North Trent Neonatal Network Clinical Guideline
|
|
|
- Madeleine Kellie Charles
- 7 years ago
- Views:
Transcription
1 North Trent Neonatal Network Clinical Guideline Title: Pulmonary Haemorrhage (neonatal) Author: Elizabeth Pilling (adapted from P Adiotomre and R Kacheroo) Date written: December 2012 Review date: April 2016 This clinical guideline has been developed to ensure appropriate evidence based standards of care throughout the North Trent Neonatal Network. The appropriate use and interpretation of this guideline in providing clinical care remains the responsibility of the individual clinician. If there is any doubt discuss with a senior colleague. Best practice recommendations represent widely used evidence-based practice and high quality standards that all Neonatal Units across the Network should implement. Subsequent suggested recommendations may be put into practice in local units. However, alternative appropriate local guidelines may also exist. A. Summary page 1. Aim of guideline The aim of this guideline is to provide evidence based management of significant pulmonary haemorrhage in infants. 2. Minimum standards where appropriate As a minimum, neonatal units should have a guideline for the management of pulmonary haemorrhage. 3. Summary Summary of management: Minor haemorrhage Close monitoring Avoidance of suctioning Major haemorrhage Immediate management: Manage airway, breathing and circulation Intubate and avoid removing ET tube Avoid suction Increase pressures and inspiratory time In shocked infants, provide circulatory support with blood product replacement Subsequent management Monitor blood gases in hypoxic infants, consider a dose of surfactant (200mg/kg)
2 Manage hypotension (as per NTNN guideline) Correct haematological parameters (see NTNN guideline) Treat for sepsis Closely monitor and manage fluid balance- consider fluid restriction and diuretics In infants with massive haemorrhage, consider endotracheal adrenaline (see text) B. Full guideline 1. Background Pulmonary haemorrhage is a relatively common but serious complication seen predominantly in preterm infants. The incidence of pulmonary haemorrhage is 1-12 per 1000 live births. The median age at onset is 46 hours for the preterm baby born at 34 weeks and below. However for the near term or full term baby born after 34 weeks of gestation the median age at onset is 6 hours 2. The 18 month outcomes of infants following a serious pulmonary haemorrhage were significantly worse (incidence of death or neurosensory impairment of 75% compared to 43% in matched infants without haemorrhage, OR 3.36) Aim The aim of this guideline is to provide evidence based management of significant pulmonary haemorrhage in infants. 3. Areas outside remit if applicable Management of insignificant pulmonary haemorrhage 4. Core guideline 4.1 Aetiology The lung effluent of infants with pulmonary haemorrhage has a low haematocrit and small molecular weight proteins, leading to the conclusion that the majority of cases, it is due to haemorrhagic oedema rather than whole blood. The pathogenesis of PH is therefore considered to be alveolar overdistension with high pulmonary capillary pressure causing epithelial breaks and leakage into the air spaces. This is thought to be caused by overdistention of the alveoli by mechanical ventilation and increased pulmonary capillary pressure due to a patent ductus arteriosis. There is circumstantial evidence to support this, with the risk factors associated with PH including ventilation, prematurity, PDA. 4.2 Risk factors 1,2 Risk factors for development of pulmonary haemorrhage are: For preterm infants Preterm birth Lack of antenatal steroids Need for positive pressure ventilation
3 Surfactant therapy Patent ductus arteriosus Thrombocytopenia (<100x10 6 ) For term infants Hypoxia o In utero (i.e. infants with growth restriction) o Intrapartum (i.e. infants with hypoxic ischaemic encephalopathy o Post partum (e.g. infants with meconium aspiration syndrome, difficult intubation leading to hypoxia) Delivery room resuscitation with positive pressure ventilation Hypotension 4.3 Prevention Antenatal Use of antenatal steroids in women at risk of preterm birth Respiratory Avoidance of hypoxia (especially in term infants who require resuscitation) Avoidance of unnecessary doses of surfactant. (see NTNN RDS guideline) Cardiovascular Management of hypotension (see NTNN hypotension guideline) Management of PDA (see NTNN guideline) Avoidance of fluid overload (as this increases risk of PDA) 4.4 Diagnosis There is considerable debate in the literature about the diagnostic criteria of pulmonary haemorrhage. Many infants have blood streaked endotracheal aspirates, however these frequently represent local trauma rather than significant haemorrhage. In the TIPPS 4 trial 15.6% of infants had some blood aspirated from the endotracheal tube, however 10.2% of infants had serious pulmonary haemorrhage, defined as requiring increase in ventilator support, oxygen requirement or blood product replacement. Table 1 describes the clinical differences and actions: Diagnosis Suction findings Clinical observations Management Significant pulmonary haemorrhage Copious amounts of fresh blood Tachycardia, BP, Pallor Acute deterioration in ventilation Minor pulmonary haemorrhage Minimal staining of ET secretions with fresh or old blood No signs of acute deterioration Most likely diagnosis - traumatic bleeding Suggest minimal suctioning and watch for clinical deterioration
4 A chest x-ray taken at the time will show patchy changes (the blood), signs consistent with heart failure. If there is a massive haemorrhage, complete white out maybe seen due to obstruction of the endotracheal tube with blood clots. 4.5 Treatment Minor pulmonary haemorrhage This may be a precursor to major haemorrhage, therefore the infant should be closely monitored and wherever possible suction and re-intubation avoided Significant pulmonary haemorrhage Infants with massive PH can be acutely unwell with hypovolaemic shock a) Assess as ABC: Airway If the infant is not intubated this will be necessary. However, this can be difficult due to haemorrhage. The most experienced intubator should perform this procedure in this situation (see NTNN guideline). Note end tidal CO 2 monitoring may be unhelpful in this situation as it may be falsely negative. In infants who are intubated, avoid removing the endotracheal tube, as replacing it can be extremely difficult. If the tube is completely blocked with blood, suction may be necessary. However, wherever possible, this should be avoided as it can precipitate further haemorrhage. Breathing There may be significant hypoxia during haemorrhage. The mean airway pressure should be increased. This can be achieved by increasing the PEEP (e.g. 6-7), inspiratory time (e.g ), PIP (or tidal volume if on VG) in steps. This helps by redistributing the lung fluid into the interstitial spaces and improving ventilation. High frequency oscillation can also be used in this situation where available. Circulation Infants with significant haemorrhage are often bradycardic and hypotensive. Blood replacement may be required urgently depending on the degree of haemorrhage. However note that the cause of PH is usually pulmonary oedema, therefore avoidance of further fluid overload is important. Wherever possible, useful fluid replacement should be given e.g. blood products, rather than saline. Hypotension should be managed as per NTNN guideline with the early use of inotropes.
5 4.5.2b) Further therapy Once the infant is acutely stabliised the following therapies can be considered: Respiratory Surfactant o There are no randomised controlled trials looking at the use of surfactant in PH, however there are a number of observational studies. A dose of 200mg/kg is used, once the infant has been stabilized if they still have a significant oxygen requirement. This is thought to act by replacing the surfactant inactivated by haemorrhage 3. o Blood gases Close monitoring of blood gases is necessary following significant pulmonary haemorrhage. Correction of acidosis may be needed, but this should be done once the other causes have been treated (e.g. hypotension). Note that bicarbonate boluses may contribute to further haemorrhage by increasing volume overload. o Sedation/muscle relaxation If ventilation is difficult, and the baby is unsettled, sedation and muscle relaxation may be required for a short period of time to allow for physiological stability to be achieved. Cardiovascular/Haematology Urgent samples should be taken for coagulation studies and full blood count. Correction may be required (see NTNN guidelines). Again, caution is needed with excessive fluid correction. Fluids Once the infant is cardiovascularly stable, fluid restriction and diuretics may be indicated to reduce the risk of fluid overload. Sepsis Sepsis may be the cause of PH, and therefore blood cultures should be taken and appropriate antibiotics commenced c) Other therapies o Adrenaline- there is one longitudinal study 5 using endotracheal adrenaline. The theoretical method of action is in constricting arterioles and reducing haemorrhage. There was a statistically significant improvement in survival in the group given adrenaline, but they were compared to historical controls and the treatment group included just 5 infants. 1:10,000 adrenaline of 0.3-1ml/kg was given via catheter advanced through the endotracheal tube (i.e. like surfactant). (REF) o Hemocoagulase- One study 6 has been published with 28 infants treated with hemocoagulase. This demonstrated a
6 significant reduction in mortality, however this drug is not currently available in the UK. o Cocaine- using a 4% cocaine spray (as used in some ENT departments) to promote vasoconstriction has been used in 1 study 7 however there is some concern regarding the use of cocaine in newborns and in addition it can be difficult to source. 6. Audit criteria None identified 7. References 1. Ductal Shunting, high pulmonary blood flow and pulmonary haemorrhage. Kluckow Journal of Pediatrics 136 (1) Antecedents of Clinically Significant Pulmonary Haemorrhage among Newborn Infants. Berger T et al. Journal of Perinatology , Surfactant for pulmonary haemorrhage in neonates (review). Aziz a et al. Cochrane database of systematic reviews Issue 7 4. Prevention and 18 month outcomes of serious pulmonary hemorrhage in extremely low birth weight infants: results from the trial of indomethacin prophylaxis in preterms. Alfaleh K et al. Pediatrics 2008; 121 e Pulmonary Hemorrhage in very low-birthweight infants: risk factors and management. Chen Y et al. Pediatrics International Role of Hemocoagulase in Pulmonary Hemorrhage in Preterm Infants: A Systematic Review. Abhay Lodha & Majeeda Kamaluddeen & Albert Akierman & Harish Amin. Indian J Pediatr (July 2011) 78(7): Pulmonary hemorrhage in neonates of early and late gestation. Bhandari V, Gagnon C, Rosenkrantz T, Hussain NJ Perinat Med. 1999;27(5): C. Appendices 1. Evidence grading
5/30/2014 OBJECTIVES THE ROLE OF A RESPIRATORY THERAPIST IN THE DELIVERY ROOM. Disclosure
 THE ROLE OF A RESPIRATORY THERAPIST IN THE DELIVERY ROOM Ona Fofah, MD FAAP Assistant Professor of Pediatrics Director, Division of Neonatology Department of Pediatrics Rutgers- NJMS, Newark OBJECTIVES
THE ROLE OF A RESPIRATORY THERAPIST IN THE DELIVERY ROOM Ona Fofah, MD FAAP Assistant Professor of Pediatrics Director, Division of Neonatology Department of Pediatrics Rutgers- NJMS, Newark OBJECTIVES
Addendum to the NRP Provider Textbook 6 th Edition Recommendations for specific modifications in the Canadian context
 Addendum to the NRP Provider Textbook 6 th Edition Recommendations for specific modifications in the Canadian context A subcommittee of the Canadian Neonatal Resuscitation Program (NRP) Steering Committee
Addendum to the NRP Provider Textbook 6 th Edition Recommendations for specific modifications in the Canadian context A subcommittee of the Canadian Neonatal Resuscitation Program (NRP) Steering Committee
NEONATAL RESUSCITATION PROVIDER (NRP) RECERTIFICATION TABLE OF CONTENTS
 NEONATAL RESUSCITATION PROVIDER (NRP) RECERTIFICATION TABLE OF CONTENTS NEONATAL FLOW ALGORITHM.2 INTRODUCTION 3 ANTICIPATION OF RESUSCITATION 4 TEMPERATURE CONTROL.4 CLEARING THE AIRWAY OF MECONIUM 5
NEONATAL RESUSCITATION PROVIDER (NRP) RECERTIFICATION TABLE OF CONTENTS NEONATAL FLOW ALGORITHM.2 INTRODUCTION 3 ANTICIPATION OF RESUSCITATION 4 TEMPERATURE CONTROL.4 CLEARING THE AIRWAY OF MECONIUM 5
Safe Zone: CV PIP < 26; HFOV: MAP < 16; HFJV: MAP < 16 Dopamine infusion up to 20 mcg/kg/min Epinephrine infusion up to 0.1 mcg /kg/min.
 Congenital Diaphragmatic Hernia: Management Guidelines 5-2006 Issued By: Division of Neonatology Reviewed: Effective Date: Categories: Chronicity Document Congenital Diaphragmatic Hernia: Management Guidelines
Congenital Diaphragmatic Hernia: Management Guidelines 5-2006 Issued By: Division of Neonatology Reviewed: Effective Date: Categories: Chronicity Document Congenital Diaphragmatic Hernia: Management Guidelines
Neonatal Emergencies. Care of the Neonate. Care of the Neonate. Care of the Neonate. Student Objectives. Student Objectives continued.
 Student Objectives Neonatal Emergencies After completing this section the student will be able to: 1. Identify three physiologic and/or anatomic features unique to the newborn 2. List three perinatal factors
Student Objectives Neonatal Emergencies After completing this section the student will be able to: 1. Identify three physiologic and/or anatomic features unique to the newborn 2. List three perinatal factors
How To Determine The Difference Between Long Versus Short Inspiratory Times In Neonates
 Long versus short inspiratory times in neonates receiving mechanical ventilation (Review) Kamlin COF, Davis PG This is a reprint of a Cochrane review, prepared and maintained by The Cochrane Collaboration
Long versus short inspiratory times in neonates receiving mechanical ventilation (Review) Kamlin COF, Davis PG This is a reprint of a Cochrane review, prepared and maintained by The Cochrane Collaboration
Acute heart failure may be de novo or it may be a decompensation of chronic heart failure.
 Management of Acute Left Ventricular Failure Acute left ventricular failure presents as pulmonary oedema due to increased pressure in the pulmonary capillaries. It is important to realise though that left
Management of Acute Left Ventricular Failure Acute left ventricular failure presents as pulmonary oedema due to increased pressure in the pulmonary capillaries. It is important to realise though that left
OET: Listening Part A: Influenza
 Listening Test Part B Time allowed: 23 minutes In this part, you will hear a talk on critical illnesses due to A/H1N1 influenza in pregnant and postpartum women, given by a medical researcher. You will
Listening Test Part B Time allowed: 23 minutes In this part, you will hear a talk on critical illnesses due to A/H1N1 influenza in pregnant and postpartum women, given by a medical researcher. You will
A8b. Resuscitation of a Term Infant with Meconium Staining. Session Summary. Session Objectives. References
 A8b Resuscitation of a Term Infant with Meconium Staining Karen Wright, PhD, NNP-BC Assistant Professor and Coordinator, Neonatal Nurse Practitioner Program Dept. of Women, Children, and Family Nursing,
A8b Resuscitation of a Term Infant with Meconium Staining Karen Wright, PhD, NNP-BC Assistant Professor and Coordinator, Neonatal Nurse Practitioner Program Dept. of Women, Children, and Family Nursing,
Emergency Fluid Therapy in Companion Animals
 Emergency Fluid Therapy in Companion Animals Paul Pitney BVSc paul.pitney@tafensw.edu.au The administration of appropriate types and quantities of intravenous fluids is the cornerstone of emergency therapy
Emergency Fluid Therapy in Companion Animals Paul Pitney BVSc paul.pitney@tafensw.edu.au The administration of appropriate types and quantities of intravenous fluids is the cornerstone of emergency therapy
11 Newborn Life Support
 11 Newborn Life Support Introduction Passage through the birth canal is a hypoxic experience for the fetus, since significant respiratory exchange at the placenta is prevented for the 50-75 s duration
11 Newborn Life Support Introduction Passage through the birth canal is a hypoxic experience for the fetus, since significant respiratory exchange at the placenta is prevented for the 50-75 s duration
SWISS SOCIETY OF NEONATOLOGY. Selective bronchial occlusion in a preterm infant with unilateral pulmonary interstitial emphysema
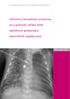 SWISS SOCIETY OF NEONATOLOGY Selective bronchial occlusion in a preterm infant with unilateral pulmonary interstitial emphysema December 2002 2 Riedel T, Pfenninger J, Pediatric Intensive Care Unit, University
SWISS SOCIETY OF NEONATOLOGY Selective bronchial occlusion in a preterm infant with unilateral pulmonary interstitial emphysema December 2002 2 Riedel T, Pfenninger J, Pediatric Intensive Care Unit, University
Update on Neonatal Resuscitation
 Update on Neonatal Resuscitation Ola Didrik Saugstad MD, PhD, FRCPE Professor of Pediatrics Director Department of Pediatric Research Rikshospitalet, Faculty of Medicine University of Oslo NORWAY 1st.
Update on Neonatal Resuscitation Ola Didrik Saugstad MD, PhD, FRCPE Professor of Pediatrics Director Department of Pediatric Research Rikshospitalet, Faculty of Medicine University of Oslo NORWAY 1st.
Mechanical Ventilators
 University of Washington Academic Medical Center Copyright 2000 Disclaimer Children's Hospital and Regional Medical Center Copyright 2002 Disclaimer Mechanical Ventilators Authors Created 07/31/95 Reviewed
University of Washington Academic Medical Center Copyright 2000 Disclaimer Children's Hospital and Regional Medical Center Copyright 2002 Disclaimer Mechanical Ventilators Authors Created 07/31/95 Reviewed
MECHINICAL VENTILATION S. Kache, MD
 MECHINICAL VENTILATION S. Kache, MD Spontaneous respiration vs. Mechanical ventilation Natural spontaneous ventilation occurs when the respiratory muscles, diaphragm and intercostal muscles pull on the
MECHINICAL VENTILATION S. Kache, MD Spontaneous respiration vs. Mechanical ventilation Natural spontaneous ventilation occurs when the respiratory muscles, diaphragm and intercostal muscles pull on the
Hummi Micro Draw Blood Transfer Device. The Next Generation System for Closed Micro Blood Sampling in the Neonate
 Hummi Micro Draw Blood Transfer Device The Next Generation System for Closed Micro Blood Sampling in the Neonate Current Methods for Umbilical Blood Sampling Current Methods for Umbilical Blood Sampling
Hummi Micro Draw Blood Transfer Device The Next Generation System for Closed Micro Blood Sampling in the Neonate Current Methods for Umbilical Blood Sampling Current Methods for Umbilical Blood Sampling
Why is prematurity a concern?
 Prematurity What is prematurity? A baby born before 37 weeks of pregnancy is considered premature. Approximately 12% of all babies are born prematurely. Terms that refer to premature babies are preterm
Prematurity What is prematurity? A baby born before 37 weeks of pregnancy is considered premature. Approximately 12% of all babies are born prematurely. Terms that refer to premature babies are preterm
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) S. Agarwal, MD, S. Kache MD
 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) S. Agarwal, MD, S. Kache MD Definition ARDS is a clinical syndrome of lung injury with hypoxic respiratory failure caused by intense pulmonary inflammation that
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) S. Agarwal, MD, S. Kache MD Definition ARDS is a clinical syndrome of lung injury with hypoxic respiratory failure caused by intense pulmonary inflammation that
Ibuprofen vs. Indomethacin in the Closure of the Patent Ductus Arteriosus (PDA)
 St. Catherine University SOPHIA Master of Arts in Nursing Theses Nursing 12-2011 Ibuprofen vs. Indomethacin in the Closure of the Patent Ductus Arteriosus (PDA) Bria James St. Catherine University Follow
St. Catherine University SOPHIA Master of Arts in Nursing Theses Nursing 12-2011 Ibuprofen vs. Indomethacin in the Closure of the Patent Ductus Arteriosus (PDA) Bria James St. Catherine University Follow
Please answer the following questions before reading the tutorial. The answers are contained in the article.
 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Author Dr D. Lacquiere Correspondence: david_lacquiere@hotmail.com Please answer the following questions before reading the tutorial. The answers are contained
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Author Dr D. Lacquiere Correspondence: david_lacquiere@hotmail.com Please answer the following questions before reading the tutorial. The answers are contained
Extracorporeal Life Support Organization (ELSO) Guidelines for Neonatal Respiratory Failure
 Extracorporeal Life Support Organization (ELSO) Guidelines for Neonatal Respiratory Failure Introduction This neonatal respiratory failure guideline is a supplement to ELSO s General Guidelines for all
Extracorporeal Life Support Organization (ELSO) Guidelines for Neonatal Respiratory Failure Introduction This neonatal respiratory failure guideline is a supplement to ELSO s General Guidelines for all
High-Frequency Oscillatory Ventilation
 High-Frequency Oscillatory Ventilation Arthur Jones EdD, RRT Learning Objectives Describe the indications and rationale and monitoring for HFOV. Identify HFOV settings and describe the effects of their
High-Frequency Oscillatory Ventilation Arthur Jones EdD, RRT Learning Objectives Describe the indications and rationale and monitoring for HFOV. Identify HFOV settings and describe the effects of their
Management of airway burns and inhalation injury PAEDIATRIC
 Management of airway burns and inhalation injury PAEDIATRIC A multidisciplinary team should provide the management of the child with inhalation injury. Childhood inhalation injury mandates transfer to
Management of airway burns and inhalation injury PAEDIATRIC A multidisciplinary team should provide the management of the child with inhalation injury. Childhood inhalation injury mandates transfer to
Resuscitation of the baby at birth
 Chapter 8 Resuscitation of the baby at birth Objectives On successfully completing this topic, you will be able to: understand the important physiological differences in the newly born baby understand
Chapter 8 Resuscitation of the baby at birth Objectives On successfully completing this topic, you will be able to: understand the important physiological differences in the newly born baby understand
3100B Clinical Training Program. 3100B HFOV VIASYS Healthcare
 3100B Clinical Training Program 3100B HFOV VIASYS Healthcare HFOV at Alveolar Level Nieman,, G, SUNY 1999 Who DO We Treat? Only Pathology studied to date has been ARDS Questions about management of adults
3100B Clinical Training Program 3100B HFOV VIASYS Healthcare HFOV at Alveolar Level Nieman,, G, SUNY 1999 Who DO We Treat? Only Pathology studied to date has been ARDS Questions about management of adults
Early Warning Scores (EWS) Clinical Sessions 2011 By Bhavin Doshi
 Early Warning Scores (EWS) Clinical Sessions 2011 By Bhavin Doshi What is EWS? After qualifying, junior doctors are expected to distinguish between the moderately sick patients who can be managed in the
Early Warning Scores (EWS) Clinical Sessions 2011 By Bhavin Doshi What is EWS? After qualifying, junior doctors are expected to distinguish between the moderately sick patients who can be managed in the
GUIDELINE 13.8 THE RESUSCITATION OF THE NEWBORN INFANT IN SPECIAL CIRCUMSTANCES
 AUSTRALIAN RESUSCITATION COUNCIL GUIDELINE 13.8 THE RESUSCITATION OF THE NEWBORN INFANT IN SPECIAL CIRCUMSTANCES PREMATURITY Temperature management Very premature infants are at particular risk of hypothermia.
AUSTRALIAN RESUSCITATION COUNCIL GUIDELINE 13.8 THE RESUSCITATION OF THE NEWBORN INFANT IN SPECIAL CIRCUMSTANCES PREMATURITY Temperature management Very premature infants are at particular risk of hypothermia.
SOUTHERN WEST MIDLANDS NEWBORN NETWORK
 SOUTHERN WEST MIDLANDS NEWBORN NETWORK Hereford, Worcester, Birmingham, Sandwell & Solihull Title Person Responsible for Review Delayed Umbilical Cord Clamping Dr Andrew Gallagher Date Guideline Agreed:
SOUTHERN WEST MIDLANDS NEWBORN NETWORK Hereford, Worcester, Birmingham, Sandwell & Solihull Title Person Responsible for Review Delayed Umbilical Cord Clamping Dr Andrew Gallagher Date Guideline Agreed:
MECHANICAL VENTILATION IN THE NEONATE
 Supplemental Resources for the PICU/NICU MECHANICAL VENTILATION IN THE NEONATE I. GENERAL PRINCIPLES A. NEONATAL VENTILATORS We use three types of neonatal ventilators in the NICU: 1. SIMV (Synchronized
Supplemental Resources for the PICU/NICU MECHANICAL VENTILATION IN THE NEONATE I. GENERAL PRINCIPLES A. NEONATAL VENTILATORS We use three types of neonatal ventilators in the NICU: 1. SIMV (Synchronized
APPENDIX B SAMPLE PEDIATRIC CRITICAL CARE NURSE PRACTITIONER GOALS AND OBJECTIVES
 APPENDIX B SAMPLE PEDIATRIC CRITICAL CARE NURSE PRACTITIONER GOALS AND OBJECTIVES The critical care nurse practitioner orientation is an individualized process based on one s previous experiences and should
APPENDIX B SAMPLE PEDIATRIC CRITICAL CARE NURSE PRACTITIONER GOALS AND OBJECTIVES The critical care nurse practitioner orientation is an individualized process based on one s previous experiences and should
Neonatal Reference Guide
 Operated by REACH Air Medical Services Assessment Heart Rate (beats/min.) Age Rate
Operated by REACH Air Medical Services Assessment Heart Rate (beats/min.) Age Rate
Recommendations: Other Supportive Therapy of Severe Sepsis*
 Recommendations: Other Supportive Therapy of Severe Sepsis* K. Blood Product Administration 1. Once tissue hypoperfusion has resolved and in the absence of extenuating circumstances, such as myocardial
Recommendations: Other Supportive Therapy of Severe Sepsis* K. Blood Product Administration 1. Once tissue hypoperfusion has resolved and in the absence of extenuating circumstances, such as myocardial
How To Treat A Heart Attack
 13 Resuscitation and preparation for anaesthesia and surgery Key Points 13.1 MANAGEMENT OF EMERGENCIES AND CARDIOPULMONARY RESUSCITATION ESSENTIAL HEALTH TECHNOLOGIES The emergency measures that are familiar
13 Resuscitation and preparation for anaesthesia and surgery Key Points 13.1 MANAGEMENT OF EMERGENCIES AND CARDIOPULMONARY RESUSCITATION ESSENTIAL HEALTH TECHNOLOGIES The emergency measures that are familiar
Update on Small Animal Cardiopulmonary Resuscitation (CPR)- is anything new?
 Update on Small Animal Cardiopulmonary Resuscitation (CPR)- is anything new? DVM, DACVA Objective: Update on the new Small animal guidelines for CPR and a discussion of the 2012 Reassessment Campaign on
Update on Small Animal Cardiopulmonary Resuscitation (CPR)- is anything new? DVM, DACVA Objective: Update on the new Small animal guidelines for CPR and a discussion of the 2012 Reassessment Campaign on
Diabetic Ketoacidosis
 Princess Margaret Hospital for Children PAEDIATRIC ACUTE CARE GUIDELINE Diabetic Ketoacidosis Scope (Staff): Scope (Area): All Emergency Department Clinicians Emergency Department This document should
Princess Margaret Hospital for Children PAEDIATRIC ACUTE CARE GUIDELINE Diabetic Ketoacidosis Scope (Staff): Scope (Area): All Emergency Department Clinicians Emergency Department This document should
KING FAISAL SPECIALIST HOSPITAL AND RESEARCH CENTRE (GEN. ORG.) NURSING AFFAIRS. Scope of Service PEDIATRIC INTENSIVE CARE UNIT (PICU)
 PICU-Jan.2012 Page 1 of 7 Number of Beds: 18 Nurse Patient Ratio: 1:1-2 : The Pediatric Intensive Care Unit (PICU) provides 24 hour intensive nursing care for patients aged neonate through adolescence.
PICU-Jan.2012 Page 1 of 7 Number of Beds: 18 Nurse Patient Ratio: 1:1-2 : The Pediatric Intensive Care Unit (PICU) provides 24 hour intensive nursing care for patients aged neonate through adolescence.
Pediatric Respiratory System: Basic Anatomy & Physiology. Jihad Zahraa Pediatric Intensivist Head of PICU, King Fahad Medical City
 Pediatric Respiratory System: Basic Anatomy & Physiology Jihad Zahraa Pediatric Intensivist Head of PICU, King Fahad Medical City Outline Introduction Developmental Anatomy Developmental Mechanics of Breathing
Pediatric Respiratory System: Basic Anatomy & Physiology Jihad Zahraa Pediatric Intensivist Head of PICU, King Fahad Medical City Outline Introduction Developmental Anatomy Developmental Mechanics of Breathing
Common Ventilator Management Issues
 Common Ventilator Management Issues William Janssen, M.D. Assistant Professor of Medicine National Jewish Health University of Colorado Denver Health Sciences Center You have just admitted a 28 year-old
Common Ventilator Management Issues William Janssen, M.D. Assistant Professor of Medicine National Jewish Health University of Colorado Denver Health Sciences Center You have just admitted a 28 year-old
A. All cells need oxygen and release carbon dioxide why?
 I. Introduction: Describe how the cardiovascular and respiratory systems interact to supply O 2 and eliminate CO 2. A. All cells need oxygen and release carbon dioxide why? B. Two systems that help to
I. Introduction: Describe how the cardiovascular and respiratory systems interact to supply O 2 and eliminate CO 2. A. All cells need oxygen and release carbon dioxide why? B. Two systems that help to
Management of Infants with BPD: Evidence-Based or Eminence-Based?
 Management of Infants with BPD: Evidence-Based or Eminence-Based? Steven M. Donn, MD, FAAP Professor of Pediatrics Division of Neonatal-Perinatal Medicine C.S. Mott Children s Hospital University of Michigan
Management of Infants with BPD: Evidence-Based or Eminence-Based? Steven M. Donn, MD, FAAP Professor of Pediatrics Division of Neonatal-Perinatal Medicine C.S. Mott Children s Hospital University of Michigan
The Sepsis Puzzle: Identification, Monitoring and Early Goal Directed Therapy
 The Sepsis Puzzle: Identification, Monitoring and Early Goal Directed Therapy Cindy Goodrich RN, MS, CCRN Content Description Sepsis is caused by widespread tissue injury and systemic inflammation resulting
The Sepsis Puzzle: Identification, Monitoring and Early Goal Directed Therapy Cindy Goodrich RN, MS, CCRN Content Description Sepsis is caused by widespread tissue injury and systemic inflammation resulting
(C) AMBULANCE VICTORIA
 The Newborn Baby: Definitions and Contacts Newborn definition 'Newborn' refers to the first min to hours post birth. For the purpose of resuscitation, AV accepts up to the first 24 hours from birth in
The Newborn Baby: Definitions and Contacts Newborn definition 'Newborn' refers to the first min to hours post birth. For the purpose of resuscitation, AV accepts up to the first 24 hours from birth in
PEDIATRIC TREATMENT GUIDELINES
 P1 Pediatric Patient Care P2 Cardiac Arrest Initial Care and CPR P3 Neonatal Resuscitation P4 Ventricular Fibrillation / Ventricular Tachycardia P5 PEA / Asystole P6 Symptomatic Bradycardia P7 Tachycardia
P1 Pediatric Patient Care P2 Cardiac Arrest Initial Care and CPR P3 Neonatal Resuscitation P4 Ventricular Fibrillation / Ventricular Tachycardia P5 PEA / Asystole P6 Symptomatic Bradycardia P7 Tachycardia
Neonatal Intubation. Purpose. Scope. Indications. Equipment Cardiorespiratory monitor SaO 2 monitor. Anatomic Considerations.
 Page 1 of 5 Purpose Scope Indications Neonatal Intubation To assure proper placement of endotracheal tubes for maximum ventilation using proper intubation procedures. The policy applies to all Respiratory
Page 1 of 5 Purpose Scope Indications Neonatal Intubation To assure proper placement of endotracheal tubes for maximum ventilation using proper intubation procedures. The policy applies to all Respiratory
AHA/AAP Neonatal Resuscitation Guidelines 2010: Summary of Major Changes and Comment on its Utility in Resource-Limited Settings
 AHA/AAP Neonatal Resuscitation Guidelines 2010: Summary of Major Changes and Comment on its Utility in Resource-Limited Settings Resuscitation step Recommendations (2005) Recommendations (2010) Comments/LOE
AHA/AAP Neonatal Resuscitation Guidelines 2010: Summary of Major Changes and Comment on its Utility in Resource-Limited Settings Resuscitation step Recommendations (2005) Recommendations (2010) Comments/LOE
Mechanical Ventilation
 Mechanical Ventilation 127 Mechanical Ventilation William Benitz, M.D. Caring for a mechanically ventilated neonate continues to unnecessarily strike fear in the heart of many a resident. This fear is
Mechanical Ventilation 127 Mechanical Ventilation William Benitz, M.D. Caring for a mechanically ventilated neonate continues to unnecessarily strike fear in the heart of many a resident. This fear is
EMBARGOED FOR RELEASE
 Systems of Care and Continuous Quality Improvement Universal elements of a system of care have been identified to provide stakeholders with a common framework with which to assemble an integrated resuscitation
Systems of Care and Continuous Quality Improvement Universal elements of a system of care have been identified to provide stakeholders with a common framework with which to assemble an integrated resuscitation
Delayed Cord Clamping
 ICEA Position Paper Delayed Cord Clamping Position The International Childbirth Education Association recognizes that the first minutes after birth are crucial to both mother and newborn. Optimal care
ICEA Position Paper Delayed Cord Clamping Position The International Childbirth Education Association recognizes that the first minutes after birth are crucial to both mother and newborn. Optimal care
Pediatrix Medical Group BabySteps and the Clinical Data Warehouse
 Pediatrix Medical Group BabySteps and the Clinical Data Warehouse Pediatrix Medical Group Reese H Clark MD Dan Ellsbury MD Alan Spitzer MD Duke Clinical Research Institute Brian Smith MD MPH MHS Danny
Pediatrix Medical Group BabySteps and the Clinical Data Warehouse Pediatrix Medical Group Reese H Clark MD Dan Ellsbury MD Alan Spitzer MD Duke Clinical Research Institute Brian Smith MD MPH MHS Danny
Quality of Birth Certificate Data. Daniela Nitcheva, PhD Division of Biostatistics PHSIS
 Quality of Birth Certificate Data Daniela Nitcheva, PhD Division of Biostatistics PHSIS Data Quality SC State Law requires that you file the birth certificate within 5 days of a child s birth. Data needs
Quality of Birth Certificate Data Daniela Nitcheva, PhD Division of Biostatistics PHSIS Data Quality SC State Law requires that you file the birth certificate within 5 days of a child s birth. Data needs
TACO vs. TRALI: Recognition, Differentiation, and Investigation of Pulmonary Transfusion Reactions
 TACO vs. TRALI: Recognition, Differentiation, and Investigation of Pulmonary Transfusion Reactions Shealynn Harris, M.D. Assistant Medical Director American Red Cross Blood Services Southern Region Case
TACO vs. TRALI: Recognition, Differentiation, and Investigation of Pulmonary Transfusion Reactions Shealynn Harris, M.D. Assistant Medical Director American Red Cross Blood Services Southern Region Case
Lothian Diabetes Handbook MANAGEMENT OF DIABETIC KETOACIDOSIS
 MANAGEMENT OF DIABETIC KETOACIDOSIS 90 MANAGEMENT OF DIABETIC KETOACIDOSIS Diagnosis elevated plasma and/or urinary ketones metabolic acidosis (raised H + /low serum bicarbonate) Remember that hyperglycaemia,
MANAGEMENT OF DIABETIC KETOACIDOSIS 90 MANAGEMENT OF DIABETIC KETOACIDOSIS Diagnosis elevated plasma and/or urinary ketones metabolic acidosis (raised H + /low serum bicarbonate) Remember that hyperglycaemia,
Oxygen - update April 2009 OXG
 PRESENTATION Oxygen (O 2 ) is a gas provided in compressed form in a cylinder. It is also available in liquid form, in a system adapted for ambulance use. It is fed via a regulator and flow meter to the
PRESENTATION Oxygen (O 2 ) is a gas provided in compressed form in a cylinder. It is also available in liquid form, in a system adapted for ambulance use. It is fed via a regulator and flow meter to the
STAGES OF SHOCK. IRREVERSIBLE SHOCK Heart deteriorates until it can no longer pump and death occurs.
 STAGES OF SHOCK SHOCK : A profound disturbance of circulation and metabolism, which leads to inadequate perfusion of all organs which are needed to maintain life. COMPENSATED NONPROGRESSIVE SHOCK 30 sec
STAGES OF SHOCK SHOCK : A profound disturbance of circulation and metabolism, which leads to inadequate perfusion of all organs which are needed to maintain life. COMPENSATED NONPROGRESSIVE SHOCK 30 sec
More detailed background information and references can be found at the end of this guideline
 Neonatal Intensive Care Unit Clinical Guideline Oxygen Over the past few years there have been significant changes, based on high quality research, in our understanding of how to give the right amount
Neonatal Intensive Care Unit Clinical Guideline Oxygen Over the past few years there have been significant changes, based on high quality research, in our understanding of how to give the right amount
Cord Blood Erythropoietin and Markers of Fetal Hypoxia
 July 21, 2011 By NeedsFixing [1] To investigating the relationship between cord blood erythropoietin and clinical markers of fetal hypoxia. Abstract Objective: To investigating the relationship between
July 21, 2011 By NeedsFixing [1] To investigating the relationship between cord blood erythropoietin and clinical markers of fetal hypoxia. Abstract Objective: To investigating the relationship between
ASSISTED VENTILATION IN NEONATES
 ASSISTED VENTILATION IN NEONATES CONTINUOUS POSITIVE AIRWAY PRESSURE (CPAP) DEFINITION Continuous Positive Airway Pressure or CPAP is a modality of respiratory support in which increased pulmonary pressure
ASSISTED VENTILATION IN NEONATES CONTINUOUS POSITIVE AIRWAY PRESSURE (CPAP) DEFINITION Continuous Positive Airway Pressure or CPAP is a modality of respiratory support in which increased pulmonary pressure
ACLS PHARMACOLOGY 2011 Guidelines
 ACLS PHARMACOLOGY 2011 Guidelines ADENOSINE Narrow complex tachycardias or wide complex tachycardias that may be supraventricular in nature. It is effective in treating 90% of the reentry arrhythmias.
ACLS PHARMACOLOGY 2011 Guidelines ADENOSINE Narrow complex tachycardias or wide complex tachycardias that may be supraventricular in nature. It is effective in treating 90% of the reentry arrhythmias.
Neonatal Reference Guide
 Operated by REACH Air Medical Services Assessment Heart Rate (beats/min.) Rate
Operated by REACH Air Medical Services Assessment Heart Rate (beats/min.) Rate
SE5h, Sepsis Education.pdf. Surviving Sepsis
 Surviving Sepsis 1 Scope and Impact of the Problem: Severe sepsis is a major healthcare problem that affects millions of people around the world each year with an extremely high mortality rate of 30 to
Surviving Sepsis 1 Scope and Impact of the Problem: Severe sepsis is a major healthcare problem that affects millions of people around the world each year with an extremely high mortality rate of 30 to
Newborn Screening Update for Health Care Practitioners
 Newborn Screening Update for Health Care Practitioners Changes in regulations affecting your practice for newborns transferred to neonatal intensive care units. Changes for newborn screening of premature,
Newborn Screening Update for Health Care Practitioners Changes in regulations affecting your practice for newborns transferred to neonatal intensive care units. Changes for newborn screening of premature,
Children's Medical Services (CMS) Regional Perinatal Intensive Care Center (RPICC) Neonatal Extracorporeal Life Support (ECLS) Centers Questionnaire
 Children's Medical Services (CMS) Regional Perinatal Intensive Care Center (RPICC) Neonatal Extracorporeal Life Support (ECLS) Centers Questionnaire Date: RPICC Facility: CMS use only Include the following
Children's Medical Services (CMS) Regional Perinatal Intensive Care Center (RPICC) Neonatal Extracorporeal Life Support (ECLS) Centers Questionnaire Date: RPICC Facility: CMS use only Include the following
Oxygen Therapy. Oxygen therapy quick guide V3 July 2012.
 PRESENTATION Oxygen (O 2 ) is a gas provided in a compressed form in a cylinder. It is also available in a liquid form. It is fed via a regulator and flow meter to the patient by means of plastic tubing
PRESENTATION Oxygen (O 2 ) is a gas provided in a compressed form in a cylinder. It is also available in a liquid form. It is fed via a regulator and flow meter to the patient by means of plastic tubing
NRP Study Guide. This packet is intended for review only. Requirements to successfully complete NRP:
 This packet is intended for review only Requirements to successfully complete NRP: Completed NRP Pretest is required for admission to the course. Score 84% on the multiplechoice posttest. You may be allowed
This packet is intended for review only Requirements to successfully complete NRP: Completed NRP Pretest is required for admission to the course. Score 84% on the multiplechoice posttest. You may be allowed
Homeostasis. The body must maintain a delicate balance of acids and bases.
 Homeostasis The body must maintain a delicate balance of acids and bases. Metabolic and respiratory processes must work together to keep hydrogen ion (H+) levels normal and stable. ph of Blood The ph of
Homeostasis The body must maintain a delicate balance of acids and bases. Metabolic and respiratory processes must work together to keep hydrogen ion (H+) levels normal and stable. ph of Blood The ph of
Airway Pressure Release Ventilation
 Page: 1 Policy #: 25.01.153 Issued: 4-1-2006 Reviewed/ Revised: Section: 10-11-2006 Respiratory Care Airway Pressure Release Ventilation Description/Definition Airway Pressure Release Ventilation (APRV)
Page: 1 Policy #: 25.01.153 Issued: 4-1-2006 Reviewed/ Revised: Section: 10-11-2006 Respiratory Care Airway Pressure Release Ventilation Description/Definition Airway Pressure Release Ventilation (APRV)
TRANSPORT OF CRITICALLY ILL PATIENTS
 TRANSPORT OF CRITICALLY ILL PATIENTS Introduction Inter-hospital and intra-hospital transport of critically ill patients places the patient at risk of adverse events and increased morbidity and mortality.
TRANSPORT OF CRITICALLY ILL PATIENTS Introduction Inter-hospital and intra-hospital transport of critically ill patients places the patient at risk of adverse events and increased morbidity and mortality.
Medical Direction and Practices Board WHITE PAPER
 Medical Direction and Practices Board WHITE PAPER Use of Pressors in Pre-Hospital Medicine: Proper Indication and State of the Science Regarding Proper Choice of Pressor BACKGROUND Shock is caused by a
Medical Direction and Practices Board WHITE PAPER Use of Pressors in Pre-Hospital Medicine: Proper Indication and State of the Science Regarding Proper Choice of Pressor BACKGROUND Shock is caused by a
Resuscitation of the baby at birth
 APPENDIX I Resuscitation of the baby at birth I.1 OBJECTIVES This will teach you: I.2 INTRODUCTION the important physiological differences in the newly born baby the equipment used for resuscitation at
APPENDIX I Resuscitation of the baby at birth I.1 OBJECTIVES This will teach you: I.2 INTRODUCTION the important physiological differences in the newly born baby the equipment used for resuscitation at
NHS FORTH VALLEY Neonatal Oxygen Saturation Guideline
 NHS FORTH VALLEY Neonatal Oxygen Saturation Guideline Date of First Issue 11/07/2011 Approved 30/09/2011 Current Issue Date 07/09/2011 Review Date July 2013 Version 1 EQIA Yes 22/10/2011 Author / Contact
NHS FORTH VALLEY Neonatal Oxygen Saturation Guideline Date of First Issue 11/07/2011 Approved 30/09/2011 Current Issue Date 07/09/2011 Review Date July 2013 Version 1 EQIA Yes 22/10/2011 Author / Contact
Milliman Guidelines NICU Levels*
 Milliman Guidelines NICU Levels* Neonatal Intensive Care Unit Level IV If the following conditions/procedures exist, in addition to the fulfillment of Level III Criteria, the approved inpatient days should
Milliman Guidelines NICU Levels* Neonatal Intensive Care Unit Level IV If the following conditions/procedures exist, in addition to the fulfillment of Level III Criteria, the approved inpatient days should
NICE Pathways bring together all NICE guidance, quality standards and other NICE information on a specific topic.
 Diabetic ketoacidosis in children and young people bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used online. They
Diabetic ketoacidosis in children and young people bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used online. They
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE. Health Technology Appraisal. Drugs for the treatment of pulmonary arterial hypertension
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Health Technology Appraisal Drugs for the treatment of Remit / Appraisal objective: Final scope To appraise the clinical and cost effectiveness of
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Health Technology Appraisal Drugs for the treatment of Remit / Appraisal objective: Final scope To appraise the clinical and cost effectiveness of
Oregon Birth Outcomes, by Planned Birth Place and Attendant Pursuant to: HB 2380 (2011)
 Oregon Birth Outcomes, by Birth Place and Attendant Pursuant to: HB 2380 (2011) In 2011, the Oregon Legislature passed House Bill 2380, which required the Oregon Public Health Division to add two questions
Oregon Birth Outcomes, by Birth Place and Attendant Pursuant to: HB 2380 (2011) In 2011, the Oregon Legislature passed House Bill 2380, which required the Oregon Public Health Division to add two questions
Brain Injury during Fetal-Neonatal Transition
 Brain Injury during Fetal-Neonatal Transition Adre du Plessis, MBChB Fetal and Transitional Medicine Children s National Medical Center Washington, DC Brain injury during fetal-neonatal transition Injury
Brain Injury during Fetal-Neonatal Transition Adre du Plessis, MBChB Fetal and Transitional Medicine Children s National Medical Center Washington, DC Brain injury during fetal-neonatal transition Injury
British Association of Perinatal Medicine. The Management of Babies born Extremely Preterm at less than 26 weeks of gestation
 Arch Dis Child - FNN Online First:Published on October 6, 2008 as 10.1136/adc.2008.143321 British Association of Perinatal Medicine The Management of Babies born Extremely Preterm at less than 26 weeks
Arch Dis Child - FNN Online First:Published on October 6, 2008 as 10.1136/adc.2008.143321 British Association of Perinatal Medicine The Management of Babies born Extremely Preterm at less than 26 weeks
CROSS HEALTH CARE BOUNDARIES MATERNITY CLINICAL GUIDELINE
 CROSS HEALTH CARE BOUNDARIES MATERNITY CLINICAL GUIDELINE Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Obstetric Early Warning Score Guideline Implementation
CROSS HEALTH CARE BOUNDARIES MATERNITY CLINICAL GUIDELINE Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Obstetric Early Warning Score Guideline Implementation
CLINICAL GUIDELINE FOR VAGINAL BIRTH AFTER CAESAREAN SECTION (VBAC)
 CLINICAL GUIDELINE FOR VAGINAL BIRTH AFTER CAESAREAN SECTION (VBAC) 1. Aim/Purpose of this Guideline 1.1. Due to a rise in the caesarean section rate there are increasing numbers of pregnant women who
CLINICAL GUIDELINE FOR VAGINAL BIRTH AFTER CAESAREAN SECTION (VBAC) 1. Aim/Purpose of this Guideline 1.1. Due to a rise in the caesarean section rate there are increasing numbers of pregnant women who
Overall Goals/Objectives - Surgical Critical Care Residency Program The goal of the Pediatric Surgical Critical Care Residency program is to provide
 Overall Goals/Objectives - Surgical Critical Care Residency Program The goal of the Pediatric Surgical Critical Care Residency program is to provide advanced proficiency in the care and management of critically
Overall Goals/Objectives - Surgical Critical Care Residency Program The goal of the Pediatric Surgical Critical Care Residency program is to provide advanced proficiency in the care and management of critically
University of Kansas. Respiratory Care Education
 University of Kansas Respiratory Care Education What is Respiratory Care? Respiratory Care is the health profession that specializes in the promotion of optimum cardiopulmonary function and health Respiratory
University of Kansas Respiratory Care Education What is Respiratory Care? Respiratory Care is the health profession that specializes in the promotion of optimum cardiopulmonary function and health Respiratory
Mechanical Ventilation for Dummies Keep It Simple Stupid
 Mechanical Ventilation for Dummies Keep It Simple Stupid Indications Airway Ventilation failure (CO2) Hypoxia Combination Airway obstruction Inability to protect airway Hypoxia (PaO 2 < 50) Hypercapnia
Mechanical Ventilation for Dummies Keep It Simple Stupid Indications Airway Ventilation failure (CO2) Hypoxia Combination Airway obstruction Inability to protect airway Hypoxia (PaO 2 < 50) Hypercapnia
Use of the A-B-C basic life support sequence.
 Basic Life Support A change in the basic life support (BLS) sequence of steps for trained rescuers from A-B-C (Airway, Breathing, Chest compressions) to C-A-B (Chest compressions, Airway, Breathing) for
Basic Life Support A change in the basic life support (BLS) sequence of steps for trained rescuers from A-B-C (Airway, Breathing, Chest compressions) to C-A-B (Chest compressions, Airway, Breathing) for
Brenda Neff MSN, RN, NE BC
 Brenda Neff MSN, RN, NE BC 1400 s newborns have a soul 1600 s estimated that only 10% of the abandoned infants reached the age of 5 years. 1857 first incubator documented in western lit 1857 first incubator
Brenda Neff MSN, RN, NE BC 1400 s newborns have a soul 1600 s estimated that only 10% of the abandoned infants reached the age of 5 years. 1857 first incubator documented in western lit 1857 first incubator
What do we mean by birth asphyxia
 Neonatal Medicine and brain injury in the Infant at term Andrew Whitelaw Professor of Neonatal Medicine University of Bristol What do we mean by birth asphyxia Interruption in oxygen delivery to the fetus
Neonatal Medicine and brain injury in the Infant at term Andrew Whitelaw Professor of Neonatal Medicine University of Bristol What do we mean by birth asphyxia Interruption in oxygen delivery to the fetus
CPT Pediatric Coding Updates 2009. The 2009 Current Procedural Terminology (CPT) codes are effective as of January 1, 2009.
 CPT Pediatric Coding Updates 2009 The 2009 Current Procedural Terminology (CPT) codes are effective as of January 1, 2009. NEW CODES Evaluation and Management Services Normal Newborn Care Codes 99431-99440
CPT Pediatric Coding Updates 2009 The 2009 Current Procedural Terminology (CPT) codes are effective as of January 1, 2009. NEW CODES Evaluation and Management Services Normal Newborn Care Codes 99431-99440
UMBILICAL CORD CLAMPING FOR TERM INFANTS 37 WEEKS
 UMBILICAL CORD CLAMPING FOR TERM INFANTS 37 WEEKS This guideline refers to umbilical cord clamping in term infants (those 37 weeks gestational age) DEFINITION Immediate (early) cord clamping (ICC): the
UMBILICAL CORD CLAMPING FOR TERM INFANTS 37 WEEKS This guideline refers to umbilical cord clamping in term infants (those 37 weeks gestational age) DEFINITION Immediate (early) cord clamping (ICC): the
Nurses Competencies in Caring for Mechanically Ventilated Patients, What does the Evidence Say? Dr. Samah Anwar Dr. Noha El-Baz
 Nurses Competencies in Caring for Mechanically Ventilated Patients, What does the Evidence Say? Dr. Samah Anwar Dr. Noha El-Baz The mechanically ventilated patient presents many challenges for the intensive
Nurses Competencies in Caring for Mechanically Ventilated Patients, What does the Evidence Say? Dr. Samah Anwar Dr. Noha El-Baz The mechanically ventilated patient presents many challenges for the intensive
!!! BOLUS DOSE IV. Use 5-10 mcg IV boluses STD ADRENALINE INFUSION. Use IM adrenaline in advance of IV dosing!
 ADRENALINE IVI BOLUS IV Open a vial of 1:1000 ADRENALINE 1 mg /ml Add 1 ml to 9 ml N/Saline = 1mg adrenaline in 10 ml (or 100 mcg/ml) Add 1 ml 1:10,000 to 9 ml N/Saline = 100 mcg adrenaline in 10 ml (or
ADRENALINE IVI BOLUS IV Open a vial of 1:1000 ADRENALINE 1 mg /ml Add 1 ml to 9 ml N/Saline = 1mg adrenaline in 10 ml (or 100 mcg/ml) Add 1 ml 1:10,000 to 9 ml N/Saline = 100 mcg adrenaline in 10 ml (or
Pediatric Airway Management
 Pediatric Airway Management Dec 2003 Dr. Shapiro I., PICU Adult Chain of Survival EMS CPR ALS Early Defibrillation Pediatric Chain of Survival Prevention CPR EMS ALS Out-of-Hospital Cardiac Arrest SIDS
Pediatric Airway Management Dec 2003 Dr. Shapiro I., PICU Adult Chain of Survival EMS CPR ALS Early Defibrillation Pediatric Chain of Survival Prevention CPR EMS ALS Out-of-Hospital Cardiac Arrest SIDS
Approved and Funded Neonatal Resuscitation Program (NRP) Research Grants and Young Investigator Awards
 Approved and Funded Neonatal Resuscitation Program (NRP) Research Grants and Young Investigator Awards 2015 Meconium aspiration syndrome and non vigorous neonates pilot study, St Louis, MO TM Identification
Approved and Funded Neonatal Resuscitation Program (NRP) Research Grants and Young Investigator Awards 2015 Meconium aspiration syndrome and non vigorous neonates pilot study, St Louis, MO TM Identification
NEWBORN LIFE SUPPORT - CLINICAL GUIDELINE 1. Aim/Purpose of this Guideline
 NEWBORN LIFE SUPPORT - CLINICAL GUIDELINE 1. Aim/Purpose of this Guideline This guideline applies to obstetric, midwifery, paediatric, and neonatal staff who may be involved in the resuscitation or stabilisation
NEWBORN LIFE SUPPORT - CLINICAL GUIDELINE 1. Aim/Purpose of this Guideline This guideline applies to obstetric, midwifery, paediatric, and neonatal staff who may be involved in the resuscitation or stabilisation
Hyperosmolar Non-Ketotic Diabetic State (HONK)
 Hyperosmolar Non-Ketotic Diabetic State (HONK) University Hospitals of Leicester NHS Trust Guidelines for Management of Acute Medical Emergencies Management is largely the same as for diabetic ketoacidosis
Hyperosmolar Non-Ketotic Diabetic State (HONK) University Hospitals of Leicester NHS Trust Guidelines for Management of Acute Medical Emergencies Management is largely the same as for diabetic ketoacidosis
NRP 2012 Putting New Resuscitation Guidelines into Practice
 Outreach Education Online Video Library for Healthcare Professionals NRP 2012 Putting New Resuscitation Guidelines into Practice. Jeanette Zaichkin, RN, MN, NNP-BC December 2, 2010 Program Handouts This
Outreach Education Online Video Library for Healthcare Professionals NRP 2012 Putting New Resuscitation Guidelines into Practice. Jeanette Zaichkin, RN, MN, NNP-BC December 2, 2010 Program Handouts This
Respiratory Care. A Life and Breath Career for You!
 Respiratory Care A Life and Breath Career for You! Respiratory Care Makes a Difference At 9:32 am, Lori Moreno brought a newborn baby struggling to breathe back to life What have you accomplished today?
Respiratory Care A Life and Breath Career for You! Respiratory Care Makes a Difference At 9:32 am, Lori Moreno brought a newborn baby struggling to breathe back to life What have you accomplished today?
Chapter 16. Learning Objectives. Learning Objectives 9/11/2012. Shock. Explain difference between compensated and uncompensated shock
 Chapter 16 Shock Learning Objectives Explain difference between compensated and uncompensated shock Differentiate among 5 causes and types of shock: Hypovolemic Cardiogenic Neurogenic Septic Anaphylactic
Chapter 16 Shock Learning Objectives Explain difference between compensated and uncompensated shock Differentiate among 5 causes and types of shock: Hypovolemic Cardiogenic Neurogenic Septic Anaphylactic
Paediatric Clinical Guidelines: Status Epilepticus
 Paediatric Clinical Guidelines: Status Epilepticus Consultant: Dr Alastair Sutcliffe, Dr Christina Petrololous, Dr Tom Bailey Pharmacist: Simon Keady/Neil Tickner To be reviewed: Autumn 2010 The following
Paediatric Clinical Guidelines: Status Epilepticus Consultant: Dr Alastair Sutcliffe, Dr Christina Petrololous, Dr Tom Bailey Pharmacist: Simon Keady/Neil Tickner To be reviewed: Autumn 2010 The following
Postoperative management in adults
 Scottish Intercollegiate Guidelines Net work 77 Postoperative management in adults A practical guide to postoperative care for clinical staff 1 Introduction 1 2 Clinical assessment and monitoring 3 3 Cardiovascular
Scottish Intercollegiate Guidelines Net work 77 Postoperative management in adults A practical guide to postoperative care for clinical staff 1 Introduction 1 2 Clinical assessment and monitoring 3 3 Cardiovascular
Congenital Diaphragmatic Hernia. Manuel A. Molina, M.D. University Hospital at Brooklyn SUNY Downstate
 Congenital Diaphragmatic Hernia Manuel A. Molina, M.D. University Hospital at Brooklyn SUNY Downstate Congenital Diaphragmatic Hernias Incidence 1 in 2000 to 5000 live births. 80% in the left side, 20%
Congenital Diaphragmatic Hernia Manuel A. Molina, M.D. University Hospital at Brooklyn SUNY Downstate Congenital Diaphragmatic Hernias Incidence 1 in 2000 to 5000 live births. 80% in the left side, 20%
F.E.E.A. FONDATION EUROPEENNE D'ENSEIGNEMENT EN ANESTHESIOLOGIE FOUNDATION FOR EUROPEAN EDUCATION IN ANAESTHESIOLOGY
 créée sous le Patronage de l'union Européenne Detailed plan of the program of six courses 1. RESPIRATORY 1. ESPIRATORY AND THORAX 1.1 Physics and principles of measurement 1.1.1 Physical laws 1.1.2 Vaporizers
créée sous le Patronage de l'union Européenne Detailed plan of the program of six courses 1. RESPIRATORY 1. ESPIRATORY AND THORAX 1.1 Physics and principles of measurement 1.1.1 Physical laws 1.1.2 Vaporizers
Management of exacerbations in chronic obstructive pulmonary disease in Primary Care
 Management of exacerbations in chronic obstructive pulmonary disease in Primary Care Acute exacerbations of chronic obstructive pulmonary disease (COPD) are associated with significant morbidity and mortality.
Management of exacerbations in chronic obstructive pulmonary disease in Primary Care Acute exacerbations of chronic obstructive pulmonary disease (COPD) are associated with significant morbidity and mortality.
