RESPIRATORY CARE OF SMA AND CHOICES I. IDENTIFYING THE PROBLEM
|
|
|
- Charleen Alexander
- 7 years ago
- Views:
Transcription
1 RESPIRATORY CARE OF SMA AND CHOICES I. IDENTIFYING THE PROBLEM Respiratory care is critically important for individuals with spinal muscular atrophy and affects both their survival and quality of life. SMA affects the muscles for breathing as well as the muscles for moving the arms and legs. NORMAL BREATHING MUSCLE FUNCTION The muscles important for breathing include the intercostal muscles and the diaphragm. The intercostal muscles are the muscles between the ribs. These muscles help to lift up and expand the shape of the rib cage thereby helping the lungs to inflate. The diaphragm is the large muscle at the bottom of the rib cage. The diaphragm works by pulling the rib cage down in an almost opposite direction of the intercostal muscles, and also helps the chest wall and lungs to expand causing air to fill the lungs. What you see in someone without SMA is that the ribcage inflates with air at the top of the ribcage as well as at the bottom of the ribcage during inhalation. SMA BREATHING MUSCLE FUNCTION SMA causes very weak intercostals muscles, the muscles between the ribs. The strongest breathing muscle in SMA is the diaphragm. As a result, children with SMA type I and type II appear to breath with their stomach muscles. The belly or abdomen pooches out while they take a breath in. The top of the rib cage does not appear to move. In infants less than a year of age, the rib cage is very soft even though it consists of the ribs, which are bones and cartilage. Over time the rib cage may appear as though the bottom of the ribcage is pulled down. This gives the appearance of a bell shaped chest meaning that the top of the chest is narrow and the bottom of the chest is much wider. Sometimes the area of the sternum or the bone in the front that the ribs attach to becomes sunken. This is called pectus excavatum and happens because the intercostals muscles are not strong enough to help pull the top of the rib cage out against the diaphragm that is pulling down. NORMAL SMA WHAT DOES THIS MEAN? Respiratory Care of SMA and Choices Page 1 of 7
2 Individuals with SMA have respiratory muscles that are at a mechanical disadvantage. Because the lungs cannot inflate fully, the lungs may not fully develop. In addition, because the muscles are weak, the cough is very weak, and it is difficult to take deep enough breaths while sleeping to maintain normal oxygen levels and normal carbon dioxide levels. LUNG UNDERDEVELOPMENT Lungs that are not fully developed may contribute to decreased lung function as an adult. Normal lung expansion helps the rib cage to grow and maintain a normal chest wall shape. A normal chest wall shape provides the best mechanical advantage for the lungs to work optimally. One of our goals for the respiratory care of children with SMA is to provide maximum lung and chest wall development. WEAK COUGH During viral respiratory infections, the nose and the lungs make a lot of secretions. In addition, everyone is weaker during a cold. If the secretions are not cleared from the lungs by coughing, the secretions will collect in the airways and cause plugging of the small breathing tubes of the lungs. If the secretions become infected this will result in pneumonia. Plugging of the small breathing tubes of the lungs results in collapse of some of the air sacs and this is called atelectasis. A consequence of atelectasis is decreased oxygen saturation, which means that there is not enough oxygen in the blood for the body to maintain normal functions. Oxygen saturation can be determined easily using a pulse oximeter. SHALLOW BREATHING DURING SLEEP During sleep, the muscles relax including the muscles for breathing. During normal breathing, we breathe in oxygen and exhale carbon dioxide. When someone who has muscle weakness falls asleep, their muscles for breathing also relax and their breaths become more shallow. Sometimes those breaths become so shallow that they do not inhale adequate oxygen and they also do not exhale enough carbon dioxide. This is called hypoventilation. As a result, their oxygen saturations during sleep may drop to less than 94% and their carbon dioxide level may increase. II. WHAT CAN BE DONE LUNG DEVELOPMENT Lung underdevelopment can be overcome by giving insufflations or big breaths daily using any of the following: a resuscitator bag and mask, or a cough machine on the inspiratory setting only or an intermittent positive pressure breathing (IPPB) device. This exercises the muscles for breathing and expands the lungs to a larger volume than the person can do on their own. 1. Using the resuscitator bag and mask, the mask is placed over the nose and mouth and a breath is given to the person while they are inhaling. Several breaths are given over several minutes to help inflate the lungs. Respiratory Care of SMA and Choices Page 2 of 7
3 2. A cough machine with an automatic cycle is a device that can be set to shift from inhalation mode to exhalation mode and then a pause before the next breath. The breaths are given by either a mask over the nose and mouth or a mouthpiece. Using the cough machine in the inhalation mode only, the lungs can be inflated to a set pressure. (Please see additional information below in Improve Cough.) 3. IPPB gives a breath in synchrony with an individual to a set pressure with a mouthpiece or a mask over the nose and mouth. A similar effect can be achieved using the cough machine. Incentive spirometers typically given to adults after a surgery are not helpful to individuals with SMA because the spirometer inflates the lungs but only to the volume the person can do already. There is no extra expansion or benefit to using this device. IMPROVE COUGH/AIRWAY CLEARANCE Coughing up secretions can be improved dramatically by using a cough machine or having someone else use their hand to cough assist. Manual cough assist means that another person uses their hand to apply pressure to the diaphragm in synchrony with the coughing person. This results in increased force of the diaphragm to move air out of the lungs. The cough machine inflates the lung to a set pressure for a set time following by sucking the air out of the lungs at a set pressure for a set time. This is very similar to what occurs during coughing in stronger people. When you cough, you inhale a big breath, close your throat, increase the pressure inside your chest, open your throat and then the air bursts out of the lungs. Typical settings for the cough machine are inhale pressure 25 to 40 cm of H20 for 1 second, exhale pressure 25 to 40 for 1 second and pause time 1 to 2 seconds. Four to 5 breaths are taken continually followed by suctioning the mouth to remove secretions coughed up and a rest period of 1 to 2 minutes. Four sets of 5 breaths is a typical treatment. The cough machine cannot be overused for the purpose of coughing and should be thought of as the way the person with SMA coughs. There is no other device that helps to clear the secretions out of the lungs. The cough machine is made by the Emerson Co. and is available through your home care durable medical equipment (DME) provider. The cough machines are known by brand as the In-exsufflator Cough Machine or the newer Cough Assist. AIRWAY SECRETION MOBILIZATION When a person with SMA has a cold, the secretions build up and are difficult to cough out. One of the ways we help remove secretions is to loosen them up in the airways before coughing. The techniques available to loosen secretions include manual or mechanical percussion, postural drainage, intrapulmonary percussive ventilation (IPV), and the Vest Airway Clearance system. 1. Manual or mechanical percussion means using your hands or palm cups to clap on different parts of the chest while positioning that part of the lung to promote maximal drainage. Mechanical percussion refers to using a vibrating device applied to the chest to loosen secretions. Respiratory Care of SMA and Choices Page 3 of 7
4 2. Postural drainage means positioning the person so that the secretions in the lungs will drain with gravity. Typically the person will lay on their tummy, back or side with their bottom higher than their chest. This allows the secretions to move with gravity out to the larger airways. This is usually done during manual or mechanical percussion. 3. IPV is a mechanical device that provides positive pressure by mask or mouthpiece into the airways at a set frequency that can be varied as tolerated. Medication or saline is nebulized with IPV. This is mechanical percussion from the inside of the lungs. The machine sounds like a choo-choo train. 4. The Vest Airway Clearance System is a mechanical device that delivers air at a set frequency and pressure to the chest through a vest that the individual wears. This device is expensive and has not been proven to be more effective than other modes of airway secretion mobilization. BREATHING SUPPORT OPTIONS Individuals with SMA type I and many individuals with SMA type II have hypoventilation while they sleep at night. This means that they exchange carbon dioxide and oxygen at lower levels than is necessary for the body to maintain normal function. Their oxygen saturations drop and their carbon dioxide levels increase. To improve this problem, patients with SMA have to receive bigger breaths during sleep. There are several options to accomplish better ventilation (bigger breaths) and oxygenation while sleeping including BiPAP, mechanical ventilator, and negative pressure ventilation. During illnesses the respiratory support device may need to be worn throughout the day also. There is no role for supplemental oxygen in patients with SMA until ALL other options have been exhausted. 1. BiPAP refers to bilevel or two level positive airway pressure. This is usually delivered through a mask over the nose. BiPAP provides a higher pressure and volume of air into the lungs during inhalation and inflates the lung greater than what the person can do without the BiPAP machine. During exhalation, the BiPAP pressure drops so that air can passively leave the lungs. The BiPAP machine can sense when the person is taking a breath and gives the breath in synchrony with the individual. A respiratory rate is also set so that the BiPAP gives a minimum number of breaths per minute. The person can breath above that rate and the BiPAP will deliver more breaths. CPAP (continuous positive airway pressure) should never be used in patients with SMA. 2. Mechanical ventilators or respirators come in a variety of models. The most portable model that is available is the LTV (laptop ventilator). This ventilator can be carried over the shoulder or placed on a wheelchair for transport. The external battery is still cumbersome, but this may improve soon. Mechanical ventilators are more complex, but also allow for control of more variables. The ventilator can be set to deliver a specific size breath at a set number of breaths per minute. Mechanical ventilation can be delivered with a nose mask, mouthpiece while awake, or through a tracheostomy tube. 3. Negative pressure ventilation refers to providing breaths into the lungs using a large chamber or tank that encircles the chest. The chamber is connected to a vacuum pump Respiratory Care of SMA and Choices Page 4 of 7
5 that takes the air out of the chamber and as a result the chest wall expands to bring air into the lungs. A Porta-Lung is an example of a negative pressure ventilator. It can be set to deliver a specific number of breaths per minute and a vacuum pressure. III. PROTOCOL FOR MANAGEMENT OF AIRWAY SECRETIONS DURING A COLD During a cold, individuals with muscle weakness can have a very hard time clearing mucus from their lower airway. You can help them by following these steps: 1. These steps should be done in the order shown below every four hours and as needed during the cold. a. Airway secretion mobilization for minutes. b. Cough machine, four sets of 5 breaths to remove the loosened secretions. c. Postural drainage for minutes, which means laying with their bottom higher than their chest so that gravity helps to move the secretions out of the lungs. d. Cough machine, four sets of 5 breaths to help remove the remaining drained secretions. 2. Use the cough machine every time your child sounds rattley or has trouble coughing out secretions. You cannot use this machine too much. If your child has difficulty getting secretions out of the back of their throat, also suction their mouth. 3. If your child is on BiPAP or breathing support by nose mask, use the machine every time that they are asleep including naps during the day. Your child is weaker than usual during colds. They may also need to use the breathing support machine while they are awake. 4. Use a pulse oximeter to check your child s oxygen saturations once per day when well and three times per day when sick. Often you may not be able to tell when your child is having difficulty breathing and the pulse oximeter may tell you there is a problem sooner and that they need help coughing. If the oxygen saturation is less than 94%, use the cough machine to clear secretions and recheck the oximetry. If the oxygen saturation is 92% or less and the cough machine is not increasing the oxygen saturation, please contact your physician. Your child may need to be in the hospital for more intense therapy. If your child is vomiting, they may become dehydrated. This can be a very serious complication in children with Spinal Muscular Atrophy. IV. CHOICES Non-invasive respiratory care management means helping a child to breathe using a mask over the nose that is connected to a BiPAP machine or a mechanical ventilator. Invasive respiratory management refers to the use of a breathing tube that is placed in the mouth and passed between the vocal cords and into the lungs. Invasive respiratory management also includes the placement of a surgical hole in the neck to the large airway (trachea) for a tracheostomy tube. A tracheostomy tube bypasses the mouth and vocal cords and goes directly from the skin to the trachea. A respirator or ventilator is connected to the endotracheal tube or tracheostomy tube. Respiratory Care of SMA and Choices Page 5 of 7
6 SMA TYPE I Children with SMA type I have a huge variation in muscle strength and their breathing support needs are difficult to predict. Almost all children with SMA type I benefit from supportive ventilation with BiPAP or a ventilator using a nasal mask while they sleep starting at an early age, 6 months for example. The breathing support needed while healthy ranges from no breathing support while sleeping to needing BiPAP while sleeping to needing breathing support 24 hours per day, 7 days per week with or without a tracheostomy tube. During colds all children require additional breathing support and may need to use their BiPAP or ventilator 24 hours per day until the cold goes away. Parents of children with SMA type I have many very difficult decisions. First is whether you wish to pursue non-invasive breathing support per nose mask for your child. The methods and equipment although generally effective are also a tremendous amount of work, especially when the child has a cold. In addition, the child may not tolerate the nose mask breathing support. Another decision is whether you desire to have your child intubated should they become very sick especially with a cold. Remember, everyone becomes weaker with a cold. One of the things you and your doctor should consider is whether the illness and difficulty breathing is a sudden change due to a cold and may be reversible, or whether it seems to be a result of the child becoming gradually weaker over all. Using an aggressive airway clearance and extubation (removal of the breathing tube) protocol followed by placing the child on breathing support by nose mask provides the greatest chance for success. Some physicians are not aware of the protocol and tools that are available. However, when a child with SMA type I has a breathing tube placed one of the risks is whether the child will succeed in having the breathing tube removed and using breathing support by nose mask when the illness has resolved. If the child does not tolerate breathing support by nose mask despite the best efforts of the doctor another difficult decision has to be made. The decision at this point is whether to: 1. Wait and see if the child will become stronger and try again. 2. Consider transferring to a hospital that has a lot of experience with non-invasive respiratory care if your hospital does not. 3. Consider tracheostomy tube placement. 4. Consider letting your child go. There are no right answers and as a parent, you will make the best decision that you can for your child. Something to keep in mind is that the non-invasive methods for respiratory care of children with SMA are not for everyone and not everyone can do this for a variety of reasons. In addition, some children do not do well with the non-invasive breathing support or require the breathing support 24 hours per day. Requiring 24 hours per day breathing support by nose mask may be very difficult for the child as well as for the family. Again, you as the parent will make the best decision you can for your child. SMA Type II Respiratory Care of SMA and Choices Page 6 of 7
7 Children with SMA type II should never require a tracheostomy, and in general are strong enough to be managed using non-invasive respiratory care techniques on a day to day basis. This means that when the child is healthy, they may use BiPAP or a ventilator with a nose mask or negative pressure ventilation while they sleep, and the Cough Assist device as needed. Some children with SMA type II do not require support for their breathing while they sleep. When a child with SMA type II develops a cold, they may need to use their nose mask breathing support more often and sometimes continuously. Remember that during a cold they are weaker than usual, but their strength improves after the cold has resolved. During a cold they need respiratory care treatments every 4 hours with airway secretion mobilization, cough machine use and postural drainage. The cough machine may be needed more often to clear the mucus. If oxygen saturation cannot be maintained at 92% or greater on BiPAP, they may need to be hospitalized and may need to have a breathing tube place and attached to a ventilator. However, through aggressive use of airway secretion mobilization and airway clearance, the tube can be removed and the child placed on ventilation by nose mask and then weaned back to using the breathing support while they sleep only. SUMMARY The respiratory care for children with SMA is critically important. The necessary tools include a cough machine, a method for airway secretion mobilization, a method for performing postural drainage, and a pulse oximeter to help monitor their oxygen saturations. In addition, a method for breathing support including a BiPAP machine or mechanical ventilator are also very important. For individuals with SMA type II, aggressive respiratory care using non-invasive techniques improves quality and quantity of life. For children with SMA type I, the non-invasive respiratory care techniques are beneficial and generally effective. Please keep in mind that not all techniques fit every child. Respiratory Care of SMA and Choices Page 7 of 7
Keeping your lungs healthy
 Keeping your lungs healthy A guide for you after spinal cord injury and other neurological conditions Regional Rehabilitation Program This booklet has been written by the health care providers who provide
Keeping your lungs healthy A guide for you after spinal cord injury and other neurological conditions Regional Rehabilitation Program This booklet has been written by the health care providers who provide
Caring Choices. For Parents of Infants Newly Diagnosed with SMA Type 1 SMA CARE SERIES
 Caring Choices For Parents of Infants Newly Diagnosed with SMA Type 1 SMA CARE SERIES SMA CARE SERIES - Caring Choices Contents Dear Parents, Friends and Family Members 3 What Decisions are Ahead 4 What
Caring Choices For Parents of Infants Newly Diagnosed with SMA Type 1 SMA CARE SERIES SMA CARE SERIES - Caring Choices Contents Dear Parents, Friends and Family Members 3 What Decisions are Ahead 4 What
Better Breathing with COPD
 Better Breathing with COPD People with Chronic Obstructive Pulmonary Disease (COPD) often benefit from learning different breathing techniques. Pursed Lip Breathing Pursed Lip Breathing (PLB) can be very
Better Breathing with COPD People with Chronic Obstructive Pulmonary Disease (COPD) often benefit from learning different breathing techniques. Pursed Lip Breathing Pursed Lip Breathing (PLB) can be very
Oxygenation. Chapter 21. Anatomy and Physiology of Breathing. Anatomy and Physiology of Breathing*
 Oxygenation Chapter 21 Anatomy and Physiology of Breathing Inspiration ~ breathing in Expiration ~ breathing out Ventilation ~ Movement of air in & out of the lungs Respiration ~ exchange of O2 & carbon
Oxygenation Chapter 21 Anatomy and Physiology of Breathing Inspiration ~ breathing in Expiration ~ breathing out Ventilation ~ Movement of air in & out of the lungs Respiration ~ exchange of O2 & carbon
What is Obstructive Sleep Apnoea?
 Patient Information Leaflet: Obstructive Sleep Apnoea Greenlane Respiratory Services, Auckland City Hospital & Greenlane Clinical Centre Auckland District Health Board What is Obstructive Sleep Apnoea?
Patient Information Leaflet: Obstructive Sleep Apnoea Greenlane Respiratory Services, Auckland City Hospital & Greenlane Clinical Centre Auckland District Health Board What is Obstructive Sleep Apnoea?
Understanding Hypoventilation and Its Treatment by Susan Agrawal
 www.complexchild.com Understanding Hypoventilation and Its Treatment by Susan Agrawal Most of us have a general understanding of what the term hyperventilation means, since hyperventilation, also called
www.complexchild.com Understanding Hypoventilation and Its Treatment by Susan Agrawal Most of us have a general understanding of what the term hyperventilation means, since hyperventilation, also called
MECHINICAL VENTILATION S. Kache, MD
 MECHINICAL VENTILATION S. Kache, MD Spontaneous respiration vs. Mechanical ventilation Natural spontaneous ventilation occurs when the respiratory muscles, diaphragm and intercostal muscles pull on the
MECHINICAL VENTILATION S. Kache, MD Spontaneous respiration vs. Mechanical ventilation Natural spontaneous ventilation occurs when the respiratory muscles, diaphragm and intercostal muscles pull on the
These factors increase your chance of developing emphysema. Tell your doctor if you have any of these risk factors:
 Emphysema Pronounced: em-fiss-see-mah by Debra Wood, RN En Español (Spanish Version) Definition Emphysema is a chronic obstructive disease of the lungs. The lungs contain millions of tiny air sacs called
Emphysema Pronounced: em-fiss-see-mah by Debra Wood, RN En Español (Spanish Version) Definition Emphysema is a chronic obstructive disease of the lungs. The lungs contain millions of tiny air sacs called
Lesson 7: Respiratory and Skeletal Systems and Tuberculosis
 Glossary 1. asthma: when the airways of the lungs narrow, making breathing difficult 2. bacteria: tiny living creatures that can only be seen with a microscope; some bacteria help the human body, and other
Glossary 1. asthma: when the airways of the lungs narrow, making breathing difficult 2. bacteria: tiny living creatures that can only be seen with a microscope; some bacteria help the human body, and other
Respiratory, Ventilator and Trach Resources
 The following excerpt has been taken from the Christopher & Dana Reeve Foundation Paralysis Resource Center website. http://www.paralysis.org/site/c.erjmjuoxfmh/b.1306557/k.a18e/respiratory.htm Respiratory,
The following excerpt has been taken from the Christopher & Dana Reeve Foundation Paralysis Resource Center website. http://www.paralysis.org/site/c.erjmjuoxfmh/b.1306557/k.a18e/respiratory.htm Respiratory,
How to Do Chest Physical Therapy (CPT) Babies and Toddlers
 How to Do Chest Physical Therapy (CPT) Babies and Toddlers (2001, 2004, 2009) The Emily Center, Phoenix Children s Hospital 1 2 (2001, 2004, 2009) The Emily Center, Phoenix Children s Hospital Name of
How to Do Chest Physical Therapy (CPT) Babies and Toddlers (2001, 2004, 2009) The Emily Center, Phoenix Children s Hospital 1 2 (2001, 2004, 2009) The Emily Center, Phoenix Children s Hospital Name of
Basic techniques of pulmonary physical therapy (I) 100/04/24
 Basic techniques of pulmonary physical therapy (I) 100/04/24 Evaluation of breathing function Chart review History Chest X ray Blood test Observation/palpation Chest mobility Shape of chest wall Accessory
Basic techniques of pulmonary physical therapy (I) 100/04/24 Evaluation of breathing function Chart review History Chest X ray Blood test Observation/palpation Chest mobility Shape of chest wall Accessory
American Heart Association
 American Heart Association Basic Life Support for Healthcare Providers Pretest April 2006 This examination to be used only as a PRECOURSE TEST For BLS for Healthcare Providers Courses 2006 American Heart
American Heart Association Basic Life Support for Healthcare Providers Pretest April 2006 This examination to be used only as a PRECOURSE TEST For BLS for Healthcare Providers Courses 2006 American Heart
Your Lungs and COPD. Patient Education Pulmonary Rehabilitation. A guide to how your lungs work and how COPD affects your lungs
 Patient Education Your Lungs and COPD A guide to how your lungs work and how COPD affects your lungs Your lungs are organs that process every breath you take. They provide oxygen (O 2 ) to the blood and
Patient Education Your Lungs and COPD A guide to how your lungs work and how COPD affects your lungs Your lungs are organs that process every breath you take. They provide oxygen (O 2 ) to the blood and
Fourth Grade The Human Body: The Respiratory System Assessment
 Fourth Grade The Human Body: The Respiratory System Assessment 1a. The brings air in and out of the body. a. respiratory system b. circulatory system 1b. The system is the part of the body responsible
Fourth Grade The Human Body: The Respiratory System Assessment 1a. The brings air in and out of the body. a. respiratory system b. circulatory system 1b. The system is the part of the body responsible
Anatomy and Physiology: Understanding the Importance of CPR
 Anatomy and Physiology: Understanding the Importance of CPR Overview This document gives you more information about the body s structure (anatomy) and function (physiology). This information will help
Anatomy and Physiology: Understanding the Importance of CPR Overview This document gives you more information about the body s structure (anatomy) and function (physiology). This information will help
Breathing and Holding Your Breath copyright, 2005, Dr. Ingrid Waldron and Jennifer Doherty, Department of Biology, University of Pennsylvania 1
 Breathing and Holding Your Breath copyright, 2005, Dr. Ingrid Waldron and Jennifer Doherty, Department of Biology, University of Pennsylvania 1 Introduction Everybody breathes all day, every day. Why?
Breathing and Holding Your Breath copyright, 2005, Dr. Ingrid Waldron and Jennifer Doherty, Department of Biology, University of Pennsylvania 1 Introduction Everybody breathes all day, every day. Why?
Pneumonia. Pneumonia is an infection that makes the tiny air sacs in your lungs inflamed (swollen and sore). They then fill with liquid.
 Pneumonia Pneumonia is an infection that makes the tiny air sacs in your lungs inflamed (swollen and sore). They then fill with liquid. People with mild (not so bad) pneumonia can usually be treated at
Pneumonia Pneumonia is an infection that makes the tiny air sacs in your lungs inflamed (swollen and sore). They then fill with liquid. People with mild (not so bad) pneumonia can usually be treated at
Whooping Cough. The Lungs Whooping cough is an infection of the lungs and breathing tubes, both of which are parts of the respiratory system.
 Whooping Cough Introduction Whooping cough is a serious bacterial infection of the lungs and breathing tubes. It is also called pertussis. About 16 million cases of whooping cough happen worldwide each
Whooping Cough Introduction Whooping cough is a serious bacterial infection of the lungs and breathing tubes. It is also called pertussis. About 16 million cases of whooping cough happen worldwide each
X-Plain Preparing For Surgery Reference Summary
 X-Plain Preparing For Surgery Reference Summary Introduction More than 25 million surgical procedures are performed each year in the US. This reference summary will help you prepare for surgery. By understanding
X-Plain Preparing For Surgery Reference Summary Introduction More than 25 million surgical procedures are performed each year in the US. This reference summary will help you prepare for surgery. By understanding
Northwestern Health Sciences University. Basic Life Support for Healthcare Providers
 Northwestern Health Sciences University Basic Life Support for Healthcare Providers Pretest May 2005 This examination to be used only as a PRECOURSE TEST for BLS for Healthcare Providers Courses Based
Northwestern Health Sciences University Basic Life Support for Healthcare Providers Pretest May 2005 This examination to be used only as a PRECOURSE TEST for BLS for Healthcare Providers Courses Based
Understanding Sleep Apnea
 Understanding Sleep Apnea www.sleepmangementsolutions.com What is Obstructive Sleep Apnea (OSA)? OSA afflicts 20 million adult men and women in the U.S. People who have OSA stop breathing repeatedly during
Understanding Sleep Apnea www.sleepmangementsolutions.com What is Obstructive Sleep Apnea (OSA)? OSA afflicts 20 million adult men and women in the U.S. People who have OSA stop breathing repeatedly during
American Heart Association. Basic Life Support for Healthcare Providers
 American Heart Association Basic Life Support for Healthcare Providers Pretest February 2001 This examination to be used only as a PRECOURSE TEST for BLS for Healthcare Providers Courses 2001 American
American Heart Association Basic Life Support for Healthcare Providers Pretest February 2001 This examination to be used only as a PRECOURSE TEST for BLS for Healthcare Providers Courses 2001 American
Human Body Vocabulary Words Week 1
 Vocabulary Words Week 1 1. arteries Any of the blood vessels that carry blood away from the heart to all parts of the body 2. heart The muscular organ inside the chest that pumps blood through the body
Vocabulary Words Week 1 1. arteries Any of the blood vessels that carry blood away from the heart to all parts of the body 2. heart The muscular organ inside the chest that pumps blood through the body
UW MEDICINE PATIENT EDUCATION. Aortic Stenosis. What is heart valve disease? What is aortic stenosis?
 UW MEDICINE PATIENT EDUCATION Aortic Stenosis Causes, symptoms, diagnosis, and treatment This handout describes aortic stenosis, a narrowing of the aortic valve in your heart. It also explains how this
UW MEDICINE PATIENT EDUCATION Aortic Stenosis Causes, symptoms, diagnosis, and treatment This handout describes aortic stenosis, a narrowing of the aortic valve in your heart. It also explains how this
Therapist Multiple-Choice Examination
 Therapist Multiple-Choice Examination Effective: January 2015 Detailed Content Outline Items are linked to open cells. Each scored form will include 20-item pretests. I. PATIENT DATA EVALUATION AND RECOMMENDATIONS
Therapist Multiple-Choice Examination Effective: January 2015 Detailed Content Outline Items are linked to open cells. Each scored form will include 20-item pretests. I. PATIENT DATA EVALUATION AND RECOMMENDATIONS
SPINAL MUSCULAR ATROPHY (SMA) is an autosomal recessive disorder and the
 SUPPLEMENT ARTICLE Special Considerations in the Respiratory Management of Spinal Muscular Atrophy Mary K. Schroth, MD Department of Pediatrics, University of Wisconsin School of Medicine and Public Health,
SUPPLEMENT ARTICLE Special Considerations in the Respiratory Management of Spinal Muscular Atrophy Mary K. Schroth, MD Department of Pediatrics, University of Wisconsin School of Medicine and Public Health,
The Take-Apart Human Body
 The Take-Apart Human Body As any teacher knows, children are naturally curious about their bodies. Their questions are endless, and present a tremendous educational opportunity: How do my ears work? Where
The Take-Apart Human Body As any teacher knows, children are naturally curious about their bodies. Their questions are endless, and present a tremendous educational opportunity: How do my ears work? Where
Support for breathing problems
 8A Support for breathing problems Information for people with or affected by motor neurone disease Motor neurone disease (MND) affects people in different ways. You are unlikely to have exactly the same
8A Support for breathing problems Information for people with or affected by motor neurone disease Motor neurone disease (MND) affects people in different ways. You are unlikely to have exactly the same
Surgery for oesophageal cancer
 Surgery for oesophageal cancer This information is an extract from the booklet Understanding oesophageal cancer (cancer of the gullet). You may find the full booklet helpful. We can send you a free copy
Surgery for oesophageal cancer This information is an extract from the booklet Understanding oesophageal cancer (cancer of the gullet). You may find the full booklet helpful. We can send you a free copy
Physiotherapy for Video Assisted Thoracic Surgery Patients
 Physio for VATS patients Royal Devon and Exeter NHS Foundation Trust Physiotherapy for Video Assisted Thoracic Surgery Patients July 2008 (Review date: July 2011) Physiotherapy Department...01392 402438
Physio for VATS patients Royal Devon and Exeter NHS Foundation Trust Physiotherapy for Video Assisted Thoracic Surgery Patients July 2008 (Review date: July 2011) Physiotherapy Department...01392 402438
CHAPTER 1: THE LUNGS AND RESPIRATORY SYSTEM
 CHAPTER 1: THE LUNGS AND RESPIRATORY SYSTEM INTRODUCTION Lung cancer affects a life-sustaining system of the body, the respiratory system. The respiratory system is responsible for one of the essential
CHAPTER 1: THE LUNGS AND RESPIRATORY SYSTEM INTRODUCTION Lung cancer affects a life-sustaining system of the body, the respiratory system. The respiratory system is responsible for one of the essential
Chapter 26. Assisting With Oxygen Needs. Elsevier items and derived items 2014, 2010 by Mosby, an imprint of Elsevier Inc. All rights reserved.
 Chapter 26 Assisting With Oxygen Needs Oxygen (O 2 ) is a gas. Oxygen It has no taste, odor, or color. It is a basic need required for life. Death occurs within minutes if breathing stops. Brain damage
Chapter 26 Assisting With Oxygen Needs Oxygen (O 2 ) is a gas. Oxygen It has no taste, odor, or color. It is a basic need required for life. Death occurs within minutes if breathing stops. Brain damage
Adult Choking and CPR Manual
 Adult Choking and CPR Manual 2009 Breath of Life Home Medical Equipment and Respiratory Services CHOKING Description: Choking is the coughing spasm and sputtering that happen when liquids or solids get
Adult Choking and CPR Manual 2009 Breath of Life Home Medical Equipment and Respiratory Services CHOKING Description: Choking is the coughing spasm and sputtering that happen when liquids or solids get
Sensory Sanctuary Staff Occupational Therapy Stress Management Program julie.greenberg@downstate.edu
 Abdominal Breathing Technique How it s done: With one hand on the chest and the other on the belly, take a deep breath in through the nose, ensuring the diaphragm (not the chest) inflates with enough air
Abdominal Breathing Technique How it s done: With one hand on the chest and the other on the belly, take a deep breath in through the nose, ensuring the diaphragm (not the chest) inflates with enough air
RSV infection. Information about RSV and how you can reduce the risk of your infant developing a severe infection.
 RSV infection Information about RSV and how you can reduce the risk of your infant developing a severe infection. What is RSV? RSV is one of the most common respiratory viruses and is spread easily. By
RSV infection Information about RSV and how you can reduce the risk of your infant developing a severe infection. What is RSV? RSV is one of the most common respiratory viruses and is spread easily. By
PATIENT HANDBOOK AND JOURNAL DAY OF SURGERY
 PATIENT HANDBOOK AND JOURNAL DAY OF SURGERY PREPARING YOUR SKIN BEFORE SURGERY PRE-OP HIBICLENS BATHING INSTRUCTIONS: General Information: Because the skin is not sterile, it is important to make sure
PATIENT HANDBOOK AND JOURNAL DAY OF SURGERY PREPARING YOUR SKIN BEFORE SURGERY PRE-OP HIBICLENS BATHING INSTRUCTIONS: General Information: Because the skin is not sterile, it is important to make sure
Pneumonia Education and Discharge Instructions
 Pneumonia Education and Discharge Instructions Pneumonia Education and Discharge Instructions Definition: Pneumonia is an infection of the lungs. Many different organisms can cause it, including bacteria,
Pneumonia Education and Discharge Instructions Pneumonia Education and Discharge Instructions Definition: Pneumonia is an infection of the lungs. Many different organisms can cause it, including bacteria,
By Casey Schmidt and Wendy Ford
 By Casey Schmidt and Wendy Ford Body systems Digestive System Circulatory System Respiratory System Excretory System Immune System Reproductive System Nervous System Muscular System Skeletal System Endocrine
By Casey Schmidt and Wendy Ford Body systems Digestive System Circulatory System Respiratory System Excretory System Immune System Reproductive System Nervous System Muscular System Skeletal System Endocrine
Physiotherapy treatment in cystic fibrosis: airway clearance techniques
 Physiotherapy treatment in cystic fibrosis: airway clearance techniques Factsheet March 2013 Physiotherapy treatment in cystic fibrosis: airway clearance techniques Introduction Looking after the chest
Physiotherapy treatment in cystic fibrosis: airway clearance techniques Factsheet March 2013 Physiotherapy treatment in cystic fibrosis: airway clearance techniques Introduction Looking after the chest
BREATHE BETTER SWIM FASTER
 BREATHE BETTER SWIM FASTER Breath control is fundamental to efficient swimming. Like singers, swimmers need to train their breathing for effective performance. Controlled breathing is the main factor contributing
BREATHE BETTER SWIM FASTER Breath control is fundamental to efficient swimming. Like singers, swimmers need to train their breathing for effective performance. Controlled breathing is the main factor contributing
Guide to Respiratory Care for Neuromuscular Disorders
 Guide to Respiratory Care for Neuromuscular Disorders National Office info@muscle.ca 2345 Yonge St. Suite 900 Toronto, ON M4P 2E5 Tel: 1-866-MUSCLE-8 416-488-0030 Fax: 416-488-7523 www.muscle.ca Vision
Guide to Respiratory Care for Neuromuscular Disorders National Office info@muscle.ca 2345 Yonge St. Suite 900 Toronto, ON M4P 2E5 Tel: 1-866-MUSCLE-8 416-488-0030 Fax: 416-488-7523 www.muscle.ca Vision
DME: Definition... 2 Life Sustaining DME... 3 Oxygen Use Policy... 4 Non-Life Sustaining DME... 7
 DME: Definition... 2 Life Sustaining DME... 3 Oxygen Use Policy... 4 Non-Life Sustaining DME... 7 A Division of Health Care Service Corporation, a Mutual Legal Reserve Company, an Independent Licensee
DME: Definition... 2 Life Sustaining DME... 3 Oxygen Use Policy... 4 Non-Life Sustaining DME... 7 A Division of Health Care Service Corporation, a Mutual Legal Reserve Company, an Independent Licensee
Oxygen AND COPD. This fact sheet talks about home oxygen, prescribed as a medicine for some people with COPD.
 Oxygen AND COPD This fact sheet talks about home oxygen, prescribed as a medicine for some people with COPD. For more information on COPD, phone 1-866-717-COPD (2673) or visit us online at www.lung.ca/copd
Oxygen AND COPD This fact sheet talks about home oxygen, prescribed as a medicine for some people with COPD. For more information on COPD, phone 1-866-717-COPD (2673) or visit us online at www.lung.ca/copd
Breathing Exercises and Clearing Your Chest
 Information for patients Breathing Exercises and Clearing Your Chest Physiotherapy Department Tel: 01473 702073 DMI ref: 1898-08.indd(RP) Issue 1: October 2008 The Ipswich Hospital NHS Trust, 2008. All
Information for patients Breathing Exercises and Clearing Your Chest Physiotherapy Department Tel: 01473 702073 DMI ref: 1898-08.indd(RP) Issue 1: October 2008 The Ipswich Hospital NHS Trust, 2008. All
Degree of Intervention
 Inglewood Care Centre Degree of Intervention Handbook for Residents and Families Index Introduction..................................................... 2 Beliefs, Values, and Wishes.........................................
Inglewood Care Centre Degree of Intervention Handbook for Residents and Families Index Introduction..................................................... 2 Beliefs, Values, and Wishes.........................................
Tracheostomy Care at Home
 Tracheostomy Care at Home Patient Education CARE AND TREATMENT This information will help you understand how to care for a person with a tracheostomy at home. It is a supplement to the teaching offered
Tracheostomy Care at Home Patient Education CARE AND TREATMENT This information will help you understand how to care for a person with a tracheostomy at home. It is a supplement to the teaching offered
Breathing Problems of Polio Survivors
 Breathing Problems of Polio Survivors People with neuromuscular disease such as post-polio often need help with breathing, not because there is something wrong with the lungs, but because the respiratory
Breathing Problems of Polio Survivors People with neuromuscular disease such as post-polio often need help with breathing, not because there is something wrong with the lungs, but because the respiratory
WHEN COPD* SYMPTOMS GET WORSE
 WHEN COPD* SYMPTOMS GET WORSE *Includes chronic bronchitis, emphysema, or both. Boehringer Ingelheim Pharmaceuticals, Inc. has no ownership interest in any other organization that advertises or markets
WHEN COPD* SYMPTOMS GET WORSE *Includes chronic bronchitis, emphysema, or both. Boehringer Ingelheim Pharmaceuticals, Inc. has no ownership interest in any other organization that advertises or markets
National Hospital for Neurology and Neurosurgery. Continuous positive airway pressure (CPAP) Sleep Respiratory Unit
 National Hospital for Neurology and Neurosurgery Continuous positive airway pressure (CPAP) Sleep Respiratory Unit If you would like this document in another language or format or if you require the services
National Hospital for Neurology and Neurosurgery Continuous positive airway pressure (CPAP) Sleep Respiratory Unit If you would like this document in another language or format or if you require the services
What You Should Know About ASTHMA
 What You Should Know About ASTHMA 200 Hospital Drive Galax, VA 24333 (276) 236-8181 www.tcrh.org WHAT IS ASTHMA? It s a lung condition that makes breathing difficult. The cause of asthma is not known.
What You Should Know About ASTHMA 200 Hospital Drive Galax, VA 24333 (276) 236-8181 www.tcrh.org WHAT IS ASTHMA? It s a lung condition that makes breathing difficult. The cause of asthma is not known.
GUIDELINES FOR THE MANAGEMENT OF OXYGEN THERAPY
 SOUTH DURHAM HEALTH CARE NHS TRUST GUIDELINES FOR THE MANAGEMENT OF OXYGEN THERAPY AIM To supplement oxygen intake using the appropriate equipment in order to correct hypoxia and relieve breathlessness.
SOUTH DURHAM HEALTH CARE NHS TRUST GUIDELINES FOR THE MANAGEMENT OF OXYGEN THERAPY AIM To supplement oxygen intake using the appropriate equipment in order to correct hypoxia and relieve breathlessness.
Respiratory Syncytial Virus (RSV)
 Respiratory Syncytial Virus (RSV) What is? is a common virus that infects the linings of the airways - the nose, throat, windpipe, bronchi and bronchioles (the air passages of the lungs). RSV is found
Respiratory Syncytial Virus (RSV) What is? is a common virus that infects the linings of the airways - the nose, throat, windpipe, bronchi and bronchioles (the air passages of the lungs). RSV is found
What is the Spasticity Clinic?
 The Spasticity Clinic This booklet can help you learn about: the Spasticity Clinic at McMaster Children s Hospital spasticity and how it may be treated Your therapist will give you more information and
The Spasticity Clinic This booklet can help you learn about: the Spasticity Clinic at McMaster Children s Hospital spasticity and how it may be treated Your therapist will give you more information and
Cardiopulmonary Physical Therapy. Haneul Lee, DSc, PT
 Cardiopulmonary Physical Therapy Haneul Lee, DSc, PT Airway ClearanceTechniques Breathing Exercise SpecialConsiderations for MechanicallyVentilated Exercise Injury Prevention and Equipment provision Patient
Cardiopulmonary Physical Therapy Haneul Lee, DSc, PT Airway ClearanceTechniques Breathing Exercise SpecialConsiderations for MechanicallyVentilated Exercise Injury Prevention and Equipment provision Patient
Tests. Pulmonary Functions
 Pulmonary Functions Tests Static lung functions volumes Dynamic lung functions volume and velocity Dynamic Tests Velocity dependent on Airway resistance Resistance of lung tissue to change in shape Dynamic
Pulmonary Functions Tests Static lung functions volumes Dynamic lung functions volume and velocity Dynamic Tests Velocity dependent on Airway resistance Resistance of lung tissue to change in shape Dynamic
Interscalene Block. Nancy A. Brown, MD
 Interscalene Block Nancy A. Brown, MD What is an Interscalene Block? An Interscalene block is a form of regional anesthesia used in conjunction with general anesthesia for surgeries of the shoulder and
Interscalene Block Nancy A. Brown, MD What is an Interscalene Block? An Interscalene block is a form of regional anesthesia used in conjunction with general anesthesia for surgeries of the shoulder and
On the Go with Oxygen
 On the Go with Oxygen Oxygen is in the air we breathe and is necessary to live. When we breathe in, oxygen enters the lungs and it goes into the blood. When the lungs cannot transfer enough oxygen into
On the Go with Oxygen Oxygen is in the air we breathe and is necessary to live. When we breathe in, oxygen enters the lungs and it goes into the blood. When the lungs cannot transfer enough oxygen into
Hysterectomy Vaginal hysterectomy Abdominal hysterectomy
 Hysterectomy A hysterectomy is a surgery to remove a woman s uterus. The uterus is one of the organs of the female reproductive system and is about the size of a closed hand. You can no longer have children
Hysterectomy A hysterectomy is a surgery to remove a woman s uterus. The uterus is one of the organs of the female reproductive system and is about the size of a closed hand. You can no longer have children
TRACHEOSTOMY TUBE PARTS
 Page1 NR 33 TRACHEOSTOMY CARE AND SUCTIONING Review ATI Basic skills videos: Tracheostomy care and Endotracheal suction using a closed suction set. TRACHEOSTOMY TUBE PARTS Match the numbers on the diagram
Page1 NR 33 TRACHEOSTOMY CARE AND SUCTIONING Review ATI Basic skills videos: Tracheostomy care and Endotracheal suction using a closed suction set. TRACHEOSTOMY TUBE PARTS Match the numbers on the diagram
Colon Cancer Surgery and Recovery. A Guide for Patients and Families
 Colon Cancer Surgery and Recovery A Guide for Patients and Families This Booklet You are receiving this booklet because you will be having surgery shortly. This booklet tells you what to do before, during,
Colon Cancer Surgery and Recovery A Guide for Patients and Families This Booklet You are receiving this booklet because you will be having surgery shortly. This booklet tells you what to do before, during,
Your Recovery After a Cesarean Delivery
 Your Recovery After a Cesarean Delivery It is normal to have many questions about your care after delivery. Cesarean delivery is surgery and your body needs time to heal and recover for the next 6 weeks,
Your Recovery After a Cesarean Delivery It is normal to have many questions about your care after delivery. Cesarean delivery is surgery and your body needs time to heal and recover for the next 6 weeks,
Why is prematurity a concern?
 Prematurity What is prematurity? A baby born before 37 weeks of pregnancy is considered premature. Approximately 12% of all babies are born prematurely. Terms that refer to premature babies are preterm
Prematurity What is prematurity? A baby born before 37 weeks of pregnancy is considered premature. Approximately 12% of all babies are born prematurely. Terms that refer to premature babies are preterm
Activity: Build Your Own Lung
 Activity: Build Your Own Lung Supplies per group: 2 liter pop bottle Scissors 2 straws 2 balloons 3 rubber bands clay piece of clear wrap paper binder clip Directions: 1. Carefully, cut the bottom off
Activity: Build Your Own Lung Supplies per group: 2 liter pop bottle Scissors 2 straws 2 balloons 3 rubber bands clay piece of clear wrap paper binder clip Directions: 1. Carefully, cut the bottom off
Ear Disorders and Problems
 Ear Disorders and Problems Introduction Your ear has three main parts: outer, middle and inner. You use all of them to hear. There are many disorders and problems that can affect the ear. The symptoms
Ear Disorders and Problems Introduction Your ear has three main parts: outer, middle and inner. You use all of them to hear. There are many disorders and problems that can affect the ear. The symptoms
Part 1: Physiology. Below is a cut-through view of a human head:
 The Frenzel Technique, Step-by-Step by Eric Fattah, Copyright 2001 efattah@interchange.ubc.ca This document should be in electronic form at: http://www.ericfattah.com/equalizing.html Feel free to distribute
The Frenzel Technique, Step-by-Step by Eric Fattah, Copyright 2001 efattah@interchange.ubc.ca This document should be in electronic form at: http://www.ericfattah.com/equalizing.html Feel free to distribute
AT HOME DR. D. K. PILLAI MUG @ UOM
 NON - INVASIVE VENTILATION AT HOME DR. D. K. PILLAI 07.09.2011 MUG @ UOM In the beginning came. OSA (HS) 1. CPAP for OSAHS (Obstructive Sleep Apnoea Hypopnoea Syndrome) 2 NIPPV 2. NIPPV (Non
NON - INVASIVE VENTILATION AT HOME DR. D. K. PILLAI 07.09.2011 MUG @ UOM In the beginning came. OSA (HS) 1. CPAP for OSAHS (Obstructive Sleep Apnoea Hypopnoea Syndrome) 2 NIPPV 2. NIPPV (Non
Guidelines for Standards of Care for Patients with Acute Respiratory Failure on Mechanical Ventilatory Support
 Guidelines for Standards of Care for Patients with Acute Respiratory Failure on Mechanical Ventilatory Support Copyright by the SOCIETY OF CRITICAL CARE MEDICINE These guidelines can also be found in the
Guidelines for Standards of Care for Patients with Acute Respiratory Failure on Mechanical Ventilatory Support Copyright by the SOCIETY OF CRITICAL CARE MEDICINE These guidelines can also be found in the
About lung cancer. Contents. The lungs
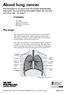 This information is an extract from the booklet Understanding lung cancer. You may find the full booklet helpful. We can send you a free copy see page 7. The lungs Contents The lungs Types of lung cancer
This information is an extract from the booklet Understanding lung cancer. You may find the full booklet helpful. We can send you a free copy see page 7. The lungs Contents The lungs Types of lung cancer
We as COPD ers have to deal with our breathing on so many levels: (1). The psychology of breathing - How anxiety affects our breathing.
 This is from a letter that a member of COPD-International and others, Filcab, developed for publication and sharing with everyone. He would like everyone either who has COPD or works with COPDers to have
This is from a letter that a member of COPD-International and others, Filcab, developed for publication and sharing with everyone. He would like everyone either who has COPD or works with COPDers to have
X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary
 X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary Introduction A Subclavian Inserted Central Catheter, or subclavian line, is a long thin hollow tube inserted in a vein under the
X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary Introduction A Subclavian Inserted Central Catheter, or subclavian line, is a long thin hollow tube inserted in a vein under the
Endoscopic Plantar Fasciotomy
 Endoscopic Plantar Fasciotomy Introduction Plantar fasciitis is a common condition that causes pain centralized around the heel. It may be severe enough to affect regular activities. Health care providers
Endoscopic Plantar Fasciotomy Introduction Plantar fasciitis is a common condition that causes pain centralized around the heel. It may be severe enough to affect regular activities. Health care providers
Position Classification Standard for Respiratory Therapist, GS-0651
 Position Classification Standard for Respiratory Therapist, GS-0651 Table of Contents SERIES DEFINITION... 2 EXCLUSIONS... 2 AUTHORIZED TITLES... 3 OCCUPATIONAL INFORMATION... 3 GRADING OF POSITIONS...
Position Classification Standard for Respiratory Therapist, GS-0651 Table of Contents SERIES DEFINITION... 2 EXCLUSIONS... 2 AUTHORIZED TITLES... 3 OCCUPATIONAL INFORMATION... 3 GRADING OF POSITIONS...
THE LUNGS IN MARFAN SYNDROME
 THE LUNGS IN MARFAN SYNDROME Many people with Marfan syndrome and some related disorders experience pulmonary complications, or problems with their lungs. If you have Marfan syndrome, it is important for
THE LUNGS IN MARFAN SYNDROME Many people with Marfan syndrome and some related disorders experience pulmonary complications, or problems with their lungs. If you have Marfan syndrome, it is important for
stretches and exercises
 stretches and exercises The enclosed sheets contain stretches and exercises which can be used to delay and minimise the development of contractures and deformities occurring in children with Duchenne muscular
stretches and exercises The enclosed sheets contain stretches and exercises which can be used to delay and minimise the development of contractures and deformities occurring in children with Duchenne muscular
Gallbladder Surgery with an Incision (Cholecystectomy)
 Gallbladder Surgery with an Incision (Cholecystectomy) It is normal to have questions about your surgery. This handout gives you information about what will happen to you before, during and after your
Gallbladder Surgery with an Incision (Cholecystectomy) It is normal to have questions about your surgery. This handout gives you information about what will happen to you before, during and after your
Nursing college, Second stage Microbiology Dr.Nada Khazal K. Hendi L14: Hospital acquired infection, nosocomial infection
 L14: Hospital acquired infection, nosocomial infection Definition A hospital acquired infection, also called a nosocomial infection, is an infection that first appears between 48 hours and four days after
L14: Hospital acquired infection, nosocomial infection Definition A hospital acquired infection, also called a nosocomial infection, is an infection that first appears between 48 hours and four days after
CHAPTER 5 - BREATHING "THE RESPIRATORY SYSTEM"
 CHAPTER 5 - BREATHING "THE RESPIRATORY SYSTEM" You have read how the blood transports oxygen from the lungs to cells and carries carbon dioxide from the cells to the lungs. It is the function of the respiratory
CHAPTER 5 - BREATHING "THE RESPIRATORY SYSTEM" You have read how the blood transports oxygen from the lungs to cells and carries carbon dioxide from the cells to the lungs. It is the function of the respiratory
A Patient s Guide to Rib Joint Pain
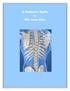 A Patient s Guide to Rib Joint Pain Anatomy Where are the rib joints? Your rib cage is made up of twelve pairs of ribs. The ribs attach to the spine in the back, and to the breastbone in the front. The
A Patient s Guide to Rib Joint Pain Anatomy Where are the rib joints? Your rib cage is made up of twelve pairs of ribs. The ribs attach to the spine in the back, and to the breastbone in the front. The
Module 4 The POLST Conversation POLST Script
 Module 4 The POLST Conversation POLST Script The POLST Script provides detailed information in order to develop comfort and competence when facilitating a POLST conversation. The POLST conversation utilizes
Module 4 The POLST Conversation POLST Script The POLST Script provides detailed information in order to develop comfort and competence when facilitating a POLST conversation. The POLST conversation utilizes
What You And Your Family Can Do About Asthma
 GLOBAL INITIATIVE FOR ASTHMA What You And Your Family Can Do About Asthma BASED ON THE GLOBAL STRATEGY FOR ASTHMA MANAGEMENT AND PREVENTION NHLBI/WHO WORKSHOP REPORT NATIONAL INSTITUTES OF HEALTH NATIONAL
GLOBAL INITIATIVE FOR ASTHMA What You And Your Family Can Do About Asthma BASED ON THE GLOBAL STRATEGY FOR ASTHMA MANAGEMENT AND PREVENTION NHLBI/WHO WORKSHOP REPORT NATIONAL INSTITUTES OF HEALTH NATIONAL
Guo Lin walking Qigong and the standing Guo Lin Qigong practices.
 Guo Lin walking Qigong and the standing Guo Lin Qigong practices. These are the forms used by Guo Lin to treat her own cancer, and used to treat the cancer of many others. If you have cancer, please consult
Guo Lin walking Qigong and the standing Guo Lin Qigong practices. These are the forms used by Guo Lin to treat her own cancer, and used to treat the cancer of many others. If you have cancer, please consult
Liver Resection. Patient Information Booklet. Delivering the best in care. UHB is a no smoking Trust
 Liver Resection Patient Information Booklet Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Liver Resection Patient Information Booklet Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Mini Medical School Lesson
 Mini Medical School Lesson The American Osteopathic Association s (AOA) Mini Medical School Lesson is designed to help educators teach children about health and fitness. This lesson is aimed towards elementary
Mini Medical School Lesson The American Osteopathic Association s (AOA) Mini Medical School Lesson is designed to help educators teach children about health and fitness. This lesson is aimed towards elementary
SANTA CLARA VALLEY MEDICAL CENTER
 Page 1 of 5 N: 11/09 C: 05/12 R-NC: A7180-08 PURPOSE/OBJECTIVE: 1. Respiratory Care/Pulmonary Diagnostic lab participates in a hospital-wide Performance Improvement (PI) Program designed to monitor, evaluate
Page 1 of 5 N: 11/09 C: 05/12 R-NC: A7180-08 PURPOSE/OBJECTIVE: 1. Respiratory Care/Pulmonary Diagnostic lab participates in a hospital-wide Performance Improvement (PI) Program designed to monitor, evaluate
Chronic Obstructive Pulmonary Disease Patient Guidebook
 Chronic Obstructive Pulmonary Disease Patient Guidebook The Respiratory System The respiratory system consists of the lungs and air passages. The lungs are the part of the body where gases are exchanged
Chronic Obstructive Pulmonary Disease Patient Guidebook The Respiratory System The respiratory system consists of the lungs and air passages. The lungs are the part of the body where gases are exchanged
Respiratory Management Following Spinal Cord Injury: What You Should Know
 SPINAL CORD MEDICINE C O N S U M E R G U I D E : R E S P I R A T O R Y M A N A G E M E N T Respiratory Management Following Spinal Cord Injury: What You Should Know A Guide for People with Spinal Cord
SPINAL CORD MEDICINE C O N S U M E R G U I D E : R E S P I R A T O R Y M A N A G E M E N T Respiratory Management Following Spinal Cord Injury: What You Should Know A Guide for People with Spinal Cord
Lung Cancer. This reference summary will help you better understand lung cancer and the treatment options that are available.
 Lung Cancer Introduction Lung cancer is the number one cancer killer of men and women. Over 165,000 people die of lung cancer every year in the United States. Most cases of lung cancer are related to cigarette
Lung Cancer Introduction Lung cancer is the number one cancer killer of men and women. Over 165,000 people die of lung cancer every year in the United States. Most cases of lung cancer are related to cigarette
CONTENTS. Note to the Reader 00. Acknowledgments 00. About the Author 00. Preface 00. Introduction 00
 Natural Therapies for Emphysema By Robert J. Green Jr., N.D. CONTENTS Note to the Reader 00 Acknowledgments 00 About the Author 00 Preface 00 Introduction 00 1 Essential Respiratory Anatomy and Physiology
Natural Therapies for Emphysema By Robert J. Green Jr., N.D. CONTENTS Note to the Reader 00 Acknowledgments 00 About the Author 00 Preface 00 Introduction 00 1 Essential Respiratory Anatomy and Physiology
Electroconvulsive Therapy - ECT
 Electroconvulsive Therapy - ECT Introduction Electroconvulsive therapy, or ECT, is a safe and effective treatment that may reduce symptoms related to depression or mental illness. During ECT, certain parts
Electroconvulsive Therapy - ECT Introduction Electroconvulsive therapy, or ECT, is a safe and effective treatment that may reduce symptoms related to depression or mental illness. During ECT, certain parts
Plantar Fascia Release
 Plantar Fascia Release Introduction Plantar fasciitis is a common condition that causes pain around the heel. It may be severe enough to affect regular activities. If other treatments are unsuccessful,
Plantar Fascia Release Introduction Plantar fasciitis is a common condition that causes pain around the heel. It may be severe enough to affect regular activities. If other treatments are unsuccessful,
Pulmonary Ventilation
 Pulmonary Ventilation Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction Pulmonary ventilation, or breathing, is the
Pulmonary Ventilation Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction Pulmonary ventilation, or breathing, is the
Department of Surgery
 What is emphysema? 2004 Regents of the University of Michigan Emphysema is a chronic disease of the lungs characterized by thinning and overexpansion of the lung-like blisters (bullae) in the lung tissue.
What is emphysema? 2004 Regents of the University of Michigan Emphysema is a chronic disease of the lungs characterized by thinning and overexpansion of the lung-like blisters (bullae) in the lung tissue.
Recovery plan: radical cystectomy Information for patients
 Recovery plan: radical cystectomy Information for patients Help for you following a bereavement 5 This leaflet will help you know what to expect during your time with us. Please take some time to read
Recovery plan: radical cystectomy Information for patients Help for you following a bereavement 5 This leaflet will help you know what to expect during your time with us. Please take some time to read
TOWN OF FAIRFIELD HEALTH DEPARTMENT PUBLIC HEALTH NURSING
 TOWN OF FAIRFIELD HEALTH DEPARTMENT PUBLIC HEALTH NURSING PROGRAM: School Health APPROVED BY: Board of Health School Medical Advisor POLICY: With Portable Suction Machine DATE: March 14, 1994 POLICY DEFINITION:
TOWN OF FAIRFIELD HEALTH DEPARTMENT PUBLIC HEALTH NURSING PROGRAM: School Health APPROVED BY: Board of Health School Medical Advisor POLICY: With Portable Suction Machine DATE: March 14, 1994 POLICY DEFINITION:
Emergency Medical Services Advanced Level Competency Checklist
 Emergency Services Advanced Level Competency Checklist EMS Service: Current License in State of Nebraska: # (Copy of license kept in file at station) Date of joining EMS Service: EMS Service Member Name:
Emergency Services Advanced Level Competency Checklist EMS Service: Current License in State of Nebraska: # (Copy of license kept in file at station) Date of joining EMS Service: EMS Service Member Name:
What If I Have a Spot on My Lung? Do I Have Cancer? Patient Education Guide
 What If I Have a Spot on My Lung? Do I Have Cancer? Patient Education Guide A M E R I C A N C O L L E G E O F C H E S T P H Y S I C I A N S Lung cancer is one of the most common cancers. About 170,000
What If I Have a Spot on My Lung? Do I Have Cancer? Patient Education Guide A M E R I C A N C O L L E G E O F C H E S T P H Y S I C I A N S Lung cancer is one of the most common cancers. About 170,000
HEALTH EFFECTS. Inhalation
 Health Effects HEALTH EFFECTS Asbestos can kill you. You must take extra precautions when you work with asbestos. Just because you do not notice any problems while you are working with asbestos, it still
Health Effects HEALTH EFFECTS Asbestos can kill you. You must take extra precautions when you work with asbestos. Just because you do not notice any problems while you are working with asbestos, it still
CPR/AED for Professional Rescuers and Health Care Providers HANDBOOK
 CPR/AED for Professional Rescuers and Health Care Providers HANDBOOK TABLE OF CONTENTS SECTION 1: THE PROFESSIONAL RESCUER The Duty to Respond 2 Preventing the Spread of Bloodborne Pathogens 3 Taking Action
CPR/AED for Professional Rescuers and Health Care Providers HANDBOOK TABLE OF CONTENTS SECTION 1: THE PROFESSIONAL RESCUER The Duty to Respond 2 Preventing the Spread of Bloodborne Pathogens 3 Taking Action
Cardio-Pulmonary Resuscitation (CPR): A Decision Aid For. KGH Patients And Their Families
 Cardio-Pulmonary Resuscitation (CPR): A Decision Aid For KGH Patients And Their Families The goal of this pamphlet is to provide information about cardiopulmonary resuscitation (CPR) so you can be adequately
Cardio-Pulmonary Resuscitation (CPR): A Decision Aid For KGH Patients And Their Families The goal of this pamphlet is to provide information about cardiopulmonary resuscitation (CPR) so you can be adequately
