GUIDELINES FOR PATIENTS HAVING A LUMBAR FUSION. Lumbar Fusion
|
|
|
- Buck Martin
- 7 years ago
- Views:
Transcription
1 ORTHOPAEDIC UNIT: / UPMC BEACON CENTRE FOR ORTHOPAEDICS: PHYSIOTHERAPY DEPARTMENT: GUIDELINES FOR PATIENTS HAVING A LUMBAR FUSION Please stick addressograph here
2 Table of Contents 1. Introduction 2. What is a Lumbar Fusion? 3. Potential Complications 4. Physiotherapy 5. Your Rehabilitation Goals 6. General recommendations 7. Discharge Instructions 8. Conclusion 9. Individual Patient Notes Introduction This information booklet has been written to give you and your family a basic understanding of what is involved when you require a lumbar fusion. Although you may have been told different information from friends or others, please follow these instructions specifically. In this booklet we provide information, including things you should know before and after your operation. It is important for you to understand the advantages but also the possible problems, which may occur after this surgery. Throughout your stay in UPMC Beacon Hospital, you will receive continuous advice and support from all members of the team. What is a Lumbar Fusion? Anatomy The lumbar spine, or lower back, is composed of 5 bones, or vertebrae. These are numbered downwards from 1-5 and, because they are part of the lumbar spine they are prefixed by the letter L. Hence, you will hear health care workers refer to L3 - L4 or L4 - L5, for example. At the very bottom of the lumbar spine is the sacrum. This bone is roughly the shape of an inverted triangle and the top part of this is referred to as S1.
3 numbness or tingling. These nerves also supply your bladder and bowel, which is why you may be asked about this. Surgery Your doctor has recommended fusion surgery on your back to correct your present condition. This surgery may be an anterior and/or posterior spinal fusion. A fusion is performed to keep separate sections of the spine secured. It s like a weld to hold bones together and involves using bone graft to cause two vertebral bodies to grow together into one long bone. Two vertebral segments need to be fused together to stop the motion at one segment, so that an L4-L5 (lumbar segment 4 and lumbar segment 5) spinal fusion is actually a one-level spinal fusion. The fusion may take six or more months to become solid and stable. Each vertebra is connected to each adjacent vertebra by 3 joints, 1 at the front and 2 at the back. The larger one at the front is where the body of a vertebra is separated from its adjacent vertebral bodies by an intervertebral disc. The 2 joints at the back are called facet joints and these lay either side of the midline. These joints also serve to connect one vertebra with its adjacent vertebra. In addition to the bony components, there are other important structures as well. The spinal canal is a bony tunnel which the spinal cord sits inside. At each level of the spine (that is between 2 individual vertebrae) a pair of nerve roots comes out (one on each side). The nerve roots that come out at the levels of the lumbar spine go on to form the nerves of the leg. These nerve roots supply the skin and muscles in your legs. Each different level of nerve root supplies different muscles and different areas of skin. This helps medical professionals decide which part of your back may be causing the trouble. This also explains why people with low back problems can suffer with leg pain, Bone graft can be taken from the patient's hip (auto graft bone) during the spinal fusion surgery, harvested from cadaver bone (allograft bone) or manufactured (synthetic bone graft substitute). Bone graft positioning
4 An incision (cut) will be made on your back. The size of the incision will depend on the extent of your problem. If bone is going to be taken from your hip, then a second incision will be made on the back of your hip on your right or left side. Bone will be removed from your hip and will be placed in your back. This will create a bone fusion. The surgery may take 3-5 hours. Your incision will be closed with either metal staples or stitches, which may be reinforced with Steri-strips, paper like strips that stick to your skin and help keep the sides of the incision together. The surgery may also involve a discectomy (removal of a herniated or damaged portion of a disk in the spine), laminectomy (removal of the back part of the bone that covers the spinal canal) or the removal of bone spurs or other spinal growths. Potential Complications of a Lumbar FusionIncidence THE MAJORITY OF PATIENTS WHO UNDERGO LUMBAR FUSION SURGERY HAVE A PLEASANT EXPERIENCE WITHOUT ANY COMPLICATIONS. THE FOLLOWING IS A LIST OF SOME OF THE PROBLEMS THAT COULD POTENTIALLY OCCUR. Infection This may occur superficially in the area of the wound or deeper, affecting the bones and soft tissues of the spine. These infections can occur in hospital or after you have been discharge home. An infection is generally treated with antibiotics. If it is a deep infection then further surgery may be required to treat the affected section of the spine. Dural Tear A thin membrane called the dura covers the spinal cord and nerves. Underneath this membrane is the cerebrospinal fluid. During spinal surgery a tear of the membrane may occur and a spinal headache may result from the spinal fluid leak. The treatment for this involves stitching the tear or sealing it with glue. If this occurs additional bed rest may be required. A leak may also increase the risk of infection of the spinal fluid (meningitis) Spinal cord/nerve root damage Rod and Screw positioning In any spinal operation there is some risk of injuring the spinal cord. Damage to the spinal cord can cause complete paralysis or paralysis in certain areas depending on which section of the spinal cord is affected. There is also the possibility of damaging one of the spinal nerves that come out of the spinal cord.
5 Persistent Pain One of the most common complications of spinal surgery is that it does not get rid of the patient s pain. In some cases, it may increase the pain. Some patients may develop scar tissue around the nerves weeks after the operation that causes pain similar to what the patient had prior to surgery Impaired Nerve Function Rarely, nerves in the vicinity of the spine level being operated on are stretched or damaged during the operation (a neuropraxia).fortunately, the majority of these neuropraxias resolve over a period of time, sometimes months, but in a very small minority the damage may be permanent. Deep Venous Thrombosis & Pulmonary Embolism There is a risk of deep venous thrombosis (DVT) after lumbar fusion. Patients are treated with medications and mechanical devices in hospital to prevent this. In most cases the measures taken are effective. However despite all these precautions some patients still develop clots and may require further treatment with medication. Pulmonary embolism (PE) may occur if the clot detaches from the vein and travels to the lung. Manage Your Pain Pain is a common occurrence following any surgical procedure. It can be well managed with medications, special pain management devices and ice. The pain will naturally reduce as your wound heals and with regular use of analgesics (pain killers). It is imperative to keep your pain well controlled so you can mobilise comfortably, perform your physiotherapy exercises and resume normal activities after your surgery. You will be asked to rate or score your pain regularly after your surgery. The score will depend on how your pain feels to you. 0= No Pain, 10= worst pain imaginable (Please point to the number that best describes your pain) STROKE OR SUDDEN DEATH Although these complications can occur following surgery they are extremely rare following spinal surgery. Assign the number you feel best describes your pain. The nurses will administer appropriate treatments/ medications depending on your pain score. The nurse will reassess your pain score after the treatment to make sure it has worked to reduce your pain.
6 Physiotherapy EXERCISE PROGRAM Exercises: The physiotherapist will teach you exercises and provide back care advice. A brace may be needed to provide extra support for your back after surgery. If required, you will be measured for the brace the morning after surgery and must wear the brace as per your consultant s specifications. The following exercises start as soon as you are able. You may feel uncomfortable at first, but these exercises will speed your recovery. 1) Ankle Pumps With your legs straight, bend your ankles up and down, towards and away from your face. Repeat 15 times. PhysioTools Ltd It is important for you to perform the exercises that your Chartered Physiotherapist prescribes for you daily. This will allow you to gently mobilise your spine and recover both motion and muscle strength. You may also be issued with additional exercises depending on your consultants request. Walking is good for you, but you should rest as needed. Do not get overtired. Try to limit going up and down stairs to once or twice a day for one to two weeks. If you have any queries in relation to these exercises do not hesitate to contact the UPMC Beacon Physiotherapy Department on (01) ) Static Gluts Tighten muscles in you bottom. Hold 5 seconds, relax. Repeat x 10. PhysioTools Ltd Preliminary Exercises- Early Postoperative Period: 0-2 weeks Frequency: You will need to do these exercises at least three to four times a day to ensure you reach your rehabilitation goals. Please be sure to read the exercises carefully and ask your physiotherapist any questions that you may have before you leave the hospital.
7 3) Quadriceps Setting. With your leg straight out in front of you, tighten the muscles at the front of your thigh, pushing the back of your knee down into the bed. The result should be straightening of the knee. Hold the contraction for 5 seconds. Repeat 15 times. PhysioTools Ltd Your Rehabilitation Goals Independent getting in and out of bed. Independent in walking with crutches or walker on a level surface. Independent walking up and down stairs. Achieve targeted joint range of motion. Achieve required muscle power and be independent with exercise programme. The physiotherapist will review you to commence activity once cleared by the consultant to start. This is usually 1 to 2 days post surgery. Day of the procedure 4) Trans Abdominal Setting Lying on your back with your knees bent. Breathe into your abdomen, and on the breath out pull gently up and in from below the belly button. Keep your breathing regular as you hold this muscle in. Hold for 5 seconds, and repeat 8 to 10 times. Before being allowed to get out of bed for the first time, it is important to do the following exercises every hour. These will help prevent complications. 1. Take 3-4 deep breaths. 2. With your knees straight move your feet vigorously up and down 20 times. PhysioTools Ltd 3. Tighten up your thigh and buttock muscles and hold for a few seconds- repeat 10 times.
8 Day One: A brace may be needed to provide extra support for your back after surgery. If required, you will be measured for the brace the morning after surgery and must wear the brace as per your consultant s specifications. Lower yourself onto your side using your arms to guide and control your body. At the same time, bend your knees and pull your legs onto the bed. The Physiotherapist will assess you and provide you with an exercise program. A log roll procedure will be practiced to carry out all transfers in and out of bed. You will walk for a short distance and may be encouraged to progress activity throughout the day. Your dressings may also be reduced. Day Two onwards: Regular exercise throughout the day is required to increase your movement and strengthen your muscles. Walking is part of your exercise programme and you should be increasing your walking distance on the ward daily. The physiotherapist will have escorted you to the stairs and by discharge you will have climbed a flight of stairs safely and independently. Keep your knees bent. Roll onto your back. Keep your shoulder and hips together as a unit as you roll. Think of yourself as a rolling log. Log Roll Method Getting into bed: Sit on your bed, closer to the head of the bed than to the foot of the bed. Scoot back onto the bed as far as you can.
9 Place your bottom hand underneath your shoulder. Place your top hand in front of you at chest level. Slowly raise your body as you lower your legs toward the floor Getting out of bed: While lying on your back, bend your knees. Roll onto your side. Keep your shoulders and hips together as a unit as you roll. Stairs Technique Going up-stairs Where using a walking aid, Maintain crutches/walking stick on the step below. Lead with the un-operated leg up onto the step above. Take your weight onto the un-operated leg by pushing on crutches/walking stick and banister. Follow with the crutch/walking stick onto the same step.
10 General Recommendations Sleeping While in hospital some patients find it harder to sleep for various reasons, i.e. different bed and environment. If you find that you are having this problem please let the nursing staff know as you may require something to help you sleep. PhysioTools Ltd Usually you sleep in any position that is comfortable. However, you should not sleep on your stomach, because this strains your back muscles. If you have a brace then this can be removed at night, unless otherwise indicated. Going Downstairs Put crutch/walking stick down onto the step below. Follow with the operated leg. Take weight onto the operated leg using the crutches and banister for support. Follow with the un-operated leg onto the same step. PhysioTools Ltd Nausea Some of the medications you can be prescribed can cause nausea. Please inform the nursing staff if you feel sick or are getting sick as your medications may need to be changed/adjusted and the nursing staff can also get a medication prescribed to help relieve this nausea. Stockings Your consultant may wish for you to go home with elasticated stockings. These can be an important part of preventing the development of deep vein thrombosis (blood clots in the legs). It is recommended to wear these for 6 weeks after surgery. Pain & Swelling Most people come round from the anaesthetic and feel an immediate relief of their leg symptoms. Pain often settles fairly quickly. Numbness and tingling sensations usually take longer to settle though - this may be days, weeks or months. It varies considerably from person to person.
11 Some people may always have an area of numbness that never fully recovers. Do not worry if your leg pain is still present - it is not a sign the surgery has failed. Nerves take time to recover from being squashed. They also have a tendency to remember what has happened to them. Also, take into consideration your recent operation. Bruising and swelling will be present which will settle, but can also irritate the delicate nerve tissue initially. Dressing Keep your dressing clean and dry, but do not remove it for 24 hours. There may be some bloody spotting on this, however this is normal. Excessive bleeding or non bloody wound drainage that soaks the dressing should be reported to nursing staff. Showering Try to keep the Opsite bandage as dry as possible when showering. Be sure to use a rubber mat in the shower, to prevent slipping. Be careful not to move your neck from side to side while the brace is off. Driving Returning to drive is at the discretion of your surgeon. Do not drive while wearing your brace. Your reaction time may be slower due to pain or certain prescribed medications. This is a safety concern as well as a legal issue Work Do not return to work until your doctor says you can. People generally get back to light work in two to four weeks and can do heavier work and sports within two to three months. General Care Do not bend from the waist to pick up things. This movement strains your back muscles-you should bend your knees and squat instead. Do not carry heavy items, such as shopping or laundry. Do not lift anything heavier than a litre of milk. Do not try to move heavy furniture until your doctor says you may. Do not lift anything over your head. Do not sit in soft or overstuffed chairs. Firm chairs with straight backs give better support. Walking is good for you, but you should rest as needed. Do not get overtired. Try to limit going up and down stairs to once a day for one to two weeks. You may resume sexual activities when your doctor says you may. Avoid strenuous exercise or activities like swimming, golfing, or running until you are advised to so by your consultant or physiotherapist. You may ride in a car from the hospital to your home. However, you should avoid longer car trips until cleared to do so by your consultant.
12 Discharge Instructions You will be discharged form hospital 2-3 days after your operation. When you leave the hospital you will be asked to make an appointment to see your consultant, usually 6 weeks after the operation. This is for a routine check-up which will make sure you are progressing satisfactorily. You will also be offered outpatient physiotherapy in the hospital and encouraged to attend this 2-3 weeks post discharge to improve your recovery. It is advisable to attend physiotherapy in this hospital as the physiotherapists will have access to all of your medical notes. The Physiotherapy team also are in direct contact with your surgeon should a problem arise. On discharge from hospital, your consultant will prescribe you some medications. One of the medications prescribed will be pain medications. Plan to take your pain medication 30 minutes before exercises. Preventing pain is easier than chasing pain. If pain control continues to be a problem, contact the orthopaedic centre or your general practitioner. Redness around the wound site Increased pain in the wound Swelling around the wound Heat at the wound site Discharge of fluid may be green or yellow Odour or smell from the wound Feeling of being generally unwell Fever or temperature Most people will have sutures that will need to removed approximately days after surgery. This may be done by the GP, Dressing clinic, consultant or in the convalescence centre. Conclusion We hope that you have found this booklet useful and that it has helped to relieve some of your fears and anxieties regarding your surgery. During your hospital stay, your medical team will be available to answer any other queries you may have. Wound Care You will leave the hospital with a simple surgical wound. Infection may occur despite your very best efforts. If any of the symptoms below occur then you will need to see your GP or liaise with the centre for orthopaedics re advice and possibly antibiotics. Signs of Infection If you develop any of the following signs of infection, it is important to report them to your doctor. The signs of infection include: Individual Patient Notes: Consultant Name: Date of Surgery: Surgery Note: Weight Bearing Status:
Guidelines for patients having a Lumbar. Discectomy. Lumbar Discectomy
 ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 Guidelines for patients having a Lumbar Discectomy Please stick addressograph
ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 Guidelines for patients having a Lumbar Discectomy Please stick addressograph
Orthopaedic Spine Center. Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs
 Orthopaedic Spine Center Graham Calvert MD James Woodall MD PhD Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs The cervical spine consists of the bony vertebrae, discs, nerves and other structures.
Orthopaedic Spine Center Graham Calvert MD James Woodall MD PhD Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs The cervical spine consists of the bony vertebrae, discs, nerves and other structures.
SPINE SURGERY - LUMBAR DECOMPRESSION
 SPINE SURGERY - LUMBAR DECOMPRESSION Information Leaflet Your Health. Our Priority. Page 2 of 7 Introduction This booklet has been compiled by the physiotherapy department to help you understand lumbar
SPINE SURGERY - LUMBAR DECOMPRESSION Information Leaflet Your Health. Our Priority. Page 2 of 7 Introduction This booklet has been compiled by the physiotherapy department to help you understand lumbar
Knee Microfracture Surgery Patient Information Leaflet
 ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 Knee Microfracture Surgery Patient Information Leaflet Table of Contents 1. Introduction
ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 Knee Microfracture Surgery Patient Information Leaflet Table of Contents 1. Introduction
Wrist Fracture. Please stick addressograph here
 ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 UPMC BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 GUIDELINES FOR PATIENTS FOLLOWING WRIST FRACTURE Please stick addressograph
ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 UPMC BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 GUIDELINES FOR PATIENTS FOLLOWING WRIST FRACTURE Please stick addressograph
Information and exercises following dynamic hip screw
 Physiotherapy Department Information and exercises following dynamic hip screw Introduction A dynamic hip screw is performed where the neck of femur has been fractured and where there is a good chance
Physiotherapy Department Information and exercises following dynamic hip screw Introduction A dynamic hip screw is performed where the neck of femur has been fractured and where there is a good chance
A Patient s Guide to Post-Operative Physiotherapy. Following Anterior Cruciate Ligament Reconstruction of the Knee
 A Patient s Guide to Post-Operative Physiotherapy Following Anterior Cruciate Ligament Reconstruction of the Knee Introduction The anterior cruciate ligament (ACL) is one of the main supporting ligaments
A Patient s Guide to Post-Operative Physiotherapy Following Anterior Cruciate Ligament Reconstruction of the Knee Introduction The anterior cruciate ligament (ACL) is one of the main supporting ligaments
Knee arthroscopy advice sheet
 Knee arthroscopy advice sheet During an arthroscopy, a camera is inserted into the knee through two or three small puncture wounds. It allows the surgeon to look at the joint surfaces, cartilage and the
Knee arthroscopy advice sheet During an arthroscopy, a camera is inserted into the knee through two or three small puncture wounds. It allows the surgeon to look at the joint surfaces, cartilage and the
Posterior Cervical Decompression
 Posterior Cervical Decompression Spinal Unit Tel: 01473 702032 or 702097 Issue 2: January 2009 Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed with a
Posterior Cervical Decompression Spinal Unit Tel: 01473 702032 or 702097 Issue 2: January 2009 Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed with a
Patient information for cervical spinal fusion.
 Patient information for cervical spinal fusion. Introduction This booklet has been compiled to help you understand spinal cervical fusion surgery and postoperative rehabilitation. Anatomy The cervical
Patient information for cervical spinal fusion. Introduction This booklet has been compiled to help you understand spinal cervical fusion surgery and postoperative rehabilitation. Anatomy The cervical
Posterior Lumbar Decompression for Spinal Stenosis
 Posterior Lumbar Decompression for Spinal Stenosis Issue 6: March 2016 Review date: February 2019 Following your recent MRI scan and consultation with your spinal surgeon you have been diagnosed with
Posterior Lumbar Decompression for Spinal Stenosis Issue 6: March 2016 Review date: February 2019 Following your recent MRI scan and consultation with your spinal surgeon you have been diagnosed with
Patient Information. Posterior Cervical Surgery. Here to help. Respond Deliver & Enable
 Here to help Our Health Information Centre (HIC) provides advice and information on a wide range of health-related topics. We also offer: Services for people with disabilities. Information in large print,
Here to help Our Health Information Centre (HIC) provides advice and information on a wide range of health-related topics. We also offer: Services for people with disabilities. Information in large print,
SHOULDER ACROMIOPLASTY/ SHOULDER DECOMPRESSION
 ORTHOPAEDIC WARD: 01-293 8687 /01-293 6602 BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 GUIDELINES FOR PATIENTS HAVING A SHOULDER ACROMIOPLASTY/ SHOULDER DECOMPRESSION
ORTHOPAEDIC WARD: 01-293 8687 /01-293 6602 BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 GUIDELINES FOR PATIENTS HAVING A SHOULDER ACROMIOPLASTY/ SHOULDER DECOMPRESSION
Lumbar Laminectomy and Interspinous Process Fusion
 Lumbar Laminectomy and Interspinous Process Fusion Introduction Low back and leg pain caused by pinched nerves in the back is a common condition that limits your ability to move, walk, and work. This condition
Lumbar Laminectomy and Interspinous Process Fusion Introduction Low back and leg pain caused by pinched nerves in the back is a common condition that limits your ability to move, walk, and work. This condition
We ve got your back. Physical Therapy After Lumbar Fusion Surgery
 We ve got your back Physical Therapy After Lumbar Fusion Surgery Physical therapy is an extremely important part of you recovery after spinal surgery. This booklet, prepared by the therapists who specialize
We ve got your back Physical Therapy After Lumbar Fusion Surgery Physical therapy is an extremely important part of you recovery after spinal surgery. This booklet, prepared by the therapists who specialize
SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS?
 SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS? The spinal canal is best imagined as a bony tube through which nerve fibres pass. The tube is interrupted between each pair of adjacent
SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS? The spinal canal is best imagined as a bony tube through which nerve fibres pass. The tube is interrupted between each pair of adjacent
Neck Surgery (Cervical spine surgery) Remember to bring this handout to the hospital with you.
 Neck Surgery (Cervical spine surgery) Remember to bring this handout to the hospital with you. 1 Neck Surgery (cervical spine surgery) Table of contents Page Why do I need neck surgery?... 2 What kinds
Neck Surgery (Cervical spine surgery) Remember to bring this handout to the hospital with you. 1 Neck Surgery (cervical spine surgery) Table of contents Page Why do I need neck surgery?... 2 What kinds
Low Back Surgery. Remember to bring this handout to the hospital with you.
 Remember to bring this handout to the hospital with you. Table of contents Page Why do I need low back surgery?... 1 What kinds of low back surgeries are there?... 2 Before your surgery... 3 After your
Remember to bring this handout to the hospital with you. Table of contents Page Why do I need low back surgery?... 1 What kinds of low back surgeries are there?... 2 Before your surgery... 3 After your
POSTOPERATIVE INSTRUCTION FOR ANTERIOR/POSTERIOR LUMBAR SPINE FUSION
 www.southerarizonaspine.com POSTOPERATIVE INSTRUCTION FOR ANTERIOR/POSTERIOR LUMBAR SPINE FUSION This handout will review the care you need to follow once you are home. If you have any questions or concerns,
www.southerarizonaspine.com POSTOPERATIVE INSTRUCTION FOR ANTERIOR/POSTERIOR LUMBAR SPINE FUSION This handout will review the care you need to follow once you are home. If you have any questions or concerns,
Posterior Lumbar Decompression for Spinal Stenosis
 Posterior Lumbar Decompression for Spinal Stenosis Spinal Unit Tel: 01473 702032 or 702097 Issue 5: August 2014 Review date: July 2017 Following your recent MRI scan and consultation with your spinal surgeon
Posterior Lumbar Decompression for Spinal Stenosis Spinal Unit Tel: 01473 702032 or 702097 Issue 5: August 2014 Review date: July 2017 Following your recent MRI scan and consultation with your spinal surgeon
ADVICE TO PATIENT DUE TO HAVE MICRODISCECTOMY / SPINAL STENOSIS DECOMPRESSION. Under the Care of Mr M Paterson - 11 -
 ADVICE TO PATIENT DUE TO HAVE MICRODISCECTOMY / SPINAL STENOSIS DECOMPRESSION Under the Care of Mr M Paterson Acknowledgement: Drawings by Jean Paterson Perth Australia 2006 Brochure: R. Grubb Amended:
ADVICE TO PATIENT DUE TO HAVE MICRODISCECTOMY / SPINAL STENOSIS DECOMPRESSION Under the Care of Mr M Paterson Acknowledgement: Drawings by Jean Paterson Perth Australia 2006 Brochure: R. Grubb Amended:
Patient Information for Lumbar Spinal Fusion. What is a lumbar spinal fusion? Page 1 of 5
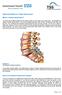 Patient Information for Lumbar Spinal Fusion What is a lumbar spinal fusion? You have been offered surgery to the lumbar region of your spine, your lower back. The operation is called a lumbar spinal fusion.
Patient Information for Lumbar Spinal Fusion What is a lumbar spinal fusion? You have been offered surgery to the lumbar region of your spine, your lower back. The operation is called a lumbar spinal fusion.
.org. Herniated Disk in the Lower Back. Anatomy. Description
 Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
Rehabilitation. Rehabilitation. Walkers, Crutches, Canes
 Walkers, Crutches, Canes These devices provide support through your arms to limit the amount of weight on your operated hip. Initially, after a total hip replacement you will use a walker to get around.
Walkers, Crutches, Canes These devices provide support through your arms to limit the amount of weight on your operated hip. Initially, after a total hip replacement you will use a walker to get around.
Anterior Cervical Discectomy and Fusion
 A Patient s Guide to Anterior Cervical Discectomy and Fusion 651 Old Country Road Plainview, NY 11803 Phone: 5166818822 Fax: 5166813332 p.lettieri@aol.com DISCLAIMER: The information in this booklet is
A Patient s Guide to Anterior Cervical Discectomy and Fusion 651 Old Country Road Plainview, NY 11803 Phone: 5166818822 Fax: 5166813332 p.lettieri@aol.com DISCLAIMER: The information in this booklet is
Total Hip Replacement Surgery Home Care Instructions
 Total Hip Replacement Surgery Home Care Instructions Surgery: Date: Doctor: This handout will review the care you need to follow once you are home. If you have any questions or concerns, please ask your
Total Hip Replacement Surgery Home Care Instructions Surgery: Date: Doctor: This handout will review the care you need to follow once you are home. If you have any questions or concerns, please ask your
Patient Information. Anterior Cervical Surgery. Here to help. Respond Deliver & Enable
 Here to help Our Health Information Centre (HIC) provides advice and information on a wide range of health-related topics. We also offer: Services for people with disabilities. Information in large print,
Here to help Our Health Information Centre (HIC) provides advice and information on a wide range of health-related topics. We also offer: Services for people with disabilities. Information in large print,
Patient Information. Lumbar Spine Segmental Decompression. Royal Devon and Exeter NHS Foundation Trust
 Lumbar Spine Segmental Decompression Royal Devon and Exeter NHS Foundation Trust Patient Information Lumbar Spine Segmental Decompression Reference Number: TO 05 004 004 (version date: June 2015) Introduction
Lumbar Spine Segmental Decompression Royal Devon and Exeter NHS Foundation Trust Patient Information Lumbar Spine Segmental Decompression Reference Number: TO 05 004 004 (version date: June 2015) Introduction
Knee Arthroscopy Post-operative Instructions
 Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Knee Arthroscopy Post-operative Instructions PLEASE READ ALL OF THESE INSTRUCTIONS CAREFULLY. THEY WILL ANSWER MOST OF YOUR QUESTIONS. 1. You may walk
Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Knee Arthroscopy Post-operative Instructions PLEASE READ ALL OF THESE INSTRUCTIONS CAREFULLY. THEY WILL ANSWER MOST OF YOUR QUESTIONS. 1. You may walk
OPERATION:... Proximal tibial osteotomy Distal femoral osteotomy
 AFFIX PATIENT DETAIL STICKER HERE Forename.. Surname NHS Organisation. Responsible surgeon. Job Title Hospital Number... D.O.B.././ No special requirements OPERATION:..... Proximal tibial osteotomy Distal
AFFIX PATIENT DETAIL STICKER HERE Forename.. Surname NHS Organisation. Responsible surgeon. Job Title Hospital Number... D.O.B.././ No special requirements OPERATION:..... Proximal tibial osteotomy Distal
Spine Surgery - Wallis Ligament Stabilisation
 Spine Surgery - Wallis Ligament Stabilisation An Information Leaflet Physiotherapy Department 0161 419 4060 August 2011 Every Patient Matters TO47 2 Introduction This booklet has been compiled by the physiotherapy
Spine Surgery - Wallis Ligament Stabilisation An Information Leaflet Physiotherapy Department 0161 419 4060 August 2011 Every Patient Matters TO47 2 Introduction This booklet has been compiled by the physiotherapy
Lumbar or Thoracic Decompression and Fusion
 Lumbar or Thoracic Decompression and Fusion DO NOT TAKE ANY ASPIRIN PRODUCTS OR NON-STEROIDAL ANTI- INFLAMMATORY DRUGS (ie NSAIDs, Advil, Celebrex, Ibuprofen, Motrin, Naprosyn, Aleve, etc) FOR 2 WEEKS
Lumbar or Thoracic Decompression and Fusion DO NOT TAKE ANY ASPIRIN PRODUCTS OR NON-STEROIDAL ANTI- INFLAMMATORY DRUGS (ie NSAIDs, Advil, Celebrex, Ibuprofen, Motrin, Naprosyn, Aleve, etc) FOR 2 WEEKS
Femoral artery bypass graft (Including femoral crossover graft)
 Femoral artery bypass graft (Including femoral crossover graft) Why do I need the operation? You have a blockage or narrowing of the arteries supplying blood to your leg. This reduces the blood flow to
Femoral artery bypass graft (Including femoral crossover graft) Why do I need the operation? You have a blockage or narrowing of the arteries supplying blood to your leg. This reduces the blood flow to
Lumbar or Thoracic Fusion +/- Decompression
 Lumbar or Thoracic Fusion +/- Decompression PLEASE DO NOT TAKE ANY NON-STEROIDAL ANTI-INFLAMMATORY DRUGS (NSAIDs like Advil, Celebrex, Ibuprofen, Motrin, Vioxx, Naprosyn, Aleve, etc) OR ASPIRIN PRODUCTS
Lumbar or Thoracic Fusion +/- Decompression PLEASE DO NOT TAKE ANY NON-STEROIDAL ANTI-INFLAMMATORY DRUGS (NSAIDs like Advil, Celebrex, Ibuprofen, Motrin, Vioxx, Naprosyn, Aleve, etc) OR ASPIRIN PRODUCTS
Open Discectomy. North American Spine Society Public Education Series
 Open Discectomy North American Spine Society Public Education Series What Is Open Discectomy? Open discectomy is the most common surgical treatment for ruptured or herniated discs of the lumbar spine.
Open Discectomy North American Spine Society Public Education Series What Is Open Discectomy? Open discectomy is the most common surgical treatment for ruptured or herniated discs of the lumbar spine.
Hip Replacement. Department of Orthopaedic Surgery Tel: 01473 702107
 Information for Patients Hip Replacement Department of Orthopaedic Surgery Tel: 01473 702107 DMI ref: 0134-08.indd(RP) Issue 3: February 2008 The Ipswich Hospital NHS Trust, 2005-2008. All rights reserved.
Information for Patients Hip Replacement Department of Orthopaedic Surgery Tel: 01473 702107 DMI ref: 0134-08.indd(RP) Issue 3: February 2008 The Ipswich Hospital NHS Trust, 2005-2008. All rights reserved.
total hip replacement
 total hip replacement EXCERCISE BOOKLET patient s name: date of surgery: physical therapist: www.jointpain.md Get Up and Go Joint Program Philosophy: With the development of newer and more sophisticated
total hip replacement EXCERCISE BOOKLET patient s name: date of surgery: physical therapist: www.jointpain.md Get Up and Go Joint Program Philosophy: With the development of newer and more sophisticated
PHYSIOTHERAPY OF HIP AND KNEE AFTER SURGERY AND INJURY BY RACHEL GEVELL PHYSIOTHERAPIST
 PHYSIOTHERAPY OF HIP AND KNEE AFTER SURGERY AND INJURY BY RACHEL GEVELL PHYSIOTHERAPIST AIMS AND OBJECTIVES To demonstrate the use of physiotherapy assessment and treatment following: Hip Arthroplasty
PHYSIOTHERAPY OF HIP AND KNEE AFTER SURGERY AND INJURY BY RACHEL GEVELL PHYSIOTHERAPIST AIMS AND OBJECTIVES To demonstrate the use of physiotherapy assessment and treatment following: Hip Arthroplasty
Premier Orthopaedic Pathway. Physiotherapy after dynamic hip screw (DHS)
 Premier Orthopaedic Pathway Physiotherapy after dynamic hip screw (DHS) The surgery After a fractured hip a dynamic hip screw (DHS) is used to hold the bones in place while the fracture heals. It allows
Premier Orthopaedic Pathway Physiotherapy after dynamic hip screw (DHS) The surgery After a fractured hip a dynamic hip screw (DHS) is used to hold the bones in place while the fracture heals. It allows
Rehabilitation. Rehabilitation. Walking after Total Knee Replacement. Continuous Passive Motion Device
 Walking after Total Knee Replacement After your TKR, continue using your walker or crutches until your surgeons tells you it is okay to stop using them. When turning with a walker or crutches DO NOT PIVOT
Walking after Total Knee Replacement After your TKR, continue using your walker or crutches until your surgeons tells you it is okay to stop using them. When turning with a walker or crutches DO NOT PIVOT
Coccydynia. (Coccyx Pain) Information for patients. Outpatients Physiotherapy Tel: 01473 703312
 Information for patients Coccydynia (Coccyx Pain) Outpatients Physiotherapy Tel: 01473 703312 DPS ref: 4508-12(RP) Issue 1: February 2013 Review date: January 2016 The Ipswich Hospital NHS Trust, 2013.
Information for patients Coccydynia (Coccyx Pain) Outpatients Physiotherapy Tel: 01473 703312 DPS ref: 4508-12(RP) Issue 1: February 2013 Review date: January 2016 The Ipswich Hospital NHS Trust, 2013.
Total knee replacement: The enhanced recovery programme
 INFORMATION FOR PATIENTS Total knee replacement: The enhanced recovery programme Aim This leaflet aims to explain the enhanced recovery programme after total knee replacement surgery, and outline what
INFORMATION FOR PATIENTS Total knee replacement: The enhanced recovery programme Aim This leaflet aims to explain the enhanced recovery programme after total knee replacement surgery, and outline what
Varicose Vein Surgery
 Information for patients Varicose Vein Surgery Northern General Hospital You have been diagnosed as having varicose veins and your specialist has recommended varicose vein surgery. This leaflet explains
Information for patients Varicose Vein Surgery Northern General Hospital You have been diagnosed as having varicose veins and your specialist has recommended varicose vein surgery. This leaflet explains
Total Hip Replacement
 NOTES Total Hip Replacement QUESTIONS DATES PHONE NOS. Compiled by Mr John F Nolan FRCS for The British Hip Society 2009. A patient s information booklet 16 1 Introduction This booklet has been produced
NOTES Total Hip Replacement QUESTIONS DATES PHONE NOS. Compiled by Mr John F Nolan FRCS for The British Hip Society 2009. A patient s information booklet 16 1 Introduction This booklet has been produced
Ankle Arthroscopy and Follow-Up Physiotherapy
 Ankle Arthroscopy and Follow-Up Physiotherapy Exceptional healthcare, personally delivered Following your consultation with a member of the Foot and Ankle team you have agreed that you might benefit from
Ankle Arthroscopy and Follow-Up Physiotherapy Exceptional healthcare, personally delivered Following your consultation with a member of the Foot and Ankle team you have agreed that you might benefit from
Knee Arthroscopy Exercise Programme
 Chester Knee Clinic & Cartilage Repair Centre Nuffield Health, The Grosvenor Hospital Chester Wrexham Road Chester CH4 7QP Hospital Telephone: 01244 680 444 CKC Website: www.kneeclinic.info Email: office@kneeclinic.info
Chester Knee Clinic & Cartilage Repair Centre Nuffield Health, The Grosvenor Hospital Chester Wrexham Road Chester CH4 7QP Hospital Telephone: 01244 680 444 CKC Website: www.kneeclinic.info Email: office@kneeclinic.info
Inguinal Hernia (Female)
 Inguinal Hernia (Female) WHAT IS AN INGUINAL HERNIA? 2 WHAT CAUSES AN INGUINAL HERNIA? 2 WHAT DOES TREATMENT / MANAGEMENT INVOLVE? 3 DAY SURGERY MANAGEMENT 3 SURGICAL REPAIR 4 WHAT ARE THE RISKS/COMPLICATIONS
Inguinal Hernia (Female) WHAT IS AN INGUINAL HERNIA? 2 WHAT CAUSES AN INGUINAL HERNIA? 2 WHAT DOES TREATMENT / MANAGEMENT INVOLVE? 3 DAY SURGERY MANAGEMENT 3 SURGICAL REPAIR 4 WHAT ARE THE RISKS/COMPLICATIONS
Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865
 Write questions or notes here: Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865 Document Title: Revision Total Hip Replacement Further Information and Feedback: Tell us how
Write questions or notes here: Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865 Document Title: Revision Total Hip Replacement Further Information and Feedback: Tell us how
Total Abdominal Hysterectomy
 What is a total abdominal hysterectomy? Is the removal of the uterus and cervix through an abdominal incision (either an up and down or bikini cut). Removal of the ovaries and tubes depends on the patient.
What is a total abdominal hysterectomy? Is the removal of the uterus and cervix through an abdominal incision (either an up and down or bikini cut). Removal of the ovaries and tubes depends on the patient.
Hip arthroscopy Frequently Asked Questions
 Hip arthroscopy Frequently Asked Questions What is a hip arthroscopy? Hip arthroscopy is key hole surgery. Usually 2-3 small incisions (about 1 cm long) are made on the side of your hip. Through these
Hip arthroscopy Frequently Asked Questions What is a hip arthroscopy? Hip arthroscopy is key hole surgery. Usually 2-3 small incisions (about 1 cm long) are made on the side of your hip. Through these
TIPS and EXERCISES for your knee stiffness. and pain
 TIPS and EXERCISES for your knee stiffness and pain KNEE EXERCISES Range of motion exercise 3 Knee bending exercises 3 Knee straightening exercises 5 STRENGTHENING EXERCISES 6 AEROBIC EXERCISE 10 ADDITIONAL
TIPS and EXERCISES for your knee stiffness and pain KNEE EXERCISES Range of motion exercise 3 Knee bending exercises 3 Knee straightening exercises 5 STRENGTHENING EXERCISES 6 AEROBIC EXERCISE 10 ADDITIONAL
Primary and revision lumbar discectomy. (nerve root decompression)
 Primary and revision lumbar discectomy (nerve root decompression) The aim of this leaflet is to help answer some of the questions you may have about having a lumbar discectomy. It explains the benefits,
Primary and revision lumbar discectomy (nerve root decompression) The aim of this leaflet is to help answer some of the questions you may have about having a lumbar discectomy. It explains the benefits,
Returning to fitness after heart surgery
 Returning to fitness after heart surgery A patient s guide 1 Increasing activity After your operation, your heart function should be improved and so your ability to exercise will also be improved. However,
Returning to fitness after heart surgery A patient s guide 1 Increasing activity After your operation, your heart function should be improved and so your ability to exercise will also be improved. However,
Guidelines for Patients having a. Total Knee Replacement
 Guidelines for Patients having a Total Knee Replacement contents introduction Introduction 3 What is a Total Knee Replacement? 4 Potential Complications 5 Preparing for Admission Checklist 7 Manage Your
Guidelines for Patients having a Total Knee Replacement contents introduction Introduction 3 What is a Total Knee Replacement? 4 Potential Complications 5 Preparing for Admission Checklist 7 Manage Your
Total Vaginal Hysterectomy with an Anterior and Posterior Repair
 Total Vaginal Hysterectomy with an Anterior and Posterior Repair What is a total vaginal hysterectomy with an anterior and posterior repair? Total vaginal hysterectomy is the removal of the uterus and
Total Vaginal Hysterectomy with an Anterior and Posterior Repair What is a total vaginal hysterectomy with an anterior and posterior repair? Total vaginal hysterectomy is the removal of the uterus and
Herniated Disk. This reference summary explains herniated disks. It discusses symptoms and causes of the condition, as well as treatment options.
 Herniated Disk Introduction Your backbone, or spine, has 24 moveable vertebrae made of bone. Between the bones are soft disks filled with a jelly-like substance. These disks cushion the vertebrae and keep
Herniated Disk Introduction Your backbone, or spine, has 24 moveable vertebrae made of bone. Between the bones are soft disks filled with a jelly-like substance. These disks cushion the vertebrae and keep
Total knee replacement
 Patient Information to be retained by patient What is a total knee replacement? In a total knee replacement the cartilage surfaces of the thigh bone (femur) and leg bone (tibia) are replaced. The cartilage
Patient Information to be retained by patient What is a total knee replacement? In a total knee replacement the cartilage surfaces of the thigh bone (femur) and leg bone (tibia) are replaced. The cartilage
A Patient s Guide to Lateral Ligament Reconstruction of the Ankle
 A Patient s Guide to Lateral Ligament Reconstruction of the Ankle The Foot and Ankle unit at the Royal National Orthopaedic Hospital (RNOH) is a multi-disciplinary team. The team consists of three specialist
A Patient s Guide to Lateral Ligament Reconstruction of the Ankle The Foot and Ankle unit at the Royal National Orthopaedic Hospital (RNOH) is a multi-disciplinary team. The team consists of three specialist
This is my information booklet: Introduction
 Hip arthroscopy is a relatively new procedure which allows the surgeon to diagnose and treat hip disorders by providing a clear view of the inside of the hip with very small incisions. This is a more complicated
Hip arthroscopy is a relatively new procedure which allows the surgeon to diagnose and treat hip disorders by providing a clear view of the inside of the hip with very small incisions. This is a more complicated
Herniated Disk in the Lower Back
 Nader M. Hebela, MD Fellow of the American Academy of Orthopaedic Surgeons http://orthodoc.aaos.org/hebela Cleveland Clinic Abu Dhabi Cleveland Clinic Abu Dhabi Neurological Institute Al Maryah Island
Nader M. Hebela, MD Fellow of the American Academy of Orthopaedic Surgeons http://orthodoc.aaos.org/hebela Cleveland Clinic Abu Dhabi Cleveland Clinic Abu Dhabi Neurological Institute Al Maryah Island
Surgery for Disc Prolapse
 Contact Details Spinal Team Nuffield Orthopaedic Centre Windmill Road Headington Oxford OX3 7LD Surgery for Disc Prolapse Phone: 01865 738051 Fax: 01865 738027 Web Site www.noc.nhs.uk Surgery for disc
Contact Details Spinal Team Nuffield Orthopaedic Centre Windmill Road Headington Oxford OX3 7LD Surgery for Disc Prolapse Phone: 01865 738051 Fax: 01865 738027 Web Site www.noc.nhs.uk Surgery for disc
A Patient s Guide to Arthritis of the Big Toe (Hallux Rigidus) With Discussion on Cheilectomy and Fusion
 A Patient s Guide to Arthritis of the Big Toe (Hallux Rigidus) With Discussion on Cheilectomy and Fusion The foot and ankle unit at the Royal National Orthopaedic Hospital (RNOH) is a multi-disciplinary
A Patient s Guide to Arthritis of the Big Toe (Hallux Rigidus) With Discussion on Cheilectomy and Fusion The foot and ankle unit at the Royal National Orthopaedic Hospital (RNOH) is a multi-disciplinary
ANTERIOR CERVICAL DECOMPRESSION AND FUSION
 ANTERIOR CERVICAL DECOMPRESSION AND FUSION NOTE: PLEASE DO NOT TAKE ANY NON-STEROIDAL ANTI-INFLAMMATORY DRUGS (NSAIDs like Advil, Celebrex, Ibuprofen, Motrin, Vioxx, etc) OR ASPIRIN PRODUCTS FOR 2 WEEKS
ANTERIOR CERVICAL DECOMPRESSION AND FUSION NOTE: PLEASE DO NOT TAKE ANY NON-STEROIDAL ANTI-INFLAMMATORY DRUGS (NSAIDs like Advil, Celebrex, Ibuprofen, Motrin, Vioxx, etc) OR ASPIRIN PRODUCTS FOR 2 WEEKS
.org. Fractures of the Thoracic and Lumbar Spine. Cause. Description
 Fractures of the Thoracic and Lumbar Spine Page ( 1 ) Spinal fractures can vary widely in severity. While some fractures are very serious injuries that require emergency treatment, other fractures can
Fractures of the Thoracic and Lumbar Spine Page ( 1 ) Spinal fractures can vary widely in severity. While some fractures are very serious injuries that require emergency treatment, other fractures can
Surgical removal of fibroids through an abdominal incision-either up and down or bikini cut. The uterus and cervix are left in place.
 What is an abdominal myomectomy? Surgical removal of fibroids through an abdominal incision-either up and down or bikini cut. The uterus and cervix are left in place. When is this surgery used? Treatment
What is an abdominal myomectomy? Surgical removal of fibroids through an abdominal incision-either up and down or bikini cut. The uterus and cervix are left in place. When is this surgery used? Treatment
Broström Lateral Ligament Reconstruction of Ankle
 Broström Lateral Ligament Reconstruction of Ankle This leaflet aims to answer your questions about having a broström lateral ligament reconstruction of ankle under the care of Mr Sam Singh. It explains
Broström Lateral Ligament Reconstruction of Ankle This leaflet aims to answer your questions about having a broström lateral ligament reconstruction of ankle under the care of Mr Sam Singh. It explains
Contents. Overview. Removing the womb (hysterectomy) Overview
 This information is an extract from the booklet Understanding womb (endometrial) cancer. You may find the full booklet helpful. We can send you a free copy see page 9. Overview Contents Overview Removing
This information is an extract from the booklet Understanding womb (endometrial) cancer. You may find the full booklet helpful. We can send you a free copy see page 9. Overview Contents Overview Removing
Total Vaginal Hysterectomy
 What is a total vaginal hysterectomy? Is the removal of the uterus and cervix through the vagina. Removal of the ovaries and tubes depends on the patient. Why is this surgery used? To treat disease of
What is a total vaginal hysterectomy? Is the removal of the uterus and cervix through the vagina. Removal of the ovaries and tubes depends on the patient. Why is this surgery used? To treat disease of
Anterior Cervical Decompression and Fusion or Anterior Cervical Corpectomy and Fusion
 Anterior Cervical Decompression and Fusion or Anterior Cervical Corpectomy and Fusion DO NOT TAKE ANY ASPIRIN PRODUCTS OR NON-STEROIDAL ANTI- INFLAMMATORY DRUGS (ie NSAIDs, Advil, Celebrex, Ibuprofen,
Anterior Cervical Decompression and Fusion or Anterior Cervical Corpectomy and Fusion DO NOT TAKE ANY ASPIRIN PRODUCTS OR NON-STEROIDAL ANTI- INFLAMMATORY DRUGS (ie NSAIDs, Advil, Celebrex, Ibuprofen,
Patient Guide to Lower Back Surgery
 The following is a sampling of products offered by Zimmer Spine for use in Open Lumbar Fusion procedures. Patient Guide to Lower Back Surgery Open Lumbar Fusion Dynesys The Dynesys Dynamic Stabilization
The following is a sampling of products offered by Zimmer Spine for use in Open Lumbar Fusion procedures. Patient Guide to Lower Back Surgery Open Lumbar Fusion Dynesys The Dynesys Dynamic Stabilization
What is the function of the spinal column?
 What is the function of the spinal column? Stability The function of the human spinal column is above all to stabilise the head, the upper body, and walking upright. Primarily responsible for this are
What is the function of the spinal column? Stability The function of the human spinal column is above all to stabilise the head, the upper body, and walking upright. Primarily responsible for this are
A Healthy Lumbar Spine... 2. A Problem Lumbar Spine... 3. Understanding Your Surgery... 4. Preparing for Surgery... 5. Day of Surgery...
 Table of Contents A Healthy Lumbar Spine................. 2 A Problem Lumbar Spine................. 3 Understanding Your Surgery.............. 4 Preparing for Surgery.................... 5 Day of Surgery.........................
Table of Contents A Healthy Lumbar Spine................. 2 A Problem Lumbar Spine................. 3 Understanding Your Surgery.............. 4 Preparing for Surgery.................... 5 Day of Surgery.........................
Elbow arthroscopy. Key points
 Patient information Elbow arthroscopy This information has been produced to help you gain the maximum benefit and understanding of your operation. It includes the following information: Key points About
Patient information Elbow arthroscopy This information has been produced to help you gain the maximum benefit and understanding of your operation. It includes the following information: Key points About
Herniated Lumbar Disc
 Herniated Lumbar Disc North American Spine Society Public Education Series What Is a Herniated Disc? The spine is made up of a series of connected bones called vertebrae. The disc is a combination of strong
Herniated Lumbar Disc North American Spine Society Public Education Series What Is a Herniated Disc? The spine is made up of a series of connected bones called vertebrae. The disc is a combination of strong
Spinal Discectomy & Decompression Surgery
 1.0 Policy Statement... 2 2.0 Purpose... 2 3.0 Scope... 2 4.0 Health & Safety... 2 5.0 Responsibilities... 2 6.0 Definitions and Abbreviations... 3 7.0 Guideline... 3 7.1 Pre-Operative... 3 7.2 Post-Operative...
1.0 Policy Statement... 2 2.0 Purpose... 2 3.0 Scope... 2 4.0 Health & Safety... 2 5.0 Responsibilities... 2 6.0 Definitions and Abbreviations... 3 7.0 Guideline... 3 7.1 Pre-Operative... 3 7.2 Post-Operative...
BRYAN. Cervical Disc System. Patient Information
 BRYAN Cervical Disc System Patient Information 3 BRYAN Cervical Disc System PATIENT INFORMATION BRYAN Cervical Disc System PATIENT INFORMATION 1 BRYAN Cervical Disc System This patient information brochure
BRYAN Cervical Disc System Patient Information 3 BRYAN Cervical Disc System PATIENT INFORMATION BRYAN Cervical Disc System PATIENT INFORMATION 1 BRYAN Cervical Disc System This patient information brochure
Physical & Occupational Therapy
 In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
Varicose Veins Operation. Patient information Leaflet
 Varicose Veins Operation Patient information Leaflet 22 nd August 2014 WHAT IS VARICOSE VEIN SURGERY (HIGH LIGATION AND MULTIPLE AVULSIONS) The operation varies from case to case, depending on where the
Varicose Veins Operation Patient information Leaflet 22 nd August 2014 WHAT IS VARICOSE VEIN SURGERY (HIGH LIGATION AND MULTIPLE AVULSIONS) The operation varies from case to case, depending on where the
Hysterectomy Vaginal hysterectomy Abdominal hysterectomy
 Hysterectomy A hysterectomy is a surgery to remove a woman s uterus. The uterus is one of the organs of the female reproductive system and is about the size of a closed hand. You can no longer have children
Hysterectomy A hysterectomy is a surgery to remove a woman s uterus. The uterus is one of the organs of the female reproductive system and is about the size of a closed hand. You can no longer have children
Anterior cervical surgery
 Anterior cervical surgery The aim of this leaflet is to help answer some of the questions you may have about having anterior cervical surgery. It explains the benefits, risks and alternatives of the procedure
Anterior cervical surgery The aim of this leaflet is to help answer some of the questions you may have about having anterior cervical surgery. It explains the benefits, risks and alternatives of the procedure
Total hip replacement
 Patient Information to be retained by patient What is a total hip replacement? In a total hip replacement both the ball (femoral or thigh bone) side of the hip joint and the socket (acetabular or pelvic
Patient Information to be retained by patient What is a total hip replacement? In a total hip replacement both the ball (femoral or thigh bone) side of the hip joint and the socket (acetabular or pelvic
Lumbar Decompression and Stabilisation for Degenerative Spondylolisthesis
 Lumbar Decompression and Stabilisation for Degenerative Spondylolisthesis Spinal Unit Tel: 01473 702032 or 702097 Issue 5: August 2014 Review date: July 2017 Following your recent investigations and consultation
Lumbar Decompression and Stabilisation for Degenerative Spondylolisthesis Spinal Unit Tel: 01473 702032 or 702097 Issue 5: August 2014 Review date: July 2017 Following your recent investigations and consultation
Arthritis of the hip. Normal hip In an x-ray of a normal hip, the articular cartilage (the area labeled normal joint space ) is clearly visible.
 Arthritis of the hip Arthritis of the hip is a condition in which the smooth gliding surfaces of your hip joint (articular cartilage) have become damaged. This usually results in pain, stiffness, and reduced
Arthritis of the hip Arthritis of the hip is a condition in which the smooth gliding surfaces of your hip joint (articular cartilage) have become damaged. This usually results in pain, stiffness, and reduced
Cast removal what to expect #3 Patient Information Leaflet
 Cast removal what to expect #3 Patient Information Leaflet SM466 Now your cast is off, self help is the key! Follow the advice given to you by your doctor and the staff in the clinic. Your skin will be
Cast removal what to expect #3 Patient Information Leaflet SM466 Now your cast is off, self help is the key! Follow the advice given to you by your doctor and the staff in the clinic. Your skin will be
Enhanced recovery programme (ERP) for patients undergoing bowel surgery
 Enhanced recovery programme (ERP) for patients undergoing bowel surgery Information for patients, relatives and carers An enhanced recovery programme (ERP) has been established at Imperial College Healthcare
Enhanced recovery programme (ERP) for patients undergoing bowel surgery Information for patients, relatives and carers An enhanced recovery programme (ERP) has been established at Imperial College Healthcare
Information for the Patient About Surgical
 Information for the Patient About Surgical Decompression and Stabilization of the Spine Aging and the Spine Daily wear and tear, along with disc degeneration due to aging and injury, are common causes
Information for the Patient About Surgical Decompression and Stabilization of the Spine Aging and the Spine Daily wear and tear, along with disc degeneration due to aging and injury, are common causes
Before Surgery You will likely be asked to see your family physician or an internal medicine doctor for a thorough medical evaluation.
 Anterior Hip Replacement - Before and After Surgery Your Hip Evaluation An orthopaedic surgeon specializes in problems affecting bones and joints. The surgeon will ask you many questions about your hip
Anterior Hip Replacement - Before and After Surgery Your Hip Evaluation An orthopaedic surgeon specializes in problems affecting bones and joints. The surgeon will ask you many questions about your hip
Femoral Hernia Repair
 Femoral Hernia Repair WHAT IS A FEMORAL HERNIA REPAIR? 2 WHAT CAUSES A FEMORAL HERNIA? 2 WHAT DOES TREATMENT/ MANAGEMENT INVOLVE? 3 DAY SURGERY MANAGEMENT 3 SURGICAL REPAIR 4 WHAT ARE THE RISKS/COMPLICATIONS
Femoral Hernia Repair WHAT IS A FEMORAL HERNIA REPAIR? 2 WHAT CAUSES A FEMORAL HERNIA? 2 WHAT DOES TREATMENT/ MANAGEMENT INVOLVE? 3 DAY SURGERY MANAGEMENT 3 SURGICAL REPAIR 4 WHAT ARE THE RISKS/COMPLICATIONS
Achilles Tendon Repair Surgery Post-operative Instructions Phase One: The First Week After Surgery
 Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Achilles Tendon Repair Surgery Post-operative Instructions Phase One: The First Week After Surgery Amon T. Ferry, MD Orthopedic Surgery / Sports Medicine
Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Achilles Tendon Repair Surgery Post-operative Instructions Phase One: The First Week After Surgery Amon T. Ferry, MD Orthopedic Surgery / Sports Medicine
Rehabilitation guidelines for patients undergoing knee arthroscopy
 Rehabilitation guidelines for patients undergoing knee arthroscopy At the RNOH, our emphasis is patient specific, which encourages recognition of those who may progress slower then others. We also want
Rehabilitation guidelines for patients undergoing knee arthroscopy At the RNOH, our emphasis is patient specific, which encourages recognition of those who may progress slower then others. We also want
Hip Replacement Surgery Understanding the Risks
 Hip Replacement Surgery Understanding the Risks Understanding the Risks of Hip Replacement Surgery Introduction This booklet is designed to help your doctor talk to you about the most common risks you
Hip Replacement Surgery Understanding the Risks Understanding the Risks of Hip Replacement Surgery Introduction This booklet is designed to help your doctor talk to you about the most common risks you
Physiotherapy for Video Assisted Thoracic Surgery Patients
 Physio for VATS patients Royal Devon and Exeter NHS Foundation Trust Physiotherapy for Video Assisted Thoracic Surgery Patients July 2008 (Review date: July 2011) Physiotherapy Department...01392 402438
Physio for VATS patients Royal Devon and Exeter NHS Foundation Trust Physiotherapy for Video Assisted Thoracic Surgery Patients July 2008 (Review date: July 2011) Physiotherapy Department...01392 402438
Excision of Vaginal Mesh
 What is excision of vaginal mesh? This procedure is done to remove mesh from the vagina. When is this surgery used? If mesh has eroded into the vagina, bladder, urethra, or bowel If there is pain associated
What is excision of vaginal mesh? This procedure is done to remove mesh from the vagina. When is this surgery used? If mesh has eroded into the vagina, bladder, urethra, or bowel If there is pain associated
Surgery for cervical disc prolapse or cervical osteophyte
 Mr Paul S. D Urso MBBS(Hons), PhD, FRACS Neurosurgeon Provider Nº: 081161DY Epworth Centre Suite 6.1 32 Erin Street Richmond 3121 Tel: 03 9421 5844 Fax: 03 9421 4186 AH: 03 9483 4040 email: paul@pauldurso.com
Mr Paul S. D Urso MBBS(Hons), PhD, FRACS Neurosurgeon Provider Nº: 081161DY Epworth Centre Suite 6.1 32 Erin Street Richmond 3121 Tel: 03 9421 5844 Fax: 03 9421 4186 AH: 03 9483 4040 email: paul@pauldurso.com
Neck Injuries and Disorders
 Neck Injuries and Disorders Introduction Any part of your neck can be affected by neck problems. These affect the muscles, bones, joints, tendons, ligaments or nerves in the neck. There are many common
Neck Injuries and Disorders Introduction Any part of your neck can be affected by neck problems. These affect the muscles, bones, joints, tendons, ligaments or nerves in the neck. There are many common
Recto-vaginal Fistula Repair
 What is a recto-vaginal fistula repair? Rectovaginal fistula repair is a procedure in which the healthy tissue between the rectum and vagina is closed in multiple tissue layers. An incision is made either
What is a recto-vaginal fistula repair? Rectovaginal fistula repair is a procedure in which the healthy tissue between the rectum and vagina is closed in multiple tissue layers. An incision is made either
You will be having surgery to remove a tumour(s) from your liver.
 Liver surgery You will be having surgery to remove a tumour(s) from your liver. This handout will help you learn about the surgery, how to prepare for surgery and your care after surgery. Surgery can be
Liver surgery You will be having surgery to remove a tumour(s) from your liver. This handout will help you learn about the surgery, how to prepare for surgery and your care after surgery. Surgery can be
Tibial Intramedullary Nailing
 Tibial Intramedullary Nailing Turnberg Building Orthopaedics 0161 206 4898 All Rights Reserved 2015. Document for issue as handout. Procedure The tibia is the long shin bone in the lower leg. It is a weight
Tibial Intramedullary Nailing Turnberg Building Orthopaedics 0161 206 4898 All Rights Reserved 2015. Document for issue as handout. Procedure The tibia is the long shin bone in the lower leg. It is a weight
X-Plain Hip Replacement Surgery - Preventing Post Op Complications Reference Summary
 X-Plain Hip Replacement Surgery - Preventing Post Op Complications Reference Summary Introduction Severe arthritis in the hip can lead to severe pain and inability to walk. To relieve the pain and improve
X-Plain Hip Replacement Surgery - Preventing Post Op Complications Reference Summary Introduction Severe arthritis in the hip can lead to severe pain and inability to walk. To relieve the pain and improve
KNEE ARTHROSCOPY. Dr C.S. Waller. Orthopaedic Surgeon
 KNEE ARTHROSCOPY Dr C.S. Waller Orthopaedic Surgeon Specializing in surgery of the hip and knee 83826199 What is Arthroscopy? Arthroscopy involves the inspection of the inside of the knee joint with a
KNEE ARTHROSCOPY Dr C.S. Waller Orthopaedic Surgeon Specializing in surgery of the hip and knee 83826199 What is Arthroscopy? Arthroscopy involves the inspection of the inside of the knee joint with a
