Prostate cancer. A guide for men who ve just been diagnosed
|
|
|
- Valentine Eric Simpson
- 8 years ago
- Views:
Transcription
1 Prostate cancer A guide for men who ve just been diagnosed
2 2 Prostate cancer A guide for men who ve just been diagnosed About this booklet This booklet is for men who ve recently been diagnosed with prostate cancer. Your partner, family and friends might also find it useful. We explain what prostate cancer is, the tests you may have to diagnose it, and the treatment options available. You can use this booklet as your personal guide. The blue shaded areas towards the back are for you to write down any contact details and information that might be helpful to you. There s also information about support to help you deal with the impact of cancer. Each hospital will do things slightly differently, so use this booklet as a guide to what to expect. Ask your doctor or nurse for more details about your care and the support available to you. You can also speak to our Specialist Nurses, in confidence, on The following symbols appear throughout the booklet to guide you to sources of further information: Prostate Cancer UK Specialist Nurses Prostate Cancer UK publications Sections for you to fill in Watch men tell their own stories in our online videos:
3 Specialist Nurses Contents About this booklet... 2 What is the prostate?... 5 What is prostate cancer?... 6 How is prostate cancer diagnosed?...8 What do my test results mean?...11 What are my treatment options?...17 Choosing a treatment...19 Dealing with prostate cancer...31 List of medical words...37 More information from us...46 Other useful organisations About Prostate Cancer UK...50 Sections for you to fill in What are my test results? Who are my team members? Appointment diary... 44
4 4 Prostate cancer A guide for men who ve just been diagnosed What is the prostate? Only men have a prostate. The prostate is usually the size and shape of a walnut. It sits underneath the bladder and surrounds the urethra, which is the tube men urinate (pee) and ejaculate through. The prostate is a gland. Its main job is to make some of the semen the fluid that carries sperm. bladder urethra penis prostate gland testicle
5 Specialist Nurses
6 6 Prostate cancer A guide for men who ve just been diagnosed What is prostate cancer? Normally the growth of all cells is carefully controlled in the body. As cells die, they are replaced in an orderly fashion. Cancer can develop when cells start to grow in an uncontrolled way. If this happens in the prostate, then prostate cancer can develop. Normal cells Cancer cells growing in an uncontrolled way Prostate cancer is the most common cancer in men in the UK. Prostate cancer can grow slowly or very quickly. Most prostate cancer is slow-growing to start with and may never cause any symptoms or problems in a man s lifetime. But some men will have cancer that s more aggressive or high risk, which means it s more likely to spread and cause problems. This needs treatment to help prevent or delay it spreading outside the prostate.
7 Specialist Nurses Some men may have symptoms, such as problems going for a pee (urinating). For others, the first noticeable symptoms are from prostate cancer which has spread to their bones. If this happens, you might notice pain in your back, hips or pelvis, that wasn t there before. In the UK, about 1 in 8 men will get prostate cancer at some point in their lives. The following things might mean you re more likely to get prostate cancer. Age prostate cancer mainly affects men over the age of 50, and your risk increases with age. Family history you are two and a half times more likely to get prostate cancer if your father or brother has been diagnosed with it, compared with a man who has no relatives with prostate cancer. There is a higher chance of developing it if your relative was under 60 when he was diagnosed, or if you have more than one close relative with prostate cancer. Ethnicity Black men are more likely to get prostate cancer than men of other ethnic backgrounds. In the UK, about 1 in 4 Black men will get prostate cancer at some point in their lives. Lifestyle no one knows how to prevent prostate cancer, but a healthy diet and lifestyle may be important in protecting against it. For more information about your risk of prostate cancer, read our booklet, Know your prostate: A guide to common prostate problems.
8 8 Prostate cancer A guide for men who ve just been diagnosed How is prostate cancer diagnosed? Prostate cancer is diagnosed using a number of tests, which we describe on the following pages. You might have already had some of these, but you may need further tests to find out whether the cancer has spread and how aggressive it is. You may not need to have all of the tests described here, and you might not have them in this order. Read more about these tests in our Tool Kit fact sheet, How prostate cancer is diagnosed. PSA test The PSA test is a blood test that measures the amount of prostate specific antigen (PSA) in your blood. PSA is a protein produced by normal cells in the prostate and also by prostate cancer cells. It s normal for all men to have a small amount of PSA in their blood. A raised PSA may show that you have a problem with your prostate, but not necessarily cancer (see page 11). Read more in our booklet, Understanding the PSA test: A guide for men concerned about prostate cancer. Digital rectal examination (DRE) This is where the doctor feels your prostate through the wall of the back passage (rectum). They ll wear gloves and put some gel onto their finger to make it more comfortable. They ll feel your prostate for any hard or irregular areas and to get an idea of its size.
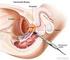
9 Specialist Nurses Prostate biopsy A prostate biopsy involves using thin needles to take small samples of tissue from the prostate to see if there is any prostate cancer. The doctor will put an ultrasound probe into your back passage, using a gel to make it more comfortable. The ultrasound probe scans the prostate and an image appears on a screen. A needle is then inserted through the wall of the back passage into the prostate, using the ultrasound image as a guide. Sometimes the biopsy is done by inserting the needles through the skin between the testicles and the back passage (perineum). The biopsy samples will be looked at under a microscope to check for any cancer cells. Your doctor will be sent a report, called a pathology report, with the results. The results will show: whether any cancer was found how many biopsy samples contained cancer how much cancer is present in each sample. You might be sent a copy of the pathology report. If you have trouble understanding any of it, ask your doctor to explain it. Or call our Specialist Nurses.
10 10 Prostate cancer A guide for men who ve just been diagnosed You may have the following tests to find out whether the cancer has spread outside the prostate. MRI scan MRI (magnetic resonance imaging) uses magnets to create a detailed picture of your prostate and the surrounding tissues, to see whether the cancer has spread. An MRI scan is often the first type of scan used as it s the most accurate way of looking at the prostate. CT scan A CT (computerised tomography) scan can also show whether the cancer has spread beyond the prostate, for instance to the lymph nodes. Lymph nodes are part of your immune system and are found throughout your body. Bone scan A bone scan can show whether any cancer cells have spread to the bone. A small amount of a safe radioactive dye is injected into a vein in your arm, and you ll have the scan two to three hours later. If there is any cancer in the bones, the dye will collect in these areas and show up on the scan.
11 Specialist Nurses What do my test results mean? Your doctor will use the results of all the tests you ve had to find out if the cancer has spread and if it s growing and how quickly. Ask your doctor to explain your test results if you don t understand them. PSA level The PSA test alone can t tell you whether you have prostate cancer. A raised PSA may show that you have a problem with your prostate, but not necessarily cancer. This is because a number of things can cause your PSA level to rise including age and an enlarged prostate as well as prostate cancer. Your PSA level rises as you get older and the prostate gets bigger. The following figures are a very rough guide to normal PSA levels, depending on your age: up to 3ng/ml for men in their 50s up to 4ng/ml for men in their 60s up to 5ng/ml for men in their 70s and over. Some men with a normal PSA level can have prostate cancer. A very high PSA level (for example, in the hundreds or thousands) normally means that a man has prostate cancer. The PSA test is also a good way of monitoring your prostate cancer after you ve been diagnosed or had treatment. You will have regular PSA tests as part of your care, and they can be used alongside other test results.
12 12 Prostate cancer A guide for men who ve just been diagnosed Gleason grade and Gleason score You may hear your doctor talk about your Gleason grade and your Gleason score when they ve looked at your biopsy results. Gleason grade If there are prostate cancer cells in your biopsy samples, they are given a Gleason grade. This grade tells you how aggressive the cancer is in other words, how likely it is to grow and spread outside the prostate. When cancer cells are looked at under the microscope, they have different patterns, depending on how quickly they re likely to grow. The pattern is given a grade from 1 to 5. This is called the Gleason grade. If a grade is given, it will usually be 3 or higher, as grade 1 and 2 are not cancer. Gleason score There may be more than one grade of cancer in the biopsy samples. An overall Gleason score is worked out by adding together two Gleason grades. The first is the most common grade in all the samples. The second is the highest grade of what s left. When the most common and the highest grade are added together, the total is called the Gleason score. Gleason score = the most common grade + the highest other grade in the samples
13 Specialist Nurses For example, if the biopsy samples show that: most of the cancer seen is grade 3 and the highest grade of any other cancer seen is grade 4, then the Gleason score will be 7 (3+4). Because grade 1 and 2 are not cancer, the combined Gleason score is normally 6 or higher. So your Gleason score will normally only be between 6 (3+3) and 10 (5+5). Some men will only be told their total Gleason score and not given their Gleason grades. What does the Gleason score mean? The higher the Gleason score, the more aggressive the cancer, and the more likely it is to spread. A Gleason score of 6 usually suggests that the cancer is slow-growing. A Gleason score of 7 suggests that the cancer may grow at a moderate rate. A Gleason score of 8, 9 or 10 suggests that the cancer may grow more quickly.
14 14 Prostate cancer A guide for men who ve just been diagnosed Staging Staging is a way of recording how far the cancer has spread. The most common method is the TNM (Tumour-Nodes- Metastases) system. T stage (tumour) The T stage shows how far the cancer has spread in and around the prostate. This is measured with a DRE (see page 8). You might also have an MRI scan to confirm your T stage. seminal vesicle bladder T1 The cancer can t be felt or seen on scans, and can only be seen under a microscope localised prostate cancer. prostate gland T1 prostate cancer seminal vesicle bladder T2 The cancer can be felt or seen on scans but it is contained within the prostate localised prostate cancer. prostate gland T2 prostate cancer
15 Specialist Nurses bladder T3 The cancer can be felt or seen breaking through the capsule of the prostate locally advanced prostate cancer. seminal vesicle prostate gland T3a prostate cancer T3a The cancer has broken through the capsule of the prostate but has not spread to the seminal vesicles (which produce some of the fluid in semen). T3b The cancer has spread to the seminal vesicles. seminal vesicle prostate gland bladder bladder neck T4 prostate cancer T4 The cancer has spread to nearby organs, such as the neck of the bladder, back passage, pelvic wall or lymph nodes locally advanced prostate cancer.
16 16 Prostate cancer A guide for men who ve just been diagnosed N stage (node) The N stage shows whether the cancer has spread to the nearby lymph nodes. Lymph nodes are part of your immune system and are found throughout your body. The lymph nodes in your groin are near the prostate and are a common place for prostate cancer to spread to. The N stage is measured using an MRI or CT scan (see page 10). This stage will only be measured if the result is likely to affect your treatment options. NX The lymph nodes were not measured. N0 No cancer cells can be seen in the lymph nodes. N1 The lymph nodes contain cancer cells. M stage (metastases) The M stage shows whether the cancer has spread (metastasised) to other parts of the body, such as the bones. This is measured using a bone scan (see page 10). Cancer that has spread to other parts of your body is called advanced prostate cancer. This stage might not be measured if the result is unlikely to affect your treatment options. MX The spread of the cancer was not measured. M0 The cancer has not spread to other parts of the body. M1 The cancer has spread to other parts of the body. Read more about how the stage of prostate cancer is measured in our Tool Kit fact sheet, How prostate cancer is diagnosed. You can record your test results on page 39.
17 Specialist Nurses What are my treatment options? Your doctor will look at all your test results to get an overall idea of how far the cancer has spread (its stage) and how quickly it may be growing. This will help you and your doctor to discuss the best possible treatments. There are different treatment options for each stage of prostate cancer. If you have localised cancer, treatments are aimed at getting rid of it completely. And even with more advanced cancer which has spread, treatments can keep it under control, sometimes for several years. Read more about treatment options on page 21. Stages of prostate cancer Localised prostate cancer Localised prostate cancer is cancer that s contained within the prostate. You may also hear it called early prostate cancer. Many localised cancers are not aggressive and grow too slowly to cause any problems in your lifetime. But, some may grow more quickly and spread to other parts of the body. There are a number of treatments for localised prostate cancer, and there is no best treatment each one has its own pros and cons. Thinking about these will help you decide which treatment is best for you. Read more in our Tool Kit fact sheet, Localised prostate cancer.
18 18 Prostate cancer A guide for men who ve just been diagnosed Locally advanced prostate cancer Locally advanced prostate cancer is cancer that s starting to break out of the prostate, or has spread to the area just outside it. It can spread to the seminal vesicles, the neck of the bladder, back passage, pelvic wall or lymph nodes in the groin. Your treatment options will depend on how far the cancer has spread. Read more in our Tool Kit fact sheet, Locally advanced prostate cancer. Advanced prostate cancer Advanced prostate cancer is cancer that has spread from the prostate to other parts of the body. It s also called metastatic prostate cancer. Prostate cancer can spread to any part of the body, but it most commonly spreads to the bones and lymph nodes. Advanced prostate cancer can cause symptoms such as bone pain and problems urinating. There are treatments available to help manage these symptoms. It s not possible to cure advanced prostate cancer, but treatments can keep it under control, sometimes for several years. Read more in our Tool Kit fact sheet, Advanced prostate cancer.
19 Specialist Nurses Choosing a treatment Your doctor or nurse will talk you through your treatment options so that you have the information you need to choose the right treatment for you. On the next few pages you ll find a summary of the different treatment options. Some of the treatments listed here might not be suitable for you, so ask your doctor or nurse to mark the treatments that are suitable. Read more about all these treatments and their pros and cons in our Tool Kit fact sheets. You can download or order them from our website at /publications or call our Specialist Nurses. What will affect my treatment choice? Which treatment you choose may depend on several things, including: how far the cancer has spread (its stage), and how quickly it may be growing your age and general health for example, if you have any other health problems such as heart disease what each treatment involves the possible side effects of each treatment the pros and cons of each treatment, including practical things like how often you would need to go to hospital, or how far away your nearest hospital is your own thoughts and feelings about different treatments for example some men prefer to have their prostate removed, while others don t like the idea of surgery how the treatment you choose now would affect your treatment options later if your cancer comes back or spreads.
20 20 Prostate cancer A guide for men who ve just been diagnosed Each treatment has side effects. These will affect each man differently, and you might not get all the possible side effects. It s important that you think about the side effects and how you would cope with them when deciding on a treatment. We ve included some information about side effects here. You can find more detailed information in our Tool Kit fact sheets. The first treatment you have may affect which treatments you can have in the future, if you need further treatment. For example, surgery is usually not an option if you ve already had radiotherapy. Read more about this for each treatment below and speak to your doctor or nurse about this. The different treatment options can be a lot to take in, especially when you ve just been diagnosed with prostate cancer. Make sure you have all the information you need, and give yourself time to think about which treatment is right for you. Your doctor or nurse will be able to help you weigh up the pros and cons. It can be a good idea to write down any questions you might want to ask at your next appointment. And you might find it useful to have someone with you at the appointment, or to make notes to help you remember what was said. What are my treatment options? The following information describes treatments for men who have just been diagnosed with prostate cancer. Men who ve had prostate cancer for some time may have different treatments and combinations of treatment. Speak to your doctor or nurse about what treatments are suitable for you. Watch men share their stories about treatments.
21 Specialist Nurses Treatment options Localised prostate cancer Surgery (radical prostatectomy) External beam radiotherapy (EBRT) Brachytherapy (either permanent seed or temporary) Active surveillance Watchful waiting High intensity focused ultrasound (in specialist centres or as part of a clinical trial) Cryotherapy (in specialist centres or as part of a clinical trial) Locally advanced prostate cancer External beam radiotherapy with hormone therapy (and sometimes with temporary brachytherapy) Hormone therapy Watchful waiting Less commonly, surgery (radical prostatectomy) with hormone therapy and/or external beam radiotherapy Advanced prostate cancer Hormone therapy Chemotherapy Pain-relieving drugs to treat pain Radiotherapy to treat symptoms Bisphosphonates to treat bone pain
22 22 Prostate cancer A guide for men who ve just been diagnosed Surgery (radical prostatectomy) This is an operation to remove the prostate and the cancer inside it. There are several types of operation: open surgery keyhole (laparoscopic) surgery robot-assisted laparoscopic surgery. Surgery is usually only suitable for men with localised prostate cancer. In men with more aggressive cancer (with higher Gleason score), the lymph nodes around the prostate are also often removed. Surgery may also be an option for some men with locally advanced prostate cancer. This can only be used in some situations as it might not be possible to remove all the cancer cells that have spread outside the prostate. In this situation, further treatment, such as radiotherapy, may also be needed afterwards. You might be offered surgery for locally advanced prostate cancer as part of a clinical trial. After surgery, if your cancer spreads outside the prostate or comes back, you will be offered a course of radiotherapy or hormone therapy. Some men have side effects after surgery. The most common side effects are leaking urine, and difficulty getting and keeping an erection (erectile dysfunction). Side effects may improve over time, and there are treatments available to help manage them. The prostate and seminal vesicles are removed during the operation. This means that you won t be able to ejaculate any semen even if you can get an erection so you will be infertile and won t be able to have children.
23 Specialist Nurses If you re planning on having children, you may be able to store your sperm before the operation for use in IVF (in vitro fertilisation). Read more about surgery, including the side effects, in our Tool Kit fact sheet, Surgery: radical prostatectomy. External beam radiotherapy (EBRT) This treatment uses high energy X-ray beams to destroy the cancer cells from outside the body. EBRT is suitable for men with localised prostate cancer, who will often have it with hormone therapy. It s also suitable for men with locally advanced prostate cancer, and is used with hormone therapy. If you have EBRT as a first treatment for prostate cancer and your cancer comes back or spreads, you may be offered high intensity focused ultrasound (HIFU), cryotherapy or hormone therapy. Surgery is rarely an option because radiotherapy changes the prostate tissue and makes it very hard for the surgeon to remove the prostate. Some men have side effects from EBRT these include problems urinating, bowel problems such as loose or watery bowel movements (diarrhoea), problems getting and keeping an erection, and tiredness (fatigue). Side effects can develop during treatment and get better with time. But for some men they can be long-term and may develop several months or years after having radiotherapy. There are treatments available to help manage side effects. Read more about EBRT, including the side effects, in our Tool Kit fact sheet, External beam radiotherapy.
24 24 Prostate cancer A guide for men who ve just been diagnosed Brachytherapy This treatment involves putting radioactive seeds or pellets into the prostate to kill the cancer cells. There are two types of brachytherapy permanent seed brachytherapy and temporary brachytherapy. Permanent seed brachytherapy, also called low dose-rate brachytherapy, involves implanting tiny radioactive seeds into the prostate. This is an option for men with localised prostate cancer. Temporary brachytherapy, also called high dose-rate brachytherapy, is where radioactive pellets are passed into the prostate for a few minutes at a time before being removed. This treatment is less common and can be used to treat localised prostate cancer, and sometimes locally advanced prostate cancer. Brachytherapy can be used together with EBRT to give higher doses of radiation to the whole gland, as well as the area just outside it. You might have hormone therapy to shrink the prostate for a few months before starting brachytherapy. If you have brachytherapy as a first treatment for prostate cancer and your cancer comes back or spreads, you may be offered cryotherapy or hormone therapy. However, you are unlikely to be able to have high intensity focused ultrasound (HIFU) or surgery. Some men may have side effects after brachytherapy including problems urinating, problems getting and keeping an erection, and tiredness (fatigue). Men who have permanent seed brachytherapy may also get bowel problems, although these tend to be mild. Problems urinating usually start to improve after a few months. Erection problems may not happen straight after treatment but can develop over several years. There are treatments available to help manage these side effects.
25 Specialist Nurses Read more about brachytherapy, including the side effects, in our Tool Kit fact sheets, Permanent seed brachytherapy and Temporary brachytherapy. Active surveillance Active surveillance is a way of monitoring slow-growing prostate cancer. The aim is to avoid or delay unnecessary treatment in men with low risk localised prostate cancer and so avoid or delay the side effects that can be caused by treatment. Active surveillance involves monitoring your cancer with regular tests, rather than treating it straight away. The tests aim to find any changes that suggest the cancer is growing. If the tests show that your cancer might be growing, you will be offered treatment with surgery (radical prostatectomy), radiotherapy or brachytherapy, with the aim of getting rid of the cancer completely. Read more in our Tool Kit fact sheet, Active surveillance. Watchful waiting Watchful waiting is a different way of monitoring prostate cancer that isn t causing any symptoms or problems. The aim is to keep an eye on the cancer over the long term. You will only start treatment if you get symptoms, such as problems urinating or bone pain. You will then be offered hormone therapy (see page 26) to manage these symptoms. Watchful waiting involves having fewer tests than active surveillance.
26 26 Prostate cancer A guide for men who ve just been diagnosed It s generally suitable for men who have other health problems and may not be fit enough for treatments such as surgery or radiotherapy. It might also be suitable if your prostate cancer isn t likely to cause problems during your lifetime, or shorten your life. Read more in our Tool Kit fact sheet, Watchful waiting. If you re offered active surveillance or watchful waiting, make sure you re clear which one your doctor is talking about. They are quite different approaches to treatment. These terms aren t always used in the same way, and some doctors use different terms such as active monitoring and wait and see. Ask your doctor to explain exactly what they mean. Hormone therapy Prostate cancer needs the male hormone testosterone to grow. Hormone therapy works by stopping testosterone from reaching prostate cancer cells. It will treat all prostate cancer cells, wherever they are in the body. Hormone therapy won t cure prostate cancer, but it can keep the cancer under control, sometimes for several years. Hormone therapy is often used with EBRT for localised prostate cancer. It can also be used with EBRT for locally advanced prostate cancer. It s the standard treatment for advanced prostate cancer. There are three main types of hormone therapy for prostate cancer: injections or implants to stop the production of testosterone surgery (orchidectomy) to remove the testicles or just the parts that make testosterone tablets to block the effects of testosterone.
27 Specialist Nurses The side effects of hormone therapy are caused by lowered testosterone levels. They can include: hot flushes loss of sex drive and problems getting and keeping an erection tiredness (fatigue) swelling and tenderness in the breast area (gynaecomastia) weight gain. The chances of getting each side effect depend on which type of hormone therapy you re having and how long you have it for. There are ways to manage them. Read more about hormone therapy, including the side effects, in our Tool Kit fact sheet, Hormone therapy, and our booklet, Living with hormone therapy: A guide for men with prostate cancer. High intensity focused ultrasound (HIFU) HIFU uses ultrasound to heat and destroy cancer cells in the prostate. HIFU is newer than some of the other treatments for prostate cancer, so we don t know as much about how well it works and the risk of side effects in the long term. Because of this, it s only available in specialist centres in the UK or as part of a clinical trial. HIFU might be a suitable option if you have localised prostate cancer. It can also be used to treat cancer that has started to grow again after radiotherapy. If you have HIFU as a first treatment for prostate cancer and your cancer comes back or spreads, you may be offered more HIFU, EBRT, cryotherapy or hormone therapy. However, you re unlikely to be able to have surgery.
28 28 Prostate cancer A guide for men who ve just been diagnosed You might have side effects after HIFU including problems urinating and difficulty getting and keeping an erection. Some men get a burning sensation or bleeding from the back passage. There are treatments available to help manage these side effects. Read more about HIFU, including the side effects, in our Tool Kit fact sheet, High intensity focused ultrasound (HIFU). Cryotherapy Cryotherapy uses freezing and thawing to destroy the prostate cancer cells. It s newer than some of the other treatments for prostate cancer, so we don t know as much about how well it works and the risk of side effects in the long term. Because of this, it s only available in specialist centres in the UK or as part of a clinical trial. Cryotherapy can be used to treat localised prostate cancer, and occasionally locally advanced prostate cancer. However, it s more often used to treat men whose cancer has come back after treatment with radiotherapy or brachytherapy. If your cancer comes back or spreads after cryotherapy, you may be offered more cryotherapy, EBRT, or hormone therapy. However, you re unlikely to be offered surgery. Some men have side effects after cryotherapy. The most common side effect is problems getting and keeping an erection. Some men also get urinary problems after cryotherapy. These side effects may improve over time, and there are ways to manage them. Read more about cryotherapy, including the side effects, in our Tool Kit fact sheet, Cryotherapy.
Locally advanced prostate cancer
 Diagnosis Specialist Nurses 0800 074 8383 prostatecanceruk.org 1 Locally advanced prostate cancer In this fact sheet: What is locally advanced prostate cancer? How is locally advanced prostate cancer diagnosed?
Diagnosis Specialist Nurses 0800 074 8383 prostatecanceruk.org 1 Locally advanced prostate cancer In this fact sheet: What is locally advanced prostate cancer? How is locally advanced prostate cancer diagnosed?
Localised prostate cancer
 Diagnosis Specialist Nurses 0800 074 8383 prostatecanceruk.org 1 Localised prostate cancer In this fact sheet: What is localised prostate cancer? How is localised prostate cancer diagnosed? What do my
Diagnosis Specialist Nurses 0800 074 8383 prostatecanceruk.org 1 Localised prostate cancer In this fact sheet: What is localised prostate cancer? How is localised prostate cancer diagnosed? What do my
Prostate cancer A guide for newly diagnosed men
 Prostate cancer A guide for newly diagnosed men 2 Prostate cancer A guide for newly diagnosed men About this booklet This booklet is for men who have recently been diagnosed with prostate cancer. It is
Prostate cancer A guide for newly diagnosed men 2 Prostate cancer A guide for newly diagnosed men About this booklet This booklet is for men who have recently been diagnosed with prostate cancer. It is
Recurrent prostate cancer A guide to treatment and support
 Recurrent prostate cancer A guide to treatment and support 2 Recurrent prostate cancer About this booklet This booklet is for you if your prostate cancer has come back after treatment that aimed to get
Recurrent prostate cancer A guide to treatment and support 2 Recurrent prostate cancer About this booklet This booklet is for you if your prostate cancer has come back after treatment that aimed to get
Advanced prostate cancer
 1 Advanced prostate cancer In this fact sheet: What is advanced (metastatic) prostate cancer? What tests are used to diagnose advanced prostate cancer? What do my test results mean? What are my treatment
1 Advanced prostate cancer In this fact sheet: What is advanced (metastatic) prostate cancer? What tests are used to diagnose advanced prostate cancer? What do my test results mean? What are my treatment
Advanced prostate cancer
 Diagnosis Helpline 0800 074 8383 prostatecanceruk.org 1 Advanced prostate cancer In this fact sheet: What is advanced (metastatic) prostate cancer? What tests are used to diagnose advanced prostate cancer?
Diagnosis Helpline 0800 074 8383 prostatecanceruk.org 1 Advanced prostate cancer In this fact sheet: What is advanced (metastatic) prostate cancer? What tests are used to diagnose advanced prostate cancer?
A guide to prostate cancer clinical trials
 1 A guide to prostate cancer clinical trials In this fact sheet: What is a clinical trial? Why are trials done? What are trials looking into at the moment? How are clinical trials done? Should I take part
1 A guide to prostate cancer clinical trials In this fact sheet: What is a clinical trial? Why are trials done? What are trials looking into at the moment? How are clinical trials done? Should I take part
A start to help you understand prostate cancer
 A start to help you understand prostate cancer If you are reading this because you have worries or concerns about yourself or someone you know then the best thing to do is make an appointment with your
A start to help you understand prostate cancer If you are reading this because you have worries or concerns about yourself or someone you know then the best thing to do is make an appointment with your
Follow-up after prostate cancer treatment What happens next?
 Follow-up after prostate cancer treatment What happens next? 2 Follow-up after prostate cancer treatment About this booklet If you ve had treatment aimed at getting rid of your prostate cancer, such as
Follow-up after prostate cancer treatment What happens next? 2 Follow-up after prostate cancer treatment About this booklet If you ve had treatment aimed at getting rid of your prostate cancer, such as
Advanced prostate cancer
 Diagnosis Specialist Nurses 0800 074 8383 prostatecanceruk.org 1 Advanced prostate cancer In this fact sheet: What is advanced prostate cancer? How is advanced prostate cancer diagnosed? What do my test
Diagnosis Specialist Nurses 0800 074 8383 prostatecanceruk.org 1 Advanced prostate cancer In this fact sheet: What is advanced prostate cancer? How is advanced prostate cancer diagnosed? What do my test
Understanding the PSA test. A guide for men concerned about prostate cancer
 Understanding the PSA test A guide for men concerned about prostate cancer Introduction This booklet is for men who want to know more about having a blood test, called a PSA test, that can help diagnose
Understanding the PSA test A guide for men concerned about prostate cancer Introduction This booklet is for men who want to know more about having a blood test, called a PSA test, that can help diagnose
Treating Localized Prostate Cancer A Review of the Research for Adults
 Treating Localized Prostate Cancer A Review of the Research for Adults Is this information right for me? Yes, this information is right for you if: Your doctor * said all tests show you have localized
Treating Localized Prostate Cancer A Review of the Research for Adults Is this information right for me? Yes, this information is right for you if: Your doctor * said all tests show you have localized
Treating Prostate Cancer
 Treating Prostate Cancer A Guide for Men With Localized Prostate Cancer Most men have time to learn about all the options for treating their prostate cancer. You have time to talk with your family and
Treating Prostate Cancer A Guide for Men With Localized Prostate Cancer Most men have time to learn about all the options for treating their prostate cancer. You have time to talk with your family and
Understanding the PSA test A guide for men concerned about prostate cancer
 Understanding the PSA test A guide for men concerned about prostate cancer 2 Understanding the PSA test A guide for men concerned about prostate cancer About this booklet This booklet is for men who want
Understanding the PSA test A guide for men concerned about prostate cancer 2 Understanding the PSA test A guide for men concerned about prostate cancer About this booklet This booklet is for men who want
How prostate cancer is diagnosed
 How prostate cancer is diagnosed This information is an extract from the booklet Having tests for prostate cancer. You may find the full booklet helpful. We can send you a free copy see page 7. Contents
How prostate cancer is diagnosed This information is an extract from the booklet Having tests for prostate cancer. You may find the full booklet helpful. We can send you a free copy see page 7. Contents
Prostate Cancer Screening. A Decision Guide
 Prostate Cancer Screening A Decision Guide This booklet was developed by the U.S. Department of Health and Human Services, Centers for Disease Control and Prevention (CDC). Is screening right for you?
Prostate Cancer Screening A Decision Guide This booklet was developed by the U.S. Department of Health and Human Services, Centers for Disease Control and Prevention (CDC). Is screening right for you?
Early Prostate Cancer: Questions and Answers. Key Points
 CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Early Prostate Cancer:
CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Early Prostate Cancer:
A Woman s Guide to Prostate Cancer Treatment
 A Woman s Guide to Prostate Cancer Treatment Supporting the man in your life Providing prostate cancer support and resources for women and families WOMEN AGAINST PROSTATE CANCER A Woman s Guide to Prostate
A Woman s Guide to Prostate Cancer Treatment Supporting the man in your life Providing prostate cancer support and resources for women and families WOMEN AGAINST PROSTATE CANCER A Woman s Guide to Prostate
How is Prostate Cancer Diagnosed?
 Prostate cancer: English Prostate cancer This fact sheet is about how prostate cancer is diagnosed and treated. We also have fact sheets in your language about chemotherapy, radiotherapy, surgery, side
Prostate cancer: English Prostate cancer This fact sheet is about how prostate cancer is diagnosed and treated. We also have fact sheets in your language about chemotherapy, radiotherapy, surgery, side
Prostate Cancer Screening. A Decision Guide for African Americans
 Prostate Cancer Screening A Decision Guide for African Americans This booklet was developed by the U.S. Department of Health and Human Services, Centers for Disease Control and Prevention (CDC). Published
Prostate Cancer Screening A Decision Guide for African Americans This booklet was developed by the U.S. Department of Health and Human Services, Centers for Disease Control and Prevention (CDC). Published
An Introduction to PROSTATE CANCER
 An Introduction to PROSTATE CANCER Being diagnosed with prostate cancer can be a life-altering experience. It requires making some very difficult decisions about treatments that can affect not only the
An Introduction to PROSTATE CANCER Being diagnosed with prostate cancer can be a life-altering experience. It requires making some very difficult decisions about treatments that can affect not only the
Radiation Therapy for Prostate Cancer
 Radiation Therapy for Prostate Cancer Introduction Cancer of the prostate is the most common form of cancer that affects men. About 240,000 American men are diagnosed with prostate cancer every year. Your
Radiation Therapy for Prostate Cancer Introduction Cancer of the prostate is the most common form of cancer that affects men. About 240,000 American men are diagnosed with prostate cancer every year. Your
How prostate cancer is diagnosed
 How prostate cancer is diagnosed In this fact sheet: How is prostate cancer diagnosed? What tests are done by my GP? What tests will I have at the hospital? What do my biopsy results mean? Will I need
How prostate cancer is diagnosed In this fact sheet: How is prostate cancer diagnosed? What tests are done by my GP? What tests will I have at the hospital? What do my biopsy results mean? Will I need
PSA Screening for Prostate Cancer Information for Care Providers
 All men should know they are having a PSA test and be informed of the implications prior to testing. This booklet was created to help primary care providers offer men information about the risks and benefits
All men should know they are having a PSA test and be informed of the implications prior to testing. This booklet was created to help primary care providers offer men information about the risks and benefits
PROSTATE CANCER 101 WHAT IS PROSTATE CANCER?
 PROSTATE CANCER 101 WHAT IS PROSTATE CANCER? Prostate cancer is cancer that begins in the prostate. The prostate is a walnut-shaped gland in the male reproductive system located below the bladder and in
PROSTATE CANCER 101 WHAT IS PROSTATE CANCER? Prostate cancer is cancer that begins in the prostate. The prostate is a walnut-shaped gland in the male reproductive system located below the bladder and in
PATIENT GUIDE. Localized Prostate Cancer
 PATIENT GUIDE Localized Prostate Cancer The prostate* is part of the male reproductive system. It is about the same size as a walnut and weighs about an ounce. As pictured in Figure 1, the prostate is
PATIENT GUIDE Localized Prostate Cancer The prostate* is part of the male reproductive system. It is about the same size as a walnut and weighs about an ounce. As pictured in Figure 1, the prostate is
CONTENTS: WHAT S IN THIS BOOKLET
 Q Questions & A & Answers About Your Prostate Having a biopsy test to find out if you may have prostate cancer can bring up a lot of questions. This booklet will help answer those questions. CONTENTS:
Q Questions & A & Answers About Your Prostate Having a biopsy test to find out if you may have prostate cancer can bring up a lot of questions. This booklet will help answer those questions. CONTENTS:
University College Hospital. Hormone therapy for prostate cancer. Radiotherapy Department Patient information series
 University College Hospital Hormone therapy for prostate cancer Radiotherapy Department Patient information series 10 2 If you need a large print, audio or translated copy of the document, please contact
University College Hospital Hormone therapy for prostate cancer Radiotherapy Department Patient information series 10 2 If you need a large print, audio or translated copy of the document, please contact
Prostate Cancer Guide. A resource to help answer your questions about prostate cancer
 Prostate Cancer Guide A resource to help answer your questions about prostate cancer Thank you for downloading this guide to prostate cancer treatment. We know that all the information provided online
Prostate Cancer Guide A resource to help answer your questions about prostate cancer Thank you for downloading this guide to prostate cancer treatment. We know that all the information provided online
Prostate Cancer. Understanding your diagnosis
 Prostate Cancer Understanding your diagnosis Prostate Cancer Understanding your diagnosis When you first hear that you have cancer, you may feel alone and afraid. You may be overwhelmed by the large amount
Prostate Cancer Understanding your diagnosis Prostate Cancer Understanding your diagnosis When you first hear that you have cancer, you may feel alone and afraid. You may be overwhelmed by the large amount
External beam radiotherapy
 Treatment Helpline 0800 074 8383 prostatecanceruk.org 1 External beam radiotherapy In this fact sheet: Who can have radiotherapy? How does radiotherapy treat prostate cancer? What are the advantages and
Treatment Helpline 0800 074 8383 prostatecanceruk.org 1 External beam radiotherapy In this fact sheet: Who can have radiotherapy? How does radiotherapy treat prostate cancer? What are the advantages and
AFTER DIAGNOSIS: PROSTATE CANCER Understanding Your Treatment Options
 AFTER DIAGNOSIS: PROSTATE CANCER Understanding Your Treatment Options INTRODUCTION This booklet describes how prostate cancer develops, how it affects the body and the current treatment methods. Although
AFTER DIAGNOSIS: PROSTATE CANCER Understanding Your Treatment Options INTRODUCTION This booklet describes how prostate cancer develops, how it affects the body and the current treatment methods. Although
Screening for Prostate Cancer
 Cancer Expert Working Group on Cancer Prevention and Screening Screening for Prostate Cancer Information for men and their families 1 What is the prostate? 2 What is prostate cancer? prostate The prostate
Cancer Expert Working Group on Cancer Prevention and Screening Screening for Prostate Cancer Information for men and their families 1 What is the prostate? 2 What is prostate cancer? prostate The prostate
Hormone therapy. In this fact sheet: How does hormone therapy treat prostate cancer? What happens next?
 1 Hormone therapy In this fact sheet: How does hormone therapy treat prostate cancer? Who can have hormone therapy? What types of hormone therapy are there? What are the advantages and disadvantages of
1 Hormone therapy In this fact sheet: How does hormone therapy treat prostate cancer? Who can have hormone therapy? What types of hormone therapy are there? What are the advantages and disadvantages of
Stereotactic Radiotherapy for Prostate Cancer using CyberKnife
 Stereotactic Radiotherapy for Prostate Cancer using CyberKnife Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Stereotactic Radiotherapy for Prostate Cancer using CyberKnife Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Tubular breast cancer
 Tubular breast cancer This booklet is for people who would like more information about tubular breast cancer. It describes what tubular breast cancer is, its symptoms, how a diagnosis is made and the possible
Tubular breast cancer This booklet is for people who would like more information about tubular breast cancer. It describes what tubular breast cancer is, its symptoms, how a diagnosis is made and the possible
Prostate Cancer. There is no known association with an enlarged prostate or benign prostatic hyperplasia (BPH).
 Prostate Cancer Definition Prostate cancer is cancer that starts in the prostate gland. The prostate is a small, walnut-sized structure that makes up part of a man's reproductive system. It wraps around
Prostate Cancer Definition Prostate cancer is cancer that starts in the prostate gland. The prostate is a small, walnut-sized structure that makes up part of a man's reproductive system. It wraps around
Prostate Cancer Action Plan: Choosing the treatment that s right for you
 Prostate Cancer Action Plan: Choosing the treatment that s right for you Segment 1: Introduction Trust me, there's a better way to choose a treatment for your prostate cancer. Watching this program is
Prostate Cancer Action Plan: Choosing the treatment that s right for you Segment 1: Introduction Trust me, there's a better way to choose a treatment for your prostate cancer. Watching this program is
PROSTATE CANCER. Get the facts, know your options. Samay Jain, MD, Assistant Professor,The University of Toledo Chief, Division of Urologic Oncology
 PROSTATE CANCER Get the facts, know your options Samay Jain, MD, Assistant Professor,The University of Toledo Chief, Division of Urologic Oncology i What is the Prostate? Unfortunately, you have prostate
PROSTATE CANCER Get the facts, know your options Samay Jain, MD, Assistant Professor,The University of Toledo Chief, Division of Urologic Oncology i What is the Prostate? Unfortunately, you have prostate
Radiotherapy for vulval cancer
 This information is an extract from the booklet Understanding cancer of the vulva. You may find the full booklet helpful. We can send you a copy free see page 6. Contents External radiotherapy Internal
This information is an extract from the booklet Understanding cancer of the vulva. You may find the full booklet helpful. We can send you a copy free see page 6. Contents External radiotherapy Internal
Prostate Specific Antigen (PSA) Blood Test
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Prostate Specific Antigen (PSA) Blood Test An information guide Prostate Specific Antigen (PSA) Blood Test Prostate Specific Antigen (PSA)
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Prostate Specific Antigen (PSA) Blood Test An information guide Prostate Specific Antigen (PSA) Blood Test Prostate Specific Antigen (PSA)
How prostate cancer is diagnosed
 How prostate cancer is diagnosed In this fact sheet: How is prostate cancer diagnosed? What tests are done by my GP? What tests will I have at the hospital? What do my biopsy results mean? Will I need
How prostate cancer is diagnosed In this fact sheet: How is prostate cancer diagnosed? What tests are done by my GP? What tests will I have at the hospital? What do my biopsy results mean? Will I need
Transrectal Ultrasound (Trus) Guided Prostate Biopsies Urology Patient Information Leaflet
 Transrectal Ultrasound (Trus) Guided Prostate Biopsies Urology Patient Information Leaflet Page 1 What is the purpose of my appointment? Your doctor has informed us that you have an elevated Prostate Specific
Transrectal Ultrasound (Trus) Guided Prostate Biopsies Urology Patient Information Leaflet Page 1 What is the purpose of my appointment? Your doctor has informed us that you have an elevated Prostate Specific
Testing for Prostate Cancer. Should I be tested? Is it the right choice for me?
 Testing for Prostate Cancer Should I be tested? Is it the right choice for me? Prostate cancer affects many men. There are tests to find it early. There may be benefits and risks with testing. Research
Testing for Prostate Cancer Should I be tested? Is it the right choice for me? Prostate cancer affects many men. There are tests to find it early. There may be benefits and risks with testing. Research
Pelvic floor muscle exercises
 Lifestyle Specialist Nurses 0800 074 8383 prostatecanceruk.org Pelvic Floor Muscles Pelvic floor muscle exercises 21 In this fact sheet: How do pelvic floor muscle exercises help? When should I start the
Lifestyle Specialist Nurses 0800 074 8383 prostatecanceruk.org Pelvic Floor Muscles Pelvic floor muscle exercises 21 In this fact sheet: How do pelvic floor muscle exercises help? When should I start the
Early Prostate Cancer
 Understanding Early Prostate Cancer Caring for people with cancer Understanding Early Prostate Cancer This booklet has been written to help you understand more about early prostate cancer. It has been
Understanding Early Prostate Cancer Caring for people with cancer Understanding Early Prostate Cancer This booklet has been written to help you understand more about early prostate cancer. It has been
to Know About Your Partner s
 What You Need to Know About Your Partner s Prostate Cancer. A Guide for Wives, Partners, and the Men They Love. Providing Support for Your Partner Prostate cancer can be a physical and emotional challenge
What You Need to Know About Your Partner s Prostate Cancer. A Guide for Wives, Partners, and the Men They Love. Providing Support for Your Partner Prostate cancer can be a physical and emotional challenge
CMScript. Member of a medical scheme? Know your guaranteed benefits! Issue 7 of 2014
 Background CMScript Member of a medical scheme? Know your guaranteed benefits! Issue 7 of 2014 Prostate cancer is second only to lung cancer as the leading cause of cancer-related deaths in men. It is
Background CMScript Member of a medical scheme? Know your guaranteed benefits! Issue 7 of 2014 Prostate cancer is second only to lung cancer as the leading cause of cancer-related deaths in men. It is
Invasive lobular breast cancer
 Invasive lobular breast cancer This booklet is about invasive lobular breast cancer. It describes what invasive lobular breast cancer is, the symptoms, how it s diagnosed and possible treatments. Diagnosed
Invasive lobular breast cancer This booklet is about invasive lobular breast cancer. It describes what invasive lobular breast cancer is, the symptoms, how it s diagnosed and possible treatments. Diagnosed
Talking about Prostate Cancer
 Talking about Prostate Cancer Talking about Prostate Cancer If I can avoid going to a doctor, I will but not when we re talking about prostate cancer. Why take chances with a condition that might be serious?
Talking about Prostate Cancer Talking about Prostate Cancer If I can avoid going to a doctor, I will but not when we re talking about prostate cancer. Why take chances with a condition that might be serious?
WHEN PROSTATE CANCER RETURNS: ADVANCED PROSTATE CANCER. How Will I Know If My Prostate Cancer Returns?
 WHEN PROSTATE CANCER RETURNS: ADVANCED PROSTATE CANCER (The following information is based on the general experiences of many prostate cancer patients. Your experience may be different.) How Will I Know
WHEN PROSTATE CANCER RETURNS: ADVANCED PROSTATE CANCER (The following information is based on the general experiences of many prostate cancer patients. Your experience may be different.) How Will I Know
Getting checked for Prostate Cancer
 Getting checked for Prostate Cancer Quick guide for men and their families and whanau Stay well for your family and whanau. doctor, nurse or health professional about prostate cancer. You should do this
Getting checked for Prostate Cancer Quick guide for men and their families and whanau Stay well for your family and whanau. doctor, nurse or health professional about prostate cancer. You should do this
Information for Men Receiving Radiation and Hormone Treatments for Prostate Cancer
 Information for Men Receiving Radiation and Hormone Treatments for Prostate Cancer Treatment Plan Stage of prostate cancer: RADIATION THERAPY Radiation Treatments: Date for planning CT: Date to start radiation
Information for Men Receiving Radiation and Hormone Treatments for Prostate Cancer Treatment Plan Stage of prostate cancer: RADIATION THERAPY Radiation Treatments: Date for planning CT: Date to start radiation
PSA. and beyond. A guide for men concerned about prostate cancer
 PSA and beyond A guide for men concerned about prostate cancer This booklet is for men who are considering having a PSA test or want to know more about PSA (Prostate Specific Antigen). It explains how
PSA and beyond A guide for men concerned about prostate cancer This booklet is for men who are considering having a PSA test or want to know more about PSA (Prostate Specific Antigen). It explains how
After Diagnosis: Prostate Cancer. Understanding Your Treatment Options
 After Diagnosis: Prostate Cancer Understanding Your Treatment Options What s inside How will this booklet help me?... 3 What is the prostate?... 4 What is prostate cancer?... 4 Who gets prostate cancer?...
After Diagnosis: Prostate Cancer Understanding Your Treatment Options What s inside How will this booklet help me?... 3 What is the prostate?... 4 What is prostate cancer?... 4 Who gets prostate cancer?...
Bard: Prostate Cancer Treatment. Bard: Pelvic Organ Prolapse. Prostate Cancer. An overview of. Treatment. Prolapse. Information and Answers
 Bard: Prostate Cancer Treatment Bard: Pelvic Organ Prolapse Prostate Cancer An overview of Pelvic Treatment Organ Prolapse Information and Answers A Brief Overview Prostate Anatomy The prostate gland,
Bard: Prostate Cancer Treatment Bard: Pelvic Organ Prolapse Prostate Cancer An overview of Pelvic Treatment Organ Prolapse Information and Answers A Brief Overview Prostate Anatomy The prostate gland,
Prostate Cancer Screening
 Prostate Cancer Screening The American Cancer Society and Congregational Health Ministry Team June Module To access this module via the Web, visit www.cancer.org and type in congregational health ministry
Prostate Cancer Screening The American Cancer Society and Congregational Health Ministry Team June Module To access this module via the Web, visit www.cancer.org and type in congregational health ministry
Prostate Cancer. Patient Information
 Prostate Cancer Patient Information 1 The Prostate & Prostate Cancer The prostate is a small gland in the male reproductive system, approximately the size and shape of a walnut. It is located directly
Prostate Cancer Patient Information 1 The Prostate & Prostate Cancer The prostate is a small gland in the male reproductive system, approximately the size and shape of a walnut. It is located directly
Breast Cancer Questions to Ask
 Ask about your medicines for primary (early) breast cancer Questions to help you get the best from your drug treatments Ask about your medicines for primary (early) breast cancer This guide is to help
Ask about your medicines for primary (early) breast cancer Questions to help you get the best from your drug treatments Ask about your medicines for primary (early) breast cancer This guide is to help
Treating Mesothelioma - A Quick Guide
 Treating Mesothelioma - A Quick Guide Contents This is a brief summary of the information on Treating mesothelioma from CancerHelp UK. You will find more detailed information on the website. In this information
Treating Mesothelioma - A Quick Guide Contents This is a brief summary of the information on Treating mesothelioma from CancerHelp UK. You will find more detailed information on the website. In this information
Understanding Locally-Advanced Prostate Cancer
 Understanding Locally-Advanced Prostate Cancer This booklet is to help you and your family understand what it means if you have been diagnosed as having locally-advanced prostate cancer. It gives an outline
Understanding Locally-Advanced Prostate Cancer This booklet is to help you and your family understand what it means if you have been diagnosed as having locally-advanced prostate cancer. It gives an outline
Dealing with Erectile Dysfunction During and After Prostate Cancer Treatment For You and Your Partner
 Dealing with Erectile Dysfunction During and After Prostate Cancer Treatment For You and Your Partner The following information is based on the general experiences of many prostate cancer patients. Your
Dealing with Erectile Dysfunction During and After Prostate Cancer Treatment For You and Your Partner The following information is based on the general experiences of many prostate cancer patients. Your
HEALTH NEWS PROSTATE CANCER THE PROSTATE
 HEALTH NEWS PROSTATE CANCER THE PROSTATE Prostate comes from the Greek meaning to stand in front of ; this is very different than prostrate which means to lie down flat. The prostate is a walnut-sized
HEALTH NEWS PROSTATE CANCER THE PROSTATE Prostate comes from the Greek meaning to stand in front of ; this is very different than prostrate which means to lie down flat. The prostate is a walnut-sized
These rare variants often act aggressively and may respond differently to therapy than the more common prostate adenocarcinoma.
 Prostate Cancer OVERVIEW Prostate cancer is the second most common cancer diagnosed among American men, accounting for nearly 200,000 new cancer cases in the United States each year. Greater than 65% of
Prostate Cancer OVERVIEW Prostate cancer is the second most common cancer diagnosed among American men, accounting for nearly 200,000 new cancer cases in the United States each year. Greater than 65% of
Patient & Family Guide 2015 Hormone Therapy for Prostate Cancer
 Patient & Family Guide 2015 Hormone Therapy for Prostate Cancer www.nshealth.ca Hormone Therapy for Prostate Cancer What is the prostate? The prostate is one of the male sex glands. It makes seminal fluid
Patient & Family Guide 2015 Hormone Therapy for Prostate Cancer www.nshealth.ca Hormone Therapy for Prostate Cancer What is the prostate? The prostate is one of the male sex glands. It makes seminal fluid
The PSA Test for Prostate Cancer Screening:
 For more information, please contact your local VA Medical Center or Health Clinic. U.S. Department of Veterans Affairs Veterans Health Administration Patient Care Services Health Promotion and Disease
For more information, please contact your local VA Medical Center or Health Clinic. U.S. Department of Veterans Affairs Veterans Health Administration Patient Care Services Health Promotion and Disease
A918: Prostate: adenocarcinoma
 A918: Prostate: adenocarcinoma General facts of prostate cancer The prostate is about the size of a walnut. It is just below the bladder and in front of the rectum. The tube that carries urine (the urethra)
A918: Prostate: adenocarcinoma General facts of prostate cancer The prostate is about the size of a walnut. It is just below the bladder and in front of the rectum. The tube that carries urine (the urethra)
LIvING WITH Prostate Cancer
 Living with Prostate Cancer A Common Cancer in Men If you ve been diagnosed with prostate cancer, it s normal to be concerned about your future. It may help you to know that this disease can often be cured
Living with Prostate Cancer A Common Cancer in Men If you ve been diagnosed with prostate cancer, it s normal to be concerned about your future. It may help you to know that this disease can often be cured
Why is radiation therapy used to treat prostate cancer? Is there anything that I have to do before my treatment planning appointment?
 2015 Information for Patients Receiving Radiation Therapy: External Beam Treatment for Prostate Cancer Why is radiation therapy used to treat prostate cancer? Prostate cancer may be treated with a combination
2015 Information for Patients Receiving Radiation Therapy: External Beam Treatment for Prostate Cancer Why is radiation therapy used to treat prostate cancer? Prostate cancer may be treated with a combination
Making the Choice. Deciding What to Do About Early Stage Prostate Cancer
 Making the Choice Deciding What to Do About Early Stage Prostate Cancer We have all faced the same tough choices you face now. We talked with our doctors and others we love and trust. We each made our
Making the Choice Deciding What to Do About Early Stage Prostate Cancer We have all faced the same tough choices you face now. We talked with our doctors and others we love and trust. We each made our
For further information on screening and early detection of prostate cancer, see the Section entitled Screening for Prostate Cancer.
 Prostate Cancer For many older men, prostate cancer may be present but never cause symptoms or problems and many men will die with their prostate cancer rather than of their prostate cancer. Yet it remains
Prostate Cancer For many older men, prostate cancer may be present but never cause symptoms or problems and many men will die with their prostate cancer rather than of their prostate cancer. Yet it remains
Talking to your consultant
 Talking to your consultant Being given a diagnosis of bladder cancer, or indeed any cancer, will likely make the world stop around you. Your brain will go into crisis mode and if you are like the majority
Talking to your consultant Being given a diagnosis of bladder cancer, or indeed any cancer, will likely make the world stop around you. Your brain will go into crisis mode and if you are like the majority
University College Hospital. Prostate high dose rate (HDR) brachytherapy. Radiotherapy Department Patient information series
 University College Hospital Prostate high dose rate (HDR) brachytherapy Radiotherapy Department Patient information series 18 2 If you need a large print, audio or translated copy of the document, please
University College Hospital Prostate high dose rate (HDR) brachytherapy Radiotherapy Department Patient information series 18 2 If you need a large print, audio or translated copy of the document, please
Testing for Prostate Cancer
 Testing for Prostate Cancer Should I be tested? Is it the right choice for me? Prostate cancer affects many men. There are tests to find it early. There may be benefits and risks with testing. Research
Testing for Prostate Cancer Should I be tested? Is it the right choice for me? Prostate cancer affects many men. There are tests to find it early. There may be benefits and risks with testing. Research
Radiation Therapy and Prostate Cancer
 Radiation Therapy and Prostate Cancer The following information is based on the general experiences of many prostate cancer patients. Your experience may be different. If you have any questions about what
Radiation Therapy and Prostate Cancer The following information is based on the general experiences of many prostate cancer patients. Your experience may be different. If you have any questions about what
Prostate Cancer. What is prostate cancer?
 Scan for mobile link. Prostate Cancer Prostate cancer is a tumor of the prostate gland, which is located in front of the rectum and below the bladder. Your doctor may perform a physical exam, prostate-specific
Scan for mobile link. Prostate Cancer Prostate cancer is a tumor of the prostate gland, which is located in front of the rectum and below the bladder. Your doctor may perform a physical exam, prostate-specific
Newly Diagnosed Prostate Cancer: Understanding Your Risk
 Newly Diagnosed Prostate Cancer: Understanding Your Risk When the urologist calls with the life-changing news that your prostate biopsy is positive for prostate cancer, an office appointment is made to
Newly Diagnosed Prostate Cancer: Understanding Your Risk When the urologist calls with the life-changing news that your prostate biopsy is positive for prostate cancer, an office appointment is made to
How treatment is planned Giving your consent The benefits and disadvantages of treatment Second opinion
 Treatment overview for lung cancer This information is an extract from the booklet Understanding lung cancer. You may find the full booklet helpful. We can send you a free copy see page 5. Contents How
Treatment overview for lung cancer This information is an extract from the booklet Understanding lung cancer. You may find the full booklet helpful. We can send you a free copy see page 5. Contents How
Short Course, Pre-operative Radiotherapy for Bowel Cancer
 Short Course, Pre-operative Radiotherapy for Bowel Cancer Patient Information Introduction This leaflet tells you about short course, pre-operative radiotherapy for the treatment of bowel cancer. It explains
Short Course, Pre-operative Radiotherapy for Bowel Cancer Patient Information Introduction This leaflet tells you about short course, pre-operative radiotherapy for the treatment of bowel cancer. It explains
University College Hospital. Metastatic spinal cord compression (MSCC) information for patients at risk of developing MSCC.
 University College Hospital Metastatic spinal cord compression (MSCC) information for patients at risk of developing MSCC Cancer Services 2 If you would like this document in another language or format,
University College Hospital Metastatic spinal cord compression (MSCC) information for patients at risk of developing MSCC Cancer Services 2 If you would like this document in another language or format,
A to Z of medical words
 Notes Specialist Nurses 0800 074 8383 A to Z of medical words 1 This fact sheet explains some of the medical words you might come across when you are finding out about prostate problems and prostate cancer.
Notes Specialist Nurses 0800 074 8383 A to Z of medical words 1 This fact sheet explains some of the medical words you might come across when you are finding out about prostate problems and prostate cancer.
Questions to Ask My Doctor About Prostate Cancer
 Questions to Ask My Doctor Being told you have prostate cancer can be scary and stressful. You probably have a lot of questions and concerns. Learning about the disease, how it s treated, and how this
Questions to Ask My Doctor Being told you have prostate cancer can be scary and stressful. You probably have a lot of questions and concerns. Learning about the disease, how it s treated, and how this
Breast Cancer. CSC Cancer Experience Registry Member, breast cancer
 ESSENTIALS Breast Cancer Take things one step at a time. Try not to be overwhelmed by the tidal wave of technical information coming your way. Finally you know your body best; you have to be your own advocate.
ESSENTIALS Breast Cancer Take things one step at a time. Try not to be overwhelmed by the tidal wave of technical information coming your way. Finally you know your body best; you have to be your own advocate.
Treatment Choices for Men
 National Cancer Institute Treatment Choices for Men With Early-Stage Prostate Cancer U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES National Institutes of Health Things to Remember Many men with prostate
National Cancer Institute Treatment Choices for Men With Early-Stage Prostate Cancer U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES National Institutes of Health Things to Remember Many men with prostate
Making the Choice Deciding What to Do About Early Stage Prostate Cancer
 Making the Choice Deciding What to Do About Early Stage Prostate Cancer We have all faced the same tough choices you face now. We talked with our doctors and others we love and trust. We each made our
Making the Choice Deciding What to Do About Early Stage Prostate Cancer We have all faced the same tough choices you face now. We talked with our doctors and others we love and trust. We each made our
Radiotherapy for breast cancer
 Radiotherapy for breast cancer This information is an extract from the booklet Understanding breast cancer. You may find the full booklet helpful. We can send you a copy free see page 6. Contents Radiotherapy
Radiotherapy for breast cancer This information is an extract from the booklet Understanding breast cancer. You may find the full booklet helpful. We can send you a copy free see page 6. Contents Radiotherapy
Ovarian cancer. Patient information from the BMJ Group. What is ovarian cancer? What are the symptoms?
 Patient information from the BMJ Group Ovarian cancer Ovarian cancer is a serious disease. If it s diagnosed at an early stage, ovarian cancer can usually be cured. But even cancers that are more advanced
Patient information from the BMJ Group Ovarian cancer Ovarian cancer is a serious disease. If it s diagnosed at an early stage, ovarian cancer can usually be cured. But even cancers that are more advanced
NHS breast screening Helping you decide
 NHS breast screening Helping you decide What is breast cancer? 2 What is breast screening? 3 Breast screening results 6 Making a choice the possible benefits 9 and risks of breast screening What are the
NHS breast screening Helping you decide What is breast cancer? 2 What is breast screening? 3 Breast screening results 6 Making a choice the possible benefits 9 and risks of breast screening What are the
Are you worried about prostate cancer? 1
 Are you worried about prostate cancer? 1 Are you worried about prostate cancer? This information is from the leaflet Are you worried about prostate cancer? You may find the full leaflet helpful. We can
Are you worried about prostate cancer? 1 Are you worried about prostate cancer? This information is from the leaflet Are you worried about prostate cancer? You may find the full leaflet helpful. We can
Prostate cancer screening. It s YOUR decision!
 Prostate cancer screening It s YOUR decision! For many years now, a test has been available to screen for. The test is called the prostate-specific antigen blood test (or PSA test). It is used in combination
Prostate cancer screening It s YOUR decision! For many years now, a test has been available to screen for. The test is called the prostate-specific antigen blood test (or PSA test). It is used in combination
Information for patients receiving short-term hormone treatment and radiotherapy for prostate cancer
 Information for patients receiving short-term hormone treatment and radiotherapy for prostate cancer Northern Centre for Cancer Care (NCCC) Freeman Hospital Introduction This leaflet has been written to
Information for patients receiving short-term hormone treatment and radiotherapy for prostate cancer Northern Centre for Cancer Care (NCCC) Freeman Hospital Introduction This leaflet has been written to
Understanding Prostate Cancer
 Understanding Prostate Cancer A guide for men with cancer, their families and friends Cancer information www.cancercouncil.com.au Understanding Prostate Cancer A guide for men with cancer, their families
Understanding Prostate Cancer A guide for men with cancer, their families and friends Cancer information www.cancercouncil.com.au Understanding Prostate Cancer A guide for men with cancer, their families
Us TOO University Presents: Understanding Diagnostic Testing
 Us TOO University Presents: Understanding Diagnostic Testing for Prostate Cancer Patients Today s speaker is Manish Bhandari, MD Program moderator is Pam Barrett, Us TOO International Made possible by
Us TOO University Presents: Understanding Diagnostic Testing for Prostate Cancer Patients Today s speaker is Manish Bhandari, MD Program moderator is Pam Barrett, Us TOO International Made possible by
Treating Oesophageal Cancer A Quick Guide
 Treating Oesophageal Cancer A Quick Guide Contents This is a brief summary of the information on Treating from our website. You will find more detailed information on the website. In this information there
Treating Oesophageal Cancer A Quick Guide Contents This is a brief summary of the information on Treating from our website. You will find more detailed information on the website. In this information there
PRIMARY LUNG CANCER TREATMENT
 PRIMARY LUNG CANCER TREATMENT Cancer Care Pathways Directorate Tailored Information in Cancer Care (TICC) Sir Anthony Mamo Oncology Centre December 2014 Contents About this booklet 1 Types of Lung Cancer
PRIMARY LUNG CANCER TREATMENT Cancer Care Pathways Directorate Tailored Information in Cancer Care (TICC) Sir Anthony Mamo Oncology Centre December 2014 Contents About this booklet 1 Types of Lung Cancer
Secondary liver cancer Patient Information Booklet
 Secondary liver cancer Patient Information Booklet Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Secondary liver cancer Patient Information Booklet Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Understanding your pathology report
 Understanding your pathology report 2 Contents Contents Introduction 3 What is a pathology report? 3 Waiting for your results 4 What s in a pathology report? 4 Information about your breast cancer 5 What
Understanding your pathology report 2 Contents Contents Introduction 3 What is a pathology report? 3 Waiting for your results 4 What s in a pathology report? 4 Information about your breast cancer 5 What
Treatment of colon cancer
 Treatment of colon cancer This information is an extract from the booklet, Understanding colon cancer. You may find the full booklet helpful. We can send you a copy free see page 5. Contents How treatment
Treatment of colon cancer This information is an extract from the booklet, Understanding colon cancer. You may find the full booklet helpful. We can send you a copy free see page 5. Contents How treatment
Prostate Cancer Treatment: What s Best for You?
 Prostate Cancer Treatment: What s Best for You? Prostate Cancer: Radiation Therapy Approaches I. Choices There is really a variety of options in prostate cancer management overall and in radiation therapy.
Prostate Cancer Treatment: What s Best for You? Prostate Cancer: Radiation Therapy Approaches I. Choices There is really a variety of options in prostate cancer management overall and in radiation therapy.
