David Logé, MD*, Sven Vanneste, MS, MA, PhD, Tim Vancamp, PT, MBA, Dirk Rijckaert, MD* OBJECTIVE. Neuromodulation: Technology at the Neural Interface
|
|
|
- Louise Stephens
- 8 years ago
- Views:
Transcription
1 Neuromodulation: Technology at the Neural Interface Received: April 26, 2012 Revised: October 18, 2012 Accepted: October 25, 2012 (onlinelibrary.wiley.com) DOI: /ner Long-Term Outcomes of Spinal Cord Stimulation With Percutaneously Introduced Paddle Leads in the Treatment of Failed Back Surgery Syndrome and Lumboischialgia David Logé, MD*, Sven Vanneste, MS, MA, PhD, Tim Vancamp, PT, MBA, Dirk Rijckaert, MD* Objective: The study aims to evaluate the long-term clinical and technical efficacy of recently developed percutaneously introducible plate electrodes for spinal cord stimulation. Methods: Twenty-one patients diagnosed with failed back surgery syndrome (FBSS) or lumboischialgia were implanted with a small profile plate-type electrode. Patients were followed-up long term and were asked at baseline, after trial, and during each follow-up visit to score their pain on a visual analog scale (VAS) for pain now, worst pain last week, least pain last week, and mean pain last week. Pain location, electrophysiologic parameters, and number of reprogrammings were collected as well. Furthermore, each patient was asked if he/she would redo the procedure post trial and at each of the follow-up visits. Results: A total of 21 patients were prospectively followed up long term. With a mean follow-up of 40.8 months, a significant mean reduction in patient self-reported pain from baseline to postoperative of 75.79% pain reduction was seen at follow-up 1 and 62.52% at follow-up 2. A significant decrease was obtained for, respectively, pain at the present moment, VAS pain worst last week, VAS pain least last week, and VAS pain mean last week in comparison with baseline VAS scores. All patients indicated that they would redo the procedure. Conclusion: Percutaneous implantation of small profile paddle leads in patients with FBSS and lumboischialgia produces favorable results over the long term that are at least comparable with surgical implanted paddle leads. The percutaneous approach also allows nonsurgically trained pain physicians to introduce paddle leads. Indices like if patients would redo the procedure may be more appropriate for analyzing long-term outcomes than the arbitrarily taking 50% reduction in VAS scores. Keywords: FBSS, long term, paddle lead, percutaneous, S-Lamitrode, SCS Conflict of interest: The authors declare that they have received no editorial or financial support for this study. T. Vancamp is an employee of St. Jude Medical and received or has no financial or other benefits related to this study. D. Logé is a paid consultant of St. Jude Medical. S. Vanneste reports no conflict of interest. D. Rijckaert reports no conflict of interest. OBJECTIVE Spinal cord stimulation (SCS) is an implantable, safe, reversible, and efficacious pain treatment option for neuropathic pain syndromes. SCS has furthermore the advantage that screening trials can be performed, evaluating the efficacy of the therapy for that patient, before it is decided to move to a permanent implantation procedure. SCS for neuropathic pain delivers mild electrical stimulation to the spinal cord, more specifically the dorsal columns, with the goal to achieve stimulation-induced paresthesias to overlap the patient s pain topography (1). SCS has to be considered a symptomatic therapy rather than a curative therapy. It has been shown that SCS has a positive effect on pain suppression, physical activity, quality of life (QOL), activities of daily living, sleep, and reduced pain medication, and is furthermore cost-effective for different chronic medical conditions (2 9). With regard to leg and back pain relief, QOL, functional capacity, and patient satisfaction, SCS has been shown to have a better success rate when compared with conventional medical management (10) and reoperation (11). In the early 1970s, the development of percutaneous leads, which could be placed epidural through a Tuohy needle, led to a simplification of the surgical implant technique, obviating the need for laminectomy. This technique allowed implantation procedures to be performed under local anesthesia by nonsurgeons and intraoperative testing of paresthesia coverage over the painful area. One of the drawbacks is that percutaneous placed cylindrical electrodes may be associated with a high rate of migration (12). Address correspondence to: David Logé, MD, A.Z. St. Lucas, Groenebriel 1, 9000, Gent, Belgium. david.loge@azstlucas.be * Department of Anesthesiology & Pain Medicine, A.Z. St. Lucas, Gent, Belgium; BRAI 2 N & Department of Neurosurgery, University Hospital Antwerp, Antwerp, Belgium; and Department of Translational Neuroscience, Faculty of Medicine, University of Antwerp, Antwerp, Belgium For more information on author guidelines, an explanation of our peer review process, and conflict of interest informed consent policies, please go to 1
2 LOGÉ ET AL. 2 Figure 1. Illustration of the S-Series 8-contact steerable paddle lead, showing contact numbering. Plate-type electrodes are placed under direct vision, and have a large surface contact area, which improves the stability. In a study by North et al., they found that a plate-type electrode implanted via laminectomy had a broader stimulation pattern and was more energy efficient compared with percutaneously placed cylindrical leads (13). Lower stimulation parameters can be partially explained as the unidirectional electrical field leads to less energy loss. Furthermore, the larger design will occupy more epidural space by which they tend to be closer to the dorsal columns. Thus, this leaves implanters with two substantially different techniques: a percutaneous introduction approach and the surgical technique to introduce larger sized plate-type electrodes. Efforts have been made in the search for less invasive approaches to introduce plate-type electrodes and enabling intraoperative testing: the minimally invasive unilateral technique as described by Vangeneugden (14) and the modified technique using a tubular retracting system as described by Beems and van Dongen (15). Still, these techniques require surgically trained implanters. In recent years, efforts have been made to bridge the gap between the percutaneous and surgical technique. Novel percutaneous techniques to implant plate-type electrodes have been developed and described by several authors, allowing nonsurgicaland surgical-trained physicians to minimally invasive position slim designed plate-type electrodes (S-Series [Fig. 1], St. Jude Medical Neuromodulation Division, St. Paul, MN, USA). One such technique is the one described by Vonhögen et al. using a 10G needle (16). Caution needs to be taken as the implantation using a large epidural needle may increase the risk for dural puncture and/or spinal cord injury if used by unskilled hands. A safer alternative may be to deliver a paddle lead through the use of the newer developed percutaneous delivery system Epiducer (St. Jude Medical Neuromodulation Division) as described by Logé et al. (17). An uncontrolled, open-label, prospective two-center study was performed to assess the safety of the Epiducer delivery system. In this study, data of 34 patients were collected. The study concluded the safe use of the Epiducer lead delivery system for percutaneous implantation and advancement of the S-Series paddle lead in the epidural canal. The slimline paddle lead was advanced four vertebral levels in most patients (61.8%). Furthermore, patient pain, satisfaction, and QOL were positively impacted throughout the study. They also found that percutaneously implanting this type of paddle lead using the Epiducer lead delivery system provides benefits to the patient without introducing any additional risk (18). In a multicenter retrospective data collection study, the feasibility and safety of percutaneously introducing and advancing a slimline plate electrode in the epidural canal has been shown in 40 patients. They found that the S-Series lead could be percutaneously implanted and advanced over multiple vertebral segments. No adverse events specifically related to the procedure were found (19). Vonhögen et al. showed a clinically relevant reduction of 52% in back pain in 17 out of the 20 patients included in this study, after 12 months using this type of electrode. Twelve months postoperatively general patient satisfaction and QOL were statistically better in comparison with preoperative, with improvements of 69% and 75%, respectively. Correlation analyses demonstrated that visual analog scale (VAS) (pre-12 months) for legs and back correlated negatively with VAS pre-12 months satisfaction and pre-12 months QOL, revealing that the more pain reduction in legs and back, the more satisfaction and QOL patients have. Acute pain recordings showed that 40% of the patients experienced no pain postoperative (16). In a prospective study conducted by de Vos et al., they found that a single hybrid lead placed over the midline was able to capture and alleviate pain in the back and legs. Forty-one patients out of the 45 eligible to a SCS trial were followed for at least 12 months. They furthermore found that pain medication was reduced in 25 patients, and 18 patients could entirely stop their medication (20). Kinfe et al. found that in their prospective trial, with a median follow-up of one year, there was improved paresthesia coverage in 87% of the 81 patients enrolled. A mean pain reduction of 73% was observed (21). In this study, we present data on the long-term efficacy of using percutaneously implanted S-Series leads in patients with failed back surgery syndrome (FBSS) and lumboischialgia. METHODS Study Design This single center study was designed to prospectively collect longterm outcomes of patients presenting with FBSS or lumboischialgia who were implanted with a percutaneously implanted S-Series lead. The same implanter performed all implantations and data were collected according to the Belgian reimbursement guidelines. Ethical committee approval was not necessary as according to the Belgian law, data collected as standard practice waive the need for Institutional Review Board approval. Pre- and posttrial data were systematically collected from patients who presented at the clinic between November 2004 and September 2008 and were subsequently implanted with an S-Series lead and had at least one follow-up visit after the trial visit. Pain scores using a VAS were recorded for pain now, worst last week, lowest last week, and mean last week at baseline, posttrial, and during each follow-up visit. Pain location, number of back surgeries, electrophysiologic parameters, lead tip location, number of reprogramming, and if patients would redo the procedure were also collected. Follow-up averaged 40.8 months (range: ) for this patient group. Posttrial visits averaged one month (range: ), follow-up 1 (FU-1): 14.0 months (range: ); follow-up 2 (FU-2): 13.9 months (range: ); and follow-up 3 (FU-3): 15.9 months (range: ). All visit intervals were counted after the former visit (see Table 1).
3 LONG-TERM OUTCOMES PERC-PADDLE LEADS Table 1. Follow-Up. Follow-up (months) Average follow-up total [range] 40.8 [ ] Average follow-up PT [range] 1.0 [ ] Average follow-up FU-1 [range] 14.0 [ ] Average follow-up FU-2 [range] 13.9 [ ] PT, Posttrial; FU, follow-up, all measured after the prior visit. Patients Twenty-one patients (female: 14 and male: 7) with a mean age of 57 years (range: 33 76) were implanted and followed over a long-term period (see Table 2). All patients met the inclusion criteria according to the Belgian reimbursement guidelines. Exclusion criteria were absent and all patients had a psychologic screening, prior to implantation and after the trial period. A bylaw mandatory minimum of 28 days trial was performed for all patients before final implantation could take place. Mean preoperative VAS pain score (mean VAS pain last week) was 7.3 (range: ). Twelve patients (57.1%) were diagnosed with FBSS and nine (42.9%) with lumboischialgia (see Table 3). Pain was respectively located as follows: 10 (47.6%) patients presented with pain in the back and both legs, seven (33.3%) in the back and left leg, three (14.3%) patients in the back and right leg, and one (4.8%) patient in the buttock and right leg (see Table 2). An average number of 0.8 (range: 0 3) back surgeries were performed in this patient group. Twelve (57.1%) patients underwent previous back surgery and nine (42.9%) were implanted without prior surgery (see Fig. 2). We looked at the number of prior surgeries and found that eight patients (38.1%) had one surgery, three patients (14.3%) had two surgeries, and one patient (4.8%) had three surgeries. Implantation Methods Patients were comfortably positioned on the operating table as usual for dorsal SCS procedures. Anesthesia monitoring was used in a standard fashion for local interventions. Fluoroscopy using a C-arm was used to identify the desired entry level and to monitor the progression of the different stages of the procedure. Disinfection, aseptic draping of the surgical field, and local anesthetics (xylocaine 2% with adrenaline 1 : ) were applied. All patients were implanted with an 8-contact S-Series lead using a percutaneous technique as described by Vönhogen et al. (16) before the availability of the Epiducer introductory system after which we started using this novel percutaneous implant technique as described by Logé et al. (17). Once the electrode was entered in the epidural canal, the lead was advanced to the anticipated level of stimulation in a cephalad direction under constant fluoroscopy. Verification of the electrodes facing the spinal cord was done looking at the built-in radiopaque marker. Once at the anticipated location, the area of paresthesia was verified through intraoperative test stimulation using a Rapid Programmer (St. Jude Medical Neuromodulation Division). If unsatisfactory coverage was noted, the lead was repositioned until a satisfactory result was achieved. The position varied with the tip between T5 and T10. Lead integrity was tested via subthreshold automated impedance measurement with the Rapid Programmer. A silastic long anchor (St. Jude Medical Neuromodulation Division) was used to secure the Lamitrode S8 to the fascia of the paravertebral musculature. The lead was then connected to a 60-cm extension and tunneled subcutaneously to the opposite site of where the implantable pulse generator (IPG) would be located in the second stage. Again, the integrity of the system was measured. A strain relief loop was applied and the connection was buried in a subcutaneous pocket lateral of the spinous process, after which the wound was closed in a multilayer fashion. Postoperatively, patients were instructed on the use of their Multiprogram Trial Stimulator (MTS, St. Jude Medical Neuromodulation Division). A trial of minimum 28 days, as mandated by the Belgian reimbursement guidelines, was performed, and a second-stage procedure was only performed after a successful trial. The externalized extension was disconnected from the lead and removed in a sterile way. After this, either the lead was directly connected to the IPG or through the use of an extension. The IPG, GenesisXP, or EON C (St. Jude Medical Neuromodulation Division) was placed in a subcutaneous pocket at the buttock (N: 19; 90%) or the abdomen (N:2; 10%). Postoperative patients were instructed on the use of their programmer. Statistical Analysis Calculations were performed using SPSS software package (IBM SPSS Statistics, IBM Co., Armonk, NY, USA). Preoperative, postoperative, and follow-up scores were compared using a repeated measures analysis of variance (ANOVA). We conducted this analysis comparing baseline with postoperative, FU-1, and FU-2. This analysis was also conducted including FU-3. However, for this latter analysis, only 14 patients were included as there were only 14 patients that already had a third follow-up. In addition, we conducted a repeated measures ANOVA with the previously described withinsubjects variables (preoperative, postoperative, and follow-up scores) and the diagnosis (failed back surgeries vs. chronic lumbioschialgia) as between-subjects variable. A similar analysis was conducted with a between-subjects variable the amount of surgeries the patient had before implantation. RESULTS A significant mean reduction in patient self-reported pain from baseline to postoperative of 75.79% was seen; 62.52% pain reduction was seen at FU-1; and 62.52% at FU-2. The obtained significant effect can be seen in Table 3. If we also include F-U3 (N = 14), a significant effect for the mean VAS scores (F = 53.93, p < 0.001) was also observed, with a 47.33% reduction in mean VAS score. The baseline mean scores of pain at present moment, VAS pain worst last week, VAS pain least last week, and VAS pain mean last week can be found in Table 3. A significant decrease was obtained for, respectively, pain at the present moment, VAS pain worst last week, VAS pain least last week, and VAS pain mean last week, indicating that over time a significant decrease in pain was perceived in comparison with baseline VAS scores (see Table 3). A comparison between patients that had chronic lumboischialgia or failed back surgery between the pain scores obtained postoperative, FU-1, FU-2, and FU-3 revealed no significant effect. In addition, an analysis was conducted to verify if the amount of surgeries before implantation had an influence on the outcome at 3
4 LOGÉ ET AL. Table 2. Patient Demographics, History of Back Surgeries, Average Mean VAS Scores at Baseline and Pain Location. Overall Female Male Patients N (%) (66.7) 7 (33.3) Age Average ( SD) 57 ( 11.4) 56,9 ( 12.6) 57,1 ( 9.4) [range] [33 78] [33 75] [50 76] Diagnosis CL (%) 9 (42.9) 7 (50.0) 2 (28.6) FBSS (%) 12 (57.1) 7 (50.0) 5 (71.4) Average prior surgeries CL FBSS [range] 1.4 [1 3] 1.4 [1 3] 1.4 [1 2] Average VAS baseline CL [range] 7.4 [ ] 7.3 [ ] 7.7 [ ] FBSS [range] 7.2 [ ] 7.0 [ ] 7.4 [ ] Pain location Back and both legs (%) 10 (47.5) 7 (50.0) 3 (42.9) Back and left leg (%) 7 (33.3) 3 (21.4) 4 (57.1) Back and right leg (%) 3 (14.3) 3 (21.4) 0 (0.0) Buttock and right leg (%) 1 (4.8) 1 (7.1) 0 (0.0) CL, chronic lumboischialgia; FBSS, failed back surgery syndrome; VAS, visual analog scale. Table 3. Mean VAS Scores for Pain Now, Worst Last Week, Lowest Last Week, Mean Last Week, and % Suppression Compared With Baseline. VAS Baseline Postoperative Follow-up 1 Follow-up 2 F Pain now Pain highest Pain lowest Pain mean All comparisons were significant at p < VAS, visual analog scale. 4 9 (43%) Number of Back Surgeries 1 (5%) 8 (38%) Figure 2. Number of back surgeries before implantation. 3 (14%) baseline, as well as the follow-up. The analysis revealed no significant results, however, indicating that the amount of surgeries before implantation had no influence on the outcome. The mean electrophysiologic parameters found were frequency: 38.4 Hz (range: Hz); pulse width: msec (range: msec); perception amplitude: 5.3 ma (range: ); comfort amplitude: 6.9 ma (range: ma); and maximum tolerable amplitude: 8.0 ma (range: ) (see Table 4). We furthermore collected the number of activated electrodes: 3.3 (range: 2 7). The mean number of anodes used was 2.0 (range: 1 5). Those that were activated as cathodes: 1.3 (range: 1 2). In total, 23 stimulation sets were used in 21 programs. In two patients, two stimulation sets were used, and in 19 patients a single stimulation set covered the patients entire pain area. Twelve (N = 23, 52.2%) bipolar combinations were used, of which six were narrow bipoles (+-) and six were other bipolar configurations. A longitudinal guarded electrode array was programmed 11 times (47.8%), of which seven were simple guarded configurations (+ -+), and four were guarded combinations with multiple anodes and/or cathodes. The number of reprogramming sessions was documented as well, with an average of 3.1 reprogrammings (range: 0 15) necessary to sustain paresthesia in the required area over the course of all visits. A median of 3.0 was found for the reprogramming sessions. All patients indicated they would redo the procedure posttrial and during all follow-ups using a descriptive scale: Definitely Yes, Yes, Maybe, Probably Not, Definitely Not (see Fig. 3). There were 90.5% of patients (N = 19) who used pain medication before the implantation and 9.5% (N = 2) used no medication prior to the trial. Of the 19 patients who took medication, five patients (26.3%) could stop their medication entirely, nine patients (47.4%) showed a reduced intake, and one (5.3%) patient had an unchanged intake of medication. Four patients (21.1%) had an increased intake of medication (see Fig. 4). The majority of the leads (N = 8, 40%) were implanted with the tip at T7, one (5%) at T5, five (25%) at T8, four (20%) at T9, and two (10%) at T10. In this study we found one lead migration (4.8%), one lead breakage (4.8%), three extension breakages (14.3%), and one IPG communication loss (4.8%). Loss of effectiveness was encountered after an average time of 2.5 years in three patients (14.3%), without an identifiable cause or apparent lead migration. A single event (4.8%) of IPG communication loss was uneventful and resolved by a replacement. No infection, dural puncture, epidural bleeding, sensory or motor deficit was observed in this patient group (see Table 5).
5 LONG-TERM OUTCOMES PERC-PADDLE LEADS Table 4. Parameter Settings for Each Patient. Patient Freq (Hz) Pulse width (msec) Perception amplitude (ma) Comfort amplitude (ma) Maximum tolerable amplitude (ma) Electrode configuration Stim Set Stim Set Stim Set Stim Set Redo Procedure? Medication Usage at Last Follow-Up 100% 80% 14% 15% 7% Unchanged 1 (4.8%) 60% 40% 20% 0% 100% Post Trial (N=21) 86% 85% 93% F-U 1 (N=21) F-U 2 (N=20) F-U 3 (N=14) Yes Definitely Yes Increased 4 (19.0%) Decreased & No medication 16 (76.2%) Decreased 9 (42.9%) No medication 7 (33.3%) Figure 3. Percentage of patients that would redo the implantation posttrial, follow-up 1 (F-U1), follow-up 2 (F-U2), and follow-up 3 (F-U3). Between brackets, the number of patients who did the respective follow-up visits is represented. DISCUSSION The SCS with a percutaneous implanted paddle lead has been shown to be feasible and safe in trained hands. This study s aim was to investigate the sustainability of SCS in patients implanted with a percutaneous implanted paddle lead. The results confirm the possibility of sustaining stimulation in the pain areas over a mean of 3.3 years, in patients with neuropathic leg and back pain. Similar results have already been published in three other studies with 12 months follow-up (16,20,21). In the study by Vonhögen et al., a correlation analysis revealed that VAS scores for legs and back correlated negatively with baseline satisfaction and QOL, showing that better pain reduction results in Figure 4. Medication usage at last follow-up of all 21 patients. improved satisfaction and QOL outcomes. They found improvements of 69% and 75% in satisfaction and QOL after one year compared with baseline (16). In the studies of de Vos et al. and Logé et al., 90% and 88.3% of the patients, respectively, rated their QOL to be improved or greatly improved (18,20). There were 85.3% of the patients in the study by Logé et al. who mentioned satisfaction or were very satisfied with the treatment outcome after implantation (18). In this study, we found that all patients indicated that they would redo the procedure. We do have to point out that in this study, only patients who received a permanent implant were followed up and this may therefore somewhat bias this result. On the other hand, this 5
6 LOGÉ ET AL. Table 5. Adverse Events Overview With Corrections Toward Events Per Year. N % Average time to event (years) Corrected events/year Migration Lead breakage Extension breakage Loss of effectiveness %/year Table 6. Comparisons of Electrophysiological Parameters and Tip Location With Other Percutaneously Introduced Lamitrode Studies. Vonhögen et al. (16) de Vos et al. (20) Kinfe et al. (21) Logé et al. (18) This study Electrophysiological parameters Frequency (Hz) 36.0 Not given Not given (30 60) (30 100) (Not given) (20 70) Pulse width (msec) Not given Not given ( ) (50 450) (Not given) ( ) Perception amplitude (ma) 3.4 Not given Not given Not given 5.3 ( ) ( ) Comfort amplitude (ma) 4.5 Not given Not given ( ) ( ) (Not given) ( ) Maximum tolerable amplitude (ma) 6.7 Not given Not given Not given 8.0 ( ) ( ) Anatomical location of the tip of the S-Series lead Tip location T8 T8 T7 Not given T7 (T6-T10) (T7-T9) (C4-T11) (T5-T10) 6 confirms that the stimulation sustainability adds to the treatment satisfaction in these patients, even long term. Vonhögen et al. found a mean reduction of 43% and 27% for the legs and back, respectively. All reductions statistical significance improved compared with baseline at one year. In 85% of the patients, they found a clinical significant reduction of the back pain component with a mean decrease of 4.3 points or 52% (16). In another study where similar leads were used, they found a decrease of VAS of 50% or more in 71% of the patients for the legs and in 51% of the patients for back pain at one year postoperatively (20). Logé et al. recently published an average patient-reported pain relief of 78.8% posttrial and Kinfe et al. found an overall median pain reduction of 73% at one year (18,21). In this study, we found statistically significant pain reduction for pain at present moment, VAS pain worst last week, VAS pain least last week, and VAS pain mean last week, at different time points: posttrial, F-U1, F-U2, and even F-U3. We excluded to time the FU-3 data as not all patients had done the third follow-up visit. We found reductions of 75.79%, 62.52%, and again 62.52% for posttrial, F-U1, and F-U2, respectively. In this study, we did not differentiate between back and leg pain, as the primary endpoint was stimulation sustainability. The significant reductions in pain, together with the sustained results at F-U1 and F-U2, show that long-term electrically induced paresthesia and pain suppression can be achieved using these leads, both for back and leg pain. An analysis of the number of prior surgeries revealed no relationship with the pain reduction outcome in this study. We did not find any statistical significance between patients with FBSS or lumboischialgia at each follow-up, indicating that both indications can benefit well of SCS when indicated. The mean electrophysiologic parameters did not differ significantly from what was found in other studies (see also Table 6) where a similar type of electrode was used. In contrast to the studies of Vonhögen et al. and de Vos et al., we found that guarded combinations were not used more than bipolar configurations. These contradictory findings in the studies indicate the interindividual differences between patients and the need to have control over the different electrophysiologic parameters to shape an optimal electrical field in order to achieve optimal paresthesia coverage for patients with chronic neuropathic pain syndromes. We found an average tip location at T7, which is slightly higher than the studies of Vonhögen et al. and de Vos et al., but similar to the findings of Kinfe et al. (Table 6). In this series, we have found one migration (4.8%), in a cranial direction. After repositioning the lead, paresthesia covered the full pain area in both legs and the low back again. The event occurred after 2.2 years and when recalculated into events per year to make it comparable with the other S-Series studies, we found an average incidence rate of 0.5 per year (2.2%/year). One lead breakage was seen so far, which happened after a trauma (fall). This happened after 3.4 years. Three extension breakages were seen (Table 7), of which one happened after a trauma (same patient as with the lead breakage). The average time of the extension breakage incidents was 3.8 years, resulting in 0.8 events per year (see also Table 5). In an evaluation of lead migration in four clinical research studies as published by Monroe et al. in 2008, they found an incidence rate of paddle lead migration of 3.0% (2 out of 67 implants) and 6.4% (15 of the 233 implants) for percutaneous leads, totaling the migration rate at 5.7% (17 out of 300) at one year follow-up (22). A literature review performed by Cameron revealed an incidence rate of 13.5% (23). With an incidence rate of 4.8% (one event), our data (2.2% when corrected for yearly incidence rate) show a lower migration rate compared with the literature. Vonhögen et al. found no migra-
7 LONG-TERM OUTCOMES PERC-PADDLE LEADS Table 7. Adverse Events: Percutaneously Implanted S-Series Studies Comparison. Vonhögen et al. (16) de Vos et al. (20) Kinfe et al. (21) Logé et al. (18) This study Total % Action N Dural puncture Bed rest Infection Explant & reimplanted Epidural bleeding N/A Neurological or motor deficit N/A Migration Repositioning, percutaneous lead added Loss of effectiveness Not mentioned Lead breakage Replaced Extension breakage Replaced Table 8. Lead Migration Comparison of Reported S-Series Studies With Literature. Author Year Lead migration rate (%) Comments Lead migration rates in literature Monroe et al. (22) Data of four prospective, multicenter, Institutional Review Board-approved clinical research studies Cameron (23) Literature review Percutaneously implanted S-Series leads Vonhögen et al (16) Retrospective data collection de Vos et al. (20) Prospective study Kinfe et al. (21) Prospective study Logé et al. (18) Prospective study Logé et al. (this study) Prospective study Averages per implant procedure type Literature: percutaneous and surgical N/A 9.6 See higher Percutaneously implanted paddle N/A 3.4 See higher tions with one-year follow-up and a comparable number of patients included in their study (16). Kinfe et al. found a 2.5% migration rate in 81 patients, with a median follow-up of one year (21). It is recommended to follow up over longer terms and with more data points, but there seems to be an increasing trend that the percutaneously implanted paddle leads behave more like surgical-implanted larger paddle leads over the longer term (see also Table 8). In contrast to these findings, the study of Logé et al. showed an incidence of 5.9% or two patients, which is around double of the earlier mentioned study of de Vos et al. (20). An explanation for this can be the initial experience with this new technique, plus the fact that the number of patients was limited, which then quickly increases the percentage. Furthermore, we have to highlight here that this study had only a follow-up of 28 days (trial period). When we compare the incidence rate of lead breakages with this type of paddle lead as reported to date with other lead studies (see also Table 9), we can conclude that the percutaneously introduced paddle lead seems to behave as a surgically introduced paddle lead. The averages even show a trend to outperform the surgically implanted leads, although we need to nuance this, as the average follow-up of the surgically introduced paddle lead studies is more than twice as long as those for the S-Series paddles to date and there is also a lot of variability seen in outcomes by the different authors. We acknowledge that this study discusses only a limited number of patients included and we therefore plan to follow up on more patients to see if the results are also sustained in larger patient groups implanted with this type of electrode. Furthermore, this study was designed as a single center study and we did not randomize with patients treated, for example, with only conventional medical treatment. Placebo-controlled studies are to date impossible with tonic stimulation, but may in the future eliminate this methodologic problem when new stimulation designs such as burst stimulation become widely available. This novel stimulation design may furthermore advance the clinical outcomes in patients with chronic pain conditions as earlier reported by De Ridder et al. (33). For example, the patients with loss of effectiveness might perhaps benefit from another stimulation design in the future to regain their benefits of SCS. Further research is warranted to compare and/or confirm these findings. CONCLUSION Percutaneous implantation of small profile paddle leads in patients with FBSS and lumboischialgia produces favorable results over the long term that are at least comparable with surgically implanted paddle leads, thus combining some favorable aspects of percutaneous as well as paddle leads. The percutaneous approach also allows nonsurgically trained pain physicians to introduce paddle leads. Indices like patients willingness to redo the procedure, QOL, or patient satisfaction may be more appropriate for analyzing 7
8 LOGÉ ET AL. Table 9. Lead Breakage Comparison of Reported S-Series Studies With Literature. Author Year N Follow-up (years) Lead failure rate (%) Cause of lead failure Lead breakage rates in literature Racz et al. (24) Lead fracture Bell and Bauer (25) Lead fracture North et al (26) Lead breakage /fatigue fracture Kumar et al (27) Lead fracture North et al (28) Lead breakage /insulation failure Anderson (29) Lead fracture Heidecke et al (30) Lead breakage /insulation failure Kumar et al (31) Lead breakage /fatigue fracture Akmal and Eljamel (32) Lead breakage /fatigue fracture Percutaneously implanted S-Series leads Vonhögen et al (16) N/A de Vos et al. (20) N/A Kinfe et al. (21) N/A Logé et al. (18) days 0.0 N/A Logé et al. (this study) Lead breakage (trauma) Averages per implant procedure type Literature percutaneous and surgical N/A See higher Percutaneously implanted paddle N/A See higher 8 outcome results, especially long term, than arbitrarily takings 50% reduction in VAS scores, as has been postulated earlier. The authors believe that the increased focus on product development, professional training and educational activities, best practice sharing, together with an expanded experience, led to improved outcomes for patients in need of a neuromodulation device. Acknowledgment The authors would like to thank Mr. Frank De Meutter from St. Jude Medical Belgium Neuromodulation Division, for his logistical and technical support during this study. Authorship Statements Drs. Logé and Vancamp were responsible for the inception and design of the study. Dr. Logé performed all the implantations and collected the data. Drs. Vancamp and Vanneste performed the statistical analysis and data interpretation. Drs. Vancamp and Logé drafted the manuscript with intellectual input from Drs. Vanneste and Rijckaert. All authors approved the final manuscript. How to Cite this Article Logé D., Vanneste S., Vancamp T., Rijckaert D Long-Term Outcomes of Spinal Cord Stimulation With Percutaneously Introduced Paddle Leads in the Treatment of FBSS and Lumboischialgia Neuromodulation 2012; e-pub ahead of print. DOI: /ner REFERENCES 1. Krames E. Spinal cord stimulation : indications, mechanism of action, and efficacy. Curr Pain Headache Rep 1999;3: Kumar K, Wilson JR. Factors affecting spinal cord stimulation outcome in chronic benign pain with suggestions to improve success rate. Acta Neurochir Suppl 2007;97: North RB, Ewend MG, Lawton MT, Piantadosi S. Spinal cord stimulation for chronic intractable pain: superiority of multi-channel devices. Pain 1991;44: Haddadan K, Krames ES. The effect of spinal cord stimulation, overall, and the effect of differing spinal cord stimulation technologies on pain, reduction in pain medication, sleep and function. Neuromodulation 2007;132: Kumar K, Toth C, Nath RK, Laing P. Epidural spinal cord stimulation for treatment of chronic pain some predictors of success. A 15-year experience. Surg Neurol 1998;50: ;discussion Kumar K, Taylor RS, Jacques L et al. The effects of spinal cord stimulation in neuropathic pain are sustained: a 24-month follow-up of the prospective randomized controlled multicenter trial of the effectiveness of spinal cord stimulation. Neurosurgery 2008;63: ;discussion North RB, Kidd DH, Farrokhi F, Piantadosi SA. Spinal cord stimulation versus repeated lumbosacral spine surgery for chronic pain: a randomized, controlled trial. Neurosurgery 2005;56:98 106;discussion Andrell P, Ekre O, Eliasson T et al. Cost-effectiveness of spinal cord stimulation versus coronary artery bypass grafting in patients with severe angina pectoris long-term results from the ESBY study. Cardiology 2003;99: Taylor RS, Taylor RJ, Van Buyten JP, Buchser E, North R, Bayliss S. The cost effectiveness of spinal cord stimulation in the treatment of pain: a systematic review of the literature. J Pain Symptom Manage 2004;27: Taylor RS, Van Buyten JP, Buchser E. Spinal cord stimulation for complex regional pain syndrome: a systematic review of the clinical and cost-effectiveness literature and assessment of prognostic factors. EurJPain2006;10: Kumar K, Taylor RS, Jacques L et al. Spinal cord stimulation versus conventional medical management for neuropathic pain: a multicentre randomised controlled trial in patients with failed back surgery syndrome. Pain 2007;132: Cameron T. Safety and efficacy of spinal cord stimulation for the treatment of chronic pain: a 20-year literature review. J Neurosurg 2004;100: North RB, Kidd DH, Olin JC, Sieracki JM. Spinal cord stimulation electrode design: prospective, randomized, controlled trial comparing percutaneous and laminectomy electrodes part I: technical outcomes. Neurosurgery 2002;51: Vangeneugden J. Implantation of surgical electrodes for spinal cord stimulation: classical midline laminotomy technique versus minimal invasive unilateral technique combined with spinal anaesthesia. Acta Neurochir Suppl 2007;97: Beems T, van Dongen RT.Minimally invasive placement of epidural plate electrodes under local anaesthesia in spinal cord stimulation. Acta Neurochir Suppl 2007;97: Vonhögen LH, Vancamp T, Vanneste S et al. Percutaneously implanted plate electrodes in failed back surgery syndrome (FBSS). Neuromodulation 2011;14: Logé D, De Coster O, Pollet W, Vancamp T. A novel percutaneous technique to implant plate-type electrodes. Min Invas Neurosurg 2011;54: Logé D, De Coster O, Washburn S. Technological innovation in spinal cord stimulation: use of a newly developed delivery device for introduction of spinal cord stimulation leads. Neuromodulation 2012;15: Logé D,De Coster O,Washburn S.A retrospective data collection study to evaluate the feasibility and safety of percutaneous introduction of a narrow paddle lead into the epidural space. New York: Poster Presented at the World Pain Congress (WIP), 2009, March 13 16,.
9 LONG-TERM OUTCOMES PERC-PADDLE LEADS 20. de Vos CC, Dijkstra C, Lenders MWPM, Holsheimer J. Spinal cord stimulation with hybrid lead relieves pain in low back and legs. Neuromodulation 2012;15: Kinfe TM,Schu S,Quack FJ,Wille C,Vesper J.Percutaneous implanted paddle lead for spinal cord stimulation: technical considerations and long-term follow-up. Neuromodulation 2012;15: Monroe CD, Washburn S, Cameron T. An evaluation of lead migration in published literature and four clinical research studies. Las Vegas: Poster Presented at the Annual Meeting of the North American Neuromodulation Society (NANS), 2008, December Cameron T. Safety and efficacy of spinal cord stimulation for the treatment of chronic pain: a 20-year literature review. J Neurosurg Spine 2004;100: Racz GB,McCarron RF,Talboys P.Percutaneous dorsal column stimulator for chronic pain control. Spine 1989;14: Bell S, Bauer BL. Dorsal column stimulation (DCS): cost to benefit analysis. Acta Neurochir 1991;52: North RB, Ewend MG, Lawton MT, Kidd DH. Failed back surgery syndrome: 5-year follow-up after SCS implantation. Neurosurgery 1991;28: Kumar K, Nath R, Wyant GM. Treatment of chronic pain by epidural spinal cord stimulation: a 10-year experience. J Neurosurg 1991;75: North RB, Kidd DH, Zahurak M et al. Spinal cord stimulation for chronic, intractable pain: experience over 2 decades. Neurosurgery 1993;32: Anderson C. Complications in spinal cord stimulation for the treatment of angina pectoris. Differences in unipolar and multipolar percutaneous inserted electrodes. Acta Cardiol 1997;55: Heidecke V, Rainov NG, Burkert W. Hardware failure in SCS for FBSS. Neuromodulation 2000;3: Kumar K, Hunter G, Demeria D. Spinal cord stimulation in treatment of chronic benign pain: challenges in treatment planning and present status, a 22-year experience. Neurosurgery 2006;58: Akmal S, Eljamel MS. Spinal cord stimulation for chronic pain: causes of long-term paddle-lead failure. Neuromodulation 2008;11: De Ridder D, Vanneste S, Plazier M, van der Loo E, Menovsky T. Burst spinal cord stimulation: toward paresthesia-free pain suppression. Neurosurgery 2010;66:
Spinal Cord Stimulation (SCS) Therapy: Fact Sheet
 Spinal Cord Stimulation (SCS) Therapy: Fact Sheet What is SCS Therapy? Spinal cord stimulation (SCS) may be a life-changing 1 surgical option for patients to control their chronic neuropathic pain and
Spinal Cord Stimulation (SCS) Therapy: Fact Sheet What is SCS Therapy? Spinal cord stimulation (SCS) may be a life-changing 1 surgical option for patients to control their chronic neuropathic pain and
NEUROMODULATION THERAPY ACCESS COALITION POSITION STATEMENT ON SPINAL CORD NEUROSTIMULATION
 NEUROMODULATION THERAPY ACCESS COALITION POSITION STATEMENT ON SPINAL CORD NEUROSTIMULATION Introduction: Spinal cord stimulation (SCS) is an established treatment for chronic neuropathic pain, which can
NEUROMODULATION THERAPY ACCESS COALITION POSITION STATEMENT ON SPINAL CORD NEUROSTIMULATION Introduction: Spinal cord stimulation (SCS) is an established treatment for chronic neuropathic pain, which can
Spinal Cord Stimulation Business Case for
 Spinal Cord Stimulation Business Case for Failed Back Surgery Syndrome Understanding How Various Stakeholders Gauge Success in Treating Chronic Pain FBSS is a subset of chronic low back pain, which is
Spinal Cord Stimulation Business Case for Failed Back Surgery Syndrome Understanding How Various Stakeholders Gauge Success in Treating Chronic Pain FBSS is a subset of chronic low back pain, which is
Economic aspects of Spinal Cord Stimulation (SCS)
 Economic aspects of Spinal Cord Stimulation (SCS) Burden of Chronic Pain Chronic pain affects one in five adults in Europe 1. Up to 10 per cent of chronic pain cases are neuropathic in origin. 2 Chronic
Economic aspects of Spinal Cord Stimulation (SCS) Burden of Chronic Pain Chronic pain affects one in five adults in Europe 1. Up to 10 per cent of chronic pain cases are neuropathic in origin. 2 Chronic
EXHIBIT C BOSTON SCIENTIFIC PRODUCTS AVAILABLE FOR NIH BRAIN INITIATIVE Page 1 of 9
 Page 1 of 9 NOTE: All systems and products should be considered as investigational-use only in the context of the NIH BRAIN Initiative. VERCISE DEEP BRAIN STIMULATION SYSTEM Description: 16-channel rechargeable
Page 1 of 9 NOTE: All systems and products should be considered as investigational-use only in the context of the NIH BRAIN Initiative. VERCISE DEEP BRAIN STIMULATION SYSTEM Description: 16-channel rechargeable
Contractor Number 11302. Oversight Region Region IV
 Local Coverage Determination (LCD): Spinal Cord Stimulators for Chronic Pain (L32549) Contractor Information Contractor Name Palmetto GBA opens in new window Contractor Number 11302 Contractor Type MAC
Local Coverage Determination (LCD): Spinal Cord Stimulators for Chronic Pain (L32549) Contractor Information Contractor Name Palmetto GBA opens in new window Contractor Number 11302 Contractor Type MAC
A New Spinal Cord Stimulation System. Effectively Relieves Chronic, Intractable Pain: A Multicenter Prospective Clinical Study
 NEUROMODULATION: TECHNOLOGY AT THE NEURAL INTERFACE Volume 10 Number 3 2007 http://www.blackwell-synergy.com/loi/ner ORIGINAL ARTICLE A New Spinal Cord Stimulation System Blackwell Publishing Inc Effectively
NEUROMODULATION: TECHNOLOGY AT THE NEURAL INTERFACE Volume 10 Number 3 2007 http://www.blackwell-synergy.com/loi/ner ORIGINAL ARTICLE A New Spinal Cord Stimulation System Blackwell Publishing Inc Effectively
Advances In Spine Care. James D. Bruffey M.D. Scripps Clinic Division of Orthopaedic Surgery Section of Spinal Surgery
 Advances In Spine Care James D. Bruffey M.D. Scripps Clinic Division of Orthopaedic Surgery Section of Spinal Surgery Introduction The Spine - A common source of problems Back pain is the #2 presenting
Advances In Spine Care James D. Bruffey M.D. Scripps Clinic Division of Orthopaedic Surgery Section of Spinal Surgery Introduction The Spine - A common source of problems Back pain is the #2 presenting
Spinal Cord Stimulators (SCS) for Injured Workers with Chronic Back and Leg
 Spinal Cord Stimulators (SCS) for Injured Workers with Chronic Back and Leg Pain after Lumbar Surgery A Prospective Study to Describe Costs, Complications, and Patient Outcomes: Final Report September
Spinal Cord Stimulators (SCS) for Injured Workers with Chronic Back and Leg Pain after Lumbar Surgery A Prospective Study to Describe Costs, Complications, and Patient Outcomes: Final Report September
Minimally Invasive Spine Surgery For Your Patients
 Minimally Invasive Spine Surgery For Your Patients Lukas P. Zebala, M.D. Assistant Professor Orthopaedic and Neurological Spine Surgery Department of Orthopaedic Surgery Washington University School of
Minimally Invasive Spine Surgery For Your Patients Lukas P. Zebala, M.D. Assistant Professor Orthopaedic and Neurological Spine Surgery Department of Orthopaedic Surgery Washington University School of
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: spinal_cord_stimulation 3/1980 10/2015 10/2016 10/2015 Description of Procedure or Service Spinal cord stimulation
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: spinal_cord_stimulation 3/1980 10/2015 10/2016 10/2015 Description of Procedure or Service Spinal cord stimulation
X Stop Spinal Stenosis Decompression
 X Stop Spinal Stenosis Decompression Am I a candidate for X Stop spinal surgery? You may be a candidate for the X Stop spinal surgery if you have primarily leg pain rather than mostly back pain and your
X Stop Spinal Stenosis Decompression Am I a candidate for X Stop spinal surgery? You may be a candidate for the X Stop spinal surgery if you have primarily leg pain rather than mostly back pain and your
Effectiveness of spinal cord stimulation for the management of neuropathic pain
 Effectiveness of spinal cord stimulation for the management of neuropathic pain August 2009 Author: Peter Larking PhD Important Note This evidence-based review summarises information on spinal cord stimulation
Effectiveness of spinal cord stimulation for the management of neuropathic pain August 2009 Author: Peter Larking PhD Important Note This evidence-based review summarises information on spinal cord stimulation
MEDICAL CONTESTED CASE HEARING NO 12090 M6-12-38043-01 DECISION AND ORDER
 MEDICAL CONTESTED CASE HEARING NO 12090 M6-12-38043-01 DECISION AND ORDER This case is decided pursuant to Chapter 410 of the Texas Workers Compensation Act and Rules of the Division of Workers Compensation
MEDICAL CONTESTED CASE HEARING NO 12090 M6-12-38043-01 DECISION AND ORDER This case is decided pursuant to Chapter 410 of the Texas Workers Compensation Act and Rules of the Division of Workers Compensation
Title: Interspinous Process Decompression with the X-Stop Device for Lumbar Spinal Stenosis: A Retrospective Review. Authors: Jennifer R.
 Title: Interspinous Process Decompression with the X-Stop Device for Lumbar Spinal Stenosis: A Retrospective Review. Authors: Jennifer R. Madonia-Barr, MS, PA-C and David L. Kramer, MD Institution: Connecticut
Title: Interspinous Process Decompression with the X-Stop Device for Lumbar Spinal Stenosis: A Retrospective Review. Authors: Jennifer R. Madonia-Barr, MS, PA-C and David L. Kramer, MD Institution: Connecticut
Neurostimulation: Orthopaedic Institute of Ohio 801 Medical Drive Lima, Ohio 45804 419-222-6622
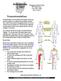 801 Medical Drive Lima, Ohio 45804 419-222-6622 Neurostimulation is the stimulation of the spinal cord by tiny electrical impulses. An implanted lead (a flexible insulated wire), which is powered by an
801 Medical Drive Lima, Ohio 45804 419-222-6622 Neurostimulation is the stimulation of the spinal cord by tiny electrical impulses. An implanted lead (a flexible insulated wire), which is powered by an
Department of Neurosciences Dorsal Root Ganglion (DRG) Stimulation Information for patients
 Oxford University Hospitals NHS Trust Department of Neurosciences Dorsal Root Ganglion (DRG) Stimulation Information for patients We have recently seen you in clinic as you have had pain for a long period
Oxford University Hospitals NHS Trust Department of Neurosciences Dorsal Root Ganglion (DRG) Stimulation Information for patients We have recently seen you in clinic as you have had pain for a long period
Spinal cord stimulation
 Spinal cord stimulation This leaflet aims to answer your questions about having spinal cord stimulation. It explains the benefits, risks and alternatives, as well as what you can expect when you come to
Spinal cord stimulation This leaflet aims to answer your questions about having spinal cord stimulation. It explains the benefits, risks and alternatives, as well as what you can expect when you come to
 Epimed Would Like To Congratulate The 20th Annual Budapest Conference The New Shape of Pain Relief SmalleST. ThiNNeST. CoNTouRed design. Precision Novi is the world s smallest, thinnest 16 contact primary
Epimed Would Like To Congratulate The 20th Annual Budapest Conference The New Shape of Pain Relief SmalleST. ThiNNeST. CoNTouRed design. Precision Novi is the world s smallest, thinnest 16 contact primary
Bionic Navigator 1.2 Software Guide
 Bionic Navigator 1.2 Software Guide 91057047-01 REV A CAUTION: Federal law restricts this device to sale, distribution and use by or on the order of a physician. Bionic Navigator 1.2 Software Guide Guarantees
Bionic Navigator 1.2 Software Guide 91057047-01 REV A CAUTION: Federal law restricts this device to sale, distribution and use by or on the order of a physician. Bionic Navigator 1.2 Software Guide Guarantees
Intrathecal Baclofen for CNS Spasticity
 Intrathecal Baclofen for CNS Spasticity Last Review Date: November 13, 2015 Number: MG.MM.ME.31bC5 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or
Intrathecal Baclofen for CNS Spasticity Last Review Date: November 13, 2015 Number: MG.MM.ME.31bC5 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or
BionicNavigator 1.2 Software Guide
 BionicNavigator 1.2 Software Guide SC-7150, SC-7150-4, SC-7150-4R, NM-7153-12, NM-7153-12R, NM-7151-30, NM-7151-30R, NM-7153-30, NM-7153-30R Clinician Programmer CAUTION: Federal law restricts this device
BionicNavigator 1.2 Software Guide SC-7150, SC-7150-4, SC-7150-4R, NM-7153-12, NM-7153-12R, NM-7151-30, NM-7151-30R, NM-7153-30, NM-7153-30R Clinician Programmer CAUTION: Federal law restricts this device
Spine Vol. 30 No. 16; August 15, 2005, pp 1799-1807
 A Randomized Controlled Trial of an Educational Intervention to Prevent the Chronic Pain of Whiplash Associated Disorders Following Rear-End Motor Vehicle Collisions 1 Spine Vol. 30 No. 16; August 15,
A Randomized Controlled Trial of an Educational Intervention to Prevent the Chronic Pain of Whiplash Associated Disorders Following Rear-End Motor Vehicle Collisions 1 Spine Vol. 30 No. 16; August 15,
ISPI Newsletter Archive Lumbar Spine Surgery
 ISPI Newsletter Archive Lumbar Spine Surgery January 2005 Effects of Charite Artificial Disc on the Implanted and Adjacent Spinal Segments Mechanics Using a Hybrid Testing Protocol Spine. 30(24):2755-2764,
ISPI Newsletter Archive Lumbar Spine Surgery January 2005 Effects of Charite Artificial Disc on the Implanted and Adjacent Spinal Segments Mechanics Using a Hybrid Testing Protocol Spine. 30(24):2755-2764,
The patient was a 48-year-old
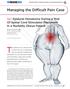 PRINTER-FRIENDLY VERSION AVAILABLE AT PAINMEDICINENEWS.COM Managing the Difficult Pain Case Case 1: Epidural Hematoma During a Trial Of Spinal Cord Stimulator Placement In a Morbidly Obese Patient SANJAY
PRINTER-FRIENDLY VERSION AVAILABLE AT PAINMEDICINENEWS.COM Managing the Difficult Pain Case Case 1: Epidural Hematoma During a Trial Of Spinal Cord Stimulator Placement In a Morbidly Obese Patient SANJAY
Local Coverage Determination (LCD): Spinal Cord Stimulation (Dorsal Column Stimulation) (L34705)
 Local Coverage Determination (LCD): Spinal Cord Stimulation (Dorsal Column Stimulation) (L34705) Contractor Information Contractor Name Novitas Solutions, Inc. LCD Information Document Information LCD
Local Coverage Determination (LCD): Spinal Cord Stimulation (Dorsal Column Stimulation) (L34705) Contractor Information Contractor Name Novitas Solutions, Inc. LCD Information Document Information LCD
Case Series on Chronic Whiplash Related Neck Pain Treated with Intraarticular Zygapophysial Joint Regeneration Injection Therapy
 Pain Physician 2007; 10:313-318 ISSN 1533-3159 Case Series Case Series on Chronic Whiplash Related Neck Pain Treated with Intraarticular Zygapophysial Joint Regeneration Injection Therapy R. Allen Hooper
Pain Physician 2007; 10:313-318 ISSN 1533-3159 Case Series Case Series on Chronic Whiplash Related Neck Pain Treated with Intraarticular Zygapophysial Joint Regeneration Injection Therapy R. Allen Hooper
Image-guided Spine Procedures for Relief of Severe Lower Back Pain:
 Image-guided Spine Procedures for Relief of Severe Lower Back Pain: A Guide to Epidural Steroid Injection, Facet Joint Injection, and Selective Nerve Root Block. PETER H TAKEYAMA MD HENRY WANG MD PhD SVEN
Image-guided Spine Procedures for Relief of Severe Lower Back Pain: A Guide to Epidural Steroid Injection, Facet Joint Injection, and Selective Nerve Root Block. PETER H TAKEYAMA MD HENRY WANG MD PhD SVEN
10801 Sixth St, Suite 120 Rancho Cucamonga, CA 91730 Tel (909) 890-2000 Fax (909) 890-2003 Visit our web site at: www.iehp.org.
 Percutaneous Image-Guided Lumbar Decompression for Lumbar Spinal Stenosis (PILD), Including the Commercial Procedure Known as Minimally Invasive Lumbar Decompression (mild -Vertos Medical) Policy: Based
Percutaneous Image-Guided Lumbar Decompression for Lumbar Spinal Stenosis (PILD), Including the Commercial Procedure Known as Minimally Invasive Lumbar Decompression (mild -Vertos Medical) Policy: Based
HEADACHES AND THE THIRD OCCIPITAL NERVE
 HEADACHES AND THE THIRD OCCIPITAL NERVE Edward Babigumira M.D. FAAPMR. Interventional Pain Management, Lincoln. B. Pain Clinic, Ltd. Diplomate ABPMR. Board Certified Pain Medicine No disclosures Disclosure
HEADACHES AND THE THIRD OCCIPITAL NERVE Edward Babigumira M.D. FAAPMR. Interventional Pain Management, Lincoln. B. Pain Clinic, Ltd. Diplomate ABPMR. Board Certified Pain Medicine No disclosures Disclosure
Present and Potential Use of Spinal Cord Stimulation to Control Chronic Pain
 Pain Physician 2014; 17:235-246 ISSN 1533-3159 Narrative Review Present and Potential Use of Spinal Cord Stimulation to Control Chronic Pain Jason J. Song, MD, PhD, Adrian Popescu, MD, and Russell L. Bell,
Pain Physician 2014; 17:235-246 ISSN 1533-3159 Narrative Review Present and Potential Use of Spinal Cord Stimulation to Control Chronic Pain Jason J. Song, MD, PhD, Adrian Popescu, MD, and Russell L. Bell,
Motiva Implant Matrix Silicone Breast Implants Summary of Clinical Data 4-Year Follow Up
 Motiva Implant Matrix Silicone Breast Implants Summary of Clinical Data 4-Year Follow Up October 2010 - March 2015 Motiva Implant Matrix Silicone Breast Implants Prospective Clinical Evaluation: 4-Year
Motiva Implant Matrix Silicone Breast Implants Summary of Clinical Data 4-Year Follow Up October 2010 - March 2015 Motiva Implant Matrix Silicone Breast Implants Prospective Clinical Evaluation: 4-Year
Precision Spinal Cord Stimulator System Clinician Manual
 Precision Spinal Cord Stimulator System Directions for Use CAUTION: Federal law restricts this device to sale, distribution and use by or on the order of a physician. 90834026-10 REV B Precision Spinal
Precision Spinal Cord Stimulator System Directions for Use CAUTION: Federal law restricts this device to sale, distribution and use by or on the order of a physician. 90834026-10 REV B Precision Spinal
Information for the Patient About Surgical
 Information for the Patient About Surgical Decompression and Stabilization of the Spine Aging and the Spine Daily wear and tear, along with disc degeneration due to aging and injury, are common causes
Information for the Patient About Surgical Decompression and Stabilization of the Spine Aging and the Spine Daily wear and tear, along with disc degeneration due to aging and injury, are common causes
Update to the Treatment of Degenerative Cervical Disc Disease
 Update to the Treatment of Degenerative Cervical Disc Disease Michael Lynn, MD Neurosurgeon, Southeastern Neurosurgical & Spine Institute Adjunct Assistant Clinical Professor of Bioengineering, Clemson
Update to the Treatment of Degenerative Cervical Disc Disease Michael Lynn, MD Neurosurgeon, Southeastern Neurosurgical & Spine Institute Adjunct Assistant Clinical Professor of Bioengineering, Clemson
Spinal Cord Stimulation
 Spinal Cord Stimulation Relieving Chronic Pain If chronic pain restricts your life, you may have tried many ways to find relief. This may include medications, nerve blocks, physical therapy, and surgery.
Spinal Cord Stimulation Relieving Chronic Pain If chronic pain restricts your life, you may have tried many ways to find relief. This may include medications, nerve blocks, physical therapy, and surgery.
Enhanced recovery programme after TKA through multi-disciplinary collaboration
 Enhanced recovery programme after TKA through multi-disciplinary collaboration ChanPK(1), ChiuKY(1), FungYK(6), YeungSS(7), NgT(8), ChanMT(5), LamR(4), WongNY(3), ChoiYY(3), ChanCW(2), NgFY(1), YanCH(1)
Enhanced recovery programme after TKA through multi-disciplinary collaboration ChanPK(1), ChiuKY(1), FungYK(6), YeungSS(7), NgT(8), ChanMT(5), LamR(4), WongNY(3), ChoiYY(3), ChanCW(2), NgFY(1), YanCH(1)
Nonoperative Management of Herniated Cervical Intervertebral Disc With Radiculopathy. Spine Volume 21(16) August 15, 1996, pp 1877-1883
 Nonoperative Management of Herniated Cervical Intervertebral Disc With Radiculopathy 1 Spine Volume 21(16) August 15, 1996, pp 1877-1883 Saal, Joel S. MD; Saal, Jeffrey A. MD; Yurth, Elizabeth F. MD FROM
Nonoperative Management of Herniated Cervical Intervertebral Disc With Radiculopathy 1 Spine Volume 21(16) August 15, 1996, pp 1877-1883 Saal, Joel S. MD; Saal, Jeffrey A. MD; Yurth, Elizabeth F. MD FROM
Ms. Jackson is the Manager of Health Finance and Reimbursement, Division of Health Policy and Practice Services, Washington, DC.
 Electrodiagnostic Testing with Same Day Evaluation Management By: Shane J. Burr, MD; Scott I. Horn, DO; Jenny J. Jackson, MPH, CPC; Joseph P. Purcell, DO Dr. Burr practices general inpatient and outpatient
Electrodiagnostic Testing with Same Day Evaluation Management By: Shane J. Burr, MD; Scott I. Horn, DO; Jenny J. Jackson, MPH, CPC; Joseph P. Purcell, DO Dr. Burr practices general inpatient and outpatient
EDUCATION: School Degree Received Year Earned University of Pittsburgh B.S. 1994 Biological Sciences Major Computer Sciences Minor
 Yeshvant Ashok Navalgund, M.D. DNA Advanced Pain Treatment Center Navalgund Consulting P.O.Box 747, Greensburg, PA 15601 (412) 561-7246 (Office) www.dnapain.com EDUCATION: School Degree Received Year Earned
Yeshvant Ashok Navalgund, M.D. DNA Advanced Pain Treatment Center Navalgund Consulting P.O.Box 747, Greensburg, PA 15601 (412) 561-7246 (Office) www.dnapain.com EDUCATION: School Degree Received Year Earned
NON SURGICAL SPINAL DECOMPRESSION. Dr. Douglas A. VanderPloeg
 NON SURGICAL SPINAL DECOMPRESSION Dr. Douglas A. VanderPloeg CONTENTS I. Incidence of L.B.P. II. Anatomy Review III. IV. Disc Degeneration, Bulge, and Herniation Non-Surgical Spinal Decompression 1. History
NON SURGICAL SPINAL DECOMPRESSION Dr. Douglas A. VanderPloeg CONTENTS I. Incidence of L.B.P. II. Anatomy Review III. IV. Disc Degeneration, Bulge, and Herniation Non-Surgical Spinal Decompression 1. History
Spine Trauma: When to Transfer. Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU
 Spine Trauma: When to Transfer Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU Disclosures Depuy Spine Consultant (teaching and courses) Department education and research funds Atlas Spine
Spine Trauma: When to Transfer Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU Disclosures Depuy Spine Consultant (teaching and courses) Department education and research funds Atlas Spine
National Coverage Determination. Vagus Nerve Stimulation (VNS)
 National Coverage Determination Vagus Nerve Stimulation (VNS) Number NEURO-004 Contractor Name Wisconsin Physicians Service Insurance Corporation AMA CPT Copyright Statement CPT codes, descriptions and
National Coverage Determination Vagus Nerve Stimulation (VNS) Number NEURO-004 Contractor Name Wisconsin Physicians Service Insurance Corporation AMA CPT Copyright Statement CPT codes, descriptions and
News and Advancements from the Department of Clinical Neurosciences. Spinal Cord Stimulation for Low Back Pain
 NeuroUpdate News and Advancements from the Department of Clinical Neurosciences Spinal Cord Stimulation for Low Back Pain Sanjay Patra, MD An estimated 70 percent to 85 percent of the adult population
NeuroUpdate News and Advancements from the Department of Clinical Neurosciences Spinal Cord Stimulation for Low Back Pain Sanjay Patra, MD An estimated 70 percent to 85 percent of the adult population
Accelerated recovery of post-operative dental implant patients by means of pulsed shortwave (SWT) therapy: An Observational Study
 Bartolomeo Operti, MD and Dr Tiziano Tealdo Accelerated recovery of post-operative dental implant patients by means of pulsed shortwave (SWT) therapy: Bartolomeo Operti, MD Chief of Anesthesia Department
Bartolomeo Operti, MD and Dr Tiziano Tealdo Accelerated recovery of post-operative dental implant patients by means of pulsed shortwave (SWT) therapy: Bartolomeo Operti, MD Chief of Anesthesia Department
Migraine and the greater occipital nerve
 Migraine and the greater occipital nerve What is the greater occipital nerve? The nerves that travel from your spine (in the neck) to the back of the head and scalp are known as the occipital nerves. There
Migraine and the greater occipital nerve What is the greater occipital nerve? The nerves that travel from your spine (in the neck) to the back of the head and scalp are known as the occipital nerves. There
Measure Title X RAY PRIOR TO MRI OR CAT SCAN IN THE EVAULATION OF LOWER BACK PAIN Disease State Back pain Indicator Classification Utilization
 Client HMSA: PQSR 2009 Measure Title X RAY PRIOR TO MRI OR CAT SCAN IN THE EVAULATION OF LOWER BACK PAIN Disease State Back pain Indicator Classification Utilization Strength of Recommendation Organizations
Client HMSA: PQSR 2009 Measure Title X RAY PRIOR TO MRI OR CAT SCAN IN THE EVAULATION OF LOWER BACK PAIN Disease State Back pain Indicator Classification Utilization Strength of Recommendation Organizations
CODING SHEETS CHRONIC INTRACTABLE SPASTICITY. Effective January 1, 2009 CODMAN 3000 NEUROMODULATION AND ONCOLOGY REIMBURSEMENT HOTLINE
 CODING SHEETS CHRONIC INTRACTABLE SPASTICITY Effective January 1, 2009 CODMAN 3000 NEUROMODULATION AND ONCOLOGY REIMBURSEMENT HOTLINE Phone: 800-609-1108 Email: codmanpump@aol.com Fax: 303-703-1572 CODMAN
CODING SHEETS CHRONIC INTRACTABLE SPASTICITY Effective January 1, 2009 CODMAN 3000 NEUROMODULATION AND ONCOLOGY REIMBURSEMENT HOTLINE Phone: 800-609-1108 Email: codmanpump@aol.com Fax: 303-703-1572 CODMAN
2.0 Synopsis. Vicodin CR (ABT-712) M05-765 Clinical Study Report R&D/07/095. (For National Authority Use Only) to Part of Dossier: Volume:
 2.0 Synopsis Abbott Laboratories Name of Study Drug: Vicodin CR Name of Active Ingredient: Hydrocodone/Acetaminophen Extended Release (ABT-712) Individual Study Table Referring to Part of Dossier: Volume:
2.0 Synopsis Abbott Laboratories Name of Study Drug: Vicodin CR Name of Active Ingredient: Hydrocodone/Acetaminophen Extended Release (ABT-712) Individual Study Table Referring to Part of Dossier: Volume:
UNILATERAL VS. BILATERAL FIRST RAY SURGERY: A PROSPECTIVE STUDY OF 186 CONSECUTIVE CASES COMPLICATIONS, PATIENT SATISFACTION, AND COST TO SOCIETY
 UNILATERAL VS. BILATERAL FIRST RAY SURGERY: A PROSPECTIVE STUDY OF 186 CONSECUTIVE CASES COMPLICATIONS, PATIENT SATISFACTION, AND COST TO SOCIETY Robert Fridman DPM, Jarrett Cain DPM, Lowell Weil Jr. DPM,
UNILATERAL VS. BILATERAL FIRST RAY SURGERY: A PROSPECTIVE STUDY OF 186 CONSECUTIVE CASES COMPLICATIONS, PATIENT SATISFACTION, AND COST TO SOCIETY Robert Fridman DPM, Jarrett Cain DPM, Lowell Weil Jr. DPM,
Marc A. Cohen, MD, FAAOS, FACS Diplomate American Board of Spinal Surgery Fellow American College of Spinal Surgery
 Marc A. Cohen, MD, FAAOS, FACS Diplomate American Board of Spinal Surgery Fellow American College of Spinal Surgery 221 Madison Ave Morristown, New Jersey 07960 (973) 538 4444 Fax (973) 538 0420 Patient
Marc A. Cohen, MD, FAAOS, FACS Diplomate American Board of Spinal Surgery Fellow American College of Spinal Surgery 221 Madison Ave Morristown, New Jersey 07960 (973) 538 4444 Fax (973) 538 0420 Patient
DIFFERENTIAL DIAGNOSIS OF LOW BACK PAIN. Arnold J. Weil, M.D., M.B.A. Non-Surgical Orthopaedics, P.C. Atlanta, GA
 DIFFERENTIAL DIAGNOSIS OF LOW BACK PAIN Arnold J. Weil, M.D., M.B.A. Non-Surgical Orthopaedics, P.C. Atlanta, GA MEDICAL ALGORITHM OF REALITY LOWER BACK PAIN Yes Patient will never get better until case
DIFFERENTIAL DIAGNOSIS OF LOW BACK PAIN Arnold J. Weil, M.D., M.B.A. Non-Surgical Orthopaedics, P.C. Atlanta, GA MEDICAL ALGORITHM OF REALITY LOWER BACK PAIN Yes Patient will never get better until case
Sample Treatment Protocol
 Sample Treatment Protocol 1 Adults with acute episode of LBP Definition: Acute episode Back pain lasting
Sample Treatment Protocol 1 Adults with acute episode of LBP Definition: Acute episode Back pain lasting
Bionic Navigator 1.2 Software Guide
 Bionic Navigator 1.2 Software Guide SC-7150, SC-7150-4, SC-7150-4R, NM-7153-12, NM-7153-12R, NM-7151-30, NM-7151-30R, NM-7153-30, NM-7153-30R Clinician Programmer CAUTION: Federal law restricts this device
Bionic Navigator 1.2 Software Guide SC-7150, SC-7150-4, SC-7150-4R, NM-7153-12, NM-7153-12R, NM-7151-30, NM-7151-30R, NM-7153-30, NM-7153-30R Clinician Programmer CAUTION: Federal law restricts this device
Thoracic Epidural Catheterization Using Ultrasound in Obese Patients for Bariatric Surgery
 IBIMA Publishing Journal of Research in Obesity http://www.ibimapublishing.com/journals/obes/obes.html Vol. 2014 (2014), Article ID 538833, 6 pages DOI: 10.5171/2014.538833 Research Article Thoracic Epidural
IBIMA Publishing Journal of Research in Obesity http://www.ibimapublishing.com/journals/obes/obes.html Vol. 2014 (2014), Article ID 538833, 6 pages DOI: 10.5171/2014.538833 Research Article Thoracic Epidural
WorkCover s physiotherapy forms: Purpose beyond paperwork?
 WorkCover s physiotherapy forms: Purpose beyond paperwork? Eva Schonstein, Dianna T Kenny and Christopher G Maher The University of Sydney We retrospectively analysed 219 consecutive treatment plans submitted
WorkCover s physiotherapy forms: Purpose beyond paperwork? Eva Schonstein, Dianna T Kenny and Christopher G Maher The University of Sydney We retrospectively analysed 219 consecutive treatment plans submitted
Promising Treatments for SCI: What s on The Horizon. SCI: A Devastating Injury. Case: Mr. MC 9/21/2015. Epidemiology: Costs:
 Promising Treatments for SCI: What s on The Horizon Shawn Song, MD SCI Fellow University of Washington/VA Puget Sound Healthcare System SCI: A Devastating Injury Epidemiology: Incidence of ~12,000 patients/year.
Promising Treatments for SCI: What s on The Horizon Shawn Song, MD SCI Fellow University of Washington/VA Puget Sound Healthcare System SCI: A Devastating Injury Epidemiology: Incidence of ~12,000 patients/year.
Pain Management. Practical Applications in Electrotherapy
 Pain Management Practical Applications in Electrotherapy The TENS Advantage Deliver Immediate Pain Relief using a unique waveform designed to help prevent nerve accommodation. Manage Dynamic Pain by adjusting
Pain Management Practical Applications in Electrotherapy The TENS Advantage Deliver Immediate Pain Relief using a unique waveform designed to help prevent nerve accommodation. Manage Dynamic Pain by adjusting
C 2 / C 3 N E RVE BLOCKS AND GREATER OCCIPITAL NERVE BLOCK IN CERV I C O G E N I C HEADACHE TREATMENT
 C 2 / C 3 N E RVE BLOCKS AND GREATER OCCIPITAL NERVE BLOCK IN CERV I C O G E N I C HEADACHE TREATMENT N u rten Inan, Aysegul Ceyhan, Levent Inan*, Ozlem Kavaklioglu, Alp Alptekin, Nurten Unal Ministry
C 2 / C 3 N E RVE BLOCKS AND GREATER OCCIPITAL NERVE BLOCK IN CERV I C O G E N I C HEADACHE TREATMENT N u rten Inan, Aysegul Ceyhan, Levent Inan*, Ozlem Kavaklioglu, Alp Alptekin, Nurten Unal Ministry
Physician Coding and Payment Guide 2015
 Targeted Drug Delivery Physician Coding and Payment Guide 2015 Flowonix Medical has compiled this coding information for your convenience. This information is gathered from third party sources and is subject
Targeted Drug Delivery Physician Coding and Payment Guide 2015 Flowonix Medical has compiled this coding information for your convenience. This information is gathered from third party sources and is subject
New York State Workers' Comp Board. Mid and Lower Back Treatment Guidelines. Summary From 1st Edition, June 30, 2010. Effective December 1, 2010
 New York State Workers' Comp Board Mid and Lower Back Treatment Guidelines Summary From 1st Edition, June 30, 2010 Effective December 1, 2010 General Principles Treatment should be focused on restoring
New York State Workers' Comp Board Mid and Lower Back Treatment Guidelines Summary From 1st Edition, June 30, 2010 Effective December 1, 2010 General Principles Treatment should be focused on restoring
Effective Date: 01/01/2012 Revision Date: 07/24/2013 Comments: Policy Accepted during 2013 Annual Review with no changes.
 Health Plan Coverage Policy ARBenefits Approval: 01/01/2012 Effective Date: 01/01/2012 Revision Date: 07/24/2013 Comments: Policy Accepted during 2013 Annual Review with no changes. Title: Minimally Invasive,
Health Plan Coverage Policy ARBenefits Approval: 01/01/2012 Effective Date: 01/01/2012 Revision Date: 07/24/2013 Comments: Policy Accepted during 2013 Annual Review with no changes. Title: Minimally Invasive,
Citation: Robertson, I.H., Gray, J.M., Pentland, B., & Waite, L.J. (1990). Microcomputerbased
 A computer-based cognitive rehabilitation program, involving scanning training twice a week for 7 weeks, did not improve cognitive function in patients with unilateral left visual neglect. Prepared by:
A computer-based cognitive rehabilitation program, involving scanning training twice a week for 7 weeks, did not improve cognitive function in patients with unilateral left visual neglect. Prepared by:
RENOWN REGIONAL MEDICAL CENTER DEPARTMENT OF ORTHOPAEDICS DELINEATION OF PRIVILEGES
 RENOWN REGIONAL MEDICAL CENTER DEPARTMENT OF THOPAEDICS DELINEATION OF PRIVILEGES BASIC EDUCATION: M.D. or D.O. MINIMAL FMAL TRAINING: ABMS Board certification or eligibility, or be able to document equivalent
RENOWN REGIONAL MEDICAL CENTER DEPARTMENT OF THOPAEDICS DELINEATION OF PRIVILEGES BASIC EDUCATION: M.D. or D.O. MINIMAL FMAL TRAINING: ABMS Board certification or eligibility, or be able to document equivalent
Does the pain radiating down your legs, buttocks or lower back prevent you from walking long distances?
 Does the pain radiating down your legs, buttocks or lower back prevent you from walking long distances? Do you experience weakness, tingling, numbness, stiffness, or cramping in your legs, buttocks or
Does the pain radiating down your legs, buttocks or lower back prevent you from walking long distances? Do you experience weakness, tingling, numbness, stiffness, or cramping in your legs, buttocks or
Adult Spine Rotation Specific Evaluation Orthopaedic Surgery Training Program School of Medicine, Queen s University
 Adult Spine Rotation Specific Evaluation Orthopaedic Surgery Training Program School of Medicine, Queen s University CanMEDS Roles / Competencies Name: PGY Rotation Dates: s s Exceeds N/A Attending Staff:
Adult Spine Rotation Specific Evaluation Orthopaedic Surgery Training Program School of Medicine, Queen s University CanMEDS Roles / Competencies Name: PGY Rotation Dates: s s Exceeds N/A Attending Staff:
Spinal Surgery Functional Status and Quality of Life Outcome Specifications 2015 (01/01/2013 to 12/31/2013 Dates of Procedure) September 2014
 Description Methodology For patients ages 18 years and older who undergo a lumbar discectomy/laminotomy or lumbar spinal fusion procedure during the measurement year, the following measures will be calculated:
Description Methodology For patients ages 18 years and older who undergo a lumbar discectomy/laminotomy or lumbar spinal fusion procedure during the measurement year, the following measures will be calculated:
Clinical Study Synopsis
 Clinical Study Synopsis This Clinical Study Synopsis is provided for patients and healthcare professionals to increase the transparency of Bayer's clinical research. This document is not intended to replace
Clinical Study Synopsis This Clinical Study Synopsis is provided for patients and healthcare professionals to increase the transparency of Bayer's clinical research. This document is not intended to replace
Important Predictors of Outcome in Patients with Cervical Spondylotic Myelopathy and Radiculopathy undergoing Surgery
 Important Predictors of Outcome in Patients with Cervical Spondylotic Myelopathy and Radiculopathy undergoing Surgery Michael G. Fehlings Professor of Neurosurgery Vice Chair Research, Department of Surgery
Important Predictors of Outcome in Patients with Cervical Spondylotic Myelopathy and Radiculopathy undergoing Surgery Michael G. Fehlings Professor of Neurosurgery Vice Chair Research, Department of Surgery
Summary and general discussion
 Chapter 7 Summary and general discussion Summary and general discussion In this thesis, treatment of vitamin K antagonist-associated bleed with prothrombin complex concentrate was addressed. In this we
Chapter 7 Summary and general discussion Summary and general discussion In this thesis, treatment of vitamin K antagonist-associated bleed with prothrombin complex concentrate was addressed. In this we
Residency Competency and Proficiency Statements
 Residency Competency and Proficiency Statements 1. REQUEST AND RESPOND TO REQUESTS FOR CONSULTATIONS Identify needs and make referrals to appropriate health care providers for the treatment of physiologic,
Residency Competency and Proficiency Statements 1. REQUEST AND RESPOND TO REQUESTS FOR CONSULTATIONS Identify needs and make referrals to appropriate health care providers for the treatment of physiologic,
SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS?
 SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS? The spinal canal is best imagined as a bony tube through which nerve fibres pass. The tube is interrupted between each pair of adjacent
SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS? The spinal canal is best imagined as a bony tube through which nerve fibres pass. The tube is interrupted between each pair of adjacent
CODING SHEETS CHRONIC INTRACTABLE PAIN MANAGEMENT. Effective January 1, 2011 CODMAN 3000 NEUROMODULATION AND ONCOLOGY REIMBURSEMENT HOTLINE
 CODING SHEETS CHRONIC INTRACTABLE PAIN MANAGEMENT Effective January 1, 2011 CODMAN 3000 NEUROMODULATION AND ONCOLOGY REIMBURSEMENT HOTLINE Phone: 800-609-1108 Email: codmanpump@aol.com Fax: 303-703-1572
CODING SHEETS CHRONIC INTRACTABLE PAIN MANAGEMENT Effective January 1, 2011 CODMAN 3000 NEUROMODULATION AND ONCOLOGY REIMBURSEMENT HOTLINE Phone: 800-609-1108 Email: codmanpump@aol.com Fax: 303-703-1572
Issued and entered this _6th_ day of October 2010 by Ken Ross Commissioner ORDER I PROCEDURAL BACKGROUND
 STATE OF MICHIGAN DEPARTMENT OF ENERGY, LABOR & ECONOMIC GROWTH OFFICE OF FINANCIAL AND INSURANCE REGULATION Before the Commissioner of Financial and Insurance Regulation In the matter of XXXXX Petitioner
STATE OF MICHIGAN DEPARTMENT OF ENERGY, LABOR & ECONOMIC GROWTH OFFICE OF FINANCIAL AND INSURANCE REGULATION Before the Commissioner of Financial and Insurance Regulation In the matter of XXXXX Petitioner
6/3/2011. High Prevalence and Incidence. Low back pain is 5 th most common reason for all physician office visits in the U.S.
 High Prevalence and Incidence Prevalence 85% of Americans will experience low back pain at some time in their life. Incidence 5% annual Timothy C. Shen, M.D. Physical Medicine and Rehabilitation Sub-specialty
High Prevalence and Incidence Prevalence 85% of Americans will experience low back pain at some time in their life. Incidence 5% annual Timothy C. Shen, M.D. Physical Medicine and Rehabilitation Sub-specialty
How To Cover Occupational Therapy
 Guidelines for Medical Necessity Determination for Occupational Therapy These Guidelines for Medical Necessity Determination (Guidelines) identify the clinical information MassHealth needs to determine
Guidelines for Medical Necessity Determination for Occupational Therapy These Guidelines for Medical Necessity Determination (Guidelines) identify the clinical information MassHealth needs to determine
THE WRIST. At a glance. 1. Introduction
 THE WRIST At a glance The wrist is possibly the most important of all joints in everyday and professional life. It is under strain not only in many blue collar trades, but also in sports and is therefore
THE WRIST At a glance The wrist is possibly the most important of all joints in everyday and professional life. It is under strain not only in many blue collar trades, but also in sports and is therefore
1 REVISOR 5223.0070. (4) Pain associated with rigidity (loss of motion or postural abnormality) or
 1 REVISOR 5223.0070 5223.0070 MUSCULOSKELETAL SCHEDULE; BACK. Subpart 1. Lumbar spine. The spine rating is inclusive of leg symptoms except for gross motor weakness, bladder or bowel dysfunction, or sexual
1 REVISOR 5223.0070 5223.0070 MUSCULOSKELETAL SCHEDULE; BACK. Subpart 1. Lumbar spine. The spine rating is inclusive of leg symptoms except for gross motor weakness, bladder or bowel dysfunction, or sexual
John E. O Toole, Marjorie C. Wang, and Michael G. Kaiser
 Hypothermia and Human Spinal Cord Injury: Updated Position Statement and Evidence Based Recommendations from the AANS/CNS Joint Sections on Disorders of the Spine & Peripheral Nerves and Neurotrauma &
Hypothermia and Human Spinal Cord Injury: Updated Position Statement and Evidence Based Recommendations from the AANS/CNS Joint Sections on Disorders of the Spine & Peripheral Nerves and Neurotrauma &
Non Surgical Management of Back pain. Dr Pankaj Wadhwa MBBS,MD(Anaesth),DNB,Dip.Acu, FIPP, Fellowship in Pain Management.
 Non Surgical Management of Back pain. Dr Pankaj Wadhwa MBBS,MD(Anaesth),DNB,Dip.Acu, FIPP, Fellowship in Pain Management. MAGNITUDE OF THE PROBLEM It is one of the commonest experiences of humankind. It
Non Surgical Management of Back pain. Dr Pankaj Wadhwa MBBS,MD(Anaesth),DNB,Dip.Acu, FIPP, Fellowship in Pain Management. MAGNITUDE OF THE PROBLEM It is one of the commonest experiences of humankind. It
.org. Herniated Disk in the Lower Back. Anatomy. Description
 Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
Failed back spine surgery
 Failed back spine surgery Presentation Definition Etiology Prevalence Evaluation Treatment Case study FBSS: Definition A constellation of conditions that describes persistent or recurring low back pain,
Failed back spine surgery Presentation Definition Etiology Prevalence Evaluation Treatment Case study FBSS: Definition A constellation of conditions that describes persistent or recurring low back pain,
Get Back to the Life You Love! The MedStar Spine Center in Chevy Chase
 Get Back to the Life You Love! The MedStar Spine Center in Chevy Chase The MedStar Spine Center in Chevy Chase Relief from Pain, Restoration of Function Non-surgical, Minimally Invasive and Complex Surgical
Get Back to the Life You Love! The MedStar Spine Center in Chevy Chase The MedStar Spine Center in Chevy Chase Relief from Pain, Restoration of Function Non-surgical, Minimally Invasive and Complex Surgical
Percutaneous Treatment of Vertebral Compression Fractures
 Percutaneous Treatment of Vertebral Compression Fractures A Meta-analysis of Complications Michael J. Lee, MD, Mark Dumonski, MD, Patrick Cahill, MD, Tom Stanley, MD, Daniel Park, MD, and Kern Singh, MD
Percutaneous Treatment of Vertebral Compression Fractures A Meta-analysis of Complications Michael J. Lee, MD, Mark Dumonski, MD, Patrick Cahill, MD, Tom Stanley, MD, Daniel Park, MD, and Kern Singh, MD
REHABILITATION SERVICES
 REHABILITATION SERVICES Table of Contents GENERAL... 2 TERMS AND ABBREVIATIONS... 2 PRIOR AUTHORIZATION REQUIREMENTS FOR MEDICAID REIMBURSEMENT OF INPATIENT REHABILITATION SERVICES (Updated 4/1/11)...
REHABILITATION SERVICES Table of Contents GENERAL... 2 TERMS AND ABBREVIATIONS... 2 PRIOR AUTHORIZATION REQUIREMENTS FOR MEDICAID REIMBURSEMENT OF INPATIENT REHABILITATION SERVICES (Updated 4/1/11)...
INTERNSHIP 1966-1967 University Hospital/Oklahoma Health Sciences Center Oklahoma City, Oklahoma
 CURRICULUM VITAE STAN PELOFSKY, M.D. BIRTHDATE April 20, 1941 BIRTHPLACE Brooklyn, New York EDUCATION 1958-1962 Long Island University Brooklyn, New York 1962-1966 University of Oklahoma College of Medicine
CURRICULUM VITAE STAN PELOFSKY, M.D. BIRTHDATE April 20, 1941 BIRTHPLACE Brooklyn, New York EDUCATION 1958-1962 Long Island University Brooklyn, New York 1962-1966 University of Oklahoma College of Medicine
Patients with pain in the neck, arm, low back, or leg (sciatica) may benefit from ESI. Specifically, those with the following conditions:
 Overview An epidural steroid injection (ESI) is a minimally invasive procedure that can help relieve neck, arm, back, and leg pain caused by inflamed spinal nerves. ESI may be performed to relieve pain
Overview An epidural steroid injection (ESI) is a minimally invasive procedure that can help relieve neck, arm, back, and leg pain caused by inflamed spinal nerves. ESI may be performed to relieve pain
Notice of Independent Review Decision DESCRIPTION OF THE SERVICE OR SERVICES IN DISPUTE:
 Notice of Independent Review Decision DATE OF REVIEW: 08/15/08 IRO CASE #: NAME: DESCRIPTION OF THE SERVICE OR SERVICES IN DISPUTE: Determine the appropriateness of the previously denied request for physical
Notice of Independent Review Decision DATE OF REVIEW: 08/15/08 IRO CASE #: NAME: DESCRIPTION OF THE SERVICE OR SERVICES IN DISPUTE: Determine the appropriateness of the previously denied request for physical
Is manual physical therapy more effective than other physical therapy approaches in reducing pain and disability in adults post whiplash injury?
 Is manual physical therapy more effective than other physical therapy approaches in reducing pain and disability in adults post whiplash injury? Clinical Bottom Line Manual therapy may have a role in the
Is manual physical therapy more effective than other physical therapy approaches in reducing pain and disability in adults post whiplash injury? Clinical Bottom Line Manual therapy may have a role in the
Y O U R S U R G E O N S. choice of. implants F O R Y O U R S U R G E R Y
 Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Your Surgeon Has Chosen the C 2 a-taper Acetabular System The
Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Your Surgeon Has Chosen the C 2 a-taper Acetabular System The
By James D. Gould, MD FACS
 By James D. Gould, MD FACS BACKGROUND Balloon devices enlarge narrowed sinus ostia and outflow tracts by remodeling the surrounding bone and paranasal sinus structures. Multiple studies have demonstrated
By James D. Gould, MD FACS BACKGROUND Balloon devices enlarge narrowed sinus ostia and outflow tracts by remodeling the surrounding bone and paranasal sinus structures. Multiple studies have demonstrated
Sacral Nerve Neuromodulation/Stimulation
 MEDICAL POLICY POLICY RELATED POLICIES POLICY GUIDELINES DESCRIPTION SCOPE BENEFIT APPLICATION RATIONALE REFERENCES CODING APPENDIX HISTORY Sacral Nerve Neuromodulation/Stimulation Number 7.01.69 Effective
MEDICAL POLICY POLICY RELATED POLICIES POLICY GUIDELINES DESCRIPTION SCOPE BENEFIT APPLICATION RATIONALE REFERENCES CODING APPENDIX HISTORY Sacral Nerve Neuromodulation/Stimulation Number 7.01.69 Effective
Open Discectomy. North American Spine Society Public Education Series
 Open Discectomy North American Spine Society Public Education Series What Is Open Discectomy? Open discectomy is the most common surgical treatment for ruptured or herniated discs of the lumbar spine.
Open Discectomy North American Spine Society Public Education Series What Is Open Discectomy? Open discectomy is the most common surgical treatment for ruptured or herniated discs of the lumbar spine.
OUTLINE. Anatomy Approach to LBP Discogenic LBP. Treatment. Herniated Nucleus Pulposus Annular Tear. Non-Surgical Surgical
 DISCOGENIC PAIN OUTLINE Anatomy Approach to LBP Discogenic LBP Herniated Nucleus Pulposus Annular Tear Treatment Non-Surgical Surgical Facet Joints: bear 20% of weight Discs bear 80% of weight Neural Foramen
DISCOGENIC PAIN OUTLINE Anatomy Approach to LBP Discogenic LBP Herniated Nucleus Pulposus Annular Tear Treatment Non-Surgical Surgical Facet Joints: bear 20% of weight Discs bear 80% of weight Neural Foramen
Direct Lateral Interbody Fusion A Minimally Invasive Approach to Spinal Stabilization
 APPROVED IRN10389-1.1-04 Direct Lateral Interbody Fusion A Minimally Invasive Approach to Spinal Stabilization Because it involves accessing the spine through the patient s side, the Direct Lateral approach
APPROVED IRN10389-1.1-04 Direct Lateral Interbody Fusion A Minimally Invasive Approach to Spinal Stabilization Because it involves accessing the spine through the patient s side, the Direct Lateral approach
Laparoscopic Repair of Incisional Hernia. Maria B. ALBUJA-CRUZ, MD University of Colorado Department of Surgery-Grand Rounds
 Laparoscopic Repair of Incisional Hernia Maria B. ALBUJA-CRUZ, MD University of Colorado Department of Surgery-Grand Rounds Overview Definition Advantages of Laparoscopic Repair Disadvantages of Open Repair
Laparoscopic Repair of Incisional Hernia Maria B. ALBUJA-CRUZ, MD University of Colorado Department of Surgery-Grand Rounds Overview Definition Advantages of Laparoscopic Repair Disadvantages of Open Repair
TASK FORCE SUPPLEMENT FOR FUNCTIONAL CAPACITY EVALUATION
 TASK FORCE SUPPLEMENT FOR FUNCTIONAL CAPACITY EVALUATION A. GENERAL PRINCIPLES Use of a Functional Capacity Evaluation (FCE) is to determine the ability of a patient to safely function within a work environment.
TASK FORCE SUPPLEMENT FOR FUNCTIONAL CAPACITY EVALUATION A. GENERAL PRINCIPLES Use of a Functional Capacity Evaluation (FCE) is to determine the ability of a patient to safely function within a work environment.
Lumbar Spinal Stenosis Materclass: Surgical management of lumbar spinal stenosis:
 Lumbar Spinal Stenosis Materclass: Surgical management of lumbar spinal stenosis: Presented By: Michelle Emsley Senior Spinal In-Patient Physiotherapist Learning objectives Indications Evidence Post operative
Lumbar Spinal Stenosis Materclass: Surgical management of lumbar spinal stenosis: Presented By: Michelle Emsley Senior Spinal In-Patient Physiotherapist Learning objectives Indications Evidence Post operative
Management of spinal cord compression
 Management of spinal cord compression (SUMMARY) Main points a) On diagnosis, all patients should receive dexamethasone 10mg IV one dose, then 4mg every 6h. then switched to oral dose and tapered as tolerated
Management of spinal cord compression (SUMMARY) Main points a) On diagnosis, all patients should receive dexamethasone 10mg IV one dose, then 4mg every 6h. then switched to oral dose and tapered as tolerated
33 % of whiplash patients develop. headaches originating from the upper. cervical spine
 33 % of whiplash patients develop headaches originating from the upper cervical spine - Dr Nikolai Bogduk Spine, 1995 1 Physical Treatments for Headache: A Structured Review Headache: The Journal of Head
33 % of whiplash patients develop headaches originating from the upper cervical spine - Dr Nikolai Bogduk Spine, 1995 1 Physical Treatments for Headache: A Structured Review Headache: The Journal of Head
