BASIC CARDIAC LIFE SUPPORT (BCLS) PROGRAMME
|
|
|
- Austin Horn
- 7 years ago
- Views:
Transcription
1 BASIC CARDIAC LIFE SUPPORT (BCLS) PROGRAMME Institute for Medical Simulation & Education
2 SAFETY IN CPR TRAINING DO s DONT s Wash your hands or use handrub before and after manikin contact. Disinfect manikin s mouth and nose with 70% methylated spirit after each participant s contact. Use a disposable face shield when performing mouth-to-mouth ventilation. Inform the staff of the training centre if you have : Wet skin rashes on your hands, in your mouth or around your lips. Hepatitis B. An upper respiratory infection. Medical problems e.g. heart, asthma or orthopaedic problems. Disinfect manikins after each practical session following guidelines provided by the training centre. Do not eat or drink during practical training to avoid contamination of manikins with food particles. Do not use pen to mark any area of the manikin. Do not attempt to force the manikin s mouth open beyond 2.5cm. Do not use lipstick if practising on the manikin. Do not perform or practise chest compression on a victim with a pulse, practise only on a manikin.
3 C o n t e n t s Module 1 INTRODUCTION 2 Module 2 The Chain of Survival 3 Module 3 The Heart Anatomy & Function 3.2 Heart Attack 3.3 Risk Factors of Heart Attack 3.4 Prudent Heart Living Module 4 ADULT CARDIO-PULMONARY RESUSCITATION (CPR) Definition 4.2 Steps of Adult One-Man CPR Module 5 ADULT RECOVERY POSITION 19 Module 6 ADULT FOREIGN BODY AIRWAY OBSTRUCTION (FBAO) Introduction 6.2 Recognition of FBAO 6.3 Relief of FBAO in the Conscious Adult 6.4 Relief of FBAO in the Unconscious Adult Module 7 INFANT CARDIO-PULMONARY RESUSCITATION (CPR) Introduction Module 8 INFANT RECOVERY POSITION 35 Module 9 INFANT FOREIGN BODY AIRWAY OBSTRUCTION (FBAO) Introduction 9.2 Relief of FBAO in the Conscious Infant 9.3 Relief of FBAO in the Unconscious Infant Module 10 APPLICATION OF POCKET MASK 43 Module 11 SUMMARY CHECKLIST 47 Copyright 2011 Produced by Institue for Medical Simulation & Education, SGH All rights reserved. No part of this publication may be reproduced, stored in a retrieval system or transmitted, in any form or by any means, electronic, mechanical, photocopying, recording or otherwise, without the prior permission of the copyright owner. 1
4 Module 1 INTRODUCTION In Singapore, heart disease is the second commonest cause of death, being responsible for about 24% of total mortality. About 2,400 persons develop an acute heart attack in Singapore. In addition, nearly 1000 people suffer from sudden cardiac arrest in the outof-hospital environment and another few hundred sustain sudden cardiac arrest after reaching hospital. The total survival rate for the group of pre-hospital collapses is about 2.6%. Public education and training in Cardio-Pulmonary Resuscitation (CPR) are crucial in reducing sudden death because the majority of these deaths occur out of hospital. One of the most startling ideas of modern medicine is that sudden death can be reversed. The actions taken during the first few minutes of an Emergency are critical to victim survival. It can be performed by any of us, anywhere. All that is needed is our two hands. REMEMBER: CPR can save lives. Do it well. Do it right. And the victim gets a chance at life. 2
5 Module 2 The Chain of Survival The concept of Chain of Survival is the best approach to the treatment of victims in cardiac arrest. The four links in this chain are: Early Recognition and Access to Emergency Care, Early CPR, Early Defibrillation and Early Advanced Cardiac Care. Early Recognition and Access Early CPR Early Defibrillation Early Advanced Care First Link : Early Recognition and Access Early recognition and access refers to shortening the time interval from onset of heart attack or cardiac arrest to arrival of a trained emergency care team. It includes: recognition of early warning signs of heart attack e.g. chest pain, sweatiness, shortness of breath, nausea or vomiting recognition of cardiac arrest e.g. unconscious, no breathing and no pulse or signs of circulation rapid call for the first response team allowing ambulances priority on the roads so that they can reach the patient quickly allowing paramedics rapid access and priority in use of elevators in high-rise buildings. Second Link : Early CPR The brain starts dying within minutes when the heart stops pumping. CPR needs to be initiated as soon as possible to provide oxygen and blood flow to the brain and heart and remove excess carbon dioxide from the lungs. CPR cannot always re-start the heart. It can however buy the valuable time needed to keep the vital organs alive until definitive help arrives. 3
6 Third Link : Early Defibrillation This procedure can frequently re-start the heart if carried out early. Studies have shown that early defibrillation is most likely to improve survival rates for out-ofhospital cardiac arrest patients. Every emergency vehicle transporting cardiac arrest patients should be equipped with a defibrillator. Defibrillation works best in the first few minutes after onset of cardiac arrest. If initiated too late, the heart will not respond to electrical therapy. For every minute of delay in delivering defibrillation following collapse, the survival rate decreases by 7 10%. Fourth Link : Early Advanced Care Advanced Cardiac Life Support stabilises the resuscitated victim s condition in the most critical phase. It consists of advanced airway management and administration of medication and is frequently carried out in the in-hospital environment. Module 3 The Heart 3.1 ANATOMY & FUNCTION The heart is a hollow, conical, muscular organ situated in the centre of the chest between the lungs and behind the sternum (breastbone). It is about the size of a clenched fist. The Heart in Relation to the Chest The Heart as a Pump Right pulmonary artery Left pulmonary artery Rib Heart Superior vena cava Left pulmonary veins Sternum Xiphoid process Inferior vena cava It receives blood depleted of oxygen from all parts of the body and pumps it to the lungs. There oxygen is taken up and the oxygen-enriched blood returns to the heart to be distributed to all parts of the body. The coronary arteries are blood vessels that send oxygen-rich blood to the muscles of the heart. 4
7 3.2 Heart ATTACK Heart attack usually occurs when a blood clot suddenly and completely blocks an already diseased coronary artery. Coronary artery disease is the end-result of a gradual build-up of fatty deposits (cholesterol plaques) and blood cells in the inner lining of the coronary arterial wall, a process also known as atherosclerosis. Over a period of years, this leads to gradual narrowing of the lumen of the vessel, thereby reducing blood flow to heart muscle. Occasionally, the surface of a plaque may split or crack, and attract blood clots, which then cause complete obstruction of the lumen, resulting in heart attacks. Coronary Arteries Right Coronary Artery Left Circumflex Artery Left Coronary Artery Left Anterior Descending Artery Symptoms of Heart Attack How to recognize a Heart Attack Chest discomfort or pain is the most common symptom. It usually has the following characteristics: uncomfortable pressure, squeezing, fullness, tightness, or pain. usually located at the centre of the chest behind the breastbone. may spread to either the shoulder, neck, lower jaw, or either arm and occasionally to the upper abdomen. usually lasts longer than 20 minutes. Other symptoms may include any or all of the following: sweating nausea (a feeling of wanting to vomit) shortness of breath weakness 5
8 Symptoms may occur suddenly and not be typical, so that some victims may not realise that they are having a heart attack. They may also think that the problem is due to indigestion. If you meet anyone with these symptoms, arrange for immediate transportation to the nearest emergency medical facility by dialling 995 for an emergency ambulance. Photo Courtesy of SCDF Common Causes Of Sudden Death Heart Attack Foreign Body Airway Obstruction Drowning Stroke Drug Overdose Suffocation Smoke Inhalation Electrocution Severe Allergic Reactions Severe Trauma, e.g. Automobile Accident Many of these deaths can be prevented if the victims get prompt help if someone trained in CPR provides proper life-saving first-aid until other medical expertise take over. 3.3 RISK FACTORS OF HEART ATTACK There are a number of well-recognised risk factors for a heart attack. All risk factors can be modified to decrease the chance of heart attack. The more risk factors are present, the greater the risk of having a heart attack. Major risk factors that cannot be changed: heredity male gender increasing age 6
9 Major risk factors that can be changed: cigarette smoking high blood pressure high blood cholesterol levels diabetes mellitus Other risk factors that can be modified: obesity physical inactivity stress 3.4 PRUDENT HEART LIVING Prudent Heart Living includes adopting a lifestyle to help minimise the risk of a future heart attack. Reducing risk factors lowers the chance of having a heart attack or stroke. Control high blood pressure treatment generally includes dietary change and medication. Take medication regularly as prescribed by your doctor. Quit smoking completely. Eat wisely reduce saturated fat and cholesterol in the diet. Eat a Balanced diet. Reduce weight if you are overweight count calories in your food intake. Exercise regularly exercise tones the muscles, stimulates blood circulation, helps avoid excess weight gain and promotes a general feeling of well being. 7
10 CARDIO-PULMONARY RESUSCITATION (CPR) Adult 8
11 Module 4 ADULT CARDIO-PULMONARY RESUSCITATION (CPR) 4.1 DEFINITION Cardio-Pulmonary Resuscitation (CPR) includes a series of assessments and interventions that support cardiac and pulmonary functions. When cardiac arrest occurs, the heart stops beating and circulation ceases. Unless the circulation is re-started quickly, organ death will begin to occur. The most sensitive organ is the brain and if its circulation to the brain is not re-started within 4 to 6 minutes, permanent and irreversible damage can occur. It is therefore important to start CPR as quickly as possible. Air contains approximately 21% oxygen at sea level. During its passage through the body, only about 5% of the oxygen is utilised and hence exhaled air contains approximately 16% oxygen. When mouth to mouth ventilation is done during CPR, there is just sufficient oxygen in the exhaled air to keep the victim alive. Chest compression squeezes the heart between the breastbone and the spine and thereby helps to circulate the blood and deliver this oxygen to the vital organs, especially the brain, heart and kidneys. If CPR is performed promptly and correctly, 1) heart function may be restored, and 2) circulation may be maintained until institution of other life support measures. The next section takes you step-by-step through the procedures needed to perform CPR or cardio-pulmonary resuscitation the basic skill needed to save life in the event of cardiac arrest. 4.2 STEPS FOR ADULT ONE-MAN CPR STEP 1 Check For Danger Look out for unsafe environment eg, electrical current, fire, possible explosion, construction works or poisonous gas. Ensure that the scene is safe for you to help. 9
12 STEP 2 ASSESS UNRESPONSIVENESS Quickly assess and determine whether the victim is responsive. The rescuer should tap or gently shake the victim on his / her shoulders and ask loudly: Hello! Hello! Are you OK? Avoid violent shaking of the victim as this might result in injury. Also, avoid unnecessary movements of the neck in the event of injury to the head and neck. If the victim does not respond, he / she is likely to be unconscious. Unconsciousness may be due to: An airway that is obstructed (blocked) by food, secretions or a tongue that has fallen backwards. Breathing that has stopped. A heart that has stopped beating, usually because of a heart attack. 10
13 STEP 3 SHOUT FOR HELP & ACTIVATE EMERGENCY MEDICAL SERVICES (EMS) If the victim does not respond, call loudly for help and immediately dial 995 for an emergency ambulance. The rescuer should activate the Emergency Medical Services (EMS) as soon as he has determined that an adult victim is unconscious and requires emergency care. If there is another person around, ask him / her to do the calling. When calling the EMS, state: Location of victim. The telephone number you are calling from. What happened (e.g. that someone is having a heart attack / is unconscious). Number of victims. Hang up only after instructed to do so by the dispatcher. In addition, there is an increasing number of AEDs (automated external defibrillators) that are currently being deployed in public areas. These can also be life saving. Thus call for an AED. Say loudly Help! Call Ambulance 995, Get AED. 11
14 STEP 4 POSITION THE victim For CPR to be effective, the victim must lie on a firm, flat surface. If the victim is lying face down, or on his / her side, you will need to roll the victim over onto his /her back. Do take care that the head, neck and body are supported and turned simultaneously during re-positioning. STEP 5 OPEN THE AIRWAY Perform a Head tilt-chin lift Manoeuvre to open the airway. In the unresponsive victim, muscle tone is impaired resulting in the tongue falling back and obstructing the airway. As the tongue is attached to the lower jaw, moving the lower jaw forward will lift the tongue away from the back of the throat and open the airway. Airway blocked Tongue falls back With head tilt-chin lift, the airway is clear 12
15 Place one hand on the victim s forehead and apply firm backward pressure with your palm to tilt the head back. Place the fingers of your other hand under the bony part of the lower jaw to lift the jaw forward. Caution Do not press deeply into the soft tissues under the chin because this might obstruct the airway. Perform a gentle chin lift if head or neck injury is suspected. STEP 6 CHECK FOR NORMAL BREATHING Place your ear and cheek over the victim s mouth and nose and assess for breathing (up to 10 seconds) : Look for the rise and fall of the chest. Listen for air escaping during exhalation. Feel for the flow of air from the victim s mouth and nose moving past your cheeks. * Gasping is NOT considered as normal breathing. 13
16 STEP 7 ASSESS FOR PULSE (FOR HEALTHCARE PROVIDERS ONLY) Maintain head tilt, locate the Adam s apple or centre of the throat of the victim with the index and middle fingers. Slide your fingers down into the groove at the side of the neck near you (This is the location of the carotid pulse). Apply gentle pressure and feel for the carotid pulse up to 10 seconds. If the victim has no pulse or if unsure of the presence of normal breathing or pulse within 10 seconds, start chest compressions. * For laypersons, it is not necessary to check for pulse. If victim has no breathing, start chest compressions. 14
17 STEP 8 LOCATE HAND POSITION FOR CHEST COMPRESSION Chest compression technique consists of serial, rhythmic applications of pressure over the lower half of the sternum (breastbone). To locate the correct hand position for chest compression : Maintain head tilt, run your middle finger from the lower margin of the victim s rib cage till you reach the Xiphi Sternum. Xiphi Sternum Place your index finger next to the middle finger. Place the heel of one hand next to the index finger. 15
18 STEP 9A PERFORM CHEST COMPRESSION Remove the index and middle fingers. Place the heel of the other hand on top of the hand on the sternum. Interlace the fingers of both hands and lift the fingers off the chest wall. Straighten both elbows and lock them in position. Position your shoulder directly over the victim s chest. Use your body weight to compress the victim s chest by at least 5cm. Count your compressions: 1 and 2 and 3 and 4 and 5 and 1 and 2 and 3 and 4 and 10 and 1 and 2 and 3 and 4 and 15 1 and 2 and 3 and 4 and 20 1 and 2 and 3 and 4 and 25 1 and 2 and 3 and 4 and 30. Perform chest compressions at a rate of at least 100 per minute. Allow complete recoil of the chest wall after each compression. The ratio of compression and ventilation is 30 compressions: 2 breaths. Healthcare Providers Check pulse after 5 cycles of 30 compressions : 2 ventilations. If no pulse or unsure presence of pulse, resume CPR. Laypersons Continue performing CPR until help arrives or victim starts moving. 16
19 GUIDELINES FOR PROPER COMPRESSION DO s Maintain your hands on the sternum (breastbone) during each upstroke. Release the pressure on the chest after each compression to allow blood to flow into the chest and heart. Use your body weight to perform the chest compression. Keep the fingers off the chest wall. Compress at rate of at least 100 per minute. DONT s Do not lift the hands from the sternum (breastbone), otherwise correct hand position may be lost. Do not bounce or jerk during compressions as these movements may cause injuries. STEP 9B MOUTH-TO-MOUTH BREATHING To perform mouth-to-mouth-breathing : Maintain head tilt-chin lift. Pinch the nose with your thumb and index finger to prevent air from escaping through the victim s nose. Seal your mouth over the victim s mouth and give 2 short breaths in quick succession one after the other. Release the nostrils to allow exhalation after each breath. Each rescue breath should make the chest rise. The duration for each breath is 1 second. Ventilation volume is between 400 to 600 ml. Note : Too great a volume of air is likely to cause air to enter the stomach and result in gastric distension. 17
20 STEP 10 RE-ASSESSMENT (FOR HEALTHCARE PROVIDES ONLY) Assess the victim for pulse and breathing after every 5 cycles of CPR 30:2. If pulse is absent (if unsure of pulse and victim has no breathing, assume cardiac arrest), continue CPR 30:2. If both the pulse and breathing are present, position the victim in the recovery position. Continue to monitor the victim s pulse and breathing every few minutes as these can stop suddenly. D R S CHECK DANGER UNRESPONSIVE? Tap shoulder firmly Ask loudly SHOUT HELP! CALL AMBULANCE 995, GET AED Activate EMS Adult 1-man CPR Flowchart courtesy of NRC A B C OPEN AIRWAY Head tilt, chin lift NOT BREATHING NORMALLY? Look, Listen, Feel Up to10 sec No No 30 CHEST COMPRESSIONS Centre of chest / lower half of sternum Depth at least 5 cm Rate at least 100 per min Allow complete chest recoil CHECK CAROTID PULSE For healthcare providers only Define pulse and normal breathing within 10 sec No OPEN AIRWAY Head tilt, chin lift 2 BREATHS 1 sec per breath, tidal volume ml till chest just rises CONTINUE UNTIL PATIENT WAKES UP AED ARRIVES AND ANALYSING HEART RHYTHM EMERGENCY TEAM TAKES OVER CPR HEALTHCARE PROVIDERS Check pulse after 5 cycles of 30 compressions : 2 ventilations. If No pulse or unsure of presence of pulse, resume CPR IF UNABLE / UNWILLING TO DO MOUTH-TO-MOUTH FOR ANY REASON DO CONTINUOUS CHEST COMPRESSIONS AT LEAST 100 / MINUTE 18
21 Module 5 ADULT RECOVERY POSITION The recovery position is used in the management of victims who are unresponsive but have breathing and pulse. When an unresponsive victim is lying supine, the airway may become obstructed by the tongue or mucus and vomit. These problems may be prevented when the victim is placed in the recovery position, because fluid can drain easily from the mouth. If there is no evidence of trauma, place the victim in the recovery position. This position keeps the airway open. The following steps are recommended : STEP 1 POSITION THE victim A) Tuck the hand nearer to you, arm straight and palm upward under the victim s thigh. B) Bring the arm further from you across the victim s chest and place the back of his hand against his cheek. C) Using your other hand, bend the victim s far knee to a 90 degrees angle. C B A 19
22 STEP 2 ROLL THE Victim TOWARDS THE RESCUER Put your palm against the victim s palm that is on the cheek and maintain position. Using your other hand, hold the victim s far hip and roll him towards you until he is lying on his side. Use your knees to support the victim s body as you turn him so as to prevent him from rolling too far forward. STEP 3 FINAL RECOVERY POSITION Ensure that the victim s head (cheek) is lying on the back of his palm. Check that the victim s other hand is lying free along side his body with palm facing upwards. The former far leg should preferably be bent at the knee at about 90 degrees. Continue to monitor the victim s pulse and breathing every few minutes as these can stop suddenly. 20
23 Module 6 ADULT FOREIGN BODY AIRWAY OBSTRUCTION (FBAO) 6.1 INTRODUCTION Complete airway obstruction is an emergency that will result in death within minutes, if not treated immediately. Complete airway obstruction indicates that the breathing passages are totally blocked. The victim is unable to speak, breathe or cough. As most choking incidents are associated with eating, and are commonly witnessed, the chance of survival increases if the rescuer is able to intervene immediately when the victim is still conscious. Techniques used to relief FBAO include the Heimlich Manoeuvre (abdominal thrusts) and chest thrusts (for pregnant and obese victims). The Heimlich Manoeuvre, also known as subdiaphragmatic abdominal thrusts or abdominal thrusts is recommended for relieve of FBAO in responsive adults and children of 1 to 8 years of age. The Heimlich Manoeuvre (abdominal thrusts) elevates the diaphragm and increase airway pressure, which force air out from the lungs. This creates an artificial cough and expels the foreign body from the airway. In obese or pregnant victims, the chest thrust is recommended. COMMON CAUSES OF FBAO Airway obstruction can result from either intrinsic, or extrinsic causes. INTRINSIC CAUSES The tongue falling backward into the pharynx in the supine unconscious victim. Blood from head and facial injuries trickle into the airway. Regurgitated stomach contents going into the airway. EXTRINSIC CAUSES Foreign bodies e.g. food, dentures etc. 21
24 6.2 RECOGNITION OF FOREIGN BODY AIRWAY OBSTRUCTION (FBAO) FBAO can cause partial or complete airway obstruction. Coughing is the body s natural defence against airway obstruction. A victim with partial airway obstruction will cough in an attempt to expel the foreign body. If the victim is wheezing (breathing noisily with a wheezing sound) or coughing, this means that the airway is partially obstructed. Do not interfere. Allow the victim to cough to expel the object himself. In complete airway obstruction, the victim is unable to speak, breathe or cough and may become cyanotic. The victim will clutch his neck with the thumb and fingers, which is the universal distress signal for choking. This requires immediate action. Universal Choking Sign 6.3 RELIEF OF FBAO IN THE CONSCIOUS ADULT Techniques used to relieve FBAO in a conscious adult include the Heimlich Manoeuvre (abdominal thrusts) and chest thrusts. A) The Heimlich Manoeuvre ( Abdominal Thrust ) Technique STEP 1 To determine whether the victim is choking, ask, Are you choking? If the victim is able to cough, ask him to cough as hard as he can to get the foreign body out of his upper airway. If the victim s airway is obstructed, he will not be able to speak, breathe or cough. The victim s face may turn blue. The rescuer should immediately proceed to the next step. STEP 2 If the victim is upright, the rescuer stands behind the victim. If the victim is sitting, the rescuer kneels down and positions himself behind the victim. Position one foot between the victim s legs. 22
25 STEP 3 Place your arms around the victim s abdomen and locate the navel. With one hand, place 2 fingers just above the navel. Make a fist with the other hand. Place the thumb-side of the fist against the abdomen above the 2 fingers. Release the 2 fingers but maintain your fist against the abdomen. Lean the victim forward and grasp your fist with the Heimlich Manoeuvre other hand. (Abdominal Thrust) Give successive inward and upward thrusts (set of 5 abdominal thrusts). Check if foreign body is expelled after every set of 5 abdominal thrusts. Repeat abdominal thrusts until the foreign body is expelled or the victim becomes unconscious. B) Chest Thrust Technique Chest thrust technique is used as an alternative to Heimlich Manoeuvre. It is performed on a conscious obese or pregnant victim. STEP 1 To determine whether the victim is choking, ask Are you choking? If the victim is choked, the victim will not be able to speak, breathe or cough. STEP 2 If the victim is upright, the rescuer stands behind the victim. If the victim is sitting, the rescuer kneels down and positions behind the victim. Position one foot between the victim s legs. 23
26 STEP 3 Place arms under the victim s armpits to encircle the chest. Make a fist with one hand. Place the thumb-side of the fist on the middle of the victim s breastbone. Grasps fist with the other hand and give successive quick backward thrusts (set of 5 chest thrusts). Check if foreign body is expelled after every set of 5 chest thrusts. If the obstruction is still not relieved, continue to deliver the set of 5 chest thrusts firmly and distinctly until the foreign body is expelled or the victim becomes unconscious. 6.4 RELIEF OF FBAO IN THE UNCONSCIOUS ADULT For an unconscious adult, proceed with the following steps: STEP 1 Position victim on a firm, flat surface and immediately activate Emergency Medical Services by dialling 995 for an emergency ambulance. STEP 2 Start 30 chest compressions (The hand position for chest compression is the same as for Adult CPR). 24
27 STEP 3 Open victim s airway by peforming head tilt-chin lift. Check victim s mouth for any visible foreign bodies. Use a hooked index finger and remove any obvious obstructing foreign bodies. STEP 4 Check for normal breathing : Look, Listen & Feel (up to 10 seconds). If breathing is absent, attempt to ventilate (1st attempt). If airway is blocked, re-position with the Head Tilt-Chin Lift procedure. Attempt 2nd ventilation. STEP 5 If airway is still blocked, perform 30 chest compressions, then proceed back to head tilt-chin lift and check for foreign body. Repeat Step 3 & 4 till help arrives or able to give 2 successful ventilation. STEP 6 Assess the victim for pulse & breathing once the airway is cleared. If pulse (for healthcare providers only) & breathing are absent, assume cardiac arrest, continue 30:2. If both pulse & breathing are present, position the victim in the recovery position Continue to monitor the victim s pulse and breathing every few minutes as these can stop suddenly. 25
28 CARDIO-PULMONARY RESUSCITATION (CPR) Infant 26
29 Module 7 INFANT CARDIO-PULMONARY RESUSCITATION (CPR) 7.1 INTRODUCTION An infant is a child who is up to 1 year old. Infants rarely collapse because of a primary heart problem. Cardiac arrest is usually secondary to other events, such as major trauma or respiratory problems. Therefore, rescuers must detect and promptly treat early signs of respiratory failure to prevent cardiac arrest. STEP 1 Check For Danger Look out for unsafe environment eg, electrical current, fire, possible explosion, construction works or poisonous gas. Ensure that the scene is safe for you to help. One should always ensure the safety of rescuer(s) and infant at the onset. STEP 2 ASSESS UNRESPONSIVENESS Quickly assess and determine whether the infant is responsive by tapping gently on the infant s shoulders. Avoid violent shaking and unnecessary movements of the infant s head and neck as this might result in injury. If the infant does not respond, he/ she is likely to be unconscious. Possible causes of unconsciousness may be: an airway that is obstructed (blocked) by food, secretions or a tongue that has fallen backwards. breathing that has stopped. a heart that has stopped beating. 27
30 STEP 3 ACTIVATE EMERGENCY MEDICAL SERVICE (EMS) When the infant does not respond : If you are alone, immediately commence CPR 30 : 2 for approximately 2 minutes before calling 995 for an ambulance. If a second rescuer is present, ask him / her to activate the EMS system by dialling the ambulance number 995. When calling EMS 995, state: Location of infant. The telephone number you are calling from. What happened Number of victims. Hang up only after instructed to do so by the dispatcher. STEP 4 POSITION THE INFANT For CPR to be effective, the infant must lie on a firm flat surface, the leg straightened and the arms placed alongside the body. 28
31 STEP 5 OPEN THE AIRWAY Perform a head tilt-chin lift manoeuvre to open the airway. In an unconscious infant, muscle tone is impaired resulting in the tongue falling back and obstructing the airway. As the tongue is attached to the lower jaw, moving the lower jaw forward will lift the tongue away from back of the throat and open the airway. Perform a head tilt-chin lift manoeuvre : Place one hand on the infant s forehead and apply firm backward pressure with your palm to tilt the head back. Place the fingers of your other hand under the bony part of the lower jaw to lift the jaw forward. Caution Do not press deeply into the soft tissues under the chin or over extend the infant s neck because this may block the airway. Perform a gentle chin lift if head or neck injury is suspected. 29
32 STEP 6 CHECK FOR NORMAL BREATHING Place your ear and cheek over the infant s mouth and nose and assess for breathing (up to 10 seconds) : Look for the rise and fall of the chest. Listen for air escaping during exhalation. Feel for the flow of air from the infant s mouth and nose moving past your cheeks. * Gasping is NOT considered as normal breathing. STEP 7 ASSESS FOR PULSE (FOR HEALTHCARE PROVIDERS ONLY) Maintain head tilt and locate the brachial pulse (which is on the inner aspect of the upper arm) with the index and middle fingers. Apply gentle pressure and feel for the brachial pulse within 10 seconds. If the infant has no pulse (if unsure of pulse) and is not breathing, start chest compressions. 30
33 STEP 8 LOCATE LANDMARK FOR CHEST COMPRESSION Chest compressions in an infant consist of serial, rhythmic applications of pressure over the lower half of the sternum (breastbone). To locate the correct landmark for chest compression: Maintain head tilt with one hand. Draw an imaginary line between the infant s nipples using your index finger of the other hand. Place the index finger on the imaginary line. Place your middle and ring fingers next to the index finger. 31
34 Move the 3 fingers to the centre of the sternum (breastbone). Position the fingers upright. Lift off the index finger but maintain the middle and ring fingers contact on the sternum (breastbone). 32
35 STEP 9A PERFORM CHEST COMPRESSION Lean forward and place your cheek near the infant s mouth and nose. Use your middle and ring fingers to compress the sternum (breastbone) 4cm. Count your compressions: 1 and 2 and 3 and 4 and 5 and 1 and 2 and 3 and 4 and 10 and 1 and 2 and 3 and 4 and 15 1 and 2 and 3 and 4 and 20 1 and 2 and 3 and 4 and 25 1 and 2 and 3 and 4 and 30. Perform chest compressions at a rate of at least 100 per minute. Healthcare Providers Check pulse after 5 cycles of 30 compressions : 2 ventilations. If no pulse or unsure presence of pulse, resume CPR. Laypersons Continue performing CPR until help arrives or infant starts moving. Note : To facilitate ventilation without delays to re-position the head, use one hand to maintain the head tilt position while performing chest compressions. 33
36 GUIDELINES FOR PROPER COMPRESSION DO s Maintain your 2 fingers on the sternum (breastbone) during each upstroke. Release the pressure on the chest after each compression to allow blood to flow into the chest and heart. Compress at rate of at least 100 per minute. DONT s Do not lift the fingers from the sternum (breastbone), otherwise correct finger position may be lost. Do not bounce or jerk during compressions as these movements may cause injuries. STEP 9B MOUTH TO MOUTH & NOSE BREATHING Perform mouth to mouth & nose breathing as follows : Maintain a head tilt-chin lift. Seal your mouth over the infant s mouth and give 2 short breaths in quick succession one after the other. Each rescue breath should make the chest rise. The duration for each breath is 1 second. Ventilation volume is approximately 30 ml per breath. Allow exhalation between breaths. STEP 10 RE-ASSESSMENT (FOR HEALTHCARE PROVIDERS ONLY) Assess the infant for pulse and breathing after every 5 cycles of CPR 30:2. If pulse is absent (if unsure of pulse and infant has no breathing, assume cardiac arrest), continue CPR 30:2. If both the pulse and breathing are present, position the infant in the recovery position. Continue to monitor the infant s pulse and breathing every few minutes as these can stop suddenly. 34
37 Module 8 INFANT RECOVERY POSITION 8.1 INTRODUCTION The recovery position is used in the management of infants who are unresponsive but are breathing. When an unresponsive infant is lying supine, the airway may become obstructed by the tongue or mucus and vomit. These problems may be prevented when the infant is placed in the recovery position, because fluid can drain easily from the mouth. The recovery position for an infant differs from the adult position. The infant is put on the lateral (side) position when pulse and breathing have resumed. This position keeps the airway open. The following steps are recommended : STEP 1 POSITION THE INFANT Place the infant s arms alongside the body. Straighten the infant s legs. 35
38 STEP 2 ROLL THE CHILD TOWARDS THE RESCUER Support the infant s head and neck with one hand. Place the other hand on the infant s hip. Gently roll or turn the infant on the side toward the rescuer. STEP 3 FINAL RECOVERY POSITION Support the infant s back with a soft pillow / cushion. Ensure that the infant s head is not over extended or flexed. Stay with the infant and continue to monitor the pulse and breathing every few minutes as these can stop suddenly. 36
39 Module 9 INFANT FOREIGN BODY AIRWAY OBSTRUCTION (FBAO) 9.1 INTRODUCTION Airway obstruction (choking) is a common cause of infant death and disability. Complete airway obstruction indicates that the breathing passages are totally blocked. The infant is unable to speak (make noises), breathe or cough. Choking in infants is commonest during eating or playing with small objects. In a witnessed choking event, the chance of survival increases if the rescuer is able to intervene when the infant is still conscious. The obstructed airway can be cleared using a combination of back blows and chest thrusts. COMMON CAUSES OF FBAO Airway obstruction can result from either intrinsic, or extrinsic causes. INTRINSIC CAUSES The tongue falling backward into the pharynx in an unconscious infant. Blood from head and facial injuries trickling into the airway. Regurgitated stomach contents going into the airway. EXTRINSIC CAUSES Foreign bodies e.g. food, small objects or toys etc. RECOGNITION OF FBAO In complete airway obstruction, the infant may exhibit the following signs: Sudden onset of respiratory /breathing distress. Cyanosis (blue lips, nail or skin). Unable to speak (make noises). Unable to breathe. Unable to cough. 37
40 9.2 RELIEF OF FBAO IN THE CONSCIOUS INFANT STEP 1 ASSESSMENT Assess for signs of complete airway obstruction e.g. unable to make noises, breathe or cough. If infant is choking, attempt to relieve the airway obstruction immediately. STEP 2 SUPPORT THE INFANT Supporting the infant s head and body between your hands and forearms using the Sandwich Manoeuvre. Hold the infant s face down and rest your forearm on your thigh. Keep the head lower than the trunk. 38
41 STEP 3 BACK BLOWS AND CHEST THRUSTS Deliver 5 back blows forcefully between the shoulder blades with the heel of your other hand. Support the infant s head and body between your hands and forearms using the Sandwich Manoeuvre after delivering the 5 back blows. Turn the infant over on his/her back, resting on your thigh. Keep the infant s head lower than the trunk. 39
42 Deliver 5 chest thrusts over the lower half of the sternum (breastbone) by counting aloud 1,2,3,4,5 (landmark for chest thrust is the same as for infant CPR). Note : Each back blow and chest thrust should be delivered with sufficient force and with the intention of expelling the foreign body. STEP 4 RE-ASSESSMENT Check if foreign body is expelled after every set of 5 back blows and 5 chest thrusts and remove it with your little finger if the foreign body is visible in the mouth. If the foreign body is expelled successfully, assess the infant for pulse and breathing. If the airway remains obstructed and the infant is still conscious, repeat the sequence of 5 back blows and 5 chest thrusts until the foreign body is expelled or the infant becomes unconscious. 40
43 9.3 RELIEF OF FBAO IN THE UNCONSCIOUS INFANT For an unconscious infant, proceed with the following steps : STEP 1 Position infant on a firm flat surface and immediately activate Emergency Medical Services by dialling 995 for an emergency ambulance, if a second rescuer is available. STEP 2 Start 30 chest compressions. (The landmark and technique is the same as for infant CPR ). STEP 3 Open infant s airway by performing head tilt-chin lift. Check the infant s mouth for visible foreign bodies. Use a hooked little finger and remove any obvious obstructing foreign bodies. STEP 4 Check for normal breathing. If breathing is absent, attempt to ventilate. If airway is blocked, re-position the infant s head and re-attempt to ventilate. Attempt 2nd ventilation. STEP 5 If airway is blocked, perform 30 chest compressions. Proceed to head tilt-chin tilt and check for foreign body. Repeat step 3 and 4 till help arrives or able to give 2 sucessful ventilations. STEP 6 Assess for pulse and breathing once the airway is cleared. If pulse and breathing are absent assume cardiac arrest & continue CPR 30:2. If both the pulse and breathing are present, position the infant in the recovery position. Continue to monitor the infant s pulse, and breathing every few minutes as these can stop suddenly. Activate EMS if it is not done earlier. 41
44 APPLICATION OF POCKET MASK 42
45 Module 10 APPLICATION OF POCKET MASK The pocket mask is a barrier device used to provide rescue breathing. It has a one-way valve that prevents exchange of secretions between the victim and rescuer. It is made of firm plastic with a cushioned rim and is roughly triangular in shape. The rim creates a flexible seal around the victim s nose and mouth. The mask fits over the victim s mouth and nose. The narrowest portion of the mask is placed over the bridge of the victim s nose. Mask connection port with one-way valve Exhalation port Mask port Filter Rim 43
46 APPLICATION STEP 1 Check that filter (if included) is snapped firmly in place. STEP 2 Push out the dome. STEP 3 Attach one-way valve to mask port. Direct exhalation port away from nose end of mask. 44
47 STEP 4 Apply the rim of the mask first between the victim s lower lip and chin. This will retract the lower lip and keep the mouth open under the mask. Position end marked nose over the victim s nose. STEP 5 Seal as illustrated. Open the airway by performing a gentle head tilt-chin lift. Blow slowly until chest rises. STEP 6 Remove your mouth and allow victim to exhale. Note: If victim vomits, remove mask and clear victim s airway. Clear mask assembly by shaking or sweeping out foreign material. Blow through valve to verify operation. Re-apply mask to victim and continue ventilation. 45
48 SUMMARY CHECKLIST 46
49 Module 11 SUMMARY CHECKLIST ADULT ONE-MAN CPR STEPS D : Danger R : Response S : Shout for Help A : Airway B : Breathing C : Circulation CPR Cycle ACTION Look out for unsafe environment, e.g. Electrical current, Fire, Possible Explosion, Construction works, or Poisonous gas Ensure that the scene is safe for you to help Establish unresponsiveness Call, tap or gently shake the victim Call out loudly: Hello! Hello! Are you OK? If no response, Call for ambulance 995 & AED Open airway : Head Tilt-Chin Lift Check for normal breathing : Look, Listen, & Feel (up to 10 seconds) Look for the rise and fall of the chest Listen for air escaping during exhalation Feel for the flow of air from the victim s mouth and nose moving past your cheeks Check for pulse up to 10 seconds (only for Healthcare providers) If no pulse and breathing, start CPR For laypersons, there is no need to check for pulse. If victim has no breathing, start CPR Locate the landmark for chest compression Proper body and hand position Compress vertically at least 5 cm downwards with complete relaxation of pressure after each compression at rate of at least 100 per minute Say mnemonic 1&2&3&4&5& 1&2&3&4&10& 1&2&3&4&15 1&2&3&4&20 1&2&3&4&25 1&2&3&4&30 Perform 30 chest compressions followed by 2 breaths The duration for each breath is 1 second. Ventilation volume is between ml/breath Allow lung deflation between each breath Reassessment Assess the victim for pulse and breathing after every 5 cycles of 30:2 (for healthcare providers only) If pulse is absent (if unsure of pulse and victim has No breathing, assume cardiac arrest), continue 30:2 For laypersons, continue performing CPR until help arrives or victim starts moving Recovery Position Place the victim in the recovery position if : Pulse and breathing are present Victim is unconscious and has no evidence of trauma Continue to monitor victim s pulse and breathing every few minutes as this can stop suddenly 47
50 ADULT FOREIGN-BODY AIRWAY OBSTRUCTION (CONSCIOUS UNCONSCIOUS) STEPS Conscious victim Assessment Heimlich Manoeuvre Technique (Normal Size) Chest Thrust Technique (Pregnant & Obese) Unconscious victim ACTION Ask: Are you choking? Victim acknowledges by nodding. Rescuer replies: I can help. Stand behind the victim. Position one foot between the victim s legs Locate the landmark : Place your arms around the victim s abdomen and locate the navel With one hand place 2 fingers just above the navel Make a fist with the other hand Place thumb-side of the fist against the abdomen above the 2 fingers Release the 2 fingers but maintain the fist on the abdomen Lean the victim forward and grasp the fist with the other hand Give successive inward-upward thrusts Check if foreign body is expelled after every set of 5 abdominal thrusts Repeat thrusts until the foreign body is dislodged or the victim becomes unconscious Stand behind the victim. Position one foot between the victim s legs Locate the landmark : Place arms under the victim s armpits to encircle the chest Make a fist with one hand Place thumb-side of fist on the middle of the victim s breastbone Grasp the fist with the other hand and give successive quick backward thrusts Check if foreign body is expelled after every set of 5 chest thrusts Repeat thrusts until the foreign body is dislodged or the victim becomes unconscious When victim becomes unconscious. Proceed with the following steps : Position the victim on a firm, flat surface Call for ambulance 995 Start 30 chest compressions (The landmark & technique is the same as for adult CPR) Open airway : Head Tilt-Chin Lift Check airway and remove any obvious foreign bodies Check for normal breathing : Look, Listen, & Feel (up to 10 seconds) If breathing is absent, attempt to ventilate (1st attempt) If airway is still blocked, re-position the victim s head and reattempt to ventilate Attempt 2nd ventilation If airway is still blocked, perform 30 chest compressions Proceed to head tilt-chin tilt and check for foreign body Repeat Step till help arrives or able to give 2 successful ventilations Check pulse (for healthcare providers only) and breathing once airway is cleared. If pulse is absent (if unsure of pulse and victim has no breathing, assume cardiac arrest), continue CPR 30:2 Recovery Position Place victim in the recovery position if : Pulse and breathing are present Continue to monitor victim s pulse and breathing every few minutes as this can stop suddenly 48
51 INFANT CPR STEPS D : Danger ACTION Look out for unsafe environment, e.g. Electrical current, Fire, Possible Explosion, Construction works, or Poisonous gas Ensure that the scene is safe for you to help R : Response Establish unresponsiveness : Call, tap or gently shake the infant s shoulder to elicit response If you are alone, immediately start CPR 30:2 for approx. 2 minutes S : Shout for Help If a second rescuer is present, ask him or her to call for ambulance 995 A : Airway B : Breathing C : Circulation Open airway : Head Tilt-Chin Lift Check for normal breathing : Look, Listen, & Feel (up to 10 seconds) Look for the rise and fall of the chest Listen for air escaping during exhalation Feel for the flow of air from the infant s mouth and nose moving past your cheeks Check for brachial pulse up to 10 seconds (only for Healthcare providers) If pulse is absent (if unsure of pulse and infant has no breathing, assume cardiac arrest), start 30:2 For laypersons, there is no need to check for pulse. If infant has no breathing, start CPR Locate landmark for chest compression: Draw an imaginary line between nipples Place index finger on the imaginary line Place your middle and ring fingers next to the index finger Move the 3 fingers to the centre of the sternum (breastbone) Position the fingers upright Lift off the index finger but maintain the middle and ring fingers contact on the sternum (breastbone) Lean forward and place your cheek near the infant s mouth and nose Use your middle and ring fingers to compress the sternum (breastbone) by 4 cm Demonstrate correct technique of compression Keep fingers contact on the sternum during each upstroke Say mnemonic 1&2&3&4&5&1&2&3&4&10&1&2&3&4&15 1&2&3&4&20 1&2&3&4&25 1&2&3&4&30 Compression rate is at least 100 per minute CPR Cycle Perform 5 cycles of 30 chest compressions followed by 2 breaths for approximately 2 minutes (For Healthcare providers only) The duration for each breath is 1 second. Ventilation volume is between 30 ml/breath Allow lung deflation between each breath Reassessment Assess for pulse and breathing after every 5 cycles of CPR 30:2 (for healthcare providers only) If pulse is absent (if unsure of pulse and infant is not breathing, assume cardiac arrest), continue CPR 30:2 For laypersons, continue performing CPR until help arrives or infant starts moving Recovery Position Recovery Position Place the infant in the recovery position if : Pulse and breathing are present Infant is unconscious and has no evidence of trauma Continue to monitor infant s pulse & breathing every few minutes as this can stop suddenly 49
52 INFANT FOREIGN-BODY AIRWAY OBSTRUCTION (CONSCIOUS UNCONSCIOUS) STEPS Conscious infant Assessment Back blows & Chest thrusts Reassessment Unconscious infant ACTION Assess for signs of complete airway obstruction (choking) If infant is choking, attempt to Assessment relieve the airway obstruction immediately Support the infant s head and body between your hands and forearms using the Sandwich Manoeuvre Hold the infant s face down and rest your forearm on your thigh Keep the head lower than the trunk Deliver 5 back blows forcefully between the shoulder blades with the heel of your other hand Support the infant s head and body between your hands and forearms after delivering the 5 back blows Turn the infant over on his/her back, resting on your thigh Keep the head lower than the trunk Deliver 5 chest thrusts over the lower half of the sternum (breastbone) by counting aloud 1,2,3,4,5.(landmark for chest thrust is the same as for infant CPR) Check if foreign body is expelled after every set of 5 back blows and 5 chest thrusts and remove if it is visible If the foreign body is expelled successfully, assess the infant for pulse & breathing If the airway remains obstructed and the infant is conscious, repeat the sequence of 5 back blows and 5 chest thrusts until the foreign body is expelled or the infant becomes unconscious When infant becomes unconscious. Proceed with the following steps : Position the infant on a firm, flat surface Call for ambulance 995 if a second rescuer is available Start 30 chest compressions (The landmark & technique is the same as for Infant CPR) Open airway : Head Tilt-Chin Lift Check airway and remove any obvious foreign bodies Check for normal breathing : Look, Listen, & Feel (up to 10 seconds) If breathing is absent, attempt to ventilate (1st attempt) If airway is still blocked, re-position the infant s head and reattempt to ventilate Attempt 2nd ventilation If airway is still blocked, perform 30 chest compressions Proceed to head tilt-chin tilt and check for foreign body Repeat Step till help arrives or able to give 2 successful ventilations Check pulse (for healthcare providers only) and breathing once airway is cleared. If pulse is absent (if unsure of pulse and infant has no breathing, assume cardiac arrest), continue CPR 30:2 Recovery Position Place the infant in the recovery position if : Pulse and breathing are present Continue to monitor infant s pulse and breathing every few minutes as this can stop suddenly Activate EMS if it is not done earlier 50
53 Notes 51
54 Notes 52
55 Notes 53
56 Singapore General Hospital Institute for Medical Simulation & Education 167 Jalan Bukit Merah, Connection One Tower 5, #03-10, Singapore Tel : / / Fax : imse@sgh.com.sg Information correct as at April 2011
Module 5 ADULT RECOvERY POSITION STEP 1 POSITION ThE victim
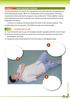 Module 5 ADULT RECOVERY POSITION The recovery position is used in the management of victims who are unresponsive but have breathing and pulse. When an unresponsive victim is lying supine, the airway may
Module 5 ADULT RECOVERY POSITION The recovery position is used in the management of victims who are unresponsive but have breathing and pulse. When an unresponsive victim is lying supine, the airway may
Adult, Child, and Infant Written Exam CPR Pro for the Professional Rescuer
 Adult, Child, and Infant Written Exam CPR Pro for the Professional Rescuer Instructions: Read each of the following questions carefully and then place an X over the correct answer on the separate answer
Adult, Child, and Infant Written Exam CPR Pro for the Professional Rescuer Instructions: Read each of the following questions carefully and then place an X over the correct answer on the separate answer
Northwestern Health Sciences University. Basic Life Support for Healthcare Providers
 Northwestern Health Sciences University Basic Life Support for Healthcare Providers Pretest May 2005 This examination to be used only as a PRECOURSE TEST for BLS for Healthcare Providers Courses Based
Northwestern Health Sciences University Basic Life Support for Healthcare Providers Pretest May 2005 This examination to be used only as a PRECOURSE TEST for BLS for Healthcare Providers Courses Based
American Heart Association. Basic Life Support for Healthcare Providers
 American Heart Association Basic Life Support for Healthcare Providers Pretest February 2001 This examination to be used only as a PRECOURSE TEST for BLS for Healthcare Providers Courses 2001 American
American Heart Association Basic Life Support for Healthcare Providers Pretest February 2001 This examination to be used only as a PRECOURSE TEST for BLS for Healthcare Providers Courses 2001 American
Heart information. CPR cardiopulmonary resuscitation
 Heart information CPR cardiopulmonary resuscitation Contents 3 What is CPR? 3 What is cardiac arrest? 4 Heart attack and cardiac arrest 4 Cardiopulmonary resuscitation (CPR) 5 Danger 6 Response 7 Send
Heart information CPR cardiopulmonary resuscitation Contents 3 What is CPR? 3 What is cardiac arrest? 4 Heart attack and cardiac arrest 4 Cardiopulmonary resuscitation (CPR) 5 Danger 6 Response 7 Send
American Heart Association
 American Heart Association Basic Life Support for Healthcare Providers Pretest April 2006 This examination to be used only as a PRECOURSE TEST For BLS for Healthcare Providers Courses 2006 American Heart
American Heart Association Basic Life Support for Healthcare Providers Pretest April 2006 This examination to be used only as a PRECOURSE TEST For BLS for Healthcare Providers Courses 2006 American Heart
Adult Choking and CPR Manual
 Adult Choking and CPR Manual 2009 Breath of Life Home Medical Equipment and Respiratory Services CHOKING Description: Choking is the coughing spasm and sputtering that happen when liquids or solids get
Adult Choking and CPR Manual 2009 Breath of Life Home Medical Equipment and Respiratory Services CHOKING Description: Choking is the coughing spasm and sputtering that happen when liquids or solids get
Success Manual and Cheat Sheet Notes to Pass Your Basic Life Support (BLS) Course
 Success Manual and Cheat Sheet Notes to Pass Your Basic Life Support (BLS) Course Written by: Jay Snaric, MS And Kimberly Hickman, RN CPR St. Louis 44 Meramec Valley Plaza St. Louis MO 63088 www.stlcpr.com
Success Manual and Cheat Sheet Notes to Pass Your Basic Life Support (BLS) Course Written by: Jay Snaric, MS And Kimberly Hickman, RN CPR St. Louis 44 Meramec Valley Plaza St. Louis MO 63088 www.stlcpr.com
CPR/AED for Professional Rescuers and Health Care Providers HANDBOOK
 CPR/AED for Professional Rescuers and Health Care Providers HANDBOOK TABLE OF CONTENTS SECTION 1: THE PROFESSIONAL RESCUER The Duty to Respond 2 Preventing the Spread of Bloodborne Pathogens 3 Taking Action
CPR/AED for Professional Rescuers and Health Care Providers HANDBOOK TABLE OF CONTENTS SECTION 1: THE PROFESSIONAL RESCUER The Duty to Respond 2 Preventing the Spread of Bloodborne Pathogens 3 Taking Action
Adult Basic Life Support
 2 Adult Basic Life Support Introduction This chapter contains the guidelines for out-of-hospital, single rescuer, adult basic life support (BLS). Like the other guidelines in this publication, it is based
2 Adult Basic Life Support Introduction This chapter contains the guidelines for out-of-hospital, single rescuer, adult basic life support (BLS). Like the other guidelines in this publication, it is based
Adult First Aid/CPR/AEd. Ready Reference
 Adult First Aid/CPR/AEd Ready Reference Contents Checking an Injured or Ill Adult 3 CPR 4 AED Adult or Child 5 Conscious Choking 7 Controlling External Bleeding 8 Burns 9 Poisoning 10 Head, Neck or Spinal
Adult First Aid/CPR/AEd Ready Reference Contents Checking an Injured or Ill Adult 3 CPR 4 AED Adult or Child 5 Conscious Choking 7 Controlling External Bleeding 8 Burns 9 Poisoning 10 Head, Neck or Spinal
Infant CPR. What You Need to Know. How to Do Infant CPR
 Infant CPR Infant CPR also called Cardiopulmonary resuscitation is emergency care given to a baby who has stopped breathing. This sheet has the steps for CPR for newborns or babies less than 1 year old.
Infant CPR Infant CPR also called Cardiopulmonary resuscitation is emergency care given to a baby who has stopped breathing. This sheet has the steps for CPR for newborns or babies less than 1 year old.
American Heart Association. BLS Instructor Course. Written Examination. July 2003
 American Heart Association BLS Instructor Course Written Examination July 2003 Basic Life Support Instructor Exam Part I Please do not mark on this examination. Record the best answer on the separate answer
American Heart Association BLS Instructor Course Written Examination July 2003 Basic Life Support Instructor Exam Part I Please do not mark on this examination. Record the best answer on the separate answer
The purpose of this course is to outline the American Heart Association s guidelines for CPR, the use of AEDs, and the Heimlich maneuver.
 CPR Cardiopulmonary Resuscitation WWW.RN.ORG Reviewed May, 2016, Expires May, 2018 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2016 RN.ORG, S.A., RN.ORG,
CPR Cardiopulmonary Resuscitation WWW.RN.ORG Reviewed May, 2016, Expires May, 2018 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2016 RN.ORG, S.A., RN.ORG,
American Heart Association. Basic Life Support for Healthcare Providers
 American Heart Association Basic Life Support for Healthcare Providers Pretest ANNOTATED ANSWER KEY February 2001 This examination to be used only as a PRECOURSE TEST for BLS for Healthcare Providers Courses
American Heart Association Basic Life Support for Healthcare Providers Pretest ANNOTATED ANSWER KEY February 2001 This examination to be used only as a PRECOURSE TEST for BLS for Healthcare Providers Courses
Anatomy and Physiology: Understanding the Importance of CPR
 Anatomy and Physiology: Understanding the Importance of CPR Overview This document gives you more information about the body s structure (anatomy) and function (physiology). This information will help
Anatomy and Physiology: Understanding the Importance of CPR Overview This document gives you more information about the body s structure (anatomy) and function (physiology). This information will help
IN CASE OF EMERGENCY. Emergency Telephone Number 112
 IN CASE OF EMERGENCY Emergency Telephone Number 112 Police, Fire, Ambulance Dial 112 in case of fire, medical emergency, serious or life threatening traffic or other accident. Tell the operator: What has
IN CASE OF EMERGENCY Emergency Telephone Number 112 Police, Fire, Ambulance Dial 112 in case of fire, medical emergency, serious or life threatening traffic or other accident. Tell the operator: What has
BLS PRETEST BASIC LIFE SUPPORT FOR HEALTHCARE PROVIDERS (CREATED BY LAST MINUTE CPR & FIRST AID)
 BLS PRETEST BASIC LIFE SUPPORT FOR HEALTHCARE PROVIDERS (CREATED BY LAST MINUTE CPR & FIRST AID) 1. THIS BLS FOR HEALTHCARE PROVIDERS COURSE IS GIVEN TO: a. Nurses, Doctors, Paramedics, & Healthcare Workers.
BLS PRETEST BASIC LIFE SUPPORT FOR HEALTHCARE PROVIDERS (CREATED BY LAST MINUTE CPR & FIRST AID) 1. THIS BLS FOR HEALTHCARE PROVIDERS COURSE IS GIVEN TO: a. Nurses, Doctors, Paramedics, & Healthcare Workers.
CPR /AED for Professional Rescuers
 CPR /AED for Professional Rescuers In-Depth Instructor Resource Contents C-A-B (Compression-Airway-Breathing) 1,3... 3 CPR Barriers... 10 Adult CPR 1,3,4... 15 Child CPR 2... 17 Infant CPR 2... 19 Special
CPR /AED for Professional Rescuers In-Depth Instructor Resource Contents C-A-B (Compression-Airway-Breathing) 1,3... 3 CPR Barriers... 10 Adult CPR 1,3,4... 15 Child CPR 2... 17 Infant CPR 2... 19 Special
U.S. ARMY MEDICAL DEPARTMENT CENTER AND SCHOOL FORT SAM HOUSTON, TEXAS 78234-6100 CARDIAC IMPAIRMENT SUBCOURSE MD0571 EDITION 100
 U.S. ARMY MEDICAL DEPARTMENT CENTER AND SCHOOL FORT SAM HOUSTON, TEXAS 78234-6100 CARDIAC IMPAIRMENT SUBCOURSE MD0571 EDITION 100 DEVELOPMENT This subcourse is approved for resident and correspondence
U.S. ARMY MEDICAL DEPARTMENT CENTER AND SCHOOL FORT SAM HOUSTON, TEXAS 78234-6100 CARDIAC IMPAIRMENT SUBCOURSE MD0571 EDITION 100 DEVELOPMENT This subcourse is approved for resident and correspondence
American Red Cross CPR Adult EXAMPLE ANSWER SHEET
 American Red Cross CPR Adult IMPORTANT: Read all instructions before beginning the exam. INSTRUCTIONS: Do not write on this exam. Mark all answers in pencil on the separate answer sheet as directed by
American Red Cross CPR Adult IMPORTANT: Read all instructions before beginning the exam. INSTRUCTIONS: Do not write on this exam. Mark all answers in pencil on the separate answer sheet as directed by
Allina Emergency Medicine Education Healthcare Provider. CPR Study Guide. American Heart Association 2010 Guidelines
 Allina Emergency Medicine Education Healthcare Provider CPR Study Guide American Heart Association 2010 Guidelines The American Heart Association strongly promotes knowledge and proficiency in BLS< ACLS
Allina Emergency Medicine Education Healthcare Provider CPR Study Guide American Heart Association 2010 Guidelines The American Heart Association strongly promotes knowledge and proficiency in BLS< ACLS
Infant CPR Skills Testing Checklist
 Infant CPR Skills Testing Checklist Student Name Date of Test Scenario: While you are pushing a baby in a stroller at the park, you notice something is wrong with the baby. You do not have a phone nearby.
Infant CPR Skills Testing Checklist Student Name Date of Test Scenario: While you are pushing a baby in a stroller at the park, you notice something is wrong with the baby. You do not have a phone nearby.
A Stretch-Break Program for Your Workplace! www.healthyworkplaceweek.ca
 www.healthyworkplaceweek.ca A Stretch-Break Program for Your Workplace! Why is stretching at work important? Sitting at a desk or computer; or standing at your work station for extended periods of time
www.healthyworkplaceweek.ca A Stretch-Break Program for Your Workplace! Why is stretching at work important? Sitting at a desk or computer; or standing at your work station for extended periods of time
Basic life support (BLS) Techniques
 module Basic life support (BLS) Techniques 1 01 04. Basic Cardio Pulmonary Resuscitation (CPR) 08. Adult basic life support sequence, according to European Resuscitation Guidelines 12. Recognition of cardiorespiratory
module Basic life support (BLS) Techniques 1 01 04. Basic Cardio Pulmonary Resuscitation (CPR) 08. Adult basic life support sequence, according to European Resuscitation Guidelines 12. Recognition of cardiorespiratory
Heart Attack: What You Need to Know
 A WorkLife4You Guide Heart Attack: What You Need to Know What is a Heart Attack? The heart works 24 hours a day, pumping oxygen and nutrient-rich blood to the body. Blood is supplied to the heart through
A WorkLife4You Guide Heart Attack: What You Need to Know What is a Heart Attack? The heart works 24 hours a day, pumping oxygen and nutrient-rich blood to the body. Blood is supplied to the heart through
BASIC LIFE SUPPORT REVISED STUDY GUIDE
 BASIC LIFE SUPPORT (Cardiopulmonary Resuscitation) REVISED STUDY GUIDE (2010 AHA Guidelines) NAME INSTRUCTOR COURSE DATE IT IS NOT THE INTENT OF THIS SUPPLEMENTAL INFORMATION PACKET TO REPLACE THE AMERICAN
BASIC LIFE SUPPORT (Cardiopulmonary Resuscitation) REVISED STUDY GUIDE (2010 AHA Guidelines) NAME INSTRUCTOR COURSE DATE IT IS NOT THE INTENT OF THIS SUPPLEMENTAL INFORMATION PACKET TO REPLACE THE AMERICAN
A proper warm-up is important before any athletic performance with the goal of preparing the athlete both mentally and physically for exercise and
 A proper warm-up is important before any athletic performance with the goal of preparing the athlete both mentally and physically for exercise and competition. A warm-up is designed to prepare an athlete
A proper warm-up is important before any athletic performance with the goal of preparing the athlete both mentally and physically for exercise and competition. A warm-up is designed to prepare an athlete
Fact sheet Exercises for older adults undergoing rehabilitation
 Fact sheet Exercises for older adults undergoing rehabilitation Flexibility refers to the amount of movement possible around a joint and is necessary for normal activities of daily living such as stretching,
Fact sheet Exercises for older adults undergoing rehabilitation Flexibility refers to the amount of movement possible around a joint and is necessary for normal activities of daily living such as stretching,
Sheet 1A. Treating short/tight muscles using MET. Pectorals. Upper trapezius. Levator scapula
 Sheet 1A Treating short/tight muscles using MET Pectorals Once daily lie at edge of bed holding a half-kilo can, arm out sideways. Raise arm and hold for 10 seconds, then allow arm to hang down, stretching
Sheet 1A Treating short/tight muscles using MET Pectorals Once daily lie at edge of bed holding a half-kilo can, arm out sideways. Raise arm and hold for 10 seconds, then allow arm to hang down, stretching
CASAID THE AIMS OF FIRST AID, INCIDENT ACTION PLAN, INITIAL ASSESSMENT AND THE RECOVERY POSITION. Airway must be open so oxygen can enter the body.
 CASAID THE AIMS OF FIRST AID, INCIDENT ACTION PLAN, INITIAL ASSESSMENT AND THE RECOVERY POSITION The Aims of First Aid The aims of first aid (the three Ps) are to: Preserve the casualty s life. Prevent
CASAID THE AIMS OF FIRST AID, INCIDENT ACTION PLAN, INITIAL ASSESSMENT AND THE RECOVERY POSITION The Aims of First Aid The aims of first aid (the three Ps) are to: Preserve the casualty s life. Prevent
BLS for Healthcare Providers Study Guide and Pretest
 BLS for Healthcare Providers Study Guide and Pretest Adult CPR 1-Rescuer CPR Sequence check for responsiveness if no response, activate 911 and get the AED open the airway look, listen, & feel for breathing
BLS for Healthcare Providers Study Guide and Pretest Adult CPR 1-Rescuer CPR Sequence check for responsiveness if no response, activate 911 and get the AED open the airway look, listen, & feel for breathing
stretches and exercises
 stretches and exercises The enclosed sheets contain stretches and exercises which can be used to delay and minimise the development of contractures and deformities occurring in children with Duchenne muscular
stretches and exercises The enclosed sheets contain stretches and exercises which can be used to delay and minimise the development of contractures and deformities occurring in children with Duchenne muscular
Pediatric Airway Management
 Pediatric Airway Management Dec 2003 Dr. Shapiro I., PICU Adult Chain of Survival EMS CPR ALS Early Defibrillation Pediatric Chain of Survival Prevention CPR EMS ALS Out-of-Hospital Cardiac Arrest SIDS
Pediatric Airway Management Dec 2003 Dr. Shapiro I., PICU Adult Chain of Survival EMS CPR ALS Early Defibrillation Pediatric Chain of Survival Prevention CPR EMS ALS Out-of-Hospital Cardiac Arrest SIDS
Self- Lymphatic Massage for Arm, Breast or Trunk Lymphedema
 Self- Lymphatic Massage for Arm, Breast or Trunk Lymphedema Patient Education Improving health through education The lymphatic system is part of our circulatory system. It helps balance the fluids of our
Self- Lymphatic Massage for Arm, Breast or Trunk Lymphedema Patient Education Improving health through education The lymphatic system is part of our circulatory system. It helps balance the fluids of our
What to do during... Medical Emergencies
 What to do during... Calling 911 Reacting in an Emergency Performing CPR Providing Rescue Breathing Delivering Abdominal Thrusts Formulating an Emergency Action Plan Assembling Your First Aid Kit Preparing
What to do during... Calling 911 Reacting in an Emergency Performing CPR Providing Rescue Breathing Delivering Abdominal Thrusts Formulating an Emergency Action Plan Assembling Your First Aid Kit Preparing
Armstrong Medical Little Joe. 1 Manikin 1 Red Cross-branded Carrying Case
 Category Ambu CPR Pal Trainer Ambu Multi Man Armstrong Medical Actar D-Fib Armstrong Medical Little Joe Laerdal Little Anne Laerdal Resusci Anne Prestan Professional Adult Manikin Retail Price $257.89/each
Category Ambu CPR Pal Trainer Ambu Multi Man Armstrong Medical Actar D-Fib Armstrong Medical Little Joe Laerdal Little Anne Laerdal Resusci Anne Prestan Professional Adult Manikin Retail Price $257.89/each
Qigong. Ba Duan Jin. The Eight Pieces of Brocade
 Qigong Ba Duan Jin The Eight Pieces of Brocade by Col and g Hamilton Yiheyuan Martial Arts Contents Page Introduction 2 Preparation 2 1. Hold up the Sky 3 2. The Archer 4 3. Join Heaven and Earth 5 4a.
Qigong Ba Duan Jin The Eight Pieces of Brocade by Col and g Hamilton Yiheyuan Martial Arts Contents Page Introduction 2 Preparation 2 1. Hold up the Sky 3 2. The Archer 4 3. Join Heaven and Earth 5 4a.
HELPFUL HINTS FOR A HEALTHY BACK
 HELPFUL HINTS FOR A HEALTHY BACK 1. Standing and Walking For correct posture, balance your head above your shoulders, eyes straight ahead, everything else falls into place. Try to point toes straight ahead
HELPFUL HINTS FOR A HEALTHY BACK 1. Standing and Walking For correct posture, balance your head above your shoulders, eyes straight ahead, everything else falls into place. Try to point toes straight ahead
Functional rehab after breast reconstruction surgery
 Functional rehab after breast reconstruction surgery UHN A guide for women who had DIEP, latissimus dorsi with a tissue expander or implant, or two-stage implant based breast reconstruction surgery Read
Functional rehab after breast reconstruction surgery UHN A guide for women who had DIEP, latissimus dorsi with a tissue expander or implant, or two-stage implant based breast reconstruction surgery Read
General Guidelines. Neck Stretch: Side. Neck Stretch: Forward. Shoulder Rolls. Side Stretch
 Stretching Exercises General Guidelines Perform stretching exercises at least 2 3 days per week and preferably more Hold each stretch for 15 20 seconds Relax and breathe normally Stretching is most effective
Stretching Exercises General Guidelines Perform stretching exercises at least 2 3 days per week and preferably more Hold each stretch for 15 20 seconds Relax and breathe normally Stretching is most effective
First Responder (FR) and Emergency Medical Responder (EMR) Progress Log
 First Responder (FR) and Emergency Medical Responder (EMR) Progress Log Note: Those competencies that are for EMR only are denoted by boldface type. For further details on the National Occupational Competencies
First Responder (FR) and Emergency Medical Responder (EMR) Progress Log Note: Those competencies that are for EMR only are denoted by boldface type. For further details on the National Occupational Competencies
2015 Interim Resources for BLS
 2015 Interim Resources for BLS Original Release: November 25, 2015 Starting in 2016, new versions of American Heart Association online courses will be released to reflect the changes published in the 2015
2015 Interim Resources for BLS Original Release: November 25, 2015 Starting in 2016, new versions of American Heart Association online courses will be released to reflect the changes published in the 2015
CPR for the Professional Rescuer
 American Red Cross Video CPR for the Professional Rescuer As a professional rescuer, you are a key part of the emergency medical service (EMS) system. Whether you are paid or volunteer, in your position
American Red Cross Video CPR for the Professional Rescuer As a professional rescuer, you are a key part of the emergency medical service (EMS) system. Whether you are paid or volunteer, in your position
CHAPTER 1 DISASTER FIRST AID INTRODUCTION
 CHAPTER 1 DISASTER FIRST AID INTRODUCTION This chapter will cover the following topics: Introduction: The basic concepts of providing disaster first aid and the equipment required to safely respond to
CHAPTER 1 DISASTER FIRST AID INTRODUCTION This chapter will cover the following topics: Introduction: The basic concepts of providing disaster first aid and the equipment required to safely respond to
CHAPTER 2 APPROACH TO THE INCIDENT
 CHAPTER 2 APPROACH TO THE INCIDENT Reassuring the casualty is very important in first aid and the best reassurance for both casualty and bystanders is a confident first aider taking decisive action. In
CHAPTER 2 APPROACH TO THE INCIDENT Reassuring the casualty is very important in first aid and the best reassurance for both casualty and bystanders is a confident first aider taking decisive action. In
Functional Firefighter Fitness
 Functional Firefighter Fitness The information provided is for informational purposes only and is not intended as a substitute for the advice of, or treatment that may be prescribed by your physician.
Functional Firefighter Fitness The information provided is for informational purposes only and is not intended as a substitute for the advice of, or treatment that may be prescribed by your physician.
Low Blood Pressure. This reference summary explains low blood pressure and how it can be prevented and controlled.
 Low Blood Pressure Introduction Low blood pressure, or hypotension, is when your blood pressure reading is 90/60 or lower. Some people have low blood pressure all of the time. In other people, blood pressure
Low Blood Pressure Introduction Low blood pressure, or hypotension, is when your blood pressure reading is 90/60 or lower. Some people have low blood pressure all of the time. In other people, blood pressure
Easy Yogic Breathing for a Restful Sleep
 YOGA POSES Enliven your days with the benefits of yoga. Discover physical and breathing poses to complement your mood, calm your mind and achieve balance in your body. Easy Yogic Breathing for a Restful
YOGA POSES Enliven your days with the benefits of yoga. Discover physical and breathing poses to complement your mood, calm your mind and achieve balance in your body. Easy Yogic Breathing for a Restful
Student Workbook. CPR & First Aid. for Childcare Providers. Emergency Response for the School and Childcare Environment.
 Student Workbook CPR & First Aid for Childcare Providers Emergency Response for the School and Childcare Environment 2010 Guidelines Emergency Index 42 65 51 35 28 49 39 7 60 33 35 20 49 43 46 42 24 26
Student Workbook CPR & First Aid for Childcare Providers Emergency Response for the School and Childcare Environment 2010 Guidelines Emergency Index 42 65 51 35 28 49 39 7 60 33 35 20 49 43 46 42 24 26
Lesson 7: Respiratory and Skeletal Systems and Tuberculosis
 Glossary 1. asthma: when the airways of the lungs narrow, making breathing difficult 2. bacteria: tiny living creatures that can only be seen with a microscope; some bacteria help the human body, and other
Glossary 1. asthma: when the airways of the lungs narrow, making breathing difficult 2. bacteria: tiny living creatures that can only be seen with a microscope; some bacteria help the human body, and other
Procedure 17: Cardiopulmonary Resuscitation
 Cardiopulmonary Resuscitation 349 Procedure 17: Cardiopulmonary Resuscitation Introduction Cardiopulmonary arrest (CPA) occurs when a patient s heart and lungs stop functioning. In children, CPA usually
Cardiopulmonary Resuscitation 349 Procedure 17: Cardiopulmonary Resuscitation Introduction Cardiopulmonary arrest (CPA) occurs when a patient s heart and lungs stop functioning. In children, CPA usually
Question-and-Answer Document 2010 AHA Guidelines for CPR & ECC As of October 18, 2010
 Question-and-Answer Document 2010 AHA Guidelines for CPR & ECC As of October 18, 2010 Q: What are the most significant changes in the 2010 AHA Guidelines for CPR & ECC? A: Major changes for all rescuers,
Question-and-Answer Document 2010 AHA Guidelines for CPR & ECC As of October 18, 2010 Q: What are the most significant changes in the 2010 AHA Guidelines for CPR & ECC? A: Major changes for all rescuers,
Spinal Exercise Program/Core Stabilization Program Adapted from The Spine in Sports: Robert G. Watkins
 Spinal Exercise Program/Core Stabilization Program Adapted from The Spine in Sports: Robert G. Watkins Below is a description of a Core Stability Program, designed to improve the strength and coordination
Spinal Exercise Program/Core Stabilization Program Adapted from The Spine in Sports: Robert G. Watkins Below is a description of a Core Stability Program, designed to improve the strength and coordination
Better Breathing with COPD
 Better Breathing with COPD People with Chronic Obstructive Pulmonary Disease (COPD) often benefit from learning different breathing techniques. Pursed Lip Breathing Pursed Lip Breathing (PLB) can be very
Better Breathing with COPD People with Chronic Obstructive Pulmonary Disease (COPD) often benefit from learning different breathing techniques. Pursed Lip Breathing Pursed Lip Breathing (PLB) can be very
Exercise 1: Knee to Chest. Exercise 2: Pelvic Tilt. Exercise 3: Hip Rolling. Starting Position: Lie on your back on a table or firm surface.
 Exercise 1: Knee to Chest Starting Position: Lie on your back on a table or firm surface. Action: Clasp your hands behind the thigh and pull it towards your chest. Keep the opposite leg flat on the surface
Exercise 1: Knee to Chest Starting Position: Lie on your back on a table or firm surface. Action: Clasp your hands behind the thigh and pull it towards your chest. Keep the opposite leg flat on the surface
Kriya for Negative Mind
 Kriya for Negative Mind Bron: The Ten Light Bodies of Conciousness van Nirvair Singh Khalsa So So So So Hung Hung Hung Hung 3 MINUTES. Let s start with this pranayam. It s going to be a 4:4 breathing pattern.
Kriya for Negative Mind Bron: The Ten Light Bodies of Conciousness van Nirvair Singh Khalsa So So So So Hung Hung Hung Hung 3 MINUTES. Let s start with this pranayam. It s going to be a 4:4 breathing pattern.
ADMINISTERING EMERGENCY OXYGEN
 FACT SHEET ADMINISTERING EMERGENCY OXYGEN Emergency oxygen can be given for many breathing and cardiac emergencies. It can help improve hypoxia (insufficient oxygen reaching the cells) and reduce pain
FACT SHEET ADMINISTERING EMERGENCY OXYGEN Emergency oxygen can be given for many breathing and cardiac emergencies. It can help improve hypoxia (insufficient oxygen reaching the cells) and reduce pain
Cardiac Rehab Program: Stretching Exercises
 Cardiac Rehab Program: Stretching Exercises Walk around the room, step side to side, ride a bike or walk on a treadmill for at least 5 minutes to warm up before doing these stretches. Stretch warm muscles
Cardiac Rehab Program: Stretching Exercises Walk around the room, step side to side, ride a bike or walk on a treadmill for at least 5 minutes to warm up before doing these stretches. Stretch warm muscles
MELT Mini Map For Motorcyclists
 MELT Mini Map For Motorcyclists The MELT Self-Treatment Tools needed for this monthʼs Mini Map can be found online at store.meltmethod.com. Depending on which tools you have on hand, you can start with
MELT Mini Map For Motorcyclists The MELT Self-Treatment Tools needed for this monthʼs Mini Map can be found online at store.meltmethod.com. Depending on which tools you have on hand, you can start with
In-hospital resuscitation. Superseded by
 6 In-hospital resuscitation Introduction These guidelines are aimed primarily at healthcare professionals who are first to respond to an in-hospital cardiac arrest and may also be applicable to healthcare
6 In-hospital resuscitation Introduction These guidelines are aimed primarily at healthcare professionals who are first to respond to an in-hospital cardiac arrest and may also be applicable to healthcare
How To Stretch Your Body
 Exercise Module A New Leaf Choices for Healthy Living University of North Carolina at Chapel Hill 2007 Center for Health Promotion and Disease Prevention Physical Activity Exercises for Keeping Active
Exercise Module A New Leaf Choices for Healthy Living University of North Carolina at Chapel Hill 2007 Center for Health Promotion and Disease Prevention Physical Activity Exercises for Keeping Active
GENERAL HEART DISEASE KNOW THE FACTS
 GENERAL HEART DISEASE KNOW THE FACTS WHAT IS Heart disease is a broad term meaning any disease affecting the heart. It is commonly used to refer to coronary heart disease (CHD), a more specific term to
GENERAL HEART DISEASE KNOW THE FACTS WHAT IS Heart disease is a broad term meaning any disease affecting the heart. It is commonly used to refer to coronary heart disease (CHD), a more specific term to
During the breathing exercises, it is important not to use your neck or shoulder muscles. Generally, ten breath cycles per session is adequate.
 Cool-Down Breathing Exercises Overview Breathing exercises help make use of the entire lung and keep the chest muscles active. They allow for more oxygen with each breath and to breathe with less effort.
Cool-Down Breathing Exercises Overview Breathing exercises help make use of the entire lung and keep the chest muscles active. They allow for more oxygen with each breath and to breathe with less effort.
Heart Attack Your quick guide
 Heart Attack Your quick guide Coronary heart disease is the UK s single biggest killer. For over 50 years we ve pioneered research that s transformed the lives of people living with heart and circulatory
Heart Attack Your quick guide Coronary heart disease is the UK s single biggest killer. For over 50 years we ve pioneered research that s transformed the lives of people living with heart and circulatory
Strengthening Exercises - Below Knee Amputation
 Strengthening Exercises - Below Knee Amputation These exercises will help you strengthen your muscles to best use your prosthetic leg. Do these exercises as directed by your therapist or doctor. Do the
Strengthening Exercises - Below Knee Amputation These exercises will help you strengthen your muscles to best use your prosthetic leg. Do these exercises as directed by your therapist or doctor. Do the
Cardiac Rehabilitation
 Cardiac Rehabilitation Introduction Experiencing heart disease should be the beginning of a new, healthier lifestyle. Cardiac rehabilitation helps you in two ways. First, it helps your heart recover through
Cardiac Rehabilitation Introduction Experiencing heart disease should be the beginning of a new, healthier lifestyle. Cardiac rehabilitation helps you in two ways. First, it helps your heart recover through
McMaster Spikeyball Therapy Drills
 BODY BLOCKS In sequencing Breathing and Tempo Flexibility / Mobility and Proprioception (feel) Upper body segment Middle body segment Lower body segment Extension / Static Posture Office / Computer Travel
BODY BLOCKS In sequencing Breathing and Tempo Flexibility / Mobility and Proprioception (feel) Upper body segment Middle body segment Lower body segment Extension / Static Posture Office / Computer Travel
First Aid as a Life Skill. Training Requirements for Quality Provision of Unit Standard-based First Aid Training
 First Aid as a Life Skill Training Requirements for Quality Provision of Unit Standard-based First Aid Training New Zealand Qualifications Authority 2010 2 Index Introduction 3 Section One: Framework outline
First Aid as a Life Skill Training Requirements for Quality Provision of Unit Standard-based First Aid Training New Zealand Qualifications Authority 2010 2 Index Introduction 3 Section One: Framework outline
Self-mobilization methods
 Self-mobilization methods 5 Muscle energy techniques, as outlined in previous chapters, provide us with an excellent series of methods for relaxation and stretching of specific tight, shortened, contracted
Self-mobilization methods 5 Muscle energy techniques, as outlined in previous chapters, provide us with an excellent series of methods for relaxation and stretching of specific tight, shortened, contracted
Emergency procedures instructions to farm staff
 Emergency procedures instructions to farm staff The first priority in the event of an emergency is for the safety of all people present. Emergency phone numbers Dial 111 for Fire/Police/Ambulance 1. Tell
Emergency procedures instructions to farm staff The first priority in the event of an emergency is for the safety of all people present. Emergency phone numbers Dial 111 for Fire/Police/Ambulance 1. Tell
Range of Motion. A guide for you after spinal cord injury. Spinal Cord Injury Rehabilitation Program
 Range of Motion A guide for you after spinal cord injury Spinal Cord Injury Rehabilitation Program This booklet has been written by the health care providers who provide care to people who have a spinal
Range of Motion A guide for you after spinal cord injury Spinal Cord Injury Rehabilitation Program This booklet has been written by the health care providers who provide care to people who have a spinal
Cardiac Catheterization
 Page 1 Cardiac Catheterization What Other Terms Are Used To Describe Cardiac Catheterization? Heart Cath (catheter) Angiogram What Is Cardiac Catheterization? This procedure is nonsurgical and is performed
Page 1 Cardiac Catheterization What Other Terms Are Used To Describe Cardiac Catheterization? Heart Cath (catheter) Angiogram What Is Cardiac Catheterization? This procedure is nonsurgical and is performed
Info. from the nurses of the Medical Service. LOWER BACK PAIN Exercise guide
 Info. from the nurses of the Medical Service LOWER BACK PAIN Exercise guide GS/ME 03/2009 EXERCISE GUIDE One of the core messages for people suffering with lower back pain is to REMAIN ACTIVE. This leaflet
Info. from the nurses of the Medical Service LOWER BACK PAIN Exercise guide GS/ME 03/2009 EXERCISE GUIDE One of the core messages for people suffering with lower back pain is to REMAIN ACTIVE. This leaflet
C-A-B. Compressions: Push hard and fast on the center of. Airway: Tilt the victim s head back and lift the chin to
 Center fr Prfessinal Practice f Nursing CPR Guidelines fr Health-Care Prviders C-A-B Cmpressins: Push hard and fast n the center f the victim s chest Airway: Tilt the victim s head back and lift the chin
Center fr Prfessinal Practice f Nursing CPR Guidelines fr Health-Care Prviders C-A-B Cmpressins: Push hard and fast n the center f the victim s chest Airway: Tilt the victim s head back and lift the chin
Keeping your lungs healthy
 Keeping your lungs healthy A guide for you after spinal cord injury and other neurological conditions Regional Rehabilitation Program This booklet has been written by the health care providers who provide
Keeping your lungs healthy A guide for you after spinal cord injury and other neurological conditions Regional Rehabilitation Program This booklet has been written by the health care providers who provide
FIRST AID HEADQUARTERS, DEPARTMENTS OF THE ARMY, THE NAVY, AND THE AIR FORCE DECEMBER 2002
 FM 4-25.11 (FM 21-11) NTRP 4-02.1 AFMAN 44-163(I) FIRST AID HEADQUARTERS, DEPARTMENTS OF THE ARMY, THE NAVY, AND THE AIR FORCE DECEMBER 2002 DISTRIBUTION RESTRICTION: Approved for public release; distribution
FM 4-25.11 (FM 21-11) NTRP 4-02.1 AFMAN 44-163(I) FIRST AID HEADQUARTERS, DEPARTMENTS OF THE ARMY, THE NAVY, AND THE AIR FORCE DECEMBER 2002 DISTRIBUTION RESTRICTION: Approved for public release; distribution
Lumbar/Core Strength and Stability Exercises
 Athletic Medicine Lumbar/Core Strength and Stability Exercises Introduction Low back pain can be the result of many different things. Pain can be triggered by some combination of overuse, muscle strain,
Athletic Medicine Lumbar/Core Strength and Stability Exercises Introduction Low back pain can be the result of many different things. Pain can be triggered by some combination of overuse, muscle strain,
Heartsaver Pediatric First Aid CPR AED Online Part 1 (90-1434) Frequently Asked Questions (FAQs) As of March 25, 2014
 Heartsaver Pediatric First Aid CPR AED Online Part 1 (90-1434) Frequently Asked Questions (FAQs) As of March 25, 2014 General Information: Q: What is Heartsaver Pediatric First Aid CPR AED Online Part
Heartsaver Pediatric First Aid CPR AED Online Part 1 (90-1434) Frequently Asked Questions (FAQs) As of March 25, 2014 General Information: Q: What is Heartsaver Pediatric First Aid CPR AED Online Part
Clinical Care Program
 Clinical Care Program Therapy for the Cardiac Patient What s CHF? Not a kind of heart disease o Heart disease is called cardiomyopathy o Heart failure occurs when the heart can t pump enough blood to meet
Clinical Care Program Therapy for the Cardiac Patient What s CHF? Not a kind of heart disease o Heart disease is called cardiomyopathy o Heart failure occurs when the heart can t pump enough blood to meet
Shoulders (free weights)
 Dumbbell Shoulder Raise Dumbbell Shoulder Raise 1) Lie back onto an incline bench (45 or less) with a DB in each hand. (You may rest each DB on the corresponding thigh.) 2) Start position: Bring the DB
Dumbbell Shoulder Raise Dumbbell Shoulder Raise 1) Lie back onto an incline bench (45 or less) with a DB in each hand. (You may rest each DB on the corresponding thigh.) 2) Start position: Bring the DB
Ho Sin Sul. Defense against wrist grabs:
 Ho Sin Sul Ho Sin Sul are ways to escape from attackers who grab, choke or attempt some other form of assault, especially one where they get hold of your body or clothes. While these moves are a memorized
Ho Sin Sul Ho Sin Sul are ways to escape from attackers who grab, choke or attempt some other form of assault, especially one where they get hold of your body or clothes. While these moves are a memorized
Rehabilitation after shoulder dislocation
 Physiotherapy Department Rehabilitation after shoulder dislocation Information for patients This information leaflet gives you advice on rehabilitation after your shoulder dislocation. It is not a substitute
Physiotherapy Department Rehabilitation after shoulder dislocation Information for patients This information leaflet gives you advice on rehabilitation after your shoulder dislocation. It is not a substitute
MEASURING AND RECORDING BLOOD PRESSURE
 MEASURING AND RECORDING BLOOD PRESSURE INTRODUCTION The blood pressure, along with the body temperature, pulse, and respirations, is one of the vital signs. These measurements are used to quickly, easily,
MEASURING AND RECORDING BLOOD PRESSURE INTRODUCTION The blood pressure, along with the body temperature, pulse, and respirations, is one of the vital signs. These measurements are used to quickly, easily,
Range of Motion Exercises
 Range of Motion Exercises Range of motion (ROM) exercises are done to preserve flexibility and mobility of the joints on which they are performed. These exercises reduce stiffness and will prevent or at
Range of Motion Exercises Range of motion (ROM) exercises are done to preserve flexibility and mobility of the joints on which they are performed. These exercises reduce stiffness and will prevent or at
BREATHE BETTER SWIM FASTER
 BREATHE BETTER SWIM FASTER Breath control is fundamental to efficient swimming. Like singers, swimmers need to train their breathing for effective performance. Controlled breathing is the main factor contributing
BREATHE BETTER SWIM FASTER Breath control is fundamental to efficient swimming. Like singers, swimmers need to train their breathing for effective performance. Controlled breathing is the main factor contributing
How to Do Self Lymphatic Massage on your Upper Body
 How to Do Self Lymphatic Massage on your Upper Body UHN For patients who were treated for breast cancer on one side of their body. For example: Lumpectomy Mastectomy Lymph node removal from an underarm
How to Do Self Lymphatic Massage on your Upper Body UHN For patients who were treated for breast cancer on one side of their body. For example: Lumpectomy Mastectomy Lymph node removal from an underarm
Tired, Aching Legs? Swollen Ankles? Varicose Veins?
 Tired, Aching Legs? Swollen Ankles? Varicose Veins? Healthy Legs 2006 http://healthylegs.com Page 1 Venous disorders are widespread Leg problems are widespread throughout the world, but what most people
Tired, Aching Legs? Swollen Ankles? Varicose Veins? Healthy Legs 2006 http://healthylegs.com Page 1 Venous disorders are widespread Leg problems are widespread throughout the world, but what most people
Training Manikin Requirements for American Red Cross Certification Courses
 Training Manikin Requirements for American Red Cross Certification Courses Introduction We are pleased to announce the release of the requirements for training manikins. These requirements apply to all
Training Manikin Requirements for American Red Cross Certification Courses Introduction We are pleased to announce the release of the requirements for training manikins. These requirements apply to all
EXERCISE INSTRUCTIONS 1
 EXERCISE INSTRUCTIONS 1 Contents ANKLE TOUCHES... 4 BACK EXTENSIONS... 4 BACK REVERSE FLYES... 4 BALL ROLL... 4 BASKETBALL SQUATS... 4 BEAR CRAWL... 4 BICEP CURL (Resistance Band)... 4 BOXING JABS... 5
EXERCISE INSTRUCTIONS 1 Contents ANKLE TOUCHES... 4 BACK EXTENSIONS... 4 BACK REVERSE FLYES... 4 BALL ROLL... 4 BASKETBALL SQUATS... 4 BEAR CRAWL... 4 BICEP CURL (Resistance Band)... 4 BOXING JABS... 5
Passive Range of Motion Exercises
 Exercise and ALS The physical or occupational therapist will make recommendations for exercise based upon each patient s specific needs and abilities. Strengthening exercises are not generally recommended
Exercise and ALS The physical or occupational therapist will make recommendations for exercise based upon each patient s specific needs and abilities. Strengthening exercises are not generally recommended
Fainting - Syncope. This reference summary explains fainting. It discusses the causes and treatment options for the condition.
 Fainting - Syncope Introduction Fainting, also known as syncope, is a temporary loss of consciousness. It is caused by a drop in blood flow to the brain. You may feel dizzy, lightheaded or nauseous before
Fainting - Syncope Introduction Fainting, also known as syncope, is a temporary loss of consciousness. It is caused by a drop in blood flow to the brain. You may feel dizzy, lightheaded or nauseous before
Low Back Pain: Exercises
 Low Back Pain: Exercises Your Kaiser Permanente Care Instructions Here are some examples of typical rehabilitation exercises for your condition. Start each exercise slowly. Ease off the exercise if you
Low Back Pain: Exercises Your Kaiser Permanente Care Instructions Here are some examples of typical rehabilitation exercises for your condition. Start each exercise slowly. Ease off the exercise if you
Don t. Hamstrings. Calf Muscles. both legs 2-3 times. stretch is felt in the back of the calf. Repeat with both legs 2-3 times.
 Remember to: Warm-up your muscles first before stretching (e.g. stretch after walking). Stretch until you feel mild discomfort, not pain. Never bounce or force a stretch. Hold the stretch for 10-30 seconds
Remember to: Warm-up your muscles first before stretching (e.g. stretch after walking). Stretch until you feel mild discomfort, not pain. Never bounce or force a stretch. Hold the stretch for 10-30 seconds
Stretching in the Office
 Stretching in the Office Legs: Quads, Hamstrings, IT band, Hip flexors, Gluts, Calves Quads: Standing @ desk maintaining upright posture, grab one leg @ a time by foot or ankle and bring it towards backside
Stretching in the Office Legs: Quads, Hamstrings, IT band, Hip flexors, Gluts, Calves Quads: Standing @ desk maintaining upright posture, grab one leg @ a time by foot or ankle and bring it towards backside
INTRODUCTION TO POSITIONING. MODULE 3: Positioning and Carrying
 MODULE 3: Positioning and Carrying Blankets, pillows and towels, sandbags, carpet on the floor, a doll with floppy limbs that can be positioned i.e. not a hard plastic doll, display materials. Icebreaker
MODULE 3: Positioning and Carrying Blankets, pillows and towels, sandbags, carpet on the floor, a doll with floppy limbs that can be positioned i.e. not a hard plastic doll, display materials. Icebreaker
12 Week Do-it-Yourself Fitness Program
 12 Week Do-it-Yourself Fitness Program Created by Brad Awalt, MS, ACSM Assistant Manager, Health Plus brad.awalt@vanderbilt.edu January 2011 Do you have a goal to begin an exercise routine, but not sure
12 Week Do-it-Yourself Fitness Program Created by Brad Awalt, MS, ACSM Assistant Manager, Health Plus brad.awalt@vanderbilt.edu January 2011 Do you have a goal to begin an exercise routine, but not sure
Routine For: OT - General Guidelines/Energy Conservation (Caregiver)
 GENERAL GUIDELINES - 9 Tips for Exercise: Body Mechanics for Helper - To protect back, stay as upright as possible and keep head in line with trunk. - Always position yourself as close as possible to the
GENERAL GUIDELINES - 9 Tips for Exercise: Body Mechanics for Helper - To protect back, stay as upright as possible and keep head in line with trunk. - Always position yourself as close as possible to the
ROTATOR CUFF HOME EXERCISE PROGRAM
 ROTATOR CUFF HOME EXERCISE PROGRAM Contact us! Vanderbilt Sports Medicine Medical Center East, South Tower, Suite 3200 1215 21st Avenue South Nashville, TN 37232-8828 For more information on this and other
ROTATOR CUFF HOME EXERCISE PROGRAM Contact us! Vanderbilt Sports Medicine Medical Center East, South Tower, Suite 3200 1215 21st Avenue South Nashville, TN 37232-8828 For more information on this and other
No Equipment Agility/Core/Strength Program for Full Body No Equip Trainer: Rick Coe
 No Equipment Agility/Core/Strength Program for Full Body No Equip Trainer: Rick Coe Introduction Program designed to be performed in a circuit. Perform exercises in sequence without rest 2-3 times. Increase
No Equipment Agility/Core/Strength Program for Full Body No Equip Trainer: Rick Coe Introduction Program designed to be performed in a circuit. Perform exercises in sequence without rest 2-3 times. Increase
