CHRONIC OBSTRUCTIVE PULMONARY DISEASE
|
|
|
- Gwendolyn Letitia Malone
- 7 years ago
- Views:
Transcription
1 CHRONIC OBSTRUCTIVE PULMONARY DISEASE Chronic obstructive pulmonary disease (COPD) is a chronic disease that affects the lungs. (The word pulmonary refers to the lungs) It is very common: more than 11 million Americans have COPD, and it is currently the fourth leading cause of death in the United States. COPD is a progressive disease, and it gets worse with each successive year. Chronic obstructive pulmonary disease can be managed with life style adjustments and medications, but there is no cure. There is evidence that some people inherit a tendency to develop COPD. Also, COPD can be caused by exposure to chemicals, pollutants, and some rare medical problems. However, environmental and medical causes of COPD are responsible for causing only a very small percentage of all cases of the disease. The great majority of cases of COPD are caused by cigarette smoking. OBJECTIVES When the student has finished this module, he/she will be able to: 1. Identify the area of the lungs where oxygen reaches the bloodstream. 2. Identify the correct definition of COPD. 3. Identify the two separate diseases that combine to cause COPD. 4. Identify the correction definition of emphysema. 5. Identify the correct definition of chronic bronchitis. 6. Identify the most common cause of COPD. 7. Identify three common signs and symptoms of COPD. 8. Identify the basic cause of the signs and symptoms of COPD. 9. Identify an important fact about the use of oxygen for patients with COPD. 10. Identify situations in which you would notify your supervisor immediately. ANATOMY AND PHYSIOLOGY OF THE PULMONARY SYSTEM The pulmonary system, also called the respiratory system, starts with the oral cavity (mouth) and the nose. Attached to the back of the mouth is a stiff but somewhat flexible tube. This is the trachea, which is more commonly called the windpipe: it is easily visible. The trachea ends at about the level of the shoulders, and it is attached to two other stiff but flexible tubes that extend down into lungs in the chest cavity. One of these extends into the left lung, the other goes into the right lung, and these are called the main stem bronchi. At the terminal ends of the main stem bronchi are many small, hollow passages called the bronchial tubes. The bronchial tubes extend from the ends of the main stem bronchi into the outer parts of the lungs. Eventually the bronchial tubes end in small clusters of air sacs called alveoli that are located at the bottom of the lungs. The alveoli look very much like clusters of grapes, and there thousands and thousands of them. They are very pliable, very elastics, and they have extremely thin walls - a feature that is very important and will be discussed later in this section.
2 When we inhale, the chest expands; air with oxygen moves through the nose and mouth; down the trachea to the main stem bronchi; through the bronchial tubes and; eventually it reaches alveoli. Immediately next to the alveoli are large numbers of extremely small blood vessels called capillaries: the alveoli and the capillaries are actually touching one another. The walls of the alveoli have tiny, tiny pores, and the inhaled air that contains oxygen moves through these pores and combines with the blood that is passing by in the capillaries. This blood is returning from the body and it contains a very low level of oxygen, but a relatively high level of another gas, carbon dioxide. After the blood in the capillaries combines with oxygen, it is pumped out of the lungs, into the heart and from there it is pumped back out to the body. This exchange of oxygen from the air to the blood happens quite easily because the alveoli and the capillaries are in such close contact, and it is so efficient because the surface area of the alveoli and the capillaries is enormous. When we exhale, harmful waste products of metabolism - most importantly the carbon dioxide - move from the blood in the capillaries into the alveoli and out through the bronchial tubes and the nose and mouth. The alveoli are where these two gases, oxygen and carbon dioxide, move in and out of the body. The basic purpose of the pulmonary system is to allow the movement of two gases, oxygen and carbon dioxide, in and out of the body. When we inhale, we take in oxygen; when we exhale, we get rid of carbon dioxide. WHAT IS COPD? The name chronic obstructive pulmonary disease is a good description for the problem. It is chronic disease - it does not go away - and it causes problems by obstructing the flow of air in and out of the lungs, which are the primary organs of the pulmonary system. Learning Break: Chronic obstructive pulmonary disease will be defined here as a chronic disease that causes permanent scarring to the lung tissue. Chronic obstructive pulmonary disease is actually a combination of two separate but closely related diseases, emphysema and chronic bronchitis. These diseases can occur by themselves, but when they are together they are called COPD. Emphysema is a disease that causes slow, progressive, and irreversible destruction of the lung tissue. In particular, emphysema damages the alveoli. In a patient with emphysema, the alveoli become weak, enlarged, and scarred. Because of this, when a patient with emphysema inhales or exhales the normal elasticity of the alveoli cannot function and they collapse under the pressure. Also, because the alveoli are scarred, oxygen and carbon dioxide cannot move into and out of the blood. The body must have oxygen and must be able to get rid of carbon dioxide to survive and the alveoli are where these processes take place, so it is obvious that if the alveoli don t function the patient s respiratory status and the normal gas exchange that takes place in the lungs will both suffer. Chronic bronchitis is the other component of COPD. Chronic bronchitis happens when the bronchial breathing passages become permanently inflamed. This is almost always a result of cigarette smoking. The chemicals and the particles in the cigarette smoke irritate the sensitive lining of the bronchial tubes. When that happens, these airway passages
3 become inflamed, they become swollen and narrowed, and large amounts of mucous are produced. As with emphysema, these changes prevent oxygen from going through to the blood when we inhale, and they prevent carbon dioxide from being expelled when we exhale. There is also a disease called acute bronchitis. This is exactly the same as chronic bronchitis, but it is caused by an infection, it can be cured with antibiotics and rest, and it does not cause permanent inflammation of the bronchial tubes. Learning Break: Chronic bronchitis is defined as permanent inflammation of the bronchial tubes. The person with COPD has bronchial tubes that are narrowed and swollen and alveoli that are scarred and have lost their elasticity. When someone with COPD inhales or exhales, air cannot effectively move in or out. Imagine trying to suck molasses through a tiny straw (the narrowed, swollen bronchial tubes) that collapses when it is stretched (the inelastic alveoli) and then trying to move it across a thick piece of cardboard that has been placed over the end of the straw (the scarred alveoli). This is what happens with the person with COPD. The air can t effectively move through the bronchial tubes because they are so narrow and when air gets to the alveoli, it can t move past them because the pores in the alveoli are covered with scar tissue and the alveoli collapse because they have lost their elasticity. WHY DOES COPD HAPPEN? The answer to this is very simple. There are a few unusual medical conditions that can cause COPD, and some cases of COPD can be caused by air pollution and chronic exposure to irritants in the air. It may also be possible to develop COPD if you are exposed to very large amounts of secondhand smoke. And there are rare cases in which someone has inherited a genetic tendency for developing COPD. For those people, small amounts of smoking or exposure to low levels of chemicals or pollution may be enough to cause COPD. However, the vast majority of cases of COPD are caused by chronic cigarette smoking. Tobacco smoking accounts for approximately 90% of all cases of COPD. Approximately 20% of all cigarettes smokers will eventually develop COPD, and the more someone smokes and the greater the number of years that person smokes the greater the risk of developing COPD. Smoking cigars and/or a pipe can also cause COPD, but the risk is much less. It is not clear why some people who smoke do not develop COPD Tobacco smoke is a very complicated compound. It contains thousands of chemicals, some of which such as carbon monoxide, cyanide, and tar are very toxic. Others act as irritants. These chemical toxins and the irritants are only present in very tiny amounts. But a smoker is exposed to them on a constant, day-to-day basis. The result of this continual exposure of the lungs to these toxins and irritants is an intense inflammation and irritation of the lung tissue that slowly but surely overwhelms the body s defenses: the lungs simply cannot heal themselves or successfully fight off the chemical assault. Given enough time, the irritation and inflammation progresses to irreversible damage, and the smoker has COPD.
4 Learning Break: What about second hand cigarette smoke? Can exposure to smokers cause COPD? The answer is not clear. Second hand smoke can damage the lungs, but it is not certain whether second hand smoke can cause damage that will progress to COPD. Cigarette smoking is the primary cause of COPD. But it is worth remembering that tobacco smoke has many other harmful health effects. Smoking increase the risk of developing heart disease by 2 to 4 times Smoking increase the risk of having a stroke by 2 to 4 times Smoking decreases circulation: You may notice that many smokers have cold hand and feet, and this is because of poor circulation. Smoking causes lung cancer Smoking has been associated with an increased risk for developing bladder cancer, cervical cancer, esophageal cancer, laryngeal cancer, pancreatic cancer, and many other malignancies Smoking has been associated with reproductive disorders such as infertility, low birth weight, stillbirth, and sudden infant death syndrome (SID) SIGNS AND SYMPTOMS OF COPD Chronic obstructive pulmonary disease is chronic and progressive. The disease gets worse and worse as the patient gets older. Because of the damage to the alveoli and the changes in the bronchial tubes, people with COPD have low levels of oxygen in their blood and high levels of carbon dioxide in their blood. These abnormal levels are the basic cause of the signs and symptoms of COPD. Some of the signs and symptoms of COPD are: Difficulty breathing Exercise intolerance Chronic cough Excessive production of sputum - also known as a productive cough Blue coloration of the fingernails - also known as cyanosis Tachypnea: Defined a rapid breathing. The normal respiratory rate is breaths a minute. This is an average, and the normal respiratory rate varies slightly from person to person. Wheezing Confusion - This would happen in advanced stages of the disease when the oxygen level in the blood gets very low Barrel chest Abnormally thick fingernails: This is called clubbing. Cough, exercise intolerance, and a productive cough are probably the most common and the most important of these signs and symptoms. In the first few years, a patient with COPD can learn to live with the disease. Medications, exercise, stopping smoking, and
5 other lifestyle changes can help. But the disease always gets worse and over time, many patients with COPD cannot even walk a few steps without becoming short of breath and needing to rest. They become more dependent on medications and oxygen, and they are also more susceptible to lung infections. EXACERBATIONS OF COPD One of the common features of COPD is an event called exacerbation of COPD: exacerbation means worsening. An exacerbation of COPD is an episode in which a patient who has been stable and breathing well suddenly becomes short of breath. The patient will also have increased coughing and increased sputum production. Other signs and symptoms such as fatigue, fever, sore throat, and weakness may develop, as well. If the patient s respiratory function and gas exchange capability are especially poor, he/she may become confused, cyanotic, and tachypneic. Exacerbations are very common, and most of them are caused by a bacterial or viral infection in the lungs. However, in many cases, there is no evidence of an infection and the reason for the sudden deterioration cannot be found. But regardless of the cause, an exacerbation of COPD is a very serious problem. People with COPD have very poor respiratory function. Their gas exchange, the oxygen delivery and carbon dioxide excretion, is very poor and there is little room for error. Any further disruption in the patient s ability to breath and she/he may need hospitalization and mechanical ventilation. EMERGENCY CARE FOR EXACERBATIONS OF COPD Most people who are having an exacerbation of COPD will have some dramatic signs and symptoms. They will be tachypneic, they will likely have a constant cough, and you may hear them wheezing. Speaking in sentences of more than a few words will be impossible, and it is likely their skin color will be bad. They may be sweaty and pale. And these people will also tell you their breathing is bad. Phrases such as I just can t catch my breath, or I feel like I can t breath are common. However, for some people the signs and symptoms of a COPD exacerbation can be a bit more difficult to detect. The patient who is having an exacerbation may not appear to be in acute distress. But if you have experience caring for this person you may notice subtle changes in behavior or appearance, small clues that indicate something s not right. In these situations, the patient s input is invaluable. The patient may not have any obvious distress, but if she/he tells you something like My breathing just doesn t feel normal, that should be taken very seriously. The patient will be the first one to know if an exacerbation is happening. If your patient appears to be having an exacerbation or you suspect that an exacerbation may be happening, immediately notify your supervisor. Some patients may have a hand-inhaled nebulizer that they have been instructed to use in these situations. This is called a rescue inhaler, and they are one of the bronchodilators such as albuterol. These inhalers provide rapid relief, usually within minutes, and if the patient has one of these you can help him/her use it.
6 Aside from notifying the supervisor and helping the patient find and use the rescue inhaler, you should encourage the patient to rest. The more active someone is the more oxygen the body needs, so activity and exacerbation of COPD are not a good combination. You should also try and maintain a calm and reassuring demeanor. Even for people who have experienced it before, an exacerbation of COPD is frightening. No matter how hard the try and no matter what is done they cannot catch their breath, and the high level of emotion can make breathing more difficult. Stay calm, and try and help the patient stay calm. Many people who have COPD use supplemental oxygen. A natural response to someone who is having difficulty breathing during an exacerbation would be to increase the flow of oxygen, and the patient may ask you to do so. Do not increase the flow of oxygen. The rate of flow is prescribed by a physician, and it can only be changed if a physician has ordered the flow to be increased or decreased. There is also some evidence that increasing oxygen flow to someone who has COPD may, at a certain point, be harmful by decreasing the respiratory rate. This last point will be discussed later in the module. TREATMENTS FOR COPD: LIFE STYLE ADJUSTMENTS There is no cure for COPD. Chronic obstructive pulmonary disease can only be treated, but as it is a progressive disease the patient s eventually succumb and will die of respiratory failure or a complication. However, COPD can be managed, life expectancy can be significantly expanded, and the quality of life can be greatly improved. The treatments for COPD can be divided into two groups: 1) Life style adjustments, and; 2) Medical treatments. Smoking Cessation Smoking cessation is the most important and the most effective treatment for COPD. Within several days of smoking cessation, the lung irritation and some of the lung damage caused by constant exposure to cigarette smoke begin to heal. Over the next few months, lung function improves, the chronic smoker s cough diminishes, and the patient s subjective complaints of shortness of breath decrease. Other health benefits - decreased risk of heart disease and stroke, for example - accumulate the longer the person goes without smoking. Of course, stopping smoking is very difficult. Nicotine is physically addictive in much the same way as illicit drugs such as cocaine and heroin. Most people will need to be enrolled in a smoking cessation program and/or use nicotine gum or patches. It can be a long difficult process to stop smoking, but for someone who has COPD, it is not an option. Unfortunately for the person with COPD, much of the damage to the bronchial tubes and the alveoli is permanent. If the patient stops smoking the harm can be limited, and areas that are damaged but not yet irreversibly so can be recovered. But even then, the decrease is pulmonary function slowly but surely worsens over time. The longer someone smokes and the more he/she smokes, the worse the damage, the less chance of recovering lung tissue, and the faster the destruction will progress.
7 Diet and Hydration Good nutrition is very important for someone who has COPD. There is evidence that clearly shows that people who have COPD and have a poor nutritional status have a decreased tolerance for exercise, their lung function is poor, and they die earlier. Poor nutrition can weaken the immune system and make the patient susceptible to infections. Unfortunately, COPD often makes people nauseated and decreases their appetite. Encourage the patient to eat well and explain the benefits of a healthy diet to them. Good hydration is also a critical part of self-care for the person who has COPD. Dehydration thickens secretions in the lungs. This increases the risk of pulmonary infections, and it also a makes it more difficult for the patient to cough up and expel those secretions. Exercise Exercise for the COPD patient can increase exercise tolerance, help prevent lung infections, and improve mood. Aerobic exercises such as bike riding, swimming, walking, etc. and strength building exercise such as weight lifting should only be initiated if the patient s physician has approved. Starting an exercise program is never easy and sticking with a program, particularly in the beginning when it is hard to see the benefits, is very difficult. This is especially so for the patient with COPD who has decreased exercise tolerance. Encourage the patient with COPD to participate in pulmonary rehabilitation as best they can. Discussing the details of an exercise program for someone with COPD is beyond the scope of this module. But if you are working with a patient who has COPD and that patient is actively exercising, part of your responsibility a CNA is patient safety. Remind the patient that if she/he develops shortness of breath or chest pain while exercising, stop exercising immediately. Some patients who have COPD may also benefit from breathing exercises. These are exercise that target the muscles involved in breathing. The number of times to do them and how often to do them will be prescribe by the patient s physician, or perhaps by a physical therapist or respiratory therapist. Examples of these breathing exercises include: Pursed lip breathing: 1) The first step is to relax the neck shoulder muscles; 2) Breathe in for two seconds through the nose while keeping the mouth closed, and; 3) Finish by breathing out for four seconds through pursed lips. If someone cannot breathe out for four seconds, simply breath out for two seconds, the same amount of time as was spent breathing in. Diaphragmatic breathing: 1) The patient should be laying on his/her back. If need be, a pillow can be placed under the knees for support; 2) Place one hand on the stomach, just below the rib cage; 3) Put the other hand on the chest; 4) While counting to three, inhale through the nose as deeply as possible. Try and keep the chest from moving during the inhalation. You should feel the stomach and the lower ribs moving up, but the chest should remain still, and; 5) Tighten the stomach muscles and exhale for a count of six through slightly pursed lips.
8 TREATMENT FOR COPD: MEDICAL CARE Oxygen Many people who have COPD require supplemental oxygen, and it has been proven that people who have COPD and use supplemental oxygen live longer and have better exercise tolerance. Oxygen therapy in a health care facility will be managed by a respiratory therapist or a registered nurse. In a home setting, a commercial service will provide delivery and equipment. Many patients can, after some instruction and initial supervision, manage their oxygen therapy at home without assistance as long as they have someone to contact if there are problems or questions. As a CNA you do not have primary responsibility for managing a patient s oxygen therapy. But you can and should be able to help your patients use oxygen safely. If your patient with COPD requires supplemental oxygen: Assess for effectiveness: If the patient is complaining of breathing difficulties or in your opinion the patient s respiratory status is declining, the oxygen therapy may not be working and someone should be notified. This does not necessarily imply the equipment is malfunctioning (That would be very be unusual), but that the patient is having an exacerbation needs an adjustment in the oxygen or perhaps medications. Use it correctly: Remember, never change rate of delivery and do not allow the patient to change the rate of delivery. Most people who are using supplemental oxygen are receiving a flow rate of 2-3 liters/minute, some less, some more. Use it safely: Oxygen supports and accelerates combustion, so oxygen must never be used near open flames or by someone who is smoking. Keep it clean: There is a variety of ways supplemental oxygen can be delivered, but the nasal cannula is probably the most common. The cannula should be washed with soap and water several times a week and it should be periodically replaced. Remember, people with COPD are susceptible to respiratory infections, and oxygen equipment that is not cleaned can become contaminated with bacteria. Keep it comfortable: Oxygen flowing directly into the nostrils can be very drying. A water-based moisturizer can be used in the nose to prevent dry and sore nasal passages. Also, you should check the skin where the cannula loops around the ears. This area can become red and irritated from the constant contact with the plastic, and bit of gauze placed there will provide protection. It was mentioned earlier that increasing the flow of oxygen could potentially harm someone who has COPD. The basis for this is that in COPD the mechanism for breathing is different than it is for someone who does not have the diseases. Here s how that works.
9 Most people often think that we breathe to take in oxygen. This is only partly true. Much of the reason we breathe is to get rid of carbon dioxide. However, because COPD damages the lungs, these patients can t eliminate carbon dioxide very efficiently and they have abnormally high levels of carbon dioxide in their blood. Eventually, these people become adapted to the high levels of carbon dioxide. At that point, the drive to breathe (which is located in a particular section of the brain) comes from the lack of oxygen in the blood, not the need to expel carbon dioxide. If the patient with COPD is given too much oxygen, the body senses that no oxygen is needed and the drive to breathe can be interfered with, and that is why oxygen must be use cautiously in the patient who has COPD. Medications Chronic obstructive pulmonary disease cannot be cured, but it can be managed with oxygen and medications. There are three types of medications that are used to treat people who have COPD. Bronchodilators: These medications open up the swollen, narrow bronchial tubes. Bronchodilators are usually used in the form of handheld inhalers. The inhalers are small, pressurized canisters that fit into the hand. The patient places the nozzle of the inhaler in his/her mouth, presses a trigger that releases the medication and inhales. Albuterol is a commonly used bronchodilator. The handheld inhalers are effective if used correctly, but the patient needs to be able to make a tight seal around the nozzle and coordinate a deep inhalation with the delivery of the medication. If the patient complains that his/her bronchodilator is not working, someone needs to make sure the patient is using it correctly. Albuterol and the other bronchodilators can also be used in nebulizers. Albuterol syrup is also available, but this is typically reserved for use in children. A commonly used brand of handheld bronchodilator inhaler is Proventil, which contains albuterol. Learning Break: The bronchodilators are designed to open the bronchial passages and provide relief for approximately 4-6 hours. Someone who is having difficulty breathing may be tempted to use a handheld bronchodilator more often than every 4-6 hours. Using a bronchodilator for rescue therapy in between the normal, scheduled use of a bronchodilator is acceptable. But if the prescribed frequency of an albuterol inhaler is not helping, more is not better and could be harmful. The patient s physician should be called if she/he feels that the bronchodilator is not providing relief. Corticosteroids: Some patients with COPD hear the word corticosteroid and associate these medications with the illegal steroids used by some athletes. Corticosteroids are different. These are oral medications or medications delivered by handheld inhalers that decrease inflammation in the lungs. A commonly used brand of corticosteroid inhaler is Flovent, which contains fluticasone. Anticholinergics: These medications are used in inhalers. They work by opening up the bronchial tubes, but in a different way than the albuterol type drugs.
10 Spiriva is a common anticholinergic used for people with COPD. Some handheld inhalers will have albuterol and an anticholinergic: Combivent is a commonly used combination brand. Antibiotics: Antibiotics should only be used if a person with COPD has a lung infection. If your patient with COPD tells you he/she has been taking an antibiotic because they have been feeling bad, and they are doing so without a doctor s orders, notify your supervisor immediately. Doing this can actually cause lung infections that are dangerous and difficult to treat. Vaccinations: People who have COPD should make sure that they have a yearly flu shot, and many patients who have COPD should receive a pneumonia vaccination. Learning Break: Lung resection is a surgical procedure that can be used to treat COPD. The damaged areas of the lung are removed - resected - and for some patients this is as close to a cure as possible. However, this procedure is only suitable for a small percentage of people who have COPD. CARING FOR THE PATIENT WITH COPD Caring for the patient with COPD can be very challenging. Many of these patients have limited ability to help themselves. Because even a little bit of physical exertion can be very tiring, the amount of activities they can perform can some times be severely limited. COPD can also be very frightening. The exacerbations may clear up with rest, oxygen, and bronchodilators, but the exacerbations can also be very severe; the patient may need to be admitted to the hospital and placed on a ventilator. Some times there is a clear reason why these exacerbations happen, but quite often there is not. Because of these unpredictable episodes of shortness of breath, many people with COPD must live with the constant fear that suddenly and without warning they will not be able to breathe. As a result of these physical and psychological issues, many people with COPD require a lot of physical assistance and emotional support. The following are the areas you will need to concentrate on and be familiar with. Emotional support: The patient with COPD often feels very vulnerable. For no apparent reason and without warning, that person may not be able to breathe. That leaves the COPD patient feeling very dependent on his/her caretakers. It is very important that you let the patient with COPD know that you understand the disease. You must also communicate to them and demonstrate to them that you are reliable and dependable. Also, because COPD exacerbations can happen unpredictably, these patients often feel a great need to establish order, regularity, and control over their environments. Doing so makes them feel secure, and it is important that you understand this and within reason, support them in this effort.
11 Physical assistance: This aspect of care of the patient with COPD is very individualized. The patient with COPD will often need help dressing and ambulating, and they may need help eating their meals. It will certainly take these patients much longer to complete any physical task. The body needs oxygen to perform physical work, and the COPD patient does not have adequate amounts of oxygen in his/her blood. It will take time for you to determine exactly what each patient with this disease is capable of doing. This is also something that you need to discuss with the patient. Many people with COPD have been living with the disease for a long time. They know exactly what they can and can t do. Health care professionals many times feel that they have to have all the answers. It is easy to forget that the patients know a lot about the disease they suffer from, and they can tell you what they are capable of doing and what they need. Monitoring for complications: this is relatively simple. Monitor the patient for any respiratory difficulties, failure to respond to therapies, or any problems with his/her cardiac or neurological status such as chest pain, confusion, or drowsiness. WHEN TO NOTIFY YOUR SUPERVISOR You should notify your supervisor if your patient with COPD is eating poorly, doesn t want to exercise, or becomes more short of breath than usual when performing his/her daily activities. When you are caring for a patient with COPD, you should notify your supervisor immediately when: The patient has a fever. The patient complains of shortness of breath. The patient has tachypnea. The patient s skin is pale or blue. The patient is requesting that you increase the flow of oxygen. The patient has used an inhaler or taken another medication but still complains of shortness of breath.
Better Breathing with COPD
 Better Breathing with COPD People with Chronic Obstructive Pulmonary Disease (COPD) often benefit from learning different breathing techniques. Pursed Lip Breathing Pursed Lip Breathing (PLB) can be very
Better Breathing with COPD People with Chronic Obstructive Pulmonary Disease (COPD) often benefit from learning different breathing techniques. Pursed Lip Breathing Pursed Lip Breathing (PLB) can be very
Emphysema. Introduction Emphysema is a type of chronic obstructive pulmonary disease, or COPD. COPD affects about 64 million people worldwide.
 Emphysema Introduction Emphysema is a type of chronic obstructive pulmonary disease, or COPD. COPD affects about 64 million people worldwide. Emphysema involves damage to the air sacs in the lungs. This
Emphysema Introduction Emphysema is a type of chronic obstructive pulmonary disease, or COPD. COPD affects about 64 million people worldwide. Emphysema involves damage to the air sacs in the lungs. This
Chronic Obstructive Pulmonary Disease Patient Guidebook
 Chronic Obstructive Pulmonary Disease Patient Guidebook The Respiratory System The respiratory system consists of the lungs and air passages. The lungs are the part of the body where gases are exchanged
Chronic Obstructive Pulmonary Disease Patient Guidebook The Respiratory System The respiratory system consists of the lungs and air passages. The lungs are the part of the body where gases are exchanged
Your Lungs and COPD. Patient Education Pulmonary Rehabilitation. A guide to how your lungs work and how COPD affects your lungs
 Patient Education Your Lungs and COPD A guide to how your lungs work and how COPD affects your lungs Your lungs are organs that process every breath you take. They provide oxygen (O 2 ) to the blood and
Patient Education Your Lungs and COPD A guide to how your lungs work and how COPD affects your lungs Your lungs are organs that process every breath you take. They provide oxygen (O 2 ) to the blood and
written by Harvard Medical School COPD It Can Take Your Breath Away www.patientedu.org/copd
 written by Harvard Medical School COPD It Can Take Your Breath Away www.patientedu.org/copd What Is COPD? COPD stands for chronic obstructive pulmonary disease. There are two major diseases included in
written by Harvard Medical School COPD It Can Take Your Breath Away www.patientedu.org/copd What Is COPD? COPD stands for chronic obstructive pulmonary disease. There are two major diseases included in
COPD It Can Take Your Breath Away www.patientedu.org
 written by Harvard Medical School COPD It Can Take Your Breath Away www.patientedu.org What Is COPD? COPD stands for chronic obstructive pulmonary disease. There are 2 major diseases included in COPD:
written by Harvard Medical School COPD It Can Take Your Breath Away www.patientedu.org What Is COPD? COPD stands for chronic obstructive pulmonary disease. There are 2 major diseases included in COPD:
These factors increase your chance of developing emphysema. Tell your doctor if you have any of these risk factors:
 Emphysema Pronounced: em-fiss-see-mah by Debra Wood, RN En Español (Spanish Version) Definition Emphysema is a chronic obstructive disease of the lungs. The lungs contain millions of tiny air sacs called
Emphysema Pronounced: em-fiss-see-mah by Debra Wood, RN En Español (Spanish Version) Definition Emphysema is a chronic obstructive disease of the lungs. The lungs contain millions of tiny air sacs called
Lesson 7: Respiratory and Skeletal Systems and Tuberculosis
 Glossary 1. asthma: when the airways of the lungs narrow, making breathing difficult 2. bacteria: tiny living creatures that can only be seen with a microscope; some bacteria help the human body, and other
Glossary 1. asthma: when the airways of the lungs narrow, making breathing difficult 2. bacteria: tiny living creatures that can only be seen with a microscope; some bacteria help the human body, and other
WHEN COPD* SYMPTOMS GET WORSE
 WHEN COPD* SYMPTOMS GET WORSE *Includes chronic bronchitis, emphysema, or both. Boehringer Ingelheim Pharmaceuticals, Inc. has no ownership interest in any other organization that advertises or markets
WHEN COPD* SYMPTOMS GET WORSE *Includes chronic bronchitis, emphysema, or both. Boehringer Ingelheim Pharmaceuticals, Inc. has no ownership interest in any other organization that advertises or markets
Lung Cancer. This reference summary will help you better understand lung cancer and the treatment options that are available.
 Lung Cancer Introduction Lung cancer is the number one cancer killer of men and women. Over 165,000 people die of lung cancer every year in the United States. Most cases of lung cancer are related to cigarette
Lung Cancer Introduction Lung cancer is the number one cancer killer of men and women. Over 165,000 people die of lung cancer every year in the United States. Most cases of lung cancer are related to cigarette
Whooping Cough. The Lungs Whooping cough is an infection of the lungs and breathing tubes, both of which are parts of the respiratory system.
 Whooping Cough Introduction Whooping cough is a serious bacterial infection of the lungs and breathing tubes. It is also called pertussis. About 16 million cases of whooping cough happen worldwide each
Whooping Cough Introduction Whooping cough is a serious bacterial infection of the lungs and breathing tubes. It is also called pertussis. About 16 million cases of whooping cough happen worldwide each
CHAPTER 1: THE LUNGS AND RESPIRATORY SYSTEM
 CHAPTER 1: THE LUNGS AND RESPIRATORY SYSTEM INTRODUCTION Lung cancer affects a life-sustaining system of the body, the respiratory system. The respiratory system is responsible for one of the essential
CHAPTER 1: THE LUNGS AND RESPIRATORY SYSTEM INTRODUCTION Lung cancer affects a life-sustaining system of the body, the respiratory system. The respiratory system is responsible for one of the essential
Objectives COPD. Chronic Obstructive Pulmonary Disease (COPD) 4/19/2011
 Objectives Discuss assessment findings and treatment for: Chronic Obstructive Pulmonary Disease Bronchitis Emphysema Asthma Anaphylaxis Other respiratory issues Provide some definitions Chronic Obstructive
Objectives Discuss assessment findings and treatment for: Chronic Obstructive Pulmonary Disease Bronchitis Emphysema Asthma Anaphylaxis Other respiratory issues Provide some definitions Chronic Obstructive
Pneumonia. Pneumonia is an infection that makes the tiny air sacs in your lungs inflamed (swollen and sore). They then fill with liquid.
 Pneumonia Pneumonia is an infection that makes the tiny air sacs in your lungs inflamed (swollen and sore). They then fill with liquid. People with mild (not so bad) pneumonia can usually be treated at
Pneumonia Pneumonia is an infection that makes the tiny air sacs in your lungs inflamed (swollen and sore). They then fill with liquid. People with mild (not so bad) pneumonia can usually be treated at
COPD What Is It? Why is it so hard to catch my breath? What does COPD feel like? What causes COPD? What is an exacerbation (ig-zas-er-bay-shun)?
 Attitudes and Beliefs 4 COPD What Is It? Why is it so hard to catch my breath? COPD is a disease that damages the lungs. In a healthy lung, the airways are open and the air sacs fill up with air. Then
Attitudes and Beliefs 4 COPD What Is It? Why is it so hard to catch my breath? COPD is a disease that damages the lungs. In a healthy lung, the airways are open and the air sacs fill up with air. Then
Your Go-to COPD Guide
 Your Go-to COPD Guide Learning how to live with chronic obstructive pulmonary disease (COPD) Inside, you ll learn: COPD facts COPD symptoms and triggers How to talk with your doctor Different treatment
Your Go-to COPD Guide Learning how to live with chronic obstructive pulmonary disease (COPD) Inside, you ll learn: COPD facts COPD symptoms and triggers How to talk with your doctor Different treatment
Understanding COPD. An educational health series from
 Understanding COPD An educational health series from Our Mission since 1899 is to heal, to discover, and to educate as a preeminent healthcare institution. We serve by providing the best integrated and
Understanding COPD An educational health series from Our Mission since 1899 is to heal, to discover, and to educate as a preeminent healthcare institution. We serve by providing the best integrated and
Asthma and COPD Awareness
 Asthma and COPD Awareness Molina Breathe with Ease sm and Chronic Obstructive Pulmonary Disease Molina Healthcare of Michigan Fall 2012 Importance of Controller Medicines Asthma is a disease that causes
Asthma and COPD Awareness Molina Breathe with Ease sm and Chronic Obstructive Pulmonary Disease Molina Healthcare of Michigan Fall 2012 Importance of Controller Medicines Asthma is a disease that causes
HEALTH EFFECTS. Inhalation
 Health Effects HEALTH EFFECTS Asbestos can kill you. You must take extra precautions when you work with asbestos. Just because you do not notice any problems while you are working with asbestos, it still
Health Effects HEALTH EFFECTS Asbestos can kill you. You must take extra precautions when you work with asbestos. Just because you do not notice any problems while you are working with asbestos, it still
There is no cure for COPD Chronic Bronchitis Emphysema
 Live Well With COPD Chronic Obstructive Pulmonary Disease, or COPD is a lung disease. People with COPD have a hard time getting air in and out of their lungs. There is no cure for COPD. COPD is also commonly
Live Well With COPD Chronic Obstructive Pulmonary Disease, or COPD is a lung disease. People with COPD have a hard time getting air in and out of their lungs. There is no cure for COPD. COPD is also commonly
Department of Surgery
 What is emphysema? 2004 Regents of the University of Michigan Emphysema is a chronic disease of the lungs characterized by thinning and overexpansion of the lung-like blisters (bullae) in the lung tissue.
What is emphysema? 2004 Regents of the University of Michigan Emphysema is a chronic disease of the lungs characterized by thinning and overexpansion of the lung-like blisters (bullae) in the lung tissue.
COPD. Information brochure for chronic obstructive pulmonary disease.
 COPD Information brochure for chronic obstructive pulmonary disease. CONTENTS What does COPD mean?...04 What are the symptoms of COPD?...06 What causes COPD?...09 Treating COPD...10 Valve therapy in COPD...12
COPD Information brochure for chronic obstructive pulmonary disease. CONTENTS What does COPD mean?...04 What are the symptoms of COPD?...06 What causes COPD?...09 Treating COPD...10 Valve therapy in COPD...12
What You Should Know About ASTHMA
 What You Should Know About ASTHMA 200 Hospital Drive Galax, VA 24333 (276) 236-8181 www.tcrh.org WHAT IS ASTHMA? It s a lung condition that makes breathing difficult. The cause of asthma is not known.
What You Should Know About ASTHMA 200 Hospital Drive Galax, VA 24333 (276) 236-8181 www.tcrh.org WHAT IS ASTHMA? It s a lung condition that makes breathing difficult. The cause of asthma is not known.
Tobacco/Marijuana. Tobacco. Short-term effects of smoking
 Tobacco/Marijuana Tobacco Nicotine, one of the more than 4,000 chemicals found in the smoke from tobacco products such as cigarettes, cigars, and pipes, is the primary component in tobacco that acts on
Tobacco/Marijuana Tobacco Nicotine, one of the more than 4,000 chemicals found in the smoke from tobacco products such as cigarettes, cigars, and pipes, is the primary component in tobacco that acts on
CONTENTS. Note to the Reader 00. Acknowledgments 00. About the Author 00. Preface 00. Introduction 00
 Natural Therapies for Emphysema By Robert J. Green Jr., N.D. CONTENTS Note to the Reader 00 Acknowledgments 00 About the Author 00 Preface 00 Introduction 00 1 Essential Respiratory Anatomy and Physiology
Natural Therapies for Emphysema By Robert J. Green Jr., N.D. CONTENTS Note to the Reader 00 Acknowledgments 00 About the Author 00 Preface 00 Introduction 00 1 Essential Respiratory Anatomy and Physiology
In case of an urgent concern or emergency, call 911 or go to the nearest emergency department right away.
 Asthma Basics Patient and Family Education This teaching sheet contains general information only. Talk with your child s doctor or a member of your child s healthcare team about specific care of your child.
Asthma Basics Patient and Family Education This teaching sheet contains general information only. Talk with your child s doctor or a member of your child s healthcare team about specific care of your child.
Pregnancy and Substance Abuse
 Pregnancy and Substance Abuse Introduction When you are pregnant, you are not just "eating for two." You also breathe and drink for two, so it is important to carefully consider what you put into your
Pregnancy and Substance Abuse Introduction When you are pregnant, you are not just "eating for two." You also breathe and drink for two, so it is important to carefully consider what you put into your
Respiratory Syncytial Virus (RSV)
 Respiratory Syncytial Virus (RSV) What is? is a common virus that infects the linings of the airways - the nose, throat, windpipe, bronchi and bronchioles (the air passages of the lungs). RSV is found
Respiratory Syncytial Virus (RSV) What is? is a common virus that infects the linings of the airways - the nose, throat, windpipe, bronchi and bronchioles (the air passages of the lungs). RSV is found
Chronic obstructive pulmonary disease (COPD)
 Chronic obstructive pulmonary disease (COPD) Chronic obstructive pulmonary disease (COPD) is the name for a group of lung diseases including chronic bronchitis, emphysema and chronic obstructive airways
Chronic obstructive pulmonary disease (COPD) Chronic obstructive pulmonary disease (COPD) is the name for a group of lung diseases including chronic bronchitis, emphysema and chronic obstructive airways
Developing Human Fetus
 Period Date LAB. DEVELOPMENT OF A HUMAN FETUS After a human egg is fertilized with human sperm, the most amazing changes happen that allow a baby to develop. This amazing process, called development, normally
Period Date LAB. DEVELOPMENT OF A HUMAN FETUS After a human egg is fertilized with human sperm, the most amazing changes happen that allow a baby to develop. This amazing process, called development, normally
400,000 people in the United States die every year due to smoking-related illnesses.
 How To Stop Smoking Ugly Facts about Smoking: 52 million Americans smoke cigarettes. 400,000 people in the United States die every year due to smoking-related illnesses. Every cigarette you smoke shortens
How To Stop Smoking Ugly Facts about Smoking: 52 million Americans smoke cigarettes. 400,000 people in the United States die every year due to smoking-related illnesses. Every cigarette you smoke shortens
How To Stop Smoking. Tamra Casper
 How To Stop Smoking Tamra Casper Ugly Facts About Smoking 52 million Americans smoke cigarettes. 400,000 people in this country die every year due to smoking related illnesses. Each cigarette you smoke
How To Stop Smoking Tamra Casper Ugly Facts About Smoking 52 million Americans smoke cigarettes. 400,000 people in this country die every year due to smoking related illnesses. Each cigarette you smoke
Stop Smoking. Key #2. It s Not Too Late to Benefit from Quitting! Health Benefits to Quitting. Other Reasons to Quit
 Key #2 Stop Smoking There are many different poisons that can be found in cigarettes, such as carbon monoxide, tar, rat poison, paint thinner, and lighter fluid, just to name a few. Any of these toxins,
Key #2 Stop Smoking There are many different poisons that can be found in cigarettes, such as carbon monoxide, tar, rat poison, paint thinner, and lighter fluid, just to name a few. Any of these toxins,
ASTHMA IN INFANTS AND YOUNG CHILDREN
 ASTHMA IN INFANTS AND YOUNG CHILDREN What is Asthma? Asthma is a chronic inflammatory disease of the airways. Symptoms of asthma are variable. That means that they can be mild to severe, intermittent to
ASTHMA IN INFANTS AND YOUNG CHILDREN What is Asthma? Asthma is a chronic inflammatory disease of the airways. Symptoms of asthma are variable. That means that they can be mild to severe, intermittent to
THERAPEUTIC USE OF HEAT AND COLD
 THERAPEUTIC USE OF HEAT AND COLD INTRODUCTION Heat and cold are simple and very effective therapeutic tools. They can be used locally or over the whole body, and the proper application of heat and cold
THERAPEUTIC USE OF HEAT AND COLD INTRODUCTION Heat and cold are simple and very effective therapeutic tools. They can be used locally or over the whole body, and the proper application of heat and cold
About one-half of all smokers die of a disease caused by smoking.the most common ones are lung cancer, heart disease, and strokes
 Patient information from the BMJ Group Stopping smoking Smoking harms your health, but it's difficult to stop. That s because most people who smoke have become addicted to nicotine, a chemical in tobacco.
Patient information from the BMJ Group Stopping smoking Smoking harms your health, but it's difficult to stop. That s because most people who smoke have become addicted to nicotine, a chemical in tobacco.
Asthma Care. Of course, your coach is there to answer any questions you have about your asthma, such as:
 Asthma Care All Health Coaches in the Asthma Care Management program are registered or certified respiratory therapists. Your coach will listen to your story of living with asthma. This will help your
Asthma Care All Health Coaches in the Asthma Care Management program are registered or certified respiratory therapists. Your coach will listen to your story of living with asthma. This will help your
Fourth Grade The Human Body: The Respiratory System Assessment
 Fourth Grade The Human Body: The Respiratory System Assessment 1a. The brings air in and out of the body. a. respiratory system b. circulatory system 1b. The system is the part of the body responsible
Fourth Grade The Human Body: The Respiratory System Assessment 1a. The brings air in and out of the body. a. respiratory system b. circulatory system 1b. The system is the part of the body responsible
Living with COPD. Chronic bronchitis. Emphysema
 Living with COPD This information is for people with chronic obstructive pulmonary disease (COPD), their families, friends and carers. It provides advice and information about COPD, including what the
Living with COPD This information is for people with chronic obstructive pulmonary disease (COPD), their families, friends and carers. It provides advice and information about COPD, including what the
Chronic Obstructive Pulmonary Disease (COPD) Programme
 Integrated Care Pathway Chronic Obstructive Pulmonary Disease (COPD) Programme Patient Handbook Contents Preface... 1 What is COPD?... 3 What causes COPD?... 4 - Smoking... 4 - Air pollution... 4 - The
Integrated Care Pathway Chronic Obstructive Pulmonary Disease (COPD) Programme Patient Handbook Contents Preface... 1 What is COPD?... 3 What causes COPD?... 4 - Smoking... 4 - Air pollution... 4 - The
Summary Guide. Living Well. Living Well. www.livingwellwithcopd.com. Chronic Obstructive Pulmonary Disease. Chronic Obstructive Pulmonary Disease
 Living Well withcopd Chronic Obstructive Pulmonary Disease BreathWorks toll-free Helpline 1-866-717-COPD (2673) www.lung.ca/breathworks Living Well withcopd Chronic Obstructive Pulmonary Disease www.livingwellwithcopd.com
Living Well withcopd Chronic Obstructive Pulmonary Disease BreathWorks toll-free Helpline 1-866-717-COPD (2673) www.lung.ca/breathworks Living Well withcopd Chronic Obstructive Pulmonary Disease www.livingwellwithcopd.com
Respiratory Disorders
 Respiratory Disorders Teaching Plan To use this lesson for self-study, the learner should read the material, do the activity, and take the test. For group study, the leader may give each learner a copy
Respiratory Disorders Teaching Plan To use this lesson for self-study, the learner should read the material, do the activity, and take the test. For group study, the leader may give each learner a copy
Frequently Asked Questions about Crab Asthma
 Frequently Asked Questions about Crab Asthma 1. Occupational asthma to snow crab: What is it? Asthma is a condition that results in breathing difficulties. These breathing difficulties occur when the breathing
Frequently Asked Questions about Crab Asthma 1. Occupational asthma to snow crab: What is it? Asthma is a condition that results in breathing difficulties. These breathing difficulties occur when the breathing
ARTHRITIS INTRODUCTION
 ARTHRITIS INTRODUCTION Arthritis is the most common disease affecting the joints. There are various forms of arthritis but the two that are the most common are osteoarthritis (OA), and rheumatoid arthritis
ARTHRITIS INTRODUCTION Arthritis is the most common disease affecting the joints. There are various forms of arthritis but the two that are the most common are osteoarthritis (OA), and rheumatoid arthritis
X-Plain Pediatric Tuberculosis Reference Summary
 X-Plain Pediatric Tuberculosis Reference Summary Introduction Tuberculosis, or TB, is a bacterial infection that causes more deaths in the world than any other infectious disease. When a child gets TB,
X-Plain Pediatric Tuberculosis Reference Summary Introduction Tuberculosis, or TB, is a bacterial infection that causes more deaths in the world than any other infectious disease. When a child gets TB,
F r e q u e n t l y As k e d Qu e s t i o n s. Lung Disease
 Lung Disease page 1 Q: What is lung disease? A: Lung disease refers to disorders that affect the lungs, the organs that allow us to breathe. Breathing problems caused by lung disease may prevent the body
Lung Disease page 1 Q: What is lung disease? A: Lung disease refers to disorders that affect the lungs, the organs that allow us to breathe. Breathing problems caused by lung disease may prevent the body
Tuberculosis: FAQs. What is the difference between latent TB infection and TB disease?
 Tuberculosis: FAQs What is TB disease? Tuberculosis (TB) is a disease caused by bacteria (germs) that are spread from person to person through the air. TB usually affects the lungs, but it can also affect
Tuberculosis: FAQs What is TB disease? Tuberculosis (TB) is a disease caused by bacteria (germs) that are spread from person to person through the air. TB usually affects the lungs, but it can also affect
2.06 Understand the functions and disorders of the respiratory system
 2.06 Understand the functions and disorders of the respiratory system 2.06 Understand the functions and disorders of the respiratory system Essential questions What are the functions of the respiratory
2.06 Understand the functions and disorders of the respiratory system 2.06 Understand the functions and disorders of the respiratory system Essential questions What are the functions of the respiratory
The flu vaccination WINTER 2016/17. Who should have it and why. Flu mmunisation 2016/17
 The flu vaccination WINTER 2016/17 Who should have it and why Flu mmunisation 2016/17 The flu vaccination 1 Winter 2016/17 Helping to protect everyone, every winter This leaflet explains how you can help
The flu vaccination WINTER 2016/17 Who should have it and why Flu mmunisation 2016/17 The flu vaccination 1 Winter 2016/17 Helping to protect everyone, every winter This leaflet explains how you can help
Anatomy and Physiology: Understanding the Importance of CPR
 Anatomy and Physiology: Understanding the Importance of CPR Overview This document gives you more information about the body s structure (anatomy) and function (physiology). This information will help
Anatomy and Physiology: Understanding the Importance of CPR Overview This document gives you more information about the body s structure (anatomy) and function (physiology). This information will help
HOW TO CARE FOR A PATIENT WITH DIABETES
 HOW TO CARE FOR A PATIENT WITH DIABETES INTRODUCTION Diabetes is one of the most common diseases in the United States, and diabetes is a disease that affects the way the body handles blood sugar. Approximately
HOW TO CARE FOR A PATIENT WITH DIABETES INTRODUCTION Diabetes is one of the most common diseases in the United States, and diabetes is a disease that affects the way the body handles blood sugar. Approximately
ACTIVITY #3: LUNG HEALTH ASTHMA AND ALLERGIES
 ACTIVITY #3: LUNG HEALTH ASTHMA AND ALLERGIES TIME 50 minutes, computer lab REQUIRED RESOURCES Activity Computer lab with internet access for student research Notepaper and pencil for research Poster board
ACTIVITY #3: LUNG HEALTH ASTHMA AND ALLERGIES TIME 50 minutes, computer lab REQUIRED RESOURCES Activity Computer lab with internet access for student research Notepaper and pencil for research Poster board
PARKINSON S DISEASE INTRODUCTION. Parkinson s disease is defined as a disease of the nervous system that affects voluntary movement.
 PARKINSON S DISEASE INTRODUCTION Parkinson s disease is a disorder of the brain and the nervous system. It is one of the more common neurological diseases in people over the age of 60, and it is more common
PARKINSON S DISEASE INTRODUCTION Parkinson s disease is a disorder of the brain and the nervous system. It is one of the more common neurological diseases in people over the age of 60, and it is more common
Call Your Home Health Nurse and/or Physician. Call 911. Self Management for COPD COMMUNITY HEALTH AND COUNSELING SERVICES
 COMMUNITY HEALTH AND COUNSELING SERVICES Self Management for COPD Call Your Home Health Nurse and/or Physician Call 911 Sputum (phlegm) that increases in amount/color or becomes thicker than usual Unrelieved
COMMUNITY HEALTH AND COUNSELING SERVICES Self Management for COPD Call Your Home Health Nurse and/or Physician Call 911 Sputum (phlegm) that increases in amount/color or becomes thicker than usual Unrelieved
Pneumonia Education and Discharge Instructions
 Pneumonia Education and Discharge Instructions Pneumonia Education and Discharge Instructions Definition: Pneumonia is an infection of the lungs. Many different organisms can cause it, including bacteria,
Pneumonia Education and Discharge Instructions Pneumonia Education and Discharge Instructions Definition: Pneumonia is an infection of the lungs. Many different organisms can cause it, including bacteria,
Influenza (Flu) Influenza is a viral infection that may affect both the upper and lower respiratory tracts. There are three types of flu virus:
 Respiratory Disorders Bio 375 Pathophysiology General Manifestations of Respiratory Disease Sneezing is a reflex response to irritation in the upper respiratory tract and is associated with inflammation
Respiratory Disorders Bio 375 Pathophysiology General Manifestations of Respiratory Disease Sneezing is a reflex response to irritation in the upper respiratory tract and is associated with inflammation
If You Smoke And Are Pregnant
 If You Smoke And Are Pregnant Or Thinking About Pregnancy, Use This Self-help Guide TAKE THE FIRST STEP FOR YOUR BABY TAKE THE FIRST STEP FOR YOUR BABY Having a plan is the most important step you can
If You Smoke And Are Pregnant Or Thinking About Pregnancy, Use This Self-help Guide TAKE THE FIRST STEP FOR YOUR BABY TAKE THE FIRST STEP FOR YOUR BABY Having a plan is the most important step you can
About lung cancer. Contents. The lungs
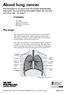 This information is an extract from the booklet Understanding lung cancer. You may find the full booklet helpful. We can send you a free copy see page 7. The lungs Contents The lungs Types of lung cancer
This information is an extract from the booklet Understanding lung cancer. You may find the full booklet helpful. We can send you a free copy see page 7. The lungs Contents The lungs Types of lung cancer
Cough, as a leading symptom, would certainly be in the top 10 of reasons for seeing a GP.
 COUGH Cough, as a leading symptom, would certainly be in the top 10 of reasons for seeing a GP. A cough in a child seems to cause more concern, even when it has not been present very long, whereas in adults
COUGH Cough, as a leading symptom, would certainly be in the top 10 of reasons for seeing a GP. A cough in a child seems to cause more concern, even when it has not been present very long, whereas in adults
COPD. (Chronic Obstructive Pulmonary Disease) (Emphysema) (Chronic Bronchitis) Education For Our Community
 COPD (Chronic Obstructive Pulmonary Disease) (Emphysema) (Chronic Bronchitis) Education For Our Community Chronic Obstructive Pulmonary Disease (COPD) Definition Chronic obstructive pulmonary disease (COPD)
COPD (Chronic Obstructive Pulmonary Disease) (Emphysema) (Chronic Bronchitis) Education For Our Community Chronic Obstructive Pulmonary Disease (COPD) Definition Chronic obstructive pulmonary disease (COPD)
Oxygen AND COPD. This fact sheet talks about home oxygen, prescribed as a medicine for some people with COPD.
 Oxygen AND COPD This fact sheet talks about home oxygen, prescribed as a medicine for some people with COPD. For more information on COPD, phone 1-866-717-COPD (2673) or visit us online at www.lung.ca/copd
Oxygen AND COPD This fact sheet talks about home oxygen, prescribed as a medicine for some people with COPD. For more information on COPD, phone 1-866-717-COPD (2673) or visit us online at www.lung.ca/copd
The Annual Direct Care of Asthma
 The Annual Direct Care of Asthma The annual direct health care cost of asthma in the United States is approximately $11.5 billion; indirect costs (e.g. lost productivity) add another $4.6 billion for a
The Annual Direct Care of Asthma The annual direct health care cost of asthma in the United States is approximately $11.5 billion; indirect costs (e.g. lost productivity) add another $4.6 billion for a
Marilyn Borkgren-Okonek, APN, CCNS, RN, MS Suburban Lung Associates, S.C. Elk Grove Village, IL
 Marilyn Borkgren-Okonek, APN, CCNS, RN, MS Suburban Lung Associates, S.C. Elk Grove Village, IL www.goldcopd.com GLOBAL INITIATIVE FOR CHRONIC OBSTRUCTIVE LUNG DISEASE GLOBAL STRATEGY FOR DIAGNOSIS, MANAGEMENT
Marilyn Borkgren-Okonek, APN, CCNS, RN, MS Suburban Lung Associates, S.C. Elk Grove Village, IL www.goldcopd.com GLOBAL INITIATIVE FOR CHRONIC OBSTRUCTIVE LUNG DISEASE GLOBAL STRATEGY FOR DIAGNOSIS, MANAGEMENT
& WHEN SHOULD I WORRY?
 WHEN SHOULD I WORRY? - Your guide to Coughs, Colds, Earache & Sore Throats Information For:- Who is this booklet for? Having an ill child can be a very scary experience for parents. If you understand more
WHEN SHOULD I WORRY? - Your guide to Coughs, Colds, Earache & Sore Throats Information For:- Who is this booklet for? Having an ill child can be a very scary experience for parents. If you understand more
Understanding COPD. Carolinas Healthcare System
 Understanding COPD Carolinas Healthcare System 2013 This self-directed learning module contains information about the pathophysiology, diagnosis, and treatment of COPD. Target Audience: All RNs and LPNs
Understanding COPD Carolinas Healthcare System 2013 This self-directed learning module contains information about the pathophysiology, diagnosis, and treatment of COPD. Target Audience: All RNs and LPNs
Oh Baby! We Want To Keep You Safe From Secondhand Smoke TAKE THE FIRST STEP FOR YOUR BABY
 Oh Baby! We Want To Keep You Safe From Secondhand Smoke TAKE THE FIRST STEP FOR YOUR BABY TAKE THE FIRST STEP FOR YOUR BABY Making a plan to avoid secondhand smoke is an important step in helping your
Oh Baby! We Want To Keep You Safe From Secondhand Smoke TAKE THE FIRST STEP FOR YOUR BABY TAKE THE FIRST STEP FOR YOUR BABY Making a plan to avoid secondhand smoke is an important step in helping your
THE LUNGS IN MARFAN SYNDROME
 THE LUNGS IN MARFAN SYNDROME Many people with Marfan syndrome and some related disorders experience pulmonary complications, or problems with their lungs. If you have Marfan syndrome, it is important for
THE LUNGS IN MARFAN SYNDROME Many people with Marfan syndrome and some related disorders experience pulmonary complications, or problems with their lungs. If you have Marfan syndrome, it is important for
PLAN OF ACTION FOR. Physician Name Signature License Date
 PLAN OF ACTION FOR Patient s copy (patient s name) I Feel Well Lignes I feel short directrices of breath: I cough up sputum daily. No Yes, colour: I cough regularly. No Yes I Feel Worse I have changes
PLAN OF ACTION FOR Patient s copy (patient s name) I Feel Well Lignes I feel short directrices of breath: I cough up sputum daily. No Yes, colour: I cough regularly. No Yes I Feel Worse I have changes
Your guide to stopping smoking for good
 Your guide to stopping smoking for good Reading this is your first step to stopping smoking for good Help2Quit gives you advice and support to help stop smoking for good. Nicotine replacement therapy and
Your guide to stopping smoking for good Reading this is your first step to stopping smoking for good Help2Quit gives you advice and support to help stop smoking for good. Nicotine replacement therapy and
If You Smoke And Are Pregnant
 If You Smoke And Are Pregnant Or Thinking About Pregnancy, Use This Self-help Guide TAKE THE FIRST STEP FOR YOUR BABY TAKE THE FIRST STEP FOR YOUR BABY Having a plan is the most important step you can
If You Smoke And Are Pregnant Or Thinking About Pregnancy, Use This Self-help Guide TAKE THE FIRST STEP FOR YOUR BABY TAKE THE FIRST STEP FOR YOUR BABY Having a plan is the most important step you can
Breathless The Whys and Wherefores Living with Alpha-1-Antitrypsin Deficiency
 Breathless The Whys and Wherefores Living with Deficiency Patient Information Program Breathlessness Short of breath after running the marathon? Short of breath after climbing a flight of stairs? Short
Breathless The Whys and Wherefores Living with Deficiency Patient Information Program Breathlessness Short of breath after running the marathon? Short of breath after climbing a flight of stairs? Short
Dental Care and Chronic Conditions. Respiratory Disease Cardiovascular Disease Diabetes
 Dental Care and Chronic Conditions Respiratory Disease Cardiovascular Disease Diabetes Shape Up Your Smile and Avoid Some Complications of Chronic Diseases When you take good care of your oral health,
Dental Care and Chronic Conditions Respiratory Disease Cardiovascular Disease Diabetes Shape Up Your Smile and Avoid Some Complications of Chronic Diseases When you take good care of your oral health,
Key Facts about Influenza (Flu) & Flu Vaccine
 Key Facts about Influenza (Flu) & Flu Vaccine mouths or noses of people who are nearby. Less often, a person might also get flu by touching a surface or object that has flu virus on it and then touching
Key Facts about Influenza (Flu) & Flu Vaccine mouths or noses of people who are nearby. Less often, a person might also get flu by touching a surface or object that has flu virus on it and then touching
Medications to help you quit smoking
 Medications to help you quit smoking How can medication help me quit smoking? Using medications can increase your chances of quitting smoking 2 to 3 times more than quitting without using medications.
Medications to help you quit smoking How can medication help me quit smoking? Using medications can increase your chances of quitting smoking 2 to 3 times more than quitting without using medications.
How To Quit Smoking
 The American College of Obstetricians and Gynecologists f AQ FREQUENTLY ASKED QUESTIONS FAQ065 WOMEN S HEALTH It s Time to Quit Smoking What are the dangers of smoking? How does smoking affect the body?
The American College of Obstetricians and Gynecologists f AQ FREQUENTLY ASKED QUESTIONS FAQ065 WOMEN S HEALTH It s Time to Quit Smoking What are the dangers of smoking? How does smoking affect the body?
What If I Have a Spot on My Lung? Do I Have Cancer? Patient Education Guide
 What If I Have a Spot on My Lung? Do I Have Cancer? Patient Education Guide A M E R I C A N C O L L E G E O F C H E S T P H Y S I C I A N S Lung cancer is one of the most common cancers. About 170,000
What If I Have a Spot on My Lung? Do I Have Cancer? Patient Education Guide A M E R I C A N C O L L E G E O F C H E S T P H Y S I C I A N S Lung cancer is one of the most common cancers. About 170,000
Smoking Cessation Program
 Smoking Cessation Program UHN Information for people who are ready to quit smoking Read this information to learn: why you should quit smoking how the Smoking Cessation Program works treatments to help
Smoking Cessation Program UHN Information for people who are ready to quit smoking Read this information to learn: why you should quit smoking how the Smoking Cessation Program works treatments to help
Compare the physiologic responses of the respiratory system to emphysema, chronic bronchitis, and asthma
 Chapter 31 Drugs Used to Treat Lower Respiratory Disease Learning Objectives Describe the physiology of respirations Compare the physiologic responses of the respiratory system to emphysema, chronic bronchitis,
Chapter 31 Drugs Used to Treat Lower Respiratory Disease Learning Objectives Describe the physiology of respirations Compare the physiologic responses of the respiratory system to emphysema, chronic bronchitis,
Keeping your lungs healthy
 Keeping your lungs healthy A guide for you after spinal cord injury and other neurological conditions Regional Rehabilitation Program This booklet has been written by the health care providers who provide
Keeping your lungs healthy A guide for you after spinal cord injury and other neurological conditions Regional Rehabilitation Program This booklet has been written by the health care providers who provide
II. ASTHMA BASICS. Overview of Asthma. Why do I need to know about asthma?
 II. ASTHMA BASICS Overview of Asthma Why do I need to know about asthma? In the United States, asthma is the most common chronic childhood illness. Asthma affects an estimated 4.8 million children nationally,
II. ASTHMA BASICS Overview of Asthma Why do I need to know about asthma? In the United States, asthma is the most common chronic childhood illness. Asthma affects an estimated 4.8 million children nationally,
Asthma Triggers. What are they and what can be done about them?
 Asthma Triggers What are they and what can be done about them? This brochure has been developed for the community by Asthma Australia It provides information about: Asthma triggers What you can do about
Asthma Triggers What are they and what can be done about them? This brochure has been developed for the community by Asthma Australia It provides information about: Asthma triggers What you can do about
Swine Flu and Common Infections to Prepare For. Rochester Recreation Club for the Deaf October 15, 2009
 Swine Flu and Common Infections to Prepare For Rochester Recreation Club for the Deaf October 15, 2009 Supporters Deaf Health Community Committee Members Julia Aggas Cathie Armstrong Michael McKee Mistie
Swine Flu and Common Infections to Prepare For Rochester Recreation Club for the Deaf October 15, 2009 Supporters Deaf Health Community Committee Members Julia Aggas Cathie Armstrong Michael McKee Mistie
IDIOPATHIC PULMONARY FIBROSIS: PATIENT INFORMATION BROCHURE. Supported by an unrestricted educational grant from
 IDIOPATHIC PULMONARY FIBROSIS: PATIENT INFORMATION BROCHURE Supported by an unrestricted educational grant from CONTENTS Understanding IPF 2-9 What is Pulmonary Fibrosis? 2 What is IPF? 2 What causes IPF?
IDIOPATHIC PULMONARY FIBROSIS: PATIENT INFORMATION BROCHURE Supported by an unrestricted educational grant from CONTENTS Understanding IPF 2-9 What is Pulmonary Fibrosis? 2 What is IPF? 2 What causes IPF?
Why is prematurity a concern?
 Prematurity What is prematurity? A baby born before 37 weeks of pregnancy is considered premature. Approximately 12% of all babies are born prematurely. Terms that refer to premature babies are preterm
Prematurity What is prematurity? A baby born before 37 weeks of pregnancy is considered premature. Approximately 12% of all babies are born prematurely. Terms that refer to premature babies are preterm
2161-1 - Page 1. Name: 1) Choose the disease that is most closely related to the given phrase. Questions 10 and 11 refer to the following:
 Name: 2161-1 - Page 1 1) Choose the disease that is most closely related to the given phrase. a disease of the bone marrow characterized by uncontrolled production of white blood cells A) meningitis B)
Name: 2161-1 - Page 1 1) Choose the disease that is most closely related to the given phrase. a disease of the bone marrow characterized by uncontrolled production of white blood cells A) meningitis B)
COPD PROTOCOL CELLO. Leiden
 COPD PROTOCOL CELLO Leiden May 2011 1 Introduction This protocol includes an explanation of the clinical picture, diagnosis, objectives and medication of COPD. The Cello way of working can be viewed on
COPD PROTOCOL CELLO Leiden May 2011 1 Introduction This protocol includes an explanation of the clinical picture, diagnosis, objectives and medication of COPD. The Cello way of working can be viewed on
Transcript for Asbestos Information for the Community
 Welcome to the lecture on asbestos and its health effects for the community. My name is Dr. Vik Kapil and I come to you from the Centers for Disease Control and Prevention, Agency for Toxic Substances
Welcome to the lecture on asbestos and its health effects for the community. My name is Dr. Vik Kapil and I come to you from the Centers for Disease Control and Prevention, Agency for Toxic Substances
RSV infection. Information about RSV and how you can reduce the risk of your infant developing a severe infection.
 RSV infection Information about RSV and how you can reduce the risk of your infant developing a severe infection. What is RSV? RSV is one of the most common respiratory viruses and is spread easily. By
RSV infection Information about RSV and how you can reduce the risk of your infant developing a severe infection. What is RSV? RSV is one of the most common respiratory viruses and is spread easily. By
SUBSTANCE ABUSE. Key Concepts. Types of Drugs
 SUBSTANCE ABUSE You have to choose who you want to be in life. This happens by making lots of decisions every day. Using substances is a choice. This is a big choice, because substances have a very real
SUBSTANCE ABUSE You have to choose who you want to be in life. This happens by making lots of decisions every day. Using substances is a choice. This is a big choice, because substances have a very real
Understanding Hypoventilation and Its Treatment by Susan Agrawal
 www.complexchild.com Understanding Hypoventilation and Its Treatment by Susan Agrawal Most of us have a general understanding of what the term hyperventilation means, since hyperventilation, also called
www.complexchild.com Understanding Hypoventilation and Its Treatment by Susan Agrawal Most of us have a general understanding of what the term hyperventilation means, since hyperventilation, also called
Information for Behavioral Health Providers in Primary Care. Asthma
 What is Asthma? Information for Behavioral Health Providers in Primary Care Asthma Asthma (AZ-ma) is a chronic (long-term) lung disease that inflames and narrows the airways. Asthma causes recurring periods
What is Asthma? Information for Behavioral Health Providers in Primary Care Asthma Asthma (AZ-ma) is a chronic (long-term) lung disease that inflames and narrows the airways. Asthma causes recurring periods
Idiopathic Pulmonary Fibrosis
 Idiopathic Pulmonary Fibrosis What is Idiopathic Pulmonary Fibrosis? Idiopathic pulmonary fibrosis (IPF) is a condition that causes persistent and progressive scarring of the tiny air sacs (alveoli) in
Idiopathic Pulmonary Fibrosis What is Idiopathic Pulmonary Fibrosis? Idiopathic pulmonary fibrosis (IPF) is a condition that causes persistent and progressive scarring of the tiny air sacs (alveoli) in
CorCap Cardiac Support Device Patient Information Booklet
 What is Heart Failure? CorCap Cardiac Support Device Patient Information Booklet Heart failure is a condition in which the heart is unable to pump enough blood to meet the needs of the body. To compensate
What is Heart Failure? CorCap Cardiac Support Device Patient Information Booklet Heart failure is a condition in which the heart is unable to pump enough blood to meet the needs of the body. To compensate
X-Plain Sinus Surgery Reference Summary
 X-Plain Sinus Surgery Reference Summary Introduction Sinus surgery is a very common and safe operation. Your doctor may recommend that you have sinus surgery. The decision whether or not to have sinus
X-Plain Sinus Surgery Reference Summary Introduction Sinus surgery is a very common and safe operation. Your doctor may recommend that you have sinus surgery. The decision whether or not to have sinus
Liver Function Essay
 Liver Function Essay Name: Quindoline Ntui Date: April 20, 2009 Professor: Dr. Danil Hammoudi Class: Anatomy and Physiology 2 Liver function The human body consist of many highly organize part working
Liver Function Essay Name: Quindoline Ntui Date: April 20, 2009 Professor: Dr. Danil Hammoudi Class: Anatomy and Physiology 2 Liver function The human body consist of many highly organize part working
MEASURING AND RECORDING BLOOD PRESSURE
 MEASURING AND RECORDING BLOOD PRESSURE INTRODUCTION The blood pressure, along with the body temperature, pulse, and respirations, is one of the vital signs. These measurements are used to quickly, easily,
MEASURING AND RECORDING BLOOD PRESSURE INTRODUCTION The blood pressure, along with the body temperature, pulse, and respirations, is one of the vital signs. These measurements are used to quickly, easily,
Health Science / Anatomy Exam 1 Study Guide
 THIS EXAM WILL ONLY COVER ALCOHOL AND TOBACCO LECTURES Alcohol What is Alcohol? Alcohol is a depressant Contains intoxicating substance called ethyl alcohol or ethanol Alcohol use Approximately 59.8% of
THIS EXAM WILL ONLY COVER ALCOHOL AND TOBACCO LECTURES Alcohol What is Alcohol? Alcohol is a depressant Contains intoxicating substance called ethyl alcohol or ethanol Alcohol use Approximately 59.8% of
Diuretics: You may get diuretic medicine to help decrease swelling in your brain. This may help your brain get better blood flow.
 Hemorrhagic Stroke GENERAL INFORMATION: What is a hemorrhagic stroke? A hemorrhagic stroke happens when a blood vessel in the brain bursts. This may happen if the blood vessel wall is weak, or sometimes
Hemorrhagic Stroke GENERAL INFORMATION: What is a hemorrhagic stroke? A hemorrhagic stroke happens when a blood vessel in the brain bursts. This may happen if the blood vessel wall is weak, or sometimes
Smoking and your lungs Why it s never too late to give up
 Smoking and your lungs Why it s never too late to give up Giving up smoking is never easy, but it s the most important thing you can do to look after your health. If you have a lung condition, you might
Smoking and your lungs Why it s never too late to give up Giving up smoking is never easy, but it s the most important thing you can do to look after your health. If you have a lung condition, you might
Disease/Illness GUIDE TO ASBESTOS LUNG CANCER. What Is Asbestos Lung Cancer? www.simpsonmillar.co.uk Telephone 0844 858 3200
 GUIDE TO ASBESTOS LUNG CANCER What Is Asbestos Lung Cancer? Like tobacco smoking, exposure to asbestos can result in the development of lung cancer. Similarly, the risk of developing asbestos induced lung
GUIDE TO ASBESTOS LUNG CANCER What Is Asbestos Lung Cancer? Like tobacco smoking, exposure to asbestos can result in the development of lung cancer. Similarly, the risk of developing asbestos induced lung
