Chemotherapy Induced Nausea and Vomiting (CINV) Anti-emetic Guidelines
|
|
|
- Clinton Melton
- 7 years ago
- Views:
Transcription
1 North of England Cancer Network Chemotherapy Induced Nausea and Vomiting (CINV) Anti-emetic Guidelines Adult Oncology & Haematology Quality and safety for every patient every time For more information regarding this document, please contact: Calum Polwart Network Pharmacist, North of England Cancer Network NE Strategic Health Authority, Waterfront 4, Goldcrest Way Newcastle Upon Tyne, NE15 7NY See last page for Document Control November 2011 (Version1.4) Page 1 of 23
2 Summary Standard Anti emetic Cover Level 1: Minimal Risk (Less than 10%) Pre-medication: No standard pre-medication normally required Level 2: Intermediate Risk (10 to 30%) Take Home Medication: No standard medication normally required. However, normally supply metoclopramide as a rescue measure with first cycle. Pre-medication: Dexamethasone 8mg IV or Oral Take Home Medication: No standard medication normally required. However, normally supply metoclopramide as a rescue measure with first cycle. Level 3: Moderate Risk (30 to 90%) Pre-medication: Dexamethasone 8mg IV or Oral Either Ondansetron 8mg IV / Oral Or Palonosetron** 0.25mg IV Take Home Medication: Dexamethasone up to 8mg Daily* Oral for 3 days Ondansetron 8mg Twice Daily Oral for 2 to 3 days (not given if using IV Palonosetron ) Metoclopramide 10-20mg TDS-QDS Oral for 3 days when required Level 4: High Risk (> 90%) Pre-medication: Dexamethasone 12mg IV or Oral Aprepitant*** 125mg Oral ( with risk factors) Either Ondansetron 8mg IV / Oral Or Palonosetron** 0.25mg IV Take Home Medication: Dexamethasone up to 8mg Daily* Oral for 2 to 3 days Aprepitant*** 80mg Daily Oral for 2 days Ondansetron 8mg Twice Daily Oral for 2 to 3 days (not given if using IV Palonosetron ) * for patients receiving pre-medication doses before 12pm, they should take a divided evening dose at 4pm on the night of chemotherapy. ** consider palonosetron where there is concern, i.e. patient has risk factors overrisk of delayed nausea and vomiting *** consider adding aprepitant where there is concern over risk of anti-emetic failure as identified by assessment of patient risk factorsalternative Agents or fosaprepitant 150mg intravenously on day 1 only (See Page 14) November 2011 (Version1.4) Page 2 of 23
3 Breakthrough Management: If patients develop acute nausea / vomiting (within 24 hours of last chemotherapy dose), which is refractory to breakthrough medication already supplied, increase to the next treatment band. If patients develop delayed nausea / vomiting (> 24hours after last chemotherapy dose), which is refractory to breakthrough medication already supplied, add additional treatment from the following (using the next available agent on the list): Metoclopramide Dexamethasone Ondansetron (or another 5HT antagonist) Levomepromazine Cyclizine (?stop metoclopramide) Prochloperazine Lorazepam Nabilone Haloperidol November 2011 (Version1.4) Page 3 of 23
4 Contents Summary Standard Anti emetic Cover... 2 Breakthrough Management:... 3 Contents... 4 Introduction... 6 Causes of Nausea & Vomiting... 8 Pathophysiology... 8 Acute... 8 Delayed... 8 Anticipatory... 8 Breakthrough... 8 Refractory... 8 Contributing Factors... 9 Gender... 9 Age... 9 Performance Status... 9 Other Medication... 9 Travel sickness... 9 Morning sickness... 9 Previous CINV Smoking Alcohol intake Drug use / misuse Individual Drug Treatment Combination Treatments Concomitant Radiotherapy Management of anti-emetic failure Exclusion of other causes Control / Treatment Metoclopramide Dexamethasone November 2011 (Version1.4) Page 4 of 23
5 Ondansetron / Granisetron Alternative 5HT 3 antagonists Aprepitant & Fosaprepitant Levomepromazine (Nozinan) Cyclizine Nabilone Benzodiazepines Haloperidol Emetogenicity of Chemotherapy Single Agent Chemotherapy Combination Chemotherapy Common Combinations Emetogenicity Credits & Acknowledgments References Appendix One: Antiemetic ladder 23 November 2011 (Version1.4) Page 5 of 23
6 Introduction Chemotherapy Induced Nausea and Vomiting (CINV) is one of the most frequently experienced side effects encountered by chemotherapy patients. Patients will often find the symptoms distressing, and develop anxiety about the potential for such symptoms to recur on future cycles of chemotherapy. Modern drug treatment can successfully control CINV for the majority of patients. Scope These guidelines are intended to support health professionals in the management and prevention of chemotherapy induced nausea and vomiting. They are not intended to address radiotherapy induced nausea and vomiting or nausea and vomiting in palliative care. This guidance applies to Adults only. Patient Group These guidelines are intended to cover adult solid tumour and haemato-oncology patients receiving cytotoxic chemotherapy within the North of England Cancer Network. Clinical Practice These guidelines are intended to provide a framework to support clinical practice, they can not cover every clinical situation and good common clinical sense and clinical experience will be required when approaching the management of individual patients. Deviation from these guidelines will be necessary in some situations and this should be appropriately documented. Drug Selection These guidelines have purposefully chosen not to recommend one specific 5HT3 antagonist, as there is limited evidence to choose between ondansetron, granisetron and palonosetron for acute CINV. Palonosetron is more effective than other 5HT3 antagonist in preventing delayed CINV but is significantly more expensive.. November 2011 (Version1.4) Page 6 of 23
7 Dexamethasone is the backbone of many of the combinations recommended here. It should be used with caution in patients with diabetes, and should not normally be used in regimens that contain high doses of alternative steroids such as prednisolone. The dose of metoclopramide recommended here exceeds the licensed dose. Many of the individual drugs or combinations of anti-emetics described within this document are out-side of product licence. For all drugs the SmPC and BNF should be consulted prior to prescribing. November 2011 (Version1.4) Page 7 of 23
8 Causes of Nausea & Vomiting Pathophysiology CINV is most commonly grouped into three phases: anticipatory, acute and delayed. Successful management requires correct identification of the phase (or combination of phases) being treated. Two further terminologies have been adopted in this document refractory and breakthrough. Acute Acute CINV is usually described as CINV presenting within the 24 hours immediately after administration of chemotherapy. Delayed Delayed CINV may present any time after the first 24 hours, and may continue for up to 6 or 7 days after chemotherapy. Anticipatory Occurs prior to administration of any chemotherapy (in this cycle). It is either a learned response following CINV on a previous cycle or an anxiety response. It is most common after 3 to 4 cycles of chemotherapy with very badly controlled acute or delayed symptoms. Breakthrough Development of symptoms (nausea or vomiting), despite standard anti-emetic therapy, which require treatment with an additional pharmacological agent Refractory Patients who have failed on both standard and rescue medication. November 2011 (Version1.4) Page 8 of 23
9 Contributing Factors Gender Women are at increased risk of CINV than males (1) (2). Age Younger patients are more susceptible than older patients, with patients under 50 years old being at the greatest risk (1) (2). Performance Status Poor performance status increases the risk of CINV Other Medication Various medications can cause nausea and vomiting and it has been proposed that when some of these are given in combination with chemotherapy that these increase the risk of CINV. Examples of these agents are listed below: Amifostine Anaesthetic Agents Anti-depressants Anti-microbials, including anti-fungals Ergot alakaloids Iron Lev and Carbo Dopa NSAIDs Travel sickness Patients who have a history of motion sickness are at increased risk of CINV (2) Morning sickness Morning sickness during pregnancy has been suggested as a predictive factor for CINV November 2011 (Version1.4) Page 9 of 23
10 Previous CINV Previous exposure to chemotherapy which has resulted in CINV increses the risk of CINV with future chemotherapy. In addition, the effectiveness of of prophylactic treatment reduces with each cycle of chemotherapy. Failure of prophylaxis in the acute setting increases the risk of failure in the delayed setting. Smoking Smoking reduces the risk of CINV. Alcohol intake Patients with a long history of alcohol consumption are at reduced risk of CINV. (3) Drug use / misuse Patients with a history of drug misuse are generally at a lower risk of CINV. Individual Drug Treatment Each individual chemotherapy drug will have a different risk factor for emetogencity ranging from drugs such as vincristine with a risk of less than 10% emetogenicity without any prophylaxis to cisplatin with a nearly 100% risk without any prophylaxis. Combination Treatments When chemotherapy agents are combined, the effect of this may be additive or synergistic. Concomitant Radiotherapy When chemotherapy agents is given in combination with radiotherapy emetogenicity will increase. November 2011 (Version1.4) Page 10 of 23
11 Management of anti-emetic failure Anti-emetic failure is described as: 4 hours of moderate to severe nausea or 2 or more episodes of vomiting and/or retching in 24 hours. There are 3 key steps for successful management 1. Exclusion of other causes, 2. Treatment, 3. Planning for the next cycle. Exclusion of other causes It is easy to assume that nausea and vomiting in a patient who has recently received chemotherapy is the result of their chemotherapy. However there are several other causes of nausea and vomiting many of which will commonly present in cancer patients and should therefore be excluded: Other medication (See Page 9) Constipation Bowel Obstruction Anxiety Metabolic Abnormalities (eg Renal Failure) Hyper-calcaemia Peptic Ulcer Disease Radiotherapy Raised Intra Cranial Pressure If another cause is identified this should be corrected or treated rather than initiating treatment for CINV. November 2011 (Version1.4) Page 11 of 23
12 Control / Treatment An additional anti-emetic should be added (from a different) therapeutic class. If necessary medication should be given rectally or parenterally to regain control. If any medication was previously being given on a 'when required' basis this should be switched to a regular dosing schedule. The use of multiple drugs may be necessary, and scheduling of treatment to avoid troughs of drug levels may be necessary. Closely monitor hydration and electrolytes and correct any abnormalities if they present. Metoclopramide Metoclopramide should be considered the first line treatment to be added to existing therapy. 20mg is usually required to achieve sufficient therapeutic levels to cross the blood brain barrier, and doses may need to be repeated 6 hourly rather than 8 hourly to maintain sufficient therapeutic levels. Metoclopramide can cause extra-pyramidal reactions in some patients and so should be used with caution in young adults and the elderly. Metoclopramide must not be given to patients with parkinson's disease. Domperidone (20mg TDS-QDS) may have similar efficacy, without causing extra-pyramidal reactions. Dexamethasone Dexamethasone is the second line treatment of choice. It is a highly effective anti-emetic when given at doses ranging from 8 to 20mg daily. Published consensus guidance, ASCO, MASSC and NCCC all favour a dose of 8mg for prevention of acute emesis in moderate risk and 20mg for prevention of acute emesis in high risk. Note the 20mg dose is reduced to 12mg when given in combination with aprepitant as the AUC of dexamethasone is increased by aprepitant. 8mg Dexamethaone is used for prevention of acute emesis in low risk as a dose usually as 4mg in the morning and at 4pm. Lower doses (4mg or 6mg) are also sometimes effective. It should not be given to patients who are already receiving another steroid as part of their chemotherapy regimen (e.g. CHOP) and should be used in care in patients who have diabetes. Doses after 6pm are likely to cause sleep disturbance. November 2011 (Version1.4) Page 12 of 23
13 Ondansetron / Granisetron 5HT3 antagonists (ondansetron or granisetron) should be considered third line, for any patient who has not already been prescribed them who is unable to be prescribed a steroid or in whom steroid treatment is inadequate. Ondansetron - 8mg twice daily (or 16mg once daily rectally) should be the normal dose prescribed. Common surgical prophylaxis schedules (eg 4mg TDS) are unlikely to be adequate. Doses of up to 32mg of ondansetron per day can be given however there is little evidence that higher doses produce additional therapeutic effect for most patients and they are more likely to cause side effects such as headache and constipation. Granisetron 1mg twice daily (or 3mg once daily) is usually considered equivalent to 8mg twice daily of ondansetron. Alternative 5HT 3 antagonists Tropisetron has less evidence to support its use in chemotherapy. Its once daily dosing schedule, anecdotally can lead to treatment failures before the next dose is due. Dolasteron 100mg. Palonosetron Palonosetron is given as a single IV dose prior to chemotherapy. It is at least as effective as ondansetron, Palonosetron - single 0.25mg IV dose prior to chemotherapy. It is at least as effective as ondansetron, and has been shown to be superior than other 5HT3 antagonists for the prevention of delayed emesis. Its extensive half life means there is no requirement to repeat the dose which may be useful in patients where compliance is a particular concern. It is more effective than standard 5HT 3 antagonists at preventing delayed CINV. However, it has no role to play in the rescue of patients with anti-emetic failure (i.e. treatment of breakthrough nausea / vomiting). Palonosetron is significantly more expensive than generic ondansetron. The 2010 MASSC Guidelines recommended palonosetron as the preferred 5-HT3 receptor antagonist in Moderately Emetogenic Chemotherapy (excluding the AC regimen). November 2011 (Version1.4) Page 13 of 23
14 Aprepitant & Fosaprepitant Aprepitant is a NK-1 receptor antagonist that has been shown to be effective for the management of delayed chemotherapy induced nausea and vomiting. Aprepitant has a known interaction with dexamethasone which may require dose reduction of dexamethasone. In clinical trials 20mg of dexamethasone was used in the control arm and 12mg in the aprepitant arm. Conventional practice within NECN would not use 20mg of dexamethasone as an antiemetic, and therefore dose reduction of steroid is probably not necessary within NECN antiemetic combinations. 125mg is given orally on day 1 an hour before treatment and 80mg on day 2 and 3, a combination pack is provided with all three doses included. Fosaprepitant is a pro-drug of aprepitant that allows it to be given intravenously. Recent data has shown that a single 150mg IV dose can be used to replace the full oral schedule (d1: 125mg and d2+3: 80mg). The SmPC recommends this is given as a 1mg/ml solution over 20 minutes, 30 minutes before chemotherapy. This is difficult to administer clinically given the size of IV infusion bags commercially available. MSD has data from clinical trials which demonstrate that the drug can be mixed in volumes from 100 to 250ml of Sodium Chloride. Where the concentration is stronger than 1mg/ml there appears to be a slightly increased risk of venous irritation therefore patients who can handle 250ml of fluid in minutes should receive their fosaprepitant in a 250ml bag rather than a 100ml bag. Clinical trails of fosaprepitant gave dexamethasone orally in doses of 12mg daily, 8mg daily, 8mg twice daily on days 1, 2, 3&4 respectively. Consideration to giving higher doses of dexamethasone should be given. Licencing studies of both aprepitant and fosaprepitant have used 32mg of ondansetron on day 1 with no other ondansetron. A single European study has used a granisetron schedule which is similar to the ondansetron schedule used in the UK. No robust data exists to confirm if aprepitant duration should be extended if chemotherapy lasts more than 1 day. In view of the cost and lack of evidence aprepitant should not be used to rescue patients with anti-emetic failure. November 2011 (Version1.4) Page 14 of 23
15 Levomepromazine (Nozinan) Levomepromazine should be added after a dopamine agonist (eg metoclopramide), a glucocorticoid steroid (eg dexamethasone) and a 5HT 3 antagonist (eg ondansetron). Leveomepromazine has a significant sedating effect which may be beneficial in achieving its antiemetic effect, however, care should be taken to avoid over sedating patients. A starting dose of 6.25mg using ¼ of a 25mg tablet (or a 6mg tablet is available but is not currently licenced) should be used, with doses repeated every 8 to 12 hours unless nausea returns sooner. Cyclizine If levomepromazine is not felt adequate, cyclizine (50mg three times a day) should be considered. However cyclizine, theoretically, inhibits the gastro-intestinal motility stimulating actions of metoclopramide. Although, in clinical practice many patients find cyclizine plus metoclopramide more effective than either alone, a small number of patients will find the combination worse than either agent alone. Patients who have reached this level of refractoryness to treatment should be considered for addition of aprepitant to the next cycle of chemotherapy. Aprepitant does not currently have any evidence to support its use in the acute management of antiemetic failure. Nabilone Consider nabilone in patients refractory to all other treatments. Benzodiazepines While benzodiazepines have limited anti-emetic properties their anxiolytic properties mean they can be a useful adjunct. They should be considered at any stage when anxiety is felt to be contributing factor to CINV. Some benzodiazepines also have a amnesiac effect which may be useful in preventing conditioning behaviors for the following cycle. Lorazepam 0.5-1mg orally (or sub-lingually) up to 12 hourly is usually sufficient. Consider staring the night before treatment, continuing on the morning of treatment. Haloperidol Haloperidol is often considered useful as an anti-emetic in palliative care, and due to its anxiolytic properties may have additional roles outside of palliative care. While not used frequently in CINV, it probably has a role in the management of patients who are refractory to other treatments. November 2011 (Version1.4) Page 15 of 23
16 Plan for next cycle North of England Cancer Network: CINV Guidelines Once adequate control has been achieved, focus can switch to careful planning for the next cycle of chemotherapy. This should include: Avoiding 'as required' scheduling Providing the most effective combination used to achieve control A rescue medication strategy in case loss of control occurs November 2011 (Version1.4) Page 16 of 23
17 Emetogenicity of Chemotherapy Single Agent Chemotherapy The individual emetogenicity of chemotherapy agents has been derived from Kris et al Americal Society of Clinical Oncology Guideline for Antiemetics in Oncology: Update Percentages refer to the level of risk if no anti-emetic cover is given at all. Carboplatin has been increased in emetogenicity on a consensus opinion of oncologists at the North of England Cancer Network Chemotherapy Group. Level 1: Minimal Risk (Less than 10%) Bevacizumab Bleomycin Busulphan Cladrabine Dasatinib Erlotinib Fludarabine Gefitinib Nilotinib Rituximab Sorafenib Level 2: Intermediate Risk (10 to 30%) Bortezomib Cetuximab Cabazitaxel* Cytarabine ( 1000mg/m²) Docetaxel* Etoposide Everolimus Level 3: Moderate Risk (30 to 90%) Azacitidine Bendamustine Carboplatin Clofarabine Cyclophosphamide (<1500mg/m²) Cytarabine > 1g/m² Daunorubicin Doxorubicin Fluorouracil Gemcitabine Lapatinib Lenalidomide Methotrexate Mitomycin (IV) Mitoxantrone Epirubicin Idarubicin Ifosfamide Imatinib Irinotecan Oxaliplatin Temozolomide Vinorelbine (Oral) Vinblastine Vincristine Vindesine Vinflunine Vinorelbine (IV) Paclitaxel* Pemetrexed* Sunitinib Tegafur Uracil Temsirolimus Topotecan Trastuzumab Moderate risk chemotherapy covers a wide range of emetogenic risk. Consideration should specifically be given to other risk factors for nausea & vomiting (See Page 9) Level 4: High Risk (> 90%) Carmustine Cisplatin Cyclophosphamide ( 1500mg/m²) Dacarbazine Dactinomycin Mechlorethamine Streptozocin *Patients receiving taxanes or pemetrexed should receive steroid cover for hypersensitivity reaction. November 2011 (Version1.4) Page 17 of 23
18 Combination Chemotherapy When assessing the emetogenicity of combination chemotherapy: 1. Identify the most emetogenic agent in the combination 2. For each drug with an emetogenic risk > 30% increase the emetogenicity by one level per drug 3. For all the drugs with an emetogenicity 10-30% the emetogenicity should be increased one level 4. For drugs with an emetogenicity < 10% no adjustment is necessary. Common Combinations Emetogenicity ABVD (Doxorubicin, Bleomycin, Vinblastine & Dacarbazine) Level 5 AC or EC (Doxorubicin or Epirubicin & Cyclophosphamide) Level 4 Carboplatin & Etoposide Level 4 Carboplatin & Gemcitabine Level 4 Carboplatin & Pemetrexed Level 4 CHOP (Cyclophosphamide, Doxorubicin, Vincristine) Level 4 Cisplatin & Etoposide Level 5 Cisplatin & Gemcitabine Level 4 Cisplatin & Pemetrexed Level 4 Cisplatin & Topotecan - Level 5 Cisplatin & Vinorelbine (IV) Level 4 CMF (Cyclophosphamide, Methotrextae & Fluorouracil) Level 4 CVP (Cyclophosphamide & Vincristine) Level 3 FC (Fludarabine & Cyclophosphamide) Level 3 FEC-100 (Fluorouracil, Epirubicin & Cyclophosphamide) Level 4 FMD (Fludarabine, Mitoxantrone & Dexamethasone) Level 2 FOLFIRI (Irinotecan & Infusional Fluorouracil) Level 4 FOLFOX (Oxaliplatin & Infusional Fluorouracil) Level 4 Modified de Grammont (Infusional Fluorouracil) Level 2 Paclitaxel & Gemcitabine Level 3 R-CHOP (Rituximab & Cyclophosphamide, Doxorubicin, Vincristine) Level 4 R-CVP (Rituximab & Cyclophosphamide & Vincristine) Level 3 XELOX (Oxaliplatin & Capecitabine) Level 4 November 2011 (Version1.4) Page 18 of 23
19 Suggested standard anti-emetics according to emetogenic risk. Level 1: Minimal Risk (Less than 10%) Pre-medication: No standard pre-medication normally required Level 2: Intermediate Risk (10 to 30%) Take Home Medication: No standard medication normally required. However, normally supply metoclopramide as a rescue measure with first cycle. Pre-medication: Dexamethasone 8mg IV or Oral Take Home Medication: No standard medication normally required. However, normally supply metoclopramide as a rescue measure with first cycle. Level 3: Moderate Risk (30 to 90%) Pre-medication: Dexamethasone 8mg IV or Oral Either Ondansetron 8mg IV / Oral Or Palonosetron** 0.25mg IV Take Home Medication: Dexamethasone up to 8mg Daily* Oral for 3 days Ondansetron 8mg Twice Daily Oral for 2 to 3 days (not given if using IV Palonosetron ) Metoclopramide 10-20mg TDS-QDS Oral for 3 days when required Level 4: High Risk (> 90%) Pre-medication: Dexamethasone 12mg IV or Oral Aprepitant*** 125mg Oral ( with risk factors) Either Ondansetron 8mg IV / Oral Or Palonosetron** 0.25mg IV Take Home Medication: Dexamethasone up to 8mg Daily* Oral for 2 to 3 days Aprepitant*** 80mg Daily Oral for 2 days Ondansetron 8mg Twice Daily Oral for 2 to 3 days (not given if using IV Palonosetron ) * for patients receiving pre-medication doses before 12pm, they should take a divided evening dose at 4pm on the night of chemotherapy. ** consider palonosetron where there is concern, i.e. patient has risk factors overrisk of delayed nausea and vomiting *** consider adding aprepitant where there is concern over risk of anti-emetic failure as identified by assessment of patient risk factorsalternative Agents or fosaprepitant 150mg intravenously on day 1 only (See Page 14) November 2011 (Version1.4) Page 19 of 23
20 5HT Antagonists Ondansetron 8mg (oral or IV) can be substituted with: - Granisetron 1mg (oral or IV) - Dolasetron 100mg (oral or IV) - Tropisetron 5mg (oral or IV) - Polanosetron 250micrograms IV (no oral required). Steroids Patients with another steroid component in their chemotherapy regimen (eg CHOP) should not normally receive additional dexamethasone. However, as most other steroids are less effective at crossing the blood brain barrier, an alternative anti-emetic agent (as for managing break through emesis: Page 8) should be added as a substitute. The same applies for patients where use of a steroid is undesirable e.g. patients with diabetes. Metoclopramide Prochloperazine 10mg every 4-6 hours as required or Cyclizine 50mg TDS can be substituted. November 2011 (Version1.4) Page 20 of 23
21 Credits & Acknowledgments This document has been developed after consultation of the following guidelines: Guideline update for MASCC and ESMO in the prevention of chemotherapy and radiotherapyinduced nausea and vomiting: results of the Perugia consensus conference. F. Roila, J. Herrstedt, M. Aapro, R.J. Gralla, et al., Annals of Oncology 21 (Supplement 5): v232 - v243, 2010 Available at NCCN Guidelines for Anti-emesis. Version available from: Kris MG, et al. American Society of Clinical Oncology Guideline for Antiemetics in Oncology: Update J Clin Oncol. 2006; 18: In addition, thanks are due to Denise Blake, Paediatric Oncology Pharmacist Newcastle Hospitals Foundation NHS Trust, upon who's paediatric guidelines some of this content has been derived. November 2011 (Version1.4) Page 21 of 23
22 References 1. Osoba D, Zee B, Pater J, et al. Determinants of post-chemotherapy nausea and Vomiting in patients with cancer. J Clin Oncol 1997; 15: Doherty KM. Closing the gap in prophylactic antiemetic therapy: patient factors in calculating the emetogenic potential of chemotherapy. Clin J Oncol Nurs 1999; 3: D'Acquisto R, Tyson LB, Gralla RJ, et al. 4. Hesketh, PJ et al A proposal for classifying the acute emetogenicity of cancer chemotherapy. J Clin Oncol. 1997; 15: Grunberg SM, et al Evaluation of new anti-emetic agents and definition of anti-neoplastic agent emetogenicity and update. Support Care Cancer 2005; 13: 80-4 Document Title: Document No: CHEMO 001 Author: Approved by: Due for Review: Summary of Changes Document Control Chemotherapy Induced Nausea Vomitting CINV 1.4- Antiemetic Guidelines NECN nov 2011 Calum Polwart, Network Pharmacist Chemotherapy Group November 2013 Current Version: Approval Signature* Date Approved: 1.1a Minor amendments per chemo group. 1.2a 1.4 Chairs Action Nov st Nov 2011 Added missing cross references. Added radiotherapy increased emetogenicty & reduced emetogenicity of carboplatin. 1.3 Updated guidance to reflect agreed changes to policy regarding dose of dexamethasone and NECDAG approval of aprepitant and palonosetron to match MASCC, ASCO and NCCN guidelines. Added antiemetic ladder as an appendix. 1.4 Updated format, added fosaprepitant and reference to MASSC 2010 guidelines updated table of emetogenicty November 2011 (Version1.4) Page 22 of 23
23 November 2011 (Version1.4) Page 23 of 23 North of England Cancer Network: CINV Guidelines
MASCC/ESMO Antiemetic Guideline 2013
 MASCC/ESMO Antiemetic Guideline 2013 Multinational Association of Supportive Care in Cancer Organizing and Overall Meeting Chairs: Richard J. Gralla, MD Fausto Roila, MD Maurizio Tonato, MD Jørn Herrstedt,
MASCC/ESMO Antiemetic Guideline 2013 Multinational Association of Supportive Care in Cancer Organizing and Overall Meeting Chairs: Richard J. Gralla, MD Fausto Roila, MD Maurizio Tonato, MD Jørn Herrstedt,
Guidelines for the Management of. Nausea and Vomiting in Cancer Patients
 Guidelines for the Management of Nausea and Vomiting in Cancer Patients Guidelines for the Management of Nausea and Vomiting in Cancer Patients Management of chemotherapy-induced nausea and vomiting includes
Guidelines for the Management of Nausea and Vomiting in Cancer Patients Guidelines for the Management of Nausea and Vomiting in Cancer Patients Management of chemotherapy-induced nausea and vomiting includes
Antiemetic Guidelines for Adult Patients Receiving Chemotherapy and Radiotherapy
 Antiemetic Guidelines f Adult Patients Receiving Chemotherapy and Radiotherapy Produced by Pinkie Chambers and Susanna Daniels University College Hospital NHS Foundation Trust November 2010 (Review date
Antiemetic Guidelines f Adult Patients Receiving Chemotherapy and Radiotherapy Produced by Pinkie Chambers and Susanna Daniels University College Hospital NHS Foundation Trust November 2010 (Review date
Chemotherapy Induced Nausea & Vomiting
 Chemotherapy Induced Nausea & Vomiting A Nurse s Perspective Michael Flynn MSc, PG Cert, RGN Chemotherapy Nurse Consultant Guy s and St Thomas NHS Foundation Trust Guy s and St Thomas NHS Foundation Trust
Chemotherapy Induced Nausea & Vomiting A Nurse s Perspective Michael Flynn MSc, PG Cert, RGN Chemotherapy Nurse Consultant Guy s and St Thomas NHS Foundation Trust Guy s and St Thomas NHS Foundation Trust
Guidelines for Prevention and Treatment of Chemotherapy-Induced Nausea and Vomiting in Adults
 Guidelines for Prevention and Treatment of Chemotherapy-Induced Nausea and Vomiting in Adults Protocol Code Tumour group Physician Contact SCNAUSEA SUPPORTIVE CARE Dr. Paul Hoskins ELIGIBILITY Adults receiving
Guidelines for Prevention and Treatment of Chemotherapy-Induced Nausea and Vomiting in Adults Protocol Code Tumour group Physician Contact SCNAUSEA SUPPORTIVE CARE Dr. Paul Hoskins ELIGIBILITY Adults receiving
Preventing and Treating Nausea and Vomiting Caused by Cancer Treatment
 A Patient s Guide Preventing and Treating Nausea and Vomiting Caused by Cancer Treatment Recommendations of the American Society of Clinical Oncology The American Society of Clinical Oncology (ASCO) is
A Patient s Guide Preventing and Treating Nausea and Vomiting Caused by Cancer Treatment Recommendations of the American Society of Clinical Oncology The American Society of Clinical Oncology (ASCO) is
Delayed emesis: moderately emetogenic chemotherapy
 Support Care Cancer (2005) 13:104 108 DOI 10.1007/s00520-004-0700-8 R E V I E W A R T I C L E Fausto Roila David Warr Rebecca A. Clark-Snow Maurizio Tonato Richard J. Gralla Lawrence H. Einhorn Jorn Herrstedt
Support Care Cancer (2005) 13:104 108 DOI 10.1007/s00520-004-0700-8 R E V I E W A R T I C L E Fausto Roila David Warr Rebecca A. Clark-Snow Maurizio Tonato Richard J. Gralla Lawrence H. Einhorn Jorn Herrstedt
11. CANCER PAIN AND PALLIATION. Jennifer Reifel, M.D.
 11. CANCER PAIN AND PALLIATION Jennifer Reifel, M.D. While supportive care was not one of the original clinical areas selected for the development of quality indicators, the Oncology and HIV Panel felt
11. CANCER PAIN AND PALLIATION Jennifer Reifel, M.D. While supportive care was not one of the original clinical areas selected for the development of quality indicators, the Oncology and HIV Panel felt
Hydration, IV Infusions, Injections and Vaccine Charge Process
 There are a number of items to be considered when billing for the Nursing service to perform drug therapy, the charge process is divided into three specific groups of codes and processes. 1. Hydration
There are a number of items to be considered when billing for the Nursing service to perform drug therapy, the charge process is divided into three specific groups of codes and processes. 1. Hydration
BREAST CANCER - METASTATIC & LOCALLY ADVANCED CHEMOTHERAPY REGIMENS Capecitabine. Capecitabine + Docetaxel. Capecitabine + Vinorelbine
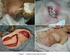 Capecitabine Capecitabine 1000-1250mg/m 2 oral TWICE daily for 14 days Until disease progression Capecitabine + Docetaxel Capecitabine 750-1000mg/m 2 oral TWICE daily for 14 days Up to 6 cycles Capecitabine
Capecitabine Capecitabine 1000-1250mg/m 2 oral TWICE daily for 14 days Until disease progression Capecitabine + Docetaxel Capecitabine 750-1000mg/m 2 oral TWICE daily for 14 days Up to 6 cycles Capecitabine
The N Factor: Prevention & Treatment of Chemotherapy-Induced Nausea & Vomiting
 The N Factor: Prevention & Treatment of Chemotherapy-Induced Nausea & Vomiting 45 TH ANNUAL GREAT LAKES CANCER NURSING CONFERENCE SOMERSET INN, TROY, MICHIGAN OCTOBER 2012 JOANNE P. MCGURN, BS PHARM, BCOP
The N Factor: Prevention & Treatment of Chemotherapy-Induced Nausea & Vomiting 45 TH ANNUAL GREAT LAKES CANCER NURSING CONFERENCE SOMERSET INN, TROY, MICHIGAN OCTOBER 2012 JOANNE P. MCGURN, BS PHARM, BCOP
Objectives PREVENTION AND TREATMENT OF CINV & VTE IN ONCOLOGY PATIENTS. Case 1. Case 1. Case 2 2/1/2015
 Objectives PREVENTION AND TREATMENT OF CINV & VTE IN ONCOLOGY PATIENTS Jennifer Gallanger, Pharm.D. Jennifer Kubert, Pharm.D. Pharmacy Practice Residents Providence Alaska Medical Center Discuss the pathophysiology
Objectives PREVENTION AND TREATMENT OF CINV & VTE IN ONCOLOGY PATIENTS Jennifer Gallanger, Pharm.D. Jennifer Kubert, Pharm.D. Pharmacy Practice Residents Providence Alaska Medical Center Discuss the pathophysiology
MOH Policy for dispensing NEOPLASTIC DISEASES DRUGS
 MOH Policy for dispensing NEOPLASTIC DISEASES DRUGS All prescriptions for antineoplastic drugs must be accompanied by the MOH special form. All the attachments mentioned on this form shall be submitted
MOH Policy for dispensing NEOPLASTIC DISEASES DRUGS All prescriptions for antineoplastic drugs must be accompanied by the MOH special form. All the attachments mentioned on this form shall be submitted
Published Ahead of Print on September 26, 2011 as 10.1200/JCO.2010.34.4614. J Clin Oncol 29. 2011 by American Society of Clinical Oncology
 Published Ahead of Print on September 26, 2011 as 10.1200/JCO.2010.34.4614 The latest version is at http://jco.ascopubs.org/cgi/doi/10.1200/jco.2010.34.4614 JOURNAL OF CLINICAL ONCOLOGY A S C O S P E C
Published Ahead of Print on September 26, 2011 as 10.1200/JCO.2010.34.4614 The latest version is at http://jco.ascopubs.org/cgi/doi/10.1200/jco.2010.34.4614 JOURNAL OF CLINICAL ONCOLOGY A S C O S P E C
MASCC/ESMO ANTIEMETIC GUIDELINE 2016
 1 MASCC/ESMO ANTIEMETIC GUIDELINE 2016 Multinational Association of Supportive Care in Cancer Organizing and Overall Meeting Chairs: Matti Aapro, MD Richard J. Gralla, MD Jørn Herrstedt, MD, DMSci Alex
1 MASCC/ESMO ANTIEMETIC GUIDELINE 2016 Multinational Association of Supportive Care in Cancer Organizing and Overall Meeting Chairs: Matti Aapro, MD Richard J. Gralla, MD Jørn Herrstedt, MD, DMSci Alex
Chapter 7: Lung Cancer
 Chapter 7: Lung Cancer Contents Chapter 7: Lung Cancer... 1 Small Cell... 2 Good PS + Limited stage... 2 Cisplatin/etoposide... 2 Concurrent chemotherapy + XRT... 2 Good / Intermediate PS... 2 Carboplatin
Chapter 7: Lung Cancer Contents Chapter 7: Lung Cancer... 1 Small Cell... 2 Good PS + Limited stage... 2 Cisplatin/etoposide... 2 Concurrent chemotherapy + XRT... 2 Good / Intermediate PS... 2 Carboplatin
Nausea and Vomiting. Understanding nausea and vomiting. What causes nausea and vomiting in people with cancer?
 Nausea and Vomiting Understanding nausea and vomiting Nausea is a subjective unpleasant feeling in the back of your throat and stomach that may lead to vomiting. There are many words that describe nausea
Nausea and Vomiting Understanding nausea and vomiting Nausea is a subjective unpleasant feeling in the back of your throat and stomach that may lead to vomiting. There are many words that describe nausea
Texas Medicaid/CHIP Vendor Drug Program Drug Utilization Criteria For Outpatient Use Guidelines
 About Information on indications for use or diagnosis is assumed to be unavailable. All criteria may be applied retrospectively; prospective application is indicated with an asterisk [*]. The information
About Information on indications for use or diagnosis is assumed to be unavailable. All criteria may be applied retrospectively; prospective application is indicated with an asterisk [*]. The information
Cycle frequency: Every four weeks Total number of cycles: 6-8
 Fludarabine Low Grade non-hodgkin s Lymphoma and CLL Fludarabine 25mg/m 2 oral Days 1-5 Cycle frequency: Every four weeks Total number of cycles: 6-8 Anti-emetic group Low Prophylactic co-trimoxazole and
Fludarabine Low Grade non-hodgkin s Lymphoma and CLL Fludarabine 25mg/m 2 oral Days 1-5 Cycle frequency: Every four weeks Total number of cycles: 6-8 Anti-emetic group Low Prophylactic co-trimoxazole and
Schedule: Drug Dose iv/infusion/oral q Carboplatin AUC 5 500mls 5% dex/1hr Day 1 Gemcitabine 1200mg/m 2 200mls N. Saline/30mins Days 1 & 8
 Carboplatin/Gemcitabine Lung Cancer (non-small cell) - Advanced Carboplatin AUC 5 500mls 5% dex/1hr Day 1 Gemcitabine 1200mg/m 2 200mls N. Saline/30mins Days 1 & 8 Cycle frequency: Every three weeks Total
Carboplatin/Gemcitabine Lung Cancer (non-small cell) - Advanced Carboplatin AUC 5 500mls 5% dex/1hr Day 1 Gemcitabine 1200mg/m 2 200mls N. Saline/30mins Days 1 & 8 Cycle frequency: Every three weeks Total
Cycle frequency: Every three weeks Total number of cycles: 3 or 4
 BEP 3-day (Bleomycin/Etoposide/Cisplatin) Germ cell tumours Bleomycin 30,000iu 200mls N. Saline/30mins Days 2, 8 & 15 Etoposide 165mg/m 2 1L N. Saline/1hr Days 1, 2 & 3 Cisplatin 50mg/m 2 1L N. Saline/4hrs
BEP 3-day (Bleomycin/Etoposide/Cisplatin) Germ cell tumours Bleomycin 30,000iu 200mls N. Saline/30mins Days 2, 8 & 15 Etoposide 165mg/m 2 1L N. Saline/1hr Days 1, 2 & 3 Cisplatin 50mg/m 2 1L N. Saline/4hrs
Cost Differences in Cancer Care Across Settings
 Cost Differences in Cancer Care Across Settings August 2013 THE MORAN COMPANY 1 Cost Differences in Cancer Care Across Settings In a prior memorandum, we presented evidence documenting the growing share
Cost Differences in Cancer Care Across Settings August 2013 THE MORAN COMPANY 1 Cost Differences in Cancer Care Across Settings In a prior memorandum, we presented evidence documenting the growing share
Implications of dose rounding intravenous chemotherapy at a community based hospital
 Implications of dose rounding intravenous chemotherapy at a community based hospital 1 2 ABSTRACT OBJECTIVES: To quantify and evaluate the total number of pharmacist interventions completed for dose rounding
Implications of dose rounding intravenous chemotherapy at a community based hospital 1 2 ABSTRACT OBJECTIVES: To quantify and evaluate the total number of pharmacist interventions completed for dose rounding
MEDICAL CENTER ADMINISTRATIVE POLICY AND PROCEDURES SCOPE KFH Hospital, City Section No.
 of 22 I. Purpose To establish safe medication practices for High Alert medications to maximize the safety of the medication processes associated with these medications. II. Policy. High alert medications
of 22 I. Purpose To establish safe medication practices for High Alert medications to maximize the safety of the medication processes associated with these medications. II. Policy. High alert medications
NURSING RESEARCH IMPORTANT POINTS COMPONENTS COMPONENTS. Proposed timeline Consent/ protection of human
 NURSING RESEARCH Implementation of a Chemotherapy-Induced Nausea and Vomiting Clinical Pathway for Moderate-high to Highly Emetogenic Chemotherapies A Nursing Research Project 2/01/2014 3/31/2015 PURPOSE:
NURSING RESEARCH Implementation of a Chemotherapy-Induced Nausea and Vomiting Clinical Pathway for Moderate-high to Highly Emetogenic Chemotherapies A Nursing Research Project 2/01/2014 3/31/2015 PURPOSE:
Cycle frequency: Every three weeks Total number of cycles: 6
 Carboplatin/Paclitaxel Ovarian Cancer Adjuvant, Advanced Paclitaxel 175mg/m 2 500mls 5% dex/3hrs Day 1 Carboplatin AUC 5 500mls 5% dex/1hr Day 1 Anti-emetic group - Moderately high Paclitaxel given first
Carboplatin/Paclitaxel Ovarian Cancer Adjuvant, Advanced Paclitaxel 175mg/m 2 500mls 5% dex/3hrs Day 1 Carboplatin AUC 5 500mls 5% dex/1hr Day 1 Anti-emetic group - Moderately high Paclitaxel given first
Applying the Principles of Antiemetic Therapy to the Management of CINV: A Case-study Approach
 Applying the Principles of Antiemetic Therapy to the Management of CINV: A Case-study Approach Applying the Principles of Antiemetic Therapy to the Management of CINV: A Case-study Approach Program Agenda
Applying the Principles of Antiemetic Therapy to the Management of CINV: A Case-study Approach Applying the Principles of Antiemetic Therapy to the Management of CINV: A Case-study Approach Program Agenda
Medications most likely to be seen in primary care
 Hazardous Medicines The majority of medicines are not classed as hazardous. The only medicinal products that are automatically deemed to be hazardous are cytotoxic and cytostatic medicines. There is no
Hazardous Medicines The majority of medicines are not classed as hazardous. The only medicinal products that are automatically deemed to be hazardous are cytotoxic and cytostatic medicines. There is no
END OF LIFE MEDICINES INFORMATION PACK
 END OF LIFE MEDICINES INFORMATION PACK Advice on end of life medication is available from the nursing and medical team at St Nicholas Hospice Care - telephone 01284 766133. Many drugs used in palliative
END OF LIFE MEDICINES INFORMATION PACK Advice on end of life medication is available from the nursing and medical team at St Nicholas Hospice Care - telephone 01284 766133. Many drugs used in palliative
Avastin in breast cancer: Summary of clinical data
 Avastin in breast cancer: Summary of clinical data Worldwide, over one million people are diagnosed with breast cancer every year 1. It is the most frequently diagnosed cancer in women 1,2, and the leading
Avastin in breast cancer: Summary of clinical data Worldwide, over one million people are diagnosed with breast cancer every year 1. It is the most frequently diagnosed cancer in women 1,2, and the leading
BCCA Protocol Summary for Advanced Therapy for Relapsed Testicular Germ Cell Cancer Using PACLitaxel, Ifosfamide and CISplatin (TIP)
 BCCA Protocol Summary for Advanced Therapy for Relapsed Testicular Germ Cell Cancer Using PACLitaxel, Ifosfamide and CISplatin (TIP) Protocol Code Tumour Group Contact Physician UGUTIP Genitourinary Dr.
BCCA Protocol Summary for Advanced Therapy for Relapsed Testicular Germ Cell Cancer Using PACLitaxel, Ifosfamide and CISplatin (TIP) Protocol Code Tumour Group Contact Physician UGUTIP Genitourinary Dr.
Lung Pathway Group Pemetrexed and Cisplatin in Non-Small Cell Lung Cancer (NSCLC)
 Indication: NICE TA181 First line treatment option in advanced or metastatic non-squamous NSCLC (histology confirmed as adenocarcinoma or large cell carcinoma) Performance status 0-1 Regimen details: Pemetrexed
Indication: NICE TA181 First line treatment option in advanced or metastatic non-squamous NSCLC (histology confirmed as adenocarcinoma or large cell carcinoma) Performance status 0-1 Regimen details: Pemetrexed
Network Chemotherapy Regimens
 Network Chemotherapy Regimens Lung Cancer Notes from the editor Thames Valley Cancer Network These protocols are available on the Network website www.tvcn.org.uk. Any correspondence about the protocols
Network Chemotherapy Regimens Lung Cancer Notes from the editor Thames Valley Cancer Network These protocols are available on the Network website www.tvcn.org.uk. Any correspondence about the protocols
I will be having surgery and radiation treatment for breast cancer. Do I need drug treatment too?
 What is node-positive breast cancer? Node-positive breast cancer means that cancer cells from the tumour in the breast have been found in the lymph nodes (sometimes called glands ) in the armpit area.
What is node-positive breast cancer? Node-positive breast cancer means that cancer cells from the tumour in the breast have been found in the lymph nodes (sometimes called glands ) in the armpit area.
Docetaxel + Carboplatin + Trastuzumab (TCH) Adjuvant Breast Cancer
 Docetaxel + Carboplatin + Trastuzumab (TCH) Adjuvant Breast Cancer Background: A non-anthracycline based regimen for high-risk, HER 2 positive breast cancer in the adjuvant setting (BCIRG 006). Patient
Docetaxel + Carboplatin + Trastuzumab (TCH) Adjuvant Breast Cancer Background: A non-anthracycline based regimen for high-risk, HER 2 positive breast cancer in the adjuvant setting (BCIRG 006). Patient
Optimizing Care for the Individual with Cancer: Counseling Patients and Families on Cancer Treatment
 Optimizing Care for the Individual with Cancer: Counseling Patients and Families on Cancer Treatment Rowena Schwartz, Pharm.D., BCOP Evaluating Care Opportunities HB is a 57 year old male with newly diagnosed
Optimizing Care for the Individual with Cancer: Counseling Patients and Families on Cancer Treatment Rowena Schwartz, Pharm.D., BCOP Evaluating Care Opportunities HB is a 57 year old male with newly diagnosed
Your A-Z of coping with nausea and vomiting A guide for patients and their carers. We care, we discover, we teach
 Your A-Z of coping with nausea and vomiting A guide for patients and their carers We care, we discover, we teach Contents What is this guide about?.... 1 What causes nausea and vomiting?... 1 Some common
Your A-Z of coping with nausea and vomiting A guide for patients and their carers We care, we discover, we teach Contents What is this guide about?.... 1 What causes nausea and vomiting?... 1 Some common
Thames Valley Chemotherapy Regimens
 Chemotherapy Regimens Lung Cancer Notes from the editor These regimens are available on the Network website www.tvcn.org.uk. Any correspondence about the regimens should be addressed to: Sally Coutts,
Chemotherapy Regimens Lung Cancer Notes from the editor These regimens are available on the Network website www.tvcn.org.uk. Any correspondence about the regimens should be addressed to: Sally Coutts,
Breast Cancer. Breast Cancer Page 1
 Breast Cancer Summary Breast cancers which are detected early are curable by local treatments. The initial surgery will give the most information about the cancer; such as size or whether the glands (or
Breast Cancer Summary Breast cancers which are detected early are curable by local treatments. The initial surgery will give the most information about the cancer; such as size or whether the glands (or
Thames Valley Cancer Network. Network Chemotherapy Protocols Breast Cancer
 Network Chemotherapy Protocols Breast Cancer Notes from the editor Thames Valley Cancer Network These protocols are available on the Network website www.tvcn.nhs.uk. Any correspondence about the protocols
Network Chemotherapy Protocols Breast Cancer Notes from the editor Thames Valley Cancer Network These protocols are available on the Network website www.tvcn.nhs.uk. Any correspondence about the protocols
1 What Zofran Solution for Injection or Infusion is and what it is used
 GlaxoSmithKline (logo) Package Leaflet: Information for the User Zofran 4 mg/2 ml (or 8mg/4 ml) Solution for Injection or Infusion ondansetron (as hydrochloride dihydrate) Read all of this leaflet carefully
GlaxoSmithKline (logo) Package Leaflet: Information for the User Zofran 4 mg/2 ml (or 8mg/4 ml) Solution for Injection or Infusion ondansetron (as hydrochloride dihydrate) Read all of this leaflet carefully
About chemotherapy for lung cancer
 About chemotherapy for lung cancer This information is about chemotherapy for lung cancer. There are sections on What is chemotherapy? Chemotherapy for small cell lung cancer Chemotherapy for non-small
About chemotherapy for lung cancer This information is about chemotherapy for lung cancer. There are sections on What is chemotherapy? Chemotherapy for small cell lung cancer Chemotherapy for non-small
Small cell Lung cancer New Chemotherapy options. Nicolas Mach, MD,PD
 Small cell Lung cancer New Chemotherapy options Nicolas Mach, MD,PD > 40 negative Phase III trials List of unsucessful drugs Pemetrexed, imatinib, bevacizumab, bcl-2 antagonist, ASCT, CASE PRESENTATION
Small cell Lung cancer New Chemotherapy options Nicolas Mach, MD,PD > 40 negative Phase III trials List of unsucessful drugs Pemetrexed, imatinib, bevacizumab, bcl-2 antagonist, ASCT, CASE PRESENTATION
West of Scotland Cancer Network Chemotherapy Protocol. Cisplatin and Pemetrexed for Malignant Mesothelioma (LUWOS 0021)
 West of Scotland Cancer Network Chemotherapy Protocol Cisplatin and Pemetrexed for Malignant Mesothelioma (LUWOS 0021) Indication Palliative chemotherapy for malignant mesothelioma of the pleura Eligibility
West of Scotland Cancer Network Chemotherapy Protocol Cisplatin and Pemetrexed for Malignant Mesothelioma (LUWOS 0021) Indication Palliative chemotherapy for malignant mesothelioma of the pleura Eligibility
Schedule: Drug Dose iv/infusion/oral q Doxorubicin 25mg/m 2 iv bolus Days 1, 2 & 3 Cisplatin 50mg/m 2 1L N. Saline/2hrs Days 1 & 2
 Doxorubicin/Cisplatin Osteosarcoma - neoadjuvant Doxorubicin 25mg/m 2 iv bolus Days 1, 2 & 3 Cisplatin 50mg/m 2 1L N. Saline/2hrs Days 1 & 2 (3 before surgery) Ensure adequate renal function Pre & post-hydration,
Doxorubicin/Cisplatin Osteosarcoma - neoadjuvant Doxorubicin 25mg/m 2 iv bolus Days 1, 2 & 3 Cisplatin 50mg/m 2 1L N. Saline/2hrs Days 1 & 2 (3 before surgery) Ensure adequate renal function Pre & post-hydration,
2014-06-10 Approved Bendamustine - Treatment of relapsed low grade NHL in patients unable to receive standard therapy 2014-05-
 Sub. Sub. Status -06-16 Approved Lenalidomide - 2nd line treatment of multiple myeloma in patients who have contraindications to the use of bortezomib -06-16 Approved Lenalidomide - 2nd line treatment
Sub. Sub. Status -06-16 Approved Lenalidomide - 2nd line treatment of multiple myeloma in patients who have contraindications to the use of bortezomib -06-16 Approved Lenalidomide - 2nd line treatment
CHEMOTHERAPY PROTOCOLS V10.1
 CHEMOTHERAPY PROTOCOLS V10.1 Issue Date: 10 th July 2014 Page 1 of 42 Filename: MCHACPROTO Issue No: 10.1 CCC Chemotherapy Protocols Haematological Malignancies... 3 Hodgkins disease...3 Non-Hodgkins Lymphoma...5
CHEMOTHERAPY PROTOCOLS V10.1 Issue Date: 10 th July 2014 Page 1 of 42 Filename: MCHACPROTO Issue No: 10.1 CCC Chemotherapy Protocols Haematological Malignancies... 3 Hodgkins disease...3 Non-Hodgkins Lymphoma...5
Prior Authorization Guideline
 Prior Authorization Guideline Guideline: PS Inj - Velcade Therapeutic Class: Antineoplastic Agents Therapeutic Sub-Class: Antineoplastic Client: PS Inj Approval Date: 10/2/2004 Revision Date: 5/22/2007
Prior Authorization Guideline Guideline: PS Inj - Velcade Therapeutic Class: Antineoplastic Agents Therapeutic Sub-Class: Antineoplastic Client: PS Inj Approval Date: 10/2/2004 Revision Date: 5/22/2007
Scottish Medicines Consortium
 Scottish Medicines Consortium pemetrexed 500mg infusion (Alimta ) No. (192/05) Eli Lilly 8 July 2005 The Scottish Medicines Consortium has completed its assessment of the above product and advises NHS
Scottish Medicines Consortium pemetrexed 500mg infusion (Alimta ) No. (192/05) Eli Lilly 8 July 2005 The Scottish Medicines Consortium has completed its assessment of the above product and advises NHS
The Pharmacological Management of Cancer Pain in Adults. Clinical Audit Tool
 The Pharmacological Management of Cancer Pain in Adults Clinical Audit Tool 2015 This clinical audit tool accompanies the Pharmacological Management of Cancer Pain in Adults NCEC National Clinical Guideline
The Pharmacological Management of Cancer Pain in Adults Clinical Audit Tool 2015 This clinical audit tool accompanies the Pharmacological Management of Cancer Pain in Adults NCEC National Clinical Guideline
Treatment of Small Cell Lung Cancer
 Chapter 5 Treatment of Small Cell Lung Cancer Ariel Lopez-Chavez MD, MS Introduction There are two main types of lung cancer, non-small cell lung cancer and small cell lung cancer. 1 It is important that
Chapter 5 Treatment of Small Cell Lung Cancer Ariel Lopez-Chavez MD, MS Introduction There are two main types of lung cancer, non-small cell lung cancer and small cell lung cancer. 1 It is important that
National Horizon Scanning Centre. Vandetanib (Zactima) for advanced or metastatic non-small cell lung cancer. December 2007
 Vandetanib (Zactima) for advanced or metastatic non-small cell lung cancer December 2007 This technology summary is based on information available at the time of research and a limited literature search.
Vandetanib (Zactima) for advanced or metastatic non-small cell lung cancer December 2007 This technology summary is based on information available at the time of research and a limited literature search.
Hydration Protocol for Cisplatin Chemotherapy
 Betsi Cadwaladr University Health Version: 1.3 CSPM2 Hydration Protocol for Cisplatin Chemotherapy Date to be reviewed: July 2018 No of pages: 9 Author(s): Tracy Parry-Jones Author(s) title: Lead Cancer
Betsi Cadwaladr University Health Version: 1.3 CSPM2 Hydration Protocol for Cisplatin Chemotherapy Date to be reviewed: July 2018 No of pages: 9 Author(s): Tracy Parry-Jones Author(s) title: Lead Cancer
Out-Patient Chemotherapy for Lung Cancer
 Lung Cancer Out-Patient Chemotherapy for Lung Cancer Principles and practice JMAJ 46(12): 542 546, 2003 Shuichi YONEDA Director, Department of Pulmonary Medicine, Saitama Cancer Center Abstract: Recent
Lung Cancer Out-Patient Chemotherapy for Lung Cancer Principles and practice JMAJ 46(12): 542 546, 2003 Shuichi YONEDA Director, Department of Pulmonary Medicine, Saitama Cancer Center Abstract: Recent
Treating myeloma. Dr Rachel Hall Royal Bournemouth Hospital
 Treating myeloma Dr Rachel Hall Royal Bournemouth Hospital Treatment overview When to treat? Aim of treatment Which treatment? Monitoring response to treatment Prevention of complications What happens
Treating myeloma Dr Rachel Hall Royal Bournemouth Hospital Treatment overview When to treat? Aim of treatment Which treatment? Monitoring response to treatment Prevention of complications What happens
Breast Pathway Group FEC 60 (Fluorouracil / Epirubicin / Cyclophosphamide) in Early Breast Cancer in Elderly / Frail
 Breast Pathway Group FEC 60 (Fluorouracil / Epirubicin / Cyclophosphamide) in Early Breast Cancer in Elderly / Frail Indication: Neoadjuvant or adjuvant therapy for elderly and frail patients with breast
Breast Pathway Group FEC 60 (Fluorouracil / Epirubicin / Cyclophosphamide) in Early Breast Cancer in Elderly / Frail Indication: Neoadjuvant or adjuvant therapy for elderly and frail patients with breast
West of Scotland Cancer Network Systemic Anti-Cancer Therapy Protocol
 West of Scotland Cancer Network Systemic Anti-Cancer Therapy Protocol FEC-DH in the adjuvant treatment of Breast Cancer (BRWOS- 031/1) Indication Adjuvant chemotherapy for HER2+ve Early Breast Cancer Eligibility
West of Scotland Cancer Network Systemic Anti-Cancer Therapy Protocol FEC-DH in the adjuvant treatment of Breast Cancer (BRWOS- 031/1) Indication Adjuvant chemotherapy for HER2+ve Early Breast Cancer Eligibility
1 PRACTICAL ISSUES IN CYTOTOXIC
 1 PRACTICAL ISSUES IN CYTOTOXIC CHEMOTHERAPY USAGE Introduction Inthischapter, theprinciplesofcytotoxicchemotherapy treatment and the appropriate use of anticancer drugs, including some of the new targeted
1 PRACTICAL ISSUES IN CYTOTOXIC CHEMOTHERAPY USAGE Introduction Inthischapter, theprinciplesofcytotoxicchemotherapy treatment and the appropriate use of anticancer drugs, including some of the new targeted
Chemotherapy for lung cancer
 This information is an extract from the booklet Understanding lung cancer. You may find the full booklet helpful. We can send you a free copy see page 8. Contents Chemoradiation Small cell lung cancer
This information is an extract from the booklet Understanding lung cancer. You may find the full booklet helpful. We can send you a free copy see page 8. Contents Chemoradiation Small cell lung cancer
Cytotoxic Therapy in Metastatic Breast Cancer
 Diagnosis and Treatment of Patients with Primary and Metastatic Breast Cancer Cytotoxic Therapy in Metastatic Breast Cancer Cytotoxic Therapy in Metastatic Breast Cancer Version 2002: von Minckwitz Versions
Diagnosis and Treatment of Patients with Primary and Metastatic Breast Cancer Cytotoxic Therapy in Metastatic Breast Cancer Cytotoxic Therapy in Metastatic Breast Cancer Version 2002: von Minckwitz Versions
Treatment strategies for breast cancer
 THE ONCOLOGY NURSE S ROLE IN THE CARE OF PATIENTS WITH BREAST CANCER * Carol S. Viele, RN, MS, CNS ABSTRACT Oncology nurses play a central role in the recognition and management of adverse events that
THE ONCOLOGY NURSE S ROLE IN THE CARE OF PATIENTS WITH BREAST CANCER * Carol S. Viele, RN, MS, CNS ABSTRACT Oncology nurses play a central role in the recognition and management of adverse events that
for Extended Stability Parenteral Drugs Third Edition Caryn M. Bing, R.Ph., M.S., FASHP Editor
 Extended Stability for Parenteral Drugs Third Edition Editor Caryn M. Bing, R.Ph., M.S., FASHP 1 American Society of Health-System Pharmacists Bethesda, Maryland Contents Preface Acknowledgments x/ Dedication
Extended Stability for Parenteral Drugs Third Edition Editor Caryn M. Bing, R.Ph., M.S., FASHP 1 American Society of Health-System Pharmacists Bethesda, Maryland Contents Preface Acknowledgments x/ Dedication
Docetaxel, Carboplatin and Trastuzumab (TCH i.e. Taxotere Carboplatin, Herceptin ) for Early Breast Cancer
 Regimen: Docetaxel, Carboplatin and Trastuzumab (TCH i.e. Taxotere Carboplatin, Herceptin ) for Early Breast Cancer Indication Approved for the treatment of early and locally advanced breast cancer in
Regimen: Docetaxel, Carboplatin and Trastuzumab (TCH i.e. Taxotere Carboplatin, Herceptin ) for Early Breast Cancer Indication Approved for the treatment of early and locally advanced breast cancer in
CHEMOTHERAPY FOR ADVANCED UROTHELIAL CANCER OF THE BLADDER. Walter Stadler, MD University of Chicago
 CHEMOTHERAPY FOR ADVANCED UROTHELIAL CANCER OF THE BLADDER Walter Stadler, MD University of Chicago Chemotherapy Doctor Terms Drugs used to treat cancer Will attack cancer no matter where it is located
CHEMOTHERAPY FOR ADVANCED UROTHELIAL CANCER OF THE BLADDER Walter Stadler, MD University of Chicago Chemotherapy Doctor Terms Drugs used to treat cancer Will attack cancer no matter where it is located
Avastin in breast cancer: Summary of clinical data
 Avastin in breast cancer: Summary of clinical data Worldwide, over one million people are diagnosed with breast cancer every year 1. It is the most frequently diagnosed cancer in women 1,2, and the leading
Avastin in breast cancer: Summary of clinical data Worldwide, over one million people are diagnosed with breast cancer every year 1. It is the most frequently diagnosed cancer in women 1,2, and the leading
Treatment of low-grade non-hodgkin lymphoma
 Produced 28.02.2011 Due for revision 28.02.2013 Treatment of low-grade non-hodgkin lymphoma Lymphomas are described as low grade if the cells appear to be dividing slowly. There are several kinds of low-grade
Produced 28.02.2011 Due for revision 28.02.2013 Treatment of low-grade non-hodgkin lymphoma Lymphomas are described as low grade if the cells appear to be dividing slowly. There are several kinds of low-grade
Analysis of Costs Associated With Administration of Intravenous Single-Drug Therapies in Metastatic Breast Cancer in a U.S.
 RESEARCH Analysis of Associated With Administration of Intravenous Single-Drug Therapies Gregory B. Kruse, MPH, MSc; Mayur M. Amonkar, PhD; Gregory Smith, BA; Dean C. Skonieczny, MBA, BSE; and Spyros Stavrakas,
RESEARCH Analysis of Associated With Administration of Intravenous Single-Drug Therapies Gregory B. Kruse, MPH, MSc; Mayur M. Amonkar, PhD; Gregory Smith, BA; Dean C. Skonieczny, MBA, BSE; and Spyros Stavrakas,
Cancer patients waiting for potentially live-saving treatments in UK
 Cancer patients waiting for potentially live-saving treatments in UK 29 May 2005 UK patients are waiting too long for new treatments, according to a 'Dossier of Delay' compiled by information charity CancerBACUP.
Cancer patients waiting for potentially live-saving treatments in UK 29 May 2005 UK patients are waiting too long for new treatments, according to a 'Dossier of Delay' compiled by information charity CancerBACUP.
Drugs Used to Treat Nausea and Vomiting
 Evaluating the Oral 5-HT3 Antagonists: Drugs Used to Treat Nausea and Vomiting Comparing Effectiveness, Safety, and Price Our Recommendations A Summary The 5-HT3 antagonists are a class of drugs often
Evaluating the Oral 5-HT3 Antagonists: Drugs Used to Treat Nausea and Vomiting Comparing Effectiveness, Safety, and Price Our Recommendations A Summary The 5-HT3 antagonists are a class of drugs often
Basics of Systemic Anticancer Therapy Prescribing and Verification
 CHAPTER 2 Basics of Systemic Anticancer Therapy Prescribing and Verification Trinh Pham Joan Rivington Learning Objectives Upon completion of the chapter, the reader will be able to: 1. Write clear and
CHAPTER 2 Basics of Systemic Anticancer Therapy Prescribing and Verification Trinh Pham Joan Rivington Learning Objectives Upon completion of the chapter, the reader will be able to: 1. Write clear and
Cancer Drug Toxicities and Anaesthesia
 Cancer Drug Toxicities and Anaesthesia 71 Cancer Drug Toxicities and Anaesthesia PAUL DE SOUZA, BSc (Med), MBBS, FRACP, MPH Senior Staff Specialist in Medical Oncology, St George Hospital, Sydney Dr de
Cancer Drug Toxicities and Anaesthesia 71 Cancer Drug Toxicities and Anaesthesia PAUL DE SOUZA, BSc (Med), MBBS, FRACP, MPH Senior Staff Specialist in Medical Oncology, St George Hospital, Sydney Dr de
CVP Chemotherapy Regimen for Lymphoma Information for Patients
 CVP Chemotherapy Regimen for Lymphoma Information for Patients The Regimen Contains: C: Cyclophosphamide (Cytoxan ) V: Vincristine (Oncovin ) P: Prednisone How Is This Regimen Given? CVP is given every
CVP Chemotherapy Regimen for Lymphoma Information for Patients The Regimen Contains: C: Cyclophosphamide (Cytoxan ) V: Vincristine (Oncovin ) P: Prednisone How Is This Regimen Given? CVP is given every
Chemotherapy Order Assessment and Review
 Chemotherapy Order Assessment and Review Contents Introduction... 2 Step 1: Verify Patient Information... 2 Step 2: Confirm Protocol Matches Clinical Indication and Eligibility for Treatment... 2 Step
Chemotherapy Order Assessment and Review Contents Introduction... 2 Step 1: Verify Patient Information... 2 Step 2: Confirm Protocol Matches Clinical Indication and Eligibility for Treatment... 2 Step
Proceedings of the World Small Animal Veterinary Association Sydney, Australia 2007
 Proceedings of the World Small Animal Sydney, Australia 2007 Hosted by: Next WSAVA Congress Rescue Chemotherapy Protocols for Dogs with Lymphoma Kenneth M. Rassnick, DVM, DACVIM (Oncology) Cornell University
Proceedings of the World Small Animal Sydney, Australia 2007 Hosted by: Next WSAVA Congress Rescue Chemotherapy Protocols for Dogs with Lymphoma Kenneth M. Rassnick, DVM, DACVIM (Oncology) Cornell University
Emerging Drug List GEFITINIB
 Generic (Trade Name): Manufacturer: Gefitinib (Iressa ) formerly referred to as ZD1839 AstraZeneca NO. 52 JANUARY 2004 Indication: Current Regulatory Status: Description: Current Treatment: Cost: Evidence:
Generic (Trade Name): Manufacturer: Gefitinib (Iressa ) formerly referred to as ZD1839 AstraZeneca NO. 52 JANUARY 2004 Indication: Current Regulatory Status: Description: Current Treatment: Cost: Evidence:
Coping With Nausea and Vomiting From Chemotherapy
 NAUSEA AND VOMITING Coping With Nausea and Vomiting From Chemotherapy Presented by Richard J. Gralla, MD Multinational Association of Supportive Care in Cancer Steven M. Grunberg, MD The University of
NAUSEA AND VOMITING Coping With Nausea and Vomiting From Chemotherapy Presented by Richard J. Gralla, MD Multinational Association of Supportive Care in Cancer Steven M. Grunberg, MD The University of
This 2-part article will discuss 9 anticancer. Commonly Used Chemotherapy Drugs Part 1. M e d i c a t i o n s. Clinician s Brief.
 M e d i c a t i o n s O N C O L O G Y Peer Reviewed Antony Moore, BVSc, MVSc, Diplomate ACVIM (Oncology) Veterinary Oncology Consultants, Sydney, Australia Commonly Used Chemotherapy Drugs Part 1 This
M e d i c a t i o n s O N C O L O G Y Peer Reviewed Antony Moore, BVSc, MVSc, Diplomate ACVIM (Oncology) Veterinary Oncology Consultants, Sydney, Australia Commonly Used Chemotherapy Drugs Part 1 This
Lung Pathway Group Nintedanib (Vargatef) in advanced Non-Small Cell Lung Cancer (NSCLC)
 Lung Pathway Group Nintedanib (Vargatef) in advanced Non-Small Cell Lung Cancer (NSCLC) Indication: In combination with docetaxel in locally advanced, metastatic or locally recurrent NSCLC of adenocarcinoma
Lung Pathway Group Nintedanib (Vargatef) in advanced Non-Small Cell Lung Cancer (NSCLC) Indication: In combination with docetaxel in locally advanced, metastatic or locally recurrent NSCLC of adenocarcinoma
Oncologic drug Exposure Risks and Prevention Guidelines 19 June 2014
 Oncologic drug Exposure Risks and Prevention Guidelines 19 June 2014 ส งค กคามซ งอาจเป นอ นตรายต อส ขภาพ HAZARD? HAZARD ส งค กคามซ งอาจเป นอ นตรายต อส ขภาพ ENCLOSURE Substitution ส งค กคามซ งอาจเป นอ นตรายต
Oncologic drug Exposure Risks and Prevention Guidelines 19 June 2014 ส งค กคามซ งอาจเป นอ นตรายต อส ขภาพ HAZARD? HAZARD ส งค กคามซ งอาจเป นอ นตรายต อส ขภาพ ENCLOSURE Substitution ส งค กคามซ งอาจเป นอ นตรายต
NORDIC. Indication Mantle cell lymphoma (for patients suitable for subsequent chemotherapy with haematopoietic stem cell rescue)
 NORDIC C) CODOX (R) CODOX M/ (R) IVAC Indication Mantle cell lymphoma (for patients suitable for subsequent chemotherapy with haematopoietic stem cell rescue) ICD-10 code C83.13 Regimen details (R) maxi-chop
NORDIC C) CODOX (R) CODOX M/ (R) IVAC Indication Mantle cell lymphoma (for patients suitable for subsequent chemotherapy with haematopoietic stem cell rescue) ICD-10 code C83.13 Regimen details (R) maxi-chop
Farmacia HOSPITALARIA
 Volumen 34. Número 1. Enero-Febrero 2010 ÓRGANO OFICIAL DE EXPRESIÓN CIENTÍFICA DE LA SOCIEDAD ESPAÑOLA DE FARMACIA HOSPITALARIA J. Hernández Martín, M. Montero Hernández, I. Font Noguera, L. Doménech
Volumen 34. Número 1. Enero-Febrero 2010 ÓRGANO OFICIAL DE EXPRESIÓN CIENTÍFICA DE LA SOCIEDAD ESPAÑOLA DE FARMACIA HOSPITALARIA J. Hernández Martín, M. Montero Hernández, I. Font Noguera, L. Doménech
SUMMARY OF RECOMMENDATIONS
 SUMMARY OF RECOMMENDATIONS FOR THE LONG- TERM TREATMENT OF RLS/WED from AN IRLSSG TASK FORCE Members of the Task Force Diego Garcia- Borreguero, MD, Madrid, Spain* Richard Allen, PhD, Baltimore, MD, USA*
SUMMARY OF RECOMMENDATIONS FOR THE LONG- TERM TREATMENT OF RLS/WED from AN IRLSSG TASK FORCE Members of the Task Force Diego Garcia- Borreguero, MD, Madrid, Spain* Richard Allen, PhD, Baltimore, MD, USA*
WM: Managing the Side Effects of Treatment
 WM: Managing the Side Effects of Treatment 2014 IWMF Educational Forum Jeffrey V. Matous, MD Colorado Blood Cancer Institute www.bloodcancerinstitute.com Tampa, FL May 17, 2014 Determining a side effect
WM: Managing the Side Effects of Treatment 2014 IWMF Educational Forum Jeffrey V. Matous, MD Colorado Blood Cancer Institute www.bloodcancerinstitute.com Tampa, FL May 17, 2014 Determining a side effect
RGN JOY LAUDE WATFORD GENERAL HOSPITAL, ENGLAND
 RGN JOY LAUDE WATFORD GENERAL HOSPITAL, ENGLAND Monitor patient on the ward to detect trends in vital signs and to manage accordingly To recognise deteriorating trends and request relevant medical/out
RGN JOY LAUDE WATFORD GENERAL HOSPITAL, ENGLAND Monitor patient on the ward to detect trends in vital signs and to manage accordingly To recognise deteriorating trends and request relevant medical/out
VAD Chemotherapy Regimen for Multiple Myeloma Information for Patients
 VAD Chemotherapy Regimen for Multiple Myeloma Information for Patients The Regimen contains: V = vincristine (Oncovin ) A = Adriamycin (doxorubicin) D = Decadron (dexamethasone) How Is This Regimen Given?
VAD Chemotherapy Regimen for Multiple Myeloma Information for Patients The Regimen contains: V = vincristine (Oncovin ) A = Adriamycin (doxorubicin) D = Decadron (dexamethasone) How Is This Regimen Given?
Treatment options for recurrent ovarian cancer
 Treatment options for recurrent ovarian cancer There are a number of treatment options for women with recurrent ovarian cancer. Chemotherapy is the treatment most commonly offered and on occasion, surgery
Treatment options for recurrent ovarian cancer There are a number of treatment options for women with recurrent ovarian cancer. Chemotherapy is the treatment most commonly offered and on occasion, surgery
Package leaflet: Information for the user. Ondemet 4mg and 8mg Tablets (Ondansetron)
 Package leaflet: Information for the user Ondemet 4mg and 8mg Tablets (Ondansetron) Read all of this leaflet carefully before you start taking this medicine because it contains important information for
Package leaflet: Information for the user Ondemet 4mg and 8mg Tablets (Ondansetron) Read all of this leaflet carefully before you start taking this medicine because it contains important information for
Regimen : Bevacizumab for metastatic colorectal cancer ICD10 codes pre-fixed with: C18, C19, C20
 Regimen : Bevacizumab for metastatic colorectal cancer ICD10 codes pre-fixed with: C18, C19, C20 Indications First or second line treatment of advanced colorectal cancer, in combination with irinotecan
Regimen : Bevacizumab for metastatic colorectal cancer ICD10 codes pre-fixed with: C18, C19, C20 Indications First or second line treatment of advanced colorectal cancer, in combination with irinotecan
Regimen: Fluorouracil, Epirubicin and Cyclophosphamide + Docetaxel (FEC/T) for Early Breast Cancer
 Regimen: Fluorouracil, Epirubicin and Cyclophosphamide + Docetaxel (FEC/T) for Early Breast Cancer Indication Adjuvant treatment for node positive early breast cancer This protocol is subject to local
Regimen: Fluorouracil, Epirubicin and Cyclophosphamide + Docetaxel (FEC/T) for Early Breast Cancer Indication Adjuvant treatment for node positive early breast cancer This protocol is subject to local
Van Cutsem E et al. Proc ASCO 2009;Abstract LBA4509.
 Efficacy Results from the ToGA Trial: A Phase III Study of Trastuzumab Added to Standard Chemotherapy in First-Line HER2- Positive Advanced Gastric Cancer Van Cutsem E et al. Proc ASCO 2009;Abstract LBA4509.
Efficacy Results from the ToGA Trial: A Phase III Study of Trastuzumab Added to Standard Chemotherapy in First-Line HER2- Positive Advanced Gastric Cancer Van Cutsem E et al. Proc ASCO 2009;Abstract LBA4509.
Effects of Smoked Cannabis and Oral 9 -Tetrahydrocannabinol on Nausea and Emesis After Cancer Chemotherapy: A Review of State Clinical Trials
 Effects of Smoked Cannabis and Oral 9 -Tetrahydrocannabinol on Nausea and Emesis After Cancer Chemotherapy: A Review of State Clinical Trials Richard E. Musty Rita Rossi ABSTRACT. Background. In 1999 the
Effects of Smoked Cannabis and Oral 9 -Tetrahydrocannabinol on Nausea and Emesis After Cancer Chemotherapy: A Review of State Clinical Trials Richard E. Musty Rita Rossi ABSTRACT. Background. In 1999 the
KING KHALID UNIVERSITY HOSPITAL PHARMACY TEAM
 KING KHALID UNIVERSITY HOSPITAL PHARMACY TEAM MINUTES OF THE MEETING Month: 29 th September Location: Director of Pharmacy office Date/Time : 29-09-2012 (13-11-1433H) 12.30pm to 2.30pm Chairman of the
KING KHALID UNIVERSITY HOSPITAL PHARMACY TEAM MINUTES OF THE MEETING Month: 29 th September Location: Director of Pharmacy office Date/Time : 29-09-2012 (13-11-1433H) 12.30pm to 2.30pm Chairman of the
ASWCS Policy for the Treatment of Extravasation Injury
 ASWCS Policy for the Treatment of Extravasation Injury Extravasation of Cytotoxic Drugs Introduction 1. The purpose of this policy is to inform practitioners of their responsibilities in relation to preventing
ASWCS Policy for the Treatment of Extravasation Injury Extravasation of Cytotoxic Drugs Introduction 1. The purpose of this policy is to inform practitioners of their responsibilities in relation to preventing
LTC Pharmacy Setting B/D Coverage. Because most LTC facilities are not considered a beneficiary s home 3
 Medicare Parts Issues This table provides a reference guide for the most frequent B/D coverage determination scenarios facing Part D plans and Part D pharmacy providers. It does not address all potential.
Medicare Parts Issues This table provides a reference guide for the most frequent B/D coverage determination scenarios facing Part D plans and Part D pharmacy providers. It does not address all potential.
Chemotherapy for non-small cell lung cancer
 Chemotherapy for non-small cell lung cancer This information is an extract from the booklet Understanding lung cancer. You may find the full booklet helpful. We can send you a free copy see page 3. Contents
Chemotherapy for non-small cell lung cancer This information is an extract from the booklet Understanding lung cancer. You may find the full booklet helpful. We can send you a free copy see page 3. Contents
Maintenance therapy in in Metastatic NSCLC. Dr Amit Joshi Associate Professor Dept. Of Medical Oncology Tata Memorial Centre Mumbai
 Maintenance therapy in in Metastatic NSCLC Dr Amit Joshi Associate Professor Dept. Of Medical Oncology Tata Memorial Centre Mumbai Definition of Maintenance therapy The U.S. National Cancer Institute s
Maintenance therapy in in Metastatic NSCLC Dr Amit Joshi Associate Professor Dept. Of Medical Oncology Tata Memorial Centre Mumbai Definition of Maintenance therapy The U.S. National Cancer Institute s
Cancer Treatments Subcommittee of PTAC Meeting held 2 March 2012. (minutes for web publishing)
 Cancer Treatments Subcommittee of PTAC Meeting held 2 March 2012 (minutes for web publishing) Cancer Treatments Subcommittee minutes are published in accordance with the Terms of Reference for the Pharmacology
Cancer Treatments Subcommittee of PTAC Meeting held 2 March 2012 (minutes for web publishing) Cancer Treatments Subcommittee minutes are published in accordance with the Terms of Reference for the Pharmacology
Drug/Drug Combination: Bevacizumab in combination with chemotherapy
 AHFS Final Determination of Medical Acceptance: Off-label Use of Bevacizumab in Combination with Chemotherapy for the Treatment of Metastatic Breast Cancer Previously Treated with Cytotoxic Chemotherapy
AHFS Final Determination of Medical Acceptance: Off-label Use of Bevacizumab in Combination with Chemotherapy for the Treatment of Metastatic Breast Cancer Previously Treated with Cytotoxic Chemotherapy
Breast Pathway Group AC (Doxorubicin / Cyclophosphamide) in Early Breast Cancer
 Breast Pathway Group AC (Doxorubicin / Cyclophosphamide) in Early Breast Cancer Indication: Neoadjuvant or adjuvant treatment of breast cancer Regimen details: Doxorubicin 60mg/m 2 IV Day 1 Cyclophosphamide
Breast Pathway Group AC (Doxorubicin / Cyclophosphamide) in Early Breast Cancer Indication: Neoadjuvant or adjuvant treatment of breast cancer Regimen details: Doxorubicin 60mg/m 2 IV Day 1 Cyclophosphamide
E. Ryan Pritchard, PharmD * ; J. Aubrey Waddell, PharmD, FAPhA, BCOP; and Dominic A. Solimando, Jr, MA, FAPhA, FASHP, BCOP
 Hosp Pharm 2015;50(2):103 107 2015 Thomas Land Publishers, Inc. www.hospital-pharmacy.com doi: 10.1310/hpj5002-103 Cancer Chemotherapy Update Gemcitabine and Carboplatin (Renally Dosed) Regimen for Bladder
Hosp Pharm 2015;50(2):103 107 2015 Thomas Land Publishers, Inc. www.hospital-pharmacy.com doi: 10.1310/hpj5002-103 Cancer Chemotherapy Update Gemcitabine and Carboplatin (Renally Dosed) Regimen for Bladder
