Chapter 12. Anatomy of Skin. Epidermis. Dermis
|
|
|
- Job Edwards
- 8 years ago
- Views:
Transcription
1 Chapter 12 SKIN GRAFTS KEY FIGURES: Skin anatomy with graft thickness Humby knife Using the dermatome Using the Humby knife Mesher Skin graft Tying the dressing in place Defatting the FTSG A skin graft involves taking a piece of skin from an uninjured area of the body (called the donor site) and using it to provide coverage for an open wound. When primary closure is impossible because of soft tissue loss and closure by secondary intention is contraindicated, a skin graft is the next rung on the reconstructive ladder. It is not a technically difficult procedure but does require some surgical skills. For a successful result, you need a thorough understanding of how skin grafts heal and how to perform the procedure. Background information Anatomy of Skin The thickness of human skin is quite variable. The eyelids have the thinnest skin (0.5 mm), and the thickest skin is found on the soles of the feet (> 5.0 mm). Epidermis The epidermis is the top portion of the skin. The outer layers of the epidermis are formed by essentially dead, nonreplicating cells. The innermost layer contains the cells capable of replication, which are responsible for wound healing and skin pigmentation. Dermis Immediately below the epidermis is the dermis. It is made primarily of collagen and is much thicker than the epidermal layer. The dermal-epidermal 97
2 98 Practical Plastic Surgery for Nonsurgeons junction is irregular and has the appearance of ridges. This anatomic arrangement accounts for the skin s strength and prevents injury from normal shear forces. Nerve endings, hair follicles, and sweat glands are located in the dermis. All skin grafts must include at least a portion of the dermal layer for survival. Subcutaneous Tissue The subcutaneous fatty tissue below the dermis provides padding for the skin. The base of many hair follicles and sweat glands, as well as many important nerves for pressure sensation, reside in the subcutaneous tissue. Because of these important skin components, I include the subcutaneous tissue as a layer of the skin. However, it is not included in a skin graft. Fat attached to the graft interferes with transport of nutrients to the important upper skin layers. Therefore, no fat should be included in the skin graft. Cross-section of human skin showing the epidermis and dermis (derived from two different germ layers). The relative thickness of skin grafts is shown. The thicker the graft, the more characteristics of normal skin it will provide. (From Cohen M (ed): Mastery of Plastic and Reconstructive Surgery. Boston, Little, Brown, 1994, with permission.) How a Skin Graft Survives When the skin graft is harvested from the donor site, it is completely separated from its blood supply. In its new position covering the open wound, the graft initially survives by diffusion of nutrients from the wound bed into the graft. Diffusion of nutrients keeps the skin graft
3 Skin Grafts 99 alive for, at most, 3 5 days. During this period, blood vessels begin to grow from the wound bed into the graft. By the time the graft is no longer able to survive by diffusion of nutrients alone, this vascular network has formed and becomes the primary mechanism for providing nutrients to the graft. In the first several weeks after the procedure, the skin graft looks quite red and irregular compared with normal surrounding skin. Reassure the patient that the appearance will improve dramatically over the next several months, but the skin-grafted area will never look completely normal. It can take at least 1 year to see the final appearance of the graft. See chapter 15, Scar Formation, for more details When is a Wound Ready for Grafting? A wound will accept a skin graft when there is no overlying dead tissue and the wound is clean, beefy red (from granulation tissue), and without surrounding infection. Skin grafts heal well over muscle. Therefore, if muscle is exposed in the wound, skin can be grafted at any time, as long as the wound is otherwise clean. Table 1. Compensating for Factors that Interfere with Graft Survival Compensation Debride the wound and treat it with wet-to-dry dressings until the wound looks clean. Use antibiotics to clear signs of surrounding infection. The skin graft can be done once the wound has improved in appearance and there are no signs of surrounding infection. Fat has a poor blood supply and may not be able to support the graft. Treat the wound with wet-to-dry dressings until granulation tissue* begins to appear. Then do the skin graft. Movement of the graft over the wound interferes with vas- cular ingrowth. The graft must be kept well secured to the wound by the dressing. If the graft is on an extremity, consider using a splint for immobilization of the limb. Fluid collection under the graft prevents the ingrowth of blood vessels necessary for graft survival. Fluid collection can be prevented by cutting holes in the graft and keeping the graft well secured to the wound. If the graft is on the leg, the patient should be kept on bedrest, with the leg elevated at all times for at least the first 4 5 days. Factor Dirty wound (e.g., surrounding infection, necrotic tissue over wound) Fat in base of wound Shear forces between graft and base of wound Blood or serum collection under graft * Granulation tissue is the beefy red tissue that develops as a wound heals. It has an excellent blood supply but also contains bacteria in its crevices. Contraindications to Wound Closure with a Skin Graft A wound that has exposed tendon or bone can be successfully covered with a skin graft only if the thin layer of tissue connecting the tendon or
4 100 Practical Plastic Surgery for Nonsurgeons bone (paratenon or periosteum, respectively) is intact. These connective tissues contain the vascular structures necessary for skin graft survival. If the paratenon or periosteum is absent, the graft will not survive. Under these circumstances, some type of flap is needed for wound closure. Split-thickness Skin Graft A split-thickness skin graft (STSG) is composed of the top layers of skin (the epidermis and part of the dermis). The graft is placed over an open wound to provide coverage and promote healing. The STSG donor site is essentially a second-degree burn because only part of the dermis is included in the graft. The donor site will heal on its own because some dermal elements remain. Indications An STSG is indicated in most wounds that cannot be closed primarily and when closure by secondary intention is contraindicated. It is also indicated for a relatively large wound (> 5 6 cm in diameter) that would take many weeks to heal secondarily. A skin graft provides more stable coverage for large wounds than the scar that results from secondary closure. A large wound also heals more quickly with a skin graft than with dressing changes alone. The wound must be clean. All necrotic tissue must be removed before skin grafting, and there should be no signs of infection in the surrounding tissues. Anesthesia of the Donor Site Because of the relatively large size of the graft to be taken, the patient usually requires either general or spinal anesthesia for adequate pain control. However, if the required graft is no more than several centimeters in diameter, the donor site can be anesthetized by local infiltration of tissues with lidocaine or bupivacaine. Preparation of the Donor Site The most common donor site is the anterior or lateral aspect of the thigh. If the wound to be covered is on the back, try to take the graft from the lateral thigh, but the posterior thigh is also acceptable. Use of the posterior thigh as a donor site is a bit more painful and difficult for the patient to care for postoperatively. Any betadine or other antibacterial solution used to prepare the donor site should be washed off with saline. Then the donor site should be dried. Apply a sterile lubricant (e.g., mineral oil, K-Y jelly) to the donor site and to the instrument you will be using to harvest the graft.
5 Skin Grafts 101 Procedure for Taking the Graft A thin layer of skin (epidermis with some underlying dermis) is taken with a dermatome or a Humby knife (sometimes called a Watson knife). A dermatome is powered by air or electricity, but it is not available in all hospitals, especially in rural settings. Remember: you are not taking full-thickness skin; some dermis must be left at the donor site. Skin-graft (Humby) knife. (From Padgett Instruments, Inc., with permission.) Both the Humby knife and dermatome have settings that can be adjusted to set the thickness of the graft. Place the settings at inch ( mm). Unfortunately, these settings are often unreliable. Another technique to ensure proper thickness of the graft is to adjust the opening of the blade so that you can snuggly fit the beveled edge of a no. 10 blade into the opening. Caution: Always check the knife settings just before you take the graft. This safety check prevents the accidental taking of too thick or too thin a graft. An assistant should help to spread and flatten out the donor site by placing tension on the skin with gauze or tongue depressors. If you have a dermatome: 1. Turn on the power while the dermatome is in the air before it comes into contact with the skin. 2. Hold the dermatome at a 45 angle with the skin and hold it firmly against the skin. 3. Slowly move down the donor site until you have taken the properly sized graft. 4. At this point do not turn off the power. Remove the dermatome from the skin with the power on so that the graft is completely freed from the donor site. 5. The entire movement is evocative of landing an airplane and taking off again right away.
6 102 Practical Plastic Surgery for Nonsurgeons Harvesting a split-thickness skin graft with a power-driven dermatome. (From Cohen M (ed): Mastery of Plastic and Reconstructive Surgery. Boston, Little, Brown, 1994, with permission.) If you have a Humby knife: 1. Hold it with the sharp edge at about a 45 angle with the skin. 2. With a back-and-forth motion run the knife over the tight skin. 3. When you have taken a large enough graft, continue the back-andforth motion, and twist your wrist into supination to remove the knife from the skin. Another option is to stop the knife movement and then use a scalpel to cut the skin graft from the donor site at the Harvesting a split-thickness graft with the Humby knife. (From McCarthy JG (ed): Plastic Surgery. Philadelphia, W.B. Saunders, 1990, with permission.)
7 Skin Grafts 103 blade edge. You may need to open the knife fully to remove the skin from the instrument. Preparation of the Skin Graft It is best to cut multiple slices in the graft to prevent blood and serum from accumulating under the graft. The cuts also help to expand the graft, allowing you to take a graft that is slightly smaller than the open wound. Use the tip of a knife or a small scissors to create the cuts in the graft. Some operating rooms have special equipment, called meshers, for this purpose. The mesher is a hand-cranked instrument that creates pie-cuts in the skin. A, The mesher, a device used to make fine cuts in skin grafts. B, The skin graft is placed on the rough side of the carrier and passed through the mesher. C, The meshed graft can now be spread over a larger area. (From Chase CA: Altas of Hand Surgery. Philadelphia, W.B. Saunders, 1973, with permission.)
8 104 Practical Plastic Surgery for Nonsurgeons How to Use the Mesher 1. Place the skin on a plastic carrier. Carriers are available in different sizes, but the best size to use is 1.5:1 (i.e., the graft is expanded 1.5 times). 2. Spread out the skin graft on the rough side of the carrier. If you put it on the smooth side, you will get spaghetti when you place the graft through the mesher. It does not matter which side of the skin faces upward on the carrier, but the dermis side is the more shiny side. 3. Pass the carrier with the skin graft through the mesher, taking care that the graft stays on the carrier and is not pulled into the blades of the mesher. Placement of the Graft onto the Recipient Site 1. Be sure that the wound is clean. Remove any small areas that appear unhealthy. 2. To decrease the amount of contamination in the top layers of the healing wound, scrape the wound with the edge of a knife. Do not push the knife edge into the wound; instead, scrape it over the wound. Rinse the wound with saline. Wound covered with a split-thickness skin graft. The graft has been meshed 1.5:1.
9 Skin Grafts Scraping the wound will make it bleed, but the bleeding is easily controlled by placing gauze over the wound and applying gentle pressure for a few minutes. Remember: hemostasis is important. 4. Place the skin graft over the wound with the dermis side (the shinier side) down, next to the raw surface of the wound. 5. Suture the graft in place with absorbable sutures. Leave a long tail on a few of these sutures so that they can be used to hold the dressing in place (see below). 6. Alternatively, the skin graft can be stapled in place, but the staples must be removed. Removal can be painful. Application of Wound Dressing 1. A layer of nonstick material, such as antibiotic-impregnated gauze, should be placed directly over the graft. If you do not have this type of gauze, apply a layer of antibiotic ointment over the graft. 2. Moisten a sterile gauze with mineral oil (if available) or saline. 3. Fluff the gauze and place it over the nonstick layer; then cover the area with dry gauze. 4. Try to keep the dressing as secure as possible, either by wrapping with gauze or by tying the dressing in place. Tying the dressing in place. In suturing the skin graft to the wound edges, leave the ends of each suture long (A). Then use the long ends to secure the dressing in place (B). This technique immobilizes the dressing and underlying graft. (From Edgerton M: The Art of Surgical Technique. Baltimore, Williams & Wilkins, 1988, with permission.)
10 106 Practical Plastic Surgery for Nonsurgeons Removal of Wound Dressing The dressing should be kept in place for 3 5 days. Check the dressing each day. If it develops an odor or has a lot of drainage, remove the dressing sooner. Be careful not to lift the graft from the wound with the dressing change. Wet the dressing with saline (mixed with a little hydrogen peroxide, if available) to prevent the dressing from sticking. Aftercare Gently apply antibiotic ointment, or use a wet-to-wet saline dressing once or twice a day for the next few days. The area can be cleansed very gently with saline at each dressing change. After days, once the wound looks like it is healing (i.e., the graft is pink and well-adherent to the wound), the dressings can be left off. A gentle moisturizer should be applied daily. The skin graft site should be kept out of the sun as much as possible. Sunscreens can be used once the graft has fully healed. Vigorously counsel the patient not to smoke during the healing period. Smoking probably will cause the skin graft to die. Care of the Donor Site At the time of surgery, the donor site should be covered with a layer of antibiotic gauze. A thick layer of gauze should be placed on top. After 24 hours, remove the outer gauze dressing not the antibiotic layer and leave the entire area open to air. The layer of antibiotic gauze will dry out over the next hours and gradually peel off as the underlying wound heals. An alternative treatment is to treat the donor site like a burn: apply antibiotic ointment twice a day until the wound has healed. Apply moisturizer regularly to the donor site once it has healed. The donor site also should be kept out of the sun. Sunscreens can be used once the wound has fully healed. Full-thickness Skin Graft A full thickness skin graft (FTSG) includes the epidermis and entire dermis but no subcutaneous fat. Because the entire thickness of skin is taken, the graft donor site must be closed primarily.
11 Skin Grafts 107 Indications FTSGs are rarely done, because the wound must be very clean for the graft to survive. Most often they are used for a small wound, usually one created surgically (such as a wound on the face created by excision of a malignant skin lesion). The other common use is for open wounds on the palmar surface of the hands and fingers. These areas may scar too tightly if the thinner STSG is used. Preparation of the Donor Site The best donor site is usually just above the inguinal crease on the lower abdomen. If the graft is needed to cover a facial wound, extra skin of a reasonable color match often can be taken from the supraclavicular area in the neck or from behind the ear. An ellipse is drawn at the donor site. Make sure that it is large enough to cover the defect but not too large to close the donor site. You can tell how large a graft you can take by seeing how much skin you can pinch or pull up at the donor site. At the inguinal area, you can flex the patient s hip to decrease tension on the closure. After a few days the patient will be able to extend the hip fully. This approach causes no long-term problems. Anesthesia of the Donor Site Because you are taking a relatively small graft, the FTSG can be harvested with a local anesthetic. Lidocaine and marcaine work equally well. Procedure for Taking the Graft 1. The ellipse of skin is excised with the full layer of dermis. To facilitate the procedure, take the graft with some underlying fat attached. 2. You must remove the attached fat, which will interfere with graft survival. How to Defat the Graft 1. The skin graft should be placed under tension. Place clamps on the ends of the graft, lay the graft over your hand, and let the clamps hang freely. 2. Use scissors to remove the fat on the dermis. Place the scissors flush with the skin, and cut away the fat. Do not worry if you take a little dermis or cut into small areas of the epidermis.
12 108 Practical Plastic Surgery for Nonsurgeons Defatting the undersurface of a full-thickness skin graft with a pair of scissors. (From McCarthy JG (ed): Plastic Surgery. Philadelphia, W.B. Saunders, 1990, with permission.) Placement of the Graft onto the Recipient Site 1. The recipient site must be very clean. 2. If you are using the FTSG for a wound on the palmar surface of the hand, decrease the amount of contamination in the top layers of the healing wound by scraping the wound with the edge of a knife. Do not push the knife edge into the wound; simply scrape it over the wound and then rinse with saline. 3. Scraping makes the wound bleed, but the bleeding is easily controlled by placing gauze over the wound and applying gentle pressure for a few minutes. Remember: hemostasis is important. 4. A few small slits can be cut in the graft to prevent fluid from accumulating under the graft. In general, the graft is placed as an intact sheet. Do not mesh a FTSG. 5. The graft is placed over the wound, dermis side down, and sutured in place with absorbable sutures. Leave a long tail on a few of these sutures so that they can be used to hold the dressing in place. Application of Wound Dressing 1. A layer of nonstick, antibiotic-impregnated gauze should be placed directly over the graft. Alternatively, place a thin layer of antibiotic ointment over the graft. 2. Moisten sterile gauze with mineral oil (if available) or saline. 3. Fluff the gauze and place it over the nonstick layer and cover with dry gauze.
13 Skin Grafts Keep the dressing as secure as possible, either by wrapping with gauze or by tying the dressing in place. Removal of Wound Dressing The dressing should be kept in place for 3 5 days. Check the dressing each day. If the wound develops an odor or has a lot of drainage, remove the dressing sooner. Be careful not to lift the graft off of the wound with dressing changes. If necessary, wet the dressing with saline (mixed with a little hydrogen peroxide if available) to prevent it from sticking. Aftercare Apply antibiotic ointment, or use a wet-to-wet saline dressing once or twice a day for the next few days. Cleanse the area gently with saline at each dressing change. The epidermis (very top layer) may become black and peel off. Do not be overly concerned. As long as the underlying dermis is attached and vascularized, the graft should heal. After 7 10 days, once the graft looks like it is healing (i.e., it is pink and well-adherent), the dressings can be left off. A gentle moisturizer should be applied. The skin graft site should be kept out of the sun as much as possible. A gentle sunscreen should be used. Vigorously counsel the patient not to smoke during the healing period. Smoking probably will cause the skin graft to die. Care of the Donor Site The donor site should be closed primarily and covered with antibiotic ointment and dry gauze. The dressing can be removed after 24 hours. Apply a small amount of antibiotic ointment and dry gauze for 2 3 days. Then the area can be left open. Clean daily with gentle soap and water. Remove the sutures after 7 10 days. Bibliography Reus WF, Mathes SJ: Wound closure. In Jurkeiwicz MJ, Krizek TJ, Mathes SJ, Ariyan S (eds): Plastic Surgery: Principles and Practice. St. Louis, Mosby, 1990, pp
Chapter 11. Everting skin edges
 Chapter 11 PRIMARY WOUND CLOSURE KEY FIGURE: Everting skin edges In primary wound closure, the skin edges of the wound are sutured together to close the defect. Whenever possible and practical, primary
Chapter 11 PRIMARY WOUND CLOSURE KEY FIGURE: Everting skin edges In primary wound closure, the skin edges of the wound are sutured together to close the defect. Whenever possible and practical, primary
FUNCTIONS OF THE SKIN
 FUNCTIONS OF THE SKIN Skin is the largest organ of the body. The average adult has 18 square feet of skin which account for 16% of the total body weight. Skin acts as a physical barrier for you to the
FUNCTIONS OF THE SKIN Skin is the largest organ of the body. The average adult has 18 square feet of skin which account for 16% of the total body weight. Skin acts as a physical barrier for you to the
APPLICATION OF DRY DRESSING
 G-100 APPLICATION OF DRY DRESSING PURPOSE To aid in the management of a wound with minimal drainage. To protect the wound from injury, prevent introduction of bacteria, reduce discomfort, and assist with
G-100 APPLICATION OF DRY DRESSING PURPOSE To aid in the management of a wound with minimal drainage. To protect the wound from injury, prevent introduction of bacteria, reduce discomfort, and assist with
Chapter 7. Expose the Injured Area
 Chapter 7 GUNSHOT WOUNDS KEY FIGURES: Entrance/exit wounds This chapter describes how to treat the external, surface wounds caused by a bullet. The evaluation for underlying injury related to gunshot wounds
Chapter 7 GUNSHOT WOUNDS KEY FIGURES: Entrance/exit wounds This chapter describes how to treat the external, surface wounds caused by a bullet. The evaluation for underlying injury related to gunshot wounds
Chapter 34. Neglected hand Escharotomy
 Chapter 34 HAND BURNS KEY FIGURES: Neglected hand Escharotomy Severe hand burns are especially problematic injuries because of their propensity for causing long-term disability. Proper treatment of the
Chapter 34 HAND BURNS KEY FIGURES: Neglected hand Escharotomy Severe hand burns are especially problematic injuries because of their propensity for causing long-term disability. Proper treatment of the
Chapter 29. Initial Care
 Chapter 29 FINGERTIP AND NAIL BED INJURIES KEY FIGURES: Digital tourniquet Bone rongeur Fingernail with hematoma Thenar flap Repair of nail bed Hand injuries are commonly encountered by health care providers
Chapter 29 FINGERTIP AND NAIL BED INJURIES KEY FIGURES: Digital tourniquet Bone rongeur Fingernail with hematoma Thenar flap Repair of nail bed Hand injuries are commonly encountered by health care providers
TAKING CARE OF WOUNDS KEY FIGURE:
 Chapter 9 TAKING CARE OF WOUNDS KEY FIGURE: Gauze Wound care represents a major area of concern for the rural health provider. This chapter discusses the treatment of open wounds, with emphasis on dressing
Chapter 9 TAKING CARE OF WOUNDS KEY FIGURE: Gauze Wound care represents a major area of concern for the rural health provider. This chapter discusses the treatment of open wounds, with emphasis on dressing
TREATMENT 1. Control bleeding by applying pressure over wound with Gauze Pads (Surgical Supply-4). 2. Contact Surgeon for laceration repair options.
 Page 1 of 8 pages NOTE Contact Surgeon before giving any medication marked with an asterisk. In an emergency or during Loss of Signal, begin appropriate treatment; then call Surgeon as soon as possible.
Page 1 of 8 pages NOTE Contact Surgeon before giving any medication marked with an asterisk. In an emergency or during Loss of Signal, begin appropriate treatment; then call Surgeon as soon as possible.
Integumentary System Individual Exercises
 Integumentary System Individual Exercises 1. A physician performs an incision and drainage of a subcutaneous abscess in his office for a particularly uncooperative established patient. How should this
Integumentary System Individual Exercises 1. A physician performs an incision and drainage of a subcutaneous abscess in his office for a particularly uncooperative established patient. How should this
Chapter 30. Rotational deformity Buddy taping Reduction of metacarpal fracture
 Chapter 30 FINGER FRACTURES AND DISLOCATIONS KEY FIGURES: Rotational deformity Buddy taping Reduction of metacarpal fracture Because we use our hands for so many things, finger fractures and dislocations
Chapter 30 FINGER FRACTURES AND DISLOCATIONS KEY FIGURES: Rotational deformity Buddy taping Reduction of metacarpal fracture Because we use our hands for so many things, finger fractures and dislocations
call 811 to get advice from a nurse, or have someone drive the patient to a hospital Emergency Department. Patients should NOT drive themselves.
 Taking Care at Home After Surgery This checklist is to help you and your support person know what to do after you go home following your surgery. If you are given instructions verbally or in writing by
Taking Care at Home After Surgery This checklist is to help you and your support person know what to do after you go home following your surgery. If you are given instructions verbally or in writing by
NIH Clinical Center Patient Education Materials Giving a subcutaneous injection
 NIH Clinical Center Patient Education Materials What is a subcutaenous injection? A subcutaneous injection is given in the fatty layer of tissue just under the skin. A subcutaneous injection into the fatty
NIH Clinical Center Patient Education Materials What is a subcutaenous injection? A subcutaneous injection is given in the fatty layer of tissue just under the skin. A subcutaneous injection into the fatty
Chapter 33. Nerve Physiology
 Chapter 33 NERVE AND VASCULAR INJURIES OF THE HAND KEY FIGURES: Digital nerve location on finger Epineurial repair Nerves and blood vessels of the hand and fingers usually are quite delicate, and some
Chapter 33 NERVE AND VASCULAR INJURIES OF THE HAND KEY FIGURES: Digital nerve location on finger Epineurial repair Nerves and blood vessels of the hand and fingers usually are quite delicate, and some
X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary
 X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary Introduction A Subclavian Inserted Central Catheter, or subclavian line, is a long thin hollow tube inserted in a vein under the
X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary Introduction A Subclavian Inserted Central Catheter, or subclavian line, is a long thin hollow tube inserted in a vein under the
Two main classes: Epithelial Connective (synovial) Epithelial. Cutaneous Mucous Serous
 Two main classes: Epithelial Connective (synovial) Epithelial Cutaneous Mucous Serous Epithelial Membranes = sheet of epithelia + connective tissue base 1. Cutaneous membrane: outer skin layer (stratified
Two main classes: Epithelial Connective (synovial) Epithelial Cutaneous Mucous Serous Epithelial Membranes = sheet of epithelia + connective tissue base 1. Cutaneous membrane: outer skin layer (stratified
X-Plain Foley Catheter Male Reference Summary
 X-Plain Foley Catheter Male Reference Summary Introduction A Foley catheter is a tube that is put through the urinary opening and into your bladder to drain urine. Your doctor may have placed or may ask
X-Plain Foley Catheter Male Reference Summary Introduction A Foley catheter is a tube that is put through the urinary opening and into your bladder to drain urine. Your doctor may have placed or may ask
TENDON INJURIES OF THE HAND KEY FIGURES:
 Chapter 32 TENDON INJURIES OF THE HAND KEY FIGURES: Extensor surface of hand Mallet finger Mallet splints Injured finger in stack splint Repair of open mallet Most hand specialists believe that the earlier
Chapter 32 TENDON INJURIES OF THE HAND KEY FIGURES: Extensor surface of hand Mallet finger Mallet splints Injured finger in stack splint Repair of open mallet Most hand specialists believe that the earlier
PATIENT TEACHING GUIDE: Wound Care Handbook
 PATIENT TEACHING GUIDE: Wound Care Handbook PATIENT TEACHING GUIDE: WOUND CARE Design by Mariscal Design, Illustrations by Lysa Hawke. The Wound Care Self Care Guide was written and prepared by: Barbara
PATIENT TEACHING GUIDE: Wound Care Handbook PATIENT TEACHING GUIDE: WOUND CARE Design by Mariscal Design, Illustrations by Lysa Hawke. The Wound Care Self Care Guide was written and prepared by: Barbara
Abdominal Pedicle Flaps To The Hand And Forearm John C. Kelleher M.D., F.A.C.S.
 Abdominal Pedicle Flaps To The Hand And Forearm John C. Kelleher M.D., F.A.C.S. Global-HELP Publications Chapter Eight: TECHNICAL REQUIREMENTS FOR FORMATION OF A TUBED PEDICLE FLAP Creating a tube pedicle
Abdominal Pedicle Flaps To The Hand And Forearm John C. Kelleher M.D., F.A.C.S. Global-HELP Publications Chapter Eight: TECHNICAL REQUIREMENTS FOR FORMATION OF A TUBED PEDICLE FLAP Creating a tube pedicle
Preparing to Suture. 6 th Annual Pediatric Advanced Practice Conference Tuesday, February 9, 2016 1:30 pm. Workshop B: Suturing for Beginners
 Preparing to Suture Kristen Devick, MPAS, PA-C University of Colorado Department of Emergency Medicine NONE! Skin Anatomy Trott, 2012, p.11 Preparing to suture Initial evaluation Hemostasis Anesthesia
Preparing to Suture Kristen Devick, MPAS, PA-C University of Colorado Department of Emergency Medicine NONE! Skin Anatomy Trott, 2012, p.11 Preparing to suture Initial evaluation Hemostasis Anesthesia
Chapter 21. How to do fasciotomy. neighboring structures
 Chapter 21 FRACTURES OF THE TIBIA AND FIBULA KEY FIGURES: Calf anatomy How to do fasciotomy Gastrocnemius and neighboring structures Longstanding open fracture Gastrocnemius flap Fractures of the tibia
Chapter 21 FRACTURES OF THE TIBIA AND FIBULA KEY FIGURES: Calf anatomy How to do fasciotomy Gastrocnemius and neighboring structures Longstanding open fracture Gastrocnemius flap Fractures of the tibia
7/11/2011. Pressure Ulcers. Moisture-NOT Pressure. Wounds NOT Caused by Pressure
 Assessment and Documentation of Pressure Ulcers Jeri Ann Lundgren, RN, BSN, PHN, CWS, CWCN Pathway Health Services July 19, 2011 Training Objectives Describe etiologies of pressure ulcers Discuss how to
Assessment and Documentation of Pressure Ulcers Jeri Ann Lundgren, RN, BSN, PHN, CWS, CWCN Pathway Health Services July 19, 2011 Training Objectives Describe etiologies of pressure ulcers Discuss how to
PHaSES: Practical Hands-on Surgical Education System
 U.S. Toll Free 866-GOLIMBS PHaSES Range PHaSES: Practical Hands-on Surgical Education System Limbs & Things is pleased to introduce the PHaSES Range. The range is based upon our well known basic & general
U.S. Toll Free 866-GOLIMBS PHaSES Range PHaSES: Practical Hands-on Surgical Education System Limbs & Things is pleased to introduce the PHaSES Range. The range is based upon our well known basic & general
BANDAGES AND BANDAGING TECHNIQUES
 BANDAGES AND BANDAGING TECHNIQUES Your role as a veterinary assistant is to understand the theory behind bandaging, as bandaging is the veterinary technician s and the veterinarian s role. You ll need
BANDAGES AND BANDAGING TECHNIQUES Your role as a veterinary assistant is to understand the theory behind bandaging, as bandaging is the veterinary technician s and the veterinarian s role. You ll need
5 Upper eyelid blepharoplasty
 5 Upper eyelid blepharoplasty INSTRUMENTS Marking pen No. 15 scalpel blade Blade handle Castroviejo needle holder Castroviejo calipers 0.5 fixation forceps Westcott scissors 6-0 prolene suture Bovie cautery
5 Upper eyelid blepharoplasty INSTRUMENTS Marking pen No. 15 scalpel blade Blade handle Castroviejo needle holder Castroviejo calipers 0.5 fixation forceps Westcott scissors 6-0 prolene suture Bovie cautery
Introduction A JP Drain is a soft tube and container used to drain fluids that build up under the skin after surgery.
 JP Drain Introduction A JP Drain is a soft tube and container used to drain fluids that build up under the skin after surgery. This reference summary explains what a JP Drain is and discusses how to take
JP Drain Introduction A JP Drain is a soft tube and container used to drain fluids that build up under the skin after surgery. This reference summary explains what a JP Drain is and discusses how to take
Position Statement: Pressure Ulcer Staging
 Position Statement: Pressure Ulcer Staging Statement of Position The Wound, Ostomy and Continence Nurses (WOCN) Society supports the use of the National Pressure Ulcer Advisory Panel Staging System (NPUAP).
Position Statement: Pressure Ulcer Staging Statement of Position The Wound, Ostomy and Continence Nurses (WOCN) Society supports the use of the National Pressure Ulcer Advisory Panel Staging System (NPUAP).
How does Diabetes Effect the Feet
 How does Diabetes Effect the Feet What Skin Changes May Occur? Diabetes can cause changes in the skin of your foot. At times your foot may become very dry. The skin may peel and crack. The problem is that
How does Diabetes Effect the Feet What Skin Changes May Occur? Diabetes can cause changes in the skin of your foot. At times your foot may become very dry. The skin may peel and crack. The problem is that
PATIENT GUIDE. Care and Maintenance Drainage Frequency: Max. Drainage Volume: Dressing Option: Clinician s Signature: Every drainage Weekly
 PATIENT GUIDE Care and Maintenance Drainage Frequency: Max. Drainage Volume: Dressing Option: Every drainage Weekly Clinician s Signature: ACCESS SYSTEMS Pleural Space Insertion Site Cuff Exit Site Catheter
PATIENT GUIDE Care and Maintenance Drainage Frequency: Max. Drainage Volume: Dressing Option: Every drainage Weekly Clinician s Signature: ACCESS SYSTEMS Pleural Space Insertion Site Cuff Exit Site Catheter
Taking Out a Tooth. Before You Begin: Ask Questions! CHAPTER11
 159 CHAPTER11 Taking Out a Tooth Not every painful tooth needs to come out. You must decide how serious the problem is, and then decide if you can treat and save the tooth. Some problems such as root canal
159 CHAPTER11 Taking Out a Tooth Not every painful tooth needs to come out. You must decide how serious the problem is, and then decide if you can treat and save the tooth. Some problems such as root canal
How To Recover From A Surgical Wound From A Cast
 Care of Your Wounds After Amputation Surgery by Paddy Rossbach, RN Depending on the reason for your amputation and the state of your limb at the time of surgery, definitive closure of the wound may take
Care of Your Wounds After Amputation Surgery by Paddy Rossbach, RN Depending on the reason for your amputation and the state of your limb at the time of surgery, definitive closure of the wound may take
STANDARD OPERATING PROCEDURE #201 RODENT SURGERY
 STANDARD OPERATING PROCEDURE #201 RODENT SURGERY 1. PURPOSE The intent of this Standard Operating Procedure (SOP) is to describe procedures for survival rodent surgery. 2. RESPONSIBILITY Principal investigators
STANDARD OPERATING PROCEDURE #201 RODENT SURGERY 1. PURPOSE The intent of this Standard Operating Procedure (SOP) is to describe procedures for survival rodent surgery. 2. RESPONSIBILITY Principal investigators
COW S EYE dissection. Dissecting a Cow s Eye Step-by-Step Instructions. Safety first!
 COW S EYE dissection Dissecting a Cow s Eye Step-by-Step Instructions One way to figure out how something works is to look inside it. To learn about how your eyes work, you can dissect, or take apart,
COW S EYE dissection Dissecting a Cow s Eye Step-by-Step Instructions One way to figure out how something works is to look inside it. To learn about how your eyes work, you can dissect, or take apart,
Care for your child s Central Venous Catheter (CVC)
 Care for your child s Central Venous Catheter (CVC) This booklet is intended for general informational purposes only. You should consult your doctor for medical advice. Please call the clinic or your home
Care for your child s Central Venous Catheter (CVC) This booklet is intended for general informational purposes only. You should consult your doctor for medical advice. Please call the clinic or your home
ARTHROSCOPIC HIP SURGERY
 ARTHROSCOPIC HIP SURGERY Hip Arthroscopy is a relatively simple procedure whereby common disorders of the hip can be diagnosed and treated using keyhole surgery. Some conditions, which previously were
ARTHROSCOPIC HIP SURGERY Hip Arthroscopy is a relatively simple procedure whereby common disorders of the hip can be diagnosed and treated using keyhole surgery. Some conditions, which previously were
Home Care for Your Wound Drain
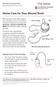 PATIENT EDUCATION patienteducation.osumc.edu When you go home after surgery, you may have one or more drains in place to help your wounds heal. Hemovac, Jackson Pratt (JP) and Blake are common drains used
PATIENT EDUCATION patienteducation.osumc.edu When you go home after surgery, you may have one or more drains in place to help your wounds heal. Hemovac, Jackson Pratt (JP) and Blake are common drains used
Your Skin. Name: Your Largest Organ
 Your Largest Organ What is the largest organ in your body? Your heart? It is the largest muscle in your body, but you do have larger organs. Your brain? The brain inside your skull is pretty big, but it's
Your Largest Organ What is the largest organ in your body? Your heart? It is the largest muscle in your body, but you do have larger organs. Your brain? The brain inside your skull is pretty big, but it's
WOUND MANAGEMENT PROTOCOLS WOUND CLEANSING: REMOVING WOUND DEBRIS FROM WOUND BASE
 WOUND MANAGEMENT PROTOCOLS PURPOSE: Provide nursing personnel with simple guidance regarding appropriate dressing selection in the absence of wound specialist expertise Identify appropriate interventions
WOUND MANAGEMENT PROTOCOLS PURPOSE: Provide nursing personnel with simple guidance regarding appropriate dressing selection in the absence of wound specialist expertise Identify appropriate interventions
Understand nurse aide skills needed to promote skin integrity.
 Unit B Resident Care Skills Essential Standard NA5.00 Understand nurse aide s role in providing residents hygiene, grooming, and skin care. Indicator Understand nurse aide skills needed to promote skin
Unit B Resident Care Skills Essential Standard NA5.00 Understand nurse aide s role in providing residents hygiene, grooming, and skin care. Indicator Understand nurse aide skills needed to promote skin
Skin biopsy. Delivering the best in care. UHB is a no smoking Trust
 Skin biopsy Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm A skin biopsy is a
Skin biopsy Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm A skin biopsy is a
Management of Burns. The burns patient has the same priorities as all other trauma patients.
 Management of Burns The burns patient has the same priorities as all other trauma patients. Assess: - Airway - Breathing: beware of inhalation and rapid airway compromise - Circulation: fluid replacement
Management of Burns The burns patient has the same priorities as all other trauma patients. Assess: - Airway - Breathing: beware of inhalation and rapid airway compromise - Circulation: fluid replacement
Peripherally Inserted Central Catheter (PICC) Patient Instructions
 Patient Care Services 300 Pasteur Drive Stanford, CA 94305 Peripherally Inserted Central Catheter (PICC) Patient Instructions A Peripherally Inserted Central Catheter (PICC) is a soft flexible tube inserted
Patient Care Services 300 Pasteur Drive Stanford, CA 94305 Peripherally Inserted Central Catheter (PICC) Patient Instructions A Peripherally Inserted Central Catheter (PICC) is a soft flexible tube inserted
Orthopaedic Spine Center. Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs
 Orthopaedic Spine Center Graham Calvert MD James Woodall MD PhD Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs The cervical spine consists of the bony vertebrae, discs, nerves and other structures.
Orthopaedic Spine Center Graham Calvert MD James Woodall MD PhD Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs The cervical spine consists of the bony vertebrae, discs, nerves and other structures.
Your Guide to Peritoneal Dialysis Module 3: Doing Peritoneal Dialysis at Home
 Your Guide to Peritoneal Dialysis Module 3: 6.0959 in Preparing to do PD One of the most important things about PD is to keep the dialysis area and anything that comes in contact with the PD equipment
Your Guide to Peritoneal Dialysis Module 3: 6.0959 in Preparing to do PD One of the most important things about PD is to keep the dialysis area and anything that comes in contact with the PD equipment
Caring for a Tenckhoff Catheter
 Caring for a Tenckhoff Catheter UHN A Patient s Guide What is a Pleural Effusion? There is a small space between the outside of your lung and the chest wall (ribs). This space is called the pleural space.
Caring for a Tenckhoff Catheter UHN A Patient s Guide What is a Pleural Effusion? There is a small space between the outside of your lung and the chest wall (ribs). This space is called the pleural space.
Wound Classification Name That Wound Sheridan, WY June 8 th 2013
 Initial Wound Care Consult Sheridan, WY June 8 th, 2013 History Physical Examination Detailed examination of the wound Photographs Cultures Procedures TCOM ABI Debridement Management Decisions A Detailed
Initial Wound Care Consult Sheridan, WY June 8 th, 2013 History Physical Examination Detailed examination of the wound Photographs Cultures Procedures TCOM ABI Debridement Management Decisions A Detailed
BARD MEDICAL DIVISION UROLOGICAL DRAINAGE. Foley Catheter Care & Maintenance. Patient Education Guide
 BARD MEDICAL DIVISION Foley Catheter Care & Maintenance Patient Education Guide WHAT IS A FOLEY CATHETER? Because of your medical problem, your body is having trouble completely emptying your bladder of
BARD MEDICAL DIVISION Foley Catheter Care & Maintenance Patient Education Guide WHAT IS A FOLEY CATHETER? Because of your medical problem, your body is having trouble completely emptying your bladder of
INJECTION TECHNIQUE. IVF NURSING OFFICE: (301) 400-2151 Darshana (301) 400-2146 Nicole
 IVF NURSING OFFICE: (301) 400-2151 Darshana (301) 400-2146 Nicole PLEASE NOTE: If you do not have medications for the next day s dose, you MUST go to the clinic that morning at 6:30 AM for more medications.
IVF NURSING OFFICE: (301) 400-2151 Darshana (301) 400-2146 Nicole PLEASE NOTE: If you do not have medications for the next day s dose, you MUST go to the clinic that morning at 6:30 AM for more medications.
Home Care for Your Nephrostomy Catheter
 Home Care for Your Nephrostomy Catheter This handout covers information about caring for your nephrostomy catheter right after placement and caring for it long term. If you have any questions, please call
Home Care for Your Nephrostomy Catheter This handout covers information about caring for your nephrostomy catheter right after placement and caring for it long term. If you have any questions, please call
Biliary Drain. What is a biliary drain?
 Biliary Drain What is a biliary drain? A biliary drain is a tube to drain bile from your liver. It is put in by a doctor called an Interventional Radiologist. The tube or catheter is placed through your
Biliary Drain What is a biliary drain? A biliary drain is a tube to drain bile from your liver. It is put in by a doctor called an Interventional Radiologist. The tube or catheter is placed through your
Central Venous Catheter (CVC) Sterile Dressing Change - The James
 PATIENT EDUCATION patienteducation.osumc.edu Central Venous Catheter (CVC) Sterile Dressing Change - The James A dressing protects your catheter site and helps reduce the risk of infection. You will need
PATIENT EDUCATION patienteducation.osumc.edu Central Venous Catheter (CVC) Sterile Dressing Change - The James A dressing protects your catheter site and helps reduce the risk of infection. You will need
Neglected Wound/Poor Wound Care
 Chapter 18 CHRONIC WOUNDS KEY FIGURES: Open wound Wound covered with skin graft Chronic wounds are open wounds that for some reason simply will not heal. They may be present for months or even years. Often,
Chapter 18 CHRONIC WOUNDS KEY FIGURES: Open wound Wound covered with skin graft Chronic wounds are open wounds that for some reason simply will not heal. They may be present for months or even years. Often,
Care of Your Hickman Catheter
 Care of Your Hickman Catheter Johns Hopkins Kimmel Cancer Center, Revised 7/11 Contents What is a Hickman Catheter? Page 3 Does the Catheter Limit My Activities? Page 4 How Do I Care for My Catheter? Page
Care of Your Hickman Catheter Johns Hopkins Kimmel Cancer Center, Revised 7/11 Contents What is a Hickman Catheter? Page 3 Does the Catheter Limit My Activities? Page 4 How Do I Care for My Catheter? Page
Laparoscopic Colectomy. What do I need to know about my laparoscopic colorectal surgery?
 Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
Glossary of Terms: www.phoenix society.org toll free 1-800-888-2876
 Glossary of Terms: Ace Bandage Wrap Elastic bandage used to wrap burned areas. It gives even pressure and support, thereby decreasing scar size, and improving circulation. Adaptic A type of gauze with
Glossary of Terms: Ace Bandage Wrap Elastic bandage used to wrap burned areas. It gives even pressure and support, thereby decreasing scar size, and improving circulation. Adaptic A type of gauze with
Arizona State University Institutional Animal Care and Use Committee STANDARD INSTITUTIONAL GUIDELINE RODENT SURGERY
 Arizona State University Institutional Animal Care and Use Committee STANDARD INSTITUTIONAL GUIDELINE RODENT SURGERY It is the policy of the IACUC that all survival surgeries involving rodents be conducted
Arizona State University Institutional Animal Care and Use Committee STANDARD INSTITUTIONAL GUIDELINE RODENT SURGERY It is the policy of the IACUC that all survival surgeries involving rodents be conducted
Caring for Your PleurX Pleural Catheter
 Caring for Your PleurX Pleural Catheter A PleurX Pleural Catheter has been placed in your chest through a small incision in your skin into the pleural space (see picture below). This allows you to drain
Caring for Your PleurX Pleural Catheter A PleurX Pleural Catheter has been placed in your chest through a small incision in your skin into the pleural space (see picture below). This allows you to drain
Safety FIRST: Infection Prevention Tips
 Reading Hospital Safety FIRST: Infection Prevention Tips Reading Hospital is committed to providing high quality care to our patients. Your healthcare team does many things to help prevent infections.
Reading Hospital Safety FIRST: Infection Prevention Tips Reading Hospital is committed to providing high quality care to our patients. Your healthcare team does many things to help prevent infections.
OASIS-C Integument Assessment: Not for Wimps! Part I: Pressure Ulcers
 OASIS-C Integument Assessment: Not for Wimps! Part I: Pressure Ulcers Presented by: Rhonda Will, RN, BS, COS-C, HCS-D Assistant Director, OASIS Competency Institute 243 King Street, Suite 246 Northampton,
OASIS-C Integument Assessment: Not for Wimps! Part I: Pressure Ulcers Presented by: Rhonda Will, RN, BS, COS-C, HCS-D Assistant Director, OASIS Competency Institute 243 King Street, Suite 246 Northampton,
MOHS MICROGRAPHIC SURGERY
 MOHS MICROGRAPHIC SURGERY UMass Memorial Medical Center 55 Lake Avenue North Worcester, MA 01655 (508) 856-1666 Dr. Mary Maloney This booklet is intended to explain Mohs surgery to you. It is not, however,
MOHS MICROGRAPHIC SURGERY UMass Memorial Medical Center 55 Lake Avenue North Worcester, MA 01655 (508) 856-1666 Dr. Mary Maloney This booklet is intended to explain Mohs surgery to you. It is not, however,
Going Home with a Urinary Catheter
 Going Home with a Urinary Catheter Doctor: Phone Number: About Your Catheter A urinary catheter is a small tube that goes through your urethra and into your bladder. This tube then drains the urine made
Going Home with a Urinary Catheter Doctor: Phone Number: About Your Catheter A urinary catheter is a small tube that goes through your urethra and into your bladder. This tube then drains the urine made
Skeletal, Muscular, and Integumentary Systems
 Chapter 36 Skeletal, Muscular, and Integumentary Systems Section 36 1 The Skeletal System (pages 921 925) This section describes the skeletal system and its functions. Introduction (page 921) 1. What forms
Chapter 36 Skeletal, Muscular, and Integumentary Systems Section 36 1 The Skeletal System (pages 921 925) This section describes the skeletal system and its functions. Introduction (page 921) 1. What forms
HICKMAN Catheter Care with a Needleless Connector
 HICKMAN Catheter Care with a Needleless Connector Table of Contents Part 1 Learning about the HICKMAN Catheter... 2 Part 2 Caring for Your Hickman Catheter... 3 A. Preventing Infection... 3 B. Bathing...
HICKMAN Catheter Care with a Needleless Connector Table of Contents Part 1 Learning about the HICKMAN Catheter... 2 Part 2 Caring for Your Hickman Catheter... 3 A. Preventing Infection... 3 B. Bathing...
INSULIN INJECTION KNOW-HOW
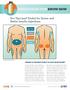 0-0- 0 INSULIN INJECTION KNOW-HOW pro tips (and tricks) for easier and better Insulin Injections ABDOMEN THIGHS BUTTOCKS ARMS recommended injection sites WHERE IS THE BEST PLACE TO GIVE INJECTIONS? 0-
0-0- 0 INSULIN INJECTION KNOW-HOW pro tips (and tricks) for easier and better Insulin Injections ABDOMEN THIGHS BUTTOCKS ARMS recommended injection sites WHERE IS THE BEST PLACE TO GIVE INJECTIONS? 0-
41 Assisting with Minor Surgery
 Learning Outcomes 41.1 Define the medical assistant s role in minor surgical procedures. 41-2 CHAPTER 41 Assisting with Minor Surgery 41.2 Describe types of wounds and explain how they heal. 41.3 Describe
Learning Outcomes 41.1 Define the medical assistant s role in minor surgical procedures. 41-2 CHAPTER 41 Assisting with Minor Surgery 41.2 Describe types of wounds and explain how they heal. 41.3 Describe
KINESIOLOGY TAPING GUIDE
 KINESIOLOGY TAPING GUIDE What is Kinesiology tape and how does Kinesiology tape work? How to apply Kinesiology tape Examples of application of UP Kinesiology tape for common injuries and conditions Introduction
KINESIOLOGY TAPING GUIDE What is Kinesiology tape and how does Kinesiology tape work? How to apply Kinesiology tape Examples of application of UP Kinesiology tape for common injuries and conditions Introduction
Eye Injuries. The Eyes The eyes are sophisticated organs. They collect light and focus it on the back of the eye, allowing us to see.
 Eye Injuries Introduction The design of your face helps protect your eyes from injury. But injuries can still damage your eyes. Sometimes injuries are severe enough that you could lose your vision. Most
Eye Injuries Introduction The design of your face helps protect your eyes from injury. But injuries can still damage your eyes. Sometimes injuries are severe enough that you could lose your vision. Most
Information for patients and nurses
 Information for patients and nurses Rocket IPC Pleural Catheter Indwelling Catheter Rocket Indwelling Pleural Catheter (IPC) Contents Contact Information...03 What s in the Rocket Dressing Pack and Bottle
Information for patients and nurses Rocket IPC Pleural Catheter Indwelling Catheter Rocket Indwelling Pleural Catheter (IPC) Contents Contact Information...03 What s in the Rocket Dressing Pack and Bottle
Facial Sports Injuries
 Facial Sports Injuries Playing catch, shooting hoops, bicycling on a scenic path or just kicking around a soccer ball have more in common than you may think. On the up side, these activities are good exercise
Facial Sports Injuries Playing catch, shooting hoops, bicycling on a scenic path or just kicking around a soccer ball have more in common than you may think. On the up side, these activities are good exercise
Insulin Pens. Basic facts. What is insulin? What are the different types of insulin?
 UW MEDICINE PATIENT EDUCATION Insulin Pens Basic facts This handout explains what insulin is, the different types of insulin, how to store it, how to give an injection with an insulin pen, and other important
UW MEDICINE PATIENT EDUCATION Insulin Pens Basic facts This handout explains what insulin is, the different types of insulin, how to store it, how to give an injection with an insulin pen, and other important
Melanoma The Skin Understanding Cancer
 Melanoma A form of cancer that begins in melanocytes (cells that make the pigment melanin). It may begin in a mole (skin melanoma), but can also begin in other pigmented tissues, such as in the eye or
Melanoma A form of cancer that begins in melanocytes (cells that make the pigment melanin). It may begin in a mole (skin melanoma), but can also begin in other pigmented tissues, such as in the eye or
Pressure Ulcers Assessing and Staging. Anne Pirzadeh RN CWOCN University of Colorado Hospital June 2010
 Pressure Ulcers Assessing and Staging Anne Pirzadeh RN CWOCN University of Colorado Hospital June 2010 Never Events: Pressure Ulcers Pressure Ulcer Codes: MD documentation of pressure ulcers determines
Pressure Ulcers Assessing and Staging Anne Pirzadeh RN CWOCN University of Colorado Hospital June 2010 Never Events: Pressure Ulcers Pressure Ulcer Codes: MD documentation of pressure ulcers determines
Bankart Repair For Shoulder Instability Rehabilitation Guidelines
 Bankart Repair For Shoulder Instability Rehabilitation Guidelines Phase I: The first week after surgery. Goals:!! 1. Control pain and swelling! 2. Protect the repair! 3. Begin early shoulder motion Activities:
Bankart Repair For Shoulder Instability Rehabilitation Guidelines Phase I: The first week after surgery. Goals:!! 1. Control pain and swelling! 2. Protect the repair! 3. Begin early shoulder motion Activities:
MOHS MICROGRAPHIC SURGERY
 Mary E. Maloney, MD Director Professor of Medicine David E. Geist, MD Assistant Professor of Medicine Dori Goldberg, MD Assistant Professor of Medicine Mark J. Scharf, MD Professor of Medicine Jason D.
Mary E. Maloney, MD Director Professor of Medicine David E. Geist, MD Assistant Professor of Medicine Dori Goldberg, MD Assistant Professor of Medicine Mark J. Scharf, MD Professor of Medicine Jason D.
IVF CLASS. IVF NURSE CONTACT INFORMATION: Darshana 301-400-2151, darshana.naik.ctr@health.mil Nicole 301-400-2146, nicole.l.sobers.ctr@health.
 IVF CLASS IVF NURSE CONTACT INFORMATION: Darshana 301-400-2151, darshana.naik.ctr@health.mil Nicole 301-400-2146, nicole.l.sobers.ctr@health.mil PLEASE NOTE: If you do not have medications for the next
IVF CLASS IVF NURSE CONTACT INFORMATION: Darshana 301-400-2151, darshana.naik.ctr@health.mil Nicole 301-400-2146, nicole.l.sobers.ctr@health.mil PLEASE NOTE: If you do not have medications for the next
Informed Consent For Laser Hair Removal
 Informed Consent For Laser Hair Removal INSTRUCTIONS This informed-consent document has been prepared to help inform you about laser procedures, its risks, as well as alternative treatment(s). It is important
Informed Consent For Laser Hair Removal INSTRUCTIONS This informed-consent document has been prepared to help inform you about laser procedures, its risks, as well as alternative treatment(s). It is important
The Use of MEDIHONEY for Wound Management in Oncology
 The Use of MEDIHONEY for Wound Management in Oncology Presenter: Patrice M. Dillow, MSN, APRN, CWOCN Cancer Treatment Centers of America Midwestern Regional Medical Center A Magnet Hospital This presentation
The Use of MEDIHONEY for Wound Management in Oncology Presenter: Patrice M. Dillow, MSN, APRN, CWOCN Cancer Treatment Centers of America Midwestern Regional Medical Center A Magnet Hospital This presentation
Anyone who has difficulty moving can get a pressure sore. But you are more likely to get one if you:
 Patient information from the BMJ Group Pressure sores Anyone can get a pressure sore if they sit or lie still for too long without moving. People who are old or very ill are most likely to get them. Careful
Patient information from the BMJ Group Pressure sores Anyone can get a pressure sore if they sit or lie still for too long without moving. People who are old or very ill are most likely to get them. Careful
Adult Forearm Fractures
 Adult Forearm Fractures Your forearm is made up of two bones, the radius and ulna. In most cases of adult forearm fractures, both bones are broken. Fractures of the forearm can occur near the wrist at
Adult Forearm Fractures Your forearm is made up of two bones, the radius and ulna. In most cases of adult forearm fractures, both bones are broken. Fractures of the forearm can occur near the wrist at
Inservice: Wound Care and Dressings. Friday, June 26, 2009. A. Closed Wounds tissue is injured but skin is not BROKEN
 f Inservice: Wound Care and Dressings Friday, June 26, 2009 WOUNDS: Are injuries of the skin and underlying subcutaneous tissues and muscles (Nursing Manual by Lippincott) Are disruptions in the integrity
f Inservice: Wound Care and Dressings Friday, June 26, 2009 WOUNDS: Are injuries of the skin and underlying subcutaneous tissues and muscles (Nursing Manual by Lippincott) Are disruptions in the integrity
Lesions, and Masses, and Tumors Oh My!!
 Lesions, and Masses, and Tumors Oh My!! Presented by: Susan Ward, CPC, CPC-H, CPC-I, CPCD, CEMC, CPRC 1 1 CPT GUIDELINES Agenda CPT DEFINITIONS OP REPORT CASES 2 Definitions Cyst - a closed sac having
Lesions, and Masses, and Tumors Oh My!! Presented by: Susan Ward, CPC, CPC-H, CPC-I, CPCD, CEMC, CPRC 1 1 CPT GUIDELINES Agenda CPT DEFINITIONS OP REPORT CASES 2 Definitions Cyst - a closed sac having
PATIENT HANDBOOK AND JOURNAL DAY OF SURGERY
 PATIENT HANDBOOK AND JOURNAL DAY OF SURGERY PREPARING YOUR SKIN BEFORE SURGERY PRE-OP HIBICLENS BATHING INSTRUCTIONS: General Information: Because the skin is not sterile, it is important to make sure
PATIENT HANDBOOK AND JOURNAL DAY OF SURGERY PREPARING YOUR SKIN BEFORE SURGERY PRE-OP HIBICLENS BATHING INSTRUCTIONS: General Information: Because the skin is not sterile, it is important to make sure
Basal Cell Carcinoma Affecting the Eye Your Treatment Explained
 Basal Cell Carcinoma Affecting the Eye Your Treatment Explained Patient Information Introduction This booklet is designed to give you information about having a Basal Cell Carcinoma near your eye and the
Basal Cell Carcinoma Affecting the Eye Your Treatment Explained Patient Information Introduction This booklet is designed to give you information about having a Basal Cell Carcinoma near your eye and the
Central Line Care for Adults
 Central Line Care for Adults Table of Contents What is a Central Venous Catheter?... 2 Central Venous Catheter Placement: What to Expect... 2 Catheter Care at a Glance... 2 Fast Facts on Central Line Care:
Central Line Care for Adults Table of Contents What is a Central Venous Catheter?... 2 Central Venous Catheter Placement: What to Expect... 2 Catheter Care at a Glance... 2 Fast Facts on Central Line Care:
2. Does the patient have one of the following appropriate indications for placing indwelling urinary catheters?
 A. Decision to Insert a Urinary Catheter: 1. Before placing an indwelling catheter, please consider if these alternatives would be more appropriate: Bladder scanner: to assess and confirm urinary retention,
A. Decision to Insert a Urinary Catheter: 1. Before placing an indwelling catheter, please consider if these alternatives would be more appropriate: Bladder scanner: to assess and confirm urinary retention,
Placement of Epidural Catheter for Pain Management Shane Bateman DVM, DVSc, DACVECC
 Placement of Epidural Catheter for Pain Management Shane Bateman DVM, DVSc, DACVECC Indications: Patients with severe abdominal or pelvic origin pain that is poorly responsive to other analgesic modalities.
Placement of Epidural Catheter for Pain Management Shane Bateman DVM, DVSc, DACVECC Indications: Patients with severe abdominal or pelvic origin pain that is poorly responsive to other analgesic modalities.
Plastic and Reconstructive Surgery
 Plastic and Reconstructive Surgery General Description Office for Clinical Affairs (515) 271-1629 FAX (515) 271-1727 Elective Rotation This elective rotation in Plastic and Reconstructive Surgery (PRS)
Plastic and Reconstructive Surgery General Description Office for Clinical Affairs (515) 271-1629 FAX (515) 271-1727 Elective Rotation This elective rotation in Plastic and Reconstructive Surgery (PRS)
Managing cavity wounds Journal of Community Nursing March 1998 Author: Rosemary Pudner
 Managing cavity wounds Journal of Community Nursing March 1998 Author: Rosemary Pudner It has been seen in recent years, that an increasing number of patients are being discharged early into the community,
Managing cavity wounds Journal of Community Nursing March 1998 Author: Rosemary Pudner It has been seen in recent years, that an increasing number of patients are being discharged early into the community,
To maintain a port of entry to venous flow when all available peripheral ports have failed.
 I. Purpose: To maintain a port of entry to venous flow when all available peripheral ports have failed. II. General Comments: Since its development, these catheters have been used with increasing frequency
I. Purpose: To maintain a port of entry to venous flow when all available peripheral ports have failed. II. General Comments: Since its development, these catheters have been used with increasing frequency
UROLOGY GROUP of PRINCETON
 UROLOGY GROUP of PRINCETON 134 STANHOPE STREET, PRINCETON, NJ 08540 PHONE 609-924-6487 FAX 609-921-7020 BARRY ROSSMAN, M.D. ALEX VUKASIN, M.D. KAREN LATZKO, D.O. ALEXEI WEDMID, M.D. VASECTOMY, THE NO SCALPEL
UROLOGY GROUP of PRINCETON 134 STANHOPE STREET, PRINCETON, NJ 08540 PHONE 609-924-6487 FAX 609-921-7020 BARRY ROSSMAN, M.D. ALEX VUKASIN, M.D. KAREN LATZKO, D.O. ALEXEI WEDMID, M.D. VASECTOMY, THE NO SCALPEL
What to Expect from your Hip Arthroscopy Surgery A Guide for Patients
 What to Expect from your Hip Arthroscopy Surgery A Guide for Patients Sources of Information: http://orthoinfo.aaos.org http://dev.aana.org/portals/0/popups/animatedsurgery.htm http://www.isha.net/ http://
What to Expect from your Hip Arthroscopy Surgery A Guide for Patients Sources of Information: http://orthoinfo.aaos.org http://dev.aana.org/portals/0/popups/animatedsurgery.htm http://www.isha.net/ http://
X-Plain Inguinal Hernia Repair Reference Summary
 X-Plain Inguinal Hernia Repair Reference Summary Introduction Hernias are common conditions that affect men and women of all ages. Your doctor may recommend a hernia operation. The decision whether or
X-Plain Inguinal Hernia Repair Reference Summary Introduction Hernias are common conditions that affect men and women of all ages. Your doctor may recommend a hernia operation. The decision whether or
All About Your Peripherally Inserted Central Catheter (PICC)
 All About Your Peripherally Inserted Central Catheter (PICC) General Information Intravenous (IV) therapy is the delivery of fluid directly into a vein. An intravenous catheter is a hollow tube that is
All About Your Peripherally Inserted Central Catheter (PICC) General Information Intravenous (IV) therapy is the delivery of fluid directly into a vein. An intravenous catheter is a hollow tube that is
Dressing and bandage
 Dressing and bandage Mihajlo Lojpur, M.D., Ph.D. INTRODUCTION The terms dressing and bandage are often used synonymously. In fact, the term dressing refers more correctly to the primary layer in contact
Dressing and bandage Mihajlo Lojpur, M.D., Ph.D. INTRODUCTION The terms dressing and bandage are often used synonymously. In fact, the term dressing refers more correctly to the primary layer in contact
Objectives At the completion of this module, unlicensed assistive personnel (UAP) should be able to:
 Objectives At the completion of this module, unlicensed assistive personnel (UAP) should be able to: 1. administer medications by subcutaneous injections. 2. document medication administration in the client
Objectives At the completion of this module, unlicensed assistive personnel (UAP) should be able to: 1. administer medications by subcutaneous injections. 2. document medication administration in the client
UW MEDICINE PATIENT EDUCATION. Using Insulin. Basic facts about insulin and self-injection. What is insulin? How does diabetes affect the body?
 UW MEDICINE PATIENT EDUCATION Using Insulin Basic facts about insulin and self-injection This handout explains what insulin is, the different types of insulin, how to store it, how to give an injection
UW MEDICINE PATIENT EDUCATION Using Insulin Basic facts about insulin and self-injection This handout explains what insulin is, the different types of insulin, how to store it, how to give an injection
Chapter 6. Hemorrhage Control UNDER FIRE KEEP YOUR HEAD DOWN
 Hemorrhage Control Chapter 6 Hemorrhage Control The hemorrhage that take[s] place when a main artery is divided is usually so rapid and so copious that the wounded man dies before help can reach him. Colonel
Hemorrhage Control Chapter 6 Hemorrhage Control The hemorrhage that take[s] place when a main artery is divided is usually so rapid and so copious that the wounded man dies before help can reach him. Colonel
Exercise and advice after breast cancer surgery
 Exercise and advice after breast cancer surgery Irving Building Physiotherapy All Rights Reserved 2015. Document for issue as handout. Role of the physiotherapist Exercises for the first week following
Exercise and advice after breast cancer surgery Irving Building Physiotherapy All Rights Reserved 2015. Document for issue as handout. Role of the physiotherapist Exercises for the first week following
Foley Catheter Placement
 Foley Catheter Placement Indications for a Foley Catheter Retention of urine leading to urinary hesitancy, straining to urinate, decrease in size and force of the urinary stream, interruption of urinary
Foley Catheter Placement Indications for a Foley Catheter Retention of urine leading to urinary hesitancy, straining to urinate, decrease in size and force of the urinary stream, interruption of urinary
MEDICAL MANAGEMENT POLICY
 TITLE: Scar Revision/Keloid PAGE: 1of 9 This Medical policy is not a guarantee of benefits or coverage, nor should it be deemed as medical advice. In the event of any conflict concerning benefit coverage,
TITLE: Scar Revision/Keloid PAGE: 1of 9 This Medical policy is not a guarantee of benefits or coverage, nor should it be deemed as medical advice. In the event of any conflict concerning benefit coverage,
