Pediatric TB. Pediatric TB. Acknowledgements & Conflict of Interest
|
|
|
- Gwendoline Chapman
- 8 years ago
- Views:
Transcription
1 Pediatric TB Paul K. Nolan, FAAP Pediatric Pulmonologist, BC Amarillo Children s Clinic #17 Care Circle Amarillo, TX TB Updates for the Community: Partnering to Eliminate TB July 23, 2009 (806) Acknowledgements & Conflict of Interest Acknowledgement for Slides: Michelle Hulse, MD Medical Director Infectious Disease/Immunology/Rheumatology Children s Hospital s and Clinics of Minnesota Conflict of Interest Dr. Nolan has no declared conflicts of interest Pediatric TB Objective: Describe current recommendations for diagnosis and treatment of pediatric TB. Content: Diagnosis Treatment strategies Case studies
2 TB Definitions: Positive tuberculin skin test (TST) result: indicates possible infection with M tuberculosis complex. (Reactivity appears in 2 to 10 weeks median interval is 3 to 4 weeks after exposure.) Positive interferon-gamma release assay (IGRA): indicates possible infection with M tuberculosis complex. Exposed person: recent contact with another person with suspected or confirmed contagious pulmonary tuberculosis disease and who has a negative TST or IGRA result, normal physical examination findings, and CXR findings that are not compatible with tuberculosis. Some exposed people become infected (and subsequently, most have a positive TST or IGRA result) and some people do not become infected after exposure (indistinguishable initially). Source case: person who has transmitted infection with M tuberculosis complex to another person who subsequently has either latent tuberculosis infection or tuberculosis disease. Latent tuberculosis infection (LTBI): M tuberculosis complex infection in a person who has a positive TST or IGRA result, no physical findings of disease, and CXRfindings that are normal or reveal evidence of healed infection (eg, calcification in the lung, hilar lymph nodes, or both). TB Definitions: Tuberculosis disease: infection with symptoms, signs, or radiographic manifestations caused by M tuberculosis complex; disease may be pulmonary, extrapulmonary, or both. Infectious tuberculosis refers to tuberculosis disease of the lungs or larynx in a person who has the potential to transmit the infection to other people. Directly observed therapy (DOT): medication is administered directly to the patient by a health care professional or trained third party (not a relative or friend), who observes and documents ingestion of each dose of medication. Multiply drug-resistant (MDR) tuberculosis: TB infection or disease caused by M tuberculosis complex resistant to at least isoniazid and rifampin. Extensively drug-resistant (XDR) tuberculosis: infection or disease caused by a strain of M tuberculosis complex resistant to isoniazid and rifampin, at least 1 fluoroquinolone, and at least 1 of parenteral drugs: amikacin, kanamycin, or capreomycin. Bacille Calmette-Guérin (BCG): attenuated vaccine strain of M bovis. BCG rarely used in United States; most widely used vaccine in the world. Figure 1. Number of reported cases of tuberculosis, by year or diagnosis United States, ATS/CDC/IDSA controlling tuberculosis in the United States. Am J Respir Crit Care Med Nov 1;172(9):
3 Figure 2. Percentage of persons infected with Mycobacterium tuberculosis, by bacteriologic status of and proximity to the source case British Columbia and Saskatchewan, Source: Reference 57. ATS/CDC/IDSA controlling tuberculosis in the United States. Am J Respir Crit Care Med Nov 1;172(9): TABLE 2. Tuberculosis rates * among five racial/ethnic populations United States, 2003 Race/Ethnicity Rate White, non-hispanic 1.4 American Indian/Alaska 8.0 (5.7) Native Hispanic 10.5 (7.5) Black, non-hispanic 11.5 (8.2) Asian/Pacific Islander 29.4 (21.0) Numbers in parentheses represent risk for tuberculosis compared with white non-hispanics. Per 100,000 population. ATS/CDC/IDSA controlling tuberculosis in the United States. Am J Respir Crit Care Med Nov 1;172(9): Figure 3. Number and percentage of cases of tuberculosis among foreign-born persons, by year of diagnosis United States, ATS/CDC/IDSA controlling tuberculosis in the United States. Am J Respir Crit Care Med Nov 1;172(9):
4 Test Microscopy for acid-fast bacilli Nucleic acid amplification assay Mycobacterial growth detection by culture Identification of cultured mycobacteria Drug susceptibility testing Drug susceptibility testing of secondline drugs TABLE 3. Essential laboratory tests for tuberculosis control ATS/CDC/IDSA controlling tuberculosis in the United States. Am J Respir Crit Care Med Nov 1;172(9): Maximum Turnaround Time Onsite 24 h from specimen collection Offsite, 24 h from laboratory receipt (time from collection to lab receipt < 24 h) < 48 h from date of specimen collection < 14 d from date of specimen collection < 21 d from date of specimen collection < 30 d from date of specimen collection < 4 wk from date of request Patient and Setting Cough of 2 3 wk duration, with at least one additional symptom, including fever, night sweats, weight loss, or hemoptysis Recommended Evaluation CXR: if suggestive of TB (or if patient has HIV infection), 3 sputums for AFB smear micro and culture High risk for TB * with an unexplained illness, including respiratory symptoms, of 2 3 wk duration HIV infection and unexplained cough and fever High risk for TB * with a diagnosis of community-acquired pneumonia no better after 7 d of treatment High risk for TB * with incidental findings on CXR (Infiltrates with or without cavitation in the upper lobes or the superior segments of the lower lobes) suggestive of TB TABLE 5. Guidelines for the evaluation of pulmonary tuberculosis in adults in five clinical scenarios ATS/CDC/IDSA controlling tuberculosis in the United States. AJRCCM Nov 1;172(9): Chest radiograph: if suggestive of TB, 3 sputums for AFB smear micro and culture CXR, 3 sputum specimens for AFB smear microscopy and culture CXR, 3 sputums for AFB smear micro and culture Review CXR, 3 sputums for AFB smear micro and culture * HIGH RISK FOR TB Recent exposure to a person with a case of infectious TB; Hx positive test result for M. tuberculosis infection; HIV infection Injection or non-injection drug use Foreign birth and immigration in 5 yr from a region in which incidence is high Residents and employees of high-risk congregate settings Membership in a medically underserved, low-income population Medical risk factor for TB (including diabetes mellitus, conditions requiring prolonged corticosteroid and other immunosuppressive therapy; chronic renal failure, certain hematologic malignancies, and carcinomas; weight more than 10% below ideal body weight, silicosis, gastrectomy, or jejunoileal bypass). ATS/CDC/IDSA controlling tuberculosis in the United States. Am J Respir Crit Care Med Nov 1;172(9):
5 TB Epidemiology Higher in urban, low-income areas 2/3rds cases in the U.S. nonwhites Foreign-born children > 1/4 newly diagnosed cases < 14 y/o Groups with higher LTBI Immigrants/adoptees/refugees/travelers highprevalence regions (eg, Asia, Africa, Latin America, and countries of the former Soviet Union) homeless people correctional facilities TB Epidemiology Higher risk for progression of LTBI to tuberculosis disease: Infants and post-pubertal adolescents Recent infection (within the past 2 years) Immunodeficiency, especially HIV infection Immunosuppressive drugs, such as prolonged or high-dose corticosteroid therapy or chemotherapy IVDA Hodgkin disease, lymphoma, diabetes mellitus, chronic renal failure, and malnutrition Treatment with tumor necrosis factor alpha (TNFalpha) antagonists, such as infliximab and etanercept. Validated Questions for Determining Risk of LTBI in Children in the United States Has a family member or contact had tuberculosis disease? Has a family member had a positive tuberculin skin test result? Was your child born in a high-risk country (countries other than the United States, Canada, Australia, New Zealand, or Western European countries)? Has your child traveled (had contact with resident populations) to a high-risk country for more than 1 week?
6 Pediatric TB Diagnostic and therapeutic challenges Less specific signs and symptoms of disease Paucibacillary resulting in fewer positive cultures Increased risk of progression of disease once infected Increased risk of dissemination TB Diagnostic Tests Tuberculin Skin Testing (TST): Most common method for diagnosing LTBI in asymptomatic people. Mantoux method consists of 5 tuberculin units of purified protein derivative (0.1ml) injected intradermally using a 27-gauge needle and a 1.0-mL syringe into the volar aspect of the forearm; Palpable induration 6 to 10 mm in dia. crucial Image 145_21. (A) Sokol ballpoint pen method, 48 to 72 hours placement, slowly approaching site until resistance is felt from induration NOT redness. Repeat on the opposite side (B) Distance between the lines in millimeters. Red Book Online Visual Library, Image 145_21. Available at: Copyright 2009 American Academy of Pediatrics
7 Definitions of Positive Tuberculin Skin Test (TST) Results in Infants, Children, and Adolescents a Induration 5 mm or greater: Close contact with known or suspected TB Case Children suspected to have TB disease: Findings on chest radiograph consistent with active or previous TB disease Clinical evidence of tuberculosis disease b Children receiving immunosuppressive therapy c or with immunosuppressive conditions, including human immunodeficiency (HIV) infection a Regardless of previous bacille Calmette-Guérin (BCG) immunization; erythema alone at TST site does not indicate a positive test result. Tests should be read at 48 to 72 hours after placement. b Evidence by physical examination or laboratory assessment that would include tuberculosis in the working differential diagnosis (eg, meningitis). c Including immunosuppressive doses of corticosteroids. Definitions of Positive Tuberculin Skin Test (TST) Results in Infants, Children, and Adolescents a Induration 10 mm or greater Children at increased risk of disseminated tuberculosis disease: Children younger than 4 years of age Children with other medical conditions, including Hodgkin disease, lymphoma, diabetes mellitus, chronic renal failure, or malnutrition (see Table 3.80, p 684) Children with likelihood of increased exposure to tuberculosis disease: Children born in high-prevalence regions of the world Children frequently exposed to adults who are HIV infected, homeless, users of illicit drugs, residents of nursing homes, incarcerated or institutionalized, or migrant farm workers Children who travel to high-prevalence regions of the world a These definitions apply regardless of previous bacille Calmette- Guérin (BCG) immunization (see also Interpretation of TST Results in Previous Recipients of BCG Vaccine, p 685); erythema alone at TST site does not indicate a positive test result. Tests should be read at 48 to 72 hours after placement. Definitions of Positive Tuberculin Skin Test (TST) Results in Infants, Children, and Adolescents a Induration 15 mm or greater Children 4 years of age or older without any risk factors a Regardless of previous bacille Calmette- Guérin (BCG) immunization; erythema alone at TST site does not indicate a positive test result. Tests should be read at 48 to 72 hours after placement.
8 TB Diagnostic Tests M tuberculosis complex culture from specimens of gastric aspirates, sputum, bronchial washings, pleural fluid, cerebrospinal fluid (CSF), urine, or other body fluids or a biopsy. M tuberculosis complex organisms isolated < 50% of children, 75% of infants w/ pulmonary TB diagnosed by other clinical criteria TB Specimen Collection Hypertonic Saline Sputum induction in > 5 y/o Cough is nonproductive or absent Early morning gastric aspirate (GA) Nasogastric tube obtained before ambulation or feeding Aspirates collected on 3 separate days GA AFB smears usually negative False-positive smear results nontuberculous mycobacteria GA highest culture yield on the first day Fluorescent staining of GA smears are more sensitive Diagnostic yield of GA < 50% TB Diagnostic Tests Immunologic-Based Testing: QuantiFERON-TB Gold and Gold In-Tube and T-SPOT.TB are IGRAs. FDA-approved tests measure ex vivo interferon-gamma production from T lymphocytes fairly specific to M tuberculosis complex cannot distinguish between latent infection and disease, negative result cannot exclude tuberculosis infection or disease in a patient with suspicious finding
9 Current recommendations for use of IGRAs in children: For immune-competent > 5 years of age and older, IGRAs can be used in place of a TST to confirm cases of tuberculosis or cases of LTBI and likely will yield fewer false-positive test results. Children with a positive result from an IGRA should be considered infected with M tuberculosis complex. A negative IGRA result cannot universally be interpreted as absence of infection. Because of their higher specificity and lack of cross-reaction with BCG, IGRAs may be useful in children who have received BCG vaccine. IGRAs may be useful to determine whether a BCGimmunized child with a reactive TST more likely has LTBI or has a false-positive TST reaction caused by the BCG. IGRAs cannot be recommended routinely for use in children younger than 5 years of age or for immune-compromised children of any age because of a lack of published data about their utility with these groups. Indeterminate IGRA results do not exclude tuberculosis infection and should not be used to make clinical decisions. Household contact with contagious teen or adult Usually > 4 hours of contact Chest 2 view PA and Lat* TWO VIEW CHEST: IMPRESSION: Airway disease. No infiltrate, adenopathy or evidence of active pulmonary tuberculosis. Pt: 2 week old infant. Adult index case: father, incarcerated during gestation, ill for several months prior to hospitalization, cavitary, smear + pulmonary disease, pericarditis, osteomyelitis. MTB pansenstive isolated TB diagnosis Risk assessment important Diagnosis in children more often based on epidemiology and clinical findings than on smear or culture
10 TB disease Clinical and radiographic findings ( ,480 US cases) Pulmonary 76.9% Primary Progressive Chronic/reactivation Extra-pulmonary Lymphatic 15.5% Meningeal 2.1% Miliary 1.1% Pleural 1.1% Bone/joint 1.4% TB in newborns TST and Pediatric Disease Positive TST with TB disease Pediatrics 89% Adults 54% Up to 20% of children with TB disease will have a negative TST at diagnosis Approximately 5% will be persistently negative Pediatric TB disease Laboratory diagnosis Adult source isolate can direct treatment Cultures need to be obtained from the child if: source case is unknown several possible source cases with different susceptibility patterns if the likely source has drug resistant TB extrapulmonary disease
11 Pediatric Exposure Treatment Window prophylaxis Window period for TST conversion: 2-12 weeks Indicated for those </=4 years Baseline TST / CXR normal INH prophylaxis recommended Children </= 4yrs Immunosuppressed pts Pts on TNF alpha blockers Follow up TST done weeks after last exposure to infectious contact induration less than 5 mm stop prophylaxis, induration greater than 5 mm treat for LTBI Pediatric TB Disease Laboratory Diagnosis Childhood pulmonary disease Inpatient early morning gastric aspirate x3 (cx + ~40%) Induced sputum x 3 in cooperative older children-first morning best Bronchoscopy: culture yield is lower than properly obtained gastric aspirate (cx + ~20%) Newer testing modalities are not used for various reasons: PCR sensitivity only slightly better than culture, specificity less, so not widely used in pediatrics NAA and IGRAs not approved for use Extrapulmonary disease Culture from affected body site (cx +~40%) Clinical Manifestations of TB Image 145_07. Tuberculosis Mycobacterium tuberculosis infection With paratracheal lymph nodes. Red Book Online Visual Library, Image 145_07. Available at: Copyright 2009 American Academy of Pediatrics
12 13 yo asymptomatic, identified as part of contact investigation PPD 20mm 6 yo PPD 15 mm Contact investigation CXR hilar and infrahilar fullness Chest CT : Multiple pulmonary nodules in the lung bases bilaterally, in the right lower lobe, one in the posterolateral right middle lobe and two in the left lower lobe. Also present is extensive adenopathy. Image 145_09. Tuberculosis A 1-year-old child with endobronchial tuberculosis with pulmonary consolidation. Red Book Online Visual Library, Image 145_09. Available at: Copyright 2009 American Academy of Pediatrics
13 TB Disease Clinical and Radiographic Findings Progressive pulmonary primary TB Associated with weight loss or FTT, anorexia, fatigue, low grade temp, intermittent cough May cause cavitation or endobronchial disease TB Disease Clinical and Radiographic Findings Chronic pulmonary/ reactivation disease Most common in adolescents with primary infection after 7 years of age Present with fever, weight loss, productive cough, hemoptysis, night sweats Xray findings include cavitations, typically upper lobe TB Disease Clinical and Radiographic Findings Chronic pulmonary/ reactivation disease US data Cavitary disease Sputum smear positive Sputum culture positive <10 years of years age of age 3.5% 11.8% (p<0.001) 1.7% 10.3% (p<0.001) % 21.3% (p<0.001
14 TB Disease Clinical and Radiographic Findings Superficial lymphadenitis Usually the anterior cervical and submandibular nodes Usually presents within 6 months of infection Affects children with median age months Nodes are firm, nontender or minimally so No systemic symptoms Chest radiographic findings may be present Image 145_26. Tuberculosis Young man with Mycobacterium tuberculosis scrofula. Red Book Online Visual Library, Image 145_26. Available at: Copyright 2009 American Academy of Pediatrics TB Disease Clinical and RadiographicFfindings Pleural effusion Most occur 3 months after primary infection Usually affect older children (mean 13.5 years) Present with fever, fatigue, respiratory distress, chest pain CXR shows unilateral pleural effusion Associated parenchymal abnormalities in about half of pts Excellent prognosis
15 Copyright 2009 American Academy of Pediatrics Image 145_13. Tuberculosis Pulmonary tuberculosis with right pleural effusion. Red Book Online Visual Library, Image 145_13. Available at: TB meningitis 8 month old East Indian girl RUL pneumonia, possible abscess or loculated pleural fluid 8 month old with pulmonary TB and TB meningitis. Chest CT with RUL dense Consolidation with multiple cavitations. Superior mediastinum findings consistent with abscess
16 TB disease Clinical and Radiographic Findings Meningeal disease Most within 3-6 months of primary infection Often associated with miliary disease, esp in < 5 yr olds Median age affected months Most severe form of disease TB disease Clinical and Radiographic Findings Meningeal disease Indolent with symptoms present 1-4 weeks before diagnosis Most common symptoms are fever, vomiting, lethargy, headache, seizure (esp in < 2 year olds) Hydrocephalus common on presentation Brain parenchymal disease (tuberculoma) in 20-37% CXR abnormal in 40-86% TB Disease Clinical and Radiographic Findings Meningeal disease Outcome depends on age and severity of symptoms at presentation Mortality <10% with effective therapy Long term sequelae are common Mental retardation Seizures hemiparesis
17 Slide: Michelle Hulse, MD Miliary disease in 18 mo Hmong male micronodular infiltrates, hilar fullness Similar to meningitis in pathogenesis, time of onset after infection, indolent presentation, and severity Median age affected is 6-11 months Often present with weeks of fever, cough, weight loss, anorexia, and malaise 21 mo Hmong male F/U CXR 3mos: improving micronodular infiltrates and hilar fullness TB Disease Clinical and Radiographic Findings Bone/joint disease Onset 6-18 months after primary infection Median age of onset 6 years Affect vertebrae, knee, hip, and elbow most commonly Present with localized inflammation, pain, swelling, decreased range of motion, and fever Xrays may show spondylitis, arthritis, and osteomyelitis 50% will have abnormal CXR
18 Copyright 2009 American Academy of Pediatrics Image 145_16. Tuberculosis Tuberculosis of the spine with paravertebral abscess (Pott disease). Red Book Online Visual Library, Image 145_16. Available at: Image 145_17. Tuberculosis Tuberculosis of the spine with paravertebral abscess (Pott disease) shown on the radiograph. This is the same patient as in image 145_16. Red Book Online Visual Library, Image 145_17. Available at: Copyright 2009 American Academy of Pediatrics 7 yo Hmong refugee Pott s disease spine MRI Destruction and collapse of L3 and L4 along with inferior L2 and Superior L5. Kyphosis and gibbus formation, mild Central stenosis
19 TB Treatment Latent tuberculosis Regimen infection (positive TST or IGRA result, no disease) Isoniazid susceptible 9 mo of isoniazid, once a day Isoniazid resistant Isoniazid-rifampin resistant a 6 mo of rifampin, once a day Consult a tuberculosis specialist Remarks If daily therapy is not possible, DOT twice a week can be used for 9 mo. If daily therapy is not possible, DOT twice a week can be used for 6 mo. Drug choice predicated on resistance pattern. a Duration of therapy is longer for human immunodeficiency virus (HIV)-infected people, and additional drugs may be indicated Pulmonary and extrapulmonary (except meningitis) TB Treatment Regimen 2 mo of isoniazid, rifampin, pyrazinamide, and ethambutol daily, followed by 4 mo of isoniazid and rifampinb by DOT for c drug-susceptible Mycobacterium tuberculosis 9 to 12 mo of isoniazid and rifampin for drug-susceptible Mycobacterium bovis Remarks If possible drug resistance is a concern, another drug (ethambutol or an aminoglycoside) is added to the initial 3-drug therapy until drug susceptibilities are determined. DOT is highly desirable. If hilar adenopathy only, a 6- mo course of isoniazid and rifampin is sufficient. Drugs can be given 2 or 3 times/wk under DOT in the initial phase if nonadherence is likely. b Medications should be administered daily for the first 2 weeks to 2 months of treatment and then can be administered 2 to 3 times per week by DOT. c If initial chest radiograph shows cavitary lesions and sputum after 2 months of therapy remains positive, duration of therapy is extended to 9 months. TB Treatment Meningitis Regimen Remarks 2 mo of isoniazid, rifampin, A fourth drug, such as an pyrazinamide, and an aminoglycoside, is given aminoglycoside or ethambutol or with initial therapy until ethionamide, once a day, drug susceptibility is followed by 7 10 mo of isoniazid known. and rifampin, once a day or twice a week (9 12 mo total) for drugsusceptible M tuberculosis At least 12 mo of therapy without pyrazinamide for drugsusceptible M bovis For patients who may have acquired tuberculosis in geographic areas where resistance to streptomycin is common, kanamycin, amikacin, or capreomycin can be used instead of streptomycin.
20 Commonly Used Drugs for Treatment of Tuberculosis in Infants, Children, and Adolescents Less Commonly Used Drugs for Treatment of Drug-Resistant Tuberculosis in Infants, Children, and Adolescents a LTBI Treatment in Pregnancy Positive TST or IGRA result, normal chest radiographic findings, and recent contact index Isoniazid for 9 months Begin after the first trimester Pyridoxine for all pregnant and breastfeeding women Isoniazid safe for nursing; no pyridoxine supplement for infant
21 TB Disease Treatment in Pregnancy Regimen of isoniazid, rifampin, and ethambutol Pyrazinamide commonly is used in a 3- or 4-drug regimen Safety during pregnancy has not established At least 6 months of therapy for drug-susceptible TB if pyrazinamide is use; At least 9 months of therapy if pyrazinamide is not used Prompt initiation of therapy is mandatory to protect mother and fetus Infant of Mother w/ TB Disease Congenital/Perinatal TB suspected? Obtain TST (usually neg) CXR Lumbar puncture Appropriate cultures Placenta Histology for granulomas and AFB Cultured for M tuberculosis complex Newborn Infant Exposed to LTBI Asymptomatic LTBI Exposure, normal CXR no separation infant & mother Household members TST or IGRA & Eval Do not delay infant s discharge
22 Newborn Infant Exposed to TB Disease Mother w/ TB Disease Eval infant for congenital TB Infant separated until the mother (contact) evaluated If TB disease confirmed separation until mother (contact) & infant on appropriate anti- TB Rx If MDR or poor addherence consider BCG immunization Infant may breastfeed after maternal 2 wks Rx and mother not contagious Criteria for Determining when a Patient with Pulmonary TB Becomes Noninfectious Negligible likelihood of multidrug-resistant TB (no known exposure to MDRTB and no history of prior episodes of TB with poor compliance during treatment). Standard multidrug anti-tb therapy for 2 3 weeks. (For AFB smear results that are negative or rarely positive, threshold for treatment is 5 7 days.) Complete adherence to treatment (e.g., is receiving directly observed therapy). Evidence of clinical improvement (e.g., reduction in the frequency of cough or reduction of the grade of the sputum AFB smear result). All contacts identified, evaluated, advised, and, if indicated, treated latent TB infection; critical, especially for close contacts: younger than 4 years; any age immunocompromised In hospital pulmonary TB should remain in airborne-infection isolation until 1. Are receiving standard multidrug anti-tb therapy 2. Demonstrated clinical improvement 3. Have had three consecutive AFB-negative smear results of sputum specimens collected 8 24 hours apart, with at least one being an early-morning specimen. Patients returning to a congregate setting (e.g., a homeless shelter or detention facility) should have three consecutive AFB-negative smear results of more than 8 hours apart before being considered noninfectious. ATS/CDC/IDSA controlling tuberculosis in the United States. Am J Respir Crit Care Med Nov 1;172(9): Case 20 mo old Somali refugee with 8 mo hx of fever, cough, chronic otitis media, constitutional symptoms +PPD Chest imaging with miliary opacities and extensive mediastinal and hilar adenopathy CNS tuberculomas Splenomegaly, retroperitoneal, and peri-portal adenopathy Mildly increased aminotransferases and inflammatory markers
23 20 months, Somali Refugee from Kenya 2 m prior 8 m hx cough, fever, poor appetite, no interest in play Chest CT Head CT
24 Case Gastric washings X3 1/3 + MTB pansensitive Induced sputum X3 all neg Left ear drainage cx +MTB Blood culture neg Urine culture neg Started therapy INH Rifampin PZA EMB B6 Steroids Ranitidine Dilantin NG feeds Case Case Rapid improvement in symptoms Defervesced More interactive and playful Improved appetite Discharged home on directly observed therapy on hospital day 11 Follow up CT one month after start of therapy
25 IMPRESSION: Improved findings of miliary tuberculosis compared to Mild cylindrical bronchiectasis right upper and middle lobes. 3. Very slight improvement in extensive necrotic mediastinal and right hilar lymphadenopathy. 4. Improved aeration right upper lobe Case Follow up chest CT: improvement in all findings except mediastinal and hilar adenopathy Head CT: marked improvement in tuberculomas Pt had been seen in clinic prior with verification that all meds were being given, TB meds by TB clinic staff, others by mom Case On repeat questioning steroids were not being given, and had not been given after the pt was discharged from the hospital Steroids are an important part of treatment in miliary disease Reduce adenopathy and potential for further airway compression and late pulmonary complications such and collapse-consolidation Bronchial erosion and endobronchial disease Reduce risk of broncho- or tracheo- esophogeal fisutala Reduce CNS inflammation
26 Case Steroids were started again, with one dose by DOT and the other verified each day Treatment for 4 weeks with 3 week taper Prolonged rx and taper reduce risk of rebound Pt did well thereafter Case Sibling: 5 yo PPD +, CXR L hilar fullness, retrocardiac LLL infiltrate, medial RUL infil vs atelectasis; GW 1/3 + MTB; induced sputum + MTB pansensitive 12/10/06 admit with chest pain, fever CXR unilateral effusion 11 yo Somali refugee PPD 18 mm 11/18/06 CXR normal
27 CXR 3 months after starting antimycobacterial meds Chest CT on admit with unilateral pleural effusion Persistent fever and rising CRP on parenteral antibiotics, BC neg, pleural fluid cx neg THANK YOU! QUESTIONS? References American Academy of Pediatrics Red Book 2009 ATS/CDC/IDSA controlling tuberculosis in the United States. Am J Respir Crit Care Med Nov 1;172(9): Mandalakas AM, Starke JMC Current Concepts of Childhood Tuberculosis Semin Pediatr Infect Dis 2005; 16:93-104
Pediatric Latent TB Diagnosis and Treatment
 Date Updated: April 2015 Guidelines Reviewed: 1. CDC Latent TB Guidelines 2. Harborview Pediatric Clinic Latent TB Management, 2010 3. Pediatric Associates Latent TB Guidelines, 2013 4. Seattle Children
Date Updated: April 2015 Guidelines Reviewed: 1. CDC Latent TB Guidelines 2. Harborview Pediatric Clinic Latent TB Management, 2010 3. Pediatric Associates Latent TB Guidelines, 2013 4. Seattle Children
Tuberculosis in Children and Adolescents
 Tuberculosis in Children and Adolescents Ritu Banerjee, MD, Ph.D TB Clinical Intensive April 8, 2015 2014 MFMER slide-1 Disclosures None 2014 MFMER slide-2 Objectives Describe the epidemiology of pediatric
Tuberculosis in Children and Adolescents Ritu Banerjee, MD, Ph.D TB Clinical Intensive April 8, 2015 2014 MFMER slide-1 Disclosures None 2014 MFMER slide-2 Objectives Describe the epidemiology of pediatric
Table. Positive Purified Protein Derivative Results (Pediatrics In Review Apr 2008)
 PPD and TB Sreening COMPETENCY- The resident should know the risk factors for TB exposure, when to screen, and the appropriate criteria for recognizing a positive PPD in children of different age groups
PPD and TB Sreening COMPETENCY- The resident should know the risk factors for TB exposure, when to screen, and the appropriate criteria for recognizing a positive PPD in children of different age groups
TUBERCULOSIS SCREENING AND TREATMENT IN PREGNANCY. Stephanie N. Lin MD 2/12/2016
 TUBERCULOSIS SCREENING AND TREATMENT IN PREGNANCY Stephanie N. Lin MD 2/12/2016 Epidemiology of TB 9.6 million new cases in 2014 12% of them are in HIV positive patients 1.5 million deaths in 2014 ~646
TUBERCULOSIS SCREENING AND TREATMENT IN PREGNANCY Stephanie N. Lin MD 2/12/2016 Epidemiology of TB 9.6 million new cases in 2014 12% of them are in HIV positive patients 1.5 million deaths in 2014 ~646
LEARNING OUTCOMES. Identify children at risk of developing TB disease. Correctly manage and refer children suspected of TB. Manage child contacts
 TB in Children 1a TB IN CHILDREN 2 LEARNING OUTCOMES Identify children at risk of developing TB disease Correctly manage and refer children suspected of TB Manage child contacts 3 TB Infection and Disease
TB in Children 1a TB IN CHILDREN 2 LEARNING OUTCOMES Identify children at risk of developing TB disease Correctly manage and refer children suspected of TB Manage child contacts 3 TB Infection and Disease
Challenges in Pediatric Tuberculosis. Mimi Emig, MD Spectrum Health Kent County Health Department
 Challenges in Pediatric Tuberculosis Mimi Emig, MD Spectrum Health Kent County Health Department Pediatric Tuberculosis: A Missed Public Health Opportunity Mimi Emig, MD Spectrum Health Kent County Health
Challenges in Pediatric Tuberculosis Mimi Emig, MD Spectrum Health Kent County Health Department Pediatric Tuberculosis: A Missed Public Health Opportunity Mimi Emig, MD Spectrum Health Kent County Health
2011 NTP Paediatric guidelines update- final draft
 Childhood TB Investigation and management of children suspected to have tuberculosis (TB) or who are close contacts of a TB case (sputum smear positive or negative) Key facts Children who are close contacts
Childhood TB Investigation and management of children suspected to have tuberculosis (TB) or who are close contacts of a TB case (sputum smear positive or negative) Key facts Children who are close contacts
Massachusetts Department of Public Health Division of Global Populations and Infectious Disease Prevention
 Massachusetts Department of Public Health Division of Global Populations and Infectious Disease Prevention Screening Infants and Children for Tuberculosis in Massachusetts Executive Summary In Massachusetts,
Massachusetts Department of Public Health Division of Global Populations and Infectious Disease Prevention Screening Infants and Children for Tuberculosis in Massachusetts Executive Summary In Massachusetts,
Self-Study Modules on Tuberculosis
 Self-Study Modules on Tuberculosis Treatment of Latent Tuberculosis Infection and Tube rc ulos is Disease U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES Centers for Disease Control and Prevention National
Self-Study Modules on Tuberculosis Treatment of Latent Tuberculosis Infection and Tube rc ulos is Disease U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES Centers for Disease Control and Prevention National
Chapter 5 Treatment for Latent Tuberculosis Infection
 Chapter 5 Treatment for Latent Tuberculosis Infection Table of Contents Chapter Objectives.... 109 Introduction.... 111 Candidates for the Treatment of LTBI.... 112 LTBI Treatment Regimens.... 118 LTBI
Chapter 5 Treatment for Latent Tuberculosis Infection Table of Contents Chapter Objectives.... 109 Introduction.... 111 Candidates for the Treatment of LTBI.... 112 LTBI Treatment Regimens.... 118 LTBI
Recent Advances in The Treatment of Mycobacterium Tuberculosis
 Recent Advances in The Treatment of Mycobacterium Tuberculosis Dr Mohd Arif Mohd Zim Senior Lecturer & Respiratory Physician Faculty of Medicine, Universiti Teknologi MARA mohdarif035@salam.uitm.edu.my
Recent Advances in The Treatment of Mycobacterium Tuberculosis Dr Mohd Arif Mohd Zim Senior Lecturer & Respiratory Physician Faculty of Medicine, Universiti Teknologi MARA mohdarif035@salam.uitm.edu.my
Chapter 3 Testing for Tuberculosis Infection and Disease
 Chapter 3 Testing for Tuberculosis Infection and Disease Table of Contents Chapter Objectives.... 45 Introduction.... 47 Identifying High-Risk Groups for M. tuberculosis Testing... 47 Testing Methods for
Chapter 3 Testing for Tuberculosis Infection and Disease Table of Contents Chapter Objectives.... 45 Introduction.... 47 Identifying High-Risk Groups for M. tuberculosis Testing... 47 Testing Methods for
Pregnancy and Tuberculosis. Information for clinicians
 Pregnancy and Tuberculosis Information for clinicians When to suspect Tuberculosis (TB)? Who is at risk of TB during pregnancy? Recent research suggests that new mothers are at an increased risk of TB
Pregnancy and Tuberculosis Information for clinicians When to suspect Tuberculosis (TB)? Who is at risk of TB during pregnancy? Recent research suggests that new mothers are at an increased risk of TB
U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES Public Health Service Centers for Disease Control and Prevention
 U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES Public Health Service Centers for Disease Control and Prevention National Center for HIV, STD, and TB Prevention Division of Tuberculosis Elimination Public
U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES Public Health Service Centers for Disease Control and Prevention National Center for HIV, STD, and TB Prevention Division of Tuberculosis Elimination Public
New York City Department of Health Protocols for Latent TB Infection Treatment
 New York City Department of Health Protocols for Latent TB Infection Treatment CONTENT A. Medical evaluation for latent TB infection (LTBI) treatment 1. Medical history and physical examination 2. Chest
New York City Department of Health Protocols for Latent TB Infection Treatment CONTENT A. Medical evaluation for latent TB infection (LTBI) treatment 1. Medical history and physical examination 2. Chest
Pediatric Tuberculosis
 Pediatric Tuberculosis Ana M. Alvarez, M.D. Division of Pediatric Infectious Diseases and Immunology University of Florida College of Medicine/Jacksonville Children are not small adults! Objectives At
Pediatric Tuberculosis Ana M. Alvarez, M.D. Division of Pediatric Infectious Diseases and Immunology University of Florida College of Medicine/Jacksonville Children are not small adults! Objectives At
Clinical description 2 Laboratory test for diagnosis 3. Incubation period 4 Mode of transmission 4 Period of communicability 4
 Tuberculosis Contents Epidemiology in New Zealand 2 Case definition 2 Clinical description 2 Laboratory test for diagnosis 3 Case classification 3 Spread of infection 4 Incubation period 4 Mode of transmission
Tuberculosis Contents Epidemiology in New Zealand 2 Case definition 2 Clinical description 2 Laboratory test for diagnosis 3 Case classification 3 Spread of infection 4 Incubation period 4 Mode of transmission
CDC TB Testing Guidelines and Recent Literature Update
 Pocket Guide QuantiFERON -TB Gold CDC TB Testing Guidelines and Recent Literature Update Using IGRAs for TB screening in your patients June 2010 A full copy of the US Centers for Disease Control and Prevention
Pocket Guide QuantiFERON -TB Gold CDC TB Testing Guidelines and Recent Literature Update Using IGRAs for TB screening in your patients June 2010 A full copy of the US Centers for Disease Control and Prevention
Tuberculosis. Subject. Goal/Objective. Instructions. Rationale. Operations Directorate, Health Branch Immigration Medical Examination Instructions
 Subject Instructions for the screening of clients to detect tuberculosis (TB) in the context of the Canadian immigration medical examination (IME). Goal/Objective These instructions are provided to ensure
Subject Instructions for the screening of clients to detect tuberculosis (TB) in the context of the Canadian immigration medical examination (IME). Goal/Objective These instructions are provided to ensure
Guideline. Treatment of tuberculosis in pregnant women and newborn infants. Version 3.0
 Guideline Treatment of tuberculosis in pregnant women and newborn infants Version 3.0 Key critical points The decision to treat tuberculosis (TB) in pregnancy must consider the potential risks to mother
Guideline Treatment of tuberculosis in pregnant women and newborn infants Version 3.0 Key critical points The decision to treat tuberculosis (TB) in pregnancy must consider the potential risks to mother
Chapter 1 Overview of Tuberculosis Epidemiology in the United States
 Chapter 1 Overview of Tuberculosis Epidemiology in the United States Table of Contents Chapter Objectives.... 1 Progress Toward TB Elimination in the United States.... 3 TB Disease Trends in the United
Chapter 1 Overview of Tuberculosis Epidemiology in the United States Table of Contents Chapter Objectives.... 1 Progress Toward TB Elimination in the United States.... 3 TB Disease Trends in the United
Childhood Tuberculosis: Diagnosis, Treatment and Prevention of TB in HIV-infected Children
 Childhood Tuberculosis: Diagnosis, Treatment and Prevention of TB in HIV-infected Children Celia DC Christie-Samuels Professor of Paediatrics (Infectious Diseases, Epidemiology and Public Health) University
Childhood Tuberculosis: Diagnosis, Treatment and Prevention of TB in HIV-infected Children Celia DC Christie-Samuels Professor of Paediatrics (Infectious Diseases, Epidemiology and Public Health) University
Maria Dalbey RN. BSN, MA, MBA March 17 th, 2015
 Maria Dalbey RN. BSN, MA, MBA March 17 th, 2015 2 Objectives Participants will be able to : Understand the Pathogenesis of Tuberculosis (TB) Identify the Goals of Public Health for TB Identify Hierarchy
Maria Dalbey RN. BSN, MA, MBA March 17 th, 2015 2 Objectives Participants will be able to : Understand the Pathogenesis of Tuberculosis (TB) Identify the Goals of Public Health for TB Identify Hierarchy
Questions and Answers About Tuberculosis
 Questions and Answers About Tuberculosis 2014 Questions and Answers About Tuberculosis 2014 Questions and Answers About Tuberculosis ( TB) was written to provide information on the diagnosis and treatment
Questions and Answers About Tuberculosis 2014 Questions and Answers About Tuberculosis 2014 Questions and Answers About Tuberculosis ( TB) was written to provide information on the diagnosis and treatment
Pediatric Tuberculosis: Pearls, Pitfalls and Progress. Amina Ahmed, MD Levine Children s Hospital June 25, 2013
 Pediatric Tuberculosis: Pearls, Pitfalls and Progress Amina Ahmed, MD Levine Children s Hospital June 25, 2013 Disclosures I have no relationships with commercial interests related to this presentation
Pediatric Tuberculosis: Pearls, Pitfalls and Progress Amina Ahmed, MD Levine Children s Hospital June 25, 2013 Disclosures I have no relationships with commercial interests related to this presentation
Introduction to TB Nurse Case Management Online February 4, 11, 18 and 25, 2015
 Introduction to TB Nurse Case Management Online February 4, 11, 18 and 25, 2015 Completion of Treatment: Case Studies or A Little Bit of Everything Presented by Cherie Fulk February 25, 2015 Cherie Fulk
Introduction to TB Nurse Case Management Online February 4, 11, 18 and 25, 2015 Completion of Treatment: Case Studies or A Little Bit of Everything Presented by Cherie Fulk February 25, 2015 Cherie Fulk
TB Prevention, Diagnosis and Treatment. Accelerating advocacy on TB/HIV 15th July, Vienna
 TB Prevention, Diagnosis and Treatment Accelerating advocacy on TB/HIV 15th July, Vienna Diagnosis Microscopy of specially stained sputum is the main test for diagnosing TB (1 2 days) TB bacilli seen in
TB Prevention, Diagnosis and Treatment Accelerating advocacy on TB/HIV 15th July, Vienna Diagnosis Microscopy of specially stained sputum is the main test for diagnosing TB (1 2 days) TB bacilli seen in
Clinical Scenarios In Childhood TB. Josefina Cadorna Carlos M.D., FPPS, FPIDSP, FSMID Associate Professor of Pediatrics U E R M M M C
 Clinical Scenarios In Childhood TB Josefina Cadorna Carlos M.D., FPPS, FPIDSP, FSMID Associate Professor of Pediatrics U E R M M M C Objectives: To present different commonly encountered clinical scenarios
Clinical Scenarios In Childhood TB Josefina Cadorna Carlos M.D., FPPS, FPIDSP, FSMID Associate Professor of Pediatrics U E R M M M C Objectives: To present different commonly encountered clinical scenarios
PEDIATRIC TUBERCULOSIS. Hot topics / Unresolved issues in Clinical Practice
 PEDIATRIC TUBERCULOSIS Hot topics / Unresolved issues in Clinical Practice Ann M. Loeffler, M.D. Legacy Emanuel Children s Hospital Portland, OR Faculty Consultant Francis J. Curry National TB Center February
PEDIATRIC TUBERCULOSIS Hot topics / Unresolved issues in Clinical Practice Ann M. Loeffler, M.D. Legacy Emanuel Children s Hospital Portland, OR Faculty Consultant Francis J. Curry National TB Center February
Tuberculosis (TB) Screening Guidelines for Substance Use Disorder Treatment Programs in California
 Tuberculosis (TB) Screening Guidelines for Substance Use Disorder Treatment Programs in California 1 of 7 Table of Contents Preface 2 TB Symptoms and TB History 2 Initial Screening 2 Follow-Up Screening
Tuberculosis (TB) Screening Guidelines for Substance Use Disorder Treatment Programs in California 1 of 7 Table of Contents Preface 2 TB Symptoms and TB History 2 Initial Screening 2 Follow-Up Screening
Tuberculosis Exposure Control Plan for Low Risk Dental Offices
 Tuberculosis Exposure Control Plan for Low Risk Dental Offices A. BACKGROUND According to the CDC, approximately one-third of the world s population, almost two billion people, are infected with tuberculosis.
Tuberculosis Exposure Control Plan for Low Risk Dental Offices A. BACKGROUND According to the CDC, approximately one-third of the world s population, almost two billion people, are infected with tuberculosis.
San Francisco Treatment Guidelines for Latent Tuberculosis Infection
 City and County of San Francisco Department of Public Health Tuberculosis Control Unit Julie Higashi, MD, PhD Director Population Health Division Edwin M. Lee Mayor Disease Prevention and Control Branch
City and County of San Francisco Department of Public Health Tuberculosis Control Unit Julie Higashi, MD, PhD Director Population Health Division Edwin M. Lee Mayor Disease Prevention and Control Branch
TUBERCULOSIS (TB) SCREENING GUIDELINES FOR RESIDENTIAL FACILITIES AND DRUG
 TUBERCULOSIS (TB) SCREENING GUIDELINES FOR RESIDENTIAL FACILITIES AND DRUG Tx CENTERS Tuberculosis Control Program Health and Human Services Agency San Diego County INTRODUCTION Reducing TB disease requires
TUBERCULOSIS (TB) SCREENING GUIDELINES FOR RESIDENTIAL FACILITIES AND DRUG Tx CENTERS Tuberculosis Control Program Health and Human Services Agency San Diego County INTRODUCTION Reducing TB disease requires
Appendix B: Provincial Case Definitions for Reportable Diseases
 Infectious Diseases Protocol Appendix B: Provincial Case Definitions for Reportable Diseases Disease: Tuberculosis Revised August 2015 Tuberculosis 1.0 Provincial Reporting Confirmed and suspect cases
Infectious Diseases Protocol Appendix B: Provincial Case Definitions for Reportable Diseases Disease: Tuberculosis Revised August 2015 Tuberculosis 1.0 Provincial Reporting Confirmed and suspect cases
San Francisco Guidelines on the Use of QuantiFERON-TB Gold (In Tube Method) for the Diagnosis of Latent TB Infection
 San Francisco Guidelines on the Use of QuantiFERON-TB Gold (In Tube Method) for the Diagnosis of Latent TB Infection Rationale When to Screen for TB Choosing the Right TB Test Patient Registration Pre-Test
San Francisco Guidelines on the Use of QuantiFERON-TB Gold (In Tube Method) for the Diagnosis of Latent TB Infection Rationale When to Screen for TB Choosing the Right TB Test Patient Registration Pre-Test
Childhood Tuberculosis Some Basic Issues. Jeffrey R. Starke, M.D. Baylor College of Medicine
 Childhood Tuberculosis Some Basic Issues Jeffrey R. Starke, M.D. Baylor College of Medicine TUBERCULOSIS IS A SOCIAL DISEASE WITH MEDICAL IMPLICATIONS THE GREAT PARADOX OF TUBERCULOSIS A CAUTIONARY TALE
Childhood Tuberculosis Some Basic Issues Jeffrey R. Starke, M.D. Baylor College of Medicine TUBERCULOSIS IS A SOCIAL DISEASE WITH MEDICAL IMPLICATIONS THE GREAT PARADOX OF TUBERCULOSIS A CAUTIONARY TALE
Targeted Testing and Treatment of Latent Tuberculosis Infection in Adults and Children
 C D H S / C T C A J O I N T G U I D E L I N E S Targeted Testing and Treatment of Latent Tuberculosis Infection in Adults and Children Targeted Skin Testing and Treatment of Latent Tuberculosis Infection
C D H S / C T C A J O I N T G U I D E L I N E S Targeted Testing and Treatment of Latent Tuberculosis Infection in Adults and Children Targeted Skin Testing and Treatment of Latent Tuberculosis Infection
TB preventive therapy in children. Introduction
 TB preventive therapy in children H S Schaaf Department of Paediatrics and Child Health, and Desmond Tutu TB Centre Stellenbosch University, and Tygerberg Children s Hospital Introduction Children are
TB preventive therapy in children H S Schaaf Department of Paediatrics and Child Health, and Desmond Tutu TB Centre Stellenbosch University, and Tygerberg Children s Hospital Introduction Children are
Primary Care Management of Latent Tuberculosis Infection in the Foreign-Born
 Primary Care Management of Latent Tuberculosis Infection in the Foreign-Born Investigators Carey Jackson MD, MPH University of Washington Jenny Pang MD, MPH, Seattle-King County Department of Public Health
Primary Care Management of Latent Tuberculosis Infection in the Foreign-Born Investigators Carey Jackson MD, MPH University of Washington Jenny Pang MD, MPH, Seattle-King County Department of Public Health
New Jersey Department of Health and Senior Services. Standards of Care for Tuberculosis Disease and Latent TB Infection
 New Jersey Department of Health and Senior Services Standards of Care for Tuberculosis Disease and Latent TB Infection Tuberculosis Medical Advisory Board March 2007 Table of Contents Standard # 1: Diagnosis
New Jersey Department of Health and Senior Services Standards of Care for Tuberculosis Disease and Latent TB Infection Tuberculosis Medical Advisory Board March 2007 Table of Contents Standard # 1: Diagnosis
Tuberculosis Prevention and Control Protocol, 2008
 Tuberculosis Prevention and Control Protocol, 2008 Preamble The Ontario Public Health Standards (OPHS) are published by the Minister of Health and Long- Term Care under the authority of the Health Protection
Tuberculosis Prevention and Control Protocol, 2008 Preamble The Ontario Public Health Standards (OPHS) are published by the Minister of Health and Long- Term Care under the authority of the Health Protection
Nevada State Health Division Technical Bulletin
 Nevada State Health Division Technical Bulletin Topic: Using QuantiFERON and Tuberculin Skin Test to Screen for TB Section/Program/Contact: Bureau of Community Health / Tuberculosis Program / Susanne Paulson,
Nevada State Health Division Technical Bulletin Topic: Using QuantiFERON and Tuberculin Skin Test to Screen for TB Section/Program/Contact: Bureau of Community Health / Tuberculosis Program / Susanne Paulson,
Screening and preventive therapy for MDR/XDR-TB exposed/infected children (and adults)
 Screening and preventive therapy for MDR/XDR-TB exposed/infected children (and adults) H S Schaaf Department of Paediatrics and Child Health, and Desmond Tutu TB Centre Stellenbosch University, and Tygerberg
Screening and preventive therapy for MDR/XDR-TB exposed/infected children (and adults) H S Schaaf Department of Paediatrics and Child Health, and Desmond Tutu TB Centre Stellenbosch University, and Tygerberg
Management of Tuberculosis
 Federal Bureau of Prisons Clinical Practice Guidelines January 2010 Clinical guidelines are being made available to the public for informational purposes only. The Federal Bureau of Prisons (BOP) does
Federal Bureau of Prisons Clinical Practice Guidelines January 2010 Clinical guidelines are being made available to the public for informational purposes only. The Federal Bureau of Prisons (BOP) does
Chapter 6 Treatment of Tuberculosis Disease
 Chapter 6 Treatment of Tuberculosis Disease Table of Contents Chapter Objectives.... 139 Introduction.... 141 Treatment and Monitoring Plan.... 143 Adherence Strategies... 143 TB Disease Treatment Regimens....
Chapter 6 Treatment of Tuberculosis Disease Table of Contents Chapter Objectives.... 139 Introduction.... 141 Treatment and Monitoring Plan.... 143 Adherence Strategies... 143 TB Disease Treatment Regimens....
X-Plain Pediatric Tuberculosis Reference Summary
 X-Plain Pediatric Tuberculosis Reference Summary Introduction Tuberculosis, or TB, is a bacterial infection that causes more deaths in the world than any other infectious disease. When a child gets TB,
X-Plain Pediatric Tuberculosis Reference Summary Introduction Tuberculosis, or TB, is a bacterial infection that causes more deaths in the world than any other infectious disease. When a child gets TB,
Management of Tuberculosis (TB)
 for Professional Health Care Providers Management of Tuberculosis (TB) USAID UNITED STATES AGENCY INTERNATIONAL DEVELOPMENT USAID FROM THE AMERICAN PEOPLE SOUTHERN AFRICA WHAT IS TB? Tuberculosis (TB)
for Professional Health Care Providers Management of Tuberculosis (TB) USAID UNITED STATES AGENCY INTERNATIONAL DEVELOPMENT USAID FROM THE AMERICAN PEOPLE SOUTHERN AFRICA WHAT IS TB? Tuberculosis (TB)
AMBULATORY TREATMENT AND PUBLIC HEALTH MEASURES FOR A PATIENT WITH UNCOMPLICATED PULMONARY TUBERCULOSIS
 AMBULATORY TREATMENT AND PUBLIC HEALTH MEASURES FOR A PATIENT WITH UNCOMPLICATED PULMONARY TUBERCULOSIS (UPDATE 2004) Internal guidelines of the Tuberculosis & Chest Service of the Department of Health
AMBULATORY TREATMENT AND PUBLIC HEALTH MEASURES FOR A PATIENT WITH UNCOMPLICATED PULMONARY TUBERCULOSIS (UPDATE 2004) Internal guidelines of the Tuberculosis & Chest Service of the Department of Health
Tuberculosis Surveillance and Screening for Long Term Care Facilities in Colorado
 Tuberculosis Surveillance and Screening for Long Term Care Facilities in Colorado Developed by the Colorado Medical Directors Association and The Colorado Department of Public Health and Environment Introduction:
Tuberculosis Surveillance and Screening for Long Term Care Facilities in Colorado Developed by the Colorado Medical Directors Association and The Colorado Department of Public Health and Environment Introduction:
Management of Tuberculosis: Indian Guidelines
 Chapter 105 Management of Tuberculosis: Indian Guidelines Kuldeep Singh Sachdeva INTRODUCTION Tuberculosis (TB) is an infectious disease caused predominantly by Mycobacterium tuberculosis and among the
Chapter 105 Management of Tuberculosis: Indian Guidelines Kuldeep Singh Sachdeva INTRODUCTION Tuberculosis (TB) is an infectious disease caused predominantly by Mycobacterium tuberculosis and among the
3. Blood and blood products such as serum, plasma, and other blood components.
 Mississippi Downloaded 01/2011 101.11 Infectious Medical Waste. The term "infectious medical waste" includes solid or liquid wastes which may contain pathogens with sufficient virulence and quantity such
Mississippi Downloaded 01/2011 101.11 Infectious Medical Waste. The term "infectious medical waste" includes solid or liquid wastes which may contain pathogens with sufficient virulence and quantity such
Latent Tuberculosis Infection: A Guide for Primary Health Care Providers
 Latent Tuberculosis Infection: A Guide for Primary Health Care Providers A B Latent Tuberculosis Infection: A Guide for Primary Health Care Providers U.S. Department of Health and Human Services Centers
Latent Tuberculosis Infection: A Guide for Primary Health Care Providers A B Latent Tuberculosis Infection: A Guide for Primary Health Care Providers U.S. Department of Health and Human Services Centers
Self-Study Modules on Tuberculosis
 Self-Study Modules on Tuberculosis Epidemiology of Tuberculosis U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES Centers for Disease Control and Prevention National Center for HIV/AIDS, Viral Hepatitis, STD,
Self-Study Modules on Tuberculosis Epidemiology of Tuberculosis U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES Centers for Disease Control and Prevention National Center for HIV/AIDS, Viral Hepatitis, STD,
Assisted Living - TB Risk Assessment
 Montana DPHHS Tuberculosis Program Assisted Living - TB Risk Assessment Assisted Living, Adult Day Care, Adult Foster Care & Transitional Living Centers Today s Date Facility Address Phone County Completed
Montana DPHHS Tuberculosis Program Assisted Living - TB Risk Assessment Assisted Living, Adult Day Care, Adult Foster Care & Transitional Living Centers Today s Date Facility Address Phone County Completed
Tuberculosis And Diabetes. Dr. hanan abuelrus Prof.of internal medicine Assiut University
 Tuberculosis And Diabetes Dr. hanan abuelrus Prof.of internal medicine Assiut University TUBERCULOSIS FACTS More than 9 million people fall sick with tuberculosis (TB) every year. Over 1.5 million die
Tuberculosis And Diabetes Dr. hanan abuelrus Prof.of internal medicine Assiut University TUBERCULOSIS FACTS More than 9 million people fall sick with tuberculosis (TB) every year. Over 1.5 million die
Long-term Care - TB Risk Assessment
 Montana DPHHS Tuberculosis Program Long-term Care - TB Risk Assessment Long-term Care, Residential Treatment, ESRD (outpatient), Hospice (inpatient) Today s Date Facility Address Phone County Completed
Montana DPHHS Tuberculosis Program Long-term Care - TB Risk Assessment Long-term Care, Residential Treatment, ESRD (outpatient), Hospice (inpatient) Today s Date Facility Address Phone County Completed
TB Intensive San Antonio, Texas November 11 14, 2014
 TB Intensive San Antonio, Texas November 11 14, 2014 TB in the HIV Patient Lisa Armitige, MD, PhD November 13, 2014 Lisa Armitige, MD, PhD has the following disclosures to make: No conflict of interests
TB Intensive San Antonio, Texas November 11 14, 2014 TB in the HIV Patient Lisa Armitige, MD, PhD November 13, 2014 Lisa Armitige, MD, PhD has the following disclosures to make: No conflict of interests
Santa Clara County Tuberculosis Screening Requirement for School Entrance Effective June 1, 2014. Frequently Asked Questions
 Frequently Asked Questions A child has history of BCG vaccination, should they have TST or IGRA? According to the American Academy of Pediatrics Red Book (2012), Interferon Gamma Release Assay (IGRA) is
Frequently Asked Questions A child has history of BCG vaccination, should they have TST or IGRA? According to the American Academy of Pediatrics Red Book (2012), Interferon Gamma Release Assay (IGRA) is
Paediatrica Indonesiana. Limitations of the Indonesian Pediatric Tuberculosis Scoring System in the context of child contact investigation
 Paediatrica Indonesiana VOLUME 51 November NUMBER 6 Original Article Limitations of the Indonesian Pediatric Tuberculosis Scoring System in the context of child contact investigation Rina Triasih 1,2,
Paediatrica Indonesiana VOLUME 51 November NUMBER 6 Original Article Limitations of the Indonesian Pediatric Tuberculosis Scoring System in the context of child contact investigation Rina Triasih 1,2,
Tuberculosis and HIV/AIDS Co-Infection: Epidemiology and Public Health Challenges
 Tuberculosis and HIV/AIDS Co-Infection: Epidemiology and Public Health Challenges John B. Kaneene, DVM, MPH, PhD University Distinguished Professor of Epidemiology Director, Center for Comparative Epidemiology
Tuberculosis and HIV/AIDS Co-Infection: Epidemiology and Public Health Challenges John B. Kaneene, DVM, MPH, PhD University Distinguished Professor of Epidemiology Director, Center for Comparative Epidemiology
Haley Blake, BA Senior Disease Investigation and Intervention Specialist Southern Nevada Health District
 Haley Blake, BA Senior Disease Investigation and Intervention Specialist Southern Nevada Health District Course Objectives Identify causes of and route of transmission of tuberculosis (TB) Explain the
Haley Blake, BA Senior Disease Investigation and Intervention Specialist Southern Nevada Health District Course Objectives Identify causes of and route of transmission of tuberculosis (TB) Explain the
American Thoracic Society Documents
 American Thoracic Society Documents American Thoracic Society/Centers for Disease Control and Prevention/Infectious Diseases Society of America: Controlling Tuberculosis in the United States This Official
American Thoracic Society Documents American Thoracic Society/Centers for Disease Control and Prevention/Infectious Diseases Society of America: Controlling Tuberculosis in the United States This Official
Health Protection Agency position statement on the use of Interferon Gamma Release Assay (IGRA) tests for Tuberculosis (TB)
 Health Protection Agency position statement on the use of Interferon Gamma Release Assay (IGRA) tests for Tuberculosis (TB) Draft Interim HPA Guidance HPA Tuberculosis Programme Board Health Protection
Health Protection Agency position statement on the use of Interferon Gamma Release Assay (IGRA) tests for Tuberculosis (TB) Draft Interim HPA Guidance HPA Tuberculosis Programme Board Health Protection
TUBERCULOSIS PLEURAL EFFUSION - MANAGEMENT
 TUBERCULOSIS PLEURAL EFFUSION - MANAGEMENT Introduction : ETB 15-20% Pleural effusion 20% in non HIV Under reporting because of AFB negative in fluid In HIV patients: EPTB 20% PTB + EPTB 50% Pleural Effusion
TUBERCULOSIS PLEURAL EFFUSION - MANAGEMENT Introduction : ETB 15-20% Pleural effusion 20% in non HIV Under reporting because of AFB negative in fluid In HIV patients: EPTB 20% PTB + EPTB 50% Pleural Effusion
Guidelines for TB Blood Testing. Minnesota Department of Health TB Prevention and Control Program June 2011
 Guidelines for TB Blood Testing Minnesota Department of Health TB Prevention and Control Program June 2011 Outline Interferon-Gamma Release Assays aka TB blood tests 1. What are they? 2. What are the current
Guidelines for TB Blood Testing Minnesota Department of Health TB Prevention and Control Program June 2011 Outline Interferon-Gamma Release Assays aka TB blood tests 1. What are they? 2. What are the current
What is an IGRA? What is an IGRA? Are they available here? How do I use them? Learning Objectives
 What is an IGRA? Are they available here? How do I use them? Debbie Staley, RN, MPH TB Nurse Consultant VDH Division of Disease Prevention TB Control Program Learning Objectives Participants will be able
What is an IGRA? Are they available here? How do I use them? Debbie Staley, RN, MPH TB Nurse Consultant VDH Division of Disease Prevention TB Control Program Learning Objectives Participants will be able
Tuberculosis Case Management in Prisoners
 Tuberculosis Case Management in Prisoners Joint Protocol for Corrections Facilities and TB Treatment Supervising Services (Regional Public Health Services and/or Clinical TB Services) in New Zealand Ministry
Tuberculosis Case Management in Prisoners Joint Protocol for Corrections Facilities and TB Treatment Supervising Services (Regional Public Health Services and/or Clinical TB Services) in New Zealand Ministry
MANAGEMENT OF TUBERCULOSIS IN PRISONS: Guidance for prison healthcare teams
 MANAGEMENT OF TUBERCULOSIS IN PRISONS: Guidance for prison healthcare teams Document control Title Type Author/s Management of tuberculosis in prisons: Guidance for prison healthcare teams Operational
MANAGEMENT OF TUBERCULOSIS IN PRISONS: Guidance for prison healthcare teams Document control Title Type Author/s Management of tuberculosis in prisons: Guidance for prison healthcare teams Operational
Transmission & Pathogenesis of Tuberculosis
 April-December, 2011: TB cases reported by the media in US Transmission & Pathogenesis of Tuberculosis Shu-Hua Wang, MD, MPH & TM Assistant Professor of Medicine The Ohio State University TB found at Seaside
April-December, 2011: TB cases reported by the media in US Transmission & Pathogenesis of Tuberculosis Shu-Hua Wang, MD, MPH & TM Assistant Professor of Medicine The Ohio State University TB found at Seaside
TuberculosisPolicies and Procedures ManualFor Public Health Authorities and Health Professionals
 TuberculosisPolicies and Procedures ManualFor Public Health Authorities and Health Professionals Introduction/Background...4 Purpose...4 Tuberculosis Program Contact Information...4 Definitions...4 Transmission
TuberculosisPolicies and Procedures ManualFor Public Health Authorities and Health Professionals Introduction/Background...4 Purpose...4 Tuberculosis Program Contact Information...4 Definitions...4 Transmission
Core Curriculum on Tuberculosis: What the Clinician Should Know Sixth Edition 2013
 Core Curriculum on Tuberculosis: What the Clinician Should Know Sixth Edition 2013 CS234269 To View or Order the Core Curriculum on Tuberculosis To view or download the Core Curriculum, please visit: www.cdc.gov/tb.
Core Curriculum on Tuberculosis: What the Clinician Should Know Sixth Edition 2013 CS234269 To View or Order the Core Curriculum on Tuberculosis To view or download the Core Curriculum, please visit: www.cdc.gov/tb.
MANAGEMENT OF COMMON SIDE EFFECTS of INH (Isoniazid), RIF (Rifampin), PZA (Pyrazinamide), and EMB (Ethambutol)
 MANAGEMENT OF COMMON SIDE EFFECTS of INH (Isoniazid), RIF (Rifampin), PZA (Pyrazinamide), and EMB (Ethambutol) 1. Hepatotoxicity: In Active TB Disease a. Background: 1. Among the 4 standard anti-tb drugs,
MANAGEMENT OF COMMON SIDE EFFECTS of INH (Isoniazid), RIF (Rifampin), PZA (Pyrazinamide), and EMB (Ethambutol) 1. Hepatotoxicity: In Active TB Disease a. Background: 1. Among the 4 standard anti-tb drugs,
TB AND M/XDR-TB: FROM CLINICAL MANAGEMENT TO CONTROL AND ELIMINATION
 ersnet.org/school TB AND M/XDR-TB: FROM CLINICAL MANAGEMENT TO CONTROL AND ELIMINATION 23-26 May 2012 - Bucharest, Romania SCHOOL COURSE 2012 Educational Material Thank you for viewing this document. We
ersnet.org/school TB AND M/XDR-TB: FROM CLINICAL MANAGEMENT TO CONTROL AND ELIMINATION 23-26 May 2012 - Bucharest, Romania SCHOOL COURSE 2012 Educational Material Thank you for viewing this document. We
Tuberculosis (TB) remains the leading cause of mortality from infectious. Tuberculosis (TB)
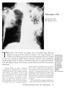 Tuberculosis (TB) John Bernardo, MD Jill S. Roncarati, PA-C Tuberculosis (TB) remains the leading cause of mortality from infectious diseases in humans in the world. In contrast to the world situation,
Tuberculosis (TB) John Bernardo, MD Jill S. Roncarati, PA-C Tuberculosis (TB) remains the leading cause of mortality from infectious diseases in humans in the world. In contrast to the world situation,
Regional Public Health or First Nations Inuit Health Branch (FNIHB):
 Public Health and Primary Health Care Communicable Disease Control 4th Floor, 300 Carlton St, Winnipeg, MB R3B 3M9 T 204 788-6737 F 204 948-2040 www.manitoba.ca November, 2015 Re: Tuberculosis Reporting
Public Health and Primary Health Care Communicable Disease Control 4th Floor, 300 Carlton St, Winnipeg, MB R3B 3M9 T 204 788-6737 F 204 948-2040 www.manitoba.ca November, 2015 Re: Tuberculosis Reporting
Lisa Y. Armitige, MD, PhD has the following disclosures to make:
 Interferon Gamma Release Assays (IGRAs) Lisa Y. Armitige, MD, PhD May 13, 2015 TB for Pulmonologist Phoenix, AZ March 13, 2015 EXCELLENCE EXPERTISE INNOVATION Lisa Y. Armitige, MD, PhD has the following
Interferon Gamma Release Assays (IGRAs) Lisa Y. Armitige, MD, PhD May 13, 2015 TB for Pulmonologist Phoenix, AZ March 13, 2015 EXCELLENCE EXPERTISE INNOVATION Lisa Y. Armitige, MD, PhD has the following
Canadian Tuberculosis Standards
 Canadian Tuberculosis Standards 7 th Edition Chapter 9: Pediatric Tuberculosis Canadian Tuberculosis Standards, 7 th Edition is available on Internet at the following address: www.phac-aspc.gc.ca Également
Canadian Tuberculosis Standards 7 th Edition Chapter 9: Pediatric Tuberculosis Canadian Tuberculosis Standards, 7 th Edition is available on Internet at the following address: www.phac-aspc.gc.ca Également
Diagnosis of Tuberculosis Infection
 Diagnosis of Tuberculosis Infection CONTENTS Introduction... 7.2 Purpose... 7.2 Policy... 7.2 High-Risk Groups... 7.3 Diagnosis of Tuberculosis Infection... 7.4 Interferon gamma release assays... 7.4 Mantoux
Diagnosis of Tuberculosis Infection CONTENTS Introduction... 7.2 Purpose... 7.2 Policy... 7.2 High-Risk Groups... 7.3 Diagnosis of Tuberculosis Infection... 7.4 Interferon gamma release assays... 7.4 Mantoux
Management of a child failing first line TB treatment.
 Management of a child failing first line TB treatment. Robert Gie Desmond Tutu Tuberculosis Centre Department of Paediatric and Child Health Stellenbosch University South Africa. Tygerberg Hospital Complex
Management of a child failing first line TB treatment. Robert Gie Desmond Tutu Tuberculosis Centre Department of Paediatric and Child Health Stellenbosch University South Africa. Tygerberg Hospital Complex
PEOSH Model Tuberculosis Infection Control Program
 PEOSH Model Tuberculosis Infection Control Program Revised November, 2004 NOTE: The information in this document is not considered to be a substitute for any provision of the PEOSH Act or for any standards
PEOSH Model Tuberculosis Infection Control Program Revised November, 2004 NOTE: The information in this document is not considered to be a substitute for any provision of the PEOSH Act or for any standards
American College Health Association (ACHA) TB Screening and Targeted Testing Recommendations Gregory Juckett, MD, MPH Professor of Family Medicine
 American College Health Association (ACHA) TB Screening and Targeted Testing Recommendations Gregory Juckett, MD, MPH Professor of Family Medicine West Virginia University gjuckett@hsc.wvu.edu Objectives
American College Health Association (ACHA) TB Screening and Targeted Testing Recommendations Gregory Juckett, MD, MPH Professor of Family Medicine West Virginia University gjuckett@hsc.wvu.edu Objectives
Tuberculousmeningitis: what is the best treatment regimen?
 Tuberculousmeningitis: what is the best treatment regimen? H S Schaaf Desmond Tutu TB Centre, Department of Paediatrics and Child Health, Faculty of Medicine and Health Sciences, Stellenbosch University
Tuberculousmeningitis: what is the best treatment regimen? H S Schaaf Desmond Tutu TB Centre, Department of Paediatrics and Child Health, Faculty of Medicine and Health Sciences, Stellenbosch University
NICE guideline Published: 13 January 2016 nice.org.uk/guidance/ng33
 Tuberculosis NICE guideline Published: 13 January 2016 nice.org.uk/guidance/ng33 NICE 2016. All rights reserved. Last updated May 2016 Your responsibility The recommendations in this guideline represent
Tuberculosis NICE guideline Published: 13 January 2016 nice.org.uk/guidance/ng33 NICE 2016. All rights reserved. Last updated May 2016 Your responsibility The recommendations in this guideline represent
Remove this cover sheet before redistributing and replace it with your own. Please ensure that DPHHS is included on your HAN distribution list.
 State of Montana Health Alert Network DPHHS HAN ADVISORY Cover Sheet DATE: May 15, 2012 SUBJECT: Pertussis INSTRUCTIONS: DISTRIBUTE to your local HAN contacts. This HAN is intended for general sharing
State of Montana Health Alert Network DPHHS HAN ADVISORY Cover Sheet DATE: May 15, 2012 SUBJECT: Pertussis INSTRUCTIONS: DISTRIBUTE to your local HAN contacts. This HAN is intended for general sharing
Tuberculosis. Clinical diagnosis and management of tuberculosis, and measures for its prevention and control
 Issue date: March 2011 Tuberculosis Clinical diagnosis and management of tuberculosis, and measures for its prevention and control This updates and replaces NICE clinical guideline 33 NICE clinical guideline
Issue date: March 2011 Tuberculosis Clinical diagnosis and management of tuberculosis, and measures for its prevention and control This updates and replaces NICE clinical guideline 33 NICE clinical guideline
QUICK REFERENCE FOR HEALTHCARE PROVIDERS
 QUICK REFERENCE FOR HEALTHCARE PROVIDERS Ministry of Health Malaysia Academy of Medicine Malaysia Malaysian Thoracic Society KEY MESSAGES 1. Tuberculosis (TB) is a notifiable infectious disease. Timely
QUICK REFERENCE FOR HEALTHCARE PROVIDERS Ministry of Health Malaysia Academy of Medicine Malaysia Malaysian Thoracic Society KEY MESSAGES 1. Tuberculosis (TB) is a notifiable infectious disease. Timely
Alberta Health Public Health Notifiable Disease Management Guidelines April 2013
 April 2013 Tuberculosis (TB) Revision Dates Case Definition Reporting Requirements Remainder of the Guideline (i.e., Etiology to References sections inclusive) April 2013 April 2013 January 2011 Case Definition
April 2013 Tuberculosis (TB) Revision Dates Case Definition Reporting Requirements Remainder of the Guideline (i.e., Etiology to References sections inclusive) April 2013 April 2013 January 2011 Case Definition
Section IV. Evaluation and Treatment of Extrapulmonary Tuberculosis
 Section IV. Evaluation and of Extrapulmonary Tuberculosis Tuberculosis Section IV. Evaluation and of Extrapulmonary Tuberculosis The basic principles that underlie the treatment of pulmonary tuberculosis
Section IV. Evaluation and of Extrapulmonary Tuberculosis Tuberculosis Section IV. Evaluation and of Extrapulmonary Tuberculosis The basic principles that underlie the treatment of pulmonary tuberculosis
Tuberculosis. Mar yland TB Guidelines for. Maryland Department of Health and Mental Hygiene
 Mar yland TB Guidelines for Pr evention and Tr eatment of Tuberculosis 2007 Maryland Department of Health and Mental Hygiene Martin O Malley, G o v e r nor Anthony G. Brown, L t. G o v er nor John M. Colmers,
Mar yland TB Guidelines for Pr evention and Tr eatment of Tuberculosis 2007 Maryland Department of Health and Mental Hygiene Martin O Malley, G o v e r nor Anthony G. Brown, L t. G o v er nor John M. Colmers,
Policy for the control and management of Tuberculosis (TB) including multi-drug resistant Tuberculosis (MDR-TB).
 Policy for the control and management of Tuberculosis (TB) including multi-drug resistant Tuberculosis (MDR-TB). Author: Responsible Lead Executive Director: Endorsing Body: Governance or Assurance Committee
Policy for the control and management of Tuberculosis (TB) including multi-drug resistant Tuberculosis (MDR-TB). Author: Responsible Lead Executive Director: Endorsing Body: Governance or Assurance Committee
Canadian Tuberculosis Standards
 Canadian Tuberculosis Standards 7 th Edition Chapter 9: Pediatric Tuberculosis To promote and protect the health of Canadians through leadership, partnership, innovation and action in public health. Public
Canadian Tuberculosis Standards 7 th Edition Chapter 9: Pediatric Tuberculosis To promote and protect the health of Canadians through leadership, partnership, innovation and action in public health. Public
GUIDELINES FOR THE MANAGEMENT OF TUBERCULOSIS IN CHILDREN
 GUIDELINES FOR THE MANAGEMENT OF TUBERCULOSIS IN CHILDREN 2013 health Department: Health REPUBLIC OF SOUTH AFRICA GUIDELINES FOR THE MANAGEMENT OF TUBERCULOSIS IN CHILDREN 2013 Published by the Department
GUIDELINES FOR THE MANAGEMENT OF TUBERCULOSIS IN CHILDREN 2013 health Department: Health REPUBLIC OF SOUTH AFRICA GUIDELINES FOR THE MANAGEMENT OF TUBERCULOSIS IN CHILDREN 2013 Published by the Department
Tuberculosis and You A Guide to Tuberculosis Treatment and Services
 Tuberculosis and You A Guide to Tuberculosis Treatment and Services Tuberculosis (TB) is a serious disease that can damage the lungs or other parts of the body like the brain, kidneys or spine. There are
Tuberculosis and You A Guide to Tuberculosis Treatment and Services Tuberculosis (TB) is a serious disease that can damage the lungs or other parts of the body like the brain, kidneys or spine. There are
MODULE THREE TB Treatment. Treatment Action Group TB/HIV Advocacy Toolkit
 MODULE THREE TB Treatment Treatment Action Group TB/HIV Advocacy Toolkit 1 Topics to be covered TB treatment fundamentals Treatment of TB infection and disease TB treatment research Advocacy issues 2 Section
MODULE THREE TB Treatment Treatment Action Group TB/HIV Advocacy Toolkit 1 Topics to be covered TB treatment fundamentals Treatment of TB infection and disease TB treatment research Advocacy issues 2 Section
Pregnancy and Tuberculosis. Patient and Public information sheet
 Pregnancy and Tuberculosis Patient and Public information sheet Who is at risk of TB? Anyone can catch TB, but it is possible that pregnant women have a slightly higher risk of TB. Some people are more
Pregnancy and Tuberculosis Patient and Public information sheet Who is at risk of TB? Anyone can catch TB, but it is possible that pregnant women have a slightly higher risk of TB. Some people are more
How To Treat Tuberculosis
 A Tuberculosis Refresher Course for Physicians A TUBERCULOSIS REFRESHER COURSE FOR PHYSICIANS The World Medical Association, with support from the Lilly MDR-TB Partnership and technical assistance from
A Tuberculosis Refresher Course for Physicians A TUBERCULOSIS REFRESHER COURSE FOR PHYSICIANS The World Medical Association, with support from the Lilly MDR-TB Partnership and technical assistance from
AMBULATORY TREATMENT AND PUBLIC HEALTH MEASURES FOR A PATIENT WITH UNCOMPLICATED PULMONARY TUBERCULOSIS
 AMBULATORY TREATMENT AND PUBLIC HEALTH MEASURES FOR A PATIENT WITH UNCOMPLICATED PULMONARY TUBERCULOSIS AN INFORMATION PAPER January 2013 AMBRX_1301 This information paper is an update of Chapter 17 of
AMBULATORY TREATMENT AND PUBLIC HEALTH MEASURES FOR A PATIENT WITH UNCOMPLICATED PULMONARY TUBERCULOSIS AN INFORMATION PAPER January 2013 AMBRX_1301 This information paper is an update of Chapter 17 of
BASIC INFORMATION ABOUT HIV, HEPATITIS B and C, and TUBERCULOSIS Adapted from the CDC
 BASIC INFORMATION ABOUT HIV, HEPATITIS B and C, and TUBERCULOSIS Adapted from the CDC HIV What are HIV and AIDS? HIV stands for Human Immunodeficiency Virus. This is the virus that causes AIDS. HIV is
BASIC INFORMATION ABOUT HIV, HEPATITIS B and C, and TUBERCULOSIS Adapted from the CDC HIV What are HIV and AIDS? HIV stands for Human Immunodeficiency Virus. This is the virus that causes AIDS. HIV is
Tuberculosis handbook for school nurses
 Tuberculosis handbook for school nurses cov1 Tuberculosis handbook for school nurses The New Jersey Medical School Global Tuberculosis Institute is designated and funded by the Centers for Disease Control
Tuberculosis handbook for school nurses cov1 Tuberculosis handbook for school nurses The New Jersey Medical School Global Tuberculosis Institute is designated and funded by the Centers for Disease Control
Disease/Illness GUIDE TO ASBESTOS LUNG CANCER. What Is Asbestos Lung Cancer? www.simpsonmillar.co.uk Telephone 0844 858 3200
 GUIDE TO ASBESTOS LUNG CANCER What Is Asbestos Lung Cancer? Like tobacco smoking, exposure to asbestos can result in the development of lung cancer. Similarly, the risk of developing asbestos induced lung
GUIDE TO ASBESTOS LUNG CANCER What Is Asbestos Lung Cancer? Like tobacco smoking, exposure to asbestos can result in the development of lung cancer. Similarly, the risk of developing asbestos induced lung
