Closing the Theory Practice Gap: Intrapartum Midwifery Management of Planned Homebirths
|
|
|
- Harriet York
- 8 years ago
- Views:
Transcription
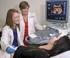
1 Closing the Theory Practice Gap: Intrapartum Midwifery Management of Planned Homebirths Saraswathi Vedam, CNM, MSN, Meredith Goff, CNM, MS, and Vicki Nolan Marnin, CNM, MSN In the United States, access to qualified homebirth providers varies by state, city, and community, and consistent, evidence-based guidelines for intrapartum management at home are not available. This article examines the similarities and differences in midwifery management of the intrapartum, postpartum, and neonatal course between planned homebirths and planned hospital births. Characteristics of qualified attendants, essential medical supplies and equipment, methods for maternal and fetal surveillance, and common intrapartum indications for transfer are discussed. Unique features of management of the healthy woman and baby in the home are described, as well as the process of consultation and/or referral for collaborative or medical management. Current evidence for the management of fetal intolerance of labor, meconium stained amniotic fluid, prolonged labor, postpartum hemorrhage, and the unstable newborn is discussed in the context of homebirth practice. Aspects of homebirth care that require cultural competency and affect the informed consent process are included. Homebirth practice may provide opportunities to increase the congruence between espoused midwifery philosophy and actual practice. J Midwifery Womens Health 2007;52: by the American College of Nurse-Midwives. keywords: collaborative care, core competencies, cultural competency, evidence-based care, home childbirth, intrapartum management, low risk obstetrics, midwifery, perinatal management, planned homebirth, risk assessment, screening criteria, transfer criteria, transfer protocols INTRODUCTION The phrase planned homebirth describes births that occur when the woman intends to deliver at home; she meets defined medical and environmental criteria for an optimal perinatal course; and she has qualified birth attendants who work within a health care system that provides access to equipment, specialized personnel, and/or hospitalization when necessary. 1 In the last decade, controlled trials and observational studies have described excellent perinatal outcomes for planned homebirths. 2 8 Women praise the increased control of the environment and process of care when delivering at home. 3,9,10 Rates of intrapartum intervention differ according to birth setting. In developed nations, outof-hospital births have been associated with the appropriate use of technology and reductions in health care expenses. 6,11,12 Several national and international advisory panels have supported informed choice for place of birth and increased access to appropriate out-of-hospital maternity services. 7,13 15 In the United States, less than 4% of members of the American College of Nurse-Midwives (ACNM) attend planned homebirths. 16 Physicians in most communities do not provide home care, and 95% of certified nursemidwives (CNMs) or certified midwives (CMs) provide intrapartum care only in the hospital. 17 The low rates of homebirth in the United States (1%) 18 may be a result of Address correspondence to Saraswathi Vedam, CNM, MSN, Division of Midwifery, University of British Columbia, B Health Sciences Mall, Vancouver, BC V6T 1Z3. saraswathi.vedam@ midwifery.ubc.ca reduced access to qualified homebirth attendants. Attendant choice of intrapartum practice site and style of management may be influenced by a lack of exposure to effective care in out-of-hospital settings. This article discusses effective intrapartum care across birth settings. The Theory Practice Gap in Contemporary Midwifery Care Recently, Lange and Kennedy 19 described a theory practice gap between espoused midwifery philosophy and professional behavior as reported by 245 newly CNMs. When asked to reflect on their final clinical rotation as students (87% hospital placements), study participants described a lack of congruity between ideal and actual midwifery practices that support normal birth in the practice(s) of the CNM preceptors they worked with just before graduation. This work suggests that there are unique competencies in perinatal management that characterize, promote, and preserve the midwifery model of care. While respondents noted very little theory practice gap in the behavior of preceptors in the dimension of caring, they observed large differences between ideal and actual midwifery practice in using low technology approaches when possible and intervening only if necessary and appropriate. Maintenance of a supportive presence in labor was found to be less congruent between professed theory and actual practice. Students in birth center settings (10%) observed the greatest congruence for respecting the normal processes of birth (P.01). Respondents also reported a gap between their perception of ideal practice and actual practice in vigilance and attention to details in homebirth practices. Authors concluded that this perception may be a function of an incongruence between how watchfulness is done Journal of Midwifery & Women s Health by the American College of Nurse-Midwives /07/$32.00 doi: /j.jmwh Issued by Elsevier Inc.
2 in a hospital setting compared with how a midwife conducts that same activity at home, further confounded by the students very limited exposure to homebirth midwifery practice (2.9% of student placements). Educational programs for CNMs and CMs in the United States rarely offer out-of-hospital clinical experiences as a core part of the curriculum. Hence, while many of the ACNM core competencies 20 are applicable to any practice setting, the translation of these competencies to an out-of-hospital setting may not be obvious. In addition, there are some screening concepts, management priorities, and therapeutic measures that assume greater significance or are different according to birth site. Increasing confidence among CNMs/CMs in the application of these concepts and methods may reduce the theory practice gap in the promotion of normal birth. If they become familiar with the realities of care at home, they may consider homebirth practice, and therefore increase access to out-of-hospital maternity services. These low technology core competencies become even more critical in an era when management of health care access and delivery outside the hospital during pandemics, natural disasters, or national crises is a palpable priority. Antepartum factors that affect birth site selection have been described in detail (Table 1). 21 This article provides a review of the aspects of intrapartum, postpartum, and neonatal midwifery management that can be provided similarly across birth sites, as well as those assessment, management, and therapeutic measures that need to be modified according to birth site. CORE COMPETENCIES ACROSS BIRTH SITES Most women will have two providers present for a planned homebirth, primarily because after the birth, both mother and baby will require attention and surveillance. Midwives may collaborate with other midwives, nurses, or trained birth assistants. Qualified homebirth attendants have the ability to monitor maternal and fetal condition and assess and treat common obstetric conditions with low technology methods. The identification of complications that would be best addressed by equipment or personnel available in the hospital and the ability to initiate a referral are essential components of professional homebirth care. When delivery is imminent or the stage or nature of the condition prohibits safe transfer, Saraswathi Vedam, CNM, MSN, is the Director of the Division of Midwifery at University of British Columbia and serves as chair of the ACNM Division of Standards and Practice Homebirth Section. Meredith Goff, CNM, MS, is on the midwifery faculty at Yale School of Nursing and provides intrapartum midwifery care in the Yale Midwifery Faculty Practice. Vicki Nolan Marnin, CNM, MSN, is clinical preceptor for Yale School of Nursing and practices in a homebirth midwifery private practice as well as a tertiary care intrapartum setting. Table 1. Antepartum Assessment Criteria for Birth Site Selection General Criteria Woman physically and mentally healthy and well-nourished Adequate social supports before and during birth Primary participants mature and able to accept responsibility for selfcare Commitment to maintaining a positive emotional environment for mother throughout process Arrangements made for emergency transport Childbirth, homebirth, and breastfeeding education secured (books/ classes) Preparation of persons planning to be present at the birth Complete records from previous provider for current and/or past pregnancies Pediatric care arranged before 36 weeks of pregnancy Obstetric consultant identified by 36 weeks Help available in home 24 hours a day for at least 1 week after the birth Commitment to birth without pharmacologic analgesia or anesthesia Understanding of and agreement to the screening criteria Open and clear communication with the midwife Recommended Indications for Consultation, Collaboration, and/or Referral of Care Anemia refractory to treatment Chronic hypertension and/or pre-eclampsia requiring management with medication Current mental illness that the midwife deems would have a harmful effect on the perinatal course Thromboembolic disease (event) requiring heparin Insulin-dependent diabetes Placenta previa at term Rh isoimmunization or positive antibody screen during current pregnancy Active preterm labor that cannot be stopped Evidence of chorioamnionitis Multiple gestation diagnosed before labor Substance abuse Non-reassuring fetal surveillance results Adapted with permission from Jackson et al., eds., the homebirth midwife may need to manage the complication independently. Hence, preparation for skills, procedures, and management during common urgent care situations is important. In reality, the competencies required for managing complications during the perinatal period are common to many midwifery practice settings. The management of immediate postpartum hemorrhage (PPH) or unexpected breech delivery, and neonatal resuscitation of the term infant are topics within core curriculum in midwifery educational programs, and prerequisite knowledge for basic certification and practice in any setting. In addition to screening for potential complications and impediments to normal birth, homebirth midwives avoid interventions that may adversely affect maternal or fetal status and precipitate a need for transfer. For example, medications for pain management can affect neonatal respiratory status, thermoregulation, glucose metabolism, and behavioral status, 22 as well as progress of labor. 22,23 In the hospital setting, the availability of naloxone (Narcan; 292 Volume 52, No. 3, May/June 2007
3 Endo Pharmaceuticals, Chadds Ford, PA) and immediate access to neonatal providers can mitigate the adverse effects of maternal administration of medications during labor. Even common procedures, such as amniotomy and vaginal exams, have potential adverse consequences if used indiscriminately. 24,25 Inviting the possibility of cord compression, chorioamnionitis, or a reduced dilution of meconium may increase the necessity of therapy only available in the hospital. Conversely, homebirth midwives and families employ a variety of intrapartum and postpartum measures to prevent complications and promote maternal and fetal well-being in an effort to avoid a change in the setting for care. The best available evidence supports continuous labor support, active hydration and nutrition, and methods to conserve energy and rest in the latent phase. Optimal maternal and fetal positioning, the use of upright positions, heat, and nonpharmacologic methods of pain management are effective, safe, and satisfying supportive and preventative measures that can be employed at home. 26 Essential Birth Supplies and Equipment The sterile tray is nearly identical for planned homebirth and planned, term hospital birth (Table 2). 27 The equipment and supplies are best organized in a limited number of carrying cases, which can be easily transported in the midwife s vehicle and carried quickly from the curb into the home. Materials that are sensitive to heat (medications) can be carried in a Thermos or package with cold packs. Hard or padded cases for oxygen tanks will protect them from damage and inadvertent release in the midwife s vehicle. The physical environment of the home may be unfamiliar to the midwife and may not provide the convenience of ergonomic examination and treatment features (adjustable beds, lighting, wall suction, neonatal warming exam tables, etc.). With a little imagination and ingenuity, all of these items can be created simply. Pillows, chair backs, stools, and human supports can be used to position both mother and midwife comfortably. Flashlights and adjustable desk lamps can be propped up with rolled washcloths to direct a beam of light. A city phone book wrapped in a folded towel and underpad makes a firm but comfortable surface to stabilize and visualize the perineum during repairs. A baking sheet or cutting board layered with soft flannel receiving blankets and an electric heating pad serves as a firm, flat, warm, portable surface for neonatal exam or resuscitation. The family supplies sources of heat, light, and water, nourishing fluids and foods for labor, and a transport vehicle for non-urgent transfer. The plan for emergency transfer is assisted with a posted written listing of emergency numbers, including transport, obstetric, and pediatric personnel, and directions to and from the Table 2. Basic Equipment for Homebirth Bag Delivery instruments Suturing instruments Gloves Cord clamps Sterile speculum Suturing supplies Urinary catheters Sterile Supplies Amniotomy device Syringes, needles Intravenous infusion fluids and supplies Sterile gauze, sterile saline Suctioning devices (e.g., DeLee mucus traps with filters, RescuVac hand powered mechanical suction) Blood and specimen collection supplies Equipment for Maternal and Fetal Assessment Scales Urine dipsticks to measure protein, glucose (Uristix) Adult stethoscope Doppler and/or fetoscope Sphygmomanometer Pediatric stethoscope Medications to control hemorrhage (oxytocin [Pitocin], ergotamine [Methergine], misoprostol [Cytotec]) Anesthesia for perineal repair (lidocaine) Portable oxygen tank Masks in varying sizes Gloves Instrument and hand cleaning solutions Nitrazine and slides for assessment of PROM Medical record forms Flashlight Mirror Disposable receptacles for contaminated sharp supplies Herbs, homeopathy as appropriate for care provider experience and education Pharmaceuticals Resuscitation Equipment Nonsterile Supplies Prophylactic agents: (e.g. AquaMEPHYTON, antibiotics for GBS prophylaxis, neonatal ophthalmic ointment) Self-inflating resuscitation bag Infant feeding tube Bendable straws Examination lubricants Newborn examination tools (e.g., tape measure, penlight, thermometer) Transport blankets and clothing Enema supplies Smelling salts Sterilization equipment Apparatus for nonpharmaceutical pain relief (e.g., heating pads, massage balls, oils, cold packs GBS Group B streptococcus; PROM premature rupture of membranes. The DeLee mucus trap is manufactured by Sherwood Medical (Saint Louis, MO). The RescueVac is manufactured by Rescue Vac Systems, Inc. (Naperville, IL). Uristix are manufactured by Bayer Diagnostics (Chicago, IL). AquaMEPHYTON is manufactured by Merck & Co., Inc. (Whitehouse Station, NJ). Adapted with permission from Jackson et al., eds. 27 nearest hospital. Organization of and access to the birth supplies, clear passageways, and clear, firm surfaces will facilitate efficient care and prompt transfer when necessary. Modifications Related to Cultural Competence Homebirth midwives often are witness to cultural and religious traditions, specific to labor and birth, that may not be practical or permissible in a hospital setting. 28,29 As invited guests in the home, it is incumbent upon midwives to be both respectful and knowledgeable about Journal of Midwifery & Women s Health 293
4 the details of these practices. The inclusion of song, prayer, or specific support persons are components that can be easily integrated into usual practice. The desire for specific environmental modifications (altar, candles, lighting, birthing room location, etc.) sometimes has to be balanced with the practicalities of access to birthing equipment, visualization, and ease of transport. Prohibitions on the use of motor vehicles (Orthodox Jewish or Amish families) may require special arrangements or exceptions when transport is necessary. Specific food and food preparation requirements (Kosher or Brahmin rules) may have an impact on the midwife s ability to prepare or serve food and fluids to the woman. Generally, the midwife can engage the client in an anticipatory discussion about how to best serve her within the context of how she interprets the aspects of her culture that interact with birth. 28,30 Anticipatory Guidance, Support, and Maternal Surveillance Once labor is established, the initial and ongoing assessment and management priorities are common to all midwifery practice regardless of anticipated birth site. Whether in home or hospital, the midwife performs a physical exam and checks the signs and symptoms of labor progress and coping abilities at regular intervals. Evidence-based measures to provide comfort and promote progress include continuous loving support, hydrotherapy, acupressure, sterile water papules, massage, maternal positioning, and heat. 26 The impact of emotional and environmental factors on the progress of labor is well documented in the literature. 31,32 Maternal anxiety engendered by the planned place of birth (either at home or in the hospital) may emerge as a reason to transfer or to initiate preventative strategies earlier. The client s psychological preparedness is a critical variable that may affect the ability to deliver in the home setting without analgesia or labor augmentation. Management of the environment at a planned homebirth has some unique challenges. The midwife s status as a guest may increase the need to balance advocacy for her patient with negotiating family dynamics and cultural expectations. For example, when the primary decision-makers are the elders in the family, they may feel more empowered to assert or insert their presence, opinions, and fears in the home than in the hospital. Fetal Surveillance In all intrapartum settings, midwifery evaluation of fetal well-being is indirectly monitored via periodic assessment of fetal heart rate pattern. In the home, intermittent auscultation is the method of fetal heart rate evaluation. Guidelines have been established outlining the frequency and interpretation of intermittent auscultation for lowrisk mothers Postpartum Follow-up At Home Follow-up postpartum care in the home involves the standard maternal postpartum evaluation of involution, bleeding, vital signs, breasts, perineum, and emotional status during each of the scheduled postpartum visits. Homebirth midwives commonly provide in-home assessments two to four times in the first week, and offer office visits subsequently. Homebirth families frequently require reminders of normal postpartum recovery needs for rest because they do not benefit from limited visiting hours and 24-hour access to nutritional and physical support in the hospital. At home, the expectations for return to normal roles and self-care activities may precede physical and emotional readiness. Many homebirth midwives encourage the mother to arrange for 24-hour in-home help during the first week. The importance of adequate postpartum rest and psychosocial support to prevent postpartum depression has been well documented. 36,37 If the midwife is willing to assume a directive role by providing written instructions and messages to the extended family, adherence may improve. Care of the Normal Neonate in the Home Unlike the hospital-based midwife, the homebirth midwife is the sole provider responsible for initial examination and care of the newborn at birth and at the early postpartum visits. In the immediate postpartum period, the midwife examines the newborn for signs of normal cardiac and respiratory transition. The newborn s vital signs, output, gross anatomy, alertness, responsiveness, and feeding/attachment behaviors inform ongoing care. Like many hospital-based midwives, the homebirth midwife also makes it her priority to assist with initial lactation. However, because there is usually no other experienced nurse or lactation consultant on site after the midwife leaves the home, many homebirth midwives will not leave until latch and adequate suck/swallow is established. Some homebirth midwives require clients to breastfeed in the initial postpartum period, as the ability to breastfeed is a marker of neonatal health, and breastfeeding improves maternal immunity, reduces stress and anxiety, and promotes uterine involution Immediate newborn care may include the administration of prophylactic therapies and medications (vitamin K or eye prophylaxis). To ensure that the family has ample opportunity to recuperate and to concentrate on establishing good parenting and breastfeeding habits, homebirth midwives often provide in-home newborn care and assessment until the child is 2 weeks of age. In addition to the physical examination, midwives can evaluate feeding behaviors, monitor family adjustment, and collect statemandated newborn screening samples. Ideally, the family will establish a relationship with a pediatric provider who is willing to be available for 294 Volume 52, No. 3, May/June 2007
5 Table 3. Reasons for Transfer From Planned Homebirth to Hospital Birth Reasons for IP Transfer Failure to progress (55% 75%) Prolonged rupture of membranes Meconium staining Nonvertex presentation Fetal distress Desire for pharmaceutical pain relief Bleeding Hypertension Reasons for PP Transfer Maternal Retained placenta Postpartum hemorrhage Laceration repair Reasons for Neonatal Transfer Inability to establish normal respirations Congenital anomalies Low birth weight Low Apgar score Birth trauma Sepsis Data taken from Ackermann-Liebrich et al. 2 ; Wiegers et al. 4 ; Davies et al. 3 ; Janssen et al. 6 ; Murphy and Fullerton 5 ; and Johnson and Daviss. 8 consultation and referral before the birth. Some pediatric providers are unaware that midwifery core competencies include newborn examination skills and may expect the family to bring the baby to their office in the first 24 hours. The midwife may inform the pediatric providers of their intention to provide care in the immediate newborn period with a letter of introduction detailing rationale for providing in-home care, and the reassurance that the midwife will provide them with copies of the records of the birth, newborn exams, postpartum course, and newborn screening results. In any situation that deviates from the normal newborn course, the midwife will contact the pediatric provider directly as well as referring the family to him/her. Frequently, care and follow-up in such cases results in collaborative care. 41,42 TRANSFER FROM HOME TO HOSPITAL Several prospective analyses of the outcomes of planned homebirths have described reasons for transfers from home to hospital before and after onset of labor at term. 2 6,8 In these studies, the rate of antepartum referrals for obstetric reasons (e.g., fetal growth restriction, previa, pregnancy-induced hypertension, twins, or preterm) for women who intended a planned homebirth ranges from 10% to 20%. Of those women who reached term without medical complications, 5% to 10% required intrapartum referrals, 1% postpartum maternal referrals, and 1% neonatal referrals. The large majority of these transfers occurred for nonemergent conditions (Table 3). The most common reason for transfer from home to hospital once labor has started is failure to progress. Johnson and Daviss 8 evaluated the outcomes of 5418 women who planned homebirths with certified professional midwives in North America. Twelve percent (n 655) were transferred to a hospital in the intrapartum or postpartum period. Of those women transferred during labor, 51.2% (n 323) were transferred for failure to progress in the first or second stage of labor. Murphy and Fullerton 5 conducted a prospective observational study describing outcomes of intended homebirths (N 1221) attended by CNMs. Of those beginning labor at home, 102 (8.3%) were transferred to the hospital in labor, more than half (n 63) for prolonged labor or rupture of membranes. Ten women (0.8%) were transferred postpartum and 14 (1.1%) infants were transferred. Intrapartum problems were positively associated with transfer to hospital-based care, and overall outcomes were consistent with expected outcomes for low-risk birth. When possible, the homebirth midwife encourages a birth site that is within 30 minutes of a hospital that provides obstetric and neonatal services. Once the woman enters the intrapartum period at home, the midwife may recommend a change in planned site of birth regardless of need for consultation or referral. The midwife must consider time required for and method of transfer, in light of whether safe and effective management would be adversely affected if maternal/fetal status changes while en route. The continuing role of the midwife will vary according to her status as a credentialed provider or a referring provider. If the woman is transferred for pain management or augmentation of labor, the midwife who is also on staff at the admitting hospital may remain as primary provider. If the same woman subsequently requires surgical intervention, the midwife will then consult and transfer care. She might provide solely supportive care or assist in the surgery recovery care. Ideally, the physician consultants are available to provide offsite consultation and assume collaborative or primary care role as necessary while still being willing to preserve as much of the birth plan as possible in the hospital setting. Joint reviews of transfers from home to hospital can inform ongoing collaboration and promote mutual respect. Families requiring an emergency transfer or prompt care for maternal or pediatric concerns will need extra support in the immediate postpartum period. Assistance with transport, physical support (rest, hydration, and food), emotional support, and guidance regarding unexpected hospital tests, routines, and treatments is invaluable. The perceived losses of normalcy and control and the loss of a low intervention birth experience can contribute to dissatisfaction and depression, especially if women are not allowed to participate in decision making. 43 Journal of Midwifery & Women s Health 295
6 Table 4. Common Intrapartum Indications for CNM/MD Consultation, Collaboration, and/or Referral During A Planned Homebirth in the United States Intrapartum and Immediate Postpartum Factors Evidence of fetal intolerance of labor Thick or particulate meconium-stained amniotic fluid with nonreassuring FHTS and/or lack of progress Breech or transverse fetus during labor Pharmaceutical induction or augmentation of labor Abnormal intrapartum bleeding Prolonged labor with no evidence of progress and/or evidence of maternal exhaustion Cord prolapse Maternal desire for pharmaceutical pain management Elevated maternal temperature with ruptured membranes Severe or persistent postpartum hemorrhage Retained placenta Congenital anomalies Newborn health status unstable Discretion of the midwife Intrapartum guidelines assume adequate time to initiate consultation. Emergent situations are stabilized and, if necessary, hospital transport is arranged. Exceptions to this list may be made taking religious exemptions into consideration. Adapted with permission from Jackson et al., eds. 27 MANAGEMENT OF INTRAPARTUM AND POSTPARTUM COMPLICATIONS Common intrapartum factors that require specialized midwifery management or consultation, collaborative care, or transfer are described in Table 4. While the reasons for most are self-explanatory, management recommendations for some conditions are affected by the evolving state of the evidence and the chosen birth place. Evidence of Fetal Intolerance of Labor Midwives in the home and in the hospital address significant fetal heart rate decelerations, tachycardia, and unexpected persistent bradycardias identically. If a nonreassuring fetal heart rate characteristic is heard, increasing the frequency and duration of auscultation is continued for several contractions to confirm if it is transitory or persistent. Simultaneously, interventions to improve uterine blood flow and fetal oxygenation are instituted, such as maternal position changes and hydration. Fetal scalp or acoustic stimulation may be performed to elicit a reassuring acceleration of the fetal heart. 44 Abdominal and/or vaginal exams may be indicated to diagnosis abruption, cord prolapse, precipitous descent, or malpresentation. If the fetal heart remains nonreassuring, the feasibility of timely transfer to a facility with continuous electronic fetal monitoring is evaluated. Consideration of stage of labor and imminence of delivery will influence the chosen course. If a persistent variant fetal heart rate pattern is identified in first-stage labor, transfer to hospital-based care may be the prudent plan. However, if delivery is imminent, preparing for possible neonatal resuscitation and encouraging delivery may be a better use of time and resources. An efficient resuscitation is best accomplished in a stable setting, not in a moving vehicle. The equipment and skill set that a homebirth midwife can provide for a term infant with a terminal bradycardia is identical to those available in most hospitals. Meconium Evidence-based management of the woman with meconium-stained amniotic fluid has evolved in the last decade. Level 1 evidence from prospective multicenter trials addressing the incidence of meconium aspiration syndrome in infants born through meconium-stained amniotic fluid suggests no benefit from amnioinfusion, endotracheal intubation, or intratracheal suctioning, especially in otherwise vigorous infants. 45,46 Potential harm associated with suctioning includes apnea, increased hypoxia, delay in resuscitation, damage of the upper airway, and cardiac arrhythmias. Community standards for care, however, may not yet acknowledge a change in recommendations. Application of the best available evidence (avoidance of suctioning) is possible and may be advisable in the home setting, but if transfer is subsequently affected, differing protocols in the receiving institution may lead to conflict. The development of meconium aspiration syndrome appears to be associated with intrauterine fetal hypoxia. In the context of thick or particulate meconium-stained amniotic fluid with nonreassuring fetal heart tones and/or lack of progress, the homebirth midwife initiates transfer unless birth is imminent. If delivery is imminent, the homebirth midwife prepares for potential resuscitation and ongoing vigilance for signs and symptoms of meconium aspiration syndrome. Typically, the infant with meconium aspiration syndrome will display symptoms of respiratory distress (e.g., nasal flaring, retractions, poor color, and an unwillingness to breastfeed), though in an otherwise vigorous term baby, these symptoms may develop over several hours. 47 Initiation of surfactant and/or nitrous oxide therapy within 12 hours of delivery may reduce hospital stays. 48 This information can guide the timing of transfer decisions when symptoms of meconium aspiration syndrome develop. Prolonged Labor Management of a long labor is another example of the gap between evidence and practice. Practice and hospital protocols frequently expect adherence to an expected partogram. The need to progress 1 cm/hour or deliver in 8 hours via active management of labor, or to deliver when staffing is available, has made time an outcome measure in itself. In the last 50 years, Friedman s definitions for normal length of labor have been widely adopted. However, Friedman s methodology has recently 296 Volume 52, No. 3, May/June 2007
7 come under scrutiny. His conclusions were based on plotting 500 individual labor curves and synthesizing them into one curve. 49 Zhang et al. 50 applied a statistical analysis to compare dilatation at various points during labor (repeated measures analysis) in nulliparous parturients who started labor spontaneously at term with singleton fetuses in a vertex presentation (N 1992). Women who had cesarean sections were excluded. 50 Labor patterns for the study subjects differed markedly from the Friedman curve, both in increased length and lack of manifestation of a deceleration phase. Several other investigators have reported that the normal lengths for each stage of labor are likely to be longer than Friedman described, without evidence of maternal or fetal compromise. 51,52 Janni 52 also noted that because the increased maternal morbidity in patients who have a prolonged second stage is partially a result of operative interventions, providers should not base active management solely on elapsed time. The evidence on maternal preference for active versus expectant management is conflicting, 26,53 but it is clear that patient involvement in decision making is associated with higher levels of satisfaction. 43 Some women experiencing a prolonged labor at home may wish to try all of the nonpharmacologic methods of augmentation before considering transfer to the hospital. Emerging evidence suggests that hydration and rest, followed by nipple stimulation, maternal position changes, acupuncture, and/or water immersion may be effective. 26,54,55 Albers 56 reviewed the conflicting data on the effects of ambulation and cited problems in methodology and confounders in many studies (e.g., randomized women switching groups, definition of ambulation, rules for bedrest, style of electronic fetal monitoring, and amniotomy). As prolonged labor is a nonurgent indication for transfer, some variation in choice can be supported. Immediate Postpartum Hemorrhage With advanced planning, immediate PPH is a complication that can usually be well managed in the home. Factors such as prolonged labor, grand multiparity, or rapid labor with a large infant may increase the risk of PPH. The homebirth midwife will have heightened sensitivity to such factors, may consider prophylactic transfer, and will have pharmaceuticals, syringes, intravenous supplies, and a urinary catheter immediately available. Evaluation and management of bleeding in the home is identical to hospital practice (e.g., digital compression and/or repair of lacerations, vaginal exploration, and assessment and treatment of atony). If there is inadequate response to therapy, emergency medical service is contacted for transport for hospital care. Transport in the case of moderate PPH is not always required. Sometimes, the midwife will summon emergency personnel but the hemorrhage will have responded to therapy before their arrival. In this case, the midwife and family will determine advisability of transport dependent on the current maternal status and prognosis. If the uterus is well contracted, the sources of bleeding have been addressed, the infant is nursing well, the vital signs are stable, and the mother is able to engage in self-care without syncope, she may remain on bed rest at home. To assure stability, the midwife usually remains in the home for several hours more than usual. Prophylactic infusion of one or two liters of intravenous fluid and/or a prescription for a postpartum oral oxytocic agent may be provided, especially in the context of homebirth and the absence of continuous nursing care. Unstable Newborn Assessment of respiratory and cardiac status of the newborn begins immediately after the birth in all settings. Both hospital and homebirth providers evaluate and treat infants with poor or absent respiratory effort according to American Academy of Pediatrics/Neonatal Resuscitation Program standards. Recent evidence indicates initiation of bag and mask ventilation with room air may be more effective than with 100% oxygen. 57 Regardless, the oxygen tank can be attached to the tubing and tested for flow before the birth. The reservoir bag can be detached and placed next to the tank with the stethoscope, so that should the addition of oxygen or cardiac assessment be necessary, they are easily accessible. Warmth can be provided continuously with the use of space heaters, the tray prepared with heating pad and receiving blankets, or with foil transport bunting. Emergency services are called for any infant who does not rapidly respond to resuscitation efforts. Signs of the inability to maintain respiratory health, thermoregulation, hypoglycemia, birth injury, or inability to suckle are all indicators for additional vigilance, supportive therapy, and pediatric consultation if unresolved. Some conditions will resolve spontaneously in the first 24 hours with supportive therapy. For example, transient tachypnea of the newborn is usually selflimiting, but may require the presence of and monitoring by the midwife for an extended period of time. In these cases, the choice of the site of care is made collaboratively between the family, the midwife, and the pediatric provider. Congenital Anomalies Some clients seeking homebirth services decline prenatal testing, such as ultrasound, first trimester screening, and/or amniocentesis. This requires the midwife to be prepared for a wide range of uncommon anomalies, which may not be immediately life-threatening but require prompt transport and evaluation. For an infant who has established adequate oxygenation and perfusion, there is usually a brief visual assessment as the infant Journal of Midwifery & Women s Health 297
8 begins to nurse. Infants with cardiac problems often have difficulty simultaneously nursing and breathing. These infants need immediate hospital care. The goal for managing newborns with anatomical anomalies, including gastroschisis, omphalocele, exstrophy of the bladder, or open spinal cord defects is to keep exposed areas moist with sterile saline and gauze, and covered with plastic wrap to maintain moisture, heat, and decrease contamination. The infant should be positioned to support the defect (e.g., prone for Pierre Robins syndrome) while transport is completed. 42 Any infant presenting significant findings outside the normal range requires a consult with the pediatric caregiver. Stable infants presenting with orthopedic anomalies or chromosomal disorders (e.g., a cleft lip/palate, Down s syndrome, or a club foot) may not need immediate pediatric evaluation but may need extra midwifery support and care during the first 24 hours. The infant s condition, the physical exam, and type of indicated therapy will help determine the timing, setting, and appropriate caregiver for care and/or consultation. INFORMED CHOICE Informed decision-making is an essential characteristic of midwifery care. CNMs/CMs who practice in the home setting need to have a clear understanding of the legal and ethical basis of informed decision making. The goal is to provide the laboring woman with the information necessary for her to make an informed choice. The core elements of informed consent include a discussion of the indications for the intervention, a description of the probable benefits and probable risks associated with the recommended intervention, a discussion of alternative interventions, and a description of the consequences of declining the recommended intervention. In the context of homebirth, the consequences may include conflict with community providers who prefer adherence to an established protocol. Truly informed choice also requires that a patient be informed when there is little or no evidence to support a particular intervention, or when there is a gap between evidence and standard community practice. This may become particularly relevant when discussing when and if to transfer to the hospital, and what can be expected. 58 Many homebirth clients will have had both the time and inclination to research all options for care, and will be aware of community standards that do not follow the best available evidence. The courts have repeatedly upheld a patient s right to refuse treatment, even if not treating may result in serious morbidity or mortality, based on the belief that only the patient can understand her own priorities. Acknowledging this, the American College of Obstetricians and Gynecologists issued a committee opinion in 2004 on informed refusal, stating that once risks, benefits, and alternatives have been explained, a woman has the right to exercise full autonomy in making an informed decision, which includes informed refusal. 59 An individual s assessment of risk is based on both fact and emotion. Risk is most effectively communicated when the informant is perceived as being both competent and caring, supportive, and empathetic, all of which engenders trust. 60 For the homebirth midwife, the development of mutual trust and a collaborative relationship with the family is an essential goal, developed over the course of pregnancy through prenatal visits that allow ample time for discussion of medical, psychosocial, and family issues. The joint plan for the intrapartum care of the woman and baby at home acknowledges the family and the midwife as the core health care team, and accounts for individual and cultural differences in priorities for management. Antepartum discussions about variations from normal, transfer protocols, and birth site selection can minimize the possibility of conflict when essential decisions need to be made during the intrapartum period. LESSONS IN PROMOTING NORMAL BIRTH ACROSS SETTINGS When midwives assume the primary management role, they are required to utilize the full scope of the ACNM core competencies. 20 Midwives in many hospitals are independently responsible for assessment, diagnosis, and initiation of therapy, even as they arrange for staff assistance, physician consultation, or collaborative care. Their competencies and judgment are deemed adequate to promote optimal outcomes. However, variations among hospitals in CNM/CM credentialing for specific procedures (e.g., repair of lacerations, manual removal of the placenta) may restrict a CNM s/cm s ability to independently manage these patients, even though such management is within her scope of practice. Within hospital settings, the ability to receive instant technologic assistance is the safety net that provides reassurance to the provider. The presence of pediatric staff at birth, required by some hospitals, may decrease the midwife s role in newborn care, resulting in a lack of confidence in applying neonatal skills. Although trained in resuscitation, without practice, a midwife may experience apprehension when required to use the skill. Regardless, instant access to technology and specialized staff has not eliminated perinatal mortality and morbidity, even for the lowest-risk women managed in the hospital. Skilled providers must use technology correctly and judiciously to improve obstetric outcomes in any setting. Familiarity with changes in midwifery practice, based upon emerging evidence that supports the reduced use of an intervention, may be difficult to acquire within an institution that has not updated its protocols. Midwives practicing in homes and midwife-managed birth centers can implement evidence-based management and new procedures more rapidly. The philosophic tenets of the 298 Volume 52, No. 3, May/June 2007
9 hallmarks of midwifery 20 include the advocacy of nonintervention in the absence of complications, the incorporation of scientific evidence into clinical practice, and advocacy for informed choice, shared decision-making, and the right to self-determination. Continuity of care and continuous labor presence is inherent in homebirth midwifery practice. Exposure to process and protocols within autonomous practices in out-of-hospital settings may provide opportunities for midwives to reduce the theory practice gap. REFERENCES 1. Vedam S. Homebirth versus hospital birth: Questioning the quality of the evidence on safety. Birth 2003;30: Ackermann-Liebrich U, Voegeli T, Gunter-Witt K, Kunz I, Zullig M, Schindler C, et al. Home versus hospital deliveries: Follow up study of matched pairs for procedures and outcome. BMJ 1996;313: Davies J, Hey E, Reid W, Young G. Prospective regional study of planned homebirths. BMJ 1996;313: Wiegers TA, Keirse MJNC, van der Zee J, Berghs GAH. Outcome of planned home and planned hospital births in low risk pregnancies: Prospective study in midwifery practices in the Netherlands. BMJ 1996;313: Murphy PA, Fullerton J. Outcomes of intended homebirths in nurse-midwifery practice: A prospective descriptive study. Obstet Gynecol 1998;92: Janssen PA, Lee SK, Ryan EM, Etches DJ, Farquharson DF, Peacock D, et al. Outcomes of planned homebirths versus planned hospital births after regulation of midwifery in British Columbia. CMAJ 2002;166: Chamberlain G, Wraight A, Crowley P. Homebirths: Report of the 1994 confidential enquiry of the National Birthday Trust Fund. Cranforth, UK: Parthenon, Johnson KC, Daviss BA. Outcomes of planned homebirths with certified professional midwives: Large prospective study in North America. BMJ 2005;330: Hodnett ED, Downe S, Edwards N, Walsh D. Home-like versus conventional institutional settings for birth. Cochrane Database Syst Rev 2005;1:CD Neuhaus W, Piroth C, Kiencke P, Gohring UJ, Mallman P. A psychosocial analysis of women planning birth outside hospital. J Obstet Gynaecol 2002;22: Olsen O. Meta-analysis of the safety of homebirth. Birth 1997;24: Anderson RE, Anderson DA. The cost-effectiveness of homebirth. J Nurse Midwifery 1999;44: World Health Organization. Care in normal birth: A practical guide. Geneva: World Health Organization, Governing Council of the American Public Health Association. Policy statement no : Increasing access to out-ofhospital maternity care services through state-regulated and nationally-certified direct-entry midwives. Washington, DC: American Public Health Association, American College of Nurse Midwives. Criteria for provision of homebirth services. ACNM Clinical Practice Bulletin #7. J Midwifery Womens Health 2003;48: Schuiling KD, Sipe TA, Fullerton J. Findings from the analysis of the American College of Nurse-Midwives membership surveys: J Midwifery Womens Health 2005;50: Declercq E. Percentage of live births attended by CNMs in the United States, J Midwifery Womens Health 2004; 49: Martin JA, Hamilton BE, Sutton PD, Ventura SJ, Menacker F, Kirmeyer S. Births: Final data for Natl Vital Stat Rep 2006;55: Lange G, Kennedy HP. Student perceptions of ideal and actual midwifery practice. J Midwifery Womens Health 2006;51: American College of Nurse-Midwives. The ACNM core competencies for basic midwifery practice. Washington, DC: ACNM, Vedam S. Birth site selection and client responsibilities. In Jackson ME, Bailes A, eds. ACNM homebirth practice handbook, 2nd edition. Silver Spring, MD: American College of Nurse- Midwives, 2004: Leighton BL, Halpern SH. The effects of epidural analgesia on labor, maternal, and neonatal outcomes: A systematic review. Am J Obstet Gynecol 2002;186:S Lieberman E, O Donoghue C. Unintended effects of epidural analgesia during labor: A systematic review. Am J Obstet Gynecol 2002;186:S Sheiner E, Segal D, Shoham-Vardi I, Ben-Tov J, Katz M, Mazor M. The impact of early amniotomy on mode of delivery and pregnancy outcome. Arch Gynecol Obstet 2000;264: Serkin M, Porte J, Monheit A. The relationship of antepartum pelvic exams to the incidence of premature rupture of membranes, maternal infection and caesarean section. Paper given at the Scientific Session of the Annual Clinical Meeting of the American College of Obstetricians and Gynecologists, Simkin P, Bolding A. Update on nonpharmacologic approaches to relieve labor pain and prevent suffering. J Midwifery Womens Health 2004;49: Equipment, skills, and birth assistants. In Jackson ME, Bailes A, eds. ACNM homebirth practice handbook, 2nd edition. Silver Spring, MD: American College of Nurse-Midwives, Cioffi J. Caring for women from culturally diverse backgrounds: Midwives experiences. J Midwifery Womens Health 2004;49: Lim R. Second stage... the chewing of angel s wings. Midwifery Today Int Midwife 2000; Esposito NW. Marginalized women s comparisons of their hospital and freestanding birth center experiences: A contrast of inner-city birthing systems. Health Care Women Int 1999;20: Saisto T. Norepinephrine, adrenocorticotropin, cortisol and beta-endorphin in women suffering from fear of labor: Responses to the cold pressor test during and after pregnancy. Acta Obstet Gynecol Scand 2004;83: Journal of Midwifery & Women s Health 299
10 32. Green JM, Baston HA. Feeling in control during labor: Concepts, correlates, and consequences. Birth 2003;30: American College of Obstetricians and Gynecologists. Intrapartum fetal heart rate monitoring. ACOG Practice Bulletin #70. Obstet Gynecol 2005;106: Mikkola C. Evidence-based midwifery: Listening to fetal heart tones. Midwifery Today 2003; American College of Nurse-Midwives. ACNM position statement: Homebirth. Silver Spring, MD: ACNM, Howell EA, Mora P, Leventhal H. Correlates of early postpartum depressive symptoms. Matern Child Health J 2006;10: Beck CT. Postpartum depression: It isn t just the blues. Am J Nurs 2006;106:40, Lawrence RA. Breastfeeding: Benefits, risks and alternatives. Curr Opin Obstet Gynecol 2000;12: Groer MW. Differences between exclusive breastfeeders, formula-feeders, and controls: A study of stress, mood, and endocrine variables. Biol Res Nurs 2005;7: Groer MW, Davis MW, Smith K, Casey K, Kramer V, Bukovsky E. Immunity, inflammation and infection in post-partum breast and formula feeders. Am J Reprod Immunol 2005;54: Townsend J, Wolke D, Hayes J, Dave S, Rogers C, Bloomfield L, et al. Routine examination of the newborn: The EMREN study. Evaluation of an extension of the midwife role including a randomised controlled trial of appropriately trained midwives and paediatric senior house officers. Health Technol Assess 2004;8: Sullivan NH, Witte M. Care of the at-risk neonate born at home. A model for nurse-midwife/physician collaboration. J Nurse Midwifery 1995;40: Hodnett ED. Pain and women s satisfaction with the experience of childbirth: A systematic review. Am J Obstet Gynecol 2002;186:S Skupski DW, Rosenberg CR, Eglinton GS. Intrapartum fetal stimulation tests: A meta-analysis. Obstet Gynecol 2002;99: Halliday HL, Sweet D. Endotracheal intubation at birth for preventing morbidity and mortality in vigorous, meconium-stained infants born at term. Cochrane Database Syst Rev 2001; 1:CD Fraser WD, Hofmeyr J, Lede R, Faron G, Alexander S, Goffinet F, et al. Amnioinfusion for the prevention of the meconium aspiration syndrome. N Engl J Med 2005;353: Kumar A, Bhat BV. Epidemiology of respiratory distress of newborns. Indian Pediatr 1996;63: Salvia-Roiges MD, Carbonell-Estrany X, Figueras-Aloy J, Rodriguez-Miguelez JM. Efficacy of three treatment schedules in severe meconium aspiration syndrome. Acta Paediatr 2004;93: Freidman EA. Labor: Clinical evaluation and management, 2nd edition. New York: Appleton-Century-Crofts, Zhang J, Troendle JF, Yancey MK. Reassessing the labor curve in nulliparous women. Am J Obstet Gynecol 2002;187: Albers LL. The duration of labor in healthy women. J Perinatol 1999;19: Janni W, Schiessl B, Peschers U, Huber S, Strobl B, Hantschmann P, et al. The prognostic impact of a prolonged second stage of labor on maternal and fetal outcome. Acta Obstet Gynecol Scand 2002;81: Lavender T, Wallymahmed AH, Walkinshaw SA. Managing labor using partograms with different action lines: A prospective study of women s views. Birth 1999;26: Cluett ER, Nikodem VC, McCandlish RE, Burns EE. Immersion in water in pregnancy, labour and birth. Cochrane Database Syst Rev 2002;2:CD Kavanagh J, Kelly AJ, Thomas J. Breast stimulation for cervical ripening and induction of labour. Cochrane Database Syst Rev 2005;3:CD Albers LL, Anderson D, Cragin L, Daniels SM, Hunter C, Sedler KD, et al. The relationship of ambulation in labor to operative delivery. J Nurse Midwifery 1997;42: Wolkoff LI, Narula P. Issues in neonatal and pediatric oxygen therapy. Respir Care Clin N Am 2000 Dec;6: Spindel PG, Suarez SH. Informed consent and homebirth. J Nurse Midwifery 1995;40: American College of Obstetricians and Gynecologists. ACOG Committee Opinion #306: Informed refusal. Obstet Gynecol 2004;104: Paling J. Strategies to help patients understand risks. BMJ 2003;327: Volume 52, No. 3, May/June 2007
Certified Professional Midwives Caring for Mothers and Babies in Virginia
 Certified Professional Midwives Caring for Mothers and Babies in Virginia Commonwealth Midwives Alliance Certified Professional Midwives in VA Licensed by the BOM since January 2006 5 member Midwifery
Certified Professional Midwives Caring for Mothers and Babies in Virginia Commonwealth Midwives Alliance Certified Professional Midwives in VA Licensed by the BOM since January 2006 5 member Midwifery
Women's Circle Nurse-Midwife Services Inc. Angela Kreider CNM, MSN 1003 Plumas Street Yuba City, CA 95991 (530)751-2273 FAX (530)751-2274
 Women's Circle Nurse-Midwife Services Inc. Angela Kreider CNM, MSN 1003 Plumas Street Yuba City, CA 95991 (530)751-2273 FAX (530)751-2274 Informed Disclosure and Consent The following consent explains
Women's Circle Nurse-Midwife Services Inc. Angela Kreider CNM, MSN 1003 Plumas Street Yuba City, CA 95991 (530)751-2273 FAX (530)751-2274 Informed Disclosure and Consent The following consent explains
Registered Midwife Clinical Privileges REAPPOINTMENT 2015-2016 Effective from July 1, 2015 to June 30, 2016
 Name: Initial privileges (initial appointment) Renewal of privileges (reappointment) All new applicants must meet the following requirements as approved by the governing body, effective: 04/Jun/2013. Applicant:
Name: Initial privileges (initial appointment) Renewal of privileges (reappointment) All new applicants must meet the following requirements as approved by the governing body, effective: 04/Jun/2013. Applicant:
Oregon Birth Outcomes, by Planned Birth Place and Attendant Pursuant to: HB 2380 (2011)
 Oregon Birth Outcomes, by Birth Place and Attendant Pursuant to: HB 2380 (2011) In 2011, the Oregon Legislature passed House Bill 2380, which required the Oregon Public Health Division to add two questions
Oregon Birth Outcomes, by Birth Place and Attendant Pursuant to: HB 2380 (2011) In 2011, the Oregon Legislature passed House Bill 2380, which required the Oregon Public Health Division to add two questions
UNMH Certified Nurse-Midwife (CNM) Clinical Privileges
 All new applicants must meet the following requirements as approved by the UNMH Board of Trustees effective: 03/27/2015 INSTRUCTIONS Applicant: Check off the "Requested" box for each privilege requested.
All new applicants must meet the following requirements as approved by the UNMH Board of Trustees effective: 03/27/2015 INSTRUCTIONS Applicant: Check off the "Requested" box for each privilege requested.
Chapter 14. Board of Certified Direct-Entry Midwives.
 Chapter 14. Board of Certified Direct-Entry Midwives. (Words in boldface and underlined indicate language being added; words [CAPITALIZED AND BRACKETED] indicate language being deleted. Complete new sections
Chapter 14. Board of Certified Direct-Entry Midwives. (Words in boldface and underlined indicate language being added; words [CAPITALIZED AND BRACKETED] indicate language being deleted. Complete new sections
Obstetrical Emergencies
 Date: July 18, 2014 Page 1 of 5 Obstetrical Emergencies Purpose: To provide the process for the assessment and management of the patient with an obstetrical related emergency. Pre-Medical Control 1. Follow
Date: July 18, 2014 Page 1 of 5 Obstetrical Emergencies Purpose: To provide the process for the assessment and management of the patient with an obstetrical related emergency. Pre-Medical Control 1. Follow
Water Birth Online Course. Women s Services
 Water Birth Online Course Women s Services 1 Water Birth Instructions for Online Class 1. Read through all the slides. 2. Print out the certificate at the end of the slides. 3. Sign and date the certificate.
Water Birth Online Course Women s Services 1 Water Birth Instructions for Online Class 1. Read through all the slides. 2. Print out the certificate at the end of the slides. 3. Sign and date the certificate.
Registered Nurse Initiated Activities Decision Support Tool No. 8A: Obstetrical Emergencies Cord Prolapse
 Registered Nurse Initiated Activities Decision Support Tool No. 8A: Obstetrical Emergencies Cord Prolapse Decision support tools are evidenced-based documents used to guide the assessment, diagnosis and
Registered Nurse Initiated Activities Decision Support Tool No. 8A: Obstetrical Emergencies Cord Prolapse Decision support tools are evidenced-based documents used to guide the assessment, diagnosis and
KENTUCKY BOARD OF NURSING 312 Whittington Parkway, Suite 300 Louisville, Kentucky 40222-5172 http://kbn.ky.gov ADVISORY OPINION STATEMENT
 (Revised 4/2016) KENTUCKY BOARD OF NURSING 312 Whittington Parkway, Suite 300 Louisville, Kentucky 40222-5172 http://kbn.ky.gov ADVISORY OPINION STATEMENT ROLES OF NURSES IN THE CARE OF PRENATAL AND INTRAPARTUM
(Revised 4/2016) KENTUCKY BOARD OF NURSING 312 Whittington Parkway, Suite 300 Louisville, Kentucky 40222-5172 http://kbn.ky.gov ADVISORY OPINION STATEMENT ROLES OF NURSES IN THE CARE OF PRENATAL AND INTRAPARTUM
Renown Regional Medical Center Department Of Obstetrics and Gynecology. Policies and Procedures Certified Nurse Midwives ( CNM S)
 1. Overview: Department Of Obstetrics and Gynecology Policies and Procedures Certified Nurse Midwives ( CNM S) supports the practice of Nurse Midwifery and will participate with Certified Nurse Midwives
1. Overview: Department Of Obstetrics and Gynecology Policies and Procedures Certified Nurse Midwives ( CNM S) supports the practice of Nurse Midwifery and will participate with Certified Nurse Midwives
PROGRAMA PART PROGRAMME Birth Plan
 PART: Programa d Atenció i Respecte al part HospiTalari Servei de Medicina Maternofetal. Institut Clínic de Ginecologia, Obstetrícia i Neonatologia (ICGON) Servei d Anestesiologia, Reanimació i Terapèutica
PART: Programa d Atenció i Respecte al part HospiTalari Servei de Medicina Maternofetal. Institut Clínic de Ginecologia, Obstetrícia i Neonatologia (ICGON) Servei d Anestesiologia, Reanimació i Terapèutica
My Birth Experience at Mercy
 My Birth Experience at Mercy This booklet provides information about labor and birth practices at Mercy and includes an optional birth plan that you can complete prior to your baby s birth. Discuss your
My Birth Experience at Mercy This booklet provides information about labor and birth practices at Mercy and includes an optional birth plan that you can complete prior to your baby s birth. Discuss your
American Academy of Pediatrics Section on Breastfeeding. Ten Steps to Support Parents Choice to Breastfeed Their Baby
 American Academy of Pediatrics Section on Breastfeeding 1 2 3 4 5 6 7 8 9 10 Ten Steps to Support Parents Choice to Breastfeed Their Baby This practice enthusiastically supports parents plans to breastfeed
American Academy of Pediatrics Section on Breastfeeding 1 2 3 4 5 6 7 8 9 10 Ten Steps to Support Parents Choice to Breastfeed Their Baby This practice enthusiastically supports parents plans to breastfeed
Clinical Policy Title: Home uterine activity monitoring
 Clinical Policy Title: Home uterine activity monitoring Clinical Policy Number: 12.01.01 Effective Date: August 19, 2015 Initial Review Date: July 17, 2013 Most Recent Review Date: July 15, 2015 Next Review
Clinical Policy Title: Home uterine activity monitoring Clinical Policy Number: 12.01.01 Effective Date: August 19, 2015 Initial Review Date: July 17, 2013 Most Recent Review Date: July 15, 2015 Next Review
Want to know. more. about. midwives? Promoting social change through policy-based research in women s health
 Want to know more midwives? about Promoting social change through policy-based research in women s health What is a midwife? A midwife is a health care professional who provides care to women throughout
Want to know more midwives? about Promoting social change through policy-based research in women s health What is a midwife? A midwife is a health care professional who provides care to women throughout
Maj Alison Baum. R3, Nellis FMR
 Maj Alison Baum R3, Nellis FMR What are some of your thoughts about birth plans? http://www.youtube.com/watch?v=hh62v0c xf04 Labor: Pain management wishes Doulas Episiotomy Intermittent fetal monitoring
Maj Alison Baum R3, Nellis FMR What are some of your thoughts about birth plans? http://www.youtube.com/watch?v=hh62v0c xf04 Labor: Pain management wishes Doulas Episiotomy Intermittent fetal monitoring
Why is prematurity a concern?
 Prematurity What is prematurity? A baby born before 37 weeks of pregnancy is considered premature. Approximately 12% of all babies are born prematurely. Terms that refer to premature babies are preterm
Prematurity What is prematurity? A baby born before 37 weeks of pregnancy is considered premature. Approximately 12% of all babies are born prematurely. Terms that refer to premature babies are preterm
MANA Home Birth Data 2004-2009: Consumer Considerations
 MANA Home Birth Data 2004-2009: Consumer Considerations By: Lauren Korfine, PhD U.S. maternity care costs continue to rise without evidence of improving outcomes for women or babies. The cesarean section
MANA Home Birth Data 2004-2009: Consumer Considerations By: Lauren Korfine, PhD U.S. maternity care costs continue to rise without evidence of improving outcomes for women or babies. The cesarean section
EmONC Training Curricula Comparison
 EmONC Training Curricula Comparison The purpose of this guide is to provide a quick resource for trainers and course administrators to decide which EmONC curriculum is most applicable to their training
EmONC Training Curricula Comparison The purpose of this guide is to provide a quick resource for trainers and course administrators to decide which EmONC curriculum is most applicable to their training
Certified Nurse-Midwife and Women s Health Care Nurse Practitioner
 Certified Nurse-Midwife and Women s Health Care Nurse Practitioner Practice Agreements at Chicago Revised March 2007 TABLE OF CONTENTS SIGNATURES OF AGREEMENT 3 ORGANIZATION RELATIONSHIPS AND MEMBERSHIP
Certified Nurse-Midwife and Women s Health Care Nurse Practitioner Practice Agreements at Chicago Revised March 2007 TABLE OF CONTENTS SIGNATURES OF AGREEMENT 3 ORGANIZATION RELATIONSHIPS AND MEMBERSHIP
Regions Hospital Delineation of Privileges Certified Nurse Midwife
 Regions Hospital Delineation of Privileges Certified Nurse Midwife Applicant s Name: Last First M. Instructions: Place a check-mark where indicated for each core group you are requesting. Review education
Regions Hospital Delineation of Privileges Certified Nurse Midwife Applicant s Name: Last First M. Instructions: Place a check-mark where indicated for each core group you are requesting. Review education
Who Is Involved in Your Care?
 Patient Education Page 3 Pregnancy and Giving Birth Who Is Involved in Your Care? Our goal is to surround you and your family with a safe environment for the birth of your baby. We look forward to providing
Patient Education Page 3 Pregnancy and Giving Birth Who Is Involved in Your Care? Our goal is to surround you and your family with a safe environment for the birth of your baby. We look forward to providing
Welcome. Client Satisfaction
 930 Martin Luther King Jr. Blvd., Suite 202, Chapel Hill, NC 27514 Tel: 919-933-3301 Fax: 919-933-3375 www.ncbirthcenter.com Welcome Welcome to Women s Birth & Wellness Center. WBWC was incorporated as
930 Martin Luther King Jr. Blvd., Suite 202, Chapel Hill, NC 27514 Tel: 919-933-3301 Fax: 919-933-3375 www.ncbirthcenter.com Welcome Welcome to Women s Birth & Wellness Center. WBWC was incorporated as
Neonatal Emergencies. Care of the Neonate. Care of the Neonate. Care of the Neonate. Student Objectives. Student Objectives continued.
 Student Objectives Neonatal Emergencies After completing this section the student will be able to: 1. Identify three physiologic and/or anatomic features unique to the newborn 2. List three perinatal factors
Student Objectives Neonatal Emergencies After completing this section the student will be able to: 1. Identify three physiologic and/or anatomic features unique to the newborn 2. List three perinatal factors
What Every Pregnant Woman Needs to Know About Cesarean Section. Be informed. Know your rights. Protect yourself. Protect your baby.
 Be informed. Know your rights. Protect yourself. Protect your baby. What Every Pregnant Woman Needs to Know About Cesarean Section 2012 Childbirth Connection If you re expecting a baby, there s a good
Be informed. Know your rights. Protect yourself. Protect your baby. What Every Pregnant Woman Needs to Know About Cesarean Section 2012 Childbirth Connection If you re expecting a baby, there s a good
A8b. Resuscitation of a Term Infant with Meconium Staining. Session Summary. Session Objectives. References
 A8b Resuscitation of a Term Infant with Meconium Staining Karen Wright, PhD, NNP-BC Assistant Professor and Coordinator, Neonatal Nurse Practitioner Program Dept. of Women, Children, and Family Nursing,
A8b Resuscitation of a Term Infant with Meconium Staining Karen Wright, PhD, NNP-BC Assistant Professor and Coordinator, Neonatal Nurse Practitioner Program Dept. of Women, Children, and Family Nursing,
Home Health Agencies. Ante & Postpartum Members
 FIRST PRIORITY HEALTH /FIRST PRIORITY LIFE INSURANCE COMPANY BLUE CROSS OF NORTHEASTERN PENNSYLVANIA CREDENTIALING CRITERIA FOR OBSTETRIC NURSES IN HOME CARE ADMINISTRATIVE PRACTICE GUIDELINE PROVIDER
FIRST PRIORITY HEALTH /FIRST PRIORITY LIFE INSURANCE COMPANY BLUE CROSS OF NORTHEASTERN PENNSYLVANIA CREDENTIALING CRITERIA FOR OBSTETRIC NURSES IN HOME CARE ADMINISTRATIVE PRACTICE GUIDELINE PROVIDER
How To Choose Between A Vaginal Birth Or A Cesarean Section
 Be informed. Know your rights. Protect yourself. Protect your baby. What Every Pregnant Woman Needs to Know About Cesarean Section 2012 Childbirth Connection If you re expecting a baby, there s a good
Be informed. Know your rights. Protect yourself. Protect your baby. What Every Pregnant Woman Needs to Know About Cesarean Section 2012 Childbirth Connection If you re expecting a baby, there s a good
Patient & Family Guide Pre-Existing Diabetes and Pregnancy
 Patient & Family Guide Pre-Existing Diabetes and Pregnancy Center for Perinatal Care Meriter Hospital 202 S. Park Street Madison, WI 53715 608.417.6667 meriter.com 09/12/1000 A Meriter Hospital and University
Patient & Family Guide Pre-Existing Diabetes and Pregnancy Center for Perinatal Care Meriter Hospital 202 S. Park Street Madison, WI 53715 608.417.6667 meriter.com 09/12/1000 A Meriter Hospital and University
POLICIES AND PROCEDURES
 Purpose: To establish guidelines for the clinical practice of Nurse Midwives. Policy: The Central California Alliance for Health (the Alliance) requires all Nurse Midwives to meet the Alliance s guidelines
Purpose: To establish guidelines for the clinical practice of Nurse Midwives. Policy: The Central California Alliance for Health (the Alliance) requires all Nurse Midwives to meet the Alliance s guidelines
Obstetric Guideline 6B ELECTRONIC FETAL MONITORING IN LABOUR, SCALP SAMPLING, & CORD BLOOD GASES
 British Columbia Reproductive Care Program Obstetric Guideline 6B ELECTRONIC FETAL MONITORING IN LABOUR, SCALP SAMPLING, & CORD BLOOD GASES 1. PREAMBLE Meta-analysis of randomized clinical trials 1,2 indicate
British Columbia Reproductive Care Program Obstetric Guideline 6B ELECTRONIC FETAL MONITORING IN LABOUR, SCALP SAMPLING, & CORD BLOOD GASES 1. PREAMBLE Meta-analysis of randomized clinical trials 1,2 indicate
Obstetrical units should develop a procedure for archiving the fetal monitoring tracings within their own institution.
 The following guidelines are intended only as a general educational resource for hospitals and clinicians, and are not intended to reflect or establish a standard of care or to replace individual clinician
The following guidelines are intended only as a general educational resource for hospitals and clinicians, and are not intended to reflect or establish a standard of care or to replace individual clinician
CDC National Survey of Maternity Practices in Infant Nutrition and Care (mpinc)
 OMB #0920-0743 EXP. DATE: 10/31/2010 CDC National Survey of Maternity Practices in Infant Nutrition and Care (mpinc) Hospital Survey Conducted for Centers for Disease Control and Prevention National Center
OMB #0920-0743 EXP. DATE: 10/31/2010 CDC National Survey of Maternity Practices in Infant Nutrition and Care (mpinc) Hospital Survey Conducted for Centers for Disease Control and Prevention National Center
Delayed Cord Clamping
 ICEA Position Paper Delayed Cord Clamping Position The International Childbirth Education Association recognizes that the first minutes after birth are crucial to both mother and newborn. Optimal care
ICEA Position Paper Delayed Cord Clamping Position The International Childbirth Education Association recognizes that the first minutes after birth are crucial to both mother and newborn. Optimal care
Newborn outcomes after cesarean section for fetal distress in BC
 Newborn outcomes after cesarean section for fetal distress in BC Patricia Janssen, PhD, UBC School of Population and Public Health Scientist, Child and Family Research Institute Kevin Jenniskens, MSc,
Newborn outcomes after cesarean section for fetal distress in BC Patricia Janssen, PhD, UBC School of Population and Public Health Scientist, Child and Family Research Institute Kevin Jenniskens, MSc,
8/27/2013 ENHANCING PHYSIOLOGIC BIRTH FOR HIGH RISK MOTHERS. Who are high risk mothers?
 ENHANCING PHYSIOLOGIC BIRTH FOR HIGH RISK MOTHERS Cecilia Jevitt, CNM, PhD, FACNM Yale School of Nursing Midwifery Specialty Coordinator Why give it a second thought? Improve labor & birth experience for
ENHANCING PHYSIOLOGIC BIRTH FOR HIGH RISK MOTHERS Cecilia Jevitt, CNM, PhD, FACNM Yale School of Nursing Midwifery Specialty Coordinator Why give it a second thought? Improve labor & birth experience for
GENERAL ASSEMBLY OF NORTH CAROLINA SESSION 2013 S 1 SENATE BILL 499. Short Title: Update/Modernize/Midwifery Practice Act.
 GENERAL ASSEMBLY OF NORTH CAROLINA SESSION S 1 SENATE BILL Short Title: Update/Modernize/Midwifery Practice Act. (Public) Sponsors: Senators Hartsell, Randleman, Stein (Primary Sponsors); Cook, D. Davis,
GENERAL ASSEMBLY OF NORTH CAROLINA SESSION S 1 SENATE BILL Short Title: Update/Modernize/Midwifery Practice Act. (Public) Sponsors: Senators Hartsell, Randleman, Stein (Primary Sponsors); Cook, D. Davis,
H-140.970 Decisions to Forgo Life-Sustaining Treatment for Incompetent Patients
 WMS policy: ETH-026 Medical Neglect and Child Abuse (Baby Doe): The Wisconsin Medical Society opposes any change to the Wisconsin Child Abuse Law that would include the federal definition of withholding
WMS policy: ETH-026 Medical Neglect and Child Abuse (Baby Doe): The Wisconsin Medical Society opposes any change to the Wisconsin Child Abuse Law that would include the federal definition of withholding
Fairview Health Services CERTIFIED NURSE MIDWIFE Delineation of Privileges CROSSWALK FOR REQUESTING FAIRVIEW PRIVILEGES
 PAGE 1 OF 4 Fairview Health Services CERTIFIED NURSE MIDWIFE Delineation of Privileges Applicant s Name (please print): CROSSWALK FOR REQUESTING FAIRVIEW PRIVILEGES I Want to Work at the Following Fairview
PAGE 1 OF 4 Fairview Health Services CERTIFIED NURSE MIDWIFE Delineation of Privileges Applicant s Name (please print): CROSSWALK FOR REQUESTING FAIRVIEW PRIVILEGES I Want to Work at the Following Fairview
General and Objectives Clinical Skills for. Nursing Students in Maternity and Gynecology. Nursing Department
 General and Objectives Clinical Skills for Nursing Students in Maternity and Gynecology Nursing Department Objectives and clinical skills of Antenatal unit Provide antenatal care to woman during normal
General and Objectives Clinical Skills for Nursing Students in Maternity and Gynecology Nursing Department Objectives and clinical skills of Antenatal unit Provide antenatal care to woman during normal
Position Paper: The Birth Doula s Contribution to Modern Maternity Care
 Position Paper: The Birth Doula s Contribution to Modern Maternity Care The birth of each baby has a long lasting impact on the physical and mental health of mother, baby and family. In the twentieth century,
Position Paper: The Birth Doula s Contribution to Modern Maternity Care The birth of each baby has a long lasting impact on the physical and mental health of mother, baby and family. In the twentieth century,
Rural Health Advisory Committee s Rural Obstetric Services Work Group
 Rural Health Advisory Committee s Rural Obstetric Services Work Group March 15 th webinar topic: Rural Obstetric Patient and Community Issues Audio: 888-742-5095, conference code 6054760826 Rural Obstetric
Rural Health Advisory Committee s Rural Obstetric Services Work Group March 15 th webinar topic: Rural Obstetric Patient and Community Issues Audio: 888-742-5095, conference code 6054760826 Rural Obstetric
Informed Consent Form for Hospital Transfer. Please carefully read this form, sign it and return it to us.
 Dear Expectant Parent: Welcome! We look forward to your stay at the Puget Sound Birth Center in Kirkland. Enclosed is some information that will assist you in pre-registering and will prepare you for your
Dear Expectant Parent: Welcome! We look forward to your stay at the Puget Sound Birth Center in Kirkland. Enclosed is some information that will assist you in pre-registering and will prepare you for your
 GUIDELINES FOR HOSPITALS WITH NEONATAL INTENSIVE CARE SERVICE : REGULATION 4 OF THE PRIVATE HOSPITALS AND MEDICAL CLINICS REGULATIONS [CAP 248, Rg 1] I Introduction 1. These Guidelines serve as a guide
GUIDELINES FOR HOSPITALS WITH NEONATAL INTENSIVE CARE SERVICE : REGULATION 4 OF THE PRIVATE HOSPITALS AND MEDICAL CLINICS REGULATIONS [CAP 248, Rg 1] I Introduction 1. These Guidelines serve as a guide
ANMC Certified-Nurse Midwife Practice Guideline
 Approved by the ANMC MCH CCBG April 2013 Reviewed Nov. 16, 2015 1. Intent of Certified Nurse-Midwife Practice Guideline 1.1. The intent of this practice guideline is to provide guidance for midwifery practice
Approved by the ANMC MCH CCBG April 2013 Reviewed Nov. 16, 2015 1. Intent of Certified Nurse-Midwife Practice Guideline 1.1. The intent of this practice guideline is to provide guidance for midwifery practice
Vanderbilt University Medical Center Policy Manual
 Key Words: OB, Obstetric, L&D, Labor and Delivery, Triage Applicable to VUH Children s VMG VMG Off-site locations VPH VUSN VUSM Sandra Smith, RN Manager, Labor and Delivery Approved by Robin Mutz, RNC,
Key Words: OB, Obstetric, L&D, Labor and Delivery, Triage Applicable to VUH Children s VMG VMG Off-site locations VPH VUSN VUSM Sandra Smith, RN Manager, Labor and Delivery Approved by Robin Mutz, RNC,
SARASOTA MEMORIAL HOSPITAL NURSING DEPARTMENT POLICY
 SARASOTA MEMORIAL HOSPITAL NURSING DEPARTMENT POLICY TITLE: MANAGEMENT OF THE PREGNANT PATIENT WITH EPIDURAL ANESTHESIA POLICY #: EFFECTIVE DATE: REVISED DATE: POLICY TYPE: PAGE: 126.722 (maternal) 10/88
SARASOTA MEMORIAL HOSPITAL NURSING DEPARTMENT POLICY TITLE: MANAGEMENT OF THE PREGNANT PATIENT WITH EPIDURAL ANESTHESIA POLICY #: EFFECTIVE DATE: REVISED DATE: POLICY TYPE: PAGE: 126.722 (maternal) 10/88
Geisinger Health System Anesthesiology Residency Program. Obstetric Anesthesia
 Geisinger Health System Anesthesiology Residency Program Obstetric Anesthesia INTRODUCTION Education and training in obstetric anesthesia will consist of attending-supervised rotations for four weeks during
Geisinger Health System Anesthesiology Residency Program Obstetric Anesthesia INTRODUCTION Education and training in obstetric anesthesia will consist of attending-supervised rotations for four weeks during
To provide safe and standardized nursing care for the patient requiring induction or augmentation of labor.
 Policy: Guidelines for the Management of Patients Undergoing Induction or Labor & Delivery Effective Date May 2012 Approval Date May 2012 Supersedes September 2011 Applicable to VUH Children s Hospital
Policy: Guidelines for the Management of Patients Undergoing Induction or Labor & Delivery Effective Date May 2012 Approval Date May 2012 Supersedes September 2011 Applicable to VUH Children s Hospital
UMBILICAL CORD CLAMPING FOR TERM INFANTS 37 WEEKS
 UMBILICAL CORD CLAMPING FOR TERM INFANTS 37 WEEKS This guideline refers to umbilical cord clamping in term infants (those 37 weeks gestational age) DEFINITION Immediate (early) cord clamping (ICC): the
UMBILICAL CORD CLAMPING FOR TERM INFANTS 37 WEEKS This guideline refers to umbilical cord clamping in term infants (those 37 weeks gestational age) DEFINITION Immediate (early) cord clamping (ICC): the
Guidelines for States on Maternity Care In the Essential Health Benefits Package
 Guidelines for States on Maternity Care In the Essential Health Benefits Package Section 2707(a) of the Patient Protection and Affordable Care Act (ACA) requires that all new health insurance plans in
Guidelines for States on Maternity Care In the Essential Health Benefits Package Section 2707(a) of the Patient Protection and Affordable Care Act (ACA) requires that all new health insurance plans in
Baltimore, MD 21225 * The Corporation Trust Inc 351 West Camden Street * Baltimore, MD 21201. KATHLEEN WARD, M.D. 3001 South Hanover Street *
 JAYLAN NORFLEET, a minor, by and through his Parents and Next Friends, SHANTIAH MOORE-NORFLEET and IN THE JOEL NORFLEET 5337 4 th Street CIRCUIT COURT Brooklyn, MD 21225 BALTIMORE CITY SHANTIAH MOORE-NORFLEET,
JAYLAN NORFLEET, a minor, by and through his Parents and Next Friends, SHANTIAH MOORE-NORFLEET and IN THE JOEL NORFLEET 5337 4 th Street CIRCUIT COURT Brooklyn, MD 21225 BALTIMORE CITY SHANTIAH MOORE-NORFLEET,
Information for you Abortion care
 Information for you Abortion care Published in February 2012 This information is for you if you are considering having an abortion. It tells you: how you can access abortion services the care you can expect
Information for you Abortion care Published in February 2012 This information is for you if you are considering having an abortion. It tells you: how you can access abortion services the care you can expect
Lorissa R. Heath RN, MSN, APRN 32 Macintosh Way Southington, CT 06489 (860) 426-1481 (H) (860) 426-1481 (Fax) E-mail: LRHeathAPRN@cox.
 Lorissa R. Heath RN, MSN, 32 Macintosh Way Southington, CT 06489 (860) 426-1481 (H) (860) 426-1481 (Fax) E-mail: LRHeath@cox.net Current Career Goal: To obtain a position as an within an established private
Lorissa R. Heath RN, MSN, 32 Macintosh Way Southington, CT 06489 (860) 426-1481 (H) (860) 426-1481 (Fax) E-mail: LRHeath@cox.net Current Career Goal: To obtain a position as an within an established private
Acute Care Pediatric Nurse Practitioner Certification Exam. Detailed Content Outline
 Acute Care Pediatric Nurse Practitioner Certification Exam Description of the Specialty This exam is for the pediatric nurse practitioner (PNP) who has graduated from a formal acute care PNP program with
Acute Care Pediatric Nurse Practitioner Certification Exam Description of the Specialty This exam is for the pediatric nurse practitioner (PNP) who has graduated from a formal acute care PNP program with
Advanced Fetal Assessment and Monitoring: Online Program. Advanced Practice Strategies, LLC
 Advanced Fetal Assessment and Monitoring: Online Program Advanced Fetal Assessment and Monitoring: Online Program Comments from the Authors As a physician who does a great deal of medical legal expert
Advanced Fetal Assessment and Monitoring: Online Program Advanced Fetal Assessment and Monitoring: Online Program Comments from the Authors As a physician who does a great deal of medical legal expert
Pain Management for Labour & Delivery
 Pain Management for Labour & Delivery Departments of Anesthesia, Obstetrics, and Obstetrical Nursing December 2008 This pamphlet has been prepared to provide you, members of your family, and others who
Pain Management for Labour & Delivery Departments of Anesthesia, Obstetrics, and Obstetrical Nursing December 2008 This pamphlet has been prepared to provide you, members of your family, and others who
YALE NEW HAVEN HOSPITAL CORE PRIVILEGES LICENSED NURSE MIDWIFE
 YALE NEW HAVEN HOSPITAL CORE PRIVILEGES LICENSED NURSE MIDWIFE Nurse Midwives are licensed in Connecticut pursuant to CGS Section 20 75a et seq. recognizes that actual midwife function will vary with training
YALE NEW HAVEN HOSPITAL CORE PRIVILEGES LICENSED NURSE MIDWIFE Nurse Midwives are licensed in Connecticut pursuant to CGS Section 20 75a et seq. recognizes that actual midwife function will vary with training
Quality of Birth Certificate Data. Daniela Nitcheva, PhD Division of Biostatistics PHSIS
 Quality of Birth Certificate Data Daniela Nitcheva, PhD Division of Biostatistics PHSIS Data Quality SC State Law requires that you file the birth certificate within 5 days of a child s birth. Data needs
Quality of Birth Certificate Data Daniela Nitcheva, PhD Division of Biostatistics PHSIS Data Quality SC State Law requires that you file the birth certificate within 5 days of a child s birth. Data needs
Breastfeeding. Nursing Education
 Breastfeeding AWHONN supports breastfeeding as the optimal method of infant nutrition. AWHONN believes that women should be encouraged to breastfeed and receive instruction and support from the entire
Breastfeeding AWHONN supports breastfeeding as the optimal method of infant nutrition. AWHONN believes that women should be encouraged to breastfeed and receive instruction and support from the entire
birth plan Use this easy fill-in-the-blank birth plan to prepare yourself for delivery and communicate your wants and needs to your medical team.
 Use this easy fill-in-the-blank birth plan to prepare yourself for delivery and communicate your wants and needs to your medical team. Full name: Today s date: Doctor s name: Partner s name: Due date/induction
Use this easy fill-in-the-blank birth plan to prepare yourself for delivery and communicate your wants and needs to your medical team. Full name: Today s date: Doctor s name: Partner s name: Due date/induction
Regions Hospital Delineation of Privileges Nurse Practitioner
 Regions Hospital Delineation of Privileges Nurse Practitioner Applicant s Last First M. Instructions: Place a check-mark where indicated for each core group you are requesting. Review education and basic
Regions Hospital Delineation of Privileges Nurse Practitioner Applicant s Last First M. Instructions: Place a check-mark where indicated for each core group you are requesting. Review education and basic
If you have any health or pregnancy related concerns contact Health Link (1-866-408-5465)
 1. When should I come in? If you think you are in labour If you think your water has broken If baby movements have stopped or you feel less than 6 fetal movements in 2 hours. If you have constant abdominal
1. When should I come in? If you think you are in labour If you think your water has broken If baby movements have stopped or you feel less than 6 fetal movements in 2 hours. If you have constant abdominal
CORD BLOOD COLLECTION / ANALYSIS- AT BIRTH
 WOMEN AND NEWBORN HEALTH SERVICE King Edward Memorial Hospital CLINICAL GUIDELINES OBSTETRICS AND MIDWIFERY King Edward Memorial Hospital WOMEN AND NEWBORN HEALTH SERVICE INTRAPARTUM CARE SPECIMEN COLLECTION
WOMEN AND NEWBORN HEALTH SERVICE King Edward Memorial Hospital CLINICAL GUIDELINES OBSTETRICS AND MIDWIFERY King Edward Memorial Hospital WOMEN AND NEWBORN HEALTH SERVICE INTRAPARTUM CARE SPECIMEN COLLECTION
Module 7 Coping with the Pain of Labor
 Module 7 Coping with the Pain of Labor Can I Have an Epidural to Help with Labor Pain? Yes. It s an effective method of pain relief. However, an epidural given early in labor can interfere with the progress
Module 7 Coping with the Pain of Labor Can I Have an Epidural to Help with Labor Pain? Yes. It s an effective method of pain relief. However, an epidural given early in labor can interfere with the progress
Birth place decisions
 Birth place decisions Information for women and partners on planning where to give birth Where can I give birth? What birth settings might be suitable for me? Who can I ask for help? Where can I find out
Birth place decisions Information for women and partners on planning where to give birth Where can I give birth? What birth settings might be suitable for me? Who can I ask for help? Where can I find out
ACNM Department of Advocacy and Government Affairs Grassroots Advocacy Resources State Fact Sheet: Alabama
 ACNM Department of Advocacy and Government Affairs Grassroots Advocacy Resources State Fact Sheet: Alabama The American College of Nurse- Midwives (ACNM) is the national organization representing the interests
ACNM Department of Advocacy and Government Affairs Grassroots Advocacy Resources State Fact Sheet: Alabama The American College of Nurse- Midwives (ACNM) is the national organization representing the interests
CURRICULUM VITAE EDUCATION. Baylor College of Medicine, Certified Nurse Midwifery Program 1987 LICENSURE/CERTIFICATIONS
 CURRICULUM VITAE Patricia Jones, CNM 1826 Portsmouth Houston, Texas 77098 EDUCATION Baylor College of Medicine, Certified Nurse Midwifery Program 1987 LICENSURE/CERTIFICATIONS Advanced Registered Nurse
CURRICULUM VITAE Patricia Jones, CNM 1826 Portsmouth Houston, Texas 77098 EDUCATION Baylor College of Medicine, Certified Nurse Midwifery Program 1987 LICENSURE/CERTIFICATIONS Advanced Registered Nurse
Effects of Pregnancy & Delivery on Pelvic Floor
 Effects of Pregnancy & Delivery on Pelvic Floor 吳 銘 斌 M.D., Ph.D. 財 團 法 人 奇 美 醫 院 婦 產 部 婦 女 泌 尿 暨 骨 盆 醫 學 科 ; 台 北 醫 學 大 學 醫 學 院 婦 產 學 科 ; 古 都 府 城 台 南 Introduction Pelvic floor disorders (PFDs) include
Effects of Pregnancy & Delivery on Pelvic Floor 吳 銘 斌 M.D., Ph.D. 財 團 法 人 奇 美 醫 院 婦 產 部 婦 女 泌 尿 暨 骨 盆 醫 學 科 ; 台 北 醫 學 大 學 醫 學 院 婦 產 學 科 ; 古 都 府 城 台 南 Introduction Pelvic floor disorders (PFDs) include
Midwifery in Manitoba Kate Abbott, RM
 Midwifery in Manitoba Kate Abbott, RM Relationships with commercial interests: Grants/Research Support: none Speakers Bureau/Honoraria: none Consulting Fees: none Other: Employee of Winnipeg Regional Health
Midwifery in Manitoba Kate Abbott, RM Relationships with commercial interests: Grants/Research Support: none Speakers Bureau/Honoraria: none Consulting Fees: none Other: Employee of Winnipeg Regional Health
NGO information to the United Nations Committee on the elimination of discrimination against Women.
 NGO information to the United Nations Committee on the elimination of discrimination against Women. For consideration when compiling the List of Issues with regard to the Combined Eighth and Ninth Periodic
NGO information to the United Nations Committee on the elimination of discrimination against Women. For consideration when compiling the List of Issues with regard to the Combined Eighth and Ninth Periodic
LECTURE OBJECTIVES & OUTLINES
 LECTURE OBJECTIVES & OUTLINES 74 I. OVERVIEW OF MATERNITY NURSING OBJECTIVES At the completion of this class the student will be able to: 1. Compare and contrast expanded nursing roles in this specialty.
LECTURE OBJECTIVES & OUTLINES 74 I. OVERVIEW OF MATERNITY NURSING OBJECTIVES At the completion of this class the student will be able to: 1. Compare and contrast expanded nursing roles in this specialty.
GUIDELINE FOR ADMINISTRATION OF FENTANYL FOR PAIN RELIEF IN LABOUR
 GUIDELINE FOR ADMINISTRATION OF FENTANYL FOR PAIN RELIEF IN LABOUR INTRODUCTION Intravenous (IV) Fentanyl is a good option for pain management during labour and should be administered in a safe and competent
GUIDELINE FOR ADMINISTRATION OF FENTANYL FOR PAIN RELIEF IN LABOUR INTRODUCTION Intravenous (IV) Fentanyl is a good option for pain management during labour and should be administered in a safe and competent
Certified Nurse Midwives in Delivery: What benefits they bring! Presented by: Deborah Johnson, CNM Jodee Gutierrez CNM
 Certified Nurse Midwives in Delivery: What benefits they bring! Presented by: Deborah Johnson, CNM Jodee Gutierrez CNM History of Midwifery Midwife means with woman French Sage femme Spanish La Partera
Certified Nurse Midwives in Delivery: What benefits they bring! Presented by: Deborah Johnson, CNM Jodee Gutierrez CNM History of Midwifery Midwife means with woman French Sage femme Spanish La Partera
LexisNexis Public Access Portal: www.lexisnexis.com/njoal
 PLEASE READ Rules and regulations of the Division of Consumer Affairs, the boards and committees in, and other units of, the Division are codified in Title 13 of the New Jersey Administrative Code, published
PLEASE READ Rules and regulations of the Division of Consumer Affairs, the boards and committees in, and other units of, the Division are codified in Title 13 of the New Jersey Administrative Code, published
Corporate Reimbursement Policy
 Corporate Reimbursement Policy Guidelines for Global Maternity Reimbursement File Name: Origination: Last Review: Next Review: guidelines_for_global_maternity_reimbursement 10/2003 7/2016 7/2017 Description
Corporate Reimbursement Policy Guidelines for Global Maternity Reimbursement File Name: Origination: Last Review: Next Review: guidelines_for_global_maternity_reimbursement 10/2003 7/2016 7/2017 Description
Inpatient Obstetric Nursing
 NCC believes the individual certified nurse is the best person to determine the specialty code for their CE, as they have the specific content of the CE program. Inpatient Obstetric Nursing NCC Maintenance
NCC believes the individual certified nurse is the best person to determine the specialty code for their CE, as they have the specific content of the CE program. Inpatient Obstetric Nursing NCC Maintenance
An exploratory study on 'Nurse Midwife Manpower' requirement in labour room, Nehru Hospital, PGIMER, Chandigarh
 An exploratory study on 'Nurse Midwife Manpower' requirement in labour room, Nehru Hospital, PGIMER, Chandigarh Gagandeep Kaur, Baljit Kaur, Seema Chopra Abstract : The aim of the study was to explore
An exploratory study on 'Nurse Midwife Manpower' requirement in labour room, Nehru Hospital, PGIMER, Chandigarh Gagandeep Kaur, Baljit Kaur, Seema Chopra Abstract : The aim of the study was to explore
BLS TREATMENT GUIDELINES - CARDIAC
 BLS TREATMENT GUIDELINES - CARDIAC CARDIOPULMONARY ARREST - NON-TRAUMATIC (SJ-B101) effective 07/01/99 Defibrillation CPR Apply S-AED and assess rhythm as trained. Defib as indicated Simultaneous OXYGEN:
BLS TREATMENT GUIDELINES - CARDIAC CARDIOPULMONARY ARREST - NON-TRAUMATIC (SJ-B101) effective 07/01/99 Defibrillation CPR Apply S-AED and assess rhythm as trained. Defib as indicated Simultaneous OXYGEN:
Vaginal or Cesarean Birth:
 Vaginal or Cesarean Birth: What Is at Stake for Women and Babies? A Best Evidence Review Executive Summary Contributors Henci Goer Amy Romano, MSN, CNM Carol Sakala, PhD, MSPH 2012, Childbirth Connection
Vaginal or Cesarean Birth: What Is at Stake for Women and Babies? A Best Evidence Review Executive Summary Contributors Henci Goer Amy Romano, MSN, CNM Carol Sakala, PhD, MSPH 2012, Childbirth Connection
Guidelines for the Management of the Obstetrical Patient for the Certified Registered Nurse Anesthetist
 American Association of Nurse Anesthetists 222 South Prospect Avenue Park Ridge, IL 60068 www.aana.com Guidelines for the Management of the Obstetrical Patient for the Certified Registered Nurse Anesthetist
American Association of Nurse Anesthetists 222 South Prospect Avenue Park Ridge, IL 60068 www.aana.com Guidelines for the Management of the Obstetrical Patient for the Certified Registered Nurse Anesthetist
Objective of This Lecture
 Component 2: The Culture of Health Care Unit 3: Health Care Settings The Places Where Care Is Delivered Lecture 5 This material was developed by Oregon Health & Science University, funded by the Department
Component 2: The Culture of Health Care Unit 3: Health Care Settings The Places Where Care Is Delivered Lecture 5 This material was developed by Oregon Health & Science University, funded by the Department
Priya Rajan, MD Northwestern University September 13, 2013
 Priya Rajan, MD Northwestern University September 13, 2013 o Study Finds Benefits in Delaying Severing of Umbilical Cord nytimes.com, 7/10/13 o Delay cord clamping for baby health, say experts bbc.com.uk,
Priya Rajan, MD Northwestern University September 13, 2013 o Study Finds Benefits in Delaying Severing of Umbilical Cord nytimes.com, 7/10/13 o Delay cord clamping for baby health, say experts bbc.com.uk,
Section 3. Innovative Models
 Section 3. Innovative Models 3. Innovative Models This section outlines the processes, methods and outcomes from five different hospitals and systems as they have worked to improve maternal and infant
Section 3. Innovative Models 3. Innovative Models This section outlines the processes, methods and outcomes from five different hospitals and systems as they have worked to improve maternal and infant
MINI - COURSE On TEMPERATURE CONTROL IN THE NEWBORN
 MINI - COURSE On TEMPERATURE CONTROL IN THE NEWBORN Instructions: Read each sheet and answer any questions as honestly as possible The first sheets have four questions to allow you to give your thoughts
MINI - COURSE On TEMPERATURE CONTROL IN THE NEWBORN Instructions: Read each sheet and answer any questions as honestly as possible The first sheets have four questions to allow you to give your thoughts
Patient Care Technician (Bridge Program)
 Patient Care Technician (Bridge Program) Introduction: At Prestige Medical Solutions we are fully vested in helping students succeed. Our vision is to be a great place to learn, where people are inspired
Patient Care Technician (Bridge Program) Introduction: At Prestige Medical Solutions we are fully vested in helping students succeed. Our vision is to be a great place to learn, where people are inspired
BRIEF REPORTS. Perceptions and Practice of Waterbirth: A Survey of Georgia Midwives
 BRIEF REPORTS Perceptions and Practice of Waterbirth: A Survey of Georgia Midwives Shaunette L. Meyer, MA, Christopher M. Weible, PhD, and Kate Woeber, CNM, MPH This study investigated the experience and
BRIEF REPORTS Perceptions and Practice of Waterbirth: A Survey of Georgia Midwives Shaunette L. Meyer, MA, Christopher M. Weible, PhD, and Kate Woeber, CNM, MPH This study investigated the experience and
CROSS HEALTH CARE BOUNDARIES MATERNITY CLINICAL GUIDELINE
 CROSS HEALTH CARE BOUNDARIES MATERNITY CLINICAL GUIDELINE Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Obstetric Early Warning Score Guideline Implementation
CROSS HEALTH CARE BOUNDARIES MATERNITY CLINICAL GUIDELINE Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Obstetric Early Warning Score Guideline Implementation
THE LABOUR ADMISSION CTG An assessment of the test s predictive values, reliability and effect How the test is perceived by practicing midwives
 THE LABOUR ADMISSION CTG An assessment of the test s predictive values, reliability and effect How the test is perceived by practicing midwives Ellen Blix Doctoral thesis at the Nordic School of Public
THE LABOUR ADMISSION CTG An assessment of the test s predictive values, reliability and effect How the test is perceived by practicing midwives Ellen Blix Doctoral thesis at the Nordic School of Public
TN Emergency Medical Services
 TN Emergency edical ODULES AND UNITS ES System ES Providers: ER and ET Safety and Wellness Body echanics System Communication Documentation Therapeutic Communication Legal and Ethical Issues Intro to Respiratory
TN Emergency edical ODULES AND UNITS ES System ES Providers: ER and ET Safety and Wellness Body echanics System Communication Documentation Therapeutic Communication Legal and Ethical Issues Intro to Respiratory
Name: www.mypregnancytoolkit.com. Copyright 2013 My Pregnancy Toolkit. All rights reserved.
 Name: Copyright 2013 by My Pregnancy Toolkit. All rights reserved. Disclaimer and Terms of Use: This guide or any portion thereof may not be reproduced or used in any manner whatsoever without the express
Name: Copyright 2013 by My Pregnancy Toolkit. All rights reserved. Disclaimer and Terms of Use: This guide or any portion thereof may not be reproduced or used in any manner whatsoever without the express
The debate about the safety of home births continues
 CMAJ Research Outcomes of planned home birth with registered midwife versus planned hospital birth or physician Patricia A. Janssen PhD, Lee Saxell MA, Lesley A. Page PhD, Michael C. Klein MD, Robert M.
CMAJ Research Outcomes of planned home birth with registered midwife versus planned hospital birth or physician Patricia A. Janssen PhD, Lee Saxell MA, Lesley A. Page PhD, Michael C. Klein MD, Robert M.
4/15/2013. Maribeth Inturrisi RN MS CNS CDE Perinatal Diabetes Educator mbturris@comcast.net
 Maribeth Inturrisi RN MS CNS CDE Perinatal Diabetes Educator mbturris@comcast.net List the potential complications associated with diabetes during labor. Identify the 2 most important interventions essential
Maribeth Inturrisi RN MS CNS CDE Perinatal Diabetes Educator mbturris@comcast.net List the potential complications associated with diabetes during labor. Identify the 2 most important interventions essential
SARASOTA MEMORIAL HOSPITAL NURSING PROCEDURE
 SARASOTA MEMORIAL HOSPITAL NURSING PROCEDURE TITLE: MAGNESIUM SULFATE ADMINISTRATION FOR ANTEPARTUM AND INTRAPARTUM PATIENTS WITH PRE-TERM LABOR DATE: REVIEWED: PAGES: 6/92 08/11 1 of 6 ISSUED FOR: Nursing
SARASOTA MEMORIAL HOSPITAL NURSING PROCEDURE TITLE: MAGNESIUM SULFATE ADMINISTRATION FOR ANTEPARTUM AND INTRAPARTUM PATIENTS WITH PRE-TERM LABOR DATE: REVIEWED: PAGES: 6/92 08/11 1 of 6 ISSUED FOR: Nursing
ARKANSAS STATE BOARD OF HEALTH ARKANSAS DEPARTMENT OF HEALTH RULES AND REGULATIONS FOR GOVERNING THE PRACTICE OF LAY MIDWIFERY IN ARKANSAS
 Agency #016.24 ARKANSAS STATE BOARD OF HEALTH ARKANSAS DEPARTMENT OF HEALTH RULES AND REGULATIONS FOR GOVERNING THE PRACTICE OF LAY MIDWIFERY IN ARKANSAS PROMULGATED UNDER THE AUTHORITY OF ARKANSAS CODE
Agency #016.24 ARKANSAS STATE BOARD OF HEALTH ARKANSAS DEPARTMENT OF HEALTH RULES AND REGULATIONS FOR GOVERNING THE PRACTICE OF LAY MIDWIFERY IN ARKANSAS PROMULGATED UNDER THE AUTHORITY OF ARKANSAS CODE
Document Classification
 Document Classification Document Title Document Type Unique Identifier Function(s) (see table) Scope (see table) Target Audience Key words Author(s) Owner (see table) Date first published 2004 Date this
Document Classification Document Title Document Type Unique Identifier Function(s) (see table) Scope (see table) Target Audience Key words Author(s) Owner (see table) Date first published 2004 Date this
CH CONSCIOUS SEDATION
 Summary: CH CONSCIOUS SEDATION It is the policy of Carondelet Health that moderate conscious sedation of patients will be undertaken with appropriate evaluation and monitoring. Effective Date: 9/4/04 Revision
Summary: CH CONSCIOUS SEDATION It is the policy of Carondelet Health that moderate conscious sedation of patients will be undertaken with appropriate evaluation and monitoring. Effective Date: 9/4/04 Revision
COLCHESTER EAST HANTS HEALTH CENTRE: WOMEN AND CHILDREN S HEALTH UNIT BIRTH PLAN
 COLCHESTER EAST HANTS HEALTH CENTRE: WOMEN AND CHILDREN S HEALTH UNIT BIRTH PLAN Name: Obstetrical Physician: Family Physician: Congratulations on your pregnancy! As your Childbirth Team we want you to
COLCHESTER EAST HANTS HEALTH CENTRE: WOMEN AND CHILDREN S HEALTH UNIT BIRTH PLAN Name: Obstetrical Physician: Family Physician: Congratulations on your pregnancy! As your Childbirth Team we want you to
NRP 2012 Putting New Resuscitation Guidelines into Practice
 Outreach Education Online Video Library for Healthcare Professionals NRP 2012 Putting New Resuscitation Guidelines into Practice. Jeanette Zaichkin, RN, MN, NNP-BC December 2, 2010 Program Handouts This
Outreach Education Online Video Library for Healthcare Professionals NRP 2012 Putting New Resuscitation Guidelines into Practice. Jeanette Zaichkin, RN, MN, NNP-BC December 2, 2010 Program Handouts This
