(PROTOCOL #18) REVERSE TOTAL SHOULDER ARTHROPLASTY PROTOCOL
|
|
|
- Christopher Dennis
- 9 years ago
- Views:
Transcription
1 The following is a set of general guidelines. It is important to remember that each patient is different. The progression of the patient depends on many factors including age and medical health of the patient and physician preferences. Any Bracing is discontinued ONLY UPON DIRECTION OF PHYSICIAN. General Information: Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH) arthritis when it is associated with irreparable rotator cuff damage, complex fractures as well as for a revision of a previously failed conventional Total Shoulder Arthroplasty (TSA) in which the rotator cuff tendons are deficient. It was initially designed and used in Europe in the late 1980 s by Grammont; and only received FDA approval for use in the United States in March of The rotator cuff is either absent or minimally involved with the rtsa; therefore, the rehabilitation for a patient following the rtsa is different than the rehabilitation following a traditional TSA. The surgeon, physical therapist and patient need to take this into consideration when establishing the postoperative treatment plan. SHOULDER DISLOCATION PERCAUTIONS: o No shoulder motion behind back. (NO combined shoulder adduction, internal rotation, and extension.) o No glenohumeral (GH) extension beyond neutral. **Precautions should be implemented for 12 weeks postoperatively unless surgeon specifically advises patient or therapist differently. Joint Protection: THERE IS A HIGHER RISK OF SHOULDER DISLOCATION FOLLOWING rtsa THAN A CONVENTIONAL TSA. o Avoidance of shoulder extension past neutral and the combination of shoulder adduction and internal rotation should be avoided for 12 weeks. o Patients with rtsa don t dislocate with the arm in abduction and external rotation. They typically dislocate with the arm in internal rotation and adduction in conjunction with extension. As such, Tucking in a shirt or performing bathroom / personal hygiene with the operative arm is a particularly dangerous activity particularly in the immediate peri-operative phase. Created on 07/01/2009 Page 1 of 8
2 Deltoid function: Stability and mobility of the shoulder joint is now dependent upon the deltoid and periscapular musculature. This concept becomes the foundation for the postoperative physical therapy management for a patient that has undergone rtsa. Typically patients achieve double the AROM from pre-op level. ROM: Expectation for range of motion gains should be set on a case-by-case basis depending upon underlying pathology. Normal/full active range of motion of the shoulder joint following rtsa is not expected. Reverse Total Shoulder Arthroplasty Biomechanics: The rtsa prosthesis reverses the orientation of the shoulder joint by replacing the glenoid fossa with a glenoid base plate and glenosphere and the humeral head with a shaft and concave cup. This prosthesis design alters the center of rotation of the shoulder joint by moving it medially and inferiorly. This subsequently increases the deltoid moment and deltoid tension, which enhances both the torque produced by the deltoid as well as the line of pull / action of the deltoid. This enhanced mechanical advantage of the deltoid compensates for the deficient RC as the deltoid becomes the primary elevator of the shoulder joint. This results in an improvement of shoulder elevation and often individuals are able to raise their upper extremity overhead. Phase I Precautions: o Sling is worn for 3-6weeks postoperatively. The use of a sling often may be extended for a total of 6 weeks, if the current rtsa procedure is a revision surgery or Tendon Transfer Procedure. o While lying supine, the distal humerus / elbow should be supported by a pillow or towel roll to avoid shoulder extension. Patients should be advised to always be able to visualize their elbow while lying supine. o No shoulder AROM. o No lifting of objects with operative extremity. o No supporting of body weight with involved extremity. o Keep incision clean and dry (no soaking/wetting for 2 weeks); No whirlpool, Jacuzzi, ocean/lake wading for 4 weeks. Created on 07/01/2009 Page 2 of 8
3 PHASE FUNCTIONAL PROGRESSION/ACTIVITIES GOALS/RESTRICTIONS Post op to 4 days OT elbow/hand ROM Putty and ADL modifications Begin PROM in supine after complete resolution of interscalene block. Forward flexion and elevation in the scapular plane in supine to 90 degrees. External rotation (ER) in scapular plane to available ROM as indicated by operative findings. Typically around degrees NO Internal Rotation Active/Active Assisted ROM (A/AAROM) of cervical spine, elbow, wrist and hand. Begin periscapular sub-maximal pain-free isometrics in the scapular plane. Frequent (4-5 times a day for about 20 minutes) cryotherapy. Continuous cryotherapy for the first 72 hours postoperatively, then frequent application (4-5 times a day for about 20 minutes). 4 days to 3 weeks Begin sub-maximal pain-free deltoid isometrics in scapular plane DASH baseline and every 4 weeks Insure patient is independent in bed mobility, transfers and ambulation. Insure proper sling fit/alignment/use. Instruct patient in proper positioning, posture, initial home exercise program. Provide patient/family with written home program including exercises and protocol information. Avoid shoulder extension when isolating posterior deltoid. Created on 07/01/2009 Page 3 of 8
4 PHASE FUNCTIONAL PROGRESSION/ACTIVITIES GOALS/RESTRICTIONS 3 weeks to 6 weeks Progress exercises listed above. Criteria for progression to the next phase (Phase II): Progress PROM: o Forward flexion and elevation in the scapular plane in supine to 120 degrees. o ER in scapular plane to tolerance, respecting soft tissue constraints. Gentle resisted exercise of elbow, wrist and hand. Tolerates shoulder PROM and isometrics; and, AROMminimally resistive program for elbow, wrist and hand. Patient demonstrates the ability to isometrically activate all components of the deltoid and periscapular musculature in the scapular plan. Continue frequent cryotherapy. 4 weeks Gradually restore AROM Begin shoulder AA/AROM as appropriate. o Forward flexion and elevation in scapular plane in supine with progression to sitting/standing. ER and IR in the scapular plane in supine with progression to sitting/standing. Control pain and inflammation. Allow continued healing of soft tissue / do not overstress healing tissue. Re-establish dynamic shoulder and scapular stability. Patient may begin to use hand of operative extremity for feeding and light activities of daily living including dressing, washing. Created on 07/01/2009 Page 4 of 8
5 Phase II Active Range of Motion / Early Strengthening Phase (Week 6 to 12): PHASE FUNCTIONAL PROGRESSION/ACTIVITIES GOALS/RESTRICTIONS 6 weeks to 8 weeks Continue progression of PROM (full PROM is not expected). Begin gentle glenohumeral IR behind back and ER sub-maximal pain free isometrics. Start PROM IR to tolerance (not to exceed 50 degrees) in the scapular plane. Initiate gentle scapulothoracic rhythmic stabilization and alternating isometrics in supine as appropriate. Begin gentle periscapular and deltoid sub-maximal pain free isotonic strengthening exercises, typically toward the end of the 8 th week. Progress strengthening of elbow, wrist and hand. Gentle glenohumeral and scapulothoracic joint mobilizations as indicated (Grade I and II). Continue use of cryotherapy as needed. BRACING DISCONTINUED UPON THE DIRECTION OF THE PHYSICIAN. Continue with PROM program. Precautions: Continue to avoid shoulder hyperextension. In the presence of poor shoulder mechanics avoid repetitive shoulder AROM exercises/activity. Restrict lifting of objects to no heavier than a coffee cup. No supporting of body weight by involved upper extremity. Created on 07/01/2009 Page 5 of 8
6 PHASE FUNCTIONAL PROGRESSION/ACTIVITIES GOALS/RESTRICTIONS 9 weeks to 12 weeks Continue with above exercises and functional activity progression. Begin AROM supine forward flexion and elevation in the plane of the scapula with light weights (1-3 lbs of kg) at varying degrees of trunk elevation as appropriate. (i.e. supine lawn chair progression with progression to sitting/standing). Progress to gentle glenohumeral IR and ER isotonic strengthening exercises in sidelying position with light weight (1-3 lbs or kg) and /or with light resistance resistive bands or sports cords. Criteria for progression to the next phase (Phase III): o Improving function of shoulder. o Patient demonstrates the ability to isotonically activate all components of the deltoid and periscapular musculature and is gaining strength. Created on 07/01/2009 Page 6 of 8
7 Phase III Moderate strengthening (Week 12+) PHASE FUNCTIONAL PROGRESSION/ACTIVITIES GOALS/RESTRICTIONS 12 weeks to 16 weeks Continue with the previous program as indicated. Progress to gentle resisted flexion, elevation in standing as appropriate. o Enhance functional use of operative extremity and advance functional activities. o Enhance shoulder mechanics, muscular strength and endurance. Precautions: o No lifting of objects heavier than 6 lbs with operative upper extremity o No sudden lifting or pushing activities. Activities: Gradually increase activity Golf: pitching wedge to start in approx 6 months Bowling: NOT RECOMMENDED Tennis: same start slow gradually increase activity Driving: able to drive, monitor meds, steer with other arm following post-op Shower: usually after first dressing with watertight dressing Throwing: 6 months Running: 3 months Refer to enclosed table for suggested exercises which optimize muscle function based on EMG activity. Created on 07/01/2009 Page 7 of 8
8 Phase IV continued Home Program (Typically 4 + months postop): Typically the patient is on a home exercise program at this stage to be performed 3-4 times per week with the focus on: o Continued strength gains o Continued progression toward a return to functional and recreational activities within limits as identified by progress made during rehabilitation and outlined by surgeon and physical therapist. Criteria for discharge from skilled therapy: o Patient is able to maintain pain free shoulder AROM demonstrating proper shoulder mechanics. (Typically degrees of elevation with functional ER of about 30 degrees.) o Typically able to complete light household and work activities. Approved By: Physician reserves the right to adjust these protocols for each patient. Signature: Date: Signature: Date: Balu Pisupati, PT Created on 07/01/2009 Page 8 of 8
Important rehabilitation management concepts to consider for a postoperative physical therapy rtsa program are:
 : General Information: Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH) arthritis when it is associated with irreparable rotator cuff
: General Information: Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH) arthritis when it is associated with irreparable rotator cuff
REVERSE SHOULDER ARTHROPLASTY
 William J. Robertson, MD UT Southwestern Orthopedics 1801 Inwood Rd. Dallas, TX 75390-8882 Office: (214) 645-3300 Fax: (214) 3301 billrobertsonmd.com REVERSE SHOULDER ARTHROPLASTY The shoulder is a ball
William J. Robertson, MD UT Southwestern Orthopedics 1801 Inwood Rd. Dallas, TX 75390-8882 Office: (214) 645-3300 Fax: (214) 3301 billrobertsonmd.com REVERSE SHOULDER ARTHROPLASTY The shoulder is a ball
ARTHROSCOPIC ROTATOR CUFF REPAIR PROTOCOL (DR. ROLF)
 ARTHROSCOPIC ROTATOR CUFF REPAIR PROTOCOL (DR. ROLF) Phase I Immediate Post Surgical Phase (Weeks 1-4): Maintain integrity of repair Diminish pain and inflammation Prevent muscular inhibition Independent
ARTHROSCOPIC ROTATOR CUFF REPAIR PROTOCOL (DR. ROLF) Phase I Immediate Post Surgical Phase (Weeks 1-4): Maintain integrity of repair Diminish pain and inflammation Prevent muscular inhibition Independent
UHealth Sports Medicine
 UHealth Sports Medicine Rehabilitation Guidelines for Arthroscopic Rotator Cuff Repair Type 2 Repairs with Bicep Tenodesis (+/- subacromial decompression) The rehabilitation guidelines are presented in
UHealth Sports Medicine Rehabilitation Guidelines for Arthroscopic Rotator Cuff Repair Type 2 Repairs with Bicep Tenodesis (+/- subacromial decompression) The rehabilitation guidelines are presented in
Orthopaedic and Spine Institute 21 Spurs Lane, Suite 245, San Antonio, TX 78240 www.saspine.com Tel# 210-487-7463
 Phase I Passive Range of Motion Phase (postop week 1-2) Minimize shoulder pain and inflammatory response Achieve gradual restoration of gentle active range of motion Enhance/ensure adequate scapular function
Phase I Passive Range of Motion Phase (postop week 1-2) Minimize shoulder pain and inflammatory response Achieve gradual restoration of gentle active range of motion Enhance/ensure adequate scapular function
Biceps Tenodesis Protocol
 Department of Rehabilitation Services Physical Therapy The intent of this protocol is to provide the clinician with a guideline of the postoperative rehabilitation course of a patient that has undergone
Department of Rehabilitation Services Physical Therapy The intent of this protocol is to provide the clinician with a guideline of the postoperative rehabilitation course of a patient that has undergone
William J. Robertson, MD UT Southwestern Orthopedics 1801 Inwood Rd. Dallas, TX 75390-8882 Office: (214) 645-3300 Fax: (214) 3301 billrobertsonmd.
 Arthroscopic Rotator Cuff Repair Postoperative Rehab Protocol Starting the first day after surgery you should remove the sling 3-4 times per day to perform pendulum exercises and elbow/wrist range of motion
Arthroscopic Rotator Cuff Repair Postoperative Rehab Protocol Starting the first day after surgery you should remove the sling 3-4 times per day to perform pendulum exercises and elbow/wrist range of motion
Rotator Cuff Surgery: Post-Operative Protocol for Mini-Open or Arthroscopic Rotator Cuff Repair
 Rotator Cuff Surgery: Post-Operative Protocol for Mini-Open or Arthroscopic Rotator Cuff Repair Considerations: 1. Mini-Open - shoulder usually assessed arthroscopically and acromioplasty is usually performed.
Rotator Cuff Surgery: Post-Operative Protocol for Mini-Open or Arthroscopic Rotator Cuff Repair Considerations: 1. Mini-Open - shoulder usually assessed arthroscopically and acromioplasty is usually performed.
Combined SLAP with Arthroscopic Rotator Cuff Repair Large to Massive Tears = or > 3 cm
 Combined SLAP with Arthroscopic Rotator Cuff Repair Large to Massive Tears = or > 3 cm *It is the treating therapist s responsibility along with the referring physician s guidance to determine the actual
Combined SLAP with Arthroscopic Rotator Cuff Repair Large to Massive Tears = or > 3 cm *It is the treating therapist s responsibility along with the referring physician s guidance to determine the actual
ROTATOR CUFF TEARS SMALL
 LOURDES MEDICAL ASSOCIATES Sean Mc Millan, DO Director of Orthopaedic Sports Medicine & Arthroscopy 2103 Burlington-Mount Holly Rd Burlington, NJ 08016 (609) 747-9200 (office) (609) 747-1408 (fax) http://orthodoc.aaos.org/drmcmillan
LOURDES MEDICAL ASSOCIATES Sean Mc Millan, DO Director of Orthopaedic Sports Medicine & Arthroscopy 2103 Burlington-Mount Holly Rd Burlington, NJ 08016 (609) 747-9200 (office) (609) 747-1408 (fax) http://orthodoc.aaos.org/drmcmillan
SLAP Repair Protocol Arthroscopic Labral Repair Protocols (Type II, IV and Complex Tears)
 SLAP Repair Protocol Arthroscopic Labral Repair Protocols (Type II, IV and Complex Tears) This protocol has been modified and is being used with permission from the BWH Sports and Shoulder Service. The
SLAP Repair Protocol Arthroscopic Labral Repair Protocols (Type II, IV and Complex Tears) This protocol has been modified and is being used with permission from the BWH Sports and Shoulder Service. The
Arthroscopic Labral Repair Protocol-Type II, IV, and Complex Tears:
 Department of Rehabilitation Services Physical Therapy This protocol has been adopted from Brotzman & Wilk, which has been published in Brotzman SB, Wilk KE, Clinical Orthopeadic Rehabilitation. Philadelphia,
Department of Rehabilitation Services Physical Therapy This protocol has been adopted from Brotzman & Wilk, which has been published in Brotzman SB, Wilk KE, Clinical Orthopeadic Rehabilitation. Philadelphia,
Rotator Cuff Repair Protocol
 Rotator Cuff Repair Protocol Anatomy and Biomechanics The shoulder is a wonderfully complex joint that is made up of the ball and socket connection between the humerus (ball) and the glenoid portion of
Rotator Cuff Repair Protocol Anatomy and Biomechanics The shoulder is a wonderfully complex joint that is made up of the ball and socket connection between the humerus (ball) and the glenoid portion of
SLAP Repair Protocol
 SLAP Repair Protocol Anatomy and Biomechanics The shoulder is a wonderfully complex joint that is made up of the ball and socket connection between the humerus (ball) and the glenoid portion of the scapula
SLAP Repair Protocol Anatomy and Biomechanics The shoulder is a wonderfully complex joint that is made up of the ball and socket connection between the humerus (ball) and the glenoid portion of the scapula
North Shore Shoulder Dr.Robert E. McLaughlin II 1-855-SHOULDER 978-969-3624 Fax: 978-921-7597 www.northshoreshoulder.com
 North Shore Shoulder Dr.Robert E. McLaughlin II 1-855-SHOULDER 978-969-3624 Fax: 978-921-7597 www.northshoreshoulder.com Physical Therapy Protocol for Patients Following Shoulder Surgery -Rotator Cuff
North Shore Shoulder Dr.Robert E. McLaughlin II 1-855-SHOULDER 978-969-3624 Fax: 978-921-7597 www.northshoreshoulder.com Physical Therapy Protocol for Patients Following Shoulder Surgery -Rotator Cuff
Postoperative Protocol For Posterior Labral Repair/ Capsular Plication-- Dr. Trueblood
 Postoperative Protocol For Posterior Labral Repair/ Capsular Plication-- Dr. Trueblood Indications: Posterior shoulder instability is a relatively uncommon finding in normal adult shoulders. The most common
Postoperative Protocol For Posterior Labral Repair/ Capsular Plication-- Dr. Trueblood Indications: Posterior shoulder instability is a relatively uncommon finding in normal adult shoulders. The most common
2. Repair of the deltoid - the amount deltoid was released and security of repair
 Johns Hopkins Shoulder Surgery Rotator Cuff Rehabilitation Program Johns Hopkins Shoulder Surgeons INTRODUCTION: This program is designed for rotator cuff repairs involving fixation of the tendon to bone,
Johns Hopkins Shoulder Surgery Rotator Cuff Rehabilitation Program Johns Hopkins Shoulder Surgeons INTRODUCTION: This program is designed for rotator cuff repairs involving fixation of the tendon to bone,
Rehabilitation Protocol: SLAP Superior Labral Lesion Anterior to Posterior
 Rehabilitation Protocol: SLAP Superior Labral Lesion Anterior to Posterior Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington
Rehabilitation Protocol: SLAP Superior Labral Lesion Anterior to Posterior Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington
REHABILITATION GUIDELINES FOR SUBSCAPULARIS (+/- SUBACROMINAL DECOMPRESSION)
 REHABILITATION GUIDELINES FOR SUBSCAPULARIS (+/- SUBACROMINAL DECOMPRESSION) The rehabilitation guidelines are presented in a criterion based progression. General time frames are given for reference to
REHABILITATION GUIDELINES FOR SUBSCAPULARIS (+/- SUBACROMINAL DECOMPRESSION) The rehabilitation guidelines are presented in a criterion based progression. General time frames are given for reference to
LOURDES MEDICAL ASSOCIATES PROFESSIONAL ORTHOPAEDICS SPORTS MEDICINE & ARTHROSCOPY
 LOURDES MEDICAL ASSOCIATES PROFESSIONAL ORTHOPAEDICS SPORTS MEDICINE & ARTHROSCOPY Sean Mc Millan, DO Director of Orthopaedic Sports Medicine & Arthroscopy 2103 Burlington-Mount Holly Rd Burlington, NJ
LOURDES MEDICAL ASSOCIATES PROFESSIONAL ORTHOPAEDICS SPORTS MEDICINE & ARTHROSCOPY Sean Mc Millan, DO Director of Orthopaedic Sports Medicine & Arthroscopy 2103 Burlington-Mount Holly Rd Burlington, NJ
Open Rotator Cuff Repair Rehabilitation Program Methodist Sports Medicine Center, Indianapolis, IN Department of Physical Therapy
 Open Rotator Cuff Repair Rehabilitation Program Methodist Sports Medicine Center, Indianapolis, IN Department of Physical Therapy Rotator Cuff Repair is a surgical procedure utilized for a tear in the
Open Rotator Cuff Repair Rehabilitation Program Methodist Sports Medicine Center, Indianapolis, IN Department of Physical Therapy Rotator Cuff Repair is a surgical procedure utilized for a tear in the
Rehabilitation Guidelines for Posterior Shoulder Reconstruction with or without Labral Repair
 Rehabilitation Guidelines for Posterior Shoulder Reconstruction with or without Labral Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on a
Rehabilitation Guidelines for Posterior Shoulder Reconstruction with or without Labral Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on a
Rehabilitation Guidelines For SLAP Lesion Repair
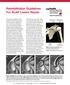 Rehabilitation Guidelines For SLAP Lesion Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on a tee. This is because the articular surface of
Rehabilitation Guidelines For SLAP Lesion Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on a tee. This is because the articular surface of
UHealth Sports Medicine
 UHealth Sports Medicine REHABILITATION GUIDELINES FOR POSTERIOR SHOULDER RECONSTRUCTION +/- LABRAL REPAIR The rehabilitation guidelines are presented in a criterion based progression. General time frames
UHealth Sports Medicine REHABILITATION GUIDELINES FOR POSTERIOR SHOULDER RECONSTRUCTION +/- LABRAL REPAIR The rehabilitation guidelines are presented in a criterion based progression. General time frames
Anterior Capsular Repair Rehabilitation Program Methodist Sports Medicine Center, Indianapolis, IN Department of Physical Therapy
 Anterior Capsular Repair Rehabilitation Program Methodist Sports Medicine Center, Indianapolis, IN Department of Physical Therapy Anterior Capsule reconstruction is a surgical procedure utilized for anterior
Anterior Capsular Repair Rehabilitation Program Methodist Sports Medicine Center, Indianapolis, IN Department of Physical Therapy Anterior Capsule reconstruction is a surgical procedure utilized for anterior
GALLAND/KIRBY UCL RECONSTRUCTION (TOMMY JOHN) POST-SURGICAL REHABILITATION PROTOCOL
 GALLAND/KIRBY UCL RECONSTRUCTION (TOMMY JOHN) POST-SURGICAL REHABILITATION PROTOCOL INTRODUCTION The ulnar collateral ligament reconstruction is a tendon transfer procedure. No muscles are transected during
GALLAND/KIRBY UCL RECONSTRUCTION (TOMMY JOHN) POST-SURGICAL REHABILITATION PROTOCOL INTRODUCTION The ulnar collateral ligament reconstruction is a tendon transfer procedure. No muscles are transected during
Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Arthroscopic Bankart Repair
 Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Arthroscopic Bankart Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on
Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Arthroscopic Bankart Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on
Shoulder Arthroscopy Combined Arthoscopic Labrum Repair Rehabilitation Protocol
 LUKE S. CHOI, M.D. 14825 N. Outer Forty Road, Suite 360 Chesterfield, MO 63017 Office: (314) 392-5063 Fax: (314) 336-2571 Shoulder Arthroscopy Combined Arthoscopic Labrum Repair Rehabilitation Protocol
LUKE S. CHOI, M.D. 14825 N. Outer Forty Road, Suite 360 Chesterfield, MO 63017 Office: (314) 392-5063 Fax: (314) 336-2571 Shoulder Arthroscopy Combined Arthoscopic Labrum Repair Rehabilitation Protocol
ROTATOR CUFF TEARS LOURDES MEDICAL ASSOCIATES PROFESSIONAL ORTHOPAEDICS SPORTS MEDICINE & ARTHROSCOPY
 LOURDES MEDICAL ASSOCIATES Sean Mc Millan, DO Director of Orthopaedic Sports Medicine & Arthroscopy 2103 Burlington-Mount Holly Rd Burlington, NJ 08016 (609) 747-9200 (office) (609) 747-1408 (fax) http://orthodoc.aaos.org/drmcmillan
LOURDES MEDICAL ASSOCIATES Sean Mc Millan, DO Director of Orthopaedic Sports Medicine & Arthroscopy 2103 Burlington-Mount Holly Rd Burlington, NJ 08016 (609) 747-9200 (office) (609) 747-1408 (fax) http://orthodoc.aaos.org/drmcmillan
POST OPERATIVE ROTATOR CUFF REPAIR PROTOCOL. Therapist Instructions
 MOON SHOULDER GROUP For information regarding the MOON Shoulder Group, speak to surgeon or contact: Rosemary Sanders 4200 Medical Center East 1215 21st Avenue South Vanderbilt University Medical Center
MOON SHOULDER GROUP For information regarding the MOON Shoulder Group, speak to surgeon or contact: Rosemary Sanders 4200 Medical Center East 1215 21st Avenue South Vanderbilt University Medical Center
THE REVERSE SHOULDER REPLACEMENT
 THE REVERSE SHOULDER REPLACEMENT The Reverse Shoulder Replacement is a newly approved implant that has been used successfully for over ten years in Europe. It was approved by the FDA for use in the U.S.A.
THE REVERSE SHOULDER REPLACEMENT The Reverse Shoulder Replacement is a newly approved implant that has been used successfully for over ten years in Europe. It was approved by the FDA for use in the U.S.A.
Rehabilitation Guidelines for Shoulder Arthroscopy
 Rehabilitation Guidelines for Shoulder Arthroscopy Front View Long head of bicep Acromion Figure 1 Shoulder anatomy Supraspinatus Image Copyright 2010 UW Health Sports Medicine Center. Short head of bicep
Rehabilitation Guidelines for Shoulder Arthroscopy Front View Long head of bicep Acromion Figure 1 Shoulder anatomy Supraspinatus Image Copyright 2010 UW Health Sports Medicine Center. Short head of bicep
POSTERIOR CAPSULAR SHIFT REHABILITATION PROTOCOL
 POSTERIOR CAPSULAR SHIFT REHABILITATION PROTOCOL The goal of this rehabilitation program is to return the patient/athlete to their activity/sport as quickly and safely as possible while maintaining a stable
POSTERIOR CAPSULAR SHIFT REHABILITATION PROTOCOL The goal of this rehabilitation program is to return the patient/athlete to their activity/sport as quickly and safely as possible while maintaining a stable
Cervical Fusion Protocol
 REHABILITATION DEPARTMENT Cervical Fusion Protocol The following protocol for physical therapy rehabilitation was designed based on the typical patient seen at the Texas Back Institute for the procedure
REHABILITATION DEPARTMENT Cervical Fusion Protocol The following protocol for physical therapy rehabilitation was designed based on the typical patient seen at the Texas Back Institute for the procedure
SHOULDER ARTHROPLASTY
 MGH Sports Medicine Center 175 Cambridge St., 4 th floor Boston, MA 02114 http://orthodoc.aaos.org/mdprice SHOULDER ARTHROPLASTY The shoulder is a ball and socket joint that enables you to raise, twist,
MGH Sports Medicine Center 175 Cambridge St., 4 th floor Boston, MA 02114 http://orthodoc.aaos.org/mdprice SHOULDER ARTHROPLASTY The shoulder is a ball and socket joint that enables you to raise, twist,
Rehabilitation Guidelines for Arthroscopic Capsular Shift
 Rehabilitation Guidelines for Arthroscopic Capsular Shift The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on a tee. This is because the articular
Rehabilitation Guidelines for Arthroscopic Capsular Shift The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on a tee. This is because the articular
SLAP Lesion Repair Rehabilitation Protocol Dr. Mark Adickes
 SLAP Lesion Repair Rehabilitation Protocol Dr. Mark Adickes Introduction: This rehabilitation protocol has been developed for the patient following a SLAP (Superior Labrum Anterior Posterior) repair. It
SLAP Lesion Repair Rehabilitation Protocol Dr. Mark Adickes Introduction: This rehabilitation protocol has been developed for the patient following a SLAP (Superior Labrum Anterior Posterior) repair. It
Rehabilitation Guidelines for Post-Operative Shoulder Instability Repair
 Rehabilitation Guidelines for Post-Operative Shoulder Instability Repair Please note that this is advisory information only. Your experiences may differ from those described. A fully qualified Physiotherapist
Rehabilitation Guidelines for Post-Operative Shoulder Instability Repair Please note that this is advisory information only. Your experiences may differ from those described. A fully qualified Physiotherapist
Progression to the next phase is based on Clinical Criteria and/or Time Frames as appropriate.
 BRIGHAM AND WOMEN S HOSPITAL Department of Rehabilitation Services Phyp Physical Therapy Total Hip Arthroplasty/ Hemiarthroplasty Protocol: The intent of this protocol is to provide the clinician with
BRIGHAM AND WOMEN S HOSPITAL Department of Rehabilitation Services Phyp Physical Therapy Total Hip Arthroplasty/ Hemiarthroplasty Protocol: The intent of this protocol is to provide the clinician with
Arthroscopic Labrum Repair of the Shoulder (SLAP)
 Anatomy Arthroscopic Labrum Repair of the Shoulder (SLAP) The shoulder joint involves three bones: the scapula (shoulder blade), the clavicle (collarbone) and the humerus (upper arm bone). The humeral
Anatomy Arthroscopic Labrum Repair of the Shoulder (SLAP) The shoulder joint involves three bones: the scapula (shoulder blade), the clavicle (collarbone) and the humerus (upper arm bone). The humeral
Copeland Surface Replacement Arthroplasty (Hannan Mullett)
 1.0 Policy Statement... 2 2.0 Purpose... 2 3.0 Scope... 2 4.0 Health & Safety... 2 5.0 Responsibilities... 2 6.0 Definitions and Abbreviations... 3 7.0 Guideline... 3 7.1 Pre-Operative... 3 7.2 Post-Operative...
1.0 Policy Statement... 2 2.0 Purpose... 2 3.0 Scope... 2 4.0 Health & Safety... 2 5.0 Responsibilities... 2 6.0 Definitions and Abbreviations... 3 7.0 Guideline... 3 7.1 Pre-Operative... 3 7.2 Post-Operative...
Rehabilitation Protocol: Total Hip Arthroplasty (THA)
 Rehabilitation Protocol: Total Hip Arthroplasty (THA) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey Medical
Rehabilitation Protocol: Total Hip Arthroplasty (THA) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey Medical
CAPPAGH NATIONAL ORTHOPAEDIC HOSPITAL, FINGLAS, DUBLIN 11. The Sisters of Mercy. Rotator Cuff Repair
 1.0 Policy Statement... 2 2.0 Purpose... 2 3.0 Scope... 2 4.0 Health & Safety... 2 5.0 Responsibilities... 2 6.0 Definitions and Abbreviations... 3 7.0 Guideline... 3 7.1 Pre-Operative... 3 7.2 Post-Operative...
1.0 Policy Statement... 2 2.0 Purpose... 2 3.0 Scope... 2 4.0 Health & Safety... 2 5.0 Responsibilities... 2 6.0 Definitions and Abbreviations... 3 7.0 Guideline... 3 7.1 Pre-Operative... 3 7.2 Post-Operative...
SHOULDER ARTHROPLASTY
 William J. Robertson, MD UT Southwestern Orthopedics 1801 Inwood Rd. Dallas, TX 75390-8882 Office: (214) 645-3300 Fax: (214) 3301 billrobertsonmd.com SHOULDER ARTHROPLASTY The shoulder is a ball and socket
William J. Robertson, MD UT Southwestern Orthopedics 1801 Inwood Rd. Dallas, TX 75390-8882 Office: (214) 645-3300 Fax: (214) 3301 billrobertsonmd.com SHOULDER ARTHROPLASTY The shoulder is a ball and socket
SHOULDER - TORN ROTATOR CUFF
 175 Cambridge Street, 4 th floor ANATOMY AND FUNCTION SHOULDER - TORN ROTATOR CUFF The shoulder joint is a ball and socket joint that connects the bone of the upper arm (humerus) with the shoulder blade
175 Cambridge Street, 4 th floor ANATOMY AND FUNCTION SHOULDER - TORN ROTATOR CUFF The shoulder joint is a ball and socket joint that connects the bone of the upper arm (humerus) with the shoulder blade
Rehabilitation Guidelines for Type I and Type II Rotator Cuff Repair and Isolated Subscapularis Repair
 UW Health SpoRTS Rehabilitation Rehabilitation Guidelines for Type I and Type II Rotator Cuff Repair and Isolated Subscapularis Repair The anatomic configuration of the shoulder joint (glenohumeral joint)
UW Health SpoRTS Rehabilitation Rehabilitation Guidelines for Type I and Type II Rotator Cuff Repair and Isolated Subscapularis Repair The anatomic configuration of the shoulder joint (glenohumeral joint)
Rehabilitation Guidelines for Post-Operative Stiff Shoulder
 Rehabilitation Guidelines for Post-Operative Stiff Shoulder Please note that this is advisory information only. Your experiences may differ from those described. A fully qualified Physiotherapist must
Rehabilitation Guidelines for Post-Operative Stiff Shoulder Please note that this is advisory information only. Your experiences may differ from those described. A fully qualified Physiotherapist must
Rotator Cuff Repair and Rehabilitation
 1 Rotator Cuff Repair and Rehabilitation Surgical Indications and Considerations Anatomical Considerations: The rotator cuff complex is comprised of four tendons from four muscles: supraspinatus, infraspinatus,
1 Rotator Cuff Repair and Rehabilitation Surgical Indications and Considerations Anatomical Considerations: The rotator cuff complex is comprised of four tendons from four muscles: supraspinatus, infraspinatus,
POSTERIOR LABRAL (BANKART) REPAIRS
 LOURDES MEDICAL ASSOCIATES Sean Mc Millan, DO Director of Orthopaedic Sports Medicine & Arthroscopy 2103 Burlington-Mount Holly Rd Burlington, NJ 08016 (609) 747-9200 (office) (609) 747-1408 (fax) http://orthodoc.aaos.org/drmcmillan
LOURDES MEDICAL ASSOCIATES Sean Mc Millan, DO Director of Orthopaedic Sports Medicine & Arthroscopy 2103 Burlington-Mount Holly Rd Burlington, NJ 08016 (609) 747-9200 (office) (609) 747-1408 (fax) http://orthodoc.aaos.org/drmcmillan
Bankart Repair Protocol
 Bankart Repair Protocol The Bankart procedure is performed to increase anterior stability of the shoulder. The following is a guideline for progression of post-operative treatment. General Information
Bankart Repair Protocol The Bankart procedure is performed to increase anterior stability of the shoulder. The following is a guideline for progression of post-operative treatment. General Information
Muscle Energy Technique. Applied to the Shoulder
 Muscle Energy Technique Applied to the Shoulder MUSCLE ENERGY Theory Muscle energy technique is a manual therapy procedure which involves the voluntary contraction of a muscle in a precisely controlled
Muscle Energy Technique Applied to the Shoulder MUSCLE ENERGY Theory Muscle energy technique is a manual therapy procedure which involves the voluntary contraction of a muscle in a precisely controlled
Rehabilitation Guidelines for Elbow Ulnar Collateral Ligament (UCL) Reconstruction
 Rehabilitation Guidelines for Elbow Ulnar Collateral Ligament (UCL) Reconstruction The elbow is a complex system of three joints formed from three bones; the humerus (the upper arm bone), the ulna (the
Rehabilitation Guidelines for Elbow Ulnar Collateral Ligament (UCL) Reconstruction The elbow is a complex system of three joints formed from three bones; the humerus (the upper arm bone), the ulna (the
SHOULDER - TORN ROTATOR CUFF
 ANATOMY AND FUNCTION SHOULDER - TORN ROTATOR CUFF The shoulder joint is a ball and socket joint that connects the bone of the upper arm (humerus) with the shoulder blade (scapula). The capsule is a broad
ANATOMY AND FUNCTION SHOULDER - TORN ROTATOR CUFF The shoulder joint is a ball and socket joint that connects the bone of the upper arm (humerus) with the shoulder blade (scapula). The capsule is a broad
Shoulder Instability. Fig 1: Intact labrum and biceps tendon
 Shoulder Instability What is it? The shoulder joint is a ball and socket joint, with the humeral head (upper arm bone) as the ball and the glenoid as the socket. The glenoid (socket) is a shallow bone
Shoulder Instability What is it? The shoulder joint is a ball and socket joint, with the humeral head (upper arm bone) as the ball and the glenoid as the socket. The glenoid (socket) is a shallow bone
Rehabilitation Guidelines for Biceps Tenodesis
 UW Health Sports Rehabilitation Rehabilitation Guidelines for Biceps Tenodesis The shoulder has two primary joints. One part of the shoulder blade, called the glenoid fossa forms a flat, shallow surface.
UW Health Sports Rehabilitation Rehabilitation Guidelines for Biceps Tenodesis The shoulder has two primary joints. One part of the shoulder blade, called the glenoid fossa forms a flat, shallow surface.
Reverse Shoulder Replacement
 Reverse Shoulder Replacement An information guide for patients Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Reverse Shoulder Replacement An information guide for patients Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Anterior Shoulder Instability Surgical Repair Protocol Dr. Mark Adickes
 Anterior Shoulder Instability Surgical Repair Protocol Dr. Mark Adickes Introduction: This rehabilitation protocol has been developed for the patient following an arthroscopic anterior stabilization procedure.
Anterior Shoulder Instability Surgical Repair Protocol Dr. Mark Adickes Introduction: This rehabilitation protocol has been developed for the patient following an arthroscopic anterior stabilization procedure.
ROTATOR CUFF HOME EXERCISE PROGRAM
 ROTATOR CUFF HOME EXERCISE PROGRAM Contact us! Vanderbilt Sports Medicine Medical Center East, South Tower, Suite 3200 1215 21st Avenue South Nashville, TN 37232-8828 For more information on this and other
ROTATOR CUFF HOME EXERCISE PROGRAM Contact us! Vanderbilt Sports Medicine Medical Center East, South Tower, Suite 3200 1215 21st Avenue South Nashville, TN 37232-8828 For more information on this and other
Shoulder Replacement Surgery
 In What Activities May I Participate After I Recover? Shoulder Replacement Surgery After undergoing shoulder replacement surgery, it is important to have realistic expectations about the types of activities
In What Activities May I Participate After I Recover? Shoulder Replacement Surgery After undergoing shoulder replacement surgery, it is important to have realistic expectations about the types of activities
MOON SHOULDER GROUP. Rotator Cuff Home Exercise Program. MOON Shoulder Group
 MOON Shoulder Group For information regarding the MOON Shoulder Group, talk to your doctor or contact: Rosemary Sanders 1215 21 st Avenue South 6100 Medical Center East Vanderbilt University Medical Center
MOON Shoulder Group For information regarding the MOON Shoulder Group, talk to your doctor or contact: Rosemary Sanders 1215 21 st Avenue South 6100 Medical Center East Vanderbilt University Medical Center
Rehabilitation after Arthroscopic Posterior Bankart Repair Phase 1: 0 to 2 weeks after surgery
 175 Cambridge Street, 4 th floor 617-726-7500 Rehabilitation after Arthroscopic Posterior Bankart Repair Phase 1: 0 to 2 weeks after surgery POSTOPERATIVE INSTRUCTIONS You will wake up in the operating
175 Cambridge Street, 4 th floor 617-726-7500 Rehabilitation after Arthroscopic Posterior Bankart Repair Phase 1: 0 to 2 weeks after surgery POSTOPERATIVE INSTRUCTIONS You will wake up in the operating
Anterior Stabilization of the Shoulder: Latarjet Protocol
 Department of Rehabilitation Services Physical Therapy Shoulder instability may be caused from congenital deformity, recurrent overuse activity, and/or traumatic dislocation. Surgical stabilization of
Department of Rehabilitation Services Physical Therapy Shoulder instability may be caused from congenital deformity, recurrent overuse activity, and/or traumatic dislocation. Surgical stabilization of
Rotator Cuff Home Exercise Program MOON SHOULDER GROUP
 Rotator Cuff Home Exercise Program MOON SHOULDER GROUP Introduction The MOON Shoulder group is a Multi-center Orthopaedic Outcomes Network. In other words, it is a group of doctors from around the country
Rotator Cuff Home Exercise Program MOON SHOULDER GROUP Introduction The MOON Shoulder group is a Multi-center Orthopaedic Outcomes Network. In other words, it is a group of doctors from around the country
Ms. Ruth Delaney ROTATOR CUFF DISEASE Orthopaedic Surgeon, Shoulder Specialist
 WHAT DOES THE ROTATOR CUFF DO? WHAT DOES THE ROTATOR CUFF DO? WHO GETS ROTATOR CUFF TEARS? HOW DO I CLINICALLY DIAGNOSE A CUFF TEAR? WHO NEEDS AN MRI? DOES EVERY CUFF TEAR NEED TO BE FIXED? WHAT DOES ROTATOR
WHAT DOES THE ROTATOR CUFF DO? WHAT DOES THE ROTATOR CUFF DO? WHO GETS ROTATOR CUFF TEARS? HOW DO I CLINICALLY DIAGNOSE A CUFF TEAR? WHO NEEDS AN MRI? DOES EVERY CUFF TEAR NEED TO BE FIXED? WHAT DOES ROTATOR
Clavicle Fracture (Broken Collarbone)
 617-726-7500 www2.massgeneral.org/sports Clavicle Fracture (Broken Collarbone) A broken collarbone is also known as a clavicle fracture. This is a very common fracture that occurs in people of all ages.
617-726-7500 www2.massgeneral.org/sports Clavicle Fracture (Broken Collarbone) A broken collarbone is also known as a clavicle fracture. This is a very common fracture that occurs in people of all ages.
Total Knee Arthroplasty. TKA - Indications. Technical Goals - TKA. Prosthesis parallel to Floor/Stance. Mechanical Axis/Center of Joint
 Total Knee Arthroplasty TKA - Indications Osteoarthritis Rheumatoid Arthritis Post Traumatic Arthritis Osteonecrosis Tumor Technical Goals - TKA Prosthesis parallel to Floor/Stance Mechanical Axis/Center
Total Knee Arthroplasty TKA - Indications Osteoarthritis Rheumatoid Arthritis Post Traumatic Arthritis Osteonecrosis Tumor Technical Goals - TKA Prosthesis parallel to Floor/Stance Mechanical Axis/Center
Arthroscopic Labrum Repair of the Shoulder (SLAP)
 617-726-7500 Anatomy Arthroscopic Labrum Repair of the Shoulder (SLAP) The shoulder joint involves three bones: the scapula (shoulder blade), the clavicle (collarbone) and the humerus (upper arm bone).
617-726-7500 Anatomy Arthroscopic Labrum Repair of the Shoulder (SLAP) The shoulder joint involves three bones: the scapula (shoulder blade), the clavicle (collarbone) and the humerus (upper arm bone).
Conventional total shoulder arthroplasty (TSA) is a widely
 [ CLINICAL COMMENTARY ] STEPHANIE BOUDREAU, PT, DPT 1 ED BOUDREAU, PT, OCS 2 LAURENCE D. HIGGINS, MD 3 REG B. WILCOX III, PT, DPT, MS, OCS 4 Rehabilitation Following Reverse Total Shoulder Arthroplasty
[ CLINICAL COMMENTARY ] STEPHANIE BOUDREAU, PT, DPT 1 ED BOUDREAU, PT, OCS 2 LAURENCE D. HIGGINS, MD 3 REG B. WILCOX III, PT, DPT, MS, OCS 4 Rehabilitation Following Reverse Total Shoulder Arthroplasty
Overhead Strength Training for the Shoulder: Guidelines for Injury Prevention and Performance Training Success
 Overhead Strength Training for the Shoulder: Guidelines for Injury Prevention and Performance Training Success Robert Panariello MS, PT, ATC, CSCS Strength training is an important component in the overall
Overhead Strength Training for the Shoulder: Guidelines for Injury Prevention and Performance Training Success Robert Panariello MS, PT, ATC, CSCS Strength training is an important component in the overall
Rotator Cuff Pathophysiology. treatment program that will effectively treat it. The tricky part about the shoulder is that it is a ball and
 Rotator Cuff Pathophysiology Shoulder injuries occur to most people at least once in their life. This highly mobile and versatile joint is one of the most common reasons people visit their health care
Rotator Cuff Pathophysiology Shoulder injuries occur to most people at least once in their life. This highly mobile and versatile joint is one of the most common reasons people visit their health care
Rehabilitation after shoulder dislocation
 Physiotherapy Department Rehabilitation after shoulder dislocation Information for patients This information leaflet gives you advice on rehabilitation after your shoulder dislocation. It is not a substitute
Physiotherapy Department Rehabilitation after shoulder dislocation Information for patients This information leaflet gives you advice on rehabilitation after your shoulder dislocation. It is not a substitute
Post-operative rehabilitation guidelines Latissimus Dorsi Transfer to Posterosuperior Cuff
 Post-operative rehabilitation guidelines Latissimus Dorsi Transfer to Posterosuperior Cuff Please note that this is advisory information only. Your experiences may differ from those described. A fully
Post-operative rehabilitation guidelines Latissimus Dorsi Transfer to Posterosuperior Cuff Please note that this is advisory information only. Your experiences may differ from those described. A fully
Arthroscopic Labrum Repair of the Shoulder (SLAP)
 Anatomy Arthroscopic Labrum Repair of the Shoulder (SLAP) The shoulder joint involves three bones: the scapula (shoulder blade), the clavicle (collarbone) and the humerus (upper arm bone). The humeral
Anatomy Arthroscopic Labrum Repair of the Shoulder (SLAP) The shoulder joint involves three bones: the scapula (shoulder blade), the clavicle (collarbone) and the humerus (upper arm bone). The humeral
Post-operative Rehabilitation Following Arthroscopic Rotator Cuff Repair
 Post-op ARCR - Ticker/Egan 1 Post-operative Rehabilitation Following Arthroscopic Rotator Cuff Repair Jonathan B. Ticker, MD Long Island Shoulder Clinic Island Orthopaedics & Sports Medicine, PC Massapequa,
Post-op ARCR - Ticker/Egan 1 Post-operative Rehabilitation Following Arthroscopic Rotator Cuff Repair Jonathan B. Ticker, MD Long Island Shoulder Clinic Island Orthopaedics & Sports Medicine, PC Massapequa,
Bankart Repair For Shoulder Instability Rehabilitation Guidelines
 Bankart Repair For Shoulder Instability Rehabilitation Guidelines Phase I: The first week after surgery. Goals:!! 1. Control pain and swelling! 2. Protect the repair! 3. Begin early shoulder motion Activities:
Bankart Repair For Shoulder Instability Rehabilitation Guidelines Phase I: The first week after surgery. Goals:!! 1. Control pain and swelling! 2. Protect the repair! 3. Begin early shoulder motion Activities:
Rehabilitation After Arthroscopic Bankart Repair And Anterior Stabilization Procedures Phase 0: 0 to 2 weeks after Surgery
 Rehabilitation After Arthroscopic Bankart Repair And Anterior Stabilization Procedures Phase 0: 0 to 2 weeks after Surgery POSTOPERATIVE INSTRUCTIONS Brett Sanders, MD Center For Sports Medicine and Orthopaedic
Rehabilitation After Arthroscopic Bankart Repair And Anterior Stabilization Procedures Phase 0: 0 to 2 weeks after Surgery POSTOPERATIVE INSTRUCTIONS Brett Sanders, MD Center For Sports Medicine and Orthopaedic
Rehabilitation Protocol: Total Knee Arthroplasty (TKA)
 Rehabilitation Protocol: Total Knee Arthroplasty (TKA) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey Medical
Rehabilitation Protocol: Total Knee Arthroplasty (TKA) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey Medical
Dr. Benjamin Hewitt. Shoulder Stabilisation
 Please contactmethroughthegoldcoasthospitaswityouhaveanyproblemsafteryoursurgery. Dr. Benjamin Hewitt Orthopaedic Surgeon Shoulder Stabilisation The shoulder is the most flexible joint in the body, allowing
Please contactmethroughthegoldcoasthospitaswityouhaveanyproblemsafteryoursurgery. Dr. Benjamin Hewitt Orthopaedic Surgeon Shoulder Stabilisation The shoulder is the most flexible joint in the body, allowing
ARTHROSCOPIC SHOULDER SURGERY REHABILITATION PROTOCOL. SLAP/Posterior Labral Repair
 ARTHROSCOPIC SHOULDER SURGERY REHABILITATION PROTOCOL SLAP/Posterior Labral Repair GENERAL GUIDELINES - The local anesthetic (similar to novacaine) in your shoulder will last 6-12 hours - Start taking
ARTHROSCOPIC SHOULDER SURGERY REHABILITATION PROTOCOL SLAP/Posterior Labral Repair GENERAL GUIDELINES - The local anesthetic (similar to novacaine) in your shoulder will last 6-12 hours - Start taking
Clavicle Fracture (Broken Collarbone)
 175 Cambridge Street 617-726-7500 www2.massgeneral.org/sports Clavicle Fracture (Broken Collarbone) A broken collarbone is also known as a clavicle fracture. This is a very common fracture that occurs
175 Cambridge Street 617-726-7500 www2.massgeneral.org/sports Clavicle Fracture (Broken Collarbone) A broken collarbone is also known as a clavicle fracture. This is a very common fracture that occurs
The Insall Scott Kelly Center for Orthopaedics and Sports Medicine 210 East 64th Street, 4 th Floor, New York, NY 10065
 ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POST-OPERATIVE REHABILITATION PROTOCOL 2003 AUTOGRAFT BONE-PATELLA TENDON-BONE and ALLOGRAFT PROTOCOL PHASE I-EARLY FUNCTIONAL (WEEKS 1-2) Goals: 1. Educate re:
ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POST-OPERATIVE REHABILITATION PROTOCOL 2003 AUTOGRAFT BONE-PATELLA TENDON-BONE and ALLOGRAFT PROTOCOL PHASE I-EARLY FUNCTIONAL (WEEKS 1-2) Goals: 1. Educate re:
B. TED MAURER, MD POSTOPERATIVE REHABILITATION PROTOCOL TOTAL KNEE ARTHROPLASTY
 B. TED MAURER, MD POSTOPERATIVE REHABILITATION PROTOCOL TOTAL KNEE ARTHROPLASTY Goals addressed prior to discharge from hospital setting: Independence with bed mobility, transfers (supine to sit and sit
B. TED MAURER, MD POSTOPERATIVE REHABILITATION PROTOCOL TOTAL KNEE ARTHROPLASTY Goals addressed prior to discharge from hospital setting: Independence with bed mobility, transfers (supine to sit and sit
1 of 6 1/22/2015 10:06 AM
 1 of 6 1/22/2015 10:06 AM 2 of 6 1/22/2015 10:06 AM This cross-section view of the shoulder socket shows a typical SLAP tear. Injuries to the superior labrum can be caused by acute trauma or by repetitive
1 of 6 1/22/2015 10:06 AM 2 of 6 1/22/2015 10:06 AM This cross-section view of the shoulder socket shows a typical SLAP tear. Injuries to the superior labrum can be caused by acute trauma or by repetitive
CAPPAGH NATIONAL ORTHOPAEDIC HOSPITAL, FINGLAS, DUBLIN 11. The Sisters of Mercy. Elbow Arthroplasty
 1.0 Policy Statement... 2 2.0 Purpose... 2 3.0 Scope... 2 4.0 Health & Safety... 2 5.0 Responsibilities... 2 6.0 Definitions and Abbreviations... 2 7.0 Guideline... 3 7.1 Indications... 3 7.2 Types of
1.0 Policy Statement... 2 2.0 Purpose... 2 3.0 Scope... 2 4.0 Health & Safety... 2 5.0 Responsibilities... 2 6.0 Definitions and Abbreviations... 2 7.0 Guideline... 3 7.1 Indications... 3 7.2 Types of
Rotator Cuff and Shoulder Conditioning Program. Purpose of Program
 Prepared for: Prepared by: OrthoInfo Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle.
Prepared for: Prepared by: OrthoInfo Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle.
Rehabilitation Protocol: Hip Arthroscopy Femoral Acetabular Impingement Debridement/Osteochondroplasty. Richard M. Wilk, M.D. Michael Kain, M.D.
 Rehabilitation Protocol: Hip Arthroscopy Femoral Acetabular Impingement Debridement/Osteochondroplasty Richard M. Wilk, M.D. Michael Kain, M.D. Department of Orthopaedic Surgery Lahey Hospital & Medical
Rehabilitation Protocol: Hip Arthroscopy Femoral Acetabular Impingement Debridement/Osteochondroplasty Richard M. Wilk, M.D. Michael Kain, M.D. Department of Orthopaedic Surgery Lahey Hospital & Medical
Shoulder Tendonitis. Brett Sanders, MD Center For Sports Medicine and Orthopaedic 2415 McCallie Ave. Chattanooga, TN (423) 624-2696
 Shoulder Tendonitis Brett Sanders, MD Center For Sports Medicine and Orthopaedic 2415 McCallie Ave. Chattanooga, TN (423) 624-2696 Shoulder tendinitis is a common overuse injury in sports (such as swimming,
Shoulder Tendonitis Brett Sanders, MD Center For Sports Medicine and Orthopaedic 2415 McCallie Ave. Chattanooga, TN (423) 624-2696 Shoulder tendinitis is a common overuse injury in sports (such as swimming,
Shoulder Joint Replacement
 Shoulder Joint Replacement Many people know someone with an artificial knee or hip joint. Shoulder replacement is less common, but it is just as successful in relieving joint pain. Shoulder replacement
Shoulder Joint Replacement Many people know someone with an artificial knee or hip joint. Shoulder replacement is less common, but it is just as successful in relieving joint pain. Shoulder replacement
J F de Beer, K van Rooyen, D Bhatia. Rotator Cuff Tears
 1 J F de Beer, K van Rooyen, D Bhatia Rotator Cuff Tears Anatomy The shoulder consists of a ball (humeral head) and a socket (glenoid). The muscles around the shoulder act to elevate the arm. The large
1 J F de Beer, K van Rooyen, D Bhatia Rotator Cuff Tears Anatomy The shoulder consists of a ball (humeral head) and a socket (glenoid). The muscles around the shoulder act to elevate the arm. The large
Knee Injuries What are the ligaments of the knee?
 As sporting participants or observers, we often hear a variety of terms used to describe sport-related injuries. Terms such as sprains, strains and tears are used to describe our aches and pains following
As sporting participants or observers, we often hear a variety of terms used to describe sport-related injuries. Terms such as sprains, strains and tears are used to describe our aches and pains following
THE SHOULDER JOINT T H E G L E N O H U M E R A L ( G H ) J O I N T
 THE SHOULDER JOINT T H E G L E N O H U M E R A L ( G H ) J O I N T CLARIFICATION OF TERMS Shoulder girdle = scapula and clavicle Shoulder joint (glenohumeral joint) = scapula and humerus Lippert, p115
THE SHOULDER JOINT T H E G L E N O H U M E R A L ( G H ) J O I N T CLARIFICATION OF TERMS Shoulder girdle = scapula and clavicle Shoulder joint (glenohumeral joint) = scapula and humerus Lippert, p115
A Patient s Guide to Shoulder Pain
 A Patient s Guide to Shoulder Pain Part 2 Evaluating the Patient James T. Mazzara, M.D. Shoulder and Elbow Surgery Sports Medicine Occupational Orthopedics Patient Education Disclaimer This presentation
A Patient s Guide to Shoulder Pain Part 2 Evaluating the Patient James T. Mazzara, M.D. Shoulder and Elbow Surgery Sports Medicine Occupational Orthopedics Patient Education Disclaimer This presentation
SHOULDER INSTABILITY IN PATIENTS WITH EDS
 EDNF 2012 CONFERENCE LIVING WITH EDS SHOULDER INSTABILITY IN PATIENTS WITH EDS Keith Kenter, MD Associate Professor Sports Medicine & Shoulder Reconstruction Director, Orthopaedic Residency Program Department
EDNF 2012 CONFERENCE LIVING WITH EDS SHOULDER INSTABILITY IN PATIENTS WITH EDS Keith Kenter, MD Associate Professor Sports Medicine & Shoulder Reconstruction Director, Orthopaedic Residency Program Department
Axillary Lymph Node Dissection: Instructions/Exercises
 Axillary Lymph Node Dissection: Instructions/Exercises The following activities have been approved by your physician to help you increase the motion and strength of your shoulder and improve your posture
Axillary Lymph Node Dissection: Instructions/Exercises The following activities have been approved by your physician to help you increase the motion and strength of your shoulder and improve your posture
Arthroscopic Labral Repair (SLAP)
 Arthroscopic Labral Repair (SLAP) Brett Sanders, MD Center For Sports Medicine and Orthopaedic 2415 McCallie Ave. Chattanooga, TN (423) 624-2696 Anatomy The shoulder joint involves three bones: the scapula
Arthroscopic Labral Repair (SLAP) Brett Sanders, MD Center For Sports Medicine and Orthopaedic 2415 McCallie Ave. Chattanooga, TN (423) 624-2696 Anatomy The shoulder joint involves three bones: the scapula
Cervical Exercise: How important is it? What can be done? The Backbone of Spine Treatment. North American Spine Society Public Education Series
 Cervical Exercise: The Backbone of Spine Treatment How important is it? What can be done? North American Spine Society Public Education Series Important: If you have had an accident that started your neck
Cervical Exercise: The Backbone of Spine Treatment How important is it? What can be done? North American Spine Society Public Education Series Important: If you have had an accident that started your neck
Physical & Occupational Therapy
 In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
Arthroscopic Rotator Cuff Repair Frequently Asked Questions:
 Department of Rehabilitation Services Physical Therapy Arthroscopic Rotator Cuff Repair Frequently Asked Questions: Are there differences between an arthroscopic and open rotator cuff repair? While the
Department of Rehabilitation Services Physical Therapy Arthroscopic Rotator Cuff Repair Frequently Asked Questions: Are there differences between an arthroscopic and open rotator cuff repair? While the
