This patient guide will help you understand:
|
|
|
- Marion Pope
- 7 years ago
- Views:
Transcription
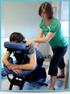
1 How to Manage Your Pain This patient guide will help you understand: What is cancer-related pain? pg 2 What causes cancer-related pain? pg 3 What can I do to manage my pain? pg 4 When should I talk to my health care team? pg 12 Where can I get more information? pg 14 This guide is for people who have pain before, during or after cancer treatment. It can be used by patients, family, friends or caregivers. It does not replace advice from your health care team. Please visit the UHN Patient Education website for more health information: This information is to be used for informational purposes only and is not intended as a substitute for professional medical advice, diagnosis or treatment. Please consult your health care provider for advice about a specific medical condition. A single copy of these materials may be reprinted for non-commercial personal use only. Author: Cancer Care Ontario Created: 05/2016 Form: D-8611
2 What is cancer-related pain? Cancer pain causes you to hurt, feel uncomfortable or suffer. You may feel pain all of the time or only some of the time. Everyone who has cancer pain will feel it differently. Only you know how much pain you feel and how it affects you. Getting relief from pain is important. Treating your pain will help you: Sleep and eat better Enjoy time with family and friends Do your work and hobbies You do not have to accept pain as a normal part of living with cancer. Tell your health care team about the pain that you feel: Bone pain can be felt as a deep throbbing pain that can be sharp at times. It may get worse when you are moving around. Neuropathic pain is from damage to your nerves. People say it is burning, shooting, piercing, stabbing or like an electric current. It might feel like pins and needles or tingling. It can hurt when things like clothing, water or wind touch your skin. Visceral pain is from damage to the organs inside your body. It might feel like a dull, deep squeezing pain. It can be hard to tell exactly where it is coming from. If you take regular medication for your pain, breakthrough pain may be felt between doses. It can happen very suddenly. 2
3 What causes cancer-related pain? Understanding the cause of your pain will help your healthcare team treat it in the best way. This picture shows things that might cause cancer-related pain: Cancer tumour or symptom Cancer treatments Stress and anxiety Medications Causes of cancerrelated pain Medical procedures and tests Other symptoms, like constipation and nausea Emotional, social and spiritual impact of cancer Other health factors 3
4 What can I do to manage my pain? Take your pain medications as prescribed Your doctor might prescribe more than one type of pain medication. The types of medications may be: Over-the-counter medications that have acetaminophen (like Tylenol) or ibuprofen (like Advil). Opioids, like codeine, morphine, hydromorphone, oxycodone, fentanyl and methadone. Medications for nerve pain like pregabalin and gabapentin. Note: these medications may take days or even weeks to start working. Speak to your doctor or pharmacist if you: Have trouble remembering to take your pills Need help figuring out the right timing Opioid pain medications Opioid medications are common to help manage cancer pain. Some are long- acting (work for a long time) and some are short-acting (work for a short time). They work together to control pain. Long-acting medication is usually taken regularly. It is released slowly into your body and works for 8-12 hours. Short-acting medication starts to work fast in about minutes. It keeps working for 2-4 hours. It is usually taken for breakthrough pain. Take your long-acting medication on schedule, even if you do not feel pain at the moment. If you are not in pain it means the medication is working well. It does not mean that you do not need to take your medication. 4
5 WHAT CAN I DO TO MANAGE MY PAIN? Keep track of when you take your medication for breakthrough pain. If you need these doses more often than normal, your doctor may need to change your medication. Be safe! Never crush or chew long-acting medications (pills or capsules). This may put too much medication into your body too fast and give you side effects. If swallowing pills is hard, ask your doctor or pharmacist about a different way to take them. Do not stop taking your pain medication suddenly. Many of these medications need to be stopped slowly. Your doctor or pharmacist will help you make a plan. Ask your health care team about what to do if you miss a dose of medication. Always check with your doctor or pharmacist before taking any over-the-counter medications. It is normal to feel nervous about taking pain medication. Some people do not take pain medications because they worry about addiction. Your family may also worry about addiction and might not want you to take your pills. If you take your medication as your doctor prescribed, you should not worry. Addiction happens when a person takes medications for reasons other than pain. Some people think they should save their pain medication in case the pain gets worse later. Pain should be treated early. If needed, your doctor can change your dose of pain medication and/ or the type of medication you take. You do not need to suffer in pain. 5
6 WHAT CAN I DO TO MANAGE MY PAIN? Side-effects of pain medication Side-effects of pain medication are common. Medication may cause: Constipation - not being able to have a bowel movement (go poo) Nausea and vomiting (throwing up) Sleepiness or drowsiness Nausea, vomiting and sleepiness usually only last for a few days and will go away on their own. Constipation from opioid medications will not go away on its own. You need to take laxatives the whole time you take opioid pain medication. Ask your health care team for more information. Be safe! Do not take fibre supplements, like Metamucil, when you are taking pain medication. They may make your constipation worse. Tell your health care team right away if you have any of these side-effects: Confusion or if you start seeing and hearing things that are not really there A skin rash Trouble breathing 6
7 WHAT CAN I DO TO MANAGE MY PAIN? Be active and exercise Even small, simple exercises may help your pain: Walk to the end of your driveway or up and down your hallway. Ride an indoor bike or do gentle yoga and stretching. Exercise Tips Start slowly and go at your own pace. If you are already active, talk to your health care team about your activities and make a plan to keep doing them. Exercise can also: Make you more hungry Give you more energy Help you get better sleep Build stronger muscles Give you a feeling of well-being Help your feelings of depression and anxiety If you need help making a plan to be more active, ask for a referral to a(n): Occupational therapist Physical therapist Exercise specialist Rehabilitation specialist Registered massage therapist 7
8 WHAT CAN I DO TO MANAGE MY PAIN? Find support It is normal to feel upset and frustrated when you are in pain. You can find support in your community and through your health care team. Talk to someone you trust about how your pain makes you feel. Talk to a trained counsellor either by yourself or as part of a group. Talk to someone at your place of worship. Join a peer support group online or in your community. Join a chronic pain self-management group. These programs have special sessions to teach you how to manage your pain. Ask your health care team about classes in your community. If you feel depressed or anxious, ask to speak to a social worker, psychologist, psychiatrist or someone who is an expert in helping people with cancer. To learn more about online support groups check out the Canadian Cancer Society s Peer Support Service and talk to someone who has been there. For more information go to: 8
9 WHAT CAN I DO TO MANAGE MY PAIN? Get physical relief Ask your health care team about other treatments before you use them, like: Transcutaneous electrical nerve stimulation (TENS) machine. Muscle relaxants and rubs like acetaminophen/methocarbamol (like Robaxacet), or diclofenac (like Voltaren Emulgel). Heat and ice may not be safe if you are getting radiation therapy, chemotherapy or if you have numbness from nerve damage. Check with your health care team. Using heat and/or ice on the body. 9
10 WHAT CAN I DO TO MANAGE MY PAIN? Relaxing activities and managing stress may help to control your pain These activities may help you relax: Breathing exercises Distraction activities like watching TV or playing computer games Healthy coping activities like walking outside, gardening, enjoying nature, reading or listening to music If you want to try complementary therapies, ask about your providers safety standards. Some therapists need a license to do their work. Be especially careful when doing things that use needles, like acupuncture. Some patients find that these complementary therapies help them take control of their pain: Meditation Hypnotism Aromatherapy Acupuncture Guided imagery (imagining yourself in a pleasant, calm place) Energy healing therapies like Healing Touch, Reiki or Qigong Yoga Massage Music therapy (from a music therapist) Reflexology (a special massage for your hands and feet) For more information on these strategies see the Canadian Cancer Society s guide to Complementary Therapies. Go to: 10
11 WHAT CAN I DO TO MANAGE MY PAIN? Keep track of your pain A pain diary can help you write down information about your pain. This will help you and your healthcare team know how your pain changes over time and what things make it better or worse. Here is a sample of a pain diary* you could use: 0 is no pain and 10 is the worst possible pain. Date & Time Pain score (0-10) Where pain is and how it feels What I was doing when it began Name and amount of medicine taken Non-drug methods I tried How long the pain lasted Notes *Pain diary from the American Cancer Society Patient Testimonial: "Keeping a pain diary is a great communication tool for me and my doctor. Together we can understand how to adjust medications to feel better. 11
12 When should I talk to my health care team? Tell your health care team right away if you have any of these symptoms: Pain that is not going away or is getting worse A new pain that you have not had before Pain when you take a deep breath Sudden leg weakness, especially if you have back pain What is symptom screening? In Ontario, patients with cancer fill out a symptom screening tool. The screen tells your health care team about your symptoms and how you are feeling. The tool is called the Edmonton Symptom Assessment System (ESAS). Doing your symptom screening helps you and your health care team to manage your symptoms. 12
13 WHEN SHOULD I TALK TO MY HEALTH CARE TEAM? Use the boxes below to help your health care team understand your pain. 0 is no pain and 10 is the worst possible pain You may have Mild pain if: You may have Moderate pain if: You may have Severe pain if: You have some pain but medications make it go away You can do regular activities like caring for yourself, cooking, cleaning or working Your pain is causing you stress Your pain medications do not always make the pain go away You find it hard to do regular activities like caring for yourself, cooking, cleaning or working You have a lot of pain everyday Your pain is causing you a lot of stress You cannot do regular activities like caring for yourself, cooking, cleaning, or working You have pain that comes on suddenly You have new pain Your muscles feel weak Your health care team wants to know about your pain. Your concerns and questions are important. Do not be afraid to share them. 13
14 Where can I get more information? For links to these and other helpful resources go to: Websites: Cancer Care Ontario Canadian Cancer Society Support services: Canadian Cancer Society Community Services Locator Canadian Cancer Society Peer Support Service Cancer Chat Canada Booklets: Pain relief: A guide for people with cancer Support for people with cancer: pain control Books: Managing Pain before it Manages You 4 th edition, Margaret A. Caudill, 2016 The pain survival guide: how to reclaim your life Dennis Turk,
15 WHERE CAN I GET MORE INFORMATION? Ask your health care team for more information about managing your pain. Self-management classes: Videos: Books: Pamphlets: Ask your health care team who you should contact if you feel that your pain is so bad that you need help right away. 15
16 This patient guide was adapted from Cancer Care Ontario s How to Manage Your Pain booklet. The recommendations in this guide are based on published evidence and expert consensus. The information in this guide was adapted from the following patient tools: Guide: Tips to help you manage your symptoms: Pain (The Ottawa Hospital) Pain we can help (Sunnybrook Health Sciences Centre) American Cancer Society s pain diary was found here at the time of print: documents/webcontent/pain-diary.pdf How to take your Opioid Pain Medication (Juravinski Cancer Centre) This patient guide was created by Cancer Care Ontario to provide patients with information about pain. It should be used for information only and does not replace medical advice. This guide does not include all information available about managing pain. Always ask your health care team if you have questions or concerns. The information in this guide does not create a physician-patient relationship between Cancer Care Ontario and you. Need this information in an accessible format? TTY (416) publicaffairs@cancercare.on.ca For other patient guides please go to: Was this patient guide helpful? Let us know at: cco.fluidsurveys.com/s/guides/ Version Cancer Care Ontario retains all copyright, trademark and all other rights in the guide, including all text and graphic images. No portion of this Resource may be used or reproduced, other than for personal use, or distributed, transmitted or "mirrored" in any form, or by any means, without the prior written permission of Cancer Care Ontario.
August Is Palliative Care and Cancer Pain Awareness Month
 August Is Palliative Care and Cancer Pain Awareness Month What Is Palliative Care? Palliative care is a growing research area that focuses on improving the quality of life of all people living with cancer,
August Is Palliative Care and Cancer Pain Awareness Month What Is Palliative Care? Palliative care is a growing research area that focuses on improving the quality of life of all people living with cancer,
Cancer Pain. What is Pain?
 Cancer Pain What is Pain? The International Association for the Study of Pain says that pain is "an unpleasant sensory and emotional experience associated with actual or potential tissue damage." Pain
Cancer Pain What is Pain? The International Association for the Study of Pain says that pain is "an unpleasant sensory and emotional experience associated with actual or potential tissue damage." Pain
Breast Cancer Surgery and Pain
 Breast Cancer Surgery and Pain Princess Margaret Information for women who have had breast surgery Read this pamphlet to learn about: Pain after surgery What you need to know about pain What you need to
Breast Cancer Surgery and Pain Princess Margaret Information for women who have had breast surgery Read this pamphlet to learn about: Pain after surgery What you need to know about pain What you need to
Manage cancer related fatigue:
 Manage cancer related fatigue: For People Affected by Cancer In this pamphlet: What can I do to manage fatigue? What is cancer related fatigue? What causes cancer related fatigue? How can my health care
Manage cancer related fatigue: For People Affected by Cancer In this pamphlet: What can I do to manage fatigue? What is cancer related fatigue? What causes cancer related fatigue? How can my health care
PAIN MANAGEMENT During Your Hospital Stay
 PAIN MANAGEMENT During Your Hospital Stay TABLE OF CONTENTS Understanding Pain...2 Pain Assessment...2 Describing Your Pain...5 Pain Treatment...5 Comfort Measures...6 Medication...7 Specialty Procedures...8
PAIN MANAGEMENT During Your Hospital Stay TABLE OF CONTENTS Understanding Pain...2 Pain Assessment...2 Describing Your Pain...5 Pain Treatment...5 Comfort Measures...6 Medication...7 Specialty Procedures...8
Weaning off your pain medicine
 Weaning off your pain medicine UHN Information for patients taking opioid pain medicines Read this booklet to learn about: why you need to wean off your pain medicine how to wean off slowly how to control
Weaning off your pain medicine UHN Information for patients taking opioid pain medicines Read this booklet to learn about: why you need to wean off your pain medicine how to wean off slowly how to control
Cancer Pain. Relief from PALLIATIVE CARE
 PALLIATIVE CARE Relief from Cancer Pain National Clinical Programme for Palliative Care For more information on the National Clinical Programme for Palliative Care, go to www.hse.ie/palliativecareprogramme
PALLIATIVE CARE Relief from Cancer Pain National Clinical Programme for Palliative Care For more information on the National Clinical Programme for Palliative Care, go to www.hse.ie/palliativecareprogramme
Questions and answers on breast cancer Guideline 10: The management of persistent pain after breast cancer treatment
 Questions and answers on breast cancer Guideline 10: The management of persistent pain after breast cancer treatment I ve had breast cancer treatment, and now I m having pain. Does this mean the cancer
Questions and answers on breast cancer Guideline 10: The management of persistent pain after breast cancer treatment I ve had breast cancer treatment, and now I m having pain. Does this mean the cancer
How to take your Opioid Pain Medication
 How to take your Opioid Pain Medication Today your doctor gave you a prescription for medication to help relieve your pain. The pain medication is called an opioid or narcotic. Taking pain medication,
How to take your Opioid Pain Medication Today your doctor gave you a prescription for medication to help relieve your pain. The pain medication is called an opioid or narcotic. Taking pain medication,
Pain Management after Surgery Patient Information Booklet
 Pain Management after Surgery Patient Information Booklet PATS 509-15-05 Your Health Care Be Involved Be involved in your healthcare. Speak up if you have questions or concerns about your care. Tell a
Pain Management after Surgery Patient Information Booklet PATS 509-15-05 Your Health Care Be Involved Be involved in your healthcare. Speak up if you have questions or concerns about your care. Tell a
Cancer-Related Pain. A Guide for Patients and Caregivers
 Cancer-Related Pain A Guide for Patients and Caregivers Copyright 2011 Conrad & Associates, LLC All Rights Reserved No part of this book may be reproduced or transmitted in any form or by any means, electronic
Cancer-Related Pain A Guide for Patients and Caregivers Copyright 2011 Conrad & Associates, LLC All Rights Reserved No part of this book may be reproduced or transmitted in any form or by any means, electronic
Controlling Pain Part 2: Types of Pain Medicines for Your Prostate Cancer
 Controlling Pain Part 2: Types of Pain Medicines for Your Prostate Cancer The following information is based on the general experiences of many prostate cancer patients. Your experience may be different.
Controlling Pain Part 2: Types of Pain Medicines for Your Prostate Cancer The following information is based on the general experiences of many prostate cancer patients. Your experience may be different.
Managing Depression after Cancer Treatment
 Managing Depression after Cancer Treatment Information for cancer survivors UHN Read this pamphlet to learn about: What depression is What causes depression and how long will it last What you can do Where
Managing Depression after Cancer Treatment Information for cancer survivors UHN Read this pamphlet to learn about: What depression is What causes depression and how long will it last What you can do Where
Objectives. Pain Management Knowing How To Help Yourself. Patients and Family Requirements. Your Rights As A Consumer
 Objectives Pain Management Knowing How To Help Yourself Jackie Carter, RN MSN CNS Become familiar with the definitions of pain Be aware of your rights to have your pain treated Become familiar with the
Objectives Pain Management Knowing How To Help Yourself Jackie Carter, RN MSN CNS Become familiar with the definitions of pain Be aware of your rights to have your pain treated Become familiar with the
Records for Keeping Track of Your Care
 Records for Keeping Track of Your Care A pain diary is an indispensable tool for making sure your pain is being adequately assessed and for helping your medical team optimize your treatment. This article
Records for Keeping Track of Your Care A pain diary is an indispensable tool for making sure your pain is being adequately assessed and for helping your medical team optimize your treatment. This article
A handbook for patients COPING WITH CANCER PAIN
 A handbook for patients COPING WITH CANCER PAIN Introduction This booklet is about pain and how to control it. Many patients with cancer fear that they will have pain. Although pain is a common problem,
A handbook for patients COPING WITH CANCER PAIN Introduction This booklet is about pain and how to control it. Many patients with cancer fear that they will have pain. Although pain is a common problem,
Managing Psychosocial and Family Distress after Cancer Treatment
 Managing Psychosocial and Family Distress after Cancer Treatment Information for cancer survivors UHN Read this pamphlet to learn: What psychosocial distress is What causes distress What you can do Where
Managing Psychosocial and Family Distress after Cancer Treatment Information for cancer survivors UHN Read this pamphlet to learn: What psychosocial distress is What causes distress What you can do Where
Epilepsy and stress / anxiety
 Epilepsy and stress / anxiety Stress is a term used to describe emotional strain and tension. When we experience stress we also can become anxious. Although stress and anxiety do not cause epilepsy, for
Epilepsy and stress / anxiety Stress is a term used to describe emotional strain and tension. When we experience stress we also can become anxious. Although stress and anxiety do not cause epilepsy, for
Pain Handbook for Cancer Patients. A Guide for Management of Pain and Side Effects
 Pain Handbook for Cancer Patients A Guide for Management of Pain and Side Effects Relief of Pain Is Important There is no benefit from suffering with pain. Pain can actually be harmful to you. It can:
Pain Handbook for Cancer Patients A Guide for Management of Pain and Side Effects Relief of Pain Is Important There is no benefit from suffering with pain. Pain can actually be harmful to you. It can:
Children s Cancer Pain Can Be Relieved A Guide for Parents and Families
 Children s Cancer Pain Can Be Relieved A Guide for Parents and Families This booklet is dedicated to Shaney Banks and all other children with cancer. Wisconsin Cancer Pain Initiative 1989 This booklet
Children s Cancer Pain Can Be Relieved A Guide for Parents and Families This booklet is dedicated to Shaney Banks and all other children with cancer. Wisconsin Cancer Pain Initiative 1989 This booklet
m y f o u n d a t i o n i n f o s h e e t
 Pain and Myeloma m y f o u n d a t i o n i n f o s h e e t Pain is the most common symptom of myeloma and can greatly affect all areas of your life, especially if it is untreated or poorly managed. This
Pain and Myeloma m y f o u n d a t i o n i n f o s h e e t Pain is the most common symptom of myeloma and can greatly affect all areas of your life, especially if it is untreated or poorly managed. This
Young Person s Guide to CFS/ME
 Young Person s Guide to CFS/ME The Royal College of Paediatrics and Child Health This leaflet has been developed as part of the Evidence based guideline for management of CFS/ME (Chronic Fatigue Syndrome
Young Person s Guide to CFS/ME The Royal College of Paediatrics and Child Health This leaflet has been developed as part of the Evidence based guideline for management of CFS/ME (Chronic Fatigue Syndrome
Opioids in Palliative Care- Patient Information Manual
 Version 2.0 with MST example Introduction The following pages explain what opioids are and what we think you may want to know about them. There is quite a lot of information here, most of it is based on
Version 2.0 with MST example Introduction The following pages explain what opioids are and what we think you may want to know about them. There is quite a lot of information here, most of it is based on
Palliative Care for Children. Support for the Whole Family When Your Child Is Living with a Serious Illness
 Palliative Care for Children Support for the Whole Family When Your Child Is Living with a Serious Illness Palliative care provides comfort and support to your child and family. When a child is seriously
Palliative Care for Children Support for the Whole Family When Your Child Is Living with a Serious Illness Palliative care provides comfort and support to your child and family. When a child is seriously
Thinking About Complementary & Alternative Medicine
 Thinking About Complementary & Alternative Medicine A guide for people with cancer PATIENT & family EDUCATION U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES National Institutes of Health National Cancer
Thinking About Complementary & Alternative Medicine A guide for people with cancer PATIENT & family EDUCATION U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES National Institutes of Health National Cancer
Constipa. tion. How to Manage Your
 How to Manage Your Constipa tion This patient guide will help you understand: What is cancer-related constipation? pg 2 What causes cancer-related constipation? pg 3 What can I do to manage my constipation?
How to Manage Your Constipa tion This patient guide will help you understand: What is cancer-related constipation? pg 2 What causes cancer-related constipation? pg 3 What can I do to manage my constipation?
A Guide to pain relief medicines For patients receiving Palliative Care
 A Guide to pain relief medicines For patients receiving Palliative Care 1 Which pain medicines are you taking? Contents Page No. Amitriptyline 8 Codeine 9 Co-codamol 10 Co-dydramol 11 Diclofenac (Voltarol
A Guide to pain relief medicines For patients receiving Palliative Care 1 Which pain medicines are you taking? Contents Page No. Amitriptyline 8 Codeine 9 Co-codamol 10 Co-dydramol 11 Diclofenac (Voltarol
Medications for chronic pain
 Medications for chronic pain When it comes to treating chronic pain with medications, there are many to choose from. Different types of pain medications are used for different pain conditions. You may
Medications for chronic pain When it comes to treating chronic pain with medications, there are many to choose from. Different types of pain medications are used for different pain conditions. You may
Understanding Your Pain
 Toll Free: 800-462-3636 Web: www.endo.com Understanding Your Pain This brochure was developed by Margo McCaffery, RN, MS, FAAN, and Chris Pasero, RN, MS, FAAN authors of Pain: Clinical Manual (2nd ed.
Toll Free: 800-462-3636 Web: www.endo.com Understanding Your Pain This brochure was developed by Margo McCaffery, RN, MS, FAAN, and Chris Pasero, RN, MS, FAAN authors of Pain: Clinical Manual (2nd ed.
Multiple Myeloma. Understanding your diagnosis
 Multiple Myeloma Understanding your diagnosis Multiple Myeloma Understanding your diagnosis When you first hear that you have cancer, you may feel alone and afraid. You may be overwhelmed by the large
Multiple Myeloma Understanding your diagnosis Multiple Myeloma Understanding your diagnosis When you first hear that you have cancer, you may feel alone and afraid. You may be overwhelmed by the large
How to Talk to Your Doctor
 Patient Series How to Talk to Your Doctor A Resource for Patients with Chronic Pain Because I have a responsibility to know the risks. Introduction CARES Alliance is dedicated to improving safety in patients
Patient Series How to Talk to Your Doctor A Resource for Patients with Chronic Pain Because I have a responsibility to know the risks. Introduction CARES Alliance is dedicated to improving safety in patients
Support for People With Cancer. National Cancer Institute. Pain Control U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES. National Institutes of Health
 National Cancer Institute Support for People With Cancer Pain Control U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES National Institutes of Health For more information... This booklet is only one of many
National Cancer Institute Support for People With Cancer Pain Control U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES National Institutes of Health For more information... This booklet is only one of many
Stress can become a problem when you are not sure how to handle it. Worry sets in, and you feel stressed.
 Stress Reduction Patient Education Improving Health Through Education What is Stress? Stress is a normal emotional and physical reaction to the demands of life. Stress comes from both the good and bad
Stress Reduction Patient Education Improving Health Through Education What is Stress? Stress is a normal emotional and physical reaction to the demands of life. Stress comes from both the good and bad
Recognizing and Understanding Pain
 Because multiple myeloma is a cancer involving the bone marrow, a common myeloma symptom is bone pain. But the good news is that most pain can be managed. This resource can help you better understand pain
Because multiple myeloma is a cancer involving the bone marrow, a common myeloma symptom is bone pain. But the good news is that most pain can be managed. This resource can help you better understand pain
Coping with chemotherapy
 This information is an extract from the booklet Understanding chemotherapy. You may find the full booklet helpful. We can send you a copy free see page 11. Contents Feelings and emotions How you can help
This information is an extract from the booklet Understanding chemotherapy. You may find the full booklet helpful. We can send you a copy free see page 11. Contents Feelings and emotions How you can help
A Patient s Guide to PAIN MANAGEMENT. After Surgery
 A Patient s Guide to PAIN MANAGEMENT After Surgery C o m p a s s i o n a n d C o m m i t m e n t A Patient s Guide to Pain Management After Surgery If you re facing an upcoming surgery, it s natural to
A Patient s Guide to PAIN MANAGEMENT After Surgery C o m p a s s i o n a n d C o m m i t m e n t A Patient s Guide to Pain Management After Surgery If you re facing an upcoming surgery, it s natural to
Managing. Cancer Pain CANCERCARE CONNECT BOOKLET SERIES. www.cancercare.org
 CANCERCARE CONNECT BOOKLET SERIES Managing Cancer Pain www.cancercare.org The CancerCare Connect Booklet Series offers up-to-date, easy-to-read information on the latest treatments, managing side effects
CANCERCARE CONNECT BOOKLET SERIES Managing Cancer Pain www.cancercare.org The CancerCare Connect Booklet Series offers up-to-date, easy-to-read information on the latest treatments, managing side effects
What you should know about treating your pain with opioids. Important information on the safe use of opioid pain medicine.
 What you should know about treating your pain with opioids Important information on the safe use of opioid pain medicine. If your healthcare provider has determined that opioid therapy is right for you,
What you should know about treating your pain with opioids Important information on the safe use of opioid pain medicine. If your healthcare provider has determined that opioid therapy is right for you,
Pain is a common symptom reported
 MULTIPLE SCLEROSIS FACT SHEET MANAGING YOUR PAIN Pain is a common symptom reported by people with multiple sclerosis (MS). Approximately 50-60% of people with MS experience acute or chronic pain at some
MULTIPLE SCLEROSIS FACT SHEET MANAGING YOUR PAIN Pain is a common symptom reported by people with multiple sclerosis (MS). Approximately 50-60% of people with MS experience acute or chronic pain at some
Helping you manage your pain
 Helping you manage your pain This booklet contains confidential personal information. If found, please mail to the address below. Personal details Name Address Telephone My health care team (please tick)
Helping you manage your pain This booklet contains confidential personal information. If found, please mail to the address below. Personal details Name Address Telephone My health care team (please tick)
Palliative Pain and Symptom Management
 Palliative Pain and Symptom Management This brochure will provide you with options about pain and symptom control, coping strategies, how to develop a pain diary and how to access resources to help you
Palliative Pain and Symptom Management This brochure will provide you with options about pain and symptom control, coping strategies, how to develop a pain diary and how to access resources to help you
Antidepressant Medicines
 Antidepressant Medicines UHN Information for patients and families Read this booklet to learn: what antidepressant medicines are how they work possible side effects important points to remember The name
Antidepressant Medicines UHN Information for patients and families Read this booklet to learn: what antidepressant medicines are how they work possible side effects important points to remember The name
PAIN JEOPARDY. I ll take INTERVENTIONS for 400 points, Alex!
 PAIN JEOPARDY I ll take INTERVENTIONS for 400 points, Alex! Fact/Myth Barriers Assessment Education Interventions 100 pt 100 pt 100 pt 100 pt 100 pt 200 pt 200 pt 200 pt 200 pt 200 pt 300 pt 300 pt 300
PAIN JEOPARDY I ll take INTERVENTIONS for 400 points, Alex! Fact/Myth Barriers Assessment Education Interventions 100 pt 100 pt 100 pt 100 pt 100 pt 200 pt 200 pt 200 pt 200 pt 200 pt 300 pt 300 pt 300
PAIN RELIEF GUIDE. Tips and advice from your pharmacist.
 PAIN RELIEF GUIDE Tips and advice from your pharmacist. Rite Aid Pharmacists: Your Pain Relief Managers Rite Aid is committed to providing everyday products and services that help our valued customers
PAIN RELIEF GUIDE Tips and advice from your pharmacist. Rite Aid Pharmacists: Your Pain Relief Managers Rite Aid is committed to providing everyday products and services that help our valued customers
The Doctor-Patient Relationship
 The Doctor-Patient Relationship It s important to feel at ease with your doctor. How well you are able to talk with your doctor is a key part of getting the care that s best for you. It s also important
The Doctor-Patient Relationship It s important to feel at ease with your doctor. How well you are able to talk with your doctor is a key part of getting the care that s best for you. It s also important
What to Expect While Receiving Radiation Therapy for Prostate Cancer
 What to Expect While Receiving Radiation Therapy for Prostate Cancer Princess Margaret Information for patients who are having radiation therapy Read this pamphlet to learn about: The main steps in planning
What to Expect While Receiving Radiation Therapy for Prostate Cancer Princess Margaret Information for patients who are having radiation therapy Read this pamphlet to learn about: The main steps in planning
Palliative Medicine, Pain Management, and Hospice. Devon Neale, MD Assistant Professor Dept of Internal Medicine UNM School of Medicine
 Palliative Medicine, Pain Management, and Hospice Devon Neale, MD Assistant Professor Dept of Internal Medicine UNM School of Medicine Pall-i- What??? Objectives: Provide information about Palliative Medicine
Palliative Medicine, Pain Management, and Hospice Devon Neale, MD Assistant Professor Dept of Internal Medicine UNM School of Medicine Pall-i- What??? Objectives: Provide information about Palliative Medicine
Studies tell us the pain will be gone or improved significantly in ¾ of patients in 4 weeks and 9/10ths of patients in 6 weeks.
 Back pain is common and ranges from mild to severe pain. Most episodes soon ease within 4 weeks and are not due to serious illness. Keeping active is the most important message along with painkillers if
Back pain is common and ranges from mild to severe pain. Most episodes soon ease within 4 weeks and are not due to serious illness. Keeping active is the most important message along with painkillers if
Home Health & Hospice. Managing Your Pain
 Home Health & Hospice Managing Your Pain Facts About Pain No pain should be accepted as normal. Pain can: Keep you from working, enjoying activity, taking pleasure in your family life. Hinder your ability
Home Health & Hospice Managing Your Pain Facts About Pain No pain should be accepted as normal. Pain can: Keep you from working, enjoying activity, taking pleasure in your family life. Hinder your ability
Collaborative Care Plan for PAIN
 1. Pain Assessment *Patient s own description of pain is the most reliable indicator for pain assessment. Pain intensity to be assessed using the ESAS (Edmonton Symptom Assessment Scale) Use 5 th Vital
1. Pain Assessment *Patient s own description of pain is the most reliable indicator for pain assessment. Pain intensity to be assessed using the ESAS (Edmonton Symptom Assessment Scale) Use 5 th Vital
My Doctor Says Stress is Bad for My Diabetes... What Can I Do About It? BD Getting Started. Stress and Diabetes
 My Doctor Says Stress is Bad for My Diabetes... What Can I Do About It? BD Getting Started Stress and Diabetes Doesn t Everyone Have Stress? It s true that stress is part of everyday life for everyone.
My Doctor Says Stress is Bad for My Diabetes... What Can I Do About It? BD Getting Started Stress and Diabetes Doesn t Everyone Have Stress? It s true that stress is part of everyday life for everyone.
Controlling Your Pain Without Medicine
 Controlling Your Pain Without Medicine The following information is based on the general experiences of many prostate cancer patients. Your experience may be different. If you have any questions about
Controlling Your Pain Without Medicine The following information is based on the general experiences of many prostate cancer patients. Your experience may be different. If you have any questions about
What to Expect While Receiving Radiation Therapy for Breast Cancer
 What to Expect While Receiving Radiation Therapy for Breast Cancer Princess Margaret Information for patients who are having radiation therapy Read this pamphlet to learn about: The main steps in planning
What to Expect While Receiving Radiation Therapy for Breast Cancer Princess Margaret Information for patients who are having radiation therapy Read this pamphlet to learn about: The main steps in planning
Physical therapies. Massage
 This information is an extract from the booklet, Understanding complementary therapies. You may find the full booklet helpful. We can send you a copy free see page 6. This information discusses eight physical
This information is an extract from the booklet, Understanding complementary therapies. You may find the full booklet helpful. We can send you a copy free see page 6. This information discusses eight physical
Doctor Discussion Guide for Osteoarthritis
 Doctor Discussion Guide for Osteoarthritis How to Talk to Your Doctor About Osteoarthritis of the Knee With more than 10 million people affected, osteoarthritis of the knee is the most common type of osteoarthritis.
Doctor Discussion Guide for Osteoarthritis How to Talk to Your Doctor About Osteoarthritis of the Knee With more than 10 million people affected, osteoarthritis of the knee is the most common type of osteoarthritis.
What might help? Informal support services
 What might help? Informal support services It will take time to adapt your life. It s fine if you have the odd duvet day when you feel upset. But if his is becoming more common or your emotions are feeling
What might help? Informal support services It will take time to adapt your life. It s fine if you have the odd duvet day when you feel upset. But if his is becoming more common or your emotions are feeling
What to Do When Receiving Radiation Therapy to the Pelvis
 What to Do When Receiving Radiation Therapy to the Pelvis UHN For patients with gynecological cancer Learn the main steps in planning radiation treatment and how to manage side effects during radiation
What to Do When Receiving Radiation Therapy to the Pelvis UHN For patients with gynecological cancer Learn the main steps in planning radiation treatment and how to manage side effects during radiation
Cancer Pain. Treatment Guidelines for Patients
 Cancer Pain Treatment Guidelines for Patients Version II/ August 2005 Current NCCN Treatment Guidelines for Patients Advanced Cancer and Palliative Care Treatment Guidelines for Patients (also available
Cancer Pain Treatment Guidelines for Patients Version II/ August 2005 Current NCCN Treatment Guidelines for Patients Advanced Cancer and Palliative Care Treatment Guidelines for Patients (also available
Cancer-Related Brain Fog
 Cancer-Related Brain Fog Information for Cancer Patients and Caregivers about Cancer-Related Brain Fog Princess Margaret Also called Chemo-Fog, Chemo-Brain, or Cancer-Related Cognitive Dysfunction Please
Cancer-Related Brain Fog Information for Cancer Patients and Caregivers about Cancer-Related Brain Fog Princess Margaret Also called Chemo-Fog, Chemo-Brain, or Cancer-Related Cognitive Dysfunction Please
How To Take A Strong Opioid Painkiller
 Using strong painkillers for cancer pain This information is an extract from the booklet Controlling cancer pain. You may find the full booklet helpful. We can send you a copy free see page 8. Contents
Using strong painkillers for cancer pain This information is an extract from the booklet Controlling cancer pain. You may find the full booklet helpful. We can send you a copy free see page 8. Contents
Personal Action / Crisis Prevention Plan
 Personal Action / Crisis Prevention Plan This Plan is meant to help clients/consumers, their support persons and providers prepare for times when life seems too hard to manage. This Plan is designed to
Personal Action / Crisis Prevention Plan This Plan is meant to help clients/consumers, their support persons and providers prepare for times when life seems too hard to manage. This Plan is designed to
Radiation Therapy for Palliative Treatment at The Carlo Fidani Peel Regional Cancer Centre
 Radiation Therapy for Palliative Treatment at The Carlo Fidani Peel Regional Cancer Centre Introduction...2 Patient Education and Information...2&3 Treatment Planning...3&4 Your Appointments...5 Radiation
Radiation Therapy for Palliative Treatment at The Carlo Fidani Peel Regional Cancer Centre Introduction...2 Patient Education and Information...2&3 Treatment Planning...3&4 Your Appointments...5 Radiation
Patient information. Using strong Opioids to control your pain
 Patient information Using strong Opioids to control your pain Published: April 2013. Date for review: April 2016 Introduction This leaflet explains what strong opioids (pronounced oh-pee-oyds) e are and
Patient information Using strong Opioids to control your pain Published: April 2013. Date for review: April 2016 Introduction This leaflet explains what strong opioids (pronounced oh-pee-oyds) e are and
Palliative Care The Relief You Need When You re Experiencing the Symptoms of Serious Illness
 Palliative Care The Relief You Need When You re Experiencing the Symptoms of Serious Illness Dealing with the symptoms of any painful or serious illness is difficult. However, special care is available
Palliative Care The Relief You Need When You re Experiencing the Symptoms of Serious Illness Dealing with the symptoms of any painful or serious illness is difficult. However, special care is available
Treating symptoms. An introduction to. Everyone diagnosed with MS can get treatment for their symptoms. The symptoms of MS. Who can get treatment?
 Everyone diagnosed with MS can get treatment for their symptoms This resource is an introduction to the treatments that are available. The symbol will point you to further resources. An introduction to
Everyone diagnosed with MS can get treatment for their symptoms This resource is an introduction to the treatments that are available. The symbol will point you to further resources. An introduction to
Anxiety and breathing difficulties
 Patient information factsheet Anxiety and breathing difficulties Breathing is something that we all automatically do and we often take this for granted. Some chronic health conditions, for example asthma
Patient information factsheet Anxiety and breathing difficulties Breathing is something that we all automatically do and we often take this for granted. Some chronic health conditions, for example asthma
Massage therapy and energy-based therapies
 Massage therapy and energy-based therapies This information is an extract from the booklet Complementary therapies and cancer. You may find the full booklet helpful. We can send you a copy free see page
Massage therapy and energy-based therapies This information is an extract from the booklet Complementary therapies and cancer. You may find the full booklet helpful. We can send you a copy free see page
A Patient s Guide to Rib Joint Pain
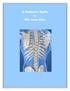 A Patient s Guide to Rib Joint Pain Anatomy Where are the rib joints? Your rib cage is made up of twelve pairs of ribs. The ribs attach to the spine in the back, and to the breastbone in the front. The
A Patient s Guide to Rib Joint Pain Anatomy Where are the rib joints? Your rib cage is made up of twelve pairs of ribs. The ribs attach to the spine in the back, and to the breastbone in the front. The
Coping with Multiple Sclerosis Strategies for you and your family
 Patient Education Coping with Multiple Sclerosis Strategies for you and your family Most people are not prepared to deal with the changes in routine and lifestyle that MS may require. Coping with MS can
Patient Education Coping with Multiple Sclerosis Strategies for you and your family Most people are not prepared to deal with the changes in routine and lifestyle that MS may require. Coping with MS can
Australian and New Zealand College of Anaesthetists and Faculty of Pain Medicine. Managing Acute Pain. A Guide for Patients.
 Australian and New Zealand College of Anaesthetists and Faculty of Pain Medicine Managing Acute Pain A Guide for Patients Approved by MANAGING ACUTE PAIN AGUIDE FOR PATIENTS Australian and New Zealand
Australian and New Zealand College of Anaesthetists and Faculty of Pain Medicine Managing Acute Pain A Guide for Patients Approved by MANAGING ACUTE PAIN AGUIDE FOR PATIENTS Australian and New Zealand
Chronic Low Back Pain
 Chronic Low Back Pain North American Spine Society Public Education Series What is Chronic Pain? Low back pain is considered to be chronic if it has been present for longer than three months. Chronic low
Chronic Low Back Pain North American Spine Society Public Education Series What is Chronic Pain? Low back pain is considered to be chronic if it has been present for longer than three months. Chronic low
Exercise. Good Weight A PT E R. Staying Healthy
 Eat Healthy Foods Keep at a Good Weight Exercise Don t Smoke Get Regular Checkups Take Care of Stress A PT E R CH Staying Healthy 6 81 How Can I Stay Healthy? You can do many things to prevent poor health
Eat Healthy Foods Keep at a Good Weight Exercise Don t Smoke Get Regular Checkups Take Care of Stress A PT E R CH Staying Healthy 6 81 How Can I Stay Healthy? You can do many things to prevent poor health
The road to recovery. The support available to help you with your recovery after stroke
 The road to recovery The road to recovery The support available to help you with your recovery after stroke We re for life after stroke Introduction Need to talk? Call our confidential Stroke Helpline
The road to recovery The road to recovery The support available to help you with your recovery after stroke We re for life after stroke Introduction Need to talk? Call our confidential Stroke Helpline
Radiation Therapy. What to expect
 Radiation Therapy What to expect This booklet was made possible through the generosity of BC Cancer Foundation donors. The BC Cancer Foundation is the fundraising partner of the BC Cancer Agency, supporting
Radiation Therapy What to expect This booklet was made possible through the generosity of BC Cancer Foundation donors. The BC Cancer Foundation is the fundraising partner of the BC Cancer Agency, supporting
Preparing for your Ultrasound-Guided Core Biopsy
 Preparing for your Ultrasound-Guided Core Biopsy UHN For patients at the Rapid Diagnostic Centre Read this resource to learn: How to prepare What to expect during the biopsy What you need to do after When
Preparing for your Ultrasound-Guided Core Biopsy UHN For patients at the Rapid Diagnostic Centre Read this resource to learn: How to prepare What to expect during the biopsy What you need to do after When
Opioid Analgesic Medication Information
 Opioid Analgesic Medication Information This handout provides information about treating pain with opioid analgesics or narcotics. Please read this entire handout. We want to be sure that you understand
Opioid Analgesic Medication Information This handout provides information about treating pain with opioid analgesics or narcotics. Please read this entire handout. We want to be sure that you understand
Pain and problem drug use
 Pain and problem drug use Information for patients Prepared by the British Pain Society in consultation with the Royal College of Psychiatrists, the Royal College of General Practitioners and the Advisory
Pain and problem drug use Information for patients Prepared by the British Pain Society in consultation with the Royal College of Psychiatrists, the Royal College of General Practitioners and the Advisory
Life with a new baby is not always what you expect
 Life with a new baby is not always what you expect Postpartum Blues or Baby Blues are COMMON. 4 in 5 mothers will have postpartum blues. POSTPARTUM BLUES OR BABY BLUES Pregnancy, the birth of a baby, or
Life with a new baby is not always what you expect Postpartum Blues or Baby Blues are COMMON. 4 in 5 mothers will have postpartum blues. POSTPARTUM BLUES OR BABY BLUES Pregnancy, the birth of a baby, or
Preventing & Treating Low Back Pain
 Preventing & Treating Low Back Pain An Introduction to Low Back Pain Low back pain is the number two reason that Americans see a health care practitioner second only to colds and flu. While most people
Preventing & Treating Low Back Pain An Introduction to Low Back Pain Low back pain is the number two reason that Americans see a health care practitioner second only to colds and flu. While most people
Fatigue Beyond Tiredness
 Fatigue Beyond Tiredness The development and printing of this booklet was sponsored by Roche Products Ltd and Chugai Pharma UK Ltd. Editorial control remains with NRAS. Have you ever: Got all dressed up
Fatigue Beyond Tiredness The development and printing of this booklet was sponsored by Roche Products Ltd and Chugai Pharma UK Ltd. Editorial control remains with NRAS. Have you ever: Got all dressed up
Dr. Kenneth A. Giraldo, MD, P.A. Patient Controlled Substance Agreement Informed Consent Form
 Dr. Kenneth A. Giraldo, MD, P.A. Patient Controlled Substance Agreement Informed Consent Form The following agreement relates to my use of controlled substance for chronic pain prescribed by Dr. Kenneth
Dr. Kenneth A. Giraldo, MD, P.A. Patient Controlled Substance Agreement Informed Consent Form The following agreement relates to my use of controlled substance for chronic pain prescribed by Dr. Kenneth
Drug treatments for neuropathic pain
 Understanding NICE guidance Information for people who use NHS services Drug treatments for neuropathic pain NICE clinical guidelines advise the NHS on caring for people with specific conditions or diseases
Understanding NICE guidance Information for people who use NHS services Drug treatments for neuropathic pain NICE clinical guidelines advise the NHS on caring for people with specific conditions or diseases
MOTOR VEHICLE ACCIDENT QUESTIONNAIRE
 MOTOR VEHICLE ACCIDENT QUESTIONNAIRE Thank you in advance for taking the time to complete this form, this will help us to better assess all of your pain concerns and provide you with the best treatment.
MOTOR VEHICLE ACCIDENT QUESTIONNAIRE Thank you in advance for taking the time to complete this form, this will help us to better assess all of your pain concerns and provide you with the best treatment.
Strong opioids (painkillers) in palliative care what you should know
 Strong opioids (painkillers) in palliative care what you should know Patient Information Author ID: JG Leaflet Number: PC 006 Version: 1 Name of Leaflet: Strong opioids (painkillers) in palliative care
Strong opioids (painkillers) in palliative care what you should know Patient Information Author ID: JG Leaflet Number: PC 006 Version: 1 Name of Leaflet: Strong opioids (painkillers) in palliative care
PAIN MANAGEMENT. Patient s name: IF YOUR INSURANCE REQUIRES A PRE AUTHORIZATION / REFERRAL FORM, PLEASE OBTAIN PRIOR TO YOUR VISIT.
 PAIN MANAGEMENT Please fill out the following questionnaire and bring it with you to your appointment. In addition, bring your medication list and Reports of any X- rays, MRI or Cat scans. Patient s name:
PAIN MANAGEMENT Please fill out the following questionnaire and bring it with you to your appointment. In addition, bring your medication list and Reports of any X- rays, MRI or Cat scans. Patient s name:
Chemotherapy Side Effects Worksheet
 Page 1 of 6 Chemotherapy Side Effects Worksheet Medicines or drugs that destroy cancer cells are called cancer chemotherapy. It is sometimes the first choice for treating many cancers. Chemotherapy differs
Page 1 of 6 Chemotherapy Side Effects Worksheet Medicines or drugs that destroy cancer cells are called cancer chemotherapy. It is sometimes the first choice for treating many cancers. Chemotherapy differs
Pain relief at home. Information for adult patients
 Pain relief at home Information for adult patients 3 Contents Page 3 Page 3 Page 5 Page 7 Page 8 Introduction to pain relief Common pain relief medicines and their side effects More information about pain
Pain relief at home Information for adult patients 3 Contents Page 3 Page 3 Page 5 Page 7 Page 8 Introduction to pain relief Common pain relief medicines and their side effects More information about pain
medicineupdate Tramadol for pain Asking the right questions about new medicines Page Section 1: What tramadol is 1 Section 2: What tramadol is for 1
 medicineupdate Asking the right questions about new medicines Tramadol for pain Page Section 1: What tramadol is 1 Section 2: What tramadol is for 1 Section 3: Who can take tramadol 2 Section 4: What does
medicineupdate Asking the right questions about new medicines Tramadol for pain Page Section 1: What tramadol is 1 Section 2: What tramadol is for 1 Section 3: Who can take tramadol 2 Section 4: What does
Questions about your pain medicines
 Questions about your pain medicines This information is an extract from the booklet Controlling cancer pain. You may find the full booklet helpful. We can send you a free copy see page 6. Contents Common
Questions about your pain medicines This information is an extract from the booklet Controlling cancer pain. You may find the full booklet helpful. We can send you a free copy see page 6. Contents Common
Because it s important to know as much as you can.
 About DEPRESSION Because it s important to know as much as you can. This booklet is designed to help you understand depression and the things you can do every day to help manage it. Taking your medicine
About DEPRESSION Because it s important to know as much as you can. This booklet is designed to help you understand depression and the things you can do every day to help manage it. Taking your medicine
Foot or Ankle Surgery
 Foot or Ankle Surgery Instructions for patients going home UHN You had a general anesthetic. Do not drive a car or drink alcohol for 24 hours. What can I eat and drink after my operation? You can go back
Foot or Ankle Surgery Instructions for patients going home UHN You had a general anesthetic. Do not drive a car or drink alcohol for 24 hours. What can I eat and drink after my operation? You can go back
Whiplash Recovery Important Facts 1
 02866328200 Whiplash Recovery Important Facts 1 What is whiplash? You can get whiplash if your head is suddenly jolted backwards and forwards in a whip-like movement. The tissues around your neck are overstretched,
02866328200 Whiplash Recovery Important Facts 1 What is whiplash? You can get whiplash if your head is suddenly jolted backwards and forwards in a whip-like movement. The tissues around your neck are overstretched,
POST-TEST Pain Resource Professional Training Program University of Wisconsin Hospital & Clinics
 POST-TEST University of Wisconsin Hospital & Clinics True/False/Don't Know - Circle the correct answer T F D 1. Changes in vital signs are reliable indicators of pain severity. T F D 2. Because of an underdeveloped
POST-TEST University of Wisconsin Hospital & Clinics True/False/Don't Know - Circle the correct answer T F D 1. Changes in vital signs are reliable indicators of pain severity. T F D 2. Because of an underdeveloped
PAIN MANAGEMENT AT UM/SYLVESTER
 PAIN MANAGEMENT AT UM/SYLVESTER W HAT IS THE PURPOSE OF THIS BROCHURE? We created this brochure for patients receiving care from the University of Miami Sylvester Comprehensive Cancer Center and their
PAIN MANAGEMENT AT UM/SYLVESTER W HAT IS THE PURPOSE OF THIS BROCHURE? We created this brochure for patients receiving care from the University of Miami Sylvester Comprehensive Cancer Center and their
Abdominal Wall Pain. What is Abdominal Wall Pain?
 Abdominal Wall Pain What is Abdominal Wall Pain? Abdominal Wall Pain is a syndrome (an experience) of abdominal pain that can occur at any time of life and is not unique to children. It is diagnosed by
Abdominal Wall Pain What is Abdominal Wall Pain? Abdominal Wall Pain is a syndrome (an experience) of abdominal pain that can occur at any time of life and is not unique to children. It is diagnosed by
Schizophrenia National Institute of Mental Health
 Schizophrenia National Institute of Mental Health U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES National Institutes of Health Schizophrenia Do you know someone who seems like he or she has lost touch with
Schizophrenia National Institute of Mental Health U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES National Institutes of Health Schizophrenia Do you know someone who seems like he or she has lost touch with
Welcome to the Pain Management Unit (PMU)
 Welcome to the Pain Management Unit (PMU) This pamphlet describes who we are and what you can expect from us, along with a few facts about chronic pain. Facts About Chronic Pain The 2 kinds of pain are:
Welcome to the Pain Management Unit (PMU) This pamphlet describes who we are and what you can expect from us, along with a few facts about chronic pain. Facts About Chronic Pain The 2 kinds of pain are:
CHPN Review Course Pain Management Part 1 Hospice and Palliative Nurses Association
 CHPN Review Course Pain Management Part 1 Disclosures Bonnie Morgan has no real or perceived conflicts of interest that relate to this presentation. Copyright 2015 by the. HPNA has the exclusive rights
CHPN Review Course Pain Management Part 1 Disclosures Bonnie Morgan has no real or perceived conflicts of interest that relate to this presentation. Copyright 2015 by the. HPNA has the exclusive rights
Diuretics: You may get diuretic medicine to help decrease swelling in your brain. This may help your brain get better blood flow.
 Hemorrhagic Stroke GENERAL INFORMATION: What is a hemorrhagic stroke? A hemorrhagic stroke happens when a blood vessel in the brain bursts. This may happen if the blood vessel wall is weak, or sometimes
Hemorrhagic Stroke GENERAL INFORMATION: What is a hemorrhagic stroke? A hemorrhagic stroke happens when a blood vessel in the brain bursts. This may happen if the blood vessel wall is weak, or sometimes
Welcome to 5 South Geriatric Psychiatry
 Welcome to 5 South Geriatric Psychiatry Toronto Rehab For patients, families and caregivers Welcome to 5 South, the Geriatric Psychiatry Program at Toronto Rehab. This booklet will give you more information
Welcome to 5 South Geriatric Psychiatry Toronto Rehab For patients, families and caregivers Welcome to 5 South, the Geriatric Psychiatry Program at Toronto Rehab. This booklet will give you more information
