Part 1 of 4: Overview of Restless Legs Syndrome
|
|
|
- Laura Stanley
- 7 years ago
- Views:
Transcription
1 SM Education Initiative in Neurology Release Date: November 17, Termination Date: January 31, Estimated time to complete Part 1: 15 minutes. Estimated time to complete this 4-part newsletter series: 1 hour. For additional updates, go to Stilling the Nighttime Intruder: Innovations in Treatment of Restless Legs Syndrome (RLS) Part 1 of 4: Overview of Restless Legs Syndrome Dear Colleague: According to the Restless Legs Foundation, despite its offbeat name, RLS is a debilitating neurologic disorder that can lead to depression and even suicide that afflicts almost 8% of the US population. Yet, only a small proportion of affected individuals seek medical care for their problem and even fewer are correctly diagnosed. People with RLS are typically sleep deprived, with profound negative effects on quality of life. Ironically, with medication RLS symptoms can be controlled for the great majority of affected individuals. This is the first of a series of four Treatment Reporters on RLS. This issue presents an overview of RLS, including diagnostic criteria, epidemiology, differential diagnosis, and burden of illness. Upcoming issues will focus on specific suggestions regarding the key clinical steps for evaluating the patient suspected of having RLS in the primary care setting. Hypotheses regarding RLS pathophysiology will be discussed and factors that may precipitate RLS will be reviewed. We will then present practical treatment strategies for patients with RLS, including special populations, such as children, pregnant women, and the elderly. We hope you find this series helpful and informative, and that the information presented can be incorporated into your clinical practice. Yours truly, Chair Arthur S. Walters, MD Staff Neurologist Director, Center for Sleep Disorders Treatment, Research & Education New Jersey Neuroscience Institute at JFK Medical Center Edison, New Jersey Professor, Department of Neuroscience Seton Hall University School of Graduate Medical Education South Orange, New Jersey Arthur S. Walters, MD Watch Your Mail for the Next Issue of Stilling the Nighttime Intruder: Innovations in Treatment of Restless Legs Syndrome (RLS) Download this 4-part series, Stilling the Nighttime Intruder: Innovations in Treatment of Restless Legs Syndrome (RLS), available at Overview of RLS Restless legs syndrome (RLS) is a troublesome neurologic disorder that is often underrecognized and mistreated. First described in 1672 and given its name in 1945, RLS has been defined as having four core features, all of which are necessary for diagnosis. 1,2 An urge to move the legs, usually accompanied or caused by uncomfortable and unpleasant sensations in the legs. (Sometimes the urge to move is present without the uncomfortable sensations and sometimes the arms or other body parts are involved in addition to the legs.) sensations begin or worsen during periods of rest or inactivity, such as lying down or sitting. sensations are partially or totally relieved by movement, such as walking or stretching, at least as long as the activity continues. sensations are worse in the evening or night than during the day or only occur in the evening or night. (When symptoms are very severe, the worsening at night may not be noticeable but must have been previously present.) Although approximately 15% of affected individuals do not experience any sensation, the majority of patients report sensations in their legs ranging from creepy, crawling, bubbling, to burning, tingling, or pain, resulting in a desire to move. Symptoms usually affect both legs simultaneously, but can be unilateral or alternating, and the arms are also involved in almost half of patients. 3,4 While symptoms may be worse at night, the key factors appear to be time of day and being supine, rather than sleep or darkness. About one fourth of patients with RLS experience symptoms on a daily basis. 5 RLS is frequently associated with two common secondary features: poor sleep and periodic limb movements of sleep (PLMS), which are repetitive, stereotypic, involuntary movements, primarily of the legs, that occur during sleep. Poor sleep is reported in almost 95% of RLS patients who experience difficulties in sleep initiation, maintenance, and efficiency. Eighty percent of RLS patients have PLMS (index >5 movements/h sleep). 4 Continued on page 2, column 2
2 REPORTER SM : NEUROLOGY Target Audience This activity is designed for neurologists, pulmonologists, sleep specialists, psychiatrists, and primary care providers who treat patients with restless legs syndrome. Activity Goal The goal of this 4-part activity is to educate clinicians on the epidemiology, diagnostic criteria, appropriate evaluation, and effective management of primary and secondary restless legs syndrome. Learning Objectives After completing this 4-part activity, the physician should be able to: Discuss the epidemiology of RLS and the burden of illness it imposes on patients and society. Identify the diagnostic criteria for restless legs syndrome, differentiate between primary and secondary RLS, and assess the presence of coexisting sleep disorders. Compare the effectiveness, risks, and benefits of various pharmacologic and nonpharmacologic RLS therapies. Summarize the differences in mechanisms of action of RLS therapies. Develop practical strategies for treating patients with RLS using pharmacologic and nonpharmacologic therapies. Tailor treatment strategies to special patient populations, including the elderly with co-morbid disease, pregnant women, and children. Statement of Accreditation Projects In Knowledge is accredited by the Accreditation Council for Continuing Medical Education to provide continuing medical education for physicians. Credit Designation Projects In Knowledge designates this educational activity for a maximum of 1.0 category 1 credit toward the AMA Physician s Recognition Award. Each physician should claim only those credits that he/she actually spent in the activity. Successful completion for 1.0 hour of CME credit requires a passing score of 70% or higher on all four posttests. Full instructions for submission are included on the posttest accompanying this CME newsletter. Disclosure Information The Disclosure Policy of Projects In Knowledge requires that faculty participating in a CME activity disclose to the audience: any significant relationship they may have with a pharmaceutical or medical equipment company, product, or service that may be mentioned as part of their presentation; any relationship with the commercial supporter of this activity; whether any drugs or products under discussion are unapproved for use or investigational, ongoing research, or preliminary data. Arthur S. Walters, MD, has received grant/research support from and is a consultant for GlaxoSmithKline. The opinions expressed in this four-part activity are those of the faculty and do not necessarily reflect those of Projects In Knowledge or the commercial supporter. This independent CME activity is planned and implemented in accordance with the ACCME Essential Areas and Policies. This CME activity is provided by Projects In Knowledge solely as an educational service. Specific patient care decisions are the responsibility of the physician caring for the patient. This independent CME activity is supported by an educational grant from GlaxoSmithKline. Copyright 2003, Projects In Knowledge, Inc. Little Falls, NJ All rights reserved. Similar involuntary movements can occur in RLS patients during wakefulness when the patient is lying down or sitting. PLMS, which frequently occur with arousals and contribute to sleep disturbance, usually affect the legs and either resemble the Babinski reflex or a triple flexion reflex affecting the ankle, knee, and hip. 3 Initially, symptoms may appear only occasionally but tend to become continuous and more severe with time. RLS can begin at any age, but most patients are middle to older age. In one study of 133 cases, the mean age for onset of RLS was 27.2 years and 43% of patients reported that their RLS symptoms began before age Interestingly, patients whose RLS symptoms begin during middle age or later tend to deteriorate more rapidly and seek medical attention sooner than those whose symptoms begin during childhood. RLS can be either primary or secondary. Primary RLS accounts for most cases and is believed to be of central nervous system origin. Secondary causes of RLS, some of which are potentially reversible, include iron-deficiency anemia, pregnancy, endstage renal disease, and medications. These causes will be discussed in greater detail in a later section of this Treatment Reporter. Burden of Illness RLS is a major cause of sleep disturbance. Patients with RLS suffer from insomnia and disrupted sleep, leading to daytime fatigue, poor functioning at home or on the job, and impaired social interactions. Their restlessness causes them to walk around for hours at night and they may find it difficult to remain sedentary in school, while traveling, or while attending the theater or movies. Patients often feel embarrassed or ashamed, and depression and anxiety secondary to sleep deprivation may arise. Epidemiology The prevalence of RLS in the adult population has been estimated as ranging from 5.5% to 15%. 6-8 Based on these estimates, between 11 million and 31 million American adults are affected by RLS symptoms. Of those, perhaps 1 out of 10 are affected seriously enough to need medical attention. RLS occurs about twice as frequently in women than men. 9 The prevalence of RLS also increases with age. In a study of 1800 people in Kentucky, RLS prevalence increased from 3% in the 18- to 29-year-old group, to 10% in the 30- to 79-year-old group, to 19% in those age 80 years and older. 7 RLS can occur in childhood and can be misdiagnosed as growing pains or attention-deficithyperactivity disorder (ADHD). 10,11 The prevalence of RLS in children and adolescents is currently unknown. Diagnosis and Work-Up of RLS RLS is underreported by patients and often misdiagnosed. For example, in a large multinational study of more than 23,000 people, less than half of the 2223 patients with RLS symptoms discussed the problem with their doctor and only 7.1% were actually diagnosed with RLS. 5 The diagnosis of RLS can be made on history alone, probing the four obligatory diagnostic features of RLS. A neurologic examination should be done to rule out secondary causes of RLS, such as peripheral neuropathy or radiculopathy. A serum ferritin level should be drawn. If the serum ferritin level is in the bottom 1/3 of normal (<50 µg/l), then iron supplementation should be considered. 2,3 Generally, referral to a sleep specialist is not necessary to make the diagnosis of RLS, although polysomnography (PSG) and the Suggested Immobilization Test (SIT) can be used to support the clinical diagnosis. Polysomnography may reveal PLMS, but PLMS are neither a sensitive nor specific enough indicator of RLS to be useful diagnostically. Only 80% of RLS patients have PLMS and PLMS are found in a high percentage of elderly individuals without RLS. PSG is warranted if there is clinical suspicion of sleep apnea or patients do not respond to RLS treatment. In the SIT, the patient sits in bed with his or her legs outstretched during wakefulness while electromyograms (EMG) are recorded from right and left anterior tibialis muscles for an hour. The patient is asked not to voluntarily move. The SIT records periodic limb movements in wakefulness. 12 Two rating scales have been developed for subjective rating of RLS symptom severity. One is a 10-point scale created by the International RLS Study Group that has been validated by comparison with independent clinician ratings in a large multicenter study. 13 The other, the Johns Hopkins Restless Legs Severity Scale, is a one-question test that focuses on the time of day symptoms appear. 14 Practically speaking, these assessment tools are used in research studies, but clinicians may find them useful for keeping track of therapeutic progress. Differential Diagnosis The most important differential diagnosis to consider is peripheral lesions, such as polyneuropathy and radiculopathy. Although peripheral neuropathy and radiculopathy may trigger RLS, the bulk of these patients do not have RLS. Although patients with peripheral neuropathy and radiculopathy may complain about paresthesias or painful sensations, those without RLS typically do not get relief of leg discomfort with activity. Nerve conduction or EMG studies may be informative for these patients. Sometimes RLS may be mistakenly misdiagnosed as leg cramps. Leg cramps are usually brief, intermittent, and severe with a localized spasm, while RLS tends 2
3 TREATMENT REPORTER Stilling the Nighttime Intruder: Innovations in Treatment of Restless Legs Syndrome (RLS) to last longer with no actual spasm. Neuroleptic-induced akathisia is also characterized by restless floor pacing. However, in neuroleptic-induced akathisia, movement is precipitated by an inner urge to move rather than the leg discomfort of RLS and, unlike RLS, there is no nighttime worsening of symptoms. Neurolepticinduced akathisia can be suspected if the patient has a history of neuroleptic use. Patients with positional pain, eg, due to arthritis of one hip, will get relief merely by shifting the weight from one hip to another while sitting and they are not compelled to walk, stretch the legs, or bend the legs as in RLS. Hypotensive akathisia and the syndrome known as Painful Legs and Moving Toes are rare conditions that can be distinguished from RLS. A comparison of these differential diagnoses and their distinguishing features from RLS are listed in Table 1. What Causes RLS? Pathophysiology The origin and pathophysiology of RLS are still under investigation. RLS is thought to result from a complex interaction between central and peripheral neurologic systems. Bara-Jimenez et al 15 observed that patients with RLS had evidence of enhanced spinal cord excitability compared with agematched controls, especially at night. Studies of cortical activity have failed to find evidence of a primary cortical involvement in RLS, and other studies suggest a subcortical dysfunction. 16 Functional MRI studies, paired transcranial magnetic stimulation studies, examination of the cortical silent period, examination of the flexor response, examination of the sequential activation of muscle groups, and evidence from spinal cord injury cases are most consistent with the hypothesis that, under normal conditions, a subcortical brain stem generator inhibits a lumbosacral generator for PLMS. The abnormal legs sensations from RLS may overcome the brain-stem inhibition and cause the lumbosacral generator to fire, thus producing PLMS. 17 A body of evidence suggests that RLS involves a disruption of subcortical dopamine systems. 16 Support for this hypothesis stems from the observation that RLS symptoms respond to dopaminergic agonist treatment and are exacerbated by centrally acting dopaminergic antagonists. 16,18-20 Small decreases in striatal dopaminergic measures have been found in four positron emission tomographic (PET) and single photon emission computed tomographic (SPECT) studies of RLS patients (see Allen and Earley 16 for a review). The observed deficits are both pre- and post-synaptic. A current hypothesis undergoing exploration is that RLS results from a deficiency of dopaminergic function based on abnormalities of iron transport and Table 1. Differential Diagnosis of RLS Paresthesias/ Movement Symptoms at Rest Worsening of Comments Dysesthesia Relieved with Activity Symptoms at Night RLS Walking, stretching bending legs to relieve paresthesias and dysesthesias Peripheral No relief neuropathy with activity Leg cramps Pushing foot against Sometimes Brief, intermittent, bed or floor to nocturnal severe, localized relieve cramp pain, spasm Neuroleptic- Walking, marching-in- No nighttime Neuroleptic use induced akathisia place, body rocking worsening Painful legs/ Involuntary movements moving toes of toes Positional pain Patient shifts weight Relieved by while sitting shifting position storage. 21 Several lines of evidence support this. Iron is linked to dopamine as it is a necessary co-factor for tyrosine hydroxylase, the rate-limiting enzyme in the conversion of levodopa to dopamine. Iron deficiency anemia is one of the secondary causes of RLS, 16 and is common in several other secondary causes, including end-stage renal disease and pregnancy. 22,23 Furthermore, correction of the peripheral iron problem often reduces or resolves RLS symptoms. 24 Even in the absence of anemia, the severity of RLS increases with serum ferritin concentrations lower than 50 µg/l. 25 MRI studies show that brain iron values appear to be particularly important, with decreased iron stores in the substantia nigra. 26 Recently, the onset of RLS was correlated with iron deficiency due to multiple blood donations. 24 Another hypothesis is that there is a hypofunction of the endogenous opioid system in RLS. Opioids improve RLS symptoms and administration of the rapidly acting opioid receptor blocker naloxone to opioid-treated patients exacerbates the symptoms of RLS. This indicates that the opiate effect is specific to the opioid receptor and implicates the endogenous opiate system in the pathogenesis of RLS. 27 Associated Conditions Table 2 28,29 lists the more well-established other medical conditions associated with and, in some cases, possibly causal to the symptoms of RLS. RLS has been noted in about 20% of women who are pregnant 22,30 and in 20% to 62% of patients with kidney failure undergoing dialysis. 31,32 Medications that can precipitate RLS include tricyclic and selective serotonin reuptake inhibitors, monoamine oxidase inhibitors, lithium, antihistamines, and typical and atypical neuroleptics. 3,6,33 Table 2. Conditions Associated with RLS 28,29 Iron-deficiency anemia Pregnancy End-stage renal disease Medications (neuroleptics/antidepressants) Rheumatoid arthritis Polyneuropathy/radiculopathy The relationship of RLS to exercise is complex. Although walking relieves RLS symptoms while the patient is actually walking, excessive exercise earlier in the day can exacerbate symptoms later that night. On the other hand, regular exercise and maintaining a good lifestyle are associated with less severe symptoms of RLS. Hypertension, heart disease, sleep apnea and arthritis are also more common in RLS, although the reasons for these associations are unclear. While the prevalence of RLS is increased in patients with rheumatoid arthritis, the reverse is not true, ie, the prevalence of rheumatoid arthritis is not increased in patients with RLS. It is still controversial as to whether or not there is a link between RLS and Parkinson s disease, a known dopaminergic deficiency disorder. 6,7,33-35 Risk Factors Several risk factors have been identified for RLS. The first is age, with increasing age associated with increasing prevalence and severity. 7 There also appears to be a genetic predisposition to developing RLS. RLS is often familial and most studies show an autosomal dominant form of inheritance. Reports have shown that up to 92% of family members of people with idiopathic RLS show RLS symptoms. 4,36 Overview of Treatment Strategies Generally nonpharmacologic therapies for RLS result in poor and temporary responses. Educating the patients about steps to improve sleep hygiene can be beneficial because poor sleep habits and sleep disruption can aggravate RLS. Some patients 3
4 find that hot baths, muscle stretching in the morning and night, delayed sleep and rise times, massage, or moderate exercise are helpful. 33 Leg vibration, nonelectric or electric stimulation, acupuncture, or sleeping on a hard floor have been tried, but most patients seeking treatment require medications. 23,37 Symptoms of RLS do respond well to pharmacologic therapy. Currently about one third of patients can achieve great relief, one third significant relief, and one third some relief. Only about 5% of patients are totally refractory to current therapies. Several pharmacologic approaches to treating RLS relate to specific deficits that contribute to RLS. For instance, iron replacement and perhaps vitamin B12 and folate supplementation can help patients with RLS. A serum ferritin in the bottom 1/3 of normal (<50 µg/l) is an indication for treatment. Earley 23 recommends 65 mg of elemental iron along with 100 mg of vitamin C on an empty stomach one to three times daily and determination of the ferritin level and iron saturation after 3 months. Oral iron supplementation should be continued until ferritin levels are at or above 50 µg/l and iron saturation is >20%. Women should be informed that RLS symptoms often diminish or disappear after pregnancy. It is better to be conservative in the treatment of RLS in pregnancy, particularly in the first trimester, although iron, vitamin B12 and folate can generally be used safely. In some cases, however, the symptoms of RLS in pregnancy are severe enough to warrant further treatment. In general, dopamine agonists and levodopa are now the first-line treatments for idiopathic or familial RLS. 38 These agents include two ergot-derived agents, bromocriptine and pergolide, and two nonergot medications, pramipexole and ropinirole. Dopaminergic agents provide symptom relief to 90% of RLS patients and reduce the frequency of PLMS by 70% to 100%. 23 Second-line options for the treatment of RLS include opiates (propoxyphene, codeine, oxycodone, methadone), benzodiazepine sedative hypnotic agents (clonazepam, diazepam) and anticonvulsants (gabapentin). The anticonvulsants are particularly appropriate for painful RLS symptoms. Summary RLS is a common, debilitating neurologic disorder that is poorly recognized by patients and physicians alike. With this in mind, it is incumbent upon clinicians to query patients about the quantity and quality of sleep, nighttime awakenings, and daytime sleepiness. A bed partner can be a key source of information about the patient s habits that may not be evident to the patient. The clinician should also inquire about risk and other dietary, metabolic, and lifestyle factors that may precipitate RLS symptoms. Once RLS is diagnosed, the clinician can utilize pharmacologic treatment strategies that focus on correcting iron deficiency or stimulating dopaminergic pathways to provide significant symptom relief. The next Treatment Reporter will review the evidence supporting specific treatment paradigms for RLS. TX References 1. Walters AS. Toward a better definition of the restless legs syndrome. The International RLS Study Group. Mov Disord. 1995;10: Allen RP, Picchietti D, Hening WA, et al. Restless legs syndrome: diagnostic criteria, special considerations, and epidemiology. A report from the restless legs syndrome diagnosis and epidemiology workshop at the National Institutes of Health. Sleep Med. 2003;4: Stiasny K, Oertel WH, Trenkwalder C. Clinical symptomatology and treatment of restless legs syndrome and periodic limb movement disorder. Sleep Med Rev. 2002;6: Montplaisir J, Boucher S, Poirier G, et al. Clinical, polysomnographic, and genetic characteristics of restless legs syndrome: a study of 133 patients diagnosed with new standard criteria. Mov Disord. 1997;12: Allen RP, Hening WA, Montplaisir J, Walters AS, Brown T, Myers A. Restless Legs Syndrome (RLS) is a common disorder rarely diagnosed in Europe or USA: the REST (RLS Epidemiology, Symptoms and Treatment) study in primary care (abstract P774). Mov Disord. 2002;17(suppl 5):S Ohayon MM, Roth T. Prevalence of restless legs syndrome and periodic limb movement disorder in the general population. J Psychosom Res. 2002;63: Phillips B, Young T, Finn L, Asher K, Hening WA, Purvis C. Epidemiology of RLS in adults. Arch Intern Med. 2000;160: Lavigne GJ, Montplaisir JY. Restless legs syndrome and sleep bruxism: prevalence and association among Canadians. Sleep. 1994;17: Rothdach AJ, Trenkwalder C, Haberstock J, Keil U, Berger K. Prevalence and risk factors of RLS in an elderly population: the MEMO study. Memory and Morbidity in Augsburg Elderly. Neurology. 2000;54: Picchietti DL, Underwood DJ, Farris WA, et. al. Further studies on periodic limb movement disorder and restless legs syndrome in children with attention-deficithyperactivity disorder. Mov Disord. 1999;14: Walters AS. Is there a subpopulation of children with growing pains who really have restless legs syndrome? A review of the literature. Sleep Med. 2002a;3: Montplaisir J, Boucher S, Nicolas A, et al. Immobilization tests and periodic leg movements in sleep for the diagnosis of restless leg syndrome. Mov Disord. 1998;13: The International Restless Legs Syndrome Study Group. Validation of the International Restless Legs Syndrome Study Group rating scale for restless legs syndrome. Sleep Med. 2003;4: Allen RP, Earley CJ. Validation of the Johns Hopkins restless legs severity scale. Sleep Med. 2001a;2: Bara-Jiminez W, Aksu M, Graham B, et al. Periodic limb movements in sleep: state-dependent excitability of the spinal flexor reflex. Neurology. 2000;55: Allen RP, Earley CJ. Restless legs syndrome: a review of clinical and pathophysiologic features. J Clin Neurophysiol. 2001b;18: Walters AS. Restless legs syndrome and periodic limb movements in sleep. Handbook of Clinical Neurophysiology. Elsevier, 2004 (In Press). 18. Akpinar S. Restless legs syndrome treatment with dopaminergic drugs. Clin Neuropharmacol. 1987;10: Wetter TC, Stiasny K, Winkelmann J, et al. A randomized controlled study of pergolide in patients with restless legs syndrome. Neurology. 1999;52: Young WB, Piovesan EJ, Biglan KM. Restless legs syndrome and drug-induced akathisia in headache patients. CNS Spectr. 2003;8: Hening WA. Restless legs syndrome: a sensorimotor disorder of sleep/wake motor regulation. Curr Neurol Neurosci Rep. 2002;2: Lee KA, Zaffke ME, Baratte-Beebe K. Restless legs syndrome and sleep disturbance during pregnancy: the role of folate and iron. J Womens Health Gend Based Med. 2001;10: Earley CJ. Clinical practice. Restless legs syndrome. N Engl J Med. 2003;348: Silber MH, Richardson JW. Multiple blood donations associated with iron deficiency in patients with restless legs syndrome. Mayo Clin Proc. 2003;78: Sun ER, Chen CA, Ho G, Earley CJ, Allen RP. Iron and the restless legs syndrome. Sleep. 1998;21: Allen RP, Barker PB, Wehrl F, Song HK, Earley CJ. MRI measurement of brain iron in patients with restless legs syndrome. Neurology. 2001;56: Walters AS. Review of the receptor agonist and antagonist studies relevant to the opiate system in restless legs syndrome. Sleep Med. 2002;3: National Heart, Lung and Blood Institute Working Group on Restless Legs Syndrome. Restless legs syndrome: detection and management in primary care. Am Fam Physician. 2000;62: Tan EK, Ondo W. Restless legs syndrome: clinical features and treatment. Am J Med Sci. 2000;319: Goodman JD, Brodie C, Ayida GA. Restless leg syndrome in pregnancy. BMJ. 1988;297: Winkelman JW, Chertow GM, Lazurus JM. Restless legs syndrome in end-stage renal disease. Am J Kidney Dis. 1996;28: Hui DS,Wong TY, Ko FW, et al. Prevalence of sleep disturbances in Chinese patients with end-stage renal failure on continuous ambulatory peritoneal dialysis. Am J Kidney Dis. 2000;36: Parker KP, Rye DB. Restless legs syndrome and periodic limb movement disorder. Nurs Clin North Am. 2002;37: Ondo WG, Vuong KD, Jankovic J. Exploring the relationship between Parkinson disease and restless leg syndrome. Arch Neurol. 2002;59: Salih AM, Gray RE, Mills KR, Webley M. A clinical, serological and neurophysiological study of restless legs syndrome in rheumatoid arthritis. Br J Rheumatol. 1994;33: Ondo W, Jankovic J. Restless legs syndrome: clinicoetiologic correlates. Neurology. 1996;47: Hu J. Acupuncture treatment of restless legs syndrome. J Tradit Chin Med. 2001;21: Comella CL. Restless legs syndrome: treatment with dopaminergic agents. Neurology. 2002;58(4 suppl 1):S
5 CME Posttest Part 1 of 4: Overview of Restless Legs Syndrome CME Instructions Stilling the Nighttime Intruder: Innovations in Treatment of Restless Legs Syndrome (RLS) To receive documentation of your participation in this 4-part CME activity (for which each newsletter equals.25 hour for a total of 1 hour of CME credit), please complete the following steps: 1. Read each Tx Reporter newsletter carefully. 2. Complete the CME Posttest included in each of the newsletters, selecting the most appropriate response to each question. 3. Complete the CME Evaluation Survey which will be included at the end of Newsletter #4. 4. Mail or fax each of your completed CME Posttests and the final CME Evaluation Survey to Projects In Knowledge, Overlook at Great Notch, 150 Clove Road, Little Falls, NJ 07424; fax: * *Successful completion for 1 hour of CME credit requires a passing score of 70% or higher on each of the 4 posttests. After you have submitted each posttest and the final CME Evaluation Survey with Newsletter #4, you will be issued a CME certificate for up to 1 hour of credit. If your score is lower than 70% on any individual posttest, you will be notified by mail and given an opportunity to retake that test. Name Degrees/Credentials Mailing Address City State ZIP Phone Fax Please select the most appropriate response to each question. 1. A 50-year-old was diagnosed with painful peripheral neuropathy. She does not feel the need to move to relieve her leg discomfort and movement does not give her relief. Does she have RLS? Yes No 2. A 70-year-old man presents with complaints of numbness, tingling, and nighttime pain in his legs. He denies any relief from walking or bending the legs, but does find shifting his weight using a pillow under his hip to be helpful. Does he have RLS? Yes No 3. Which of the following is necessary to make the diagnosis of RLS? Polysomnography Serum ferritin level Sensory/motor physical exam None of the above 4. Which of the following are not considered a secondary cause of RLS? Pregnancy End-stage kidney disease Hypoxia Medications 5. What are some strategies to consider when treating RLS? Resolve iron deficiency Use a benzodiazepine, hypnotic or opioid Treat with a dopaminergic agonist or L-DOPA. Treat with an anticonvulsant like gabapentin All of the above 1671PT Page 1 of 1
1/25/2015. Idiopathic restless legs syndrome: clinical definition, pathophysiology and treatment. Five essential criteria (all must be met)
 Idiopathic restless legs syndrome: clinical definition, pathophysiology and treatment Joan Santamaria, MD Neurology service, Multidisciplinary Sleep Disorders Unit Hospital Clínic de Barcelona University
Idiopathic restless legs syndrome: clinical definition, pathophysiology and treatment Joan Santamaria, MD Neurology service, Multidisciplinary Sleep Disorders Unit Hospital Clínic de Barcelona University
SUMMARY OF RECOMMENDATIONS
 SUMMARY OF RECOMMENDATIONS FOR THE LONG- TERM TREATMENT OF RLS/WED from AN IRLSSG TASK FORCE Members of the Task Force Diego Garcia- Borreguero, MD, Madrid, Spain* Richard Allen, PhD, Baltimore, MD, USA*
SUMMARY OF RECOMMENDATIONS FOR THE LONG- TERM TREATMENT OF RLS/WED from AN IRLSSG TASK FORCE Members of the Task Force Diego Garcia- Borreguero, MD, Madrid, Spain* Richard Allen, PhD, Baltimore, MD, USA*
Sleep Difficulties. Insomnia. By Thomas Freedom, MD and Johan Samanta, MD
 Sleep Difficulties By Thomas Freedom, MD and Johan Samanta, MD For most people, night is a time of rest and renewal; however, for many people with Parkinson s disease nighttime is a struggle to get the
Sleep Difficulties By Thomas Freedom, MD and Johan Samanta, MD For most people, night is a time of rest and renewal; however, for many people with Parkinson s disease nighttime is a struggle to get the
Restless Legs Syndrome: Who are Willis and Ekbom?
 Restless Legs Syndrome: Who are Willis and Ekbom? Rochelle Goldberg, MD, FAASM, FCCP Associate Professor, Sidney Kimmel Medical Center, Thomas Jefferson University Director, Sleep Medicine Services Main
Restless Legs Syndrome: Who are Willis and Ekbom? Rochelle Goldberg, MD, FAASM, FCCP Associate Professor, Sidney Kimmel Medical Center, Thomas Jefferson University Director, Sleep Medicine Services Main
RESTLESS LEGS SYNDROME FOUNDATION
 RESTLESS LEGS SYNDROME Causes, diagnosis and treatment for the patient living with Restless Legs Syndrome (RLS) RESTLESS LEGS SYNDROME FOUNDATION DO I HAVE RESTLESS LEGS SYNDROME? Chances are, if you are
RESTLESS LEGS SYNDROME Causes, diagnosis and treatment for the patient living with Restless Legs Syndrome (RLS) RESTLESS LEGS SYNDROME FOUNDATION DO I HAVE RESTLESS LEGS SYNDROME? Chances are, if you are
SLEEP AND PARKINSON S DISEASE
 A Practical Guide on SLEEP AND PARKINSON S DISEASE MICHAELJFOX.ORG Introduction Many people with Parkinson s disease (PD) have trouble falling asleep or staying asleep at night. Some sleep problems are
A Practical Guide on SLEEP AND PARKINSON S DISEASE MICHAELJFOX.ORG Introduction Many people with Parkinson s disease (PD) have trouble falling asleep or staying asleep at night. Some sleep problems are
Restless Legs Syndrome Creepy-Crawly Legs Causing Distress?
 written by Harvard Medical School Restless Legs Syndrome Creepy-Crawly Legs Causing Distress? www.patientedu.org Although many of us take it for granted, sleep is very important for health. For some 12
written by Harvard Medical School Restless Legs Syndrome Creepy-Crawly Legs Causing Distress? www.patientedu.org Although many of us take it for granted, sleep is very important for health. For some 12
SLEEP DISTURBANCE AND PSYCHIATRIC DISORDERS
 E-Resource December, 2013 SLEEP DISTURBANCE AND PSYCHIATRIC DISORDERS Between 10-18% of adults in the general population and up to 50% of adults in the primary care setting have difficulty sleeping. Sleep
E-Resource December, 2013 SLEEP DISTURBANCE AND PSYCHIATRIC DISORDERS Between 10-18% of adults in the general population and up to 50% of adults in the primary care setting have difficulty sleeping. Sleep
Restless Legs Syndrome
 CLINICAL REVIEW Restless Legs Syndrome Mathew M. Clark, MD Background: Restless legs syndrome is a common but not well-recognized central nervous system disorder that leads to insomnia and daytime distress.
CLINICAL REVIEW Restless Legs Syndrome Mathew M. Clark, MD Background: Restless legs syndrome is a common but not well-recognized central nervous system disorder that leads to insomnia and daytime distress.
What is PD? Dr Catherine Dotchin MD MRCP Consultant Geriatrician
 What is PD? Dr Catherine Dotchin MD MRCP Consultant Geriatrician Overview of presentation Case history Video example pre and post treatment Historical review PD in the UK Epidemiology and aetiology Making
What is PD? Dr Catherine Dotchin MD MRCP Consultant Geriatrician Overview of presentation Case history Video example pre and post treatment Historical review PD in the UK Epidemiology and aetiology Making
CPAP Treats Muscle Cramps in Patients with Obstructive Sleep Apnea
 CPAP Treats Muscle Cramps in Patients with Obstructive Sleep Apnea Andrew J Westwood, M.D., MRCP(UK) 1, Andrew R Spector, M.D., 2 Sanford H Auerbach, M.D. 3 1 Columbia University College of Physicians
CPAP Treats Muscle Cramps in Patients with Obstructive Sleep Apnea Andrew J Westwood, M.D., MRCP(UK) 1, Andrew R Spector, M.D., 2 Sanford H Auerbach, M.D. 3 1 Columbia University College of Physicians
Medical Massage Client Intake Form Medical Massage Client Intake Form
 Medical Massage Client Intake Form Medical Massage Client Intake Form Client Name: Date: Please note: The more information you are able to provide, the better equipped our therapists will be to help you.
Medical Massage Client Intake Form Medical Massage Client Intake Form Client Name: Date: Please note: The more information you are able to provide, the better equipped our therapists will be to help you.
Corporate Medical Policy
 Corporate Medical Policy Polysomnography for Non Respiratory Sleep Disorders File Name: Origination: Last CAP Review: Next CAP Review: Last Review: polysomnography_for_non_respiratory_sleep_disorders 10/2015
Corporate Medical Policy Polysomnography for Non Respiratory Sleep Disorders File Name: Origination: Last CAP Review: Next CAP Review: Last Review: polysomnography_for_non_respiratory_sleep_disorders 10/2015
Restless Legs Syndrome
 Max Bayard, MD; Thomas Avonda, MD; and James Wadzinski, MD, East Tennessee State University, Quillen College of Medicine, Johnson City, Tennessee Restless legs syndrome is a common neurologic movement
Max Bayard, MD; Thomas Avonda, MD; and James Wadzinski, MD, East Tennessee State University, Quillen College of Medicine, Johnson City, Tennessee Restless legs syndrome is a common neurologic movement
Sample Treatment Protocol
 Sample Treatment Protocol 1 Adults with acute episode of LBP Definition: Acute episode Back pain lasting
Sample Treatment Protocol 1 Adults with acute episode of LBP Definition: Acute episode Back pain lasting
Sleep Disorders in Geriatrics. Beth A. Malow, M.D., M.S. Associate Professor of Neurology Director, Vanderbilt Sleep Disorders Center
 Sleep Disorders in Geriatrics Beth A. Malow, M.D., M.S. Associate Professor of Neurology Director, Vanderbilt Sleep Disorders Center Presentation Goals To recognize the prevalence and impact of treating
Sleep Disorders in Geriatrics Beth A. Malow, M.D., M.S. Associate Professor of Neurology Director, Vanderbilt Sleep Disorders Center Presentation Goals To recognize the prevalence and impact of treating
Don t just dream of higher-quality sleep. How health care should be
 Don t just dream of higher-quality sleep. How health care should be Many of our patients with sleep disorders don t realize there s another way of life, a better way, until they are treated. Robert Israel,
Don t just dream of higher-quality sleep. How health care should be Many of our patients with sleep disorders don t realize there s another way of life, a better way, until they are treated. Robert Israel,
SLEEP DIFFICULTIES AND PARKINSON S DISEASE Julie H. Carter, R.N., M.S., A.N.P.
 SLEEP DIFFICULTIES AND PARKINSON S DISEASE Julie H. Carter, R.N., M.S., A.N.P. Problems with sleep are common in Parkinson s disease. They can sometimes interfere with quality of life. It is helpful to
SLEEP DIFFICULTIES AND PARKINSON S DISEASE Julie H. Carter, R.N., M.S., A.N.P. Problems with sleep are common in Parkinson s disease. They can sometimes interfere with quality of life. It is helpful to
Amino Acid Therapy to Restore Neurotransmitter Function
 Amino Acid Therapy to Restore Neurotransmitter Function Alvin Stein, MD Neurotransmitters are chemicals manufactured by our bodies that allow our nervous system to function properly. When the body requires
Amino Acid Therapy to Restore Neurotransmitter Function Alvin Stein, MD Neurotransmitters are chemicals manufactured by our bodies that allow our nervous system to function properly. When the body requires
Tara Leigh Taylor, MD, FCCP Intensivist, Wyoming Medical Center
 Tara Leigh Taylor, MD, FCCP Intensivist, Wyoming Medical Center Objectives Define the magnitude of the problem Define diagnostic criteria of insomnia Understand the risk factors and consequences of insomnia
Tara Leigh Taylor, MD, FCCP Intensivist, Wyoming Medical Center Objectives Define the magnitude of the problem Define diagnostic criteria of insomnia Understand the risk factors and consequences of insomnia
ALL ABOUT SPASTICITY. www.almirall.com. Solutions with you in mind
 ALL ABOUT SPASTICITY www.almirall.com Solutions with you in mind WHAT IS SPASTICITY? The muscles of the body maintain what is called normal muscle tone, a level of muscle tension that allows us to hold
ALL ABOUT SPASTICITY www.almirall.com Solutions with you in mind WHAT IS SPASTICITY? The muscles of the body maintain what is called normal muscle tone, a level of muscle tension that allows us to hold
National Hospital for Neurology and Neurosurgery. Managing Spasticity. Spasticity Service
 National Hospital for Neurology and Neurosurgery Managing Spasticity Spasticity Service If you would like this document in another language or format, or require the services of an interpreter please contact
National Hospital for Neurology and Neurosurgery Managing Spasticity Spasticity Service If you would like this document in another language or format, or require the services of an interpreter please contact
LUMBAR. Hips R L B R L B LUMBAR. Hips R L B R L B LUMBAR. Hips R L B R L B
 1 Patient Name In order to properly assess your condition, we must understand how much your BACK/LEG (SCIATIC) PAIN has affected your ability to manage everyday activities. For each item below, please
1 Patient Name In order to properly assess your condition, we must understand how much your BACK/LEG (SCIATIC) PAIN has affected your ability to manage everyday activities. For each item below, please
Clinical guidance for MRI referral
 MRI for cervical radiculopathy Referral by a medical practitioner (excluding a specialist or consultant physician) for a scan of spine for a patient 16 years or older for suspected: cervical radiculopathy
MRI for cervical radiculopathy Referral by a medical practitioner (excluding a specialist or consultant physician) for a scan of spine for a patient 16 years or older for suspected: cervical radiculopathy
Disordered sleep at night has long been
 Neurology 59 Excessive daytime sleepiness in PD Excessive Daytime Sleepiness (EDS) in Parkinson s disease (PD) is an important issue that warrants serious attention because it can have adverse effects
Neurology 59 Excessive daytime sleepiness in PD Excessive Daytime Sleepiness (EDS) in Parkinson s disease (PD) is an important issue that warrants serious attention because it can have adverse effects
Nursing Interventions for Sleep Disorders Following TBI
 Nursing Interventions for Sleep Disorders Following TBI Kadesha Clark, RN BSN When you sleep, your body rests and restores its energy levels. A good night's sleep is often the best way to help you cope
Nursing Interventions for Sleep Disorders Following TBI Kadesha Clark, RN BSN When you sleep, your body rests and restores its energy levels. A good night's sleep is often the best way to help you cope
Chapter 28. Drug Treatment of Parkinson s Disease
 Chapter 28 Drug Treatment of Parkinson s Disease 1. Introduction Parkinsonism Tremors hands and head develop involuntary movements when at rest; pin rolling sign (finger and thumb) Muscle rigidity arthritis
Chapter 28 Drug Treatment of Parkinson s Disease 1. Introduction Parkinsonism Tremors hands and head develop involuntary movements when at rest; pin rolling sign (finger and thumb) Muscle rigidity arthritis
Lewy body dementia Referral for a Diagnosis
 THE Lewy Body society The more people who know, the fewer people who suffer Lewy body dementia Referral for a Diagnosis Lewy Body Dementias REFERRAL FOR A DIAGNOSIS In the UK people with all forms of dementia
THE Lewy Body society The more people who know, the fewer people who suffer Lewy body dementia Referral for a Diagnosis Lewy Body Dementias REFERRAL FOR A DIAGNOSIS In the UK people with all forms of dementia
Recognition and Treatment of Depression in Parkinson s Disease
 Recognition and Treatment of Depression in Parkinson s Disease Web Ross VA Pacific Islands Health Care System What is depression? Depression is a serious medical condition that affects a person s feelings,
Recognition and Treatment of Depression in Parkinson s Disease Web Ross VA Pacific Islands Health Care System What is depression? Depression is a serious medical condition that affects a person s feelings,
Aetna Nerve Conduction Study Policy
 Aetna Nerve Conduction Study Policy Policy Aetna considers nerve conduction velocity (NCV) studies medically necessary when both of the following criteria are met: 1. Member has any of the following indications:
Aetna Nerve Conduction Study Policy Policy Aetna considers nerve conduction velocity (NCV) studies medically necessary when both of the following criteria are met: 1. Member has any of the following indications:
PARKINSON S DISEASE INTRODUCTION. Parkinson s disease is defined as a disease of the nervous system that affects voluntary movement.
 PARKINSON S DISEASE INTRODUCTION Parkinson s disease is a disorder of the brain and the nervous system. It is one of the more common neurological diseases in people over the age of 60, and it is more common
PARKINSON S DISEASE INTRODUCTION Parkinson s disease is a disorder of the brain and the nervous system. It is one of the more common neurological diseases in people over the age of 60, and it is more common
A Healthy Life RETT SYNDROME AND SLEEP. Exercise. Sleep. Diet 1. WHY SLEEP? 4. ARE SLEEP PROBLEMS A COMMON PARENT COMPLAINT?
 Diet Sleep Exercise RETT SYNDROME AND SLEEP DR. DANIEL GLAZE, MEDICAL DIRECTOR THE BLUE BIRD CIRCLE RETT CENTER A good night s sleep promotes learning, improved mood, general good health, and a better
Diet Sleep Exercise RETT SYNDROME AND SLEEP DR. DANIEL GLAZE, MEDICAL DIRECTOR THE BLUE BIRD CIRCLE RETT CENTER A good night s sleep promotes learning, improved mood, general good health, and a better
FUNCTIONAL EEG ANALYZE IN AUTISM. Dr. Plamen Dimitrov
 FUNCTIONAL EEG ANALYZE IN AUTISM Dr. Plamen Dimitrov Preamble Autism or Autistic Spectrum Disorders (ASD) is a mental developmental disorder, manifested in the early childhood and is characterized by qualitative
FUNCTIONAL EEG ANALYZE IN AUTISM Dr. Plamen Dimitrov Preamble Autism or Autistic Spectrum Disorders (ASD) is a mental developmental disorder, manifested in the early childhood and is characterized by qualitative
Depression in Older Persons
 Depression in Older Persons How common is depression in later life? Depression affects more than 6.5 million of the 35 million Americans aged 65 or older. Most people in this stage of life with depression
Depression in Older Persons How common is depression in later life? Depression affects more than 6.5 million of the 35 million Americans aged 65 or older. Most people in this stage of life with depression
Sleep Medicine. Maintenance of Certification Examination Blueprint. Purpose of the exam
 Sleep Medicine Maintenance of Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of the
Sleep Medicine Maintenance of Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of the
PARKINSON S DISEASE IN LONG-TERM-CARE SETTINGS
 PARKINSON S DISEASE IN LONG-TERM-CARE SETTINGS De Anna Looper, RN CHPN Corporate Clinical Consultant / Legal Nurse Consultant Carrefour Associates L.L.C. PARKINSON S DISEASE IN LONG-TERM-CARE SETTINGS
PARKINSON S DISEASE IN LONG-TERM-CARE SETTINGS De Anna Looper, RN CHPN Corporate Clinical Consultant / Legal Nurse Consultant Carrefour Associates L.L.C. PARKINSON S DISEASE IN LONG-TERM-CARE SETTINGS
Some people with Parkinson s experience restless legs syndrome.
 Symptoms and lifestyle Restless legs syndrome and Parkinson s Some people with Parkinson s experience restless legs syndrome. This information sheet explains what restless legs syndrome is, what the symptoms
Symptoms and lifestyle Restless legs syndrome and Parkinson s Some people with Parkinson s experience restless legs syndrome. This information sheet explains what restless legs syndrome is, what the symptoms
Steps to getting a diagnosis: Finding out if it s Alzheimer s Disease.
 Steps to getting a diagnosis: Finding out if it s Alzheimer s Disease. Memory loss and changes in mood and behavior are some signs that you or a family member may have Alzheimer s disease. If you have
Steps to getting a diagnosis: Finding out if it s Alzheimer s Disease. Memory loss and changes in mood and behavior are some signs that you or a family member may have Alzheimer s disease. If you have
A 34-year-old female with a history of multiple sclerosis (MS) returns to the neurology clinic for follow-up.
 Complementary and Alternative Medicine in Multiple Sclerosis Case Presentation: A 34-year-old female with a history of multiple sclerosis (MS) returns to the neurology clinic for follow-up. The patient
Complementary and Alternative Medicine in Multiple Sclerosis Case Presentation: A 34-year-old female with a history of multiple sclerosis (MS) returns to the neurology clinic for follow-up. The patient
CLINICAL PRACTICE GUIDELINES FOR MANAGEMENT OF LOW BACK PAIN
 CLINICAL PRACTICE GUIDELINES FOR MANAGEMENT OF LOW BACK PAIN Low back pain is very common, up to 90+% of people are affected by back pain at some time in their lives. Most often back pain is benign and
CLINICAL PRACTICE GUIDELINES FOR MANAGEMENT OF LOW BACK PAIN Low back pain is very common, up to 90+% of people are affected by back pain at some time in their lives. Most often back pain is benign and
Paxil/Paxil-CR (paroxetine)
 Generic name: Paroxetine Available strengths: 10 mg, 20 mg, 30 mg, 40 mg tablets; 10 mg/5 ml oral suspension; 12.5 mg, 25 mg, 37.5 mg controlled-release tablets (Paxil-CR) Available in generic: Yes, except
Generic name: Paroxetine Available strengths: 10 mg, 20 mg, 30 mg, 40 mg tablets; 10 mg/5 ml oral suspension; 12.5 mg, 25 mg, 37.5 mg controlled-release tablets (Paxil-CR) Available in generic: Yes, except
Emergency Room Treatment of Psychosis
 OVERVIEW The term Lewy body dementias (LBD) represents two clinical entities dementia with Lewy bodies (DLB) and Parkinson s disease dementia (PDD). While the temporal sequence of symptoms is different
OVERVIEW The term Lewy body dementias (LBD) represents two clinical entities dementia with Lewy bodies (DLB) and Parkinson s disease dementia (PDD). While the temporal sequence of symptoms is different
SLEEP DISORDERS IN ASBESTOS-RELATED DISEASES
 SLEEP DISORDERS IN ASBESTOS-RELATED DISEASES Asbestos pleural diseases ie benign asbestos pleural plaques, diffuse pleural thickening, benign asbestos pleurisy, benign asbestos pleural effusions and asbestosis
SLEEP DISORDERS IN ASBESTOS-RELATED DISEASES Asbestos pleural diseases ie benign asbestos pleural plaques, diffuse pleural thickening, benign asbestos pleurisy, benign asbestos pleural effusions and asbestosis
Fibromyalgia. Factsheet
 Factsheet Fibromyalgia Fibromyalgia can cause similar symptoms to multiple sclerosis (MS) including muscle weakness and pain in the arms and legs. In fibromyalgia, the pain is musclespecific, and not in
Factsheet Fibromyalgia Fibromyalgia can cause similar symptoms to multiple sclerosis (MS) including muscle weakness and pain in the arms and legs. In fibromyalgia, the pain is musclespecific, and not in
Upper Arm. Shoulder Blades R L B R L B WHICH SIDE IS MORE PAINFUL? (CERVICAL PAIN SIDE) RIGHT LEFT EQUAL NOT APPLICABLE (N/A) CERVICAL.
 1 NECK PAIN Patient Name In order to properly assess your condition, we must understand how much your NECK/ARM problems has affected your ability to manage everyday activities. For each item below, please
1 NECK PAIN Patient Name In order to properly assess your condition, we must understand how much your NECK/ARM problems has affected your ability to manage everyday activities. For each item below, please
Multifocal Motor Neuropathy. Jonathan Katz, MD Richard Lewis, MD
 Multifocal Motor Neuropathy Jonathan Katz, MD Richard Lewis, MD What is Multifocal Motor Neuropathy? Multifocal Motor Neuropathy (MMN) is a rare condition in which multiple motor nerves are attacked by
Multifocal Motor Neuropathy Jonathan Katz, MD Richard Lewis, MD What is Multifocal Motor Neuropathy? Multifocal Motor Neuropathy (MMN) is a rare condition in which multiple motor nerves are attacked by
PLANTAR FASCITIS (Heel Spur Syndrome)
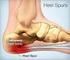 PLANTAR FASCITIS (Heel Spur Syndrome) R. Amadeus Mason MD Description Plantar fascitis is characterized by stiffness and inflammation of the main fascia (fibrous connective [ligament-like] tissue) on the
PLANTAR FASCITIS (Heel Spur Syndrome) R. Amadeus Mason MD Description Plantar fascitis is characterized by stiffness and inflammation of the main fascia (fibrous connective [ligament-like] tissue) on the
Coping with Symptoms of Multiple Sclerosis
 Coping with Symptoms of Multiple Sclerosis Josée Poirier B. Sc. Nursing, MSCN Outline What Is a Pseudo exacerbation? Awareness Advancement of Treatments Treatment of Symptoms Uhthoff s Phenomenon What
Coping with Symptoms of Multiple Sclerosis Josée Poirier B. Sc. Nursing, MSCN Outline What Is a Pseudo exacerbation? Awareness Advancement of Treatments Treatment of Symptoms Uhthoff s Phenomenon What
Dementia & Movement Disorders
 Dementia & Movement Disorders A/Prof Michael Davis Geriatrician ACT Health & GSAHS ANU Medical School Eastern Dementia Network Aged and Dementia Care Symposium Bateman s Bay, 22 October 2010 Types of Dementia
Dementia & Movement Disorders A/Prof Michael Davis Geriatrician ACT Health & GSAHS ANU Medical School Eastern Dementia Network Aged and Dementia Care Symposium Bateman s Bay, 22 October 2010 Types of Dementia
Introduction: Anatomy of the spine and lower back:
 Castleknock GAA club member and Chartered Physiotherapist, James Sherry MISCP, has prepared an informative article on the common causes of back pain and how best it can be treated. To book a physiotherapy
Castleknock GAA club member and Chartered Physiotherapist, James Sherry MISCP, has prepared an informative article on the common causes of back pain and how best it can be treated. To book a physiotherapy
Medical Information to Support the Decisions of TUECs INTRINSIC SLEEP DISORDERS
 Introduction Excessive daytime sleepiness (EDS) is a common complaint. Causes of EDS are numerous and include: o Intrinsic sleep disorders (e.g. narcolepsy, obstructive sleep apnoea/hypopnea syndrome (OSAHS)
Introduction Excessive daytime sleepiness (EDS) is a common complaint. Causes of EDS are numerous and include: o Intrinsic sleep disorders (e.g. narcolepsy, obstructive sleep apnoea/hypopnea syndrome (OSAHS)
A Physical Therapist s Perspective
 You Can Do Something About INCONTINENCE A Physical Therapist s Perspective American Physical Therapy Association 1 You Can Do Something About Urinary Incontinence Incontinence, involuntary loss of bladder
You Can Do Something About INCONTINENCE A Physical Therapist s Perspective American Physical Therapy Association 1 You Can Do Something About Urinary Incontinence Incontinence, involuntary loss of bladder
Understanding. Peripheral Neuropathy. Lois, diagnosed in 1998, with her husband, Myron.
 Understanding Peripheral Neuropathy Lois, diagnosed in 1998, with her husband, Myron. What Is Peripheral Neuropathy? Peripheral neuropathy is a nerve disorder. It may cause numbness, tingling, and weakness.
Understanding Peripheral Neuropathy Lois, diagnosed in 1998, with her husband, Myron. What Is Peripheral Neuropathy? Peripheral neuropathy is a nerve disorder. It may cause numbness, tingling, and weakness.
Alcohol Overuse and Abuse
 Alcohol Overuse and Abuse ACLI Medical Section CME Meeting February 23, 2015 Daniel Z. Lieberman, MD Professor and Vice Chair Department of Psychiatry George Washington University Alcohol OVERVIEW Definitions
Alcohol Overuse and Abuse ACLI Medical Section CME Meeting February 23, 2015 Daniel Z. Lieberman, MD Professor and Vice Chair Department of Psychiatry George Washington University Alcohol OVERVIEW Definitions
Depression & Multiple Sclerosis
 Depression & Multiple Sclerosis Managing specific issues Aaron, diagnosed in 1995. The words depressed and depression are used so casually in everyday conversation that their meaning has become murky.
Depression & Multiple Sclerosis Managing specific issues Aaron, diagnosed in 1995. The words depressed and depression are used so casually in everyday conversation that their meaning has become murky.
Lauren Schrock, M.D Assistant Professor of Neurology University of Utah Co-Director, Movement Disorders Program
 Lauren Schrock, M.D Assistant Professor of Neurology University of Utah Co-Director, Movement Disorders Program Brief clinical overview What are tics? Definition of TS and related tic disorders What we
Lauren Schrock, M.D Assistant Professor of Neurology University of Utah Co-Director, Movement Disorders Program Brief clinical overview What are tics? Definition of TS and related tic disorders What we
BACK PAIN MEASURES GROUP OVERVIEW
 2014 PQRS OPTIONS F MEASURES GROUPS: BACK PAIN MEASURES GROUP OVERVIEW 2014 PQRS MEASURES IN BACK PAIN MEASURES GROUP: #148. Back Pain: Initial Visit #149. Back Pain: Physical Exam #150. Back Pain: Advice
2014 PQRS OPTIONS F MEASURES GROUPS: BACK PAIN MEASURES GROUP OVERVIEW 2014 PQRS MEASURES IN BACK PAIN MEASURES GROUP: #148. Back Pain: Initial Visit #149. Back Pain: Physical Exam #150. Back Pain: Advice
The Burden of Pain Among Adults in the United States
 P F I Z E R F A C T S The Burden of Pain Among Adults in the United States Findings from the National Health and Nutrition Examination Survey, the National Health Care Surveys, and the National Health
P F I Z E R F A C T S The Burden of Pain Among Adults in the United States Findings from the National Health and Nutrition Examination Survey, the National Health Care Surveys, and the National Health
F r e q u e n t l y A s k e d Q u e s t i o n s
 Myasthenia Gravis Q: What is myasthenia gravis (MG)? A: Myasthenia gravis (meye-uhss- THEEN-ee-uh GRAV uhss) (MG) is an autoimmune disease that weakens the muscles. The name comes from Greek and Latin
Myasthenia Gravis Q: What is myasthenia gravis (MG)? A: Myasthenia gravis (meye-uhss- THEEN-ee-uh GRAV uhss) (MG) is an autoimmune disease that weakens the muscles. The name comes from Greek and Latin
Sciatica Yuliya Mutsa PTA 236
 Sciatica Yuliya Mutsa PTA 236 Sciatica is a common type of pain affecting the sciatic nerve, which extends from the lower back all the way through the back of the thigh and down through the leg. Depending
Sciatica Yuliya Mutsa PTA 236 Sciatica is a common type of pain affecting the sciatic nerve, which extends from the lower back all the way through the back of the thigh and down through the leg. Depending
National Hospital for Neurology and Neurosurgery. Migraine associated dizziness Department of Neuro-otology
 National Hospital for Neurology and Neurosurgery Migraine associated dizziness Department of Neuro-otology If you would like this document in another language or format or if you require the services of
National Hospital for Neurology and Neurosurgery Migraine associated dizziness Department of Neuro-otology If you would like this document in another language or format or if you require the services of
NEW PATIENT CLINICAL INFORMATION FORM. Booth Gardner Parkinson s Care & Movement Disorders Center Evergreen Neuroscience Institute
 NEW PATIENT CLINICAL INFORMATION FORM Booth Gardner Parkinson s Care & Movement Disorders Center Evergreen Neuroscience Institute Date: Name: Referring Doctor: How did you hear about us? NWPF Your Physician:
NEW PATIENT CLINICAL INFORMATION FORM Booth Gardner Parkinson s Care & Movement Disorders Center Evergreen Neuroscience Institute Date: Name: Referring Doctor: How did you hear about us? NWPF Your Physician:
Tone Management in Cerebral Palsy. Jenny Wilson, MD wilsjen@ohsu.edu OHSU and Shriners Hospital for Children October, 2015
 Tone Management in Cerebral Palsy Jenny Wilson, MD wilsjen@ohsu.edu OHSU and Shriners Hospital for Children October, 2015 Disclosures I am involved in a Dysport sponsored research study Goals Describe
Tone Management in Cerebral Palsy Jenny Wilson, MD wilsjen@ohsu.edu OHSU and Shriners Hospital for Children October, 2015 Disclosures I am involved in a Dysport sponsored research study Goals Describe
Chemobrain. Halle C.F. Moore, MD The Cleveland Clinic October 3, 2015
 Chemobrain Halle C.F. Moore, MD The Cleveland Clinic October 3, 2015 Terminology Chemotherapy-associated cognitive dysfunction Post-chemotherapy cognitive impairment Cancer treatment-associated cognitive
Chemobrain Halle C.F. Moore, MD The Cleveland Clinic October 3, 2015 Terminology Chemotherapy-associated cognitive dysfunction Post-chemotherapy cognitive impairment Cancer treatment-associated cognitive
Clinical and Therapeutic Cannabis Information. Written by Cannabis Training University (CTU) All rights reserved
 Clinical and Therapeutic Cannabis Information Written by Cannabis Training University (CTU) All rights reserved Contents Introduction... 3 Chronic Pain... 6 Neuropathic Pain... 8 Movement Disorders...
Clinical and Therapeutic Cannabis Information Written by Cannabis Training University (CTU) All rights reserved Contents Introduction... 3 Chronic Pain... 6 Neuropathic Pain... 8 Movement Disorders...
Depression is a common biological brain disorder and occurs in 7-12% of all individuals over
 Depression is a common biological brain disorder and occurs in 7-12% of all individuals over the age of 65. Specific groups have a much higher rate of depression including the seriously medically ill (20-40%),
Depression is a common biological brain disorder and occurs in 7-12% of all individuals over the age of 65. Specific groups have a much higher rate of depression including the seriously medically ill (20-40%),
The type of cancer Your specific treatment Your pre training levels before diagnose (your current strength and fitness levels)
 Exercise and Breast Cancer: Things you can do! Cancer within the fire service is one of the most dangerous threats to our firefighter s health & wellness. According to the latest studies firefighters are
Exercise and Breast Cancer: Things you can do! Cancer within the fire service is one of the most dangerous threats to our firefighter s health & wellness. According to the latest studies firefighters are
SUMMARY. White finger disease; Rheumatoid arthritis; Disablement (vibrations) (tools).
 SUMMARY DECISION NO. 1242/99 White finger disease; Rheumatoid arthritis; Disablement (vibrations) (tools). The worker was a jackleg driller until 1976 and then a hoist man until he retired in 1991. The
SUMMARY DECISION NO. 1242/99 White finger disease; Rheumatoid arthritis; Disablement (vibrations) (tools). The worker was a jackleg driller until 1976 and then a hoist man until he retired in 1991. The
Sleepless After TBI. MEDICAL News. Page 1
 Sleepless After TBI Why is it important to treat sleep disorders in TBI? Over 5 million people in the United States are currently living with a disability associated with brain injury. Although the major
Sleepless After TBI Why is it important to treat sleep disorders in TBI? Over 5 million people in the United States are currently living with a disability associated with brain injury. Although the major
Amitriptyline. Drug information Amitriptyline
 Drug information Amitriptyline Amitriptyline This leaflet provides information on amitriptyline and will answer any questions you have about the treatment. Arthritis Research UK produce and print our booklets
Drug information Amitriptyline Amitriptyline This leaflet provides information on amitriptyline and will answer any questions you have about the treatment. Arthritis Research UK produce and print our booklets
Cervical Spondylosis (Arthritis of the Neck)
 Copyright 2009 American Academy of Orthopaedic Surgeons Cervical Spondylosis (Arthritis of the Neck) Neck pain is extremely common. It can be caused by many things, and is most often related to getting
Copyright 2009 American Academy of Orthopaedic Surgeons Cervical Spondylosis (Arthritis of the Neck) Neck pain is extremely common. It can be caused by many things, and is most often related to getting
The Role of the Haematology Specialist Nurse. Catherine Chapman RN. BSc (Hons)
 The Role of the Haematology Specialist Nurse Catherine Chapman RN. BSc (Hons) Key Roles Information Support Advice Patient advocate Education Coordination of care Information Patient Family Carers Health
The Role of the Haematology Specialist Nurse Catherine Chapman RN. BSc (Hons) Key Roles Information Support Advice Patient advocate Education Coordination of care Information Patient Family Carers Health
TUE Physician Guidelines Medical Information to Support the Decisions of TUE Committees Neuropathic Pain. Neuropathic Pain
 1. Medical Condition Neuropathic pain is defined as pain arising from a lesion or any disease that causes dysfunction of the somatosensory system. Neuropathic pain is frequently difficult to treat, and
1. Medical Condition Neuropathic pain is defined as pain arising from a lesion or any disease that causes dysfunction of the somatosensory system. Neuropathic pain is frequently difficult to treat, and
What is Multiple Sclerosis? Gener al information
 What is Multiple Sclerosis? Gener al information Kim, diagnosed in 1986 What is MS? Multiple sclerosis (or MS) is a chronic, often disabling disease that attacks the central nervous system (brain and spinal
What is Multiple Sclerosis? Gener al information Kim, diagnosed in 1986 What is MS? Multiple sclerosis (or MS) is a chronic, often disabling disease that attacks the central nervous system (brain and spinal
Insomnia affects 1 in 3 adults every year in the U.S. and Canada.
 Insomnia What is insomnia? Having insomnia means you often have trouble falling or staying asleep or going back to sleep if you awaken. Insomnia can be either a short-term or a long-term problem. Insomnia
Insomnia What is insomnia? Having insomnia means you often have trouble falling or staying asleep or going back to sleep if you awaken. Insomnia can be either a short-term or a long-term problem. Insomnia
symptoms of Incontinence
 Types, causes and symptoms of Urinary Incontinence Aims and Objectives Aim: To have an understanding of the types and causes of urinary incontinence. Objectives: To be aware of the incidence and prevalence
Types, causes and symptoms of Urinary Incontinence Aims and Objectives Aim: To have an understanding of the types and causes of urinary incontinence. Objectives: To be aware of the incidence and prevalence
CHPN Review Course Pain Management Part 1 Hospice and Palliative Nurses Association
 CHPN Review Course Pain Management Part 1 Disclosures Bonnie Morgan has no real or perceived conflicts of interest that relate to this presentation. Copyright 2015 by the. HPNA has the exclusive rights
CHPN Review Course Pain Management Part 1 Disclosures Bonnie Morgan has no real or perceived conflicts of interest that relate to this presentation. Copyright 2015 by the. HPNA has the exclusive rights
DIFFERENTIAL DIAGNOSIS OF LOW BACK PAIN. Arnold J. Weil, M.D., M.B.A. Non-Surgical Orthopaedics, P.C. Atlanta, GA
 DIFFERENTIAL DIAGNOSIS OF LOW BACK PAIN Arnold J. Weil, M.D., M.B.A. Non-Surgical Orthopaedics, P.C. Atlanta, GA MEDICAL ALGORITHM OF REALITY LOWER BACK PAIN Yes Patient will never get better until case
DIFFERENTIAL DIAGNOSIS OF LOW BACK PAIN Arnold J. Weil, M.D., M.B.A. Non-Surgical Orthopaedics, P.C. Atlanta, GA MEDICAL ALGORITHM OF REALITY LOWER BACK PAIN Yes Patient will never get better until case
Spine Care Centre (SCC) protocols for Multiple Sclerosis Update 1 August 2015
 Spine Care Centre (SCC) protocols for Multiple Sclerosis Update 1 August 2015 Introduction Multiple sclerosis (MS) affects nerves in the brain and spinal cord, causing a wide range of symptoms including
Spine Care Centre (SCC) protocols for Multiple Sclerosis Update 1 August 2015 Introduction Multiple sclerosis (MS) affects nerves in the brain and spinal cord, causing a wide range of symptoms including
The majority of parkinsonism (approx. 80%) is due to idiopathic PD other causes include drug therapy (Table 1),toxins and trauma.
 THE TREATMENT OF PARKINSON S DISEASE SUMMARY Levodopa (L-dopa) administered in conjunction with a dopa decarboxylase inhibitor (DDCI) remains the mainstay of therapy for Parkinson s disease. New drugs
THE TREATMENT OF PARKINSON S DISEASE SUMMARY Levodopa (L-dopa) administered in conjunction with a dopa decarboxylase inhibitor (DDCI) remains the mainstay of therapy for Parkinson s disease. New drugs
New England Pain Management Consultants At New England Baptist Hospital
 New England Pain Management Consultants At New England Baptist Hospital Pain Management Center Health Assessment Dear New Pain Management Patient, Welcome to the New England Pain Management Consultants
New England Pain Management Consultants At New England Baptist Hospital Pain Management Center Health Assessment Dear New Pain Management Patient, Welcome to the New England Pain Management Consultants
.org. Herniated Disk in the Lower Back. Anatomy. Description
 Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
Parkinson s Disease Symptoms Guide
 Parkinson s Disease Symptoms Guide Some symptoms of Parkinson s disease (PD) are hard for even specialists to detect. Others are obvious even to an untrained eye. Parkinson s symptoms are different for
Parkinson s Disease Symptoms Guide Some symptoms of Parkinson s disease (PD) are hard for even specialists to detect. Others are obvious even to an untrained eye. Parkinson s symptoms are different for
Update and Review of Medication Assisted Treatments
 Update and Review of Medication Assisted Treatments for Opiate and Alcohol Use Disorders Richard N. Whitney, MD Medical Director Addiction Services Shepherd Hill Newark, Ohio Medication Assisted Treatment
Update and Review of Medication Assisted Treatments for Opiate and Alcohol Use Disorders Richard N. Whitney, MD Medical Director Addiction Services Shepherd Hill Newark, Ohio Medication Assisted Treatment
Changes in the Evaluation and Treatment of Sleep Apnea
 Changes in the Evaluation and Treatment of Sleep Apnea Joseph DellaValla, MD FACP Medical Director Center for Sleep Medicine At Androscoggin Valley Hospital Sleep Related Breathing Problems Obstructive
Changes in the Evaluation and Treatment of Sleep Apnea Joseph DellaValla, MD FACP Medical Director Center for Sleep Medicine At Androscoggin Valley Hospital Sleep Related Breathing Problems Obstructive
Fibromyalgia: The Information and the Care You Deserve PATIENT HANDBOOK
 Fibromyalgia: The Information and the Care You Deserve PATIENT HANDBOOK Fibromyalgia: You Need the Facts Fibromyalgia (fi bro-mi-al je- ) affects more than 6 million people in the United States. e Most
Fibromyalgia: The Information and the Care You Deserve PATIENT HANDBOOK Fibromyalgia: You Need the Facts Fibromyalgia (fi bro-mi-al je- ) affects more than 6 million people in the United States. e Most
Preferred Practice Guidelines Bipolar Disorder in Children and Adolescents
 These Guidelines are based in part on the following: American Academy of Child and Adolescent Psychiatry s Practice Parameter for the Assessment and Treatment of Children and Adolescents With Bipolar Disorder,
These Guidelines are based in part on the following: American Academy of Child and Adolescent Psychiatry s Practice Parameter for the Assessment and Treatment of Children and Adolescents With Bipolar Disorder,
HEADACHES IN CHILDREN AND ADOLESCENTS. Brian D. Ryals, M.D.
 HEADACHES IN CHILDREN AND ADOLESCENTS Brian D. Ryals, M.D. Frequency and Type of Headaches in Schoolchildren 8993 children age 7-15 in Sweden Migraine in 4% Frequent Nonmigrainous in 7% Infrequent Nonmigrainous
HEADACHES IN CHILDREN AND ADOLESCENTS Brian D. Ryals, M.D. Frequency and Type of Headaches in Schoolchildren 8993 children age 7-15 in Sweden Migraine in 4% Frequent Nonmigrainous in 7% Infrequent Nonmigrainous
Multiple System Atrophy guide (http://www.msaweb.co.uk/msaguide.htm)
 Multiple System Atrophy guide (http://www.msaweb.co.uk/msaguide.htm) Accessing information on Multiple System Atrophy (MSA) can be hard work. The Sarah Matheson Trust (SMT) produces a guide to MSA that
Multiple System Atrophy guide (http://www.msaweb.co.uk/msaguide.htm) Accessing information on Multiple System Atrophy (MSA) can be hard work. The Sarah Matheson Trust (SMT) produces a guide to MSA that
This continuing education activity is co-sponsored by Indiana University School of Medicine and by CME Outfitters, LLC.
 This continuing education activity is co-sponsored by Indiana University School of Medicine and by CME Outfitters, LLC. Indiana University School of Medicine and CME Outfitters, LLC, gratefully acknowledge
This continuing education activity is co-sponsored by Indiana University School of Medicine and by CME Outfitters, LLC. Indiana University School of Medicine and CME Outfitters, LLC, gratefully acknowledge
Why are you being seen at Frontier Diagnostic Sleep Center?
 8425 South 84th Street Suite B Omaha, NE 68127 Phone: 402.339.7378 Fax: 402.339.9455 SLEEP QUESTIONNAIRE NAME: ADDRESS: Last First MI Street Address DATE City State Zip PHONE: ( ) BIRTHDATE: HEIGHT: WEIGHT:
8425 South 84th Street Suite B Omaha, NE 68127 Phone: 402.339.7378 Fax: 402.339.9455 SLEEP QUESTIONNAIRE NAME: ADDRESS: Last First MI Street Address DATE City State Zip PHONE: ( ) BIRTHDATE: HEIGHT: WEIGHT:
Chronic Low Back Pain
 Chronic Low Back Pain North American Spine Society Public Education Series What is Chronic Pain? Low back pain is considered to be chronic if it has been present for longer than three months. Chronic low
Chronic Low Back Pain North American Spine Society Public Education Series What is Chronic Pain? Low back pain is considered to be chronic if it has been present for longer than three months. Chronic low
Migraine The Problem: Common Symptoms:
 Migraine The Problem: A combination of genetic and environmental factors alter pain mechanisms in your brain Transient changes in brain chemicals such as serotonin and neuropeptides affect the membranes
Migraine The Problem: A combination of genetic and environmental factors alter pain mechanisms in your brain Transient changes in brain chemicals such as serotonin and neuropeptides affect the membranes
Post Traumatic Stress Disorder (PTSD) Karen Elmore MD Robert K. Schneider MD Revised 5-11-2001 by Robert K. Schneider MD
 Post Traumatic Stress Disorder (PTSD) Karen Elmore MD Robert K. Schneider MD Revised 5-11-2001 by Robert K. Schneider MD Definition and Criteria PTSD is unlike any other anxiety disorder. It requires that
Post Traumatic Stress Disorder (PTSD) Karen Elmore MD Robert K. Schneider MD Revised 5-11-2001 by Robert K. Schneider MD Definition and Criteria PTSD is unlike any other anxiety disorder. It requires that
IMR ISSUES, DECISIONS AND RATIONALES The Final Determination was based on decisions for the disputed items/services set forth below:
 Case Number: CM13-0018009 Date Assigned: 10/11/2013 Date of Injury: 06/11/2004 Decision Date: 01/13/2014 UR Denial Date: 08/16/2013 Priority: Standard Application Received: 08/29/2013 HOW THE IMR FINAL
Case Number: CM13-0018009 Date Assigned: 10/11/2013 Date of Injury: 06/11/2004 Decision Date: 01/13/2014 UR Denial Date: 08/16/2013 Priority: Standard Application Received: 08/29/2013 HOW THE IMR FINAL
Learn the steps to identify pediatric muscle weakness and signs of neuromuscular disease.
 Learn the steps to identify pediatric muscle weakness and signs of neuromuscular disease. Guide for therapists/specialists Questions and comments to: info@childmuscleweakness.org Surveillance and Referral
Learn the steps to identify pediatric muscle weakness and signs of neuromuscular disease. Guide for therapists/specialists Questions and comments to: info@childmuscleweakness.org Surveillance and Referral
Comorbid Conditions in Autism Spectrum Illness. David Ermer MD June 13, 2014
 Comorbid Conditions in Autism Spectrum Illness David Ermer MD June 13, 2014 Overview Diagnosing comorbidities in autism spectrum illnesses Treatment issues specific to autism spectrum illnesses Treatment
Comorbid Conditions in Autism Spectrum Illness David Ermer MD June 13, 2014 Overview Diagnosing comorbidities in autism spectrum illnesses Treatment issues specific to autism spectrum illnesses Treatment
Depression and Anxiety in Parkinson s disease
 Depression and Anxiety in Parkinson s disease Greg Pontone, MD Director, Movement Disorders Psychiatry Clinical Programs at Johns Hopkins Morris K. Udall Parkinson's Disease Research Center Johns Hopkins
Depression and Anxiety in Parkinson s disease Greg Pontone, MD Director, Movement Disorders Psychiatry Clinical Programs at Johns Hopkins Morris K. Udall Parkinson's Disease Research Center Johns Hopkins
REHABILITATION MEDICINE by PROFESSOR ANTHONY WARD
 REHABILITATION MEDICINE by PROFESSOR ANTHONY WARD What is Rehabilitation Medicine? Rehabilitation Medicine (RM) is the medical specialty with rehabilitation as its primary strategy. It provides services
REHABILITATION MEDICINE by PROFESSOR ANTHONY WARD What is Rehabilitation Medicine? Rehabilitation Medicine (RM) is the medical specialty with rehabilitation as its primary strategy. It provides services

 More information >>> HERE
More information >>> HERE