Rehabilitation guidelines for patients undergoing Pes Cavus Correction
|
|
|
- Blake Hardy
- 7 years ago
- Views:
Transcription
1 Rehabilitation guidelines for patients undergoing Pes Cavus Correction At the RNOH, our emphasis is patient specific, which encourages recognition of those who may progress slower than others. We also want to encourage clinical reasoning. Milestone driven These are milestone driven guidelines designed to provide an equitable rehabilitation service to all our patients. They will also limit unnecessary visits to the outpatient clinic at RNOH by helping the patient and therapist to identify which specialist review is required. Team contact details: Unit secretary Foot.ankle@rnoh.nhs.uk Physiotherapy Dept Indications for surgery: Pain and decreased function not responsive to conservative treatment Instability To prevent further deterioration / deformity Causes of pes cavus include: Neurological Traumatic Idiopathic Residual Clubfoot Possible complications: Infection Wound healing problems Persistent swelling Persistent / recurrent pain Non-union / mal-union / delayed union Bleeding Nerve damage Deep Vein Thrombosis Pulmonary Embolism Recurrent heel varus Callosities Contractures
2 Degenerative changes at other joints Stiffness May require subsequent revision surgery If neurological cause for pes cavus, progression of neurological symptoms may limit outcome, e.g. progressive weakness Surgical techniques Commonly at RONH, the surgery includes: Calcaneal osteotomy 1 st metatarsal osteotomy Peroneal tenodesis Tibialis posterior Z-lengthening However, depending upon the clinical presentation of the patient, surgery may also include one or more of the following: Soft tissue releases Tendon transfers Other osteotomies Joint fusions Expected outcome: Stable, plantargrade foot Improved function / mobility Improved pain relief Increased walking tolerance and improved gait pattern with decreased walking aid and orthotic requirement Decreased muscle imbalance Decreased callosities / pressure areas Maintenance / improvement of range of movement Return to low-impact sports may be possible but strenuous sport unlikely Full recovery may take up to twelve months Pre-operatively When practical the patient will be seen pre-operatively, and with consent, the following assessed: Current functional levels General health Social / work / hobbies Functional Range of Movement Gait / mobility, including walking aids and orthoses Post-operative expectations Patient information leaflet issued
3 Post-operative management explained Post-operatively: Always check the operation notes, and the post-operative instructions. Discuss any deviation from routine guidelines with the team concerned. This is very important as the patient may have had a combination of techniques which may affect weight-bearing status and progressions.
4 Initial rehabilitation Phase: 0-6 weeks Goals: To be safely and independently mobile with appropriate walking aid, adhering to weight bearing status To be independent with home exercise programme as appropriate To understand self management / monitoring, e.g. skin sensation, colour, swelling, temperature, circulation Restrictions Ensure that weight bearing restrictions are adhered to: Standard RNOH pes cavus surgery: Full Plaster of Paris (POP) with ankle plantargrade for 2 weeks Non Weight Bearing (NWB) POP changed at 2 weeks. Progress to Full Weight Bearing (FWB) in POP POP removed at 6 weeks. May require aircast boot or other orthosis. FWB If any other surgical techniques used ensure you check any restrictions with team as these may differ Elevation If sedentary employment, may be able to return to work from 4 weeks post-operatively, as long as provisions to elevate leg, and no complications Treatment: Likely to be in POP Pain-relief: Ensure adequate analgesia Elevation: ensure elevating leg with foot higher than waist Exercises: teach circulatory exercises Education: teach how to monitor sensation, colour, circulation, temperature, swelling, and advise what to do if concerned Mobility: ensure patient independent with transfers and mobility, including stairs if necessary On discharge from ward: Independent and safe mobilising, including stairs if appropriate Independent with transfers Independent and safe with home exercise programme / monitoring
5 Milestones to progress to next phase: Out of POP. Team to refer to physiotherapy at 6 weeks from clinic. Progression from NWB to FWB phase. Team to refer to physiotherapy if required to review safety of mobility / use of walking aids Adequate analgesia
6 Recovery rehabilitation phase: 6 weeks 12 weeks Goals: To be independently mobile out of aircast boot To achieve full range of movement To optimise normal movement Restrictions: Ensure adherence to weight bearing status No strengthening against resistance until at least 3 months postoperatively of tenodesis / any tendon transfers if performed Do not stretch any tendon transfers / ligament reconstructions if performed. They will naturally lengthen over a 6 month period Treatment: Pain relief Advice / Education Posture advice / education Mobility: ensure safely and independently mobile adhering to appropriate weight bearing restrictions. Progress off walking aids as able once reaches FWB stage Gait Re-education Wean out of aircast boot once advised to do so, and provision of plaster shoe as appropriate, if patient unable to get into normal footwear Exercises: Passive range of movement (PROM) Active assisted range of movement (AAROM) Active range of movement (AROM) Strengthening exercises as appropriate Core stability work Balance / proprioception work once appropriate Stretches of tight structures as appropriate (e.g. Achilles Tendon), not of tendon transfers / ligament reconstructions if performed Review lower limb biomechanics. Address issues as appropriate If tendon transfer performed, encourage isolation of transfer activation without overuse of other muscles. Biofeedback likely to be useful Swelling Management
7 Manual therapy: Soft tissue techniques as appropriate Joint mobilisations as appropriate ensuring awareness of osteotomy sites and those joints which may be fused, and therefore not appropriate to mobilise Monitor sensation, swelling, colour, temperature, circulation Orthotics if required via surgical team Hydrotherapy if appropriate Pacing advice as appropriate Milestones to progress to next phase: Full range of movement Independently mobilising out of aircast boot Neutral foot position when weight bearing / mobilising Tendon transfers activating if performed Failure to meet milestones: Refer back to team / Discuss with team Continue with outpatient physiotherapy if still progressing
8 Intermediate Rehabilitation Phase 12 weeks 6 months Goals: Independently mobile unaided Wearing normal footwear Optimise normal movement Grade 4 or 5 muscle strength around ankle (NB. This may vary if neurological cause for pes cavus) Treatment Further progression of the above treatment: Pain relief Advice / Education Posture advice / education Mobility: Progression of mobility and function Gait Re-education Exercises: Range of movement Strengthening exercises as appropriate Core stability work Balance / proprioception work Stretches of tight structures as appropriate (e.g. Achilles tendon), not of transfers / ligament reconstructions if performed. Review lower limb biomechanics. Address issues as appropriate If tendon transfer performed progress isolation of transfer activation without overuse of other muscles. Biofeedback likely to be useful Swelling Management Manual therapy: Soft tissue techniques as appropriate Joint mobilisations as appropriate ensuring awareness of those which may be fused and therefore not appropriate to mobilise Monitor sensation, swelling, colour, temperature, circulation Orthotics if required via surgical team Hydrotherapy if appropriate Pacing advice as appropriate Milestones to progress to next phase: Independently mobile unaided Wearing normal footwear Adequate analgesia Tendon transfers to be activating if performed
9 Failure to meet milestones: Refer back to team / Discuss with team Continue with outpatient physiotherapy if still progressing
10 Final rehabilitation phase 6 months 1 year Goals: Return to gentle low-impact sports Establish long term maintenance programme Grade 5 muscle strength around ankle and grade 4 or 5 of tendon transfers if performed (NB. This may vary if neurological cause for pes cavus) Treatment: Mobility / function: Progression of mobility and function, increasing dynamic control with specific training to functional goals Gait Re-education Exercises: Progression of exercises including range of movement, strengthening, transfer activation, balance and proprioception, core stability Swelling Management Manual therapy Soft tissue techniques as appropriate Joint mobilisations as appropriate ensuring awareness of those which may be fused and therefore not appropriate to mobilise Pacing advice Milestones for discharge Independently mobile unaided Appropriate patient-specific functional goals achieved Independent with long term maintenance programme
11 Failure to progress If a patient is failing to progress, then consider the following: POSSIBLE PROBLEM Swelling Pain Breakdown of wound e.g. inflammation, bleeding, infection Transfer not activating Numbness/altered sensation ACTION Ensure elevating leg regularly Use ice as appropriate if normal skin sensation and no contraindications Decrease amount of time on feet Pacing Use walking aids Circulatory exercises If decreases overnight, monitor closely If does not decrease overnight, refer back to surgical team or to GP Decrease activity Ensure adequate analgesia Elevate regularly Decrease weight bearing and use walking aids as appropriate Pacing Modify exercise programme as appropriate If persists, refer back to surgical team or to GP Refer to surgical team or to GP Start working in NWB gravity eliminated position with AAROM and then build up as able Biofeedback Ensure adequate analgesia as appropriate Ensure swelling under control as appropriate Ensure foot neutral when mobilising to avoid excessive shear. Consider orthotics referral via surgical team if unable to keep neutral Refer back to surgical team if no improvement Review immediate post-operative status if possible Ensure swelling under control If new onset or increasing refer back to surgical team or GP
12 If static, monitor closely, but inform surgical team and refer back if deteriorates or if concerned Summary of evidence for physiotherapy guidelines A comprehensive literature search was carried out to identify research relating to surgery for pes cavus and subsequent rehabilitation. After reviewing the articles and information, the physiotherapy guidelines were produced on the best available evidence. Azmaipairashvili et al (2005) Correction of cavovarus foot deformity in Charcot-Marie-Tooth disease Journal of Pediatric Orthopaedics 25, (3): Giannini et al (2002) Surgical treatment of adult idiopathic cavus foot with plantar fasciotomy, naviculocuneiform arthrodesis, and cuboid osteotomy: a review of thirty-nine cases American Journal of Bone and Joint Surgery 84-A Supplement 2, Sanmarco G & Taylor R (2001) Cavovarus foot treated with combined calcaneal and metatarsal osteotomies Foot and Ankle International 22, (1): Sizensky J (2007) The pes cavovarus foot: update on current advances Current opinion in Orthopaedics 18, (2): Younger et al (2005) Adult Cavovarus Foot Journal of American Academy of Orthopaedic Surgeons 13, (5): October 2007 JB
Rehabilitation guidelines for patients undergoing knee arthroscopy
 Rehabilitation guidelines for patients undergoing knee arthroscopy At the RNOH, our emphasis is patient specific, which encourages recognition of those who may progress slower then others. We also want
Rehabilitation guidelines for patients undergoing knee arthroscopy At the RNOH, our emphasis is patient specific, which encourages recognition of those who may progress slower then others. We also want
sealant without sutures (occasionally sutures may be required). This can be performed via a mini-arthrotomy, a less invasive approach.
 Rehabilitation guidelines for patients undergoing surgery for autologous chondrocyte implantation (ACI), matrix induced autologous chondrocyte implantation (MACI) and autologous matrix induced chondrogenesis
Rehabilitation guidelines for patients undergoing surgery for autologous chondrocyte implantation (ACI), matrix induced autologous chondrocyte implantation (MACI) and autologous matrix induced chondrogenesis
RNOH Physiotherapy Department (020 8909 5820) Rehabilitation guidelines for patients undergoing spinal surgery
 RNOH Physiotherapy Department (020 8909 5820) Rehabilitation guidelines for patients undergoing spinal surgery As a specialist orthopaedic hospital, we recognise that our broad and often complex patient
RNOH Physiotherapy Department (020 8909 5820) Rehabilitation guidelines for patients undergoing spinal surgery As a specialist orthopaedic hospital, we recognise that our broad and often complex patient
RNOH Physiotherapy Department (020 8909 5820) Rehabilitation guidelines for patients undergoing spinal surgery
 RNOH Physiotherapy Department (020 8909 5820) Rehabilitation guidelines for patients undergoing spinal surgery As a specialist orthopaedic hospital we recognise that our broad and often complex patient
RNOH Physiotherapy Department (020 8909 5820) Rehabilitation guidelines for patients undergoing spinal surgery As a specialist orthopaedic hospital we recognise that our broad and often complex patient
.org. Posterior Tibial Tendon Dysfunction. Anatomy. Cause. Symptoms
 Posterior Tibial Tendon Dysfunction Page ( 1 ) Posterior tibial tendon dysfunction is one of the most common problems of the foot and ankle. It occurs when the posterior tibial tendon becomes inflamed
Posterior Tibial Tendon Dysfunction Page ( 1 ) Posterior tibial tendon dysfunction is one of the most common problems of the foot and ankle. It occurs when the posterior tibial tendon becomes inflamed
A Patient s Guide to Arthritis of the Big Toe (Hallux Rigidus) With Discussion on Cheilectomy and Fusion
 A Patient s Guide to Arthritis of the Big Toe (Hallux Rigidus) With Discussion on Cheilectomy and Fusion The foot and ankle unit at the Royal National Orthopaedic Hospital (RNOH) is a multi-disciplinary
A Patient s Guide to Arthritis of the Big Toe (Hallux Rigidus) With Discussion on Cheilectomy and Fusion The foot and ankle unit at the Royal National Orthopaedic Hospital (RNOH) is a multi-disciplinary
A Patient s Guide to Post-Operative Physiotherapy. Following Anterior Cruciate Ligament Reconstruction of the Knee
 A Patient s Guide to Post-Operative Physiotherapy Following Anterior Cruciate Ligament Reconstruction of the Knee Introduction The anterior cruciate ligament (ACL) is one of the main supporting ligaments
A Patient s Guide to Post-Operative Physiotherapy Following Anterior Cruciate Ligament Reconstruction of the Knee Introduction The anterior cruciate ligament (ACL) is one of the main supporting ligaments
A Patient s Guide to Lateral Ligament Reconstruction of the Ankle
 A Patient s Guide to Lateral Ligament Reconstruction of the Ankle The Foot and Ankle unit at the Royal National Orthopaedic Hospital (RNOH) is a multi-disciplinary team. The team consists of three specialist
A Patient s Guide to Lateral Ligament Reconstruction of the Ankle The Foot and Ankle unit at the Royal National Orthopaedic Hospital (RNOH) is a multi-disciplinary team. The team consists of three specialist
Arthroscopic Ankle Fusion (Arthrodesis)
 Arthroscopic Ankle Fusion (Arthrodesis) Exceptional healthcare, personally delivered Following your consultation with a member of the Foot and Ankle team you have been diagnosed with ankle arthritis and
Arthroscopic Ankle Fusion (Arthrodesis) Exceptional healthcare, personally delivered Following your consultation with a member of the Foot and Ankle team you have been diagnosed with ankle arthritis and
.org. Achilles Tendinitis. Description. Cause. Achilles tendinitis is a common condition that causes pain along the back of the leg near the heel.
 Achilles Tendinitis Page ( 1 ) Achilles tendinitis is a common condition that causes pain along the back of the leg near the heel. The Achilles tendon is the largest tendon in the body. It connects your
Achilles Tendinitis Page ( 1 ) Achilles tendinitis is a common condition that causes pain along the back of the leg near the heel. The Achilles tendon is the largest tendon in the body. It connects your
Heel pain and Plantar fasciitis
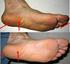 A patient s guide Heel pain and Plantar fasciitis Fred Robinson BSc FRCS FRCS(orth) Consultant Trauma & Orthopaedic Surgeon Alex Wee BSc FRCS(orth) Consultant Trauma & Orthopaedic Surgeon. What causes
A patient s guide Heel pain and Plantar fasciitis Fred Robinson BSc FRCS FRCS(orth) Consultant Trauma & Orthopaedic Surgeon Alex Wee BSc FRCS(orth) Consultant Trauma & Orthopaedic Surgeon. What causes
Calcaneus (Heel Bone) Fractures
 Copyright 2010 American Academy of Orthopaedic Surgeons Calcaneus (Heel Bone) Fractures Fractures of the heel bone, or calcaneus, can be disabling injuries. They most often occur during high-energy collisions
Copyright 2010 American Academy of Orthopaedic Surgeons Calcaneus (Heel Bone) Fractures Fractures of the heel bone, or calcaneus, can be disabling injuries. They most often occur during high-energy collisions
This is my information booklet: Introduction
 Hip arthroscopy is a relatively new procedure which allows the surgeon to diagnose and treat hip disorders by providing a clear view of the inside of the hip with very small incisions. This is a more complicated
Hip arthroscopy is a relatively new procedure which allows the surgeon to diagnose and treat hip disorders by providing a clear view of the inside of the hip with very small incisions. This is a more complicated
Endoscopic Plantar Fasciotomy
 Endoscopic Plantar Fasciotomy Introduction Plantar fasciitis is a common condition that causes pain centralized around the heel. It may be severe enough to affect regular activities. Health care providers
Endoscopic Plantar Fasciotomy Introduction Plantar fasciitis is a common condition that causes pain centralized around the heel. It may be severe enough to affect regular activities. Health care providers
Plantar Fascia Release
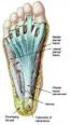 Plantar Fascia Release Introduction Plantar fasciitis is a common condition that causes pain around the heel. It may be severe enough to affect regular activities. If other treatments are unsuccessful,
Plantar Fascia Release Introduction Plantar fasciitis is a common condition that causes pain around the heel. It may be severe enough to affect regular activities. If other treatments are unsuccessful,
Milestone Driven. Team Contact Details
 REHABILITATION GUIDELINES FOR PATIENTS UNDERGOING A UNICONDYLAR KNEE REPLACEMENT (UKR) PATELLOFEMORAL JOINT REPLACEMENT (PFJR) OR TOTAL KNEE REPLACEMENT (TKR) At The RNOH our emphasis is on patient specific
REHABILITATION GUIDELINES FOR PATIENTS UNDERGOING A UNICONDYLAR KNEE REPLACEMENT (UKR) PATELLOFEMORAL JOINT REPLACEMENT (PFJR) OR TOTAL KNEE REPLACEMENT (TKR) At The RNOH our emphasis is on patient specific
Podo Pediatrics Identifying Biomechanical Pathologies
 Podo Pediatrics Identifying Biomechanical Pathologies David Lee, D.P.M., D. A.B.P.S. Purpose Identification of mechanical foot and ankle conditions Base treatments Knowing when to refer to a podiatrist
Podo Pediatrics Identifying Biomechanical Pathologies David Lee, D.P.M., D. A.B.P.S. Purpose Identification of mechanical foot and ankle conditions Base treatments Knowing when to refer to a podiatrist
Ankle Stabilisation Procedure
 Ankle Stabilisation Procedure Exceptional healthcare, personally delivered Following your consultation with a member of the Foot and Ankle team you have been diagnosed with an unstable ankle. This leaflet
Ankle Stabilisation Procedure Exceptional healthcare, personally delivered Following your consultation with a member of the Foot and Ankle team you have been diagnosed with an unstable ankle. This leaflet
Predislocation syndrome
 Predislocation syndrome Sky Ridge Medical Center, Aspen Building Pre-dislocation syndrome, capsulitis, and metatarsalgia are all similar problems usually at the ball of the foot near the second and third
Predislocation syndrome Sky Ridge Medical Center, Aspen Building Pre-dislocation syndrome, capsulitis, and metatarsalgia are all similar problems usually at the ball of the foot near the second and third
A compressive dressing that you apply around your ankle, and
 Ankle Injuries & Treatment The easiest way to remember this is: R.I.C.E. Each of these letters stands for: Rest. Rest your ankle. Do not place weight on it if it is very tender. Avoid walking long distances.
Ankle Injuries & Treatment The easiest way to remember this is: R.I.C.E. Each of these letters stands for: Rest. Rest your ankle. Do not place weight on it if it is very tender. Avoid walking long distances.
Rehabilitation Guidelines for Post-Operative Shoulder Instability Repair
 Rehabilitation Guidelines for Post-Operative Shoulder Instability Repair Please note that this is advisory information only. Your experiences may differ from those described. A fully qualified Physiotherapist
Rehabilitation Guidelines for Post-Operative Shoulder Instability Repair Please note that this is advisory information only. Your experiences may differ from those described. A fully qualified Physiotherapist
Knee Microfracture Surgery Patient Information Leaflet
 ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 Knee Microfracture Surgery Patient Information Leaflet Table of Contents 1. Introduction
ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 Knee Microfracture Surgery Patient Information Leaflet Table of Contents 1. Introduction
Rehabilitation Guidelines for Post-Operative Stiff Shoulder
 Rehabilitation Guidelines for Post-Operative Stiff Shoulder Please note that this is advisory information only. Your experiences may differ from those described. A fully qualified Physiotherapist must
Rehabilitation Guidelines for Post-Operative Stiff Shoulder Please note that this is advisory information only. Your experiences may differ from those described. A fully qualified Physiotherapist must
Physiotherapy in Rheumatoid Arthritis. Information for patients Gina Wall Senior Physiotherapist
 Physiotherapy in Rheumatoid Arthritis Information for patients Gina Wall Senior Physiotherapist What do Physiotherapists do? We conduct assessments by asking detailed questions about your symptoms, medical
Physiotherapy in Rheumatoid Arthritis Information for patients Gina Wall Senior Physiotherapist What do Physiotherapists do? We conduct assessments by asking detailed questions about your symptoms, medical
Plantar fascia. Plantar Fasciitis (pain in the heel of the foot)
 ! Plantar fascia Plantar Fasciitis (pain in the heel of the foot) Plantar Fasciitis is the most common foot problem seen in runners and is often associated with an increase in running mileage. Typically
! Plantar fascia Plantar Fasciitis (pain in the heel of the foot) Plantar Fasciitis is the most common foot problem seen in runners and is often associated with an increase in running mileage. Typically
ACCELERATED REHABILITATION PROTOCOL FOR POST OPERATIVE POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION DR LEO PINCZEWSKI DR JUSTIN ROE
 ACCELERATED REHABILITATION PROTOCOL FOR POST OPERATIVE POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION DR LEO PINCZEWSKI DR JUSTIN ROE January 2005 Rationale of Accelerated Rehabilitation Rehabilitation after
ACCELERATED REHABILITATION PROTOCOL FOR POST OPERATIVE POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION DR LEO PINCZEWSKI DR JUSTIN ROE January 2005 Rationale of Accelerated Rehabilitation Rehabilitation after
Combined SLAP with Arthroscopic Rotator Cuff Repair Large to Massive Tears = or > 3 cm
 Combined SLAP with Arthroscopic Rotator Cuff Repair Large to Massive Tears = or > 3 cm *It is the treating therapist s responsibility along with the referring physician s guidance to determine the actual
Combined SLAP with Arthroscopic Rotator Cuff Repair Large to Massive Tears = or > 3 cm *It is the treating therapist s responsibility along with the referring physician s guidance to determine the actual
Arthroscopic rotator cuff repair
 Arthroscopic rotator cuff repair The aim of this leaflet is to help answer some of the questions you may have about having an arthroscopic rotator cuff repair. It explains the benefits, risks and alternatives
Arthroscopic rotator cuff repair The aim of this leaflet is to help answer some of the questions you may have about having an arthroscopic rotator cuff repair. It explains the benefits, risks and alternatives
PLANTAR FASCITIS (Heel Spur Syndrome)
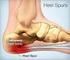 PLANTAR FASCITIS (Heel Spur Syndrome) R. Amadeus Mason MD Description Plantar fascitis is characterized by stiffness and inflammation of the main fascia (fibrous connective [ligament-like] tissue) on the
PLANTAR FASCITIS (Heel Spur Syndrome) R. Amadeus Mason MD Description Plantar fascitis is characterized by stiffness and inflammation of the main fascia (fibrous connective [ligament-like] tissue) on the
APPENDIX 1: INTERDISCIPLINARY APPROACH TO PREVENTION AND MANAGEMENT OF DIABETIC FOOT COMPLICATIONS
 APPENDIX 1: INTERDISCIPLINARY APPROACH TO PREVENTION AND MANAGEMENT OF DIABETIC FOOT COMPLICATIONS Template: Regional Foot Programs should develop a list of available health professionals in the following
APPENDIX 1: INTERDISCIPLINARY APPROACH TO PREVENTION AND MANAGEMENT OF DIABETIC FOOT COMPLICATIONS Template: Regional Foot Programs should develop a list of available health professionals in the following
Broström Lateral Ligament Reconstruction of Ankle
 Broström Lateral Ligament Reconstruction of Ankle This leaflet aims to answer your questions about having a broström lateral ligament reconstruction of ankle under the care of Mr Sam Singh. It explains
Broström Lateral Ligament Reconstruction of Ankle This leaflet aims to answer your questions about having a broström lateral ligament reconstruction of ankle under the care of Mr Sam Singh. It explains
Plantar Fasciitis. Plantar Fascia
 Plantar Fasciitis Introduction Plantar fasciitis is an inflammation of the thick band of tissue that connects your heel bone to your toes. This thick band of tissue is called the plantar fascia. Plantar
Plantar Fasciitis Introduction Plantar fasciitis is an inflammation of the thick band of tissue that connects your heel bone to your toes. This thick band of tissue is called the plantar fascia. Plantar
Forefoot deformity correction
 Contact us Pharmacy Medicines Helpline If you have any questions or concerns about your medicines, please speak to the staff caring for you or call our helpline. t: 020 7188 8748 9am to 5pm, Monday to
Contact us Pharmacy Medicines Helpline If you have any questions or concerns about your medicines, please speak to the staff caring for you or call our helpline. t: 020 7188 8748 9am to 5pm, Monday to
RX: Custom Thermoplastic AFO Compliance Documentation
 RX: Custom Thermoplastic AFO Compliance Documentation Doctor Name: Phone: Patient Name: HICN: DOB: Indicate Quality ARIZONA THERMOPLASTIC ARTICULATED AFO, DORSI-ASSIST CROW L4631 A bivalved custom molded
RX: Custom Thermoplastic AFO Compliance Documentation Doctor Name: Phone: Patient Name: HICN: DOB: Indicate Quality ARIZONA THERMOPLASTIC ARTICULATED AFO, DORSI-ASSIST CROW L4631 A bivalved custom molded
Treatment of Spastic Foot Deformities
 Penn Comprehensive Neuroscience Center Treatment of Spastic Foot Deformities Penn Neuro-Orthopaedics Service 1 Table of Contents Overview Overview 1 Treatment 2 Procedures 4 Achilles Tendon Lengthening
Penn Comprehensive Neuroscience Center Treatment of Spastic Foot Deformities Penn Neuro-Orthopaedics Service 1 Table of Contents Overview Overview 1 Treatment 2 Procedures 4 Achilles Tendon Lengthening
Mary LaBarre, PT, DPT,ATRIC
 Aquatic Therapy and the ACL Current Concepts on Prevention and Rehab Mary LaBarre, PT, DPT,ATRIC Anterior Cruciate Ligament (ACL) tears are a common knee injury in athletic rehab. Each year, approximately
Aquatic Therapy and the ACL Current Concepts on Prevention and Rehab Mary LaBarre, PT, DPT,ATRIC Anterior Cruciate Ligament (ACL) tears are a common knee injury in athletic rehab. Each year, approximately
Arthritis of the Big Toe
 Arthritis of the Big Toe A patient s guide Fred Robinson BSc FRCS FRCS(orth) Consultant Trauma & Orthopaedic Surgeon www.cambridgefootandankle.com Arthritis of the Big Toe - Hallux Rigidus Fred Robinson
Arthritis of the Big Toe A patient s guide Fred Robinson BSc FRCS FRCS(orth) Consultant Trauma & Orthopaedic Surgeon www.cambridgefootandankle.com Arthritis of the Big Toe - Hallux Rigidus Fred Robinson
.org. Lisfranc (Midfoot) Injury. Anatomy. Description
 Lisfranc (Midfoot) Injury Page ( 1 ) Lisfranc (midfoot) injuries result if bones in the midfoot are broken or ligaments that support the midfoot are torn. The severity of the injury can vary from simple
Lisfranc (Midfoot) Injury Page ( 1 ) Lisfranc (midfoot) injuries result if bones in the midfoot are broken or ligaments that support the midfoot are torn. The severity of the injury can vary from simple
Eastern Suburbs Sports Medicine Centre
 Eastern Suburbs Sports Medicine Centre ACCELERATED ANTERIOR CRUCIATE LIGAMENT REHABILITATION PROGRAM Alan Davies Diane Long Mark Kenna (APA Sports Physiotherapists) The following ACL reconstruction rehabilitation
Eastern Suburbs Sports Medicine Centre ACCELERATED ANTERIOR CRUCIATE LIGAMENT REHABILITATION PROGRAM Alan Davies Diane Long Mark Kenna (APA Sports Physiotherapists) The following ACL reconstruction rehabilitation
Tibial Intramedullary Nailing
 Tibial Intramedullary Nailing Turnberg Building Orthopaedics 0161 206 4898 All Rights Reserved 2015. Document for issue as handout. Procedure The tibia is the long shin bone in the lower leg. It is a weight
Tibial Intramedullary Nailing Turnberg Building Orthopaedics 0161 206 4898 All Rights Reserved 2015. Document for issue as handout. Procedure The tibia is the long shin bone in the lower leg. It is a weight
Post Operative Total Knee Replacement Protocol Brian White, MD www.western-ortho.com
 Post Operative Total Knee Replacement Protocol Brian White, MD www.western-ortho.com The intent of this protocol is to provide guidelines for progression of rehabilitation. It is not intended to serve
Post Operative Total Knee Replacement Protocol Brian White, MD www.western-ortho.com The intent of this protocol is to provide guidelines for progression of rehabilitation. It is not intended to serve
OPERATION:... Proximal tibial osteotomy Distal femoral osteotomy
 AFFIX PATIENT DETAIL STICKER HERE Forename.. Surname NHS Organisation. Responsible surgeon. Job Title Hospital Number... D.O.B.././ No special requirements OPERATION:..... Proximal tibial osteotomy Distal
AFFIX PATIENT DETAIL STICKER HERE Forename.. Surname NHS Organisation. Responsible surgeon. Job Title Hospital Number... D.O.B.././ No special requirements OPERATION:..... Proximal tibial osteotomy Distal
Rehabilitation Guidelines for Lateral Ankle Reconstruction
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Lateral Ankle Reconstruction The ankle is a very complex joint. There are actually three joints that make up the ankle complex: the tibiotalar
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Lateral Ankle Reconstruction The ankle is a very complex joint. There are actually three joints that make up the ankle complex: the tibiotalar
CAPPAGH NATIONAL ORTHOPAEDIC HOSPITAL, FINGLAS, DUBLIN 11. The Sisters of Mercy. Plantar Fascitis
 1.0 Policy Statement... 2 2.0 Purpose... 2 3.0 Scope... 2 4.0 Health & Safety... 2 5.0 Responsibilities... 2 6.0 Definitions and Abbreviations... 2 7.0 Guideline... 3 7.1 Assessment... 3 7.2 Treatment...
1.0 Policy Statement... 2 2.0 Purpose... 2 3.0 Scope... 2 4.0 Health & Safety... 2 5.0 Responsibilities... 2 6.0 Definitions and Abbreviations... 2 7.0 Guideline... 3 7.1 Assessment... 3 7.2 Treatment...
Sports Injuries of the Foot and Ankle. Dr. Travis Kieckbusch August 7, 2014
 Sports Injuries of the Foot and Ankle Dr. Travis Kieckbusch August 7, 2014 Foot and Ankle Injuries in Athletes Lateral ankle sprains Syndesmosis sprains high ankle sprain Achilles tendon injuries Lisfranc
Sports Injuries of the Foot and Ankle Dr. Travis Kieckbusch August 7, 2014 Foot and Ankle Injuries in Athletes Lateral ankle sprains Syndesmosis sprains high ankle sprain Achilles tendon injuries Lisfranc
PHYSIOTHERAPY OF HIP AND KNEE AFTER SURGERY AND INJURY BY RACHEL GEVELL PHYSIOTHERAPIST
 PHYSIOTHERAPY OF HIP AND KNEE AFTER SURGERY AND INJURY BY RACHEL GEVELL PHYSIOTHERAPIST AIMS AND OBJECTIVES To demonstrate the use of physiotherapy assessment and treatment following: Hip Arthroplasty
PHYSIOTHERAPY OF HIP AND KNEE AFTER SURGERY AND INJURY BY RACHEL GEVELL PHYSIOTHERAPIST AIMS AND OBJECTIVES To demonstrate the use of physiotherapy assessment and treatment following: Hip Arthroplasty
Progression to the next phase is based on Clinical Criteria and/or Time Frames as appropriate.
 BRIGHAM AND WOMEN S HOSPITAL Department of Rehabilitation Services Phyp Physical Therapy Total Hip Arthroplasty/ Hemiarthroplasty Protocol: The intent of this protocol is to provide the clinician with
BRIGHAM AND WOMEN S HOSPITAL Department of Rehabilitation Services Phyp Physical Therapy Total Hip Arthroplasty/ Hemiarthroplasty Protocol: The intent of this protocol is to provide the clinician with
.org. Plantar Fasciitis and Bone Spurs. Anatomy. Cause
 Plantar Fasciitis and Bone Spurs Page ( 1 ) Plantar fasciitis (fashee-eye-tiss) is the most common cause of pain on the bottom of the heel. Approximately 2 million patients are treated for this condition
Plantar Fasciitis and Bone Spurs Page ( 1 ) Plantar fasciitis (fashee-eye-tiss) is the most common cause of pain on the bottom of the heel. Approximately 2 million patients are treated for this condition
Cheilectomy. For more information please go to Mr Singh s Website: http://www.footandanklesurgeon.co.uk
 Cheilectomy This leaflet aims to answer your questions about having surgery for a cheilectomy procedure under the care of Mr Sam Singh. It explains the benefits, risks and alternatives, as well as what
Cheilectomy This leaflet aims to answer your questions about having surgery for a cheilectomy procedure under the care of Mr Sam Singh. It explains the benefits, risks and alternatives, as well as what
Rehabilitation Protocol: Total Knee Arthroplasty (TKA)
 Rehabilitation Protocol: Total Knee Arthroplasty (TKA) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey Medical
Rehabilitation Protocol: Total Knee Arthroplasty (TKA) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey Medical
Integra. MCP Joint Replacement PATIENT INFORMATION
 Integra MCP Joint Replacement PATIENT INFORMATION Integra MCP Patient Information This brochure summarizes information about the use, risks, and benefits of the Integra MCP finger implant. Be sure to discuss
Integra MCP Joint Replacement PATIENT INFORMATION Integra MCP Patient Information This brochure summarizes information about the use, risks, and benefits of the Integra MCP finger implant. Be sure to discuss
Outline. The Agony of the Foot: Disclosure. Plantar Fasciitis. Top 5 Foot and Ankle Problems in Primary Care. Daniel Thuillier, M.D.
 The Agony of the Foot: Top 5 Foot and Ankle Problems in Primary Care Daniel Thuillier, M.D. Assistant Professor of Clinical Orthopaedics University of California San Francisco Plantar Fasciitis Achilles
The Agony of the Foot: Top 5 Foot and Ankle Problems in Primary Care Daniel Thuillier, M.D. Assistant Professor of Clinical Orthopaedics University of California San Francisco Plantar Fasciitis Achilles
Post-operative rehabilitation guidelines Latissimus Dorsi Transfer to Posterosuperior Cuff
 Post-operative rehabilitation guidelines Latissimus Dorsi Transfer to Posterosuperior Cuff Please note that this is advisory information only. Your experiences may differ from those described. A fully
Post-operative rehabilitation guidelines Latissimus Dorsi Transfer to Posterosuperior Cuff Please note that this is advisory information only. Your experiences may differ from those described. A fully
ACL RECONSTRUCTION POST-OPERATIVE REHABILITATION PROGRAMME
 ACL RECONSTRUCTION POST-OPERATIVE REHABILITATION PROGRAMME ABOUT THE OPERATION The aim of your operation is to reconstruct the Anterior Cruciate Ligament (ACL) to restore knee joint stability. A graft,
ACL RECONSTRUCTION POST-OPERATIVE REHABILITATION PROGRAMME ABOUT THE OPERATION The aim of your operation is to reconstruct the Anterior Cruciate Ligament (ACL) to restore knee joint stability. A graft,
The Ankle Sprain That Won t Get Better. By: George E. Quill, Jr., M.D. With springtime in Louisville upon us, the primary care physician and the
 The Ankle Sprain That Won t Get Better By: George E. Quill, Jr., M.D. With springtime in Louisville upon us, the primary care physician and the orthopaedist alike can expect to see more than his or her
The Ankle Sprain That Won t Get Better By: George E. Quill, Jr., M.D. With springtime in Louisville upon us, the primary care physician and the orthopaedist alike can expect to see more than his or her
Copeland Surface Replacement Arthroplasty (Hannan Mullett)
 1.0 Policy Statement... 2 2.0 Purpose... 2 3.0 Scope... 2 4.0 Health & Safety... 2 5.0 Responsibilities... 2 6.0 Definitions and Abbreviations... 3 7.0 Guideline... 3 7.1 Pre-Operative... 3 7.2 Post-Operative...
1.0 Policy Statement... 2 2.0 Purpose... 2 3.0 Scope... 2 4.0 Health & Safety... 2 5.0 Responsibilities... 2 6.0 Definitions and Abbreviations... 3 7.0 Guideline... 3 7.1 Pre-Operative... 3 7.2 Post-Operative...
Integra. Subtalar MBA Implant
 Integra Subtalar MBA Implant Patient EDUCATION Overview: What is Flatfoot? Flatfoot is a physical deformity where there is an absence of the arch that runs from the heel of the foot to the toes. A common
Integra Subtalar MBA Implant Patient EDUCATION Overview: What is Flatfoot? Flatfoot is a physical deformity where there is an absence of the arch that runs from the heel of the foot to the toes. A common
FORGET ME NOT: The Triple Arthrodesis
 C H A P T E R 1 5 FORGET ME NOT: The Triple Arthrodesis Andrea D. Cass, DPM INTRODUCTION The triple arthrodesis is a procedure that is performed much less commonly for the same conditions as it was 20
C H A P T E R 1 5 FORGET ME NOT: The Triple Arthrodesis Andrea D. Cass, DPM INTRODUCTION The triple arthrodesis is a procedure that is performed much less commonly for the same conditions as it was 20
Plantar Fasciitis Information Leaflet. Maneesh Bhatia. Consultant Orthopaedic Surgeon
 Plantar Fasciitis Information Leaflet Maneesh Bhatia Consultant Orthopaedic Surgeon What is plantar fasciitis? The plantar fascia is a strong band of tissue that stretches from the heel to the toes. It
Plantar Fasciitis Information Leaflet Maneesh Bhatia Consultant Orthopaedic Surgeon What is plantar fasciitis? The plantar fascia is a strong band of tissue that stretches from the heel to the toes. It
Knowing about your Ankle Sprain
 Knowing about your Ankle Sprain Knowing about ankle sprain Ankle sprain is a common injury amongst sports such as netball, basketball, rugby and soccer. Sprains can also happen with everyday activities
Knowing about your Ankle Sprain Knowing about ankle sprain Ankle sprain is a common injury amongst sports such as netball, basketball, rugby and soccer. Sprains can also happen with everyday activities
Osteoarthritis progresses slowly and the pain and stiffness it causes worsens over time.
 Arthritis of the Foot and Ankle Arthritis is the leading cause of disability in the United States. It can occur at any age, and literally means "pain within a joint." As a result, arthritis is a term used
Arthritis of the Foot and Ankle Arthritis is the leading cause of disability in the United States. It can occur at any age, and literally means "pain within a joint." As a result, arthritis is a term used
Recent Injuries. www.physiofirst.org.uk
 Recent Injuries www.physiofirst.org.uk A recent or acute injury can occur suddenly during any activity, from tripping over the kerb, to making the bed, to playing sport. In some cases, an acute injury
Recent Injuries www.physiofirst.org.uk A recent or acute injury can occur suddenly during any activity, from tripping over the kerb, to making the bed, to playing sport. In some cases, an acute injury
Anterior Cruciate Ligament Reconstruction Delayed Rehab Dr. Walter R. Lowe
 Anterior Cruciate Ligament Reconstruction Delayed Rehab Dr. Walter R. Lowe This rehabilitation protocol has been designed for patients who have undergone an ACL reconstruction (HS graft/ptg/allograft)
Anterior Cruciate Ligament Reconstruction Delayed Rehab Dr. Walter R. Lowe This rehabilitation protocol has been designed for patients who have undergone an ACL reconstruction (HS graft/ptg/allograft)
KNEE LIGAMENT REPAIR AND RECONSTRUCTION INFORMED CONSENT INFORMATION
 KNEE LIGAMENT REPAIR AND RECONSTRUCTION INFORMED CONSENT INFORMATION The purpose of this document is to provide written information regarding the risks, benefits and alternatives of the procedure named
KNEE LIGAMENT REPAIR AND RECONSTRUCTION INFORMED CONSENT INFORMATION The purpose of this document is to provide written information regarding the risks, benefits and alternatives of the procedure named
RNOH Physiotherapy Department Rehabilitation guidelines for patients undergoing spinal surgery
 RNOH Physiotherapy Department Rehabilitation guidelines for patients undergoing spinal surgery Please note that this is advisory information only. Your experiences may differ from those described. All
RNOH Physiotherapy Department Rehabilitation guidelines for patients undergoing spinal surgery Please note that this is advisory information only. Your experiences may differ from those described. All
CAPPAGH NATIONAL ORTHOPAEDIC HOSPITAL, FINGLAS, DUBLIN 11. The Sisters of Mercy. Rotator Cuff Repair
 1.0 Policy Statement... 2 2.0 Purpose... 2 3.0 Scope... 2 4.0 Health & Safety... 2 5.0 Responsibilities... 2 6.0 Definitions and Abbreviations... 3 7.0 Guideline... 3 7.1 Pre-Operative... 3 7.2 Post-Operative...
1.0 Policy Statement... 2 2.0 Purpose... 2 3.0 Scope... 2 4.0 Health & Safety... 2 5.0 Responsibilities... 2 6.0 Definitions and Abbreviations... 3 7.0 Guideline... 3 7.1 Pre-Operative... 3 7.2 Post-Operative...
.org. Ankle Fractures (Broken Ankle) Anatomy
 Ankle Fractures (Broken Ankle) Page ( 1 ) A broken ankle is also known as an ankle fracture. This means that one or more of the bones that make up the ankle joint are broken. A fractured ankle can range
Ankle Fractures (Broken Ankle) Page ( 1 ) A broken ankle is also known as an ankle fracture. This means that one or more of the bones that make up the ankle joint are broken. A fractured ankle can range
SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS?
 SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS? The spinal canal is best imagined as a bony tube through which nerve fibres pass. The tube is interrupted between each pair of adjacent
SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS? The spinal canal is best imagined as a bony tube through which nerve fibres pass. The tube is interrupted between each pair of adjacent
Rehabilitation Program for Achilles Tendon Rupture/Repair
 Rehabilitation Program for Achilles Tendon Rupture/Repair This protocol is designed to assist you with your rehabilitation after surgery and should be followed under the direction of a physiotherapist
Rehabilitation Program for Achilles Tendon Rupture/Repair This protocol is designed to assist you with your rehabilitation after surgery and should be followed under the direction of a physiotherapist
George E. Quill, Jr., M.D. Louisville Orthopaedic Clinic Louisville, KY
 George E. Quill, Jr., M.D. Louisville Orthopaedic Clinic Louisville, KY The Ankle Sprain That Won t Get Better With springtime in Louisville upon us, the primary care physician and the orthopaedist alike
George E. Quill, Jr., M.D. Louisville Orthopaedic Clinic Louisville, KY The Ankle Sprain That Won t Get Better With springtime in Louisville upon us, the primary care physician and the orthopaedist alike
Spinal Discectomy & Decompression Surgery
 1.0 Policy Statement... 2 2.0 Purpose... 2 3.0 Scope... 2 4.0 Health & Safety... 2 5.0 Responsibilities... 2 6.0 Definitions and Abbreviations... 3 7.0 Guideline... 3 7.1 Pre-Operative... 3 7.2 Post-Operative...
1.0 Policy Statement... 2 2.0 Purpose... 2 3.0 Scope... 2 4.0 Health & Safety... 2 5.0 Responsibilities... 2 6.0 Definitions and Abbreviations... 3 7.0 Guideline... 3 7.1 Pre-Operative... 3 7.2 Post-Operative...
Total knee replacement
 Patient Information to be retained by patient What is a total knee replacement? In a total knee replacement the cartilage surfaces of the thigh bone (femur) and leg bone (tibia) are replaced. The cartilage
Patient Information to be retained by patient What is a total knee replacement? In a total knee replacement the cartilage surfaces of the thigh bone (femur) and leg bone (tibia) are replaced. The cartilage
Y O U R S U R G E O N S. choice of. implants F O R Y O U R S U R G E R Y
 Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Your Surgeon Has Chosen the C 2 a-taper Acetabular System The
Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Your Surgeon Has Chosen the C 2 a-taper Acetabular System The
Musculoskeletal System
 CHAPTER 3 Impact of SCI on the Musculoskeletal System Voluntary movement of the body is dependent on a number of systems. These include: The brain initiates the movement and receives feedback to assess
CHAPTER 3 Impact of SCI on the Musculoskeletal System Voluntary movement of the body is dependent on a number of systems. These include: The brain initiates the movement and receives feedback to assess
Orthopaedic and Spine Institute 21 Spurs Lane, Suite 245, San Antonio, TX 78240 www.saspine.com Tel# 210-487-7463
 Phase I Passive Range of Motion Phase (postop week 1-2) Minimize shoulder pain and inflammatory response Achieve gradual restoration of gentle active range of motion Enhance/ensure adequate scapular function
Phase I Passive Range of Motion Phase (postop week 1-2) Minimize shoulder pain and inflammatory response Achieve gradual restoration of gentle active range of motion Enhance/ensure adequate scapular function
Knee Arthroscopy Exercise Programme
 Chester Knee Clinic & Cartilage Repair Centre Nuffield Health, The Grosvenor Hospital Chester Wrexham Road Chester CH4 7QP Hospital Telephone: 01244 680 444 CKC Website: www.kneeclinic.info Email: office@kneeclinic.info
Chester Knee Clinic & Cartilage Repair Centre Nuffield Health, The Grosvenor Hospital Chester Wrexham Road Chester CH4 7QP Hospital Telephone: 01244 680 444 CKC Website: www.kneeclinic.info Email: office@kneeclinic.info
Total knee replacement: The enhanced recovery programme
 INFORMATION FOR PATIENTS Total knee replacement: The enhanced recovery programme Aim This leaflet aims to explain the enhanced recovery programme after total knee replacement surgery, and outline what
INFORMATION FOR PATIENTS Total knee replacement: The enhanced recovery programme Aim This leaflet aims to explain the enhanced recovery programme after total knee replacement surgery, and outline what
Information and exercises following dynamic hip screw
 Physiotherapy Department Information and exercises following dynamic hip screw Introduction A dynamic hip screw is performed where the neck of femur has been fractured and where there is a good chance
Physiotherapy Department Information and exercises following dynamic hip screw Introduction A dynamic hip screw is performed where the neck of femur has been fractured and where there is a good chance
Wrist and Hand. Patient Information Guide to Bone Fracture, Bone Reconstruction and Bone Fusion: Fractures of the Wrist and Hand: Carpal bones
 Patient Information Guide to Bone Fracture, Bone Reconstruction and Bone Fusion: Wrist and Hand Fractures of the Wrist and Hand: Fractures of the wrist The wrist joint is made up of the two bones in your
Patient Information Guide to Bone Fracture, Bone Reconstruction and Bone Fusion: Wrist and Hand Fractures of the Wrist and Hand: Fractures of the wrist The wrist joint is made up of the two bones in your
Knee arthroscopy advice sheet
 Knee arthroscopy advice sheet During an arthroscopy, a camera is inserted into the knee through two or three small puncture wounds. It allows the surgeon to look at the joint surfaces, cartilage and the
Knee arthroscopy advice sheet During an arthroscopy, a camera is inserted into the knee through two or three small puncture wounds. It allows the surgeon to look at the joint surfaces, cartilage and the
Hip Replacement. Department of Orthopaedic Surgery Tel: 01473 702107
 Information for Patients Hip Replacement Department of Orthopaedic Surgery Tel: 01473 702107 DMI ref: 0134-08.indd(RP) Issue 3: February 2008 The Ipswich Hospital NHS Trust, 2005-2008. All rights reserved.
Information for Patients Hip Replacement Department of Orthopaedic Surgery Tel: 01473 702107 DMI ref: 0134-08.indd(RP) Issue 3: February 2008 The Ipswich Hospital NHS Trust, 2005-2008. All rights reserved.
CUSTOM ORTHOTICS/SHOES FAQ AND GLOSSARY
 CUSTOM ORTHOTICS/SHOES FAQ AND GLOSSARY What is GSC s new orthotics and orthopedic shoe policy? Only certain health professionals can prescribe and provide you with custom orthotics, orthopedic shoes,
CUSTOM ORTHOTICS/SHOES FAQ AND GLOSSARY What is GSC s new orthotics and orthopedic shoe policy? Only certain health professionals can prescribe and provide you with custom orthotics, orthopedic shoes,
ACL Reconstruction: Patellar Tendon Graft/Hamstring Tendon Graft
 ACL Reconstruction: Patellar Tendon Graft/Hamstring Tendon Graft Patellar Tendon Graft/Hamstring Tendon Graft General Information: The intent of these guidelines is to provide the therapist with direction
ACL Reconstruction: Patellar Tendon Graft/Hamstring Tendon Graft Patellar Tendon Graft/Hamstring Tendon Graft General Information: The intent of these guidelines is to provide the therapist with direction
Varicose Veins Operation. Patient information Leaflet
 Varicose Veins Operation Patient information Leaflet 22 nd August 2014 WHAT IS VARICOSE VEIN SURGERY (HIGH LIGATION AND MULTIPLE AVULSIONS) The operation varies from case to case, depending on where the
Varicose Veins Operation Patient information Leaflet 22 nd August 2014 WHAT IS VARICOSE VEIN SURGERY (HIGH LIGATION AND MULTIPLE AVULSIONS) The operation varies from case to case, depending on where the
Frequently Asked Questions about Foot and Ankle Surgery. Foot & Ankle Clinic. Cambridge. A patient s guide. Fred Robinson
 Frequently Asked Questions about Foot and Ankle Surgery A patient s guide Fred Robinson BSc FRCS FRCS(orth) Consultant Trauma & Orthopaedic Surgeon www.cambridgefootandankle.com Frequently Asked Questions
Frequently Asked Questions about Foot and Ankle Surgery A patient s guide Fred Robinson BSc FRCS FRCS(orth) Consultant Trauma & Orthopaedic Surgeon www.cambridgefootandankle.com Frequently Asked Questions
Ankle Arthroscopy and Follow-Up Physiotherapy
 Ankle Arthroscopy and Follow-Up Physiotherapy Exceptional healthcare, personally delivered Following your consultation with a member of the Foot and Ankle team you have agreed that you might benefit from
Ankle Arthroscopy and Follow-Up Physiotherapy Exceptional healthcare, personally delivered Following your consultation with a member of the Foot and Ankle team you have agreed that you might benefit from
Physical Therapy for Shoulder. Joseph Lorenzetti PT, DPT, MTC Catholic Health Athleticare Kenmore 1495 Military Road Kenmore, NY 14217
 Physical Therapy for Shoulder and Knee Pain Joseph Lorenzetti PT, DPT, MTC Catholic Health Athleticare Kenmore 1495 Military Road Kenmore, NY 14217 Physical Therapy for Shoulder and Knee Pain GOALS: Explain
Physical Therapy for Shoulder and Knee Pain Joseph Lorenzetti PT, DPT, MTC Catholic Health Athleticare Kenmore 1495 Military Road Kenmore, NY 14217 Physical Therapy for Shoulder and Knee Pain GOALS: Explain
Biceps Tenodesis Protocol
 Department of Rehabilitation Services Physical Therapy The intent of this protocol is to provide the clinician with a guideline of the postoperative rehabilitation course of a patient that has undergone
Department of Rehabilitation Services Physical Therapy The intent of this protocol is to provide the clinician with a guideline of the postoperative rehabilitation course of a patient that has undergone
SCRIPT NUMBER 82 SPRAINED ANKLE (TWO SPEAKERS)
 SCRIPT NUMBER 82 SPRAINED ANKLE (TWO SPEAKERS) PROGRAM NAME: HEALTH NUGGETS PROGRAM TITLE: SPRAINED ANKLE PROGRAM NUMBER: 82 SUBJECT: PATHOLOGY, CAUSES, DIAGNOSIS, TREATMENT, PREVENTION OF SPRAINED ANKLES
SCRIPT NUMBER 82 SPRAINED ANKLE (TWO SPEAKERS) PROGRAM NAME: HEALTH NUGGETS PROGRAM TITLE: SPRAINED ANKLE PROGRAM NUMBER: 82 SUBJECT: PATHOLOGY, CAUSES, DIAGNOSIS, TREATMENT, PREVENTION OF SPRAINED ANKLES
Understanding. Heel Pain
 Understanding Heel Pain What Causes Heel Pain? Heel pain is a common problem that occurs when the heel is placed under too much stress. Heel pain is most often caused by walking in ways that irritate tissues
Understanding Heel Pain What Causes Heel Pain? Heel pain is a common problem that occurs when the heel is placed under too much stress. Heel pain is most often caused by walking in ways that irritate tissues
Posttraumatic medial ankle instability
 Posttraumatic medial ankle instability Alexej Barg, Markus Knupp, Beat Hintermann Orthopaedic Department University Hospital of Basel, Switzerland Clinic of Orthopaedic Surgery, Kantonsspital Baselland
Posttraumatic medial ankle instability Alexej Barg, Markus Knupp, Beat Hintermann Orthopaedic Department University Hospital of Basel, Switzerland Clinic of Orthopaedic Surgery, Kantonsspital Baselland
Podiatric Medicine. What is a Podiatrist?
 Page 3 Podiatric Medicine Podiatric Medicine is the profession that strives to improve the overall health and wellbeing of patients by focusing on preventing, diagnosing, and treating conditions associated
Page 3 Podiatric Medicine Podiatric Medicine is the profession that strives to improve the overall health and wellbeing of patients by focusing on preventing, diagnosing, and treating conditions associated
DROP FOOT AND TREATMENTS YOUNGMEE PARK
 DROP FOOT AND TREATMENTS YOUNGMEE PARK WHAT IS FOOT DROP Foot drop / Drop foot the inability to lift the front part of the foot not a disease a symptom of some other medical problems a sign of an underlying
DROP FOOT AND TREATMENTS YOUNGMEE PARK WHAT IS FOOT DROP Foot drop / Drop foot the inability to lift the front part of the foot not a disease a symptom of some other medical problems a sign of an underlying
Ankle Injury/Sprains in Youth Soccer Players Elite Soccer Community Organization (ESCO) November 14, 2013
 Ankle Injury/Sprains in Youth Soccer Players Elite Soccer Community Organization (ESCO) November 14, 2013 Jeffrey R. Baker, DPM, FACFAS Weil Foot and Ankle Institute Des Plaines, IL Ankle Injury/Sprains
Ankle Injury/Sprains in Youth Soccer Players Elite Soccer Community Organization (ESCO) November 14, 2013 Jeffrey R. Baker, DPM, FACFAS Weil Foot and Ankle Institute Des Plaines, IL Ankle Injury/Sprains
.org. Arthritis of the Hand. Description
 Arthritis of the Hand Page ( 1 ) The hand and wrist have multiple small joints that work together to produce motion, including the fine motion needed to thread a needle or tie a shoelace. When the joints
Arthritis of the Hand Page ( 1 ) The hand and wrist have multiple small joints that work together to produce motion, including the fine motion needed to thread a needle or tie a shoelace. When the joints
ILIOTIBIAL BAND SYNDROME
 ILIOTIBIAL BAND SYNDROME Description The iliotibial band is the tendon attachment of hip muscles into the upper leg (tibia) just below the knee to the outer side of the front of the leg. Where the tendon
ILIOTIBIAL BAND SYNDROME Description The iliotibial band is the tendon attachment of hip muscles into the upper leg (tibia) just below the knee to the outer side of the front of the leg. Where the tendon
Dr Doron Sher MB.BS. MBiomedE, FRACS(Orth)
 Dr Doron Sher MB.BS. MBiomedE, FRACS(Orth) Knee, Shoulder, Elbow Surgery ACL REHABILITATION PROGRAM (With thanks to the Eastern Suburbs Sports Medicine Centre) The time frames in this program are a guide
Dr Doron Sher MB.BS. MBiomedE, FRACS(Orth) Knee, Shoulder, Elbow Surgery ACL REHABILITATION PROGRAM (With thanks to the Eastern Suburbs Sports Medicine Centre) The time frames in this program are a guide
Total hip replacement
 Patient Information to be retained by patient What is a total hip replacement? In a total hip replacement both the ball (femoral or thigh bone) side of the hip joint and the socket (acetabular or pelvic
Patient Information to be retained by patient What is a total hip replacement? In a total hip replacement both the ball (femoral or thigh bone) side of the hip joint and the socket (acetabular or pelvic
.org. Herniated Disk in the Lower Back. Anatomy. Description
 Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
ORIGINAL ARTICLE. EXCISION OF RETROCALCANEAL SPUR BY A LATERAL APPROACH FOR RELIEF OF HEEL PAIN. Nandivada V.S. Kiran Kumar
 EXCISION OF RETROCALCANEAL SPUR BY A LATERAL APPROACH FOR RELIEF OF HEEL PAIN. Nandivada V.S. Kiran Kumar 1. Assistant Professor. Department of Orthopaedics, King George Hospital. Visakhapatnam. CORRESPONDING
EXCISION OF RETROCALCANEAL SPUR BY A LATERAL APPROACH FOR RELIEF OF HEEL PAIN. Nandivada V.S. Kiran Kumar 1. Assistant Professor. Department of Orthopaedics, King George Hospital. Visakhapatnam. CORRESPONDING
