A Guide for Completion of the British Columbia Neonatal Daily Classification
|
|
|
- Alfred Mathews
- 8 years ago
- Views:
Transcription
1 A Guide for Completion of the British Columbia Neonatal Daily Classification May 2014 Contents Introduction Guiding Principles General Guidelines Classification Levels West Tower, Suite West 12th Avenue Vancouver, BC Canada V5Z 3X7 Tel: Variables Postmenstrual Age (PMA) Today s Weight Respiratory Status Cardiovascular Status Neurological Status Nutritional Requirements Other Abbreviations Appendix A: Neonatal Daily Classification Tool Appendix B: Classification Algorithm While every attempt has been made to ensure that the information contained herein is clinically accurate and current, acknowledges that many issues remain controversial, and therefore may be subject to practice interpretation., 2014
2 Introduction A common neonatal classification system across British Columbia which classifies babies according to their needs is critical for planning regionalized services. The Neonatal Daily Classification tool has been developed to facilitate the assessment of newborns in a structured, logical and standardized manner. It is a tool to facilitate communication and planning of care among health care providers. The Neonatal Daily Classification tool: supports matching the care the baby requires with the level of care available and makes efficient use of provincial service capacity; facilitates transfers of patients from one facility to another through a common understanding of the baby s needs; reduces/eliminates transfers of mothers and babies out of province/country by optimizing capacity management; supports longer term planning by determining numbers of level 1a (normal), 1b, 2a, 2b, 3a, and 3b babies requiring care in facilities across the province; and supports the availability of appropriate funding and other resources for facilities. coordinated the development of the daily classification tool. It is the result of extensive consultation with provincial stakeholders and is based on expert clinical consensus. This completion guide will help the health care provider determine the classification level the baby should be given. Explanations are given for some of the more complex variables on the daily classification. Guiding Principles Several key principles guided the design and development: Applicable for all maternity (including single room maternity care), postpartum, pediatric, special care or neonatal intensive care units providing newborn care; Facilitate early recognition, timely communication, and intervention for changes in newborn well-being; Utilize standardized terminology and abbreviations; Facilitate provincial and regional data analyses of babies requiring neonatal care in the BC Perinatal Data Registry in; and Allow for possible future electronic archiving or formatting. 2
3 General Guidelines The Neonatal Daily Classification is based on the needs of the baby and not on the maximum level of care that can be provided at the facility, actual bed assignment, or available staffing. It is appropriate that occasionally an infant will be assessed and classified higher than the services and resources available at that site. The daily classification tool is not a workload measurement tool. WHO gets Classified? any baby admitted at birth to a maternity (including single room maternity care), postpartum, pediatric, special care, or neonatal intensive care unit; any baby who is transferred from a facility to a maternity (including single room maternity care), postpartum, pediatric, special care, or neonatal intensive care unit at a different facility; any baby readmitted from home and who is up to 28 days old at the time of admission to a maternity (including single room maternity care), postpartum, pediatric, special care, or neonatal intensive care unit. WHEN and for HOW LONG is Classification done? on admission and daily at the start of the day shift; once in a 24 hour period; daily for the entirety of the baby s stay. HOW is Classification done and charted? by performing a newborn physical, feeding, and behavioral assessment; the classification level reflects the highest classification variable assessed for the baby in the past 24 hours; once all the variables have been assessed and the Neonatal Daily Classification level determined, the healthcare provider (most often the nurse) enters the Neonatal Daily Classification level onto the baby s Neonatal Daily Classification Monthly Record, which then becomes part of the permanent chart. Note: A new version of the BC Newborn Clinical Path (v3 May 2014 PSBC 1593) will include an area where the daily classification level can be entered EXCLUSIONS? daily classification is not required if the baby has been readmitted from home and is 29 or more days old at the time of admission; does not reflect resuscitation/stabilization within the first hour of life or rescue interventions. Classification Levels Level 1a (normal) baby requires routine newborn care. Level 1b baby requires increased observation. Level 2a baby requires increased observation and increased care. Level 2b baby requires acute management. Level 3a baby has high acuity. Level 3b baby has or is at risk for high acuity and requires multi-specialty care. A Guide for Completion of the British Columbia Neonatal Daily Classification 3
4 Variables System Variables Postmenstrual Age (PMA) Formerly referred to as Corrected Age Today s Weight Respiratory Status Description Determine the infant s postmenstrual age (PMA). The PMA takes into account the baby s gestational age at birth plus the postnatal age (days of life). Age is always in completed weeks. Example: a baby born at 26 weeks + 5 days and is now 5 days old; the PMA is 27 weeks + 3 days which is then rounded down to 27 weeks. Postmenstrual age is an important indicator of risk. For example: babies whose gestational age is less than 26 weeks are at significant risk of morbidity and mortality. These risks differ on day one versus day 10 of life. Consider the most recent weight obtained on the baby. A loss in the baby s weight from his/her previous weight may result in a change in classification, even if it still falls within the expected weight loss range. Assess the baby s respiratory status to appropriately reflect the highest respiratory requirement in the past 24 hours. Under observation with continuous cardiorespiratory and/or SpO 2 monitoring by itself is a Level 1b procedure. (Classify as Level 1b) Any time oxygen is administered, the concentration must be measured continuously with an oxygen analyzer. Babies are classified into one of the following: Supplemental O 2 less than 30% and less than 4 hours of age. Anticipate resolution of respiratory distress within 24 hours. (Classify as Level 1b) Supplemental O 2 30% or greater. Anticipate escalation of care. (Classify as Level 2a) Continuous supplemental O 2 at more than 4 hours of age. Anticipate escalation of care. (Classify as Level 2a) CPAP (including biphasic CPAP) versus Heated Humidified High Flow by Nasal Cannula: As opposed to CPAP, heated humidified high flow by nasal cannula is a form of respiratory support administered with nasal cannula where the pressure delivered is not measured and where there is a large leak between the cannula and nostrils. *Please Note: High flow should never be administered without adequate warming humidification and outside of a protocol. Heated humidified high flow by nasal cannula. (Classify as Level 2a) CPAP. (Classify as Level 2b) On caffeine, or off within past 5 days considers the ongoing risk of apnea. (Classify as Level 2a) The term ventilation includes all modes of ventilation. A baby with respiratory distress who is intubated for administration of surfactant falls within this indicator. (Classify as Level 3a) The term extubated for less than 24 hours considers the increased risk of requiring reintubation. (Classify as Level 3a) Inhaled nitric oxide (ino) is administered to babies with severe respiratory failure. (Classify as Level 3a) 4
5 System Variables Respiratory Status (cont d) Description Chest tube whether inserted to drain air or fluid. (Classify as Level 3a) The term unstable airway indicates the baby is at risk for airway obstruction but does not require intervention beyond laryngoscopic intubation to stabilize the airway. Examples include choanal atresia and bilateral vocal cord paralysis. (Classify as Level 3a) OI greater than 25 if greater than 34 weeks: OI refers to oxygenation index. It is a marker of severity of respiratory illness. Babies whose OI exceeds 25 are in severe respiratory failure and should be transferred to an ECMO/ECLS center. (Classify as Level 3b) The OI should not be calculated for babies whose gestational age is less than 34 weeks. The OI should be calculated after initial stabilization in any ventilated late-preterm or term baby needing more than 60% oxygen. percent of oxygen x mean airway pressure = OI PaO 2 The term critical airway indicates there is a risk of severe airway obstruction and respiratory decompensation (may or may not be ventilated) that may require intervention beyond a laryngoscopic intubation (such as a bronchoscopy) to stabilize the airway. Examples include babies who may need an airway procedure, including a tracheostomy for subglottic stenosis, or extreme mandibular hypoplasia. (Classify as Level 3b) Tracheostomy: These babies, even if stable, have a high incidence of complications including death and therefore require immediate access to subspecialty services. (Classify as Level 3b) ECMO/ECLS is a technical procedure performed on babies requiring specialized intensive care whereby blood is circulated through a pump and oxygenator, external to the body, in order to support a failing heart and/or lung incapable of maintaining life. (Classify as Level 3b) Cardiovascular Status Assess the cardiovascular status by identifying the relevant cardiovascular condition or care requirement of the baby *Please Note: A patent ductus arteriosus (PDA) is not a CHD. The presence of a PDA is not used in classification as other system variables will appropriately capture that baby. Babies with a congenital heart defect are classified into one of the following: Diagnosed, stabilized, and considered hemodynamically stable, including those awaiting eventual cardiac surgery: These babies are deemed stable by pediatric cardiology and the immediate presence of pediatric cardiology services is not needed. Examples: babies not in failure who have an ASD, VSD or AVSD. (Classify as Level 2b) The baby is on inotropic/vasopressic support. Examples of this include: Dopamine, Dobutamine, Epinephrine, and Hydrocortisone. (Classify as Level 3a) A baby who does not stabilize and requires assessment for management by cardiology. (Classify as level 3b) A Guide for Completion of the British Columbia Neonatal Daily Classification 5
6 System Variables Cardiovascular Status (cont d) Neurological Status Nutritional Requirements Description Unstable or stable, including arrhythmia, during diagnosis and stabilization: These babies require the immediate presence of pediatric cardiology services to confirm the diagnosis and determine the level of service required. (Classify as Level 3b) Prostaglandin dependent: These babies require the immediate presence of pediatric cardiology services. (Classify as Level 3b) Assess the baby s neurological status and identify any variable that applies. Prenatal substance exposure includes maternal SSRI/SNRI use. Babies can be classified into one of the following: Prenatal substance exposure and is asymptomatic and not requiring drug therapy. (Classify as Level 1a) Prenatal substance exposure and is symptomatic but not requiring drug therapy. (Classify as Level 1b) Prenatal substance exposure, requiring drug therapy. (Classify as Level 2a) Hypoxic Ischemic Encephalopathy (HIE): Babies are classified into one of the following: HIE stage 1 (mild) less than 72 hours. The baby s condition is expected to resolve but special observation/monitoring is required. (Classify as Level 2a) HIE stage 2 (moderate) or 3 (severe), older than 10 days. These babies are likely to require feeding support by OT, PT, speech therapy and/or others. (Classify as Level 2b) HIE stage 2 (moderate) or 3 (severe), less than 10 days of age. These babies require resources including therapeutic hypothermia and specialized neuroimaging. (Classify as Level 3a) Seizures: Babies are classified into one of the following: On anticonvulsant therapy for less than 10 days with controlled seizures. (Classify as Level 3a) Uncontrolled seizures despite anticonvulsants. These babies require ongoing support of neurology, EEG and other subspecialties for investigation. (Classify as Level 3b) Neurosurgical (1st week postop): Conditions such as spina bifida, VP shunt or hydrocephalus require the immediate availability of pediatric surgical services. (Classify as Level 3b) Determine the baby s nutritional requirements and identify the most appropriate variable(s). Ad lib feeds (feeding on demand). (Classify as Level 1a) At-risk for hypoglycemia with glucose greater than 2.6 mmol/l. Healthy term babies who require blood glucose monitoring for risk of hypoglycemia and their blood glucose is greater than 2.6 mmol/l do not need a higher classification. (Classify as Level 1a) Measured oral feeds. This includes babies who are being fed a measured amount for hypoglycemia. (Classify as Level 1b) 6
7 System Variables Nutritional Requirements (cont d) Description Gavage feeds by gravity. (Classify as Level 1b) Intravenous fluids whether for an infusion or TKVO. This also includes babies who have an IV infusion initiated for hypoglycemia. (Classify as Level 2a) *Please Note: If a baby with a consistent history of hypoglycemia requires an intravenous infusion rate greater than 100 ml/kg/d in order to maintain glycemia, he/she is classified higher. (Classify as Level 3a) Gavage feeds by pump. A feed administered by an infusion pump is a more complex procedure than a feed by gravity and reflects a baby with increased needs. (Classify as Level 2a) Colostomy. (Classify as Level 2a) Parenteral nutrition. Babies on parenteral nutrition require acute management regardless of the standard solution administered. (Classify as Level 2b) Specialized additives beyond human milk fortifiers (HMF). (Classify as Level 2b) Subspecialty feeding support by OT, PT, speech therapy and/or others. This term does not include lactation consultants. (Classify as Level 2b) Babies with a stable gastrostomy tube greater than 10 days post-op. (Classify as Level 2b) Dextrose concentration greater than 12.5% for hypoglycemia, even if under subspecialty care. (Classify as Level 3a) Medications for hypoglycemia such as glucagon or diazoxide, even if under subspecialty care. (Classify as Level 3a) Post-op with enteral feeds less than full feeds. These are post-op babies whose enteral feeds are less than 100 % but more than 50% of total fluid volume. (Classify as Level 3a) Gastrostomy tube less than 10 days post-op. (Classify as Level 3a) Jejunal tube. (Classify as Level 3a) Ileostomy. Babies with an ileostomy are at risk for fluid-electrolyte imbalance. (Classify as Level 3a) Jejunostomy. Babies with a jejunostomy have complex nutritional needs and require immediate access to subspecialty and surgical services because of medical and surgical complexities. (Classify as Level 3b) Post-op with enteral feeds less than 50%. These are post-op babies whose enteral feeds are at less than 50% of their total fluid volume. (Classify as Level 3b) Mucous fistula refeeds. Babies with mucous fistula refeeds have a high complication rate and require immediate access to subspecialty and surgical services. (Classify as Level 3b) A Guide for Completion of the British Columbia Neonatal Daily Classification 7
8 System Variables Other Description Determine if there are other variables, which when assessed, classify a baby at a specific level. Phototherapy, regardless of how intensive. (Classify as Level 1a) Please refer to: Canadian Paediatric Society Guidelines for detection, management and prevention of hyperbilirubinemia in term and late preterm newborn infants Figure 2 - Guideline for Intensive Phototherapy in Infants of 35 or More Weeks Gestation Paediatr Child Health 2007;12(Suppl B):1B-12B Post-cesarean section. (Classify as Level 1a) Terminal palliative care, with no invasive interventions required. Palliative measures are as per local protocols. (Classify as Level 1a) Boarder baby. A boarder baby is a healthy term baby who is not discharged because of social or maternal medical reasons. (Classify as Level 1a) Antibiotics. Babies who are clinically asymptomatic who have risk factors are classified as follows: Prophylactic antibiotics for a well baby with risk factors; this includes babies awaiting blood culture results. (Classify as Level 1b) Therapeutic antibiotics for a baby with positive cultures. (Classify as Level 2a) Retinopathy of prematurity (ROP). Less than weekly checks. (Classify as Level 2a) Weekly checks. (Classify as Level 3a) More than weekly checks by ophthalmologist. (Classify as Level 3b) Transfusion of blood/ IVIG: includes blood products such as fresh frozen plasma and packed red blood cells. (Classify as Level 2a) Babies diagnosed with hemolytic disease of the newborn under phototherapy, including those who receive IVIG. (Classify as Level 2a) Wound care: includes babies who require frequent dressing changes by nursing. (Classify as Level 2a) PICC/CVC/UVCs require acute management; although in themselves do not increase classification level beyond 2b. (Classify as Level 2b) Hyperbilirubinemia: at phototherapy level in the first 24 hours of life. (Classify as Level 3a) Day of and up to 24 hours after exchange blood transfusion. (Classify as Level 3a) Total serum bilirubin at exchange level (Appendix A Canadian Paediatric Society Guideline for Intensive Phototherapy in Infants of 35 or More Weeks Gestation). (Classify as Level 3a) Day of advanced diagnostic imaging refers to diagnostic imaging, usually in the radiology department with/without anesthesia/ sedation. Examples include MRI, GI studies with contrast, and cystourethrograms. Excluded are non-contrast radiology, ultrasound and ECHO. (Classify as Level 3a) 8
9 System Variables Other (cont d) Description Day of surgery and up to 48 hours after surgery. (Classify as Level 3a) Acute pre-surgical and surgical NEC, GI obstructions (includes any interruption between the esophagus and anus), urologic, etc. if daily access to surgical services is required. (Classify as Level 3b) Acute metabolic disorder being stabilized with daily visits by metabolic services. (Classify as Level 3b) Others requiring immediate in-unit access to multispecialty care beyond neonatology. (Classify as Level 3b) A Guide for Completion of the British Columbia Neonatal Daily Classification 9
10 Abbreviations ASD atrial septal defect AVSD atrioventricular septal defect CPAP continuous positive airway pressure CHD congenital heart defect CVC central venous catheter ECHO echocardiogram ECLS extracorporeal life support ECMO extracorporeal membrane oxygenation EEG electroencephalography HMF human milk fortifier ino inhaled nitric oxide IVIG intravenous immunoglobulin MRI magnetic resonance imaging NEC necrotizing enterocolitis OI oxygenation index PICC peripherally inserted central catheter PMA post menstrual age PT physiotherapy ROP retinopathy of prematurity SNRI serotonin norepinephrine reuptake inhibitors SSRI selective serotonin re-uptake inhibitors TKVO to keep vein open OT occupational therapy UVC umbilical venous catheter VP ventriculoperitoneal VSD ventricular septal defect 10
11 Appendix A: Neonatal Daily Classification Tool Neonatal Daily Classification The nurse enters the daily classification score onto the baby s Neonatal Daily Classification Monthly Record SYSTEM VARIABLES LEVEL Ia Baby requires normal newborn care LEVEL Ib Baby requires increased observation LEVEL 2a Baby requires increased observation and increased care LEVEL 2b Baby requires acute management LEVEL 3a Baby has high acuity LEVEL 3b Baby has high acuity, or is at risk of high acuity, and requires multispecialty care Post Menstrual Age Greater than or equal to 37 weeks Today s Weight Greater than or equal to 2500 g 35 to weeks 32 to weeks 30 to weeks 26 to weeks Less than 26 weeks 1800 to 2499 g 1500 to 1799 g 1200 to 1499 g Less than 1200 g Respiratory Status Under observation with continuous cardiorespiratory and / or SpO 2 monitoring Supplemental O 2 less than 30% and less than 4 hours of age Supplemental O 2 30% or greater Continuous supplemental O 2 at more than 4 hours of age Heated humidified high flow by nasal cannula On caffeine, or off within past 5 days CPAP Ventilated (includes IPPV) Extubated for less than 24 hours Inhaled nitric oxide Chest tube Unstable airway OI greater than 25 if greater than 34 weeks Critical airway Tracheostomy ECMO / ECLS Cardiovascular Status CHD: diagnosed, stabilized and considered hemodynamically stable, including those awaiting eventual cardiac surgery Inotropes / vasopressors CHD: unstable or stable, including arrhythmia, during diagnostic and stabilization phase Prostaglandin dependent Neurological Status Prenatal substance exposure not requiring drug therapy and is asymptomatic Prenatal substance exposure and is symptomatic HIE stage 1 (mild) less than 72 hours Prenatal substance exposure requiring drug therapy HIE stage 2 (moderate) or 3 (severe) older than 10 days HIE stage 2 (moderate) or 3 (severe) less than 10 days of age Anticonvulsant therapy less than 10 days Neurosurgical (1st week post-op) Uncontrolled seizures despite anticonvulsants Nutritional Requirements Ad-lib feeds At-risk of hypoglycemia with blood glucose greater than 2.6 mmol / L Measured oral feeds Gavage feeds by gravity Intravenous fluids HMF Gavage feeds by pump Colostomy Parenteral nutrition Specialized additives beyond HMF Subspecialty support for nipple feeding Stable gastrostomy greater than 10 days post-op Dextrose concentration greater than D12.5%W for hypoglycemia Medications for hypoglycemia Post-op with enteral feeds less than full feeds Gastrostomy less than 10 days post-op Jejeunal tube Ileostomy Jejunostomy Post-op with enteral feeds less than 50% Mucous fistula refeeds Other Phototherapy Post cesarean section Terminal palliative care, no invasive interventions required Boarder baby Antibiotics in a well baby with risk factors Classification does not reflect resuscitation / stabilization within first hour of life ROP: less than weekly checks Antibiotics in a baby with positive cultures Transfusion of blood / IVIG Hemolytic disease of the newborn under phototherapy Wound care PICC / CVC / UVC ROP: weekly checks Bili at exchange level At phototherapy level in first 24 hours of life per CPS charts Day of and up to 24 hours after exchange transfusion Day of advanced diagnostic imaging OR day and up to 48 hours post-op ROP: more than weekly check by ophthalmologist Acute pre-surgical and surgical NEC, GI obstructions, urologic, etc (daily access to surgical services) Acute metabolic disorder being stabilized Others requiring immediate in-unit access to multispecialty care MAY 2013 A Guide for Completion of the British Columbia Neonatal Daily Classification 11
12 Appendix B: Classification Algorithm Neonatal Daily Classification Every Baby, Every Day, No Matter Where Baby born and admitted to a maternity (including single room maternity care), postpartum, pediatric, special care or neonatal intensive care unit Baby born and transferred from another facility to a maternity (including single room maternity care), postpartum, pediatric, special care or neonatal intensive care unit Assess Neonatal Daily Classification every day for the entirety of baby s stay Discharged home Readmitted to a maternity (including single room maternity care), postpartum, pediatric, special care or neonatal intensive care unit 29 days old or older 28 days old or younger Neonatal Daily Classification NOT required 12
13 West Tower, Suite West 12th Avenue Vancouver, BC Canada V5Z 3X7 Tel: While every attempt has been made to ensure that the information contained herein is clinically accurate and current, Perinatal Services BC acknowledges that many issues remain controversial, and therefore may be subject to practice interpretation., 2014
Milliman Guidelines NICU Levels*
 Milliman Guidelines NICU Levels* Neonatal Intensive Care Unit Level IV If the following conditions/procedures exist, in addition to the fulfillment of Level III Criteria, the approved inpatient days should
Milliman Guidelines NICU Levels* Neonatal Intensive Care Unit Level IV If the following conditions/procedures exist, in addition to the fulfillment of Level III Criteria, the approved inpatient days should
Why is prematurity a concern?
 Prematurity What is prematurity? A baby born before 37 weeks of pregnancy is considered premature. Approximately 12% of all babies are born prematurely. Terms that refer to premature babies are preterm
Prematurity What is prematurity? A baby born before 37 weeks of pregnancy is considered premature. Approximately 12% of all babies are born prematurely. Terms that refer to premature babies are preterm
Children's Medical Services (CMS) Regional Perinatal Intensive Care Center (RPICC) Neonatal Extracorporeal Life Support (ECLS) Centers Questionnaire
 Children's Medical Services (CMS) Regional Perinatal Intensive Care Center (RPICC) Neonatal Extracorporeal Life Support (ECLS) Centers Questionnaire Date: RPICC Facility: CMS use only Include the following
Children's Medical Services (CMS) Regional Perinatal Intensive Care Center (RPICC) Neonatal Extracorporeal Life Support (ECLS) Centers Questionnaire Date: RPICC Facility: CMS use only Include the following
 GUIDELINES FOR HOSPITALS WITH NEONATAL INTENSIVE CARE SERVICE : REGULATION 4 OF THE PRIVATE HOSPITALS AND MEDICAL CLINICS REGULATIONS [CAP 248, Rg 1] I Introduction 1. These Guidelines serve as a guide
GUIDELINES FOR HOSPITALS WITH NEONATAL INTENSIVE CARE SERVICE : REGULATION 4 OF THE PRIVATE HOSPITALS AND MEDICAL CLINICS REGULATIONS [CAP 248, Rg 1] I Introduction 1. These Guidelines serve as a guide
Objective of This Lecture
 Component 2: The Culture of Health Care Unit 3: Health Care Settings The Places Where Care Is Delivered Lecture 5 This material was developed by Oregon Health & Science University, funded by the Department
Component 2: The Culture of Health Care Unit 3: Health Care Settings The Places Where Care Is Delivered Lecture 5 This material was developed by Oregon Health & Science University, funded by the Department
Institutional Handbook of Operating Procedures Policy 9.1.10
 Section: Clinical Policies Institutional Handbook of Operating Procedures Policy 9.1.10 Responsible Vice President: EVP & CEO Health System Subject: Admission, Discharge, and Transfer Responsible Entity:
Section: Clinical Policies Institutional Handbook of Operating Procedures Policy 9.1.10 Responsible Vice President: EVP & CEO Health System Subject: Admission, Discharge, and Transfer Responsible Entity:
Feeding in Infants with Complex Congenital Heart Disease. Rachel Torok, MD Southeastern Pediatric Cardiology Society Conference September 6, 2014
 Feeding in Infants with Complex Congenital Heart Disease Rachel Torok, MD Southeastern Pediatric Cardiology Society Conference September 6, 2014 Objectives Discuss common feeding issues in patients with
Feeding in Infants with Complex Congenital Heart Disease Rachel Torok, MD Southeastern Pediatric Cardiology Society Conference September 6, 2014 Objectives Discuss common feeding issues in patients with
Levels of Critical Care for Adult Patients
 LEVELS OF CARE 1 Levels of Critical Care for Adult Patients STANDARDS AND GUIDELINES LEVELS OF CARE 2 Intensive Care Society 2009 All rights reserved. No reproduction, copy or transmission of this publication
LEVELS OF CARE 1 Levels of Critical Care for Adult Patients STANDARDS AND GUIDELINES LEVELS OF CARE 2 Intensive Care Society 2009 All rights reserved. No reproduction, copy or transmission of this publication
2008 Coding Questions and Answers
 2008 Coding Questions and Answers 1. An infant is born at 29 wks gestation and has RDS. His birthweight is 1200 gms. He is admitted to the NICU. It is evident that he has severe RDS and a decision is made
2008 Coding Questions and Answers 1. An infant is born at 29 wks gestation and has RDS. His birthweight is 1200 gms. He is admitted to the NICU. It is evident that he has severe RDS and a decision is made
Overall Goals/Objectives - Surgical Critical Care Residency Program The goal of the Pediatric Surgical Critical Care Residency program is to provide
 Overall Goals/Objectives - Surgical Critical Care Residency Program The goal of the Pediatric Surgical Critical Care Residency program is to provide advanced proficiency in the care and management of critically
Overall Goals/Objectives - Surgical Critical Care Residency Program The goal of the Pediatric Surgical Critical Care Residency program is to provide advanced proficiency in the care and management of critically
APPENDIX B SAMPLE PEDIATRIC CRITICAL CARE NURSE PRACTITIONER GOALS AND OBJECTIVES
 APPENDIX B SAMPLE PEDIATRIC CRITICAL CARE NURSE PRACTITIONER GOALS AND OBJECTIVES The critical care nurse practitioner orientation is an individualized process based on one s previous experiences and should
APPENDIX B SAMPLE PEDIATRIC CRITICAL CARE NURSE PRACTITIONER GOALS AND OBJECTIVES The critical care nurse practitioner orientation is an individualized process based on one s previous experiences and should
BRITISH ASSOCIATION OF PERINATAL MEDICINE
 BRITISH ASSOCIATION OF PERINATAL MEDICINE Categories of Care 2011 Introduction The 2001 categories of care replaced the 1996 categories of care. In the subsequent 10 years, neonatal care changed and it
BRITISH ASSOCIATION OF PERINATAL MEDICINE Categories of Care 2011 Introduction The 2001 categories of care replaced the 1996 categories of care. In the subsequent 10 years, neonatal care changed and it
KING FAISAL SPECIALIST HOSPITAL AND RESEARCH CENTRE (GEN. ORG.) NURSING AFFAIRS. Scope of Service PEDIATRIC INTENSIVE CARE UNIT (PICU)
 PICU-Jan.2012 Page 1 of 7 Number of Beds: 18 Nurse Patient Ratio: 1:1-2 : The Pediatric Intensive Care Unit (PICU) provides 24 hour intensive nursing care for patients aged neonate through adolescence.
PICU-Jan.2012 Page 1 of 7 Number of Beds: 18 Nurse Patient Ratio: 1:1-2 : The Pediatric Intensive Care Unit (PICU) provides 24 hour intensive nursing care for patients aged neonate through adolescence.
11.0 SERVICE DEPARTMENTS
 Horizon NJ Health is available to assist you in providing health care services to our members. This section describes each of the service departments by function. 11.1 Professional Contracting & Servicing
Horizon NJ Health is available to assist you in providing health care services to our members. This section describes each of the service departments by function. 11.1 Professional Contracting & Servicing
Human Capital Development & Education Program Proposal
 Human Capital Development & Education Program Proposal Cardiology & Cardiovascular Surgery Emergency Medicine Respiratory Medicine Infection Control HMIS 1 (15 Courses) Module 1/2 1/15 Course Title : Management
Human Capital Development & Education Program Proposal Cardiology & Cardiovascular Surgery Emergency Medicine Respiratory Medicine Infection Control HMIS 1 (15 Courses) Module 1/2 1/15 Course Title : Management
NICU Level of Care Criteria
 Introduction The NICU Criteria were developed to assist in the authorization for various levels of Neonatal Intensive Care Unit (NICU), as well as assistance in determining the appropriate level of care.
Introduction The NICU Criteria were developed to assist in the authorization for various levels of Neonatal Intensive Care Unit (NICU), as well as assistance in determining the appropriate level of care.
NORTH WALES CRITICAL CARE NETWORK
 NORTH WALES CRITICAL CARE NETWORK LEVELS OF CRITICAL CARE FOR ADULT PATIENTS Throughout the work of the North Wales Critical Care Network reference to Levels of Care for the critically ill are frequently
NORTH WALES CRITICAL CARE NETWORK LEVELS OF CRITICAL CARE FOR ADULT PATIENTS Throughout the work of the North Wales Critical Care Network reference to Levels of Care for the critically ill are frequently
ELSO GUIDELINES FOR ECMO CENTERS
 ELSO GUIDELINES FOR ECMO CENTERS PURPOSE These guidelines developed by the Extracorporeal Life Support Organization, outline the ideal institutional requirements needed for effective use of extracorporeal
ELSO GUIDELINES FOR ECMO CENTERS PURPOSE These guidelines developed by the Extracorporeal Life Support Organization, outline the ideal institutional requirements needed for effective use of extracorporeal
Regions Hospital Delineation of Privileges Nurse Practitioner
 Regions Hospital Delineation of Privileges Nurse Practitioner Applicant s Last First M. Instructions: Place a check-mark where indicated for each core group you are requesting. Review education and basic
Regions Hospital Delineation of Privileges Nurse Practitioner Applicant s Last First M. Instructions: Place a check-mark where indicated for each core group you are requesting. Review education and basic
Nutrition in Paediatric Cardiology. Karen Hayes Paediatric Dietitian Addenbrooke s Hospital
 Nutrition in Paediatric Cardiology Karen Hayes Paediatric Dietitian Addenbrooke s Hospital Topics Who needs Nutrition support? Energy Requirements Meeting Energy and growth requirements Feeding Issues
Nutrition in Paediatric Cardiology Karen Hayes Paediatric Dietitian Addenbrooke s Hospital Topics Who needs Nutrition support? Energy Requirements Meeting Energy and growth requirements Feeding Issues
Extracorporeal Life Support Organization (ELSO) Guidelines for Neonatal Respiratory Failure
 Extracorporeal Life Support Organization (ELSO) Guidelines for Neonatal Respiratory Failure Introduction This neonatal respiratory failure guideline is a supplement to ELSO s General Guidelines for all
Extracorporeal Life Support Organization (ELSO) Guidelines for Neonatal Respiratory Failure Introduction This neonatal respiratory failure guideline is a supplement to ELSO s General Guidelines for all
Brenda Neff MSN, RN, NE BC
 Brenda Neff MSN, RN, NE BC 1400 s newborns have a soul 1600 s estimated that only 10% of the abandoned infants reached the age of 5 years. 1857 first incubator documented in western lit 1857 first incubator
Brenda Neff MSN, RN, NE BC 1400 s newborns have a soul 1600 s estimated that only 10% of the abandoned infants reached the age of 5 years. 1857 first incubator documented in western lit 1857 first incubator
CURRICULUM VITAE. Business Address: 3020 Children s Way, RCHSD MC 5008, San Diego, CA 92123 Phone: 858 966-5818 email: blane@rchsd.
 CURRICULUM VITAE Date: April 3, 2014 Name: Brian P. Lane, M.D. Business Address: 3020 Children s Way, RCHSD MC 5008, San Diego, CA 92123 Phone: 858 966-5818 email: blane@rchsd.org Place of Birth: Greene
CURRICULUM VITAE Date: April 3, 2014 Name: Brian P. Lane, M.D. Business Address: 3020 Children s Way, RCHSD MC 5008, San Diego, CA 92123 Phone: 858 966-5818 email: blane@rchsd.org Place of Birth: Greene
BOARD OF PHARMACY SPECIALITIES 2215 Constitution Avenue, NW Washington, DC 20037-2985 202-429-7591 FAX 202-429-6304 info@bpsweb.org www.bpsweb.
 BOARD OF PHARMACY SPECIALITIES 2215 Constitution Avenue, NW Washington, DC 20037-2985 202-429-7591 FAX 202-429-6304 info@bpsweb.org www.bpsweb.org Content Outline for the CRITICAL PHARMACY SPECIALTY CERTIFICATION
BOARD OF PHARMACY SPECIALITIES 2215 Constitution Avenue, NW Washington, DC 20037-2985 202-429-7591 FAX 202-429-6304 info@bpsweb.org www.bpsweb.org Content Outline for the CRITICAL PHARMACY SPECIALTY CERTIFICATION
Patient Care Technician (Bridge Program)
 Patient Care Technician (Bridge Program) Introduction: At Prestige Medical Solutions we are fully vested in helping students succeed. Our vision is to be a great place to learn, where people are inspired
Patient Care Technician (Bridge Program) Introduction: At Prestige Medical Solutions we are fully vested in helping students succeed. Our vision is to be a great place to learn, where people are inspired
CLINICAL QUALITY MEASURES FINALIZED FOR ELIGIBLE HOSPITALS AND CRITICAL ACCESS HOSPITALS BEGINNING WITH FY 2014
 CLINICAL QUALITY MEASURES FINALIZED FOR ELIGIBLE HOSPITALS AND CRITICAL ACCESS HOSPITALS BEGINNING WITH FY 2014 e 55 0495 2 Emergency Department (ED)- 1 Emergency Department Throughput Median time from
CLINICAL QUALITY MEASURES FINALIZED FOR ELIGIBLE HOSPITALS AND CRITICAL ACCESS HOSPITALS BEGINNING WITH FY 2014 e 55 0495 2 Emergency Department (ED)- 1 Emergency Department Throughput Median time from
RESPIRATORY CRITICAL CARE UNIT STUDENT INTERNSHIP SKILLS LIST Provo School District
 RESPIRATORY CRITICAL CARE UNIT STUDENT INTERNSHIP SKILLS LIST Provo School District The following procedures and items of equipment should be noted, observed and studied during this clinical rotation period.
RESPIRATORY CRITICAL CARE UNIT STUDENT INTERNSHIP SKILLS LIST Provo School District The following procedures and items of equipment should be noted, observed and studied during this clinical rotation period.
She was 39 years old, gravida 4, para 2. She had an Idiopathic Pulmonary. Arterial Hypertension (PAH) revealed during pregnancy by a New York Heart
 Case #1 (year 1992): She was 39 years old, gravida 4, para 2. She had an Idiopathic Pulmonary Arterial Hypertension (PAH) revealed during pregnancy by a New York Heart Association (NYHA) functional class
Case #1 (year 1992): She was 39 years old, gravida 4, para 2. She had an Idiopathic Pulmonary Arterial Hypertension (PAH) revealed during pregnancy by a New York Heart Association (NYHA) functional class
Newborn Screening Update for Health Care Practitioners
 Newborn Screening Update for Health Care Practitioners Changes in regulations affecting your practice for newborns transferred to neonatal intensive care units. Changes for newborn screening of premature,
Newborn Screening Update for Health Care Practitioners Changes in regulations affecting your practice for newborns transferred to neonatal intensive care units. Changes for newborn screening of premature,
Safe Zone: CV PIP < 26; HFOV: MAP < 16; HFJV: MAP < 16 Dopamine infusion up to 20 mcg/kg/min Epinephrine infusion up to 0.1 mcg /kg/min.
 Congenital Diaphragmatic Hernia: Management Guidelines 5-2006 Issued By: Division of Neonatology Reviewed: Effective Date: Categories: Chronicity Document Congenital Diaphragmatic Hernia: Management Guidelines
Congenital Diaphragmatic Hernia: Management Guidelines 5-2006 Issued By: Division of Neonatology Reviewed: Effective Date: Categories: Chronicity Document Congenital Diaphragmatic Hernia: Management Guidelines
Veteran s/lpn Bridge Course 8 didactic credits (120 hours); 4 lab/simulation/clinical/pharm/iv credits (180 hours) Total of 12 credits/300 clock hours
 Veteran s/lpn Bridge Course 8 didactic credits (120 hours); 4 lab/simulation/clinical/pharm/iv credits (180 hours) Total of 12 credits/300 clock hours Course Description: Designed to bridge previously
Veteran s/lpn Bridge Course 8 didactic credits (120 hours); 4 lab/simulation/clinical/pharm/iv credits (180 hours) Total of 12 credits/300 clock hours Course Description: Designed to bridge previously
Neonatal Intensive Care Unit (NICU)
 Neonatal Intensive Care Unit (NICU) Integrated Care for Newborns with Critical or Special Needs startstrongbaby.org A World Leader in Neonatal Research and Care Innovation As a birthplace of modern neonatology
Neonatal Intensive Care Unit (NICU) Integrated Care for Newborns with Critical or Special Needs startstrongbaby.org A World Leader in Neonatal Research and Care Innovation As a birthplace of modern neonatology
SARASOTA MEMORIAL HOSPITAL NURSING DEPARTMENT POLICY
 PS1006 SARASOTA MEMORIAL HOSPITAL NURSING DEPARTMENT POLICY TITLE: NEONATAL INTENSIVE CARE UNIT: ADMISSION AND TRANSFER PROCEDURE AND ACUITY GUIDELINES Job Title of Reviewer: EFFECTIVE DATE: REVISED DATE:
PS1006 SARASOTA MEMORIAL HOSPITAL NURSING DEPARTMENT POLICY TITLE: NEONATAL INTENSIVE CARE UNIT: ADMISSION AND TRANSFER PROCEDURE AND ACUITY GUIDELINES Job Title of Reviewer: EFFECTIVE DATE: REVISED DATE:
Cardiac Catheterisation. Cardiology
 Cardiac Catheterisation Cardiology Name: Cardiac catheterisation Version: 1 Page 1 of 7 Contents Page Number(s) 1. Introduction 3 2. Management pre operative 3 3. Management post operative 5 4. Discharge
Cardiac Catheterisation Cardiology Name: Cardiac catheterisation Version: 1 Page 1 of 7 Contents Page Number(s) 1. Introduction 3 2. Management pre operative 3 3. Management post operative 5 4. Discharge
Universal Fetal Cardiac Ultrasound At the Heart of Newborn Well-being
 Universal Fetal Cardiac Ultrasound At the Heart of Newborn Well-being Optimizes detection of congenital heart disease (chd) in the general low risk obstetrical population Daniel J. Cohen, M.D. danjcohen@optonline.net
Universal Fetal Cardiac Ultrasound At the Heart of Newborn Well-being Optimizes detection of congenital heart disease (chd) in the general low risk obstetrical population Daniel J. Cohen, M.D. danjcohen@optonline.net
5/30/2014 OBJECTIVES THE ROLE OF A RESPIRATORY THERAPIST IN THE DELIVERY ROOM. Disclosure
 THE ROLE OF A RESPIRATORY THERAPIST IN THE DELIVERY ROOM Ona Fofah, MD FAAP Assistant Professor of Pediatrics Director, Division of Neonatology Department of Pediatrics Rutgers- NJMS, Newark OBJECTIVES
THE ROLE OF A RESPIRATORY THERAPIST IN THE DELIVERY ROOM Ona Fofah, MD FAAP Assistant Professor of Pediatrics Director, Division of Neonatology Department of Pediatrics Rutgers- NJMS, Newark OBJECTIVES
PROPOSED AMENDMENTS NURSES (REGISTERED) AND NURSE PRACTITIONERS REGULATION. Health Professions Act
 Health Professions Act NURSES (REGISTERED) AND NURSE PRACTITIONERS REGULATION PROPOSED AMENDMENTS TO B.C. REG. 284/2008 abc abc text to be removed text to be added Contents 1 Definitions 2 College name
Health Professions Act NURSES (REGISTERED) AND NURSE PRACTITIONERS REGULATION PROPOSED AMENDMENTS TO B.C. REG. 284/2008 abc abc text to be removed text to be added Contents 1 Definitions 2 College name
Disclosures. Not as Pink as You Think 3/17/2014. Not As Pink As You Think: Pulse Oximetry Screening For Critical Congenital Heart Disease
 March of Dimes New York State Chapter 36th Annual Perinatal Nurses Conference Promoting Perinatal Health Through Evidence Based Practice Not As Pink As You Think: Pulse Oximetry Screening For Critical
March of Dimes New York State Chapter 36th Annual Perinatal Nurses Conference Promoting Perinatal Health Through Evidence Based Practice Not As Pink As You Think: Pulse Oximetry Screening For Critical
Board of Directors. 28 January 2015
 Executive Summary Purpose: Board of Directors 28 January 2015 Briefing on the requirements for the Trust to comply with Hard Truths Commitments Regarding the Publishing of Staffing Data Director of Nursing
Executive Summary Purpose: Board of Directors 28 January 2015 Briefing on the requirements for the Trust to comply with Hard Truths Commitments Regarding the Publishing of Staffing Data Director of Nursing
Requirements for Provision of Outreach Paediatric Cardiology Service
 Requirements for Provision of Outreach Paediatric Cardiology Service Dr Shakeel A Qureshi, Consultant Paediatric Cardiologist, Evelina Children s Hospital, London, UK On behalf of British Congenital Cardiac
Requirements for Provision of Outreach Paediatric Cardiology Service Dr Shakeel A Qureshi, Consultant Paediatric Cardiologist, Evelina Children s Hospital, London, UK On behalf of British Congenital Cardiac
PROPOSED AMENDMENTS - NURSES (REGISTERED) AND NURSE PRACTITIONERS REGULATION. Health Professions Act
 Health Professions Act NURSES (REGISTERED) AND NURSE PRACTITIONER REGULATION PROPOSED TO REPLACE B.C. REG. 284/2008 Contents 1 Definitions 2 College name 3 Reserved titles 4 Scope of practice 5 Patient
Health Professions Act NURSES (REGISTERED) AND NURSE PRACTITIONER REGULATION PROPOSED TO REPLACE B.C. REG. 284/2008 Contents 1 Definitions 2 College name 3 Reserved titles 4 Scope of practice 5 Patient
College of Applied Medical Sciences\ Department of Nursing
 2 nd Edition 2014/2015 College of Applied Medical Sciences\ Department of Nursing CAMS/ Department of Nursing/ Internship Training Logbook 2 nd Edition 1 INTERNSHIP TRAINING LOGBOOK Nurse Intern Name:
2 nd Edition 2014/2015 College of Applied Medical Sciences\ Department of Nursing CAMS/ Department of Nursing/ Internship Training Logbook 2 nd Edition 1 INTERNSHIP TRAINING LOGBOOK Nurse Intern Name:
NEONATAL NURSE PRACTITIONER MODEL OF CARE WERRIBEE MERCY HOSPITAL
 NEONATAL NURSE PRACTITIONER MODEL OF CARE WERRIBEE MERCY HOSPITAL Background Neonatal Nurse practitioners provide an additional model of care for neonates and their families. They have been educated to
NEONATAL NURSE PRACTITIONER MODEL OF CARE WERRIBEE MERCY HOSPITAL Background Neonatal Nurse practitioners provide an additional model of care for neonates and their families. They have been educated to
Prior Authorization Requirements for Florida Effective March 1, 2015
 for Florida Effective March 1, 215 General Information The following list represents our prior authorization requirements for UnitedHealthcare in Florida. All services rendered by a non-contracted physician,
for Florida Effective March 1, 215 General Information The following list represents our prior authorization requirements for UnitedHealthcare in Florida. All services rendered by a non-contracted physician,
Neural Tube Defects - NTDs
 Neural Tube Defects - NTDs Introduction Neural tube defects are also known as NTDs. They happen when the spine and brain do not fully develop while the fetus is forming in the uterus. Worldwide, there
Neural Tube Defects - NTDs Introduction Neural tube defects are also known as NTDs. They happen when the spine and brain do not fully develop while the fetus is forming in the uterus. Worldwide, there
Neonatal Outreach Education Program Course Catalog
 2012 Neonatal Outreach Education Program Course Catalog Photo by Brian Redden (559) 353-5615 (559) 353-6255 Table of Contents Program Overview... 2 General Course Information... 3 Save The Date Children
2012 Neonatal Outreach Education Program Course Catalog Photo by Brian Redden (559) 353-5615 (559) 353-6255 Table of Contents Program Overview... 2 General Course Information... 3 Save The Date Children
Documentation Guidelines for Physicians Interventional Pain Services
 Documentation Guidelines for Physicians Interventional Pain Services Pamela Gibson, CPC Assistant Director, VMG Coding Anesthesia and Surgical Divisions 343.8791 1 General Principles of Medical Record
Documentation Guidelines for Physicians Interventional Pain Services Pamela Gibson, CPC Assistant Director, VMG Coding Anesthesia and Surgical Divisions 343.8791 1 General Principles of Medical Record
A8b. Resuscitation of a Term Infant with Meconium Staining. Session Summary. Session Objectives. References
 A8b Resuscitation of a Term Infant with Meconium Staining Karen Wright, PhD, NNP-BC Assistant Professor and Coordinator, Neonatal Nurse Practitioner Program Dept. of Women, Children, and Family Nursing,
A8b Resuscitation of a Term Infant with Meconium Staining Karen Wright, PhD, NNP-BC Assistant Professor and Coordinator, Neonatal Nurse Practitioner Program Dept. of Women, Children, and Family Nursing,
CONGENITAL HEART DISEASE
 CONGENITAL HEART DISEASE Introduction Congenital heart disease (CHD) is the most common congenital disorder in newborns [1]. Due to definitional issues, there are large variations in prevalence estimates.
CONGENITAL HEART DISEASE Introduction Congenital heart disease (CHD) is the most common congenital disorder in newborns [1]. Due to definitional issues, there are large variations in prevalence estimates.
Acute Care Pediatric Nurse Practitioner Certification Exam. Detailed Content Outline
 Acute Care Pediatric Nurse Practitioner Certification Exam Description of the Specialty This exam is for the pediatric nurse practitioner (PNP) who has graduated from a formal acute care PNP program with
Acute Care Pediatric Nurse Practitioner Certification Exam Description of the Specialty This exam is for the pediatric nurse practitioner (PNP) who has graduated from a formal acute care PNP program with
LOUISIANA STATE UNIVERSITY HEALTH SCIENCES CENTER - SHREVEPORT MEDICAL RECORDS CONTENT/DOCUMENTATION
 LOUISIANA STATE UNIVERSITY HEALTH SCIENCES CENTER - SHREVEPORT MEDICAL RECORDS CONTENT/DOCUMENTATION Hospital Policy Manual Purpose: To define the components of the paper and electronic medical record
LOUISIANA STATE UNIVERSITY HEALTH SCIENCES CENTER - SHREVEPORT MEDICAL RECORDS CONTENT/DOCUMENTATION Hospital Policy Manual Purpose: To define the components of the paper and electronic medical record
VOCATIONAL NURSE PROGRAM EXPECTED CLINICAL ROTATION PERFORMANCE GUIDELINES
 VN: Objective 01 EXPECTED CLINICAL ROTATION PERFORMANCE GUIDELINES Clinical rotation expected performances are reflected in the clinical objectives. Clinical objectives are posted by instructor at each
VN: Objective 01 EXPECTED CLINICAL ROTATION PERFORMANCE GUIDELINES Clinical rotation expected performances are reflected in the clinical objectives. Clinical objectives are posted by instructor at each
DISCHARGE ABSTRACTS DATABASE (HOSPITAL SEPARATIONS) DATA DICTIONARY
 DISCHARGE ABSTRACTS DATABASE (HOSPITAL SEPARATIONS) DATA DICTIONARY Includes discharges, transfers and deaths of in-patients from acute care hospitals in BC, including day surgeries. Fields are available
DISCHARGE ABSTRACTS DATABASE (HOSPITAL SEPARATIONS) DATA DICTIONARY Includes discharges, transfers and deaths of in-patients from acute care hospitals in BC, including day surgeries. Fields are available
Guidelines for Specialized Health Care Procedures (Revision 2004)
 Guidelines for Specialized Health Care Procedures (Revision 2004) Vickie H. Southall, MSN, RN Family, Community, and Mental Health Systems Department School of Nursing University of Virginia for the Virginia
Guidelines for Specialized Health Care Procedures (Revision 2004) Vickie H. Southall, MSN, RN Family, Community, and Mental Health Systems Department School of Nursing University of Virginia for the Virginia
ALS INTERFACILITY TRANSFERS. SUPERSEDES: January 8, 2009
 EFFECTIVE: September 8, 2010 AUTHORIZATION: AR PAGE: 1 of 7 *This Administrative Requirement may be effectuated by an ambulance service only upon appropriate training of its EMS personnel.* Minimum Standards
EFFECTIVE: September 8, 2010 AUTHORIZATION: AR PAGE: 1 of 7 *This Administrative Requirement may be effectuated by an ambulance service only upon appropriate training of its EMS personnel.* Minimum Standards
GENERAL ADMISSION CRITERIA INPATIENT REHABILITATION PROGRAMS
 Originator: Case Management Original Date: 9/94 Review/Revision: 6/96, 2/98, 1/01, 4/02, 8/04, 3/06, 03/10, 3/11, 3/13 Stakeholders: Case Management, Medical Staff, Nursing, Inpatient Therapy GENERAL ADMISSION
Originator: Case Management Original Date: 9/94 Review/Revision: 6/96, 2/98, 1/01, 4/02, 8/04, 3/06, 03/10, 3/11, 3/13 Stakeholders: Case Management, Medical Staff, Nursing, Inpatient Therapy GENERAL ADMISSION
JOB DESCRIPTION NURSE PRACTITIONER
 JOB DESCRIPTION NURSE PRACTITIONER Related documents: Nurse Practitioner Process Protocol Authorization for Individuals to Provide Services as Allied Health Personnel in the LPCH/SCH Administrative Manual
JOB DESCRIPTION NURSE PRACTITIONER Related documents: Nurse Practitioner Process Protocol Authorization for Individuals to Provide Services as Allied Health Personnel in the LPCH/SCH Administrative Manual
Innovative use of Neonatal Nurse Practitioners in Rural Hawaii
 Innovative use of Neonatal Nurse Practitioners in Rural Hawaii Petri Pate Pieron, MSN, MPH, APRN Rx, CPNP, NNP Presentation was supported by NIH 1 R25 RR019321 Clinical Research Education and Career Development
Innovative use of Neonatal Nurse Practitioners in Rural Hawaii Petri Pate Pieron, MSN, MPH, APRN Rx, CPNP, NNP Presentation was supported by NIH 1 R25 RR019321 Clinical Research Education and Career Development
The Pattern of Congenital Heart Disease among Neonates Referred for Echocardiography
 Bahrain Medical Bulletin, Vol. 36, No. 2, June 2014 ABSTRACT The Pattern of Congenital Heart Disease among Neonates Referred for Echocardiography Hussain Al Khawahur, MD* Hussain Al Sowaiket, MD** Thuria
Bahrain Medical Bulletin, Vol. 36, No. 2, June 2014 ABSTRACT The Pattern of Congenital Heart Disease among Neonates Referred for Echocardiography Hussain Al Khawahur, MD* Hussain Al Sowaiket, MD** Thuria
Newborns with Trisomy 18: To Treat or not to Treat? Have Times Changed?
 Newborns with Trisomy 18: To Treat or not to Treat? Have Times Changed? George Hardart, MD MPH Chair, Morgan Stanley Children s Hospital of New York Ethics Committee March 11, 2010 12:00 noon 1:30 pm Introduction
Newborns with Trisomy 18: To Treat or not to Treat? Have Times Changed? George Hardart, MD MPH Chair, Morgan Stanley Children s Hospital of New York Ethics Committee March 11, 2010 12:00 noon 1:30 pm Introduction
Screening for Critical Congenital Heart Disease in the Apparently Healthy Newborn
 Screening for Critical Congenital Heart Disease in the Apparently Healthy Newborn A presentation of Texas Pulse Oximetry Project: A Joint Educational Initiative of The University of Texas Health Science
Screening for Critical Congenital Heart Disease in the Apparently Healthy Newborn A presentation of Texas Pulse Oximetry Project: A Joint Educational Initiative of The University of Texas Health Science
Rural Health Advisory Committee s Rural Obstetric Services Work Group
 Rural Health Advisory Committee s Rural Obstetric Services Work Group March 15 th webinar topic: Rural Obstetric Patient and Community Issues Audio: 888-742-5095, conference code 6054760826 Rural Obstetric
Rural Health Advisory Committee s Rural Obstetric Services Work Group March 15 th webinar topic: Rural Obstetric Patient and Community Issues Audio: 888-742-5095, conference code 6054760826 Rural Obstetric
OKLAHOMA BOARD OF NURSING 2915 North Classen Boulevard, Suite 524 Oklahoma City, OK 73106 (405) 962-1800
 OKLAHOMA BOARD OF NURSING 2915 North Classen Boulevard, Suite 524 Oklahoma City, OK 73106 (405) 962-1800 Medic Veteran to Licensed Practical Nurse Bridge Course I. Introduction/Purpose: Per 59 O.S. Section
OKLAHOMA BOARD OF NURSING 2915 North Classen Boulevard, Suite 524 Oklahoma City, OK 73106 (405) 962-1800 Medic Veteran to Licensed Practical Nurse Bridge Course I. Introduction/Purpose: Per 59 O.S. Section
Feeding infants with congenital heart disease with breast milk: Findings from the Norwegian Mother and Child Cohort Study
 Feeding infants with congenital heart disease with breast milk: Findings from the Norwegian Mother and Child Cohort Study Bente Silnes Tandberg (1), Margarete Vollrath (2,3), Eivind Ystrom (2), Henrik
Feeding infants with congenital heart disease with breast milk: Findings from the Norwegian Mother and Child Cohort Study Bente Silnes Tandberg (1), Margarete Vollrath (2,3), Eivind Ystrom (2), Henrik
CCS - Does CCS provide Counseling or Support Services? CCS - Are there any costs to me? CCS - What papers should I bring?
 CCS - Does CCS provide Counseling or Support Services? CCS - Are there any costs to me? CCS - What papers should I bring? CCS - What are the steps to CCS services? CCS - How is my privacy protected? CCS
CCS - Does CCS provide Counseling or Support Services? CCS - Are there any costs to me? CCS - What papers should I bring? CCS - What are the steps to CCS services? CCS - How is my privacy protected? CCS
NEONATAL CLINICAL PRACTICE GUIDELINE
 NEONATAL CLINICAL PRACTICE GUIDELINE Title: Routine Screening of Neonates Approval Date: January 2015 Approved by: Neonatal Patient Care Teams, HSC & SBH Child Health Standards Committee Pages: 1 of 6
NEONATAL CLINICAL PRACTICE GUIDELINE Title: Routine Screening of Neonates Approval Date: January 2015 Approved by: Neonatal Patient Care Teams, HSC & SBH Child Health Standards Committee Pages: 1 of 6
California Children s Services Program Analysis Final Report
 California Children s Services Program Analysis Final Report Paul H. Wise, MD, MPH Vandana Sundaram, MPH Lisa Chamberlain, MD, MPH Ewen Wang, MD Olga Saynina, MS Jia Chan, MS Kristen Chan, MASc Beate Danielsen,
California Children s Services Program Analysis Final Report Paul H. Wise, MD, MPH Vandana Sundaram, MPH Lisa Chamberlain, MD, MPH Ewen Wang, MD Olga Saynina, MS Jia Chan, MS Kristen Chan, MASc Beate Danielsen,
Title/Description: Admission Criteria, Discharge Criteria, and Standards of Operation of the Pediatric Intensive Care Unit.
 University of Kentucky / UK HealthCare Policy and Procedure Policy # CH02-02 Title/Description: Admission Criteria, Discharge Criteria, and Standards of Operation of the Pediatric Intensive Care Unit.
University of Kentucky / UK HealthCare Policy and Procedure Policy # CH02-02 Title/Description: Admission Criteria, Discharge Criteria, and Standards of Operation of the Pediatric Intensive Care Unit.
STS Congenital Quality Module - Center Data
 STS Congenital Quality Module - Center Data Version 1.0 This document current as of: 05/21/2012 2:00:11 PM STS Congenital Quality Module - Center Data Version: 1.0 Bedside multidisciplinary rounds BedRounds
STS Congenital Quality Module - Center Data Version 1.0 This document current as of: 05/21/2012 2:00:11 PM STS Congenital Quality Module - Center Data Version: 1.0 Bedside multidisciplinary rounds BedRounds
Airway and Breathing Skills Levels Interpretive Guidelines
 Office of Emergency Medical Services and Trauma INDEX EFFECTIVE LAST REVIEW PAGES VERSION R-P11A 7/1/2011 7/1/2011 5 2011 Scope of Practice for EMS Personnel Emergency Medical Personnel are permitted to
Office of Emergency Medical Services and Trauma INDEX EFFECTIVE LAST REVIEW PAGES VERSION R-P11A 7/1/2011 7/1/2011 5 2011 Scope of Practice for EMS Personnel Emergency Medical Personnel are permitted to
PARAMEDIC TRAINING CLINICAL OBJECTIVES
 Page 1 of 21 GENERAL PATIENT UNIT When assigned to the General Patient unit paramedic student should gain knowledge and experience in the following: 1. Appropriate communication with patients and members
Page 1 of 21 GENERAL PATIENT UNIT When assigned to the General Patient unit paramedic student should gain knowledge and experience in the following: 1. Appropriate communication with patients and members
Recommendations: Other Supportive Therapy of Severe Sepsis*
 Recommendations: Other Supportive Therapy of Severe Sepsis* K. Blood Product Administration 1. Once tissue hypoperfusion has resolved and in the absence of extenuating circumstances, such as myocardial
Recommendations: Other Supportive Therapy of Severe Sepsis* K. Blood Product Administration 1. Once tissue hypoperfusion has resolved and in the absence of extenuating circumstances, such as myocardial
BORN Ontario: Clinical Reports Hospitals Part 1 May 2012
 BORN Ontario: Clinical Reports Hospitals Part 1 May 2012 Hospital Reports Release dates Report types Use and interpretation Access Questions and Answers 2 Clinical Reports Release Dates Available in the
BORN Ontario: Clinical Reports Hospitals Part 1 May 2012 Hospital Reports Release dates Report types Use and interpretation Access Questions and Answers 2 Clinical Reports Release Dates Available in the
Facts about Congenital Heart Defects
 Facts about Congenital Heart Defects Joseph A. Sweatlock, Ph.D., DABT New Jersey Department of Health Early Identification & Monitoring Program Congenital heart defects are conditions that are present
Facts about Congenital Heart Defects Joseph A. Sweatlock, Ph.D., DABT New Jersey Department of Health Early Identification & Monitoring Program Congenital heart defects are conditions that are present
Common types of congenital heart defects
 Common types of congenital heart defects Congenital heart defects are abnormalities that develop before birth. They can occur in the heart's chambers, valves or blood vessels. A baby may be born with only
Common types of congenital heart defects Congenital heart defects are abnormalities that develop before birth. They can occur in the heart's chambers, valves or blood vessels. A baby may be born with only
F.E.E.A. FONDATION EUROPEENNE D'ENSEIGNEMENT EN ANESTHESIOLOGIE FOUNDATION FOR EUROPEAN EDUCATION IN ANAESTHESIOLOGY
 créée sous le Patronage de l'union Européenne Detailed plan of the program of six courses 1. RESPIRATORY 1. ESPIRATORY AND THORAX 1.1 Physics and principles of measurement 1.1.1 Physical laws 1.1.2 Vaporizers
créée sous le Patronage de l'union Européenne Detailed plan of the program of six courses 1. RESPIRATORY 1. ESPIRATORY AND THORAX 1.1 Physics and principles of measurement 1.1.1 Physical laws 1.1.2 Vaporizers
RGN JOY LAUDE WATFORD GENERAL HOSPITAL, ENGLAND
 RGN JOY LAUDE WATFORD GENERAL HOSPITAL, ENGLAND Monitor patient on the ward to detect trends in vital signs and to manage accordingly To recognise deteriorating trends and request relevant medical/out
RGN JOY LAUDE WATFORD GENERAL HOSPITAL, ENGLAND Monitor patient on the ward to detect trends in vital signs and to manage accordingly To recognise deteriorating trends and request relevant medical/out
Maryland MOLST. Guide for Authorized Decision Makers. Maryland MOLST Training Task Force
 Maryland MOLST Guide for Authorized Decision Makers Maryland MOLST Training Task Force May 2012 Health Care Decision Making: Goals and Treatment Options Guide for Authorized Decision Makers Contents Introduction
Maryland MOLST Guide for Authorized Decision Makers Maryland MOLST Training Task Force May 2012 Health Care Decision Making: Goals and Treatment Options Guide for Authorized Decision Makers Contents Introduction
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: skilled_nursing_facility_care 02/2008 2/2015 2/2016 2/2015 Description of Procedure or Service A skilled
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: skilled_nursing_facility_care 02/2008 2/2015 2/2016 2/2015 Description of Procedure or Service A skilled
Newborn outcomes after cesarean section for fetal distress in BC
 Newborn outcomes after cesarean section for fetal distress in BC Patricia Janssen, PhD, UBC School of Population and Public Health Scientist, Child and Family Research Institute Kevin Jenniskens, MSc,
Newborn outcomes after cesarean section for fetal distress in BC Patricia Janssen, PhD, UBC School of Population and Public Health Scientist, Child and Family Research Institute Kevin Jenniskens, MSc,
Emergency Medical Services Advanced Level Competency Checklist
 Emergency Services Advanced Level Competency Checklist EMS Service: Current License in State of Nebraska: # (Copy of license kept in file at station) Date of joining EMS Service: EMS Service Member Name:
Emergency Services Advanced Level Competency Checklist EMS Service: Current License in State of Nebraska: # (Copy of license kept in file at station) Date of joining EMS Service: EMS Service Member Name:
Lorissa R. Heath RN, MSN, APRN 32 Macintosh Way Southington, CT 06489 (860) 426-1481 (H) (860) 426-1481 (Fax) E-mail: LRHeathAPRN@cox.
 Lorissa R. Heath RN, MSN, 32 Macintosh Way Southington, CT 06489 (860) 426-1481 (H) (860) 426-1481 (Fax) E-mail: LRHeath@cox.net Current Career Goal: To obtain a position as an within an established private
Lorissa R. Heath RN, MSN, 32 Macintosh Way Southington, CT 06489 (860) 426-1481 (H) (860) 426-1481 (Fax) E-mail: LRHeath@cox.net Current Career Goal: To obtain a position as an within an established private
Evaluation and treatment of emphysema in a preterm infant
 ISPUB.COM The Internet Journal of Pediatrics and Neonatology Volume 11 Number 1 Evaluation and treatment of emphysema in a preterm infant T Saad, P Chess, W Pegoli, P Katzman Citation T Saad, P Chess,
ISPUB.COM The Internet Journal of Pediatrics and Neonatology Volume 11 Number 1 Evaluation and treatment of emphysema in a preterm infant T Saad, P Chess, W Pegoli, P Katzman Citation T Saad, P Chess,
Addendum to the NRP Provider Textbook 6 th Edition Recommendations for specific modifications in the Canadian context
 Addendum to the NRP Provider Textbook 6 th Edition Recommendations for specific modifications in the Canadian context A subcommittee of the Canadian Neonatal Resuscitation Program (NRP) Steering Committee
Addendum to the NRP Provider Textbook 6 th Edition Recommendations for specific modifications in the Canadian context A subcommittee of the Canadian Neonatal Resuscitation Program (NRP) Steering Committee
Resuscitation in congenital heart disease. Peter C. Laussen MBBS FCICM Department Critical Care Medicine Hospital for Sick Children Toronto
 Resuscitation in congenital heart disease Peter C. Laussen MBBS FCICM Department Critical Care Medicine Hospital for Sick Children Toronto Evolution of Congenital Heart Disease Extraordinary success: Overall
Resuscitation in congenital heart disease Peter C. Laussen MBBS FCICM Department Critical Care Medicine Hospital for Sick Children Toronto Evolution of Congenital Heart Disease Extraordinary success: Overall
Medical Surgical Nursing Skills List
 Medical Surgical Nursing Skills List Read each of the required clinical skills for a Registered Nurse working on a typical acute medical-surgical unit. Write the number that corresponds to the level of
Medical Surgical Nursing Skills List Read each of the required clinical skills for a Registered Nurse working on a typical acute medical-surgical unit. Write the number that corresponds to the level of
PROPOSED CHANGES TO THE NURSING REGULATIONS
 PROPOSED CHANGES TO THE NURSING REGULATIONS This guidance document provides general information about the proposed regulations that have been posted for the 3 regulated nursing colleges. It is intended
PROPOSED CHANGES TO THE NURSING REGULATIONS This guidance document provides general information about the proposed regulations that have been posted for the 3 regulated nursing colleges. It is intended
SWISS SOCIETY OF NEONATOLOGY. Selective bronchial occlusion in a preterm infant with unilateral pulmonary interstitial emphysema
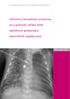 SWISS SOCIETY OF NEONATOLOGY Selective bronchial occlusion in a preterm infant with unilateral pulmonary interstitial emphysema December 2002 2 Riedel T, Pfenninger J, Pediatric Intensive Care Unit, University
SWISS SOCIETY OF NEONATOLOGY Selective bronchial occlusion in a preterm infant with unilateral pulmonary interstitial emphysema December 2002 2 Riedel T, Pfenninger J, Pediatric Intensive Care Unit, University
V: Infusion Therapy. Alberta Licensed Practical Nurses Competency Profile 217
 V: Infusion Therapy Alberta Licensed Practical Nurses Competency Profile 217 Competency: V-1 Knowledge of Intravenous Therapy V-1-1 V-1-2 V-1-3 V-1-4 V-1-5 Demonstrate knowledge and ability to apply critical
V: Infusion Therapy Alberta Licensed Practical Nurses Competency Profile 217 Competency: V-1 Knowledge of Intravenous Therapy V-1-1 V-1-2 V-1-3 V-1-4 V-1-5 Demonstrate knowledge and ability to apply critical
Virginia Office of Emergency Medical Services Scope of Practice - Procedures for EMS Personnel
 Specific tasks in this document shall refer to the Virginia Education Standards. AIRWAY TECHNIQUES Airway Adjuncts Airway Maneuvers Alternate Airway Devices Cricothyrotomy Obstructed Airway Clearance Intubation
Specific tasks in this document shall refer to the Virginia Education Standards. AIRWAY TECHNIQUES Airway Adjuncts Airway Maneuvers Alternate Airway Devices Cricothyrotomy Obstructed Airway Clearance Intubation
Delayed Cord Clamping
 ICEA Position Paper Delayed Cord Clamping Position The International Childbirth Education Association recognizes that the first minutes after birth are crucial to both mother and newborn. Optimal care
ICEA Position Paper Delayed Cord Clamping Position The International Childbirth Education Association recognizes that the first minutes after birth are crucial to both mother and newborn. Optimal care
Hummi Micro Draw Blood Transfer Device. The Next Generation System for Closed Micro Blood Sampling in the Neonate
 Hummi Micro Draw Blood Transfer Device The Next Generation System for Closed Micro Blood Sampling in the Neonate Current Methods for Umbilical Blood Sampling Current Methods for Umbilical Blood Sampling
Hummi Micro Draw Blood Transfer Device The Next Generation System for Closed Micro Blood Sampling in the Neonate Current Methods for Umbilical Blood Sampling Current Methods for Umbilical Blood Sampling
Guidelines for Core Clinical Privileges Certified Registered Nurse Anesthetists
 Guidelines for Core Clinical Privileges Certified Registered Nurse Anesthetists Copyright 2005 222 South Prospect Park Ridge, IL 60068 www.aana.com Guidelines for Core Clinical Privileges Certified Registered
Guidelines for Core Clinical Privileges Certified Registered Nurse Anesthetists Copyright 2005 222 South Prospect Park Ridge, IL 60068 www.aana.com Guidelines for Core Clinical Privileges Certified Registered
NICE Pathways bring together all NICE guidance, quality standards and other NICE information on a specific topic.
 Safe staffing for nursing in adult inpatient wards in acute hospitals overview bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed
Safe staffing for nursing in adult inpatient wards in acute hospitals overview bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed
Epidemiology 521. Epidemiology of Maternal and Child Health Problems. Winter / Spring, 2010
 Extended MPH Degree Program School of Public Health Department of Epidemiology University of Washington Epidemiology 521 Epidemiology of Maternal and Child Health Problems Winter / Spring, 2010 Instructor:
Extended MPH Degree Program School of Public Health Department of Epidemiology University of Washington Epidemiology 521 Epidemiology of Maternal and Child Health Problems Winter / Spring, 2010 Instructor:
ELSO GUIDELINES FOR TRAINING AND CONTINUING EDUCATION OF ECMO SPECIALISTS
 ELSO GUIDELINES FOR TRAINING AND CONTINUING EDUCATION OF ECMO SPECIALISTS PURPOSE The "" is a document developed by the Extracorporeal Life Support Organization (ELSO) as a reference for current and future
ELSO GUIDELINES FOR TRAINING AND CONTINUING EDUCATION OF ECMO SPECIALISTS PURPOSE The "" is a document developed by the Extracorporeal Life Support Organization (ELSO) as a reference for current and future
a guide to understanding pierre robin sequence
 a guide to understanding pierre robin sequence a publication of children s craniofacial association a guide to understanding pierre robin sequence this parent s guide to Pierre Robin Sequence is designed
a guide to understanding pierre robin sequence a publication of children s craniofacial association a guide to understanding pierre robin sequence this parent s guide to Pierre Robin Sequence is designed
8.470 HOSPITAL BACK UP LEVEL OF CARE PAGE 1 OF 10. Complex wound care means that the client meets the following criteria:
 8.470 HOSPITAL BACK UP LEVEL OF CARE PAGE 1 OF 10 8.470 HOSPITAL BACK UP LEVEL OF CARE 8.470.1 DEFINITIONS Complex wound care means that the client meets the following criteria: 1. Has at least one of
8.470 HOSPITAL BACK UP LEVEL OF CARE PAGE 1 OF 10 8.470 HOSPITAL BACK UP LEVEL OF CARE 8.470.1 DEFINITIONS Complex wound care means that the client meets the following criteria: 1. Has at least one of
The ASA defines anesthesiology as the practice of medicine dealing with but not limited to:
 1570 Midway Pl. Menasha, WI 54952 920-720-1300 Procedure 1205- Anesthesia Lines of Business: All Purpose: This guideline describes Network Health s reimbursement of anesthesia services. Procedure: Anesthesia
1570 Midway Pl. Menasha, WI 54952 920-720-1300 Procedure 1205- Anesthesia Lines of Business: All Purpose: This guideline describes Network Health s reimbursement of anesthesia services. Procedure: Anesthesia
Common Conditions, Concerns, and Equipment in the NICU
 Common Conditions, Concerns, and Equipment in the NICU Babies in the NICU are carefully monitored because of their health risk. While the following is a comprehensive list of common conditions found in
Common Conditions, Concerns, and Equipment in the NICU Babies in the NICU are carefully monitored because of their health risk. While the following is a comprehensive list of common conditions found in
