ACLS for the Clinical Pharmacist
|
|
|
- Clementine Nancy Cunningham
- 7 years ago
- Views:
Transcription
1 ACLS for the Clinical Pharmacist Krista A. Wahby, Pharm.D. Dale Tucker, RPh, MEd, BCPS June 2007
2 Objectives To review the importance of having a pharmacist attend codes To familiarize the pharmacist with the ACLS protocols To review routes of administration for medications used in code blue emergencies To introduce several common ECG rhythms To identify and discuss the most common drugs used by the ACLS algorithms
3 Why Involve Pharmacist? Improves outcomes in Code Blue Pharmacotherapy Apr 27(4); Pharmacotherapy (5); Calculate drug doses Drug information Preparation of drugs Source of quick access for medications not on crash cart Assessment of patient s allergies and medication usage
4 Common Principles in New ACLS Guidelines Early, effective bystander CPR 2. Early defibrillation - Public Access Defibrillation 3. Minimal interruptions in chest compressions 4. Establishing a specific diagnosis by ECG 5. Choose one antiarrhythmic agent One, and only one antiarrhythmic should be used. 6. If IV access is not established, Intraosseous cannulation is the first line alternative and endotracheal is an alternative.
5 Pharmacist Involvement Pharmacists should KNOW: How? Why? to use an agent we use an agent When? to use an agent What?...to watch for
6 How To Use the Medication?
7 Routes of Medications IV Push (IVP) Preferred route fast, convenient,+ bioavailability Peripheral flush w/ 20cc bolus and elevate arm for seconds. Peak effect takes minutes Central line should be placed (however, keep in mind it is a relative contraindication for thrombolytic therapy) V - vasopressin A amiodarone, atropine, adenosine L lidocaine E epinephrine
8 Intravenous Infusion Intravenous infusion Medications for continuous IV infusion only P procainamide I isoproterenol N norepinephrine D dopamine Central line preferred, however, peripheral OK in emergency
9 Intraosseous Administration When IV access not available Gives access to a noncollapsible venous access route Important when patients are in shock with peripheral vasoconstriction
10 Endotracheal Administration When IV access is not available Doses usually times higher Absorption occurs at alveolar capillary interface Dilute drugs with 10ml 0.9% NaCl or Water to allow for adequate delivery (H2O preferred) L lidocaine (2-4 4 mg/kg) E epinephrine ( mg) A atropine (2-3 3 mg) N naloxone ( mg) V vasopressin ( Units)
11 HOW? Medication Administration Do not interrupt chest compressions Time to maximum effect of drug may depend on the distance from the heart Administer 10-20ml NS after each drug administered (20ml if peripheral administration & elevate arm) Have medications labeled and ready in advance Best to give immediately after shock
12 WHEN To Use WHAT Medication?
13 Use of Algorithms Meant to treat broadest range of patients Memory aids Use wisely, not blindly Not meant to replace clinical judgment Where to find? American Heart Association Attached to crash cart Included in DMC Tier 2 policy acls.net on the web
14 Wave forms Check Rhythm ECG Rhythms healthcentral.org
15 ECG Rhythms Normal sinus rhythm healthcentral.org
16 ECG Rhythms Asystole Bradycardia healthcentral.org
17 ECG Rhythms Ventricular Tachycardia Ventricular Fibrillation healthcentral.org
18 ECG Rhythms Artifact (waveform interference) healthcentral.org
19 Cardiac Arrest Management 1. Pulseless Cardiac Arrest i.e. ASYSTOLE and PEA 2. VENTRICULAR FIBRILLATION and PULSELESS V.TACH
20 Pulseless Arrest Algorithm Minimize interruptions in chest compressions Limit pulse and rhythm checks Do not check pulse immediately after shock give 5 cycles, then check! Once advanced airway in place do not interrupt compressions
21 Asystole and Pulseless Electrical Activity (PEA) Asystole is a cardiac standstill PEA-pt has mechanical contractions but no pulse. Any rhythm possible Both are non-shockable rhythms Most do not survive Asystole means the patient s life has ended
22 Asystole & PEA Algorithm BLS Algorithm: Call for help, give CPR Give oxygen when available Attach monitor/defibrillator when available Check rhythm: shockable? YES or NO If NO and problem is asystole/pea Resume CPR immediately for 5 cycles Give vasopressor: Epinephrine or vasopressin Consider Atropine for asystole or slow PEA rate Give 5 cycles of CPR Check rhythm: shockable? If no:
23 Asystole and PEA Algorithm P E A Interventions Problem search via Differential Diagnosis table; treat accordingly. (PATCH 4MDs) Continue algorithm if indicated. Epinephrine 1 mg IVP/IO q3-5 5 min. OR Vasopressin 40 units IV/IO, once, in place of the first or second dose of epinephrine. Atropine 1 mg IVP/IO q3-5 5 minutes; 3mg maximum.
24 Problem Search: Differential Diagnosis PATCH(4) MDs Pulmonary embolism Acidosis Thrombolytics Bicarb./hyperventilation Tension pneumothorax Thoracostomy Cardiac tamponade Pericardiocentesis Hyperkalemia HCO3, CaCl,, Ins/Glc Glc,, HD, diuresis, kayexylate Hypokalemia Hypovolemia Hypoxia Myocardial infarct ACS protocol Avoid BB if cocaine Drugs Shivering
25 Basic Pharmacology Review
26 Vasoactive Receptor Effects α1 VASOCONSTRICTION of arteries and veins α2 Feedback and Vasoconstriction Decreases NE release β1 INOTROPE & CHRONOTROPE β2 VASODILATION (skin, kidneys, skeletal muscles, visceral and pulmonary arteries) and BRONCHODILATION
27 Vasopressor Therapy Increases SBP by increasing preload and ventricular filling pressure Enhance organ perfusion, increase cerebral and coronary perfusion pressures (increases success of defibrillation) Mostly via α 1 stimulation and V 1 stimulation List the Vasopressors: Epinephrine Vasopressin Norepinephrine Phenylephrine Dopamine
28 Inotropic Therapy Increase cardiac contractility and increase cardiac output (CO) Work via β1 1 stimulation and/or by increasing camp and Calcium influx List the Inotropes: Dobutamine Milrinone (or inamrinone) Digoxin Glucagon
29 Catecholamine Pharmacology Bind to β adrenoreceptor and stimulate Gs protein Stimulates adenylate cyclase, camp camp acts to INCREASE Ca INFLUX VASOCONSTRICTION, INOTROPY
30 E = Epinephrine 1mg IVP/IO every minutes. GOAL Improve Perfusion to Essential Organs (Heart, Brain). Shifts blood centrally. MOA Alpha and Beta Adrenergic Agonist α1 Vasoconstriction. Increases BP; improves cerebral and coronary perfusion pressures β Stimulates the cardiac muscle increasing the strength of ventricular contraction. + inotrope and chronotrope. Does increase myocardial work
31 Epinephrine Side Effects Nervous system: anxiety, agitation Cardiovascular: dilated CM, LV dysfunction Psychiatric: disorientation, hallucinations Metabolic: acidosis, hypokalemia Renal: renal insufficiency Other: extravasation, skin necrosis
32 Vasopresssin Vasopressin 40 units IVP/IO x 1 (2 vials required. Each vial = 20 Units) May replace 1st or 2 nd dose of epinephrine Pharmacology: : Endogenous ADH Causes vasoconstriction at high doses by directly stimulating smooth muscle V 1 receptors Dilates cerebral blood vessels Coronary & renal vasoconstriction
33 Vasopressin Rationale Enhance organ perfusion Advantages over epinephrine? Longer half-life life (10-20 minutes) Not affected by acidosis Unique MOA - nonadrenergic Best outcomes in ASYSTOLE? Pharmacotherapy 2006;26(6):
34 Vasopressin Side Effects GI: nausea, intestinal cramps Increased mesenteric vascular resistance Bronchial constriction Uterine contractions Extravasation - necrosis
35 A = Atropine 1mg IVP/IO every minutes up to a maximum of 3 mg Excessive parasympathetic tone may play a role in stopping ventricular and supraventricular pacemaker activity Avoid if lack of cardiac activity has a clear explanation such as hypothermia
36 Atropine Pharmacology Competitive antagonist of acetylcholine Vagolytic action causes restoration of heart rate and blood pressure Reverses cholinergic-mediated decreases in: Heart rate Systemic vascular resistance Blood pressure
37 Atropine Side Effects Anticholinergic Confusion Blurred vision Dry mouth, skin, nose Constipation Urinary retention Lightheadedness
38 VF and PVT VF = ventricular fibrillation Fibrillary contractions of the ventricular muscle due to rapid repetitive excitation of myocardial fibers without coordinated contraction of the ventricle PVT = pulseless ventricular tachycardia An abnormally rapid ventricular rhythm with aberrant ventricular excitation most commonly associated with atrioventricular dissociation The patient has no pulse
39 ECG Rhythms Ventricular fibrillation healthcentral.org
40 ECG Rhythms Ventricular tachycardia healthcentral.org
41 VF/PVT Algorithm: SCREAM Give 1 shock Resume CPR immediately for 5 cycles Check rhythm: : Shockable? YES or NO? YES - Continue CPR while defibrillator is charging Give 1 shock Resume CPR immediately after the shock When IV/PO available give vasopressor (epinephrine( or vasopressin) during CPR before or after the shock Check rhythm: if shockable Continue CPR while defibrillator is charging Give 1 shock Resume CPR immediately after the shock Consider antiarrhythmic medications (amiodarone, lidocaine, magnesium): give during CPR before or after the shock After 5 cycles of CPR
42 Shock Manual biphasic Device specific Typically J If unknown, use 200 J AED Device specific Monophasic 360 J
43 VF/PVT Algorithm: SCREAM S Shock 360J monophasic, 1 st and subsequent shocks. Shock every 2 minutes if indicated. C R CPR Rhythm After shock, immediately begin chest compressions followed by respirations for 2 minutes. Do not check rhythm or pulse. Rhythm check after 2 minutes of CPR (and after every 2 minutes of CPR thereafter) and shock again if indicated. Check pulse only if an organized or non-shockable rhythm is present Implement the Secondary ABCD Survey. Continue this algorithm if indicated. Give drugs during CPR before or after shocking. Minimize imize interruptions in chest compressions to < 10 seconds. Consider differential diagnosis.
44 VF/PVT Algorithm: SCREAM E Epinephrine 1mg IVP/IO q3-5 5 minutes or vasopressin 40 units IV/IO, once, in place of the 1 st or 2 nd dose of epinephrine. A M Antiarrhythmic Medications Consider antiarrhythmics: Any ny Legitimate Medication Amiodarone 300mg IVP/IO, may repeat once at 150mg in minutes if VF/PVT persists or Lidocaine (if amiodarone unavailable) mg/kg IVP/IO, may repeat X2, q5-10 min at mg/kg 0.75mg/kg Max LD= 3mg/kg Magnesium Sulfate 1-22 gm IVP/IO diluted in 10m D5/W (5-20 min push) for torsades de pointes or suspected/known hypomagnesemia.
45 Amiodarone 300mg IVP/IO once, then consider additional 150mg IVP/IO once If pt is pulseless, give IVP, otherwise dilution with 20-30ml and a slower infusion results in less bradycardia, hypotension and phlebitis Infusion OK peripherally if < 2mg/ml Not for ET administration
46 Amiodarone MOA: Inhibits conduction through Sodium, Potassium and Calcium channels and α & β adrenergic blocking ability Inhibits adrenergic stimulation, prolongs the action potential and refractory period in myocardial tissue, and decreases AV conduction and sinus node function Based on ARREST and ALIVE Trials Side effects: hypotension, bradycardia, nausea, vomiting, tremor, dizziness, headache, phlebitis
47 Lidocaine mg/kg first dose then mg/kg 0.75mg/kg IVP/IO q5-10 minutes Maximum of 3 doses or 3 mg/kg After return of ROSC infuse at mg/min (50% reduction if cardiac or liver failure) Suppresses automaticity of conduction tissue and blocks both the initiation and conduction of nerve impulses Side effects: hypotension, headache, shivering
48 Magnesium 1-22 grams IVP/IO diluted in 10ml D5W over minutes. If patient has pulse, can slow down infusion to min INDICATION: torsades de pointes Low magnesium causes inhibition of conduction through K+ channels in heart prolongs AP and QT prolongation Side effects: flushing, somnolence, complete heart block, respiratory paralysis
49 Arrhythmia Management Bradycardia Tachycardia: SVT
50 Bradycardia Bradycardia: HR < 60 beats/minute or when the heart rate is slower than expected Signs and symptoms might include: Chest pain, shortness of breath Hypotension, pulmonary edema, congestive heart failure
51 ECG Rhythms Sinus bradycardia healthcentral.org
52 Bradycardia Algorithm: Pacing Always Ends Danger Maintain patient airway; assist breathing as needed Give oxygen Monitor ECG, blood pressure, oximetry Establish IV access Signs/symptoms of poor perfusion caused by the bradycardia? If yes: Prepare for transcutaneous pacing Consider atropine IV while awaiting pacer; if ineffective begin pacing Consider epinephrine or dopamine infusion while awaiting pacer or if pacing ineffective Prepare for transvenous pacing Treat contributing causes Consider expert consultation
53 Bradycardia Algorithm: Pacing Always Ends Danger Mnemonic Pacing Intervention TCP Note Immediately prepare for TCP with serious circulatory compromise due to bradycardia (especially high-degree blocks) or if atropine failed to increase rate Consider medications while pacing is readied. Always Ends Danger Atropine Epinephrine 2-10mcg/min Dopamine 2-10 mcg/kg/min First line drug, 0.5mg IV/IO q3-5 5 min (maximum 3mg) Second line drugs to consider if atropine and/or TCP are ineffective. Use with extreme caution
54 Transcutaneous Pacing Used to speed up a cardiac rhythm that is too slow If considered, start immediately To be effective, must be performed early and combined with drug therapy
55 Transcutaneous Pacing Apparatus
56 Atropine Atropine 0.5 mg IV while awaiting pacer 50% reduction in dose when compared with PEA algorithm May repeat to a total dose of 3 mg If ineffective, begin pacing
57 Epinephrine Consider epinephrine mcg/min continuous infusion while awaiting pacer Use 1ml of the 1:1000 or 10 ml of the 1:10,000 in 500ml D5W Alternatively, 0.5 mg IVP boluses To avoid tachyarrhythmias Until continuous infusion available Until pacemaker available Or if pacing ineffective
58 Dopamine Or consider dopamine mcg/kg/min infusion while awaiting pacer or if pacing ineffective MOA: Precursor of norepinephrine, stimulates heart through both alpha- and beta-adrenergic adrenergic receptors Increases both cardiac output and arterial perfusion pressure
59 Dopamine Side Effects Cardiovascular: ectopic heartbeats, tachycardia, vasoconstriction, hypotension, ventricular arrhythimas CNS: headache GI: nausea, vomiting Respiratory: dyspnea Other: Adrenal insufficiency
60 Tachycardia Algorithm Assess and support ABCs as needed Give oxygen Monitor ECG, blood pressure, oximetry Identify and treat reversible causes Symptoms persist and patient stable Establish IV access Obtain 12-lead ECG or rhythm strip Is QRS narrow or wide? Narrow QRS (<0.12 sec) with regular rhythm Narrow QRS (<0.12 sec) with regular rhythm
61 Tachycardia Algorithm (continued) Attempt vagal maneuvers Give adenosine 6mg rapid IVP If no conversion, give 12mg rapid IVP May repeat 12mg dose once Does rhythm convert? Note: Consider expert consultation Yes: Probable reentry SVT. Observe for recurrence. Treat recurrence with adenosine or diltiazem (Cardizem( Cardizem) ) or beta- blockers. or No: Possible atrial flutter, ectopic atrial tachycardia, or junctional tachycardia. Control rate with diltiazem (Cardizem)) or beta-blockers. blockers. Treat underlying cause. Consider expert consultation.
62 Tachycardia Algorithm Tachycardia is stable, narrow, and regular: Yes Yes 1-2-3, 1 think SVT, then V-A-C 1. Stable? 2. Narrow? 3. Regular? Yes: see question 2 Yes: see question 3 Yes: see mnemonic No: unstable = immediate electrical cardioversion No: wide = consult an expert with QRS 0.12 sec No: irregular = consult an expert
63 Tachycardia Algorithm Yes 1-2-3, 1 think SVT, then V-A-C Vagal maneuvers, if this fails Adenosine 6 mg rapid IVP (may repeat X2, q1-2 2 min at 12mg) Cardizem (diltiazem) managed by an expert if stable, narrow, regular tachyarrhythmia continues
64 Vagal Maneuvers Valsalva s maneuver A forcible exhalation effort against a closed glottis which results in an increase in intrathoracic pressure which interferes with venous return to the heart Carotid sinus massage Firm rotatory pressure applied to one side of the neck over the carotid sinus in a supine patient to cause vagal stimulation in order to slow or terminate tachycardia
65 Adenosine To convert SVT: 6 mg rapid IVP over 1-1 3sec followed by 20ml saline flush; if rate dose not convert in min give 12mg IVP & repeat 12mg in minutes again Larger doses required for patients with significant blood levels of theophylline, caffeine, or theobromine Reduce initial dose to 3 mg in patients taking dipyridamole or carbamazepine or those with transplanted hearts or if given by central venous access
66 Adenosine Slows conduction time through AV node, interrupts reentry pathways through AVN and restores NSR Side effects common but transient: flushing, dyspnea, chest pain
67 Diltiazem (Cardizem) Use if adenosine fails 15-20mg (0.25mg/kg) IVP over 2 min; if needed in 15 minutes give an IVP dose of 20-25mg 25mg (0.35mg/kg) Maintenance infusion dose is 5-15mg/hr5 Blocks conduction through the AV node Harmful if given to patients with atrial fibrillation or atrial flutter associated with known pre-excitation excitation such as Wolf- Parkinson-White
68 Cases: Rhythm: What is this? Algorithm? Drugs/Doses? Ventricular Fibrillation SCREAM Epi 1 mg q3-5min Amiodarone 300mg IVP, may repeat with 150mg
69 Cases: Rhythm: What is this? Algorithm? Drugs/Doses? Asystole PEA Epi 1 mg q3-5min (or vasopressin 40 Units IVP) Atropine 1mg q3-5 5 min to max dose = 3mg
70 Cases: Rhythm: What is this? Algorithm? Drugs/Doses? Bradycardia Pacing Always Ends Danger Atropine 0.5 mg q3-5min to max = 3mg Epi mcg/min Dopamine mcg/kg/min
71 Cases: Rhythm: What is this? Algorithm? Drugs/Doses? SVT Yes 1, 2, 3, then think VAC Adenosine 6mg IVP then 12mg IVP, then 12mg IVP Cardizem mg IVP then 5-15 mg/hr
72 Other Code Situations Anaphylaxis: Epi mg IV, steroids, ranitidine, diphenhydramine AFib: diltiazem, βb, digoxin, amiodarone, ibutilide Hyperkalemia: Insulin + D50; CaCl; Bicarb; albuterol, dialysis, kayexylate, furosemide Hypotension: Norepinephrine mcg/min, Phenylephrine mcg/min; Vasopressin Units/min, Dopamine mcg/kg/min
73 Other Code Situations Pulmonary Embolism: Massive PE with shock or hemodynamic instability should receive tpa 100mg IVPB over 2 hr Status Epilepticus: Lorazepam 0.1mg/kg IVP, Phenytoin mg/kg IVPB or Fosphenytoin Prolonged Code: Systemic acidosis ensues NaBicarb may be appropriate
74 Induced Hypothermia Hypothermia for 24 hr Hypothermia After Cardiac Arrest (HACA) NEJM 2002;346: Ice packs, Artic Sun Protocol, Cooling blankets Requires continuous sedative and analgesic infusions, meperidine for shivering and avoidance of anticoagulation
75 Take Away Points Most frequently used medications Epinephrine: asystole, bradycardia, PEA, VF/PVT Atropine: asystole, bradycardia, PEA Vasopressin: asystole, PEA, VF/PVT
76 Take Away Points Medications IVPB only P - procainamide I - isoproterenol N - norepinephrine D - dopamine Medications IVP or IVPB V - vasopressin A amiodarone, adenosine, atropine L - lidocaine E - epinephrine Tracheal administration L lidocaine E epinephrine A atropine N naloxone V - vasopressin Doses usually times those given IVP Follow each dose with 10 ml NS flush down tracheal tube if not diluted to that volume for administration
77 Supplemental Reading Cardiovascular complications of cocaine use. N Engl J Med 2001;345(5): Evolving role of vasopressin in the treatment of cardiac arrest. Pharmacotherapy 2006;26(6): Pharmacotherapy considerations in advanced cardiac life support. Pharmacotherapy 2006;26(12):
78
ACLS PHARMACOLOGY 2011 Guidelines
 ACLS PHARMACOLOGY 2011 Guidelines ADENOSINE Narrow complex tachycardias or wide complex tachycardias that may be supraventricular in nature. It is effective in treating 90% of the reentry arrhythmias.
ACLS PHARMACOLOGY 2011 Guidelines ADENOSINE Narrow complex tachycardias or wide complex tachycardias that may be supraventricular in nature. It is effective in treating 90% of the reentry arrhythmias.
ACLS Cardiac Arrest Algorithm Neumar, R. W. et al. Circulation 2010;122:S729-S767
 ACLS Cardiac Arrest Algorithm Neumar, R. W. et al. Circulation 2010;122:S729-S767 Copyright 2010 American Heart Association ACLS Cardiac Arrest Circular Algorithm Neumar, R. W. et al. Circulation 2010;122:S729-S767
ACLS Cardiac Arrest Algorithm Neumar, R. W. et al. Circulation 2010;122:S729-S767 Copyright 2010 American Heart Association ACLS Cardiac Arrest Circular Algorithm Neumar, R. W. et al. Circulation 2010;122:S729-S767
PRO-CPR. 2015 Guidelines: PALS Algorithm Overview. (Non-AHA supplementary precourse material)
 PRO-CPR 2015 Guidelines: PALS Algorithm Overview (Non-AHA supplementary precourse material) Please reference Circulation (from our website), the ECC Handbook, or the 2015 ACLS Course Manual for correct
PRO-CPR 2015 Guidelines: PALS Algorithm Overview (Non-AHA supplementary precourse material) Please reference Circulation (from our website), the ECC Handbook, or the 2015 ACLS Course Manual for correct
Crash Cart Drugs Drugs used in CPR. Dr. Layla Borham Professor of Clinical Pharmacology Umm Al Qura University
 Crash Cart Drugs Drugs used in CPR Dr. Layla Borham Professor of Clinical Pharmacology Umm Al Qura University Introduction A list of the drugs kept in the crash carts. This list has been approved by the
Crash Cart Drugs Drugs used in CPR Dr. Layla Borham Professor of Clinical Pharmacology Umm Al Qura University Introduction A list of the drugs kept in the crash carts. This list has been approved by the
ANNE ARUNDEL MEDICAL CENTER CRITICAL CARE MEDICATION MANUAL DEPARTMENT OF NURSING AND PHARMACY. Guidelines for Use of Intravenous Isoproterenol
 ANNE ARUNDEL MEDICAL CENTER CRITICAL CARE MEDICATION MANUAL DEPARTMENT OF NURSING AND PHARMACY Guidelines for Use of Intravenous Isoproterenol Major Indications Status Asthmaticus As a last resort for
ANNE ARUNDEL MEDICAL CENTER CRITICAL CARE MEDICATION MANUAL DEPARTMENT OF NURSING AND PHARMACY Guidelines for Use of Intravenous Isoproterenol Major Indications Status Asthmaticus As a last resort for
MEDICATIONS USED IN ADULT CODE BLUE EMERGENCIES. Source: ACLS Provider Manual. American Heart Association. 2001, 2002. Updated 2003.
 MEDICATIONS USED IN ADULT CODE BLUE EMERGENCIES Source: ACLS Provider Manual. American Heart Association. 2001, 2002. Updated 2003. 1 ET Administration Atropine o First drug for symptomatic sinus bradycardia
MEDICATIONS USED IN ADULT CODE BLUE EMERGENCIES Source: ACLS Provider Manual. American Heart Association. 2001, 2002. Updated 2003. 1 ET Administration Atropine o First drug for symptomatic sinus bradycardia
Cardiac Arrest VF/Pulseless VT Learning Station Checklist
 Cardiac Arrest VF/Pulseless VT Learning Station Checklist VF/VT 00 American Heart Association Adult Cardiac Arrest Shout for Help/Activate Emergency Response Epinephrine every - min Amiodarone Start CPR
Cardiac Arrest VF/Pulseless VT Learning Station Checklist VF/VT 00 American Heart Association Adult Cardiac Arrest Shout for Help/Activate Emergency Response Epinephrine every - min Amiodarone Start CPR
Present : PGY 王 淳 峻 Supervisor: F1 王 德 皓 991109
 Present : PGY 王 淳 峻 Supervisor: F1 王 德 皓 991109 Interventions to prevent cardiac arrest + Airway management + Ventilation support + Treatment of bradyarrhythmias & Tachyarrhythmias Treat cardiac arrest
Present : PGY 王 淳 峻 Supervisor: F1 王 德 皓 991109 Interventions to prevent cardiac arrest + Airway management + Ventilation support + Treatment of bradyarrhythmias & Tachyarrhythmias Treat cardiac arrest
ACLS PRE-TEST ANNOTATED ANSWER KEY
 ACLS PRE-TEST ANNOTATED ANSWER KEY June, 2011 Question 1: Question 2: There is no pulse with this rhythm. Question 3: Question 4: Question 5: Question 6: Question 7: Question 8: Question 9: Question 10:
ACLS PRE-TEST ANNOTATED ANSWER KEY June, 2011 Question 1: Question 2: There is no pulse with this rhythm. Question 3: Question 4: Question 5: Question 6: Question 7: Question 8: Question 9: Question 10:
Inotropes/Vasoactive Agents Hina N. Patel, Pharm.D., BCPS Cathy Lawson, Pharm.D., BCPS
 Inotropes/Vasoactive Agents Hina N. Patel, Pharm.D., BCPS Cathy Lawson, Pharm.D., BCPS 1. Definition -an agent that affects the contractility of the heart -may be positive (increases contractility) or
Inotropes/Vasoactive Agents Hina N. Patel, Pharm.D., BCPS Cathy Lawson, Pharm.D., BCPS 1. Definition -an agent that affects the contractility of the heart -may be positive (increases contractility) or
ACLS Study Guide BLS Overview CAB
 ACLS Study Guide The ACLS Provider exam is 50-mutiple choice questions. Passing score is 84%. Student may miss 8 questions. For students taking ACLS for the first time or renewing students with a current
ACLS Study Guide The ACLS Provider exam is 50-mutiple choice questions. Passing score is 84%. Student may miss 8 questions. For students taking ACLS for the first time or renewing students with a current
If you do not wish to print the entire pre-test you may print Page 2 only to write your answers, score your test, and turn in to your instructor.
 This is a SAMPLE of the pretest you can access with your AHA PALS Course Manual at Heart.org/Eccstudent using your personal code that comes with your PALS Course Manual The American Heart Association strongly
This is a SAMPLE of the pretest you can access with your AHA PALS Course Manual at Heart.org/Eccstudent using your personal code that comes with your PALS Course Manual The American Heart Association strongly
American Heart Association ACLS Pre-Course Self Assessment Dec., 2006. ECG Analysis. Name the following rhythms from the list below:
 American Heart Association ACLS Pre-Course Self Assessment Dec., 2006 ECG Analysis This pre-test is exactly the same as the pretest on the ACLS Provider manual CD. This paper version can be completed in
American Heart Association ACLS Pre-Course Self Assessment Dec., 2006 ECG Analysis This pre-test is exactly the same as the pretest on the ACLS Provider manual CD. This paper version can be completed in
IU Health ACLS Study Guide
 IU Health ACLS Study Guide Preparing for your upcoming ACLS Class REVISED SEPTEMBER 2011 ON APRIL 1, 2011 WE BEGAN TEACHING THE 2010 AHA GUIDELINES. WE HIGHLY RECOMMEND REVIEWING THE NEW ALGORYHMS FOUND
IU Health ACLS Study Guide Preparing for your upcoming ACLS Class REVISED SEPTEMBER 2011 ON APRIL 1, 2011 WE BEGAN TEACHING THE 2010 AHA GUIDELINES. WE HIGHLY RECOMMEND REVIEWING THE NEW ALGORYHMS FOUND
Atrial & Junctional Dysrhythmias
 Atrial & Junctional Dysrhythmias Atrial & Junctional Dysrhythmias Atrial Premature Atrial Complex Wandering Atrial Pacemaker Atrial Tachycardia (ectopic) Multifocal Atrial Tachycardia Atrial Flutter Atrial
Atrial & Junctional Dysrhythmias Atrial & Junctional Dysrhythmias Atrial Premature Atrial Complex Wandering Atrial Pacemaker Atrial Tachycardia (ectopic) Multifocal Atrial Tachycardia Atrial Flutter Atrial
Stimulates HR, BP, CO, and vasoconstriction. Stimulates renal, venous, mesenteric arterial. basic chart below) (alpha receptors) vasoconstriction
 Bolus Alternate Range Drip ACLS Drugs and Drips Amiodarone / Cordarone Lidocaine Procainamide / Pronestyl Dopamine / Intropin CARDIAC ARREST PULSELESS VT/VF Arrest Kit: (300mg bolus) Amiodarone 6 Vial
Bolus Alternate Range Drip ACLS Drugs and Drips Amiodarone / Cordarone Lidocaine Procainamide / Pronestyl Dopamine / Intropin CARDIAC ARREST PULSELESS VT/VF Arrest Kit: (300mg bolus) Amiodarone 6 Vial
ACLS Provider Manual Comparison Sheet Based on 2010 AHA Guidelines for CPR and ECC. BLS Changes
 ACLS Provider Manual Comparison Sheet Based on 2010 AHA Guidelines for CPR and ECC CPR Chest compressions, Airway, Breathing (C-A-B) BLS Changes New Old Rationale New science indicates the following order:
ACLS Provider Manual Comparison Sheet Based on 2010 AHA Guidelines for CPR and ECC CPR Chest compressions, Airway, Breathing (C-A-B) BLS Changes New Old Rationale New science indicates the following order:
Arrest. What s a Nurse to do?
 Benzo s, Blockers, Coma & Cardiac Arrest What s a Nurse to do? Objectives Review of ACLS Algorithms for Cardiac Arrest Management Discuss the toxicology of Beta Blocker Poisoning Describe the clinical
Benzo s, Blockers, Coma & Cardiac Arrest What s a Nurse to do? Objectives Review of ACLS Algorithms for Cardiac Arrest Management Discuss the toxicology of Beta Blocker Poisoning Describe the clinical
Here is a drug list that you need to know before taking the NREMT-P exam!! Taken from the book EMS NOTES.com
 Here is a drug list that you need to know before taking the NREMT-P exam!! Taken from the book EMS NOTES.com Special thanks to the number #1 internet training site id44.com and also to (NOTE) Please remember
Here is a drug list that you need to know before taking the NREMT-P exam!! Taken from the book EMS NOTES.com Special thanks to the number #1 internet training site id44.com and also to (NOTE) Please remember
New resuscitation science and American Heart Association treatment guidelines were released October 28, 2010!
 ACLS Study Guide 2010 Bulletin: New resuscitation science and American Heart Association treatment guidelines were released October 28, 2010! The new AHA Handbook of Emergency Cardiac Care (ECC) contains
ACLS Study Guide 2010 Bulletin: New resuscitation science and American Heart Association treatment guidelines were released October 28, 2010! The new AHA Handbook of Emergency Cardiac Care (ECC) contains
E C C. American Heart Association. Advanced Cardiovascular Life Support. Written Precourse Self-Assessment. May 2011. 2011 American Heart Association
 E C C American Heart Association Advanced Cardiovascular Life Support Written Precourse Self-Assessment May 2011 2011 American Heart Association 2011 ACLS Written Precourse Self-Assessment 1. Ten minutes
E C C American Heart Association Advanced Cardiovascular Life Support Written Precourse Self-Assessment May 2011 2011 American Heart Association 2011 ACLS Written Precourse Self-Assessment 1. Ten minutes
www.cprtrainingfast.com
 ADVANCED CARDIAC LIFE SUPPORT (ACLS) RECERTIFICATION EXAMINATION 1. Ten minutes after an 85 year old woman collapses, paramedics arrive and start CPR for the first time. The monitor shows fine (low amplitude)
ADVANCED CARDIAC LIFE SUPPORT (ACLS) RECERTIFICATION EXAMINATION 1. Ten minutes after an 85 year old woman collapses, paramedics arrive and start CPR for the first time. The monitor shows fine (low amplitude)
8 Peri-arrest arrhythmias
 8 Peri-arrest arrhythmias Introduction Cardiac arrhythmias are relatively common in the peri-arrest period. They are common in the setting of acute myocardial infarction and may precipitate ventricular
8 Peri-arrest arrhythmias Introduction Cardiac arrhythmias are relatively common in the peri-arrest period. They are common in the setting of acute myocardial infarction and may precipitate ventricular
GUIDELINE 11.9 MANAGING ACUTE DYSRHYTHMIAS. (To be read in conjunction with Guideline 11.7 Post-Resuscitation Therapy in Adult Advanced Life Support)
 AUSTRALIAN RESUSCITATION COUNCIL GUIDELINE 11.9 MANAGING ACUTE DYSRHYTHMIAS (To be read in conjunction with Guideline 11.7 Post-Resuscitation Therapy in Adult Advanced Life Support) The term cardiac arrhythmia
AUSTRALIAN RESUSCITATION COUNCIL GUIDELINE 11.9 MANAGING ACUTE DYSRHYTHMIAS (To be read in conjunction with Guideline 11.7 Post-Resuscitation Therapy in Adult Advanced Life Support) The term cardiac arrhythmia
Update on Small Animal Cardiopulmonary Resuscitation (CPR)- is anything new?
 Update on Small Animal Cardiopulmonary Resuscitation (CPR)- is anything new? DVM, DACVA Objective: Update on the new Small animal guidelines for CPR and a discussion of the 2012 Reassessment Campaign on
Update on Small Animal Cardiopulmonary Resuscitation (CPR)- is anything new? DVM, DACVA Objective: Update on the new Small animal guidelines for CPR and a discussion of the 2012 Reassessment Campaign on
Official Online ACLS Exam
 \ Official Online ACLS Exam Please fill out this form before you take the exam. Name : Email : Phone : 1. Hypovolemia initially produces which arrhythmia? A. PEA B. Sinus tachycardia C. Symptomatic bradyarrhythmia
\ Official Online ACLS Exam Please fill out this form before you take the exam. Name : Email : Phone : 1. Hypovolemia initially produces which arrhythmia? A. PEA B. Sinus tachycardia C. Symptomatic bradyarrhythmia
Community Ambulance Service of Minot ALS Standing Orders Legend
 Legend Indicates General Information and Guidelines Indicates Procedures Indicates Medication Administration Indicates Referral to Other Protocol Indicates Referral to Online Medical Direction Pediatric
Legend Indicates General Information and Guidelines Indicates Procedures Indicates Medication Administration Indicates Referral to Other Protocol Indicates Referral to Online Medical Direction Pediatric
Alabama Medications. Christopher J. Colvin January 2010
 Alabama Medications Christopher J. Colvin p January 2010 Activated Charcoal Used to absorb toxins ingested before they can be absorbed in the GI system. Contraindicated in AMS patients who cannot control
Alabama Medications Christopher J. Colvin p January 2010 Activated Charcoal Used to absorb toxins ingested before they can be absorbed in the GI system. Contraindicated in AMS patients who cannot control
Cardiac Arrest Pediatric Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008
 Cardiac Arrest Pediatric Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008 Preamble In contrast to cardiac arrest in adults, cardiopulmonary arrest in pediatric
Cardiac Arrest Pediatric Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008 Preamble In contrast to cardiac arrest in adults, cardiopulmonary arrest in pediatric
Advanced Cardiac Life Support
 Advanced Cardiac Life Support Dr Teo Wee Siong NATIONAL RESUSCITATION COUNCIL Singapore Guidelines 2006 Prof Anantharaman A/Prof Lim Swee Han Dr Chee Tek Siong A/Prof Peter Manning A/Prof Eillyne Seow
Advanced Cardiac Life Support Dr Teo Wee Siong NATIONAL RESUSCITATION COUNCIL Singapore Guidelines 2006 Prof Anantharaman A/Prof Lim Swee Han Dr Chee Tek Siong A/Prof Peter Manning A/Prof Eillyne Seow
Cardiac Arrest - Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008
 Cardiac Arrest - Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008 Preamble Survival from cardiorespiratory arrest for patients who present with ventricular fibrillation
Cardiac Arrest - Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008 Preamble Survival from cardiorespiratory arrest for patients who present with ventricular fibrillation
Pulseless Emergencies
 Pulseless Emergencies Nicole M. Acquisto, Pharm.D., BCPS Emergency Medicine Clinical Pharmacy Specialist University of Rochester Medical Center Nothing to disclose Disclosures Objectives Understand the
Pulseless Emergencies Nicole M. Acquisto, Pharm.D., BCPS Emergency Medicine Clinical Pharmacy Specialist University of Rochester Medical Center Nothing to disclose Disclosures Objectives Understand the
PALS Interim Study Guide
 PALS Interim Study Guide 2006 Bulletin: New resuscitation science and American Heart Association treatment guidelines were released November 28, 2005! The new AHA Handbook of Emergency Cardiac Care (ECC)
PALS Interim Study Guide 2006 Bulletin: New resuscitation science and American Heart Association treatment guidelines were released November 28, 2005! The new AHA Handbook of Emergency Cardiac Care (ECC)
Adult Drug Reference. Dopamine Drip Chart. Pediatric Drug Reference. Pediatric Drug Dosage Charts DRUG REFERENCES
 Adult Drug Reference Dopamine Drip Chart Pediatric Drug Reference Pediatric Drug Dosage Charts DRUG REFERENCES ADULT DRUG REFERENCE Drug Indication Adult Dosage Precautions / Comments ADENOSINE Paroxysmal
Adult Drug Reference Dopamine Drip Chart Pediatric Drug Reference Pediatric Drug Dosage Charts DRUG REFERENCES ADULT DRUG REFERENCE Drug Indication Adult Dosage Precautions / Comments ADENOSINE Paroxysmal
DIPHENHYDRAMINE (Benadryl)
 DIPHENHYDRAMINE (Benadryl) Classification: Antihistamine (H1 blocker) Antihistamine; appear to compete with histamine for cell receptor sites on effector cells. Therapeutic Relieves effects of histamine
DIPHENHYDRAMINE (Benadryl) Classification: Antihistamine (H1 blocker) Antihistamine; appear to compete with histamine for cell receptor sites on effector cells. Therapeutic Relieves effects of histamine
Bradycardia CHAPTER 12 CODE SCENARIO
 Senecal-12.qxd 14/04/2005 09:44 AM Page 69 CHAPTER 12 Bradycardia CODE SCENARIO A code is called for a 78-year-old man who was admitted to the hospital for syncope of unknown etiology. He was resting comfortably
Senecal-12.qxd 14/04/2005 09:44 AM Page 69 CHAPTER 12 Bradycardia CODE SCENARIO A code is called for a 78-year-old man who was admitted to the hospital for syncope of unknown etiology. He was resting comfortably
Vasopressors. Judith Hellman, M.D. Associate Professor Anesthesia and Perioperative Care University of California, San Francisco
 Vasopressors Judith Hellman, M.D. Associate Professor Anesthesia and Perioperative Care University of California, San Francisco Overview Define shock states Review drugs commonly used to treat hypotension
Vasopressors Judith Hellman, M.D. Associate Professor Anesthesia and Perioperative Care University of California, San Francisco Overview Define shock states Review drugs commonly used to treat hypotension
Pediatric Pharmacotherapy A Monthly Newsletter for Health Care Professionals Children s Medical Center at the University of Virginia
 Pediatric Pharmacotherapy A Monthly Newsletter for Health Care Professionals Children s Medical Center at the University of Virginia Volume 2 Number 12 December 1996 Medications for Neonatal and Pediatric
Pediatric Pharmacotherapy A Monthly Newsletter for Health Care Professionals Children s Medical Center at the University of Virginia Volume 2 Number 12 December 1996 Medications for Neonatal and Pediatric
Wilson County Emergency Management Agency Protocol Manual Protocols
 Asystole No pulse or respirations Confirm cardiac rhythm with combo pads or electrodes Record in two leads to confirm Asystole and to rule out fine V-Fib. Basic assessment and management (up to your scope
Asystole No pulse or respirations Confirm cardiac rhythm with combo pads or electrodes Record in two leads to confirm Asystole and to rule out fine V-Fib. Basic assessment and management (up to your scope
Septic Shock: Pharmacologic Agents for Hemodynamic Support. Nathan E Cope, PharmD PGY2 Critical Care Pharmacy Resident
 Septic Shock: Pharmacologic Agents for Hemodynamic Support Nathan E Cope, PharmD PGY2 Critical Care Pharmacy Resident Objectives Define septic shock and briefly review pathophysiology Outline receptor
Septic Shock: Pharmacologic Agents for Hemodynamic Support Nathan E Cope, PharmD PGY2 Critical Care Pharmacy Resident Objectives Define septic shock and briefly review pathophysiology Outline receptor
E C C. American Heart Association. Advanced Cardiovascular Life Support. Written Exams. May 2011
 E C C American Heart Association Advanced Cardiovascular Life Support Written Exams Contents: Exam Memo Student Answer Sheet Version A Exam Version A Answer Key Version A Reference Sheet Version B Exam
E C C American Heart Association Advanced Cardiovascular Life Support Written Exams Contents: Exam Memo Student Answer Sheet Version A Exam Version A Answer Key Version A Reference Sheet Version B Exam
table of contents drug reference
 table of contents drug reference ADULT DRUG REFERENCE...155 161 PEDIATRIC DRUG REFERENCE...162 164 PEDIATRIC WEIGHT-BASED DOSING CHARTS...165 180 Adenosine...165 Amiodarone...166 Atropine...167 Defibrillation...168
table of contents drug reference ADULT DRUG REFERENCE...155 161 PEDIATRIC DRUG REFERENCE...162 164 PEDIATRIC WEIGHT-BASED DOSING CHARTS...165 180 Adenosine...165 Amiodarone...166 Atropine...167 Defibrillation...168
DEBRIEFING GUIDE. The key components of an optimal code response: 1. Early recognition that the patient is deteriorating or has become unresponsive.
 DEBRIEFING GUIDE I N T R O D U C T I O N Debriefing has been shown to improve clinical behavior during cardiac resuscitation and, as such, has become a recommended procedure in the 2010 American Heart
DEBRIEFING GUIDE I N T R O D U C T I O N Debriefing has been shown to improve clinical behavior during cardiac resuscitation and, as such, has become a recommended procedure in the 2010 American Heart
Team Leader. Ensures high-quality CPR at all times Assigns team member roles Ensures that team members perform well. Bradycardia Management
 ACLS Megacode Case 1: Sinus Bradycardia (Bradycardia VF/Pulseless VT Asystole Out-of-Hospital Scenario You are a paramedic and arrive on the scene to find a 57-year-old woman complaining of indigestion.
ACLS Megacode Case 1: Sinus Bradycardia (Bradycardia VF/Pulseless VT Asystole Out-of-Hospital Scenario You are a paramedic and arrive on the scene to find a 57-year-old woman complaining of indigestion.
Atrial Fibrillation Management Across the Spectrum of Illness
 Disclosures Atrial Fibrillation Management Across the Spectrum of Illness NONE Barbara Birriel, MSN, ACNP-BC, FCCM The Pennsylvania State University Objectives AF Discuss the pathophysiology, diagnosis,
Disclosures Atrial Fibrillation Management Across the Spectrum of Illness NONE Barbara Birriel, MSN, ACNP-BC, FCCM The Pennsylvania State University Objectives AF Discuss the pathophysiology, diagnosis,
Management of Adult Cardiac Arrest
 73991_CH27_page68-73.qxd 6/6/11 3:54 PM Page 68 27.68 Section 5 Medical Guidelines for Performing a 12-Lead ECG The only way to learn how to obtain a 12-lead ECG is to practice with the equipment itself.
73991_CH27_page68-73.qxd 6/6/11 3:54 PM Page 68 27.68 Section 5 Medical Guidelines for Performing a 12-Lead ECG The only way to learn how to obtain a 12-lead ECG is to practice with the equipment itself.
The Pharmacist s Role in Advanced Cardiac Life Support (ACLS) Pharmacist Objectives. Pharmacists in the ER. Background
 The Pharmacist s Role in Advanced Cardiac Life Support (ACLS) I have no actual or potential conflict of interest in relation to this activity. it James Jensen B.S., Pharm.D., BCPS Pharmacist Objectives
The Pharmacist s Role in Advanced Cardiac Life Support (ACLS) I have no actual or potential conflict of interest in relation to this activity. it James Jensen B.S., Pharm.D., BCPS Pharmacist Objectives
Chapter 16. Learning Objectives. Learning Objectives 9/11/2012. Shock. Explain difference between compensated and uncompensated shock
 Chapter 16 Shock Learning Objectives Explain difference between compensated and uncompensated shock Differentiate among 5 causes and types of shock: Hypovolemic Cardiogenic Neurogenic Septic Anaphylactic
Chapter 16 Shock Learning Objectives Explain difference between compensated and uncompensated shock Differentiate among 5 causes and types of shock: Hypovolemic Cardiogenic Neurogenic Septic Anaphylactic
ANZCOR Guideline 12.4 Medications and Fluids in Paediatric Advanced Life Support
 ANZCOR Guideline 12. Medications and Fluids in Paediatric Advanced Life Support Who does this guideline apply to? This guideline applies to infants and children. Summary Who is the audience for this guideline?
ANZCOR Guideline 12. Medications and Fluids in Paediatric Advanced Life Support Who does this guideline apply to? This guideline applies to infants and children. Summary Who is the audience for this guideline?
PREPARATIONS: Adrenaline 1mg in 1ml (1:1000) Adrenaline 100micrograms in 1ml (1:10,000)
 ADRENALINE Acute hypotension Via a CENTRAL venous line Initially 100-300 nanograms/kg/minute 0.1-0.3 microgram/kg/minute adjusted according to response up to a maximum of 1.5 micrograms/kg/minute. Increase
ADRENALINE Acute hypotension Via a CENTRAL venous line Initially 100-300 nanograms/kg/minute 0.1-0.3 microgram/kg/minute adjusted according to response up to a maximum of 1.5 micrograms/kg/minute. Increase
Adding IV Amiodarone to the EMS Algorithm for Cardiac Arrest Due to VF/Pulseless VT
 Adding IV Amiodarone to the EMS Algorithm for Cardiac Arrest Due to VF/Pulseless VT Introduction Before the year 2000, the traditional antiarrhythmic agents (lidocaine, bretylium, magnesium sulfate, procainamide,
Adding IV Amiodarone to the EMS Algorithm for Cardiac Arrest Due to VF/Pulseless VT Introduction Before the year 2000, the traditional antiarrhythmic agents (lidocaine, bretylium, magnesium sulfate, procainamide,
The management of cardiac arrest
 CHAPTER 6 The management of cardiac arrest LEARNING OBJECTIVES In this chapter you will learn: How to assess the cardiac arrest rhythm and perform advanced life support 6.1. INTRODUCTION Cardiac arrest
CHAPTER 6 The management of cardiac arrest LEARNING OBJECTIVES In this chapter you will learn: How to assess the cardiac arrest rhythm and perform advanced life support 6.1. INTRODUCTION Cardiac arrest
Quiz 4 Arrhythmias summary statistics and question answers
 1 Quiz 4 Arrhythmias summary statistics and question answers The correct answers to questions are indicated by *. All students were awarded 2 points for question #2 due to no appropriate responses for
1 Quiz 4 Arrhythmias summary statistics and question answers The correct answers to questions are indicated by *. All students were awarded 2 points for question #2 due to no appropriate responses for
What is the Future of Epinephrine in Cardiac Arrest? Pros and Cons
 What is the Future of Epinephrine in Cardiac Arrest? Pros and Cons Melissa L. Thompson Bastin, PharmD., BCPS Komal A. Pandya, PharmD., BCPS 0 Presenter Disclosure Information Melissa L. Thompson Bastin,
What is the Future of Epinephrine in Cardiac Arrest? Pros and Cons Melissa L. Thompson Bastin, PharmD., BCPS Komal A. Pandya, PharmD., BCPS 0 Presenter Disclosure Information Melissa L. Thompson Bastin,
Jeopardy Topics: THE CLOT STOPS HERE (anticoagulants) SUGAR, SUGAR, HOW D YOU GET SO HIGH (insulins)
 Jeopardy Topics: THE CLOT STOPS HERE (anticoagulants) SUGAR, SUGAR, HOW D YOU GET SO HIGH (insulins) I HEAR YA KNOCKING BUT YOU CAN T COME IN (electrolytes) TAKE MY BREATH AWAY (Opiates-morphine) OUT WITH
Jeopardy Topics: THE CLOT STOPS HERE (anticoagulants) SUGAR, SUGAR, HOW D YOU GET SO HIGH (insulins) I HEAR YA KNOCKING BUT YOU CAN T COME IN (electrolytes) TAKE MY BREATH AWAY (Opiates-morphine) OUT WITH
Medical Direction and Practices Board WHITE PAPER
 Medical Direction and Practices Board WHITE PAPER Use of Pressors in Pre-Hospital Medicine: Proper Indication and State of the Science Regarding Proper Choice of Pressor BACKGROUND Shock is caused by a
Medical Direction and Practices Board WHITE PAPER Use of Pressors in Pre-Hospital Medicine: Proper Indication and State of the Science Regarding Proper Choice of Pressor BACKGROUND Shock is caused by a
Current Management of Atrial Fibrillation DISCLOSURES. Heart Beat Anatomy. I have no financial conflicts to disclose
 Current Management of Atrial Fibrillation Mary Macklin, MSN, APRN Concord Hospital Cardiac Associates DISCLOSURES I have no financial conflicts to disclose Book Women: Fit at Fifty. A Guide to Living Long.
Current Management of Atrial Fibrillation Mary Macklin, MSN, APRN Concord Hospital Cardiac Associates DISCLOSURES I have no financial conflicts to disclose Book Women: Fit at Fifty. A Guide to Living Long.
HTEC 91. Topic for Today: Atrial Rhythms. NSR with PAC. Nonconducted PAC. Nonconducted PAC. Premature Atrial Contractions (PACs)
 HTEC 91 Medical Office Diagnostic Tests Week 4 Topic for Today: Atrial Rhythms PACs: Premature Atrial Contractions PAT: Paroxysmal Atrial Tachycardia AF: Atrial Fibrillation Atrial Flutter Premature Atrial
HTEC 91 Medical Office Diagnostic Tests Week 4 Topic for Today: Atrial Rhythms PACs: Premature Atrial Contractions PAT: Paroxysmal Atrial Tachycardia AF: Atrial Fibrillation Atrial Flutter Premature Atrial
Paediatric Advanced Life Support
 Paediatric Advanced Life Support Introduction There is concern that resuscitation from cardiac arrest is not performed as well as it might because the variations in guidelines for different age groups
Paediatric Advanced Life Support Introduction There is concern that resuscitation from cardiac arrest is not performed as well as it might because the variations in guidelines for different age groups
Pediatric Advanced Life Support (PALS) Recertification Preparatory Materials
 Pediatric Advanced Life Support (PALS) Recertification Preparatory Materials 1 PEDIATRIC ADVANCED LIFE SUPPORT (PALS) RECERTIFICATION TABLE OF CONTENTS CYCLIC APPROACH 03 PEDIATRIC ASSESSMENT FLOWCHART
Pediatric Advanced Life Support (PALS) Recertification Preparatory Materials 1 PEDIATRIC ADVANCED LIFE SUPPORT (PALS) RECERTIFICATION TABLE OF CONTENTS CYCLIC APPROACH 03 PEDIATRIC ASSESSMENT FLOWCHART
PEDIATRIC TREATMENT GUIDELINES
 P1 Pediatric Patient Care P2 Cardiac Arrest Initial Care and CPR P3 Neonatal Resuscitation P4 Ventricular Fibrillation / Ventricular Tachycardia P5 PEA / Asystole P6 Symptomatic Bradycardia P7 Tachycardia
P1 Pediatric Patient Care P2 Cardiac Arrest Initial Care and CPR P3 Neonatal Resuscitation P4 Ventricular Fibrillation / Ventricular Tachycardia P5 PEA / Asystole P6 Symptomatic Bradycardia P7 Tachycardia
ROC CONTINUOUS CHEST COMPRESSIONS STUDY (CCC): MEDICAL CARDIAC ARREST MEDICAL DIRECTIVE
 ROC CONTINUOUS CHEST COMPRESSIONS STUDY (CCC): MEDICAL CARDIAC ARREST MEDICAL DIRECTIVE An Advanced Care Paramedic will provide the treatment based on the randomization scheme and as prescribed in this
ROC CONTINUOUS CHEST COMPRESSIONS STUDY (CCC): MEDICAL CARDIAC ARREST MEDICAL DIRECTIVE An Advanced Care Paramedic will provide the treatment based on the randomization scheme and as prescribed in this
ADVANCED LIFE SUPPORT LEARNING PACKAGE
 SOUTH WEST HEALTHCARE WARRNAMBOOL ADVANCED LIFE SUPPORT LEARNING PACKAGE Prepared by: J. Brown, ICU Last revised February, 2010. C. Joseph, Nursing Education. CONTENTS: Page: Objectives 3-5 Basic Life
SOUTH WEST HEALTHCARE WARRNAMBOOL ADVANCED LIFE SUPPORT LEARNING PACKAGE Prepared by: J. Brown, ICU Last revised February, 2010. C. Joseph, Nursing Education. CONTENTS: Page: Objectives 3-5 Basic Life
Glucagon stimulates adenyl cyclase. Amrinone and milrinone inhibit phosphodiesteras e
 Beta-Adrenergic Blocker Poisoning John Gualtieri, PharmD Clinical Assistant Professor Dept. of Experimental and Clinical Pharmacology College of Pharmacy, Univ of Minnesota I. Objectives 1.) Described
Beta-Adrenergic Blocker Poisoning John Gualtieri, PharmD Clinical Assistant Professor Dept. of Experimental and Clinical Pharmacology College of Pharmacy, Univ of Minnesota I. Objectives 1.) Described
Dysrhythmia Assessment and Management Scenarios
 Dysrhythmia Assessment and Management Scenarios Authors: John Guerriero, EMT-P, Gene Iannuzzi, RN, CCRN, EMT-P, Arther Romano, EMT-P, Kevin Brown, MD, EMT-P 1 An Important Word About the Therapies Discussed
Dysrhythmia Assessment and Management Scenarios Authors: John Guerriero, EMT-P, Gene Iannuzzi, RN, CCRN, EMT-P, Arther Romano, EMT-P, Kevin Brown, MD, EMT-P 1 An Important Word About the Therapies Discussed
Tachyarrhythmias (fast heart rhythms)
 Patient information factsheet Tachyarrhythmias (fast heart rhythms) The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
Patient information factsheet Tachyarrhythmias (fast heart rhythms) The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
ADRENERGIC AND ANTI-ADRENERGIC DRUGS. Mr. D.Raju, M.pharm, Lecturer
 ADRENERGIC AND ANTI-ADRENERGIC DRUGS Mr. D.Raju, M.pharm, Lecturer SYMPATHETIC NERVOUS SYSTEM Fight or flight response results in: 1. Increased BP 2. Increased blood flow to brain, heart and skeletal muscles
ADRENERGIC AND ANTI-ADRENERGIC DRUGS Mr. D.Raju, M.pharm, Lecturer SYMPATHETIC NERVOUS SYSTEM Fight or flight response results in: 1. Increased BP 2. Increased blood flow to brain, heart and skeletal muscles
Adrenergic agonists:-
 Adrenergic agonists:- A.) Catecholamines They are called catecholamines because they contain a catechol group, they are water-soluble and are 50% bound to plasma proteins, so they circulate in the bloodstream.
Adrenergic agonists:- A.) Catecholamines They are called catecholamines because they contain a catechol group, they are water-soluble and are 50% bound to plasma proteins, so they circulate in the bloodstream.
Paramedic Pediatric Medical Math Test
 Paramedic Pediatric Medical Math Test Name: Date: Problem 1 Your 4 year old pediatric patient weighs 40 pounds. She is febrile. You need to administer acetaminophen (Tylenol) 15mg/kg. How many mg will
Paramedic Pediatric Medical Math Test Name: Date: Problem 1 Your 4 year old pediatric patient weighs 40 pounds. She is febrile. You need to administer acetaminophen (Tylenol) 15mg/kg. How many mg will
Advanced Cardiovascular Life Support Case Scenarios
 Advanced Cardiovascular Life Support Case Scenarios ACLS Respiratory Arrest Case Out-of-Hospital Scenario You are a paramedic and respond to the scene of a possible cardiac arrest. A young man lies motionless
Advanced Cardiovascular Life Support Case Scenarios ACLS Respiratory Arrest Case Out-of-Hospital Scenario You are a paramedic and respond to the scene of a possible cardiac arrest. A young man lies motionless
Sign up to receive ATOTW weekly email worldanaesthesia@mac.com
 INTRODUCTION TO CARDIOVASCULAR PHYSIOLOGY ANAESTHESIA TUTORIAL OF THE WEEK 125 16 TH MARCH 2009 Toby Elkington, Specialist Registrar Carl Gwinnutt, Consultant Department of Anaesthesia, Salford Royal NHS
INTRODUCTION TO CARDIOVASCULAR PHYSIOLOGY ANAESTHESIA TUTORIAL OF THE WEEK 125 16 TH MARCH 2009 Toby Elkington, Specialist Registrar Carl Gwinnutt, Consultant Department of Anaesthesia, Salford Royal NHS
Physiology and Pharmacology
 Pharmacokinetics Physiology and Pharmacology Pharmacokinetics of Local Anesthetics Uptake Oral Route Topical Route Injection Distribution Metabolism (Biotransformation) Excretion Uptake So what? Vasoactivity
Pharmacokinetics Physiology and Pharmacology Pharmacokinetics of Local Anesthetics Uptake Oral Route Topical Route Injection Distribution Metabolism (Biotransformation) Excretion Uptake So what? Vasoactivity
American Heart Association. Pediatric Advanced Life Support. Written Precourse Self-Assessment. Questions and Answer Key for Students.
 E C C American Heart Association Pediatric Advanced Life Support Written Precourse Self-Assessment Questions and Answer Key for Students January 2012 PALS Written 2011 Precourse Self-Assessment ECG Rhythm
E C C American Heart Association Pediatric Advanced Life Support Written Precourse Self-Assessment Questions and Answer Key for Students January 2012 PALS Written 2011 Precourse Self-Assessment ECG Rhythm
Essential facts for med-surg nurses
 Emergency cardiac drugs: Essential facts for med-surg nurses Emergencies on a med-surg unit can be daunting. By Ira Gene Reynolds, MSNEd, RN, PCCN-CMC IN THE HOSPITAL SETTING, emergencies typically occur
Emergency cardiac drugs: Essential facts for med-surg nurses Emergencies on a med-surg unit can be daunting. By Ira Gene Reynolds, MSNEd, RN, PCCN-CMC IN THE HOSPITAL SETTING, emergencies typically occur
OBJECTIVES. When the student has finished this module, he/she will be able to:
 Advanced Cardiac Life Support (ACLS) Review WWW.RN.ORG Reviewed September, 2015, Expires September, 2017 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited
Advanced Cardiac Life Support (ACLS) Review WWW.RN.ORG Reviewed September, 2015, Expires September, 2017 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited
10. An infant with a history of vomiting and diarrhea arrives by ambulance. During your primary assessment the infant responds only to painful stimula
 1. You are called to help resuscitate an infant with severe symptomatic bradycardia associated with respiratory distress. The bradycardia persists despite establishment of an effective airway, oxygenation,
1. You are called to help resuscitate an infant with severe symptomatic bradycardia associated with respiratory distress. The bradycardia persists despite establishment of an effective airway, oxygenation,
Normal Sinus Rhythm. Sinus Bradycardia. Sinus Tachycardia. Rhythm ECG Characteristics Example (NSR) & consistent. & consistent.
 Normal Sinus Rhythm (NSR) Rate: 60-100 per minute Rhythm: R- R = P waves: Upright, similar P-R: 0.12-0.20 second & consistent P:qRs: 1P:1qRs Sinus Tachycardia Exercise Hypovolemia Medications Fever Hypoxia
Normal Sinus Rhythm (NSR) Rate: 60-100 per minute Rhythm: R- R = P waves: Upright, similar P-R: 0.12-0.20 second & consistent P:qRs: 1P:1qRs Sinus Tachycardia Exercise Hypovolemia Medications Fever Hypoxia
Wide-Complex Tachycardias in the ED: Myths and Pitfalls
 Wide-Complex Tachycardias in the ED: Myths and Pitfalls, FACEP, FAAEM Professor and Vice Chair Director, Emergency Cardiology Fellowship Department of Emergency Medicine University of Maryland School of
Wide-Complex Tachycardias in the ED: Myths and Pitfalls, FACEP, FAAEM Professor and Vice Chair Director, Emergency Cardiology Fellowship Department of Emergency Medicine University of Maryland School of
Episode 20 Atrial fibrillation Prepared by Dr. Lucas Chartier
 Episode 20 Atrial fibrillation Prepared by Dr. Lucas Chartier Most common dysrhythmia seen in ED, and incidence increasing with ageing population Presentation Common presentations: younger patients often
Episode 20 Atrial fibrillation Prepared by Dr. Lucas Chartier Most common dysrhythmia seen in ED, and incidence increasing with ageing population Presentation Common presentations: younger patients often
ACLS Rhythms for the ACLS Algorithms
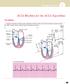 ACLS Rhythms for the ACLS Algorithms The Basics 1. Anatomy of the cardiac conduction system: relationship to the ECG cardiac cycle. A, Heart: anatomy of conduction system. B, P-QRS-T complex: lines to
ACLS Rhythms for the ACLS Algorithms The Basics 1. Anatomy of the cardiac conduction system: relationship to the ECG cardiac cycle. A, Heart: anatomy of conduction system. B, P-QRS-T complex: lines to
Cardiac Arrest: General Considerations
 Andrea Gabrielli, MD, FCCM Cardiac Arrest: General Considerations Cardiopulmonary resuscitation (CPR) is described as a series of assessments and interventions performed during a variety of acute medical
Andrea Gabrielli, MD, FCCM Cardiac Arrest: General Considerations Cardiopulmonary resuscitation (CPR) is described as a series of assessments and interventions performed during a variety of acute medical
!!! BOLUS DOSE IV. Use 5-10 mcg IV boluses STD ADRENALINE INFUSION. Use IM adrenaline in advance of IV dosing!
 ADRENALINE IVI BOLUS IV Open a vial of 1:1000 ADRENALINE 1 mg /ml Add 1 ml to 9 ml N/Saline = 1mg adrenaline in 10 ml (or 100 mcg/ml) Add 1 ml 1:10,000 to 9 ml N/Saline = 100 mcg adrenaline in 10 ml (or
ADRENALINE IVI BOLUS IV Open a vial of 1:1000 ADRENALINE 1 mg /ml Add 1 ml to 9 ml N/Saline = 1mg adrenaline in 10 ml (or 100 mcg/ml) Add 1 ml 1:10,000 to 9 ml N/Saline = 100 mcg adrenaline in 10 ml (or
RESPONDING TO ANESTHETIC COMPLICATIONS
 RESPONDING TO ANESTHETIC COMPLICATIONS General anesthesia poses minimal risk to most patients when performed by a capable anesthetist using appropriate protocols and proper monitoring. However, it is vitally
RESPONDING TO ANESTHETIC COMPLICATIONS General anesthesia poses minimal risk to most patients when performed by a capable anesthetist using appropriate protocols and proper monitoring. However, it is vitally
Atrial Fibrillation in the ICU: Attempting to defend 4 controversial statements
 Atrial Fibrillation in the ICU: Attempting to defend 4 controversial statements Salmaan Kanji, Pharm.D. The Ottawa Hospital The Ottawa Hospital Research Institute Conflict of Interest No financial, proprietary
Atrial Fibrillation in the ICU: Attempting to defend 4 controversial statements Salmaan Kanji, Pharm.D. The Ottawa Hospital The Ottawa Hospital Research Institute Conflict of Interest No financial, proprietary
Cardiovascular System & Its Diseases. Lecture #4 Heart Failure & Cardiac Arrhythmias
 Cardiovascular System & Its Diseases Lecture #4 Heart Failure & Cardiac Arrhythmias Dr. Derek Bowie, Department of Pharmacology & Therapeutics, Room 1317, McIntyre Bldg, McGill University derek.bowie@mcgill.ca
Cardiovascular System & Its Diseases Lecture #4 Heart Failure & Cardiac Arrhythmias Dr. Derek Bowie, Department of Pharmacology & Therapeutics, Room 1317, McIntyre Bldg, McGill University derek.bowie@mcgill.ca
Allergy Emergency Treatment Protocol
 Allergy Emergency Treatment Protocol I. Initial evaluation of possible allergic reaction a. Cease administration of allergenic extracts b. Notify physician c. Record vital signs: blood pressure, pulse,
Allergy Emergency Treatment Protocol I. Initial evaluation of possible allergic reaction a. Cease administration of allergenic extracts b. Notify physician c. Record vital signs: blood pressure, pulse,
Intravenous Infusions
 Intravenous Infusions 1 Intravenous Infusions This course will cover different types of common intravenous medication infusions including insulin, heparin, vasopressors, vasodilators, and anti-arrhythmics.
Intravenous Infusions 1 Intravenous Infusions This course will cover different types of common intravenous medication infusions including insulin, heparin, vasopressors, vasodilators, and anti-arrhythmics.
New Approaches for Prehospital Cardiac Arrest Management 2010 NCEMSF Conference
 New Approaches for Prehospital Cardiac Arrest Management 2010 NCEMSF Conference Mark E. Pinchalk, MS, EMT-P Paramedic Crew Chief City of Pittsburgh EMS Out of Hospital Cardiac Arrest Poor outcomes: Arizona
New Approaches for Prehospital Cardiac Arrest Management 2010 NCEMSF Conference Mark E. Pinchalk, MS, EMT-P Paramedic Crew Chief City of Pittsburgh EMS Out of Hospital Cardiac Arrest Poor outcomes: Arizona
Adrenergic agonists. R. A. Nimmi Dilsha Department of pharmacy Faculty of Health Sciences The Open University of Sri Lanka
 Adrenergic agonists R. A. Nimmi Dilsha Department of pharmacy Faculty of Health Sciences The Open University of Sri Lanka Outline Recall Introduction to adrenergic agonists Classification of adrenergic
Adrenergic agonists R. A. Nimmi Dilsha Department of pharmacy Faculty of Health Sciences The Open University of Sri Lanka Outline Recall Introduction to adrenergic agonists Classification of adrenergic
Adult Cardiac Life Support (ACLS) Recertification Preparatory Materials
 Adult Cardiac Life Support (ACLS) Recertification Preparatory Materials 1 ADULT CARDIAC LIFE SUPPORT (ACLS) RECERTIFICATION TABLE OF CONTENTS PRIMARY AND SECONDARY ABCDs I. Primary ABCD s 03 II. Secondary
Adult Cardiac Life Support (ACLS) Recertification Preparatory Materials 1 ADULT CARDIAC LIFE SUPPORT (ACLS) RECERTIFICATION TABLE OF CONTENTS PRIMARY AND SECONDARY ABCDs I. Primary ABCD s 03 II. Secondary
Recurrent AF: Choosing the Right Medication.
 In the name of God Shiraz E-Medical Journal Vol. 11, No. 3, July 2010 http://semj.sums.ac.ir/vol11/jul2010/89015.htm Recurrent AF: Choosing the Right Medication. Basamad Z. * Assistant Professor, Department
In the name of God Shiraz E-Medical Journal Vol. 11, No. 3, July 2010 http://semj.sums.ac.ir/vol11/jul2010/89015.htm Recurrent AF: Choosing the Right Medication. Basamad Z. * Assistant Professor, Department
PHENYLEPHRINE HYDROCHLORIDE INJECTION USP
 PRESCRIBING INFORMATION PHENYLEPHRINE HYDROCHLORIDE INJECTION USP 10 mg/ml Sandoz Canada Inc. Date of Preparation: September 1992 145 Jules-Léger Date of Revision : January 13, 2011 Boucherville, QC, Canada
PRESCRIBING INFORMATION PHENYLEPHRINE HYDROCHLORIDE INJECTION USP 10 mg/ml Sandoz Canada Inc. Date of Preparation: September 1992 145 Jules-Léger Date of Revision : January 13, 2011 Boucherville, QC, Canada
Sign up to receive ATOTW weekly - email worldanaesthesia@mac.com
 ADRENALINE (EPINEPHRINE) ANAESTHESIA TUTORIAL OF THE WEEK 226 6 TH JUNE 2011 Prof. John Kinnear Southend University Hospital NHS Foundation Trust, UK Correspondence to John.Kinnear@southend.nhs.uk QUESTIONS
ADRENALINE (EPINEPHRINE) ANAESTHESIA TUTORIAL OF THE WEEK 226 6 TH JUNE 2011 Prof. John Kinnear Southend University Hospital NHS Foundation Trust, UK Correspondence to John.Kinnear@southend.nhs.uk QUESTIONS
Milwaukee School of Engineering Gerrits@msoe.edu. Case Study: Factors that Affect Blood Pressure Instructor Version
 Case Study: Factors that Affect Blood Pressure Instructor Version Goal This activity (case study and its associated questions) is designed to be a student-centered learning activity relating to the factors
Case Study: Factors that Affect Blood Pressure Instructor Version Goal This activity (case study and its associated questions) is designed to be a student-centered learning activity relating to the factors
Exchange solutes and water with cells of the body
 Chapter 8 Heart and Blood Vessels Three Types of Blood Vessels Transport Blood Arteries Carry blood away from the heart Transport blood under high pressure Capillaries Exchange solutes and water with cells
Chapter 8 Heart and Blood Vessels Three Types of Blood Vessels Transport Blood Arteries Carry blood away from the heart Transport blood under high pressure Capillaries Exchange solutes and water with cells
Guideline for the management of arrhythmias
 Guideline for the management of arrhythmias The following guideline is approved only for use at University College London Hospitals NHS Foundation Trust. It is provided as supporting information for the
Guideline for the management of arrhythmias The following guideline is approved only for use at University College London Hospitals NHS Foundation Trust. It is provided as supporting information for the
ACID- BASE and ELECTROLYTE BALANCE. MGHS School of EMT-Paramedic Program 2011
 ACID- BASE and ELECTROLYTE BALANCE MGHS School of EMT-Paramedic Program 2011 ACID- BASE BALANCE Ions balance themselves like a see-saw. Solutions turn into acids when concentration of hydrogen ions rises
ACID- BASE and ELECTROLYTE BALANCE MGHS School of EMT-Paramedic Program 2011 ACID- BASE BALANCE Ions balance themselves like a see-saw. Solutions turn into acids when concentration of hydrogen ions rises
Pharmacology - Problem Drill 06: Autonomic Pharmacology - Adrenergic System
 Pharmacology - Problem Drill 06: Autonomic Pharmacology - Adrenergic System Question No. 1 of 10 Instructions: (1) Read the problem and answer choices carefully, (2) Work the problems on paper as 1. What
Pharmacology - Problem Drill 06: Autonomic Pharmacology - Adrenergic System Question No. 1 of 10 Instructions: (1) Read the problem and answer choices carefully, (2) Work the problems on paper as 1. What
Purpose To guide registered nurses who may manage clients experiencing sudden or unexpected life-threatening cardiac emergencies.
 Emergency Cardiac Care: Decision Support Tool #1 RN-Initiated Emergency Cardiac Care Without Cardiac Monitoring/Manual Defibrillator or Emergency Cardiac Drugs Decision support tools are evidence-based
Emergency Cardiac Care: Decision Support Tool #1 RN-Initiated Emergency Cardiac Care Without Cardiac Monitoring/Manual Defibrillator or Emergency Cardiac Drugs Decision support tools are evidence-based
ACLS RHYTHM TEST. 2. A 74-year-old woman with chest pain. Blood pressure 192/90 and rates her pain 9/10.
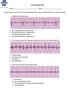 ACLS RHYTHM TEST Name Date Choose the best answer for each of the following questions. Each of the following strips is 6 seconds in length. 1. Identify the following rhythm a. Sinus bradycardia with 2
ACLS RHYTHM TEST Name Date Choose the best answer for each of the following questions. Each of the following strips is 6 seconds in length. 1. Identify the following rhythm a. Sinus bradycardia with 2
