Proceeding of the NAVC North American Veterinary Conference Jan. 8-12, 2005, Orlando, Florida
|
|
|
- Charla Black
- 7 years ago
- Views:
Transcription
1 Proceeding of the NAVC North American Veterinary Conference Jan. 8-12, 2005, Orlando, Florida Reprinted in the IVIS website with the permission of the NAVC
2 The North American Veterinary Conference 2005 Proceedings CARDIAC ARRHYTHMIAS: WHAT TO TREAT, WHEN AND HOW Rebecca L. Stepien, DVM, MS, DACVIM School of Veterinary Medicine University of Wisconsin, Madison, WI THE PATIENT-ARRHYTHMIA INTERACTIONS Cardiovascular pathology and clinical situations interact to cause or aggravate arrhythmias. A frequent cause of arrhythmias is primary cardiovascular disease, but other systemic abnormalities may directly cause or contribute to the occurrence of arrhythmias. In any case, the best therapy for most arrhythmias is to eliminate the underlying cause (e.g. therapy of pulmonary edema to reduce hypoxiarelated arrhythmias). In the case of systemic disease-related arrhythmias, it is especially important to treat the disease, not necessarily the arrhythmia (e.g. hyperkalemia-related bradyarrhythmias require fluid therapy and sodium bicarbonate or calcium, not a pacemaker). The clinician can usually define the cause of arrhythmias based on history, clinical examination findings, blood tests and other routine diagnostic tests. The presence of heart disease does not always mean it is the cause of the arrhythmia, but chronic heart disease patients may have more risk factors for arrhythmia development than other patients. Systemic derangements common in chronic heart failure patients (e.g. acid/base or electrolyte disorders and alterations in renal function due to medications given for heart failure management) may make drug toxicity more likely (e.g. hypokalemia) or may lead to decreased elimination of medications and accumulations of toxic plasma drug concentrations. APPROACH TO ANTIARRHYTHMIC THERAPY Correct identification of the arrhythmia is the most important step in the process, but given the rhythm a name is just part of the puzzle. Some characteristics of arrhythmias (e.g. bradycardia vs. tachycardia, supraventricular vs. ventricular origin of ectopic complexes) lead the clinician to a specific choice of medication. Other characteristics (e.g. effect on cardiac output, probability of sudden death) help the clinician to decide if an arrhythmia is life-threatening (i.e. should be treated immedicately), symptom-aggravating (i.e. may be involved in clinical signs of other disease) or clinically unimportant (i.e. requires only monitoring). This information is used to decide if complete resolution is needed to avert death (e.g. high rate ventricular tachycardia) or control but not complete resolution is sufficient (e.g. decrease in frequency or repetitiveness of paroxysmal tachycardia or administration of anticholinergics in vagally-induced bradcardias) A final and important step in therapy of arrhythmia occurs if the therapy does not appear to be working. At this point, the diagnosis should also be reconsidered. If the diagnosis is correct, factors that limit response to medication (e.g. hypokalemia) should be investigated. On occasion, a change in the arrhythmia during therapy can lead the clinician to reconsider the original diagnosis. Choice of antiarrhythmic therapy Beyond therapy or resolution of any contributory clinical situation, antiarrhythmic therapy can include direct treatment of the arrhythmia with medical (drug) or mechanical (e.g. electrical conversion) therapy or palliative methods that control the clinical signs without attempting to address the origin of the arrhythmia directly (e.g. pacemaker implantation for 3 rd degree AVB). The clinician can choose the optimal therapy based on origin (e.g. supraventricular vs. ventricular) or proposed mechanism of the arrhythmia (e.g. reentry vs. increased automaticity). In addition, choices regarding choice of medication and route of delivery are affected by rapidity of onset of effect. THERAPY OF BRADYCARDIC ARRHYTHMIAS Sinus Bradycardia Bradycardias are heart rhythms that occur at a rate slower than the normal rate. Sinus bradycardias are frequently associated with identifiable physical causes including use of sedatives or anesthetic agents, antiarrhythmic medications (e.g. beta blockers) and medications or conditions that alter electrolyte balance. In addition, conditions that intensify vagal tone (hypothermia, deep sleep, neurologic, gastrointestinal or pulmonary diseases) may be associated with slow but normally conducted heart rhythms. These sinus bradycardias are usually self-limiting, not associated with over clinical signs of low cardiac output and resolve with removal of the underlying cause. If sinus bradycardia is associated with clinical signs of weakness or known hypotension, the heart rate (HR) can be supported with medications (e.g anticholinergics, IV catecholamines, Table 1) until diagnostics can be pursued. If the clinical importance of a bradycardic rhythm is in doubt, an atropine response test may be helpful. A baseline ECG is recorded, 0.04 mg/kg of atropine is given IM and a follow-up ECG recorded 30 minutes later. A normal response includes a HR increase of 50% with normal conduction. If this response does not occur, sinus node disease rather than high vagal tone may be suspected as the cause of bradycardia. Sinus Arrest, Bradycardia/Tachycardia Syndromes (Sick Sinus Syndrome) Periods of sinus arrest without development of an escape rhythm for greater than approximately 3-5 seconds lead to neurologic signs (e.g. staggering, syncope) in dogs with sick sinus syndrome. The sinus arrest seldom leads to sudden death, but frequency of events may severely affect quality of life. Short-term therapy is the same as that for sinus bradycardia, but immediate pacing may be required if nonresponsive to anticholinergics or if the animal is severely symptomatic. Although theophylline or terbutaline therapy are frequently recommended for management of this disease, therapy with these drugs alone is usually not effective. In the long term, sinus arrest and bradycardia/tachycardia syndromes are most effectively treated with pacemaker implantation. Atrial Standstill (Atrial Asystole) Atrial standstill (asystole) may be associated primary disease of the atrial muscle (atrial myopathies) or occur more commonly secondary to hyperkalemia. The atrial myopathyrelated atrial standstill is treated with pacemaker implantation if the rhythm is bradycardic. Hyperkalemia at a concentration high enough to lead to atrial standstill is an emergency. Immediate therapy includes anticholinergics, IV saline and IV calcium administration along with definitive therapy to reduce potassium concentrations (sodium bicarbonate, insulin etc.). A rare cause of atrial standstill is toxic concentrations of digoxin; these cases respond to therapy for digoxin toxicity. 140
3 Small Animal - Cardiology Bizarre escape rhythms associated with atrial standstill should not be mistaken for ventricular tachycardia; suppression of these life-sustaining rhythms may be lethal. Atrioventricular Blocks (AVB) The most common cause of 1 st or 2 nd degree AVB is high vagal tone or use of vagomimetic drugs (e.g. digoxin). In these cases, the underlying cause should be treated, rather than the AV block. If second degree AV block is symptomatic and does not respond to anticholinergics, pacing may be required. Symptomatic high grade 2 nd degree AVB (long strings of P waves without any QRS complexes) require immediate pacing. Third degree AVB usually reflects primary nodal disease and anticholinergics are typically ineffective. Immediate therapy is warranted because 3 rd degree AVB can lead to sudden death if the escape focus fails. If the patient is symptomatic, IV catecholamines may induce subsidiary pacemaker activity in the short term but immediate temporary or permanent pacemaker implantation is recommended. Therapy of Tachyarrhythmias (Table 1) The clinical importance of an arrhythmia is partly related to origin of abnormal rhythm. Supraventricular arrhythmias (narrow QRS with or without P waves) tend to carry a low risk of sudden death but the risk of clinical signs is high, especially with very high HR. Ventricular arrhythmias (wide QRS without associated P waves) carry a variable risk of sudden death and the clinical signs seen are likewise variable, often depending on the HR. When treating any tachyarrhythmia, the correct dose should be administered (use of lower doses may have no effect). The overall clinical situation should be monitored closely and continue to be monitored after the drug has had its desired effect. In any situation, if the diagnosis is in doubt, consider faxing the ECG to a specialist for help the diagnosis and advice on therapy. Figure 1: Atrial standstill due to severe hyperkalemia Table 1: Medications Commonly Used in the Therapy of Arrhythmias (2004)* Parasympatholytics: Atropine: (D,C) mg/kg IV, IM, SC Glycopyrrolate: (D,C) mg/kg IV,IM,SC Sympathomimetics: Dobutamine: (D) 2-15 mcg/kg/min (start low and titrate up) Dopamine: (D) 2-10 mcg/kg/min (start low and titrate up) Epinephrine: (D) 5 mcg/kg IV, mcg/kg/min (start low and titrate up) Isoproterenol: (D) Dilute 1 mg in 500 cc of 5% dextrose or Ringer s, infuse IV at ml/min (1-2 ug/min) or to effect Antiarrhythmics: Amiodarone: Atenolol: Diltiazem Esmolol: Lidocaine: Mexiletine: Procainamide: Propranolol: Sotalol: Verapamil: (D) mg/kg q 12 hr (D) mg q hr, start low/titrate, (C) mg q hr (NOT sustained release): (D): mg/kg PO q 8 hr, 0.25 mg/kg IV (over 3 min), (C): mg/kg PO q 8hr (D/C) 0.5 mg/kg IV bolus, mcg/kg/min (D) 2-4 mg/kg IV bolus, mcg/kg/min, (C) mg/kg IV slow bolus (D) 5-8 mg/kg q 8 hr (D) 5-15 mg/kg IV, IM q 6 hr, mg/kg PO q 6 hr, mcg/kg/min (D) mg/kg PO q 8 hr, start low/titrate, mg/kg IV slowly, (C) mg total dose q 8 hrs, start low/titrate (D,C) 1-2 mg/kg PO q 12 hr (D/C) 0.05 mg/kg q 30 min up to 0.15 to 0.5 mg/kg total *The most recent editions of Current Veterinary Therapy (X, XI, XII) are recommended as references for drug doses and additional medical information. These doses are suggestions only and any medical therapy must be tailored to the patient based on the clinician s judgement. 141
4 The North American Veterinary Conference 2005 Proceedings SUPRAVENTRICULAR TACHYARRHYTHMIAS Sinus Tachycardia Sinus tachycardia is almost always the result of clinical derangements not related to primary cardiac disease. The underlying situation commonly involved hypotension, but pain may also contribute. The underlying disease should be treated; sinus tachycardia is not a fatal arrhythmia and usually resolves without direct therapy. Atrial Premature Complexes, Atrial Tachycardia (AT), Supraventricular Tachycardia (SVT) Single atrial ectopic depolarizations (APCs) may not require therapy if they occur at low frequency, are not related to CHF or known structural heart disease and are not associated with clinical signs. They often resolve with systemic problem resolution. Supraventricular tachycardia or atrial tachycardia often occurs at extremely rapid HR (~400 bpm in dog) and may severely decrease cardiac output. A vagal maneuver (ocular pressure or carotid sinus stimulation) may abruptly abolish the tachycardia, but recurrence is common if no other method is used. The first choice in medical therapy of AT or SVT is IV beta-blockers (BB, esmolol or propranolol) or calcium channel blockers (CCB, diltiazem or verapamil). These medications may be given orally if no IV access is available. Chronic medical therapy of frequent APCs, SVT or AT usually consists of BB or CCB (do not combine) if no definable underlying disease is present, or digoxin plus BB OR CCB (one or the other) if cardiac disease present. Atrial Fibrillation (AF) If spontaneous AF is diagnosed, underlying heart disease is usually present. A new diagnosis of AF may be the cause of sudden decompensation in a previously stable CHF patient. The therapeutic goal is control of the ventricular response to AF. Acute decreases in HR are recommended if ventricular rate is > 180 bpm (dogs) or > 200 bpm (cats). The most rapid and effective therapy presently used is IV diltiazem. Oral diltiazem or BB can be used if IV is not available. BB may lead to acute worsening of CHF and should be use with caution in patients without CHF and should not be used when overt CHF is present. Oral digoxin therapy can be started concurrently with either BB or CCB. The chronic therapy of AF is the same as that used for SVT. In severe heart failure, the patient may be dependent on an elevated HR to support cardiac output; antiarrhythmic drugs used to slow the ventricular response rate to atrial fibrillation are often titrated to the desired clinical effect. A typical acceptable HR in AF is bpm (dogs) or bpm (cats). Table 2: Differentiation of accelerated idioventricular rhythm vs. ventricular tachycardia. Ventricular Tachycardia Accelerated Idioventricular Rhythm Depolarization Rate Usually > 160 bpm Usually < 160 bpm First abnormal complex Premature (early diastolic) Late diastolic Relationship to sinus rhythm Significantly faster Within ~ 5-10 bpm Associated with pulse deficits Yes Usually no Figure 2: Ventricular tachycardia in a dog Figure 3: Accelerated idioventricular tachycardia in a dog 142
5 Small Animal - Cardiology VENTRICULAR ARRHYTHMIAS: Accelerated Idioventricular Rhythms (AIR) Accelerated idioventricular rhythms (alternative terms: fast idioventricular rhythm slow ventricular tachycardia or idioventricular tachycardia ) are very common in canine critical care patients, and are commonly confused with ventricular tachycardia. Misdiagnosis may lead to administration of toxic doses of antiarrhythmic medication in an unsuccessful attempt to convert VT. Because AIR is frequently noted as a complication of severe systemic illness and is usually not associated with evidence of impaired cardiac performance, therapy is aimed at the underlying problem. Hydration, oxygenation, electrolyte and acid-base abnormalities should be rectified and specific therapy for the underlying disease instituted. Pain should be assessed and managed appropriately. No direct antiarrhythmic therapy is indicated if ALL of the following criteria apply: If HR and blood pressure are within normal ranges and stable If no clinical signs are apparent If no other ventricular ectopics interrupt AIR Direct antiarrhythmic therapy (as for VT) may be indicated if ANY of the following occur: HR > bpm If hypotension or unstable blood pressure If premature ventricular ectopics initiate or interrupt AIR, or if R wave of ectopic occurs on the T waves of the previous depolarization ( R-on-T ) Clinical signs of poor cardiac output present VENTRICULAR PREMATURE COMPLEXES (VPCS) OR VENTRICULAR TACHYCARDIA (VT) The decision to treat ventricular arrhythmias depend on the arrhythmia s effect on cardiac output and electrical instability of the arrhythmia. Ventricular arrhythmias significantly decrease cardiac output if they occur concurrently with CHF, in the setting of severe myocardial dysfunction or if the arrhythmia is highly repetitive or provides large proportion of total HR. Ventricular arrhythmias may be electrical unstable (and lead to sudden death) if the ventricular ectopics occur at such a high HR that the ectopic falls on the T wave of the previous sinus complex ( R on T ). If cardiac output is compromised or electrical instability is suspected, therapy is warranted. The cornerstone of acute therapy of ventricular arrhythmias remains IV lidocaine. If lidocaine is unsuccessful or contraindicated, IV procainamide or BB may be used. Be sure to administer significant doses of the medication before diagnosing lack of response. If lidocaine is administered as a bolus and is effective, a continuous rate infusion (CRI) should be started immediately. Intermittent boluses of lidocaine may be needed until CRI reaches therapeutic blood levels. When the patient is stable and can tolerate oral medications, these drugs can be started while the CRI is still running. Once oral medications are started, the rate of the CRI can be decreased by 50% every 6 hours. In cats, lidocaine can be used but with great caution. IV or oral BB may be a better choice in cats that are not critically unstable. Choices for therapy of chronic therapy of ventricular arrhythmias include oral drugs such as sotalol (class II [betablocker] and Class III [K channel blocker] effects) and mexiletine (class I effects, similar to lidocaine). Sotalol is very effective and usually well-tolerated, but should be used with caution with patients with heart failure or that are hypotensive. Mexiletine is effective against many ventricular arrhythmias, especially in short term, and may be combined with oral BB (e.g. atenolol) for added efficacy. Amiodarone is used less frequently to treat ventricular arrhythmias; amiodarone is highly effective against resistant arrhythmias but more worrisome toxicity profile than the other medications suggested. 143
ACLS PHARMACOLOGY 2011 Guidelines
 ACLS PHARMACOLOGY 2011 Guidelines ADENOSINE Narrow complex tachycardias or wide complex tachycardias that may be supraventricular in nature. It is effective in treating 90% of the reentry arrhythmias.
ACLS PHARMACOLOGY 2011 Guidelines ADENOSINE Narrow complex tachycardias or wide complex tachycardias that may be supraventricular in nature. It is effective in treating 90% of the reentry arrhythmias.
ANNE ARUNDEL MEDICAL CENTER CRITICAL CARE MEDICATION MANUAL DEPARTMENT OF NURSING AND PHARMACY. Guidelines for Use of Intravenous Isoproterenol
 ANNE ARUNDEL MEDICAL CENTER CRITICAL CARE MEDICATION MANUAL DEPARTMENT OF NURSING AND PHARMACY Guidelines for Use of Intravenous Isoproterenol Major Indications Status Asthmaticus As a last resort for
ANNE ARUNDEL MEDICAL CENTER CRITICAL CARE MEDICATION MANUAL DEPARTMENT OF NURSING AND PHARMACY Guidelines for Use of Intravenous Isoproterenol Major Indications Status Asthmaticus As a last resort for
Atrial & Junctional Dysrhythmias
 Atrial & Junctional Dysrhythmias Atrial & Junctional Dysrhythmias Atrial Premature Atrial Complex Wandering Atrial Pacemaker Atrial Tachycardia (ectopic) Multifocal Atrial Tachycardia Atrial Flutter Atrial
Atrial & Junctional Dysrhythmias Atrial & Junctional Dysrhythmias Atrial Premature Atrial Complex Wandering Atrial Pacemaker Atrial Tachycardia (ectopic) Multifocal Atrial Tachycardia Atrial Flutter Atrial
TOP 5. The term cardiac arrhythmia encompasses all cardiac. Arrhythmias in Dogs & Cats. Sinus Arrhythmia. TOP 5 Arrhythmias Seen in Dogs & Cats
 Top 5 ardiology Peer reviewed TOP 5 rrhythmias in Dogs & ats shley Jones, DVM mara Estrada, DVM, DVIM (ardiology) University of Florida The term cardiac arrhythmia encompasses all cardiac rhythms other
Top 5 ardiology Peer reviewed TOP 5 rrhythmias in Dogs & ats shley Jones, DVM mara Estrada, DVM, DVIM (ardiology) University of Florida The term cardiac arrhythmia encompasses all cardiac rhythms other
Crash Cart Drugs Drugs used in CPR. Dr. Layla Borham Professor of Clinical Pharmacology Umm Al Qura University
 Crash Cart Drugs Drugs used in CPR Dr. Layla Borham Professor of Clinical Pharmacology Umm Al Qura University Introduction A list of the drugs kept in the crash carts. This list has been approved by the
Crash Cart Drugs Drugs used in CPR Dr. Layla Borham Professor of Clinical Pharmacology Umm Al Qura University Introduction A list of the drugs kept in the crash carts. This list has been approved by the
Cardiac Arrest VF/Pulseless VT Learning Station Checklist
 Cardiac Arrest VF/Pulseless VT Learning Station Checklist VF/VT 00 American Heart Association Adult Cardiac Arrest Shout for Help/Activate Emergency Response Epinephrine every - min Amiodarone Start CPR
Cardiac Arrest VF/Pulseless VT Learning Station Checklist VF/VT 00 American Heart Association Adult Cardiac Arrest Shout for Help/Activate Emergency Response Epinephrine every - min Amiodarone Start CPR
ACLS Cardiac Arrest Algorithm Neumar, R. W. et al. Circulation 2010;122:S729-S767
 ACLS Cardiac Arrest Algorithm Neumar, R. W. et al. Circulation 2010;122:S729-S767 Copyright 2010 American Heart Association ACLS Cardiac Arrest Circular Algorithm Neumar, R. W. et al. Circulation 2010;122:S729-S767
ACLS Cardiac Arrest Algorithm Neumar, R. W. et al. Circulation 2010;122:S729-S767 Copyright 2010 American Heart Association ACLS Cardiac Arrest Circular Algorithm Neumar, R. W. et al. Circulation 2010;122:S729-S767
GUIDELINE 11.9 MANAGING ACUTE DYSRHYTHMIAS. (To be read in conjunction with Guideline 11.7 Post-Resuscitation Therapy in Adult Advanced Life Support)
 AUSTRALIAN RESUSCITATION COUNCIL GUIDELINE 11.9 MANAGING ACUTE DYSRHYTHMIAS (To be read in conjunction with Guideline 11.7 Post-Resuscitation Therapy in Adult Advanced Life Support) The term cardiac arrhythmia
AUSTRALIAN RESUSCITATION COUNCIL GUIDELINE 11.9 MANAGING ACUTE DYSRHYTHMIAS (To be read in conjunction with Guideline 11.7 Post-Resuscitation Therapy in Adult Advanced Life Support) The term cardiac arrhythmia
8 Peri-arrest arrhythmias
 8 Peri-arrest arrhythmias Introduction Cardiac arrhythmias are relatively common in the peri-arrest period. They are common in the setting of acute myocardial infarction and may precipitate ventricular
8 Peri-arrest arrhythmias Introduction Cardiac arrhythmias are relatively common in the peri-arrest period. They are common in the setting of acute myocardial infarction and may precipitate ventricular
HTEC 91. Topic for Today: Atrial Rhythms. NSR with PAC. Nonconducted PAC. Nonconducted PAC. Premature Atrial Contractions (PACs)
 HTEC 91 Medical Office Diagnostic Tests Week 4 Topic for Today: Atrial Rhythms PACs: Premature Atrial Contractions PAT: Paroxysmal Atrial Tachycardia AF: Atrial Fibrillation Atrial Flutter Premature Atrial
HTEC 91 Medical Office Diagnostic Tests Week 4 Topic for Today: Atrial Rhythms PACs: Premature Atrial Contractions PAT: Paroxysmal Atrial Tachycardia AF: Atrial Fibrillation Atrial Flutter Premature Atrial
Medical management of CHF: A New Class of Medication. Al Timothy, M.D. Cardiovascular Institute of the South
 Medical management of CHF: A New Class of Medication Al Timothy, M.D. Cardiovascular Institute of the South Disclosures Speakers Bureau for Amgen Background Chronic systolic congestive heart failure remains
Medical management of CHF: A New Class of Medication Al Timothy, M.D. Cardiovascular Institute of the South Disclosures Speakers Bureau for Amgen Background Chronic systolic congestive heart failure remains
PRO-CPR. 2015 Guidelines: PALS Algorithm Overview. (Non-AHA supplementary precourse material)
 PRO-CPR 2015 Guidelines: PALS Algorithm Overview (Non-AHA supplementary precourse material) Please reference Circulation (from our website), the ECC Handbook, or the 2015 ACLS Course Manual for correct
PRO-CPR 2015 Guidelines: PALS Algorithm Overview (Non-AHA supplementary precourse material) Please reference Circulation (from our website), the ECC Handbook, or the 2015 ACLS Course Manual for correct
MEDICATIONS USED IN ADULT CODE BLUE EMERGENCIES. Source: ACLS Provider Manual. American Heart Association. 2001, 2002. Updated 2003.
 MEDICATIONS USED IN ADULT CODE BLUE EMERGENCIES Source: ACLS Provider Manual. American Heart Association. 2001, 2002. Updated 2003. 1 ET Administration Atropine o First drug for symptomatic sinus bradycardia
MEDICATIONS USED IN ADULT CODE BLUE EMERGENCIES Source: ACLS Provider Manual. American Heart Association. 2001, 2002. Updated 2003. 1 ET Administration Atropine o First drug for symptomatic sinus bradycardia
Recurrent AF: Choosing the Right Medication.
 In the name of God Shiraz E-Medical Journal Vol. 11, No. 3, July 2010 http://semj.sums.ac.ir/vol11/jul2010/89015.htm Recurrent AF: Choosing the Right Medication. Basamad Z. * Assistant Professor, Department
In the name of God Shiraz E-Medical Journal Vol. 11, No. 3, July 2010 http://semj.sums.ac.ir/vol11/jul2010/89015.htm Recurrent AF: Choosing the Right Medication. Basamad Z. * Assistant Professor, Department
Normal Sinus Rhythm. Sinus Bradycardia. Sinus Tachycardia. Rhythm ECG Characteristics Example (NSR) & consistent. & consistent.
 Normal Sinus Rhythm (NSR) Rate: 60-100 per minute Rhythm: R- R = P waves: Upright, similar P-R: 0.12-0.20 second & consistent P:qRs: 1P:1qRs Sinus Tachycardia Exercise Hypovolemia Medications Fever Hypoxia
Normal Sinus Rhythm (NSR) Rate: 60-100 per minute Rhythm: R- R = P waves: Upright, similar P-R: 0.12-0.20 second & consistent P:qRs: 1P:1qRs Sinus Tachycardia Exercise Hypovolemia Medications Fever Hypoxia
Atrial Fibrillation Management Across the Spectrum of Illness
 Disclosures Atrial Fibrillation Management Across the Spectrum of Illness NONE Barbara Birriel, MSN, ACNP-BC, FCCM The Pennsylvania State University Objectives AF Discuss the pathophysiology, diagnosis,
Disclosures Atrial Fibrillation Management Across the Spectrum of Illness NONE Barbara Birriel, MSN, ACNP-BC, FCCM The Pennsylvania State University Objectives AF Discuss the pathophysiology, diagnosis,
Tachyarrhythmias (fast heart rhythms)
 Patient information factsheet Tachyarrhythmias (fast heart rhythms) The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
Patient information factsheet Tachyarrhythmias (fast heart rhythms) The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
Equine Cardiovascular Disease
 Equine Cardiovascular Disease 3 rd most common cause of poor performance in athletic horses (after musculoskeletal and respiratory) Cardiac abnormalities are rare Clinical Signs: Poor performance/exercise
Equine Cardiovascular Disease 3 rd most common cause of poor performance in athletic horses (after musculoskeletal and respiratory) Cardiac abnormalities are rare Clinical Signs: Poor performance/exercise
Official Online ACLS Exam
 \ Official Online ACLS Exam Please fill out this form before you take the exam. Name : Email : Phone : 1. Hypovolemia initially produces which arrhythmia? A. PEA B. Sinus tachycardia C. Symptomatic bradyarrhythmia
\ Official Online ACLS Exam Please fill out this form before you take the exam. Name : Email : Phone : 1. Hypovolemia initially produces which arrhythmia? A. PEA B. Sinus tachycardia C. Symptomatic bradyarrhythmia
Presenter Disclosure Information
 2:15 3 pm Managing Arrhythmias in Primary Care Presenter Disclosure Information The following relationships exist related to this presentation: Raul Mitrani, MD, FACC, FHRS: Speakers Bureau for Medtronic.
2:15 3 pm Managing Arrhythmias in Primary Care Presenter Disclosure Information The following relationships exist related to this presentation: Raul Mitrani, MD, FACC, FHRS: Speakers Bureau for Medtronic.
The Emerging Atrial Fibrillation Epidemic: Treat It, Leave It or Burn It?
 The Emerging Atrial Fibrillation Epidemic: Treat It, Leave It or Burn It? Indiana Chapter-ACC 17 th Annual Meeting Indianapolis, Indiana October 19, 2013 Deepak Bhakta MD FACC FACP FAHA FHRS CCDS Associate
The Emerging Atrial Fibrillation Epidemic: Treat It, Leave It or Burn It? Indiana Chapter-ACC 17 th Annual Meeting Indianapolis, Indiana October 19, 2013 Deepak Bhakta MD FACC FACP FAHA FHRS CCDS Associate
ACLS PRE-TEST ANNOTATED ANSWER KEY
 ACLS PRE-TEST ANNOTATED ANSWER KEY June, 2011 Question 1: Question 2: There is no pulse with this rhythm. Question 3: Question 4: Question 5: Question 6: Question 7: Question 8: Question 9: Question 10:
ACLS PRE-TEST ANNOTATED ANSWER KEY June, 2011 Question 1: Question 2: There is no pulse with this rhythm. Question 3: Question 4: Question 5: Question 6: Question 7: Question 8: Question 9: Question 10:
Present : PGY 王 淳 峻 Supervisor: F1 王 德 皓 991109
 Present : PGY 王 淳 峻 Supervisor: F1 王 德 皓 991109 Interventions to prevent cardiac arrest + Airway management + Ventilation support + Treatment of bradyarrhythmias & Tachyarrhythmias Treat cardiac arrest
Present : PGY 王 淳 峻 Supervisor: F1 王 德 皓 991109 Interventions to prevent cardiac arrest + Airway management + Ventilation support + Treatment of bradyarrhythmias & Tachyarrhythmias Treat cardiac arrest
Bradycardia CHAPTER 12 CODE SCENARIO
 Senecal-12.qxd 14/04/2005 09:44 AM Page 69 CHAPTER 12 Bradycardia CODE SCENARIO A code is called for a 78-year-old man who was admitted to the hospital for syncope of unknown etiology. He was resting comfortably
Senecal-12.qxd 14/04/2005 09:44 AM Page 69 CHAPTER 12 Bradycardia CODE SCENARIO A code is called for a 78-year-old man who was admitted to the hospital for syncope of unknown etiology. He was resting comfortably
COVERAGE GUIDANCE: ABLATION FOR ATRIAL FIBRILLATION
 COVERAGE GUIDANCE: ABLATION FOR ATRIAL FIBRILLATION Question: How should the EGBS Coverage Guidance regarding ablation for atrial fibrillation be applied to the Prioritized List? Question source: Evidence
COVERAGE GUIDANCE: ABLATION FOR ATRIAL FIBRILLATION Question: How should the EGBS Coverage Guidance regarding ablation for atrial fibrillation be applied to the Prioritized List? Question source: Evidence
Novartis Gilenya FDO Program Clinical Protocol and Highlights from Prescribing Information (PI)
 Novartis Gilenya FDO Program Clinical Protocol and Highlights from Prescribing Information (PI) Highlights from Prescribing Information - the link to the full text PI is as follows: http://www.pharma.us.novartis.com/product/pi/pdf/gilenya.pdf
Novartis Gilenya FDO Program Clinical Protocol and Highlights from Prescribing Information (PI) Highlights from Prescribing Information - the link to the full text PI is as follows: http://www.pharma.us.novartis.com/product/pi/pdf/gilenya.pdf
PRACTICAL APPROACH TO SVT. Graham C. Wong MD MPH Division of Cardiology Vancouver General Hospital University of British Columbia
 PRACTICAL APPROACH TO SVT Graham C. Wong MD MPH Division of Cardiology Vancouver General Hospital University of British Columbia CONDUCTION SYSTEM OF THE HEART SA node His bundle Left bundle AV node Right
PRACTICAL APPROACH TO SVT Graham C. Wong MD MPH Division of Cardiology Vancouver General Hospital University of British Columbia CONDUCTION SYSTEM OF THE HEART SA node His bundle Left bundle AV node Right
Guideline for the management of arrhythmias
 Guideline for the management of arrhythmias The following guideline is approved only for use at University College London Hospitals NHS Foundation Trust. It is provided as supporting information for the
Guideline for the management of arrhythmias The following guideline is approved only for use at University College London Hospitals NHS Foundation Trust. It is provided as supporting information for the
Adult Drug Reference. Dopamine Drip Chart. Pediatric Drug Reference. Pediatric Drug Dosage Charts DRUG REFERENCES
 Adult Drug Reference Dopamine Drip Chart Pediatric Drug Reference Pediatric Drug Dosage Charts DRUG REFERENCES ADULT DRUG REFERENCE Drug Indication Adult Dosage Precautions / Comments ADENOSINE Paroxysmal
Adult Drug Reference Dopamine Drip Chart Pediatric Drug Reference Pediatric Drug Dosage Charts DRUG REFERENCES ADULT DRUG REFERENCE Drug Indication Adult Dosage Precautions / Comments ADENOSINE Paroxysmal
ACLS RHYTHM TEST. 2. A 74-year-old woman with chest pain. Blood pressure 192/90 and rates her pain 9/10.
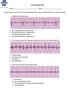 ACLS RHYTHM TEST Name Date Choose the best answer for each of the following questions. Each of the following strips is 6 seconds in length. 1. Identify the following rhythm a. Sinus bradycardia with 2
ACLS RHYTHM TEST Name Date Choose the best answer for each of the following questions. Each of the following strips is 6 seconds in length. 1. Identify the following rhythm a. Sinus bradycardia with 2
ATRIAL FIBRILLATION (RATE VS RHYTHM CONTROL)
 ATRIAL FIBRILLATION (RATE VS RHYTHM CONTROL) By Prof. Dr. Helmy A. Bakr Mansoura Universirty 2014 AF Classification: Mechanisms of AF : Selected Risk Factors and Biomarkers for AF: WHY AF? 1. Atrial fibrillation
ATRIAL FIBRILLATION (RATE VS RHYTHM CONTROL) By Prof. Dr. Helmy A. Bakr Mansoura Universirty 2014 AF Classification: Mechanisms of AF : Selected Risk Factors and Biomarkers for AF: WHY AF? 1. Atrial fibrillation
ACCIDENT AND EMERGENCY DEPARTMENT/CARDIOLOGY
 Care Pathway Triage category ATRIAL FIBRILLATION PATHWAY ACCIDENT AND EMERGENCY DEPARTMENT/CARDIOLOGY AF/ FLUTTER IS PRIMARY REASON FOR PRESENTATION YES NO ONSET SYMPTOMS OF AF./../ TIME DURATION OF AF
Care Pathway Triage category ATRIAL FIBRILLATION PATHWAY ACCIDENT AND EMERGENCY DEPARTMENT/CARDIOLOGY AF/ FLUTTER IS PRIMARY REASON FOR PRESENTATION YES NO ONSET SYMPTOMS OF AF./../ TIME DURATION OF AF
Current Management of Atrial Fibrillation DISCLOSURES. Heart Beat Anatomy. I have no financial conflicts to disclose
 Current Management of Atrial Fibrillation Mary Macklin, MSN, APRN Concord Hospital Cardiac Associates DISCLOSURES I have no financial conflicts to disclose Book Women: Fit at Fifty. A Guide to Living Long.
Current Management of Atrial Fibrillation Mary Macklin, MSN, APRN Concord Hospital Cardiac Associates DISCLOSURES I have no financial conflicts to disclose Book Women: Fit at Fifty. A Guide to Living Long.
table of contents drug reference
 table of contents drug reference ADULT DRUG REFERENCE...155 161 PEDIATRIC DRUG REFERENCE...162 164 PEDIATRIC WEIGHT-BASED DOSING CHARTS...165 180 Adenosine...165 Amiodarone...166 Atropine...167 Defibrillation...168
table of contents drug reference ADULT DRUG REFERENCE...155 161 PEDIATRIC DRUG REFERENCE...162 164 PEDIATRIC WEIGHT-BASED DOSING CHARTS...165 180 Adenosine...165 Amiodarone...166 Atropine...167 Defibrillation...168
Atrial Fibrillation Peter Santucci, MD Revised May, 2008
 Atrial Fibrillation Peter Santucci, MD Revised May, 2008 Atrial fibrillation (AF) is an irregular, disorganized rhythm characterized by a lack of organized mechanical atrial activity. The atrial rate is
Atrial Fibrillation Peter Santucci, MD Revised May, 2008 Atrial fibrillation (AF) is an irregular, disorganized rhythm characterized by a lack of organized mechanical atrial activity. The atrial rate is
Cardiac Arrest Pediatric Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008
 Cardiac Arrest Pediatric Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008 Preamble In contrast to cardiac arrest in adults, cardiopulmonary arrest in pediatric
Cardiac Arrest Pediatric Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008 Preamble In contrast to cardiac arrest in adults, cardiopulmonary arrest in pediatric
Atrial Fibrillation in the ICU: Attempting to defend 4 controversial statements
 Atrial Fibrillation in the ICU: Attempting to defend 4 controversial statements Salmaan Kanji, Pharm.D. The Ottawa Hospital The Ottawa Hospital Research Institute Conflict of Interest No financial, proprietary
Atrial Fibrillation in the ICU: Attempting to defend 4 controversial statements Salmaan Kanji, Pharm.D. The Ottawa Hospital The Ottawa Hospital Research Institute Conflict of Interest No financial, proprietary
Update on Small Animal Cardiopulmonary Resuscitation (CPR)- is anything new?
 Update on Small Animal Cardiopulmonary Resuscitation (CPR)- is anything new? DVM, DACVA Objective: Update on the new Small animal guidelines for CPR and a discussion of the 2012 Reassessment Campaign on
Update on Small Animal Cardiopulmonary Resuscitation (CPR)- is anything new? DVM, DACVA Objective: Update on the new Small animal guidelines for CPR and a discussion of the 2012 Reassessment Campaign on
American Heart Association ACLS Pre-Course Self Assessment Dec., 2006. ECG Analysis. Name the following rhythms from the list below:
 American Heart Association ACLS Pre-Course Self Assessment Dec., 2006 ECG Analysis This pre-test is exactly the same as the pretest on the ACLS Provider manual CD. This paper version can be completed in
American Heart Association ACLS Pre-Course Self Assessment Dec., 2006 ECG Analysis This pre-test is exactly the same as the pretest on the ACLS Provider manual CD. This paper version can be completed in
Ngaire has Palpitations
 Ngaire has Palpitations David Heaven Cardiac Electrophysiologist/Heart Rhythm Specialist Middlemore, Auckland City and Mercy Hospitals Auckland Heart Group MCQ Ms A is 45, and a healthy marathon runner.
Ngaire has Palpitations David Heaven Cardiac Electrophysiologist/Heart Rhythm Specialist Middlemore, Auckland City and Mercy Hospitals Auckland Heart Group MCQ Ms A is 45, and a healthy marathon runner.
Electrolyte Physiology. Something in the way she moves
 Electrolyte Physiology Something in the way she moves me Electrolyte Movement CONCENTRATION GRADIENT ELECTRICAL GRADIENT DRIVING FORCE NERNST NUMBER (E-ion) CONDUCTANCE (G-ion) PERMEABILITY CHANNELS: small
Electrolyte Physiology Something in the way she moves me Electrolyte Movement CONCENTRATION GRADIENT ELECTRICAL GRADIENT DRIVING FORCE NERNST NUMBER (E-ion) CONDUCTANCE (G-ion) PERMEABILITY CHANNELS: small
Diagnosis Code Crosswalk : ICD-9-CM to ICD-10-CM Cardiac Rhythm and Heart Failure Diagnoses
 Diagnosis Code Crosswalk : to 402.01 Hypertensive heart disease, malignant, with heart failure 402.11 Hypertensive heart disease, benign, with heart failure 402.91 Hypertensive heart disease, unspecified,
Diagnosis Code Crosswalk : to 402.01 Hypertensive heart disease, malignant, with heart failure 402.11 Hypertensive heart disease, benign, with heart failure 402.91 Hypertensive heart disease, unspecified,
ACLS Study Guide BLS Overview CAB
 ACLS Study Guide The ACLS Provider exam is 50-mutiple choice questions. Passing score is 84%. Student may miss 8 questions. For students taking ACLS for the first time or renewing students with a current
ACLS Study Guide The ACLS Provider exam is 50-mutiple choice questions. Passing score is 84%. Student may miss 8 questions. For students taking ACLS for the first time or renewing students with a current
Atrial Fibrillation An update on diagnosis and management
 Dr Arvind Vasudeva Consultant Cardiologist Atrial Fibrillation An update on diagnosis and management Atrial fibrillation (AF) remains the commonest disturbance of cardiac rhythm seen in clinical practice.
Dr Arvind Vasudeva Consultant Cardiologist Atrial Fibrillation An update on diagnosis and management Atrial fibrillation (AF) remains the commonest disturbance of cardiac rhythm seen in clinical practice.
Treating AF: The Newest Recommendations. CardioCase presentation. Ethel s Case. Wayne Warnica, MD, FACC, FACP, FRCPC
 Treating AF: The Newest Recommendations Wayne Warnica, MD, FACC, FACP, FRCPC CardioCase presentation Ethel s Case Ethel, 73, presents with rapid heart beating and mild chest discomfort. In the ED, ECG
Treating AF: The Newest Recommendations Wayne Warnica, MD, FACC, FACP, FRCPC CardioCase presentation Ethel s Case Ethel, 73, presents with rapid heart beating and mild chest discomfort. In the ED, ECG
NAME OF THE HOSPITAL: 1. Coronary Balloon Angioplasty: M7F1.1/ Angioplasty with Stent(PTCA with Stent): M7F1.3
 1. Coronary Balloon Angioplasty: M7F1.1/ Angioplasty with Stent(PTCA with Stent): M7F1.3 1. Name of the Procedure: Coronary Balloon Angioplasty 2. Select the Indication from the drop down of various indications
1. Coronary Balloon Angioplasty: M7F1.1/ Angioplasty with Stent(PTCA with Stent): M7F1.3 1. Name of the Procedure: Coronary Balloon Angioplasty 2. Select the Indication from the drop down of various indications
Paramedic Pediatric Medical Math Test
 Paramedic Pediatric Medical Math Test Name: Date: Problem 1 Your 4 year old pediatric patient weighs 40 pounds. She is febrile. You need to administer acetaminophen (Tylenol) 15mg/kg. How many mg will
Paramedic Pediatric Medical Math Test Name: Date: Problem 1 Your 4 year old pediatric patient weighs 40 pounds. She is febrile. You need to administer acetaminophen (Tylenol) 15mg/kg. How many mg will
Cardiac Arrest - Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008
 Cardiac Arrest - Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008 Preamble Survival from cardiorespiratory arrest for patients who present with ventricular fibrillation
Cardiac Arrest - Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008 Preamble Survival from cardiorespiratory arrest for patients who present with ventricular fibrillation
Community Ambulance Service of Minot ALS Standing Orders Legend
 Legend Indicates General Information and Guidelines Indicates Procedures Indicates Medication Administration Indicates Referral to Other Protocol Indicates Referral to Online Medical Direction Pediatric
Legend Indicates General Information and Guidelines Indicates Procedures Indicates Medication Administration Indicates Referral to Other Protocol Indicates Referral to Online Medical Direction Pediatric
Assessment, diagnosis and specialist referral of adults (>16 years) with an episode of transient loss of consciousness (TLoC) or a blackout.
 Assessment, diagnosis and specialist referral of adults (>16 years) with an episode of transient loss of consciousness (TLoC) or a blackout. TLoC is common huge variation in management range of clinicians
Assessment, diagnosis and specialist referral of adults (>16 years) with an episode of transient loss of consciousness (TLoC) or a blackout. TLoC is common huge variation in management range of clinicians
If you do not wish to print the entire pre-test you may print Page 2 only to write your answers, score your test, and turn in to your instructor.
 This is a SAMPLE of the pretest you can access with your AHA PALS Course Manual at Heart.org/Eccstudent using your personal code that comes with your PALS Course Manual The American Heart Association strongly
This is a SAMPLE of the pretest you can access with your AHA PALS Course Manual at Heart.org/Eccstudent using your personal code that comes with your PALS Course Manual The American Heart Association strongly
Palpitations & AF. Richard Grocott Mason Consultant Cardiologist THH NHS Foundation Trust & Royal Brompton & Harefield NHS Foundation Trust
 Palpitations & AF Richard Grocott Mason Consultant Cardiologist THH NHS Foundation Trust & Royal Brompton & Harefield NHS Foundation Trust Palpitations Frequent symptom Less than 50% associated with arrhythmia
Palpitations & AF Richard Grocott Mason Consultant Cardiologist THH NHS Foundation Trust & Royal Brompton & Harefield NHS Foundation Trust Palpitations Frequent symptom Less than 50% associated with arrhythmia
QRS Complexes. Fast & Easy ECGs A Self-Paced Learning Program
 6 QRS Complexes Fast & Easy ECGs A Self-Paced Learning Program Q I A ECG Waveforms Normally the heart beats in a regular, rhythmic fashion producing a P wave, QRS complex and T wave I Step 4 of ECG Analysis
6 QRS Complexes Fast & Easy ECGs A Self-Paced Learning Program Q I A ECG Waveforms Normally the heart beats in a regular, rhythmic fashion producing a P wave, QRS complex and T wave I Step 4 of ECG Analysis
Wide-Complex Tachycardias in the ED: Myths and Pitfalls
 Wide-Complex Tachycardias in the ED: Myths and Pitfalls, FACEP, FAAEM Professor and Vice Chair Director, Emergency Cardiology Fellowship Department of Emergency Medicine University of Maryland School of
Wide-Complex Tachycardias in the ED: Myths and Pitfalls, FACEP, FAAEM Professor and Vice Chair Director, Emergency Cardiology Fellowship Department of Emergency Medicine University of Maryland School of
ATRIAL FIBRILLATION IN THE 21 ST CENTURY TIMOTHY DOWLING, D.O. FAMILY PHYSICIAN
 ATRIAL FIBRILLATION IN THE 21 ST CENTURY TIMOTHY DOWLING, D.O. FAMILY PHYSICIAN GOALS AND OBJECTIVES At The end of this talk you should understand: What is Atrial Fibrillation Causes of Atrial Fibrillation
ATRIAL FIBRILLATION IN THE 21 ST CENTURY TIMOTHY DOWLING, D.O. FAMILY PHYSICIAN GOALS AND OBJECTIVES At The end of this talk you should understand: What is Atrial Fibrillation Causes of Atrial Fibrillation
MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question.
 Exam Name MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) What term is used to refer to the process of electrical discharge and the flow of electrical
Exam Name MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) What term is used to refer to the process of electrical discharge and the flow of electrical
DEPARTMENT OF HEALTH AND HUMAN SERVICES Centers for Medicare & Medicaid Services
 DEPARTMENT OF HEALTH AND HUMAN SERVICES Centers for Medicare & Medicaid Services NEW product from the Medicare Learning Network (MLN) Provider Compliance Tips for Computed Tomography (CT) Scans Podcast,
DEPARTMENT OF HEALTH AND HUMAN SERVICES Centers for Medicare & Medicaid Services NEW product from the Medicare Learning Network (MLN) Provider Compliance Tips for Computed Tomography (CT) Scans Podcast,
How to control atrial fibrillation in 2013 The ideal patient for a rate control strategy
 How to control atrial fibrillation in 2013 The ideal patient for a rate control strategy L. Pison, MD Advances in Cardiac Arrhythmias and Great Innovations in Cardiology - Torino, September 28 th 2013
How to control atrial fibrillation in 2013 The ideal patient for a rate control strategy L. Pison, MD Advances in Cardiac Arrhythmias and Great Innovations in Cardiology - Torino, September 28 th 2013
DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) MANAGEMENT of Atrial Fibrillation (AF)
 DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) MANAGEMENT of Atrial Fibrillation (AF) Key priorities Identification and diagnosis Treatment for persistent AF Treatment for permanent AF Antithrombotic
DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) MANAGEMENT of Atrial Fibrillation (AF) Key priorities Identification and diagnosis Treatment for persistent AF Treatment for permanent AF Antithrombotic
School of Health Sciences
 School of Health Sciences Cardiology Teaching Package A Beginners Guide to Normal Heart Function, Sinus Rhythm & Common Cardiac Arrhythmias Welcome This document extends subjects covered in the Cardiology
School of Health Sciences Cardiology Teaching Package A Beginners Guide to Normal Heart Function, Sinus Rhythm & Common Cardiac Arrhythmias Welcome This document extends subjects covered in the Cardiology
Stimulates HR, BP, CO, and vasoconstriction. Stimulates renal, venous, mesenteric arterial. basic chart below) (alpha receptors) vasoconstriction
 Bolus Alternate Range Drip ACLS Drugs and Drips Amiodarone / Cordarone Lidocaine Procainamide / Pronestyl Dopamine / Intropin CARDIAC ARREST PULSELESS VT/VF Arrest Kit: (300mg bolus) Amiodarone 6 Vial
Bolus Alternate Range Drip ACLS Drugs and Drips Amiodarone / Cordarone Lidocaine Procainamide / Pronestyl Dopamine / Intropin CARDIAC ARREST PULSELESS VT/VF Arrest Kit: (300mg bolus) Amiodarone 6 Vial
Quiz 4 Arrhythmias summary statistics and question answers
 1 Quiz 4 Arrhythmias summary statistics and question answers The correct answers to questions are indicated by *. All students were awarded 2 points for question #2 due to no appropriate responses for
1 Quiz 4 Arrhythmias summary statistics and question answers The correct answers to questions are indicated by *. All students were awarded 2 points for question #2 due to no appropriate responses for
NEW ONSET ATRIAL FIBRILLATION IN THE SURGICAL PATIENT
 DISCLAIMER: These guidelines were prepared by the Department of Surgical Education, Orlando Regional Medical Center. They are intended to serve as a general statement regarding appropriate patient care
DISCLAIMER: These guidelines were prepared by the Department of Surgical Education, Orlando Regional Medical Center. They are intended to serve as a general statement regarding appropriate patient care
ACLS Provider Manual Comparison Sheet Based on 2010 AHA Guidelines for CPR and ECC. BLS Changes
 ACLS Provider Manual Comparison Sheet Based on 2010 AHA Guidelines for CPR and ECC CPR Chest compressions, Airway, Breathing (C-A-B) BLS Changes New Old Rationale New science indicates the following order:
ACLS Provider Manual Comparison Sheet Based on 2010 AHA Guidelines for CPR and ECC CPR Chest compressions, Airway, Breathing (C-A-B) BLS Changes New Old Rationale New science indicates the following order:
Banner Staff Service ECG Study Guide
 Banner Staff Service ECG Study Guide Edited by Larry H. Lybbert, MS, RN Table of Contents ECG STUDY GUIDE... 3 ECG INTERPRETATION BASICS... 4 EKG GRAPH PAPER...4 RATE MEASUREMENT...9 The Six Second Method...9
Banner Staff Service ECG Study Guide Edited by Larry H. Lybbert, MS, RN Table of Contents ECG STUDY GUIDE... 3 ECG INTERPRETATION BASICS... 4 EKG GRAPH PAPER...4 RATE MEASUREMENT...9 The Six Second Method...9
NEONATAL & PEDIATRIC ECG BASICS RHYTHM INTERPRETATION
 NEONATAL & PEDIATRIC ECG BASICS & RHYTHM INTERPRETATION VIKAS KOHLI MD FAAP FACC SENIOR CONSULATANT PEDIATRIC CARDIOLOGY APOLLO HOSPITAL MOB: 9891362233 ECG FAX LINE: 011-26941746 THE BASICS: GRAPH PAPER
NEONATAL & PEDIATRIC ECG BASICS & RHYTHM INTERPRETATION VIKAS KOHLI MD FAAP FACC SENIOR CONSULATANT PEDIATRIC CARDIOLOGY APOLLO HOSPITAL MOB: 9891362233 ECG FAX LINE: 011-26941746 THE BASICS: GRAPH PAPER
Diagnosis and Management of Life Threatening Cardiac Emergencies
 Diagnosis and Management of Life Threatening Cardiac Emergencies Carley Saelinger,VMD, DACVIM (Cardiology) Providing the best quality care and service for the patient, the client, and the referring veterinarian.
Diagnosis and Management of Life Threatening Cardiac Emergencies Carley Saelinger,VMD, DACVIM (Cardiology) Providing the best quality care and service for the patient, the client, and the referring veterinarian.
Atrial Fibrillation The High Risk Obese Patient
 Atrial Fibrillation The High Risk Obese Patient Frederick Schaller, D.O.,F.A.C.O.I. Professor and Vice Dean Touro University Nevada A 56 year old male with a history of hypertension and chronic stable
Atrial Fibrillation The High Risk Obese Patient Frederick Schaller, D.O.,F.A.C.O.I. Professor and Vice Dean Touro University Nevada A 56 year old male with a history of hypertension and chronic stable
E C C. American Heart Association. Advanced Cardiovascular Life Support. Written Precourse Self-Assessment. May 2011. 2011 American Heart Association
 E C C American Heart Association Advanced Cardiovascular Life Support Written Precourse Self-Assessment May 2011 2011 American Heart Association 2011 ACLS Written Precourse Self-Assessment 1. Ten minutes
E C C American Heart Association Advanced Cardiovascular Life Support Written Precourse Self-Assessment May 2011 2011 American Heart Association 2011 ACLS Written Precourse Self-Assessment 1. Ten minutes
www.cprtrainingfast.com
 ADVANCED CARDIAC LIFE SUPPORT (ACLS) RECERTIFICATION EXAMINATION 1. Ten minutes after an 85 year old woman collapses, paramedics arrive and start CPR for the first time. The monitor shows fine (low amplitude)
ADVANCED CARDIAC LIFE SUPPORT (ACLS) RECERTIFICATION EXAMINATION 1. Ten minutes after an 85 year old woman collapses, paramedics arrive and start CPR for the first time. The monitor shows fine (low amplitude)
Management of ATRIAL FIBRILLATION. in general practice. 22 BPJ Issue 39
 Management of ATRIAL FIBRILLATION in general practice 22 BPJ Issue 39 What is atrial fibrillation? Atrial fibrillation (AF) is the most common cardiac arrhythmia encountered in primary care. It is often
Management of ATRIAL FIBRILLATION in general practice 22 BPJ Issue 39 What is atrial fibrillation? Atrial fibrillation (AF) is the most common cardiac arrhythmia encountered in primary care. It is often
Efficacy and Safety of Pharmacological Options for Rate Control in Atrial Fibrillation
 AACN Advanced Critical Care Volume 23, Number 2, pp.120 125 2012, AACN ECG Challenges Earnest Alexander, PharmD, and Gregory M. Susla, PharmD Department Editors Efficacy and Safety of Pharmacological Options
AACN Advanced Critical Care Volume 23, Number 2, pp.120 125 2012, AACN ECG Challenges Earnest Alexander, PharmD, and Gregory M. Susla, PharmD Department Editors Efficacy and Safety of Pharmacological Options
RUSSELLS HALL HOSPITAL EMERGENCY DEPARTMENT
 RUSSELLS HALL HOSPITAL EMERGENCY DEPARTMENT CLINICAL GUIDELINE ATRIAL FIBRILLATION March 2011 For quick links to AF algorithms: UNSTABLE PATIENT STABLE PATIENT - 1 - Introduction Atrial fibrillation is
RUSSELLS HALL HOSPITAL EMERGENCY DEPARTMENT CLINICAL GUIDELINE ATRIAL FIBRILLATION March 2011 For quick links to AF algorithms: UNSTABLE PATIENT STABLE PATIENT - 1 - Introduction Atrial fibrillation is
ACUTE ATRIAL FIBRILLATION TREATMENT IN THE SURGICAL PATIENT
 DISCLAIMER: These guidelines were prepared by the Department of Surgical Education, Orlando Regional Medical Center. They are intended to serve as a general statement regarding appropriate patient care
DISCLAIMER: These guidelines were prepared by the Department of Surgical Education, Orlando Regional Medical Center. They are intended to serve as a general statement regarding appropriate patient care
Cardiovascular System & Its Diseases. Lecture #4 Heart Failure & Cardiac Arrhythmias
 Cardiovascular System & Its Diseases Lecture #4 Heart Failure & Cardiac Arrhythmias Dr. Derek Bowie, Department of Pharmacology & Therapeutics, Room 1317, McIntyre Bldg, McGill University derek.bowie@mcgill.ca
Cardiovascular System & Its Diseases Lecture #4 Heart Failure & Cardiac Arrhythmias Dr. Derek Bowie, Department of Pharmacology & Therapeutics, Room 1317, McIntyre Bldg, McGill University derek.bowie@mcgill.ca
Atrial Fibrillation The Basics
 Atrial Fibrillation The Basics Family Practice Symposium Tim McAveney, M.D. 10/23/09 Objectives Review the fundamentals of managing afib Discuss the risks for stroke and the indications for anticoagulation
Atrial Fibrillation The Basics Family Practice Symposium Tim McAveney, M.D. 10/23/09 Objectives Review the fundamentals of managing afib Discuss the risks for stroke and the indications for anticoagulation
New resuscitation science and American Heart Association treatment guidelines were released October 28, 2010!
 ACLS Study Guide 2010 Bulletin: New resuscitation science and American Heart Association treatment guidelines were released October 28, 2010! The new AHA Handbook of Emergency Cardiac Care (ECC) contains
ACLS Study Guide 2010 Bulletin: New resuscitation science and American Heart Association treatment guidelines were released October 28, 2010! The new AHA Handbook of Emergency Cardiac Care (ECC) contains
Atrial fibrillation (AF) care pathways. for the primary care physicians
 Atrial fibrillation (AF) care pathways for the primary care physicians by University of Minnesota Physicians Heart, October, 2011 Evaluation by the primary care physician: 1. Comprehensive history and
Atrial fibrillation (AF) care pathways for the primary care physicians by University of Minnesota Physicians Heart, October, 2011 Evaluation by the primary care physician: 1. Comprehensive history and
Management of Pacing Wires After Cardiac Surgery
 Management of Pacing Wires After Cardiac Surgery David E. Lizotte, Jr. PA C, MPAS, FAPACVS President, Association of Physician Assistants in Cardiovascular Surgery Conflicts: None Indications 2008 Journal
Management of Pacing Wires After Cardiac Surgery David E. Lizotte, Jr. PA C, MPAS, FAPACVS President, Association of Physician Assistants in Cardiovascular Surgery Conflicts: None Indications 2008 Journal
RATE VERSUS RHYTHM CONTROL OF ATRIAL FIBRILLATION: SPECIAL CONSIDERATION IN ELDERLY. Charles Jazra
 RATE VERSUS RHYTHM CONTROL OF ATRIAL FIBRILLATION: SPECIAL CONSIDERATION IN ELDERLY Charles Jazra NO CONFLICT OF INTEREST TO DECLARE Relationship Between Atrial Fibrillation and Age Prevalence, percent
RATE VERSUS RHYTHM CONTROL OF ATRIAL FIBRILLATION: SPECIAL CONSIDERATION IN ELDERLY Charles Jazra NO CONFLICT OF INTEREST TO DECLARE Relationship Between Atrial Fibrillation and Age Prevalence, percent
Atrial Fibrillation: Drugs, Ablation, or Benign Neglect. Robert Kennedy, MD October 10, 2015
 Atrial Fibrillation: Drugs, Ablation, or Benign Neglect Robert Kennedy, MD October 10, 2015 Definitions 2014 AHA/ACC/HRS Guideline for the Management of Patients With Atrial Fibrillation: Executive Summary.
Atrial Fibrillation: Drugs, Ablation, or Benign Neglect Robert Kennedy, MD October 10, 2015 Definitions 2014 AHA/ACC/HRS Guideline for the Management of Patients With Atrial Fibrillation: Executive Summary.
An Introduction to Tachyarrhythmias R. A. Seyon MN, NP, CCN(C) & Dr. R. G. Williams
 Arrhythmias 1 An Introduction to Tachyarrhythmias R. A. Seyon MN, NP, CCN(C) & Dr. R. G. Williams Things to keep in mind when analyzing arrhythmias: Electrical activity recorded in 12 and 15 leads Examine
Arrhythmias 1 An Introduction to Tachyarrhythmias R. A. Seyon MN, NP, CCN(C) & Dr. R. G. Williams Things to keep in mind when analyzing arrhythmias: Electrical activity recorded in 12 and 15 leads Examine
Adding IV Amiodarone to the EMS Algorithm for Cardiac Arrest Due to VF/Pulseless VT
 Adding IV Amiodarone to the EMS Algorithm for Cardiac Arrest Due to VF/Pulseless VT Introduction Before the year 2000, the traditional antiarrhythmic agents (lidocaine, bretylium, magnesium sulfate, procainamide,
Adding IV Amiodarone to the EMS Algorithm for Cardiac Arrest Due to VF/Pulseless VT Introduction Before the year 2000, the traditional antiarrhythmic agents (lidocaine, bretylium, magnesium sulfate, procainamide,
Megacode Testing Checklist 1/2 Bradycardia VF/Pulseless VT Asystole ROSC
 Megacode Testing Checklist 1/2 Bradycardia VF/Pulseless VT Asystole ROSC Student Name: Test Bradycardia Management Recognizes symptomatic bradycardia Administers correct dose of atropine Prepares for second-line
Megacode Testing Checklist 1/2 Bradycardia VF/Pulseless VT Asystole ROSC Student Name: Test Bradycardia Management Recognizes symptomatic bradycardia Administers correct dose of atropine Prepares for second-line
Electrophysiology Daymar College. Lisa H. Young, RN, BSN, MAE 2011
 Electrophysiology Daymar College Lisa H. Young, RN, BSN, MAE 2011 Electrical Conduction Pathway Chemical Basis for Impulse Formation Cardiac Action Potential Phases http://www.youtube.com/watch?v=oqpffilde0e
Electrophysiology Daymar College Lisa H. Young, RN, BSN, MAE 2011 Electrical Conduction Pathway Chemical Basis for Impulse Formation Cardiac Action Potential Phases http://www.youtube.com/watch?v=oqpffilde0e
Interpretation of Laboratory Values
 Interpretation of Laboratory Values Konrad J. Dias PT, DPT, CCS Overview Electrolyte imbalances Renal Function Tests Complete Blood Count Coagulation Profile Fluid imbalance Sodium Electrolyte Imbalances
Interpretation of Laboratory Values Konrad J. Dias PT, DPT, CCS Overview Electrolyte imbalances Renal Function Tests Complete Blood Count Coagulation Profile Fluid imbalance Sodium Electrolyte Imbalances
PHENYLEPHRINE HYDROCHLORIDE INJECTION USP
 PRESCRIBING INFORMATION PHENYLEPHRINE HYDROCHLORIDE INJECTION USP 10 mg/ml Sandoz Canada Inc. Date of Preparation: September 1992 145 Jules-Léger Date of Revision : January 13, 2011 Boucherville, QC, Canada
PRESCRIBING INFORMATION PHENYLEPHRINE HYDROCHLORIDE INJECTION USP 10 mg/ml Sandoz Canada Inc. Date of Preparation: September 1992 145 Jules-Léger Date of Revision : January 13, 2011 Boucherville, QC, Canada
Atrial fibrillation. Quick reference guide. Issue date: June 2006. The management of atrial fibrillation
 Quick reference guide Issue date: June 2006 Atrial fibrillation The management of atrial fibrillation Developed by the National Collaborating Centre for Chronic Conditions Contents Contents Patient-centred
Quick reference guide Issue date: June 2006 Atrial fibrillation The management of atrial fibrillation Developed by the National Collaborating Centre for Chronic Conditions Contents Contents Patient-centred
Inpatient Heart Failure Management: Risks & Benefits
 Inpatient Heart Failure Management: Risks & Benefits Dr. Kenneth L. Baughman Professor of Medicine Harvard Medical School Director, Advanced Heart Disease Section Brigham & Women's Hospital Harvard Medical
Inpatient Heart Failure Management: Risks & Benefits Dr. Kenneth L. Baughman Professor of Medicine Harvard Medical School Director, Advanced Heart Disease Section Brigham & Women's Hospital Harvard Medical
Episode 20 Atrial fibrillation Prepared by Dr. Lucas Chartier
 Episode 20 Atrial fibrillation Prepared by Dr. Lucas Chartier Most common dysrhythmia seen in ED, and incidence increasing with ageing population Presentation Common presentations: younger patients often
Episode 20 Atrial fibrillation Prepared by Dr. Lucas Chartier Most common dysrhythmia seen in ED, and incidence increasing with ageing population Presentation Common presentations: younger patients often
Cardioversion for. Atrial Fibrillation. Your Heart s Electrical System Cardioversion Living with Atrial Fibrillation
 Cardioversion for Atrial Fibrillation Your Heart s Electrical System Cardioversion Living with Atrial Fibrillation When You Have Atrial Fibrillation You ve been told you have a heart condition called atrial
Cardioversion for Atrial Fibrillation Your Heart s Electrical System Cardioversion Living with Atrial Fibrillation When You Have Atrial Fibrillation You ve been told you have a heart condition called atrial
Essential facts for med-surg nurses
 Emergency cardiac drugs: Essential facts for med-surg nurses Emergencies on a med-surg unit can be daunting. By Ira Gene Reynolds, MSNEd, RN, PCCN-CMC IN THE HOSPITAL SETTING, emergencies typically occur
Emergency cardiac drugs: Essential facts for med-surg nurses Emergencies on a med-surg unit can be daunting. By Ira Gene Reynolds, MSNEd, RN, PCCN-CMC IN THE HOSPITAL SETTING, emergencies typically occur
INFORMATION FOR PATIENTS AND FAMILIES A Patient s Guide to Living with Atrial Fibrillation
 INFORMATION FOR PATIENTS AND FAMILIES A Patient s Guide to Living with Atrial Fibrillation 30 Bond Street, Toronto, ON M5B 1W8 Canada 416.864.6060 stmichaelshospital.com Form No. XXXXX Dev. XX/XXXX GOALS
INFORMATION FOR PATIENTS AND FAMILIES A Patient s Guide to Living with Atrial Fibrillation 30 Bond Street, Toronto, ON M5B 1W8 Canada 416.864.6060 stmichaelshospital.com Form No. XXXXX Dev. XX/XXXX GOALS
Addendum to the Guideline on antiarrhythmics on atrial fibrillation and atrial flutter
 22 July 2010 EMA/CHMP/EWP/213056/2010 Addendum to the Guideline on antiarrhythmics on atrial fibrillation and atrial flutter Draft Agreed by Efficacy Working Party July 2008 Adoption by CHMP for release
22 July 2010 EMA/CHMP/EWP/213056/2010 Addendum to the Guideline on antiarrhythmics on atrial fibrillation and atrial flutter Draft Agreed by Efficacy Working Party July 2008 Adoption by CHMP for release
Alabama Medications. Christopher J. Colvin January 2010
 Alabama Medications Christopher J. Colvin p January 2010 Activated Charcoal Used to absorb toxins ingested before they can be absorbed in the GI system. Contraindicated in AMS patients who cannot control
Alabama Medications Christopher J. Colvin p January 2010 Activated Charcoal Used to absorb toxins ingested before they can be absorbed in the GI system. Contraindicated in AMS patients who cannot control
Basic Cardiac Rhythms Identification and Response
 Basic Cardiac Rhythms Identification and Response Module 1 ANATOMY, PHYSIOLOGY, & ELECTRICAL CONDUCTION Objectives Describe the normal cardiac anatomy and physiology and normal electrical conduction through
Basic Cardiac Rhythms Identification and Response Module 1 ANATOMY, PHYSIOLOGY, & ELECTRICAL CONDUCTION Objectives Describe the normal cardiac anatomy and physiology and normal electrical conduction through
Interpreting AV (Heart) Blocks: Breaking Down the Mystery
 Interpreting AV (Heart) Blocks: Breaking Down the Mystery 2 Contact Hours Copyright 2012 by RN.com. All Rights Reserved. Reproduction and distribution of these materials is prohibited without the express
Interpreting AV (Heart) Blocks: Breaking Down the Mystery 2 Contact Hours Copyright 2012 by RN.com. All Rights Reserved. Reproduction and distribution of these materials is prohibited without the express
HEART HEALTH WEEK 3 SUPPLEMENT. A Beginner s Guide to Cardiovascular Disease HEART FAILURE. Relatively mild, symptoms with intense exercise
 WEEK 3 SUPPLEMENT HEART HEALTH A Beginner s Guide to Cardiovascular Disease HEART FAILURE Heart failure can be defined as the failing (insufficiency) of the heart as a mechanical pump due to either acute
WEEK 3 SUPPLEMENT HEART HEALTH A Beginner s Guide to Cardiovascular Disease HEART FAILURE Heart failure can be defined as the failing (insufficiency) of the heart as a mechanical pump due to either acute
Inotropes/Vasoactive Agents Hina N. Patel, Pharm.D., BCPS Cathy Lawson, Pharm.D., BCPS
 Inotropes/Vasoactive Agents Hina N. Patel, Pharm.D., BCPS Cathy Lawson, Pharm.D., BCPS 1. Definition -an agent that affects the contractility of the heart -may be positive (increases contractility) or
Inotropes/Vasoactive Agents Hina N. Patel, Pharm.D., BCPS Cathy Lawson, Pharm.D., BCPS 1. Definition -an agent that affects the contractility of the heart -may be positive (increases contractility) or
Protocol for the management of atrial fibrillation in primary care
 Protocol for the management of atrial fibrillation in primary care Protocol for the management of atrial fibrillation in primary care Contents Page no Definition 2 Classification of AF 2 3 Identification
Protocol for the management of atrial fibrillation in primary care Protocol for the management of atrial fibrillation in primary care Contents Page no Definition 2 Classification of AF 2 3 Identification
