Usefulness of emergency ultrasound in nontraumatic cardiac arrest
|
|
|
- Giles Dixon
- 8 years ago
- Views:
Transcription
1 American Journal of Emergency Medicine (2011) 29, Review Usefulness of emergency ultrasound in nontraumatic cardiac arrest Giovanni Volpicelli MD Department of Emergency Medicine, San Luigi Gonzaga Hospital, Orbassano (Torino), Italy Received 14 March 2009; accepted 19 March 2009 Abstract Treatment of nontraumatic cardiac arrest in the hospital setting depends on the recognition of heart rhythm and differential diagnosis of the underlying condition while maintaining a constant oxygenated blood flow by ventilation and chest compression. Diagnostic process relies only on patient's history, physical findings, and active electrocardiography. Ultrasound is not currently scheduled in the resuscitation guidelines. Nevertheless, the use of real-time ultrasonography during resuscitation has the potential to improve diagnostic accuracy and allows the physician a greater confidence in deciding aggressive life-saving therapeutic procedures. This article reviews the current opinions and literature about the use of emergency ultrasound during resuscitation of nontraumatic cardiac arrest. Cardiac and lung ultrasound have a great potential in identifying the reversible mechanical causes of pulseless electrical activity or asystole. Brief examination of the heart can even detect a real cardiac standstill regardless of electrical activity displayed on the monitor, which is a crucial prognostic indicator. Moreover, ultrasound can be useful to verify and monitor the tracheal tube placement. Limitation to the use of ultrasound is the need to minimize the no-flow intervals during mechanical cardiopulmonary resuscitation. However, real-time ultrasound can be successfully applied during brief pausing of chest compression and first pulse-check. Finally, lung sonographic examination targeted to the detection of signs of pulmonary congestion has the potential to allow hemodynamic noninvasive monitoring before and after mechanical cardiopulmonary maneuvers Elsevier Inc. All rights reserved. 1. Introduction The American and European resuscitation guidelines provide algorithms for managing cardiac arrest whose main objectives are to ensure a constant blood flow to the brain while identifying the causes of the condition, and treating them, if possible [1-3]. The ability to succeed in resolving S.C.D.O. Medicina d'urgenza, Ospedale San Luigi Gonzaga, Torino, Italy. Tel.: ( ); fax: address: gio.volpicelli@tin.it. cardiac arrest is strictly time-dependent. The critical points to be pursued to improve prognosis are the early initiation of resuscitation maneuvers, the quick identification and treatment of underlying causes, and also the reduction of the duration of no-flow intervals. For these reasons, the only diagnostic technology recommended by the Advanced Cardiac Life Support (ACLS) protocols during resuscitation is active electrocardiography. Except for the evaluation of cardiac rhythm, all the other diagnostic procedures are based only on physical examination and patient's history. The need for quick initiation of resuscitation and strict limitation of pauses during chest compression prevents the use of sophisticated diagnostic devices /$ see front matter 2011 Elsevier Inc. All rights reserved. doi: /j.ajem
2 Emergency ultrasound during cardiac arrest In recent years, emergency ultrasound has gained broader acceptance as a clinical tool for the clinician, and this has led to several new applications. Point-of-care focused ultrasound results in a narrower differential diagnosis and improved outcome in adult patients with undifferentiated hypotension [4]. Clinician's ability to assess bedside cardiac function by gross visual sonographic estimates is adequately accurate [5-8]. Moreover, sonographic evaluation of lung diseases has been proved to be extremely useful and accurate in the emergency settings [9-11]. Finally, newly developed, highly portable ultrasound devices have sufficient quality and resolution to assess cardiac status and performance: thus, they may deeply affect bedside diagnostic procedures. For these reasons, many recent studies and case reports have examined the application of emergency ultrasound to different scenarios of cardiac arrest [12-20]. Particularly, the ability of clinicians to rapidly obtain adequate images of the heart using subxiphoid approach in the cardiac arrest setting has been widely tested [12,13,15,17]. The general purpose of these studies is to find a compromise between the need to limit the pauses during chest compression coupled with the need for an increased diagnostic clarity. This article reviews and discusses current knowledge on the diagnostic application of emergency ultrasound during cardiac arrest. We have identified some issues that have been mostly discussed in literature. 2. Diagnostic usefulness of sonography during pulseless electrical activity Cardiac arrest can occur with 3 different rhythms: shockable rhythms, asystole, or pulseless electrical activity (PEA). The ACLS guidelines provide 3 different algorithms for the resuscitative procedures in cardiac arrest, depending on the rhythm that is recorded during the event. In recent years, major efforts have been made to show the usefulness of emergency ultrasound during PEA [12,13,16]. There are at least 2 main reasons explaining the interest of researchers on this application: the possibility of a more accurate and prompt differential diagnosis of the underlying potentially reversible condition and the opportunity to perform ultrasound during time intervals of chest compression Differential diagnosis of PEA 217 Pulseless electrical activity may result from a list of conditions that are potentially reversible. The importance of accurate and timely diagnosis of a reversible underlying cause is highly stressed in the ACLS algorithm of PEA, whereas in ventricular fibrillation the shock is the mainstay of treatment. Among the causes of PEA, some are easily recognizable by emergency ultrasound [4,8,16,21,22]. All of Fig. 1 Sonographic image of the heart of a patient with tamponade as a cause of cardiac arrest. This subxiphoid view, performed during pausing of chest compression and checking carotid pulse, shows some pericardial effusion (upper white arrow). In real time, the mechanical collapse of the right ventricle was clearly visible. RV indicates right ventricle; LV, left ventricle.
3 218 G. Volpicelli these are mechanical reversible conditions including severe hypovolemia, cardiac tamponade, pulmonary embolism, and tension pneumothorax. Diagnosis can be made by sonographic examination of the heart and lungs. Sonography can be performed with convex, microconvex, or cardiac probe, and the first organ to be examined is the heart. The usual window is subxiphoid, but parasternal and apical views can also be used depending on patient's constitution and presence of bandages, wounds, or others. The aim is to obtain a glimpse of the ventricles, possibly gaining a complete 4-chamber cardiac view. Once the heart is visualized and severe hypovolemia, cardiac tamponade, or pulmonary massive embolism are excluded, the same probe can be moved to obtain a parasternal anterior view of the lungs to rule out pneumothorax. Even a negative ultrasound examination is useful because it eliminates many conditions from the differential Severe hypovolemia Reduction of intravascular volume is well detected by measuring sonographic left ventricular end-diastolic area [23]. In the most severe cases that may lead to cardiac arrest, the sonographic pattern of underfilled right ventricle in the presence of a small dynamic left ventricle is easy to detect [15,20]. In this case, the resuscitation maneuvers should be directed toward prompt fluid replacement while continuing chest compression. A valuable adjunct to cardiac imaging could be venous assessment. Sonography of the inferior vena cava by subxiphoid transverse scan represents fluid status [24]. Visualization of collapsed venous walls should confirm hypovolemia and the need for aggressive fluid resuscitation [25]. A common cause of PEA due to hypovolemia is the rupture of an abdominal aortic aneurysm. In case of a cardiac and venous sonographic pattern suggestive of hypovolemia, the probe should be slightly moved downward from the subxiphoid approach to evaluate the diameter of the abdominal aorta [20]. A dilated aorta up to 30 mm makes vascular rupture a likely cause of PEA. In this case, blood loss can be confirmed by a sonographic quick search of effusion in the pleural and peritoneal spaces [20] Cardiac tamponade Pericardial effusion causing cardiac tamponade is commonly encountered in cardiac arrest with PEA. Potentially, it is readily reversible if treated invasively with immediate pericardiocentesis. Diagnostic certainty by emergency cardiac ultrasound is crucial to guide the resuscitation team toward the rescue drainage [16]. Only effusion in the pericardial sac coupled with right chamber collapse demonstrates real cardiac tamponade, irrespective of the thickness of the fluid layer (Fig. 1). Emergency cardiac ultrasound by any thoracic window is highly accurate in detecting this association, even if performed by emergency physicians [26]. Fig. 2 This anterior oblique lung scan shows multiple vertical echogenic artefacts, named B lines (asterisks). They are a sign of properly aerated lung (thus, ruling out pneumothorax) and can be a sign of pulmonary congestion. White arrow indicates pleural line.
4 Emergency ultrasound during cardiac arrest 219 Fig. 3 Anterior oblique lung scan recorded during cardiac arrest due to tension pneumothorax with parietal subcutaneous emphysema. The scan is similar to that of Fig. 2. Notice some vertical echogenic artefacts (asterisks) that can mislead the sonographer because they may be confused with B lines. In this case, the echogenic horizontal line (white arrow) is not the pleural line but the muscular layer of the chest wall Massive pulmonary embolus Another highly prevalent mechanic cause of PEA arrest is pulmonary embolus. Prompt administration of thrombolytic agents can be rapidly effective, and it is recommended in the ACLS guidelines because it has the potential of greatly impact outcomes [19]. The ability to immediately diagnose acute pulmonary embolus can be dramatically increased by the use of emergency echocardiography [19,21,22,27]. The finding of an engorged and dilated right ventricle with flattened left chambers is the sonographic pattern identifying acute obstruction of the pulmonary arterial bed as the cause of cardiac arrest [12,19] Tension pneumothorax In recent years, lung sonography has gained increasing diagnostic potential in detecting signs of pneumothorax [28]. The ability of sonography in allowing a prompt diagnosis of tension pneumothorax relies on 2 signs: the absence of lung sliding and B lines when the lung is visualized anteromedially along the mid-clavicular line [9,28,29]. The lung sliding is a slight to-and-fro movement of the echogenic pleural line during active or passive respiration [28]. The B lines are vertical echogenic rays that arise from the plural line, reach the lower edge of the screen without fading, and move synchronous with respiratory movements (Fig. 2) [29]. The sonographic lung pattern of absence of lung sliding and B lines is accurate in detecting pneumothorax, but some possible pitfalls should be remembered [30]. The presence of parietal emphysema may prevent the diagnosis of pneumothorax as it may lead into a false view of pleural motion and vertical artefacts very similar to B lines (Fig. 3). In this circumstance, safe detection of the pleural line by searching for the bat sign (Fig. 4) and bilateral comparison of lung scans are essential steps (Fig. 5A and B). Despite this limitation, emergency lung ultrasound is often critical to guide the physician toward the diagnosis and consequent prompt drainage of pneumothorax during PEA. Sonographic intercostal scans of both lungs can be performed in a few seconds by the same probe used for cardiac evaluation, just moving it from the subxiphoid to the anterior chest wall Pulse-check pausing The other reason why researchers are testing the diagnostic application of sonography in PEA arrest is the possibility to perform it during pulse-check pausing of chest compression. The need to limit the no-flow intervals during resuscitation frustrates the use of emergency
5 220 G. Volpicelli 3. Diagnosis of cardiac standstill Fig. 4 This longitudinal lung scan shows the bat sign : 2 adjacent ribs (white arrows) and the echogenic pleural line between and below them (gray arrow). Visualization of this sign is fundamental for the safe detection of the pleural line. Protocols for treating patients in cardiac arrest provide hints for cessation of resuscitative efforts. Time limit is commonly used to cease maneuvers, when the patient does not appear to be responding to treatment. Despite these indications, stopping resuscitation procedures is problematic, especially when electrical activity is still noted on a cardiac monitor [31]. Early abortion of resuscitative efforts can have catastrophic consequences, but also perpetuation on a patient who has already died has deleterious effects because a great deal of time and ED resources are wasted [14]. Current guidelines do not provide any accurate method for predicting certain death and real cardiac electromechanical dissociation. Sonography has the potential of providing information about the real contractility of the heart in pulseless patients, regardless of the rhythm displayed in the monitor. The sonographic pattern of cardiac standstill and complete absence of any motion indicate a poor outcome despite resuscitation [14]. Some authors noted that 100% of patients presenting with cardiac standstill detected by ultrasound did not survive the arrest despite resuscitative efforts [14-16,32]. Most of the patients of these studies presented with cardiac electrical activity, either PEA or ventricular fibrillation. These observations may help in the future in the implementation of existing guidelines with sonographic evaluation of real cardiac kinetic activity, which may be added to the criteria used to limit resuscitation efforts for cardiac arrest patients. ultrasound in other conditions of cardiac arrest (asystole and shockable rhythm), where chest compressions are not allowed to be interrupted. On the contrary, the algorithm of PEA provides repeated pauses, up to 10 seconds each, during the resuscitative effort. Pauses during chest compression, while PEA persists, are essential to palpate a possible carotid pulse in presence of a cardiac rhythm potentially compatible with a spontaneous circulation [1-3]. These brief interruptions can be used to repeatedly perform real-time cardiac, vascular, and lung ultrasound targeted to the search of the above-mentioned sonographic signs. On discontinuation of chest compression, the probe must be positioned as fast as possible to gain a complete 4-chamber view of the heart and then moved to the lungs to check for pleural sliding and B lines. These targets can be achieved using even more than a pause for pulse-check during the cyclic algorithm of resuscitation [12,13]. 4. Application of sonography during continuous chest compression Studies about the usefulness of emergency echocardiography performed during chest compression in cardiac arrest are not numerous. The reason is obvious, because accuracy of emergency ultrasound is likely to be too low when the hands of the rescuer push hardly on the thorax and hinder the search for an optimal acoustic window. Moreover, because of external compression, the real cardiac motion can be misdiagnosed. For these reasons, most of the trials on the use of sonography during cardiac arrest have been performed during pulse-check pausing of PEA algorithm or first pulsecheck at presentation in the ED [12-14,32]. Nevertheless, some authors published their experience of sonography approach during continuous chest compression [18]. This approach is desirable, but the detection of most of the above- Fig. 5 Bilateral anterior lung scans of a patient with cardiac arrest: the presence of echogenic horizontal lines at different heights allows diagnosis of right-sided parietal emphysema. In the right side, the echogenic horizontal line is the sonographic representation of the muscular layer of the chest wall (A, white arrow) and should not be confounded with the pleural line. Subcutaneous emphysema hides the pleural line, making detection of sonographic signs of pneumothorax impossible. The left lung shows a deeper echogenic horizontal line, that is the regular pleural imaging (B, white arrow).
6 Emergency ultrasound during cardiac arrest 221
7 222 G. Volpicelli mentioned sonographic signs presents a number of potential pitfalls [24]. When regular and effective chest compression is being performed at the usual rate of 100 min 1, distinguishing between spontaneous or induced cardiac motion may be challenging. Moreover, assessment of severe impairment of intravascular volume is difficult even if the sonographic evaluation of the inferior vena cava is added to cardiac imaging. External compression could cause a confounding collapse of the venous walls and even flattened right and left ventricles, leading to a possible misdiagnosis. Finally, during compressions, thoracic acoustic windows are reduced and only the subxiphoid approach can be used. Even if preferable most of the time, this window does not always allow sufficient visualization of the heart chambers, and sometimes parasternal or apical sonographic approaches should be attempted. Further studies are needed to evaluate the exact accuracy of sonography during chest compression. 5. Hemodynamic evaluation by lung ultrasound In recent years, the usefulness of lung ultrasound in the assessment of pulmonary congestion and extravascular lung water has been shown [33,34]. The sonographic method relies on detection of some vertical artefatcts named B lines, which are constant in cardiogenic pulmonary edema (Fig. 2) [35]. The number and diffusion of these artefacts correlate with extravascular lung water assessed by invasive determinations [34]. Implication is the possible use of real-time lung ultrasound in the monitoring of the hemodynamic state before and after a mechanical cardiopulmonary resuscitation. Moreover, pulmonary congestion could be monitored during fluid replacement in hypovolemic patients. The appearance of pulmonary B lines during volume resuscitation warns the clinician that a patient was becoming volume overloaded before he became dyspneic. Moreover, the absence of B lines could suggest euvolemia or hypovolemia more appropriately than physical findings. Lung ultrasound monitoring is a relatively simple and cost-saving diagnostic skill compared to echocardiography that is relatively complex and expensive. 6. Verification of tracheal intubation Tracheal tube insertion is one of the major elements of resuscitation. A failed intubation can have catastrophic consequences in the management of patients with cardiac arrest. After insertion of the tube, the ACLS guidelines suggest a confirmatory procedure to exclude esophageal or endobronchial intubation. Moreover, once the tube has been inserted correctly and verified, position should be continuously monitored to avoid lung atelectasis due to accidental endobronchial displacement. The routine methods for confirmation of endotracheal tube are auscultation and end-tidal carbon dioxide detection, but the accuracy of both is limited [36,37]. Emergency ultrasound of the lung can be useful to verify and monitor tube position and can be proposed as a real-time method to be performed immediately after tube placement during cardiac arrest [38]. Lung ultrasound provides an indirect indicator of lung expansion by visualization of the pleural motion. This method is easy to perform during the resuscitation procedures and requires a few seconds. The probe should be positioned at the same anterior chest areas where the emergency physicians usually perform auscultation after tube placement, corresponding to the 2 to 3 intercostal spaces along the midclavicular line. Endotracheal position of the tube gives bilateral equal motion of the pleural line synchronized with ventilation (lung sliding). A regular lung sliding visualized on the left lung or on both sides is a sign of correct positioning of the tube and regular bilateral ventilation. During assisted ventilation, main bronchus position of the tube is suggested by absence of lung sliding of the left lung while the right pleural line is regularly moving. This sign indicates the need to move the tube backward. The bilateral absence of lung sliding is a sign of esophageal position of the tube and should urge the physician to perform a new attempt [28,39]. 7. Conclusion Cardiac arrest scenarios are often sudden chaotic, and physicians who attempt resuscitation need prompt diagnostic certainties. Sonographic evaluation can be applied during resuscitative maneuvers: it provides physicians with some novel items to take proper decisions. Procedural limitations are due to the need of continuous chest compressions necessary to generate blood flow during cardiac arrest. Nevertheless, trained personnel can apply sonography during the brief interruptions of chest compression provided by the ACLS guidelines. On the other hand, application of emergency ultrasound during chest compression deserves further careful evaluation by specifically designed clinical trials. Echocardiography and lung ultrasound can be used to clarify the cause of cardiac arrest. Moreover, the diagnosis of cardiac standstill can be confirmed by sonography with high accuracy. Real-time lung ultrasound can be useful to assess pulmonary congestion before and after cardiac arrest, having the potential to drive resuscitative fluid replacement. Finally, the role of lung ultrasound in verification of correct tracheal tube position may lead to its routine use during resuscitation. These and other items about the appropriateness of diagnostic emergency ultrasound during cardiac arrest deserve further studies. Particularly, the proper timing of sonographic evaluation during the resuscitative effort of cardiac arrest should be further examined.
8 Emergency ultrasound during cardiac arrest References [1] Cummins RO, editor. ACLS provider manual, Dallas (Tex): American Heart Association; p [2] Nolan JP, Deakin CD, Soar J, Bottiger BW, Smith G. European Resuscitation Council Guidelines for resuscitation Section 4: adult advanced life support. Resuscitation 2005;67(Suppl 1):S39-S86. [3] International Liaison Committee on Resuscitation International consensus on cardiopulmonary resuscitation and emergency cardiovascular care science with treatment reccomendations. Resuscitation 2005;67: [4] Jones AE, Tayal VS, Sullivan DM, Kline JA. Randomized, controlled trial of immediate versus delayed goal-directed ultrasound to identify the cause of nontraumatic hypotension in emergency department patients. Crit Care Med 2004;32: [5] Moore CL, Rose GA, Tayal VS, Sullivan DM, Arrowood JA, Kline JA. Determination of left ventricular function by emergency physician echocardiography of hypotensive patients. Acad Emerg Med 2002;9: [6] Randazzo MR, Snoey ER, Levitt MA, Binder K. Accuracy of emergency physician assessment of left ventricular ejection fraction and central venous pressure using echocardiography. Acad Emerg Med 2003;10: [7] Mueller X, Stauffer JC, Jaussi A, Goy JJ, Kappenberger L. Subjective visual echocardiographic estimate of left ventricular ejection fraction as an alternative to conventional echocardiographic methods: comparison with contrast angiography. Clin Cardiol 1991;14: [8] Levitt MA, Jan BA. The effect of real time 2-D-echocardiography on medical decision-making in the emergency department. J Emerg Med 2002;22: [9] Lichtenstein DA. Ultrasound in the management of thoracic disease. Crit Care Med 2007;35:S [10] Volpicelli G, Cardinale L, Garofalo G, Veltri A. Usefulness of lung ultrasound in the bedside distinction between pulmonary edema and exacerbation of COPD. Emerg Radiol 2008;15: [11] Volpicelli G, Silva F, Radeos M. Real-time lung ultrasound for the diagnosis of alveolar consolidation and interstitial syndrome in the emergency department. Eur J Emerg Med [in press]. [12] Niendorff DF, Rassias AJ, Palac R, Beach ML, Costa S, Greenberg M. Rapid cardiac ultrasound of inpatients suffering PEA arrest performed by nonexpert sonographers. Resuscitation 2005;67:81-7. [13] Breitkreutz R, Walcher F, Seeger FH. Focused echocardiographic evaluation in resuscitation management: concept of an advanced life support-conformed algorithm. Crit Care Med 2007;35(5 Suppl): S [14] Blaivas M, Fox JC. Outcome in cardiac arrest patients found to have cardiac standstill on the bedside emergency department echocardiogram. Acad Emerg Med 2001;8: [15] Varriale P, Maldonado JM. Echocardiographic observations during in hospital cardiopulmonary resuscitation. Crit Care Med 1997;25: [16] Tayal VS, Kline JA. Emergency echocardiography to detect pericardial effusion in patients in PEA and near-pea states. Resuscitation 2003;59: [17] Bocka JJ, Overton DT, Hauser A. Electromechanical dissociation in human beings: an echocardiographic evaluation. Ann Emerg Med 1988;17: [18] Hernandez C, Shuler K, Hannan H, Sonyika C, Likourezos A, Marshall J. CAUSE: Cardiac arrest ultra-sound exam a better approach to managing patients in primary non-arrhythmogenic cardiac arrest. Resuscitation 2008;76: [19] MacCarthy P, Worrall A, McCarthy G, Davies J. The use of transthoracic echocardiography to guide thrombolytic therapy during cardiac arrest due to massive pulmonary embolism. Emerg Med J 2002;19: [20] Hendrickson RG, Dean AJ, Costantino TG. A novel use of ultrasound in pulseless electrical activity: the diagnosis of an acute abdominal aortic aneurysm rupture. J Emerg Med 2001;21: [21] McConnell MV, Solomon SD, Rayan M, et al. Regional right ventricular dysfunction detected by echocardiography in acute pulmonary embolism. Am J Cardiol 1996;78: [22] Jardin F, Dubourg O, Bourdarias J. Echocardiographic pattern of acute cor pulmonale. Chest 1997;111: [23] Brown JM. Use of echocardiography for hemodynamic monitoring. Crit Care Med 2002;30: [24] Breitkreutz R, Walcher F, Seeger FH.. Resuscitation 2008;77: [25] Lyon M, Blaivas M, Brannam L. Sonographic measurement of the inferior vena cava as a marker of blood loss. Am J Emerg Med 2005; 23: [26] Mandavia DP, Hoffner RJ, Mahaney K, Henderson SO. Bedside echocardiography by emergency physicians. Ann Emerg Med 2001;38: [27] Leibowitz D. Role of echocardiography in the diagnosis and treatment of acute pulmonary thromboembolism. J Am Soc Echocardiogr 2001; 14: [28] Lichtenstein D, Menu Y. A bedside ultrasound sign ruling out pneumothorax in the critically ill: lung sliding. Chest 1995;108: [29] Lichtenstein D, Meziere G, Biderman P, Gepner A. The comet-tail artifact, an ultrasound sign ruling out pneumothorax. Intensive Care Med 1999;25: [30] Volpicelli G. Towards an appropriate use of ultrasound in resuscitation. Resuscitation 2008;79: [31] Marco CA, Bessman ES, Schoenfeld CN, Kelen GD. Ethical issues of cardiopulmonary resuscitation: current practice among emergency physicians. Acad Emerg Med 1997;4: [32] Salen P, Melniker L, Chooljian C, Rose JS, Alteveer J, Reed J, et al. Does the presence or absence of sonographically identified cardiac activity predict resuscitation outcomes of cardiac arrest patients? Am J Emerg Med 2005;23: [33] Volpicelli G, Caramello V, Cardinale L, Mussa A, Bar F, Frascisco MF. Bedside ultrasound of the lung for the monitoring of acute decompensated heart failure. Am J Emerg Med 2008;26: [34] Agricola E, Bove T, Oppizzi M, Marino G, Zangrillo A, Margonato A, et al. Ultrasound comet-tail images : a marker of pulmonary edema: a comparative study with wedge pressure and extravascular lung water. Chest 2005;127: [35] Lichtenstein DA, Mezière GA. Relevance of lung ultrasound in the diagnosis of acute respiratory failure: the BLUE protocol. Chest 2008;134: [36] Grmec S. Comparison of three different methods to confirm tracheal tube placement in emergency intubation. Intensive Care Med 2002;28: [37] Knapp S, Kofler J, Stoiser B, et al. The assessment of four methods to verify tracheal tube placement in the critical care setting. Anesth Analg 1999;88: [38] Sustić A. Role of ultrasound in the airway management of critically ill patients. Crit Care Med 2007;35(5 Suppl):S [39] Chun R, Kirkpatrick AW, Sirois M, et al. Where's the tube? Evaluation of hand-held ultrasound in confirming endotracheal tube placement. Prehospital Disaster Med 2004;19:366-9.
Case III. Disscussion. the UHP ultrasound protocol. Novel Ultrasound Approach to the Empiric Evaluation of the Undifferentiated Hypotensive Patient
 The UHP Ultrasound Protocol: A Novel Ultrasound Approach to the Empiric Evaluation of the Undifferentiated Hypotensive Patient JOHN S. ROSE, MD,* AARON E. BAIR, MD,* DIKU MANDAVIA, MD, AND DONNA J. KINSER,
The UHP Ultrasound Protocol: A Novel Ultrasound Approach to the Empiric Evaluation of the Undifferentiated Hypotensive Patient JOHN S. ROSE, MD,* AARON E. BAIR, MD,* DIKU MANDAVIA, MD, AND DONNA J. KINSER,
CARDIAC ARREST ULTRASOUND
 ADIA AEST ULTASOUND Phillip Andrus, MD, FAEP Department of Emergency Medicine Division of Emergency Ultrasound Mount Sinai School of Medicine Point of are Ultrasound provides important diagnostic, procedural
ADIA AEST ULTASOUND Phillip Andrus, MD, FAEP Department of Emergency Medicine Division of Emergency Ultrasound Mount Sinai School of Medicine Point of are Ultrasound provides important diagnostic, procedural
CARDIAC MOVEMENT IDENTIFIED ON PREHOSPITAL ECHOCARDIOGRAPHY PREDICTS OUTCOME IN CARDIAC ARREST PATIENTS
 CARDIAC MOVEMENT IDENTIFIED ON PREHOSPITAL ECHOCARDIOGRAPHY PREDICTS OUTCOME IN CARDIAC ARREST PATIENTS Gernot Aichinger, MD, Peter Michael Zechner, MD, Gerhard Prause, MD, Florian Sacherer, Gernot Wildner,
CARDIAC MOVEMENT IDENTIFIED ON PREHOSPITAL ECHOCARDIOGRAPHY PREDICTS OUTCOME IN CARDIAC ARREST PATIENTS Gernot Aichinger, MD, Peter Michael Zechner, MD, Gerhard Prause, MD, Florian Sacherer, Gernot Wildner,
FALLS-protocol: lung ultrasound in hemodynamic assessment of shock
 Review article Heart, Lung and Vessels. 2013; 5(3): 142-147 142 FALLS-protocol: lung ultrasound in hemodynamic assessment of shock D. Lichtenstein Service de Réanimation Médicale, Hôpital Ambroise-Paré,
Review article Heart, Lung and Vessels. 2013; 5(3): 142-147 142 FALLS-protocol: lung ultrasound in hemodynamic assessment of shock D. Lichtenstein Service de Réanimation Médicale, Hôpital Ambroise-Paré,
Ultrasound Use in Resuscitation
 Critical Decisions in Emergency Medicine Lesson 23 Ultrasound Use in Resuscitation Michael Herndon, DO, and Catherine Erickson, MD Objectives On completion of this lesson, you should be able to: 1. Explain
Critical Decisions in Emergency Medicine Lesson 23 Ultrasound Use in Resuscitation Michael Herndon, DO, and Catherine Erickson, MD Objectives On completion of this lesson, you should be able to: 1. Explain
Ultrasound Assessment for Extravascular Lung Water in Patients Undergoing Hemodialysis*
 Original Research CHEST ULTRASONOGRAPHY Ultrasound Assessment for Extravascular Lung Water in Patients Undergoing Hemodialysis* Time Course for Resolution Vicki E. Noble, MD, RDMS; Alice F. Murray, MBChB;
Original Research CHEST ULTRASONOGRAPHY Ultrasound Assessment for Extravascular Lung Water in Patients Undergoing Hemodialysis* Time Course for Resolution Vicki E. Noble, MD, RDMS; Alice F. Murray, MBChB;
ACLS Provider Manual Comparison Sheet Based on 2010 AHA Guidelines for CPR and ECC. BLS Changes
 ACLS Provider Manual Comparison Sheet Based on 2010 AHA Guidelines for CPR and ECC CPR Chest compressions, Airway, Breathing (C-A-B) BLS Changes New Old Rationale New science indicates the following order:
ACLS Provider Manual Comparison Sheet Based on 2010 AHA Guidelines for CPR and ECC CPR Chest compressions, Airway, Breathing (C-A-B) BLS Changes New Old Rationale New science indicates the following order:
Sonography for Trauma
 Sonography for Trauma Christine Butts and Justin Cook 9 KEY POINTS Focused abdominal sonography for trauma (FAST) is sensitive and specific for the detection of intraperitoneal free fluid, but it has poor
Sonography for Trauma Christine Butts and Justin Cook 9 KEY POINTS Focused abdominal sonography for trauma (FAST) is sensitive and specific for the detection of intraperitoneal free fluid, but it has poor
The RUSH Exam: Rapid Ultrasound in SHock in the Evaluation of the Critically lll
 The RUSH Exam: Rapid Ultrasound in SHock in the Evaluation of the Critically lll Phillips Perera, MD, RDMS, FACEP a, *, Thomas Mailhot, MD, RDMS b, David Riley, MD, MS, RDMS a, Diku Mandavia, MD, FACEP,
The RUSH Exam: Rapid Ultrasound in SHock in the Evaluation of the Critically lll Phillips Perera, MD, RDMS, FACEP a, *, Thomas Mailhot, MD, RDMS b, David Riley, MD, MS, RDMS a, Diku Mandavia, MD, FACEP,
Bedside ultrasound of the lung for the monitoring of acute decompensated heart failure
 American Journal of Emergency Medicine (2008) 26, 585 591 www.elsevier.com/locate/ajem Original Contribution Bedside ultrasound of the lung for the monitoring of acute decompensated heart failure Giovanni
American Journal of Emergency Medicine (2008) 26, 585 591 www.elsevier.com/locate/ajem Original Contribution Bedside ultrasound of the lung for the monitoring of acute decompensated heart failure Giovanni
RACE I Rapid Assessment by Cardiac Echo. Intensive Care Training Program Radboud University Medical Centre NIjmegen
 RACE I Rapid Assessment by Cardiac Echo Intensive Care Training Program Radboud University Medical Centre NIjmegen RACE Goal-directed study with specific questions Excludes Doppler ultrasound Perform 50
RACE I Rapid Assessment by Cardiac Echo Intensive Care Training Program Radboud University Medical Centre NIjmegen RACE Goal-directed study with specific questions Excludes Doppler ultrasound Perform 50
How To Teach An Integrated Ultrasound
 University of South Carolina School of Medicine Integrated Ultrasound Curriculum iusc Richard Hoppmann The Integrated Ultrasound Curriculum Initiated 2006 First (M1) and Second (M2) Year Medical Students
University of South Carolina School of Medicine Integrated Ultrasound Curriculum iusc Richard Hoppmann The Integrated Ultrasound Curriculum Initiated 2006 First (M1) and Second (M2) Year Medical Students
Review Article Bedside Ultrasound in Resuscitation and the Rapid Ultrasound in Shock Protocol
 Hindawi Publishing Corporation Critical Care Research and Practice Volume 2012, Article ID 503254, 14 pages doi:10.1155/2012/503254 Review Article Bedside Ultrasound in Resuscitation and the Rapid Ultrasound
Hindawi Publishing Corporation Critical Care Research and Practice Volume 2012, Article ID 503254, 14 pages doi:10.1155/2012/503254 Review Article Bedside Ultrasound in Resuscitation and the Rapid Ultrasound
Focused assessment of sonography in trauma
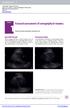 Chapter1 Focused assessment of sonography in trauma Patricia Fermin and John Christian Fox Epicardial fat pad When imaging the heart, careful attention must be made in identifying any surrounding fluid.
Chapter1 Focused assessment of sonography in trauma Patricia Fermin and John Christian Fox Epicardial fat pad When imaging the heart, careful attention must be made in identifying any surrounding fluid.
Section Four: Pulmonary Artery Waveform Interpretation
 Section Four: Pulmonary Artery Waveform Interpretation All hemodynamic pressures and waveforms are generated by pressure changes in the heart caused by myocardial contraction (systole) and relaxation/filling
Section Four: Pulmonary Artery Waveform Interpretation All hemodynamic pressures and waveforms are generated by pressure changes in the heart caused by myocardial contraction (systole) and relaxation/filling
Michigan Adult Cardiac Protocols CARDIAC ARREST GENERAL. Date: May 31, 2012 Page 1 of 5
 Date: May 31, 2012 Page 1 of 5 Cardiac Arrest General This protocol should be followed for all adult cardiac arrests. Medical cardiac arrest patients undergoing attempted resuscitation should not be transported
Date: May 31, 2012 Page 1 of 5 Cardiac Arrest General This protocol should be followed for all adult cardiac arrests. Medical cardiac arrest patients undergoing attempted resuscitation should not be transported
ACLS Study Guide BLS Overview CAB
 ACLS Study Guide The ACLS Provider exam is 50-mutiple choice questions. Passing score is 84%. Student may miss 8 questions. For students taking ACLS for the first time or renewing students with a current
ACLS Study Guide The ACLS Provider exam is 50-mutiple choice questions. Passing score is 84%. Student may miss 8 questions. For students taking ACLS for the first time or renewing students with a current
THE ABSENCE of a palpable central pulse CLINICAL INVESTIGATIONS
 60 CAPNOGRAPHY Salen et al. SONOGRAPHY AND CAPNOGRAPHY TO PREDICT OUTCOMES CLINICAL INVESTIGATIONS Can Cardiac Sonography and Capnography Be Used Independently and in Combination to Predict Resuscitation
60 CAPNOGRAPHY Salen et al. SONOGRAPHY AND CAPNOGRAPHY TO PREDICT OUTCOMES CLINICAL INVESTIGATIONS Can Cardiac Sonography and Capnography Be Used Independently and in Combination to Predict Resuscitation
Update on Small Animal Cardiopulmonary Resuscitation (CPR)- is anything new?
 Update on Small Animal Cardiopulmonary Resuscitation (CPR)- is anything new? DVM, DACVA Objective: Update on the new Small animal guidelines for CPR and a discussion of the 2012 Reassessment Campaign on
Update on Small Animal Cardiopulmonary Resuscitation (CPR)- is anything new? DVM, DACVA Objective: Update on the new Small animal guidelines for CPR and a discussion of the 2012 Reassessment Campaign on
INTERNATIONAL TRAUMA LIFE SUPPORT
 INTERNATIONAL TRAUMA LIFE SUPPORT NEEDLE DECOMPRESSION OF TENSION PNEUMOTHORAX Roy Alson, MD, PhD, FACEP, FAAEM and Sabina Braithwaite, MD, MPH, FACEP INTRODUCTION The purpose of this document is to update
INTERNATIONAL TRAUMA LIFE SUPPORT NEEDLE DECOMPRESSION OF TENSION PNEUMOTHORAX Roy Alson, MD, PhD, FACEP, FAAEM and Sabina Braithwaite, MD, MPH, FACEP INTRODUCTION The purpose of this document is to update
How To Learn To Perform An Ultrasound
 CAE ICCU E-Learning CAE VIMEDIX Ultrasound Simulator Master Ultrasonography of the Thoracic, Abdominal and Pelvic Cavities An Engaging Learning Solution for Ultrasound Hands-on Simulation, Multimedia Content,
CAE ICCU E-Learning CAE VIMEDIX Ultrasound Simulator Master Ultrasonography of the Thoracic, Abdominal and Pelvic Cavities An Engaging Learning Solution for Ultrasound Hands-on Simulation, Multimedia Content,
Cardiac Arrest: General Considerations
 Andrea Gabrielli, MD, FCCM Cardiac Arrest: General Considerations Cardiopulmonary resuscitation (CPR) is described as a series of assessments and interventions performed during a variety of acute medical
Andrea Gabrielli, MD, FCCM Cardiac Arrest: General Considerations Cardiopulmonary resuscitation (CPR) is described as a series of assessments and interventions performed during a variety of acute medical
Traumatic Cardiac Tamponade. Shane KF Seal 19 November 2003 POS
 Traumatic Cardiac Tamponade Shane KF Seal 19 November 2003 POS Objectives Definition Pathophysiology Diagnosis Treatment Cardiac Tamponade The decompensated phase of cardiac compression resulting from
Traumatic Cardiac Tamponade Shane KF Seal 19 November 2003 POS Objectives Definition Pathophysiology Diagnosis Treatment Cardiac Tamponade The decompensated phase of cardiac compression resulting from
Sonography in Cardiac Arrest
 Sonography in Cardiac Arrest Real-time Assessment and Evaluation with Sonography - Outcomes Network (REASON) Dr. Paul Atkinson MB MA FRCEM Professor and Research Program Director Emergency Medicine Dalhousie
Sonography in Cardiac Arrest Real-time Assessment and Evaluation with Sonography - Outcomes Network (REASON) Dr. Paul Atkinson MB MA FRCEM Professor and Research Program Director Emergency Medicine Dalhousie
The importance of the initial assessment in trauma patients /in a prehospital setting: Therapeutic decisions Patient outcomes
 The importance of the initial assessment in trauma patients /in a prehospital setting: Therapeutic decisions Patient outcomes Reporter: Intern 鄭 琬 蓉 Supervisor: Dr. 朱 健 銘 Date: Sep. 16th, 2014 The nonspecific
The importance of the initial assessment in trauma patients /in a prehospital setting: Therapeutic decisions Patient outcomes Reporter: Intern 鄭 琬 蓉 Supervisor: Dr. 朱 健 銘 Date: Sep. 16th, 2014 The nonspecific
Caval Sonography in Shock
 SOUND JUDGMENT SERIES Caval Sonography in Shock A Noninvasive Method for Evaluating Intravascular Volume in Critically Ill Patients Dina Seif, MD, MBA, RDMS, Thomas Mailhot, MD, RDMS, Phillips Perera,
SOUND JUDGMENT SERIES Caval Sonography in Shock A Noninvasive Method for Evaluating Intravascular Volume in Critically Ill Patients Dina Seif, MD, MBA, RDMS, Thomas Mailhot, MD, RDMS, Phillips Perera,
Question-and-Answer Document 2010 AHA Guidelines for CPR & ECC As of October 18, 2010
 Question-and-Answer Document 2010 AHA Guidelines for CPR & ECC As of October 18, 2010 Q: What are the most significant changes in the 2010 AHA Guidelines for CPR & ECC? A: Major changes for all rescuers,
Question-and-Answer Document 2010 AHA Guidelines for CPR & ECC As of October 18, 2010 Q: What are the most significant changes in the 2010 AHA Guidelines for CPR & ECC? A: Major changes for all rescuers,
Emergency Ultrasound Course
 Emergency Ultrasound Course Dr Justin Bowra ED Course Manual 5: Credentialing 1 Why all the fuss? Why credential in point-of-care US (POCUS)? POCUS is quite a different skill to traditional US in the Radiology
Emergency Ultrasound Course Dr Justin Bowra ED Course Manual 5: Credentialing 1 Why all the fuss? Why credential in point-of-care US (POCUS)? POCUS is quite a different skill to traditional US in the Radiology
Bedside Lung Ultrasound in Critical Care Units
 Med. J. Cairo Univ., Vol. 78, No. 2, September: 197-203, 2010 www.medicaljournalofcairouniversity.com Bedside Lung Ultrasound in Critical Care Units MOHAMED TALAAT ELKHOLY, M.D. *; HATEM S. ABDELHAMID,
Med. J. Cairo Univ., Vol. 78, No. 2, September: 197-203, 2010 www.medicaljournalofcairouniversity.com Bedside Lung Ultrasound in Critical Care Units MOHAMED TALAAT ELKHOLY, M.D. *; HATEM S. ABDELHAMID,
Emergency Ultrasound Course
 Emergency Ultrasound Course Dr Justin Bowra ED Course Manual 2: EFAST Extended Focused Assessment with Sonography in Trauma JUSTIN BOWRA 1 The Questions: 1. Is there free fluid (FF) a. In the pleural space?
Emergency Ultrasound Course Dr Justin Bowra ED Course Manual 2: EFAST Extended Focused Assessment with Sonography in Trauma JUSTIN BOWRA 1 The Questions: 1. Is there free fluid (FF) a. In the pleural space?
APPENDIX B SAMPLE PEDIATRIC CRITICAL CARE NURSE PRACTITIONER GOALS AND OBJECTIVES
 APPENDIX B SAMPLE PEDIATRIC CRITICAL CARE NURSE PRACTITIONER GOALS AND OBJECTIVES The critical care nurse practitioner orientation is an individualized process based on one s previous experiences and should
APPENDIX B SAMPLE PEDIATRIC CRITICAL CARE NURSE PRACTITIONER GOALS AND OBJECTIVES The critical care nurse practitioner orientation is an individualized process based on one s previous experiences and should
Anatomy and Physiology: Understanding the Importance of CPR
 Anatomy and Physiology: Understanding the Importance of CPR Overview This document gives you more information about the body s structure (anatomy) and function (physiology). This information will help
Anatomy and Physiology: Understanding the Importance of CPR Overview This document gives you more information about the body s structure (anatomy) and function (physiology). This information will help
The American Heart Association released new resuscitation science and treatment guidelines on October 19, 2010.
 ACLS Study Guide The American Heart Association released new resuscitation science and treatment guidelines on October 19, 2010. Please read the below information carefully This letter is to confirm your
ACLS Study Guide The American Heart Association released new resuscitation science and treatment guidelines on October 19, 2010. Please read the below information carefully This letter is to confirm your
Edwards FloTrac Sensor & Edwards Vigileo Monitor. Understanding Stroke Volume Variation and Its Clinical Application
 Edwards FloTrac Sensor & Edwards Vigileo Monitor Understanding Stroke Volume Variation and Its Clinical Application 1 Topics System Configuration Pulsus Paradoxes Reversed Pulsus Paradoxus What is Stroke
Edwards FloTrac Sensor & Edwards Vigileo Monitor Understanding Stroke Volume Variation and Its Clinical Application 1 Topics System Configuration Pulsus Paradoxes Reversed Pulsus Paradoxus What is Stroke
Teaching Med-5 Students Point-of-Care Transthoracic Echocardiography
 Teaching Med-5 Students Point-of-Care Transthoracic Echocardiography Anthony M.-H. Ho, Lester A. H. Critchley, Patricia Kan, Sylvia Au, Siu Keung Ng, Simon K. C. Chan, Philip Lam, Gordon Choi, Alex Lee,
Teaching Med-5 Students Point-of-Care Transthoracic Echocardiography Anthony M.-H. Ho, Lester A. H. Critchley, Patricia Kan, Sylvia Au, Siu Keung Ng, Simon K. C. Chan, Philip Lam, Gordon Choi, Alex Lee,
Impact of Manual CPR on Increasing Coronary Perfusion Pressure
 Impact of Manual CPR on Increasing Coronary Perfusion Pressure In sudden cardiac arrest cases, the ability to adequately perfuse the brain and heart during resuscitation is of critical importance. The
Impact of Manual CPR on Increasing Coronary Perfusion Pressure In sudden cardiac arrest cases, the ability to adequately perfuse the brain and heart during resuscitation is of critical importance. The
Convincing Deans that Ultrasound should be in the Medical Student Curriculum. Richard Hoppmann Dean University of South Carolina School of Medicine
 Convincing Deans that Ultrasound should be in the Medical Student Curriculum Richard Hoppmann Dean University of South Carolina School of Medicine Convincing Deans that Ultrasound should be in the Medical
Convincing Deans that Ultrasound should be in the Medical Student Curriculum Richard Hoppmann Dean University of South Carolina School of Medicine Convincing Deans that Ultrasound should be in the Medical
Cardiac and Pulmonary Issues in the Elite Athlete. Keep Your Edge Hockey Sports Medicine 2015 Toronto August 28-30 2015
 Cardiac and Pulmonary Issues in the Elite Athlete Keep Your Edge Hockey Sports Medicine 2015 Toronto August 28-30 2015 THORACIC EMERGENCIES Hockey related thoracic trauma is blunt Injury to the boney
Cardiac and Pulmonary Issues in the Elite Athlete Keep Your Edge Hockey Sports Medicine 2015 Toronto August 28-30 2015 THORACIC EMERGENCIES Hockey related thoracic trauma is blunt Injury to the boney
Resuscitation in congenital heart disease. Peter C. Laussen MBBS FCICM Department Critical Care Medicine Hospital for Sick Children Toronto
 Resuscitation in congenital heart disease Peter C. Laussen MBBS FCICM Department Critical Care Medicine Hospital for Sick Children Toronto Evolution of Congenital Heart Disease Extraordinary success: Overall
Resuscitation in congenital heart disease Peter C. Laussen MBBS FCICM Department Critical Care Medicine Hospital for Sick Children Toronto Evolution of Congenital Heart Disease Extraordinary success: Overall
Cardiac Arrest Pediatric Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008
 Cardiac Arrest Pediatric Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008 Preamble In contrast to cardiac arrest in adults, cardiopulmonary arrest in pediatric
Cardiac Arrest Pediatric Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008 Preamble In contrast to cardiac arrest in adults, cardiopulmonary arrest in pediatric
Official Online ACLS Exam
 \ Official Online ACLS Exam Please fill out this form before you take the exam. Name : Email : Phone : 1. Hypovolemia initially produces which arrhythmia? A. PEA B. Sinus tachycardia C. Symptomatic bradyarrhythmia
\ Official Online ACLS Exam Please fill out this form before you take the exam. Name : Email : Phone : 1. Hypovolemia initially produces which arrhythmia? A. PEA B. Sinus tachycardia C. Symptomatic bradyarrhythmia
Purpose To guide registered nurses who may manage clients experiencing sudden or unexpected life-threatening cardiac emergencies.
 Emergency Cardiac Care: Decision Support Tool #1 RN-Initiated Emergency Cardiac Care Without Cardiac Monitoring/Manual Defibrillator or Emergency Cardiac Drugs Decision support tools are evidence-based
Emergency Cardiac Care: Decision Support Tool #1 RN-Initiated Emergency Cardiac Care Without Cardiac Monitoring/Manual Defibrillator or Emergency Cardiac Drugs Decision support tools are evidence-based
The Fatal Pulmonary Artery Involvement in Behçet s Disease
 The Fatal Pulmonary Artery Involvement in Behçet s Disease Dr. Vedat Hamuryudan Div. Rheumatology, Dept. Internal Medicine Cerrahpasa Medical Faculty, University of Istanbul 33 years old man Sept 2011:
The Fatal Pulmonary Artery Involvement in Behçet s Disease Dr. Vedat Hamuryudan Div. Rheumatology, Dept. Internal Medicine Cerrahpasa Medical Faculty, University of Istanbul 33 years old man Sept 2011:
CHEST TUBES AND CHEST DRAINAGE SYSTEMS
 CHEST TUBES AND CHEST DRAINAGE SYSTEMS Central Nursing Orientation April 2008 Revised September 2011 OBJECTIVES Describe common tubes and indications for use at LHSC Review indications and contraindications,
CHEST TUBES AND CHEST DRAINAGE SYSTEMS Central Nursing Orientation April 2008 Revised September 2011 OBJECTIVES Describe common tubes and indications for use at LHSC Review indications and contraindications,
2015 Interim Resources for BLS
 2015 Interim Resources for BLS Original Release: November 25, 2015 Starting in 2016, new versions of American Heart Association online courses will be released to reflect the changes published in the 2015
2015 Interim Resources for BLS Original Release: November 25, 2015 Starting in 2016, new versions of American Heart Association online courses will be released to reflect the changes published in the 2015
Documenting & Coding. Chronic Obstructive Pulmonary Disease (COPD) Presented by: David S. Brigner, MLA, CPC
 Documenting & Coding Chronic Obstructive Pulmonary Disease (COPD) Presented by: David S. Brigner, MLA, CPC Sr. Provider Training & Development Consultant Professional Profile David Brigner currently performs
Documenting & Coding Chronic Obstructive Pulmonary Disease (COPD) Presented by: David S. Brigner, MLA, CPC Sr. Provider Training & Development Consultant Professional Profile David Brigner currently performs
PRO-CPR. 2015 Guidelines: PALS Algorithm Overview. (Non-AHA supplementary precourse material)
 PRO-CPR 2015 Guidelines: PALS Algorithm Overview (Non-AHA supplementary precourse material) Please reference Circulation (from our website), the ECC Handbook, or the 2015 ACLS Course Manual for correct
PRO-CPR 2015 Guidelines: PALS Algorithm Overview (Non-AHA supplementary precourse material) Please reference Circulation (from our website), the ECC Handbook, or the 2015 ACLS Course Manual for correct
MECHINICAL VENTILATION S. Kache, MD
 MECHINICAL VENTILATION S. Kache, MD Spontaneous respiration vs. Mechanical ventilation Natural spontaneous ventilation occurs when the respiratory muscles, diaphragm and intercostal muscles pull on the
MECHINICAL VENTILATION S. Kache, MD Spontaneous respiration vs. Mechanical ventilation Natural spontaneous ventilation occurs when the respiratory muscles, diaphragm and intercostal muscles pull on the
STATE OF CONNECTICUT
 STATE OF CONNECTICUT DEPARTMENT OF PUBLIC HEALTH June 7, 2010 The Following Will Be Policy For Emergency Medical Service Care Providers: GUIDELINES FOR EMR, EMT, AEMT, and Paramedic DETERMINATION OF DEATH/DISCONTINUATION
STATE OF CONNECTICUT DEPARTMENT OF PUBLIC HEALTH June 7, 2010 The Following Will Be Policy For Emergency Medical Service Care Providers: GUIDELINES FOR EMR, EMT, AEMT, and Paramedic DETERMINATION OF DEATH/DISCONTINUATION
How To Know If A Patient Is Preload Sensitive
 The Open Critical Care Medicine Journal, 2010, 3, 33-37 33 Open Access Use of Ultrasound to Assess Fluid Responsiveness in the Intensive Care Unit Moses M. Kitakule * and Paul Mayo * The Division of Pulmonary,
The Open Critical Care Medicine Journal, 2010, 3, 33-37 33 Open Access Use of Ultrasound to Assess Fluid Responsiveness in the Intensive Care Unit Moses M. Kitakule * and Paul Mayo * The Division of Pulmonary,
Management of Adult Cardiac Arrest
 73991_CH27_page68-73.qxd 6/6/11 3:54 PM Page 68 27.68 Section 5 Medical Guidelines for Performing a 12-Lead ECG The only way to learn how to obtain a 12-lead ECG is to practice with the equipment itself.
73991_CH27_page68-73.qxd 6/6/11 3:54 PM Page 68 27.68 Section 5 Medical Guidelines for Performing a 12-Lead ECG The only way to learn how to obtain a 12-lead ECG is to practice with the equipment itself.
The Sepsis Puzzle: Identification, Monitoring and Early Goal Directed Therapy
 The Sepsis Puzzle: Identification, Monitoring and Early Goal Directed Therapy Cindy Goodrich RN, MS, CCRN Content Description Sepsis is caused by widespread tissue injury and systemic inflammation resulting
The Sepsis Puzzle: Identification, Monitoring and Early Goal Directed Therapy Cindy Goodrich RN, MS, CCRN Content Description Sepsis is caused by widespread tissue injury and systemic inflammation resulting
Adding IV Amiodarone to the EMS Algorithm for Cardiac Arrest Due to VF/Pulseless VT
 Adding IV Amiodarone to the EMS Algorithm for Cardiac Arrest Due to VF/Pulseless VT Introduction Before the year 2000, the traditional antiarrhythmic agents (lidocaine, bretylium, magnesium sulfate, procainamide,
Adding IV Amiodarone to the EMS Algorithm for Cardiac Arrest Due to VF/Pulseless VT Introduction Before the year 2000, the traditional antiarrhythmic agents (lidocaine, bretylium, magnesium sulfate, procainamide,
Acute heart failure may be de novo or it may be a decompensation of chronic heart failure.
 Management of Acute Left Ventricular Failure Acute left ventricular failure presents as pulmonary oedema due to increased pressure in the pulmonary capillaries. It is important to realise though that left
Management of Acute Left Ventricular Failure Acute left ventricular failure presents as pulmonary oedema due to increased pressure in the pulmonary capillaries. It is important to realise though that left
A t h e n s I n s t i t u t e o f U l t r a s o u n d 8 6 4 S u n s e t D r i v e A t h e n s G A 3 0 6 0 6
 Student Catalog 2013 A t h e n s I n s t i t u t e o f U l t r a s o u n d 8 6 4 S u n s e t D r i v e A t h e n s G A 3 0 6 0 6 Table of Contents GENERAL INFORMATION 2 Mission 2 Vision 2 Facilities 2
Student Catalog 2013 A t h e n s I n s t i t u t e o f U l t r a s o u n d 8 6 4 S u n s e t D r i v e A t h e n s G A 3 0 6 0 6 Table of Contents GENERAL INFORMATION 2 Mission 2 Vision 2 Facilities 2
Oxygen Therapy. Oxygen therapy quick guide V3 July 2012.
 PRESENTATION Oxygen (O 2 ) is a gas provided in a compressed form in a cylinder. It is also available in a liquid form. It is fed via a regulator and flow meter to the patient by means of plastic tubing
PRESENTATION Oxygen (O 2 ) is a gas provided in a compressed form in a cylinder. It is also available in a liquid form. It is fed via a regulator and flow meter to the patient by means of plastic tubing
CODE BLUE IN HOUSE (UGH!!!) We only have ONE shot at this!!!
 CODE BLUE IN HOUSE (UGH!!!) We only have ONE shot at this!!! Realities We are all nervous! What happens What should happen Room is Chaotic Everyone is yelling, screaming Strict order must be kept Only
CODE BLUE IN HOUSE (UGH!!!) We only have ONE shot at this!!! Realities We are all nervous! What happens What should happen Room is Chaotic Everyone is yelling, screaming Strict order must be kept Only
UNIVERSITA' DEGLI STUDI DI ROMA TOR VERGATA
 SYSTEMATIC PATHOLOGY I IIIYear Scientific Field DISCIPLINE TUTOR Systematic Pathology I MED/21 MED/10 Thoracic Surgery Respiratory Diseases Tommaso Claudio Mineo Paola Rogliani MED/10 Respiratory Diseases
SYSTEMATIC PATHOLOGY I IIIYear Scientific Field DISCIPLINE TUTOR Systematic Pathology I MED/21 MED/10 Thoracic Surgery Respiratory Diseases Tommaso Claudio Mineo Paola Rogliani MED/10 Respiratory Diseases
Heart Failure EXERCISES. Ⅰ. True or false questions (mark for true question, mark for false question. If it is false, correct it.
 Heart Failure EXERCISES Ⅰ. True or false questions (mark for true question, mark for false question. If it is false, correct it. ) 1. Heart rate increase is a kind of economic compensation, which should
Heart Failure EXERCISES Ⅰ. True or false questions (mark for true question, mark for false question. If it is false, correct it. ) 1. Heart rate increase is a kind of economic compensation, which should
DEBRIEFING GUIDE. The key components of an optimal code response: 1. Early recognition that the patient is deteriorating or has become unresponsive.
 DEBRIEFING GUIDE I N T R O D U C T I O N Debriefing has been shown to improve clinical behavior during cardiac resuscitation and, as such, has become a recommended procedure in the 2010 American Heart
DEBRIEFING GUIDE I N T R O D U C T I O N Debriefing has been shown to improve clinical behavior during cardiac resuscitation and, as such, has become a recommended procedure in the 2010 American Heart
Resuscitation Could this new model of CPR hold promise for better rates of neurologically intact survival?
 Cover report by Gordon A. Ewy, MD, Michael J. Kellum, MD, & Bentley J. Bobrow, MD CARDIOCEREBRAL Resuscitation Could this new model of CPR hold promise for better rates of neurologically intact survival?
Cover report by Gordon A. Ewy, MD, Michael J. Kellum, MD, & Bentley J. Bobrow, MD CARDIOCEREBRAL Resuscitation Could this new model of CPR hold promise for better rates of neurologically intact survival?
Vasopressors. Judith Hellman, M.D. Associate Professor Anesthesia and Perioperative Care University of California, San Francisco
 Vasopressors Judith Hellman, M.D. Associate Professor Anesthesia and Perioperative Care University of California, San Francisco Overview Define shock states Review drugs commonly used to treat hypotension
Vasopressors Judith Hellman, M.D. Associate Professor Anesthesia and Perioperative Care University of California, San Francisco Overview Define shock states Review drugs commonly used to treat hypotension
Australian and New Zealand College of Anaesthetists (ANZCA) Guidelines on Training and Practice of Perioperative Cardiac Ultrasound in Adults
 PS46 2014 Australian and New Zealand College of Anaesthetists (ANZCA) Guidelines on Training and Practice of Perioperative Cardiac Ultrasound in Adults 1. INTRODUCTION Ultrasound imaging of the heart is
PS46 2014 Australian and New Zealand College of Anaesthetists (ANZCA) Guidelines on Training and Practice of Perioperative Cardiac Ultrasound in Adults 1. INTRODUCTION Ultrasound imaging of the heart is
Oxygen - update April 2009 OXG
 PRESENTATION Oxygen (O 2 ) is a gas provided in compressed form in a cylinder. It is also available in liquid form, in a system adapted for ambulance use. It is fed via a regulator and flow meter to the
PRESENTATION Oxygen (O 2 ) is a gas provided in compressed form in a cylinder. It is also available in liquid form, in a system adapted for ambulance use. It is fed via a regulator and flow meter to the
New Cardiothoracic Surgery CPT Codes for 2013
 New Cardiothoracic Surgery CPT Codes for 2013 There were several changes to the cardiothoracic surgery CPT codes for 2013. There are five new codes in the general thoracic surgery section, with one revised
New Cardiothoracic Surgery CPT Codes for 2013 There were several changes to the cardiothoracic surgery CPT codes for 2013. There are five new codes in the general thoracic surgery section, with one revised
Thoracic Ultrasound. Joel P. Turner, MD, MSc, FRCP a,b,c,d, *, Jerrald Dankoff, MDCM, CSPQ e
 Thoracic Ultrasound Joel P. Turner, MD, MSc, FRCP a,b,c,d, *, Jerrald Dankoff, MDCM, CSPQ e KEYWORDS Ultrasound Thoracic Pneumothorax Pleural effusion Pneumonia Blue B-lines Pleural line Patients with
Thoracic Ultrasound Joel P. Turner, MD, MSc, FRCP a,b,c,d, *, Jerrald Dankoff, MDCM, CSPQ e KEYWORDS Ultrasound Thoracic Pneumothorax Pleural effusion Pneumonia Blue B-lines Pleural line Patients with
Ultrasound Credentialing & Curriculum for CCRMC FM Residency
 1. Purpose: Ultrasound Credentialing & Curriculum for CCRMC FM Residency To establish a credentialing process and a curriculum for an ultrasound program in the family medicine residency program at Contra
1. Purpose: Ultrasound Credentialing & Curriculum for CCRMC FM Residency To establish a credentialing process and a curriculum for an ultrasound program in the family medicine residency program at Contra
Chest Pain. Acute Myocardial Infarction: Differential Diagnosis and Patient Management. Common complaint in ED. Wide range of etiologies
 Acute Myocardial Infarction: Differential Diagnosis and Patient Management Presented By: Barbara Furry, RN-BC, MS, CCRN, FAHA Director The Center of Excellence in Education Director of HERO Chest Pain
Acute Myocardial Infarction: Differential Diagnosis and Patient Management Presented By: Barbara Furry, RN-BC, MS, CCRN, FAHA Director The Center of Excellence in Education Director of HERO Chest Pain
Bayfront. Heart Center. www.bayfrontheart.org
 Bayfront Heart Center www.bayfrontheart.org THE HEART OF THE MATTER At the Bayfront Heart Center, the leading cardiac facility in the area, we are fully equipped to treat all aspects of cardiovascular
Bayfront Heart Center www.bayfrontheart.org THE HEART OF THE MATTER At the Bayfront Heart Center, the leading cardiac facility in the area, we are fully equipped to treat all aspects of cardiovascular
Cardiac Arrest - Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008
 Cardiac Arrest - Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008 Preamble Survival from cardiorespiratory arrest for patients who present with ventricular fibrillation
Cardiac Arrest - Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008 Preamble Survival from cardiorespiratory arrest for patients who present with ventricular fibrillation
HEALTH CARE FOR EXPOSURE TO ASBESTOS. 2010 The SafetyNet Centre for Occupational Health and Safety Research Memorial University www.safetynet.mun.
 HEALTH CARE FOR PATIENTS WITH EXPOSURE TO ASBESTOS 2010 The SafetyNet Centre for Occupational Health and Safety Research Memorial University www.safetynet.mun.ca HEALTH CARE FOR PATIENTS WITH EXPOSURE
HEALTH CARE FOR PATIENTS WITH EXPOSURE TO ASBESTOS 2010 The SafetyNet Centre for Occupational Health and Safety Research Memorial University www.safetynet.mun.ca HEALTH CARE FOR PATIENTS WITH EXPOSURE
Pericardium. Pericardial Diseases. Function of Pericardium 10/1/2012
 NO LASIX, PLEASE! PERICARDIAL DISEASE IN THE DOG Pericardium Michael Luethy, DVM Diplomate ACVIM Cardiology September 13 th, 2012 Tough, outer, parietal pericardium Delicate, serous, visceral pericardium
NO LASIX, PLEASE! PERICARDIAL DISEASE IN THE DOG Pericardium Michael Luethy, DVM Diplomate ACVIM Cardiology September 13 th, 2012 Tough, outer, parietal pericardium Delicate, serous, visceral pericardium
Educational Goals & Objectives
 Educational Goals & Objectives The Cardiology rotation will provide the resident with an understanding of cardiovascular physiology and its broad systemic manifestations. The resident will have the opportunity
Educational Goals & Objectives The Cardiology rotation will provide the resident with an understanding of cardiovascular physiology and its broad systemic manifestations. The resident will have the opportunity
Survival rates for victims of traumatic cardiac arrest range
 ORIGINAL ARTICLE The heart of the matter: Utility of ultrasound of cardiac activity during traumatic arrest Elizabeth L. Cureton, MD, Louise Y. Yeung, MD, Rita O. Kwan, MD, MPH, Emily J. Miraflor, MD,
ORIGINAL ARTICLE The heart of the matter: Utility of ultrasound of cardiac activity during traumatic arrest Elizabeth L. Cureton, MD, Louise Y. Yeung, MD, Rita O. Kwan, MD, MPH, Emily J. Miraflor, MD,
Cardiopulmonary Physical Therapy. Haneul Lee, DSc, PT
 Cardiopulmonary Physical Therapy Haneul Lee, DSc, PT Airway ClearanceTechniques Breathing Exercise SpecialConsiderations for MechanicallyVentilated Exercise Injury Prevention and Equipment provision Patient
Cardiopulmonary Physical Therapy Haneul Lee, DSc, PT Airway ClearanceTechniques Breathing Exercise SpecialConsiderations for MechanicallyVentilated Exercise Injury Prevention and Equipment provision Patient
FVMA 2015: Diagnosis and Management of Pericardial Disease PERICARDIAL EFFUSION Pathophysiology of Cardiac Tamponade
 FVMA 2015: Diagnosis and Management of Pericardial Disease Jonathan A. Abbott, DVM, Dipl. ACVIM (Cardiology) VA-MD College of Veterinary Medicine Virginia Tech, Blacksburg, Virginia Pericardial disease
FVMA 2015: Diagnosis and Management of Pericardial Disease Jonathan A. Abbott, DVM, Dipl. ACVIM (Cardiology) VA-MD College of Veterinary Medicine Virginia Tech, Blacksburg, Virginia Pericardial disease
Ventilation Perfusion Relationships
 Ventilation Perfusion Relationships VENTILATION PERFUSION RATIO Ideally, each alveolus in the lungs would receive the same amount of ventilation and pulmonary capillary blood flow (perfusion). In reality,
Ventilation Perfusion Relationships VENTILATION PERFUSION RATIO Ideally, each alveolus in the lungs would receive the same amount of ventilation and pulmonary capillary blood flow (perfusion). In reality,
BASIC LIFE SUPPORT - ADULT
 BASIC LIFE SUPPORT - ADULT First Issued by/date BKW PCT May 2003 Issue Version Purpose of Issue/Description of Change 3 Policy reviewed. No changes in procedure or legislation since policy revised 12 months
BASIC LIFE SUPPORT - ADULT First Issued by/date BKW PCT May 2003 Issue Version Purpose of Issue/Description of Change 3 Policy reviewed. No changes in procedure or legislation since policy revised 12 months
Ultrasound in Vascular Surgery. Torbjørn Dahl
 Ultrasound in Vascular Surgery Torbjørn Dahl 1 The field of vascular surgery Veins dilatation and obstruction (varicose veins and valve dysfunction) Arteries dilatation and narrowing (aneurysms and atherosclerosis)
Ultrasound in Vascular Surgery Torbjørn Dahl 1 The field of vascular surgery Veins dilatation and obstruction (varicose veins and valve dysfunction) Arteries dilatation and narrowing (aneurysms and atherosclerosis)
Patient Schematic. Perkins GD et al The Lancet, 385, 2015, 947-955
 Lancet March 2015 Patient Schematic Perkins GD et al The Lancet, 385, 2015, 947-955 Background Adequate CPR is critical for survival for CA patients Maintenance of high-quality compressions during OHCA
Lancet March 2015 Patient Schematic Perkins GD et al The Lancet, 385, 2015, 947-955 Background Adequate CPR is critical for survival for CA patients Maintenance of high-quality compressions during OHCA
2015 Interim Resources for HeartCode ACLS
 2015 Interim Resources for HeartCode ACLS Original Release: November 25, 2015 Starting in 2016, new versions of American Heart Association online courses will be released to reflect the changes published
2015 Interim Resources for HeartCode ACLS Original Release: November 25, 2015 Starting in 2016, new versions of American Heart Association online courses will be released to reflect the changes published
NEEDLE THORACENTESIS Pneumothorax / Hemothorax
 NEEDLE THORACENTESIS Pneumothorax / Hemothorax By: Steven Jones, NREMT-P Pneumothorax Pneumothorax is a collection of air or gas in the pleural space of the lung, causing the lung to collapse. Pneumothorax
NEEDLE THORACENTESIS Pneumothorax / Hemothorax By: Steven Jones, NREMT-P Pneumothorax Pneumothorax is a collection of air or gas in the pleural space of the lung, causing the lung to collapse. Pneumothorax
AIUM Practice Guideline for the Performance of the Focused Assessment With Sonography for Trauma (FAST) Examination
 AIUM Practice Guideline for the Performance of the Focused Assessment With Sonography for Trauma (FAST) Examination 2007 by the American Institute of Ultrasound in Medicine The American Institute of Ultrasound
AIUM Practice Guideline for the Performance of the Focused Assessment With Sonography for Trauma (FAST) Examination 2007 by the American Institute of Ultrasound in Medicine The American Institute of Ultrasound
ARKANSAS TECH UNIVERSITY
 ARKANSAS TECH UNIVERSITY DEPARTMENT OF NURSING PRINCIPLES OF ACLS NUR 4502 MT1 Fall 2013 ARKANSAS TECH UNIVERSITY DEPARTMENT OF NURSING Course: NUR 4502 Course Title: Credit Hours: SELECTED TOPICS: SURVIVING
ARKANSAS TECH UNIVERSITY DEPARTMENT OF NURSING PRINCIPLES OF ACLS NUR 4502 MT1 Fall 2013 ARKANSAS TECH UNIVERSITY DEPARTMENT OF NURSING Course: NUR 4502 Course Title: Credit Hours: SELECTED TOPICS: SURVIVING
National Guidelines for Statewide Implementation of EMS "Do Not Resuscitate" (DNR) Programs
 National Guidelines for Statewide Implementation of EMS "Do Not Resuscitate" (DNR) Programs National Association of Emergency Medical Services Directors (NASEMSD) 1 and the National Association of Emergency
National Guidelines for Statewide Implementation of EMS "Do Not Resuscitate" (DNR) Programs National Association of Emergency Medical Services Directors (NASEMSD) 1 and the National Association of Emergency
N26 Chest Tubes 5/9/2012
 Thoracic cavity, pleural space 1 Conditions requiring chest drainage_1 Air between the pleurae is a pneumothorax Occurs when there is an opening on the surface of the lung or in the airways, y, in the
Thoracic cavity, pleural space 1 Conditions requiring chest drainage_1 Air between the pleurae is a pneumothorax Occurs when there is an opening on the surface of the lung or in the airways, y, in the
Diseases. Inflammations Non-inflammatory pleural effusions Pneumothorax Tumours
 Pleura Visceral pleura covers lungs and extends into fissures Parietal pleura limits mediastinum and covers dome of diaphragm and inner aspect of chest wall. Two layers between them (pleural cavity) contains
Pleura Visceral pleura covers lungs and extends into fissures Parietal pleura limits mediastinum and covers dome of diaphragm and inner aspect of chest wall. Two layers between them (pleural cavity) contains
Guidelines for Standards of Care for Patients with Acute Respiratory Failure on Mechanical Ventilatory Support
 Guidelines for Standards of Care for Patients with Acute Respiratory Failure on Mechanical Ventilatory Support Copyright by the SOCIETY OF CRITICAL CARE MEDICINE These guidelines can also be found in the
Guidelines for Standards of Care for Patients with Acute Respiratory Failure on Mechanical Ventilatory Support Copyright by the SOCIETY OF CRITICAL CARE MEDICINE These guidelines can also be found in the
BUNDLES IN 2013: SURVIVING SEPSIS CAMPAIGN
 BUNDLES IN 2013: SURVIVING SEPSIS CAMPAIGN R. Phillip Dellinger MD, MSc, MCCM Professor of Medicine Cooper Medical School of Rowan University Professor of Medicine University Medicine and Dentistry of
BUNDLES IN 2013: SURVIVING SEPSIS CAMPAIGN R. Phillip Dellinger MD, MSc, MCCM Professor of Medicine Cooper Medical School of Rowan University Professor of Medicine University Medicine and Dentistry of
SPONTANEOUS PNEUMOTHORAX AS A COMPLICATION OF SEPTIC PULMONARY EMBOLISM IN AN INTRAVENOUS DRUG USER: A CASE REPORT
 Spontaneous pneumothorax in an IV drug user SPONTANEOUS PNEUMOTHORAX AS A COMPLICATION OF SEPTIC PULMONARY EMBOLISM IN AN INTRAVENOUS DRUG USER: A CASE REPORT Chau-Chyun Sheu, Jhi-Jhu Hwang, Jong-Rung
Spontaneous pneumothorax in an IV drug user SPONTANEOUS PNEUMOTHORAX AS A COMPLICATION OF SEPTIC PULMONARY EMBOLISM IN AN INTRAVENOUS DRUG USER: A CASE REPORT Chau-Chyun Sheu, Jhi-Jhu Hwang, Jong-Rung
UW MEDICINE PATIENT EDUCATION. Aortic Stenosis. What is heart valve disease? What is aortic stenosis?
 UW MEDICINE PATIENT EDUCATION Aortic Stenosis Causes, symptoms, diagnosis, and treatment This handout describes aortic stenosis, a narrowing of the aortic valve in your heart. It also explains how this
UW MEDICINE PATIENT EDUCATION Aortic Stenosis Causes, symptoms, diagnosis, and treatment This handout describes aortic stenosis, a narrowing of the aortic valve in your heart. It also explains how this
404 Section 5 Shock and Resuscitation. Scene Size-up. Primary Assessment. History Taking
 404 Section 5 and Resuscitation Scene Size-up Scene Safety Mechanism of Injury (MOI)/ Nature of Illness (NOI) Ensure scene safety and address hazards. Standard precautions should include a minimum of gloves
404 Section 5 and Resuscitation Scene Size-up Scene Safety Mechanism of Injury (MOI)/ Nature of Illness (NOI) Ensure scene safety and address hazards. Standard precautions should include a minimum of gloves
Medicare C/D Medical Coverage Policy
 Medicare C/D Medical Coverage Policy Oxygen and Oxygen Supplements Origination: April 10, 1992 Review Date: July 15, 2015 Next Review: July, 2017 DESCRIPTION OF PROCEDURE OR SERVICE USP Oxygen is a gaseous
Medicare C/D Medical Coverage Policy Oxygen and Oxygen Supplements Origination: April 10, 1992 Review Date: July 15, 2015 Next Review: July, 2017 DESCRIPTION OF PROCEDURE OR SERVICE USP Oxygen is a gaseous
How you can help save lives
 How you can help save lives Through Life Support Training Courses with THE INTERNATIONAL LIFE SUPPORT TRAINING CENTER (ILSTC) TABLE OF CONTENTS Introduction Page 3 Basic Life Support for Healthcare Provider
How you can help save lives Through Life Support Training Courses with THE INTERNATIONAL LIFE SUPPORT TRAINING CENTER (ILSTC) TABLE OF CONTENTS Introduction Page 3 Basic Life Support for Healthcare Provider
Respiratory Care. A Life and Breath Career for You!
 Respiratory Care A Life and Breath Career for You! Respiratory Care Makes a Difference At 9:32 am, Lori Moreno brought a newborn baby struggling to breathe back to life What have you accomplished today?
Respiratory Care A Life and Breath Career for You! Respiratory Care Makes a Difference At 9:32 am, Lori Moreno brought a newborn baby struggling to breathe back to life What have you accomplished today?
Lung Sonography. Giovanni Volpicelli, MD, FCCP
 REVIEW ARTICLE Lung Sonography Giovanni Volpicelli, MD, FCCP Article includes CME test Videos online at www.jultrasoundmed.org Lung sonography represents an emerging and useful technique in the management
REVIEW ARTICLE Lung Sonography Giovanni Volpicelli, MD, FCCP Article includes CME test Videos online at www.jultrasoundmed.org Lung sonography represents an emerging and useful technique in the management
Ultrasound Billing CPT Codes Summary and Notes
 Ultrasound Billing CPT Codes Summary and Notes CPT codes for ultrasound examinations are considered to be complete studies unless specified as limited studies in their code definitions. A limited study
Ultrasound Billing CPT Codes Summary and Notes CPT codes for ultrasound examinations are considered to be complete studies unless specified as limited studies in their code definitions. A limited study
ACLS PRE-TEST ANNOTATED ANSWER KEY
 ACLS PRE-TEST ANNOTATED ANSWER KEY June, 2011 Question 1: Question 2: There is no pulse with this rhythm. Question 3: Question 4: Question 5: Question 6: Question 7: Question 8: Question 9: Question 10:
ACLS PRE-TEST ANNOTATED ANSWER KEY June, 2011 Question 1: Question 2: There is no pulse with this rhythm. Question 3: Question 4: Question 5: Question 6: Question 7: Question 8: Question 9: Question 10:
Heart of America Medical Center EMR, EMT, EMT-Intermediate & AEMT Protocols
 USE OF THE LUCAS DEVICE TO PROVIDE EXTERNAL CHEST COMPRESSIONS IN PATIENTS SUFFERING CARDIAC ARREST Purpose This procedure describes the appropriate methods to apply, operate, and discontinue the LUCAS
USE OF THE LUCAS DEVICE TO PROVIDE EXTERNAL CHEST COMPRESSIONS IN PATIENTS SUFFERING CARDIAC ARREST Purpose This procedure describes the appropriate methods to apply, operate, and discontinue the LUCAS
School of Diagnostic Medical Sonography
 Semester 1 Orientation - 101 This class is an introduction to sonography which includes a basic anatomy review, introduction to sonographic scanning techniques and physical principles. This curriculum
Semester 1 Orientation - 101 This class is an introduction to sonography which includes a basic anatomy review, introduction to sonographic scanning techniques and physical principles. This curriculum
