Anesthesia at the Ambulatory Surgery Center (ASC)
|
|
|
- Allyson Jacobs
- 7 years ago
- Views:
Transcription
1 Anesthesia at the Ambulatory Surgery Center (ASC) The MGH Orthopaedic ASC Anesthesia Department is made up of Anesthesiologists, Certified Registered Nurse Anesthetists and a rotating senior MGH anesthesia resident. Our goal at the ASC is to make your anesthetic and surgical experience the safest it can be and to discharge you home in the most comfortable manner possible. During your pre-operative visit with your surgeon, you may discuss the different anesthetic options for your surgery and you will be instructed to fill out your One Medical Passport (OMP) questionnaire online. This needs to be done prior to your pre-op nursing and anesthesia evaluations. Once OMP is completed and your surgery is scheduled, you will receive a phone call from a nurse. If a regional anesthesia, also known as a nerve block, is an option for your surgery, you will receive a call from an anesthesiologist. There are several different options available for orthopaedic surgical procedures including general anesthesia, MAC (local anesthesia with IV sedation), IV regional anesthesia (Bier Block), regional anesthesia (nerve block) or a combination of the options. The type of anesthesia you will receive for your surgical procedure will be dependent on the several factors: the particular surgical procedure, the surgeon's preference for that procedure, your medical condition, the anesthesiologist's recommendation and the patient's preference.
2 General Anesthesia Sedation Types of Anesthesia General Anesthesia is an anesthetic technique in which the patient's body is cannot feel surgical pain, and the patient is totally unconscious. It may be used as the primary anesthetic or in conjunction with a regional anesthesia based on the surgeon or the patient's preference. At the ASC, sedation plays an important role in making your anesthetic and surgical experience less stressful. The anesthesiologist will use IV sedation either during the performance of a regional block or in the OR during the surgical procedure. Regional Anesthesia Regional Anesthesia, also known as a nerve block, is an anesthetic technique in which a part or area of the patient's body is made numb (put to sleep) using a local anesthetic or numbing medicine. Because orthopedic surgeries involve the extremities, (e.g. shoulder to hand or hip to foot) regional anesthesia can be a good anesthetic option. Ankle Block o The ankle block is a regional anesthetic technique used in conjunction with sedation or a light general anesthesia for surgeries of the foot. Axillary Block o The axillary block is a regional anesthetic technique used in conjunction with sedation or a light general anesthesia for surgeries of the elbow, forearm, wrist and hand. Bier Block o The Bier Block or IV Regional is a regional anesthetic technique used for surgery of the forearm, wrist and hand. Unlike the other regional techniques the Bier block or IV regional is a short lasting regional technique and is performed in the operating room itself. Femoral Nerve Block o The femoral nerve block is a regional anesthetic technique used in conjunction with general anesthesia for ACL reconstruction surgery, tibial osteotomies and other more painful complex surgeries involving the knee joint. Infraclavicular Block o The infraclavicular block is a regional anesthetic technique used in conjunction with sedation or a light general anesthesia for surgeries of the upper arm, elbow, forearm, wrist and hand. Interscalene Block o The interscalene block is a regional anesthetic technique usually used in conjunction with sedation or a light general anesthesia for surgeries of the shoulder and upper arm. Popliteal Block o The popliteal nerve block is a regional anesthetic technique used in conjunction with sedation or a light general anesthesia for surgery of the lower leg, ankle and foot. Supraclavicular Block o The supraclavicular block is a regional anesthetic technique usually used in conjunction with a light general anesthesia for surgeries of the upper arm, elbow, forearm, wrist and hand. Adductor Canal/Saphenous Nerve Block o The adductor canal/saphenous nerve block is a regional anesthetic technique used in conjunction with general anesthesia for ACL reconstruction surgery, tibial osteotomies and other more painful complex surgeries involving the knee joint.
3 General Anesthesia General Anesthesia is an anesthetic technique in which the patient's body cannot feel surgical pain, and the patient is totally unconscious. It may be used as the primary anesthetic or in conjunction with a regional anesthesia. This is based on the surgeon or the patient's preference. On arrival to the prep area at the ASC you will meet the members of the anesthesia care team, a certified registered nurse anesthetist (CRNA) and the attending anesthesiologist. The risks and benefits of the procedure will be discussed with you before you sign your consent. Once the surgeon, operating room (OR) and OR team are ready, you will then be transferred to the OR. You will receive some sedation through your IV prior to your transfer to the OR, which will help you. Once in the OR, you will be asked to move onto the OR table, and then a few monitors will be attached: a blood pressure cuff, a light sensor to measure your blood oxygen level will be attached to your finger and EKG leads will be placed on your chest. The Anesthesia care team will ask you to take a couple of deep breaths of oxygen. They will then place medication into your IV to start the general anesthesia. You may feel a warm burning sensation at the IV site when this medicine is injected, which is normal. Once you are asleep, an airway will be placed into the back of your mouth, which moves your tongue aside so you can breathe on your own, and in rare instances a breathing tube will be placed in your windpipe. The general anesthesia will then be maintained with a mixture of anesthetic gases you breathe into your lungs and IV pain medication. Your vital signs will be monitored continually throughout the surgery. Once the surgical procedure is complete, the airway or the breathing tube will be removed and the anesthetic gases shut off. As you breathe off the anesthetic gases, you will gradually wake up. You will be transferred to the Post-Anesthesia Care Unit (PACU) and your care will be transferred to the PACU nurses. What patients remember of the experience can vary. You may or may not remember waking up in the OR, or you may not even recall your PACU stay due to the amnestic effects of the anesthetic medications. As with any anesthesia, there are inherent risks associated with general anesthesia. Fortunately, serious complications are extremely rare. Prior to signing your consent, the anesthesiologist will ask if you understand the common and uncommon risks, side effects and possible complications of general anesthesia listed on the consent form. He or she will also answer any questions you may have.
4 IV Sedation With surgery under regional anesthesia or local anesthesia, patients are often concerned about what they will feel or hear while receiving a regional anesthetic block or in the operating room (OR) during surgery. At the ASC, sedation plays a significant role in making your anesthetic and surgical experience as easy and comfortable as possible. The anesthesiologist will use IV sedation either while administering a regional block or in the OR during the surgical procedure. When the anesthesiologist is administering a regional anesthetic block, he or she will also give IV medications that relieve anxiety and any minor discomfort before the block. Patients usually are unaware that they have experienced an anesthetic procedure. Once patients understand that they will not feel discomfort during the placement of the regional anesthetic block, most of their anxiety is eliminated. Once in the OR and during the surgical procedure, sedation also plays a major role. There is a broad spectrum of sedation you could receive in the OR. This spectrum ranges from "light sedation' (aware of what is going but without anxiety) to "heavy sedation" (totally unaware like sleeping at home). In addition, the level of sedation experienced varies from patient to patient. Some patients may remember every detail of the surgery, while others may not remember anything until they wake up in the recovery room. There are many factors that determine how awake or asleep the patient is during the surgery, including the type of surgery, the patient's position, medical condition and the comfort level of the surgeon and anesthesiologist. In the end, it is the joint decision between the patient, surgeon and the attending anesthesiologist as to how to manage the patient's sedation and awareness during regional anesthesia in order to provide the safest anesthetic and surgical experience possible.
5 Regional Anesthesia Regional Anesthesia, also known as a nerve block, is an anesthetic technique in which a part or area of the patient's body is made numb (put to sleep) using a local anesthetic or numbing medicine. Because orthopedic surgeries involve the extremities, (e.g. shoulder to hand or hip to foot), regional anesthesia can be a good anesthetic option. This type of surgery may also be associated with significant post-operative pain. Regional anesthesia can also be used to provide excellent long lasting post-operative pain relief, in addition to providing intra-operative pain relief, making it very appealing for use with outpatient orthopedic surgical procedures. Many of our surgeons will discuss regional anesthesia with you during your pre-op visit. If regional anesthesia is an option for your surgical procedure, you will receive a pre-operative phone call from an anesthesiologist. He/she will review your medical history to determine if you are a candidate for a regional anesthetic technique/nerve block. The anesthesiologist will also explain how the nerve block is performed, the risks and benefits of the nerve block as well as what to expect from the block. This will also give you an opportunity to address any questions or concerns you may have about regional anesthesia. There are several regional options available depending on the type of surgery, location of the surgery, duration of surgery, amount of expected post-operative pain and surgeon preference. Regional anesthesia can be divided into two basic categories. 1. Peripheral nerve blocks in which local anesthesia or numbing medicine is placed next to the nerves that supply the extremity. These blocks provide both good intra-operative pain relief and occasionally up to 24 hours of post-operative pain control. These blocks are used primarily for longer surgical procedures and ones in which a large amount of post-operative pain is expected. 2. Bier block/iv regional is a short-acting regional anesthetic technique in which the local anesthetic is injected into a vein in the extremity. The bier block/iv regional provides good intra-operative pain relief. However unlike the peripheral nerve block, it does not provide post-operative pain relief. This technique is used for shorter procedures in which little post-operative pain is anticipated. Combined with the regional anesthesia, the patient receives either sedation through an IV to provide different levels of relaxation and sedation, or a light general anesthetic depending on the patient and surgeon preference. Patients can react differently to sedation and regional anesthetics. Therefore, from the moment the patient receives his/her block until the time the patient is comfortable in the recovery room, a member of the anesthesia care team will be caring for the patient the entire time. This is done to ensure the anesthetic is working perfectly, and the patient is calm, comfortable and stable. As with any anesthetic, there are inherent risks associated with regional anesthesia. Fortunately, serious complications are extremely rare. Prior to signing your consent, the anesthesiologist will ask you if you understand the common and uncommon risks, side effects and possible complications of the regional anesthesia technique listed on the consent form. He or she will also answer any questions you may have.
6 Ankle Block The ankle block is a regional anesthetic technique used in conjunction with sedation or a light general anesthesia for surgeries of the foot. It is a safe and effective block that provides excellent surgical anesthesia and post-operative pain control. During a preoperative call with an anesthesiologist, you will discuss the procedure, as well as its risks and benefits. On arrival to the ASC prep area, you will be asked to sign a consent for the procedure. You will then be attached to a few monitors: a blood pressure cuff, a light sensor to measure your blood oxygen level will be attached to your finger and EKG leads will be placed on your chest. You will receive some sedation through your IV prior to placement of the block, which both relaxes you and will likely cause you to have little or no recollection of the block placement. Next, the anesthesiologist will cleanse your ankle and foot on the operative side with an antiseptic solution. He or she will use both anatomical landmarks and an ultrasound machine to find the desired location for the ankle block. Once the best locations are found, the anesthesiologist will numb the skin with some local anesthetic. Next, a needle will be inserted, and using an ultrasound to guide the needle, your anesthesiologist will find the proper locations near the nerves. The ankle block requires a series of 3 to 5 injections of a long acting Novocain-like medicine around the ankle just below the skin. Placing the block usually only takes a few minutes. After the block is in place, it takes approximately minutes to work. You will notice your foot gradually becoming numb. Once in the operating room, you will again be attached to monitors and positioned by the surgeon. You will receive relatively deep levels of sedation or a light general anesthetic because it allows for better blood pressure control, less bleeding and ultimately more patient comfort. After the surgery and transport to the recovery room, the sedation or general anesthesia will begin to wear off. You will notice that you will have little or no pain in your foot. The numbness and weakness from the block should last from 6-18 hours. As it begins to wear off, you should start the pain medicine that was prescribed by your surgeon.
7 Axillary Block The axillary block is a regional anesthetic technique used in conjunction with sedation or a light general anesthesia for surgeries of the elbow, forearm, wrist and hand. It is a safe and effective block that provides excellent surgical anesthesia and post-operative pain control. During a preoperative call with an anesthesiologist, you will discuss the procedure as well as its risks and benefits. On arrival to the ASC prep area, you will be asked to sign a consent for the procedure. You will then be attached to a few monitors: a blood pressure cuff, a light sensor to measure your blood oxygen level will be attached to your finger and EKG leads will be placed on your chest. You will receive some sedation through your IV prior to placement of the block, which both relaxes you and will likely cause you to have little or no recollection of the block placement. Next, the anesthesiologist will cleanse your upper chest, axilla (armpit) and upper arm region on the operative side with an antiseptic solution. He or she will use both anatomical landmarks and an ultrasound machine to find the desired location for the axillary nerve block near the collarbone/shoulder region. Once the best location is found, the anesthesiologist will numb the skin with some local anesthetic. Next, a needle will be inserted, and using an ultrasound to guide the needle, your anesthesiologist will find the proper locations near the nerves. In addition to the ultrasound, occasionally, a process called nerve stimulation will be used to assist in verifying the location of the nerves to your arm/hand and optimizing needle placement. If nerve stimulation is used, a very small amount of electrical current will be put through the needle and you will feel the sensation of involuntary twitches or movements in your arm and hand. Do not try to stop these movements because they tell the anesthesiologist if he/she is in the right location with the needle. When the location and/or response is optimal, the anesthesiologist will inject the long acting Novocain-like medicine in multiple small doses which will numb your arm and hand. Placing the block usually only takes a few minutes. The block takes approximately minutes to work. You will notice your arm and hand becoming gradually more weak and numb. Once in the operating room, you will once again be attached to monitors and positioned by the surgeon. You will receive relatively deep levels of sedation or a light general anesthetic because it allows for better blood pressure control, less bleeding and ultimately more patient comfort. After the surgery and transport to the recovery room, the sedation or general anesthesia will begin to wear off. You may notice a few things. First you will have little or no pain, and secondly you will not be able to move or feel your arm and hand. The numbness and weakness from the block should last from 6-18 hours. As it begins to wear off, you should start the pain medicine that was prescribed by your surgeon.
8 Bier Block/IV Regional The Bier Block or IV Regional is a regional anesthetic technique used for surgery of the forearm, wrist and hand. It is an effective block that provides excellent surgical anesthesia for short and less painful surgeries. Unlike the other regional techniques, the Bier block or IV regional is a short-lasting regional technique and is performed in the operating room (OR) itself. When you arrive at the prep area of the ASC, you will discuss the regional procedure as well as the risks and benefits. Your questions will be answered at that time before you sign your consent. An IV catheter will be place on the back of the hand to be operated on. Once the surgeon, OR and OR team are ready, you will be transferred to the OR. You will be attached to a few monitors: a blood pressure cuff, a light sensor to measure your blood oxygen level will be attached to your finger and EKG leads will be placed on your chest. You will receive some sedation through your IV prior to placement of the block, which will both relax you and likely cause you to have little or no recollection of the block placement. Next, the anesthetist will position you for the block. He or she will ask you to remain lying on your back. A deflated tourniquet will then be place around the operative side upper arm or forearm. An assistant will hold the hand of the operative side above you. A large rubber band will be wrapped from your hand to the tourniquet forcing the blood out of your arm. Then the tourniquet will be inflated. This prevents blood from coming back into the arm and also prevents local anesthetic from leaving the arm during the surgery. Once it is confirmed that the tourniquet is functioning properly, Lidocaine - the local anesthetic - will be injected into the IV on the back of the hand. After the injection of local anesthetic, the IV catheter will be removed. The block takes about 5 to 10 minutes to work. As the block begins to work, you may experience a short-lived burning or warm sensation in your arm and hand. Then your arm, wrist and hand will become numb. You will receive additional IV sedation once the block is in, which will make you more relaxed and you most likely will not recall the surgery. The surgeon may place additional local anesthetic in the incision to help with post-operative pain. Upon completion of the surgery, the tourniquet is deflated and the blood flow returns to your arm and hand washing out the Lidocaine. Normal feelings and movement will return very shortly thereafter. After the surgery, you will be transported to the recovery room. The block will have worn off, and the sedation will begin to wear off too. If you need it, you will receive supplemental post-operative pain medicine in the recovery room.
9 Femoral Nerve Block The femoral nerve block is a regional anesthetic technique used in conjunction with general anesthesia for ACL reconstruction surgery, tibial osteotomies and other more painful complex surgeries involving the knee joint. It is a safe and effective block that provides excellent post-operative pain control for the inside and front of the knee. During a preoperative call with an anesthesiologist, you will discuss the procedure, as well as its risks and benefits. On arrival to the ASC prep area, you will be asked to sign a consent form for the procedure. You will then be attached to a few monitors: a blood pressure cuff, a light sensor to measure your blood oxygen level will be attached to your finger and EKG leads will be placed on your chest. You will receive some sedation through your IV prior to placement of the block, which both relaxes you and likely cause you to have little or no recollection of the block placement. Next, while maintaining modesty, the anesthesiologist will cleanse your groin region on the operative side with an antiseptic solution. He or she will use both anatomical landmarks and an ultrasound machine to find the desired location for the femoral nerve block in the groin region. Once the best location is found, the anesthesiologist will numb the skin with local anesthetic and insert a needle through your skin. Your anesthesiologist will use ultrasound to guide the needle to the proper location near the nerve. In addition to the ultrasound, occasionally, a process called nerve stimulation, will be used to assist verifying the location of the nerve to your thigh and knee. If nerve stimulation is used, a very small amount of electrical current will be put through the needle and you will feel the sensation of involuntary twitches or movements in your upper leg and kneecap. Do not try to stop these movements because they tell the anesthesiologist if s/he has found the correct location with the needle. When the location and/or response is optimal, the anesthesiologist will inject the long acting Novocain-like medicine in multiple small doses which will numb the front of your thigh and knee. This procedure takes only a few minutes to perform. The block takes approximately minutes to work. You will notice upper leg weakness and numbness over your thigh area. Once in the operating room, you will once again be attached to monitors and positioned by the surgeon. You will receive a light general anesthetic, in addition to the femoral nerve block as your anesthetic, because the femoral nerve block does not numb the back of the knee. After the surgery and transport to the recovery room, the general anesthesia will begin to wear off. You will have little or no pain in the front of your leg or knee. However you will probably have some discomfort behind your knee. That is expected. You will receive pain medicine in the recovery room as you need it. The numbness and weakness from the block usually lasts from hours and occasionally greater than 24 hours. As it begins to wear off, you should start the pain medicine prescribed by your surgeon.
10 Infraclavicular Block The infraclavicular block is a regional anesthetic technique used in conjunction with sedation or a light general anesthesia for surgeries of the upper arm, elbow, forearm, wrist and hand. It is a safe and effective block that provides excellent surgical anesthesia and post-operative pain control. During a preoperative call with an anesthesiologist, you will discuss the procedure, as well as its risks and benefits. On arrival to the ASC prep area, you will be asked to sign a consent form for the procedure. You will then be attached to a few monitors: a blood pressure cuff, a light sensor to measure your blood oxygen level will be attached to your finger and EKG leads will be placed on your chest. You will receive some sedation through your IV prior to placement of the block, which both relaxes you and likely cause you to have little or no recollection of the block placement. Next, the anesthesiologist will cleanse your upper chest, collarbone and shoulder region on the operative side with an antiseptic solution. He or she will use both anatomical landmarks and an ultrasound machine to find the desired location for the infraclavicular nerve block near the collarbone/shoulder region. Once the best location is found, the anesthesiologist will numb the skin with some local anesthetic and insert a needle through the skin. Your anesthesiologist will utilize ultrasound to guide the needle to the proper location near the nerves. In addition to the ultrasound, occasionally, a process called nerve stimulation will be used to assist verifying the location of the nerves to your arm/hand and optimizing needle placement. If nerve stimulation is used, a very small amount of electrical current will be put through the needle and you will feel the sensation of involuntary twitches or movements in your arm and hand. Do not try to stop these movements because they tell the anesthesiologist if s/he is in the right location with the needle. When the location and/or response is optimal, the anesthesiologist will inject the long acting Novocain-like medicine in multiple small doses, which will numb your arm and hand. This procedure takes only a few minutes to perform. The block takes approximately minutes to work. You will notice your arm and hand becoming gradually more weak and numb. Once in the operating room, you will once again be attached to monitors and positioned by the surgeon. You will receive relatively deep levels of sedation or a light general anesthetic because it allows for better blood pressure control and ultimately more patient comfort. After the surgery and transport to the recovery room, the sedation or general anesthesia will begin to wear off. You may notice a few things. You will have little or no pain, and you will not be able to move or feel your arm and hand. The numbness and weakness from the block should last from 6-18 hours. As it begins to wear off, you should start the pain medicine prescribed by your surgeon.
11 Interscalene Block The interscalene block is a regional anesthetic technique usually used in conjunction with sedation or a light general anesthesia for surgeries of the shoulder and upper arm. It is a safe and effective block that provides excellent surgical anesthesia and post-operative pain control. During a preoperative call with an anesthesiologist, you will discuss the procedure, as well as its risks and benefits. On arrival to the ASC prep area, you will be asked to sign a consent form for the procedure. You will be attached to a fewmonitors: a blood pressure cuff, a light sensor to measure your blood oxygen level will be attached to your finger and EKG leads will be placed on your chest. You will receive sedation through your IV prior to placement of the block, which will both relax you and likely cause you to have little or no recollection of the block placement. Next, the anesthesiologist will cleanse your neck on the operative side with an antiseptic solution. He or she will use both anatomical landmarks and an ultrasound machine to find the desired location for the interscalene block an inch or two above the collarbone on your neck. Once the best location is found, the anesthesiologist will numb the skin with local anesthetic and insert a needle through the skin. Your anesthesiologist will utilize ultrasound to guide the needle to the proper location near the nerves. In addition to the ultrasound, occasionally a process called nerve stimulation will used to assist verifying the location of the nerves to your shoulder/upper arm and optimizing needle placement. If nerve stimulation is used, a very small amount of electrical current will be put through the needle and you will feel the sensation of involuntary twitches or movements in your chest, shoulder or arm. Do not try to stop these movements these are what tell the anesthesiologist if s/he is in the right location with the needle. When the location and/or response is optimal, the anesthesiologist will inject the long acting Novocain-like medicine in multiple small doses which will to numb your shoulder and arm. This procedure takes only a few minutes to perform. The block takes approximately minutes to work. You will notice shoulder and arm weakness and numbness. Once in the operating room, you will once again be attached to monitors and positioned by the surgeon. You usually will receive a light general anesthetic because it allows for better blood pressure control and ultimately more patient comfort. Most of the shoulder surgeons prefer general anesthesia to prevent any patient movement during the surgery. After the surgery and transport to the recovery room, the anesthesia will begin to wear off. You will have little or no pain. You will not be able to move or feel your shoulder, arm and sometimes your hand. Your voice may be hoarse and you may feel like you are not taking as deep a breath as you did before the surgery. These are normal and expected side effects from the interscalene block, and they are short lived. The numbness from the block usually lasts from hours. As it begins to wear off, you should start the pain medicine prescribed by your surgeon.
12 Poplietal Block The popliteal nerve block is a regional anesthetic technique used in conjunction with sedation or a light general anesthesia for surgery of the lower leg, ankle and foot. It is a safe and effective block that provides excellent surgical anesthesia and post-operative pain control. During a preoperative call with an anesthesiologist, you will discuss the procedure, as well as its risks and benefits. On arrival to the ASC prep area, you will be asked to sign a consent form for the procedure. You will be attached to a few monitors: a blood pressure cuff, a light sensor to measure your blood oxygen level will be attached to your finger and EKG leads will be placed on your chest. You will receive sedation through your IV prior to placement of the block, which will relax you and likely cause you to have little or no recollection of the block placement. Next, the anesthesiologist will position you for the block. You may be asked to remain lying on your back or to turn onto your side or your belly. He or she will cleanse either the side of your thigh or behind your knee with an antiseptic solution. He or she will use both anatomical landmarks and an ultrasound machine to find the desired location behind your knee for the popliteal block. Once the best location is found, the anesthesiologist will numb the skin with local anesthetic and insert a needle through the skin. Your anesthesiologist will utilize ultrasound to guide the needle to the proper location near the nerve. In addition to the ultrasound, occasionally a process called nerve stimulation is used to assist in verifying the location of the nerves to your lower leg/ankle/foot and optimizing needle placement. If nerve stimulation is used, a very small amount of electrical current will be put through the needle and you will feel the sensation of involuntary twitches or movements in your foot. Do not try to stop these movements because they tell the anesthesiologist if s/he is in the right location with the needle. When the location and/or response is optimal, the anesthesiologist will inject the long acting Novocain-like medicine in multiple small doses which will numb your lower leg, ankle and foot. This procedure takes only a few minutes to perform. Because the popliteal block only numbs-up approximately the outer 90% of the lower leg, ankle and foot, the anesthesiologist will also do a saphenous nerve block to numb up the remaining inner part of the lower leg, ankle or foot. While positioned lying on your back, the ultrasound machine will be used to locate the saphenous nerve. The lower inner thigh will be cleansed with an aseptic solution and the anesthesiologist will use the same method of locating the nerve with ultrasoundalternatively, the anesthesiologist may make a simple injection under the skin near the kneecap or ankle. Both blocks take up to 30 minutes or more to work. You will notice foot and ankle numbness or weakness. Once in the operating room, you will once again be attached to monitors and positioned by the surgeon. You will receive a relatively deep level of sedation or a light general anesthetic in addition to the popliteal nerve block. It allows for better blood pressure control and more patient comfort. After the surgery and transport to the recovery room, the sedation or general anesthesia will begin to wear off. You will have little or no pain in the ankle or foot, and you will be unable to move your ankle or foot. You will receive pain medicine in the recovery room, if you need it. The numbness and weakness from the block usually lasts from 6-18 hours. As it begins to wear off, you should start the pain medicine prescribed by your surgeon.
13 Supraclavicular Block The supraclavicular block is a regional anesthetic technique usually used in conjunction with a light general anesthesia for surgeries of the upper arm, elbow, forearm, wrist and hand. It is a safe and effective block that provides excellent surgical anesthesia and post-operative pain control. During a preoperative call with an anesthesiologist, you will discuss the procedure, as well as its risks and benefits. On arrival to the ASC prep area, you will be asked to sign a consent form for the procedure. You will be attached to a few monitors: a blood pressure cuff, a light sensor to measure your blood oxygen level will be attached to your finger and EKG leads will be placed on your chest. You will receive sedation through your IV prior to placement of the block, which will relax you and likely cause you to have little or no recollection of the block placement. Next, the anesthesiologist will cleanse your upper chest, collarbone and lower neck region on the operative side with an antiseptic solution. He or she will use both anatomical landmarks and an ultrasound machine to find the desired location for the supraclavicular block near the collarbone/neck region. Once the best location is found, the anesthesiologist will numb the skin with some local anesthetic and insert a needle through the skin. Your anesthesiologist will utilize ultrasound to guide the needle to the proper location near the nerves. In addition to the ultrasound, occasionally a process called nerve stimulation will be used to assist in verifying the location of the nerves to your arm/hand and optimizing needle placement. If nerve stimulation is used, a very small amount of electrical current will be put through the needle and you will feel the sensation of involuntary twitches or movements in your arm and hand. Do not try to stop these movements because they tell the anesthesiologist if s/he is in the right location with the needle. When the location and/or response is, optimal the anesthesiologist will inject the long acting Novocain-like medicine in multiple small doses which will numb your arm and hand. This procedure takes only a few minutes to perform. The block takes approximately minutes to work. You will notice your arm and hand becoming gradually more weak and numb. Once in the operating room, you will once again be attached to monitors and positioned by the surgeon. You will usually receive a light general anesthetic because it allows for better blood pressure control and more patient comfort. Most surgeons prefer general anesthesia to prevent any movement during the surgery. After the surgery and transport to the recovery room, the sedation or general anesthesia will begin to wear off. You will have little or no pain, and you will not be able to move or feel your arm and hand. The numbness and weakness from the block should last from 6-14 hours. As it begins to wear off, you should start the pain medicine prescribed by the surgeon.
14 Adductor Canal/Saphenous Nerve Block The adductor canal/saphenous nerve block is a regional anesthetic technique used in conjunction with general anesthesia for ACL reconstruction surgery, tibial osteotomies and other more painful complex surgeries involving the knee joint. Some surgeons prefer it over a femoral nerve block because it is purely a sensory nerve block, providing good pain relief, and there is no weakness of the muscles associated with it. It is a safe and effective block that provides excellent post-operative pain control for the inside and front of the knee. During a preoperative call with an anesthesiologist, you will discuss the procedure, as well as its risks and benefits. On arrival to the ASC prep area, you will be asked to sign a consent form for the procedure. You will be attached to a few monitors: a blood pressure cuff, a light sensor to measure your blood oxygen level will be attached to your finger and EKG leads will be placed on your chest. You will receive sedation through your IV prior to placement of the block, which will relax you and likely cause you to have little or no recollection of the block placement. Next, while maintaining modesty, the anesthesiologist will cleanse the inner mid-thigh region on the operative side with an antiseptic solution. He or she will use both anatomical landmarks and an ultrasound machine to find the desired location for the adductor canal/saphenous nerve block in the groin region. Once the best location is found, the anesthesiologist will numb the skin with local anesthetic. Next the anesthesiologist will slowly insert a needle the size of a paperclip through the skin. Your anesthesiologist will utilize ultrasound to guide the needle to the proper location near the nerve. When the location and/or response are optimal, the anesthesiologist will inject the long acting Novocain-like medicine in multiple small doses which will numb the front of your thigh and knee. This procedure takes only a few minutes to perform. The block takes approximately minutes to work. You will notice numbness over knee and inner calf area. Once in the operating room, you will once again be attached to the monitors and positioned by the surgeon. You will receive a light general anesthetic in addition to the adductor canal/saphenous nerve block as your anesthetic because this nerve block does not numb-up the entire knee, especially not back of the knee. After the surgery and transport to the recovery room, the general anesthesia will begin to wear off. You will have little or no pain in the front of your leg or knee. However you will probably have some discomfort behind and below your knee. That is expected. You will receive pain medicine in the recovery room, as you need it. The numbness and weakness from the block usually lasts from hours and occasionally greater than 24 hours. As it begins to wear off, you should start the pain medicine prescribed by the surgeon.
Interscalene Block. Nancy A. Brown, MD
 Interscalene Block Nancy A. Brown, MD What is an Interscalene Block? An Interscalene block is a form of regional anesthesia used in conjunction with general anesthesia for surgeries of the shoulder and
Interscalene Block Nancy A. Brown, MD What is an Interscalene Block? An Interscalene block is a form of regional anesthesia used in conjunction with general anesthesia for surgeries of the shoulder and
ANESTHESIA. Anesthesia for Ambulatory Surgery
 ANESTHESIA & YOU Anesthesia for Ambulatory Surgery T oday the majority of patients who undergo surgery or diagnostic tests do not need to stay overnight in the hospital. In most cases, you will be well
ANESTHESIA & YOU Anesthesia for Ambulatory Surgery T oday the majority of patients who undergo surgery or diagnostic tests do not need to stay overnight in the hospital. In most cases, you will be well
Epidural Continuous Infusion. Patient information Leaflet
 Epidural Continuous Infusion Patient information Leaflet April 2015 Introduction You may already know that epidural s are often used to treat pain during childbirth. This same technique can also used as
Epidural Continuous Infusion Patient information Leaflet April 2015 Introduction You may already know that epidural s are often used to treat pain during childbirth. This same technique can also used as
Common Regional Nerve Blocks Quick Guide developed by UWHC Acute Pain Service Jan 2011
 Common Regional Nerve Blocks Quick Guide developed by UWHC Acute Pain Service Jan 2011 A single shot nerve block is the injection of local anesthetic to block a specific nerve distribution. It can be placed
Common Regional Nerve Blocks Quick Guide developed by UWHC Acute Pain Service Jan 2011 A single shot nerve block is the injection of local anesthetic to block a specific nerve distribution. It can be placed
Femoral artery bypass graft (Including femoral crossover graft)
 Femoral artery bypass graft (Including femoral crossover graft) Why do I need the operation? You have a blockage or narrowing of the arteries supplying blood to your leg. This reduces the blood flow to
Femoral artery bypass graft (Including femoral crossover graft) Why do I need the operation? You have a blockage or narrowing of the arteries supplying blood to your leg. This reduces the blood flow to
Varicose Veins Operation. Patient information Leaflet
 Varicose Veins Operation Patient information Leaflet 22 nd August 2014 WHAT IS VARICOSE VEIN SURGERY (HIGH LIGATION AND MULTIPLE AVULSIONS) The operation varies from case to case, depending on where the
Varicose Veins Operation Patient information Leaflet 22 nd August 2014 WHAT IS VARICOSE VEIN SURGERY (HIGH LIGATION AND MULTIPLE AVULSIONS) The operation varies from case to case, depending on where the
OPERATION:... Proximal tibial osteotomy Distal femoral osteotomy
 AFFIX PATIENT DETAIL STICKER HERE Forename.. Surname NHS Organisation. Responsible surgeon. Job Title Hospital Number... D.O.B.././ No special requirements OPERATION:..... Proximal tibial osteotomy Distal
AFFIX PATIENT DETAIL STICKER HERE Forename.. Surname NHS Organisation. Responsible surgeon. Job Title Hospital Number... D.O.B.././ No special requirements OPERATION:..... Proximal tibial osteotomy Distal
LASER TREATMENT FOR VARICOSE VEINS
 LASER TREATMENT FOR VARICOSE VEINS How can varicose veins be treated by laser? Laser treatment of varicose veins, Endovascular Laser Ablation (known as EVLA), is a minimally invasive procedure for treating
LASER TREATMENT FOR VARICOSE VEINS How can varicose veins be treated by laser? Laser treatment of varicose veins, Endovascular Laser Ablation (known as EVLA), is a minimally invasive procedure for treating
Your spinal Anaesthetic
 Your spinal Anaesthetic Information for patients Your spinal anaesthetic This information leaflet explains what to expect when you have an operation with a spinal anaesthetic. It has been written by patients,
Your spinal Anaesthetic Information for patients Your spinal anaesthetic This information leaflet explains what to expect when you have an operation with a spinal anaesthetic. It has been written by patients,
Thyroid Surgery at Massachusetts General Hospital Frequently Asked Questions
 Thyroid Surgery at Massachusetts General Hospital Frequently Asked Questions Q: What is the thyroid gland? A: The thyroid is a butterfly-shaped gland located in the front of the neck. It is one of the
Thyroid Surgery at Massachusetts General Hospital Frequently Asked Questions Q: What is the thyroid gland? A: The thyroid is a butterfly-shaped gland located in the front of the neck. It is one of the
X-Plain Preparing For Surgery Reference Summary
 X-Plain Preparing For Surgery Reference Summary Introduction More than 25 million surgical procedures are performed each year in the US. This reference summary will help you prepare for surgery. By understanding
X-Plain Preparing For Surgery Reference Summary Introduction More than 25 million surgical procedures are performed each year in the US. This reference summary will help you prepare for surgery. By understanding
Pain Relief Options for Labor. Providing You with Quality Care, Information and Support
 Pain Relief Options for Labor Providing You with Quality Care, Information and Support What can I expect during my labor and delivery? As a patient in the Labor and Delivery Suite at Lucile Packard Children
Pain Relief Options for Labor Providing You with Quality Care, Information and Support What can I expect during my labor and delivery? As a patient in the Labor and Delivery Suite at Lucile Packard Children
Colon Cancer Surgery and Recovery. A Guide for Patients and Families
 Colon Cancer Surgery and Recovery A Guide for Patients and Families This Booklet You are receiving this booklet because you will be having surgery shortly. This booklet tells you what to do before, during,
Colon Cancer Surgery and Recovery A Guide for Patients and Families This Booklet You are receiving this booklet because you will be having surgery shortly. This booklet tells you what to do before, during,
X-Plain Trigeminal Neuralgia Reference Summary
 X-Plain Trigeminal Neuralgia Reference Summary Introduction Trigeminal neuralgia is a condition that affects about 40,000 patients in the US every year. Its treatment mostly involves the usage of oral
X-Plain Trigeminal Neuralgia Reference Summary Introduction Trigeminal neuralgia is a condition that affects about 40,000 patients in the US every year. Its treatment mostly involves the usage of oral
Preparing for Your Surgery
 Preparing for Your Surgery Welcome As you get ready for surgery, you may have a lot of questions. This booklet will help you know what to expect before, during and after surgery. You and your family are
Preparing for Your Surgery Welcome As you get ready for surgery, you may have a lot of questions. This booklet will help you know what to expect before, during and after surgery. You and your family are
The science of medicine. The compassion to heal.
 A PATIENT S GUIDE TO ELECTROPHYSIOLOGY STUDIES OF THE HEART The science of medicine. The compassion to heal. This teaching booklet is designed to introduce you to electrophysiology studies of the heart.
A PATIENT S GUIDE TO ELECTROPHYSIOLOGY STUDIES OF THE HEART The science of medicine. The compassion to heal. This teaching booklet is designed to introduce you to electrophysiology studies of the heart.
X-Plain Hip Replacement Surgery - Preventing Post Op Complications Reference Summary
 X-Plain Hip Replacement Surgery - Preventing Post Op Complications Reference Summary Introduction Severe arthritis in the hip can lead to severe pain and inability to walk. To relieve the pain and improve
X-Plain Hip Replacement Surgery - Preventing Post Op Complications Reference Summary Introduction Severe arthritis in the hip can lead to severe pain and inability to walk. To relieve the pain and improve
Significant nerve damage is uncommonly associated with a general anaesthetic
 Risks associated with your anaesthetic Section 10: Nerve damage associated with an operation under general anaesthetic Section 10: Significant nerve damage is uncommonly associated with a general anaesthetic
Risks associated with your anaesthetic Section 10: Nerve damage associated with an operation under general anaesthetic Section 10: Significant nerve damage is uncommonly associated with a general anaesthetic
Endoscopic Plantar Fasciotomy
 Endoscopic Plantar Fasciotomy Introduction Plantar fasciitis is a common condition that causes pain centralized around the heel. It may be severe enough to affect regular activities. Health care providers
Endoscopic Plantar Fasciotomy Introduction Plantar fasciitis is a common condition that causes pain centralized around the heel. It may be severe enough to affect regular activities. Health care providers
Pain Management for Labour & Delivery
 Pain Management for Labour & Delivery Departments of Anesthesia, Obstetrics, and Obstetrical Nursing December 2008 This pamphlet has been prepared to provide you, members of your family, and others who
Pain Management for Labour & Delivery Departments of Anesthesia, Obstetrics, and Obstetrical Nursing December 2008 This pamphlet has been prepared to provide you, members of your family, and others who
Cardiac Catheterization
 Page 1 Cardiac Catheterization What Other Terms Are Used To Describe Cardiac Catheterization? Heart Cath (catheter) Angiogram What Is Cardiac Catheterization? This procedure is nonsurgical and is performed
Page 1 Cardiac Catheterization What Other Terms Are Used To Describe Cardiac Catheterization? Heart Cath (catheter) Angiogram What Is Cardiac Catheterization? This procedure is nonsurgical and is performed
Epidurals for pain relief after surgery
 Epidurals for pain relief after surgery This information leaflet is for anyone who may benefit from an epidural for pain relief after surgery. We hope it will help you to ask questions and direct you to
Epidurals for pain relief after surgery This information leaflet is for anyone who may benefit from an epidural for pain relief after surgery. We hope it will help you to ask questions and direct you to
Local anaesthesia for your eye operation
 Local anaesthesia for your eye operation Information for patients and families. www.anaesthesia.ie 1 This information leaflet is for anyone expecting to have an eye operation with a local anaesthetic.
Local anaesthesia for your eye operation Information for patients and families. www.anaesthesia.ie 1 This information leaflet is for anyone expecting to have an eye operation with a local anaesthetic.
Oxford Centre for Respiratory Medicine Bronchial-Artery Embolisation Information for patients
 Oxford Centre for Respiratory Medicine Bronchial-Artery Embolisation Information for patients This leaflet tells you about the bronchial-artery embolisation procedure. It explains what is involved and
Oxford Centre for Respiratory Medicine Bronchial-Artery Embolisation Information for patients This leaflet tells you about the bronchial-artery embolisation procedure. It explains what is involved and
Plantar Fascia Release
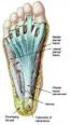 Plantar Fascia Release Introduction Plantar fasciitis is a common condition that causes pain around the heel. It may be severe enough to affect regular activities. If other treatments are unsuccessful,
Plantar Fascia Release Introduction Plantar fasciitis is a common condition that causes pain around the heel. It may be severe enough to affect regular activities. If other treatments are unsuccessful,
Gallbladder Surgery with an Incision (Cholecystectomy)
 Gallbladder Surgery with an Incision (Cholecystectomy) It is normal to have questions about your surgery. This handout gives you information about what will happen to you before, during and after your
Gallbladder Surgery with an Incision (Cholecystectomy) It is normal to have questions about your surgery. This handout gives you information about what will happen to you before, during and after your
PATIENT HANDBOOK AND JOURNAL DAY OF SURGERY
 PATIENT HANDBOOK AND JOURNAL DAY OF SURGERY PREPARING YOUR SKIN BEFORE SURGERY PRE-OP HIBICLENS BATHING INSTRUCTIONS: General Information: Because the skin is not sterile, it is important to make sure
PATIENT HANDBOOK AND JOURNAL DAY OF SURGERY PREPARING YOUR SKIN BEFORE SURGERY PRE-OP HIBICLENS BATHING INSTRUCTIONS: General Information: Because the skin is not sterile, it is important to make sure
YOU AND YOUR ANAESTHETIC
 YOU AND YOUR ANAESTHETIC Information Leaflet Your Health. Our Priority. Page 2 of 8 This leaflet aims to answer some of the questions you may have about your anaesthetic and contains fasting instructions.
YOU AND YOUR ANAESTHETIC Information Leaflet Your Health. Our Priority. Page 2 of 8 This leaflet aims to answer some of the questions you may have about your anaesthetic and contains fasting instructions.
Total hip replacement
 Patient Information to be retained by patient What is a total hip replacement? In a total hip replacement both the ball (femoral or thigh bone) side of the hip joint and the socket (acetabular or pelvic
Patient Information to be retained by patient What is a total hip replacement? In a total hip replacement both the ball (femoral or thigh bone) side of the hip joint and the socket (acetabular or pelvic
Total Knee Replacement
 Total Knee Replacement Contents Introduction Total Knee Replacement Preparing for surgery Pre-op visit Day of surgery After surgery (In Hospital) After surgery (In Rehab) Exercise Program and Physical
Total Knee Replacement Contents Introduction Total Knee Replacement Preparing for surgery Pre-op visit Day of surgery After surgery (In Hospital) After surgery (In Rehab) Exercise Program and Physical
A PATIENT S GUIDE TO CARDIAC CATHETERIZATION
 A PATIENT S GUIDE TO CARDIAC CATHETERIZATION The science of medicine. The compassion to heal. This teaching booklet is designed to introduce you to cardiac catheterization. In the following pages, we will
A PATIENT S GUIDE TO CARDIAC CATHETERIZATION The science of medicine. The compassion to heal. This teaching booklet is designed to introduce you to cardiac catheterization. In the following pages, we will
A Patient s Guide to Post-Operative Physiotherapy. Following Anterior Cruciate Ligament Reconstruction of the Knee
 A Patient s Guide to Post-Operative Physiotherapy Following Anterior Cruciate Ligament Reconstruction of the Knee Introduction The anterior cruciate ligament (ACL) is one of the main supporting ligaments
A Patient s Guide to Post-Operative Physiotherapy Following Anterior Cruciate Ligament Reconstruction of the Knee Introduction The anterior cruciate ligament (ACL) is one of the main supporting ligaments
Elbow Joint Replacement A guide for patients
 Elbow Joint Replacement A guide for patients GATESHEAD UPPER LIMB UNIT Mr Andreas Hinsche Mr John Harrison Mr Jagannath Chakravarthy Page 1 of 7 The elbow joint The elbow consists of three bones; the humerus
Elbow Joint Replacement A guide for patients GATESHEAD UPPER LIMB UNIT Mr Andreas Hinsche Mr John Harrison Mr Jagannath Chakravarthy Page 1 of 7 The elbow joint The elbow consists of three bones; the humerus
Total knee replacement
 Patient Information to be retained by patient What is a total knee replacement? In a total knee replacement the cartilage surfaces of the thigh bone (femur) and leg bone (tibia) are replaced. The cartilage
Patient Information to be retained by patient What is a total knee replacement? In a total knee replacement the cartilage surfaces of the thigh bone (femur) and leg bone (tibia) are replaced. The cartilage
Peripherally Inserted Central Catheter (PICC) for Outpatient
 Peripherally Inserted Central Catheter (PICC) for Outpatient Introduction A Peripherally Inserted Central Catheter, or PICC line, is a thin, long, soft plastic tube inserted into a vein of the arm. It
Peripherally Inserted Central Catheter (PICC) for Outpatient Introduction A Peripherally Inserted Central Catheter, or PICC line, is a thin, long, soft plastic tube inserted into a vein of the arm. It
Hip Replacement. Department of Orthopaedic Surgery Tel: 01473 702107
 Information for Patients Hip Replacement Department of Orthopaedic Surgery Tel: 01473 702107 DMI ref: 0134-08.indd(RP) Issue 3: February 2008 The Ipswich Hospital NHS Trust, 2005-2008. All rights reserved.
Information for Patients Hip Replacement Department of Orthopaedic Surgery Tel: 01473 702107 DMI ref: 0134-08.indd(RP) Issue 3: February 2008 The Ipswich Hospital NHS Trust, 2005-2008. All rights reserved.
PATIENT HANDBOOK AND JOURNAL POST SURGERY
 PATIENT HANDBOOK AND JOURNAL POST SURGERY POST ANESTHESIA CARE UNIT (PACU) After surgery you will be moved from the Operating Room directly to a special recovery room, called the Post Anesthesia Care Unit
PATIENT HANDBOOK AND JOURNAL POST SURGERY POST ANESTHESIA CARE UNIT (PACU) After surgery you will be moved from the Operating Room directly to a special recovery room, called the Post Anesthesia Care Unit
The degree of liver inflammation or damage (grade) Presence and extent of fatty liver or other metabolic liver diseases
 ilearning about your health Liver Biopsy www.cpmc.org/learning What is a Liver Biopsy? A liver biopsy is a procedure where a specially trained doctor (typically a hepatologist, radiologist, or gastroenterologist)
ilearning about your health Liver Biopsy www.cpmc.org/learning What is a Liver Biopsy? A liver biopsy is a procedure where a specially trained doctor (typically a hepatologist, radiologist, or gastroenterologist)
Endovascular Abdominal Aortic Aneurysm Repair Surgery
 Endovascular Abdominal Aortic Aneurysm Repair Surgery You are scheduled for an admission to Cooper University Hospital for Endovascular Abdominal Aortic Aneurysm surgery (EVAR). Please read this handout,
Endovascular Abdominal Aortic Aneurysm Repair Surgery You are scheduled for an admission to Cooper University Hospital for Endovascular Abdominal Aortic Aneurysm surgery (EVAR). Please read this handout,
Understanding your Peripherally Inserted Central Catheter (PICC) Patient Information
 Understanding your Peripherally Inserted Central Catheter (PICC) Patient Information The Purpose of this Information Sheet This information sheet has been written by patients, members of the public and
Understanding your Peripherally Inserted Central Catheter (PICC) Patient Information The Purpose of this Information Sheet This information sheet has been written by patients, members of the public and
A Patient s Guide to PAIN MANAGEMENT. After Surgery
 A Patient s Guide to PAIN MANAGEMENT After Surgery C o m p a s s i o n a n d C o m m i t m e n t A Patient s Guide to Pain Management After Surgery If you re facing an upcoming surgery, it s natural to
A Patient s Guide to PAIN MANAGEMENT After Surgery C o m p a s s i o n a n d C o m m i t m e n t A Patient s Guide to Pain Management After Surgery If you re facing an upcoming surgery, it s natural to
Inferior Vena Cava filter and removal
 Inferior Vena Cava filter and removal What is Inferior Vena Cava Filter Placement and Removal? An inferior vena cava filter placement procedure involves an interventional radiologist (a specialist doctor)
Inferior Vena Cava filter and removal What is Inferior Vena Cava Filter Placement and Removal? An inferior vena cava filter placement procedure involves an interventional radiologist (a specialist doctor)
An Informative Guide for Heart Catheterization Patients & Families
 An Informative Guide for Heart Catheterization Patients & Families What is a Cardiac Cath? Cardiac catheterization is a procedure used to diagnose and treat patients who have various forms of heart disease.
An Informative Guide for Heart Catheterization Patients & Families What is a Cardiac Cath? Cardiac catheterization is a procedure used to diagnose and treat patients who have various forms of heart disease.
UW MEDICINE PATIENT EDUCATION. Aortic Stenosis. What is heart valve disease? What is aortic stenosis?
 UW MEDICINE PATIENT EDUCATION Aortic Stenosis Causes, symptoms, diagnosis, and treatment This handout describes aortic stenosis, a narrowing of the aortic valve in your heart. It also explains how this
UW MEDICINE PATIENT EDUCATION Aortic Stenosis Causes, symptoms, diagnosis, and treatment This handout describes aortic stenosis, a narrowing of the aortic valve in your heart. It also explains how this
Electroconvulsive Therapy - ECT
 Electroconvulsive Therapy - ECT Introduction Electroconvulsive therapy, or ECT, is a safe and effective treatment that may reduce symptoms related to depression or mental illness. During ECT, certain parts
Electroconvulsive Therapy - ECT Introduction Electroconvulsive therapy, or ECT, is a safe and effective treatment that may reduce symptoms related to depression or mental illness. During ECT, certain parts
Spinal Injections. North American Spine Society Public Education Series
 Spinal Injections North American Spine Society Public Education Series What Is a Spinal Injection? Your doctor has suggested that you have a spinal injection to help reduce pain and improve function. This
Spinal Injections North American Spine Society Public Education Series What Is a Spinal Injection? Your doctor has suggested that you have a spinal injection to help reduce pain and improve function. This
Your Recovery After a Cesarean Delivery
 Your Recovery After a Cesarean Delivery It is normal to have many questions about your care after delivery. Cesarean delivery is surgery and your body needs time to heal and recover for the next 6 weeks,
Your Recovery After a Cesarean Delivery It is normal to have many questions about your care after delivery. Cesarean delivery is surgery and your body needs time to heal and recover for the next 6 weeks,
Arthroscopic shoulder stabilisation. Patient Information to be retained by patient
 PLEASE PRINT WHOLE FORM DOUBLE SIDED ON YELLOW PAPER Patient Information to be retained by patient affix patient label Shoulder instability The shoulder is the most common joint in the body to dislocate.
PLEASE PRINT WHOLE FORM DOUBLE SIDED ON YELLOW PAPER Patient Information to be retained by patient affix patient label Shoulder instability The shoulder is the most common joint in the body to dislocate.
Peripherally Inserted Central Catheter (PICC)
 Peripherally Inserted Central Catheter (PICC) Disclaimer This is general information developed by The Ottawa Hospital. It is not intended to replace the advice of a qualified healthcare provider. Please
Peripherally Inserted Central Catheter (PICC) Disclaimer This is general information developed by The Ottawa Hospital. It is not intended to replace the advice of a qualified healthcare provider. Please
Undergoing an Oesophageal Endoscopic Resection (ER)
 Contact Information If you have an enquiry about your appointment time/date please contact the Booking Office on 0300 422 6350. For medication enquiries please call 0300 422 8232, this is an answer machine
Contact Information If you have an enquiry about your appointment time/date please contact the Booking Office on 0300 422 6350. For medication enquiries please call 0300 422 8232, this is an answer machine
Pain Relief during Labour and Delivery: What Are My Options?
 Pain Relief during Labour and Delivery: What Are My Options? To help you prepare for the birth of your baby, this booklet answers some of the questions you may have about pain relief options. You should
Pain Relief during Labour and Delivery: What Are My Options? To help you prepare for the birth of your baby, this booklet answers some of the questions you may have about pain relief options. You should
Informed Patient Tutorial Copyright 2012 by the American Academy of Orthopaedic Surgeons
 Informed Patient Tutorial Copyright 2012 by the American Academy of Orthopaedic Surgeons Informed Patient - Carpal Tunnel Release Surgery Introduction Welcome to the American Academy of Orthopaedic Surgeons'
Informed Patient Tutorial Copyright 2012 by the American Academy of Orthopaedic Surgeons Informed Patient - Carpal Tunnel Release Surgery Introduction Welcome to the American Academy of Orthopaedic Surgeons'
Elbow arthroscopy. Key points
 Patient information Elbow arthroscopy This information has been produced to help you gain the maximum benefit and understanding of your operation. It includes the following information: Key points About
Patient information Elbow arthroscopy This information has been produced to help you gain the maximum benefit and understanding of your operation. It includes the following information: Key points About
.org. Knee Arthroscopy. Description. Preparing for Surgery. Surgery
 Knee Arthroscopy Page ( 1 ) Arthroscopy is a common surgical procedure in which a joint (arthro-) is viewed (-scopy) using a small camera. Arthroscopy gives doctors a clear view of the inside of the knee.
Knee Arthroscopy Page ( 1 ) Arthroscopy is a common surgical procedure in which a joint (arthro-) is viewed (-scopy) using a small camera. Arthroscopy gives doctors a clear view of the inside of the knee.
Dr. Kenneth A. Giraldo, MD, P.A. Patient Controlled Substance Agreement Informed Consent Form
 Dr. Kenneth A. Giraldo, MD, P.A. Patient Controlled Substance Agreement Informed Consent Form The following agreement relates to my use of controlled substance for chronic pain prescribed by Dr. Kenneth
Dr. Kenneth A. Giraldo, MD, P.A. Patient Controlled Substance Agreement Informed Consent Form The following agreement relates to my use of controlled substance for chronic pain prescribed by Dr. Kenneth
Knee Conditioning Program. Purpose of Program
 Prepared for: Prepared by: OrthoInfo Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle.
Prepared for: Prepared by: OrthoInfo Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle.
Parathyroidectomy An operation to remove overactive parathyroid glands Information for patients
 Oxford University Hospitals NHS Trust Parathyroidectomy An operation to remove overactive parathyroid glands Information for patients What are the parathyroid glands? There are four parathyroid glands
Oxford University Hospitals NHS Trust Parathyroidectomy An operation to remove overactive parathyroid glands Information for patients What are the parathyroid glands? There are four parathyroid glands
Provided by the American Venous Forum: veinforum.org
 CHAPTER 17 SURGICAL THERAPY FOR DEEP VALVE INCOMPETENCE Original author: Seshadri Raju Abstracted by Gary W. Lemmon Introduction Deep vein valvular incompetence happens when the valves in the veins (tubes
CHAPTER 17 SURGICAL THERAPY FOR DEEP VALVE INCOMPETENCE Original author: Seshadri Raju Abstracted by Gary W. Lemmon Introduction Deep vein valvular incompetence happens when the valves in the veins (tubes
THE RECOVERY PROCESS
 THE RECOVERY PROCESS PART 1 This information will help you get ready for your surgery AND prepare for the days, weeks, and months following your surgery. You may need to adjust your work schedule, ask
THE RECOVERY PROCESS PART 1 This information will help you get ready for your surgery AND prepare for the days, weeks, and months following your surgery. You may need to adjust your work schedule, ask
Cardiac catheterization Information for patients
 Cardiac catheterization Information for patients You have been scheduled for a cardiac catheterization. Your procedure is scheduled for:. Someone will call you the day before your procedure to tell you
Cardiac catheterization Information for patients You have been scheduled for a cardiac catheterization. Your procedure is scheduled for:. Someone will call you the day before your procedure to tell you
A Stretch-Break Program for Your Workplace! www.healthyworkplaceweek.ca
 www.healthyworkplaceweek.ca A Stretch-Break Program for Your Workplace! Why is stretching at work important? Sitting at a desk or computer; or standing at your work station for extended periods of time
www.healthyworkplaceweek.ca A Stretch-Break Program for Your Workplace! Why is stretching at work important? Sitting at a desk or computer; or standing at your work station for extended periods of time
Ankle Block. Indications The ankle block is suitable for the following: Orthopedic and podiatry surgical procedures of the distal foot.
 Ankle Block The ankle block is a common peripheral nerve block. It is useful for procedures of the foot and toes, as long as a tourniquet is not required above the ankle. It is a safe and effective technique.
Ankle Block The ankle block is a common peripheral nerve block. It is useful for procedures of the foot and toes, as long as a tourniquet is not required above the ankle. It is a safe and effective technique.
Corporate Medical Policy
 File Name: anesthesia_services Origination: 8/2007 Last CAP Review: 1/2016 Next CAP Review: 1/2017 Last Review: 1/2016 Corporate Medical Policy Description of Procedure or Service There are three main
File Name: anesthesia_services Origination: 8/2007 Last CAP Review: 1/2016 Next CAP Review: 1/2017 Last Review: 1/2016 Corporate Medical Policy Description of Procedure or Service There are three main
Shoulder Arthroscopy
 Copyright 2011 American Academy of Orthopaedic Surgeons Shoulder Arthroscopy Arthroscopy is a procedure that orthopaedic surgeons use to inspect, diagnose, and repair problems inside a joint. The word
Copyright 2011 American Academy of Orthopaedic Surgeons Shoulder Arthroscopy Arthroscopy is a procedure that orthopaedic surgeons use to inspect, diagnose, and repair problems inside a joint. The word
.org. Clavicle Fracture (Broken Collarbone) Anatomy. Description. Cause. Symptoms
 Clavicle Fracture (Broken Collarbone) Page ( 1 ) A broken collarbone is also known as a clavicle fracture. This is a very common fracture that occurs in people of all ages. Anatomy The collarbone (clavicle)
Clavicle Fracture (Broken Collarbone) Page ( 1 ) A broken collarbone is also known as a clavicle fracture. This is a very common fracture that occurs in people of all ages. Anatomy The collarbone (clavicle)
Functional rehab after breast reconstruction surgery
 Functional rehab after breast reconstruction surgery UHN A guide for women who had DIEP, latissimus dorsi with a tissue expander or implant, or two-stage implant based breast reconstruction surgery Read
Functional rehab after breast reconstruction surgery UHN A guide for women who had DIEP, latissimus dorsi with a tissue expander or implant, or two-stage implant based breast reconstruction surgery Read
Your Nerve Block &Home Pump For Arm/Hand Surgery
 Your Nerve Block &Home Pump For Arm/Hand Surgery Department of Anesthesiology and Perioperative Medicine www.happypatient.org Updated 5/10 Why? To Help Control Postoperative Pain at Home A pump connected
Your Nerve Block &Home Pump For Arm/Hand Surgery Department of Anesthesiology and Perioperative Medicine www.happypatient.org Updated 5/10 Why? To Help Control Postoperative Pain at Home A pump connected
Total Hip Replacement
 Please contactmethroughthegoldcoasthospitaswityouhaveanyproblemsafteryoursurgery. Dr. Benjamin Hewitt Orthopaedic Surgeon Total Hip Replacement The hip joint is a ball and socket joint that connects the
Please contactmethroughthegoldcoasthospitaswityouhaveanyproblemsafteryoursurgery. Dr. Benjamin Hewitt Orthopaedic Surgeon Total Hip Replacement The hip joint is a ball and socket joint that connects the
Local anaesthesia for your eye operation
 Local anaesthesia for your eye operation A short guide for patients and families. This is for anyone expecting to have an eye operation with a local anaesthetic. It does not give detailed information about
Local anaesthesia for your eye operation A short guide for patients and families. This is for anyone expecting to have an eye operation with a local anaesthetic. It does not give detailed information about
A Patient s Guide to Guyon s Canal Syndrome
 A Patient s Guide to DISCLAIMER: The information in this booklet is compiled from a variety of sources. It may not be complete or timely. It does not cover all diseases, physical conditions, ailments or
A Patient s Guide to DISCLAIMER: The information in this booklet is compiled from a variety of sources. It may not be complete or timely. It does not cover all diseases, physical conditions, ailments or
Orthopaedic Spine Center. Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs
 Orthopaedic Spine Center Graham Calvert MD James Woodall MD PhD Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs The cervical spine consists of the bony vertebrae, discs, nerves and other structures.
Orthopaedic Spine Center Graham Calvert MD James Woodall MD PhD Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs The cervical spine consists of the bony vertebrae, discs, nerves and other structures.
Understanding and Preparing for a CAtHeteRIZAtIon PRoCeDURe
 Understanding and Preparing for a CAtHeteRIZAtIon PRoCeDURe The Massachusetts General Hospital Heart Center and Vascular Center welcome you to the Knight Center for Interventional Cardiovascular Therapy.
Understanding and Preparing for a CAtHeteRIZAtIon PRoCeDURe The Massachusetts General Hospital Heart Center and Vascular Center welcome you to the Knight Center for Interventional Cardiovascular Therapy.
Having denervation of the renal arteries for treatment of high blood pressure
 Having denervation of the renal arteries for treatment of high blood pressure The aim of this information sheet is to help answer some of the questions you may have about having denervation of the renal
Having denervation of the renal arteries for treatment of high blood pressure The aim of this information sheet is to help answer some of the questions you may have about having denervation of the renal
Passive Range of Motion Exercises
 Exercise and ALS The physical or occupational therapist will make recommendations for exercise based upon each patient s specific needs and abilities. Strengthening exercises are not generally recommended
Exercise and ALS The physical or occupational therapist will make recommendations for exercise based upon each patient s specific needs and abilities. Strengthening exercises are not generally recommended
Urinary Diversion: Ileovesicostomy/Ileal Loop/Colon Loop
 Urinary Diversion: Ileovesicostomy/Ileal Loop/Colon Loop Why do I need this surgery? A urinary diversion is a surgical procedure that is performed to allow urine to safely pass from the kidneys into a
Urinary Diversion: Ileovesicostomy/Ileal Loop/Colon Loop Why do I need this surgery? A urinary diversion is a surgical procedure that is performed to allow urine to safely pass from the kidneys into a
Renal Vascular Access Having a Fistula For Haemodialysis
 Renal Vascular Access Having a Fistula For Haemodialysis Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Renal Vascular Access Having a Fistula For Haemodialysis Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Treating your abdominal aortic aneurysm by open repair (surgery)
 Patient information Abdominal aortic aneurysm open surgery Treating your abdominal aortic aneurysm by open repair (surgery) Introduction This leaflet tells you about open repair of abdominal aortic aneurysm,
Patient information Abdominal aortic aneurysm open surgery Treating your abdominal aortic aneurysm by open repair (surgery) Introduction This leaflet tells you about open repair of abdominal aortic aneurysm,
Presence and extent of fatty liver or other metabolic liver diseases
 UC San Diego Health System Patient Information Sheet: Liver Biopsy What is a Liver Biopsy? A liver biopsy is a procedure where a qualified doctor (typically a hepatologist, radiologist or gastroenterologist)
UC San Diego Health System Patient Information Sheet: Liver Biopsy What is a Liver Biopsy? A liver biopsy is a procedure where a qualified doctor (typically a hepatologist, radiologist or gastroenterologist)
Range of Motion Exercises
 Range of Motion Exercises Range of motion (ROM) exercises are done to preserve flexibility and mobility of the joints on which they are performed. These exercises reduce stiffness and will prevent or at
Range of Motion Exercises Range of motion (ROM) exercises are done to preserve flexibility and mobility of the joints on which they are performed. These exercises reduce stiffness and will prevent or at
Arterio-Venous Fistula or Arterio-Venous Graft for Haemodialysis
 Department of Nephrology Care of your Fistula Nephrology Department Lower Lane Liverpool L9 7AL Tel:0151-525-5980 Arterio-Venous Fistula or Arterio-Venous Graft for Haemodialysis Haemodialysis access In
Department of Nephrology Care of your Fistula Nephrology Department Lower Lane Liverpool L9 7AL Tel:0151-525-5980 Arterio-Venous Fistula or Arterio-Venous Graft for Haemodialysis Haemodialysis access In
Tibial Intramedullary Nailing
 Tibial Intramedullary Nailing Turnberg Building Orthopaedics 0161 206 4898 All Rights Reserved 2015. Document for issue as handout. Procedure The tibia is the long shin bone in the lower leg. It is a weight
Tibial Intramedullary Nailing Turnberg Building Orthopaedics 0161 206 4898 All Rights Reserved 2015. Document for issue as handout. Procedure The tibia is the long shin bone in the lower leg. It is a weight
Laparoscopic Surgery for Inguinal Hernia Repair
 Laparoscopic Surgery for Inguinal Hernia Repair What is an Inguinal Hernia Repair? 2 What is a Laparoscopic Inguinal Hernia Repair? 2 Are there any alternatives to Laparoscopic Hernia Repair? 3 Am I a
Laparoscopic Surgery for Inguinal Hernia Repair What is an Inguinal Hernia Repair? 2 What is a Laparoscopic Inguinal Hernia Repair? 2 Are there any alternatives to Laparoscopic Hernia Repair? 3 Am I a
Electrophysiology study (EPS)
 Patient information factsheet Electrophysiology study (EPS) The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
Patient information factsheet Electrophysiology study (EPS) The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
Department of Surgery
 Thoracic Surgery After Your Lung Surgery Patient Education Discharge Information You have just had lung surgery. The following are definitions of terms you may hear in connection with your surgery: THORACOTOMY
Thoracic Surgery After Your Lung Surgery Patient Education Discharge Information You have just had lung surgery. The following are definitions of terms you may hear in connection with your surgery: THORACOTOMY
Cardiac Catheterization Lab Procedures
 UW MEDICINE PATIENT EDUCATION Cardiac Catheterization Lab Procedures This handout describes how cardiac catheterization works. It also explains how to prepare for your procedure and the self-care needed
UW MEDICINE PATIENT EDUCATION Cardiac Catheterization Lab Procedures This handout describes how cardiac catheterization works. It also explains how to prepare for your procedure and the self-care needed
M A T E R N I T Y C A R E. Managing Pain. During Labor & Delivery
 M A T E R N I T Y C A R E Managing Pain During Labor & Delivery Managing Your Pain One of the most common concerns about labor and delivery is pain. How much will it hurt? How will I cope? At MidMichigan
M A T E R N I T Y C A R E Managing Pain During Labor & Delivery Managing Your Pain One of the most common concerns about labor and delivery is pain. How much will it hurt? How will I cope? At MidMichigan
Mesenteric Angiography
 Information for patients Mesenteric Angiography Sheffield Vascular Institute Northern General Hospital You have been given this leaflet because you need a procedure known as a Mesenteric Angiogram. This
Information for patients Mesenteric Angiography Sheffield Vascular Institute Northern General Hospital You have been given this leaflet because you need a procedure known as a Mesenteric Angiogram. This
SHOULDER INSTABILITY. E. Edward Khalfayan, MD
 SHOULDER INSTABILITY E. Edward Khalfayan, MD Instability of the shoulder can occur from a single injury or as the result of repetitive activity such as overhead sports. Dislocations of the shoulder are
SHOULDER INSTABILITY E. Edward Khalfayan, MD Instability of the shoulder can occur from a single injury or as the result of repetitive activity such as overhead sports. Dislocations of the shoulder are
You will be having surgery to remove a tumour(s) from your liver.
 Liver surgery You will be having surgery to remove a tumour(s) from your liver. This handout will help you learn about the surgery, how to prepare for surgery and your care after surgery. Surgery can be
Liver surgery You will be having surgery to remove a tumour(s) from your liver. This handout will help you learn about the surgery, how to prepare for surgery and your care after surgery. Surgery can be
PICC/Midclavicular/Midline Catheter
 47 PICC/Midclavicular/Midline Catheter Introduction- PICC/ MCV/ Midline You have a PICC/Midclavicular/Midline (peripherally inserted) catheter. This catheter should make receiving I.V. medicines or solutions
47 PICC/Midclavicular/Midline Catheter Introduction- PICC/ MCV/ Midline You have a PICC/Midclavicular/Midline (peripherally inserted) catheter. This catheter should make receiving I.V. medicines or solutions
Michael A. Boss, M.D. FMH Plastic, Reconstructive und Aesthetic Surgery
 Michael A. Boss, M.D. FMH Plastic, Reconstructive und Aesthetic Surgery Boss Aesthetic Center Schauplatzgasse 23 CH-3011 Bern Switzerland +41 31 311 7691 www.aesthetic-center.com B r e a s t A u g m e
Michael A. Boss, M.D. FMH Plastic, Reconstructive und Aesthetic Surgery Boss Aesthetic Center Schauplatzgasse 23 CH-3011 Bern Switzerland +41 31 311 7691 www.aesthetic-center.com B r e a s t A u g m e
Department of Neurosciences Dorsal Root Ganglion (DRG) Stimulation Information for patients
 Oxford University Hospitals NHS Trust Department of Neurosciences Dorsal Root Ganglion (DRG) Stimulation Information for patients We have recently seen you in clinic as you have had pain for a long period
Oxford University Hospitals NHS Trust Department of Neurosciences Dorsal Root Ganglion (DRG) Stimulation Information for patients We have recently seen you in clinic as you have had pain for a long period
LAW ANESTHESIA. the. Nerve Damage from Regional Blocks Placed In Anesthetized/Sedated Patients
 ANESTHESIA & the LAW A RISK MANAGEMENT NEWSLETTER DON T SETTLE. OWN. ISSUE 28 Nerve Damage from Regional Blocks Placed In Anesthetized/Sedated Patients W hether regional blocks should be placed in adult
ANESTHESIA & the LAW A RISK MANAGEMENT NEWSLETTER DON T SETTLE. OWN. ISSUE 28 Nerve Damage from Regional Blocks Placed In Anesthetized/Sedated Patients W hether regional blocks should be placed in adult
You have been advised by your GP or hospital doctor to have an investigation known as a Gastroscopy.
 Gastroscopy (OGD) The Procedure Explained You have been advised by your GP or hospital doctor to have an investigation known as a Gastroscopy. This procedure requires your formal consent. If you are unable
Gastroscopy (OGD) The Procedure Explained You have been advised by your GP or hospital doctor to have an investigation known as a Gastroscopy. This procedure requires your formal consent. If you are unable
Human Body Vocabulary Words Week 1
 Vocabulary Words Week 1 1. arteries Any of the blood vessels that carry blood away from the heart to all parts of the body 2. heart The muscular organ inside the chest that pumps blood through the body
Vocabulary Words Week 1 1. arteries Any of the blood vessels that carry blood away from the heart to all parts of the body 2. heart The muscular organ inside the chest that pumps blood through the body
Your Guide to Outpatient Surgery
 Your Guide to Outpatient Surgery An entire team of professionals will be involved in preparing you for your surgery. Welcome Memorial s mission is to provide you, the patient, with the highest quality
Your Guide to Outpatient Surgery An entire team of professionals will be involved in preparing you for your surgery. Welcome Memorial s mission is to provide you, the patient, with the highest quality
X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary
 X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary Introduction A Subclavian Inserted Central Catheter, or subclavian line, is a long thin hollow tube inserted in a vein under the
X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary Introduction A Subclavian Inserted Central Catheter, or subclavian line, is a long thin hollow tube inserted in a vein under the
What you Need to Know about Sleep Apnea and Surgery
 What you Need to Know about Sleep Apnea and Surgery UHN For patients with sleep apnea who are going to have surgery Read this brochure to learn: What sleep apnea is Risks of having sleep apnea when going
What you Need to Know about Sleep Apnea and Surgery UHN For patients with sleep apnea who are going to have surgery Read this brochure to learn: What sleep apnea is Risks of having sleep apnea when going
Laparoscopic Colectomy. What do I need to know about my laparoscopic colorectal surgery?
 Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
PERIACETABULAR OSTEOTOMY SURGERY
 1 PERIACETABULAR OSTEOTOMY SURGERY It is important to us that all of our patients know what to expect before surgery, during their hospitalization and after surgery. Office Visits Planning begins with
1 PERIACETABULAR OSTEOTOMY SURGERY It is important to us that all of our patients know what to expect before surgery, during their hospitalization and after surgery. Office Visits Planning begins with
