the Learning Environment, June 11, 2002; ( accessed July 16, 2004).
|
|
|
- Dustin Joseph
- 7 years ago
- Views:
Transcription
1 Accreditation Council for Graduate Medical Education (ACGME) The ACGME s Approach to Limit Resident Duty Hours 12 Months After Implementation: A Summary of Achievements Rationale for the Duty Hour Limits Changes in health care delivery, and concerns that restricted sleep has a negative effect on performance resulted in a need to limit resident duty hours. As the accrediting body for more than 7,900 residency programs, the Accreditation Council for Graduate Medical Education is the entity charged with setting and enforcing duty hour limits. In July 2003, ACGME instituted a comprehensive approach that includes: (1) standards for resident hours and institutional oversight; (2) promoting compliance; and (3) increasing knowledge on the effect of the standards and on innovative ways to conduct education and patient care under limited resident hours. ACGME considers duty hour limits an important element of its comprehensive approach to promote high-quality education and safe patient care. The Standards ACGME s common duty hour standards acknowledge scientific evidence that long hours and sleep loss have a negative effect on resident performance, learning and well-being. The duty hour standards include: An 80-hour weekly limit, averaged over four weeks; An adequate rest period, which should consist of 10 hours of rest between duty periods; A 24-hour limit on continuous duty, and up to six added hours for continuity of care and education; One day in seven free from patient care and educational obligations, averaged over four weeks; In-house call no more than once every three nights, averaged over four weeks; The option for programs in some specialties to request an increase of up to 8 hours in the weekly hours, if this benefits resident education, with approval by their sponsoring institution and the Residency Review Committee (RRC) in the given specialty. ACGME chose 80-hours as the upper limit to safeguard against the negative effects of chronic sleep loss, and selected a limit of 24 hours plus up to six hours to address the effects of acute sleep loss, and to allow for adequate time for patient hand-off and didactic learning. 1 Achievements in the first 12 Months In the first 12 months after the July 2003 implementation, ACGME, the RRCs and the residency education community rose to the challenge of applying the duty hour standards to 7,973 accredited specialty and subspecialty programs. Programs and sponsoring institutions made changes in the clinical training of residents, their patient care activities and the mechanisms for duty hour monitoring and oversight. Many programs used schedule changes, night float and other rotation changes to bring duty hours below the common limits. Others replaced resident services with care by nurse practitioners, physician assistants or hospitalists. A few programs completely re-engineered their patient care and education system to function well under reduced hours. Virtually all programs increased the clinical responsibilities of faculty physicians. Highlights from the first year under the new standards include: ACGME collected data on duty hour compliance from the program directors of all accredited programs, with more than 98% of ACGME-accredited programs responding by the March 2004 deadline. Senior officials at each sponsoring institution verified this information. ACGME instituted systems to track compliance, including the number of programs cited for duty hour violations, complaints related to resident hours, and programs applying for duty hour exceptions. During accreditation reviews conducted between July 2003 and June 2004, ACGME site visitors interviewed program directors, faculty, residents and sponsoring institution representatives and conducted primary reviews of documents that detail resident duty hours, including rotation schedules, call rosters and some institutional duty hour surveys to verify compliance with the standards. Of the 2,235 programs reviewed during Academic Year , 208 were applications for new programs. Of 2,027 existing programs that received full reviews, 101 programs (5.0%) received one or more citations related to non-compliance with the duty hour standards. The majority of citations related to compliance with the 80-hour weekly limit (52 citations), followed by the requirement for one day in seven free of program duties and the 24 + up to 6-hour limit on continuous duty (29 and 27 1 Accreditation Council for Graduate Medical Education, Report of the Work Group on Resident Duty Hours and the Learning Environment, June 11, 2002; ( accessed July 16, 2004).
2 citations, respectively). RRCs requested that 42 programs provide them with dedicated reports that detail their efforts to bring duty hours into compliance or general progress reports that included information on duty hours. Detailed information on duty hour citations, including duty hour citations and time to next RRC review by specialty, is shown at Exhibit 1. ACGME interviewed between 11,000 and 13,000 residents during scheduled accreditation site visits, and via an electronic resident survey collected data on duty hour compliance from 25,176 residents in 1,489 programs. Among the respondents, 834 residents (3.3% of the responding residents) in 370 programs (24.8% of responding programs) reported working more than 80 hours per week during the previous 4 weeks. That a small group of residents work beyond the duty hour limits likely relates to factors associated with individual residents learning and practice performance, rather than program level non-compliance with the standards. At the same time, the survey found a few programs where the majority of residents worked significantly beyond the duty hour limits. ACGME is following up with programs where the resident survey data suggests a potential program-level compliance problem. ACGME received 53 complaints related to non-compliance related to resident hours. Eleven were dismissed as unfounded. For the remainder ACGME instituted appropriate follow-up activities, including its procedure for Rapid Response to Alleged Egregious Accreditation Violations or Catastrophic Institutional Events for the most serious complaints. Details are shown at Exhibit 2. The RRCs approved 75 requests by individual programs to extend the weekly limit to 88 hours, and denied another 14 requests. Exhibit 3 shows requests by specialty. ACGME denied a request by the surgical RRCs to increase the weekly limit for the surgical chief resident year to 88 hours, due a lack of data thus far showing a negative effect of the limits, and ability of programs to request an increase in their weekly limit for chief residents to 88-hours, with the approval of their institution and RRC. Eleven RRCs have standards that are more restrictive than the common duty hour limits or do not permit programs to apply for the increase in the weekly duty hour limit, as shown at Exhibit 4. ACGME communicated its approach to limit resident duty hours and its compliance efforts to the academic community and the public through published articles, interviews and information presented on the ACGME Web site and in the quarterly ACGME Bulletin. In August 2003, ACGME communicated with approximately 100,000 residents in accredited programs through the officials at their sponsoring institution, informing them about the duty hour standards and compliance monitoring activities, including residents rights to raise concerns about violations of the standards with their institutions and, ultimately, ACGME. ACGME is sensitive to the issue that reporting alleged non-compliance with the standards may place such whistleblowers at risk for retaliation or retribution, and its confidential complaint management process and institutional requirements seek to safeguard these individuals. In addition, ACGME has emphasized to program directors and institutional leaders the need to protect confidential reporters, beginning with an article in the fall 2003 ACGME Bulletin. ACGME kept the academic community informed about compliance activities and innovative ideas for meeting the standards thorough articles in the ACGME Bulletin, question and answer sections on the ACGME Web site and presentations to the academic community. Successful approaches for reducing hours that preserve a balance between education and service could be adopted or adapted by other programs and institutions. A sampling of innovative ideas is presented at Exhibit 5. Potential Future Refinements to the Standards ACGME has solicited feedback on the elements of the standards that may reduce educational quality or have other unintended effects, with the goal of assessing the need for future refinements. It is aware that public attention is focused on the issue of resident hours and the mechanisms to ensure compliance and believes that a period of at least 12 to 18 months without changes to the standards is needed to give programs time to adapt education and patient care activities to the limits and to collect data on their effect. ACGME may make future refinements in areas where key indices suggest the standards may be problematic from an educational or patient care perspective. Revisions to the standards would be made only in response to convincing data that they are necessary and would benefit education and/or patient care, and after a process of soliciting broad input and support for any changes from the education community and the general public. 2
3 - Programs with Duty Hour Citations, July 1, 2003 June 30, 2004 Exhibit 1 No Continous Call no more Total Duty Avg. Avg. Total No. of programs hours Day hour than Hour Cycle Citat- Duty Hour % programs per in 7 rest duty every 3rd Moon- Cita- Length ions Reports Specialty reviewed cited Cited week free period 24h + 6 night lighting tions (1) (1) Requested Allergy and Immunology % Clin. Lab. Immunol % Anesthesiology % Anesth. Subspec % Colon and Rectal Surgery % Dermatology % Dermatology Subspec % Emergency Medicine % Emerg. Med. Subspec % Family Practice % Family Practice Subspec % Internal Medicine % Internal Med. Subspec % Medical Genetics % Molec. Genetic Pathol % Neurological Surgery % Neurology % Neurology Subspecialties % Nuclear Medicine % Obstetrics and Gynecology % Ophthalmology % Orthopaedic Surgery % Ortho. Surg. Subspec % Otolaryngology % Otolaryngology Subspec % Pathology % Pathology Subspec % Pediatrics % Pediatrics Subspecialties % Phys. Med. & Rehab % PM and R Subspec % Plastic Surgery % Plastic Surgery Subspec % Preventive Medicine % Prev. Med. Subsp % Psychiatry % Psychiatry Subspecialties % Radiation Oncology % Diagnostic Radiology % Diagn. Radiol. Subspec % General Surgery % General Surgery Subspec % Thoracic Surgery % Transitional Year % Urology % Urology Subspecialties % Overall Citations %
4 Exhibit 2 Specialty Complaints about Alleged Non-Compliance with the Duty Hour Standards and their Disposition July 1, 2003 through June 30, 2004 No. of Complaints % of all Complaints Residents in specialty % of all residents Internal Medicine % 21, % Pulmonary/Critical Care Medicine 2 3.8% 1, % Gastroenterology 1 1.9% 1, % General Surgery % 7, % Orthopaedic Surgery 4 7.5% 3, % Obstetrics Gynecology 3 5.7% 4, % Family Practice 3 5.7% 9, % Diagnostic Radiology 3 5.7% 4, % Anesthesiology 2 3.8% 4, % Pediatrics 2 3.8% 7, % Psychiatry 2 3.8% 4, % Child and Adolescent Psychiatry 1 1.9% % Emergency Medicine 2 3.8% 3, % Transitional Year 2 3.8% 1, % Neurology 1 1.9% 1, % Neurosurgery 1 1.9% % Plastic Surgery 1 1.9% % Thoracic Surgery 1 1.9% % Total, Specialties with complaints % 79,570 Residents in Specialties without duty hour complaints 0 20,944 Grand Total ,514.05% Disposition of Complaint Number % of all complaints Monitor at time of next site visit % Site visit scheduled % Disposition pending % Reviewed by RRC without a site visit % Requested progress report % Proposed Probation % Confirmed Probation % Program warned and time to site visit shortened % Complaint dismissed as unfounded % Total % 4
5 Exhibit 3 Requests for Extend the Weekly Limit to 88 Hours By Specialty: Total Number of Programs Requests for Duty Hour Exceptions Requested Denied Approved Allergy and Immunology (1) 83 Anesthesiology (1) 324 Colon and rectal surgery 37 0 Dermatology (1) Emergency Medicine (1) 163 Family Practice (1) 569 Internal Medicine (1) 1,842 Medical Genetics (1) 58 0 Neurological surgery Neurology (1) 301 Nuclear medicine 64 Obstetrics and Gynecology Ophthalmology Orthopaedic Surgery (1) Otolaryngology (1) Pathology (1) Pediatrics (1) 842 Phys. Med. And Rehabilitation (1) Plastic Surgery (1) Preventive Medicine (1) 86 Psychiatry (1) 446 Radiation oncology 77 0 Radiology - Diagnostic (1) 464 Surgery - General (1) Thoracic surgery Urology (1) Transitional year Totals 7, Shaded: RRC does not permit an increase to 88 weekly hours (1) Includes subspecialty programs Source: ACGME Accreditation Database, June
6 Exhibit 4 Specialty-Specific Duty Hour Requirements that Exceed the Common Duty Hour Requirements July 1, 2003 Allergy and Immunology: V.F.6. The RRC for Allergy & Immunology will not consider requests for an exception to the limit to 80 hours per week, averaged monthly. Anesthesiology: V.F.3.b: During the 6 additional hours (after the end of the on-call period), residents may not administer anesthesia in the operating room for a new operative case or manage new admissions to the ICU. The resident should not manage non-continuity patients in the 6 hours post-call. V.F.2.d. The RRC will not consider requests for a rest period of less than 10 hours. V.F.6. The RRC for Anesthesiology will not consider requests for an exception to the limit to 80 hours per week, averaged monthly. Emergency Medicine: IV.A. 7.a.2) While on duty in the emergency department, residents may not work longer than 12 continuous scheduled hours. There must be at least an equivalent period of continuous time off between scheduled work periods. IV.A. 7.a. 3) A resident should not work more than 60 scheduled hours per week seeing patients in the emergency department and no more than 72 duty hours per week. Duty hours comprise all clinical duty time and conferences, whether spent within or outside the educational program, including all on-call hours. V.F.6. The RRC for Emergency Medicine will not consider requests for an exception to the limit to 80 hours per week, averaged monthly. Family Practice: V.F.2.d. The RRC will not consider requests for a rest period of less than 10 hours. V.D.6. The RRC for Family Practice will not consider requests for an exception to the limit to 80 hours per week, averaged monthly. Internal Medicine: In-house call must occur no more frequently than every third night (this standard does not permit averaging the frequency of in-house call). V.D.6. The RRC for Internal Medicine will not consider requests for an exception to the limit to 80 hours week, averaged monthly. Neurology: V.F.6. The RRC for Neurology will not consider requests for exceptions to the limit to 80 hours per week, averaged monthly. Nuclear Medicine: V.F.6. The RRC for Nuclear Medicine will not consider requests for exceptions to the limit to 80 hours per week, averaged monthly. Pediatrics: V.F.6. The RRC for Pediatrics will not consider requests for exceptions to the limit to 80 hours per week, averaged monthly. Preventive Medicine: V.F.6. The RRC for Preventive Medicine will not consider requests for an exception to the limit to 80 hours per week, averaged monthly. Psychiatry: V.F.6. The RRC for Psychiatry will not consider requests for exceptions to the limit to 80 hours per week, averaged monthly. Diagnostic Radiology: V.F.6. The RRC for Diagnostic Radiology will not consider requests for exceptions to the limit to 80 hours per week, averaged monthly. 6
7 Exhibit 5 Selected Innovative Approaches Internal Medicine: Reducing Internal Medicine Duty Hours at the University of Virginia In March of 2002, information on resident hours at this major university teaching hospital showed that 25% oft the residents worked more than 80 hours per week. A volunteer resident task force developed options to bring the program into compliance and the residents chose a plan which maintained a schedule of call every fourth night, but mandated that one member of the intern-resident team go home at 10 pm, when the admitting cycle ended. This schedule resulted in residents taking overnight call every eight night, and decreased the percentage of residents working over the 80-hour limit from 25% to 8%. To bring all residents into compliance, an additional day off was added to each four-week ward block. Each team member takes off Thursday or Friday during the week the team has Saturday call. This adds a fifth day off to each four-week inpatient rotation and produced 100% compliance with the duty hour limits. It also maintains continuity of care. Since the implementation of this plan, documented attendance at conferences has not decreased, suggesting that the structured educational experiences have not been affected by the changes in residents scheduling patterns. Neurological Surgery: The Neurological Surgery Program at the University of Florida In this neurological surgery program, faculty and residents have worked together to create and refine a system that complies with the common duty hour requirements, while preserving and maximizing the educational mission of the residency program. To make up for the reduced availability of residents the department hired nurse practitioners (NPs) for each of two services where residents train. Despite the added financial burden, the NPs have worked out well. They handle many of the less educational aspects of residency, such as routine consults, preoperative histories and physicals, routine labs, lumbar punctures and discharge orders. Patient and family satisfaction has increased significantly, especially in the area of discharge teaching. The department has also begun to include residents who are off service or in the laboratory in the call rotation, and has moved to home call for chief residents who back up junior residents, and for two clinical services that are smaller and have less medical acuity. Residents are required to complete and return a weekly time card. A few residents were caught falsifying their time cards early in this process, and the department informed them that severe consequences would follow if duty hours were not accurately reported. The program director and all residents meet monthly to discuss duty hour issues, and explore the need for adjustments to the system. Neurology: Reducing Neurology Resident Hours at UT Medical Branch, Galveston In early 2003, this neurology program revised its resident scheduling patterns to conform to the ACGME duty hour limits. The program s nine residents all take night call with no differences between senior and junior residents. Rotating residents do not participate in call. At the heart of the system is that each resident is scheduled for a two-week long night float rotation three times per year. The other residents are on a regular rotation with more limited call. No resident works more than 80 hours per week or 24 hours of continuous duty. The primary benefit is that residents no longer complain of being post-call and do not fall asleep in conferences. Residents and faculty consider the plan a success. Surgery: Models for Surgical Resident Education at Northwestern University, Chicago A think tank at the McGaw Medical Center of Northwestern University developed four resident rotation models the surgery residency program currently uses. The goal was to develop models programs can adopt to comply with the standards while maintaining or enhancing resident education. In the Stretch Model, residents take call every fourth night (or less) and leave the next morning. This is the easiest approach to get to an 80-hour week, but it has no real educational advantages other than reducing duty hours, presumably giving residents more time to read. The Night Float Model consists of a traditional resident team system, except that a percentage of the program's residents are designated to a night-float shift, usually for a month at a time. Each resident rotates on night float two to three months per year. The day team has one hour of overlap with the night- float team to allow for a robust "sign-out." Teams 7
8 working during the day would take no in-house night call. The "night float" team works a night shift six days per week, although larger programs may be able to accommodate a five nights per week schedule. The Apprentice Model involves one resident working exclusively with one or two faculty members over several months. Residents work side-by-side with their mentors in the operating room and outpatient setting and take home call when their mentor is on call, and participate only in the care of their mentors' patients. Faculty members are selected carefully based on dedication to education and an appropriate practice profile. This model lends itself well to subspecialty areas like colorectal or breast surgery, but also can be used for general surgery rotations. Apprentices take no in-house call, and are on duty less than 80 hours, even if they have to come in at night once or twice a week. In the Mastery (Case-Based) Model, cases are assigned to residents solely based on their learning needs. Knowledge and skills associated with diagnoses and operations are measured by personal progress, not by time. Proficiency is verified through formal assessment, and residents are allowed to advance to other areas and are not required to scrub on operations they have mastered unless they want to refresh their knowledge. Residents are responsible for making arrangements to review the cases with the appropriate attending. They round on their own patients in the morning and go to the clinic or operating room depending on their assignments for that week. They are not required to take night call, but could take call from home. Learning expectations are made clear at the start and are mastery-based, but broken down by year of training for planning purposes. Surgery: From more than 110 to less than 80 hours at St. Luke s Hospital, Bethlehem After analyzing the responsibilities and tasks of its residents and the service requirements of their various clinical rotations, the leadership of this surgery program instituted a modified night float system. From Sunday through Thursday one resident is on a night-float rotation from 6 pm to 8 am and to 11 am for Friday morning conferences. Two different residents are on call Friday night, Saturday day and night, and Sunday during the day. The night-float resident changes weekly. Chief residents take call from home and come to the hospital when needed. The modified night float system has advantages in a small surgery program: (1) residents miss few clinical opportunities; (2) residents are able to attend surgical clinics and attending faculty office hours; (3) residents can participate in time-protected conferences during the morning; (4) residents have more time for rest and personal learning; (5) the night float resident is still involved in operative procedures in that he/she participates in late elective surgical cases and is involved in emergency surgical cases at night. Making the modified night float system a success requires a commitment by the faculty, nursing and administration to make the residency primarily an educational experience. It also requires understanding on the part of residents and faculty that the ACGME duty hour standards improve the educational experience of residents. Finally, a robust sign-out of patients at the beginning and end of the night-float period is a key element of a successful night-float model. 8
Specialty-specific References for DIOs: Expected Time for Program Director ACGME
 -specific References for DIOs: Expected Time for Program Director ACGME Specialty Allergy and Immunology Anesthesiology (effective: July 1, 2016) Adult Cardiothoracic Anesthesiology Critical Care Anesthesiology
-specific References for DIOs: Expected Time for Program Director ACGME Specialty Allergy and Immunology Anesthesiology (effective: July 1, 2016) Adult Cardiothoracic Anesthesiology Critical Care Anesthesiology
Responsibilities of the Program Coordinator. Presentation Goals. What is a Program Coordinator?
 Responsibilities of the Program Coordinator New Coordinators Pre-Course 2008 ACGME Annual Educational Conference Grapevine, Texas Norma R. de Yagcier Senior Accreditation Administrator Presentation Goals
Responsibilities of the Program Coordinator New Coordinators Pre-Course 2008 ACGME Annual Educational Conference Grapevine, Texas Norma R. de Yagcier Senior Accreditation Administrator Presentation Goals
Specialty-specific References for DIOs: Program Director Qualifications ACGME
 -specific References for DIOs: Program Director Qualifications ACGME Common Program Requirements are in BOLD Specialty Allergy and Immunology Anesthesiology II.A.3.b) current certification in the specialty
-specific References for DIOs: Program Director Qualifications ACGME Common Program Requirements are in BOLD Specialty Allergy and Immunology Anesthesiology II.A.3.b) current certification in the specialty
MGMA PROVIDER COMPENSATION 2015
 Physicians Allergy/Immunology 203 86 Anesthesiology 2,146 120 Anesthesiology: Pain Management 127 59 Cardiology: Electrophysiology 327 126 Cardiology: Invasive 424 148 Cardiology: Invasive-Interventional
Physicians Allergy/Immunology 203 86 Anesthesiology 2,146 120 Anesthesiology: Pain Management 127 59 Cardiology: Electrophysiology 327 126 Cardiology: Invasive 424 148 Cardiology: Invasive-Interventional
Physician Practice Acquisitions
 Trend Watch: Physician Practice Acquisitions Tracking Which Physician Practices Hospitals are Acquiring Introduction Are hospitals actively acquiring physician practices? If so, which specialties? In this
Trend Watch: Physician Practice Acquisitions Tracking Which Physician Practices Hospitals are Acquiring Introduction Are hospitals actively acquiring physician practices? If so, which specialties? In this
(A) Information needed to identify and classify the hospital, include the following: (b) The hospital number assigned by the department;
 3701-59-05 Hospital registration and reporting requirements. Every hospital, public or private, shall, by the first of March of each year, register with and report to the department of health the following
3701-59-05 Hospital registration and reporting requirements. Every hospital, public or private, shall, by the first of March of each year, register with and report to the department of health the following
REQUEST FOR MEMBERSHIP AND CLINICAL PRIVILEGES
 REQUEST FOR MEMBERSHIP AND CLINICAL PRIVILEGES *Applicant Printed Name: *Denotes required fields (Last) (First) (M.I) (Degree) Maiden Name (Alias): (Last) (First) *DOB: *SSN Sex: Male Female *Applicant
REQUEST FOR MEMBERSHIP AND CLINICAL PRIVILEGES *Applicant Printed Name: *Denotes required fields (Last) (First) (M.I) (Degree) Maiden Name (Alias): (Last) (First) *DOB: *SSN Sex: Male Female *Applicant
CURRICULUM ON MEDICAL KNOWLEDGE I. Educational Purpose and Goals Physicians must demonstrate knowledge about both established and evolving
 CURRICULUM ON MEDICAL KNOWLEDGE I. Educational Purpose and Goals Physicians must demonstrate knowledge about both established and evolving biomedical, clinical, and cognate (e.g. epidemiological and social-behavioral)
CURRICULUM ON MEDICAL KNOWLEDGE I. Educational Purpose and Goals Physicians must demonstrate knowledge about both established and evolving biomedical, clinical, and cognate (e.g. epidemiological and social-behavioral)
Perceived and Actual Competitiveness of the Canadian Residency Programs by Specialty
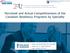 Perceived and Actual Competitiveness of the Canadian Residency Programs by Specialty Author: Alexander Bilbily MD Candidate Supervisor: Dr. Robert Bleakney Date: October 20 th 2012 I do not have an affiliation
Perceived and Actual Competitiveness of the Canadian Residency Programs by Specialty Author: Alexander Bilbily MD Candidate Supervisor: Dr. Robert Bleakney Date: October 20 th 2012 I do not have an affiliation
2012 Physician Specialty Data Book. Center for Workforce Studies. November 2012. Association of American Medical Colleges
 Center for Workforce Studies November 2012 Association of American Medical Colleges Table of Contents Introduction... 1 Acknowledgments... 1 Key Findings... 2 Key Definitions... 3 Commonly Used Acronyms...
Center for Workforce Studies November 2012 Association of American Medical Colleges Table of Contents Introduction... 1 Acknowledgments... 1 Key Findings... 2 Key Definitions... 3 Commonly Used Acronyms...
DRAFT. Select VHA ENTERPRISE STANDARD TITLE:??
 Select VHA ENTERPRISE STANDARD TITLE:?? Choose from: ACUPUNCTURE CONSULT ACUPUNCTURE NOTE ADDENDUM ADDICTION PSYCHIATRY ADDICTION SEVERITY INDEX NOTE ADDICTION PSYCHIATRY ADMINISTRATIVE NOTE ADDICTION
Select VHA ENTERPRISE STANDARD TITLE:?? Choose from: ACUPUNCTURE CONSULT ACUPUNCTURE NOTE ADDENDUM ADDICTION PSYCHIATRY ADDICTION SEVERITY INDEX NOTE ADDICTION PSYCHIATRY ADMINISTRATIVE NOTE ADDICTION
Teaching Physician Billing Compliance. Effective Date: March 27, 2012. Office of Origin: UCSF Clinical Enterprise Compliance Program. I.
 Teaching Physician Billing Compliance Effective Date: March 27, 2012 Office of Origin: UCSF Clinical Enterprise Compliance Program I. Purpose These Policies and Procedures are intended to clarify the Medicare
Teaching Physician Billing Compliance Effective Date: March 27, 2012 Office of Origin: UCSF Clinical Enterprise Compliance Program I. Purpose These Policies and Procedures are intended to clarify the Medicare
Careers in Medicine: The U.S. Approach to Career Planning in Medical School. George V. Richard, Ph.D. Director, Careers in Medicine Program
 Careers in Medicine: The U.S. Approach to Career Planning in Medical School George V. Richard, Ph.D. Director, Careers in Medicine Program January 18, 2007 The Structure of U.S. Medical Education Baccalaureate
Careers in Medicine: The U.S. Approach to Career Planning in Medical School George V. Richard, Ph.D. Director, Careers in Medicine Program January 18, 2007 The Structure of U.S. Medical Education Baccalaureate
Policy and Procedures ACLS & PALS Certification Courses
 Policy and Procedures & PALS Courses UMHS Clinical Simulation Center Training of American Heart Association Advanced Cardiac Life Support The Clinical Simulation Center is the primary provider for Advanced
Policy and Procedures & PALS Courses UMHS Clinical Simulation Center Training of American Heart Association Advanced Cardiac Life Support The Clinical Simulation Center is the primary provider for Advanced
Mississippi Medicaid Enrollment Application (Ordering/Referring/Prescribing Provider)
 This application is for the sole purpose of ordering/referring/prescribing items and services for MS Medicaid beneficiaries. This type of enrollment does not allow MS Medicaid to reimburse the applicant/provider
This application is for the sole purpose of ordering/referring/prescribing items and services for MS Medicaid beneficiaries. This type of enrollment does not allow MS Medicaid to reimburse the applicant/provider
August 13, 2014. Dear Administrator Tavenner:
 Marilyn B. Tavenner Administrator Centers for Medicare & Medicaid Services U.S. Department of Health and Human Services Hubert H. Humphrey Building, Room 445 G 200 Independence Avenue, SW Washington, DC
Marilyn B. Tavenner Administrator Centers for Medicare & Medicaid Services U.S. Department of Health and Human Services Hubert H. Humphrey Building, Room 445 G 200 Independence Avenue, SW Washington, DC
REPORT TO THE 2015 LEGISLATURE. Report on Findings from the Hawai i Physician Workforce Assessment Project
 REPORT TO THE 2015 LEGISLATURE Report on Findings from the Hawai i Physician Workforce Assessment Project Act 18, SSLH 2009 (Section 5), as amended by Act 186, SLH 2012 January 2015 Hawai i Physician Workforce
REPORT TO THE 2015 LEGISLATURE Report on Findings from the Hawai i Physician Workforce Assessment Project Act 18, SSLH 2009 (Section 5), as amended by Act 186, SLH 2012 January 2015 Hawai i Physician Workforce
Survey PRACTICE AND COMPENSATION EXPECTATIONS FOR PHYSICIAN ASSISTANTS. 800.780.3500 mdainc.com
 Survey PRACTICE AND COMPENSATION EXPECTATIONS FOR PHYSICIAN ASSISTANTS 800.780.3500 mdainc.com Overview OBJECTIVE The objective of this survey was to collect and quantify practice and compensation expectations
Survey PRACTICE AND COMPENSATION EXPECTATIONS FOR PHYSICIAN ASSISTANTS 800.780.3500 mdainc.com Overview OBJECTIVE The objective of this survey was to collect and quantify practice and compensation expectations
You re Invited About Us Distinctions Education Executive Education. Graduate Training Technology Contact Us
 You re Invited About Us Distinctions Education Executive Education Graduate Training Technology Contact Us You re Invited Cleveland Clinic Global Physician Associate Program You re Invited Cleveland Clinic
You re Invited About Us Distinctions Education Executive Education Graduate Training Technology Contact Us You re Invited Cleveland Clinic Global Physician Associate Program You re Invited Cleveland Clinic
The following departments have submitted a guide for course choices that would be beneficial for a student interested in their specialty:
 Career Guides Career Guides for Selection of Senior Coursework The following departments have submitted a guide for course choices that would be beneficial for a student interested in their specialty:
Career Guides Career Guides for Selection of Senior Coursework The following departments have submitted a guide for course choices that would be beneficial for a student interested in their specialty:
Accredited Schools and Programs
 A.B. Freeman School of Business Bachelor of Science in Management (BSM), Master of Business Administration (MBA), Master of Global Management (MGM), Master of Management, Master of Finance (MFIN), Master
A.B. Freeman School of Business Bachelor of Science in Management (BSM), Master of Business Administration (MBA), Master of Global Management (MGM), Master of Management, Master of Finance (MFIN), Master
Frequently Asked Questions: ACGME Common Duty Hour Requirements Effective July 1, 2011 Updated June 18, 2014
 Frequently Asked Questions: ACGME Common Duty Hour Requirements Effective July 1, 2011 Updated June 18, 2014 Note: The term resident in this document refers to both specialty residents and subspecialty
Frequently Asked Questions: ACGME Common Duty Hour Requirements Effective July 1, 2011 Updated June 18, 2014 Note: The term resident in this document refers to both specialty residents and subspecialty
Selection of Future Medical Practice: Using the Australian Medical Schools Outcomes Database to inform national workforce planning
 Selection of Future Medical Practice: Using the Australian Medical Schools Outcomes Database to inform national workforce planning Author: David A Kandiah Date: 19 October 2012 I do not have an affiliation
Selection of Future Medical Practice: Using the Australian Medical Schools Outcomes Database to inform national workforce planning Author: David A Kandiah Date: 19 October 2012 I do not have an affiliation
What do ACO s and Hospitals want from SNF s and CCRC s
 What do ACO s and Hospitals want from SNF s and CCRC s Presented to the Institute of Senior Living, April 11, 2013 A Division of Kindred Healthcare 1 Assessing the match: What hospitals and ACO s currently
What do ACO s and Hospitals want from SNF s and CCRC s Presented to the Institute of Senior Living, April 11, 2013 A Division of Kindred Healthcare 1 Assessing the match: What hospitals and ACO s currently
PHYSICIAN ASSISTANT. Education and Practice Donna DeGracia MPAS, PA-C St. Catherine University MPAS Program
 PHYSICIAN ASSISTANT Education and Practice Donna DeGracia MPAS, PA-C St. Catherine University MPAS Program History of PA Profession Started in the mid 1960s to address shortage of primary care physicians
PHYSICIAN ASSISTANT Education and Practice Donna DeGracia MPAS, PA-C St. Catherine University MPAS Program History of PA Profession Started in the mid 1960s to address shortage of primary care physicians
Joint Surgery/Thoracic Surgery Program Review Committees for Surgery and Thoracic Surgery
 I. Introduction Joint Surgery/Thoracic Surgery Program Review Committees for Surgery and Thoracic Surgery The Joint Surgery/Thoracic Surgery program is approved by both the American Board of Surgery (ABS)
I. Introduction Joint Surgery/Thoracic Surgery Program Review Committees for Surgery and Thoracic Surgery The Joint Surgery/Thoracic Surgery program is approved by both the American Board of Surgery (ABS)
Medical Council of New Zealand List of approved qualifications for locum tenens specialist appointments (showing amendments)
 Anaesthesia Fellowship of the Australian and New Zealand College of Anaesthetists Fellowship of the Faculty of Anaesthetists, Royal Australasian College of Surgeons Fellowship of the Royal College of Physicians
Anaesthesia Fellowship of the Australian and New Zealand College of Anaesthetists Fellowship of the Faculty of Anaesthetists, Royal Australasian College of Surgeons Fellowship of the Royal College of Physicians
January 13, 2016. Lois M. Nora MD JD MBA President and CEO American board of Medical Specialties. Dear Dr. Nora,
 January 13, 2016 Lois M. Nora MD JD MBA President and CEO American board of Medical Specialties Dear Dr. Nora, CMSS is pleased to comment on the proposed ABMS Standards for Focused Expertise. We have uploaded
January 13, 2016 Lois M. Nora MD JD MBA President and CEO American board of Medical Specialties Dear Dr. Nora, CMSS is pleased to comment on the proposed ABMS Standards for Focused Expertise. We have uploaded
Charting Outcomes in the Match
 ing Outcomes in the Match Characteristics of Applicants Who to Their Preferred Specialty in the 29 Main Residency Match 3rd Edition Prepared by: National Resident Matching Program and Association of American
ing Outcomes in the Match Characteristics of Applicants Who to Their Preferred Specialty in the 29 Main Residency Match 3rd Edition Prepared by: National Resident Matching Program and Association of American
AAPA ANNUAL SURVEY REPORT
 2013 AAPA ANNUAL SURVEY REPORT PHYSICIAN ASSISTANTS AT A GLANCE HIGHLIGHTS OF THE MEDIAN AGE CLINICALLY PRACTICING PAS BY PRIMARY SPECIALTY PRACTICE SETTING Primary Care 32.0% Surgical Subspecialties 27.0%
2013 AAPA ANNUAL SURVEY REPORT PHYSICIAN ASSISTANTS AT A GLANCE HIGHLIGHTS OF THE MEDIAN AGE CLINICALLY PRACTICING PAS BY PRIMARY SPECIALTY PRACTICE SETTING Primary Care 32.0% Surgical Subspecialties 27.0%
Elenco dei periodici elettronici in Ovid Full text
 Academic Medicine Addictive Disorders & Their Treatment Advances in Anatomic Pathology Age & Ageing AIDS AIDS Patient Care & Stds AJN, American Journal of Nursing Alzheimer Disease & Associated Disorders
Academic Medicine Addictive Disorders & Their Treatment Advances in Anatomic Pathology Age & Ageing AIDS AIDS Patient Care & Stds AJN, American Journal of Nursing Alzheimer Disease & Associated Disorders
EXHIBIT 3 SPECIALTY CLASSIFICATION CODES FOR PHYSICIANS, SURGEONS AND OTHER HEALTH CARE PROVIDERS (JUA)
 EXHIBIT 3 SPECIALTY CLASSIFICATION FOR PHYSICIANS, SURGEONS AND OTHER HEALTH CARE PROVIDERS () CLASS 005 PHYSICIANS - NO SURGERY 00534 Administrative Medicine No Surgery 00508 Hematology No Surgery 00582
EXHIBIT 3 SPECIALTY CLASSIFICATION FOR PHYSICIANS, SURGEONS AND OTHER HEALTH CARE PROVIDERS () CLASS 005 PHYSICIANS - NO SURGERY 00534 Administrative Medicine No Surgery 00508 Hematology No Surgery 00582
cleveland Clinic global solutions, riyadh Global Healthcare, Consulting and Education Services
 cleveland Clinic global solutions, riyadh Global Healthcare, Consulting and Education Services About Cleveland Clinic clevelandclinic.org Cleveland Clinic, a not-for-profit multispecialty academic medical
cleveland Clinic global solutions, riyadh Global Healthcare, Consulting and Education Services About Cleveland Clinic clevelandclinic.org Cleveland Clinic, a not-for-profit multispecialty academic medical
Michigan Department of Community Health Survey of Physician Assistants Frequency Report by School 1
 Michigan Department of Community Health Survey of Physician Assistants Frequency Report by School 1 INTRODUCTION Since 2007, the Michigan Department of Community Health (MDCH) has conducted annual surveys
Michigan Department of Community Health Survey of Physician Assistants Frequency Report by School 1 INTRODUCTION Since 2007, the Michigan Department of Community Health (MDCH) has conducted annual surveys
Appendix 1 Current list of approved qualifications for Locum Tenens registration
 Appendix 1 Current list of approved qualifications for Locum Tenens registration Anaesthesia Fellowship of the Australian and New Zealand College of Anaesthetists Fellowship of the Faculty of Anaesthetists,
Appendix 1 Current list of approved qualifications for Locum Tenens registration Anaesthesia Fellowship of the Australian and New Zealand College of Anaesthetists Fellowship of the Faculty of Anaesthetists,
4. Clinton Memorial Hospital Family Practice Program ACGME# 1203821626
 CLOSED RESIDENCY PROGRAMS 1. Cabrini Medical Center Cardiovascular Disease Fellowship Program ACGME# 1413531114 Internal Medicine Program ACGME# 1403531266 Infectious Disease Program ACGME# 146351097 Podiatry
CLOSED RESIDENCY PROGRAMS 1. Cabrini Medical Center Cardiovascular Disease Fellowship Program ACGME# 1413531114 Internal Medicine Program ACGME# 1403531266 Infectious Disease Program ACGME# 146351097 Podiatry
Specialty-specific Duty Hour Definitions
 Specialty-specific Duty Hour Definitions The Common Program Requirements include revised duty hour standards, effective July 1, 2011. The Review Committees have provided clarification of the following
Specialty-specific Duty Hour Definitions The Common Program Requirements include revised duty hour standards, effective July 1, 2011. The Review Committees have provided clarification of the following
THE UNIVERSITY OF IOWA CARVER COLLEGE OF MEDICINE ADVANCED CLERKSHIPS/COURSES 2016-2017
 THE UNIVERSITY OF IOWA CARVER COLLEGE OF MEDICINE ADVANCED CLERKSHIPS/COURSES 2016-2017 Course descriptions are available at: http://www.medicine.uiowa.edu/md/fourthyear/ INTERDISCIPLINARY Weeks Blocks
THE UNIVERSITY OF IOWA CARVER COLLEGE OF MEDICINE ADVANCED CLERKSHIPS/COURSES 2016-2017 Course descriptions are available at: http://www.medicine.uiowa.edu/md/fourthyear/ INTERDISCIPLINARY Weeks Blocks
Official Accreditation Report Academic Year 2014-15 (As of July 1, 2014)
 Official Report Introduction This report is a listing of accredited degree and certificate programs at The University of Kansas Medical Center (KUMC) for which a national accrediting agency exists. In
Official Report Introduction This report is a listing of accredited degree and certificate programs at The University of Kansas Medical Center (KUMC) for which a national accrediting agency exists. In
Our faculty has been hand-picked for their knowledge, experience, and enthusiasm for teaching
 We welcome your interest in Advocate Lutheran General Hospital s Psychiatry Residency Program. ALGH is a 638-bed teaching hospital located adjacent to Chicago on the northwest side. We proudly provide
We welcome your interest in Advocate Lutheran General Hospital s Psychiatry Residency Program. ALGH is a 638-bed teaching hospital located adjacent to Chicago on the northwest side. We proudly provide
Campaign Participation May 10, 2012
 Campaign Participation May 10, 2012 *Note: "Other Departments" reflects a combined total of departments within the Division having 5 or less employees. Division/Departments % Participation Memorial Art
Campaign Participation May 10, 2012 *Note: "Other Departments" reflects a combined total of departments within the Division having 5 or less employees. Division/Departments % Participation Memorial Art
Full name/ Title of Medical Qualifications Eligible for Conditional Registration. American Board of Obstetrics and Gynaecology
 Conferred by s in the United States of America: Board Cert (Anaesthesiology) Board Cert (Anatomic Pathology) Board Cert (Cardiology) Board Cert (Cardiovascular Disease) Board Cert (Clinical Pathology)
Conferred by s in the United States of America: Board Cert (Anaesthesiology) Board Cert (Anatomic Pathology) Board Cert (Cardiology) Board Cert (Cardiovascular Disease) Board Cert (Clinical Pathology)
MEDICAL PRACTITIONER PROFESSIONAL INDEMNITY APPLICATION FORM
 MEDICAL PRACTITIONER PROFESSIONAL INDEMNITY APPLICATION FORM 1. PERSONAL DETAILS Intended Start Date of Policy: Title: Given Names: Last Name: Gender: M F Date of Birth: Email: Telephone: Mobile: Home
MEDICAL PRACTITIONER PROFESSIONAL INDEMNITY APPLICATION FORM 1. PERSONAL DETAILS Intended Start Date of Policy: Title: Given Names: Last Name: Gender: M F Date of Birth: Email: Telephone: Mobile: Home
MeSH Tree Structures - 2015
 MeSH Tree Structures - 2015 H2 - HEALTH OCCUPATIONS SON ITAPUCOC HTLAHE - 2H H2 Acupuncture H2.04 Allied H2.10 Audiology H2.10.150 Medical Laboratory Science H2.10.450 J1.897. Occupational Therapy H2.10.500
MeSH Tree Structures - 2015 H2 - HEALTH OCCUPATIONS SON ITAPUCOC HTLAHE - 2H H2 Acupuncture H2.04 Allied H2.10 Audiology H2.10.150 Medical Laboratory Science H2.10.450 J1.897. Occupational Therapy H2.10.500
UB Graduate Medical Education Supervision Policy
 UB Graduate Medical Education Supervision Policy Approved: December 2011 General Statements The graduate training programs of the University at Buffalo School of Medicine and Biomedical Sciences (UB) will
UB Graduate Medical Education Supervision Policy Approved: December 2011 General Statements The graduate training programs of the University at Buffalo School of Medicine and Biomedical Sciences (UB) will
Frequently Asked Questions: Physical Medicine and Rehabilitation Review Committee for Physical Medicine and Rehabilitation ACGME
 Frequently Asked Questions: Physical Medicine and Rehabilitation Review Committee for Physical Medicine and Rehabilitation ACGME Questions Program Personnel and Resources Does the Review Committee grant
Frequently Asked Questions: Physical Medicine and Rehabilitation Review Committee for Physical Medicine and Rehabilitation ACGME Questions Program Personnel and Resources Does the Review Committee grant
INDUSTRY PERSPECTIVES
 INDUSTRY PERSPECTIVES Behavioral Health: Staying ahead of the shortage As the demand for behavioral health professionals increases, facilities should consider what implications this may have on facility
INDUSTRY PERSPECTIVES Behavioral Health: Staying ahead of the shortage As the demand for behavioral health professionals increases, facilities should consider what implications this may have on facility
McLAUGHLIN & ASSOCIATES GEORGIA PHYSICIAN SURVEY DECEMBER 11, 2013
 McLAUGHLIN & ASSOCIATES GEORGIA PHYSICIAN SURVEY DECEMBER 11, 2013 1. ARE YOU A CURRENT MEMBER OF THE MEDICAL ASSOCIATION OF GEORGIA, ALSO KNOWN AS MAG? YES 46.5 NO 48.4 DK/REFUSED 5.1 2. HAVE YOU EVER
McLAUGHLIN & ASSOCIATES GEORGIA PHYSICIAN SURVEY DECEMBER 11, 2013 1. ARE YOU A CURRENT MEMBER OF THE MEDICAL ASSOCIATION OF GEORGIA, ALSO KNOWN AS MAG? YES 46.5 NO 48.4 DK/REFUSED 5.1 2. HAVE YOU EVER
Evolving UM SOM Clinical Practice as the Healthcare Environment Changes
 Evolving UM SOM Clinical Practice as the Healthcare Environment Changes Introduction to the UM SOM Medical Service Plan This section will cover the following elements: 1. FPI creation, organization, and
Evolving UM SOM Clinical Practice as the Healthcare Environment Changes Introduction to the UM SOM Medical Service Plan This section will cover the following elements: 1. FPI creation, organization, and
2013 REGISTERED NURSE
 2013 REGISTERED NURSE OHIO WORKFORCE DATA SUMMARY REPORT OCTOBER 2013 Ohio Board of Nursing 17 S. High Street, Suite 400 Columbus, Ohio 43215 TABLE OF CONTENTS Introduction.................................................
2013 REGISTERED NURSE OHIO WORKFORCE DATA SUMMARY REPORT OCTOBER 2013 Ohio Board of Nursing 17 S. High Street, Suite 400 Columbus, Ohio 43215 TABLE OF CONTENTS Introduction.................................................
University of North Dakota School of Medicine & Health Sciences Internal Medicine Residency Program
 University of North Dakota School of Medicine & Health Sciences Internal Medicine Residency Program Required Clinical Rotations and Other Learning Experiences 2015-16 Academic Year The curriculum for the
University of North Dakota School of Medicine & Health Sciences Internal Medicine Residency Program Required Clinical Rotations and Other Learning Experiences 2015-16 Academic Year The curriculum for the
UIC College of Medicine Compliance Plan/Program
 UIC College of Medicine Compliance Plan/Program Updated for Calendar Year 2010 Policy: Each designated operating unit within the University of Illinois Medical Center at Chicago and its associated clinical
UIC College of Medicine Compliance Plan/Program Updated for Calendar Year 2010 Policy: Each designated operating unit within the University of Illinois Medical Center at Chicago and its associated clinical
Aggregate Indemnity and Medical Costs for Calendar Year 2012 (CA-IM-2012) Due Date: April 2, 2013
 February 1, 2013 525 Market Street, Suite 800 San Francisco, CA 94105-2767 Voice 415.778.7008 www.wcirbonline.org escad@wcirbonline.org David M. Bellusci Executive Vice President, COO & Chief Actuary To:
February 1, 2013 525 Market Street, Suite 800 San Francisco, CA 94105-2767 Voice 415.778.7008 www.wcirbonline.org escad@wcirbonline.org David M. Bellusci Executive Vice President, COO & Chief Actuary To:
What Are the Pathology Education Requirements for All Nonpathology ACGME-Accredited Programs in an Academic Center?
 What Are the Pathology Education Requirements for All Nonpathology ACGME-Accredited Programs in an Academic Center? Sarah M. Bean, MD, 1 Alisa Nagler, JD, EdD, 2 and Patrick J. Buckley, MD, PhD 1 Key Words:
What Are the Pathology Education Requirements for All Nonpathology ACGME-Accredited Programs in an Academic Center? Sarah M. Bean, MD, 1 Alisa Nagler, JD, EdD, 2 and Patrick J. Buckley, MD, PhD 1 Key Words:
CMS SPECIALTY CODES/HEALTHCARE PROVIDER TAXONOMY CROSSWALK. This table reflects Medicare Specialty Codes as of April 1, 2003.
 CMS SPECIALTY CODE CMS SPECIALTY CODES/HEALTHCARE PROVIDER TAXONOMY CROSSWALK This table reflects Medicare Specialty Codes as of April 1, 2003. This table reflects Healthcare Provider Taxonomy Codes (HPTC)
CMS SPECIALTY CODE CMS SPECIALTY CODES/HEALTHCARE PROVIDER TAXONOMY CROSSWALK This table reflects Medicare Specialty Codes as of April 1, 2003. This table reflects Healthcare Provider Taxonomy Codes (HPTC)
Master of Physician Assistant Studies Course Descriptions for Year I
 FALL TERM COURSES: Master of Physician Assistant Studies Course Descriptions for Year I PHAC 7230 Fundamentals in Pharmacology for Health Care I Credit Hrs: 3 This course will build on foundational knowledge
FALL TERM COURSES: Master of Physician Assistant Studies Course Descriptions for Year I PHAC 7230 Fundamentals in Pharmacology for Health Care I Credit Hrs: 3 This course will build on foundational knowledge
2013 R-1 MAIN RESIDENCY MATCH REPORT
 2013 R-1 MAIN RESIDENCY MATCH REPORT carms.ca August 2013 Executive Summary The Canadian Resident Matching Service (CaRMS) is a national, not-for-profit, fee-for-service organization that provides medical
2013 R-1 MAIN RESIDENCY MATCH REPORT carms.ca August 2013 Executive Summary The Canadian Resident Matching Service (CaRMS) is a national, not-for-profit, fee-for-service organization that provides medical
APPLICATION FOR A NEW AOA OSTEOPATHIC RESIDENCY TRAINING PROGRAM TABLE OF CONTENTS
 APPLICATION FOR A NEW AOA OSTEOPATHIC RESIDENCY TRAINING PROGRAM TABLE OF CONTENTS SECTION A INSTRUCTIONS... 2 SECTION B - PROGRAM INFORMATION... 4 SECTION C REQUIRED DOCUMENTATION... 5 SECTION D APPROVAL
APPLICATION FOR A NEW AOA OSTEOPATHIC RESIDENCY TRAINING PROGRAM TABLE OF CONTENTS SECTION A INSTRUCTIONS... 2 SECTION B - PROGRAM INFORMATION... 4 SECTION C REQUIRED DOCUMENTATION... 5 SECTION D APPROVAL
Wisconsin Department of Safety and Professional Services
 PLAN AHEAD: Wisconsin Department of Safety and Professional Services Mail To: P.O. Box 8935 Madison, WI 53708-8935 1400 E. Washington Avenue Madison, WI 53703 FAX #: (608) 261-7083 Phone #: (608) 266-2112
PLAN AHEAD: Wisconsin Department of Safety and Professional Services Mail To: P.O. Box 8935 Madison, WI 53708-8935 1400 E. Washington Avenue Madison, WI 53703 FAX #: (608) 261-7083 Phone #: (608) 266-2112
Palm Beach Gardens Community Hospital, Inc.
 Quality Report Palm Beach Gardens Community Hospital, Inc. DBA: Palm Beach Gardens Medical Center HCO ID: 6884 3360 Burns Road (561 694-7200 w w w.pbgmc.com Summary of Quality Information Accreditation
Quality Report Palm Beach Gardens Community Hospital, Inc. DBA: Palm Beach Gardens Medical Center HCO ID: 6884 3360 Burns Road (561 694-7200 w w w.pbgmc.com Summary of Quality Information Accreditation
The Perfect Answer Medical Answering Service
 Medical Answering Service Website: drsansweringservice.com Email: DrsAnsweringService.com PHONE: 770.448.3799 FAX: 770.448.6696 EMAIL: perfectanswertas@gmail.com Exclusively Serving The Health Care Community
Medical Answering Service Website: drsansweringservice.com Email: DrsAnsweringService.com PHONE: 770.448.3799 FAX: 770.448.6696 EMAIL: perfectanswertas@gmail.com Exclusively Serving The Health Care Community
Specific Standards of Accreditation for Residency Programs in General Surgery
 Specific Standards of Accreditation for Residency Programs in General Surgery 2010 INTRODUCTION The purpose of this document is to provide program directors and surveyors with an interpretation of the
Specific Standards of Accreditation for Residency Programs in General Surgery 2010 INTRODUCTION The purpose of this document is to provide program directors and surveyors with an interpretation of the
Compare your plan options
 SMALL BUSINESS GROUP Compare your plan options 2014 plans for businesses with 1 50 employees I SMALL BUSINESS GROUP Group Health plans offer value, choice, and more A well-run business takes a lot of time,
SMALL BUSINESS GROUP Compare your plan options 2014 plans for businesses with 1 50 employees I SMALL BUSINESS GROUP Group Health plans offer value, choice, and more A well-run business takes a lot of time,
WEST VIRGINIA UNIVERSITY HOSPITALS, INC. ORGANIZATIONAL MANUAL
 WEST VIRGINIA UNIVERSITY HOSPITALS, INC. ORGANIZATIONAL MANUAL June 1999 Revised: June 2000 July 2001 December 2002 August 2003 February 2007 June 2007 April 2008 June 2008 June 2009 September 2009 November
WEST VIRGINIA UNIVERSITY HOSPITALS, INC. ORGANIZATIONAL MANUAL June 1999 Revised: June 2000 July 2001 December 2002 August 2003 February 2007 June 2007 April 2008 June 2008 June 2009 September 2009 November
Application for Pediatric Dermatology Fellowship Training Programs
 Application for Pediatric Dermatology Fellowship Training Programs The American Board of Dermatology Henry Ford Health System One Ford Place Detroit, Michigan 48202-3450 1-313-874-1088 E-Mail: abderm@hfhs.org
Application for Pediatric Dermatology Fellowship Training Programs The American Board of Dermatology Henry Ford Health System One Ford Place Detroit, Michigan 48202-3450 1-313-874-1088 E-Mail: abderm@hfhs.org
Pediatric General Surgery Fellowship
 Pediatric General Surgery Fellowship Fellowship Objectives: This fellowship has been developed to produce an individual who is: Clinically proficient in the assessment and management of surgical problems
Pediatric General Surgery Fellowship Fellowship Objectives: This fellowship has been developed to produce an individual who is: Clinically proficient in the assessment and management of surgical problems
Charting Outcomes in the Match
 ing Outcomes in the Match Characteristics of Applicants Who to Their Preferred Specialty in the 4 Main Residency Match 5th Edition Prepared by: National Resident Matching Program www.nrmp.org August 4
ing Outcomes in the Match Characteristics of Applicants Who to Their Preferred Specialty in the 4 Main Residency Match 5th Edition Prepared by: National Resident Matching Program www.nrmp.org August 4
Step 3: Planning a 4 th year curriculum for your career
 Step 3: Planning a 4 th year curriculum for your career There are six tasks to accomplish in fourth year: Step 1: Write your CV. Document what you have done thus far. Step 2: Choose a career. Choose wisely:
Step 3: Planning a 4 th year curriculum for your career There are six tasks to accomplish in fourth year: Step 1: Write your CV. Document what you have done thus far. Step 2: Choose a career. Choose wisely:
Introduction There are two approved residency training models for plastic surgery, the Independent Model and the Integrated Model.
 TRAINING REQUIREMENTS Introduction There are two approved residency training models for plastic surgery, the Independent Model and the Integrated Model. A plastic surgery program director may choose to
TRAINING REQUIREMENTS Introduction There are two approved residency training models for plastic surgery, the Independent Model and the Integrated Model. A plastic surgery program director may choose to
AMA/Specialty Society RVS Update Committee (RUC) Barbara S. Levy, MD AMA/Specialty Society RVS Update Committee, Chair
 AMA/Specialty Society RVS Update Committee (RUC) Barbara S. Levy, MD AMA/Specialty Society RVS Update Committee, Chair The RUC An Overview The RUC is an independent group exercising its First Amendment
AMA/Specialty Society RVS Update Committee (RUC) Barbara S. Levy, MD AMA/Specialty Society RVS Update Committee, Chair The RUC An Overview The RUC is an independent group exercising its First Amendment
APPLICATION FOR HOSPITALS PROFESSIONAL AND/OR GENERAL LIABILITY INSURANCE
 APPLICATION FOR HOSPITALS PROFESSIONAL AND/OR GENERAL LIABILITY INSURANCE (Claims Made Basis) APPLICANT S INSTRUCTIONS: 1. Answer all questions. If the answer requires detail, please attach a separate
APPLICATION FOR HOSPITALS PROFESSIONAL AND/OR GENERAL LIABILITY INSURANCE (Claims Made Basis) APPLICANT S INSTRUCTIONS: 1. Answer all questions. If the answer requires detail, please attach a separate
2010 Physician Survey
 Vermont Department of Health 2010 Physician Survey Statistical Report 2010 Physician Survey Statistical Report State of Vermont Peter Shumlin, Governor Agency of Human Services Douglas Racine, Secretary
Vermont Department of Health 2010 Physician Survey Statistical Report 2010 Physician Survey Statistical Report State of Vermont Peter Shumlin, Governor Agency of Human Services Douglas Racine, Secretary
December 7, 2010. Dear Dr. Michaels:
 December 7, 2010 The Honorable David Michaels, PhD, MPH Assistant Secretary for Occupational Safety and Health U.S. Department of Labor Occupational Safety and Health Administration 200 Constitution Avenue,
December 7, 2010 The Honorable David Michaels, PhD, MPH Assistant Secretary for Occupational Safety and Health U.S. Department of Labor Occupational Safety and Health Administration 200 Constitution Avenue,
VACAVILLE MEDICAL CENTER. Staff Navigator
 VACAVILLE MEDICAL CENTER Staff Navigator VACAVILLE MEDICAL CENTER Hospital VACAVILLE MEDICAL CENTER - Hospital Department Floor Bldg Pg Administration - HIMS 4 H 9 Admitting 1 H 6 Bed Repair B H 5 Cafeteria
VACAVILLE MEDICAL CENTER Staff Navigator VACAVILLE MEDICAL CENTER Hospital VACAVILLE MEDICAL CENTER - Hospital Department Floor Bldg Pg Administration - HIMS 4 H 9 Admitting 1 H 6 Bed Repair B H 5 Cafeteria
Taxonomy Code Mapping Professional Providers
 Mapping Professional s Adult Care Nurse Adult Psychiatric Mental Health Nursing 363LA2200X 364SP0809X Adult Health Practice Nursing s Clinical Nurse Specialist Adult Psychiatric/Mental Health Allergy and
Mapping Professional s Adult Care Nurse Adult Psychiatric Mental Health Nursing 363LA2200X 364SP0809X Adult Health Practice Nursing s Clinical Nurse Specialist Adult Psychiatric/Mental Health Allergy and
QUESTIONS FOR The Commonwealth Medical College
 Page 1 QUESTIONS FOR The Commonwealth Medical College PROCESS OF CURRICULUM REDESIGN Why did you redesign your curriculum? What were your goals? What was the timeframe? What lessons were learned while
Page 1 QUESTIONS FOR The Commonwealth Medical College PROCESS OF CURRICULUM REDESIGN Why did you redesign your curriculum? What were your goals? What was the timeframe? What lessons were learned while
Physician Assistant Census Report: Results from the 2010 AAPA Census
 Physician Assistant Census Report: Results from the 2010 AAPA Census PHYSICIAN ASSISTANTS AT A GLANCE: HIGHLIGHTS OF THE 2010 ANNUAL PHYSICIAN ASSISTANT CENSUS REPORT Median Age: 38 years Percent in Clinical
Physician Assistant Census Report: Results from the 2010 AAPA Census PHYSICIAN ASSISTANTS AT A GLANCE: HIGHLIGHTS OF THE 2010 ANNUAL PHYSICIAN ASSISTANT CENSUS REPORT Median Age: 38 years Percent in Clinical
CMS SPECIALTY CODES/HEALTHCARE PROVIDER TAXONOMY CROSSWALK
 CMS SPECIALTY CODES/HEALTHCARE PROVIDER TAXONOMY CROSSWALK This document walks the CMS Medicare specialty codes to the taxonomy codes currently maintained by the Washington Publishing Company as mandated
CMS SPECIALTY CODES/HEALTHCARE PROVIDER TAXONOMY CROSSWALK This document walks the CMS Medicare specialty codes to the taxonomy codes currently maintained by the Washington Publishing Company as mandated
New Expectations for Single Program and Small Institutions: Accreditation and CLER
 Accreditation Council for Graduate Medical Education SES 003 ACGME Annual Education Conference February 27, 2015 New Expectations for Single Program and Small Institutions: Accreditation and CLER Baretta
Accreditation Council for Graduate Medical Education SES 003 ACGME Annual Education Conference February 27, 2015 New Expectations for Single Program and Small Institutions: Accreditation and CLER Baretta
Frequently Asked Questions: Physical Medicine and Rehabilitation Review Committee for Physical Medicine and Rehabilitation ACGME
 Frequently Asked Questions: Physical Medicine and Rehabilitation Review Committee for Physical Medicine and Rehabilitation ACGME Questions Program Personnel and Resources Does the Review Committee grant
Frequently Asked Questions: Physical Medicine and Rehabilitation Review Committee for Physical Medicine and Rehabilitation ACGME Questions Program Personnel and Resources Does the Review Committee grant
SCHEDULING GUIDE. April 15, 2016. FOR CHANGES TO THE SCHEDULING DIRECTORY, PLEASE EMAIL gainer@musc.edu.
 SCHEDULING GUIDE April 15, 2016 FOR CHANGES TO THE SCHEDULING DIRECTORY, PLEASE EMAIL gainer@musc.edu. Service Telephone Fax Adolescent Medicine 876-0444 876-1493 Allergy & Immunology 876-8282 876-8181
SCHEDULING GUIDE April 15, 2016 FOR CHANGES TO THE SCHEDULING DIRECTORY, PLEASE EMAIL gainer@musc.edu. Service Telephone Fax Adolescent Medicine 876-0444 876-1493 Allergy & Immunology 876-8282 876-8181
Provider Network Adequacy Instructions
 Provider Network Adequacy Instructions Table of Contents Regulatory Overview...1 Creating an Account under the MDH Provider Network Adequacy (PNA) System...2 Provider Network Adequacy Recertification Requirements...2
Provider Network Adequacy Instructions Table of Contents Regulatory Overview...1 Creating an Account under the MDH Provider Network Adequacy (PNA) System...2 Provider Network Adequacy Recertification Requirements...2
ForwardHealth-Required Taxonomy Codes
 ForwardHealth-Required s Provider Type Ambulance Air Ambulance 3416A0800X Air Transport Ambulance Land Ambulance 3416L0300X Land Transport Federally Qualified Health Ambulance Water Ambulance 3416S0300X
ForwardHealth-Required s Provider Type Ambulance Air Ambulance 3416A0800X Air Transport Ambulance Land Ambulance 3416L0300X Land Transport Federally Qualified Health Ambulance Water Ambulance 3416S0300X
BMA SURVEY OF CONSULTANT WORKING PATTERNS AND ON CALL SERVICES
 BMA SURVEY OF CONSULTANT WORKING PATTERNS AND ON CALL SERVICES Health Policy and Economic Research Unit Report author: Duncan Bland Ocber 2014 bma.org.uk British Medical Association, 2014 Index Executive
BMA SURVEY OF CONSULTANT WORKING PATTERNS AND ON CALL SERVICES Health Policy and Economic Research Unit Report author: Duncan Bland Ocber 2014 bma.org.uk British Medical Association, 2014 Index Executive
Taxonomy Code Mapping Professional Providers
 Professional s Adult Care Nurse Adult Psychiatric Mental Health Nursing 363LA2200X 364SP0809X Adult Health Nursing s Clinical Nurse Specialist Adult Psychiatric/Mental Health Allergy and Immunology 207K00000X
Professional s Adult Care Nurse Adult Psychiatric Mental Health Nursing 363LA2200X 364SP0809X Adult Health Nursing s Clinical Nurse Specialist Adult Psychiatric/Mental Health Allergy and Immunology 207K00000X
PRINCIPLES OF ORGANIZING A NEUROLOGY RESIDENCY PROGRAM. Ralph F. Józefowicz, M.D. University of Rochester, NY
 PRINCIPLES OF ORGANIZING A NEUROLOGY RESIDENCY PROGRAM Ralph F. Józefowicz, M.D. University of Rochester, NY The following twelve principles should be kept in mind when organizing a Neurology residency
PRINCIPLES OF ORGANIZING A NEUROLOGY RESIDENCY PROGRAM Ralph F. Józefowicz, M.D. University of Rochester, NY The following twelve principles should be kept in mind when organizing a Neurology residency
What Does it Mean When Patients Choose Wisely? David Ansley Senior Analyst, Health Product Development Consumer Reports
 What Does it Mean When Patients Choose Wisely? David Ansley Senior Analyst, Health Product Development Consumer Reports People are realizing that more medicine is not necessarily better. And that we re
What Does it Mean When Patients Choose Wisely? David Ansley Senior Analyst, Health Product Development Consumer Reports People are realizing that more medicine is not necessarily better. And that we re
December 21, 2012. The Honorable Harry Reid Majority Leader U.S. Senate S-221 U.S. Capitol Washington, DC 20510
 December 21, 2012 The Honorable Harry Reid Majority Leader U.S. Senate S-221 U.S. Capitol Washington, DC 20510 The Honorable Mitch McConnell Republican Leader U.S. Senate S-230 U.S. Capitol Washington,
December 21, 2012 The Honorable Harry Reid Majority Leader U.S. Senate S-221 U.S. Capitol Washington, DC 20510 The Honorable Mitch McConnell Republican Leader U.S. Senate S-230 U.S. Capitol Washington,
WHY BECOME AN AIR FORCE PHYSICIAN? READ ON...
 WHY BECOME AN AIR FORCE PHYSICIAN? READ ON... RESPECT AND PRESTIGE The Air Force has one of the best healthcare systems in the world. Through continuing research and development of new technology, our
WHY BECOME AN AIR FORCE PHYSICIAN? READ ON... RESPECT AND PRESTIGE The Air Force has one of the best healthcare systems in the world. Through continuing research and development of new technology, our
How To Become A Royal Perth Hospital Graduate Nurse
 www.nursingwa.com.au > graduate info 1...the Career of a Lifetime > Graduate Nurse Programs > graduate info AT RPH, WE OFFER OUR NURSES EXCEPTIONAL CAREER OPPORTUNITIES ACROSS A COMPREHENSIVE RANGE OF
www.nursingwa.com.au > graduate info 1...the Career of a Lifetime > Graduate Nurse Programs > graduate info AT RPH, WE OFFER OUR NURSES EXCEPTIONAL CAREER OPPORTUNITIES ACROSS A COMPREHENSIVE RANGE OF
TRAINING IN SURGERY IN GREECE
 TRAINING IN SURGERY IN GREECE George N Zografos Consultant Surgeon, Athens General Hospital General Secretary Hellenic Surgical Association National Delegate, UEMS Division of General Surgery STATISTICAL
TRAINING IN SURGERY IN GREECE George N Zografos Consultant Surgeon, Athens General Hospital General Secretary Hellenic Surgical Association National Delegate, UEMS Division of General Surgery STATISTICAL
Robert Englander, MD Laura Edgar, EdD Lois Margaret Nora, MD, JD, MBA
 Robert Englander, MD Laura Edgar, EdD Lois Margaret Nora, MD, JD, MBA Competency-based Medical Education Robert Englander, MD, MPH March 27 th, 2015 Definitions CBME: An outcomes-based approach to the
Robert Englander, MD Laura Edgar, EdD Lois Margaret Nora, MD, JD, MBA Competency-based Medical Education Robert Englander, MD, MPH March 27 th, 2015 Definitions CBME: An outcomes-based approach to the
Roles, Responsibilities and Patient Care Activities of Residents Family Medicine-Sports Medicine Fellowship
 Roles, Responsibilities and Patient Care Activities of Residents Family Medicine-Sports Medicine Fellowship University of Washington Medical Center Harborview Medical Center Seattle Cancer Care Alliance
Roles, Responsibilities and Patient Care Activities of Residents Family Medicine-Sports Medicine Fellowship University of Washington Medical Center Harborview Medical Center Seattle Cancer Care Alliance
Specialty-specific Duty Hour Definitions (06/10/2012)
 Specialty-specific Duty Hour Definitions (06/10/2012) Below is the updated list of specialty-specific duty hour definitions. Definitions that were approved in June 2012 are underlined and will be incorporated
Specialty-specific Duty Hour Definitions (06/10/2012) Below is the updated list of specialty-specific duty hour definitions. Definitions that were approved in June 2012 are underlined and will be incorporated
CURRICULUM OF BACHELOR'S DEGREE IN MEDICINE SCHOOL OF MEDICINE CURRICULUM
 CURRICULUM OF BACHELOR'S DEGREE IN MEDICINE SCHOOL OF MEDICINE CURRICULUM Minimum Duration of Course: 12 Semesters Maximum Duration of Course: 24 Semesters Average Duration of Course: 12 Semesters Curriculum
CURRICULUM OF BACHELOR'S DEGREE IN MEDICINE SCHOOL OF MEDICINE CURRICULUM Minimum Duration of Course: 12 Semesters Maximum Duration of Course: 24 Semesters Average Duration of Course: 12 Semesters Curriculum
League of Women Voters. November 20, 2012
 League of Women Voters November 20, 2012 Palo Alto Medical Foundation Multi-Specialty Medical Group for past 82 years. Outpatient Medical Centers not a hospital Community based, not-for-profit Physician-led
League of Women Voters November 20, 2012 Palo Alto Medical Foundation Multi-Specialty Medical Group for past 82 years. Outpatient Medical Centers not a hospital Community based, not-for-profit Physician-led
List of Australian Recognised Medical Specialties
 List of Australian Recognised Medical Specialties The List of Australian Recognised Medical Specialties includes those organisations, specialties and qualifications that are recognised as medical specialties
List of Australian Recognised Medical Specialties The List of Australian Recognised Medical Specialties includes those organisations, specialties and qualifications that are recognised as medical specialties
Community Medical School October 26, 2010
 Community Medical School October 26, 2010 Who is Taking Care of You? Paul A. Taheri MD, MBA President / CEO University of Vermont Medical Group Sr. Associate Dean for Clinical Affairs Health Care is Complex
Community Medical School October 26, 2010 Who is Taking Care of You? Paul A. Taheri MD, MBA President / CEO University of Vermont Medical Group Sr. Associate Dean for Clinical Affairs Health Care is Complex
Neurodegenerative diseases Includes multiple sclerosis, Parkinson s disease, postpolio syndrome, rheumatoid arthritis, lupus
 TIRR Memorial Hermann is a nationally recognized rehabilitation hospital that returns lives interrupted by neurological illness, trauma or other debilitating conditions back to independence. Some of the
TIRR Memorial Hermann is a nationally recognized rehabilitation hospital that returns lives interrupted by neurological illness, trauma or other debilitating conditions back to independence. Some of the
UNC Hospitals Graduate Medical Education Application 2014/2015 Page 1 of 5
 Instruction for Completion of Application for Appointment to Graduate Medical Education at University of North Carolina Hospitals Chapel Hill, North Carolina 27514 Complete all required information on
Instruction for Completion of Application for Appointment to Graduate Medical Education at University of North Carolina Hospitals Chapel Hill, North Carolina 27514 Complete all required information on
