How To Pay For Health Care Benefits
|
|
|
- Betty Jordan
- 3 years ago
- Views:
Transcription
1 Blue Shield PPO Plan Benefit Booklet Stanford University Group Number: Effective Date: January 1, 2013 An independent member of the Blue Shield Association Claims Administered by Blue Shield of California
2
3 PLEASE NOTE Some hospitals and other providers do not provide one or more of the following services that may be covered under your Plan and that you or your family member might need: family planning; contraceptive services, including emergency contraception; sterilization, including tubal ligation at the time of labor and delivery; infertility treatments; or abortion. You should obtain more information before you enroll. Call your prospective doctor, medical group, independent practice association, or clinic, or call the health Plan at the Customer Service telephone number listed at the back of this booklet to ensure that you can obtain the health care services that you need. aso (1/13)
4 The Comprehensive Preferred Medical Plan Participant Bill of Rights As a Comprehensive Preferred Medical Plan Participant, you have the right to: 1. Receive considerate and courteous care, with respect for your right to personal privacy and dignity. 2. Receive information about all health Services available to you, including a clear explanation of how to obtain them. 3. Receive information about your rights and responsibilities. 4. Receive information about your Preferred Medical Plan, the Services we offer you, the Physicians and other practitioners available to care for you. 5. Have reasonable access to appropriate medical services. 6. Participate actively with your Physician in decisions regarding your medical care. To the extent permitted by law, you also have the right to refuse treatment. 7. A candid discussion of appropriate or Medically Necessary treatment options for your condition, regardless of cost or benefit coverage. 8. Receive from your Physician an understanding of your medical condition and any proposed appropriate or Medically Necessary treatment alternatives, including available success/outcomes information, regardless of cost or benefit coverage, so you can make an informed decision before you receive treatment. 9. Receive preventive health Services. 10. Know and understand your medical condition, treatment plan, expected outcome, and the effects these have on your daily living. 11. Have confidential health records, except when disclosure is required by law or permitted in writing by you. With adequate notice, you have the right to review your medical record with your Physician. 12. Communicate with and receive information from Customer Service in a language you can understand. 13. Know about any transfer to another Hospital, including information as to why the transfer is necessary and any alternatives available. 14. Be fully informed about Blue Shield dispute procedure and understand how to use it without fear of interruption of health care. 15. Voice complaints or grievances about the Preferred Medical Plan or the care provided to you. 16. Make recommendations regarding Blue Shield s Member rights responsibilities policy. 2
5 The Comprehensive Preferred Medical Plan Participant Responsibilities As a Comprehensive Preferred Medical Plan Participant, you have the responsibility to: 1. Carefully read all Blue Shield of California Preferred Medical Plan materials immediately after you are enrolled so you understand how to use your Benefits and how to minimize your out of pocket costs. Ask questions when necessary. You have the responsibility to follow the provisions of your Blue Shield of California Preferred Medical Plan as explained in this booklet. 2. Maintain your good health and prevent illness by making positive health choices and seeking appropriate care when it is needed. 3. Provide, to the extent possible, information that your Physician, and/or the Plan need to provide appropriate care for you. 4. Understand your health problems and take an active role in developing treatment goals with your medical provider, whenever possible. 5. Follow the treatment plans and instructions you and your Physician have agreed to and consider the potential consequences if you refuse to comply with treatment plans or recommendations. 6. Ask questions about your medical condition and make certain that you understand the explanations and instructions you are given. 7. Make and keep medical appointments and inform your Physician ahead of time when you must cancel. 8. Communicate openly with the Physician you choose so you can develop a strong partnership based on trust and cooperation. 9. Offer suggestions to improve the Blue Shield Preferred Medical Plan. 10. Help Blue Shield to maintain accurate and current medical records by providing timely information regarding changes in address, family status and other health plan coverage. 11. Notify Blue Shield as soon as possible if you are billed inappropriately or if you have any complaints. 12. Treat all Plan personnel respectfully and courteously as partners in good health care. 13. Pay your fees, Copayments and charges for noncovered services on time. 14. For all Mental Health Services, follow the treatment plans and instructions agreed to by you and the Mental Health Service Administrator (MHSA) and obtain prior authorization for all Inpatient Mental Health Services, Intensive Outpatient Care, Outpatient Partial Hospitalization, Outpatient electroconvulsive therapy (ECT) Services and Non-routine Outpatient Care. 15. Follow the provisions of Blue Shield s Benefits Management Program. 3
6 TABLE OF CONTENTS PREFERRED SUMMARY OF BENEFITS... 7 INTRODUCTION Preferred Providers Continuity of Care by a Terminated Provider Financial Responsibility for Continuity of Care Services Submitting a Claim Form ELIGIBILITY EFFECTIVE DATE OF COVERAGE RENEWAL OF PLAN DOCUMENT SERVICES FOR EMERGENCY CARE UTILIZATION REVIEW SECOND MEDICAL OPINION POLICY HEALTH EDUCATION AND HEALTH PROMOTION SERVICES RETAIL-BASED HEALTH CLINICS NURSEHELP 24/7 SM BLUE SHIELD ONLINE BENEFITS MANAGEMENT PROGRAM Prior Authorization Hospital and Skilled Nursing Facility Admissions Emergency Admission Notification Hospital Inpatient Review Discharge Planning Case Management ADDITIONAL AND REDUCED PAYMENTS FOR FAILURE TO USE THE BENEFITS MANAGEMENT PROGRAM DEDUCTIBLE Calendar Year Deductible (Medical Plan Deductible) Services Not Subject to the Deductible Prior Carrier Deductible Credit NO MEMBER MAXIMUM LIFETIME BENEFITS NO ANNUAL DOLLAR LIMIT ON ESSENTIAL BENEFITS PAYMENT Participant s Maximum Calendar Year Copayment Responsibility PRINCIPAL BENEFITS AND COVERAGES (COVERED SERVICES) Acupuncture Benefits Allergy Testing and Treatment Benefits Ambulance Benefits Ambulatory Surgery Center Benefits Bariatric Surgery Benefits for Residents of Designated Counties in California Chiropractic Benefits Clinical Trial for Cancer Benefits Diabetes Care Benefits Dialysis Centers Benefits Durable Medical Equipment Benefits Emergency Room Benefits Family Planning Benefits Home Health Care Benefits Home Infusion/Home Injectable Therapy Benefits Hospice Program Benefits Hospital Benefits (Facility Services) Infertility Benefits Medical Treatment of the Teeth, Gums, Jaw Joints or Jaw Bones Benefits Mental Health Benefits Orthotics Benefits Outpatient X-ray, Pathology and Laboratory Benefits PKU Related Formulas and Special Food Products Benefits Podiatric Benefits Pregnancy and Maternity Care Benefits Preventive Health Benefits Professional (Physician) Benefits
7 TABLE OF CONTENTS Prosthetic Appliances Benefits Radiological and Nuclear Imaging Benefits Rehabilitation Benefits (Physical, Occupational and Respiratory Therapy) Skilled Nursing Facility Benefits Speech Therapy Benefits Transplant Benefits Cornea, Kidney or Skin Transplant Benefits - Special PRINCIPAL LIMITATIONS, EXCEPTIONS, EXCLUSIONS AND REDUCTIONS General Exclusions and Limitations Medical Necessity Exclusion Limitations for Duplicate Coverage Exception for Other Coverage Claims Review Reductions Third Party Liability Coordination of Benefits TERMINATION OF BENEFITS Extension of Benefits GROUP CONTINUATION COVERAGE AND INDIVIDUAL PLAN Continuation of Group Coverage Continuation of Group Coverage for Members on Military Leave Availability of Blue Shield of California s Individual Plans GENERAL PROVISIONS Liability of Participants in the Event of Non-Payment by Blue Shield Independent Contractors Non-Assignability Plan Interpretation Confidentiality of Personal and Health Information Access to Information CUSTOMER SERVICE SETTLEMENT OF DISPUTES ERISA INFORMATION DEFINITIONS Plan Provider Definitions All Other Definitions SUPPLEMENT A OUTPATIENT PRESCRIPTION DRUG BENEFITS SUPPLEMENT B SUBSTANCE ABUSE CONDITION BENEFITS
8 This booklet constitutes only a summary of the health Plan. The health Plan document must be consulted to determine the exact terms and conditions of coverage. The Plan Document is on file with your Employer and a copy will be furnished upon request. This is a Preferred Medical Plan. Be sure you understand the Benefits of this Plan before Services are received. NOTICE Please read this Benefit Booklet carefully to be sure you understand the Benefits, exclusions and general provisions. It is your responsibility to keep informed about any changes in your health coverage. Should you have any questions regarding your health Plan, see your Employer or contact any of the Blue Shield offices listed on the last page of this booklet. IMPORTANT No Member has the right to receive the Benefits of this Plan for Services or supplies furnished following termination of coverage, except as specifically provided under the Extension of Benefits provision, and when applicable, the Group Continuation Coverage provision in this booklet. Benefits of this Plan are available only for Services and supplies furnished during the term it is in effect and while the individual claiming Benefits is actually covered by this Plan. Benefits may be modified during the term of this Plan as specifically provided under the terms of the plan document or upon renewal. If Benefits are modified, the revised Benefits (including any reduction in Benefits or the elimination of Benefits) apply for Services or supplies furnished on or after the effective date of modification. There is no vested right to receive the Benefits of this Plan. Stanford University is the Employer. Blue Shield of California has been appointed the Claims Administrator. Blue Shield of California processes and reviews the claims submitted under this Plan. Blue Shield of California provides administrative claims payment services only and does not assume any financial risk or obligation with respect to claims. Note: The following Summary of Benefits contains the Benefits and applicable Copayments of your Plan. The Summary of Benefits represents only a brief description of the Benefits. Please read this booklet carefully for a complete description of provisions, Benefits and exclusions of the Plan. 6
9 Preferred Summary of Benefits Note: See the end of this Summary of Benefits for important benefit footnotes. Summary of Benefits Member Calendar Year Deductible 1 (Medical Plan Deductible) Calendar Year Medical Deductible Member Maximum Calendar Year Copayment Responsibility 2 Calendar Year Copayment Maximum Member Maximum Lifetime Benefits Lifetime Benefit Maximum Deductible Responsibility Services by Preferred, Participating, and Other Providers $500 per Member / $1,500 per Family Preferred Plan Services by Non-Preferred and Non-Participating Providers $1,000 per Member / $3,000 per Family Member Maximum Calendar Year Copayment 2, 3 Services by Preferred, Participating, and Other Providers $3,500 per Member / $7,000 per Family Maximum Blue Shield Payment Services by Preferred, Participating, and Other Providers No maximum Services by any combination of Preferred, Participating, Other Providers, Non-Preferred and Non-Participating Providers $7,500 per Member / $15,000 per Family Services by Non-Preferred and Non-Participating Providers Additional Payment(s) Additional Payment(s) for Failure to Use the Benefits Management Program Refer to the Benefits Management Program section for any additional payments which may apply. 7
10 Benefit Member Copayment 3 Services by Preferred, Participating, and Other Providers 4 Acupuncture Benefits Acupuncture Not covered Not covered Allergy Testing and Treatment Benefits Allergy serum purchased separately for treatment 20% 40% Office visits (includes visits for allergy serum injections) $35 per visit 40% Ambulance Benefits Emergency or authorized transport 20% 7 20% 7 Ambulatory Surgery Center Benefits Note: Participating Ambulatory Surgery Centers may not be available in all areas. Outpatient ambulatory surgery Services may also be obtained from a Hospital or an ambulatory surgery center that is affiliated with a Hospital, and will be paid according to the Hospital Benefits (Facility Services) section of this Summary of Benefits. Ambulatory surgery center Outpatient surgery facility Services 20% 40% Ambulatory surgery center Outpatient surgery Physician Services 20% 40% Bariatric Surgery Benefits All bariatric surgery Services must be prior authorized, in writing, from Blue Shield's Medical Director. Prior authorization is required for all Members. Hospital Inpatient Services 20% 40% Hospital Outpatient Services 20% 40% Physician bariatric surgery Services 20% 40% Chiropractic Benefits Chiropractic Services Covered Services rendered by a chiropractor Up to a Benefit maximum of $1,500 per Member per Calendar Year Clinical Trial for Cancer Benefits Clinical trial for cancer Services Covered Services for Members who have been accepted into an approved clinical trial for cancer when prior authorized by the Plan. Note: Services for routine patient care will be paid on the same basis and at the same Benefit levels as other covered Services shown in this Summary of Benefits. 20% 40% You pay nothing Diabetes Care Benefits Devices, equipment and supplies 20% 7 40% Diabetes self-management training provided by a Physician in an office setting Diabetes self-management training provided by a registered dietician or registered nurse that are certified diabetes educators Dialysis Center Benefits Dialysis Services Note: Dialysis Services may also be obtained from a Hospital. Dialysis Services obtained from a Hospital will be paid at the Preferred or Non-Preferred level as specified under Hospital Benefits (Facility Services) of this Summary of Benefits. $20 per visit 40% $35 per visit 40% 20% 40% Services by Non-Preferred and Non- Participating Providers 5 You pay nothing Durable Medical Equipment Benefits Breast pump You pay nothing Not covered Other Durable Medical Equipment 20% 40% 8
11 Benefit Member Copayment 3 Services by Preferred, Participating, and Other Providers 4 Emergency Room Benefits Emergency room Physician Services 20% 20% Note: After Services have been provided, Blue Shield may conduct a retrospective review. If this review determines that Services were provided for a medical condition that a person would not have reasonably believed was an emergency medical condition, Benefits will be paid at the applicable Preferred and Non-Preferred Provider levels as specified under Outpatient Physician Services Benefit in the Professional (Physician) Benefits in this Summary of Benefits and will be subject to any Calendar Year medical Deductible. Emergency room Services not resulting in admission $50 per visit $50 per visit Note: After Services have been provided, Blue Shield may conduct a retrospective review. If this review determines that Services were provided for a medical condition that a person would not have reasonably believed was an emergency medical condition, Benefits will be paid at the applicable Preferred and Non-Preferred Provider levels as specified under Hospital Benefits (Facility Services), Outpatient Services for treatment of illness or illness, or injury, radiation therapy, chemotherapy and necessary supplies in this Summary of Benefits and will be subject to any Calendar Year medical Deductible. Emergency room Services resulting in admission 20% 20% 8 (Billed as part of Inpatient Hospital Services) Family Planning Benefits Note: Copayments listed in this section are for Outpatient Physician Services only. If Services are performed at a facility (Hospital, ambulatory surgery center, etc.), the facility Copayment listed under the appropriate facility Benefit in this Summary of Benefits will also apply, except for insertion and/or removal of intrauterine device (IUD), intrauterine device (IUD), and tubal ligation. Counseling and consulting You pay nothing 40% (Including Physician office visits for diaphragm fitting, injectable contraceptives, or implantable contraceptives) Diaphragm fitting procedure You pay nothing 40% Elective abortion 20% 40% Implantable contraceptives You pay nothing 40% Injectable contraceptives You pay nothing 40% Insertion and/or removal of intrauterine device (IUD) You pay nothing 40% Intrauterine device (IUD) You pay nothing 40% Tubal ligation You pay nothing 40% Vasectomy 20% 40% Home Health Care Benefits Services by Non-Preferred and Non- Participating Providers 5 Home health care agency Services (including home visits by a 20% Not covered 9 nurse, home health aide, medical social worker, physical therapist, speech therapist, or occupational therapist) Medical supplies and laboratory Services 20% Not covered 9 9
12 Benefit Member Copayment 3 Services by Preferred, Participating, and Other Providers 4 Services by Non-Preferred and Non- Participating Providers 5 Home Infusion/Home Injectable Therapy Benefits Hemophilia home infusion Services provided by a hemophilia infusion 20% Not covered provider and prior authorized by the Plan Home infusion/home intravenous injectable therapy provided by a 20% Not covered 9 Home Infusion Agency (Home infusion agency visits are not subject to the visit limitation under Home Health Care Benefits.) Note: Home non-intravenous self-administered injectable drugs are covered under the Outpatient Prescription Drug Benefit if selected as an optional Benefit by your Employer, and are described in a Supplement included with this booklet. Home visits by an infusion nurse 20% Not covered 9 Home infusion agency nursing visits are not subject to the Home Health Care Calendar Year visit limitation Hospice Program Benefits Covered Services for Members who have been accepted into an approved Hospice Program All Hospice Program Benefits must be prior authorized by the Plan and must be received from a Participating Hospice Agency. 24-hour Continuous Home Care 20% Not covered 10 General Inpatient care 20% Not covered 10 Inpatient Respite Care 20% Not covered 10 Pre-hospice consultation 20% Not covered 10 Routine home care 20% Not covered 10 Hospital Benefits (Facility Services) Inpatient Emergency Facility Services 20% 20% 11 Inpatient non-emergency Facility Services 20% 40% Semi-private room and board, and Medically Necessary Services and supplies, including Subacute Care Inpatient Medically Necessary skilled nursing Services including 20% 40% Subacute Care Up to a maximum of 120 days per Calendar Year per Member except when received through a Hospice Program provided by a Participating Hospice Agency. This day maximum is a combined Benefit maximum for all skilled nursing services whether rendered in a Hospital or a free-standing Skilled Nursing Facility. If your Plan has a Calendar Year medical Deductible, the number of days start counting toward the maximum when Services are first provided even if the Calendar Year medical Deductible has not been met. Inpatient Services to treat acute medical complications of detoxification 20% 40% Outpatient diagnostic testing X-ray, diagnostic examination and 20% 40% 11 clinical laboratory Services Note: These Benefits are for diagnostic, non-preventive Health Services. For Benefits for Preventive Health Services, see the Preventive Health Benefits section of this Summary of Benefits. Outpatient dialysis Services 20% 40% 11 Outpatient Services for surgery and necessary supplies 20% 40% 11 Outpatient Services for treatment of illness or injury, radiation therapy, chemotherapy and necessary supplies 20% 40% 11 10
13 Infertility Benefits Benefit Member Copayment 3 Services by Preferred, Participating, and Other Providers 4 Diagnosis and treatment of cause of Infertility (GIFT, IVF and 50% Not covered ZIFT are not covered). This Benefit is limited to 3 cycles per lifetime. Note: Infertility drugs are limited to a Plan payment maximum of $5,000 per lifetime Medical Treatment of the Teeth, Gums, Jaw Joints or Jaw Bones Benefits Treatment of gum tumors, damaged natural teeth resulting from Accidental Injury, TMJ as specifically stated and orthognathic surgery for skeletal deformity (Be sure to read the Principal Benefits and Coverages (Covered Services) section for a complete description.) Inpatient Hospital Services 20% 40% 11 Office location $35 per visit 40% Outpatient department of a Hospital 20% 40% 11 Services by Non-Preferred and Non- Participating Providers 5 Mental Health Benefits 12 Services by Services by Non- Participating Providers Participating Providers 13 Inpatient Hospital Services 14 You pay nothing 40% 15 Behavioral Health Treatment - home or other setting (noninstitutional) 20% Not covered 14 Behavioral Health Treatment - office location 14 $35 per visit 40% Inpatient Professional (Physician) Services You pay nothing 40% Outpatient Mental Health Services, Intensive Outpatient Care and $20 per visit 16 40% 16 Outpatient electroconvulsive therapy (ECT) 14 Outpatient Partial Hospitalization 14 20% per episode 17 40% 17 Psychological testing 20% 40% 11
14 Benefit Member Copayment 3 Services by Preferred, Participating, and Other Providers 4 Orthotics Benefits Office location for Services from Doctors of Medicine who are doctors $20 per visit 40% of internal medicine, family doctors, general practitioners, gy- necologists, obstetricians or pediatricians Office location for Services from Doctors of Medicine who are other $35 per visit 40% than doctors of internal medicine, family doctors, general practi- tioners, gynecologists, obstetricians or pediatricians Orthotic equipment and devices 20% 40% Outpatient Prescription Drug Benefits Outpatient Prescription Drug Benefits are described in Supplement A. Outpatient X-ray, Pathology, and Laboratory Benefits Note: Benefits in this section are for diagnostic, non-preventive Health Services. For Benefits for Preventive Health Services, see the Preventive Health Benefits section of this Summary of Benefits. For Benefits for diagnostic radiological procedures such as CT scans, MRIs, MRAs, PET scans, etc. see the Radiological and Nuclear Imaging Benefits section of this Summary of Benefits. Outpatient diagnostic X-ray, pathology, diagnostic examination and clinical laboratory Services, including mammography and Papanicolaou test. Outpatient Laboratory Center or Outpatient Radiology Center Note: Preferred Laboratory Centers and Preferred Radiology Centers may not be available in all areas. Laboratory and radiology Services may also be obtained from a Hospital or from a laboratory and radiology center that is affiliated with a Hospital. Laboratory and radiology Services obtained from a Hospital or Hospitalaffiliated laboratory and radiology center will be paid at the Preferred or Non-Preferred level as specified under Hospital Benefits (Facility Services) of this Summary of Benefits. 20% 6, 18 6, 18 40% PKU Related Formulas and Special Food Products Benefits PKU Related Formulas and Special Food Products 20% 20% Podiatric Benefits Podiatric Services provided by a licensed doctor of podiatric medicine Pregnancy and Maternity Care Benefits Note: Routine newborn circumcision is only covered as described in the Principal Benefits and Coverages (Covered Services) section. When covered, Services will pay as any other surgery as noted in this Summary of Benefits. All necessary Inpatient Hospital Services for normal delivery, Cesarean section, and complications of pregnancy Prenatal and postnatal Physician office visits (including prenatal diagnosis of genetic disorders of the fetus by means of diagnostic procedures in cases of high-risk pregnancy) $35 per visit 40% 20% 40% 11 $20 for initial visit then you pay nothing Services by Non-Preferred and Non- Participating Providers 5 40% 12
15 Benefit Member Copayment 3 Services by Preferred, Participating, and Other Providers 4 Preventive Health Benefits 19 Annual routine gynecological office visit, including the gynecological You pay nothing Not covered examination office visit, routine mammography, routine Papanicolaou (Pap) test or other FDA approved cervical cancer screening test, human papillomavirus (HPV) screening tests. Annual routine physical examination office visit, including the You pay nothing Not covered physical examination office visit, routine eye/ear screening for Members through age 18 and pediatric and adult immunizations and the immunization agent. Colorectal cancer screening You pay nothing Not covered Eye refraction You pay nothing Not covered Note: One self-referred exam every 12 months. Osteoporosis screening You pay nothing Not covered Routine laboratory Services including well baby laboratory Services You pay nothing Not covered Well baby office visits, including well baby examination office visit, pediatric immunizations and the immunization agent, well baby vision and hearing screening for Members through age 2. Professional (Physician) Benefits You pay nothing Inpatient Physician Services 20% 40% Services by Non-Preferred and Non- Participating Providers 5 Not covered Internet based consultations $10 per consultation Not covered Outpatient Physician Services, other than an office setting 20% 40% Physician home visits $20 per visit 40% Specialist home visits $35 per visit 40% Physician office visits $20 per visit 40% Specialist office visits Note: For other Services with the office visit, you may incur an additional Benefit Copayment as listed for that Service within this Summary of Benefits. This additional Benefit Copayment may be subject to the Plan's medical Deductible. Additionally, certain Physician office visits may have a Copayment amount that is different from the one stated here. For those Physician office visits, the Copayment will be as stated elsewhere in this Summary of Benefits. $35 per visit 40% Prosthetic Appliances Benefits Office location for Services from Doctors of Medicine who are doctors $20 per visit 40% of internal medicine, family doctors, general practitioners, gy- necologists, obstetricians or pediatricians Office location for Services from Doctors of Medicine who are other $35 per visit 40% than doctors of internal medicine, family doctors, general practi- tioners, gynecologists, obstetricians or pediatricians Prosthetic equipment and devices 20% 40% 13
16 Benefit Member Copayment 3 Radiological and Nuclear Imaging Benefits Note: Benefits in this section are for diagnostic, non-preventive Health Services. For Benefits for Preventive Health Services, see the Preventive Health Benefits section of this Summary of Benefits. Outpatient non-emergency radiological and nuclear imaging procedures including CT scans, MRIs, MRAs, PET scans, and cardiac diagnostic procedures utilizing nuclear medicine. Prior authorization required by the Plan. Outpatient department of a Hospital Prior authorization required by the Plan. Radiology Center Note: Preferred Radiology Centers may not be available in all areas. Services by Preferred, Participating, and Other Providers 4 20% 40% 18 20% 18 40% 18 Prior authorization required by the Plan. Rehabilitation Benefits (Physical, Occupational and Respiratory Therapy) Rehabilitation Services by a physical, occupational, or respiratory therapist in the following settings: Office location $35 per visit 6, 20 40% Outpatient department of a Hospital $35 per visit 6, 20 40% Rehabilitation unit of a Hospital for Medically Necessary days In an Inpatient facility, this Copayment is billed as part of Inpatient Hospital Services Skilled Nursing Facility rehabilitation unit for Medically Necessary days. Up to a maximum of 120 days per Calendar Year per Member except when received through a Hospice Program provided by a Participating Hospice Agency. This day maximum is a combined Benefit maximum for all skilled nursing services whether rendered in a Hospital or a free-standing Skilled Nursing Facility. If your Plan has a Calendar Year medical Deductible, the number of days start counting toward the maximum when Services are first provided even if the Calendar Year medical Deductible has not been met. Skilled Nursing Facility Benefits Services by a free-standing Skilled Nursing Facility Up to a maximum of 120 days per Calendar Year per Member except when received through a Hospice Program provided by a Participating Hospice Agency. This day maximum is a combined Benefit maximum for all skilled nursing services whether rendered in a Hospital or a free-standing Skilled Nursing Facility. If your Plan has a Calendar Year medical Deductible, the number of days start counting toward the maximum when Services are first provided even if the Calendar Year medical Deductible has not been met. 20% 40% 20% 21 20% 21 20% 21 20% 21 Services by Non-Preferred and Non- Participating Providers 5 14
17 Benefit Member Copayment 3 Services by Preferred, Participating, and Other Providers 4 Speech Therapy Benefits Speech Therapy Services by a licensed speech pathologist or certified speech therapist in the following settings: Office location $35 per visit 6, 22 40% Outpatient department of a Hospital $35 per visit 6, 22 40% Rehabilitation unit of a Hospital for Medically Necessary days 20% 40% In an Inpatient facility, this Copayment is billed as part of Inpatient Hospital Services Skilled Nursing Facility rehabilitation unit for Medically Necessary 20% 21 20% 21 days. Up to a maximum of 100 days per Calendar Year per Member except when received through a Hospice Program provided by a Participating Hospice Agency. This day maximum is a combined Benefit maximum for all skilled nursing services whether rendered in a Hospital or a free-standing Skilled Nursing Facility. If your Plan has a Calendar Year medical Deductible, the number of days start counting toward the maximum when Services are first provided even if the Calendar Year medical Deductible has not been met. Transplant Benefits - Cornea, Kidney or Skin Organ Transplant Benefits for transplant of a cornea, kidney or skin Hospital Services 20% 40% Professional (Physician) Services 20% 40% Transplant Benefits - Special 23 Note: Blue Shield requires prior authorization from Blue Shield's Medical Director for all Special Transplant Services. Also, all Services must be provided at a Special Transplant Facility designated by Blue Shield. Special Transplant Benefits for transplant of human heart, lung, heart and lung in combination, human bone marrow transplants, pediatric human small bowel transplants, pediatric and adult human small bowel and liver transplants in combination. Facility Services in a Special Transplant Facility 20% Not covered Professional (Physician) Services 20% Not covered Services by Non-Preferred and Non- Participating Providers 5 15
18 Summary of Benefits Footnotes The Calendar Year Deductible (Medical Plan Deductible) may include Services on both a dollar Copayment or Copayment percentage basis and applies to all applicable Services except the Services listed below. Covered travel expenses for bariatric surgery Services; Emergency room Facility Services not resulting in an admission; Family planning counseling and consultation Services, diaphragm fitting procedure, injectable contraceptives by a Physician, implantable contraceptives, insertion and/or removal of intrauterine device, intrauterine device, and tubal ligation; Internet based consultations; Breast pump as listed under Durable Medical Equipment Benefits; Preferred Physician office and home visits: However, covered Services received during or in connection with a Preferred Physician office or home visit are subject to the Calendar Year Deductible; Preventive health Benefits; Services provided under the Outpatient Prescription Drug Benefits Supplement. The following are not included in the maximum Calendar Year Copayment amount: Additional and reduced payments under the Benefits Management Program; Charges by Non-Preferred Providers in excess of covered amounts; Charges in excess of specified benefit maximums; Covered travel expenses for bariatric surgery Services; Services provided under the Outpatient Prescription Drug Benefits Supplement; The Calendar Year Deductible. Note: Copayments and charges for Services not accruing to the maximum Calendar Year Copayment responsibility continue to be the Member's responsibility after the Calendar Year Copayment maximum is reached. Unless otherwise specified, Copayments are calculated based on the Allowable Amount. Other Providers are not Preferred Providers and so for Services by Other Providers you are responsible for all charges above the Allowable Amount. Other Providers include acupuncturists, nursing homes and certain labs (for a complete list of Other Providers see the Definitions section). For Services by Non-Preferred and Non-Participating Providers you are responsible for all charges above the Allowable Amount. The Copayment will be calculated based upon the provider's billed charges or the amount the provider has otherwise agreed to accept as payment in full from the Plan, whichever is less. If billed by your provider, you will also be responsible for an office visit Copayment. For emergency room Services directly resulting in admission as an Inpatient to a Non-Preferred Hospital which the Plan determines are not emergencies, your Copayment will be the Non-Preferred Hospital Inpatient Services Copayment. Services by Non-Participating Home Health Care/Home Infusion Agencies are not covered unless prior authorized by the Plan. When authorized by the Plan, these Non-Participating Agencies will be reimbursed at a rate determined by the Plan and the agency and your Copayment will be the Participating Agency Copayment. Services by Non-Participating Hospice Agencies are not covered unless prior authorized by the Plan. When authorized by the Plan, these Non-Participating Agencies will be reimbursed at a rate determined by the Plan and the agency and your Copayment will be the Participating Agency Copayment. For Emergency Services by Non-Preferred Providers, your Copayment will be the Preferred Provider Copayment. No benefits are provided for Substance Abuse Conditions, unless substance abuse coverage is selected as an optional Benefit by your Employer. Note: Inpatient Services which are Medically Necessary to treat the acute medical complications of detoxification are covered as part of the medical Benefits and are not considered to be treatment of the Substance Abuse Condition itself. For Services by Non-Participating Providers you are responsible for all charges above the Allowable Amount. All Behavioral Health Treatment, Inpatient Mental Health Services, Outpatient Partial Hospitalization, Intensive Outpatient Care and Outpatient electroconvulsive therapy Services (except for Emergency and urgent Services) must be prior authorized by Blue Shield. For Emergency Services by Non-Participating Hospitals your Copayment will be the Participating Hospital Copayment based on the Allowable Amount. 16
19 This Copayment includes both Outpatient facility and Professional (Physician) Services. For Outpatient Partial Hospitalization Services, an episode of care is the date from which the patient is admitted to the Partial Hospitalization Program to the date the patient is discharged or leaves the Partial Hospitalization Program. Any Services received between these two dates would constitute the episode of care. If the patient needs to be readmitted at a later date, this would constitute another episode of care. Your Copayment will be assessed per provider per date of service. No benefits are provided for preventive health Benefits by Non-Preferred or Non-Participating Providers. For Services by certified occupational therapists and certified respiratory therapists, which are Other Providers, you are responsible for all charges above the Allowable Amount. For Services by free-standing Skilled Nursing Facilities (nursing homes), which are Other Providers, you are responsible for all charges above the Allowable Amount. For Services by licensed speech therapists, which are Other Providers, you are responsible for all charges above the Allowable Amount. Special Transplant Benefits are limited to the procedures listed in the Principal Benefits and Coverages (Covered Services) section. See the Transplant Benefits - Special Covered Services section for information on Services and requirements. 17
20 INTRODUCTION If you have questions about your Benefits, contact Blue Shield of California before Hospital or medical Services are received. This Plan is designed to reduce the cost of health care to you, the Participant. In order to reduce your costs, much greater responsibility is placed on you. You should read your Benefit Booklet carefully. Your booklet tells you which services are covered by your health Plan and which are excluded. It also lists your Copayment and Deductible responsibilities. When you need health care, present your Blue Shield ID card to your Physician, Hospital, or other licensed healthcare provider. Your ID card has your Participant and group numbers on it. Be sure to include these numbers on all claims you submit to Blue Shield of California. In order to receive the highest level of Benefits, you should assure that your provider is a Preferred Provider (see the Preferred Providers section). You are responsible for following the provisions shown in the Benefits Management Program section of this booklet, including: 1. You or your Physician must obtain Blue Shield approval at least 5 working days before Hospital or Skilled Nursing Facility admissions for all non-emergency Inpatient Hospital or Skilled Nursing Facility Services or, obtain approval from the MHSA for all Inpatient Mental Health Services, Outpatient Partial Hospitalization, Intensive Outpatient Care, Outpatient ECT Services (except for Emergency and urgent Services) and Nonroutine Outpatient Care.. (See the Preferred Providers section for information.) 2. You or your Physician must notify Blue Shield (or the MHSA in the case of Mental Health Services) within 24 hours or by the end of the first business day following emergency admissions, or as soon as it is reasonably possible to do so. 3. You or your Physician must obtain prior authorization in order to determine if contemplated services are covered. See Prior Authorization in the Benefits Management Program section for a listing of Services requiring prior authorization. Failure to meet these responsibilities may result in your incurring a substantial financial liability. Some Services may not be covered unless prior review and other requirements are met. Note: Blue Shield or the MHSA will render a decision on all requests for prior authorization within 5 business days from receipt of the request. The treating provider will be notified of the decision within 24 hours followed by written notice to the provider and Participant within 2 business days of the decision. For urgent services in situations in which the routine decision making process might seriously jeopardize the life or health of a Member or when the Member is experiencing severe pain, Blue Shield will respond as soon as possible to accommodate the Member s condition not to exceed 72 hours from receipt of the request. PLEASE READ THE FOLLOWING INFORMATION SO YOU WILL KNOW FROM WHOM OR WHAT GROUP OF PROVIDERS HEALTH CARE MAY BE OBTAINED. PREFERRED PROVIDERS The Blue Shield of California Preferred Plan is specifically designed for you to use Blue Shield of California Preferred Providers. Preferred Providers include certain Physicians, Hospitals, Alternate Care Services Providers, and other Providers. Preferred Providers are listed in the Preferred Provider Directories. All Blue Shield of California Physician Members are Preferred Providers. So are selected Hospitals in your community. Many other healthcare professionals, including dentists, podiatrists, optometrists, audiologists, licensed clinical psychologists and licensed marriage and family therapists are also Preferred Providers. They are all listed in your Preferred Provider Directories. To determine whether a provider is a Preferred Provider, consult the Preferred Provider Directory. You may also verify this information by accessing Blue Shield s Internet site located at or by calling Customer Service at the telephone number shown on the last page of this booklet. Note: A Preferred Provider s status may change. It is your obligation to verify whether the Physician, Hospital or Alternate Care Services provider you choose is a Preferred Provider, in case there have been any changes since your Preferred Provider Directory was published. Note: In some instances services are covered only if rendered by a Preferred Provider. Using a Non-Preferred Provider could result in lower or no payment by Blue Shield for services. Preferred Providers agree to accept Blue Shield's payment, plus your payment of any applicable Deductibles, Copayments, or amounts in excess of specified Benefit maximums, as payment in full for covered Services, except for the Deductibles, Copayments, and amounts in excess of specified Benefit maximums, or as provided under the Exception for Other Coverage provision and the Reductions section regarding Third Party Liability. This is not true of non-preferred Providers. You are not responsible to Participating and Preferred Providers for payment for covered Services, except for the Deductibles, Copayments, and amounts in excess of specified Benefit maximums, and except as provided under the Exception for Other Coverage provision. Blue Shield of California contracts with Hospitals and Physicians to provide Services to Members for specified rates. This contractual arrangement may include incentives to manage all services provided to Members in an appropriate manner consistent with the contract. If you want to know 18
21 more about this payment system, contact Customer Service at the number provided on the back page of this booklet. If you go to a Non-Preferred Provider, Blue Shield's payment for a Service by that Non-Preferred Provider may be substantially less than the amount billed. You are responsible for the difference between the amount Blue Shield pays and the amount billed by Non-Preferred Providers. It is therefore to your advantage to obtain medical and Hospital Services from Preferred Providers. Payment for Emergency Services rendered by a Physician or Hospital who is not a Preferred Provider will be based on the Allowable Amount but will be paid at the Preferred level of benefits. You are responsible for notifying Blue Shield within 24 hours, or by the end of the first business day following emergency admission at a Non-Preferred Hospital, or as soon as it is reasonably possible to do so. Directories of Preferred Providers located in your area have been provided to you. Extra copies are available from Blue Shield. If you do not have the directories, please contact Blue Shield immediately and request them at the telephone number listed on the last page of this booklet. CONTINUITY OF CARE BY A TERMINATED PROVIDER Members who are being treated for acute conditions, serious chronic conditions, pregnancies (including immediate postpartum care), or terminal illness; or who are children from birth to 36 months of age; or who have received authorization from a now-terminated provider for surgery or another procedure as part of a documented course of treatment can request completion of care in certain situations with a provider who is leaving the Blue Shield of California provider network. Contact Customer Service to receive information regarding eligibility criteria and the policy and procedure for requesting continuity of care from a terminated provider. FINANCIAL RESPONSIBILITY FOR CONTINUITY OF CARE SERVICES If a Member is entitled to receive Services from a terminated provider under the preceding Continuity of Care provision, the responsibility of the Member to that provider for Services rendered under the Continuity of Care provisions shall be no greater than for the same Services rendered by a Preferred Provider in the same geographic area. SUBMITTING A CLAIM FORM Preferred Providers submit claims for payment after their Services have been received. You or your Non-Preferred Providers also submit claims for payment after Services have been received. You are paid directly by Blue Shield if Services are rendered by a Non-Preferred Provider. Payments to you for covered Services are in amounts identical to those made directly to providers. Requests for payment must be submitted to Blue Shield within 1 year after the month Services were provided. Special claim forms are not necessary, but each claim submission must contain your name, home address, Plan number, Participant's number, a copy of the provider's billing showing the Services rendered, dates of treatment and the patient's name. Blue Shield will notify you of its determination within 30 days after receipt of the claim. To submit a claim for payment, send a copy of your itemized bill, along with a completed Blue Shield of California Participant's Statement of Claim form to theblue Shield service center listed on the last page of this booklet. Claim forms are available on Blue Shield s Internet site located at or you may call Customer Service at the number listed on the last page of this booklet to ask for forms. If necessary, you may use a photocopy of the Blue Shield claim form. Be sure to send in a claim for all covered Services even if you have not yet met your Calendar Year Deductible. Blue Shield will keep track of the Deductible for you. Blue Shield uses an Explanation of Benefits to describe how your claim was processed and to inform you of your financial responsibility. ELIGIBILITY 1. To enroll and continue enrollment, a Member must meet all of the eligibility requirements of the Plan. If you are an Employee, you are eligible for coverage as a Participant the day following the date you complete the waiting period established by your Employer. Your spouse or Domestic Partner and all your Dependent children are eligible at the same time. When you decline coverage for yourself or your Dependents during the initial enrollment period and later request enrollment, you and your Dependents will be considered to be Late Enrollees. When Late Enrollees decline enrollment during the initial enrollment period, they will be eligible the earlier of 12 months from the date of the request for enrollment or at the Employer s next Open Enrollment Period. Blue Shield will not consider applications for earlier effective dates. You and your Dependents will not be considered to be Late Enrollees if either you or your Dependents lose coverage under another employer s health plan and you apply for coverage under this Plan within 31 days of the date of loss of coverage. You will be required to furnish Blue Shield written proof of the loss of coverage. Newborn infants of the Participant, spouse, or his or her Domestic Partner will be eligible immediately after birth for the first 31 days. A child placed for adoption will be eligible immediately upon the date the Participant, spouse or Domestic Partner has the right to control the child s health care. Enrollment requests for children who have been placed for adoption must be accompanied by evidence of the Participant s, spouse s or Domestic Partner s right to control 19
22 the child s health care. Evidence of such control includes a health facility minor release report, a medical authorization form or a relinquishment form. In order to have coverage continue beyond the first 31 days without lapse, an application must be submitted to and received by Blue Shield within 31 days from the date of birth or placement for adoption of such Dependent. A child acquired by legal guardianship will be eligible on the date of the court ordered guardianship, if an application is submitted within 31 days of becoming eligible. You may add newly acquired Dependents and yourself to the Plan by submitting an application within 31 days from the date of acquisition of the Dependent: a. to continue coverage of a newborn or child placed for adoption; b. to add a spouse after marriage, or add a Domestic Partner after establishing a domestic partnership; c. to add yourself and spouse following the birth of a newborn or placement of a child for adoption; d. to add yourself and spouse after marriage; e. to add yourself and your newborn or child placed for adoption, following birth or placement for adoption. A completed health statement may be required with the application. Coverage is never automatic; an application is always required. If both partners in a marriage or domestic partnership are both eligible to be Participants, children may be eligible and may be enrolled as a Dependent of either parent, but not both. Enrolled Dependent children who would normally lose their eligibility under this Plan solely because of age, but who are incapable of self-sustaining employment by reason of a physically or mentally disabling injury, illness, or condition, may have their eligibility extended under the following conditions: (1) the child must be chiefly dependent upon the Employee for support and maintenance, and (2) the Employee must submit a Physician s written certification of such disabling condition. Blue Shield or the Employer will notify you at least 90 days prior to the date the Dependent child would otherwise lose eligibility. You must submit the Physician s written certification within 60 days of the request for such information by the Employer or by Blue Shield. Proof of continuing disability and dependency must be submitted by the Employee as requested by Blue Shield but not more frequently than 2 years after the initial certification and then annually thereafter. Subject to the requirements described under the Continuation of Group Coverage provision in this booklet, if applicable, an Employee and his or her Dependents will be eligible to continue group coverage under this Plan when coverage would otherwise terminate. 2. If a Member commits any of the following acts, they will immediately lose eligibility to continue enrollment: a. Abusive or disruptive behavior which: (1) threatens the life or well-being of Plan personnel, or providers of services; (2) substantially impairs the ability of Blue Shield to arrange for services to the Member; or (3) substantially impairs the ability of providers of Services to furnish Services to the Member or to other patients. b. Failure or refusal to provide Blue Shield access to documents and other information necessary to determine eligibility or to administer benefits under the Plan. 3. Employer eligibility The Employer must meet specified Employer eligibility, participation and contribution requirements to be eligible for this group Plan. See your Employer for further information. Active Employees Faculty and staff of Stanford University and the SLAC National Accelerator Laboratory as well as certain family members are eligible for benefits coverage if the criteria below are met: When you add a family member to your coverage, you need to confirm they are eligible. You have 30 days from the date you add your family member to submit the documentation. You will receive a request for the documents that includes instructions on how to submit them. If you do not submit documentation by the deadline, your dependent s enrollment is cancelled and you must wait until another life event, or annual Open Enrollment Period, to add them again. See the Educated Choices Plan Document for detailed information You are eligible for Stanford's benefits program if you are scheduled to work in a benefits-eligible position for 6 months or more (4 months or more for bargaining unit employees) and you are a: Part-time employee working between 50% and 74% time (FTE), or Full-time employee working between 75% and 100% time (FTE) Eligible family members include: 1. Spouse, unless legally separated 2. Domestic Partner registered with the state of California 3. Dependent children to age Unmarried children over the age limit if: a. They are dependent on you for primary financial support and maintenance due to a physical or mental disability b. They are incapable of self-support, and c. The disability existed before reaching age
UC Care Plan. Benefit Booklet. University of California. Group Number: W0051612 Plan ID: PPOX0001 Effective Date: January 1, 2016
 UC Care Plan Benefit Booklet University of California Group Number: W0051612 Plan ID: PPOX0001 Effective Date: January 1, 2016 An independent member of the Blue Shield Association Claims Administered by
UC Care Plan Benefit Booklet University of California Group Number: W0051612 Plan ID: PPOX0001 Effective Date: January 1, 2016 An independent member of the Blue Shield Association Claims Administered by
Blue Shield of California Life & Health Insurance Company
 Active Start SM Plan 25 - G Blue Shield of California Life & Health Insurance Company Policy Individual Plan An independent licensee of the Blue Shield Association (Intentionally left blank) Active Start
Active Start SM Plan 25 - G Blue Shield of California Life & Health Insurance Company Policy Individual Plan An independent licensee of the Blue Shield Association (Intentionally left blank) Active Start
Shield Savings 3500 - G. Blue Shield of California Life & Health Insurance Company
 Shield Savings 3500 - G Blue Shield of California Life & Health Insurance Company Policy Individual and Family Plan An independent licensee of the Blue Shield Association (Intentionally left blank) Shield
Shield Savings 3500 - G Blue Shield of California Life & Health Insurance Company Policy Individual and Family Plan An independent licensee of the Blue Shield Association (Intentionally left blank) Shield
CDHP (Consumer Driven Health Plan)
 CDHP (Consumer Driven Health Plan) Benefit Booklet Group Number: 976208 & 976209 Effective Date: January 1, 2013 An Independent Member of the Blue Shield Association Claims Administered by Blue Shield
CDHP (Consumer Driven Health Plan) Benefit Booklet Group Number: 976208 & 976209 Effective Date: January 1, 2013 An Independent Member of the Blue Shield Association Claims Administered by Blue Shield
Stanford Health Care Alliance (SHCA)
 Stanford Health Care Alliance (SHCA) Benefit Booklet Stanford University Group Number: 976248 Effective Date: January 1, 2015 An independent member of the Blue Shield Association Claims Administered by
Stanford Health Care Alliance (SHCA) Benefit Booklet Stanford University Group Number: 976248 Effective Date: January 1, 2015 An independent member of the Blue Shield Association Claims Administered by
SISC Custom SaveNet Zero Admit 10 Benefit Summary (Uniform Health Plan Benefits and Coverage Matrix)
 SISC Custom SaveNet Zero Admit 10 Benefit Summary (Uniform Health Plan Benefits and Coverage Matrix) Blue Shield of California Highlights: A description of the prescription drug coverage is provided separately
SISC Custom SaveNet Zero Admit 10 Benefit Summary (Uniform Health Plan Benefits and Coverage Matrix) Blue Shield of California Highlights: A description of the prescription drug coverage is provided separately
Ultimate Full PPO for Small Business 0 Benefit Summary (For groups 1 to 50) (Uniform Health Plan Benefits and Coverage Matrix)
 Ultimate Full PPO for Small Business 0 Benefit Summary (For groups 1 to 50) (Uniform Health Plan Benefits and Coverage Matrix) Blue Shield of California Effective January 1, 2014 THIS MATRIX IS INTENDED
Ultimate Full PPO for Small Business 0 Benefit Summary (For groups 1 to 50) (Uniform Health Plan Benefits and Coverage Matrix) Blue Shield of California Effective January 1, 2014 THIS MATRIX IS INTENDED
CSAC/EIA Health Small Group Access+ HMO 15-0 Inpatient Benefit Summary
 CSAC/EIA Health Small Group Access+ HMO 15-0 Inpatient Benefit Summary (Uniform Health Plan Benefits and Coverage Matrix) Blue Shield of California THIS MATRIX IS INTENDED TO BE USED TO HELP YOU COMPARE
CSAC/EIA Health Small Group Access+ HMO 15-0 Inpatient Benefit Summary (Uniform Health Plan Benefits and Coverage Matrix) Blue Shield of California THIS MATRIX IS INTENDED TO BE USED TO HELP YOU COMPARE
No Charge (Except as described under "Rehabilitation Benefits" and "Speech Therapy Benefits")
 An Independent Licensee of the Blue Shield Association Custom Access+ HMO Plan Certificated & Management Benefit Summary (For groups of 300 and above) (Uniform Health Plan Benefits and Coverage Matrix)
An Independent Licensee of the Blue Shield Association Custom Access+ HMO Plan Certificated & Management Benefit Summary (For groups of 300 and above) (Uniform Health Plan Benefits and Coverage Matrix)
Summary of Services and Cost Shares
 Summary of Services and Cost Shares This summary does not describe benefits. For the description of a benefit, including any limitations or exclusions, please refer to the identical heading in the Benefits
Summary of Services and Cost Shares This summary does not describe benefits. For the description of a benefit, including any limitations or exclusions, please refer to the identical heading in the Benefits
NATIONWIDE INSURANCE $20-40 / 250A NATIONAL MANAGED CARE SCHEDULE OF BENEFITS
 WASHINGTON NATIONWIDE INSURANCE $20-40 / 250A NATIONAL MANAGED CARE SCHEDULE OF BENEFITS General Features Calendar Year Deductible Lifetime Benefit Maximum (Does not apply to Chemical Dependency) ($5,000.00
WASHINGTON NATIONWIDE INSURANCE $20-40 / 250A NATIONAL MANAGED CARE SCHEDULE OF BENEFITS General Features Calendar Year Deductible Lifetime Benefit Maximum (Does not apply to Chemical Dependency) ($5,000.00
2015 OPEN ENROLLMENT MEDICAL PLANS
 2015 OPEN ENROLLMENT MEDICAL PLANS Table of Contents Section I. Enrollment Guidelines Page 3 Health Plan Comparison Chart Page 4 Health Plan Premiums and Employee Cost-Sharing Page 5 Section II. Blue Shield
2015 OPEN ENROLLMENT MEDICAL PLANS Table of Contents Section I. Enrollment Guidelines Page 3 Health Plan Comparison Chart Page 4 Health Plan Premiums and Employee Cost-Sharing Page 5 Section II. Blue Shield
CENTRAL MICHIGAN UNIVERSITY - Premier Plan (PPO1) 007000285-0002 0004 Effective Date: July 1, 2015 Benefits-at-a-Glance
 CENTRAL MICHIGAN UNIVERSITY - Premier Plan (PPO1) 007000285-0002 0004 Effective Date: July 1, 2015 Benefits-at-a-Glance This is intended as an easy-to-read summary and provides only a general overview
CENTRAL MICHIGAN UNIVERSITY - Premier Plan (PPO1) 007000285-0002 0004 Effective Date: July 1, 2015 Benefits-at-a-Glance This is intended as an easy-to-read summary and provides only a general overview
S c h o o l s I n s u r a n c e G r o u p Health Net Plan Comparison Fiscal Year 7/1/14-6/30/15
 S c h o o l s I n s u r a n c e G r o u p Health Net Plan Comparison Fiscal Year 7/1/14-6/30/15 This information sheet is for reference only. Please refer to Evidence of Coverage requirements, limitations
S c h o o l s I n s u r a n c e G r o u p Health Net Plan Comparison Fiscal Year 7/1/14-6/30/15 This information sheet is for reference only. Please refer to Evidence of Coverage requirements, limitations
County of San Bernardino - Retiree Shield Signature High Option
 An Independent Member of the Blue Shield Association County of San Bernardino - Retiree Shield Signature High Option Benefit Summary (Uniform Health Plan Benefits and Coverage Matrix) Blue Shield of California
An Independent Member of the Blue Shield Association County of San Bernardino - Retiree Shield Signature High Option Benefit Summary (Uniform Health Plan Benefits and Coverage Matrix) Blue Shield of California
S c h o o l s I n s u r a n c e G r o u p Health Net Plan Comparison Fiscal Year 7/1/15-6/30/16
 S c h o o l s I n s u r a n c e G r o u p Health Net Plan Comparison Fiscal Year 7/1/15-6/30/16 This information sheet is for reference only. Please refer to Evidence of Coverage requirements, limitations
S c h o o l s I n s u r a n c e G r o u p Health Net Plan Comparison Fiscal Year 7/1/15-6/30/16 This information sheet is for reference only. Please refer to Evidence of Coverage requirements, limitations
SMALL GROUP PLAN DESIGN AND BENEFITS OPEN CHOICE OUT-OF-STATE PPO PLAN - $1,000
 PLAN FEATURES PREFERRED CARE NON-PREFERRED CARE Deductible (per calendar year; applies to all covered services) $1,000 Individual $3,000 Family $2,000 Individual $6,000 Family Plan Coinsurance ** 80% 60%
PLAN FEATURES PREFERRED CARE NON-PREFERRED CARE Deductible (per calendar year; applies to all covered services) $1,000 Individual $3,000 Family $2,000 Individual $6,000 Family Plan Coinsurance ** 80% 60%
PREFERRED CARE. All covered expenses, including prescription drugs, accumulate toward both the preferred and non-preferred Payment Limit.
 PLAN FEATURES Deductible (per plan year) $300 Individual $300 Individual None Family None Family All covered expenses, excluding prescription drugs, accumulate toward both the preferred and non-preferred
PLAN FEATURES Deductible (per plan year) $300 Individual $300 Individual None Family None Family All covered expenses, excluding prescription drugs, accumulate toward both the preferred and non-preferred
Important Questions Answers Why this Matters:
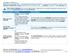 Minimum Coverage PPO Network Name: Exclusive Coverage Period: Beginning on or after 1/1/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual + Family Plan
Minimum Coverage PPO Network Name: Exclusive Coverage Period: Beginning on or after 1/1/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual + Family Plan
Medical Plan - Healthfund
 18 Medical Plan - Healthfund Oklahoma City Community College Effective Date: 07-01-2010 Aetna HealthFund Open Choice (PPO) - Oklahoma PLAN DESIGN AND BENEFITS PROVIDED BY AETNA LIFE INSURANCE COMPANY -
18 Medical Plan - Healthfund Oklahoma City Community College Effective Date: 07-01-2010 Aetna HealthFund Open Choice (PPO) - Oklahoma PLAN DESIGN AND BENEFITS PROVIDED BY AETNA LIFE INSURANCE COMPANY -
California Small Group MC Aetna Life Insurance Company
 PLAN FEATURES Deductible (per calendar year) $3,000 Individual $6,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. All covered expenses accumulate separately
PLAN FEATURES Deductible (per calendar year) $3,000 Individual $6,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. All covered expenses accumulate separately
Blue Cross Premier Bronze Extra
 An individual PPO health plan from Blue Cross Blue Shield of Michigan. You will have a broad choice of doctors and hospitals within Blue Cross Blue Shield of Michigan s unsurpassed statewide PPO network
An individual PPO health plan from Blue Cross Blue Shield of Michigan. You will have a broad choice of doctors and hospitals within Blue Cross Blue Shield of Michigan s unsurpassed statewide PPO network
Commercial. Individual & Family Plan. Health Net California Farm Bureau and PPO. Insurance Plans. Outline of Coverage and Exclusions and Limitations
 Commercial Individual & Family Plan Health Net California Farm Bureau and PPO Insurance Plans Outline of Coverage and Exclusions and Limitations Table of Contents Health Plans Outline of coverage 1 Read
Commercial Individual & Family Plan Health Net California Farm Bureau and PPO Insurance Plans Outline of Coverage and Exclusions and Limitations Table of Contents Health Plans Outline of coverage 1 Read
SUMMARY OF BENEFITS. Cigna Health and Life Insurance Co. Laramie County School District 2 Open Access Plus Base - Effective 7/1/2015
 SUMMARY OF BENEFITS Cigna Health and Life Insurance Co. Laramie County School District 2 Open Access Plus Base - Effective General Services In-Network Out-of-Network Physician office visit Urgent care
SUMMARY OF BENEFITS Cigna Health and Life Insurance Co. Laramie County School District 2 Open Access Plus Base - Effective General Services In-Network Out-of-Network Physician office visit Urgent care
California Small Group MC Aetna Life Insurance Company
 PLAN FEATURES Deductible (per calendar year) $1,000 per member $1,000 per member Unless otherwise indicated, the Deductible must be met prior to benefits being payable. All covered expenses accumulate
PLAN FEATURES Deductible (per calendar year) $1,000 per member $1,000 per member Unless otherwise indicated, the Deductible must be met prior to benefits being payable. All covered expenses accumulate
The Deductible is applicable to all covered services except for flat dollar Copayment services.
 PRIORITY HEALTH www.priorityhealth.com/mpsers PRIORITYHMO SM PLUS PLAN MICHIGAN PUBLIC SCHOOL EMPLOYEES RETIREMENT SYSTEM (MPSERS) Effective January 1, 2016 through December 31, 2016 The HMO Plus plan
PRIORITY HEALTH www.priorityhealth.com/mpsers PRIORITYHMO SM PLUS PLAN MICHIGAN PUBLIC SCHOOL EMPLOYEES RETIREMENT SYSTEM (MPSERS) Effective January 1, 2016 through December 31, 2016 The HMO Plus plan
PPO Schedule of Payments (Maryland Large Group) Qualified High Deductible Health Plan National QA2000-20
 PPO Schedule of Payments (Maryland Large Group) Qualified High Health Plan National QA2000-20 Benefit Year Individual Family (Amounts for Participating and s services are separated in calculating when
PPO Schedule of Payments (Maryland Large Group) Qualified High Health Plan National QA2000-20 Benefit Year Individual Family (Amounts for Participating and s services are separated in calculating when
PLAN DESIGN AND BENEFITS - Tx OAMC 2500 08 PREFERRED CARE
 PLAN FEATURES Deductible (per calendar year) $2,500 Individual $5,000 Individual $7,500 3 Individuals per $15,000 3 Individuals per Unless otherwise indicated, the Deductible must be met prior to benefits
PLAN FEATURES Deductible (per calendar year) $2,500 Individual $5,000 Individual $7,500 3 Individuals per $15,000 3 Individuals per Unless otherwise indicated, the Deductible must be met prior to benefits
SUMMARY OF BENEFITS. Cigna Health and Life Insurance Co. Grand County Open Access Plus Effective 1/1/2015
 SUMMARY OF BENEFITS Cigna Health and Life Insurance Co. Grand County Open Access Plus Effective General Services In-Network Out-of-Network Primary care physician You pay $25 copay per visit Physician office
SUMMARY OF BENEFITS Cigna Health and Life Insurance Co. Grand County Open Access Plus Effective General Services In-Network Out-of-Network Primary care physician You pay $25 copay per visit Physician office
OverVIEW of Your Eligibility Class by determineing Benefits
 OVERVIEW OF YOUR BENEFITS IMPORTANT PHONE NUMBERS Benefit Fund s Member Services Department (646) 473-9200 For answers to questions about your eligibility or prescription drug benefit. You can also visit
OVERVIEW OF YOUR BENEFITS IMPORTANT PHONE NUMBERS Benefit Fund s Member Services Department (646) 473-9200 For answers to questions about your eligibility or prescription drug benefit. You can also visit
STATE STANDARD 20-40/400D HMO SCHEDULE OF BENEFITS
 CALIFORNIA STATE STANDARD 20-40/400D HMO SCHEDULE OF BENEFITS These services are covered as indicated when authorized through your Primary Care Physician in your Participating Medical Group. General Features
CALIFORNIA STATE STANDARD 20-40/400D HMO SCHEDULE OF BENEFITS These services are covered as indicated when authorized through your Primary Care Physician in your Participating Medical Group. General Features
PLAN DESIGN AND BENEFITS AETNA LIFE INSURANCE COMPANY - Insured
 PLAN FEATURES Deductible (per calendar year) Individual $750 Individual $1,500 Family $2,250 Family $4,500 All covered expenses accumulate simultaneously toward both the preferred and non-preferred Deductible.
PLAN FEATURES Deductible (per calendar year) Individual $750 Individual $1,500 Family $2,250 Family $4,500 All covered expenses accumulate simultaneously toward both the preferred and non-preferred Deductible.
National PPO 1000. PPO Schedule of Payments (Maryland Small Group)
 PPO Schedule of Payments (Maryland Small Group) National PPO 1000 The benefits outlined in this Schedule are in addition to the benefits offered under Coventry Health & Life Insurance Company Small Employer
PPO Schedule of Payments (Maryland Small Group) National PPO 1000 The benefits outlined in this Schedule are in addition to the benefits offered under Coventry Health & Life Insurance Company Small Employer
Senate Bill 91 (2011) Standard Plan - EHB and Cost Share Matrix - Updated for 2016 ***NOT INTENDED AS A STATEMENT OF COVERAGE***
 Deductible Medical: $1,250; Medical: $2,500; Integrated Medical/Rx: Rx: $0 Rx: $0 $5,000 Maximum OOP Combined Medical Combined Medical Combined Medical and and Drug: $6,350 and Drug: $6,350 Drug: $6,350
Deductible Medical: $1,250; Medical: $2,500; Integrated Medical/Rx: Rx: $0 Rx: $0 $5,000 Maximum OOP Combined Medical Combined Medical Combined Medical and and Drug: $6,350 and Drug: $6,350 Drug: $6,350
Reliability and predictable costs for individuals and families
 INDIVIDUAL & FAMILY PLANS HEALTH NET HMO PLANS Reliability and predictable costs for individuals and families If you re looking for a health plan that s simple to use and easy to understand, you ve found
INDIVIDUAL & FAMILY PLANS HEALTH NET HMO PLANS Reliability and predictable costs for individuals and families If you re looking for a health plan that s simple to use and easy to understand, you ve found
UnitedHealthcare Choice Plus. UnitedHealthcare Insurance Company. Certificate of Coverage
 UnitedHealthcare Choice Plus UnitedHealthcare Insurance Company Certificate of Coverage For the Plan 7EG of Educators Benefit Services, Inc. Enrolling Group Number: 717578 Effective Date: January 1, 2012
UnitedHealthcare Choice Plus UnitedHealthcare Insurance Company Certificate of Coverage For the Plan 7EG of Educators Benefit Services, Inc. Enrolling Group Number: 717578 Effective Date: January 1, 2012
UnitedHealthcare Choice Plus. UnitedHealthcare Insurance Company. Certificate of Coverage
 UnitedHealthcare Choice Plus UnitedHealthcare Insurance Company Certificate of Coverage For the Health Savings Account (HSA) Plan 7PD of Educators Benefit Services, Inc. Enrolling Group Number: 717578
UnitedHealthcare Choice Plus UnitedHealthcare Insurance Company Certificate of Coverage For the Health Savings Account (HSA) Plan 7PD of Educators Benefit Services, Inc. Enrolling Group Number: 717578
PLAN DESIGN AND BENEFITS HMO Open Access Plan 912
 PLAN FEATURES Deductible (per calendar year) $1,000 Individual $2,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. Member cost sharing for certain services
PLAN FEATURES Deductible (per calendar year) $1,000 Individual $2,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. Member cost sharing for certain services
Schedule of Benefits HARVARD PILGRIM LAHEY HEALTH VALUE HMO MASSACHUSETTS MEMBER COST SHARING
 Schedule of s HARVARD PILGRIM LAHEY HEALTH VALUE HMO MASSACHUSETTS ID: MD0000003378_ X Please Note: In this plan, Members have access to network benefits only from the providers in the Harvard Pilgrim-Lahey
Schedule of s HARVARD PILGRIM LAHEY HEALTH VALUE HMO MASSACHUSETTS ID: MD0000003378_ X Please Note: In this plan, Members have access to network benefits only from the providers in the Harvard Pilgrim-Lahey
Plans. Who is eligible to enroll in the Plan? Blue Care Network (BCN) Health Alliance Plan (HAP) Health Plus. McLaren Health Plan
 Who is eligible to enroll in the Plan? All State of Michigan Employees who reside in the coverage area determined by zip code. All State of Michigan Employees who reside in the coverage area determined
Who is eligible to enroll in the Plan? All State of Michigan Employees who reside in the coverage area determined by zip code. All State of Michigan Employees who reside in the coverage area determined
University of Michigan Group: 007005187-0000, 0001 Comprehensive Major Medical (CMM) Benefits-at-a-Glance
 University of Michigan Group: 007005187-0000, 0001 Comprehensive Major Medical (CMM) Benefits-at-a-Glance This is intended as an easy-to-read summary and provides only a general overview of your benefits.
University of Michigan Group: 007005187-0000, 0001 Comprehensive Major Medical (CMM) Benefits-at-a-Glance This is intended as an easy-to-read summary and provides only a general overview of your benefits.
CIGNA HEALTH AND LIFE INSURANCE COMPANY, a Cigna company (hereinafter called Cigna)
 Home Office: Bloomfield, Connecticut Mailing Address: Hartford, Connecticut 06152 CIGNA HEALTH AND LIFE INSURANCE COMPANY, a Cigna company (hereinafter called Cigna) CERTIFICATE RIDER No CR7SI006-1 Policyholder:
Home Office: Bloomfield, Connecticut Mailing Address: Hartford, Connecticut 06152 CIGNA HEALTH AND LIFE INSURANCE COMPANY, a Cigna company (hereinafter called Cigna) CERTIFICATE RIDER No CR7SI006-1 Policyholder:
Member s responsibility (deductibles, copays, coinsurance and dollar maximums)
 MICHIGAN CATHOLIC CONFERENCE January 2015 Benefit Summary This is intended as an easy-to-read summary and provides only a general overview of your benefits. It is not a contract. Additional limitations
MICHIGAN CATHOLIC CONFERENCE January 2015 Benefit Summary This is intended as an easy-to-read summary and provides only a general overview of your benefits. It is not a contract. Additional limitations
100% Fund Administration
 FUND FEATURES HealthFund Amount $500 Employee $750 Employee + Spouse $750 Employee + Child(ren) $1,000 Family Amount contributed to the Fund by the employer Fund Coinsurance Percentage at which the Fund
FUND FEATURES HealthFund Amount $500 Employee $750 Employee + Spouse $750 Employee + Child(ren) $1,000 Family Amount contributed to the Fund by the employer Fund Coinsurance Percentage at which the Fund
Employee + 2 Dependents
 FUND FEATURES HealthFund Amount $500 Individual $1,000 Employee + 1 Dependent $1,000 Employee + 2 Dependents $1,000 Family Amount contributed to the Fund by the employer Fund Coinsurance Percentage at
FUND FEATURES HealthFund Amount $500 Individual $1,000 Employee + 1 Dependent $1,000 Employee + 2 Dependents $1,000 Family Amount contributed to the Fund by the employer Fund Coinsurance Percentage at
Hawaii Benchmarks Benefits under the Affordable Care Act (ACA)
 Hawaii Benchmarks Benefits under the Affordable Care Act (ACA) 10/2012 Coverage for Newborn and Foster Children Coverage Outside the Provider Network Adult Routine Physical Exams Well-Baby and Well-Child
Hawaii Benchmarks Benefits under the Affordable Care Act (ACA) 10/2012 Coverage for Newborn and Foster Children Coverage Outside the Provider Network Adult Routine Physical Exams Well-Baby and Well-Child
PDS Tech, Inc Proposed Effective Date: 01-01-2012 Aetna HealthFund Aetna Choice POS ll - ASC
 FUND FEATURES HealthFund Amount $500 Individual $1,000 Employee + 1 Dependent $1,000 Employee + 2 Dependents $1,000 Family Amount contributed to the Fund by the employer Fund Coinsurance 100% Percentage
FUND FEATURES HealthFund Amount $500 Individual $1,000 Employee + 1 Dependent $1,000 Employee + 2 Dependents $1,000 Family Amount contributed to the Fund by the employer Fund Coinsurance 100% Percentage
2015 Medical Plan Summary
 2015 Medical Plan Summary AVMED POS PLAN This Schedule of Benefits reflects the higher provider and prescription copayments for 2015. This is not a contract, it s a summary of the plan highlights and is
2015 Medical Plan Summary AVMED POS PLAN This Schedule of Benefits reflects the higher provider and prescription copayments for 2015. This is not a contract, it s a summary of the plan highlights and is
PLAN DESIGN AND BENEFITS POS Open Access Plan 1944
 PLAN FEATURES PARTICIPATING Deductible (per calendar year) $3,000 Individual $9,000 Family $4,000 Individual $12,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being
PLAN FEATURES PARTICIPATING Deductible (per calendar year) $3,000 Individual $9,000 Family $4,000 Individual $12,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being
Cost Sharing Definitions
 SU Pro ( and ) Annual Deductible 1 Coinsurance Cost Sharing Definitions $200 per individual with a maximum of $400 for a family 5% of allowable amount for inpatient hospitalization - or - 50% of allowable
SU Pro ( and ) Annual Deductible 1 Coinsurance Cost Sharing Definitions $200 per individual with a maximum of $400 for a family 5% of allowable amount for inpatient hospitalization - or - 50% of allowable
Business Life Insurance - Health & Medical Billing Requirements
 PLAN FEATURES Deductible (per plan year) $2,000 Employee $2,000 Employee $3,000 Employee + Spouse $3,000 Employee + Spouse $3,000 Employee + Child(ren) $3,000 Employee + Child(ren) $4,000 Family $4,000
PLAN FEATURES Deductible (per plan year) $2,000 Employee $2,000 Employee $3,000 Employee + Spouse $3,000 Employee + Spouse $3,000 Employee + Child(ren) $3,000 Employee + Child(ren) $4,000 Family $4,000
UnitedHealthcare Insurance Company of the River Valley Attachment D - Schedule of Benefits
 UnitedHealthcare Insurance Company of the River Valley Attachment D - Schedule of Benefits Please refer to your Provider Directory for listings of Participating Physicians, Hospitals, and other Providers.
UnitedHealthcare Insurance Company of the River Valley Attachment D - Schedule of Benefits Please refer to your Provider Directory for listings of Participating Physicians, Hospitals, and other Providers.
California PCP Selected* Not Applicable
 PLAN FEATURES Deductible (per calendar ) Member Coinsurance * Not Applicable ** Not Applicable Copay Maximum (per calendar ) $3,000 per Individual $6,000 per Family All member copays accumulate toward
PLAN FEATURES Deductible (per calendar ) Member Coinsurance * Not Applicable ** Not Applicable Copay Maximum (per calendar ) $3,000 per Individual $6,000 per Family All member copays accumulate toward
AVMED POS PLAN. Allergy Injections No charge 30% co-insurance after deductible Allergy Skin Testing $30 per visit 30% co-insurance after deductible
 AVMED POS PLAN This Schedule of Benefits reflects the higher provider and prescription copays for 2015. This is not a contract, it s a summary of the plan highlights and is subject to change. For specific
AVMED POS PLAN This Schedule of Benefits reflects the higher provider and prescription copays for 2015. This is not a contract, it s a summary of the plan highlights and is subject to change. For specific
Benefit Summary - A, G, C, E, Y, J and M
 Benefit Summary - A, G, C, E, Y, J and M Benefit Year: Calendar Year Payment for Services Deductible Individual $600 $1,200 Family (Embedded*) $1,200 $2,400 Coinsurance (the percentage amount the Covered
Benefit Summary - A, G, C, E, Y, J and M Benefit Year: Calendar Year Payment for Services Deductible Individual $600 $1,200 Family (Embedded*) $1,200 $2,400 Coinsurance (the percentage amount the Covered
Independence Blue Cross Plan Summary PPO Core Medical Plan
 TO: FROM: SUBJECT: MLH Medical Plan Participants MLH Human Resources Benefits Team Independence Blue Cross Plan Summary PPO Core Medical Plan Attached you will find the Independence Blue Cross (IBC) Plan
TO: FROM: SUBJECT: MLH Medical Plan Participants MLH Human Resources Benefits Team Independence Blue Cross Plan Summary PPO Core Medical Plan Attached you will find the Independence Blue Cross (IBC) Plan
Health Net Life Insurance Company California Farm Bureau Members Health Insurance Plans Major Medical Expense Coverage Outline of Coverage
 Health Net Life Insurance Company California Farm Bureau Members Health Insurance Plans Major Medical Expense Coverage Outline of Coverage Read Your Certificate Carefully This outline of coverage provides
Health Net Life Insurance Company California Farm Bureau Members Health Insurance Plans Major Medical Expense Coverage Outline of Coverage Read Your Certificate Carefully This outline of coverage provides
Individual. Employee + 1 Family
 FUND FEATURES HealthFund Amount Individual Employee + 1 Family $750 $1,125 $1,500 Amount contributed to the Fund by the employer is reflected above. Fund Amount reflected is on a per calendar year basis.
FUND FEATURES HealthFund Amount Individual Employee + 1 Family $750 $1,125 $1,500 Amount contributed to the Fund by the employer is reflected above. Fund Amount reflected is on a per calendar year basis.
Dickinson Wright, PLLC 03956-006
 Dickinson Wright, PLLC 03956-006 Flexible Blue SM Plan 3 Medical Coverage with Preventive Care and Mammography Benefits Benefits-at-a-Glance This is intended as an easy-to-read summary and provides only
Dickinson Wright, PLLC 03956-006 Flexible Blue SM Plan 3 Medical Coverage with Preventive Care and Mammography Benefits Benefits-at-a-Glance This is intended as an easy-to-read summary and provides only
PRIORITY HEALTH priorityhealth.com HealthbyChoice Incentives Summary of Benefits TRINITY HEALTH -HbCI 2 1/1/13 12/31/13
 PRIORITY HEALTH priorityhealth.com Healthby Incentives Summary of Benefits TRINITY HEALTH -HbCI 2 1/1/13 12/31/13 The Healthby Incentives HMO plan is a Consumer Engaged Health plan that offers a choice
PRIORITY HEALTH priorityhealth.com Healthby Incentives Summary of Benefits TRINITY HEALTH -HbCI 2 1/1/13 12/31/13 The Healthby Incentives HMO plan is a Consumer Engaged Health plan that offers a choice
Baltimore City Public Schools Health Plan Comparison Chart Benefits Effective January 1, 2015
 Baltimore City Public Schools Health Plan Comparison Chart Benefits Effective January 1, 2015 About this chart: This chart is to be used as a guide only and does not contain all details or exclusions.
Baltimore City Public Schools Health Plan Comparison Chart Benefits Effective January 1, 2015 About this chart: This chart is to be used as a guide only and does not contain all details or exclusions.
Health Plans Coverage Summary
 www.hr.msu.edu/openenrollment Faculty & Staff Health Plans Coverage Summary PREVENTIVE SERVICES Health Maintenance Exam (1) Annual Gynecological Exam Pap Smear Screening (lab services only) Mammography
www.hr.msu.edu/openenrollment Faculty & Staff Health Plans Coverage Summary PREVENTIVE SERVICES Health Maintenance Exam (1) Annual Gynecological Exam Pap Smear Screening (lab services only) Mammography
Alternative Benefit Plan (ABP) ABP Cost-Sharing & Comparison to Standard Medicaid Services
 Alternative Benefit Plan (ABP) ABP Cost-Sharing & Comparison to Standard Medicaid Services Most adults who qualify for the Medicaid category known as the Other Adult Group receive services under the New
Alternative Benefit Plan (ABP) ABP Cost-Sharing & Comparison to Standard Medicaid Services Most adults who qualify for the Medicaid category known as the Other Adult Group receive services under the New
SERVICES IN-NETWORK COVERAGE OUT-OF-NETWORK COVERAGE
 COVENTRY HEALTH AND LIFE INSURANCE COMPANY 3838 N. Causeway Blvd. Suite 3350 Metairie, LA 70002 1-800-341-6613 SCHEDULE OF BENEFITS BENEFITS AND PRIOR AUTHORIZATION REQUIREMENTS ARE SET FORTH IN ARTICLES
COVENTRY HEALTH AND LIFE INSURANCE COMPANY 3838 N. Causeway Blvd. Suite 3350 Metairie, LA 70002 1-800-341-6613 SCHEDULE OF BENEFITS BENEFITS AND PRIOR AUTHORIZATION REQUIREMENTS ARE SET FORTH IN ARTICLES
Harvard Pilgrim Health Care of New England, Inc. THE HARVARD PILGRIM BEST BUY TIERED COPAYMENT HMO - LP NEW HAMPSHIRE
 ID: MD0000003228_B3 X Schedule of s Harvard Pilgrim Health Care of New England, Inc. THE HARVARD PILGRIM BEST BUY TIERED COPAYMENT HMO - LP NEW HAMPSHIRE Coverage under this Plan is under the jurisdiction
ID: MD0000003228_B3 X Schedule of s Harvard Pilgrim Health Care of New England, Inc. THE HARVARD PILGRIM BEST BUY TIERED COPAYMENT HMO - LP NEW HAMPSHIRE Coverage under this Plan is under the jurisdiction
UnitedHealthcare Choice Plus. United HealthCare Insurance Company. Certificate of Coverage
 UnitedHealthcare Choice Plus United HealthCare Insurance Company Certificate of Coverage For Westminster College Enrolling Group Number: 715916 Effective Date: January 1, 2009 Offered and Underwritten
UnitedHealthcare Choice Plus United HealthCare Insurance Company Certificate of Coverage For Westminster College Enrolling Group Number: 715916 Effective Date: January 1, 2009 Offered and Underwritten
Summary of PNM Resources Health Care Benefits Active Employees 2011
 of PNM Resources Health Care Benefits Active Employees 2011 The following charts show deductibles, limits, benefit levels and amounts for the PNM Resources medical, dental and vision programs. For more
of PNM Resources Health Care Benefits Active Employees 2011 The following charts show deductibles, limits, benefit levels and amounts for the PNM Resources medical, dental and vision programs. For more
Important Questions Answers Why this Matters: What is the overall deductible? Are there other deductibles for specific services?
 Gold 80 PPO Network Name: Exclusive Coverage Period: Beginning on or after 1/1/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual + Family Plan Type:
Gold 80 PPO Network Name: Exclusive Coverage Period: Beginning on or after 1/1/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual + Family Plan Type:
PLAN DESIGN & BENEFITS - CONCENTRIC MODEL
 PLAN FEATURES Deductible (per calendar year) Rice University None Family Member Coinsurance Applies to all expenses unless otherwise stated. Payment Limit (per calendar year) $1,500 Individual $3,000 Family
PLAN FEATURES Deductible (per calendar year) Rice University None Family Member Coinsurance Applies to all expenses unless otherwise stated. Payment Limit (per calendar year) $1,500 Individual $3,000 Family
Unlimited except where otherwise indicated.
 PLAN FEATURES Deductible (per calendar year) $1,250 Individual $5,000 Individual $2,500 Family $10,000 Family All covered expenses including prescription drugs accumulate separately toward both the preferred
PLAN FEATURES Deductible (per calendar year) $1,250 Individual $5,000 Individual $2,500 Family $10,000 Family All covered expenses including prescription drugs accumulate separately toward both the preferred
PLAN DESIGN AND BENEFITS Basic HMO Copay Plan 1-10
 PLAN FEATURES Deductible (per calendar year) Member Coinsurance Not Applicable Not Applicable Out-of-Pocket Maximum $5,000 Individual (per calendar year) $10,000 Family Once the Family Out-of-Pocket Maximum
PLAN FEATURES Deductible (per calendar year) Member Coinsurance Not Applicable Not Applicable Out-of-Pocket Maximum $5,000 Individual (per calendar year) $10,000 Family Once the Family Out-of-Pocket Maximum
Bates College Effective date: 01-01-2010 HMO - Maine PLAN DESIGN AND BENEFITS PROVIDED BY AETNA HEALTH INC. - FULL RISK PLAN FEATURES
 PLAN FEATURES Deductible (per calendar year) $500 Individual $1,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. Once Family Deductible is met, all family
PLAN FEATURES Deductible (per calendar year) $500 Individual $1,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. Once Family Deductible is met, all family
IL Small Group PPO Aetna Life Insurance Company Plan Effective Date: 04/01/2009 PLAN DESIGN AND BENEFITS- PPO HSA HDHP $2,500 100/80 (04/09)
 PLAN FEATURES OUT-OF- Deductible (per calendar ) $2,500 Individual $5,000 Individual $5,000 Family $10,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable.
PLAN FEATURES OUT-OF- Deductible (per calendar ) $2,500 Individual $5,000 Individual $5,000 Family $10,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable.
Greater Tompkins County Municipal Health Insurance Consortium
 WHO IS COVERED Requires both Medicare A & B enrollment. Type of Coverage Offered Single only Single only MEDICAL NECESSITY Pre-Certification Requirement None None Medical Benefit Management Program Not
WHO IS COVERED Requires both Medicare A & B enrollment. Type of Coverage Offered Single only Single only MEDICAL NECESSITY Pre-Certification Requirement None None Medical Benefit Management Program Not
LOCKHEED MARTIN AERONAUTICS COMPANY PALMDALE 2011 IAM NEGOTIATIONS UNDER AGE 65 LM HEALTHWORKS SUMMARY
 Annual Deductibles, Out-of-Pocket Maximums, Lifetime Maximum Benefits Calendar Year Deductible Calendar Year Out-of- Pocket Maximum Lifetime Maximum Per Individual Physician Office Visits Primary Care
Annual Deductibles, Out-of-Pocket Maximums, Lifetime Maximum Benefits Calendar Year Deductible Calendar Year Out-of- Pocket Maximum Lifetime Maximum Per Individual Physician Office Visits Primary Care
California Ironworkers Field Welfare Plan 1/1/2014 Open Enrollment Benefit Plan Comparison Non-Medicare Retired Participants Residing in Nevada
 Non- Choice of Providers Calendar Year Deductible *The Fund s Calendar Year Deductible is never waived. However, some services are not subject to the Deductible. If you live in Nevada, your network of
Non- Choice of Providers Calendar Year Deductible *The Fund s Calendar Year Deductible is never waived. However, some services are not subject to the Deductible. If you live in Nevada, your network of
Schedule of Benefits for the MoDOT/MSHP Medical Plan Medicare ASO PPO 20088 Effective 1/1/2016
 Schedule of Benefits for the MoDOT/MSHP Medical Plan Medicare ASO PPO 20088 Effective 1/1/2016 This Schedule of Benefits summarizes your obligation towards the cost of certain covered services. Refer to
Schedule of Benefits for the MoDOT/MSHP Medical Plan Medicare ASO PPO 20088 Effective 1/1/2016 This Schedule of Benefits summarizes your obligation towards the cost of certain covered services. Refer to
SPIN Effective Date: 01-01-2013 Aetna HealthFund Aetna Choice POS ll - ASC PLAN DESIGN & BENEFITS ADMINISTERED BY AETNA LIFE INSURANCE COMPANY
 HealthFund Amount $1,500 Employee $1,500 Employee + 1 Dependent $1,500 Employee + 2 Dependents $1,500 Family Amount contributed to Fund by employer Fund Coinsurance 100% Percentage at which Fund will reimburse
HealthFund Amount $1,500 Employee $1,500 Employee + 1 Dependent $1,500 Employee + 2 Dependents $1,500 Family Amount contributed to Fund by employer Fund Coinsurance 100% Percentage at which Fund will reimburse
PLAN DESIGN AND BENEFITS - PA Health Network Option AHF HRA 1.3. Fund Pays Member Responsibility
 HEALTHFUND PLAN FEATURES HealthFund Amount (Per plan year. Fund changes between tiers requires a life status change qualifying event.) Fund Coinsurance (Percentage at which the Fund will reimburse) Fund
HEALTHFUND PLAN FEATURES HealthFund Amount (Per plan year. Fund changes between tiers requires a life status change qualifying event.) Fund Coinsurance (Percentage at which the Fund will reimburse) Fund
PLAN DESIGN AND BENEFITS - New York Open Access EPO 1-10/10
 PLAN FEATURES Deductible (per calendar year) $1,000 Individual $3,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. Member cost sharing for certain services,
PLAN FEATURES Deductible (per calendar year) $1,000 Individual $3,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. Member cost sharing for certain services,
FEATURES NETWORK OUT-OF-NETWORK
 Schedule of Benefits Employer: The Vanguard Group, Inc. ASA: 697478-A Issue Date: January 1, 2014 Effective Date: January 1, 2014 Schedule: 3B Booklet Base: 3 For: Choice POS II - 950 Option - Retirees
Schedule of Benefits Employer: The Vanguard Group, Inc. ASA: 697478-A Issue Date: January 1, 2014 Effective Date: January 1, 2014 Schedule: 3B Booklet Base: 3 For: Choice POS II - 950 Option - Retirees
Preauthorization Requirements * (as of January 1, 2016)
 OFFICE VISITS Primary Care Office Visits Primary Care Home Visits Specialist Office Visits No Specialist Home Visits PREVENTIVE CARE Well Child Visits and Immunizations Adult Annual Physical Examinations
OFFICE VISITS Primary Care Office Visits Primary Care Home Visits Specialist Office Visits No Specialist Home Visits PREVENTIVE CARE Well Child Visits and Immunizations Adult Annual Physical Examinations
PLAN DESIGN AND BENEFITS - Tx OAMC Basic 2500-10 PREFERRED CARE
 PLAN FEATURES Deductible (per calendar year) $2,500 Individual $4,000 Individual $7,500 Family $12,000 Family 3 Individuals per Family 3 Individuals per Family Unless otherwise indicated, the Deductible
PLAN FEATURES Deductible (per calendar year) $2,500 Individual $4,000 Individual $7,500 Family $12,000 Family 3 Individuals per Family 3 Individuals per Family Unless otherwise indicated, the Deductible
New York Small Group Indemnity Aetna Life Insurance Company Plan Effective Date: 10/01/2010. PLAN DESIGN AND BENEFITS - NY Indemnity 1-10/10*
 PLAN FEATURES Deductible (per calendar year) $2,500 Individual $7,500 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. Member cost sharing for certain services,
PLAN FEATURES Deductible (per calendar year) $2,500 Individual $7,500 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. Member cost sharing for certain services,
Services and supplies required by Health Care Reform Age and frequency guidelines apply to covered preventive care Not subject to deductible if PPO
 Page 1 of 5 Individual Deductible Calendar year $400 COMBINED Individual / Family OOP Calendar year $4,800 Individual $12,700 per family UNLIMITED Annual Maximum July 1 st to June 30 th UNLIMITED UNLIMITED
Page 1 of 5 Individual Deductible Calendar year $400 COMBINED Individual / Family OOP Calendar year $4,800 Individual $12,700 per family UNLIMITED Annual Maximum July 1 st to June 30 th UNLIMITED UNLIMITED
What is the overall deductible? Are there other deductibles for specific services?
 : MyPriority POS RxPlus Silver 1800 Coverage Period: Beginning on or after 01/01/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Subscriber/Dependent Plan Type:
: MyPriority POS RxPlus Silver 1800 Coverage Period: Beginning on or after 01/01/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Subscriber/Dependent Plan Type:
100% Percentage at which the Fund will reimburse Fund Administration
 FUND FEATURES HealthFund Amount $500 Employee $1,000 Employee + 1 Dependent $1,000 Employee + 2 Dependents $1,000 Family Amount contributed to the Fund by the employer Fund amount reflected is on a per
FUND FEATURES HealthFund Amount $500 Employee $1,000 Employee + 1 Dependent $1,000 Employee + 2 Dependents $1,000 Family Amount contributed to the Fund by the employer Fund amount reflected is on a per
PREVENTIVE CARE See the REHP Benefits Handbook for a list of preventive benefits* MATERNITY SERVICES Office visits Covered in full including first
 Network Providers Non Network Providers** DEDUCTIBLE (Per Calendar Year) None $250 per person $500 per family OUT-OF-POCKET MAXIMUM (When the out-of-pocket maximum is reached, benefits are paid at 100%
Network Providers Non Network Providers** DEDUCTIBLE (Per Calendar Year) None $250 per person $500 per family OUT-OF-POCKET MAXIMUM (When the out-of-pocket maximum is reached, benefits are paid at 100%
CA Group Business 2-50 Employees
 PLAN FEATURES Network Primary Care Physician Selection Deductible (per calendar year) Member Coinsurance Copay Maximum (per calendar year) Lifetime Maximum Referral Requirement PHYSICIAN SERVICES Primary
PLAN FEATURES Network Primary Care Physician Selection Deductible (per calendar year) Member Coinsurance Copay Maximum (per calendar year) Lifetime Maximum Referral Requirement PHYSICIAN SERVICES Primary
BENEFIT PLAN. What Your Plan Covers and How Benefits are Paid. Appendix A. Prepared Exclusively for The Dow Chemical Company
 Appendix A BENEFIT PLAN Prepared Exclusively for The Dow Chemical Company What Your Plan Covers and How Benefits are Paid Choice POS II (MAP Plus Option 2 - High Deductible Health Plan (HDHP) with Prescription
Appendix A BENEFIT PLAN Prepared Exclusively for The Dow Chemical Company What Your Plan Covers and How Benefits are Paid Choice POS II (MAP Plus Option 2 - High Deductible Health Plan (HDHP) with Prescription
UnitedHealthcare Choice. UnitedHealthcare Insurance Company. Certificate of Coverage
 UnitedHealthcare Choice UnitedHealthcare Insurance Company Certificate of Coverage For the Plan 9DF of District of Columbia Government Enrolling Group Number: 712971 Effective Date: January 1, 2013 Offered
UnitedHealthcare Choice UnitedHealthcare Insurance Company Certificate of Coverage For the Plan 9DF of District of Columbia Government Enrolling Group Number: 712971 Effective Date: January 1, 2013 Offered
Iowa Wellness Plan Benefits Coverage List
 Iowa Wellness Plan Benefits Coverage List Service Category Covered Duration, Scope, exclusions, and Limitations Excluded Coding 1. Ambulatory Services Primary Care Illness/injury Physician Services Should
Iowa Wellness Plan Benefits Coverage List Service Category Covered Duration, Scope, exclusions, and Limitations Excluded Coding 1. Ambulatory Services Primary Care Illness/injury Physician Services Should
THE MITRE CORPORATION PPO High Deductible Plan with a Health Saving Account (HSA)
 THE MITRE CORPORATION PPO High Deductible Plan with a Health Saving Account (HSA) Effective Date: 01-01-2016 PLAN FEATURES Annual Deductible $1,500 Employee $3,000 Employee $3,000 Employee + 1 Dependent
THE MITRE CORPORATION PPO High Deductible Plan with a Health Saving Account (HSA) Effective Date: 01-01-2016 PLAN FEATURES Annual Deductible $1,500 Employee $3,000 Employee $3,000 Employee + 1 Dependent
$6,350 Individual $12,700 Individual
 PLAN FEATURES IN-NETWORK OUT-OF-NETWORK Deductible $5,000 Individual $10,000 Individual $10,000 Family $20,000 Family All covered expenses accumulate separately toward the preferred or non-preferred Deductible.
PLAN FEATURES IN-NETWORK OUT-OF-NETWORK Deductible $5,000 Individual $10,000 Individual $10,000 Family $20,000 Family All covered expenses accumulate separately toward the preferred or non-preferred Deductible.
Western Health Advantage: City of Sacramento HSA ABHP Coverage Period: 1/1/2016-12/31/2016
 Coverage For: Self Plan Type: HMO This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.westernhealth.com or
Coverage For: Self Plan Type: HMO This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.westernhealth.com or
SECTION A. Summary of Benefits LW-V, 10/09
 SECTION A. Summary of Benefits LW-V, 10/09 This Summary is part of your Benefit Handbook. It states the Cost Sharing amounts that you must pay for Covered Benefits and some important limitations on your
SECTION A. Summary of Benefits LW-V, 10/09 This Summary is part of your Benefit Handbook. It states the Cost Sharing amounts that you must pay for Covered Benefits and some important limitations on your
Coventry Health and Life Insurance Company PPO Schedule of Benefits
 State(s) of Issue: Oklahoma PPO Plan: OI08C30050 30 Coventry Health and Life Insurance Company PPO Schedule of Benefits Covered Services Contract Year Deductible For All Eligible Expenses (unless otherwise
State(s) of Issue: Oklahoma PPO Plan: OI08C30050 30 Coventry Health and Life Insurance Company PPO Schedule of Benefits Covered Services Contract Year Deductible For All Eligible Expenses (unless otherwise
Health Insurance Benefits Summary
 Independent licensee of the Blue Cross and Blue Shield Association Health Insurance Benefits Summary Community Blue SM PPO Health Maintenance Exam (1) Covered 100%, one per calendar year, includes select
Independent licensee of the Blue Cross and Blue Shield Association Health Insurance Benefits Summary Community Blue SM PPO Health Maintenance Exam (1) Covered 100%, one per calendar year, includes select
PLAN DESIGN AND BENEFITS - Tx OAMC 1500-10 PREFERRED CARE
 PLAN FEATURES Deductible (per calendar year) $1,500 Individual $3,000 Individual $4,500 Family $9,000 Family 3 Individuals per Family 3 Individuals per Family Unless otherwise indicated, the Deductible
PLAN FEATURES Deductible (per calendar year) $1,500 Individual $3,000 Individual $4,500 Family $9,000 Family 3 Individuals per Family 3 Individuals per Family Unless otherwise indicated, the Deductible
