AANA Journal Course 3
|
|
|
- Lionel Weaver
- 7 years ago
- Views:
Transcription
1 AANA Journal Course 3 Update for nurse anesthetists Aspiration prophylaxis: Is it time for changes in our practice? *6 CE Credits John J. Nagelhout, CRNA, PhD Pasadena, California Pulmonary aspiration of gastric contents during anesthesia is a complication that is fortunately rare, yet potentially catastrophic. Despite its infrequency, techniques geared toward preventing this serious outcome influence many of our routine practices and beliefs. Reports on large-scale clinical studies have opened new insights and questions about the effectiveness of long-standing anesthetic practices. These include conventional beliefs about preoperative fasting guidelines, acceptable gastric fluid volumes and ph, effective pharmacologic interventions, risk factors for pulmonary aspiration, and preventative anesthetic techniques such as rapidsequence induction. This AANA Journal course outlines current knowledge as to the incidence, risk factors, and efficacy of practices geared toward preventing aspiration. It is anticipated that this review will stimulate discussions regarding possible changes in the anesthetic management of patients in individual practice settings. Key words: Aspiration, cricoid pressure, preoperative fasting, preoperative medications, rapid-sequence induction. Objectives At the completion of the course, the reader should be able to: 1. Identify the patient groups that have an increased risk for aspiration. 2. Discuss the controversies regarding standard anesthetic practices to reduce aspiration. 3. Outline patient management and treatment of aspiration. 4. Describe current preoperative fasting and drug prophylaxis recommendations. 5. Contrast the various techniques for rapidsequence induction. Introduction Aspiration is a rare yet serious complication of general anesthesia. Much effort is given to prevention of this untoward event and minimization of sequelae if it does occur. New information is emerging that questions many long-standing practices and beliefs and may change routine clinical practice. This article reviews the incidence, risk factors, prevention, and treatment of this anesthetic complication. Incidence By definition, pulmonary aspiration has 2 compo- nents. First, gastric contents escape from the stomach into the pharynx and, second, enter the lungs. This results from preexisting disease, airway manipulation, and the inevitable compromise in protective reflexes that accompanies the anesthetic process. Aspirates are commonly categorized as contaminated, acidic, particulate, or nonparticulate. Fewer than half of all aspirations lead to pneumonia. 1 Pneumonia occurs most often in patients with pulmonary ingestion of virulent material or who are immunocompromised. Ingestion of highly acidic or particulate aspirate may cause severe respiratory damage without an infectious component. Patients who initially show no signs of infection, however, may develop pneumonia over the longterm due to the severity of the lung injury and prolonged respiratory support. 1 Several major reviews have been published regarding the incidence of aspiration during anesthesia. Olsson et al 2 retrospectively studied 185,358 anesthetics in Sweden and found 83 cases of aspiration for an incidence of 4.7 per 10,000 cases. Of the patients, 53% required no treatment; 47% of the cases were confirmed by x-ray. Of this 47%, 15 patients (17%) required mechanical ventilation and 4 patients died. Factors associated with significant morbidity were *AANA Journal Course No. 23: The American Association of Nurse Anesthetists is accredited as a provider of continuing education in nursing by the American Nurses Credentialing Center Commission on Accreditation. The AANA Journal course will consist of 6 successive articles, each with objectives for the reader and sources for additional reading. At the conclusion of the 6-part series, a final examination will be printed in the AANA Journal. Successful completion will yield the participant 6 CE credits (6 contact hours), code number: 25468, expiration date: July 31, AANA Journal/August 2003/Vol. 71, No
2 emergency procedures, pregnancy, obesity, gastrointestinal disease, elevated intracranial pressure, extremes of age, and airway difficulties. They concluded that clinically significant aspiration occurs in 1 per 35,000 anesthetics. In a multicenter, prospective study in France involving infants and children, the aspiration incidence rate was 5 cases in 40,240 anesthetics. High ASA physical status and emergency procedures were noted as risk factors. 3 The Australian Anaesthetic Incident Monitoring Study noted 133 cases of aspiration in 5,000 reported anesthesia incidents. 4 There were 5 deaths. Aspiration was confirmed by clinical signs or radiography. Predisposing factors included abdominal disease, obesity, diabetes, neurological deficit, lithotomy position, difficult intubation, reflux disease, hiatal hernia, and inadequate anesthesia leading to straining and bucking. Ezri et al 5 studied general anesthesia by mask in obstetric patients who required surgery immediately following vaginal delivery. Procedures included placental extraction; repair of vaginal, cervical, and perineal tears; and uterine manipulation. This database in Israel involved 1,705 anesthetics with 1 case of mild aspiration diagnosed by observation and follow-up chest x-ray. Warner et al 6 from the Mayo Clinic reviewed 215,488 general anesthetics. Pulmonary aspiration defined by particulates visualized in the tracheobronchial tree or radiographic confirmation occurred in 67 patients. Of the 66 patients who survived the surgery, 42 (63%) did not develop symptoms and were discharged the same day. Of the 24 (36%) who did develop symptoms, 13 required mechanical ventilatory support for more than 6 hours. Three of these patients died. The overall mortality was 1 per 71,829 anesthetics. Complications developed in equal percentages among those who received or did not receive pharmacological acid aspiration prophylaxis. Patients who aspirated did not develop problems and could be discharged within 2 hours of the incident if they met these 3 criteria: (1) They did not develop symptoms that included a new cough or a wheeze. (2) There was no decrease in SpO 2 of 10% or more of preoperative levels while breathing room air. (3) There was no radiographic evidence of pulmonary aspiration. Not surprisingly, the largest number of aspirations occurred during induction and intubation or on emergence within 5 minutes of extubation. They found no serious morbidity from pulmonary aspiration in nearly 120,000 elective procedures in patients classified as ASA physical status 1 or 2. In a later study, Warner et al 7 reported on the incidence of aspiration in infants and children. Unlike other reports they found there was no increased incidence in young patients. They noted 24 aspirations in a series of 63,180 general anesthetics. Fifteen of the 24 children did not develop symptoms within 2 hours, and no treatment was required. Five children required respiratory support, 3 for more than 48 hours. There were no deaths. Risk factors Numerous factors have been postulated as increasing the risk of aspiration during anesthesia. A list of the commonly noted factors is given in Table 1. Table 1. Risk factors for aspiration Emergency surgery Full stomach Obstetrics Gastrointestinal obstruction Ascites Diabetic gastroparesis Gastroesophageal reflux disease (GERD) Hiatal hernia Peptic ulcer disease Difficult airway management High gastric pressure/lower esophageal sphincter tone Impaired reflexes Head injury Depression of consciousness Seizures Obesity Scleroderma Trauma or stress Nausea and vomiting Opioids Cricoid pressure Cardiac arrest Severe hypotension Inadequate anesthesia Gastric volume and ph. It has long been thought that gastric fluid volume (GFV) of more than 0.4 ml/kg (25 ml/70 kg) and a ph of less than 2.5 are significant indicators of risk for aspiration sequelae. In 1974, Roberts and Shirley 8 published a classic article advocating these arbitrarily defined surrogate end points in patients undergoing cesarean section. These markers became widely accepted in clinical practice, and efforts to reach these levels preoperatively in many patient groups included insertion of nasogastric tubes and multidrug pharmacologic intervention. Questions are being raised as to the validity of the data behind these recommendations with the suggestion that a reappraisal is in order. 9 Since GFVs of more than 0.4 ml/kg are common, even with fasting, and 300 AANA Journal/August 2003/Vol. 71, No. 4
3 aspiration rarely accompanies these higher levels, the use of this marker seems less than realistic. In a report comparing gastric content differences in healthy obese vs lean patients, a GFV of more than 25 ml/70 kg and a ph of less than 2.5 were noted in 27% of obese and 42% of lean patients. 10 These data suggest that healthy obese patients do not exhibit delayed gastric emptying, and many patients routinely fall into the surrogate range of GFV of more than 25 ml/70 kg and a ph of less than 2.5 without aspiration. Acidity has a role in aspiration-induced lung damage; however, preoperative pharmacologic manipulation of gastric ph has not been proven clinically effective. 6,9,11 It has been suggested that the focus be shifted away from GFV and ph toward patient characteristics, condition, and anesthetic practices that place the patient at risk of pulmonary aspiration. Cricoid pressure. The use of cricoid pressure is another standard practice being questioned. It is difficult to apply properly and may impede intubation due to distortion of the airway, and application of cricoid pressure during rapid-sequence induction reduces upper and lower esophageal sphincter tone. 12,13 It is interesting to note that aspiration occurred despite the use of cricoid pressure in the Mayo Clinic study of 215,488 anesthetics discussed previously. 6 Upon failed intubation, cricoid pressure impedes insertion of a laryngeal mask airway for airway rescue and makes it more difficult to intubate through an in-place laryngeal mask airway. As one author noted in a recent review: There is no convincing evidence to suggest that cricoid pressure has reduced the incidence of aspiration or mortality. 14 Others believe that continued use with safer application and better training is warranted. 15 Laryngeal mask airway. The advent of the laryngeal mask airway has brought into question whether the increasing use of this airway-management technique leads to a greater frequency of aspiration. Several reports addressing this question support the conclusion that there is no increase in aspiration risk compared with the risk associated with a face mask. 16 An endotracheal tube remains the safest technique to ensure airway integrity. Positive pressure ventilation. Sellick 17 in his original article did not describe the need for apnea during rapidsequence induction. The practice of intentional apnea during rapid-sequence induction likely became popular with the 15-step description by Stept and Safar 18 in Concern regarding gastric distention and regurgitation during positive pressure ventilation and cricoid pressure was sufficient to recommend apnea before intubation. This recommendation is clearly opinionbased and not the result of clear data or evidence that the practice ever was or remains warranted. Clinicians are aware of the possibility of straining or bucking during light anesthesia. The rapid effect of modern induction drugs and improved techniques lead to the question of whether a reappraisal is in order. Light ventilation using what is commonly referred to as a modified rapid-sequence induction has not been shown to increase the risk of aspiration. As recently noted: Few things seem more counterintuitive to an anesthesiologist whose main responsibility is to maintain adequate oxygenation than to willfully cause apnea, drop oxygen reserves and reduce oxygen saturation, thereby handicapping themselves with a time constraint to intubate and oxygenate. 19 Prevention Pharmacologic prophylaxis for aspiration has been common practice for many years. Much of the concern arose from the finding that large volumes of acidic gastric contents, if aspirated, caused lung damage and increased the risk of serious morbidity and mortality. Agents such as gastrokinetics, histamine blockers, anticholinergics, antacids, proton pump inhibitors, and antiemetics are used alone or in various combinations to raise the gastric ph and lower gastric volume. Recent evidence questioning the benefit of this practice of routine administration of these agents in healthy patients without an increased aspiration risk has led to new practice guidelines. A task force appointed by the American Society of Anesthesiologists reviewed data with an evidence-based approach to the current fasting guidelines and drug prophylaxis. Their fasting guidelines are given in Table 2, and drug prophylaxis guidelines are in Table Evidence does not support the practice of routine preoperative administration of these gastric-related agents. Use in patients thought to exhibit risk factors should be continued. Table 2. Fasting guidelines* Ingested material Minimum fasting period (h) Clear liquid 2 Breast milk 4 Infant formula 6 Nonhuman milk 6 Light meal 6 * In the United Kingdom, pediatric anesthetists have encouraged 4-hour fasting times for breast milk and 6 hours for formula milk in neonates and nonhuman milk in children. 20 (Adapted from Practice guidelines for preoperative fasting and the use of pharmacologic agents to reduce the risk of pulmonary aspiration: application to healthy patients undergoing elective procedures: a report by the American Society of Anesthesiologists Task Force on Preoperative Fasting. 21 ) AANA Journal/August 2003/Vol. 71, No
4 Table 3. Drug prophylaxis for anesthesia Medication type and common examples Recommendation Gastrointestinal stimulants Metoclopramide Gastric acid secretion blockers Cimetidine Famotidine Omeprazole Lansoprazole Antacids Sodium citrate Sodium bicarbonate Magnesium trisilicate Antiemetics Droperidol Ondansetron Anticholinergics No use Atropine Scopolamine Glycopyrrolate Combinations of the above medications * The routine preoperative use of these medications to decrease aspiration risk in patients with no apparent increased risk is not recommended. The use of anticholinergics to decrease aspiration risk is not recommended. (Adapted from Practice guidelines for preoperative fasting and the use of pharmacologic agents to reduce the risk of pulmonary aspiration: application to healthy patients undergoing elective procedures: a report by the American Society of Anesthesiologists Task Force on Preoperative Fasting. 21 ) Treatment Treatment for the management of aspiration depends on the severity of the incident, type of aspirant, and rapidity of symptom development As noted earlier, if no significant symptoms develop within 2 hours of the aspiration, the patient is considered unlikely to become seriously compromised and may be discharged safely following a period of observation. Patients with evidence of particulate aspiration may benefit from bronchopulmonary lavage. Those with nonparticulate acid aspiration do not benefit from lavage or instillation of neutralizing solutions. Evidence indicates that the damage is immediate; 23 therefore, efforts to neutralize the aspirant are ineffective. Symptomatic chemical pneumonitis may require mechanical respiratory support to maintain blood gases at normal levels, and radiographic evidence may take a few hours to appear. Steroids that have been used commonly in the past have little efficacy and might, in fact, promote infection. Antibiotics may be used when there is direct evidence of infection. If the infiltrate clears within 24 to 48 hours, it is likely due to a noninfectious origin and antibiotic therapy is not warranted. Summary Synthesis of the data from several large-scale clinical studies and revised practice recommendations indicate that a review of many standard practices with regard to aspiration prophylaxis may be in order. These include the following: 1. The use of GFV of more than 0.4 ml/kg (25 ml/ 70 kg) and a ph of less than 2.5 should be abandoned as surrogate end points for aspiration risk. 2. Cricoid pressure as a requirement for rapidsequence induction may be beneficial as long as it is performed properly and does not impede effective airway management. 3. Patients should be ventilated during rapidsequence induction. There is no evidence that smooth, controlled light ventilation increases the incidence of aspiration. Prolonged periods of apnea should be abandoned. 4. Routine pharmacologic gastric prophylaxis in healthy patients with minimal risk for aspiration should not be given. 5. Realistic preoperative fasting guidelines should be instituted with respect to types of food or liquids ingested, patient age and characteristics, type of anesthetic and surgical procedure, and presence of risk factors. The rule of nothing by mouth after midnight for all patients should be modified. REFERENCES 1. Cassiere HA. Aspiration pneumonia: current concepts and approach to management. Medscape General Medicine. 1998;2:1:1-11. Available at: Accessed April, 12, Olsson GL, Hallen B, Hambraeus-Jonzon K. Aspiration during anaesthesia: a computer-aided study of 185,385 anaesthetics. Acta Anaesthesiol Scand. 1986;30: Tiret L, Nivoche Y, Hatton F, et al. Complications related to anaesthesia in infants and children: a prospective survey of 40,240 anaesthetics. Br J Anaesth. 1986;61: Kluger MT, Short TG. Aspiration during anaesthesia: a review of 133 cases from the Australian Anaesthetic Incident Monitoring Study (AIMS). Anaesthesia. 1999;54: Ezri T, Szmuck P, Stein A, et al. Peripartum general anaesthesia without tracheal intubation: incidence of aspiration pneumonia. Anaesthesia. 2000;55: Warner MA, Warner ME, Weber JG. Clinical significance of pulmonary aspiration during the perioperative period. Anesthesiology. 1993;78: Warner MA, Warner ME, Warner DO, et al. Perioperative pulmonary aspiration in infants and children. Anesthesiology. 1999;90: Roberts RB, Shirley MA. Reducing the risk of acid aspiration during cesarean section. Anesth Analg. 1974;53: Schreiner MS. Gastric fluid volume: is it really a risk factor for pulmonary aspiration [editorial[? Anesth Analg. 1998;87: Harter RL, Kelly WB, Kramer MG, et al. A comparison of the volume and ph of gastric contents of obese and lean surgical patients. Anesth Analg. 1998;86: Stoelting RK. NPO and Aspiration: New Perspectives in ASA Refresher Course Lectures. Park Ridge, Ill: American Society of Anesthesiologists; 2002;274: Brimacombe JR, Berry AM. Cricoid pressure. Can J Anaesth. 1997;44:4: AANA Journal/August 2003/Vol. 71, No. 4
5 13. Chassard D, Tournadre JP, Berrada KR, et al. Cricoid pressure decreases lower oesaphageal sphincter tone in anaesthetized pigs. Can J Anaesth. 1996;43: Ng A, Smith G. Gastroesophageal reflux and aspiration of gastric contents in anesthetic practice. Anesth Analg. 2001;93: Vanner RG, Asai T. Safe use of cricoid pressure. Anaesthesia. 1999;54: Brimacombe JR, Berry A. The incidence of aspiration associated with the laryngeal mask airway: a meta-analysis of published literature. J Clin Anesth. 1995;4: Sellick BA. Cricoid pressure to prevent regurgitation of stomach contents during induction of anaesthesia. Lancet. 1961;ii: Stept WJ, Safar P. Rapid induction-intubation for prevention of gastric-content aspiration. Anesth Analg. 1970;49: Vadhera RB. Airway management in patients at high risk of aspiration. In: Ovssapian A, Coalson DW, eds. Problems in Anesthesia. Vol. 13. Philadelphia Pa: Lippincott Williams & Wilkins, Inc; 2001: Emerson BM, Wrigley SR, Newton M. Preoperative fasting in paediatric anaesthesia: a survey of current practice. Anaesthesia. 1998;53: Practice guidelines for preoperative fasting and the use of pharmacologic agents to reduce the risk of pulmonary aspiration: application to healthy patients undergoing elective procedures: a report by the American Society of Anesthesiologists Task Force on Preoperative Fasting. Anesthesiology. 1999;90: Tasch MD. Pulmonary aspiration. In: Atlee JL, ed. Complications of Anesthesia. Philadelphia, Pa: WB Saunders; 1999: Levison ME. Pneumonia. In: Braunwald E, Fauci AS, Kasper DL, Hauser SL, Longo DL, Jameson JL, eds. Harrison s Principles of Internal Medicine. 15th ed. New York, NY: McGraw-Hill; 2001: Glover ML, Reed MD. Lower respiratory tract infections. In: Dipiro JT, Talbert RL, Yee GC, Matzke GR, Wells BG, Posey LM, eds. Pharmacotherapy: A Pathophysiologic Approach. 5th ed. New York, NY: McGraw-Hill; 2002: AUTHOR John J. Nagelhout, CRNA, PhD, is the director of the Kaiser Permanente School of Anesthesia/California State University Fullerton, Pasadena, Calif. AANA Journal/August 2003/Vol. 71, No
PRACTICE Guidelines are systematically developed recommendations
 for Preoperative Fasting and the Use of Pharmacologic Agents to Reduce the Risk of Pulmonary Aspiration: Application to Healthy Patients Undergoing Elective Procedures An Updated Report by the American
for Preoperative Fasting and the Use of Pharmacologic Agents to Reduce the Risk of Pulmonary Aspiration: Application to Healthy Patients Undergoing Elective Procedures An Updated Report by the American
GASTROESOPHAGEAL REFLUX DISEASE (GERD)
 GASTROESOPHAGEAL REFLUX DISEASE (GERD) Gastroesophageal reflux disease is a clinical scenario where the gastric or duodenal contents reflux back up into the esophagus. Reflux esophagitis, however, is a
GASTROESOPHAGEAL REFLUX DISEASE (GERD) Gastroesophageal reflux disease is a clinical scenario where the gastric or duodenal contents reflux back up into the esophagus. Reflux esophagitis, however, is a
Medical Nutrition Therapy for Upper Gastrointestinal Tract Disorders. By: Jalal Hejazi PhD, MSc.
 Medical Nutrition Therapy for Upper Gastrointestinal Tract Disorders By: Jalal Hejazi PhD, MSc. Digestive Disorders Common problem; more than 50 million outpatient visits per year Dietary habits and nutrition
Medical Nutrition Therapy for Upper Gastrointestinal Tract Disorders By: Jalal Hejazi PhD, MSc. Digestive Disorders Common problem; more than 50 million outpatient visits per year Dietary habits and nutrition
The University of Hong Kong Department of Surgery Division of Esophageal and Upper Gastrointestinal Surgery
 Program Overview The University of Hong Kong Department of Surgery Division of Esophageal and Upper Gastrointestinal Surgery Weight Control and Metabolic Surgery Program The Weight Control and Metabolic
Program Overview The University of Hong Kong Department of Surgery Division of Esophageal and Upper Gastrointestinal Surgery Weight Control and Metabolic Surgery Program The Weight Control and Metabolic
Upper Endoscopy (EGD)
 Upper Endoscopy (EGD) Appointment Information: Patient Name: MRN: Physician Name: Location: _ For information on Directions, please visit: http://www.brighamandwomens.org/general/directions/directions.aspx
Upper Endoscopy (EGD) Appointment Information: Patient Name: MRN: Physician Name: Location: _ For information on Directions, please visit: http://www.brighamandwomens.org/general/directions/directions.aspx
Perioperative Management of Patients with Obstructive Sleep Apnea. Kalpesh Ganatra,MD Diplomate, American Board of Sleep Medicine
 Perioperative Management of Patients with Obstructive Sleep Apnea Kalpesh Ganatra,MD Diplomate, American Board of Sleep Medicine Disclosures. This activity is supported by an education grant from Trivalley
Perioperative Management of Patients with Obstructive Sleep Apnea Kalpesh Ganatra,MD Diplomate, American Board of Sleep Medicine Disclosures. This activity is supported by an education grant from Trivalley
PROCEDURAL SEDATION/ANALGESIA NCBON Position Statement for RN Practice
 PROCEDURAL SEDATION/ANALGESIA NCBON Position Statement for RN Practice P.O. BOX 2129 Raleigh, NC 27602 (919) 782-3211 FAX (919) 781-9461 Nurse Aide II Registry (919) 782-7499 www.ncbon.com Issue: Administration
PROCEDURAL SEDATION/ANALGESIA NCBON Position Statement for RN Practice P.O. BOX 2129 Raleigh, NC 27602 (919) 782-3211 FAX (919) 781-9461 Nurse Aide II Registry (919) 782-7499 www.ncbon.com Issue: Administration
Laparoscopic Anti-Reflux (GERD) Surgery Patient Information from SAGES
 Laparoscopic Anti-Reflux (GERD) Surgery Patient Information from SAGES Surgery for "Heartburn" If you suffer from moderate to severe "heartburn" your surgeon may have recommended Laparoscopic Antireflux
Laparoscopic Anti-Reflux (GERD) Surgery Patient Information from SAGES Surgery for "Heartburn" If you suffer from moderate to severe "heartburn" your surgeon may have recommended Laparoscopic Antireflux
5/30/2014 OBJECTIVES THE ROLE OF A RESPIRATORY THERAPIST IN THE DELIVERY ROOM. Disclosure
 THE ROLE OF A RESPIRATORY THERAPIST IN THE DELIVERY ROOM Ona Fofah, MD FAAP Assistant Professor of Pediatrics Director, Division of Neonatology Department of Pediatrics Rutgers- NJMS, Newark OBJECTIVES
THE ROLE OF A RESPIRATORY THERAPIST IN THE DELIVERY ROOM Ona Fofah, MD FAAP Assistant Professor of Pediatrics Director, Division of Neonatology Department of Pediatrics Rutgers- NJMS, Newark OBJECTIVES
DRAFT 7/17/07. Procedural Sedation and Rapid Sequence Intubation (RSI) Consensus Statement
 Procedural Sedation and Rapid Sequence Intubation (RSI) Consensus Statement Many patients with emergency medical conditions in emergency and critical care settings frequently experience treatable pain,
Procedural Sedation and Rapid Sequence Intubation (RSI) Consensus Statement Many patients with emergency medical conditions in emergency and critical care settings frequently experience treatable pain,
Digestive System (continued) Digestive System. Stomach. Peptic Ulcer Disease
 Digestive System Digestive System (continued) Responsible for breaking down food, absorbing nutrients, eliminating wastes Alimentary canal Also known as gastrointestinal tract Reaches from mouth to anus
Digestive System Digestive System (continued) Responsible for breaking down food, absorbing nutrients, eliminating wastes Alimentary canal Also known as gastrointestinal tract Reaches from mouth to anus
POLICIES AND PROCEDURES GOVERNING ANESTHESIA PRIVILEGING IN HOSPITALS
 POLICIES AND PROCEDURES GOVERNING ANESTHESIA PRIVILEGING IN HOSPITALS **Hospitals must review and revise with legal counsel and ensure compliance with State and federal laws and regulations. ASA intends
POLICIES AND PROCEDURES GOVERNING ANESTHESIA PRIVILEGING IN HOSPITALS **Hospitals must review and revise with legal counsel and ensure compliance with State and federal laws and regulations. ASA intends
CLINICAL PRIVILEGES- NURSE ANESTHETIST
 Name: Page 1 Initial Appointment Reappointment All new applicants must meet the following requirements as approved by the governing body effective: 8/5/2015. Applicant: Check off the Requested box for
Name: Page 1 Initial Appointment Reappointment All new applicants must meet the following requirements as approved by the governing body effective: 8/5/2015. Applicant: Check off the Requested box for
Paediatric fluids 13/06/05
 Dr Catharine Wilson Consultant Paediatric Anaesthetist Sheffield Children s Hospital. UK Paediatric fluids 13/06/05 Self assessment: Complete these questions before reading the tutorial. Discuss the answers
Dr Catharine Wilson Consultant Paediatric Anaesthetist Sheffield Children s Hospital. UK Paediatric fluids 13/06/05 Self assessment: Complete these questions before reading the tutorial. Discuss the answers
Guidelines for the Management of the Obstetrical Patient for the Certified Registered Nurse Anesthetist
 American Association of Nurse Anesthetists 222 South Prospect Avenue Park Ridge, IL 60068 www.aana.com Guidelines for the Management of the Obstetrical Patient for the Certified Registered Nurse Anesthetist
American Association of Nurse Anesthetists 222 South Prospect Avenue Park Ridge, IL 60068 www.aana.com Guidelines for the Management of the Obstetrical Patient for the Certified Registered Nurse Anesthetist
Informed Consent for Laparoscopic Vertical Sleeve Gastrectomy. Patient Name
 Informed Consent for Laparoscopic Vertical Sleeve Gastrectomy Patient Name Please read this form carefully and ask about anything you may not understand. I consent to have a laparoscopic Vertical Sleeve
Informed Consent for Laparoscopic Vertical Sleeve Gastrectomy Patient Name Please read this form carefully and ask about anything you may not understand. I consent to have a laparoscopic Vertical Sleeve
The ASA defines anesthesiology as the practice of medicine dealing with but not limited to:
 1570 Midway Pl. Menasha, WI 54952 920-720-1300 Procedure 1205- Anesthesia Lines of Business: All Purpose: This guideline describes Network Health s reimbursement of anesthesia services. Procedure: Anesthesia
1570 Midway Pl. Menasha, WI 54952 920-720-1300 Procedure 1205- Anesthesia Lines of Business: All Purpose: This guideline describes Network Health s reimbursement of anesthesia services. Procedure: Anesthesia
Preoperative Laboratory and Diagnostic Studies
 Preoperative Laboratory and Diagnostic Studies Preoperative Labratorey and Diagnostic Studies The concept of standardized testing in all presurgical patients regardless of age or medical condition is no
Preoperative Laboratory and Diagnostic Studies Preoperative Labratorey and Diagnostic Studies The concept of standardized testing in all presurgical patients regardless of age or medical condition is no
An Overview of Asthma - Diagnosis and Treatment
 An Overview of Asthma - Diagnosis and Treatment Asthma is a common chronic disorder of the airways that is complex and characterized by variable and recurring symptoms, airflow obstruction, bronchial hyperresponsiveness,
An Overview of Asthma - Diagnosis and Treatment Asthma is a common chronic disorder of the airways that is complex and characterized by variable and recurring symptoms, airflow obstruction, bronchial hyperresponsiveness,
Understanding Hypoventilation and Its Treatment by Susan Agrawal
 www.complexchild.com Understanding Hypoventilation and Its Treatment by Susan Agrawal Most of us have a general understanding of what the term hyperventilation means, since hyperventilation, also called
www.complexchild.com Understanding Hypoventilation and Its Treatment by Susan Agrawal Most of us have a general understanding of what the term hyperventilation means, since hyperventilation, also called
PRACTICE Advisories are systematically developed reports
 for Preanesthesia Evaluation An Updated Report by the American Society of Anesthesiologists Task Force on Preanesthesia Evaluation Updated by the Committee on Standards and Practice Parameters, Jeffrey
for Preanesthesia Evaluation An Updated Report by the American Society of Anesthesiologists Task Force on Preanesthesia Evaluation Updated by the Committee on Standards and Practice Parameters, Jeffrey
Respiratory Concerns in Children with Down Syndrome
 Respiratory Concerns in Children with Down Syndrome Paul E. Moore, M.D. Associate Professor of Pediatrics and Pharmacology Director, Pediatric Allergy, Immunology, and Pulmonary Medicine Vanderbilt University
Respiratory Concerns in Children with Down Syndrome Paul E. Moore, M.D. Associate Professor of Pediatrics and Pharmacology Director, Pediatric Allergy, Immunology, and Pulmonary Medicine Vanderbilt University
High Impact Intervention Care bundle to reduce ventilation-association pneumonia
 High Impact Intervention Care bundle to reduce ventilation-association pneumonia Aim To reduce the incidence of ventilation-associated pneumonia (VAP). Context The aim of the care bundle, as set out in
High Impact Intervention Care bundle to reduce ventilation-association pneumonia Aim To reduce the incidence of ventilation-associated pneumonia (VAP). Context The aim of the care bundle, as set out in
PATIENT CONSENT TO PROCEDURE - ROUX-EN-Y GASTRIC BYPASS
 As a patient you must be adequately informed about your condition and the recommended surgical procedure. Please read this document carefully and ask about anything you do not understand. Please initial
As a patient you must be adequately informed about your condition and the recommended surgical procedure. Please read this document carefully and ask about anything you do not understand. Please initial
G E R D. (Gastroesophageal Reflux Disease)
 G E R D (Gastroesophageal Reflux Disease) What is GERD? Gastroesophageal reflux disease (GERD) is a disorder caused by gastric acid flowing from the stomach into the esophagus. What are the symptoms of
G E R D (Gastroesophageal Reflux Disease) What is GERD? Gastroesophageal reflux disease (GERD) is a disorder caused by gastric acid flowing from the stomach into the esophagus. What are the symptoms of
Pediatric Airway Management
 Pediatric Airway Management Dec 2003 Dr. Shapiro I., PICU Adult Chain of Survival EMS CPR ALS Early Defibrillation Pediatric Chain of Survival Prevention CPR EMS ALS Out-of-Hospital Cardiac Arrest SIDS
Pediatric Airway Management Dec 2003 Dr. Shapiro I., PICU Adult Chain of Survival EMS CPR ALS Early Defibrillation Pediatric Chain of Survival Prevention CPR EMS ALS Out-of-Hospital Cardiac Arrest SIDS
Over 660 Contact Hours of Online Continuing Nursing Education!
 Over 660 of Online Continuing Nursing Education! Choose from Four Great Series: Clinical Health Care Clinical & Continuing Education MedSenses AACN NetLearning is committed to providing you with the very
Over 660 of Online Continuing Nursing Education! Choose from Four Great Series: Clinical Health Care Clinical & Continuing Education MedSenses AACN NetLearning is committed to providing you with the very
Nursing college, Second stage Microbiology Dr.Nada Khazal K. Hendi L14: Hospital acquired infection, nosocomial infection
 L14: Hospital acquired infection, nosocomial infection Definition A hospital acquired infection, also called a nosocomial infection, is an infection that first appears between 48 hours and four days after
L14: Hospital acquired infection, nosocomial infection Definition A hospital acquired infection, also called a nosocomial infection, is an infection that first appears between 48 hours and four days after
Mississippi Board of Nursing
 Mississippi Board of Nursing Regulating Nursing Practice www.msbn.state.ms.us 713 Pear Orchard Road, Suite 300 Ridgeland, MS 39157 Administration and Management of Intravenous (IV) Moderate Sedation POSITION
Mississippi Board of Nursing Regulating Nursing Practice www.msbn.state.ms.us 713 Pear Orchard Road, Suite 300 Ridgeland, MS 39157 Administration and Management of Intravenous (IV) Moderate Sedation POSITION
Scope and Standards for Nurse Anesthesia Practice
 Scope and Standards for Nurse Anesthesia Practice Copyright 2010 222 South Prospect Ave. Park Ridge, IL 60068 www.aana.com Scope and Standards for Nurse Anesthesia Practice The AANA Scope and Standards
Scope and Standards for Nurse Anesthesia Practice Copyright 2010 222 South Prospect Ave. Park Ridge, IL 60068 www.aana.com Scope and Standards for Nurse Anesthesia Practice The AANA Scope and Standards
Neonatal Intubation. Purpose. Scope. Indications. Equipment Cardiorespiratory monitor SaO 2 monitor. Anatomic Considerations.
 Page 1 of 5 Purpose Scope Indications Neonatal Intubation To assure proper placement of endotracheal tubes for maximum ventilation using proper intubation procedures. The policy applies to all Respiratory
Page 1 of 5 Purpose Scope Indications Neonatal Intubation To assure proper placement of endotracheal tubes for maximum ventilation using proper intubation procedures. The policy applies to all Respiratory
Why is prematurity a concern?
 Prematurity What is prematurity? A baby born before 37 weeks of pregnancy is considered premature. Approximately 12% of all babies are born prematurely. Terms that refer to premature babies are preterm
Prematurity What is prematurity? A baby born before 37 weeks of pregnancy is considered premature. Approximately 12% of all babies are born prematurely. Terms that refer to premature babies are preterm
Iatrogenesis. Suzanne Beyea,, RN, PhD, FAAN Associate Director: Centers for Health and Aging
 Iatrogenesis Suzanne Beyea,, RN, PhD, FAAN Associate Director: Centers for Health and Aging Iatrogenesis Definition from the Greek word, iatros,, meaning healer, iatrogenesis means brought forth by a healer
Iatrogenesis Suzanne Beyea,, RN, PhD, FAAN Associate Director: Centers for Health and Aging Iatrogenesis Definition from the Greek word, iatros,, meaning healer, iatrogenesis means brought forth by a healer
National Digestive Diseases Information Clearinghouse
 Barrett s Esophagus National Digestive Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is Barrett s esophagus? Barrett s esophagus is
Barrett s Esophagus National Digestive Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is Barrett s esophagus? Barrett s esophagus is
Heart Failure: Diagnosis and Treatment
 Heart Failure: Diagnosis and Treatment Approximately 5 million people about 2 percent of the U.S. population are affected by heart failure. Diabetes affects 20.8 million Americans and 65 million Americans
Heart Failure: Diagnosis and Treatment Approximately 5 million people about 2 percent of the U.S. population are affected by heart failure. Diabetes affects 20.8 million Americans and 65 million Americans
Common Surgical Procedures in the Elderly
 Common Surgical Procedures in the Elderly From hip and knee replacements to cataract and heart surgery, America s elderly undergo 20% of all surgical procedures. For a group that comprises only 13% of
Common Surgical Procedures in the Elderly From hip and knee replacements to cataract and heart surgery, America s elderly undergo 20% of all surgical procedures. For a group that comprises only 13% of
Title/Subject Procedural Sedation and Analgesia Page 1 of 10
 Policy Procedural Sedation and Analgesia Page 1 of 10 Scope: Providers and nurses (M.D., D.O., D.M.D., D.D.S., A.P.R.N., P.A., R.N.) with appropriate privileges and who have successfully demonstrated adequate
Policy Procedural Sedation and Analgesia Page 1 of 10 Scope: Providers and nurses (M.D., D.O., D.M.D., D.D.S., A.P.R.N., P.A., R.N.) with appropriate privileges and who have successfully demonstrated adequate
The etiology of obesity is multifactorial,
 The frequency of respiratory failure in patients with morbid obesity undergoing gastric bypass Eleanor L. Blouw, CRNA, MNA Anne D. Rudolph, CRNA, MNA Bradley J. Narr, MD Michael G. Sarr, MD Rochester,
The frequency of respiratory failure in patients with morbid obesity undergoing gastric bypass Eleanor L. Blouw, CRNA, MNA Anne D. Rudolph, CRNA, MNA Bradley J. Narr, MD Michael G. Sarr, MD Rochester,
A BIBLIOGRAPHY OF PEER-REVIEWED JOURNAL ARTICLES
 ANESTHESIA CLOSED CLAIMS PROJECT A BIBLIOGRAPHY OF PEER-REVIEWED JOURNAL ARTICLES PROJECT OFFICE Anesthesia Closed Claims Project Department of Anesthesiology and Pain Medicine University of Washington
ANESTHESIA CLOSED CLAIMS PROJECT A BIBLIOGRAPHY OF PEER-REVIEWED JOURNAL ARTICLES PROJECT OFFICE Anesthesia Closed Claims Project Department of Anesthesiology and Pain Medicine University of Washington
GASTRIC BYPASS SURGERY CONSENT FORM
 Page 1 of 6 I, have been asked to read carefully all of the (name of patient or substitute decision-maker) information contained in this consent form and to consent to the procedure described below on
Page 1 of 6 I, have been asked to read carefully all of the (name of patient or substitute decision-maker) information contained in this consent form and to consent to the procedure described below on
Oxygen Therapy. Oxygen therapy quick guide V3 July 2012.
 PRESENTATION Oxygen (O 2 ) is a gas provided in a compressed form in a cylinder. It is also available in a liquid form. It is fed via a regulator and flow meter to the patient by means of plastic tubing
PRESENTATION Oxygen (O 2 ) is a gas provided in a compressed form in a cylinder. It is also available in a liquid form. It is fed via a regulator and flow meter to the patient by means of plastic tubing
Laparoscopic Gallbladder Removal (Cholecystectomy) Patient Information from SAGES
 Laparoscopic Gallbladder Removal (Cholecystectomy) Patient Information from SAGES Gallbladder removal is one of the most commonly performed surgical procedures. Gallbladder removal surgery is usually performed
Laparoscopic Gallbladder Removal (Cholecystectomy) Patient Information from SAGES Gallbladder removal is one of the most commonly performed surgical procedures. Gallbladder removal surgery is usually performed
INTRAPERITONEAL HYPERTHERMIC CHEMOTHERAPY (IPHC) FOR PERITONEAL CARCINOMATOSIS AND MALIGNANT ASCITES. INFORMATION FOR PATIENTS AND FAMILY MEMBERS
 INTRAPERITONEAL HYPERTHERMIC CHEMOTHERAPY (IPHC) FOR PERITONEAL CARCINOMATOSIS AND MALIGNANT ASCITES. INFORMATION FOR PATIENTS AND FAMILY MEMBERS Description of Treatment A major difficulty in treating
INTRAPERITONEAL HYPERTHERMIC CHEMOTHERAPY (IPHC) FOR PERITONEAL CARCINOMATOSIS AND MALIGNANT ASCITES. INFORMATION FOR PATIENTS AND FAMILY MEMBERS Description of Treatment A major difficulty in treating
Gastroschisis and My Baby
 Patient and Family Education Gastroschisis and My Baby Gastroschisis is a condition where a baby is born with the intestine outside the body. Learning about the diagnosis What is gastroschisis? (pronounced
Patient and Family Education Gastroschisis and My Baby Gastroschisis is a condition where a baby is born with the intestine outside the body. Learning about the diagnosis What is gastroschisis? (pronounced
PRE-ASSESSMENT. Surgical Anesthesia Delivered by Non-physicians
 CCOHTA No. 37 July 2004 Before CCOHTA decides to undertake a health technology assessment, a pre-assessment of the literature is performed. Pre-assessments are based on a limited literature search; they
CCOHTA No. 37 July 2004 Before CCOHTA decides to undertake a health technology assessment, a pre-assessment of the literature is performed. Pre-assessments are based on a limited literature search; they
Scope and Standards for Nurse Anesthesia Practice
 Scope and Standards for Nurse Anesthesia Practice Copyright 2013 222 South Prospect Ave. Park Ridge, IL 60068 www.aana.com Scope and Standards for Nurse Anesthesia Practice The AANA Scope and Standards
Scope and Standards for Nurse Anesthesia Practice Copyright 2013 222 South Prospect Ave. Park Ridge, IL 60068 www.aana.com Scope and Standards for Nurse Anesthesia Practice The AANA Scope and Standards
Tuberculosis Exposure Control Plan for Low Risk Dental Offices
 Tuberculosis Exposure Control Plan for Low Risk Dental Offices A. BACKGROUND According to the CDC, approximately one-third of the world s population, almost two billion people, are infected with tuberculosis.
Tuberculosis Exposure Control Plan for Low Risk Dental Offices A. BACKGROUND According to the CDC, approximately one-third of the world s population, almost two billion people, are infected with tuberculosis.
Anesthesia Guidelines
 Anesthesia Guidelines Updated April 2012 Anesthesia BlueCross requires anesthesiologists and certified registered nurse anesthetists (CRNAs) to file claims using CPT anesthesia codes. We cover general
Anesthesia Guidelines Updated April 2012 Anesthesia BlueCross requires anesthesiologists and certified registered nurse anesthetists (CRNAs) to file claims using CPT anesthesia codes. We cover general
Department of Veterans Affairs VHA DIRECTIVE 2012-032 Veterans Health Administration Washington, DC 20420 October 26, 2012
 Department of Veterans Affairs VHA DIRECTIVE 2012-032 Veterans Health Administration Washington, DC 20420 OUT OF OPERATING ROOM AIRWAY MANAGEMENT 1. PURPOSE: This Veterans Health Administration (VHA) Directive
Department of Veterans Affairs VHA DIRECTIVE 2012-032 Veterans Health Administration Washington, DC 20420 OUT OF OPERATING ROOM AIRWAY MANAGEMENT 1. PURPOSE: This Veterans Health Administration (VHA) Directive
Series 1 Case Studies Adverse Events that Represent Unanticipated Problems: Reporting Required
 Welcome! This document contains three (3) series of Case Study examples that will demonstrate all four OHSU reporting categories (#1 4) as well as examples of events that are considered not reportable.
Welcome! This document contains three (3) series of Case Study examples that will demonstrate all four OHSU reporting categories (#1 4) as well as examples of events that are considered not reportable.
Overall Goals/Objectives - Surgical Critical Care Residency Program The goal of the Pediatric Surgical Critical Care Residency program is to provide
 Overall Goals/Objectives - Surgical Critical Care Residency Program The goal of the Pediatric Surgical Critical Care Residency program is to provide advanced proficiency in the care and management of critically
Overall Goals/Objectives - Surgical Critical Care Residency Program The goal of the Pediatric Surgical Critical Care Residency program is to provide advanced proficiency in the care and management of critically
*Reflex withdrawal from a painful stimulus is NOT considered a purposeful response.
 Analgesia and Moderate Sedation This Nebraska Board of Nursing advisory opinion is issued in accordance with Nebraska Revised Statute (NRS) 71-1,132.11(2). As such, this advisory opinion is for informational
Analgesia and Moderate Sedation This Nebraska Board of Nursing advisory opinion is issued in accordance with Nebraska Revised Statute (NRS) 71-1,132.11(2). As such, this advisory opinion is for informational
Pain Relief Options for Labor. Providing You with Quality Care, Information and Support
 Pain Relief Options for Labor Providing You with Quality Care, Information and Support What can I expect during my labor and delivery? As a patient in the Labor and Delivery Suite at Lucile Packard Children
Pain Relief Options for Labor Providing You with Quality Care, Information and Support What can I expect during my labor and delivery? As a patient in the Labor and Delivery Suite at Lucile Packard Children
Gastroesophageal Reflux Disease (GERD) and Barrett s Esophagus (BE)
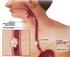 Gastroesophageal Reflux Disease (GERD) and Barrett s Esophagus (BE) Hashem El-Serag, M.D., M.P.H. Dan L. Duncan Professor of Medicine Chief, Gastroenterology and Hepatology Baylor College of Medicine Houston,
Gastroesophageal Reflux Disease (GERD) and Barrett s Esophagus (BE) Hashem El-Serag, M.D., M.P.H. Dan L. Duncan Professor of Medicine Chief, Gastroenterology and Hepatology Baylor College of Medicine Houston,
Program Specification for Master Degree Anesthesia, ICU and Pain Management
 Cairo University Faculty of Medicine Program type: Single Program Specification for Master Degree Anesthesia, ICU and Pain Management Department offering program: Anesthesia, intensive care and pain management
Cairo University Faculty of Medicine Program type: Single Program Specification for Master Degree Anesthesia, ICU and Pain Management Department offering program: Anesthesia, intensive care and pain management
The Sepsis Puzzle: Identification, Monitoring and Early Goal Directed Therapy
 The Sepsis Puzzle: Identification, Monitoring and Early Goal Directed Therapy Cindy Goodrich RN, MS, CCRN Content Description Sepsis is caused by widespread tissue injury and systemic inflammation resulting
The Sepsis Puzzle: Identification, Monitoring and Early Goal Directed Therapy Cindy Goodrich RN, MS, CCRN Content Description Sepsis is caused by widespread tissue injury and systemic inflammation resulting
Laparoscopic Antireflux Surgery Information Sheet
 Laparoscopic Antireflux Surgery Information Sheet What is Laparoscopic Antireflux Surgery? Antireflux surgery (also known as fundoplication) is the standard surgical method of treating gastro-oesophageal
Laparoscopic Antireflux Surgery Information Sheet What is Laparoscopic Antireflux Surgery? Antireflux surgery (also known as fundoplication) is the standard surgical method of treating gastro-oesophageal
DISCHARGE CRITERIA FOR PHASE I & II- POST ANESTHESIA CARE
 REFERENCES: The Joint Commission Accreditation Manual for Hospitals American Society of Post Anesthesia Nurses: Standards of Post Anesthesia Nursing Practice (1991, 2002). RELATED DOCUMENTS: SHC Administrative
REFERENCES: The Joint Commission Accreditation Manual for Hospitals American Society of Post Anesthesia Nurses: Standards of Post Anesthesia Nursing Practice (1991, 2002). RELATED DOCUMENTS: SHC Administrative
What You Need to Know About Anesthesia Filing Guidelines
 What You Need to Know About Anesthesia Filing Guidelines 2015 Edition Published by Provider Relations and Education Your Partners in Outstanding Quality, Satisfaction and Service This document provides
What You Need to Know About Anesthesia Filing Guidelines 2015 Edition Published by Provider Relations and Education Your Partners in Outstanding Quality, Satisfaction and Service This document provides
Local Anaesthetic Systemic Toxicity. Dr Thomas Engelhardt, MD, PhD, FRCA Royal Aberdeen Children s Hospital, Scotland
 Local Anaesthetic Systemic Toxicity Dr Thomas Engelhardt, MD, PhD, FRCA Royal Aberdeen Children s Hospital, Scotland Conflict of interest None Overview Local anesthetic systemic toxicity (LAST) Background
Local Anaesthetic Systemic Toxicity Dr Thomas Engelhardt, MD, PhD, FRCA Royal Aberdeen Children s Hospital, Scotland Conflict of interest None Overview Local anesthetic systemic toxicity (LAST) Background
1.4.4 Oxyhemoglobin desaturation
 Critical Care Therapy and Respiratory Care Section Category: Clinical Section: Clinical Monitoring Title: Monitoring of Patients Undergoing Conscious Sedation Policy #: 09 Revised: 05/00 1.0 DESCRIPTION
Critical Care Therapy and Respiratory Care Section Category: Clinical Section: Clinical Monitoring Title: Monitoring of Patients Undergoing Conscious Sedation Policy #: 09 Revised: 05/00 1.0 DESCRIPTION
What You Need to know about Your Pet s Upcoming Dentistry and Periodontal Treatment
 What You Need to know about Your Pet s Upcoming Dentistry and Periodontal Treatment We are sending this packet of information in anticipation of your pet s upcoming dental procedure. Many people have questions
What You Need to know about Your Pet s Upcoming Dentistry and Periodontal Treatment We are sending this packet of information in anticipation of your pet s upcoming dental procedure. Many people have questions
Geisinger Health System Anesthesiology Residency Program. Obstetric Anesthesia
 Geisinger Health System Anesthesiology Residency Program Obstetric Anesthesia INTRODUCTION Education and training in obstetric anesthesia will consist of attending-supervised rotations for four weeks during
Geisinger Health System Anesthesiology Residency Program Obstetric Anesthesia INTRODUCTION Education and training in obstetric anesthesia will consist of attending-supervised rotations for four weeks during
RGN JOY LAUDE WATFORD GENERAL HOSPITAL, ENGLAND
 RGN JOY LAUDE WATFORD GENERAL HOSPITAL, ENGLAND Monitor patient on the ward to detect trends in vital signs and to manage accordingly To recognise deteriorating trends and request relevant medical/out
RGN JOY LAUDE WATFORD GENERAL HOSPITAL, ENGLAND Monitor patient on the ward to detect trends in vital signs and to manage accordingly To recognise deteriorating trends and request relevant medical/out
ECG may be indicated for patients with cardiovascular risk factors
 eappendix A. Summary for Preoperative ECG American College of Cardiology/ American Heart Association, 2007 A1 2002 A2 European Society of Cardiology and European Society of Anaesthesiology, 2009 A3 Improvement,
eappendix A. Summary for Preoperative ECG American College of Cardiology/ American Heart Association, 2007 A1 2002 A2 European Society of Cardiology and European Society of Anaesthesiology, 2009 A3 Improvement,
NICE Pathways bring together all NICE guidance, quality standards and other NICE information on a specific topic.
 Diabetic ketoacidosis in children and young people bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used online. They
Diabetic ketoacidosis in children and young people bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used online. They
What is the Sleeve Gastrectomy?
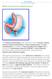 What is the Sleeve Gastrectomy? The Sleeve Gastrectomy (also referred to as the Gastric Sleeve, Vertical Sleeve Gastrectomy, Partial Gastrectomy, or Tube Gastrectomy) is a relatively new procedure for
What is the Sleeve Gastrectomy? The Sleeve Gastrectomy (also referred to as the Gastric Sleeve, Vertical Sleeve Gastrectomy, Partial Gastrectomy, or Tube Gastrectomy) is a relatively new procedure for
Guidelines for Core Clinical Privileges Certified Registered Nurse Anesthetists
 Guidelines for Core Clinical Privileges Certified Registered Nurse Anesthetists Copyright 2005 222 South Prospect Park Ridge, IL 60068 www.aana.com Guidelines for Core Clinical Privileges Certified Registered
Guidelines for Core Clinical Privileges Certified Registered Nurse Anesthetists Copyright 2005 222 South Prospect Park Ridge, IL 60068 www.aana.com Guidelines for Core Clinical Privileges Certified Registered
Chapter 7. Ideally, educational preparation for childbirth begins prior to conception
 Chapter 7 Nursing Management of Pain During Labor and Birth Key Terms Cleansing breath Effleurage Endorphins Pain threshold Focal point Pain tolerance Education for Childbearing Ideally, educational preparation
Chapter 7 Nursing Management of Pain During Labor and Birth Key Terms Cleansing breath Effleurage Endorphins Pain threshold Focal point Pain tolerance Education for Childbearing Ideally, educational preparation
Weight Loss before Hernia Repair Surgery
 Weight Loss before Hernia Repair Surgery What is an abdominal wall hernia? The abdomen (commonly called the belly) holds many of your internal organs. In the front, the abdomen is protected by a tough
Weight Loss before Hernia Repair Surgery What is an abdominal wall hernia? The abdomen (commonly called the belly) holds many of your internal organs. In the front, the abdomen is protected by a tough
Oxygen - update April 2009 OXG
 PRESENTATION Oxygen (O 2 ) is a gas provided in compressed form in a cylinder. It is also available in liquid form, in a system adapted for ambulance use. It is fed via a regulator and flow meter to the
PRESENTATION Oxygen (O 2 ) is a gas provided in compressed form in a cylinder. It is also available in liquid form, in a system adapted for ambulance use. It is fed via a regulator and flow meter to the
Public Assessment Report. Pharmacy to General Sales List Reclassification. Nexium Control 20mg Gastro-Resistant Tablets.
 Public Assessment Report Pharmacy to General Sales List Reclassification Nexium Control 20mg Gastro-Resistant Tablets (Esomeprazole) EMA Agency number: Pfizer Consumer Healthcare Ltd TABLE OF CONTENTS
Public Assessment Report Pharmacy to General Sales List Reclassification Nexium Control 20mg Gastro-Resistant Tablets (Esomeprazole) EMA Agency number: Pfizer Consumer Healthcare Ltd TABLE OF CONTENTS
Surgical Safety Checklists and Briefings Clinician s User Guidelines
 Surgical Safety Checklists and Briefings Clinician s User Guidelines 3/15/2009 Surrey Memorial Hospital Author: Keith Martinsen Before Induction Checklist Surgeon s Team Briefing Before Skin Incision Checklist
Surgical Safety Checklists and Briefings Clinician s User Guidelines 3/15/2009 Surrey Memorial Hospital Author: Keith Martinsen Before Induction Checklist Surgeon s Team Briefing Before Skin Incision Checklist
Acute Abdominal Pain following Bariatric Surgery. Disclosure. Objectives 8/17/2015. I have nothing to disclose
 Acute Abdominal Pain following Bariatric Surgery Kathy J. Morris, DNP, APRN, FNP C, FAANP University of Nebraska Medical Center College of Nursing Disclosure I have nothing to disclose Objectives Pathophysiology
Acute Abdominal Pain following Bariatric Surgery Kathy J. Morris, DNP, APRN, FNP C, FAANP University of Nebraska Medical Center College of Nursing Disclosure I have nothing to disclose Objectives Pathophysiology
Surgical removal of fibroids through an abdominal incision-either up and down or bikini cut. The uterus and cervix are left in place.
 What is an abdominal myomectomy? Surgical removal of fibroids through an abdominal incision-either up and down or bikini cut. The uterus and cervix are left in place. When is this surgery used? Treatment
What is an abdominal myomectomy? Surgical removal of fibroids through an abdominal incision-either up and down or bikini cut. The uterus and cervix are left in place. When is this surgery used? Treatment
International Training Program for Nurse Anesthetist The program: International training program for nurse anesthetist Name of certificate:
 International Training Program for Nurse Anesthetist Department of Anesthesiology Faculty of Medicine Siriraj Hospital Mahidol University, Bangkok, Thailand The program: International training program
International Training Program for Nurse Anesthetist Department of Anesthesiology Faculty of Medicine Siriraj Hospital Mahidol University, Bangkok, Thailand The program: International training program
Blood Transfusion. There are three types of blood cells: Red blood cells. White blood cells. Platelets.
 Blood Transfusion Introduction Blood transfusions can save lives. Every second, someone in the world needs a blood transfusion. Blood transfusions can replace the blood lost from a serious injury or surgery.
Blood Transfusion Introduction Blood transfusions can save lives. Every second, someone in the world needs a blood transfusion. Blood transfusions can replace the blood lost from a serious injury or surgery.
Gastroesophageal Reflux
 Gastroesophageal Reflux What is Gastroesophageal Reflux? Gastroesophageal reflux (GER) is involuntary regurgitation of stomach contents into the esophagus. Reflux causes a number of problems: 1. Chemical
Gastroesophageal Reflux What is Gastroesophageal Reflux? Gastroesophageal reflux (GER) is involuntary regurgitation of stomach contents into the esophagus. Reflux causes a number of problems: 1. Chemical
Evaluating MSDS First Aid Advice
 Evaluating MSDS First Aid Advice Senior Technical Specialist Evidence-Based Approach Identify specific questions Search for relevant literature Critically evaluate quality of evidence Determine best answer
Evaluating MSDS First Aid Advice Senior Technical Specialist Evidence-Based Approach Identify specific questions Search for relevant literature Critically evaluate quality of evidence Determine best answer
CH CONSCIOUS SEDATION
 Summary: CH CONSCIOUS SEDATION It is the policy of Carondelet Health that moderate conscious sedation of patients will be undertaken with appropriate evaluation and monitoring. Effective Date: 9/4/04 Revision
Summary: CH CONSCIOUS SEDATION It is the policy of Carondelet Health that moderate conscious sedation of patients will be undertaken with appropriate evaluation and monitoring. Effective Date: 9/4/04 Revision
Omega-3 fatty acids improve the diagnosis-related clinical outcome. Critical Care Medicine April 2006;34(4):972-9
 Omega-3 fatty acids improve the diagnosis-related clinical outcome 1 Critical Care Medicine April 2006;34(4):972-9 Volume 34(4), April 2006, pp 972-979 Heller, Axel R. MD, PhD; Rössler, Susann; Litz, Rainer
Omega-3 fatty acids improve the diagnosis-related clinical outcome 1 Critical Care Medicine April 2006;34(4):972-9 Volume 34(4), April 2006, pp 972-979 Heller, Axel R. MD, PhD; Rössler, Susann; Litz, Rainer
Peptic Ulcer. Anatomy The stomach is a hollow organ. It is located in the upper abdomen, under the ribs.
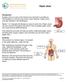 Peptic Ulcer Introduction A peptic ulcer is a sore in the lining of your stomach or duodenum. The duodenum is the first part of your small intestine. Peptic ulcers may also develop in the esophagus. Nearly
Peptic Ulcer Introduction A peptic ulcer is a sore in the lining of your stomach or duodenum. The duodenum is the first part of your small intestine. Peptic ulcers may also develop in the esophagus. Nearly
Gastrointestinal Bleeding
 Gastrointestinal Bleeding Introduction Gastrointestinal bleeding is a symptom of many diseases rather than a disease itself. A number of different conditions can cause gastrointestinal bleeding. Some causes
Gastrointestinal Bleeding Introduction Gastrointestinal bleeding is a symptom of many diseases rather than a disease itself. A number of different conditions can cause gastrointestinal bleeding. Some causes
Levels of Critical Care for Adult Patients
 LEVELS OF CARE 1 Levels of Critical Care for Adult Patients STANDARDS AND GUIDELINES LEVELS OF CARE 2 Intensive Care Society 2009 All rights reserved. No reproduction, copy or transmission of this publication
LEVELS OF CARE 1 Levels of Critical Care for Adult Patients STANDARDS AND GUIDELINES LEVELS OF CARE 2 Intensive Care Society 2009 All rights reserved. No reproduction, copy or transmission of this publication
What can I eat? Peptic ulcers. What are peptic ulcers? What tests are needed? Will the ulcer come back? What causes a peptic ulcer?
 In association with: INFORMATION ABOUT Peptic ulcers www.corecharity.org.uk What are peptic ulcers? What causes a peptic ulcer? How are NSAIDs and aspirin involved? How do I know if I ve got an ulcer?
In association with: INFORMATION ABOUT Peptic ulcers www.corecharity.org.uk What are peptic ulcers? What causes a peptic ulcer? How are NSAIDs and aspirin involved? How do I know if I ve got an ulcer?
National Digestive Diseases Information Clearinghouse
 Gastritis National Digestive Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is gastritis? Gastritis is a condition in which the stomach
Gastritis National Digestive Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is gastritis? Gastritis is a condition in which the stomach
MODEL SEDATION PROTOCOL FOR MODERATE SEDATION AND ANALGESIA PERFORMED BY NON-ANESTHESIA PROVIDERS DURING PROCEDURES
 MODEL SEDATION PROTOCOL FOR MODERATE SEDATION AND ANALGESIA PERFORMED BY NON-ANESTHESIA PROVIDERS DURING PROCEDURES ON ADULTS AND CHILDREN OLDER THAN 10 YEARS OF AGE. PURPOSE This policy has been established
MODEL SEDATION PROTOCOL FOR MODERATE SEDATION AND ANALGESIA PERFORMED BY NON-ANESTHESIA PROVIDERS DURING PROCEDURES ON ADULTS AND CHILDREN OLDER THAN 10 YEARS OF AGE. PURPOSE This policy has been established
You have been advised by your GP or hospital doctor to have an investigation known as a Gastroscopy.
 Gastroscopy (OGD) The Procedure Explained You have been advised by your GP or hospital doctor to have an investigation known as a Gastroscopy. This procedure requires your formal consent. If you are unable
Gastroscopy (OGD) The Procedure Explained You have been advised by your GP or hospital doctor to have an investigation known as a Gastroscopy. This procedure requires your formal consent. If you are unable
Congenital Diaphragmatic Hernia. Manuel A. Molina, M.D. University Hospital at Brooklyn SUNY Downstate
 Congenital Diaphragmatic Hernia Manuel A. Molina, M.D. University Hospital at Brooklyn SUNY Downstate Congenital Diaphragmatic Hernias Incidence 1 in 2000 to 5000 live births. 80% in the left side, 20%
Congenital Diaphragmatic Hernia Manuel A. Molina, M.D. University Hospital at Brooklyn SUNY Downstate Congenital Diaphragmatic Hernias Incidence 1 in 2000 to 5000 live births. 80% in the left side, 20%
OET: Listening Part A: Influenza
 Listening Test Part B Time allowed: 23 minutes In this part, you will hear a talk on critical illnesses due to A/H1N1 influenza in pregnant and postpartum women, given by a medical researcher. You will
Listening Test Part B Time allowed: 23 minutes In this part, you will hear a talk on critical illnesses due to A/H1N1 influenza in pregnant and postpartum women, given by a medical researcher. You will
F.E.E.A. FONDATION EUROPEENNE D'ENSEIGNEMENT EN ANESTHESIOLOGIE FOUNDATION FOR EUROPEAN EDUCATION IN ANAESTHESIOLOGY
 créée sous le Patronage de l'union Européenne Detailed plan of the program of six courses 1. RESPIRATORY 1. ESPIRATORY AND THORAX 1.1 Physics and principles of measurement 1.1.1 Physical laws 1.1.2 Vaporizers
créée sous le Patronage de l'union Européenne Detailed plan of the program of six courses 1. RESPIRATORY 1. ESPIRATORY AND THORAX 1.1 Physics and principles of measurement 1.1.1 Physical laws 1.1.2 Vaporizers
Explore the World of a Nurse Anesthetist!
 Continuing Education Explore the World of a Nurse Anesthetist! Sherly Shaji, CRNA, documents a blood transfusion in the anesthesia chart. Photograph by Lee McClelland, CRNA The purpose of this educational
Continuing Education Explore the World of a Nurse Anesthetist! Sherly Shaji, CRNA, documents a blood transfusion in the anesthesia chart. Photograph by Lee McClelland, CRNA The purpose of this educational
Section 2. Overview of Obesity, Weight Loss, and Bariatric Surgery
 Section 2 Overview of Obesity, Weight Loss, and Bariatric Surgery What is Weight Loss? How does surgery help with weight loss? Short term versus long term weight loss? Conditions Improved with Weight Loss
Section 2 Overview of Obesity, Weight Loss, and Bariatric Surgery What is Weight Loss? How does surgery help with weight loss? Short term versus long term weight loss? Conditions Improved with Weight Loss
OB PBLD L117 Labor and Delivery in the Age of Ebola Upper 20B-20C. PI PBLD L120 He's 15, Needs This Operation, and He's DNR!
 ETHICS - Saturday, October 24 OB PBLD L117 Labor and Delivery in the Age of Ebola PI PBLD L120 He's 15, Needs This Operation, and He's DNR! PD PBLD L118 Sex, Drugs, and Rock 'N' Roll: An Anxious Adolescent
ETHICS - Saturday, October 24 OB PBLD L117 Labor and Delivery in the Age of Ebola PI PBLD L120 He's 15, Needs This Operation, and He's DNR! PD PBLD L118 Sex, Drugs, and Rock 'N' Roll: An Anxious Adolescent
Caring Choices. For Parents of Infants Newly Diagnosed with SMA Type 1 SMA CARE SERIES
 Caring Choices For Parents of Infants Newly Diagnosed with SMA Type 1 SMA CARE SERIES SMA CARE SERIES - Caring Choices Contents Dear Parents, Friends and Family Members 3 What Decisions are Ahead 4 What
Caring Choices For Parents of Infants Newly Diagnosed with SMA Type 1 SMA CARE SERIES SMA CARE SERIES - Caring Choices Contents Dear Parents, Friends and Family Members 3 What Decisions are Ahead 4 What
National Learning Objectives for COPD Educators
 National Learning Objectives for COPD Educators National Learning Objectives for COPD Educators The COPD Educator will be able to achieve the following objectives. Performance objectives, denoted by the
National Learning Objectives for COPD Educators National Learning Objectives for COPD Educators The COPD Educator will be able to achieve the following objectives. Performance objectives, denoted by the
The literature on emergency management of the pediatric
 Original Article Incidence of Reflex Bradycardia and Effects of Pretreatment With Atropine Rebecca K. Fastle, MD and Mark G. Roback, MD Background: The American College of Emergency Physicians (ACEP) recommends
Original Article Incidence of Reflex Bradycardia and Effects of Pretreatment With Atropine Rebecca K. Fastle, MD and Mark G. Roback, MD Background: The American College of Emergency Physicians (ACEP) recommends
St. Louis Eye Care Specialists, LLC Andrew N. Blatt, MD
 St. Louis Eye Care Specialists, LLC Andrew N. Blatt, MD 675 Old Ballas Rd. Suite 220 St. Louis, MO 63141 Phone: 314-997-3937 Fax: 314997-3911 Toll Free: 866-869-3937 PEDIACTRIC CATARACT SURGERY A cataract
St. Louis Eye Care Specialists, LLC Andrew N. Blatt, MD 675 Old Ballas Rd. Suite 220 St. Louis, MO 63141 Phone: 314-997-3937 Fax: 314997-3911 Toll Free: 866-869-3937 PEDIACTRIC CATARACT SURGERY A cataract
Why would we want to change a practice with a track record that has proven safe and that works well?
 Good morning, Mr. Chairman and distinguished members of the House Professional Licensure Committee. My name is Dr. Erin Sullivan. I am president of the Pennsylvania Society of Anesthesiologists and a board
Good morning, Mr. Chairman and distinguished members of the House Professional Licensure Committee. My name is Dr. Erin Sullivan. I am president of the Pennsylvania Society of Anesthesiologists and a board
NURSING SERVICES DEPARTMENT
 NURSING SERVICES DEPARTMENT TITLE: Mechanical Ventilation PATIENT CARE PLAN DIAGNOSIS: DISCHARGE CRITERIA: 1 The patient will: Maintain adequate mechanics of PERTINENT INFORMATION:. ventilation as demonstrated
NURSING SERVICES DEPARTMENT TITLE: Mechanical Ventilation PATIENT CARE PLAN DIAGNOSIS: DISCHARGE CRITERIA: 1 The patient will: Maintain adequate mechanics of PERTINENT INFORMATION:. ventilation as demonstrated
