RESEARCH ARTICLE. On the Added Value of Baseline FDG-PET in Malignant Lymphoma
|
|
|
- Iris Alexander
- 7 years ago
- Views:
Transcription
1 B The Author(s), 2009 Published Online: 7 October 2009 Mol Imaging Biol (2010) 12:225Y232 DOI: /s RESEARCH ARTICLE On the Added Value of Baseline FDG-PET in Malignant Lymphoma Henriette Quarles van Ufford, 1,2 Otto Hoekstra, 3 Marie de Haas, 4 Rob Fijnheer, 5 Shulamiet Wittebol, 5 Bianca Tieks, 4 Mark Kramer, 6 John de Klerk 4 1 Radiology, University Medical Center Utrecht, Utrecht, The Netherlands 2 Radiology and Nuclear Medicine, Meander Medical Center, Utrecht, The Netherlands 3 Nuclear Medicine & PET research, Vrije University Medical Center, Amsterdam, The Netherlands 4 Nuclear Medicine, Meander Medical Center, Amersfoort, The Netherlands 5 Internal Medicine, Meander Medical Center, Amersfoort, The Netherlands 6 Internal Medicine, Vrije University Medical Centre, Amsterdam, The Netherlands Abstract Purpose: The added value of baseline positron emission tomography (PET) scans in therapy evaluation in malignant lymphoma is unclear. In guidelines, baseline PET is recommended but not mandatory except in lymphoma types with variable fluoro-d-glucose uptake. The aim of the present study was to test the hypothesis that adding baseline PET information decreases false positive readings with posttreatment PET and improves observer agreement. Methods: Forty-four patients (mean age 56 years, standard deviation 14) with malignant lymphoma were included. Two nuclear medicine physicians retrospectively and independently evaluated the posttreatment PET, 3 weeks later followed by paired reading of baseline and posttreatment PET. For each PET, 22 regions were classified as positive, negative, or equivocal, resulting in an overall PET score of positive, unclear, or negative. In case of discrepancies, consensus was reached. Results: Addition of baseline to posttreatment PET evaluation affected the classification of metabolic response in 34% of malignant lymphoma patients treated with first-line chemotherapy. In one out of seven patients, addition of the baseline PET lead to opposite conclusions (95% confidence interval 4 14). False positivity was reduced by adding the baseline scan information, but the effect on false negativity was similar. In addition, the amount of unclear classifications halved after paired reading. Observer agreement did not improve upon adding the baseline PET data. Conclusion: Without any other clinical information, pretreatment PET facilitates changes the interpretation of a posttreatment PET in a third of the patients, resulting in both upgrading and downgrading of the posttreatment situation of a malignant lymphoma patient. If these results are confirmed for PET computed tomography systems, they favor the addition of baseline PET to the current work-up of patients with malignant lymphoma. Key words: FDG PET, Malignant lymphoma, Therapy evaluation, Baseline PET, Hodgkin s disease, Non-Hodgkin s lymphoma Introduction Prognosis and survival of patients with Hodgkin s disease (HD) and non-hodgkin s lymphoma (NHL) depend on Correspondence to: Henriette Quarles van Ufford; h.m.e.quarlesv anufford@umcutrecht.nl both histological grade and clinical stage at the moment of diagnosis and furthermore on the response to treatment [1]. The Ann Arbor classification with Cotswolds revision is the guideline for radiological staging of HD and most types of NHL [2, 3]. In the past, the Ann Arbor staging system was based on physical examination and bone marrow evaluation, later to include the computed tomography (CT) scan. With the
2 226 Quarles van Ufford, et al.: On the Added Value of Baseline FDG-PET in Malignant Lymphoma Table 1. Patient characteristics of NHL and HD patients Patient NHL HD Number 35 9 M:F 16:19 7:2 Mean age (years; range) 58 (24 87) 40 (19 71) Pathological subtypes DLBCL, 18 Nodular sclerosis, 7 Follicular, 9 Mixed cellularity, 2 Burkitt, 1 MCL, 2 MZL, 1 MALT, 1 SLL, 2 ACL, 1 NHL non-hodgkin s lymphoma, HD Hodgkin s disease, M male, F female, DLBCL diffuse large B cell lymphoma, MCL mantle cell lymphoma, MZL marginal zone lymphoma, MALT mucosa-associated lymphoid tissue, SLL small lymphocytic lymphoma, ACL anaplastic cell lymphoma implementation of the positron emission tomography (PET) scan and later the integrated PET/CT scan, several studies concluded that a baseline 2-deoxy-2-[18F]fluoro-D-glucose (FDG) PET scan provides significant more information than conventional CT, with subsequent therapeutic consequences [4 6]. Whereas the application of PET in therapy evaluation in malignant lymphoma is rapidly emerging, the added value of baseline PET scans in this context is less clear. In guidelines, baseline PET is recommended but not mandatory except in lymphoma types with variable FDG uptake. Baseline scans may facilitate interpretation of PET at therapy evaluation, increase reader confidence, and perhaps avoid misinterpretation. Guidelines on PET reading after therapy refer to previously involved lesions to avoid false positivity [7 9]. The aim of the present study was to test the hypothesis that adding baseline PET information decreases false positive readings with therapy evaluation PET and improves observer agreement. Materials and Methods Subjects We retrospectively studied baseline and posttreatment PET scans of 44 patients with newly diagnosed malignant lymphoma undergoing firstline therapy between January 2005 and July In all patients, malignant lymphoma had been histopathologically proven, and initial staging was done according to the Ann Arbor classification (with supplementary baseline PET scan). The posttreatment PET scan was performed at least 4 6 weeks after completion of therapy, and patients were at least 10 days off granulocyte colony-stimulating factor (G- CSF) therapy [7, 10]. The study was approved by the ethical board, and informed consent was waived. PET Imaging PET was performed with a mobile scanner (ECAT-ACCEL, Siemens/CTI, Knoxville, TN, USA). Patients fasted for 6 h before the scan. Prior to injection, blood glucose levels were within the normal range (G11 mmol/l). One hour after injection of FDG (5 MBq/kg body weight), patients were scanned from mid femur to Table 2. Agreement of isolated posttreatment and reference PET classification (a), as a function of PET positivity criteria (b), and observer agreement (c) (a) Consensus-isolated posttreatment PET (b) Conservative: consensus-isolated posttreatment PET Sensitive: consensus-isolated posttreatment PET (c) Observer 1 isolated posttreatment PET Observer 2 isolated posttreatment PET Consensus-paired reading (reference standard) Negative Unclear Positive Total Conservative: consensus-paired reading (reference standard) Negative Positive Total Negative Positive Total Sensitive: consensus-paired reading (reference standard) Negative Positive Total Negative Positive Total Observer 1 posttreatment PET (paired reading) Negative Unclear Positive Total Observer 2 posttreatment PET (paired reading) Negative Unclear Positive Total
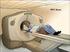
3 Quarles van Ufford, et al.: On the Added Value of Baseline FDG-PET in Malignant Lymphoma 227 Fig. 1. Posttreatment and pretreatment PET scan of a 51-year-old male with follicular non-hodgkin lymphoma. Both interpreters scored complete metabolic response on the isolated posttreatment PET scan. a Posttreatment PET scan: coronal images with an b axial and c sagittal image at the level of the described lesion. d Pretreatment PET scan: coronal images with an e axial and f sagittal image at the level of the described lesion. The pretreatment PET scan displays multiple regions with pathologic FDG uptake: multiple regions above (neck and mediastinum) and below (intra abdominal and inguinal) diaphragm and diffuse bone marrow involvement. With this knowledge, the initial interpretation of the posttreatment PET scan was changed to a positive posttreatment PET scan: In the right inguinal region, there is increased FDG uptake. Without the pretreatment PET scan, this was considered physiologic. the base of the skull. Acquisition time was 5 min per bed position, with a transmission time of 60 s each. Patients were scanned in seven bed positions. PET images were reconstructed with and without attenuation correction using a weighted iterative ordered subsets expectation maximization algorithm (OSEM, two iterations, eight subsets). In the final step, a three-dimensional isotropic gauss filter was applied to a final image resolution with 8 9-mm full width at half maximum.
4 228 Quarles van Ufford, et al.: On the Added Value of Baseline FDG-PET in Malignant Lymphoma Fig. 1. (continued). PET Analysis Two nuclear medicine physicians with >5-year clinical PET experience (MJH, JMHK) independently evaluated the PET scans. First, they interpreted all 44 posttreatment PET scans, 3 weeks later followed by another session in which the same posttreatment PET scans were presented together with the baseline PET scans (paired reading). The observers were aware that the patients had malignant lymphoma but unaware of the type and grade of lymphoma and results of baseline or posttreatment conventional staging. For each scan, they analyzed 22 regions using a standardized form, classifying FDG uptake as positive, negative, or equivocal. Criteria for PET positivity were as follows: A region with FDG uptake above background in a location incompatible with normal anatomy or physiology was considered positive [7]. After evaluation of the forms of the posttreatment PET scans in both sessions, the observers were requested to assign a consensus score in case of discrepancies. Consensus was reached for the
5 Quarles van Ufford, et al.: On the Added Value of Baseline FDG-PET in Malignant Lymphoma 229 regions of the posttreatment PET without presentation of the baseline PET, followed by the posttreatment PET in combination with the baseline PET. Besides this lesion-based analysis, the observers provided per patient evaluations. In each patient, all scores of the 22 different regions were taken together resulting in a negative posttreatment PET scan (all regions negative, indicating complete metabolic remission), or a positive posttreatment PET scan ( 1 positive region). Patients with only equivocal scores, besides negative scores, were classified as unclear. Because both observers evaluated the PET scans without clinical information, the positive or equivocal classified regions of the posttreatment PET scans were compared with the initially affected regions reported in the clinical database (baseline CT, PET scan, bone marrow biopsy). Statistical Analysis We considered the consensus scores of the paired reading as the gold standard for presence or absence of viable tumor after therapy. To measure the impact of adding a baseline PET scan as a function of sensitivity of PET readings, the posttreatment PET results (isolated and paired reading) were dichotomized by assigning the unclear classification to either the PET-negative (complete responders) or to the PET-positive classification. Sensitivity, specificity, positive predictive value, and negative predictive value were determined for either strategy. To analyze interobserver variability and agreement of isolated and combined baseline and posttreatment PET readings, we used linear-weighted kappa (κ w ;SAS 9.1; SAS Institute, Cary, NC), considering kappa G0.20 as poor observer agreement, as fair, as moderate, as good, and as very good [11]. Ninety-five percent confidence intervals of proportions were calculated with Confidence Interval Analysis Results Subjects We included 44 patients with a mean age of 56 years (SD 14), diagnosed with NHL in 35 (80%), and HD in nine (20%) patients, further details are provided in Table 1. All patients had FDG avid lymphoma at baseline and had been clinically staged (including PET) according to the Ann Arbor classification as stage 1 (n=3, 7%), stage 2 (n=15, 34%), stage 3 (n=16, 36%), and stage 4 (n=10, 23%). Per Patient Analysis For each patient, the initial stage of disease and type of lymphoma as reported in the clinical digital database, the scores of the isolated posttreatment PET scans, and the paired posttreatment PET readings for either observer or their consensus scores are provided in Appendix (Table 4). In the consensus reading of the isolated posttreatment PET scans, 24 PET scans were classified as negative, six as unclear, Table 3. Per region analysis of the agreement of isolated posttreatment and reference PET classifications (a), as a function of PET positivity criteria (b), and observer agreement (c) (a) Consensus-isolated posttreatment PET (b) Conservative: consensus-isolated posttreatment PET Sensitive: consensus-isolated posttreatment PET (c) Observer 1 isolated posttreatment PET Observer 2 isolated posttreatment PET Consensus-paired reading (reference standard) Negative Unclear Positive Total Conservative: consensus-paired reading (reference standard) Negative Positive Total Negative Positive Total Sensitive: consensus-paired reading (reference standard) Negative Positive Total Negative Positive Total Observer 1 posttreatment PET (paired reading) Negative Unclear Positive Total Observer 2 posttreatment PET (paired reading) Negative Unclear Positive Total
6 230 Quarles van Ufford, et al.: On the Added Value of Baseline FDG-PET in Malignant Lymphoma and 14 as positive. In the consensus reading of the paired reading, 25 posttherapy PET scans were classified as negative, three as unclear, and 16 as positive (Table 2). The consensus scores of the isolated posttreatment PET scans vs paired reference standard were concordant in 29/44 cases (66%, 95% CI 54 77%) resulting in a good correlation (κ w =0.73, 95% CI , pg0.0001). The proportion of unclear readings was 6.8% in the paired reading vs 13.6% in the isolated reading. Adding the baseline PET scan altered the PET classification in 15 cases but in either direction of suspicion: in eight patients the level of suspicion increased, in seven decreasing (Table 2a). In six cases (13.6%) the conclusion was opposite, with three false positive and three false negative (Fig. 1) isolated PET readings. Dichotomization did not clearly affect the results with accuracies of 75% (95% CI 63 84%) and 77% (95% CI 65 86%) for sensitive and conservative reading strategies, respectively (kappa s: 0.49, 95% CI vs 0.50, 95% CI , respectively). False positivity rates of the isolated posttreatment PET interpretations prevailed in 4/14 (29%, 95% CI 14 51%) and 6/20 (30%, 95% CI 16 48%) for conservative and sensitive readings, respectively (Table 2b). The interobserver agreement of paired baseline and posttreatment evaluations was similar compared to the isolated PET evaluations (linear weighted kappa s: 0.64, 95% CI vs 0.67, 95% CI , respectively). Per Lesion Analysis As expected, the large majority of regions were FDG negative: in the consensus setting, 95% of both isolated posttreatment scans and paired readings (Table 3a); of the nonnegative readings, 22% and 17% were classified as unclear, respectively (NS). Twentyfour of the isolated posttherapy PET classifications altered after addition of the baseline scan (similar to the patient-based analysis), and the change was in either direction of suspicion (12 towards lower level). Dichotomization yielded kappa s of 0.75 (95% CI ) and 0.71 (95% CI ) for conservative and sensitive reading strategies, respectively. The false positivity rates of isolated PET readings were 17% (95 %CI 9 30%) and 24% (95% CI 16 36%) with conservative and sensitive readings, respectively. The interobserver agreement for the per lesion evaluation of the isolated posttreatment PET scans was good (κ w =0.71, 95% CI , pg0.0001). Adding the baseline PET information did not further improve the observer agreement (κ w =0.66, 95% CI , pg0.0001). Discrepant lesional scores were randomly divided over the 22 different regions, the number of different scores ranging from 1 to 7 for each region in 20 of 22 regions. lymphoma patients treated with first-line chemotherapy. In one out of seven patients, addition of the baseline PET lead to opposite conclusions (95% CI 4 14). False positivity was reduced by adding the baseline scan information, but the effect on false negativity was similar. In addition, the amount of unclear classifications reduced (50%) after paired reading. Observer agreement did not improve upon adding the baseline PET data. In malignant lymphoma, baseline PET information is essential to be able to assess response in lymphoma types with variable FDG avidity. In routinely FDG-avid lymphoma, baseline scans are recommended but not mandatory [8]. The intrinsic paradox flows from a lack of evidence, primarily at the level of effectiveness. Obvious disadvantages of routine baseline scanning are costs and unnecessary radiation (typically about 3.5 msv) added by FDG to the standard CT work-up [12, 13]. In case of adding low-dose CT to PET, augmented with another 2 3 msv[14]. Even though diagnostic CT (typically extending from neck to perineum in these patients) yields most of the radiation dose, adding PET should be justified by an impact on disease classification. Our study has some limitations. First, PET scans in this study were performed with a stand-alone PET scanner rather than with PET-CT. Second, the observers were blinded for type and grade of lymphoma, pretreatment, or posttreatment situation and CT findings. An argument favoring interpreting diagnostic tests with clinical information is that the accuracy of the read may be improved by the additional information. It could be argued that the added value of the pretreatment PET scan may have been less, when this information had been provided. An argument favoring interpreting diagnostic tests without clinical information is that it may bias the reading and that clinical information should be incorporated into decision-making only after an unbiased read [15]. In three patients, one region which was initially not affected according to the clinical digital database was classified as equivocal in the first session. After pairedreading, these scores were changed into negative. In this situation the pretreatment scan provided the same information as the knowledge of the initial clinical information and instead of 34% (15/44), 27% (12/44) of the overall results differed. In conclusion, without any other clinical information, a pretreatment PET facilitates and changes the interpretation of a posttreatment PET in a third of the patients, resulting in both upgrading and downgrading of the posttreatment situation of a malignant lymphoma patient. Adding a baseline PET scan did not improve observer agreement. If these results are confirmed for PET/CT systems, they favor the addition of baseline PET to the current work-up of patients with malignant lymphoma. Discussion The addition of baseline to posttreatment PET evaluation affected the classification of metabolic response in 34% of malignant Open Access. This article is distributed under the terms of the Creative Commons Attribution Noncommercial License which permits any noncommercial use, distribution, and reproduction in any medium, provided the original author(s) and source are credited.
7 Quarles van Ufford, et al.: On the Added Value of Baseline FDG-PET in Malignant Lymphoma 231 Appendix Table 4. Results per case of the PET evaluation Cases Initial stage and PA Post a Post and pre b Difference c O 1 O 2 C O 1 O 2 C 1 4, NHL; small lymphocytic lymphoma No 2 2, NHL; diffuse large B cell lymphoma U d U U Yes 3 3, NHL; diffuse large B cell lymphoma No 4 2, HD; nodular sclerosis U U U Yes 5 2, NHL; diffuse large B cell lymphoma U No 6 4, NHL; Burkitt No 7 2, NHL; follicular No 8 3, HD; nodular sclerosis U U U Yes 9 4, NHL; diffuse large B cell lymphoma + U + Yes 10 4, NHL; diffuse large B cell lymphoma No 11 1, HD; mixed cellularity U U + Yes 12 4, NHL; follicular + + Yes 13 3, NHL; diffuse large B cell lymphoma No 14 2, NHL; diffuse large B cell lymphoma U U Yes 15 2, HD; nodular sclerosis No 16 4, NHL; mucose related lymphoid tissue No 17 3, NHL; diffuse large B cell lymphoma Yes 18 2, NHL; diffuse large B cell lymphoma No 19 4, NHL; follicular No 20 2, HD; mixed cellularity No 21 2, HD; nodular sclerosis No 22 3, NHL; diffuse large B cell lymphoma + U U Yes 23 3, NHL; diffuse large B cell lymphoma U + U Yes 24 2, NHL; anaplastic cell lymphoma + U + U + + No 25 3, NHL; diffuse large B cell lymphoma U U Yes 26 4, HD; nodular sclerosis No 27 3, NHL; diffuse large B cell lymphoma No 28 3, NHL; follicular No 29 1, NHL; diffuse large B cell lymphoma No 30 3, NHL; diffuse large B cell lymphoma No 31 3, NHL; mantle cell lymphoma No 32 3, NHL; follicular No 33 2, NHL; follicular No 34 2, HD; nodular sclerosis No 35 4, HD; nodular sclerosis U No 36 3, NHL; diffuse large B cell lymphoma No 37 3, NHL; mantle cell lymphoma U U U Yes 38 3, NHL; follicular U U No 39 2, NHL; marginal zone lymphoma No 40 3, NHL; small lymphocytic lymphoma U U U U Yes 41 1, NHL; follicular Yes 42 4, NHL; diffuse large B cell lymphoma No 43. 2, NHL; follicular U Yes 44 2, NHL; diffuse large B cell lymphoma No a Post: per patient evaluation of the posttreatment PET scan without knowledge of the pretreatment PET scan b Post and pre: per patient evaluation of the posttreatment PET scan after visualization of the pretreatment PET scan, i.e., paired reading c Difference: if there is a difference in interpretation of the posttreatment PET with and without the knowledge of the pretreatment PET d Unclear: when one or more regions are scored equivocal and all other regions are classified negative in the PET scan, it is not possible to determine whether the scan is positive or negative, and the conclusion is unclear References 1. Hoskin PJ (2003) PET in lymphoma: what are the oncologist s needs? Eur J Nucl Med Mol Imaging 30(Suppl 1):S37 S41 2. Carbone PP, Kaplan HS, Musshoff K et al (1971) Report of the committee on Hodgkin s disease staging classification. Cancer Res 31: Armitage JO (2005) Staging non-hodgkin lymphoma. CA Cancer J Clin 55: Hoh CK, Glaspy J, Rosen P et al (1997) Whole-body FDG-PET imaging for staging of Hodgkin s disease and lymphoma. J Nucl Med 38: Buchmann I, Reinhardt M, Elsner K et al (2001) 2-(fluorine-18)fluoro- 2-deoxy-D-glucose positron emission tomography in the detection and staging of malignant lymphoma. A bicenter trial. Cancer 91: Seam P, Juweid ME, Cheson BD (2007) The role of FDG-PET scans in patients with lymphoma. Blood 110:
8 232 Quarles van Ufford, et al.: On the Added Value of Baseline FDG-PET in Malignant Lymphoma 7. Juweid ME, Stroobants S, Hoekstra OS et al (2007) Use of positron emission tomography for response assessment of lymphoma: consensus of the imaging subcommittee of International Harmonization Project in Lymphoma. J Clin Oncol 25: Cheson BD, Pfistner B, Juweid ME et al (2007) Revised response criteria for malignant lymphoma. J Clin Oncol 25: Manning K, Tepfer B, Goldklang G et al (2007) Clinical practice guidelines for the utilization of positron emission tomography/computed tomography imaging in selected oncologic applications: suggestions from a provider group. Mol Imaging Biol 9: Lister TA, Crowther D, Sutcliffe SB et al (1989) Report of a committee convened to discuss the evaluation and staging of patients with Hodgkin s disease: cotswolds meeting. J Clin Oncol 7: Altman DG (1999) Inter-rater agreement. In: Altman DG (ed) Practical statistics for medical research. Chapman & Hall, London, pp Wu TH, Huang YH, Lee JJ et al (2004) Radiation exposure during transmission measurements: comparison between CT- and germaniumbased techniques with a current PET scanner. Eur J Nucl Med Mol Imaging 31: Brix G, Lechel U, Glatting G et al (2005) Radiation exposure of patients undergoing whole-body dual-modality 18F-FDG PET/CT examinations. J Nucl Med 46: Kinahan PE, Townsend DW, Beyer T et al (1998) Attenuation correction for a combined 3D PET/CT scanner. Med Phys 25: Griscom NT (2002) A suggestion: look at the images first, before you read the history. Radiology 223:9 10
False positive PET in lymphoma
 False positive PET in lymphoma Thomas Krause Introduction and conclusion 2 3 Introduction 4 FDG-PET in staging of lymphoma 34 studies with 2227 Patients CT FDG-PET Sensitivity 63 % 89 % (58%-100%) (63%-100%)
False positive PET in lymphoma Thomas Krause Introduction and conclusion 2 3 Introduction 4 FDG-PET in staging of lymphoma 34 studies with 2227 Patients CT FDG-PET Sensitivity 63 % 89 % (58%-100%) (63%-100%)
PET/CT in Lymphoma. Ur Metser, M.D. Division Head, Molecular Imaging Joint Department of Medical Imaging, UHN- MSH- WCH University of Toronto
 PET/CT in Lymphoma Ur Metser, M.D. Division Head, Molecular Imaging Joint Department of Medical Imaging, UHN- MSH- WCH University of Toronto Outline 1. Introduction: PET/CT, how does it work? 2.Current
PET/CT in Lymphoma Ur Metser, M.D. Division Head, Molecular Imaging Joint Department of Medical Imaging, UHN- MSH- WCH University of Toronto Outline 1. Introduction: PET/CT, how does it work? 2.Current
Response Criteria for Malignant Lymphoma 2007. Cheson Criteria. Quick Reference Guide
 Response Criteria for Malignant Lymphoma 2007 Cheson Criteria Quick Reference Guide Table of Contents Summary of Assessments...3 Baseline Lesion Burden...4 What isameasurable Lesion?...5 Choosing Target
Response Criteria for Malignant Lymphoma 2007 Cheson Criteria Quick Reference Guide Table of Contents Summary of Assessments...3 Baseline Lesion Burden...4 What isameasurable Lesion?...5 Choosing Target
PET. Can we afford PET-CT. Positron annihilation. PET-CT scanner. PET detection
 PET-CT Can we afford PET-CT John Buscombe New technology Combines functional information-pet anatomical information-ct Machine able to perform both studies in single imaging episode PET imaging depends
PET-CT Can we afford PET-CT John Buscombe New technology Combines functional information-pet anatomical information-ct Machine able to perform both studies in single imaging episode PET imaging depends
Aggressive lymphomas. Michael Crump Princess Margaret Hospital
 Aggressive lymphomas Michael Crump Princess Margaret Hospital What are the aggressive lymphomas? Diffuse large B cell Mediastinal large B cell Anaplastic large cell Burkitt lymphoma (transformed lymphoma:
Aggressive lymphomas Michael Crump Princess Margaret Hospital What are the aggressive lymphomas? Diffuse large B cell Mediastinal large B cell Anaplastic large cell Burkitt lymphoma (transformed lymphoma:
Hodgkin Lymphoma Disease Specific Biology and Treatment Options. John Kuruvilla
 Hodgkin Lymphoma Disease Specific Biology and Treatment Options John Kuruvilla My Disclaimer This is where I work Objectives Pathobiology what makes HL different Diagnosis Staging Treatment Philosophy
Hodgkin Lymphoma Disease Specific Biology and Treatment Options John Kuruvilla My Disclaimer This is where I work Objectives Pathobiology what makes HL different Diagnosis Staging Treatment Philosophy
PET/CT: Basic Principles, Applications in Oncology
 PET/CT: Basic Principles, Applications in Oncology Mabel Djang, HMS III Overview PET Basics and Limitations PET/CT - Advantages and Limitations Applications of PET/CT in oncology Summary 2 Principles of
PET/CT: Basic Principles, Applications in Oncology Mabel Djang, HMS III Overview PET Basics and Limitations PET/CT - Advantages and Limitations Applications of PET/CT in oncology Summary 2 Principles of
MALIGNANT LYMPHOMAS. Dr. Olga Vujovic (Updated August 2010)
 MALIGNANT LYMPHOMAS Dr. Olga Vujovic (Updated August 2010) Malignant lymphomas consist of Hodgkin and non-hodgkin lymphomas. The current management of these diseases involves a multi-disciplinary approach.
MALIGNANT LYMPHOMAS Dr. Olga Vujovic (Updated August 2010) Malignant lymphomas consist of Hodgkin and non-hodgkin lymphomas. The current management of these diseases involves a multi-disciplinary approach.
Malignant Pleural Diseases Advances Clinicians Should Know F Gleeson
 Malignant Pleural Diseases Advances Clinicians Should Know F Gleeson The following relevant disclosures, conflicts of interest and/ or financial relationships exist related to this presentation: Consultant
Malignant Pleural Diseases Advances Clinicians Should Know F Gleeson The following relevant disclosures, conflicts of interest and/ or financial relationships exist related to this presentation: Consultant
Malignant Lymphomas and Plasma Cell Myeloma
 Malignant Lymphomas and Plasma Cell Myeloma Dr. Bruce F. Burns Dept. of Pathology and Lab Medicine Overview definitions - lymphoma lymphoproliferative disorder plasma cell myeloma pathogenesis - translocations
Malignant Lymphomas and Plasma Cell Myeloma Dr. Bruce F. Burns Dept. of Pathology and Lab Medicine Overview definitions - lymphoma lymphoproliferative disorder plasma cell myeloma pathogenesis - translocations
Lauren Berger: Why is it so important for patients to get an accurate diagnosis of their blood cancer subtype?
 Hello, I m Lauren Berger and I m the Senior Director of Patient Services Programs at The Leukemia & Lymphoma Society. I m pleased to welcome Dr. Rebecca Elstrom. Dr. Elstrom is an Assistant Professor in
Hello, I m Lauren Berger and I m the Senior Director of Patient Services Programs at The Leukemia & Lymphoma Society. I m pleased to welcome Dr. Rebecca Elstrom. Dr. Elstrom is an Assistant Professor in
PET/CT in Lung Cancer
 PET/CT in Lung Cancer Rodolfo Núñez Miller, M.D. Nuclear Medicine and Diagnostic Imaging Section Division of Human Health International Atomic Energy Agency Vienna, Austria GLOBOCAN 2012 #1 #3 FDG-PET/CT
PET/CT in Lung Cancer Rodolfo Núñez Miller, M.D. Nuclear Medicine and Diagnostic Imaging Section Division of Human Health International Atomic Energy Agency Vienna, Austria GLOBOCAN 2012 #1 #3 FDG-PET/CT
Collaboration to collect Autologous transplant outcomes in Lymphoma and Myeloma (CALM) Additional Questionnaire (MED C) INCLUSION CRITERIA CALM STUDY
 Additional Questionnaire (MED C) CALM study Inclusion period: 01/01/2008 to 31/12/2011 PATIENT REGISTRATION FORM Disease Diagnosis Lymphoma S Non Hodgkin Lymphoma (NHL) Mature B-cell neoplasm Follicular
Additional Questionnaire (MED C) CALM study Inclusion period: 01/01/2008 to 31/12/2011 PATIENT REGISTRATION FORM Disease Diagnosis Lymphoma S Non Hodgkin Lymphoma (NHL) Mature B-cell neoplasm Follicular
Outline of thesis and future perspectives.
 Outline of thesis and future perspectives. This thesis is divided into two different sections. The B- section involves reviews and studies on B- cell non- Hodgkin lymphoma [NHL] and radioimmunotherapy
Outline of thesis and future perspectives. This thesis is divided into two different sections. The B- section involves reviews and studies on B- cell non- Hodgkin lymphoma [NHL] and radioimmunotherapy
Uso della PET nella valutazione della risposta
 La diagnostica per immagini e la radioterapia: una cooperazione nel nostro futuro Uso della PET nella valutazione della risposta Cagliari, 21 giugno 2008 Arturo Chiti Medicina Nucleare, Istituto Clinico
La diagnostica per immagini e la radioterapia: una cooperazione nel nostro futuro Uso della PET nella valutazione della risposta Cagliari, 21 giugno 2008 Arturo Chiti Medicina Nucleare, Istituto Clinico
Lymphoma. Measurability of Quality Performance Indicators Version 2.0
 Lymphoma Measurability of Quality Performance Indicators Version 2.0 To be read in conjunction with: Lymphoma Clinical Quality Performance Indicators (September 2013) Lymphoma Data Definitions V2.0 (September
Lymphoma Measurability of Quality Performance Indicators Version 2.0 To be read in conjunction with: Lymphoma Clinical Quality Performance Indicators (September 2013) Lymphoma Data Definitions V2.0 (September
Frequency of NHL Subtypes in Adults
 Chemotherapy Options Stephanie A. Gregory, M.D. The Elodia Kehm Professor of Medicine Director, Section of Hematology Rush University Medical Center Chicago, Illinois Frequency of NHL Subtypes in Adults
Chemotherapy Options Stephanie A. Gregory, M.D. The Elodia Kehm Professor of Medicine Director, Section of Hematology Rush University Medical Center Chicago, Illinois Frequency of NHL Subtypes in Adults
A new score predicting the survival of patients with spinal cord compression from myeloma
 A new score predicting the survival of patients with spinal cord compression from myeloma (1) Sarah Douglas, Department of Radiation Oncology, University of Lubeck, Germany; sarah_douglas@gmx.de (2) Steven
A new score predicting the survival of patients with spinal cord compression from myeloma (1) Sarah Douglas, Department of Radiation Oncology, University of Lubeck, Germany; sarah_douglas@gmx.de (2) Steven
Continuing Medical Education Article Imaging of Multiple Myeloma and Related Plasma Cell Dyscrasias JNM, July 2012, Volume 53, Number 7
 Continuing Medical Education Article Imaging of Multiple Myeloma and Related Plasma Cell Dyscrasias JNM, July 2012, Volume 53, Number 7 Authors Ronald C. Walker 1,2, Tracy L. Brown 3, Laurie B. Jones-Jackson
Continuing Medical Education Article Imaging of Multiple Myeloma and Related Plasma Cell Dyscrasias JNM, July 2012, Volume 53, Number 7 Authors Ronald C. Walker 1,2, Tracy L. Brown 3, Laurie B. Jones-Jackson
PROTOCOLS FOR TREATMENT OF MALIGNANT LYMPHOMA
 2012 1 31,, PROTOCOLS FOR TREATMENT OF MALIGNANT LYMPHOMA Version 1.0 2012 DIVISION OF HAEMATOLOGY / ONCOLOGY DEPARTMENT OF MEDICINE KAOHSING VETERAN GENERAL HOSPTIAL General Guide Diagnosis 1.Adequate
2012 1 31,, PROTOCOLS FOR TREATMENT OF MALIGNANT LYMPHOMA Version 1.0 2012 DIVISION OF HAEMATOLOGY / ONCOLOGY DEPARTMENT OF MEDICINE KAOHSING VETERAN GENERAL HOSPTIAL General Guide Diagnosis 1.Adequate
Non-Hodgkin s Lymphoma
 Non-Hodgkin s Lymphoma Luis Fayad, MD Assistant Professor Clinical Medical Director Lymphoma/Myeloma Department Non-Hodgkin s Lymphoma Non-Hodgkin s lymphomas (NHL) are a heterogeneous group of malignant
Non-Hodgkin s Lymphoma Luis Fayad, MD Assistant Professor Clinical Medical Director Lymphoma/Myeloma Department Non-Hodgkin s Lymphoma Non-Hodgkin s lymphomas (NHL) are a heterogeneous group of malignant
RT for Recurrent, Bulky, and Chemotherapy-Refractory Follicular Lymphoma: A Treatment Modality for Both Alleviating Symptoms and Potential Cure
 RT for Recurrent, Bulky, and Chemotherapy-Refractory Follicular Lymphoma: A Treatment Modality for Both Alleviating Symptoms and Potential Cure Case Number: RT2009-04(M) Potential Audiences: Intent Doctor,
RT for Recurrent, Bulky, and Chemotherapy-Refractory Follicular Lymphoma: A Treatment Modality for Both Alleviating Symptoms and Potential Cure Case Number: RT2009-04(M) Potential Audiences: Intent Doctor,
Incidence of Incidental Thyroid Nodules on Computed Tomography (CT) Scan of the Chest Performed for Reasons Other than Thyroid Disease
 International Journal of Clinical Medicine, 2011, 2, 264-268 doi:10.4236/ijcm.2011.23042 Published Online July 2011 (http://www.scirp.org/journal/ijcm) Incidence of Incidental Thyroid Nodules on Computed
International Journal of Clinical Medicine, 2011, 2, 264-268 doi:10.4236/ijcm.2011.23042 Published Online July 2011 (http://www.scirp.org/journal/ijcm) Incidence of Incidental Thyroid Nodules on Computed
In Practice Whole Body MR for Visualizing Metastatic Prostate Cancer
 In Practice Whole Body MR for Visualizing Metastatic Prostate Cancer Prostate cancer is the second most common cancer in men worldwide, accounting for 15% of all new cancer cases. 1 Great strides have
In Practice Whole Body MR for Visualizing Metastatic Prostate Cancer Prostate cancer is the second most common cancer in men worldwide, accounting for 15% of all new cancer cases. 1 Great strides have
LYMPHOMA. BACHIR ALOBEID, M.D. HEMATOPATHOLOGY DIVISION PATHOLOGY DEPARTMENT Columbia University/ College of Physicians & Surgeons
 LYMPHOMA BACHIR ALOBEID, M.D. HEMATOPATHOLOGY DIVISION PATHOLOGY DEPARTMENT Columbia University/ College of Physicians & Surgeons Normal development of lymphocytes Lymphocyte proliferation and differentiation:
LYMPHOMA BACHIR ALOBEID, M.D. HEMATOPATHOLOGY DIVISION PATHOLOGY DEPARTMENT Columbia University/ College of Physicians & Surgeons Normal development of lymphocytes Lymphocyte proliferation and differentiation:
Low-dose CT Imaging. Edgar Fearnow, M.D. Section Chief, Computed Tomography, Lancaster General Hospital
 Lung Cancer Screening with Low-dose CT Imaging Edgar Fearnow, M.D. Section Chief, Computed Tomography, Lancaster General Hospital Despite recent declines in the incidence of lung cancer related to the
Lung Cancer Screening with Low-dose CT Imaging Edgar Fearnow, M.D. Section Chief, Computed Tomography, Lancaster General Hospital Despite recent declines in the incidence of lung cancer related to the
Analysis of Prostate Cancer at Easter Connecticut Health Network Using Cancer Registry Data
 The 2014 Cancer Program Annual Public Reporting of Outcomes/Annual Site Analysis Statistical Data from 2013 More than 70 percent of all newly diagnosed cancer patients are treated in the more than 1,500
The 2014 Cancer Program Annual Public Reporting of Outcomes/Annual Site Analysis Statistical Data from 2013 More than 70 percent of all newly diagnosed cancer patients are treated in the more than 1,500
NEW HYBRID IMAGING TECHNOLOGY MAY HAVE BIG POTENTIAL FOR IMPROVING DIAGNOSIS OF PROSTATE CANCER
 Media Release April 7, 2009 For Immediate Release NEW HYBRID IMAGING TECHNOLOGY MAY HAVE BIG POTENTIAL FOR IMPROVING DIAGNOSIS OF PROSTATE CANCER London, Ontario Improved hybrid imaging techniques developed
Media Release April 7, 2009 For Immediate Release NEW HYBRID IMAGING TECHNOLOGY MAY HAVE BIG POTENTIAL FOR IMPROVING DIAGNOSIS OF PROSTATE CANCER London, Ontario Improved hybrid imaging techniques developed
Comparison of radiation dose from X-ray, CT, and PET/ CT in paediatric patients with neuroblastoma using a dose monitoring program
 Comparison of radiation dose from X-ray, CT, and PET/ CT in paediatric patients with neuroblastoma using a dose monitoring program Poster No.: C-0591 Congress: ECR 2015 Type: Authors: Keywords: DOI: Scientific
Comparison of radiation dose from X-ray, CT, and PET/ CT in paediatric patients with neuroblastoma using a dose monitoring program Poster No.: C-0591 Congress: ECR 2015 Type: Authors: Keywords: DOI: Scientific
Leukemias and Lymphomas: A primer
 Leukemias and Lymphomas: A primer Normal blood contains circulating white blood cells, red blood cells and platelets 700 red cells (oxygen) 1 white cell Neutrophils (60%) bacterial infection Lymphocytes
Leukemias and Lymphomas: A primer Normal blood contains circulating white blood cells, red blood cells and platelets 700 red cells (oxygen) 1 white cell Neutrophils (60%) bacterial infection Lymphocytes
Case Report: Whole-body Oncologic Imaging with syngo TimCT
 Case Report: Whole-body Oncologic Imaging with syngo TimCT Eric Hatfield, M.D. 1 ; Agus Priatna, Ph.D. 2 ; John Kotyk, Ph.D. 1 ; Benjamin Tan, M.D. 1 ; Alto Stemmer 3 ; Stephan Kannengiesser, Ph.D. 3 ;
Case Report: Whole-body Oncologic Imaging with syngo TimCT Eric Hatfield, M.D. 1 ; Agus Priatna, Ph.D. 2 ; John Kotyk, Ph.D. 1 ; Benjamin Tan, M.D. 1 ; Alto Stemmer 3 ; Stephan Kannengiesser, Ph.D. 3 ;
Variations in PET/CT Methodology for Oncologic Imaging at U.S. Academic Medical Centers: An Imaging Response Assessment Team Survey
 Variations in PET/CT Methodology for Oncologic Imaging at U.S. Academic Medical Centers: An Imaging Response Assessment Team Survey Michael M. Graham 1, Ramsey D. Badawi 2, and Richard L. Wahl 3 1 University
Variations in PET/CT Methodology for Oncologic Imaging at U.S. Academic Medical Centers: An Imaging Response Assessment Team Survey Michael M. Graham 1, Ramsey D. Badawi 2, and Richard L. Wahl 3 1 University
Cutaneous Lymphoma FAST FACTS
 Cutaneous Lymphoma FAST FACTS What is Cutaneous Lymphoma? Cutaneous lymphomas are types of non-hodgkin s lymphomas (NHL) that originate in the lymphocytes (white blood cells). Unlike most other types of
Cutaneous Lymphoma FAST FACTS What is Cutaneous Lymphoma? Cutaneous lymphomas are types of non-hodgkin s lymphomas (NHL) that originate in the lymphocytes (white blood cells). Unlike most other types of
Summary & Conclusion
 The prognostic value of angiogenesis markers in patients with non-hodgkin lymphoma. Summary & Conclusion The current study aims to asses the prognostic value of some angiogenesis markers in patients with
The prognostic value of angiogenesis markers in patients with non-hodgkin lymphoma. Summary & Conclusion The current study aims to asses the prognostic value of some angiogenesis markers in patients with
Interview with David Djang, MD On PET Scan in Oncology: Principles and Practice
 Interview with David Djang, MD On PET Scan in Oncology: Principles and Practice By Howard (Jack) West, MD May, 2009 Hello and welcome to the GRACE audio podcast on PET scanning. This one is with Dr. David
Interview with David Djang, MD On PET Scan in Oncology: Principles and Practice By Howard (Jack) West, MD May, 2009 Hello and welcome to the GRACE audio podcast on PET scanning. This one is with Dr. David
Mantle Cell Lymphoma Understanding Your Treatment Options
 New Developments in Mantle Cell Lymphoma John P. Leonard, M.D. Richard T. Silver Distinguished Professor of Hematology and Medical Oncology Associate Dean for Clinical Research Vice Chairman, Department
New Developments in Mantle Cell Lymphoma John P. Leonard, M.D. Richard T. Silver Distinguished Professor of Hematology and Medical Oncology Associate Dean for Clinical Research Vice Chairman, Department
Comparison of Threshold-Based Segmentation Methods on Pre- and Post- Therapy PET Scans
 M. Phillips, S.F. Barrington, D.L.G. Hill, P.K. Marsden 1 Comparison of Threshold-Based Segmentation Methods on Pre- and Post- Therapy PET Scans Michael Phillips 1 Michael.Phillips.1@city.ac.uk Sally F.
M. Phillips, S.F. Barrington, D.L.G. Hill, P.K. Marsden 1 Comparison of Threshold-Based Segmentation Methods on Pre- and Post- Therapy PET Scans Michael Phillips 1 Michael.Phillips.1@city.ac.uk Sally F.
Positron Emission Tomography - For Patients
 Positron Emission Tomography - For Patients A physician s written order is required for any PET-CT tests. How should I prepare for my PET-CT? PET-CT is more complicated than most other tests you may be
Positron Emission Tomography - For Patients A physician s written order is required for any PET-CT tests. How should I prepare for my PET-CT? PET-CT is more complicated than most other tests you may be
Mississippi Medicaid. Provider Reference Guide. For Part 220. Radiology Services
 Mississippi Medicaid Provider Reference Guide For Part 220 Radiology Services This is a companion document to the Mississippi Administrative Code Title 23 and must be utilized as a reference only. Table
Mississippi Medicaid Provider Reference Guide For Part 220 Radiology Services This is a companion document to the Mississippi Administrative Code Title 23 and must be utilized as a reference only. Table
UMHS-PUHSC JOINT INSTITUTE
 Imaging Biomarkers for Staging and Assessing Response to Therapy in Multiple Myeloma Qian Dong, MD. Radiology University of Michigan Wei Guo, MD. Orthopedic Oncology Peking University Second Hospital Team
Imaging Biomarkers for Staging and Assessing Response to Therapy in Multiple Myeloma Qian Dong, MD. Radiology University of Michigan Wei Guo, MD. Orthopedic Oncology Peking University Second Hospital Team
Us TOO University Presents: Understanding Diagnostic Testing
 Us TOO University Presents: Understanding Diagnostic Testing for Prostate Cancer Patients Today s speaker is Manish Bhandari, MD Program moderator is Pam Barrett, Us TOO International Made possible by
Us TOO University Presents: Understanding Diagnostic Testing for Prostate Cancer Patients Today s speaker is Manish Bhandari, MD Program moderator is Pam Barrett, Us TOO International Made possible by
Post-PET Restaging Cancer Form National Oncologic PET Registry
 Post-PET Restaging Cancer Form National Oncologic PET Registry Facility ID #: Registry Case Number: Patient Name: Your patient had a PET scan on: mm/dd/yyyy. The PET scan was done for restaging of (cancer
Post-PET Restaging Cancer Form National Oncologic PET Registry Facility ID #: Registry Case Number: Patient Name: Your patient had a PET scan on: mm/dd/yyyy. The PET scan was done for restaging of (cancer
Treating Thyroid Cancer using I-131 Maximum Tolerable Dose Method
 Treating Thyroid Cancer using I-131 Maximum Tolerable Dose Method Christopher Martel, M.Sc., CHP Lisa Thornhill,, NRRPT, RT(NM) Boston University Medical Center Thyroid Carcinoma New cases and deaths in
Treating Thyroid Cancer using I-131 Maximum Tolerable Dose Method Christopher Martel, M.Sc., CHP Lisa Thornhill,, NRRPT, RT(NM) Boston University Medical Center Thyroid Carcinoma New cases and deaths in
QUANTITATIVE IMAGING IN MULTICENTER CLINICAL TRIALS: PET
 Centers for Quantitative Imaging Excellence (CQIE) LEARNING MODULE QUANTITATIVE IMAGING IN MULTICENTER CLINICAL TRIALS: PET American College of Radiology Clinical Research Center v.1 Centers for Quantitative
Centers for Quantitative Imaging Excellence (CQIE) LEARNING MODULE QUANTITATIVE IMAGING IN MULTICENTER CLINICAL TRIALS: PET American College of Radiology Clinical Research Center v.1 Centers for Quantitative
TAMPERE UNIVERSITY OF TECHNOLOGY
 TAMPERE UNIVERSITY OF TECHNOLOGY ABHISEK DEV BHATTARAI SIDE-EFFECT OF CHEMOTHERAPY ON LIVER IN LYMPHOMA PATIENTS STUDIED BY STANDARD UPTAKE VALUE Master s Thesis Examiner: Professor Hannu Eskola Examiner
TAMPERE UNIVERSITY OF TECHNOLOGY ABHISEK DEV BHATTARAI SIDE-EFFECT OF CHEMOTHERAPY ON LIVER IN LYMPHOMA PATIENTS STUDIED BY STANDARD UPTAKE VALUE Master s Thesis Examiner: Professor Hannu Eskola Examiner
Social inequalities impacts of care management and survival in patients with non-hodgkin lymphomas (ISO-LYMPH)
 Session 3 : Epidemiology and public health Social inequalities impacts of care management and survival in patients with non-hodgkin lymphomas (ISO-LYMPH) Le Guyader-Peyrou Sandra Bergonie Institut Context:
Session 3 : Epidemiology and public health Social inequalities impacts of care management and survival in patients with non-hodgkin lymphomas (ISO-LYMPH) Le Guyader-Peyrou Sandra Bergonie Institut Context:
Oncology Best Practice Documentation
 Oncology Best Practice Documentation Click on the desired Diagnoses link or press Enter to view all information. Diagnoses: Solid Tumors Lymphomas Leukemias Myelodysplastic Syndrome Pathology Findings
Oncology Best Practice Documentation Click on the desired Diagnoses link or press Enter to view all information. Diagnoses: Solid Tumors Lymphomas Leukemias Myelodysplastic Syndrome Pathology Findings
PET and PET/CT in Clinical Trials
 PET and PET/CT in Clinical Trials Nathan C. Hall, M.D., Ph.D. The Ohio State University Medical Center CALGB Imaging Core Lab CALGB Imaging Committee Outline Introduction to PET Positron Emitter Physics
PET and PET/CT in Clinical Trials Nathan C. Hall, M.D., Ph.D. The Ohio State University Medical Center CALGB Imaging Core Lab CALGB Imaging Committee Outline Introduction to PET Positron Emitter Physics
Quantitative Imaging In Clinical Trials Using PET/CT: Update
 Quantitative Imaging In Clinical Trials Using PET/CT: Update Paul Kinahan, Robert Doot Imaging Research Laboratory Department of Radiology University of Washington, Seattle, WA Supported by RSNA Quantitative
Quantitative Imaging In Clinical Trials Using PET/CT: Update Paul Kinahan, Robert Doot Imaging Research Laboratory Department of Radiology University of Washington, Seattle, WA Supported by RSNA Quantitative
Lymphoma Diagnosis and Classification
 Lymphoma Diagnosis and Classification By Atef Shrit, MD, Pathology B- and T/NK-cell lymphomas are clonal neoplasms of immature and mature B-lymphocytes, T-lymphocytes or natural killer cells at various
Lymphoma Diagnosis and Classification By Atef Shrit, MD, Pathology B- and T/NK-cell lymphomas are clonal neoplasms of immature and mature B-lymphocytes, T-lymphocytes or natural killer cells at various
IF AT FIRST YOU DON T SUCCEED: TRIAL, TRIAL AGAIN
 + IF AT FIRST YOU DON T SUCCEED: TRIAL, TRIAL AGAIN Rena Buckstein MD FRCPC Head Hematology Site Group Sunnybrook Odette Cancer Center (OCC) Head of Hematology Clinical Trials Group at OCC + Outline Start
+ IF AT FIRST YOU DON T SUCCEED: TRIAL, TRIAL AGAIN Rena Buckstein MD FRCPC Head Hematology Site Group Sunnybrook Odette Cancer Center (OCC) Head of Hematology Clinical Trials Group at OCC + Outline Start
What is non-hodgkin lymphoma, how is it treated, and what is the unmet need?
 What is non-hodgkin lymphoma, how is it treated, and what is the unmet need? Tim Illidge BSc PhD MRCP FRCR FRCPath Institute of Cancer Sciences, University of Manchester Manchester Cancer Research Centre,
What is non-hodgkin lymphoma, how is it treated, and what is the unmet need? Tim Illidge BSc PhD MRCP FRCR FRCPath Institute of Cancer Sciences, University of Manchester Manchester Cancer Research Centre,
Supplementary appendix
 Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Farooqui MZH, Valdez J, Martyr S, et al. Ibrutinib
Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Farooqui MZH, Valdez J, Martyr S, et al. Ibrutinib
The Center for Prostate Cancer. Personalized Treatment. Clinical Excellence.
 The Center for Prostate Cancer Personalized Treatment. Clinical Excellence. The Center for Prostate Cancer Leaders in Prostate Cancer Treatment and Research The Center for Prostate Cancer at the North
The Center for Prostate Cancer Personalized Treatment. Clinical Excellence. The Center for Prostate Cancer Leaders in Prostate Cancer Treatment and Research The Center for Prostate Cancer at the North
Non Hodgkin Lymphoma:
 Non Hodgkin Lymphoma: Non Hodgkin Lymphoma, often referred to as NHL, is a cancer originating in the lymphocytes, a type of blood cell, which are integral to the body s immune system. Non Hodgkin Lymphoma
Non Hodgkin Lymphoma: Non Hodgkin Lymphoma, often referred to as NHL, is a cancer originating in the lymphocytes, a type of blood cell, which are integral to the body s immune system. Non Hodgkin Lymphoma
Many people with non-hodgkin lymphoma have found an educational support group helpful. Support
 Track 2: Treatment Options [Narrator] Many people with non-hodgkin lymphoma have found an educational support group helpful. Support groups take many forms: some meet the needs of people with all kinds
Track 2: Treatment Options [Narrator] Many people with non-hodgkin lymphoma have found an educational support group helpful. Support groups take many forms: some meet the needs of people with all kinds
PET and PET/CT in Lymphoma and Monitoring Therapy
 PET and PET/CT in Lymphoma and Monitoring Therapy Dominique Delbeke, MD, PhD VUMC PET/CT Conference 2009 Classification of Lymphomas Working Formulation = outdated REAL Classification (Revised European
PET and PET/CT in Lymphoma and Monitoring Therapy Dominique Delbeke, MD, PhD VUMC PET/CT Conference 2009 Classification of Lymphomas Working Formulation = outdated REAL Classification (Revised European
Houston Cancer Institute
 Houston Cancer Institute A personal path to healing Memorial-West Houston Katy Northwest Houston Southeast Houston Sugar Land Convenience for Patients State of the Art Therapies and Diagnosis Real Support
Houston Cancer Institute A personal path to healing Memorial-West Houston Katy Northwest Houston Southeast Houston Sugar Land Convenience for Patients State of the Art Therapies and Diagnosis Real Support
CHAPTER 26 LATE BREAKING DEVELOPMENTS: IMPACT OF ANTI-CD20 MONOCLONAL ANTIBODIES ON LYMPHOMA THERAPY
 CHAPTER 26 LATE BREAKING DEVELOPMENTS: IMPACT OF ANTI-CD20 MONOCLONAL ANTIBODIES ON LYMPHOMA THERAPY 26.1 Introduction rituximab Subsequent to the completion of drafts for the guidelines earlier in 2004,
CHAPTER 26 LATE BREAKING DEVELOPMENTS: IMPACT OF ANTI-CD20 MONOCLONAL ANTIBODIES ON LYMPHOMA THERAPY 26.1 Introduction rituximab Subsequent to the completion of drafts for the guidelines earlier in 2004,
Case Number: RT2009-124(M) Potential Audiences: Intent Doctor, Oncology Special Nurse, Resident Doctor
 Renal Cell Carcinoma of the Left Kidney Post Radical Surgery with pt4 Classification with Multiple Lung and Single Brain Metastases: the Role and Treatment Consideration of Radiotherapy Case Number: RT2009-124(M)
Renal Cell Carcinoma of the Left Kidney Post Radical Surgery with pt4 Classification with Multiple Lung and Single Brain Metastases: the Role and Treatment Consideration of Radiotherapy Case Number: RT2009-124(M)
Test Request Tip Sheet
 With/Without Contrast CT, MRI Studies should NOT be ordered simultaneously as dual studies (i.e., with and without contrast). Radiation exposure is doubled and both views are rarely necessary. The study
With/Without Contrast CT, MRI Studies should NOT be ordered simultaneously as dual studies (i.e., with and without contrast). Radiation exposure is doubled and both views are rarely necessary. The study
HOVON Staging and Response Criteria for Non-Hodgkin s Lymphomas Page 1
 HOVON Staging and Response Criteria for Non-Hodgkin s Lymphomas Page 1 This document describes the minimally required staging and evaluation procedures and response criteria that will be applied in all
HOVON Staging and Response Criteria for Non-Hodgkin s Lymphomas Page 1 This document describes the minimally required staging and evaluation procedures and response criteria that will be applied in all
Infrared Thermography Not a Useful Breast Cancer Screening Tool
 Contact: Jeanne-Marie Phillips Sharon Grutman HealthFlash Marketing The American Society of Breast Surgeons 203-977-3333 877-992-5470 Infrared Thermography Not a Useful Breast Cancer Screening Tool Mammography
Contact: Jeanne-Marie Phillips Sharon Grutman HealthFlash Marketing The American Society of Breast Surgeons 203-977-3333 877-992-5470 Infrared Thermography Not a Useful Breast Cancer Screening Tool Mammography
Chemobrain. Halle C.F. Moore, MD The Cleveland Clinic October 3, 2015
 Chemobrain Halle C.F. Moore, MD The Cleveland Clinic October 3, 2015 Terminology Chemotherapy-associated cognitive dysfunction Post-chemotherapy cognitive impairment Cancer treatment-associated cognitive
Chemobrain Halle C.F. Moore, MD The Cleveland Clinic October 3, 2015 Terminology Chemotherapy-associated cognitive dysfunction Post-chemotherapy cognitive impairment Cancer treatment-associated cognitive
Detection and staging of recurrent prostate cancer is still one of the important clinical problems in prostate cancer. A rise in PSA or biochemical
 Summary. 111 Detection and staging of recurrent prostate cancer is still one of the important clinical problems in prostate cancer. A rise in PSA or biochemical recurrence (BCR) is the first sign of recurrent
Summary. 111 Detection and staging of recurrent prostate cancer is still one of the important clinical problems in prostate cancer. A rise in PSA or biochemical recurrence (BCR) is the first sign of recurrent
GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER
 GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER BY Ali Shamseddine, MD (Coordinator); as04@aub.edu.lb Fady Geara, MD Bassem Shabb, MD Ghassan Jamaleddine, MD CLINICAL PRACTICE GUIDELINES FOR THE TREATMENT
GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER BY Ali Shamseddine, MD (Coordinator); as04@aub.edu.lb Fady Geara, MD Bassem Shabb, MD Ghassan Jamaleddine, MD CLINICAL PRACTICE GUIDELINES FOR THE TREATMENT
Interesting Case Series. Periorbital Richter Syndrome
 Interesting Case Series Periorbital Richter Syndrome MarkGorman,MRCS,MSc, a Julia Ruston, MRCS, b and Sarath Vennam, BMBS a a Division of Plastic Surgery, Royal Devon and Exeter Hospital, Exeter, Devon,
Interesting Case Series Periorbital Richter Syndrome MarkGorman,MRCS,MSc, a Julia Ruston, MRCS, b and Sarath Vennam, BMBS a a Division of Plastic Surgery, Royal Devon and Exeter Hospital, Exeter, Devon,
Objectives. Mylene T. Truong, MD. Malignant Pleural Mesothelioma Background
 Imaging of Pleural Tumors Mylene T. Truong, MD Imaging of Pleural Tumours Mylene T. Truong, M. D. University of Texas M.D. Anderson Cancer Center, Houston, TX Objectives To review tumors involving the
Imaging of Pleural Tumors Mylene T. Truong, MD Imaging of Pleural Tumours Mylene T. Truong, M. D. University of Texas M.D. Anderson Cancer Center, Houston, TX Objectives To review tumors involving the
Elements of PET/CT Reporting
 Elements of PET/CT Reporting 1. Clinical History a. Indication i. tumor type ii. abnormality to be evaluated iii. specific clinical question b. Relevent history i. biopsy results ii. chemotherapy iii.
Elements of PET/CT Reporting 1. Clinical History a. Indication i. tumor type ii. abnormality to be evaluated iii. specific clinical question b. Relevent history i. biopsy results ii. chemotherapy iii.
RESEARCH EDUCATE ADVOCATE. Just Diagnosed with Melanoma Now What?
 RESEARCH EDUCATE ADVOCATE Just Diagnosed with Melanoma Now What? INTRODUCTION If you are reading this, you have undergone a biopsy (either of a skin lesion or a lymph node) or have had other tests in which
RESEARCH EDUCATE ADVOCATE Just Diagnosed with Melanoma Now What? INTRODUCTION If you are reading this, you have undergone a biopsy (either of a skin lesion or a lymph node) or have had other tests in which
BAISHIDENG PUBLISHING GROUP INC
 Reviewer s code: 01714224 Reviewer s country: Italy Date reviewed: 2015-01-30 20:36 [ Y] Grade A: Priority publishing [ ] Accept [ ] Grade C: Good [ Y] Grade D: Fair language [ Y] Major revision The article
Reviewer s code: 01714224 Reviewer s country: Italy Date reviewed: 2015-01-30 20:36 [ Y] Grade A: Priority publishing [ ] Accept [ ] Grade C: Good [ Y] Grade D: Fair language [ Y] Major revision The article
Report series: General cancer information
 Fighting cancer with information Report series: General cancer information Eastern Cancer Registration and Information Centre ECRIC report series: General cancer information Cancer is a general term for
Fighting cancer with information Report series: General cancer information Eastern Cancer Registration and Information Centre ECRIC report series: General cancer information Cancer is a general term for
Crosswalk for Positron Emission Tomography (PET) Imaging Codes G0230 G0030, G0032, G0034, G0036, G0038, G0040, G0042, G0044, G0046
 Positron Emission Tomography (PET) CPT to HCPCS Level Crosswalk Changes below from CMS Change Request 3741 Transmittals 518 & 31 published on April 1, 2005; mplementation of CPT codes are effective January
Positron Emission Tomography (PET) CPT to HCPCS Level Crosswalk Changes below from CMS Change Request 3741 Transmittals 518 & 31 published on April 1, 2005; mplementation of CPT codes are effective January
Disease/Illness GUIDE TO ASBESTOS LUNG CANCER. What Is Asbestos Lung Cancer? www.simpsonmillar.co.uk Telephone 0844 858 3200
 GUIDE TO ASBESTOS LUNG CANCER What Is Asbestos Lung Cancer? Like tobacco smoking, exposure to asbestos can result in the development of lung cancer. Similarly, the risk of developing asbestos induced lung
GUIDE TO ASBESTOS LUNG CANCER What Is Asbestos Lung Cancer? Like tobacco smoking, exposure to asbestos can result in the development of lung cancer. Similarly, the risk of developing asbestos induced lung
Recommendations for cross-sectional imaging in cancer management, Second edition
 www.rcr.ac.uk Recommendations for cross-sectional imaging in cancer management, Second edition Breast cancer Faculty of Clinical Radiology www.rcr.ac.uk Contents Breast cancer 2 Clinical background 2 Who
www.rcr.ac.uk Recommendations for cross-sectional imaging in cancer management, Second edition Breast cancer Faculty of Clinical Radiology www.rcr.ac.uk Contents Breast cancer 2 Clinical background 2 Who
Metastatic Renal Cell Carcinoma: Staging and Prognosis of Three Separate Cases.
 Metastatic Renal Cell Carcinoma: Staging and Prognosis of Three Separate Cases. Abstract This paper describes the staging, imaging, treatment, and prognosis of renal cell carcinoma. Three case studies
Metastatic Renal Cell Carcinoma: Staging and Prognosis of Three Separate Cases. Abstract This paper describes the staging, imaging, treatment, and prognosis of renal cell carcinoma. Three case studies
A new score predicting the survival of patients with spinal cord compression from myeloma
 A new score predicting the survival of patients with spinal cord compression from myeloma (1) Sarah Douglas, Department of Radiation Oncology, University of Lubeck, Germany; sarah_douglas@gmx.de (2) Steven
A new score predicting the survival of patients with spinal cord compression from myeloma (1) Sarah Douglas, Department of Radiation Oncology, University of Lubeck, Germany; sarah_douglas@gmx.de (2) Steven
First floor, Main Hospital North Services provided 24/7 365 days per year
 First floor, Main Hospital North Services provided 24/7 365 days per year General Radiology (X-ray) Fluoroscopy Ultrasound (Sonography) Nuclear Medicine P.E.T. imaging Computed Tomography (CT scan) Magnetic
First floor, Main Hospital North Services provided 24/7 365 days per year General Radiology (X-ray) Fluoroscopy Ultrasound (Sonography) Nuclear Medicine P.E.T. imaging Computed Tomography (CT scan) Magnetic
FDG-PET/CT in Lymphoma 3rd IPET Meeting, Vienna, October 2015. Ora Israel, MD Department of Nuclear Medicine Rambam Health Care Campus Haifa, Israel
 FDG-PET/CT in Lymphoma 3rd IPET Meeting, Vienna, October 2015 Ora Israel, MD Department of Nuclear Medicine Rambam Health Care Campus Haifa, Israel Lymphoma Clinical Data & Challenges Broad spectrum, heterogeneous
FDG-PET/CT in Lymphoma 3rd IPET Meeting, Vienna, October 2015 Ora Israel, MD Department of Nuclear Medicine Rambam Health Care Campus Haifa, Israel Lymphoma Clinical Data & Challenges Broad spectrum, heterogeneous
A new predictive algorithm for aiding clinical decision-making in lung cancer
 Better Care. Faster A new predictive algorithm for aiding clinical decision-making in lung cancer Y Kogan, I Sela, Y Kheiffetz, M Kleiman, Z Agur, Optimata Ltd., O Liran, N Peled, Sheba hospital, I Lazarev,
Better Care. Faster A new predictive algorithm for aiding clinical decision-making in lung cancer Y Kogan, I Sela, Y Kheiffetz, M Kleiman, Z Agur, Optimata Ltd., O Liran, N Peled, Sheba hospital, I Lazarev,
Multiple Myeloma. Abstract. Introduction
 Multiple Myeloma Abstract Multiple Myeloma is a plasma cell cancer that causes an overproduction of plasma cells. Multiple Myeloma is a difficult disease to diagnosis because symptoms might not be present
Multiple Myeloma Abstract Multiple Myeloma is a plasma cell cancer that causes an overproduction of plasma cells. Multiple Myeloma is a difficult disease to diagnosis because symptoms might not be present
Radiotherapy in Plasmacytoma and Myeloma. David Cutter Multiple Myeloma NSSG Annual Meeting 14 th September 2015
 Radiotherapy in Plasmacytoma and Myeloma David Cutter Multiple Myeloma NSSG Annual Meeting 14 th September 2015 Contents Indications for radiotherapy: Palliation in Multiple Myeloma Solitary Bone Plasmacytoma
Radiotherapy in Plasmacytoma and Myeloma David Cutter Multiple Myeloma NSSG Annual Meeting 14 th September 2015 Contents Indications for radiotherapy: Palliation in Multiple Myeloma Solitary Bone Plasmacytoma
Bone Marrow/Stem Cell Transplant
 Blue Distinction Centers for Transplants Program Selection Criteria for 2010 Mid-Point Designations To qualify as a Blue Distinction Center for Transplants (), each facility must satisfy s quality based
Blue Distinction Centers for Transplants Program Selection Criteria for 2010 Mid-Point Designations To qualify as a Blue Distinction Center for Transplants (), each facility must satisfy s quality based
RADIOLOGY SERVICES. By Dr Lim Eng Kok 1
 INTRODUCTION RADIOLOGY SERVICES By Dr Lim Eng Kok 1 Radiology is the branch of medicine that deals with the use of ionising (e.g. x- rays and radio-isotopes) and non-ionising radiation (e.g. ultrasound
INTRODUCTION RADIOLOGY SERVICES By Dr Lim Eng Kok 1 Radiology is the branch of medicine that deals with the use of ionising (e.g. x- rays and radio-isotopes) and non-ionising radiation (e.g. ultrasound
Patterns of nodal spread in thoracic malignancies
 Patterns of nodal spread in thoracic malignancies Poster No.: C-0977 Congress: ECR 2010 Type: Educational Exhibit Topic: Chest Authors: R. dos Santos, M. Duarte, J. Alpendre, J. Castaño, Z. Seabra, Â.
Patterns of nodal spread in thoracic malignancies Poster No.: C-0977 Congress: ECR 2010 Type: Educational Exhibit Topic: Chest Authors: R. dos Santos, M. Duarte, J. Alpendre, J. Castaño, Z. Seabra, Â.
Pediatric Oncology for Otolaryngologists
 Pediatric Oncology for Otolaryngologists Frederick S. Huang, M.D. Division of Hematology/Oncology Department of Pediatrics The University of Texas Medical Branch Grand Rounds Presentation to Department
Pediatric Oncology for Otolaryngologists Frederick S. Huang, M.D. Division of Hematology/Oncology Department of Pediatrics The University of Texas Medical Branch Grand Rounds Presentation to Department
Proton Therapy for Pediatric Cancers
 Proton Therapy for Pediatric Cancers Christine Hill- Kayser, MD Editor- in- Chief, OncoLink Assistant Professor of Radiation Oncology, Pediatrics Service, University of Pennsylvania Melanie Eisenhower,
Proton Therapy for Pediatric Cancers Christine Hill- Kayser, MD Editor- in- Chief, OncoLink Assistant Professor of Radiation Oncology, Pediatrics Service, University of Pennsylvania Melanie Eisenhower,
Molecular Imaging in Early Phase Oncology Trials
 Molecular Imaging in Early Phase Oncology Trials Lessons Learned Potential Role for SNM Network Susan Galbraith MB BChir PhD Vice-President Oncology Discovery Medicine & Clinical Biomarkers Bristol-Myers
Molecular Imaging in Early Phase Oncology Trials Lessons Learned Potential Role for SNM Network Susan Galbraith MB BChir PhD Vice-President Oncology Discovery Medicine & Clinical Biomarkers Bristol-Myers
Salute to Dr. Saul Hertz Diagnostic and Therapeutic Uses of Radioiodine
 Salute to Dr. Saul Hertz Diagnostic and Therapeutic Uses of Radioiodine Salute to Dr. Saul Hertz Diagnostic and Therapeutic Uses of Radioiodine Douglas Van Nostrand, MD, FACP, FACNM Director, Nuclear Medicine
Salute to Dr. Saul Hertz Diagnostic and Therapeutic Uses of Radioiodine Salute to Dr. Saul Hertz Diagnostic and Therapeutic Uses of Radioiodine Douglas Van Nostrand, MD, FACP, FACNM Director, Nuclear Medicine
Prostate cancer is the most common cause of death from cancer in men over age 75. Prostate cancer is rarely found in men younger than 40.
 A.D.A.M. Medical Encyclopedia. Prostate cancer Cancer - prostate; Biopsy - prostate; Prostate biopsy; Gleason score Last reviewed: October 2, 2013. Prostate cancer is cancer that starts in the prostate
A.D.A.M. Medical Encyclopedia. Prostate cancer Cancer - prostate; Biopsy - prostate; Prostate biopsy; Gleason score Last reviewed: October 2, 2013. Prostate cancer is cancer that starts in the prostate
Rotation Specific Goals & Objectives: University Health Network-Princess Margaret Hospital/ Sunnybrook Breast/Melanoma
 Rotation Specific Goals & Objectives: University Health Network-Princess Margaret Hospital/ Sunnybrook Breast/Melanoma Medical Expert: Breast Rotation Specific Competencies/Objectives 1.0 Medical History
Rotation Specific Goals & Objectives: University Health Network-Princess Margaret Hospital/ Sunnybrook Breast/Melanoma Medical Expert: Breast Rotation Specific Competencies/Objectives 1.0 Medical History
SMALL CELL LUNG CANCER
 Protocol for Planning and Treatment The process to be followed in the management of: SMALL CELL LUNG CANCER Patient information given at each stage following agreed information pathway 1. DIAGNOSIS New
Protocol for Planning and Treatment The process to be followed in the management of: SMALL CELL LUNG CANCER Patient information given at each stage following agreed information pathway 1. DIAGNOSIS New
Standardized MRI Protocol for Brain Tumor Clinical Trials. Benjamin M. Ellingson, Ph.D. Assistant Professor of Radiology at UCLA
 Standardized MRI Protocol for Brain Tumor Clinical Trials Benjamin M. Ellingson, Ph.D. Assistant Professor of Radiology at UCLA Standardized MRI Protocol for Therapeutic Studies FDA Meeting in January
Standardized MRI Protocol for Brain Tumor Clinical Trials Benjamin M. Ellingson, Ph.D. Assistant Professor of Radiology at UCLA Standardized MRI Protocol for Therapeutic Studies FDA Meeting in January
Sodium Fluoride PET/CT Bone Imaging: Theory and Practice
 Sodium Fluoride PET/CT Bone Imaging: Theory and Practice George Segall, M.D. Stanford University Why F-18 Fluoride? Faster Higher Resolution Anatomic Correlation Chemiadsorption Hydroxyapatite Ca10(PO4)6(OH)2
Sodium Fluoride PET/CT Bone Imaging: Theory and Practice George Segall, M.D. Stanford University Why F-18 Fluoride? Faster Higher Resolution Anatomic Correlation Chemiadsorption Hydroxyapatite Ca10(PO4)6(OH)2
Role of taxanes in the treatment of advanced NHL patients: A randomized study of 87 cases
 Role of taxanes in the treatment of advanced NHL patients: A randomized study of 87 cases R. Shraddha, P.N. Pandit Radium Institute, Patna Medical College and Hospital, Patna, India Abstract NHL is a highly
Role of taxanes in the treatment of advanced NHL patients: A randomized study of 87 cases R. Shraddha, P.N. Pandit Radium Institute, Patna Medical College and Hospital, Patna, India Abstract NHL is a highly
Measure #405: Appropriate Follow-up Imaging for Incidental Abdominal Lesions National Quality Strategy Domain: Effective Clinical Care
 Measure #405: Appropriate Follow-up Imaging for Incidental Abdominal Lesions National Quality Strategy Domain: Effective Clinical Care 2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES: CLAIMS, REGISTRY DESCRIPTION:
Measure #405: Appropriate Follow-up Imaging for Incidental Abdominal Lesions National Quality Strategy Domain: Effective Clinical Care 2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES: CLAIMS, REGISTRY DESCRIPTION:
Radiotherapy in locally advanced & metastatic NSC lung cancer
 Radiotherapy in locally advanced & metastatic NSC lung cancer Dr Raj Hegde. MD. FRANZCR Consultant Radiation Oncologist. William Buckland Radiotherapy Centre. Latrobe Regional Hospital. Locally advanced
Radiotherapy in locally advanced & metastatic NSC lung cancer Dr Raj Hegde. MD. FRANZCR Consultant Radiation Oncologist. William Buckland Radiotherapy Centre. Latrobe Regional Hospital. Locally advanced
Cancer. 9p21.3 deletion. t(12;21) t(15;17)
 CANCER FISH PROBES INDIVIDUAL AND PANEL S Acute Lymphoblastic Leukemia (ALL) ALL FISH Panel (includes all probes below) 8010 LSI MYB/CEP6 LSI p16 (CDKN2A) LSI BCR/ABL with ASS LSI ETV6 (TEL)/AML1 (RUNX1)
CANCER FISH PROBES INDIVIDUAL AND PANEL S Acute Lymphoblastic Leukemia (ALL) ALL FISH Panel (includes all probes below) 8010 LSI MYB/CEP6 LSI p16 (CDKN2A) LSI BCR/ABL with ASS LSI ETV6 (TEL)/AML1 (RUNX1)
Global Business Unit Address. Siemens Medical Solutions USA, Inc. 2501 N. Barrington Road Hoffman Estates, IL 60192-5203. Telephone: +1847 304 7700
 Trademarks and service marks used in this material are property of Siemens Medical Solutions USA or Siemens AG. All other company, brand, product and service names may be trademarks or registered trademarks
Trademarks and service marks used in this material are property of Siemens Medical Solutions USA or Siemens AG. All other company, brand, product and service names may be trademarks or registered trademarks
