Original Article Effect of anterior cervical decompression fusion at different cervical segments on C5 nerve root palsy
|
|
|
- Scarlett Carr
- 7 years ago
- Views:
Transcription
1 Int J Clin Exp Med 2016;9(2): /ISSN: /IJCEM Original Article Effect of anterior cervical decompression fusion at different cervical segments on C5 nerve root palsy Gang Duan 1, Hongliang Chen 2, Ziqiang Zhu 1, Changming Yan 1, Gang Liu 1, Bin Wang 1, Xinghai Jia 1 1 Department of Orthopedics, Second Affiliated Hospital of Xuzhou Medical College, Xuzhou , China; 2 Department of Orthopedics, Affiliated Hospital of Xuzhou Medical College, Xuzhou , Jiangsu, China Received September ; Accepted December ; Epub February 15, 2016; Published February 29, 2016 Abstract: Objective: This study aimed to investigate the effect of anterior cervical decompression fusion at different cervical segments on C5 nerve root palsy. Methods: A total of 78 patients who received anterior cervical decompression and bone graft fusion due to cervical disease and ossification of the posterior longitudinal ligament of the spine between March 2009 and August 2013 were retrospectively reviewed. Patients were divided into 2 groups: In Group A, patients underwent 1- or 2-segment decompression, and those in Group B underwent 3- or 4-segment decompression. The Japanese Orthopedic Association (JOA) scoring system was used to evaluate the clinical efficacy. The preoperative and postoperative cervical curvature indexes (CCI) and cervical lordosis angle (Cobb angle) were measured. Results: The incidence of C5 nerve root palsy was 2% in Group A and 15.8% in Group B, showing a significant difference (P<0.05). In addition, the postoperative CCI change rate was 18.0±16.6% in Group B, which was significantly higher than in Group A (11.5±7.9%), and the postoperative cervical Cobb angle and CCI increased markedly in Group B, as compared to those before surgery (P<0.05). The JOA score was comparable between two groups before and after surgery (P>0.05). Conclusion: Decompression fusion at several segments may increase the intervertebral disc gap and significantly change postoperative cervical curvature, which is an important cause of C5 nerve root injury. Keywords: Anterior approach, cervical curvature, C5 nerve root palsy Introduction C5 nerve root palsy is a common and important complication of anterior or posterior cervical decompressive surgery, and its pathogenesis has not yet been elucidated. It is imperative to reduce the incidence of post-operative C5 nerve root palsy because it significantly affects the quality of life of patients. To date, most studies focus on the C5 nerve root palsy following posterior cervical decompression, and the C5 nerve root palsy after anterior cervical decompression is less studied. This study summarized the clinical information of patients who received anterior cervical decompression fusion in our department, and the cervical curvature and C5 nerve root palsy were investigated. Patients and methods Patients and grouping A total of 78 patients received the anterior cervical decompression and bone graft fusion due to cervical disease and ossification of the posterior longitudinal ligament (OPLL) of the spine between March 2009 and August There were 45 men and 33 women with the median age of 45 years (range: years). Of these patients, 39 were diagnosed with cervical spondylotic myelopathy, 21 with nerve root cervical spondylosis, and 18 with OPLL of the spine. Patients with cervical tumor and cervical trauma were excluded from this study. Patients were followed up for a median of 15.5 months (range: 8-22 months). Patients were divided into 2 groups. in Group A, patients underwent 1- or 2-segment decompression; there were 23 men and 17 women; the mean age was 53 years (range: years); 20 patients were diagnosed with cervical spondylotic myelopathy, 12 with nerve root cervical spondylosis, 8 with OPLL of the spine; 13 received single-segment intervertebral disc decompression, cage bone grafting and titanium plate fixation, and 27 underwent double-segment (C3-C5, C4-C6 and C5-C7) cervical vertebral disc decompression
2 Table 1. General characteristics of patients in both groups Group n Sex Minimal width of C4/C5 intervertebral foramen (mm) C3/C4 C4/C5 C5/C6 Patients with hyperintense-signal Age (yrs) M F C6/C7 Patients with OPLL (n) A ± ± B ± ± Figure 1. Measurement of cervical Cobb angle: In the neutral position, a cervical lateral radiograph was obtained, and 2 straight lines parallel to the edge of the C3 and C7 vertebral bodies were drawn. The angle between 2 straight lines was measured as Cobb angle. Preoperative (A) and postoperative (B) Cobb angles. and internal fixation. In Group B, patients underwent 3- or 4-segment decompression; there were 25 men and 13 women; the median age was 56.7 years (range: years); 19 patients were diagnosed with cervical spondylotic myelopathy, 9 with nerve root cervical spondylosis, and 10 with OPLL of the spine; 37 patients received 3-segment (C3-C6 or C4-C7) cervical vertebral disc decompression and internal fixation, and 1 underwent 4-segment cervical vertebral disc decompression and internal fixation (C3-C7). A cervical gear was used for 3 months after surgery for all the patients. Before surgery, there were no significant differences in the age, sex, width of intervertebral foramen at C4/C5 for men, number of patients with hyperintense signals at C3/C4, C4/C5, C5/C6 and C6/C7 and number of OPLL of the spine between two groups (P>0.05; Table 1). Diagnostic criteria for C5 nerve root palsy In cases without serious spinal symptoms, the muscle force of the deltoid and bicipital muscles of the arm declined 1 level or more. C5 nerve root palsy was diagnosed according to the diagnostic criteria developed by Kim et al. [1]: the muscle strength of the deltoid and/ or biceps reduced by 1 or more grades after 3718 Int J Clin Exp Med 2016;9(2):
3 Figure 2. CCI measurement: a lateral radiograph was obtained, and a line connecting the posterior lower corner of C2 and C7 was drawn. The length of this line was A; the distance between the posterior lower corner of different vertebral bodies (C3 and C6) and the former line was al, a2, a3 and a4, respectively; CCI was calculated: CCI = (a1 + a2 + a3 + a4)/a 100%. A. Preoperative CCI; B. Postoperative CCI. surgery, with or without hypoesthesia at the shoulder and lateral upper arm and uncontrollable shoulder pain in the absence of deterioration of spinal symptoms. Neurological function The Japanese Orthopedic Association (JOA) [2] scoring system was used to assess the neurological function before surgery and at the last follow-up, and the improvement of neurological function was determined as follow: improvement rate = (postoperative score-preoperative score)/(17-preoperative score) 100%. Cervical cobb angle [3] In the neutral position, a cervical lateral radiograph was obtained, 2 straight lines were drawn parallel to the edge of the C3 and C7 vertebral bodies independently, and then the angle between 2 straight lines (Cobb angle) was measured before and after surgery (Figure 1). Cervical curvature index (CCI) [4] CCI was measured as follows: a lateral radiograph was obtained, and a line connecting the posterior lower corner of C2 and C7 was drawn. The length of this line was A; the distance between the posterior lower corner of different vertebral bodies (C3 and C6) and the former line was a1, a2, a3 and a4, respectively; CCI was calculated: CCI = (a1 + a2 + a3 + a4)/a 100% (Figure 2). Statistical analysis Data with normal distribution are expressed as mean ± standard deviation ( _ x! s). Quantitative data were compared with t test and qualitative data with chi square test. A value of P<0.05 was considered statistically significant. Statistical analysis was performed with SPSS version Results Incidence of C5 nerve root palsy In Group, C5 nerve root palsy was found in 1 patient (2.5%, 1/40) and only involved the deltoid muscle. In Group B, C5 nerve root palsy was found in 6 patients (15.8%, 6/38) and affected both deltoid muscle and biceps in Int J Clin Exp Med 2016;9(2):
4 Table 2. Cervical curvature in both groups before and after surgery Group n Patients with 5 nerve root palsy (n) Cobb angle (degrees) CCI (%) Preoperative Postoperative Preoperative Postoperative CCI change rate A ± ± ± ± ±7.9 B ± ± ± ± ±16.6 Table 3. JOA score before surgery Group n patients, and only involved deltoid muscle in 4 patients. Significant difference was observed in the incidence of C5 nerve root palsy between groups (χ 2 = 4.21, P<0.05; Table 2). In both groups, only unilateral C5 nerve root palsy was found, and the muscle strength was I-IV. At the last follow up, the muscle strength recovered to IV-V. C5 nerve root palsy occurred at 1 day to 1 week after surgery. Cervical cobb angle and CCI After surgery, the cervical Cobb angle was 15.6 ±2.9, and the CCI change and CCI change rate were 15.2%±1.8% and 18.0%±16.6%, respectively, in Group B, which were significantly higher than in Group A (13.8 ±3.1, 12.9%±2.5%, and 11.5%±7.9%, respectively) (P<0.05; Table 2). JOA score The preoperative and postoperative JOA score was 10.1±2.3 and 13.4±1.7, respectively in Group A, and 10.2±2.3 and 13.7±1.4, respectively in Group B. The postoperative improvement rate in JOA score was 45.8%±18.3% in Group A and 50.7%±19.3% in Group B, although significant difference was not observed (P> 0.05; Table 3). Discussion Patients with C5 nerve root palsy (n) JOA score Preoperative Postoperative Improvement rate A ± ± ±18.3 B ± ± ±19.3 C5 nerve root palsy is frequently found after a cervical decompression. Its classic symptom includes the movement dysfunction of the deltoid and or biceps without deterioration of spinal symptoms. Most patients develop mild amyasthenia, and a few patients have concomitant sensory disturbance and/or pain at the C5 innervated area [4]. In 1961, Scoville et al. [5] and Stoops et al. [6] for the first time reported C5 nerve root palsy. Since then, increasing studies have been conducted to investigate C5 nerve root palsy. It has been reported that the incidence of C5 nerve root palsy as a complication of anterior or posterior cervical decompression is 0-30% [4, 7]. C5 nerve root palsy may occur immediately after surgery, but often occurs within 1 week after surgery. Several patients may develop C5 nerve root palsy at 2 to 4 weeks after surgery. It is also possible that patients develop C5 nerve root palsy at 2 months after surgery. In addition, 92% of patients have unilateral involvement and 8% develop bilateral C5 nerve root palsy [4, 8]. Currently, the pathogenesis of C5 nerve root palsy is still poorly understood. There are 5 possible causes: 1) intraoperative direct injury to the nerve root; 2) retraction of the nerve root due to spinal cord drift after decompression results in the tethered effect; 3) the reduced blood supply to radicular arteries leads to spinal cord ischemia; 4) segmental spinal cord dysfunction; 5) spinal cord ischemia-reperfusion injury. Posterior cervical decompression is the first surgery used for the therapy of cervical spondylosis. For patients with spinal cord lesions involving 3 or more segments, Posterior cervical decompression is recommended. The backward shift of the spinal cord drift may avoid the pressure due to the anterior spinal cord. However, the posterior cervical decompression fail to relieve the anterior spinal cord compression, spinal epidural scar is easy to form on the spinal cord after lamina excision leading to the dynamic compression and retraction of the spinal cord [9]. Moreover, the backward shift may cause the retraction of nerve root, resulting in tethered effect [10]. Anatomically, the C5 nerve root is shorter than other nerve roots and C5 is the highest site of decompression regions. Thus, the spinal cord shift is larger which is easy to cause C5 nerve root 3720 Int J Clin Exp Med 2016;9(2):
5 injury [11]. Therefore, available studies on C5 nerve root palsy mainly focus on the posterior cervical decompression, and anterior cervical decompression is less reported. In view of the disadvantages of posterior cervical decompression, anterior cervical decompression is introduced for the therapy of cervical spondylosis. However, C5 nerve root palsy is also present after anterior cervical decompression as in posterior cervical decompression, and the reported incidence of C5 nerve root palsy after anterior cervical decompression varies between studies. In particular, Li et al. [12] reported an incidence of 5.2% (1.4%- 10.6%) for C5 nerve root palsy after anterior decompression, which was lower than that after posterior cervical decompression. However, Gandhoke et al. [13] found there was no marked difference in the incidence of C5 nerve root palsy between anterior vertebral body subtotal resection and posterior laminoplasty in patients with cervical stenosis. Liu et al. [14] treated cervical spondylotic myelopathy with 3 reconstruction methods: long segmental anterior cervical corpectomy and fusion, mixed n anterior cervical decompression and fusion and anterior cervical decompression and fusion, and the incidence of C5 nerve root palsy was compared. Their results showed that the incidence of C5 nerve root palsy was the highest after long segmental anterior cervical corpectomy and fusion (11.49%). Yonenobu et al. [15] also reported that the incidence of C5 nerve root palsy increased after anterior subtotal corpectomy of 3 vertebral bodies, which was mainly ascribed to the increased forward drift of the spinal cord after expanded cervical decompression and subsequent shift of the bone graft or the intervertebral foramen stenosis due to cervical hyperextension. However, the mechanism underlying the effect of forward drift of the cervical spinal cord on the C5 nerve root is still unclear. Theoretically, anterior cervical decompression relieve the anterior compression, leading to the forward shift of the spinal cord, which reduces the tension of the C5 nerve root and thus decreases the incidence of C5 nerve root palsy. However, Saunders et al. [16] proposed that the forward displacement of the spinal cord to a certain extent could easily lead to the retraction and entangling of C5 nerve root, eventually resulting in C5 nerve root palsy. When the vertebral body slot width decreases, the ventral drift of the spinal cord reduces, which significantly decreases the incidence of C5 nerve root palsy [17]. In the present study, there were no marked differences in the age, sex and preoperative characteristics between two groups (P>0.05). After surgery, C5 nerve root palsy was found in 1 patient of Group A (2.5%) in which patients received 1- or 2-segment decompression-fusion. C5 nerve root palsy was noted in 6 patients (15.8%) in Group B in which patients received 3- and 4- segment decompression-fusion. Significant difference was observed between 2 groups (P<0.05). With the increase in the cervical segments undergoing decompression and fusion, the change in the cervical curvature also increased. In Group B, the post-operative CCI change rate was greater than in Group A, and the cervical Cord angle and CCI in Group B increased significantly after surgery when compared with those before surgery (P<0.05). However, the JOA score before and after surgery was comparable between two groups (P>0.05). We speculate that the anterior cervical titanium plate increase the change in cervical curvature with the increase in the number of segments undergoing decompression, and the increased intervertebral space may increase the ventral drift of the spinal cord, resulting in the nerve root retraction and injury to the C5 nerve root. Our results indicate that the anterior cervical decompression is an effective modality for the treatment of cervical spondylosis. C5 nerve root palsy is a complication of cervical decompression and caused by many factors. The increased cervical curvature secondary to decompression-fusion at several cervical segments is a major cause of C5 nerve root palsy and the tethering of C5 nerve root is one of important mechanisms underlying the pathogenesis of C5 nerve root palsy. However, this study was a retrospective one, and the sample size was still small. Thus, further prospective studies with large sample size are required to investigate and elucidate the risk factors related to C5 nerve root palsy. Disclosure of conflict of interest None. Address correspondence to: Hongliang Chen, Department of Orthopedics, Affiliated Hospital of Xuzhou Medical College, Xuzhou , Jiangsu, China. chenhongliangdd@sina.com 3721 Int J Clin Exp Med 2016;9(2):
6 References [1] Kim S, Lee SH, Kim ES and Eoh W. Clinical and radiographic analysis of c5 palsy after anterior cervical decompression and fusion for cervical degenerative disease. J Spinal Disord Tech 2014; 27: [2] Morimoto T, Ohtsuka H, Sakaki T and Kawaguchi M. Postlaminectomy cervical spinal cord compression demonstrated by dynamic magnetic resonance imaging. Case report. J Neurosurg 1998; 88: [3] Ishihara A. [Roentgenographic studies on the normal pattern of the cervical curvature]. Nihon Seikeigeka Gakkai Zasshi 1968; 42: [4] Sakaura H, Hosono N, Mukai Y, Ishii T and Yoshikawa H. C5 palsy after decompression surgery for cervical myelopathy: review of the literature. Spine (Phila Pa 1976) 2003; 28: [5] Scoville WB. Cervical spondylosis treated by bilateral facetectomy and laminectomy. J Neurosurg 1961; 18: [6] Stoops WL and King RB. Neural complications of cervical spondylosis: their response to laminectomy and foramenotomy. J Neurosurg 1962; 19: [7] Hojo Y, Ito M, Abumi K, Kotani Y, Sudo H, Takahata M and Minami A. A late neurological complication following posterior correction surgery of severe cervical kyphosis. Eur Spine J 2011; 20: [8] Nassr A, Eck JC, Ponnappan RK, Zanoun RR, Donaldson WF 3rd and Kang JD. The incidence of C5 palsy after multilevel cervical decompression procedures: a review of 750 consecutive cases. Spine (Phila Pa 1976) 2012; 37: [9] Liu T, Zou W, Han Y and Wang Y. Correlative study of nerve root palsy and cervical posterior decompression laminectomy and internal fixation. Orthopedics 2010; 33. [10] Shiozaki T, Otsuka H, Nakata Y, Yokoyama T, Takeuchi K, Ono A, Numasawa T, Wada K and Toh S. Spinal cord shift on magnetic resonance imaging at 24 hours after cervical laminoplasty. Spine (Phila Pa 1976) 2009; 34: [11] Currier BL. Neurological complications of cervical spine surgery: C5 palsy and intraoperative monitoring. Spine (Phila Pa 1976) 2012; 37: E [12] Li H and Dai LY. A systematic review of complications in cervical spine surgery for ossification of the posterior longitudinal ligament. Spine J 2011; 11: [13] Gandhoke G, Wu JC, Rowland NC, Meyer SA, Gupta C and Mummaneni PV. Anterior corpectomy versus posterior laminoplasty: is the risk of postoperative C-5 palsy different? Neurosurg Focus 2011; 31: E12. [14] Liu Y, Qi M, Chen H, Yang L, Wang X, Shi G, Gao R, Wang C and Yuan W. Comparative analysis of complications of different reconstructive techniques following anterior decompression for multilevel cervical spondylotic myelopathy. Eur Spine J 2012; 21: [15] Yonenobu K, Hosono N, Iwasaki M, Asano M and Ono K. Neurologic complications of surgery for cervical compression myelopathy. Spine (Phila Pa 1976) 1991; 16: [16] Saunders RL. On the pathogenesis of the radiculopathy complicating multilevel corpectomy. Neurosurgery 1995; 37: ; discussion [17] Odate S, Shikata J, Yamamura S and Soeda T. Extremely wide and asymmetric anterior decompression causes postoperative C5 palsy: an analysis of 32 patients with postoperative C5 palsy after anterior cervical decompression and fusion. Spine (Phila Pa 1976) 2013; 38: Int J Clin Exp Med 2016;9(2):
Cervical Spondylotic Myelopathy Associated with Kyphosis or Sagittal Sigmoid Alignment: Outcome after Anterior or Posterior Decompression
 Cervical Spondylotic Myelopathy Associated with Kyphosis or Sagittal Sigmoid Alignment: Outcome after Anterior or Posterior Decompression 1 Journal of Neurosurgery: Spine November 2009, Volume 11, pp.
Cervical Spondylotic Myelopathy Associated with Kyphosis or Sagittal Sigmoid Alignment: Outcome after Anterior or Posterior Decompression 1 Journal of Neurosurgery: Spine November 2009, Volume 11, pp.
Postoperative C5 palsy in consequence of anterior cervical discectomy and fusion (ACDF)
 Postoperative C5 palsy in consequence of anterior cervical discectomy and fusion (ACDF) *Takeshi Aoyama, *Kazutoshi Hida, *:Shunsuke Yano, *Tomohiro Yamauchi, **Motoyuki Iwasaki, *Kiyohiro Houkin *Department
Postoperative C5 palsy in consequence of anterior cervical discectomy and fusion (ACDF) *Takeshi Aoyama, *Kazutoshi Hida, *:Shunsuke Yano, *Tomohiro Yamauchi, **Motoyuki Iwasaki, *Kiyohiro Houkin *Department
CERVICAL DISC HERNIATION
 CERVICAL DISC HERNIATION Most frequent at C 5/6 level but also occur at C 6 7 & to a lesser extent at C4 5 & other levels In relatively younger persons soft disk protrusion is more common than hard disk
CERVICAL DISC HERNIATION Most frequent at C 5/6 level but also occur at C 6 7 & to a lesser extent at C4 5 & other levels In relatively younger persons soft disk protrusion is more common than hard disk
1 REVISOR 5223.0070. (4) Pain associated with rigidity (loss of motion or postural abnormality) or
 1 REVISOR 5223.0070 5223.0070 MUSCULOSKELETAL SCHEDULE; BACK. Subpart 1. Lumbar spine. The spine rating is inclusive of leg symptoms except for gross motor weakness, bladder or bowel dysfunction, or sexual
1 REVISOR 5223.0070 5223.0070 MUSCULOSKELETAL SCHEDULE; BACK. Subpart 1. Lumbar spine. The spine rating is inclusive of leg symptoms except for gross motor weakness, bladder or bowel dysfunction, or sexual
Cervical Spine Surgery. Orthopaedic Nursing Seminar. Dr Michelle Atkinson. Friday October 21 st 2011. Cervical Disc Herniation
 Cervical Spine Surgery Dr Michelle Atkinson The Sydney and Dalcross Adventist Hospitals Orthopaedic Nursing Seminar Friday October 21 st 2011 Cervical disc herniation The most frequently treated surgical
Cervical Spine Surgery Dr Michelle Atkinson The Sydney and Dalcross Adventist Hospitals Orthopaedic Nursing Seminar Friday October 21 st 2011 Cervical disc herniation The most frequently treated surgical
Spinal Surgery Functional Status and Quality of Life Outcome Specifications 2015 (01/01/2013 to 12/31/2013 Dates of Procedure) September 2014
 Description Methodology For patients ages 18 years and older who undergo a lumbar discectomy/laminotomy or lumbar spinal fusion procedure during the measurement year, the following measures will be calculated:
Description Methodology For patients ages 18 years and older who undergo a lumbar discectomy/laminotomy or lumbar spinal fusion procedure during the measurement year, the following measures will be calculated:
Cervical Conditions: Diagnosis and Treatments
 Cervical Conditions: Diagnosis and Treatments Mark R Mikles, M.D. Cervical Conditions: Diagnosis and Treatment Cervical conditions Neck Pain Radiculopathy Myelopathy 1 Cervical Conditions: Diagnosis and
Cervical Conditions: Diagnosis and Treatments Mark R Mikles, M.D. Cervical Conditions: Diagnosis and Treatment Cervical conditions Neck Pain Radiculopathy Myelopathy 1 Cervical Conditions: Diagnosis and
visualized. The correct level is then identified again. With the use of a microscope and
 SURGERY FOR SPINAL STENOSIS Laminectomy A one inch (or longer for extensive stenosis) incision is made in the middle of the back over the effected region of the spine. The muscles over the bone are moved
SURGERY FOR SPINAL STENOSIS Laminectomy A one inch (or longer for extensive stenosis) incision is made in the middle of the back over the effected region of the spine. The muscles over the bone are moved
White Paper: Reducing Utilization Concerns Regarding Spinal Fusion and Artificial Disc Implants
 White Paper: Reducing Utilization Concerns Regarding Spinal Fusion and Artificial Disc Implants For Health Plans, Medical Management Organizations and TPAs Executive Summary Back pain is one of the most
White Paper: Reducing Utilization Concerns Regarding Spinal Fusion and Artificial Disc Implants For Health Plans, Medical Management Organizations and TPAs Executive Summary Back pain is one of the most
Bin Yue, Bohua Chen, Xue-Xiao Ma, Yong-Ming Xi, Hong-Fei Xiang, You-Gu Hu, Guoqing Zhang
 Int J Clin Exp Med 2015;8(6):9565-9569 www.ijcem.com /ISSN:1940-5901/IJCEM0005168 Original Article One stage laminoplasty and posterior herniotomy for the treatment of myelopathy caused by cervical stenosis
Int J Clin Exp Med 2015;8(6):9565-9569 www.ijcem.com /ISSN:1940-5901/IJCEM0005168 Original Article One stage laminoplasty and posterior herniotomy for the treatment of myelopathy caused by cervical stenosis
Surgical Procedures and Clinical Results of Endoscopic Decompression for Lumbar Canal Stenosis
 Surgical Procedures and Clinical Results of Endoscopic Decompression for Lumbar Canal Stenosis Munehito Yoshida, Akitaka Ueyoshi, Kazuhiro Maio, Masaki Kawai, and Yukihiro Nakagawa Summary. The purpose
Surgical Procedures and Clinical Results of Endoscopic Decompression for Lumbar Canal Stenosis Munehito Yoshida, Akitaka Ueyoshi, Kazuhiro Maio, Masaki Kawai, and Yukihiro Nakagawa Summary. The purpose
If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time.
 If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time. You may be worried about your future, both in respect of finances and
If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time. You may be worried about your future, both in respect of finances and
Nonoperative Management of Herniated Cervical Intervertebral Disc With Radiculopathy. Spine Volume 21(16) August 15, 1996, pp 1877-1883
 Nonoperative Management of Herniated Cervical Intervertebral Disc With Radiculopathy 1 Spine Volume 21(16) August 15, 1996, pp 1877-1883 Saal, Joel S. MD; Saal, Jeffrey A. MD; Yurth, Elizabeth F. MD FROM
Nonoperative Management of Herniated Cervical Intervertebral Disc With Radiculopathy 1 Spine Volume 21(16) August 15, 1996, pp 1877-1883 Saal, Joel S. MD; Saal, Jeffrey A. MD; Yurth, Elizabeth F. MD FROM
Soft-tissue injuries of the neck in automobile accidents: Factors influencing prognosis
 Soft-tissue injuries of the neck in automobile accidents: Factors influencing prognosis 1 Mason Hohl, MD FROM ABSTRACT: Journal of Bone and Joint Surgery (American) December 1974;56(8):1675-1682 Five years
Soft-tissue injuries of the neck in automobile accidents: Factors influencing prognosis 1 Mason Hohl, MD FROM ABSTRACT: Journal of Bone and Joint Surgery (American) December 1974;56(8):1675-1682 Five years
ANTERIOR CERVICAL DISCECTOMY AND FUSION. Basic Anatomical Landmarks: Anterior Cervical Spine
 Anterior In the human anatomy, referring to the front surface of the body or position of one structure relative to another Cervical Relating to the neck, in the spine relating to the first seven vertebrae
Anterior In the human anatomy, referring to the front surface of the body or position of one structure relative to another Cervical Relating to the neck, in the spine relating to the first seven vertebrae
Minimally Invasive Spine Surgery For Your Patients
 Minimally Invasive Spine Surgery For Your Patients Lukas P. Zebala, M.D. Assistant Professor Orthopaedic and Neurological Spine Surgery Department of Orthopaedic Surgery Washington University School of
Minimally Invasive Spine Surgery For Your Patients Lukas P. Zebala, M.D. Assistant Professor Orthopaedic and Neurological Spine Surgery Department of Orthopaedic Surgery Washington University School of
Important Predictors of Outcome in Patients with Cervical Spondylotic Myelopathy and Radiculopathy undergoing Surgery
 Important Predictors of Outcome in Patients with Cervical Spondylotic Myelopathy and Radiculopathy undergoing Surgery Michael G. Fehlings Professor of Neurosurgery Vice Chair Research, Department of Surgery
Important Predictors of Outcome in Patients with Cervical Spondylotic Myelopathy and Radiculopathy undergoing Surgery Michael G. Fehlings Professor of Neurosurgery Vice Chair Research, Department of Surgery
Patient Information. Anterior Cervical Discectomy and Fusion Surgery (ACDF).
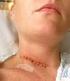 Patient Information. Anterior Cervical Discectomy and Fusion Surgery (ACDF). Understanding your spine Disc Between each pair of vertebrae there is a disc that acts as a cushion to protect the vertebra,
Patient Information. Anterior Cervical Discectomy and Fusion Surgery (ACDF). Understanding your spine Disc Between each pair of vertebrae there is a disc that acts as a cushion to protect the vertebra,
Brown-Sequard Syndrome Caused by Cervical Disc Herniation
 62 CASE REPORT Brown-Sequard Syndrome Caused by Cervical Disc Herniation Chih-Hsiu Wang, Chun-Chung Chen, Der-Yang Cho Department of Neurosurgery, China Medical University Hospital, Taichung, Taiwan, R.O.C.
62 CASE REPORT Brown-Sequard Syndrome Caused by Cervical Disc Herniation Chih-Hsiu Wang, Chun-Chung Chen, Der-Yang Cho Department of Neurosurgery, China Medical University Hospital, Taichung, Taiwan, R.O.C.
Options for Cervical Disc Degeneration A Guide to the Fusion Arm of the M6 -C Artificial Disc Study
 Options for Cervical Disc Degeneration A Guide to the Fusion Arm of the M6 -C Artificial Disc Study Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine
Options for Cervical Disc Degeneration A Guide to the Fusion Arm of the M6 -C Artificial Disc Study Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine
BRYAN. Cervical Disc System. Patient Information
 BRYAN Cervical Disc System Patient Information 3 BRYAN Cervical Disc System PATIENT INFORMATION BRYAN Cervical Disc System PATIENT INFORMATION 1 BRYAN Cervical Disc System This patient information brochure
BRYAN Cervical Disc System Patient Information 3 BRYAN Cervical Disc System PATIENT INFORMATION BRYAN Cervical Disc System PATIENT INFORMATION 1 BRYAN Cervical Disc System This patient information brochure
Patient Information. Lateral Lumbar Interbody Fusion Surgery (LLIF).
 Patient Information. Lateral Lumbar Interbody Fusion Surgery (LLIF). Understanding your spine Disc Between each pair of vertebrae there is a disc that acts as a cushion to protect the vertebra, allows
Patient Information. Lateral Lumbar Interbody Fusion Surgery (LLIF). Understanding your spine Disc Between each pair of vertebrae there is a disc that acts as a cushion to protect the vertebra, allows
Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, The Cervical Spine. What is the Cervical Spine?
 Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine condition that can cause pain and numbness in the neck, shoulders, arms, and even hands. This patient
Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine condition that can cause pain and numbness in the neck, shoulders, arms, and even hands. This patient
Anterior Approach Burn s Space Esophagus
 Cervical Complications Complications after Cervical Spine Surgery Dr. Rock Patel University of Michigan, Ann Arbor APPROACH RELATED Anterior Posterior PROCEDURE RELATED ACDF Disc Arthroplasty Laminectomy/Fusion
Cervical Complications Complications after Cervical Spine Surgery Dr. Rock Patel University of Michigan, Ann Arbor APPROACH RELATED Anterior Posterior PROCEDURE RELATED ACDF Disc Arthroplasty Laminectomy/Fusion
Minimally Invasive Spine Surgery What is it and how will it benefit patients?
 Minimally Invasive Spine Surgery What is it and how will it benefit patients? Dr Raoul Pope MBChB, FRACS, Neurosurgeon and Minimally Invasive Spine Surgeon Concord Hospital and Mater Private Hospital Sydney
Minimally Invasive Spine Surgery What is it and how will it benefit patients? Dr Raoul Pope MBChB, FRACS, Neurosurgeon and Minimally Invasive Spine Surgeon Concord Hospital and Mater Private Hospital Sydney
A Patient s Guide to the Disorders of the Cervical and Upper Thoracic Spine
 A Patient s Guide to the Disorders of the Cervical and Upper Thoracic Spine General Anatomy of the Spine The spine can be divided into four regions based on vertebral shape and sagittal plane curve.» CERVICAL:
A Patient s Guide to the Disorders of the Cervical and Upper Thoracic Spine General Anatomy of the Spine The spine can be divided into four regions based on vertebral shape and sagittal plane curve.» CERVICAL:
A Patient s Guide to Artificial Cervical Disc Replacement
 A Patient s Guide to Artificial Cervical Disc Replacement Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine condition that can cause pain and numbness
A Patient s Guide to Artificial Cervical Disc Replacement Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine condition that can cause pain and numbness
Three-level cervical disc herniation Case report and review of the literature
 Romanian Neurosurgery (2015) XXIX 3: 305-311 305 Three-level cervical disc herniation Case report and review of the literature Andrei St. Iencean 1,3, Ion Poeata 2,3 1 PhD Student, Grigore T. Popa University
Romanian Neurosurgery (2015) XXIX 3: 305-311 305 Three-level cervical disc herniation Case report and review of the literature Andrei St. Iencean 1,3, Ion Poeata 2,3 1 PhD Student, Grigore T. Popa University
Spine Anatomy and Spine General The purpose of the spine is to help us stand and sit straight, move, and provide protection to the spinal cord.
 Spine Anatomy and Spine General The purpose of the spine is to help us stand and sit straight, move, and provide protection to the spinal cord. Normal List Kyphosis The human spine has 7 Cervical vertebra
Spine Anatomy and Spine General The purpose of the spine is to help us stand and sit straight, move, and provide protection to the spinal cord. Normal List Kyphosis The human spine has 7 Cervical vertebra
Do you have Back Pain? Associated with:
 Do you have Back Pain? Associated with: Herniated Discs? Protruding Discs? Degenerative Disk Disease? Posterior Facet Syndrome? Sciatica? You may be a candidate for Decompression Therapy The Dynatronics
Do you have Back Pain? Associated with: Herniated Discs? Protruding Discs? Degenerative Disk Disease? Posterior Facet Syndrome? Sciatica? You may be a candidate for Decompression Therapy The Dynatronics
X Stop Spinal Stenosis Decompression
 X Stop Spinal Stenosis Decompression Am I a candidate for X Stop spinal surgery? You may be a candidate for the X Stop spinal surgery if you have primarily leg pain rather than mostly back pain and your
X Stop Spinal Stenosis Decompression Am I a candidate for X Stop spinal surgery? You may be a candidate for the X Stop spinal surgery if you have primarily leg pain rather than mostly back pain and your
LOW BACK PAIN; MECHANICAL
 1 ORTHO 16 LOW BACK PAIN; MECHANICAL Background This case definition was developed by the Armed Forces Health Surveillance Center (AFHSC) for the purpose of epidemiological surveillance of a condition
1 ORTHO 16 LOW BACK PAIN; MECHANICAL Background This case definition was developed by the Armed Forces Health Surveillance Center (AFHSC) for the purpose of epidemiological surveillance of a condition
CERVICAL PROCEDURES PHYSICIAN CODING
 CERVICAL PROCEDURES PHYSICIAN CODING Anterior Cervical Discectomy with Interbody Fusion (ACDF) Anterior interbody fusion, with discectomy and decompression; cervical below C2 22551 first interspace 22552
CERVICAL PROCEDURES PHYSICIAN CODING Anterior Cervical Discectomy with Interbody Fusion (ACDF) Anterior interbody fusion, with discectomy and decompression; cervical below C2 22551 first interspace 22552
Low Back Injury in the Industrial Athlete: An Anatomic Approach
 Low Back Injury in the Industrial Athlete: An Anatomic Approach Earl J. Craig, M.D. Assistant Professor Indiana University School of Medicine Department of Physical Medicine and Rehabilitation Epidemiology
Low Back Injury in the Industrial Athlete: An Anatomic Approach Earl J. Craig, M.D. Assistant Professor Indiana University School of Medicine Department of Physical Medicine and Rehabilitation Epidemiology
James A. Sanfilippo, M.D. CONSENT FOR SPINAL SURGERY PATIENT: DATE:
 James A. Sanfilippo, M.D. CONSENT FOR SPINAL SURGERY PATIENT: DATE: 1. I have been strongly advised to carefully read and consider this operative permit. I realize that it is important that I understand
James A. Sanfilippo, M.D. CONSENT FOR SPINAL SURGERY PATIENT: DATE: 1. I have been strongly advised to carefully read and consider this operative permit. I realize that it is important that I understand
Cervical Spine Radiculopathy: Convervative Treatment. Christos K. Yiannakopoulos, MD Orthopaedic Surgeon
 Cervical Spine Radiculopathy: Convervative Treatment Christos K. Yiannakopoulos, MD Orthopaedic Surgeon Laboratory for the Research of the Musculoskeletal System, University of Athens & IASO General Hospital,
Cervical Spine Radiculopathy: Convervative Treatment Christos K. Yiannakopoulos, MD Orthopaedic Surgeon Laboratory for the Research of the Musculoskeletal System, University of Athens & IASO General Hospital,
White Paper: Cervical Disc Replacement: When is the Mobi-C Cervical Disc Medically Necessary?
 White Paper: Cervical Disc Replacement: When is the Mobi-C Cervical Disc Medically Necessary? For Health Plans, Medical Management Organizations and TPAs Cervical Disc Disease: An Overview The cervical
White Paper: Cervical Disc Replacement: When is the Mobi-C Cervical Disc Medically Necessary? For Health Plans, Medical Management Organizations and TPAs Cervical Disc Disease: An Overview The cervical
Temple Physical Therapy
 Temple Physical Therapy A General Overview of Common Neck Injuries For current information on Temple Physical Therapy related news and for a healthy and safe return to work, sport and recreation Like Us
Temple Physical Therapy A General Overview of Common Neck Injuries For current information on Temple Physical Therapy related news and for a healthy and safe return to work, sport and recreation Like Us
Title: Interspinous Process Decompression with the X-Stop Device for Lumbar Spinal Stenosis: A Retrospective Review. Authors: Jennifer R.
 Title: Interspinous Process Decompression with the X-Stop Device for Lumbar Spinal Stenosis: A Retrospective Review. Authors: Jennifer R. Madonia-Barr, MS, PA-C and David L. Kramer, MD Institution: Connecticut
Title: Interspinous Process Decompression with the X-Stop Device for Lumbar Spinal Stenosis: A Retrospective Review. Authors: Jennifer R. Madonia-Barr, MS, PA-C and David L. Kramer, MD Institution: Connecticut
Complications in Adult Deformity Surgery
 Complications in Adult Deformity Surgery Proximal Junctional Kyphosis: Thoracolumbar and Cervicothoracic Sigurd Berven, MD Professor in Residence UC San Francisco Disclosures Research/Institutional Support:
Complications in Adult Deformity Surgery Proximal Junctional Kyphosis: Thoracolumbar and Cervicothoracic Sigurd Berven, MD Professor in Residence UC San Francisco Disclosures Research/Institutional Support:
CERVICAL SPONDYLOSIS
 CERVICAL SPONDYLOSIS Dr. Sahni B.S Dy. Chief Medical Officer, ONGC Hospital Panvel-410221,Navi Mumbai,India Introduction The cervical spine consists of the top 7 vertebrae of the spine. These are referred
CERVICAL SPONDYLOSIS Dr. Sahni B.S Dy. Chief Medical Officer, ONGC Hospital Panvel-410221,Navi Mumbai,India Introduction The cervical spine consists of the top 7 vertebrae of the spine. These are referred
Pathoanatomical Changes of the Brachial Plexus and of C5-C6 Following Whiplash-Type Injury: A Case Report
 Pathoanatomical Changes of the Brachial Plexus and of C5-C6 Following Whiplash-Type Injury: A Case Report 1 Journal Of Whiplash & Related Disorders Vol. 1, No, 1, 2002 Gunilla Bring, Halldor Jonsson Jr.,
Pathoanatomical Changes of the Brachial Plexus and of C5-C6 Following Whiplash-Type Injury: A Case Report 1 Journal Of Whiplash & Related Disorders Vol. 1, No, 1, 2002 Gunilla Bring, Halldor Jonsson Jr.,
Spinal Surgery Clinical Coverage Policy No: 1A-30 Revised Date: DRAFT Table of Contents
 Clinical Coverage Policy No: 1A-30 Table of Contents 1.0 Description of the Procedure, Product, or Service... 1 1.1 Definitions... 1 2.0 Eligible Recipients... 2 2.1 General Provisions... 2 2.2 EPSDT Special
Clinical Coverage Policy No: 1A-30 Table of Contents 1.0 Description of the Procedure, Product, or Service... 1 1.1 Definitions... 1 2.0 Eligible Recipients... 2 2.1 General Provisions... 2 2.2 EPSDT Special
Options for Cervical Disc Degeneration A Guide to the M6-C. clinical study
 Options for Cervical Disc Degeneration A Guide to the M6-C clinical study Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine condition that can cause
Options for Cervical Disc Degeneration A Guide to the M6-C clinical study Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine condition that can cause
HEADACHES AND THE THIRD OCCIPITAL NERVE
 HEADACHES AND THE THIRD OCCIPITAL NERVE Edward Babigumira M.D. FAAPMR. Interventional Pain Management, Lincoln. B. Pain Clinic, Ltd. Diplomate ABPMR. Board Certified Pain Medicine No disclosures Disclosure
HEADACHES AND THE THIRD OCCIPITAL NERVE Edward Babigumira M.D. FAAPMR. Interventional Pain Management, Lincoln. B. Pain Clinic, Ltd. Diplomate ABPMR. Board Certified Pain Medicine No disclosures Disclosure
.org. Cervical Spondylosis (Arthritis of the Neck) Anatomy. Cause
 Cervical Spondylosis (Arthritis of the Neck) Page ( 1 ) Neck pain can be caused by many things but is most often related to getting older. Like the rest of the body, the disks and joints in the neck (cervical
Cervical Spondylosis (Arthritis of the Neck) Page ( 1 ) Neck pain can be caused by many things but is most often related to getting older. Like the rest of the body, the disks and joints in the neck (cervical
Value Analysis Brief MIS Lateral Approach to Interbody Fusion
 Value Analysis Brief MIS Lateral Approach to Interbody Fusion Methods This value analysis brief presents information on the clinical and economic benefits of the minimally invasive lateral approach to
Value Analysis Brief MIS Lateral Approach to Interbody Fusion Methods This value analysis brief presents information on the clinical and economic benefits of the minimally invasive lateral approach to
SPINE SERVICE ROTATION ROTATION SPECIFIC OBJECTIVES (RSO) DEPT. OF ORTHOPEDICS AND PHYSICAL REHABILITATION UNIVERSITY OF MASSACHUSETTS
 SPINE SERVICE ROTATION ROTATION SPECIFIC OBJECTIVES (RSO) DEPT. OF ORTHOPEDICS AND PHYSICAL REHABILITATION UNIVERSITY OF MASSACHUSETTS The purpose of this RSO is to outline and clarify the objectives of
SPINE SERVICE ROTATION ROTATION SPECIFIC OBJECTIVES (RSO) DEPT. OF ORTHOPEDICS AND PHYSICAL REHABILITATION UNIVERSITY OF MASSACHUSETTS The purpose of this RSO is to outline and clarify the objectives of
Standard of Care: Cervical Radiculopathy
 Department of Rehabilitation Services Physical Therapy Diagnosis: Cervical radiculopathy, injury to one or more nerve roots, has multiple presentations. Symptoms may include pain in the cervical spine
Department of Rehabilitation Services Physical Therapy Diagnosis: Cervical radiculopathy, injury to one or more nerve roots, has multiple presentations. Symptoms may include pain in the cervical spine
SPINE ANATOMY AND PROCEDURES. Tulsa Spine & Specialty Hospital 6901 S. Olympia Avenue Tulsa, Oklahoma 74132
 SPINE ANATOMY AND PROCEDURES Tulsa Spine & Specialty Hospital 6901 S. Olympia Avenue Tulsa, Oklahoma 74132 SPINE ANATOMY The spine consists of 33 bones called vertebrae. The top 7 are cervical, or neck
SPINE ANATOMY AND PROCEDURES Tulsa Spine & Specialty Hospital 6901 S. Olympia Avenue Tulsa, Oklahoma 74132 SPINE ANATOMY The spine consists of 33 bones called vertebrae. The top 7 are cervical, or neck
How To Write An Icd10
 Crosswalk of Common Spine ICD-9-CM Codes to ICD-10 Codes As of October 1, 2015, all health care entities covered by the Health Insurance Portability and Accountability Act (HIPAA) will be required to use
Crosswalk of Common Spine ICD-9-CM Codes to ICD-10 Codes As of October 1, 2015, all health care entities covered by the Health Insurance Portability and Accountability Act (HIPAA) will be required to use
EXPERIMENTAL AND THERAPEUTIC MEDICINE 5: 567-571, 2013
 EXPERIMENTAL AND THERAPEUTIC MEDICINE 5: 567-571, 2013 Treatment of multilevel degenerative lumbar spinal stenosis with spondylolisthesis using a combination of microendoscopic discectomy and minimally
EXPERIMENTAL AND THERAPEUTIC MEDICINE 5: 567-571, 2013 Treatment of multilevel degenerative lumbar spinal stenosis with spondylolisthesis using a combination of microendoscopic discectomy and minimally
Posterior Surgery for Cervical Myelopathy: Laminectomy, Laminectomy with Fusion, and Laminoplasty
 Asian Spine Journal Vol. 2, No. 2, pp 114~126, 2008 Posterior Surgery for Cervical Myelopathy: Laminectomy, Laminectomy with Fusion, and Laminoplasty John M. Rhee, Sushil Basra The Emory Spine Center,
Asian Spine Journal Vol. 2, No. 2, pp 114~126, 2008 Posterior Surgery for Cervical Myelopathy: Laminectomy, Laminectomy with Fusion, and Laminoplasty John M. Rhee, Sushil Basra The Emory Spine Center,
Update to the Treatment of Degenerative Cervical Disc Disease
 Update to the Treatment of Degenerative Cervical Disc Disease Michael Lynn, MD Neurosurgeon, Southeastern Neurosurgical & Spine Institute Adjunct Assistant Clinical Professor of Bioengineering, Clemson
Update to the Treatment of Degenerative Cervical Disc Disease Michael Lynn, MD Neurosurgeon, Southeastern Neurosurgical & Spine Institute Adjunct Assistant Clinical Professor of Bioengineering, Clemson
Treating Bulging Discs & Sciatica. Alexander Ching, MD
 Treating Bulging Discs & Sciatica Alexander Ching, MD Disclosures Depuy Spine Teaching and courses K2 Spine Complex Spine Study Group Disclosures Take 2 I am a spine surgeon I like spine surgery I believe
Treating Bulging Discs & Sciatica Alexander Ching, MD Disclosures Depuy Spine Teaching and courses K2 Spine Complex Spine Study Group Disclosures Take 2 I am a spine surgeon I like spine surgery I believe
CONCOMITANT COMBINED DEGENERATIVE COMPRESSION OF THE SPINAL CORD AND CAUDA EQUINA: A REPORT ON THREE CASES
 CASE REPORT CONCOMITANT COMBINED DEGENERATIVE COMPRESSION OF THE SPINAL CORD AND CAUDA EQUINA: A REPORT ON THREE CASES Atanas Davarski 1, Ivo Kehayov 1, Tanya Kitova 2, Christo Zhelyazkov 1, Borislav Kitov
CASE REPORT CONCOMITANT COMBINED DEGENERATIVE COMPRESSION OF THE SPINAL CORD AND CAUDA EQUINA: A REPORT ON THREE CASES Atanas Davarski 1, Ivo Kehayov 1, Tanya Kitova 2, Christo Zhelyazkov 1, Borislav Kitov
ISPI Newsletter Archive Lumbar Spine Surgery
 ISPI Newsletter Archive Lumbar Spine Surgery January 2005 Effects of Charite Artificial Disc on the Implanted and Adjacent Spinal Segments Mechanics Using a Hybrid Testing Protocol Spine. 30(24):2755-2764,
ISPI Newsletter Archive Lumbar Spine Surgery January 2005 Effects of Charite Artificial Disc on the Implanted and Adjacent Spinal Segments Mechanics Using a Hybrid Testing Protocol Spine. 30(24):2755-2764,
Cervical Stenosis & Myelopathy
 Cervical Stenosis & Myelopathy North American Spine Society Public Education Series What Are Cervical Stenosis and Myelopathy? The cervical spine (neck) is made up of a series of connected bones called
Cervical Stenosis & Myelopathy North American Spine Society Public Education Series What Are Cervical Stenosis and Myelopathy? The cervical spine (neck) is made up of a series of connected bones called
Spine Trauma: When to Transfer. Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU
 Spine Trauma: When to Transfer Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU Disclosures Depuy Spine Consultant (teaching and courses) Department education and research funds Atlas Spine
Spine Trauma: When to Transfer Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU Disclosures Depuy Spine Consultant (teaching and courses) Department education and research funds Atlas Spine
Diagnosis and Treatment of Lumbar Spinal Canal Stenosis
 Low Back Pains Diagnosis and Treatment of Lumbar Spinal Canal Stenosis JMAJ 46(10): 439 444, 2003 Katsuro TOMITA Department of Orthopedic Surgery, Kanazawa University Abstract: Lumbar spinal canal stenosis
Low Back Pains Diagnosis and Treatment of Lumbar Spinal Canal Stenosis JMAJ 46(10): 439 444, 2003 Katsuro TOMITA Department of Orthopedic Surgery, Kanazawa University Abstract: Lumbar spinal canal stenosis
Marc A. Cohen, MD, FAAOS, FACS Diplomate American Board of Spinal Surgery Fellow American College of Spinal Surgery
 Marc A. Cohen, MD, FAAOS, FACS Diplomate American Board of Spinal Surgery Fellow American College of Spinal Surgery 221 Madison Ave Morristown, New Jersey 07960 (973) 538 4444 Fax (973) 538 0420 Patient
Marc A. Cohen, MD, FAAOS, FACS Diplomate American Board of Spinal Surgery Fellow American College of Spinal Surgery 221 Madison Ave Morristown, New Jersey 07960 (973) 538 4444 Fax (973) 538 0420 Patient
A Patient's Guide to Neck Pain (Overview)
 Neck Pain Overview A Patient's Guide to Neck Pain (Overview) Introduction Over many years, our necks are subjected to repeated stress and minor injury. These injuries may not cause pain at the time of
Neck Pain Overview A Patient's Guide to Neck Pain (Overview) Introduction Over many years, our necks are subjected to repeated stress and minor injury. These injuries may not cause pain at the time of
Presented by Zoran Maric, M.D. Orthopaedic Spine Surgeon May 22, 2010
 Presented by Zoran Maric, M.D. Orthopaedic Spine Surgeon May 22, 2010 1 cervical area thoracic area lumbar area sacrum coccyx Mayfield Clinic 2 3 4 5 Zoran Maric, MD Spine Surgery Procedures How to Document
Presented by Zoran Maric, M.D. Orthopaedic Spine Surgeon May 22, 2010 1 cervical area thoracic area lumbar area sacrum coccyx Mayfield Clinic 2 3 4 5 Zoran Maric, MD Spine Surgery Procedures How to Document
Surgery for cervical disc prolapse or cervical osteophyte
 Mr Paul S. D Urso MBBS(Hons), PhD, FRACS Neurosurgeon Provider Nº: 081161DY Epworth Centre Suite 6.1 32 Erin Street Richmond 3121 Tel: 03 9421 5844 Fax: 03 9421 4186 AH: 03 9483 4040 email: paul@pauldurso.com
Mr Paul S. D Urso MBBS(Hons), PhD, FRACS Neurosurgeon Provider Nº: 081161DY Epworth Centre Suite 6.1 32 Erin Street Richmond 3121 Tel: 03 9421 5844 Fax: 03 9421 4186 AH: 03 9483 4040 email: paul@pauldurso.com
J of Evolution of Med and Dent Sci/ eissn- 2278-4802, pissn- 2278-4748/ Vol. 4/ Issue 55/ July 09, 2015 Page 9518
 POST-OPERATIVE NEUROLOGICAL RECOVERY PATTERN IN DEGENERATIVE CERVICAL MYELOPATHY AND RADICULOPATHY Raju B. Mundhe 1, Arvind B. Goregaonkar 2, Anuraag G. Gupta 3 HOW TO CITE THIS ARTICLE: Raju B. Mundhe,
POST-OPERATIVE NEUROLOGICAL RECOVERY PATTERN IN DEGENERATIVE CERVICAL MYELOPATHY AND RADICULOPATHY Raju B. Mundhe 1, Arvind B. Goregaonkar 2, Anuraag G. Gupta 3 HOW TO CITE THIS ARTICLE: Raju B. Mundhe,
ICD 10 CM IMPLEMENTATION DATE OCT 1, 2015
 Presented by: Teri Romano, RN, MBA, CPC, CMDP ICD 10 CM IMPLEMENTATION DATE OCT 1, 2015 Source: http://journal.ahima.org/2015/02/04/us house committee to hold hearing on icd 10 implementation/ 2 2015 Web_Non
Presented by: Teri Romano, RN, MBA, CPC, CMDP ICD 10 CM IMPLEMENTATION DATE OCT 1, 2015 Source: http://journal.ahima.org/2015/02/04/us house committee to hold hearing on icd 10 implementation/ 2 2015 Web_Non
Minimally Invasive Spine Surgery
 Chapter 1 Minimally Invasive Spine Surgery 1 H.M. Mayer Primum non nocere First do no harm In the long history of surgery it always has been a basic principle to restrict the iatrogenic trauma done to
Chapter 1 Minimally Invasive Spine Surgery 1 H.M. Mayer Primum non nocere First do no harm In the long history of surgery it always has been a basic principle to restrict the iatrogenic trauma done to
Posterior Cervical Decompression
 Posterior Cervical Decompression Spinal Unit Tel: 01473 702032 or 702097 Issue 2: January 2009 Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed with a
Posterior Cervical Decompression Spinal Unit Tel: 01473 702032 or 702097 Issue 2: January 2009 Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed with a
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Interspinous Fixation (Fusion) Devices Page 1 of 6 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: See Also: Interspinous Fixation (Fusion) Devices Lumbar Spine
Interspinous Fixation (Fusion) Devices Page 1 of 6 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: See Also: Interspinous Fixation (Fusion) Devices Lumbar Spine
A review of spinal problems
 Dr Ulrich R Hähnle MD, FCS Orthopaedic Surgeon, Wits Facharzt für Orthopädie, Berlin Phone: +27 11 485 3236 Fax: +27 11 485 2446 Suite 102, Medical Centre, Linksfield Park Clinic P.O. Box 949, Johannesburg
Dr Ulrich R Hähnle MD, FCS Orthopaedic Surgeon, Wits Facharzt für Orthopädie, Berlin Phone: +27 11 485 3236 Fax: +27 11 485 2446 Suite 102, Medical Centre, Linksfield Park Clinic P.O. Box 949, Johannesburg
www.backandspinefl.com Back and Spine Center 509 Riverside Dr., Suite 203 Stuart, FL 34994 Phone: (772) 288-5862
 Non-Profit ORG. U.S. Postage PAID West Palm BCH. FL. PERMIT NO. 4709 www.backandspinefl.com Back and Spine Center 509 Riverside Dr., Suite 203 Stuart, FL 34994 Phone: (772) 288-5862 The evolution of neurosurgery
Non-Profit ORG. U.S. Postage PAID West Palm BCH. FL. PERMIT NO. 4709 www.backandspinefl.com Back and Spine Center 509 Riverside Dr., Suite 203 Stuart, FL 34994 Phone: (772) 288-5862 The evolution of neurosurgery
APSS YANGON OPERATIVE SPINE COURSE. Local Organizing Chairman: Prof Myint Thaung. Venue: Yangon Orthopaedic Hospital
 5 th - 8 th Feb 2015 Pls insert Hospital Logo here Local Organizing Chairman: Prof Myint Thaung Venue: Yangon Orthopaedic Hospital Invited International and Local Faculties Arvind Jayaswal (India) Chung-Chek
5 th - 8 th Feb 2015 Pls insert Hospital Logo here Local Organizing Chairman: Prof Myint Thaung Venue: Yangon Orthopaedic Hospital Invited International and Local Faculties Arvind Jayaswal (India) Chung-Chek
Anterior Lumbar Interbody Fusion (ALIF). Instrument set supports placement of ALIF spacers using anterior or anterolateral approach.
 Anterior Lumbar Interbody Fusion (ALIF). Instrument set supports placement of ALIF spacers using anterior or anterolateral approach. Technique Guide Instruments and implants approved by the AO Foundation
Anterior Lumbar Interbody Fusion (ALIF). Instrument set supports placement of ALIF spacers using anterior or anterolateral approach. Technique Guide Instruments and implants approved by the AO Foundation
Spinal Decompression
 Spinal Decompression Spinal decompression is just one more tool we have to treat radiculopathy. With appropriate education and exercises, this modality has been proven to assist in the resolution of symptoms
Spinal Decompression Spinal decompression is just one more tool we have to treat radiculopathy. With appropriate education and exercises, this modality has been proven to assist in the resolution of symptoms
Advances In Spine Care. James D. Bruffey M.D. Scripps Clinic Division of Orthopaedic Surgery Section of Spinal Surgery
 Advances In Spine Care James D. Bruffey M.D. Scripps Clinic Division of Orthopaedic Surgery Section of Spinal Surgery Introduction The Spine - A common source of problems Back pain is the #2 presenting
Advances In Spine Care James D. Bruffey M.D. Scripps Clinic Division of Orthopaedic Surgery Section of Spinal Surgery Introduction The Spine - A common source of problems Back pain is the #2 presenting
Does the pain radiating down your legs, buttocks or lower back prevent you from walking long distances?
 Does the pain radiating down your legs, buttocks or lower back prevent you from walking long distances? Do you experience weakness, tingling, numbness, stiffness, or cramping in your legs, buttocks or
Does the pain radiating down your legs, buttocks or lower back prevent you from walking long distances? Do you experience weakness, tingling, numbness, stiffness, or cramping in your legs, buttocks or
Sample Treatment Protocol
 Sample Treatment Protocol 1 Adults with acute episode of LBP Definition: Acute episode Back pain lasting
Sample Treatment Protocol 1 Adults with acute episode of LBP Definition: Acute episode Back pain lasting
Effects of Vertebral Axial Decompression (VAX-D) On Intradiscal Pressure
 Effects of Vertebral Axial Decompression (VAX-D) On Intradiscal Pressure Gustavo Ramos, M.D., William Marin, M.D. Journal of Neursurgery 81:35-353 1994 Departments of Neurosurgery and Radiology, Rio Grande
Effects of Vertebral Axial Decompression (VAX-D) On Intradiscal Pressure Gustavo Ramos, M.D., William Marin, M.D. Journal of Neursurgery 81:35-353 1994 Departments of Neurosurgery and Radiology, Rio Grande
Subject: Implanted Devices for Spinal Stenosis Policy #: SURG.00092 Current Effective Date: 07/13/2011 Status: Reviewed Last Review Date: 05/19/2011
 1 of 5 6/18/2012 11:08 AM Medical Policy Subject: Implanted Devices for Spinal Stenosis Policy #: SURG.00092 Current Effective Date: 07/13/2011 Status: Reviewed Last Review Date: 05/19/2011 Description/Scope
1 of 5 6/18/2012 11:08 AM Medical Policy Subject: Implanted Devices for Spinal Stenosis Policy #: SURG.00092 Current Effective Date: 07/13/2011 Status: Reviewed Last Review Date: 05/19/2011 Description/Scope
.org. Fractures of the Thoracic and Lumbar Spine. Cause. Description
 Fractures of the Thoracic and Lumbar Spine Page ( 1 ) Spinal fractures can vary widely in severity. While some fractures are very serious injuries that require emergency treatment, other fractures can
Fractures of the Thoracic and Lumbar Spine Page ( 1 ) Spinal fractures can vary widely in severity. While some fractures are very serious injuries that require emergency treatment, other fractures can
Spine Clinic Neurospine Specialists, Orthopaedics and Neurosurgery
 Spine Clinic Neurospine Specialists, Orthopaedics and Neurosurgery REVISION SPINE SURGERY Revision surgery is a very complex field which requires experience, training and evaluation in a very individual
Spine Clinic Neurospine Specialists, Orthopaedics and Neurosurgery REVISION SPINE SURGERY Revision surgery is a very complex field which requires experience, training and evaluation in a very individual
The Petrylaw Lawsuits Settlements and Injury Settlement Report
 The Petrylaw Lawsuits Settlements and Injury Settlement Report BACK INJURIES How Minnesota Juries Decide the Value of Pain and Suffering in Back Injury Cases The Petrylaw Lawsuits Settlements and Injury
The Petrylaw Lawsuits Settlements and Injury Settlement Report BACK INJURIES How Minnesota Juries Decide the Value of Pain and Suffering in Back Injury Cases The Petrylaw Lawsuits Settlements and Injury
IN THE COMMONWEALTH COURT OF PENNSYLVANIA
 IN THE COMMONWEALTH COURT OF PENNSYLVANIA Advanced Dermatology Associates : (Selective Insurance Company of : America), : Petitioners : : v. : No. 2186 C.D. 2014 : Submitted: May 22, 2015 Workers Compensation
IN THE COMMONWEALTH COURT OF PENNSYLVANIA Advanced Dermatology Associates : (Selective Insurance Company of : America), : Petitioners : : v. : No. 2186 C.D. 2014 : Submitted: May 22, 2015 Workers Compensation
Adult Spine Rotation Specific Evaluation Orthopaedic Surgery Training Program School of Medicine, Queen s University
 Adult Spine Rotation Specific Evaluation Orthopaedic Surgery Training Program School of Medicine, Queen s University CanMEDS Roles / Competencies Name: PGY Rotation Dates: s s Exceeds N/A Attending Staff:
Adult Spine Rotation Specific Evaluation Orthopaedic Surgery Training Program School of Medicine, Queen s University CanMEDS Roles / Competencies Name: PGY Rotation Dates: s s Exceeds N/A Attending Staff:
.org. Cervical Radiculopathy (Pinched Nerve) Anatomy. Cause
 Cervical Radiculopathy (Pinched Nerve) Page ( 1 ) Cervical radiculopathy, commonly called a pinched nerve occurs when a nerve in the neck is compressed or irritated where it branches away from the spinal
Cervical Radiculopathy (Pinched Nerve) Page ( 1 ) Cervical radiculopathy, commonly called a pinched nerve occurs when a nerve in the neck is compressed or irritated where it branches away from the spinal
Cervical-Spine Injuries: Catastrophic Injury to Neck Sprain. Seth Cheatham, MD
 Cervical-Spine Injuries: Catastrophic Injury to Neck Sprain Seth Cheatham, MD 236 Seth A. Cheatham, MD VCU Sports Medicine I have no financial disclosures Contact sports, specifically football, places
Cervical-Spine Injuries: Catastrophic Injury to Neck Sprain Seth Cheatham, MD 236 Seth A. Cheatham, MD VCU Sports Medicine I have no financial disclosures Contact sports, specifically football, places
Mid-Cervical Spine Fusion
 1 Mid-Cervical Spine Fusion Anatomical Considerations: The cervical spine consists of several joints. It is an area where stability has been sacrificed for mobility, making the cervical spine particularly
1 Mid-Cervical Spine Fusion Anatomical Considerations: The cervical spine consists of several joints. It is an area where stability has been sacrificed for mobility, making the cervical spine particularly
TABLE OF CONTENTS. Surgical Technique 2. Indications 4. Product Information 5. 1. Patient Positioning and Approach 2
 Surgical Technique TABLE OF CONTENTS Surgical Technique 2 1. Patient Positioning and Approach 2 2. Intervertebral Device Implanted 2 3. Buttress Plate Selection 2 4. Awl Insertion 2 5. Screw Insertion
Surgical Technique TABLE OF CONTENTS Surgical Technique 2 1. Patient Positioning and Approach 2 2. Intervertebral Device Implanted 2 3. Buttress Plate Selection 2 4. Awl Insertion 2 5. Screw Insertion
Artificial Intervertebral Disc: Cervical Spine
 dapplies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
dapplies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH)
 A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH) Introduction Diffuse Idiopathic Skeletal Hyperostosis (DISH) is a phenomenon that more commonly affects older males. It is associated
A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH) Introduction Diffuse Idiopathic Skeletal Hyperostosis (DISH) is a phenomenon that more commonly affects older males. It is associated
Lumbar Spinal Stenosis
 Lumbar Spinal Stenosis Introduction Lumbar spinal stenosis is defined as reduction in the diameter of the spinal canal, lateral nerve canals or neural foramina. The stenosis may involve multiple level
Lumbar Spinal Stenosis Introduction Lumbar spinal stenosis is defined as reduction in the diameter of the spinal canal, lateral nerve canals or neural foramina. The stenosis may involve multiple level
Contents. Introduction 1. Anatomy of the Spine 1. 2. Spinal Imaging 7. 3. Spinal Biomechanics 23. 4. History and Physical Examination of the Spine 33
 Contents Introduction 1. Anatomy of the Spine 1 Vertebrae 1 Ligaments 3 Intervertebral Disk 4 Intervertebral Foramen 5 2. Spinal Imaging 7 Imaging Modalities 7 Conventional Radiographs 7 Myelography 9
Contents Introduction 1. Anatomy of the Spine 1 Vertebrae 1 Ligaments 3 Intervertebral Disk 4 Intervertebral Foramen 5 2. Spinal Imaging 7 Imaging Modalities 7 Conventional Radiographs 7 Myelography 9
Neck Pain Overview Causes, Diagnosis and Treatment Options
 Neck Pain Overview Causes, Diagnosis and Treatment Options Neck pain is one of the most common forms of pain for which people seek treatment. Most individuals experience neck pain at some point during
Neck Pain Overview Causes, Diagnosis and Treatment Options Neck pain is one of the most common forms of pain for which people seek treatment. Most individuals experience neck pain at some point during
Spinal cord injury secondary to cervical disc herniation in ambulatory patients with cerebral palsy
 Spinal Cord (1998) 36, 288 ± 292 1998 International Medical Society of Paraplegia All rights reserved 1362 ± 4393/98 $12.00 http://www.stockton-press.co.uk/sc Spinal cord injury secondary to cervical disc
Spinal Cord (1998) 36, 288 ± 292 1998 International Medical Society of Paraplegia All rights reserved 1362 ± 4393/98 $12.00 http://www.stockton-press.co.uk/sc Spinal cord injury secondary to cervical disc
ICD-10-PCS Documentation and Coding for Spinal Procedures October 22, 2015
 Questions and Answers 1. We have a question regarding a spinal surgical procedure. The diagnosis was bilateral lateral recess stenosis and central stenosis from L2-L5. The procedure was an open lumbar
Questions and Answers 1. We have a question regarding a spinal surgical procedure. The diagnosis was bilateral lateral recess stenosis and central stenosis from L2-L5. The procedure was an open lumbar
Patient Information. Posterior Cervical Surgery. Here to help. Respond Deliver & Enable
 Here to help Our Health Information Centre (HIC) provides advice and information on a wide range of health-related topics. We also offer: Services for people with disabilities. Information in large print,
Here to help Our Health Information Centre (HIC) provides advice and information on a wide range of health-related topics. We also offer: Services for people with disabilities. Information in large print,
Information for the Patient About Surgical
 Information for the Patient About Surgical Decompression and Stabilization of the Spine Aging and the Spine Daily wear and tear, along with disc degeneration due to aging and injury, are common causes
Information for the Patient About Surgical Decompression and Stabilization of the Spine Aging and the Spine Daily wear and tear, along with disc degeneration due to aging and injury, are common causes
MEDICAL POLICY No. 91591-R2 LUMBAR LAMINECTOMY Including Discectomy or Microdiscectomy, Foraminotomy, Laminotomy
 LUMBAR LAMINECTOMY Effective Date: June 4, 2015 Review Dates: 4/11, 4/12, 4/13, 5/14, 5/15 Date Of Origin: April 13, 2011 Status: Current Note: The prior authorization requirement was removed effective
LUMBAR LAMINECTOMY Effective Date: June 4, 2015 Review Dates: 4/11, 4/12, 4/13, 5/14, 5/15 Date Of Origin: April 13, 2011 Status: Current Note: The prior authorization requirement was removed effective
Lumbar Spinal Stenosis Materclass: Surgical management of lumbar spinal stenosis:
 Lumbar Spinal Stenosis Materclass: Surgical management of lumbar spinal stenosis: Presented By: Michelle Emsley Senior Spinal In-Patient Physiotherapist Learning objectives Indications Evidence Post operative
Lumbar Spinal Stenosis Materclass: Surgical management of lumbar spinal stenosis: Presented By: Michelle Emsley Senior Spinal In-Patient Physiotherapist Learning objectives Indications Evidence Post operative
Disorders of the Spine & Peripheral Nerves
 Disorders of the Spine & Peripheral Nerves An Introduction The LSU-Shreveport Department of Neurosurgery Presenting Authors: Neurosurgery Residents & Faculty Spine Disorders & Neurosurgery Neurosurgery
Disorders of the Spine & Peripheral Nerves An Introduction The LSU-Shreveport Department of Neurosurgery Presenting Authors: Neurosurgery Residents & Faculty Spine Disorders & Neurosurgery Neurosurgery
