Prognostic stratification of patients with T3N1M0 non-small cell lung cancer: which phase should it be?
|
|
|
- Jayson Horton
- 8 years ago
- Views:
Transcription
1 DOI /s y ORIGINAL PAPER Prognostic stratification of patients with T3N1M0 non-small cell lung cancer: which phase should it be? Ali Kilicgun Ozgur Tanriverdi Akif Turna Muzaffer Metin Adnan Sayar Okan Solak Nur Urer Atilla Gurses Received: 30 December 2010 / Accepted: 9 March 2011 Ó Springer Science+Business Media, LLC 2011 Abstract In the 1997 revision of the TNM staging system for lung cancer, patients with T3N0M0 disease were moved from stage IIIA to stage IIB since these patients have a better prognosis. Despite this modification, the local lymph node metastasis remained the most important prognostic factor in patients with lung cancer. The present study aimed to evaluate the prognosis of patients with T3N1 disease as compared with that of patients with stages IIIA and IIB disease. During 7-year period, 313 patients with non-small cell lung cancer (297 men, 16 women) who had resection were enrolled. The patients were staged according the 2007 revision of Lung Cancer Staging by American Joint Committee on Cancer. The Kaplan Meier statistics was used for survival analysis, and comparisons were made using Cox proportional hazard method. The 5-year survival of patients with stage IIIA disease A. Kilicgun Department of Thoracic Surgery, Izzet Baysal University Faculty of Medicine, Bolu, Turkey O. Tanriverdi (&) Department of Medical Oncology, Adnan Menderes University Faculty of Medicine, Aydin, Turkey ozgurtanriverdi@hotmail.com A. Turna M. Metin A. Sayar A. Gurses Department of Thoracic Surgery, Yedikule Chest Diseases and Thoracic Surgery Training and Research Hospital, Istanbul, Turkey O. Solak Department of Thoracic Surgery, Kocatepe University Faculty of Medicine, Afyonkarahisar, Turkey N. Urer Department of Pathology, Yedikule Chest Diseases and Thoracic Surgery Training and Research Hospital, Istanbul, Turkey excluding T3N1 patients was 40%, whereas the survival of the patients with stage IIB disease was 66% at 5 years. The 5-year survival rates of stage III T3N1 patients (singlestation N1) was found to be higher than those of patients with stage IIIA disease (excluding pt3n1 patients, P = 0.04), while those were found to be similar with those of patients with stage IIB disease (P = 0.4). Survival of the present cohort of patients with T3N1M0 disease represented the survival of IIB disease rather than IIIA non-small cell lung cancer. Further studies are needed to suggest further revisions in the recent staging system regarding T3N1MO disease. Keywords Lung cancer Neoplasm staging Lymphatic metastasis Survival Carcinoma Non-small cell Introduction Surgical-pathologic stage N2 (pn2) disease involving the mediastinal lymph nodes at the advanced stage is associated with a poor surgical outcome with a 5-year survival ranging from 7 to 23% [1 5]. Patients with pn1 disease can be considered an intermediate group with respect to disease progression between patients with pn0 and pn2 diseases. However, the surgical outcome of pn1 disease is controversial. In a collected series that included previously untreated patients with non-small cell lung cancer (NSCLC), Mountain reported [1] that 5-year surgical-pathologic stage survival was 23% for stage IIIA patients (all patients with pt1-2-3n2m0), while it was reported to be 25% in patients with only pt3n1m0 disease. Similarly, Inoue et al. [3] and Jassem et al. [5] reported 5-year survival of T3N1M0 patients to be 38 and 35%, respectively.
2 We previously evaluated the significance of N1 involvement in multiple- or single stations and reported that 5-year survival was significantly higher in patients with single-station N1 disease [6]. Theoretically, it could be suggested that reclassification of T3N0M0 patients as stage IIB could have led this stage of patients with worse prognosis than previously reported in The present study aimed to evaluate the prognosis of patients with T3N1M0 disease as compared with that of patients with stage IIIA and IIB diseases. This information should help to reconsider the classification of patients with T3N1M0 disease. Materials and methods Study design and patients This was a retrospective study in which patients who had received their primary surgical treatment for NSCLC are examined. Three hundred and thirteen consecutive patients (297 men, 16 women) diagnosed as NSCLC histopathological after complete pulmonary resection and lymph node dissection between January 1997 and December 2004 were enrolled in the study. Routine systematic sampling of the hilar and mediastinal lymph nodes was performed in each case, even if the preoperative evaluation was N0 or N1. All patients underwent posteroanterior and lateral chest radiography and bronchoscopy. All patients hemoglobin, serum alkaline phosphatase, and calcium levels were determined preoperatively. Preoperative and postoperative staging Computed tomographical or ultrasonographical imagings of the thorax, abdomen, and cranium with whole-body bone scintigraphical imagings were performed in all patients for pretreatment staging. In the years, the patients were operated, positron emission tomography scan (PET/ CT) was rarely used in our country, and thus it was used only in a small number of patients for preoperative staging. Since we did not have the opportunity for PET/CT and we had ample clinical experiences in the past, mediastinal lymph node samplings using cervical mediastinoscopy were performed in all patients. The mediastinal exploration was achieved by a left anterior mediastinotomy or an extended mediastinoscopy in tumors located in the left upper lobe or in the left main bronchus and in tumors associated with enlarged ([1 cm) anterior mediastinal and/ or aorticopulmonary lymph nodes. Staging was determined according to the New International Staging System for Lung Cancer in construction of a final surgical-pathologic stage (ptnm) [7]. A systematic lymph node dissection was performed following resection. Data obtained from thoracotomy and pathological examinations were used. Exclusion criteria Patients with multiple lung tumors or low-grade malignancy such as bronchial carcinoid, mediastinal node or T3 involvement, and chest wall invasion and patients who underwent partial resection or segmentectomy and got neoadjuvant therapy were excluded from the study. Ethics All patients were informed before the operation by patient consent form. Informed patient consent forms could not be obtained from the patients since the study was conducted retrospectively. Pathological examination Resection materials of primary tumor or resected lymph nodes were fixed in 10% formalin. Samples were sliced using cryostat and treated in the standard manner. Lymph nodes that could potentially alter the borders of resection were examined by frozen section. Afterward, routine follow-up and histopathological examinations of paraffin sections were carried out. The pathologist sampled lymph nodes on resection material and did paraffin blocks, routine follow-up, and microscopic examination. There were no disconcordances observed between frozen examinations and routine follow-up. Sections were stained with hematoxylin eosin and then examined. Limited numbers of immunohistochemical examinations were being carried out in our center during the period when patients were operated. Immunohistochemical examinations were carried out when necessary and in doubt. Patients with histologic subtype of adenocarcinoma, squamous cell carcinoma, and large cell neuroendocrine carcinoma were included in the study. Tumors like adenosquamous cell carcinoma comprised of mixed cells histopathologically were named as not otherwise specified (NOS). Special attention was paid to N1 and N2 stations according to the recent revision of lymph node mapping. Single-station N1 metastasis was considered if only one station in the N1 region was involved, whereas multiple-station N1 metastasis was considered if more than one station in the N1 region was involved. Follow-up All patients discovered to have single- or multiple-station N2 disease postoperatively were referred to adjuvant chemotherapy and radiotherapy. Patients had been followed by
3 different centers and oncology experts. Follow-ups and treatment data were not homogenous in this retrospective study. Therefore, the relation between survival and treatment modalities with disease-free survival times was not defined as study goals. Statistical evaluation Survival analysis was performed by the method of Kaplan and Meier, using time zero as the date of thoracotomy and time death as the end point. The mean survival time with 95% confidence intervals (CI) was given for patients with different nodal stage classification. Initially, a univariate analysis was performed and the factors identified as significant were included in a multivariate analysis. Univariate analysis for the prognostic variables (age, gender, co- morbidity, smoking, clinical and surgical-pathologic T and N status, histological type of tumor, stage, resection type, and curability) was performed using a Cox proportional hazard regression model. All analyses were performed using the statistical program for social sciences (SPSS) version 11. Results were evaluated in 95% confidence intervals (CI). P values \ 0.05 were considered significant. Results The clinical and surgical characteristics of 313 patients enrolled in the study are presented in Table 1. According to the postoperative pathologic evaluation, there were 32 (10%), 67 (21%), 18 (6%), 93 (30%), 83 (27%), and 20 (6%) patients with stages IA, IB, IIA, IIB, IIIA, and IIIB diseases, respectively (Table 1). For the entire patient population, the mean follow-up period was 24 months (range months) and the median survival time was 49 months (95% CI months). The 1-, 3-, and 5-year survival rates were 79, 59, and 53%, respectively. The median survival times were 77, 44, 46, and 21 months in patients with surgicalpathologic stages I, II, IIIA and IIIB, respectively (Fig. 1). Table 1 Demographic, surgical and pathologic characteristics of patients SD: SCC squamous cell carcinoma, LCNEC large cell neuroendocrine carcinoma, NOS not otherwise specified (the patient group includes mixed pathologies such as adenosquamous carcinoma) Variables Features Patient count (n) % Age (all patients, year) 57 ± Gender Men Women 16 5 Smokers/non-smokers Men 211/86 71/29 Women 2/14 12/88 Comorbidity (present/absent) Men 16/281 5/95 Women 2/14 12/88 Histology Adenocarcinoma SCC LCNEC 9 3 NOS Postoperative T status T T T T Postoperative N status N N N Stage Stage IA Stage IB Stage IIA 18 6 Stage IIB Stage IIIA Stage IIIB 20 6 Operation Pneumonectomy Bilobectomy 29 9 Lobectomy Curability Complete Incomplete (R1, R2) 35 11
4 Table 2 Univariate and multivariate analyses of the factors for overall survival Hazard ratio (95% CI) P value Fig. 1 The median survival curves according to the stages (the median survival times were 77, 44, 46, and 21 months in patients with surgical- pathologic stages I, II, IIIA, and IIIB, respectively) There were significant differences between patients with stage IA and IB disease (P = 0.04), patients with stage IB and IIA disease (P = 0.03), and patients with stage IIA and IIB disease (P = 0.01) with respect to cumulative survival. In addition, a significant difference was found between patients with stage IIIA and IIIB (P = 0.02) with respect to cumulative survival. Initially, univariate analysis was performed to enable identification of the factors that were significant for survival. The variables that showed significance in the analysis were as follows: surgical-pathologic nodal status (P = 0.002), histologic type (P = 0.013), stage (P = 0.048), and T status (P = 0.02). Patients with histopathological subtype adenocarcinoma histopathology were defined to have worse prognosis than patients with squamous cell carcinoma (P = 0.041). NOS group had the best survival among all histologic types (P = 0.043). The type of resection was found to be a significant prognostic factor, and the outcome of lobectomy/bilobectomy was a better survival compared with those who had pneumonectomy (P = 0.039). Incomplete resection (R1 or R2) resulted in a lower survival rate (P = ). The following factors were found to be non-significant: age (P = 0.497), smoking (P = 0.235), and comorbidity (P = 0.458; Table 2). After grouping the variables in steps, multivariate analysis was performed. Presence of metastatic lymph nodes (N0/N1 vs. N2) was found to be an independent prognostic factor (P = , Hazard ratio % CI ). Multivariate analysis resulted that histopathology type, T status, stage, operation type, and incomplete resection had no effects on survival (Table 2). There were 34 patients (11%) who were found to have T3N1 NSCLC. The 5-year survival rate of these patients Univariate factors Age 1.52 ( ) Comorbidity 1.56 ( ) Smoke 1.74 ( ) Histology 0.31 ( ) 0.013* T status 0.28 ( ) 0.025* N status ( ) 0.002* Stage 1.04 ( ) 0.048* Resection type 3.47 ( ) 0.039* Curability 0.42 ( ) 0.012* Multıvarıate factors Histology 1.03 ( ) T status 2.33 ( ) N status ( ) 0.013* Stage 0.29 ( ) Resection type 2.34 ( ) Curability 2.55 ( ) Cox proportional hazards model of overall survival The variables that showed significance in the analysis were; surgicalpathologic nodal status (P = 0.002), histologic type (P = 0.013), stage (P = 0.048), T status (P = 0.02), resection type (P = 0.039), and curability (P = 0.012). Presence of metastatic lymph nodes (N0/N1 vs. N2) was found to be independent prognostic factor (P = ) *P values \ 0.05 were considered significant (single-station and multiple-station N1 patients) was 58%, and the mean survival time was 66 ± 12 months (95% CI, months). Of these patients, five had multiple-station N1 disease. The 5-year survival rate of the remaining T3N1 patients (n = 29, single station) was calculated to be 65%, and the mean survival time was 69 ± 12 months (95% CI = months). The number of patients with hilar (station 10), interlobar (station 11), lobar (station 12), segmental (station 13), and subsegmental (station 14) metastases were 5, 16, 2, 1, and 5, respectively. In the present study, the median number of examined N1 nodes (removed from resected material by both the surgeon and the pathologist) was eight. Findings related to clinical and pathologic features of patients at T3N1, stage IIB, and stage IIIA (excluding T3N1 patients) were shown in Table 3. The 5-year survival rate of patients with stage IIIA disease excluding T3N1 patients was 40%, whereas the survival of the patients with stage IIB disease was 66% at 5 years. The 5-year survival of T3N1 (single-station N1) patients (65%) was found to be higher than that of patients with stage IIIA (excluding T3N1 patients) disease (40%, P = 0.04), whereas it was found to be similar to that of patients with stage IIB disease (66%, P = 0.4; Fig. 2).
5 Table 3 Demographic, surgical and pathologic characteristics of patients with stage IIB, stage IIIA (excluding T3N1), and pt3n1 (single-station N1) NSCLC Variables pt3n1 (single-station N1) Stage IIB Stage IIIA (excluding T3N1) P Patients (n) Histology ACA SCC LCNEC NOS Smoking Present Absent Comorbidity Present Absent Operation Lobectomy Bilobectomy Pneumonectomy year survival 65% 66% a 40% a ACA adenocarcinoma, SCC squamous cell carcinoma, LCNEC large cell neuroendocrine carcinoma, NOS not otherwise specified (the patient group includes mixed pathologies such as adenosquamous carcinoma) a The 5-year survival rate of T3N1 (single-station N1) patients (65%) was found to be higher than that of patients with stage IIIA (excluding T3N1 patients) disease (40%, P = 0.04), whereas it was found to be similar to that of patients with stage IIB disease (66%, P = 0.4) Discussion Approximately one in every three cancer deaths occurs due to lung cancer. The proportion of patients with lung cancer who survive longer than 5 years after the diagnosis is only 15% [7]. To determine the best treatment modality in light of recent data, the clinical stage of these patients, who have a poor survival after surgical operation, should be determined. In fact, tumor stage is the most important prognostic factor in patients with lung cancer [7 11]. Thus, TNM (tumor, node, metastasis) staging system used for staging of the malignant tumors was first devised by Pierre Denoix in 1946 and modified for lung cancer by the American Joint Committee on Cancer (AJCC) in 1973 [7]. Of the staging studies to date, the last was published in 2007 as the seventh edition of the TNM classification for malignant tumors [11, 12]. This classification system has provided a precise discussion of tumor size, which was not focused before [11, 12]. Considering the survival of T3N0M0 patients, it was suggested that T3N0M0 patients be moved to stage IIB in the fifth edition of TNM Fig. 2 The 5-year survival curves according to the patients with stage IIB, stage IIIA disease (excluding pt3n1 patients with single station) and pt3n1 (single-station N1) (the 5-year survival rate of patients with stage IIIA disease excluding T3N1 patients was 40%, whereas the survival of patients with stage IIB disease was 66% at 5 years. The 5-year survival rate of T3N1 patients with single-station N1 was 65%) classification, and in the sixth edition, no modification was established with regard to this suggestion. Although this suggestion was not changed in the seventh edition, tumors [7 cm in size was classified as T3 independent from invasion criteria [11]. In the seventh edition of TNM classification, in which no changes was proposed with respect to N descriptors, it was suggested that each T stage and N subgroups should be evaluated together. However, the fact that local lymph node metastasis is the most important prognostic factor in NSCLC patients has not changed [12]. In the sixth version of the TNM staging system, N1 tumors were categorized as two stage groups for T1 to T3 tumors without distant disease: stage II (T1N1, T2N1) and stage IIIA (T3N1) [9]. However, in the 1997 revision of the TNM staging system, N1 tumors were divided into three stage groups as stage IIA (T1N1), stage IIB (T2N1), and stage IIIA (T3N1) [1]. In addition, T3N0 disease was reclassified as stage IIB rather than stage IIIA. Thus, it could be speculated that stage IIIA disease now consists of patients who have slightly worse prognosis than it was before We recently found that N1 disease consisted of two subgroups: one involving single node and the other involving multiple nodes (i.e., multiple-station N1 disease or multiple N1 disease) of which the postoperative prognosis was not statistically different from that of N2 disease [6]. Therefore, we hypothesized that the T3 tumors with single-station N1 involvement must be revisited in terms of staging. We found that the survival of patients with T3N1 disease was similar to that of patients with stage IIB
6 disease rather than the patients with stage IIIA disease (P = 0.4 and P = 0.04, respectively). It is generally accepted that patients with T3N1M0 and T3N2M0 diseases had similar prognoses [1, 2, 13]. However, there are also studies reporting better prognoses for patients with T3N1M0 disease as compared to patients with T3N2M0 diseases [14]. Obviously, a need for reconsideration of stage IIB was declared soon after the new classification [15]. Mediastinal nodal involvement, which is one of the most important prognostic factors, significantly affects survival of patients with lung cancer [1 6]. In an analysis of stage III NSCLC patients by Ichinose et al. [16], 5-year survival rates for N0/N1 and N2 diseases have been reported as 62 and 23%, respectively. As a result, stage III in NSCLC N2 disease was reported to be an independent prognostic factor. T3N1M0 may be another subgroup candidate for stage IIB; however, further studies are required to find the correct classification. The survival rates of patients with NSCLC in the present study were comparable with the rates reported previously [1, 3 5, 14, 16]. However, the survival rates of patients with stage IIIB disease in the present study was found to be relatively better than the survival rates reported in previous studies [1, 14, 16]. This may be attributed to patient selection criteria, since this group consisted of patients with T4 disease rather than N3 disease, and each institution used its own criteria for the inclusion of selected T4 tumors [5, 14, 16]. It could be suggested that multiple N1 disease might be an ignored N2 disease [17]. It can also be proposed that a more extensive lymph node dissection might provide a more accurate lymph node staging postoperatively. However, we did not analyze time trends in patients undergoing surgical resection for NSCLC. Nevertheless, exclusion of multiple-station N1 disease may lead to decrease in the number of ignored N2 disease. In the study by Tanaka et al. [18], involvement of the hilar node and aberrant p53 expression was reported to be significant factors predicting a worse prognosis in resected T1-2N1M0 NSCLC. Although its biological meaning remains unclear, nodal status could be an indicator of invasiveness of tumor in terms of lymphatic and/or blood vessel involvement. Thus, multiple-station N1 or N2 disease (e.g., T3N1 vs. T3N2 disease) could be proposed to have more invasive/metastatic carcinoma than those with single-station N1 disease. Therefore, further molecular analysis of biologic differences in different nodal statuses has to be accomplished. There are some limitations of the present study that must be addressed. The number of patients with T3N1M0 disease is relatively small. Moreover, we did not assess the micrometastatic disease involving mediastinal nodes which may have been overlooked. In addition, the observed statistical difference between the survival curves of patients with stage IIIA and T3N1 was minor in the present study. Moreover, the single-station N1 entity has not been universally accepted and seemed to depend on the appropriate and adequate effort in the isolation of N1 nodes from the resected material by a pathologist. In conclusion, we suggest that the prognosis of T3N1 disease among the present cohort of patients is similar to that of stage IIB disease rather than that of stage IIIA NSCLC. As this retrospective study has been carried out in a limited geographic region with a restricted technical setup, it should be supported by multicenter studies in which more patients are included, different clinical and histopathological features as well as different treatment modalities are compared. References 1. Mountain CF. Revisions in the international system for staging lung cancer. Chest. 1997;111: Suzuki K, Nagai K, Yoshida J, Nishimura M, Takahashi K, et al. Conventional clinicopathologic factors in surgically resected nonsmall cell lung carcinoma. A Comparison of prognostic factors for each pathologic TNM stage based on multivariate analyses. Cancer. 1999;86: Inoue K, Sato M, Fujimura S, Sakurada A, Takahashi S, et al. Prognostic assessment of 1310 patients with non-small-cell lung cancer who underwent complete resection from 1980 to J Thorac Cardiovasc Surg. 1998;116: van Rens MT, de la Riviere AB, Elbers HR, van Den Bosch JM. Prognostic assessment of 2, 361 patients who underwent pulmonary resection for non-small cell lung cancer, stage I, II, and IIIA. Chest. 2000;117: Jassem J, Skokowski J, Dziadziuszko R, Jassem E, Szymanowska A, et al. Results of surgical treatment of non-small cell lung cancer: validation of the new postoperative pathologic TNM classification. J Thorac Cardiovasc Surg. 2000;119: Sayar A, Turna A, Kilicgun A, Solak O, Urer N, et al. Prognostic significance of surgical-pathologic multiple-station N1 disease in non-small cell carcinoma of the lung. Eur J Cardiothorac Surg. 2004;25: Robinson LA, Ruckdeschel JC, Wagner H Jr, Stevens CW. Treatment of non- small cell lung cancer- stage IIIA: ACCP evidence- based clinical practice guidelines (second edition). Chest. 2007;132(Supp 3):243S 65S. 8. Tsim S, O Dowd CA, Milroy R, Davidson S. Staging of nonsmall cell lung cancer (NSCLC): a review. Respir Med. 2010; 104: Mountain CF. A new international system for staging lung cancer. Chest. 1986;89(4 Suppl):225S 32S. 10. Ramon-Rami P, Crowley JJ, Goldstraw P. The revised TNM staging system for lung cancer. Ann Thorac Cardiovasc Surg. 2009;15: Rusch VW, Crowley J, Giroux DJ, Goldstraw P, Im JG, et al. The IASLC lung cancer staging project: proposals for the revision of the N descriptors in the forthcoming seventh edition of the TNM classification for lung cancer. J Thorac Oncol. 2007;2: Goldstraw P, Crowley J, Chansky K, Giroux DJ, Groome PA, et al. The IASLC lung cancer staging project: proposals for the
7 revision of the TNM stage groupings in the forthcoming (seventh) edition of the TNM classification for malignant tumors. J Thorac Oncol. 2007;2: Sabanathan S, Richardson J, Mearns AJ, Goulden C. Results of surgical treatment of stage III lung cancer. Eur J Cardiothorac Surg. 1994;8: Naruke T, Goya T, Tsuchiya R, Suemasu K. Prognosis and survival in resected lung carcinoma based on the new international staging system. J Thorac Cardiovasc Surg. 1988;96: Detterbeck FC, Socinski MA. IIB or not IIB: the current question in staging non-small cell lung cancer. Chest. 1997;112: Ichinose Y, Yano T, Asoh H, Yokoyama H, Yoshino I, et al. Prognostic factors obtained by a pathologic examination in completely resected non small-cell lung cancer. An analysis in each pathologic stage. J Thorac Cardiovasc Surg. 1995;110: Lee JG, Lee CY, Park IK, Kim JK, Park YP, et al. Number of metastatic lymph nodes in resected non- small cell lung cancer predicts patients survival. Ann Thorac Surg. 2008;85: Tanaka F, Yanagihara K, Otake Y, Yamada T, Shoji T, et al. Prognostic factors in patients with resected pathologic (p-) T1 2N1M0 non-small cell lung cancer. Eur J Cardiothorac Surg. 2001;19:
Survival analysis of 220 patients with completely resected stage II non small cell lung cancer
 窑 Original Article 窑 Chinese Journal of Cancer Survival analysis of 22 patients with completely resected stage II non small cell lung cancer Yun Dai,2,3, Xiao Dong Su,2,3, Hao Long,2,3, Peng Lin,2,3, Jian
窑 Original Article 窑 Chinese Journal of Cancer Survival analysis of 22 patients with completely resected stage II non small cell lung cancer Yun Dai,2,3, Xiao Dong Su,2,3, Hao Long,2,3, Peng Lin,2,3, Jian
Post-recurrence survival in completely resected stage I non-small cell lung cancer with local recurrence
 Post- survival in completely resected stage I non-small cell lung cancer with local J-J Hung, 1,2,3 W-H Hsu, 3 C-C Hsieh, 3 B-S Huang, 3 M-H Huang, 3 J-S Liu, 2 Y-C Wu 3 See Editorial, p 185 c A supplementary
Post- survival in completely resected stage I non-small cell lung cancer with local J-J Hung, 1,2,3 W-H Hsu, 3 C-C Hsieh, 3 B-S Huang, 3 M-H Huang, 3 J-S Liu, 2 Y-C Wu 3 See Editorial, p 185 c A supplementary
A Practical Guide to Advances in Staging and Treatment of NSCLC
 A Practical Guide to Advances in Staging and Treatment of NSCLC Robert J. Korst, M.D. Director, Thoracic Surgery Medical Director, The Blumenthal Cancer Center The Valley Hospital Objectives Revised staging
A Practical Guide to Advances in Staging and Treatment of NSCLC Robert J. Korst, M.D. Director, Thoracic Surgery Medical Director, The Blumenthal Cancer Center The Valley Hospital Objectives Revised staging
Stage I Non-Small Cell Lung Cancer: Recurrence Patterns, Prognostic Factors and Survival
 16 Stage I Non-Small Cell Lung Cancer: Recurrence Patterns, Prognostic Factors and Survival Jung-Jyh Hung and Yu-Chung Wu Division of Thoracic Surgery, Department of Surgery, Taipei Veterans General Hospital
16 Stage I Non-Small Cell Lung Cancer: Recurrence Patterns, Prognostic Factors and Survival Jung-Jyh Hung and Yu-Chung Wu Division of Thoracic Surgery, Department of Surgery, Taipei Veterans General Hospital
The New International Staging System Lung Cancer
 The New International Staging System Lung Cancer Valerie W. Rusch, MD Chief, Thoracic Surgery Memorial Sloan-Kettering Cancer Center Chair, Lung and Esophagus Task Force, American Joint Commission on Cancer
The New International Staging System Lung Cancer Valerie W. Rusch, MD Chief, Thoracic Surgery Memorial Sloan-Kettering Cancer Center Chair, Lung and Esophagus Task Force, American Joint Commission on Cancer
PET/CT in Lung Cancer
 PET/CT in Lung Cancer Rodolfo Núñez Miller, M.D. Nuclear Medicine and Diagnostic Imaging Section Division of Human Health International Atomic Energy Agency Vienna, Austria GLOBOCAN 2012 #1 #3 FDG-PET/CT
PET/CT in Lung Cancer Rodolfo Núñez Miller, M.D. Nuclear Medicine and Diagnostic Imaging Section Division of Human Health International Atomic Energy Agency Vienna, Austria GLOBOCAN 2012 #1 #3 FDG-PET/CT
The Need for Accurate Lung Cancer Staging
 The Need for Accurate Lung Cancer Staging Peter Baik, DO Thoracic Surgery Cancer Treatment Centers of America Oklahoma Osteopathic Association 115th Annual Convention Financial Disclosures: None 2 Objectives
The Need for Accurate Lung Cancer Staging Peter Baik, DO Thoracic Surgery Cancer Treatment Centers of America Oklahoma Osteopathic Association 115th Annual Convention Financial Disclosures: None 2 Objectives
CANCER PULMON: ESTADIOS INICIALES POSTMUNDIAL PULMON DENVER 2015. 8-10-2015.Manuel Cobo Dols S. Oncología Médica HU Málaga Regional y VV
 CANCER PULMON: ESTADIOS INICIALES POSTMUNDIAL PULMON DENVER 2015 8-10-2015.Manuel Cobo Dols S. Oncología Médica HU Málaga Regional y VV Meta-analisis LACE: adyuvancia vs no adyuvancia Pignon JP, et al.
CANCER PULMON: ESTADIOS INICIALES POSTMUNDIAL PULMON DENVER 2015 8-10-2015.Manuel Cobo Dols S. Oncología Médica HU Málaga Regional y VV Meta-analisis LACE: adyuvancia vs no adyuvancia Pignon JP, et al.
GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER
 GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER BY Ali Shamseddine, MD (Coordinator); as04@aub.edu.lb Fady Geara, MD Bassem Shabb, MD Ghassan Jamaleddine, MD CLINICAL PRACTICE GUIDELINES FOR THE TREATMENT
GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER BY Ali Shamseddine, MD (Coordinator); as04@aub.edu.lb Fady Geara, MD Bassem Shabb, MD Ghassan Jamaleddine, MD CLINICAL PRACTICE GUIDELINES FOR THE TREATMENT
Non-Small Cell Lung Cancer Treatment Comparison to NCCN Guidelines
 Non-Small Cell Lung Cancer Treatment Comparison to NCCN Guidelines April 2008 (presented at 6/12/08 cancer committee meeting) By Shelly Smits, RHIT, CCS, CTR Conclusions by Dr. Ian Thompson, MD Dr. James
Non-Small Cell Lung Cancer Treatment Comparison to NCCN Guidelines April 2008 (presented at 6/12/08 cancer committee meeting) By Shelly Smits, RHIT, CCS, CTR Conclusions by Dr. Ian Thompson, MD Dr. James
Temporal Trends in Demographics and Overall Survival of Non Small-Cell Lung Cancer Patients at Moffitt Cancer Center From 1986 to 2008
 Special Report Temporal Trends in Demographics and Overall Survival of Non Small-Cell Lung Cancer Patients at Moffitt Cancer Center From 1986 to 2008 Matthew B. Schabath, PhD, Zachary J. Thompson, PhD,
Special Report Temporal Trends in Demographics and Overall Survival of Non Small-Cell Lung Cancer Patients at Moffitt Cancer Center From 1986 to 2008 Matthew B. Schabath, PhD, Zachary J. Thompson, PhD,
General Information About Non-Small Cell Lung Cancer
 General Information About Non-Small Cell Lung Cancer Non-small cell lung cancer is a disease in which malignant (cancer) cells form in the tissues of the lung. The lungs are a pair of cone-shaped breathing
General Information About Non-Small Cell Lung Cancer Non-small cell lung cancer is a disease in which malignant (cancer) cells form in the tissues of the lung. The lungs are a pair of cone-shaped breathing
The National Clinical Lung Cancer Audit (LUCADA)
 The National Clinical Lung Cancer Audit (LUCADA) DATA MANUAL Title: Version: 3.1.5 Date: September 2013 LUCADA Lung Cancer Audit VERSION HISTORY Version Date Issued Brief Summary of Change Owner s Name
The National Clinical Lung Cancer Audit (LUCADA) DATA MANUAL Title: Version: 3.1.5 Date: September 2013 LUCADA Lung Cancer Audit VERSION HISTORY Version Date Issued Brief Summary of Change Owner s Name
How To Know When To Stage Lung Cancer
 WHITE PAPER - SBRT for Non Small Cell Lung Cancer I. Introduction This white paper will focus on non-small cell lung carcinoma with sections one though six comprising a general review of lung cancer from
WHITE PAPER - SBRT for Non Small Cell Lung Cancer I. Introduction This white paper will focus on non-small cell lung carcinoma with sections one though six comprising a general review of lung cancer from
Lung Cancer Treatment Guidelines
 Updated June 2014 Derived and updated by consensus of members of the Providence Thoracic Oncology Program with the aid of evidence-based National Comprehensive Cancer Network (NCCN) national guidelines,
Updated June 2014 Derived and updated by consensus of members of the Providence Thoracic Oncology Program with the aid of evidence-based National Comprehensive Cancer Network (NCCN) national guidelines,
Protein kinase C alpha expression and resistance to neo-adjuvant gemcitabine-containing chemotherapy in non-small cell lung cancer
 Protein kinase C alpha expression and resistance to neo-adjuvant gemcitabine-containing chemotherapy in non-small cell lung cancer Dan Vogl Lay Abstract Early stage non-small cell lung cancer can be cured
Protein kinase C alpha expression and resistance to neo-adjuvant gemcitabine-containing chemotherapy in non-small cell lung cancer Dan Vogl Lay Abstract Early stage non-small cell lung cancer can be cured
Table of Contents. Data Supplement 1: Summary of ASTRO Guideline Statements. Data Supplement 2: Definition of Terms
 Definitive and Adjuvant Radiotherapy in Locally Advanced Non-Small-Cell Lung Cancer: American Society of Clinical Oncology Clinical Practice Guideline Endorsement of the American Society for Radiation
Definitive and Adjuvant Radiotherapy in Locally Advanced Non-Small-Cell Lung Cancer: American Society of Clinical Oncology Clinical Practice Guideline Endorsement of the American Society for Radiation
Small Cell Lung Cancer
 Small Cell Lung Cancer Types of Lung Cancer Non-small cell carcinoma (NSCC) (87%) Adenocarcinoma (38%) Squamous cell (20%) Large cell (5%) Small cell carcinoma (13%) Small cell lung cancer is virtually
Small Cell Lung Cancer Types of Lung Cancer Non-small cell carcinoma (NSCC) (87%) Adenocarcinoma (38%) Squamous cell (20%) Large cell (5%) Small cell carcinoma (13%) Small cell lung cancer is virtually
Regular follow-up after curative resection of nonsmall cell lung cancer: a real benefit for patients?
 Eur Respir J 2002; 19: 464 468 DOI: 10.1183/09031936.02.00231802 Printed in UK all rights reserved Copyright #ERS Journals Ltd 2002 European Respiratory Journal ISSN 0903-1936 Regular follow-up after curative
Eur Respir J 2002; 19: 464 468 DOI: 10.1183/09031936.02.00231802 Printed in UK all rights reserved Copyright #ERS Journals Ltd 2002 European Respiratory Journal ISSN 0903-1936 Regular follow-up after curative
ORIGINAL ARTICLE THORACIC ONCOLOGY
 Ann Surg Oncol (2013) 20:1934 1940 DOI 10.1245/s10434-012-2800-x ORIGINAL ARTICLE THORACIC ONCOLOGY Predictors for Locoregional Recurrence for Clinical Stage III-N2 Non-small Cell Lung Cancer with Nodal
Ann Surg Oncol (2013) 20:1934 1940 DOI 10.1245/s10434-012-2800-x ORIGINAL ARTICLE THORACIC ONCOLOGY Predictors for Locoregional Recurrence for Clinical Stage III-N2 Non-small Cell Lung Cancer with Nodal
Chapter 2 Staging of Breast Cancer
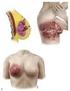 Chapter 2 Staging of Breast Cancer Zeynep Ozsaran and Senem Demirci Alanyalı 2.1 Introduction Five decades ago, Denoix et al. proposed classification system (tumor node metastasis [TNM]) based on the dissemination
Chapter 2 Staging of Breast Cancer Zeynep Ozsaran and Senem Demirci Alanyalı 2.1 Introduction Five decades ago, Denoix et al. proposed classification system (tumor node metastasis [TNM]) based on the dissemination
Epidemiology, Staging and Treatment of Lung Cancer. Mark A. Socinski, MD
 Epidemiology, Staging and Treatment of Lung Cancer Mark A. Socinski, MD Associate Professor of Medicine Multidisciplinary Thoracic Oncology Program Lineberger Comprehensive Cancer Center University of
Epidemiology, Staging and Treatment of Lung Cancer Mark A. Socinski, MD Associate Professor of Medicine Multidisciplinary Thoracic Oncology Program Lineberger Comprehensive Cancer Center University of
Adjuvant Therapy Non Small Cell Lung Cancer. Sunil Nagpal MD Director, Thoracic Oncology Jan 30, 2015
 Adjuvant Therapy Non Small Cell Lung Cancer Sunil Nagpal MD Director, Thoracic Oncology Jan 30, 2015 No Disclosures Number of studies Studies Per Month 12 10 8 6 4 2 0 1 2 3 4 5 6 7 8 9 10 11 12 1 2 3
Adjuvant Therapy Non Small Cell Lung Cancer Sunil Nagpal MD Director, Thoracic Oncology Jan 30, 2015 No Disclosures Number of studies Studies Per Month 12 10 8 6 4 2 0 1 2 3 4 5 6 7 8 9 10 11 12 1 2 3
Non-Small Cell Lung Cancer
 Non-Small Cell Lung Cancer John delcharco, MD (Statistics based on CVMC data 2009-2013) Statistics Lung cancer is the leading cause of cancer deaths in the United States. The American Cancer Society estimates
Non-Small Cell Lung Cancer John delcharco, MD (Statistics based on CVMC data 2009-2013) Statistics Lung cancer is the leading cause of cancer deaths in the United States. The American Cancer Society estimates
A912: Kidney, Renal cell carcinoma
 A912: Kidney, Renal cell carcinoma General facts of kidney cancer Renal cell carcinoma, a form of kidney cancer that involves cancerous changes in the cells of the renal tubule, is the most common type
A912: Kidney, Renal cell carcinoma General facts of kidney cancer Renal cell carcinoma, a form of kidney cancer that involves cancerous changes in the cells of the renal tubule, is the most common type
Primary -Benign - Malignant Secondary
 TUMOURS OF THE LUNG Primary -Benign - Malignant Secondary The incidence of lung cancer has been increasing almost logarithmically and is now reaching epidemic levels. The overall cure rate is very low
TUMOURS OF THE LUNG Primary -Benign - Malignant Secondary The incidence of lung cancer has been increasing almost logarithmically and is now reaching epidemic levels. The overall cure rate is very low
Lung Cancer: Diagnosis, Staging and Treatment
 PATIENT EDUCATION patienteducation.osumc.edu Lung Cancer: Diagnosis, Staging and Treatment Cancer begins in our cells. Cells are the building blocks of our tissues. Tissues make up the organs of the body.
PATIENT EDUCATION patienteducation.osumc.edu Lung Cancer: Diagnosis, Staging and Treatment Cancer begins in our cells. Cells are the building blocks of our tissues. Tissues make up the organs of the body.
Surgical Outcomes in Resected Non-small Cell Lung Cancer 1 cm in Diameter
 ORIGINAL ARTICLE Surgical Outcomes in Resected Non-small Cell Lung Cancer 1 cm in Diameter Bing-Yen Wang 1, Jung-Jyh Hung 1,2,3, Wen-Juei Jeng 4, Wen-Hu Hsu 1, Chih-Cheng Hsieh 1, Min-Hsiung Huang 1, Biing-Shiun
ORIGINAL ARTICLE Surgical Outcomes in Resected Non-small Cell Lung Cancer 1 cm in Diameter Bing-Yen Wang 1, Jung-Jyh Hung 1,2,3, Wen-Juei Jeng 4, Wen-Hu Hsu 1, Chih-Cheng Hsieh 1, Min-Hsiung Huang 1, Biing-Shiun
Treatment Algorithms for the Management of Lung Cancer in NSW Guide for Clinicians
 Treatment Algorithms for the Management of Lung Cancer in NSW Guide for Clinicians Background The Cancer Institute New South Wales Oncology Group Lung (NSWOG Lung) identified the need for the development
Treatment Algorithms for the Management of Lung Cancer in NSW Guide for Clinicians Background The Cancer Institute New South Wales Oncology Group Lung (NSWOG Lung) identified the need for the development
Malignant Pleural Mesothelioma in Singapore
 RESEARCH COMMUNICATION C SP Yip 1, HN Koong 2, CM Loo 3, KW Fong 1* Abstract Aim: To examine the clinical characteristics and outcomes of malignant pleural mesothelioma (MPM) in Singapore. Methods and
RESEARCH COMMUNICATION C SP Yip 1, HN Koong 2, CM Loo 3, KW Fong 1* Abstract Aim: To examine the clinical characteristics and outcomes of malignant pleural mesothelioma (MPM) in Singapore. Methods and
Lung Cancer. Public Outcomes Report. Submitted by Omar A. Majid, MD
 Public Outcomes Report Lung Cancer Submitted by Omar A. Majid, MD Lung cancer is the most common cancer-related cause of death among men and women. It has been estimated that there will be 226,1 new cases
Public Outcomes Report Lung Cancer Submitted by Omar A. Majid, MD Lung cancer is the most common cancer-related cause of death among men and women. It has been estimated that there will be 226,1 new cases
The lungs What is lung cancer? How common is it? Risks & symptoms Diagnosis & treatment options
 Why We re Here The lungs What is lung cancer? How common is it? Risks & symptoms Diagnosis & treatment options What Are Lungs? What Do They Do? 1 Located in the chest Allow you to breathe Provide oxygen
Why We re Here The lungs What is lung cancer? How common is it? Risks & symptoms Diagnosis & treatment options What Are Lungs? What Do They Do? 1 Located in the chest Allow you to breathe Provide oxygen
Extrapleural Pneumonectomy for Malignant Mesothelioma: Pro. Joon H. Lee 9/17/2012
 Extrapleural Pneumonectomy for Malignant Mesothelioma: Pro Joon H. Lee 9/17/2012 Malignant Pleural Mesothelioma (Epidemiology) Incidence: 7/mil (Japan) to 40/mil (Australia) Attributed secondary to asbestos
Extrapleural Pneumonectomy for Malignant Mesothelioma: Pro Joon H. Lee 9/17/2012 Malignant Pleural Mesothelioma (Epidemiology) Incidence: 7/mil (Japan) to 40/mil (Australia) Attributed secondary to asbestos
Although many reports on the prognostic factors of non small cell
 Carbone et al T2 tumors larger than five centimeters in diameter can be upgraded to T3 in non small cell lung cancer Emanuela Carbone, MD a,b Hisao Asamura, MD a Hidefumi Takei, MD a Haruhiko Kondo, MD
Carbone et al T2 tumors larger than five centimeters in diameter can be upgraded to T3 in non small cell lung cancer Emanuela Carbone, MD a,b Hisao Asamura, MD a Hidefumi Takei, MD a Haruhiko Kondo, MD
Neoplasms of the LUNG and PLEURA
 Neoplasms of the LUNG and PLEURA 2015-2016 FCDS Educational Webcast Series Steven Peace, BS, CTR September 19, 2015 2015 Focus o Anatomy o SSS 2000 o MPH Rules o AJCC TNM 1 Case 1 Case Vignette HISTORY:
Neoplasms of the LUNG and PLEURA 2015-2016 FCDS Educational Webcast Series Steven Peace, BS, CTR September 19, 2015 2015 Focus o Anatomy o SSS 2000 o MPH Rules o AJCC TNM 1 Case 1 Case Vignette HISTORY:
L Lang-Lazdunski, A Bille, S Marshall, R Lal, D Landau, J Spicer
 Pleurectomy/decortication, hyperthermic pleural lavage with povidone-iodine and systemic chemotherapy in malignant pleural mesothelioma. A 10-year experience. L Lang-Lazdunski, A Bille, S Marshall, R Lal,
Pleurectomy/decortication, hyperthermic pleural lavage with povidone-iodine and systemic chemotherapy in malignant pleural mesothelioma. A 10-year experience. L Lang-Lazdunski, A Bille, S Marshall, R Lal,
Definitive Treatment of Poor-Risk Patients with Stage I Lung Cancer. A Single Institution Experience
 ORIGINAL ARTICLE Definitive Treatment of Poor-Risk Patients with Stage I Lung Cancer A Single Institution Experience Michael Hsie, MD,* Stefania Morbidini-Gaffney, MD,* Leslie J. Kohman, MD, Elisabeth
ORIGINAL ARTICLE Definitive Treatment of Poor-Risk Patients with Stage I Lung Cancer A Single Institution Experience Michael Hsie, MD,* Stefania Morbidini-Gaffney, MD,* Leslie J. Kohman, MD, Elisabeth
Treatment and prognosis of primary esophageal small cell carcinoma
 [Chinese Journal of Cancer 28:3, 254-258; March 2009]; 2009 Landes Bioscience Clinical Research Paper Treatment and prognosis of primary esophageal small cell carcinoma A report of 151 cases Yan Song,
[Chinese Journal of Cancer 28:3, 254-258; March 2009]; 2009 Landes Bioscience Clinical Research Paper Treatment and prognosis of primary esophageal small cell carcinoma A report of 151 cases Yan Song,
Lung Cancer: An Overview
 VOL. I Issue 2 2010 Lung Cancer: An Overview By Matthew F. Koscielski, M.D. Lung cancer is the most common cause of cancer mortality worldwide. In the United States there are about 220,000 new cases of
VOL. I Issue 2 2010 Lung Cancer: An Overview By Matthew F. Koscielski, M.D. Lung cancer is the most common cause of cancer mortality worldwide. In the United States there are about 220,000 new cases of
Understanding Your Surgical Options for Lung Cancer
 Information Booklet for Patients Understanding Your Surgical Options for Lung Cancer Understanding Lung Cancer If you have just been diagnosed with lung cancer, this booklet will serve as an informational
Information Booklet for Patients Understanding Your Surgical Options for Lung Cancer Understanding Lung Cancer If you have just been diagnosed with lung cancer, this booklet will serve as an informational
Lung cancer is a disease of the elderly. National
 Similar Long-term Survival of Elderly Patients With Non-small Cell Lung Cancer Treated With Lobectomy or Wedge Resection Within the Surveillance, Epidemiology, and End Results Database* Carlos M. Mery,
Similar Long-term Survival of Elderly Patients With Non-small Cell Lung Cancer Treated With Lobectomy or Wedge Resection Within the Surveillance, Epidemiology, and End Results Database* Carlos M. Mery,
Clinical Indications and Results Following Chest Wall Resection
 Clinical Indications and Results Following Chest Wall Resection for Recurrent Malignant Pleural Mesothelioma Ali SO, Burt BM, Groth SS, DaSilva MC, Yeap BY, Richards WG, Baldini EH and Sugarbaker DJ. Division
Clinical Indications and Results Following Chest Wall Resection for Recurrent Malignant Pleural Mesothelioma Ali SO, Burt BM, Groth SS, DaSilva MC, Yeap BY, Richards WG, Baldini EH and Sugarbaker DJ. Division
Male. Female. Death rates from lung cancer in USA
 Male Female Death rates from lung cancer in USA Smoking represents an interesting combination of an entrenched industry and a clearly drug-induced cancer Tobacco Use in the US, 1900-2000 5000 100 Per Capita
Male Female Death rates from lung cancer in USA Smoking represents an interesting combination of an entrenched industry and a clearly drug-induced cancer Tobacco Use in the US, 1900-2000 5000 100 Per Capita
This factsheet aims to outline the characteristics of some rare lung cancers, and highlight where each type of lung cancer may be different.
 There are several different kinds of lung cancer, often referred to as lung cancer subtypes. Some of these occur more often than others. In this factsheet we will specifically look at the subtypes of cancers
There are several different kinds of lung cancer, often referred to as lung cancer subtypes. Some of these occur more often than others. In this factsheet we will specifically look at the subtypes of cancers
Surgical Treatment of Stage I Non-small Cell Lung Carcinoma
 Review Surgical Treatment of Stage I Non-small Cell Lung Carcinoma Chiaki Endo, MD, PhD, 1 Motoyasu Sagawa, MD, PhD, 2 Akira Sakurada, MD, PhD, 1 Masami Sato, MD, PhD, 1 Takashi Kondo, MD, PhD, 1 and Shigefumi
Review Surgical Treatment of Stage I Non-small Cell Lung Carcinoma Chiaki Endo, MD, PhD, 1 Motoyasu Sagawa, MD, PhD, 2 Akira Sakurada, MD, PhD, 1 Masami Sato, MD, PhD, 1 Takashi Kondo, MD, PhD, 1 and Shigefumi
Lung Cancer and Mesothelioma
 Lung Cancer and Mesothelioma Robert Kratzke, M.D. John C. Skoglund Professor of Lung Cancer Research Section of Heme/Onc/Transplant Department of Medicine University of Minnesota Medical School Malignant
Lung Cancer and Mesothelioma Robert Kratzke, M.D. John C. Skoglund Professor of Lung Cancer Research Section of Heme/Onc/Transplant Department of Medicine University of Minnesota Medical School Malignant
Radiation Therapy in the Treatment of
 Lung Cancer Radiation Therapy in the Treatment of Lung Cancer JMAJ 46(12): 537 541, 2003 Kazushige HAYAKAWA Professor and Chairman, Department of Radiology, Kitasato University School of Medicine Abstract:
Lung Cancer Radiation Therapy in the Treatment of Lung Cancer JMAJ 46(12): 537 541, 2003 Kazushige HAYAKAWA Professor and Chairman, Department of Radiology, Kitasato University School of Medicine Abstract:
Lungenkrebs. Lungenkrebs Häufigkeit
 Lungenkrebs Prof. Dr. E.W. Russi Pneumologie 1.9.2008 Lungenkrebs Häufigkeit The Principles and Practice of Medicine William Osler New York D. Appleton and Company 1892 Section IV DISEASE OF THE RESPIRATORY
Lungenkrebs Prof. Dr. E.W. Russi Pneumologie 1.9.2008 Lungenkrebs Häufigkeit The Principles and Practice of Medicine William Osler New York D. Appleton and Company 1892 Section IV DISEASE OF THE RESPIRATORY
Targeted Therapy What the Surgeon Needs to Know
 Targeted Therapy What the Surgeon Needs to Know AATS Focus in Thoracic Surgery 2014 David R. Jones, M.D. Professor & Chief, Thoracic Surgery Memorial Sloan Kettering Cancer Center I have no disclosures
Targeted Therapy What the Surgeon Needs to Know AATS Focus in Thoracic Surgery 2014 David R. Jones, M.D. Professor & Chief, Thoracic Surgery Memorial Sloan Kettering Cancer Center I have no disclosures
How To Stage Non-Small Cell Lung Cancer
 CHAPTER 7: TREATMENT FOR NON-SMALL CELL LUNG CANCER INTRODUCTION This chapter provides an overview of treatment for non-small cell lung cancer (NSCLC). Treatment options are discussed according to the
CHAPTER 7: TREATMENT FOR NON-SMALL CELL LUNG CANCER INTRODUCTION This chapter provides an overview of treatment for non-small cell lung cancer (NSCLC). Treatment options are discussed according to the
How To Treat Lung Cancer At Cleveland Clinic
 Treatment Guide Lung Cancer Management The Chest Cancer Center at Cleveland Clinic, which includes specialists from the Respiratory Institute, Taussig Cancer Institute and Miller Family Heart & Vascular
Treatment Guide Lung Cancer Management The Chest Cancer Center at Cleveland Clinic, which includes specialists from the Respiratory Institute, Taussig Cancer Institute and Miller Family Heart & Vascular
Lung Cancer Workup and Staging
 CHAPTER 16 Lung Cancer Workup and Staging Bernard J. Park and Valerie W. Rusch The Staging System Diagnosis and Staging History and Physical Examination Noninvasive Modalities Chest Radiography Sputum
CHAPTER 16 Lung Cancer Workup and Staging Bernard J. Park and Valerie W. Rusch The Staging System Diagnosis and Staging History and Physical Examination Noninvasive Modalities Chest Radiography Sputum
SUNY DOWNSTATE MEDICAL CENTER SURGERY GRAND ROUNDS February 28, 2013 VERENA LIU, MD ROSEANNA LEE, MD
 SUNY DOWNSTATE MEDICAL CENTER SURGERY GRAND ROUNDS February 28, 2013 VERENA LIU, MD ROSEANNA LEE, MD Case Presentation 35 year old male referred from PMD with an asymptomatic palpable right neck mass PMH/PSH:
SUNY DOWNSTATE MEDICAL CENTER SURGERY GRAND ROUNDS February 28, 2013 VERENA LIU, MD ROSEANNA LEE, MD Case Presentation 35 year old male referred from PMD with an asymptomatic palpable right neck mass PMH/PSH:
RESEARCH EDUCATE ADVOCATE. Just Diagnosed with Melanoma Now What?
 RESEARCH EDUCATE ADVOCATE Just Diagnosed with Melanoma Now What? INTRODUCTION If you are reading this, you have undergone a biopsy (either of a skin lesion or a lymph node) or have had other tests in which
RESEARCH EDUCATE ADVOCATE Just Diagnosed with Melanoma Now What? INTRODUCTION If you are reading this, you have undergone a biopsy (either of a skin lesion or a lymph node) or have had other tests in which
Mesothelioma. 1. Introduction. 1.1 General Information and Aetiology
 Mesothelioma 1. Introduction 1.1 General Information and Aetiology Mesotheliomas are tumours that arise from the mesothelial cells of the pleura, peritoneum, pericardium or tunica vaginalis [1]. Most are
Mesothelioma 1. Introduction 1.1 General Information and Aetiology Mesotheliomas are tumours that arise from the mesothelial cells of the pleura, peritoneum, pericardium or tunica vaginalis [1]. Most are
Metastatic Renal Cell Carcinoma: Staging and Prognosis of Three Separate Cases.
 Metastatic Renal Cell Carcinoma: Staging and Prognosis of Three Separate Cases. Abstract This paper describes the staging, imaging, treatment, and prognosis of renal cell carcinoma. Three case studies
Metastatic Renal Cell Carcinoma: Staging and Prognosis of Three Separate Cases. Abstract This paper describes the staging, imaging, treatment, and prognosis of renal cell carcinoma. Three case studies
Tumor Budding as a Useful Prognostic Marker in T1-Stage Squamous Cell Carcinoma of the Esophagus
 2013;108:42 46 Tumor Budding as a Useful Prognostic Marker in T1-Stage Squamous Cell Carcinoma of the Esophagus HITOSHI TERAMOTO, MD, 1 * MASAHIKO KOIKE, MD, PhD, 1 CHIE TANAKA, MD, PhD, 1 SUGURU YAMADA,
2013;108:42 46 Tumor Budding as a Useful Prognostic Marker in T1-Stage Squamous Cell Carcinoma of the Esophagus HITOSHI TERAMOTO, MD, 1 * MASAHIKO KOIKE, MD, PhD, 1 CHIE TANAKA, MD, PhD, 1 SUGURU YAMADA,
SMALL CELL LUNG CANCER
 Protocol for Planning and Treatment The process to be followed in the management of: SMALL CELL LUNG CANCER Patient information given at each stage following agreed information pathway 1. DIAGNOSIS New
Protocol for Planning and Treatment The process to be followed in the management of: SMALL CELL LUNG CANCER Patient information given at each stage following agreed information pathway 1. DIAGNOSIS New
Survey on the treatment of non-small cell lung cancer (NSCLC) in England and Wales
 Eur Respir J 1997; 10: 1552 1558 DOI: 10.1183/09031936.97.10071552 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1997 European Respiratory Journal ISSN 0903-1936 Survey on the treatment
Eur Respir J 1997; 10: 1552 1558 DOI: 10.1183/09031936.97.10071552 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1997 European Respiratory Journal ISSN 0903-1936 Survey on the treatment
9. Discuss guidelines for follow-up post-thyroidectomy for cancer (labs/tests) HH
 9. Discuss guidelines for follow-up post-thyroidectomy for cancer (labs/tests) HH Differentiated thyroid cancer expresses the TSH receptor on the cell membrane and responds to TSH stimulation by increasing
9. Discuss guidelines for follow-up post-thyroidectomy for cancer (labs/tests) HH Differentiated thyroid cancer expresses the TSH receptor on the cell membrane and responds to TSH stimulation by increasing
Non-Small Cell Lung Cancer
 Non-Small Cell Lung Cancer About Your Lungs and Lung Cancer How do your lungs work? To understand lung cancer it is helpful to understand your lungs. Your lungs put oxygen into the blood, which the heart
Non-Small Cell Lung Cancer About Your Lungs and Lung Cancer How do your lungs work? To understand lung cancer it is helpful to understand your lungs. Your lungs put oxygen into the blood, which the heart
A new score predicting the survival of patients with spinal cord compression from myeloma
 A new score predicting the survival of patients with spinal cord compression from myeloma (1) Sarah Douglas, Department of Radiation Oncology, University of Lubeck, Germany; sarah_douglas@gmx.de (2) Steven
A new score predicting the survival of patients with spinal cord compression from myeloma (1) Sarah Douglas, Department of Radiation Oncology, University of Lubeck, Germany; sarah_douglas@gmx.de (2) Steven
Integrating Chemotherapy and Liver Surgery for the Management of Colorectal Metastases
 I Congresso de Oncologia D Or July 5-6, 2013 Integrating Chemotherapy and Liver Surgery for the Management of Colorectal Metastases Michael A. Choti, MD, MBA, FACS Department of Surgery Johns Hopkins University
I Congresso de Oncologia D Or July 5-6, 2013 Integrating Chemotherapy and Liver Surgery for the Management of Colorectal Metastases Michael A. Choti, MD, MBA, FACS Department of Surgery Johns Hopkins University
PET. Can we afford PET-CT. Positron annihilation. PET-CT scanner. PET detection
 PET-CT Can we afford PET-CT John Buscombe New technology Combines functional information-pet anatomical information-ct Machine able to perform both studies in single imaging episode PET imaging depends
PET-CT Can we afford PET-CT John Buscombe New technology Combines functional information-pet anatomical information-ct Machine able to perform both studies in single imaging episode PET imaging depends
3.0 With final Comments for presentation at Sub Group Meeting 24. 24.11.10
 Guideline for the Treatment of Lung Cancer Version History 2.0 Endorsed by the Governance Committee as treatment of lung cancer 27.07.09 with radiotherapy and chemotherapy. 2.1 Re-written to include the
Guideline for the Treatment of Lung Cancer Version History 2.0 Endorsed by the Governance Committee as treatment of lung cancer 27.07.09 with radiotherapy and chemotherapy. 2.1 Re-written to include the
Characterization of lung cancer patients, their actual treatment and survival: experience in Slovenia
 Characterization of lung cancer patients, their actual treatment and survival: experience in Slovenia Lučka Debevec 1, Andrej Debeljak 1, Janez Eržen 2, Viljem Kovač 3, Izidor Kern 1 1 University Clinic
Characterization of lung cancer patients, their actual treatment and survival: experience in Slovenia Lučka Debevec 1, Andrej Debeljak 1, Janez Eržen 2, Viljem Kovač 3, Izidor Kern 1 1 University Clinic
NCCN Non-Small Cell Lung Cancer V.1.2011 Update Meeting 07/09/10
 Guideline Page and Request NSCL-3 Stage IA, margins positive delete the recommendation for chemoradiation. Stage IB, IIA, margins positive delete the recommendation for chemoradiation + Stage IIA, Stage
Guideline Page and Request NSCL-3 Stage IA, margins positive delete the recommendation for chemoradiation. Stage IB, IIA, margins positive delete the recommendation for chemoradiation + Stage IIA, Stage
Multidisciplinary Therapy of Stage IIIA Non Small-Cell Lung Cancer: Long-term Outcome of Chemoradiation With or Without Surgery
 Special Report Multidisciplinary Therapy of Stage IIIA Non Small-Cell Lung Cancer: Long-term Outcome of Chemoradiation With or Without Surgery Charu Aggarwal, MD, Linna Li, MD, Hossein Borghaei, DO, Ranee
Special Report Multidisciplinary Therapy of Stage IIIA Non Small-Cell Lung Cancer: Long-term Outcome of Chemoradiation With or Without Surgery Charu Aggarwal, MD, Linna Li, MD, Hossein Borghaei, DO, Ranee
TNM Classification for Lung Cancer
 Review TNM Classification for Lung Cancer Yoh Watanabe, MD 1,2,3 The international tumor-node-metastasis (TNM) staging system is the international language in cancer diagnosis and treatment. Six revisions
Review TNM Classification for Lung Cancer Yoh Watanabe, MD 1,2,3 The international tumor-node-metastasis (TNM) staging system is the international language in cancer diagnosis and treatment. Six revisions
INTERNATIONAL ASSOCIATION FOR THE STUDY OF LUNG CANCER Prospective Mesothelioma Staging Project
 INTERNATIONAL ASSOCIATION FOR THE STUDY OF LUNG CANCER Prospective Mesothelioma Staging Project Data Forms and Fields in CRAB Electronic Data Capture System - Reduced Set - Pivotal data elements for developing
INTERNATIONAL ASSOCIATION FOR THE STUDY OF LUNG CANCER Prospective Mesothelioma Staging Project Data Forms and Fields in CRAB Electronic Data Capture System - Reduced Set - Pivotal data elements for developing
Klaus Junker, MD; Kathrin Langner, MD; Folker Klinke, MD; Ulrich Bosse, MD; and Michael Thomas, MD
 Grading of Tumor Regression in Non-small Cell Lung Cancer* Morphology and Prognosis Klaus Junker, MD; Kathrin Langner, MD; Folker Klinke, MD; Ulrich Bosse, MD; and Michael Thomas, MD Objective: Different
Grading of Tumor Regression in Non-small Cell Lung Cancer* Morphology and Prognosis Klaus Junker, MD; Kathrin Langner, MD; Folker Klinke, MD; Ulrich Bosse, MD; and Michael Thomas, MD Objective: Different
Finding an Appropriate Treatment
 Focus on CME at the University of Toronto Early Detected Lung Cancer: Finding an Appropriate Treatment Thanks to modern technology, subcentimeter tumors are now being identified. As with other malignant
Focus on CME at the University of Toronto Early Detected Lung Cancer: Finding an Appropriate Treatment Thanks to modern technology, subcentimeter tumors are now being identified. As with other malignant
Sentinel Lymph Node Mapping for Endometrial Cancer. Locke Uppendahl, MD Grand Rounds
 Sentinel Lymph Node Mapping for Endometrial Cancer Locke Uppendahl, MD Grand Rounds Endometrial Cancer Most common gynecologic malignancy in US estimated 52,630 new cases in 2014 estimated 8,590 deaths
Sentinel Lymph Node Mapping for Endometrial Cancer Locke Uppendahl, MD Grand Rounds Endometrial Cancer Most common gynecologic malignancy in US estimated 52,630 new cases in 2014 estimated 8,590 deaths
J Clin Oncol 26:5113-5118. 2008 by American Society of Clinical Oncology INTRODUCTION
 VOLUME 26 NUMBER 31 NOVEMBER 1 2008 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T Outcome After Surgical Resections of Chest Wall Sarcomas Michael W. Wouters, Albert N. van Geel, Lotte Nieuwenhuis,
VOLUME 26 NUMBER 31 NOVEMBER 1 2008 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T Outcome After Surgical Resections of Chest Wall Sarcomas Michael W. Wouters, Albert N. van Geel, Lotte Nieuwenhuis,
Outcome of Early Cervical Carcinoma Treated by Wertheim Hysterectomy with Selective Postoperative Radiotherapy
 ORIGINAL ARTICLES 613 Outcome of Early Cervical Carcinoma Treated by Wertheim Hysterectomy with Selective Postoperative Radiotherapy S K Tay,*FAMS, MD, FRCOG, L K Tan,**MBBS, M Med (O & G), MRCOG Abstract
ORIGINAL ARTICLES 613 Outcome of Early Cervical Carcinoma Treated by Wertheim Hysterectomy with Selective Postoperative Radiotherapy S K Tay,*FAMS, MD, FRCOG, L K Tan,**MBBS, M Med (O & G), MRCOG Abstract
An Overview of Lung Cancer Symptoms, Pathophysiology, And Treatment Linda H. Yoder
 CE Objectives and Evaluation Form appear on page 235. An Overview of Lung Cancer Symptoms, Pathophysiology, And Treatment Linda H. Yoder Patients with lung cancer can provide treatment challenges for even
CE Objectives and Evaluation Form appear on page 235. An Overview of Lung Cancer Symptoms, Pathophysiology, And Treatment Linda H. Yoder Patients with lung cancer can provide treatment challenges for even
Prognostic and Predictive Factors in Oncology. Mustafa Benekli, M.D.
 Prognostic and Predictive Factors in Oncology Mustafa Benekli, M.D. NCI Definitions ESMO Course -Essentials of Medical Oncology -Istanbul 2 Prognostic factor: NCI Definition A situation or condition, or
Prognostic and Predictive Factors in Oncology Mustafa Benekli, M.D. NCI Definitions ESMO Course -Essentials of Medical Oncology -Istanbul 2 Prognostic factor: NCI Definition A situation or condition, or
What is neuroendocrine cervical cancer?
 Key Points: 1. Neuroendocrine cancer of the uterine cervix is a rare and aggressive disease. 2. Treatment for neuroendocrine cervical cancer is usually more intensive than that for most other types of
Key Points: 1. Neuroendocrine cancer of the uterine cervix is a rare and aggressive disease. 2. Treatment for neuroendocrine cervical cancer is usually more intensive than that for most other types of
Image. 3.11.3 SW Review the anatomy of the EAC and how this plays a role in the spread of tumors.
 Neoplasms of the Ear and Lateral Skull Base Image 3.11.1 SW What are the three most common neoplasms of the auricle? 3.11.2 SW What are the four most common neoplasms of the external auditory canal (EAC)
Neoplasms of the Ear and Lateral Skull Base Image 3.11.1 SW What are the three most common neoplasms of the auricle? 3.11.2 SW What are the four most common neoplasms of the external auditory canal (EAC)
Moving forward, where are we with Clinical Trials?
 Moving forward, where are we with Clinical Trials? Dennis A. Wigle Division of Thoracic Surgery Mayo Clinic AATS/STS General Thoracic Surgery Symposium Sunday, April 27 th 2014 2012 MFMER slide-1 Where
Moving forward, where are we with Clinical Trials? Dennis A. Wigle Division of Thoracic Surgery Mayo Clinic AATS/STS General Thoracic Surgery Symposium Sunday, April 27 th 2014 2012 MFMER slide-1 Where
Do we need a revised staging system for malignant pleural mesothelioma? Analysis of the IASLC database
 Featured Article Do we need a revised staging system for malignant pleural mesothelioma? Analysis of the IASLC database Valerie W. Rusch 1, Dorothy Giroux 2 1 Memorial Sloan-Kettering Cancer Center, New
Featured Article Do we need a revised staging system for malignant pleural mesothelioma? Analysis of the IASLC database Valerie W. Rusch 1, Dorothy Giroux 2 1 Memorial Sloan-Kettering Cancer Center, New
Avastin: Glossary of key terms
 Avastin: Glossary of key terms Adenocarcinoma Adenoma Adjuvant therapy Angiogenesis Anti-angiogenics Antibody Antigen Avastin (bevacizumab) Benign A form of carcinoma that originates in glandular tissue.
Avastin: Glossary of key terms Adenocarcinoma Adenoma Adjuvant therapy Angiogenesis Anti-angiogenics Antibody Antigen Avastin (bevacizumab) Benign A form of carcinoma that originates in glandular tissue.
Treatment of mesothelioma in Bloemfontein, South Africa
 European Journal of Cardio-thoracic Surgery 24 (2003) 434 440 www.elsevier.com/locate/ejcts Treatment of mesothelioma in Bloemfontein, South Africa W.J. de Vries*, M.A. Long Cardiothoracic Department,
European Journal of Cardio-thoracic Surgery 24 (2003) 434 440 www.elsevier.com/locate/ejcts Treatment of mesothelioma in Bloemfontein, South Africa W.J. de Vries*, M.A. Long Cardiothoracic Department,
2009 Cancer Committee
 2009 Cancer Committee Lung (non-small cell) Cancer Study Stage IIIA and IIIB John Clouse, M.D. Alicia Stark, RHIT Jeff Robinson Table of Cont ent s Table of Contents... 1 Lung (non-small cell) Cancer Facts.2
2009 Cancer Committee Lung (non-small cell) Cancer Study Stage IIIA and IIIB John Clouse, M.D. Alicia Stark, RHIT Jeff Robinson Table of Cont ent s Table of Contents... 1 Lung (non-small cell) Cancer Facts.2
Objectives. Mylene T. Truong, MD. Malignant Pleural Mesothelioma Background
 Imaging of Pleural Tumors Mylene T. Truong, MD Imaging of Pleural Tumours Mylene T. Truong, M. D. University of Texas M.D. Anderson Cancer Center, Houston, TX Objectives To review tumors involving the
Imaging of Pleural Tumors Mylene T. Truong, MD Imaging of Pleural Tumours Mylene T. Truong, M. D. University of Texas M.D. Anderson Cancer Center, Houston, TX Objectives To review tumors involving the
SMALL. 1-800-298-2436 LungCancerAlliance.org
 UNDERSTANDING Non- SMALL CELL LUNG CANCER 1-800-298-2436 LungCancerAlliance.org A guide for the patient I ANATOMY OF THE LUNGS The following image shows different parts that make up the lungs. Please use
UNDERSTANDING Non- SMALL CELL LUNG CANCER 1-800-298-2436 LungCancerAlliance.org A guide for the patient I ANATOMY OF THE LUNGS The following image shows different parts that make up the lungs. Please use
Diagnosis and Prognosis of Pancreatic Cancer
 Main Page Risk Factors Reducing Your Risk Screening Symptoms Diagnosis Treatment Overview Chemotherapy Radiation Therapy Surgical Procedures Lifestyle Changes Managing Side Effects Talking to Your Doctor
Main Page Risk Factors Reducing Your Risk Screening Symptoms Diagnosis Treatment Overview Chemotherapy Radiation Therapy Surgical Procedures Lifestyle Changes Managing Side Effects Talking to Your Doctor
NEOPLASMS OF KIDNEY (RENAL CELL CARCINOMA) And RENAL PELVIS (TRANSITIONAL CELL CARCINOMA)
 NEOPLASMS OF KIDNEY (RENAL CELL CARCINOMA) And RENAL PELVIS (TRANSITIONAL CELL CARCINOMA) Merat Esfahani, MD Medical Oncologist, Hematologist Cancer Liaison Physician SwedishAmerican Regional Cancer Center
NEOPLASMS OF KIDNEY (RENAL CELL CARCINOMA) And RENAL PELVIS (TRANSITIONAL CELL CARCINOMA) Merat Esfahani, MD Medical Oncologist, Hematologist Cancer Liaison Physician SwedishAmerican Regional Cancer Center
Accelerated hemithoracic radiation followed by extrapleural pneumonectomy for malignant pleural mesothelioma
 Accelerated hemithoracic radiation followed by extrapleural pneumonectomy for malignant pleural mesothelioma Marc de Perrot, Ronald Feld, Natasha B Leighl, Andrew Hope, Thomas K Waddell, Shaf Keshavjee,
Accelerated hemithoracic radiation followed by extrapleural pneumonectomy for malignant pleural mesothelioma Marc de Perrot, Ronald Feld, Natasha B Leighl, Andrew Hope, Thomas K Waddell, Shaf Keshavjee,
Komorbide brystkræftpatienter kan de tåle behandling? Et registerstudie baseret på Danish Breast Cancer Cooperative Group
 Komorbide brystkræftpatienter kan de tåle behandling? Et registerstudie baseret på Danish Breast Cancer Cooperative Group Lotte Holm Land MD, ph.d. Onkologisk Afd. R. OUH Kræft og komorbiditet - alle skal
Komorbide brystkræftpatienter kan de tåle behandling? Et registerstudie baseret på Danish Breast Cancer Cooperative Group Lotte Holm Land MD, ph.d. Onkologisk Afd. R. OUH Kræft og komorbiditet - alle skal
Malignant pleural mesothelioma P/D vs. EPP
 3 rd International Thoracic Oncology Congress Dresden, September 13 15, 2012 Malignant pleural mesothelioma P/D vs. EPP Walter Weder, MD Professor of Surgery Dokumentenname Datum Seite 1 Extrapleural Pneumonectomy
3 rd International Thoracic Oncology Congress Dresden, September 13 15, 2012 Malignant pleural mesothelioma P/D vs. EPP Walter Weder, MD Professor of Surgery Dokumentenname Datum Seite 1 Extrapleural Pneumonectomy
REPORT ASCO 1998 LOS ANGELES : LUNG CANCER Johan F. Vansteenkiste, MD, PhD, Univ. Hospital and Leuven Lung Cancer Group
 REPORT ASCO 1998 LOS ANGELES : LUNG CANCER Johan F. Vansteenkiste, MD, PhD, Univ. Hospital and Leuven Lung Cancer Group Educational session Treatment of stage III non-small cell lung cancer (NSCLC) in
REPORT ASCO 1998 LOS ANGELES : LUNG CANCER Johan F. Vansteenkiste, MD, PhD, Univ. Hospital and Leuven Lung Cancer Group Educational session Treatment of stage III non-small cell lung cancer (NSCLC) in
Results of Surgery in a New Lung Institute in South Texas Focused on the Treatment of Lung Cancer
 Results of Surgery in a New Lung Institute in South Texas Focused on the Treatment of Lung Cancer Lung cancer accounts for 13% of all cancer diagnoses and is the leading cause of cancer death in both males
Results of Surgery in a New Lung Institute in South Texas Focused on the Treatment of Lung Cancer Lung cancer accounts for 13% of all cancer diagnoses and is the leading cause of cancer death in both males
Medullary Renal Cell Carcinoma Case Report
 Bahrain Medical Bulletin, Vol. 27, No. 4, December 2005 Medullary Renal Cell Carcinoma Case Report Mohammed Abdulla Al-Tantawi MBBCH, CABS* Abdul Amir Issa MBBCH, CABS*** Mohammed Abdulla MBBCH, CABS**
Bahrain Medical Bulletin, Vol. 27, No. 4, December 2005 Medullary Renal Cell Carcinoma Case Report Mohammed Abdulla Al-Tantawi MBBCH, CABS* Abdul Amir Issa MBBCH, CABS*** Mohammed Abdulla MBBCH, CABS**
Rotation Specific Goals & Objectives: University Health Network-Princess Margaret Hospital/ Sunnybrook Breast/Melanoma
 Rotation Specific Goals & Objectives: University Health Network-Princess Margaret Hospital/ Sunnybrook Breast/Melanoma Medical Expert: Breast Rotation Specific Competencies/Objectives 1.0 Medical History
Rotation Specific Goals & Objectives: University Health Network-Princess Margaret Hospital/ Sunnybrook Breast/Melanoma Medical Expert: Breast Rotation Specific Competencies/Objectives 1.0 Medical History
Results of Surgical Treatment for Small Cell Lung Cancers
 NAOSITE: Nagasaki University's Ac Title Author(s) Results of Surgical Treatment for S Ayabe, Hiroyoshi; Nakamura, Akihiro Hara, Shinsuke; Tagawa, Yutaka; Kaw Citation Acta medica Nagasakiensia. 1994, 39
NAOSITE: Nagasaki University's Ac Title Author(s) Results of Surgical Treatment for S Ayabe, Hiroyoshi; Nakamura, Akihiro Hara, Shinsuke; Tagawa, Yutaka; Kaw Citation Acta medica Nagasakiensia. 1994, 39
Thoracic 18F-FDG PETCT
 Thoracic 18F-FDG PETCT RAD Magazine, 41, 482, 13-16 Dr Allanah arker Specialist registrar radiology Dr Nagmi Qureshi Consultant cardiothoracic radiologist Papworth Hospital, Cambridge email: allanahbarker@nhs.net
Thoracic 18F-FDG PETCT RAD Magazine, 41, 482, 13-16 Dr Allanah arker Specialist registrar radiology Dr Nagmi Qureshi Consultant cardiothoracic radiologist Papworth Hospital, Cambridge email: allanahbarker@nhs.net
Management of Non-Small Cell Lung Cancer Guide for General Practitioners
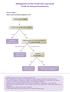 Management of n-small Cell Lung Cancer Guide for General Practitioners Clinical Stage I Cancer only in one lobe of lung and
Management of n-small Cell Lung Cancer Guide for General Practitioners Clinical Stage I Cancer only in one lobe of lung and
Non-small cell lung cancer (NSCLC) accounts for approximately
 Diagn Interv Radiol 2012; 18:435 440 Turkish Society of Radiology 2012 CHEST IMAGING ORIGINAL ARTICLE Contrast enhanced CT versus integrated PET-CT in pre-operative nodal staging of non-small cell lung
Diagn Interv Radiol 2012; 18:435 440 Turkish Society of Radiology 2012 CHEST IMAGING ORIGINAL ARTICLE Contrast enhanced CT versus integrated PET-CT in pre-operative nodal staging of non-small cell lung
