Evaluation of the North Carolina Stroke Care Program
|
|
|
- Claire Barber
- 8 years ago
- Views:
Transcription
1 382 Evaluation of the North Carolina Stroke Care Program MARK B. DIGNAN, PH.D., M.P.H.,* GEORGE HOWARD, M.S.P.H.,t JAMES F. TOOLE, M.D.,t CAROLINE BECKER, M.D.,t AND KENNETH R. MCLEROY, PH.D. SUMMARY A study of 774 patients in eastern North Carolina was undertaken to determine the effects of a coordinated program of care and follow-up on recovery from stroke. The program was designed to coordinate and improve in-hospital stroke care and rehabilitation, to provide for education and training of the family for post-hospital care, and to coordinate and facilitate continued access to services after discharge. As measured by the Barthel Index at discharge, three, six and 12, the impact of the program was found to be minimal. Patients' scores throughout follow-up were influenced by age, whether the stroke event was new or recurrent, and the state of consciousness at admission. Follow-up Barthel scores were also related to scores obtained at discharge. Stroke Vol 17, No 3, 1986 THIS PAPER REPORTS RESULTS from the evaluation of a program designed to improve recovery following stroke, a major cause of disability among adults in the United States.' In spite of an overall reduction in mortality from stroke, there is no evidence of a decline in the prevalence of this condition. 2 Since this condition primarily affects the elderly, the increasing average age of Americans foreshadows an increasing problem. The value of stroke rehabilitation has been accepted for some time. 3 However, the mode of delivery of rehabilitative services, whether through specialized stroke units or integration with 'regular' medical units, as well as the range and intensity of services have been subjects of continued debate. 4 " 6 Most reports of stroke rehabilitation have dealt with specific hospital populations. 7-8 Community settings rarely have been studied, and we found no reports of American efforts to provide coordinated stroke care and rehabilitation using a network of community hospitals and home health agencies. 9 In North Carolina, 15 contiguous, primarily rural counties in the eastern part of the state were selected for study. These counties are part of the "stroke belt"; an area of documented excess stroke incidence. l0 This report concerns evaluation of the effects of a program designed to coordinate stroke diagnostic and rehabilitative services on post-stroke function as measured by the Barthel Index. The Stroke Care Program The program was a community-based effort designed to improve in-hospital care of stroke patients as well as to coordinate provision of post-hospitalization From the Departments of Family and Community Medicine,* and Neurology,t Bowman Gray School of Medicine,* Department of Epidemiology, School of Public Health,t University of North Carolina, Chapel Hill, and the Division of Public Health, Education, University of North Carolina, Greensboro. This work was supported by contract number NO1-NS2386 from the North Carolina Heart Association. Address correspondence to: Dr. Mark B. Dignan, Assistant Professor, Department of Family and Community Medicine, Bowman Gray School of Medicine, Winston-Salem, North Carolina Received June 21, 1985; revision 2 accepted March 27, services. To reach the primary goal of the project, the participating hospitals agreed to a uniform system for the provision of coordinated care to stroke patients. Stroke team members from the hospital staffs, as well as nurses performing data collection, were given special training provided by the staff of the Stroke Care Program. The second goal of the project was met through coordination of follow-up care. To accomplish this, agreements were established with home health agencies serving the target population. Formal presentations to home health agency administration and staff, as well as identification and training of key personnel to facilitate follow-up, were carried out. Follow-up personnel were employed and kept administratively independent of the home health agency. Physicians' orders were developed to direct effective, coordinated care in each phase. During the acute illness, in addition to basic medical care, status of neurological function was assessed and physical therapy was begun for passive range of motion. The nursing staff was instructed to evaluate the family's understanding of stroke, provide emotional support, and begin basic education about the stroke. After the acute phase, physical therapists began active exercises and evaluated sitting and standing balance. Social worker evaluation and speech therapy were begun. Nursing staff began teaching the family about skin care, positioning, how to move the patient and other aspects of care of the stroke victim. At this point, assessment of Activities of Daily Living (ADL), using the Barthel Index was done. In the convalescent phase, medical rehabilitation was intensified. Physical therapists trained patients to use the walker, cane, and wheelchair as needed. Family teaching continued regarding skin care, positioning, bowel and bladder training and other necessary techniques. ADL evaluation was completed and the home health nurse, who was to coordinate post-hospitalization care, evaluated the home setting. During rehabilitation, the physical therapist taught transfer techniques to the patient and family, and the nursing staff involved the family with basic care, gradually transferring responsibility from the nursing staff to the family. Final evaluations and modifications were carried out by the speech therapist, social worker and home health nurse; referrals were
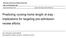
2 NORTH CAROLINA STROKE CARE PROGRAM/Dignan et al 383 made to necessary home health agencies. ADL evaluation was reassessed by project staff at three, six and 12 after discharge. Methods The entry period was January 1979 through January Nineteen hospitals in Eastern North Carolina were included. Identification of strokes, interviews with patients, follow-up diagnoses, and completion of stroke forms were carried out by trained registered nurses. Neurologists validated all stroke diagnoses. For the intervention, the participating hospitals were divided into three groups, A, B and C. During the first six, the community stroke program was established in the A hospitals, while the B and C hospitals served as controls. During the next six both A and B hospitals were provided the community stroke program while the C hospitals served as controls. During the subsequent six, all hospitals were providing the community stroke program. A patient was considered as being "on" the program if the hospital to which he was admitted was providing the community stroke program at the time of his admission. These admissions were to the 19 hospitals in the survey area. Data were provided by the patient, or the family if the patient was unable to communicate. Data collected on hospitalized stroke admissions included: (1) standard demographic measures (age, race, sex, marital status, employment status, and education); (2) diagnostic and disease-related information including type of stroke, the presence or absence of specific risk factors and comorbid diseases, consciousness level at admission and discharge from hospital, length of hospital stay, type of diagnostic procedure administered; and (3) a measure of functional status using the Barthel Index at discharge from the hospital and at three, six and 12 post-discharge."' 12 The Barthel Index is a widely used ADL evaluation instrument that has been used to assess the impact of stroke. It can also be used to assess the relative effectiveness of different ways of treating stroke victims. We evaluated the impact of the Community Stroke Care Program on independence in ADL as measured by the Barthel Index, after controlling for age, race, sex, first versus recurrent stroke and admission consciousness level. We evaluated the impact of the program on continuing improvement, as measured by the Barthel Index at three, six, and 12 month follow-ups, after controlling for the above factors as well as the Barthel Index score at discharge. The impact of the individual factors on the Barthel Index scores at each time period (discharge, three, six, and 12 ) was determined using linear regression. Forward stepwise regression was used. Any missing data eliminated a patient from the analysis, but to obtain the best possible estimates, and use as much patient data as possible, separate analyses were rerun after the regression equations had been developed. These analyses included all patients with complete data for the variables included in the regression equations. Results Data were collected on a total of 774 admissions to the 19 study hospitals with a diagnosis of stroke. Of the 744 admissions, 482 (62%) were white and 364 (47%) were male. A total of 614 (79%) were admitted for a first stroke. Table 1 presents descriptive data on the patients at discharge, divided into program and control groups. As shown in table 1, at discharge, the program and control patients were alike in all ways except admission consciousness. There were approximately twice as many patients admitted in a comatose state to the program hospitals as to the controls. Thus, because the general prognosis for recovery from stroke is strongly related to consciousness, the program and control groups were not equivalent at the outset of the evaluation and the program group was therefore at some disadvantage. Effectiveness of the Stroke Care Program was measured by the Barthel Index scores. Figure 1 depicts the Barthel Index scores, over the course of the study, including measurements at discharge, three, six and 12. As seen in figure 1, the Barthel Index scores, for the program and control groups, showed the controls having better scores, on average, at discharge. This difference disappeared by the three month evaluation, reappeared at a lower magnitude at the six month evaluation, and became even smaller at the twelve month follow-up. Stepwise linear regression was used to estimate the impact of the Stroke Care Program on the patients' recovery, as measured by the Barthel Index. This choice of analytic procedure allowed us to control for difference between the groups while testing for program effect. Like analysis of covariance, this procedure allows for "adjustment" for the documented significant difference in consciousness levels between the control and program groups, as well as for nonsignificant differences that may influence the comparison of TABLE 1 Stroke Care Program Patients and Controls at Discharge Group Measure Program Control p value Age Mean Median Percent white Percent male Admission consciousness Percent alert Percent stuperous Percent comatose Percent first stroke Percent hypertensive Percent cardiac disease Percent diabetic Notes: p values for differences in means were via the t test, for difference in median were via the median test, and between proportions were via the chi-square test.
3 384 STROKE VOL 17, No 3, MAY-JUNE Discharge 3 Months 6 Months Group Control Program FIGURE 1. The Barthel Index scores, including measurements at discharge, three, six and twelve, for program and control patients. program versus control. The significance of the factors predicting statistically significant regression (p <.05) are shown in table 2. If a factor was found to be statistically significant (p <.05) in the stepwise procedure, the significance level in the reduced model is provided. The factors that did not contribute to regression are also indicated. At discharge, the Barthel Index score was found to be significantly affected by age (p < ), sex (p =.013), admission consciousness level (p < ), and whether the stroke was a first or recurrent event (p =.0002). The fact that admission consciousness contributes to regression verifies our aim to control for its effects on program results. With each yearly increase in age, the average discharge Barthel Index score was found to be about one-half point lower. This one-half point difference is estimated after "control" for other significant factors in the final model; adjustment for sex, admission consciousness level, and whether the event was afirstversus recurrent event. Females were found to have an average discharge Barthel Index score 5.3 points lower than males. Patients with recurrent strokes had scores that averaged about 10 points lower than those with first strokes. The admission consciousness level had a major impact on the discharge Barthel Index score, with disoriented patients having scores averaging 18 points below their alert counterparts and lethargic or comatose patients having scores which averaged 15 points lower. The scores of the disoriented, lethargic or comatose patients were significantly lower than those of the alert patients. After controlling for age, sex, admission consciousness, and the first vs. recurrent stroke episode, the Barthel Index scores, as measured at discharge, were not affected by the community stroke program (p =.9833). At three the Barthel Index score was found to be affected only by the age of the patient (p < ) and the Barthel Index score (p < ) obtained at discharge. The impact of admission consciousness disappeared. With each yearly increase in age, the three month score was lowered, on average, by 0.4. Also, with each decrease in the Barthel score at discharge, the three month Barthel score was 0.7 lower. After controlling for age and the discharge Barthel Index score, the three month Barthel Index score was not affected by the community stroke program (p =.07). At six, the Barthel Index score was affected by age (p = ), race (p =.012), whether the stroke was afirstor a repeat event (p =.017), admission consciousness (p =.035), and the discharge Barthel Index score (p = ). For each yearly increase in age, the six month Barthel Index score decreased by approximately one-half point. Nonwhite patients had six month scores which averaged 6.2 points higher than whites and victims ofrepeatstrokes had six month scores averaging 7.6 points below first stroke victims. Patients who were disoriented at admission had average scores that were 7.7 points below the alert patients (p =.01); however, patients who were stuporous or comatose had scores which, while 3.1 points higher than the alert patients, were not found to be statistically different. Discharge Barthel scores continued to exert a significant impact on Barthel Index scores at follow-up periods, where for each point of decrease in the discharge score the six month score averaged one-half point lower. At 12, the Barthel Index score was affected by only first vs. recurrent stroke episode (p = ), and the discharge Barthel Index score (p = ). Twelve month Barthel Index scores decreased an average of.46 for each year increase in age. Patients experiencing arecurrentstroke averaged 14.6 points lower on their 12 month Barthel Index score. The discharge Barthel Index scores were again related to the followup scores, where the 12 month score was.54 points TABLE 2 Probability ValuesfromStepwise Linear Regression of Selected Factors on Barthel Scale Scores at Discharge, Three, Six and 12 Months Follow-up period Age Sex Factor First vs recurrent stroke episode Consciousness Program vs control Race Diabetes Hypertension Cardiac disease Previous TIA Discharge Barthel Scale score Discharge * *A11 underlined values are those that were judged to significantly contribute to the "best" model predicting ADL.
4 NORTH CAROLINA STROKE CARE PROGRAMJDignan et al 385 lower for each point decrease in the discharge scores. After controlling for the above factors, program participation still did not affect Barthel scores (p =.8). As a further test for program impact, the data were also analyzed after eliminating those subjects with the worst prognosis. Those admitted in stuporous or comatose states of consciousness and those with a recurrent stroke were eliminated from this analysis. The results of this analysis still showed no program effect. Discussion The primary goal of this study was to assess the impact of a program intended to coordinate care of stroke patients, hospital and home-health, as well as educate the family about stroke care. Because the groups differed in admission consciousness, with more of the program patients unconscious, the prospect for the program showing any difference was diminished at the outset. The fact that the program patients, on average, did not fare significantly worse than the controls is a possible argument for the Stroke Care Program's effectiveness. However, the statistical approach undertaken in this report provided an "adjustment" for this difference in admission consciousness, and after controlling for factors found to affect the outcome of stroke patients, the impact of the community stroke program (as measured by Barthel Index scores), was negligible at discharge and did not change through 12 of follow-up. That is, with other factors affecting recovery held constant, there were no differences in the Barthel Index scores of patients who had the benefit of the program from those who were denied the program. The factors related to the ADL status varied with the time period. Patient age seemed to influence the Barthel Index score at discharge and at all three followup periods with older patients generally having poorer scores. At each of the four follow-up periods, with other factors held constant, the Barthel Index score decreased approximately one-half point with each year increase in age. The second factor influencing Barthel Index scores at the follow-up periods was the discharge Barthel Index score. For each point change in the discharge score, the scores at three, six, and 12 also changed approximately one-half to three-fourths of a point. Not surprisingly, patients with high discharge Barthel Index scores also tended to have high Barthel Index scores at the follow-up assessments. However, the differences in patients' Barthel Index scores (all other factors held constant) tended to decrease through the follow-up time periods. Third, whether the stroke was the first or a recurrent episode made a difference in the Barthel Index scores at discharge, six, and 12 and had a marginally significant effect on the three month score. At discharge, the Barthel scores of those patients with repeat strokes averaged 9 points lower than their first stroke counterparts; at three, the difference averaged 5 points, 7 points at six, and 14 points at 12. We speculate that this pattern in which differences at discharge decreased at three, and then increased at six and 12, was due to worsening in the status of patients suffering a repeat stroke compared to those suffering an initial stroke. In addition to age, discharge Barthel Index scores andrecurrentversus first strokes, several other factors played significant roles during selected time periods. Admission consciousness strongly affected discharge Barthel Index scores, with alert patients having scores averaging over 15 points higher than patients with some disturbance in consciousness level. Because the effect of admission consciousness would be contained in the Barthel Index score at discharge, after controlling for the discharge scores, we would not expect admission consciousness to be reflected at the three, six or 12 month follow-up assessments. While admission consciousness did not affect the three or 12 month Barthel Index score, it was found to have a significant impact on the six month score. The six month Barthel Index scores of those patients disoriented at admission were significantly below those who were alert. However, there was no difference between the alert and stuporous or comatose patients. This apparent inconsistency could be due to differential mortality, removing the worst patients from the stuporous or comatose group, leaving patients who had a reasonable chance of recovery, despite their consciousness level. Sex affected only the discharge Barthel Index score, with females averaging approximately 5 points lower than males. Race had an effect only on the six month score, in that nonwhite patients had scores averaging six points higher than their white counterparts (0.1 < p < 0.05). History of risk factors had no effect on Barthel Index scores at any of the four follow-up periods. This would suggest that once an individual has developed a stroke, risk factors are not related to the recovery of the patient as measured by the Barthel Index. It has been well accepted that rehabilitation following stroke is essential and should begin as soon as possible. 13 " 17 Numerous reports have shown positive correlations between early introduction of rehabilitation efforts and better recovery. What has remained unresolved is whether the recovery was due to the efforts or timing of rehabilitation, spontaneous recovery, or early rehabilitation interacting with characteristics of the patient and his/her disease to produce a superior outcome. 18 " 20 Our program sought to provide high quality care to stroke patients through enhanced professional communication; professional and family education; planning of stroke care in 19 community hospitals; and coordinated, informed and well-trained post-hospitalization care andrehabilitation.by working closely together in an organized manner, it was planned that the stroke teams would be able to overcome any barriers that might exist between hospital medical care and long term rehabilitation. This approach would insure continuous, high quality rehabilitative services whether from long term care facilities, home health nurses, the family, or some combination of the three. 21 " 23 This
5 386 STROKE VOL 17, No 3, MAY-JUNE 1986 approach was used to seek answers to two primary questions: (1) Was the organized approach that included professional organization and family education any better than the standard community level care in helping stroke victims to recover to their maximum potential? and (2) which patients would or would not become functionally independent if they were served by a coordinated stroke team? The impact of the community stroke program was found to be minimal as assessed at discharge, three, six and 12. The Barthel Index scores varied specifically with the age of the patients at every assessment; older patients had lower scores. In addition, patients experiencing recurrences of stroke fared worse than those with initial strokes and this difference increased through the 12 month follow-up period. Those patients admitted in a stuporous or comatose state of consciousness also did more poorly than those admitted alert or lethargic. If we assume that spontaneous recovery was a major factor influencing the outcome of the study, we would not expect to find any difference in the Barthel Index scores between the program and control patients. Our results supported this postulate and, given the effects of age, discharge Barthel scores and consciousness, showed no significant difference between the program and control groups through the 12 month follow-up. Thus spontaneous recovery, which is assumed to have equal impact on program and control hospitals and their patients, is a plausible explanation for the lack of significant difference between the two groups of patients. In conclusion, although the Community Stroke Care Program included extensive education of the patient and family about rehabilitation and physical therapy in addition to coordination of all medical services, the benefit to patients in terms of recovery was minimal. The Barthel Index scores were clearly influenced by the age of the patients and, at follow-up, by the score that was obtained at discharge. In addition, patients suffering from repeat episodes of stroke fared worse than their first stroke counterparts, with the difference apparently increasing through the course of the followup period. These findings make it apparent that the use of a coordinated stroke team provided no special advantage for patients' recovery as measured by the Barthel Index. Though not measured, the effects of the educational efforts and close cooperation among stroke care team members on the patient and the family can be assumed to have been positive in terms of perceptions of quality of care. This study, like most others, limited the measurement of progress to Activities of Daily Living and did not focus on other measures of the program's activities such as family education, sensitivity to stroke patient's needs, attitude towards rehabilitation, and other psychosocial variables related to the quality of life. Further research is needed to explore these dimensions of the care of stroke patients and other patients with similar long-term rehabilitative needs. References 1. USDHHS: Advance report of final mortality statistics, Vital Statistics Report. NCHS Monthly. 33(9 Suppl). Dec. 20, DHHSPubNo. (PHS) Gairaway WM, Whisant JP, Dniry 1: The changing pattern of survival following stroke. Stroke 14: , Garraway M: Stroke rehabilitation units: concepts, evaluation, and unresolved issues. Stroke 16(2): , Johnston MV, Keister M: Early rehabilitation for stroke patients: a new look. Arch Phys Med Rehabil 65: , Herman JM, Culpepper L, Franks P: Patterns of utilization, disposition, and length of stay among stroke patients in a community hospital setting. JI Am Geriatr Soc 31(6): , Johnston MV, Keith RA: Cost-benefits of medical rehabilitation: review and critique. Arch Phys Med Rehabil 64: , Lind K: A synthesis of studies on stroke rehabilitation. J Chron Dis 35: , Sivenius J, Pyorala K, Heinonen OP, Salonen JT, Reikkinen P: The significance of intensity of rehabilitation of stroke A controlled trial. Stroke 13: , Waylonis GW, Keith MW, Aseff JN: Stroke rehabilitation in a midwestem county. Arch Phys Med Rehabil 54: , Howard G, Till JS, Toole JF, Matthews C, Truscott BL: Factors influencing return to work following cerebral infarction. JAMA 253(2): , Mahoney FL, Barthel DW: Rehabilitation of hemiplegic patient: clinical evaluation. Arch Phys Med Rehabil 35: , Granger CV, Dewis LS, Peters NC, Sherwood CC, Barrett JE: Stroke rehabilitation: analysis of repeated Barthel Index measures. Arch Phys Med Rehabil 60: 14-17, Granger CV, Greer DS, Liset E, Coulombe J, O'Brien E: Measurement of outcomes of care for stroke patients. Stroke 6: 34-41, Dinken H: Evaluation of disability and treatment in hemiplegia. Arch Phys Med Rehabil 28: , Wylie CM: Value of early rehabilitation in stroke. Geriatrics 25: , Feigenson JS: Stroke rehabilitation: effectiveness, benefits and cost: some practical considerations. Stroke 10: 1-4, Truscott BL, Kretschmann CM, Toole JF, PajakTF: Early rehabilitative care in community hospitals: effective on quality of survivorship following stroke. Stroke 5: , Feigenson JS, McCarthy ML, Meese PD, Feigenson WD, Greenberg SD, Rubin E, McDowell FH: Stroke rehabilitation: factors predicting outcome and length of stay an overview. NY State J Med 77: , Johnston MV, Keister M: Cost-benefits of medical rehabilitation: review and critique. Arch Phys Med Rehabil 564: , Isaacs B, Marks R: Determinants of outcome of stroke rehabilitation. Age and Ageing 2: , Feigenson JS, Gitlow HS, Greenbert SD: The disability oriented rehabilitation unit a major factor influencing stroke outcome. Stroke 10: 5-8, Bryant NH, Cantland L, Loewenstein R: Comparison of care and cost outcomes for stroke patients with and without home care. Stroke 5: 54-59, Strand T, AsplundK, Eriksson S, Hagg E, Lithner F, WesterPO: A non-intensive stroke unit reduces functional disability and the need for long-term hospitalization. Stroke 16(1): 29-34, 1985
Efficiency, Effectiveness, and Duration of Stroke Rehabilitation
 241 Efficiency, Effectiveness, and Duration of Stroke Rehabilitation Surya Shah, MEd OTR/L, Frank Vanclay, MSocSci, and Betty Cooper, BAppSc This prospective multicenter study identifies the variables
241 Efficiency, Effectiveness, and Duration of Stroke Rehabilitation Surya Shah, MEd OTR/L, Frank Vanclay, MSocSci, and Betty Cooper, BAppSc This prospective multicenter study identifies the variables
Functional outcomes and rehabilitation: An acute care field study
 W. Department of Veterans Affairs Journal of Rehabilitation Research and Development Vol. 26 No. 3 Pages 17 26 Functional outcomes and rehabilitation: An acute care field study Patricia Ostrow, MA, OTR
W. Department of Veterans Affairs Journal of Rehabilitation Research and Development Vol. 26 No. 3 Pages 17 26 Functional outcomes and rehabilitation: An acute care field study Patricia Ostrow, MA, OTR
Factors Influencing Outcome and Length of Stay in a Stroke Rehabilitation Unit
 Factors Influencing Outcome and Length Stay in a Stroke Rehabilitation Unit 657 Part 2. Comparison 318 Screened and 248 Unscreened Patients JOEL S. FEIGENSON, M.D., MARY LOU MCCARTHY, R.N., SUSAN D. GREENBERG,
Factors Influencing Outcome and Length Stay in a Stroke Rehabilitation Unit 657 Part 2. Comparison 318 Screened and 248 Unscreened Patients JOEL S. FEIGENSON, M.D., MARY LOU MCCARTHY, R.N., SUSAN D. GREENBERG,
ESTABLISHMENT OF COMMUNITY STROKE PROGRAMS. DEVELOPMENT OF THE NORTH CAROLINA COMPREHENSIVE STROKE PROGRAM
 Establishment of community stroke programs depend on the solution of many interrelated problems. The development of such programs in North Carolina is explored, and the factors involved are examined. Improved
Establishment of community stroke programs depend on the solution of many interrelated problems. The development of such programs in North Carolina is explored, and the factors involved are examined. Improved
Comparison of Care and Cost Outcomes for Stroke Patients With and Without Home Care
 Comparison of Care and Cost Outcomes for Stroke Patients With and Without Home Care BY NANCY H. BRYANT, R.N., B.S.,* LOUISE CANDLAND, R.N., M.A.,t AND REGINA LOEWENSTEIN, A.M Abstract: Comparison of Care
Comparison of Care and Cost Outcomes for Stroke Patients With and Without Home Care BY NANCY H. BRYANT, R.N., B.S.,* LOUISE CANDLAND, R.N., M.A.,t AND REGINA LOEWENSTEIN, A.M Abstract: Comparison of Care
Malnutrition and outcome after acute stroke: using the Malnutrition Universal Screening Tool
 Malnutrition and outcome after acute stroke: using the Malnutrition Universal Screening Tool L Choy, A Bhalla Department of Elderly Care St Helier Hospital, Carshalton, Surrey Prevalence of malnutrition
Malnutrition and outcome after acute stroke: using the Malnutrition Universal Screening Tool L Choy, A Bhalla Department of Elderly Care St Helier Hospital, Carshalton, Surrey Prevalence of malnutrition
ISSUED BY: TITLE: ISSUED BY: TITLE: President
 CLINICAL PRACTICE GUIDELINE PROFESSIONAL PRACTICE TITLE: Stroke Care Rehabilitation Unit DATE OF ISSUE: 2005, 05 PAGE 1 OF 7 NUMBER: CPG 20-3 SUPERCEDES: New ISSUED BY: TITLE: Chief of Medical Staff ISSUED
CLINICAL PRACTICE GUIDELINE PROFESSIONAL PRACTICE TITLE: Stroke Care Rehabilitation Unit DATE OF ISSUE: 2005, 05 PAGE 1 OF 7 NUMBER: CPG 20-3 SUPERCEDES: New ISSUED BY: TITLE: Chief of Medical Staff ISSUED
Chapter 3: Review of Literature Stroke
 Chapter 3: Review of Literature Stroke INTRODUCTION Cerebrovascular accident (also known as stroke) is a serious health problem in the United States and a leading cause of long-term disability. In this
Chapter 3: Review of Literature Stroke INTRODUCTION Cerebrovascular accident (also known as stroke) is a serious health problem in the United States and a leading cause of long-term disability. In this
The TeleHealth Model
 The Model CareCycle Solutions The Solution Calendar Year 2011 Company Overview CareCycle Solutions (CCS) specializes in managing the needs of chronically ill patients through the use of Interventional
The Model CareCycle Solutions The Solution Calendar Year 2011 Company Overview CareCycle Solutions (CCS) specializes in managing the needs of chronically ill patients through the use of Interventional
DEPRESSION CARE PROCESS STEP EXPECTATIONS RATIONALE
 1 DEPRESSION CARE PROCESS STEP EXPECTATIONS RATIONALE ASSESSMENT/PROBLEM RECOGNITION 1. Did the staff and physician seek and document risk factors for depression and any history of depression? 2. Did staff
1 DEPRESSION CARE PROCESS STEP EXPECTATIONS RATIONALE ASSESSMENT/PROBLEM RECOGNITION 1. Did the staff and physician seek and document risk factors for depression and any history of depression? 2. Did staff
Audit on treatment and recovery of ankle sprain
 Hong Kong Journal of Emergency Medicine Audit on treatment and recovery of ankle sprain WY Lee Study Objectives: The object of this study is to audit the care of ankle sprain of different severity and
Hong Kong Journal of Emergency Medicine Audit on treatment and recovery of ankle sprain WY Lee Study Objectives: The object of this study is to audit the care of ankle sprain of different severity and
Nebraska Health Data Reporter
 Nebraska Health Data Reporter Volume 3, Number 1 May 2000 Demographic, health, and functional status characteristics of new residents to Nebraska nursing homes: A summary Joan Penrod, Ph.D. Jami Fletcher,
Nebraska Health Data Reporter Volume 3, Number 1 May 2000 Demographic, health, and functional status characteristics of new residents to Nebraska nursing homes: A summary Joan Penrod, Ph.D. Jami Fletcher,
Timing it Right to Support Families as they Transition
 Timing it Right to Support Families as they Transition Jill Cameron, PhD Canadian Institutes of Health Research New Investigator Assistant Professor Adjunct Scientist, Toronto Rehabilitation Institute
Timing it Right to Support Families as they Transition Jill Cameron, PhD Canadian Institutes of Health Research New Investigator Assistant Professor Adjunct Scientist, Toronto Rehabilitation Institute
Marina Richardson, M.Sc. Deb Willems, BSc.PT David Ure, OT Robert Teasell, MD FRCPC
 Assessing the Impact of Southwestern Ontario s Community Stroke Rehabilitation Teams: An Economic Analysis Presenters: Laura Allen, M.Sc. (cand.) Matthew Meyer, Ph.D (cand.) Marina Richardson, M.Sc. Deb
Assessing the Impact of Southwestern Ontario s Community Stroke Rehabilitation Teams: An Economic Analysis Presenters: Laura Allen, M.Sc. (cand.) Matthew Meyer, Ph.D (cand.) Marina Richardson, M.Sc. Deb
Hamilton Health Sciences Integrated Stroke Model of Care. Rhonda Whiteman, Stroke Best Practices Coordinator, Hamilton Health Sciences
 Hamilton Health Sciences Integrated Stroke Model of Care Rhonda Whiteman, Stroke Best Practices Coordinator, Hamilton Health Sciences Integrated Stroke Model of Care Goals To provide a more comprehensive
Hamilton Health Sciences Integrated Stroke Model of Care Rhonda Whiteman, Stroke Best Practices Coordinator, Hamilton Health Sciences Integrated Stroke Model of Care Goals To provide a more comprehensive
HealthCare Partners of Nevada. Heart Failure
 HealthCare Partners of Nevada Heart Failure Disease Management Program 2010 HF DISEASE MANAGEMENT PROGRAM The HealthCare Partners of Nevada (HCPNV) offers a Disease Management program for members with
HealthCare Partners of Nevada Heart Failure Disease Management Program 2010 HF DISEASE MANAGEMENT PROGRAM The HealthCare Partners of Nevada (HCPNV) offers a Disease Management program for members with
Functional recovery differs between ischemic and hemorrhagic stroke patients
 6 Functional recovery differs between ischemic and hemorrhagic stroke patients Vera Schepers, Marjolijn Ketelaar, Anne Visser-Meily, Vincent de Groot, Jos Twisk, Eline Lindeman Submitted Chapter 6 Abstract
6 Functional recovery differs between ischemic and hemorrhagic stroke patients Vera Schepers, Marjolijn Ketelaar, Anne Visser-Meily, Vincent de Groot, Jos Twisk, Eline Lindeman Submitted Chapter 6 Abstract
Handling the Handoff: Rural and Race-Based Disparities in Post-Hospitalization. Follow-up Care Among Medicare Beneficiaries with Diabetes.
 Handling the Handoff: Rural and Race-Based Disparities in Post-Hospitalization Follow-up Care Among Medicare Beneficiaries with Diabetes South Carolina Rural Health Research Center At the Heart of Health
Handling the Handoff: Rural and Race-Based Disparities in Post-Hospitalization Follow-up Care Among Medicare Beneficiaries with Diabetes South Carolina Rural Health Research Center At the Heart of Health
Using Objective Measures to Facilitate Rehabilitation Referral
 Using Objective Measures to Facilitate Rehabilitation Referral Mark Bayley MD, FRCPC Medical Director, Neuro Rehabilitation Program, Toronto Rehabilitation Institute Associate Professor, Division of Physiatry,
Using Objective Measures to Facilitate Rehabilitation Referral Mark Bayley MD, FRCPC Medical Director, Neuro Rehabilitation Program, Toronto Rehabilitation Institute Associate Professor, Division of Physiatry,
Predicting nursing home length of stay : implications for targeting pre-admission review efforts
 Scholarly Commons at Miami University http://sc.lib.miamioh.edu Scripps Gerontology Center Scripps Gerontology Center Publications Predicting nursing home length of stay : implications for targeting pre-admission
Scholarly Commons at Miami University http://sc.lib.miamioh.edu Scripps Gerontology Center Scripps Gerontology Center Publications Predicting nursing home length of stay : implications for targeting pre-admission
Summary chapter 2 chapter 2
 Summary Multiple Sclerosis (MS) is a chronic disease of the brain and the spinal cord. The cause of MS is unknown. MS usually starts in young adulthood. In the course of the disease progression of neurological
Summary Multiple Sclerosis (MS) is a chronic disease of the brain and the spinal cord. The cause of MS is unknown. MS usually starts in young adulthood. In the course of the disease progression of neurological
SAM KARAS ACUTE REHABILITATION CENTER
 SAM KARAS ACUTE REHABILITATION CENTER 1 MEDICAL CARE Sam Karas Acute Rehabilitation The Sam Karas Acute Rehabilitation Center is a comprehensive and interdisciplinary inpatient unit. Medical care is directed
SAM KARAS ACUTE REHABILITATION CENTER 1 MEDICAL CARE Sam Karas Acute Rehabilitation The Sam Karas Acute Rehabilitation Center is a comprehensive and interdisciplinary inpatient unit. Medical care is directed
Assessment of Patient Outcomes of Rehabilitative Care Provided in Inpatient Rehabilitation Facilities (IRFs) and After Discharge
 Assessment of Patient Outcomes of Rehabilitative Care Provided in Inpatient Rehabilitation Facilities (IRFs) and After Discharge PREPARED FOR: ARA Research Institute PRESENTED BY: Al Dobson, Ph.D. PREPARED
Assessment of Patient Outcomes of Rehabilitative Care Provided in Inpatient Rehabilitation Facilities (IRFs) and After Discharge PREPARED FOR: ARA Research Institute PRESENTED BY: Al Dobson, Ph.D. PREPARED
Attachment A Minnesota DHS Community Service/Community Services Development
 Attachment A Minnesota DHS Community Service/Community Services Development Applicant Organization: First Plan of Minnesota Project Title: Implementing a Functional Daily Living Skills Assessment to Predict
Attachment A Minnesota DHS Community Service/Community Services Development Applicant Organization: First Plan of Minnesota Project Title: Implementing a Functional Daily Living Skills Assessment to Predict
Stakeholder s Report. 2525 SW 75 th Ave Miami, Florida 33155 305.262.6800 www.westgablesrehabhospital.com
 212 Stakeholder s Report 2525 SW 75 th Ave Miami, Florida 33155 35.262.68 www.westgablesrehabhospital.com PROFILE REPORT For more than 25 years, West Gables Rehabilitation Hospital has made a mission of
212 Stakeholder s Report 2525 SW 75 th Ave Miami, Florida 33155 35.262.68 www.westgablesrehabhospital.com PROFILE REPORT For more than 25 years, West Gables Rehabilitation Hospital has made a mission of
SECTION B THE SERVICES COMMUNITY STROKE REHABILITATION SPECIFICATION 20XX/YY
 SECTION B THE SERVICES COMMUNITY STROKE REHABILITATION SPECIFICATION 20XX/YY SECTION B PART 1 - SERVICE SPECIFICATIONS Service specification number Service Commissioner Lead Provider Lead Period Date of
SECTION B THE SERVICES COMMUNITY STROKE REHABILITATION SPECIFICATION 20XX/YY SECTION B PART 1 - SERVICE SPECIFICATIONS Service specification number Service Commissioner Lead Provider Lead Period Date of
Progress Review Rehabilitation for Stroke: A Review
 363 Progress Review Rehabilitation for Stroke: A Review MARY L. DOMBOVY, M.D., BURTON A. SANDOK, M.D., AND JEFFREY R. BASFORD, M.D. SUMMARY Survivors of stroke are often left with severe mental and physical
363 Progress Review Rehabilitation for Stroke: A Review MARY L. DOMBOVY, M.D., BURTON A. SANDOK, M.D., AND JEFFREY R. BASFORD, M.D. SUMMARY Survivors of stroke are often left with severe mental and physical
Reducing Readmissions with Predictive Analytics
 Reducing Readmissions with Predictive Analytics Conway Regional Health System uses analytics and the LACE Index from Medisolv s RAPID business intelligence software to identify patients poised for early
Reducing Readmissions with Predictive Analytics Conway Regional Health System uses analytics and the LACE Index from Medisolv s RAPID business intelligence software to identify patients poised for early
HEALTH CHARACTERISTICS OF PATIENTS IN NURSING AND PERSONAL CARE HOMES
 168 HEALTH CHARACTERISTICS OF PATIENTS IN NURSING AND PERSONAL CARE HOMES E. Earl Bryant, National Center for Health Statistics Arne B. Nelson, National Center for Health Statistics Carl A. Taube, National
168 HEALTH CHARACTERISTICS OF PATIENTS IN NURSING AND PERSONAL CARE HOMES E. Earl Bryant, National Center for Health Statistics Arne B. Nelson, National Center for Health Statistics Carl A. Taube, National
Best Practice Recommendations for Inpatient Stroke Care: Rationale and Evidence for Integrated Stroke Units in North Simcoe Muskoka LHIN
 Best Practice Recommendations for Inpatient Stroke Care: Rationale and Evidence for Integrated Stroke Units in North Simcoe Muskoka LHIN Physician Education Session May 24, 2013 Dr. Mark Bayley,, Cheryl
Best Practice Recommendations for Inpatient Stroke Care: Rationale and Evidence for Integrated Stroke Units in North Simcoe Muskoka LHIN Physician Education Session May 24, 2013 Dr. Mark Bayley,, Cheryl
October 2013 Family Choice: Best Practices in Care for Nursing Home Residents
 SNP Alliance Best Practices October 2013 Family Choice: Best Practices in Care for Nursing Home Residents Overview of Family Choice of New York I-SNP Independent Health s Medicare Advantage Family Choice
SNP Alliance Best Practices October 2013 Family Choice: Best Practices in Care for Nursing Home Residents Overview of Family Choice of New York I-SNP Independent Health s Medicare Advantage Family Choice
Administration of Emergency Medicine
 doi:10.1016/j.jemermed.2005.07.008 The Journal of Emergency Medicine, Vol. 30, No. 4, pp. 455 460, 2006 Copyright 2006 Elsevier Inc. Printed in the USA. All rights reserved 0736-4679/06 $ see front matter
doi:10.1016/j.jemermed.2005.07.008 The Journal of Emergency Medicine, Vol. 30, No. 4, pp. 455 460, 2006 Copyright 2006 Elsevier Inc. Printed in the USA. All rights reserved 0736-4679/06 $ see front matter
Stroke Rehabilitation Triage Severe Strokes
 The London Stroke Rehab Data Base Project Robert Teasell MD FRCPC Professor and Chair-Chief Department of Phys Med Rehab London Ontario Retrospective Data Bases In stroke rehab limited funding for clinical
The London Stroke Rehab Data Base Project Robert Teasell MD FRCPC Professor and Chair-Chief Department of Phys Med Rehab London Ontario Retrospective Data Bases In stroke rehab limited funding for clinical
Seton Medical Center Hepatocellular Carcinoma Patterns of Care Study Rate of Treatment with Chemoembolization 2007 2012 N = 50
 General Data Seton Medical Center Hepatocellular Carcinoma Patterns of Care Study Rate of Treatment with Chemoembolization 2007 2012 N = 50 The vast majority of the patients in this study were diagnosed
General Data Seton Medical Center Hepatocellular Carcinoma Patterns of Care Study Rate of Treatment with Chemoembolization 2007 2012 N = 50 The vast majority of the patients in this study were diagnosed
Rehabilitation. Care
 Rehabilitation Care Bruyère Continuing Care is the champion of well-being for aging Canadians and those requiring Continuing Care, helping them to become and remain as healthy and independent as possible
Rehabilitation Care Bruyère Continuing Care is the champion of well-being for aging Canadians and those requiring Continuing Care, helping them to become and remain as healthy and independent as possible
Does referral from an emergency department to an. alcohol treatment center reduce subsequent. emergency room visits in patients with alcohol
 Does referral from an emergency department to an alcohol treatment center reduce subsequent emergency room visits in patients with alcohol intoxication? Robert Sapien, MD Department of Emergency Medicine
Does referral from an emergency department to an alcohol treatment center reduce subsequent emergency room visits in patients with alcohol intoxication? Robert Sapien, MD Department of Emergency Medicine
Where Should Rehabilitation Take Place?!
 Where Should Rehabilitation Take Place?! Three Basic Questions! 1. Is rehabilitation effective in improving a patient s functional abilities?!yes" yes" 2. Is rehabilitation cost effective?!yes" where"
Where Should Rehabilitation Take Place?! Three Basic Questions! 1. Is rehabilitation effective in improving a patient s functional abilities?!yes" yes" 2. Is rehabilitation cost effective?!yes" where"
The remarkable decline in stroke mortality in
 Comments, Opinions, and Reviews 1081 A Review of Stroke Rehabilitation and Physiotherapy Edzard Ernst, MD, PhD Most of the members of the therapeutic team in stroke rehabilitation take the effectiveness
Comments, Opinions, and Reviews 1081 A Review of Stroke Rehabilitation and Physiotherapy Edzard Ernst, MD, PhD Most of the members of the therapeutic team in stroke rehabilitation take the effectiveness
Bryant T. Aldridge Rehabilitation Center Unit Specific Inclusive Diversity Analysis: CULTURAL COMPETENCY AND DIVERSITY PLAN February 2015
 Bryant T. Aldridge Rehabilitation Center Unit Specific Inclusive Diversity Analysis: CULTURAL COMPETENCY AND DIVERSITY PLAN February 2015 Prepared by Brian Agan A Cultural Competency and Inclusive Diversity
Bryant T. Aldridge Rehabilitation Center Unit Specific Inclusive Diversity Analysis: CULTURAL COMPETENCY AND DIVERSITY PLAN February 2015 Prepared by Brian Agan A Cultural Competency and Inclusive Diversity
Stroke is a common cause of premature death and disability
 Does the Organization of Postacute Stroke Care Really Matter? Peter Langhorne, PhD, FRCP; Pamela Duncan, PhD, PT Background and Purpose Postacute rehabilitation stroke services represent a large component
Does the Organization of Postacute Stroke Care Really Matter? Peter Langhorne, PhD, FRCP; Pamela Duncan, PhD, PT Background and Purpose Postacute rehabilitation stroke services represent a large component
How can registries contribute to guidelines? Nicolas DANCHIN, HEGP, Paris
 How can registries contribute to guidelines? Nicolas DANCHIN, HEGP, Paris Pros and cons of registers Prospective randomised trials constitute the cornerstone of "evidence-based" medicine, and they therefore
How can registries contribute to guidelines? Nicolas DANCHIN, HEGP, Paris Pros and cons of registers Prospective randomised trials constitute the cornerstone of "evidence-based" medicine, and they therefore
STROKE PREVENTION AND TREATMENT MARK FISHER, MD PROFESSOR OF NEUROLOGY UC IRVINE
 STROKE PREVENTION AND TREATMENT MARK FISHER, MD PROFESSOR OF NEUROLOGY UC IRVINE CASE REPORT: ACUTE STROKE MANAGEMENT 90 YEAR OLD WOMAN, PREVIOUSLY ACTIVE AND INDEPENDENT, CHRONIC ATRIAL FIBRILLATION,
STROKE PREVENTION AND TREATMENT MARK FISHER, MD PROFESSOR OF NEUROLOGY UC IRVINE CASE REPORT: ACUTE STROKE MANAGEMENT 90 YEAR OLD WOMAN, PREVIOUSLY ACTIVE AND INDEPENDENT, CHRONIC ATRIAL FIBRILLATION,
CARE MANAGEMENT FOR LATE LIFE DEPRESSION IN URBAN CHINESE PRIMARY CARE CLINICS
 CARE MANAGEMENT FOR LATE LIFE DEPRESSION IN URBAN CHINESE PRIMARY CARE CLINICS Dept of Public Health Sciences February 6, 2015 Yeates Conwell, MD Dept of Psychiatry, University of Rochester Shulin Chen,
CARE MANAGEMENT FOR LATE LIFE DEPRESSION IN URBAN CHINESE PRIMARY CARE CLINICS Dept of Public Health Sciences February 6, 2015 Yeates Conwell, MD Dept of Psychiatry, University of Rochester Shulin Chen,
Outcome of in-patient Treatment for Severe Motor Conversion Disorder - does it work? A.S.David, R.McCormack and Lishman Unit MDT
 Outcome of in-patient Treatment for Severe Motor Conversion Disorder - does it work? A.S.David, R.McCormack and Lishman Unit MDT Evidence to date: inpatient rehab Inpatient multi-disciplinary intervention
Outcome of in-patient Treatment for Severe Motor Conversion Disorder - does it work? A.S.David, R.McCormack and Lishman Unit MDT Evidence to date: inpatient rehab Inpatient multi-disciplinary intervention
Jon S. Howell, LNHA President & CEO Georgia Health Care Association November 18, 2013
 Jon S. Howell, LNHA President & CEO Georgia Health Care Association November 18, 2013 GEORGIA HEALTH CARE ASSOCIATION Represents 336 skilled nursing facilities 13 SOURCE agencies 15 assisted living communities
Jon S. Howell, LNHA President & CEO Georgia Health Care Association November 18, 2013 GEORGIA HEALTH CARE ASSOCIATION Represents 336 skilled nursing facilities 13 SOURCE agencies 15 assisted living communities
Atrial Fibrillation 2014 How to Treat How to Anticoagulate. Allan Anderson, MD, FACC, FAHA Division of Cardiology
 Atrial Fibrillation 2014 How to Treat How to Anticoagulate Allan Anderson, MD, FACC, FAHA Division of Cardiology Projection for Prevalence of Atrial Fibrillation: 5.6 Million by 2050 Projected number of
Atrial Fibrillation 2014 How to Treat How to Anticoagulate Allan Anderson, MD, FACC, FAHA Division of Cardiology Projection for Prevalence of Atrial Fibrillation: 5.6 Million by 2050 Projected number of
Karen R. Waters. Advanced Nurse Practitioner and Professor Martin Johnson, University of Salford
 Dying with dementia: A retrospective case note analysis of nursing and care home residents who died in hospital. Karen R. Waters. Advanced Nurse Practitioner and Professor Martin Johnson, University of
Dying with dementia: A retrospective case note analysis of nursing and care home residents who died in hospital. Karen R. Waters. Advanced Nurse Practitioner and Professor Martin Johnson, University of
isn t Nursing as Usual
 Why Rehabilitation ti Nursing isn t Nursing as Usual Terri Gately, RN, MS, CRRN Providence Holy Cross Medical Center The Specialty Practice of Rehabilitation Nursing Providence Holy Cross Medical Center
Why Rehabilitation ti Nursing isn t Nursing as Usual Terri Gately, RN, MS, CRRN Providence Holy Cross Medical Center The Specialty Practice of Rehabilitation Nursing Providence Holy Cross Medical Center
In-patient Rehabilitation Outcomes Following Lower Extremity Fracture in Patients with Pneumonia
 In-patient Rehabilitation Outcomes Following Lower Extremity Fracture in Patients with Pneumonia Ijaz Ahmed MD RRT, James E Graham PhD, Amol M Karmarkar PhD, Carl V Granger MD, and Kenneth J Ottenbacher
In-patient Rehabilitation Outcomes Following Lower Extremity Fracture in Patients with Pneumonia Ijaz Ahmed MD RRT, James E Graham PhD, Amol M Karmarkar PhD, Carl V Granger MD, and Kenneth J Ottenbacher
Navigating Depression:
 Navigating Depression: A roadmap for health professionals and patients AH National Conference, 8 th -20 th July, 2007, Hobart, Tasmania Principal investigator: Project Manager: Acknowledgements: Kirsten
Navigating Depression: A roadmap for health professionals and patients AH National Conference, 8 th -20 th July, 2007, Hobart, Tasmania Principal investigator: Project Manager: Acknowledgements: Kirsten
Hospitalizations and Medical Care Costs of Serious Traumatic Brain Injuries, Spinal Cord Injuries and Traumatic Amputations
 Hospitalizations and Medical Care Costs of Serious Traumatic Brain Injuries, Spinal Cord Injuries and Traumatic Amputations FINAL REPORT JUNE 2013 J. Mick Tilford, PhD Professor and Chair Department of
Hospitalizations and Medical Care Costs of Serious Traumatic Brain Injuries, Spinal Cord Injuries and Traumatic Amputations FINAL REPORT JUNE 2013 J. Mick Tilford, PhD Professor and Chair Department of
Impact of Osteoarthritis on Rehabilitation for Persons With Hip Fracture
 Arthritis & Rheumatism (Arthritis Care & Research) Vol. 55, No. 6, December 15, 2006, pp 920 924 DOI 10.1002/art.22345 2006, American College of Rheumatology ORIGINAL ARTICLE Impact of Osteoarthritis on
Arthritis & Rheumatism (Arthritis Care & Research) Vol. 55, No. 6, December 15, 2006, pp 920 924 DOI 10.1002/art.22345 2006, American College of Rheumatology ORIGINAL ARTICLE Impact of Osteoarthritis on
MULTI-FACTORIAL FALL RISK ASSESSMENT AND INTERVENTION FOR COMMUNITY DWELLING SENIORS: THE ROLE OF HOME HEALTH AGENCIES. Caring Choices.
 MULTI-FACTORIAL FALL RISK ASSESSMENT AND INTERVENTION FOR COMMUNITY DWELLING SENIORS: THE ROLE OF HOME HEALTH AGENCIES Caring Choices April 2006 Caring Choices Page 1 Multi-Factorial Fall Risk Assessment
MULTI-FACTORIAL FALL RISK ASSESSMENT AND INTERVENTION FOR COMMUNITY DWELLING SENIORS: THE ROLE OF HOME HEALTH AGENCIES Caring Choices April 2006 Caring Choices Page 1 Multi-Factorial Fall Risk Assessment
EXPANDING THE EVIDENCE BASE IN OUTCOMES RESEARCH: USING LINKED ELECTRONIC MEDICAL RECORDS (EMR) AND CLAIMS DATA
 EXPANDING THE EVIDENCE BASE IN OUTCOMES RESEARCH: USING LINKED ELECTRONIC MEDICAL RECORDS (EMR) AND CLAIMS DATA A CASE STUDY EXAMINING RISK FACTORS AND COSTS OF UNCONTROLLED HYPERTENSION ISPOR 2013 WORKSHOP
EXPANDING THE EVIDENCE BASE IN OUTCOMES RESEARCH: USING LINKED ELECTRONIC MEDICAL RECORDS (EMR) AND CLAIMS DATA A CASE STUDY EXAMINING RISK FACTORS AND COSTS OF UNCONTROLLED HYPERTENSION ISPOR 2013 WORKSHOP
Community Liaison Path for Stroke in Kumamoto Prefecture, Japan
 Research and Reviews Community Liaison Path for Stroke in Kumamoto Prefecture, Japan JMAJ 53(5): 301 305, 2010 Susumu WATANABE,* 1 Makoto TOKUNAGA,* 2 Yoichiro HASHIMOTO,* 3 Yoshifumi HIRATA* 4 Abstract
Research and Reviews Community Liaison Path for Stroke in Kumamoto Prefecture, Japan JMAJ 53(5): 301 305, 2010 Susumu WATANABE,* 1 Makoto TOKUNAGA,* 2 Yoichiro HASHIMOTO,* 3 Yoshifumi HIRATA* 4 Abstract
Elderly males, especially white males, are the people at highest risk for suicide in America.
 Statement of Ira R. Katz, MD, PhD Professor of Psychiatry Director, Section of Geriatric Psychiatry University of Pennsylvania Director, Mental Illness Research Education and Clinical Center Philadelphia
Statement of Ira R. Katz, MD, PhD Professor of Psychiatry Director, Section of Geriatric Psychiatry University of Pennsylvania Director, Mental Illness Research Education and Clinical Center Philadelphia
Early mortality rate (EMR) in Acute Myeloid Leukemia (AML)
 Early mortality rate (EMR) in Acute Myeloid Leukemia (AML) George Yaghmour, MD Hematology Oncology Fellow PGY5 UTHSC/West cancer Center, Memphis, TN May,1st,2015 Off-Label Use Disclosure(s) I do not intend
Early mortality rate (EMR) in Acute Myeloid Leukemia (AML) George Yaghmour, MD Hematology Oncology Fellow PGY5 UTHSC/West cancer Center, Memphis, TN May,1st,2015 Off-Label Use Disclosure(s) I do not intend
Evaluations. Viewer Call-In. www.t2b2.org. Phone: 800-452-0662 Fax: 518-426-0696. Geriatric Mental Health. Thanks to our Sponsors: Guest Speaker
 Geriatric Mental Health June 1, 7 Guest Speaker Michael B. Friedman, LMSW Chairperson Geriatric Mental Health Alliance of New York Thanks to our Sponsors: School of Public Health, University at Albany
Geriatric Mental Health June 1, 7 Guest Speaker Michael B. Friedman, LMSW Chairperson Geriatric Mental Health Alliance of New York Thanks to our Sponsors: School of Public Health, University at Albany
Medical Care Costs for Diabetes Associated with Health Disparities Among Adults Enrolled in Medicaid in North Carolina
 No. 160 August 2009 Among Adults Enrolled in Medicaid in North Carolina by Paul A. Buescher, Ph.D. J. Timothy Whitmire, Ph.D. Barbara Pullen-Smith, M.P.H. A Joint Report from the and the Office of Minority
No. 160 August 2009 Among Adults Enrolled in Medicaid in North Carolina by Paul A. Buescher, Ph.D. J. Timothy Whitmire, Ph.D. Barbara Pullen-Smith, M.P.H. A Joint Report from the and the Office of Minority
The use of text messaging to improve asthma control: a pilot study using the mobile phone short messaging service (SMS)
 RESEARCH Original article... Q The use of text messaging to improve asthma control: a pilot study using the mobile phone short messaging service (SMS) Lathy Prabhakaran*, Wai Yan Chee*, Kia Chong Chua,
RESEARCH Original article... Q The use of text messaging to improve asthma control: a pilot study using the mobile phone short messaging service (SMS) Lathy Prabhakaran*, Wai Yan Chee*, Kia Chong Chua,
Professor Keith Hill, School of Physiotherapy and Exercise Science Curtin University Keith.Hill@Curtin.edu.au
 Professor Keith Hill, School of Physiotherapy and Exercise Science Curtin University Keith.Hill@Curtin.edu.au Curtin University is a trademark of Curtin University of Technology CRICOS Provider Code 00301J
Professor Keith Hill, School of Physiotherapy and Exercise Science Curtin University Keith.Hill@Curtin.edu.au Curtin University is a trademark of Curtin University of Technology CRICOS Provider Code 00301J
Physician House Calls. vanishing practice, have experience a remarkable resurgence in interest in the last decade. 1
 Wayne Liang MPHP 439 Online Chapter Physician House Calls Outline: I. Introduction II. Why House Calls? Why Now? III. Comparing Physician House Calls & Home-Health Agencies IV. Modern House Call Programs
Wayne Liang MPHP 439 Online Chapter Physician House Calls Outline: I. Introduction II. Why House Calls? Why Now? III. Comparing Physician House Calls & Home-Health Agencies IV. Modern House Call Programs
The Outcome of Stroke at Hospital Discharge in New York City Blacks
 The Outcome of Stroke at Hospital Discharge in New York City Blacks BY STEPHEN Q. SHAFER, M.D., BERTEL BRUUN, M.D., AND RALPH W. RICHTER, M.D. Abstract: The Outcome of Stroke at Hospital Discharge in New
The Outcome of Stroke at Hospital Discharge in New York City Blacks BY STEPHEN Q. SHAFER, M.D., BERTEL BRUUN, M.D., AND RALPH W. RICHTER, M.D. Abstract: The Outcome of Stroke at Hospital Discharge in New
Rehabilitation Integrated Transition Tracking System (RITTS)
 Rehab Criteria The patient must have a physical impairment requiring rehabilitation OR have a known cognitive impairment requiring ongoing rehabilitation support or services. The patient is medically stable:
Rehab Criteria The patient must have a physical impairment requiring rehabilitation OR have a known cognitive impairment requiring ongoing rehabilitation support or services. The patient is medically stable:
Nurse Use of a Clinical Decision Support Tool and Patient Outcomes
 Nurse Use of a Clinical Decision Support Tool and Patient Outcomes Penny Hollander Feldman, PhD Margaret McDonald, MSW Yolanda Barron, MS Timothy Peng, PhD Sridevi Sridharan, MS Melissa Trachtenberg, BS
Nurse Use of a Clinical Decision Support Tool and Patient Outcomes Penny Hollander Feldman, PhD Margaret McDonald, MSW Yolanda Barron, MS Timothy Peng, PhD Sridevi Sridharan, MS Melissa Trachtenberg, BS
TORONTO STROKE FLOW INITIATIVE - Outpatient Rehabilitation Best Practice Recommendations Guide (updated July 26, 2013)
 Objective: To enhance system-wide performance and outcomes for persons with stroke in Toronto. Goals: Timely access to geographically located acute stroke unit care with a dedicated interprofessional team
Objective: To enhance system-wide performance and outcomes for persons with stroke in Toronto. Goals: Timely access to geographically located acute stroke unit care with a dedicated interprofessional team
D. Clinical indicators for psychiatric evaluation are established by one or more of the following criteria. The consumer is:
 MCCMH MCO Policy 2-015 Date: 4/21/11 V. Standards A. A psychiatric evaluation shall be done as an integral part of the assessment process. It serves as the guide to the identification of medical and psychiatric
MCCMH MCO Policy 2-015 Date: 4/21/11 V. Standards A. A psychiatric evaluation shall be done as an integral part of the assessment process. It serves as the guide to the identification of medical and psychiatric
Importance of Integrating Stroke Rehabilitation Across the Continuum of Care
 Importance of Integrating Stroke Rehabilitation Across the Continuum of Care Dori Tooke, MHA, PT, CSCS Manager-Inpatient Rehab Program St. Luke s Medical Center Milwaukee, WI Disclosure Nothing to disclose
Importance of Integrating Stroke Rehabilitation Across the Continuum of Care Dori Tooke, MHA, PT, CSCS Manager-Inpatient Rehab Program St. Luke s Medical Center Milwaukee, WI Disclosure Nothing to disclose
Rural Disparities in posthospitalization. after traumatic brain injury.
 Rural Disparities in posthospitalization rehabilitation after traumatic brain injury. Ashley D Meagher MD, Jennifer Doorey MS, Christopher Beadles MD PhD, Anthony Charles MD MPH University of North Carolina
Rural Disparities in posthospitalization rehabilitation after traumatic brain injury. Ashley D Meagher MD, Jennifer Doorey MS, Christopher Beadles MD PhD, Anthony Charles MD MPH University of North Carolina
A Primer on Ratio Analysis and the CAH Financial Indicators Report
 A Primer on Ratio Analysis and the CAH Financial Indicators Report CAH Financial Indicators Report Team North Carolina Rural Health Research and Policy Analysis Center Cecil G. Sheps Center for Health
A Primer on Ratio Analysis and the CAH Financial Indicators Report CAH Financial Indicators Report Team North Carolina Rural Health Research and Policy Analysis Center Cecil G. Sheps Center for Health
Discharge Planning. Home Care 1. Objectives. Where are they Going?
 Discharge Planning Heidi White, MD Associate Professor of Medicine Yvonne Spurney, RN Associate Chief Nurse Cristina C. Hendrix, DNS, GNP-BC Associate Professor of Nursing Objectives Describe challenges
Discharge Planning Heidi White, MD Associate Professor of Medicine Yvonne Spurney, RN Associate Chief Nurse Cristina C. Hendrix, DNS, GNP-BC Associate Professor of Nursing Objectives Describe challenges
TECHNICAL/CLINICAL TOOLS BEST PRACTICE 7: Depression Screening and Management
 TECHNICAL/CLINICAL TOOLS BEST PRACTICE 7: Depression Screening and Management WHY IS THIS IMPORTANT? Depression causes fluctuations in mood, low self esteem and loss of interest or pleasure in normally
TECHNICAL/CLINICAL TOOLS BEST PRACTICE 7: Depression Screening and Management WHY IS THIS IMPORTANT? Depression causes fluctuations in mood, low self esteem and loss of interest or pleasure in normally
David Eubanks, RN, MSN Billie Papasifakis, RN-BC, MSN, AACC. Describe model of care most appropriate
 THE BRIDGE PROGRAM David Eubanks, RN, MSN Billie Papasifakis, RN-BC, MSN, AACC Pamela Teenier, RN, MBA, COC-C, C HCS-D HCSD 1 Objectives Describe model of care most appropriate for a Bridge program from
THE BRIDGE PROGRAM David Eubanks, RN, MSN Billie Papasifakis, RN-BC, MSN, AACC Pamela Teenier, RN, MBA, COC-C, C HCS-D HCSD 1 Objectives Describe model of care most appropriate for a Bridge program from
Success factors in Behavioral Medicine
 Success factors in Behavioral Medicine interventions post myocardial infarction Depression Gunilla post myocardial Burell, PhD infarction Department of Public Health, Uppsala University, Sweden XIII Svenska
Success factors in Behavioral Medicine interventions post myocardial infarction Depression Gunilla post myocardial Burell, PhD infarction Department of Public Health, Uppsala University, Sweden XIII Svenska
648 Predicting the Stroke Patient's Ability to Live Independently
 648 Predicting the Stroke Patient's Ability to Live Independently GERBEN DEJONG, PH.D. * AND LAURENCE G. BRANCH, PH.D.** SUMMARY The objective of this paper is to identify those variables that best predict
648 Predicting the Stroke Patient's Ability to Live Independently GERBEN DEJONG, PH.D. * AND LAURENCE G. BRANCH, PH.D.** SUMMARY The objective of this paper is to identify those variables that best predict
One step closer to home
 One step closer to home Post-hospital short-term rehabilitation and sub-acute care at The Valley View Center for Nursing Care and Rehabilitation Helping to ensure a smooth transition Prior to discharge,
One step closer to home Post-hospital short-term rehabilitation and sub-acute care at The Valley View Center for Nursing Care and Rehabilitation Helping to ensure a smooth transition Prior to discharge,
Prediction of the MoCA and the MMSE in Out-patients with the risks of cognitive impairment
 Prediction of the MoCA and the MMSE in Out-patients with the risks of cognitive impairment Teresa Leung Therapist Prince of Wales Hospital 7 th May, 2012 Outline of Presentation Introduction Study Objectives,
Prediction of the MoCA and the MMSE in Out-patients with the risks of cognitive impairment Teresa Leung Therapist Prince of Wales Hospital 7 th May, 2012 Outline of Presentation Introduction Study Objectives,
THE CORRELATION BETWEEN PHYSICAL HEALTH AND MENTAL HEALTH
 HENK SWINKELS (STATISTICS NETHERLANDS) BRUCE JONAS (US NATIONAL CENTER FOR HEALTH STATISTICS) JAAP VAN DEN BERG (STATISTICS NETHERLANDS) THE CORRELATION BETWEEN PHYSICAL HEALTH AND MENTAL HEALTH IN THE
HENK SWINKELS (STATISTICS NETHERLANDS) BRUCE JONAS (US NATIONAL CENTER FOR HEALTH STATISTICS) JAAP VAN DEN BERG (STATISTICS NETHERLANDS) THE CORRELATION BETWEEN PHYSICAL HEALTH AND MENTAL HEALTH IN THE
Multidisciplinary Rehabilitation Daycare Center in the Community in Kiryat Bialik: Evaluation Study
 C E N T E R F O R R E S E A R C H O N A G I N G Multidisciplinary Rehabilitation Daycare Center in the Community in Kiryat Bialik: Evaluation Study Shirli Resnizky Netta Bentur The study was commissioned
C E N T E R F O R R E S E A R C H O N A G I N G Multidisciplinary Rehabilitation Daycare Center in the Community in Kiryat Bialik: Evaluation Study Shirli Resnizky Netta Bentur The study was commissioned
In the mid-1960s, the need for greater patient access to primary care. Physician Assistants in Primary Care: Trends and Characteristics
 Physician Assistants in Primary Care: Trends and Characteristics Bettie Coplan, MPAS, PA-C 1 James Cawley, MPH, PA-C 2 James Stoehr, PhD 1 1 Physician Assistant Program, College of Health Sciences, Midwestern
Physician Assistants in Primary Care: Trends and Characteristics Bettie Coplan, MPAS, PA-C 1 James Cawley, MPH, PA-C 2 James Stoehr, PhD 1 1 Physician Assistant Program, College of Health Sciences, Midwestern
CART Community Assessment of Risk Tool
 CART Community Assessment of Risk Tool 0 3-0 7. 2 0 1 2 D E M E N T I A L E A R N I N G E V E N T M U L L I N G A R PA R K H O T E L T U E S D AY 3 R D J U LY 2 0 1 2 D R R Ó N Á N O C A O I M H P R O
CART Community Assessment of Risk Tool 0 3-0 7. 2 0 1 2 D E M E N T I A L E A R N I N G E V E N T M U L L I N G A R PA R K H O T E L T U E S D AY 3 R D J U LY 2 0 1 2 D R R Ó N Á N O C A O I M H P R O
Pressure Ulcers Among Nursing Home Residents: United States, 2004
 Pressure Ulcers Among Nursing Home Residents: United States, 2004 Eunice Park-Lee, Ph.D., and Christine Caffrey, Ph.D., Division of Health Care Statistics Key findings Data from the National Nursing Home
Pressure Ulcers Among Nursing Home Residents: United States, 2004 Eunice Park-Lee, Ph.D., and Christine Caffrey, Ph.D., Division of Health Care Statistics Key findings Data from the National Nursing Home
Taming Of The Queue VI. Christine Struthers APN Cardiac Telehealth University of Ottawa Heart Institute
 Taming Of The Queue VI Christine Struthers APN Cardiac Telehealth University of Ottawa Heart Institute March 2009 The Heart Failure Continuum 2 Leadership. Knowledge. Community. HF Readmissions Hospital
Taming Of The Queue VI Christine Struthers APN Cardiac Telehealth University of Ottawa Heart Institute March 2009 The Heart Failure Continuum 2 Leadership. Knowledge. Community. HF Readmissions Hospital
Serious Mental Illness: Symptoms, Treatment and Causes of Relapse
 Serious Mental Illness: Symptoms, Treatment and Causes of Relapse Bipolar Disorder, Schizophrenia and Schizoaffective Disorder Symptoms and Prevalence of Bipolar Disorder Bipolar disorder, formerly known
Serious Mental Illness: Symptoms, Treatment and Causes of Relapse Bipolar Disorder, Schizophrenia and Schizoaffective Disorder Symptoms and Prevalence of Bipolar Disorder Bipolar disorder, formerly known
UCare provides case management for all UCare members not affiliated with one of the above listed care systems. 2011 UCare for Seniors
 Case Requirements Updated 3/16/2011 According to the Case Society of America (CMSA), Case Model Act of 2009, Case management is a collaborative process of assessment, planning, facilitation, care coordination,
Case Requirements Updated 3/16/2011 According to the Case Society of America (CMSA), Case Model Act of 2009, Case management is a collaborative process of assessment, planning, facilitation, care coordination,
Ruchika D. Husa, MD, MS Assistant t Professor of Medicine in the Division of Cardiology The Ohio State University Wexner Medical Center
 Modified Early Warning Score (MEWS) Ruchika D. Husa, MD, MS Assistant t Professor of Medicine i in the Division of Cardiology The Ohio State University Wexner Medical Center MEWS Simple physiological scoring
Modified Early Warning Score (MEWS) Ruchika D. Husa, MD, MS Assistant t Professor of Medicine i in the Division of Cardiology The Ohio State University Wexner Medical Center MEWS Simple physiological scoring
Understanding the Structures of Home-Based Care Delivery: Developing a Picture of the Home Care Team. Research Team and Funder
 Understanding the Structures of Home-Based Care Delivery: Developing a Picture of the Home Care Team Margaret Saari PhD Candidate & Erin Patterson PhD Candidate CHCA 2015 Home Care Summit Research Team
Understanding the Structures of Home-Based Care Delivery: Developing a Picture of the Home Care Team Margaret Saari PhD Candidate & Erin Patterson PhD Candidate CHCA 2015 Home Care Summit Research Team
PCHC FACTS ABOUT HEALTH CONDITIONS AND MOOD DIFFICULTIES
 PCHC FACTS ABOUT HEALTH CONDITIONS AND MOOD DIFFICULTIES Why should mood difficulties in individuals with a health condition be addressed? Many people with health conditions also experience mood difficulties
PCHC FACTS ABOUT HEALTH CONDITIONS AND MOOD DIFFICULTIES Why should mood difficulties in individuals with a health condition be addressed? Many people with health conditions also experience mood difficulties
Summary Evaluation of the Medicare Lifestyle Modification Program Demonstration and the Medicare Cardiac Rehabilitation Benefit
 The Centers for Medicare & Medicaid Services' Office of Research, Development, and Information (ORDI) strives to make information available to all. Nevertheless, portions of our files including charts,
The Centers for Medicare & Medicaid Services' Office of Research, Development, and Information (ORDI) strives to make information available to all. Nevertheless, portions of our files including charts,
How To Write A Nursing Home Self Assessment Survey On Patient Transitions And Family Caregivers
 How Are We Doing? A Nursing Home Self Assessment Survey on Patient Transitions and Family Caregivers Well-planned and managed transitions are essential for high quality care and patient safety. Transitions
How Are We Doing? A Nursing Home Self Assessment Survey on Patient Transitions and Family Caregivers Well-planned and managed transitions are essential for high quality care and patient safety. Transitions
Conjoint Professor Brian Draper
 Chronic Serious Mental Illness and Dementia Optimising Quality Care Psychiatry Conjoint Professor Brian Draper Academic Dept. for Old Age Psychiatry, Prince of Wales Hospital, Randwick Cognitive Course
Chronic Serious Mental Illness and Dementia Optimising Quality Care Psychiatry Conjoint Professor Brian Draper Academic Dept. for Old Age Psychiatry, Prince of Wales Hospital, Randwick Cognitive Course
Care of Persons With AIDS in the Nursing Home
 436 June 1998 Family Medicine Clinical Research and Methods Care of Persons With AIDS in the Nursing Home John Michael Heath, MD Background: AIDS is becoming a chronic illness for some patients whose significant
436 June 1998 Family Medicine Clinical Research and Methods Care of Persons With AIDS in the Nursing Home John Michael Heath, MD Background: AIDS is becoming a chronic illness for some patients whose significant
CLINICAL PRACTICE GUIDELINES Treatment of Schizophrenia
 CLINICAL PRACTICE GUIDELINES Treatment of Schizophrenia V. Service Delivery Service Delivery and the Treatment System General Principles 1. All patients should have access to a comprehensive continuum
CLINICAL PRACTICE GUIDELINES Treatment of Schizophrenia V. Service Delivery Service Delivery and the Treatment System General Principles 1. All patients should have access to a comprehensive continuum
How many RCTs in Stroke Rehab?
 Evidence Based Stroke Rehabilitation: Maximizing Recovery and Improving Outcomes Robert Teasell MD FRCPC Professor and Chair Chief Physical Medicine & Rehabilitation St. Joseph s Health Care London University
Evidence Based Stroke Rehabilitation: Maximizing Recovery and Improving Outcomes Robert Teasell MD FRCPC Professor and Chair Chief Physical Medicine & Rehabilitation St. Joseph s Health Care London University
Objectives. Objectives 4/5/2014
 Session: T32 A True Person Centered Restorative Nursing Program- Individualized Care at it s Best! Presented By: Sue LaGrange, RN, BSN, NHA Director of Education Pathway Health (651) 964-4946 Objectives
Session: T32 A True Person Centered Restorative Nursing Program- Individualized Care at it s Best! Presented By: Sue LaGrange, RN, BSN, NHA Director of Education Pathway Health (651) 964-4946 Objectives
Patient / Carer Empowerment in Rehabilitation: Challenges and Success Factors
 東 華 三 院 黃 大 仙 醫 院 Tung Wah Group of Hospitals Wong Tai Sin Hospital Patient / Carer Empowerment in Rehabilitation: Challenges and Success Factors HA Convention 2015 Li KY, Tang IFK, Kwong MWY, Chan RWH,
東 華 三 院 黃 大 仙 醫 院 Tung Wah Group of Hospitals Wong Tai Sin Hospital Patient / Carer Empowerment in Rehabilitation: Challenges and Success Factors HA Convention 2015 Li KY, Tang IFK, Kwong MWY, Chan RWH,
 SUMMARY This PhD thesis addresses the long term recovery of hemiplegic gait in severely affected stroke patients. It first reviews current rehabilitation research developments in functional recovery after
SUMMARY This PhD thesis addresses the long term recovery of hemiplegic gait in severely affected stroke patients. It first reviews current rehabilitation research developments in functional recovery after
REHABILITATION. begins right here
 REHABILITATION begins right here Select Rehabilitation Hospital of Denton offers you a new direction in medical rehabilitation. Our 44-bed, state-of-the-science hospital offers unparalleled treatment to
REHABILITATION begins right here Select Rehabilitation Hospital of Denton offers you a new direction in medical rehabilitation. Our 44-bed, state-of-the-science hospital offers unparalleled treatment to
A Phase II RCT of Stroke Navigators to Improve Compliance with Secondary Stroke Prevention: PROTECT DC
 A Phase II RCT of Stroke Navigators to Improve Compliance with Secondary Stroke Prevention: PROTECT DC Alexander W. Dromerick, MD National Rehabilitation Hospital Georgetown University Departments of Neurology
A Phase II RCT of Stroke Navigators to Improve Compliance with Secondary Stroke Prevention: PROTECT DC Alexander W. Dromerick, MD National Rehabilitation Hospital Georgetown University Departments of Neurology
Caring About Palliative Care An overview
 Caring About Palliative Care An overview Developed by the Palliative Care Consultation Team at VH and C. Talbot, Palliative Care Consultation Team at UH Presented by: Lee Ann Craig NP, Palliative Care
Caring About Palliative Care An overview Developed by the Palliative Care Consultation Team at VH and C. Talbot, Palliative Care Consultation Team at UH Presented by: Lee Ann Craig NP, Palliative Care
