F322 Feeding Tubes Handouts
|
|
|
- Dulcie Horn
- 7 years ago
- Views:
Transcription
1 Slide Naso-Gastric Tubes (F322 Feeding Tubes) Surveyor Train the Trainer: Investigative Protocol 1 Slide 2 Presented by: Miriam Thornquist R.N. HFE Nurse Evaluator II Minnesota Department of Health 2 Slide 3 OBJECTIVES Following the presentation the participant will be able to: Identify the change from F tag 321 to 322 State the definitions of tube feeding terms State the considerations prior to decision to use a feeding tube Describe benefits of tube feeding for resident Describe possible complications of feeding tube use 3 Page 1 of 22
2 Slide 4 OBJECTIVES cont. Describe investigative protocol regarding feeding tubes Describe determination of compliance or noncompliance with F tag Slide 5 Federal Regulatory Language (g) Naso-Gastric Tubes* - Based on the comprehensive assessment of a resident, the facility must ensure that (g)(1) - A resident who has been able to eat enough alone or with assistance is not fed by naso-gastric tube unless the resident s clinical condition demonstrates that use of a naso-gastric tube was unavoidable; and 5 Slide 6 Federal Regulatory Language (cont) (g)(2) - A resident who is fed by a nasogastric or gastrostomy tube receives the appropriate treatment and services to prevent aspiration pneumonia, diarrhea, vomiting, dehydration, metabolic abnormalities, and nasal-pharyngeal ulcers and to restore, if possible, normal eating skills. 6 Page 2 of 22
3 Slide 7 Merging Tags F321 and F322 The revisions to appendix PP Interpretive Guidelines for Long Term Care Facilities at (g)(1)(2) combines F321 and F322, and incorporated the guidance into F Slide (g) Naso-Gastric Tubes* *For the purpose of the interpretative guidelines at F tag 322 the regulatory title (g) Naso-gastric tubes is considered to include any feeding tube used to provide enteral nutrition to a resident by bypassing oral intake. 8 Slide 9 Intent The intent of this regulation is that: The feeding tube is utilized only after adequate assessment determines that the resident's clinical condition makes this intervention medically necessary; A feeding tube is utilized in accordance with current clinical standards of practice and services are provided to prevent complications to the extent possible; and Services are provided to restore normal eating skills to the extent possible. 9 Page 3 of 22
4 Slide 10 Definitions Avoidable/Unavoidable use of a feeding tube Avoidable -- there is not a clear indication for using a feeding tube, and there is insufficient evidence that it provides a benefit that outweighs associated risks. Unavoidable -- there is a clear indication for using a feeding tube, and there is sufficient evidence that it provides a benefit that outweighs associated risks. 10 Slide 11 Definitions (cont d) Bolus feeding means the administration of a limited volume of enteral formula over brief periods of time. Continuous feeding means the uninterrupted administration of enteral formula over extended periods of time. 11 Slide 12 Definitions (cont d) Enteral nutrition (a.k.a. tube feeding ) means the delivery of nutrients through a feeding tube directly into the stomach, duodenum, or jejunum. Feeding tube means a medical device used to provide enteral nutrition to a resident by bypassing oral intake. 12 Page 4 of 22
5 Slide 13 Definitions (cont d) Gastrostomy tube ( G-tube ) means a tube that is placed directly into the stomach through an abdominal wall incision for administration of food, fluids, and medications. The most common type is a percutaneous endoscopic gastrostomy (PEG) tube. 13 Slide 14 PEG tube 14 Slide 15 Definitions Jejunostomy tube (a.k.a. percutaneous endoscopic jejunostomy (PEJ) or J-tube ) means a feeding tube placed directly into the small intestine. Nasogastric feeding tube ( NG tube ) means a tube that is passed through the nose and down through the nasopharynx and esophagus into the stomach. 15 Page 5 of 22
6 Slide 16 Definitions Transgastric jejunal feeding tube ( G-J tube ) means a feeding tube that is placed through the stomach into the jejunum and that has dual ports to access both the stomach and the small intestine. Tube feeding (a.k.a. enteral feeding ) means the delivery of nutrients through a feeding tube directly into the stomach, duodenum, or jejunum. 16 Slide 17 Transgastric jejunal tube G-J tube 17 Slide 18 Overview The decision to use a feeding tube: Has a major impact on a resident and his or her quality of life; and Is based on the resident s clinical condition and wishes and federal and state laws. Use of feeding tubes varies widely among states depending on opinions about non-oral nutrition and varied facility policies and usual practices. 18 Page 6 of 22
7 Slide 19 Considerations Regarding The Use of Feeding Tubes The resident s clinical condition must demonstrate the use of a feeding tube to be unavoidable : No viable alternative to maintain adequate nutrition and/or hydration; and Use is consistent with the clinical need to maintain or improve nutritional /hydration parameters. 19 Slide 20 Other factors that may be associated with use: Medical conditions that impair nutrition; Considerations Regarding The Use of Feeding Tubes (cont d.) Need to improve nutritional status or comfort; To provide comfort; and Desire to prolong life. 20 Slide 21 Considerations Regarding The Use of Feeding Tubes (cont d.) Clinical rationale supporting the use of a feeding tube includes: Assessment of the resident s nutritional and clinical status; Relevant functional and psychosocial factors (such as potential ability to maintain activities of daily living ADL); and Prior interventions (nutrition therapy and medical intervention tried) and the resident s response. 21 Page 7 of 22
8 Slide 22 Considerations Regarding The Use of Feeding Tubes Potential benefits of feeding tube use include: Addressing malnutrition and dehydration; Promoting wound healing; Allowing the resident to gain strength (for ADL) including appropriate interventions that may help to restore the residents ability to eat; and Improving the resident s ability to make decisions about their care and ability to interact with others. 22 Slide 23 Considerations Regarding The Use of Feeding Tubes (cont d.) Possible adverse effects of feeding tube use include: Diminished socialization; Decreased opportunity to experience taste, texture and chewing of foods; Complications related to the tube; and Restricted movement. 23 Slide 24 Decisions to Use Feeding tube Decisions to continue or discontinue the use of a feeding tube: Are collaborative and involve the resident (or legal representative), physician and interdisciplinary team; and Include the relevance of a feeding tube to the resident s treatment goals and wishes. 24 Page 8 of 22
9 Slide 25 Technical and Nutritional Aspects of Feeding Tubes Facility protocols assure that staff implement and provide care and services related to feeding tubes according to the resident s need and clinical standards of practice. Protocols regarding some technical aspects include: Location where inserted, when to verify; Care secured externally, cleaning insertion site; and Replacement when, by whom. 25 Slide 26 Technical and Nutritional Aspects of Feeding Tubes (cont d.) Protocols regarding some nutritional aspects include: Enteral nutrition meeting the resident's nutritional needs; Feeding flow managing and monitoring the rate of flow. The practitioner s feeding tube order typically include: kind of feeding, caloric value, volume, duration, mechanism of administration, and frequency of flush. 26 Slide 27 Significant Complications Related to the Feeding Tube Aspiration Leakage around the insertion site Stomach or Intestinal perforation Abdominal wall abscess Erosion at the insertion site (including nasal area) 27 Page 9 of 22
10 Slide 28 Esophageal Complications Related to the Feeding Tube Peritonitis Esophagitis Ulcerations Strictures Tracheoesophageal fistulas Clogged tube 28 Slide 29 Complications Related to the Administration of the Enteral Nutrition Product Nausea; Vomiting; Diarrhea; Abdominal cramping; Inadequate nutrition; Aspiration; Reduced effectiveness of various medications; or Metabolic complications. 29 Slide 30 Aspiration Can be dependent on other risk factors; Is not necessarily related to gastric residual volumes; and Should be assessed individually to implement interventions accordingly (e.g., positioning). 30 Page 10 of 22
11 Slide 31 Enteral Formula May Reduce the Effectiveness of Some Medications For example: The effectiveness of phenytoin sodium may be reduced by the drug binding with the enteral feeding's protein component, leading to less free drug availability and possibly inadequate therapeutic levels. 31 Slide 32 Metabolic Complications Metabolic complications related to tube feeding may include inadequate calorie or protein intake, altered hydration, hypo- or hyperglycemia, and altered electrolyte and nutrient levels. 32 Slide 33 The facility is expected to: Complications Management Identify and address actual or potential complications related to the feeding tube or tube feeding; and Notify and involve the practitioner in evaluating and managing care to address these complications and risk factors. 33 Page 11 of 22
12 Slide 34 To determine if: Objectives Investigative Protocol A feeding tube is utilized only after adequate assessment determines that the resident's clinical condition makes this intervention medically necessary; A feeding tube is utilized in accordance with current clinical standards of practice and if services are provided to prevent complications to the extent possible; and Services are provided to restore normal eating skills to the extent possible. 34 Slide 35 Observations Interviews Record Review Procedures Investigative Protocol 35 Slide 36 Investigative Protocol Observations During various shifts, observe staff interactions with the resident and provision of care including: Initiation, continuation, and termination of feedings; Care of the tube site and equipment; and Medication administration via the feeding tube. 36 Page 12 of 22
13 Slide 37 Investigative Protocol Observations (cont d) To determine whether staff follow: Clinical standards of practice; Facility policy; Resident care plan; and Prescriber s orders. 37 Slide 38 Observations (cont d) Investigative Protocol Use to determine whether staff try to minimize the risk for complications. For example: Providing mouth care, including teeth, gums, and tongue; Checking that the tubing remains in the correct location; and Properly positioning the resident consistent with the resident s individual needs. 38 Slide 39 Investigative Protocol Interviews: Resident/representative Determine if the facility has involved the resident (or legal representative) in the care plan process to reflect the resident s choices, preferences, and response to tube feeding. For example, determine whether: The resident (or legal representative) was informed about benefits and risks of tube feeding and possible alternatives; and/or There has been reassessment and discussion with the resident (or legal representative) re: continued appropriateness/necessity of the feeding tube. 39 Page 13 of 22
14 Slide 40 Investigative Protocol Interviews: Facility Staff Interview the facility staff, who provide direct care, to determine, for example: Whether the resident has voiced any complaints or exhibited any physical or psychosocial complications that may be associated with the tube feeding: o Nausea and/or vomiting o Diarrhea o Pain associated with the tube o Abdominal discomfort o Depression and/or withdrawal 40 Slide 41 Investigative Protocol Interviews: Facility Staff (cont d) Interview the facility staff, who provide direct care, to determine, for example: How these problems have been addressed; and To whom a staff member has reported the resident s signs or symptoms. 41 Slide 42 Investigative Protocol Interviews: Facility Staff (cont d) Interview staff with responsibility for overseeing or training regarding care related to feeding tubes to determine, for example: How does staff calculate nutritional needs for the resident and ensure that the resident receives close to the calculated amount of nutrition daily? How are staff trained and directed regarding management of feeding tubes and tube feedings in general, and in addressing any specific issues related to this individual resident? 42 Page 14 of 22
15 Slide 43 Record review Investigative Protocol Review the resident s record for evidence of rationale for feeding tube insertion (including interventions tried), and the potential to restore normal eating skills. For example, did the staff: Verify that the feeding tube was properly placed? Monitor the resident for possible complications related to a feeding tube and the tube feeding? 43 Slide 44 Review of Facility Practices Related concerns may have been identified that would suggest the need for interviews with staff (including facility management) and a review of: Facility practices; Staffing; Staff training; and Functional responsibilities. 44 Slide 45 Review of Facility Practices (cont d.) If there is a pattern of residents who have issues related to the indications, utilization, complications, process or performance issues with feeding tubes, determine whether the facility has incorporated into its quality assurance activities a review of appropriateness and management of tube feedings. 45 Page 15 of 22
16 Slide 46 Synopsis of F322 Regulation The regulation requires that the facility: Determination of Compliance Utilize a feeding tube only after it determines that a resident s clinical condition demonstrates this intervention was unavoidable; and Provides the resident who is fed by a tube services to prevent complications and restore normal eating skills to the extent possible. 46 Slide 47 Criteria for Compliance with F322 The facility is in compliance if staff: Determination of Compliance Use a feeding tube to provide nutrition and hydration only when the resident s clinical condition makes this intervention necessary based on adequate assessment and after other efforts to maintain or improve the resident s nutritional status have failed; 47 Slide 48 Criteria for Compliance with F322 (cont d.) The facility is in compliance if staff: Determination of Compliance Manage all aspects of a feeding tube and enteral feeding consistent with current clinical standards of practice in order to meet the resident s nutritional and hydration needs and to prevent complications; and Identify and address the potential risks and /or complications associated with feeding tubes, and provide treatment and services to restore, if possible, adequate oral intake. 48 Page 16 of 22
17 Slide 49 Determination of Compliance Noncompliance at F322 Noncompliance with F322 may include, but is not limited to, failure to do one or more of the following: Appropriately assess a resident s nutritional status and needs, and identify a clinically pertinent rationale for the use of a feeding tube; Identify nutritional requirements for a resident fed by a feeding tube and ensure that a tube feeding meets those needs; 49 Slide 50 Failure to: Determination of Compliance Noncompliance at F322 (cont d) Adequately address the nutritional aspects of enteral feeding and the management of the feeding tube, including prevention of related complications; or Use and monitor a feeding tube per facility protocol and pertinent clinical standards of practice, provide services to attempt to restore, if possible, normal eating skills, or identify and manage tube-related or enteral feeding-related complications. 50 Slide 51 DEFICIENCY CATEGORIZATION (Part IV, Appendix P) Severity Determination Key Components Harm/negative outcome(s) or potential for negative outcomes due to a failure of care and services, Degree of harm (actual or potential) related to noncompliance, and Immediacy of correction required. 51 Page 17 of 22
18 Slide 52 Deficiency Categorization Determining Actual or Potential Harm Actual or potential harm/negative outcome at F322 may include: Failure to adequately identify nutritional requirements for a resident fed by a feeding tube and ensure that the tube feeding met those needs (if clinically feasible), resulting in the resident experiencing malnutrition and dehydration; and Failure to verify the location of the tube in accordance with current clinical standards, facility protocols, and resident condition; therefore increasing the risk for complications such as aspiration. 52 Slide 53 Deficiency Categorization Determining Degree of Harm How the facility practices caused, resulted in, allowed, or contributed to harm (actual/potential) If harm has occurred, determine if the harm is at the level of serious injury, impairment, death, compromise, or discomfort; and If harm has not yet occurred, determine how likely the potential is for serious injury, impairment, death, compromise or discomfort to occur to the resident. 53 Slide 54 Deficiency Categorization The Immediacy of Correction Required Determine whether the noncompliance requires immediate correction in order to prevent serious injury, harm, impairment, or death to one or more residents. 54 Page 18 of 22
19 Slide 55 Severity Levels Deficiency Categorization Level 4: Immediate Jeopardy to Resident Health or Safety Level 3: Actual Harm that is Not Immediate Jeopardy Level 2: No Actual Harm with Potential for More than Minimal Harm that is Not Immediate Jeopardy Level 1: No Actual Harm with Potential for Minimal Harm 55 Slide 56 Deficiency Categorization Severity Level 4 Immediate Jeopardy Has allowed/caused/resulted in, or is likely to cause serious injury, harm, impairment, or death to a resident; and 56 Slide 57 Deficiency Categorization Severity Level 4: Immediate Jeopardy (cont d) Requires immediate correction, as the facility either created the situation or allowed the situation to continue by failing to implement preventative or corrective measures. 57 Page 19 of 22
20 Slide 58 Severity Level 4 Example Severity Level 4 Example As a result of the facility routinely keeping a resident lying almost flat in bed while administering the resident s tube feeding, the resident aspirated some of the tube feeding and got aspiration pneumonia. 58 Slide 59 Severity Determination Severity Level 3: Actual Harm that is not Immediate Jeopardy The negative outcome may include but may not be limited to clinical compromise, decline, or the resident s inability to maintain and/or reach his/her highest practicable level of well-being. 59 Slide 60 Severity Determination Severity Level 3 Example Severity Level 3 Example The facility failed to monitor for complications related to a resident s feeding tube and tube feeding. As a result, the resident experienced significant but not lifethreatening tube feeding-related complications. 60 Page 20 of 22
21 Slide 61 Severity Determination Severity Level 2: No Actual Harm with potential for more than minimal harm that is not Immediate Jeopardy Noncompliance that results in a resident outcome of no more than minimal discomfort, and/or Has the potential to compromise the resident s ability to maintain or reach his or her highest practicable level of well-being. 61 Slide 62 Severity Determination Severity Level 2 Example Severity Level 2 Example As a result of staff failure to manage a tube feeding pump properly, the resident did not receive the calculated amount of tube feeding, without resulting in significant weight loss or other GI complications. 62 Slide 63 Severity Determination Severity Level 1: No Actual Harm with Potential for Minimal Harm The failure of the facility to provide appropriate care and services for feeding tubes, places the resident at risk for more than minimal harm. Therefore, Severity Level 1 does not apply for this regulatory requirement. 63 Page 21 of 22
22 Slide 64 QIS Critical Element Pathway Observation Interview Document review 64 Slide 65 QIS CE pathway (cont ) Assessment Care planning implementation Care planning revision Provision of care and services Concern with associated requirements 65 Slide 66 CONCLUSION The federal regulatory language for feeding tubes has not changed Regulatory language from F tag 321 has been incorporated into F tag 322 Additional definitions, interpretive guidance and investigative protocol have been added 66 Page 22 of 22
483.25(i) Nutrition (F325) Surveyor Training: Interpretive Guidance Investigative Protocol
 483.25(i) Nutrition (F325) Surveyor Training: 1 With regard to the revised guidance F325 Nutrition, there have been significant changes. Specifically, F325 and F326 were merged. However, the regulatory
483.25(i) Nutrition (F325) Surveyor Training: 1 With regard to the revised guidance F325 Nutrition, there have been significant changes. Specifically, F325 and F326 were merged. However, the regulatory
Care of Gastrostomy Tubes for Adults with IDD in Community Settings: The Nurse s Role. Lillian Khalil, BSN, RN Volunteers of America, Chesapeake
 Care of Gastrostomy Tubes for Adults with IDD in Community Settings: The Nurse s Role Lillian Khalil, BSN, RN Volunteers of America, Chesapeake Objectives The participants will be able to identify the
Care of Gastrostomy Tubes for Adults with IDD in Community Settings: The Nurse s Role Lillian Khalil, BSN, RN Volunteers of America, Chesapeake Objectives The participants will be able to identify the
Patients First. Tube Feeding Guidelines. Careful handwashing and a clean work surface help prevent infection. Patient Education CARE AND TREATMENT
 Patient Education CARE AND TREATMENT Careful handwashing and a clean work surface help prevent infection. Tube Feeding Guidelines This information will guide you in learning about the procedure for tube
Patient Education CARE AND TREATMENT Careful handwashing and a clean work surface help prevent infection. Tube Feeding Guidelines This information will guide you in learning about the procedure for tube
Center for Medicaid and State Operations/Survey and Certification Group Ref: S&C-07-30 DATE: August 10, 2007 (revised)
 DEPARTMENT OF HEALTH & HUMAN SERVICES Centers for Medicare & Medicaid Services 7500 Security Boulevard, Mail Stop S2-12-25 Baltimore, Maryland 21244-1850 Center for Medicaid and State Operations/Survey
DEPARTMENT OF HEALTH & HUMAN SERVICES Centers for Medicare & Medicaid Services 7500 Security Boulevard, Mail Stop S2-12-25 Baltimore, Maryland 21244-1850 Center for Medicaid and State Operations/Survey
42 CFR 483.25 (F309) QUALITY OF CARE. Changes to Interpretive Guidance. Training Objectives. *Overview of changes
 42 CFR 483.25 (F309) QUALITY OF CARE Changes to Interpretive Guidance 1 Training Objectives Review guidance for hospice and/or ESRD services, formerly in the SOM in Appendix P; Describe when to use F309
42 CFR 483.25 (F309) QUALITY OF CARE Changes to Interpretive Guidance 1 Training Objectives Review guidance for hospice and/or ESRD services, formerly in the SOM in Appendix P; Describe when to use F309
PATIENT CONSENT TO PROCEDURE - ROUX-EN-Y GASTRIC BYPASS
 As a patient you must be adequately informed about your condition and the recommended surgical procedure. Please read this document carefully and ask about anything you do not understand. Please initial
As a patient you must be adequately informed about your condition and the recommended surgical procedure. Please read this document carefully and ask about anything you do not understand. Please initial
DEPARTMENT OF HEALTH AND HUMAN SERVICES CENTERS FOR MEDICARE & MEDICAID SERVICES
 Facility Name: Facility ID: Date: Surveyor Name: Resident Name: Resident ID: Initial Admission Date: Interviewable: Yes No Resident Room: Care Area(s): Use Use this protocol for a sampled resident receiving
Facility Name: Facility ID: Date: Surveyor Name: Resident Name: Resident ID: Initial Admission Date: Interviewable: Yes No Resident Room: Care Area(s): Use Use this protocol for a sampled resident receiving
Interviewable: Yes No Resident Room: Initial Admission Date: Care Area(s): Use
 Facility Name: Facility ID: Date: Surveyor Name: Resident Name: Resident ID: Initial Admission Date: Care Area(s): Interviewable: Yes No Resident Room: Use Use this protocol to determine whether the facility
Facility Name: Facility ID: Date: Surveyor Name: Resident Name: Resident ID: Initial Admission Date: Care Area(s): Interviewable: Yes No Resident Room: Use Use this protocol to determine whether the facility
Interviewable: Yes No Resident Room: Initial Admission Date: Care Area(s): Use
 Facility Name: Facility ID: Date: Surveyor Name: Resident Name: Resident ID: Initial Admission Date: Care Area(s): Interviewable: Yes No Resident Room: Use Use this protocol for a sampled resident receiving
Facility Name: Facility ID: Date: Surveyor Name: Resident Name: Resident ID: Initial Admission Date: Care Area(s): Interviewable: Yes No Resident Room: Use Use this protocol for a sampled resident receiving
What s new? INVESTIGATIVE PROTOCOL FOR URINARY INCONTINENCE & CATHETERS. The Revised Guidance Includes: Interpretive Guidelines
 INVESTIGATIVE PROTOCOL FOR URINARY INCONTINENCE & CATHETERS The Revised Guidance Includes: Interpretive Guidelines Investigative Protocols Compliance & Severity Guidance What s new? The new guidance for
INVESTIGATIVE PROTOCOL FOR URINARY INCONTINENCE & CATHETERS The Revised Guidance Includes: Interpretive Guidelines Investigative Protocols Compliance & Severity Guidance What s new? The new guidance for
Medicines & Enteral Feeding Tubes A DELA V IDICKI-MASTILOVICH C LINICAL P HARMACIST R OYAL C HILDREN S H OSPITAL
 Medicines & Enteral Feeding Tubes A DELA V IDICKI-MASTILOVICH C LINICAL P HARMACIST R OYAL C HILDREN S H OSPITAL Introduction Types of Tubes Choosing a formulation Crushing tablets/opening capsules Administration
Medicines & Enteral Feeding Tubes A DELA V IDICKI-MASTILOVICH C LINICAL P HARMACIST R OYAL C HILDREN S H OSPITAL Introduction Types of Tubes Choosing a formulation Crushing tablets/opening capsules Administration
Delivering nutrition, fluids & medication via a PEG. By Julia Pointer & Caroline Ross, Staff Nurses, Hospice Day Service
 Delivering nutrition, fluids & medication via a PEG By Julia Pointer & Caroline Ross, Staff Nurses, Hospice Day Service Aims of this session? To give an explanation of the theory and practice of a Percutaneous
Delivering nutrition, fluids & medication via a PEG By Julia Pointer & Caroline Ross, Staff Nurses, Hospice Day Service Aims of this session? To give an explanation of the theory and practice of a Percutaneous
My patient has a feeding tube
 My patient has a feeding tube What does that mean? Martha Kliebenstein, MSN, RN Clinical Educator (December, 2014) Types of tubes Gastrostomy (G-tube) Gastrostomy jejunostomy (G-J tube) Naso gastric (NG
My patient has a feeding tube What does that mean? Martha Kliebenstein, MSN, RN Clinical Educator (December, 2014) Types of tubes Gastrostomy (G-tube) Gastrostomy jejunostomy (G-J tube) Naso gastric (NG
DATE DUE: RESIDENT NAME: DATE(S) OF COMPLETION: STAFF COMPLETING RESIDENT REVIEW:
 483.25 QUALITY OF CARE F309 CARE AND SERVICES FOR RESIDENT WITH PAIN Based on QIS CE Pathway CMS-20076 - Pain Recognition and Management http://www.aging.ks.gov/manuals/qismanual.htm Use of this tool is
483.25 QUALITY OF CARE F309 CARE AND SERVICES FOR RESIDENT WITH PAIN Based on QIS CE Pathway CMS-20076 - Pain Recognition and Management http://www.aging.ks.gov/manuals/qismanual.htm Use of this tool is
TPN/ Enteral nutrition. Salsabil HADIRE Dietitian in Oncology Hematology Center of University Hospital Mohammed VI Marrakech-
 TPN/ Enteral nutrition Salsabil HADIRE Dietitian in Oncology Hematology Center of University Hospital Mohammed VI Marrakech- Work plan Part 1: Total Parenteral Nutrition (TPN) Part 2: Enteral Nutrition
TPN/ Enteral nutrition Salsabil HADIRE Dietitian in Oncology Hematology Center of University Hospital Mohammed VI Marrakech- Work plan Part 1: Total Parenteral Nutrition (TPN) Part 2: Enteral Nutrition
Information for people being discharged with a naso-gastric (NG) feeding tube
 Information for people being discharged with a naso-gastric (NG) feeding tube The aim of this leaflet is to provide patients with the relevant information for the use of a nasogastric tube. It will include:
Information for people being discharged with a naso-gastric (NG) feeding tube The aim of this leaflet is to provide patients with the relevant information for the use of a nasogastric tube. It will include:
Are any artificial parts used in the ACE Malone surgery?
 ACE Malone (Antegrade Continence Enema) What is the ACE Malone? The Antegrade Continence Enema (ACE) is a type of surgery designed for the child who has chronic bowel problems with bouts of constipation,
ACE Malone (Antegrade Continence Enema) What is the ACE Malone? The Antegrade Continence Enema (ACE) is a type of surgery designed for the child who has chronic bowel problems with bouts of constipation,
Colic is one of the most dreaded conditions horse owners and trainers encounter with
 Impaction Colic and Hydration Michele Frazer, DVM, DACVIM, DACVECC Impaction Colic Colic is one of the most dreaded conditions horse owners and trainers encounter with their horses. The term colic, however,
Impaction Colic and Hydration Michele Frazer, DVM, DACVIM, DACVECC Impaction Colic Colic is one of the most dreaded conditions horse owners and trainers encounter with their horses. The term colic, however,
Long Term Tube Feeding. Sunnybrook. A Guide for Patients and Substitute Decision Makers VETERANS & COMMUNITY
 Long Term Tube Feeding A Guide for Patients and Substitute Decision Makers Sunnybrook VETERANS & COMMUNITY Sunnybrook VETERANS & COMMUNITY This brochure has been produced by: Sunnybrook Health Sciences
Long Term Tube Feeding A Guide for Patients and Substitute Decision Makers Sunnybrook VETERANS & COMMUNITY Sunnybrook VETERANS & COMMUNITY This brochure has been produced by: Sunnybrook Health Sciences
The Anorexic Cat For this reason, any cat that stops eating for any reason is considered an emergency situation.
 The Anorexic Cat Introduction Any cat that stops eating (anorexic) or begins to eat much less than their normal amount should be seen by a veterinarian right away. The primary reason why a cat stops eating
The Anorexic Cat Introduction Any cat that stops eating (anorexic) or begins to eat much less than their normal amount should be seen by a veterinarian right away. The primary reason why a cat stops eating
Section II When you are finished with this section, you will be able to: Define medication (p 2) Describe how medications work (p 3)
 Section II When you are finished with this section, you will be able to: Define medication (p 2) Describe how medications work (p 3) List the different medication effects (p5) List the ways that medications
Section II When you are finished with this section, you will be able to: Define medication (p 2) Describe how medications work (p 3) List the different medication effects (p5) List the ways that medications
Initial Admission Date: Interviewable: Yes No Resident Room: Care Area(s):
 Facility Name: Facility ID: Date: Surveyor Name: Resident Name: Resident ID: Initial Admission Date: Interviewable: Yes No Resident Room: Care Area(s): Use Use this protocol for a sampled resident with
Facility Name: Facility ID: Date: Surveyor Name: Resident Name: Resident ID: Initial Admission Date: Interviewable: Yes No Resident Room: Care Area(s): Use Use this protocol for a sampled resident with
Nutritional Management in Esophageal Cancer. Kurt Boeykens Nutrition Nurse Specialist
 Nutritional Management in Esophageal Cancer Kurt Boeykens Nutrition Nurse Specialist 1 Are these patients nutritionally at risk? If surgery: Major surgery Preoperative treatment Chemotherapy and radiation
Nutritional Management in Esophageal Cancer Kurt Boeykens Nutrition Nurse Specialist 1 Are these patients nutritionally at risk? If surgery: Major surgery Preoperative treatment Chemotherapy and radiation
Gastrostomy Feeding CARE GUIDELINES FOR PATIENTS & CARERS. Accessory items. Freka UK Funnel Adapter. Fixation Plate CH9. Male Luer Lock Adapter
 Accessory items Freka UK Funnel Adapter Fixation Plate CH9 Code: 7755681 Code: 7903002 Male Luer Lock Adapter CH9 Fixation Plate CH15 Code: 7981311 Code: 7904002 Male Luer Lock Adapter CH15 Code: 798137Y
Accessory items Freka UK Funnel Adapter Fixation Plate CH9 Code: 7755681 Code: 7903002 Male Luer Lock Adapter CH9 Fixation Plate CH15 Code: 7981311 Code: 7904002 Male Luer Lock Adapter CH15 Code: 798137Y
Tube Feeding at Home Gravity or Syringe Feeding
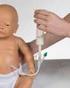 Tube Feeding at Home Gravity or Syringe Feeding Adapted from the former Taming the Feeding Tube, North Shore Hospital. 1 Where do I find information in this booklet? Subject Page How do I contact my health
Tube Feeding at Home Gravity or Syringe Feeding Adapted from the former Taming the Feeding Tube, North Shore Hospital. 1 Where do I find information in this booklet? Subject Page How do I contact my health
Karen Schoeneman Consul5ng 1
 + Spring Cleaning The Rules in Our Heads Karen Schoeneman, Owner Karen Schoeneman Consulting + What Do We Desire in Long Term 2 Care? Quality of Care FOR SURE! That s what we are there for, isn t it? But,
+ Spring Cleaning The Rules in Our Heads Karen Schoeneman, Owner Karen Schoeneman Consulting + What Do We Desire in Long Term 2 Care? Quality of Care FOR SURE! That s what we are there for, isn t it? But,
Medication Guide. Serious loss of body fluid (dehydration) and changes in blood salts (electrolytes) in your blood.
 Medication Guide MoviPrep (moo-vee-prěp) (PEG 3350, sodium sulfate, sodium chloride, potassium chloride, sodium ascorbate, and ascorbic acid for oral solution) Read this Medication Guide before you start
Medication Guide MoviPrep (moo-vee-prěp) (PEG 3350, sodium sulfate, sodium chloride, potassium chloride, sodium ascorbate, and ascorbic acid for oral solution) Read this Medication Guide before you start
Activities of Daily Living F 311 Minnesota Department of Health Nursing Home Surveyor Training Resource
 2/2006 1 Objectives Activities of Daily Living F 311 Minnesota Department of Health Use To determine if the facility is providing maintenance and restorative programs that will not only maintain, but improve,
2/2006 1 Objectives Activities of Daily Living F 311 Minnesota Department of Health Use To determine if the facility is providing maintenance and restorative programs that will not only maintain, but improve,
G E R D. (Gastroesophageal Reflux Disease)
 G E R D (Gastroesophageal Reflux Disease) What is GERD? Gastroesophageal reflux disease (GERD) is a disorder caused by gastric acid flowing from the stomach into the esophagus. What are the symptoms of
G E R D (Gastroesophageal Reflux Disease) What is GERD? Gastroesophageal reflux disease (GERD) is a disorder caused by gastric acid flowing from the stomach into the esophagus. What are the symptoms of
Surgical Weight Loss. Mission Bariatrics
 Surgical Weight Loss Mission Bariatrics Obesity is a major health problem in the United States, with more than one in every three people suffering from this chronic condition. Obese adults are at an increased
Surgical Weight Loss Mission Bariatrics Obesity is a major health problem in the United States, with more than one in every three people suffering from this chronic condition. Obese adults are at an increased
STAY-PUT Nasojejunal Feeding Tubes. Nursing Manual/ Patient Information
 SPECIALTY FEEDING TUBES STAY-PUT Nasojejunal Feeding Tubes Nursing Manual/ Patient Information Manual contains important care and maintenance information and should accompany patient NURSING CONSIDERATIONS
SPECIALTY FEEDING TUBES STAY-PUT Nasojejunal Feeding Tubes Nursing Manual/ Patient Information Manual contains important care and maintenance information and should accompany patient NURSING CONSIDERATIONS
AHLA. CC. The Intersection of Regulatory and Personal Injury Litigation Practical Considerations
 AHLA CC. The Intersection of Regulatory and Personal Injury Litigation Practical Considerations Joseph L. Bianculli Health Care Lawyers PLC Arlington, VA T. Andrew Graham Hall Booth Smith PC Atlanta, GA
AHLA CC. The Intersection of Regulatory and Personal Injury Litigation Practical Considerations Joseph L. Bianculli Health Care Lawyers PLC Arlington, VA T. Andrew Graham Hall Booth Smith PC Atlanta, GA
NPO until Dysphagia Screen
 NPO until Dysphagia Screen Nancy B. Swigert, M.A., CCC/SLP, BRS-S Speech-Language Pathologist Board Recognized Specialist in Swallowing and Swallowing Disorders Director Speech-Language Pathology & Respiratory
NPO until Dysphagia Screen Nancy B. Swigert, M.A., CCC/SLP, BRS-S Speech-Language Pathologist Board Recognized Specialist in Swallowing and Swallowing Disorders Director Speech-Language Pathology & Respiratory
Consent for Treatment/Procedure Laparoscopic Sleeve Gastrectomy
 Patient's Name: Today's Date: / / The purpose of this document is to confirm, in the presence of witnesses, your informed request to have Surgery for obesity. You are asked to read the following document
Patient's Name: Today's Date: / / The purpose of this document is to confirm, in the presence of witnesses, your informed request to have Surgery for obesity. You are asked to read the following document
Learning Objectives. Introduction to Medical Careers. Vocabulary: Chapter 16 FACTS. Functions. Organs. Digestive System Chapter 16
 Learning Objectives Introduction to Medical Careers Digestive System Chapter 16 Define at least 10 terms relating to the digestive Describe the four functions of the digestive Identify different structures
Learning Objectives Introduction to Medical Careers Digestive System Chapter 16 Define at least 10 terms relating to the digestive Describe the four functions of the digestive Identify different structures
Degree of Intervention
 Inglewood Care Centre Degree of Intervention Handbook for Residents and Families Index Introduction..................................................... 2 Beliefs, Values, and Wishes.........................................
Inglewood Care Centre Degree of Intervention Handbook for Residents and Families Index Introduction..................................................... 2 Beliefs, Values, and Wishes.........................................
Use of stents in esophageal cancer" Hans Gerdes, M.D. Director, GI Endoscopy Unit Memorial Sloan-Kettering Cancer Center
 Use of stents in esophageal cancer" Hans Gerdes, M.D. Director, GI Endoscopy Unit Memorial Sloan-Kettering Cancer Center Features of esophageal cancer Esophageal cancer is an abnormal growth that arises
Use of stents in esophageal cancer" Hans Gerdes, M.D. Director, GI Endoscopy Unit Memorial Sloan-Kettering Cancer Center Features of esophageal cancer Esophageal cancer is an abnormal growth that arises
INTERDISCIPLINARY CLINICAL MANUAL Policy & Procedure
 INTERDISCIPLINARY CLINICAL MANUAL Policy & Procedure TITLE: Section: Nasogastric Tube Insertion, Gastrointestinal/Nutrition NUMBER: CC 25-015 Date Issued: May 2007 Source: Distribution: Surgical Specialties
INTERDISCIPLINARY CLINICAL MANUAL Policy & Procedure TITLE: Section: Nasogastric Tube Insertion, Gastrointestinal/Nutrition NUMBER: CC 25-015 Date Issued: May 2007 Source: Distribution: Surgical Specialties
Frequently Asked Questions: Gastric Bypass Surgery at CMC
 Frequently Asked Questions: Gastric Bypass Surgery at CMC Please feel free to talk with any member of the Obesity Treatment Center team at Catholic Medical Center regarding any questions, concerns or comments
Frequently Asked Questions: Gastric Bypass Surgery at CMC Please feel free to talk with any member of the Obesity Treatment Center team at Catholic Medical Center regarding any questions, concerns or comments
Assessment Day Bariatric Surgery. 12266 DePaul Drive, Suite 310 Bridgeton, MO 63044 (P) 1-877-477-6954 ssmweightloss.com
 Assessment Day Bariatric Surgery 12266 DePaul Drive, Suite 310 Bridgeton, MO 63044 (P) 1-877-477-6954 ssmweightloss.com Assessment Day Agenda Types of Surgery Complications Expectations Next Steps Questions
Assessment Day Bariatric Surgery 12266 DePaul Drive, Suite 310 Bridgeton, MO 63044 (P) 1-877-477-6954 ssmweightloss.com Assessment Day Agenda Types of Surgery Complications Expectations Next Steps Questions
Care of Persons With Jejunostomy Tubes Or Gastrojejunal Tubes
 STATE OF CONNECTICUT DEPARTMENT OF DEVELOPMENTAL SERVICES NURSING PROTOCOL # NP 09-2 Care of Persons With Jejunostomy Tubes Or Gastrojejunal Tubes Issue Date: March 2009 Implementation Date: May 1, 2009
STATE OF CONNECTICUT DEPARTMENT OF DEVELOPMENTAL SERVICES NURSING PROTOCOL # NP 09-2 Care of Persons With Jejunostomy Tubes Or Gastrojejunal Tubes Issue Date: March 2009 Implementation Date: May 1, 2009
Upper Gastrointestinal Tract KNH 406
 Upper Gastrointestinal Tract KNH 406 Upper GI A&P GI tract long tube ~ 15 ft. Upper GI mouth, pharynx, esophagus, stomach Accessory organs pancreas, biliary system, liver Four basic functions: motility,
Upper Gastrointestinal Tract KNH 406 Upper GI A&P GI tract long tube ~ 15 ft. Upper GI mouth, pharynx, esophagus, stomach Accessory organs pancreas, biliary system, liver Four basic functions: motility,
TUBE FEEDING AT HOME
 TUBE FEEDING AT HOME Adapted from the former Taming the Feeding Tube, Royal North Shore Hospital. Revised 2005, 2007, Jan 2009 1 Where do I find information in this booklet? Only the pages that you need
TUBE FEEDING AT HOME Adapted from the former Taming the Feeding Tube, Royal North Shore Hospital. Revised 2005, 2007, Jan 2009 1 Where do I find information in this booklet? Only the pages that you need
Maryland MOLST. Guide for Authorized Decision Makers. Maryland MOLST Training Task Force
 Maryland MOLST Guide for Authorized Decision Makers Maryland MOLST Training Task Force May 2012 Health Care Decision Making: Goals and Treatment Options Guide for Authorized Decision Makers Contents Introduction
Maryland MOLST Guide for Authorized Decision Makers Maryland MOLST Training Task Force May 2012 Health Care Decision Making: Goals and Treatment Options Guide for Authorized Decision Makers Contents Introduction
Laparoscopic Colectomy. What do I need to know about my laparoscopic colorectal surgery?
 Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
Common Questions and Answers About Artificial Nutrition and Hydration
 Common Questions and Answers About Artificial Nutrition and Hydration Artificial nutrition and hydration There often comes a time when patients are so ill that they may only be kept alive by artificial
Common Questions and Answers About Artificial Nutrition and Hydration Artificial nutrition and hydration There often comes a time when patients are so ill that they may only be kept alive by artificial
Quality Measures for Long-stay Residents Percent of residents whose need for help with daily activities has increased.
 Quality Measures for Long-stay Residents Percent of residents whose need for help with daily activities has increased. This graph shows the percent of residents whose need for help doing basic daily tasks
Quality Measures for Long-stay Residents Percent of residents whose need for help with daily activities has increased. This graph shows the percent of residents whose need for help doing basic daily tasks
Depression: Facility Assessment Checklists
 Depression: Facility Assessment Checklists A facility system assessment is a starting point for a quality improvement project. The checklists included in this booklet will be most useful if you take a
Depression: Facility Assessment Checklists A facility system assessment is a starting point for a quality improvement project. The checklists included in this booklet will be most useful if you take a
Rehab and Restorative Critical Element Pathway
 Use this pathway for a sampled resident who has had a lack of improvement in any areas of functional ability to determine if the resident received necessary rehabilitative services. Review the following
Use this pathway for a sampled resident who has had a lack of improvement in any areas of functional ability to determine if the resident received necessary rehabilitative services. Review the following
Bariatric Surgery 101
 Bariatric Surgery 101 Dr. Brent Bell, MD Bariatric / General Surgeon Medical Conditions Caused By Morbid Obesity Type 2 DM Hypertension Cholesterol Sleep Apnea Fatty Liver Asthma Osteoarthritis Reduced
Bariatric Surgery 101 Dr. Brent Bell, MD Bariatric / General Surgeon Medical Conditions Caused By Morbid Obesity Type 2 DM Hypertension Cholesterol Sleep Apnea Fatty Liver Asthma Osteoarthritis Reduced
Medical Nutrition Therapy for Upper Gastrointestinal Tract Disorders. By: Jalal Hejazi PhD, MSc.
 Medical Nutrition Therapy for Upper Gastrointestinal Tract Disorders By: Jalal Hejazi PhD, MSc. Digestive Disorders Common problem; more than 50 million outpatient visits per year Dietary habits and nutrition
Medical Nutrition Therapy for Upper Gastrointestinal Tract Disorders By: Jalal Hejazi PhD, MSc. Digestive Disorders Common problem; more than 50 million outpatient visits per year Dietary habits and nutrition
Preschool Learning Center
 Preschool Learning Center GUIDELINES AND INFORMATION ON FEEDING AND SAFE MEALTIME PRACTICES FOR STUDENTS IN A SCHOOL SETTING I. RATIONALE FOR FEEDING GUIDELINES The number of children with severe disabilities
Preschool Learning Center GUIDELINES AND INFORMATION ON FEEDING AND SAFE MEALTIME PRACTICES FOR STUDENTS IN A SCHOOL SETTING I. RATIONALE FOR FEEDING GUIDELINES The number of children with severe disabilities
Cancer Treatment Centers of America Treating the Whole Patient. Presented by: Jill Schuman, RD, CNSC, CSP, LCN Date: Spring 2012
 Cancer Treatment Centers of America Treating the Whole Patient Presented by: Jill Schuman, RD, CNSC, CSP, LCN Date: Spring 2012 What is Cancer Two types of tumors Liquid tumor Leukemia Lymphoma Aplastic
Cancer Treatment Centers of America Treating the Whole Patient Presented by: Jill Schuman, RD, CNSC, CSP, LCN Date: Spring 2012 What is Cancer Two types of tumors Liquid tumor Leukemia Lymphoma Aplastic
Dehydration in Long Term Care: The Nurse s Role in Guiding the Interdisciplinary Team
 Dehydration in Long Term Care: The Nurse s Role in Guiding the Interdisciplinary Team Welcome to the Elizabeth McGown Training Institute Cell Phones and Pagers Please turn your cell phones off or turn
Dehydration in Long Term Care: The Nurse s Role in Guiding the Interdisciplinary Team Welcome to the Elizabeth McGown Training Institute Cell Phones and Pagers Please turn your cell phones off or turn
Care and Problems of the Digestive System. Chapter 18 Lesson 2
 Care and Problems of the Digestive System Chapter 18 Lesson 2 Care of the Digestive System Good eating habits are the best way to avoid or minimize digestive system problems. Eat a variety of foods Avoid
Care and Problems of the Digestive System Chapter 18 Lesson 2 Care of the Digestive System Good eating habits are the best way to avoid or minimize digestive system problems. Eat a variety of foods Avoid
NHRMC General Surgery Specialists. Minimally Invasive Gastrointestinal Surgery Phone: 910-662-9300 Fax: 910-662-9303
 Minimally Invasive Gastrointestinal Surgery Phone: 910-662-9300 Fax: 910-662-9303 W. Borden Hooks III, MD 1725 New Hanover Medical Park Drive Wilmington, NC 28403 Thank you for choosing NHRMC General Surgery
Minimally Invasive Gastrointestinal Surgery Phone: 910-662-9300 Fax: 910-662-9303 W. Borden Hooks III, MD 1725 New Hanover Medical Park Drive Wilmington, NC 28403 Thank you for choosing NHRMC General Surgery
Emergencies in Post- Bariatric Surgery Patients
 Emergencies in Post- Patients Disclosures Dr. Birnbaumer has no financial disclosures Diane M. Birnbaumer, M.D., FACEP Professor of Medicine University of California, Los Angeles Senior Clinical Educator
Emergencies in Post- Patients Disclosures Dr. Birnbaumer has no financial disclosures Diane M. Birnbaumer, M.D., FACEP Professor of Medicine University of California, Los Angeles Senior Clinical Educator
Gastroschisis and My Baby
 Patient and Family Education Gastroschisis and My Baby Gastroschisis is a condition where a baby is born with the intestine outside the body. Learning about the diagnosis What is gastroschisis? (pronounced
Patient and Family Education Gastroschisis and My Baby Gastroschisis is a condition where a baby is born with the intestine outside the body. Learning about the diagnosis What is gastroschisis? (pronounced
11/10/2014. I have nothing to Disclose. Covered Stents discussed are NOT FDA approved for the indications covered in my presentation
 I have nothing to Disclose Ramsey Dallal, MD, FACS Vice Chair Department of Surgery Chief Bariatric i and Minimally i Invasive Surgery Einstein Healthcare Network Nemacolin, PA 2014 Covered Stents discussed
I have nothing to Disclose Ramsey Dallal, MD, FACS Vice Chair Department of Surgery Chief Bariatric i and Minimally i Invasive Surgery Einstein Healthcare Network Nemacolin, PA 2014 Covered Stents discussed
TUBE-FEEDING INSTRUCTIONS FOR HOME
 Name Clinic Number Room: TUBE-FEEDING INSTRUCTIONS FOR HOME CENTER FOR HUMAN NUTRITION, M17/ DIGESTIVE DISEASE INSTITUTE 9500 Euclid Avenue Cleveland, OH 44195 1.800.CCF.CARE 1.216.444.3046 YOUR TUBE-FEEDING
Name Clinic Number Room: TUBE-FEEDING INSTRUCTIONS FOR HOME CENTER FOR HUMAN NUTRITION, M17/ DIGESTIVE DISEASE INSTITUTE 9500 Euclid Avenue Cleveland, OH 44195 1.800.CCF.CARE 1.216.444.3046 YOUR TUBE-FEEDING
Nutr 341: Medical Nutrition Therapy: A Case Study Approach 3 rd ed. Case 32 Esophageal Cancer Treated with Surgery and Radiation
 Nutr 341: Medical Nutrition Therapy: A Case Study Approach 3 rd ed. Case 32 Esophageal Cancer Treated with Surgery and Radiation Name: Julianne Edwards Instructions: This is not a group case study; it
Nutr 341: Medical Nutrition Therapy: A Case Study Approach 3 rd ed. Case 32 Esophageal Cancer Treated with Surgery and Radiation Name: Julianne Edwards Instructions: This is not a group case study; it
Acute Abdominal Pain following Bariatric Surgery. Disclosure. Objectives 8/17/2015. I have nothing to disclose
 Acute Abdominal Pain following Bariatric Surgery Kathy J. Morris, DNP, APRN, FNP C, FAANP University of Nebraska Medical Center College of Nursing Disclosure I have nothing to disclose Objectives Pathophysiology
Acute Abdominal Pain following Bariatric Surgery Kathy J. Morris, DNP, APRN, FNP C, FAANP University of Nebraska Medical Center College of Nursing Disclosure I have nothing to disclose Objectives Pathophysiology
Restorative Care. Policy, Procedures and Training Package
 Restorative Care Policy, Procedures and Training Package Release Date: December 17, 2010 Disclaimer The Ontario Association of Non-Profit Homes and Services for Seniors (OANHSS) Long-Term Care Homes Act
Restorative Care Policy, Procedures and Training Package Release Date: December 17, 2010 Disclaimer The Ontario Association of Non-Profit Homes and Services for Seniors (OANHSS) Long-Term Care Homes Act
Nurse Initiated Medications Procedure
 1. Purpose This Procedure is performed as a means of ensuring the safe administration of therapeutic medication to patients in accordance with all legislative and regulatory requirements. 2. Application
1. Purpose This Procedure is performed as a means of ensuring the safe administration of therapeutic medication to patients in accordance with all legislative and regulatory requirements. 2. Application
CUESTA COLLEGE REGISTERED NURSING PROGRAM CRITICAL ELEMENTS
 CUESTA COLLEGE REGISTERED NURSING PROGRAM CRITICAL ELEMENTS LEVELS I through IV A. OVERRIDING CRITICAL ELEMENTS Violation of an overriding area will result in termination and failure of the particular
CUESTA COLLEGE REGISTERED NURSING PROGRAM CRITICAL ELEMENTS LEVELS I through IV A. OVERRIDING CRITICAL ELEMENTS Violation of an overriding area will result in termination and failure of the particular
GASTRIC BYPASS SURGERY CONSENT FORM
 Page 1 of 6 I, have been asked to read carefully all of the (name of patient or substitute decision-maker) information contained in this consent form and to consent to the procedure described below on
Page 1 of 6 I, have been asked to read carefully all of the (name of patient or substitute decision-maker) information contained in this consent form and to consent to the procedure described below on
Sleeve Gastrectomy Surgery & Follow Up Care
 Sleeve Gastrectomy Surgery & Follow Up Care Sleeve Gastrectomy Restrictive surgical weight loss procedure Able to eat a smaller amount of food to feel satiety, less than 6 ounces at a meal Surgery The
Sleeve Gastrectomy Surgery & Follow Up Care Sleeve Gastrectomy Restrictive surgical weight loss procedure Able to eat a smaller amount of food to feel satiety, less than 6 ounces at a meal Surgery The
Urinary Diversion: Ileovesicostomy/Ileal Loop/Colon Loop
 Urinary Diversion: Ileovesicostomy/Ileal Loop/Colon Loop Why do I need this surgery? A urinary diversion is a surgical procedure that is performed to allow urine to safely pass from the kidneys into a
Urinary Diversion: Ileovesicostomy/Ileal Loop/Colon Loop Why do I need this surgery? A urinary diversion is a surgical procedure that is performed to allow urine to safely pass from the kidneys into a
Ohio Department of Health Division of Quality Assurance Quarterly Nursing Home Report Issue 4, April 2012
 Ohio Department of Health Division of Quality Assurance Quarterly Nursing Home Report Issue 4, April 2012 Quarterly Nursing Home Report April 2012 This report provides information on selected indicators
Ohio Department of Health Division of Quality Assurance Quarterly Nursing Home Report Issue 4, April 2012 Quarterly Nursing Home Report April 2012 This report provides information on selected indicators
V: Infusion Therapy. Alberta Licensed Practical Nurses Competency Profile 217
 V: Infusion Therapy Alberta Licensed Practical Nurses Competency Profile 217 Competency: V-1 Knowledge of Intravenous Therapy V-1-1 V-1-2 V-1-3 V-1-4 V-1-5 Demonstrate knowledge and ability to apply critical
V: Infusion Therapy Alberta Licensed Practical Nurses Competency Profile 217 Competency: V-1 Knowledge of Intravenous Therapy V-1-1 V-1-2 V-1-3 V-1-4 V-1-5 Demonstrate knowledge and ability to apply critical
Having a PEG tube inserted?
 Having a PEG tube inserted? Information for Patients and Carers Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Having a PEG tube inserted? Information for Patients and Carers Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Acute abdominal conditions Key Points
 7 Acute abdominal conditions Key Points 7.1 ASSESSMENT AND DIAGNOSIS Referred abdominal pain Fore gut pain (stomach, duodenum, gall bladder) is referred to the upper abdomen Mid gut pain (small intestine,
7 Acute abdominal conditions Key Points 7.1 ASSESSMENT AND DIAGNOSIS Referred abdominal pain Fore gut pain (stomach, duodenum, gall bladder) is referred to the upper abdomen Mid gut pain (small intestine,
NAUSEA AND VOMITING. Ryan F. Porter, M.D. and C. Prakash Gyawali, M.D., MRCP Division of Gastroenterology Washington University St.
 NAUSEA AND VOMITING Ryan F. Porter, M.D. and C. Prakash Gyawali, M.D., MRCP Division of Gastroenterology Washington University St. Louis, MO What is nausea and vomiting? Nausea is the unpleasant urge to
NAUSEA AND VOMITING Ryan F. Porter, M.D. and C. Prakash Gyawali, M.D., MRCP Division of Gastroenterology Washington University St. Louis, MO What is nausea and vomiting? Nausea is the unpleasant urge to
Effective Date: No later than November 30, 2012. The State Agency should disseminate this information within 30 days of the date of this memorandum.
 DEPA RTM EN T OF H EA LTH & H UMA N SERVICES Centers for M edicare & M edicaid Services 7500 Security Boulevard, M ail Stop C2-21-16 Baltimore, M aryland 21244-1850 Center for Clinical Standards and Quality/
DEPA RTM EN T OF H EA LTH & H UMA N SERVICES Centers for M edicare & M edicaid Services 7500 Security Boulevard, M ail Stop C2-21-16 Baltimore, M aryland 21244-1850 Center for Clinical Standards and Quality/
Update: Medical Necessity Documentation. Kerry Dunning, MHA, MSH, CPAR, RAC-CT GPS HEALTHCARE CONSULTANTS November 2013
 Update: Medical Necessity Documentation Kerry Dunning, MHA, MSH, CPAR, RAC-CT GPS HEALTHCARE CONSULTANTS November 2013 REMINDER Many claim denials occur because the providers or suppliers do not submit
Update: Medical Necessity Documentation Kerry Dunning, MHA, MSH, CPAR, RAC-CT GPS HEALTHCARE CONSULTANTS November 2013 REMINDER Many claim denials occur because the providers or suppliers do not submit
Undergoing an Oesophageal Endoscopic Resection (ER)
 Contact Information If you have an enquiry about your appointment time/date please contact the Booking Office on 0300 422 6350. For medication enquiries please call 0300 422 8232, this is an answer machine
Contact Information If you have an enquiry about your appointment time/date please contact the Booking Office on 0300 422 6350. For medication enquiries please call 0300 422 8232, this is an answer machine
Compliance Tip Sheet CMS FY 2010 TOP TEN HOSPICE SURVEY DEFICIENCIES COMPLIANCE RECOMMENDATIONS CMS TOP TEN HOSPICE SURVEY DEFICIENCIES
 Compliance Tip Sheet National Hospice and Palliative Care Organization www.nhpco.org/regulatory CMS FY 2010 TOP TEN HOSPICE SURVEY DEFICIENCIES COMPLIANCE RECOMMENDATIONS INTRODUCTION The Centers for Medicare
Compliance Tip Sheet National Hospice and Palliative Care Organization www.nhpco.org/regulatory CMS FY 2010 TOP TEN HOSPICE SURVEY DEFICIENCIES COMPLIANCE RECOMMENDATIONS INTRODUCTION The Centers for Medicare
ADVANCE DIRECTIVE. A LIVING WILL A Directive To Withhold Or To Provide Treatment. A Durable Power Of Attorney FOR HEALTH CARE
 ADVANCE DIRECTIVE A LIVING WILL A Directive To Withhold Or To Provide Treatment and A Durable Power Of Attorney FOR HEALTH CARE Name Date of Birth Form # 8-0553 (7-07) LIVING WILL AND DURABLE POWER OF
ADVANCE DIRECTIVE A LIVING WILL A Directive To Withhold Or To Provide Treatment and A Durable Power Of Attorney FOR HEALTH CARE Name Date of Birth Form # 8-0553 (7-07) LIVING WILL AND DURABLE POWER OF
Weight-Loss Surgery for Adults With Diabetes or Prediabetes Who Are at the Lower Levels of Obesity
 Weight-Loss Surgery for Adults With Diabetes or Prediabetes Who Are at the Lower Levels of Obesity A Review of the Research for Adults With a BMI Between 30 and 35 Is This Information Right for Me? If
Weight-Loss Surgery for Adults With Diabetes or Prediabetes Who Are at the Lower Levels of Obesity A Review of the Research for Adults With a BMI Between 30 and 35 Is This Information Right for Me? If
Pressure Ulcers: Facility Assessment Checklists
 Pressure Ulcers: Facility Assessment Checklists This is a series of self-assessment checklists for nursing home staff to use to assess processes related to managing pressure ulcers in the facility, in
Pressure Ulcers: Facility Assessment Checklists This is a series of self-assessment checklists for nursing home staff to use to assess processes related to managing pressure ulcers in the facility, in
BILIOPANCREATIC DIVERSION WITH DUODENAL SWITCH SURGERY
 WITH DUODENAL SWITCH SURGERY Disclaimer This movie is an educational resource only and should not be used to manage Obesity. All decisions about surgical management of Obesity must be made in conjunction
WITH DUODENAL SWITCH SURGERY Disclaimer This movie is an educational resource only and should not be used to manage Obesity. All decisions about surgical management of Obesity must be made in conjunction
Minnesota s Call to Action Quality of Life Initiative for Activities F248/249 An Interdisciplinary Approach. F248 Deficiency Severity Guidance
 Severity Level 4 Considerations: Immediate jeopardy to resident health or safety Severity Level 3 Considerations: Actual harm that is not immediate jeopardy Severity Level 2 Considerations: No actual Harm
Severity Level 4 Considerations: Immediate jeopardy to resident health or safety Severity Level 3 Considerations: Actual harm that is not immediate jeopardy Severity Level 2 Considerations: No actual Harm
Restorative Nursing Teleconference Script
 Slide 1 Slide 2 Slide 3 Maintaining independence in ADLs and mobility is very important to most of us. In fact, functional decline can lead to depression, withdrawal, social isolation, and complications
Slide 1 Slide 2 Slide 3 Maintaining independence in ADLs and mobility is very important to most of us. In fact, functional decline can lead to depression, withdrawal, social isolation, and complications
Nutritional Challenges After Surgery
 Nutritional Challenges After Surgery L I N D A P A T A K I M S R D C S O L D C N S C M D A N D E R S O N C A N C E R C E N T E R H O U S T O N, T E X A S Objectives Identify the reasons that GIST and its
Nutritional Challenges After Surgery L I N D A P A T A K I M S R D C S O L D C N S C M D A N D E R S O N C A N C E R C E N T E R H O U S T O N, T E X A S Objectives Identify the reasons that GIST and its
7/1/2014 REGISTERED NURSE CONSULTATION PURPOSE & KEY TERMS OBJECTIVES
 REGISTERED NURSE CONSULTATION June 2012 DHS Office of Licensing and Regulatory Oversight 1 PURPOSE & KEY TERMS The purpose of this section is to assist the learner in understanding the role of a Registered
REGISTERED NURSE CONSULTATION June 2012 DHS Office of Licensing and Regulatory Oversight 1 PURPOSE & KEY TERMS The purpose of this section is to assist the learner in understanding the role of a Registered
Multiple Sclerosis (MS)
 Multiple Sclerosis (MS) Purpose/Goal: Care partners will have an understanding of Multiple Sclerosis and will demonstrate safety and promote independence while providing care to the client with MS. Introduction
Multiple Sclerosis (MS) Purpose/Goal: Care partners will have an understanding of Multiple Sclerosis and will demonstrate safety and promote independence while providing care to the client with MS. Introduction
OCCUPATIONAL GROUP: Health Services. CLASS FAMILY: Nursing CLASS FAMILY DESCRIPTION:
 OCCUPATIONAL GROUP: Health Services CLASS FAMILY: Nursing CLASS FAMILY DESCRIPTION: This family of positions includes those whose purpose is to perform professional nursing services that directly and/or
OCCUPATIONAL GROUP: Health Services CLASS FAMILY: Nursing CLASS FAMILY DESCRIPTION: This family of positions includes those whose purpose is to perform professional nursing services that directly and/or
Iatrogenesis. Suzanne Beyea,, RN, PhD, FAAN Associate Director: Centers for Health and Aging
 Iatrogenesis Suzanne Beyea,, RN, PhD, FAAN Associate Director: Centers for Health and Aging Iatrogenesis Definition from the Greek word, iatros,, meaning healer, iatrogenesis means brought forth by a healer
Iatrogenesis Suzanne Beyea,, RN, PhD, FAAN Associate Director: Centers for Health and Aging Iatrogenesis Definition from the Greek word, iatros,, meaning healer, iatrogenesis means brought forth by a healer
After Radiation Therapy
 After Radiation Therapy CHRISTOPHER G. JORDAN, DO, FACOI UNIVERSITY OF NORTH TEXAS HEALTH SCIENCE CENTER DIRECTOR, SECTION OF HEMATOLOGY & ONCOLOGY MAY 1, 2015 A brief Understanding of Radiation Multiple
After Radiation Therapy CHRISTOPHER G. JORDAN, DO, FACOI UNIVERSITY OF NORTH TEXAS HEALTH SCIENCE CENTER DIRECTOR, SECTION OF HEMATOLOGY & ONCOLOGY MAY 1, 2015 A brief Understanding of Radiation Multiple
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES HEAD AND NECK ONCOLOGY NURSING FOR HEAD AND NECK CANCERS Head & Neck Site Group Oncology Nursing for Head and Neck Cancers Specialized Oncology
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES HEAD AND NECK ONCOLOGY NURSING FOR HEAD AND NECK CANCERS Head & Neck Site Group Oncology Nursing for Head and Neck Cancers Specialized Oncology
Registered Nurse Series Final Classification Standards December 2007
 Final Classification Standards December 2007 Series Overview This series is comprised of three classifications with progressive responsibility for nursing care and services and administrative duties within
Final Classification Standards December 2007 Series Overview This series is comprised of three classifications with progressive responsibility for nursing care and services and administrative duties within
RESTORATIVE. Yvonne Russell RN Long Term Care Nursing Coalition of Mississippi-1 st Teleconference Restorative Nursing
 RESTORATIVE Yvonne Russell RN Long Term Care Nursing Coalition of Mississippi-1 st Teleconference Restorative Nursing OVERVIEW Restorative Nursing is not a new concept Techniques have been taught in nursing
RESTORATIVE Yvonne Russell RN Long Term Care Nursing Coalition of Mississippi-1 st Teleconference Restorative Nursing OVERVIEW Restorative Nursing is not a new concept Techniques have been taught in nursing
CHAPTER 4: CARE AREA TRIGGERS (CATs) AND CARE PLANNING
 The information below is provided only as an example of what Chapter 4 of the RAI User s Manual, Version 3.0 and a CAT will resemble final information will be included in the RAI manual for MDS 3.0 available
The information below is provided only as an example of what Chapter 4 of the RAI User s Manual, Version 3.0 and a CAT will resemble final information will be included in the RAI manual for MDS 3.0 available
GUIDELINES ON PREVENTING MEDICATION ERRORS IN PHARMACIES AND LONG-TERM CARE FACILITIES THROUGH REPORTING AND EVALUATION
 GUIDELINES GUIDELINES ON PREVENTING MEDICATION ERRORS IN PHARMACIES AND LONG-TERM CARE FACILITIES THROUGH REPORTING AND EVALUATION Preamble The purpose of this document is to provide guidance for the pharmacist
GUIDELINES GUIDELINES ON PREVENTING MEDICATION ERRORS IN PHARMACIES AND LONG-TERM CARE FACILITIES THROUGH REPORTING AND EVALUATION Preamble The purpose of this document is to provide guidance for the pharmacist
Nursing college, Second stage Microbiology Dr.Nada Khazal K. Hendi L14: Hospital acquired infection, nosocomial infection
 L14: Hospital acquired infection, nosocomial infection Definition A hospital acquired infection, also called a nosocomial infection, is an infection that first appears between 48 hours and four days after
L14: Hospital acquired infection, nosocomial infection Definition A hospital acquired infection, also called a nosocomial infection, is an infection that first appears between 48 hours and four days after
Over 50% of hospitalized patients are malnourished. Coding for Malnutrition in the Adult Patient: What the Physician Needs to Know
 Carol Rees Parrish, M.S., R.D., Series Editor Coding for Malnutrition in the Adult Patient: What the Physician Needs to Know Wendy Phillips At least half of all hospitalized patients are malnourished,
Carol Rees Parrish, M.S., R.D., Series Editor Coding for Malnutrition in the Adult Patient: What the Physician Needs to Know Wendy Phillips At least half of all hospitalized patients are malnourished,
Continuing Care Health Service Standards
 Continuing Care Health Service Standards July 2008 and Amended March 5, 2013 For further information For additional copies of this document contact: Alberta Health Communications Phone: 780-427-7164 Fax:
Continuing Care Health Service Standards July 2008 and Amended March 5, 2013 For further information For additional copies of this document contact: Alberta Health Communications Phone: 780-427-7164 Fax:
ENTERAL FORMULAE AND PARENTERAL NUTRITIONAL SOLUTIONS, DME
 ENTERAL FORMULAE AND PARENTERAL NUTRITIONAL SOLUTIONS, DME Policy NHP only reimburses participating DME vendors for the provision of medically necessary enteral and parenteral formulae and nutritional
ENTERAL FORMULAE AND PARENTERAL NUTRITIONAL SOLUTIONS, DME Policy NHP only reimburses participating DME vendors for the provision of medically necessary enteral and parenteral formulae and nutritional
Peptic Ulcer. Anatomy The stomach is a hollow organ. It is located in the upper abdomen, under the ribs.
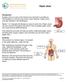 Peptic Ulcer Introduction A peptic ulcer is a sore in the lining of your stomach or duodenum. The duodenum is the first part of your small intestine. Peptic ulcers may also develop in the esophagus. Nearly
Peptic Ulcer Introduction A peptic ulcer is a sore in the lining of your stomach or duodenum. The duodenum is the first part of your small intestine. Peptic ulcers may also develop in the esophagus. Nearly
New York State Office of Alcoholism & Substance Abuse Services Addiction Services for Prevention, Treatment, Recovery
 New York State Office of Alcoholism & Substance Abuse Services Addiction Services for Prevention, Treatment, Recovery USING THE 48 HOUR OBSERVATION BED USING THE 48 HOUR OBSERVATION BED Detoxification
New York State Office of Alcoholism & Substance Abuse Services Addiction Services for Prevention, Treatment, Recovery USING THE 48 HOUR OBSERVATION BED USING THE 48 HOUR OBSERVATION BED Detoxification
