Central non-tunneled closed end or valved (i.e., Bard Solo Power PICC) Pediatrics: 1.9 F 0.06 ml F ml 4 F 0.6 ml
|
|
|
- Asher Stafford
- 8 years ago
- Views:
Transcription
1 Second Edition
2 Standardizing Central Venous Catheter Care: Hospital to Home Introduction This is the second edition of the guidelines for out of hospital care of central venous access devices (CVAD). The purpose of the guidelines is to standardize the out of hospital care of patients with central venous catheters in order to optimize safe medication administration across the continuum of care and improve patient outcomes. The development of these guidelines has been a joint effort of the organizations listed below. In May 2011, this group convened and began developing the guidelines, assigning themselves and the project the acronym SCORCH Standardizing Central Catheter Care in the Omaha Region: Care from Hospital to Home. We hope that the information in these guidelines will be useful in the provision of best practices to patients dismissed from hospital with central venous catheters in place. These guidelines are for guidance only and are not a substitute for physician or nursing judgment or consultation with experts with respect to individual patients. Contributing Authors Bibliography The Nebraska Medical Center Regina E. Nailon, RN, PhD, Project Lead Clinical Nurse Researcher, Nursing Research and Quality Outcomes rnailon@nebraskamed.com Susan O Neill, RN Staff Nurse, Peggy Cowdery Patient Care Center Sue Wardian Hartung, RN, MSN, OCN Nurse Coordinator, Patient Education Cancer Service Line L. Kate Tyner, RN, BSN, CIC Infection Preventionist Patti Tomb, RN, BSN Vascular Access Specialist University of Nebraska Medical Center Mark E. Rupp, MD, Project Co-Lead Professor and Chief, Division of Infectious Diseases Medical Director, Healthcare Epidemiology merupp@unmc.edu Kari A. Simonsen, MD Assistant Professor of Pediatrics, Section of Pediatric Infectious Diseases Program Director, Pediatric Infectious Diseases Fellowship Medical Advisor, Douglas County Health Department Children s Home Healthcare Children s Hospital & Medical Center Sarah J. Ciriaco, RN, CPN Clinical Services Manager Kimberly A. Peterson, MSN, APRN-PCNS-BC, CPN Clinical Nurse Specialist Amy Phillips, MSN, APRN-CNS, CCRN Clinical Nurse Specialist Alegent Health at Home DeAnn Wintle, RN, BSN Home Care/Infusion Team Coordinator Home Nursing with Heart Julie Harding, RN, BSN President InfuScience, a Bioscrip Company Paul Wettengel, PharmD General Manager Methodist Home Health and Hospice Cindy Harris, RN, BSN Regulatory Compliance Coordinator Diane Randolph, RN, BSN Director of Home Services Debra Yarges, RN, BSN, BC Supervisor of Home Services Visiting Nurse Association of the Midlands Wanda J. Bowles, RN, BSN Infusion Clinical Manager Bridget Caniglia, BSN, CRRN Vice President of Home Care Cheryl Havekost, RN, BSN Clinical Liaison Specialist Lorraine Johnson, RN, BSN, CRNI Clinical Liaison Specialist Bridget Young, RN, BSN, MBA Vice President of Operations Consultant Ruth VanGerpen, RN, MS, APRN-CNS, AOCNS Clinical Nurse Specialist The development of these guidelines was supported by the Cardinal Health Foundation. 1. O Grady, N., et al. (2011). Guidelines for the prevention of intravascular catheter-related infections [CDC Guidelines]. Clinical Infectious Diseases. 2. Infusion Nurses Society (2011). Infusion Nursing Standards of Practice. Journal of Infusion Nursing, 34(1S), S1-S Cope, D. et al. (2011). Vascular access devices (VADS). In D. Camp-Sorrell (Ed.), Access device guidelines: Recommendations for nursing practice and education. Oncology Nursing Society, Pittsburgh, Penn. 4. SCORCH Consensus agreed upon content based on clinical experience and judgment of committee members in absence of definitive or conclusive research or other evidence. 5. Rupp, M., Yu, S., Huerta, T., Cavalieri, J., Alter, R., Fey, P., Van Schooneveld, T., Anderson, J. (2012). Adequate disinfection of a split-septum needleless intravascular connector with a 5- second alcohol scrub. Infection Control and Hospital Epidemiology 33(7), Chernecky, C., Macklin, D., Casella, L., & Jarvis, E. (2009). Caring for patients with cancer through nursing knowledge of IV connectors. Clinical Journal of Oncology Nursing 13(6), Hadaway, L., Richardson, D. (2010). Needleless connectors: A primer on terminology. Journal of Infusion Nursing, 33(1), Infusion Nurses Society. Flushing Protocols 2008 (rev. 2011). Norwood, Mass. 9. Children s Hospital & Medical Center (2012). Venous Access Device Flushing Policy. Omaha, Neb. To order additional copies contact: Regina Nailon RN, PhD Clinical Nurse Researcher Nursing Research and Quality Outcomes The Nebraska Medical Center Nebraska Medical Center Omaha, NE Phone:
3 Standardizing Central Venous Catheter Care: Hospital to Home Second Edition ACCESSING A CVAD Assessment FLUSHING (SEE TABLE AT END OF GUIDELINES FOR SCHEDULE OF FLUSHING AND/OR USE OF HEPARIN) General flushing A single use syringe should never be used more than once (even on the same lumen) (4). A 10 ml syringe filled with normal saline should not be divided into several doses and used for multiple lumens (2). Syringe size To prevent catheter damage, and unless otherwise directed by the manufacturer, the minimum syringe size that should be used when flushing a CVAD and for subsequent flush (post-medication administration) is 10 ml (2). Volume A minimum volume of twice the internal volume of the catheter should be used to flush the CVAD (2). In general, for the adult population, 10 ml is sufficient; for the pediatric population, 1-5 ml is sufficient for the majority of catheters (4). Technique Flushing technique will depend upon the type of catheter and type of connector valve being used. For catheters with negative pressure connector valves, the catheter should be flushed vigorously using a pulsatile motion, maintaining pressure at the end of the flush to prevent reflux back into the catheter (positive pressure technique). Positive pressure is maintained while flushing a catheter by clamping the extension tubing while still flushing the line (3, 6, 7). For catheters with positive pressure connector valves, the catheter should be flushed vigorously using a pulsatile motion. Disconnect syringe from injection port after flushing and then close the clamp (6, 7). For catheters with neutral pressure connector valves, the catheter should be flushed vigorously using a pulsatile motion. Clamp sequence is not required; clamping can be done before or after disconnection of syringe (6, 7). Solution and frequency for CVAD in intermittent use and in maintenance mode For peripherally inserted central venous catheters and midline catheters, verify external catheter length (i.e., exit site markings) before accessing (2). Follow agency policy regarding accessing line if exit markings differ from information documented upon insertion (4). The assessment and treatment of phlebitis, infiltration or extravsation shall be established per agency policy (2). Hand hygiene Hand hygiene should be performed before and after accessing an intravascular catheter (1, 2, 3). Perform hand hygiene procedures either by washing hands with conventional soap and water or with alcohol-based hand gel (1). Glove use is required per standard precautions per Occupational Safety and Health Administration (4). Scrub time for the access cap In the absence of definitive data, we suggest scrubbing the access cap for a time of no less than 5 seconds, using 70% alcohol solution and vigorous scrubbing (1, 2, 4, 5). Implanted Port Access in addition to all of the above Use aseptic technique and sterile gloves when accessing an implanted port (2). The RN will wear a mask when accessing an implanted port (4). Skin preparation for accessing the implanted port to be determined by agency policy (4). Cover the noncoring needle and access site of an implanted port with a transparent semipermeable membrane (TSM) dressing or gauze dressing (2). If gauze is used to support the access needle and it does not prevent visualization of the needle insertion site under a transparent dressing, it can be considered a transparent dressing and changed every 7 days (2). Replace the noncoring needle at least every 7 days or if it becomes dislodged (2, 4). 0.9% NaCl (normal saline [NS]) solution should be used to flush lines before and after each use (2). (SEE TABLE AT END OF GUIDELINES FOR SCHEDULE OF FLUSHING AND/OR USE OF HEPARIN) 3
4 Standardizing Central Venous Catheter Care: Hospital to Home Second Edition DRAWING BLOOD FOR LABORATORY TESTING Pre-draw For pediatric patients, draw blood samples per physician order. Drawing blood samples peripherally is the preferred method (4). When drawing blood for therapeutic drug levels, draw blood from a lumen other than the lumen being used for the drug infusion when possible (2). Refer to and follow troubleshooting steps to the extent that time permits and the patient care situation allows if other lumen is problematic (4). Use caution in interpreting results when therapeutic drug levels are drawn from same lumen being used to administer the medications (2, 3). If laboratory values appear to be grossly inaccurate, redraw a blood sample from a peripheral vein (2, 3). If CVAD is connected to an infusion, stop all infusates for at least one minute before drawing blood sample (3). For adult patients, flush CVAD with 10 ml NS before blood sample is drawn (2). For pediatric patients, flush CVAD with 3-5 ml NS or as directed by the physician before blood sample is drawn (4). If total parenteral nutrition (TPN) is infusing in the lumen from which blood is to be drawn, flush line with 20 ml NS before blood is drawn in adults (2, 3) and 5 ml NS in pediatric patients (4). Discard To avoid contamination and blood clot formation, do not reinfuse the discard specimen following blood draw (2). Discard times the volume of the internal catheter lumen (5 ml is sufficient for adult patients; 3 ml is sufficient for pediatric patients) before drawing blood sample (3). Post-draw Following blood draw, flush CVAD with 20 ml NS for adults, and 3-5 ml NS or as directed by the physician for pediatric patients, using vigorous, pulsating technique (3, 4). DRAWING BLOOD CULTURES General information Pre-draw and obtaining specimen Use of blood drawn from a CVAD is not recommended for blood cultures, unless the CVAD is suspected to be the source of infection (4). There are two methods appropriate for drawing blood from a CVAD for blood cultures. A) Remove the access the cap, scrub the catheter hub vigorously with a 70% alcohol pad for a minimum of 5 seconds, and replace with a new access cap. Draw the blood culture specimen from the new access cap after scrubbing the access cap for a minimum of 5 seconds with a 70% alcohol pad (3). OR B) Remove the access cap, scrub the catheter hub vigorously with a 70% alcohol pad for a minimum of 5 seconds. Draw the blood culture specimen directly from the catheter hub (3). Discard Do not discard blood sample when obtaining specimen for blood cultures (4). Post-draw Replace with new access cap when blood draw is complete (unless new cap was placed immediately before specimen was drawn) (4). Following blood draw, flush CVAD with 20 ml NS for adults, and 3-5 ml NS or as directed by the physician for pediatric patients, using vigorous, pulsating technique (3, 4). Document the site (specifying lumen used, if multiple lumen CVAD) and the time when the blood culture specimen was drawn on the lab specimen container and/or on the specimen label (4). 4
5 Standardizing Central Venous Catheter Care: Hospital to Home Second Edition Dressing Change General information With a well-healed tunneled CVAD, consideration may be given to no dressing (2, 3). Assess every CVAD within 24 hours of insertion to verify integrity and assess for post insertion complications (4). Replace catheter site dressing if the dressing becomes damp, loosened, or visibly soiled (1, 2, 3). Replace catheter site dressing at least every 7 days for transparent dressings, and every 2 days for gauze dressings (1, 2) except in those pediatric patients in which the risk for dislodging the catheter may outweigh the benefit of changing the dressing (1). When guaze is placed under a transparent dressing, it should be considered a gauze dressing and therefore changed every 2 days (2). Placement of a gauze dressing under a transparent dressing should be considered a gauze dressing and changed every 2 days. If gauze is used underneath a transparent dressing to support the noncoring needle in an implanted port and does not prevent visualization of the insertion site, it is not considered a gauze dressing (2). Access cap change Change the access cap at least every 7 days or per manufacturer s recommendations and in the presence of any of the following: Access cap is removed to initiate an infusion or draw blood (4). Blood cannot be completely flushed from the access cap after blood draw (2). Signs of blood, precipitate, cracks, leaks, or other defects are noted (3). Access cap septum is no longer intact (e.g., after multiple uses) (3, 4). If access cap change is performed with dressing change, the provider should don a mask and have the patient don a mask during the access cap change unless the patient is able to turn their head away and maintain this position throughout the procedure (4). There is conflicting evidence regarding wearing a mask when accessing a CVAD catheter hub or changing an access cap (2). If the access cap change is done at a time other than the time of a dressing change, the use of a mask should be compliant with agency policy (4). Dressing change procedure Perform hand hygiene (see hand hygiene guidelines) and don clean gloves to remove old dressing. After the dressing is removed, remove gloves, perform hand hygiene. Don a mask and have the patient don a mask unless the patient is able to turn their head away and maintain this position throughout the procedure (4). Change dressing per sterile technique using sterile gloves (2, 4). Use chlorhexidine solution for skin antisepsis as part of CVAD site care, for patients older than 2 months of age (1, 2). When cleansing the insertion or exit site, use gentle friction for 30 seconds to ensure that the disinfectant has adequate skin penetration and contact time (3). Allow the antiseptic to air dry completely. Do not fan (4). There is conflicting evidence regarding the use of chlorhexidine in infants aged < 2 months (4). Use of chlorhexidine in infants younger than 2 months should comply with agency policy or physician order (4). If chlorhexidine is used with a patient younger than 2 months of age, clean the exit site for 30 seconds using gentle friction, allow to air dry completely. Wipe with sterile NS (4). Chlorhexidine solution is preferred for skin antisepsis as part of CVAD site care. If there is a contraindication to the use of chlorhexidine, there is no directive to use one specific product over another. One should preferentially, use: A povidone-iodine with alcohol combination solution. If this is not available, Iodophor (povidone-iodine), 70% alcohol, or one percent to two percent tincture of iodine may be used (2, 3). Dried povidone-iodine used with infants younger than 2 months of age or with patients with compromised skin integrity should be removed with NS wipes or sterile water (2). 5
6 Standardizing Central Venous Catheter Care: Hospital to Home Second Edition Dressing Change >> cont d Dressing change with chlorhexidine-impregnated dressings There are no specific clinical indications or relevant studies that detail the need to change a soiled chlorhexidine-impregnated dressing before the seven-day dressing cycle ends (4). Change the chlorhexidine-impregnated dressing if it is approximately 2/3 saturated with organic matter (4). TROUBLESHOOTING ACCESS BARRIERS When a provider assesses for and identifies signs of CVAD occlusion, including the inability to withdraw blood, sluggish flow, and/or inability to flush or infuse through the device, the following steps should be taken: 1. Assess for potential causes of catheter occlusion; 2. Have the patient change position by lifting arm on the side of the body of the insertion site, turning from side-to-side, coughing, or other maneuvers to change body/cvad position. If this does not alleviate the problem, 3. Remove the access cap and attempt to flush/withdraw blood using the direct method of connecting the 10 ml syringe to the catheter hub, and then replace with a new access cap. If it is an implanted port, consider changing the access needle. If steps in #3 do not alleviate the problem, 4. Consider changing the CVAD site dressing. If this does not alleviate the problem, 5. Consult with a physician for further orders, which may involve use of a fibrinolytic agent. If a fibrinolytic agent is ordered, repeat x1 if first attempt is ineffective (for total of 2 doses). Leave 2nd dose of the fibrinolytic agent indwelling up to 24 hours before proceeding with next steps in troubleshooting. If the fibrinolytic agent is ineffective, 6. Consult with a physician and consider next steps in troubleshooting the occluded CVAD such as obtaining an X-ray to verify line integrity and/or a cathetergram (2, 4). OTHER INFORMATION Equipment Minimize connections (i.e., number of extension sets) in infusion administration sets (1, 4). Change the needleless components at least as frequently as the administration set (1). A new sterile compatible covering device (i.e., a new needleless connector) should be attached using aseptic technique to the end of the administration set after each intermittent use (2). Primary continuous infusion administration sets Secondary continuous infusion administration sets Intravenous fat emulsions Heparin use Primary administration sets used for continuous infusions that enhance microbial growth (i.e., lipids, TPN with lipids) should be changed every 24 hours after initiation of therapy (1, 2, 3). Primary administration sets used for continuous infusions that do not enhance microbial growth should be changed twice weekly and at least every 96 hours, unless contraindicated by medication being administered (1, 2, 3). Scheduled weekdays of administration set change to be determined per agency policy (4). Primary administration sets used for intermittent infusions should be changed every 24 hours (2). A secondary administration set that is detached from the primary administration set is considered a primary intermittent administration set and should be changed every 24 hours (2). When administering lipids intermittently, the administration set should be changed with each new container (2). There is conflicting evidence regarding the use of heparin to maintain patency. Consider individualized patient needs for indications for heparin use (2). If heparin is to be used, the least amount of heparin needed to maintain patency is desired (4). If heparin is being used, the preferred concentration is 10 units/ml for adults unless otherwise indicated or per physician order (3). 6
7 Flushing Frequencies and Use of Heparin CVAD TYPE and Approximate Priming Volume (8) Implanted port Internal Diameter (I.D.) 0.8 mm I.D. 0.8 ml 1.0 mm I.D ml 1.1 mm I.D. 1.2 ml 1.4 mm I.D. 1.7 ml 1.6 mm I.D. 2 ml Centrally tunneled open end (i.e., Hickman, Broviac) 2-3 F ml 4 F 0.3 ml 5 F 0.5 ml 6 F ml 7 F ml 9 F ml Centrally tunneled closed end (i.e., Groshong) 2-3 F ml 4 F 0.3 ml 5 F 0.5 ml 6 F ml 7 F ml 9 F ml Central non-tunneled open end (PICC, SC) 1.9 F 0.06 ml F ml 4 F 0.6 ml 5 F ml 6 F ml Heparin Use/NS Flushing Frequency for CVAD in Intermittent Mode For implanted port (open and closed) being used a minimum of every 8 hours, flush with 10 ml NS after each use or every 24 hours (or per mfr. recommendations) (4). For implanted port (open and closed) flush with 3-5 ml NS (or amount specified per physician order) before and after each use (8). After flushing with NS (for implanted port open and closed), flush with heparin (10 units/ml) after each use or every 24 hours (or per physician order) If being used a minimum of every 8 hours, flush with 10 ml NS after each use or every 24 hours (or per mfr. recommendations) (4). If line is being flushed with NS every 24 hours only, flush with heparin (10 units/ml) following NS flush (3,4) ^#*. Heparin is not needed if flushing line every 8 hours with NS (4). Flush with 1-3 ml NS (or amount specified per physician order) before and after each use (8). units/ ml) after each use or every 24 hours (or per physician order) Flush with 10 ml NS before and after each use or every 24 hours (or per physician order or mfr. recommendations) (3). Flush with 1-3 ml NS (or amount specified per physician order) before and after each use (8). units/ml) after each use or every 24 hours (or per physician order) If being used a minimum of every 8 hours, flush with 10 ml NS before and after each use or every 24 hours (or per or mfr. recommendations) (4). If PICC > 2FR flush with 2-3 ml NS (or amount specified per physician order) before and after each use or every 12 hours (or per physician order) (8). units/ml) after each use or every 12 hours (or per physician order) Heparin Use/NS Flushing Frequency for CVAD in Maintenance Mode For implanted port (closed), flush with 10 ml NS every 4 weeks (or per physician order) (2, 3, 4). For implanted port (open) flush with 10 ml NS followed by 5 ml of heparin (100 units/ml) administered via 5 ml syringe every 4 weeks (or per physician order) (2). For implanted port (open and closed) flush with 3-5 ml NS (or amount specified per physician order) every 4 weeks (8, 9). After flushing with NS (for implanted port open and closed), flush with heparin (100 units/ml) every 4 weeks and prior to de-accessing (or per physician order) Flush with 10 ml NS once weekly (or per physician order) (3). After flushing with NS, flush with 3-5 ml of heparin (10 units/ml) once weekly (3). Flush with1-3 ml NS (or amount specified per physician order) every 24 hours (or per physician order) (8). units/ml) every 24 hours (or per physician order) Flush with 10 ml NS once weekly (or per physician order or mfr. recommendations) (3, 4). Flush with 1-3 ml NS (or amount specified per physician order) every 24 hours (or per physician order) (8). units/ml) every 24 hours (or per physician order Flush with 10 ml NS every 24 hours (or per physician order or mfr. recommendations) (3, 4). If PICC > 2FR flush with 2-3 ml NS (or amount specified per physician order) every 12 hours (or per physician order) (8). units/ml) every 12 hours (or per physician order) 7
8 Flushing Frequencies and Use of Heparin <cont d> CVAD TYPE and Approximate Priming Volume (8) Central non-tunneled closed end or valved (i.e., Bard Solo Power PICC) 1.9 F 0.06 ml F ml 4 F 0.6 ml 5 F ml 6 F ml Heparin Use/NS Flushing Frequency for CVAD in Intermittent Mode Flush with 10 ml NS before and after each use or every 24 hours (or per mfr. recommendations) (4). If PICC > 2FR flush with 2-3 ml NS (or amount specified per physician order) before and after each use or every 12 hours (or per physician order) (8). units/ml) after each use or every 12 hours (or per physician order) Heparin Use/NS Flushing Frequency for CVAD in Maintenance Mode Flush with 10 ml NS once weekly (or per physician order or mfr. recommendations) (3, 4). If PICC > 2FR flush with 2-3 ml NS (or amount specified per physician order) every 12 hours (or per physician order) (8). units/ml) every 12 hours (or per physician order) Non-Centrally Inserted Venous Access Device and Approximate Priming Volume (8) Midline catheter open or closed end, or valved 3 F 0.16 ml 4 F 0.19 ml 5 F 0.22 ml Heparin Use/NS Flushing Frequency for Device in Intermittent Mode If being used a minimum of every 8 hours, flush with 10 ml NS before and after each use or every 24 hours (or per mfr. recommendations) (4). If Midline > 2 FR flush with 2-3 ml NS (or amount specified per physician order) before and after each use or every 12 hours (or per physician order) (4, 8). units/ ml) after each use or every 12 hours (or per physician order) Heparin Use/NS Flushing Frequency for Device in Maintenance Mode Flush with 10 ml NS every 24 hours (or per physician order or mfr. recommendations) (3, 4). If Midline > 2 FR flush with 2-3 ml NS (or amount specified per physician order) every 12 hours (or per physician order) (4, 8). units/ml) every 12 hours (or per physician order) ^ When administering pediatric medications the SASH technique should be used: Saline, Antibiotic/ Medication, Saline, Heparin. If dextrose is to be used in place of 0.9% NS, for compatibility, pharmacy should have instructions on label(s) (4, 9). # Heparin volume should be determined by physician order (4). Consideration must be given to approximate priming volume of device and tubing configurations when determining appropriate heparin volume to be administered (8, 9). * In an effort to avoid systemic anticoagulation of the patient during use of heparin flushes in pediatric patients, multiple doses of heparin over a short time period (defined here as 4 hours), that result in an average total of heparin dosage greater than 25 units/kg/hour may constitute systemic anticoagulation. All administrations of heparin must be considered when calculating total heparin dosage: heparin in running IV lines, and administration through all lines and lumens of central lines being flushed (4, 9). 8
Management of Catheters Infectious Diseases Working Party/Nurses Group
 Management of Catheters Infectious Diseases Working Party/Nurses Group Arno Mank RN PhD, Amsterdam (NL) www.ebmt.org London 09/04/2012 Content Background Management of CVC Types of CVC Care aspect of CVC
Management of Catheters Infectious Diseases Working Party/Nurses Group Arno Mank RN PhD, Amsterdam (NL) www.ebmt.org London 09/04/2012 Content Background Management of CVC Types of CVC Care aspect of CVC
Policies & Procedures. ID Number: 1118
 Policies & Procedures Title: INTRAVENOUS AND/OR PERIPHERAL SALINE LOCK INSERTION AND MAINTENANCE ID Number: 1118 Authorization [X] SHR Nursing Practice Committee Source: Nursing Date Revised: September
Policies & Procedures Title: INTRAVENOUS AND/OR PERIPHERAL SALINE LOCK INSERTION AND MAINTENANCE ID Number: 1118 Authorization [X] SHR Nursing Practice Committee Source: Nursing Date Revised: September
Policy and Procedure Flushing and / or Blood withdrawal Aspiration Procedure For PICC Line and Midline Catheters
 Policy and Procedure Flushing and / or Blood withdrawal Aspiration Procedure For PICC Line and Midline Catheters Purpose: Blood Withdrawal: To obtain blood samples for laboratory evaluation, eliminating
Policy and Procedure Flushing and / or Blood withdrawal Aspiration Procedure For PICC Line and Midline Catheters Purpose: Blood Withdrawal: To obtain blood samples for laboratory evaluation, eliminating
Patient Information Guide Morpheus CT Peripherally Inserted Central Catheter
 Patient Information Guide Morpheus CT Peripherally Inserted Central Catheter IC 192 Rev C A measure of flexibility and strength. Table of Contents 1. Introduction 2. What is the Morpheus CT PICC? 3. What
Patient Information Guide Morpheus CT Peripherally Inserted Central Catheter IC 192 Rev C A measure of flexibility and strength. Table of Contents 1. Introduction 2. What is the Morpheus CT PICC? 3. What
I-140 Venipuncture for Blood Specimen Collection
 I-140 Venipuncture for Blood Specimen Collection Purpose Obtain a blood specimen by venipuncture for laboratory analysis using aseptic technique. Applies To Registered Nurses Licensed Practical/Vocational
I-140 Venipuncture for Blood Specimen Collection Purpose Obtain a blood specimen by venipuncture for laboratory analysis using aseptic technique. Applies To Registered Nurses Licensed Practical/Vocational
To maintain a port of entry to venous flow when all available peripheral ports have failed.
 I. Purpose: To maintain a port of entry to venous flow when all available peripheral ports have failed. II. General Comments: Since its development, these catheters have been used with increasing frequency
I. Purpose: To maintain a port of entry to venous flow when all available peripheral ports have failed. II. General Comments: Since its development, these catheters have been used with increasing frequency
If viewing a printed copy of this policy, please note it could be expired. Got to www.fairview.org/fhipolicies to view current policies.
 If viewing a printed copy of this policy, please note it could be expired. Got to www.fairview.org/fhipolicies to view current policies. Entity: Fairview Pharmacy Services Department: Fairview Home Infusion
If viewing a printed copy of this policy, please note it could be expired. Got to www.fairview.org/fhipolicies to view current policies. Entity: Fairview Pharmacy Services Department: Fairview Home Infusion
Providing optimal care
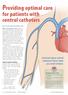 Providing optimal care for patients with central catheters By Ann Earhart, MSN, RN, ACNS-BC, CRNI WHEN REGISTERED NURSE Andrea arrives on shift for report, she learns that her patient, a 62-year-old male,
Providing optimal care for patients with central catheters By Ann Earhart, MSN, RN, ACNS-BC, CRNI WHEN REGISTERED NURSE Andrea arrives on shift for report, she learns that her patient, a 62-year-old male,
PERIPHERALLY INSERTED CENTRAL CATHETERS (PICC) Fong So Kwan APN, Haematology unit Medical Department, QMH
 PERIPHERALLY INSERTED CENTRAL CATHETERS (PICC) Fong So Kwan APN, Haematology unit Medical Department, QMH 1 What is a PICC catheter? Primary vascular access device since their introduction in the mid-1970s,
PERIPHERALLY INSERTED CENTRAL CATHETERS (PICC) Fong So Kwan APN, Haematology unit Medical Department, QMH 1 What is a PICC catheter? Primary vascular access device since their introduction in the mid-1970s,
Flushing and Dressing a Peripherally Inserted Central Catheter (PICC Line): a Guide for Nurses
 Flushing and Dressing a Peripherally Inserted Central Catheter (PICC Line): a Guide for Nurses Information for Nurses Introduction This information is for community nursing staffs who have been asked to
Flushing and Dressing a Peripherally Inserted Central Catheter (PICC Line): a Guide for Nurses Information for Nurses Introduction This information is for community nursing staffs who have been asked to
Appendix L: Accessing/Deaccessing Implanted Central Venous Access Port
 Effective Date: 03/01/2008 Page 1 of 5 Recommendations for Use Insertion Considerations Implanted Port Dressing Access/ Reaccess An implanted port is strongly recommended for patients in whom more than
Effective Date: 03/01/2008 Page 1 of 5 Recommendations for Use Insertion Considerations Implanted Port Dressing Access/ Reaccess An implanted port is strongly recommended for patients in whom more than
PICC & Midline Catheters Patient Information Guide
 PICC & Midline Catheters Patient Information Guide medcompnet.com 1 table of contents Introduction 4 What is a PICC or Midline Catheter? 4 How is the PICC or Midline Catheter Inserted? 6 Catheter Care
PICC & Midline Catheters Patient Information Guide medcompnet.com 1 table of contents Introduction 4 What is a PICC or Midline Catheter? 4 How is the PICC or Midline Catheter Inserted? 6 Catheter Care
PICC and Midline Catheters
 PICC and Midline Catheters Infusion RN s Deb Bucher RN BSN CRNI Dawn Finch RN CRNI Marianne Hansen RN BSN CRNI Karman Youngblood RN BS CRNI Infusion Pharmacist Kathy Cimakasky Pharm D Tamara Migut RPh
PICC and Midline Catheters Infusion RN s Deb Bucher RN BSN CRNI Dawn Finch RN CRNI Marianne Hansen RN BSN CRNI Karman Youngblood RN BS CRNI Infusion Pharmacist Kathy Cimakasky Pharm D Tamara Migut RPh
PATIENT GUIDE. Understand and care for your peripherally inserted central venous catheter (PICC). MEDICAL
 PATIENT GUIDE Understand and care for your peripherally inserted central venous catheter (PICC). MEDICAL Introduction The following information is presented as a guideline for your reference. The best
PATIENT GUIDE Understand and care for your peripherally inserted central venous catheter (PICC). MEDICAL Introduction The following information is presented as a guideline for your reference. The best
Care of Your Hickman Catheter
 Care of Your Hickman Catheter Johns Hopkins Kimmel Cancer Center, Revised 7/11 Contents What is a Hickman Catheter? Page 3 Does the Catheter Limit My Activities? Page 4 How Do I Care for My Catheter? Page
Care of Your Hickman Catheter Johns Hopkins Kimmel Cancer Center, Revised 7/11 Contents What is a Hickman Catheter? Page 3 Does the Catheter Limit My Activities? Page 4 How Do I Care for My Catheter? Page
Policies & Procedures. I.D. Number: 1073
 Policies & Procedures Title:: CENTRAL VENOUS CATHETERS INSERTION ASSISTING I.D. Number: 1073 Authorization [] Pharmacy Nursing Committee [] MAC Motion #: [x] SHR Nursing Practice Committee Source: Nursing
Policies & Procedures Title:: CENTRAL VENOUS CATHETERS INSERTION ASSISTING I.D. Number: 1073 Authorization [] Pharmacy Nursing Committee [] MAC Motion #: [x] SHR Nursing Practice Committee Source: Nursing
Within the Scope of Practice/Role of APRN RN _ X_LPN CNA
 Wyoming State Board of Nursing 130 Hobbs Avenue, Suite B Cheyenne, WY 82002 Phone (307) 777-7601 Fax (307) 777-3519 E-Mail: wsbn-info-licensing@wyo.gov Home Page: https://nursing-online.state.wy.us/ OPINION:
Wyoming State Board of Nursing 130 Hobbs Avenue, Suite B Cheyenne, WY 82002 Phone (307) 777-7601 Fax (307) 777-3519 E-Mail: wsbn-info-licensing@wyo.gov Home Page: https://nursing-online.state.wy.us/ OPINION:
Central Line-Associated Bloodstream Infection (CLABSI) Prevention. Basics of Infection Prevention 2-Day Mini-Course 2013
 Central Line-Associated Bloodstream Infection (CLABSI) Prevention Basics of Infection Prevention 2-Day Mini-Course 2013 2 Objectives Describe the etiology and epidemiology of central line associated bloodstream
Central Line-Associated Bloodstream Infection (CLABSI) Prevention Basics of Infection Prevention 2-Day Mini-Course 2013 2 Objectives Describe the etiology and epidemiology of central line associated bloodstream
Managing Your Non-Tunneled (Percutaneous) Catheter: PICC, SICC, and JCC. What is a PICC catheter?
 Managing Your Non-Tunneled The staff of the Procedure, Vascular Access, Conscious Sedation Service has written this information to explain your new PICC (peripherally inserted central catheter), SICC (subclavian
Managing Your Non-Tunneled The staff of the Procedure, Vascular Access, Conscious Sedation Service has written this information to explain your new PICC (peripherally inserted central catheter), SICC (subclavian
Aspirating a blood return from a catheter
 Questions have been grouped together based on their content or focus. Aspirating a blood return from a catheter Can we use CVC with no blood return? If a CVAD has no blood return should studies be made
Questions have been grouped together based on their content or focus. Aspirating a blood return from a catheter Can we use CVC with no blood return? If a CVAD has no blood return should studies be made
Guardian Pharmacy IV Policy & Procedures TABLE OF CONTENTS
 TABLE OF CONTENTS.Introduction...3 Ordering and Receiving Medications Ordering Medications and Supplies...4 Obtaining Interim Infusion Medication and Supplies...6 STAT Orders...7 Infusion Device/Pump and
TABLE OF CONTENTS.Introduction...3 Ordering and Receiving Medications Ordering Medications and Supplies...4 Obtaining Interim Infusion Medication and Supplies...6 STAT Orders...7 Infusion Device/Pump and
Care for your child s Central Venous Catheter (CVC)
 Care for your child s Central Venous Catheter (CVC) This booklet is intended for general informational purposes only. You should consult your doctor for medical advice. Please call the clinic or your home
Care for your child s Central Venous Catheter (CVC) This booklet is intended for general informational purposes only. You should consult your doctor for medical advice. Please call the clinic or your home
Peripherally Inserted Central Catheter (PICC) Benefits Long-term access - dwell time varies (can be > one year) Decreased length of stay in hospital a
 Nursing Management of Venous Access Devices: Peripherally Inserted Central Catheter (PICC) Mimi Bartholomay, RN, MSN, AOCN Denise Dreher, RN, CRNI, VA-BC Theresa Evans, RN, MSN Susan Finn, RN, MSN, AOCNS
Nursing Management of Venous Access Devices: Peripherally Inserted Central Catheter (PICC) Mimi Bartholomay, RN, MSN, AOCN Denise Dreher, RN, CRNI, VA-BC Theresa Evans, RN, MSN Susan Finn, RN, MSN, AOCNS
TITLE CLIN_216 HEMODIALYSIS/PLASMAPHERESIS PROCEDURE AND CATHETER MANAGEMENT FOR THE ADULT AND PEDIATRIC PATIENT
 Policies and procedures are guidelines and are not a substitute for the exercise of individual judgment. If you are reading a printed copy of this policy, make sure it is the most current by checking the
Policies and procedures are guidelines and are not a substitute for the exercise of individual judgment. If you are reading a printed copy of this policy, make sure it is the most current by checking the
Vaxcel PICCs Valved and Non-Valved. A Patient s Guide
 Vaxcel PICCs Valved and Non-Valved A Patient s Guide Information about your Vaxcel PICC is available by calling the Navilyst Medical Vascular Access Information Line 800.513.6876 Vaxcel Peripherally Inserted
Vaxcel PICCs Valved and Non-Valved A Patient s Guide Information about your Vaxcel PICC is available by calling the Navilyst Medical Vascular Access Information Line 800.513.6876 Vaxcel Peripherally Inserted
Infection Control Manual. Table of Contents
 Infection Control Manual Policy Name The Prevention of Intravascular Catheter-Related Infections Policy Number IC 0032 Date this Version Effective May 2013 Responsible for Content Hospital Epidemiology
Infection Control Manual Policy Name The Prevention of Intravascular Catheter-Related Infections Policy Number IC 0032 Date this Version Effective May 2013 Responsible for Content Hospital Epidemiology
PICCs and Midline Catheters
 Patient Education PICCs and Midline Catheters Patient s guide to PICC (peripherally inserted central catheter) and midline catheters What are PICCs and midline catheters used for? Any medicine given over
Patient Education PICCs and Midline Catheters Patient s guide to PICC (peripherally inserted central catheter) and midline catheters What are PICCs and midline catheters used for? Any medicine given over
VUMC Guidelines for Management of Indwelling Urinary Catheters. UC Access/ Maintenance
 VUMC Guidelines for Management of Indwelling Urinary Catheters UC Insertion Preparation & Procedure Indications for insertion and continued use of indwelling urinary catheters include: Urinary retention
VUMC Guidelines for Management of Indwelling Urinary Catheters UC Insertion Preparation & Procedure Indications for insertion and continued use of indwelling urinary catheters include: Urinary retention
Medications or therapeutic solutions may be injected directly into the bloodstream
 Intravenous Therapy Medications or therapeutic solutions may be injected directly into the bloodstream for immediate circulation and use by the body. State practice acts designate which health care professionals
Intravenous Therapy Medications or therapeutic solutions may be injected directly into the bloodstream for immediate circulation and use by the body. State practice acts designate which health care professionals
Peripherally Inserted Central Catheter (PICC) for Outpatient
 Peripherally Inserted Central Catheter (PICC) for Outpatient Introduction A Peripherally Inserted Central Catheter, or PICC line, is a thin, long, soft plastic tube inserted into a vein of the arm. It
Peripherally Inserted Central Catheter (PICC) for Outpatient Introduction A Peripherally Inserted Central Catheter, or PICC line, is a thin, long, soft plastic tube inserted into a vein of the arm. It
A4.7 Management of a totally occluded central catheter and persistent withdrawal occlusion (PWO)
 A4.7 Management of a totally occluded central catheter and persistent withdrawal occlusion (PWO) Types of Catheter Related Thrombotic A catheter-related thrombus may be intraluminal (inside the catheter)
A4.7 Management of a totally occluded central catheter and persistent withdrawal occlusion (PWO) Types of Catheter Related Thrombotic A catheter-related thrombus may be intraluminal (inside the catheter)
Implanted Central Venous Access Devices (Ports)
 Nursing Management of Venous Access Devices: Implanted Central Venous Access Devices (Ports) Mimi Bartholomay, RN, MSN, AOCN Denise Dreher,, RN, CRNI, VA-BC Theresa Evans, RN, MSN Susan Finn, RN, MSN,
Nursing Management of Venous Access Devices: Implanted Central Venous Access Devices (Ports) Mimi Bartholomay, RN, MSN, AOCN Denise Dreher,, RN, CRNI, VA-BC Theresa Evans, RN, MSN Susan Finn, RN, MSN,
MISSISSIPPI BOARD OF NURSING IV THERAPY COURSE FOR THE EXPANDED ROLE LICENSED PRACTICAL NURSE COURSE OUTLINE
 THEORY MINIMUM 40 HOURS COURSE OUTLINE UNIT TOPIC HOURS* I LEGAL ASPECTS AND PRACTICE OF IV THERAPY 1 II REVIEW OF ANATOMY AND PHYSIOLOGY 6 III FLUID AND ELECTROLYTE BALANCE 10 IV EQUIPMENT AND PROCEDURES
THEORY MINIMUM 40 HOURS COURSE OUTLINE UNIT TOPIC HOURS* I LEGAL ASPECTS AND PRACTICE OF IV THERAPY 1 II REVIEW OF ANATOMY AND PHYSIOLOGY 6 III FLUID AND ELECTROLYTE BALANCE 10 IV EQUIPMENT AND PROCEDURES
Changing Your Central Line Catheter Cap
 Changing Your Central Line Catheter Cap The catheter cap on each lumen of your central line needs to be changed once a week. A lumen is a small tube within your catheter. These same steps can be used for
Changing Your Central Line Catheter Cap The catheter cap on each lumen of your central line needs to be changed once a week. A lumen is a small tube within your catheter. These same steps can be used for
Flushing and Dressing a Peripherally Inserted Central Catheter (PICC Line)
 Flushing and Dressing a Peripherally Inserted Central Catheter (PICC Line) Patient Information Introduction This booklet has been written to provide information to patients with a Peripherally Inserted
Flushing and Dressing a Peripherally Inserted Central Catheter (PICC Line) Patient Information Introduction This booklet has been written to provide information to patients with a Peripherally Inserted
Central Line Blood Draw
 Central Line Blood Draw Welcome to the Central Line dressing blood draw refresher. Please use the navigation below to advance to the next page. The Central Line blood draw module is also available as a
Central Line Blood Draw Welcome to the Central Line dressing blood draw refresher. Please use the navigation below to advance to the next page. The Central Line blood draw module is also available as a
Central venous catheters. Care of the site 88 CVP measurement 90 Removal of CVC (non-tunnelled) 93 Care of long-term CVCs 95
 4 Central venous catheters Care of the site 88 CVP measurement 90 Removal of CVC (non-tunnelled) 93 Care of long-term CVCs 95 CARE OF THE SITE Preparation Patient Equipment/Environment Nurse Explain the
4 Central venous catheters Care of the site 88 CVP measurement 90 Removal of CVC (non-tunnelled) 93 Care of long-term CVCs 95 CARE OF THE SITE Preparation Patient Equipment/Environment Nurse Explain the
I. Questions for VAD slide program
 I. Questions for VAD slide program 1. The rate of central line associated blood stream infections (CLABSI) in the adult ICUs in Johns Hopkins Hospital is lower than the national average. 2. The mortality
I. Questions for VAD slide program 1. The rate of central line associated blood stream infections (CLABSI) in the adult ICUs in Johns Hopkins Hospital is lower than the national average. 2. The mortality
BestPractice. Evidence Based Practice Information Sheets for Health Professionals. This Practice Information Sheet Covers The Following Concepts:
 Volume 2, Issue 1, 1998 ISSN 1329-1874 BestPractice Evidence Based Practice Information Sheets for Health Professionals Purpose The purpose of this practice information sheet is to provide summarised best
Volume 2, Issue 1, 1998 ISSN 1329-1874 BestPractice Evidence Based Practice Information Sheets for Health Professionals Purpose The purpose of this practice information sheet is to provide summarised best
Bard Access Systems, Inc. How to Care For Your. Nursing Guide
 Bard Access Systems, Inc. How to Care For Your Nursing Guide Table of Contents Introduction 1 Product Description Placement PowerPICC SOLO* Catheter Valve Function Indications for Use Catheter Irrigation
Bard Access Systems, Inc. How to Care For Your Nursing Guide Table of Contents Introduction 1 Product Description Placement PowerPICC SOLO* Catheter Valve Function Indications for Use Catheter Irrigation
Guy s, King s and St Thomas Cancer Centre The Cancer Outpatient Clinic Central venous catheter: Peripherally inserted central catheter
 Guy s, King s and St Thomas Cancer Centre The Cancer Outpatient Clinic Central venous catheter: Peripherally inserted central catheter This information leaflet aims to help answer some of the questions
Guy s, King s and St Thomas Cancer Centre The Cancer Outpatient Clinic Central venous catheter: Peripherally inserted central catheter This information leaflet aims to help answer some of the questions
Care of your peripherally inserted central catheter
 Care of your peripherally inserted central catheter A guide for patients and their carers We care, we discover, we teach Contents What is a PICC?.... 1 How is it put in?.... 1 What are the benefits of
Care of your peripherally inserted central catheter A guide for patients and their carers We care, we discover, we teach Contents What is a PICC?.... 1 How is it put in?.... 1 What are the benefits of
Intravenous (IV) Catheter Care: Peripheral & Central (Adult)
 Policy No: 1007 Approved: 05/07 Effective: 08/07 Revised: 12/11; 04/12 Intravenous (IV) Catheter Care: Peripheral & Central (Adult) TABLE OF CONTENTS I. Purpose II. Scope III. Definitions IV. Policy Statements
Policy No: 1007 Approved: 05/07 Effective: 08/07 Revised: 12/11; 04/12 Intravenous (IV) Catheter Care: Peripheral & Central (Adult) TABLE OF CONTENTS I. Purpose II. Scope III. Definitions IV. Policy Statements
Community Nurse Referral Letter (Hickman Line Care)
 Community Nurse Referral Letter (Hickman Line Care) Name of nurse making the referral: Name Signature.. Date Ward.Tel 0845 1555 000 Ext. Dear Community Nurse The following patient requires care for a Hickman
Community Nurse Referral Letter (Hickman Line Care) Name of nurse making the referral: Name Signature.. Date Ward.Tel 0845 1555 000 Ext. Dear Community Nurse The following patient requires care for a Hickman
X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary
 X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary Introduction A Subclavian Inserted Central Catheter, or subclavian line, is a long thin hollow tube inserted in a vein under the
X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary Introduction A Subclavian Inserted Central Catheter, or subclavian line, is a long thin hollow tube inserted in a vein under the
PROCEDURE FOR SUBCUTANEOUS INSERTION, REMOVAL, MEDICATION ADMINISTRATION AND FLUID ADMINISTRATION FOR COMMUNITY PALLIATIVE CARE PATIENTS
 PROCEDURE FOR SUBCUTANEOUS INSERTION, REMOVAL, MEDICATION ADMINISTRATION AND FLUID ADMINISTRATION FOR COMMUNITY PALLIATIVE CARE PATIENTS Approved: February 2010 Date for review: February 2010 1 PROCEDURE
PROCEDURE FOR SUBCUTANEOUS INSERTION, REMOVAL, MEDICATION ADMINISTRATION AND FLUID ADMINISTRATION FOR COMMUNITY PALLIATIVE CARE PATIENTS Approved: February 2010 Date for review: February 2010 1 PROCEDURE
Continuing Education. CVAD Guidelines for Home Infusion: Creating a Resource to Address Our Unique Site of Care for Adult Patients
 Continuing Education CVAD Guidelines for Home Infusion: Creating a Resource to Address Our Unique Site of Care for Adult Patients By Nancy Kramer, R.N., B.S.N., CRNI, Melissa Leone R.N., B.S.N., Kevin
Continuing Education CVAD Guidelines for Home Infusion: Creating a Resource to Address Our Unique Site of Care for Adult Patients By Nancy Kramer, R.N., B.S.N., CRNI, Melissa Leone R.N., B.S.N., Kevin
Your Guide to Peritoneal Dialysis Module 3: Doing Peritoneal Dialysis at Home
 Your Guide to Peritoneal Dialysis Module 3: 6.0959 in Preparing to do PD One of the most important things about PD is to keep the dialysis area and anything that comes in contact with the PD equipment
Your Guide to Peritoneal Dialysis Module 3: 6.0959 in Preparing to do PD One of the most important things about PD is to keep the dialysis area and anything that comes in contact with the PD equipment
Section 6: Your Hemodialysis Catheter
 Section 6: Your Hemodialysis Catheter What you should know about your dialysis catheter How to change your catheter TEGO connectors Starting dialysis using a catheter End of dialysis using a catheter Changing
Section 6: Your Hemodialysis Catheter What you should know about your dialysis catheter How to change your catheter TEGO connectors Starting dialysis using a catheter End of dialysis using a catheter Changing
Syringe. Product Usage Information: Precautions:
 Syringe Standard Draw Procedure In-Patient, Automated Retraction Non-Reusable. Prepare and give injection using aseptic technique according to institutional policy.. For injection into patients, continue
Syringe Standard Draw Procedure In-Patient, Automated Retraction Non-Reusable. Prepare and give injection using aseptic technique according to institutional policy.. For injection into patients, continue
Ward 29 guide to the safe preparation and administration of intravenous (IV) antibiotics at home
 Ward 29 guide to the safe preparation and administration of intravenous (IV) antibiotics at home Contents Page Important contact numbers 1 General information on preparing and administering IV antibiotics
Ward 29 guide to the safe preparation and administration of intravenous (IV) antibiotics at home Contents Page Important contact numbers 1 General information on preparing and administering IV antibiotics
HICKMAN Catheter Care with a Needleless Connector
 HICKMAN Catheter Care with a Needleless Connector Table of Contents Part 1 Learning about the HICKMAN Catheter... 2 Part 2 Caring for Your Hickman Catheter... 3 A. Preventing Infection... 3 B. Bathing...
HICKMAN Catheter Care with a Needleless Connector Table of Contents Part 1 Learning about the HICKMAN Catheter... 2 Part 2 Caring for Your Hickman Catheter... 3 A. Preventing Infection... 3 B. Bathing...
V: Infusion Therapy. Alberta Licensed Practical Nurses Competency Profile 217
 V: Infusion Therapy Alberta Licensed Practical Nurses Competency Profile 217 Competency: V-1 Knowledge of Intravenous Therapy V-1-1 V-1-2 V-1-3 V-1-4 V-1-5 Demonstrate knowledge and ability to apply critical
V: Infusion Therapy Alberta Licensed Practical Nurses Competency Profile 217 Competency: V-1 Knowledge of Intravenous Therapy V-1-1 V-1-2 V-1-3 V-1-4 V-1-5 Demonstrate knowledge and ability to apply critical
Community Nurse Referral Letter (PICC Care)
 Community Nurse Referral Letter (PICC Care) Name of nurse making the referral: Name Signature.. Date Ward.Tel 0845 1555 000 Ext. Dear Community Nurse The following patient requires care for a PICC (Peripherally
Community Nurse Referral Letter (PICC Care) Name of nurse making the referral: Name Signature.. Date Ward.Tel 0845 1555 000 Ext. Dear Community Nurse The following patient requires care for a PICC (Peripherally
Central Line Care for Adults
 Central Line Care for Adults Table of Contents What is a Central Venous Catheter?... 2 Central Venous Catheter Placement: What to Expect... 2 Catheter Care at a Glance... 2 Fast Facts on Central Line Care:
Central Line Care for Adults Table of Contents What is a Central Venous Catheter?... 2 Central Venous Catheter Placement: What to Expect... 2 Catheter Care at a Glance... 2 Fast Facts on Central Line Care:
Central Venous Catheter (CVC) Sterile Dressing Change - The James
 PATIENT EDUCATION patienteducation.osumc.edu Central Venous Catheter (CVC) Sterile Dressing Change - The James A dressing protects your catheter site and helps reduce the risk of infection. You will need
PATIENT EDUCATION patienteducation.osumc.edu Central Venous Catheter (CVC) Sterile Dressing Change - The James A dressing protects your catheter site and helps reduce the risk of infection. You will need
Administration of Medications & Fluids via a Peripheral Intravenous Cannula
 Administration of Medications & Fluids via a Peripheral Intravenous Cannula Clinical S.O.P. No.: 22.0 Compiled by: Approved by: Review date: November 2016 Administration of Medications & Fluids via S.O.P.
Administration of Medications & Fluids via a Peripheral Intravenous Cannula Clinical S.O.P. No.: 22.0 Compiled by: Approved by: Review date: November 2016 Administration of Medications & Fluids via S.O.P.
III-701 Urinary Catheterization/Bladder Irrigation Original Date: 3/1/1977 Last Review Date: 10/28/2004
 III-701 Urinary Catheterization/Bladder Irrigation Original Date: 3/1/1977 Last Review Date: 10/28/2004 Purpose A. Allow for precise measurement of urine output. B. Collect a sterile urine specimen. C.
III-701 Urinary Catheterization/Bladder Irrigation Original Date: 3/1/1977 Last Review Date: 10/28/2004 Purpose A. Allow for precise measurement of urine output. B. Collect a sterile urine specimen. C.
02 DEPARTMENT OF PROFESSIONAL AND FINANCIAL REGULATION REGULATIONS RELATING TO ADMINISTRATION OF INTRAVENOUS THERAPY BY LICENSED NURSES
 02 DEPARTMENT OF PROFESSIONAL AND FINANCIAL REGULATION 380 BOARD OF NURSING Chapter 10: REGULATIONS RELATING TO ADMINISTRATION OF INTRAVENOUS THERAPY BY LICENSED NURSES SUMMARY: This chapter identifies
02 DEPARTMENT OF PROFESSIONAL AND FINANCIAL REGULATION 380 BOARD OF NURSING Chapter 10: REGULATIONS RELATING TO ADMINISTRATION OF INTRAVENOUS THERAPY BY LICENSED NURSES SUMMARY: This chapter identifies
Care of your central venous catheter A guide for patients and their carers. We care, we discover, we teach
 Care of your central venous catheter A guide for patients and their carers We care, we discover, we teach This booklet contains information about central venous catheters (CVC). These are sometimes called
Care of your central venous catheter A guide for patients and their carers We care, we discover, we teach This booklet contains information about central venous catheters (CVC). These are sometimes called
A. ADMINISTERING SUBCUTANEOUS MEDICATIONS INTERMITTENTLY/CONTINUOUSLY B. (SUBCUTANEOUS INFUSION) HYDRODERMOCLYSIS
 SUBCUTANEOUS THERAPY A. ADMINISTERING SUBCUTANEOUS MEDICATIONS INTERMITTENTLY/CONTINUOUSLY B. (SUBCUTANEOUS INFUSION) HYDRODERMOCLYSIS PARTS I. Purposes II. General Information III. Responsibilities IV.
SUBCUTANEOUS THERAPY A. ADMINISTERING SUBCUTANEOUS MEDICATIONS INTERMITTENTLY/CONTINUOUSLY B. (SUBCUTANEOUS INFUSION) HYDRODERMOCLYSIS PARTS I. Purposes II. General Information III. Responsibilities IV.
Caring for a Tenckhoff Catheter
 Caring for a Tenckhoff Catheter UHN A Patient s Guide What is a Pleural Effusion? There is a small space between the outside of your lung and the chest wall (ribs). This space is called the pleural space.
Caring for a Tenckhoff Catheter UHN A Patient s Guide What is a Pleural Effusion? There is a small space between the outside of your lung and the chest wall (ribs). This space is called the pleural space.
PICC/Midclavicular/Midline Catheter
 47 PICC/Midclavicular/Midline Catheter Introduction- PICC/ MCV/ Midline You have a PICC/Midclavicular/Midline (peripherally inserted) catheter. This catheter should make receiving I.V. medicines or solutions
47 PICC/Midclavicular/Midline Catheter Introduction- PICC/ MCV/ Midline You have a PICC/Midclavicular/Midline (peripherally inserted) catheter. This catheter should make receiving I.V. medicines or solutions
INS Position Paper. Recommendations for Frequency of Assessment of the Short Peripheral Catheter Site
 INS Position Paper Recommendations for Frequency of Assessment of the Short Peripheral Catheter Site Background As many organizations choose to follow the Infusion Nurses Society (INS) recommendations
INS Position Paper Recommendations for Frequency of Assessment of the Short Peripheral Catheter Site Background As many organizations choose to follow the Infusion Nurses Society (INS) recommendations
1-800-862-2731 Administration of Meropenem For Child
 1 Drug Name: _Meropenem 1-800-862-2731 Administration of Meropenem For Child Dosage: milligrams every hours over 5 minutes Key Points: FLUSHING: Meropenem Heparin flush 1. Always wash your hands with an
1 Drug Name: _Meropenem 1-800-862-2731 Administration of Meropenem For Child Dosage: milligrams every hours over 5 minutes Key Points: FLUSHING: Meropenem Heparin flush 1. Always wash your hands with an
Best Practices in Pediatric Central Venous Catheter Care: A Case Study from Children s Medical Center of Dallas
 Best Practices in Pediatric Central Venous Catheter Care: A Case Study from Children s Medical Center of Dallas Author: Darcy Doellman, RN, BSN, CRNI, VA-BC Darcy Doellman serves as a national speaker
Best Practices in Pediatric Central Venous Catheter Care: A Case Study from Children s Medical Center of Dallas Author: Darcy Doellman, RN, BSN, CRNI, VA-BC Darcy Doellman serves as a national speaker
CUESTA COLLEGE REGISTERED NURSING PROGRAM CRITICAL ELEMENTS
 CUESTA COLLEGE REGISTERED NURSING PROGRAM CRITICAL ELEMENTS LEVELS I through IV A. OVERRIDING CRITICAL ELEMENTS Violation of an overriding area will result in termination and failure of the particular
CUESTA COLLEGE REGISTERED NURSING PROGRAM CRITICAL ELEMENTS LEVELS I through IV A. OVERRIDING CRITICAL ELEMENTS Violation of an overriding area will result in termination and failure of the particular
NURSING PRACTICE & SKILL
 NURSING PRACTICE & SKILL Vascular Access Devices: Assessing to Reduce Risk of Complications What is Performing an Assessment to Reduce the Risk of Complications for Vascular Access Devices? The function
NURSING PRACTICE & SKILL Vascular Access Devices: Assessing to Reduce Risk of Complications What is Performing an Assessment to Reduce the Risk of Complications for Vascular Access Devices? The function
Nursing Management of Venous Access Devices: Peripheral IV lines
 Nursing Management of Venous Access Devices: Peripheral IV lines Mimi Bartholomay, RN, MSN, AOCN Denise Dreher,, RN, CRNI, VA-BC Theresa Evans, RN, MSN Susan Finn, RN, MSN, AOCNS Debra Guthrie, RN, CRNI
Nursing Management of Venous Access Devices: Peripheral IV lines Mimi Bartholomay, RN, MSN, AOCN Denise Dreher,, RN, CRNI, VA-BC Theresa Evans, RN, MSN Susan Finn, RN, MSN, AOCNS Debra Guthrie, RN, CRNI
Lifecath Midline. A Nurses Guide to Lifecath Midline
 Lifecath Midline A Nurses Guide to Lifecath Midline vygon@vygon.co.uk www.vygon.co.uk Lifecath Midline A Nurses Guide to Lifecath Midline This booklet provides guidance in the care and maintenance of Midline
Lifecath Midline A Nurses Guide to Lifecath Midline vygon@vygon.co.uk www.vygon.co.uk Lifecath Midline A Nurses Guide to Lifecath Midline This booklet provides guidance in the care and maintenance of Midline
POSSIBLE NURSING DIAGNOSIS: Pain Potential for Infection / Infection Fluid volume deficit
 1 Procedure for Subcutaneous Over-the-needle Cannula Insertion, Removal, Medication Administration, and Fluid Administration for the Individual in the Home PURPOSE: To provide medication via the subcutaneous
1 Procedure for Subcutaneous Over-the-needle Cannula Insertion, Removal, Medication Administration, and Fluid Administration for the Individual in the Home PURPOSE: To provide medication via the subcutaneous
Peripherally Inserted Central Catheter (PICC) Patient Instructions
 Patient Care Services 300 Pasteur Drive Stanford, CA 94305 Peripherally Inserted Central Catheter (PICC) Patient Instructions A Peripherally Inserted Central Catheter (PICC) is a soft flexible tube inserted
Patient Care Services 300 Pasteur Drive Stanford, CA 94305 Peripherally Inserted Central Catheter (PICC) Patient Instructions A Peripherally Inserted Central Catheter (PICC) is a soft flexible tube inserted
Site Care of Your Central Venous Catheter Sterile
 Site Care of Your Central Venous Catheter Sterile Dressing Change Sterile Technique The skin surrounding your catheter s exit site must be kept clean, and a new sterile dressing should be applied on a
Site Care of Your Central Venous Catheter Sterile Dressing Change Sterile Technique The skin surrounding your catheter s exit site must be kept clean, and a new sterile dressing should be applied on a
Objectives At the completion of this module, unlicensed assistive personnel (UAP) should be able to:
 Objectives At the completion of this module, unlicensed assistive personnel (UAP) should be able to: 1. administer medications by subcutaneous injections. 2. document medication administration in the client
Objectives At the completion of this module, unlicensed assistive personnel (UAP) should be able to: 1. administer medications by subcutaneous injections. 2. document medication administration in the client
A PROCEDURAL GUIDE TO MIDLINE CATHETER INSERTION
 A PROCEDURAL GUIDE TO MIDLINE CATHETER INSERTION See Also CPG midline catheters for indications, contraindications and post insertion management What is a midline A midline catheter is an 8-12 cm catheter
A PROCEDURAL GUIDE TO MIDLINE CATHETER INSERTION See Also CPG midline catheters for indications, contraindications and post insertion management What is a midline A midline catheter is an 8-12 cm catheter
Page 1 of 10 MC1482 Peripherally-Inserted Central Catheter. Peripherally-Inserted Central Catheter (PICC)
 Page 1 of 10 MC1482 Peripherally-Inserted Central Catheter Peripherally-Inserted Central Catheter (PICC) Page 2 of 10 MC1482 Peripherally-Inserted Central Catheter Introduction A peripherally-inserted
Page 1 of 10 MC1482 Peripherally-Inserted Central Catheter Peripherally-Inserted Central Catheter (PICC) Page 2 of 10 MC1482 Peripherally-Inserted Central Catheter Introduction A peripherally-inserted
IV 03 CRAIG HOSPITAL POLICY/PROCEDURE
 CRAIG HOSPITAL POLICY/PROCEDURE Approved: NPC, P&P 12/06; P&T 2/07; Effective Date: 10/78 IC, MEC 03/07; NPC, P&P 08/09; MEC 9/09 P&T 12/10; MEC, P&P 01/11, 04/11 Attachments: Revised Date: 12/02, 07/04,
CRAIG HOSPITAL POLICY/PROCEDURE Approved: NPC, P&P 12/06; P&T 2/07; Effective Date: 10/78 IC, MEC 03/07; NPC, P&P 08/09; MEC 9/09 P&T 12/10; MEC, P&P 01/11, 04/11 Attachments: Revised Date: 12/02, 07/04,
Clinician Competency:
 Thanks to CR Bard Clinician Competency: INS (Intravenous Nursing Society) recommends that an institution create a set criteria to evaluate the competency of nurses learning to place PICC Line / Midline
Thanks to CR Bard Clinician Competency: INS (Intravenous Nursing Society) recommends that an institution create a set criteria to evaluate the competency of nurses learning to place PICC Line / Midline
Title: Greater Manchester and Cheshire Cancer Network Policy for the Care of long term Central Venous Catheters
 Title: Greater Manchester and Cheshire Cancer Network Policy for the Care of long term Central Venous Catheters Purpose: For staff to be aware of policies and guidelines for the care of long term Central
Title: Greater Manchester and Cheshire Cancer Network Policy for the Care of long term Central Venous Catheters Purpose: For staff to be aware of policies and guidelines for the care of long term Central
NURSING PRACTICE & SKILL
 NURSING PRACTICE & SKILL ICD-9 99.29 Author Carita Caple, RN, BSN, MSHS Reviewers Eliza Schub, RN, BSN Sara Richards, MSN, RN Nursing Practice Council Glendale Adventist Medical Center, Glendale, CA Editor
NURSING PRACTICE & SKILL ICD-9 99.29 Author Carita Caple, RN, BSN, MSHS Reviewers Eliza Schub, RN, BSN Sara Richards, MSN, RN Nursing Practice Council Glendale Adventist Medical Center, Glendale, CA Editor
Clinical Guideline for: Aseptic Technique
 Clinical Guideline for: Technique Summary This guideline provides the principles of, Non Touch, and Clean Techniques to be implemented in the hospital environment. Key Points The essential elements of
Clinical Guideline for: Technique Summary This guideline provides the principles of, Non Touch, and Clean Techniques to be implemented in the hospital environment. Key Points The essential elements of
SAFE HANDLING OF HAZARDOUS MEDICATIONS. Cytotoxic and Non-Cytotoxic. Winnipeg Regional Health Authority Policy # 110.160.010
 SAFE HANDLING OF HAZARDOUS MEDICATIONS Cytotoxic and Non-Cytotoxic Winnipeg Regional Health Authority Policy # 110.160.010 By the end of this presentation staff should be able to 1. Understand what information
SAFE HANDLING OF HAZARDOUS MEDICATIONS Cytotoxic and Non-Cytotoxic Winnipeg Regional Health Authority Policy # 110.160.010 By the end of this presentation staff should be able to 1. Understand what information
Intravenous Line Maintenance. The care of intravenous devices is standardized
 Seattle Children's (Clinical Policy/Procedure) Intravenous Line Maintenance POLICY: The care of intravenous devices is standardized PURPOSE: Describes general line care maintenance practices for all venous
Seattle Children's (Clinical Policy/Procedure) Intravenous Line Maintenance POLICY: The care of intravenous devices is standardized PURPOSE: Describes general line care maintenance practices for all venous
Tunneled Central Venous Catheter (CVC) Placement
 PATIENT EDUCATION patienteducation.osumc.edu Tunneled Central Venous Catheter (CVC) Placement A tunneled Central Venous Catheter (CVC) is a special type of intravenous (IV) line that is placed into a large
PATIENT EDUCATION patienteducation.osumc.edu Tunneled Central Venous Catheter (CVC) Placement A tunneled Central Venous Catheter (CVC) is a special type of intravenous (IV) line that is placed into a large
TITLE: ANTIBIOTIC (ALT) AND ETHANOL (ELT) LOCK THERAPY FOR THE MANAGEMENT OF CENTRAL VENOUS CATHETER-RELATED INFECTIONS
 Page 1 of 11 TITLE: ANTIBIOTIC (ALT) AND ETHANOL (ELT) LOCK THERAPY FOR THE MANAGEMENT OF CENTRAL VENOUS CATHETER-RELATED INFECTIONS GUIDELINES: Antibiotic lock therapy (ALT) and ethanol lock therapy (ELT)
Page 1 of 11 TITLE: ANTIBIOTIC (ALT) AND ETHANOL (ELT) LOCK THERAPY FOR THE MANAGEMENT OF CENTRAL VENOUS CATHETER-RELATED INFECTIONS GUIDELINES: Antibiotic lock therapy (ALT) and ethanol lock therapy (ELT)
National Patient Safety Goals Effective January 1, 2015
 National Patient Safety Goals Goal 1 Nursing are enter ccreditation Program Improve the accuracy of patient and resident identification. NPSG.01.01.01 Use at least two patient or resident identifiers when
National Patient Safety Goals Goal 1 Nursing are enter ccreditation Program Improve the accuracy of patient and resident identification. NPSG.01.01.01 Use at least two patient or resident identifiers when
Aspira* Peritoneal Drainage Catheter
 Aspira* Peritoneal Drainage Catheter Instructions For Use Access Systems Product Description: The Aspira* Peritoneal Drainage Catheter is a tunneled, long-term catheter used to drain accumulated fluid
Aspira* Peritoneal Drainage Catheter Instructions For Use Access Systems Product Description: The Aspira* Peritoneal Drainage Catheter is a tunneled, long-term catheter used to drain accumulated fluid
National Patient Safety Goals Effective January 1, 2015
 National Patient Safety Goals Effective January 1, 2015 Goal 1 Improve the accuracy of resident identification. NPSG.01.01.01 Long Term are ccreditation Program Medicare/Medicaid ertification-based Option
National Patient Safety Goals Effective January 1, 2015 Goal 1 Improve the accuracy of resident identification. NPSG.01.01.01 Long Term are ccreditation Program Medicare/Medicaid ertification-based Option
Procedure for Inotrope Administration in the home
 Procedure for Inotrope Administration in the home Purpose This purpose of this procedure is to define the care used when administering inotropic agents intravenously in the home This includes: A. Practice
Procedure for Inotrope Administration in the home Purpose This purpose of this procedure is to define the care used when administering inotropic agents intravenously in the home This includes: A. Practice
REMOVAL OF A PICC. Possible Cause Nursing Actions Prevention
 REMOVAL OF A PICC PICC lines are removed following a physician order, when therapy is completed or complications such as line sepsis, thrombosis or phlebitis, require removal. The removal of a PICC line
REMOVAL OF A PICC PICC lines are removed following a physician order, when therapy is completed or complications such as line sepsis, thrombosis or phlebitis, require removal. The removal of a PICC line
An Infusion of Quality and Safety STAT!
 Quality is not an act, it is a habit. Aristotle An Infusion of Quality and Safety STAT! Quality is not an act, it is a habit. Mary Kakenmaster MSN, RN, CNE Oakton Community College mkakenma@oakton.edu
Quality is not an act, it is a habit. Aristotle An Infusion of Quality and Safety STAT! Quality is not an act, it is a habit. Mary Kakenmaster MSN, RN, CNE Oakton Community College mkakenma@oakton.edu
ADMINISTRATION OF INTRAVENOUS PUSH/DIRECT MEDICATIONS
 SASKATOON DISTRICT HEALTH Department of Nursing Affairs ADMINISTRATION OF INTRAVENOUS PUSH/DIRECT MEDICATIONS SPECIAL NURSING PROCEDURE LEARNING PACKAGE This package provides the basic information necessary
SASKATOON DISTRICT HEALTH Department of Nursing Affairs ADMINISTRATION OF INTRAVENOUS PUSH/DIRECT MEDICATIONS SPECIAL NURSING PROCEDURE LEARNING PACKAGE This package provides the basic information necessary
Sterile Dressing Change with Tegaderm CHG for Central Venous Catheter (CVC)
 Sterile Dressing Change with Tegaderm CHG for Central Venous Catheter (CVC) The dressing protects your catheter site. It also helps prevent infection at the site. Keep your dressing clean and dry at all
Sterile Dressing Change with Tegaderm CHG for Central Venous Catheter (CVC) The dressing protects your catheter site. It also helps prevent infection at the site. Keep your dressing clean and dry at all
Promoting safer use of injectable medicines
 Promoting safer use of injectable medicines A template standard operating procedure for: prescribing, preparing and administering injectable medicines in clinical areas Introduction The use of injectable
Promoting safer use of injectable medicines A template standard operating procedure for: prescribing, preparing and administering injectable medicines in clinical areas Introduction The use of injectable
How to safely collect blood samples from persons suspected to be infected with highly infectious blood-borne pathogens (e.g.
 How to safely collect blood samples from persons suspected to be infected with highly infectious blood-borne pathogens (e.g. Ebola) Step 1: Before entering patient room, assemble all equipment (1 st part)
How to safely collect blood samples from persons suspected to be infected with highly infectious blood-borne pathogens (e.g. Ebola) Step 1: Before entering patient room, assemble all equipment (1 st part)
BLOOD CULTURE COLLECTION GUIDELINES FOR PHLEBOTOMISTS (WITHIN REGION 6)
 BLOOD CULTURE COLLECTION GUIDELINES FOR PHLEBOTOMISTS (WITHIN REGION 6) The rate of isolation of micro-organisms from blood is directly related to the volume of blood collected. Therefore, it is recommended
BLOOD CULTURE COLLECTION GUIDELINES FOR PHLEBOTOMISTS (WITHIN REGION 6) The rate of isolation of micro-organisms from blood is directly related to the volume of blood collected. Therefore, it is recommended
Procedure -8. Intraosseous Infusion Adult and Pediatric EZIO. Page 1 of 7 APPROVED:
 Page 1 of 7 Intraosseous Infusion Adult and Pediatric APPROVED: EMS Medical Director EMS Administrator 1. Goals/Introduction: 1.1 Intraosseous (IO) infusion provides an effective alternative means of providing
Page 1 of 7 Intraosseous Infusion Adult and Pediatric APPROVED: EMS Medical Director EMS Administrator 1. Goals/Introduction: 1.1 Intraosseous (IO) infusion provides an effective alternative means of providing
PICC Catheter for IV Therapy
 PICC Catheter for IV Therapy A Patient Guide for: PATIENT PICC A PICC is defined as a Peripherally Inserted Central Catheter. A PICC is a special IV Catheter. It is put in an arm vein and ends in a large
PICC Catheter for IV Therapy A Patient Guide for: PATIENT PICC A PICC is defined as a Peripherally Inserted Central Catheter. A PICC is a special IV Catheter. It is put in an arm vein and ends in a large
Central Venous Catheter Care For Haemodialysis
 Central Venous Catheter Care For Haemodialysis Information For Parents and Carers Haemodialysis Unit 01 878 4757 Main Hospital Number 01 878 4200 Central Venous Catheters We hope this booklet will help
Central Venous Catheter Care For Haemodialysis Information For Parents and Carers Haemodialysis Unit 01 878 4757 Main Hospital Number 01 878 4200 Central Venous Catheters We hope this booklet will help
Patient Information. PORT-A-CATH Implantable Venous Access Systems
 Patient Information PORT-A-CATH Implantable Venous Access Systems Your doctor has prescribed treatment that requires the frequent administration of medications or other fluids directly into your bloodstream
Patient Information PORT-A-CATH Implantable Venous Access Systems Your doctor has prescribed treatment that requires the frequent administration of medications or other fluids directly into your bloodstream
