Hysteroscopic Metroplasty for the Septate Uterus: Review and Meta-Analysis
|
|
|
- Bruce Manning
- 8 years ago
- Views:
Transcription
1 Review Article Hysteroscopic Metroplasty for the Septate Uterus: Review and Meta-Analysis Rafael F. Valle, MD*, and Geraldine E. Ekpo, MD From the Department of Obstetrics and Gynecology, Northwestern University Feinberg School of Medicine, Chicago, Illinois (both authors). ABSTRACT Keywords: The introduction of hysteroscopy to diagnose and treat intrauterine conditions, specifically to divide the uterine septum, or metroplasty, has replaced the traditional laparotomy approach, and objective results demonstrate its salutary effects in women treated. Hysteroscopic metroplasty averts the implications of major invasive abdominal surgery, with good and satisfactory results in pregnancy and live-birth rates, despite the lack of prospective, randomized, controlled studies. A careful review of the published results supports this type of treatment when the uterine septum adversely affects normal reproductive function. Journal of Minimally Invasive Gynecology (2013) 20, Ó 2013 AAGL. All rights reserved. Uterine anomalies; Uterine septum; Pregnancy wastage; Hysteroscopy; Hysteroscopic metroplasty DISCUSS You can discuss this article with its authors and with other AAGL members at Use your Smartphone to scan this QR code and connect to the discussion forum for this article now* * Download a free QR Code scanner by searching for QR scanner in your smartphone s app store or app marketplace. Errors of arrest in the development of the embryologic m ullerian ducts are conducive to uterine anomalies. The lack of fusion of the original ducts or lack of reabsorption of the embryologic septum can result in a bicornuate or a septate uterus. While not all uterine anomalies may impair normal uterine reproductive function, some do, and may require surgical treatment. One common uterine anomaly that benefits from treatment by metroplasty is the septate uterus. Congenital Uterine Malformations Incidence It is difficult to determine the incidence of congenital uterine malformations in the general population because most affected women do not experience reproductive problems. The incidence has been calculated to be 1 or 2 per The authors have no commercial, proprietary, or financial interest in the products or companies described in this article. Corresponding author: Rafael F. Valle, MD, Department of Obstetrics and Gynecology, Northwestern University Feinberg School of Medicine, 880 N Lake Shore Dr, Ste 20-C, Chicago, IL rafaelvalle1@aol.com Submitted September 18, Accepted for publication September 22, Available at and women and as high as 15 per 1000 women. Some studies have reported a 12% incidence [1 5]. Genetic Factors The occurrence of congenital uterine malformations seems to be influenced by a genetic heterogeneity and/or polygenic multifactorial inheritance. Inasmuch as these anomalies develop early in embryonic life, a short review of this crucial period is appropriate [6]. The m ullerian ducts arise from the urogenital ridge of the embryo as an invagination of the celomic epithelium at about 5 to 6 weeks of embryonic life. The ducts grow downward immediately to fuse in the midline at about 9 weeks and then are united with the endodermal bulbs of the urogenital sinus to form the remainder of the vagina. This process is completed by 12 to 14 weeks of gestation, and reabsorption of the septum is completed by week 19 to 20 embryonic life. In the absence of m ullerian inhibiting factor produced by the testes, the paramesonephric m ullerian ducts progress to normal female development. The different stages of arrest in m ullerian ducts differentiation are manifested in various clinical entities. Unilateral absence of a m ullerian duct results in a unicornuate uterus, and medial absence of the ducts results in absence of the uterus. Lack of fusion at various stages results in a didelphic /$ - see front matter Ó 2013 AAGL. All rights reserved.
2 Valle and Ekpo. Hysteroscopic Metroplasty for Septate Uterus 23 Fig. 1 Septate uterus: partial (1 and 2), complete (3), complete with septate cervix (4), and complete with cervical and vaginal septation (5). uterus with a double cervix and septate vagina. Failure of reabsorption of the medial septum in the uterus results in a septate uterus [7 10] (Fig. 1). Classification of Uterine Anomalies There are many classifications of developmental anomalies of the uterus. In 1979, Buttram and Gibbons [11] proposed a classification that was further revised in 1988 by the American Society of Reproductive Medicine, then known as the American Fertility Society [12] (Fig. 2). This classification groups anomalies in categories on the basis of similarities in clinical features, obstetric outcome, and treatment options [12]. While the American Society of Reproductive Medicine classification has gained widespread acceptance, subclassifications have been proposed to further differentiate uterine anomalies previously classified as class V (septate) and class VI (arcuate) [13]. Alternative grouping systems include vaginal anomalies and separate uterovaginal anomalies in 3 separate groups on the basis of embryonic developmental defects and clinical features. Such is the classification proposed by Jones and Rock [14] and Jones [15], which is based on lateral or vertical defects of fusion, both with or without obstruction. However, a simpler, easy to remember, and clinically useful classification of uterine anomalies is that proposed in 1966 by Strassman [3], based on the various stages of embryologic developmental arrest that occur during embryogenesis, and that by Lindeman et al [16]. These classifications are given in Table 1. Because of the close relationship and common embryologic origins of the genital tract and urinary systems, with both developing from the mesonephric system, m ullerian anomalies are frequently associated with urologic malformations. Various urinary tract anomalies have been described in patients with septate uterus and other m ullerian anomalies including unilateral renal agenesis, unilateral or bilateral pelvic kidneys, malrotation of the kidney, and duplication of the collecting system, hydroureter, or extrophy of the bladder. Conventional management of any uterine anomaly should therefore include imaging to rule out renal and urinary tract malformations. In addition, anomalies of the spine and skeletal system have been reported in patients with m ullerian anomalies independently or as part of a syndrome [17]. Vascularization and Muscular Components of the Uterine Septum Few histologic evaluations of the uterine septum have been performed. It is clear that the composition of the septum varies according to site and level at which the tissue samples are obtained for study. In addition, the width of the septum is important inasmuch as some are very thin and others very thick; thus, the results obtained from studies vary considerably. The uterine septum, in general, is
3 24 Journal of Minimally Invasive Gynecology, Vol 20, No 1, January/February 2013 Fig. 2 American Fertility Society classification of m ullerian anomalies. composed of fibromuscular tissue and may borrow vascularization from the adjacent uterine walls. When hysteroscopic metroplasty is performed, the uterine cavity is distended, and the septum becomes apparent as it stretches away from the uterine walls. This effect enables the medial portion of the septum to be practically free of vascularization, except with a thick septum, thus enabling its division in the middle without substantial bleeding. Studies in which samples were obtained at hysteroscopy or laparotomy (Tompkins procedure) to evaluate the components of the uterine septum have challenged the concept of poor vascularization of the septum; however, the evaluations were performed using resected portions of the septum or hysteroscopic selected biopsy samples, which do not represent the totality of the septum [18,19]. Further and more systematic evaluations of different types of septum will be valuable to better elicit the true composition of the different septae. Kupesic and Kurjak [20] have used transvaginal color and pulsed Doppler sonography and 3-dimensional (3-D) sonography in the evaluation of the uterine septum, showing septal vascularity in 71% of patients studied, which suggests that most uterine septae carry myometrial vessels. They also concluded that most obstetric problems could be due to higher and uncoordinated activity of the septum muscular tissue [20]. In addition, magnetic resonance imaging (MRI) is a useful and accurate method for evaluating the muscular and vascular components of the uterine septum. It is not clear the role uterine motility has, if any, in septate uterus as a cause of pregnancy loss, although motility has been studied in the bicornuate uterus and showed dissimilar responses when the 2 uterine horns were asymmetric. No such studies have been performed on the septate uterus [21]. Diagnosis and Evaluation Although the diagnosis of a malformed uterus can be made during physical examination when obvious anomalies of the vagina and cervix are present, the subtlest uterine anomalies can be discovered and confirmed only by other methods of evaluation such as hysterosalpingography, sonography in all its modes, and hysteroscopy (Figs. 3 and 4). Differentiation of a bicornuate from a septate uterusmay require additional evaluation via ultrasonography and/ or laparoscopy. Imaging techniques are discussed later in this review (see Preoperative Evaluation and Diagnosis. ). Reproductive Problems Caused by Uterine Septum Most women with m ullerian anomalies, specifically of the septum, have efficient reproductive function; only about 20% to 25% may experience recurrent spontaneous abortions [22,23]. Of all of the uterine anomalies encountered, septate uterus is most often associated with reproductive wastage. The classic clinical finding is of repeated early mid-trimester pregnancy wastage with obvious signs of labor, including bleeding. Infertility rarely results from a uterine anomaly alone. Therefore, the mere recognition of a uterine anomaly does not dictate surgical therapy. Furthermore, in patients who have demonstrated pregnancy wastage, a complete workup is necessary to rule out other possible extrauterine causes of the reproductive failures [23].
4 Valle and Ekpo. Hysteroscopic Metroplasty for Septate Uterus 25 Table 1 Classifications of uterine anomalies Strassman Classification [3] Symmetric With external division of uterus (2 cavities) Complete Incomplete Without external division but with midline septum Complete Incomplete Asymmetric With rudimentary horn Communicating Noncommunicating Jones Classification [14,15] Agenesis Problems of vertical fusion Obstructive Nonobstructive Problems of lateral fusion Obstructive Nonobstructive Buttram and Gibbons Classification [11] Segmental m ullerian agenesis/hypoplasia Vaginal Cervical Fundal Tubal Combined anomalies Unicornuate With rudimentary horn With endometrial cavity Communicating Noncommunicating Without endometrial cavity Without rudimentary horn Didelphys Bicornuate Complete (division down to internal os) Partial Arcuate Septate Complete (septum to internal os) Partial Diethylstilbestrol related Fig. 3 Hysteroscopic view of septate uterus. Obstetric problems associated with uterine anomalies include breech presentation (25% 30%), oblique and transverse positions (5%), and premature labor (20%). In the postpartum period, retained placenta can occur in 5% to 10% of patients [24]. In recent studies by Hua et al [24] and Agostini et al [25], the presence of a uterine anomaly was associated with a 6-fold increased risk of preterm birth, 3-fold preterm premature rupture of the membranes, breech presentation, and cesarean section performed in the presence of a fetus not in the breech position. In some patients, a uterine anomaly is diagnosed if there is incomplete uterine evacuation in association with voluntary pregnancy interruption. Because of the significant association of urinary tract anomalies with uterine anomalies (30% 40%), in particular in the asymmetric forms, evaluation of renal function via sonography and intravenous pyelography should be performed routinely [5,11]. Why Do Some Women With Uterine Septum Abort? Several theories have been offered to explain why repetitive abortions occur in women with uterine septum. These include decreased luminal space, impaired development of the endometrium such that it cannot support the pregnancy, decreased steroid estrogens receptors, decreased serum cystine aminopeptidase, and decreasing neutralization of circulating oxytocin [26]. Other theories include an alteration in cervical fibromuscular/connective tissue ratios. The Fig. 4 Sonographic view of septate uterus.
5 26 Journal of Minimally Invasive Gynecology, Vol 20, No 1, January/February 2013 hypermuscular cervix, with increased cervical fibromuscular tissue and decreased connective tissue, results in less resistance to cervical dilation, leading to pregnancy wastage [27]. A decrease in growth factors such as vascular endothelial growth factor has been noted in women with septate uterus and repeated abortions as compared with women without reproductive problems [28]. Although all of these factors may have a synergistic role, the most generally accepted cause has been decreased vascularization of the septal area, as demonstrated during surgical division of the septum when the uterus is distended, therefore affecting blastocyst implantation and nutrition of the implanted embryo. Fedele et al [29] conducted serial sonographic studies of implanted embryos in patients with known septate uterus and found that when implantation in the septum occurred, most of these patients aborted as compared with those with implantation occurring in the lateral uterine walls. Endometrial biopsy samples obtained at hysteroscopy in the preovulatory phase of the cycle from uterine septal areas and evaluated via scanning electron microscopy have demonstrated decreased sensitivity of this endometrium to preovulatory hormonal changes as compared with biopsy samples obtained from the lateral walls of the uterus, which suggests a possible role in and pregnancy wastage [30]. Indications for Metroplasty Most women with septate uterus reproduce successfully; only 20% to 25% may have pregnancy wastage, late firsttrimester abortion, or early second-trimester abortion initiated with mini-labor and bleeding. This problem seems to correlate with the length of the septum, with longer septae posing the greatest risk. The most genuine indication for treatment is repeated abortion. However, with the advances in minimally invasive procedures such as hysteroscopy, other relative indications include requiring special treatment for induction of ovulation, insemination, or other assisted-reproduction technologies. The role of metroplasty in patients with primary continues to be controversial, and although some patients have been treated solely for this reason, with subsequent postoperative pregnancies, the pregnancy rate in general has been much lower than when the indication for metroplasty is pregnancy wastage. Because the septate uterus seldom causes, other uterine and extrauterine causes of the should be ruled out before metroplasty is performed [31]. A rough pregnancy rate of 48% was obtained after metroplasty in 84 infertile patients gathered from 7 reports [32]. In a study by Shokeir et al [33], the pregnancy rate after hysteroscopic metroplasty in 88 patients with primary unexplained was 40.7%, with 80% of patients conceiving spontaneously. Of 44 pregnancies in 42 women, 36 live newborns were delivered [33]. Pabuccu and Gomel [34] reported on the reproductive outcomes after hysteroscopic metroplasty in women with septate uterus and unexplained. Of 61 women who underwent hysteroscopic metroplasty, 25 (41%) conceived after metroplasty. Of the 25 patients who conceived, 18 (29.5% of the total group) delivered live infants and 7 (11.5% of the total group) had spontaneous abortions. The authors concluded that hysteroscopic metroplasty had a beneficial effect in these women [34]. In a similar study, which was retrospective and controlled, 127 women with septate uterus and unexplained were evaluated, 102 after metroplasty (group 1) and 25 before metroplasty (group 2). Forty-four patients (43.1%) achieved pregnancy in group 1, compared with only 5 (20%) in group 2. The abortion rate was 11.4% in group 1, and 60% in group 2. It was concluded that hysteroscopic metroplasty improved reproductive outcome in patients with septate uterus and unexplained [35,36]. Other observational studies have reported similar findings [37]. To evaluate the role of septate uterus in the reproductive performance of patients requiring in vitro fertilization (IVF), a retrospective, matched, controlled study was performed that evaluated 2481 embryo transfers in stimulated IVF/intracytoplasmic sperm injection cycles in women with known septate uterus. Two hundred eighty-nine embryo transfers were performed before metroplasty, and 538 after metroplasty, and were compared with 2 consecutive embryo transfers in the control group. The pregnancy rate before metroplasty was lower than after metroplasty, and the abortion rate was higher. These results show that the presence of septate uterus decreases the pregnancy rate and may increase the abortion rate after embryo transfers for IVF/intracytoplasmatic sperm injection [38]. Preoperative Evaluation and Diagnosis Multiple imaging methods have been used to delineate uterine anomalies. Because most women with uterine anomalies have normal external genitalia, most uterine anomalies are not apparent until the time of expected menarche or at work-up because of or pregnancy loss. Laparoscopy and Hysteroscopy Evaluation of the septate uterus is frequently performed via laparoscopy or hysteroscopy, in particular when the laparoscope is used to monitor the hysteroscopic performance of the metroplasty. This approach also enables evaluation of the adnexae and pelvic cavity for possible pelvic adhesions, tubal or ovarian distortions, and endometriosis that could be treated during the same session. The accuracy of these methods has been reported as 100%, and they have been the criterion standard in the evaluation of the septate and bicornuate uterus before and during metroplasty. Hysterosalpingography and Virtual Hysterosalpingography Hysterosalpingography (HSG) is the most accurate method of diagnosing a division of the uterine cavity.
6 Valle and Ekpo. Hysteroscopic Metroplasty for Septate Uterus 27 Table 2 Outcome after abdominal metroplasty Source, year No. of patients Method Rock and Jones [62], 1977 Musich and Behrman [67], 1978 Mercer et al [68], 1981 Kessler et al [69], 1986 Candiani et al [70], 1990 Ayhan et al [71], 1992 Kirk et al [72], Bicornuate, septate, didelphys Septate, 6 bicornuate, 3 arcuate Septate, 1 bicornuate, 1 didelphys 17 4 Septate, 12 bicornuate, 1 didelphys Septate, 2 bicornuate Septate, 40 bicornuate 22 Patients, 44 Pregnancies Jones Tompkins, Jones, Strassman 15 Jones, 2 Strassman 13 Strassman, 3 Tompkins, 1 Jones 55 Tompkins, 6 Jones, 5 Te Linde, 5 Strassman 44 Jones, 40 Strassman, 5 Tompkins 18 Tompkins, 5 Jones, 3 Strassman Postoperative outcome a Complications 1 Intrauterine synechiae Pregnancy rate/no. of pregnancies 37/39 (58 pregnancies) Live-birth rate Term Preterm Abortion 41/58 42/58 4/58 12/58 NR 16/21 12/16 12/16 NA 14/16 NR 12/16 14/15 14/15 NA 1/15 NR 4 2/4 2/4 NA 2/4 NR 56 45/56 45/56 NR 11/56 NR 46 30/46 16/30 22/30 8/30 NR 44 33/44 31/44 4/44 9/44 NA 5 not applicable; NR 5 none reported. a When provided, listed outcomes are only for metroplasty to treat septate uterus. However, to avoid confusing the anomaly with a bicornuate uterus, laparoscopy or sonography is added to determine the external uterine configuration and to evaluate other tuboperitoneal factors. Diagnostic accuracy of HSG in differentiating septate from bicornuate uterus has been reported to be as low as 55%. Limitations of HSG also include exposure to ionizing radiation, postprocedural pain, and risk of pelvic inflammatory disease [39]. Virtual HSG is another imaging method that enables visualization of the uterine cavity, cervix, and fallopian tubes, and has several advantages over standard HSG. It seems to be better tolerated by patients, with less discomfort; offers minimal radiation exposure; and takes less time to complete. Furthermore, it provides a variety of visual findings such as coronal and sagittal multiplanar reconstruction. In addition, it gives a 3-D volume rendering and virtual endoscopic images, showing an inner view of the lumen of the uterine cavity, cervix, and fallopian tubes. It can accurately differentiate bicornuate uterus from septate uterus [40]. Ultrasonography Two-dimensional (2-D) ultrasonography is an excellent noninvasive method of evaluation of the uterine cavity and surrounding uterine walls. It has several advantages over HSG because no radiation is used, the procedure is not uncomfortable for the patient, it is quick, and it is relatively inexpensive. It can be used as the first line for evaluating the uterus. The sensitivity of 2-D ultrasonography in detecting uterine malformations ranges from 88% to 93% in some studies, and the specificity from 94% to 99%. The positive predictive value ranges from 50% to 55%, and the negative predictive value from 88% to 100%. For detection of the septate uterus, sensitivity has been reported as 81%. With the instillation of saline solution, the sensitivity of transabdominal ultrasonography increases to 56% to 92%, and specificity from 56% to 100% [41 44]. Three-dimensional ultrasonography can provide a coronal view of the uterine surface and contour, therefore adding
7 28 Journal of Minimally Invasive Gynecology, Vol 20, No 1, January/February 2013 precision in the diagnosis and differentiation of bicornuate and septate uterus. Furthermore, the images obtained can be stored and evaluated later. Three-dimensional ultrasonography has been evaluated and proved reproducible for the diagnosis of uterine anomalies including uterine cavity measurements in all 3 dimensions. The accuracy of 3-D ultrasonography for detection of septate uterus has been reported as 92% and 100% for bicornuate uterus, with positive and negative predictive values of 100%. The combined use of hysteroscopic evaluation and 3-D ultrasonography seem to be a reliable and simple strategy to determine septate uterus for performance of metroplasty without laparoscopic investigation of the uterine fundus. Threedimensional ultrasonography may become the only method needed for assessment of the uterine cavity in patients with a suspected septate or bicornuate uterus before performing surgical correction [45 47]. The diagnostic value of 3-D sonohysterography (SHG) is comparable to hysteroscopy for detecting intrauterine lesions, and both are superior to 2-D SHG [48]. Sonohysterography By infusing saline solution into the uterine cavity as a contrast medium, excellent appraisal of the uterine cavity can be obtained, most useful in delineating uterine anomalies with sensitivity of 97% and specificity of 11%. When saline solution is infused into the uterine cavity, sensitivity increases to 98%, and specificity to 100%. Three-dimensional SHG is perhaps the most accurate imaging method for evaluation of septate uterus. In one study, compared with hysteroscopy, 3-D SHG had a sensitivity of 100% and a positive predictive value of 92% in diagnosing intrauterine lesions [48 52]. Magnetic Resonance Imaging Although MRI is not frequently used for evaluation of uterine anomalies because of its cost, its accuracy and lack of ionizing radiation make this method invaluable, in particular in difficult and complex situations and when HSG or sonography fail to provide the proper and precise diagnosis. Some septate uterus may not be well delineated via HSG or sonography or even via laparoscopy or hysteroscopy because one of the chambers of the divided cavity may not be enlarged and the entrance to the hemi-cavity may be obscured at hysteroscopy. In such situations, MRI becomes invaluable in establishing the diagnosis before metroplasty. In one report, MRI to detect intrauterine lesions had sensitivity of 100% and specificity of 79% [53 55]. It is important to evaluate other factors that may cause pregnancy wastage before surgically correcting septate uterus. A karyotype of both partners should be obtained, and normal maturation of the endometrium should be evaluated during the late luteal phase (days of the cycle) via serum progesterone and transvaginal ultrasound to measure endometrial thickness in lieu of endometrial biopsy in the middle or late luteal phase, which has not proved reliable in predicting fertility [56]. Endocrine conditions such as hypothyroidism should be evaluated via a thyroid-stimulating hormone assay. Autoimmune conditions must be ruled out via a lupus anticoagulant factor study, partial thromboplastin time, and anti-cardiolipin antibodies. Alloimmune conditions should be evaluated only in selected individuals via tissue typing for histocompatibility leukocyte antigens. Chronic endometritis should be ruled out via endometrial biopsy [57 61]. Treatment of Uterine Septum Because the original metroplastic procedures via laparotomy paved the way to the modern approach via hysteroscopy, a brief review of those methods is in order. Abdominal Metroplasty The original surgical treatments of the septate uterus were all via laparotomy and hysterotomy and were performed only in habitual aborters. Noninvasive methods such as cerclage, bed rest, and tocolytic agents were frequently used to preserve the ongoing pregnancy before any surgical procedure was undertaken. Abdominal metroplasty procedures performed were of the Jones type, involving transfundal uterine excision of the septate uterus by removing a cuneiform portion of the fundal myometrium and septum with subsequent repair [62]. The other method used was the Bret-Tomkins metroplasty with division of the uterus in the anteroposterior plane and transverse division of the septum in the middle without excision of myometrial tissue. Both methods achieved 70% to 80% rate of viable pregnancies [63,64]. Nonetheless, because they required laparotomy and hysterotomy, abdominal metroplasty exposed the patient to formation of postoperative adhesions, prolonged recovery, and longer waiting time before attempting conception (3 6 months), with a mandatory cesarean section as the route of delivery in subsequent pregnancies [65]. In 1976, El Magoub [66] introduced another approach using small fundal, transverse incisions in the uterus along the septum and removal of the uterus transfundally using long scissors. However, this method did not gain much acceptance. Experience with and outcomes of abdominal metroplasty are given in Table 2. Hysteroscopic Metroplasty In 1884, Ruge [73] attempted transcervical division of septate uterus blindly; however, this technique did not gain clinical acceptance because of its blind approach. In 1974, Edstrom [74] attempted removal of a uterine septum using a biopsy forceps guided by hysteroscopy; in the following years, hysteroscopic scissors were introduced and markedly facilitated the procedure. The generally avascular central portion of the fibrotic septum, enhanced by uterine distention, facilitates its central division without substantial
8 Valle and Ekpo. Hysteroscopic Metroplasty for Septate Uterus 29 Fig. 5 Hysteroscopic division of septum with semi-rigid scissors. bleeding. Furthermore, the hysteroscopic approach reduces the adverse effects and morbidity of the procedure, enabling prompt resumption of patient activities and earlier possibility of conception (4 5 weeks) after the procedure. Patients who conceive do not require mandatory cesarean section [75]. Hysteroscopic metroplasty can be accomplished via several methods including use of mechanical scissors; electrosurgery with specially designed electrodes fitted to the hysteroscope or resectoscope; vaporizing or bipolar electrodes; lasers of the fiber type such as the neodymium- YAG, the KTP-532, and the argon laser with extruded tips; and mechanical morcellators [76 83] (Figs. 5 7). The most commonly used instruments are the hysteroscopic scissors and the resectoscope fitted with an appropriately designed electrode. All require experience and knowledge of their properties and specific requirements in the use of uterine distending fluids and energies. Although the best time for performance of these procedures is in the early follicular phase when the endometrium is thin, alternatively they can be performed after hormone therapy Fig. 6 Resectoscopic division of uterine septum with knife-electrode. to artificially thin the endometrium, as with the use of gonadotropin-releasing hormone analogues. Concomitant laparoscopic or ultrasonic monitoring of the procedure is an option to increase safety and security during septal division. Other approaches to septal division have been described including use of fluoroscopy, sonographically guided septal division, and even tactile sensation guidance of a thin scissors [84 90]. However, these methods are less effective and precise, and because the uterus is not distended, it exposes the patient to significant intraoperative bleeding, which may be difficult to control except with tamponade and may prohibit completion of the treatment in one setting or stage. The results achieved with hysteroscopic metroplasty not only compare well with those of abdominal metroplasty, they seem to surpass them with an 80% to 90% rate of viable pregnancies in patients treated because of repeated abortion and no sequelae of secondary due to subsequent pelvic adhesions, as with laparotomy. Furthermore, the patient is spared the inconveniences of hospitalization, laparotomy and hysterotomy, mandatory cesarean section in future pregnancies, and cost [91,92]. It has been proposed that performance of hysteroscopic metroplasty be moved to the office setting to make it more acceptable to the patient and less invasive [93 95]. Nonetheless, although division of a uterine septum via hysteroscopy or resectoscopy is easy, in particular if it is partial and thin and the procedure can be performed in an ambulatory surgical center, certain precautions and availability of additional instrumentation are important such as those required for laparoscopy and supportive anesthesia personnel, should the need arise. These are important aspects of safety and supportive team measures that should be available to approach the procedure with Fig. 7 Hysteroscopic view of unified uterine cavity after hysteroscopic laser metroplasty.
9 30 Journal of Minimally Invasive Gynecology, Vol 20, No 1, January/February 2013 Table 3 Adjunctive therapy and complications of hysteroscopic metroplasty Source, year No. of patients Technique Routine preoperative or postoperative therapy Danazol/ GnRH) Estrogen Progesterone IUD/Foley catheter Antibiotics Complications Valle and Sciarra 12 Flexible, semi-rigid None [104], 1986 or rigid scissors Fayez [92], Rigid scissors Perforations Corson and Batzer [105], Resectosocope Perforation, 1 delayed postoperative bleed DeCherney et al 72 Resectoscope Perforation [80], 1986 March and Israel [77], Flexible scissors Perforation, 3 postoperative significant bleeding Perino et al 24 Semi-rigid scissors None [106], 1989 Daly et al 51 Flexible scissors None [107], 1989 Guarino et al 29 Semi-rigid scissors None [108], 1989 Choe and Baggish [82], Nd:YAG laser Perforation, 1 postoperative uterine synechiae Fedele et al Semi-rigid scissors, NR [110], argon laser, 12 resectoscope Marabini et al [111], Resectoscope None Cararach et al [90], Hysteroscopic scissors, 53 resectoscope Perforations, 1 pulmonary edema Colacurci et al 69 Resectoscope None [112], 1996 Valle [109], Semi-rigid scissors, 20 resectoscope, 6 Nd: YAG laser Admission because of possible pulmonary aspiration Romer and Lober 6 Resectoscope Perforation [113], 1997 Jourdain et al 15 Nd:YAG laser with None [114], 1998 flexible hysteroscopy Grimbizis et al 42 Resectoscope Perforations [115], 1998 Porcu et al [116], Resectoscope, 5 Nd:YAG laser, Perforation 1 abnormal bleeding 3 endoscopic scissors Venturoli et al 141 Resectoscope None [117], 2002 Saygiili-Yilmaz 361 Resectoscope None et al [118], 2002 Jakiel et al 31 Resectoscope None [119], 2004 Pabuccu and Gomel 61 Resectoscope None [34], 2004 Pace et al [120], Resectoscope, rigid scissors None Hollett-Caines et al [121], 2006 Yang et al [122], Versapoint bipolar needle, 20 resectoscope None 28 Nd:YAG laser None (Continued)
10 Valle and Ekpo. Hysteroscopic Metroplasty for Septate Uterus 31 Table 3 Continued Source, year Zlopasa et al [123], 2006 Colacurci et al [124], 2007 Litta et al [125], 2008 Mollo et al [126], 2009 Wang et al [127], 2009 Pai et al [128], 2009 Roy et al [129], 2009 Nouri et al [130], 2010 Sendag et al [131], 2010 Tonguc et al [35], 2011 No. of patients Technique Routine preoperative or postoperative therapy Danazol/ GnRH) Estrogen Progesterone IUD/Foley catheter Antibiotics 25 Resectoscope None Resectoscope, 65 Versapoint bipolar system Resectoscope, 42 Versapoint bipolar system Complications Significant intraoperative blood loss Cervical lacerations 44 Resectoscope None 18 Resectoscope None 64 Resectoscope, Versapoint bipolar system 152 Hysteroscopic monopolar knife None Perforations, 1 cervical injury, 2 excessive bleeding Uterine perforations 49 Monopolar electrosurgery 30 Resectoscope None 102 Resectoscope None GnRH 5 gonadotropin-releasing hormone; IUD 5 intrauterine device; Nd:YAG 5 neodynium:yttrium-aluminum-garnet; NR 5 none reported; 1 5 yes; 2 5 no. safety and efficiency. Although in some selected cases, hysteroscopic metroplasty may be performed in the office setting, the unpredictable nature of this type of procedure demands caution and selection to avoid failure, frustration, and possible complications. Furthermore, health regulations at local, state, and national levels for performance of surgical procedures in the office setting should be respected and followed. Role of Various Adjuncts Before and After Metroplasty Prophylactic Antibiotic Therapy Although various antibiotic regimens are used perioperatively with hysteroscopic metroplasty, no prospective randomized studies have been performed to demonstrate their efficacy. Hormone Therapy Because hysteroscopic metroplasty is ideally performed in the early follicular phase of the menstrual cycle, when the endometrium is thin, occasionally hormone therapy may be required, and among the various options, gonadotropin-releasing hormone analogues are well suited for this task [96,97]. Postoperative hormone therapy using estrogen and terminal progesterone is controversial because their efficacy has not been demonstrated in well-designed, prospective, randomized studies. Nonetheless, artificial stimulation of endometrial growth postoperatively may assist in the overall healing process by artificially enhancing endometrial growth by use of estrogen and subsequent shedding by use of terminal progesterone, paving the way to normal endometrial growth and subsequent spontaneous ovulation. Once withdrawal bleeding occurs, the uterine cavity is evaluated at HSG, hysteroscopy, or ultrasonography to assess its symmetry and normality [98]. The HSG has the advantage of enabling inspection of the uterine cavity in a perpendicular axis and direction, as compared with hysteroscopy, which evaluates the uterine cavity from a cervical axis, therefore better appraising symmetry of the uterine cavity. However, ultrasonography is gaining in acceptance because it enables evaluation not only of the uterine cavity but also the entire uterine body. Stents The use of stents postoperatively to prevent formation of adhesions was an adaptation of the treatment used for intrauterine adhesions. However, being of different pathophysiology and manner of healing, stents never were adopted as
11 32 Journal of Minimally Invasive Gynecology, Vol 20, No 1, January/February 2013 Table 4 Uterine rupture after hysteroscopic metroplasty Source, year Patient age, yr Method of metroplasty Uterine perforation recognized Time from metroplasty to pregnancy Gestational age at rupture, wk Israel and March [156], Scissors No 2 Mo 39 a Creinin and Chen [157], Resectoscope Yes 5 Mo 37 (twin gestation) Howe [158], Rigid scissors Yes 12 Mo 33 Halvorson et al [159], Scissors Yes 1 Mo 19 Lobaugh et al [160], KTP laser No 1.6 Yr 32 Tannous et al [161], Resectoscope Yes 2 Mo 39 Alatas et al [162], Resectoscope No 18 Wk 33 (placenta accreta) Gabriele et al [163], Scissors with electrosurgery Yes 11 Mo 37 (rupture during induction of labor) Chokri et al [164], Resectoscope No 2 Yr 35 b Angell et al [165], 2002 NR Rigid scissors No NR 37 Kerimis et al [166], Scissors with No 3 Mo 41 (spontaneous labor) electrosurgery Conturso et al [167], Resectoscope Yes 12 Mo 28 Ducarme et al [168], Resectoscope No 1 Yr 32 Kucera et al [169], Resectoscope Yes 14 Mo 40 (rupture during labor) Sanchez et al [170], Resectoscope Yes 17 Mo 37 Satiroglu et al [171], Resectoscope No 2 Mo 29 Gultekin et al [172], Resectoscope No 8 Mo 37 (cesarean section, fetus alive) 26 Resectoscope No 11 Mo 34 (cesarean section, fetus dead) NR 5 not reported. a At 18 months after uterine rupture and repair, the patient became pregnant, and delivered at term via elective cesarean section. b At 7 months after uterine rupture and repair, the patient became pregnant; however, at 27 weeks, uterine rupture occurred again. a standard treatment after metroplasty. The postoperative use of intrauterine devices, catheters, inflated balloons, and such has been found to be unnecessary because division of the uterine septum does not lead to formation of adhesions. When fundal defects are discovered postoperatively, they usually are due to remnants of septal tissue left behind [99 102]. Anti-adhesive Agents Many attempts have been made to place gels and other anti-adhesive substances in the uterine cavity after metroplasty; nonetheless, contrary to intrauterine adhesions, their use seems unnecessary because of the high potential for regeneration innate in normal endometrium [103]. Experience with adjunctive therapy with metroplasty are given in Table 3. Healing of the Uterus After Hysteroscopic Metroplasty The high regenerative capacity of the normal endometrium helps in the healing process of the defect from septal division. Fedele et al [132] demonstrated the centripetal and centrifugal directions of the endometrial repair that occurs after division of the uterine septum. At 13 days after the procedure, they studied, via light microscopy and scanning electron microscopy, the histologic changes of the defect left after resection of the septum. Re-epithelialization of the defect proceeded centripetally via proliferation of the surrounding endometrium and centrifugally from the bottom of the glands present at the center, therefore expediting repair [132]. Candiani et al [133] further studied healing of the uterus after hysteroscopic metroplasty via multiple biopsy samples obtained after surgery in 19 women. Complete healing occurred within 8 weeks after metroplasty [133]. Treatment of Complete Septate Uterus With Septate Cervix Treatment of complete septate uterus with septate cervix may be somewhat more challenging than treatment of the corporeal septum alone [109,113, ]. With the background of the embryologic origin of the uterus and arrest of reabsorption of the medial septum, the complete septum is thinner in the lower segment, close to the internal cervical os, where the original reabsorption begins. Therefore, by inserting a probe or indwelling catheter through one of the cervical openings and just above the internal cervical os, the area is made to slightly bulge into the opposite uterine chamber of the divided cavity, and fenestration is performed using either a hysteroscopic scissors or an electrode guided by the resectoscope introduced in the opposite chamber of the
12 Valle and Ekpo. Hysteroscopic Metroplasty for Septate Uterus 33 divided cavity. The indwelling catheter is slightly deflated and pulled down to occlude the hemi-cavity, or if a probe has been used, the probe is removed after fenestration, and the cervix on that side is occluded using a tenaculum to enable better uterine distention without reflux of the distention medium. The reminder of the corporeal septal division is then completed. An alternative treatment of a complete septate uterus with septate cervix is to remove the cervical septum first, using a straight scissors and with division of the corporeal septum using a resectoscope [138]. The results obtained using this method apparently have been satisfactory, with no untoward sequelae such as bleeding or incompetent cervix. However, experience and follow-up are limited, and more experience is needed before accepting routine use of this method, in particular with a thick septum. Nonetheless, this method is a good alternative when preservation of the cervical septum is difficult or fenestration of the corporeal septum fails, rather than proceeding with abdominal metroplasty. Vercellini et al [139] proposed resecting initially the cervical portion of the septum using a straight scissors and then proceeding with division of the corporeal septum via endoscopy. Although the results of this method have been satisfactory, it should be approached with caution, in particular when the cervical septum is thick, because bleeding may occur, and the possibility of an incompetent cervix should also be kept in mind [140,141]. Endoscopic Treatment of Bicornuate Uterus or Strassman Metroplasty Bicornuate uterus is a defect that results from lack of fusion of the m ullerian ducts and can be the cause of pregnancy wastage. The original treatment proposed by Strassman was laparotomy and hysterotomy. A transverse uterine fundal incision between the round ligaments is made to divide the uterine fundus until the uterine cavity is entered; then the incision is closed anteroposteriorly. Attempts have been made to perform this operation less invasively by using endoscopes. The methods used are laparoscopy alone or laparoscopy and hysteroscopy with or without the aid of minilaparotomy for closure of the defect. With the laparoscope in place and using the resectoscope, the uterine nadir of the defect is divided transversally until the serosal layer is observed; then the transverse incision is performed laparoscopically until the uterine cavity is reached. The repair anteroposteriorly is then completed via laparoscopy. Because of the difficulty of achieving a secure closure at laparoscopy, mini-laparotomy can be performed and the uterine repair completed through this small incision. However, these techniques have not been used frequently, and experience with their use is limited [ ]. Occasionally, bicornuate uterus is combined with the septum, and the treatment, if required, does not vary from that of the septum alone; however, it benefits from concomitant laparoscopic or ultrasonographic monitoring to prevent inadvertently entering the muscular layer of the uterine wall [146]. Early and Late Complications of Hysteroscopic Metroplasty As with any surgical procedure, hysteroscopic metroplasty may have its complications. These include bleeding, fluid overload, uterine perforation, formation of adhesions, and uterine rupture in subsequent pregnancy. Bleeding Bleeding during hysteroscopic metroplasty can occur, in particular if uterine distention is insufficient to adequately visualize the septum and enable the accompanying vessels from the uterine wall to be deflected from the central portion of the uterine septum. In addition, risk of bleeding is increased if the operator drifts close to the uterine wall rather than keeping the division in the midline portion of the septum. Postoperative bleeding may occur when the procedure is performed in the luteal phase of the menstrual cycle rather than in the early follicular phase, sometimes mixing with impending menstruation [147,148]. Fluid Overload Excessive fluid absorption may occur if the duration of the operation is prolonged and intake and output of the fluids used is not closely monitored. This is especially important during monopolar electrosurgery because the fluids used are devoid of electrolytes, potentially triggering hyponatremia [ ]. Uterine Perforation Division of the uterine septum requires awareness of the uterine anatomy, and some type of monitoring of the procedure is advantageous to prevent uterine perforations, if not totally, at least substantially decreased. Laparoscopy will help to assess the diaphanoscopy or translucency of the hysteroscopic/resectoscopic light through the uterine wall and will also aid in evaluation of the adnexae and pelvic cavity for additional deleterious factors such as adhesions and endometriosis that can be treated concomitantly. In addition, it can warn the hysteroscopist early of possible perforation [152]. An alternative to laparoscopy is sonography, which can warn of deep penetration of the dissection into the myometrium and possible perforation [153]. Postoperative Intrauterine Adhesions Postoperative intrauterine adhesions have not been a problem with hysteroscopic metroplasty when the procedure is performed systematically and completely without leaving untreated septal remnants that can be confused with adhesions at subsequent examinations.
13 Table 5 Reproductive outcome after hysteroscopic metroplasty Source, year Valle and Sciarra [104], 1986 Canadian task force classification No. of patients Technique Indication Pregnancy rate II-3 12 Flexible, semi-rigid and rigid scissors Fayez [92], 1986 II-1 19 Rigid scissors primary Corson and Batzer [105], 1986 DeCherney et al [80], 1986 March and Israel [77], 1987 Perino et al [106], 1987 III 18 Resectoscope DES-related malformation Recurrent miscarriage 10/12 7/12 (3 ongoing) Live-birth rate Term Preterm Abortion 5/10 2/10 2/10 16/19 14/19 14/16 NA 2/16 13/18 (17 pregnancies) II-3 72 Resectoscope Recurrent miscarriage 67/72 58/72 (5 ongoing) III 79 (66 Flexible scissors III 24 Semi-rigid scissors Daly et al [107], 1989 III 70 (60 Guarino et al [108], 1989 Choe and Baggish [82], 1992 II-3 35 (29 III 19 (14 Flexible scissors Semi-rigid scissors Nd:YAG laser with bare or sculpted fibers Fedele et al [110], 1993 III Semi-rigid scissors, 10 argon laser, 12 resectoscope Marabini et al [111], 1994 III 40 (26 Resectoscope Cararach et al [90], 1994 II-1 81 (70 Colacurci et al [112], Hysteroscopic scissors, 53 resectoscope primary primary, dysmenorrhea III 69 Resectoscope primary Valle [109], 1996 III Semi-rigid scissors, 20 resectoscope, 6 Nd:YAG laser Romer and Lober [113], 1997 Kupesic and Kurjak [175], 1998 III 6 Resectoscope III 116 Operative hysteroscopy, secondary, spontaneous abortion, preterm delivery Jourdain et al [114], 1998 III 17 (15 Nd:YAG laser with flexible hysteroscopy 57/66 (63 pregnancies) 11/18 10/13 1/13 2/13 48/63 (7 ongoing) 16/24 14/24 (1 lost to follow-up) 47/51 (79 pregnancies) 58/79 (4 ongoing) 22/29 13/29 (4 ongoing) 13/15 10/15 (3 ongoing) 58/67 NA 4/67 44/63 4/63 8/63 14/16 NA 1/16 55/79 5/79 15/79 13/22 1/22 4/22 10/15 1/15 1/15 66/102 55/102 45/66 10/66 11/66 19/26 13/26 (4 ongoing) 13/15 13/15 0/15 51/70 29/70 29/51 29/51 NA (10 ongoing) 46/69 36/69 31/46 31/46 5/46 (4 ongoing) 101/124 91/124 84/101 84/101 7/101 3/6 3/6 3/3 3/3 NA 59/116 48/116 44/59 44/59 4/59 12/15 10/15 10/12 10/12 NA 34 Journal of Minimally Invasive Gynecology, Vol 20, No 1, January/February 2013
14 Grimbizis et al [115], 1998 III 57 (42 Resectoscope Porcu et al [116], 2000 III Resectoscope, 5 Nd:YAG laser, 3 endoscopic scissors Preutthipan and Linasmita [176], 2001 Venturoli et al [117], 2002 Saygiili-Yilmaz et al [118], 2002 III 28 (19 7 Scissors, 10 Versapoint system, 11 resectoscope Infertility, spontaneous abortion II Resectoscope II Resectoscope Recurrent miscarriage 19 patients (20 pregnancies) 30/42 (44 pregnancies) 30/42 28/44 28/44 2/44 45/56 28/56 26/43 26/43 2/43 (2 ongoing) 15/20 (2 ongoing) 15/20 15/20 0/20 92/141 57/141 45/92 45/92 12/92 (14 ongoing) 180/ / / /180 34/180 Jakiel et al [119], 2004 III 26 Resectoscope Infertility 18/31 10/31 7/18 7/18 4/18 Pabuccu and Gomel III 61 Resectoscope Primary 25/61 18/61 13/25 13/25 5/25 [34], 2004 Pace et al [120], 2006 III 75 (40 Resectoscope, semi-rigid scissors, preterm delivery 30/40 27/40 22/30 22/30 5/30 Hollett-Caines et al [121], 2006 III 26 6 Versapoint bipolar, 19 resectoscope, 1 Nd: YAG laser Yang et al [122], 2006 III 45 (28 Zlopasa et al [123], 2007 Colacurci et al [124], 2007 Nd:YAG laser, preterm delivery III 25 Resectoscope Recurrent miscarriage 25 patients (52 pregnancies) I 180 (135 Litta et al [125], 2008 II-1 63 (45 followed up) Mollo et al [126], 2009 Wang et al [127], Resectoscope, 65 Versapoint bipolar 21 Resectoscope, 42 Versapoint bipolar primary 21/26 15/26 12/21 12/21 3/21 20/28 16/28 16/20 16/20 NR 32/52 23/52 23/52 9/52 99/135 82/135 66/99 66/99 16/99 Spontaneous abortion 36/45 27/45 22/36 22/36 5/36 II-1 44 Resectoscope Infertility 17/44 15/44 12/17 12/17 3/17 III 25 (18 Resectoscope Paietal[128], 2009 III 64 Resectoscope, Versapoint bipolar Roy et al [129], 2009 III 152 Hysteroscopic monopolar knife Nouri et al [130], 2010 Sendag et al [131], 2010 Tonguc et al [35], 2011 III 64 (49 Monopolar electrosurgery 15/18 6/18 (7 ongoing) 5/15 5/15 1/15 Infertility 33/64 29/64 24/33 24/33 5/33, preterm delivery 142/152 (186 pregnancies) 162/ / /186 14/186 34/49 24/49 15/34 15/34 9/34 III 30 Resectoscope Spontaneous abortion, 20/30 13/30 11/20 11/20 2/20 preterm delivery II Resectoscope Infertility 44/102 36/102 31/44 31/44 8/44 DES 5 diethylstilbestrol; NA 5 not available; Nd:YAG 5 neodynium:yttrium-aluminum-garnet; NR 5 not reported. Valle and Ekpo. Hysteroscopic Metroplasty for Septate Uterus 35
15 36 Journal of Minimally Invasive Gynecology, Vol 20, No 1, January/February 2013 Fig. 8 Pregnancy rate after hysteroscopic metroplasty. Initial meta-analysis was performed on all studies (groups 1 and 2) with pregnancy rate reported as percentage. After excluding studies with inconsistent definition of pregnancy rate (i.e., all post-metroplasty pregnancies reported, not just index pregnancy) and studies with a substantial number of subjects lost to follow-up or with ongoing pregnancies, a second analysis was performed on the clean studies (group 1). Statistics for each study Source, Year Event 95% CI Z Value p Value Rate (%) Group 1 Fayez, Fedele et al, Valle, Romer and Loper, Kupesic and Kurjak, Jourdain et al, Saygiili-Yilmaz et al, Jakiel et al, Pabuccu and Gomel, Pace et al, Hollet-Caines et al, Yang et al, Colacurci et al, Litta et al, Mollo et al, Pai et al, Nouri et al, Sendag et al, Tonguc et al, Group 2 Valle, Decherney et al, Perino et al, Guarino et al, Choe and Baggish, Marabini et al, Cararach et al, Colacurci et al, Porcu et al, Venturoli et al, Overall Event Rate and 95% CI Favors A Favors B Uterine Rupture With Subsequent Pregnancy The literature includes 18 confirmed reports of uterine rupture during pregnancy or delivery after hysteroscopic metroplasty (Table 4). All describe some complication during the procedure such as excessive or overzealous excision, with substantial penetration of the myometrium and even perforation of the uterine wall, and excessive use of electrosurgical or laser energy [ ]. Therefore, regardless of the treatment method used, meticulous attention to technique should always be exercised. Published Surgical Results of Hysteroscopic Metroplasty and Their Level of Evidence Many reports in the literature have detailed the salutary effects of treatment of septate uterus on subsequent reproduction[173,174]. However, all have uniformly used the patients as their own control, without prospective randomization or sufficient number of patients for comparison of treatment vs no treatment. Nonetheless, the accumulated experience and favorable results indicate the beneficial effect of surgery. Thus, perhaps a prospective randomized study comparing treatment vs no treatment becomes moot or even unnecessary because it would be difficult to perform due to the ethical implications and willingness of patients to participate in a randomized trial because of the urgency sometimes associated with childbearing. The overall rate of pregnancy and viable pregnancies after surgery is 80% to 90% (Table 5). Meta-analysis of Reproductive Outcomes After Hysteroscopic Metroplasty We identified studies that reported outcomes after hysteroscopic metroplasty from 1986 to 2011 by performing an extensive search of Medline and by hand searching cross-references and review articles. Keywords used in the
16 Valle and Ekpo. Hysteroscopic Metroplasty for Septate Uterus 37 Fig. 9 Live-birth rate after hysteroscopic metroplasty. Initial meta-analysis was performed on all studies (groups 1 and 2) with live-birth rate reported as percentage. After excluding studies with inconsistent definition of pregnancy rate (i.e., all post-metroplasty pregnancies reported, not just index pregnancy) and studies with a substantial number of subjects lost to follow-up or with ongoing pregnancies, a second analysis was performed on the clean studies (group 1). Statistics for each study Source, Year Event 95% CI Z Value p Value Rate (%) Group 1 Fayez, Fedele etal, Valle, Romer and Loper, Kupesic and Kurjak, Jourdain et al, Saygiili-Yilmaz et al, Jakiel et al, Pabuccu and Gomel, Pace et al, Hollet-Caines et al, Yang et al, Colacurci et al, Litta et al, Mollo et al, Pai et al, Nouri et al, Sendag et al, Tonguc et al, Group 2 Valle, Decherney et al, Perino et al, Guarino et al, Choe and Baggish, Marabini et al, Cararach et al, Colacurci et al, Porcu et al, Venturoli et al, Overall Event Rate and 95% CI Favors A Favors B search included hysteroscopy, metroplasty, uterine septum, recurrent miscarriage,, and uterine anomalies. No randomized controlled trials were identified; thus, all included studies in the meta-analysis were categorized as Canadian Task Force classification II or III. The outcome measures of interest were pregnancy rate and live-birth rate after hysteroscopic metroplasty. Studies were excluded if both outcome measures were not reported or if full article text could not be obtained. To avoid duplication, studies describing the same study population were included only once. We did not include studies of hysteroscopic metroplasty in patients undergoing IVF. Data were extracted by one of us (G.E.E.) with population information including number of patients, indication, and interventional technique (Table 5). The data were then analyzed using Comprehensive Metaanalysis software (version 2; Biostat, Inc., Englewood, NJ). After eliminating studies using exclusion criteria as described above, 29 studies remained and were used for initial meta-analysis (groups 1 and 2). Given the substantially different populations, a random-effects model was used for the calculations. The calculated overall pregnancy rate was 67.8% (95% confidence interval [CI], ), and live birth rate was 53.5% (95% CI, ) (Figs. 8 and 9). There was significant heterogeneity between studies (p,.01). Significant within study variability was also noted. After eliminating 10 studies in which the reported pregnancy rate included more than 1 pregnancy per patient and/or unreliable live-birth rates as a result of patients being lost to follow-up before giving birth, a second analysis was performed of the remaining 19 clean studies (group 1), which showed a lower overall pregnancy rate of 63.5% (95% CI, ) and live-birth rate of 50.2% (95% CI, ) (Figs. 8 and 9). This difference is not surprising inasmuch as some studies in the larger group likely reported falsely elevated pregnancy rates because subsequent pregnancies in the same subject were included in the pregnancy
17 38 Journal of Minimally Invasive Gynecology, Vol 20, No 1, January/February 2013 rate and also because the live-birth rate was reported as the number of births divided by this exaggerated number of pregnancies. The test of heterogeneity using subgroup analysis was significant when calculating the pregnancy rate (p 5.02); thus, the reported event rates (63.5% pregnancy rate and 50.2% live-birth rate) from group 1 are more reliable. In a review of 12 published retrospective studies, Homer et al [32] compared reproductive outcome before and after hysteroscopic surgery. Such comparison is less than ideal, but showed a pooled postoperative pregnancy rate of 80% in women with miscarriage or. In addition, the term birth rate increased from 0% to 7% to 73% to 100% after the operation. In another systematic review and pooled analysis of 1501 women in 18 studies, Nouri et al [130] reported an overall pregnancy rate of 60.1% and a live-birth rate of 45% after hysteroscopic metroplasty, which is similar to findings from our meta-analysis. The present meta-analysis is limited by predominantly observational studies because there are no published prospective randomized trials that compared metroplasty with no intervention, which could provide the highest level of evidence. The realities of performing a randomized controlled trial and the possible ethical implications leave only observational studies for analysis and interpretation. Methods were quite varied in the selected studies despite an attempt to define clear inclusion criteria, and indications also varied. Some studies contained inconsistent follow-up data, with findings published before reaching the outcome of live birth in some individuals, which could be a source of confounding bias. No comparisons of pregnancy and live birth rates before metroplasty were made. Perhaps the most important inference from this metaanalysis is the clinical heterogeneity within and between studies. This reflects the controversy in the indications for performing hysteroscopic metroplasty, with current indications ranging from history of R1 pregnancy loss to preterm labor, unexplained, and even removal of identified septum in the absence of any adverse pregnancy outcomes. A random-effects model was used for the calculations to adjust for this heterogeneity, and perhaps inclusion of different populations enables generalization to a broader range of patients. On the basis of data from the current literature, findings from our descriptive meta-analysis show a 63.5% pregnancy rate and a 50.2% live-birth rate after hysteroscopic metroplasty of septate uterus. These rates may certainly be higher in subjects with exclusively recurrent miscarriages in whom their septum has been removed, and lower in those with other causes of. The focus of further research studies should be on specific populations with clear indications, to draw reasonable and meaningful conclusions about the outcomes of hysteroscopic metroplasty. Adequate time after the procedure should be allowed so that subjects have ample time to attempt conception and also to give birth, to allow for accurate live-birth rate calculations. Future of Hysteroscopic Metroplasty Innovations in instrumentation and safe energy sources will continue to improve the safety and simplicity of hysteroscopic metroplasty. The hysteroscopic scissors should be made sturdier without compromising diameter and semirigidity. They also should maintain their ability to cut after several uses. On the horizon is the introduction of endoscopes that are also capable of sonographic evaluation with sufficient resolution and penetration to aid in the safe, precise, and efficient division of the uterine septum, eventually simplifying the procedure and adding precision to its performance. These and other advances may eventually become reality, even further simplifying hysteroscopic metroplasty. Summary and Conclusions Septate uterus resulting from failure of reabsorption of the embryologic original fusion of the m ullerian ducts may impair reproductive function in 20% to 25% of women with this anomaly. When this occurs, the septum may be amenable to surgical correction now performed via hysteroscopic or resectoscopic division. The limitations and inconveniences of laparotomy and hysterotomy are thus averted, and preservation of the integrity of the uterine walls does not require cesarean section in subsequent viable pregnancies. Hysteroscopic treatment of a symptomatic septate uterus can be accomplished via various methods including scissors, electrosurgical electrodes guided through the hysteroscope, or resectoscopy, which are the most commonly used methods. Fiber lasers have been used, although their use has markedly decreased because of cost and the simplification of electrosurgery using vaporizing and bipolar electrodes. Mechanical morcellators have also been tried, although the shape of the morcellators does not seem to surpass the available electrosurgical electrodes and the mechanical hysteroscopic scissors. In patients with a history of reproductive failure manifested by repeated abortions, it is important to rule out other potential causes such as genetic, metabolic, and endocrine abnormalities before proceeding with surgical treatment. The results achieved with hysteroscopic metroplasty surpass those of previous invasive abdominal metroplasty procedures, with a rate of viable pregnancies.80% in patients with a history of repeated abortion. It is expected that in the future, research will focus on specific populations with clear indications, to draw meaningful conclusions on the outcomes of hysteroscopic metroplasty. Although no prospective randomized studies have been performed with an adequate number of patients to demonstrate the efficacy of treatment vs no treatment, the overall success reported indicates its efficacy and reaffirms the place of minimally invasive treatment such as hysteroscopic metroplasty as the criterion standard and method of choice for treatment of this septate uterus.
18 Valle and Ekpo. Hysteroscopic Metroplasty for Septate Uterus 39 Acknowledgments We thank Drs. Alfred W. Rademaker (Professor, Department of Preventive Medicine) and Amy Wong (Fellow, Maternal-Fetal Medicine, Department of Obstetrics and Gynecology) at Northwestern University for assistance with the statistical analysis. References 1. Wallach EE. Evaluation and management of uterine causes of. Clin Obstet Gynecol. 1979;22: Semmens JP. Congenital anomalies of female genital tract: functional classification based on review of 56 personal cases and 500 reported cases. Obstet Gynecol. 1962;19: Strassman EO. Fertility and unification of double uterus. Fertil Steril. 1966;17: Hay D. Uterus unicollis and its relationship to pregnancy. BJOG. 1961;68: Uterine anomalies. In: Buttram VC, Reiter RC, editors. Surgical Treatment of the Infertile Female. Chapter 6. Baltimore, MD: Williams & Wilkins; p Elias S, Simpson JL, Carson SA, Malinak LR, Buttram VC Jr. Genetic studies in incomplete Mullerian fusion. Obstet Gynecol. 1984;63: Moore KL. The urogenital system. In: Moore KL, Persuad TVN, editors. The Developing Human: Clinically Oriented Embryology. 4th ed. Philadelphia: WB Saunders; p Larsen WJ. Human Embryology. New York: Churchill Livingstone; Lin PC, Bhatnagar KP, Nettleton GS, Nakajima ST. Female genital anomalies affecting reproduction. Fertil Steril. 2002;78: Patton PE. Anatomic uterine defects. Clin Obstet Gynecol. 1994;37: Buttram VC Jr, Gibbons WE. Mullerian anomalies: a proposed classification (an analysis of 144 cases). Fertil Steril. 1979;32: American Fertility Society. The American Fertility Society classifications of adnexal adhesions, distal tubal occlusion, tubal occlusion secondary to tubal ligation, tubal pregnancies, Mullerian anomalies and intrauterine adhesions. Fertil Steril. 1988;49: Gubbini G, Sardo AD, Nascetti D, et al. New outpatient subclassification system for American Fertility Society classes V and VI uterine anomalies. J Minim Invasive Gynecol. 2009;16: Jones HW, Rock JA. Reparative and Constructive Surgery of the Female Genital Tract. Baltimore, MD: Williams & Wilkins; 1983: Jones HW. Reproductive impairment and the malformed uterus. Fertil Steril. 1981;36: Lindeman E, Shepard MK, Pescovitz OH. Mullerian agenesis: an update. Obstet Gynecol. 1997;90: Fore SR, Hammond CB, Parker RT, Anderson EE. Urologic and genital anomalies in patients with congenital absence of the vagina. Obstet Gynecol. 1975;46: Sparac V, Kupesic S, Ilijas M, Zodan T, Kurjak A. Histologic architecture and vascularization of hysteroscopically excised intrauterine septum. J Am Assoc Gynecol Laparosc. 2001;8: Dabirashrafi H, Bahadori M, Mohammad K, et al. Septate uterus: new idea on the histologic features of the septum in this abnormal uterus. Am J Obstet Gynecol. 1995;172: Kupesic S, Karjak A. Septate uterus detection and prediction of obstetrical complications by different forms of ultrasonography. J Ultrasound Med. 1998;17: Oliva GC, Fratoni A, Genova M, Romanini C. Uterine motility in patients with bicornuate uterus. Int J Obstet Gynecol. 1992;37: Green LK, Harris RE. Uterine anomalies: frequency of diagnosis and associated obstetric complications. Obstet Gynecol. 1976;47: Valle RF. Clinical management of uterine factors in infertile patients. Semin Reprod Med. 1985;3: Hua M, Odibo AO, Longman RE, Macones GA, Roehl KA, Cahill AG. Congenital uterine anomalies and adverse pregnancy outcomes. Am J Obstet Gynecol. 2011;205:558.e1 e Agostini A, De Guibert F, Salari K, Crochet P, Bretelle F, Gamerre M. Adverse obstetric outcomes at term after hysteroscopic metroplasty. J Minim Invasive Gynecol. 2009;16: Blum M. Comparative study of serum CAP activity during pregnancy in malformed and normal uterus. J Perinat Med. 1978;6: Roddick JW, Buckingham JC, Danforth DN. The muscular cervix: a cause of incompetency in pregnancy. Obstet Gynecol. 1961;17: Raga F, Casan EM, Bonilla-Musoles F. Expression of vascular endothelial growth factor receptors in the endometrium of septate uterus. Fertil Steril. 2009;92: Fedele L, Dorta M, Brioschi D, Giudici MN, Candiani GB. Pregnancies in septate uteri: outcome in relation to site of uterine implantation as determined by sonography. AJR Am J Roentgenol. 1989;152: Fedele L, Bianchi S, Marchini M, Franchi D, Tozzi L, Dorta M. Ultrastructural aspects of endometrium in infertile women with septate uterus. Fertil Steril. 1996;65: Heinonen PK, Pystynen PP. Primary and uterine anomalies. Fertil Steril. 1983;40: Homer HA, Li TC, Cooke ID. The septate uterus: a review of management and reproductive outcome. Fertil Steril. 2000;73: Shokeir T, Abdelshaheed M, El-Shafie M, Sherif L, Badawy A. Determinants of fertility and reproductive success after hysteroscopic septoplasty for women with unexplained primary : a prospective analysis of 88 cases. Eur J Obstet Gynecol Reprod Biol. 2011;155: Pabuccu R, Gomel V. Reproductive outcome after hysteroscopic metroplasty in women with septate uterus and otherwise unexplained. Fertil Steril. 2004;81: Tonguc EA, Var T, Batioglu S. Hysteroscopic metroplasty in patients with a uterine septum and otherwise unexplained. Int J Gynaecol Obstet. 2011;113: Ayas S, Gurbuz A, Tuna G, Sargin M, Alkan A, Eren S. Hysteroscopic resection of uterine septum improves reproductive performance in women with unexplained. Turk J Med Sci. 2011;41: Paradisi R, Barzani R, Natali F, et al. Metroplasty in a large population of women with septate uterus. J Minim Invasive Gynecol. 2011;18: Tomazevic T, Ban-Frangez H, Virant-Klun I, Verdenik I, Pozlep B, Vrtacnik-Bokal E. Septate, subseptate and arcuate uterus decrease pregnancy and live birth rates in IVF/ICSI. Reprod Biomed Online. 2010;21: Reuter K, Daly DC, Cohen SM. Septate versus bicornuate uteri: errors in imaging diagnosis. Radiology. 1989;172: Carrascosa P, Sueldo C, Capunay C, Baronio M, Papier S. Virtual hysterosalpingography in the diagnosis of bicornuate versus septate uterus. Fertil Steril. 2011;96: Nicolini U, Bellotti M, Bonazzi B, Zamberletti D, Candiani GB. Can ultrasound be used to screen uterine malformations? Fertil Steril. 1987;47: Fedele L, Ferrazzi E, Dorta M, Vercellini P, Candiani GB. Ultrasonography in the differential diagnosis of double uteri. Fertil Steril. 1988;50: Salle B, Sergeant P, Gaucherand P, Guimont I, de Saint Hillaire P, Rudigoz RC. Transvaginal hysterosonographic evaluation of septate uteri: a preliminary report. Hum Reprod. 1996;11:
19 40 Journal of Minimally Invasive Gynecology, Vol 20, No 1, January/February Storment JM, Kaiser JR, Sites CK. Transvaginal ultrasonographic diagnosis of uterine septa. J Reprod Med. 1998;43: Jurkovic D, Geipel A, Gruboeck K, Haniaux M, Natucci M, Campbell S. Three-dimensional ultrasound for the assessment of uterine anatomy and detection of congenital anomalies: a comparison with hysterosalpingography and two-dimensional sonography. Ultrasound Obstet Gynecol. 1995;5: Woelfer B, Salim R, Banerjee S, Elson J, Regan L, Jurkovic D. Reproductive outcomes in women with congenital uterine anomalies detected by three-dimensional ultrasound screening. Obstet Gynecol. 2001;98: Salim R, Woelfer B, Backos M, Regan L, Jurkovic D. Reproducibility of three-dimensional ultrasound diagnosis of congenital uterine anomalies. Ultrasound Obstet Gynecol. 2003;21: Alborzi S, Dehbashi S, Parsanezhad ME. Differential diagnosis of septate and bicornuate uterus by sonohysterography eliminates the need for laparoscopy. Fertil Steril. 2002;78: Raga F, Bonilla-Musoles F, Blanes J, Osborne NG. Congenital Mullerian anomalies: diagnostic accuracy of three-dimensional ultrasound. Fertil Steril. 1996;65: El-Sherbiny W, Nasr AS. Value of 3-dimensional sonohysterography in work-up. J Minim Invasive Gynecol. 2011;18: Faivre E, Fernandez H, Deffieux X, Gervaise A, Frydman R, Levaillant JM. Accuracy of three-dimensional ultrasonography in differential diagnosis of septate and bicornuate uterus compared with office hysteroscopy and pelvic magnetic resonance imaging. J Minim Invasive Gynecol. 2012;19: Mollo A, Nazzaro G, Granata M, et al. Combined hysteroscopic findings and 3-dimensional reconstructed coronal view of the uterus to avoid laparoscopic assessment for inpatient hysteroscopic metroplasty: pilot study. J Minim Invasive Gynecol. 2011;18: Pellerito JS, McCarthy SM, Doyle MB, Glickman MG, DeCherney AH. Diagnosis of uterine anomalies: relative accuracy of MR imaging, endovaginal sonography, and hysterosalpingography. Radiology. 1992;183: Yoder IC. Diagnosis of uterine anomalies: relative accuracy of MRI imaging, endovaginal sonography, and hysterosalpingography [Devil s Advocate]. Radiology. 1992;183: Pellerito JS, McCarthy SM, Glickman M, DeCherney AH. Diagnosis of uterine anomalies-relative accuracy of MRI imaging, endovaginal sonography, and hysterosalpingography [Response]. Radiology. 1992;185: Coutifaris C, Myers ER, Guzick DS, et al. Histological dating of timed endometrial biopsy tissue is not related to fertility status. Fertil Steril. 2004;82: Branch DW, Gibson M, Silver RM. Recurrent Miscarriage [Clinical Practice]. N Engl J Med. 2010;363: Carp H, Toder V, Aviram A, Daniely M, Mashiach S, Barkai G. Karyotype of the abortus in recurrent miscarriage. Fertil Steril. 2001;75: Jones HW Jr, Jones GES. Double uterus as an etiologic factor in repeated abortion: indications for surgical repair. Am J Obstet Gynecol. 1953;65: Carp HJ, Toder V, Mashiach S, Nebel L, Serr DM. Recurrent miscarriage: a review of current concepts, immune mechanisms, and results of treatment. Obstet Gynecol Surv. 1990;45: Rock JA, Zacur HA. The clinical management of repeated early pregnancy wastage. Fertil Steril. 1983;39: Rock JA, Jones HW Jr. The clinical management of the double uterus. Fertil Steril. 1977;28: Bret AJ, Guillet B. Reconstructive hysteroplasty without muscular resection in uterine malformations: a cause of repeated abortion. Presse Med. 1959;67: Tompkins P. Comments on the bicornuate uterus and twinning. Surg Clin North Am. 1962;42: McShane PM, Reilly RJ, Schiff I. Pregnancy outcomes following Tompkins metroplasty. Fertil Steril. 1983;40: El-Mahgoub S. Unification of a septate uterus: Mahgoub s operation. Int J Gynaecol Obstet. 1978;15: Musich JR, Behrman SJ. Obstetric outcome before and after metroplasty in women with uterine anomalies. Obstet Gynecol. 1978;52: Mercer CA, Long WN, Thompson JD. Uterine unification: indications and techniques. Clin Obstet Gynecol. 1981;24: Kessler I, Lancet M, Appelman Z, Borenstein R. Indications and results of metroplasty in uterine malformations. Int J Gynaecol Obstet. 1986;24: Candiani GB, Fedele L, Parazzini F, Zamberletti D. Reproductive prognosis after abdominal metroplasty in bicornuate or septate uterus: a life table analysis. Br J Obstet Gynaecol. 1990;97: Ayhan A, Yucel I, Tuncer ZS, Kisnisci HA. Reproductive performance after conventional metroplasty: an evaluation of 102 cases. Fertil Steril. 1992;57: Kirk EP, Chuong CJ, Coulam CB, Williams TJ. Pregnancy after metroplasty for uterine anomalies. Fertil Steril. 1993;59: Ruge P. Einen fall von schwangerschaft bei uterus septus. Z Geburtshilfe Gynakol. 1884;10: Edstrom KGB. Intrauterine surgical procedures during hysteroscopy. Endoscopy. 1974;6: Valle RF. Uterine septa. In: Bieber EG, Loffer FD, editors. Gynecologic Resectoscopy. Cambridge: Blackwell Science; p Daly DC, Walters CA, Soto-Albors CD, Riddick DH. Hysteroscopic metroplasty: surgical technique and obstetric outcome. Fertil Steril. 1983;39: March CM, Israel R. Hysteroscopic management of recurrent abortion caused by septate uterus. Am J Obstet Gynecol. 1987;156: Vilos GA. Intrauterine surgery using a new coaxial bipolar electrode in normal saline solution (Versapoint): a pilot study. Fertil Steril. 1999; 72: Shawki HE. Reproductive outcomes after Versapoint hysteroscopic metroplasty. Middle East Fertil Soc J. 2010;15: DeCherney AH, Russell JB, Graebe RA, Polan ML. Resectoscopic management of Mullerian fusion defects. Fertil Steril. 1986;45: Daniell JF, Osher S, Miller W. Hysteroscopic resection of uterine septa with visible light laser surgery. Colposc Gynecol Laser Surg. 1987;3: Choe JK, Baggish MS. Hysteroscopic treatment of septate uterus with neodymium-yag laser. Fertil Steril. 1992;57: Candiani GB, Vercellini P, Fedele L, Garsia S, Brioschi D, Villa L. Argon laser versus microscissors for hysteroscopic incision of uterine septa. Am J Obstet Gynecol. 1991;164: Querleu D, Brasme TL, Parmentier D. Ultrasound-guided transcervical metroplasty. Fertil Steril. 1990;54: Ohl D, Bettahar-Lebugle K. Ultrasound-guided transcervical resection of uterine septa: 7 years experience. Ultrasound Obstet Gynecol. 1996;7: Valle JA, Lifchez AS, Moise J. A simpler technique for reduction of uterine septum. Fertil Steril. 1992;56: Simons M, Hamerlynck TW, Abdulkadir L, Schoot BC. Hysteroscopic morcellator system can be used for removal of a uterine septum. Fertil Steril. 2011;96:e118 e El Saman AM, Darwish AM, Zakherah MS, Hamed HO, Bedaiwy MA, Nasr AM. Tactile cold scissor metroplasty as a novel back up method for hysteroscopic metroplasty. Fertil Steril. 2010;94: Vercellini P, Vendola N, Colombo A, et al. Hysteroscopic metroplasty with resectoscope or microscissors for the correction of septate uterus. Surg Gynecol Obstet. 1993;178: Cararach M, Penella J, Ubeda A, Labastida R. Hysteroscopic division of septate uterus: scissors versus resectoscope. Hum Reprod. 1994;9:
20 Valle and Ekpo. Hysteroscopic Metroplasty for Septate Uterus Spirtos NJ, Evans TN, Magyar DM, Moghissi KS. The reproductive performance of women before and after metroplasty. Int J Fertil. 1987;32: Fayez JA. Comparison between abdominal and hysteroscopic metroplasty. Obstet Gynecol. 1986;68: Bettocchi S, Ceci O, Nappi L, Pontrelli G, Pinto L, Vicino M. Office hysteroscopic metroplasty: three diagnostic criteria to differentiate between septate and bicornuate uterus. J Minim Invasive Gynecol. 2007;14: Scuderi G, Gallea MR, Giuca R, et al. Office hysteroscopy: golden standard in diagnosis and treatment of uterine septa. Giorn Ital Ostet Ginecol. 2011;33: De Frumarsis P, De Biazio G, Toro G, et al. Office hysteroscopy vs. resectoscope for the treatment of septate uterus. Giorn Ital Ostet Ginecol. 2009;31: Colacurci N, De Franciscis P, Mollo A, Mele D, Fortunato N, Zarcone R. Preoperative GnRH analogue in hysteroscopic metroplasty. Panminerva Med. 1998;40: Vercellini P, Ragni G, Colombo A, et al. Gonadotropin releasing hormone agonist treatment before hysteroscopic metroplasty. Gynaecol Endosc. 1993;2: Milad MP, Valle RF. Does hormone therapy after hysteroscopic metroplasty hasten endometrial healing? J Am Assoc Gynecol Laparosc. 1995;2: Shawki OA, Ebrashi AN, Kandeel HO, Soliman EM, Saleet ME. Evaluation of different approaches for prevention of intrauterine adhesions following hysteroscopic metroplasty for septate uterus. Middle East Fertil Soc J. 1999;4: Vercellini P, Fedele L, Arcaini L, Rognoni MT, Candiani GB. Value of intrauterine device insertion and estrogen administration after hysteroscopic metroplasty. J Reprod Med. 1989;34: Dabirashrafi H, Mohammad K, Moghadami-Tabrizi N, Zandinejad K, Moghadami-Tabrizi M. Is estrogen necessary after hysteroscopic incision of the uterine septum? J Am Assoc Gynecol Laparosc. 1996; Tonguc EA, Var T, Yilmaz N, Balioglu S. Intrauterine device or estrogen treatment after hysteroscopic uterine septum resection. Int J Gynecol Obstet. 2010;109: Di Spiezio SA, Spinelli M, Bramante S, Scognamiglio M. Efficacy of a polyethylene oxide-sodium carboxymethylcellulose gel in prevention of intrauterine adhesions after hysteroscopic surgery. J Minim Invasive Gynecol. 2011;18: Valle RF, Sciarra JJ. Hysteroscopic treatment of the septate uterus. Obstet Gynecol. 1986;67: Corson SL, Batzer FR. CO 2 uterine distension for hysteroscopic septal incision. J Reprod Med. 1986;31: Perino A, Mencaglia L, Hamou J, Cittadini E. Hysteroscopy for metroplasty of uterine septa: report of 24 cases. Fertil Steril. 1987;48: Daly DC, Maier D, Soto-Albors C. Hysteroscopic metroplasty: six years experience. Obstet Gynecol. 1989;73: Guarino S, Incandela S, Maneschi M, et al. Hysteroscopic treatment of uterine septum. Acta Eur Fertil. 1989;20: Valle RF. Hysteroscopic treatment of partial and complete uterine septum. Int J Fertil Menopausal Studies. 1996;41: Fedele L, Vercellini P, Arcaini L, Di Nola, Parazzini F. Reproductive prognosis after hysteroscopic metroplasty in 102 women: life-table analysis. Fertil Steril. 1993;59: Marabini A, Gubbini G, Stagnozzi R, Stefanetti M, Filoni M, Bovicelli A. Hysteroscopic metroplasty. Ann NY Acad Sci. 1994; 734: Colacurci N, De Placido G, Mollo A, Carravetta C, De Francisicis P. Reproductive outcome after hysteroscopic metroplasty. Eur J Obstet Gynecol Reprod Biol. 1996;66: Romer T, Lober R. Hysteroscopic correction of a complete septate uterus using a balloon technique. Hum Reprod. 1997;12: Jourdain O, Dabysing F, Harle T, Lajus C, Roux D, Dallay D. Management of septate uterus by flexible hysteroscopy and Nd:YAG laser. Int J Gynaecol Obstet. 1998;63: Grimbizis G, Camus M, Clasen K, Tournaye H, De Munck L, Devroey P. Hysteroscopic septum resection in patients with recurrent abortions or. Hum Reprod. 1998;13: Porcu G, Cravello L, D Ercole C, et al. Hysteroscopic metroplasty for septate uterus and repetitive abortions: reproductive outcome. Eur J Obstet Gynecol Reprod Biol. 2000;88: Venturoli S, Colombo FM, Vianello F, Seracchioli R, Possati G, Parasidi R. A study of hysteroscopic metroplasty in 141 women with a septate uterus. Arch Gynecol Obstet. 2002;266: Saygiili-Yilmaz ES, Erman-Akar Z, Yilmaz Z. A retrospective study on the reproductive outcome of the septate uterus corrected by hysteroscopic metroplasty. Int J Gynaecol Obstet. 2002;78: Jakiel G, Robak-Cholubek D, Przytula-Pilat M. Two-year studies of women with fertility problems following uterine septum hysteroscopic treatment. Ann Univ Mariae Curie Sklodowska Med. 2004; 59: Pace S, Cipriano L, Pace G, Catania R, Montanino G. Septate uterus: reproductive outcome after hysteroscopic metroplasty. Clin Exp Obstet Gynecol. 2006;33: Hollett-Caines J, Vilos GA, Abu-Rafea B, Ahmad R. Fertility and pregnancy outcomes following hysteroscopic septum division. J Obstet Gynaecol Can. 2006;28: Yang J, Yin TU, Xu WM, Xia LG, Li AB, Hu J. Reproductive outcome of septate uterus after hysteroscopic treatment with neodymium:yag laser. Photomed Laser Surg. 2006;24: Zlopasa G, Skrablin S, Kalafatic D, Banovic V, Lesin J. Uterine anomalies and pregnancy outcome following resectoscope metroplasty. Int J Gynaecol Obstet. 2007;98: Colacurci N, De Franciscis P, Mollo A, et al. Small-diameter hysteroscopy with Versapoint versus resectoscopy with a unipolar knife for the treatment of septate uterus: a prospective randomized study. J Minim Invasive Gynecol. 2007;14: Litta P, Spiller E, Saccardi C, Ambrosini G, Caserta D, Cosmi E. Resectoscope or Versapoint for hysteroscopic metroplasty. Int J Gynaecol Obstet. 2008;101: Mollo A, De Franciscis P, Colacurci N, et al. Hysteroscopic resection of the septum improves the pregnancy rate of women with unexplained : a prospective controlled trial. Fertil Steril. 2009;91: Wang JH, Xu K-H, Lin J, Chen XZ. Hysteroscopic septum resection of complete septate uterus with cervical duplication, sparing the double cervix in patients with recurrent spontaneous abortions or. Fertil Steril. 2009;91: Pai HD, Kundnani MT, Palshetkar NP, Pai RD, Saxena N. Reproductive performance after hysteroscopic metroplasty in women with primary and septate uterus. J Gynecol Endosc Surg. 2009;1: Roy KK, Singla S, Baruah J, Kumar S, Sharma JB, Karmakar D. Reproductive outcome following hysteroscopic septal resection in patients with and recurrent abortions. Arch Gynecol Obstet. 2011;283: Nouri K, Ott J, Huber JC, Fischer E. Reproductive outcome after hysteroscopic septoplasty in patients with septate uterus: a retrospective cohort study and systematic review of the literature. Reprod Biol Endocrinol. 2010;8: Sendag F, Mermer T, Yucebilgin S, Oztekin K, Bilgin O. Reproductive outcomes after hysteroscopic metroplasty for uterine septum. Clin Exp Obstet Gynecol. 2010;37: Fedele L, Marchini M, Baglioni A, Carinelli SG, Candiani GB. Endometrial reconstruction after hysteroscopic incisional metroplasty. Obstet Gynecol. 1989;73: Candiani GB, Vercellini P, Fedele L, et al. Repair of the uterine cavity after hysteroscopic septal incision. Fertil Steril. 1990;54:
The position of hysteroscopy in current fertility practice is under debate.
 The position of hysteroscopy in current fertility practice is under debate. The procedure is well tolerated. No consensus on effectiveness of HSC in improving prognosis of subfertile women. systematic
The position of hysteroscopy in current fertility practice is under debate. The procedure is well tolerated. No consensus on effectiveness of HSC in improving prognosis of subfertile women. systematic
Ultrasound and Hysteroscopy in Infertility
 Ultrasound and Hysteroscopy in Infertility James M. Shwayder, M.D., J.D. Professor and Chair Department of Obstetrics and Gynecology University of Mississippi Medical Center Jackson, Mississippi Ultrasound
Ultrasound and Hysteroscopy in Infertility James M. Shwayder, M.D., J.D. Professor and Chair Department of Obstetrics and Gynecology University of Mississippi Medical Center Jackson, Mississippi Ultrasound
SUBSEROSAL FIBROIDS TREATMENT
 INTRODUCTION Uterine fibroids, also known as leiomyomas, are the most common pelvic mass found in women. Fibroids are benign tumors that arise from the uterine muscular tissue (myometrium). They occur
INTRODUCTION Uterine fibroids, also known as leiomyomas, are the most common pelvic mass found in women. Fibroids are benign tumors that arise from the uterine muscular tissue (myometrium). They occur
The following chapter is called The Role of Endoscopy, Laparoscopy, and Hysteroscopy in Infertility.
 Welcome to Chapter 14. The following chapter is called The Role of Endoscopy, Laparoscopy, and Hysteroscopy in Infertility. The authors are Dr. Jose Remohi and Dr. Jaime Ferro. 1 There are several tools
Welcome to Chapter 14. The following chapter is called The Role of Endoscopy, Laparoscopy, and Hysteroscopy in Infertility. The authors are Dr. Jose Remohi and Dr. Jaime Ferro. 1 There are several tools
CHAPTER 10 Uterine Synechiae
 CHAPTER 10 Uterine Synechiae Uterine synechiae are intrauterine adhesions. They may involve small focal areas of the endometrium (Figures 10.1a e), or they can be so extensive that they obliterate the
CHAPTER 10 Uterine Synechiae Uterine synechiae are intrauterine adhesions. They may involve small focal areas of the endometrium (Figures 10.1a e), or they can be so extensive that they obliterate the
Lecture 2 Advanced Hysteroscopic Surgery
 Lecture 2 Advanced Hysteroscopic Surgery Dubai BSGE Approved Course Mr N Panay Consultant Gynaecologist & Honorary Senior Lecturer Hammersmith Hospitals NHS Trust & Imperial College London Advanced Hysteroscopic
Lecture 2 Advanced Hysteroscopic Surgery Dubai BSGE Approved Course Mr N Panay Consultant Gynaecologist & Honorary Senior Lecturer Hammersmith Hospitals NHS Trust & Imperial College London Advanced Hysteroscopic
Laparoscopy and Hysteroscopy
 AMERICAN SOCIETY FOR REPRODUCTIVE MEDICINE Laparoscopy and Hysteroscopy A Guide for Patients PATIENT INFORMATION SERIES Published by the American Society for Reproductive Medicine under the direction of
AMERICAN SOCIETY FOR REPRODUCTIVE MEDICINE Laparoscopy and Hysteroscopy A Guide for Patients PATIENT INFORMATION SERIES Published by the American Society for Reproductive Medicine under the direction of
Uterine fibroids (Leiomyoma)
 Uterine fibroids (Leiomyoma) What are uterine fibroids? Uterine fibroids are fairly common benign (not cancer) growths in the uterus. They occur in about 25 50% of all women. Many women who have fibroids
Uterine fibroids (Leiomyoma) What are uterine fibroids? Uterine fibroids are fairly common benign (not cancer) growths in the uterus. They occur in about 25 50% of all women. Many women who have fibroids
A Guide to Hysteroscopy. Patient Education
 A Guide to Hysteroscopy Patient Education QUESTIONS AND ANSWERS ABOUT HYSTEROSCOPY Your doctor has recommended that you have a procedure called a hysteroscopy. Naturally, you may have questions about
A Guide to Hysteroscopy Patient Education QUESTIONS AND ANSWERS ABOUT HYSTEROSCOPY Your doctor has recommended that you have a procedure called a hysteroscopy. Naturally, you may have questions about
Patient Information: Endometriosis Disease Process and Treatment
 1 William N. Burns, M. D. Associate Professor Department of Obstetrics & Gynecology Joan C. Edwards School of Medicine Marshall University Huntington, West Virginia, USA Patient Information: Endometriosis
1 William N. Burns, M. D. Associate Professor Department of Obstetrics & Gynecology Joan C. Edwards School of Medicine Marshall University Huntington, West Virginia, USA Patient Information: Endometriosis
Abnormal Uterine Bleeding FAQ Sheet
 Abnormal Uterine Bleeding FAQ Sheet What is abnormal uterine bleeding? Under normal circumstances, a woman's uterus sheds a limited amount of blood during each menstrual period. Bleeding that occurs between
Abnormal Uterine Bleeding FAQ Sheet What is abnormal uterine bleeding? Under normal circumstances, a woman's uterus sheds a limited amount of blood during each menstrual period. Bleeding that occurs between
Hysteroscopic septum resection in patients with recurrent abortions or infertility
 Human Reproduction vol.13 no.5 pp.1188 1193, 1998 Hysteroscopic septum resection in patients with recurrent abortions or infertility Grigoris Grimbizis, Michel Camus, Koen Clasen, Herman Tournaye, Luc
Human Reproduction vol.13 no.5 pp.1188 1193, 1998 Hysteroscopic septum resection in patients with recurrent abortions or infertility Grigoris Grimbizis, Michel Camus, Koen Clasen, Herman Tournaye, Luc
In - Vitro Fertilization Handbook
 In - Vitro Fertilization Handbook William F. Ziegler, D.O. Medical Director Scott Kratka, ELD, TS Embryology Laboratory Director Lauren F. Lucas, P.A.-C, M.S. Physician Assistant Frances Cerniak, R.N.
In - Vitro Fertilization Handbook William F. Ziegler, D.O. Medical Director Scott Kratka, ELD, TS Embryology Laboratory Director Lauren F. Lucas, P.A.-C, M.S. Physician Assistant Frances Cerniak, R.N.
Abnormal Uterine Bleeding
 Abnormal Uterine Bleeding WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 Abnormal uterine bleeding is one of the most common reasons women see their doctors. It can occur at any age and has
Abnormal Uterine Bleeding WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 Abnormal uterine bleeding is one of the most common reasons women see their doctors. It can occur at any age and has
Treating heavy menstrual bleeding caused by fibroids or polyps
 Treating heavy menstrual bleeding caused by fibroids or polyps With today s medical advances the outlook for successful treatment of fibroids and polyps has never been better. You don t have to live with
Treating heavy menstrual bleeding caused by fibroids or polyps With today s medical advances the outlook for successful treatment of fibroids and polyps has never been better. You don t have to live with
Septate Uterus: Detection and Prediction of Obstetrical Complications by Different Forms of Ultrasonography
 Septate Uterus: Detection and Prediction of Obstetrical Complications by Different Forms of Ultrasonography Sanja Kupesic, MD, PhD, Asim Kurjak, MD, PhD The aims of the study were to compare the accuracy
Septate Uterus: Detection and Prediction of Obstetrical Complications by Different Forms of Ultrasonography Sanja Kupesic, MD, PhD, Asim Kurjak, MD, PhD The aims of the study were to compare the accuracy
Specialists In Reproductive Medicine & Surgery, P.A.
 Specialists In Reproductive Medicine & Surgery, P.A. Craig R. Sweet, M.D. www.dreamababy.com Fertility@DreamABaby.com Excellence, Experience & Ethics Endometriosis Awareness Week/Month Common Questions
Specialists In Reproductive Medicine & Surgery, P.A. Craig R. Sweet, M.D. www.dreamababy.com Fertility@DreamABaby.com Excellence, Experience & Ethics Endometriosis Awareness Week/Month Common Questions
A potential treatment for your abnormal uterine bleeding
 TRUCLEAR System A potential treatment for your abnormal uterine bleeding Do You Suffer from Abnormal Uterine Bleeding? What is a Hysteroscopy? What is the TRUCLEAR Procedure? What Happens Before Your
TRUCLEAR System A potential treatment for your abnormal uterine bleeding Do You Suffer from Abnormal Uterine Bleeding? What is a Hysteroscopy? What is the TRUCLEAR Procedure? What Happens Before Your
GYNAECOLOGY. Ahmed Mohamed Abbas*, Mohamed Khalaf*, Abd El-Aziz E. Tammam**, Ahmed H. Abdellah**, Ahmed Mwafy**. Introduction ABSTRACT
 Thai Journal of Obstetrics and Gynaecology April 2015, Vol. 23, pp. 113-117 GYNAECOLOGY The Diagnostic Value of Saline Infusion Sonohysterography Versus Hysteroscopy in Evaluation of Uterine Cavity in
Thai Journal of Obstetrics and Gynaecology April 2015, Vol. 23, pp. 113-117 GYNAECOLOGY The Diagnostic Value of Saline Infusion Sonohysterography Versus Hysteroscopy in Evaluation of Uterine Cavity in
Asherman syndrome is an acquired
 Comprehensive management of severe Asherman syndrome and amenorrhea Erinn M. Myers, M.D., a and Bradley S. Hurst, M.D. a,b a Department of Obstetrics and Gynecology and b Division of Reproductive Endocrinology,
Comprehensive management of severe Asherman syndrome and amenorrhea Erinn M. Myers, M.D., a and Bradley S. Hurst, M.D. a,b a Department of Obstetrics and Gynecology and b Division of Reproductive Endocrinology,
In Vitro Fertilization
 Patient Education In Vitro Fertilization What to expect This handout describes how to prepare for and what to expect when you have in vitro fertilization. It provides written information about this process,
Patient Education In Vitro Fertilization What to expect This handout describes how to prepare for and what to expect when you have in vitro fertilization. It provides written information about this process,
About the Uterus. Hysterectomy may be done to treat conditions that affect the uterus. Some reasons a hysterectomy may be needed include:
 Hysterectomy removal of the uterus is a way of treating problems that affect the uterus. Many conditions can be cured with hysterectomy. Because it is major surgery, your doctor may suggest trying other
Hysterectomy removal of the uterus is a way of treating problems that affect the uterus. Many conditions can be cured with hysterectomy. Because it is major surgery, your doctor may suggest trying other
טופס הסכמה לטיפולי הפרייה חוץ גופית
 טופס הסכמה לטיפולי הפרייה חוץ גופית CONSENT FORM: IN-VITRO FERTILIZATION (IVF) 1. General In-vitro fertilization is performed in cases of impaired fertility, which may be caused by the following: Obstruction
טופס הסכמה לטיפולי הפרייה חוץ גופית CONSENT FORM: IN-VITRO FERTILIZATION (IVF) 1. General In-vitro fertilization is performed in cases of impaired fertility, which may be caused by the following: Obstruction
Understanding Your Diagnosis of Endometrial Cancer A STEP-BY-STEP GUIDE
 Understanding Your Diagnosis of Endometrial Cancer A STEP-BY-STEP GUIDE Introduction This guide is designed to help you clarify and understand the decisions that need to be made about your care for the
Understanding Your Diagnosis of Endometrial Cancer A STEP-BY-STEP GUIDE Introduction This guide is designed to help you clarify and understand the decisions that need to be made about your care for the
TREATMENT OF UTERINE ANOMALIES AND REPRODUCTIVE OUTCOME
 TREATMENT OF UTERINE ANOMALIES AND REPRODUCTIVE OUTCOME Danie Botha The Dalmeyer Fertility Unit Port Elizabeth SASOG 2014 Uterine anomalies are any abnormality of the uterus that may result from defective
TREATMENT OF UTERINE ANOMALIES AND REPRODUCTIVE OUTCOME Danie Botha The Dalmeyer Fertility Unit Port Elizabeth SASOG 2014 Uterine anomalies are any abnormality of the uterus that may result from defective
Assisted Reproductive Technologies at IGO
 9339 Genesee Avenue, Suite 220 San Diego, CA 92121 858 455 7520 Assisted Reproductive Technologies at IGO Although IGO no longer operates an IVF laboratory or program as such, we work closely with area
9339 Genesee Avenue, Suite 220 San Diego, CA 92121 858 455 7520 Assisted Reproductive Technologies at IGO Although IGO no longer operates an IVF laboratory or program as such, we work closely with area
Reproductive Health Group
 Gynaecology Services & Treatments 2015 Fee Schedule Consultations - Assessment Initial gynaecology consultation 200-250 Follow-up gynaecology consultation 150-175 Initial fertility consultation *Harley
Gynaecology Services & Treatments 2015 Fee Schedule Consultations - Assessment Initial gynaecology consultation 200-250 Follow-up gynaecology consultation 150-175 Initial fertility consultation *Harley
AMERICAN SOCIETY FOR REPRODUCTIVE MEDICINE
 AMERICAN SOCIETY FOR REPRODUCTIVE MEDICINE UTERINE FIBROIDS A Guide for Patients PATIENT INFORMATION SERIES Published by the American Society for Reproductive Medicine under the direction of the Patient
AMERICAN SOCIETY FOR REPRODUCTIVE MEDICINE UTERINE FIBROIDS A Guide for Patients PATIENT INFORMATION SERIES Published by the American Society for Reproductive Medicine under the direction of the Patient
WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500. Endometriosis
 Endometriosis WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 The lining of the uterus is called the endometrium. Sometimes, endometrial tissue grows elsewhere in the body. When this happens
Endometriosis WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 The lining of the uterus is called the endometrium. Sometimes, endometrial tissue grows elsewhere in the body. When this happens
All you need to know about Endometriosis. Nordica Fertility Centre, Lagos, Asaba, Abuja
 All you need to know about Endometriosis October, 2015 About The Author Nordica Lagos Fertility Centre is one of Nigeria's leading centres for world class Assisted Reproductive Services, with comfort centres
All you need to know about Endometriosis October, 2015 About The Author Nordica Lagos Fertility Centre is one of Nigeria's leading centres for world class Assisted Reproductive Services, with comfort centres
Summa Health System. A Woman s Guide to Hysterectomy
 Summa Health System A Woman s Guide to Hysterectomy Hysterectomy A hysterectomy is a surgical procedure to remove a woman s uterus (womb). The uterus is the organ which shelters and nourishes a baby during
Summa Health System A Woman s Guide to Hysterectomy Hysterectomy A hysterectomy is a surgical procedure to remove a woman s uterus (womb). The uterus is the organ which shelters and nourishes a baby during
Ovarian Cyst. Homoeopathy Clinic. Introduction. Types of Ovarian Cysts. Contents. Case Reports. 21 August 2002
 Case Reports 21 August 2002 Ovarian Cyst Homoeopathy Clinic Check Yourself If you have any of the following symptoms call your doctor. Sense of fullness or pressure or a dull ache in the abdomen Pain during
Case Reports 21 August 2002 Ovarian Cyst Homoeopathy Clinic Check Yourself If you have any of the following symptoms call your doctor. Sense of fullness or pressure or a dull ache in the abdomen Pain during
Ovarian Cystectomy / Oophorectomy
 Cystectomy and Ovarian Cysts Ovarian cysts are sacs filled with fluids or pockets located on or in an ovary. In some cases, these cysts need to be removed surgically. Types of Cysts Ovarian cysts are quite
Cystectomy and Ovarian Cysts Ovarian cysts are sacs filled with fluids or pockets located on or in an ovary. In some cases, these cysts need to be removed surgically. Types of Cysts Ovarian cysts are quite
Uterus myomatosus. 10-May-15. Clinical presentation. Incidence. Causes? 3 out of 4 women. Growth rate vary. Most common solid pelvic tumor in women
 Uterus myomatosus A.J. Henriquez March 14, 2015 Uterus myomatosus Definition, incidence, clinical presentation and diagnosis. New FIGO classification for uterine leiomyomas Brief description on treatment
Uterus myomatosus A.J. Henriquez March 14, 2015 Uterus myomatosus Definition, incidence, clinical presentation and diagnosis. New FIGO classification for uterine leiomyomas Brief description on treatment
Introduction Ovarian cysts are a very common female condition. An ovarian cyst is a fluid-filled sac on an ovary in the female reproductive system.
 Ovarian Cysts Introduction Ovarian cysts are a very common female condition. An ovarian cyst is a fluid-filled sac on an ovary in the female reproductive system. Most women have ovarian cysts sometime
Ovarian Cysts Introduction Ovarian cysts are a very common female condition. An ovarian cyst is a fluid-filled sac on an ovary in the female reproductive system. Most women have ovarian cysts sometime
Gynecology Abnormal Pelvic Anatomy and Physiology: Cervix. Cervix. Nabothian cysts. cervical polyps. leiomyomas. Cervical stenosis
 Gynecology Abnormal Pelvic Anatomy and Physiology: (Effective February 2007) pediatric, reproductive, and perimenopausal/postmenopausal (24-28 %) Cervix Nabothian cysts result from chronic cervicitis most
Gynecology Abnormal Pelvic Anatomy and Physiology: (Effective February 2007) pediatric, reproductive, and perimenopausal/postmenopausal (24-28 %) Cervix Nabothian cysts result from chronic cervicitis most
A report of 300 cases using vacuum aspiration for the termination of pregnancy
 A report of 300 cases using vacuum aspiration for the termination of pregnancy Wu, Yuantai and Wu, Xianzhen Chinese Journal of Obstetrics and Gynaecology (1958:447-9) More than 100 years after Recamier
A report of 300 cases using vacuum aspiration for the termination of pregnancy Wu, Yuantai and Wu, Xianzhen Chinese Journal of Obstetrics and Gynaecology (1958:447-9) More than 100 years after Recamier
OVARIAN CYSTS. Types of Ovarian Cysts There are many types of ovarian cysts and these can be categorized into functional and nonfunctional
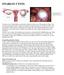 OVARIAN CYSTS Follicular Cyst Ovarian cysts are fluid-filled sacs that form within or on the ovary. The majority of these cysts are functional meaning they usually form during a normal menstrual cycle.
OVARIAN CYSTS Follicular Cyst Ovarian cysts are fluid-filled sacs that form within or on the ovary. The majority of these cysts are functional meaning they usually form during a normal menstrual cycle.
Implementation of hysteroscopy in an infertility clinic: The one-stop uterine diagnosis and treatment
 Facts Views Vis Obgyn, 2014, 6 (4): 235-239 Short communication Implementation of hysteroscopy in an infertility clinic: The one-stop uterine diagnosis and treatment R. Campo 1,2,3, R. Meier,2, N. Dhont
Facts Views Vis Obgyn, 2014, 6 (4): 235-239 Short communication Implementation of hysteroscopy in an infertility clinic: The one-stop uterine diagnosis and treatment R. Campo 1,2,3, R. Meier,2, N. Dhont
Interrupted Pregnancy Coding
 Interrupted Pregnancy Coding American College of Obstetricians and Gynecologists Terry Tropin, RHIA, CPC, CCS-P, ACS-OB, PCS Content Development Expert, DecisionHealth ACOG Committee on Coding and Nomenclature
Interrupted Pregnancy Coding American College of Obstetricians and Gynecologists Terry Tropin, RHIA, CPC, CCS-P, ACS-OB, PCS Content Development Expert, DecisionHealth ACOG Committee on Coding and Nomenclature
CONFIDENT CODING FOR OB/GYN CONFIDENT CODING FOR OB/GYN
 Arlene J. Smith, CPC AAPC National Advisory Board 2007-2009 1 So when exactly does the global period start? Unraveling the confusion in antepartum care coding Correct coding for multiple gestations! Vaginal
Arlene J. Smith, CPC AAPC National Advisory Board 2007-2009 1 So when exactly does the global period start? Unraveling the confusion in antepartum care coding Correct coding for multiple gestations! Vaginal
Review Article What Is the Role of Hysteroscopic Surgery in the Management of Female Infertility? A Review of the Literature
 Surgery Research and Practice, Article ID 105412, 6 pages http://dx.doi.org/10.1155/2014/105412 Review Article What Is the Role of Hysteroscopic Surgery in the Management of Female Infertility? A Review
Surgery Research and Practice, Article ID 105412, 6 pages http://dx.doi.org/10.1155/2014/105412 Review Article What Is the Role of Hysteroscopic Surgery in the Management of Female Infertility? A Review
Ectopic Pregnancy. A Guide for Patients PATIENT INFORMATION SERIES
 Ectopic Pregnancy A Guide for Patients PATIENT INFORMATION SERIES Published by the American Society for Reproductive Medicine under the direction of the Patient Education Committee and the Publications
Ectopic Pregnancy A Guide for Patients PATIENT INFORMATION SERIES Published by the American Society for Reproductive Medicine under the direction of the Patient Education Committee and the Publications
Welcome to chapter 2. The following chapter is called "Indications For IVF". The author is Dr Kamini A. Rao.
 Welcome to chapter 2. The following chapter is called "Indications For IVF". The author is Dr Kamini A. Rao. The indications for an IVF treatment have increased since the birth of the first IVF baby. The
Welcome to chapter 2. The following chapter is called "Indications For IVF". The author is Dr Kamini A. Rao. The indications for an IVF treatment have increased since the birth of the first IVF baby. The
Frequently Asked Questions About Ovarian Cancer
 Media Contact: Gerri Gomez Howard Cell: 303-748-3933 gerri@gomezhowardgroup.com Frequently Asked Questions About Ovarian Cancer What is ovarian cancer? Ovarian cancer is a cancer that forms in tissues
Media Contact: Gerri Gomez Howard Cell: 303-748-3933 gerri@gomezhowardgroup.com Frequently Asked Questions About Ovarian Cancer What is ovarian cancer? Ovarian cancer is a cancer that forms in tissues
STUDY OF MORPHOLOGY OF UTERUS USING ULTRASOUND SCAN
 Original Article STUDY OF MORPHOLOGY OF UTERUS USING ULTRASOUND SCAN P. Priya 1, S. Vijayalakshmi * 2. 1 Associate Professor, Dept. of Anatomy, Saveetha Medical College, Chennai, Tamil Nadu, India. *2
Original Article STUDY OF MORPHOLOGY OF UTERUS USING ULTRASOUND SCAN P. Priya 1, S. Vijayalakshmi * 2. 1 Associate Professor, Dept. of Anatomy, Saveetha Medical College, Chennai, Tamil Nadu, India. *2
Risks and complications of assisted conception
 Risks and complications of assisted conception August 005 Richard Kennedy British Fertility Society Factsheet www.fertility.org.uk No medical treatment is entirely free from risk and infertility treatment
Risks and complications of assisted conception August 005 Richard Kennedy British Fertility Society Factsheet www.fertility.org.uk No medical treatment is entirely free from risk and infertility treatment
Hysterosalpingography
 Scan for mobile link. Hysterosalpingography Hysterosalpingography uses a real-time form of x-ray called fluoroscopy to examine the uterus and fallopian tubes of a woman who is having difficulty becoming
Scan for mobile link. Hysterosalpingography Hysterosalpingography uses a real-time form of x-ray called fluoroscopy to examine the uterus and fallopian tubes of a woman who is having difficulty becoming
Laparoscopic management of endometriosis in infertile women and outcome
 International Journal of Reproduction, Contraception, Obstetrics and Gynecology Sahu L et al. Int J Reprod Contracept Obstet Gynecol. 2013 Jun;2(2):177-181 www.ijrcog.org pissn 2320-1770 eissn 2320-1789
International Journal of Reproduction, Contraception, Obstetrics and Gynecology Sahu L et al. Int J Reprod Contracept Obstet Gynecol. 2013 Jun;2(2):177-181 www.ijrcog.org pissn 2320-1770 eissn 2320-1789
CASE REPORT Double Cervix and Vagina with Septate Uterus: An Uncommon Müllerian Malformation
 CASE REPORT Double Cervix and Vagina with Septate Uterus: An Uncommon Müllerian Malformation Andrew F. Hundley, M.D., Julia R. Fielding, M.D.*, Lennox Hoyte, M.D. Departments of Obstetrics and Gynecology
CASE REPORT Double Cervix and Vagina with Septate Uterus: An Uncommon Müllerian Malformation Andrew F. Hundley, M.D., Julia R. Fielding, M.D.*, Lennox Hoyte, M.D. Departments of Obstetrics and Gynecology
Three-Dimensional Inversion Rendering
 Image Presentation Three-Dimensional Inversion Rendering New Sonographic Technique and Its Use in Gynecology Ilan E. Timor-Tritsch, MD, RDMS, na Monteagudo, MD, RDMS, Tanya Tsymbal,, RDMS, Irina Strok,
Image Presentation Three-Dimensional Inversion Rendering New Sonographic Technique and Its Use in Gynecology Ilan E. Timor-Tritsch, MD, RDMS, na Monteagudo, MD, RDMS, Tanya Tsymbal,, RDMS, Irina Strok,
Women s Health Laparoscopy Information for patients
 Women s Health Laparoscopy Information for patients This leaflet is for women who have been advised to have a laparoscopy. It outlines the common reasons doctors recommend this operation, what will happen
Women s Health Laparoscopy Information for patients This leaflet is for women who have been advised to have a laparoscopy. It outlines the common reasons doctors recommend this operation, what will happen
WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500. Ovarian Cysts
 Ovarian Cysts WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 The ovaries are two small organs located on either side of a woman s uterus. An ovarian cyst is a sac or pouch filled with fluid
Ovarian Cysts WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 The ovaries are two small organs located on either side of a woman s uterus. An ovarian cyst is a sac or pouch filled with fluid
CONSENT TO PARTICIPATE IN THE IN VITRO FERTILIZATION-EMBRYO TRANSFER PROGRAM
 CONSENT TO PARTICIPATE IN THE IN VITRO FERTILIZATION-EMBRYO TRANSFER PROGRAM I, after consultation with my physician, request to participate in the In Vitro Fertilization (IVF)-Embryo Transfer (ET) procedures
CONSENT TO PARTICIPATE IN THE IN VITRO FERTILIZATION-EMBRYO TRANSFER PROGRAM I, after consultation with my physician, request to participate in the In Vitro Fertilization (IVF)-Embryo Transfer (ET) procedures
FAMILY PLANNING AND PREGNANCY
 FAMILY PLANNING AND PREGNANCY Decisions about family planning can be difficult and very emotional when one of the prospective parents has a genetic disorder, such as Marfan syndrome. Before making any
FAMILY PLANNING AND PREGNANCY Decisions about family planning can be difficult and very emotional when one of the prospective parents has a genetic disorder, such as Marfan syndrome. Before making any
The following chapter is called "Follow-ups with a Positive or a Negative Pregnancy Test".
 Slide 1 Welcome to chapter 7. The following chapter is called "Follow-ups with a Positive or a Negative Pregnancy Test". The author is Professor Pasquale Patrizio. Slide 2 This chapter has the following
Slide 1 Welcome to chapter 7. The following chapter is called "Follow-ups with a Positive or a Negative Pregnancy Test". The author is Professor Pasquale Patrizio. Slide 2 This chapter has the following
In Vitro Fertilization (IVF) Page 1 of 11
 In Vitro Fertilization (IVF) Page 1 of 11 This document is a part of your informed consent process. Both partners should read the entire document carefully. In vitro fertilization (IVF) is a treatment
In Vitro Fertilization (IVF) Page 1 of 11 This document is a part of your informed consent process. Both partners should read the entire document carefully. In vitro fertilization (IVF) is a treatment
Migration of an intrauterine contraceptive device to the sigmoid colon: a case report
 The European Journal of Contraception and Reproductive Health Care 2003;8:229 232 Case Report Migration of an intrauterine contraceptive device to the sigmoid colon: a case report Ü. S. nceboz, H. T. Özçakir,
The European Journal of Contraception and Reproductive Health Care 2003;8:229 232 Case Report Migration of an intrauterine contraceptive device to the sigmoid colon: a case report Ü. S. nceboz, H. T. Özçakir,
Welcome to chapter 8. The following chapter is called "Monitoring IVF Cycle & Oocyte Retrieval". The author is Professor Jie Qiao.
 Welcome to chapter 8. The following chapter is called "Monitoring IVF Cycle & Oocyte Retrieval". The author is Professor Jie Qiao. The learning objectives of this chapter are 2 fold. The first section
Welcome to chapter 8. The following chapter is called "Monitoring IVF Cycle & Oocyte Retrieval". The author is Professor Jie Qiao. The learning objectives of this chapter are 2 fold. The first section
Ultrasound in the First Trimester of Pregnancy. Elizabeth Lipson, HMS III
 Ultrasound in the First Trimester of Pregnancy Elizabeth Lipson, HMS III First Trimester Sonography Localization of Gestational Sac Intrauterine vs. ectopic Identification of abnormalities Embryonic demise
Ultrasound in the First Trimester of Pregnancy Elizabeth Lipson, HMS III First Trimester Sonography Localization of Gestational Sac Intrauterine vs. ectopic Identification of abnormalities Embryonic demise
Endometriosis Obstetrics & Gynaecology Women and Children s Group
 Endometriosis Obstetrics & Gynaecology Women and Children s Group This leaflet has been designed to give you important information about your condition / procedure, and to answer some common queries that
Endometriosis Obstetrics & Gynaecology Women and Children s Group This leaflet has been designed to give you important information about your condition / procedure, and to answer some common queries that
Considering Endometriosis Surgery? Learn about minimally invasive da Vinci Surgery
 Considering Endometriosis Surgery? Learn about minimally invasive da Vinci Surgery The Condition: Endometriosis Endometriosis is a condition in which the tissue that lines your uterus (the endometrium)
Considering Endometriosis Surgery? Learn about minimally invasive da Vinci Surgery The Condition: Endometriosis Endometriosis is a condition in which the tissue that lines your uterus (the endometrium)
Transvaginal Endoscopy TVE GYN 18 7.0 02/2015-E
 Transvaginal Endoscopy TVE GYN 18 7.0 02/2015-E TRANSVAGINAL ENDOSCOPY Leuven Institute for Fertility and Embryology Prof. Dr. S. Gordts, Dr. R. Campo, Dr. P. Puttemans, Prof. Em. Dr. I. Brosens 2 Transvaginal
Transvaginal Endoscopy TVE GYN 18 7.0 02/2015-E TRANSVAGINAL ENDOSCOPY Leuven Institute for Fertility and Embryology Prof. Dr. S. Gordts, Dr. R. Campo, Dr. P. Puttemans, Prof. Em. Dr. I. Brosens 2 Transvaginal
Hysteroscopic evaluation in infertile patients: a prospective study
 International Journal of Reproduction, Contraception, Obstetrics and Gynecology Sahu L et al. Int J Reprod Contracept Obstet Gynecol. 2012 Dec;1(1):37-41 www.ijrcog.org pissn 2320-1770 eissn 2320-1789
International Journal of Reproduction, Contraception, Obstetrics and Gynecology Sahu L et al. Int J Reprod Contracept Obstet Gynecol. 2012 Dec;1(1):37-41 www.ijrcog.org pissn 2320-1770 eissn 2320-1789
The main surgical options for treating early stage cervical cancer are:
 INFORMATION LEAFLET ON TOTAL LAPAROSCOPIC RADICAL HYSTERECTOMY (TLRH) FOR EARLY STAGE CERVICAL CANCER (TREATING EARLY STAGE CERVICAL CANCER BY RADICAL HYSTERECTOMY THROUGH KEYHOLE SURGERY) Aim of the leaflet
INFORMATION LEAFLET ON TOTAL LAPAROSCOPIC RADICAL HYSTERECTOMY (TLRH) FOR EARLY STAGE CERVICAL CANCER (TREATING EARLY STAGE CERVICAL CANCER BY RADICAL HYSTERECTOMY THROUGH KEYHOLE SURGERY) Aim of the leaflet
Artificial insemination with donor sperm
 Artificial insemination with donor sperm Ref. 123 / 2009 Reproductive Medicine Unit Servicio de Medicina de la Reproducción Gran Vía Carlos III 71-75 08028 Barcelona Tel. (+34) 93 227 47 00 Fax. (+34)
Artificial insemination with donor sperm Ref. 123 / 2009 Reproductive Medicine Unit Servicio de Medicina de la Reproducción Gran Vía Carlos III 71-75 08028 Barcelona Tel. (+34) 93 227 47 00 Fax. (+34)
Glossary. amenorrhea, primary - from the beginning and lifelong; menstruation never begins at puberty.
 Glossary amenorrhea - absence or cessation of menstrual periods. amenorrhea, primary - from the beginning and lifelong; menstruation never begins at puberty. A amenorrhea, secondary - due to some physical
Glossary amenorrhea - absence or cessation of menstrual periods. amenorrhea, primary - from the beginning and lifelong; menstruation never begins at puberty. A amenorrhea, secondary - due to some physical
WHAT YOU SHOULD KNOW ABOUT ABORTION
 WHAT YOU SHOULD KNOW ABOUT ABORTION It is the public policy of the state of Idaho to prefer live childbirth over abortion: "The Supreme Court of the United States having held that the states have a "profound
WHAT YOU SHOULD KNOW ABOUT ABORTION It is the public policy of the state of Idaho to prefer live childbirth over abortion: "The Supreme Court of the United States having held that the states have a "profound
Clinical Interruption of Pregnancy (Medical/Surgical Abortion)
 Clinical Interruption of Pregnancy (Medical/Surgical Abortion) Approximately one fifth of all pregnancies in the United States end in abortion (Ventura et al., 2009). According to the CDC (2011a), there
Clinical Interruption of Pregnancy (Medical/Surgical Abortion) Approximately one fifth of all pregnancies in the United States end in abortion (Ventura et al., 2009). According to the CDC (2011a), there
Understanding Endometriosis - Information Pack
 What is endometriosis? Endometriosis (pronounced en- doh mee tree oh sis) is the name given to the condition where cells like the ones in the lining of the womb (uterus) are found elsewhere in the body.
What is endometriosis? Endometriosis (pronounced en- doh mee tree oh sis) is the name given to the condition where cells like the ones in the lining of the womb (uterus) are found elsewhere in the body.
, hereby agree to a form of treatment known
 Patient Consent for Therapy Human In Vitro Fertilization and Embryo Transfer This is to certify that I, as In Vitro Fertilization and Embryo Transfer., hereby agree to a form of treatment known I have
Patient Consent for Therapy Human In Vitro Fertilization and Embryo Transfer This is to certify that I, as In Vitro Fertilization and Embryo Transfer., hereby agree to a form of treatment known I have
Infertility: An Overview
 AMERICAN SOCIETY FOR REPRODUCTIVE MEDICINE Infertility: An Overview A Guide for Patients PATIENT INFORMATION SERIES Published by the American Society for Reproductive Medicine under the direction of the
AMERICAN SOCIETY FOR REPRODUCTIVE MEDICINE Infertility: An Overview A Guide for Patients PATIENT INFORMATION SERIES Published by the American Society for Reproductive Medicine under the direction of the
Get the Facts, Be Informed, Make YOUR Best Decision. Pelvic Organ Prolapse
 Pelvic Organ Prolapse ETHICON Women s Health & Urology, a division of ETHICON, INC., a Johnson & Johnson company, is dedicated to providing innovative solutions for common women s health problems and to
Pelvic Organ Prolapse ETHICON Women s Health & Urology, a division of ETHICON, INC., a Johnson & Johnson company, is dedicated to providing innovative solutions for common women s health problems and to
Hysterectomy. What is a hysterectomy? Why is hysterectomy done? Are there alternatives to hysterectomy?
 ROBERT LEVITT, MD JESSICA BERGER-WEISS, MD ADRIENNE POTTS, MD HARTAJ POWELL, MD, MPH COURTNEY LEVENSON, MD LAUREN BURNS, MSN, RN, WHNP OBGYNCWC.COM What is a hysterectomy? Hysterectomy Hysterectomy is
ROBERT LEVITT, MD JESSICA BERGER-WEISS, MD ADRIENNE POTTS, MD HARTAJ POWELL, MD, MPH COURTNEY LEVENSON, MD LAUREN BURNS, MSN, RN, WHNP OBGYNCWC.COM What is a hysterectomy? Hysterectomy Hysterectomy is
Three-Dimensional Sonography of the Endometrium and Adjacent Myometrium
 Technical dvance Three-Dimensional Sonography of the Endometrium and djacent Myometrium Preliminary Observations Rochelle F. ndreotti, MD, rthur C. Fleischer, MD, Lawrence E. Mason, Jr, MD Objective. y
Technical dvance Three-Dimensional Sonography of the Endometrium and djacent Myometrium Preliminary Observations Rochelle F. ndreotti, MD, rthur C. Fleischer, MD, Lawrence E. Mason, Jr, MD Objective. y
3D in Gynecology: Luxury or necessity?
 ISUOG 2011 Los Angeles September 16-22 3D in Gynecology: Luxury or necessity? Ilan E. Timor-Tritsch Educational objectives To describe the 3D US tools available to complement 2D US To apply these tools
ISUOG 2011 Los Angeles September 16-22 3D in Gynecology: Luxury or necessity? Ilan E. Timor-Tritsch Educational objectives To describe the 3D US tools available to complement 2D US To apply these tools
Management fertility sparing degli endometriomi Errico Zupi
 Management fertility sparing degli endometriomi Errico Zupi Università Tor Vergata Roma Management of endometrioma Pain Infertility Surgical treatment Medical treatment Infertility clinic Both medical
Management fertility sparing degli endometriomi Errico Zupi Università Tor Vergata Roma Management of endometrioma Pain Infertility Surgical treatment Medical treatment Infertility clinic Both medical
Uterine Fibroids. More than half of all women have fibroids. They are a common, benign, uterine growth.
 Uterine Fibroids More than half of all women have fibroids. They are a common, benign, uterine growth. Fibroids are not a disease. Much like the genetic blueprint that determines the color of your eyes
Uterine Fibroids More than half of all women have fibroids. They are a common, benign, uterine growth. Fibroids are not a disease. Much like the genetic blueprint that determines the color of your eyes
WHAT YOU SHOULD KNOW ABOUT ABORTION
 WHAT YOU SHOULD KNOW ABOUT ABORTION It is the public policy of the state of Idaho to prefer live childbirth over abortion: "The Supreme Court of the United States having held that the states have a "profound
WHAT YOU SHOULD KNOW ABOUT ABORTION It is the public policy of the state of Idaho to prefer live childbirth over abortion: "The Supreme Court of the United States having held that the states have a "profound
The causes of infertility include abnormalities of any portion of the male or female reproductive system.
 Harvard-MIT Division of Health Sciences and Technology HST.071: Human Reproductive Biology Course Director: Professor Henry Klapholz IN SUMMARY Defined as 1 year of unprotected intercourse during which
Harvard-MIT Division of Health Sciences and Technology HST.071: Human Reproductive Biology Course Director: Professor Henry Klapholz IN SUMMARY Defined as 1 year of unprotected intercourse during which
Laser Procedure Note
 Laser Procedure Note Patient Name Date 1. Pre procedure diagnosis 2. Procedure and Eye Eye: 3. Pre procedure topical medications administered (and time) 4. Vital signs BP / HR Acuity OD: OS: 5. IOP: OD
Laser Procedure Note Patient Name Date 1. Pre procedure diagnosis 2. Procedure and Eye Eye: 3. Pre procedure topical medications administered (and time) 4. Vital signs BP / HR Acuity OD: OS: 5. IOP: OD
Consent for Frozen Donor Oocyte In Vitro Fertilization and Embryo Transfer (Recipient)
 Name of Patient: Name of Partner: We, the Patient and Partner (if applicable) named above, are each over the age of twenty-one (21) years. By our signatures below, I/we request and authorize the performance
Name of Patient: Name of Partner: We, the Patient and Partner (if applicable) named above, are each over the age of twenty-one (21) years. By our signatures below, I/we request and authorize the performance
IMAP Statement on Safe Abortion
 International Planned Parenthood Federation IMAP Statement on Safe Abortion Key points: When performed early in pregnancy by trained health personnel in adequate facilities, abortion is a very safe procedure
International Planned Parenthood Federation IMAP Statement on Safe Abortion Key points: When performed early in pregnancy by trained health personnel in adequate facilities, abortion is a very safe procedure
LIPPES LOOP TRADEMARK. your intrauterine contraceptive
 LIPPES LOOP TRADEMARK your intrauterine contraceptive LIPPES LOOP Patient Information This brochure provides information on the use of In trauterine Contraceptive Devices (lud s). There are other birth
LIPPES LOOP TRADEMARK your intrauterine contraceptive LIPPES LOOP Patient Information This brochure provides information on the use of In trauterine Contraceptive Devices (lud s). There are other birth
HYDROSALPINX PATIENT INFORMATION
 What is a Hydrosalpinx? Hydrosalpinx, derived from Greek, is a word literally meaning water tube. A Hydrosalpinx is a blocked, dilated, fluid filled-fallopian tube usually caused by a previous tubal infection.
What is a Hydrosalpinx? Hydrosalpinx, derived from Greek, is a word literally meaning water tube. A Hydrosalpinx is a blocked, dilated, fluid filled-fallopian tube usually caused by a previous tubal infection.
POST MENOPAUSAL BLEEDING CHECKLIST. Ultrasound. Information folder given to patient. Booking form faxed/emailed
 POST MENOPAUSAL BLEEDING CHECKLIST Ultrasound Information folder given to patient Booking form faxed/emailed 1 BOOKING FORM - HYSTEROSCOPY FOR POST MENOPAUSAL BLEEDING Patient s Name: Surname: DOB: / /
POST MENOPAUSAL BLEEDING CHECKLIST Ultrasound Information folder given to patient Booking form faxed/emailed 1 BOOKING FORM - HYSTEROSCOPY FOR POST MENOPAUSAL BLEEDING Patient s Name: Surname: DOB: / /
Facing a Hysterectomy? If you ve been diagnosed with early stage gynecologic cancer, learn about minimally invasive da Vinci Surgery
 Facing a Hysterectomy? If you ve been diagnosed with early stage gynecologic cancer, learn about minimally invasive da Vinci Surgery The Condition: Early Stage Gynecologic Cancer A variety of gynecologic
Facing a Hysterectomy? If you ve been diagnosed with early stage gynecologic cancer, learn about minimally invasive da Vinci Surgery The Condition: Early Stage Gynecologic Cancer A variety of gynecologic
LOG BOOK Approved by The European Board and College of Obstetrics and Gynaecology
 Training in Obstetrics and Gynaecology LOG BOOK Approved by The European Board and College of Obstetrics and Gynaecology TO BE COMPLETED AFTER EACH YEAR OF TRAINING AND SENT WITH WITHIN THREE MONTHS THEREAFTER
Training in Obstetrics and Gynaecology LOG BOOK Approved by The European Board and College of Obstetrics and Gynaecology TO BE COMPLETED AFTER EACH YEAR OF TRAINING AND SENT WITH WITHIN THREE MONTHS THEREAFTER
Endometriosis & Infertility& Treatments. A. Musa Zamah, MD, PhD
 Endometriosis & Infertility& Treatments A. Musa Zamah, MD, PhD Full Disclosure of Faculty Financial Interests or Relationships I agree to follow the UIC and ACCME policies and declare that I do not have
Endometriosis & Infertility& Treatments A. Musa Zamah, MD, PhD Full Disclosure of Faculty Financial Interests or Relationships I agree to follow the UIC and ACCME policies and declare that I do not have
Laparoscopic Assisted Vaginal Hysterectomy
 Department of Obstetrics and Gynecology, Chang Gung Memorial Hospital at ChiaYi 嘉 義 長 庚 紀 念 醫 院 婦 產 科 Clinical Guideline Laparoscopic Assisted Vaginal Hysterectomy By Dr. CJ Tseng Laparoscopic assisted
Department of Obstetrics and Gynecology, Chang Gung Memorial Hospital at ChiaYi 嘉 義 長 庚 紀 念 醫 院 婦 產 科 Clinical Guideline Laparoscopic Assisted Vaginal Hysterectomy By Dr. CJ Tseng Laparoscopic assisted
Antibiotic prophylaxis during obstetric and gynaecology surgery in adults: background information
 Antibiotic prophylaxis during obstetric and gynaecology surgery in adults: background information Pages 1 to 3 provide available evidence and references to support the surgical prophylaxis recommendations.
Antibiotic prophylaxis during obstetric and gynaecology surgery in adults: background information Pages 1 to 3 provide available evidence and references to support the surgical prophylaxis recommendations.
Lippes Loop intrauterine device left in the uterus for 50 years. Case report
 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 Lippes Loop intrauterine device left in the uterus for 50 years Case report Background.The first Lippes Loop intrauterine device was distributed in 1962. It was a
1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 Lippes Loop intrauterine device left in the uterus for 50 years Case report Background.The first Lippes Loop intrauterine device was distributed in 1962. It was a
Symposium on RECENT ADVANCES IN ASSISTED REPRODUCTIVE TECHNOLOGY
 Symposium on RECENT ADVANCES IN ASSISTED REPRODUCTIVE TECHNOLOGY Dr Niel Senewirathne Senior Consultant of Obstetrician & Gynaecologist De zoyza Maternity Hospita 1 ART - IVF & ICSI 2 Infertility No pregnancy
Symposium on RECENT ADVANCES IN ASSISTED REPRODUCTIVE TECHNOLOGY Dr Niel Senewirathne Senior Consultant of Obstetrician & Gynaecologist De zoyza Maternity Hospita 1 ART - IVF & ICSI 2 Infertility No pregnancy
Infertility Services Medical Policy For University of Vermont Medical Center and Central Vermont Medical Center employer groups
 Infertility Services Medical Policy For University of Vermont Medical Center and Central Vermont Medical Center employer groups File name: Infertility Services File code: UM.REPRO.01 Last Review: 02/2016
Infertility Services Medical Policy For University of Vermont Medical Center and Central Vermont Medical Center employer groups File name: Infertility Services File code: UM.REPRO.01 Last Review: 02/2016
Reproductive Technology. Chapter 21
 Reproductive Technology Chapter 21 Assisted Reproduction When a couple is sub-fertile or infertile they may need Assisted Reproduction to become pregnant: Replace source of gametes Sperm, oocyte or zygote
Reproductive Technology Chapter 21 Assisted Reproduction When a couple is sub-fertile or infertile they may need Assisted Reproduction to become pregnant: Replace source of gametes Sperm, oocyte or zygote
THE CENTER FOR ADVANCED REPRODUCTIVE SERVICES (CARS) (The Center) CONSENT FOR IN VITRO FERTILIZATION AND EMBRYO TRANSFER
 THE CENTER FOR ADVANCED REPRODUCTIVE SERVICES (CARS) (The Center) CONSENT FOR IN VITRO FERTILIZATION AND EMBRYO TRANSFER Partner #1 Last Name (Surname): Partner #1 First Name: Partner #1 Last 5 Digits
THE CENTER FOR ADVANCED REPRODUCTIVE SERVICES (CARS) (The Center) CONSENT FOR IN VITRO FERTILIZATION AND EMBRYO TRANSFER Partner #1 Last Name (Surname): Partner #1 First Name: Partner #1 Last 5 Digits
Heavy menstrual bleeding and what you can do about it!
 Heavy menstrual bleeding and what you can do about it! The intrauterine system as an alternative to hysterectomy. What is heavy menstrual bleeding? Do I have it? A woman s menstrual periods are considered
Heavy menstrual bleeding and what you can do about it! The intrauterine system as an alternative to hysterectomy. What is heavy menstrual bleeding? Do I have it? A woman s menstrual periods are considered
Assisted reproductive technologies (ART) in Canada: 2011 results from the Canadian ART Register
 1 Assisted reproductive technologies (ART) in Canada: 2011 results from the Canadian ART Register Joanne Gunby, M.Sc. CARTR Co-ordinator Email: gunbyj@mcmaster.ca Supported by the IVF Directors Group of
1 Assisted reproductive technologies (ART) in Canada: 2011 results from the Canadian ART Register Joanne Gunby, M.Sc. CARTR Co-ordinator Email: gunbyj@mcmaster.ca Supported by the IVF Directors Group of
ESSURE REIMBURSEMENT GUIDE
 ESSURE REIMBURSEMENT GUIDE A CODING AND COVERAGE RESOURCE Indication Essure is indicated for women who desire permanent birth control (female sterilization) by bilateral occlusion of the fallopian tubes.
ESSURE REIMBURSEMENT GUIDE A CODING AND COVERAGE RESOURCE Indication Essure is indicated for women who desire permanent birth control (female sterilization) by bilateral occlusion of the fallopian tubes.
Diagnosis Codes for Pregnancy and Complications of Pregnancy
 This list is for informational purposes only and is not a binding or definitive list of covered conditions. It is not a guarantee of coverage; coverage depends on the available benefits and eligibility
This list is for informational purposes only and is not a binding or definitive list of covered conditions. It is not a guarantee of coverage; coverage depends on the available benefits and eligibility
