Comparison of surgical procedures for degenerative lumbar spinal stenosis: a meta-analysis of the literature from 1975 to 1995
|
|
|
- Lesley Holmes
- 8 years ago
- Views:
Transcription
1 Eur Spine J (1997) 6 : Springer-Verlag 1997 O. Niggemeyer J. M. Strauss K. P. Schulitz Comparison of surgical procedures for degenerative lumbar spinal stenosis: a meta-analysis of the literature from 1975 to 1995 Received: 8 March 1997 Revised: 18 June 1997 Accepted: 30 June 1997 O. Niggemeyer (~). J. M. Strauss K. P. Schulitz Department of Orthopaedics, Heinrich Heine University, Moorenstrasse 5, D Dtisseldorf, Germany Fax i Abstract Therapy for spinal stenosis remains difficult. The possibilities for conservative management are limited and not satisfactory in the more severe cases. Various surgical procedures are possible, such as decompression, decompression and fusion without instrumentation and decompression and fusion with instrumentation. The aim of our metaanalysis was to compare the postoperative results of these three surgical techniques in the literature and, thus, to establish a treatment of choice for degenerative lumbar spinal stenosis. Via Medline, 30 articles met the inclusion criteria for our study, leading to a total number of 1668 cases being included in the meta-analysis. The evaluation was made according to our own definition of outcomes, based on criteria most commonly used in the studies reviewed. We found that in patients suffering degenerative spinal stenosis for up to 8 years, decompression without fusion showed the best results. For a dura- tion of symptoms of 15 years or more, decompression with instrumented fusion had the best results. Analysing all postoperative outcomes, decompression is the surgical procedure with the highest rate of success and the fewest complications, followed by decompression with instrumented fusion. In surgery for degenerative lumbar spinal stenosis, decompression and fusion without instrumentation was the least successful procedure. As patients suffering from a degenerative spinal stenosis often are elderly, operations are risky and place a strain on them. This review of the literature shows that the least invasive surgical procedure can obtain the best results if the correct diagnosis is made and if the operation is carried out within the first years of the disease. Key words Meta-analysis Degenerative lumbar spinal stenosis Decompression- Fusion Introduction Spinal stenosis of the lumbar spine is described as one of the end processes in the pathogenesis of low back pain [27]. The initial concept of spinal stenosis was developed in However, it was only after 1954, when Verbiest [26] set out definitive clinical and pathological findings, that spinal stenosis could adequately be diagnosed [18]. Lumbar spinal stenosis has been defined as a condition in- volving any type of narrowing of the spinal canal, nerve root canals, or tunnels of intervertebral foramina [1]. The most common form is the degenerative lumbar spinal stenosis due to hypertrophy of the facet joint, with or without developmental changes, leading eventually to protrusions of the intervertebral discs resulting in a narrowing of the spinal canal [17]. The therapeutic choices remain difficult and controversial. The possibilities for conservative therapy are limited
2 424 and their effect is lasting only in mild cases [2, 27]. Surgical intervention should be considered when medical management fails or in cases of initial signs of cauda equina dysfunction or progressive neurologic deterioration [3]. Many surgical techniques have been described [5, 8, 10, 13, 15, 20-23, 29], all based on the principles of decompression alone or decompression and fusion with or without instrumentation. These different surgical techniques show a wide range of good, fair and poor results and they all have specific complications; spinal instability after decompression operations and pseudarthrosis after lumbar fusions are particular problems. However, a reference procedure has not yet been established. One way to compare the different surgical techniques described in the literature is to conduct a meta-analysis. The aim of our meta-analysis was to compare the the postoperative outcomes for the following three surgical techniques: decompression; decompression and instrumented fusion; and decompression and fusion without instrumentation. Materials and methods A Medline database search was conducted using the key words: 1. Lumbar spinal stenosis 2. Fusion/decompression of the spine 3. Claudicatio spinalis 4. Radicular signs Literature included in our study fitted the following inclusion criteria: 1. Published between 1975 and 1995 in English, French or German 2. Reported cases of degenerative lumbar stenosis with no precedent operations of the lumbar spine ("virgin backs") 3. Covered a minimum of seven patients in the original study We did not include degenerative spondylolisthesis with resulting spinal stenosis in our study because it has a different etiology from pure degenerative spinal stenosis. Furthermore, there is already a therapeutic concept for the treatment of the degenerative spondylolisthesis with good results. Each article selected was read independently by two clinicians with training in research methods. The raters extracted specific information concerning the study morphology, preoperative patient Table 1 Outcome rating criteria of the meta-analysis Outcome Good Fair Poor Criteria No or occasional mild pain Able to work at usual job No or minimal restriction of physical activity Mild persistant back/leg pain; occasional moderate pain Able to work with some restrictions Able to perform most normal activities Persistent moderate and/or occasional severe pain Little or no pain relief from surgery Persistent root symptoms Unable to work Severe activity restrictions characteristics, surgical methods and patient outcomes, recording these data on standardised coding forms. They then met to review information from each paper, and all disagreements were discussed until a consensus could be reached. When agreement could not be reachedl the article was sent to a third rater for arbitration. This was particularly necessary regarding the evaluation of the postoperative patient clinical outcome. Our literature review revealed a wide range of definitions of "good", "fair" and "poor" overall outcome. We therefore used our own definitions. This procedure is usual in meta-anatyses [16, 24, 25]. We used outcome rating criteria similar to those of Turner et al. [24] (see Table 1). Whenever enough information was provided in an article, we classified the outcomes according to our own criteria so that we could compare outcomes across studies. We also rated outcomes for each of the measured variables separately, such as leg pain, back pain, job functioning, functional disability and preoperative duration of symptoms. Finally, we recorded the authors' own overall ratings of good, fair and poor outcome. Unlike Turner et al. [24], we maximized the total number of studies available for the meta-analysis with the use of a weighting factor. In studies including a wider set of preoperative diagnoses than our study, where an overall outcome was presented for all the different diagnoses, we first weighted the whole study as follows: relevant patients of the (i)th study wf= all patients of the (i)th study with the weighting factor wfcalculated by dividing the number of relevant patients of the (i)th study by the total number of patients in that study. The meta-analysis was performed according to the procedures described by Mosteller and Chalmers, Glass et al. and Fleiss [6, 7, 19]. To calculate simple proportions p(i) for each study, the number of patients with a certain surgical procedure and the number of patients with satisfactory results in the (i)th study were divided by the total number of patients n(i) in that study. The standard error SE(i) for a proportion p(i) was computed using the binomial distribution: SEi.~/Pi (lni- Pl ) The weighting w(i) for a proportion p(i) is the reciprocal of the squared standard error for the proportion: 1 w i -- SEi2 For combined estimate based on all studies, the weighted pooled proportion P, was calculated as follows: p _ wi Pi Y~w i where p(i) is the proportion for the ith study and w(i) is the weight for p(i). The variance of P was computed as follows: vat(p) - y-"wi2 SEi2 (Y~Wi) 2 The Z value for comparing two weighted pooled proportions p(1) and p(2) based on two different sets of studies is computed according to the formula: Z= [1-f'2 ~/var(p 1 ) + var(p2) The Z value indicates whether there is a statistically significant difference between the two different sets of studies. The comparison of the different factors predicting patient outcome was made with the Student t-test, the level of significance was fixed at.
3 425 Table 2 Preoperative symptoms of the patients. The third, fourth and fifth colmnns indicate the maximum and minimum values of each study and the average value for all studies, respectively Symptoms % of the articles Minimum Maximum Average reporting symptom value value value Duration 38 3 months 30 years 7.9 years Leg pain 50 18% 100% 51% Claudication 54 14% 74% 28% Back pain 54 1% 92% 47% No root signs 19 0% 0% 0% Paresis 46 9% 38% 22% Dysaesthesia 35 12% 73% 29% Bladder dysfunction 19 1% 6% 3 % Straight leg raising pain 23 8% 19% 11% One of the general problems when conducting a meta-analysis is that one has to deal with the data that is provided from the authors of the original article. Only in a very few cases is it possible to find data about every single patient. Thus, we sometimes had to integrate all the patients of the original article into our meta-analysis, so that individual outcomes were not noted. For example, in the case of the patient age - which is mostly reported as an age range - exclusion of single patients of an inappropriate age was not possible. The reason for the number of original papers included in our study being so small is that most authors reported on patients suffering from low back pain, but with different diagnoses such as spondylolisthesis, degenerative spinal stenosis, disc herniation and others. As outcomes are mostly not differentiated for the different primary diagnoses, inclusion in our meta-analysis was not possible for statistical reasons in these cases. Results Using the above-mentioned key words for the Medline search, 247 articles were identified. Only 30 of these articles met all the inclusion criteria, so we conducted the meta-analysis with these studies (see Appendix). The sample sizes ranged from 8 to 184 patients (mean 67.5 patients), leading to a total of 1668 patients. The youngest patient was 19 years old and the oldest 87, with a mean age of 55.7 years. The sex ratio varied a lot, from 29% to 85% male patients (mean 58.2%). The time of follow-up ranged from 1 to 32 years (mean 4.7 years). The diagnosis of lumbar spinal stenosis was established in the studies with the help of physical examination, CT (reported in 23% of the studies), myelography (50% of the studies) and electrophysiological neurologic investigations (3% of the studies). The diameter of the spinal canal was reported in 27% of the original articles, with a range of mm found to be the limit for a diagnosis of spinal stenosis. The preoperative symptoms of the patients were reported only in some of the articles (see Table 2). Most of the patients had back or leg pain (47% and 51%, respectively), but only alzout 30% of patients, on average, were reported to have any neurologic deficits. Straight leg raising was abnormal in an average of 11% of subjects. We divided the different surgical techniques performed into three groups in order not to have too few patients in Table 3 Postoperative results of the patients with decompression. The third, fourth and fifth columns show the good, fair and poor results of the patients of all the articles that reported on these symptoms (second column) Symptoms after % of articles Good Fair Poor decompression reporting results results results symptom (%) (%) (%) Leg/back pain Neurologic symptoms Ability to work Table 4 Postoperative results of the patients after decompression and fusion without instrumentation Symptoms after % of articles Good Fair Poor decompression reporting results results results and fusion without syndrom (%) (%) (%) instrumentation Leg/back pain Neurologic symptoms Ability to work Table 5 Postoperative results of the patients after decompression and fusion with instrumentation Symptoms after % of articles Good Fair Poor decompression reporting results results results and fusion without syndrom (%) (%) (%) instrumentation Leg/back pain Neurologic symptoms Ability to work each group. We included in the group of patients with decompression only, all patients with hemilaminectomies (n = 299) and those with complete laminectomies (n = 1177). Fusion without instrumentation was a posterolateral fusion in all cases (n = 49). The group of patients with instrumented fusion included those instrumented with pedicle screws and a rod (n = 169), with pedicle screws and a plate fixation (n = 29) or with various other techniques (n = 45). All patients with fusion of the lumbar spine had a
4 426 Table 6 Comparison of the results of the different surgical techniques. The Z value indicates whether there is a statistically significant difference between the two sets of studies Decompression vs. decompression and fusion Z = without instrumentation (n. s.) Decompression vs. decompression and fusion Z = with instrumentation (n. s.) Decompression and fusion with instrumentation vs. Z = decompression and fusion without instrumentation (n.s.) Good Fair Poor Z = Z = (n. s.) (n. s.) Z = M-.478 Z = (n. s.) (n. s.) Z = Z= (n.s.) (n.s.) Table 7 Complications following the operations as reported in the articles Complications % of articles Minimum total Maximum total Average reporting symptom no. no. no. Deep vein thrombosis Infections Operative mortality Neurologic disorders Others, e.g. reoperation Table 8 Comparison of the good versus the fair and poor postoperative outcomes for the different surgical techniques for all patients with a history of degenerative spinal stenosis of less than 7 years Surgical technique Good results Fair + poor results Decompression only Instrumented fusion Uninstrumented fusion Decompression only Instrumented fusion Uninstrumented fusion P < 0.78 Table 9 Comparison of the good versus the fair and poor postoperative outcomes for the different surgical techniques for all patients with a history of degenerative spinal stenosis of at least 15 years Surgical technique Good results Fair + poor results Decompression only Instrumented fusion Uninstrumented fusion Decompression only P < 0.45 Instrumented fusion Uninstrumented fusion complete laminectomy and none underwent anterior fusion of the spine. The postoperative results were presented very differently in each study. We tried to assess the results presented in the articles with the help of the criteria mentioned in Table 1. This was only possible in cases where information additional to the authors' rating was provided, such as a description of the postoperative clinical symptoms of the patient in comparison to the preoperative clinical symptoms. Such information was provided in 0%--42% of the studies, depending on the criterion (Tables 3-5). The comparison of the three surgical techniques did not reveal a statistically significant superioritiy of any one of them. Decompression only was the procedure with the highest rate of good postoperative results, followed by decompression and instrumented fusion. Decompression and fusion without instrumentation showed the lowest rate of good postoperative results (see Table 6). Reported complications of surgery are shown in Table 7. The accuracy of these data are unknown. Typically, ar- ticles did not report the absence of specific complications. If a particular complication was not mentioned in an article, it is unknown whether it occurred or not. None of the studies reported death as a direct result of the surgery. We also analysed preoperative clinical symptoms as factors predicting the surgical outcome of the patients. None of the factors leg pain, back pain, claudicatio spinalis or neurologic symptoms showed any influence on the postoperative result for any of the symptoms. In patients with multiple symptoms surgery was less successful than in those with only few clinical symptoms prior to operation. This finding did not depend on which surgical technique was used and the difference in outcome between the different groups was not statistically significant. The duration of preoperative symptoms had an important influence on the rates of success. In those patients that underwent surgery in the first 7 years of the disease, the best results were obtained by decompression only (P0.01, see Table 8); in those with a duration of symptoms of 15 years or more, instrumented fusion showed the best postoperative outcome (P0.01, see Table 9). For a dura-
5 427 tion of symptoms of 8-15 years none of the three analysed surgical procedures was superior. Discussion Conservative management of degenerative lumbar spinal stenosis is very seldom mentioned in literature [12, 27]. A randomised study comparing the surgical and the natural outcome of patients with degenerative spinal stenosis has not been reported so far, but would be highly interesting. We compared only the different surgical approaches to this disease. For patients with degenerative lumbar spinal stenosis a treatment of choice has not yet been established. Therefore, which of the different possible forms of surgical interventions is used mostly depends on the progress and experience of the surgeon. Furthermore, most of the articles in the literature report on more specific problems and deal with few patients, so that information regarding a treatment of choice cannot be obtained. That is why we tried to evaluate the different surgical techniques used for degenerative lumbar spinal stenosis with the aid of a metaanalysis in order to give some orientation marks for the best possible treatment. A similar meta-analysis by Turner et al. was unsatisfactory because of the poor scientific quality of the literature and major deficits in study design, analysis and reporting [24]. We encountered the problem of quality as well, but with the help of a weighting factor for the studies we were able to incorporate more literature into our meta-analysis. Nevertheless some of the integrated articles did not provide enough information about the postoperative outcome of the patients, so we were obliged to use the authors' rating in the meta-analysis. Like previous studies, we also analysed the clinical factors influencing the outcome after surgery for spinal stenosis. Some authors reported factors predisposing patients to worse outcomes as: female sex, greater severity and duration of symptoms before surgery, younger age (30-50 years), prior back surgery, compensation and ligitation issues and multilevel decompression [4, 8, 9, 11, 14, 28]. We were unable to analyse whether previous surgery of the spine influenced the postoperative outcome, since these patients were not included in the analysis. In our metaanalysis we found none of the clinical symptoms to be a predicting factor for the surgical outcome where there was only one of the mentioned symptoms. In cases of severe illness with more severe and multiple symptoms the surgical outcome of the patients was less successful, but showed similar results for the three surgical techniques compared. A difference was found in relation to the preoperative duration of the clinical symptoms, so that this was the only predicting factor for the postoperative outcome. These findings are probably due to the natural course of spinal stenosis leading to an increased instability of the spine and advanced facet joint degeneration. Therefore, different durations of symptoms may require different surgical techniques, and the decision of which technique to use should be made taking the duration of symptoms into consideration. Improvements in the means of diagnosing spinal stenosis will surely lead to fewer patients with a long duration of symptoms before surgery, since the diagnosis can be established earlier. Patients will thus be operated at an earlier state of the disease, so that decompression only will be of increasing value for patients suffering from degenerative spinal stenosis. This is a benefit, since most patients undergoing surgery for degenerative spinal stenosis are aged over 60 years (in our study 901 patients = 54%), with many aged over 80 years (in our study 517 patients = 31%) and there is an increased morbidity associated with fusions [24]. In conclusion, we found that decompressive laminectomy only shows the best results for patients with degenerative spinal stenosis if the duration of symptoms is less than 8 years, so the clinician should aim to establish the diagnosis early and offer the operation to the patient early as well. Then patients can have maximum benefit from the operation, especially since it is associated with an acceptably low rate of complications. References 1. Arnoldi CC, Brodsky AE, Chauchoix J, Crock HV, Dommisse GF, Edgar MA, Gargano FP, Jacobson RE, Kirkaldy-Willis WH, Kurihara A, Lan-- genski^ld A, Macnab I, McIvor GWD, Newman PH, Paine KWE, Russin LA, Sheldon J, Tile M, Urist MR, Wilson WE, Wiltse LL (1976) Lumbar spinal stenosis and nerve root entrapment syndromes. Definition and classification. Clin Orthop 115: Baumgartner H (1993) Klinik der Spinalstenose. Orthopfide 22: Circillo SF, Weinstein PR (1993) Lumbar spinal stenosis. West J Med 158: Echeverria T, Lockwood RC (1979) Lumbar spinal stenosis: experience at a community hospital. NY State Med 79: Ehni G (1977) Surgical treatment of spondylotic caudal radiculopathy. In: Weinstein PR, Ehni G, Wilson CB (eds) Lumbar spondylosis: diagnosis, management and surgical treatment. Year Book Medical Publishers, Chicago, pp Fleiss JL (1993) The statistical basis of meta-analysis. Stat Meth Med Res 2: Glass GV, McGaw B, Smith ML (1981) Meta-analysis in social research. Sage, Beverly Hills 8. Grabias S (1980) The treatment of spinal stenosis. J Bone Joint Surg [Am] 62: Herron L, Mangelsdorf C ( 1991) Lumbar spinal stenosis: results of surgical treatment. J Spinal Disord 4:26-33
6 Hutter CG (1985) Spinal stenosis and posterior lumbar interbody fusion. Clin Orthop 193: Johnsson KE, Redlund-Jonell I, Uden A, Willner S (1989) Preoperative and postoperative instability in lumbar spinal stenosis. Spine 14: Johnsson KE, Rosen I, Uden A (1992) The natural course of lumbar spinal stenosis. Clin Orthop 279: Kawai S, Hattori S, Oda H, Yamaguchi Y, Yoshida Y (1981) Enlargement of the lumbar vertebral canal in lumbar canal stenosis. Spine 6: Lee CK, Hansen HT, Weiss AB (1978) Developmental spinal stenosis: pathology and surgical treatment. Spine 3: Lin PM (1982) Internal decompression for multiple levels of lumbar spinal stenosis: a technical note. Neurosurgery 11 : Mardjetko SM, Conolly PJ, Shott S (1994) Degenerative lumbar spondylolisthesis: a meta-analysis of literature Spine 19:$2256-$ McIvor GWD, Kirkaldy-Willis WH (1976) Pathologic and myelographic changes in the major types of lumbar spinal stenosis. Clin Orthop 115: Meerkotter DV, Craig J (1988) Spinal stenosis at Baragwanath Hospital, Johannesburg. S Afr J Surg 26: Mosteller F, Chalmers TC (1992) Some progress and problems in metaanalysis of clinical trials. Stat Sci 7: Pennal GF, Shatzker J (1971) Stenosis of the lumbar spinal canal. Clin Neurosurg 18: Ray CD (1982) New techniques for decompression of lumbar spinal stenosis. Neurosurgery 10: Rosomoff HL (1981) Neural arch resection for lumbar spinal stenosis. Clin Orthop 154: Shenkin HA, Hash CJ (1976) A new approach to the surgical treatment of lumbar spondylosis. J Neurosurg 44: Turner JA, Ersek M, Herron L, Deyo R (1992) Surgery for lumbar spinal stenosis attempted meta-analysis of the literature. Spine 17: Turner JA, Ersek M, Herron L, Haselkorn J, Kent D, Ciol MA, Deyo R (1992) Patient outcomes after lumbar spinal fusions. JAMA 268: Verbiest H (1954) A radicular syndrome from developmental narrowness of the bony lumbar vertebral canal. J Bone Joint Surg [Br] 36: Wedge JH (1983) The natural history of spinal degeneration. In: Kirkaldy- Willis WH (ed) Managing low back pain. Churchill Livingstone, New York, pp Wiltse LL (1977) Surgery for intervertebral disc disease of the lumbar spine. Clin Orthop 129: Wiltse LL, Kirkaldy-Willis WH, Mc- Ivor GWD (1976) The treatment of spinal stenosis. Clin Orthop 115: Appendix Studies included in the meta-analysis M l.bitan F, Bex M, Lassale B, Rocolle J, Deburge A, de la Chaffiniere J (1984) Facteurs de r6ussite de l'arthrodbse post6ro-laterale du rachis lombo-sacrfi. Rev Chir Orthop 70: M 2. Boccanera L, Pellicioni S, Laus M (1984) Stenosis of the lumbar spinal canal. Ital J Orthop Traumatol 10: M 3. Brodsky A, Hendricks R, Khalil M, Darden B, Brotzman T (1989) Segmental ("floating") lumbar spine fusions. Spine 14: M 4. Caputy A, Luessenhop A (1992) Long-term evaluation of decompressive surgery for degenerative lumbar spinal stenosis. J Neurosurg 77: M 5. Chahal C, Mundkur Y, Sanchetti H, Ortho D, Arora R, Rastogi P (1982): Lumbar canal stenosis. Paraplegia 20: M 6. Ciric I, Mikhael M, Tarkington J, Vick N (1980) The lateral recess syndrome. J Neurosurg 53: M 7.Dick W, Widmer H (1993) Degenerative Lumbalskoliose und Spinalstenose. Orthop~ide 22: M 8.Ganz J (1990) Lumbar spinal stenosis: postoperative results in terms of preoperative-related pain. J Neurosurg 72:71-74 M 9.Getty C (1980) Lumbar spinal stenosis. J Bone Joint Surg [Br] 62: M10. Grob D, Humke T, Dvorak J (1993) Die Bedeutung der simultanen Fusion bei operierter Dekompression der lumbalen Spinalstenose. Orthop~tde 22: M11.Herno A, Airaksinen O, Saari T (1993) Long-term results of surgical treatment of lumbar spinal stenosis. Spine 18: M 12. Herron L, Mangelsdorf C ( 1991) Lumbar spinal stenosis: results of surgical treatment. J Spinal Disord 4: M 13. Hirabayashi S, Kumano K, Kuroki T (1991) Cotrel-Dubousset pedicle screw system for various spinal disorders. Spine 16: M14. Jalovaara P, L~ihde P, Iikko E, Ninim/iki T, Puranen J, Lindholm R (1989) The significance of residual stenosis after decompression for lumbar spinal stenosis. Ann Chir Gyn 78: M15. Johnson K, Willner S, Petterson H (1981) Analysis of operated cases with lumbar spinal stenosis. Acta Orthop Scand 52: M16.Kawai S, Hattori S, Oda H, Yamaguchi Y, Yoshida Y (1981) Enlargement of the lumbar vertebral canal in lumbar canal stenosis. Spine 6: M17. Kirkaldy-Willis WH, Wedge J, Yong-Hing K, Tchang S, de Korompay V, Shannon R (1982) Lumbar spinal nerve lateral entrapment. Clin Orthop 169: M18. Kurihara A, Tanaka Y, Tsumura N, Iwasaki Y (1988) Hyperostotic lumbar spinal stenosis. Spine 13: M19. Lassale B, Deburge A, Benoist M (1985) Resultats a long terme du traitement chirurgical des stenoses lombaires oper~es. Rev Rhum 52: M20. Nasca R (1989) Rationale for spinal fusion in lumbar spinal stenosis. Spine 14: M21.Onel D, Sari S, D?nmez C (1993) Lumbar spinal stenosis: clinical/radiologic therapeutic evaluation in 145 patients. Spine 18: M22. Petropoulos B (1989) Lumbar spinal stenosis syndrome. Clin Orthop 246: M23. Postacchini F, Cinotti G (1992) Bone regrowth after surgical decompression for lumbar spinal stenosis. J Bone Joint Surg [Br] 74:
7 429 M24. Salibi B (1976) Neurogenic intermittent claudication and stenosis of the lumbar spinal canal. Surg Neurol 5: M25. Sanderson P, Wood P (1993) Surgery for lumbar spinal stenosis in old people. J Bone Joint Surg [Br] 75: M26. San Martino A, D'Andria F, San Martino C (1983) The surgical treatment of nerve root compression caused by scoliosis of the lumbar spine. Spine 8: M27. Spanu G, Messina A, Assietti R, Sangiovanni G, Rodriguez Y, Barnea R (1988) Lumbar canal stenosis: results in 40 patients surgically treated. Acta Neurochir 94: M28. Turner J, Ersek M, Herron L, Haselkorn J, Kent D, Marcia C, Deyo R (1992) Patient outcomes after lumbar spinal fusions. JAMA 268: M29.Weir B, De Leo R (1981) Lumbar stenosis: analysis of factors affecting outcome in 81 surgical cases. J Can Sci Neurol 8: M30. Zdeblick T (1993) A prospective randomized study of lumbar fusion. Spine 18:
The outcome of Microscopic Selective Decompression of Degenerative Lumbar Spinal Stenosis
 Bahrain Medical Bulletin, Vol.28, No.4, December 2006 The outcome of Microscopic Selective Decompression of Degenerative Lumbar Spinal Stenosis A.Aziz Mohammed, CABS, FRCS (Ortho, Tr)* Tariq El Kalifa,
Bahrain Medical Bulletin, Vol.28, No.4, December 2006 The outcome of Microscopic Selective Decompression of Degenerative Lumbar Spinal Stenosis A.Aziz Mohammed, CABS, FRCS (Ortho, Tr)* Tariq El Kalifa,
Minimally Invasive Spine Surgery For Your Patients
 Minimally Invasive Spine Surgery For Your Patients Lukas P. Zebala, M.D. Assistant Professor Orthopaedic and Neurological Spine Surgery Department of Orthopaedic Surgery Washington University School of
Minimally Invasive Spine Surgery For Your Patients Lukas P. Zebala, M.D. Assistant Professor Orthopaedic and Neurological Spine Surgery Department of Orthopaedic Surgery Washington University School of
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: lumbar_spine_fusion_surgery 9/2010 5/2015 5/2016 5/2015 Description of Procedure or Service Low back pain
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: lumbar_spine_fusion_surgery 9/2010 5/2015 5/2016 5/2015 Description of Procedure or Service Low back pain
We carried out a retrospective review of 155
 Surgical treatment of lumbar spinal stenosis FIVE-YEAR FOLLOW-UP B. M. Jolles, F. Porchet, N. Theumann From the Central University Hospital of Vaudois, Lausanne, Switzerland We carried out a retrospective
Surgical treatment of lumbar spinal stenosis FIVE-YEAR FOLLOW-UP B. M. Jolles, F. Porchet, N. Theumann From the Central University Hospital of Vaudois, Lausanne, Switzerland We carried out a retrospective
1 REVISOR 5223.0070. (4) Pain associated with rigidity (loss of motion or postural abnormality) or
 1 REVISOR 5223.0070 5223.0070 MUSCULOSKELETAL SCHEDULE; BACK. Subpart 1. Lumbar spine. The spine rating is inclusive of leg symptoms except for gross motor weakness, bladder or bowel dysfunction, or sexual
1 REVISOR 5223.0070 5223.0070 MUSCULOSKELETAL SCHEDULE; BACK. Subpart 1. Lumbar spine. The spine rating is inclusive of leg symptoms except for gross motor weakness, bladder or bowel dysfunction, or sexual
Lumbar Spinal Stenosis Materclass: Surgical management of lumbar spinal stenosis:
 Lumbar Spinal Stenosis Materclass: Surgical management of lumbar spinal stenosis: Presented By: Michelle Emsley Senior Spinal In-Patient Physiotherapist Learning objectives Indications Evidence Post operative
Lumbar Spinal Stenosis Materclass: Surgical management of lumbar spinal stenosis: Presented By: Michelle Emsley Senior Spinal In-Patient Physiotherapist Learning objectives Indications Evidence Post operative
Spinal Surgery Functional Status and Quality of Life Outcome Specifications 2015 (01/01/2013 to 12/31/2013 Dates of Procedure) September 2014
 Description Methodology For patients ages 18 years and older who undergo a lumbar discectomy/laminotomy or lumbar spinal fusion procedure during the measurement year, the following measures will be calculated:
Description Methodology For patients ages 18 years and older who undergo a lumbar discectomy/laminotomy or lumbar spinal fusion procedure during the measurement year, the following measures will be calculated:
Nonoperative Management of Herniated Cervical Intervertebral Disc With Radiculopathy. Spine Volume 21(16) August 15, 1996, pp 1877-1883
 Nonoperative Management of Herniated Cervical Intervertebral Disc With Radiculopathy 1 Spine Volume 21(16) August 15, 1996, pp 1877-1883 Saal, Joel S. MD; Saal, Jeffrey A. MD; Yurth, Elizabeth F. MD FROM
Nonoperative Management of Herniated Cervical Intervertebral Disc With Radiculopathy 1 Spine Volume 21(16) August 15, 1996, pp 1877-1883 Saal, Joel S. MD; Saal, Jeffrey A. MD; Yurth, Elizabeth F. MD FROM
White Paper: Reducing Utilization Concerns Regarding Spinal Fusion and Artificial Disc Implants
 White Paper: Reducing Utilization Concerns Regarding Spinal Fusion and Artificial Disc Implants For Health Plans, Medical Management Organizations and TPAs Executive Summary Back pain is one of the most
White Paper: Reducing Utilization Concerns Regarding Spinal Fusion and Artificial Disc Implants For Health Plans, Medical Management Organizations and TPAs Executive Summary Back pain is one of the most
Surgical Procedures and Clinical Results of Endoscopic Decompression for Lumbar Canal Stenosis
 Surgical Procedures and Clinical Results of Endoscopic Decompression for Lumbar Canal Stenosis Munehito Yoshida, Akitaka Ueyoshi, Kazuhiro Maio, Masaki Kawai, and Yukihiro Nakagawa Summary. The purpose
Surgical Procedures and Clinical Results of Endoscopic Decompression for Lumbar Canal Stenosis Munehito Yoshida, Akitaka Ueyoshi, Kazuhiro Maio, Masaki Kawai, and Yukihiro Nakagawa Summary. The purpose
Spinal Surgery 2. Teaching Aims. Common Spinal Pathologies. Disc Degeneration. Disc Degeneration. Causes of LBP 8/2/13. Common Spinal Conditions
 Teaching Aims Spinal Surgery 2 Mr Mushtaque A. Ishaque BSc(Hons) BChir(Cantab) DM FRCS FRCS(Ed) FRCS(Orth) Hunterian Professor at The Royal College of Surgeons of England Consultant Orthopaedic Spinal
Teaching Aims Spinal Surgery 2 Mr Mushtaque A. Ishaque BSc(Hons) BChir(Cantab) DM FRCS FRCS(Ed) FRCS(Orth) Hunterian Professor at The Royal College of Surgeons of England Consultant Orthopaedic Spinal
Measure Title X RAY PRIOR TO MRI OR CAT SCAN IN THE EVAULATION OF LOWER BACK PAIN Disease State Back pain Indicator Classification Utilization
 Client HMSA: PQSR 2009 Measure Title X RAY PRIOR TO MRI OR CAT SCAN IN THE EVAULATION OF LOWER BACK PAIN Disease State Back pain Indicator Classification Utilization Strength of Recommendation Organizations
Client HMSA: PQSR 2009 Measure Title X RAY PRIOR TO MRI OR CAT SCAN IN THE EVAULATION OF LOWER BACK PAIN Disease State Back pain Indicator Classification Utilization Strength of Recommendation Organizations
Low Back Pain (LBP) Prevalence. Low Back Pain (LBP) Prevalence. Lumbar Fusion: Where is the Evidence?
 15 th Annual Cleveland Clinic Pain Management Symposium Sarasota, Florida Lumbar Fusion: Where is the Evidence? Gordon R. Bell, M.D. Director, Cleveland Clinic Low Back Pain (LBP) Prevalence Lifetime prevalence:
15 th Annual Cleveland Clinic Pain Management Symposium Sarasota, Florida Lumbar Fusion: Where is the Evidence? Gordon R. Bell, M.D. Director, Cleveland Clinic Low Back Pain (LBP) Prevalence Lifetime prevalence:
Surgical Guideline for Lumbar Fusion (Arthrodesis)
 I. Introduction Surgical Guideline for Lumbar Fusion (Arthrodesis) The purpose of this guideline is: A. To provide utilization review staff with the information necessary to make recommendations about
I. Introduction Surgical Guideline for Lumbar Fusion (Arthrodesis) The purpose of this guideline is: A. To provide utilization review staff with the information necessary to make recommendations about
visualized. The correct level is then identified again. With the use of a microscope and
 SURGERY FOR SPINAL STENOSIS Laminectomy A one inch (or longer for extensive stenosis) incision is made in the middle of the back over the effected region of the spine. The muscles over the bone are moved
SURGERY FOR SPINAL STENOSIS Laminectomy A one inch (or longer for extensive stenosis) incision is made in the middle of the back over the effected region of the spine. The muscles over the bone are moved
Diagnosis and Treatment of Lumbar Spinal Canal Stenosis
 Low Back Pains Diagnosis and Treatment of Lumbar Spinal Canal Stenosis JMAJ 46(10): 439 444, 2003 Katsuro TOMITA Department of Orthopedic Surgery, Kanazawa University Abstract: Lumbar spinal canal stenosis
Low Back Pains Diagnosis and Treatment of Lumbar Spinal Canal Stenosis JMAJ 46(10): 439 444, 2003 Katsuro TOMITA Department of Orthopedic Surgery, Kanazawa University Abstract: Lumbar spinal canal stenosis
Motion Preservation. Hansen Yuan, MD President, Spine Arthroplasty Society
 Motion Preservation Procedure Codes Hansen Yuan, MD President, Spine Arthroplasty Society Who are we? The Spine Arthroplasty Society (SAS) is a group of medical and associated specialists devoted to the
Motion Preservation Procedure Codes Hansen Yuan, MD President, Spine Arthroplasty Society Who are we? The Spine Arthroplasty Society (SAS) is a group of medical and associated specialists devoted to the
DUKE ORTHOPAEDIC SURGERY GOALS AND OBJECTIVES SPINE SERVICE
 GOALS AND OBJECTIVES PATIENT CARE Able to perform a complete musculoskeletal and neurologic examination on the patient including cervical spine, thoracic spine, and lumbar spine. The neurologic examination
GOALS AND OBJECTIVES PATIENT CARE Able to perform a complete musculoskeletal and neurologic examination on the patient including cervical spine, thoracic spine, and lumbar spine. The neurologic examination
Lumbar Stenosis Without Spondylolift - A Review
 J Neurosurg: Spine 2:686 691, 2005 Guidelines for the performance of fusion procedures for degenerative disease of the lumbar spine. Part 10: fusion following decompression in patients with stenosis without
J Neurosurg: Spine 2:686 691, 2005 Guidelines for the performance of fusion procedures for degenerative disease of the lumbar spine. Part 10: fusion following decompression in patients with stenosis without
Cervical Spine Surgery. Orthopaedic Nursing Seminar. Dr Michelle Atkinson. Friday October 21 st 2011. Cervical Disc Herniation
 Cervical Spine Surgery Dr Michelle Atkinson The Sydney and Dalcross Adventist Hospitals Orthopaedic Nursing Seminar Friday October 21 st 2011 Cervical disc herniation The most frequently treated surgical
Cervical Spine Surgery Dr Michelle Atkinson The Sydney and Dalcross Adventist Hospitals Orthopaedic Nursing Seminar Friday October 21 st 2011 Cervical disc herniation The most frequently treated surgical
X Stop Spinal Stenosis Decompression
 X Stop Spinal Stenosis Decompression Am I a candidate for X Stop spinal surgery? You may be a candidate for the X Stop spinal surgery if you have primarily leg pain rather than mostly back pain and your
X Stop Spinal Stenosis Decompression Am I a candidate for X Stop spinal surgery? You may be a candidate for the X Stop spinal surgery if you have primarily leg pain rather than mostly back pain and your
Operative treatment for degenerative lumbar spinal canal stenosis
 Acta Orthop. Belg., 2004, 70, 337-343 Operative treatment for degenerative lumbar spinal canal stenosis Hans TROUILLIER, Christof BIRKENMAIER, Jan KLUZIK, Thomas KAUSCHKE, Hans Jürgen REFIOR From Franziskus
Acta Orthop. Belg., 2004, 70, 337-343 Operative treatment for degenerative lumbar spinal canal stenosis Hans TROUILLIER, Christof BIRKENMAIER, Jan KLUZIK, Thomas KAUSCHKE, Hans Jürgen REFIOR From Franziskus
Research Article Partial Facetectomy for Lumbar Foraminal Stenosis
 Advances in Orthopedics, Article ID 534658, 4 pages http://dx.doi.org/10.1155/2014/534658 Research Article Partial Facetectomy for Lumbar Foraminal Stenosis Kevin Kang, 1 Juan Carlos Rodriguez-Olaverri,
Advances in Orthopedics, Article ID 534658, 4 pages http://dx.doi.org/10.1155/2014/534658 Research Article Partial Facetectomy for Lumbar Foraminal Stenosis Kevin Kang, 1 Juan Carlos Rodriguez-Olaverri,
OUTLINE. Anatomy Approach to LBP Discogenic LBP. Treatment. Herniated Nucleus Pulposus Annular Tear. Non-Surgical Surgical
 DISCOGENIC PAIN OUTLINE Anatomy Approach to LBP Discogenic LBP Herniated Nucleus Pulposus Annular Tear Treatment Non-Surgical Surgical Facet Joints: bear 20% of weight Discs bear 80% of weight Neural Foramen
DISCOGENIC PAIN OUTLINE Anatomy Approach to LBP Discogenic LBP Herniated Nucleus Pulposus Annular Tear Treatment Non-Surgical Surgical Facet Joints: bear 20% of weight Discs bear 80% of weight Neural Foramen
Lumbar spinal stenosis JA Shipley MMed(Orth) Department Orthopaedic Surgery, University of the Free State, Bloemfontein
 Page 42 / SA ORTHOPAEDIC JOURNAL Autumn 2008 CLINICAL ARTICLE C L I N I C A L A RT I C L E Lumbar spinal stenosis JA Shipley MMed(Orth) Department Orthopaedic Surgery, University of the Free State, Bloemfontein
Page 42 / SA ORTHOPAEDIC JOURNAL Autumn 2008 CLINICAL ARTICLE C L I N I C A L A RT I C L E Lumbar spinal stenosis JA Shipley MMed(Orth) Department Orthopaedic Surgery, University of the Free State, Bloemfontein
The Furcal nerve. Ronald L L Collins,MB,BS(UWI),FRCS(Edin.),FICS (Fort Lee Surgical Center, Fort Lee,NJ)
 The Furcal nerve. Ronald L L Collins,MB,BS(UWI),FRCS(Edin.),FICS (Fort Lee Surgical Center, Fort Lee,NJ) The furcal nerve is regarded as an anomalous nerve root, and has been found with significant frequency
The Furcal nerve. Ronald L L Collins,MB,BS(UWI),FRCS(Edin.),FICS (Fort Lee Surgical Center, Fort Lee,NJ) The furcal nerve is regarded as an anomalous nerve root, and has been found with significant frequency
ISPI Newsletter Archive Lumbar Spine Surgery
 ISPI Newsletter Archive Lumbar Spine Surgery January 2005 Effects of Charite Artificial Disc on the Implanted and Adjacent Spinal Segments Mechanics Using a Hybrid Testing Protocol Spine. 30(24):2755-2764,
ISPI Newsletter Archive Lumbar Spine Surgery January 2005 Effects of Charite Artificial Disc on the Implanted and Adjacent Spinal Segments Mechanics Using a Hybrid Testing Protocol Spine. 30(24):2755-2764,
CERVICAL DISC HERNIATION
 CERVICAL DISC HERNIATION Most frequent at C 5/6 level but also occur at C 6 7 & to a lesser extent at C4 5 & other levels In relatively younger persons soft disk protrusion is more common than hard disk
CERVICAL DISC HERNIATION Most frequent at C 5/6 level but also occur at C 6 7 & to a lesser extent at C4 5 & other levels In relatively younger persons soft disk protrusion is more common than hard disk
LOW BACK PAIN; MECHANICAL
 1 ORTHO 16 LOW BACK PAIN; MECHANICAL Background This case definition was developed by the Armed Forces Health Surveillance Center (AFHSC) for the purpose of epidemiological surveillance of a condition
1 ORTHO 16 LOW BACK PAIN; MECHANICAL Background This case definition was developed by the Armed Forces Health Surveillance Center (AFHSC) for the purpose of epidemiological surveillance of a condition
Lumbar Spinal Stenosis
 Lumbar Spinal Stenosis Introduction Lumbar spinal stenosis is defined as reduction in the diameter of the spinal canal, lateral nerve canals or neural foramina. The stenosis may involve multiple level
Lumbar Spinal Stenosis Introduction Lumbar spinal stenosis is defined as reduction in the diameter of the spinal canal, lateral nerve canals or neural foramina. The stenosis may involve multiple level
Title: Interspinous Process Decompression with the X-Stop Device for Lumbar Spinal Stenosis: A Retrospective Review. Authors: Jennifer R.
 Title: Interspinous Process Decompression with the X-Stop Device for Lumbar Spinal Stenosis: A Retrospective Review. Authors: Jennifer R. Madonia-Barr, MS, PA-C and David L. Kramer, MD Institution: Connecticut
Title: Interspinous Process Decompression with the X-Stop Device for Lumbar Spinal Stenosis: A Retrospective Review. Authors: Jennifer R. Madonia-Barr, MS, PA-C and David L. Kramer, MD Institution: Connecticut
Instrumented in situ posterolateral fusion for low-grade lytic spondylolisthesis in adults
 Acta Orthop. Belg., 2005, 71, 83-87 ORIGINAL STUDY Instrumented in situ posterolateral fusion for low-grade lytic spondylolisthesis in adults Mohamed A. EL MASRY, Walaa I. EL ASSUITY, Youssry K. EL HAWARY,
Acta Orthop. Belg., 2005, 71, 83-87 ORIGINAL STUDY Instrumented in situ posterolateral fusion for low-grade lytic spondylolisthesis in adults Mohamed A. EL MASRY, Walaa I. EL ASSUITY, Youssry K. EL HAWARY,
LUMBAR SPINAL STENOSIS OBSERVATIONS, EVIDENCE, AND TRENDS FULILLING THE UNMET CLINICAL NEED WRITTEN BY: HALLETT MATHEWS, MD, MBA
 LUMBAR SPINAL STENOSIS OBSERVATIONS, EVIDENCE, AND TRENDS FULILLING THE UNMET CLINICAL NEED WRITTEN BY: HALLETT MATHEWS, MD, MBA Overview of Lumbar Spinal Stenosis Spine stabilization, which has equated
LUMBAR SPINAL STENOSIS OBSERVATIONS, EVIDENCE, AND TRENDS FULILLING THE UNMET CLINICAL NEED WRITTEN BY: HALLETT MATHEWS, MD, MBA Overview of Lumbar Spinal Stenosis Spine stabilization, which has equated
Spine Trauma: When to Transfer. Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU
 Spine Trauma: When to Transfer Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU Disclosures Depuy Spine Consultant (teaching and courses) Department education and research funds Atlas Spine
Spine Trauma: When to Transfer Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU Disclosures Depuy Spine Consultant (teaching and courses) Department education and research funds Atlas Spine
Does the pain radiating down your legs, buttocks or lower back prevent you from walking long distances?
 Does the pain radiating down your legs, buttocks or lower back prevent you from walking long distances? Do you experience weakness, tingling, numbness, stiffness, or cramping in your legs, buttocks or
Does the pain radiating down your legs, buttocks or lower back prevent you from walking long distances? Do you experience weakness, tingling, numbness, stiffness, or cramping in your legs, buttocks or
Sample Treatment Protocol
 Sample Treatment Protocol 1 Adults with acute episode of LBP Definition: Acute episode Back pain lasting
Sample Treatment Protocol 1 Adults with acute episode of LBP Definition: Acute episode Back pain lasting
Advances In Spine Care. James D. Bruffey M.D. Scripps Clinic Division of Orthopaedic Surgery Section of Spinal Surgery
 Advances In Spine Care James D. Bruffey M.D. Scripps Clinic Division of Orthopaedic Surgery Section of Spinal Surgery Introduction The Spine - A common source of problems Back pain is the #2 presenting
Advances In Spine Care James D. Bruffey M.D. Scripps Clinic Division of Orthopaedic Surgery Section of Spinal Surgery Introduction The Spine - A common source of problems Back pain is the #2 presenting
Subject: BlueCross BlueShield of North Carolina Lumbar Spine Fusion Surgery Notification
 , 2010 Don W. Bradley, M.D. Senior Vice President, Healthcare & Chief Medical Officer Blue Cross and Blue Shield of North Carolina 5901 Chapel Hill Road Durham, NC 27707 Subject: BlueCross BlueShield of
, 2010 Don W. Bradley, M.D. Senior Vice President, Healthcare & Chief Medical Officer Blue Cross and Blue Shield of North Carolina 5901 Chapel Hill Road Durham, NC 27707 Subject: BlueCross BlueShield of
Presenter : Dr Yashpal Singh Rathore
 Presenter : Dr Yashpal Singh Rathore 1 Narrowing of the spinal canal/lateral recess/ intervertebral foramen. Verbiest (1954) first established LCS as a clinical entity Annual incidence 5 cases / 100,000
Presenter : Dr Yashpal Singh Rathore 1 Narrowing of the spinal canal/lateral recess/ intervertebral foramen. Verbiest (1954) first established LCS as a clinical entity Annual incidence 5 cases / 100,000
EXPERIMENTAL AND THERAPEUTIC MEDICINE 5: 567-571, 2013
 EXPERIMENTAL AND THERAPEUTIC MEDICINE 5: 567-571, 2013 Treatment of multilevel degenerative lumbar spinal stenosis with spondylolisthesis using a combination of microendoscopic discectomy and minimally
EXPERIMENTAL AND THERAPEUTIC MEDICINE 5: 567-571, 2013 Treatment of multilevel degenerative lumbar spinal stenosis with spondylolisthesis using a combination of microendoscopic discectomy and minimally
Complications in Adult Deformity Surgery
 Complications in Adult Deformity Surgery Proximal Junctional Kyphosis: Thoracolumbar and Cervicothoracic Sigurd Berven, MD Professor in Residence UC San Francisco Disclosures Research/Institutional Support:
Complications in Adult Deformity Surgery Proximal Junctional Kyphosis: Thoracolumbar and Cervicothoracic Sigurd Berven, MD Professor in Residence UC San Francisco Disclosures Research/Institutional Support:
Etiology of Long-term Failures of Lumbar Spine Surgery
 PAIN MEDICINE Volume 3 Number 1 2002 Etiology of Long-term Failures of Lumbar Spine Surgery Alexis Waguespack, MD, Jerome Schofferman, MD, Paul Slosar, MD, and James Reynolds, MD SpineCare Medical Group,
PAIN MEDICINE Volume 3 Number 1 2002 Etiology of Long-term Failures of Lumbar Spine Surgery Alexis Waguespack, MD, Jerome Schofferman, MD, Paul Slosar, MD, and James Reynolds, MD SpineCare Medical Group,
SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS?
 SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS? The spinal canal is best imagined as a bony tube through which nerve fibres pass. The tube is interrupted between each pair of adjacent
SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS? The spinal canal is best imagined as a bony tube through which nerve fibres pass. The tube is interrupted between each pair of adjacent
Advanced Practice Provider Academy
 (+)Dean T. Harrison, MPAS,PA C,DFAAPA Director of Mid Level Practitioners; Assistant Medical Director Clinical Evaluation Unit, Division of Emergency Medicine, Department of Surgery, Duke University Medical
(+)Dean T. Harrison, MPAS,PA C,DFAAPA Director of Mid Level Practitioners; Assistant Medical Director Clinical Evaluation Unit, Division of Emergency Medicine, Department of Surgery, Duke University Medical
https://www.laserspineinstitute.com/back_problems/foraminal_stenosis/e...
 Questions? Call toll free 1-866-249-1627 Contact us today. We're here for you seven days a week. MRI Review Consultation Live help Call 1-866-249-1627 Chat Live Home Laser Spine Institute Laser Spine Institute's
Questions? Call toll free 1-866-249-1627 Contact us today. We're here for you seven days a week. MRI Review Consultation Live help Call 1-866-249-1627 Chat Live Home Laser Spine Institute Laser Spine Institute's
STATE OF WEST VIRGINIA SUPREME COURT OF APPEALS MEMORANDUM DECISION
 STATE OF WEST VIRGINIA GARY E. GOSNELL, Claimant Below, Petitioner SUPREME COURT OF APPEALS FILED March 27, 2015 RORY L. PERRY II, CLERK SUPREME COURT OF APPEALS OF WEST VIRGINIA vs.) No. 14-0614 (BOR
STATE OF WEST VIRGINIA GARY E. GOSNELL, Claimant Below, Petitioner SUPREME COURT OF APPEALS FILED March 27, 2015 RORY L. PERRY II, CLERK SUPREME COURT OF APPEALS OF WEST VIRGINIA vs.) No. 14-0614 (BOR
Effective Date: 01/01/2012 Revision Date: 07/24/2013 Comments: Policy Accepted during 2013 Annual Review with no changes.
 Health Plan Coverage Policy ARBenefits Approval: 01/01/2012 Effective Date: 01/01/2012 Revision Date: 07/24/2013 Comments: Policy Accepted during 2013 Annual Review with no changes. Title: Minimally Invasive,
Health Plan Coverage Policy ARBenefits Approval: 01/01/2012 Effective Date: 01/01/2012 Revision Date: 07/24/2013 Comments: Policy Accepted during 2013 Annual Review with no changes. Title: Minimally Invasive,
EPIDURAL STEROID AND FACET INJECTIONS FOR SPINAL PAIN
 MEDICAL POLICY EPIDURAL STEROID AND FACET INJECTIONS FOR SPINAL PAIN Policy Number: 2015T0004W Effective Date: December 1, 2015 Table of Contents BENEFIT CONSIDERATIONS COVERAGE RATIONALE APPLICABLE CODES..
MEDICAL POLICY EPIDURAL STEROID AND FACET INJECTIONS FOR SPINAL PAIN Policy Number: 2015T0004W Effective Date: December 1, 2015 Table of Contents BENEFIT CONSIDERATIONS COVERAGE RATIONALE APPLICABLE CODES..
Medical Research Institute, Pusan National University School of Medicine, Busan, Korea 2
 Asian Spine Journal Vol. 5, No. 2, pp 100~106, 2011 doi:10.4184/asj.2011.5.2.100 Posterior Decompression and Fusion in Patients with Multilevel Lumbar Foraminal Stenosis: A Comparison of Segmental Decompression
Asian Spine Journal Vol. 5, No. 2, pp 100~106, 2011 doi:10.4184/asj.2011.5.2.100 Posterior Decompression and Fusion in Patients with Multilevel Lumbar Foraminal Stenosis: A Comparison of Segmental Decompression
Effects of vertebral axial decompression on intradiscal pressure
 This article is reprinted with the permission of the authors from the Journal of Neurosurgery, Volume 81. J Neurosurg 81:350-353, 1994 Effects of vertebral axial decompression on intradiscal pressure GUSTAVO
This article is reprinted with the permission of the authors from the Journal of Neurosurgery, Volume 81. J Neurosurg 81:350-353, 1994 Effects of vertebral axial decompression on intradiscal pressure GUSTAVO
Patient Guide to Lower Back Surgery
 The following is a sampling of products offered by Zimmer Spine for use in Open Lumbar Fusion procedures. Patient Guide to Lower Back Surgery Open Lumbar Fusion Dynesys The Dynesys Dynamic Stabilization
The following is a sampling of products offered by Zimmer Spine for use in Open Lumbar Fusion procedures. Patient Guide to Lower Back Surgery Open Lumbar Fusion Dynesys The Dynesys Dynamic Stabilization
SPINE SERVICE ROTATION ROTATION SPECIFIC OBJECTIVES (RSO) DEPT. OF ORTHOPEDICS AND PHYSICAL REHABILITATION UNIVERSITY OF MASSACHUSETTS
 SPINE SERVICE ROTATION ROTATION SPECIFIC OBJECTIVES (RSO) DEPT. OF ORTHOPEDICS AND PHYSICAL REHABILITATION UNIVERSITY OF MASSACHUSETTS The purpose of this RSO is to outline and clarify the objectives of
SPINE SERVICE ROTATION ROTATION SPECIFIC OBJECTIVES (RSO) DEPT. OF ORTHOPEDICS AND PHYSICAL REHABILITATION UNIVERSITY OF MASSACHUSETTS The purpose of this RSO is to outline and clarify the objectives of
Treating Bulging Discs & Sciatica. Alexander Ching, MD
 Treating Bulging Discs & Sciatica Alexander Ching, MD Disclosures Depuy Spine Teaching and courses K2 Spine Complex Spine Study Group Disclosures Take 2 I am a spine surgeon I like spine surgery I believe
Treating Bulging Discs & Sciatica Alexander Ching, MD Disclosures Depuy Spine Teaching and courses K2 Spine Complex Spine Study Group Disclosures Take 2 I am a spine surgeon I like spine surgery I believe
Presented by Zoran Maric, M.D. Orthopaedic Spine Surgeon May 22, 2010
 Presented by Zoran Maric, M.D. Orthopaedic Spine Surgeon May 22, 2010 1 cervical area thoracic area lumbar area sacrum coccyx Mayfield Clinic 2 3 4 5 Zoran Maric, MD Spine Surgery Procedures How to Document
Presented by Zoran Maric, M.D. Orthopaedic Spine Surgeon May 22, 2010 1 cervical area thoracic area lumbar area sacrum coccyx Mayfield Clinic 2 3 4 5 Zoran Maric, MD Spine Surgery Procedures How to Document
If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time.
 If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time. You may be worried about your future, both in respect of finances and
If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time. You may be worried about your future, both in respect of finances and
SPINAL STENOSIS, A CAUSE OF CAUDA EQUINA COMPRESSION*
 SPINAL STENOSIS, A CAUSE OF CAUDA EQUINA COMPRESSION* JOSEPH SCHATZKER and GEORGE F. PENNAL, TORONTO, ONTARIO, CANADA In 1934 Mixter and Barr described the syndrome of the ruptured intervertebral disc
SPINAL STENOSIS, A CAUSE OF CAUDA EQUINA COMPRESSION* JOSEPH SCHATZKER and GEORGE F. PENNAL, TORONTO, ONTARIO, CANADA In 1934 Mixter and Barr described the syndrome of the ruptured intervertebral disc
The Surgical Spine. Sergio Rivero M.D.
 The Surgical Spine Sergio Rivero M.D. Goals: Review Current literature in spinal surgery. To utilize evidence based medicine to treat spinal pathology. It is much more important to know what sort of a
The Surgical Spine Sergio Rivero M.D. Goals: Review Current literature in spinal surgery. To utilize evidence based medicine to treat spinal pathology. It is much more important to know what sort of a
Health Benchmarks Program Clinical Quality Indicator Specification 2013
 Health Benchmarks Program Clinical Quality Indicator Specification 2013 Measure Title USE OF IMAGING STUDIES FOR LOW BACK PAIN Disease State Musculoskeletal Indicator Classification Utilization Strength
Health Benchmarks Program Clinical Quality Indicator Specification 2013 Measure Title USE OF IMAGING STUDIES FOR LOW BACK PAIN Disease State Musculoskeletal Indicator Classification Utilization Strength
ICD-10-PCS Documentation and Coding for Spinal Procedures October 22, 2015
 Questions and Answers 1. We have a question regarding a spinal surgical procedure. The diagnosis was bilateral lateral recess stenosis and central stenosis from L2-L5. The procedure was an open lumbar
Questions and Answers 1. We have a question regarding a spinal surgical procedure. The diagnosis was bilateral lateral recess stenosis and central stenosis from L2-L5. The procedure was an open lumbar
Polymethylmethacrylate (PMMA) Augmentation Of A Cannulated And Fenestrated Pedicle
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 13, Issue 5 Ver. III. (May. 2014), PP 77-81 Polymethylmethacrylate (PMMA) Augmentation Of A Cannulated
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 13, Issue 5 Ver. III. (May. 2014), PP 77-81 Polymethylmethacrylate (PMMA) Augmentation Of A Cannulated
Spine Clinic Neurospine Specialists, Orthopaedics and Neurosurgery
 Spine Clinic Neurospine Specialists, Orthopaedics and Neurosurgery REVISION SPINE SURGERY Revision surgery is a very complex field which requires experience, training and evaluation in a very individual
Spine Clinic Neurospine Specialists, Orthopaedics and Neurosurgery REVISION SPINE SURGERY Revision surgery is a very complex field which requires experience, training and evaluation in a very individual
Evidence-based lumbar spine surgery
 34 Acta Orthop Scand (Suppl 5) 02; 73 Evidence-based lumbar spine surgery The role of national registration Björn Strömqvist Department of Orthopedics, Lund University Hospital, SE-221 85 Lund, Sweden,
34 Acta Orthop Scand (Suppl 5) 02; 73 Evidence-based lumbar spine surgery The role of national registration Björn Strömqvist Department of Orthopedics, Lund University Hospital, SE-221 85 Lund, Sweden,
Minimally Invasive Spine Surgery What is it and how will it benefit patients?
 Minimally Invasive Spine Surgery What is it and how will it benefit patients? Dr Raoul Pope MBChB, FRACS, Neurosurgeon and Minimally Invasive Spine Surgeon Concord Hospital and Mater Private Hospital Sydney
Minimally Invasive Spine Surgery What is it and how will it benefit patients? Dr Raoul Pope MBChB, FRACS, Neurosurgeon and Minimally Invasive Spine Surgeon Concord Hospital and Mater Private Hospital Sydney
How To Understand The Anatomy Of A Lumbar Spine
 Sciatica: Low back and Leg Pain Diagnosis and Treatment Options Presented by Devesh Ramnath, MD Orthopaedic Associates Of Dallas Baylor Spine Center Sciatica Compression of the spinal nerves in the back
Sciatica: Low back and Leg Pain Diagnosis and Treatment Options Presented by Devesh Ramnath, MD Orthopaedic Associates Of Dallas Baylor Spine Center Sciatica Compression of the spinal nerves in the back
Balloon Kyphoplasty. Balloon Kyphoplasty is a minimally invasive procedure to treat vertebral body compression fractures.
 Balloon Kyphoplasty Overview Balloon Kyphoplasty is a minimally invasive procedure to treat vertebral body compression fractures. The technique is designed to: Reduce and stabilise the fracture in a controlled
Balloon Kyphoplasty Overview Balloon Kyphoplasty is a minimally invasive procedure to treat vertebral body compression fractures. The technique is designed to: Reduce and stabilise the fracture in a controlled
Employees Compensation Appeals Board
 U. S. DEPARTMENT OF LABOR Employees Compensation Appeals Board In the Matter of DEBORAH R. EVANS and U.S. POSTAL SERVICE, POST OFFICE, Orlando, FL Docket No. 02-1888; Submitted on the Record; Issued December
U. S. DEPARTMENT OF LABOR Employees Compensation Appeals Board In the Matter of DEBORAH R. EVANS and U.S. POSTAL SERVICE, POST OFFICE, Orlando, FL Docket No. 02-1888; Submitted on the Record; Issued December
EPIDURAL STEROID AND FACET INJECTIONS FOR SPINAL PAIN
 CLINICAL POLICY EPIDURAL STEROID AND FACET INJECTIONS FOR SPINAL PAIN Policy Number: PAIN 019.16 T2 Effective Date: December 1, 2015 Table of Contents CONDITIONS OF COVERAGE... BENEFIT CONSIDERATIONS..
CLINICAL POLICY EPIDURAL STEROID AND FACET INJECTIONS FOR SPINAL PAIN Policy Number: PAIN 019.16 T2 Effective Date: December 1, 2015 Table of Contents CONDITIONS OF COVERAGE... BENEFIT CONSIDERATIONS..
Information for the Patient About Surgical
 Information for the Patient About Surgical Decompression and Stabilization of the Spine Aging and the Spine Daily wear and tear, along with disc degeneration due to aging and injury, are common causes
Information for the Patient About Surgical Decompression and Stabilization of the Spine Aging and the Spine Daily wear and tear, along with disc degeneration due to aging and injury, are common causes
Evidence Based Medicine in Spinal Surgery
 Evidence Based Medicine in Spinal Surgery Roger Härtl, MD Associate Professor of Neurosurgery Chief of Spinal Surgery Neurosurgeon to the GIANTS Football team Brain & Spine Center Weill Cornell Medical
Evidence Based Medicine in Spinal Surgery Roger Härtl, MD Associate Professor of Neurosurgery Chief of Spinal Surgery Neurosurgeon to the GIANTS Football team Brain & Spine Center Weill Cornell Medical
Three-level cervical disc herniation Case report and review of the literature
 Romanian Neurosurgery (2015) XXIX 3: 305-311 305 Three-level cervical disc herniation Case report and review of the literature Andrei St. Iencean 1,3, Ion Poeata 2,3 1 PhD Student, Grigore T. Popa University
Romanian Neurosurgery (2015) XXIX 3: 305-311 305 Three-level cervical disc herniation Case report and review of the literature Andrei St. Iencean 1,3, Ion Poeata 2,3 1 PhD Student, Grigore T. Popa University
Cervical Spondylotic Myelopathy Associated with Kyphosis or Sagittal Sigmoid Alignment: Outcome after Anterior or Posterior Decompression
 Cervical Spondylotic Myelopathy Associated with Kyphosis or Sagittal Sigmoid Alignment: Outcome after Anterior or Posterior Decompression 1 Journal of Neurosurgery: Spine November 2009, Volume 11, pp.
Cervical Spondylotic Myelopathy Associated with Kyphosis or Sagittal Sigmoid Alignment: Outcome after Anterior or Posterior Decompression 1 Journal of Neurosurgery: Spine November 2009, Volume 11, pp.
Update to the Treatment of Degenerative Cervical Disc Disease
 Update to the Treatment of Degenerative Cervical Disc Disease Michael Lynn, MD Neurosurgeon, Southeastern Neurosurgical & Spine Institute Adjunct Assistant Clinical Professor of Bioengineering, Clemson
Update to the Treatment of Degenerative Cervical Disc Disease Michael Lynn, MD Neurosurgeon, Southeastern Neurosurgical & Spine Institute Adjunct Assistant Clinical Professor of Bioengineering, Clemson
r1 is well known that the general population is aging and
 Journal of Gervntology: MEDICAL SCIENCES 1998, Vol. S3A, No. I, M72-M75 Copyright 1998 by The Cerontological Society of America Lumbar Spinal Stenosis in an Elderly Patient Daniel M. Clinchot, 1 Paul E.
Journal of Gervntology: MEDICAL SCIENCES 1998, Vol. S3A, No. I, M72-M75 Copyright 1998 by The Cerontological Society of America Lumbar Spinal Stenosis in an Elderly Patient Daniel M. Clinchot, 1 Paul E.
The conservative surgical treatment of lumbar spinal stenosis in the elderly
 REVIEW Robert Gunzburg Marek Szpalski The conservative surgical treatment of lumbar spinal stenosis in the elderly R. Gunzburg ( ) Department of Orthopaedics, Eeuwfeestkliniek, Harmoniestraat 68, 2018
REVIEW Robert Gunzburg Marek Szpalski The conservative surgical treatment of lumbar spinal stenosis in the elderly R. Gunzburg ( ) Department of Orthopaedics, Eeuwfeestkliniek, Harmoniestraat 68, 2018
Effects of Vertebral Axial Decompression (VAX-D) On Intradiscal Pressure
 Effects of Vertebral Axial Decompression (VAX-D) On Intradiscal Pressure Gustavo Ramos, M.D., William Marin, M.D. Journal of Neursurgery 81:35-353 1994 Departments of Neurosurgery and Radiology, Rio Grande
Effects of Vertebral Axial Decompression (VAX-D) On Intradiscal Pressure Gustavo Ramos, M.D., William Marin, M.D. Journal of Neursurgery 81:35-353 1994 Departments of Neurosurgery and Radiology, Rio Grande
Minimally Invasive Lumbar Fusion
 Minimally Invasive Lumbar Fusion Biomechanical Evaluation (1) coflex-f screw Biomechanical Evaluation (1) coflex-f intact Primary Stability intact Primary Stability Extension Neutral Position Flexion Coflex
Minimally Invasive Lumbar Fusion Biomechanical Evaluation (1) coflex-f screw Biomechanical Evaluation (1) coflex-f intact Primary Stability intact Primary Stability Extension Neutral Position Flexion Coflex
The economic burden of musculoskeletal disorders is
 The Effect of Surgical and Nonsurgical Treatment on Longitudinal Outcomes of Lumbar Spinal Stenosis Over 1 Years Yuchiao Chang, PhD, Daniel E. Singer, MD, Yen A. Wu, MPH, Robert B. Keller, MD, w and Steven
The Effect of Surgical and Nonsurgical Treatment on Longitudinal Outcomes of Lumbar Spinal Stenosis Over 1 Years Yuchiao Chang, PhD, Daniel E. Singer, MD, Yen A. Wu, MPH, Robert B. Keller, MD, w and Steven
Treatment pathways in lumbar spinal stenosis. By Prof. Dr. H. Michael Mayer
 Treatment pathways in lumbar spinal stenosis By Prof. Dr. H. Michael Mayer Content The pathology of spinal stenosis 4 The treatment of spinal stenosis 6 Spinal stenosis treatment options and outcomes 8
Treatment pathways in lumbar spinal stenosis By Prof. Dr. H. Michael Mayer Content The pathology of spinal stenosis 4 The treatment of spinal stenosis 6 Spinal stenosis treatment options and outcomes 8
Nerve root decompression without fusion in spondylolytic spondylolisthesis: long-term results of Gill s procedure
 DOI 10.1007/s00586-006-0115-y ORIGINAL ARTICLE Nerve root decompression without fusion in spondylolytic spondylolisthesis: long-term results of Gill s procedure Mark Arts Æ Willem Pondaag Æ Wilco Peul
DOI 10.1007/s00586-006-0115-y ORIGINAL ARTICLE Nerve root decompression without fusion in spondylolytic spondylolisthesis: long-term results of Gill s procedure Mark Arts Æ Willem Pondaag Æ Wilco Peul
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Interspinous Fixation (Fusion) Devices Page 1 of 6 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: See Also: Interspinous Fixation (Fusion) Devices Lumbar Spine
Interspinous Fixation (Fusion) Devices Page 1 of 6 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: See Also: Interspinous Fixation (Fusion) Devices Lumbar Spine
Decompressive Surgery Alone for Lumbar Spinal Stenosis in Elderly Patients
 CLINICAL ARTICLE Kor J Spine 5(2):83-88, 2008 Decompressive Surgery Alone for Lumbar Spinal Stenosis in Elderly Patients Il-Tae Jang, M.D., Sang-Won Lee, M.D., Paul M. Atienza, M.D., Jang-Seon You, M.D.
CLINICAL ARTICLE Kor J Spine 5(2):83-88, 2008 Decompressive Surgery Alone for Lumbar Spinal Stenosis in Elderly Patients Il-Tae Jang, M.D., Sang-Won Lee, M.D., Paul M. Atienza, M.D., Jang-Seon You, M.D.
Imaging degenerative disk disease in the lumbar spine. Elaine Besancon MS III Dr. Gillian Lieberman
 Imaging degenerative disk disease in the lumbar spine Elaine Besancon MS III Dr. Gillian Lieberman Learning Objectives Anatomy review Pathophysiology of degenerative disc disease Common sequelae of disk
Imaging degenerative disk disease in the lumbar spine Elaine Besancon MS III Dr. Gillian Lieberman Learning Objectives Anatomy review Pathophysiology of degenerative disc disease Common sequelae of disk
How To Get An Mri Of The Lumbar Spine W/O Contrast
 Date notice sent to all parties: May 27, 2014 IRO CASE #: ReviewTex, Inc. 1818 Mountjoy Drive San Antonio, TX 78232 (phone) 210-598-9381 (fax) 210-598-9382 reviewtex@hotmail.com Notice of Independent Review
Date notice sent to all parties: May 27, 2014 IRO CASE #: ReviewTex, Inc. 1818 Mountjoy Drive San Antonio, TX 78232 (phone) 210-598-9381 (fax) 210-598-9382 reviewtex@hotmail.com Notice of Independent Review
Management of spinal cord compression
 Management of spinal cord compression (SUMMARY) Main points a) On diagnosis, all patients should receive dexamethasone 10mg IV one dose, then 4mg every 6h. then switched to oral dose and tapered as tolerated
Management of spinal cord compression (SUMMARY) Main points a) On diagnosis, all patients should receive dexamethasone 10mg IV one dose, then 4mg every 6h. then switched to oral dose and tapered as tolerated
Cervical Spine Radiculopathy: Convervative Treatment. Christos K. Yiannakopoulos, MD Orthopaedic Surgeon
 Cervical Spine Radiculopathy: Convervative Treatment Christos K. Yiannakopoulos, MD Orthopaedic Surgeon Laboratory for the Research of the Musculoskeletal System, University of Athens & IASO General Hospital,
Cervical Spine Radiculopathy: Convervative Treatment Christos K. Yiannakopoulos, MD Orthopaedic Surgeon Laboratory for the Research of the Musculoskeletal System, University of Athens & IASO General Hospital,
Spinal Decompression: Laminectomy & Laminotomy
 Spinal Decompression: Laminectomy & Laminotomy Overview Narrowing of the spinal canal, a condition called spinal stenosis can cause chronic pain, numbness, and muscle weakness in your arms or legs (Fig.
Spinal Decompression: Laminectomy & Laminotomy Overview Narrowing of the spinal canal, a condition called spinal stenosis can cause chronic pain, numbness, and muscle weakness in your arms or legs (Fig.
Adult Spine Rotation Specific Evaluation Orthopaedic Surgery Training Program School of Medicine, Queen s University
 Adult Spine Rotation Specific Evaluation Orthopaedic Surgery Training Program School of Medicine, Queen s University CanMEDS Roles / Competencies Name: PGY Rotation Dates: s s Exceeds N/A Attending Staff:
Adult Spine Rotation Specific Evaluation Orthopaedic Surgery Training Program School of Medicine, Queen s University CanMEDS Roles / Competencies Name: PGY Rotation Dates: s s Exceeds N/A Attending Staff:
Degenerative Lumbar Scoliosis with Stenosis Successfully Treated with Cox Distraction Manipulation
 Cox Technic Case Report #92 (sent February 2011 2/8/11 ) 1 Degenerative Lumbar Scoliosis with Stenosis Successfully Treated with Cox Distraction Manipulation Presented By Robert E. Patterson Jr., D.C.
Cox Technic Case Report #92 (sent February 2011 2/8/11 ) 1 Degenerative Lumbar Scoliosis with Stenosis Successfully Treated with Cox Distraction Manipulation Presented By Robert E. Patterson Jr., D.C.
Patient Information. Lateral Lumbar Interbody Fusion Surgery (LLIF).
 Patient Information. Lateral Lumbar Interbody Fusion Surgery (LLIF). Understanding your spine Disc Between each pair of vertebrae there is a disc that acts as a cushion to protect the vertebra, allows
Patient Information. Lateral Lumbar Interbody Fusion Surgery (LLIF). Understanding your spine Disc Between each pair of vertebrae there is a disc that acts as a cushion to protect the vertebra, allows
Overview Anatomy of the spinal canal What is spinal stenosis? > 1
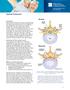 Spinal Stenosis Overview Spinal stenosis is the narrowing of your spinal canal and nerve root canal along with the enlargement of your facet joints. Most commonly it is caused by osteoarthritis and your
Spinal Stenosis Overview Spinal stenosis is the narrowing of your spinal canal and nerve root canal along with the enlargement of your facet joints. Most commonly it is caused by osteoarthritis and your
Spine conditionsnew treatments. Ben Okafor FRCS FRCS.orth Consultant Orthopaedic Surgeon
 Spine conditionsnew treatments Ben Okafor FRCS FRCS.orth Consultant Orthopaedic Surgeon Certainties of life Death Taxes Back pain New Advances Minimal access surgery Indirect Lumbar decompression Dynamic
Spine conditionsnew treatments Ben Okafor FRCS FRCS.orth Consultant Orthopaedic Surgeon Certainties of life Death Taxes Back pain New Advances Minimal access surgery Indirect Lumbar decompression Dynamic
Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, The Cervical Spine. What is the Cervical Spine?
 Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine condition that can cause pain and numbness in the neck, shoulders, arms, and even hands. This patient
Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine condition that can cause pain and numbness in the neck, shoulders, arms, and even hands. This patient
Spine University s Guide to Cauda Equina Syndrome
 Spine University s Guide to Cauda Equina Syndrome 2 Introduction Your spine is a very complicated part of your body. It s made up of the bones (vertebrae) that keep it aligned, nerves that channel down
Spine University s Guide to Cauda Equina Syndrome 2 Introduction Your spine is a very complicated part of your body. It s made up of the bones (vertebrae) that keep it aligned, nerves that channel down
WORKPLACE SAFETY AND INSURANCE APPEALS TRIBUNAL DECISION NO. 1708/15
 WORKPLACE SAFETY AND INSURANCE APPEALS TRIBUNAL DECISION NO. 1708/15 BEFORE: E. Kosmidis : Vice-Chair E. Tracey : Member Representative of Employers C. Salama : Member Representative of Workers HEARING:
WORKPLACE SAFETY AND INSURANCE APPEALS TRIBUNAL DECISION NO. 1708/15 BEFORE: E. Kosmidis : Vice-Chair E. Tracey : Member Representative of Employers C. Salama : Member Representative of Workers HEARING:
Lumbar Laminectomy and Interspinous Process Fusion
 Lumbar Laminectomy and Interspinous Process Fusion Introduction Low back and leg pain caused by pinched nerves in the back is a common condition that limits your ability to move, walk, and work. This condition
Lumbar Laminectomy and Interspinous Process Fusion Introduction Low back and leg pain caused by pinched nerves in the back is a common condition that limits your ability to move, walk, and work. This condition
Spine DJD Nomenclature. Sonia K Ghei, MD
 Spine DJD Nomenclature Sonia K Ghei, MD Recommendations of the Combined Task Forces of the North American Spine Society, American Society of Spine Radiology, and American Society of Neuroradiology http://www.asnr.org/spine_nomenclature/
Spine DJD Nomenclature Sonia K Ghei, MD Recommendations of the Combined Task Forces of the North American Spine Society, American Society of Spine Radiology, and American Society of Neuroradiology http://www.asnr.org/spine_nomenclature/
LOW BACK PAIN. common of these conditions include: muscle strain ( pulled muscle ), weak core muscles
 LOW BACK PAIN Most episodes of low back pain are caused by relatively harmless conditions. The most common of these conditions include: muscle strain ( pulled muscle ), weak core muscles (abdominal and
LOW BACK PAIN Most episodes of low back pain are caused by relatively harmless conditions. The most common of these conditions include: muscle strain ( pulled muscle ), weak core muscles (abdominal and
Options for Cervical Disc Degeneration A Guide to the Fusion Arm of the M6 -C Artificial Disc Study
 Options for Cervical Disc Degeneration A Guide to the Fusion Arm of the M6 -C Artificial Disc Study Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine
Options for Cervical Disc Degeneration A Guide to the Fusion Arm of the M6 -C Artificial Disc Study Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine
Spinal Decompression
 Spinal Decompression Spinal decompression is just one more tool we have to treat radiculopathy. With appropriate education and exercises, this modality has been proven to assist in the resolution of symptoms
Spinal Decompression Spinal decompression is just one more tool we have to treat radiculopathy. With appropriate education and exercises, this modality has been proven to assist in the resolution of symptoms
Marc A. Cohen, MD, FAAOS, FACS Diplomate American Board of Spinal Surgery Fellow American College of Spinal Surgery
 Marc A. Cohen, MD, FAAOS, FACS Diplomate American Board of Spinal Surgery Fellow American College of Spinal Surgery 221 Madison Ave Morristown, New Jersey 07960 (973) 538 4444 Fax (973) 538 0420 Patient
Marc A. Cohen, MD, FAAOS, FACS Diplomate American Board of Spinal Surgery Fellow American College of Spinal Surgery 221 Madison Ave Morristown, New Jersey 07960 (973) 538 4444 Fax (973) 538 0420 Patient
