Guidelines for the management of eczema in children under 12 years
|
|
|
- Alan Jefferson
- 7 years ago
- Views:
Transcription
1 Contents: select ctrl and click to follow page links Page Definition, Assess and Treatment recommendations 2 Treatment of trunk and limbs 3 Treatment of face and neck 4 Topical calcineurin inhibitors (TCI) Algorithm 5 Topical infections formulary 6 Appendix 1: Safe use of topical corticosteroids and Finger Tip Unit (FTU) Guide 7 Appendix 2: Recommended Corticosteroid Products 8 Appendix 3: Further supporting clinical information 9 References 10 1
2 Definition: Assessment Eczema (atopic eczema/dermatitis) is the commonest inflammatory condition of the skin, characterised by itching, diffuse redness and dry skin, as well as sometimes oozing, crusting, scaling, skin thickening and changes in skin pigmentation (not all of these symptoms will necessarily occur together). Images can be viewed on the Primary Care Dermatology Society website. Diagnose and assess the physical severity of eczema. Remember to consider the impact on quality of life and psychological wellbeing of the child and family when choosing treatment options (the CDLQI children s DLQI) can be used if necessary. The following descriptors can be used as a guide 1 : Physical severity of disease CLEAR - Normal skin, no evidence of active atopic eczema MILD - Areas of dry skin, infrequent itching (with or without small areas of redness) MODERATE - Areas of dry skin, frequent itching, redness (with or without excoriation and localised skin thickening) SEVERE - Widespread areas of dry skin, incessant itching, redness (with or without excoriation, extensive skin thickening, bleeding, oozing, cracking and alteration of pigmentation) NONE no impact Impact on quality of life and psychological well-being MILD little impact on everyday activities, sleep and psychosocial wellbeing MODERATE moderate impact on everyday activities and psychosocial wellbeing, frequently disturbed sleep SEVERE severe limitation on everyday activities and psychosocial functioning, nightly loss of sleep Treatment recommendations 1, 2,3 Treat according to the recommendations in the flow charts and/or formulary that follow. Hyperlinks to the eczema NICE pathway are provided in the flowcharts. Remember that patient education on preventative measures and on how to use treatments effectively is crucial in the management of eczema (see appendices 1 and 2 for supporting information and links to external websites). Provide an information leaflet (click on hyperlink or access via EMISweb) and signpost to patient support groups (see appendix 2) as useful resources to reinforce key messages. Various factors may play an important role as triggers of eczema. NICE recommends identifying and managing suspected triggers 3. Patients are advised to avoid suspected/identified triggers, such as: o irritants (soaps/detergents, wool or synthetic clothing, chemical products, perspiration) use emollients as a soap substitute o contact allergens o food/dietary factors: suspect in those who have reacted previously to a food with immediate symptoms, or in infants and young children with moderate or severe atopic eczema not optimally managed particularly when associated with gut dysmotility or failure to thrive. See separate NICE recommendations and Cow s Milk Protein Allergy guidelines o inhalant allergens particularly in those with seasonal flares, asthma, allergic rhinitis, atopic eczema on the face over the age of 3; o climate and environmental factors (e.g. extremes of temperature/humidity, air pollution, tobacco smoke, sun-/ultraviolet- light); o microbial colonisation/infection; concurrent illness and disruption to family life. 2
3 Treatment of TRUNK and LIMBS Emollients Use regularly even when skin is clear. Use as soap substitute also. Offer a range of emollients. Most effective emollient is the one the patient will use please refer to Emollient prescribing guidelines for further detail including choices. Educate patient on regular use of emollients to prevent flares. Patient presents with mild disease Check for infection Treatment Options: (1) Mild potency steroid - Hydrocortisone 1% cream or ointment applied once daily (2) Moderate potency steroid - Clobetasone butyrate 0.05% ointment /cream applied once daily Reinforce key messages on safe use of topical corticosteroids Refer to specialist Phototherapy Systemic therapy Consider twice weekly use of mild to moderate potency steroid to previously affected skin to prevent flares Step down to twice weekly application to normal skin to prevent flares Patient presents with moderate disease Check for infection Treatment Options: (1) Moderate potency steroid - Clobetasone butyrate 0.05% cream or ointment once daily or if needed: (2) Potent steroid Betamethasone valerate 0.1% cream/ointment once daily or (3) Potent steroid - Mometasone Furoate 0.1% cream or ointment once daily Avoid potent steroids in children <12 months NB: Only use for 7-14 days on vulnerable sites e.g. axillae/groin Review & reinforce key messages on safe use of topical corticosteroids Topical calcineurin inhibitors(tci) Pimecrolimus 1% cream or Tacrolimus ointment 0.03%. Apply twice daily (see TCI algorithm (9) ) Bandages and dressings wet wrap technique Consider twice weekly use of moderate potency steroid to previously affected skin to prevent flares See TCI algorithm Unable to reduce daily topical steroids See TCI algorithm Consider referral using checklist Patient presents with severe disease Check for infection Treatment Options: (1) Potent steroid - Betamethasone valerate 0.1% cream/ointment once daily NB: Only use for 7-14 days on vulnerable sites e.g. axillae/groin (2) Potent steroid - Mometasone Furoate 0.1% cream or ointment applied once daily Avoid use of potent steroids in children <12 months old Review after 7-14 days and reinforce key messages on safe use of topical corticosteroids Check triggers Ensure infection is treated Always educate patient on use of product Refer to most recent BNF / BNFc or the Summary of Product Characteristics for up-to-date prescribing information 3
4 Treatment of FACE and NECK Emollients Use regularly even when skin is clear. Use as soap substitute also. Offer a range of emollients from formulary. Most effective emollient is the one the patient will use please refer to Emollient prescribing guidelines for further detail including choices. Educate patient on regular use of emollients to prevent flares. Consider twice weekly use of mild potency steroid to normal skin to prevent flares Patient presents with mild disease Treatment Options: Mild potency steroid - Hydrocortisone 1% ointment applied once daily Reinforce key messages on safe use of topical corticosteroids. Consider TCIs if needing ongoing mild corticosteroids In older children consider twice weekly use of mild -moderate potency steroid to normal skin to prevent flares; review within 3months, consider need for TCIs Patient presents with moderate or severe disease Treatment Options: Moderate potency steroid - Clobetasone butyrate 0.05% ointment applied once daily Review after 5 days; Reinforce key messages on safe use of topical corticosteroids Refer to specialist Potent corticosteroids Systemic therapy Phototherapy Step down to twice weekly application Topical calcineurin inhibitors (TCIs) (9) Pimecrolimus cream 1% (Licence: for mild to moderate eczema from 2 years of age) or Tacrolimus 0.03% ointment (Licence: moderate- severe eczema, 2-16 years Apply twice daily Encourage use of sunscreens Consider use in those requiring long-term or frequent use of mild or moderate topical corticosteroid or whose eczema is not well controlled by corticosteroids (>4 flares/year) (see TCI algorithm (9) ) Consider referral using checklist Always educate patient on use of product Refer to most recent BNF / BNFc or the Summary of Product Characteristics for up-todate prescribing information 4
5 TCI Algorithm The place of topical calcineurin inhibitors in the management of atopic eczema in children and young people Diagnosis of mild-moderate atopic dermatitis Consider 2 nd line treatment with Pimecrolimus cream 1% in those requiring long-term or frequent use of a mild or moderate topical corticosteroid especially at vulnerable sites Diagnosis of moderate severe eczema Emollients plus appropriate potency corticosteroids Steroid related concerns: concerns about atrophy, lesions on eyelids/ ocular side effects, other side effects Topical steroid failure in absence of infection: No or inadequate response after 5 days of moderate potency steroids (face) or after 14 days of potent steroids (trunk, limbs, body flexures) Review and treat active infection. Exclude cold sores nearby Patient advice and counselling on rationale and risk: benefit of treatment with TCIs Consider Topical calcineurin inhibitors (TCIs) (9) Pimecrolimus cream 1% (Licence: for mild to moderate eczema from 2 years of age) or Tacrolimus 0.03% ointment (Licence: moderate- severe eczema, 2-16 years or 0.1% Licence: >16 years) Apply minutes before or after emollients; may cause tingling after application. Do NOT use under occlusive dressings. Advise use of sunscreens. TCIs should be initiated (2 nd line) by practitioners experienced/confident in using them, following the use of moderate topical corticosteroids. Refer to specialist for further advice/management. Refer to secondary care if: Diagnostic concerns GP not confident to prescribe TCIs Inadequate response Recalcitrant infection Psychosocial issues Review need for treatment: reduce to once daily after 3 weeks in children. If no improvement is seen after two weeks, consider other treatment options. Stop therapy after 12 months and review need for ongoing treatment Flares: ; Initiate twice-daily Topical calcineurin inhibitors therapy for up to three weeks (children); this may cause tingling initially. Add appropriate strength topical corticosteroids once daily if needed Maintenance: (>4 flares per year): initiate twice-weekly therapy (Leave 2-3 days between applications eg Monday and Thursdays) Treat flare using twice-daily therapy. Add appropriate strength topical corticosteroids once daily if needed Once lesions have cleared, return to maintenance regime. 5
6 TOPICAL INFECTIONS FORMULARY INFECTION TYPE TREATMENT DURATION Flexures: Hydrocortisone 1% and Fusidic acid (Fucidin H ) cream (mild potency steroid) Trunk / limbs: Betamethasone valerate 0.1% and Fusidic acid (Fucibet ) cream (potent steroid) Maximum of 2 Topical/localised infections Face / neck: weeks Hydrocortisone 1% and Fusidic acid (Fucidin H ) cream or ointment (mild potency steroid) Timodine cream (mild potency steroid) For severe infection unresponsive to topical and oral treatment seek specialist advice. Systemic treatment of Staphylococcus aureus and streptococcal infections Adjunct therapy (at appropriate dilutions) to decrease bacterial load in cases of recurrent infected atopic eczema swab nose and axillae for culture (swab family members also if positive for Staphylococcus aureus and recurrent despite treatment) Consider referral to specialist if recurrent infection despite optimising topical therapy 1 st LINE TREATMENT PENICILLIN ALLERGY / RESISTANCE Flucloxacillin (oral) (usually for 7 days) refer to latest BNFc / BNF for dose and available formulations 1 st line - Clarithromycin twice daily(oral) for 7 days 2 nd line Erythromycin four times daily (oral) for 7 days refer to latest BNFc / BNF for dose and available formulations Dermol cream Eczmol cream (lotion) Dermol 500 lotion Dermol 600 bath emollient with antimicrobial Treat nasal carriage with Naseptin four times daily application to each nostril for 7 days (contains peanut oil) OR Mupirocin nasal ointment twice daily in each nostril for 7 days Refer to latest BNFc/ BNF for treatment duration Avoid long-term use Herpes Infection: If a child with atopic eczema has a lesion on the skin suspected to be herpes simplex virus, an emergency referral to a dermatologist or paediatrician for same-day/next-day review should be arranged by telephone where there is clinical suspicion of eczema herpeticum 5. Signs of eczema herpeticum: areas of rapidly worsening, painful eczema clustered blisters consistent with early-stage cold sores punched-out erosions (circular, depressed, ulcerated lesions) usually 1 3 mm that are uniform in appearance (these may coalesce to form larger areas of erosion with crusting) possible fever, lethargy or distress 6
7 APPENDIX 1 Safe use of topical corticosteroids and Finger Tip Unit (FTU) Guide Continuous use of topical corticosteroids may result in permanent skin damage and other adverse effects, causing: irreversible skin atrophy and striae psoriasis to become unstable systemic side effects when applied continuously to extensive psoriasis (for example more than 10% of body surface area affected). It is important that patients and their families / carers are educated on the risks of overuse of topical corticosteroids and discuss how to avoid them: Very potent topical corticosteroids should not be used continuously at any site for longer than 4 weeks Potent topical corticosteroids should not be used continuously at any site for longer than 8 weeks Do not use very potent corticosteroids in children and young people A break of at least 4 weeks should be observed between courses of topical corticosteroid Offer an annual review to assess for adverse effects in (1) children using any topical corticosteroids on a regular basis and (2) for adults using potent or very potent topical corticosteroids either as short courses or intermittent use. Topical corticosteroids should always be used for the least amount of time necessary to control symptoms, and should be applied thinly, avoiding normal skin. The quantity to be applied is specified by the amount of cream/ointment squeezed out of the tube nozzle in a line from the tip of an adult finger to the crease of the first joint (~2.5cm); equivalent to 0.5g of cream/ointment. As a guide, one Finger Tip Unit is enough to cover the palms of both hands. Various areas of the skin may be affected differently ensure that potency of treatment is tailored according to the severity of each affected part 1, 6. Number of fingertip dosage units recommended for a single application are listed below (this guide indicates how much is required to cover the entire area specified. Smaller areas will need correspondingly lower amounts of cream/ointment). [NB the patient.co.uk patient information leaflet repeats this information] Age Face & neck Arm & hand Leg & foot Trunk (front) Trunk (back) including buttocks 3-6 mths yrs yrs yrs Adults Remember: Always educate patient about the use of products Table to show number of adult finger tip units (FTU) per body parts for children Diagram to show an adult finger tip and adults unit (FTU) = 0.5g Corticosteroid formulations Always apply thinly in accordance with finger tip unit guide Apply once daily Topical corticosteroid treatment for flares should be started as soon as signs and symptoms appear Continue for +/- 48 hours after symptoms subside. Always check for and reinforce avoidance of trigger factors (e.g. soap) Ointment preparations are always to be preferred when available, use cream if ointment is unacceptable to the patient They can be applied twice weekly to prevent flares but if they are need daily to prevent flares, consider topical calcineurin inhibitors (see TCI algorithm). Twice weekly use to prevent flares must be monitored and appropriate Prescribing and dispensing: best practice recommendations When prescribing or dispensing topical corticosteroids, the potency of the preparation should be specified on the prescription and the dispensing label. 1,3 This aids both patient and healthcare professional education and also medicines reconciliation processes when patient care is transferred to another setting 7
8 APPENDIX 2: Recommended Corticosteroids Products POTENCY RECOMMENDED PRODUCTS (formulary approved) once daily COST (BNF 65 pricing) COST / gram COMMENTS MILD CORTICOSTEROID Hydrocortisone 1% cream and ointment 30g (Cream) = g (Ointment) = p 8p Avoid prescribing Hydrocortisone 0.1% cream which may be confused with Locoid, see below As recommended by the BNF for children, topical corticosteroids may be prescribed children under 1 year. For mild to moderate eczema, flexural or facial eczema Hydrocortisone 1% is listed as an appropriate topical corticosteroid to use. MODERATE CORTICOSTEROID POTENT CORTICOSTEROID Clobetasone Butyrate 0.05% (Eumovate) cream or ointment 1 st Line Betamethasone valerate 0.1% (Betnovate) Ointment 2 nd Line - Mometasone Furoate 0.1% (Elocon) Ointment 100g = g (Cream) = g (Ointment) = g = g = p 6.2p 6.2p 8p 12p Prescribe Clobetasone in preference to Hydrocortisone 2.5% Cream/Ointment No robust trial evidence for preferring one over the other, therefore prescribe product with the lowest acquisition cost first. Clinical experience suggests some patients prefer mometasone, finding it more effective either in terms of speed of response or reduced frequency of application; therefore consider a trial of it. Mometasone may sting on initial application. It can be used twice weekly, with review within 3-6 months, to prevent flares Avoid prescribing these items if possible Betamethasone RD (0.025%) Hydrocortisone butyrate 0.1% (Locoid ) 100g = g = p 5p NB: This is a steroid of moderate potency NB: This is a potent steroid Fluocinolone 0.025% (Synalar ) 100g = p Prescribe Clobetasone in preference Avoid Hydrocortisone 2.5% cream or ointment 30g (Cream) = g Ointment) = p 156p Educate patient on use of product Refer to most recent BNF / BNFc or the Summary of Product Characteristics for up-to-date prescribing information 8
9 APPENDIX 3 - Further supporting clinical information Emollients - Please refer to the Emollients prescribing guidelines for full information and recommended products Application of more than one topical preparation - When applying more than one topical formulation to the affected part(s) (e.g. emollient and topical corticosteroid), do not mix the preparations this can lead to altered properties of the formulations, which could impact on the efficacy of the preparations. Rather, allow several minutes between applications of different formulations. 1,7 Systemic therapy for urticaria / severe itching: o Sedating antihistamines: Trial for 7 14 days in: Children aged 6 months or over during acute flares, if sleep disturbance has a significant impact on the child or parents or carers. This can be repeated during subsequent flares if successful If longer duration treatment required, ensure topical therapy has been optimised. NB: Do not routinely use oral antihistamines in the management of atopic eczema in children 1 st line: hydroxyzine (no younger than 6 months; see BNFC/BNF for 2 nd Line: chlorphenamine or refer to BNFC/BNF dosing information) o Non-Sedating antihistamines: Trial for 1 month in: children with severe atopic eczema children with mild or moderate atopic eczema where there is severe itching or urticaria/ dermographism children with co-existent allergic rhinitis, asthma or food sensitivity If successful, continue treatment while symptoms persist. Review 3 monthly. NB: Do not routinely use oral antihistamines in the management of atopic eczema in children 1 st line: Loratadine (from age 2 years and above; see BNFC/BNF) 2 nd l ine: Cetirizine (from age 1 year and above; see BNFC/BNF; see Paediatric Formulary) Topical calcineurin inhibitors - only to be used by practitioners experienced/confident in use, following use of moderate topical corticosteroids. Do NOT use under occlusive dressings. Do NOT use if skin is infected. Refer to specialist for further advice/management. Paste bandages or wet wrap garments only to be used in patients with non-infected moderate to severe eczema, where an adequate trial of corticosteroids alone or topical calcineurin inhibitors has not adequately controlled the eczema. Parents will require instruction on how to safely apply and use paste bandages or wet wrap garments. A referral should be considered if these interventions donot then adequately control eczema. Patient Education GSTFT provide an eczema education programme for Lambeth patients. The Southwark Community dermatology service provides a programme for Southwark patients. Specialist nurses support is also available in the specialist Paediatric Dermatology clinics at KCH Web-links for healthcare professionals: NICE eczema pathway Map of Medicine (select patient option when viewing content) Primary Care Dermatology Society (PCDS) British Association of Dermatologists (BAD) Clinical Knowledge Summaries from NICE Web-links for patient information: British Association of Dermatologists (with links to NES and other patient materials) NHS Choices National Eczema Society (NES) 9
10 References 1. National Institute for Health and Clinical Excellence (NICE). CG57 Atopic Eczema in children: quick reference guide Care Pathway for atopic eczema in children, stepped care plan. London: December 2007, p Available online at: (date accessed: 22 Nov 2012). 2. National Institute for Health and Clinical Excellence (NICE). NICE Pathways: Treatments for atopic eczema in children. London: August 2012, p1-14. Available online at: (date accessed: 22 Nov 2012). 3. National Institute for Health and Care Excellence (NICE). NICE Pathways: Assessment of children with atopic eczema. London: August Available online at: (last updated: March 2012, date accessed: 22 Nov 2012) 4. National Eczema Society. Eczema and its management: A guide for Pharmacists Measuring topical steroid application p16. London: Available online at: (free registration required) (Date accessed 4 Dec 2012). 5. The British Association of Dermatologists. British Association of Dermatologists Patient Information Leaflet: Eczema. August 2004 (last updated: April 2009). Available at: (date accessed: 4 Dec 2012) 6. BMJ Group and Royal Pharmaceutical Society. British National Formulary 64. London: March Primary Care Dermatology Society. Atopic eczema clinical guideline. February 2012 (last updated: March 2013). Available at: (date accessed 19 Jun 2013) 8. National Institute for Health and Clinical Excellence (NICE). TA81 Frequency of application of topical corticosteroids for atopic eczema. London: August Available online at: (date accessed: 31 July 2013). 9. C Charman, M J Cork, W I Henderson,B Page, D Paige, T Poyner. The place of Tacrolimus ointment in the management of atopic eczema. Dermatology in Practice 2013 Vol 19 S 3 10
Atopic eczema in children
 Issue date: December 2007 Atopic eczema in children Management of atopic eczema in children from birth up to the age of 12 years NICE clinical guideline 57 Developed by the National Collaborating Centre
Issue date: December 2007 Atopic eczema in children Management of atopic eczema in children from birth up to the age of 12 years NICE clinical guideline 57 Developed by the National Collaborating Centre
Atopic eczema in children: management of atopic eczema in children from birth up to the age of 12 years
 Atopic eczema in children: management of atopic eczema in children from birth up to the age of 12 years NICE guideline Draft for consultation, June 2007 If you wish to comment on this version of the guideline,
Atopic eczema in children: management of atopic eczema in children from birth up to the age of 12 years NICE guideline Draft for consultation, June 2007 If you wish to comment on this version of the guideline,
Prescribing advice for the management and treatment of psoriasis
 Prescribing advice for the management and treatment of psoriasis This guidance contains suggested advice for the management and treatment of patients presenting with psoriasis. This guidance applies to
Prescribing advice for the management and treatment of psoriasis This guidance contains suggested advice for the management and treatment of patients presenting with psoriasis. This guidance applies to
Topical Tacrolimus or Pimecrolimus for the treatment of mild, moderate or severe atopic eczema. Effective Shared Care Agreement
 Topical Tacrolimus or Pimecrolimus for the treatment of mild, moderate or severe atopic eczema. Effective Shared Care Agreement A Copy of this page signed by all three parties should be retained in the
Topical Tacrolimus or Pimecrolimus for the treatment of mild, moderate or severe atopic eczema. Effective Shared Care Agreement A Copy of this page signed by all three parties should be retained in the
TOP TIPS FOR TREATING
 TOP TIPS FOR TREATING Sandra Lawton OBE (Nurse Consultant Dermatology and Queen s Nurse, Nottingham University Hospitals NHS Trust) suggests practical ways to manage eczema. Caring for eczema can present
TOP TIPS FOR TREATING Sandra Lawton OBE (Nurse Consultant Dermatology and Queen s Nurse, Nottingham University Hospitals NHS Trust) suggests practical ways to manage eczema. Caring for eczema can present
Management of atopic eczema in children
 PRESCRIBING IN CHILDREN n Management of atopic eczema in children REBECCA PHILLIPS, HYWEL WILLIAMS and JANE RAVENSCROFT Atopic eczema is a common condition, affecting about a fifth of children in the UK.
PRESCRIBING IN CHILDREN n Management of atopic eczema in children REBECCA PHILLIPS, HYWEL WILLIAMS and JANE RAVENSCROFT Atopic eczema is a common condition, affecting about a fifth of children in the UK.
March 2011. Management of atopic eczema in primary care. A national clinical guideline. Scottish Intercollegiate Guidelines Network
 SIGN Scottish Intercollegiate Guidelines Network Part of NHS Quality Improvement Scotland Help us to improve SIGN guidelines click here to complete our survey 125 Management of atopic eczema in primary
SIGN Scottish Intercollegiate Guidelines Network Part of NHS Quality Improvement Scotland Help us to improve SIGN guidelines click here to complete our survey 125 Management of atopic eczema in primary
Atopic Dermatitis/Eczema
 Atopic Dermatitis/Eczema Symptoms Eczema, also known as atopic eczema or atopic dermatitis, is a skin condition causing inflammation and intense irritation. Eczema symptoms tend to be caused by dry skin.
Atopic Dermatitis/Eczema Symptoms Eczema, also known as atopic eczema or atopic dermatitis, is a skin condition causing inflammation and intense irritation. Eczema symptoms tend to be caused by dry skin.
Caring for children and young people with atopic eczema
 Royal college of nursing Caring for children and young people with atopic eczema Guidance for nurses This publication is supported by the pharmaceutical industry Caring for children and young people with
Royal college of nursing Caring for children and young people with atopic eczema Guidance for nurses This publication is supported by the pharmaceutical industry Caring for children and young people with
PACKAGE LEAFLET: INFORMATION FOR THE USER. Elidel 10 mg/g Cream. pimecrolimus
 PACKAGE LEAFLET: INFORMATION FOR THE USER Elidel 10 mg/g Cream pimecrolimus Read all of this leaflet carefully before you start using Elidel cream Keep this leaflet. You may need to read it again. If you
PACKAGE LEAFLET: INFORMATION FOR THE USER Elidel 10 mg/g Cream pimecrolimus Read all of this leaflet carefully before you start using Elidel cream Keep this leaflet. You may need to read it again. If you
Treatments for allergy are usually straightforward, safe and effective. Common treatments include:
 Allergy Medications The treatments prescribed for allergy control the symptoms and reactions; they do not cure the condition. However, using treatments as prescribed can show a huge change in a patient
Allergy Medications The treatments prescribed for allergy control the symptoms and reactions; they do not cure the condition. However, using treatments as prescribed can show a huge change in a patient
Scottish Medicines Consortium
 Scottish Medicines Consortium betamethasone valerate 2.25mg medicated plaster (Betesil ) No. (622/10) Genus Pharmaceuticals 09 July 2010 The Scottish Medicines Consortium (SMC) has completed its assessment
Scottish Medicines Consortium betamethasone valerate 2.25mg medicated plaster (Betesil ) No. (622/10) Genus Pharmaceuticals 09 July 2010 The Scottish Medicines Consortium (SMC) has completed its assessment
Public Assessment Report. Pharmacy to General Sales List Reclassification. Pirinase Hayfever Relief for Adults 0.05% Nasal Spray.
 Public Assessment Report Pharmacy to General Sales List Reclassification Pirinase Hayfever Relief for Adults 0.05% Nasal Spray (Fluticasone) PL 00079/0688 Glaxo Wellcome UK Limited TABLE OF CONTENTS Introduction
Public Assessment Report Pharmacy to General Sales List Reclassification Pirinase Hayfever Relief for Adults 0.05% Nasal Spray (Fluticasone) PL 00079/0688 Glaxo Wellcome UK Limited TABLE OF CONTENTS Introduction
MEDICATION GUIDE. PROTOPIC [pro-top-ik] (tacrolimus) Ointment 0.03% Ointment 0.1%
![MEDICATION GUIDE. PROTOPIC [pro-top-ik] (tacrolimus) Ointment 0.03% Ointment 0.1% MEDICATION GUIDE. PROTOPIC [pro-top-ik] (tacrolimus) Ointment 0.03% Ointment 0.1%](/thumbs/27/10084771.jpg) MEDICATION GUIDE PROTOPIC [pro-top-ik] (tacrolimus) Ointment 0.03% Ointment 0.1% Read the Medication Guide every time you or a family member gets PROTOPIC Ointment. There may be new information. This Medication
MEDICATION GUIDE PROTOPIC [pro-top-ik] (tacrolimus) Ointment 0.03% Ointment 0.1% Read the Medication Guide every time you or a family member gets PROTOPIC Ointment. There may be new information. This Medication
COMMON BACTERIAL SKIN INFECTIONS IN GENERAL PRACTICE
 COMMON BACTERIAL SKIN INFECTIONS IN GENERAL PRACTICE The two most common bacteria to cause skin infections are staphylococcus aureus (staph aureus ) and streptococcus pyogenes ( strep) (see Table 1). Staphylococcus
COMMON BACTERIAL SKIN INFECTIONS IN GENERAL PRACTICE The two most common bacteria to cause skin infections are staphylococcus aureus (staph aureus ) and streptococcus pyogenes ( strep) (see Table 1). Staphylococcus
TOPICAL THERAPY. ADVANTAGES - increased dose of medication to affected area. - reduced systemic side effects and toxicity
 TOPICAL THERAPY ADVANTAGES - increased dose of medication to affected area. - reduced systemic side effects and toxicity DISADVANTAGES - takes time - may be greasy or messy - may have different preparations
TOPICAL THERAPY ADVANTAGES - increased dose of medication to affected area. - reduced systemic side effects and toxicity DISADVANTAGES - takes time - may be greasy or messy - may have different preparations
Dry skin, eczema, psoriasis and flare-ups
 Dry skin, eczema, psoriasis and flare-ups Let s feel comfortable in our skin FL4368_1000031525 BTS LFGT Specialist Skin A5LFT 12pp V7.indd 1 21/02/2014 09:58 Some of us live with a dry or sore skin condition.
Dry skin, eczema, psoriasis and flare-ups Let s feel comfortable in our skin FL4368_1000031525 BTS LFGT Specialist Skin A5LFT 12pp V7.indd 1 21/02/2014 09:58 Some of us live with a dry or sore skin condition.
Atopic eczema is a relapsing and remitting disease.
 Vol 2 September 2010 Clinical Pharmacist 291 The education of patients and their carers on avoiding trigger factors, using emollients effectively and adopting a stepped management plan is essential for
Vol 2 September 2010 Clinical Pharmacist 291 The education of patients and their carers on avoiding trigger factors, using emollients effectively and adopting a stepped management plan is essential for
Medicines Use Review Supporting Information for Asthma Patients
 Medicines Use Review Supporting Information for Asthma Patients What is asthma? Asthma is a chronic inflammatory disorder of the airways. The inflammation causes an associated increase in airway hyper-responsiveness,
Medicines Use Review Supporting Information for Asthma Patients What is asthma? Asthma is a chronic inflammatory disorder of the airways. The inflammation causes an associated increase in airway hyper-responsiveness,
SHINGLES (Herpes zoster infection)
 SHINGLES (Herpes zoster infection) What are the aims of this leaflet? This leaflet has been written to help you understand more about shingles. It will tell you what it is, what causes it, what can be
SHINGLES (Herpes zoster infection) What are the aims of this leaflet? This leaflet has been written to help you understand more about shingles. It will tell you what it is, what causes it, what can be
Pre-operative M.R.S.A. Screening Information for Patients
 Infection Prevention and Control Pre-operative M.R.S.A. Screening Information for Patients This information is designed for patients undergoing MRSA screening before coming into hospital for a planned
Infection Prevention and Control Pre-operative M.R.S.A. Screening Information for Patients This information is designed for patients undergoing MRSA screening before coming into hospital for a planned
Pharmacists improving care in care homes
 The Royal Pharmaceutical Society believes that better utilisation of pharmacists skills in care homes will bring significant benefits to care home residents, care homes providers and the NHS. Introduction
The Royal Pharmaceutical Society believes that better utilisation of pharmacists skills in care homes will bring significant benefits to care home residents, care homes providers and the NHS. Introduction
ECZEMA: YOUR GP THE SECRETS WON T TELL YOU
 ECZEMA: THE SECRETS YOUR GP WON T TELL YOU As a sufferer of eczema or dry skin, it s likely that you ll understand the frustrations associated with trying various creams and lotions that are supposed to
ECZEMA: THE SECRETS YOUR GP WON T TELL YOU As a sufferer of eczema or dry skin, it s likely that you ll understand the frustrations associated with trying various creams and lotions that are supposed to
TOPICAL TREATMENTS FOR PSORIASIS
 TOPICAL TREATMENTS FOR PSORIASIS What are the aims of this leaflet? Patients with psoriasis are usually treated with preparations that are applied to the skin. This leaflet has been written to help you
TOPICAL TREATMENTS FOR PSORIASIS What are the aims of this leaflet? Patients with psoriasis are usually treated with preparations that are applied to the skin. This leaflet has been written to help you
What are the symptoms of a vulval skin condition?
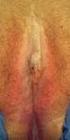 Information for you Published in December 2013 (next review date: 2016) Skin conditions of the vulva About this information This information is for you if you want to know about skin conditions affecting
Information for you Published in December 2013 (next review date: 2016) Skin conditions of the vulva About this information This information is for you if you want to know about skin conditions affecting
Guide to. Allergies 020 8742 7042. A guide to allergies
 If you need advice on taking over-the-counter medicines speak to a pharmacist or call the Consumer Health Information Centre s Over-the-Counter Medicines Advice Line on 020 8742 7042. The advice line is
If you need advice on taking over-the-counter medicines speak to a pharmacist or call the Consumer Health Information Centre s Over-the-Counter Medicines Advice Line on 020 8742 7042. The advice line is
DIET AND ECZEMA IN CHILDREN
 DIET AND ECZEMA IN CHILDREN It has been known for many years that what children eat may have an effect on their eczema. There has been an ever-increasing interest in the part that diet plays in the development
DIET AND ECZEMA IN CHILDREN It has been known for many years that what children eat may have an effect on their eczema. There has been an ever-increasing interest in the part that diet plays in the development
Psoriasis Treatment Transition Pathway
 Psoriasis Treatment Transition Pathway A Treatment Support Tool Adapted from Circle Nottingham NHS Treatment Centre Psoriasis Pathway (under consultation) with support from Abbvie Ltd Treatment Pathways
Psoriasis Treatment Transition Pathway A Treatment Support Tool Adapted from Circle Nottingham NHS Treatment Centre Psoriasis Pathway (under consultation) with support from Abbvie Ltd Treatment Pathways
A guide for people with genital herpes
 A guide for people with genital herpes Contents Getting the facts 4 The key facts 6 What is genital herpes? 8 Genital herpes symptoms 10 Getting tested 12 The first outbreak 14 Recurrent outbreaks 16 Common
A guide for people with genital herpes Contents Getting the facts 4 The key facts 6 What is genital herpes? 8 Genital herpes symptoms 10 Getting tested 12 The first outbreak 14 Recurrent outbreaks 16 Common
ASTHMA IN INFANTS AND YOUNG CHILDREN
 ASTHMA IN INFANTS AND YOUNG CHILDREN What is Asthma? Asthma is a chronic inflammatory disease of the airways. Symptoms of asthma are variable. That means that they can be mild to severe, intermittent to
ASTHMA IN INFANTS AND YOUNG CHILDREN What is Asthma? Asthma is a chronic inflammatory disease of the airways. Symptoms of asthma are variable. That means that they can be mild to severe, intermittent to
PSORIASIS AND ITS. Learn how vitamin D medications play an important role in managing plaque psoriasis
 PLAQUE PSORIASIS AND ITS TREATMENTS Learn how vitamin D medications play an important role in managing plaque psoriasis 2 Understanding Plaque Psoriasis WHAT CAUSES PLAQUE PSORIASIS? No one knows exactly
PLAQUE PSORIASIS AND ITS TREATMENTS Learn how vitamin D medications play an important role in managing plaque psoriasis 2 Understanding Plaque Psoriasis WHAT CAUSES PLAQUE PSORIASIS? No one knows exactly
Protection for hand eczema
 Oxford University Hospitals NHS Trust Department of Dermatology Protection for hand eczema Information for patients What can I do to help my hand eczema? Hand eczema (the same as hand dermatitis) is normally
Oxford University Hospitals NHS Trust Department of Dermatology Protection for hand eczema Information for patients What can I do to help my hand eczema? Hand eczema (the same as hand dermatitis) is normally
Seasonal Allergies. 1995-2012 The Patient Education Institute, Inc. www.x-plain.com im010101 Last reviewed: 05/30/2012 1
 Seasonal Allergies Introduction Seasonal allergies are allergies that develop during certain times of the year. Seasonal allergies are usually a response to pollen from trees, grasses, and weeds. Constant
Seasonal Allergies Introduction Seasonal allergies are allergies that develop during certain times of the year. Seasonal allergies are usually a response to pollen from trees, grasses, and weeds. Constant
Lichen Sclerosus. Exceptional healthcare, personally delivered
 Lichen Sclerosus Exceptional healthcare, personally delivered Lichen Sclerosus (LS) is an itchy skin condition usually affecting genital skin, but it can occur elsewhere. It affects women more often than
Lichen Sclerosus Exceptional healthcare, personally delivered Lichen Sclerosus (LS) is an itchy skin condition usually affecting genital skin, but it can occur elsewhere. It affects women more often than
Hydrozole Cream Hydrocortisone (microfine) 1% w/w and Clotrimazole 1% w/w
 CONSUMER MEDICINE INFORMATION What is in this leaflet? This leaflet answers some common questions about Hydrozole It does not contain all the available information. It does not take the place of talking
CONSUMER MEDICINE INFORMATION What is in this leaflet? This leaflet answers some common questions about Hydrozole It does not contain all the available information. It does not take the place of talking
Staff Skin Care Policy
 This is an official Northern Trust policy and should not be edited in any way Staff Skin Care Policy Reference Number: NHSCT/10/350 Target audience: All Trust staff and in particular those involved in
This is an official Northern Trust policy and should not be edited in any way Staff Skin Care Policy Reference Number: NHSCT/10/350 Target audience: All Trust staff and in particular those involved in
FastTest. You ve read the book... ... now test yourself
 FastTest You ve read the book...... now test yourself To ensure you have learned the key points that will improve your patient care, read the authors questions below. Please refer back to relevant sections
FastTest You ve read the book...... now test yourself To ensure you have learned the key points that will improve your patient care, read the authors questions below. Please refer back to relevant sections
Subject ID: Subject Initials Date completed Interviewer. Person answering questions. 1 yes 2 no
 COAST III Childhood Origins of ASThma Asthma Allergy Symptoms COAST 3 year visit Subject ID Subject ID: Subject Initials Date completed Interviewer Person answering questions 99. This form was completed
COAST III Childhood Origins of ASThma Asthma Allergy Symptoms COAST 3 year visit Subject ID Subject ID: Subject Initials Date completed Interviewer Person answering questions 99. This form was completed
Pimecrolimus cream (Elidel) for facial atopic dermatitis
 for facial atopic dermatitis (pi-me-kro-ly-mus) Summary Pimecrolimus 1% cream is PBS listed for treating facial atopic dermatitis in adults and children when topical corticosteroids are contraindicated
for facial atopic dermatitis (pi-me-kro-ly-mus) Summary Pimecrolimus 1% cream is PBS listed for treating facial atopic dermatitis in adults and children when topical corticosteroids are contraindicated
Allergy Shots and Allergy Drops for Adults and Children. A Review of the Research
 Allergy Shots and Allergy Drops for Adults and Children A Review of the Research Is This Information Right for Me? This information may be helpful to you if: Your doctor* has said that you or your child
Allergy Shots and Allergy Drops for Adults and Children A Review of the Research Is This Information Right for Me? This information may be helpful to you if: Your doctor* has said that you or your child
Treatment options a simple guide
 Guide Treatment options a simple guide To decide which treatment is right for you, a good starting point is to know what options you have and to understand the pros and cons of each one. People respond
Guide Treatment options a simple guide To decide which treatment is right for you, a good starting point is to know what options you have and to understand the pros and cons of each one. People respond
PATIENT INFORMATION ABOUT TREATMENTS FOR ASTHMA AND ALLERGIC RHINITIS, PRESCRIPTIONS & OVER THE COUNTER MEDICINE
 PATIENT INFORMATION ABOUT TREATMENTS FOR ASTHMA AND ALLERGIC RHINITIS, PRESCRIPTIONS & OVER THE COUNTER MEDICINE The content of this booklet was developed by Allergy UK. MSD reviewed this booklet to comment
PATIENT INFORMATION ABOUT TREATMENTS FOR ASTHMA AND ALLERGIC RHINITIS, PRESCRIPTIONS & OVER THE COUNTER MEDICINE The content of this booklet was developed by Allergy UK. MSD reviewed this booklet to comment
EBMT Education Day for Nurses and AHPs April 2012 Skin care: not every rash is GVHD
 EBMT Education Day for Nurses and AHPs April 2012 Skin care: not every rash is GVHD Eileen Parry Consultant Dermatologist Tameside Hospital Foundation Trust Overview How to assess a patient with a rash
EBMT Education Day for Nurses and AHPs April 2012 Skin care: not every rash is GVHD Eileen Parry Consultant Dermatologist Tameside Hospital Foundation Trust Overview How to assess a patient with a rash
Common Skin Conditions in Children. Liz Moore and Emma King Dermatology Nurse Consultants
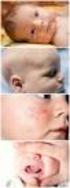 Common Skin Conditions in Children Liz Moore and Emma King Dermatology Nurse Consultants Diagnosis? Nummular Dermatitis Disc pattern rash (discoid eczema) Clearly demarcated edges Occurs at any age Can
Common Skin Conditions in Children Liz Moore and Emma King Dermatology Nurse Consultants Diagnosis? Nummular Dermatitis Disc pattern rash (discoid eczema) Clearly demarcated edges Occurs at any age Can
1g cream or ointment contains 1 mg methylprednisolone aceponate.
 CONSUMER MEDICINE INFORMATION ADVANTAN 1g cream or ointment contains 1 mg methylprednisolone aceponate. What is in this leaflet Please read this leaflet carefully before you start using ADVANTAN. It will
CONSUMER MEDICINE INFORMATION ADVANTAN 1g cream or ointment contains 1 mg methylprednisolone aceponate. What is in this leaflet Please read this leaflet carefully before you start using ADVANTAN. It will
FAQs on Influenza A (H1N1-2009) Vaccine
 FAQs on Influenza A (H1N1-2009) Vaccine 1) What is Influenza A (H1N1-2009) (swine flu) 1? Influenza A (H1N1-2009), previously known as "swine flu", is a new strain of influenza virus that spreads from
FAQs on Influenza A (H1N1-2009) Vaccine 1) What is Influenza A (H1N1-2009) (swine flu) 1? Influenza A (H1N1-2009), previously known as "swine flu", is a new strain of influenza virus that spreads from
X-Plain Psoriasis Reference Summary
 X-Plain Psoriasis Reference Summary Introduction Psoriasis is a long-lasting skin disease that causes the skin to become inflamed. Patches of thick, red skin are covered with silvery scales. It affects
X-Plain Psoriasis Reference Summary Introduction Psoriasis is a long-lasting skin disease that causes the skin to become inflamed. Patches of thick, red skin are covered with silvery scales. It affects
Withycombe Raleigh C of E Primary School Administering Medication in Schools 2015
 K.Lee - 2009 Revised August 2012/Sept 2013/July 2014 Latest Review July 2015 Withycombe Raleigh C of E Primary School Administering Medication in Schools 2015 At Withycombe Raleigh Church of England Primary
K.Lee - 2009 Revised August 2012/Sept 2013/July 2014 Latest Review July 2015 Withycombe Raleigh C of E Primary School Administering Medication in Schools 2015 At Withycombe Raleigh Church of England Primary
Lambeth and Southwark Action on Malnutrition Project (LAMP) Dr Liz Weekes Project Lead Guy s & St Thomas NHS Foundation Trust
 Lambeth and Southwark Action on Malnutrition Project (LAMP) Dr Liz Weekes Project Lead Guy s & St Thomas NHS Foundation Trust Page 0 What is the problem? Page 1 3 million (5 % population) at risk of malnutrition
Lambeth and Southwark Action on Malnutrition Project (LAMP) Dr Liz Weekes Project Lead Guy s & St Thomas NHS Foundation Trust Page 0 What is the problem? Page 1 3 million (5 % population) at risk of malnutrition
Frequency of application of topical corticosteroids for atopic eczema
 Frequency of application of topical corticosteroids for Issued: August 2004 guidance.nice.org.uk/ta81 NICE 2004 Contents 1 Guidance... 3 2 Clinical need and practice... 4 3 The technology... 8 4 Evidence
Frequency of application of topical corticosteroids for Issued: August 2004 guidance.nice.org.uk/ta81 NICE 2004 Contents 1 Guidance... 3 2 Clinical need and practice... 4 3 The technology... 8 4 Evidence
Allergies: ENT and Allergy Center of Missouri YOUR GUIDE TO TESTING AND TREATMENT. University of Missouri Health Care
 Allergies: YOUR GUIDE TO TESTING AND TREATMENT ENT and Allergy Center of Missouri University of Missouri Health Care 812 N. Keene St., Columbia, MO 65201 (573) 817-3000 www.muhealth.org WHAT CAUSES ALLERGIES
Allergies: YOUR GUIDE TO TESTING AND TREATMENT ENT and Allergy Center of Missouri University of Missouri Health Care 812 N. Keene St., Columbia, MO 65201 (573) 817-3000 www.muhealth.org WHAT CAUSES ALLERGIES
Childhood Asthma / Wheeze
 Childhood Asthma / Wheeze Symptoms Asthma causes a range of breathing problems. These include wheezing, feeling of tightness in the lungs/chest and a cough (often in the night or early morning). The most
Childhood Asthma / Wheeze Symptoms Asthma causes a range of breathing problems. These include wheezing, feeling of tightness in the lungs/chest and a cough (often in the night or early morning). The most
On completion of this chapter you should be able to: discuss the stepwise approach to the pharmacological management of asthma in children
 7 Asthma Asthma is a common disease in children and its incidence has been increasing in recent years. Between 10-15% of children have been diagnosed with asthma. It is therefore a condition that pharmacists
7 Asthma Asthma is a common disease in children and its incidence has been increasing in recent years. Between 10-15% of children have been diagnosed with asthma. It is therefore a condition that pharmacists
For Mild to Moderate Plaque Psoriasis and Moderate to Severe Atopic Dermatitis
 For Mild to Moderate Plaque Psoriasis and Moderate to Severe Atopic Dermatitis OLUX-E (clobetasol propionate) Foam, 0.05% Please see Important Safety Information on back page and accompanying Full Prescribing
For Mild to Moderate Plaque Psoriasis and Moderate to Severe Atopic Dermatitis OLUX-E (clobetasol propionate) Foam, 0.05% Please see Important Safety Information on back page and accompanying Full Prescribing
A ragweed pollen as a treatment for a ragweed allergy? It s called immunotherapy.
 A ragweed pollen as a treatment for a ragweed allergy? It s called immunotherapy. RAGWITEK is a prescription medicine used for sublingual (under the tongue) immunotherapy to treat ragweed pollen allergies
A ragweed pollen as a treatment for a ragweed allergy? It s called immunotherapy. RAGWITEK is a prescription medicine used for sublingual (under the tongue) immunotherapy to treat ragweed pollen allergies
These guidelines are intended to support General Practitioners in the care of their patients with dementia both in the community and in care homes.
 This is a new guideline. These guidelines are intended to support General Practitioners in the care of their patients with dementia both in the community and in care homes. It incorporates NICE clinical
This is a new guideline. These guidelines are intended to support General Practitioners in the care of their patients with dementia both in the community and in care homes. It incorporates NICE clinical
Informed Consent For Laser Hair Removal
 Informed Consent For Laser Hair Removal INSTRUCTIONS This informed-consent document has been prepared to help inform you about laser procedures, its risks, as well as alternative treatment(s). It is important
Informed Consent For Laser Hair Removal INSTRUCTIONS This informed-consent document has been prepared to help inform you about laser procedures, its risks, as well as alternative treatment(s). It is important
How to care for a Midline Catheter
 How to care for a Midline Catheter Developed by the health care professionals of the IV Program with assistance from the Department of Learning and Development. All rights reserved. No part of this book
How to care for a Midline Catheter Developed by the health care professionals of the IV Program with assistance from the Department of Learning and Development. All rights reserved. No part of this book
Lung Pathway Group Nintedanib (Vargatef) in advanced Non-Small Cell Lung Cancer (NSCLC)
 Lung Pathway Group Nintedanib (Vargatef) in advanced Non-Small Cell Lung Cancer (NSCLC) Indication: In combination with docetaxel in locally advanced, metastatic or locally recurrent NSCLC of adenocarcinoma
Lung Pathway Group Nintedanib (Vargatef) in advanced Non-Small Cell Lung Cancer (NSCLC) Indication: In combination with docetaxel in locally advanced, metastatic or locally recurrent NSCLC of adenocarcinoma
Professor Andrew Wright,
 Professor Andrew Wright, Systemic treatments are drugs taken as tablets or injections that travel through the bloodstream, dampening down the immune system to reach and treat eczema all over the body.
Professor Andrew Wright, Systemic treatments are drugs taken as tablets or injections that travel through the bloodstream, dampening down the immune system to reach and treat eczema all over the body.
Poison Ivy, Oak & Sumac: A Rash of Information About Identification, Treatment and Prevention
 Poison Ivy, Oak & Sumac: A Rash of Information About Identification, Treatment and Prevention The American Academy of Family Physicians Foundation has favorably reviewed this material through 2007. Favorable
Poison Ivy, Oak & Sumac: A Rash of Information About Identification, Treatment and Prevention The American Academy of Family Physicians Foundation has favorably reviewed this material through 2007. Favorable
NEHSNORTH EASTERN HEALTH SPECIALISTS
 COSMETIC DERMATOLOGY NEHSNORTH EASTERN HEALTH SPECIALISTS nehs.com.au CONSENT FORM ACNE Treatment I, DOB:, of authorize of North Eastern Health Specialist to perform hair removal with the BBL / Nd-Yag
COSMETIC DERMATOLOGY NEHSNORTH EASTERN HEALTH SPECIALISTS nehs.com.au CONSENT FORM ACNE Treatment I, DOB:, of authorize of North Eastern Health Specialist to perform hair removal with the BBL / Nd-Yag
D.RIGOPOULOS, D.IOANNIDES,* D.KALOGEROMITROS, S.GREGORIOU AND A.KATSAMBAS
 British Journal of Dermatology 24; 151: 171 175. DOI: 1.1111/j.1365-2133.24.628.x Therapeutics Pimecrolimus cream 1% vs. betamethasone 17-valerate Æ1% cream in the treatment of seborrhoeic dermatitis.
British Journal of Dermatology 24; 151: 171 175. DOI: 1.1111/j.1365-2133.24.628.x Therapeutics Pimecrolimus cream 1% vs. betamethasone 17-valerate Æ1% cream in the treatment of seborrhoeic dermatitis.
Local Enhanced Service Specification for the Supply of Pharmaceutical Services to Care Homes through Community Pharmacy
 Local Enhanced Service Specification for the Supply of Pharmaceutical Services to Care Homes through Community Pharmacy Contents: 1. Introduction and purpose 2. Period of Service 3. Aim of the Service
Local Enhanced Service Specification for the Supply of Pharmaceutical Services to Care Homes through Community Pharmacy Contents: 1. Introduction and purpose 2. Period of Service 3. Aim of the Service
READ THIS LEAFLET VERY CAREFULLY, AND KEEP IT IN A SAFE PLACE. FLU IS SPREADING IN IRELAND, AND THIS INFORMATION IS IMPORTANT FOR YOU AND YOUR FAMILY.
 READ THIS LEAFLET VERY CAREFULLY, AND KEEP IT IN A SAFE PLACE. FLU IS SPREADING IN IRELAND, AND THIS INFORMATION IS IMPORTANT FOR YOU AND YOUR FAMILY. Information and medical advice for the public on Pandemic
READ THIS LEAFLET VERY CAREFULLY, AND KEEP IT IN A SAFE PLACE. FLU IS SPREADING IN IRELAND, AND THIS INFORMATION IS IMPORTANT FOR YOU AND YOUR FAMILY. Information and medical advice for the public on Pandemic
Humulin R (U500) insulin: Prescribing Guidance
 Leeds Humulin R (U500) insulin: Prescribing Guidance Amber Drug Level 2 We have started your patient on Humulin R (U500) insulin for the treatment of diabetic patients with marked insulin resistance requiring
Leeds Humulin R (U500) insulin: Prescribing Guidance Amber Drug Level 2 We have started your patient on Humulin R (U500) insulin for the treatment of diabetic patients with marked insulin resistance requiring
A t f e t r e r th t is s lec e t c u t re r e t h t e e st s u t den e t t sh s ould b e e a b a le e t o t :
 Dermatopharmacology Prof Werner Sinclair Department of Dermatology University of the Free State Outcomes for this Lecture After this lecture the student should be able to: Name the most important characteristics
Dermatopharmacology Prof Werner Sinclair Department of Dermatology University of the Free State Outcomes for this Lecture After this lecture the student should be able to: Name the most important characteristics
treat nasal congestion that happens with seasonal allergic rhinitis in adults and children 2 years of age and older.
 Patient Information NASONEX [nā-zə-neks] (mometasone furoate monohydrate) Nasal Spray, 50 mcg FOR INTRANASAL USE ONLY Read the Patient Information that comes with NASONEX before you start using it and
Patient Information NASONEX [nā-zə-neks] (mometasone furoate monohydrate) Nasal Spray, 50 mcg FOR INTRANASAL USE ONLY Read the Patient Information that comes with NASONEX before you start using it and
Protecting your child against flu
 Protecting your child against flu Information for parents Flu mmunisation 2015/16 Helping to protect everyone, every winter This year, the flu vaccine is being offered to: children aged two, three and
Protecting your child against flu Information for parents Flu mmunisation 2015/16 Helping to protect everyone, every winter This year, the flu vaccine is being offered to: children aged two, three and
FUNGAL INFECTIONS OF THE NAILS
 FUNGAL INFECTIONS OF THE NAILS What are the aims of this leaflet? This leaflet has been written to help you understand more about fungal infections of the nails. It tells you what they are, what causes
FUNGAL INFECTIONS OF THE NAILS What are the aims of this leaflet? This leaflet has been written to help you understand more about fungal infections of the nails. It tells you what they are, what causes
Medication Policy and Procedures
 Medication Policy and Procedures Policy Number: 2009/10 Approved by: Heritage Management Committee 10 November 2009 Last reviewed: October 2009 Next review due: November 2011 Policy Statement Studies of
Medication Policy and Procedures Policy Number: 2009/10 Approved by: Heritage Management Committee 10 November 2009 Last reviewed: October 2009 Next review due: November 2011 Policy Statement Studies of
Medicines reconciliation on admission and discharge from hospital policy April 2013. WHSCT medicines reconciliation policy 1
 Medicines reconciliation on admission and discharge from hospital policy April 2013 WHSCT medicines reconciliation policy 1 Policy Title Policy Reference Number Medicines reconciliation on admission and
Medicines reconciliation on admission and discharge from hospital policy April 2013 WHSCT medicines reconciliation policy 1 Policy Title Policy Reference Number Medicines reconciliation on admission and
See, Think, and Act! Anaphylaxis (Severe Allergies)
 See, Think, and Act! Anaphylaxis (Severe Allergies) California After School Resource Center (CASRC) Administered for the California Department of Education (C.D.E.) Hello. My name is Robyn Sakamoto. Welcome
See, Think, and Act! Anaphylaxis (Severe Allergies) California After School Resource Center (CASRC) Administered for the California Department of Education (C.D.E.) Hello. My name is Robyn Sakamoto. Welcome
All Wales Prescription Writing Standards
 All Wales Prescription Writing Standards These standards should be read in conjunction with completing the All Wales Medication Chart e- learning package, available on the Learning@NHSWales internet site
All Wales Prescription Writing Standards These standards should be read in conjunction with completing the All Wales Medication Chart e- learning package, available on the Learning@NHSWales internet site
Guidance to support the stepwise review of combination inhaled corticosteroid therapy for adults ( 18yrs) in asthma
 Guidance to support the stepwise review of combination inhaled corticosteroid therapy for adults ( 18yrs) in asthma Important Complete asthma control needs to be achieved for at least 12 weeks before attempting
Guidance to support the stepwise review of combination inhaled corticosteroid therapy for adults ( 18yrs) in asthma Important Complete asthma control needs to be achieved for at least 12 weeks before attempting
Chickenpox in pregnancy: what you need to know
 Chickenpox in pregnancy: what you need to know First published December 2003 Revised edition published November 2008 What is chickenpox? Chickenpox is a very infectious illness caused by a virus called
Chickenpox in pregnancy: what you need to know First published December 2003 Revised edition published November 2008 What is chickenpox? Chickenpox is a very infectious illness caused by a virus called
Guidelines for Hand Foot and Mouth Disease HFMD
 Guidelines for Hand Foot and Mouth Disease HFMD Hand, foot, and mouth disease, or HFMD, is a contagious illness caused by different viruses. Infants and children younger than 5 years are more likely to
Guidelines for Hand Foot and Mouth Disease HFMD Hand, foot, and mouth disease, or HFMD, is a contagious illness caused by different viruses. Infants and children younger than 5 years are more likely to
Hand Dermatitis in Health Care Workers
 Hand in Health Care Workers Safety and Health Assessment and Research for Prevention (SHARP) Program Washington Department of Labor and Industries PO Box 44330 Olympia, WA 98504-4330 1-888-66-SHARP www.lni.wa.gov/sharp/derm
Hand in Health Care Workers Safety and Health Assessment and Research for Prevention (SHARP) Program Washington Department of Labor and Industries PO Box 44330 Olympia, WA 98504-4330 1-888-66-SHARP www.lni.wa.gov/sharp/derm
HEALTH SERVICES PROGRAM
 HEALTH SERVICES PROGRAM The Board of Education will provide for the health and physical well being of students through the establishment of a district wide student Health Services Program in the school
HEALTH SERVICES PROGRAM The Board of Education will provide for the health and physical well being of students through the establishment of a district wide student Health Services Program in the school
Policy for Screening Patients for MRSA Colonisation
 Policy for Screening Patients for MRSA Colonisation To whom this document applies: All staff in Colchester Hospital University Foundation Trust screening Patients for MRSA Procedural Documents Approval
Policy for Screening Patients for MRSA Colonisation To whom this document applies: All staff in Colchester Hospital University Foundation Trust screening Patients for MRSA Procedural Documents Approval
Intravenous Methyl Prednisolone in Multiple Sclerosis
 Intravenous Methyl Prednisolone in Multiple Sclerosis Exceptional healthcare, personally delivered Relapse management in multiple sclerosis Relapses in multiple sclerosis (MS) are common and caused by
Intravenous Methyl Prednisolone in Multiple Sclerosis Exceptional healthcare, personally delivered Relapse management in multiple sclerosis Relapses in multiple sclerosis (MS) are common and caused by
Patient Information Leaflet for Flixonase Aqueous Nasal Spray (fluticasone propionate)
 Patient Information Leaflet for Flixonase Aqueous Nasal Spray (fluticasone propionate) Your doctor has decided to prescribe Flixonase Aqueous Nasal Spray as part of your treatment. This leaflet tells you
Patient Information Leaflet for Flixonase Aqueous Nasal Spray (fluticasone propionate) Your doctor has decided to prescribe Flixonase Aqueous Nasal Spray as part of your treatment. This leaflet tells you
For more information, please contact the National Psoriasis Foundation at 800-723-9166 or
 For more information, please contact the National Psoriasis Foundation at 800-723-9166 or www.psoriasis.org. PSORIASIS 101: LEARNING TO LIVE IN THE SKIN YOU RE IN is part of an awareness program to educate
For more information, please contact the National Psoriasis Foundation at 800-723-9166 or www.psoriasis.org. PSORIASIS 101: LEARNING TO LIVE IN THE SKIN YOU RE IN is part of an awareness program to educate
Manchester Triage System A global solution
 Manchester Triage System A global solution Jill Windle Lecturer Practitioner in Emergency Nursing Salford Royal Hospital, Manchester University of Salford This session will contain.. Explanation Clarification
Manchester Triage System A global solution Jill Windle Lecturer Practitioner in Emergency Nursing Salford Royal Hospital, Manchester University of Salford This session will contain.. Explanation Clarification
BRITISH DERMATOLOGICAL NURSING GROUP
 Nurse Led systemic monitoring clinics guidance on setting up this service Introduction Nurse led systemic monitoring clinics are an innovative approach to improving care delivery and maintaining both a
Nurse Led systemic monitoring clinics guidance on setting up this service Introduction Nurse led systemic monitoring clinics are an innovative approach to improving care delivery and maintaining both a
Antibiotic Guidelines: Ear Nose and Throat (ENT) Infections. Contents
 Antibiotic Guidelines: Ear Nose and Throat (ENT) Infections. Classification: Clinical Guideline Lead Author: Antibiotic Steering Committee Additional author(s): Authors Division: DCSS & Tertiary Medicine
Antibiotic Guidelines: Ear Nose and Throat (ENT) Infections. Classification: Clinical Guideline Lead Author: Antibiotic Steering Committee Additional author(s): Authors Division: DCSS & Tertiary Medicine
Conjunctivitis - Pink Eye
 Conjunctivitis - Pink Eye Introduction Conjunctivitis is often called pink eye. It causes inflammation of the thin, clear lining inside the eyelid and on the white of the eye. The inflammation gives the
Conjunctivitis - Pink Eye Introduction Conjunctivitis is often called pink eye. It causes inflammation of the thin, clear lining inside the eyelid and on the white of the eye. The inflammation gives the
Anaphylaxis and Epinephrine Auto-Injector
 Lesson Guide Anaphylaxis and Epinephrine Auto-Injector Lesson Length: 45 minutes Guidance for the Instructor To complete this lesson and meet the lesson objectives, you must: Welcome participants and explain
Lesson Guide Anaphylaxis and Epinephrine Auto-Injector Lesson Length: 45 minutes Guidance for the Instructor To complete this lesson and meet the lesson objectives, you must: Welcome participants and explain
Consumers. Allergic rhinitis. and your. Asthma. What you should know
 Consumers Allergic rhinitis and your Asthma What you should know Contents Allergic rhinitis facts...3 How allergic rhinitis can affect your asthma...3 What are the symptoms of allergic rhinitis?...4 What
Consumers Allergic rhinitis and your Asthma What you should know Contents Allergic rhinitis facts...3 How allergic rhinitis can affect your asthma...3 What are the symptoms of allergic rhinitis?...4 What
Cough, as a leading symptom, would certainly be in the top 10 of reasons for seeing a GP.
 COUGH Cough, as a leading symptom, would certainly be in the top 10 of reasons for seeing a GP. A cough in a child seems to cause more concern, even when it has not been present very long, whereas in adults
COUGH Cough, as a leading symptom, would certainly be in the top 10 of reasons for seeing a GP. A cough in a child seems to cause more concern, even when it has not been present very long, whereas in adults
Hormone. Replacement. Therapy. Information leaflet. This information is also available on request in other formats by phoning 01387 241053.
 Hormone Replacement Therapy This information is also available on request in other formats by phoning 01387 241053. Information leaflet Produced by Dr H Currie & Sr. K Martin May 2005 Updated Dec. 2013
Hormone Replacement Therapy This information is also available on request in other formats by phoning 01387 241053. Information leaflet Produced by Dr H Currie & Sr. K Martin May 2005 Updated Dec. 2013
Anaphylaxis: a severe, life threatening allergic reaction usually involving swelling, trouble breathing, and can progress to shock
 Allergy is a condition in which the immune system causes sneezing, itching, rashes, and wheezing, or sometimes even life-threatening allergic reactions. The more you know about allergies, the better prepared
Allergy is a condition in which the immune system causes sneezing, itching, rashes, and wheezing, or sometimes even life-threatening allergic reactions. The more you know about allergies, the better prepared
DERMATITIS ECZEMA JOHN L. BEZZANT, M.D.
 DERMATITIS ECZEMA JOHN L. BEZZANT, M.D. THE PHYSICIAN IS PRIMARILY A PROBLEM SOLVER FACULTY TEACHING HANDBOOK UNIVERSITY OF UTAH SCHOOL OF MEDICINE, FALL 2005, p 62. THE GODS ARE MORE WILLING TO HELP US
DERMATITIS ECZEMA JOHN L. BEZZANT, M.D. THE PHYSICIAN IS PRIMARILY A PROBLEM SOLVER FACULTY TEACHING HANDBOOK UNIVERSITY OF UTAH SCHOOL OF MEDICINE, FALL 2005, p 62. THE GODS ARE MORE WILLING TO HELP US
Your psoriasis story. Print this out, answer the questions, then share it with your doctor
 Your psoriasis story Print this out, answer the questions, then share it with your doctor 1 SYMPTOMS Surface Area Your doctor will use a variety of different factors to measure the severity of your disease,
Your psoriasis story Print this out, answer the questions, then share it with your doctor 1 SYMPTOMS Surface Area Your doctor will use a variety of different factors to measure the severity of your disease,
BOHRF BOHRF BOHRF BOHRF
 Occupational Contact Dermatitis and Urticaria A Guide for Occupational Health and Safety Representatives Professionals, Safety Professionals March 2010 British Occupational Health Research Foundat ion
Occupational Contact Dermatitis and Urticaria A Guide for Occupational Health and Safety Representatives Professionals, Safety Professionals March 2010 British Occupational Health Research Foundat ion
Going home after an AV Fistula or AV Graft
 Going home after an AV Fistula or AV Graft TGH Information for patients and families During your hospital stay, your surgeon created an: AV Fistula AV Graft Read this booklet to learn: how to care for
Going home after an AV Fistula or AV Graft TGH Information for patients and families During your hospital stay, your surgeon created an: AV Fistula AV Graft Read this booklet to learn: how to care for
NHS FORTH VALLEY Multiple Sclerosis Service Management of MS Relapses
 NHS FORTH VALLEY Multiple Sclerosis Service Management of MS Relapses Approved 22/06/2010 Version Version 2 Date of First Issue 2002 Review Date 10/05/2016 Date of Issue 01/02/2010 EQIA Yes 22.06.10 Author
NHS FORTH VALLEY Multiple Sclerosis Service Management of MS Relapses Approved 22/06/2010 Version Version 2 Date of First Issue 2002 Review Date 10/05/2016 Date of Issue 01/02/2010 EQIA Yes 22.06.10 Author
Oral allergy syndrome
 Oxford University Hospitals NHS Trust Children s Allergy Clinic Oral allergy syndrome Information for parents What is oral allergy syndrome? In the common form, oral allergy syndrome usually causes redness,
Oxford University Hospitals NHS Trust Children s Allergy Clinic Oral allergy syndrome Information for parents What is oral allergy syndrome? In the common form, oral allergy syndrome usually causes redness,
Peninsula Commissioning Priorities Group. Commissioning Policy Varicose Vein Referral
 NHS Devon NHS Plymouth Torbay Care Trust Peninsula Commissioning Priorities Group Commissioning Policy Varicose Vein Referral Varicose Vein Referral Guidelines 1. Description of service/treatment Most
NHS Devon NHS Plymouth Torbay Care Trust Peninsula Commissioning Priorities Group Commissioning Policy Varicose Vein Referral Varicose Vein Referral Guidelines 1. Description of service/treatment Most
Raynaud s Disease. What is Raynaud s Disease? Raynaud s disease is also sometimes known as Raynaud s phenomenon or Raynaud s syndrome.
 Raynaud s Disease Introduction Raynaud s disease is a rare disorder of the blood vessels. It usually affects the fingers and toes. This disorder causes the blood vessels to narrow which turns the affected
Raynaud s Disease Introduction Raynaud s disease is a rare disorder of the blood vessels. It usually affects the fingers and toes. This disorder causes the blood vessels to narrow which turns the affected
