Extravasation guidelines Implementation Toolkit
|
|
|
- Marylou Conley
- 8 years ago
- Views:
Transcription
1 Extravasation guidelines 2007 Guidelines Implementation Toolkit
2 Contents Extravasation guidelines 2007 Introduction to the Extravasation guidelines Introduction 4 Overall Goal 4 Specific Targets and Aims 4 The Nurse s Role 5 Key points to understand from the extravasation guidelines What is extravasation? 6 Types of extravasation 6 When does extravasation occur? 8 Prevalence 8 Risk factors 8 What are the implications of extravasation? 10 Initial symptoms 10 Tissue damage 10 Surgery 11 Impact on cancer therapy 11 Other consequences 11 How is extravasation recognised? 12 Patient reporting 12 Visual assessment 13 Checking the infusion line 13 Distinguishing extravasation vs. other conditions 14 How is extravasation prevented? 15 Standard procedures 15 Training 15 Patient education 16 Equipment selection 16 Vein selection in peripheral administration 17 Administering intravenous treatment 17 2
3 How is extravasation managed? 19 Procedures and protocols 19 Management initial steps 20 Management next steps 21 Antidotes 24 Anthracycline extravasation 26 Extravasation kit 26 Surgery and debridement 26 Documentation and reporting 27 Summary 29 Appendices 30 List of drugs: vesicants, irritants and non-vesicants 30 Distinguishing extravasation from other conditions 31 Vein selection procedure 32 Administering Savene (dexrazoxane) 33 Administering dimethylsulfoxide 34 Administering hyaluronidase 35 Extravasation kit 36 Documentation template 37 References 41 We would like to thank the following people for their guidance in helping to develop these documents: Yvonne Wengström Jan Foubert Anita Margulies Helen Roe Sebastien Bugeia OCN, PhD, Past President of the European Oncology Nursing Society (EONS) RPN, PhD, Senior Lecturer in Nursing and Midwifery, Erasmushogeschool, Department of Healthcare, Brussels, Belgium BSN, RN, Clinical Nurse and Lecturer, Board Member of EONS, Klinik und Poliklinik für Onkologie, Universitätsspital, Zürich, Switzerland RN, BSc(Hons), Consultant Cancer Nurse / Lead Chemotherapy Nurse, North Cumbria Acute Hospitals NHS Trust; Chair of the United Kingdom Oncology Nursing Society (UKONS) North Zone Chemotherapy Group, United Kingdom Oncology Nurse at the Institut Gustave Roussy (Villejuif, FRANCE), Board Member of the French Oncology Nursing Society (AFIC). 3
4 Introduction With over 100,000 doses of chemotherapy and in excess of 1,000,000 intravenous (IV) infusions given every day around the world, keeping adverse events and complications of these procedures to a minimum is important both for the patients receiving them and the healthcare systems in which they take place. Extravasation is a serious condition that warrants special attention from the healthcare professionals involved in administering intravenous medications. This educational module summarises and explains the most recent literature and recommendations on extravasation in the clinical setting from prevention and recognition to possible treatment with antidotes. It also provides an outline of the pivotal role that nurses play in the patient management process. The scope of this document is to describe and explain the prevention, recognition and management of extravasation in general terms. More detailed descriptions of techniques for proper cannulation or phlebotomy (an important skill for the prevention of extravasation) will not be dealt with in this guideline. Overall Goal Specific Targets and Aims The Nurse s Role Overall Goal The overall goal of these guidelines is to help nurses understand and recognise extravasation, and improve the prevention and overall management of extravasations in cancer patients. Specific Targets and Aims The targets and aims of this module are to: Increase nurses knowledge of specific elements of extravasation: Causes and risk factors for extravasation Features and symptoms of extravasation Differences vs. flare and other reactions Consequences of extravasation Prevention measures The use of antidotes in treating extravasation Encourage successful management of extravasation Update and inform nurses of the current standards from different guidelines and protocols Encourage adoption of procedures for extravasation that fit with the current guidelines 4
5 The Nurse s Role Nurses are among the best placed professionals to recognise and deal with extravasation in the clinical setting. The nurses who routinely provide cancer therapies intravenously (either peripherally or through central venous access devices (CVADs) are particularly important in the ongoing management of this possibly serious complication of therapy. Nurses have a key role to play in identification and management of extravasation, and, of course, in preventing it. From maintaining a high standard of care in the delivery of IV drugs to managing the treatment strategy for extravasation, they have many important duties in this area. Nurses represent an important link for ensuring that extravasation is prevented, diagnosed and managed where possible. Their role in providing information and providing ongoing support for patients relating to cancer therapy (and the need to be vigilant for any symptoms) is critical in cutting the incidence of extravasation. This module will discuss the role of the nurse in extravasation management and highlight information and issues that will assist nurses to perform these roles more efficiently. 5
6 What is extravasation? In a general sense, extravasation refers to the process by which one substance (e.g., fluid, drug) leaks into the surrounding tissue. 1 In terms of cancer therapy, extravasation is defined as the accidental leakage from its intended compartment (the vein) into the surrounding tissue. 2 Usually, this occurs when intravenous (IV) medication passes from the blood vessel into the tissue around the blood vessels and beyond. 1 4 A broader definition of extravasation includes the resulting injury. Depending on the substance that extravasates into the tissue, the degree of injury can range from a very mild skin reaction to severe necrosis. 4 Types of extravasation Types of extravasation Extravasation can be classified according to the reaction that is caused by the substance passing into the surrounding tissue. Many different drugs have been classified according to the type of reaction they cause; however, for the purpose of this discussion, we will refer only to cancer therapies. It should be noted, however, that cancer therapies are not the only drugs that cause damage when extravasated, and non-cancer therapies (e.g., aminophylline, calcium solutions, hypertonic glucose, phenytoin, total parenteral nutrition, X-ray contrast media) can be equally as destructive. 5 Cancer drugs can be grouped into 3 broad categories, based on their potential to cause tissue damage upon extravasation: 3 Non-vesicants Irritants Vesicants Non-vesicants do not cause ulceration. In fact, if they are extravasated, they rarely produce an acute reaction or progress to necrosis. 3 Irritants, on the other hand, do tend to cause pain at, and around the injection site, and along the vein. They may or may not also cause inflammation. Some irritants do also have the potential to cause ulceration, but only in the case that a very large amount of the drug is extravasated into the tissue. 3 6
7 Vesicants are drugs that have the potential to cause blistering and ulceration and which when left untreated, can lead to the more serious side effects of extravasation such as tissue destruction and necrosis. 3 These drugs can be sub-classified according to the mechanism by which they cause damage, which is also important since it affects the management strategy. 3 DNA-binding: These drugs are absorbed locally and enter the cells, bind to nucleic acids (i.e., DNA) and precipitate the death of the cell. Following cell death these agents can be rereleased to destroy non-cancer cells. They can be divided into 3 categories: 3 Anthracyclines Alkylating agents Others Non-DNA-binding: These drugs initiate cancer cell death by mechanisms other than binding DNA. They can be divided into 2 groups: 3 Vinca alkaloids Taxanes For a comprehensive list of vesicants (including all subcategories), irritants and non-vesicants please refer to Appendix 1. 7
8 When does extravasation occur? In an ideal situation, extravasation of vesicant cancer therapies would never occur. Despite the many precautionary measures in place, accidental extravasation does still occur, both from peripheral lines and from CVADs. Prevalence Risk factors Prevalence Extravasation is not as rare as some people may think. In cancer therapy experts estimate that it accounts for 0.5% to 6.0% of all adverse events associated with treatment. 4 But, when you consider that adverse events with cancer therapy are quite common, the absolute number of extravasations which take place is significant. 6 Data regarding extravasation from CVADs is more limited. One small study estimated that extravasation occurs about 6% of the time. 4 Risk factors Some extravasations can be accounted for by error in the IV procedure, etc. 4,7 However, patients receiving these cancer therapies may have multiple risk factors that make IV infusion very difficult. For example, cancer patients with a tendency for thin, fragile and mobile veins are at higher risk of extravasation than the general population. 4 In addition to factors relating to the procedure and to the patient, factors associated with the equipment/material used, concomitant medications and the treatments themselves can also increase the likelihood of extravasation. Some the most common factors known to increase the risk of extravasation are listed below: 4,8-10 Patient factors Small blood vessels (e.g., infants and young children) Fragile veins (e.g., elderly, cancer patients) Hard, sclerosed veins Mobile veins Impaired circulation (e.g., cannula sited on side of mastectomy, lymphoedema) Obstructed vena cava (elevated venous pressure can cause leakage) Pre-existing conditions (diabetes, peripheral circulatory conditions like Raynaud s syndrome, radiation damage) Obesity 8
9 Trouble reporting symptoms early Inability to report stinging/discomfort (e.g., sedated, confused) Decreased sensation (e.g., as a result of neuropathy, diabetes, peripheral vascular disease) Cannulation and infusion procedure Untrained or inexperienced staff Multiple attempts at cannulation Unfavourable cannulation site (e.g., back of hand vs. forearm, close to bone) Bolus injection High flow pressure Equipment Steel butterfly needle Catheter size and type Treatment Ability to bind directly to DNA Ability to kill replicating cells Ability to cause tissue or vascular dilatation ph Osmolality Characteristics of diluent 9
10 What are the implications of extravasation? In general, extravasation is to be avoided. Even in patients who do not progress to ulcerative and necrotic tissue damage may still experience pain and discomfort, as well as indirect consequences, such as disruption of treatment and committing hospital resources to the management of extravasation. 3,4 The specific symptoms of extravasation, as well as their wider consequences, are discussed in this section. Initial symptoms Tissue damage Surgery Impact on cancer therapy Other consequences Initial symptoms The initial symptoms of extravasation occur immediately after the blood vessel has been breached. Depending on the agent and the patient extravasation may be accompanied by discomfort or pain, which can range from mild to intense. Patients often describe the pain as a burning sensation. 4 The pain may be followed, in the next few hours, by erythema and oedema near the injection site. 3 In addition, there may be discolouration or redness of the skin near the site. 4 The initial symptoms of extravasation are subtle, however, and can be similar for the extravasation of different agents (i.e., irritants vs. vesicants). The progression from these initial symptoms, however, differs greatly for irritants and vesicants particularly relating to permanent damage to the tissue. 3 Tissue damage Vesicants, by definition, have the potential to cause tissue damage upon extravasation from the vein. Like the initial symptoms, the extent of tissue damage can vary greatly between different treatment regimens and patients. 4 Tissue destruction caused by leakage of vesicants into surrounding tissue may be progressive in nature, and may happen quite slowly with little pain. Induration or ulcer formation is by no means an immediate phenomenon as it takes time to develop. 5 In general, tissue damage begins with the appearance of inflammation and blisters at or near the site of injection. Depending on the drug and other factors, this can then progress to ulceration, and then in some 10
11 cases may progress to necrosis of the local tissue. 5 Necrosis can occasionally be so severe that function in the affected area cannot be recovered and surgery is required. 5 If extravasation occurs in the forearm, the damage to tissue includes skin and subcutaneous tissue damage. If the extravasation occurs next to a nerve, ligament or tendon, then the damage can extend to that tissue and have an impact on sensation and function. 11 Surgery If vesicant extravasation is not recognised and dealt with promptly, the tissue damage can become so severe that surgical debridement and plastic surgery (possibly including skin grafting) may become necessary. 5 In the event that extravasation does affect nerves, ligaments or tendons, the damage may necessitate more extensive surgery. 4 It is estimated that one third of vesicant extravasations give rise to ulceration. This ulceration, in combination with pain and necrosis, can be an indication for surgical intervention. 5,12 Impact on cancer therapy Most extravasation protocols call for the immediate cessation of the drug delivery, followed by measures to prevent further spread of the cancer drug into the tissue. 8,13 16 As a result, the delivery of cancer therapy may be delayed until the extravasation is resolved. Some guidelines specifically address the issue of re-establishment of IV cancer therapy recommending the establishment of an IV site in another limb. 13 However, most guidelines do not specifically address this process. 8,14 16 Other consequences Apart from the physical consequences, extravasation can lead to longer hospital stay, more consultations and increased length of follow-up care; the need for physical therapy; high treatment costs; psychological consequences (e.g., distress, anxiety); and even lost wages. 4 In addition, it is not uncommon for hospitals and their staff to be faced with a lawsuit following an extravasation. 5 All of these factors contribute to the seriousness of an extravasation, and can add to the toll on the patient, their family and the healthcare system. One of the primary goals of extravasation protocols and guidelines is to educate healthcare professionals about the avoidance of serious complications and preventions of extravasations before patients require surgical processes. 11
12 How is extravasation recognised? It is critical that an extravasation is recognised and diagnosed early. The most effective way to recognise and detect extravasation in its early stages is to be aware of and act on all relevant signs and symptoms. Telltale signs and symptoms can be gathered from patient reports, simple visual assessment of the injection site, and careful monitoring of the IV device. Then, once an extravasation is suspected, it will also be important to rule out other possible conditions, such as flare reaction. 4,7 The quality of the nursing assessment during administration can play a key role in minimising frequency and severity, since delays in the recognition and treatment of vesicant extravasation increase the likelihood of developing tissue damage and necrosis. 4,17 Since extravasation could have serious consequences, a second opinion is always warranted. If there is any doubt as to whether or not it has occurred, stop and ask for help. Patient reporting Visual assessment Checking the infusion line Distinguishing extravasation vs. other conditions Patient reporting Patients need to know the possible side effects of the treatments they are receiving. In the case of extravasation, it is recommended that the patient be told about the possible complications and to be aware of any pain/sensation at the site of infusion. Patients should feel that they can report any strange sensations as soon as they arise, so the healthcare team can take these symptoms into account. The most important patient-reported symptoms for assessing extravasation relate to the sensation around the site of injection or, in the case of a central line, around the CVAD and surrounding area. Typically these complaints include: 8,18 Pain Swelling Redness Discomfort Burning Stinging Other acute changes at the site of extravasation None of these are confirmation of an extravasation on their own, but should be treated with concern and warrant further examination, such as testing the patency of the infusion with blood return. In addition, the nature of the complaints should be verified against the signs and symptoms of other possible diagnoses. 12
13 Visual assessment Visual signs, while by no means exclusive to extravasation, do provide useful confirmation for patient reports in suspected extravasation. The common signs, occurring at or around the site of the cannula or, in the case of central line around the CVAD and the surrounding area include: 8,18,19 Early symptoms Swelling/oedema Redness/erythema Later symptoms Inflammation Induration Blistering Importantly, many of these symptoms do not occur immediately upon infusion. Induration and blistering, in particular, tend to appear later in the extravasation process. Therefore, careful monitoring of the site should continue during the infusion time and for some time following an infusion. 7 Checking the infusion line Apart from patient reporting and visible symptoms of extravasation, it is possible to determine whether extravasation has occurred by checking the infusion line itself. Verification of the line should be used to help confirm any suspected extravasation (peripheral or central line), if possible. Signs of extravasation, in relation to the cannula, include: 8,18 Increased resistance when administering IV drugs Slow or sluggish infusion Change in infusion flow Lack or loss of blood return from the cannula Look for blood return (flashback) upon insertion of the needle. If the needle is in the lumen of the vein, you should notice some blood return. If you confirm blood return, the cannula can be glided carefully into position, ready to stop if met with any resistance. Brief blood return may be seen if the needle passes through the lumen of the vein and then out the other wall. However, the return will halt once the needle has passed the posterior venous wall. 20 If this occurs, the needle has passed through the lumen and anything infused will be administered straight into the surrounding tissue. The cannula should be removed and the procedure recommenced using another vein, if necessary in another vein above the original site on the same vein (closer to the heart). 7 13
14 Distinguishing extravasation vs. other conditions Distinguishing between extravasation and other local reactions is an important step in diagnosis. Initially, making the distinction can be very difficult and requires sound clinical judgment. Familiarity with the different symptoms increases the likelihood of appropriate treatment. In the case of extravasation, that means that interventions and management will be initiated at an early stage and help to prevent some of the more serious consequences associated with it. 4,8 Other conditions that resemble extravasation include: 4,7,8,18 Flare reaction Vessel irritation Venous shock Phlebitis Hypersensitivity The principal differences between extravasation and these conditions relate to the nature and timing of the patient s complaints, the type and extent of erythema noted and the location and presence of swelling. 4,8 A guide describing symptoms and differences between conditions commonly associated with IV infusion can be found in Appendix 2. 14
15 How is extravasation prevented? The most important approach to minimising the consequences of extravasation is prevention. 12 Healthcare professionals involved in the handling and administration of IV cancer therapies should become familiar with their local procedures and protocols and develop an understanding of the important precautionary steps that should be taken to avoid extravasation and the resulting injuries. Given this cautious and systematic approach, most episodes of extravasation can be avoided altogether. 21 The following sections provide advice for good practice and may help prevent extravasation and minimise injury. Standard procedures Training Patient education Equipment selection Vein selection in peripheral administration Administering intravenous treatment Standard procedures Local policies and protocols for preventing, identifying risk factors, diagnosis, and managing extravasation represent one of the best ways with which to combat extravasation in the clinical setting. The protocols should be drug specific and be developed with input from the whole healthcare team involved. If they are already in place, efforts should be taken to make them readily available to all who require them (i.e., those healthcare professionals involved in the administration of IV cancer therapy). 22 If protocols do not exist, efforts should be made to formally document the local procedures for dealing with extravasations. There are several examples of existing policies and protocols; some of them can even be found online (see references section). 2,13 16 Training As mentioned above, local policies and protocols are very important for the delivery of quality cancer care. As well as making these documents available, active education of the relevant staff members including doctors, would help to keep the standard of care at a consistently high level across the board. 18 All staff should be encouraged to regularly review the relevant literature on cytotoxics handling and relating to new agents, as part of their ongoing training
16 Those involved in the administration of IV cancer therapies should be educated on the techniques of IV infusion as well as the local organisational policies for: 18 Venous access Venous assessment Administration of chemotherapy Management of extravasation Management of hypersensitivity, etc. Patient education With regard to extravasation, communication with the patient is very important, since they are being relied upon to report symptoms critical in its recognition. Using positive language, patients should be told about the nature of the cancer therapy they are receiving and the real possibility of side effects. They should be asked to report any change in sensation, stinging or burning, no matter how insignificant it appears to them. An informed patient can then help to recognise extravasation early and should always be listened to. 11 In addition, training relating to meeting the information needs of patients within cancer care, for example presenting a positive approach to delivering information vs. a negative one: XXX is a possible side effect, but we can t predict your reaction; most patients take these drugs and tolerate them well. 11 Equipment selection The choice of equipment/material for administering cancer therapy is important when trying to minimise the risk of extravasation. Important considerations include the size and type of cannula or catheter, and whether to use a subcutaneous device or a central line. In general, the goal is to choose a needle that is least likely to become dislodged, and one that allows the blood to flow around it. As a rule, it is advisable to use the smallest gauge cannula in the largest vein possible. Specific recommendations include: 4,7,12,20 Use of a small bore plastic cannula ( cm long) For peripheral access, short, flexible polyethylene or Teflon Use a clear dressing to secure the cannula to allow for constant inspection Secure the infusion line, but never cover the line with a bandage (the insertion point must always be visible) 16
17 Vein selection in peripheral administration The choice of vein for the infusion is an equally important consideration for the prevention of extravasation. Finding the largest, softest and most pliable vein is the best choice to avoid complications. 9 Some general guidelines include: 8,12,18 Try to use the forearm, not the back of the hand Avoid small and fragile veins Avoid insertion on limbs with lymphoedema or with neurological weakness Avoid veins next to joints, tendons, nerves or arteries Avoid the antecubital fossa (area near the elbow) For a more detailed overview of vein selection please refer to Appendix 3. If a first attempt to insert a cannula failed, the second insertion should be made above (closer to the heart) the original site if possible. In general, it is thought that it is best to avoid administering cytotoxic drugs below a previous venepuncture site. 7 Administering intravenous treatment In addition to careful selection of equipment and veins for administration of IV cancer therapy, there are many precautions that can be considered during the infusion to help reduce the risk of extravasation. 8,12,18,22 Starting IV treatment: 8,12,18,22 Become familiar with the manufacturers' recommendations for administration of each treatment Dilute drugs to the recommended concentrations and give at the appropriate rate Check blood return from the cannula, or CVAD, prior to administration Before administering therapy, flush the line with saline (sodium chloride 0.9%) or glucose 5% (as well as between infusions) Ensure that the cannula is secure during the administration of drugs the appropriate dressing (e.g., IV OPSITE 3000, VecaFix or Tegaderm IV) should be used Never cover the insertion point (i.e., cover cannula site with a bandage) If in doubt, re-cannulate Monitoring IV treatment: 8,12,18 Check for swelling, inflammation, redness and pain around cannula site during administration of IV drugs Check blood return from the cannula when vesicants are administered Question the patient about any possible symptoms (i.e., heat, pain and swelling during administration) Do not allow patients receiving intravenous infusions of vesicant drugs to leave clinical area 17
18 Considerations for vesicants: 8,12 Whenever possible, always give vesicant drugs into a recently inserted cannula Patients receiving repeated doses of potentially harmful drugs peripherally should have the cannula resited at regular intervals every few days (depending on hospital recommendations) Consider the order of the infusions being given attempt to administer treatments so vesicants present the least risk to the patient A CVAD could be considered if veins are very difficult to access. This might minimise the risk of extravasation In no case should a butterfly needle be used for any chemotherapeutic infusion 18
19 How is extravasation managed? If extravasation does occur, prevention of serious injury and tissue damage becomes the main focus of those involved in the patient management. Swift action is important to limit the damage caused by the extravasated drug. 22 In general the management of extravasation includes detection (covered in the How is extravasation recognised? section), analysis and action. 23 Procedures and protocols Management initial steps Management next steps Antidotes Anthracycline extravasation Extravasation kit Surgery and debridement Documentation and reporting Procedures and protocols Just as they play a key role in the prevention of extravasation, local procedures and protocols are paramount in the timely recognition and management of extravasation and the prevention of serious tissue damage. If they are already existing, efforts should be made to make them readily available to all who need them (i.e., those healthcare professionals involved in the administration of IV cancer therapy). 22 If protocols do not exist, efforts must be made to formally document the local procedures for dealing with extravasations. It is highly recommended that all healthcare professionals involved in the administration of IV cancer therapy should be aware of: 22 The extravasation policy The contents and whereabouts of the extravasation kit and a replacement kit There are several examples of existing policies and protocols which can be found online. 2,
20 Management initial steps Specific courses of action depend on the nature of the drug, how much of it has extravasated and where. 3 Delays in recognition and treatment can increase the risk of tissue necrosis. If extravasation is suspected, treatment should begin as soon as possible as commencing treatment within 24 hours can reduce damage to tissues, however, extravasation may only become apparent 1 4 weeks after the administration. 3 No matter what the nature of the drug, if extravasation is suspected the initial response remains the same. The most important thing initially is to limit the amount of drug extravasating into the surrounding tissue ,22 Depending on your hospital or centre, there may be prescribed steps and procedures to undertake before any action is taken (i.e., getting a physician s signature on the extravasation protocol). In general, the first course of action is to stop the infusion, aspirate as much of the infusate as possible, mark the site and then remove the cannula (while continuing to aspirate from the extravasation site). Elevate the affected limb and administer analgesia if required. 8,15 If possible take a digital image of the extravasated area. Then, depending on the drug being infused, the correct protocol should be followed to determine the next steps. An example protocol is illustrated in Figure 1. Figure 1. Management of extravasation. 8 Step 1 Stop the infusion immediately. DO NOT remove the cannula at this point. Step 2 Disconnect the infusion (not the cannula/needle). Step 3 Leave the cannula/needle in place and try to aspirate as much of the drug as possible from the cannula with a 10 ml syringe. Avoid applying direct manual pressure to suspected extravasation site. Step 4 Mark the affected area and take digital images of the site. Step 5 Remove the cannula/ needle. Step 6 Collect the extravasation kit (if available), notify the physician on service and seek advice from the chemotherapy team or Senior Medical Staff. Step 7 Administer pain relief if required. Complete required documentation. NOTE: STEP 8 onwards appear in Figures 3, 4 and 5, depending on whether the extravasation requires Localisation and neutralisation or Dispersion and dilution. How to determine which pathway to follow is described in the following sections. 20
21 Management next steps From this point forward, the nature of the treatment prescribed by the presiding physician or hospital policy will depend on the drug, which has extravasated. Figure 2 shows the decision pathway as it relates to individual treatments. Figure 2. Decide on appropriate treatment. 8 Decide on appropriate treatment Amsacrine Actinomycin D Carmustine Dacarbazine Daunorubicin Doxorubicin Epirubicin Idarubicin Mitomycin C Mustine Streptozotocin Vinblastine Vincristine Vindesine Vinorelbine Aminophilline Calcium solutions Hypertonic glucose Phenytoin TPN X-ray contrast media Localise and neutralise Disperse and dilute If the drug is a non-vesicant, application of a simple cold compress and elevation of the limb may be sufficient to limit the swelling etc. 8 In contrast, the extravasation of a vesicant requires several steps and differs for the various classes of drug. There are two broad approaches to limiting the damage caused by extravasation: localisation and neutralisation; or dispersion and dilution. 8 Localise and neutralise strategy (Figure 3): 8 Use cold compresses to limit the spread of infusate. It used to be thought that cold limited spread through vasoconstriction. In animal models, it appears that cold prevents spread by a mechanism other than vasoconstriction suggested to be decreased cellular uptake of drug at lower temperatures Consider using antidotes to counteract vesicant actions. 21
22 Figure 3. Localise and neutralise. 8 NOTE: The initial steps leading to STEP 7 are described in Figure 1. Step 8 LOCALISE Apply a cold pack to the affected area for 20 minutes 4 times daily for 1 2 days. Step 9 NEUTRALISE Neutralise the drug by using the specific antidote (if available).the antidote should be given as per the specific directions provided by the manufacturer. (N.B. Only anthracyclines*, mitomycin C and mustine have specific antidotes for drugs without antidotes omit step 9) LOCALISE AND NEUTRALISE STEP 10 Remove the cannula (delivering the antidote) after confirming no more antidote will be prescribed or given. STEP 11 Elevate the limb. STEP 12 Document the incident using extravasation documentation sheet. STEP 13 Arrange follow up for the patient as appropriate. *For a detailed list of anthracyclines, please refer to Appendix 1) 22
23 Disperse and dilute strategy (Figure 4): 8 Appropriate for the extravasation of vinca alkaloids Use warm compresses to prompt vasodilation and encourage blood flow in the tissues, thereby spreading the infusate around Consider using hyaluronidase to dilute infusate Figure 4. Disperse and dilute. 8 NOTE: The initial steps leading to STEP 7 are described in Figure 1. STEP 8 DISPERSE Apply a warm compress to the affected area for 20 minutes 4 times daily for 1 2 days. DILUTE AND DISPERSE STEP 9 DILUTE Give several subcutaneous injections of IU of hyaluronidase diluted in 1 ml sterile water around the extravasated area to dilute the infusate. STEP 10 Document the incident using extravasation documentation sheet. STEP 11 Arrange follow up for the patient as appropriate. In addition, measures can be taken to limit inflammation, discomfort and pain. 22 A saline flush out technique could also be used but this approach requires specialist advice Corticosteroids can be given to treat inflammation although there is little evidence to support their use in extravasation Antihistamines and analgesics may be required for relief of pain and other symptoms If the infusate is a non-vesicant, the procedure is similar to localise and neutralise, but does not involve any antidotes. 8 A step-by-step approach for non-vesicants is shown in Figure 5. It is worth noting that beyond the measures described here, unfortunately, the management of extravasation is not well standardised due to a lack of documented evidence. As such, extravasation and often calls for specialist advice. 23
24 Figure 5. Treatment for non-vesicants. 8 STEP 8 Elevate the limb. NON-VESICANTS STEP 9 Consider applying a cold pack if local symptoms occur. STEP 10 Document the incident using extravasation documentation sheet. STEP 11 Arrange follow up for the patient as appropriate. Antidotes Antidotes are agents applied or injected to the extravasated area to counteract the effects of the infiltrated agent usually vesicants. They form an important part of the localise and neutralise and the disperse and dilute strategies. For example, Savene (dexrazoxane) can help to neutralise anthracyclines; whereas hyaluronidase helps to facilitate the dilution of vinca alkaloids into the surrounding tissues. Provided they are used in the appropriate way and for the appropriate infusate they might help to prevent progression to ulceration, blistering and necrosis. The evidence supporting the use of different antidotes is often inconclusive and their use (including pros and cons) should be carefully considered. Antidotes currently available used for treating extravasation (and their proposed mechanism) include: 12,24 28 Savene (dexrazoxane): The only registered antidote for anthracyclines, inhibits DNA topoisomerase II, which is the target of anthracycline chemotherapy, blocking the enzyme so it is no longer affected by anthracyclines and damage to the cells is averted Dimethylsulfoxide (DMSO): Prevents ulceration. May work by virtue of its free radical scavenging property Sodium thiosulfate: Prevents alkylation and subsequent destruction in subcutaneous tissue by providing a substrate for alkylation Hyaluronidase: Breaks down hyaluronic acid ("cement") in connective/soft tissue, allowing for dispersion of the extravasated drug, thereby reducing the local concentration of the damaging agent and increasing its rate of absorption 24
25 Table 1. Antidote use after extravasation. 12* Extravasated drug Suggested antidote Level of evidence Advice Anthracyclines Savene (dexrazoxane) Efficacy in biopsy-verified anthracycline extravasation has been confirmed in clinical trials 3 day course of Savene treatment: 1000 mg/m 2 IV as soon as possible (no later than 6 hours) after extravasation on day 1; 1000 mg/m 2 on day 2; and 500 mg/m 2 on day 3 See Appendix 4 for full details Anthracyclines Topical DMSO (99%) Suggested as a possible antidote in many literature sources. Due to lack of evidence it is recommended that this is further studied Mitomycin C Topical DMSO (99%) Suggested as a possible antidote in many literature sources. Due to lack of evidence it is recommended that this is further studied Apply locally as soon as possible. Repeat every 8 hours for 7 days See Appendix 5 for full details Apply locally as soon as possible. Repeat every 8 hours for 7 days See Appendix 5 for full details Mechlorethamine (Nitrogen mustard) Sodium thiosulfate Due to lack of evidence, this antidote is not recommended 2 ml of a solution made from 4 ml sodium thiosulfate + 6 ml sterile water for subcutaneous injection Vinca alkaloids Hyaluronidase Suggested as a possible antidote in many literature sources. Due to lack of evidence it is recommended that this is further studied Taxanes Hyaluronidase Suggested as a possible antidote in many literature sources. Due to lack of evidence it is recommended that this is further studied IU subcutaneously around the area of extravasation See Appendix 6 for full details IU subcutaneously around the area of extravasation See Appendix 6 for full details *For a detailed list of vesicants, please refer to Appendix 1) 25
26 Anthracycline extravasation For anthracycline extravasation, a new treatment, Savene, and the data supporting it is changing the way antidotes are recommended in the localise and neutralise strategy. In the past, several protocols and policies suggested the use of topical DMSO (99%) to stop the development of ulcers in anthracycline extravasation. 12 In the past few years, new data from preclinical and clinical studies has changed the way antidotes are used in anthracycline extravasation, particularly that for Savene And, it has since become the only licensed specific antidote to anthracycline extravasation. As a result, more recent guidance in this area recommends the use of Savene in the treatment of anthracycline extravasation from both a central- and a peripheral line. 2 Extravasation kit The idea behind the extravasation kit is to store all the drugs and equipment that would be used in an emergency situation. The kit should be put together to deal with any eventuality, including extravasation of a variety of vesicant drugs. 19 The kit should be checked regularly and restocked from pharmacy following use. 22 An example of a recommended extravasation kit can be found in Appendix 7. Surgery and debridement Even if extravasation is identified early, progressive extravasation can give rise to ulcerated and necrotic tissue over time. However, the early steps to prevent and manage extravasation help to limit the need for surgery. 5 Ulcerative cases caused by anthracycline extravasations are common (about 1 3 of all cases), therefore surgery should not be considered as the initial primary treatment of choice. 4 When there is ulceration or continued pain, surgical intervention is indicated to excise the damaged tissue. In general, the goal of surgery is to remove the damaged tissue and the vesicant infusate to prevent progression of the extravasation, as well as to restore function and reduce pain to the affected area. 5 Once this tissue is removed, the remaining wound often needs to be closed. The options for wound closure include skin flap and skin grafts (from other areas of the body). 5 In most cases, the surgeon would opt for a wait and see conservative approach to establish whether ulceration will occur naturally and to attempt to avoid surgery and skin grafting. 12 However, in cases where there is pain, surgical debridement of the extravasated area must be considered 24 hours to 1 week after an extravasation
27 Documentation and reporting Each incident of extravasation must be thoroughly documented and reported. 23 Documentation serves several purposes: To provide an accurate account of what happened (in the event that there is litigation) To protect the healthcare professionals involved (showing they followed procedure) To gather information on extravasations, how and when they occurs for audit purposes Highlight any possible deficits in practice which require review In different centres, the documentation procedure may differ slightly between organisations, however the information collected will be very similar. Following an extravasation, the following details should be documented: 15,18,23 Patient name and number Clinical area Date and time of extravasation Name of drug which has extravasated Signs and symptoms Colour of surrounding skin Size of extravasation Description of the IV access Venepuncture site Size and position of cannula Number of attempts at obtaining venous access and positions Drugs administered and the sequence Drug administration technique (bolus or infusion) Blood return Extravasation area Approximate amount of the drug extravasated Photograph of extravasated area Size (diameter, length and width) of extravasation area Appearance of extravasation area Step-by step management with date and time of each step performed and medical notification Aspiration possible (including amount) or not, location (venous and/or subcutaneous), and amount Cold/heat Antidote Referral details (if any) 27
28 Patient s complaints, comments, statements Indication that patient s information sheet given to patient Follow-up instructions given (to patient, nurse, physician, etc.) Names of all professionals involved in the patient management Signature of nurse In addition to the initial documentation, the extravasated area should be checked and any changes documented every 8 hours. Any oedema, erythema, stinging, burning, pain, or fluid leakage at insertion site should be included in this report. 15 A couple of examples of extravasation documentation forms have been included for your reference in Appendix 8. 28
29 Summary Managing extravasation in accordance with the latest scientific understanding and medical consensus allows for optimal treatment to be delivered across different regions. By following the example set out in this module, which includes the latest information on extravasation and a selection of current protocols and policies from prominent centres, 8,13 16 nurses and other healthcare can help to raise the standard of care in cancer therapy. Nurses have a key role to play in implementing these improvements to practice. As outlined in this module, they have a unique interaction with the patient and play a large part in the administration of IV cancer therapy. By learning how to effectively recognise extravasation and by becoming familiar with all the local protocols for dealing with it, including the use of antidotes nurses can help to minimise the incidence of this complication of cancer treatment. Nurses also have the opportunity to play a lead role in expanding the use of best practice in this area. They can help to initiate and develop local protocols and policies where there aren t any due to their role in administration of the drugs and thanks to their knowledge of the patient and unique perspective regarding extravasation management. By helping to broaden the understanding of extravasation and its management across the nursing and other healthcare professions, it is hoped that this educational module will achieve its objective of improving prevention and overall management of extravasations in cancer patients by utilising the latest available evidence. 29
30 Appendix 1. List of drugs: vesicants, irritants and non-vesicants 8,12,15 Vesicants DNA-binding Alkylating agents Mechlorethamine (Nitrogen mustard) Anthracyclines Daunorubicin Doxorubicin Epirubicin Idarubicin Others Dactinomycin Mitomycin C Non-DNA-binding Vinca alkaloids Vinblastine Vincristine Vindesine Vinorelbine Irritants Carmustine Cyclophosphamide Dacarbazine Etoposide Fluorouracil Ifosfamide Mephalan Mitoxantron Streptozocin Possible irritants 2 Carboplatin Cisplatin Docetaxel Irinotecan Oxaliplatin Paclitaxel Topotecan Non-vesicants 1 Asparaginase Bleomycin Bortezumib Cladribine Cytarabine Etoposide phosphate Gemcitabine Interferons Interleukin-2 Methotrexate Monoclonal antibodies Pemetrexed Raltitrexed Thiothepa 1 Any agent extravasated in high enough concentration may be an irritant. 2 There have been few reports of these agents acting as irritants, but there is no clear evidence for this. NOTE: For those medications that are not considered a vesicant but cause prolonged patient discomfort at the infusion site, it is strongly recommended that a central line be placed. Return to text, page 7 Return to text, page 22 Return to text, page 25 30
31 Appendix 2. Distinguishing extravasation from other conditions 4,7,8 Characteristic Flare reaction Vessel irritation Venous shock Extravasation Presenting symptoms Itchy blotches or hives; pain and burning uncommon Aching and tightness Muscular wall of the blood vessel in spasm Pain and burning are common at injection site; stinging may occur during infusion Colouration Raised red streak, blotches or hive-like erythema along the vessel; diffuse or irregular pattern Erythema or dark discolouration along vessel Erythema around area of needle or around the venepuncture site Timing Usually appears suddenly and dissipates within minutes Usually appears within minutes after injection. Colouration may only appear later in the process Usually appears right after injection Symptoms start to appear right after injection, symptoms endure Swelling Unlikely Unlikely Occurs often; does not dissipate for several days Blood return Usually, but not always intact Usually, but not always intact Often absent Usually absent or sluggish Return to text 31
32 Appendix 3.Vein selection procedure 11 Assess veins in both arms and hands Do not use veins in compromised limbs/lower extremities Most desirable Least desirable Criteria for vein selection IDEAL VEIN / BEST LOCATION large, soft, resilient veins in forearm IDEAL VEIN / LESS DESIRABLE LOCATION large, soft, resilient veins in hand/antecubital fossa SATISFACTORY VEIN / BEST LOCATION small, thin veins in forearm SATISFACTORY VEIN / UNDESIRABLE LOCATION small, thin veins in hand; veins in forearm not palpable or visible UNSATISFACTORY VEIN / UNDESIRABLE LOCATION small, fragile veins, which easily rupture in forearm/hand UNSATISFACTORY VEIN / UNDESIRABLE LOCATION veins in forearm/hand not palpable or visible Appropriate choice of venepuncture site Forearm Hand Forearm Hand Consider central venous line Consider central venous line Return to text 32
33 Appendix 4. Administering Savene (dexrazoxane) 2,26 Savene is the only licensed treatment for anthracycline extravasation (doxorubicin, epirubicin, daunorubicin, idarubicin). Steps for administration: 1) Follow steps for localisation and neutralisation of extravasation (Figure 1 and Figure 3) 2) Administration of Savene should begin as soon as possible and no later than 6 hours after the accident 3) Remove ice packs (or other cooling procedures) from the area at least 15 minutes before the administration of Savene 4) Reconstitute Savene with 25 ml sterile water before further dilution in diluent 5) Give Savene as an intravenous infusion once daily for 3 consecutive days according to body surface area: a. Day 1: 1000 mg/m 2 b. Day 2: 1000 mg/m 2 c. Day 3: 500 mg/m 2 6) For patients with a body surface area of more than 2.0 m 2 the single dose should not exceed 2000 mg on day 1 and day 2 and 1000 mg on day 3 Please refer to Savene prescribing information for a full list of contraindications, precautions and warnings. Return to text 33
34 Appendix 5. Administering dimethylsulfoxide 25 Dimethylsulfoxide (DMSO 99%) is an option for the treatment of extravasation with anthracyclines, mitomycin C, doxorubicin, idarubicin, epirubicin and actinomycin D. DMSO/corticosteorids should not be used. Steps for administration: 1) Follow steps for localisation and neutralisation of extravasation (Figure 1 and Figure 3) 2) Draw around area with indelible pen 3) Put gloves on 4) Apply thin layer of DMSO topically to the marked area 5) Allow it to dry 6) Apply a non-occlusive dressing 7) This should be applied within minutes 8) Check for erythema caused by DMSO Please refer to DMSO 99% prescribing information for a full list of contraindications, precautions and warnings. Return to text 34
35 Appendix 6. Administering hyaluronidase* 27 Hyaluronidase may be indicated for suspected or known extravasation of: dextrose in concentration of >10%; parenteral alimentation solution (glucose or protein); solutions containing calcium or potassium; aminophylline; antibiotics. In addition, there are recommendations for hyaluronidase in response to vinca alkaloid extravasation. 12 Steps for administration: 1) Follow steps for dispersion and dilution of extravasation (Figure 1 and Figure 4) 2) Administration of hyaluronidase should begin within 1 hour of extravasation for best results 3) Dilute IU of hyaluronidase in 1 ml sterile water 4) If there is no blood return in the affected IV catheter, consider infusing 0.4 CC of dose directly through the affected IV catheter before removing the catheter and administering the remainder of the dose subcutaneously around the periphery extravasation 5) Use 25 or 27 gauge needle and change after each injection 6) Subcutaneously (or intradermally) inject 1 ml (150 IU) of hyaluronidase as 5 separate 0.2 ml injections around the periphery of extravasation site * Hyaluronidase is not available in all countries Please refer to hyaluronidase prescribing information for a full list of contraindications, precautions and warnings. Return to text 35
Medications or therapeutic solutions may be injected directly into the bloodstream
 Intravenous Therapy Medications or therapeutic solutions may be injected directly into the bloodstream for immediate circulation and use by the body. State practice acts designate which health care professionals
Intravenous Therapy Medications or therapeutic solutions may be injected directly into the bloodstream for immediate circulation and use by the body. State practice acts designate which health care professionals
Coversheet for Network Site Specific Group Agreed Documentation
 Coversheet for Network Site Specific Group Agreed Documentation This sheet is to accompany all documentation agreed by Pan Birmingham Cancer Network Site Specific Groups. This will assist the Network Governance
Coversheet for Network Site Specific Group Agreed Documentation This sheet is to accompany all documentation agreed by Pan Birmingham Cancer Network Site Specific Groups. This will assist the Network Governance
Extravasation. Monique Ackermann. EAHP Foundation seminar in Krakow 23-25 Mai 2008
 Extravasation Monique Ackermann EAHP Foundation seminar in Krakow 23-25 Mai 2008 Pharmacie Interhospitalière de la Côte, Morges Pharmacie des Hôpitaux Universitaires de Genève PLAN 1. Introduction 1. Definition
Extravasation Monique Ackermann EAHP Foundation seminar in Krakow 23-25 Mai 2008 Pharmacie Interhospitalière de la Côte, Morges Pharmacie des Hôpitaux Universitaires de Genève PLAN 1. Introduction 1. Definition
Flushing and Dressing a Peripherally Inserted Central Catheter (PICC Line): a Guide for Nurses
 Flushing and Dressing a Peripherally Inserted Central Catheter (PICC Line): a Guide for Nurses Information for Nurses Introduction This information is for community nursing staffs who have been asked to
Flushing and Dressing a Peripherally Inserted Central Catheter (PICC Line): a Guide for Nurses Information for Nurses Introduction This information is for community nursing staffs who have been asked to
ASWCS Policy for the Treatment of Extravasation Injury
 ASWCS Policy for the Treatment of Extravasation Injury Extravasation of Cytotoxic Drugs Introduction 1. The purpose of this policy is to inform practitioners of their responsibilities in relation to preventing
ASWCS Policy for the Treatment of Extravasation Injury Extravasation of Cytotoxic Drugs Introduction 1. The purpose of this policy is to inform practitioners of their responsibilities in relation to preventing
Peripherally Inserted Central Catheter (PICC) for Outpatient
 Peripherally Inserted Central Catheter (PICC) for Outpatient Introduction A Peripherally Inserted Central Catheter, or PICC line, is a thin, long, soft plastic tube inserted into a vein of the arm. It
Peripherally Inserted Central Catheter (PICC) for Outpatient Introduction A Peripherally Inserted Central Catheter, or PICC line, is a thin, long, soft plastic tube inserted into a vein of the arm. It
Cytotoxic and Biotherapies Credentialing Programme Module 6
 Cytotoxic and Biotherapies Credentialing Programme Module 6 1. Safe Handling and Administration of Cytotoxic and Biotherapies 2. Waste and Spill Management At the completion of this module the RN will
Cytotoxic and Biotherapies Credentialing Programme Module 6 1. Safe Handling and Administration of Cytotoxic and Biotherapies 2. Waste and Spill Management At the completion of this module the RN will
Guideline for the Management of Extravasation
 Guideline for the Management of Extravasation Version History Version Date Brief Summary of Change Issued 1.0 19.03.07 Endorsed by the Governance Committee 1.1 21.08.08 Prepared for review 1.2 09.02.09
Guideline for the Management of Extravasation Version History Version Date Brief Summary of Change Issued 1.0 19.03.07 Endorsed by the Governance Committee 1.1 21.08.08 Prepared for review 1.2 09.02.09
Patient Information Guide Morpheus CT Peripherally Inserted Central Catheter
 Patient Information Guide Morpheus CT Peripherally Inserted Central Catheter IC 192 Rev C A measure of flexibility and strength. Table of Contents 1. Introduction 2. What is the Morpheus CT PICC? 3. What
Patient Information Guide Morpheus CT Peripherally Inserted Central Catheter IC 192 Rev C A measure of flexibility and strength. Table of Contents 1. Introduction 2. What is the Morpheus CT PICC? 3. What
A4.7 Management of a totally occluded central catheter and persistent withdrawal occlusion (PWO)
 A4.7 Management of a totally occluded central catheter and persistent withdrawal occlusion (PWO) Types of Catheter Related Thrombotic A catheter-related thrombus may be intraluminal (inside the catheter)
A4.7 Management of a totally occluded central catheter and persistent withdrawal occlusion (PWO) Types of Catheter Related Thrombotic A catheter-related thrombus may be intraluminal (inside the catheter)
Vaxcel PICCs Valved and Non-Valved. A Patient s Guide
 Vaxcel PICCs Valved and Non-Valved A Patient s Guide Information about your Vaxcel PICC is available by calling the Navilyst Medical Vascular Access Information Line 800.513.6876 Vaxcel Peripherally Inserted
Vaxcel PICCs Valved and Non-Valved A Patient s Guide Information about your Vaxcel PICC is available by calling the Navilyst Medical Vascular Access Information Line 800.513.6876 Vaxcel Peripherally Inserted
Guy s, King s and St Thomas Cancer Centre The Cancer Outpatient Clinic Central venous catheter: Peripherally inserted central catheter
 Guy s, King s and St Thomas Cancer Centre The Cancer Outpatient Clinic Central venous catheter: Peripherally inserted central catheter This information leaflet aims to help answer some of the questions
Guy s, King s and St Thomas Cancer Centre The Cancer Outpatient Clinic Central venous catheter: Peripherally inserted central catheter This information leaflet aims to help answer some of the questions
PICC & Midline Catheters Patient Information Guide
 PICC & Midline Catheters Patient Information Guide medcompnet.com 1 table of contents Introduction 4 What is a PICC or Midline Catheter? 4 How is the PICC or Midline Catheter Inserted? 6 Catheter Care
PICC & Midline Catheters Patient Information Guide medcompnet.com 1 table of contents Introduction 4 What is a PICC or Midline Catheter? 4 How is the PICC or Midline Catheter Inserted? 6 Catheter Care
IV Contrast Extravasation PQI Project Feed-Back Document from the Society of Abdominal Radiology & American College of Radiology
 IV Contrast Extravasation PQI Project Feed-Back Document from the Society of Abdominal Radiology & American College of Radiology This performance feedback document and the accompanying spreadsheet include
IV Contrast Extravasation PQI Project Feed-Back Document from the Society of Abdominal Radiology & American College of Radiology This performance feedback document and the accompanying spreadsheet include
Administration of Medications & Fluids via a Peripheral Intravenous Cannula
 Administration of Medications & Fluids via a Peripheral Intravenous Cannula Clinical S.O.P. No.: 22.0 Compiled by: Approved by: Review date: November 2016 Administration of Medications & Fluids via S.O.P.
Administration of Medications & Fluids via a Peripheral Intravenous Cannula Clinical S.O.P. No.: 22.0 Compiled by: Approved by: Review date: November 2016 Administration of Medications & Fluids via S.O.P.
Lifecath Midline. A Nurses Guide to Lifecath Midline
 Lifecath Midline A Nurses Guide to Lifecath Midline vygon@vygon.co.uk www.vygon.co.uk Lifecath Midline A Nurses Guide to Lifecath Midline This booklet provides guidance in the care and maintenance of Midline
Lifecath Midline A Nurses Guide to Lifecath Midline vygon@vygon.co.uk www.vygon.co.uk Lifecath Midline A Nurses Guide to Lifecath Midline This booklet provides guidance in the care and maintenance of Midline
Beaumont Hospital. Varicose Veins. and their TREATMENT. Professor Austin Leahy, MCh, FRCS, FRCSI WWW.VEINCLINICSOFIRELAND.COM
 Beaumont Hospital Varicose Veins and their TREATMENT Professor Austin Leahy, MCh, FRCS, FRCSI WWW.VEINCLINICSOFIRELAND.COM Department of Surgery Beaumont Hospital and Royal College of Surgeons in Ireland
Beaumont Hospital Varicose Veins and their TREATMENT Professor Austin Leahy, MCh, FRCS, FRCSI WWW.VEINCLINICSOFIRELAND.COM Department of Surgery Beaumont Hospital and Royal College of Surgeons in Ireland
Treating Mesothelioma - A Quick Guide
 Treating Mesothelioma - A Quick Guide Contents This is a brief summary of the information on Treating mesothelioma from CancerHelp UK. You will find more detailed information on the website. In this information
Treating Mesothelioma - A Quick Guide Contents This is a brief summary of the information on Treating mesothelioma from CancerHelp UK. You will find more detailed information on the website. In this information
Policies & Procedures. ID Number: 1118
 Policies & Procedures Title: INTRAVENOUS AND/OR PERIPHERAL SALINE LOCK INSERTION AND MAINTENANCE ID Number: 1118 Authorization [X] SHR Nursing Practice Committee Source: Nursing Date Revised: September
Policies & Procedures Title: INTRAVENOUS AND/OR PERIPHERAL SALINE LOCK INSERTION AND MAINTENANCE ID Number: 1118 Authorization [X] SHR Nursing Practice Committee Source: Nursing Date Revised: September
Breast Pathway Group FEC 60 (Fluorouracil / Epirubicin / Cyclophosphamide) in Early Breast Cancer in Elderly / Frail
 Breast Pathway Group FEC 60 (Fluorouracil / Epirubicin / Cyclophosphamide) in Early Breast Cancer in Elderly / Frail Indication: Neoadjuvant or adjuvant therapy for elderly and frail patients with breast
Breast Pathway Group FEC 60 (Fluorouracil / Epirubicin / Cyclophosphamide) in Early Breast Cancer in Elderly / Frail Indication: Neoadjuvant or adjuvant therapy for elderly and frail patients with breast
Severe rheumatoid arthritis (a disease that causes inflammation of the joints),where MabThera is given intravenously together with methotrexate.
 EMA/614203/2010 EMEA/H/C/000165 EPAR summary for the public rituximab This is a summary of the European public assessment report (EPAR) for. It explains how the Committee for Medicinal Products for Human
EMA/614203/2010 EMEA/H/C/000165 EPAR summary for the public rituximab This is a summary of the European public assessment report (EPAR) for. It explains how the Committee for Medicinal Products for Human
Hydration, IV Infusions, Injections and Vaccine Charge Process
 There are a number of items to be considered when billing for the Nursing service to perform drug therapy, the charge process is divided into three specific groups of codes and processes. 1. Hydration
There are a number of items to be considered when billing for the Nursing service to perform drug therapy, the charge process is divided into three specific groups of codes and processes. 1. Hydration
X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary
 X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary Introduction A Subclavian Inserted Central Catheter, or subclavian line, is a long thin hollow tube inserted in a vein under the
X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary Introduction A Subclavian Inserted Central Catheter, or subclavian line, is a long thin hollow tube inserted in a vein under the
Intravenous Therapy. Marjorie Wiltshire, RN
 Intravenous Therapy Marjorie Wiltshire, RN :OBJECTIVES Define key terms related to intravenous therapy. Demonstrate the procedure for IV insertion, conversion to a saline lock, administration of IV fluids,
Intravenous Therapy Marjorie Wiltshire, RN :OBJECTIVES Define key terms related to intravenous therapy. Demonstrate the procedure for IV insertion, conversion to a saline lock, administration of IV fluids,
Carla Duff, CPNP MSN CCRP Clinical Advanced Registered Nurse Practitioner University of South Florida Division of Allergy, Immunology, and
 Carla Duff, CPNP MSN CCRP Clinical Advanced Registered Nurse Practitioner University of South Florida Division of Allergy, Immunology, and Rheumatology Intravenous Subcutaneous IVIg SCIg What should you
Carla Duff, CPNP MSN CCRP Clinical Advanced Registered Nurse Practitioner University of South Florida Division of Allergy, Immunology, and Rheumatology Intravenous Subcutaneous IVIg SCIg What should you
Epidural Continuous Infusion. Patient information Leaflet
 Epidural Continuous Infusion Patient information Leaflet April 2015 Introduction You may already know that epidural s are often used to treat pain during childbirth. This same technique can also used as
Epidural Continuous Infusion Patient information Leaflet April 2015 Introduction You may already know that epidural s are often used to treat pain during childbirth. This same technique can also used as
A PROCEDURAL GUIDE TO MIDLINE CATHETER INSERTION
 A PROCEDURAL GUIDE TO MIDLINE CATHETER INSERTION See Also CPG midline catheters for indications, contraindications and post insertion management What is a midline A midline catheter is an 8-12 cm catheter
A PROCEDURAL GUIDE TO MIDLINE CATHETER INSERTION See Also CPG midline catheters for indications, contraindications and post insertion management What is a midline A midline catheter is an 8-12 cm catheter
3% Sodium Chloride Injection, USP 5% Sodium Chloride Injection, USP
 PRESCRIBING INFORMATION 3% Sodium Chloride Injection, USP 5% Sodium Chloride Injection, USP IV Fluid and Electrolyte Replenisher Baxter Corporation Mississauga, Ontario L5N 0C2 Canada Date of Revision:
PRESCRIBING INFORMATION 3% Sodium Chloride Injection, USP 5% Sodium Chloride Injection, USP IV Fluid and Electrolyte Replenisher Baxter Corporation Mississauga, Ontario L5N 0C2 Canada Date of Revision:
Questions and answers on breast cancer Guideline 10: The management of persistent pain after breast cancer treatment
 Questions and answers on breast cancer Guideline 10: The management of persistent pain after breast cancer treatment I ve had breast cancer treatment, and now I m having pain. Does this mean the cancer
Questions and answers on breast cancer Guideline 10: The management of persistent pain after breast cancer treatment I ve had breast cancer treatment, and now I m having pain. Does this mean the cancer
Eastern Health MS Service. Tysabri Therapy. Information for People with MS and their Families
 Eastern Health MS Service Tysabri Therapy Information for People with MS and their Families The Eastern Health MS Service has developed this information for you as a guide through what will happen to you
Eastern Health MS Service Tysabri Therapy Information for People with MS and their Families The Eastern Health MS Service has developed this information for you as a guide through what will happen to you
Thyroid Eye Disease. Anatomy: There are 6 muscles that move your eye.
 Thyroid Eye Disease Your doctor thinks you have thyroid orbitopathy. This is an autoimmune condition where your body's immune system is producing factors that stimulate enlargement of the muscles that
Thyroid Eye Disease Your doctor thinks you have thyroid orbitopathy. This is an autoimmune condition where your body's immune system is producing factors that stimulate enlargement of the muscles that
PATIENT GUIDE. Understand and care for your peripherally inserted central venous catheter (PICC). MEDICAL
 PATIENT GUIDE Understand and care for your peripherally inserted central venous catheter (PICC). MEDICAL Introduction The following information is presented as a guideline for your reference. The best
PATIENT GUIDE Understand and care for your peripherally inserted central venous catheter (PICC). MEDICAL Introduction The following information is presented as a guideline for your reference. The best
Chemotherapy for lung cancer
 This information is an extract from the booklet Understanding lung cancer. You may find the full booklet helpful. We can send you a free copy see page 8. Contents Chemoradiation Small cell lung cancer
This information is an extract from the booklet Understanding lung cancer. You may find the full booklet helpful. We can send you a free copy see page 8. Contents Chemoradiation Small cell lung cancer
MISSISSIPPI BOARD OF NURSING IV THERAPY COURSE FOR THE EXPANDED ROLE LICENSED PRACTICAL NURSE COURSE OUTLINE
 THEORY MINIMUM 40 HOURS COURSE OUTLINE UNIT TOPIC HOURS* I LEGAL ASPECTS AND PRACTICE OF IV THERAPY 1 II REVIEW OF ANATOMY AND PHYSIOLOGY 6 III FLUID AND ELECTROLYTE BALANCE 10 IV EQUIPMENT AND PROCEDURES
THEORY MINIMUM 40 HOURS COURSE OUTLINE UNIT TOPIC HOURS* I LEGAL ASPECTS AND PRACTICE OF IV THERAPY 1 II REVIEW OF ANATOMY AND PHYSIOLOGY 6 III FLUID AND ELECTROLYTE BALANCE 10 IV EQUIPMENT AND PROCEDURES
VARICOSE VEINS. Information Leaflet. Your Health. Our Priority. VTE Ambulatory Clinic Stepping Hill Hospital
 VARICOSE VEINS Information Leaflet Your Health. Our Priority. Page 2 of 7 Varicose Veins There are no accurate figures for the number of people with varicose veins. Some studies suggest that 3 in 100 people
VARICOSE VEINS Information Leaflet Your Health. Our Priority. Page 2 of 7 Varicose Veins There are no accurate figures for the number of people with varicose veins. Some studies suggest that 3 in 100 people
Intraosseous Vascular Access and Lidocaine
 Intraosseous Vascular Access and Lidocaine Intraosseous (IO) needles provide access to the medullary cavity of a bone. It is a technique primarily used in emergency situations to administer fluid and medication
Intraosseous Vascular Access and Lidocaine Intraosseous (IO) needles provide access to the medullary cavity of a bone. It is a technique primarily used in emergency situations to administer fluid and medication
Information for patients who require Foam Sclerotherapy for Varicose Veins.
 Information for patients who require Foam Sclerotherapy for Varicose Veins. Why do I need this procedure? Everybody has two sets of veins in the legs. These include the superficial and deep veins. Their
Information for patients who require Foam Sclerotherapy for Varicose Veins. Why do I need this procedure? Everybody has two sets of veins in the legs. These include the superficial and deep veins. Their
About chemotherapy for lung cancer
 About chemotherapy for lung cancer This information is about chemotherapy for lung cancer. There are sections on What is chemotherapy? Chemotherapy for small cell lung cancer Chemotherapy for non-small
About chemotherapy for lung cancer This information is about chemotherapy for lung cancer. There are sections on What is chemotherapy? Chemotherapy for small cell lung cancer Chemotherapy for non-small
Chapter 4 Physiological Therapeutics. 1 Cryotherapy
 Chapter 4 Physiological Therapeutics 1 Cryotherapy CRYOTHERAPY PHYSIOLOGIC EFFECTS OF ICE APPLICATION 1. Decreased circulation 5. Increased tissue stiffness 2. Local vasoconstriction 6. Decreased muscle
Chapter 4 Physiological Therapeutics 1 Cryotherapy CRYOTHERAPY PHYSIOLOGIC EFFECTS OF ICE APPLICATION 1. Decreased circulation 5. Increased tissue stiffness 2. Local vasoconstriction 6. Decreased muscle
Breast Cancer. Breast Cancer Page 1
 Breast Cancer Summary Breast cancers which are detected early are curable by local treatments. The initial surgery will give the most information about the cancer; such as size or whether the glands (or
Breast Cancer Summary Breast cancers which are detected early are curable by local treatments. The initial surgery will give the most information about the cancer; such as size or whether the glands (or
PERIPHERALLY INSERTED CENTRAL CATHETERS (PICC) Fong So Kwan APN, Haematology unit Medical Department, QMH
 PERIPHERALLY INSERTED CENTRAL CATHETERS (PICC) Fong So Kwan APN, Haematology unit Medical Department, QMH 1 What is a PICC catheter? Primary vascular access device since their introduction in the mid-1970s,
PERIPHERALLY INSERTED CENTRAL CATHETERS (PICC) Fong So Kwan APN, Haematology unit Medical Department, QMH 1 What is a PICC catheter? Primary vascular access device since their introduction in the mid-1970s,
INS Position Paper. Recommendations for Frequency of Assessment of the Short Peripheral Catheter Site
 INS Position Paper Recommendations for Frequency of Assessment of the Short Peripheral Catheter Site Background As many organizations choose to follow the Infusion Nurses Society (INS) recommendations
INS Position Paper Recommendations for Frequency of Assessment of the Short Peripheral Catheter Site Background As many organizations choose to follow the Infusion Nurses Society (INS) recommendations
Beaumont Hospital Department of Nephrology and Renal Nursing. Guideline for administering Ferinject
 Beaumont Hospital Department of Nephrology and Renal Nursing Guideline Name: Guideline for administering Ferinject Guideline Number: 18 Guideline Version: a Developed By: Louise Kelly CNM 1 Renal Day Care
Beaumont Hospital Department of Nephrology and Renal Nursing Guideline Name: Guideline for administering Ferinject Guideline Number: 18 Guideline Version: a Developed By: Louise Kelly CNM 1 Renal Day Care
Inferior Vena Cava filter and removal
 Inferior Vena Cava filter and removal What is Inferior Vena Cava Filter Placement and Removal? An inferior vena cava filter placement procedure involves an interventional radiologist (a specialist doctor)
Inferior Vena Cava filter and removal What is Inferior Vena Cava Filter Placement and Removal? An inferior vena cava filter placement procedure involves an interventional radiologist (a specialist doctor)
Guideline for the use of subcutaneous hydration in palliative care (hypodermoclysis)
 Guideline for the use of subcutaneous hydration in palliative care (hypodermoclysis) Date Approved by Network Governance September 2012 Date for Review September 2015 Page 1 of 7 1 Scope of Guideline 1.1
Guideline for the use of subcutaneous hydration in palliative care (hypodermoclysis) Date Approved by Network Governance September 2012 Date for Review September 2015 Page 1 of 7 1 Scope of Guideline 1.1
PHENYLEPHRINE HYDROCHLORIDE INJECTION USP
 PRESCRIBING INFORMATION PHENYLEPHRINE HYDROCHLORIDE INJECTION USP 10 mg/ml Sandoz Canada Inc. Date of Preparation: September 1992 145 Jules-Léger Date of Revision : January 13, 2011 Boucherville, QC, Canada
PRESCRIBING INFORMATION PHENYLEPHRINE HYDROCHLORIDE INJECTION USP 10 mg/ml Sandoz Canada Inc. Date of Preparation: September 1992 145 Jules-Léger Date of Revision : January 13, 2011 Boucherville, QC, Canada
Advanced Lung Cancer Treatment - Chemotherapy vs Radiotherapy
 Which treatment for advanced lung cancer This information tells you about the treatments for advanced lung cancer. Chemotherapy and radiotherapy can both be used to treat advanced lung cancer. They can
Which treatment for advanced lung cancer This information tells you about the treatments for advanced lung cancer. Chemotherapy and radiotherapy can both be used to treat advanced lung cancer. They can
What are spider veins? What is the best treatment for spider veins?
 Laser Spider/Leg Vein Q & A What are spider veins? Millions of women and men are bothered by unsightly spider veins on their faces and legs. Spider veins or telangiectasias are those small red, blue and
Laser Spider/Leg Vein Q & A What are spider veins? Millions of women and men are bothered by unsightly spider veins on their faces and legs. Spider veins or telangiectasias are those small red, blue and
Intravenous Therapy Principles of Care. Breege Smithers Practice Educator
 Intravenous Therapy Principles of Care Breege Smithers Practice Educator Objectives State indications for intravenous therapy List the advantages and disadvantages of intravenous therapy Identify the principles
Intravenous Therapy Principles of Care Breege Smithers Practice Educator Objectives State indications for intravenous therapy List the advantages and disadvantages of intravenous therapy Identify the principles
IAC 1/12/11 Nursing Board[655] Ch 6, p.1 CHAPTER 6 NURSING PRACTICE FOR REGISTERED NURSES/LICENSED PRACTICAL NURSES
![IAC 1/12/11 Nursing Board[655] Ch 6, p.1 CHAPTER 6 NURSING PRACTICE FOR REGISTERED NURSES/LICENSED PRACTICAL NURSES IAC 1/12/11 Nursing Board[655] Ch 6, p.1 CHAPTER 6 NURSING PRACTICE FOR REGISTERED NURSES/LICENSED PRACTICAL NURSES](/thumbs/27/10150251.jpg) IAC 1/12/11 Nursing Board[655] Ch 6, p.1 CHAPTER 6 NURSING PRACTICE FOR REGISTERED NURSES/LICENSED PRACTICAL NURSES 655 6.1(152) Definitions. Accountability means being obligated to answer for one s acts,
IAC 1/12/11 Nursing Board[655] Ch 6, p.1 CHAPTER 6 NURSING PRACTICE FOR REGISTERED NURSES/LICENSED PRACTICAL NURSES 655 6.1(152) Definitions. Accountability means being obligated to answer for one s acts,
Orthopaedic Spine Center. Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs
 Orthopaedic Spine Center Graham Calvert MD James Woodall MD PhD Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs The cervical spine consists of the bony vertebrae, discs, nerves and other structures.
Orthopaedic Spine Center Graham Calvert MD James Woodall MD PhD Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs The cervical spine consists of the bony vertebrae, discs, nerves and other structures.
PICCs and Midline Catheters
 Patient Education PICCs and Midline Catheters Patient s guide to PICC (peripherally inserted central catheter) and midline catheters What are PICCs and midline catheters used for? Any medicine given over
Patient Education PICCs and Midline Catheters Patient s guide to PICC (peripherally inserted central catheter) and midline catheters What are PICCs and midline catheters used for? Any medicine given over
PAEDIATRIC PERIPHERAL INTRAVENOUS CANNULA CARE
 12.1 PROTOCOL SUBJECT: PAEDIATRIC PERIPHERAL INTRAVENOUS CANNULA CARE DOCUMENT NUMBER: 12.1 DATE DEVELOPED: 11/06 LAST REVISED DATE: NEW PLANNED REVIEW DATE: 11/09 DISTRIBUTION: All Clinical Areas Kaleidoscope
12.1 PROTOCOL SUBJECT: PAEDIATRIC PERIPHERAL INTRAVENOUS CANNULA CARE DOCUMENT NUMBER: 12.1 DATE DEVELOPED: 11/06 LAST REVISED DATE: NEW PLANNED REVIEW DATE: 11/09 DISTRIBUTION: All Clinical Areas Kaleidoscope
Positron Emission Tomography - For Patients
 Positron Emission Tomography - For Patients A physician s written order is required for any PET-CT tests. How should I prepare for my PET-CT? PET-CT is more complicated than most other tests you may be
Positron Emission Tomography - For Patients A physician s written order is required for any PET-CT tests. How should I prepare for my PET-CT? PET-CT is more complicated than most other tests you may be
IVC Filter Insertion PROCEDURAL CONSENT FORM. A. Interpreter / cultural needs. B. Procedure. C. Risks of the procedure
 DO NOT WRITE IN THIS BINDING MARGIN V4.00-03/2011 SW9264 Facility: A. Interpreter / cultural needs An Interpreter Service is required? Yes No If Yes, is a qualified Interpreter present? Yes No A Cultural
DO NOT WRITE IN THIS BINDING MARGIN V4.00-03/2011 SW9264 Facility: A. Interpreter / cultural needs An Interpreter Service is required? Yes No If Yes, is a qualified Interpreter present? Yes No A Cultural
In non-hodgkin s lymphoma, MabThera is used to treat two types of the disease, both of which affect B-lymphocytes:
 EMA/614203/2010 EMEA/H/C/000165 EPAR summary for the public rituximab This is a summary of the European public assessment report (EPAR) for. It explains how the Committee for Medicinal Products for Human
EMA/614203/2010 EMEA/H/C/000165 EPAR summary for the public rituximab This is a summary of the European public assessment report (EPAR) for. It explains how the Committee for Medicinal Products for Human
PERIPHERAL STEM CELL TRANSPLANT INTRODUCTION
 PERIPHERAL STEM CELL TRANSPLANT INTRODUCTION This booklet was designed to help you and the important people in your life understand the treatment of high dose chemotherapy with stem cell support: a procedure
PERIPHERAL STEM CELL TRANSPLANT INTRODUCTION This booklet was designed to help you and the important people in your life understand the treatment of high dose chemotherapy with stem cell support: a procedure
Understanding Your Diagnosis of Endometrial Cancer A STEP-BY-STEP GUIDE
 Understanding Your Diagnosis of Endometrial Cancer A STEP-BY-STEP GUIDE Introduction This guide is designed to help you clarify and understand the decisions that need to be made about your care for the
Understanding Your Diagnosis of Endometrial Cancer A STEP-BY-STEP GUIDE Introduction This guide is designed to help you clarify and understand the decisions that need to be made about your care for the
MOH Policy for dispensing NEOPLASTIC DISEASES DRUGS
 MOH Policy for dispensing NEOPLASTIC DISEASES DRUGS All prescriptions for antineoplastic drugs must be accompanied by the MOH special form. All the attachments mentioned on this form shall be submitted
MOH Policy for dispensing NEOPLASTIC DISEASES DRUGS All prescriptions for antineoplastic drugs must be accompanied by the MOH special form. All the attachments mentioned on this form shall be submitted
PACKAGE LEAFLET: INFORMATION FOR THE USER. PARACETAMOL MACOPHARMA 10 mg/ml, solution for infusion. Paracetamol
 PACKAGE LEAFLET: INFORMATION FOR THE USER PARACETAMOL MACOPHARMA 10 mg/ml, solution for infusion Paracetamol Read all of this leaflet carefully before you start using this medicine. Keep this leaflet.
PACKAGE LEAFLET: INFORMATION FOR THE USER PARACETAMOL MACOPHARMA 10 mg/ml, solution for infusion Paracetamol Read all of this leaflet carefully before you start using this medicine. Keep this leaflet.
PERIPHERAL INTRAVENOUS CATHETER MANAGEMENT Adult & Paed
 Auckland District BOARD Clinical Practice Health Board (Section 1) Manual Overview This Document This document covers recommended best practices relating to the selection, insertion, care and management
Auckland District BOARD Clinical Practice Health Board (Section 1) Manual Overview This Document This document covers recommended best practices relating to the selection, insertion, care and management
The Radiotherapy Department Radiotherapy to the chest wall and lymph nodes
 Oxford University Hospitals NHS Trust The Radiotherapy Department Radiotherapy to the chest wall and lymph nodes Information for patients Introduction This leaflet is for people who have had surgery for
Oxford University Hospitals NHS Trust The Radiotherapy Department Radiotherapy to the chest wall and lymph nodes Information for patients Introduction This leaflet is for people who have had surgery for
Breast Implants: Local Complications and Adverse Outcomes
 Breast Implants: Local Complications and Adverse Outcomes This booklet highlights the most common problems associated with silicone gel-filled and saline-filled breast implants: those that occur in the
Breast Implants: Local Complications and Adverse Outcomes This booklet highlights the most common problems associated with silicone gel-filled and saline-filled breast implants: those that occur in the
Stepping toward a different treatment option LEARN WHAT ACTHAR CAN DO FOR YOU
 FOR MS RELAPSES Stepping toward a different treatment option LEARN WHAT ACTHAR CAN DO FOR YOU As a person with multiple sclerosis (MS), you know firsthand the profound impact MS relapses can have on your
FOR MS RELAPSES Stepping toward a different treatment option LEARN WHAT ACTHAR CAN DO FOR YOU As a person with multiple sclerosis (MS), you know firsthand the profound impact MS relapses can have on your
X-Plain Varicose Veins Reference Summary
 X-Plain Varicose Veins Reference Summary Introduction Varicose veins are very common, in both women and men. Varicose veins can be painful and unattractive. Vein doctors use non-invasive ultrasound imaging
X-Plain Varicose Veins Reference Summary Introduction Varicose veins are very common, in both women and men. Varicose veins can be painful and unattractive. Vein doctors use non-invasive ultrasound imaging
The Radiotherapy Department Radiotherapy to the breast Information for patients
 Oxford University Hospitals NHS Trust The Radiotherapy Department Radiotherapy to the breast Information for patients page 2 Introduction This leaflet is for people who have had surgery for breast cancer
Oxford University Hospitals NHS Trust The Radiotherapy Department Radiotherapy to the breast Information for patients page 2 Introduction This leaflet is for people who have had surgery for breast cancer
02 DEPARTMENT OF PROFESSIONAL AND FINANCIAL REGULATION REGULATIONS RELATING TO ADMINISTRATION OF INTRAVENOUS THERAPY BY LICENSED NURSES
 02 DEPARTMENT OF PROFESSIONAL AND FINANCIAL REGULATION 380 BOARD OF NURSING Chapter 10: REGULATIONS RELATING TO ADMINISTRATION OF INTRAVENOUS THERAPY BY LICENSED NURSES SUMMARY: This chapter identifies
02 DEPARTMENT OF PROFESSIONAL AND FINANCIAL REGULATION 380 BOARD OF NURSING Chapter 10: REGULATIONS RELATING TO ADMINISTRATION OF INTRAVENOUS THERAPY BY LICENSED NURSES SUMMARY: This chapter identifies
Dehydration and Fluid Therapy Guide
 Dehydration and Fluid Therapy Guide Background: Dehydration occurs when the loss of body fluids (mainly water) exceeds the amount taken in. Fluid loss can be caused by numerous factors such as: fever,
Dehydration and Fluid Therapy Guide Background: Dehydration occurs when the loss of body fluids (mainly water) exceeds the amount taken in. Fluid loss can be caused by numerous factors such as: fever,
How To Treat A Heart Attack
 13 Resuscitation and preparation for anaesthesia and surgery Key Points 13.1 MANAGEMENT OF EMERGENCIES AND CARDIOPULMONARY RESUSCITATION ESSENTIAL HEALTH TECHNOLOGIES The emergency measures that are familiar
13 Resuscitation and preparation for anaesthesia and surgery Key Points 13.1 MANAGEMENT OF EMERGENCIES AND CARDIOPULMONARY RESUSCITATION ESSENTIAL HEALTH TECHNOLOGIES The emergency measures that are familiar
Heat Illnesses. Common Heat Rash Sites
 Heat Illnesses Introduction Heat illnesses happen when the body becomes too hot and cannot cool itself. There are several different types of heat-related illnesses. This includes heat cramps, heat exhaustion,
Heat Illnesses Introduction Heat illnesses happen when the body becomes too hot and cannot cool itself. There are several different types of heat-related illnesses. This includes heat cramps, heat exhaustion,
MEDICAL CENTER ADMINISTRATIVE POLICY AND PROCEDURES SCOPE KFH Hospital, City Section No.
 of 22 I. Purpose To establish safe medication practices for High Alert medications to maximize the safety of the medication processes associated with these medications. II. Policy. High alert medications
of 22 I. Purpose To establish safe medication practices for High Alert medications to maximize the safety of the medication processes associated with these medications. II. Policy. High alert medications
Caring for a Tenckhoff Catheter
 Caring for a Tenckhoff Catheter UHN A Patient s Guide What is a Pleural Effusion? There is a small space between the outside of your lung and the chest wall (ribs). This space is called the pleural space.
Caring for a Tenckhoff Catheter UHN A Patient s Guide What is a Pleural Effusion? There is a small space between the outside of your lung and the chest wall (ribs). This space is called the pleural space.
Treatment of low-grade non-hodgkin lymphoma
 Produced 28.02.2011 Due for revision 28.02.2013 Treatment of low-grade non-hodgkin lymphoma Lymphomas are described as low grade if the cells appear to be dividing slowly. There are several kinds of low-grade
Produced 28.02.2011 Due for revision 28.02.2013 Treatment of low-grade non-hodgkin lymphoma Lymphomas are described as low grade if the cells appear to be dividing slowly. There are several kinds of low-grade
ARTHROSCOPIC HIP SURGERY
 ARTHROSCOPIC HIP SURGERY Hip Arthroscopy is a relatively simple procedure whereby common disorders of the hip can be diagnosed and treated using keyhole surgery. Some conditions, which previously were
ARTHROSCOPIC HIP SURGERY Hip Arthroscopy is a relatively simple procedure whereby common disorders of the hip can be diagnosed and treated using keyhole surgery. Some conditions, which previously were
POSSIBLE NURSING DIAGNOSIS: Pain Potential for Infection / Infection Fluid volume deficit
 1 Procedure for Subcutaneous Over-the-needle Cannula Insertion, Removal, Medication Administration, and Fluid Administration for the Individual in the Home PURPOSE: To provide medication via the subcutaneous
1 Procedure for Subcutaneous Over-the-needle Cannula Insertion, Removal, Medication Administration, and Fluid Administration for the Individual in the Home PURPOSE: To provide medication via the subcutaneous
What You Should Know About Cerebral Aneurysms
 What You Should Know About Cerebral Aneurysms From the Cerebrovascular Imaging and Interventions Committee of the American Heart Association Cardiovascular Radiology Council Randall T. Higashida, M.D.,
What You Should Know About Cerebral Aneurysms From the Cerebrovascular Imaging and Interventions Committee of the American Heart Association Cardiovascular Radiology Council Randall T. Higashida, M.D.,
Disease/Illness GUIDE TO ASBESTOS LUNG CANCER. What Is Asbestos Lung Cancer? www.simpsonmillar.co.uk Telephone 0844 858 3200
 GUIDE TO ASBESTOS LUNG CANCER What Is Asbestos Lung Cancer? Like tobacco smoking, exposure to asbestos can result in the development of lung cancer. Similarly, the risk of developing asbestos induced lung
GUIDE TO ASBESTOS LUNG CANCER What Is Asbestos Lung Cancer? Like tobacco smoking, exposure to asbestos can result in the development of lung cancer. Similarly, the risk of developing asbestos induced lung
A. ADMINISTERING SUBCUTANEOUS MEDICATIONS INTERMITTENTLY/CONTINUOUSLY B. (SUBCUTANEOUS INFUSION) HYDRODERMOCLYSIS
 SUBCUTANEOUS THERAPY A. ADMINISTERING SUBCUTANEOUS MEDICATIONS INTERMITTENTLY/CONTINUOUSLY B. (SUBCUTANEOUS INFUSION) HYDRODERMOCLYSIS PARTS I. Purposes II. General Information III. Responsibilities IV.
SUBCUTANEOUS THERAPY A. ADMINISTERING SUBCUTANEOUS MEDICATIONS INTERMITTENTLY/CONTINUOUSLY B. (SUBCUTANEOUS INFUSION) HYDRODERMOCLYSIS PARTS I. Purposes II. General Information III. Responsibilities IV.
Varicose veins - 1 -
 Varicose veins - 1 - Varicose Veins About 3 in 10 adults develop varicose veins at some time in their life. Most people with varicose veins do not have an underlying disease and they usually occur for
Varicose veins - 1 - Varicose Veins About 3 in 10 adults develop varicose veins at some time in their life. Most people with varicose veins do not have an underlying disease and they usually occur for
Radiotherapy to the chest wall
 Oxford University Hospitals NHS Trust The Radiotherapy Department Radiotherapy to the chest wall Information for patients Introduction This leaflet is for people who have had surgery for breast cancer
Oxford University Hospitals NHS Trust The Radiotherapy Department Radiotherapy to the chest wall Information for patients Introduction This leaflet is for people who have had surgery for breast cancer
Inflammatory breast cancer
 april 2007 information about Inflammatory breast cancer What is inflammatory breast cancer? Inflammatory breast cancer is a rare and rapidly growing form of breast cancer. Unlike other breast cancers which
april 2007 information about Inflammatory breast cancer What is inflammatory breast cancer? Inflammatory breast cancer is a rare and rapidly growing form of breast cancer. Unlike other breast cancers which
Note that the following document is copyright, details of which are provided on the next page.
 Please note that the following document was created by the former Australian Council for Safety and Quality in Health Care. The former Council ceased its activities on 31 December 2005 and the Australian
Please note that the following document was created by the former Australian Council for Safety and Quality in Health Care. The former Council ceased its activities on 31 December 2005 and the Australian
Other treatments for chronic myeloid leukaemia
 Other treatments for chronic myeloid leukaemia This information is an extract from the booklet Understanding chronic myeloid leukaemia. You may find the full booklet helpful. We can send you a copy free
Other treatments for chronic myeloid leukaemia This information is an extract from the booklet Understanding chronic myeloid leukaemia. You may find the full booklet helpful. We can send you a copy free
Within the Scope of Practice/Role of APRN RN _ X_LPN CNA
 Wyoming State Board of Nursing 130 Hobbs Avenue, Suite B Cheyenne, WY 82002 Phone (307) 777-7601 Fax (307) 777-3519 E-Mail: wsbn-info-licensing@wyo.gov Home Page: https://nursing-online.state.wy.us/ OPINION:
Wyoming State Board of Nursing 130 Hobbs Avenue, Suite B Cheyenne, WY 82002 Phone (307) 777-7601 Fax (307) 777-3519 E-Mail: wsbn-info-licensing@wyo.gov Home Page: https://nursing-online.state.wy.us/ OPINION:
PICC- Peripherally Inserted Central Catheter PROCEDURAL CONSENT FORM. A. Interpreter / cultural needs. B. Procedure. C. Risks of the procedure
 DO NOT WRITE IN THIS BINDING MARGIN v3.00-03/2011 SW9266 Facility: PICC- Peripherally Inserted Central Catheter A. Interpreter / cultural needs An Interpreter Service is required? Yes No If Yes, is a qualified
DO NOT WRITE IN THIS BINDING MARGIN v3.00-03/2011 SW9266 Facility: PICC- Peripherally Inserted Central Catheter A. Interpreter / cultural needs An Interpreter Service is required? Yes No If Yes, is a qualified
Care of Gastrostomy Tubes for Adults with IDD in Community Settings: The Nurse s Role. Lillian Khalil, BSN, RN Volunteers of America, Chesapeake
 Care of Gastrostomy Tubes for Adults with IDD in Community Settings: The Nurse s Role Lillian Khalil, BSN, RN Volunteers of America, Chesapeake Objectives The participants will be able to identify the
Care of Gastrostomy Tubes for Adults with IDD in Community Settings: The Nurse s Role Lillian Khalil, BSN, RN Volunteers of America, Chesapeake Objectives The participants will be able to identify the
Policy and Procedure Flushing and / or Blood withdrawal Aspiration Procedure For PICC Line and Midline Catheters
 Policy and Procedure Flushing and / or Blood withdrawal Aspiration Procedure For PICC Line and Midline Catheters Purpose: Blood Withdrawal: To obtain blood samples for laboratory evaluation, eliminating
Policy and Procedure Flushing and / or Blood withdrawal Aspiration Procedure For PICC Line and Midline Catheters Purpose: Blood Withdrawal: To obtain blood samples for laboratory evaluation, eliminating
I will be having surgery and radiation treatment for breast cancer. Do I need drug treatment too?
 What is node-positive breast cancer? Node-positive breast cancer means that cancer cells from the tumour in the breast have been found in the lymph nodes (sometimes called glands ) in the armpit area.
What is node-positive breast cancer? Node-positive breast cancer means that cancer cells from the tumour in the breast have been found in the lymph nodes (sometimes called glands ) in the armpit area.
Acute Low Back Pain. North American Spine Society Public Education Series
 Acute Low Back Pain North American Spine Society Public Education Series What Is Acute Low Back Pain? Acute low back pain (LBP) is defined as low back pain present for up to six weeks. It may be experienced
Acute Low Back Pain North American Spine Society Public Education Series What Is Acute Low Back Pain? Acute low back pain (LBP) is defined as low back pain present for up to six weeks. It may be experienced
Raynaud s phenomenon, Scleroderma and associated disorders
 Patient information Raynaud s phenomenon, Scleroderma and associated disorders Vascular Surgery Surgical Division PIF 202/V5 What is Raynaud s phenomenon? Raynaud s phenomenon is a condition where the
Patient information Raynaud s phenomenon, Scleroderma and associated disorders Vascular Surgery Surgical Division PIF 202/V5 What is Raynaud s phenomenon? Raynaud s phenomenon is a condition where the
Surgery. Wedge resection only part of the lung, not. not a lobe, is removed. Cancer Council NSW
 The treatment you receive will depend on your lung cancer type, for example, whether you have a non-small cell lung cancer Adenocarcinoma or Squamous cell carcinoma, and if this is a sub-type with a mutation.
The treatment you receive will depend on your lung cancer type, for example, whether you have a non-small cell lung cancer Adenocarcinoma or Squamous cell carcinoma, and if this is a sub-type with a mutation.
Varicose Veins Operation. Patient information Leaflet
 Varicose Veins Operation Patient information Leaflet 22 nd August 2014 WHAT IS VARICOSE VEIN SURGERY (HIGH LIGATION AND MULTIPLE AVULSIONS) The operation varies from case to case, depending on where the
Varicose Veins Operation Patient information Leaflet 22 nd August 2014 WHAT IS VARICOSE VEIN SURGERY (HIGH LIGATION AND MULTIPLE AVULSIONS) The operation varies from case to case, depending on where the
Guidelines for the Use of Naloxone in Palliative Care in Adult Patients
 Guidelines for the Use of Naloxone in Palliative Care in Adult Patients Date Approved by Network Governance May 2012 Date for Review May 2015 Changes between Version 1 and 2 1. Guideline background 2.
Guidelines for the Use of Naloxone in Palliative Care in Adult Patients Date Approved by Network Governance May 2012 Date for Review May 2015 Changes between Version 1 and 2 1. Guideline background 2.
PICC and Midline Catheters
 PICC and Midline Catheters Infusion RN s Deb Bucher RN BSN CRNI Dawn Finch RN CRNI Marianne Hansen RN BSN CRNI Karman Youngblood RN BS CRNI Infusion Pharmacist Kathy Cimakasky Pharm D Tamara Migut RPh
PICC and Midline Catheters Infusion RN s Deb Bucher RN BSN CRNI Dawn Finch RN CRNI Marianne Hansen RN BSN CRNI Karman Youngblood RN BS CRNI Infusion Pharmacist Kathy Cimakasky Pharm D Tamara Migut RPh
X-Plain Hip Replacement Surgery - Preventing Post Op Complications Reference Summary
 X-Plain Hip Replacement Surgery - Preventing Post Op Complications Reference Summary Introduction Severe arthritis in the hip can lead to severe pain and inability to walk. To relieve the pain and improve
X-Plain Hip Replacement Surgery - Preventing Post Op Complications Reference Summary Introduction Severe arthritis in the hip can lead to severe pain and inability to walk. To relieve the pain and improve
Informed Patient Tutorial Copyright 2012 by the American Academy of Orthopaedic Surgeons
 Informed Patient Tutorial Copyright 2012 by the American Academy of Orthopaedic Surgeons Informed Patient - Carpal Tunnel Release Surgery Introduction Welcome to the American Academy of Orthopaedic Surgeons'
Informed Patient Tutorial Copyright 2012 by the American Academy of Orthopaedic Surgeons Informed Patient - Carpal Tunnel Release Surgery Introduction Welcome to the American Academy of Orthopaedic Surgeons'
ALLERGENIC EXTRACT. Prescription Set of Serial Dilutions (or Maintenance Vial (s)) INSTRUCTIONS FOR USE. U.S. Government License No.
 ALLERGENIC EXTRACT Prescription Set of Serial Dilutions (or Maintenance Vial (s)) INSTRUCTIONS FOR USE U.S. Government License No. 308 Revised 07/04 PO Box 800 Lenoir, NC 28645 USA DESCRIPTION This set
ALLERGENIC EXTRACT Prescription Set of Serial Dilutions (or Maintenance Vial (s)) INSTRUCTIONS FOR USE U.S. Government License No. 308 Revised 07/04 PO Box 800 Lenoir, NC 28645 USA DESCRIPTION This set
Ward 29 guide to the safe preparation and administration of intravenous (IV) antibiotics at home
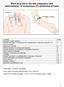 Ward 29 guide to the safe preparation and administration of intravenous (IV) antibiotics at home Contents Page Important contact numbers 1 General information on preparing and administering IV antibiotics
Ward 29 guide to the safe preparation and administration of intravenous (IV) antibiotics at home Contents Page Important contact numbers 1 General information on preparing and administering IV antibiotics
VAD Chemotherapy Regimen for Multiple Myeloma Information for Patients
 VAD Chemotherapy Regimen for Multiple Myeloma Information for Patients The Regimen contains: V = vincristine (Oncovin ) A = Adriamycin (doxorubicin) D = Decadron (dexamethasone) How Is This Regimen Given?
VAD Chemotherapy Regimen for Multiple Myeloma Information for Patients The Regimen contains: V = vincristine (Oncovin ) A = Adriamycin (doxorubicin) D = Decadron (dexamethasone) How Is This Regimen Given?
Guidance for the Safe Use of Cytotoxic Chemotherapy in Grampian, Orkney and Shetland
 Guidance for the Safe Use of Cytotoxic Chemotherapy in Grampian, Orkney and Shetland Co-ordinator: Lynn Adams Reviewer: Pharmacists Aberdeen Royal Infirmary Approver: Dr M Nicolson Signature: Signature:
Guidance for the Safe Use of Cytotoxic Chemotherapy in Grampian, Orkney and Shetland Co-ordinator: Lynn Adams Reviewer: Pharmacists Aberdeen Royal Infirmary Approver: Dr M Nicolson Signature: Signature:
