WA Cancer & Palliative Care Network. Colorectal Cancer Model of Care
|
|
|
- Lorin Hudson
- 7 years ago
- Views:
Transcription
1 WA Cancer & Palliative Care Network Colorectal Cancer Model of Care 1
2 Department of Health, State of Western Australia (2008). Copyright to this material produced by the Western Australian Department of Health belongs to the State of Western Australia, under the provisions of the Copyright Act 1968 (Commonwealth Australia). Apart from any fair dealing for personal, academic, research or non-commercial use, no part may be reproduced without written permission of the WA Cancer & Palliative Care Network, Western Australian Department of Health. The Department of Health is under no obligation to grant this permission. Please acknowledge the WA Department of Health when reproducing or quoting material from this source. Suggested Citation Department of Health, Western Australia. Colorectal Model of Care. Perth: WA Cancer & Palliative Care Network, Department of Health, Western Australia; Important Disclaimer: All information and content in this Material is provided in good faith by the WA Department of Health, and is based on sources believed to be reliable and accurate at the time of development. The State of Western Australia, the WA Department of Health and their respective officers, employees and agents, do not accept legal liability or responsibility for the Material, or any consequences arising from its use. 2
3 Table of Contents Introduction Screening & Prevention Initial Diagnosis and Referral Diagnostic Pathways MDT Assessment and Plan of Treatment Treatment Surveillance (Follow-Up Care) Survivorship Relapse and Retreatment Palliative Care Recommendations...19 References...20 Acknowledgements...20 Index of Figures Figure 1. Appropriate access to specialist care...6 3
4 Introduction Cancer is the leading cause of death in Western Australia, representing 30.6 per cent of all deaths in Population ageing will significantly increase the number of new cases of cancer over the next ten years, with an estimated 10,000 more cases per annum in Western Australia by In 2006, 1080 Western Australians were diagnosed with colorectal cancer and there were 400 deaths due to this type of cancer in Cancer is a complex disease to diagnose and treat and represents a significant burden to patients and their families, the health system, and the community at large. Western Australia s strategic and planned approach to cancer reform includes the establishment of a Ministerial Taskforce for Cancer, the implementation of the Fighting cancer policy and a cancer services framework for Western Australia. Two significant directions of the Cancer Services Framework are the establishment of integrated cancer services in metropolitan and regional Western Australia, and the development of service delivery and improvement through a tumour streams model. Since 2004, eight integrated cancer services have been established in metropolitan and regional Western Australia based on specified geographic populations. The philosophy of an integrated cancer service is that hospitals and primary and community health services develop integrated care and defined referral pathways for the populations they serve. This requires effective collaboration between hospitals and community-based services, including general practitioners. This will promote more effective local coordination of care for cancer patients, and a more rational, evidence-based approach to cancer service planning and delivery. The Cancer Services Framework also recommended that organ or system-specific tumour streams be adopted to support the delivery and improvement of care. The reasoning behind the tumour streams is that a consistent approach to clinical management based on evidence-based practice will reduce unacceptable variations in care across the state. Data Collection and Audit Data collection regarding treatment and outcomes is essential to monitor the quality and safety of care. An appropriate clinical database for colorectal cancer treatment and outcomes should be available and adequately resourced. Treatment outcomes including morbidity and survival data should be readily available in the public domain. Model of Care The WA Cancer and Palliative Care Network (WACPCN) Model of Care for Cancer ( l_of_care.pdf) provides the basis for this tumour site specific model of care. This document describes how Colorectal Cancer care should be delivered in WA. The eight steps in figure 1 describe the patient centred journey that provides safe, quality, evidence based, and multidisciplinary care resulting in optimum outcomes. 4
5 Underpinning this journey is the integration of primary care, supportive care, psychooncology and palliative care. 1 The Western Australian Cancer Registry, Cancer incidence and mortality in Western Australia,
6 Figure 1. Appropriate access to specialist care Every cancer patient should have appropriate access to specialist cancer care Prevention & Screening Symptomatic Presentation Initial Diagnosis & Referral Diagnostic Pathways (Fast Track / Staging) MDT Assessment & Plan of Treatment Treatment Surveillance (follow up care) Survivorship Relapse & Retreatment Palliative Care 6
7 1. Screening & Prevention Screening The early detection of colorectal cancer, especially at an asymptomatic stage, is associated with improved patient outcomes. To this end, the National Health and Medical Research Council (NHMRC) strongly recommends organised screening with faecal occult blood testing (FOBT) every 2 years for all Australians over 50 years of age. Attempts to fulfil these recommendations have begun with the Commonwealth funded National Bowel Cancer Screening Program (NBCSP), although it is currently only available to individuals aged 50, 55 and 65 years. Invitations to participate and FOBT kits are delivered to eligible individuals by letter directly from the Commonwealth. Participants found to have a positive FOBT are advised to contact their nominated general practitioner, who is then responsible for organising appropriate further investigations, usually a colonoscopy. The Department of Health, Western Australia (DoH,WA) in conjunction with the WA Cancer and Palliative Care Network (WACPCN), Colorectal Tumour Collaborative (CRTC), WA Bowel Cancer Screening Implementation Team and the Cancer Council WA have provided supplementary professional and community education regarding this Program. It is essential that FOBT positive participants are able to access timely follow-up colonoscopies provided by credentialed colonoscopists in approved facilities. This can be provided through the private or public system, or through the Ambulatory Surgery Initiative which allows access for uninsured patients in secondary hospitals. Individuals not eligible for the NBCSP are encouraged to participate in FOBT screening privately, by purchasing kits from pharmacists, via selected general practices or online, until such time that the NBCSP is extended to all individuals as recommended by the NHMRC. Surveillance for High Risk Subjects Individuals who are at significantly increased risk of colorectal cancer (> 3x average risk) should enter an appropriate surveillance program, usually involving regular colonoscopy. Such individuals include those with a strong family history of bowel cancer, those belonging to inherited autosomal dominant genetic bowel cancer families (e.g., Familial Adenomatous Polyposis and Lynch syndrome (hereditary nonpolyposis colorectal cancer syndrome)) and those with long history of inflammatory bowel disease. Surveillance programs for these individuals must include review by appropriate specialists such as the Familial Cancer Clinic of the Genetic Services of WA, gastroenterologists and surgeons. Prevention The burden of colorectal cancer in our society can be substantially reduced by primary prevention. This involves acting on recommendations in relation to physical activity, body weight, dietary modifications, alcohol consumption and smoking. Evidence-based guidelines have been published by the NHMRC. Health promotion information should be provided by Government, through health professionals or organisations such as the Cancer Council WA. 7
8 2. Initial Diagnosis and Referral 1. Symptoms and signs the common symptoms of colorectal cancer are rectal bleeding, altered bowel habit, abdominal discomfort and bloating, iron deficiency anaemia and the general symptoms of cancer. a. Patients present to the General Practitioner (GP) for assessment and appropriate diagnostic tests in order to diagnose (or exclude) cancer. b. In some circumstances the patient s symptoms, signs or general condition will warrant urgent referral to a specialist rather than being investigated further by the GP. Patients with suspicious symptoms may be referred by the GP for a diagnostic colonoscopy without the necessity of specialist consultation. On diagnosis of a colorectal cancer the patient should be referred to a specialist surgeon for further management. c. Patients may present to an Emergency Department (ED) with acute bowel obstruction/acute abdomen necessitating urgent surgical intervention. In less urgent cases patients seen in the ED need fast tracked referral to an appropriate specialist for urgent assessment and diagnostic investigations. Appropriate referral pathways should be available or developed. 2. Timeframe to see a specialist a. The aim is to see a specialist and begin treatment within 4-6 weeks of (proven or strongly suspected) cancer diagnosis. b. Verbal referral essential in urgent cases and should be confirmed by urgent written (fax, ) referral. 3. Type of specialist a. A patient with a confirmed diagnosis of colorectal cancer should be referred directly to a colorectal surgeon, specialist surgeon or colorectal cancer care team who participate in a multidisciplinary team (MDT) approach to colorectal cancer care. b. A patient with a suspected diagnosis of colorectal cancer may be referred to a relevant specialist (gastroenterologist or surgeon or colorectal cancer care team for further investigation). 8
9 3. Diagnostic Pathways This step deals with the investigations that may be required to confirm the diagnosis of cancer and assess the extent (staging) of the cancer. This may involve complex tests in different departments/locations and wherever possible should be coordinated to improve patient convenience and well being. Fast track, coordinated diagnostic pathways should be implemented at a system level. Colonoscopy An important investigation in the diagnosis of colorectal cancer is colonoscopy. This must be performed by appropriately trained and credentialed practitioners. It is the responsibility of the DoH,WA to ensure there are sufficient colonoscopists to provide a timely service. The DoH,WA should ensure that training programs and credentialing protocols are provided. In rural and regional centres it will be appropriate for colonoscopy to be performed in appropriately staffed facilities, usually a secondary hospital. An important strategy to increase colonoscopy availability is to reduce the numbers of procedures being performed for inappropriate indications, including excessively frequent surveillance colonoscopies. Computed Tomography Scan (CAT Scan) CAT scan of the chest abdomen and pelvis is the most useful imaging study to determine the presence of locoregional and distant metastasis. This must be and is available in both the public and private community setting, and in both metro and regional areas. It is appropriate for GPs or specialists to organise a CAT scan in a private radiology community setting as this will expedite this investigation. Discussion with the specialist at the time of referral may lead to this investigation being performed so that it is available at the time of initial specialist consultation. Timely access to CAT scanning should be available in metro and regional centres. Magnetic Resonance Imaging (MRI) MRI is used in the assessment of rectal cancers to determine whether preoperative chemoradiotherapy is indicated. The need for this investigation is usually determined by the colorectal surgeon and the MDT as part of the comprehensive assessment prior to determining the type of treatment. When required, decision planning is dependant on the result, otherwise treatment is delayed. It is expected that MRI will be available in a timely fashion so that treatment delay does not occur. Pathology Assessment of tissue specimens by appropriately qualified histopathologists is critical to the diagnostic process. Fine Needle Aspiration (FNA) specimens for cytology may be obtained from sites of potential metastasis and expert cytopathologists are required to assess this material. Timely provision of these services will usually be carried out by the state pathology service, PathWest or by private pathology providers. 9
10 4. MDT Assessment and Plan of Treatment All patients should have access to a MDT to plan the management of their cancer. It is essential that a cancer specialist lead the MDT approach and that this be available to all patients no matter where they live. It is expected that patients in rural and remote areas will have access to this care and that this will be co-ordinated by their GP, local specialist or cancer nurse coordinator using video-conferencing or assisted travel where appropriate. MDT Team The multidisciplinary team comprises (in alphabetical order): Medical Oncologist Nurse Coordinator Pathologist Radiation Oncologist Radiologist with expertise in MRI Social Worker Surgeon (colorectal for rectal cancer) Stomal therapist With access to: Allied health services including Dietician, where appropriate Palliative care service for patients with locally advanced cancers and metastatic disease. Psycho-oncology services as required (psychologist/psychiatrist) Hepatobiliary Surgeon Gastroenterologist with colorectal expertise The lead role in the multidisciplinary team will be determined by the team and must take responsibility for the activity of the team. MDT Treatment Care Plan Treatment will be planned after all relevant investigations have been reviewed. Ideally, all patients with rectal cancer should at the very least be discussed in a MDT setting where there is expertise in rectal cancer (see below). Discussion should take place before surgery, because multimodality neoadjuvant therapy is often optimal. Patients with uncomplicated colon cancer will usually be presented for MDT planning after surgery, particularly with respect to follow up chemotherapy. The primary specialist who makes the referral to the MDT is responsible for the patient until care is passed to another practitioner. 10
11 The MDT must be adequately resourced to undertake the following responsibilities and should: Specify and document who will be the primary treating specialist. Fully document the agreed care plan. Circulate the agreed care plan to all relevant members of the team. The progression of care within the MDT should be coordinated ensuring that the patient and all care givers understand their responsibilities for delivering this care. The GP should be informed of the planned treatment and their role in this plan. The patient and their family should be centrally involved in arriving at the preferred treatment plan. 11
12 5. Treatment This step is concerned with the type of treatment that will be delivered, who will provide it and where it should be provided to ensure safe, high quality and effective care. Surgery Nearly all patients will be offered surgery if appropriate. Surgery should be performed by surgeons (FRACS or equivalent) with adequate training and experience in colon or rectal surgery that enables institutional credentialing and agreed scope of practice within this area. Patients with rectal cancer should, wherever possible, have their surgery performed by specialist colorectal surgeons with adequate training and experience that enables institutional credentialing and agreed scope of practice within this area. Surgery should be performed in institutions (usually tertiary and secondary hospitals) that provide appropriate facilities including: Surgeon, stomal therapist and anaesthetic services Intensive care and/or high dependency care unit 24 hours medical staff availability 24 hours operating room access Diagnostic imaging Radiation Treatment For high risk rectal cancer, adjuvant pre-operative or post-operative radiation treatment is commonly indicated. In colon cancer it has a limited role. Radiation treatment should be given by a radiation oncologist (FRANZCR or equivalent) with adequate training and experience that enables institutional credentialing and agreed scope of practice within this area. Radiation treatment should be performed in accredited institutions with experience in complex treatment planning. Drug Therapy Drug therapy including chemotherapy is usually given to patients who are at high risk of relapse and who may benefit from adjuvant therapy. Drug therapy may be given to those patients with locally advanced or metastatic disease. Drug therapy is usually given by a Medical Oncologist (FRACP or equivalent) with adequate training and experience that enables institutional credentialing and agreed scope of practice within this area. Drug therapy is usually given in an institution with the following characteristics: Staff including a medical oncologist, nurses with adequate training in chemotherapy administration, handling and disposal of cytotoxic waste, pharmacist with adequate training in chemotherapy medications and preparation. 12
13 Less complex therapies may be given in secondary, regional or primary care settings (where no medical oncologist is locally available) by another medical practitioner or nurse chemotherapy provider with training and experience that enables credentialing and agreed scope of practice. This should be in accordance with a detailed treatment plan arising from a MDT setting, and should be under the supervision of a medical oncologist with communication as required. Facilities for safe administration of drug therapy include: Emergency care and advice after hours Care for neutropenic patients Access to haematology testing Cytotoxic drugs are prepared in a pharmacy with appropriate facilities, including provision and transport of such drugs from a tertiary or secondary institution Guidelines and protocols for the safe administration of drugs including management of extravasation Intensive care/high dependency unit availability Combined therapy with chemotherapy and radiation therapy needs effective coordination, especially where the facilities are not co-located. 13
14 6. Surveillance (Follow-Up Care) This step concerns the monitoring of the patient following initial treatment. The aim is the early detection of disease relapse and /or the management of symptoms arising from treatment or the disease. It also provides reassurance to patients who appear to be free of disease. A clear documented plan of surveillance should be established and be available to the patient. This should avoid multiple visits to multiple specialists. What follow up care is needed: Patients who are medically fit should undergo regular surveillance as they are at increased risk of second primary colorectal cancers. Patients who are medically fit, who are at moderate to high risk of metastatic or recurrent disease, should undergo surveillance to identify potentially resectable metastases (often hepatic). A surveillance/follow up plan should be agreed by the patient and the coordinating MDT clinician and clearly documented in the patient record. The surveillance plan must be communicated to the patient s general practitioner. The surveillance plan should be individualised according to risk of recurrence and patient needs. Clinical examination and investigations such as colonoscopy, CT scan, Chest Xray and Tumour markers should be available in tertiary, secondary and primary care settings as recommended in established clinical practice guidelines (ref : ACN colorectal cancer guidelines 2005). The exact location of follow up will be decided in consultation with the patient, GP and lead clinician. Who should provide the follow up care: The MDT team should decide whether the patient is medically fit for intensive follow-up and communicate this appropriately to avoid unnecessary investigations in those patients who would not be fit for further procedures. The MDT team in consultation with the GP will decide who should lead the follow up care. Responsibility for follow up investigations (colonoscopy, CT scan) should be agreed by the lead clinician, GP and patient and should be documented. Patient failure to attend for follow up should be notified to the responsible clinicians. Every effort must be made to reduce multiple visits to different treatment disciplines. Patient specific follow up may require involvement of occupational therapists, physiotherapists, dieticians, stomal therapists, social work, psycho-oncology support and nurses. 14
15 Where should follow up be provided: Follow up should be provided in public hospitals (tertiary and secondary), private hospitals, private specialist consulting rooms or general practitioner rooms. Imaging studies can be provided by any appropriately credentialed facility as long as results are delivered to the appropriate responsible clinician. Regional centres should be encouraged to provide coordinated follow up according to protocol, with input from the lead clinician as required, if necessary by videoconference. The GP has a key role in the coordination of follow up. 15
16 7. Survivorship The transition from active to post treatment care is critical to long term health. Care should be planned and coordinated. Survivors should have knowledge of their increased risk of second/ recurrent cancers or treatment related morbidities. This encourages them to actively participate in their continuing post treatment care. This approach is essential so that routine follow up visits become opportunities to promote a healthy life style, check for cancer recurrence and manage lasting effects of the cancer experience. Survivorship may be medically led, particularly through primary care, nurse-led or patient-led. Cancer Councils across Australia are developing and evaluating approaches that are patient centred. 16
17 8. Relapse and Retreatment This step concerns the diagnosis and management of patients who have recurrence of the disease (local or metastatic) and who need assessment regarding further treatment. This assessment may be made by the GP initially with subsequent involvement of the specialist and the MDT. Clinical evaluation and patient discussion will determine the most appropriate treatment which may be curative or palliative in intent. Patients who relapse require expert opinion as to the best plan of management and this will usually be provided by the colorectal MDT. Treatment for relapse may require drug therapy, radiation therapy or surgery. What should be provided: The diagnosis of relapse will usually be made by the GP or the specialist surgeon/physician coordinating follow up. Referral for full assessment and discussion by the MDT is recommended. Access to appropriate investigations is important including: Haematology and Biochemistry Chest X ray Ultrasound CAT scan MRI pelvis where appropriate Positron Emission Tomography (PET) where appropriate Colonoscopy Biopsy or FNA Management should be discussed by: The lead clinician in liaison with the GP and with involvement of one or more relevant members of the multidisciplinary team with input from a hepatobiliary surgeon if necessary. The management plan should be decided in consultation with the patient and fully documented in the patient record. Where appropriate, participation by the GP and palliative care team is essential. Where should assessment and retreatment occur: Following diagnosis and confirmation of relapse, assessment should occur in a setting that involves the lead clinician and the MDT, often in a tertiary cancer centre but could be in a secondary or regional centre with input by the relevant clinician/oncologist and the MDT. Telehealth may be of assistance in some cases. Surgical treatment for relapse often involves complex therapy and is usually carried out in a tertiary cancer centre. Patients receiving palliative chemotherapy could be treated at public tertiary or secondary hospitals or large private hospitals with appropriate infrastructure. The extent of disease and the patient s health may lead to a process of disease control or palliation rather than a curative approach. 17
18 9. Palliative Care The WA Palliative Care model defines the appropriate approach to symptom management and end of life care. It is important that patients and their families receive optimal palliative care and early referral for assessment and advice is recommended. It is also important to recognise that a major component of palliative care involves symptom relief and this may require surgical intervention, radiation therapy or chemotherapy. ( del_of_care.pdf) 18
19 10. Recommendations 1. MRI for rectal cancers is currently not covered by a Medicare rebate. It is recommended that this is highlighted as an area of concern and that public patients accessing MRI in the private setting be eligible for a full rebate from the Department of Health. 2. Data collection regarding treatment and outcomes is essential to monitor the quality and safety of care. An appropriate clinical database for colorectal cancer treatment and outcomes should be available and adequately resourced. 3. Patients with rectal cancer should, wherever possible, have their surgery performed by specialist colorectal surgeons with adequate training and experience. 4. Multidisciplinary team assessment and treatment planning should be available to all patients with a diagnosis of colon or rectal cancer. It is recommended that support be given to this essential activity with particular emphasis on rural patients who may be disadvantaged due to location. 19
20 References 1. The Western Australian Cancer Registry, Cancer incidence and mortality in Western Australia, Australian Cancer Network Colorectal Cancer Guidelines Review Committee (ACNCCGRC) 2005, Clinical practice guidelines for the prevention, early detection and management of colorectal cancer, The Cancer Council Australia and Australian Cancer Network, Sydney. Acknowledgements The WA Cancer & Palliative Care Network have used, with permission, some of the content and template, used in the "Victorian Government Cancer Initiatives Cancer Services Framework Overview " to produce this Model of Care for Colorectal Cancer 20
21 WA Cancer & Palliative Care Network Level 1, 1 Centro Ave Subiaco Western Australia 6008
National Bowel Cancer Audit Report 2008 Public and Executive Summary
 National Bowel Cancer Audit Report 2008 Public and Executive Summary Prepared in association with: Healthcare Quality Improvement Partnership HQIP Association of Coloproctology of Great Britain and Ireland
National Bowel Cancer Audit Report 2008 Public and Executive Summary Prepared in association with: Healthcare Quality Improvement Partnership HQIP Association of Coloproctology of Great Britain and Ireland
Cancer services children s CSCF v3.2
 Cancer services children s CSCF v3.2 Module overview Please note: This module should be read in conjunction with the Fundamentals of the Framework (including glossary and acronym list), Children s Services
Cancer services children s CSCF v3.2 Module overview Please note: This module should be read in conjunction with the Fundamentals of the Framework (including glossary and acronym list), Children s Services
Rotation Specific Goals & Objectives: University Health Network-Princess Margaret Hospital/ Sunnybrook Breast/Melanoma
 Rotation Specific Goals & Objectives: University Health Network-Princess Margaret Hospital/ Sunnybrook Breast/Melanoma Medical Expert: Breast Rotation Specific Competencies/Objectives 1.0 Medical History
Rotation Specific Goals & Objectives: University Health Network-Princess Margaret Hospital/ Sunnybrook Breast/Melanoma Medical Expert: Breast Rotation Specific Competencies/Objectives 1.0 Medical History
Colorectal Cancer Care A Cancer Care Map for Patients
 Colorectal Cancer Care A Cancer Care Map for Patients Understanding the process of care that a patient goes through in the diagnosis and treatment of colorectal cancer in BC. Colorectal Cancer Care Map
Colorectal Cancer Care A Cancer Care Map for Patients Understanding the process of care that a patient goes through in the diagnosis and treatment of colorectal cancer in BC. Colorectal Cancer Care Map
Surgical guidelines for the management of breast cancer
 Available online at www.sciencedirect.com EJSO xx (2009) S1eS22 www.ejso.com Guidelines Surgical guidelines for the management of breast cancer Contents Association of Breast Surgery at BASO 2009 Introduction...
Available online at www.sciencedirect.com EJSO xx (2009) S1eS22 www.ejso.com Guidelines Surgical guidelines for the management of breast cancer Contents Association of Breast Surgery at BASO 2009 Introduction...
Colorectal Cancer Treatment
 Scan for mobile link. Colorectal Cancer Treatment Colorectal cancer overview Colorectal cancer, also called large bowel cancer, is the term used to describe malignant tumors found in the colon and rectum.
Scan for mobile link. Colorectal Cancer Treatment Colorectal cancer overview Colorectal cancer, also called large bowel cancer, is the term used to describe malignant tumors found in the colon and rectum.
This vision does not represent government policy but provides useful insight into how breast cancer services might develop over the next 5 years
 Breast Cancer 2015 Annex C Background 1. Breast cancer is the most common cancer in women in England with (not including cases of ductal carcinoma in situ (DCIS) 1 ) 39,681 new cases diagnosed in 2008
Breast Cancer 2015 Annex C Background 1. Breast cancer is the most common cancer in women in England with (not including cases of ductal carcinoma in situ (DCIS) 1 ) 39,681 new cases diagnosed in 2008
PRACTICE FRAMEWORK AND COMPETENCY STANDARDS FOR THE PROSTATE CANCER SPECIALIST NURSE
 PRACTICE FRAMEWORK AND COMPETENCY STANDARDS FOR THE PROSTATE CANCER SPECIALIST NURSE MARCH 2013 MONOGRAPHS IN PROSTATE CANCER OUR VISION, MISSION AND VALUES Prostate Cancer Foundation of Australia (PCFA)
PRACTICE FRAMEWORK AND COMPETENCY STANDARDS FOR THE PROSTATE CANCER SPECIALIST NURSE MARCH 2013 MONOGRAPHS IN PROSTATE CANCER OUR VISION, MISSION AND VALUES Prostate Cancer Foundation of Australia (PCFA)
STATEMENT ON THE DELINEATION OF EMERGENCY DEPARTMENTS
 STATEMENT Document No: S12 Approved: Jul-97 Last Revised: Nov-12 Version No: 05 STATEMENT ON THE DELINEATION OF EMERGENCY DEPARTMENTS 1. PURPOSE This document defines the minimum requirement for a health
STATEMENT Document No: S12 Approved: Jul-97 Last Revised: Nov-12 Version No: 05 STATEMENT ON THE DELINEATION OF EMERGENCY DEPARTMENTS 1. PURPOSE This document defines the minimum requirement for a health
Palliative Care Role Delineation Framework
 Director-General Palliative Care Role Delineation Framework Document Number GL2007_022 Publication date 26-Nov-2007 Functional Sub group Clinical/ Patient Services - Medical Treatment Clinical/ Patient
Director-General Palliative Care Role Delineation Framework Document Number GL2007_022 Publication date 26-Nov-2007 Functional Sub group Clinical/ Patient Services - Medical Treatment Clinical/ Patient
Cancer Screening and Early Detection Guidelines
 Cancer Screening and Early Detection Guidelines Guillermo Tortolero Luna, MD, PhD Director Cancer Control and Population Sciences Program University of Puerto Rico Comprehensive Cancer Center ASPPR Clinical
Cancer Screening and Early Detection Guidelines Guillermo Tortolero Luna, MD, PhD Director Cancer Control and Population Sciences Program University of Puerto Rico Comprehensive Cancer Center ASPPR Clinical
Breast Cancer Pathway
 Breast Cancer Pathway Risk Stratified Follow Up Dr Dorothy Goddard, Associate Medical Director for Cancer Macmillan Consultant Medical Advisor Survivorship What is risk stratified follow up? Refers to
Breast Cancer Pathway Risk Stratified Follow Up Dr Dorothy Goddard, Associate Medical Director for Cancer Macmillan Consultant Medical Advisor Survivorship What is risk stratified follow up? Refers to
Cancer: Pancreatic (Adult)
 A02/S/b 2013/14 NHS STANDARD CONTRACT FOR CANCER: PANCREATIC (ADULT) SECTION B PART 1 - SERVICE SPECIFICATIONS Service Specification No. Service Commissioner Lead Provider Lead Period Date of Review A02/S/b
A02/S/b 2013/14 NHS STANDARD CONTRACT FOR CANCER: PANCREATIC (ADULT) SECTION B PART 1 - SERVICE SPECIFICATIONS Service Specification No. Service Commissioner Lead Provider Lead Period Date of Review A02/S/b
Recommendations for cross-sectional imaging in cancer management, Second edition
 www.rcr.ac.uk Recommendations for cross-sectional imaging in cancer management, Second edition Breast cancer Faculty of Clinical Radiology www.rcr.ac.uk Contents Breast cancer 2 Clinical background 2 Who
www.rcr.ac.uk Recommendations for cross-sectional imaging in cancer management, Second edition Breast cancer Faculty of Clinical Radiology www.rcr.ac.uk Contents Breast cancer 2 Clinical background 2 Who
Follow-up care plan after treatment for breast cancer. A guide for General Practitioners
 Follow-up care plan after treatment for breast cancer A guide for General Practitioners This leaflet provides information for GPs on the follow-up care required by women who had breast cancer. It is for
Follow-up care plan after treatment for breast cancer A guide for General Practitioners This leaflet provides information for GPs on the follow-up care required by women who had breast cancer. It is for
The Scottish Public Services Ombudsman Act 2002
 Scottish Public Services Ombudsman The Scottish Public Services Ombudsman Act 2002 Investigation Report UNDER SECTION 15(1)(a) SPSO 4 Melville Street Edinburgh EH3 7NS Tel 0800 377 7330 SPSO Information
Scottish Public Services Ombudsman The Scottish Public Services Ombudsman Act 2002 Investigation Report UNDER SECTION 15(1)(a) SPSO 4 Melville Street Edinburgh EH3 7NS Tel 0800 377 7330 SPSO Information
Colorectal cancer. A guide for journalists on colorectal cancer and its treatment
 Colorectal cancer A guide for journalists on colorectal cancer and its treatment Contents Contents 2 3 Section 1: Colorectal cancer 4 i. What is colorectal cancer? 4 ii. Causes and risk factors 4 iii.
Colorectal cancer A guide for journalists on colorectal cancer and its treatment Contents Contents 2 3 Section 1: Colorectal cancer 4 i. What is colorectal cancer? 4 ii. Causes and risk factors 4 iii.
Lung Cancer Multidisciplinary Meeting Toolkit. National Lung Cancer Working Group
 Lung Cancer Multidisciplinary Meeting Toolkit National Lung Cancer Working Group September 2014 Contents Introduction 1 Multidisciplinary meetings 1 Toolkit for implementing high-quality lung cancer MDMs
Lung Cancer Multidisciplinary Meeting Toolkit National Lung Cancer Working Group September 2014 Contents Introduction 1 Multidisciplinary meetings 1 Toolkit for implementing high-quality lung cancer MDMs
Breast Cancer Follow-Up
 Diagnosis and Treatment of Patients with Primary and Metastatic Breast Cancer Breast Cancer Follow-Up Breast Cancer Follow-Up Version 2002: Thomssen / Scharl Version 2003 2009: Bauerfeind / Bischoff /
Diagnosis and Treatment of Patients with Primary and Metastatic Breast Cancer Breast Cancer Follow-Up Breast Cancer Follow-Up Version 2002: Thomssen / Scharl Version 2003 2009: Bauerfeind / Bischoff /
Strategic Directions for Multidisciplinary Cancer Care
 Achieving best practice cancer care A guide for implementing multidisciplinary care 4 Clinical review of area mental health services 1997-2004 Intensive care for adults in Victorian public hospitals 2003
Achieving best practice cancer care A guide for implementing multidisciplinary care 4 Clinical review of area mental health services 1997-2004 Intensive care for adults in Victorian public hospitals 2003
How To Prepare A Meeting For A Health Care Conference
 THORACIC ONCOLOGY MULTIDISCIPLINARY TEAM MEETINGS: OPERATIONAL POLICY EXECUTIVE SUMMARY 1. All patients in Lothian with thoracic malignancies should be discussed at designated times in pathway (see App
THORACIC ONCOLOGY MULTIDISCIPLINARY TEAM MEETINGS: OPERATIONAL POLICY EXECUTIVE SUMMARY 1. All patients in Lothian with thoracic malignancies should be discussed at designated times in pathway (see App
POSITION PAPER: Occupational therapy in oncology
 POSITION PAPER: Occupational therapy in oncology Occupational Therapy Australia 2015 About Occupational Therapy Australia Occupational Therapy Australia is the professional association for occupational
POSITION PAPER: Occupational therapy in oncology Occupational Therapy Australia 2015 About Occupational Therapy Australia Occupational Therapy Australia is the professional association for occupational
Cancer research in the Midland Region the prostate and bowel cancer projects
 Cancer research in the Midland Region the prostate and bowel cancer projects Ross Lawrenson Waikato Clinical School University of Auckland MoH/HRC Cancer Research agenda Lung cancer Palliative care Prostate
Cancer research in the Midland Region the prostate and bowel cancer projects Ross Lawrenson Waikato Clinical School University of Auckland MoH/HRC Cancer Research agenda Lung cancer Palliative care Prostate
Development of strategies for maximising the benefits of the Medicare Benefits Schedule multidisciplinary care item numbers SUMMARY REPORT
 Development of strategies for maximising the benefits of the Medicare Benefits Schedule multidisciplinary care item numbers SUMMARY REPORT Project Sponsor: Associate Professor John Seymour Project Officers:
Development of strategies for maximising the benefits of the Medicare Benefits Schedule multidisciplinary care item numbers SUMMARY REPORT Project Sponsor: Associate Professor John Seymour Project Officers:
Inova. Breast Care Institute
 Inova Breast Care Institute At the Inova Breast Care Institute, our commitment is to provide expert care for you, every step of the way. Our multidisciplinary team of more than 80 experts provides a full
Inova Breast Care Institute At the Inova Breast Care Institute, our commitment is to provide expert care for you, every step of the way. Our multidisciplinary team of more than 80 experts provides a full
How common is bowel cancer?
 information Primary Care Society for Gastroenterology Bowel Cancer (1 of 6) How common is bowel cancer? Each year 35,000 people in Britain are diagnosed with cancer of the bowel, that is to say cancer
information Primary Care Society for Gastroenterology Bowel Cancer (1 of 6) How common is bowel cancer? Each year 35,000 people in Britain are diagnosed with cancer of the bowel, that is to say cancer
Diagnosis and Prognosis of Pancreatic Cancer
 Main Page Risk Factors Reducing Your Risk Screening Symptoms Diagnosis Treatment Overview Chemotherapy Radiation Therapy Surgical Procedures Lifestyle Changes Managing Side Effects Talking to Your Doctor
Main Page Risk Factors Reducing Your Risk Screening Symptoms Diagnosis Treatment Overview Chemotherapy Radiation Therapy Surgical Procedures Lifestyle Changes Managing Side Effects Talking to Your Doctor
The Role of the MDT Coordinator. Laura Throssell
 The Role of the MDT Coordinator Laura Throssell NHS Cancer Plan (2000) the care of all patients with cancer should be formally reviewed by a specialist team. all patients have the benefit of the range
The Role of the MDT Coordinator Laura Throssell NHS Cancer Plan (2000) the care of all patients with cancer should be formally reviewed by a specialist team. all patients have the benefit of the range
SUBMISSION TO THE MEDICARE BENEFITS SCHEDULE REVIEW TASKFORCE
 SUBMISSION November 2015 SUBMISSION TO THE MEDICARE BENEFITS SCHEDULE REVIEW TASKFORCE Submission by the Chiropractors Association of Australia Page 1 of 10 About the Chiropractors Association of Australia
SUBMISSION November 2015 SUBMISSION TO THE MEDICARE BENEFITS SCHEDULE REVIEW TASKFORCE Submission by the Chiropractors Association of Australia Page 1 of 10 About the Chiropractors Association of Australia
REPORT ON STOMA SERVICE AND PRACTICE. MM / YY to MM / YY. Name: Title: Centre:
 REPORT ON STOMA SERVICE AND PRACTICE MM / YY to MM / YY Name: Title: Centre: 1 Contents 1.0 Introduction 2.0 Aims of the Stoma Care Service 3.0 Clinical Activity 4.0 Cost Saving Measures 5.0 Education
REPORT ON STOMA SERVICE AND PRACTICE MM / YY to MM / YY Name: Title: Centre: 1 Contents 1.0 Introduction 2.0 Aims of the Stoma Care Service 3.0 Clinical Activity 4.0 Cost Saving Measures 5.0 Education
Optimal care pathway for people with lung cancer
 Optimal care pathway for people with lung cancer Optimal care pathway for people with lung cancer To receive this publication in an accessible format phone 03 9096 2136 using the National Relay Service
Optimal care pathway for people with lung cancer Optimal care pathway for people with lung cancer To receive this publication in an accessible format phone 03 9096 2136 using the National Relay Service
Clinical Governance for Nurse Practitioners in Queensland
 Office of the Chief Nursing Officer Clinical Governance for Nurse Practitioners in Queensland A guide Clinical Governance for Nurse Practitioners in Queensland: A guide Queensland Health Office of the
Office of the Chief Nursing Officer Clinical Governance for Nurse Practitioners in Queensland A guide Clinical Governance for Nurse Practitioners in Queensland: A guide Queensland Health Office of the
Cancer Care Delivered Locally by Physicians You Know and Trust
 West Florida Physician Office Building Johnson Ave. University Pkwy. Olive Road N. Davis Hwy. For more information on West Florida Cancer Center: 850-494-5404 2130 East Johnson Avenue Pensacola, Florida
West Florida Physician Office Building Johnson Ave. University Pkwy. Olive Road N. Davis Hwy. For more information on West Florida Cancer Center: 850-494-5404 2130 East Johnson Avenue Pensacola, Florida
An Integrated Approach to Lung Cancer in a Community Setting
 An Integrated Approach to Lung Cancer in a Community Setting The multidisciplinary thoracic clinic at Erie Regional Cancer Center by Jan M. Rothman, MD, and Shelley D. KuBaney, RN, OCN 40 OI May June 2013
An Integrated Approach to Lung Cancer in a Community Setting The multidisciplinary thoracic clinic at Erie Regional Cancer Center by Jan M. Rothman, MD, and Shelley D. KuBaney, RN, OCN 40 OI May June 2013
Guidelines for Management of Renal Cancer
 Guidelines for Management of Renal Cancer Date Approved by Network Governance July 2012 Date for Review July 2015 Changes Between Versions 2 and 3 Section 5 updated bullets 5.3 and 5.4 Section 6 updated
Guidelines for Management of Renal Cancer Date Approved by Network Governance July 2012 Date for Review July 2015 Changes Between Versions 2 and 3 Section 5 updated bullets 5.3 and 5.4 Section 6 updated
Multidisciplinary team members views about MDT working:
 National Cancer Action Team Multidisciplinary team members views about MDT working: Results from a survey commissioned by the National Cancer Action Team September 2009 Report prepared by: Cath Taylor,
National Cancer Action Team Multidisciplinary team members views about MDT working: Results from a survey commissioned by the National Cancer Action Team September 2009 Report prepared by: Cath Taylor,
Guideline for the Follow Up of Patients Following Treatment for Breast Cancer
 Guideline for the Follow Up of Patients Following Treatment for Breast Cancer Date Approved by Network Governance July 2012 Date for Review July 2015 Page 1 of 6 1 Scope of the Guideline This guideline
Guideline for the Follow Up of Patients Following Treatment for Breast Cancer Date Approved by Network Governance July 2012 Date for Review July 2015 Page 1 of 6 1 Scope of the Guideline This guideline
2015/16 NHS STANDARD CONTRACT FOR ACUTE, AMBULANCE, COMMUNITY AND MENTAL HEALTH AND LEARNING DISABILITY SERVICES (MULTILATERAL)-
 2015/16 NHS STANDARD CONTRACT FOR ACUTE, AMBULANCE, COMMUNITY AND MENTAL HEALTH AND LEARNING DISABILITY SERVICES (MULTILATERAL)- SECTION B PART 1 - SERVICE SPECIFICATION FOR LUNG CANCER Service specification
2015/16 NHS STANDARD CONTRACT FOR ACUTE, AMBULANCE, COMMUNITY AND MENTAL HEALTH AND LEARNING DISABILITY SERVICES (MULTILATERAL)- SECTION B PART 1 - SERVICE SPECIFICATION FOR LUNG CANCER Service specification
.org. Metastatic Bone Disease. Description
 Metastatic Bone Disease Page ( 1 ) Cancer that begins in an organ, such as the lungs, breast, or prostate, and then spreads to bone is called metastatic bone disease (MBD). More than 1.2 million new cancer
Metastatic Bone Disease Page ( 1 ) Cancer that begins in an organ, such as the lungs, breast, or prostate, and then spreads to bone is called metastatic bone disease (MBD). More than 1.2 million new cancer
The Center for Prostate Cancer. Personalized Treatment. Clinical Excellence.
 The Center for Prostate Cancer Personalized Treatment. Clinical Excellence. The Center for Prostate Cancer Leaders in Prostate Cancer Treatment and Research The Center for Prostate Cancer at the North
The Center for Prostate Cancer Personalized Treatment. Clinical Excellence. The Center for Prostate Cancer Leaders in Prostate Cancer Treatment and Research The Center for Prostate Cancer at the North
Frequently Asked Questions About Ovarian Cancer
 Media Contact: Gerri Gomez Howard Cell: 303-748-3933 gerri@gomezhowardgroup.com Frequently Asked Questions About Ovarian Cancer What is ovarian cancer? Ovarian cancer is a cancer that forms in tissues
Media Contact: Gerri Gomez Howard Cell: 303-748-3933 gerri@gomezhowardgroup.com Frequently Asked Questions About Ovarian Cancer What is ovarian cancer? Ovarian cancer is a cancer that forms in tissues
MANCHESTER Lung Cancer Screening Program Dartmouth-Hitchcock Manchester 100 Hitchcock Way Manchester, NH 03104 (603) 695-2850
 LEBANON Lung Cancer Screening Program One Medical Center Drive Lebanon, NH 03756 (603) 650-4400 (866) 966-1601 Toll-free cancer.dartmouth.edu/lungscreening MANCHESTER Lung Cancer Screening Program Dartmouth-Hitchcock
LEBANON Lung Cancer Screening Program One Medical Center Drive Lebanon, NH 03756 (603) 650-4400 (866) 966-1601 Toll-free cancer.dartmouth.edu/lungscreening MANCHESTER Lung Cancer Screening Program Dartmouth-Hitchcock
Bowel (Colorectal) Cancer Diagnosis and Treatment
 Bowel (Colorectal) Cancer Diagnosis and Treatment Introduction The information in this document has been reproduced with the permission of the Colorectal and Stoma Care Team, Barts & the London NHS Trust.
Bowel (Colorectal) Cancer Diagnosis and Treatment Introduction The information in this document has been reproduced with the permission of the Colorectal and Stoma Care Team, Barts & the London NHS Trust.
Smoking and misuse of certain pain medicines can affect the risk of developing renal cell cancer.
 Renal cell cancer Renal cell cancer is a disease in which malignant (cancer) cells form in tubules of the kidney. Renal cell cancer (also called kidney cancer or renal adenocarcinoma) is a disease in which
Renal cell cancer Renal cell cancer is a disease in which malignant (cancer) cells form in tubules of the kidney. Renal cell cancer (also called kidney cancer or renal adenocarcinoma) is a disease in which
An Action Guide for Engaging Employers and Professional Medical Organizations
 Increasing Quality Colorectal Cancer Screening and Promoting Screen Quality: An Action Guide for Engaging Employers and Professional Medical Organizations U.S. Department of Health and Human Services,
Increasing Quality Colorectal Cancer Screening and Promoting Screen Quality: An Action Guide for Engaging Employers and Professional Medical Organizations U.S. Department of Health and Human Services,
PSA Screening for Prostate Cancer Information for Care Providers
 All men should know they are having a PSA test and be informed of the implications prior to testing. This booklet was created to help primary care providers offer men information about the risks and benefits
All men should know they are having a PSA test and be informed of the implications prior to testing. This booklet was created to help primary care providers offer men information about the risks and benefits
Lung Cancer & Mesothelioma 2011-2015
 Lung Cancer & Mesothelioma 2011-2015 Annex G Mesothelioma 1. The vision for mesothelioma services is set out in the Mesothelioma Framework issued by DH on 26 February 2007 (supported by the British Thoracic
Lung Cancer & Mesothelioma 2011-2015 Annex G Mesothelioma 1. The vision for mesothelioma services is set out in the Mesothelioma Framework issued by DH on 26 February 2007 (supported by the British Thoracic
NICE Pathways bring together all NICE guidance, quality standards and other NICE information on a specific topic.
 bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published.
bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published.
Post-PET Restaging Cancer Form National Oncologic PET Registry
 Post-PET Restaging Cancer Form National Oncologic PET Registry Facility ID #: Registry Case Number: Patient Name: Your patient had a PET scan on: mm/dd/yyyy. The PET scan was done for restaging of (cancer
Post-PET Restaging Cancer Form National Oncologic PET Registry Facility ID #: Registry Case Number: Patient Name: Your patient had a PET scan on: mm/dd/yyyy. The PET scan was done for restaging of (cancer
Breast Health Program
 Breast Health Program Working together, for your health. Breast Health Program The Breast Health Program at The University of Arizona Cancer Center offers patients a personalized approach to breast cancer,
Breast Health Program Working together, for your health. Breast Health Program The Breast Health Program at The University of Arizona Cancer Center offers patients a personalized approach to breast cancer,
Cancer Expert Working Group on Cancer Prevention and Screening. Prevention and Screening for Colorectal Cancer
 Cancer Expert Working Group on Cancer Prevention and Screening Prevention and Screening for Colorectal Cancer 1 What is colorectal cancer? Colorectum (colon and rectum, or the large bowel or large intestine)
Cancer Expert Working Group on Cancer Prevention and Screening Prevention and Screening for Colorectal Cancer 1 What is colorectal cancer? Colorectum (colon and rectum, or the large bowel or large intestine)
Approved: Acute Stroke Ready Hospital Advanced Certification Program
 Approved: Acute Stroke Ready Hospital Advanced Certification Program The Joint Commission recently developed a new Disease- Specific Care Advanced Certification program for Acute Stroke Ready Hospitals
Approved: Acute Stroke Ready Hospital Advanced Certification Program The Joint Commission recently developed a new Disease- Specific Care Advanced Certification program for Acute Stroke Ready Hospitals
B10/S/a Cancer: Malignant Mesothelioma (Adult)
 B10/S/a 2013/14 NHS STANDARD CONTRACT FOR CANCER: MALIGNANT MESOTHELIOMA (ADULT) SECTION B PART 1 - SERVICE SPECIFICATIONS Service Specification No. Service Commissioner Lead Provider Lead Period Date
B10/S/a 2013/14 NHS STANDARD CONTRACT FOR CANCER: MALIGNANT MESOTHELIOMA (ADULT) SECTION B PART 1 - SERVICE SPECIFICATIONS Service Specification No. Service Commissioner Lead Provider Lead Period Date
National Professional Development Framework for Cancer Nursing in New Zealand
 National Professional Development Framework for Cancer Nursing in New Zealand Adapted from: National Cancer Education Project (EdCan). 2008. National Education Framework: Cancer nursing A national professional
National Professional Development Framework for Cancer Nursing in New Zealand Adapted from: National Cancer Education Project (EdCan). 2008. National Education Framework: Cancer nursing A national professional
Treatment of colon cancer
 Treatment of colon cancer This information is an extract from the booklet, Understanding colon cancer. You may find the full booklet helpful. We can send you a copy free see page 5. Contents How treatment
Treatment of colon cancer This information is an extract from the booklet, Understanding colon cancer. You may find the full booklet helpful. We can send you a copy free see page 5. Contents How treatment
Bowel cancer: should I be screened?
 Patient information from the BMJ Group Bowel cancer: should I be screened? Bowel cancer is a serious condition, but there are good treatments. Treatment works best if it's started early.to pick up early
Patient information from the BMJ Group Bowel cancer: should I be screened? Bowel cancer is a serious condition, but there are good treatments. Treatment works best if it's started early.to pick up early
adult services between 1 January and 31 December 2013 had an operation where the
 Organisational audit: round 4 Adult services audit tool Section 1: Demographics DEM 1.1 How many IBD patients does your service manage? DEM 1.2 Is this figure: an estimate (enter e ) or from a database/register
Organisational audit: round 4 Adult services audit tool Section 1: Demographics DEM 1.1 How many IBD patients does your service manage? DEM 1.2 Is this figure: an estimate (enter e ) or from a database/register
Analysis of Prostate Cancer at Easter Connecticut Health Network Using Cancer Registry Data
 The 2014 Cancer Program Annual Public Reporting of Outcomes/Annual Site Analysis Statistical Data from 2013 More than 70 percent of all newly diagnosed cancer patients are treated in the more than 1,500
The 2014 Cancer Program Annual Public Reporting of Outcomes/Annual Site Analysis Statistical Data from 2013 More than 70 percent of all newly diagnosed cancer patients are treated in the more than 1,500
Information for Men Diagnosed with Testicular Cancer
 Patient Information Service Information for Men Diagnosed with Testicular Cancer Bristol Haematology and Oncology Centre Bristol Testicular Cancer Service Patient Information is supported by September
Patient Information Service Information for Men Diagnosed with Testicular Cancer Bristol Haematology and Oncology Centre Bristol Testicular Cancer Service Patient Information is supported by September
This publication was developed and produced with funding from the Centers for Disease Control and Prevention under a cooperative agreement.
 This publication was developed and produced with funding from the Centers for Disease Control and Prevention under a cooperative agreement. Suggested Citation Centers for Disease Control and Prevention.
This publication was developed and produced with funding from the Centers for Disease Control and Prevention under a cooperative agreement. Suggested Citation Centers for Disease Control and Prevention.
OBJECTIVES By the end of this segment, the community participant will be able to:
 Cancer 101: Cancer Diagnosis and Staging Linda U. Krebs, RN, PhD, AOCN, FAAN OCEAN Native Navigators and the Cancer Continuum (NNACC) (NCMHD R24MD002811) Cancer 101: Diagnosis & Staging (Watanabe-Galloway
Cancer 101: Cancer Diagnosis and Staging Linda U. Krebs, RN, PhD, AOCN, FAAN OCEAN Native Navigators and the Cancer Continuum (NNACC) (NCMHD R24MD002811) Cancer 101: Diagnosis & Staging (Watanabe-Galloway
Guide to Abdominal or Gastroenterological Surgery Claims
 What are the steps towards abdominal surgery? Investigation and Diagnosis It is very important that all necessary tests are undertaken to investigate the patient s symptoms appropriately and an accurate
What are the steps towards abdominal surgery? Investigation and Diagnosis It is very important that all necessary tests are undertaken to investigate the patient s symptoms appropriately and an accurate
Key Priority Area 1: Key Direction for Change
 Key Priority Areas Key Priority Area 1: Improving access and reducing inequity Key Direction for Change Primary health care is delivered through an integrated service system which provides more uniform
Key Priority Areas Key Priority Area 1: Improving access and reducing inequity Key Direction for Change Primary health care is delivered through an integrated service system which provides more uniform
PREPARING FOR YOUR STOMA REVERSAL
 PREPARING FOR YOUR STOMA REVERSAL Information Leaflet Your Health. Our Priority. Page 2 of 6 Introduction- What you need to know As part of your bowel operation you may have had a temporary stoma formed.
PREPARING FOR YOUR STOMA REVERSAL Information Leaflet Your Health. Our Priority. Page 2 of 6 Introduction- What you need to know As part of your bowel operation you may have had a temporary stoma formed.
Examples of good screening tests include: mammography for breast cancer screening and Pap smears for cervical cancer screening.
 CANCER SCREENING Dr. Tracy Sexton (updated July 2010) What is screening? Screening is the identification of asymptomatic disease or risk factors by history taking, physical examination, laboratory tests
CANCER SCREENING Dr. Tracy Sexton (updated July 2010) What is screening? Screening is the identification of asymptomatic disease or risk factors by history taking, physical examination, laboratory tests
What If I Have a Spot on My Lung? Do I Have Cancer? Patient Education Guide
 What If I Have a Spot on My Lung? Do I Have Cancer? Patient Education Guide A M E R I C A N C O L L E G E O F C H E S T P H Y S I C I A N S Lung cancer is one of the most common cancers. About 170,000
What If I Have a Spot on My Lung? Do I Have Cancer? Patient Education Guide A M E R I C A N C O L L E G E O F C H E S T P H Y S I C I A N S Lung cancer is one of the most common cancers. About 170,000
How To Manage A Cancer Oncology Clinic
 GYNAECOLOGICAL ONCOLOGY MULTIDISCIPLINARY TEAM MEETINGS: OPERATIONAL POLICY Version 3 Policy agreed Sept 2009 (updated Jan/Feb 2013) Agreed by: SCAN gynae group 2009 Update agreed SCAN gynae group May
GYNAECOLOGICAL ONCOLOGY MULTIDISCIPLINARY TEAM MEETINGS: OPERATIONAL POLICY Version 3 Policy agreed Sept 2009 (updated Jan/Feb 2013) Agreed by: SCAN gynae group 2009 Update agreed SCAN gynae group May
Clinical Management Guideline Management of locally advanced or recurrent Renal cell carcinoma. Protocol for Planning and Treatment
 Protocol for Planning and Treatment The process to be followed in the management of: LOCALLY ADVANCED OR METASTATIC RENAL CELL CARCINOMA Patient information given at each stage following agreed information
Protocol for Planning and Treatment The process to be followed in the management of: LOCALLY ADVANCED OR METASTATIC RENAL CELL CARCINOMA Patient information given at each stage following agreed information
CMScript. Member of a medical scheme? Know your guaranteed benefits! Issue 7 of 2014
 Background CMScript Member of a medical scheme? Know your guaranteed benefits! Issue 7 of 2014 Prostate cancer is second only to lung cancer as the leading cause of cancer-related deaths in men. It is
Background CMScript Member of a medical scheme? Know your guaranteed benefits! Issue 7 of 2014 Prostate cancer is second only to lung cancer as the leading cause of cancer-related deaths in men. It is
Clinical Training Profile: Nursing. March 2014. HWA Clinical Training Profile: Nursing
 Clinical Training Profile: Nursing March 2014 1 Health Workforce Australia. This work is copyright. It may be reproduced in whole or part for study or training purposes. Subject to an acknowledgement of
Clinical Training Profile: Nursing March 2014 1 Health Workforce Australia. This work is copyright. It may be reproduced in whole or part for study or training purposes. Subject to an acknowledgement of
A PATIENT S GUIDE TO ABLATION THERAPY
 A PATIENT S GUIDE TO ABLATION THERAPY THE DIVISION OF VASCULAR/INTERVENTIONAL RADIOLOGY THE ROBERT WOOD JOHNSON UNIVERSITY HOSPITAL Treatment options for patients with cancer continue to expand, providing
A PATIENT S GUIDE TO ABLATION THERAPY THE DIVISION OF VASCULAR/INTERVENTIONAL RADIOLOGY THE ROBERT WOOD JOHNSON UNIVERSITY HOSPITAL Treatment options for patients with cancer continue to expand, providing
Better bowel cancer care in Scotland
 Better bowel cancer care in Scotland October 2013 Page 1 of 27 Contents Table of Figures 3 Foreword 4 Executive summary and recommendations 5 Introduction 7 Incidence, mortality and survival rates for
Better bowel cancer care in Scotland October 2013 Page 1 of 27 Contents Table of Figures 3 Foreword 4 Executive summary and recommendations 5 Introduction 7 Incidence, mortality and survival rates for
Endometrial Cancer. Measurability of Quality Performance Indicators Version 2.0
 Endometrial Cancer Measurability of Quality Performance Indicators Version 2.0 To be read in conjunction with: Endometrial Cancer QPIs Final Publication v2 Endometrial QPI Dataset (latest published version)
Endometrial Cancer Measurability of Quality Performance Indicators Version 2.0 To be read in conjunction with: Endometrial Cancer QPIs Final Publication v2 Endometrial QPI Dataset (latest published version)
Hosts. New Methods for Treating Colorectal Cancer
 Hosts Anees Chagpar MD Associate Professor of Surgical Oncology Francine MD Professor of Medical Oncology New Methods for Treating Colorectal Cancer Guest Expert: Scott, MD Associate Professor in the Department
Hosts Anees Chagpar MD Associate Professor of Surgical Oncology Francine MD Professor of Medical Oncology New Methods for Treating Colorectal Cancer Guest Expert: Scott, MD Associate Professor in the Department
Transurethral Resection of Bladder Tumour (T.U.R.B.T)
 Transurethral Resection of Bladder Tumour (T.U.R.B.T) Patient Information Introduction This booklet has been written to help you understand the surgery you are about to undergo. It will give you information
Transurethral Resection of Bladder Tumour (T.U.R.B.T) Patient Information Introduction This booklet has been written to help you understand the surgery you are about to undergo. It will give you information
Measure #405: Appropriate Follow-up Imaging for Incidental Abdominal Lesions National Quality Strategy Domain: Effective Clinical Care
 Measure #405: Appropriate Follow-up Imaging for Incidental Abdominal Lesions National Quality Strategy Domain: Effective Clinical Care 2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES: CLAIMS, REGISTRY DESCRIPTION:
Measure #405: Appropriate Follow-up Imaging for Incidental Abdominal Lesions National Quality Strategy Domain: Effective Clinical Care 2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES: CLAIMS, REGISTRY DESCRIPTION:
Breast Cancer Care & Research
 Breast Cancer Care & Research Professor John FR Robertson University of Nottingham Nottingham City Hospital Breast Cancer (BC) 15,000 BC deaths in the UK each year 20% female cancer deaths 5% all female
Breast Cancer Care & Research Professor John FR Robertson University of Nottingham Nottingham City Hospital Breast Cancer (BC) 15,000 BC deaths in the UK each year 20% female cancer deaths 5% all female
LIVER CANCER AND TUMOURS
 LIVER CANCER AND TUMOURS LIVER CANCER AND TUMOURS Healthy Liver Cirrhotic Liver Tumour What causes liver cancer? Many factors may play a role in the development of cancer. Because the liver filters blood
LIVER CANCER AND TUMOURS LIVER CANCER AND TUMOURS Healthy Liver Cirrhotic Liver Tumour What causes liver cancer? Many factors may play a role in the development of cancer. Because the liver filters blood
QS114. NICE quality standard for irritable bowel syndrome in adults (QS114)
 NICE quality standard for irritable bowel syndrome in adults (QS114) QS114 NICE approved the reproduction of its content for this booklet. The production of this booklet is sponsored by Thermo Fisher Scientific,
NICE quality standard for irritable bowel syndrome in adults (QS114) QS114 NICE approved the reproduction of its content for this booklet. The production of this booklet is sponsored by Thermo Fisher Scientific,
Hugh Sanderson, Andrew Walker and Denise Young
 [This page: 449] 6 Colorectal Cancer Hugh Sanderson, Andrew Walker and Denise Young 1 Summary Occurrence Colorectal cancer is a major cause of mortality and morbidity in the UK and care for this disease
[This page: 449] 6 Colorectal Cancer Hugh Sanderson, Andrew Walker and Denise Young 1 Summary Occurrence Colorectal cancer is a major cause of mortality and morbidity in the UK and care for this disease
Guide to Understanding Breast Cancer
 An estimated 220,000 women in the United States are diagnosed with breast cancer each year, and one in eight will be diagnosed during their lifetime. While breast cancer is a serious disease, most patients
An estimated 220,000 women in the United States are diagnosed with breast cancer each year, and one in eight will be diagnosed during their lifetime. While breast cancer is a serious disease, most patients
Patient management framework. Lung tumour stream: non-small cell lung cancer. a guide to consistent cancer care
 Patient management framework Lung tumour stream: non-small cell lung cancer a guide to consistent cancer care Patient management framework Lung tumour stream: non-small cell lung cancer ii Patient management
Patient management framework Lung tumour stream: non-small cell lung cancer a guide to consistent cancer care Patient management framework Lung tumour stream: non-small cell lung cancer ii Patient management
Kidney Cancer OVERVIEW
 Kidney Cancer OVERVIEW Kidney cancer is the third most common genitourinary cancer in adults. There are approximately 54,000 new cancer cases each year in the United States, and the incidence of kidney
Kidney Cancer OVERVIEW Kidney cancer is the third most common genitourinary cancer in adults. There are approximately 54,000 new cancer cases each year in the United States, and the incidence of kidney
Salisbury Lung Cancer Service (1 of 5)
 Salisbury Lung Cancer Service (1 of 5) i If you need this information in another language or medium (audio, large print, etc) please contact Customer Care on 0800 374 208 email: customercare@ salisbury.nhs.uk.
Salisbury Lung Cancer Service (1 of 5) i If you need this information in another language or medium (audio, large print, etc) please contact Customer Care on 0800 374 208 email: customercare@ salisbury.nhs.uk.
Best practice approaches to the management of lung cancer in Australia. Final report
 Best practice approaches to the management of lung cancer in Australia Final report Best practice approaches to the management of lung cancer in Australia Final report November 2013 Best practice approaches
Best practice approaches to the management of lung cancer in Australia Final report Best practice approaches to the management of lung cancer in Australia Final report November 2013 Best practice approaches
Guideline for the Imaging of Patients Presenting with Breast Symptoms incorporating the guideline for the use of MRI in breast cancer
 Guideline for the Imaging of Patients Presenting with Breast Symptoms incorporating the guideline for the use of MRI in breast cancer Version History Version Date Summary of Change/Process 0.1 09.01.11
Guideline for the Imaging of Patients Presenting with Breast Symptoms incorporating the guideline for the use of MRI in breast cancer Version History Version Date Summary of Change/Process 0.1 09.01.11
Management of Non-Small Cell Lung Cancer Guide for General Practitioners
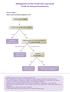 Management of n-small Cell Lung Cancer Guide for General Practitioners Clinical Stage I Cancer only in one lobe of lung and
Management of n-small Cell Lung Cancer Guide for General Practitioners Clinical Stage I Cancer only in one lobe of lung and
Cancer Association of South Africa (CANSA)
 Cancer Association of South Africa (CANSA) Fact Sheet on Metastatic Breast Cancer Introduction Metastatic breast cancer is cancer that has spread beyond the breast and lymph nodes under the arm. It occurs
Cancer Association of South Africa (CANSA) Fact Sheet on Metastatic Breast Cancer Introduction Metastatic breast cancer is cancer that has spread beyond the breast and lymph nodes under the arm. It occurs
One out of every two men and one out of every three women will have some type of cancer at some point during their lifetime. 3
 1. What is cancer? 2. What causes cancer?. What causes cancer? 3. Can cancer be prevented? The Facts One out of every two men and one out of every three women will have some type of cancer at some point
1. What is cancer? 2. What causes cancer?. What causes cancer? 3. Can cancer be prevented? The Facts One out of every two men and one out of every three women will have some type of cancer at some point
GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER
 GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER BY Ali Shamseddine, MD (Coordinator); as04@aub.edu.lb Fady Geara, MD Bassem Shabb, MD Ghassan Jamaleddine, MD CLINICAL PRACTICE GUIDELINES FOR THE TREATMENT
GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER BY Ali Shamseddine, MD (Coordinator); as04@aub.edu.lb Fady Geara, MD Bassem Shabb, MD Ghassan Jamaleddine, MD CLINICAL PRACTICE GUIDELINES FOR THE TREATMENT
AMERICAN BURN ASSOCIATION BURN CENTER VERIFICATION REVIEW PROGRAM Verificatoin Criterea EFFECTIVE JANUARY 1, 2015. Criterion. Level (1 or 2) Number
 Criterion AMERICAN BURN ASSOCIATION BURN CENTER VERIFICATION REVIEW PROGRAM Criterion Level (1 or 2) Number Criterion BURN CENTER ADMINISTRATION 1. The burn center hospital is currently accredited by The
Criterion AMERICAN BURN ASSOCIATION BURN CENTER VERIFICATION REVIEW PROGRAM Criterion Level (1 or 2) Number Criterion BURN CENTER ADMINISTRATION 1. The burn center hospital is currently accredited by The
About McGrath Foundation
 POSITION: LEVEL: GROUP: SYNOPSIS: REPORTS TO: McGrath Clinical Nurse Educator Equivalent to Clinical Nurse Consultant Grade 3 or Nursing Educator Grade 3 Co-located at Head Office and Westmead Breast Cancer
POSITION: LEVEL: GROUP: SYNOPSIS: REPORTS TO: McGrath Clinical Nurse Educator Equivalent to Clinical Nurse Consultant Grade 3 or Nursing Educator Grade 3 Co-located at Head Office and Westmead Breast Cancer
Chapter 13. The hospital-based cancer registry
 Chapter 13. The hospital-based cancer registry J.L. Young California Tumor Registry, 1812 14th Street, Suite 200, Sacramento, CA 95814, USA Introduction The purposes of a hospital-based cancer registry
Chapter 13. The hospital-based cancer registry J.L. Young California Tumor Registry, 1812 14th Street, Suite 200, Sacramento, CA 95814, USA Introduction The purposes of a hospital-based cancer registry
Specific Standards of Accreditation for Residency Programs in Pediatric Hematology/Oncology
 Specific Standards of Accreditation for Residency Programs in Pediatric Hematology/Oncology INTRODUCTION 2009 A university wishing to have an accredited program in Pediatric Hematology/Oncology must also
Specific Standards of Accreditation for Residency Programs in Pediatric Hematology/Oncology INTRODUCTION 2009 A university wishing to have an accredited program in Pediatric Hematology/Oncology must also
Small cell lung cancer
 Small cell lung cancer Small cell lung cancer is a disease in which malignant (cancer) cells form in the tissues of the lung. The lungs are a pair of cone-shaped breathing organs that are found within
Small cell lung cancer Small cell lung cancer is a disease in which malignant (cancer) cells form in the tissues of the lung. The lungs are a pair of cone-shaped breathing organs that are found within
Breast Cancer Network Australia. Submission to the Medicare Benefits Schedule Review Taskforce. November 2015
 Submission to the Medicare Benefits Schedule Review Taskforce November 2015 About (BCNA) is the peak national consumer organisation for Australians personally affected by breast cancer. We support, inform,
Submission to the Medicare Benefits Schedule Review Taskforce November 2015 About (BCNA) is the peak national consumer organisation for Australians personally affected by breast cancer. We support, inform,
Treatment Algorithms for the Management of Lung Cancer in NSW Guide for Clinicians
 Treatment Algorithms for the Management of Lung Cancer in NSW Guide for Clinicians Background The Cancer Institute New South Wales Oncology Group Lung (NSWOG Lung) identified the need for the development
Treatment Algorithms for the Management of Lung Cancer in NSW Guide for Clinicians Background The Cancer Institute New South Wales Oncology Group Lung (NSWOG Lung) identified the need for the development
Nurse Practitioner Frequently Asked Questions
 HEALTH SERVICES Nurse Practitioner Frequently Asked Questions The Frequently Asked Questions (FAQs) have been designed to increase awareness and understanding of the Nurse Practitioner role within the
HEALTH SERVICES Nurse Practitioner Frequently Asked Questions The Frequently Asked Questions (FAQs) have been designed to increase awareness and understanding of the Nurse Practitioner role within the
Consultation. Review of the scopes of practice for registration in the profession of medical radiation technology
 Consultation Review of the scopes of practice for registration in the profession of medical radiation technology CONTENTS Page Consultation Information... 3 Context of the Consultation... 4-7 Legislative
Consultation Review of the scopes of practice for registration in the profession of medical radiation technology CONTENTS Page Consultation Information... 3 Context of the Consultation... 4-7 Legislative
