Issue date: December Quick reference guide
|
|
|
- Adela Johnston
- 7 years ago
- Views:
Transcription
1 Issue date: December 2004 Quick reference guide Anxiety: management of anxiety (panic disorder, with or without agoraphobia, and generalised anxiety disorder) in adults in primary, secondary and community care Clinical Guideline 22 Developed by the National Collaborating Centre for Primary Care
2 Key messages about anxiety disorders Key messages about anxiety disorders Anxiety disorders are common chronic the cause of considerable distress and disability often unrecognised and untreated. If left untreated, they are costly to both the individual and society. A range of effective interventions is available to treat anxiety disorders, including medication, psychological therapies and self-help. Individuals do get better and remain better. Involving individuals in an effective partnership with healthcare professionals, with all decisionmaking being shared, improves outcomes. Access to information, including support groups, is a valuable part of any package of care. Clinical Guideline 22 Anxiety: management of anxiety (panic disorder, with or without agoraphobia, and generalised anxiety disorder) in adults in primary, secondary and community care Issue date: December 2004 This guidance is written in the following context: This guidance represents the view of the Institute, which was arrived at after careful consideration of the evidence available. Health professionals are expected to take it fully into account when exercising their clinical judgement. The guidance does not, however, override the individual responsibility of health professionals to make decisions appropriate to the circumstances of the individual patient, in consultation with the patient and/or guardian or carer. National Institute for Clinical Excellence MidCity Place 71 High Holborn London WC1V 6NA ISBN: Published by the National Institute for Clinical Excellence December 2004 Artwork by LIMA Graphics Ltd, Frimley, Surrey Printed by Abba Litho Sales Limited, London National Institute for Clinical Excellence, December All rights reserved. This material may be freely reproduced for educational and not-for-profit purposes within the NHS. reproduction by or for commercial organisations is allowed without the express written permission of the National Institute for Clinical Excellence. 2 NICE Guideline: quick reference guide anxiety
3 Which NICE guideline? What are the patient s symptoms? Low mood or loss of interest, usually accompanied by one or more of the following: low energy, changes in appetite, weight or sleep pattern, poor concentration, feelings of guilt or worthlessness and suicidal ideas? Enter NICE clinical guideline on depression ( CG023) Which NICE guideline? Apprehension, cued panic attacks, spontaneous panic attacks, irritability, poor sleeping, avoidance, poor concentration? Enter anxiety guideline (this guideline) Intermittent episodes of panic or anxiety, and taking avoiding action to prevent these feelings? Episodes of anxiety triggered by external stimuli? Panic disorder with or without agoraphobia (go to Step 1) Agoraphobia, social phobia or simple phobia (not covered by this guideline) Over-arousal, irritability, poor concentration, poor sleeping and worry about several areas most of the time? Generalised anxiety disorder (go to Step 1) Stepped approaches to care The guideline provides recommendations for care at different stages of the patient journey, represented as different steps: Panic Generalised disorder anxiety disorder See page: See page: Step 1: Recognition and diagnosis 5 5 Step 2: Treatment in primary care Step 3: Review and consideration of alternative treatments Step 4: Review and referral to specialist mental health services Step 5: Care in specialist mental health services NICE Guideline: quick reference guide anxiety 3
4 Key priorities for implementation Key priorities for implementation General management Shared decision-making between the individual and healthcare professionals should take place during the process of diagnosis and in all phases of care. Patients, and where appropriate, families and carers should be provided with information on the nature, course and treatment of panic disorder or generalised anxiety disorder, including information on the use and likely side-effect profile of medication. Patients, families and carers should be informed of self-help groups and support groups and be encouraged to participate in such programmes where appropriate. All patients prescribed antidepressants should be informed that, although the drugs are not associated with tolerance and craving, discontinuation/withdrawal symptoms may occur on stopping or missing doses or, occasionally, on reducing the dose of the drug. These symptoms are usually mild and self-limiting but occasionally can be severe, particularly if the drug is stopped abruptly. Step 1: Recognition and diagnosis of panic disorder and generalised anxiety disorder The diagnostic process should elicit necessary relevant information such as personal history, any self-medication, and cultural or other individual characteristics that may be important considerations in subsequent care. (See also Which NICE guideline?, page 3.) Step 2: Offer treatment in primary care There are positive advantages of services based in primary care practice (for example, lower dropout rates) and these services are often preferred by patients. The treatment of choice should be available promptly. Panic disorder Benzodiazepines are associated with a less good outcome in the long term and should not be prescribed for the treatment of individuals with panic disorder. Any of the following types of intervention should be offered and the preference of the person should be taken into account. The interventions that have evidence for the longest duration of effect, in descending order, are: (a) psychological therapy (cognitive behavioural therapy [CBT]); (b) pharmacological therapy (a selective serotonin reuptake inhibitor [SSRI] licensed for panic disorder; or if an SSRI is unsuitable or there is no improvement, imipramine a or clomipramine a may be considered); (c) self-help (bibliotherapy the use of written material to help people understand their psychological problems and learn ways to overcome them by changing their behaviour based on CBT principles). Generalised anxiety disorder Benzodiazepines should not usually be used beyond 2 4 weeks. In the longer-term care of individuals with generalised anxiety disorder, any of the following types of intervention should be offered and the preference of the person with generalised anxiety disorder should be taken into account. The interventions that have evidence for the longest duration of effect, in descending order, are: (a) psychological therapy (CBT); (b) pharmacological therapy (an SSRI); (c) self-help (bibliotherapy based on CBT principles). Step 3: Review and offer alternative treatment If one type of intervention does not work, the patient should be reassessed and consideration given to trying one of the other types of intervention. Step 4: Review and offer referral from primary care In most instances, if there have been two interventions provided (any combination of psychological therapy, medication or bibliotherapy) and the person still has significant symptoms, then referral to specialist mental health services should be offered. Step 5: Care in specialist mental health services Specialist mental health services should conduct a thorough, holistic, reassessment of the individual, their environment and their social circumstances. Short, self-complete questionnaires (such as the panic subscale of the agoraphobic mobility inventory for individuals with panic disorder) should be used to monitor outcomes wherever possible. a Imipramine and clomipramine are not licensed for panic disorder but have been shown to be effective in its management. 4 NICE Guideline: quick reference guide anxiety
5 For details of recommendation grading, see page 11. General principles of care all steps Shared decision-making and information provision Shared decision-making between the individual and healthcare professionals should take place during diagnosis and all phases of care. D To facilitate shared decision-making: provide evidence-based information about treatments D provide information on the nature, course and treatment of panic disorder or generalised anxiety disorder, including the use and likely side-effect profile of medication D discuss concerns about taking medication, such as fears of addiction D consider patient preference and experience and outcome of previous treatments D offer information about self-help groups and support groups for patients, families and carers encourage participation in self-help and support groups. D D General principles of care all steps Language Use everyday, jargon-free language, and explain any technical terms. D Where appropriate, provide written material in the language of the patient, and seek interpreters for people whose first language is not English. D Where available, consider providing psychotherapies in the patient s own language if this is not English. D Step 1: Recognition and diagnosis of panic disorder and generalised anxiety disorder Consultation skills A high standard of consultation skills is needed so that a structured approach can be taken to the diagnosis and management plan a. D Diagnosis Ask about relevant information such as personal history, any self-medication, and cultural or other individual characteristics that may be important considerations in subsequent care. D Comorbidities Be alert to comorbidity, which is common (particularly anxiety with depression and anxiety with substance abuse). D Identify the main problem(s) through discussion with the patient. D Clarify the sequence of the problems to determine the priorities of the comorbidities drawing up a timeline to show when different problems developed can help with this. D If the patient has depression or anxiety with depression, follow the NICE guideline on management of depression (Clinical Guideline 23, see D Presentation in A&E or other settings with a panic attack If a patient presents with a panic attack, he or she should: D be asked if they are already receiving treatment for panic disorder undergo the minimum investigations necessary to exclude acute physical problems not usually be admitted to a medical or psychiatric bed be referred to primary care for subsequent care, even if assessment has been undertaken in A&E be given appropriate written information about panic attacks and why they are being referred to primary care be offered appropriate written information about sources of support, including local and national voluntary and self-help groups. a The standards detailed in the video workbook Summative Assessment For General Practice Training: Assessment Of Consulting Skills the MRCGP/Summative Assessment Single Route (see NICE Guideline: quick reference guide anxiety 5 Step 1: Recognition and diagnosis of panic disorder and generalised anxiety disorder
6 Management of panic disorder in primary care: Steps 2 4 Management of panic disorder in primary care: S Psychological therapy CBT should be used A It should be delivered by trained and supervised people, closely adhering to empirically grounded treatment protocols A For most people, CBT should be in weekly sessions of 1 2 hours and be completed within 4 months B The optimal range is 7 14 hours in total A If offering briefer CBT, it should be about 7 hours, should be designed to integrate with structured self-help materials, D and should be supplemented with appropriate focused information and tasks A Sometimes, more intensive CBT over a very short period might be appropriate C Pharmacological therapy Before prescribing, consider: age D previous treatment response D risks of deliberate self-harm or accidental overdose D tolerability D the patient s preference D cost, where equal effectiveness D Step 2: Offer treatmen Following discussion with patient and taking acc listed in descending order of evidence for the lo psychological therapy A or pharmacological therapy A or self-help A The chosen treatment option should be available When prescribing Offer an SSRI licensed for panic If an SSRI is not suitable or ther appropriate, consider imipramin Inform patients, at the time tre potential side effects (includ possible discontinuation/wit delay in onset of effect D time course of treatment D need to take medication as medication in order to avoid Written information appropriat Side effects on initiation may be satisfactory therapeutic respons Long-term treatment and doses Benzodiazepines, A sedating treatment of panic disorder a Imipramine and clomipramine are n effective in its management Assess progress according to process within the practice determine the nature of the process on a case-by-case basis Use short, self-complete questionnaires to monitor outcomes wherever possible D Review efficacy and side effects within 2 weeks o 12 weeks D Review at 8 12 week intervals if drug used for m Follow Summary of Product Characteristics for all Use short, self-complete questionnaires to monito Is there improvement after a course of treatment? Has there been an improvement after 12 weeks of treatment? Ye If appropriate, continue care and monitoring Step 3: Review Reassess the patient and consider trying another intervention D Is this at least the second intervention tried? Y If appropriate 6 NICE Guideline: quick reference guide anxiety (Management of panic disorder: Steps 2 4)
7 teps 2 4 t in primary care ount of patient preference, offer (interventions ngest duration of effect): promptly D disorder, unless otherwise indicated A e is no improvement after a 12-week course, and if further medication is e a or clomipramine a A atment is initiated, about: ing transient increase in anxiety at the start of treatment) C hdrawal symptoms (see box on page 10) C prescribed (this may be particularly important with short half-life discontinuation/withdrawal symptoms) C e for the patient s needs should be made available. D minimised by starting at a low dose and slowly increasing the dose until a e is achieved D at the upper end of the indicated dose range may be necessary B antihistamines or antipsychotics D should not be prescribed for the ot licensed for the treatment of panic disorder but have been shown to be f starting treatment and again at 4, 6 and ore than 12 weeks D other monitoring required D r outcomes wherever possible D Self-help Offer bibliotherapy based on CBT principles A Offer information about support groups, where available D Discuss the benefits of exercise as part of good general health B Computerised cognitive behaviour therapy may be of value, but a NICE technology appraisal b found the evidence was an insufficient basis on which to recommend its general introduction into the NHS N b See Offer contact with primary healthcare professionals to monitor progress and review; determine on a case-by-case basis but likely to be every 4 8 weeks D Use short, self-complete questionnaires to monitor outcomes wherever possible D Management of panic disorder in primary care: Steps 2 4 continued Ongoing management s Use with appropriate monitoring for 6 months after optimal dose reached: then dose can be tapered D When stopping, reduce the dose gradually over an extended period C If appropriate, continue care and monitoring Is there improvement after a course of treatment? If appropriate, continue care and monitoring es Step 4: Review and offer referral to specialist mental health services (see page 10) If appropriate and the person still has significant symptoms D NICE Guideline: quick reference guide anxiety (Management of panic disorder: Steps 2 4) 7
8 Management of generalised anxiety disorder in primary care: Steps 2 4 Step 2: Offer treatment in primary care Consider offering: support and information D problem solving C benzodiazepines A do not use for more than 2 4 weeks sedative antihistamines A self-help D Psychological therapy CBT should be used A It should be delivered by trained and supervised people, closely adhering to empirically grounded treatment protocols A For most people, CBT should be in weekly sessions of 1 2 hours and be completed within 4 months B The optimal range is hours in total A If offering briefer CBT, it should be about 8 10 hours, should be designed to integrate with structured self-help materials, D and should be supplemented with appropriate focused information and tasks A Assess progress according to process within the practice determine the nature of the process on a case-by-case basis Use short, self-complete questionnaires to monitor outcomes wherever possible D Management of genera Pharmacological therapy Before prescribing, consider: age D previous treatment response D risks of deliberate self-harm or accidental overdose D tolerability D the patient s preference D cost, where equal effectiveness D Is immediate management necessary? Following discussion with patient and taking acc listed in descending order of evidence for the lo psychological therapy A or pharmacological therapy A or self-help A The chosen treatment option should be available When prescribing Offer an SSRI, unless otherwise indic If one SSRI is not suitable or there is is appropriate, another SSRI should b Inform patients, at the time treatme potential side effects (including t possible discontinuation/withdraw delay in onset of effect D time course of treatment D need to take medication as presc medication in order to avoid disc Written information appropriate for Side effects on initiation may be min a satisfactory therapeutic response is Long-term treatment and doses at th a Paroxetine has a licence for the treatmen Review efficacy and side effects within 2 weeks o 12 weeks D Review at 8 12 week intervals if drug used for m Follow Summary of Product Characteristics for all Use short, self-complete questionnaires to monito Is there improvement after a course of treatment? Has there been an improvement after 12 weeks of treatment? Ye If appropriate, continue care and monitoring Step 3: Review Reassess the patient and consider trying another intervention D Is this at least the second intervention tried? Y If appropriate 8 NICE Guideline: quick reference guide anxiety (Management of GAD in primary care: Steps 2 4)
9 lised anxiety disorder in primary care: Steps 2 4 ount of patient preference, offer interventions ngest duration of effect: promptly D ated a B no improvement after a 12-week course, and if a further medication e offered D nt is initiated, about: ransient increase in anxiety at the start of treatment) C al symptoms (see box on page 10) C ribed (this may be particularly important with short half-life ontinuation/withdrawal symptoms) C the patient s needs should be made available D imised by starting at a low dose and slowly increasing the dose until achieved D e upper end of the indicated dose range may be necessary B t of generalised anxiety disorder s f starting treatment and again at 4, 6 and ore than 12 weeks D other monitoring required D r outcomes wherever possible D Ongoing management Use with appropriate monitoring for 6 months after optimal dose reached: then dose can be tapered D When stopping, reduce the dose gradually over an extended period C If appropriate, continue care and monitoring Self-help Offer bibliotherapy based on CBT principles A Consider large-group CBT C Offer information about support groups, where available D Discuss the benefits of exercise as part of good general health B Computerised cognitive behaviour therapy may be of value, but a NICE technology appraisal b found the evidence was an insufficient basis on which to recommend its general introduction into the NHS N b See Offer contact with primary healthcare professionals to monitor progress and review; determine on a case-by-case basis but likely to be every 4 8 weeks D Use short, self-complete questionnaires to monitor outcomes wherever possible D Is there improvement after a course of treatment? Management of generalised anxiety disorder in primary care: Steps 2 4 continued es Step 4: Review and offer referral to specialist mental health services (see page 10) If appropriate and the person still has significant symptoms D If venlafaxine is being considered Venlafaxine treatment should: only be initiated by specialist mental health medical practitioners including General Practitioners with a Special Interest in Mental Health ; D only be managed under the supervision of specialist mental health medical practitioners including General Practitioners with a Special Interest in Mental Health D Before prescribing venlafaxine an initial ECG and blood pressure measurement should be undertaken. There should be regular monitoring of blood pressure, and monitoring of cardiac status as clinically appropriate. D The dose of venlafaxine should be no higher than 75 mg per day. A If appropriate, continue care and monitoring NICE Guideline: quick reference guide anxiety (Management of GAD in primary care: Steps 2 4) 9
10 Step 5: Care for people with panic disorder and GAD in specialist mental health services Step 5: Care for people with panic disorder and generalised anxiety disorder in specialist mental health services Reassess the patient, their environment and their social circumstances. Evaluate: previous treatments, including effectiveness and concordance D any substance use, including nicotine, alcohol, caffeine and recreational drugs D comorbidities D day-to-day functioning D social networks D continuing chronic stressors D the role of agoraphobic and other avoidant symptoms. D Undertake a comprehensive risk assessment. D Develop an appropriate risk management plan. D To carry out these evaluations, and to develop and share a full formulation, more than one session may be required and should be available. D Consider: treatment of comorbid conditions D CBT with an experienced therapist if not offered already, including home-based CBT if attendance at clinic is difficult D structured problem solving D full exploration of pharmaco-therapy D day support to relieve carers and family members D referral for advice, assessment or management to tertiary centres. D Ensure accurate and effective communication between all healthcare professionals particularly between primary care clinicians (GP and teams) and secondary care clinicians (community mental health teams) if there are existing physical health conditions that also require active management. D Antidepressant discontinuation/ withdrawal symptoms Antidepressant discontinuation/withdrawal symptoms Inform patients that: although antidepressants are not associated with tolerance and craving, discontinuation/withdrawal symptoms may occur on stopping or missing doses or, occasionally, on reducing the dose of the drug. These symptoms are usually mild and self-limiting but occasionally can be severe, particularly if the drug is stopped abruptly C the most commonly experienced discontinuation/withdrawal symptoms are dizziness, numbness and tingling, gastrointestinal disturbances (particularly nausea and vomiting), headache, sweating, anxiety and sleep disturbances D they should seek advice from their medical practitioner if they experience significant discontinuation/withdrawal symptoms. D Stopping antidepressants abruptly can cause discontinuation/withdrawal symptoms. To minimise the risk of discontinuation/withdrawal symptoms when stopping antidepressants, the dose should be reduced gradually over an extended period of time. C Mild discontinuation/withdrawal symptoms: reassure the patient and monitor symptoms. D Severe discontinuation/withdrawal symptoms: consider reintroducing the antidepressant (or prescribing another from the same class that has a longer half-life) and gradually reducing the dose while monitoring symptoms. D 10 NICE Guideline: quick reference guide anxiety
11 Grading of the recommendations The recommendations on pages 5 10 are evidence-based. The grading system used is shown below. Further information on the grading of the recommendations and the evidence used to develop the guideline is presented in the full guideline (see the back cover for details). A B C D N Based on category I evidence (meta-analysis of randomised controlled trials [RCTs] or at least one RCT) Directly based on category II evidence (at least one controlled study without randomisation or at least one other quasi-experimental study) or extrapolated from category I evidence Directly based on category III evidence (non-experimental descriptive studies) or extrapolated from category I or II evidence Directly based on category IV evidence (expert committee reports or opinions and/or clinical experience of respected authorities) or extrapolated from category I, II or III evidence Evidence from NICE technology appraisal guidance See the NICE guideline for further information ( Implementation Local health communities should review their existing practice for the care of individuals with panic disorder or generalised anxiety disorder against this guideline. The review should consider the resources required to implement the recommendations set out in Section 1 of the NICE guideline ( the people and processes involved and the timeline over which full implementation is envisaged. It is in the interests of patients that the implementation timeline is as rapid as possible. Relevant local clinical guidelines and protocols should be reviewed in the light of this guidance and revised accordingly. The implementation of this guideline will build on the National Service Frameworks for Mental Health in England and Wales and should form part of the service development plans for each local health community in England and Wales. The National Service Frameworks are available for England from HealthAndSocialCareTopics/MentalHealth/fs/en, and for Wales from The National Institute for Mental Health in England (NIMHE), which is part of the NHS Modernisation Agency, is able to support the implementation of NICE guidelines through its regional development centres. More details can be found at The introduction of the new general medical services (GMS) contract for primary care on 1 April 2004 provides a further opportunity to implement these guidelines. A draft quality and outcome framework is provided in the NICE guideline ( Suggested audit criteria are listed in Appendix D of the NICE guideline. These can be used as the basis for local clinical audit, at the discretion of those in practice. Implementation/grading of the recommendations NICE Guideline: quick reference guide anxiety 11
12 Further information Distribution The distribution list for this quick reference guide is available from NICE guideline The NICE guideline, Anxiety: management of anxiety (panic disorder, with or without agoraphobia, and generalised anxiety disorder) in adults in primary, secondary and community care, is available from the NICE website ( The NICE guideline contains the following sections: Key priorities for implementation; 1 Guidance; 2 tes on the scope of the guidance; 3 Implementation in the NHS; 4 Key research recommendations; 5 Other versions of this guideline; 6 Related NICE guidance; 7 Review date. It also gives details of the grading scheme for the evidence and recommendations, the Guideline Development Group, the Guideline Review Panel and technical detail on the criteria for audit. Information for the public NICE has produced a version of this guidance for people with people with panic disorder or generalised anxiety disorder, their carers and the public. The information is available, in English and Welsh, from the NICE website ( Printed versions are also available see below for ordering information. Full guideline The full guideline includes the evidence on which the recommendations are based, in addition to information in the NICE guideline. It is published by the National Collaborating Centre for Primary Care. It is available from from and on the website of the National Electronic Library for Health ( Related guidance For information about NICE guidance that has been issued or is in development, see the website ( Guidance on the use of computerised cognitive behavioural therapy for anxiety and depression. NICE Technology Appraisal Guidance. 51 (2002). Available from Depression: management of depression in primary and secondary care. NICE Clinical Guideline. 23 (2004). Available from NICE is in the process of developing clinical guidelines on the following: the management of post-traumatic stress disorder in adults and children in primary, secondary and community care (publication expected March 2005) core interventions in the treatment of obsessive compulsive disorder and body dysmorphic disorder (publication expected September 2005). Review date The process of reviewing the evidence is expected to begin 4 years after the date of issue of this guideline. Reviewing may begin earlier than 4 years if significant evidence that affects the guideline recommendations is identified sooner. The updated guideline will be available within 2 years of the start of the review process. Ordering information Copies of this quick reference guide can be obtained from the NICE website at or from the NHS Response Line by telephoning and quoting reference number N0763. Information for the public is also available from the NICE website or from the NHS Response Line (quote reference number N0764 for a version in English and N0765 for a version in English and Welsh). N0763 1P 80k Dec 04 (ABA) National Institute for Clinical Excellence MidCity Place 71 High Holborn London WC1V 6NA
Anxiety Care Pathway Panic Disorder and Generalised Anxiety Disorder
 Anxiety Care Pathway Panic Disorder and Generalised Anxiety Disorder December 2009 Instructions: Throughout this pathway if you click on the Bookmarks tab to the left of the screen and then click on the
Anxiety Care Pathway Panic Disorder and Generalised Anxiety Disorder December 2009 Instructions: Throughout this pathway if you click on the Bookmarks tab to the left of the screen and then click on the
Depression: management of depression in primary and secondary care
 Issue date: December 2004 Quick reference guide Depression: management of depression in primary and secondary care Clinical Guideline 23 Developed by the National Collaborating Centre for Mental Health
Issue date: December 2004 Quick reference guide Depression: management of depression in primary and secondary care Clinical Guideline 23 Developed by the National Collaborating Centre for Mental Health
Post-traumatic stress disorder (PTSD): the treatment of PTSD in adults and children
 Post-traumatic stress disorder (PTSD): the treatment of PTSD in adults and children Understanding NICE guidance information for people with PTSD, their advocates and carers, and the public March 2005 Information
Post-traumatic stress disorder (PTSD): the treatment of PTSD in adults and children Understanding NICE guidance information for people with PTSD, their advocates and carers, and the public March 2005 Information
Amendments to recommendations concerning venlafaxine
 Amendments to recommendations concerning venlafaxine On 31 May 2006 the MHRA issued revised prescribing advice for venlafaxine*. This amendment brings the guideline into line with the new advice but does
Amendments to recommendations concerning venlafaxine On 31 May 2006 the MHRA issued revised prescribing advice for venlafaxine*. This amendment brings the guideline into line with the new advice but does
Clinical guideline Published: 29 November 2005 nice.org.uk/guidance/cg31
 Obsessive-compulsive e disorder and body dysmorphic disorder: treatment Clinical guideline Published: 29 November 2005 nice.org.uk/guidance/cg31 NICE 2005. All rights reserved. Contents Introduction...
Obsessive-compulsive e disorder and body dysmorphic disorder: treatment Clinical guideline Published: 29 November 2005 nice.org.uk/guidance/cg31 NICE 2005. All rights reserved. Contents Introduction...
NICE Clinical guideline 23
 NICE Clinical guideline 23 Depression Management of depression in primary and secondary care Consultation on amendments to recommendations concerning venlafaxine On 31 May 2006 the MHRA issued revised
NICE Clinical guideline 23 Depression Management of depression in primary and secondary care Consultation on amendments to recommendations concerning venlafaxine On 31 May 2006 the MHRA issued revised
`çããçå=jéåí~ä= aáëçêçéêëw=^åñáéíó=~åç= aééêéëëáçå. aêk=`=f=lâçåü~ jéçáå~ä=aáêéåíçê lñäé~ë=kep=cçìåç~íáçå=qêìëí=
 `çããçå=jéåí~ä= aáëçêçéêëw=^åñáéíó=~åç= aééêéëëáçå aêk=`=f=lâçåü~ jéçáå~ä=aáêéåíçê lñäé~ë=kep=cçìåç~íáçå=qêìëí= Overview: Common Mental What are they? Disorders Why are they important? How do they affect
`çããçå=jéåí~ä= aáëçêçéêëw=^åñáéíó=~åç= aééêéëëáçå aêk=`=f=lâçåü~ jéçáå~ä=aáêéåíçê lñäé~ë=kep=cçìåç~íáçå=qêìëí= Overview: Common Mental What are they? Disorders Why are they important? How do they affect
Borderline personality disorder
 Issue date: January 2009 Borderline personality disorder Borderline personality disorder: treatment and management NICE clinical guideline 78 Developed by the National Collaborating Centre for Mental Health
Issue date: January 2009 Borderline personality disorder Borderline personality disorder: treatment and management NICE clinical guideline 78 Developed by the National Collaborating Centre for Mental Health
Borderline personality disorder
 Understanding NICE guidance Information for people who use NHS services Borderline personality disorder NICE clinical guidelines advise the NHS on caring for people with specific conditions or diseases
Understanding NICE guidance Information for people who use NHS services Borderline personality disorder NICE clinical guidelines advise the NHS on caring for people with specific conditions or diseases
Depression in children and young people. Quick reference guide. Issue date: September 2005
 Quick reference guide Issue date: September 2005 Depression in children and young people Identification and management in primary, community and secondary care Clinical Guideline 28 Developed by the National
Quick reference guide Issue date: September 2005 Depression in children and young people Identification and management in primary, community and secondary care Clinical Guideline 28 Developed by the National
Post-traumatic stress disorder overview
 Post-traumatic stress disorder overview A NICE pathway brings together all NICE guidance, quality standards and materials to support implementation on a specific topic area. The pathways are interactive
Post-traumatic stress disorder overview A NICE pathway brings together all NICE guidance, quality standards and materials to support implementation on a specific topic area. The pathways are interactive
Clinical guideline Published: 28 January 2009 nice.org.uk/guidance/cg78
 Borderline personality disorder: recognition and management Clinical guideline Published: 28 January 2009 nice.org.uk/guidance/cg78 NICE 2009. All rights reserved. Your responsibility The recommendations
Borderline personality disorder: recognition and management Clinical guideline Published: 28 January 2009 nice.org.uk/guidance/cg78 NICE 2009. All rights reserved. Your responsibility The recommendations
NICE Pathways bring together all NICE guidance, quality standards and other NICE information on a specific topic.
 bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published.
bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published.
Common mental health disorders
 Issue date: May 2011 Common mental health disorders Identification and pathways to care NICE clinical guideline 123 Developed by the National Collaborating Centre for Mental Health NICE clinical guideline
Issue date: May 2011 Common mental health disorders Identification and pathways to care NICE clinical guideline 123 Developed by the National Collaborating Centre for Mental Health NICE clinical guideline
Generalised anxiety disorder in adults
 www.bpac.org.nz keyword: anxiety Generalised anxiety disorder in adults diagnosis and management Key concepts: Anxiety disorders are the most frequently seen mental disorders in primary care Generalised
www.bpac.org.nz keyword: anxiety Generalised anxiety disorder in adults diagnosis and management Key concepts: Anxiety disorders are the most frequently seen mental disorders in primary care Generalised
and body dysmorphic disorder (BDD) in adults, children and young people Issue date: November 2005
 Issue date: November 2005 Treating obsessivecompulsive disorder (OCD) and body dysmorphic disorder (BDD) in adults, children and young people Understanding NICE guidance information for people with OCD
Issue date: November 2005 Treating obsessivecompulsive disorder (OCD) and body dysmorphic disorder (BDD) in adults, children and young people Understanding NICE guidance information for people with OCD
Borderline personality disorder
 Borderline personality disorder Treatment and management Issued: January 2009 NICE clinical guideline 78 guidance.nice.org.uk/cg78 NICE 2009 Contents Introduction... 3 Person-centred care... 5 Key priorities
Borderline personality disorder Treatment and management Issued: January 2009 NICE clinical guideline 78 guidance.nice.org.uk/cg78 NICE 2009 Contents Introduction... 3 Person-centred care... 5 Key priorities
Depression Pathway. Patient Education Box 4. Guided self help Box 18. pg 11
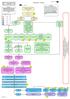 LCFT localised Map pathway June 2009 Depression Pathway Instructions: Throughout this pathway if you click on the Bookmarks tab to the left of the screen and then click on the various documents you will
LCFT localised Map pathway June 2009 Depression Pathway Instructions: Throughout this pathway if you click on the Bookmarks tab to the left of the screen and then click on the various documents you will
Step 4: Complex and severe depression in adults
 Step 4: Complex and severe depression in adults A NICE pathway brings together all NICE guidance, quality standards and materials to support implementation on a specific topic area. The pathways are interactive
Step 4: Complex and severe depression in adults A NICE pathway brings together all NICE guidance, quality standards and materials to support implementation on a specific topic area. The pathways are interactive
Rehabilitation after critical illness
 Quick reference guide Issue date: March 2009 Rehabilitation after critical illness NICE clinical guideline 83 Developed by the Centre for Clinical Practice at NICE Patient-centred care This is a quick
Quick reference guide Issue date: March 2009 Rehabilitation after critical illness NICE clinical guideline 83 Developed by the Centre for Clinical Practice at NICE Patient-centred care This is a quick
Sunderland Psychological Wellbeing Service
 Sunderland Psychological Wellbeing Service Information for Referrers Offering a range of psychological therapies across Sunderland. To make a referral call 0191 566 5454 A partnership between Northumberland,
Sunderland Psychological Wellbeing Service Information for Referrers Offering a range of psychological therapies across Sunderland. To make a referral call 0191 566 5454 A partnership between Northumberland,
Costing statement: Generalised anxiety disorder and panic disorder (with or without agoraphobia) in adults
 Costing statement: Generalised anxiety disorder and panic disorder (with or without agoraphobia) in adults Introduction The partial update of the guideline on Generalised anxiety disorder and panic disorder
Costing statement: Generalised anxiety disorder and panic disorder (with or without agoraphobia) in adults Introduction The partial update of the guideline on Generalised anxiety disorder and panic disorder
Depression. The treatment and management of depression in adults. This is a partial update of NICE clinical guideline 23
 Issue date: October 2009 Depression The treatment and management of depression in adults This is a partial update of NICE clinical guideline 23 NICE clinical guideline 90 Developed by the National Collaborating
Issue date: October 2009 Depression The treatment and management of depression in adults This is a partial update of NICE clinical guideline 23 NICE clinical guideline 90 Developed by the National Collaborating
Managing depression after stroke. Presented by Maree Hackett
 Managing depression after stroke Presented by Maree Hackett After stroke Physical changes We can see these Depression Emotionalism Anxiety Confusion Communication problems What is depression? Category
Managing depression after stroke Presented by Maree Hackett After stroke Physical changes We can see these Depression Emotionalism Anxiety Confusion Communication problems What is depression? Category
Depression in adults with a chronic physical health problem
 Depression in adults with a chronic physical health problem Treatment and management Issued: October 2009 NICE clinical guideline 91 guidance.nice.org.uk/cg91 NICE has accredited the process used by the
Depression in adults with a chronic physical health problem Treatment and management Issued: October 2009 NICE clinical guideline 91 guidance.nice.org.uk/cg91 NICE has accredited the process used by the
Low back pain. Quick reference guide. Issue date: May 2009. Early management of persistent non-specific low back pain
 Issue date: May 2009 Low back pain Early management of persistent non-specific low back pain Developed by the National Collaborating Centre for Primary Care About this booklet This is a quick reference
Issue date: May 2009 Low back pain Early management of persistent non-specific low back pain Developed by the National Collaborating Centre for Primary Care About this booklet This is a quick reference
Antisocial personality disorder
 Understanding NICE guidance Information for people who use NHS services Antisocial personality disorder NICE clinical guidelines advise the NHS on caring for people with specific conditions or diseases
Understanding NICE guidance Information for people who use NHS services Antisocial personality disorder NICE clinical guidelines advise the NHS on caring for people with specific conditions or diseases
Treatment and management of depression in adults, including adults with a chronic physical health problem
 Issue date: October 2009 Depression Treatment and management of depression in adults, including adults with a chronic physical health problem This is an update of NICE clinical guideline 23 Developed by
Issue date: October 2009 Depression Treatment and management of depression in adults, including adults with a chronic physical health problem This is an update of NICE clinical guideline 23 Developed by
Costing report. Drug misuse: psychosocial interventions and opioid detoxification. Implementing NICE guidance. July 2007
 Drug misuse: psychosocial interventions and opioid detoxification Costing report Implementing NICE guidance July 2007 NICE clinical guidelines 51 and 52 National costing report: Drug misuse guidelines
Drug misuse: psychosocial interventions and opioid detoxification Costing report Implementing NICE guidance July 2007 NICE clinical guidelines 51 and 52 National costing report: Drug misuse guidelines
Clinical guideline Published: 28 October 2009 nice.org.uk/guidance/cg90
 Depression in adults: recognition and management Clinical guideline Published: 28 October 2009 nice.org.uk/guidance/cg90 NICE 2009. All rights reserved. Last updated April 2016 Your responsibility The
Depression in adults: recognition and management Clinical guideline Published: 28 October 2009 nice.org.uk/guidance/cg90 NICE 2009. All rights reserved. Last updated April 2016 Your responsibility The
in young people Management of depression in primary care Key recommendations: 1 Management
 Management of depression in young people in primary care Key recommendations: 1 Management A young person with mild or moderate depression should typically be managed within primary care services A strength-based
Management of depression in young people in primary care Key recommendations: 1 Management A young person with mild or moderate depression should typically be managed within primary care services A strength-based
Anxiety, Panic and Other Disorders
 Methodist Assistance Program Anxiety, Panic and Other Disorders Anxiety, panic and other disorders such as agoraphobia, social phobia, compulsive disorder and posttraumatic stress disorder are all very
Methodist Assistance Program Anxiety, Panic and Other Disorders Anxiety, panic and other disorders such as agoraphobia, social phobia, compulsive disorder and posttraumatic stress disorder are all very
Depression in children and young people. Identification and management in primary, community and secondary care
 NICE guideline May 2005 Issue date: September 2005 Depression in children and young people Identification and management in primary, community and secondary care Clinical Guideline 28 Developed by the
NICE guideline May 2005 Issue date: September 2005 Depression in children and young people Identification and management in primary, community and secondary care Clinical Guideline 28 Developed by the
Post-traumatic stress disorder (PTSD)
 Post-traumatic stress disorder (PTSD) The management of PTSD in adults and children in primary and secondary care Clinical Guideline 26 March 2005 Developed by the National Collaborating Centre for Mental
Post-traumatic stress disorder (PTSD) The management of PTSD in adults and children in primary and secondary care Clinical Guideline 26 March 2005 Developed by the National Collaborating Centre for Mental
Mental Health Needs Assessment Personality Disorder Prevalence and models of care
 Mental Health Needs Assessment Personality Disorder Prevalence and models of care Introduction and definitions Personality disorders are a complex group of conditions identified through how an individual
Mental Health Needs Assessment Personality Disorder Prevalence and models of care Introduction and definitions Personality disorders are a complex group of conditions identified through how an individual
Treatments for drug misuse
 Understanding NICE guidance Information for people who use NHS services Treatments for drug misuse NICE clinical guidelines advise the NHS on caring for people with specific conditions or diseases and
Understanding NICE guidance Information for people who use NHS services Treatments for drug misuse NICE clinical guidelines advise the NHS on caring for people with specific conditions or diseases and
Asthma, anxiety & depression
 Anxiety and are common in people with asthma. The good news is that there are effective treatments both for asthma and for anxiety and. With careful management, the symptoms of anxiety and can be treated
Anxiety and are common in people with asthma. The good news is that there are effective treatments both for asthma and for anxiety and. With careful management, the symptoms of anxiety and can be treated
Alcohol use disorders: sample chlordiazepoxide dosing regimens for use in managing alcohol withdrawal
 Alcohol use disorders: sample chlordiazepoxide dosing regimens for use in managing alcohol withdrawal February 2010 NICE clinical guidelines 100 and 115 1 These sample chlordiazepoxide dosing regimens
Alcohol use disorders: sample chlordiazepoxide dosing regimens for use in managing alcohol withdrawal February 2010 NICE clinical guidelines 100 and 115 1 These sample chlordiazepoxide dosing regimens
IAPT OUTLINE SERVICE SPECIFICATION
 IAPT OUTLINE SERVICE SPECIFICATION Improving Access to Psychological Therapies Programme (IAPT) The IAPT Programme is a Department of Health initiative to improve access to psychological therapies. It
IAPT OUTLINE SERVICE SPECIFICATION Improving Access to Psychological Therapies Programme (IAPT) The IAPT Programme is a Department of Health initiative to improve access to psychological therapies. It
Adefovir dipivoxil and peginterferon alfa-2a for the treatment of chronic hepatitis B. Issue date: February 2006
 Issue date: February 2006 Adefovir dipivoxil and peginterferon alfa-2a for the treatment of chronic Understanding NICE guidance information for people with chronic, their families and carers, and the public
Issue date: February 2006 Adefovir dipivoxil and peginterferon alfa-2a for the treatment of chronic Understanding NICE guidance information for people with chronic, their families and carers, and the public
Assessment of depression in adults in primary care
 Assessment of depression in adults in primary care Adapted from: Identification of Common Mental Disorders and Management of Depression in Primary care. New Zealand Guidelines Group 1 The questions and
Assessment of depression in adults in primary care Adapted from: Identification of Common Mental Disorders and Management of Depression in Primary care. New Zealand Guidelines Group 1 The questions and
Mild depression: Few, if any, symptoms in excess of the 5 required to make the diagnosis, and symptoms result in only minor functional impairment.
 6.1 Anxiety Depression - Adults Anxiety is a condition characterized by persistent worry or unease and is usually accompanied by fear, panic, irritability, poor sleep, poor concentration and avoidance,
6.1 Anxiety Depression - Adults Anxiety is a condition characterized by persistent worry or unease and is usually accompanied by fear, panic, irritability, poor sleep, poor concentration and avoidance,
TREATING MAJOR DEPRESSIVE DISORDER
 TREATING MAJOR DEPRESSIVE DISORDER A Quick Reference Guide Based on Practice Guideline for the Treatment of Patients With Major Depressive Disorder, Second Edition, originally published in April 2000.
TREATING MAJOR DEPRESSIVE DISORDER A Quick Reference Guide Based on Practice Guideline for the Treatment of Patients With Major Depressive Disorder, Second Edition, originally published in April 2000.
Naltrexone Shared Care Guideline for the treatment of alcohol dependence and opioid dependance
 Naltrexone Shared Care Guideline for the treatment of alcohol dependence and opioid dependance Introduction Indication/Licensing information: Naltrexone is licensed for use as an additional therapy, within
Naltrexone Shared Care Guideline for the treatment of alcohol dependence and opioid dependance Introduction Indication/Licensing information: Naltrexone is licensed for use as an additional therapy, within
DEPRESSION Depression Assessment PHQ-9 Screening tool Depression treatment Treatment flow chart Medications Patient Resource
 E-Resource March, 2015 DEPRESSION Depression Assessment PHQ-9 Screening tool Depression treatment Treatment flow chart Medications Patient Resource Depression affects approximately 20% of the general population
E-Resource March, 2015 DEPRESSION Depression Assessment PHQ-9 Screening tool Depression treatment Treatment flow chart Medications Patient Resource Depression affects approximately 20% of the general population
NICE Pathways bring together all NICE guidance, quality standards and other NICE information on a specific topic.
 bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published.
bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published.
SLEEP DISTURBANCE AND PSYCHIATRIC DISORDERS
 E-Resource December, 2013 SLEEP DISTURBANCE AND PSYCHIATRIC DISORDERS Between 10-18% of adults in the general population and up to 50% of adults in the primary care setting have difficulty sleeping. Sleep
E-Resource December, 2013 SLEEP DISTURBANCE AND PSYCHIATRIC DISORDERS Between 10-18% of adults in the general population and up to 50% of adults in the primary care setting have difficulty sleeping. Sleep
MOH CLINICAL PRACTICE GUIDELINES 6/2011 DEPRESSION
 MOH CLINICAL PRACTICE GUIDELINES 6/2011 DEPRESSION Executive summary of recommendations Details of recommendations can be found in the main text at the pages indicated. Clinical evaluation D The basic
MOH CLINICAL PRACTICE GUIDELINES 6/2011 DEPRESSION Executive summary of recommendations Details of recommendations can be found in the main text at the pages indicated. Clinical evaluation D The basic
Step 2: Recognised depression in adults persistent subthreshold depressive symptoms or mild to moderate depression
 Step 2: Recognised depression in adults persistent subthreshold depressive symptoms or mild to moderate depression A NICE pathway brings together all NICE guidance, quality standards and materials to support
Step 2: Recognised depression in adults persistent subthreshold depressive symptoms or mild to moderate depression A NICE pathway brings together all NICE guidance, quality standards and materials to support
MOH CLINICAL PRACTICE GUIDELINES 2/2008 Prescribing of Benzodiazepines
 MOH CLINICL PRCTICE GUIELINES 2/2008 Prescribing of Benzodiazepines College of Family Physicians, Singapore cademy of Medicine, Singapore Executive summary of recommendations etails of recommendations
MOH CLINICL PRCTICE GUIELINES 2/2008 Prescribing of Benzodiazepines College of Family Physicians, Singapore cademy of Medicine, Singapore Executive summary of recommendations etails of recommendations
Depression Flow Chart
 Depression Flow Chart SCREEN FOR DEPRESSION ANNUALLY Assess for depression annually with the PHQ-9. Maintain a high index of suspicion in high risk older adults. Consider suicide risk and contributing
Depression Flow Chart SCREEN FOR DEPRESSION ANNUALLY Assess for depression annually with the PHQ-9. Maintain a high index of suspicion in high risk older adults. Consider suicide risk and contributing
NICE Pathways bring together all NICE guidance, quality standards and other NICE information on a specific topic.
 bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published.
bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published.
NICE clinical guideline 90
 Depression in adults The treatment and management of depression in adults Issued: October 2009 NICE clinical guideline 90 guidance.nice.org.uk/cg90 NHS Evidence has accredited the process used by the Centre
Depression in adults The treatment and management of depression in adults Issued: October 2009 NICE clinical guideline 90 guidance.nice.org.uk/cg90 NHS Evidence has accredited the process used by the Centre
Costing statement: Depression: the treatment and management of depression in adults. (update) and
 Costing statement: Depression: the treatment and management of depression in adults (update) and Depression in adults with a chronic physical health problem: treatment and management Summary It has not
Costing statement: Depression: the treatment and management of depression in adults (update) and Depression in adults with a chronic physical health problem: treatment and management Summary It has not
Recognition and Treatment of Depression in Parkinson s Disease
 Recognition and Treatment of Depression in Parkinson s Disease Web Ross VA Pacific Islands Health Care System What is depression? Depression is a serious medical condition that affects a person s feelings,
Recognition and Treatment of Depression in Parkinson s Disease Web Ross VA Pacific Islands Health Care System What is depression? Depression is a serious medical condition that affects a person s feelings,
SPECIFICATION FOR THE LOCAL COMMISSIONED SERVICE FOR THE MANAGEMENT ALCOHOL MISUSE
 SPECIFICATION FOR THE LOCAL COMMISSIONED SERVICE FOR THE MANAGEMENT OF ALCOHOL MISUSE Date: March 2015 1 1. Introduction Alcohol misuse is a major public health problem in Camden with high rates of hospital
SPECIFICATION FOR THE LOCAL COMMISSIONED SERVICE FOR THE MANAGEMENT OF ALCOHOL MISUSE Date: March 2015 1 1. Introduction Alcohol misuse is a major public health problem in Camden with high rates of hospital
Diagnosis and management of ADHD in children, young people and adults
 Issue date: September 2008 Attention deficit hyperactivity disorder Diagnosis and management of ADHD in children, young people and adults NICE clinical guideline 72 Developed by the National Collaborating
Issue date: September 2008 Attention deficit hyperactivity disorder Diagnosis and management of ADHD in children, young people and adults NICE clinical guideline 72 Developed by the National Collaborating
CPD sample profile. 1.1 Full name: Counselling Psychologist early career 1.2 Profession: Counselling Psychologist 1.3 Registration number: PYLxxxxx
 CPD sample profile 1.1 Full name: Counselling Psychologist early career 1.2 Profession: Counselling Psychologist 1.3 Registration number: PYLxxxxx 2. Summary of recent work experience/practice. I have
CPD sample profile 1.1 Full name: Counselling Psychologist early career 1.2 Profession: Counselling Psychologist 1.3 Registration number: PYLxxxxx 2. Summary of recent work experience/practice. I have
Care Manager Resources: Common Questions & Answers about Treatments for Depression
 Care Manager Resources: Common Questions & Answers about Treatments for Depression Questions about Medications 1. How do antidepressants work? Antidepressants help restore the correct balance of certain
Care Manager Resources: Common Questions & Answers about Treatments for Depression Questions about Medications 1. How do antidepressants work? Antidepressants help restore the correct balance of certain
SOMERSET DUAL DIAGNOSIS PROTOCOL OCTOBER 2011
 SOMERSET DUAL DIAGNOSIS PROTOCOL OCTOBER 2011 This document is intended to be used with the Somerset Dual Diagnosis Operational Working guide. This document provides principles governing joint working
SOMERSET DUAL DIAGNOSIS PROTOCOL OCTOBER 2011 This document is intended to be used with the Somerset Dual Diagnosis Operational Working guide. This document provides principles governing joint working
POST-TRAUMATIC STRESS DISORDER PTSD Diagnostic Criteria PTSD Detection and Diagnosis PC-PTSD Screen PCL-C Screen PTSD Treatment Treatment Algorithm
 E-Resource March, 2014 POST-TRAUMATIC STRESS DISORDER PTSD Diagnostic Criteria PTSD Detection and Diagnosis PC-PTSD Screen PCL-C Screen PTSD Treatment Treatment Algorithm Post-traumatic Stress Disorder
E-Resource March, 2014 POST-TRAUMATIC STRESS DISORDER PTSD Diagnostic Criteria PTSD Detection and Diagnosis PC-PTSD Screen PCL-C Screen PTSD Treatment Treatment Algorithm Post-traumatic Stress Disorder
Algorithm for Initiating Antidepressant Therapy in Depression
 Algorithm for Initiating Antidepressant Therapy in Depression Refer for psychotherapy if patient preference or add cognitive behavioural office skills to antidepressant medication Moderate to Severe depression
Algorithm for Initiating Antidepressant Therapy in Depression Refer for psychotherapy if patient preference or add cognitive behavioural office skills to antidepressant medication Moderate to Severe depression
mpv`elildf`^i=qob^qjbkqp=ñçê= ^åñáéíó=~åç=aééêéëëáçå h~íó=dê~òéäêççâ `äáåáå~ä=ié~çi=dêééåïáåü=qáãé=qç=q~äâ `çåëìäí~åí=`äáåáå~ä=mëóåüçäçöáëí
 mpv`elildf`^i=qob^qjbkqp=ñçê= ^åñáéíó=~åç=aééêéëëáçå h~íó=dê~òéäêççâ `äáåáå~ä=ié~çi=dêééåïáåü=qáãé=qç=q~äâ `çåëìäí~åí=`äáåáå~ä=mëóåüçäçöáëí Plan of the presentation Summary of NICE recommended psychological
mpv`elildf`^i=qob^qjbkqp=ñçê= ^åñáéíó=~åç=aééêéëëáçå h~íó=dê~òéäêççâ `äáåáå~ä=ié~çi=dêééåïáåü=qáãé=qç=q~äâ `çåëìäí~åí=`äáåáå~ä=mëóåüçäçöáëí Plan of the presentation Summary of NICE recommended psychological
SPECIALIST ARTICLE A BRIEF GUIDE TO PSYCHOLOGICAL THERAPIES
 SPECIALIST ARTICLE A BRIEF GUIDE TO PSYCHOLOGICAL THERAPIES Psychological therapies are increasingly viewed as an important part of both mental and physical healthcare, and there is a growing demand for
SPECIALIST ARTICLE A BRIEF GUIDE TO PSYCHOLOGICAL THERAPIES Psychological therapies are increasingly viewed as an important part of both mental and physical healthcare, and there is a growing demand for
Paxil/Paxil-CR (paroxetine)
 Generic name: Paroxetine Available strengths: 10 mg, 20 mg, 30 mg, 40 mg tablets; 10 mg/5 ml oral suspension; 12.5 mg, 25 mg, 37.5 mg controlled-release tablets (Paxil-CR) Available in generic: Yes, except
Generic name: Paroxetine Available strengths: 10 mg, 20 mg, 30 mg, 40 mg tablets; 10 mg/5 ml oral suspension; 12.5 mg, 25 mg, 37.5 mg controlled-release tablets (Paxil-CR) Available in generic: Yes, except
Eating Disorder Treatment Protocol
 Eating Disorder Treatment Protocol All Team Members: Patient Self-Management Education & Support Eating Disorders are incredibly debilitating and are associated with significant medical and psychosocial
Eating Disorder Treatment Protocol All Team Members: Patient Self-Management Education & Support Eating Disorders are incredibly debilitating and are associated with significant medical and psychosocial
Antidepressant treatment in adults
 Antidepressant treatment in adults A NICE pathway brings together all NICE guidance, quality standards and materials to support implementation on a specific topic area. The pathways are interactive and
Antidepressant treatment in adults A NICE pathway brings together all NICE guidance, quality standards and materials to support implementation on a specific topic area. The pathways are interactive and
These guidelines are intended to support General Practitioners in the care of their patients with dementia both in the community and in care homes.
 This is a new guideline. These guidelines are intended to support General Practitioners in the care of their patients with dementia both in the community and in care homes. It incorporates NICE clinical
This is a new guideline. These guidelines are intended to support General Practitioners in the care of their patients with dementia both in the community and in care homes. It incorporates NICE clinical
Learning Disabilities
 Learning Disabilities Positive Practice Guide January 2009 Relieving distress, transforming lives Learning Disabilities Positive Practice Guide January 2009 Contents 1. Background and policy framework
Learning Disabilities Positive Practice Guide January 2009 Relieving distress, transforming lives Learning Disabilities Positive Practice Guide January 2009 Contents 1. Background and policy framework
Elizabeth A. Crocco, MD Assistant Clinical Professor Chief, Division of Geriatric Psychiatry Department of Psychiatry and Behavioral Sciences Miller
 Elizabeth A. Crocco, MD Assistant Clinical Professor Chief, Division of Geriatric Psychiatry Department of Psychiatry and Behavioral Sciences Miller School of Medicine/University of Miami Question 1 You
Elizabeth A. Crocco, MD Assistant Clinical Professor Chief, Division of Geriatric Psychiatry Department of Psychiatry and Behavioral Sciences Miller School of Medicine/University of Miami Question 1 You
TREATMENT-RESISTANT DEPRESSION AND ANXIETY
 University of Washington 2012 TREATMENT-RESISTANT DEPRESSION AND ANXIETY Catherine Howe, MD, PhD University of Washington School of Medicine Definition of treatment resistance Failure to remit after 2
University of Washington 2012 TREATMENT-RESISTANT DEPRESSION AND ANXIETY Catherine Howe, MD, PhD University of Washington School of Medicine Definition of treatment resistance Failure to remit after 2
Understanding anxiety and depression
 Understanding anxiety and depression www.beyondblue.org.au 1300 22 4636 Anxiety Over two million people in Australia experience anxiety each year. On average, one in three women and one in fve men will
Understanding anxiety and depression www.beyondblue.org.au 1300 22 4636 Anxiety Over two million people in Australia experience anxiety each year. On average, one in three women and one in fve men will
Post-Traumatic Stress Disorder (PTSD)
 Post-Traumatic Stress Disorder (PTSD) Post traumatic stress disorder is a condition where you have recurring distressing memories, flashbacks, and other symptoms after suffering a traumatic event. Treatment
Post-Traumatic Stress Disorder (PTSD) Post traumatic stress disorder is a condition where you have recurring distressing memories, flashbacks, and other symptoms after suffering a traumatic event. Treatment
Anxiety. Providing services we would be happy for our own families to use
 Anxiety Providing services we would be happy for our own families to use An information guide for Anxiety This booklet aim to: Give you an understanding of Anxiety, it s causes and symptoms Provide information
Anxiety Providing services we would be happy for our own families to use An information guide for Anxiety This booklet aim to: Give you an understanding of Anxiety, it s causes and symptoms Provide information
Alcohol-use disorders
 Issue date: February 2011 Alcohol-use disorders Diagnosis, assessment and management of harmful drinking and alcohol dependence Alcohol dependence: NICE guideline FINAL DRAFT (February 2011) 1 NICE clinical
Issue date: February 2011 Alcohol-use disorders Diagnosis, assessment and management of harmful drinking and alcohol dependence Alcohol dependence: NICE guideline FINAL DRAFT (February 2011) 1 NICE clinical
Social Phobia. Fact sheet 39. What is Social Phobia? Signs and symptoms. How common is Social Phobia and who experiences it?
 Social Phobia Fact sheet 39 What is Social Phobia? It is normal to feel nervous in situations in which we could possibly come under the scrutiny of others, whether they are strangers or people we know.
Social Phobia Fact sheet 39 What is Social Phobia? It is normal to feel nervous in situations in which we could possibly come under the scrutiny of others, whether they are strangers or people we know.
Eating disorders: anorexia nervosa, bulimia nervosa and related eating disorders
 Eating disorders: anorexia nervosa, bulimia nervosa and related eating disorders Understanding NICE guidance: a guide for people with eating disorders, their advocates and carers, and the public January
Eating disorders: anorexia nervosa, bulimia nervosa and related eating disorders Understanding NICE guidance: a guide for people with eating disorders, their advocates and carers, and the public January
Depression and anxiety
 alzheimers.org.uk Depression and anxiety Depression and anxiety are common conditions that are frequently experienced by people with dementia and their carers. They are known as psychological conditions
alzheimers.org.uk Depression and anxiety Depression and anxiety are common conditions that are frequently experienced by people with dementia and their carers. They are known as psychological conditions
What are Cognitive and/or Behavioural Psychotherapies?
 What are Cognitive and/or Behavioural Psychotherapies? Paper prepared for a UKCP/BACP mapping psychotherapy exercise Katy Grazebrook, Anne Garland and the Board of BABCP July 2005 Overview Cognitive and
What are Cognitive and/or Behavioural Psychotherapies? Paper prepared for a UKCP/BACP mapping psychotherapy exercise Katy Grazebrook, Anne Garland and the Board of BABCP July 2005 Overview Cognitive and
Bipolar disorder. Understanding NICE guidance
 Understanding NICE guidance Information for people who use NHS services Bipolar disorder NICE clinical guidelines advise the NHS on caring for people with specific conditions or diseases and the treatments
Understanding NICE guidance Information for people who use NHS services Bipolar disorder NICE clinical guidelines advise the NHS on caring for people with specific conditions or diseases and the treatments
Eating disorders: core interventions in the treatment and management of anorexia nervosa, bulimia nervosa, and related eating disorders
 Eating disorders: core interventions in the treatment and management of anorexia nervosa, bulimia nervosa, and related eating disorders A guide for people with eating disorders, their advocates and carers,
Eating disorders: core interventions in the treatment and management of anorexia nervosa, bulimia nervosa, and related eating disorders A guide for people with eating disorders, their advocates and carers,
Benzodiazepine Detoxification and Reduction of Long term Use
 Benzodiazepine Detoxification and Reduction of Long term Use Malcolm Lader 1 Model of general drug misuse and dependence. Tactical interventional options Social dimension Increasing breaking of social
Benzodiazepine Detoxification and Reduction of Long term Use Malcolm Lader 1 Model of general drug misuse and dependence. Tactical interventional options Social dimension Increasing breaking of social
Bipolar disorder. The management of bipolar disorder in adults, children and adolescents, in primary and secondary care
 Issue date: July 2006 Bipolar disorder The management of bipolar disorder in adults, children and adolescents, in primary and secondary care NICE clinical guideline 38 Developed by the National Collaborating
Issue date: July 2006 Bipolar disorder The management of bipolar disorder in adults, children and adolescents, in primary and secondary care NICE clinical guideline 38 Developed by the National Collaborating
Alcohol-use disorders: alcohol dependence. Costing report. Implementing NICE guidance
 Alcohol-use disorders: alcohol dependence Costing report Implementing NICE guidance February 2011 (February 2011) 1 of 37 NICE clinical guideline 115 This costing report accompanies the clinical guideline:
Alcohol-use disorders: alcohol dependence Costing report Implementing NICE guidance February 2011 (February 2011) 1 of 37 NICE clinical guideline 115 This costing report accompanies the clinical guideline:
Depression is a common biological brain disorder and occurs in 7-12% of all individuals over
 Depression is a common biological brain disorder and occurs in 7-12% of all individuals over the age of 65. Specific groups have a much higher rate of depression including the seriously medically ill (20-40%),
Depression is a common biological brain disorder and occurs in 7-12% of all individuals over the age of 65. Specific groups have a much higher rate of depression including the seriously medically ill (20-40%),
Alcohol-use disorders
 Issue date: February 2011 Alcohol-use disorders Diagnosis, assessment and management of harmful drinking and alcohol dependence Alcohol dependence: NICE guideline FINAL DRAFT (February 2011) 1 NICE clinical
Issue date: February 2011 Alcohol-use disorders Diagnosis, assessment and management of harmful drinking and alcohol dependence Alcohol dependence: NICE guideline FINAL DRAFT (February 2011) 1 NICE clinical
DEPRESSION CARE PROCESS STEP EXPECTATIONS RATIONALE
 1 DEPRESSION CARE PROCESS STEP EXPECTATIONS RATIONALE ASSESSMENT/PROBLEM RECOGNITION 1. Did the staff and physician seek and document risk factors for depression and any history of depression? 2. Did staff
1 DEPRESSION CARE PROCESS STEP EXPECTATIONS RATIONALE ASSESSMENT/PROBLEM RECOGNITION 1. Did the staff and physician seek and document risk factors for depression and any history of depression? 2. Did staff
COUNTY OF LOS ANGELES - DEPARTMENT OF MENTAL HEALTH OFFICE OF THE MEDICAL DIRECTOR. 3.4 PARAMETERS FOR THE USE OF ANXIOLYTIC MEDICATIONS October 2014
 COUNTY OF LOS ANGELES - DEPARTMENT OF MENTAL HEALTH OFFICE OF THE MEDICAL DIRECTOR 3.4 PARAMETERS FOR THE USE OF ANXIOLYTIC MEDICATIONS October 2014 I. GENERAL CONSIDERATIONS A. Definition: Anxiolytic
COUNTY OF LOS ANGELES - DEPARTMENT OF MENTAL HEALTH OFFICE OF THE MEDICAL DIRECTOR 3.4 PARAMETERS FOR THE USE OF ANXIOLYTIC MEDICATIONS October 2014 I. GENERAL CONSIDERATIONS A. Definition: Anxiolytic
Obsessive Compulsive Disorder: a pharmacological treatment approach
 Obsessive Compulsive Disorder: a pharmacological treatment approach Professor Alasdair Vance Head, Academic Child Psychiatry Department of Paediatrics University of Melbourne Royal Children s Hospital
Obsessive Compulsive Disorder: a pharmacological treatment approach Professor Alasdair Vance Head, Academic Child Psychiatry Department of Paediatrics University of Melbourne Royal Children s Hospital
Obsessive-Compulsive Disorder and Body Dysmorphic Disorder
 South West London and St George s Mental Health NHS Trust A National Service for Obsessive-Compulsive Disorder and Body Dysmorphic Disorder Springfield University Hospital A Referrer s Guide 1 Who we are
South West London and St George s Mental Health NHS Trust A National Service for Obsessive-Compulsive Disorder and Body Dysmorphic Disorder Springfield University Hospital A Referrer s Guide 1 Who we are
Donepezil, galantamine, rivastigmine and memantine for Alzheimer s disease
 Understanding NICE guidance Information for people who use NHS services Donepezil, galantamine, rivastigmine and memantine for Alzheimer s disease NICE technology appraisal guidance advises on when and
Understanding NICE guidance Information for people who use NHS services Donepezil, galantamine, rivastigmine and memantine for Alzheimer s disease NICE technology appraisal guidance advises on when and
TREATING PANIC DISORDER
 TREATING PANIC DISORDER A Quick Reference Guide Based on Practice Guideline for the Treatment of Patients With Panic Disorder, originally published in May 1998. A guideline watch, summarizing significant
TREATING PANIC DISORDER A Quick Reference Guide Based on Practice Guideline for the Treatment of Patients With Panic Disorder, originally published in May 1998. A guideline watch, summarizing significant
Withdrawal Symptoms: How Long Do They Last?
 Withdrawal Symptoms: How Long Do They Last? Posted by First Step Medical Detox on November 24, 2015 When considering stopping drugs or alcohol, many addicts and alcoholics are concerned about the withdrawal
Withdrawal Symptoms: How Long Do They Last? Posted by First Step Medical Detox on November 24, 2015 When considering stopping drugs or alcohol, many addicts and alcoholics are concerned about the withdrawal
Traumatic Stress. and Substance Use Problems
 Traumatic Stress and Substance Use Problems The relation between substance use and trauma Research demonstrates a strong link between exposure to traumatic events and substance use problems. Many people
Traumatic Stress and Substance Use Problems The relation between substance use and trauma Research demonstrates a strong link between exposure to traumatic events and substance use problems. Many people
Update on guidelines on biological treatment of depressive disorder. Dr. Henry CHEUNG Psychiatrist in private practice
 Update on guidelines on biological treatment of depressive disorder Dr. Henry CHEUNG Psychiatrist in private practice 2013 update International Task Force of World Federation of Societies of Biological
Update on guidelines on biological treatment of depressive disorder Dr. Henry CHEUNG Psychiatrist in private practice 2013 update International Task Force of World Federation of Societies of Biological
IMR ISSUES, DECISIONS AND RATIONALES The Final Determination was based on decisions for the disputed items/services set forth below:
 Case Number: CM13-0018009 Date Assigned: 10/11/2013 Date of Injury: 06/11/2004 Decision Date: 01/13/2014 UR Denial Date: 08/16/2013 Priority: Standard Application Received: 08/29/2013 HOW THE IMR FINAL
Case Number: CM13-0018009 Date Assigned: 10/11/2013 Date of Injury: 06/11/2004 Decision Date: 01/13/2014 UR Denial Date: 08/16/2013 Priority: Standard Application Received: 08/29/2013 HOW THE IMR FINAL
Mental Health in the Workplace. Kate Hubl- Occupational Therapist
 Mental Health in the Workplace Kate Hubl- Occupational Therapist So what does the workplace have to do with mental health and mental health issues? Its not abnormal, weird, strange or weak to experience
Mental Health in the Workplace Kate Hubl- Occupational Therapist So what does the workplace have to do with mental health and mental health issues? Its not abnormal, weird, strange or weak to experience
Amphetamines Addiction
 Introduction Amphetamines, which are classified as stimulants, work by using the dopamine reward system of the brain. When these drugs are used, the user s central nervous system is simulated which causes
Introduction Amphetamines, which are classified as stimulants, work by using the dopamine reward system of the brain. When these drugs are used, the user s central nervous system is simulated which causes
Postnatal depression is an illness. It is not a sign that you don't love your baby or can't look after your baby properly.
 Patient information from the BMJ Group Postnatal depression Postnatal depression is an illness that women can get after having a baby. If you have it, you may feel sad and anxious, and find it hard to
Patient information from the BMJ Group Postnatal depression Postnatal depression is an illness that women can get after having a baby. If you have it, you may feel sad and anxious, and find it hard to
Depression in Adults
 Depression in Adults A chapter of Croydon s mental health Joint Strategic Needs Assessment 2012/13 Health and Wellbeing Board 5 December 2012 Bernadette Alves, Locum Consultant in Public Health Croydon
Depression in Adults A chapter of Croydon s mental health Joint Strategic Needs Assessment 2012/13 Health and Wellbeing Board 5 December 2012 Bernadette Alves, Locum Consultant in Public Health Croydon
