors; their expression and functions Transcription Onset and site of Mouse & human References factor pancreatic expression mutations Homeodomain factors Pdx1 e8.5, early pancreatic heterozygous human Guz et al., epithelium, beta and delta mutation: MODY4 1995; Jonsson cells of mature pancreas Pancreatic agenesis, et al., 1994; Stoffers et al.1997a,b Ahlgren et al. 1998; Pbx1 e10.5, ubiquitous Hypoplastic pancreas Kim et al., 2002 HNF6 e9.5, throughout the Impaired endocrine Jacquemin et pancreatic buds differentiation al.,2000 Pax4 e9.5, in developing Deficiency of beta & Dohrmann et endocrine cells, not delta cells, increase al.,2000; Sosafound in mature pancreas in alpha cells Pineda et al., 1997 Pax6 e9, in endocrine cells No alpha cells, decrease St-Onge et al., in other endocrine 1997 cell types Nkx2.2 e9.5, throughout pancreatic Lack of beta cells, decrease Sussel et. al, bud, later in endocrine cells in alpha and PP cells 1998 Nkx6.1 e9.5, in beta cells Decrease in beta cells Sander et al., 2000 Isl1 e9, in all islet cells No differentiated islet cells Ahlgren et al., 1997
26 Introduction 23 HNF1a e10.5, dorsal pancreas, Heterozygous human Nammo et al., mature beta cells mutation and homozygous 2002; mouse mutation: MODY3 Pontoglio et al., 1998 HNF4a e5.5, in visceral endoderm, Early embryonic lethal Ferrer, 2002; e9.5 in pancreatic Heterozygous human Duncan et al., primordium mutation: MODY Basic helix-loop-helix factors Ngn3 e9.5, endocrine precursors No endocrine cells Gradwohl et al., 2000; Gu et al., 2002 NeuroD e9.5, endocrine precursors Impaired islet Jensen et al., and adult islet cells development 2000a; Naya et al., 1997 Ptf1-p48 e10, exocrine, endocrine No exocrine cells Kawaguchi et and ductal progenitors al., 2002; Krapp et al., 1996; Krapp et al., 1998 Forkhead / winged helix factors Foxa2 / e , early foregut Lack of foregut Lee et al., HNF3b endoderm, adult acinar and formation 2002; islet tissue Sund et al., 2001 Foxa1 / e7.5, notochord, later in Reduced proglucagon Kaestner et al., HNF3a all islet cell types expression 1999
27 Introduction Pancreatic diseases A number of diseases relate to the pancreas. The most frequently occurring diseases are pancreatic carcinoma, pancreatitis (acute or chronic), pancreatic enzyme insufficiency and diabetes mellitus. Some 30,000 Americans are diagnosed with pancreatic cancer each year, and nearly all will succumb to the disease. Pancreatitis is a rapid and severe inflammation of pancreas; it can be acute or chronic. Binge alcohol drinking is a common cause of acute pancreatitis. Gallstones lodged in the main bile duct next to the pancreas also cause this condition. Accidents, such as the upper abdomen hitting the steering wheel during a car accident, can cause pancreatitis. Certain drugs, such as diuretics, can produce the disorder, as can extremely high blood fat levels (triglycerides). Heredity seems to play a role since, in some families; the condition develops in several members of the family. In pancreatitis, the digestive enzymes of the pancreas break out into the tissues of the organ rather than staying within the tubes (ducts). Severe damage to the pancreas then results. Pancreas enzyme insufficiency occurs when there is deficiency in the digestive enzymes that are necessary to break down protein, fat, and carbohydrates in foods that are ingested. The nutrients are not broken down, resulting in malnutrition and weight loss. This condition is also called malabsorption because the intestine is unable to absorb these vital nutrients.
28 Introduction Diabetes mellitus According to the World Health Organization in 2006, at least 171 million people worldwide suffer from diabetes. Diabetes mellitus is characterized by abnormally high levels of glucose in blood. This may be because of the inadequate secretion or action of insulin, an inadequate response by the body s cells to insulin, or a combination of all these factors. The most common forms of diabetes are type 1 and type 2 diabetes. Gestational diabetes occurs at the time of pregnancy, and other forms of diabetes are rare and are caused by a single gene mutation. Figure 1.5 Epideomology of diabetes Number of persons with diabetes in the year 2000 and estimated for the year (This figure is adopted from Yach et al., 2006.)
29 Introduction Type 1 diabetes Type 1 diabetes affects 700,000 people in the United States and is the most common chronic metabolic disorder to affect children. Type 1 diabetes (10% of cases) is caused by autoimmune destruction of β-cells of the islets of Langerhans resulting in absolute insulin deficiency. The gene thought to be responsible for this reaction is located within a region of the major histocompatibility complex (MHC) HLA class 2 gene, called IDDM1. The role of this gene in the immune response is the presentation of foreign molecules to T cells; however, the detailed action of the gene is still under investigation. The onset is usually acute, the disease developing over a period of a few days to weeks. Over 95% of persons with type 1 diabetes mellitus develop the disease before the age of 25, with an equal incidence in both sexes Type 2 diabetes An important factor in type 2 diabetes is the body s resistance to insulin, and another factor is the falling production of insulin by the β-cells of pancreas. Thus, type 2 diabetes may be a combination of the deficient secretion and deficient action of insulin. Defective β-cells become exhausted, further fueling the cycle of glucose intolerance and hyperglycemia. This is the most common form of diabetes mellitus, and the etiology is multifactorial. It is highly associated with a family history of diabetes, older age, obesity, and lack of exercise. Type 2 diabetes accounts for 90-95% of all cases of diabetes. The prevalence of type 2 diabetes is increasing dramatically across the globe and in some areas has reached epidemic proportions. This increase in prevalence is primarily being driven by environmental factors, through modern age dietary and exercise habits.
Diabetes mellitus. Lecture Outline
 Diabetes mellitus Lecture Outline I. Diagnosis II. Epidemiology III. Causes of diabetes IV. Health Problems and Diabetes V. Treating Diabetes VI. Physical activity and diabetes 1 Diabetes Disorder characterized
Diabetes mellitus Lecture Outline I. Diagnosis II. Epidemiology III. Causes of diabetes IV. Health Problems and Diabetes V. Treating Diabetes VI. Physical activity and diabetes 1 Diabetes Disorder characterized
Regulation of Metabolism. By Dr. Carmen Rexach Physiology Mt San Antonio College
 Regulation of Metabolism By Dr. Carmen Rexach Physiology Mt San Antonio College Energy Constant need in living cells Measured in kcal carbohydrates and proteins = 4kcal/g Fats = 9kcal/g Most diets are
Regulation of Metabolism By Dr. Carmen Rexach Physiology Mt San Antonio College Energy Constant need in living cells Measured in kcal carbohydrates and proteins = 4kcal/g Fats = 9kcal/g Most diets are
Department Of Biochemistry. Subject: Diabetes Mellitus. Supervisor: Dr.Hazim Allawi & Dr.Omar Akram Prepared by : Shahad Ismael. 2 nd stage.
 Department Of Biochemistry Subject: Diabetes Mellitus Supervisor: Dr.Hazim Allawi & Dr.Omar Akram Prepared by : Shahad Ismael. 2 nd stage. Diabetes mellitus : Type 1 & Type 2 What is diabestes mellitus?
Department Of Biochemistry Subject: Diabetes Mellitus Supervisor: Dr.Hazim Allawi & Dr.Omar Akram Prepared by : Shahad Ismael. 2 nd stage. Diabetes mellitus : Type 1 & Type 2 What is diabestes mellitus?
DRUGS FOR GLUCOSE MANAGEMENT AND DIABETES
 Page 1 DRUGS FOR GLUCOSE MANAGEMENT AND DIABETES Drugs to know are: Actrapid HM Humulin R, L, U Penmix SUNALI MEHTA The three principal hormones produced by the pancreas are: Insulin: nutrient metabolism:
Page 1 DRUGS FOR GLUCOSE MANAGEMENT AND DIABETES Drugs to know are: Actrapid HM Humulin R, L, U Penmix SUNALI MEHTA The three principal hormones produced by the pancreas are: Insulin: nutrient metabolism:
Insulin is a hormone produced by the pancreas to control blood sugar. Diabetes can be caused by too little insulin, resistance to insulin, or both.
 Diabetes Definition Diabetes is a chronic (lifelong) disease marked by high levels of sugar in the blood. Causes Insulin is a hormone produced by the pancreas to control blood sugar. Diabetes can be caused
Diabetes Definition Diabetes is a chronic (lifelong) disease marked by high levels of sugar in the blood. Causes Insulin is a hormone produced by the pancreas to control blood sugar. Diabetes can be caused
STEM CELL FELLOWSHIP
 Module I: The Basic Principles of Stem Cells 1. Basics of Stem Cells a. Understanding the development of embryonic stem cells i. Embryonic stem cells ii. Embryonic germ cells iii. Differentiated stem cell
Module I: The Basic Principles of Stem Cells 1. Basics of Stem Cells a. Understanding the development of embryonic stem cells i. Embryonic stem cells ii. Embryonic germ cells iii. Differentiated stem cell
PowerPoint Lecture Outlines prepared by Dr. Lana Zinger, QCC CUNY. 12a. FOCUS ON Your Risk for Diabetes. Copyright 2011 Pearson Education, Inc.
 PowerPoint Lecture Outlines prepared by Dr. Lana Zinger, QCC CUNY 12a FOCUS ON Your Risk for Diabetes Your Risk for Diabetes! Since 1980,Diabetes has increased by 50 %. Diabetes has increased by 70 percent
PowerPoint Lecture Outlines prepared by Dr. Lana Zinger, QCC CUNY 12a FOCUS ON Your Risk for Diabetes Your Risk for Diabetes! Since 1980,Diabetes has increased by 50 %. Diabetes has increased by 70 percent
Chapter 25: Metabolism and Nutrition
 Chapter 25: Metabolism and Nutrition Chapter Objectives INTRODUCTION 1. Generalize the way in which nutrients are processed through the three major metabolic fates in order to perform various energetic
Chapter 25: Metabolism and Nutrition Chapter Objectives INTRODUCTION 1. Generalize the way in which nutrients are processed through the three major metabolic fates in order to perform various energetic
1333 Plaza Blvd, Suite E, Central Point, OR 97502 * www.mountainviewvet.net
 1333 Plaza Blvd, Suite E, Central Point, OR 97502 * www.mountainviewvet.net Diabetes Mellitus (in cats) Diabetes, sugar Affected Animals: Most diabetic cats are older than 10 years of age when they are
1333 Plaza Blvd, Suite E, Central Point, OR 97502 * www.mountainviewvet.net Diabetes Mellitus (in cats) Diabetes, sugar Affected Animals: Most diabetic cats are older than 10 years of age when they are
ETIOLOGIC CLASSIFICATION. Type I diabetes Type II diabetes
 DIABETES MELLITUS DEFINITION It is a common, chronic, metabolic syndrome characterized by hyperglycemia as a cardinal biochemical feature. Resulting from absolute lack of insulin. Abnormal metabolism of
DIABETES MELLITUS DEFINITION It is a common, chronic, metabolic syndrome characterized by hyperglycemia as a cardinal biochemical feature. Resulting from absolute lack of insulin. Abnormal metabolism of
Abdulaziz Al-Subaie. Anfal Al-Shalwi
 Abdulaziz Al-Subaie Anfal Al-Shalwi Introduction what is diabetes mellitus? A chronic metabolic disorder characterized by high blood glucose level caused by insulin deficiency and sometimes accompanied
Abdulaziz Al-Subaie Anfal Al-Shalwi Introduction what is diabetes mellitus? A chronic metabolic disorder characterized by high blood glucose level caused by insulin deficiency and sometimes accompanied
Disability Evaluation Under Social Security
 Disability Evaluation Under Social Security Revised Medical Criteria for Evaluating Endocrine Disorders Effective June 7, 2011 Why a Revision? Social Security revisions reflect: SSA s adjudicative experience.
Disability Evaluation Under Social Security Revised Medical Criteria for Evaluating Endocrine Disorders Effective June 7, 2011 Why a Revision? Social Security revisions reflect: SSA s adjudicative experience.
Causes, incidence, and risk factors
 Causes, incidence, and risk factors Insulin is a hormone produced by the pancreas to control blood sugar. Diabetes can be caused by too little insulin, resistance to insulin, or both. To understand diabetes,
Causes, incidence, and risk factors Insulin is a hormone produced by the pancreas to control blood sugar. Diabetes can be caused by too little insulin, resistance to insulin, or both. To understand diabetes,
INJEX Self Study Program Part 1
 INJEX Self Study Program Part 1 What is Diabetes? Diabetes is a disease in which the body does not produce or properly use insulin. Diabetes is a disorder of metabolism -- the way our bodies use digested
INJEX Self Study Program Part 1 What is Diabetes? Diabetes is a disease in which the body does not produce or properly use insulin. Diabetes is a disorder of metabolism -- the way our bodies use digested
7 Answers to end-of-chapter questions
 7 Answers to end-of-chapter questions Multiple choice questions 1 B 2 B 3 A 4 B 5 A 6 D 7 C 8 C 9 B 10 B Structured questions 11 a i Maintenance of a constant internal environment within set limits i Concentration
7 Answers to end-of-chapter questions Multiple choice questions 1 B 2 B 3 A 4 B 5 A 6 D 7 C 8 C 9 B 10 B Structured questions 11 a i Maintenance of a constant internal environment within set limits i Concentration
Diabetes and Insulin Signaling
 Diabetes and Insulin Signaling NATIONAL CENTER FOR CASE STUDY TEACHING IN SCIENCE by Kristy J. Wilson School of Mathematics and Sciences Marian University, Indianapolis, IN Part I Research Orientation
Diabetes and Insulin Signaling NATIONAL CENTER FOR CASE STUDY TEACHING IN SCIENCE by Kristy J. Wilson School of Mathematics and Sciences Marian University, Indianapolis, IN Part I Research Orientation
GLUCOSE HOMEOSTASIS-II: An Overview
 GLUCOSE HOMEOSTASIS-II: An Overview University of Papua New Guinea School of Medicine & Health Sciences, Division of Basic Medical Sciences Discipline of Biochemistry & Molecular Biology, M Med Part I
GLUCOSE HOMEOSTASIS-II: An Overview University of Papua New Guinea School of Medicine & Health Sciences, Division of Basic Medical Sciences Discipline of Biochemistry & Molecular Biology, M Med Part I
X-Plain Hypoglycemia Reference Summary
 X-Plain Hypoglycemia Reference Summary Introduction Hypoglycemia is a condition that causes blood sugar level to drop dangerously low. It mostly shows up in diabetic patients who take insulin. When recognized
X-Plain Hypoglycemia Reference Summary Introduction Hypoglycemia is a condition that causes blood sugar level to drop dangerously low. It mostly shows up in diabetic patients who take insulin. When recognized
Liver, Gallbladder, Exocrine Pancreas KNH 406
 Liver, Gallbladder, Exocrine Pancreas KNH 406 2007 Thomson - Wadsworth LIVER Anatomy - functions With disease blood flow becomes obstructed Bile All bile drains into common hepatic duct Liver Bile complex
Liver, Gallbladder, Exocrine Pancreas KNH 406 2007 Thomson - Wadsworth LIVER Anatomy - functions With disease blood flow becomes obstructed Bile All bile drains into common hepatic duct Liver Bile complex
Compartmentalization of the Cell. Objectives. Recommended Reading. Professor Alfred Cuschieri. Department of Anatomy University of Malta
 Compartmentalization of the Cell Professor Alfred Cuschieri Department of Anatomy University of Malta Objectives By the end of this session the student should be able to: 1. Identify the different organelles
Compartmentalization of the Cell Professor Alfred Cuschieri Department of Anatomy University of Malta Objectives By the end of this session the student should be able to: 1. Identify the different organelles
Understanding Diabetes
 Understanding Diabetes What is diabetes? Diabetes is a condition where there is too much glucose (a type of sugar) in your blood. Your blood glucose level is regulated with the help of insulin, a hormone
Understanding Diabetes What is diabetes? Diabetes is a condition where there is too much glucose (a type of sugar) in your blood. Your blood glucose level is regulated with the help of insulin, a hormone
Control of Gene Expression
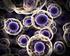 Control of Gene Expression What is Gene Expression? Gene expression is the process by which informa9on from a gene is used in the synthesis of a func9onal gene product. What is Gene Expression? Figure
Control of Gene Expression What is Gene Expression? Gene expression is the process by which informa9on from a gene is used in the synthesis of a func9onal gene product. What is Gene Expression? Figure
DIABETES A chronic, debilitating and often deadly disease A global epidemic Diabetes in Africa
 DIABETES A chronic, debilitating and often deadly disease Diabetes is a chronic condition that arises when the pancreas does not produce enough insulin, or when the body cannot effectively use the insulin
DIABETES A chronic, debilitating and often deadly disease Diabetes is a chronic condition that arises when the pancreas does not produce enough insulin, or when the body cannot effectively use the insulin
Is Insulin Effecting Your Weight Loss and Your Health?
 Is Insulin Effecting Your Weight Loss and Your Health? Teressa Alexander, M.D., FACOG Women s Healthcare Associates www.rushcopley.com/whca 630-978-6886 Obesity is Epidemic in the US 2/3rds of U.S. adults
Is Insulin Effecting Your Weight Loss and Your Health? Teressa Alexander, M.D., FACOG Women s Healthcare Associates www.rushcopley.com/whca 630-978-6886 Obesity is Epidemic in the US 2/3rds of U.S. adults
glucose and fatty acids to raise your blood sugar levels.
 Endocrine & Cell Communication Part IV: Maintaining Balance (Homeostasis) TEACHER NOTES needs coding 1 Endocrine & Cell Communication Part IV: Maintaining Balance (Homeostasis) 2 AP Biology Curriculum
Endocrine & Cell Communication Part IV: Maintaining Balance (Homeostasis) TEACHER NOTES needs coding 1 Endocrine & Cell Communication Part IV: Maintaining Balance (Homeostasis) 2 AP Biology Curriculum
Describe how these hormones exert control quickly by changes in phosphorylation state of enzyme, and more slowly by changes of gene expression
 Section VIII. Section VIII. Tissue metabolism Many tissues carry out specialized functions: Ch. 43 look at different hormones affect metabolism of fuels, especially counter-insulin Ch. 44 Proteins and
Section VIII. Section VIII. Tissue metabolism Many tissues carry out specialized functions: Ch. 43 look at different hormones affect metabolism of fuels, especially counter-insulin Ch. 44 Proteins and
Control of Gene Expression
 Control of Gene Expression (Learning Objectives) Explain the role of gene expression is differentiation of function of cells which leads to the emergence of different tissues, organs, and organ systems
Control of Gene Expression (Learning Objectives) Explain the role of gene expression is differentiation of function of cells which leads to the emergence of different tissues, organs, and organ systems
The diagram below summarizes the effects of the compounds that cells use to regulate their own metabolism.
 Regulation of carbohydrate metabolism Intracellular metabolic regulators Each of the control point steps in the carbohydrate metabolic pathways in effect regulates itself by responding to molecules that
Regulation of carbohydrate metabolism Intracellular metabolic regulators Each of the control point steps in the carbohydrate metabolic pathways in effect regulates itself by responding to molecules that
INSULIN PRODUCTS. Jack DeRuiter
 INSULIN PRODUCTS Jack DeRuiter The number and types of insulin preparations available in the United States is constantly changing, thus students should refer to recent drug resources for a current list
INSULIN PRODUCTS Jack DeRuiter The number and types of insulin preparations available in the United States is constantly changing, thus students should refer to recent drug resources for a current list
Diabetes Fundamentals
 Diabetes Fundamentals Prevalence of Diabetes in the U.S. Undiagnosed 10.7% of all people 20+ 23.1% of all people 60+ (12.2 million) Slide provided by Roche Diagnostics Sources: ADA, WHO statistics Prevalence
Diabetes Fundamentals Prevalence of Diabetes in the U.S. Undiagnosed 10.7% of all people 20+ 23.1% of all people 60+ (12.2 million) Slide provided by Roche Diagnostics Sources: ADA, WHO statistics Prevalence
1. What has a higher stored energy potential per gram, glycogen or triglycerides? Explain.
 Lipid Metabolism 1. What has a higher stored energy potential per gram, glycogen or triglycerides? Explain. 2. How can excess acetyl CoA trapped in the mitochondria, be utilized as a substrate for fatty
Lipid Metabolism 1. What has a higher stored energy potential per gram, glycogen or triglycerides? Explain. 2. How can excess acetyl CoA trapped in the mitochondria, be utilized as a substrate for fatty
Lecture 8. Protein Trafficking/Targeting. Protein targeting is necessary for proteins that are destined to work outside the cytoplasm.
 Protein Trafficking/Targeting (8.1) Lecture 8 Protein Trafficking/Targeting Protein targeting is necessary for proteins that are destined to work outside the cytoplasm. Protein targeting is more complex
Protein Trafficking/Targeting (8.1) Lecture 8 Protein Trafficking/Targeting Protein targeting is necessary for proteins that are destined to work outside the cytoplasm. Protein targeting is more complex
Endocrine Responses to Resistance Exercise
 chapter 3 Endocrine Responses to Resistance Exercise Chapter Objectives Understand basic concepts of endocrinology. Explain the physiological roles of anabolic hormones. Describe hormonal responses to
chapter 3 Endocrine Responses to Resistance Exercise Chapter Objectives Understand basic concepts of endocrinology. Explain the physiological roles of anabolic hormones. Describe hormonal responses to
HOW TO CARE FOR A PATIENT WITH DIABETES
 HOW TO CARE FOR A PATIENT WITH DIABETES INTRODUCTION Diabetes is one of the most common diseases in the United States, and diabetes is a disease that affects the way the body handles blood sugar. Approximately
HOW TO CARE FOR A PATIENT WITH DIABETES INTRODUCTION Diabetes is one of the most common diseases in the United States, and diabetes is a disease that affects the way the body handles blood sugar. Approximately
Cardiovascular Disease Risk Factors Part XII Insulin Resistance By James L. Holly, MD Your Life Your Health The Examiner September 15, 2005
 Cardiovascular Disease Risk Factors Part XII By James L. Holly, MD Your Life Your Health The Examiner September 15, 2005 As we approach the end of our extended series on cardiovascular disease risk factors,
Cardiovascular Disease Risk Factors Part XII By James L. Holly, MD Your Life Your Health The Examiner September 15, 2005 As we approach the end of our extended series on cardiovascular disease risk factors,
N E B R A S K A JAIL BULLETIN NUMBER 102 OCTOBER 1993
 N E B R A S K A JAIL BULLETIN NUMBER 102 OCTOBER 1993 The Jail Bulletin is a monthly feature of the Crime Commission Update. The Bulletin may be used as a supplement to your jail in-service training program
N E B R A S K A JAIL BULLETIN NUMBER 102 OCTOBER 1993 The Jail Bulletin is a monthly feature of the Crime Commission Update. The Bulletin may be used as a supplement to your jail in-service training program
Overview of Metabolism. Peds 231 April 9, 2009 Julie Theriot
 Overview of Metabolism Peds 231 April 9, 2009 Julie Theriot Outline What is metabolism and why should you care about it? Summary of human carbohydrate metabolism and connections to diabetes Metabolism
Overview of Metabolism Peds 231 April 9, 2009 Julie Theriot Outline What is metabolism and why should you care about it? Summary of human carbohydrate metabolism and connections to diabetes Metabolism
Version 1 2015. Module guide. Preliminary document. International Master Program Cardiovascular Science University of Göttingen
 Version 1 2015 Module guide International Master Program Cardiovascular Science University of Göttingen Part 1 Theoretical modules Synopsis The Master program Cardiovascular Science contains four theoretical
Version 1 2015 Module guide International Master Program Cardiovascular Science University of Göttingen Part 1 Theoretical modules Synopsis The Master program Cardiovascular Science contains four theoretical
Mind the Gap: Navigating the Underground World of DKA. Objectives. Back That Train Up! 9/26/2014
 Mind the Gap: Navigating the Underground World of DKA Christina Canfield, MSN, RN, ACNS-BC, CCRN Clinical Nurse Specialist Cleveland Clinic Respiratory Institute Objectives Upon completion of this activity
Mind the Gap: Navigating the Underground World of DKA Christina Canfield, MSN, RN, ACNS-BC, CCRN Clinical Nurse Specialist Cleveland Clinic Respiratory Institute Objectives Upon completion of this activity
Stem Cell Quick Guide: Stem Cell Basics
 Stem Cell Quick Guide: Stem Cell Basics What is a Stem Cell? Stem cells are the starting point from which the rest of the body grows. The adult human body is made up of hundreds of millions of different
Stem Cell Quick Guide: Stem Cell Basics What is a Stem Cell? Stem cells are the starting point from which the rest of the body grows. The adult human body is made up of hundreds of millions of different
Control of Gene Expression
 Home Gene Regulation Is Necessary? Control of Gene Expression By switching genes off when they are not needed, cells can prevent resources from being wasted. There should be natural selection favoring
Home Gene Regulation Is Necessary? Control of Gene Expression By switching genes off when they are not needed, cells can prevent resources from being wasted. There should be natural selection favoring
Stem Cell Therapy In Diabetes Mellitus. Professor Megahid Abuelmagd Diabetes And Endocrine Unit. Mansoura Faculty Of Medicine
 Stem Cell Therapy In Diabetes Mellitus Professor Megahid Abuelmagd Diabetes And Endocrine Unit. Mansoura Faculty Of Medicine For many years, there has been great interest in approaches to the replacement
Stem Cell Therapy In Diabetes Mellitus Professor Megahid Abuelmagd Diabetes And Endocrine Unit. Mansoura Faculty Of Medicine For many years, there has been great interest in approaches to the replacement
Stem Cell Information
 Stem Cell Information The official National Institutes of Health resource for stem cell research Stem Cell Basics Stem cells have the remarkable potential to develop into many different cell types in the
Stem Cell Information The official National Institutes of Health resource for stem cell research Stem Cell Basics Stem cells have the remarkable potential to develop into many different cell types in the
X-Plain Diabetes - Introduction Reference Summary
 X-Plain Diabetes - Introduction Reference Summary Introduction Diabetes is a disease that affects millions of Americans every year. Your doctor may have informed you that you have diabetes. Although there
X-Plain Diabetes - Introduction Reference Summary Introduction Diabetes is a disease that affects millions of Americans every year. Your doctor may have informed you that you have diabetes. Although there
Endocrine System: Practice Questions #1
 Endocrine System: Practice Questions #1 1. Removing part of gland D would most likely result in A. a decrease in the secretions of other glands B. a decrease in the blood calcium level C. an increase in
Endocrine System: Practice Questions #1 1. Removing part of gland D would most likely result in A. a decrease in the secretions of other glands B. a decrease in the blood calcium level C. an increase in
Diabetes Mellitus Type 2
 Diabetes Mellitus Type 2 What is it? Diabetes is a common health problem in the U.S. and the world. In diabetes, the body does not use the food it digests well. It is hard for the body to use carbohydrates
Diabetes Mellitus Type 2 What is it? Diabetes is a common health problem in the U.S. and the world. In diabetes, the body does not use the food it digests well. It is hard for the body to use carbohydrates
Liver Function Tests. Dr Stephen Butler Paediatric Advance Trainee TDHB
 Liver Function Tests Dr Stephen Butler Paediatric Advance Trainee TDHB Introduction Case presentation What is the liver? Overview of tests used to measure liver function RJ 10 month old European girl
Liver Function Tests Dr Stephen Butler Paediatric Advance Trainee TDHB Introduction Case presentation What is the liver? Overview of tests used to measure liver function RJ 10 month old European girl
10.1 The function of Digestion pg. 402
 10.1 The function of Digestion pg. 402 Macromolecules and Living Systems The body is made up of more than 60 % water. The water is found in the cells cytoplasm, the interstitial fluid and the blood (5
10.1 The function of Digestion pg. 402 Macromolecules and Living Systems The body is made up of more than 60 % water. The water is found in the cells cytoplasm, the interstitial fluid and the blood (5
CME Test for AMDA Clinical Practice Guideline. Diabetes Mellitus
 CME Test for AMDA Clinical Practice Guideline Diabetes Mellitus Part I: 1. Which one of the following statements about type 2 diabetes is not accurate? a. Diabetics are at increased risk of experiencing
CME Test for AMDA Clinical Practice Guideline Diabetes Mellitus Part I: 1. Which one of the following statements about type 2 diabetes is not accurate? a. Diabetics are at increased risk of experiencing
Type 2 Diabetes. What is diabetes? Understanding blood glucose and insulin. What is Type 2 diabetes? Page 1 of 5
 Page 1 of 5 Type 2 Diabetes Type 2 diabetes occurs mainly in people aged over 40. The 'first-line' treatment is diet, weight control and physical activity. If the blood glucose level remains high despite
Page 1 of 5 Type 2 Diabetes Type 2 diabetes occurs mainly in people aged over 40. The 'first-line' treatment is diet, weight control and physical activity. If the blood glucose level remains high despite
Markham Stouffville Hospital
 Markham Stouffville Hospital Adult Diabetes Education Frequently Asked Questions What is diabetes? Diabetes is a disease in which blood glucose levels are above normal. Most of the food we eat is turned
Markham Stouffville Hospital Adult Diabetes Education Frequently Asked Questions What is diabetes? Diabetes is a disease in which blood glucose levels are above normal. Most of the food we eat is turned
Blood glucose levels have important health effects, which is why it is important for people with diabetes to control their blood glucose.
 Lesson 4: The Biology of Diabetes Inquiry Focus: Who can have diabetes? Student Learning Objectives: By the end of the lesson, students will be able to do the following: Describe diabetes as a disorder
Lesson 4: The Biology of Diabetes Inquiry Focus: Who can have diabetes? Student Learning Objectives: By the end of the lesson, students will be able to do the following: Describe diabetes as a disorder
Types of Diabetes
 Anti-Diabetic Drugs Bassim I Mohammad Specialist Physician-Assistant Professor College of Pharmacy/ Al Qadisiyah University Iraq Diabetes Mellitus (Definition) DM is an elevated blood glucose level associated
Anti-Diabetic Drugs Bassim I Mohammad Specialist Physician-Assistant Professor College of Pharmacy/ Al Qadisiyah University Iraq Diabetes Mellitus (Definition) DM is an elevated blood glucose level associated
Anatomy and Physiology Placement Exam 2 Practice with Answers at End!
 Anatomy and Physiology Placement Exam 2 Practice with Answers at End! General Chemical Principles 1. bonds are characterized by the sharing of electrons between the participating atoms. a. hydrogen b.
Anatomy and Physiology Placement Exam 2 Practice with Answers at End! General Chemical Principles 1. bonds are characterized by the sharing of electrons between the participating atoms. a. hydrogen b.
Unit 1 Higher Human Biology Summary Notes
 Unit 1 Higher Human Biology Summary Notes a. Cells tissues organs body systems Division of labour occurs in multicellular organisms (rather than each cell carrying out every function) Most cells become
Unit 1 Higher Human Biology Summary Notes a. Cells tissues organs body systems Division of labour occurs in multicellular organisms (rather than each cell carrying out every function) Most cells become
Regenerative Medicine : A Promising Approach In Overcoming Diabetes As An Increasing Economic Health Burden
 Journal of Emerging Economies and Islamic Research www.jeeir.com Regenerative Medicine : A Promising Approach In Overcoming Diabetes As An Increasing Economic Health Burden Nafeeza Mohd Ismail a, Renu
Journal of Emerging Economies and Islamic Research www.jeeir.com Regenerative Medicine : A Promising Approach In Overcoming Diabetes As An Increasing Economic Health Burden Nafeeza Mohd Ismail a, Renu
Actions of Hormones on Target Cells Page 1. Actions of Hormones on Target Cells Page 2. Goals/ What You Need to Know Goals What You Need to Know
 Actions of Hormones on Target Cells Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Actions of Hormones on Target Cells Hormones
Actions of Hormones on Target Cells Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Actions of Hormones on Target Cells Hormones
Introduction. Pathogenesis of type 2 diabetes
 Introduction Type 2 diabetes mellitus (t2dm) is the most prevalent form of diabetes worldwide. It is characterised by high fasting and high postprandial blood glucose concentrations (hyperglycemia). Chronic
Introduction Type 2 diabetes mellitus (t2dm) is the most prevalent form of diabetes worldwide. It is characterised by high fasting and high postprandial blood glucose concentrations (hyperglycemia). Chronic
DIABETES MELLITUS. By Tracey Steenkamp Biokineticist at the Institute for Sport Research, University of Pretoria
 DIABETES MELLITUS By Tracey Steenkamp Biokineticist at the Institute for Sport Research, University of Pretoria What is Diabetes Diabetes Mellitus (commonly referred to as diabetes ) is a chronic medical
DIABETES MELLITUS By Tracey Steenkamp Biokineticist at the Institute for Sport Research, University of Pretoria What is Diabetes Diabetes Mellitus (commonly referred to as diabetes ) is a chronic medical
Biotechnology. Srivatsan Kidambi, Ph.D.
 Stem Stem Cell Cell Engineering-What, Biology and it Application Why, How?? to Biotechnology Srivatsan Kidambi, Ph.D. Assistant Professor Department of Chemical & Biomolecular Engineering University of
Stem Stem Cell Cell Engineering-What, Biology and it Application Why, How?? to Biotechnology Srivatsan Kidambi, Ph.D. Assistant Professor Department of Chemical & Biomolecular Engineering University of
Tuberculosis And Diabetes. Dr. hanan abuelrus Prof.of internal medicine Assiut University
 Tuberculosis And Diabetes Dr. hanan abuelrus Prof.of internal medicine Assiut University TUBERCULOSIS FACTS More than 9 million people fall sick with tuberculosis (TB) every year. Over 1.5 million die
Tuberculosis And Diabetes Dr. hanan abuelrus Prof.of internal medicine Assiut University TUBERCULOSIS FACTS More than 9 million people fall sick with tuberculosis (TB) every year. Over 1.5 million die
Digestion, Absorption. How & where?
 Digestion, Absorption How & where? What happens to food? Three processes Digestion Absorption Elimination Where do they occur? GI tract Overview of Digestion GI tract Gastrointestinal (GI) tract: series
Digestion, Absorption How & where? What happens to food? Three processes Digestion Absorption Elimination Where do they occur? GI tract Overview of Digestion GI tract Gastrointestinal (GI) tract: series
Basal Insulin Analogues Where are We Now?
 232 Medicine Update 41 Basal Insulin Analogues Where are We Now? S CHANDRU, V MOHAN Insulin is a polypeptide secreted by the beta cells of pancreas and consists of 51 amino acids (AA). It has two polypeptide
232 Medicine Update 41 Basal Insulin Analogues Where are We Now? S CHANDRU, V MOHAN Insulin is a polypeptide secreted by the beta cells of pancreas and consists of 51 amino acids (AA). It has two polypeptide
Endocrine Glands and the General Principles of Hormone Action
 Endocrine Glands and the General Principles of Hormone Action Cai Li, Ph.D. Assistant professor Touchstone Center for Diabetes Research Departments of Physiology and Internal Medicine The University of
Endocrine Glands and the General Principles of Hormone Action Cai Li, Ph.D. Assistant professor Touchstone Center for Diabetes Research Departments of Physiology and Internal Medicine The University of
A disaccharide is formed when a dehydration reaction joins two monosaccharides. This covalent bond is called a glycosidic linkage.
 CH 5 Structure & Function of Large Molecules: Macromolecules Molecules of Life All living things are made up of four classes of large biological molecules: carbohydrates, lipids, proteins, and nucleic
CH 5 Structure & Function of Large Molecules: Macromolecules Molecules of Life All living things are made up of four classes of large biological molecules: carbohydrates, lipids, proteins, and nucleic
Management of Clients with Diabetes Mellitus
 Management of Clients with Diabetes Mellitus Black, J.M. & Hawks, J.H. (2005) Chapters 47, (pp 1243-1288) 1288) Baptist Health School of Nursing NSG 4037: Adult Nursing III Carole Mackey, MNSc,, RN, PNP
Management of Clients with Diabetes Mellitus Black, J.M. & Hawks, J.H. (2005) Chapters 47, (pp 1243-1288) 1288) Baptist Health School of Nursing NSG 4037: Adult Nursing III Carole Mackey, MNSc,, RN, PNP
Lesson 3: Blood glucose
 Lesson 3: Blood glucose Inquiry Focus: How does the body deliver the energy in food to its parts? Student Learning Objectives: By the end of the lesson, students will be able to do the following: Describe
Lesson 3: Blood glucose Inquiry Focus: How does the body deliver the energy in food to its parts? Student Learning Objectives: By the end of the lesson, students will be able to do the following: Describe
Treatment of diabetes In order to survive, people with type 1 diabetes must have insulin delivered by a pump or injections.
 National Diabetes Statistics What is diabetes? Diabetes mellitus is a group of diseases characterized by high levels of blood glucose resulting from defects in insulin production, insulin action, or both.
National Diabetes Statistics What is diabetes? Diabetes mellitus is a group of diseases characterized by high levels of blood glucose resulting from defects in insulin production, insulin action, or both.
Complex multicellular organisms are produced by cells that switch genes on and off during development.
 Home Control of Gene Expression Gene Regulation Is Necessary? By switching genes off when they are not needed, cells can prevent resources from being wasted. There should be natural selection favoring
Home Control of Gene Expression Gene Regulation Is Necessary? By switching genes off when they are not needed, cells can prevent resources from being wasted. There should be natural selection favoring
1. The diagram below represents a biological process
 1. The diagram below represents a biological process 5. The chart below indicates the elements contained in four different molecules and the number of atoms of each element in those molecules. Which set
1. The diagram below represents a biological process 5. The chart below indicates the elements contained in four different molecules and the number of atoms of each element in those molecules. Which set
Disaccharides consist of two monosaccharide monomers covalently linked by a glycosidic bond. They function in sugar transport.
 1. The fundamental life processes of plants and animals depend on a variety of chemical reactions that occur in specialized areas of the organism s cells. As a basis for understanding this concept: 1.
1. The fundamental life processes of plants and animals depend on a variety of chemical reactions that occur in specialized areas of the organism s cells. As a basis for understanding this concept: 1.
Eating, pooping, and peeing THE DIGESTIVE SYSTEM
 THE DIGESTIVE SYSTEM Ingested food is not technically in the body until it is absorbed so it needs to be: Mechanically and chemically reduced Transported by the blood to the cells Large portions are not
THE DIGESTIVE SYSTEM Ingested food is not technically in the body until it is absorbed so it needs to be: Mechanically and chemically reduced Transported by the blood to the cells Large portions are not
Bile Duct Diseases and Problems
 Bile Duct Diseases and Problems Introduction A bile duct is a tube that carries bile between the liver and gallbladder and the intestine. Bile is a substance made by the liver that helps with digestion.
Bile Duct Diseases and Problems Introduction A bile duct is a tube that carries bile between the liver and gallbladder and the intestine. Bile is a substance made by the liver that helps with digestion.
Stem Cell Research: Adult or Somatic Stem Cells
 Chiang 1 Stem Cell Research: Adult or Somatic Stem Cells Abstract Kelly Chiang Cluster 7 Dr. LeFebvre 07/26/10 Over the past few decades, stem cells have been a controversial topic in the scientific field.
Chiang 1 Stem Cell Research: Adult or Somatic Stem Cells Abstract Kelly Chiang Cluster 7 Dr. LeFebvre 07/26/10 Over the past few decades, stem cells have been a controversial topic in the scientific field.
SMALL AND LARGE INTESTINE SECRETIONS
 SMALL AND LARGE INTESTINE SECRETIONS Objectives At the end of lecture student should be able to know, Digestive system Digestive system secretions Small intestine Component of small intestine Intestinal
SMALL AND LARGE INTESTINE SECRETIONS Objectives At the end of lecture student should be able to know, Digestive system Digestive system secretions Small intestine Component of small intestine Intestinal
Sweet-taste receptors, glucose absorption and insulin release: Are LCS nutritionally active?
 Sweet-taste receptors, glucose absorption and insulin release: Are LCS nutritionally active? Samuel V. Molinary, Ph.D. Consultant, Scientific & Regulatory Affairs ILSI/NA April 6, 2011 Washington, DC Why
Sweet-taste receptors, glucose absorption and insulin release: Are LCS nutritionally active? Samuel V. Molinary, Ph.D. Consultant, Scientific & Regulatory Affairs ILSI/NA April 6, 2011 Washington, DC Why
The chemical reactions inside cells are controlled by enzymes. Cells may be specialised to carry out a particular function.
 12.1 What are animals and plants built from? All living things are made up of cells. The structures of different types of cells are related to their functions. to relate the structure of different types
12.1 What are animals and plants built from? All living things are made up of cells. The structures of different types of cells are related to their functions. to relate the structure of different types
Questions on The Nervous System and Gas Exchange
 Name: Questions on The Nervous System and Gas Exchange Directions: The following questions are taken from previous IB Final Papers on Topics 6.4 (Gas Exchange) and 6.5 (Nerves, hormones and homeostasis).
Name: Questions on The Nervous System and Gas Exchange Directions: The following questions are taken from previous IB Final Papers on Topics 6.4 (Gas Exchange) and 6.5 (Nerves, hormones and homeostasis).
The Digestive System. You are what you eat!
 The Digestive System You are what you eat! Try to label the diagram (PENCIL!!) What is Digestion? Digestion: the breakdown of large macromolecules (proteins, fats, carbohydrates) into smaller molecules
The Digestive System You are what you eat! Try to label the diagram (PENCIL!!) What is Digestion? Digestion: the breakdown of large macromolecules (proteins, fats, carbohydrates) into smaller molecules
Chapter 18 Regulation of Gene Expression
 Chapter 18 Regulation of Gene Expression 18.1. Gene Regulation Is Necessary By switching genes off when they are not needed, cells can prevent resources from being wasted. There should be natural selection
Chapter 18 Regulation of Gene Expression 18.1. Gene Regulation Is Necessary By switching genes off when they are not needed, cells can prevent resources from being wasted. There should be natural selection
10.2 The Human Digestive System pg. 411
 10.2 The Human Digestive System pg. 411 The human digestive system is made up of a group of organs working together. The digestive tract is made up of the mouth, esophagus, stomach, small intestine, and
10.2 The Human Digestive System pg. 411 The human digestive system is made up of a group of organs working together. The digestive tract is made up of the mouth, esophagus, stomach, small intestine, and
Diabetes Mellitus. Melissa Meredith M.D. Diabetes Mellitus
 Melissa Meredith M.D. Diabetes mellitus is a group of metabolic diseases characterized by high blood glucose resulting from defects in insulin secretion, insulin action, or both Diabetes is a chronic,
Melissa Meredith M.D. Diabetes mellitus is a group of metabolic diseases characterized by high blood glucose resulting from defects in insulin secretion, insulin action, or both Diabetes is a chronic,
How To Understand The Chemistry Of Organic Molecules
 CHAPTER 3 THE CHEMISTRY OF ORGANIC MOLECULES 3.1 Organic Molecules The chemistry of carbon accounts for the diversity of organic molecules found in living things. Carbon has six electrons, four of which
CHAPTER 3 THE CHEMISTRY OF ORGANIC MOLECULES 3.1 Organic Molecules The chemistry of carbon accounts for the diversity of organic molecules found in living things. Carbon has six electrons, four of which
The digestive system eliminated waste from the digestive tract. But we also need a way to eliminate waste from the rest of the body.
 Outline Urinary System Urinary System and Excretion Bio105 Lecture 20 Chapter 16 I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of the urinary system 1
Outline Urinary System Urinary System and Excretion Bio105 Lecture 20 Chapter 16 I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of the urinary system 1
Absorption of Drugs. Transport of a drug from the GI tract
 Absorption of Drugs Absorption is the transfer of a drug from its site of administration to the bloodstream. The rate and efficiency of absorption depend on the route of administration. For IV delivery,
Absorption of Drugs Absorption is the transfer of a drug from its site of administration to the bloodstream. The rate and efficiency of absorption depend on the route of administration. For IV delivery,
Calculating and Graphing Glucose, Insulin, and GFR HASPI Medical Biology Activity 19c
 Calculating and Graphing Glucose, Insulin, and GFR HASPI Medical Biology Activity 19c Name: Period: Date: Part A Background The Pancreas and Insulin The following background information has been provided
Calculating and Graphing Glucose, Insulin, and GFR HASPI Medical Biology Activity 19c Name: Period: Date: Part A Background The Pancreas and Insulin The following background information has been provided
PHOSPHATE-SANDOZ Tablets (High dose phosphate supplement)
 1 PHOSPHATE-SANDOZ Tablets (High dose phosphate supplement) PHOSPHATE-SANDOZ PHOSPHATE-SANDOZ Tablets are a high dose phosphate supplement containing sodium phosphate monobasic. The CAS registry number
1 PHOSPHATE-SANDOZ Tablets (High dose phosphate supplement) PHOSPHATE-SANDOZ PHOSPHATE-SANDOZ Tablets are a high dose phosphate supplement containing sodium phosphate monobasic. The CAS registry number
Diagnosis, classification and prevention of diabetes
 Diagnosis, classification and prevention of diabetes Section 1 1 of 4 Curriculum Module II 1 Diagnosis, classification and presentation of diabetes Slide 2 of 48 Polyurea Definition of diabetes Slide 3
Diagnosis, classification and prevention of diabetes Section 1 1 of 4 Curriculum Module II 1 Diagnosis, classification and presentation of diabetes Slide 2 of 48 Polyurea Definition of diabetes Slide 3
Cells. Structure, Function and Homeostasis
 Cells Structure, Function and Homeostasis Characteristics of Cells Basic unit of life anything alive is made of cells Plasma membrane (skin) that separates them from the environment. Skeletonsfor protection
Cells Structure, Function and Homeostasis Characteristics of Cells Basic unit of life anything alive is made of cells Plasma membrane (skin) that separates them from the environment. Skeletonsfor protection
Diabetes may be classified as. i) Type - I Diabetes mellitus. Type - II Diabetes mellitus. Type - 1.5 Diabetes mellitus. Gestational Diabetes INSULIN
 HYPOGLYCEMIC AGENT Diabetes mellitus is a chronic metabolic disorder of multiple aetiology characterized by chronic hyperglycaemia with disturbances of carbohydrate, fat and protein metabolism resulting
HYPOGLYCEMIC AGENT Diabetes mellitus is a chronic metabolic disorder of multiple aetiology characterized by chronic hyperglycaemia with disturbances of carbohydrate, fat and protein metabolism resulting
BIO 137: CHAPTER 1 OBJECTIVES
 BIO 137: CHAPTER 1 OBJECTIVES 1. Define the terms anatomy and physiology, and explain their relationship using an example of a human structure with its corresponding function. A. ANATOMY = the study of
BIO 137: CHAPTER 1 OBJECTIVES 1. Define the terms anatomy and physiology, and explain their relationship using an example of a human structure with its corresponding function. A. ANATOMY = the study of
Baskets of Care Diabetes Subcommittee
 Baskets of Care Diabetes Subcommittee Disclaimer: This background information is not intended to be a comprehensive scientific discussion of the topic, but rather an attempt to provide a baseline level
Baskets of Care Diabetes Subcommittee Disclaimer: This background information is not intended to be a comprehensive scientific discussion of the topic, but rather an attempt to provide a baseline level
Diabetic Emergencies. David Hill, D.O.
 Diabetic Emergencies David Hill, D.O. Class Outline Diabetic emergency/glucometer training Identify the different signs of insulin shock Diabetic coma, and HHNK Participants will understand the treatment
Diabetic Emergencies David Hill, D.O. Class Outline Diabetic emergency/glucometer training Identify the different signs of insulin shock Diabetic coma, and HHNK Participants will understand the treatment
NUTRITION OF THE BODY
 5 Training Objectives:! Knowledge of the most important function of nutrients! Description of both, mechanism and function of gluconeogenesis! Knowledge of the difference between essential and conditionally
5 Training Objectives:! Knowledge of the most important function of nutrients! Description of both, mechanism and function of gluconeogenesis! Knowledge of the difference between essential and conditionally
Diabetes Mellitus: Type 1
 Diabetes Mellitus: Type 1 What is type 1 diabetes mellitus? Type 1 diabetes is a disorder that happens when your body produces little or no insulin. The lack of insulin causes the level of sugar in your
Diabetes Mellitus: Type 1 What is type 1 diabetes mellitus? Type 1 diabetes is a disorder that happens when your body produces little or no insulin. The lack of insulin causes the level of sugar in your
RAD 223. Radiography physiology. Lecture Notes. First lecture: Cell and Tissue
 RAD 223 Radiography physiology Lecture Notes First lecture: Cell and Tissue Physiology: the word physiology derived from a Greek word for study of nature. It is the study of how the body and its part work
RAD 223 Radiography physiology Lecture Notes First lecture: Cell and Tissue Physiology: the word physiology derived from a Greek word for study of nature. It is the study of how the body and its part work
Insulin s Effects on Testosterone, Growth Hormone and IGF I Following Resistance Training
 Insulin s Effects on Testosterone, Growth Hormone and IGF I Following Resistance Training By: Jason Dudley Summary Nutrition supplements with a combination of carbohydrate and protein (with a ratio of
Insulin s Effects on Testosterone, Growth Hormone and IGF I Following Resistance Training By: Jason Dudley Summary Nutrition supplements with a combination of carbohydrate and protein (with a ratio of
Carbohydrates, proteins and lipids
 Carbohydrates, proteins and lipids Chapter 3 MACROMOLECULES Macromolecules: polymers with molecular weights >1,000 Functional groups THE FOUR MACROMOLECULES IN LIFE Molecules in living organisms: proteins,
Carbohydrates, proteins and lipids Chapter 3 MACROMOLECULES Macromolecules: polymers with molecular weights >1,000 Functional groups THE FOUR MACROMOLECULES IN LIFE Molecules in living organisms: proteins,
Nutrition. Type 2 Diabetes: A Growing Challenge in the Healthcare Setting NAME OF STUDENT
 1 Nutrition Type 2 Diabetes: A Growing Challenge in the Healthcare Setting NAME OF STUDENT 2 Type 2 Diabetes: A Growing Challenge in the Healthcare Setting Introduction and background of type 2 diabetes:
1 Nutrition Type 2 Diabetes: A Growing Challenge in the Healthcare Setting NAME OF STUDENT 2 Type 2 Diabetes: A Growing Challenge in the Healthcare Setting Introduction and background of type 2 diabetes:
