Emergency Neurological Life Support: Intracranial Hypertension and Herniation
|
|
|
- Amos Patterson
- 8 years ago
- Views:
Transcription
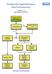
1 DOI /s REVIEW ARTICLE Emergency Neurological Life Support: Intracranial Hypertension and Herniation Robert D. Stevens J. Stephen Huff Josh Duckworth Alexander Papangelou Scott D. Weingart Wade S. Smith Ó Neurocritical Care Society 2012 Abstract Sustained intracranial hypertension and acute brain herniation are brain codes, signifying catastrophic neurological events that require immediate recognition and treatment to prevent irreversible injury and death. As in cardiac arrest, evidence supports the organized implementation of a stepwise management algorithm. Because there are multiple etiologies and many treatments that can potentially reverse cerebral herniation, intracranial hypertension and herniation was chosen as an Emergency Neurological Life Support (ENLS) protocol. R. D. Stevens J. Duckworth A. Papangelou Department of Anesthesiology and Critical Care Medicine, Johns Hopkins University School of Medicine, Baltimore, MD, USA R. D. Stevens J. Duckworth A. Papangelou Department of Neurology, Johns Hopkins University School of Medicine, Baltimore, MD, USA R. D. Stevens J. Duckworth Department of Neurosurgery, Johns Hopkins University School of Medicine, Baltimore, MD, USA R. D. Stevens J. Duckworth Department of Radiology, Johns Hopkins University School of Medicine, Baltimore, MD, USA J. S. Huff (&) Department of Emergency Medicine and Neurology, University of Virginia School of Medicine, Charlottesville, VA, USA jshuff505@me.com S. D. Weingart ENLS Course Co-Chair, Division of ED Critical Care, Mount Sinai School of Medicine, New York, NY, USA W. S. Smith ENLS Course Co-Chair, Department of Neurology, University of California, San Francisco, CA, USA smithw@neurology.ucsf.edu Keywords ICP Cerebral perfusion pressure Mass effect Ventriculostomy Osmotherapy hypertonic saline Protocol Introduction The ENLS-suggested algorithm for the initial management of intracranial hypertension or herniation is shown in Fig. 1. The sum of intracranial contents brain, blood, and cerebrospinal fluid (CSF) represents a fixed volume determined by the invariant constraints of the cranial vault [1, 2]. Relative volumes of these contents will change to accommodate a space-occupying mass; however, this compensation is lost once a critical volume change has occurred, as demonstrated by the inflection point of the pressure volume relationship (Fig. 2). Intracranial hypertension and cerebral herniation are brain codes lifethreatening neurological emergencies signifying that that intracranial compliance adaptive mechanisms have been overwhelmed. Although frequently linked, elevations of intracranial pressure (ICP) and brain herniation can occur independently. Intracranial hypertension is defined as a sustained (>5 min) elevation of ICP of >20 mmhg [3]. Detection requires invasive monitoring, but certain clinical and physiological signs may suggest elevated ICP prior to instrumentation. Herniation syndromes result from intracranial compartmental pressure gradients leading to parenchymal tissue shifts that compress or displace the brainstem, cranial nerves, or cerebral vasculature. Ischemia or infarction from vascular compression may cause edema and further deterioration in compliance.
2 Table 1 Etiologies of brain code Fig. 1 ENLS intracranial hypertension or herniation protocol Extra-axial process Epidural hemorrhage Subdural hemorrhage Subdural empyema Extra-axial brain tumor Pneumocephalus Focal brain process Brain tumor (primary, metastatic) Ischemic stroke Primary intracerebral hemorrhage Brain abscess Traumatic brain injury Hydrocephalus Diffuse brain process Traumatic brain injury Aneurysmal subarachnoid hemorrhage Infectious meningitides and encephalitides Non-infectious neuroinflammatory disorders Hepatic encephalopathy Toxic-metabolic encephalopathies Intracranial pressure The etiologies of brain code are classified anatomically as extra-axial or intraparenchymal processes which can be focal or diffuse (Table 1). In the emergent setting of a brain code, resuscitative measures are pursued even if the etiological mechanism has not been fully characterized. Presentation Total intracranial volume Fig. 2 Intracranial compliance is biphasic Clinically, increased ICP may be signaled by the presence of headache, hypertension, bradycardia, and irregular respirations or apnea (Cushing s triad), though the concurrence of three signs is uncommon [4]. Common sites for herniation are the cingulum (subfalcine herniation), medial temporal lobe (uncal herniation), and inferior cerebellum (tonsillar herniation). The cardinal signs of transtentorial (uncal) herniation are an acute loss of consciousness associated with ipsilateral pupillary dilation and contralateral hemiparesis, resulting respectively from compression or displacement of ascending arousal pathways, oculomotor nerve (III), and corticospinal tract [5, 6]. Transtentorial herniation may cause ipsilateral cerebral infarction because of occlusion of the posterior cerebral artery. In a subset of patients, herniation-associated shift of the midbrain compresses the contralateral anterior cerebral peduncle (crus cerebri) against the tentorium, resulting in hemiparesis that is ipsilateral to the lesion (Kernohan s false localizing sign) [7]. Neuroimaging In the emergent setting of a brain code, a cranial-computed tomography (CT) scan should be obtained without delay to identify a process that may require surgical intervention. Initial resuscitative measures and stabilization, including airway interventions and provision of circulatory and ventilatory support, must occur prior to transport to the radiology suite. Cranial CT is preferred over magnetic resonance imaging (MRI) due to availability and speed of imaging. In the majority of cases, CT will identify the underlying process (see Table 1), though MRI may
3 subsequently be needed for characterization. MRI should only be sought if the risk of an additional brain code has been addressed by medical and/or surgical intervention. ICP Monitoring ICP monitors are invasive and are of several different types, including intraventricular catheters as well as intraparenchymal, subdural, and epidural devices. The decision to proceed with ICP monitoring is determined by the underlying process and the likelihood of its progression. In traumatic brain injury (TBI), neurosurgical guidelines recommended placement of an ICP monitor in patients with severe TBI who are comatose after resuscitation (Glasgow Coma Scale, or GCS, of 3 8) and have either (1) abnormalities on cranial CT scan or (2) meet at least two of the following three criteria: age older than 40 years, systolic blood pressure <90 mmhg, or abnormal posturing [8]. Cerebral perfusion pressure (CPP), used as a surrogate for global cerebral blood flow (CBF), is approximated by the equation: CPP ¼ mean arterial pressure ðmapþ ICP In patients with TBI, available data support maintaining CPP >50 60 mmhg to prevent cerebral ischemia [3]. Aggressive efforts to maintain CPP >60 mmhg may elevate the risk of systemic complications, including acute respiratory distress syndrome [9]. Indications for ICP monitoring and CPP targets for patients with nontraumatic intracranial hypertension have not been adequately studied. Tier Zero Brain code resuscitation begins with an assessment for adequate circulation, airway patency, and ventilation. The head of the bed should be elevated to 30 degrees or higher to facilitate cerebral venous drainage [10, 11]. Stimuli, such as tracheal suctioning that may elevate ICP, should be minimized. If hyperthermia is present, measures should be taken to lower body and brain temperature. Only iso- or hyperosmotic fluids should be used as intravenous solutions. If hyponatremia is present, steps should be initiated for correction. High-dose corticosteroid therapy is initiated for vasogenic edema resulting from brain tumors, abscesses, or non-infectious neuroinflammatory conditions [12, 13]. If the brain has not yet been imaged, a non-contrast head CT scan should be performed when the patient can be safely transported. Tier One If acute obstructive hydrocephalus is present as determined by neuroimaging, an external ventricular drainage (EVD) system should be placed emergently. If a ventricular shunt or an EVD system is in place, drain 5 10 ml of cerebrospinal fluid [14]. Mannitol is administered as g/kg intravenous (IV) bolus and may be repeated every 4 6 h if serum osmolality is monitored [15]. No therapeutic benefit is appreciable with osmolality >320 mosm/kg. As a temporizing measure, a brief course (<2 h) of hyperventilation to a PaCO 2 of mmhg may be considered [16, 17]. If ICP is not controlled, and/or clinical signs of herniation do not resolve with Tier One interventions, review decompressive surgical options [18, 19]. If surgery is not appropriate or not undertaken, move to Tier Two. If ICP is controlled with Tier One interventions, consider repeating the head CT scan to rule out new processes. Head CT After Tier One or Tier Two (the following), if brain imaging has not yet been performed, a head CT scan should be performed to determine the cause of herniation or intracranial hypertension, for the reasons explained in the Neuroimaging section earlier. Tier Two If Tier One interventions have failed to control ICP, Tier Two should be engaged. Brain edema and ICP are treatable with hypertonic saline in concentrations ranging from 2 to 23.4 %. Concentrations >3 % are preferably administered via a central venous catheter (when using concentrations lower than this, peripheral lines may be used, but the infusion should be in a large vessel, and the IV site should be carefully monitored for infiltration). However, because two prehospital trials using 7.5 and 3 % saline solutions via peripheral lines had no negative local effects, these treatments should not be withheld simply because central access is not yet available [20, 21]. Bolus 23.4 % saline has been associated with ICP reduction and reversal of transtentorial herniation [22]. When infusing hypertonic saline, a target serum sodium concentration should be identified and serum sodium level checked every 4 6 h. The therapeutic benefit of achieving serum sodium levels >160 mmol/l is not known. Propofol reduces CMRO 2 and CBF volume and, consequently, ICP [23]. It is administered as a bolus of 1 3 mg/kg and may be continued as an infusion (titrate to maximium 200 lg/kg/min). Propofol is associated with
4 circulatory depression, which should be corrected with IV fluids and/or vasopressors/inotropes to maintain CPP goal. A subset of patients receiving infusions of propofol develop a syndrome of metabolic acidosis, cardiac dysfunction, rhabdomyolysis, and hypertriglyceridemia, often with a fatal outcome [24, 25]. If ICP is not responsive to Tier Two interventions, rescue decompressive surgery should be considered. If the patient is ineligible for surgery, Tier Three should be engaged. Decompression Surgery is considered for brain code patients who have failed medical management. Decompressive surgical interventions for the management of brain code include (a) placement of a ventricular drain, (b) evacuation of extra-axial lesion (e.g., epidural hematoma), (c) resection of intracerebral lesion (e.g., lobar hemorrhage), (d) removal brain parenchyma (e.g., cerebellar mass), and (d) uni- or bilateral craniectomies. Selected patients with rapid neurological deterioration from focal space-occupying lesions may benefit from surgical decompression. This includes patients with brain tumors, brain abscesses, and parenchymal hemorrhages, particularly when the hemorrhages are lobar [26] or cerebellar [27, 28] in location. Decompressive craniectomy may also be considered in patients with diffuse brain swelling associated with traumatic brain injury [29 32]; stroke with massive brain edema, the process in which hemicraniectomy has been most extensively studied [33, 34]; meningoencephalitis; or non-infectious neuroinflammatory conditions (e.g., acute demyelinating encephalomyelitis). Tier Three Tier Three measures represent the most aggressive level of management and carry the highest risk of adverse effects. Rigorous randomized prospective studies are lacking, and recommendations are driven by consensus. This tier includes administration of pentobarbital (bolus 10 mg/kg over 30 min, then 5 mg/kg/h 9 3 h; maintenance infusion of 1 4 mg/kg/h titrated to ICP goal). The electroencephalogram (EEG) should be continuously monitored and pentobarbital titrated either to ICP or to EEG burst suppression of 5 20 s. The pentobarbital infusion is continued for h while the underlying processes driving ICP are treated [35 37]. Pentobarbital is associated with respiratory depression, circulatory instability, immune suppression, and paralytic ileus; neurological examination is limited to an assessment of pupillary reactivity, and drug clearance may take several days after discontinuation of infusion. Moderate hypothermia (target core temperature C) is induced with external cooling devices or with IV infusion of cooled fluids [38 43]. Treatment may be associated with shivering, cardiac arrhythmias, sepsis, coagulopathy, and electrolyte disturbances. Hyperventilation to achieve moderate hypocapnia (PaCO mmhg) may be considered in selected patients who have failed other management. Aggressive hyperventilation should be accomplished in conjunction with a cerebral oxygenation monitor (e.g., jugular venous oximetry, brain tissue oxygen probe), to minimize the risk of cerebral ischemia. Prolonging hyperventilation for >6 h is unlikely to be beneficial and may cause ischemic brain injury [17]. Consider Additional Monitoring Patients who have had or are at risk for a brain code may benefit from additional neuromonitoring, including jugular venous oximetry, brain tissue oxygenation, and cerebral microdialysis. Treatment based on ICP and CPP alone overlooks significant information on the physiologic and metabolic state of the injured brain. Furthermore, assumptions regarding CPP may not hold if CBF autoregulation is impaired. Complementary neuromonitoring techniques should be considered to optimize medical management in selected patients with severe brain injury. Studies using brain tissue oxygen sensors indicate that significant parenchymal hypoxia may occur even when ICP and CPP are normal [44, 45]. Cerebral microdialysis measures brain interstitial lactate, pyruvate, glucose, and glutamate indicators of cerebral metabolic distress whose levels may be altered independently of ICP and CPP [46]. Dynamic indices of cerebral auto-regulation express the correlation between a systemic hemodynamic parameter (arterial blood pressure or CPP) and an intracranial physiological parameter such as ICP (PRx), transcranial Doppler-derived CBF velocity (Mx), or brain tissue PO 2 (Orx). High degrees of correlation suggest a failure of autoregulation and an increased risk of injury because of hypo or hyperperfusion [47, 48]. Revise ICP/MAP Goals Depending on the specific circumstances and the invasive or non-invasive monitoring that is available, the standard goals of MAP and ICP should be reconsidered and customized to the patient. For example, a patient who is
5 neurologically intact, but has an ICP in excess of 20 mmhg or a CPP <60 mmhg, may not require intervention. References 1. Monro A. Observations on the structure and functions of the nervous system. Edinburgh: Printed for, and sold by, W. Creech; Kellie G. Appearances observed in the dissection of two individuals; death from cold and congestion of the brain. Trans Med Chir Soc Edinburgh. 1824;1: Brain Trauma Foundation, American Association of Neurological Surgeons, Congress of Neurological Surgeons, et al. Guidelines for the management of severe traumatic brain injury. VIII. Intracranial pressure thresholds. J Neurotrauma. 2007;24 Suppl 1: S Cushing H. Concerning a definite regulatory mechanism of the vasomotor centre which controls blood pressure during cerebral compression. Bull Johns Hopkins Hosp. 1901;126: Meyer A. Herniation of the brain. Arch Neurol Psychiatry. 1920; 4: Ropper AH. Lateral displacement of the brain and level of consciousness in patients with an acute hemispheral mass. N Engl J Med. 1986;314: Kernohan JW, Woltman HW. Incisura of the crus due to contralateral brain tumour. Arch Neurol Psychiatry. 1929;21: Brain Trauma Foundation, American Association of Neurological Surgeons, Congress of Neurological Surgeons, et al. Guidelines for the management of severe traumatic brain injury. VI. Indications for intracranial pressure monitoring. J Neurotrauma. 2007;24 Suppl 1:S Contant CF, Valadka AB, Gopinath SP, Hannay HJ, Robertson CS. Adult respiratory distress syndrome: a complication of induced hypertension after severe head injury. J Neurosurg. 2001; 95: Feldman Z, Kanter MJ, Robertson CS, et al. Effect of head elevation on intracranial pressure, cerebral perfusion pressure, and cerebral blood flow in head-injured patients. J Neurosurg. 1992; 76: Ng I, Lim J, Wong HB. Effects of head posture on cerebral hemodynamics: its influences on intracranial pressure, cerebral perfusion pressure, and cerebral oxygenation. Neurosurgery. 2004;54:593 7: Discussion: Galicich JH, French LA, Melby JC. Use of dexamethasone in treatment of cerebral edema associated with brain tumors. J Lancet. 1961;81: Quartey GR, Johnston JA, Rozdilsky B. Decadron in the treatment of cerebral abscess. An experimental study. J Neurosurg. 1976;45: Kerr EM, Marion D, Sereika MS, et al. The effect of cerebrospinal fluid drainage on cerebral perfusion in traumatic brain injured adults. J Neurosurg Anesthesiol. 2000;12: Francony G, Fauvage B, Falcon D, et al. Equimolar doses of mannitol and hypertonic saline in the treatment of increased intracranial pressure. Crit Care Med. 2008;36: Coles JP, Minhas PS, Fryer TD, et al. Effect of hyperventilation on cerebral blood flow in traumatic head injury: clinical relevance and monitoring correlates. Crit Care Med. 2002;30: Muizelaar JP, Marmarou A, Ward JD, et al. Adverse effects of prolonged hyperventilation in patients with severe head injury: a randomized clinical trial. J Neurosurg. 1991;75: Eberle BM, Schnuriger B, Inaba K, Gruen JP, Demetriades D, Belzberg H. Decompressive craniectomy: surgical control of traumatic intracranial hypertension may improve outcome. Injury. 2010;41: Johnson RD, Maartens NF, Teddy PJ. Decompressive craniectomy for malignant middle cerebral artery infarction: evidence and controversies. J Clin Neurosci. 2011;18: Bulger EM, May S, Brasel KJ, et al. Out-of-hospital hypertonic resuscitation following severe traumatic brain injury: a randomized controlled trial. JAMA. 2012;304: Dubick MA, Wade CE. A review of the efficacy and safety of 7.5 % NaCl/6 % dextran 70 in experimental animals and in humans. J Trauma. 1994;36: Koenig MA, Bryan M, Lewin JL 3rd, Mirski MA, Geocadin RG, Stevens RD. Reversal of transtentorial herniation with hypertonic saline. Neurology. 2008;70: Kelly DF, Goodale DB, Williams J, et al. Propofol in the treatment of moderate and severe head injury: a randomized, prospective double-blinded pilot trial. J Neurosurg. 1999;90: Roberts RJ, Barletta JF, Fong JJ, et al. Incidence of propofolrelated infusion syndrome in critically ill adults: a prospective, multicenter study. Crit Care. 2009;13:R Fong JJ, Sylvia L, Ruthazer R, Schumaker G, Kcomt M, Devlin JW. Predictors of mortality in patients with suspected propofol infusion syndrome. Crit Care Med. 2008;36: Mendelow AD, Gregson BA, Fernandes HM, et al. Early surgery versus initial conservative treatment in patients with spontaneous supratentorial intracerebral haematomas in the International Surgical Trial in Intracerebral Haemorrhage (STICH): a randomised trial. Lancet. 2005;365: Pfefferkorn T, Eppinger U, Linn J, et al. Long-term outcome after suboccipital decompressive craniectomy for malignant cerebellar infarction. Stroke. 2009;40: Raco A, Caroli E, Isidori A, Salvati M. Management of acute cerebellar infarction: one institution s experience. Neurosurgery. 2003;53:1061 5: Discussion: Jiang JY, Xu W, Li WP, et al. Efficacy of standard trauma craniectomy for refractory intracranial hypertension with severe traumatic brain injury: a multicenter, prospective, randomized controlled study. J Neurotrauma. 2005;22: Olivecrona M, Rodling-Wahlstrom M, Naredi S, Koskinen LO. Effective ICP reduction by decompressive craniectomy in patients with severe traumatic brain injury treated by an ICPtargeted therapy. J Neurotrauma. 2007;24: Taylor A, Butt W, Rosenfeld J, et al. A randomized trial of very early decompressive craniectomy in children with traumatic brain injury and sustained intracranial hypertension. Childs Nerv Syst. 2001;17: Cooper DJ, Rosenfeld JV, Murray L, et al. Decompressive craniectomy in diffuse traumatic brain injury. N Engl J Med. 2011;364: Hofmeijer J, Kappelle LJ, Algra A, et al. Surgical decompression for space-occupying cerebral infarction (the Hemicraniectomy After Middle Cerebral Artery infarction with Life-threatening Edema Trial [HAMLET]): a multicentre, open, randomised trial. Lancet Neurol. 2009;8: Vahedi K, Hofmeijer J, Juettler E, et al. Early decompressive surgery in malignant infarction of the middle cerebral artery: a pooled analysis of three randomised controlled trials. Lancet Neurol. 2007;6: Brain Trauma Foundation. The use of barbiturates in the control of intracranial hypertension. J Neurotrauma. 1996;13: Eisenberg HM, Frankowski RF, Contant CF, Marshall LF, Walker MD. High-dose barbiturate control of elevated intracranial pressure in patients with severe head injury. J Neurosurg. 1988;69:15 23.
6 37. Perez-Barcena J, Llompart-Pou JA, Homar J, et al. Pentobarbital versus thiopental in the treatment of refractory intracranial hypertension in patients with traumatic brain injury: a randomized controlled trial. Crit Care. 2008;12:R Jiang J, Yu M, Zhu C. Effect of long-term mild hypothermia therapy in patients with severe traumatic brain injury: 1-year follow-up review of 87 cases. J Neurosurg. 2000;93: Liu WG, Qiu WS, Zhang Y, Wang WM, Lu F, Yang XF. Effects of selective brain cooling in patients with severe traumatic brain injury: a preliminary study. J Int Med Res. 2006;34: Marion DW, Obrist WD, Carlier PM, Penrod LE, Darby JM. The use of moderate therapeutic hypothermia for patients with severe head injuries: a preliminary report. J Neurosurg. 1993;79: Marion DW, Penrod LE, Kelsey SF, et al. Treatment of traumatic brain injury with moderate hypothermia. N Engl J Med. 1997; 336: Qiu W, Zhang Y, Sheng H, et al. Effects of therapeutic mild hypothermia on patients with severe traumatic brain injury after craniotomy. J Crit Care. 2007;22: Shiozaki T, Sugimoto H, Taneda M, et al. Effect of mild hypothermia on uncontrollable intracranial hypertension after severe head injury. J Neurosurg. 1993;79: Chang JJ, Youn TS, Benson D, et al. Physiologic and functional outcome correlates of brain tissue hypoxia in traumatic brain injury. Crit Care Med. 2009;37: Longhi L, Pagan F, Valeriani V, et al. Monitoring brain tissue oxygen tension in brain-injured patients reveals hypoxic episodes in normal-appearing and in peri-focal tissue. Intensive Care Med. 2007;33: Chen HI, Stiefel MF, Oddo M, et al. Detection of cerebral compromise with multimodality monitoring in patients with subarachnoid hemorrhage. Neurosurgery. 2011;69:53 63: Discussion. 47. Schmidt B, Czosnyka M, Raabe A, et al. Adaptive noninvasive assessment of intracranial pressure and cerebral autoregulation. Stroke. 2003;34: Brady K, Joshi B, Zweifel C, et al. Real-time continuous monitoring of cerebral blood flow autoregulation using near-infrared spectroscopy in patients undergoing cardiopulmonary bypass. Stroke. 2010;41:
THERAPY INTENSITY LEVEL
 THERAPY INTENSITY LEVEL TILBasic = TIL Basic. CDE Variable TILBasic = TIL Basic; Global summary measure of Therapy Intensity Level for control of Intracranial Pressure (ICP).. CDE Definition This summary
THERAPY INTENSITY LEVEL TILBasic = TIL Basic. CDE Variable TILBasic = TIL Basic; Global summary measure of Therapy Intensity Level for control of Intracranial Pressure (ICP).. CDE Definition This summary
Constituents within the skull include the brain (80%/1400ml), blood (10%/150ml) and cerebrospinal fluid (CSF 10%/150ml)
 Cerebral Blood Flow and Intracranial Pressure Dr Lisa Hill, SpR Anaesthesia, Royal Oldham Hospital, UK. Email lambpie10@hotmail.com Dr Carl Gwinnutt, Consultant Neuroanaesthetist, Hope Hospital, UK. Part
Cerebral Blood Flow and Intracranial Pressure Dr Lisa Hill, SpR Anaesthesia, Royal Oldham Hospital, UK. Email lambpie10@hotmail.com Dr Carl Gwinnutt, Consultant Neuroanaesthetist, Hope Hospital, UK. Part
The Clinical Evaluation of the Comatose Patient in the Emergency Department
 The Clinical Evaluation of the Comatose Patient in the Emergency Department patients with altered mental status (AMS) and coma. treat patients who present to the Emergency Department with altered mental
The Clinical Evaluation of the Comatose Patient in the Emergency Department patients with altered mental status (AMS) and coma. treat patients who present to the Emergency Department with altered mental
Using the Pupillometer in Clinical Practice
 Using the Pupillometer in Clinical Practice Claude Hemphill MD M.A.S. chmephill@sfgh.ucsf.edu Kathy Johnson RN, MSN KJOHNSON@queens.org Mary Kay Bader RN, MSN, CCNS Badermk@aol.com Pupillometry: How It
Using the Pupillometer in Clinical Practice Claude Hemphill MD M.A.S. chmephill@sfgh.ucsf.edu Kathy Johnson RN, MSN KJOHNSON@queens.org Mary Kay Bader RN, MSN, CCNS Badermk@aol.com Pupillometry: How It
Head Injury. Dr Sally McCarthy Medical Director ECI
 Head Injury Dr Sally McCarthy Medical Director ECI Head injury in the emergency department A common presentation 80% Mild Head Injury = GCS 14 15 10% Moderate Head Injury = GCS 9 13 10% Severe Head Injury
Head Injury Dr Sally McCarthy Medical Director ECI Head injury in the emergency department A common presentation 80% Mild Head Injury = GCS 14 15 10% Moderate Head Injury = GCS 9 13 10% Severe Head Injury
6.0 Management of Head Injuries for Maxillofacial SHOs
 6.0 Management of Head Injuries for Maxillofacial SHOs As a Maxillofacial SHO you are not required to manage established head injury, however an awareness of the process is essential when dealing with
6.0 Management of Head Injuries for Maxillofacial SHOs As a Maxillofacial SHO you are not required to manage established head injury, however an awareness of the process is essential when dealing with
Pressure reactivity: Relationship between ICP and arterial blood pressure (ABP). Pressure-reactivity index, computational methods. Clinical examples.
 Pressure reactivity: Relationship between ICP and arterial blood pressure (ABP). Pressure-reactivity index, computational methods. Clinical examples. Optimization of cerebral perfusion pressure: Relationship
Pressure reactivity: Relationship between ICP and arterial blood pressure (ABP). Pressure-reactivity index, computational methods. Clinical examples. Optimization of cerebral perfusion pressure: Relationship
KING FAISAL SPECIALIST HOSPITAL AND RESEARCH CENTRE (GEN. ORG.) NURSING AFFAIRS. Scope of Service PEDIATRIC INTENSIVE CARE UNIT (PICU)
 PICU-Jan.2012 Page 1 of 7 Number of Beds: 18 Nurse Patient Ratio: 1:1-2 : The Pediatric Intensive Care Unit (PICU) provides 24 hour intensive nursing care for patients aged neonate through adolescence.
PICU-Jan.2012 Page 1 of 7 Number of Beds: 18 Nurse Patient Ratio: 1:1-2 : The Pediatric Intensive Care Unit (PICU) provides 24 hour intensive nursing care for patients aged neonate through adolescence.
The Sepsis Puzzle: Identification, Monitoring and Early Goal Directed Therapy
 The Sepsis Puzzle: Identification, Monitoring and Early Goal Directed Therapy Cindy Goodrich RN, MS, CCRN Content Description Sepsis is caused by widespread tissue injury and systemic inflammation resulting
The Sepsis Puzzle: Identification, Monitoring and Early Goal Directed Therapy Cindy Goodrich RN, MS, CCRN Content Description Sepsis is caused by widespread tissue injury and systemic inflammation resulting
Brain Cooling in Traumatic Brain Injury and Stroke
 Brain Cooling in Traumatic Brain Injury and Stroke Bridget Harris, PhD, RGN Clinical Research Specialist, NHS Lothian Research Fellow, University of Edinburgh Content Therapeutic temperature reduction
Brain Cooling in Traumatic Brain Injury and Stroke Bridget Harris, PhD, RGN Clinical Research Specialist, NHS Lothian Research Fellow, University of Edinburgh Content Therapeutic temperature reduction
PE finding: Left side extremities mild weakness No traumatic wound No bloody otorrhea, nor rhinorrhea
 Case report A 82-year-old man was suffered from sudden onset spasm of extremities then he fell down to the ground with loss of consciousness. He recovered his consciousness 7-8 mins later but his conscious
Case report A 82-year-old man was suffered from sudden onset spasm of extremities then he fell down to the ground with loss of consciousness. He recovered his consciousness 7-8 mins later but his conscious
Cerebral blood flow (CBF) is dependent on a number of factors that can broadly be divided into:
 Cerebral Blood Flow and Intracranial Pressure Dr Lisa Hill, SpR Anaesthesia, Royal Oldham Hospital, UK. Email lambpie10@hotmail.com Dr Carl Gwinnutt, Consultant Neuroanaesthetist, Hope Hospital, UK. The
Cerebral Blood Flow and Intracranial Pressure Dr Lisa Hill, SpR Anaesthesia, Royal Oldham Hospital, UK. Email lambpie10@hotmail.com Dr Carl Gwinnutt, Consultant Neuroanaesthetist, Hope Hospital, UK. The
 Approximately 70-80% of all strokes are ischemic and 20-30% are hemorrhagic Hemorrhagic stroke is defined as an acute neurologic injury resulting from bleeding in the brain There are two distinct types
Approximately 70-80% of all strokes are ischemic and 20-30% are hemorrhagic Hemorrhagic stroke is defined as an acute neurologic injury resulting from bleeding in the brain There are two distinct types
NORTH WALES CRITICAL CARE NETWORK
 NORTH WALES CRITICAL CARE NETWORK LEVELS OF CRITICAL CARE FOR ADULT PATIENTS Throughout the work of the North Wales Critical Care Network reference to Levels of Care for the critically ill are frequently
NORTH WALES CRITICAL CARE NETWORK LEVELS OF CRITICAL CARE FOR ADULT PATIENTS Throughout the work of the North Wales Critical Care Network reference to Levels of Care for the critically ill are frequently
The Initial and 24 h (After the Patient Rehabilitation) Deficit of Arterial Blood Gases as Predictors of Patients Outcome
 Biomedical & Pharmacology Journal Vol. 6(2), 259-264 (2013) The Initial and 24 h (After the Patient Rehabilitation) Deficit of Arterial Blood Gases as Predictors of Patients Outcome Vadod Norouzi 1, Ali
Biomedical & Pharmacology Journal Vol. 6(2), 259-264 (2013) The Initial and 24 h (After the Patient Rehabilitation) Deficit of Arterial Blood Gases as Predictors of Patients Outcome Vadod Norouzi 1, Ali
Discovery of an Aneurysm Following a Motorcycle Accident. Maya Babu, MSIII Gillian Lieberman, M.D.
 Discovery of an Aneurysm Following a Motorcycle Accident Maya Babu, MSIII Gillian Lieberman, M.D. Patient CC: July 2004 65 yo male transferred to the BI from an OSH s/p motorcycle crash w/o a helmet CC
Discovery of an Aneurysm Following a Motorcycle Accident Maya Babu, MSIII Gillian Lieberman, M.D. Patient CC: July 2004 65 yo male transferred to the BI from an OSH s/p motorcycle crash w/o a helmet CC
MANAGEMENT OF HEAD INJURY & INTRACRANIAL PRESSURE D. Franzon, MD, S. Kache, MD
 MANAGEMENT OF HEAD INJURY & INTRACRANIAL PRESSURE D. Franzon, MD, S. Kache, MD Etiologies of elevated ICP: Increased ICP can occur with any CNS pathology that results in a space occupying mass lesion,
MANAGEMENT OF HEAD INJURY & INTRACRANIAL PRESSURE D. Franzon, MD, S. Kache, MD Etiologies of elevated ICP: Increased ICP can occur with any CNS pathology that results in a space occupying mass lesion,
Raised intracranial pressure (ICP) is a common problem in neurosurgical and neurological
 RAISED INTRACRANIAL PRESSURE Laurence T Dunn *i23 J Neurol Neurosurg Psychiatry 2002;73(Suppl I):i23 i27 Raised intracranial pressure (ICP) is a common problem in neurosurgical and neurological practice.
RAISED INTRACRANIAL PRESSURE Laurence T Dunn *i23 J Neurol Neurosurg Psychiatry 2002;73(Suppl I):i23 i27 Raised intracranial pressure (ICP) is a common problem in neurosurgical and neurological practice.
10. Monitoring of pressure-volume compensation- VPR and RAP
 10. Monitoring of pressure-volume compensation- VPR and RAP Various shapes of Pressure-Volume curves J.Neurosurg 1975, Vol 42 Volume pressure response is proportional to mean ICP but not always Avezaat
10. Monitoring of pressure-volume compensation- VPR and RAP Various shapes of Pressure-Volume curves J.Neurosurg 1975, Vol 42 Volume pressure response is proportional to mean ICP but not always Avezaat
Traumatic Head Injuries
 Traumatic Brain Injury (TBI) Traumatic Head Injuries Major contributing cause of trauma deaths Many survivors have permanent disability Commonly occurs in young adults (mostly males) Spokane County EMS
Traumatic Brain Injury (TBI) Traumatic Head Injuries Major contributing cause of trauma deaths Many survivors have permanent disability Commonly occurs in young adults (mostly males) Spokane County EMS
Short Communications. Alcoholic Intracerebral Hemorrhage
 Short Communications 1565 Alcoholic Intracerebral Hemorrhage Leon A. Weisberg, MD Six alcoholic patients developed extensive cerebral hemispheric hemorrhages with both intraventricular and subarachnoid
Short Communications 1565 Alcoholic Intracerebral Hemorrhage Leon A. Weisberg, MD Six alcoholic patients developed extensive cerebral hemispheric hemorrhages with both intraventricular and subarachnoid
SERVICE: Neurosurgery - Sinai, PGY 1
 SERVICE: Neurosurgery - Sinai, PGY 1 General description: The Sinai surgical residents will rotate in the Department of Neurosurgery at Sinai Hospital during their intern year. The duration of this rotation
SERVICE: Neurosurgery - Sinai, PGY 1 General description: The Sinai surgical residents will rotate in the Department of Neurosurgery at Sinai Hospital during their intern year. The duration of this rotation
A First Class Emergency: Headache in Flight. David Bordo, MD
 A First Class Emergency: Headache in Flight A 41 year-old flight attendant boarded a plane in London to return to Chicago, complaining of her typical migraine headache. A co-worker gave her a sumatriptan
A First Class Emergency: Headache in Flight A 41 year-old flight attendant boarded a plane in London to return to Chicago, complaining of her typical migraine headache. A co-worker gave her a sumatriptan
TRAUMATIC BRAIN INJURY Chapter 8
 TRAUMATIC BRAIN INJURY Chapter 8 Contributing Authors Scott A. Marshall, MD Randy Bell, MD Rocco A. Armonda, MD, LTC, MC, US Army Eric Savitsky, MD Geoffrey S.F. Ling, MD, PhD, COL, MC, US Army All figures
TRAUMATIC BRAIN INJURY Chapter 8 Contributing Authors Scott A. Marshall, MD Randy Bell, MD Rocco A. Armonda, MD, LTC, MC, US Army Eric Savitsky, MD Geoffrey S.F. Ling, MD, PhD, COL, MC, US Army All figures
Levels of Critical Care for Adult Patients
 LEVELS OF CARE 1 Levels of Critical Care for Adult Patients STANDARDS AND GUIDELINES LEVELS OF CARE 2 Intensive Care Society 2009 All rights reserved. No reproduction, copy or transmission of this publication
LEVELS OF CARE 1 Levels of Critical Care for Adult Patients STANDARDS AND GUIDELINES LEVELS OF CARE 2 Intensive Care Society 2009 All rights reserved. No reproduction, copy or transmission of this publication
APPENDIX B SAMPLE PEDIATRIC CRITICAL CARE NURSE PRACTITIONER GOALS AND OBJECTIVES
 APPENDIX B SAMPLE PEDIATRIC CRITICAL CARE NURSE PRACTITIONER GOALS AND OBJECTIVES The critical care nurse practitioner orientation is an individualized process based on one s previous experiences and should
APPENDIX B SAMPLE PEDIATRIC CRITICAL CARE NURSE PRACTITIONER GOALS AND OBJECTIVES The critical care nurse practitioner orientation is an individualized process based on one s previous experiences and should
1. Cerebrospainal Fluid (CSF) circulation in brain: Sites and mechanisms of CSF secretion, circulation and reabsorption. Physiological and modelling
 1. Cerebrospainal Fluid (CSF) circulation in brain: Sites and mechanisms of CSF secretion, circulation and reabsorption. Physiological and modelling description. Cerebrospinal space Brain lump in a box?
1. Cerebrospainal Fluid (CSF) circulation in brain: Sites and mechanisms of CSF secretion, circulation and reabsorption. Physiological and modelling description. Cerebrospinal space Brain lump in a box?
FERNE / EMRA 2009 Mid-Atlantic Emergency Medicine Medical Student Symposium: ABCs of Head CT Interpretation; Heather M. Prendergast MD, MPH.
 ABCs of Head CT Interpretation in the Emergency Department: CT Interpretation Workshop Guide Heather M. Prendergast, MD, MPH, FACEP Associate Professor Department of Emergency Medicine University of Illinois
ABCs of Head CT Interpretation in the Emergency Department: CT Interpretation Workshop Guide Heather M. Prendergast, MD, MPH, FACEP Associate Professor Department of Emergency Medicine University of Illinois
Update on Small Animal Cardiopulmonary Resuscitation (CPR)- is anything new?
 Update on Small Animal Cardiopulmonary Resuscitation (CPR)- is anything new? DVM, DACVA Objective: Update on the new Small animal guidelines for CPR and a discussion of the 2012 Reassessment Campaign on
Update on Small Animal Cardiopulmonary Resuscitation (CPR)- is anything new? DVM, DACVA Objective: Update on the new Small animal guidelines for CPR and a discussion of the 2012 Reassessment Campaign on
Types of Brain Injury
 Types of Brain Injury The bones of your skull are hard and they protect your brain. Your brain is soft, like firm Jell-O. When your head moves, your brain moves inside your skull. When your head is hit
Types of Brain Injury The bones of your skull are hard and they protect your brain. Your brain is soft, like firm Jell-O. When your head moves, your brain moves inside your skull. When your head is hit
EMS Management of Stroke. Deaver Shattuck, M.D. Brian Wiseman, M.D. Keith Woodward, M.D.
 EMS Management of Stroke Deaver Shattuck, M.D. Brian Wiseman, M.D. Keith Woodward, M.D. Financial Disclosure: No relevant financial relationship exists Working Together to End Stroke Formed in 2013 Identified
EMS Management of Stroke Deaver Shattuck, M.D. Brian Wiseman, M.D. Keith Woodward, M.D. Financial Disclosure: No relevant financial relationship exists Working Together to End Stroke Formed in 2013 Identified
THERAPEUTIC INDUCED HYPOTHERMIA GUIDELINES
 THERAPEUTIC INDUCED HYPOTHERMIA GUIDELINES Guidelines for Inclusion: (check all that apply) Cardiac arrest patients with any of the following: Ventricular fibrillation Pulseless Ventricular tachycardia
THERAPEUTIC INDUCED HYPOTHERMIA GUIDELINES Guidelines for Inclusion: (check all that apply) Cardiac arrest patients with any of the following: Ventricular fibrillation Pulseless Ventricular tachycardia
TRAUMATIC BRAIN INJURY (TBI)
 Background: Traumatic Brain Injury (TBI) is one of the leading causes of trauma related disability and death in the U.S. TBIs can occur as either blunt, penetrating, or a combination of both depending
Background: Traumatic Brain Injury (TBI) is one of the leading causes of trauma related disability and death in the U.S. TBIs can occur as either blunt, penetrating, or a combination of both depending
perfusion pressure: Definitions. Implication on management protocols. What happens when CPP is too low, and when it is too high? Non-invasive CPP?
 7. Cerebral perfusion pressure: Definitions. Implication on management protocols. What happens when CPP is too low, and when it is too high? Non-invasive CPP? Definitions of CPP Thanks to Dr. E. Schmidt
7. Cerebral perfusion pressure: Definitions. Implication on management protocols. What happens when CPP is too low, and when it is too high? Non-invasive CPP? Definitions of CPP Thanks to Dr. E. Schmidt
ICTUS CEREBELOSOS. Carlos S. Kase, M.D. Department of Neurology Boston University Boston, MA
 ICTUS CEREBELOSOS Carlos S. Kase, M.D. Department of Neurology Boston University Boston, MA CEREBELLAR STROKES CEREBELLAR INFARCTION CEREBELLAR HEMORRHAGE Distribution of Pathologically Confirmed Cerebellar
ICTUS CEREBELOSOS Carlos S. Kase, M.D. Department of Neurology Boston University Boston, MA CEREBELLAR STROKES CEREBELLAR INFARCTION CEREBELLAR HEMORRHAGE Distribution of Pathologically Confirmed Cerebellar
Guidelines for the Triage and Transfer of Patients with Brain Injury to The Queen s Medical Center. April 2007. Revised September 2007
 Guidelines for the Triage and Transfer of Patients with Brain Injury to The Queen s Medical Center April 2007 Revised September 2007 Reviewed March 2012 2 The Queen s Medical Center (QMC) is the only trauma
Guidelines for the Triage and Transfer of Patients with Brain Injury to The Queen s Medical Center April 2007 Revised September 2007 Reviewed March 2012 2 The Queen s Medical Center (QMC) is the only trauma
Neurology Clerkship Learning Objectives
 Neurology Clerkship Learning Objectives Clinical skills Perform a neurological screening examination of the cranial nerves, motor system, reflexes, and sensory system under the observation and guidance
Neurology Clerkship Learning Objectives Clinical skills Perform a neurological screening examination of the cranial nerves, motor system, reflexes, and sensory system under the observation and guidance
Treatment of Ischemic Stroke in the Neuro-ICU
 Treatment of Ischemic Stroke in the Neuro-ICU Gary L. Bernardini, MD, PhD Professor of Neurology Director, Stroke and Neurocritical Care Departments of Neurology and Neurosurgery Albany Medical Center
Treatment of Ischemic Stroke in the Neuro-ICU Gary L. Bernardini, MD, PhD Professor of Neurology Director, Stroke and Neurocritical Care Departments of Neurology and Neurosurgery Albany Medical Center
Appendix. Costing Case Samples for OOHCA
 Appendix Costing Case Samples for OOHCA The patient (ICD-1) Treatment Codes (OPCS 4) Patient 27 Admitted to ICU following percutaneous cardiac intervention (PCI) with 2 drugeluting stents following a VF
Appendix Costing Case Samples for OOHCA The patient (ICD-1) Treatment Codes (OPCS 4) Patient 27 Admitted to ICU following percutaneous cardiac intervention (PCI) with 2 drugeluting stents following a VF
John E. O Toole, Marjorie C. Wang, and Michael G. Kaiser
 Hypothermia and Human Spinal Cord Injury: Updated Position Statement and Evidence Based Recommendations from the AANS/CNS Joint Sections on Disorders of the Spine & Peripheral Nerves and Neurotrauma &
Hypothermia and Human Spinal Cord Injury: Updated Position Statement and Evidence Based Recommendations from the AANS/CNS Joint Sections on Disorders of the Spine & Peripheral Nerves and Neurotrauma &
CURRENT CONTROVERSIES IN TRAUMATIC BRAIN INJURY
 Annual Queenstown Update in Anaesthesia, 2011 Current Controversies in Traumatic Brain Injury CURRENT CONTROVERSIES IN TRAUMATIC BRAIN INJURY Dr Hamish Gray Christchurch Hospital, Christchurch 51 This
Annual Queenstown Update in Anaesthesia, 2011 Current Controversies in Traumatic Brain Injury CURRENT CONTROVERSIES IN TRAUMATIC BRAIN INJURY Dr Hamish Gray Christchurch Hospital, Christchurch 51 This
ICMB: software for on-line analysis of bedside monitoring data after severe head trauma
 Acta Neurochir (2005) [Suppl] 95: 43 49 6 Springer-Verlag 2005 Printed in Austria ICMB: software for on-line analysis of bedside monitoring data after severe head trauma P. Smielewski1,2, M. Czosnyka1,
Acta Neurochir (2005) [Suppl] 95: 43 49 6 Springer-Verlag 2005 Printed in Austria ICMB: software for on-line analysis of bedside monitoring data after severe head trauma P. Smielewski1,2, M. Czosnyka1,
ACLS PHARMACOLOGY 2011 Guidelines
 ACLS PHARMACOLOGY 2011 Guidelines ADENOSINE Narrow complex tachycardias or wide complex tachycardias that may be supraventricular in nature. It is effective in treating 90% of the reentry arrhythmias.
ACLS PHARMACOLOGY 2011 Guidelines ADENOSINE Narrow complex tachycardias or wide complex tachycardias that may be supraventricular in nature. It is effective in treating 90% of the reentry arrhythmias.
IVTMTM Intravascular Temperature
 IVTMTM Intravascular Temperature Management T e m p e r a t u r e i s V i t a l Intravascular Temperature Management (IVTM) Temperature Management Is Vital to Life Temperature is one of the four main vital
IVTMTM Intravascular Temperature Management T e m p e r a t u r e i s V i t a l Intravascular Temperature Management (IVTM) Temperature Management Is Vital to Life Temperature is one of the four main vital
Acute Myocardial Infarction (the formulary thrombolytic for AMI at AAMC is TNK, please see the TNK monograph in this manual for information)
 ANNE ARUNDEL MEDICAL CENTER CRITICAL CARE MEDICATION MANUAL DEPARTMENT OF NURSING AND PHARMACY Guidelines for Use of Intravenous Alteplase (Tissue Plasminogen Activator (t-pa)), Activase in the Treatment
ANNE ARUNDEL MEDICAL CENTER CRITICAL CARE MEDICATION MANUAL DEPARTMENT OF NURSING AND PHARMACY Guidelines for Use of Intravenous Alteplase (Tissue Plasminogen Activator (t-pa)), Activase in the Treatment
Head and Spinal Cord Injury: Diagnosis and Management
 Head and Spinal Cord Injury: Diagnosis and Management Prashant Chittiboina, MD, MPH a, Hugo Cuellar-Saenz, MD b, Christina Notarianni, MD a, Raul Cardenas, MD c, Bharat Guthikonda, MD a, * KEYWORDS Traumatic
Head and Spinal Cord Injury: Diagnosis and Management Prashant Chittiboina, MD, MPH a, Hugo Cuellar-Saenz, MD b, Christina Notarianni, MD a, Raul Cardenas, MD c, Bharat Guthikonda, MD a, * KEYWORDS Traumatic
Intrathecal Baclofen for CNS Spasticity
 Intrathecal Baclofen for CNS Spasticity Last Review Date: November 13, 2015 Number: MG.MM.ME.31bC5 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or
Intrathecal Baclofen for CNS Spasticity Last Review Date: November 13, 2015 Number: MG.MM.ME.31bC5 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or
OHTAC Recommendation
 OHTAC Recommendation Multiple Sclerosis and Chronic Cerebrospinal Venous Insufficiency Presented to the Ontario Health Technology Advisory Committee in May 2010 May 2010 Issue Background A review on the
OHTAC Recommendation Multiple Sclerosis and Chronic Cerebrospinal Venous Insufficiency Presented to the Ontario Health Technology Advisory Committee in May 2010 May 2010 Issue Background A review on the
The Treatment of Brain Ischemia With Vasopressor Drugs
 The Treatment of Brain Ischemia With Vasopressor Drugs BY GARY WISE, M.D., ROBERT SUTTER, M.D., AND JAMES BURKHOLDER, M.D. Abstract: The Treat me nl of Brain Ischemia With Vasopressor Drugs Vasopressor
The Treatment of Brain Ischemia With Vasopressor Drugs BY GARY WISE, M.D., ROBERT SUTTER, M.D., AND JAMES BURKHOLDER, M.D. Abstract: The Treat me nl of Brain Ischemia With Vasopressor Drugs Vasopressor
Medical Direction and Practices Board WHITE PAPER
 Medical Direction and Practices Board WHITE PAPER Use of Pressors in Pre-Hospital Medicine: Proper Indication and State of the Science Regarding Proper Choice of Pressor BACKGROUND Shock is caused by a
Medical Direction and Practices Board WHITE PAPER Use of Pressors in Pre-Hospital Medicine: Proper Indication and State of the Science Regarding Proper Choice of Pressor BACKGROUND Shock is caused by a
Adding IV Amiodarone to the EMS Algorithm for Cardiac Arrest Due to VF/Pulseless VT
 Adding IV Amiodarone to the EMS Algorithm for Cardiac Arrest Due to VF/Pulseless VT Introduction Before the year 2000, the traditional antiarrhythmic agents (lidocaine, bretylium, magnesium sulfate, procainamide,
Adding IV Amiodarone to the EMS Algorithm for Cardiac Arrest Due to VF/Pulseless VT Introduction Before the year 2000, the traditional antiarrhythmic agents (lidocaine, bretylium, magnesium sulfate, procainamide,
ACS TQIP BEST PRACTICES IN THE MANAGEMENT OF TRAUMATIC BRAIN INJURY
 ACS TQIP BEST PRACTICES IN THE MANAGEMENT OF TRAUMATIC BRAIN INJURY Table of Contents Introduction... 3 Using the Glasgow Coma Scale... 3 Triage and Transport... 5 Goals of Treatment... 5 Intracranial
ACS TQIP BEST PRACTICES IN THE MANAGEMENT OF TRAUMATIC BRAIN INJURY Table of Contents Introduction... 3 Using the Glasgow Coma Scale... 3 Triage and Transport... 5 Goals of Treatment... 5 Intracranial
Management of Acute Traumatic Brain Injury
 Management of Acute Traumatic Brain Injury By G. Christopher Wood, Pharm.D., FCCP, BCPS (AQ Infectious Diseases); and Bradley A. Boucher, Pharm.D., FCCP, FCCM, BCPS Reviewed by Teresa A. Allison, Pharm.D.,
Management of Acute Traumatic Brain Injury By G. Christopher Wood, Pharm.D., FCCP, BCPS (AQ Infectious Diseases); and Bradley A. Boucher, Pharm.D., FCCP, FCCM, BCPS Reviewed by Teresa A. Allison, Pharm.D.,
Traumatic Brain Injury (TBI)
 Traumatic Brain Injury (TBI) Overview Traumatic brain injury (TBI) is sudden damage to the brain caused by a blow or jolt to the head. Common causes include car or motorcycle crashes, falls, sports injuries,
Traumatic Brain Injury (TBI) Overview Traumatic brain injury (TBI) is sudden damage to the brain caused by a blow or jolt to the head. Common causes include car or motorcycle crashes, falls, sports injuries,
ST. ROSE HOSPITAL EMERGENCY SERVICES THERAPEUTIC HYPOTHERMIA AFTER CARDIAC ARREST PROTOCOL PURPOSE
 PURPOSE To outline the management of therapeutic hypothermia for the patient following cardiac arrest. LEVEL SUPPORTIVE DATA EFFECTS OF THERAPEUTIC HYPOTHERMIA Interdependent. Requires MD order. Cardiac
PURPOSE To outline the management of therapeutic hypothermia for the patient following cardiac arrest. LEVEL SUPPORTIVE DATA EFFECTS OF THERAPEUTIC HYPOTHERMIA Interdependent. Requires MD order. Cardiac
It is recommended that the reader review each medical directive presented in this presentation along with the actual PCP Core medical directive.
 It is recommended that the reader review each medical directive presented in this presentation along with the actual PCP Core medical directive. This presentation will highlight the changes and any new
It is recommended that the reader review each medical directive presented in this presentation along with the actual PCP Core medical directive. This presentation will highlight the changes and any new
Advances in Stroke Care
 Advances in Stroke Care 2015 Friday October 2 7 a.m. to 4:30 p.m. Hyatt Regency New Brunswick Two Albany Street New Brunswick, NJ 08901 Jointly sponsored by the Comprehensive Stroke Center Robert Wood
Advances in Stroke Care 2015 Friday October 2 7 a.m. to 4:30 p.m. Hyatt Regency New Brunswick Two Albany Street New Brunswick, NJ 08901 Jointly sponsored by the Comprehensive Stroke Center Robert Wood
What You Should Know About Cerebral Aneurysms
 What You Should Know About Cerebral Aneurysms From the Cerebrovascular Imaging and Interventions Committee of the American Heart Association Cardiovascular Radiology Council Randall T. Higashida, M.D.,
What You Should Know About Cerebral Aneurysms From the Cerebrovascular Imaging and Interventions Committee of the American Heart Association Cardiovascular Radiology Council Randall T. Higashida, M.D.,
Reversibility of Acute Demyelinating Lesions in relapsingremitting
 Reversibility of Acute Demyelinating Lesions in relapsingremitting Multiple Sclerosis Omar A. Khan ( Division of Neuroimmunology, Department of Neurology, Neurology and Research Services. Veterans Affairs
Reversibility of Acute Demyelinating Lesions in relapsingremitting Multiple Sclerosis Omar A. Khan ( Division of Neuroimmunology, Department of Neurology, Neurology and Research Services. Veterans Affairs
THE INTERNET STROKE CENTER PRESENTATIONS AND DISCUSSIONS ON STROKE MANAGEMENT
 THE INTERNET STROKE CENTER PRESENTATIONS AND DISCUSSIONS ON STROKE MANAGEMENT Stroke Prevention in Atrial Fibrillation Gregory Albers, M.D. Director Stanford Stroke Center Professor of Neurology and Neurological
THE INTERNET STROKE CENTER PRESENTATIONS AND DISCUSSIONS ON STROKE MANAGEMENT Stroke Prevention in Atrial Fibrillation Gregory Albers, M.D. Director Stanford Stroke Center Professor of Neurology and Neurological
*Reflex withdrawal from a painful stimulus is NOT considered a purposeful response.
 Analgesia and Moderate Sedation This Nebraska Board of Nursing advisory opinion is issued in accordance with Nebraska Revised Statute (NRS) 71-1,132.11(2). As such, this advisory opinion is for informational
Analgesia and Moderate Sedation This Nebraska Board of Nursing advisory opinion is issued in accordance with Nebraska Revised Statute (NRS) 71-1,132.11(2). As such, this advisory opinion is for informational
May 20, 2016. May 21, 2016. The 5th Annual Comprehensive Stroke and Neurocritical Care Symposium. Comprehensive Stroke Symposium
 The 5th Annual Comprehensive Stroke and Neurocritical Care Symposium May 20, 2016 Comprehensive Stroke Symposium May 21, 2016 Emergency Neurological Life Support Course and Certification The Richmond Marriott
The 5th Annual Comprehensive Stroke and Neurocritical Care Symposium May 20, 2016 Comprehensive Stroke Symposium May 21, 2016 Emergency Neurological Life Support Course and Certification The Richmond Marriott
Emergency Neurological Life Support. Spinal Cord Compression. Version: 1.0 Last Updated: 8/3/2014. Checklist & Communication
 Emergency Neurological Life Support 18 Spinal Cord Compression Version: 1.0 Last Updated: 8/3/2014 17 5 10 12 9 7 13 6 15 4 Checklist & Communication Spinal Cord Compression Page 2 Checklist Quadriplegia?
Emergency Neurological Life Support 18 Spinal Cord Compression Version: 1.0 Last Updated: 8/3/2014 17 5 10 12 9 7 13 6 15 4 Checklist & Communication Spinal Cord Compression Page 2 Checklist Quadriplegia?
Resuscitation in congenital heart disease. Peter C. Laussen MBBS FCICM Department Critical Care Medicine Hospital for Sick Children Toronto
 Resuscitation in congenital heart disease Peter C. Laussen MBBS FCICM Department Critical Care Medicine Hospital for Sick Children Toronto Evolution of Congenital Heart Disease Extraordinary success: Overall
Resuscitation in congenital heart disease Peter C. Laussen MBBS FCICM Department Critical Care Medicine Hospital for Sick Children Toronto Evolution of Congenital Heart Disease Extraordinary success: Overall
Septic Shock: Pharmacologic Agents for Hemodynamic Support. Nathan E Cope, PharmD PGY2 Critical Care Pharmacy Resident
 Septic Shock: Pharmacologic Agents for Hemodynamic Support Nathan E Cope, PharmD PGY2 Critical Care Pharmacy Resident Objectives Define septic shock and briefly review pathophysiology Outline receptor
Septic Shock: Pharmacologic Agents for Hemodynamic Support Nathan E Cope, PharmD PGY2 Critical Care Pharmacy Resident Objectives Define septic shock and briefly review pathophysiology Outline receptor
What do we mean by birth asphyxia
 Neonatal Medicine and brain injury in the Infant at term Andrew Whitelaw Professor of Neonatal Medicine University of Bristol What do we mean by birth asphyxia Interruption in oxygen delivery to the fetus
Neonatal Medicine and brain injury in the Infant at term Andrew Whitelaw Professor of Neonatal Medicine University of Bristol What do we mean by birth asphyxia Interruption in oxygen delivery to the fetus
Edwards FloTrac Sensor & Edwards Vigileo Monitor. Understanding Stroke Volume Variation and Its Clinical Application
 Edwards FloTrac Sensor & Edwards Vigileo Monitor Understanding Stroke Volume Variation and Its Clinical Application 1 Topics System Configuration Pulsus Paradoxes Reversed Pulsus Paradoxus What is Stroke
Edwards FloTrac Sensor & Edwards Vigileo Monitor Understanding Stroke Volume Variation and Its Clinical Application 1 Topics System Configuration Pulsus Paradoxes Reversed Pulsus Paradoxus What is Stroke
Brain Injury during Fetal-Neonatal Transition
 Brain Injury during Fetal-Neonatal Transition Adre du Plessis, MBChB Fetal and Transitional Medicine Children s National Medical Center Washington, DC Brain injury during fetal-neonatal transition Injury
Brain Injury during Fetal-Neonatal Transition Adre du Plessis, MBChB Fetal and Transitional Medicine Children s National Medical Center Washington, DC Brain injury during fetal-neonatal transition Injury
Common Surgical Procedures in the Elderly
 Common Surgical Procedures in the Elderly From hip and knee replacements to cataract and heart surgery, America s elderly undergo 20% of all surgical procedures. For a group that comprises only 13% of
Common Surgical Procedures in the Elderly From hip and knee replacements to cataract and heart surgery, America s elderly undergo 20% of all surgical procedures. For a group that comprises only 13% of
Guideline Statement for the Treatment of Disseminated Intravascular Coagulation
 Guideline Statement for the Treatment of Disseminated Intravascular Coagulation Introduction Though a rare occurrence in the perioperative setting, disseminated intravascular coagulation (DIC) is a syndrome
Guideline Statement for the Treatment of Disseminated Intravascular Coagulation Introduction Though a rare occurrence in the perioperative setting, disseminated intravascular coagulation (DIC) is a syndrome
Outcome Prediction after Moderate and Severe Head Injury Using an Artificial Neural Network
 241 Outcome Prediction after Moderate and Severe Head Injury Using an Artificial Neural Network Min-Huei Hsu a,b, Yu-Chuan Li c, Wen-Ta Chiu d, Ju-Chuan Yen e a Department of Neurosurgery, e Department
241 Outcome Prediction after Moderate and Severe Head Injury Using an Artificial Neural Network Min-Huei Hsu a,b, Yu-Chuan Li c, Wen-Ta Chiu d, Ju-Chuan Yen e a Department of Neurosurgery, e Department
LECTURE 16 NEUROPATHOPHYSIOLOGY (HEAD INJURY)
 LECTURE 16 Copyright 2000 by Bowman O. Davis, Jr. The approach and organization of this material was developed by Bowman O. Davis, Jr. for specific use in online instruction. All rights reserved. No part
LECTURE 16 Copyright 2000 by Bowman O. Davis, Jr. The approach and organization of this material was developed by Bowman O. Davis, Jr. for specific use in online instruction. All rights reserved. No part
PRACTICE PARAMETERS: ASSESSMENT AND MANAGEMENT OF PATIENTS IN THE PERSISTENT VEGETATIVE STATE. (Summary Statement)
 PRACTICE PARAMETERS: ASSESSMENT AND MANAGEMENT OF PATIENTS IN THE PERSISTENT VEGETATIVE STATE (Summary Statement) Report of the Quality Standards Subcommittee of the American Academy of Neurology Overview.
PRACTICE PARAMETERS: ASSESSMENT AND MANAGEMENT OF PATIENTS IN THE PERSISTENT VEGETATIVE STATE (Summary Statement) Report of the Quality Standards Subcommittee of the American Academy of Neurology Overview.
CH CONSCIOUS SEDATION
 Summary: CH CONSCIOUS SEDATION It is the policy of Carondelet Health that moderate conscious sedation of patients will be undertaken with appropriate evaluation and monitoring. Effective Date: 9/4/04 Revision
Summary: CH CONSCIOUS SEDATION It is the policy of Carondelet Health that moderate conscious sedation of patients will be undertaken with appropriate evaluation and monitoring. Effective Date: 9/4/04 Revision
The 5 Most Important EMS Articles EAGLES 2014
 The 5 Most Important EMS Articles EAGLES 2014 Corey M. Slovis, M.D. Vanderbilt University Medical Center Metro Nashville Fire Department Nashville International Airport Nashville, TN VanderbiltEM.com
The 5 Most Important EMS Articles EAGLES 2014 Corey M. Slovis, M.D. Vanderbilt University Medical Center Metro Nashville Fire Department Nashville International Airport Nashville, TN VanderbiltEM.com
Epinephrine in CPR. The 5 Most Important EMS Articles EAGLES 2014. Epi vs No-Epi Take Homes 2/28/2014. VF/VT (1990 Pairs) Epi vs No-Epi
 The 5 Most Important EMS Articles EAGLES 214 Corey M. Slovis, M.D. Vanderbilt University Medical Center Metro Nashville Fire Department Nashville International Airport Nashville, TN nephrine in CPR VF/VT
The 5 Most Important EMS Articles EAGLES 214 Corey M. Slovis, M.D. Vanderbilt University Medical Center Metro Nashville Fire Department Nashville International Airport Nashville, TN nephrine in CPR VF/VT
The focus of this article is the early recognition
 CURRENT CONCEPTS CURRENT CONCEPTS Emergent Treatment of Athletes With Brain Injury Saint-Aaron Morris, MD* Wesley H. Jones, MD* Mark R. Proctor, MD Arthur L. Day, MD Department of Neurosurgery, University
CURRENT CONCEPTS CURRENT CONCEPTS Emergent Treatment of Athletes With Brain Injury Saint-Aaron Morris, MD* Wesley H. Jones, MD* Mark R. Proctor, MD Arthur L. Day, MD Department of Neurosurgery, University
All Intraosseous Sites Are Not Equal
 All Intraosseous Sites Are Not Equal Clinical Data Suggests the Sternal IO Route Improves Patient Outcomes Current Guidelines, (such as AHA) indicate that Intraosseous Infusion (IO) is a rapid, safe and
All Intraosseous Sites Are Not Equal Clinical Data Suggests the Sternal IO Route Improves Patient Outcomes Current Guidelines, (such as AHA) indicate that Intraosseous Infusion (IO) is a rapid, safe and
GUIDELINES FOR ACTIVATING INTER-FACILITY AIR MEDICAL TRANSPORT - V1.1
 GUIDELINES FOR ACTIVATING INTER-FACILITY AIR MEDICAL TRANSPORT - V1.1 Instructions: Contact your respective receiving facility / transfer center to arrange for patient transfer and acceptance. Most transfer
GUIDELINES FOR ACTIVATING INTER-FACILITY AIR MEDICAL TRANSPORT - V1.1 Instructions: Contact your respective receiving facility / transfer center to arrange for patient transfer and acceptance. Most transfer
Appendix L: HQO Year 1 Implementation Priorities
 Appendix L: HQO Year 1 Implementation Priorities Chronic Obstructive Pulmonary Disease (Source: COPD Chairs) Non-Invasive Positive Pressure Ventilation Early Ambulation If possible, seek patient preferences
Appendix L: HQO Year 1 Implementation Priorities Chronic Obstructive Pulmonary Disease (Source: COPD Chairs) Non-Invasive Positive Pressure Ventilation Early Ambulation If possible, seek patient preferences
APPENDIX A NEUROLOGIST S GUIDE TO USING ICD-9-CM CODES FOR CEREBROVASCULAR DISEASES INTRODUCTION
 APPENDIX A NEUROLOGIST S GUIDE TO USING ICD-9-CM CODES FOR CEREBROVASCULAR DISEASES INTRODUCTION ICD-9-CM codes for cerebrovascular diseases is not user friendly. This presentation is designed to assist
APPENDIX A NEUROLOGIST S GUIDE TO USING ICD-9-CM CODES FOR CEREBROVASCULAR DISEASES INTRODUCTION ICD-9-CM codes for cerebrovascular diseases is not user friendly. This presentation is designed to assist
Functions of the Brain
 Objectives 0 Participants will be able to identify 4 characteristics of a healthy brain. 0 Participants will be able to state the functions of the brain. 0 Participants will be able to identify 3 types
Objectives 0 Participants will be able to identify 4 characteristics of a healthy brain. 0 Participants will be able to state the functions of the brain. 0 Participants will be able to identify 3 types
Therapeutic Hypothermia after Cardiac Arrest General Guideline
 Therapeutic Hypothermia after Cardiac Arrest General Guideline I. Associated Guidelines and Appendices 1. Neurological Prognosis after Cardiac Arrest 2. Hypothermia after Cardiac Arrest Algorithm 3. Effect
Therapeutic Hypothermia after Cardiac Arrest General Guideline I. Associated Guidelines and Appendices 1. Neurological Prognosis after Cardiac Arrest 2. Hypothermia after Cardiac Arrest Algorithm 3. Effect
LIFEFLIGHT OF MAINE GUIDELINES FOR HELICOPTER TRANSPORT
 LIFEFLIGHT OF MAINE GUIDELINES FOR HELICOPTER TRANSPORT I. GENERAL GUIDELINES Many patients who require transport to centers with specialized or tertiary level resources are appropriate for transport by
LIFEFLIGHT OF MAINE GUIDELINES FOR HELICOPTER TRANSPORT I. GENERAL GUIDELINES Many patients who require transport to centers with specialized or tertiary level resources are appropriate for transport by
Extracorporeal Life Support Organization (ELSO) Guidelines for Neonatal Respiratory Failure
 Extracorporeal Life Support Organization (ELSO) Guidelines for Neonatal Respiratory Failure Introduction This neonatal respiratory failure guideline is a supplement to ELSO s General Guidelines for all
Extracorporeal Life Support Organization (ELSO) Guidelines for Neonatal Respiratory Failure Introduction This neonatal respiratory failure guideline is a supplement to ELSO s General Guidelines for all
Headache: Differential diagnosis and Evaluation. Raymond Rios PGY-1 Pediatrics
 Headache: Differential diagnosis and Evaluation Raymond Rios PGY-1 Pediatrics You are evaluating a 9 year old male patient at the ED brought by his mother, who says that her son has had a fever, cough,
Headache: Differential diagnosis and Evaluation Raymond Rios PGY-1 Pediatrics You are evaluating a 9 year old male patient at the ED brought by his mother, who says that her son has had a fever, cough,
Cardiac Arrest: General Considerations
 Andrea Gabrielli, MD, FCCM Cardiac Arrest: General Considerations Cardiopulmonary resuscitation (CPR) is described as a series of assessments and interventions performed during a variety of acute medical
Andrea Gabrielli, MD, FCCM Cardiac Arrest: General Considerations Cardiopulmonary resuscitation (CPR) is described as a series of assessments and interventions performed during a variety of acute medical
The ASA defines anesthesiology as the practice of medicine dealing with but not limited to:
 1570 Midway Pl. Menasha, WI 54952 920-720-1300 Procedure 1205- Anesthesia Lines of Business: All Purpose: This guideline describes Network Health s reimbursement of anesthesia services. Procedure: Anesthesia
1570 Midway Pl. Menasha, WI 54952 920-720-1300 Procedure 1205- Anesthesia Lines of Business: All Purpose: This guideline describes Network Health s reimbursement of anesthesia services. Procedure: Anesthesia
What Is an Arteriovenous Malformation (AVM)?
 What Is an Arteriovenous Malformation (AVM)? From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall T. Higashida, M.D., Chair 1 What
What Is an Arteriovenous Malformation (AVM)? From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall T. Higashida, M.D., Chair 1 What
Recommendations: Other Supportive Therapy of Severe Sepsis*
 Recommendations: Other Supportive Therapy of Severe Sepsis* K. Blood Product Administration 1. Once tissue hypoperfusion has resolved and in the absence of extenuating circumstances, such as myocardial
Recommendations: Other Supportive Therapy of Severe Sepsis* K. Blood Product Administration 1. Once tissue hypoperfusion has resolved and in the absence of extenuating circumstances, such as myocardial
Emergency Fluid Therapy in Companion Animals
 Emergency Fluid Therapy in Companion Animals Paul Pitney BVSc paul.pitney@tafensw.edu.au The administration of appropriate types and quantities of intravenous fluids is the cornerstone of emergency therapy
Emergency Fluid Therapy in Companion Animals Paul Pitney BVSc paul.pitney@tafensw.edu.au The administration of appropriate types and quantities of intravenous fluids is the cornerstone of emergency therapy
Sepsis: Identification and Treatment
 Sepsis: Identification and Treatment Daniel Z. Uslan, MD Associate Clinical Professor Division of Infectious Diseases Medical Director, UCLA Sepsis Task Force Severe Sepsis: A Significant Healthcare Challenge
Sepsis: Identification and Treatment Daniel Z. Uslan, MD Associate Clinical Professor Division of Infectious Diseases Medical Director, UCLA Sepsis Task Force Severe Sepsis: A Significant Healthcare Challenge
Oxygen Therapy. Oxygen therapy quick guide V3 July 2012.
 PRESENTATION Oxygen (O 2 ) is a gas provided in a compressed form in a cylinder. It is also available in a liquid form. It is fed via a regulator and flow meter to the patient by means of plastic tubing
PRESENTATION Oxygen (O 2 ) is a gas provided in a compressed form in a cylinder. It is also available in a liquid form. It is fed via a regulator and flow meter to the patient by means of plastic tubing
Pseudoabducens palsy: When a VI nerve palsy is not a VI nerve palsy
 Pseudoabducens palsy: When a VI nerve palsy is not a VI nerve palsy Emily S. Birkholz, MD, and Michael Wall, MD December 30, 2009 CC: 44 year old male with diplopia HPI: This 44 year old man with a history
Pseudoabducens palsy: When a VI nerve palsy is not a VI nerve palsy Emily S. Birkholz, MD, and Michael Wall, MD December 30, 2009 CC: 44 year old male with diplopia HPI: This 44 year old man with a history
Pain Management in the Critically ill Patient
 Pain Management in the Critically ill Patient Jim Ducharme MD CM, FRCP President-Elect, IFEM Clinical Professor of Medicine, McMaster University Adjunct Professor of Family Medicine, Queens University
Pain Management in the Critically ill Patient Jim Ducharme MD CM, FRCP President-Elect, IFEM Clinical Professor of Medicine, McMaster University Adjunct Professor of Family Medicine, Queens University
With approximately 50,000 patients dying each year of
 Direct Transport Within An Organized State Trauma System Reduces Mortality in Patients With Severe Traumatic Brain Injury Roger Härtl, MD, Linda M. Gerber, PhD, Laura Iacono, RN, MSN, Quanhong Ni, MS,
Direct Transport Within An Organized State Trauma System Reduces Mortality in Patients With Severe Traumatic Brain Injury Roger Härtl, MD, Linda M. Gerber, PhD, Laura Iacono, RN, MSN, Quanhong Ni, MS,
Chiari Malformation: An Overview
 Chiari Malformation: An Overview SYMPTOMS DIAGNOSIS LIVING WITH CHIARI TREATMENT Rick Labuda, Executive Director director@conquerchiari.org 724-940-0116 Disclaimer: This presentation is intended for informational
Chiari Malformation: An Overview SYMPTOMS DIAGNOSIS LIVING WITH CHIARI TREATMENT Rick Labuda, Executive Director director@conquerchiari.org 724-940-0116 Disclaimer: This presentation is intended for informational
UBC Pain Medicine Residency Program: CanMEDS Goals and Objectives of the Neurology Rotation
 UBC Pain Medicine Residency Program: CanMEDS Goals and Objectives of the Neurology Rotation Goals of the Program To acquire the knowledge and skills necessary to assess and provide a management plan for
UBC Pain Medicine Residency Program: CanMEDS Goals and Objectives of the Neurology Rotation Goals of the Program To acquire the knowledge and skills necessary to assess and provide a management plan for
ACLS Provider Manual Comparison Sheet Based on 2010 AHA Guidelines for CPR and ECC. BLS Changes
 ACLS Provider Manual Comparison Sheet Based on 2010 AHA Guidelines for CPR and ECC CPR Chest compressions, Airway, Breathing (C-A-B) BLS Changes New Old Rationale New science indicates the following order:
ACLS Provider Manual Comparison Sheet Based on 2010 AHA Guidelines for CPR and ECC CPR Chest compressions, Airway, Breathing (C-A-B) BLS Changes New Old Rationale New science indicates the following order:
Aktuelle Literatur aus der Notfallmedizin
 05.02.2014 Aktuelle Literatur aus der Notfallmedizin prä- und innerklinisch Aktuelle Publikationen aus 2012 / 2013 PubMed hits zu emergency medicine 12,599 Abstract OBJECTIVES: Current American Heart
05.02.2014 Aktuelle Literatur aus der Notfallmedizin prä- und innerklinisch Aktuelle Publikationen aus 2012 / 2013 PubMed hits zu emergency medicine 12,599 Abstract OBJECTIVES: Current American Heart
