Having your bladder removed a robotic-assisted laparoscopic cystectomy Information for men
|
|
|
- Lenard Cox
- 7 years ago
- Views:
Transcription
1 Having your bladder removed a robotic-assisted laparoscopic cystectomy Information for men Your doctor has recommended that you have a cystectomy as treatment for your condition. This leaflet explains: what a robotic-assisted cystectomy involves what happens during the operation the possible risks, benefits and side effects your recovery after the surgery. If you have any questions, please ask a member of staff caring for you. What is a cystectomy? Cystectomy is the medical term for removing the entire bladder. It is sometimes referred to as radical cystectomy, a cystoprostatectomy or a cysto-prostato-urethrectomy, depending on which organs are removed. bladder tail bone pelvic floor muscle pubic bone prostate gland penis anus urethra The male urinary system. Image supplied by the Prostate Cancer Charity. 1 of 10
2 What does the operation involve? The operation is performed under a general anaesthetic. This means that you will be asleep for the whole operation, so you will not feel any pain. The anaesthetic is given through a small injection into the back of your hand. For more information on having an anaesthetic, ask your nurse for a leaflet. The type of cystectomy you will have will depend on your individual circumstances. Usually the surgeon will remove your bladder, prostate, seminal vesicles (where semen is stored) and lymph glands within the pelvis. In some cases, your surgeon will also remove your urethra (tube that urine passes down from the bladder before leaving the body). Your surgeon will discuss the operation with you in detail. It is important that you understand what is going to happen, so please ask questions if you are uncertain. What is robotic-assisted laparoscopic surgery? Laparoscopic surgery is also often called keyhole surgery. It is carried out using several small incisions (also called keyholes or port holes) rather than the one large incision used for traditional surgery. For this operation, your surgeon will make six small incisions or cuts (about 1cm) to your abdomen (tummy) and one slightly longer incision (5cm) to remove the bladder. Traditional open surgery would involve a single 15cm-18cm long incision. Robotic-assisted surgery is a laparoscopic technique that uses a robotic console (the davinci system) to help your surgeon during the operation. Your surgeon is in the same room, but away from you and controls the robotic arms to perform the operation. It is important to understand that the robot is not performing the surgery. The surgeon still carries out the procedure, but the robotic console allows more controlled and precise movements during the operation. The robotic console has three arms; one holds a high magnification 3D camera, which is inserted into your abdomen through one of the keyholes. This allows your surgeon to see inside your abdomen. The other robotic arms can hold various instruments, which your surgeon will use to carry out the operation. The instruments are smaller than those used for traditional open surgery. Robotic-assisted surgery has a number of advantages over traditional open surgery: Average blood loss is around 200ml to 500ml compared to 500ml to 1,500ml for traditional open surgery. You are generally able to start eating and drinking more quickly after robotic assisted surgery. You are often able to leave hospital a day or two sooner than if you have traditional open surgery. 2 of 10
3 Why should I have a cystectomy? The benefits of this operation will be discussed with you in more detail, but your doctor may be recommending surgery for you because: you have cancer in your bladder, which would be best managed by complete removal of the bladder your bladder may be damaged from radiation treatment your bladder may be bleeding after chemotherapy or radiotherapy your bladder may be damaged or may be bleeding uncontrollably from other causes or treatments. What are the alternatives? Possible alternative treatments will depend on the reason you are being recommended a cystectomy. However, examples include: having radiation therapy with or without chemotherapy, or other forms of cancer treatment if you have cancer choosing not to have treatment while recognising the risks of your condition. Your doctor or nurse will explain your choices and any alternative treatments to you in more detail. How will the surgery affect me? This is a major operation, which permanently changes your body in several ways. It affects how you pass urine, your ability to have children, to have sex and to some extent, your bowel function. Passing urine During the operation, your surgeon will carry out a procedure called a urinary diversion. The tubes that connect your kidneys to your bladder (the ureters) are disconnected from the bladder. They are joined to a short segment of your bowel that is isolated from the rest of your intestines. This is then brought to the skin surface, usually on the right hand side of your abdomen. This is known as an ileal conduit. The part of your bowel that opens on to your abdomen is known as a stoma or a urostomy. Your urine then empties through this stoma into a small bag, which you need to empty and change regularly. Image source: Christie Hospital 3 of 10
4 In some cases, an artificial bladder can be created from a section of your bowel, removing the need for a stoma. This is only suitable for a small proportion of patients your consultant will discuss this with you if it is suitable for you. A leaflet on this type of surgery called Bladder removal (cystectomy) and bladder reconstruction (neo bladder) is available. Ability to get an erection The organs, nerves and blood vessels all lie close together within the pelvis. Therefore, when a cystectomy is carried out, the nerves that supply your penis are affected. This means that you may not be able to achieve an erection after your operation without additional treatment. You should also be aware that if you are able to get an erection, you will not ejaculate any semen, so you will be infertile. If you want to have a family, please discuss this with your doctor before your surgery as you will need to have semen stored. Some men find that treatments to restore erections, such as tablets, injections or vacuum devices are helpful, but not all do. If you would like further information about this, please speak to a member of staff looking after you before you come into hospital for your surgery. Bowel function As a small portion of the bowel is used to make the urostomy, your bowel may also be affected by the operation. The remaining part of your bowel left for digestion and absorption of your food will be slightly shorter. This means that you may find that you go to the toilet more frequently or notice that your bowel movements are more loose than before. Alternatively, you may experience some constipation for which you may require laxatives to help you open your bowels. This may last for up to a year. Your doctor can discuss this in more detail with you if this applies to you. These are all major changes for you. It is important to us that you are able to return to as active a lifestyle as possible after this operation. This depends on how you feel mentally as well as physically. There are people you can talk to at the hospital. Some patients who have had this type of surgery are also willing to answer questions that you might have. Please ask your doctor or nurse specialist for more details. Alternatively there is a Bladder Cancer Support Group held every month where you can meet other people with bladder cancer. Ask the nurse specialist for details. What are the risks of a cystectomy? Your surgeon will discuss the possible risks of this operation with you in more detail before asking you to sign a consent form. Please ask questions if you are uncertain about anything. Possible early complications of any major operation Problems that can occur while you are in hospital recovering are similar to those for any major operation. These include: bleeding requiring the need for a blood transfusion or re-operation injury to nearby nerves or tissues a chest infection blood clots in your lower leg (deep vein thrombosis or DVT), which could pass to your lung wound infection bruising around your wounds, poor wound healing or weakness at the wound sites. 4 of 10
5 Specific risks for a robotic-assisted cystectomy Damage to structures inside your abdomen or to your rectum. This risk is higher when the instruments are inserted, so the telescopic instrument (the high magnification 3D camera) is inserted first and then used to help insert the other instruments. Leakage from, or narrowing of, your intestine where the section of bowel was removed, which may need surgery. Urine could leak out where the ureters are joined to the section of your intestine. Blockage of the ureters, preventing urine from passing to your urostomy. This may require treatment in the future. Carbon dioxide (used during surgery) could become trapped in your abdomen. This can cause pain in one or both shoulders, but disappears as the gas is reabsorbed by your body. The need to convert to traditional open surgery. Nerve compression, where the pressure from the positioning of your body during the operation can reduce the blood flow supplying your nerves and cause damage. This may require further treatment. The operation may not remove all of your cancer or it may become apparent once surgery has begun, that the cancer is not operable (if cancer was the reason for your surgery) Your sexual function (ability to get an erection) may be affected. There is a small risk of dying from this surgery (one to two in a hundred men). This is no higher than for traditional open surgery. Preparing for your surgery You will have a pre-operative assessment or an appointment with the Proactive Care of Older People undergoing Surgery (POPS) team before your surgery. It is important that you come to this appointment, as this is when we will assess your suitability for surgery and the anaesthetic. We will also make sure you have had the relevant tests and examinations. If you do not come to this appointment, we may have to cancel your surgery. The urology department currently runs an Enhanced Recovery Programme (ERP) for patients undergoing cystectomy. This programme aims to help you recover from your surgery and regain your independence as quickly as possible. There is researched evidence that eating, drinking, moving around soon after your operation and having good control of your pain helps with, and speeds up, your recovery. Therefore, the programme emphasises these aspects of your recovery and focuses on how you can help yourself after your surgery. Please ask staff for more details. As part of the ERP you will also come to a pre-cystectomy preparation clinic where you will meet one of the clinical nurse specialists (CNS) for bladder cancer, the dietician, the physiotherapist and the stoma nurse specialist. The CNS will prepare you for your surgery and your hospital stay, answering any questions you may have and talking you through the ERP pathway. The dietician will give you instructions on what you are allowed to eat and drink prior to your admission for surgery. He/she will also give you some nutritional supplement drinks to have at home prior to your admission. 5 of 10
6 The physiotherapist will focus on two elements. The first will be your physical function before your operation and the second will be what to expect physically after it. He/she will provide you with advice on your physical preparation for surgery and will explain their role in helping your recovery after your surgery. He/she will also discuss what is available after your surgery to help in your recovery. The stoma nurse specialist will help prepare you for the formation of your urostomy/stoma and will teach you how to manage your stoma and change your urostomy bags. He/she will also make a mark on your tummy to help guide the surgeon as to the most suitable place for your stoma to be sited. This is usually away from skin creases when you sit, away from previous operation scars and somewhere that you can see easily. He/she will answer any questions you have regarding the stoma and stoma care and will provide you with some written information. If you smoke, you should try to stop smoking, as this increases the risk of developing a chest infection or deep vein thrombosis (DVT), explained in the risks section. Smoking can also delay wound healing. For help giving up smoking, please speak to your nurse, or call the Trust stop smoking service on , or call the NHS Smoking Helpline on If you take any medicines that thin your blood, such as aspirin, warfarin, clopidogrel or rivaroxaban please tell your doctor or the nurse in pre-assessment/pops. They will give you special instructions. If you take any of these medicines, you may need to come into hospital earlier. This will be arranged at your pre-admission clinic appointment if it is needed. Please continue to take all your medicines unless you are told otherwise and remember to bring them into hospital with you. Coming into hospital Generally you will come into hospital on the day of your operation and will be admitted via the Surgical Admissions Lounge (SAL). On admission you will be asked for a urine sample. Some patients will need to be admitted via a ward the day before. We will let you know if this is the case for you. You should expect to stay in hospital for seven to 10 days after your surgery. Giving my consent (permission) We want to involve you in decisions about your care and treatment. If you decide to go ahead, you will be asked to sign a consent form. This states that you agree to have the treatment and you understand what it involves. If you would like more information about our consent process, please speak to a member of staff caring for you. 6 of 10
7 The day of your operation You will not be able to eat or drink anything for six hours before you go to theatre. If you have prescription medicines, you can take these with a small sip of water. The anaesthetist will discuss with you exactly which tablets you are able to take. On the morning of your surgery you should have a shower either at home if admitted on day of surgery, or on the ward if admitted the day before surgery. You will be given a clean gown and anti-thrombus stockings to put on. These help to prevent blood clots forming in your legs during surgery. You may take them off to shower during your hospital stay, but you must keep them on at all other times to help reduce the risk of blood clots. You should continue to wear them for two weeks after you leave hospital. From the Surgical Admissions Lounge or ward you will be taken to the anaesthetic room where you will be seen by the anaesthetic nurse and doctors. Once anaesthetised, you will be taken through to the operating theatre. After your operation After the surgery is finished, we will transfer you to the Guy s Critical Care Unit (GCCU) on the 1 st floor of Tower Wing. In GCCU we will monitor your blood pressure, heart rate and fluid levels using very accurate equipment. You will usually stay there for 24 hours until you are ready to return to your ward. In exceptional circumstances you may need to stay on GCCU a little longer (24 48 hours). On the day of your surgery, friends and family members can visit you afterwards but you should try to limit your visitors on the first night as you will still feel tired from the anaesthetic. Your urologist will come to see you following your surgery. To reduce the pain post-operatively, the anaesthetist will discuss pain control with you before your surgery. You will usually have: an injection into your back (directly into your spinal nerve system) of painkillers and local anaesthetic. The injection is given in theatre whilst you are still under anaesthetic and the pain relief lasts for about half a day. a device that you control, that releases painkillers into your blood stream via a drip in your arm (patient-controlled analgesia, PCA). After two to four days you should not usually need this level of pain relief and the ward staff will give you tablets or injections instead. Please tell the staff looking after you if you are still in pain or discomfort. After your operation you will also have: a drip running into a vein in your arm or neck to give you fluids until you are able to drink normally. This will be removed about three to five days after your operation). Soon after you are able to drink normally, you will be able to start eating again. a fine plastic tube from your nose through to your stomach to stop you from being sick. This is rarely needed and will be inserted while you are in theatre and is usually removed before you wake up. dressings over your wounds on your abdomen and a stoma bag collecting urine from your new urostomy. 7 of 10
8 one small plastic tube (drain) from your abdomen to drain away excess fluid. We will remove this five to seven days after your operation, but sometimes it will stay in a little longer if it continues to drain fluid. a tube (catheter) from your penis, also draining excess fluid. We will remove this one to two days after your operation. You will also have two thin tubes (stents) coming through the urostomy. The stoma nurse specialist will remove these about days after you leave hospital. Sometimes they may be removed before you leave hospital. These tubes are inserted to make sure the join between the ureters and the piece of bowel forming the ileal conduit has healed and will not leak if urine passes over this join. The doctors will check your stomach with a stethoscope every day, listening for any bowel sounds or gurgling. They may also ask you whether you have passed any wind. Please do not be embarrassed these are both signs that your bowel is recovering from the surgery and that you will be able to start drinking again. If you start to eat or drink before this, you will feel nauseous and may be sick. You may notice some swelling around your eyelids and face. This is because of the position you were in during surgery (head down). This usually disappears within 48 hours. Your recovery The ward staff will help you to get out of bed on the first or second day after your operation and to start walking soon after this. Usually, people are independently up and about around four to five days after surgery. A physiotherapist will help you with this. For the first few days whilst you are recovering from your surgery, the ward staff and stoma nurses will provide stoma care for you. As you improve you will be able to start caring for your own urostomy and the ward staff and stoma nurses will teach you how to do this. The stoma nurse will make sure that you have everything you need for your urostomy before you leave hospital and will explain how to get further supplies. He/she will also ensure that you have follow-up arranged with the stoma team on discharge. We will arrange a date for you to leave hospital (your discharge date) when you, and the team looking after you, feel that you are fit for discharge and are able to look after your urostomy yourself. This is usually about seven to 10 days after your surgery. Before you leave hospital, we will: arrange for a district nurse to visit you while you are recovering send a letter to your GP and give you at least two weeks supply of any new medication that we have supplied for you and a replacement of your own medicines, (if these have been used in hospital and you have less than 14 days of treatment with you or at home) give you a date for your follow-up appointment, which is usually made for about two weeks after you leave hospital. We will also arrange for you to go home with 28 days of medicine (injections) to prevent blood clots. You will be taught how to self administer these or the District Nurse will do it for you. 8 of 10
9 Getting back to normal In the first few weeks after your surgery, you might experience blood-stained urine, bruising around your incision sites and/or red or sore areas around your stoma site. Recovery time after abdominal surgery varies but you should generally start to feel back to normal about six to 12 weeks after your surgery. Do not attempt to drive a car during the first six weeks after your surgery. Before you start driving again, make sure you feel able to do an emergency stop and check with your insurance provider that you are covered. Do not attempt to lift or move heavy objects, start digging the garden or do housework for the first six weeks after your surgery. Build up your activities slowly and only do as much as you feel able to. To help aid your recovery you should slowly increase your activity levels back to normal. Within the first six weeks this will be through slowly increasing the amount of walking you do or your activities around the house. During your stay on the ward you will see a physiotherapist who may discuss coming to an exercise class following your first six weeks of recovery. This is an eight week course aimed at increasing your strength and ability to do more. If you would like to attend this class please discuss with your physiotherapist or CNS. When you can return to work will depend on the type of job you do. Please ask your surgeon if you are unsure how much time off you will need. Your follow-up appointment You will have a follow-up appointment in the outpatient clinic two to three weeks after leaving hospital. Three and six months after your surgery you may have further follow-up appointments. These may involve blood tests or scans. Follow-up after that will be every six to twelve months depending on your final results. Your follow-up may be different to this if you need more treatment. Cancer support organisations Dimbleby Cancer Care is the cancer support service for Guy s and St Thomas. They have drop-in information centres, and also offer complementary therapies, psychological support and benefits advice. Drop-in information centres are located at Guy s in Oncology Outpatients (Ground floor, Tabard Annexe) and at St Thomas on the Lower Ground Floor, Lambeth Wing. t: e: RichardDimblebyCentre@gstt.nhs.uk Macmillan Cancer Support provides information and support to anyone affected by cancer. t: w: Cancer Research UK has a patient information website, with information on all types of cancer and treatment options, as well as a book list for further information. t: w: Sections of this leaflet have been adapted, with permission from Christie Hospital s leaflet, Cystectomy for men information about your operation (removal of the bladder). 9 of 10
10 Contact us If you want any further information or any help, do not hesitate to contact the urology department. Ring to speak to the bladder cancer clinical nurse specialist, Monday to Friday, 9am to 5pm. Alternatively, ring switchboard on and ask the operator to bleep 2840 or Out of hours call Aston Key Ward on or Florence Ward on Pharmacy Medicines Helpline If you have any questions or concerns about your medicines, please speak to the staff caring for you or call our helpline. t: am to 5pm, Monday to Friday Your comments and concerns For advice, support or to raise a concern, contact our Patient Advice and Liaison Service (PALS). To make a complaint, contact the complaints department. t: (PALS) e: pals@gstt.nhs.uk t: (complaints) e: complaints2@gstt.nhs.uk Language Support Services If you need an interpreter or information about your care in a different language or format, please get in touch: t: e: languagesupport@gstt.nhs.uk NHS 111 Offers medical help and advice from fully trained advisers supported by experienced nurses and paramedics. Available over the phone 24 hours a day. t: 111 NHS Choices Provides online information and guidance on all aspects of health and healthcare, to help you make choices about your health. w: Get involved and have your say: become a member of the Trust Members of Guy s and St Thomas NHS Foundation Trust contribute to the organisation on a voluntary basis. We count on them for feedback, local knowledge and support. Membership is free and it is up to you how much you get involved. To find out more, and to become a member: t: e: members@gstt.nhs.uk w: 10 of 10 Leaflet number 2030/VER4 Date published: July 2016 Review date: July Guy s and St Thomas NHS Foundation Trust
Bladder reconstruction (neo-bladder)
 Bladder reconstruction (neo-bladder) We have written this leaflet to help you understand about your operation. It is designed to help you answer any questions you may have. The leaflet contains the following
Bladder reconstruction (neo-bladder) We have written this leaflet to help you understand about your operation. It is designed to help you answer any questions you may have. The leaflet contains the following
Laparoscopic Nephrectomy
 Laparoscopic Nephrectomy Information for Patients This leaflet explains: What is a Nephrectomy?... 2 Why do I need a nephrectomy?... 3 What are the risks and side effects of laparoscopic nephrectomy?...
Laparoscopic Nephrectomy Information for Patients This leaflet explains: What is a Nephrectomy?... 2 Why do I need a nephrectomy?... 3 What are the risks and side effects of laparoscopic nephrectomy?...
Treating your enlarged prostate gland HoLEP (holmium laser enucleation of the prostate)
 Treating your enlarged prostate gland HoLEP (holmium laser enucleation of the prostate) This leaflet is designed to answer any questions you may have about having holmium laser treatment for your enlarged
Treating your enlarged prostate gland HoLEP (holmium laser enucleation of the prostate) This leaflet is designed to answer any questions you may have about having holmium laser treatment for your enlarged
Information sheet: Robotic-Assisted Laparoscopic Radical Prostatectomy
 6 Pages, English Information sheet: Robotic-Assisted Laparoscopic Radical Prostatectomy This information sheet is to provide you and your family with information regarding your treatment and recovery from
6 Pages, English Information sheet: Robotic-Assisted Laparoscopic Radical Prostatectomy This information sheet is to provide you and your family with information regarding your treatment and recovery from
Treatment for bladder tumours - transurethral resection of a bladder tumour (TURBT)
 Treatment for bladder tumours - transurethral resection of a bladder tumour (TURBT) You have had a cystoscopy or other examination that has shown that you have an abnormal area (tumour) in your bladder.
Treatment for bladder tumours - transurethral resection of a bladder tumour (TURBT) You have had a cystoscopy or other examination that has shown that you have an abnormal area (tumour) in your bladder.
Having a circumcision information for men
 Having a circumcision information for men This leaflet aims to answer your questions about having a circumcision. It explains the benefits, risks and alternatives, as well as what you can expect when you
Having a circumcision information for men This leaflet aims to answer your questions about having a circumcision. It explains the benefits, risks and alternatives, as well as what you can expect when you
Enhanced recovery programme (ERP) for patients undergoing bowel surgery
 Enhanced recovery programme (ERP) for patients undergoing bowel surgery Information for patients, relatives and carers An enhanced recovery programme (ERP) has been established at Imperial College Healthcare
Enhanced recovery programme (ERP) for patients undergoing bowel surgery Information for patients, relatives and carers An enhanced recovery programme (ERP) has been established at Imperial College Healthcare
Contents. Overview. Removing the womb (hysterectomy) Overview
 This information is an extract from the booklet Understanding womb (endometrial) cancer. You may find the full booklet helpful. We can send you a free copy see page 9. Overview Contents Overview Removing
This information is an extract from the booklet Understanding womb (endometrial) cancer. You may find the full booklet helpful. We can send you a free copy see page 9. Overview Contents Overview Removing
Having a tension-free vaginal tape (TVT) operation for stress urinary incontinence
 Having a tension-free vaginal tape (TVT) operation for stress urinary incontinence This leaflet explains more about tension-free vaginal tape (TVT) including the benefits, risks and any alternatives, and
Having a tension-free vaginal tape (TVT) operation for stress urinary incontinence This leaflet explains more about tension-free vaginal tape (TVT) including the benefits, risks and any alternatives, and
Surgery for oesophageal cancer
 Surgery for oesophageal cancer This information is an extract from the booklet Understanding oesophageal cancer (cancer of the gullet). You may find the full booklet helpful. We can send you a free copy
Surgery for oesophageal cancer This information is an extract from the booklet Understanding oesophageal cancer (cancer of the gullet). You may find the full booklet helpful. We can send you a free copy
The main surgical options for treating early stage cervical cancer are:
 INFORMATION LEAFLET ON TOTAL LAPAROSCOPIC RADICAL HYSTERECTOMY (TLRH) FOR EARLY STAGE CERVICAL CANCER (TREATING EARLY STAGE CERVICAL CANCER BY RADICAL HYSTERECTOMY THROUGH KEYHOLE SURGERY) Aim of the leaflet
INFORMATION LEAFLET ON TOTAL LAPAROSCOPIC RADICAL HYSTERECTOMY (TLRH) FOR EARLY STAGE CERVICAL CANCER (TREATING EARLY STAGE CERVICAL CANCER BY RADICAL HYSTERECTOMY THROUGH KEYHOLE SURGERY) Aim of the leaflet
Having a trans-urethral resection of the prostate (TURP)
 Having a trans-urethral resection of the prostate (TURP) This leaflet gives you information about having a trans-urethral resection of your prostate (TURP), which is an operation to treat an enlarged prostate
Having a trans-urethral resection of the prostate (TURP) This leaflet gives you information about having a trans-urethral resection of your prostate (TURP), which is an operation to treat an enlarged prostate
Preparing for your laparoscopic pyeloplasty
 Preparing for your laparoscopic pyeloplasty Welcome We look forward to welcoming you to The Royal London Hospital. You have been referred to us for a laparoscopic pyeloplasty, which is an operation using
Preparing for your laparoscopic pyeloplasty Welcome We look forward to welcoming you to The Royal London Hospital. You have been referred to us for a laparoscopic pyeloplasty, which is an operation using
PROCEDURE- SPECIFIC INFORMATION FOR PATIENTS
 The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E- mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk admin@baus.org.uk PROCEDURE-
The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E- mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk admin@baus.org.uk PROCEDURE-
Femoral artery bypass graft (Including femoral crossover graft)
 Femoral artery bypass graft (Including femoral crossover graft) Why do I need the operation? You have a blockage or narrowing of the arteries supplying blood to your leg. This reduces the blood flow to
Femoral artery bypass graft (Including femoral crossover graft) Why do I need the operation? You have a blockage or narrowing of the arteries supplying blood to your leg. This reduces the blood flow to
Enhanced recovery after laparoscopic surgery (ERALS) programme: patient information and advice 2
 This booklet is funded by, and developed in collaboration between University Hospital Southampton NHS Foundation Trust and Pfizer Limited. NPKAM0198 March 2014 Enhanced recovery after laparoscopic surgery
This booklet is funded by, and developed in collaboration between University Hospital Southampton NHS Foundation Trust and Pfizer Limited. NPKAM0198 March 2014 Enhanced recovery after laparoscopic surgery
Subtotal Colectomy. Delivering the best in care. UHB is a no smoking Trust
 Subtotal Colectomy Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm This leaflet
Subtotal Colectomy Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm This leaflet
Treating your abdominal aortic aneurysm by open repair (surgery)
 Patient information Abdominal aortic aneurysm open surgery Treating your abdominal aortic aneurysm by open repair (surgery) Introduction This leaflet tells you about open repair of abdominal aortic aneurysm,
Patient information Abdominal aortic aneurysm open surgery Treating your abdominal aortic aneurysm by open repair (surgery) Introduction This leaflet tells you about open repair of abdominal aortic aneurysm,
Arthroscopic rotator cuff repair
 Arthroscopic rotator cuff repair The aim of this leaflet is to help answer some of the questions you may have about having an arthroscopic rotator cuff repair. It explains the benefits, risks and alternatives
Arthroscopic rotator cuff repair The aim of this leaflet is to help answer some of the questions you may have about having an arthroscopic rotator cuff repair. It explains the benefits, risks and alternatives
Laparoscopic Hysterectomy
 Any further questions? Please contact the matron for Women s Health on 020 7288 5161 (answerphone) Monday - Thursday 9am - 5pm. For more information: Royal College of Obstetrics and Gynaecology Recovering
Any further questions? Please contact the matron for Women s Health on 020 7288 5161 (answerphone) Monday - Thursday 9am - 5pm. For more information: Royal College of Obstetrics and Gynaecology Recovering
PROCEDURE- SPECIFIC INFORMATION FOR PATIENTS
 The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E- mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk admin@baus.org.uk PROCEDURE-
The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E- mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk admin@baus.org.uk PROCEDURE-
Total Abdominal Hysterectomy
 What is a total abdominal hysterectomy? Is the removal of the uterus and cervix through an abdominal incision (either an up and down or bikini cut). Removal of the ovaries and tubes depends on the patient.
What is a total abdominal hysterectomy? Is the removal of the uterus and cervix through an abdominal incision (either an up and down or bikini cut). Removal of the ovaries and tubes depends on the patient.
Having denervation of the renal arteries for treatment of high blood pressure
 Having denervation of the renal arteries for treatment of high blood pressure The aim of this information sheet is to help answer some of the questions you may have about having denervation of the renal
Having denervation of the renal arteries for treatment of high blood pressure The aim of this information sheet is to help answer some of the questions you may have about having denervation of the renal
Trans Urethral Resection of the Prostate (TURP) Trans Urethral Incision of the Prostate (TUIP) Department of Urology
 Trans Urethral Resection of the Prostate (TURP) Trans Urethral Incision of the Prostate (TUIP) Department of Urology Where is the Prostate Gland? The prostate gland sits below the bladder which lies behind
Trans Urethral Resection of the Prostate (TURP) Trans Urethral Incision of the Prostate (TUIP) Department of Urology Where is the Prostate Gland? The prostate gland sits below the bladder which lies behind
Surgical removal of fibroids through an abdominal incision-either up and down or bikini cut. The uterus and cervix are left in place.
 What is an abdominal myomectomy? Surgical removal of fibroids through an abdominal incision-either up and down or bikini cut. The uterus and cervix are left in place. When is this surgery used? Treatment
What is an abdominal myomectomy? Surgical removal of fibroids through an abdominal incision-either up and down or bikini cut. The uterus and cervix are left in place. When is this surgery used? Treatment
Urinary Diversion: Ileovesicostomy/Ileal Loop/Colon Loop
 Urinary Diversion: Ileovesicostomy/Ileal Loop/Colon Loop Why do I need this surgery? A urinary diversion is a surgical procedure that is performed to allow urine to safely pass from the kidneys into a
Urinary Diversion: Ileovesicostomy/Ileal Loop/Colon Loop Why do I need this surgery? A urinary diversion is a surgical procedure that is performed to allow urine to safely pass from the kidneys into a
Recto-vaginal Fistula Repair
 What is a recto-vaginal fistula repair? Rectovaginal fistula repair is a procedure in which the healthy tissue between the rectum and vagina is closed in multiple tissue layers. An incision is made either
What is a recto-vaginal fistula repair? Rectovaginal fistula repair is a procedure in which the healthy tissue between the rectum and vagina is closed in multiple tissue layers. An incision is made either
What should I expect before the procedure?
 The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E- mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk admin@baus.org.uk PROCEDURE-
The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E- mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk admin@baus.org.uk PROCEDURE-
SUPRAPUBIC CATHETER INSERTION INFORMATION FOR PATIENTS
 The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E-mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk admin@baus.org.uk INFORMATION
The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E-mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk admin@baus.org.uk INFORMATION
REPAIR OF A URINARY VAGINAL FISTULA
 Procedure Specific Information What is the evidence base for this information? This publication includes advice from consensus panels, the British Association of Urological Surgeons, the Department of
Procedure Specific Information What is the evidence base for this information? This publication includes advice from consensus panels, the British Association of Urological Surgeons, the Department of
Excision of Vaginal Mesh
 What is excision of vaginal mesh? This procedure is done to remove mesh from the vagina. When is this surgery used? If mesh has eroded into the vagina, bladder, urethra, or bowel If there is pain associated
What is excision of vaginal mesh? This procedure is done to remove mesh from the vagina. When is this surgery used? If mesh has eroded into the vagina, bladder, urethra, or bowel If there is pain associated
Elective Laparoscopic Cholecystectomy
 General Surgery Elective Laparoscopic Cholecystectomy This information aims to explain what will happen before, during and after your surgery to remove your gallbladder. It includes information about the
General Surgery Elective Laparoscopic Cholecystectomy This information aims to explain what will happen before, during and after your surgery to remove your gallbladder. It includes information about the
Total Vaginal Hysterectomy with an Anterior and Posterior Repair
 Total Vaginal Hysterectomy with an Anterior and Posterior Repair What is a total vaginal hysterectomy with an anterior and posterior repair? Total vaginal hysterectomy is the removal of the uterus and
Total Vaginal Hysterectomy with an Anterior and Posterior Repair What is a total vaginal hysterectomy with an anterior and posterior repair? Total vaginal hysterectomy is the removal of the uterus and
Forefoot deformity correction
 Contact us Pharmacy Medicines Helpline If you have any questions or concerns about your medicines, please speak to the staff caring for you or call our helpline. t: 020 7188 8748 9am to 5pm, Monday to
Contact us Pharmacy Medicines Helpline If you have any questions or concerns about your medicines, please speak to the staff caring for you or call our helpline. t: 020 7188 8748 9am to 5pm, Monday to
Recovery plan: radical cystectomy Information for patients
 Recovery plan: radical cystectomy Information for patients Help for you following a bereavement 5 This leaflet will help you know what to expect during your time with us. Please take some time to read
Recovery plan: radical cystectomy Information for patients Help for you following a bereavement 5 This leaflet will help you know what to expect during your time with us. Please take some time to read
Total Vaginal Hysterectomy
 What is a total vaginal hysterectomy? Is the removal of the uterus and cervix through the vagina. Removal of the ovaries and tubes depends on the patient. Why is this surgery used? To treat disease of
What is a total vaginal hysterectomy? Is the removal of the uterus and cervix through the vagina. Removal of the ovaries and tubes depends on the patient. Why is this surgery used? To treat disease of
AMPUTATION OF THE PENIS (PARTIAL OR COMPLETE) FOR CANCER INFORMATION FOR PATIENTS
 The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E-mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk admin@baus.org.uk AMPUTATION
The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E-mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk admin@baus.org.uk AMPUTATION
Ulnar Nerve Decompression/Transposition
 Department of Neurosurgery Ulnar Nerve Decompression/Transposition What happens when you are in hospital page 2 Ulnar Nerve Decompression/Transposition This leaflet explains what to expect when you are
Department of Neurosurgery Ulnar Nerve Decompression/Transposition What happens when you are in hospital page 2 Ulnar Nerve Decompression/Transposition This leaflet explains what to expect when you are
Name of procedure: Laparoscopic (key-hole) ovarian surgery. Left/ Right unilateral salpingo-oophorectomy* (removal of one fallopian tube and ovary)
 For staff use only: Patient Details: Surname: First names: Date of birth: Hospital no: Female: (Use hospital identification label) Gynaecology Patient agreement to treatment Name of procedure: Laparoscopic
For staff use only: Patient Details: Surname: First names: Date of birth: Hospital no: Female: (Use hospital identification label) Gynaecology Patient agreement to treatment Name of procedure: Laparoscopic
Having an open partial nephrectomy
 Having an open partial nephrectomy Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Having an open partial nephrectomy Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Patient Information and Daily Programme for Patients Having Whipple s Surgery (Pancreatico duodenectomy)
 Patient Information and Daily Programme for Patients Having Whipple s Surgery (Pancreatico duodenectomy) Date of admission Date of surgery Expected Length of Stay in hospital We will aim to discharge you
Patient Information and Daily Programme for Patients Having Whipple s Surgery (Pancreatico duodenectomy) Date of admission Date of surgery Expected Length of Stay in hospital We will aim to discharge you
Hysterectomy for womb cancer
 Gynaecology Oncology Service Hysterectomy for womb cancer April 2014 Great Staff Great Care Great Future INTRODUCTION This leaflet has been produced to provide you with general information about your operation.
Gynaecology Oncology Service Hysterectomy for womb cancer April 2014 Great Staff Great Care Great Future INTRODUCTION This leaflet has been produced to provide you with general information about your operation.
Surgery and cancer of the pancreas
 Surgery and cancer of the pancreas This information is an extract from the booklet Understanding cancer of the pancreas. You may find the full booklet helpful. We can send you a free copy see page 8. Introduction
Surgery and cancer of the pancreas This information is an extract from the booklet Understanding cancer of the pancreas. You may find the full booklet helpful. We can send you a free copy see page 8. Introduction
Lymph Node Dissection for Penile Cancer
 Lymph Node Dissection for Penile Cancer Exceptional healthcare, personally delivered Removal of Lymph Nodes Why are the Lymph Nodes so important when I have penile cancer? Lymph nodes are small bean shaped
Lymph Node Dissection for Penile Cancer Exceptional healthcare, personally delivered Removal of Lymph Nodes Why are the Lymph Nodes so important when I have penile cancer? Lymph nodes are small bean shaped
An operation for prolapse Colpocleisis
 Saint Mary s Hospital Gynaecology Service Warrell Unit An operation for prolapse Colpocleisis Information for Patients What is a prolapse? A prolapse is a bulge or lump in the vagina caused by sagging
Saint Mary s Hospital Gynaecology Service Warrell Unit An operation for prolapse Colpocleisis Information for Patients What is a prolapse? A prolapse is a bulge or lump in the vagina caused by sagging
Laparoscopic Cholecystectomy
 Laparoscopic Cholecystectomy Removal of Gall Bladder Page 12 Patient Information Further Information We endeavour to provide an excellent service at all times, but should you have any concerns please,
Laparoscopic Cholecystectomy Removal of Gall Bladder Page 12 Patient Information Further Information We endeavour to provide an excellent service at all times, but should you have any concerns please,
Anterior Resection Your Operation Explained
 Anterior Resection Your Operation Explained Patient Information Introduction This leaflet tells you about the procedure known as an anterior resection. It explains what is involved, and some of the common
Anterior Resection Your Operation Explained Patient Information Introduction This leaflet tells you about the procedure known as an anterior resection. It explains what is involved, and some of the common
Vaginal Repair- with Mesh A. Interpreter / cultural needs B. Condition and treatment C. Risks of a vaginal repair- with mesh
 The State of Queensland (Queensland Health), 2011 Permission to reproduce should be sought from ip_officer@health.qld.gov.au DO NOT WRITE IN THIS BINDING MARGIN v2.00-03/2011 SW9226 Facility: A. Interpreter
The State of Queensland (Queensland Health), 2011 Permission to reproduce should be sought from ip_officer@health.qld.gov.au DO NOT WRITE IN THIS BINDING MARGIN v2.00-03/2011 SW9226 Facility: A. Interpreter
Women s Health. The TVT procedure. Information for patients
 Women s Health The TVT procedure Information for patients What is a TVT procedure? A TVT (Tension-free Vaginal Tape) procedure is an operation to help women with stress incontinence the leakage of urine
Women s Health The TVT procedure Information for patients What is a TVT procedure? A TVT (Tension-free Vaginal Tape) procedure is an operation to help women with stress incontinence the leakage of urine
Primary and revision lumbar discectomy. (nerve root decompression)
 Primary and revision lumbar discectomy (nerve root decompression) The aim of this leaflet is to help answer some of the questions you may have about having a lumbar discectomy. It explains the benefits,
Primary and revision lumbar discectomy (nerve root decompression) The aim of this leaflet is to help answer some of the questions you may have about having a lumbar discectomy. It explains the benefits,
Laparoscopic Surgery for Inguinal Hernia Repair
 Laparoscopic Surgery for Inguinal Hernia Repair What is an Inguinal Hernia Repair? 2 What is a Laparoscopic Inguinal Hernia Repair? 2 Are there any alternatives to Laparoscopic Hernia Repair? 3 Am I a
Laparoscopic Surgery for Inguinal Hernia Repair What is an Inguinal Hernia Repair? 2 What is a Laparoscopic Inguinal Hernia Repair? 2 Are there any alternatives to Laparoscopic Hernia Repair? 3 Am I a
An operation for prolapse Laparoscopic Sacrohysteropexy
 Saint Mary s Hospital Gynaecology Service Warrell Unit An operation for prolapse Laparoscopic Sacrohysteropexy Information for Patients What is a prolapse? Uterine prolapse is a bulge or lump in the vagina
Saint Mary s Hospital Gynaecology Service Warrell Unit An operation for prolapse Laparoscopic Sacrohysteropexy Information for Patients What is a prolapse? Uterine prolapse is a bulge or lump in the vagina
Femoral Hernia Repair
 Femoral Hernia Repair WHAT IS A FEMORAL HERNIA REPAIR? 2 WHAT CAUSES A FEMORAL HERNIA? 2 WHAT DOES TREATMENT/ MANAGEMENT INVOLVE? 3 DAY SURGERY MANAGEMENT 3 SURGICAL REPAIR 4 WHAT ARE THE RISKS/COMPLICATIONS
Femoral Hernia Repair WHAT IS A FEMORAL HERNIA REPAIR? 2 WHAT CAUSES A FEMORAL HERNIA? 2 WHAT DOES TREATMENT/ MANAGEMENT INVOLVE? 3 DAY SURGERY MANAGEMENT 3 SURGICAL REPAIR 4 WHAT ARE THE RISKS/COMPLICATIONS
Vesico-Vaginal Fistula
 Saint Mary s Hospital The Warrell Unit Vesico-Vaginal Fistula Information For Patients Contents Page What is a vesico-vaginal fistula? 3 How does a fistula develop? 3 What tests will I need? 3 How can
Saint Mary s Hospital The Warrell Unit Vesico-Vaginal Fistula Information For Patients Contents Page What is a vesico-vaginal fistula? 3 How does a fistula develop? 3 What tests will I need? 3 How can
Having a urinary catheter information for men
 Having a urinary catheter information for men This leaflet explains what a catheter is, why you need it and how you should look after it. If you have any further questions, please contact your district
Having a urinary catheter information for men This leaflet explains what a catheter is, why you need it and how you should look after it. If you have any further questions, please contact your district
Guy s, King s and St Thomas Cancer Centre The Cancer Outpatient Clinic Maintenance BCG for nonmuscle invasive bladder cancer
 Guy s, King s and St Thomas Cancer Centre The Cancer Outpatient Clinic Maintenance BCG for nonmuscle invasive bladder cancer This information sheet has been given to you to explain the use of maintenance
Guy s, King s and St Thomas Cancer Centre The Cancer Outpatient Clinic Maintenance BCG for nonmuscle invasive bladder cancer This information sheet has been given to you to explain the use of maintenance
Procedure Information Guide
 Procedure Information Guide Surgery to remove the pancreas (whipple's procedure) Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made
Procedure Information Guide Surgery to remove the pancreas (whipple's procedure) Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made
Epidural Continuous Infusion. Patient information Leaflet
 Epidural Continuous Infusion Patient information Leaflet April 2015 Introduction You may already know that epidural s are often used to treat pain during childbirth. This same technique can also used as
Epidural Continuous Infusion Patient information Leaflet April 2015 Introduction You may already know that epidural s are often used to treat pain during childbirth. This same technique can also used as
Biliary Stone Disease
 Biliary Stone Disease Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm You have
Biliary Stone Disease Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm You have
GreenLight laser prostatectomy
 Ambulatory Care & Local Networks GreenLight laser prostatectomy Information for day surgery patients This information sheet answers some of the questions you may have about having a GreenLight laser prostatectomy.
Ambulatory Care & Local Networks GreenLight laser prostatectomy Information for day surgery patients This information sheet answers some of the questions you may have about having a GreenLight laser prostatectomy.
The ovaries are part of a woman s reproductive system. There are two ovaries, the size and shape of almonds, one on either side of the womb.
 Surgery for Suspicious Ovarian Cysts Patient Information sheet The Ovaries The ovaries are part of a woman s reproductive system. There are two ovaries, the size and shape of almonds, one on either side
Surgery for Suspicious Ovarian Cysts Patient Information sheet The Ovaries The ovaries are part of a woman s reproductive system. There are two ovaries, the size and shape of almonds, one on either side
Keyhole (Laparoscopic) Surgery
 Patient Information leaflet Keyhole (Laparoscopic) Surgery Produced by: Department of Obstetrics & Gynaecology December 2002 Reviewed April 2010 1 What is keyhole (laparoscopic) surgery? Laparoscopic surgery
Patient Information leaflet Keyhole (Laparoscopic) Surgery Produced by: Department of Obstetrics & Gynaecology December 2002 Reviewed April 2010 1 What is keyhole (laparoscopic) surgery? Laparoscopic surgery
Inguinal (Groin) Hernia Repair
 Information for patients Inguinal (Groin) Hernia Repair General Surgery Tel: 01473 712233 DMI ref: 11582-09.indd(RP) Issue 1: February 2010 The Ipswich Hospital NHS Trust, 2010. All rights reserved. Not
Information for patients Inguinal (Groin) Hernia Repair General Surgery Tel: 01473 712233 DMI ref: 11582-09.indd(RP) Issue 1: February 2010 The Ipswich Hospital NHS Trust, 2010. All rights reserved. Not
An operation for prolapse Sacrospinous Fixation Sacrospinous Hysteropexy
 Saint Mary s Hospital Gynaecology Service Warrell Unit An operation for prolapse Sacrospinous Fixation Sacrospinous Hysteropexy Information For Patients 1 What is a prolapse? Prolapse is a bulge or lump
Saint Mary s Hospital Gynaecology Service Warrell Unit An operation for prolapse Sacrospinous Fixation Sacrospinous Hysteropexy Information For Patients 1 What is a prolapse? Prolapse is a bulge or lump
Laparoscopic Bilateral Salpingo-Oophorectomy
 Laparoscopic Bilateral Salpingo-Oophorectomy What is a? This is a surgery where your doctor uses a thin, lighted camera and small surgical tool placed through a small (1/2 inch) incision usually in the
Laparoscopic Bilateral Salpingo-Oophorectomy What is a? This is a surgery where your doctor uses a thin, lighted camera and small surgical tool placed through a small (1/2 inch) incision usually in the
Information for Patients
 Notes Information for Patients Sling procedure for urinary stress incontinence Aysha Qureshi Version 1, June 2010 Review date June 2013 Date of publication: June 2010 Ref: RUH GYN/002 Royal United Hospital
Notes Information for Patients Sling procedure for urinary stress incontinence Aysha Qureshi Version 1, June 2010 Review date June 2013 Date of publication: June 2010 Ref: RUH GYN/002 Royal United Hospital
However, each person may be managed in a different way as bowel pattern is different in each person.
 Department of colorectal surgery Reversal of ileostomy A guide for patients Introduction This booklet is designed to tell you about your reversal of ileostomy operation and how your bowels might work after
Department of colorectal surgery Reversal of ileostomy A guide for patients Introduction This booklet is designed to tell you about your reversal of ileostomy operation and how your bowels might work after
Vaginal hysterectomy and vaginal repair
 Women s Service Vaginal hysterectomy and vaginal repair Information for patients Vaginal hysterectomy and vaginal repair This leaflet is for women who have been advised to have a vaginal hysterectomy.
Women s Service Vaginal hysterectomy and vaginal repair Information for patients Vaginal hysterectomy and vaginal repair This leaflet is for women who have been advised to have a vaginal hysterectomy.
Hysteroscopy. What is a hysteroscopy? When is this surgery used? How do I prepare for surgery?
 What is a hysteroscopy? This is a procedure where a doctor uses a thin tube with a tiny camera to look inside the uterus. There are no incisions. Saline solution is used to expand the uterus in order to
What is a hysteroscopy? This is a procedure where a doctor uses a thin tube with a tiny camera to look inside the uterus. There are no incisions. Saline solution is used to expand the uterus in order to
Guy s, King s and St Thomas Cancer Centre The Cancer Outpatient Clinic Central venous catheter: Peripherally inserted central catheter
 Guy s, King s and St Thomas Cancer Centre The Cancer Outpatient Clinic Central venous catheter: Peripherally inserted central catheter This information leaflet aims to help answer some of the questions
Guy s, King s and St Thomas Cancer Centre The Cancer Outpatient Clinic Central venous catheter: Peripherally inserted central catheter This information leaflet aims to help answer some of the questions
Types of surgery for kidney cancer
 Useful information for cancer patients Contents This information is about the different operations that you may have for kidney cancer. Surgery can be used to treat almost any stage of kidney cancer. There
Useful information for cancer patients Contents This information is about the different operations that you may have for kidney cancer. Surgery can be used to treat almost any stage of kidney cancer. There
University College Hospital. Prostate high dose rate (HDR) brachytherapy. Radiotherapy Department Patient information series
 University College Hospital Prostate high dose rate (HDR) brachytherapy Radiotherapy Department Patient information series 18 2 If you need a large print, audio or translated copy of the document, please
University College Hospital Prostate high dose rate (HDR) brachytherapy Radiotherapy Department Patient information series 18 2 If you need a large print, audio or translated copy of the document, please
Patient Information Sheet
 TRANSURETHRAL RESECTION OF PROSTATE (TURP) Patient Information Sheet Department of Urology Homerton University Hospital NHS Foundation Trust Homerton Row, London, E9 6SR Reviewed: June 2012 Next date:
TRANSURETHRAL RESECTION OF PROSTATE (TURP) Patient Information Sheet Department of Urology Homerton University Hospital NHS Foundation Trust Homerton Row, London, E9 6SR Reviewed: June 2012 Next date:
Sigmoid Colectomy Your Operation Explained
 Sigmoid Colectomy Your Operation Explained Patient Information Information for patients This leaflet tells you about the procedure known as a sigmoid colectomy. It explains what is involved, and some of
Sigmoid Colectomy Your Operation Explained Patient Information Information for patients This leaflet tells you about the procedure known as a sigmoid colectomy. It explains what is involved, and some of
Total Hip Replacement
 NOTES Total Hip Replacement QUESTIONS DATES PHONE NOS. Compiled by Mr John F Nolan FRCS for The British Hip Society 2009. A patient s information booklet 16 1 Introduction This booklet has been produced
NOTES Total Hip Replacement QUESTIONS DATES PHONE NOS. Compiled by Mr John F Nolan FRCS for The British Hip Society 2009. A patient s information booklet 16 1 Introduction This booklet has been produced
GASTRIC BYPASS SURGERY
 GASTRIC BYPASS SURGERY This leaflet gives you general information about your surgery. Please read it carefully. Share the information with your partner and family (if you wish) so that they are able to
GASTRIC BYPASS SURGERY This leaflet gives you general information about your surgery. Please read it carefully. Share the information with your partner and family (if you wish) so that they are able to
Transobturator tape sling Female sling system
 Transobturator tape sling Female sling system Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Transobturator tape sling Female sling system Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Having a Mitrofanoff continent urinary diversion
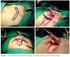 Having a Mitrofanoff continent urinary diversion Your surgeon has recommended that you need a continent urinary diversion. This leaflet aims to answer your questions about having a Mitrofanoff continent
Having a Mitrofanoff continent urinary diversion Your surgeon has recommended that you need a continent urinary diversion. This leaflet aims to answer your questions about having a Mitrofanoff continent
Preparing for your Surgery:
 Preparing for your Surgery: Information for Patients Undergoing a: UHN Minimally Invasive Radical Hysterectomy Possible removal of one or both ovaries and tubes Possible removal of pelvic lymph nodes Patient
Preparing for your Surgery: Information for Patients Undergoing a: UHN Minimally Invasive Radical Hysterectomy Possible removal of one or both ovaries and tubes Possible removal of pelvic lymph nodes Patient
Surgery for rectal cancer
 This information is an extract from the booklet Understanding rectal cancer. You may find the full booklet helpful. We can send you a free copy see page 12. Contents Enhanced recovery programme (ERP) Before
This information is an extract from the booklet Understanding rectal cancer. You may find the full booklet helpful. We can send you a free copy see page 12. Contents Enhanced recovery programme (ERP) Before
Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865
 Write questions or notes here: Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865 Document Title: Revision Total Hip Replacement Further Information and Feedback: Tell us how
Write questions or notes here: Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865 Document Title: Revision Total Hip Replacement Further Information and Feedback: Tell us how
Radical Hysterectomy and Pelvic Lymph Node Dissection
 Radical Hysterectomy and Pelvic Lymph Node Dissection Tena koutou katoa, Kia orana, Talofa lava, Malo e lelei, Fakaalofa lahi atu, Taloha Ni, Ni Sa Bula Vinaka, Greetings and Welcome to National Women's
Radical Hysterectomy and Pelvic Lymph Node Dissection Tena koutou katoa, Kia orana, Talofa lava, Malo e lelei, Fakaalofa lahi atu, Taloha Ni, Ni Sa Bula Vinaka, Greetings and Welcome to National Women's
Laparoscopic Colectomy. What do I need to know about my laparoscopic colorectal surgery?
 Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
Varicose Vein Surgery
 Information for patients Varicose Vein Surgery Northern General Hospital You have been diagnosed as having varicose veins and your specialist has recommended varicose vein surgery. This leaflet explains
Information for patients Varicose Vein Surgery Northern General Hospital You have been diagnosed as having varicose veins and your specialist has recommended varicose vein surgery. This leaflet explains
Liver Resection. Patient Information Booklet. Delivering the best in care. UHB is a no smoking Trust
 Liver Resection Patient Information Booklet Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Liver Resection Patient Information Booklet Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Inguinal Hernia (Female)
 Inguinal Hernia (Female) WHAT IS AN INGUINAL HERNIA? 2 WHAT CAUSES AN INGUINAL HERNIA? 2 WHAT DOES TREATMENT / MANAGEMENT INVOLVE? 3 DAY SURGERY MANAGEMENT 3 SURGICAL REPAIR 4 WHAT ARE THE RISKS/COMPLICATIONS
Inguinal Hernia (Female) WHAT IS AN INGUINAL HERNIA? 2 WHAT CAUSES AN INGUINAL HERNIA? 2 WHAT DOES TREATMENT / MANAGEMENT INVOLVE? 3 DAY SURGERY MANAGEMENT 3 SURGICAL REPAIR 4 WHAT ARE THE RISKS/COMPLICATIONS
Total hip replacement
 Patient Information to be retained by patient What is a total hip replacement? In a total hip replacement both the ball (femoral or thigh bone) side of the hip joint and the socket (acetabular or pelvic
Patient Information to be retained by patient What is a total hip replacement? In a total hip replacement both the ball (femoral or thigh bone) side of the hip joint and the socket (acetabular or pelvic
Ilioinguinal dissection (removal of lymph nodes in the groin and pelvis)
 Ilioinguinal dissection (removal of lymph nodes in the groin and pelvis) This sheet answers common questions about ilio-inguinal dissection. If you would like further information, or have any particular
Ilioinguinal dissection (removal of lymph nodes in the groin and pelvis) This sheet answers common questions about ilio-inguinal dissection. If you would like further information, or have any particular
Information for men considering a male sling procedure
 Information for men considering a male sling procedure Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Information for men considering a male sling procedure Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Patient Information for Lumbar Spinal Fusion. What is a lumbar spinal fusion? Page 1 of 5
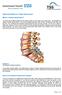 Patient Information for Lumbar Spinal Fusion What is a lumbar spinal fusion? You have been offered surgery to the lumbar region of your spine, your lower back. The operation is called a lumbar spinal fusion.
Patient Information for Lumbar Spinal Fusion What is a lumbar spinal fusion? You have been offered surgery to the lumbar region of your spine, your lower back. The operation is called a lumbar spinal fusion.
GASTRIC BYPASS SURGERY
 GASTRIC BYPASS SURGERY This leaflet gives you general information about your surgery. Please read it carefully. Share the information with your partner and family (if you wish) so that they are able to
GASTRIC BYPASS SURGERY This leaflet gives you general information about your surgery. Please read it carefully. Share the information with your partner and family (if you wish) so that they are able to
Arthroscopic subacromial decompression and rotator cuff repair
 Further sources of information http://www.patient.co.uk/showdoc/553/ http://www.shoulderdoc.co.uk/article.asp?section=11 http://www.medic8.com/healthguide/articles/painfulshoulder.html http://www.cks.nhs.uk/patientinformationleaflet/shoulderpainarc/st
Further sources of information http://www.patient.co.uk/showdoc/553/ http://www.shoulderdoc.co.uk/article.asp?section=11 http://www.medic8.com/healthguide/articles/painfulshoulder.html http://www.cks.nhs.uk/patientinformationleaflet/shoulderpainarc/st
SlEEvE GASTRECTomY SURGERY What is a sleeve gastrectomy operation? BARIATRIC SURGERY
 Sleeve gastrectomy surgery This leaflet gives you general information about your surgery. Please read carefully. Share the information with your partner and family (if you wish) so that they are able to
Sleeve gastrectomy surgery This leaflet gives you general information about your surgery. Please read carefully. Share the information with your partner and family (if you wish) so that they are able to
GreenLight Laser Therapy for Treating Benign Prostatic Hyperplasia (BPH)
 GreenLight Laser Therapy for Treating Benign Prostatic Hyperplasia (BPH) To learn about this procedure it helps to know these words: The prostate is the sexual gland that makes a fluid which helps sperm
GreenLight Laser Therapy for Treating Benign Prostatic Hyperplasia (BPH) To learn about this procedure it helps to know these words: The prostate is the sexual gland that makes a fluid which helps sperm
Colposuspension for stress urinary incontinence
 Colposuspension for stress urinary incontinence Information for patients This leaflet sheet answers some of the questions you may have about colposuspension. It explains the benefits, the risks and the
Colposuspension for stress urinary incontinence Information for patients This leaflet sheet answers some of the questions you may have about colposuspension. It explains the benefits, the risks and the
Transurethral Resection of Bladder Tumour (T.U.R.B.T)
 Transurethral Resection of Bladder Tumour (T.U.R.B.T) Patient Information Introduction This booklet has been written to help you understand the surgery you are about to undergo. It will give you information
Transurethral Resection of Bladder Tumour (T.U.R.B.T) Patient Information Introduction This booklet has been written to help you understand the surgery you are about to undergo. It will give you information
Periurethral bulking agent for stress urinary incontinence (macroplastique)
 PLEASE PRINT WHOLE FORM DOUBLE SIDED ON YELLOW PAPER Patient Information to be retained by patient affix patient label Who is this leaflet for? This leaflet provides information about having an injection
PLEASE PRINT WHOLE FORM DOUBLE SIDED ON YELLOW PAPER Patient Information to be retained by patient affix patient label Who is this leaflet for? This leaflet provides information about having an injection
Dental care for patients with head and neck cancer
 Dental care for patients with head and neck cancer This leaflet explains why it is important to see a dentist before and after your treatment for head and neck cancer. It also explains what you can expect
Dental care for patients with head and neck cancer This leaflet explains why it is important to see a dentist before and after your treatment for head and neck cancer. It also explains what you can expect
Total knee replacement: The enhanced recovery programme
 INFORMATION FOR PATIENTS Total knee replacement: The enhanced recovery programme Aim This leaflet aims to explain the enhanced recovery programme after total knee replacement surgery, and outline what
INFORMATION FOR PATIENTS Total knee replacement: The enhanced recovery programme Aim This leaflet aims to explain the enhanced recovery programme after total knee replacement surgery, and outline what
Transrectal Ultrasound (Trus) Guided Prostate Biopsies Urology Patient Information Leaflet
 Transrectal Ultrasound (Trus) Guided Prostate Biopsies Urology Patient Information Leaflet Page 1 What is the purpose of my appointment? Your doctor has informed us that you have an elevated Prostate Specific
Transrectal Ultrasound (Trus) Guided Prostate Biopsies Urology Patient Information Leaflet Page 1 What is the purpose of my appointment? Your doctor has informed us that you have an elevated Prostate Specific
