Polyhematoporphyrin-mediated photodynamic therapy and decortication in palliation of malignant pleural mesothelioma: a clinical pilot study q
|
|
|
- Erin Cook
- 8 years ago
- Views:
Transcription
1 Interactive Cardiovascular and Thoracic Surgery 3 (2004) Work in progress report - Thoracic general Polyhematoporphyrin-mediated photodynamic therapy and decortication in palliation of malignant pleural mesothelioma: a clinical pilot study q Veronika Matzi a, Alfred Maier a, *, Michael Woltsche b, Freyja Maria Smolle-Jüttner a a Department of Surgery, Division of Thoracic and Hyperbaric Surgery, University Medical School, Auenbruggerplatz 29, A-8036 Graz, Austria b Department of Pneumology, LKH Hörgas-Enzenbach, Austria Received 11 April 2003; received in revised form 24 July 2003; accepted 26 August Abstract The aim of this study was to evaluate the additional effect of intraoperative photodynamic therapy (PDT) under hyperbaric oxygenation (HBO) when compared with decortication alone. From 1/1993 to 8/2002, palliation with decortication was done in 25 patients suffering from advanced malignant pleural mesothelioma. Fourteen patients received additional intraoperative PDT under HBO. The surgery and PDT/HBO was done 48 h after photosensitization with a polyhematoporphyrin, 2 mg/kg/bw using a diode laser delivering red light at 630 nm through a microlens. The light dose was calculated for 300 J with a distance of 1 cm from the tumor surface. At 6-month follow up local tumor control and survival showed a significant difference in both groups. Although the study only includes a small number of patients not allowing definite conclusions, it indicates that the additional PDT/HBO represents a safe and technically feasible approach in the palliative setting of advanced malignant mesothelioma of the pleura. q 2003 Elsevier B.V. All rights reserved. Keywords: Pleural mesothelioma; Photodynamic therapy 1. Introduction Because of the lack of sufficient treatments [1,2], malignant pleural mesothelioma has become a model disease for the development of adjunctive treatment modalities. The efficacy of photodynamic therapy as a treatment protocol of malignant pleural mesothelioma has been described and established in several clinical studies [3 6]. Photodynamic therapy is based on the illumination of malignant tissue after selective accumulation of photosensitizers in tumor cells. Photosensitizing agents can absorb photons of appropriate wavelength and become excited to a triplet species. The photon energy is transferred to ground state triplet oxygen producing the excited singlet oxygen (type II photo-oxygenation reaction). In the other type of photo-oxidative process (type I photo-oxygenation reaction) the excited sensitizer itself initiates a free radical reaction. q Presented at the 10th Annual Meeting of the European Society of Thoracic Surgeons, Istanbul, Turkey, October 26 28, * Corresponding author. Tel.: þ ; fax: þ address: alf.maier@kfunigraz.ac.at (A. Maier). Both types of reaction are associated with photodynamic therapy (PDT). Potentially, they cause an acute necrosis of tumor in the illuminated tumor region [7]. In vitro experiments, however, have shown that oxygen is a key component in PDT [8,9]. Under hyperbaric oxygenation (HBO) oxygen physically dissolves in all fluid components of the body, resulting in the fact, that oxygenation is no longer dependent on the presence of red blood cells. The use of HBO in this particular field of cancer treatment could be the key to obtain high levels of molecular oxygen in tumor tissue in order to increase cytotoxicity. According to the experimental studies by Dong et al. [8], use of HBO in PDT accelerates the photodynamic reaction by raising the transmission efficiency of light energy, increasing the quantum amount of oxygen and extending its radius of effective distance. In an experimental animal model, Jirsa et al. [9] studied the influence of HBO and PDT in tumor-bearing nude mice. They concluded that combining HBO and PDT improves the efficiency of PDT by increasing the depth of tumor cell damage, and/or by reducing the doses of sensitizers. The rationale of this clinical trial was to study both the technical feasibility and the efficacy of combined decortication of the pleura and intraoperative PDT under HBO. Main /$ - see front matter q 2003 Elsevier B.V. All rights reserved. doi: /s (03)
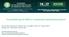
2 V. Matzi et al. / Interactive Cardiovascular and Thoracic Surgery 3 (2004) Diagnostic work-up Fig. 1. Intraoperative view after tumorectomy/decortication and lymphadenectotomy of the upper mediastinum and the paracaval region. variables were considered as PDT associated side effects, morbidity/or mortality and survival time compared to debulking procedure alone. 2. Patients and methods In a prospective non-randomized clinical trial from January 1993 to August 2002, tumorectomy/decortication was done in 25 patients (21 male, four female; mean age: 64.3 years, range: years), suffering from advanced malignant mesothelioma of the pleura. Fourteen patients received additional intraoperative photodynamic therapy under HBO. In case of palliation, decortication combined with additional intracavitary PDT of residual tumor tissue was offered to all patients. However, since additional intracavitary PDT represents an experimental treatment and the disadvantage of long lasting skin photosensitization (8 12 weeks) only 14 patients agreed additional PDT. Therefore, patient selection for additional PDT was done according signed informed consent. All patients suffered from dyspnea and chest pain caused by direct tumor expansion and pleural effusion associated to the tumor. Twenty-one patients had a history of asbestos exposure and 18 patients were heavy cigarette smokers. In presence of a tentative diagnosis made after initial radiological work-up including conventional chest roentgenograms and computed tomography (CT)-scan of the thorax. Video-assisted diagnostic thoracoscopy (VATS) with pleural biopsy, confirming the diagnosis in all patients. Ipsilateral mediastinal lymphnode biopsy during the VATS procedure was done if technically feasible. Clinical staging revealed UICC III (T 2 n ¼ 15; T 3 n ¼ 10; N 1 n ¼ 7; N 2 n ¼ 18). Histological examination revealed 14 epithelial, nine biphasic and two sarcomatous subtypes. After establishing the definitive diagnosis CT scan of the abdomen and bone-scan completed the staging procedure. Additional positron emission tomography (PET) scan was done in six patients Surgery In 25 patients, debulking and decortication was done through a posterolateral thoracotomy. All gross disease (up to 1200 g) was removed, leaving as little residual tumor as possible and mediastinal lymph nodes were sampled routinely (Fig. 1). In two cases subtotal pericardiectomy followed by synthetic mesh reconstruction was done. In 14 cases, the treatment was completed with intraoperative photodynamic therapy enhanced by hyperbaric oxygenation applied to all residual tumor surfaces (Fig. 2). Fig. 2. Intraoperative PDT under HBO in a walk-in hyperbaric chamber. Fig. 3. Kaplan Meier survival distribution.
3 54 V. Matzi et al. / Interactive Cardiovascular and Thoracic Surgery 3 (2004) Pathological staging confirmed UICC stage III in all patients Intraoperative photodynamic therapy (PDT) under hyperbaric oxygenation (HBO) In order to achieve an optimum effect of the photosensitizer the operation was scheduled 48 h after intravenous application of 2 mg/kg BW of a polyhematoporphyrin (Photosan-3, Seehof Laboratory, Wesselburenkoog, Germany). The operation was done in a hyperbaric chamber fully equipped as an operating theatre. After finishing decortication and lymphadenectomy, PDT was done by one surgeon, under hyperbaric oxygenation (100% oxygen, 2ATA pressure). Transcutaneous po 2 -levels were used as an indirect indicator of the oxygen load. They rose from 59 to 77 mmhg (mean: 68 mmhg) under normobaric conditions to mmhg (mean: 580 mmhg) tcpo 2 - levels under 2 ata [10,11]. After a steady state of transcutaneous po 2 had been reached, PDT/HBO was started. Using a diode laser system (Ceramoptec w, Bonn, Germany) delivering red light at 630 nm through a microlens (PhotoDynamicTherapy w, Vienna, Austria), the light dose at the tumor surface was calculated as 300 J with a distance of 1 cm from the tumor surface. Illumination of the tumor area was done cm 2 per cm 2 of tumor surface using a microlens that was moved stepwise along a flexible sterile plastic grid. Depending on the topography and extent of the tumor area, the delivery time ranged from min (median time: 50 min) Follow-up Follow-up investigations were scheduled 3, 6 and 12 months after combined surgical resection ^ intraoperative PDT/HBO comprising CT-scans of the thorax and abdomen and assessment of changes in the quality of life, by using the Karnofsky index. Table 1 Six-month follow-up PDT/surgery (n ¼ 14) Surgery (n ¼ 11) Local tumor regrowth n ¼ 4 n ¼ 8 P ¼,0.05 KPS 95 (90 100) 92 (85 100) n.s. Decrease of dyspnea n ¼ 14 n ¼ 11 n.s. Decrease of pain n ¼ 11 n ¼ 7 n.s. FVC1 1.6 l ( ) 1.7 l ( ) n.s Statistical workup The Chi-square test was used to compare paired values as well as the Kaplan Meier survival table and log-rank test. 3. Results At 6-month follow-up, dyspnea, pain, Kanofsky performance status, FVC1 and tumor regrowth was checked (Table 1). Comparison of CT scans 1 and 6 months post operative documented focal regrowth of the tumor in eight/11 cases of the non-pdt group. However, in the PDT group tumor regrowth was detected in four/14 cases Survival (Fig. 3) In the non-pdt group nine patients died from their disease due to local tumor progression and distant metastases. Two patients are still alive 6 and 8 months from the date of operation. In the PDT group 10/14 patients died from their disease, due to local tumor progression and/or distant metastases. Four patients are still alive from the date of operation at 6, 7, 12 and 18 months, respectively, postoperatively Complications There were no major intra- or postoperative complications. The mean stay at the intensive care unit was 3 days (range from 1 to 7 days) and the mean estimated blood loss was 640 ml (range from 300 to 2400 ml). Sixteen patients required blood transfusions to maintain a hemoglobin of at least 12 g/l. Two patients needed mechanical respiratory support for more than 24 h (40 and 46 h). Air leaks could be observed in 21 patients, however, these closed spontaneously within 3 6 days. The patients were discharged from hospital between days 9 and 20 (mean 14 days). In two cases with additional PDT a superficial dehiscence of the thoracotomy wound was present which, however, closed spontaneously under outpatient wound care. In one patient, re-admission, 4 weeks after discharge due to empyema became necessary. He could be successfully managed by open window thoracostomy. No major complications related to either to photosensitization, to PDT or to HBO were observed during or after the intervention. Side effects included mild skin photosensensitivity in two patients who had neglected the instructions to avoid sunlight after PDT and use a sun blocker for at least 12 weeks [10]. A single episode of fever up to 39 8C in the afternoon after the PDT-procedure was observed in four patients. None of these effects required specific treatment.
4 V. Matzi et al. / Interactive Cardiovascular and Thoracic Surgery 3 (2004) Discussion Debulking and decortication are frequently used as palliative treatment in case of advanced malignant pleural mesothelioma. Local recurrences are almost unavoidable, as surrounding structures and the diffuse character of the tumor preclude an actually radical resection. Because of the low chemosensitivity of mesothelioma, and the difficulty of radiotherapy to include all areas, the additive use of radio- and/or chemotherapy conveys little benefit [1,2]. Several reports suggested that malignant mesothelioma of the pleura responds to PDT [3 6], an attractive antitumor treatment characterized by high potential for selectivity, destroying tumor tissue along the path of monochromatic light, while sparing adjacent healthy structures. Therefore it might be reasonable to use it in addition to debulking and/or pleuropneumonectomy to improve local control of the tumor. However, as mentioned in several reports [5,6], the esophagus and bronchial stump should be protected to prevent fistula formation. PDT involves the interaction of photosensitizers, light and oxygen. Sensitizers originally in a low energy state are excited to a maximum by absorption of monochromatic light of appropriate wavelength and energy. In this energetic state, they react directly through a free radical mechanism, or indirectly via molecular oxygen which undergoes a spin-state transition to reactive singlet oxygen. The depth of penetration of monochromatic light about 5 7 mm limits the active range of the cytotoxic effect. Both pathways yield potentially cytotoxic compounds, although the singlet oxygen process is thought to be predominant in PDT [12,13] and oxygen has been shown to be fuelling the polyhematoporphyrin based photodynamic action in vitro [14]. Considering the interactions of photosensitizer, light and oxygen, with singlet oxygen as the final common mediator of photodynamic cytotoxicity, an enhanced tumoricidal effect may be achieved by increasing the amount of oxygen available for the photochemical reaction. This concept is of crucial importance, as PDT by itself induces reduced blood flow and causes a shutdown of tumor vessels resulting in hypoxia with decreased oxygen tension [15]. Therefore the use of HBO in this concept increased the oxygen tension from below 75 mmhg of up to 750 mmhg. Side effects of HBO may affect the central nervous system and the lung but they subside spontaneously and are very rarely seen at pressures below 2 ATA and exposure times less than 90 min. Accordingly, we did not observe them in our patients. From the technical point of view, combined surgical treatment followed by PDT and HBO did not include any problems provided the laser light generator was positioned outside the hyperbaric chamber with only the fiber being exposed to the hyperbaric atmosphere. We did not observe any complications specifically related to intraoperative PDT and HBO. Because of the residual tumor in case of tumor debulking in advanced malignant mesothelioma, PDT represents a safe additional tool in tumor reduction. Even radical and aggressive surgical procedures could not serve the purpose of oncological success, associated by severe morbidity and mortality. Therefore PDT seems to be an additional option in palliative surgery of malignant mesothelioma to achieve respectable results and clinical outcome in consideration of low morbidity and treatment associated complications. The statistically significant survival benefit as well as the longer interval of tumor recurrence in patients receiving additional PDT/HBO are explicable due to: (a) the treatment of non-resected involved parts of the thoracic cavity, i.e. the phrenic nerve, the pericardium, the diaphragm, the hilus and the lung; and (b) the treatment of the mediastinum after systematic lymphadenectomy. In conclusion, the poor prognosis of advanced malignant mesothelioma of the pleura necessitates new treatment protocols. PDT represents a highly selective tumoricidal tool, whereby oxygen seems to be one of the keys to improve this additive therapy. Although the study only includes a small number of patients not allowing definite conclusions, it indicates that the additional PDT under HBO represents a safe and technically feasible approach in the palliative setting of advanced malignant mesothelioma of the pleura. References [1] Aisner J. Current approach to malignant mesothelioma of the pleura. Chest 1995;107: [2] Sugarbaker D, Garcia J, Richards W. Extrapleural pneumonectomy in the multimodality therapy for malignant pleural mesothelioma: results in 120 consecutive patients. Ann Surg 1996;224: [3] Baas P, Murrer L, Zoetmulder FA. Photodynamic therapy as adjuvant therapy in surgically treated pleural malignancies. Br J Cancer 1997; 76: [4] Pass HI, Temeck BK, Kranda K. Phase III randomized trial of surgery with or without intraoperative photodynamic therapy and postoperative immunochemotherapy for malignant pleural mesothelioma. Ann Surg Oncol 1997;4: [5] Ris H, Altermatt H, Nachbur B. Intraoperative photodynamic therapy with m-tetrahydroxypheylchlorin for chest malignancies. Lasers Surg Med 1996;18: [6] Friedberg JS, Mick R, Stevenson J, Metz J, Zhu T, Buyske J, Sterman DH, Pass HI, Glatstein E, Hahn SM. A phase I study of foscanmediated photodynamic therapy and surgery in patients with mesothelioma. Ann Thorac Surg 2003;75: [7] Moan J, Peng Q, Sorensen R, Jani V, Nesland JM. Biophysical foundations of photodynamic therapy. Endoscopy 1998;30: [8] Dong GC, Hu SX, Zhao GY, Gao SZ, Wu LR. Experimental study on cytotoxic effects of hyperbaric oxygen and photodynamic therapy on mouse transplanted tumours. Chin Med J Engl 1987; 100:
5 56 V. Matzi et al. / Interactive Cardiovascular and Thoracic Surgery 3 (2004) [9] Jirsa Jr M, Pouckiva P, Dolezal J, Pospisil J, Jirsa M. Hyperbaric oxygen and photodynamic therapy in tumour bearing nude mice. Eur J Cancer 1991;27: [10] Maier A, Anegg U, Fell B, Rehak P, Ratzenhofer B, Tomaselli F, Sankin O, Pinter H, Smolle-Jüttner FM. Hyperbaric oxygen and photodynamic therapy in the treatment of advanced carcinoma of the cardia and the esophagus. Lasers Surg Med 2000;26:1 7. [11] Gray BJ, Heaton RW, Henderson A, Hutchinson DCS. In vivo calibration of a transcutaneous oxygen electrode in adult patients. Advances in experimental medicine and biology. New York and London: Plenum Press; p [12] Foote CS. Mechanism of photooxygenation. In: Doiron DR, Alan R, editors. Porphyrin localization and treatment of tumours. New York: Liss; p. 3. [13] Cortese DA, Kinsey GH. Endoscopic treatment of lung cancer with hematoporphyrin phototherapy. Mayo Clin Proc 1982;57: [14] Diamond I, Granelli SG, McDonough AF, Nielson S, Wilson CB, Jaenicke R. Photodynamic therapy of malignant tumours. Lancet 1972;2:117. [15] Wiemann TJ, Mang TS, Fingar VH. Effect of photodynamic therapy on blood flow in normal and tumour vessels. Surgery 1988;194:
MesoPDT. Photodynamic Therapy for malignant pleural mesothelioma ONCO-THAI. Image Assisted Laser Therapy for Oncology
 MesoPDT Photodynamic Therapy for malignant pleural mesothelioma ONCO-THAI Image Assisted Laser Therapy for Oncology Unité Inserm ONCO-THAI «Image Assisted Laser Therapy for Oncology» Inserm ONCO-THAI "Image
MesoPDT Photodynamic Therapy for malignant pleural mesothelioma ONCO-THAI Image Assisted Laser Therapy for Oncology Unité Inserm ONCO-THAI «Image Assisted Laser Therapy for Oncology» Inserm ONCO-THAI "Image
Accelerated hemithoracic radiation followed by extrapleural pneumonectomy for malignant pleural mesothelioma
 Accelerated hemithoracic radiation followed by extrapleural pneumonectomy for malignant pleural mesothelioma Marc de Perrot, Ronald Feld, Natasha B Leighl, Andrew Hope, Thomas K Waddell, Shaf Keshavjee,
Accelerated hemithoracic radiation followed by extrapleural pneumonectomy for malignant pleural mesothelioma Marc de Perrot, Ronald Feld, Natasha B Leighl, Andrew Hope, Thomas K Waddell, Shaf Keshavjee,
Malignant pleural mesothelioma P/D vs. EPP
 3 rd International Thoracic Oncology Congress Dresden, September 13 15, 2012 Malignant pleural mesothelioma P/D vs. EPP Walter Weder, MD Professor of Surgery Dokumentenname Datum Seite 1 Extrapleural Pneumonectomy
3 rd International Thoracic Oncology Congress Dresden, September 13 15, 2012 Malignant pleural mesothelioma P/D vs. EPP Walter Weder, MD Professor of Surgery Dokumentenname Datum Seite 1 Extrapleural Pneumonectomy
L Lang-Lazdunski, A Bille, S Marshall, R Lal, D Landau, J Spicer
 Pleurectomy/decortication, hyperthermic pleural lavage with povidone-iodine and systemic chemotherapy in malignant pleural mesothelioma. A 10-year experience. L Lang-Lazdunski, A Bille, S Marshall, R Lal,
Pleurectomy/decortication, hyperthermic pleural lavage with povidone-iodine and systemic chemotherapy in malignant pleural mesothelioma. A 10-year experience. L Lang-Lazdunski, A Bille, S Marshall, R Lal,
Extrapleural Pneumonectomy for Malignant Mesothelioma: Pro. Joon H. Lee 9/17/2012
 Extrapleural Pneumonectomy for Malignant Mesothelioma: Pro Joon H. Lee 9/17/2012 Malignant Pleural Mesothelioma (Epidemiology) Incidence: 7/mil (Japan) to 40/mil (Australia) Attributed secondary to asbestos
Extrapleural Pneumonectomy for Malignant Mesothelioma: Pro Joon H. Lee 9/17/2012 Malignant Pleural Mesothelioma (Epidemiology) Incidence: 7/mil (Japan) to 40/mil (Australia) Attributed secondary to asbestos
Mesothelioma. Malignant Pleural Mesothelioma
 Mesothelioma William G. Richards, PhD Brigham and Women s Hospital Malignant Pleural Mesothelioma 2,000-3,000 cases per year (USA) Increasing incidence Asbestos (50-80%, decreasing) 30-40 year latency
Mesothelioma William G. Richards, PhD Brigham and Women s Hospital Malignant Pleural Mesothelioma 2,000-3,000 cases per year (USA) Increasing incidence Asbestos (50-80%, decreasing) 30-40 year latency
PRODYNOV. Targeted Photodynamic Therapy of Ovarian Peritoneal Carcinomatosis ONCO-THAI. Image Assisted Laser Therapy for Oncology
 PRODYNOV Targeted Photodynamic Therapy of Ovarian Peritoneal Carcinomatosis ONCO-THAI Image Assisted Laser Therapy for Oncology Inserm ONCO-THAI «Image Assisted Laser Therapy for Oncology» Inserm ONCO-THAI
PRODYNOV Targeted Photodynamic Therapy of Ovarian Peritoneal Carcinomatosis ONCO-THAI Image Assisted Laser Therapy for Oncology Inserm ONCO-THAI «Image Assisted Laser Therapy for Oncology» Inserm ONCO-THAI
بسم هللا الرحمن الرحيم
 بسم هللا الرحمن الرحيم Updates in Mesothelioma By Samieh Amer, MD Professor of Cardiothoracic Surgery Faculty of Medicine, Cairo University History Wagner and his colleagues (1960) 33 cases of mesothelioma
بسم هللا الرحمن الرحيم Updates in Mesothelioma By Samieh Amer, MD Professor of Cardiothoracic Surgery Faculty of Medicine, Cairo University History Wagner and his colleagues (1960) 33 cases of mesothelioma
Mesothelioma. 1. Introduction. 1.1 General Information and Aetiology
 Mesothelioma 1. Introduction 1.1 General Information and Aetiology Mesotheliomas are tumours that arise from the mesothelial cells of the pleura, peritoneum, pericardium or tunica vaginalis [1]. Most are
Mesothelioma 1. Introduction 1.1 General Information and Aetiology Mesotheliomas are tumours that arise from the mesothelial cells of the pleura, peritoneum, pericardium or tunica vaginalis [1]. Most are
A Case of Advanced Malignant Pleural Mesothelioma Treatment with Chemotherapy and Photodynamic Therapy
 CASE REPORT http://dx.doi.org/10.4046/trd.2015.78.1.36 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2015;78:36-40 A Case of Advanced Malignant Pleural Mesothelioma Treatment with Chemotherapy
CASE REPORT http://dx.doi.org/10.4046/trd.2015.78.1.36 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2015;78:36-40 A Case of Advanced Malignant Pleural Mesothelioma Treatment with Chemotherapy
Treatment of mesothelioma in Bloemfontein, South Africa
 European Journal of Cardio-thoracic Surgery 24 (2003) 434 440 www.elsevier.com/locate/ejcts Treatment of mesothelioma in Bloemfontein, South Africa W.J. de Vries*, M.A. Long Cardiothoracic Department,
European Journal of Cardio-thoracic Surgery 24 (2003) 434 440 www.elsevier.com/locate/ejcts Treatment of mesothelioma in Bloemfontein, South Africa W.J. de Vries*, M.A. Long Cardiothoracic Department,
Objectives. Mylene T. Truong, MD. Malignant Pleural Mesothelioma Background
 Imaging of Pleural Tumors Mylene T. Truong, MD Imaging of Pleural Tumours Mylene T. Truong, M. D. University of Texas M.D. Anderson Cancer Center, Houston, TX Objectives To review tumors involving the
Imaging of Pleural Tumors Mylene T. Truong, MD Imaging of Pleural Tumours Mylene T. Truong, M. D. University of Texas M.D. Anderson Cancer Center, Houston, TX Objectives To review tumors involving the
Multimodal therapy of malignant pleural mesothelioma: is the replacement of radical surgery imminent?
 Interactive CardioVascular and Thoracic Surgery Advance Access published November 21, 2012 Interactive CardioVascular and Thoracic Surgery (2012) 1 7 doi:10.1093/icvts/ivs465 ORIGINAL ARTICLE Multimodal
Interactive CardioVascular and Thoracic Surgery Advance Access published November 21, 2012 Interactive CardioVascular and Thoracic Surgery (2012) 1 7 doi:10.1093/icvts/ivs465 ORIGINAL ARTICLE Multimodal
Sternotomy and removal of the tumor
 Sternotomy and removal of the tumor All thymomas originate from epithelial thymic cells 4% of them consist of a pure population of epithelial cells Most have mixed populations of lymphoid cells to a
Sternotomy and removal of the tumor All thymomas originate from epithelial thymic cells 4% of them consist of a pure population of epithelial cells Most have mixed populations of lymphoid cells to a
Malignant Mesothelioma
 Malignant Malignant mesothelioma is a tumour originating from mesothelial cells. 85 95% of mesotheliomas are caused by asbestos exposure. It occurs much more commonly in the chest (malignant pleural mesothelioma)
Malignant Malignant mesothelioma is a tumour originating from mesothelial cells. 85 95% of mesotheliomas are caused by asbestos exposure. It occurs much more commonly in the chest (malignant pleural mesothelioma)
Malignant Mesothelioma
 Malignant mesothelioma is a tumour originating from mesothelial cells. 85 95% of mesotheliomas are caused by asbestos exposure. It occurs much more commonly in the chest (malignant pleural mesothelioma)
Malignant mesothelioma is a tumour originating from mesothelial cells. 85 95% of mesotheliomas are caused by asbestos exposure. It occurs much more commonly in the chest (malignant pleural mesothelioma)
Malignant pleural mesothelioma: outcome of limited surgical management
 Interactive Cardiovascular and Thoracic Surgery 2 (2003) 30 34 Institutional review Thoracic general Malignant pleural mesothelioma: outcome of limited surgical management Peter G. Phillips a, George Asimakopoulos
Interactive Cardiovascular and Thoracic Surgery 2 (2003) 30 34 Institutional review Thoracic general Malignant pleural mesothelioma: outcome of limited surgical management Peter G. Phillips a, George Asimakopoulos
General Information About Non-Small Cell Lung Cancer
 General Information About Non-Small Cell Lung Cancer Non-small cell lung cancer is a disease in which malignant (cancer) cells form in the tissues of the lung. The lungs are a pair of cone-shaped breathing
General Information About Non-Small Cell Lung Cancer Non-small cell lung cancer is a disease in which malignant (cancer) cells form in the tissues of the lung. The lungs are a pair of cone-shaped breathing
Surgical therapy of. who should be operated
 SAMO Interdisciplinary Workshop on Chest Tumors Lucerne, 13th and 14th January 2012 Surgical therapy of mesothelioma, who should be operated Walter Weder MD Professor of Surgery University Hospital Zurich
SAMO Interdisciplinary Workshop on Chest Tumors Lucerne, 13th and 14th January 2012 Surgical therapy of mesothelioma, who should be operated Walter Weder MD Professor of Surgery University Hospital Zurich
Clinical cases in Malignant Pleural Mesothelioma: Adherence to the ESMO Clinical Practice Guidelines
 Clinical cases in Malignant Pleural Mesothelioma: Adherence to the ESMO Clinical Practice Guidelines Wieneke Buikhuisen The Netherlands Cancer Institute Amsterdam The Netherlands Case (1) Male, 56 year
Clinical cases in Malignant Pleural Mesothelioma: Adherence to the ESMO Clinical Practice Guidelines Wieneke Buikhuisen The Netherlands Cancer Institute Amsterdam The Netherlands Case (1) Male, 56 year
A Practical Guide to Advances in Staging and Treatment of NSCLC
 A Practical Guide to Advances in Staging and Treatment of NSCLC Robert J. Korst, M.D. Director, Thoracic Surgery Medical Director, The Blumenthal Cancer Center The Valley Hospital Objectives Revised staging
A Practical Guide to Advances in Staging and Treatment of NSCLC Robert J. Korst, M.D. Director, Thoracic Surgery Medical Director, The Blumenthal Cancer Center The Valley Hospital Objectives Revised staging
Screening, early referral and treatment for asbestos related cancer
 Screening, early referral and treatment for asbestos related cancer Marc de Perrot, MD, MSc, FRCSC Toronto Mesothelioma Research Program University of Toronto Asbestos related diseases Mesothelioma Lung
Screening, early referral and treatment for asbestos related cancer Marc de Perrot, MD, MSc, FRCSC Toronto Mesothelioma Research Program University of Toronto Asbestos related diseases Mesothelioma Lung
SMALL CELL LUNG CANCER
 Protocol for Planning and Treatment The process to be followed in the management of: SMALL CELL LUNG CANCER Patient information given at each stage following agreed information pathway 1. DIAGNOSIS New
Protocol for Planning and Treatment The process to be followed in the management of: SMALL CELL LUNG CANCER Patient information given at each stage following agreed information pathway 1. DIAGNOSIS New
Mesothelioma: Questions and Answers
 CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Mesothelioma: Questions
CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Mesothelioma: Questions
Photodynamic Therapy for Malignant Pleural Mesothelioma
 S-75 Photodynamic Therapy for Malignant Pleural Mesothelioma Presented by Joseph S. Friedberg, MD, University of Pennsylvania Health System, Philadelphia, Pennsylvania Abstract Surgery is the treatment
S-75 Photodynamic Therapy for Malignant Pleural Mesothelioma Presented by Joseph S. Friedberg, MD, University of Pennsylvania Health System, Philadelphia, Pennsylvania Abstract Surgery is the treatment
Columbia University Mesothelioma Applied Research Foundation - 2009 - www.curemeso.org. Mesothelioma Center www.mesocenter.org
 Columbia University Mesothelioma Center www.mesocenter.org Multimodal clinical trials, treatment (surgery, radiation, chemotherapy) Peritoneal mesothelioma program Immunotherapy translational, experimental
Columbia University Mesothelioma Center www.mesocenter.org Multimodal clinical trials, treatment (surgery, radiation, chemotherapy) Peritoneal mesothelioma program Immunotherapy translational, experimental
Malignant Pleural Mesothelioma in Singapore
 RESEARCH COMMUNICATION C SP Yip 1, HN Koong 2, CM Loo 3, KW Fong 1* Abstract Aim: To examine the clinical characteristics and outcomes of malignant pleural mesothelioma (MPM) in Singapore. Methods and
RESEARCH COMMUNICATION C SP Yip 1, HN Koong 2, CM Loo 3, KW Fong 1* Abstract Aim: To examine the clinical characteristics and outcomes of malignant pleural mesothelioma (MPM) in Singapore. Methods and
Post-operative intrapleural chemotherapy for mesothelioma
 Post-operative intrapleural chemotherapy for mesothelioma Robert Kratzke, MD John Skoglund Chair for Lung Cancer Research Section of Heme-Onc-Transplant University of Minnesota Medical School Efficacy
Post-operative intrapleural chemotherapy for mesothelioma Robert Kratzke, MD John Skoglund Chair for Lung Cancer Research Section of Heme-Onc-Transplant University of Minnesota Medical School Efficacy
Clinical Indications and Results Following Chest Wall Resection
 Clinical Indications and Results Following Chest Wall Resection for Recurrent Malignant Pleural Mesothelioma Ali SO, Burt BM, Groth SS, DaSilva MC, Yeap BY, Richards WG, Baldini EH and Sugarbaker DJ. Division
Clinical Indications and Results Following Chest Wall Resection for Recurrent Malignant Pleural Mesothelioma Ali SO, Burt BM, Groth SS, DaSilva MC, Yeap BY, Richards WG, Baldini EH and Sugarbaker DJ. Division
Disease/Illness GUIDE TO ASBESTOS LUNG CANCER. What Is Asbestos Lung Cancer? www.simpsonmillar.co.uk Telephone 0844 858 3200
 GUIDE TO ASBESTOS LUNG CANCER What Is Asbestos Lung Cancer? Like tobacco smoking, exposure to asbestos can result in the development of lung cancer. Similarly, the risk of developing asbestos induced lung
GUIDE TO ASBESTOS LUNG CANCER What Is Asbestos Lung Cancer? Like tobacco smoking, exposure to asbestos can result in the development of lung cancer. Similarly, the risk of developing asbestos induced lung
Malignant Mesothelioma Current Approaches to a Difficult Problem. Raja M Flores, MD Thoracic Surgery Memorial Sloan-Kettering Cancer Center
 Malignant Mesothelioma Current Approaches to a Difficult Problem Raja M Flores, MD Thoracic Surgery Memorial Sloan-Kettering Cancer Center Malignant Pleural Mesothelioma Clinical Presentation Insidious
Malignant Mesothelioma Current Approaches to a Difficult Problem Raja M Flores, MD Thoracic Surgery Memorial Sloan-Kettering Cancer Center Malignant Pleural Mesothelioma Clinical Presentation Insidious
International Journal of Case Reports in Medicine
 International Journal of Case Reports in Medicine Vol. 2013 (2013), Article ID 409830, 15 minipages. DOI:10.5171/2013.409830 www.ibimapublishing.com Copyright 2013 Andrew Thomas Low, Iain Smith and Simon
International Journal of Case Reports in Medicine Vol. 2013 (2013), Article ID 409830, 15 minipages. DOI:10.5171/2013.409830 www.ibimapublishing.com Copyright 2013 Andrew Thomas Low, Iain Smith and Simon
Protein kinase C alpha expression and resistance to neo-adjuvant gemcitabine-containing chemotherapy in non-small cell lung cancer
 Protein kinase C alpha expression and resistance to neo-adjuvant gemcitabine-containing chemotherapy in non-small cell lung cancer Dan Vogl Lay Abstract Early stage non-small cell lung cancer can be cured
Protein kinase C alpha expression and resistance to neo-adjuvant gemcitabine-containing chemotherapy in non-small cell lung cancer Dan Vogl Lay Abstract Early stage non-small cell lung cancer can be cured
Treating Mesothelioma - A Quick Guide
 Treating Mesothelioma - A Quick Guide Contents This is a brief summary of the information on Treating mesothelioma from CancerHelp UK. You will find more detailed information on the website. In this information
Treating Mesothelioma - A Quick Guide Contents This is a brief summary of the information on Treating mesothelioma from CancerHelp UK. You will find more detailed information on the website. In this information
This factsheet aims to outline the characteristics of some rare lung cancers, and highlight where each type of lung cancer may be different.
 There are several different kinds of lung cancer, often referred to as lung cancer subtypes. Some of these occur more often than others. In this factsheet we will specifically look at the subtypes of cancers
There are several different kinds of lung cancer, often referred to as lung cancer subtypes. Some of these occur more often than others. In this factsheet we will specifically look at the subtypes of cancers
Mesothelioma. 1995-2013, The Patient Education Institute, Inc. www.x-plain.com ocft0101 Last reviewed: 03/21/2013 1
 Mesothelioma Introduction Mesothelioma is a type of cancer. It starts in the tissue that lines your lungs, stomach, heart, and other organs. This tissue is called mesothelium. Most people who get this
Mesothelioma Introduction Mesothelioma is a type of cancer. It starts in the tissue that lines your lungs, stomach, heart, and other organs. This tissue is called mesothelium. Most people who get this
Primary -Benign - Malignant Secondary
 TUMOURS OF THE LUNG Primary -Benign - Malignant Secondary The incidence of lung cancer has been increasing almost logarithmically and is now reaching epidemic levels. The overall cure rate is very low
TUMOURS OF THE LUNG Primary -Benign - Malignant Secondary The incidence of lung cancer has been increasing almost logarithmically and is now reaching epidemic levels. The overall cure rate is very low
Therapy of pleural effusions Modern techniques
 Therapy of pleural effusions Modern techniques Dr. Melanie Toffel Sugery of the chest Pleural effusion Ethiology In the normal pleural space there is a steady state in which there is a roughly equal rate
Therapy of pleural effusions Modern techniques Dr. Melanie Toffel Sugery of the chest Pleural effusion Ethiology In the normal pleural space there is a steady state in which there is a roughly equal rate
Malignant Mesothelioma State of the Art
 Malignant Mesothelioma State of the Art Paul Baas The Netherlands Cancer Institute August 12, 2011, Carlsbad, CA Summary Diagnosis; epithelial type subdivided Pleiomorphic vs other Staging: IASLC-IMIG
Malignant Mesothelioma State of the Art Paul Baas The Netherlands Cancer Institute August 12, 2011, Carlsbad, CA Summary Diagnosis; epithelial type subdivided Pleiomorphic vs other Staging: IASLC-IMIG
Lung Cancer and Mesothelioma
 Lung Cancer and Mesothelioma Robert Kratzke, M.D. John C. Skoglund Professor of Lung Cancer Research Section of Heme/Onc/Transplant Department of Medicine University of Minnesota Medical School Malignant
Lung Cancer and Mesothelioma Robert Kratzke, M.D. John C. Skoglund Professor of Lung Cancer Research Section of Heme/Onc/Transplant Department of Medicine University of Minnesota Medical School Malignant
Surgical Management of Malignant Pleural Mesothelioma: A Clinical Practice Guideline
 Evidence-based Series #7-14-2: Section 1 Surgical Management of Malignant Pleural Mesothelioma: A Clinical Practice Guideline D.E. Maziak, A. Gagliardi, A.E. Haynes, J.A. Mackay, W.K. Evans, and members
Evidence-based Series #7-14-2: Section 1 Surgical Management of Malignant Pleural Mesothelioma: A Clinical Practice Guideline D.E. Maziak, A. Gagliardi, A.E. Haynes, J.A. Mackay, W.K. Evans, and members
Understanding Pleural Mesothelioma
 Understanding Pleural Mesothelioma UHN Information for patients and families Read this booklet to learn about: What is pleural mesothelioma? What causes it? What are the symptoms? What tests are done to
Understanding Pleural Mesothelioma UHN Information for patients and families Read this booklet to learn about: What is pleural mesothelioma? What causes it? What are the symptoms? What tests are done to
Surgeons Role in Symptom Management. A/Prof Cliff K. C. Choong Consultant Thoracic Surgeon Latrobe Regional Hospital GIPPSLAND
 Surgeons Role in Symptom Management A/Prof Cliff K. C. Choong Consultant Thoracic Surgeon Latrobe Regional Hospital GIPPSLAND Conditions PLEURAL Pleural effusion Pneumothorax ENDOBRONCHIAL Haemoptysis
Surgeons Role in Symptom Management A/Prof Cliff K. C. Choong Consultant Thoracic Surgeon Latrobe Regional Hospital GIPPSLAND Conditions PLEURAL Pleural effusion Pneumothorax ENDOBRONCHIAL Haemoptysis
Surgery. Wedge resection only part of the lung, not. not a lobe, is removed. Cancer Council NSW
 The treatment you receive will depend on your lung cancer type, for example, whether you have a non-small cell lung cancer Adenocarcinoma or Squamous cell carcinoma, and if this is a sub-type with a mutation.
The treatment you receive will depend on your lung cancer type, for example, whether you have a non-small cell lung cancer Adenocarcinoma or Squamous cell carcinoma, and if this is a sub-type with a mutation.
ASBESTOS EXPOSURE AND SARCOMATOID MALIGNANT PLEURAL MESOTHELIOMA Gorantla Sambasivarao 1, Namballa Usharani 2, Tupakula Suresh Babu 3
 ASBESTOS EXPOSURE AND SARCOMATOID MALIGNANT PLEURAL MESOTHELIOMA Gorantla Sambasivarao 1, Namballa Usharani 2, Tupakula Suresh Babu 3 HOW TO CITE THIS ARTICLE: Gorantla Sambasivarao, Namballa Usharani,
ASBESTOS EXPOSURE AND SARCOMATOID MALIGNANT PLEURAL MESOTHELIOMA Gorantla Sambasivarao 1, Namballa Usharani 2, Tupakula Suresh Babu 3 HOW TO CITE THIS ARTICLE: Gorantla Sambasivarao, Namballa Usharani,
Round Table with Drs. Anne Tsao and Alex Farivar, Case 2: Mesothelioma
 Round Table with Drs. Anne Tsao and Alex Farivar, Case 2: Mesothelioma I d like to welcome everyone, thanks for coming out to our lunch with experts. The faculty today are great people in the thoracic
Round Table with Drs. Anne Tsao and Alex Farivar, Case 2: Mesothelioma I d like to welcome everyone, thanks for coming out to our lunch with experts. The faculty today are great people in the thoracic
Post-recurrence survival in completely resected stage I non-small cell lung cancer with local recurrence
 Post- survival in completely resected stage I non-small cell lung cancer with local J-J Hung, 1,2,3 W-H Hsu, 3 C-C Hsieh, 3 B-S Huang, 3 M-H Huang, 3 J-S Liu, 2 Y-C Wu 3 See Editorial, p 185 c A supplementary
Post- survival in completely resected stage I non-small cell lung cancer with local J-J Hung, 1,2,3 W-H Hsu, 3 C-C Hsieh, 3 B-S Huang, 3 M-H Huang, 3 J-S Liu, 2 Y-C Wu 3 See Editorial, p 185 c A supplementary
Small cell lung cancer
 Small cell lung cancer Small cell lung cancer is a disease in which malignant (cancer) cells form in the tissues of the lung. The lungs are a pair of cone-shaped breathing organs that are found within
Small cell lung cancer Small cell lung cancer is a disease in which malignant (cancer) cells form in the tissues of the lung. The lungs are a pair of cone-shaped breathing organs that are found within
Rotation Specific Goals & Objectives: University Health Network-Princess Margaret Hospital/ Sunnybrook Breast/Melanoma
 Rotation Specific Goals & Objectives: University Health Network-Princess Margaret Hospital/ Sunnybrook Breast/Melanoma Medical Expert: Breast Rotation Specific Competencies/Objectives 1.0 Medical History
Rotation Specific Goals & Objectives: University Health Network-Princess Margaret Hospital/ Sunnybrook Breast/Melanoma Medical Expert: Breast Rotation Specific Competencies/Objectives 1.0 Medical History
Update on Mesothelioma
 November 8, 2012 Update on Mesothelioma Intro incidence and nomenclature Update on Classification Diagnostic specimens Morphologic features Epithelioid Histology Biphasic Histology Immunohistochemical
November 8, 2012 Update on Mesothelioma Intro incidence and nomenclature Update on Classification Diagnostic specimens Morphologic features Epithelioid Histology Biphasic Histology Immunohistochemical
How To Treat Lung Cancer At Cleveland Clinic
 Treatment Guide Lung Cancer Management The Chest Cancer Center at Cleveland Clinic, which includes specialists from the Respiratory Institute, Taussig Cancer Institute and Miller Family Heart & Vascular
Treatment Guide Lung Cancer Management The Chest Cancer Center at Cleveland Clinic, which includes specialists from the Respiratory Institute, Taussig Cancer Institute and Miller Family Heart & Vascular
Targeting Specific Cell Signaling Pathways for the Treatment of Malignant Peritoneal Mesothelioma
 The Use of Kinase Inhibitors: Translational Lab Results Targeting Specific Cell Signaling Pathways for the Treatment of Malignant Peritoneal Mesothelioma Sheelu Varghese, Ph.D. H. Richard Alexander, M.D.
The Use of Kinase Inhibitors: Translational Lab Results Targeting Specific Cell Signaling Pathways for the Treatment of Malignant Peritoneal Mesothelioma Sheelu Varghese, Ph.D. H. Richard Alexander, M.D.
PET/CT in Lung Cancer
 PET/CT in Lung Cancer Rodolfo Núñez Miller, M.D. Nuclear Medicine and Diagnostic Imaging Section Division of Human Health International Atomic Energy Agency Vienna, Austria GLOBOCAN 2012 #1 #3 FDG-PET/CT
PET/CT in Lung Cancer Rodolfo Núñez Miller, M.D. Nuclear Medicine and Diagnostic Imaging Section Division of Human Health International Atomic Energy Agency Vienna, Austria GLOBOCAN 2012 #1 #3 FDG-PET/CT
Survival analysis of 220 patients with completely resected stage II non small cell lung cancer
 窑 Original Article 窑 Chinese Journal of Cancer Survival analysis of 22 patients with completely resected stage II non small cell lung cancer Yun Dai,2,3, Xiao Dong Su,2,3, Hao Long,2,3, Peng Lin,2,3, Jian
窑 Original Article 窑 Chinese Journal of Cancer Survival analysis of 22 patients with completely resected stage II non small cell lung cancer Yun Dai,2,3, Xiao Dong Su,2,3, Hao Long,2,3, Peng Lin,2,3, Jian
Treatment of Mesothelioma with Radiotherapy
 41 Treatment of Mesothelioma with Radiotherapy Ryan P. Smith and Stephen M. Hahn General Principles of Radiation Therapy Radiation therapy is a therapeutic modality that uses ionizing radiation to treat
41 Treatment of Mesothelioma with Radiotherapy Ryan P. Smith and Stephen M. Hahn General Principles of Radiation Therapy Radiation therapy is a therapeutic modality that uses ionizing radiation to treat
Avastin: Glossary of key terms
 Avastin: Glossary of key terms Adenocarcinoma Adenoma Adjuvant therapy Angiogenesis Anti-angiogenics Antibody Antigen Avastin (bevacizumab) Benign A form of carcinoma that originates in glandular tissue.
Avastin: Glossary of key terms Adenocarcinoma Adenoma Adjuvant therapy Angiogenesis Anti-angiogenics Antibody Antigen Avastin (bevacizumab) Benign A form of carcinoma that originates in glandular tissue.
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES LUNG SITE MESOTHELIOMA Lung Site Group Mesothelioma Date Guideline Created: April 2013 Authors: Dr. Meredith Giuliani, Dr. Andrea Bezjak 1.
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES LUNG SITE MESOTHELIOMA Lung Site Group Mesothelioma Date Guideline Created: April 2013 Authors: Dr. Meredith Giuliani, Dr. Andrea Bezjak 1.
B10/S/a Cancer: Malignant Mesothelioma (Adult)
 B10/S/a 2013/14 NHS STANDARD CONTRACT FOR CANCER: MALIGNANT MESOTHELIOMA (ADULT) SECTION B PART 1 - SERVICE SPECIFICATIONS Service Specification No. Service Commissioner Lead Provider Lead Period Date
B10/S/a 2013/14 NHS STANDARD CONTRACT FOR CANCER: MALIGNANT MESOTHELIOMA (ADULT) SECTION B PART 1 - SERVICE SPECIFICATIONS Service Specification No. Service Commissioner Lead Provider Lead Period Date
Lung Cancer & Mesothelioma 2011-2015
 Lung Cancer & Mesothelioma 2011-2015 Annex G Mesothelioma 1. The vision for mesothelioma services is set out in the Mesothelioma Framework issued by DH on 26 February 2007 (supported by the British Thoracic
Lung Cancer & Mesothelioma 2011-2015 Annex G Mesothelioma 1. The vision for mesothelioma services is set out in the Mesothelioma Framework issued by DH on 26 February 2007 (supported by the British Thoracic
Medullary Renal Cell Carcinoma Case Report
 Bahrain Medical Bulletin, Vol. 27, No. 4, December 2005 Medullary Renal Cell Carcinoma Case Report Mohammed Abdulla Al-Tantawi MBBCH, CABS* Abdul Amir Issa MBBCH, CABS*** Mohammed Abdulla MBBCH, CABS**
Bahrain Medical Bulletin, Vol. 27, No. 4, December 2005 Medullary Renal Cell Carcinoma Case Report Mohammed Abdulla Al-Tantawi MBBCH, CABS* Abdul Amir Issa MBBCH, CABS*** Mohammed Abdulla MBBCH, CABS**
Summary of treatment benefits
 Risk Management Plan PEMETREXED Powder for concentrate for Solution for infusion Pemetrexed is also indicated as monotherapy for the maintenance treatment of locally advanced or metastatic non small cell
Risk Management Plan PEMETREXED Powder for concentrate for Solution for infusion Pemetrexed is also indicated as monotherapy for the maintenance treatment of locally advanced or metastatic non small cell
Adiuwantowe i neoadiuwantowe leczenie chorych na zaawansowanego raka żołądka
 Adiuwantowe i neoadiuwantowe leczenie chorych na zaawansowanego raka żołądka Neoadiuvant and adiuvant therapy for advanced gastric cancer Franco Roviello, IT Neoadjuvant and adjuvant therapy for advanced
Adiuwantowe i neoadiuwantowe leczenie chorych na zaawansowanego raka żołądka Neoadiuvant and adiuvant therapy for advanced gastric cancer Franco Roviello, IT Neoadjuvant and adjuvant therapy for advanced
How TARGIT Intra-operative Radiotherapy can help Older Patients with Breast cancer
 How TARGIT Intra-operative Radiotherapy can help Older Patients with Breast cancer Jeffrey S Tobias, Jayant S Vaidya, Frederik Wenz and Michael Baum, University College Hospital, London, UK - on behalf
How TARGIT Intra-operative Radiotherapy can help Older Patients with Breast cancer Jeffrey S Tobias, Jayant S Vaidya, Frederik Wenz and Michael Baum, University College Hospital, London, UK - on behalf
Metastatic Renal Cell Carcinoma: Staging and Prognosis of Three Separate Cases.
 Metastatic Renal Cell Carcinoma: Staging and Prognosis of Three Separate Cases. Abstract This paper describes the staging, imaging, treatment, and prognosis of renal cell carcinoma. Three case studies
Metastatic Renal Cell Carcinoma: Staging and Prognosis of Three Separate Cases. Abstract This paper describes the staging, imaging, treatment, and prognosis of renal cell carcinoma. Three case studies
MESOTHELIOMA. Not Just a Late Night Commercial. Graciela Hoal, RN, MSN, ACNP-BC
 MESOTHELIOMA Not Just a Late Night Commercial Graciela Hoal, RN, MSN, ACNP-BC Saturday Session Thoracic Surgery Nurse Practitioner Greater Los Angeles Veteran Affairs Objectives Course Objectives: Discuss
MESOTHELIOMA Not Just a Late Night Commercial Graciela Hoal, RN, MSN, ACNP-BC Saturday Session Thoracic Surgery Nurse Practitioner Greater Los Angeles Veteran Affairs Objectives Course Objectives: Discuss
INTERNATIONAL ASSOCIATION FOR THE STUDY OF LUNG CANCER Prospective Mesothelioma Staging Project
 INTERNATIONAL ASSOCIATION FOR THE STUDY OF LUNG CANCER Prospective Mesothelioma Staging Project Data Forms and Fields in CRAB Electronic Data Capture System - Reduced Set - Pivotal data elements for developing
INTERNATIONAL ASSOCIATION FOR THE STUDY OF LUNG CANCER Prospective Mesothelioma Staging Project Data Forms and Fields in CRAB Electronic Data Capture System - Reduced Set - Pivotal data elements for developing
Lung Cancer Understanding your diagnosis
 Lung Cancer Understanding your diagnosis Lung Cancer Understanding your diagnosis When you first hear that you have cancer you may feel alone and afraid. You may be overwhelmed by the large amount of information
Lung Cancer Understanding your diagnosis Lung Cancer Understanding your diagnosis When you first hear that you have cancer you may feel alone and afraid. You may be overwhelmed by the large amount of information
Current Status and Perspectives of Radiation Therapy for Breast Cancer
 Breast Cancer Current Status and Perspectives of Radiation Therapy for Breast Cancer JMAJ 45(10): 434 439, 2002 Masahiro HIRAOKA, Masaki KOKUBO, Chikako YAMAMOTO and Michihide MITSUMORI Department of Therapeutic
Breast Cancer Current Status and Perspectives of Radiation Therapy for Breast Cancer JMAJ 45(10): 434 439, 2002 Masahiro HIRAOKA, Masaki KOKUBO, Chikako YAMAMOTO and Michihide MITSUMORI Department of Therapeutic
Cytoreduction and hyperthermic intraperitoneal chemotherapy for the treatment of pseudomyxoma
 Medical Policy Cytoreduction and Hyperthermic Intraperitoneal Chemotherapy for the Treatment of Pseudomyxoma Peritonei and Peritoneal Carcinomatosis of Gastrointestinal Origin, and Peritoneal Mesothelioma
Medical Policy Cytoreduction and Hyperthermic Intraperitoneal Chemotherapy for the Treatment of Pseudomyxoma Peritonei and Peritoneal Carcinomatosis of Gastrointestinal Origin, and Peritoneal Mesothelioma
What is Mesothelioma?
 What is Mesothelioma? Mesothelioma is a rare type of cancer that develops in the mesothelial cells found in one s body. These cells form membranous linings that surround and protect the body s organs and
What is Mesothelioma? Mesothelioma is a rare type of cancer that develops in the mesothelial cells found in one s body. These cells form membranous linings that surround and protect the body s organs and
Lung Cancer. This reference summary will help you better understand lung cancer and the treatment options that are available.
 Lung Cancer Introduction Lung cancer is the number one cancer killer of men and women. Over 165,000 people die of lung cancer every year in the United States. Most cases of lung cancer are related to cigarette
Lung Cancer Introduction Lung cancer is the number one cancer killer of men and women. Over 165,000 people die of lung cancer every year in the United States. Most cases of lung cancer are related to cigarette
Malignant Pleural Diseases Advances Clinicians Should Know F Gleeson
 Malignant Pleural Diseases Advances Clinicians Should Know F Gleeson The following relevant disclosures, conflicts of interest and/ or financial relationships exist related to this presentation: Consultant
Malignant Pleural Diseases Advances Clinicians Should Know F Gleeson The following relevant disclosures, conflicts of interest and/ or financial relationships exist related to this presentation: Consultant
Radiation therapy involves using many terms you may have never heard before. Below is a list of words you could hear during your treatment.
 Dictionary Radiation therapy involves using many terms you may have never heard before. Below is a list of words you could hear during your treatment. Applicator A device used to hold a radioactive source
Dictionary Radiation therapy involves using many terms you may have never heard before. Below is a list of words you could hear during your treatment. Applicator A device used to hold a radioactive source
A succesfull case of HIPEC in a peritoneal mesothelioma patient
 A succesfull case of HIPEC in a peritoneal mesothelioma patient Firmino, NLJ¹²; Miranda, E¹³; Oliveira, DA ²; Lima, MBA ¹²; Diniz, AF ¹²; Gomes, GES ¹²; Azevedo, LW ¹²; Soares,MC¹²; Gomes, ASA³. ¹Pernambuco
A succesfull case of HIPEC in a peritoneal mesothelioma patient Firmino, NLJ¹²; Miranda, E¹³; Oliveira, DA ²; Lima, MBA ¹²; Diniz, AF ¹²; Gomes, GES ¹²; Azevedo, LW ¹²; Soares,MC¹²; Gomes, ASA³. ¹Pernambuco
J of Evidence Based Med & Hlthcare, pissn- 2349-2562, eissn- 2349-2570/ Vol. 2/Issue 33/Aug. 17, 2015 Page 5063
 PERITONEAL MALIGNANT MESOTHELIOMA: A RARE S. R. Dhamotharan 1, S. Shanthi Nirmala 2, F. Celine Foustina Mary 3, M. Arul Raj Kumar 4, R. Vinothprabhu 5 HOW TO CITE THIS ARTICLE: S. R. Dhamotharan, S. Shanthi
PERITONEAL MALIGNANT MESOTHELIOMA: A RARE S. R. Dhamotharan 1, S. Shanthi Nirmala 2, F. Celine Foustina Mary 3, M. Arul Raj Kumar 4, R. Vinothprabhu 5 HOW TO CITE THIS ARTICLE: S. R. Dhamotharan, S. Shanthi
Malignant mesothelioma (MM) is an uncommon
 Intraoperative Photodynamic Therapy After Pleuropneumonectomy in Patients With Malignant Pleural Mesothelioma* Dose Finding and Toxicity Results Hugo Schouwink, MD ; Emiel T. Rutgers, MD, PhD; Joost van
Intraoperative Photodynamic Therapy After Pleuropneumonectomy in Patients With Malignant Pleural Mesothelioma* Dose Finding and Toxicity Results Hugo Schouwink, MD ; Emiel T. Rutgers, MD, PhD; Joost van
Cancer treatment. TOP EUROPEAN CANCER EXPERTISE The path to recovery
 Cancer treatment TOP EUROPEAN CANCER EXPERTISE The path to recovery 0% LAND OF HIGH QUALITY HEALTHCARE Located in Finland, a land of high quality healthcare, Helsinki University Hospital is regarded as
Cancer treatment TOP EUROPEAN CANCER EXPERTISE The path to recovery 0% LAND OF HIGH QUALITY HEALTHCARE Located in Finland, a land of high quality healthcare, Helsinki University Hospital is regarded as
Neoplasms of the LUNG and PLEURA
 Neoplasms of the LUNG and PLEURA 2015-2016 FCDS Educational Webcast Series Steven Peace, BS, CTR September 19, 2015 2015 Focus o Anatomy o SSS 2000 o MPH Rules o AJCC TNM 1 Case 1 Case Vignette HISTORY:
Neoplasms of the LUNG and PLEURA 2015-2016 FCDS Educational Webcast Series Steven Peace, BS, CTR September 19, 2015 2015 Focus o Anatomy o SSS 2000 o MPH Rules o AJCC TNM 1 Case 1 Case Vignette HISTORY:
How To Treat A Cancer With A Radical
 Management of mesothelioma Jan.vanmeerbeeck@ugent.be Amsterdam, March 6, 2010 1 management Palliation Symptomatic care Pain Breathlessness Radiotherapy Chemotherapy Surgery Radical (intention to cure)
Management of mesothelioma Jan.vanmeerbeeck@ugent.be Amsterdam, March 6, 2010 1 management Palliation Symptomatic care Pain Breathlessness Radiotherapy Chemotherapy Surgery Radical (intention to cure)
Malignant Mesothelioma: an Update
 Malignant Mesothelioma: an Update Nico van Zandwijk Asbestos Diseases Research Institute Bernie Banton Centre University of Sydney Australia Physicians Week RACP 19-5-2009 Health Risks of Asbestos Fibers
Malignant Mesothelioma: an Update Nico van Zandwijk Asbestos Diseases Research Institute Bernie Banton Centre University of Sydney Australia Physicians Week RACP 19-5-2009 Health Risks of Asbestos Fibers
PANCREATIC AND PERIAMPULLARY TUMORS: PANCREATICODUODENECTOMY. Dr. Shailesh V. Shrikhande
 PANCREATIC AND PERIAMPULLARY TUMORS: PANCREATICODUODENECTOMY Dr. Shailesh V. Shrikhande Associate Professor & Consultant Surgeon GI and HPB Surgical Oncology Tata Memorial Hospital, Mumbai INDIA HELICAL
PANCREATIC AND PERIAMPULLARY TUMORS: PANCREATICODUODENECTOMY Dr. Shailesh V. Shrikhande Associate Professor & Consultant Surgeon GI and HPB Surgical Oncology Tata Memorial Hospital, Mumbai INDIA HELICAL
Lung Cancer Treatment Guidelines
 Updated June 2014 Derived and updated by consensus of members of the Providence Thoracic Oncology Program with the aid of evidence-based National Comprehensive Cancer Network (NCCN) national guidelines,
Updated June 2014 Derived and updated by consensus of members of the Providence Thoracic Oncology Program with the aid of evidence-based National Comprehensive Cancer Network (NCCN) national guidelines,
Non-Small Cell Lung Cancer
 Non-Small Cell Lung Cancer About Your Lungs and Lung Cancer How do your lungs work? To understand lung cancer it is helpful to understand your lungs. Your lungs put oxygen into the blood, which the heart
Non-Small Cell Lung Cancer About Your Lungs and Lung Cancer How do your lungs work? To understand lung cancer it is helpful to understand your lungs. Your lungs put oxygen into the blood, which the heart
GRANT APPLICATION FORM: ORGANISING AN ESO EDUCATIONAL EVENT
 GRANT APPLICATION FORM: ORGANISING AN ESO EDUCATIONAL EVENT 1) TOPIC OF THE EVENT MALIGNANT PLEURAL DISEASE 2) SUGGESTED TITLE : Approach to Pleural Cancer: State-of-the-Art 3) TYPE OF EVENT Course Native
GRANT APPLICATION FORM: ORGANISING AN ESO EDUCATIONAL EVENT 1) TOPIC OF THE EVENT MALIGNANT PLEURAL DISEASE 2) SUGGESTED TITLE : Approach to Pleural Cancer: State-of-the-Art 3) TYPE OF EVENT Course Native
Colorectal Cancer Treatment
 Scan for mobile link. Colorectal Cancer Treatment Colorectal cancer overview Colorectal cancer, also called large bowel cancer, is the term used to describe malignant tumors found in the colon and rectum.
Scan for mobile link. Colorectal Cancer Treatment Colorectal cancer overview Colorectal cancer, also called large bowel cancer, is the term used to describe malignant tumors found in the colon and rectum.
Non-Small Cell Lung Cancer Treatment Comparison to NCCN Guidelines
 Non-Small Cell Lung Cancer Treatment Comparison to NCCN Guidelines April 2008 (presented at 6/12/08 cancer committee meeting) By Shelly Smits, RHIT, CCS, CTR Conclusions by Dr. Ian Thompson, MD Dr. James
Non-Small Cell Lung Cancer Treatment Comparison to NCCN Guidelines April 2008 (presented at 6/12/08 cancer committee meeting) By Shelly Smits, RHIT, CCS, CTR Conclusions by Dr. Ian Thompson, MD Dr. James
1 page Overview. CONCURRENT 1D, 1E, 1F Biology & Pathogenesis Multi-Modality Immunology 1
 1 page Overview 21 Oct Tuesday 1500 on REGISTRATION 1800 Welcome Reception & Cocktails at the Cape Town International Conference Centre (CTICC) 22 Oct Wednesday 0730 REGISTRATION 0830 OPENING 0900 PLENARY
1 page Overview 21 Oct Tuesday 1500 on REGISTRATION 1800 Welcome Reception & Cocktails at the Cape Town International Conference Centre (CTICC) 22 Oct Wednesday 0730 REGISTRATION 0830 OPENING 0900 PLENARY
Table of Contents. Data Supplement 1: Summary of ASTRO Guideline Statements. Data Supplement 2: Definition of Terms
 Definitive and Adjuvant Radiotherapy in Locally Advanced Non-Small-Cell Lung Cancer: American Society of Clinical Oncology Clinical Practice Guideline Endorsement of the American Society for Radiation
Definitive and Adjuvant Radiotherapy in Locally Advanced Non-Small-Cell Lung Cancer: American Society of Clinical Oncology Clinical Practice Guideline Endorsement of the American Society for Radiation
Lung cancer forms in tissues of the lung, usually in the cells lining air passages.
 Scan for mobile link. Lung Cancer Lung cancer usually forms in the tissue cells lining the air passages within the lungs. The two main types are small-cell lung cancer (usually found in cigarette smokers)
Scan for mobile link. Lung Cancer Lung cancer usually forms in the tissue cells lining the air passages within the lungs. The two main types are small-cell lung cancer (usually found in cigarette smokers)
Is pleurectomy and decortication superior to palliative care in the treatment of malignant pleural mesothelioma?
 doi:10.1510/icvts.2010.256271 Interactive CardioVascular and Thoracic Surgery 12 (2011) 812 817 www.icvts.org Best evidence topic - Thoracic oncologic Is pleurectomy and decortication superior to palliative
doi:10.1510/icvts.2010.256271 Interactive CardioVascular and Thoracic Surgery 12 (2011) 812 817 www.icvts.org Best evidence topic - Thoracic oncologic Is pleurectomy and decortication superior to palliative
Cancer is the leading cause of death for Canadians aged 35 to 64 and is also the leading cause of critical illness claims in Canada.
 Underwriting cancer In this issue of the Decision, we provide an overview of Canadian cancer statistics and the information we use to make an underwriting decision. The next few issues will deal with specific
Underwriting cancer In this issue of the Decision, we provide an overview of Canadian cancer statistics and the information we use to make an underwriting decision. The next few issues will deal with specific
Management of Postmenopausal Women with T1 ER+ Tumors: Options and Tradeoffs. Case Study. Surgery. Lumpectomy and Radiation
 Management of Postmenopausal Women with T1 ER+ Tumors: Options and Tradeoffs Michael Alvarado, MD Associate Professor of Surgery University of California San Francisco Case Study 59 yo woman with new palpable
Management of Postmenopausal Women with T1 ER+ Tumors: Options and Tradeoffs Michael Alvarado, MD Associate Professor of Surgery University of California San Francisco Case Study 59 yo woman with new palpable
Male. Female. Death rates from lung cancer in USA
 Male Female Death rates from lung cancer in USA Smoking represents an interesting combination of an entrenched industry and a clearly drug-induced cancer Tobacco Use in the US, 1900-2000 5000 100 Per Capita
Male Female Death rates from lung cancer in USA Smoking represents an interesting combination of an entrenched industry and a clearly drug-induced cancer Tobacco Use in the US, 1900-2000 5000 100 Per Capita
Radiation Therapy in the Treatment of
 Lung Cancer Radiation Therapy in the Treatment of Lung Cancer JMAJ 46(12): 537 541, 2003 Kazushige HAYAKAWA Professor and Chairman, Department of Radiology, Kitasato University School of Medicine Abstract:
Lung Cancer Radiation Therapy in the Treatment of Lung Cancer JMAJ 46(12): 537 541, 2003 Kazushige HAYAKAWA Professor and Chairman, Department of Radiology, Kitasato University School of Medicine Abstract:
How To Understand How Cancer Works
 Mesothelioma Understanding your diagnosis Mesothelioma Understanding your diagnosis When you first hear that you have cancer, you may feel alone and afraid. You may be overwhelmed by the large amount of
Mesothelioma Understanding your diagnosis Mesothelioma Understanding your diagnosis When you first hear that you have cancer, you may feel alone and afraid. You may be overwhelmed by the large amount of
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: microwave_tumor_ablation 12/2011 11/2015 11/2016 11/2015 Description of Procedure or Service Microwave ablation
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: microwave_tumor_ablation 12/2011 11/2015 11/2016 11/2015 Description of Procedure or Service Microwave ablation
Exploring the Role of Vitamins in Achieving a Healthy Heart
 Exploring the Role of Vitamins in Achieving a Healthy Heart There are many avenues you can take to keep your heart healthy. The first step you should take is to have a medical professional evaluate the
Exploring the Role of Vitamins in Achieving a Healthy Heart There are many avenues you can take to keep your heart healthy. The first step you should take is to have a medical professional evaluate the
Diseases. Inflammations Non-inflammatory pleural effusions Pneumothorax Tumours
 Pleura Visceral pleura covers lungs and extends into fissures Parietal pleura limits mediastinum and covers dome of diaphragm and inner aspect of chest wall. Two layers between them (pleural cavity) contains
Pleura Visceral pleura covers lungs and extends into fissures Parietal pleura limits mediastinum and covers dome of diaphragm and inner aspect of chest wall. Two layers between them (pleural cavity) contains
Asbestos and your lungs
 This information describes what asbestos is and the lung conditions that are caused by exposure to it. It also includes information about what to do if you have been exposed to asbestos, and the benefits
This information describes what asbestos is and the lung conditions that are caused by exposure to it. It also includes information about what to do if you have been exposed to asbestos, and the benefits
H. Richard Alexander, Jr., M.D. Department of Surgery and The Greenebaum Cancer Center University of Maryland School of Medicine Baltimore, Md
 Major Advances in Cancer Prevention, Diagnosis and Treatment~ Why Mesothelioma Leads the Way H. Richard Alexander, Jr., M.D. Department of Surgery and The Greenebaum Cancer Center University of Maryland
Major Advances in Cancer Prevention, Diagnosis and Treatment~ Why Mesothelioma Leads the Way H. Richard Alexander, Jr., M.D. Department of Surgery and The Greenebaum Cancer Center University of Maryland
