Protocol for the Examination of Specimens From Patients With Tumors of Soft Tissue
|
|
|
- Amie Davis
- 7 years ago
- Views:
Transcription
1 Protocol for the Examination of Specimens From Patients With Tumors of Soft Tissue Protocol applies to soft tissue tumors of intermediate (locally aggressive) and intermediate (rarely metastasizing) potential and malignant soft tissue tumors. Based on AJCC/UICC TNM, 7 th edition Protocol web posting date: June 2012 Procedures Biopsy Resection Authors Brian P. Rubin, MD, PhD, FCAP* Department of Anatomic Pathology, Cleveland Clinic, Lerner Research Institute and Taussig Cancer Center, Cleveland, Ohio Kumarasen Cooper, MBChB, DPhil, FRCPath Department of Pathology, University of Vermont, Fletcher Allen Health Care, Burlington, Vermont Christopher D.M. Fletcher, MD, FRCPath Department of Pathology, Brigham and Women s Hospital, Boston, Massachusetts Andrew Lawrence Folpe, MD, FCAP Department of Anatomic Pathology, Mayo Clinic, Rochester, Minnesota Francis H. Gannon, MD, FCAP Department of Pathology, Baylor College of Medicine, Houston, Texas Jennifer Leigh Hunt, MD, FCAP Department of Anatomic Pathology, Cleveland Clinic Foundation, Cleveland, Ohio Alexander J. Lazar, MD PhD, FCAP Department of Pathology, Sarcoma Research Center, The University of Texas M. D. Anderson Cancer Center, Houston, Texas Anthony G. Montag, MD Department of Pathology, University of Chicago Medical Center, Chicago, Illinois Terrance D. Peabody, MD Department of Orthopedic Surgery, University of Chicago Medical Center, Chicago, Illinois Raphael E. Pollock, MD, PhD Department of Surgical Oncology, Sarcoma Research Center, The University of Texas M D Anderson Cancer Center, Houston, Texas John D. Reith, MD, FCAP Department of Pathology, Immunology, and Laboratory Medicine, University of Florida, Gainesville, Florida Stephen J. Qualman, MD, FCAP** Department of Laboratory Medicine, Children s Hospital, Columbus, Ohio Andrew E. Rosenberg, MD, FCAP Department of Pathology, Massachusetts General Hospital, Boston, Massachusetts Sharon W. Weiss, MD, FCAP Department of Pathology and Laboratory Medicine, Emory University School of Medicine, Atlanta, Georgia Thomas Krausz, MD, FRCPath Department of Pathology, University of Chicago Medical Center, Chicago, Illinois For the Members of the Cancer Committee, College of American Pathologists * Denotes primary author. Denotes senior author. All other contributing authors are listed alphabetically. ** Deceased.
2 2012 College of American Pathologists (CAP). All rights reserved. The College does not permit reproduction of any substantial portion of these protocols without its written authorization. The College hereby authorizes use of these protocols by physicians and other health care providers in reporting on surgical specimens, in teaching, and in carrying out medical research for nonprofit purposes. This authorization does not extend to reproduction or other use of any substantial portion of these protocols for commercial purposes without the written consent of the College. The CAP also authorizes physicians and other health care practitioners to make modified versions of the Protocols solely for their individual use in reporting on surgical specimens for individual patients, teaching, and carrying out medical research for non-profit purposes. The CAP further authorizes the following uses by physicians and other health care practitioners, in reporting on surgical specimens for individual patients, in teaching, and in carrying out medical research for non-profit purposes: (1) Dictation from the original or modified protocols for the purposes of creating a text-based patient record on paper, or in a word processing document; (2) Copying from the original or modified protocols into a text-based patient record on paper, or in a word processing document; (3) The use of a computerized system for items (1) and (2), provided that the Protocol data is stored intact as a single text-based document, and is not stored as multiple discrete data fields. Other than uses (1), (2), and (3) above, the CAP does not authorize any use of the Protocols in electronic medical records systems, pathology informatics systems, cancer registry computer systems, computerized databases, mappings between coding works, or any computerized system without a written license from CAP. Applications for such a license should be addressed to the SNOMED Terminology Solutions division of the CAP. Any public dissemination of the original or modified Protocols is prohibited without a written license from the CAP. The College of American Pathologists offers these protocols to assist pathologists in providing clinically useful and relevant information when reporting results of surgical specimen examinations of surgical specimens. The College regards the reporting elements in the Surgical Pathology Cancer Case Summary portion of the protocols as essential elements of the pathology report. However, the manner in which these elements are reported is at the discretion of each specific pathologist, taking into account clinician preferences, institutional policies, and individual practice. The College developed these protocols as an educational tool to assist pathologists in the useful reporting of relevant information. It did not issue the protocols for use in litigation, reimbursement, or other contexts. Nevertheless, the College recognizes that the protocols might be used by hospitals, attorneys, payers, and others. Indeed, effective January 1, 2004, the Commission on Cancer of the American College of Surgeons mandated the use of the required data elements of the protocols as part of its Cancer Program Standards for Approved Cancer Programs. Therefore, it becomes even more important for pathologists to familiarize themselves with these documents. At the same time, the College cautions that use of the protocols other than for their intended educational purpose may involve additional considerations that are beyond the scope of this document. The inclusion of a product name or service in a CAP publication should not be construed as an endorsement of such product or service, nor is failure to include the name of a product or service to be construed as disapproval. 2
3 CAP Soft Tissue Protocol Revision History Version Code The definition of version code can be found at Version: Summary of Changes The following changes have been made since the November 2011 release. Biopsy Ancillary Studies Added required only if applicable to this element. Resection Ancillary Studies Added required only if applicable to this element. Treatment Effect Specify percentage of viable tumor: added compared with pretreatment biopsy, if available. Explanatory Notes M Category Considerations The word checklist was changed to case summary. Important Note These recommendations are designed to be applied principally to soft tissue sarcomas in teenagers and adults, since pediatric sarcomas are, in general, treated under strict protocols that may differ significantly from the recommendations supplied herein. 1 3
4 CAP Approved Surgical Pathology Cancer Case Summary Protocol web posting date: June 2012 SOFT TISSUE: Biopsy Select a single response unless otherwise indicated. Procedure (Note A) Core needle biopsy Incisional biopsy Excisional biopsy Other (specify): Not specified Tumor Site Specify (if known): Not specified Tumor Size (Note B) Greatest dimension: cm + Additional dimensions: x cm Cannot be determined (see Comment ) Macroscopic Extent of Tumor (select all that apply) Superficial Dermal Subcutaneous/suprafascial Deep Fascial Subfascial Intramuscular Mediastinal Intra-abdominal Retroperitoneal Head and neck Other (specify): Cannot be determined Histologic Type (World Health Organization [WHO] classification of soft tissue tumors) (Note C) Specify: Cannot be determined Mitotic Rate (Note D) Specify: /10 high-power fields (HPF) (1 HPF x 400 = mm 2 ; X40 objective; most proliferative area) + Data elements preceded by this symbol are not required. However, these elements may be clinically important, but are not yet validated or regularly used in patient management. 4
5 CAP Approved Necrosis (Note D) Not identified Present Extent: % Cannot be determined Histologic Grade (French Federation of Cancer Centers Sarcoma Group [FNCLCC]) (Note D) Grade 1 Grade 2 Grade 3 Ungraded sarcoma Cannot be determined Margins (for excisional biopsy only) (Note E) Cannot be assessed Margins negative for sarcoma Distance of sarcoma from closest margin: cm Specify margin: Specify other close (less than 2.0 cm) margin(s): Margin(s) positive for sarcoma Specify margin(s): + Lymph-Vascular Invasion (Note F) + Not identified + Present + Indeterminate + Additional Pathologic Findings + Specify: Ancillary Studies (required only if applicable) Immunohistochemistry Specify: Not performed Cytogenetics Specify: Not performed Molecular Pathology Specify: Not performed Prebiopsy Treatment (select all that apply) No therapy Chemotherapy performed Radiation therapy performed Therapy performed, type not specified Unknown + Data elements preceded by this symbol are not required. However, these elements may be clinically important, but are not yet validated or regularly used in patient management. 5
6 CAP Approved Treatment Effect (Note G) Not identified Present + Specify percentage of viable tumor: % Cannot be determined + Comment(s) + Data elements preceded by this symbol are not required. However, these elements may be clinically important, but are not yet validated or regularly used in patient management. 6
7 CAP Approved Surgical Pathology Cancer Case Summary Protocol web posting date: June 2012 SOFT TISSUE: Resection Select a single response unless otherwise indicated. Procedure (Note H) Intralesional resection Marginal resection Wide resection Radical resection Other (specify): Not specified Tumor Site Specify (if known): Not specified Tumor Size Greatest dimension: cm + Additional dimensions: x cm Cannot be determined (see Comment ) Macroscopic Extent of Tumor (select all that apply) Superficial Dermal Subcutaneous/suprafascial Deep Fascial Subfascial Intramuscular Mediastinal Intra-abdominal Retroperitoneal Head and neck Other (specify): Cannot be determined Histologic Type (World Health Organization [WHO] classification of soft tissue tumors) (Note C, Note I) Specify: Cannot be determined + Data elements preceded by this symbol are not required. However, these elements may be clinically important, but are not yet validated or regularly used in patient management. 7
8 CAP Approved Mitotic Rate (Note D) Specify: /10 high-power fields (HPF) (1 HPF x 400 = mm 2 ; X40 objective; most proliferative area) Necrosis (macroscopic or microscopic) (Note D) Not identified Present Extent: % Histologic Grade (French Federation of Cancer Centers Sarcoma Group [FNCLCC]) (Note D) Grade 1 Grade 2 Grade 3 Ungraded sarcoma Cannot be determined Margins (Note E) Cannot be assessed Margins negative for sarcoma Distance of sarcoma from closest margin: cm Specify margin: Specify other close (less than 2.0 cm) margin(s): Margin(s) positive for sarcoma Specify margin(s): + Lymph-Vascular Invasion (Note F) + Not identified + Present + Indeterminate Pathologic Staging (ptnm) (Note J) TNM Descriptors (required only if applicable) (select all that apply) m (multiple) r (recurrent) y (posttreatment) Primary Tumor (pt) ptx: Primary tumor cannot be assessed pt0: No evidence of primary tumor pt1a: Tumor 5 cm or less in greatest dimension, superficial tumor pt1b: Tumor 5 cm or less in greatest dimension, deep tumor pt2a: Tumor more than 5 cm in greatest dimension, superficial tumor pt2b: Tumor more than 5 cm in greatest dimension, deep tumor + Data elements preceded by this symbol are not required. However, these elements may be clinically important, but are not yet validated or regularly used in patient management. 8
9 CAP Approved Regional Lymph Nodes (pn) (Notes J and K) pnx: Regional lymph nodes cannot be assessed pn0: No regional lymph node metastasis pn1: Regional lymph node metastasis No nodes submitted or found Number of Lymph Nodes Examined Specify: Number cannot be determined (explain): Number of Lymph Nodes Involved Specify: Number cannot be determined (explain): Distant Metastasis (pm) (Note J) Not applicable pm1: Distant metastasis + Specify site(s), if known: + Additional Pathologic Findings + Specify: Ancillary Studies (required only if applicable) Immunohistochemistry Specify: Not performed Cytogenetics Specify: Not performed Molecular Pathology Specify: Not performed Preresection Treatment (select all that apply) No therapy Chemotherapy performed Radiation therapy performed Therapy performed, type not specified Unknown Treatment Effect (Note G) Not identified Present + Specify percentage of viable tumor (compared with pretreatment biopsy, if available): % Cannot be determined + Comment(s) + Data elements preceded by this symbol are not required. However, these elements may be clinically important, but are not yet validated or regularly used in patient management. 9
10 Explanatory Notes A. Tissue Processing Fixation Tissue specimens from soft tissue tumors optimally are received fresh/unfixed because of the importance of ancillary studies, such as cytogenetics, which require fresh tissue. Tissue Submission for Histologic Evaluation One section per centimeter of maximum dimension is usually recommended, although fewer sections per centimeter are needed for very large tumors, especially if they are homogeneous. Tumors known to be high grade from a previous biopsy do not require as many sections as those that were previously diagnosed as low grade, as documentation of a high-grade component will change stage and prognosis in the latter case. Sections should be taken of grossly heterogeneous areas, and there is no need to submit more than 1 section of necrotic tumor (always with a transition to viable tumor). Occasionally, gross pathology can be misleading, and areas that appear to be grossly necrotic may actually be myxoid or edematous. When this happens, additional sections of these areas should be submitted for histologic examination. When estimates of gross necrosis exceed those of histologic necrosis, the greater percentage of necrosis should be recorded on the surgical pathology report. In general, most tumors require 12 sections or fewer, excluding margins. Tumors with greater areas of heterogeneity may need to be sampled more thoroughly. Fresh tissue for special studies should be submitted at the time the specimen is received. Note that classification of many subtypes of sarcoma is not dependent upon special studies, such as cytogenetics or molecular genetics, but frozen tissue may be needed to enter patients into treatment protocols. Discretion should be used in triaging tissue from sarcomas. Adequate tissue should be submitted for conventional light microscopy before tissue has been taken for cytogenetics, electron microscopy, or molecular analysis. Molecular Studies It is important to snap freeze a small portion of tissue whenever possible. This tissue can be used for a variety of molecular analyses for tumor-specific molecular translocations (see Table 1) that help in classifying soft tissue tumors. 2,3 In addition, treatment protocols increasingly require fresh tissue for correlative studies. Approximately 1 cm 3 of fresh tissue (less is acceptable for small specimens, including core biopsies) should be cut into small, 0.2-cm fragments, reserving sufficient tissue for histologic examination. This frozen tissue should ideally be stored at 70 o C and can be shipped on dry ice to facilities that perform molecular analysis. Table 1. Characteristic Cytogenetic and Molecular Events of Soft Tissue Tumors Histologic Type Cytogenetic Events Molecular Events Alveolar soft part sarcoma t(x;17)(p11;q25) TFE3-ASPL fusion Aneurysmal bone cyst t(16;17)q22;p13) CDH11-USP6 fusion Angiomatoid fibrous histiocytoma t(12;16)(q13;p11) FUS-ATF1 fusion t(12;22)(q13;q12) t(2;22)(q33;q12) EWSR1-ATF1 fusion EWSR1-CREB1 fusion Extraskeletal myxoid chondrosarcoma t(9;22)(q22;q12) EWS-NR4A3 fusion t(9;17)(q22;q11) TAF2N-NR4A3 fusion t(9;15)(q22;q21) TCF12-NR4A3 fusion 10
11 Histologic Type Cytogenetic Events Molecular Events Clear cell sarcoma t(12;22)(q13;q12) EWSR1-ATF1 fusion t(2;22(q33;q12) EWSR1-CREB1 fusion Desmoplastic small round cell tumor t(11;22)(p13;q12) EWSR1-WT1 fusion Dermatofibrosarcoma protuberans Ring form of chromosomes 17 and 22 COL1A1-PDGFB fusion t(17;22)(q21;q13) COL1A1-PDGFB fusion Ewing sarcoma/pnet t(11;22)(q24;q12) EWSR1-FLI1 fusion t(21;22)(q12;q12) EWSR1-ERG fusion t(2;22)(q33;q12) EWSR1-FEV fusion t(7;22)(p22;q12) EWSR1-ETV1 fusion t(17;22)(q12;q12) EWSR1-E1AF fusion inv(22)(q12q12) EWSR1-ZSG fusion t(16;21)(p11;q22) FUS-ERG fusion Fibrosarcoma, infantile t(12;15)(p13;q26) ETV6-NTRK3 fusion Trisomies 8, 11, 17, and 20 Inflammatory myofibroblastic tumor t(1;2)(q22;p23) TPM3-ALK fusion Leiomyosarcoma t(2;19)(p23;p13) t(2;17)(p23;q23) t(2;2)(p23;q13) Complex with frequent deletion of 1p TPM4-ALK fusion CLTC-ALK fusion RANB2-ALK fusion Liposarcoma Well-differentiated Ring form of chromosome 12 Amplification of MDM2, CDK4, and others Myxoid/Round cell t(12;16)(q13;p11) TLS-DDIT3 fusion t(12;22)(q13;q12) EWSR1-DDIT3 fusion Pleomorphic Complex Low-grade fibromyxoid sarcoma t(7;16)(q33;p11) FUS-CREB3L2 fusion Malignant peripheral nerve sheath tumor Complex Myxofibrosarcoma (myxoid MFH) Ring form of chromosome 12 Rhabdoid tumor Deletion of 22q INI1 inactivation Rhabdomyosarcoma Alveolar t(2;13)(q35;q14) PAX3-FOXO1A fusion t(1;13)(p36;q14), double minutes PAX7-FOXO1A fusion t(2 ;2)(q35 ;p23) PAX3-NCOA1 fusion PAX3-AFX fusion Embryonal Trisomies 2q, 8 and 20 Loss of heterozygosity at 11p15 Synovial sarcoma Monophasic t(x;18)(p11;q11) SS18-SSX1, SS18-SSX2 or SS18-SSX4 fusion Biphasic t(x;18)(p11;q11) Predominantly SS18-SSX1 fusion MFH, malignant fibrous histiocytoma; PNET, primitive neuroectodermal tumor. 11
12 B. Tumor Size In cases of nonexcisional biopsy (eg, core biopsy, incisional biopsy) the tumor size cannot be determined on pathologic grounds; therefore, imaging data (computed tomography [CT], magnetic resonance imaging [MRI], etc) can be used instead. C. Histologic Classification Intraoperative Consultation Histologic classification of soft tissue tumors is sufficiently complex that, in many cases, it is unreasonable to expect a precise classification of these tumors based on an intraoperative consultation. A complete understanding of the surgeon s treatment algorithm is recommended before rendering a frozen section diagnosis. Intraoperative consultation is useful in assessing if lesional tissue is present and in constructing a differential diagnosis that can direct the proper triage of tissue for flow cytometry (lymphoma), electron microscopy, and molecular studies/cytogenetics. Tissue triage optimally is performed at the time of frozen section. In many cases, it is important that a portion of tissue be submitted for ancillary studies, even from fine-needle aspiration (FNA) and core needle biopsy specimens, after sufficient tissue has been submitted for histologic evaluation. Tumor Classification from Biopsies It is not always possible to classify soft tissue tumors precisely based on biopsy material, especially FNA and core needle biopsy specimens. Although pathologists should make every attempt to classify lesions in small biopsy specimens, on occasion stratification into very basic diagnostic categories, such as lymphoma, carcinoma, melanoma, and sarcoma, is all that is possible. In some cases, precise classification is only possible in open biopsies or resection specimens. WHO Classification of Tumors Classification of tumors should be made according to the World Health Organization (WHO) classification of soft tissue tumors listed below. 4 As part of the latest WHO classification of soft tissue tumors, a recommendation was made to divide tumors into 4 categories: benign, intermediate (locally aggressive), intermediate (rarely metastasizing), and malignant. WHO Classification of Soft Tissue Tumors of Intermediate Malignant Potential and Malignant Soft Tissue Tumors Adipocytic Tumors Intermediate (locally aggressive) Atypical lipomatous tumor / Well-differentiated liposarcoma Malignant Dedifferentiated liposarcoma Myxoid/round cell liposarcoma Pleomorphic liposarcoma Mixed-type liposarcoma Liposarcoma, not otherwise specified Fibroblastic / Myofibroblastic Tumors Intermediate (locally aggressive) Superficial fibromatoses (palmar / plantar) Desmoid-type fibromatoses Lipofibromatosis Intermediate (rarely metastasizing) Solitary fibrous tumor and hemangiopericytoma (including lipomatous hemangiopericytoma) Inflammatory myofibroblastic tumor 12
13 Low-grade myofibroblastic sarcoma Myxoinflammatory fibroblastic sarcoma Infantile fibrosarcoma Malignant Adult fibrosarcoma Myxofibrosarcoma Low grade fibromyxoid sarcoma/hyalinizing spindle cell tumor Sclerosing epithelioid fibrosarcoma So-called Fibrohistiocytic Tumors Intermediate (rarely metastasizing) Plexiform fibrohistiocytic tumor Giant cell tumor of soft tissues Malignant Pleomorphic malignant fibrous histiocytoma (MFH) / Undifferentiated pleomorphic sarcoma Giant cell MFH / Undifferentiated pleomorphic sarcoma with giant cells Inflammatory MFH / Undifferentiated pleomorphic sarcoma with prominent inflammation Smooth Muscle Tumors Malignant Leiomyosarcoma Skeletal Muscle Tumors Malignant Embryonal rhabdomyosarcoma (including spindle cell, botryoid, anaplastic) Alveolar rhabdomyosarcoma (including solid, anaplastic) Pleomorphic rhabdomyosarcoma Vascular Tumors Intermediate (locally aggressive) Kaposiform hemangioendothelioma # Intermediate (rarely metastasizing) Retiform hemangioendothelioma Papillary intralymphatic angioendothelioma Composite hemangioendothelioma Malignant Epithelioid hemangioendothelioma Angiosarcoma of soft tissue Tumors of Peripheral Nerves Malignant Malignant peripheral nerve sheath tumor Epithelioid malignant peripheral nerve sheath tumor Chondro-osseous Tumors Malignant Mesenchymal chondrosarcoma Extraskeletal osteosarcoma Tumors of Uncertain Differentiation Intermediate (rarely metastasizing) Angiomatoid fibrous histiocytoma 13
14 Ossifying fibromyxoid tumor (including atypical / malignant) Mixed tumour / Myoepithelioma / Parachordoma Malignant Synovial sarcoma Epithelioid sarcoma Alveolar soft part sarcoma Clear cell sarcoma of soft tissue Extraskeletal myxoid chondrosarcoma ( chordoid type) Primitive neuroectodermal tumor (PNET) / Extraskeletal Ewing tumor Peripheral primitive neuroectodermal tumor (ppnet) Extraskeletal Ewing tumor Desmoplastic small round cell tumor Extra-renal rhabdoid tumor Malignant mesenchymoma Neoplasms with perivascular epithelioid cell differentiation (PEComa) Clear cell myomelanocytic tumor Intimal sarcoma # Since the last edition of the WHO classification, 2 cases of well-documented regional metastasis of kaposiform hemangioendothelioma have been reported, 5 raising the issue of whether or not kaposiform hemangioendothelioma might be more appropriately included in the category of intermediate (rarely metastasizing) instead of intermediate (locally aggressive). This will undoubtedly be addressed in the next WHO classification of tumors of soft tissue. D. Grading Unlike with other organ systems, the staging of soft tissue sarcomas is largely determined by grade. Unfortunately, there is no generally agreed-upon scheme for grading soft tissue tumors. 6 The most widely used soft tissue grading systems are the French Federation of Cancer Centers Sarcoma Group (FNCLCC) and National Cancer Institute (NCI) systems. 7,8 Both systems have 3 grades and are based on mitotic activity, necrosis, and differentiation, and are highly correlated with prognosis. 9 However, in addition to these criteria, the NCI system requires the quantification of cellularity and pleomorphism for certain subtypes of sarcomas, which is difficult to determine objectively. The FNCLCC system is easier to use in our opinion, and it may be slightly better in predicting prognosis than the NCI system. 9 Other systems with 2 or 4 grades also have been used. The seventh edition of the AJCC Cancer Staging Manual 10 adopted the FNCLCC grading system. The revison of the American Joint Committee on Cancer (AJCC) staging system incorporates a 3-tiered grading system; however, grade 1 and grades 2 to 3 (effectively low and high) are used for staging groups. Accurate grading requires an adequate sample of tissue, which is not always available from FNA or core needle biopsy or in tumors previously treated with radiation or chemotherapy. However, given the importance of grade in staging and treatment, efforts to separate sarcomas on the basis of needle biopsies into at least 2 tiers (ie, low and high grade) is encouraged. In many instances the histologic type of sarcoma will readily permit this distinction (ie, Ewing sarcoma/pnet, pleomorphic liposarcoma), whereas in less obvious instances the difficulty of assigning grade should be noted. In general, multiple needle core biopsies exhibiting a highgrade sarcoma can be regarded as high grade, since the probability of subsequent downgrading is remote, but limited core biopsies of low-grade sarcoma carry a risk of upgrading. FNCLCC Grading The FNCLCC grade is based on 3 parameters: differentiation, mitotic activity, and necrosis. Each of these parameters receives a score: differentiation (1 to 3), mitotic activity (1 to 3), and necrosis (0 to 2). The scores are summed to produce a grade. Grade 1: 2 or 3 14
15 Grade 2: 4 or 5 Grade 3: 6 to 8 Differentiation: Tumor differentiation is scored as follows (see Table 2). Score 1: Score 2: Score 3: Sarcomas closely resembling normal, adult mesenchymal tissue Sarcomas of certain histologic type Synovial sarcomas, embryonal sarcomas, undifferentiated sarcomas, and sarcomas of doubtful tumor type Tumor differentiation is the most problematic aspect of the FNCLCC system. Its use is subjective and does not include every subtype of sarcoma. Nevertheless, it is an integral part of the system, and an attempt should be made to assign a differentiation score. Table 2. Tumor Differentiation Score According to Histologic Type in the Updated Version of the French Federation of Cancer Centers Sarcoma Group System Tumor Differentiation Histologic Type Score Well-differentiated liposarcoma 1 Myxoid liposarcoma 2 Round cell liposarcoma 3 Pleomorphic liposarcoma 3 Dedifferentiated liposarcoma 3 Fibrosarcoma 2 Myxofibrosarcoma (malignant fibrous histiocytoma [MFH]) 2 MFH, pleomorphic type (patternless pleomorphic sarcoma) 3 Giant cell and inflammatory MFH (pleomorphic sarcoma, NOS, with giant cells or inflammatory cells) 3 Well-differentiated leiomyosarcoma 1 Conventional leiomyosarcoma 2 Poorly differentiated / pleomorphic / epithelioid leiomyosarcoma 3 Biphasic / monophasic synovial sarcoma 3 Poorly differentiated synovial sarcoma 3 Pleomorphic rhabdomyosarcoma 3 Mesenchymal chondrosarcoma 3 Extraskeletal osteosarcoma 3 Ewing sarcoma / primitive neuroectodermal tumor 3 Malignant rhabdoid tumor 3 Undifferentiated sarcoma 3 Note: Grading of malignant peripheral nerve sheath tumor, embryonal and alveolar rhabdomyosarcoma, angiosarcoma, extraskeletal myxoid chondrosarcoma, alveolar soft part sarcoma, clear cell sarcoma, and epithelioid sarcoma is not recommended. 4 From Guillou et al. 9 Modified with permission American Society of Clinical Oncology. All rights reserved. 15
16 Mitosis Count: The count is made in the most mitotically active area in 10 successive high-power fields (HPF) (1 HPF X 400 = mm 2 ) (use the X40 objective). Score 1: Score 2: Score 3: 0 to 9 mitoses per 10 HPF 10 to19 mitoses per 10 HPF 20 or more mitoses per 10 HPF Tumor Necrosis: Determined on histologic sections. Score 0: Score 1: Score 2: No tumor necrosis Less than or equal to 50% tumor necrosis More than 50% tumor necrosis TNM Grading The seventh edition of the American Joint Committee on Cancer (AJCC) and International Union Against Cancer (UICC) staging system for soft tissue tumors recommends the FNCLCC 3-grade system but effectively collapses into high grade and low grade. 10,11 This means that FNCLCC grade 2 tumors are considered high grade for the purposes of stage grouping. E. Margins It has been recommended that for all margins <2 cm, the distance of the tumor from the margin be reported in centimeters. 12 However, there is a lack of agreement on this issue. We recommend specifying the location of all margins <2 cm and the distance of the closest margin that is <2 cm. Margins from soft tissue tumors should be taken as perpendicular sections, if possible. If bones are present in the specimen and are not involved by tumor, or the tumor is >2 cm from the margin, the marrow can be scooped out and submitted as a margin. F. Lymph-Vascular Invasion Lymph-vascular invasion (LVI) indicates whether microscopic lymph-vascular invasion is identified. LVI includes lymphatic invasion, vascular invasion, or lymph-vascular invasion. By AJCC/UICC convention, LVI does not affect the T category indicating local extent of tumor unless specifically included in the definition of a T category. G. Response to Chemotherapy/Radiation Therapy Effect Although agreement has not been reached about measuring the effect of preoperative (neoadjuvant) chemotherapy/radiation therapy in soft tissue tumors, an attempt should be made to quantify these effects, especially in the research setting. Therapy response is expressed as a percentage of total tumor area that is viable. Nonliquefied tumor tissue from a cross-section through the longest axis of the tumor should be sampled. At least 1 section of necrotic tumor (always with a transition to viable tumor) should be sampled to verify the gross impression of necrosis. Nonsampled necrotic areas should be included in the estimate of necrosis and the percentage of tumor necrosis reported. The gross appearance can be misleading, and areas that appear grossly necrotic may actually be myxoid or edematous. Additional sections from these areas should be submitted for histologic examination. When estimates of gross necrosis exceed those of histologic necrosis, the greater percentage of necrosis should be recorded on the surgical pathology report. H. Definition of Procedures The following is a list of guidelines to be used in defining what type of procedure has been performed. Intralesional Resection Leaving gross or microscopic tumor behind. Partial debulking or curettage are examples or when microscopic tumor is left at the margin unintententionally in an attempted marginal resection. 16
17 Marginal Resection Removing the tumor and its pseudocapsule with a relatively small amount of adjacent tissue. There is no gross tumor at the margin; however, there is a high likelihood that microscopic tumor is present. If microscopic disease is identified at the margin, then it is an intralesional resection. Note that occasionally a surgeon will perform an excisional biopsy, which effectively accomplishes the same thing as a marginal resection. Wide Resection An intracompartmental resection. The tumor is removed with pseudocapsule and a cuff of normal tissue surrounding the neoplasm, but without the complete removal of an entire muscle group, compartment, or bone. Radical Resection The removal of an entire soft tissue compartment (for example, anterior compartment of the thigh, the quadriceps) or bone, or the excision of the adjacent muscle groups if the tumor is extracompartmental. I. Histological Classification of Treated Lesions Because of extensive treatment effects, such as necrosis, fibrosis, and chemotherapy-induced and radiation-induced pleomorphism, it may not be possible to classify some lesions that were either never biopsied or where the biopsy was insufficient for a precise diagnosis. J. TNM and Stage Groupings The TNM staging system for soft tissue tumors of the AJCC and UICC is recommended. 10,11 The staging system applies to all soft tissue sarcomas except Kaposi sarcoma, gastrointestinal stromal tumors, fibromatosis (desmoid tumor), and infantile fibrosarcoma. In addition, sarcomas arising within the confines of the dura mater, including the brain, and sarcomas arising in parenchymatous organs and from hollow viscera are not optimally staged by this system. Pathologic (ptnm) staging consists of the removal and pathologic evaluation of the primary tumor and clinical/radiologic evaluation for regional and distant metastases. In circumstances where it is not possible to obtain accurate measurements of the excised primary sarcoma specimen, it is acceptable to use radiologic assessment of tumor size to assign a pt category. In examining the primary tumor, the pathologist should subclassify the lesion and assign a histopathologic grade. Definition of pt Although size currently is designated within the TNM system as 5 cm or smaller versus larger than 5 cm, particular emphasis should be placed on providing size measurements. Size should be regarded as a continuous variable, with 5 cm as merely an arbitrary division that makes it possible to dichotomize patient populations. Depth Depth is evaluated relative to the investing fascia of the extremity and trunk. Superficial is defined as lack of any involvement of the superficial investing muscular fascia in extremity or trunk lesions. For staging, all retroperitoneal and visceral lesions are considered to be deep lesions. Depth is also an independent variable and is defined as follows. 1. Superficial a. Tumor is located entirely in the subcutaneous tissues without any involvement of the muscular fascia. In these cases, pretreatment imaging studies demonstrate a subcutaneous tumor without involvement of muscle, and excisional biopsy pathology specimen demonstrate a tumor 17
18 located within the subcutaneous tissues without invasion into fascia (adopted from the seventh edition of the AJCC Cancer Staging Manual). 2. Deep a. Tumor is located partly or completely within 1 or more muscle groups within the extremity. Deep tumors may extend through the muscular fascia into the subcutaneous tissues or even to the skin, but the critical criterion is location of any portion of the tumor within the muscular compartments of the extremity or invasion of the muscular fascia. In these cases, pretreatment imaging studies demonstrate a tumor located completely or partly within the muscular compartments of the extremity. Finally, on pathologic evaluation, any tumor that is superficial to the muscular fasica, but invades the fascia, is considered deep (adopted from the seventh edition of the AJCC Cancer Staging Manual). b. All intraperitoneal visceral lesions, retroperitoneal lesions, intrathoracic lesions, and the majority of head and neck tumors are considered deep. 3. Depth is evaluated in relation to tumor size (T) a. Tumor 5 cm or less: T1a = superficial; T1b = deep. b. Tumor greater than 5 cm: T2a = superficial; T2b = deep. Regional Lymph Nodes (pn) Nodal involvement is rare in adult soft tissue sarcomas but, when present, has a very poor prognosis. N1 disease is classified as stage III. Patients whose nodal status is not determined to be positive for tumor, either clinically or pathologically, should be designated as N0. Restaging of Recurrent Tumors The same staging should be used when a patient requires restaging of sarcoma recurrence. Such reports should specify whether patients have primary lesions or lesions that were previously treated and have subsequently recurred. Reporting of possible etiologic factors, such as radiation exposure and inherited or genetic syndromes, is encouraged. Appropriate workup for recurrent sarcoma usually includes cross-sectional imaging (computed tomography [CT] scan or magnetic resonance imaging [MRI] scan) of the tumor, a CT scan of the chest, and a tissue biopsy to confirm diagnosis prior to initiation of therapy. TNM Descriptors For identification of special cases of TNM or ptnm classifications, the m suffix and the y and r prefixes are used. Although they do not affect the stage grouping, they indicate cases needing separate analysis. The m suffix indicates the presence of multiple primary tumors in a single site and is recorded in parentheses: pt(m)nm. The y prefix indicates those cases in which classification is performed during or following initial multimodality therapy (ie, neoadjuvant chemotherapy, radiation therapy, or both chemotherapy and radiation therapy). The ctnm or ptnm category is identified by a y prefix. The yctnm or yptnm categorizes the extent of tumor actually present at the time of that examination. The y categorization is not an estimate of tumor prior to multimodality therapy (ie, before initiation of neoadjuvant therapy). The r prefix indicates a recurrent tumor when staged after a documented disease-free interval, and is identified by the r prefix: rtnm. 18
19 T Category Considerations Superficial tumor is located exclusively above the superficial fascia without invasion of the fascia; deep tumor is located either exclusively beneath the superficial fascia or superficial to the fascia with invasion of or through the fascia. Retroperitoneal, mediastinal, and pelvic sarcomas are classified as deep tumors. N Category Considerations Presence of positive nodes (N1) is considered stage III. M Category Considerations pmx and pm0 (no distant metastasis) are no longer case summary options as the use of pmx provides no meaningful information to the clinician or cancer registrar and at times may create confusion in tumor staging. Stage Groupings Stage IA T1a N0 NX M0 G1 Low T1b N0 NX M0 G1 Low Stage IB T2a N0 NX M0 G1 Low T2b N0 NX M0 G1 Low Stage IIA T1a N0 NX M0 G2 High T1b N0 NX M0 G2 High Stage IIB T2a N0 NX M0 G2 High Stage III T2b N0-1 NX M0 G3 High Stage IV Any T Any N M1 Any G High or Low Additional Descriptors Residual Tumor (R) Tumor remaining in a patient after therapy with curative intent (eg, surgical resection for cure) is categorized by a system known as R classification, shown below. RX R0 R1 R2 Presence of residual tumor cannot be assessed No residual tumor Microscopic residual tumor Macroscopic residual tumor For the surgeon, the R classification may be useful to indicate the known or assumed status of the completeness of a surgical excision. For the pathologist, the R classification is relevant to the status of the margins of a surgical resection specimen. That is, tumor involving the resection margin on pathologic examination may be assumed to correspond to residual tumor in the patient and may be classified as macroscopic or microscopic according to the findings at the specimen margin(s). K. Lymph Nodes With the exception of epithelioid sarcoma and clear cell sarcoma of soft parts, regional lymph node metastasis is uncommon in adult soft tissue sarcomas. Nodes are not sampled routinely, and it usually is not necessary to exhaustively search for nodes. When present, regional lymph node metastasis has prognostic importance and should be reported. The seventh edition of the AJCC Cancer Manual recommends that N1 M0 disease to be regarded as stage III rather than stage IV disease. 19
20 References 1. Qualman SJ, Bowen J, Parham DM, Branton PA, Meyer WH. Protocol for the examination of specimens from patients (children and young adults) with rhabdomyosarcoma. Arch Pathol Lab Med. 2003;127(10): Ladanyi M, Bridge JA. Contribution of molecular genetic data to the classification of sarcomas. Hum Pathol. 2000;31(5): Tomescu O, Barr FG. Chromosomal translocations in sarcomas: prospects for therapy. Trends Mol Med. 2001;7(12): Fletcher CDM, Unni KK, Mertens F, eds. Pathology and Genetics of Tumours of Soft Tissue and Bone. Lyon, France: IARC Press; World Health Organization Classification of Tumours, Vol Lyons LL, North PE, Mac-Moune Lai F, Stoler MH, Folpe AL, Weiss SW. Kaposiform hemangioendothelioma: a study of 33 cases emphasizing its pathologic, immunophenotypic, and biologic uniqueness from juvenile hemangioma. Am J Surg Pathol. 2004;28(5): Oliveira AM, Nascimento AG. Grading in soft tissue tumors: principles and problems. Skeletal Radiol. 2001;30(10): Coindre JM, Trojani M, Contesso G, et al. Reproducibility of a histopathologic grading system for adult soft tissue sarcoma. Cancer. 1986;58(2): Costa J, Wesley RA, Glatstein E, Rosenberg SA. The grading of soft tissue sarcomas: results of a clinicohistopathologic correlation in a series of 163 cases. Cancer. 1984;53(3): Guillou L, Coindre JM, Bonichon F, et al. Comparative study of the National Cancer Institute and French Federation of Cancer Centers Sarcoma Group grading systems in a population of 410 adult patients with soft tissue sarcoma. J Clin Oncol. 1997;15(1): Edge SE, Byrd DR, Carducci MA, Compton CC, eds. AJCC Cancer Staging Manual. 7th ed. New York, NY: Springer; Sobin LH, Gospodarowicz M, Wittekind Ch, eds. UICC TNM Classification of Malignant Tumours. 7th ed. New York, NY: Wiley-Liss; Recommendations for the reporting of soft tissue sarcomas. Association of Directors of Anatomic and Surgical Pathology. Mod Pathol. 1998;11(12):
The evolving pathology of solitary fibrous tumours. Luciane Dreher Irion MREH / CMFT / NSOPS
 The evolving pathology of solitary fibrous tumours Luciane Dreher Irion MREH / CMFT / NSOPS Historical review Haemangiopericytoma (HPC) first described primarily as a soft tissue vascular tumour of pericytic
The evolving pathology of solitary fibrous tumours Luciane Dreher Irion MREH / CMFT / NSOPS Historical review Haemangiopericytoma (HPC) first described primarily as a soft tissue vascular tumour of pericytic
WHO Classification of Soft Tissue Tumours
 WHO Classification of Soft Tissue Tumours This new WHO classification of soft tissue tumours, in line with other volumes in this new series, incorporates detailed clinical, histological and genetic data.
WHO Classification of Soft Tissue Tumours This new WHO classification of soft tissue tumours, in line with other volumes in this new series, incorporates detailed clinical, histological and genetic data.
Immunohistochemistry of soft tissue tumors
 Immunohistochemistry of soft tissue tumors Immunohistochemistry Major advances : antigen retrieval techniques (HIER) sensitive detection systems numerous antibodies of good quality Standardization : automated
Immunohistochemistry of soft tissue tumors Immunohistochemistry Major advances : antigen retrieval techniques (HIER) sensitive detection systems numerous antibodies of good quality Standardization : automated
Tumor Patterns. Common Morphologic Patterns in Soft Tissue Tumors. Update on Lipomatous Tumors. MFH-like. Highly cellular spindle cell pattern
 Common Morphologic Patterns in Soft Tissue Tumors John R. Goldblum, M.D. Chairman, Department of Anatomic Pathology The Cleveland Clinic Professor of Pathology Cleveland Clinic Lerner College of Medicine
Common Morphologic Patterns in Soft Tissue Tumors John R. Goldblum, M.D. Chairman, Department of Anatomic Pathology The Cleveland Clinic Professor of Pathology Cleveland Clinic Lerner College of Medicine
Update on Mesothelioma
 November 8, 2012 Update on Mesothelioma Intro incidence and nomenclature Update on Classification Diagnostic specimens Morphologic features Epithelioid Histology Biphasic Histology Immunohistochemical
November 8, 2012 Update on Mesothelioma Intro incidence and nomenclature Update on Classification Diagnostic specimens Morphologic features Epithelioid Histology Biphasic Histology Immunohistochemical
Protocol for the Examination of Specimens From Patients With Malignant Pleural Mesothelioma
 Protocol for the Examination of Specimens From Patients With Malignant Pleural Mesothelioma Based on AJCC/UICC TNM, 7th edition Protocol web posting date: February 1, 2011 Procedures Resection Authors
Protocol for the Examination of Specimens From Patients With Malignant Pleural Mesothelioma Based on AJCC/UICC TNM, 7th edition Protocol web posting date: February 1, 2011 Procedures Resection Authors
World Health Organization Classification of Tumours. Pathology and Genetics of Tumours of Soft Tissue and Bone
 World Health Organization Classification of Tumours WHO OMS International Agency for Research on Cancer (IARC) Pathology and Genetics of Tumours of Soft Tissue and one Edited by Christopher D.M. Fletcher
World Health Organization Classification of Tumours WHO OMS International Agency for Research on Cancer (IARC) Pathology and Genetics of Tumours of Soft Tissue and one Edited by Christopher D.M. Fletcher
Chapter 2 Staging of Breast Cancer
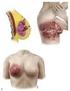 Chapter 2 Staging of Breast Cancer Zeynep Ozsaran and Senem Demirci Alanyalı 2.1 Introduction Five decades ago, Denoix et al. proposed classification system (tumor node metastasis [TNM]) based on the dissemination
Chapter 2 Staging of Breast Cancer Zeynep Ozsaran and Senem Demirci Alanyalı 2.1 Introduction Five decades ago, Denoix et al. proposed classification system (tumor node metastasis [TNM]) based on the dissemination
Malcolm Mattes, MD Ajay Tejwani, MD, MPH New York Methodist Hospital
 Malcolm Mattes, MD Ajay Tejwani, MD, MPH New York Methodist Hospital 39 year old female patient who felt a mass in the right gluteal area. Slowly growing over the course of 2 3 months. The mass is associated
Malcolm Mattes, MD Ajay Tejwani, MD, MPH New York Methodist Hospital 39 year old female patient who felt a mass in the right gluteal area. Slowly growing over the course of 2 3 months. The mass is associated
7 th Edition Staging. AJCC 7 th Edition Staging. Disease Site Webinar. Melanoma of Skin. Overview. This webinar is sponsored by
 AJCC 7 th Edition Staging Melanoma of Skin Donna M. Gress, RHIT, CTR Validating science. Improving patient care. This presentation was supported by the Cooperative Agreement Number DP13-1310 from The Centers
AJCC 7 th Edition Staging Melanoma of Skin Donna M. Gress, RHIT, CTR Validating science. Improving patient care. This presentation was supported by the Cooperative Agreement Number DP13-1310 from The Centers
Something Old, Something New.
 Something Old, Something New. Michelle A. Fajardo, D.O. Loma Linda University Medical Center Clinical Presentation 6 year old boy, presented with hematuria Renal mass demonstrated by ultrasound & CT scan
Something Old, Something New. Michelle A. Fajardo, D.O. Loma Linda University Medical Center Clinical Presentation 6 year old boy, presented with hematuria Renal mass demonstrated by ultrasound & CT scan
9. Discuss guidelines for follow-up post-thyroidectomy for cancer (labs/tests) HH
 9. Discuss guidelines for follow-up post-thyroidectomy for cancer (labs/tests) HH Differentiated thyroid cancer expresses the TSH receptor on the cell membrane and responds to TSH stimulation by increasing
9. Discuss guidelines for follow-up post-thyroidectomy for cancer (labs/tests) HH Differentiated thyroid cancer expresses the TSH receptor on the cell membrane and responds to TSH stimulation by increasing
Protocol for the Examination of Specimens From Patients With Tumors of the Peritoneum
 Protocol for the Examination of Specimens From Patients With Tumors of the Peritoneum Protocol applies to all primary borderline and malignant epithelial tumors and malignant mesothelial neoplasms of the
Protocol for the Examination of Specimens From Patients With Tumors of the Peritoneum Protocol applies to all primary borderline and malignant epithelial tumors and malignant mesothelial neoplasms of the
MODERN IMMUNOHISTOCHEMISTRY
 MODERN IMMUNOHISTOCHEMISTRY Cambridge Illustrated Surgical Pathology Peiguo G. Chu City of Hope National Medical Center, Duarte, California Lawrence M. Weiss City of Hope National Medical Center, Duarte,
MODERN IMMUNOHISTOCHEMISTRY Cambridge Illustrated Surgical Pathology Peiguo G. Chu City of Hope National Medical Center, Duarte, California Lawrence M. Weiss City of Hope National Medical Center, Duarte,
OBJECTIVES By the end of this segment, the community participant will be able to:
 Cancer 101: Cancer Diagnosis and Staging Linda U. Krebs, RN, PhD, AOCN, FAAN OCEAN Native Navigators and the Cancer Continuum (NNACC) (NCMHD R24MD002811) Cancer 101: Diagnosis & Staging (Watanabe-Galloway
Cancer 101: Cancer Diagnosis and Staging Linda U. Krebs, RN, PhD, AOCN, FAAN OCEAN Native Navigators and the Cancer Continuum (NNACC) (NCMHD R24MD002811) Cancer 101: Diagnosis & Staging (Watanabe-Galloway
Soft tissue sarcoma of the extremities. SUNY Downstate Medical Center Brooklyn Veterans Hospital Valery Dronsky, M.D.
 Soft tissue sarcoma of the extremities SUNY Downstate Medical Center Brooklyn Veterans Hospital Valery Dronsky, M.D. Soft Tissue Sarcomas of the Extremities Soft Tissue Sarcomas: Definition Sarcomas are
Soft tissue sarcoma of the extremities SUNY Downstate Medical Center Brooklyn Veterans Hospital Valery Dronsky, M.D. Soft Tissue Sarcomas of the Extremities Soft Tissue Sarcomas: Definition Sarcomas are
CASE OF THE MONTH AUGUST-2015 DR. GURUDUTT GUPTA HEAD HISTOPATHOLOGY
 CASE OF THE MONTH AUGUST-2015 DR. GURUDUTT GUPTA HEAD HISTOPATHOLOGY CASE HISTORY 52Y MALE RIGHT RADICAL NEPHERECTOMY Case of right renal mass with IVC thrombus. History of surgery and RT for right occipital
CASE OF THE MONTH AUGUST-2015 DR. GURUDUTT GUPTA HEAD HISTOPATHOLOGY CASE HISTORY 52Y MALE RIGHT RADICAL NEPHERECTOMY Case of right renal mass with IVC thrombus. History of surgery and RT for right occipital
Pathology of lung cancer
 Pathology of lung cancer EASO COURSE ON LUNG CANCER AND MESOTHELIOMA DAMASCUS (SYRIA), MAY 3-4, 2007 Gérard ABADJIAN MD Pathologist Associate Professor, Saint Joseph University Pathology Dept. Hôtel-Dieu
Pathology of lung cancer EASO COURSE ON LUNG CANCER AND MESOTHELIOMA DAMASCUS (SYRIA), MAY 3-4, 2007 Gérard ABADJIAN MD Pathologist Associate Professor, Saint Joseph University Pathology Dept. Hôtel-Dieu
Changes in Breast Cancer Reports After Second Opinion. Dr. Vicente Marco Department of Pathology Hospital Quiron Barcelona. Spain
 Changes in Breast Cancer Reports After Second Opinion Dr. Vicente Marco Department of Pathology Hospital Quiron Barcelona. Spain Second Opinion in Breast Pathology Usually requested when a patient is referred
Changes in Breast Cancer Reports After Second Opinion Dr. Vicente Marco Department of Pathology Hospital Quiron Barcelona. Spain Second Opinion in Breast Pathology Usually requested when a patient is referred
Kidney Cancer OVERVIEW
 Kidney Cancer OVERVIEW Kidney cancer is the third most common genitourinary cancer in adults. There are approximately 54,000 new cancer cases each year in the United States, and the incidence of kidney
Kidney Cancer OVERVIEW Kidney cancer is the third most common genitourinary cancer in adults. There are approximately 54,000 new cancer cases each year in the United States, and the incidence of kidney
Recommendations for the Reporting of Pleural Mesothelioma
 Recommendations for the Reporting of Pleural Mesothelioma Association of Directors of Anatomic and Surgical Pathology * DOI: 10.1309/6A30YQHBMTHEJTEM It has been evident for decades that pathology reports
Recommendations for the Reporting of Pleural Mesothelioma Association of Directors of Anatomic and Surgical Pathology * DOI: 10.1309/6A30YQHBMTHEJTEM It has been evident for decades that pathology reports
Breast Cancer: from bedside and grossing room to diagnoses and beyond. Adriana Corben, M.D.
 Breast Cancer: from bedside and grossing room to diagnoses and beyond Adriana Corben, M.D. About breast anatomy Breasts are special organs that develop in women during puberty when female hormones are
Breast Cancer: from bedside and grossing room to diagnoses and beyond Adriana Corben, M.D. About breast anatomy Breasts are special organs that develop in women during puberty when female hormones are
The Diagnosis of Cancer in the Pathology Laboratory
 The Diagnosis of Cancer in the Pathology Laboratory Dr Edward Sheffield Christmas Select 74 Meeting, Queen s Hotel Cheltenham, 3 rd December 2014 Agenda Overview of the pathology of cancer How specimens
The Diagnosis of Cancer in the Pathology Laboratory Dr Edward Sheffield Christmas Select 74 Meeting, Queen s Hotel Cheltenham, 3 rd December 2014 Agenda Overview of the pathology of cancer How specimens
Report series: General cancer information
 Fighting cancer with information Report series: General cancer information Eastern Cancer Registration and Information Centre ECRIC report series: General cancer information Cancer is a general term for
Fighting cancer with information Report series: General cancer information Eastern Cancer Registration and Information Centre ECRIC report series: General cancer information Cancer is a general term for
Introduction: Tumor Swelling / new growth / mass. Two types of growth disorders: Non-Neoplastic. Secondary / adaptation due to other cause.
 Disorders of Growth Introduction: Tumor Swelling / new growth / mass Two types of growth disorders: Non-Neoplastic Secondary / adaptation due to other cause. Neoplastic. Primary growth abnormality. Non-Neoplastic
Disorders of Growth Introduction: Tumor Swelling / new growth / mass Two types of growth disorders: Non-Neoplastic Secondary / adaptation due to other cause. Neoplastic. Primary growth abnormality. Non-Neoplastic
Diagnosis and Prognosis of Pancreatic Cancer
 Main Page Risk Factors Reducing Your Risk Screening Symptoms Diagnosis Treatment Overview Chemotherapy Radiation Therapy Surgical Procedures Lifestyle Changes Managing Side Effects Talking to Your Doctor
Main Page Risk Factors Reducing Your Risk Screening Symptoms Diagnosis Treatment Overview Chemotherapy Radiation Therapy Surgical Procedures Lifestyle Changes Managing Side Effects Talking to Your Doctor
Protocol for the Examination of Specimens From Patients With Hepatocellular Carcinoma
 Protocol for the Examination of Specimens From Patients With Hepatocellular Carcinoma Cholangiocarcinoma, mixed hepatocellular-cholangiocarcinoma, and hepatoblastoma are not included. Based on AJCC/UICC
Protocol for the Examination of Specimens From Patients With Hepatocellular Carcinoma Cholangiocarcinoma, mixed hepatocellular-cholangiocarcinoma, and hepatoblastoma are not included. Based on AJCC/UICC
Rotation Specific Goals & Objectives: University Health Network-Princess Margaret Hospital/ Sunnybrook Breast/Melanoma
 Rotation Specific Goals & Objectives: University Health Network-Princess Margaret Hospital/ Sunnybrook Breast/Melanoma Medical Expert: Breast Rotation Specific Competencies/Objectives 1.0 Medical History
Rotation Specific Goals & Objectives: University Health Network-Princess Margaret Hospital/ Sunnybrook Breast/Melanoma Medical Expert: Breast Rotation Specific Competencies/Objectives 1.0 Medical History
Cardiac Masses and Tumors
 Cardiac Masses and Tumors Question: What is the diagnosis? A. Aortic valve myxoma B. Papillary fibroelastoma C. Vegetation from Infective endocarditis D. Thrombus in transit E. None of the above Answer:
Cardiac Masses and Tumors Question: What is the diagnosis? A. Aortic valve myxoma B. Papillary fibroelastoma C. Vegetation from Infective endocarditis D. Thrombus in transit E. None of the above Answer:
SUNY DOWNSTATE MEDICAL CENTER SURGERY GRAND ROUNDS February 28, 2013 VERENA LIU, MD ROSEANNA LEE, MD
 SUNY DOWNSTATE MEDICAL CENTER SURGERY GRAND ROUNDS February 28, 2013 VERENA LIU, MD ROSEANNA LEE, MD Case Presentation 35 year old male referred from PMD with an asymptomatic palpable right neck mass PMH/PSH:
SUNY DOWNSTATE MEDICAL CENTER SURGERY GRAND ROUNDS February 28, 2013 VERENA LIU, MD ROSEANNA LEE, MD Case Presentation 35 year old male referred from PMD with an asymptomatic palpable right neck mass PMH/PSH:
How to report Upper GI EMR/ESD specimens
 Section of Pathology and Tumour Biology How to report Upper GI EMR/ESD specimens Dr.H.Grabsch Warning. Most of the criteria, methodologies, evidence presented in this talk are based on studies in early
Section of Pathology and Tumour Biology How to report Upper GI EMR/ESD specimens Dr.H.Grabsch Warning. Most of the criteria, methodologies, evidence presented in this talk are based on studies in early
General Rules SEER Summary Stage 2000. Objectives. What is Staging? 5/8/2014
 General Rules SEER Summary Stage 2000 Linda Mulvihill Public Health Advisor NCRA Annual Meeting May 2014 National Center for Chronic Disease Prevention and Health Promotion Division of Cancer Prevention
General Rules SEER Summary Stage 2000 Linda Mulvihill Public Health Advisor NCRA Annual Meeting May 2014 National Center for Chronic Disease Prevention and Health Promotion Division of Cancer Prevention
Chapter 13. The hospital-based cancer registry
 Chapter 13. The hospital-based cancer registry J.L. Young California Tumor Registry, 1812 14th Street, Suite 200, Sacramento, CA 95814, USA Introduction The purposes of a hospital-based cancer registry
Chapter 13. The hospital-based cancer registry J.L. Young California Tumor Registry, 1812 14th Street, Suite 200, Sacramento, CA 95814, USA Introduction The purposes of a hospital-based cancer registry
Soft tissue sarcoma. 329 Soft tissue sarcoma Page 1 of 11
 Soft tissue sarcoma Page 1 of 11 Introduction This booklet is to give you, your family and your friends some information about this group of illnesses, and how we treat them at The Christie. Introduction:
Soft tissue sarcoma Page 1 of 11 Introduction This booklet is to give you, your family and your friends some information about this group of illnesses, and how we treat them at The Christie. Introduction:
TUMORS OF THE TESTICULAR ADNEXA and SPERMATIC CORD
 TUMORS OF THE TESTICULAR ADNEXA and SPERMATIC CORD Victor E. Reuter, MD Memorial Sloan-Kettering Cancer Center reuterv@mskcc.org 66 th Annual Pathology Seminar California Society of Pathologists Short
TUMORS OF THE TESTICULAR ADNEXA and SPERMATIC CORD Victor E. Reuter, MD Memorial Sloan-Kettering Cancer Center reuterv@mskcc.org 66 th Annual Pathology Seminar California Society of Pathologists Short
Thyroid and Adrenal Gland
 Thyroid and Adrenal Gland NAACCR 2011 2012 Webinar Series 12/1/11 Q&A Please submit all questions concerning webinar content through the Q&A panel. Reminder: If you have participants watching this webinar
Thyroid and Adrenal Gland NAACCR 2011 2012 Webinar Series 12/1/11 Q&A Please submit all questions concerning webinar content through the Q&A panel. Reminder: If you have participants watching this webinar
Image. 3.11.3 SW Review the anatomy of the EAC and how this plays a role in the spread of tumors.
 Neoplasms of the Ear and Lateral Skull Base Image 3.11.1 SW What are the three most common neoplasms of the auricle? 3.11.2 SW What are the four most common neoplasms of the external auditory canal (EAC)
Neoplasms of the Ear and Lateral Skull Base Image 3.11.1 SW What are the three most common neoplasms of the auricle? 3.11.2 SW What are the four most common neoplasms of the external auditory canal (EAC)
Understanding Metastatic Disease
 Supported by an unrestricted educational grant from Pfizer Understanding Metastatic Disease Metastatic disease or metastases are phrases that mean the same as Secondary cancer. This means that the cancer
Supported by an unrestricted educational grant from Pfizer Understanding Metastatic Disease Metastatic disease or metastases are phrases that mean the same as Secondary cancer. This means that the cancer
Post-PET Restaging Cancer Form National Oncologic PET Registry
 Post-PET Restaging Cancer Form National Oncologic PET Registry Facility ID #: Registry Case Number: Patient Name: Your patient had a PET scan on: mm/dd/yyyy. The PET scan was done for restaging of (cancer
Post-PET Restaging Cancer Form National Oncologic PET Registry Facility ID #: Registry Case Number: Patient Name: Your patient had a PET scan on: mm/dd/yyyy. The PET scan was done for restaging of (cancer
Protocol applies to all primary borderline and malignant epithelial tumors, and malignant mesothelial neoplasms of the peritoneum.
 Peritoneum Protocol applies to all primary borderline and malignant epithelial tumors, and malignant mesothelial neoplasms of the peritoneum. Protocol revision date: January 2004 No AJCC/UICC staging system
Peritoneum Protocol applies to all primary borderline and malignant epithelial tumors, and malignant mesothelial neoplasms of the peritoneum. Protocol revision date: January 2004 No AJCC/UICC staging system
Objectives. Mylene T. Truong, MD. Malignant Pleural Mesothelioma Background
 Imaging of Pleural Tumors Mylene T. Truong, MD Imaging of Pleural Tumours Mylene T. Truong, M. D. University of Texas M.D. Anderson Cancer Center, Houston, TX Objectives To review tumors involving the
Imaging of Pleural Tumors Mylene T. Truong, MD Imaging of Pleural Tumours Mylene T. Truong, M. D. University of Texas M.D. Anderson Cancer Center, Houston, TX Objectives To review tumors involving the
Osteosarcoma What are the differences between cancers in adults and children?
 Osteosarcoma What are the differences between cancers in adults and children? The types of cancers that develop in children and teens are often different from the types that develop in adults. Childhood
Osteosarcoma What are the differences between cancers in adults and children? The types of cancers that develop in children and teens are often different from the types that develop in adults. Childhood
YOUR LUNG CANCER PATHOLOGY REPORT
 UNDERSTANDING YOUR LUNG CANCER PATHOLOGY REPORT 1-800-298-2436 LungCancerAlliance.org A GUIDE FOR THE PATIENT 1 CONTENTS What is a Pathology Report?...3 The Basics...4 Sections of a Pathology Report...7
UNDERSTANDING YOUR LUNG CANCER PATHOLOGY REPORT 1-800-298-2436 LungCancerAlliance.org A GUIDE FOR THE PATIENT 1 CONTENTS What is a Pathology Report?...3 The Basics...4 Sections of a Pathology Report...7
How To Treat A Uterine Sarcoma
 EVERYONE S GUIDE FOR CANCER THERAPY Malin Dollinger, MD, Ernest H. Rosenbaum, MD, Margaret Tempero, MD, and Sean Mulvihill, MD 4 th Edition 2001 Uterus: Uterine Sarcomas Jeffrey L. Stern, MD Uterine sarcomas
EVERYONE S GUIDE FOR CANCER THERAPY Malin Dollinger, MD, Ernest H. Rosenbaum, MD, Margaret Tempero, MD, and Sean Mulvihill, MD 4 th Edition 2001 Uterus: Uterine Sarcomas Jeffrey L. Stern, MD Uterine sarcomas
Pediatric Oncology for Otolaryngologists
 Pediatric Oncology for Otolaryngologists Frederick S. Huang, M.D. Division of Hematology/Oncology Department of Pediatrics The University of Texas Medical Branch Grand Rounds Presentation to Department
Pediatric Oncology for Otolaryngologists Frederick S. Huang, M.D. Division of Hematology/Oncology Department of Pediatrics The University of Texas Medical Branch Grand Rounds Presentation to Department
1400 Telegraph Bloomfield Hills, MI 48302 248-334-6877-Phone number/248-334-6877-fax Number CANCER TREATMENT
 1400 Telegraph Bloomfield Hills, MI 48302 248-334-6877-Phone number/248-334-6877-fax Number CANCER TREATMENT Learning that your pet has a diagnosis of cancer can be overwhelming. We realize that your pet
1400 Telegraph Bloomfield Hills, MI 48302 248-334-6877-Phone number/248-334-6877-fax Number CANCER TREATMENT Learning that your pet has a diagnosis of cancer can be overwhelming. We realize that your pet
Non-Small Cell Lung Cancer Treatment Comparison to NCCN Guidelines
 Non-Small Cell Lung Cancer Treatment Comparison to NCCN Guidelines April 2008 (presented at 6/12/08 cancer committee meeting) By Shelly Smits, RHIT, CCS, CTR Conclusions by Dr. Ian Thompson, MD Dr. James
Non-Small Cell Lung Cancer Treatment Comparison to NCCN Guidelines April 2008 (presented at 6/12/08 cancer committee meeting) By Shelly Smits, RHIT, CCS, CTR Conclusions by Dr. Ian Thompson, MD Dr. James
THYROID CANCER. I. Introduction
 THYROID CANCER I. Introduction There are over 11,000 new cases of thyroid cancer each year in the US. Females are more likely to have thyroid cancer than men by a ratio of 3:1, and it is more common in
THYROID CANCER I. Introduction There are over 11,000 new cases of thyroid cancer each year in the US. Females are more likely to have thyroid cancer than men by a ratio of 3:1, and it is more common in
Pathologic Assessment Of The Breast And Axilla After Preoperative Therapy
 Pathologic Assessment Of The Breast And Axilla After Preoperative Therapy W. Fraser Symmans, M.D. Associate Professor of Pathology UT M.D. Anderson Cancer Center Pathologic Complete Response (pcr) Proof
Pathologic Assessment Of The Breast And Axilla After Preoperative Therapy W. Fraser Symmans, M.D. Associate Professor of Pathology UT M.D. Anderson Cancer Center Pathologic Complete Response (pcr) Proof
Bone forming and Cartilage forming tumours. Pancras C.W. Hogendoorn Department of Pathology Leiden University Medical Center The Netherlands
 Bone forming and Cartilage forming tumours Pancras C.W. Hogendoorn Department of Pathology Leiden University Medical Center The Netherlands Surgeon Surgeon Lesion Lesion Pathologist Radiologist Pathologist
Bone forming and Cartilage forming tumours Pancras C.W. Hogendoorn Department of Pathology Leiden University Medical Center The Netherlands Surgeon Surgeon Lesion Lesion Pathologist Radiologist Pathologist
Staging Head and Neck Cancers Transitioning to the Seventh Edition of The AJCC Cancer Staging Manual
 Staging Head and Neck Cancers Transitioning to the Seventh Edition of The AJCC Cancer Staging Manual Jatin P. Shah, MD, PhD (Hon) Memorial Sloan-Kettering Cancer Center New York, New York The American
Staging Head and Neck Cancers Transitioning to the Seventh Edition of The AJCC Cancer Staging Manual Jatin P. Shah, MD, PhD (Hon) Memorial Sloan-Kettering Cancer Center New York, New York The American
Protocol for the Examination of Specimens From Patients With Invasive Carcinoma of Renal Tubular Origin
 Protocol for the Examination of Specimens From Patients With Invasive Carcinoma of Renal Tubular Origin Wilms tumors and tumors of urothelial origin are not included. Based on AJCC/UICC TNM, 7th edition
Protocol for the Examination of Specimens From Patients With Invasive Carcinoma of Renal Tubular Origin Wilms tumors and tumors of urothelial origin are not included. Based on AJCC/UICC TNM, 7th edition
INTERNATIONAL ASSOCIATION FOR THE STUDY OF LUNG CANCER Prospective Mesothelioma Staging Project
 INTERNATIONAL ASSOCIATION FOR THE STUDY OF LUNG CANCER Prospective Mesothelioma Staging Project Data Forms and Fields in CRAB Electronic Data Capture System - Reduced Set - Pivotal data elements for developing
INTERNATIONAL ASSOCIATION FOR THE STUDY OF LUNG CANCER Prospective Mesothelioma Staging Project Data Forms and Fields in CRAB Electronic Data Capture System - Reduced Set - Pivotal data elements for developing
Aggressive lymphomas. Michael Crump Princess Margaret Hospital
 Aggressive lymphomas Michael Crump Princess Margaret Hospital What are the aggressive lymphomas? Diffuse large B cell Mediastinal large B cell Anaplastic large cell Burkitt lymphoma (transformed lymphoma:
Aggressive lymphomas Michael Crump Princess Margaret Hospital What are the aggressive lymphomas? Diffuse large B cell Mediastinal large B cell Anaplastic large cell Burkitt lymphoma (transformed lymphoma:
A912: Kidney, Renal cell carcinoma
 A912: Kidney, Renal cell carcinoma General facts of kidney cancer Renal cell carcinoma, a form of kidney cancer that involves cancerous changes in the cells of the renal tubule, is the most common type
A912: Kidney, Renal cell carcinoma General facts of kidney cancer Renal cell carcinoma, a form of kidney cancer that involves cancerous changes in the cells of the renal tubule, is the most common type
Lesions, and Masses, and Tumors Oh My!!
 Lesions, and Masses, and Tumors Oh My!! Presented by: Susan Ward, CPC, CPC-H, CPC-I, CPCD, CEMC, CPRC 1 1 CPT GUIDELINES Agenda CPT DEFINITIONS OP REPORT CASES 2 Definitions Cyst - a closed sac having
Lesions, and Masses, and Tumors Oh My!! Presented by: Susan Ward, CPC, CPC-H, CPC-I, CPCD, CEMC, CPRC 1 1 CPT GUIDELINES Agenda CPT DEFINITIONS OP REPORT CASES 2 Definitions Cyst - a closed sac having
Ewing Family of Tumors
 Ewing Family of Tumors What is the Ewing family of tumors? Cancer starts when cells in the body begin to grow out of control. Cells in nearly any part of the body can become cancer, and can spread to other
Ewing Family of Tumors What is the Ewing family of tumors? Cancer starts when cells in the body begin to grow out of control. Cells in nearly any part of the body can become cancer, and can spread to other
Seattle. Case Presentations. Case 1. 76 year old female with a history of breast cancer 12 years ago. Now presents with a pleural effusion.
 Seattle Montreal IAP September 2006 Case Presentations Allen M. Gown, M.D. Medical Director and Chief Pathologist PhenoPath Laboratories Clinical Professor of Pathology University of British Columbia Case
Seattle Montreal IAP September 2006 Case Presentations Allen M. Gown, M.D. Medical Director and Chief Pathologist PhenoPath Laboratories Clinical Professor of Pathology University of British Columbia Case
DESMOPLASTIC SMALL ROUND CELL TUMOR: A RARE PATHOLOGY PUZZLE
 DESMOPLASTIC SMALL ROUND CELL TUMOR: A RARE PATHOLOGY PUZZLE Ryan Granger University of Rhode Island Cytotechnology program May 2, 2015 ASCT Annual Meeting Nashville, Tennessee DESMOPLASTIC SMALL ROUND
DESMOPLASTIC SMALL ROUND CELL TUMOR: A RARE PATHOLOGY PUZZLE Ryan Granger University of Rhode Island Cytotechnology program May 2, 2015 ASCT Annual Meeting Nashville, Tennessee DESMOPLASTIC SMALL ROUND
Protocol for the Examination of Specimens From Patients With Ductal Carcinoma In Situ (DCIS) of the Breast
 Protocol for the Examination of Specimens From Patients With Ductal Carcinoma In Situ (DCIS) of the Breast Protocol applies to DCIS without invasive carcinoma or microinvasion. Based on AJCC/UICC TNM,
Protocol for the Examination of Specimens From Patients With Ductal Carcinoma In Situ (DCIS) of the Breast Protocol applies to DCIS without invasive carcinoma or microinvasion. Based on AJCC/UICC TNM,
.org. Osteochondroma. Solitary Osteochondroma
 Osteochondroma Page ( 1 ) An osteochondroma is a benign (noncancerous) tumor that develops during childhood or adolescence. It is an abnormal growth that forms on the surface of a bone near the growth
Osteochondroma Page ( 1 ) An osteochondroma is a benign (noncancerous) tumor that develops during childhood or adolescence. It is an abnormal growth that forms on the surface of a bone near the growth
A918: Prostate: adenocarcinoma
 A918: Prostate: adenocarcinoma General facts of prostate cancer The prostate is about the size of a walnut. It is just below the bladder and in front of the rectum. The tube that carries urine (the urethra)
A918: Prostate: adenocarcinoma General facts of prostate cancer The prostate is about the size of a walnut. It is just below the bladder and in front of the rectum. The tube that carries urine (the urethra)
Thoracic Mesothelium. Protocol applies to malignant thoracic mesothelioma. Procedures Cytology (No Accompanying Checklist) Incisional Biopsy Resection
 Thoracic Mesothelium Protocol applies to malignant thoracic mesothelioma. Protocol revision date: January 2004 Based on AJCC/UICC TNM, 6 th edition Procedures Cytology (No Accompanying Checklist) Incisional
Thoracic Mesothelium Protocol applies to malignant thoracic mesothelioma. Protocol revision date: January 2004 Based on AJCC/UICC TNM, 6 th edition Procedures Cytology (No Accompanying Checklist) Incisional
Extrapleural Pneumonectomy for Malignant Mesothelioma: Pro. Joon H. Lee 9/17/2012
 Extrapleural Pneumonectomy for Malignant Mesothelioma: Pro Joon H. Lee 9/17/2012 Malignant Pleural Mesothelioma (Epidemiology) Incidence: 7/mil (Japan) to 40/mil (Australia) Attributed secondary to asbestos
Extrapleural Pneumonectomy for Malignant Mesothelioma: Pro Joon H. Lee 9/17/2012 Malignant Pleural Mesothelioma (Epidemiology) Incidence: 7/mil (Japan) to 40/mil (Australia) Attributed secondary to asbestos
The TV Series. www.healthybodyhealthymind.com INFORMATION TELEVISION NETWORK
 The TV Series www.healthybodyhealthymind.com Produced By: INFORMATION TELEVISION NETWORK ONE PARK PLACE 621 NW 53RD ST BOCA RATON, FL 33428 1-800-INFO-ITV www.itvisus.com 2005 Information Television Network.
The TV Series www.healthybodyhealthymind.com Produced By: INFORMATION TELEVISION NETWORK ONE PARK PLACE 621 NW 53RD ST BOCA RATON, FL 33428 1-800-INFO-ITV www.itvisus.com 2005 Information Television Network.
Medullary Renal Cell Carcinoma Case Report
 Bahrain Medical Bulletin, Vol. 27, No. 4, December 2005 Medullary Renal Cell Carcinoma Case Report Mohammed Abdulla Al-Tantawi MBBCH, CABS* Abdul Amir Issa MBBCH, CABS*** Mohammed Abdulla MBBCH, CABS**
Bahrain Medical Bulletin, Vol. 27, No. 4, December 2005 Medullary Renal Cell Carcinoma Case Report Mohammed Abdulla Al-Tantawi MBBCH, CABS* Abdul Amir Issa MBBCH, CABS*** Mohammed Abdulla MBBCH, CABS**
MALIGNANT MESOTHELIOMA UPDATE ON PATHOLOGY AND IMMUNOHISTOCHEMISTRY
 MALIGNANT MESOTHELIOMA CLASSIFICATION MALIGNANT MESOTHELIOMA UPDATE ON PATHOLOGY AND IMMUNOHISTOCHEMISTRY Sisko Anttila, MD, PhD Jorvi Hospital Laboratory of Pathology Helsinki University Hospital Espoo,
MALIGNANT MESOTHELIOMA CLASSIFICATION MALIGNANT MESOTHELIOMA UPDATE ON PATHOLOGY AND IMMUNOHISTOCHEMISTRY Sisko Anttila, MD, PhD Jorvi Hospital Laboratory of Pathology Helsinki University Hospital Espoo,
Diagnosis of Mesothelioma Pitfalls and Practical Information
 Diagnosis of Mesothelioma Pitfalls and Practical Information Mary Beth Beasley, M.D. Mt Sinai Medical Ctr Dept of Pathology One Gustave L Levy Place New York, NY 10029 (212) 241-5307 mbbeasleymd@yahoo.com
Diagnosis of Mesothelioma Pitfalls and Practical Information Mary Beth Beasley, M.D. Mt Sinai Medical Ctr Dept of Pathology One Gustave L Levy Place New York, NY 10029 (212) 241-5307 mbbeasleymd@yahoo.com
MALIGNANT MESOTHELIOMA UPDATE ON PATHOLOGY AND IMMUNOHISTOCHEMISTRY
 MALIGNANT MESOTHELIOMA UPDATE ON PATHOLOGY AND IMMUNOHISTOCHEMISTRY Sisko Anttila, MD, PhD Jorvi Hospital Laboratory of Pathology Helsinki University Hospital Espoo, Finland 2nd Nordic Conference on Applied
MALIGNANT MESOTHELIOMA UPDATE ON PATHOLOGY AND IMMUNOHISTOCHEMISTRY Sisko Anttila, MD, PhD Jorvi Hospital Laboratory of Pathology Helsinki University Hospital Espoo, Finland 2nd Nordic Conference on Applied
General Information About Non-Small Cell Lung Cancer
 General Information About Non-Small Cell Lung Cancer Non-small cell lung cancer is a disease in which malignant (cancer) cells form in the tissues of the lung. The lungs are a pair of cone-shaped breathing
General Information About Non-Small Cell Lung Cancer Non-small cell lung cancer is a disease in which malignant (cancer) cells form in the tissues of the lung. The lungs are a pair of cone-shaped breathing
A practical guide to understanding cancer
 A practical guide to understanding cancer Contents Contents About this booklet 4 What is cancer? 5 The lymphatic system 7 Soft tissue sarcomas 8 Types of soft tissue sarcoma 10 Risk factors and causes
A practical guide to understanding cancer Contents Contents About this booklet 4 What is cancer? 5 The lymphatic system 7 Soft tissue sarcomas 8 Types of soft tissue sarcoma 10 Risk factors and causes
PROTOCOL OF THE RITA DATA QUALITY STUDY
 PROTOCOL OF THE RITA DATA QUALITY STUDY INTRODUCTION The RITA project is aimed at estimating the burden of rare malignant tumours in Italy using the population based cancer registries (CRs) data. One of
PROTOCOL OF THE RITA DATA QUALITY STUDY INTRODUCTION The RITA project is aimed at estimating the burden of rare malignant tumours in Italy using the population based cancer registries (CRs) data. One of
PATHOLOGY OF THE PLEURA: Mesothelioma and mimickers Necessity of Immunohistochemistry. M. Praet
 PATHOLOGY OF THE PLEURA: Mesothelioma and mimickers Necessity of Immunohistochemistry M. Praet Pathology of the Pleura Normal serosa: visceral and parietal layers Inflammation Neoplasia: Primary: mesothelioma
PATHOLOGY OF THE PLEURA: Mesothelioma and mimickers Necessity of Immunohistochemistry M. Praet Pathology of the Pleura Normal serosa: visceral and parietal layers Inflammation Neoplasia: Primary: mesothelioma
Nicole Kounalakis, MD
 Breast Disease: Diagnosis and Management Nicole Kounalakis, MD Assistant Professor of Surgery Goal of Breast Evaluation The goal of breast evaluation is to classify findings as: normal physiologic variations
Breast Disease: Diagnosis and Management Nicole Kounalakis, MD Assistant Professor of Surgery Goal of Breast Evaluation The goal of breast evaluation is to classify findings as: normal physiologic variations
Lung Cancer: Diagnosis, Staging and Treatment
 PATIENT EDUCATION patienteducation.osumc.edu Lung Cancer: Diagnosis, Staging and Treatment Cancer begins in our cells. Cells are the building blocks of our tissues. Tissues make up the organs of the body.
PATIENT EDUCATION patienteducation.osumc.edu Lung Cancer: Diagnosis, Staging and Treatment Cancer begins in our cells. Cells are the building blocks of our tissues. Tissues make up the organs of the body.
The National Clinical Lung Cancer Audit (LUCADA)
 The National Clinical Lung Cancer Audit (LUCADA) DATA MANUAL Title: Version: 3.1.5 Date: September 2013 LUCADA Lung Cancer Audit VERSION HISTORY Version Date Issued Brief Summary of Change Owner s Name
The National Clinical Lung Cancer Audit (LUCADA) DATA MANUAL Title: Version: 3.1.5 Date: September 2013 LUCADA Lung Cancer Audit VERSION HISTORY Version Date Issued Brief Summary of Change Owner s Name
The Ontario Cancer Registry moves to the 21 st Century
 The Ontario Cancer Registry moves to the 21 st Century Rebuilding the OCR Public Health Ontario Grand Rounds Oct. 14, 2014 Diane Nishri, MSc Mary Jane King, MPH, CTR Outline 1. What is the Ontario Cancer
The Ontario Cancer Registry moves to the 21 st Century Rebuilding the OCR Public Health Ontario Grand Rounds Oct. 14, 2014 Diane Nishri, MSc Mary Jane King, MPH, CTR Outline 1. What is the Ontario Cancer
LYMPHOMA IN DOGS. Diagnosis/Initial evaluation. Treatment and Prognosis
 LYMPHOMA IN DOGS Lymphoma is a relatively common cancer in dogs. It is a cancer of lymphocytes (a type of white blood cell) and lymphoid tissues. Lymphoid tissue is normally present in many places in the
LYMPHOMA IN DOGS Lymphoma is a relatively common cancer in dogs. It is a cancer of lymphocytes (a type of white blood cell) and lymphoid tissues. Lymphoid tissue is normally present in many places in the
The treatment and outcome of patients with soft tissue sarcomas and synchronous metastases
 Sarcoma (2002) 6, 69 73 ORIGINAL ARTICLE The treatment and outcome of patients with soft tissue sarcomas and synchronous metastases JOHN M. KANE III, J. WILLIAM FINLEY, DEBORAH DRISCOLL, WILLIAM G. KRAYBILL
Sarcoma (2002) 6, 69 73 ORIGINAL ARTICLE The treatment and outcome of patients with soft tissue sarcomas and synchronous metastases JOHN M. KANE III, J. WILLIAM FINLEY, DEBORAH DRISCOLL, WILLIAM G. KRAYBILL
RESEARCH EDUCATE ADVOCATE. Just Diagnosed with Melanoma Now What?
 RESEARCH EDUCATE ADVOCATE Just Diagnosed with Melanoma Now What? INTRODUCTION If you are reading this, you have undergone a biopsy (either of a skin lesion or a lymph node) or have had other tests in which
RESEARCH EDUCATE ADVOCATE Just Diagnosed with Melanoma Now What? INTRODUCTION If you are reading this, you have undergone a biopsy (either of a skin lesion or a lymph node) or have had other tests in which
HOVON Staging and Response Criteria for Non-Hodgkin s Lymphomas Page 1
 HOVON Staging and Response Criteria for Non-Hodgkin s Lymphomas Page 1 This document describes the minimally required staging and evaluation procedures and response criteria that will be applied in all
HOVON Staging and Response Criteria for Non-Hodgkin s Lymphomas Page 1 This document describes the minimally required staging and evaluation procedures and response criteria that will be applied in all
A Practical Guide to Advances in Staging and Treatment of NSCLC
 A Practical Guide to Advances in Staging and Treatment of NSCLC Robert J. Korst, M.D. Director, Thoracic Surgery Medical Director, The Blumenthal Cancer Center The Valley Hospital Objectives Revised staging
A Practical Guide to Advances in Staging and Treatment of NSCLC Robert J. Korst, M.D. Director, Thoracic Surgery Medical Director, The Blumenthal Cancer Center The Valley Hospital Objectives Revised staging
Analysis of Prostate Cancer at Easter Connecticut Health Network Using Cancer Registry Data
 The 2014 Cancer Program Annual Public Reporting of Outcomes/Annual Site Analysis Statistical Data from 2013 More than 70 percent of all newly diagnosed cancer patients are treated in the more than 1,500
The 2014 Cancer Program Annual Public Reporting of Outcomes/Annual Site Analysis Statistical Data from 2013 More than 70 percent of all newly diagnosed cancer patients are treated in the more than 1,500
RENAL CANCER PATHOLOGY WHAT REALLY MATTERS? STEWART FLEMING UNIVERSITY OF DUNDEE
 RENAL CANCER PATHOLOGY WHAT REALLY MATTERS? STEWART FLEMING UNIVERSITY OF DUNDEE MAJOR PARADIGM SHIFT IN EARLY 1990S IN UNDERSTANDING RENAL CANCER Molecular differential pathology of renal cell tumours
RENAL CANCER PATHOLOGY WHAT REALLY MATTERS? STEWART FLEMING UNIVERSITY OF DUNDEE MAJOR PARADIGM SHIFT IN EARLY 1990S IN UNDERSTANDING RENAL CANCER Molecular differential pathology of renal cell tumours
Breast Cancer. Sometimes cells keep dividing and growing without normal controls, causing an abnormal growth called a tumor.
 Breast Cancer Introduction Cancer of the breast is the most common form of cancer that affects women but is no longer the leading cause of cancer deaths. About 1 out of 8 women are diagnosed with breast
Breast Cancer Introduction Cancer of the breast is the most common form of cancer that affects women but is no longer the leading cause of cancer deaths. About 1 out of 8 women are diagnosed with breast
Protocol for the Examination of Specimens From Patients With Carcinoma of the Esophagus
 Protocol for the Examination of Specimens From Patients With Carcinoma of the Esophagus Protocol applies to all carcinomas of the esophagus, including esophagogastric junction carcinomas. Well-differentiated
Protocol for the Examination of Specimens From Patients With Carcinoma of the Esophagus Protocol applies to all carcinomas of the esophagus, including esophagogastric junction carcinomas. Well-differentiated
Smoking and misuse of certain pain medicines can affect the risk of developing renal cell cancer.
 Renal cell cancer Renal cell cancer is a disease in which malignant (cancer) cells form in tubules of the kidney. Renal cell cancer (also called kidney cancer or renal adenocarcinoma) is a disease in which
Renal cell cancer Renal cell cancer is a disease in which malignant (cancer) cells form in tubules of the kidney. Renal cell cancer (also called kidney cancer or renal adenocarcinoma) is a disease in which
A PATIENT S GUIDE TO ABLATION THERAPY
 A PATIENT S GUIDE TO ABLATION THERAPY THE DIVISION OF VASCULAR/INTERVENTIONAL RADIOLOGY THE ROBERT WOOD JOHNSON UNIVERSITY HOSPITAL Treatment options for patients with cancer continue to expand, providing
A PATIENT S GUIDE TO ABLATION THERAPY THE DIVISION OF VASCULAR/INTERVENTIONAL RADIOLOGY THE ROBERT WOOD JOHNSON UNIVERSITY HOSPITAL Treatment options for patients with cancer continue to expand, providing
Plueral Malignancy: Radiologic-pathologic
 Plueral Malignancy: Radiologic-pathologic Correlation Ritu R. Gill, MD Pleural Malignancies: Radiologic-Pathologic Correlation Ritu R Gill MD Brigham and Women s Hospital Boston, Massachusetts Pleural
Plueral Malignancy: Radiologic-pathologic Correlation Ritu R. Gill, MD Pleural Malignancies: Radiologic-Pathologic Correlation Ritu R Gill MD Brigham and Women s Hospital Boston, Massachusetts Pleural
Breast Cancer. The Pathology report gives an outline on direction of treatment. It tells multiple stories to help us understand the patient s cancer.
 Breast Cancer What Does the Pathology Report Say Normal Cells The Pathology report gives an outline on direction of treatment. It tells multiple stories to help us understand the patient s cancer. Non-Invasive
Breast Cancer What Does the Pathology Report Say Normal Cells The Pathology report gives an outline on direction of treatment. It tells multiple stories to help us understand the patient s cancer. Non-Invasive
Individual Prediction
 Individual Prediction Michael W. Kattan, Ph.D. Professor of Medicine, Epidemiology and Biostatistics, Cleveland Clinic Lerner College of Medicine of Case Western Reserve University Chairman, Department
Individual Prediction Michael W. Kattan, Ph.D. Professor of Medicine, Epidemiology and Biostatistics, Cleveland Clinic Lerner College of Medicine of Case Western Reserve University Chairman, Department
Breast cancer close to the nipple: Does this carry a higher risk ofaxillary node metastasesupon diagnosis?
 Breast cancer close to the nipple: Does this carry a higher risk ofaxillary node metastasesupon diagnosis? Erin I. Lewis, BUSM 2010 Cheri Nguyen, BUSM 2008 Priscilla Slanetz, M.D., MPH Al Ozonoff, Ph.d.
Breast cancer close to the nipple: Does this carry a higher risk ofaxillary node metastasesupon diagnosis? Erin I. Lewis, BUSM 2010 Cheri Nguyen, BUSM 2008 Priscilla Slanetz, M.D., MPH Al Ozonoff, Ph.d.
TNM Staging of Head and Neck Cancer and Neck Dissection Classification
 QUICK REFERENCE GUIDE TO TNM Staging of Head and Neck Cancer and Neck Dissection Classification Fourth Edition 2014 All materials in this ebook are copyrighted by the American Academy of Otolaryngology
QUICK REFERENCE GUIDE TO TNM Staging of Head and Neck Cancer and Neck Dissection Classification Fourth Edition 2014 All materials in this ebook are copyrighted by the American Academy of Otolaryngology
Corporate Medical Policy Molecular Markers in Fine Needle Aspirates of the Thyroid
 Corporate Medical Policy Molecular Markers in Fine Needle Aspirates of the Thyroid File Name: Origination: Last CAP Review: Next CAP Review: Last Review: molecular_markers_in_fine_needle_aspirates_of_the_thyroid
Corporate Medical Policy Molecular Markers in Fine Needle Aspirates of the Thyroid File Name: Origination: Last CAP Review: Next CAP Review: Last Review: molecular_markers_in_fine_needle_aspirates_of_the_thyroid
FRIEND TO FRIEND CPT CODES 2015 2016. Diagnostic digital breast tomosynthesis, unilateral (list separately in addition to code for primary procedure)
 FRIEND TO FRIEND CPT CODES 2015 2016 CPT CODE SERVICE DESCRIPTION FEE EFFECTIVE G0101 Screening pelvic examination $36.69 01 Jan 16 G0202 Mammography, screening, digital, bilateral (2 view film study of
FRIEND TO FRIEND CPT CODES 2015 2016 CPT CODE SERVICE DESCRIPTION FEE EFFECTIVE G0101 Screening pelvic examination $36.69 01 Jan 16 G0202 Mammography, screening, digital, bilateral (2 view film study of
Oncology Quarterly. Corky and Kaylee Smith
 Oncology Quarterly Volume 2 Winter 2007 Corky and Kaylee Smith For Richard and Monica Smith, it started simply as a small area of hair loss on their eight yearold Shetland Sheepdog, Corky s, left tarsus.
Oncology Quarterly Volume 2 Winter 2007 Corky and Kaylee Smith For Richard and Monica Smith, it started simply as a small area of hair loss on their eight yearold Shetland Sheepdog, Corky s, left tarsus.
Surgical Staging of Endometrial Cancer
 Surgical Staging of Endometrial Cancer I. Endometrial Cancer Surgical Staging Overview Uterine cancer types: carcinomas type I and type II, sarcomas, carcinosarcomas Hysterectomy with BSO Surgical Staging
Surgical Staging of Endometrial Cancer I. Endometrial Cancer Surgical Staging Overview Uterine cancer types: carcinomas type I and type II, sarcomas, carcinosarcomas Hysterectomy with BSO Surgical Staging
Frozen Section Diagnosis
 Frozen Section Diagnosis Dr Catherine M Corbishley Honorary Consultant Histopathologist St George s Healthcare NHS Trust and lead examiner final FRCPath Practical 2008-2011 Frozen Section Diagnosis The
Frozen Section Diagnosis Dr Catherine M Corbishley Honorary Consultant Histopathologist St George s Healthcare NHS Trust and lead examiner final FRCPath Practical 2008-2011 Frozen Section Diagnosis The
Early Prostate Cancer: Questions and Answers. Key Points
 CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Early Prostate Cancer:
CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Early Prostate Cancer:
