Efficacy of conventional and implant-supported mandibular resection prostheses: Study overview and treatment outcomes
|
|
|
- Aubrey Horton
- 8 years ago
- Views:
Transcription
1 Efficacy of conventional and implant-supported mandibular resection prostheses: Study overview and treatment outcomes Neal Garrett, PhD, a EleniD.Roumanas,DDS, b Keith E. Blackwell, MD, c Earl Freymiller, MD, DMD, d Elliot Abemayor, MD, PhD, e Weng Kee Wong, PhD, f Bruce Gerratt, PhD, g Gerald Berke, MD, h John Beumer III, DDS, MS, i and Krishan K. Kapur, DDS, MS j The Jane and Jerry Weintraub Center of Reconstructive Biotechnology, UCLA School of Dentistry; David Geffen School of Medicine at UCLA; UCLA School of Public Health, Los Angeles, Calif; Veterans Administration Greater Los Angeles Healthcare System, Los Angeles, Calif Statement of problem. While surgical restoration of mandibular resections has advanced dramatically with free-flap techniques, oral function and patient perceptions of function, as well as treatment outcomes, often indicate significant impairment. Purpose. This longitudinal prospective study was designed to determine whether conventional prostheses (CP) or implant-supported prostheses (IP) and current surgical reconstructive procedures restore patients oral functions and quality of life to their status prior to segmental mandibulectomy with immediate fibula free-flap reconstruction. Study design and implementation, characteristics of the study sample, treatment completion rates, and selected presurgical and postsurgical functional and perceptual outcomes are presented. Material and methods. Forty-six subjects were enrolled. Longitudinal evaluations of medical and dental histories, oromaxillofacial examinations, questionnaires, and sensory and functional tests were planned before and after surgery and after CP and IP treatment. Sample characteristics are described with descriptive statistics and comparisons of subject responses to questionnaire items at entry and postsurgical intervals were made with Fisher exact tests (a=.05). Results. Conventional prostheses were completed in 33 of 46 subjects, and 16 of 33 CP subjects were treated with IP. Reasons for noncompletion of IP were recurrent/metastatic disease (16), refusal of implant therapy (7), lost to follow-up (4), treatment with a reconstruction plate (1), excessive radiation at implant sites (1), and death (1). All 16 recurrences/metastases occurred within 13 months of surgery. Only 3 of the 58 implants placed in 17 participants were considered failures. One failed due to lack of integration 31 weeks following placement, and 2 were buried due to unacceptable positioning for prosthetic restoration during denture fabrication. The remaining 55 implants were successful at final evaluation, ranging from 58 to 123 weeks following implant placement (mean duration= weeks). Conclusions. While 72% (33/46) of the subjects enrolled were able and willing to complete treatment with CP, only 35% (16/46) completed IP treatment. Careful consideration must be given to selection of the type of prosthetic rehabilitation and the timing of implant placement if an IP is planned. (J Prosthet Dent 2006; 96:13-24.) This study was supported by the National Institute of Dental and Craniofacial Research (grant No. 1RO1DE11255), Department of Veteran Affairs Medical Research Service, and UCLA Maxillofacial Prosthetics Clinic. This investigation was conducted in a facility constructed with support from Research Facilities Improvement Program Grant No. CO6 RR from the National Center for Research Resources, National Institutes of Health. Preliminary results presented at the International Association for Dental Research Annual Meeting, June 2003, Goteborg, Sweden, and the International Society for Maxillofacial Rehabilitation, June 2004, Maastricht, Netherlands. a Professor, Division of Advanced Prosthodontics, Biomaterials and Hospital Dentistry, and Director, The Jane and Jerry Weintraub Center for Reconstructive Biotechnology, UCLA School of Dentistry; Director, Dental Research Laboratory, Veterans Administration Greater Los Angeles Healthcare System. b Professor, Division of Advanced Prosthodontics, Biomaterials and Hospital Dentistry, and Chair, Section of Removable Prosthodontics, The Jane and Jerry Weintraub Center for Reconstructive Biotechnology, UCLA School of Dentistry. c Associate Professor, Division of Head and Neck Surgery, David Geffen School of Medicine at UCLA. d Clinical Professor, Division of Diagnostic and Surgical Sciences, and Chair, Section of Oral and Maxillofacial Surgery, UCLA School of Dentistry. e Professor In-Residence, Division of Head and Neck Surgery, David Geffen School of Medicine at UCLA. f Professor, Department of Biostatistics, UCLA School of Public Health. g Professor In-Residence, Division of Head and Neck Surgery, and Chair, Speech Pathology and Audiology, David Geffen School of Medicine at UCLA. h Professor and Chair, Division of Head and Neck Surgery, David Geffen School of Medicine at UCLA. i Professor and Chair, Division of Advanced Prosthodontics, Biomaterials and Hospital Dentistry, The Jane and Jerry Weintraub Center for Reconstructive Biotechnology, UCLA School of Dentistry. j Professor Emeritus, Division of Advanced Prosthodontics, Biomaterials and Hospital Dentistry, The Jane and Jerry Weintraub Center for Reconstructive Biotechnology, UCLA School of Dentistry. JULY 2006 THE JOURNAL OF PROSTHETIC DENTISTRY 13
2 THE JOURNAL OF PROSTHETIC DENTISTRY GARRETT ET AL CLINICAL IMPLICATIONS Due to the high rate of recurrence/metastasis within the first year following ablative surgery, consideration of extensive implant therapy, particularly in partially dentate patients, should be delayed for at least a year. Oral cancer represents 2.5% of all cancers and 1.5% of cancer deaths in the United States. Approximately 30,200 people were diagnosed for oral cancer, and 7800 died of this disease in the United States in Estimated 5-year survival rates of 53% in whites and 32% in blacks have been reported in the United States. 1-3 High mortality rates and possible physical disfigurement and functional impairments 4,5 associated with tumor ablative surgery are a challenge to health care providers treating patients with oral cancer. Only minimal longitudinal evidence exists to describe the functional and perceptual impairments resulting from ablative oncologic surgery and the rehabilitative effect of current surgical reconstructive techniques and dental restorative procedures In 1990, a review 12 of 32 articles described outcomes of various mandibular reconstruction techniques and indicated that functional rehabilitation was rarely addressed. Assessments of functional outcomes in terms of deglutition, mastication, and esthetics were provided for only 4% of the 782 patients evaluated. Prosthetic rehabilitation was presented for only 16 patients (2%) of all mandibular reconstructions. The same paper included a retrospective evaluation of a small number of patients who had undergone mandibular resection with and without mandibular reconstruction and concluded that restoration of mandibular continuity does not enhance functional rehabilitation of the majority of patients. Significant strides in microvascular surgical approaches during the past decade have permitted predictable restoration of bony and soft tissue orofacial defects However, limited studies indicate only varying degrees of improvement in terms of esthetics, speech intelligibility, swallowing, and masticatory performance. 9,10,18-22 It appears that even new surgical reconstructive techniques may not sufficiently restore sensory-motor functions, and in most instances they fail to provide adequate support for dental prostheses. Poor tissue support after mandibular reconstruction has hindered prosthodontists in constructing stable and functional dental prostheses for these patients. Based on dentition status and soft and hard tissue configuration, dental implants are used to increase support, stability, and retention of prostheses. Treatment with implant-supported prostheses has been described for oral cancer patients with mandibular reconstruction, and there is limited indication that levels of masticatory function and occlusal forces similar to normal individuals with implant dentures may be achieved Although dental implants are used in selected patients at a number of healthcare centers, neither the functional efficacy nor the treatment success rates of conventional and implant prostheses have been established in oral cancer patients with reconstructed mandibles. To provide assessment of the effects of surgical and dental rehabilitation in patients undergoing partial mandibulectomy, a longitudinal prospective clinical study was designed to compare functional and perceptual outcomes between conventional and implant-supported dental prostheses in patients requiring segmental mandibulectomy and surgical reconstruction. The primary purpose was to test 2 hypotheses: (1) that the 2 types of prostheses each restore specified oral functions and oral perceptions to presurgical levels, and (2) that both types of prostheses are equally effective in restoring specified oral functions and perceptions. The aim of this paper is to describe the study design and implementation, sample characteristics, and treatment completion rates for the conventional and implant-supported prostheses and selected oral functional and perceptual outcomes following surgical mandibular reconstruction but prior to prosthetic rehabilitation. Extensive evaluation of treatment effects on oral functions and subject perceptions will be presented in subsequent reports. MATERIAL AND METHODS Study sample Masticatory performance (MP) was selected as the primary variable for sample size determination because of its possible effects on ingestion, dietary intake, and social behavior. Furthermore, masticatory performance is the outcome of several other proposed key measures, including the ability to clear particles from the mouth (oral clearance), oral stereognosis, occlusal force, and masticatory muscle effort. Unfortunately, no pre- or postsurgical estimates were available in the literature for the proposed study population to provide the basis for power analysis to determine sample size. Estimates of anticipated impairments in masticatory function were based on extensive data on populations ranging from completely edentulous to completely dentate and selected limited studies of function in partial 14 VOLUME 96 NUMBER 1
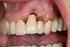
3 GARRETT ET AL THE JOURNAL OF PROSTHETIC DENTISTRY mandibulectomy patients. 7,9,31 Masticatory performance was estimated from pilot data of pre- and postsurgical dentition status for this patient population. To test the hypotheses that the 2 treatments are equally effective in restoring function, a change of 10 in MP from the estimated presurgical performance score of 44.5 (on a scale) was considered clinically significant. Based on these estimates, a sample of 33 was required to provide a power of 0.8 (alpha 0.05, effect size 0.71). Assuming a 20% patient loss during the first year of participation, 40 patients were planned to be enrolled. An additional 6 patients were later added to offset the greater than anticipated loss of study subjects. Recruitment The study protocol and use of human subjects was approved by University of California at Los Angeles (UCLA) Human Subjects Protection Committee. Subjects requiring segmental mandibulectomy were recruited from the UCLA Maxillofacial Prosthetics Clinic and the UCLA Head and Neck Surgery Clinic, including referrals from affiliated medical centers in Los Angeles (VA Greater Los Angeles Healthcare System, West Los Angeles; Olive View-UCLA Medical Center; Harbor-UCLA Medical Center, and Kaiser Permanente Medical Centers in Greater Los Angeles). The purpose of the study was explained to patients and all subjects signed an approved informed consent form. Only patients planning to receive segmental mandibulectomy involving the ramus (R), body (B), or symphysis (S), as classified by the Urken classification, 38 were accepted for the study. Patients with defects expected to involve the mandibular condyle were excluded. Exclusion criteria are listed in Table I. Present treatment practices at UCLA and its affiliated institutions The treatment of a patient with oral cancer is a collaborative team effort among head and neck surgeons, reconstructive surgeons, radiation oncologists, and maxillofacial prosthodontists. Free tissue transfers are routinely used to reconstruct both the soft tissue and bone defect immediately following the ablative surgery. A large percent of patients receive radiation 4 to 6 weeks postoperatively. The total radiation dose to the tumor bed depends on the presence or absence of microscopic disease at the surgical margin. The tumor dose is generally limited to 55 Gy for patients with clear margins, and up to 65 to 70 Gy in patients with close margins. Radiation positioners are used extensively, and radiation fields are configured to minimize exposure of the major salivary glands to high doses of irradiation; however, intensity-modulated radiation therapy (IMRT) was not employed. With careful planning, radiation dose to bone can often be minimized in areas of proposed implant sites. Although hyperbaric oxygen (HBO) Table I. Exclusion and treatment failure criteria Exclusion criteria d Unable to perform tests due to lesion size or restrictive opening d More than 55 Gy radiation at potential implant sites d Defects involving mandibular condyle d Total glossectomy d Bilateral resection of motor and sensory nerves d Need for implants to be placed at time of mandibular reconstruction d Insufficient bone to accommodate implants $10 mm in length after reconstructive surgery Treatment failure criteria d Patient does not use prosthesis frequently during eating d Implant-supported prostheses becomes tissue-supported due to loss of implant therapy has been proposed to improve vascularity and quality of the tissues, 39,43 issues related to cost and potential complications precluded use of HBO in this study. Treatment and research protocol The complete sequence and projected timing of clinical and research procedures performed for subjects with and without postsurgical radiation are shown in Figure 1. Immediately after enrollment in the study, participants completed a series of objective and subjective functional tests, questionnaires, and examinations (Table II). Within 1 to 7 days after testing, participants underwent composite resection and immediate fibula free-flap reconstruction. Approximately 6 weeks after the ablative surgery, it was anticipated that 60% of subjects would receive radiation therapy for 5 to 7 weeks. New conventional prostheses were fabricated as soon as the healing from reconstructive surgery and radiotherapy would permit. Cast frameworks were used for conventional removable partial dentures (RPDs) (Fig. 2). It was planned that implants would be placed 4 to 6 months after reconstruction, depending on the need for postoperative radiation therapy. Although primary implant placement has been advocated in some reports, 44,45 all implants were placed secondarily 46 following healing of the osteotomy sites and resolution of acute radiation therapy effects. Two to 4 dental implants (3i Implant Innovations, Inc, Palm Beach Gardens, Fla), 10 mm or longer and 3.75 mm in diameter, were placed. Implants were located in the available native bone and/or in the free vascularized bone of the reconstructed mandible. Surgical guides were fabricated for each subject to assist the surgeon in positioning implants for ideal prosthetic restoration. 24,46 Segments of impeding reconstruction plates were removed at this surgery prior to the placement of implants. The planned healing time prior to implant exposure (Stage II surgery) was 6 months (Fig. 1). A peri-implant JULY
4 THE JOURNAL OF PROSTHETIC DENTISTRY GARRETT ET AL Fig. 1. Timeline for treatment and testing. Table II. Examinations, tests and questionnaires administered at baseline and follow-up intervals Examinations: Medical and social history Orofacial and dental exams, diagnostic casts Radiographs One week dietary intake log Objective assessments (physiological) Masticatory performance, right and left sides (key variable) Swallowing threshold performance Oral clearance: with and without tongue sweep Oral sensation: stereognosis, two-point discrimination thresholds, tactile thresholds Salivary secretion rates (whole and parotid): resting and stimulated Subjective assessment (psychological) Overall patient satisfaction - questionnaire Chewing preference - questionnaire Food preference questionnaire Facial attractiveness (panel rated) Standardized speech recording: naturalness evaluation Postsurgical, post-cp and post-ip intervals: All evaluations above, plus: Occlusal force on defect and non-defect sides Bilateral masseter muscle activity (right and left side mastication) At rest During occlusal force evaluation During masticatory performance tests Mandibular movement patterns During masticatory performance tests Teeth and prosthesis evaluation submucosal resection was performed at the time of implant uncovering to assure a thin layer (3-4 mm) of attached tissue around the implants. Depending on remaining mandibular dentition, participants were provided with an implant-supported (partial overdenture) or implant-assisted (complete overdenture) prosthesis retained by a tissue bar and clips (Hader; Sterngold ImplaMed, Attleboro, Mass) or resilient attachments (ERA; Sterngold ImplaMed) (Fig. 3). The same series of tests and subjective assessments made before surgery were repeated after recovery from reconstructive surgery and radiation (postsurgical), and 16 weeks after insertion of the conventional prosthesis (CP) and implant-supported prosthesis (IP). Objective and subjective evaluations The series of examinations, tests, and questionnaires administered at baseline and follow-up intervals is listed in Table II. Although most of the results of these outcomes will be presented in future reports, the methods are briefly described. Medical and social histories include demographic, medical (medical problems and medications), and social information retrieved from the medical record and verified with the participant. One investigator (ER) conducted orofacial examination of the face, lips, oral cavity, and temporomandibular joints. Because of the limited access to the participants prior to surgery, the dental examination at entry was restricted to simple counts of teeth, their current status, and a general assessment of oral hygiene and gingival health. A detailed caries and periodontal health evaluation of each tooth and an assessment of the CP and IP were made at the completion of dental reconstruction. Determination of primary tumor staging was made according to published guidelines. 47 Panoramic radiographs and lateral cephalometric radiographs were made at entry as required for surgical treatment. Lateral cephalometric films were repeated on completion of dental reconstruction. Mandibular 16 VOLUME 96 NUMBER 1
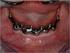
5 GARRETT ET AL THE JOURNAL OF PROSTHETIC DENTISTRY Fig. 2. Conventional removable prosthesis. A, Lateral edentulous space to be restored. B, Removable prosthesis with cast framework and retentive clasps. and maxillary diagnostic casts in white plaster (#2; Kerrlab, Orange, Calif) were made at pre- and postsurgical reconstruction. Participants recorded a 1-week log of food intake at each evaluation interval for analysis of intake, nutritional value, and masticatory difficulty of diet. Three questionnaires were presented to the participants, both verbally and in written form, with responses recorded by a trained research assistant. The first questionnaire included 20 items for participants to rate their experience related to mastication, speech, odor, denture hygiene, comfort, security, and general satisfaction (Table III). Items 1-18 were rated on a 4-point Likert scale (1, most positive; 4, most negative response), and items were rated on a 6-point scale (1, complete satisfaction; 6, complete dissatisfaction). These questionnaire items were adapted from a similar questionnaire used in previous studies of CPs and IPs. 48 A food preference questionnaire elicited the subject s preferences in terms of taste, texture, frequency of eating, and ease of mastication for 13 common foods A third set of question items was designed for this study, Fig. 3. Implant-supported prosthesis. A, Lateral edentulous space restored with implant-supported milled bar. B, Removable partial denture with cast suprastucture with Hader clips and milled bar. C, Implant-supported prosthesis in position over milled bar. based on the authors experience, to evaluate the effects of surgery and dental rehabilitation on the side preferred by the participant to masticate food. Frontal and profile 35-mm color slides were made with the participant s head in a standardized upright position. Panel evaluations will be made using a visual analog scale of 0 mm (least attractive) to 100 mm (most attractive). 54 JULY
6 THE JOURNAL OF PROSTHETIC DENTISTRY GARRETT ET AL Table III. Patient satisfaction questionnaire items Do you experience any discomfort when you chew: 1. I experience no discomfort when chewing 2. I experience slight discomfort when chewing 3. I experience moderate discomfort when chewing 4. I experience great discomfort when I chew How well can you chew? Do you enjoy eating? Does your chewing ability affect your choice of foods?..your social life? Do you find food particles collecting under your tongue?..sticking inside your cheeks? Do you experience any problem in the taste of food? How satisfied are you with your speech? Do you experience any bad mouth odor? Do you experience any difficulty cleaning your teeth? After cleaning, are you satisfied with the cleanliness of your teeth? How satisfied are you with your facial appearance? Do you feel that your facial appearance affects your social life? Do you experience any mouth dryness? Do you experience problems with oral continence (drooling)? Do you use your dentures for eating? How secure do you feel with your dentures? How satisfied are you with your teeth? How satisfied are you with your dentures? Whole saliva secretion rates were collected at rest and while masticating a standardized bolus (rubber bands). 55 In separate tests, parotid saliva was collected using a modified Carlson-Crittenden vacuum cup (custom-made; Maxillofacial Prosthetics Laboratory, UCLA School of Dentistry) on the opening of Stenson s duct on the nonsurgical side. 56 Specimens were obtained at rest and while a gustastory stimulus (sucrose solution) was placed on the dorsum and lateral surfaces of the tongue. Taste discrimination and perception thresholds for the sweet modality were established using a forced choice method. 55 Tactile thresholds on the cheeks, tongue, and palate were determined using a method of limits procedure. 57 Two-point discrimination thresholds were established for the tip of the tongue, lateral tongue, and buccal mucosa. Stereognostic ability was assessed using a series of 10 distinct shapes of approximately 5 mm in diameter made from raw carrots. Participants identified each figure from an enlarged drawing following oral manipulation of the item. 58 Two measures of oral clearance ability were made separately for the right and left sides of the mouth. Controlled specimens of ground peanuts were placed in the participant s right or left lower buccal cavity. In one test, the subjects were asked to expectorate as much of the ground food as possible in a 20-second period without using the tongue to sweep the buccal cavity. In the second test, they were instructed to use the tongue to sweep the buccal cavity in each lower quadrant only 2 times and expectorate the food in a cup. The remaining food was retrieved separately. The cleared and Table IV. General sample characteristics at entry (prior to surgery), CP evaluation, and IP evaluation Entry CP IP Male (N) Female (N) Total (N) Mean (SD) Mean (SD) Mean (SD) Age (y) 60.0 (15.6) 60.2 (13.0) 58.1 (10.4) No. principal medical 2.8 (1.8) 1.7 (1.0) 1.9 (1.0) diagnoses No. medication categories 1.7 (1.6) 1.3 (1.3) 1.3 (1.4) Years smoked cigarettes 31.0 (16.1) 33.9 (10.6) 31.7 (9.1) Packs per day 1.1 (0.6) 1.0 (0.2) 1.0 (0.2) % % % Smokers Currently smokes cigarettes Currently drinks alcohol Education. high school Disease status N (%) N (%) N (%) Primary tumor 25 (54) 13 (52) 9 (60) Recurrent tumor 10 (22) 3 (12) 1 (7) Benign neoplasm 5 (11) 3 (12) 2 (13) Osteoradionecrosis 4 (9) 4 (16) 2 (13) Plate fracture 1 (2) 1 (4) 1 (7) Metastatic disease 1 (2) 1 (4) 0 (0) retrieved particles were separately dried and weighed. The ratios of weights of cleared particles to total particles recovered were calculated and expressed as percents. 34 Standardized masticatory tests were performed by participants on the right and left sides separately, with peanuts as the test food. 34 Three test portions, 3 grams each, were masticated on the directed side by the subject for 20 strokes. The masticated food was expectorated into a cup, the mouth rinsed to clear the remaining particles, and the rinsing (liquid) added to the cup. The masticated food for all 3 portions for a given test food was pooled for a single measurement. For analysis, the masticated food was sieved into coarse and fine particles using a US standard sieve #12 mesh (Fisher Scientific Intl, Hampton, NH). The particles were centrifuged (Dynac Centrifuge; Clay Adams, Div of Becton, Dickinson & Co, Parsippany, NJ) for 3 minutes at 1500 rpm, and the volume of the test materials was recorded. Masticatory performance scores were calculated by dividing the volume of the fine particles by the total volume of test food recovered and expressed as a percent. A swallowing threshold test with raw carrots provided additional assessment of the participants routine mastication. 34 A 3-g carrot portion was divided into 4 equal parts. Subjects were instructed to chew normally, without regard to side or number of strokes, until ready for swallowing. The masticated food was expectorated, 18 VOLUME 96 NUMBER 1
7 GARRETT ET AL THE JOURNAL OF PROSTHETIC DENTISTRY Fig. 4. Distribution of mandibular bony defects. Sh, Unilateral half of the symphysis. and the remaining particles were retrieved for particle size analyses as described for masticatory performance tests. Participants not able to attempt the masticatory or swallowing threshold tests at an evaluation interval received a score of zero performance for that interval. Electromyographic (EMG) recordings were made from the left and right superior masseter muscles with the mandible in resting position, during occlusal force measurements, and during the standardized right and left side masticatory tests. 59 Mandibular jaw movements were concurrently recorded (Biopak 1.7R; BioResearch Associates, Inc, Milwaukee, Wis) during the masticatory tests. Variables quantified included total EMG activity, peak EMG activity, cycle duration, and for jaw movement, the maximum velocity and the maximum range of excursion on each of the axes (vertical, lateral, and anteroposterior). Occlusal force measurements were made with an interleaving beam strain gauge transducer. The transducer vertical dimension was approximately 4 mm and was placed in the area of the second premolar/first molar on each side. Participants were asked to bite as hard as possible without discomfort. The peak amplitudes from 3 trials on each side were averaged to provide measures of occlusal force. Speech was recorded while subjects read the Rainbow Passage (a phonetically balanced reading passage) and 10 sentences generated by The Computerized Assessment of Intelligibility of Dysarthric Speech (computer software; C.C. Publications, Tigard, Ore). A trained rater evaluated the speech quality on a 4-point scale. The rater was blinded with regard to speaker identity and time of testing. For this overview of the study design and treatment, subject and treatment characteristics are presented with descriptive statistics (mean values and SDs, percentages, and frequency distributions) based on the level of measurement. For comparisons of subject responses to questionnaire items at entry and postsurgical intervals, Fisher exact tests were used (a=.05). RESULTS Subject recruitment began July 30, 1997 and continued to November 5, Forty-six participants with oral lesions, requiring segmental mandibulectomy with and without partial glossectomy, were enrolled. Sample characteristics at entry Participants ranged in age from 19 to 83 years, with a mean age of 60 years (Table IV). A positive tobacco smoking history ($5 years) was found in 50% (23/46) of the sample, averaging 31 years of smoking, and only 13% (6/46) of participants were currently smoking. Alcohol was consumed by 28% (13/46) of the sample, and 1 additional subject reported a positive drinking history but had been abstinent for 4 years. Education levels were relatively high, with over 90% (42/46) having completed high school. At entry into the study, 54.3% (25/46) of the participants presented with primary malignant tumors, 21.7% (10/46) with recurrent tumors, 10.8% (6/46) with benign neoplasms, 8.7% (4/46) with osteoradionecroses, 2.2% (1/46) with plate fracture, and 2.2% (1/46) with metastatic tumors (Table IV). The predominant defects (Fig. 4) involved the body (B) in combination with either the symphysis ([S] 43.5%, 20/46) or the ramus ([R] 28.3%, 13/46). Very large defects combining multiple segments (S-B-R, S h -B-R, RBSB, CRBS h ; S h denotes a unilateral half of the symphysis) occurred in 10 subjects (21.7%). Prior to surgery, 7 subjects were edentulous and 39 were dentate, with the dentate subjects having a mean of 12.5 teeth in the maxilla and 11.8 in the mandible. After ablative and reconstructive surgery, the total JULY
8 THE JOURNAL OF PROSTHETIC DENTISTRY GARRETT ET AL Table V. Subjects unable to complete treatment and evaluation Evaluation period Prior to PS evaluation N Prior to CP completion N Prior to CP evaluation N Prior to IP completion N Prior to IP evaluation N Recurrence/metastasis Death 1 Lost to follow-up Refused implants 2 5 Requested implants buried 1 Excluded due to radiation 1 Not a candidate (reconstruction plate) 1 Total number of teeth for those that were dentate decreased by a mean of 4.6 teeth, from 24.2 to 19.6, due in whole to the loss of teeth in the resected mandible. The 25 subjects who completed CP treatment and evaluation and the 15 who completed IP treatment and evaluation (Table IV) showed little difference in general characteristics or disease status from the total 46 who were enrolled. Participants treated with CP Only 33 subjects completed CP treatment. The loss of 28% (13/46) of the subjects prior to CP completion was greater than original estimates of a 25% loss through completion of the IP phase (Table V). This loss was due to a higher than anticipated rate of recurrent and metastatic disease. Following ablative surgery and prior to treatment with the CP, 1 subject died due to medical complications, and 10 subjects had a recurrence or metastasis. Two subjects were lost to follow-up prior to CP insertion. Of the 33 subjects completing CP treatment, 5 received complete mandibular dentures, and the remaining received RPDs. In the 28 subjects treated with an RPD, 3 to 11 mandibular teeth were present (mean ). Following treatment with the CP and before the evaluation period, 5 additional subjects had recurrences. Two subjects refused additional treatment and evaluation, and 1 was lost to follow-up. Evaluations of the CP were completed for 25 subjects, with a mean duration after CP insertion of weeks and weeks after reconstructive surgery. Failure of the CP treatment due to lack of use of the prosthesis occurred in 2 (6%) subjects. Although not considered failures, 3 prostheses had to be remade one due to further surgical intervention, another due to a change in alignment of the abutment teeth, and a third due to loss of the prosthesis. Participants treated with IP Following evaluation of the CP and prior to treatment with the IP, 1 subject had a recurrence, 1 received excessive radiation treatment (.55 Gy) precluding implants, 1 was lost to follow-up, and 5 refused implant placement (previously, 2 refused implant therapy prior to CP evaluation) (Table V). While it was planned that implants would be placed soon after healing of the osteotomy sites (4-6 months) (Fig. 1), the mean duration for Stage I implant placement was 51 weeks after reconstructive surgery. The extended duration was primarily due to delays in patient acceptance of further surgical procedures. One subject did not have implants placed until 27 months after initial surgery due to personal time constraints. A total of 58 implants were placed in 17 subjects. Nine subjects (52.9%) had 4 implants each, 6 subjects (35.3%) had 3 implants each, and 2 subjects (11.8%) had 2 implants each. One subject had implants placed, completed CP treatment, and did not return for further testing or treatment. The implant prostheses inserted were primarily unilateral removable implant-supported prostheses with milled bar attachments (81.3%, 13/ 16), with only 3 subjects (18.7%, 3/16) receiving complete mandibular implant-assisted overdentures. Three implants were considered failures due to loss of osseointegration (N=1) or unacceptable position for prosthetic restoration (N=2). No prosthesis failures were due to implant loss. Failure of the IP treatment was seen in only 1 subject (6%, 1/16), who elected to have the milled bar removed and return to a conventional prosthesis. Of the 46 participants enrolled, completion of both CP and IP treatments and follow-up evaluations were achieved for 15 (32.6%) subjects. Distribution of subjects able to attempt masticatory tests The standardized masticatory performance tests with peanuts as a test food were difficult for many participants to complete prior to surgery (Table VI), with only 28.3% able to masticate the test food on the side dominated by the defect (defect side). After recovery from reconstructive surgery but prior to definitive CP treatment, only 5.1% of the remaining 39 subjects were able to 20 VOLUME 96 NUMBER 1
9 GARRETT ET AL THE JOURNAL OF PROSTHETIC DENTISTRY Table VI. Distribution of subjects able to masticate test food Evaluation period Entry PS CP IP Defect side 28.3% (13/46) 5.1% (2/39) 44.0% (11/25) 92.9% (14/15) Nondefect side 69.6% (32/46) 61.5% (24/39) 88.0% (22/25) 92.9% (14/15) masticate the test food on the defect side, and more than one third could not masticate the food on the nondefect side. After treatment with the CP, 88% of the 25 subjects completing evaluation were able to masticate the test food on the nondefect side, while half of these continued to not be able to masticate on the defect side. After treatment with the IP, 14 of the 15 subjects completing evaluation could masticate the test food on both sides. Comparisons of subject perceptions From the questionnaire given to assess subject perceptions of their function with teeth and dentures, the percent of favorable responses to selected questions at entry and postsurgery prior to prosthetic treatment are compared in Table VII. Prior to ablative surgery, 43.5% of the subjects reported having difficulty with chewing, and over 60% indicated that their food choices were moderately to greatly limited. Social life and satisfaction with facial appearance were not strongly impacted prior to ablative surgery for 67% of the sample, and only 15% indicated their social life was moderately to strongly limited. At the postsurgical interval, the percentages of subjects having a favorable response to questions related to chewing ability, effects of chewing ability and appearance on social life, and satisfaction with facial appearance were not significantly different from entry. However, the percentage of subjects experiencing moderate to severe limitations in food choices increased from 60.9% to 78.9% (P,.05). DISCUSSION Recent advancements in facial reconstructive surgery and osseointegrated dental implants provide a treatment modality that may adequately rehabilitate oral cancer patients so that they can return to a healthy, productive life. However, functional and perceptual evaluations of these efforts are necessary before such costly procedures can be accepted for application to large numbers of patients at various health care institutions. The need for such evaluations has been stressed by health care providers and is equally important for policy makers to properly prioritize health care resources. This prospective longitudinal study was designed to assess the functional and perceptual losses following surgery and the benefits of prosthodontic treatments. Tests made prior to the ablative surgery provide initial functional estimates and assessments (presurgical), although it is recognized that impairments exist in most subjects Table VII. Percents of favorable responses (score of 1 or 2) for selected patient perception Question Entry Postsurgery 1. Chewing ability Chewing doesn t effect food choices Chewing doesn t affect social life Facial appearance satisfaction Appearance affects social life at this time due to their medical condition. 22 The second interval (postsurgical), prior to the insertion of conventional prosthesis, was selected to provide time for adaptation to the outcomes of ablative surgery and any adjunctive postoperative radiation therapy. The third test interval, 16 weeks after the insertion of the CP, was chosen to provide sufficient adaptation time to the new prosthesis. The same adaptation time, 16 weeks after insertion of the IP, was maintained for the fourth interval. The adaptation period of 4 months was selected because previous longitudinal studies on complete dentures and RPDs, including implant-supported prostheses, have shown minimal functional changes after 4 months of the insertion of a prosthesis. 34,36,59 There were significant difficulties with this population in meeting the targeted treatment and evaluation intervals. Enrollment was expected to be 10 to 12 patients per year for the first 42 months of the study, permitting treatment completion and data collection for both types of prostheses in all patients within 5 years. However, accrual of the predetermined study sample required 52 months. In terms of treatment, extended durations for implant placements were required due to adjunctive therapies and healing intervals for the grafted bone. Additionally, the extensive ablative and reconstructive surgeries delayed the patient s desire to proceed with additional surgical procedures for implant placement. This led to a much longer than expected average interval after reconstructive surgery for implant placement (mean of weeks) and for completion of the IP ( weeks). In this study and in most of the clinical applications in similar patients at UCLA, overdentures are used instead of fixed prostheses for several reasons: (1) the sacrifice of the marginal mandibular and inferior alveolar nerves during lateral composite surgery results in retraction of the lower lip, which compromises speech articulation and a patient s ability to control the confinement of JULY
10 THE JOURNAL OF PROSTHETIC DENTISTRY GARRETT ET AL saliva to the oral cavity. These problems can be resolved or minimized when the denture flange of an overlay denture repositions the lower lip labially to interact properly with the upper lip; (2) the denture flange helps to improve the facial appearance by replacing both the missing teeth as well as the alveolar segment; (3) the overdenture provides critical daily access for hygiene maintenance of implant abutments to minimize periimplant soft tissue problems; (4) the removable denture permits the placement of teeth more posteriorly than the fixed denture, thereby enabling a compromised tongue to better manage the food bolus; and (5) the initial and maintenance costs for removable prostheses are less than for fixed denture prostheses. A CP or IP was considered a failure if the patient did not use it frequently during meals, if they rejected the prosthesis, or if the IP became tissue-supported due to the loss of all implants. The decision to consider an IP a failure on the loss of all implants was made because the prosthesis support becomes similar to that of a CP. Such an outcome is clear cut. Other choices based on the number or percent of implant losses or failures would be difficult because of the wide variability in prosthesis design among patients. Only 3 prostheses that were inserted were considered failures 2 conventional prostheses and 1 implant prosthesis. Clearly, the more significant treatment issue was not the failure of implants (5.2%, 3/58) or implant prostheses (6%, 1/16 prosthesis failure), but the rejection of implant therapy by 7 of the 24 eligible subjects (29%, 7/24). While intent on being treated with the implant prosthesis at study enrollment, these subjects rejected implant treatment primarily due to difficulties coping with additional surgery, time constraints, and acceptance of the CP as being adequate. The significant loss of subjects prior to completion of the IP leads to questions regarding primary placement of implants at the time of reconstructive surgery versus secondary placement after the patient has stabilized and determined if they have a need for additional stabilization/ retention of the CP for function, esthetics, or comfort. With 35% (16 of 46) of the sample suffering recurrence, metastasis, or death within 13 months following the ablative and reconstructive surgery, there would be significant additional cost, effort, and potential complications to patients that would result in a prosthesis that would never be used. This loss would be even greater if the study sample was limited to only cancer resection patients. It should be noted that of the patients who suffered recurrences, 9 were initially treated for T 4 47 primary tumors, 1 for a T 3, and the remaining 6 for recurrent disease. In contrast, the 15 patients that completed all treatment and evaluation phases of the study included 2 treated for osteoradionecrosis, 2 for benign tumors, 1 for plate fracture, one T 1, five T 2, one T 3, two T 4, and 1 recurrent tumor. Considering that only 36 of the 46 subjects were treated for malignant tumors, the actual recurrence rate in this sample was 44% (16/36). In addition, 7 subjects were satisfied with their CPs and remaining natural dentition and indicated the potential to improve the fit of the prosthesis did not offset the additional time, surgery, and inconvenience required for implant therapy. The fact that 88% of the subjects treated with the CP could complete a masticatory test with a difficult-to-masticate food (peanuts) on the nondefect side indicates that the CP may meet at least minimal functional needs. The choices regarding further treatment with the IP were made without the consideration of cost, which was covered by the study. It is quite likely that the average cost of IP therapy of approximately $15,000 (US) for the implants and prostheses, not including hospital costs, would have deterred others from completing this treatment. IP therapy could be given at an earlier stage with primary implant placement at the time of reconstructive surgery, and the issue of additional surgery would not be a major factor in rejecting IP therapy, since only minor stage II surgery would be required. Primary implant placement also has been advocated by some groups as an alternative option to overcome the problems of implant placement in irradiated bone, 44,45 including higher implant failures and possible osteoradionecrosis. Hyperbaric oxygen therapy is generally prescribed when the implant sites are exposed to greater than 50 Gy radiation in the hopes of improving the vascularity and quality of the bone and irradiated soft tissues In this study protocol, HBO was not used due to issues related to the relatively high costs in time, dollars, and potential complications. 39,43 Additionally, it has not been unequivocally demonstrated that primary implant placement or HBO obviates all or any of the problems or issues discussed previously. 23,29,46 Limitations in the number of subjects enrolled from a single institution indicate that future studies would benefit from multi-institutional participation. Greater sample size would permit an increase in the number of participants completing both conventional and implantbased prosthetic treatments, resulting in greater ability to evaluate subgroups of patients. Even with the restrictive inclusion/exclusion requirements, large differences in defects and dentition status occurred in the present study. It is difficult to assess the effects of treatment type on small subgroups of 2 to 3 subjects with similar characteristics. In addition, the relatively small participant pool necessitated a within-subject design without randomization of treatment order. The effect of a longer adaptation period to the surgical interventions at the time of evaluation of the IP compared to the CP is unknown. CONCLUSIONS Conventional prosthesis treatment was completed in 72% (33/46) of the subjects enrolled in this study. 22 VOLUME 96 NUMBER 1
11 GARRETT ET AL THE JOURNAL OF PROSTHETIC DENTISTRY However, due to high rates of recurrence/metastasis (44%) during the first year following ablative surgery for subjects treated for malignant tumors, and rejection of implant therapy by 7 of the 33 subjects treated with a CP, only 16 subjects were treated with the IP. Treatment failures of either the CP (6%, 2/33) or IP (6%, 1/16) were limited and were related to lack of use or subject preference for alternative treatment. In the reconstructed mandibulectomy patient, initial treatment with a CP and secondary implant placement permit the assessment of the functional level of the patient prior to recommending further treatment options, including use of IPs. Secondary placement also allows for a disease-free period before the initiation of extensive dental procedures. REFERENCES 1. Jemal A, Thomas A, Murray T, Thun M. Cancer statistics, CA Cancer J Clin 2002;52: Silverman S Jr. Demographics and occurrence of oral and pharyngeal cancers. The outcomes, the trends, the challenge. J Am Dent Assoc 2001; 132(Suppl):7S-11S. 3. Silverberg E, Boring CC, Squires TS. Cancer statistics, CA Cancer J Clin 1990;40: Logemann JA, Bytell DE. Swallowing disorders in three types of head and neck surgical patients. Cancer 1979;44: Beumer J, Marunick MT, Curtis TA, Roumanas E. Acquired defects of the mandible: aetiology, treatment and rehabilitation. In: Beumer J, Curtis TA, Marunick MT, editors. Maxillofacial rehabilitation: prosthodontic and surgical considerations. St. Louis: Ishiyaku EuroAmerica; p Finlay PM, Dawson F, Robertson AG, Soutar DS. An evaluation of functional outcome after surgery and radiotherapy for intraoral cancer. Br J Oral Maxillofac Surg 1992;30: Marunick M, Mahmassani O, Siddoway J, Klein B. Prospective analysis of masticatory function following lateral mandibulotomy. J Surg Oncol 1991;47: Marunick M, Mathes BE, Klein BB, Seyedsadr M. Occlusal force after partial mandibular resection. J Prosthet Dent 1992;67: Marunick MT, Mathes BE, Klein BB. Masticatory function in hemimandibulectomy patients. J Oral Rehabil 1992;19: McConnel FM, Pauloski BR, Logemann JA, Rademaker AW, Colangelo L, Shedd D, et al. Functional results of primary closure vs flaps in oropharyngeal reconstruction: a prospective study of speech and swallowing. Arch Otolaryngol Head Neck Surg 1998;124: Schliephake H, Schmelzeisen R, Schonweiler R, Schneller T, Altenbernd C. Speech, deglutition and life quality after intraoral tumour resection. A prospective study. Int J Oral Maxillofac Surg 1998;27: Komisar A. The functional result of mandibular reconstruction. Laryngoscope 1990;100: Hidalgo DA. Fibula free flap: a new method of mandible reconstruction. Plast Reconstr Surg 1989;84: Hidalgo DA. Aesthetic improvements in free-flap mandible reconstruction. Plast Reconstr Surg 1991;88:574-85; discussion Jewer DD, Boyd JB, Manktelow RT, Zuker RM, Rosen IB, Gullane PJ, et al. Orofacial and mandibular reconstruction with the iliac crest free flap: a review of 60 cases and a new method of classification. Plast Reconstr Surg 1989;84: ; discussion Soutar DS, Widdowson WP. Immediate reconstruction of the mandible using a vascularized segment of radius. Head Neck Surg 1986;8: Matloub HS, Larson DL, Kuhn JC, Yousif NJ, Sanger JR. Lateral arm free flap in oral cavity reconstruction: a functional evaluation. Head Neck 1989;11: Hsiao HT, Leu YS, Lin CC. Primary closure versus radial forearm flap reconstruction after hemiglossectomy: functional assessment of swallowing and speech. Ann Plast Surg 2002;49: McConnel FM, Teichgraeber JF, Adler RK. A comparison of three methods of oral reconstruction. Arch Otolaryngol Head Neck Surg 1987;113: Pauloski BR, Rademaker AW, Logemann JA, McConnel FM, Heiser MA, Cardinale S, et al. Surgical variables affecting swallowing in patients treated for oral/oropharyngeal cancer. Head Neck 2004;26: Hsiao HT, Leu YS, Chang SH, Lee JT. Swallowing function in patients who underwent hemiglossectomy: comparison of primary closure and free radial forearm flap reconstruction with videofluoroscopy. Ann Plast Surg 2003;50: Wagner JD, Coleman JJ 3rd, Weisberger E, Righi PD, Radpour S, McGarvey S, et al. Predictive factors for functional recovery after free tissue transfer oromandibular reconstruction. Am J Surg 1998;176: Schliephake H, Neukam FW, Schmelzeisen R, Wichmann M. Long-term results of endosteal implants used for restoration of oral function after oncologic surgery. Int J Oral Maxillofac Surg 1999;28: Roumanas ED, Markowitz BL, Lorant JA, Calcaterra TC, Jones NF, Beumer J 3rd. Reconstructed mandibular defects: fibula free flaps and osseointegrated implants. Plast Reconstr Surg 1997;99: Urken ML, Buchbinder D, Weinberg H, Vickery C, Sheiner A, Biller HF. Primary placement of osseointegrated implants in microvascular mandibular reconstruction. Otolaryngol Head Neck Surg 1989;101: Riediger D. Restoration of masticatory function by microsurgically revascularized iliac crest bone grafts using enosseous implants. Plast Reconstr Surg 1988;81: Lukash FN, Sachs SA, Fischman B, Attie JN. Osseointegrated denture in a vascularized bone transfer: functional jaw reconstruction. Ann Plast Surg 1987;19: Barber HD, Seckinger RJ, Hayden RE, Weinstein GS. Evaluation of osseointegration of endosseous implants in radiated, vascularized fibula flaps to the mandible: a pilot study. J Oral Maxillofac Surg 1995;53: 640-4; discussion Schmelzeisen R, Neukam FW, Shirota T, Specht B, Wichmann M. Postoperative function after implant insertion in vascularized bone grafts in maxilla and mandible. Plast Reconstr Surg 1996;97: Curtis DA, Plesh O, Miller AJ, Curtis TA, Sharma A, Schweitzer R, et al. A comparison of masticatory function in patients with or without reconstruction of the mandible. Head Neck 1997;19: Urken ML, Buchbinder D, Weinberg H, Vickery C, Sheiner A, Parker R, et al. Functional evaluation following microvascular oromandibular reconstruction of the oral cancer patient: a comparative study of reconstructed and nonreconstructed patients. Laryngoscope 1991;101: Matsui Y, Neukam FW, Schmelzeisen R, Ohno K. Masticatory function of postoperative tumor patients rehabilitated with osseointegrated implants. J Oral Maxillofac Surg 1996;54: Curtis DA, Plesh O, Hannam AG, Sharma A, Curtis TA. Modeling of jaw biomechanics in the reconstructed mandibulectomy patient. J Prosthet Dent 1999;81: Garrett NR, Kapur KK, Hamada MO, Roumanas ED, Freymiller E, Han T, et al. A randomized clinical trial comparing the efficacy of mandibular implant-supported overdentures and conventional dentures in diabetic patients. Part II. Comparisons of masticatory performance. J Prosthet Dent 1998;79: Garrett NR, Perez P, Elbert C, Kapur KK. Effects of improvements of poorly fitting dentures and new dentures on masticatory performance. J Prosthet Dent 1996;75: Kapur KK. Veterans Administration Cooperative Dental Implant Study comparisons between fixed partial dentures supported by blade-vent implants and removable partial dentures. Part III: comparisons of masticatory scores between two treatment modalities. J Prosthet Dent 1991;65: Kapur KK, Garrett NR. Studies of biologic parameters for denture design. Part II: comparison of masseter muscle activity, masticatory performance, and salivary secretion rates between denture and natural dentition groups. J Prosthet Dent 1984;52: Urken ML, Weinberg H, Vickery C, Buchbinder D, Lawson W, Biller HF. Oromandibular reconstruction using microvascular composite free flaps. Report of 71 cases and a new classification scheme for bony, soft-tissue, and neurologic defects. Arch Otolaryngol Head Neck Surg 1991;117: Granstrom G, Jacobsson M, Tjellstrom A. Titanium implants in irradiated tissue: benefits from hyperbaric oxygen. Int J Oral Maxillofac Implants 1992;7: JULY
12 THE JOURNAL OF PROSTHETIC DENTISTRY GARRETT ET AL 40. Granstrom G, Tjellstrom A, Branemark PI, Fornander J. Bone-anchored reconstruction of the irradiated head and neck cancer patient. Otolaryngol Head Neck Surg 1993;108: Johnsson K, Hansson A, Granstrom G, Jacobsson M, Turesson I. The effects of hyperbaric oxygenation on bone-titanium implant interface strength with and without preceding irradiation. Int J Oral Maxillofac Implants 1993;8: Larsen PE, Stronczek MJ, Beck FM, Rohrer M. Osteointegration of implants in radiated bone with and without adjunctive hyperbaric oxygen. J Oral Maxillofac Surg 1993;51: Marx RE, Ames JR. The use of hyperbaric oxygen therapy in bony reconstruction of the irradiated and tissue-deficient patient. J Oral Maxillofac Surg 1982;40: Buchbinder D, Urken ML, Vickery C, Weinberg H, Sheiner A, Biller H. Functional mandibular reconstruction of patients with oral cancer. Oral Surg Oral Med Oral Pathol 1989;68: ; discussion Sclaroff A, Haughey B, Gay WD, Paniello R. Immediate mandibular reconstruction and placement of dental implants. At the time of ablative surgery. Oral Surg Oral Med Oral Pathol 1994;78: Marunick MT, Roumanas ED. Functional criteria for mandibular implant placement post resection and reconstruction for cancer. J Prosthet Dent 1999;82: Greene FL, Page DL, Fleming ID, Fritz A, Balch CM, editors. AJCC cancer staging handbook. 6th ed. Hoboken (NJ): Springer; p Kapur KK, Garrett NR, Hamada MO, Roumanas ED, Freymiller E, Han T, et al. Randomized clinical trial comparing the efficacy of mandibular implant-supported overdentures and conventional dentures in diabetic patients. Part III: comparisons of patient satisfaction. J Prosthet Dent 1999;82: Wayler AH, Kapur KK, Feldman RS, Chauncey HH. Effects of age and dentition status on measures of food acceptability. J Gerontol 1982;37: Kapur KK. Veterans administration cooperative implant study. Comparisons between fixed partial dentures supported by blade-vent implants and removable partial dentures. Part I: methodology and comparisons between treatment groups at baseline. J Prosthet Dent 1987;58: Chauncey HH, Muench ME, Kapur KK, Wayler AH. The effect of the loss of teeth on diet and nutrition. Int Dent J 1984;34: Feldman RS, Kapur KK, Alman JE, Chauncey HH. Aging and mastication: changes in performance and in the swallowing threshold with natural dentition. J Am Geriatr Soc 1980;28: Roumanas ED, Garrett NR, Hamada MO, Diener RM, Kapur KK. A randomized clinical trial comparing the efficacy of mandibular implantsupported overdentures and conventional dentures in diabetic patients. Part V: food preference comparisons. J Prosthet Dent 2002;87: Phillips C, Trentini CJ, Douvartzidis N. The effect of treatment on facial attractiveness. J Oral Maxillofac Surg 1992;50: Kapur KK, Collister T, Fischer EE. Masticatory and gustatory salivary reflex secretion rates and taste thresholds of denture wearers. J Prosthet Dent 1967;18: Kapur KK, Collister T. A study of food textural discrimination in persons with natural and artificial dentitions. In: Bosman LJ, editor. Second symposium on oral sensation and perception. Springfield (IL): Charles C. Thomas; p Garrett NR, Hasse AL, Kapur KK. Comparisons of tactile thresholds between implant-supported fixed partial dentures and removable partial dentures. Int J Prosthodont 1992;5: Garrett NR, Kapur KK, Jochen DG. Oral stereognostic ability and masticatory performance in denture wearers. Int J Prosthodont 1994;7: Garrett NR, Perez P, Elbert C, Kapur KK. Effects of improvements of poorly fitting dentures and new dentures on masseter activity during chewing. J Prosthet Dent 1996;76: Reprint requests to: DR NEAL GARRETT UCLA SCHOOL OF DENTISTRY LE CONTE AVE, B3-087 CHS LOS ANGELES, CA FAX: ngarrett@ucla.edu /$32.00 Copyright Ó 2006 by The Editorial Council of The Journal of Prosthetic Dentistry. doi: /j.prosdent Noteworthy Abstracts of the Current Literature Temporomandibular disorders among smokers and nonsmokers: A longitudinal cohort study Wanman A. J Orofac Pain 2005;19: Aims: To evaluate whether smoking influences the presence and/or development of signs and symptoms of temporomandibular disorders (TMD) among adults. Methods: A random sample of subjects 35, 50, and 65 years of age was drawn from the general population and examined with the aid of a questionnaire and a clinical examination. Within the sample, smokers were identified based on reported current smoking and nonsmokers were matched to the smokers based on age, gender, educational level, area of residence, and number of teeth. In total, 268 subjects were matched (134 pairs). Six years after the baseline examination, 122 matched pairs were re-examined. Results: Mild symptoms of TMD were reported by approximately 30% of the sample both at baseline and at the follow-up examination 6 years later. Pain in the jaws and/or more severe symptoms of TMD were reported by approximately 15% on both occasions. No significant differences between smokers and nonsmokers were found regarding symptoms of TMD. In both examinations, mild signs (dysfunction index I) were found in approximately 40% of the sample and moderate to severe signs (dysfunction index II to III) in approximately 20%; no statistically significant differences were found between smokers and nonsmokers. No significant differences were found between smokers and nonsmokers regarding the course of symptoms or signs of TMD during the study period. Conclusion: Smoking is not a factor related to the presence or development of signs and symptoms of TMD. Reprinted with permission of Quintessence Publishing. 24 VOLUME 96 NUMBER 1
IMPLANT DENTISTRY EXAM BANK
 IMPLANT DENTISTRY EXAM BANK 1. Define osseointegration. (4 points, 1/4 2. What are the critical components of an acceptable clinical trial? (10 points) 3. Compare the masticatory performance of individuals
IMPLANT DENTISTRY EXAM BANK 1. Define osseointegration. (4 points, 1/4 2. What are the critical components of an acceptable clinical trial? (10 points) 3. Compare the masticatory performance of individuals
Ridge Reconstruction for Implant Placement
 Volume 1, No. 5 July/August 2009 The Journal of Implant & Advanced Clinical Dentistry Ridge Reconstruction for Implant Placement 2 Hours of CE Credit Oral Implications of Cancer Chemotherapy Immediate
Volume 1, No. 5 July/August 2009 The Journal of Implant & Advanced Clinical Dentistry Ridge Reconstruction for Implant Placement 2 Hours of CE Credit Oral Implications of Cancer Chemotherapy Immediate
The Impact of Dental Implants on Maxillofacial Patient s Quality of Life
 46 The Open Pathology Journal, 2011, 5, 46-51 Open Access The Impact of Dental Implants on Maxillofacial Patient s Quality of Life Jorge Gonzalez * Center for Maxillofacial Prosthodontics, Baylor College
46 The Open Pathology Journal, 2011, 5, 46-51 Open Access The Impact of Dental Implants on Maxillofacial Patient s Quality of Life Jorge Gonzalez * Center for Maxillofacial Prosthodontics, Baylor College
IMPLANT CONSENT FORM WHAT ARE DENTAL IMPLANTS?
 IMPLANT CONSENT FORM WHAT ARE DENTAL IMPLANTS? Dental implants are a very successful and accepted treatment option to replace lost or missing teeth. A dental implant is essentially an artificial tooth
IMPLANT CONSENT FORM WHAT ARE DENTAL IMPLANTS? Dental implants are a very successful and accepted treatment option to replace lost or missing teeth. A dental implant is essentially an artificial tooth
Improving Esthetics with Sequential Treatment Planning and Implant-Retained Dentures
 Improving Esthetics with Sequential Treatment Planning and Implant-Retained Dentures by Timothy F. Kosinski, DDS, MAGD While oral function is the primary concern for most patients, the importance of esthetics
Improving Esthetics with Sequential Treatment Planning and Implant-Retained Dentures by Timothy F. Kosinski, DDS, MAGD While oral function is the primary concern for most patients, the importance of esthetics
Australian Dental Journal
 Australian Dental Journal The official journal of the Australian Dental Association SCIENTIFIC ARTICLE Australian Dental Journal 2011; 56: 160 165 doi: 10.1111/j.1834-7819.2011.01318.x Oral rehabilitation
Australian Dental Journal The official journal of the Australian Dental Association SCIENTIFIC ARTICLE Australian Dental Journal 2011; 56: 160 165 doi: 10.1111/j.1834-7819.2011.01318.x Oral rehabilitation
UNMH Oral and Maxillofacial Surgery Clinical Privileges
 All new applicants must meet the following requirements as approved by the UNMH Board of Trustees effective: 09/26/2014 INSTRUCTIONS Applicant: Check off the "Requested" box for each privilege requested.
All new applicants must meet the following requirements as approved by the UNMH Board of Trustees effective: 09/26/2014 INSTRUCTIONS Applicant: Check off the "Requested" box for each privilege requested.
SCD Case Study. Treatment Considerations for Implant Rehabilitation
 SCD Case Study Treatment Considerations for Implant Rehabilitation Multiple surgical and restorative factors play a role in the treatment planning of implant restorations for the edentulous patient (Ali
SCD Case Study Treatment Considerations for Implant Rehabilitation Multiple surgical and restorative factors play a role in the treatment planning of implant restorations for the edentulous patient (Ali
Case Report Mandibular Rehabilitation with Dental Implants: A case report
 Mandibular Rehabilitation with Dental Implants: A case report Yueh-Ling Chao, DDS School of Dentistry, National Taiwan University, Taipei, Taiwan Graduate student, Graduate Institute of Clinical Dentistry,
Mandibular Rehabilitation with Dental Implants: A case report Yueh-Ling Chao, DDS School of Dentistry, National Taiwan University, Taipei, Taiwan Graduate student, Graduate Institute of Clinical Dentistry,
Residency Competency and Proficiency Statements
 Residency Competency and Proficiency Statements 1. REQUEST AND RESPOND TO REQUESTS FOR CONSULTATIONS Identify needs and make referrals to appropriate health care providers for the treatment of physiologic,
Residency Competency and Proficiency Statements 1. REQUEST AND RESPOND TO REQUESTS FOR CONSULTATIONS Identify needs and make referrals to appropriate health care providers for the treatment of physiologic,
Supervisors: Dr. Farhan Raza Khan
 1 Presenter: Dr. Sana Ehsen Supervisors: Dr. Farhan Raza Khan 2 A dental implant (also known as an endosseous implant or fixture) is a surgical component that interfaces with the bone of the jaw to support
1 Presenter: Dr. Sana Ehsen Supervisors: Dr. Farhan Raza Khan 2 A dental implant (also known as an endosseous implant or fixture) is a surgical component that interfaces with the bone of the jaw to support
Clinical and Laboratory Procedures for Fixed Margin Implant Abutments
 Clinical and Laboratory Procedures for Fixed Margin Implant Abutments Dr. Carl Drago DDS, MS, American Board of Prosthodontics Director, Dental Research BIOMET 3i, Adjunct Faculty Department of Prosthodontics,
Clinical and Laboratory Procedures for Fixed Margin Implant Abutments Dr. Carl Drago DDS, MS, American Board of Prosthodontics Director, Dental Research BIOMET 3i, Adjunct Faculty Department of Prosthodontics,
Oftentimes, as implant surgeons, we are
 CLINICAL AVOIDING INJURY TO THE INFERIOR ALVEOLAR NERVE BY ROUTINE USE OF INTRAOPERATIVE RADIOGRAPHS DURING IMPLANT PLACEMENT Jeffrey Burstein, DDS, MD; Chris Mastin, DMD; Bach Le, DDS, MD Injury to the
CLINICAL AVOIDING INJURY TO THE INFERIOR ALVEOLAR NERVE BY ROUTINE USE OF INTRAOPERATIVE RADIOGRAPHS DURING IMPLANT PLACEMENT Jeffrey Burstein, DDS, MD; Chris Mastin, DMD; Bach Le, DDS, MD Injury to the
What Dental Implants Can Do For You!
 What Dental Implants Can Do For You! Putting Smiles into Motion About Implants 01. What if a Tooth is Lost and the Area is Left Untreated? 02. Do You Want to Restore Confidence in Your Appearance? 03.
What Dental Implants Can Do For You! Putting Smiles into Motion About Implants 01. What if a Tooth is Lost and the Area is Left Untreated? 02. Do You Want to Restore Confidence in Your Appearance? 03.
Long-term success of osseointegrated implants
 Against All Odds A No Bone Solution Long-term success of osseointegrated implants depends on the length of the implants used and the quality and quantity of bone surrounding these implants. As surgical
Against All Odds A No Bone Solution Long-term success of osseointegrated implants depends on the length of the implants used and the quality and quantity of bone surrounding these implants. As surgical
PATIENT INFORM CONSENT for IMPLANT RESTORATION Rev 04.2012
 PATIENT INFORM CONSENT for IMPLANT RESTORATION Rev 04.2012 Implant placement and restoration involves two major stages: surgical placement of the implant(s) followed by the restoration of the implant after
PATIENT INFORM CONSENT for IMPLANT RESTORATION Rev 04.2012 Implant placement and restoration involves two major stages: surgical placement of the implant(s) followed by the restoration of the implant after
Resorptive Changes of Maxillary and Mandibular Bone Structures in Removable Denture Wearers
 Resorptive Changes of Maxillary and Mandibular Bone Structures in Removable Denture Wearers Dubravka KnezoviÊ-ZlatariÊ Asja»elebiÊ Biserka LaziÊ Department of Prosthodontics School of Dental Medicine University
Resorptive Changes of Maxillary and Mandibular Bone Structures in Removable Denture Wearers Dubravka KnezoviÊ-ZlatariÊ Asja»elebiÊ Biserka LaziÊ Department of Prosthodontics School of Dental Medicine University
Dental care and treatment for patients with head and neck cancer. Department of Restorative Dentistry Information for patients
 Dental care and treatment for patients with head and neck cancer Department of Restorative Dentistry Information for patients i Why have I been referred to the Restorative Dentistry Team? Treatment of
Dental care and treatment for patients with head and neck cancer Department of Restorative Dentistry Information for patients i Why have I been referred to the Restorative Dentistry Team? Treatment of
Regions Hospital Delineation of Privileges Oral & Maxillofacial Surgery
 Regions Hospital Delineation of Privileges al & Maxillofacial Surgery Applicant s Name: Last First M. Instructions: Place a check-mark where indicated for each core group you are requesting. Review education
Regions Hospital Delineation of Privileges al & Maxillofacial Surgery Applicant s Name: Last First M. Instructions: Place a check-mark where indicated for each core group you are requesting. Review education
Replacement of the upper left central incisor with a Straumann Bone Level Implant and a Straumann Customized Ceramic Abutment
 Replacement of the upper left central incisor with a Straumann Bone Level Implant and a Straumann Customized Ceramic Abutment by Dr. Ronald Jung and Master Dental Technician Xavier Zahno Initial situation
Replacement of the upper left central incisor with a Straumann Bone Level Implant and a Straumann Customized Ceramic Abutment by Dr. Ronald Jung and Master Dental Technician Xavier Zahno Initial situation
CLINICAL GOALS OF PATIENT CARE AND CLINIC MANAGEMENT. Philosophical Basis of the Patient Care System. Patient Care Goals
 University of Washington School of Dentistry CLINICAL GOALS OF PATIENT CARE AND CLINIC MANAGEMENT Philosophical Basis of the Patient Care System The overall mission of the patient care system in the School
University of Washington School of Dentistry CLINICAL GOALS OF PATIENT CARE AND CLINIC MANAGEMENT Philosophical Basis of the Patient Care System The overall mission of the patient care system in the School
Dr Ansgar C Cheng BDS, MS, FRCDC, FRACDS, FAM(S), FCDSS, MRACDS, Cert. Pros., Cert. MaxFac. Pros.
 I M P L A N T S in IRRADIATED TISSUES Dr Ansgar C Cheng BDS, MS, FRCDC, FRACDS, FAM(S), FCDSS, MRACDS, Cert. Pros., Cert. MaxFac. Pros. Adj Associate Professor, National University of Singapore Chair,
I M P L A N T S in IRRADIATED TISSUES Dr Ansgar C Cheng BDS, MS, FRCDC, FRACDS, FAM(S), FCDSS, MRACDS, Cert. Pros., Cert. MaxFac. Pros. Adj Associate Professor, National University of Singapore Chair,
PREPARATION OF MOUTH FOR REMOVABLE PARTIAL DENTURES Dr. Mazen kanout
 PREPARATION OF MOUTH FOR REMOVABLE PARTIAL DENTURES Dr. Mazen kanout Mouth preparation includes procedures in four categories: 1. Oral Surgical Preparation. 2. Conditioning of Abused and Irritated Tissue.
PREPARATION OF MOUTH FOR REMOVABLE PARTIAL DENTURES Dr. Mazen kanout Mouth preparation includes procedures in four categories: 1. Oral Surgical Preparation. 2. Conditioning of Abused and Irritated Tissue.
Life Table Analysis for Evaluating Curative-effect of One-stage Non-submerged Dental Implant in Taiwan
 Journal of Data Science 6(2008), 591-599 Life Table Analysis for Evaluating Curative-effect of One-stage Non-submerged Dental Implant in Taiwan Miin-Jye Wen 1, Chuen-Chyi Tseng 2 and Cheng K. Lee 3 1 National
Journal of Data Science 6(2008), 591-599 Life Table Analysis for Evaluating Curative-effect of One-stage Non-submerged Dental Implant in Taiwan Miin-Jye Wen 1, Chuen-Chyi Tseng 2 and Cheng K. Lee 3 1 National
Retention of maxillary implant overdenture bars of different designs
 Retention of maxillary implant overdenture bars of different designs Brian H. Williams, DDS, a Kent T. Ochiai, DDS, b Satoru Hojo, DDS, PhD, c Russell Nishimura, DDS, d and Angelo A. Caputo, PhD e School
Retention of maxillary implant overdenture bars of different designs Brian H. Williams, DDS, a Kent T. Ochiai, DDS, b Satoru Hojo, DDS, PhD, c Russell Nishimura, DDS, d and Angelo A. Caputo, PhD e School
BIOMECHANICAL ANALYSIS OF NORMAL AND IMPLANTED TOOTH USING BITING FORCE MEASUREMENT
 BIOMECHANICAL ANALYSIS OF NORMAL AND IMPLANTED TOOTH USING BITING FORCE MEASUREMENT B K Biswas 1 S Bag 2 & S Pal 3 1. Dept. of Dental Surgery, Associate Professor, KPC Medical College & Hospital, Kolkata,
BIOMECHANICAL ANALYSIS OF NORMAL AND IMPLANTED TOOTH USING BITING FORCE MEASUREMENT B K Biswas 1 S Bag 2 & S Pal 3 1. Dept. of Dental Surgery, Associate Professor, KPC Medical College & Hospital, Kolkata,
Ideal treatment of the impaired
 RESEARCH IMPLANTS AS ANCHORAGE IN ORTHODONTICS: ACLINICAL CASE REPORT Dale B. Herrero, DDS KEY WORDS External anchorage Pneumatized Often, in dental reconstruction, orthodontics is required for either
RESEARCH IMPLANTS AS ANCHORAGE IN ORTHODONTICS: ACLINICAL CASE REPORT Dale B. Herrero, DDS KEY WORDS External anchorage Pneumatized Often, in dental reconstruction, orthodontics is required for either
Don t Let Life Pass You By Because Of Missing Teeth
 Don t Let Life Pass You By Because Of Missing Teeth Ask For Dental Implant Solutions From BIOMET 3i Scan With Your Smartphone! In order to scan QR codes, your mobile device must have a QR code reader installed.
Don t Let Life Pass You By Because Of Missing Teeth Ask For Dental Implant Solutions From BIOMET 3i Scan With Your Smartphone! In order to scan QR codes, your mobile device must have a QR code reader installed.
More than a fixed rehabilitation.
 More than a fixed rehabilitation. A reason to smile. In combination with: Patient expectations drive dental treatments for fixed edentulous immediate restorations. Patients today have increasingly high
More than a fixed rehabilitation. A reason to smile. In combination with: Patient expectations drive dental treatments for fixed edentulous immediate restorations. Patients today have increasingly high
There When You Need Them: 10 Principles of Successful RPD Treatment
 There When You Need Them: 10 Principles of Successful RPD Treatment Jeff Scott, DMD Jeff.Scott@jeffscottdentistry.com 239 2 nd Ave South Suite 100 St. Petersburg, FL 33701 The West Coast District Dental
There When You Need Them: 10 Principles of Successful RPD Treatment Jeff Scott, DMD Jeff.Scott@jeffscottdentistry.com 239 2 nd Ave South Suite 100 St. Petersburg, FL 33701 The West Coast District Dental
Osseointegrated craniofacial implants in the rehabilitation of orbital defects: An update of a retrospective experience in the United States
 Osseointegrated craniofacial implants in the rehabilitation of orbital defects: An update of a retrospective experience in the United States Joseph A. Toljanic, DDS, a Steven E. Eckert, DDS, MS, b Eleni
Osseointegrated craniofacial implants in the rehabilitation of orbital defects: An update of a retrospective experience in the United States Joseph A. Toljanic, DDS, a Steven E. Eckert, DDS, MS, b Eleni
Tuition and Fees Dentists - Full time (per annum): 20,000
 Diploma of Oral Surgery Residency Training Program in preparation for the Fachzahnarzt in Oral Surgery Specialty Examination in the Republic of Germany Degree awarded: - Diploma of Oral Surgery - Fachzahnarzt
Diploma of Oral Surgery Residency Training Program in preparation for the Fachzahnarzt in Oral Surgery Specialty Examination in the Republic of Germany Degree awarded: - Diploma of Oral Surgery - Fachzahnarzt
Restoring quality to life. Dental implants. A naturally better solution. Patient Education
 Restoring quality to life. Dental implants. A naturally better solution. Patient Education Dental implants: A better treatment option. What are dental implants? Dental implants are a safe, medically proven,
Restoring quality to life. Dental implants. A naturally better solution. Patient Education Dental implants: A better treatment option. What are dental implants? Dental implants are a safe, medically proven,
Placement of Dental Implants in Irradiated Bone: The Case for Using Hyperbaric Oxygen
 CLINICAL CONTROVERSIES IN ORAL AND MAXILLOFACIAL SURGERY: PART ONE J Oral Maxillofac Surg 64:812-818, 2006 Placement of Dental Implants in Irradiated Bone: The Case for Using Hyperbaric Oxygen Gösta Granström,
CLINICAL CONTROVERSIES IN ORAL AND MAXILLOFACIAL SURGERY: PART ONE J Oral Maxillofac Surg 64:812-818, 2006 Placement of Dental Implants in Irradiated Bone: The Case for Using Hyperbaric Oxygen Gösta Granström,
Position Classification Standard for Dental Officer Series, GS-0680
 Position Classification Standard for Dental Officer Series, GS-0680 Table of Contents SERIES DEFINITION... 2 BACKGROUND... 2 TITLES... 3 GRADE-LEVEL EVALUATION CRITERIA... 3 NOTES ON THE USE OF THE STANDARDS...
Position Classification Standard for Dental Officer Series, GS-0680 Table of Contents SERIES DEFINITION... 2 BACKGROUND... 2 TITLES... 3 GRADE-LEVEL EVALUATION CRITERIA... 3 NOTES ON THE USE OF THE STANDARDS...
Current Concepts in American Dentistry: Advances in Implantology and Oral Rehabilitation
 2009 New York University College Of Dentistry Linhart Continuing Dental Education Program Presents Current Concepts in American Dentistry: Advances in Implantology and Oral Rehabilitation International
2009 New York University College Of Dentistry Linhart Continuing Dental Education Program Presents Current Concepts in American Dentistry: Advances in Implantology and Oral Rehabilitation International
05 - DENTAL SURGERY. (02) MS (Oral Surgery) Part II Examination
 05 - DENTAL SURGERY (02) MS (Oral Surgery) Part II Examination 01. October 1990 02. October 1991 03. October 1992 04. October 1993 05. October 1994 06. November 1995 07. October 1996 08. November 1997
05 - DENTAL SURGERY (02) MS (Oral Surgery) Part II Examination 01. October 1990 02. October 1991 03. October 1992 04. October 1993 05. October 1994 06. November 1995 07. October 1996 08. November 1997
LATERAL BONE EXPANSION FOR IMMEDIATE PLACEMENT OF ENDOSSEOUS DENTAL IMPLANTS
 LATERAL BONE EXPANSION FOR IMMEDIATE PLACEMENT OF ENDOSSEOUS DENTAL IMPLANTS Department of Oral Maxillofacial Surgery, Chisinau Abstract: The study included 10 using the split control expansion technique
LATERAL BONE EXPANSION FOR IMMEDIATE PLACEMENT OF ENDOSSEOUS DENTAL IMPLANTS Department of Oral Maxillofacial Surgery, Chisinau Abstract: The study included 10 using the split control expansion technique
A Comprehensive Explanation
 Dental Implants A Comprehensive Explanation Overview Since the 1980s, dental implants have become more popular among dentists and patients. 1 In some clinical situations, implants may be the best treatment
Dental Implants A Comprehensive Explanation Overview Since the 1980s, dental implants have become more popular among dentists and patients. 1 In some clinical situations, implants may be the best treatment
Tooth Replacement Options
 Dr. Jordan Johnson Johnson Dental Associates http://www.beta.mydentalhub.com/ada/test/ (800) 947-4746 Tooth Replacement Options If you re missing one or more teeth, you may be all too aware of their importance
Dr. Jordan Johnson Johnson Dental Associates http://www.beta.mydentalhub.com/ada/test/ (800) 947-4746 Tooth Replacement Options If you re missing one or more teeth, you may be all too aware of their importance
Straumann Bone Level Tapered Implant Peer-to-peer communication
 Straumann Bone Level Tapered Implant Peer-to-peer communication Clinical cases April, 2015 Clinical Cases Case No. Site 1 Single unit; Anterior Maxilla 2 Multi-unit; Anterior Maxilla Implant placement
Straumann Bone Level Tapered Implant Peer-to-peer communication Clinical cases April, 2015 Clinical Cases Case No. Site 1 Single unit; Anterior Maxilla 2 Multi-unit; Anterior Maxilla Implant placement
A New Beginning with Dental Implants. A Guide to Understanding Your Treatment Options
 A New Beginning with Dental Implants A Guide to Understanding Your Treatment Options Why Should I Replace My Missing Teeth? Usually, when you lose a tooth, it is best for your oral health to have it replaced.
A New Beginning with Dental Implants A Guide to Understanding Your Treatment Options Why Should I Replace My Missing Teeth? Usually, when you lose a tooth, it is best for your oral health to have it replaced.
GIVE YOUR PATIENTS THE FREEDOM TO EAT, SPEAK AND LAUGH AGAIN.
 Now Distributed By GIVE YOUR PATIENTS THE FREEDOM TO EAT, SPEAK AND LAUGH AGAIN. OPENING MINDS AND EXPANDING PRACTICE REVENUE OPPORTUNITIES Since the McGill Consensus in 2002, the dental industry has recognized
Now Distributed By GIVE YOUR PATIENTS THE FREEDOM TO EAT, SPEAK AND LAUGH AGAIN. OPENING MINDS AND EXPANDING PRACTICE REVENUE OPPORTUNITIES Since the McGill Consensus in 2002, the dental industry has recognized
2016 Buy Up Dental Care Plan Procedure List
 * This is in addition to the embedded Preventive Plan (see procedure list at deltadentalco.com/kp_preventive. BASIC SERVICES Minor Restorative Services D2140 Amalgam 1 surface, primary or permanent D2150
* This is in addition to the embedded Preventive Plan (see procedure list at deltadentalco.com/kp_preventive. BASIC SERVICES Minor Restorative Services D2140 Amalgam 1 surface, primary or permanent D2150
Understanding Dental Implants
 Understanding Dental Implants Comfort and Confidence Again A new smile It s no fun when you re missing teeth. You may not feel comfortable eating or speaking. You might even avoid smiling in public. Fortunately,
Understanding Dental Implants Comfort and Confidence Again A new smile It s no fun when you re missing teeth. You may not feel comfortable eating or speaking. You might even avoid smiling in public. Fortunately,
Dr. Little received his doctorate degree in dentistry from UT Health at San Antonio Dental
 Implant Solutions for the Implant Patient: Diagnosis and Treatment Planning for Predictable Results David Little, DDS 6961 U.S. Highway 87 East San Antonio, TX 78263 Phone: (210)648-4411 Fax: (210) 648-6498
Implant Solutions for the Implant Patient: Diagnosis and Treatment Planning for Predictable Results David Little, DDS 6961 U.S. Highway 87 East San Antonio, TX 78263 Phone: (210)648-4411 Fax: (210) 648-6498
1 The Single Tooth Implant. The Ultimate Aesthetic Challenge
 1 The Single Tooth Implant The Ultimate Aesthetic Challenge by Daniel G. Pompa, D.D.S. 2 Before starting any Maxillary Anterior Single Implant, or any case in the esthetic zone: TAKE A PHOTO OF YOUR PATIENT
1 The Single Tooth Implant The Ultimate Aesthetic Challenge by Daniel G. Pompa, D.D.S. 2 Before starting any Maxillary Anterior Single Implant, or any case in the esthetic zone: TAKE A PHOTO OF YOUR PATIENT
Course Curriculum for the Master Degree in Dentistry/Orthodontics
 Jordan University of Science and Technology Faculty of Graduate Studies Course Curriculum for the Master Degree in Dentistry/Orthodontics The Master Degree in Dentistry/ Orthodontics is awarded by the
Jordan University of Science and Technology Faculty of Graduate Studies Course Curriculum for the Master Degree in Dentistry/Orthodontics The Master Degree in Dentistry/ Orthodontics is awarded by the
DENT IMPLANT restoring qualit S: of LIfE
 DENTAL IMPLANTS: restoring quality of life Dental Implants: A Better Treatment Option. What are dental implants? Dental implants are a safe, esthetic alternative to traditional crowns, bridgework, and
DENTAL IMPLANTS: restoring quality of life Dental Implants: A Better Treatment Option. What are dental implants? Dental implants are a safe, esthetic alternative to traditional crowns, bridgework, and
MINI IMPLANTS FOR LOWER DENTURE STABLIZATION
 MINI IMPLANTS FOR LOWER DENTURE STABLIZATION From the Office of Dr. Michael J. Guy 511A Lakeshore Drive, North Bay ON, P1A 2E3 Mini dental implants (MDI) have become increasingly popular in the past decade
MINI IMPLANTS FOR LOWER DENTURE STABLIZATION From the Office of Dr. Michael J. Guy 511A Lakeshore Drive, North Bay ON, P1A 2E3 Mini dental implants (MDI) have become increasingly popular in the past decade
Don t Let Life Pass You By Because Of Oral Bone Loss
 Don t Let Life Pass You By Because Of Oral Bone Loss Ask For Dental Implant Solutions From BIOMET 3i Scan With Your Smartphone! In order to scan QR codes, your mobile device must have a QR code reader
Don t Let Life Pass You By Because Of Oral Bone Loss Ask For Dental Implant Solutions From BIOMET 3i Scan With Your Smartphone! In order to scan QR codes, your mobile device must have a QR code reader
Telescopic Denture A Treatment Modality for Minimizing the Conventional Removable Complete Denture Problems: A Case Report
 Dentistry Section Case Report ID: JCDR/2012/3886:2351 Telescopic Denture A Treatment Modality for Minimizing the Conventional Removable Complete Denture Problems: A Case Report Kunwarjeet Singh, Nidhi
Dentistry Section Case Report ID: JCDR/2012/3886:2351 Telescopic Denture A Treatment Modality for Minimizing the Conventional Removable Complete Denture Problems: A Case Report Kunwarjeet Singh, Nidhi
education Although demographic factors and growing patient awareness of the benefits of dental implants
 education Increasing implant dentistry in undergraduate education using new technology: A pilot project Hugo De Bruyn, MDS, MsC, PhD ± & Stefan Vandeweghe, DDS Although demographic factors and growing
education Increasing implant dentistry in undergraduate education using new technology: A pilot project Hugo De Bruyn, MDS, MsC, PhD ± & Stefan Vandeweghe, DDS Although demographic factors and growing
Prosthetic treatment planning on the basis of scientific evidence.
 Prosthetic treatment planning on the basis of scientific evidence. Pjetursson BE, Lang NP. J Oral Rehabil. 2008 Jan;35 Suppl 1:72-9. Faculty of Odontology, University of Iceland, Reykjavik, Iceland, and
Prosthetic treatment planning on the basis of scientific evidence. Pjetursson BE, Lang NP. J Oral Rehabil. 2008 Jan;35 Suppl 1:72-9. Faculty of Odontology, University of Iceland, Reykjavik, Iceland, and
RESIDENT TRAINING GOALS AND OBJECTIVES STATEMENTS
 RESIDENT TRAINING GOALS AND OBJECTIVES STATEMENTS Evaluation and treatment of dental emergencies Recognize, anticipate and manage emergency problems related to the oral cavity. Differentiate between those
RESIDENT TRAINING GOALS AND OBJECTIVES STATEMENTS Evaluation and treatment of dental emergencies Recognize, anticipate and manage emergency problems related to the oral cavity. Differentiate between those
Dental Implants - the tooth replacement solution
 Dental Implants - the tooth replacement solution Are missing teeth causing you to miss out on life? Missing teeth and loose dentures make too many people sit on the sidelines and let life pass them by.
Dental Implants - the tooth replacement solution Are missing teeth causing you to miss out on life? Missing teeth and loose dentures make too many people sit on the sidelines and let life pass them by.
TMJ. Problems. Certain headaches and pain in. the ear, jaw, neck, tooth, and. sinus can be the result of a. temporomandibular joint (TMJ)
 DIVISION OF ORAL AND MAXILLOFACIAL SURGERY TMJ Problems Certain headaches and pain in the ear, jaw, neck, tooth, and sinus can be the result of a temporomandibular joint (TMJ) problem. People with TMJ
DIVISION OF ORAL AND MAXILLOFACIAL SURGERY TMJ Problems Certain headaches and pain in the ear, jaw, neck, tooth, and sinus can be the result of a temporomandibular joint (TMJ) problem. People with TMJ
What is a dental implant?
 What is a dental implant? Today, the preferred method of tooth replacement is a dental implant. They replace missing tooth roots and form a stable foundation for replacement teeth that look, feel and function
What is a dental implant? Today, the preferred method of tooth replacement is a dental implant. They replace missing tooth roots and form a stable foundation for replacement teeth that look, feel and function
Tooth Supported Overdentures
 Unless otherwise noted, the content of this course material is licensed under a Creative Commons Attribution - Non-Commercial - Share Alike 3.0 License. Copyright 2008, Dr. Jeff Shotwell. The following
Unless otherwise noted, the content of this course material is licensed under a Creative Commons Attribution - Non-Commercial - Share Alike 3.0 License. Copyright 2008, Dr. Jeff Shotwell. The following
Coding and Payment Guide for Dental Services. A comprehensive coding, billing, and reimbursement resource for dental services
 Coding and Payment Guide for Dental Services A comprehensive coding, billing, and reimbursement resource for dental services 2011 Contents Introduction...1 Coding Systems... 1 Claim Forms... 2 Contents
Coding and Payment Guide for Dental Services A comprehensive coding, billing, and reimbursement resource for dental services 2011 Contents Introduction...1 Coding Systems... 1 Claim Forms... 2 Contents
INTRODUCTION. most popular stud attachment available to the dental profession to increase the retention of implant complete
 CLINICAL AN OVERVIEW OF THE O-RING IMPLANT OVERDENTURE ATTACHMENT: CLINICAL REPORTS Sheldon Winkler, DDS Jack Piermatti, DMD Amy Rothman, DMD, MA Georgios Siamos, DDS, MS KEY WORDS O-ring Implant overdenture
CLINICAL AN OVERVIEW OF THE O-RING IMPLANT OVERDENTURE ATTACHMENT: CLINICAL REPORTS Sheldon Winkler, DDS Jack Piermatti, DMD Amy Rothman, DMD, MA Georgios Siamos, DDS, MS KEY WORDS O-ring Implant overdenture
Taking the Mystique out of Implant Dentistry. Dr. Michael Weinberg B.Sc., DDS, FICOI
 Taking the Mystique out of Implant Dentistry Dr. Michael Weinberg B.Sc., DDS, FICOI What is Restorative Implant Dentistry? Restorative implant dentistry involves taking a few simple mechanical principles
Taking the Mystique out of Implant Dentistry Dr. Michael Weinberg B.Sc., DDS, FICOI What is Restorative Implant Dentistry? Restorative implant dentistry involves taking a few simple mechanical principles
Dental Implants in Edentulism
 Academy of Medicine, Singapore Dental Implants in Edentulism AMS-MOH Clinical Practice Guidelines 1/2012 Aug 2012 Levels of evidence and grades of recommendation Levels of evidence Level Type of Evidence
Academy of Medicine, Singapore Dental Implants in Edentulism AMS-MOH Clinical Practice Guidelines 1/2012 Aug 2012 Levels of evidence and grades of recommendation Levels of evidence Level Type of Evidence
!Financial agreement COST / RISK / BENEFIT
 COMPLETE DENTURES 1 2 Oral Examination, Diagnosis and Treatment Planning Initial Appointment! Get to know your patient! Personally, experiences, expectations! Past medical history! Past dental history!
COMPLETE DENTURES 1 2 Oral Examination, Diagnosis and Treatment Planning Initial Appointment! Get to know your patient! Personally, experiences, expectations! Past medical history! Past dental history!
BEST DENTAL ASSOCIATES / DRSTONEDDS.COM THE DENTAL IMPLANT GUIDE
 THE DENTAL IMPLANT GUIDE We specialize in the most advanced technologies in dental restoration, reconstruction and replacement. We d love to help you to improve your comfort, lifestyle, & confidence with
THE DENTAL IMPLANT GUIDE We specialize in the most advanced technologies in dental restoration, reconstruction and replacement. We d love to help you to improve your comfort, lifestyle, & confidence with
SCD Case Study. Most malignant lesions of the tonsil are either lymphosarcoma or carcinoma.
 SCD Case Study Dry Mouth This case study details a patient who has experienced xerostomia as a result of treatment for squamous cell carcinoma of the left tonsil involving surgery followed by deep x-ray
SCD Case Study Dry Mouth This case study details a patient who has experienced xerostomia as a result of treatment for squamous cell carcinoma of the left tonsil involving surgery followed by deep x-ray
Powertome Assisted Atraumatic Tooth Extraction
 Powertome Assisted Atraumatic Tooth Extraction White et al Jason White, DDS 1 2 3 Abstract Background: While traditional dental extraction techniques encourage minimal trauma, luxated elevation and forceps
Powertome Assisted Atraumatic Tooth Extraction White et al Jason White, DDS 1 2 3 Abstract Background: While traditional dental extraction techniques encourage minimal trauma, luxated elevation and forceps
Ando A., Nakamura Y., Kanbara R., Kumano H., Miyata T., Masuda T., Ohno Y. and Tanaka Y.
 11. The Effect of Abutment Tooth Connection with Extracoronal Attachment using the Three Dimensional Finite Element Method - Part 2. The Construction of Finite Element Model from CT Data - Ando A., Nakamura
11. The Effect of Abutment Tooth Connection with Extracoronal Attachment using the Three Dimensional Finite Element Method - Part 2. The Construction of Finite Element Model from CT Data - Ando A., Nakamura
CDT 2015 Code Change Summary New codes effective 1/1/2015
 CDT 2015 Code Change Summary New codes effective 1/1/2015 Code Nomenclature Delta Dental Policy D0171 Re-Evaluation Post Operative Office Visit Not a Covered Benefit D0351 3D Photographic Image Not a Covered
CDT 2015 Code Change Summary New codes effective 1/1/2015 Code Nomenclature Delta Dental Policy D0171 Re-Evaluation Post Operative Office Visit Not a Covered Benefit D0351 3D Photographic Image Not a Covered
ANGEL DENTAL CARE Implant Consent
 This information is to help you make an informed decision about having implant treatment. You should take as much time as you wish to make the decision in relation to signing the following consent form.
This information is to help you make an informed decision about having implant treatment. You should take as much time as you wish to make the decision in relation to signing the following consent form.
CLINICAL IMPLICATIONS
 A randomized clinical trial comparing the efficacy of mandibular implantsupported overdentures and conventional dentures in diabetic patients. Part I: Methodology and clinical outcomes Krishan K. Kapur,
A randomized clinical trial comparing the efficacy of mandibular implantsupported overdentures and conventional dentures in diabetic patients. Part I: Methodology and clinical outcomes Krishan K. Kapur,
dental implants for tooth replacement be a confident you
 dental implants for tooth replacement be a confident you smile big Anyone missing one or more teeth understands how tooth loss can make you feel uncomfortable about smiling or eating in public. You may
dental implants for tooth replacement be a confident you smile big Anyone missing one or more teeth understands how tooth loss can make you feel uncomfortable about smiling or eating in public. You may
Porous surface of extraoral implants: report of two cases rehabilitated with a new Brazilian extraoral implant
 Braz J Oral Sci. October/December 2004 - Vol. 3 - Number 11 Luciano Lauria Dib 1 Joaquim Augusto Piras de Oliveira 2 Renata Lazari Sandoval 3 Ulf Nannmark 4 1 Professor of Stomatology at UNIP, São Paulo,
Braz J Oral Sci. October/December 2004 - Vol. 3 - Number 11 Luciano Lauria Dib 1 Joaquim Augusto Piras de Oliveira 2 Renata Lazari Sandoval 3 Ulf Nannmark 4 1 Professor of Stomatology at UNIP, São Paulo,
To provide care for the partially-dentate or edentulous
 The shortened dental arch: A review of the literature Debora Armellini, DDS, MS, a and J. Anthony von Fraunhofer, MSc, PhD b School of Dentistry, University of Maryland, Baltimore, Md The functional demands
The shortened dental arch: A review of the literature Debora Armellini, DDS, MS, a and J. Anthony von Fraunhofer, MSc, PhD b School of Dentistry, University of Maryland, Baltimore, Md The functional demands
The Most Frequently Asked Questions About Dental Implants... A Consumer s Guide to Understanding Implant Treatment
 Number 3 $1.25 The Most Frequently Asked Questions About Dental Implants... A Consumer s Guide to Understanding Implant Treatment If you are like most people considering dental implants, you probably have
Number 3 $1.25 The Most Frequently Asked Questions About Dental Implants... A Consumer s Guide to Understanding Implant Treatment If you are like most people considering dental implants, you probably have
Modern Tooth Replacement Strategies & Digital Workflow
 Modern Tooth Replacement Strategies & Digital Workflow Case Studies by Dr Maurice Salama, DMD AS PUBLISHED BY Dentistry Today, June 2014 Complete Implant Restoration System FACTS: Implant Dentistry Has
Modern Tooth Replacement Strategies & Digital Workflow Case Studies by Dr Maurice Salama, DMD AS PUBLISHED BY Dentistry Today, June 2014 Complete Implant Restoration System FACTS: Implant Dentistry Has
Dental Implant Treatment after Improvement of Oral Environment by Orthodontic Therapy
 Dental implant treatment after impr Title environment by orthodontic therapy. Sekine, H; Miyazaki, H; Takanashi, Author(s) Matsuzaki, F; Taguchi, T; Katada, H Journal Bulletin of Tokyo Dental College,
Dental implant treatment after impr Title environment by orthodontic therapy. Sekine, H; Miyazaki, H; Takanashi, Author(s) Matsuzaki, F; Taguchi, T; Katada, H Journal Bulletin of Tokyo Dental College,
Dental Implants. Change Your Life & Smile with. Kingston Kitchener Newmarket Oshawa Scarborough Toronto Waterloo
 Change Your Life & Smile with Dental Implants Page 1 Dental Implants 101 3 What To Expect 5 Fees & Financing 6 FAQ Aurora Barrie Brooklin Cambridge Hanover Guelph Kingston Kitchener Newmarket Oshawa Scarborough
Change Your Life & Smile with Dental Implants Page 1 Dental Implants 101 3 What To Expect 5 Fees & Financing 6 FAQ Aurora Barrie Brooklin Cambridge Hanover Guelph Kingston Kitchener Newmarket Oshawa Scarborough
E. Richard Hughes, D.D.S.
 E. Richard Hughes, D.D.S. Docket No. FDA-2012-N-0677 Blade Form Endosseous Dental Implants E. Richard Hughes, D.D.S. 46440 Benedict Dr.,# 201 Sterling, Va. 20164 USA 703-444-1152 erhughesdds@aol.com Diplomate,
E. Richard Hughes, D.D.S. Docket No. FDA-2012-N-0677 Blade Form Endosseous Dental Implants E. Richard Hughes, D.D.S. 46440 Benedict Dr.,# 201 Sterling, Va. 20164 USA 703-444-1152 erhughesdds@aol.com Diplomate,
BICON DENTAL IMPLANTS
 BICON DENTAL IMPLANTS The Bicon Dental Implant System, since 1985, has offered discerning dentists the ability to provide secure implant restorations that look, feel, and function like natural teeth. With
BICON DENTAL IMPLANTS The Bicon Dental Implant System, since 1985, has offered discerning dentists the ability to provide secure implant restorations that look, feel, and function like natural teeth. With
ADA Insurance Codes for Laboratory Procedures:
 ADA Insurance Codes for Laboratory Procedures: Inlay/Onlay Restorations D2510 Inlay - metallic - one surface D2520 Inlay - metallic - two surfaces D2530 Inlay - metallic - three or more surfaces D2542
ADA Insurance Codes for Laboratory Procedures: Inlay/Onlay Restorations D2510 Inlay - metallic - one surface D2520 Inlay - metallic - two surfaces D2530 Inlay - metallic - three or more surfaces D2542
CRANIOMAXILLOFACIAL DEFORMITIES/COSMETIC SURGERY. Reza Movahed, DMD,* Marcus Teschke, DMD, MD,y and Larry M. Wolford, DMDz
 CRANIOMAXILLOFACIAL DEFORMITIES/COSMETIC SURGERY Protocol for Concomitant Temporomandibular Joint Custom-Fitted Total Joint Reconstruction and Orthognathic Surgery Utilizing Computer-Assisted Surgical
CRANIOMAXILLOFACIAL DEFORMITIES/COSMETIC SURGERY Protocol for Concomitant Temporomandibular Joint Custom-Fitted Total Joint Reconstruction and Orthognathic Surgery Utilizing Computer-Assisted Surgical
deltadentalins.com/usc
 Plan Benefit Highlights for: UNIVERSITY OF SOUTHERN CALIFORNIA STUDENT PLAN Group No: 05008 The Delta Dental PPO table plan provides you great dental benefits at a reasonable cost. With a table of allowance
Plan Benefit Highlights for: UNIVERSITY OF SOUTHERN CALIFORNIA STUDENT PLAN Group No: 05008 The Delta Dental PPO table plan provides you great dental benefits at a reasonable cost. With a table of allowance
Appropriate soft tissue closure represents a critical
 Periosteoplasty for Soft Tissue Closure and Augmentation in Preprosthetic Surgery: A Surgical Report Albino Triaca, Dr Med, Dr Med Dent 1 /Roger Minoretti, Dr Med, Dr Med Dent 1 / Mauro Merli, DMD 2 /Beat
Periosteoplasty for Soft Tissue Closure and Augmentation in Preprosthetic Surgery: A Surgical Report Albino Triaca, Dr Med, Dr Med Dent 1 /Roger Minoretti, Dr Med, Dr Med Dent 1 / Mauro Merli, DMD 2 /Beat
GUIDELINES. Educational Requirements & Professional Responsibilities for Implant Dentistry CONTENTS. The Guidelines of the Royal College of
 Educational Requirements & Professional GUIDELINES Approved by Council May 2013 This is replacing the document last published in August 2002. Educational Requirements & Professional The Guidelines of the
Educational Requirements & Professional GUIDELINES Approved by Council May 2013 This is replacing the document last published in August 2002. Educational Requirements & Professional The Guidelines of the
Full Mouth Restoration with Screw-Retained Zirconia Bridges
 Full Mouth Restoration with Screw-Retained Zirconia Bridges A DENTIST-LAB RELATIONSHIP THAT WORKS Dentist: Steven P. Stern, DMD Windsor Dental Center New Windsor, NY Dental Laboratory: InnoDDS Dental Laboratory
Full Mouth Restoration with Screw-Retained Zirconia Bridges A DENTIST-LAB RELATIONSHIP THAT WORKS Dentist: Steven P. Stern, DMD Windsor Dental Center New Windsor, NY Dental Laboratory: InnoDDS Dental Laboratory
Teeth and Dental Implants: When to save, and when to extract.
 Teeth and Dental Implants: When to save, and when to extract. One of the most difficult decisions a restorative dentist has to make is when to refer a patient for extraction and placement of dental implants.
Teeth and Dental Implants: When to save, and when to extract. One of the most difficult decisions a restorative dentist has to make is when to refer a patient for extraction and placement of dental implants.
HEALTH SERVICES POLICY & PROCEDURE MANUAL. SUBJECT: Types of Dental Treatments Provided EFFECTIVE DATE: July 2014 SUPERCEDES DATE: January 2014
 PAGE 1 of 5 References Related ACA Standards 4 th Edition Standards for Adult Correctional Institutions 4-4369, 4-4375 PURPOSE To provide guidelines for determining appropriate levels of care and types
PAGE 1 of 5 References Related ACA Standards 4 th Edition Standards for Adult Correctional Institutions 4-4369, 4-4375 PURPOSE To provide guidelines for determining appropriate levels of care and types
Osseo-integrated Dental Implant Policy and Guidelines
 Osseo-integrated Dental Implant Policy and Guidelines 1. PURPOSE The purpose of this document is to outline the Department of Veterans Affairs (DVA) policy regarding the provision of dental implant treatment
Osseo-integrated Dental Implant Policy and Guidelines 1. PURPOSE The purpose of this document is to outline the Department of Veterans Affairs (DVA) policy regarding the provision of dental implant treatment
Page 1 of 10 BDS FINAL PROFESSIONAL EXAMINATION 2007 Prosthodontics (MCQs) Model Paper SECTION I
 Page 1 of 10 COMPLETE DENTURES ANATOMICAL LANDMARKS SECTION I 1. There are many landmarks in the oral cavity which helps in designing complete dentures. One of the important landmarks is fovea palatini.
Page 1 of 10 COMPLETE DENTURES ANATOMICAL LANDMARKS SECTION I 1. There are many landmarks in the oral cavity which helps in designing complete dentures. One of the important landmarks is fovea palatini.
Saudi Fellowship In Dental Implant (SF-DI)
 Saudi Fellowship In Dental Implant (SF-DI) Prepared and Updated by Dr. Arwa AL-Sayed Consultant Periodontics and Dental Implants M E M B E R S Dr. Arwa AL-Sayed Dr. Abdulhadi Abanmy Dr. Ali AL-Ghamdi Dr.
Saudi Fellowship In Dental Implant (SF-DI) Prepared and Updated by Dr. Arwa AL-Sayed Consultant Periodontics and Dental Implants M E M B E R S Dr. Arwa AL-Sayed Dr. Abdulhadi Abanmy Dr. Ali AL-Ghamdi Dr.
Lateral pterygoid muscle Medial pterygoid muscle
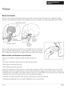 PATIENT INFORMATION BOOKLET Trismus Normal Jaw Function The jaw is a pair of bones that form the framework of the mouth and teeth. The upper jaw is called the maxilla. The lower jaw is called the mandible.
PATIENT INFORMATION BOOKLET Trismus Normal Jaw Function The jaw is a pair of bones that form the framework of the mouth and teeth. The upper jaw is called the maxilla. The lower jaw is called the mandible.
TREATMENT REFUSAL FORMS
 TREATMENT REFUSAL FORMS These forms are intended to be used when a patient refuses the treatment. These forms help confirm that the patient is informed and aware of the risks involved with not proceeding
TREATMENT REFUSAL FORMS These forms are intended to be used when a patient refuses the treatment. These forms help confirm that the patient is informed and aware of the risks involved with not proceeding
CUSTOMIZED PROVISIONAL ABUTMENT AND PROVISIONAL RESTORATION FOR AN IMMEDIATELY-PLACED IMPLANT
 CONTINUING EDUCATION 1 4 CUSTOMIZED PROVISIONAL ABUTMENT AND PROVISIONAL RESTORATION FOR AN IMMEDIATELY-PLACED IMPLANT Gerard J. Lemongello, Jr, DMD* LEMONGELLO 19 7 AUGUST The use of immediate implant
CONTINUING EDUCATION 1 4 CUSTOMIZED PROVISIONAL ABUTMENT AND PROVISIONAL RESTORATION FOR AN IMMEDIATELY-PLACED IMPLANT Gerard J. Lemongello, Jr, DMD* LEMONGELLO 19 7 AUGUST The use of immediate implant
Coding and Payment Guide for Dental Services. A comprehensive coding, billing, and reimbursement resource for dental services
 Coding and Payment Guide for Dental Services A comprehensive coding, billing, and reimbursement resource for dental services 2014 Contents Introduction...1 Coding Systems... 1 Claim Forms... 2 Contents
Coding and Payment Guide for Dental Services A comprehensive coding, billing, and reimbursement resource for dental services 2014 Contents Introduction...1 Coding Systems... 1 Claim Forms... 2 Contents
Dental Implant Options in Atrophic Jaws
 Dental Implant Options in Atrophic Jaws Orthopedic Application Jay B. Reznick, D.M.D., M.D. Diplomate, American Board of Oral and Maxillofacial Surgery Tarzana, CA Endopore Dental Implant System Screw-Type
Dental Implant Options in Atrophic Jaws Orthopedic Application Jay B. Reznick, D.M.D., M.D. Diplomate, American Board of Oral and Maxillofacial Surgery Tarzana, CA Endopore Dental Implant System Screw-Type
European Academy of DentoMaxilloFacial Radiology
 European Academy of DentoMaxilloFacial Radiology Framework for Specialist Training in Dental and Maxillofacial Radiology Background The scope of DentoMaxilloFacial Radiology DMFR (Dental and Maxillofacial
European Academy of DentoMaxilloFacial Radiology Framework for Specialist Training in Dental and Maxillofacial Radiology Background The scope of DentoMaxilloFacial Radiology DMFR (Dental and Maxillofacial
Condylar position in children with functional posterior crossbites: before and after crossbite correction*
 PEDIATRIC DENTISTRY/Copyright 1980 by The American Academy of Pedodontics/Vol. 2, No. 3 Condylar position in children with functional posterior crossbites: before and after crossbite correction* David
PEDIATRIC DENTISTRY/Copyright 1980 by The American Academy of Pedodontics/Vol. 2, No. 3 Condylar position in children with functional posterior crossbites: before and after crossbite correction* David
TRI Product NewsFlash. December 2015
 TRI Product NewsFlash December 2015 Study Overview 2015 Dear Partners Year in, year out, we are screening all major scientific journals to ensure that our TRI Performance Concept still reflects the latest
TRI Product NewsFlash December 2015 Study Overview 2015 Dear Partners Year in, year out, we are screening all major scientific journals to ensure that our TRI Performance Concept still reflects the latest
Long-Term Outcome of Trigeminal Nerve Injuries Related to Dental Treatment
 DENTOALVEOLAR SURGERY J Oral Maxillofac Surg 69:2284-2288, 2011 Long-Term Outcome of Trigeminal Nerve Injuries Related to Dental Treatment M. Anthony Pogrel, DDS, MD, FACS, FRCS,* Ryan Jergensen, DDS,
DENTOALVEOLAR SURGERY J Oral Maxillofac Surg 69:2284-2288, 2011 Long-Term Outcome of Trigeminal Nerve Injuries Related to Dental Treatment M. Anthony Pogrel, DDS, MD, FACS, FRCS,* Ryan Jergensen, DDS,
