Chronic Aortic and Mitral Regurgitation
|
|
|
- Joshua Gilbert
- 7 years ago
- Views:
Transcription
1 32 nd Annual Advances in Heart Disease Chronic Aortic and Mitral Regurgitation When Should We Intervene? Gabriel Gregoratos, MD, FACC Disclosure Statement Nothing to Disclose 1
2 Valvular Regurgitation: When Should we Intervene? A complex Issue 1. Regurgitant lesions are mostly well tolerated and patients remain asymptomatic for many years while irreparable ventricular dysfunction develops-which may not improve after intervention 2. Limited data comparing interventions vs. medical therapies or timing of intervention and most data obtained from retrospective studies or prospective non-randomized registries. Therefore most guideline recommendations have evidence level B or C (Not robust evidence) 3. Some conflicting conclusions in different studies 4. Valve replacement exchanges one disease for another Factors Affecting Decision and Timing of Intervention Severity (quantified objectively by TTE, Cath, etc.) Etiology and chronicity of regurgitation Natural history of chronic regurgitation Presence or absence of symptoms Ventricular function and other predictors of outcome such as pulmonary hypertension, atrial fibrillation Patient status (age, co-morbidities, etc) Type of intervention and durability: Repair vs. Replacement and Surgical vs. Transcatheter 2
3 The Heart Valve Team and Heart Valve Centers of Excellence Recommendations COR LOE Patients with severe VHD should be evaluated by a multidisciplinary Heart Valve Team when I C intervention is considered Consultation with or referral to a Heart Valve Center of Excellence is reasonable when discussing treatment options for 1) asymptomatic patients with severe VHD, 2) patients who may benefit from valve repair versus valve replacement, or 3) patients with multiple comorbidities for whom valve intervention is considered IIa C Heart Valve Centers of Excellence Composed of experienced providers from multiple disciplines Offer all available options for diagnosis and management (surgery, valve repair, trans-catheter therapies) Participate in outcome registries (regional or national) Demonstrate adherence to Guidelines Participate in continual evaluation and QI processes Publicly report mortality and success rates 3
4 Stages of Progression of VHD Stage Definition Description A At risk Patients with risk factors for the development of VHD B Progressive Patients with progressive VHD (mild-to-moderate severity and asymptomatic) C ** Asymptomatic severe Asymptomatic patients who have reached the criteria for severe VHD C1: Asymptomatic patients with severe VHD in whom the left or right ventricle remains compensated C2: Asymptomatic patients who have severe VHD, with decompensation of the left or right ventricle D Symptomatic severe Patients who have developed symptoms as a result of VHD Chronic Aortic Regurgitation 4
5 Natural History of Chronic Asymptomatic AR Bonow, Circulation 1991 and Borer, Circulation 1998 } Survival without Surgery - Chronic AR Significance of Symptoms Dujardin et al. Circulation
6 Natural History of Chronic AR Based on 9 Studies / 593 Patients Asymptomatic patients with normal LV systolic function: Progression to symptoms and/or LV dysfunction: 6%/ year Progression to asymptomatic LV dysfunction: 3.5% /year Sudden death: < 0.2% per year Asymptomatic patients with LV systolic dysfunction: Progression to cardiac symptoms: >25% per year Symptomatic patients: Mortality rate: >10% per year JACC 2008:52:e1-e142 Predictors of Sub-optimal Surgical Outcomes in Chronic AR Patients LVEF < 50% LVESD 55 mm LVEDD 75 mm LVESV 200 ml/m 2 Prolonged LV dysfunction (>12 mos.) Age>80 yrs. Ventricular response to exercise (??) Advanced symptoms (class III & IV) JACC 2008:52:e1-e142 JACC 1997;30(3):746 6
7 Serial Evaluation in Asymptomatic Chronic AR Clinical evaluation: annually TTE evaluation: Stage B (progressive, mild AR): every 3-5 years Stage B (progressive, moderate AR): every 1-2 years Stage C (severe AR): annually Stage C (severe AR, dilating LV): more frequently Quantification of Severe AR by TTE * Jet width 65% of LVOT Vena contracta >0.6 cm Holodiastolic flow reversal in the proximal abdominal aorta Reg. Vol 60 ml/beat Reg. Fraction 50% ERO 0.3 cm2 Angiography grade 3+ to 4+ Plus evidence of LV dilation 7
8 Severe AR Role of Exercise Testing in Evaluating Chronic AR * Exercise LVEF and change in LVEF from rest to exercise are often abnormal even in asymptomatic patients, but these changes have not been shown to be of independent prognostic value above that provided by LV function and dimensions Sedentary patients and/or those with no or equivocal symptoms to assess true functional capacity useful No specific recommendation in current guideline Change from prior version where indications for exercise testing were class IIa (reasonable) 8
9 Interventions for Severe AR ** Medical therapy Aortic valve replacement (>90%) Aortic valve repair for insufficient bicuspid valves Decalcification of Ao. Valve pretty much abandoned For AR due to root dilatation/aneurysm: Root replacement by graft and valve re-suspension Percutaneous replacement for AR still under investigation Medical Therapy for Chronic Severe AR * Results of vasodilator therapy inconsistent Current guideline recommendations: Treatment of Hypertension with Dihydropyridine CCB and ACE-I/ARBs (Class I, LOE B) Treatment with ACE-I/ARB and Beta Blockers in patients with severe AR and symptoms and/or LV dysfunction when surgery not feasible because of comorbidities (Class IIa, LOE B) 9
10 ACC/AHA Class I Recommendations for Aortic Valve Surgery (AVR) 1. AVR is indicated for symptomatic patients with severe AR (stage D) regardless of LV systolic function. (LOE: B) 2. AVR is indicated for asymptomatic patients with chronic severe AR and LV systolic dysfunction (LVEF<0.50) at rest. (LOE: B) 3. AVR is indicated for patients with chronic severe AR (stage C or D) while undergoing cardiac surgery for other indications (LOE: C) ACC/AHA Class IIa Recommendations for Aortic Valve Surgery 1. AVR is reasonable for asymptomatic patients with severe AR with normal LV systolic function (EF 0.50) but with severe LV dilatation, defined as LVESD>50 mm (stage C2) (LOE: B) 2. AVR is reasonable in patients with moderate AR (stage B) undergoing cardiac surgery for other indications. (LOE B) 10
11 ACC/AHA Class IIb Recommendations for Aortic Valve Surgery 1. AVR may be considered for asymptomatic pts. with severe AR, normal LV systolic function (LVEF 0.50, stage C1) and progressive severe LV dilatation, defined as LVEDD>65 mm if surgical risk is low (LOE: C) Intervention for Chronic Severe AR Conclusions Optimal outcomes from Aortic valve surgery can be achieved if AVR takes place.. Before NYHA Class III / IV HF symptoms develop Before LV dysfunction ( EF<0.50) develops Before LVESD exceeds 50 mm Before LVEDD exceeds 65 mm Close clinical and echo follow-up (per guidelines) is necessary Quantification of AR severity by TTE is essential Exercise testing may be useful in few selected cases 11
12 Is it Ever too Late for AVR in Aortic Regurgitation? Very few patients should be denied AVR even when they have missed the opportunity for best surgical results (even if LVESD>50mm and/or EF severely depressed) because AVR reduces LV afterload and leads to LVEF and forward Cardiac Output However, preliminary and unconfirmed data suggest that patients in this setting who cannot generate systolic LV pressure>120 mmhg are likely to experience less afterload reduction after AVR and are probably poor surgical candidates (Carabello, JACC 2004) Comorbidities and advanced physiologic age must be considered Bicuspid Aortic Valve & Aortopathy * Bicuspid Ao. Valves frequently associated with aortic root dilatation Result of structural aortic wall changes and abnormal hemodynamics of the bicuspid valve Aortopathy more frequent with fusion of Right and Noncoronary cusps and less frequent with the more common fusion phenotype of Right and Left cusps Specific genetic cause not identified Risk of dissection when Ao. Root Diameter>4.5 cm 12
13 Repair of Aortic Sinuses or Replacement * of Ascending Aorta: Class I, LOE B: Diameter of ascending aorta or aortic sinuses >5.5 cm Class IIa, LOE C: Diameter of ascending aorta or aortic sinuses > 5 cm plus dissection risk (FH of dissection or rate of diameter increase 0.5 cm/year) Class IIa, LOE C: Ascending aorta diameter > 4.5 cm in patient undergoing AVR for severe AS or AR Hot off the Press Clarification JACC December 2015, published ahead of print * Class IIa, LOE C: Diameter of ascending aorta or aortic sinuses cm plus dissection risk (FH of dissection or rate of diameter increase 0.5 cm/year) OR if patient is at low risk and surgery is performed by an experienced surgical team Low surgical risk is defined as STS mortality risk<4% 13
14 Chronic Mitral Regurgitation Chronic Mitral Regurgitation * Primary (degenerative) MR MV prolapse Infective Endocarditis CT diseases Rheumatic heart disease Congenital MV cleft Radiation heart disease Secondary (functional) MR Severe LV dysfunction CAD with/without MI (ischemic secondary MR) Primary myocardial disease (non ischemic secondary MR) These two conditions have more differences than similarities 14
15 Typical Myxomatous MV * Chronic Primary MR Pathophysiology Mild/moderate MR may remain asymptomatic for many years Even with severe chronic MR, due to favorable loading conditions the LVEF is maintained in low normal range of 50% to 60% and forward CO is maintained, despite the presence of significant myocardial (contractile) dysfunction This is the key consideration in current thinking that intervention should be carried out before overt LV dysfunction develops 15
16 Natural History of Severe Chronic MR (Enriquez-Sarano et al. NEJM 1996 & Rosen et al. AJC 1994) Survival post MV Surgery as a Function of LVEF (Enriquez-Sarano, et al. Circulation 1994) 16
17 Predictors of Sub-optimal Surgical Outcomes in Chronic Severe Primary MR Advanced symptoms Functional status NYHA III-IV LVEF<60% LVESD 40 mm RV dysfunction Pulmonary hypertension Atrial Fibrillation LA dimensions/volume BNP level? Serial Evaluation of Asymptomatic Patients with Chronic Primary MR (JACC 2014;63(22):e57-e185) Mild MR (with no evidence of LV enlargement, dysfunction, or PH): Annual clinical evaluation. TTE every 2-3 years Moderate MR (with no evidence of LV enlargement, dysfunction or PH): Annual clinical and TTE Severe MR: Annual or Semiannual clinical and TTE With careful monitoring of LVEF, LVESD, and PA pressure 17
18 Quantification of Severe MR by TTE * * Central jet MR > 40% LA or holosystolic eccentric jet MR Vena contracta 0.7 cm Regurgitant volume 60 cc Regurgitant fraction 50% ERO 0.40 cm 2 Angiographic grade 3 4+ Severe MR 18
19 Exercise Testing Recommendations Class IIa Exercise hemodynamics with either Doppler echocardiography or cardiac catheterization is reasonable in symptomatic patients with chronic primary MR where there is a discrepancy between symptoms and the severity of MR at rest (stages B and C) Exercise treadmill testing can be useful in patients with chronic primary MR to establish symptom status and exercise tolerance (stages B and C) Exercise Testing in Evaluating Chronic Primary MR * Assess symptomatic status, especially if good history of exercise capacity cannot be obtained - useful Functional capacity on Cardiopulmonary testing (<84% of expected for age and sex). Griffin, Circulation 2006 ECHO parameters to be assessed with exercise: Severity of MR during exercise - useful PA pressure during exercise - useful Changes in LVEF during exercise - not very useful due to loading conditions 19
20 Medical Therapy for Chronic Primary MR Medical therapy for systolic LV dysfunction is reasonable in symptomatic patients with chronic primary MR (stage D) and LVEF less than 60% in whom surgery is not contemplated (Class IIa, LOE:B) Vasodilator therapy is not indicated for normotensive asymptomatic patients with chronic primary MR (stages B and C1) and normal systolic LV function (Class III, No Benefit, LOE B) Interventions for Severe Primary MR Types of Surgery: MV replacement with preservation of MV apparatus MV repair ± annuloplasty MV replacement with removal of MV apparatus is rarely, if ever, indicated Mitral Valve repair is preferable to MVR in most cases of primary MR if a successful and durable repair can be achieved which depends on valve morphology and surgical expertise (JACC, 2014;63(22):e57-e185) Percutaneous repair (Mitraclip) 20
21 Interventions for Chronic Primary Severe MR (Class I, LOE:B) MV surgery is recommended for symptomatic patients with chronic severe primary MR (stage D) and LVEF >30% MV surgery is recommended for asymptomatic patients with chronic severe primary MR and LV dysfunction (LVEF 30% 60% and/or LVESD 40 mm, stage C2) Concomitant MV repair or replacement is indicated in patients with chronic severe primary MR undergoing other cardiac surgery Interventions for Chronic Primary MR (Class I, LOE:B) MV Repair is recommended in preference to MV Replacement when surgical treatment is indicated for patients with chronic severe primary MR limited to the posterior leaflet MV Repair is recommended in preference to MV Replacement when surgical treatment is indicated for patients with chronic severe primary MR involving the anterior leaflet or both leaflets when a successful and durable repair can be accomplished 21
22 Interventions for Chronic Primary MR (Class IIa, LOE:B) MV Repair is reasonable in asymptomatic patients with chronic severe primary MR (stage C1) with preserved LV function (LVEF >60% and LVESD <40 mm) provided the likelihood of a successful and durable repair without residual MR is >95%, with an expected mortality <1% when performed at a Heart Valve Center of Excellence OR there is a high likelihood of a successful and durable repair of a non rheumatic MV with 1) new onset of AF or 2) resting pulmonary hypertension (PA systolic arterial pressure >50 mm Hg) * Interventions for Chronic Primary MR (Class IIa, LOE:B) Concomitant MV Repair is reasonable in patients with chronic moderate primary MR (stage B) undergoing other cardiac surgery 22
23 Interventions for Chronic Primary MR (Class IIb) MV surgery may be considered in symptomatic patients with chronic severe primary MR and LVEF 30% (stage D)(LOE:C) MV repair may be considered in patients with rheumatic mitral valve disease when surgical treatment is indicated if a durable and successful repair is likely or if the reliability of long-term anticoagulation management is questionable (LOE:B) Interventions for Chronic Primary MR Percutaneous MV repair may be considered for severely symptomatic patients (NYHA class III-IV) with chronic severe primary MR (stage D) who have a reasonable life expectancy, prohibitive surgical risk because of severe comorbidities (Class IIb, LOE:B) MV Replacement should not be performed for the treatment of isolated severe primary MR limited to less than one half of the posterior leaflet unless MV repair has been attempted and was unsuccessful (Class III-Harm, LOE:B) 23
24 The Argument for Early Surgery in Asymptomatic Patients * Surgery is almost inevitable in severe primary MR Surgery in patients with advanced symptoms has inferior outcomes. Early surgery has low operative mortality of % (when performed by expert surgeons) and restores patients to survival almost identical to that of the general population Good preoperative imaging predicts reparability with high degree of confidence Severe primary MR has serious consequences if not corrected No alternative therapies have been established Long-term Outcomes of Patients with Severe Degenerative (Primary) MR (Montant P et al. J Thor & CV Surg 2009; 138(6): ) (n=67) OVERALL SURVIVAL (%) (n=125) Follow-up in years 24
25 Long-term Outcomes in Severe Primary MR Suri RM et al. JAMA 2013;310(6): patients 446 patients (<3m.) Long-term Outcomes in Severe Primary MR Suri RM et al. JAMA 2013;310(6):
26 Intervention for Chronic Severe Primary MR - Conclusions MV repair superior to replacement Severity of MR must be quantified objectively MV surgery for severely symptomatic MR and LV dysfunction is Rescue Surgery necessary but not desirable with inferior long-term outcomes MV surgery outcomes best before major symptoms develop, before LVEF<60%, before LVESD>40 mm and before AF and/or PH develop, if likelihood of repair is very high (>90%--98%) Close follow-up important (Heart Valve Center) ** Interventions for Chronic Secondary Severe MR Standard HF therapy for patients with secondary MR, HF and reduced LVEF (Class I, LOE A) MV surgery is reasonable for patients with severe secondary MR who are undergoing CABG or AVR (Class IIa, LOE C) MV surgery may be considered for severely symptomatic patients (NYHA class III-IV) with chronic severe secondary MR (Class IIb, LOE B) MV repair may be considered for patients with chronic moderate secondary MR who are undergoing other cardiac surgery (Class IIb, LOE C) 26
27 Funct. Class III/IV Results of Surgery for Severe, Secondary Symptomatic MR (JACC 2010;55:271) LVEF (%) EDD (mm) Operation 30-day M % Survival % Yrs F-U N/A 30±9 63±8 MVA (2.5y) 49/51 27±7 N/A MVA, MVR (5 y) 72/5 (ACORN)** 24±9 70±9 MVA, MVR (2 y) 75/25 28±4 68 MVA, MVR (2.7 y) N/A 23±7 65±8 MVA (5 y) 68/30 37±12 N/A MVA, MVR (5 y) 21/10 23±7 66±8 MVA, MVR (5 y) Thank You! 27
28 Supplemental Slides Stages of Chronic Aortic Regurgitation Stage Definition Valve Anatomy Valve Hemodynamics A At risk of AR Bicuspid aortic valve AR severity (or other congenital none or trace valve anomaly) Aortic valve sclerosis Diseases of the aortic sinuses or ascending aorta History of rheumatic fever or known rheumatic heart disease IE Hemodynamic Symptoms Consequences None None 28
29 Stages of Chronic Aortic Regurgitation (cont.) Stage Definition Valve Anatomy Valve Hemodynamics Hemodynamic Consequences B Progressive AR Mild-tomoderate calcification of a trileaflet valve bicuspid aortic valve (or other congenital valve anomaly) Dilated aortic sinuses Rheumatic valve changes Previous IE Mild AR: o Jet width <25% of LVOT o Vena contracta <0.3 cm o RVol <30 ml/beat o RF <30% o ERO <0.10 cm 2 o Angiography grade 1+ Moderate AR: o Jet width 25% 64% of LVOT o Vena contracta cm o RVol ml/beat o RF 30% 49% o ERO cm 2 o Angiography grade 2+ Normal LV systolic function Normal LV volume or mild LV dilation Symptoms None Stages of Chronic Aortic Regurgitation (cont.) Stage Definition Valve Anatomy Valve Hemodynamics Hemodynamic Consequences C Asymptomatic severe AR Calcific aortic valve disease Bicuspid valve (or other congenital abnormality) Dilated aortic sinuses or ascending aorta Rheumatic valve changes IE with abnormal leaflet closure or perforation Severe AR: o Jet width 65% of LVOT o Vena contracta >0.6 cm o Holodiastolic flow reversal in the proximal abdominal aorta o RVol 60 ml/beat o RF 50% o ERO 0.3 cm 2 o Angiography grade 3+ to 4+ o In addition, diagnosis of chronic severe AR requires evidence of LV dilation C1: Normal LVEF ( 50%) and mild-tomoderate LV dilation (LVESD 50 mm) C2: Abnormal LV systolic function with depressed LVEF (<50%) or severe LV dilatation (LVESD >50 mm or indexed LVESD >25 mm/m 2 ) Symptoms None; exercise testing is reasonable to confirm symptom status 29
30 Stages of Chronic Aortic Regurgitation (cont.) Stage Definition Valve Anatomy Valve Hemodynamics Hemodynamic Consequences D Symptomatic severe AR Calcific valve disease Bicuspid valve (or other congenital abnormality) Dilated aortic sinuses or ascending aorta Rheumatic valve changes Previous IE with abnormal leaflet closure or perforation Severe AR: o Doppler jet width 65% of LVOT; o Vena contracta >0.6 cm, o Holodiastolic flow reversal in the proximal abdominal aorta, o RVol 60 ml/beat; o RF 50%; o ERO 0.3 cm 2 ; o Angiography grade 3+ to 4+ o In addition, diagnosis of chronic severe AR requires evidence of LV dilation Symptomatic severe AR may occur with normal systolic function (LVEF 50%), mild-tomoderate LV dysfunction (LVEF 40% to 50%) or severe LV dysfunction (LVEF <40%); Moderate-to-severe LV dilation is present. Symptoms Exertional dyspnea or angina, or more severe HF symptoms Indications for Aortic Valve Replacement for Chronic Aortic Regurgitation 30
31 Stages of Primary Mitral Regurgitation Stage Definition Valve Anatomy Valve Hemodynamics Hemodynamic Consequences A At risk of None MR B Progressive MR Mild mitral valve prolapse with normal coaptation Mild valve thickening and leaflet restriction Severe mitral valve prolapse with normal coaptation Rheumatic valve changes with leaflet restriction and loss of central coaptation Prior IE No MR jet or small central jet area <20% LA on Doppler Small vena contracta <0.3 cm Central jet MR 20% 40% LA or late systolic eccentric jet MR Vena contracta <0.7 cm Regurgitant volume <60 cc Regurgitant fraction <50% ERO <0.40 cm 2 Angiographic grade 1 2+ Mild LA enlargement No LV enlargement Normal pulmonary pressure Symptoms None None Stages of Primary Mitral Regurgitation (cont.) Stage Definition Valve Anatomy Valve Hemodynamics C Asymptomatic severe MR Severe mitral valve prolapse with loss of coaptation or flail leaflet Rheumatic valve changes with leaflet restriction and loss of central coaptation Prior IE Thickening of leaflets with radiation heart disease Central jet MR >40% LA or holosystolic eccentric jet MR Vena contracta 0.7 cm Regurgitant volume 60 cc Regurgitant fraction 50% ERO 0.40 cm 2 Angiographic grade 3 4+ Hemodynamic Consequences Moderate or severe LA enlargement LV enlargement Pulmonary hypertension may be present at rest or with exercise C1: LVEF >60% and LVESD <40 mm C2: LVEF 60% and LVESD 40 mm Symptoms None 31
32 Stages of Primary Mitral Regurgitation (cont.) Stage Definition Valve Anatomy Valve Hemodynamics D Symptomatic severe MR Severe mitral valve prolapse with loss of coaptation or flail leaflet Rheumatic valve changes with leaflet restriction and loss of central coaptation Prior IE Thickening of leaflets with radiation heart disease Central jet MR >40% LA or holosystolic eccentric jet MR Vena contracta 0.7 cm Regurgitant volume 60 cc Regurgitant fraction 50% ERO 0.40 cm 2 Angiographic grade 3 4+ Hemodynamic Consequences Moderate or severe LA enlargement LV enlargement Pulmonary hypertension present Symptoms Decreased exercise tolerance Exertional dyspnea Indications for Surgery for Mitral Regurgitation 32
33 Stages of Secondary Mitral Regurgitation (cont.) Grade Definition Valve Anatomy Valve Hemodynamics Associated Cardiac Findings Symptoms A At risk of MR Normal valve leaflets, chords, and annulus in a patient with coronary disease or a cardiomyopathy No MR jet or small central jet area <20% LA on Doppler Small vena contracta <0.30 cm Normal or mildly dilated LV size with fixed (infarction) or inducible (ischemia) regional wall motion abnormalities Primary myocardial disease with LV dilation and systolic dysfunction Symptoms due to coronary ischemia or HF may be present that respond to revascularization and appropriate medical therapy Stages of Secondary Mitral Regurgitation (cont.) Grade Definition Valve Anatomy Valve Hemodynamics B Progressive MR Regional wall motion abnormalities with mild tethering of mitral leaflet Annular dilation with mild loss of central coaptation of the mitral leaflets ERO <0.20 cm 2 Regurgitant volume <30 cc Associated Cardiac Findings Regional wall motion abnormalities with reduced LV systolic function LV dilation and systolic dysfunction due to primary myocardial disease Symptoms Symptoms due to coronary ischemia or HF may be present that respond to revascularization and appropriate medical therapy 33
34 Stages of Secondary Mitral Regurgitation (cont.) Grade Definition Valve Anatomy Valve Hemodynamics C Asymptomatic severe MR Regional wall motion abnormalities and/or LV dilation with severe tethering of mitral leaflet Annular dilation with severe loss of central coaptation of the mitral leaflets ERO 0.20 cm 2 Regurgitant volume 30 cc Associated Cardiac Findings Regional wall motion abnormalities with reduced LV systolic function LV dilation and systolic dysfunction due to primary myocardial disease Symptoms Symptoms due to coronary ischemia or HF may be present that respond to revascularization and appropriate medical therapy Stages of Secondary Mitral Regurgitation (cont.) Grade Definition Valve Anatomy Valve Hemodynamics D Symptomatic severe MR Regional wall motion abnormalities and/or LV dilation with severe tethering of mitral leaflet Annular dilation with severe loss of central coaptation of the mitral leaflets ERO 0.20 cm 2 Regurgitant volume 30 cc Associated Cardiac Findings Regional wall motion abnormalities with reduced LV systolic function LV dilation and systolic dysfunction due to primary myocardial disease. Symptoms HF symptoms due to MR persist even after revascularization and optimization of medical therapy Decreased exercise tolerance Exertional dyspnea 34
Managing Mitral Regurgitation: Repair, Replace, or Clip? Michael Howe, MD Traverse Heart & Vascular
 Managing Mitral Regurgitation: Repair, Replace, or Clip? Michael Howe, MD Traverse Heart & Vascular Mitral Regurgitation Anatomy Mechanisms of MR Presentation Evaluation Management Repair Replace Clip
Managing Mitral Regurgitation: Repair, Replace, or Clip? Michael Howe, MD Traverse Heart & Vascular Mitral Regurgitation Anatomy Mechanisms of MR Presentation Evaluation Management Repair Replace Clip
How To Treat Aortic Stenosis
 2014 AHA/ACC Guideline for the Management of Patients With Valvular Heart Disease Developed in Collaboration with the American Association for Thoracic Surgery, American Society of Echocardiography, Society
2014 AHA/ACC Guideline for the Management of Patients With Valvular Heart Disease Developed in Collaboration with the American Association for Thoracic Surgery, American Society of Echocardiography, Society
5. Management of rheumatic heart disease
 5. Management of rheumatic heart disease The fundamental goal in the long-term management of RHD is to prevent ARF recurrences, and therefore, prevent the progression of RHD, and in many cases allow for
5. Management of rheumatic heart disease The fundamental goal in the long-term management of RHD is to prevent ARF recurrences, and therefore, prevent the progression of RHD, and in many cases allow for
Management of the Patient with Aortic Stenosis undergoing Non-cardiac Surgery
 Management of the Patient with Aortic Stenosis undergoing Non-cardiac Surgery Srinivasan Rajagopal M.D. Assistant Professor Division of Cardiothoracic Anesthesia Objectives Describe the pathophysiology
Management of the Patient with Aortic Stenosis undergoing Non-cardiac Surgery Srinivasan Rajagopal M.D. Assistant Professor Division of Cardiothoracic Anesthesia Objectives Describe the pathophysiology
2/20/2015. Cardiac Evaluation of Potential Solid Organ Transplant Recipients. Issues Specific to Transplantation. Kidney Transplantation.
 DISCLOSURES I have no relevant financial relationships to disclose. Cardiac Evaluation of Potential Solid Organ Transplant Recipients Michele Hamilton, MD Director, Heart Failure Program Cedars Sinai Heart
DISCLOSURES I have no relevant financial relationships to disclose. Cardiac Evaluation of Potential Solid Organ Transplant Recipients Michele Hamilton, MD Director, Heart Failure Program Cedars Sinai Heart
Mitral valve repair current Status and the modern Sternotomy
 Mitral valve repair current Status and the modern Sternotomy David L Saint MD, FACS Tallahassee Memorial Hospital Clinical Assistant Professor Florida State University School of Medicine History of Mitral
Mitral valve repair current Status and the modern Sternotomy David L Saint MD, FACS Tallahassee Memorial Hospital Clinical Assistant Professor Florida State University School of Medicine History of Mitral
Low-gradient severe aortic stenosis with normal LVEF: A disturbing clinical entity
 Low-gradient severe aortic stenosis with normal LVEF: A disturbing clinical entity Jean-Luc MONIN, MD, PhD Henri Mondor University Hospital Créteil, FRANCE Disclosures : None 77-year-old woman, mild dyspnea
Low-gradient severe aortic stenosis with normal LVEF: A disturbing clinical entity Jean-Luc MONIN, MD, PhD Henri Mondor University Hospital Créteil, FRANCE Disclosures : None 77-year-old woman, mild dyspnea
Cardiac Assessment for Renal Transplantation: Pre-Operative Clearance is Only the Tip of the Iceberg
 Cardiac Assessment for Renal Transplantation: Pre-Operative Clearance is Only the Tip of the Iceberg 2 nd Annual Duke Renal Transplant Symposium March 1, 2014 Durham, NC Joseph G. Rogers, M.D. Associate
Cardiac Assessment for Renal Transplantation: Pre-Operative Clearance is Only the Tip of the Iceberg 2 nd Annual Duke Renal Transplant Symposium March 1, 2014 Durham, NC Joseph G. Rogers, M.D. Associate
Aortic Valve Stenosis and CAD
 EUROECHO 14, Copenhagen 2010 Aortic Valve Stenosis and CAD Aleksandar N. Neskovic Clinical Hospital Center Zemun Belgrade University School of Medicine Aortic Stenosis and CAD Important facts Links AS/CAD
EUROECHO 14, Copenhagen 2010 Aortic Valve Stenosis and CAD Aleksandar N. Neskovic Clinical Hospital Center Zemun Belgrade University School of Medicine Aortic Stenosis and CAD Important facts Links AS/CAD
Mitral Valve Repair versus Replacement for Severe Ischemic Mitral Regurgitation. Michael Acker, MD For the CTSN Investigators AHA November 2013
 Mitral Valve Repair versus Replacement for Severe Ischemic Mitral Regurgitation Michael Acker, MD For the CTSN Investigators AHA November 2013 Acknowledgements Supported by U01 HL088942 Cardiothoracic
Mitral Valve Repair versus Replacement for Severe Ischemic Mitral Regurgitation Michael Acker, MD For the CTSN Investigators AHA November 2013 Acknowledgements Supported by U01 HL088942 Cardiothoracic
Clinical Commissioning Policy Statement: Percutaneous mitral valve leaflet repair for mitral regurgitation April 2013. Reference: NHSCB/A09/PS/b
 Clinical Commissioning Policy Statement: Percutaneous mitral valve leaflet repair for mitral regurgitation April 2013 Reference: NHS Commissioning Board Clinical Commissioning Policy Statement: Percutaneous
Clinical Commissioning Policy Statement: Percutaneous mitral valve leaflet repair for mitral regurgitation April 2013 Reference: NHS Commissioning Board Clinical Commissioning Policy Statement: Percutaneous
Diagnostic and Therapeutic Procedures
 Diagnostic and Therapeutic Procedures Diagnostic and therapeutic cardiovascular s are central to the evaluation and management of patients with cardiovascular disease. Consistent with the other sections,
Diagnostic and Therapeutic Procedures Diagnostic and therapeutic cardiovascular s are central to the evaluation and management of patients with cardiovascular disease. Consistent with the other sections,
Provider Checklist-Outpatient Imaging. Checklist: Nuclear Stress Test, Thallium/Technetium/Sestamibi (CPT Code 78451-78454 78469)
 Provider Checklist-Outpatient Imaging Checklist: Nuclear Stress Test, Thallium/Technetium/Sestamibi (CPT Code 78451-78454 78469) Medical Review Note: Per InterQual, if any of the following are present,
Provider Checklist-Outpatient Imaging Checklist: Nuclear Stress Test, Thallium/Technetium/Sestamibi (CPT Code 78451-78454 78469) Medical Review Note: Per InterQual, if any of the following are present,
RACE I Rapid Assessment by Cardiac Echo. Intensive Care Training Program Radboud University Medical Centre NIjmegen
 RACE I Rapid Assessment by Cardiac Echo Intensive Care Training Program Radboud University Medical Centre NIjmegen RACE Goal-directed study with specific questions Excludes Doppler ultrasound Perform 50
RACE I Rapid Assessment by Cardiac Echo Intensive Care Training Program Radboud University Medical Centre NIjmegen RACE Goal-directed study with specific questions Excludes Doppler ultrasound Perform 50
2014 AHA/ACC Guideline for the Management of Patients With Valvular Heart Disease: Executive Summary
 2014 AHA/ACC Guideline for the Management of Patients With Valvular Heart Disease: Executive Summary A Report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines
2014 AHA/ACC Guideline for the Management of Patients With Valvular Heart Disease: Executive Summary A Report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines
Perioperative Cardiac Evaluation
 Perioperative Cardiac Evaluation Caroline McKillop Advisor: Dr. Tam Psenka 10-3-2007 Importance of Cardiac Guidelines -Used multiple times every day -Patient Safety -Part of Surgical Care Improvement Project
Perioperative Cardiac Evaluation Caroline McKillop Advisor: Dr. Tam Psenka 10-3-2007 Importance of Cardiac Guidelines -Used multiple times every day -Patient Safety -Part of Surgical Care Improvement Project
Read It, Code It, See It
 Read It, Code It, See It Richard L. Prager, M.D. University of Michigan Ann Arbor, Michigan Dorothy Latham, R.N. Port Huron Hospital Port Huron, Michigan Nothing to Disclose Disclosure Preoperative diagnosis:
Read It, Code It, See It Richard L. Prager, M.D. University of Michigan Ann Arbor, Michigan Dorothy Latham, R.N. Port Huron Hospital Port Huron, Michigan Nothing to Disclose Disclosure Preoperative diagnosis:
38 year old female with mild obesity. She is planning an exercise program to loose weight. She has no other known risk factors for CAD.
 Stress Testing: Wael A. Jaber, MD,FACC 38 year old female with mild obesity She is planning an exercise program to loose weight. She has no other known risk factors for CAD. You recommend: A. Exercise
Stress Testing: Wael A. Jaber, MD,FACC 38 year old female with mild obesity She is planning an exercise program to loose weight. She has no other known risk factors for CAD. You recommend: A. Exercise
Treating AF: The Newest Recommendations. CardioCase presentation. Ethel s Case. Wayne Warnica, MD, FACC, FACP, FRCPC
 Treating AF: The Newest Recommendations Wayne Warnica, MD, FACC, FACP, FRCPC CardioCase presentation Ethel s Case Ethel, 73, presents with rapid heart beating and mild chest discomfort. In the ED, ECG
Treating AF: The Newest Recommendations Wayne Warnica, MD, FACC, FACP, FRCPC CardioCase presentation Ethel s Case Ethel, 73, presents with rapid heart beating and mild chest discomfort. In the ED, ECG
Medical management of CHF: A New Class of Medication. Al Timothy, M.D. Cardiovascular Institute of the South
 Medical management of CHF: A New Class of Medication Al Timothy, M.D. Cardiovascular Institute of the South Disclosures Speakers Bureau for Amgen Background Chronic systolic congestive heart failure remains
Medical management of CHF: A New Class of Medication Al Timothy, M.D. Cardiovascular Institute of the South Disclosures Speakers Bureau for Amgen Background Chronic systolic congestive heart failure remains
Steven J. Yakubov, MD FACC For the CoreValve US Clinical Investigators
 Long-Term Outcomes Using a Self- Expanding Bioprosthesis in Patients With Severe Aortic Stenosis Deemed Extreme Risk for Surgery: Two-Year Results From the CoreValve US Pivotal Trial Steven J. Yakubov,
Long-Term Outcomes Using a Self- Expanding Bioprosthesis in Patients With Severe Aortic Stenosis Deemed Extreme Risk for Surgery: Two-Year Results From the CoreValve US Pivotal Trial Steven J. Yakubov,
Minimally Invasive Mitral Valve Surgery
 Minimally Invasive Mitral Valve Surgery Stanford Health Care offers leading, superior options in cardiac surgery, including the latest techniques and research for Minimally Invasive Cardiac surgery. Advanced
Minimally Invasive Mitral Valve Surgery Stanford Health Care offers leading, superior options in cardiac surgery, including the latest techniques and research for Minimally Invasive Cardiac surgery. Advanced
How should we treat atrial fibrillation in heart failure
 Advances in Cardiac Arrhhythmias and Great Innovations in Cardiology Torino, 23/24 Ottobre 2015 How should we treat atrial fibrillation in heart failure Matteo Anselmino Dipartimento Scienze Mediche Città
Advances in Cardiac Arrhhythmias and Great Innovations in Cardiology Torino, 23/24 Ottobre 2015 How should we treat atrial fibrillation in heart failure Matteo Anselmino Dipartimento Scienze Mediche Città
Real-Time 3-Dimensional Transesophageal Echocardiography in the Evaluation of Post-Operative Mitral Annuloplasty Ring and Prosthetic Valve Dehiscence
 Journal of the American College of Cardiology Vol. 53, No. 17, 2009 2009 by the American College of Cardiology Foundation ISSN 0735-1097/09/$36.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2008.12.059
Journal of the American College of Cardiology Vol. 53, No. 17, 2009 2009 by the American College of Cardiology Foundation ISSN 0735-1097/09/$36.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2008.12.059
HISTORY. Questions: 1. What diagnosis is suggested by this history? 2. How do you explain her symptoms during pregnancy?
 HISTORY 33-year-old woman. CHIEF COMPLAINT: months duration. Dyspnea, fatigue and nocturnal wheezing of six PRESENT ILLNESS: At ages 5 and 9, she had migratory arthritis. At age 29, in the third trimester
HISTORY 33-year-old woman. CHIEF COMPLAINT: months duration. Dyspnea, fatigue and nocturnal wheezing of six PRESENT ILLNESS: At ages 5 and 9, she had migratory arthritis. At age 29, in the third trimester
Objectives. Preoperative Cardiac Risk Stratification for Noncardiac Surgery. History
 Preoperative Cardiac Risk Stratification for Noncardiac Surgery Kimberly Boddicker, MD FACC Essentia Health Heart and Vascular Center 27 th Heart and Vascular Conference May 13, 2011 Objectives Summarize
Preoperative Cardiac Risk Stratification for Noncardiac Surgery Kimberly Boddicker, MD FACC Essentia Health Heart and Vascular Center 27 th Heart and Vascular Conference May 13, 2011 Objectives Summarize
Heart Sounds and Murmurs. Objectives. Valves. Wright, 2012 1
 Heart Sounds and Murmurs Wendy L. Wright, MS, RN, ARNP, FNP, FAANP Family Nurse Practitioner Owner Wright & Associates Family Healthcare Partner Partners in Healthcare Education 1 Objectives Upon completion
Heart Sounds and Murmurs Wendy L. Wright, MS, RN, ARNP, FNP, FAANP Family Nurse Practitioner Owner Wright & Associates Family Healthcare Partner Partners in Healthcare Education 1 Objectives Upon completion
Heart Sounds & Murmurs
 Cardiovascular Physiology Heart Sounds & Murmurs Dr. Abeer A. Al-Masri MBBS, MSc, PhD Associate Professor Consultant Cardiovascular Physiologist Faculty of Medicine, KSU Detected over anterior chest wall
Cardiovascular Physiology Heart Sounds & Murmurs Dr. Abeer A. Al-Masri MBBS, MSc, PhD Associate Professor Consultant Cardiovascular Physiologist Faculty of Medicine, KSU Detected over anterior chest wall
Dysfunction of aortic valve prostheses
 Dysfunction of aortic valve prostheses Kai Andersen Oslo University Hospital Rikshospitalet, Norway Dysfunction of aortic valve prostheses Kai Andersen Oslo University Hospital Rikshospitalet, Norway No
Dysfunction of aortic valve prostheses Kai Andersen Oslo University Hospital Rikshospitalet, Norway Dysfunction of aortic valve prostheses Kai Andersen Oslo University Hospital Rikshospitalet, Norway No
Non Invasive Testing for CAD
 Non Invasive Testing for CAD Wael A. Jaber, MD Section of Cardiac Imaging Heart and Vascular Institute Cleveland Clinic 38 year old female with mild obesity She is planning an exercise program to loose
Non Invasive Testing for CAD Wael A. Jaber, MD Section of Cardiac Imaging Heart and Vascular Institute Cleveland Clinic 38 year old female with mild obesity She is planning an exercise program to loose
Surgeons Role in Atrial Fibrillation
 Atrial Fibrillation Surgeons Role in Atrial Fibrillation Steven J Feldhaus, MD, FACS 2015 Cardiac Symposium September 18, 2015 Stages of Atrial Fibrillation Paroxysmal (Intermittent) Persistent (Continuous)
Atrial Fibrillation Surgeons Role in Atrial Fibrillation Steven J Feldhaus, MD, FACS 2015 Cardiac Symposium September 18, 2015 Stages of Atrial Fibrillation Paroxysmal (Intermittent) Persistent (Continuous)
5. Diagnosis and management of rheumatic heart disease
 5. Diagnosis and management of rheumatic heart disease Introduction Chronic rheumatic valvular heart disease is the long-term result of ARF. It is a disease of poverty and disadvantage. In Australia, the
5. Diagnosis and management of rheumatic heart disease Introduction Chronic rheumatic valvular heart disease is the long-term result of ARF. It is a disease of poverty and disadvantage. In Australia, the
Aortic Stenosis and Comorbidities: the clinical challenge. P. Faggiano Cardiology Division Spedali Civili, Brescia - Italy
 Aortic Stenosis and Comorbidities: the clinical challenge P. Faggiano Cardiology Division Spedali Civili, Brescia - Italy 1 Factors affecting decision-making in patients with symptomatic severe aortic
Aortic Stenosis and Comorbidities: the clinical challenge P. Faggiano Cardiology Division Spedali Civili, Brescia - Italy 1 Factors affecting decision-making in patients with symptomatic severe aortic
Listen to your heart: Good Cardiovascular Health for Life
 Listen to your heart: Good Cardiovascular Health for Life Luis R. Castellanos MD, MPH Assistant Clinical Professor of Medicine University of California San Diego School of Medicine Sulpizio Family Cardiovascular
Listen to your heart: Good Cardiovascular Health for Life Luis R. Castellanos MD, MPH Assistant Clinical Professor of Medicine University of California San Diego School of Medicine Sulpizio Family Cardiovascular
4/7/2015. Cardiac Rehabilitation: From the other side of the glass door. Chicago, circa 1999. Objectives. No disclosures, no conflicts
 Cardiac Rehabilitation: From the other side of the glass door No disclosures, no conflicts Charles X. Kim, MD, FACC, ABVM Objectives 1. Illustrate common CV benefits of CV rehab in real world practice.
Cardiac Rehabilitation: From the other side of the glass door No disclosures, no conflicts Charles X. Kim, MD, FACC, ABVM Objectives 1. Illustrate common CV benefits of CV rehab in real world practice.
Updated Cardiac Resynchronization Therapy Guidelines
 The Ohio State University Heart and Vascular Center Updated Cardiac Resynchronization Therapy Guidelines William T. Abraham, MD, FACP, FACC, FAHA, FESC Professor of Medicine, Physiology, and Cell Biology
The Ohio State University Heart and Vascular Center Updated Cardiac Resynchronization Therapy Guidelines William T. Abraham, MD, FACP, FACC, FAHA, FESC Professor of Medicine, Physiology, and Cell Biology
Management of Atrial Fibrillation in Heart Failure
 Disadvantages of AV Junction Ablation Persistent AFib- no AV synchrony Ongoing risk of thromboembolism Life-long dependency on pacemaker Comparison of LA Ablation vs. AVN Ablation LA Ablation AVN Ablation
Disadvantages of AV Junction Ablation Persistent AFib- no AV synchrony Ongoing risk of thromboembolism Life-long dependency on pacemaker Comparison of LA Ablation vs. AVN Ablation LA Ablation AVN Ablation
Medical Policy Manual. Topic: Transcatheter Mitral Valve Repair Date of Origin: November 2015. Section: Surgery Last Reviewed Date: November 2015
 Medical Policy Manual Topic: Transcatheter Mitral Valve Repair Date of Origin: November 2015 Section: Surgery Last Reviewed Date: November 2015 Policy No: 199 Effective Date: January 1, 2016 IMPORTANT
Medical Policy Manual Topic: Transcatheter Mitral Valve Repair Date of Origin: November 2015 Section: Surgery Last Reviewed Date: November 2015 Policy No: 199 Effective Date: January 1, 2016 IMPORTANT
Automatic External Defibrillators
 Last Review Date: May 27, 2016 Number: MG.MM.DM.10dC2 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary care provider must submit to EmblemHealth
Last Review Date: May 27, 2016 Number: MG.MM.DM.10dC2 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary care provider must submit to EmblemHealth
DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) MANAGEMENT of Atrial Fibrillation (AF)
 DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) MANAGEMENT of Atrial Fibrillation (AF) Key priorities Identification and diagnosis Treatment for persistent AF Treatment for permanent AF Antithrombotic
DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) MANAGEMENT of Atrial Fibrillation (AF) Key priorities Identification and diagnosis Treatment for persistent AF Treatment for permanent AF Antithrombotic
EAE TEACHING COURSE Aorta and aortic valve 2012
 EAE TEACHING COURSE Aorta and aortic valve 2012 31th March 2012 Szczecin, Poland EP EAE TEACHING COURSE: aorta and aortic valve Szczecin, 31st March 2012 Prof. Luigi Badano, Italy Prof. Patrizio Lancellotti,
EAE TEACHING COURSE Aorta and aortic valve 2012 31th March 2012 Szczecin, Poland EP EAE TEACHING COURSE: aorta and aortic valve Szczecin, 31st March 2012 Prof. Luigi Badano, Italy Prof. Patrizio Lancellotti,
COVERAGE GUIDANCE: ABLATION FOR ATRIAL FIBRILLATION
 COVERAGE GUIDANCE: ABLATION FOR ATRIAL FIBRILLATION Question: How should the EGBS Coverage Guidance regarding ablation for atrial fibrillation be applied to the Prioritized List? Question source: Evidence
COVERAGE GUIDANCE: ABLATION FOR ATRIAL FIBRILLATION Question: How should the EGBS Coverage Guidance regarding ablation for atrial fibrillation be applied to the Prioritized List? Question source: Evidence
Guidelines on the management of valvular heart disease
 European Heart Journal doi:10.1093/eurheartj/ehl428 Guidelines on the management of valvular heart disease The Task Force on the Management of Valvular Heart Disease of the European Society of Cardiology
European Heart Journal doi:10.1093/eurheartj/ehl428 Guidelines on the management of valvular heart disease The Task Force on the Management of Valvular Heart Disease of the European Society of Cardiology
Potential Causes of Sudden Cardiac Arrest in Children
 Potential Causes of Sudden Cardiac Arrest in Children Project S.A.V.E. When sudden death occurs in children, adolescents and younger adults, heart abnormalities are likely causes. These conditions are
Potential Causes of Sudden Cardiac Arrest in Children Project S.A.V.E. When sudden death occurs in children, adolescents and younger adults, heart abnormalities are likely causes. These conditions are
2014 AHA/ACC Guideline for the Management of Patients With Valvular Heart Disease
 Accepted Manuscript 2014 AHA/ACC Guideline for the Management of Patients With Valvular Heart Disease Rick A. Nishimura, MD, MACC, FAHA Catherine M. Otto, MD, FACC, FAHA Robert O. Bonow, MD, MACC, FAHA
Accepted Manuscript 2014 AHA/ACC Guideline for the Management of Patients With Valvular Heart Disease Rick A. Nishimura, MD, MACC, FAHA Catherine M. Otto, MD, FACC, FAHA Robert O. Bonow, MD, MACC, FAHA
Resuscitation in congenital heart disease. Peter C. Laussen MBBS FCICM Department Critical Care Medicine Hospital for Sick Children Toronto
 Resuscitation in congenital heart disease Peter C. Laussen MBBS FCICM Department Critical Care Medicine Hospital for Sick Children Toronto Evolution of Congenital Heart Disease Extraordinary success: Overall
Resuscitation in congenital heart disease Peter C. Laussen MBBS FCICM Department Critical Care Medicine Hospital for Sick Children Toronto Evolution of Congenital Heart Disease Extraordinary success: Overall
ATRIAL FIBRILLATION (RATE VS RHYTHM CONTROL)
 ATRIAL FIBRILLATION (RATE VS RHYTHM CONTROL) By Prof. Dr. Helmy A. Bakr Mansoura Universirty 2014 AF Classification: Mechanisms of AF : Selected Risk Factors and Biomarkers for AF: WHY AF? 1. Atrial fibrillation
ATRIAL FIBRILLATION (RATE VS RHYTHM CONTROL) By Prof. Dr. Helmy A. Bakr Mansoura Universirty 2014 AF Classification: Mechanisms of AF : Selected Risk Factors and Biomarkers for AF: WHY AF? 1. Atrial fibrillation
CTA OF THE EXTRACORONARY HEART
 CTA OF THE EXTRACORONARY HEART Charles White MD Director of Thoracic Imaging Department of Radiology University of Maryland NO DISCLOSURES CWHITE@UMM.EDU CARDIAC CASE DISTRIBUTION Coronary CTA 30% ED chest
CTA OF THE EXTRACORONARY HEART Charles White MD Director of Thoracic Imaging Department of Radiology University of Maryland NO DISCLOSURES CWHITE@UMM.EDU CARDIAC CASE DISTRIBUTION Coronary CTA 30% ED chest
Section 8: Clinical Exercise Testing. a maximal GXT?
 Section 8: Clinical Exercise Testing Maximal GXT ACSM Guidelines: Chapter 5 ACSM Manual: Chapter 8 HPHE 4450 Dr. Cheatham Outline What is the purpose of a maximal GXT? Who should have a maximal GXT (and
Section 8: Clinical Exercise Testing Maximal GXT ACSM Guidelines: Chapter 5 ACSM Manual: Chapter 8 HPHE 4450 Dr. Cheatham Outline What is the purpose of a maximal GXT? Who should have a maximal GXT (and
Recommendations for Evaluation of the Severity of Native Valvular Regurgitation with Two-dimensional and Doppler Echocardiography
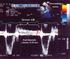 AMERICAN SOCIETY OF ECHOCARDIOGRAPHY REPORT Recommendations for Evaluation of the Severity of Native Valvular Regurgitation with Two-dimensional and Doppler Echocardiography A report from the American
AMERICAN SOCIETY OF ECHOCARDIOGRAPHY REPORT Recommendations for Evaluation of the Severity of Native Valvular Regurgitation with Two-dimensional and Doppler Echocardiography A report from the American
Main Effect of Screening for Coronary Artery Disease Using CT
 Main Effect of Screening for Coronary Artery Disease Using CT Angiography on Mortality and Cardiac Events in High risk Patients with Diabetes: The FACTOR-64 Randomized Clinical Trial Joseph B. Muhlestein,
Main Effect of Screening for Coronary Artery Disease Using CT Angiography on Mortality and Cardiac Events in High risk Patients with Diabetes: The FACTOR-64 Randomized Clinical Trial Joseph B. Muhlestein,
TAVR: A New Treatment Option for Aortic Stenosis. Alexis Auger, MSN, NP-BC
 TAVR: A New Treatment Option for Aortic Stenosis Alexis Auger, MSN, NP-BC 22nd Annual Northeast Regional Nurse Practitioner Conference May 6-8, 2015 DISCLOSURES There has been no commercial support or
TAVR: A New Treatment Option for Aortic Stenosis Alexis Auger, MSN, NP-BC 22nd Annual Northeast Regional Nurse Practitioner Conference May 6-8, 2015 DISCLOSURES There has been no commercial support or
Cardiovascular Guidelines for DOT Physical Exams By Maureen Collins MSN, APRN, BC
 Cardiovascular Guidelines for DOT Physical Exams By Maureen Collins MSN, APRN, BC The Federal Motor Carrier Safety Administration (FMCSA) administers the Federal Motor Carrier Safety Regulations (FMCSRs)
Cardiovascular Guidelines for DOT Physical Exams By Maureen Collins MSN, APRN, BC The Federal Motor Carrier Safety Administration (FMCSA) administers the Federal Motor Carrier Safety Regulations (FMCSRs)
The Difficult Mitral Valve Repair in Children, Leave with Stenosis or Regurgitation
 The Difficult Mitral Valve Repair in Children, Leave with Stenosis or Regurgitation Abdullah A. Alghamdi, MD, MSc, FRCSC King Abdulaziz Cardiac Center, National Guard Riyadh, Saudi Arabia Outlines Not
The Difficult Mitral Valve Repair in Children, Leave with Stenosis or Regurgitation Abdullah A. Alghamdi, MD, MSc, FRCSC King Abdulaziz Cardiac Center, National Guard Riyadh, Saudi Arabia Outlines Not
Auscultation of the Heart
 Review of Clinical Signs uscultation of the Heart Series Editor: Bernard Karnath, MD Bernard Karnath, MD William Thornton, MD uscultation of the heart can provide clues to the diagnosis of many cardiac
Review of Clinical Signs uscultation of the Heart Series Editor: Bernard Karnath, MD Bernard Karnath, MD William Thornton, MD uscultation of the heart can provide clues to the diagnosis of many cardiac
Press conference: Rheumatic Heart Disease a forgotten but devastating disease
 www.worldcardiocongress.org Chairpersons: Bongani M. Mayosi Jonathan Carapetis Press conference: Rheumatic Heart Disease a forgotten but devastating disease www.worldcardiocongress.org www.worldcardiocongress.org
www.worldcardiocongress.org Chairpersons: Bongani M. Mayosi Jonathan Carapetis Press conference: Rheumatic Heart Disease a forgotten but devastating disease www.worldcardiocongress.org www.worldcardiocongress.org
Heart Murmurs. Outline. Basic Pathophysiology
 Heart Murmurs David Leder Outline I. Basic Pathophysiology II. Describing murmurs III. Systolic murmurs IV. Diastolic murmurs V. Continuous murmurs VI. Summary Basic Pathophysiology Murmurs = Math Q =
Heart Murmurs David Leder Outline I. Basic Pathophysiology II. Describing murmurs III. Systolic murmurs IV. Diastolic murmurs V. Continuous murmurs VI. Summary Basic Pathophysiology Murmurs = Math Q =
Renovascular Hypertension
 Renovascular Hypertension Philip Stockwell, MD Assistant Professor of Medicine (Clinical) Warren Alpert School of Medicine Cardiology for the Primary Care Provider September 28, 201 Renovascular Hypertension
Renovascular Hypertension Philip Stockwell, MD Assistant Professor of Medicine (Clinical) Warren Alpert School of Medicine Cardiology for the Primary Care Provider September 28, 201 Renovascular Hypertension
Durability of mitral valve repair for mitral regurgitation due to degenerative mitral valve disease
 Keynote Lecture Series Durability of mitral valve repair for mitral regurgitation due to degenerative mitral valve disease Tirone E. David Division of Cardiovascular Surgery, Peter Munk Cardiac Centre,
Keynote Lecture Series Durability of mitral valve repair for mitral regurgitation due to degenerative mitral valve disease Tirone E. David Division of Cardiovascular Surgery, Peter Munk Cardiac Centre,
UPMC HEALTH PLAN MANAGEMENT OF HEART FAILURE WITH LEFT VENTRICULAR SYSTOLIC DYSFUNCTION: CLINICAL PRACTICE GUIDELINE
 General Statement on UPMC Health Plan Clinical Practice Guidelines: UPMC Health Plan develops clinical practice guidelines to support the practice of evidence-based medicine. The guidelines are from recognized
General Statement on UPMC Health Plan Clinical Practice Guidelines: UPMC Health Plan develops clinical practice guidelines to support the practice of evidence-based medicine. The guidelines are from recognized
NAME OF THE HOSPITAL: 1. Coronary Balloon Angioplasty: M7F1.1/ Angioplasty with Stent(PTCA with Stent): M7F1.3
 1. Coronary Balloon Angioplasty: M7F1.1/ Angioplasty with Stent(PTCA with Stent): M7F1.3 1. Name of the Procedure: Coronary Balloon Angioplasty 2. Select the Indication from the drop down of various indications
1. Coronary Balloon Angioplasty: M7F1.1/ Angioplasty with Stent(PTCA with Stent): M7F1.3 1. Name of the Procedure: Coronary Balloon Angioplasty 2. Select the Indication from the drop down of various indications
PHARMACOLOGICAL Stroke Prevention in Atrial Fibrillation STROKE RISK ASSESSMENT SCORES Vs. BLEEDING RISK ASSESSMENT SCORES.
 PHARMACOLOGICAL Stroke Prevention in Atrial Fibrillation STROKE RISK ASSESSMENT SCORES Vs. BLEEDING RISK ASSESSMENT SCORES. Hossam Bahy, MD (1992 2012), 19 tools have been identified 11 stroke scores 1
PHARMACOLOGICAL Stroke Prevention in Atrial Fibrillation STROKE RISK ASSESSMENT SCORES Vs. BLEEDING RISK ASSESSMENT SCORES. Hossam Bahy, MD (1992 2012), 19 tools have been identified 11 stroke scores 1
Transcatheter Mitral Valve Repair
 MEDICAL POLICY POLICY RELATED POLICIES POLICY GUIDELINES DESCRIPTION SCOPE BENEFIT APPLICATION RATIONALE REFERENCES CODING APPENDIX HISTORY Transcatheter Mitral Valve Repair Number 2.02.30 Effective Date
MEDICAL POLICY POLICY RELATED POLICIES POLICY GUIDELINES DESCRIPTION SCOPE BENEFIT APPLICATION RATIONALE REFERENCES CODING APPENDIX HISTORY Transcatheter Mitral Valve Repair Number 2.02.30 Effective Date
Inpatient Heart Failure Management: Risks & Benefits
 Inpatient Heart Failure Management: Risks & Benefits Dr. Kenneth L. Baughman Professor of Medicine Harvard Medical School Director, Advanced Heart Disease Section Brigham & Women's Hospital Harvard Medical
Inpatient Heart Failure Management: Risks & Benefits Dr. Kenneth L. Baughman Professor of Medicine Harvard Medical School Director, Advanced Heart Disease Section Brigham & Women's Hospital Harvard Medical
The road to mitral valve repair with live 3D transesophageal echocardiography (TEE)
 Clinical applications The road to mitral valve repair with live 3D transesophageal echocardiography (T) R.M. Lang I.S. Salgo A.C. Anyanwu D.H. Adams Professor of Medicine; Director, Noninvasive Cardiac
Clinical applications The road to mitral valve repair with live 3D transesophageal echocardiography (T) R.M. Lang I.S. Salgo A.C. Anyanwu D.H. Adams Professor of Medicine; Director, Noninvasive Cardiac
Presenter Disclosure Information
 2:15 3 pm Managing Arrhythmias in Primary Care Presenter Disclosure Information The following relationships exist related to this presentation: Raul Mitrani, MD, FACC, FHRS: Speakers Bureau for Medtronic.
2:15 3 pm Managing Arrhythmias in Primary Care Presenter Disclosure Information The following relationships exist related to this presentation: Raul Mitrani, MD, FACC, FHRS: Speakers Bureau for Medtronic.
INHERIT. The Lancet Diabetes & Endocrinology In press
 INHibition of the renin angiotensin system in hypertrophic cardiomyopathy and the Effect on hypertrophy a Randomized Intervention Trial with losartan Anna Axelsson, Kasper Iversen, Niels Vejlstrup, Carolyn
INHibition of the renin angiotensin system in hypertrophic cardiomyopathy and the Effect on hypertrophy a Randomized Intervention Trial with losartan Anna Axelsson, Kasper Iversen, Niels Vejlstrup, Carolyn
FFR CT : Clinical studies
 FFR CT : Clinical studies Bjarne Nørgaard Department Cardiology B Aarhus University Hospital Skejby, Denmark Disclosures: Research grants: Edwards and Siemens Coronary CTA: High diagnostic sensitivity
FFR CT : Clinical studies Bjarne Nørgaard Department Cardiology B Aarhus University Hospital Skejby, Denmark Disclosures: Research grants: Edwards and Siemens Coronary CTA: High diagnostic sensitivity
on behalf of the AUGMENT-HF Investigators
 One Year Follow-Up Results from AUGMENT-HF: A Multicenter Randomized Controlled Clinical Trial of the Efficacy of Left Ventricular Augmentation with Algisyl-LVR in the Treatment of Heart Failure* Douglas
One Year Follow-Up Results from AUGMENT-HF: A Multicenter Randomized Controlled Clinical Trial of the Efficacy of Left Ventricular Augmentation with Algisyl-LVR in the Treatment of Heart Failure* Douglas
RATE VERSUS RHYTHM CONTROL OF ATRIAL FIBRILLATION: SPECIAL CONSIDERATION IN ELDERLY. Charles Jazra
 RATE VERSUS RHYTHM CONTROL OF ATRIAL FIBRILLATION: SPECIAL CONSIDERATION IN ELDERLY Charles Jazra NO CONFLICT OF INTEREST TO DECLARE Relationship Between Atrial Fibrillation and Age Prevalence, percent
RATE VERSUS RHYTHM CONTROL OF ATRIAL FIBRILLATION: SPECIAL CONSIDERATION IN ELDERLY Charles Jazra NO CONFLICT OF INTEREST TO DECLARE Relationship Between Atrial Fibrillation and Age Prevalence, percent
CARDIAC RISKS OF NON CARDIAC SURGERY
 CARDIAC RISKS OF NON CARDIAC SURGERY N E W S T U D I E S & N E W G U I D E L I N E S W. B. C A L H O U N, M D, F A C C 2014 ACC/AHA Guideline on perioperative cardiovascular evaluation and management
CARDIAC RISKS OF NON CARDIAC SURGERY N E W S T U D I E S & N E W G U I D E L I N E S W. B. C A L H O U N, M D, F A C C 2014 ACC/AHA Guideline on perioperative cardiovascular evaluation and management
one of the most prevalent cardiac in almost 2.4 percent of the population. 1 Although the incidence of infective
 Case Report Hellenic J Cardiol 2011; 52: 177-181 Successful Surgical Repair of Mitral Valve Prolapse Endocarditis: Case Report and Review of the Current Literature Pavlos N. Stougiannos 1, Dimitrios Z.
Case Report Hellenic J Cardiol 2011; 52: 177-181 Successful Surgical Repair of Mitral Valve Prolapse Endocarditis: Case Report and Review of the Current Literature Pavlos N. Stougiannos 1, Dimitrios Z.
How To Understand What You Know
 Heart Disorders Glossary ABG (Arterial Blood Gas) Test: A test that measures how much oxygen and carbon dioxide are in the blood. Anemia: A condition in which there are low levels of red blood cells in
Heart Disorders Glossary ABG (Arterial Blood Gas) Test: A test that measures how much oxygen and carbon dioxide are in the blood. Anemia: A condition in which there are low levels of red blood cells in
Richtlijn voor de chirurgische behandeling van hartklep-aandoeningen
 Richtlijn voor de chirurgische behandeling van hartklep-aandoeningen Nederlandse Vereniging voor Thoraxchirurgie Deze richtlijn is mede gebaseerd op de ESC-richtlijnen over de behandeling van aandoeningen
Richtlijn voor de chirurgische behandeling van hartklep-aandoeningen Nederlandse Vereniging voor Thoraxchirurgie Deze richtlijn is mede gebaseerd op de ESC-richtlijnen over de behandeling van aandoeningen
Percutaneous closure of paravalvular leaks EULOGIO GARCIA MD MADRID ~ SPAIN
 Percutaneous closure of paravalvular leaks EULOGIO GARCIA MD MADRID ~ SPAIN BACKGROUND The incidente of paravalvular leaks is variable ( from 2% up to 17% ). More frequent in mechanical valves. Surgical
Percutaneous closure of paravalvular leaks EULOGIO GARCIA MD MADRID ~ SPAIN BACKGROUND The incidente of paravalvular leaks is variable ( from 2% up to 17% ). More frequent in mechanical valves. Surgical
Chronic Thromboembolic Disease. Chronic Thromboembolic Disease Definition. Diagnosis Prevention Treatment Surgical Nonsurgical
 Chronic Thromboembolic Disease Diagnosis Prevention Treatment Surgical Nonsurgical Chronic Thromboembolic Disease Definition Pulmonary Hypertension due to chronic thromboembolism 6 months post acute PE:
Chronic Thromboembolic Disease Diagnosis Prevention Treatment Surgical Nonsurgical Chronic Thromboembolic Disease Definition Pulmonary Hypertension due to chronic thromboembolism 6 months post acute PE:
Perioperative Risk Stratification for Noncardiac Surgical Patients with Cardiac Diagnosis. Michael A. Blazing
 Perioperative Risk Stratification for Noncardiac Surgical Patients with Cardiac Diagnosis Michael A. Blazing Outline The coming crush A practical approach to clinical risk assessment Classic approach to
Perioperative Risk Stratification for Noncardiac Surgical Patients with Cardiac Diagnosis Michael A. Blazing Outline The coming crush A practical approach to clinical risk assessment Classic approach to
Atrial Fibrillation The High Risk Obese Patient
 Atrial Fibrillation The High Risk Obese Patient Frederick Schaller, D.O.,F.A.C.O.I. Professor and Vice Dean Touro University Nevada A 56 year old male with a history of hypertension and chronic stable
Atrial Fibrillation The High Risk Obese Patient Frederick Schaller, D.O.,F.A.C.O.I. Professor and Vice Dean Touro University Nevada A 56 year old male with a history of hypertension and chronic stable
Atrial Fibrillation Peter Santucci, MD Revised May, 2008
 Atrial Fibrillation Peter Santucci, MD Revised May, 2008 Atrial fibrillation (AF) is an irregular, disorganized rhythm characterized by a lack of organized mechanical atrial activity. The atrial rate is
Atrial Fibrillation Peter Santucci, MD Revised May, 2008 Atrial fibrillation (AF) is an irregular, disorganized rhythm characterized by a lack of organized mechanical atrial activity. The atrial rate is
17 Endocarditis. Infective endocarditis
 17 Endocarditis 234 Endocarditis refers to inflammation of the endocardium, the inner layer of the heart (including the heart valves). Endocarditis can be: infective (e.g. bacterial, fungal) non-infective
17 Endocarditis 234 Endocarditis refers to inflammation of the endocardium, the inner layer of the heart (including the heart valves). Endocarditis can be: infective (e.g. bacterial, fungal) non-infective
Utilizing the Cath Lab for Cardiac Arrest
 Utilizing the Cath Lab for Cardiac Arrest Khaled M. Ziada, MD Director, Cardiovascular Catheterization Laboratories Gill Heart Institute, University of Kentucky UK/AHA Strive to Revive Symposium May 2013
Utilizing the Cath Lab for Cardiac Arrest Khaled M. Ziada, MD Director, Cardiovascular Catheterization Laboratories Gill Heart Institute, University of Kentucky UK/AHA Strive to Revive Symposium May 2013
2012 Scientific Sessions of the ACC March 24, 2012. Emerson C Perin, MD, PhD
 Effect of Transendocardial Delivery of Autologous Bone Marrow Mononuclear Cells on Functional Capacity, Left Ventricular Function, and Perfusion in Chronic Ischemic Heart Failure: The FOCUS CCTRN Trial
Effect of Transendocardial Delivery of Autologous Bone Marrow Mononuclear Cells on Functional Capacity, Left Ventricular Function, and Perfusion in Chronic Ischemic Heart Failure: The FOCUS CCTRN Trial
Ottavio Alfieri S. Raffaele University Hospital, Milano
 The future of mitral surgery: revolution versus involution Ottavio Alfieri S. Raffaele University Hospital, Milano Future The trouble with the future is that it s so much less knowable than the past. John
The future of mitral surgery: revolution versus involution Ottavio Alfieri S. Raffaele University Hospital, Milano Future The trouble with the future is that it s so much less knowable than the past. John
The Cardiac Society of Australia and New Zealand
 The Cardiac Society of Australia and New Zealand Guidelines on Support Facilities for Coronary Angiography and Percutaneous Coronary Intervention (PCI) including Guidelines on the Performance of Procedures
The Cardiac Society of Australia and New Zealand Guidelines on Support Facilities for Coronary Angiography and Percutaneous Coronary Intervention (PCI) including Guidelines on the Performance of Procedures
1p36 and the Heart. John Lynn Jefferies, MD, MPH, FACC, FAHA
 1p36 and the Heart John Lynn Jefferies, MD, MPH, FACC, FAHA Director, Advanced Heart Failure and Cardiomyopathy Services Associate Professor, Pediatric Cardiology and Adult Cardiovascular Diseases Associate
1p36 and the Heart John Lynn Jefferies, MD, MPH, FACC, FAHA Director, Advanced Heart Failure and Cardiomyopathy Services Associate Professor, Pediatric Cardiology and Adult Cardiovascular Diseases Associate
Chest Pain. Acute Myocardial Infarction: Differential Diagnosis and Patient Management. Common complaint in ED. Wide range of etiologies
 Acute Myocardial Infarction: Differential Diagnosis and Patient Management Presented By: Barbara Furry, RN-BC, MS, CCRN, FAHA Director The Center of Excellence in Education Director of HERO Chest Pain
Acute Myocardial Infarction: Differential Diagnosis and Patient Management Presented By: Barbara Furry, RN-BC, MS, CCRN, FAHA Director The Center of Excellence in Education Director of HERO Chest Pain
Contemporary Management of Cardiovascular Disease
 Contemporary Management of Cardiovascular Disease FRIDAY, OCTOBER 30, 2015 Baltimore Hilton Hotel Baltimore, Maryland Register Today! ccfcme.org/gocvddc Contemporary Management of Cardiovascular Disease
Contemporary Management of Cardiovascular Disease FRIDAY, OCTOBER 30, 2015 Baltimore Hilton Hotel Baltimore, Maryland Register Today! ccfcme.org/gocvddc Contemporary Management of Cardiovascular Disease
PRECOMBAT Trial. Seung-Whan Lee, MD, PhD On behalf of the PRECOMBAT Investigators
 Premier of Randomized Comparison of Bypass Surgery versus Angioplasty Using Sirolimus-Eluting Stent in Patients with Left Main Coronary Artery Disease PRECOMBAT Trial Seung-Whan Lee, MD, PhD On behalf
Premier of Randomized Comparison of Bypass Surgery versus Angioplasty Using Sirolimus-Eluting Stent in Patients with Left Main Coronary Artery Disease PRECOMBAT Trial Seung-Whan Lee, MD, PhD On behalf
Atrial Fibrillation: Drugs, Ablation, or Benign Neglect. Robert Kennedy, MD October 10, 2015
 Atrial Fibrillation: Drugs, Ablation, or Benign Neglect Robert Kennedy, MD October 10, 2015 Definitions 2014 AHA/ACC/HRS Guideline for the Management of Patients With Atrial Fibrillation: Executive Summary.
Atrial Fibrillation: Drugs, Ablation, or Benign Neglect Robert Kennedy, MD October 10, 2015 Definitions 2014 AHA/ACC/HRS Guideline for the Management of Patients With Atrial Fibrillation: Executive Summary.
Heart valve repair and replacement
 16 Heart valve repair and replacement 222 Valvular heart disease can be treated in a variety of ways: valve replacement, in which an artificial (prosthetic) heart valve is implanted surgically to replace
16 Heart valve repair and replacement 222 Valvular heart disease can be treated in a variety of ways: valve replacement, in which an artificial (prosthetic) heart valve is implanted surgically to replace
May 1 6, 2016 Loews Atlanta Hotel Atlanta, GA PRELIMINARY PROGRAM AT A GLANCE
 Sunday, May 1 7:00-8:30 pm Image Optimization Workshop: 2D Echocardiography Moderators: Fabio De Vasconelos Papa, MD; Mark A. Taylor, MD : Annemarie Thompson, MD Speakers: Gregg S. Hartman, MD Lori B.
Sunday, May 1 7:00-8:30 pm Image Optimization Workshop: 2D Echocardiography Moderators: Fabio De Vasconelos Papa, MD; Mark A. Taylor, MD : Annemarie Thompson, MD Speakers: Gregg S. Hartman, MD Lori B.
Section Four: Pulmonary Artery Waveform Interpretation
 Section Four: Pulmonary Artery Waveform Interpretation All hemodynamic pressures and waveforms are generated by pressure changes in the heart caused by myocardial contraction (systole) and relaxation/filling
Section Four: Pulmonary Artery Waveform Interpretation All hemodynamic pressures and waveforms are generated by pressure changes in the heart caused by myocardial contraction (systole) and relaxation/filling
Atrial Fibrillation and Heart Failure: A Cause or a Consequence
 Atrial Fibrillation and Heart Failure: A Cause or a Consequence Rajat Deo, MD, MTR Assistant Professor of Medicine Division of Cardiology, Electrophysiology Section University of Pennsylvania November
Atrial Fibrillation and Heart Failure: A Cause or a Consequence Rajat Deo, MD, MTR Assistant Professor of Medicine Division of Cardiology, Electrophysiology Section University of Pennsylvania November
INTRODUCTION TO EECP THERAPY
 INTRODUCTION TO EECP THERAPY is an FDA cleared, Medicare approved, non-invasive medical therapy for the treatment of stable and unstable angina, congestive heart failure, acute myocardial infarction, and
INTRODUCTION TO EECP THERAPY is an FDA cleared, Medicare approved, non-invasive medical therapy for the treatment of stable and unstable angina, congestive heart failure, acute myocardial infarction, and
How do you decide on rate versus rhythm control?
 How do you decide on rate versus rhythm control? Dr. Mark O Neill Consultant Cardiologist & Electrophysiologist Assumptions Camm et al. EHJ 2010;Sept 25 epub Choice of strategy: Criteria for consideration
How do you decide on rate versus rhythm control? Dr. Mark O Neill Consultant Cardiologist & Electrophysiologist Assumptions Camm et al. EHJ 2010;Sept 25 epub Choice of strategy: Criteria for consideration
Pulmonary Atresia With Intact Ventricular Septum - Anatomy, Physiology, and Diagnostic Imaging
 Pulmonary Atresia With Intact Ventricular Septum - Anatomy, Physiology, and Diagnostic Imaging Larry Latson MD Director of Pediatric Interventional Cardiology and Adult CHD Joe DiMaggio Children s Hospital
Pulmonary Atresia With Intact Ventricular Septum - Anatomy, Physiology, and Diagnostic Imaging Larry Latson MD Director of Pediatric Interventional Cardiology and Adult CHD Joe DiMaggio Children s Hospital
Nikos Kouris a, *, Ignatios Ikonomidis b, Dimitra Kontogianni a, Peter Smith b, Petros Nihoyannopoulos b
 Eur J Echocardiography (2005) 6, 435e442 Mitral valve repair versus replacement for isolated non-ischemic mitral regurgitation in patients with preoperative left ventricular dysfunction. A long-term follow-up
Eur J Echocardiography (2005) 6, 435e442 Mitral valve repair versus replacement for isolated non-ischemic mitral regurgitation in patients with preoperative left ventricular dysfunction. A long-term follow-up
Cilostazol versus Clopidogrel after Coronary Stenting
 Cilostazol versus Clopidogrel after Coronary Stenting Seong-Wook Park, MD, PhD, FACC Division of Cardiology, Asan Medical Center University of Ulsan College of Medicine Seoul, Korea AMC, 2004 Background
Cilostazol versus Clopidogrel after Coronary Stenting Seong-Wook Park, MD, PhD, FACC Division of Cardiology, Asan Medical Center University of Ulsan College of Medicine Seoul, Korea AMC, 2004 Background
123 Main St NY, New York 12345 ph: (202) 555 5555 fax: (202) 555 5555
 Patient Name: DOE, JOHN D. Gender: M Date of Study: 4/2/2013 Date of birth: 6/28/1962 Age: 50 Medical Record #: 45869725 Ordering Physician: JANE INTERNIST, MD History: Atypical Angina, Abn ECG, High Cholesterol,
Patient Name: DOE, JOHN D. Gender: M Date of Study: 4/2/2013 Date of birth: 6/28/1962 Age: 50 Medical Record #: 45869725 Ordering Physician: JANE INTERNIST, MD History: Atypical Angina, Abn ECG, High Cholesterol,
Cardiac Catheterization Curriculum for Fellows in Cardiology Dartmouth-Hitchcock Medical Center Level 1 and Level 2 Training 2008-2009
 Cardiac Catheterization Curriculum for Fellows in Cardiology Dartmouth-Hitchcock Medical Center Level 1 and Level 2 Training 2008-2009 I. Overview of Training in Cardiac Catheterization Cardiac catheterization
Cardiac Catheterization Curriculum for Fellows in Cardiology Dartmouth-Hitchcock Medical Center Level 1 and Level 2 Training 2008-2009 I. Overview of Training in Cardiac Catheterization Cardiac catheterization
